Blood pressure. Arterial and venous circulation 1
|
|
|
- Jared Glenn
- 6 years ago
- Views:
Transcription
1 Blood pressure. Arterial and venous circulation 1 Introduction Hales first measured blood pressure in 1733 by inserting tubes directly into the arteries of animals. Non invasive techniques for the measurement of blood pressure have been in existence since the early 1800s, although Scipione Riva Rocci, an Italian physician, is credited with developing the first conventional sphygmomanometer in In 1905, Nicolai Korotkoff described various sounds while auscultating over the brachial artery during deflation of a Riva Rocci cuff. [1] Although the System International d'unites (SI) unit of pressure is the Pascal [equivalent to 1 Newton per square meter (N/m 2 )], by convention, blood pressure is measured in millimeters of mercury (mm Hg). Blood pressure (BP) is the force exerted by circulating blood on the walls of blood vessels, and constitutes one of the principal vital signs. The pressure of the circulating blood decreases as blood moves through arteries, arterioles, capillaries, and veins; the term blood pressure generally refers to arterial pressure, i.e., the pressure in the larger arteries, the blood vessels that take blood away from the heart. Fig. 1 As blood travels through the arterial system, resistance from the walls of the blood vessels reduces the pressure and velocity of the blood. Systolic and Diastolic Blood Pressure For each heartbeat, blood pressure varies between systolic and diastolic pressures. Systolic pressure (SBP) is peak pressure in the arteries, which occurs near the beginning of the cardiac cycle when the ventricles are contracting. Diastolic pressure (DBP) is minimum pressure in the arteries, which occurs near the end of the cardiac cycle when the ventricles are filled with blood. An example of normal measured values for a resting, healthy adult human is 115 mmhg systolic and 75 mmhg diastolic (written as 115/75 mmhg). Pulse pressure is the difference between systolic and diastolic pressures. Systolic and diastolic arterial blood pressures are not static but undergo natural variations from one heartbeat to another and throughout the day (in a circadian rhythm). They also change in response to stress, nutritional factors, drugs, disease, exercise, and momentarily from standing up. Sometimes the variations are large. Hypertension refers to arterial pressure being abnormally high, as opposed to hypotension, when it is abnormally low. 1 Practical Notes of the Physiology Department II, Carol Davila Univ. of Medicine and Pharmacy, Bucharest Dr. Ana Maria Zagrean, Coordinator, 2 nd Year English Module
2 'Normal' blood pressure varies with age, state of health and clinical situation. At birth, a typical blood pressure is 80/50 mmhg. It rises steadily throughout childhood, so that in a young adult it might be 120/80 mmhg. As we get older, blood pressure continues to rise and a rule of thumb is that normal systolic pressure is age in years Blood pressure is lower in late pregnancy and during sleep. From this, you can see that a systolic pressure of 160mmHg for an elderly man or 90 mmhg for a pregnant woman may be quite normal. To judge whether any particular reading is too high or too low, we must compare the reading with the 'normal' for that patient. Mean Arterial Pressure The mean arterial pressure (MAP) is a term used in medicine to describe an average blood pressure in an individual. It is defined as the average arterial pressure during a single cardiac cycle. The mean arterial pressure (MAP) is determined by the cardiac output (CO), systemic vascular resistance (SVR), and central venous pressure (CVP) according to the following relationship, which is based upon the relationship between flow, pressure and resistance: MAP = (CO SVR) + CVP Therefore, changes in either CO or SVR will affect MAP. If CO and SVR change reciprocally and proportionately, then MAP will not change. For example, if CO doubles and SVR decreases by onehalf, MAP does not change (if CVP = 0). In practice, MAP is not determined by knowing the CO and SVR, but rather by direct or indirect measurements of arterial pressure. At normal resting heart rates, MAP can be approximated by the following equation: MAP = DBP + 1/3(SBP DBP) Likewise to SBP and DBP, MAP varies during lifetime at birth 70 mmhg, adults 100 mmhg, elder 110 mmhg, and elder with atherosclerosis 140 mmhg. Differential Pressure (Pulse Pressure) The pulse pressure or differential pressure is the difference between systolic and diastolic blood pressure and represents the force that your heart generates each time it contracts. Pulse Pressure = Systolic Pressure Diastolic Pressure In a person with a systolic blood pressure of 120 mmhg and a diastolic pressure of 80 mmhg, the pulse pressure would be 40 mmhg. The rise in aortic pressure from its diastolic to systolic value is determined by the compliance of the aorta as well as the ventricular stroke volume. In the arterial system, the aorta has the highest compliance, due in part to a relatively greater proportion of elastin fibers versus smooth muscle and collagen. This serves the important function of dampening the pulsatile output of the left ventricle, thereby reducing the pulse pressure (systolic minus diastolic arterial pressure). If the aorta were a rigid tube, the pulse pressure would be very high. Because the aorta is compliant, as blood is ejected into the aorta, the walls of the aorta expand to accommodate the increase in blood volume. As the aorta expands, the increase in pressure is determined by the compliance of the aorta at that particular range of volumes. The more compliant the aorta, the
3 smaller the pressure change during ventricular ejection (i.e., smaller pulse pressure). Therefore, aortic compliance is a major determinant, along with stroke volume, of the pulse pressure. Arterial pulse. Sphygmogram. The ejection of blood in the aorta by the left ventricle systole generates two different processes. The first process consists in the propulsion of the blood volume along the arteries at a velocity of m/s. The other process occurs in the walls of the arteries, as a wave initiated at the root of the aorta that travels distally and propagates through the arterial wall of all arteries. This wave is called the arterial pulse or pressure of pulse (not to be mistaken for pulse pressure) and can be perceived as a pulsatile wave when taking the pulse. This wave travels 15 times faster than blood at a velocity of 3 5 m/s in the aorta, 7 10 m/s in large arteries and m/s in small arteries. The velocity can change with age due to arteriosclerosis. The pulse can also be recorded as an expansion of the arterial wall or as a wave of pressure. The sphygmogram represents the recording of the pulsatile wave at the level of large arteries. Recorded simultaneously with ECG and phonocardiogram, the sphygmogram can offer information on the cardiac output and the duration of heart systole phases. The sphygmogram can be recorded: Invasively through the catheterization of a large artery Non invasively using a pressure transducer, a piezoelectric sensor (arteriopiezogram) or a photoelectric (infrared) transducer The sphygmogram has the following components: Systolic ascending slope or anacrotic slope rises at to the horizontal plane. Gives rise to the Percussion wave (P wave). The height of P wave and the fast ejection time (which lasts for s) of the left ventricle is related to the ejection ability of heart and the compliance index of aorta. A larger slope indicates a better performance of the heart ejection function and aorta compliance. Thus it is used as a quantitative feature to evaluate the cardiovascular system. The second peak, called the Tidal wave (T wave), appears when blood hits the artery wall and rebounds. As a result, T wave manifest if the artery possesses excellent elasticity that reflects low peripheral resistance of the circulatory system. On the other hand, an artery with a stiff wall makes the T wave propagate fast. Accordingly, the T wave will merge with the P wave, which results in a wider P wave. The time between the peaks of the P and T wave is also known as the systolic plateau, lasting 0.14s. Finally, when the aortic valve is closed, the Dicrotic wave (D wave) is generated. The height of the D wave will decrease due to a stiff aorta or aortic regurgitation. The descending slope of the sphygmogram is also called catacrotic slope. The sphygmogram can change in pathological conditions (some examples are given below): pulsus tardus et parvus It is seen in aortic valve stenosis. With respect to aortic stenosis, "typical findings include a narrow pulse pressure.
