Computer Model of Mechanisms Underlying Dynamic Electrocardiographic T-wave Changes. Ashish Nikhil Doshi
|
|
|
- Felicity Garrett
- 6 years ago
- Views:
Transcription
1 Computer Model of Mechanisms Underlying Dynamic Electrocardiographic T-wave Changes by Ashish Nikhil Doshi Department of Biomedical Engineering Duke University Date: Approved: Salim F. Idriss, Supervisor Craig S. Henriquez Wanda K. Neu Patrick D. Wolf Warren M. Grill Dissertation submitted in partial fulfillment of the requirements for the degree of Doctor of Philosophy in the Department of Biomedical Engineering in the Graduate School of Duke University 2010
2 ABSTRACT Computer Model of Mechanisms Underlying Dynamic Electrocardiographic T-wave Changes by Ashish Nikhil Doshi Department of Biomedical Engineering Duke University Date: Approved: Salim F. Idriss, Supervisor Craig S. Henriquez Wanda K. Neu Patrick D. Wolf Warren M. Grill An abstract of a dissertation submitted in partial fulfillment of the requirements for the degree of Doctor of Philosophy in the Department of Biomedical Engineering in the Graduate School of Duke University 2010
3 Copyright by Ashish Nikhil Doshi 2010
4 Abstract Sudden death from arrhythmia is a major cause of mortality in the United States. Unfortunately, no current diagnostic test can accurately predict risk for sudden arrhythmic death. Because ventricular arrhythmias often result from abnormalities of repolarization, assessment of myocardial repolarization using the electrocardiogram (ECG) can aid in prediction of arrhythmia risk. Non-linear, rate-dependent changes in myocardial repolarization can promote the development of arrhythmia, but few studies examine how these dynamic changes in repolarization affect the ECG. This dissertation describes the use of a computer model to investigate the effect of dynamic changes in myocardial repolarization on the ECG T wave. To simulate action potential conduction from the endocardium to the epicardium of the free wall of the canine left ventricle, 1-dimensional multicellular computer fiber models were created. Each fiber model was composed of endocardial, midmyocardial, and epicardial cells. For each cell type, existing mathematical models were modified to approximate experimental data for four types of dynamic repolarization behavior: (1) dynamic restitution, the response to steady-state pacing; (2) S1-S2 restitution, the response to a premature or postmature stimulus; (3) short-term memory (STM), the response to an abrupt change in pacing rate; and (4) repolarization alternans, beat-to-beat alternation in cellular repolarization time. Repolarization times were obtained from endocardial, midmyocardial, and epicardial regions in the fiber model and compared to parameters measured from a computed transmural ECG. iv
5 Spatial differences in repolarization created two voltage gradients that influenced the ECG: an endocardial-midmyocardial (endo-mid) gradient and a midmyocardialepicardial (mid-epi) gradient. Epicardial dynamic restitution changes altered the mid-epi gradient, influencing the rising phase of the ECG T wave, and endocardial dynamic restitution changes altered the endo-mid gradient, influencing the falling phase of the T wave. Changes in epicardial or endocardial repolarization due to S1-S2 restitution or STM caused transient changes in the rising or falling phase of the T wave, respectively. During repolarization alternans, an alternating, asymmetric distribution of extracellular potential around the fiber influenced the measurement of T-wave alternans (TWA) in the ECG. Presence of a resistive barrier in the fiber model altered the magnitude of repolarization alternans as well as the TWA amplitude in the ECG with effects dependent on barrier location. The resistive barrier also modified the relationship between cellular repolarization alternans magnitude and TWA amplitude. The results presented in this dissertation explain basic mechanisms by which dynamic changes in myocardial repolarization affect the ECG T wave. These mechanisms form the foundation for the development of techniques to identify arrhythmogenic, dynamic changes in the myocardium using the ECG. Future studies in higher-dimensional, more complex models will build upon these results by considering the influence of additional voltage gradients, more realistic tissue geometries, and heterogeneities in the volume conductor. v
6 Contents Abstract... iv List of Tables... x List of Figures... xi List of Abbreviations... xv 1. Introduction Significance of Research in Cardiac Electrophysiology Dynamic Repolarization of Cardiac Tissue Electrical Restitution: The 1:1 Domain Action Potential Duration Alternans: The 2:2 Rhythm Dynamic ECG Changes Motivation for Using a Computer Model Advantages of Using a Computer Model Limitations of Using a Computer Model Research Goals and Specific Aims Methods Computer Fiber Model Overview Fiber Model for Restitution Studies Fiber Model for Repolarization Alternans Studies Models of Cellular Electrical Activity Model for Dynamic Restitution Study vi
7 2.2.2 Model for S1-S2 Restitution and Short-Term Memory Study Model for Repolarization Alternans Studies Numerical Methods and Simulation Simulation Tools Numerical Methods Pacing Protocols Generation of the Computed ECG Measurement of Cellular and ECG Parameters Cellular Measures of Activation and Repolarization ECG Parameters Measured ECG Manifestations of Dynamic Restitution Introduction Results Cellular Activation and Repolarization ECG Characteristics Cellular Repolarization Relation to T-Wave Parameters Intercellular Voltage Gradients Responsible for ECG Waveforms Discussion Effect of Spatial Differences in Dynamic Restitution on the ECG Implications for the Use of ECG Parameters to Assess Myocardial Repolarization Limitations ECG Manifestations of S1-S2 Restitution and Short-Term Memory vii
8 4.1 Introduction Results Cellular Activation and Repolarization Effects of Cellular Short-Term Memory Changes on the ECG Effects of Cellular S1-S2 Responses on the ECG Discussion Limitations Effect of Electrode Placement on T-Wave Alternans Measurement Introduction Results Cellular Repolarization Alternans and Tissue Repolarization Gradients T-Wave Alternans Amplitude Relation to Repolarization Alternans T-Wave Amplitude and T-Wave Alternans Amplitude as a Function of Electrode Position Extracellular Potential Distributions Produced by Alternating Repolarization Gradients Discussion Limitations Effect of a Resistive Barrier on Repolarization Alternans and T-Wave Alternans Introduction Results Cellular Activation and Conduction Resistive Barrier Effects on Cellular Repolarization Resistive Barrier Effects on Alternans of ECG Time Parameters viii
9 6.2.4 Resistive Barrier Effects on Repolarization Alternans and T-wave Alternans Discussion Limitations Conclusions Summary of Findings Limitations and Future Directions Appendix A. Modification of Models of Cellular Electrical Activity A.1 Model for Dynamic Restitution Study A.2 Model for S1-S2 Restitution and Short-Term Memory Study A.3 Model for Repolarization Alternans Studies References Biography ix
10 List of Tables Table 4.1: STM beat constants for cellular repolarization times and ECG parameters for a fiber with control mean conductivity Table 4.2: STM beat constants for cellular repolarization times and ECG parameters for a fiber with reduced mean conductivity Table 4.3: STM beat constants for cellular repolarization times and ECG parameters for a fiber with enhanced mean conductivity Table 4.4: Repolarization times and ECG parameters for S1 (steady-state) pacing and S2 (premature) stimuli. Results are for a fiber with control conductivity Table 4.5: Repolarization times and ECG parameters for S1 (steady-state) pacing and S2 (premature) stimuli. Results are for a fiber with reduced conductivity Table 4.6: Repolarization times and ECG parameters for S1 (steady-state) pacing and S2 (premature) stimuli. Results are for a fiber with enhanced conductivity Table 5.1: T-wave measurements for representative electrode distances Table 5.2: T-wave measurements for representative lead angles x
11 List of Figures Figure 1.1: Illustration of APD response to steady-state pacing (dynamic restitution). Stimuli are applied at a fixed interval (BCL) and produce a fixed APD and fixed DI... 4 Figure 1.2: Dynamic restitution curves for simulated canine endocardial, midmyocardial, and epicardial cells. Data are shown for the modifications of the MV model described in section in the fiber described in section used to investigate dynamic restitution at control conductivity Figure 1.3: Illustration of APD response to a premature stimulus during steady-state pacing (S1-S2 restitution). A premature stimulus applied to a system previously at steady state produces an APD that is different from steady-state APD... 5 Figure 1.4: STM response of endocardial, midmyocardial, and epicardial cells in response to an abrupt change in BCL from 1000 to 600 ms. Data are shown for the modifications of the FMG model described in section in the fiber described in section used to investigate S1-S2 restitution and STM at reduced conductivity... 6 Figure 1.5: Two types of repolarization alternans. Red lines indicate a long alternating action potential, and blue lines indicate a short alternating action potential. APD in different regions of the myocardium alternate in phase with each other during concordant alternans and out of phase with each other during discordant alternans... 8 Figure 2.1: Schematic of fiber model with distinct cellular regions and ECG electrodes, being paced from the endocardial end Figure 2.2: Core conductor model for the fiber model Figure 2.3: Axial conductivity values along the length of fiber models used in (A) dynamic restitution study and (B) S1-S2 restitution and short-term memory study Figure 2.4: Conductivity of fiber with resistive barrier (black) and conductivity of fiber of equivalent, homogeneous mean conductivity (blue) Figure 2.5: (A) Endocardial, midmyocardial, and epicardial APD as a function of BCL for modified MV model. Experimental values are indicated with X s. (B) Endocardial, midmyocardial, and epicardial AP tracings at BCL of 4000, 1000, 800, and 500 ms Figure 2.6: APD and APD alternans magnitude along the fiber model for repolarization alternans studies at a BCL of 220 ms xi
12 Figure 2.7: Electrodes for study of effect of electrode location on T-wave alternans placed at distance d from fiber center and angle θ with respect to fiber axis Figure 2.8: Parameters measured from ECG Figure 3.1: Local CV measured at a BCL of 1000 ms for fiber at control, reduced, and enhanced conductivity Figure 3.2: Epicardial AP tracings plotted with ECG tracings showing the correspondence between epicardial AP downstroke time and T-wave upstroke time for (A) representative BCL and (B) different levels of tissue conductivity Figure 3.3: Epicardial AP tracings plotted with ECG tracings showing the correspondence between epicardial repolarization time and QT peak intervals for (A) representative BCL and (B) different levels of tissue conductivity Figure 3.4: Endocardial AP tracings plotted with ECG tracings showing the correspondence between endocardial AP downstroke time and T-wave downstroke time for (A) representative BCL and (B) different levels of tissue conductivity Figure 3.5: Midmyocardial AP tracings plotted with ECG tracings showing the correspondence between midmyocardial repolarization time and threshold-approximated QT interval for (A) representative BCL and (B) different levels of tissue conductivity.. 45 Figure 3.6: Midmyocardial AP tracings plotted with ECG tracings showing the correspondence between midmyocardial repolarization time and tangent-approximated QT interval for (A) representative BCL and (B) different levels of tissue conductivity.. 46 Figure 3.7: TDR and (A) threshold-approximated T peak -T end interval or (B) tangentapproximated T peak -T end interval plotted as a function of BCL at control, enhanced and reduced conductivity. TDR is defined at degrees of repolarization that best match each approximation method for T peak -T end interval at control conductivity and a BCL of 1000 ms Figure 3.8: Midmyocardial-epicardial (mid-epi) and endocardial-midmyocardial (endomid) voltage gradients shown for (A) representative BCL and (B) different levels of tissue conductivity. The sum of the two gradients closely approximates the transmural ECG. (C) Maximum magnitude of voltage gradient as a function of BCL at different levels of tissue conductivity. (D) Magnitude of gradient of repolarization time between midmyocardial node and epicardial node (mid-epi) and between endocardial node and midmyocardial node (endo-mid) as a function of BCL at different levels of tissue conductivity xii