4 pulsus bisferiens Bisferious means striking twice. Classically, it is detected when aortic insufficiency exists in association with aortic stenosis, or in severe Ao. insufficiency pulsus alternans is a physical finding with arterial pulse waveform showing alternating strong and weak beats. It is almost always indicative of left ventricular systolic impairment, and carries a poor prognosis. pulsus paradoxus (Kussmaul sign) is an exaggeration of the normal variation in the pulse during the inspiratory phase of respiration, in which the pulse becomes weaker as one inhales and stronger (>10mmHg) as one exhales. It is a sign that is indicative of several conditions including cardiac tamponade, pericarditis, chronic sleep apnea, croup, and obstructive lung disease Blood Pressure Measurement Methods Arterial pressures are usually measured non invasively (indirectly), without penetrating skin or artery. Measuring pressure invasively (directly), by penetrating the arterial wall to take the measurement, is much less common, and usually restricted to a hospital setting. Non Invasive Blood Pressure Measurement A. Auscultatory method The auscultatory method was described for the first time by Nikolai Korotkoff in 1905 being currently the most widely used method for BP measurement. It uses a stethoscope and a sphygmomanometer. This comprises an inflatable (Riva Rocci) cuff placed around the upper arm at roughly the same vertical height as the heart, attached to a mercury or aneroid manometer. The mercury manometer measures the height of a column of mercury, giving an absolute result without need for calibration, and consequently not subject to the errors and drift of calibration which affect other methods. The use of mercury manometers is often required in clinical trials and for the clinical measurement of hypertension in high risk patients, such as pregnant women. Fig. 2 Types of sphygmomanometers. Left: mercury sphygmomanometer; Right aneroid sphygmomanometer. The principle on which the auscultatory method relies is the inflation of the cuff compressing the brachial artery hence causing the artery to collapse once the systolic pressure (the maximum pressure exerted by the blood against the wall of the brachial artery when the heart beats) has been exceeded. The valve on the pump is loosened slowly to allow the pressure of the sphygmomanometer cuff to decrease. Once the systolic pressure is reached the brachial artery opens causing volatile
5 blood flow, which causes vibrations against the artery walls. These noises are called Korotkoff sounds (named after their discoverer) and can be heard through a stethoscope as the pressure exerted onto the brachial artery falls. The blood flow through the brachial artery increases steadily, until the pressure of the sphygmomanometer cuff falls below the diastolic pressure. This is the point where the blood flow through the artery is laminar. The Korotkoff sounds are first heard when the cuff pressure equals the systolic pressure, and cease to be heard once the cuff has deflated past the diastolic pressure. It is generally accepted that there are five phases of Korotkoff sounds. Each phase is characterized by the volume and quality of sound heard. Phase 1. With the pressure cuff inflated to beyond the systolic pressure, the artery is completely occluded and no blood can flow through it. Consequently, no sounds are heard above the systolic pressure. At the point where cuff pressure equals the systolic pressure, a sharp tapping sound is heard. We recall that the blood pressure oscillates between systolic and diastolic pressure. At systolic, the pressure is great enough to force the artery walls open and for blood to spurt through. As the pressure dips to diastolic, however, the artery walls bang shut again. It is the closing shut of the artery walls that results in the tapping sound. Phase 2. This phase is characterized by a swishing sound, caused by the swirling currents in the blood as the flow through the artery increases. Sometimes, if the cuff is deflated too slowly, the sounds vanish temporarily. This happens when the blood vessels beneath the cuff become congested, and is often a sign of hypertension. The congestion eventually clears, and sounds resume. The intervening period is called the auscultatory gap. Phase 3. In this phase, there is a resumption of crisp tapping sounds, similar to those heard in phase 1. At this stage, the increased flow of blood is pounding against the artery walls. Phase 4. At this point, there is an abrupt muffling of sound. The blood flow is becoming less turbulent. Some medical practitioners choose to record this point as the diastolic pressure. Phase 5. This is the point at which sounds cease to be heard all together. The blood flow has returned to normal and is now laminar. The pressure cuff is deflated entirely and removed. Fig. 3 A. Cuff inflated above the systolic blood pressure (SBP), no flow occurs distally to the cuff; B. Once the pressure in the cuff descends below the SBP, soft intermittent tapping sounds are being heard; C. The pressure in the cuff approaches the diastolic blood pressure (DBP) value, muffled sound are being heard; D. The cuff is deflated below DBP no sounds are heard. Preparation for measurement Before the blood pressure measurement begins the following conditions should be met: 1. Subjects should abstain from eating, drinking (anything else than water), smoking and taking drugs that affect the blood pressure one hour before measurement. 2. Because a full bladder affects the blood pressure it should have been emptied.
6 3. Painful procedures and exercise should not have occurred within one hour. 4. Subject should have been sitting quietly for about 5 minutes. 5. Subject should have removed outer garments and all other tight clothes. The sleeve of shirts, blouses, etc. should have been rolled up so that the upper right arm is bare. The remaining garments should not be constrictive and the blood pressure cuff should not be placed over the garment. 6. Blood pressure should be measured in a quiet room with comfortable temperature. The room temperature should have been recorded. 7. The time of day should have been recorded. Position of the subject Measurements should be taken in sitting position so that the arm and back are supported. Subject's feet should be resting firmly on the floor, not dangling. If the subject's feet do not reach the floor, a platform should be used to support them. Position of the arm The subject's arm should be resting on the desk so that the antecubital fossa (a triangular cavity of the elbow joint that contains a tendon of the biceps, the median nerve, and the brachial artery) is at the level of the heart and palm is facing up. To achieve this position, either the chair should be adjusted or the arm on the desk should be raised, e.g. by using a pillow. The subject must always feel comfortable. The measurements should be made on the right arm whenever possible. However, Measure BP in both arms at first consult of a subject/patient to detect possible differences due to peripheral vascular disease. In this instance, take the higher value as the reference one. Selection of the cuff The greatest circumference of the upper arm is measured, with the arm relaxed and in the normal blood pressure measurement position (antecubital fossa at the level of the heart), using a nonelastic tape. The measurement should be read to the nearest centimeter. Select the correct cuff for the arm circumference: Cuff width 8 cm 12 cm 16 cm Arm circumference less than 25 cm 25 cm 35 cm over 35 cm The cuff should be placed on the right arm so that its bottom edge is 2 3 cm above the antecubital fossa, allowing sufficient room for the bell of the stethoscope. The top edge of the cuff should not be restricted by clothing. Number of measurements Three measurements should be taken one minute apart. If three measurements are not feasible, two will suffice with a certain loss in data stability. Procedure of the pulse rate and blood pressure measurement 1. The radial pulse is palpated and the pulse rate is counted for 30 seconds, measured by a digital wrist watch or one with second hand. Record 30 second pulse count and whether pulse was regular. 2. The manometer should be placed so that the scale is at eye level and the column perfectly vertical. The subject should not be able to see the column of the manometer. 3. Determining the peak inflation level: a. The mercury column has to be at 0 level. b. The subject's radial pulse is again palpated. c. The cuff is inflated and the level of the top of the meniscus of the mercury column is noted at the point when the radial pulse disappears. The cuff is immediately deflated by completely opening the valve. d. The peak inflation level is determined by adding 30 mm to the pressure where the radial pulse disappeared.
7 4. Venous blood pool in the forearm is normalized by waiting at least 30 seconds or by raising the arm for 5 6 seconds. 5. The brachial pulse is located and the bell of the stethoscope is placed immediately below the cuff at the point of maximal pulsation. If it is not possible to feel the brachial pulse, the bell of the stethoscope should be placed over the area of the upper arm immediately inside the biceps muscle tendon. The bell should not touch the cuff, rubber or clothing. The bell of the stethoscope should be used because it gives clearer sounds than the diaphragm. 6. The cuff is rapidly inflated to the peak inflation level and then deflated at a rate of 2 mmhg per second. 7. The pressure should be reduced steadily at this rate until the occurrence of the systolic level at the first appearance of a clear, repetitive tapping sound (Korotkoff Phase 1) and diastolic level at disappearance of repetitive sounds (Phase 5) have been observed. Then the cuff should be rapidly deflated by fully opening the valve of the inflation bulb. Note: There may be a brief period (auscultatory gap) between systolic and diastolic pressure, when no Korotkoff sounds are heard. Therefore, the 2mmHg/second deflation should be continued until the diastolic blood pressure is definitely established. If Korotkoff sounds persist until the cuff is completely deflated, a diastolic blood pressure of 0 should be recorded. 8. The measurements should be recorded to the nearest 2 mmhg. If the top of the meniscus falls half way between two markings, the marking immediately above is chosen. The subject is not told the blood pressure values at this point. 9. After one minute of wait to allow redistribution of blood in the forearm a second measurement is made by repeating steps 6 to 8. The subject should not change position during the wait. 10. After another one minute a third measurement is made by repeating steps 6 to The subject may now be told the measurement values. B. Doppler ultrasound method The Doppler method uses a Doppler ultrasound transducer instead of a stethoscope in order to detect flow past the pressurized cuff attached to an aneroid or mercury manometer. The Doppler transducer uses an ultrasound beam to detect blood flow, the signal being displayed on a screen or heard in speakers. This method is useful when the Korotkoff sounds cannot be heard due to very low blood pressures (i.e. hemodynamic shock) or small size arteries (i.e. pediatric patients). Another disadvantage of the method is that diastolic blood pressure cannot be determined. The use of ultrasound gel is essential to allow the passage of ultrasound waves between the transducer and the subcutaneous structures. C. Photoplethysmography method This method is also based on the Riva Rocci principle like the two previously described methods. The device used to detect blood flow distally to the cuff is a pulse plethysmograph sensor. The blood flow signal is usually displayed on a monitor. The method is mainly used in intensive care and research setups. Fig. 3 Pulseplethysmography recording D. Palpatory method The palpatory method is another method based on the Riva Rocci principle. It is mainly used when no devices are available to detect blood flow (i.e. stethoscope, Doppler transducer, etc). Place the cuff of the sphygmomanometer around the arm (as described previously). With one hand, palpate (feel) the radial pulse in the wrist. Slowly inflate the cuff by pumping the bulb with the other hand and note the pressure reading when the radial pulse is first lost. Then increase the pressure to
8 around 20 mm Hg above this point. Slowly reduce the pressure in the cuff by turning the valve counterclockwise slightly to let air out of the bag. Note the pressure when the radial pulse first reappears. This is systolic blood pressure, the highest pressure in the systemic artery. The systolic pressure recorded with the palpatory method is usually around 5 mm Hg lower than that obtained using the auscultatory method. A major disadvantage of the palpatory method is that it cannot be used to measure the diastolic pressure. E. Ankle brachial pressure index An ankle brachial pressure index (ABPI) is a simple non invasive method of identifying arterial insufficiency within a limb. It represents the ratio of the blood pressure in the lower legs to the blood pressure in the arms. Compared to the arm, lower blood pressure in the leg is a symptom of blocked arteries (peripheral vascular disease). The ABPI is calculated by dividing the systolic blood pressure in the arteries at the ankle and foot by the higher of the two systolic blood pressures in the arms. Fig. 4 Illustration of the ABPI test. The ABPI gives the ratio of the systolic blood pressure in the ankle to the systolic blood pressure in the brachial artery of the arm. A Doppler ultrasound blood flow transducer is used to register the peripheral pulse while the cuff of a sphygmomanometer is inflated over the artery until the pulse ceases, proximal to the Doppler probe. The cuff is slowly deflated, and the corresponding sphygmomanometer pressure at the instant the pulse returns provides the systolic blood pressure reading, for the given artery. The higher of the left and right arm brachial artery pressure is generally used in the assessment. The pressures in each foot's posterior tibial artery and dorsalis pedis artery are measured with the higher of the two values used as the ABPI for that leg. ABPI = SBP Leg / SBP Arm The ABPI is a useful tool for the non invasive assessment of peripheral vascular disease. Studies have shown the sensitivity of ABPI is 90% with a corresponding 98% specificity for detecting hemodynamically significant stenosis >50% in major leg arteries, defined by angiogram. In a normal subject the pressure at the ankle is slightly higher than at the elbow (there is reflection of the pulse pressure from the vascular bed of the feet, whereas at the elbow the artery continues on some distance to the wrist). ABPI value Interpretation above 1.2 Abnormal Vessel hardening from peripheral vascular disease Normal range Acceptable Some arterial disease Moderate arterial disease under 0.5 Severe arterial disease
9 F. Oscillation based methods Oscillometric method. The method was developed by Victor Pachon, a French physician, in Pachon s Oscillometer was a master piece of creative engineering, which was reputed to be indestructible. The device is difficult to use as the good use of the device is dependant on the user's ability to recognize and analyze the difference in amplitude between the minima and maxima, which is amplified on the larger of the two displays by a needle linked directly to the pressure in the cuff. The smaller display indicates the constant pressure inside the actual device. To use the device, one has to inflate the cuff to about 200 mmhg (using a little bicycle pump), then slowly let the pressure drop by the using beautifully crafted release valves. As the pressure in the cuff drops, the amplitude of the signal gets greater as more blood flows through the arteries. The point of the device is to judge at what point the amplitude of the signal is greatest. This point is referred to as the Oscillometric Index. In this way, the oscillometer allows the user to estimate the elasticity of the arterial walls and the strength of the pulse wave through the arteries. Pachon's oscillometer is an improvement over the oscillometer devised by Heinrich von Recklinghausen. Oscillotonometry. The Von Recklinghausen Oscillotonometer is a device which allows both systolic and diastolic blood pressure to be read without a stethoscope. It consists of two overlapping cuffs (one large, one small) a large dial for reading pressure, a bleed valve and a control lever. The large cuff performs the usual function of the sphygmomanometer cuff. The job of the smaller cuff is basically to amplify the pulsations which occur as the larger cuff is deflated, so that instead of listening for the Korotkoff sounds, they are seen as oscillations of the needle on the pressure gauge. The lever simply switches the dial between the two cuffs. Wrap the cuff round the arm in the usual way, and inflate it. Adjust the bleed valve so that the pressure falls slowly. Pull the control lever towards you. The needle will jump slightly in time with the pulse. As the cuff pressure approaches systolic, the needle suddenly starts to jump more vigorously. At this point, let go of the lever, and the needle will display systolic pressure. Pull the lever forward again. As the pressure is reduced, the needle jumps more vigorously. If the lever is released at the point of maximum needle oscillations, the dial will read the mean arterial pressure. If it is released at the point when the needle jumps get suddenly smaller, the dial reads diastolic pressure. Both oscillometric and oscillotonometric methods are nowadays rarely used in their initial form, the principle being applied on automated BP measurement devices. G. Automatic measurement Automatic devices which essentially apply the same principle as the oscillotonometer have been produced. They require a supply of electricity. A single cuff is applied to the patients arm, and the machine inflates it to a level assumed to be greater than systolic pressure. The cuff is deflated gradually. A sensor then measures the tiny oscillations in the pressure of the cuff caused by the pulse. Systolic is taken to be when the pulsations start, mean pressure is when they are maximal, and diastolic is when they disappear. They can produce fairly accurate readings and free the hands of the investigator for other tasks. There are important sources of inaccuracy, however. Such devices tend to over read at low blood pressure, and under read very high blood pressure. The cuff should be an appropriate size. The patient should be still during measurement. The technique relies heavily on a constant pulse volume, so in a patient with an irregular heart beat (especially atrial fibrillation) readings can be inaccurate. Sometimes an automatic blood pressure measuring device inflates and deflates repeatedly "hunting" without displaying the blood pressure successfully. If the pulse is palpated as the cuff is being inflated and deflated the blood pressure may be estimated by palpation and reading the cuff pressure on the display. Invasive Blood Pressure Measurement
10 Direct BP measurement involves placing a needle or catheter into the lumen of an artery. The catheter is then connected via saline filled tubing to a pressure transducer. The transducer converts the mechanical fluctuations in the fluid into an electrical signal that can be displayed on an oscilloscope or charted on a paper trace. Direct monitoring is considered the gold standard of BP measurement. Generally, this method requires sedation or anesthesia for catheter placement. Therefore, although this technique is very useful for intraoperative monitoring, it is less practical for conscious patients. Complications include infection of the catheter, thromboembolism, or serious hemorrhage if the catheter becomes dislodged. Other limiting factors include the technical difficulty of arterial catheterization and the constant attention needed to keep the catheter patent. These complications generally render direct BP measurement unsuitable for routine or outpatient use. Physiological Variation of Blood Pressure Many physiological conditions can influence the systolic and diastolic blood pressure values. SBP can be increased in emotional states (i.e. anger), cold environment, and physical effort. It can be decreased during sleep, digestion, after physical effort and in professional sportsmen, hot environment, constitutionally. BP can be pathologically increased in situations like hypertension, fever, hyperthyroidism, and decreased in shock, syncope, etc. Postural change. BP changes depending on the posture: lying down (supine/clinostatism), sitting, and standing (orthostatism). The SBP decreases slightly or remains unchanged, meanwhile the DBP increases. Measure your partner's blood pressure while she or he is lying down (supine), sitting, and standing. Record your results on your worksheet and also think about what might cause the changes in pressure that accompany these changes in body position. Thermal stress test. Classically the test is known as the cold pressure test, although hot stimuli produce the same effect. This test is used to demonstrate the effect of a sensory stimulus (cold/hot) on blood pressure. A normal reflex response to such a cold/hot stimulus is an increase in blood pressure (both systolic and diastolic). In a normal individual the systolic pressure will rise no more than 10 mm Hg, but in a hypertensive individual the rise may be 30 to 40 mm Hg. This is why this test is used in some medical systems for hypertension screening purposes. 1. Have the subject sit down comfortably or lie supine in a comfortable environment. 2. Record the systolic and diastolic blood pressure every 5 minutes until a constant level is obtained. 3. Immerse the subject's free hand in ice water (approximately 0 4 C) to a depth well above the wrist. 4. After a lapse of 10 to 15 seconds, obtain the blood pressure every 20 seconds for 1 or 2 minutes and record. If there is insufficient time to obtain both systolic and diastolic pressure, just measure the systolic value. Instead of cold water a hot stimulus can be used (40 45 C) like hot water or a Peltier element. Explain the mechanism by which thermal stress influences blood pressure. Physical Effort. This test examines the short term effects of exercise on blood pressure. Note The subject should be in good health, with no known cardiovascular or respiratory problems. 1. Have the subject sit comfortably. 2. Record the systolic and diastolic blood pressure every 5 minutes until a constant level is obtained. 3. Have the subject run up and down several flights of stairs, and then return to the sitting position. 4. Obtain and record the blood pressure immediately, then every minute for 5 minutes. Normally SBP increases instantly with mmhg and returns to basal values 2 3 minutes after the effort ceased. DBP remains unchanged or decreases slightly. White coat hypertension. For some patients, BP measurements taken in a doctor's office may not correctly characterize their typical BP. In up to 25% of patients, the office measurement is higher than their typical BP. This type of error is called white coat hypertension (WCH) and can result from
11 anxiety related to an examination by a health care professional. The misdiagnosis of hypertension for these patients can result in needless and possibly harmful medication. WCH can be reduced (but not eliminated) with automated BP measurements over 15 to 20 minutes in a quiet part of the office or clinic. References Guidelines for the management of arterial hypertension. The Task Force for the Management of Arterial Hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). European Heart Journal (2007) 28: Klabunde, Richard (2005). Cardiovascular Physiology Concepts. Lippincott Williams & Wilkins. ISBN National Heart, Lung and Blood Institute. Blood Pressure Tables for Children and Adolescents Sacks D, Bakal CW, Beatty PT, et al. Position statement on the use of the Ankle Brachial Index in the evaluation of patients with peripheral vascular disease: a consensus statement developed by the standards division of the society of cardiovascular and interventional radiology. J Vasc Interv Radiol (2002) 13: Textbook of Medical Physiology, 11th Ed., Guyton & Hall, Elsevier Saunders, ISBN X 6. The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC 7). Hypertension (2003) 42: Wesseling KH. A century of non invasive arterial pressure measurement: from Marey to Penaz and Finapres. Homeostasis (1995) 36:50 66.