13 Figure 4.1: Repolarization phase of endocardial (endo), midmyocardial (mid), and epicardial (epi) cellular action potentials, ECG T waves, and tissue voltage gradients for a fiber with homogeneous STM beat constant (black) and (A) reduced endocardial STM beat constant (red) or (B) reduced epicardial STM beat constant (red). Results shown here are for a fiber with control mean conductivity Figure 4.2: Repolarization phase of endocardial (endo), midmyocardial (mid), and epicardial (epi) cellular action potentials, ECG T waves, and tissue voltage gradients for a fiber with homogeneous STM beat constant (black) and (A) reduced endocardial STM beat constant (red) or (B) reduced epicardial STM beat constant (red). Results shown here are for a fiber with reduced mean conductivity Figure 4.3: Repolarization phase of endocardial (endo), midmyocardial (mid), and epicardial (epi) cellular action potentials, ECG T waves, and tissue voltage gradients for a fiber with homogeneous STM beat constant (black) and (A) reduced endocardial STM beat constant (red) or (B) reduced epicardial STM beat constant (red). Results shown here are for a fiber with enhanced mean conductivity Figure 5.1: Repolarization times of endocardial, midmyocardial, and epicardial nodes in fiber model for two alternating beats at various repolarization alternans magnitudes Figure 5.2: Gradient of repolarization times in the fiber model for two alternating beats at various repolarization alternans magnitudes Figure 5.3: T-wave amplitude plotted as a function of repolarization gradient. A regression line highlights the linear relationship between T-wave amplitude and repolarization gradient Figure 5.4: TWA amplitude plotted as a function of repolarization gradient alternans. A regression line highlights the linear relationship between TWA amplitude and repolarization gradient alternans Figure 5.5: Potential distribution around fiber model at instant of peak of (A) tall T wave and (B) short T wave. Representative electrode locations are marked with a black X. 88 Figure 6.1: Cellular repolarization times, tissue voltage gradients, and T waves for two consecutive beats during alternans for a fiber with homogeneous conductivity of 1.25 ms/cm (red lines) and a fiber with homogeneous conductivity of ms/cm (black lines) Figure 6.2: Cellular repolarization times, tissue voltage gradients, and T waves for two consecutive beats for a fiber with a resistive barrier (red lines) or a fiber of equivalent, homogeneous mean conductivity (black lines) xiii
14 Figure 6.3: (A) Maximum cellular alternans magnitude and (B) TWA amplitude for various resistive barrier strengths as a function of barrier location in the fiber. Values given for the fiber with no barrier are for a fiber of homogeneous conductivity equivalent to the mean conductivity of a fiber with a barrier. (C) TWA amplitude as a function of maximum cellular alternans magnitude for representative barrier locations. A regression line illustrates the quasi-linear relationship between TWA and cellular alternans. (D) Gain (slope) of the relationship between TWA amplitude and maximum cellular alternans magnitude as a function of barrier location. Gain for the data plotted in panel C is indicated xiv
15 List of Abbreviations APD BCL CV DI ECG FMG LV MV STM TDR TWA action potential duration (measured in ms) basic cycle length (measured in ms) conduction velocity (measured in cm/s) diastolic interval (measured in ms) electrocardiogram Fox-McHarg-Gilmour (model) left ventricle minimal ventricular (model) short-term memory transmural dispersion of repolarization (measured in ms) T-wave alternans xv
16 Acknowledgements I have been incredibly fortunate to pursue my doctoral degree in such a nurturing and supportive environment. First and foremost, I would like to thank my thesis advisor, Dr. Salim Idriss, for encouraging me to think beyond the results, for granting me the independence to learn from my mistakes, and especially for teaching me how to write and present effectively, skills that I will carry with me for the rest of my life. I would also like to thank my departmental advisor, Dr. Craig Henriquez, who graciously agreed to help me write a fellowship grant proposal and who provided crucial advice on mathematical models and computer simulations. I have also appreciated the constructive feedback and suggestions of my other committee members. Dr. Wanda Krassowska Neu was instrumental in influencing and refining my dissertation project. Dr. Patrick Wolf provided his expertise on extracellular signals and wrote supporting documents for my fellowship grant proposal. Finally, Dr. Warren Grill provided useful critiques from someone outside of my field of study and gave me opportunities to share my knowledge by allowing me to give guest lectures in his classes. I have benefitted from the helpful advice and camaraderie of current and previous members of the Cardiac Dynamics Group: Dr. Daniel Gauthier, Dr. David Schaeffer, Dr. Xiaopeng Zhao, Carolyn Martsberger, Jonathan Cranford, Caroline Ring, Jamie Bell, and especially Ann Pitruzzello, whose advice for the preliminary exam and for dissertation writing has been invaluable. xvi
17 Several members of the Henriquez lab were incredibly kind to share their expertise in computer simulation with me. Marjorie Letitia Hubbard taught me several useful hints and tricks for CardioWave. Jong Kim provided me with code to fit experimental data for the minimal ventricular model used in chapter 3. Dr. Vincent Jacquemet taught me how to create new membrane models and how to use other many other features of CardioWave. I would also like to thank a former Henriquez lab member, Dr. John Pormann, for creating CardioWave. In doing so, he simplified the process of computer simulation, allowing me to accomplish much more during my graduate studies than if I had to design each simulation from scratch. I would be remiss if I didn t mention the exceptionally committed and friendly Biomedical Engineering department staff, including Erica Clayton, Joyce Franklin, Angie Luan, Amy Norstrud, Ellen Ray, and Susan Story-Hill. I would especially like to thank Kathy Barbour, who has been my main point of contact since before I matriculated, and Ned Daniely, who welcomed all of my computing concerns with a smile and a sympathetic ear. I d also like to thank Matt Brown, Dianne Kindel, and Marcus Henderson, who made the teaching assistantship requirement easy and fun. I would like to thank my former research mentors, who triggered my interest in research. Dr. Ravi Bellamkonda and Dr. Marc Levenston introduced me to the world of research and taught me basic principles of investigation. Dr. Kathe Derwin gave me the independence to pursue my own project and work through problems and also was kind enough to write a letter of recommendation for my fellowship grant proposal. I also am xvii
18 indebted to the research assistants and (then) graduate students in those labs: Justin Saul, Stacy Imler, and Andrew Baker, all of whom patiently taught me laboratory techniques and data analysis skills that I use to this day. The Duke Medical Scientist Training Program and the American Heart Association Mid-Atlantic Affiliate have provided funding during the course of my graduate studies, and I am grateful to these institutions for their support. Most importantly, I would like to thank my parents and sister for their endless love and encouragement, for always being proud of me, and for always checking to make sure that I m getting enough sleep. Finally, I d like to thank my niece, whose pictures adorned my workspace and gave me a reason to smile every day. xviii
19 1. Introduction 1.1 Significance of Research in Cardiac Electrophysiology Sudden death from arrhythmia kills roughly 310,000 Americans per year (46). Unfortunately, no current diagnostic test can accurately predict which individuals are most at risk for sudden arrhythmic death. Since basic research has shown that the development of arrhythmia is tied to abnormalities in repolarization, methods that assess repolarization have the potential to evaluate susceptibility to sudden arrhythmic death. Given the risk and expense involved in invasive electrophysiologic testing, assessment of repolarization using noninvasive signals such as the body surface electrocardiogram (ECG) is ideal. Several studies have attempted to assess repolarization and spatial heterogeneity of repolarization using ECG techniques, such as QT dispersion (12, 22, 49, 86), T-wave lability (3, 37, 54), and various forms of T-wave morphology analysis (20, 56, 57, 97-99). However, none of these methods assess the rate-dependent, nonlinear changes in repolarization due to electrical restitution. Currently, the effects of dynamic changes in myocardial repolarization on extracellular signals such as the ECG are largely unknown. The main focus of this study is to determine how spatial and temporal dynamic changes in repolarization within myocardial tissue affect the ECG. This work is significant in that new knowledge has been obtained that can form the foundation to develop novel noninvasive methods of sudden death risk stratification using ECG measurements. 1
20 1.2 Dynamic Repolarization of Cardiac Tissue Abnormalities in repolarization, particularly in temporal and spatial dispersion of repolarization, are associated with increased susceptibility to arrhythmia. A large degree of repolarization dispersion in tissue results in some areas repolarizing and becoming available for subsequent activation before others. A premature stimulus can then result in unidirectional block: activation propagates in the direction in which tissue has repolarized and blocks in the direction in which tissue has not yet repolarized. The activation wave may then propagate around the region of block and activate the previously refractory region, leading to reentry, a self-sustaining, spiral wavefront that can degenerate to arrhythmia. Several studies have demonstrated that intrinsic heterogeneity in action potential duration (APD) (i.e. dispersion of repolarization) exists across the free wall of the left ventricle (LV) in several species, including rabbits (39, 69), dogs (75-77, 96), and man (33). However, the APD within each ventricular layer is not static but is dependent upon stimulation rate through a phenomenon known as electrical restitution. Since each cardiac myocyte can exhibit unique restitution behavior, spatial variation of APD heterogeneity within tissue, and by extension susceptibility to arrhythmia, could change drastically in response to changes in stimulation rate Electrical Restitution: The 1:1 Domain Electrical restitution is often described using the APD restitution curve (RC), which relates the APD to the preceding diastolic interval (DI), the period during which transmembrane voltage remained at rest. However, APD restitution is more complex than this sole nonlinear relationship. In this study, I investigated three different types of 2
21 restitution behavior: dynamic restitution, S1-S2 restitution, and short-term memory (STM). Dynamic restitution describes the relationship between APD and DI during steady-state pacing at a constant basic cycle length (BCL), where the BCL is the period of time between successive stimuli. After pacing at a single BCL for some period of time, the APD and DI at a specific tissue site reach steady state, producing a unique APD for a given DI (Figure 1.1). This relationship is described by the dynamic RC, a plot of steadystate APD value as a function of steady-state DI (Figure 1.2). Each cardiac cell has a single dynamic RC that is largely determined by the cell s ion channel distribution and intracellular calcium-handling mechanism. Although the mechanisms underlying dynamic restitution are not completely understood, the shortening of APD with decreasing BCL is thought to be due to time-dependent activity of ion channels (13). After an action potential, the state of ion channel gates return to steady state over time. Pacing at a shorter BCL allows less time for ion channel gates to return to steady state, and ion channel current is different than at steady state. Because each ion channel species has different kinetics, pacing at a different BCL alters the contribution of each ion channel current to the action potential, resulting in a different APD at each BCL. 3
22 Figure 1.1: Illustration of APD response to steady-state pacing (dynamic restitution). Stimuli are applied at a fixed interval (BCL) and produce a fixed APD and fixed DI. Figure 1.2: Dynamic restitution curves for simulated canine endocardial, midmyocardial, and epicardial cells. Data are shown for the modifications of the MV model described in section in the fiber described in section used to investigate dynamic restitution at control conductivity. S1-S2 restitution describes the APD response of a system previously at steady state to a perturbation in cycle length. An S1-S2 restitution response is elicited by steadystate pacing at a fixed BCL (S1 stimuli) followed by a single premature or postmature stimulus (known as the S2 stimulus) delivered after a certain duration (the S1-S2 4
23 coupling interval) (Figure 1.3). The resulting S1-S2 response is dependent on the BCL and, like dynamic restitution, can vary between cells. As with dynamic restitution, the mechanism behind S1-S2 restitution is not known but is likely due to time-dependent activity of ion channels (13). Pacing at an S1-S2 coupling interval that is shorter than the preceding BCL allows less time for ion channel gates to return to steady state, and ion channel current is different than when paced at a fixed BCL. Pacing at a different S1-S2 coupling interval thus alters the contribution of each ion channel current to the action potential, resulting in a different APD for each S1-S2 coupling interval. Figure 1.3: Illustration of APD response to a premature stimulus during steady-state pacing (S1-S2 restitution). A premature stimulus applied to a system previously at steady state produces an APD that is different from steady-state APD. Short-term memory, also known as accommodation, refers to the transient process by which APD monotonically approaches a stable steady-state value in response to an abrupt change in BCL. The plot of APD as a function of time or beat number is a decaying monoexponential (Figure 1.4), and the short-term memory (STM) response can be fit to equations 1.1 or 1.2: APD(t) = APD old + (ΔAPD)e t τ (1.1) 5
24 APD(n) = APD old + (ΔAPD)e n τ beat (1.2) STM response is therefore defined by the time constant, τ, or beat constant, τ beat. Time constant and beat constant are related by equation 1.3: τ = (BCL new )(τ beat ) (1.3) STM time constant is site-dependent in rabbit ventricle (52, 63), but limited data exists on spatial differences in STM in the dog and human. Simulation studies suggest that the mechanism responsible for STM is a slow change in intracellular sodium concentration due to slow dynamics of the sodium-potassium pump current (23). Figure 1.4: STM response of endocardial, midmyocardial, and epicardial cells in response to an abrupt change in BCL from 1000 to 600 ms. Data are shown for the modifications of the FMG model described in section in the fiber described in section used to investigate S1-S2 restitution and STM at reduced conductivity. Dynamic restitution, S1-S2 restitution, and STM have profound effects on susceptibility to arrhythmia. Nolasco and Dahlen used a mapping model of dynamic APD restitution and found that APD instability (and thus increased potential for arrhythmia) occurred for BCLs at which the S1-S2 RC slope is greater than one (55). This 6
25 dependence of APD instability on increased RC slope has been supported by experimental (42, 43) and modeling (5, 6, 41, 68) studies that demonstrate induction of APD alternans, an unstable and arrhythmogenic APD response, for dynamic and S1-S2 RC slopes greater than one. However, several other studies have demonstrated a stable APD at points where the dynamic RC slope is greater than one (5, 6, 40). Since Nolasco and Dahlen only investigated dynamic and S1-S2 restitution, one possible reason for this discrepancy in results is the effect of STM. Cherry and Fenton demonstrated that APD alternans could be suppressed at steep restitution by adding STM to an ionic model (18). However, STM is not always antiarrhythmic. Fenton and coworkers found that stable reentry in a computer model degenerated to arrhythmia when STM behavior was added to the model (31). Thus, the effects of steady-state restitution, S1-S2 restitution, and short-term memory should all be considered when investigating restitution behavior Action Potential Duration Alternans: The 2:2 Rhythm APD alternans is a beat-to-beat alternation in APD that typically occurs at fast pacing rates. It can be a result of alternation in conduction velocity (CV), alternation in cellular repolarization, or both. Experimental studies have shown that APD alternans may be arrhythmogenic (59). Two types of APD alternans exist: concordant alternans and discordant alternans (Figure 1.5). During concordant alternans, APD from all regions alternate in phase with each other. Concordant alternans can degenerate to discordant alternans (89), in which APD of one region alternates out phase with another region. Because it involves a higher degree of spatiotemporal dispersion of repolarization, 7
26 discordant alternans is thought to be more arrhythmogenic than concordant alternans (59). Figure 1.5: Two types of repolarization alternans. Red lines indicate a long alternating action potential, and blue lines indicate a short alternating action potential. APD in different regions of the myocardium alternate in phase with each other during concordant alternans and out of phase with each other during discordant alternans. T-wave alternans (TWA) is the ECG manifestation of APD alternans. Beat-tobeat alternation in myocardial repolarization causes beat-to-beat changes in the amplitude and morphology of the ECG T wave (59). TWA is therefore a useful risk stratification tool because of the association between APD alternans and arrhythmia (53). In my studies, I chose to investigate the relationship between concordant repolarization alternans and TWA. Although discordant alternans is more arrhythmogenic, the large temperospatial dispersion of repolarization causes alternation in T-wave polarity in my models, making comparison of T wave parameters difficult. 1.3 Dynamic ECG Changes No ECG analysis method currently exists that assesses the rate-dependent, nonlinear changes in repolarization due to electrical restitution. Prolongation of the QT interval of the ECG is widely associated with an increased risk for sudden death (70, 73, 8
27 74). Physiologically, the QT interval lengthens at low heart rates and shortens at high heart rates. Thus, the QT interval is a dynamic ECG change: its value changes due to changes in pacing rate. However, in typical clinical use, the QTc ( QT corrected ) interval is calculated to correct for this rate-dependence in QT interval, either by dividing QT interval by the square root (7) or the cube root (34) of the RR interval on the ECG (i.e., the heart rate). These correction methods are based on data nearly a century old that were not designed for correction of QT interval for risk stratification purposes. Furthermore, the use of rate-correction methods assumes that there is a fixed relationship between ECG parameters and heart rate. From experimental studies, it has been established that myocardial electrical activity is nonlinear, rate-dependent, and timedependent due to electrical restitution. Because the ECG is reflective of myocardial electrical activity, ECG parameters should similarly be nonlinear, rate-dependent, and time-dependent. Methods such as QT interval correction ignore or distort these dynamic changes in the ECG. The goal of this study, therefore, is to clarify the link between dynamic changes in cellular repolarization and dynamic changes in the ECG T wave. 1.4 Motivation for Using a Computer Model Advantages of Using a Computer Model In investigating the relationship between cellular dynamics and the ECG, a computer model has several advantages over an experimental preparation. Simplicity Because this study seeks to uncover basic mechanisms by which cellular repolarization dynamics affect the ECG, a simple model is the best choice to provide 9
28 general insights on this relationship. Effects that are predominant in a simple computer model may be lost in an experimental preparation due to the presence of confounding variables such as inter-animal variability and inaccuracies in measurement. Manipulation of settings A computer model allows manipulation of settings that would be difficult or impossible to achieve in an experimental preparation. For example, in chapter 4, the STM properties of one region of tissue are altered to determine the effect of regional STM changes on the ECG. Settings can also be manipulated to mimic pathologic or physiologic states. Access to output parameters Because all input settings are defined, a computer model provides output data that may be experimentally inaccessible. These data are useful for postulating mechanisms that can later be tested with more advanced experimental techniques Limitations of Using a Computer Model Proper use of a computer model involves acknowledgement of its limitations. Processing power As model complexity increases, computational time also increases. For my simulations, which consisted of a simple 1-dimensional structural model and ionic models of moderate complexity, two minutes of simulated pacing took two to five hours of real time. Therefore, studies that require long-term pacing are time-consuming. However, this limitation is somewhat mitigated by the use of parallel processing to simultaneously run multiple simulations with different settings. For example, rather than 10
29 running one simulation with a pacing protocol involving a decrease in BCL every 20 s, separate simulations can be run that each consist of 20 s of pacing at a particular BCL. Model approximation of physiology A computer model relies on experimentally-obtained data to use as inputs and simulation settings. Unfortunately, experimental data are often not available for all parameters that are modeled. For example, in chapter 4, STM time constants were not available for all regions of the canine LV free wall. Input data must then be based on approximations from other tissues. Although the results from such simulations are not as accurate as results from an experimental preparation, they can still provide insight on important mechanisms that contribute to the modeled phenomenon. 1.5 Research Goals and Specific Aims The effects of temporal and spatial differences in cellular repolarization dynamics on the ECG are not well known. The goal of my research was to investigate the ECG manifestations of temporal and spatial differences in dynamic restitution, S1-S2 restitution, STM, and repolarization alternans and to explore the mechanisms that modify the relationship between cellular dynamics and ECG dynamics. I hypothesize that spatial differences in repolarization dynamics alter voltage gradients that influence the ECG. My specific aims to investigate this hypothesis were as follows: Specific Aim 1: Determine how spatial heterogeneity of APD and of dynamic restitution, S1-S2 restitution, and STM affect the T wave of the ECG. Specific Aim 2: Determine how changes in electrode position alter the measurement of TWA. 11
30 Specific Aim 3: Determine how presence and location of a resistive barrier alter TWA and repolarization alternans. My approach used 1-dimensional computer fiber models to approximate conduction from the endocardium to the epicardium of the canine LV free wall. The canine LV free wall was selected because of the availability of data on APD dynamics throughout the wall as well as the electrophysiologic similarity of the canine LV to human LV. I modified models of cellular electrical activity to approximate spatial differences in dynamic restitution, S1-S2 restitution, STM, and repolarization alternans. I paced the fiber models to elicit dynamic behavior, and I analyzed the dynamic behavior in the ECG. I also investigated the effects of changes in tissue conductivity, which can alter temporal and spatial differences in repolarization. Because no current model approximates dynamic restitution, S1-S2 restitution, STM, and repolarization alternans for different regions of the canine LV free wall, these effects were studied separately. The results of specific aim 1 are described in chapter 3 (dynamic restitution) and chapter 4 (S1-S2 restitution and STM). The results of specific aim 2 are described in chapter 5. The results of specific aim 3 are described in chapter 6. 12