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE. MEASURING BLOOD PRESSURE - MANUAL (equ04)
 SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: MEASURING BLOOD PRESSURE - MANUAL Nursing DATE: REVIEWED: PAGES: 2/80 7/17 1 of 5 RESPONSIBILITY: RN, LPN, Patient Care Technician Multi-skilled
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: MEASURING BLOOD PRESSURE - MANUAL Nursing DATE: REVIEWED: PAGES: 2/80 7/17 1 of 5 RESPONSIBILITY: RN, LPN, Patient Care Technician Multi-skilled
PLANK 1 Direct Care Staff Trained in Accurate BP Measurement
 Direct Care Staff Trained in Accurate BP Measurement 1. 2. 3. 5. 22 to 26 cm Small adult (12X22 cm) 27 to 34 cm Adult (16X30 cm) 35 to 44 cm Large adult (16X36 cm) 45 to 52 cm Adult thigh (16X42 cm) widths
Direct Care Staff Trained in Accurate BP Measurement 1. 2. 3. 5. 22 to 26 cm Small adult (12X22 cm) 27 to 34 cm Adult (16X30 cm) 35 to 44 cm Large adult (16X36 cm) 45 to 52 cm Adult thigh (16X42 cm) widths
#6 - Cardiovascular III Heart Sounds, Pulse Rate, Hemoglobin Saturation, and Blood Pressure
 #6 - Cardiovascular III Heart Sounds, Pulse Rate, Hemoglobin Saturation, and Blood Pressure Objectives: Observe slide of artery and vein cross-section Auscultate heart sounds using a stethoscope Measure
#6 - Cardiovascular III Heart Sounds, Pulse Rate, Hemoglobin Saturation, and Blood Pressure Objectives: Observe slide of artery and vein cross-section Auscultate heart sounds using a stethoscope Measure
LAB: Blood Pressure Measurable Indicator of the Health of the Circulatory System!
 LAB: Blood Measurable Indicator of the Health of the Circulatory System! Lab Objectives. At the completion of the lab, you should be able to: measure pulse or heart rate (HR) and respiratory rate (RR);
LAB: Blood Measurable Indicator of the Health of the Circulatory System! Lab Objectives. At the completion of the lab, you should be able to: measure pulse or heart rate (HR) and respiratory rate (RR);
Taking and recording blood pressure and pulse. City Gate Training Centre all rights reserved
 Taking and recording blood pressure and pulse City Gate Training Centre all rights reserved Course Content: Definition of Blood Pressure Normal Blood Pressure Readings Systolic and Diastolic Blood Pressure
Taking and recording blood pressure and pulse City Gate Training Centre all rights reserved Course Content: Definition of Blood Pressure Normal Blood Pressure Readings Systolic and Diastolic Blood Pressure
Ambulatory Services Orientation & Skill Review Skill Performance Checklist: Vital Signs. Name: Date:
 Evaluation Levels Behavior Level 3 Met Performed all skills competently. No behaviors omitted. Level 2 Satisfactory Omitted no more than three (3) non-critical behaviors. Level 1 Unsatisfactory Omitted
Evaluation Levels Behavior Level 3 Met Performed all skills competently. No behaviors omitted. Level 2 Satisfactory Omitted no more than three (3) non-critical behaviors. Level 1 Unsatisfactory Omitted
Vital Signs. Vital Signs. Pulse. Temperature. Respiration. Blood Pressure
 Vital Signs Jarvis, Chapter 9 Vital Signs Classic Vital Signs TPR/BP Temperature Pulse Respirations Blood Pressure Additional Vital Signs Height Weight BMI (Kg/m2) or (702Xlbs/in2) Supine, orthostatic
Vital Signs Jarvis, Chapter 9 Vital Signs Classic Vital Signs TPR/BP Temperature Pulse Respirations Blood Pressure Additional Vital Signs Height Weight BMI (Kg/m2) or (702Xlbs/in2) Supine, orthostatic
CAMOSUN COLLEGE BIOLOGY 144 (2010) LABS
 LAB 8: CARDIOVASCULAR PHYSIOLOGY PART 1. HEART SOUNDS AND PULSE DETERMINATIONS Introduction Two distinct sounds can be heard during each cardiac cycle. These sounds are commonly described as lub and dup
LAB 8: CARDIOVASCULAR PHYSIOLOGY PART 1. HEART SOUNDS AND PULSE DETERMINATIONS Introduction Two distinct sounds can be heard during each cardiac cycle. These sounds are commonly described as lub and dup
Human Cardiovascular Physiology: Blood Pressure and Pulse Determinations
 ighapmlre33apg269_274 5/12/04 3:10 PM Page 269 impos03 302:bjighapmL:ighapmLrevshts:layouts: NAME Human Cardiovascular Physiology: Blood Pressure and Pulse Determinations LAB TIME/DATE REVIEW SHEET exercise
ighapmlre33apg269_274 5/12/04 3:10 PM Page 269 impos03 302:bjighapmL:ighapmLrevshts:layouts: NAME Human Cardiovascular Physiology: Blood Pressure and Pulse Determinations LAB TIME/DATE REVIEW SHEET exercise
Lab #10 Physiology of the Circulatory System
 Lab #10 Physiology of the Circulatory System Introduction The circulatory system functions to deliver oxygen an nutrients to tissues for growth and metabolism, and to remove metabolic wastes. The heart
Lab #10 Physiology of the Circulatory System Introduction The circulatory system functions to deliver oxygen an nutrients to tissues for growth and metabolism, and to remove metabolic wastes. The heart
Section 03: Pre Exercise Evaluations and Risk Factor Assessment
 Section 03: Pre Exercise Evaluations and Risk Factor Assessment ACSM Guidelines: Chapter 3 Pre Exercise Evaluations ACSM Manual: Chapter 3 Risk Factor Assessments HPHE 4450 Dr. Cheatham Purpose The extent
Section 03: Pre Exercise Evaluations and Risk Factor Assessment ACSM Guidelines: Chapter 3 Pre Exercise Evaluations ACSM Manual: Chapter 3 Risk Factor Assessments HPHE 4450 Dr. Cheatham Purpose The extent
LEARNING OUTCOME The students will be able to elicit vital signs correctly on human volunteers/patients
 Vital signs (pulse, blood pressure, temperature, respiratory rate, pain) are physiological parameters that a healthcare professional requires when dealing with patients. Accurate measurement of vital signs
Vital signs (pulse, blood pressure, temperature, respiratory rate, pain) are physiological parameters that a healthcare professional requires when dealing with patients. Accurate measurement of vital signs
Chapter 15: Measuring Height, Weight, and Vital Signs. Copyright 2012 Wolters Kluwer Health Lippincott Williams & Wilkins
 Chapter 15: Measuring Height, Weight, and Vital Signs Height and Weight Weight Baseline measurement at patient s first visit Measured in kg or lbs Common types of scales Balance beam Dial Digital Height
Chapter 15: Measuring Height, Weight, and Vital Signs Height and Weight Weight Baseline measurement at patient s first visit Measured in kg or lbs Common types of scales Balance beam Dial Digital Height
Physiology of the Circulatory System modified from
 Physiology of the Circulatory System modified from http://www.ekcsk12.org/science/aplabreview/aplab10.htm Introduction The circulatory system functions to deliver oxygen and nutrients to tissues for growth
Physiology of the Circulatory System modified from http://www.ekcsk12.org/science/aplabreview/aplab10.htm Introduction The circulatory system functions to deliver oxygen and nutrients to tissues for growth
LAB 9: Metabolic Rates
 LAB 9: Metabolic Rates Introduction: The cardiovascular (circulatory) system functions to deliver oxygen and nutrients to tissues for growth and metabolism, and to remove metabolic wastes. The heart pumps
LAB 9: Metabolic Rates Introduction: The cardiovascular (circulatory) system functions to deliver oxygen and nutrients to tissues for growth and metabolism, and to remove metabolic wastes. The heart pumps
2. Measure a subject's blood pressure and heart rate both at rest and during exercise.
 Lab Activity 11 The Cardiovascular System Student Learning Objectives After completing this lab, you should be able to: 1. Define, explain and correctly use the key terms. 2. Measure a subject's blood
Lab Activity 11 The Cardiovascular System Student Learning Objectives After completing this lab, you should be able to: 1. Define, explain and correctly use the key terms. 2. Measure a subject's blood
Blood Pressure Laboratory
 Introduction The blood that circulates throughout the body maintains a flow and pressure. The nervous system can change the flow and pressure based on the particular needs at a given time. For example,
Introduction The blood that circulates throughout the body maintains a flow and pressure. The nervous system can change the flow and pressure based on the particular needs at a given time. For example,
1 Non-invasive measurement of arterial pressure
 Non-invasive measurement of arterial pressure I. Background A. Circulatory systems Human circulation takes place in a closed system that consists of two subsystems, pulmonary circulation and systemic circulation,
Non-invasive measurement of arterial pressure I. Background A. Circulatory systems Human circulation takes place in a closed system that consists of two subsystems, pulmonary circulation and systemic circulation,
5.2. MEASUREMENT OF BLOOD PRESSURE
 5.2. MEASUREMENT OF BLOOD PRESSURE Purpose of experiment To examine a person s blood pressure. Tasks of experiment To record the pressure changes in the vascular system: using the traditional method measure
5.2. MEASUREMENT OF BLOOD PRESSURE Purpose of experiment To examine a person s blood pressure. Tasks of experiment To record the pressure changes in the vascular system: using the traditional method measure
HUMAN ANATOMY AND PHYSIOLOGY
 HUMAN ANATOMY AND PHYSIOLOGY NAME Detection of heart sounds. Clean the ear pieces of the stethoscope before using. The ear pieces should be pointing slightly forward when inserted into the ears because
HUMAN ANATOMY AND PHYSIOLOGY NAME Detection of heart sounds. Clean the ear pieces of the stethoscope before using. The ear pieces should be pointing slightly forward when inserted into the ears because
AN INTRODUCTION TO DOPPLER. Sarah Gardner, Clinical lead, Tissue viability service. Oxford Health NHS Foundation Trust.