31 2. Methods This chapter describes the components and implementation of the computer simulations used to study the relationship between dynamic behavior in the electrocardiogram (ECG) and cellular repolarization dynamics in underlying myocardium. The general setup is similar among all studies performed (Figure 2.1). Modifications made to this general approach for each study are described in detail below and are summarized in each chapter. Briefly, a multicellular, 1-dimensional computer fiber model was created to simulate the free wall of the canine left ventricle (LV). Modifications of existing mathematical models were used to simulate electrical activity of each cell in the fiber model and to approximate experimentally-observed cellular repolarization dynamics. The fiber model was simulated with different pacing protocols to elicit various types of dynamic behavior. A computed ECG was calculated using cellular voltage data from the fiber model. Measurements of cellular repolarization were compared with ECG parameters to determine the relationship between cellular repolarization dynamics and dynamic behavior in the ECG. Figure 2.1: Schematic of fiber model with distinct cellular regions and ECG electrodes, being paced from the endocardial end. 13
32 2.1 Computer Fiber Model Overview To simulate action potential (AP) conduction from the endocardium to the epicardium of the free wall of the canine LV, a 1-dimensional, monodomain, multicellular fiber model was created. The model consisted of either 100 or 130 nodes (study-dependent, see below), each representing a 100-µm-long cylindrical cardiac myocyte, placed 0.01 cm (100 µm) apart in a 2-dimensional Cartesian coordinate system from x = 0 to x = Previous computer modeling studies have used a 1-dimensional model to simulate planar conduction from the endocardium to the epicardium of the LV free wall (35, 87, 88). For our purposes, use of a 1-dimensional fiber model as a surrogate for transmural propagation in the canine LV free wall involves several assumptions: 1. The assumption that conduction occurs primarily in a planar fashion from the endocardial surface to the epicardial surface of the LV free wall. This conduction pattern is supported by data from Durrer and coworkers, who suggested that activation of the Purkinje system rapidly activated the endocardial LV surface, resulting in a broad planar activation wavefront that propagates towards the epicardial surface (29). 2. The assumption that the major gradient of repolarization is in the transmural direction. This assumption has been supported by numerous experimental studies of the canine LV wedge preparation demonstrating a large non-monotonic 14
33 gradient of repolarization time from the endocardium to the epicardium (79, 80, 95, 96). 3. The assumption that the gradient of repolarization in the transmural direction is the main source of the ECG T wave. Although the source of the T wave in the whole heart is debated (58), the source of the T wave in an isolated canine LV wedge preparation has been shown to be largely due to this transmural repolarization gradient (95). An equation for current flow through the fiber model can be derived using the cable equations (64). Figure 2.2 shows the core conductor model, an electrical representation of the fiber model, in which Φ i is potential along the intracellular path, Φ e is potential along the extracellular path, r i is the resistance per unit length along the intracellular path, r e is the resistance per unit length along the intracellular path, I i is the axial current in the intracellular path, I e is the axial current in the extracellular path, and i m is the transmembrane current per unit length. Figure 2.2: Core conductor model for the fiber model. 15
34 By Ohm s law, the decrease in potential along the fiber is equivalent to the axial resistance multiplied by the axial current: φ e x = I er e (2.1) φ i x = I ir i (2.2) Assuming conservation of current, the following equations can be derived for transmembrane current: I e x = i m (2.3) Transmembrane voltage, V m, is defined as follows: I i x = i m (2.4) V m = Φ i Φ e (2.5) The spatial derivative of V m can be found by taking the spatial derivative of equation 2.5 and substituting equations 2.1 and 2.2: Deriving equation 2.6 by x gives the following: V m x = Φ i x Φ e x = I i r i + I e r e (2.6) 2 V m x 2 I = r i i x + r I e e x (2.7) Substituting equations 2.3 and 2.4 gives the following: 2 V m x 2 = (r i + r e )i m (2.8) 16
35 In all simulations in this dissertation, the fiber model is taken to be in a large, unbounded volume conductor, and r e can be assumed to be equal to zero: 2 V m x 2 = r i i m (2.9) Resistance per unit length, r i, can be expressed in terms of resistivity, R i, or conductivity, σ i, where a in the following equation is fiber radius: r i = Combining equations 2.9 and 2.10 gives the following: R i πa = 1 2 σ i πa (2.10) 2 i m = σ i πa 2 2 V m x 2 (2.11) Transmembrane current per unit length, i m, can be converted to transmembrane current per unit area, I m, by dividing by the circumference of the fiber cross section: I m = i m 2πa (2.12) Substituting equation 2.12 into equation 2.11 yields the following: I m = σ a i 2 V m 2 x (2.13) 2 Equation 2.14 below shows that 2/a is the surface area to volume ratio of the fiber, which will be designated with the letter β (l denotes fiber length in equation 2.14): Substituting β into equation 2.13 gives the following: SA V = 2πal πa 2 l = 2 a β (2.14) I m = σ i 2 V m β x (2.15) 2 17
36 Transmembrane current per unit area is a result of ionic currents (I ion ) as well as the capacitive current: I m = I ion + C m V m t (2.16) Combining equations 2.15 and 2.16 and rearranging gives equation 2.17, the equation solved in all computer simulations in this dissertation, σ i 2 V m x 2 V = β C m m t + I ion (2.17) where x is distance along the fiber, t is time, σ i is axial conductivity (study-dependent, see below), β is surface-area-to-volume ratio (study-dependent, see below), C m is membrane capacitance (1 µf/cm 2 ), V m is the cellular transmembrane voltage in mv, and I ion is the sum of ionic currents in µa/cm 2 defined by the chosen model of cellular electrical activity (study-dependent, see section 2.2). For all simulations, no-flux ( sealed end ) boundary conditions were used. The fiber model was considered to be surrounded by an unbounded, homogeneous volume conductor of conductivity 20 ms/cm, equal to that of 0.9% saline at 37 Celsius (51) Fiber Model for Restitution Studies Fiber models for the restitution studies (chapters 3 and 4) were based on experimental values for canine LV wall thickness and LV tissue conductivity from the endocardium to the epicardium (96). Each fiber model consisted of 130 nodes, spaced 0.01 cm apart from x = 0 to x = This setup resulted in fiber models of length 1.3 cm, closely approximating the experimental value of mean canine LV wall thickness, 1.29 cm 18
37 (96). Each node represented a 100-µm-long cylindrical cardiac myocyte with diameter 20 µm, giving surface-area-to-volume ratio, β, of 2000 cm -1. Axial conductivity, σ i, varied as a function of length along the fiber to model physiologic heterogeneity in tissue conductivity from the endocardial surface to the epicardial surface. Each fiber model consisted of 10 regions with conductivity based on experimental values of tissue resistivity across the canine LV wall. Experimental resistivity values ranged from to kω*cm, giving conductivity values that ranged from to ms/cm (96). When used in the fiber model, these values produced mean conduction velocity (CV) that was much higher than physiologic CV. Therefore, the conductivity values used in the model were decreased from the experimental values until the mean conduction velocity (CV) along the fiber was comparable to LV transmural CV recorded in vitro (29, 65, 66, 96). The study of dynamic restitution (chapter 3) and the study of S1-S2 restitution and short-term memory (STM) (chapter 4) used different models of cellular electrical activity, which had different AP conduction properties. Therefore, the actual conductivity values used for the fiber model for each study were different (Figure 2.3). To study the effects of reduction or enhancement in tissue conductivity, tissue conductivity values throughout each fiber were either halved (conductivity reduction) or doubled (conductivity enhancement). By modifying conductivity values throughout the fiber, overall fiber conductivity was reduced or enhanced while maintaining heterogeneity in conductivity. 19
38 Figure 2.3: Axial conductivity values along the length of fiber models used in (A) dynamic restitution study and (B) S1-S2 restitution and short-term memory study. To model transmural heterogeneity in repolarization, the fiber models used in restitution studies consisted of three regions. Each fiber region consisted of nodes with ionic currents determined by a regional modification of the model for cellular electrical activity. The first 13 nodes (0.13 cm) of the fiber consisted of endocardial-type nodes, the middle 78 nodes (0.78 cm) of the fiber consisted of midmyocardial-type nodes, and the final 39 nodes (0.39 cm) consisted of epicardial-type nodes. Sections and describe in detail the modifications and properties of these models of cellular electrical activity. 20
39 2.1.3 Fiber Model for Repolarization Alternans Studies Fiber models for the repolarization alternans studies (chapters 5 and 6) consisted of 100 nodes, spaced 0.01 cm apart. Each node represented a 100-µm-long cylindrical cardiac myocyte. For the study of electrode placement and T-wave alternans (chapter 5), each myocyte had diameter 22 µm, giving surface-area-to-volume ratio, β, of 1818 cm -1. For the study of a resistive barrier and T-wave alternans (chapter 6), each myocyte had diameter 20 µm, giving β of 2000 cm -1. For the study of electrode placement and T-wave alternans (chapter 5), axial conductivity, σ i, was constant at 1.5 ms/cm throughout the length along the fiber. A homogeneous conductivity was chosen to ensure that the effects observed were due to intrinsic spatial differences in cellular repolarization alternans rather than spatial alternans differences modulated by conductivity heterogeneity. The effects of spatial alternans differences modulated by conductivity heterogeneity were examined in the study of a resistive barrier and T-wave alternans (chapter 6). For the fiber model used in this study, axial conductivity was constant at 1.25 ms/cm throughout most of the fiber. A resistive barrier was placed in one of ten successive 1-mm blocks between the endocardial end and the epicardial end. The barrier consisted of a 10-50% decrease in local conductivity from the control value of 1.25 ms/cm (Figure 2.4). For comparison, fiber models were created with homogeneous conductivity equal to the mean conductivity of each barrier fiber. For example, the mean conductivity of a fiber with a barrier of a 50% decrease in local conductivity is
40 ms/cm. Therefore, a corresponding fiber model was created with homogeneous conductivity of ms/cm. Figure 2.4: Conductivity of fiber with resistive barrier (black) and conductivity of fiber of equivalent, homogeneous mean conductivity (blue) Fiber models for both repolarization alternans studies consisted of three fiber regions. The first 33 nodes (0.33 cm) of the fiber consisted of endocardial-type nodes, the middle 34 nodes (0.34 cm) of the fiber consisted of midmyocardial-type nodes, and the final 33 nodes (0.33 cm) consisted of epicardial-type nodes. Section describes in detail the modifications and properties of these models of cellular electrical activity. 2.2 Models of Cellular Electrical Activity No models of cellular electrical activity exist that approximate cellular repolarization dynamics of the endocardium, midmyocardium, and epicardium of the canine LV. Therefore, to model these phenomena, existing models were modified to approximate experimental values of action potential duration (APD), STM beat constant, and APD alternans magnitude for each region of the canine LV. 22