 AN INTRODUCTION TO DOPPLER Sarah Gardner, Clinical lead, Tissue viability service. Oxford Health NHS Foundation Trust. THE DOPPLER EFFECT The Doppler Principle was described by Physicist and mathematician
AN INTRODUCTION TO DOPPLER Sarah Gardner, Clinical lead, Tissue viability service. Oxford Health NHS Foundation Trust. THE DOPPLER EFFECT The Doppler Principle was described by Physicist and mathematician
Data Collection Worksheet
 Data Collection Worksheet 1. Has a doctor or nurse ever said that you have: High blood pressure or hypertension? [ ] No [ ] Yes [ ] Not Sure 1.a. If Yes, then at what age were you first told this? Age
Data Collection Worksheet 1. Has a doctor or nurse ever said that you have: High blood pressure or hypertension? [ ] No [ ] Yes [ ] Not Sure 1.a. If Yes, then at what age were you first told this? Age
Biomedical Instrumentation E. Blood Pressure
 Biomedical Instrumentation E. Blood Pressure Dr Gari Clifford Adapted from slides by Prof. Lionel Tarassenko Blood pressure Blood is pumped around the body by the heart. It makes its way around the body
Biomedical Instrumentation E. Blood Pressure Dr Gari Clifford Adapted from slides by Prof. Lionel Tarassenko Blood pressure Blood is pumped around the body by the heart. It makes its way around the body
External Oscillatory Blood Pressure - EOBPTM
 External Oscillatory Blood Pressure - EOBPTM Development of Novel Principle To Measure Blood Pressure Mindaugas Pranevicius, M.D., Osvaldas Pranevicius, M.D., Ph.D. Pranevicius Biotech Inc., Forest Hills,
External Oscillatory Blood Pressure - EOBPTM Development of Novel Principle To Measure Blood Pressure Mindaugas Pranevicius, M.D., Osvaldas Pranevicius, M.D., Ph.D. Pranevicius Biotech Inc., Forest Hills,
AP Biology Lab 10 PHYSIOLOGY OF THE CIRCULATORY SYSTEM
 AP Biology Laboratory Date: Name and Period: AP Biology Lab 10 PHYSIOLOGY OF THE CIRCULATORY SYSTEM OVERVIEW In this lab you will: 1. in Exercise 10A you will learn how to measure blood pressure. 2. in
AP Biology Laboratory Date: Name and Period: AP Biology Lab 10 PHYSIOLOGY OF THE CIRCULATORY SYSTEM OVERVIEW In this lab you will: 1. in Exercise 10A you will learn how to measure blood pressure. 2. in
Techniques of Vital Signs. John Gazewood, MD, MSPH Department of Family Medicine
 Techniques of Vital Signs John Gazewood, MD, MSPH Department of Family Medicine Objectives Define normal in several ways. Describe correct technique of measuring vital signs. Describe correct technique
Techniques of Vital Signs John Gazewood, MD, MSPH Department of Family Medicine Objectives Define normal in several ways. Describe correct technique of measuring vital signs. Describe correct technique
AFFORDABLE TECHNOLOGY
 World Health Organization AFFORDABLE TECHNOLOGY BLOOD PRESSURE MEASURING DEVICES FOR LOW RESOURCE SETTINGS CARDIOVASCULAR DISEASES Blood Pressure Measurement in Low Resource Settings Annex 1: Blood Pressure
World Health Organization AFFORDABLE TECHNOLOGY BLOOD PRESSURE MEASURING DEVICES FOR LOW RESOURCE SETTINGS CARDIOVASCULAR DISEASES Blood Pressure Measurement in Low Resource Settings Annex 1: Blood Pressure
Protocol 4: Measuring Blood Pressure
 Zool 430L Protocols Page 8 of 12 Protocol 4: Measuring Blood Pressure 4.1 Via Auscultation (listening through stethoscope) The estimate of blood pressure is obtained by cutting off blood flow with a known
Zool 430L Protocols Page 8 of 12 Protocol 4: Measuring Blood Pressure 4.1 Via Auscultation (listening through stethoscope) The estimate of blood pressure is obtained by cutting off blood flow with a known
a central pulse located at the apex of the heart Apical pulse Apical-radial pulse a complete absence of respirations Apnea
 Afebrile absence of a fever Apical pulse a central pulse located at the apex of the heart Apical-radial pulse measurement of the apical beat and the radial pulse at the same time Apnea a complete absence
Afebrile absence of a fever Apical pulse a central pulse located at the apex of the heart Apical-radial pulse measurement of the apical beat and the radial pulse at the same time Apnea a complete absence
IB TOPIC 6.2 THE BLOOD SYSTEM
 IB TOPIC 6.2 THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein THE BLOOD SYSTEM 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
IB TOPIC 6.2 THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein THE BLOOD SYSTEM 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
How To Measure Vital Signs
 How To Measure Vital Signs How to Use This Tutorial This tutorial is intended for healthcare providers or students to teach basic vital signs skills Use the navigation buttons below to move through the
How To Measure Vital Signs How to Use This Tutorial This tutorial is intended for healthcare providers or students to teach basic vital signs skills Use the navigation buttons below to move through the
The measurement of blood pressure and hypertension. Handout Fenyvesi Tamás III.Department of Medicine
 The measurement of blood pressure and hypertension Handout Fenyvesi Tamás III.Department of Medicine 1 2 History of the blood pressure measurement direct Stephen HALES 1726 horse carotid indirect Riva-Rocci
The measurement of blood pressure and hypertension Handout Fenyvesi Tamás III.Department of Medicine 1 2 History of the blood pressure measurement direct Stephen HALES 1726 horse carotid indirect Riva-Rocci
IB TOPIC 6.2 THE BLOOD SYSTEM
 IB TOPIC 6.2 THE BLOOD SYSTEM THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
IB TOPIC 6.2 THE BLOOD SYSTEM THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
CHAPTER 4 ESTIMATION OF BLOOD PRESSURE USING PULSE TRANSIT TIME
 64 CHAPTER 4 ESTIMATION OF BLOOD PRESSURE USING PULSE TRANSIT TIME 4.1 GENERAL This chapter presents the methodologies that are usually adopted for the measurement of blood pressure, heart rate and pulse
64 CHAPTER 4 ESTIMATION OF BLOOD PRESSURE USING PULSE TRANSIT TIME 4.1 GENERAL This chapter presents the methodologies that are usually adopted for the measurement of blood pressure, heart rate and pulse
BLOOD PRESSURE ASSESSMENT
 BLOOD PRESSURE ASSESSMENT Course Principles of Health Science Unit X Vital Signs Course Health Science Unit VI CPR / AED & First Aid Essential Question How do health care skills help to promote health
BLOOD PRESSURE ASSESSMENT Course Principles of Health Science Unit X Vital Signs Course Health Science Unit VI CPR / AED & First Aid Essential Question How do health care skills help to promote health
Lecture #3 - Blood Pressure Recording Procedure. Equipment
 Lecture #3 - Blood Pressure Recording Procedure CKiD Blood Pressure Training Equipment Mabis Medic-Kit aneroid sphygmomanometer Mabis Medic-Kit assortment of cuff sizes Stethoscope with bell (pediatric
Lecture #3 - Blood Pressure Recording Procedure CKiD Blood Pressure Training Equipment Mabis Medic-Kit aneroid sphygmomanometer Mabis Medic-Kit assortment of cuff sizes Stethoscope with bell (pediatric
PART I: HEART ANATOMY
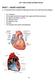 Lab 7: Heart Sounds and Blood Pressure PART I: HEART ANATOMY a) You should be able to identify the following structures on an adult human heart diagram. the 4 chambers the bicuspid (mitral) and tricuspid
Lab 7: Heart Sounds and Blood Pressure PART I: HEART ANATOMY a) You should be able to identify the following structures on an adult human heart diagram. the 4 chambers the bicuspid (mitral) and tricuspid
Blood Pressure and Exercise Lab
 Blood Pressure and Exercise Lab Rob MacLeod March 9, 2006 1 Purpose and Background Purpose: To learn about external means to measure blood pressure, observe features of venous circulation, and observe
Blood Pressure and Exercise Lab Rob MacLeod March 9, 2006 1 Purpose and Background Purpose: To learn about external means to measure blood pressure, observe features of venous circulation, and observe
Heart Rate and Blood Pressure as Vital Signs
 Heart Rate and Blood Pressure as Vital Signs Computer 10 Since the earliest days of medicine heart rate has been recognized as a vital sign an indicator of health, disease, excitement, and stress. Medical
Heart Rate and Blood Pressure as Vital Signs Computer 10 Since the earliest days of medicine heart rate has been recognized as a vital sign an indicator of health, disease, excitement, and stress. Medical
High Blood Pressure Blood Pressure Monitoring at Home -- F...
 Return to Web version High Blood Pressure Blood Pressure Monitoring at Home Why should I measure my blood pressure at home and keep a record of it? Measuring your blood pressure at home and keeping a record
Return to Web version High Blood Pressure Blood Pressure Monitoring at Home Why should I measure my blood pressure at home and keep a record of it? Measuring your blood pressure at home and keeping a record
Blood Pressure Competency Training
 Blood Pressure Competency Training WORKBOOK Table of Contents 3..... Introduction 4..... Background 6..... Equipment Accurate blood pressure What impacts a patient s blood pressure Strategies for proper
Blood Pressure Competency Training WORKBOOK Table of Contents 3..... Introduction 4..... Background 6..... Equipment Accurate blood pressure What impacts a patient s blood pressure Strategies for proper
Managing Blood Pressure: It Takes a Team
 Managing Blood Pressure: It Takes a Team Module Two How to Take Blood Pressure October 2011 MODULE TWO: How to Take Blood Pressure Module Two: HOW TO TAKE BLOOD PRESSURE Objectives Demonstrate proper technique
Managing Blood Pressure: It Takes a Team Module Two How to Take Blood Pressure October 2011 MODULE TWO: How to Take Blood Pressure Module Two: HOW TO TAKE BLOOD PRESSURE Objectives Demonstrate proper technique
Chapter 12 - Vital_Signs_and_Monitoring_Devices
 Introduction to Emergency Medical Care 1 OBJECTIVES 12.1 Define key terms introduced in this chapter. Slides 13 15, 17, 21 22, 26, 28, 30, 32 33, 35, 44, 47 48, 50, 55, 60 12.2 Identify the vital signs
Introduction to Emergency Medical Care 1 OBJECTIVES 12.1 Define key terms introduced in this chapter. Slides 13 15, 17, 21 22, 26, 28, 30, 32 33, 35, 44, 47 48, 50, 55, 60 12.2 Identify the vital signs
Cardiovascular Physiology
 Cardiovascular Physiology The mammalian heart is a pump that pushes blood around the body and is made of four chambers: right and left atria and right and left ventricles. The two atria act as collecting
Cardiovascular Physiology The mammalian heart is a pump that pushes blood around the body and is made of four chambers: right and left atria and right and left ventricles. The two atria act as collecting
Physiology lecture 15 Hemodynamic
 Physiology lecture 15 Hemodynamic Dispensability (D) : proportional change in volume per unit change in pressure D = V/ P*V It is proportional (divided by the original volume). Compliance (C) : total change
Physiology lecture 15 Hemodynamic Dispensability (D) : proportional change in volume per unit change in pressure D = V/ P*V It is proportional (divided by the original volume). Compliance (C) : total change
Vital Signs. Temperature. Pulse. Respirations. Blood Pressure. O2 Saturation
 Vital Signs Temperature Pulse Respirations Blood Pressure O2 Saturation Vital Signs Temperature, pulse, respiration, blood pressure (B/P) & oxygen saturation are the most frequent measurements taken by
Vital Signs Temperature Pulse Respirations Blood Pressure O2 Saturation Vital Signs Temperature, pulse, respiration, blood pressure (B/P) & oxygen saturation are the most frequent measurements taken by
AMERICAN ASSOCIATION OF SLEEP TECHNOLOGISTS TECHNICAL GUIDELINE FOR PATIENT ASSESSMENT AND VITAL SIGNS MEASUREMENT AND DOCUMENTATION
 AMERICAN ASSOCIATION OF SLEEP TECHNOLOGISTS TECHNICAL GUIDELINE FOR PATIENT ASSESSMENT AND VITAL SIGNS MEASUREMENT AND DOCUMENTATION SUMMARY: Sleep technologists observe and monitor physical signs and
AMERICAN ASSOCIATION OF SLEEP TECHNOLOGISTS TECHNICAL GUIDELINE FOR PATIENT ASSESSMENT AND VITAL SIGNS MEASUREMENT AND DOCUMENTATION SUMMARY: Sleep technologists observe and monitor physical signs and
Cardiovascular Physiology Laboratory Clive M. Baumgarten, Ph.D.
 Cardiovascular Physiology Laboratory Clive M. Baumgarten, Ph.D. To pump blood, the heart has a rhythmical sequence of both electrical and mechanical events, the cardiac cycle. The electrical activity,
Cardiovascular Physiology Laboratory Clive M. Baumgarten, Ph.D. To pump blood, the heart has a rhythmical sequence of both electrical and mechanical events, the cardiac cycle. The electrical activity,
Lesson 16 BLOOD PRESSURE
 Physiology Lessons for use with the Lesson 16 BLOOD PRESSURE Indirect measurement Ventricular Systole & Diastole Korotkoff sounds Mean Arterial pressure Manual Revision 3.7.3 061808 Richard Pflanzer, Ph.D.
Physiology Lessons for use with the Lesson 16 BLOOD PRESSURE Indirect measurement Ventricular Systole & Diastole Korotkoff sounds Mean Arterial pressure Manual Revision 3.7.3 061808 Richard Pflanzer, Ph.D.
CATCH A WAVE.. INTRODUCTION NONINVASIVE HEMODYNAMIC MONITORING 4/12/2018
 WAVES CATCH A WAVE.. W I S C O N S I N P A R A M E D I C S E M I N A R A P R I L 2 0 1 8 K E R I W Y D N E R K R A U S E R N, C C R N, E M T - P Have you considered that if you don't make waves, nobody
WAVES CATCH A WAVE.. W I S C O N S I N P A R A M E D I C S E M I N A R A P R I L 2 0 1 8 K E R I W Y D N E R K R A U S E R N, C C R N, E M T - P Have you considered that if you don't make waves, nobody
PHONOCARDIOGRAPHY (PCG)
 PHONOCARDIOGRAPHY (PCG) The technique of listening to sounds produced by the organs and vessels of the body is called auscultation. The areas at which the heart sounds are heard better are called auscultation
PHONOCARDIOGRAPHY (PCG) The technique of listening to sounds produced by the organs and vessels of the body is called auscultation. The areas at which the heart sounds are heard better are called auscultation
BIOE221. Session 2. Vital Signs. Biosciences Dept.
 BIOE221 Session 2 Vital Signs Biosciences Dept. www.endeavour.edu.au Session Objectives cont o Understand the physiology related to the vital signs of temperature, pulse, respiration and blood pressure.
BIOE221 Session 2 Vital Signs Biosciences Dept. www.endeavour.edu.au Session Objectives cont o Understand the physiology related to the vital signs of temperature, pulse, respiration and blood pressure.
Dual-Cuff Method Improves Accuracy of Blood Pressure and Hemodynamics Determination
 Dual-Cuff Method Improves Accuracy of Blood Pressure and Hemodynamics Determination JIRI JILEK 1, MILAN STORK 2 1 Carditech, Culver City, California, USA jilekj@usa.net 2 Dept. of Applied Electronics and
Dual-Cuff Method Improves Accuracy of Blood Pressure and Hemodynamics Determination JIRI JILEK 1, MILAN STORK 2 1 Carditech, Culver City, California, USA jilekj@usa.net 2 Dept. of Applied Electronics and
SECTION 16: BLOOD PRESSURE MEASUREMENT
 CHRONIC KIDNEY DISEASE IN CHILDREN COHORT STUDY SECTION 16: BLOOD PRESSURE MEASUREMENT 16.1 OVERVIEW OF BLOOD PRESSURE MEASUREMENT This section describes the procedures that are to be performed to obtain
CHRONIC KIDNEY DISEASE IN CHILDREN COHORT STUDY SECTION 16: BLOOD PRESSURE MEASUREMENT 16.1 OVERVIEW OF BLOOD PRESSURE MEASUREMENT This section describes the procedures that are to be performed to obtain
science-u.org What affects blood Blood Pressure Directions You Will Need BEST FOR GRADES 5-8 ESTIMATED TIME Minutes
 What affects blood pressure? BEST FOR GRADES 5-8 ESTIMATED TIME 25-60 Minutes You Will Need Sphygmomanometer (blood pressure cuff) Stethoscope Blood pressure cuffs and stethoscopes can be found online
What affects blood pressure? BEST FOR GRADES 5-8 ESTIMATED TIME 25-60 Minutes You Will Need Sphygmomanometer (blood pressure cuff) Stethoscope Blood pressure cuffs and stethoscopes can be found online
Biology 236 Spring 2002 Campos/Wurdak/Fahey Laboratory 4. Cardiovascular and Respiratory Adjustments to Stationary Bicycle Exercise.