A tale of two dogs: analyzing two models of canine ventricular electrophysiology
 Am J Physiol Heart Circ Physiol 292: H43 H55, 2007. First published September 22, 2006; doi:10.1152/ajpheart.00955.2006. CALL FOR PAPERS Computational Analyses in Ion Channelopathies A tale of two dogs:
Am J Physiol Heart Circ Physiol 292: H43 H55, 2007. First published September 22, 2006; doi:10.1152/ajpheart.00955.2006. CALL FOR PAPERS Computational Analyses in Ion Channelopathies A tale of two dogs:
Shock-induced termination of cardiac arrhythmias
 Shock-induced termination of cardiac arrhythmias Group members: Baltazar Chavez-Diaz, Chen Jiang, Sarah Schwenck, Weide Wang, and Jinglei Zhang Abstract: Cardiac arrhythmias occur when blood flow to the
Shock-induced termination of cardiac arrhythmias Group members: Baltazar Chavez-Diaz, Chen Jiang, Sarah Schwenck, Weide Wang, and Jinglei Zhang Abstract: Cardiac arrhythmias occur when blood flow to the
Shock-induced termination of cardiac arrhythmias
 Shock-induced termination of cardiac arrhythmias Group members: Baltazar Chavez-Diaz, Chen Jiang, Sarah Schwenck, Weide Wang, and Jinglei Zhang Cardiac arrhythmias, also known as irregular heartbeat, occur
Shock-induced termination of cardiac arrhythmias Group members: Baltazar Chavez-Diaz, Chen Jiang, Sarah Schwenck, Weide Wang, and Jinglei Zhang Cardiac arrhythmias, also known as irregular heartbeat, occur
Principles and Applications of Electrical Circuits and Signal Theories in EP
 Principles and Applications of Electrical Circuits and Signal Theories in EP Graydon Beatty, VP Therapy Development Atrial Fibrillation Division, St. Jude Medical, Inc. CardioRhythm 2009 Background Biophysics
Principles and Applications of Electrical Circuits and Signal Theories in EP Graydon Beatty, VP Therapy Development Atrial Fibrillation Division, St. Jude Medical, Inc. CardioRhythm 2009 Background Biophysics
A Dynamic model of Pulmonary Vein Electrophysiology. Harry Green 2 nd year Ph.D. student University of Exeter
 A Dynamic model of Pulmonary Vein Electrophysiology Harry Green 2 nd year Ph.D. student University of Exeter Background to the Project Cardiac disease is the leading cause of death in most developed countries
A Dynamic model of Pulmonary Vein Electrophysiology Harry Green 2 nd year Ph.D. student University of Exeter Background to the Project Cardiac disease is the leading cause of death in most developed countries
Quantitative Electrophysiology
 ECE 795: Quantitative Electrophysiology Notes for Lecture #10 Wednesday, November 22, 2006 14. FUNDAMENTALS OF FUNCTIONAL ELECTRICAL STIMULATION (FES) We will look at: Design issues for FES Subthreshold
ECE 795: Quantitative Electrophysiology Notes for Lecture #10 Wednesday, November 22, 2006 14. FUNDAMENTALS OF FUNCTIONAL ELECTRICAL STIMULATION (FES) We will look at: Design issues for FES Subthreshold
Phase 2 Early Afterdepolarization as a Trigger of Polymorphic Ventricular Tachycardia in Acquired Long-QT Syndrome
 Phase 2 Early Afterdepolarization as a Trigger of Polymorphic Ventricular Tachycardia in Acquired Long-QT Syndrome Direct Evidence From Intracellular Recordings in the Intact Left Ventricular Wall Gan-Xin
Phase 2 Early Afterdepolarization as a Trigger of Polymorphic Ventricular Tachycardia in Acquired Long-QT Syndrome Direct Evidence From Intracellular Recordings in the Intact Left Ventricular Wall Gan-Xin
PART I. Disorders of the Heart Rhythm: Basic Principles
 PART I Disorders of the Heart Rhythm: Basic Principles FET01.indd 1 1/11/06 9:53:05 AM FET01.indd 2 1/11/06 9:53:06 AM CHAPTER 1 The Cardiac Electrical System The heart spontaneously generates electrical
PART I Disorders of the Heart Rhythm: Basic Principles FET01.indd 1 1/11/06 9:53:05 AM FET01.indd 2 1/11/06 9:53:06 AM CHAPTER 1 The Cardiac Electrical System The heart spontaneously generates electrical
Systems Biology Across Scales: A Personal View XXVII. Waves in Biology: Cardiac Arrhythmia. Sitabhra Sinha IMSc Chennai
 Systems Biology Across Scales: A Personal View XXVII. Waves in Biology: Cardiac Arrhythmia Sitabhra Sinha IMSc Chennai The functional importance of biological waves Spiral Waves Cardiac Arrhythmias Arrhythmias:
Systems Biology Across Scales: A Personal View XXVII. Waves in Biology: Cardiac Arrhythmia Sitabhra Sinha IMSc Chennai The functional importance of biological waves Spiral Waves Cardiac Arrhythmias Arrhythmias:
Sample Lab Report 1 from 1. Measuring and Manipulating Passive Membrane Properties
 Sample Lab Report 1 from http://www.bio365l.net 1 Abstract Measuring and Manipulating Passive Membrane Properties Biological membranes exhibit the properties of capacitance and resistance, which allow
Sample Lab Report 1 from http://www.bio365l.net 1 Abstract Measuring and Manipulating Passive Membrane Properties Biological membranes exhibit the properties of capacitance and resistance, which allow
Chapter 12: Cardiovascular Physiology System Overview
 Chapter 12: Cardiovascular Physiology System Overview Components of the cardiovascular system: Heart Vascular system Blood Figure 12-1 Plasma includes water, ions, proteins, nutrients, hormones, wastes,
Chapter 12: Cardiovascular Physiology System Overview Components of the cardiovascular system: Heart Vascular system Blood Figure 12-1 Plasma includes water, ions, proteins, nutrients, hormones, wastes,
The Effect of Ischaemic Region Shape on ST Potentials using a Half-Ellipsoid Model of the Left Ventricle
 The Effect of Ischaemic Region Shape on ST Potentials using a Half-Ellipsoid Model of the Left Ventricle Author Barnes, Josef, Johnston, Peter Published 2012 Conference Title Computing in Cardiology (CinC)
The Effect of Ischaemic Region Shape on ST Potentials using a Half-Ellipsoid Model of the Left Ventricle Author Barnes, Josef, Johnston, Peter Published 2012 Conference Title Computing in Cardiology (CinC)
Dynamic Origin of Spatially Discordant Alternans in Cardiac Tissue
 448 Biophysical Journal Volume 92 January 2007 448 460 Dynamic Origin of Spatially Discordant Alternans in Cardiac Tissue Hideki Hayashi,* Yohannes Shiferaw, y Daisuke Sato, z Motoki Nihei,* Shien-Fong
448 Biophysical Journal Volume 92 January 2007 448 460 Dynamic Origin of Spatially Discordant Alternans in Cardiac Tissue Hideki Hayashi,* Yohannes Shiferaw, y Daisuke Sato, z Motoki Nihei,* Shien-Fong
ELECTROCARDIOGRAPHY (ECG)
 ELECTROCARDIOGRAPHY (ECG) The heart is a muscular organ, which pumps blood through the blood vessels of the circulatory system. Blood provides the body with oxygen and nutrients, as well as assists in
ELECTROCARDIOGRAPHY (ECG) The heart is a muscular organ, which pumps blood through the blood vessels of the circulatory system. Blood provides the body with oxygen and nutrients, as well as assists in
A Cellular Automata Model For Dynamics and Control of Cardiac Arrhythmias DANNY GALLENBERGER (CARROLL UNIVERSITY) XIAOPENG ZHAO (UTK) KWAI WONG (UTK)
 A Cellular Automata Model For Dynamics and Control of Cardiac Arrhythmias DANNY GALLENBERGER (CARROLL UNIVERSITY) XIAOPENG ZHAO (UTK) KWAI WONG (UTK) Introduction Sudden cardiac arrest is responsible for
A Cellular Automata Model For Dynamics and Control of Cardiac Arrhythmias DANNY GALLENBERGER (CARROLL UNIVERSITY) XIAOPENG ZHAO (UTK) KWAI WONG (UTK) Introduction Sudden cardiac arrest is responsible for
Where are the normal pacemaker and the backup pacemakers of the heart located?
 CASE 9 A 68-year-old woman presents to the emergency center with shortness of breath, light-headedness, and chest pain described as being like an elephant sitting on her chest. She is diagnosed with a
CASE 9 A 68-year-old woman presents to the emergency center with shortness of breath, light-headedness, and chest pain described as being like an elephant sitting on her chest. She is diagnosed with a
Death, dynamics and disorder: Terminating reentry in excitable media by dynamically-induced inhomogeneities
 PRAMANA c Indian Academy of Sciences Vol. 64, No. 4 journal of April 2005 physics pp. 553 562 Death, dynamics and disorder: Terminating reentry in excitable media by dynamically-induced inhomogeneities
PRAMANA c Indian Academy of Sciences Vol. 64, No. 4 journal of April 2005 physics pp. 553 562 Death, dynamics and disorder: Terminating reentry in excitable media by dynamically-induced inhomogeneities
Simulation of T-Wave Alternans and its Relation to the Duration of Ventricular Action Potentials Disturbance
 The Open Pacing, Electrophysiology & Therapy Journal, 2010, 3, 21-27 21 Open Access Simulation of T-Wave Alternans and its Relation to the Duration of Ventricular Action Potentials Disturbance Dariusz
The Open Pacing, Electrophysiology & Therapy Journal, 2010, 3, 21-27 21 Open Access Simulation of T-Wave Alternans and its Relation to the Duration of Ventricular Action Potentials Disturbance Dariusz
CASE 10. What would the ST segment of this ECG look like? On which leads would you see this ST segment change? What does the T wave represent?
 CASE 10 A 57-year-old man presents to the emergency center with complaints of chest pain with radiation to the left arm and jaw. He reports feeling anxious, diaphoretic, and short of breath. His past history
CASE 10 A 57-year-old man presents to the emergency center with complaints of chest pain with radiation to the left arm and jaw. He reports feeling anxious, diaphoretic, and short of breath. His past history
The roles of mid myocardial and epicardial cells in T wave alternans development: a simulation study
 https://doi.org/10.1186/s12938-018-0492-6 BioMedical Engineering OnLine RESEARCH Open Access The roles of mid myocardial and epicardial cells in T wave alternans development: a simulation study D. Janusek
https://doi.org/10.1186/s12938-018-0492-6 BioMedical Engineering OnLine RESEARCH Open Access The roles of mid myocardial and epicardial cells in T wave alternans development: a simulation study D. Janusek
Sheet 5 physiology Electrocardiography-
 *questions asked by some students Sheet 5 physiology Electrocardiography- -why the ventricles lacking parasympathetic supply? if you cut both sympathetic and parasympathetic supply of the heart the heart
*questions asked by some students Sheet 5 physiology Electrocardiography- -why the ventricles lacking parasympathetic supply? if you cut both sympathetic and parasympathetic supply of the heart the heart
Modeling of Anatomy, Electrophysiology and Tension Development in the Human Heart
 European Functional Cardiac Modeling Meeting Modeling of Anatomy, Electrophysiology and Tension Development in the Human Heart Dr.-Ing. Gunnar Seemann Overview Electrophysiology Tension development Anatomy
European Functional Cardiac Modeling Meeting Modeling of Anatomy, Electrophysiology and Tension Development in the Human Heart Dr.-Ing. Gunnar Seemann Overview Electrophysiology Tension development Anatomy
Mathematical modeling of ischemia and infarction
 Mathematical modeling of ischemia and infarction Mostly based on Cimponeriu, Starmer and Bezerianos: A theoretical analysis of acute ischemia and infarction using ECG reconstruction on a 2-D model of myocardium
Mathematical modeling of ischemia and infarction Mostly based on Cimponeriu, Starmer and Bezerianos: A theoretical analysis of acute ischemia and infarction using ECG reconstruction on a 2-D model of myocardium
Systolic and Diastolic Currents of Injury
 Systolic and Diastolic Currents of Injury Figure 1 Action Potentials of Normal and Ischemic Tissue In Figure 1 above, the action potential of normal myocardium is represented by the solid lines and the
Systolic and Diastolic Currents of Injury Figure 1 Action Potentials of Normal and Ischemic Tissue In Figure 1 above, the action potential of normal myocardium is represented by the solid lines and the
Alternans and spiral breakup in a human ventricular tissue model
 Alternans and spiral breakup in a human ventricular tissue model K. H. W. J. ten Tusscher and A. V. Panfilov Am J Physiol Heart Circ Physiol 291:H1088-H1100, 2006. First published 24 March 2006; doi: 10.1152/ajpheart.00109.2006
Alternans and spiral breakup in a human ventricular tissue model K. H. W. J. ten Tusscher and A. V. Panfilov Am J Physiol Heart Circ Physiol 291:H1088-H1100, 2006. First published 24 March 2006; doi: 10.1152/ajpheart.00109.2006
Questions. Question 1!