 BACKGROUND: Cardiovascular and Respiratory Adjustments to Stationary Bicycle Exercise. The integration of cardiovascular and respiratory adjustments occurring in response to varying levels of metabolic
BACKGROUND: Cardiovascular and Respiratory Adjustments to Stationary Bicycle Exercise. The integration of cardiovascular and respiratory adjustments occurring in response to varying levels of metabolic
Experiment HC-1: Blood Pressure, Peripheral Circulation, and Body Position
 Experiment HC-1: Blood Pressure, Peripheral Circulation, and Body Position Exercise 1: Blood Pressures from the Left Arm Aim: To determine the systolic and diastolic blood pressures in a reclining subject,
Experiment HC-1: Blood Pressure, Peripheral Circulation, and Body Position Exercise 1: Blood Pressures from the Left Arm Aim: To determine the systolic and diastolic blood pressures in a reclining subject,
Clinical Research Coordinator Skills Program
 Clinical Research Coordinator Skills Program Vital Signs This Skill Requires Provider direction Standard Precautions Using purell before and after contact with the patient or the patient s environment
Clinical Research Coordinator Skills Program Vital Signs This Skill Requires Provider direction Standard Precautions Using purell before and after contact with the patient or the patient s environment
Bio& 242, Unit 3/ Lab 4 Blood Vessels, Lymphatic System and Blood Pressure G. Blevins/ G. Brady Summer 2009
 Bio& 242, Unit 3/ Lab 4 Blood Vessels, Lymphatic System and Blood Pressure G. Blevins/ G. Brady Summer 2009 Major Arteries and for arteries and veins with common names your answer must include either artery
Bio& 242, Unit 3/ Lab 4 Blood Vessels, Lymphatic System and Blood Pressure G. Blevins/ G. Brady Summer 2009 Major Arteries and for arteries and veins with common names your answer must include either artery
A GUIDE TO OUR NIBP TECHNOLOGY
 GE Healthcare THE DINAMAP DIFFERENCE A GUIDE TO OUR NIBP TECHNOLOGY OUR TECHNOLOGICAL ADVANTAGES THE OSCILLOMETRIC METHODOLOGY Oscillometry is the most commonly used means of indirect blood pressure measurement
GE Healthcare THE DINAMAP DIFFERENCE A GUIDE TO OUR NIBP TECHNOLOGY OUR TECHNOLOGICAL ADVANTAGES THE OSCILLOMETRIC METHODOLOGY Oscillometry is the most commonly used means of indirect blood pressure measurement
Lectures on Medical Biophysics Department of Biophysics, Medical Faculty, Masaryk University in Brno. Biophysics of cardiovascular system
 Lectures on Medical Biophysics Department of Biophysics, Medical Faculty, Masaryk University in Brno Biophysics of cardiovascular system 1 Lecture outline Mechanical properties of blood vessels Reynolds
Lectures on Medical Biophysics Department of Biophysics, Medical Faculty, Masaryk University in Brno Biophysics of cardiovascular system 1 Lecture outline Mechanical properties of blood vessels Reynolds
ECG, Blood Pressure, and Exercise Lab
 ECG, Blood Pressure, and Exercise Lab Rob MacLeod March 31, 2006 1 Purpose and Background Purpose: The purpose of the lab is to learn about measuring the ECG and blood pressures and observing the effects
ECG, Blood Pressure, and Exercise Lab Rob MacLeod March 31, 2006 1 Purpose and Background Purpose: The purpose of the lab is to learn about measuring the ECG and blood pressures and observing the effects
VITAL SIGNS. Academic Success Center
 VITAL SIGNS Academic Success Center Because of the importance of these measurements they are referred to as Vital Signs. They are important indicators of the body s response to physical, environmental,
VITAL SIGNS Academic Success Center Because of the importance of these measurements they are referred to as Vital Signs. They are important indicators of the body s response to physical, environmental,
Hemodynamic Monitoring
 Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
MANUAL BLOOD PRESSURE MONITOR BPM 168B Contents Blood Pressure Monitor Intended Use What is blood pressure?
 MANUAL BLOOD PRESSURE MONITOR BPM 168B Contents 01... Blood Pressure Monitor Intended Use 02... 1. What is blood pressure? 02... 2. Why is it useful measure blood pressure at home?... A. WHO blood pressure
MANUAL BLOOD PRESSURE MONITOR BPM 168B Contents 01... Blood Pressure Monitor Intended Use 02... 1. What is blood pressure? 02... 2. Why is it useful measure blood pressure at home?... A. WHO blood pressure
2. The heart sounds are produced by a summed series of mechanical events, as follows:
 Heart Sounds. Phonocardiography 1 Objectives 1. Phonocardiography - Definition 2. What produces the heart sounds 3. Where to listen for the heart sounds 4. How to record a phonocardiogram 5. Normal heart
Heart Sounds. Phonocardiography 1 Objectives 1. Phonocardiography - Definition 2. What produces the heart sounds 3. Where to listen for the heart sounds 4. How to record a phonocardiogram 5. Normal heart
HEART SOUNDS & BLOOD PRESSURE
 LABORATORY HANDBOOK HEART SOUNDS & BLOOD PRESSURE For the course Systems Biology Karolinska Institutet Department of Physiology and Pharmacology Physiology Education Postal address: 171 77 Stockholm Visiting
LABORATORY HANDBOOK HEART SOUNDS & BLOOD PRESSURE For the course Systems Biology Karolinska Institutet Department of Physiology and Pharmacology Physiology Education Postal address: 171 77 Stockholm Visiting
1 Ankle Brachial Pressure Index
 1 Ankle Brachial Pressure Index Stuart Wind Video Time 3 mins 42 s Overview The Ankle-Brachial Pressure Index (ABPI) is a very useful non-invasive test which can quickly identify the presence and severity
1 Ankle Brachial Pressure Index Stuart Wind Video Time 3 mins 42 s Overview The Ankle-Brachial Pressure Index (ABPI) is a very useful non-invasive test which can quickly identify the presence and severity
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Physics of the Cardiovascular System
 Dentistry College Medical Physics Physics of the Cardiovascular System The cells of the body act like individual engines. In order for them to function they must have: - 1. Fuel from our food to supply
Dentistry College Medical Physics Physics of the Cardiovascular System The cells of the body act like individual engines. In order for them to function they must have: - 1. Fuel from our food to supply
Measuring Vital Signs. Copyright 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved.
 Measuring Vital Signs Copyright 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Five Vital Signs Temperature, pulse, respiration, blood pressure, and pain Vital signs give indications
Measuring Vital Signs Copyright 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Five Vital Signs Temperature, pulse, respiration, blood pressure, and pain Vital signs give indications
Chapter 15: The Cardiovascular System
 Chapter 15: The Cardiovascular System McArdle, W. D., Katch, F. I., & Katch, V. L. (2010). Exercise Physiology: Nutrition, Energy, and Human Performance (7 ed.). Baltimore, MD.: Lippincott Williams and
Chapter 15: The Cardiovascular System McArdle, W. D., Katch, F. I., & Katch, V. L. (2010). Exercise Physiology: Nutrition, Energy, and Human Performance (7 ed.). Baltimore, MD.: Lippincott Williams and
Lab #3: Electrocardiogram (ECG / EKG)
 Lab #3: Electrocardiogram (ECG / EKG) An introduction to the recording and analysis of cardiac activity Introduction The beating of the heart is triggered by an electrical signal from the pacemaker. The
Lab #3: Electrocardiogram (ECG / EKG) An introduction to the recording and analysis of cardiac activity Introduction The beating of the heart is triggered by an electrical signal from the pacemaker. The
Chapter 24 Vital Signs. Copyright 2011 Wolters Kluwer Health Lippincott Williams & Wilkins
 Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
Vital Signs and Oxygen Administration
 Vital Signs and Oxygen Administration By Dr. Mohsen Dashti Patient Care and Management (202) May-9-2010 Vital Signs and Oxygen Administration What are the vital signs? Why do we need to know them? How
Vital Signs and Oxygen Administration By Dr. Mohsen Dashti Patient Care and Management (202) May-9-2010 Vital Signs and Oxygen Administration What are the vital signs? Why do we need to know them? How
Investigation and evaluation of arterial pulses, blood pressure, and jugular venous pressure
 Investigation and evaluation of arterial pulses, blood pressure, and jugular venous pressure Dr. András Tislér October 2013. Objectives To understand the principles of Assessing vital signs Examination
Investigation and evaluation of arterial pulses, blood pressure, and jugular venous pressure Dr. András Tislér October 2013. Objectives To understand the principles of Assessing vital signs Examination
AP Biology Lab 10 Physiology of the Circulatory System Lab Activity Student Study Guide
 TM AP Biology Lab 10 Physiology of the Circulatory System Lab Activity Student Study Guide BACKGROUND Some of your arteries and veins are as big around as your thumb, and some are almost too small to see.
TM AP Biology Lab 10 Physiology of the Circulatory System Lab Activity Student Study Guide BACKGROUND Some of your arteries and veins are as big around as your thumb, and some are almost too small to see.
Medical Electronics Dr. Neil Townsend Michaelmas Term 2001 ( The story so far.
 Medical Electronics Dr Neil Townsend Michaelmas Term 2001 (wwwrobotsoxacuk/~neil/teaching/lectures/med_elec) Blood Pressure has been measured (in some way) for centuries However, clinical interpretation
Medical Electronics Dr Neil Townsend Michaelmas Term 2001 (wwwrobotsoxacuk/~neil/teaching/lectures/med_elec) Blood Pressure has been measured (in some way) for centuries However, clinical interpretation
Assessment of techniques for measurement of blood pressure in infants and children
 Archives of Disease in Childhood, 1973, 48, 932. Assessment of techniques for measurement of blood pressure in infants and children A. M. ELSEED, E. A. SHINEBOURNE, and M. C. JOSEPH From the Paediatric
Archives of Disease in Childhood, 1973, 48, 932. Assessment of techniques for measurement of blood pressure in infants and children A. M. ELSEED, E. A. SHINEBOURNE, and M. C. JOSEPH From the Paediatric
Lab #3: Electrocardiogram (ECG / EKG)
 Lab #3: Electrocardiogram (ECG / EKG) An introduction to the recording and analysis of cardiac activity Introduction The beating of the heart is triggered by an electrical signal from the pacemaker. The
Lab #3: Electrocardiogram (ECG / EKG) An introduction to the recording and analysis of cardiac activity Introduction The beating of the heart is triggered by an electrical signal from the pacemaker. The
9/27/2016. Adherence and Monitoring of Hypertensive Patients. Conflicts of Interest. Brought to you though a partnership:
 Adherence and Monitoring of Hypertensive Patients. Conflicts of Interest Speaker has no conflicts of interest to disclose I have had no financial relationship over the past 12 months with any commercial
Adherence and Monitoring of Hypertensive Patients. Conflicts of Interest Speaker has no conflicts of interest to disclose I have had no financial relationship over the past 12 months with any commercial
Technique. Technique. Technique. Monitoring 1. Local anesthetic? Aseptic technique Hyper-extend (if radial)
 Critical Care Monitoring Hemodynamic Monitoring Arterial Blood Pressure Cannulate artery Uses 2 Technique Sites Locate artery, prep 3 1 Technique Local anesthetic? Aseptic technique Hyper-extend (if radial)
Critical Care Monitoring Hemodynamic Monitoring Arterial Blood Pressure Cannulate artery Uses 2 Technique Sites Locate artery, prep 3 1 Technique Local anesthetic? Aseptic technique Hyper-extend (if radial)
Measuring body temperature, blood pressure, pulse, respiratory rate and oxygen saturation
 Vital Signs Measuring body temperature, blood pressure, pulse, respiratory rate and oxygen saturation Aims To ensure that students are able to demonstrate the safe and correct technique for setting up
Vital Signs Measuring body temperature, blood pressure, pulse, respiratory rate and oxygen saturation Aims To ensure that students are able to demonstrate the safe and correct technique for setting up
ADVANCED PATIENT MONITORING DURING ANAESTHESIA: PART ONE
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk ADVANCED PATIENT MONITORING DURING ANAESTHESIA: PART ONE Author : CARL BRADBROOK Categories : Vets Date : October 7, 2013
Vet Times The website for the veterinary profession https://www.vettimes.co.uk ADVANCED PATIENT MONITORING DURING ANAESTHESIA: PART ONE Author : CARL BRADBROOK Categories : Vets Date : October 7, 2013
SMALL GROUP SESSION 18A January 17th or January 19th. Groups 1-12: VS and Chest Exam and Harvey Stethophone Session
 SMALL GROUP SESSION 18A January 17th or January 19th Groups 1-12: VS and Chest Exam and Harvey Stethophone Session Readings: Complete the cardiac examination web module. Mosby s Physical Examination, 4
SMALL GROUP SESSION 18A January 17th or January 19th Groups 1-12: VS and Chest Exam and Harvey Stethophone Session Readings: Complete the cardiac examination web module. Mosby s Physical Examination, 4
An Indian Journal FULL PAPER ABSTRACT KEYWORDS. Trade Science Inc.
 [Type text] [Type text] [Type text] ISSN : 0974-7435 Volume 10 Issue 16 BioTechnology 2014 An Indian Journal FULL PAPER BTAIJ, 10(16), 2014 [8944-8948] Clinical study on the relationship between blood
[Type text] [Type text] [Type text] ISSN : 0974-7435 Volume 10 Issue 16 BioTechnology 2014 An Indian Journal FULL PAPER BTAIJ, 10(16), 2014 [8944-8948] Clinical study on the relationship between blood
Unit 1: Human Systems. The Circulatory System
 Unit 1: Human Systems The Circulatory System nourish all cells with oxygen, glucose, amino acids and other nutrients and carry away carbon dioxide, urea and other wastes Purposes Transport chemical messengers
Unit 1: Human Systems The Circulatory System nourish all cells with oxygen, glucose, amino acids and other nutrients and carry away carbon dioxide, urea and other wastes Purposes Transport chemical messengers
Heart Rate, Blood Pressure, and Exercise. Evaluation copy
 Heart Rate, Blood Pressure, and Exercise Computer 11 The adaptability of the heart can be observed during exercise, when the metabolic activity of skeletal muscles increases. The cardiovascular system,
Heart Rate, Blood Pressure, and Exercise Computer 11 The adaptability of the heart can be observed during exercise, when the metabolic activity of skeletal muscles increases. The cardiovascular system,
Measuring and Recording Temperature
 Measuring and Recording Temperature Measurement of balance between heat lost and produced by the body. Lost through: Perspiration Respiration Excretion Produced by: Metabolism of food Muscle and gland
Measuring and Recording Temperature Measurement of balance between heat lost and produced by the body. Lost through: Perspiration Respiration Excretion Produced by: Metabolism of food Muscle and gland
Physiological Measurements Training for Care/Nursing & LD Small Group Home Staff
 Physiological Measurements Training for Care/Nursing & LD Small Group Home Staff CONTENTS 1. The National Early Warning Score 2. Respiratory Rate 3. Oxygen Saturations 4. Temperature 5. Blood Pressure
Physiological Measurements Training for Care/Nursing & LD Small Group Home Staff CONTENTS 1. The National Early Warning Score 2. Respiratory Rate 3. Oxygen Saturations 4. Temperature 5. Blood Pressure
UNIVERSITY OF UTAH HEALTH CARE HOSPITALS AND CLINICS
 UNIVERSITY OF UTAH HEALTH CARE HOSPITALS AND CLINICS CARDIAC MECHANICAL SUPPORT PROGRAM GUIDELINES CARDIAC MECHANICAL SUPPORT: LVAD BASICS FREQUENT SCENARIOS AND TROUBLESHOOTING Review Date: July 2011
UNIVERSITY OF UTAH HEALTH CARE HOSPITALS AND CLINICS CARDIAC MECHANICAL SUPPORT PROGRAM GUIDELINES CARDIAC MECHANICAL SUPPORT: LVAD BASICS FREQUENT SCENARIOS AND TROUBLESHOOTING Review Date: July 2011
!"#$ Blood Pressure Monitor. Instruction manual page 1 Gebrauchsanweisung Seite 17 Gebruiksaanwijzing pagina 33
 !"#$ Blood Pressure Monitor Instruction manual page 1 Gebrauchsanweisung Seite 17 Gebruiksaanwijzing pagina 33 Mode d emploi page 49 Manuale de instructone pagina 65 Manual de instrucciones pagina 81 Introduction
!"#$ Blood Pressure Monitor Instruction manual page 1 Gebrauchsanweisung Seite 17 Gebruiksaanwijzing pagina 33 Mode d emploi page 49 Manuale de instructone pagina 65 Manual de instrucciones pagina 81 Introduction
GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND
 GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND AIM To provide evidence based principles for the measurement of Ankle Brachial Pressure Index (ABPI) using a BACKGROUND/EVIDENCE
GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND AIM To provide evidence based principles for the measurement of Ankle Brachial Pressure Index (ABPI) using a BACKGROUND/EVIDENCE
Non-Invasive Method of Blood Pressure Measurement Validated in a Mathematical Model
 Non-Invasive Method of Blood Pressure Measurement Validated in a Mathematical Model Instrumentation and Control Department, JSS Academy of Technical Education, Noida (U.P.), India Abstract- The non-invasive
Non-Invasive Method of Blood Pressure Measurement Validated in a Mathematical Model Instrumentation and Control Department, JSS Academy of Technical Education, Noida (U.P.), India Abstract- The non-invasive
Chapter 29 1/8/2018. Vital Signs. Measuring and Reporting Vital Signs. Key Terms
 Chapter 29 Vital Signs Key Terms Blood pressure Body temperature Diastolic pressure Hypertension Hypotension Pulse Pulse rate Respiration Sphygmomanometer Stethoscope Systolic pressure Vital signs Measuring
Chapter 29 Vital Signs Key Terms Blood pressure Body temperature Diastolic pressure Hypertension Hypotension Pulse Pulse rate Respiration Sphygmomanometer Stethoscope Systolic pressure Vital signs Measuring
Peripheral Vascular Examination. Dr. Gary Mumaugh Western Physical Assessment
 Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
CARDIOVASCULAR PHYSIOLOGY
 CARDIOVASCULAR PHYSIOLOGY LECTURE 4 Cardiac cycle Polygram - analysis of cardiac activity Ana-Maria Zagrean MD, PhD The Cardiac Cycle - definitions: the sequence of electrical and mechanical events that
CARDIOVASCULAR PHYSIOLOGY LECTURE 4 Cardiac cycle Polygram - analysis of cardiac activity Ana-Maria Zagrean MD, PhD The Cardiac Cycle - definitions: the sequence of electrical and mechanical events that
CARDIOVASCULAR MONITORING. Prof. Yasser Mostafa Kadah
 CARDIOVASCULAR MONITORING Prof. Yasser Mostafa Kadah Introduction Cardiovascular monitoring covers monitoring of heart and circulatory functions It makes it possible to commence interventions quickly in
CARDIOVASCULAR MONITORING Prof. Yasser Mostafa Kadah Introduction Cardiovascular monitoring covers monitoring of heart and circulatory functions It makes it possible to commence interventions quickly in