 Questions Question 1 In a laboratory, scientists often study neurons in isolation, outside of a living creature, in a dish. In this setting, one can have a good deal of control over the local ionic environment
Questions Question 1 In a laboratory, scientists often study neurons in isolation, outside of a living creature, in a dish. In this setting, one can have a good deal of control over the local ionic environment
Comparison of Different ECG Signals on MATLAB
 International Journal of Electronics and Computer Science Engineering 733 Available Online at www.ijecse.org ISSN- 2277-1956 Comparison of Different Signals on MATLAB Rajan Chaudhary 1, Anand Prakash 2,
International Journal of Electronics and Computer Science Engineering 733 Available Online at www.ijecse.org ISSN- 2277-1956 Comparison of Different Signals on MATLAB Rajan Chaudhary 1, Anand Prakash 2,
Effects of I Kr and I Ks Heterogeneity on Action Potential Duration and Its Rate Dependence
 Effects of I Kr and I Ks Heterogeneity on Action Potential Duration and Its Rate Dependence A Simulation Study Prakash C. Viswanathan, BE; Robin M. Shaw, PhD; Yoram Rudy, PhD Background A growing body
Effects of I Kr and I Ks Heterogeneity on Action Potential Duration and Its Rate Dependence A Simulation Study Prakash C. Viswanathan, BE; Robin M. Shaw, PhD; Yoram Rudy, PhD Background A growing body
Cardiac physiology. b. myocardium -- cardiac muscle and fibrous skeleton of heart
 I. Heart anatomy -- general gross. A. Size/orientation - base/apex B. Coverings D. Chambers 1. parietal pericardium 2. visceral pericardium 3. Layers of heart wall a. epicardium Cardiac physiology b. myocardium
I. Heart anatomy -- general gross. A. Size/orientation - base/apex B. Coverings D. Chambers 1. parietal pericardium 2. visceral pericardium 3. Layers of heart wall a. epicardium Cardiac physiology b. myocardium
J-wave syndromes: update on ventricular fibrillation mechanisms
 J-wave syndromes: update on ventricular fibrillation mechanisms Michael Nabauer University of Munich, Germany 28.8.2011 I have no conflicts of interest ECG labelling by Einthoven Circ 1998 Osborn wave
J-wave syndromes: update on ventricular fibrillation mechanisms Michael Nabauer University of Munich, Germany 28.8.2011 I have no conflicts of interest ECG labelling by Einthoven Circ 1998 Osborn wave
Ameen Alsaras. Ameen Alsaras. Mohd.Khatatbeh
 9 Ameen Alsaras Ameen Alsaras Mohd.Khatatbeh Nerve Cells (Neurons) *Remember: The neural cell consists of: 1-Cell body 2-Dendrites 3-Axon which ends as axon terminals. The conduction of impulse through
9 Ameen Alsaras Ameen Alsaras Mohd.Khatatbeh Nerve Cells (Neurons) *Remember: The neural cell consists of: 1-Cell body 2-Dendrites 3-Axon which ends as axon terminals. The conduction of impulse through
Introduction. Circulation
 Introduction Circulation 1- Systemic (general) circulation 2- Pulmonary circulation carries oxygenated blood to all parts of the body carries deoxygenated blood to the lungs From Lt. ventricle aorta From
Introduction Circulation 1- Systemic (general) circulation 2- Pulmonary circulation carries oxygenated blood to all parts of the body carries deoxygenated blood to the lungs From Lt. ventricle aorta From
PHASE RESPONSE OF MODEL SINOATRIAL NODE CELLS - AN INVESTIGATION OF THE INFLUENCE OF STIMULUS PARAMETERS
 PHASE RESPONSE OF MODEL SINOATRIAL NODE CELLS - AN INVESTIGATION OF THE INFLUENCE OF STIMULUS PARAMETERS A. C. F. Coster, B. G. Celler Biomedical Systems Laboratory, School of Electrical Engineering, University
PHASE RESPONSE OF MODEL SINOATRIAL NODE CELLS - AN INVESTIGATION OF THE INFLUENCE OF STIMULUS PARAMETERS A. C. F. Coster, B. G. Celler Biomedical Systems Laboratory, School of Electrical Engineering, University
Chapter 13 The Cardiovascular System: Cardiac Function
 Chapter 13 The Cardiovascular System: Cardiac Function Overview of the Cardiovascular System The Path of Blood Flow through the Heart and Vasculature Anatomy of the Heart Electrical Activity of the Heart
Chapter 13 The Cardiovascular System: Cardiac Function Overview of the Cardiovascular System The Path of Blood Flow through the Heart and Vasculature Anatomy of the Heart Electrical Activity of the Heart
Arrhythmias By Dimension or Heart Attacks can give you Mathematics
 Arrhythmias By Dimension or Heart Attacks can give you Mathematics J. P. Keener Mathematics Department Arrhythmias By DimensionorHeart Attacks can give you Mathematics p.1/26 The Medical Problem Sudden
Arrhythmias By Dimension or Heart Attacks can give you Mathematics J. P. Keener Mathematics Department Arrhythmias By DimensionorHeart Attacks can give you Mathematics p.1/26 The Medical Problem Sudden
Microstructural Basis of Conduction II Introduction to Experimental Studies
 Bioeng 6460 Electrophysiology and Bioelectricity Microstructural Basis of Conduction II Introduction to Experimental Studies Frank B. Sachse fs@cvrti.utah.edu Overview Microstructural Basis of Conduction
Bioeng 6460 Electrophysiology and Bioelectricity Microstructural Basis of Conduction II Introduction to Experimental Studies Frank B. Sachse fs@cvrti.utah.edu Overview Microstructural Basis of Conduction
V. TACHYCARDIAS Rapid rhythm abnormalities
 V. TACHYCARDIAS Rapid rhythm abnormalities Tachyarrhythmias currently account for up to 350,000 deaths annually in the US. In addition to these clearly dangerous rhythm disturbances, other forms of more
V. TACHYCARDIAS Rapid rhythm abnormalities Tachyarrhythmias currently account for up to 350,000 deaths annually in the US. In addition to these clearly dangerous rhythm disturbances, other forms of more
ECGSIM; AN INTERACTIVE TOOL FOR STUDYING THE GENESIS OF QRST WAVEFORMS
 ECGSIM; AN INTERACTIVE TOOL FOR STUDYING THE GENESIS OF QRST WAVEFORMS A. van Oosterom, PhD. Professor of Medical Physics Department of Medical Physics; University of Nijmegen; The Netherlands T.F. Oostendorp,
ECGSIM; AN INTERACTIVE TOOL FOR STUDYING THE GENESIS OF QRST WAVEFORMS A. van Oosterom, PhD. Professor of Medical Physics Department of Medical Physics; University of Nijmegen; The Netherlands T.F. Oostendorp,
Physiology sheet #2. The heart composed of 3 layers that line its lumen and cover it from out side, these layers are :
 Physiology sheet #2 * We will talk in this lecture about cardiac muscle physiology, the mechanism and the energy sources of their contraction and intracellular calcium homeostasis. # Slide 4 : The heart
Physiology sheet #2 * We will talk in this lecture about cardiac muscle physiology, the mechanism and the energy sources of their contraction and intracellular calcium homeostasis. # Slide 4 : The heart
QT Interval: The Proper Measurement Techniques.
 In the name of God Shiraz E-Medical Journal Vol. 11, No. 2, April 2010 http://semj.sums.ac.ir/vol11/apr2010/88044.htm QT Interval: The Proper Measurement Techniques. Basamad Z*. * Assistant Professor,
In the name of God Shiraz E-Medical Journal Vol. 11, No. 2, April 2010 http://semj.sums.ac.ir/vol11/apr2010/88044.htm QT Interval: The Proper Measurement Techniques. Basamad Z*. * Assistant Professor,
Assessment of Reliability of Hamilton-Tompkins Algorithm to ECG Parameter Detection
 Proceedings of the 2012 International Conference on Industrial Engineering and Operations Management Istanbul, Turkey, July 3 6, 2012 Assessment of Reliability of Hamilton-Tompkins Algorithm to ECG Parameter
Proceedings of the 2012 International Conference on Industrial Engineering and Operations Management Istanbul, Turkey, July 3 6, 2012 Assessment of Reliability of Hamilton-Tompkins Algorithm to ECG Parameter
SUPPLEMENTARY INFORMATION. Supplementary Figure 1
 SUPPLEMENTARY INFORMATION Supplementary Figure 1 The supralinear events evoked in CA3 pyramidal cells fulfill the criteria for NMDA spikes, exhibiting a threshold, sensitivity to NMDAR blockade, and all-or-none
SUPPLEMENTARY INFORMATION Supplementary Figure 1 The supralinear events evoked in CA3 pyramidal cells fulfill the criteria for NMDA spikes, exhibiting a threshold, sensitivity to NMDAR blockade, and all-or-none
Enhanced Cellular Automation Model For Detecting Heart Fibrillation
 Enhanced Cellular Automation Model For Detecting Heart Fibrillation R. Touqan, A. Nasser & N. Hamdy Arab Academy for Science and Technology (AAST), email< rtouqan@hotmail.com Abstract: A new technique
Enhanced Cellular Automation Model For Detecting Heart Fibrillation R. Touqan, A. Nasser & N. Hamdy Arab Academy for Science and Technology (AAST), email< rtouqan@hotmail.com Abstract: A new technique
Body surface electrocardiograms and electrograms recorded
 Ionic Current Basis of Electrocardiographic Waveforms A Model Study Kazutaka Gima, Yoram Rudy Abstract Body surface electrocardiograms and electrograms recorded from the surfaces of the heart are the basis
Ionic Current Basis of Electrocardiographic Waveforms A Model Study Kazutaka Gima, Yoram Rudy Abstract Body surface electrocardiograms and electrograms recorded from the surfaces of the heart are the basis
Journal of Chemical and Pharmaceutical Sciences Print ISSN: Abnormal Calcium Channels: Role on Generation of ST Segment Depression, T-wave
 Abnormal Calcium Channels: Role on Generation of ST Segment Depression, T-wave Alternant and T- wave Inversion A Computational Study Gulothungan G*, Malathi R Department of Electronics and Instrumentation
Abnormal Calcium Channels: Role on Generation of ST Segment Depression, T-wave Alternant and T- wave Inversion A Computational Study Gulothungan G*, Malathi R Department of Electronics and Instrumentation
J Wave Syndromes. Osama Diab Lecturer of Cardiology Ain Shams University
 J Wave Syndromes Osama Diab Lecturer of Cardiology Ain Shams University J Wave Syndromes Group of electric disorders characterized by > 1 mm elevation of the J point or prominent J wave with or without
J Wave Syndromes Osama Diab Lecturer of Cardiology Ain Shams University J Wave Syndromes Group of electric disorders characterized by > 1 mm elevation of the J point or prominent J wave with or without
Chapter 7 Nerve Cells and Electrical Signaling
 Chapter 7 Nerve Cells and Electrical Signaling 7.1. Overview of the Nervous System (Figure 7.1) 7.2. Cells of the Nervous System o Neurons are excitable cells which can generate action potentials o 90%
Chapter 7 Nerve Cells and Electrical Signaling 7.1. Overview of the Nervous System (Figure 7.1) 7.2. Cells of the Nervous System o Neurons are excitable cells which can generate action potentials o 90%
EE 791 Lecture 2 Jan 19, 2015
 EE 791 Lecture 2 Jan 19, 2015 Action Potential Conduction And Neural Organization EE 791-Lecture 2 1 Core-conductor model: In the core-conductor model we approximate an axon or a segment of a dendrite
EE 791 Lecture 2 Jan 19, 2015 Action Potential Conduction And Neural Organization EE 791-Lecture 2 1 Core-conductor model: In the core-conductor model we approximate an axon or a segment of a dendrite
STRUCTURAL ELEMENTS OF THE NERVOUS SYSTEM
 STRUCTURAL ELEMENTS OF THE NERVOUS SYSTEM STRUCTURE AND MAINTENANCE OF NEURONS (a) (b) Dendrites Cell body Initial segment collateral terminals (a) Diagrammatic representation of a neuron. The break in
STRUCTURAL ELEMENTS OF THE NERVOUS SYSTEM STRUCTURE AND MAINTENANCE OF NEURONS (a) (b) Dendrites Cell body Initial segment collateral terminals (a) Diagrammatic representation of a neuron. The break in
NEURONS Chapter Neurons: specialized cells of the nervous system 2. Nerves: bundles of neuron axons 3. Nervous systems
 NEURONS Chapter 12 Figure 12.1 Neuronal and hormonal signaling both convey information over long distances 1. Nervous system A. nervous tissue B. conducts electrical impulses C. rapid communication 2.
NEURONS Chapter 12 Figure 12.1 Neuronal and hormonal signaling both convey information over long distances 1. Nervous system A. nervous tissue B. conducts electrical impulses C. rapid communication 2.
Lab #3: Electrocardiogram (ECG / EKG)
 Lab #3: Electrocardiogram (ECG / EKG) An introduction to the recording and analysis of cardiac activity Introduction The beating of the heart is triggered by an electrical signal from the pacemaker. The
Lab #3: Electrocardiogram (ECG / EKG) An introduction to the recording and analysis of cardiac activity Introduction The beating of the heart is triggered by an electrical signal from the pacemaker. The
University of Bristol - Explore Bristol Research. Publisher's PDF, also known as Version of record
 Adeniran, I., McPate, M. J. W., Witchel, H. J., Hancox, J. C., & Zhang, H. (2011). Increased vulnerability of human ventricle to re-entrant excitation in herg-linked variant 1 short QT syndrome. PLoS Computational
Adeniran, I., McPate, M. J. W., Witchel, H. J., Hancox, J. C., & Zhang, H. (2011). Increased vulnerability of human ventricle to re-entrant excitation in herg-linked variant 1 short QT syndrome. PLoS Computational
A POSSIBLE LINK BETWEEN R-WAVE AMPLITUDE ALTERNANS AND T-WAVE ALTERNANS IN ECGs
 University of Kentucky UKnowledge Theses and Dissertations--Biomedical Engineering Biomedical Engineering 2019 A POSSIBLE LINK BETWEEN R-WAVE AMPLITUDE ALTERNANS AND T-WAVE ALTERNANS IN ECGs Sahar Alaei
University of Kentucky UKnowledge Theses and Dissertations--Biomedical Engineering Biomedical Engineering 2019 A POSSIBLE LINK BETWEEN R-WAVE AMPLITUDE ALTERNANS AND T-WAVE ALTERNANS IN ECGs Sahar Alaei
Department of medical physiology 7 th week and 8 th week
 Department of medical physiology 7 th week and 8 th week Semester: winter Study program: Dental medicine Lecture: RNDr. Soňa Grešová, PhD. Department of medical physiology Faculty of Medicine PJŠU Cardiovascular
Department of medical physiology 7 th week and 8 th week Semester: winter Study program: Dental medicine Lecture: RNDr. Soňa Grešová, PhD. Department of medical physiology Faculty of Medicine PJŠU Cardiovascular
Nerve. (2) Duration of the stimulus A certain period can give response. The Strength - Duration Curve
 Nerve Neuron (nerve cell) is the structural unit of nervous system. Nerve is formed of large numbers of nerve fibers. Types of nerve fibers Myelinated nerve fibers Covered by myelin sheath interrupted
Nerve Neuron (nerve cell) is the structural unit of nervous system. Nerve is formed of large numbers of nerve fibers. Types of nerve fibers Myelinated nerve fibers Covered by myelin sheath interrupted
Arrhythmias. 1. beat too slowly (sinus bradycardia). Like in heart block
 Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
Medical Electronics Dr. Neil Townsend Michaelmas Term 2001 (www.robots.ox.ac.uk/~neil/teaching/lectures/med_elec) The story so far
 Medical Electronics Dr. Neil Townsend Michaelmas Term 2001 (www.robots.ox.ac.uk/~neil/teaching/lectures/med_elec) The story so far The heart pumps blood around the body. It has four chambers which contact
Medical Electronics Dr. Neil Townsend Michaelmas Term 2001 (www.robots.ox.ac.uk/~neil/teaching/lectures/med_elec) The story so far The heart pumps blood around the body. It has four chambers which contact
Introduction to ECG Gary Martin, M.D.
 Brief review of basic concepts Introduction to ECG Gary Martin, M.D. The electrical activity of the heart is caused by a sequence of rapid ionic movements across cell membranes resulting first in depolarization
Brief review of basic concepts Introduction to ECG Gary Martin, M.D. The electrical activity of the heart is caused by a sequence of rapid ionic movements across cell membranes resulting first in depolarization
PCA Enhanced Kalman Filter for ECG Denoising
 IOSR Journal of Electronics & Communication Engineering (IOSR-JECE) ISSN(e) : 2278-1684 ISSN(p) : 2320-334X, PP 06-13 www.iosrjournals.org PCA Enhanced Kalman Filter for ECG Denoising Febina Ikbal 1, Prof.M.Mathurakani
IOSR Journal of Electronics & Communication Engineering (IOSR-JECE) ISSN(e) : 2278-1684 ISSN(p) : 2320-334X, PP 06-13 www.iosrjournals.org PCA Enhanced Kalman Filter for ECG Denoising Febina Ikbal 1, Prof.M.Mathurakani
TdP Mechanisms and CiPA
 TdP Mechanisms and CiPA Craig T. January, MD, PhD Division of Cardiovascular Medicine University of Wisconsin-Madison Cardiac Safety Research Consortium Hilton Washington DC December 6, 2016 Disclosures
TdP Mechanisms and CiPA Craig T. January, MD, PhD Division of Cardiovascular Medicine University of Wisconsin-Madison Cardiac Safety Research Consortium Hilton Washington DC December 6, 2016 Disclosures
ADRENERGIC STIMULATION IN ACUTE HYPERGLYCEMIA: EFFECTS ON CELLULAR AND TISSUE LEVEL MURINE CARDIAC ELECTROPHYSIOLOGY
 University of Kentucky UKnowledge Theses and Dissertations--Biomedical Engineering Biomedical Engineering 2018 ADRENERGIC STIMULATION IN ACUTE HYPERGLYCEMIA: EFFECTS ON CELLULAR AND TISSUE LEVEL MURINE
University of Kentucky UKnowledge Theses and Dissertations--Biomedical Engineering Biomedical Engineering 2018 ADRENERGIC STIMULATION IN ACUTE HYPERGLYCEMIA: EFFECTS ON CELLULAR AND TISSUE LEVEL MURINE
Dynamic Role of the Cardiac Jelly
 61 Chapter 6 Dynamic Role of the Cardiac Jelly Before looping, when the embryonic heart is still a straight tube, the cardiac jelly occupies the bulk of the heart tube walls. Despite its preeminence in
61 Chapter 6 Dynamic Role of the Cardiac Jelly Before looping, when the embryonic heart is still a straight tube, the cardiac jelly occupies the bulk of the heart tube walls. Despite its preeminence in
ARTICLE IN PRESS. Journal of Theoretical Biology
 Journal of Theoretical Biology ] (]]]]) ]]] ]]] Contents lists available at ScienceDirect Journal of Theoretical Biology journal homepage: www.elsevier.com/locate/yjtbi Minimal model for human ventricular
Journal of Theoretical Biology ] (]]]]) ]]] ]]] Contents lists available at ScienceDirect Journal of Theoretical Biology journal homepage: www.elsevier.com/locate/yjtbi Minimal model for human ventricular
Simulating the Effect of Global Cardiac Ischaemia on the Dynamics of Ventricular Arrhythmias in the Human Heart
 Simulating the Effect of Global Cardiac Ischaemia on the Dynamics of Ventricular Arrhythmias in the Human Heart Mitra Abbasi Department of Computer Science September 2016 A thesis submitted in partial
Simulating the Effect of Global Cardiac Ischaemia on the Dynamics of Ventricular Arrhythmias in the Human Heart Mitra Abbasi Department of Computer Science September 2016 A thesis submitted in partial
Effect of an Increase in Coronary Perfusion on Transmural Ventricular Repolarization
 Physiol. Res. 56: 285-290, 2007 Effect of an Increase in Coronary Perfusion on Transmural Ventricular Repolarization Y.-Z. ZHANG 1, B. HE 1, L.-X. WANG 2 1 Department of Cardiology, Renji Hospital, Medical
Physiol. Res. 56: 285-290, 2007 Effect of an Increase in Coronary Perfusion on Transmural Ventricular Repolarization Y.-Z. ZHANG 1, B. HE 1, L.-X. WANG 2 1 Department of Cardiology, Renji Hospital, Medical
Effect of an increase in coronary perfusion on transmural. ventricular repolarization
 Effect of an increase in coronary perfusion on transmural ventricular repolarization Yan-Zhou Zhang 1, MD, PhD, Ben He 1, MD, Le-Xin Wang 2, MD, PhD. From: 1 Department of Cardiology, Renji Hospital, Medical
Effect of an increase in coronary perfusion on transmural ventricular repolarization Yan-Zhou Zhang 1, MD, PhD, Ben He 1, MD, Le-Xin Wang 2, MD, PhD. From: 1 Department of Cardiology, Renji Hospital, Medical
Effects of adrenergic activation to the action potentials and ionic currents of cardiac cells. by Ferenc Ruzsnavszky MD
 SHORT THESIS FOR THE DEGREE OF DOCTOR OF PHILOSOPHY (PhD) Effects of adrenergic activation to the action potentials and ionic currents of cardiac cells by Ferenc Ruzsnavszky MD Supervisor: Prof. János
SHORT THESIS FOR THE DEGREE OF DOCTOR OF PHILOSOPHY (PhD) Effects of adrenergic activation to the action potentials and ionic currents of cardiac cells by Ferenc Ruzsnavszky MD Supervisor: Prof. János
ENTRAINMENT OF ELECTRICAL ACTIVATION BY SPATIO-TEMPORAL DISTRIBUTED PACING DURING VENTRICULAR FIBRILLATION
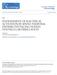 University of Kentucky UKnowledge University of Kentucky Master's Theses Graduate School 2003 ENTRAINMENT OF ELECTRICAL ACTIVATION BY SPATIO-TEMPORAL DISTRIBUTED PACING DURING VENTRICULAR FIBRILLATION
University of Kentucky UKnowledge University of Kentucky Master's Theses Graduate School 2003 ENTRAINMENT OF ELECTRICAL ACTIVATION BY SPATIO-TEMPORAL DISTRIBUTED PACING DURING VENTRICULAR FIBRILLATION
Factors Determining Vulnerability to Ventricular Fibrillation Induced by 60-CPS Alternating Current
 Factors Determining Vulnerability to Ventricular Fibrillation Induced by 60-CPS Alternating Current By Tsuneoki Sugimoto, M.D., Stephen F. School, M.D., and Andrew G. Wallace, M.D. ABSTRACT Very weak,
Factors Determining Vulnerability to Ventricular Fibrillation Induced by 60-CPS Alternating Current By Tsuneoki Sugimoto, M.D., Stephen F. School, M.D., and Andrew G. Wallace, M.D. ABSTRACT Very weak,
THE EFFECT OF EXCITATION CURRENT ON REFRACTORY PERIOD OF ACTION POTENTIAL AND ITS SIMULATION BY MATLAB SOFTWARE
 THE EFFECT OF EXCITATION CURRENT ON REFRACTORY PERIOD OF ACTION POTENTIAL AND ITS SIMULATION BY MATLAB SOFTWARE Mostafa Mohammadi Department of Electrical Engineering Islamic Azad University of Central
THE EFFECT OF EXCITATION CURRENT ON REFRACTORY PERIOD OF ACTION POTENTIAL AND ITS SIMULATION BY MATLAB SOFTWARE Mostafa Mohammadi Department of Electrical Engineering Islamic Azad University of Central
Full file at
 MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What electrical event must occur for atrial kick to occur? 1) A) Atrial repolarization B) Ventricular
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What electrical event must occur for atrial kick to occur? 1) A) Atrial repolarization B) Ventricular
CARDIOVASCULAR SYSTEM
 CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
Antiarrhythmic Drugs
 Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Arrhythmias. Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium.
 Arrhythmias Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium. However, in clinic it present as a complex family of disorders that show variety of symptoms, for
Arrhythmias Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium. However, in clinic it present as a complex family of disorders that show variety of symptoms, for
BIONB/BME/ECE 4910 Neuronal Simulation Assignments 1, Spring 2013
 BIONB/BME/ECE 4910 Neuronal Simulation Assignments 1, Spring 2013 Tutorial Assignment Page Due Date Week 1/Assignment 1: Introduction to NIA 1 January 28 The Membrane Tutorial 9 Week 2/Assignment 2: Passive
BIONB/BME/ECE 4910 Neuronal Simulation Assignments 1, Spring 2013 Tutorial Assignment Page Due Date Week 1/Assignment 1: Introduction to NIA 1 January 28 The Membrane Tutorial 9 Week 2/Assignment 2: Passive
Electrocardiography Biomedical Engineering Kaj-Åge Henneberg
 Electrocardiography 31650 Biomedical Engineering Kaj-Åge Henneberg Electrocardiography Plan Function of cardiovascular system Electrical activation of the heart Recording the ECG Arrhythmia Heart Rate
Electrocardiography 31650 Biomedical Engineering Kaj-Åge Henneberg Electrocardiography Plan Function of cardiovascular system Electrical activation of the heart Recording the ECG Arrhythmia Heart Rate
ECG. Prepared by: Dr.Fatima Daoud Reference: Guyton and Hall Textbook of Medical Physiology,12 th edition Chapters: 11,12,13
 ECG Prepared by: Dr.Fatima Daoud Reference: Guyton and Hall Textbook of Medical Physiology,12 th edition Chapters: 11,12,13 The Concept When the cardiac impulse passes through the heart, electrical current
ECG Prepared by: Dr.Fatima Daoud Reference: Guyton and Hall Textbook of Medical Physiology,12 th edition Chapters: 11,12,13 The Concept When the cardiac impulse passes through the heart, electrical current
Subject-Specific Modeling of Cardiac Ischemia
 Subject-Specific Modeling of Cardiac Ischemia Darrell Swenson PhD. Proposal Advisor Dr. Rob MacLeod Biomedical Engineering, University of Utah Scientific Computing and Imaging Institute What is the leading
Subject-Specific Modeling of Cardiac Ischemia Darrell Swenson PhD. Proposal Advisor Dr. Rob MacLeod Biomedical Engineering, University of Utah Scientific Computing and Imaging Institute What is the leading
Structural Determinants of T Wave Alternans in Patients with Cardiomyopathy
 Structural Determinants of T Wave Alternans in Patients with Cardiomyopathy by Adrian M Suszko A thesis submitted in conformity with the requirements for the degree of Master of Science Graduate Department
Structural Determinants of T Wave Alternans in Patients with Cardiomyopathy by Adrian M Suszko A thesis submitted in conformity with the requirements for the degree of Master of Science Graduate Department
Electrophysiology. General Neurophysiology. Action Potentials
 5 Electrophysiology Cochlear implants should aim to reproduce the coding of sound in the auditory system as closely as possible, for best sound perception. The cochlear implant is in part the result of
5 Electrophysiology Cochlear implants should aim to reproduce the coding of sound in the auditory system as closely as possible, for best sound perception. The cochlear implant is in part the result of
Modeling Chaos in the Heart
 Modeling Chaos in the Heart S. M. Haider Aejaz haider_aejaz@yahoo.com PIMCS, Lahore, Pakistan Abstract: Chaos theory describes the dynamics of a deterministic system whose dynamics show extreme dependence
Modeling Chaos in the Heart S. M. Haider Aejaz haider_aejaz@yahoo.com PIMCS, Lahore, Pakistan Abstract: Chaos theory describes the dynamics of a deterministic system whose dynamics show extreme dependence
WHAT S THAT RHYTHM I AM HEARING? GUIDE TO AUSCULTATION OF ARRHYTHMIAS IN HORSES
 WHAT S THAT RHYTHM I AM HEARING? GUIDE TO AUSCULTATION OF ARRHYTHMIAS IN HORSES Michelle Henry Barton DVM, PhD, DACVIM University of Georgia, Athens, GA INTRODUCTION The purpose of this talk is to review
WHAT S THAT RHYTHM I AM HEARING? GUIDE TO AUSCULTATION OF ARRHYTHMIAS IN HORSES Michelle Henry Barton DVM, PhD, DACVIM University of Georgia, Athens, GA INTRODUCTION The purpose of this talk is to review
Benchmarking In Silico Models and Candidate Metrics for Assessing the Risk of Torsade de Pointes
 Benchmarking In Silico Models and Candidate Metrics for Assessing the Risk of Torsade de Pointes Sara Dutta Division of Applied Regulatory Science/OCP/CDER CRSC/HESI/SPS/FDA Meeting December 11, 2014 Silver
Benchmarking In Silico Models and Candidate Metrics for Assessing the Risk of Torsade de Pointes Sara Dutta Division of Applied Regulatory Science/OCP/CDER CRSC/HESI/SPS/FDA Meeting December 11, 2014 Silver
798 Biophysical Journal Volume 96 February
 798 iophysical Journal Volume 96 February 2009 798 817 Mechanisms of Transition from Normal to Reentrant Electrical ctivity in a Model of Rabbit trial Tissue Interaction of Tissue Heterogeneity and nisotropy
798 iophysical Journal Volume 96 February 2009 798 817 Mechanisms of Transition from Normal to Reentrant Electrical ctivity in a Model of Rabbit trial Tissue Interaction of Tissue Heterogeneity and nisotropy
Cardiac Arrhythmia Mapping!
 Cardiac Arrhythmia Mapping! Challenges and Opportunities" Derek J. Dosdall, Ph.D. 22 October, 2010 OUTLINE!! Historical perspective! Current mapping techniques!optical mapping!electrical mapping (Purkinje
Cardiac Arrhythmia Mapping! Challenges and Opportunities" Derek J. Dosdall, Ph.D. 22 October, 2010 OUTLINE!! Historical perspective! Current mapping techniques!optical mapping!electrical mapping (Purkinje
Showkat Hamid Mentor: Dr. Mrinalini Meesala MD, FACC. University at Buffalo; State University of New York; Sisters Hospital IMTP June 12 th 2013
 Showkat Hamid Mentor: Dr. Mrinalini Meesala MD, FACC. University at Buffalo; State University of New York; Sisters Hospital IMTP June 12 th 2013 Disclosures: None Topic: Evaluation of electrogenic properties
Showkat Hamid Mentor: Dr. Mrinalini Meesala MD, FACC. University at Buffalo; State University of New York; Sisters Hospital IMTP June 12 th 2013 Disclosures: None Topic: Evaluation of electrogenic properties
NONLINEAR DYNAMICS OF HEART RHYTHMS
 Proceedings of COBEM 007 Copyright 007 by ABCM 9th International Congress of Mechanical Engineering November -9, 007, Brasília, DF NONLINEAR DYNAMICS OF HEART RHYTHMS Sandra R.F.S.M. Gois, sandrarregina@hotmail.com
Proceedings of COBEM 007 Copyright 007 by ABCM 9th International Congress of Mechanical Engineering November -9, 007, Brasília, DF NONLINEAR DYNAMICS OF HEART RHYTHMS Sandra R.F.S.M. Gois, sandrarregina@hotmail.com
- why the T wave is deflected upwards although it's a repolarization wave?
 Cardiac Electrograph: - why the T wave is deflected upwards although it's a repolarization wave? After depolarization the ventricle contracts but since the heart is a volume conductor (3D not 2D), when
Cardiac Electrograph: - why the T wave is deflected upwards although it's a repolarization wave? After depolarization the ventricle contracts but since the heart is a volume conductor (3D not 2D), when
An electrocardiogram (ECG) is a recording of the electricity of the heart. Analysis of ECG
 Introduction An electrocardiogram (ECG) is a recording of the electricity of the heart. Analysis of ECG data can give important information about the health of the heart and can help physicians to diagnose
Introduction An electrocardiogram (ECG) is a recording of the electricity of the heart. Analysis of ECG data can give important information about the health of the heart and can help physicians to diagnose
Age: 39. Reported Symptom Status: Snapshot (10 sec) 12-lead ECG
 Age: 39 Gender: Male Reported Symptom Status: Not stated A-ECG Report For: Chambers, MT (Date/Time of ECG): Type of Test: (11-25-14 13.12 PM) Snapshot (10 sec) 12-lead ECG Study / Physician: ECG Research
Age: 39 Gender: Male Reported Symptom Status: Not stated A-ECG Report For: Chambers, MT (Date/Time of ECG): Type of Test: (11-25-14 13.12 PM) Snapshot (10 sec) 12-lead ECG Study / Physician: ECG Research
Chapter 20: Cardiovascular System: The Heart
 Chapter 20: Cardiovascular System: The Heart I. Functions of the Heart A. List and describe the four functions of the heart: 1. 2. 3. 4. II. Size, Shape, and Location of the Heart A. Size and Shape 1.
Chapter 20: Cardiovascular System: The Heart I. Functions of the Heart A. List and describe the four functions of the heart: 1. 2. 3. 4. II. Size, Shape, and Location of the Heart A. Size and Shape 1.
MASSACHUSETTS INSTITUTE OF TECHNOLOGY
 Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Clinical Cardiac Electrophysiology
 Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
Electrocardiographic Markers Associated with Sotalol-induced Torsades de Pointes
 Electrocardiographic Markers Associated with Sotalol-induced Torsades de Pointes Based on Data from the Telemetric and Holter ECG Warehouse (THEW) Initiative Jean-PhiIippe Couderc, PhD Center for Quantitative
Electrocardiographic Markers Associated with Sotalol-induced Torsades de Pointes Based on Data from the Telemetric and Holter ECG Warehouse (THEW) Initiative Jean-PhiIippe Couderc, PhD Center for Quantitative
An activation-repolarization time metric to predict localized regions of high susceptibility to reentry
 An activation-repolarization time metric to predict localized regions of high susceptibility to reentry Nicholas Child, Martin J. Bishop, Ben Hanson, Ruben Coronel, Tobias Opthof, Bastiaan J. Boukens,
An activation-repolarization time metric to predict localized regions of high susceptibility to reentry Nicholas Child, Martin J. Bishop, Ben Hanson, Ruben Coronel, Tobias Opthof, Bastiaan J. Boukens,
Dispersion of myocardial repolarization results in regional
 Imaging Dispersion of Myocardial Repolarization, II Noninvasive Reconstruction of Epicardial Measures Raja N. Ghanem, MS; John E. Burnes, PhD; Albert L. Waldo, MD; Yoram Rudy, PhD Background Dispersion
Imaging Dispersion of Myocardial Repolarization, II Noninvasive Reconstruction of Epicardial Measures Raja N. Ghanem, MS; John E. Burnes, PhD; Albert L. Waldo, MD; Yoram Rudy, PhD Background Dispersion
1908 Biophysical Journal Volume 108 April
 1908 Biophysical Journal Volume 108 April 2015 1908 1921 Article Calcium-Voltage Coupling in the Genesis of Early and Delayed Afterdepolarizations in Cardiac Myocytes Zhen Song, 1,2 Christopher Y. Ko,
1908 Biophysical Journal Volume 108 April 2015 1908 1921 Article Calcium-Voltage Coupling in the Genesis of Early and Delayed Afterdepolarizations in Cardiac Myocytes Zhen Song, 1,2 Christopher Y. Ko,
V4, V5 and V6 follow the 5 th intercostal space and are NOT horizontal as indicated in the image. Page 1 of 7
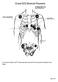 V4, V5 and V6 follow the 5 th intercostal space and are NOT horizontal as indicated in the image. Page 1 of 7 "Is it correct to place the electrodes under the female breasts?" Placement of electrodes directly
V4, V5 and V6 follow the 5 th intercostal space and are NOT horizontal as indicated in the image. Page 1 of 7 "Is it correct to place the electrodes under the female breasts?" Placement of electrodes directly
