ABSTRACT. Sweden; 1 Department of Plastic Surgery, Uppsala University Hospital, Uppsala, 2 Jack Brockhoff Reconstructive Plastic Surgery Research
|
|
|
- Emil Holt
- 6 years ago
- Views:
Transcription
1 Postoperative Monitoring of Free Flaps in Autologous Breast Reconstruction: A Multicenter Comparison of 398 Flaps Using Clinical Monitoring, Microdialysis, and the Implantable Doppler Probe Iain S. Whitaker, B.A. (Hons.), M.A. Cantab., M.B.B.Chir., M.R.C.S., Ph.D., 1 Warren M. Rozen, M.B.B.S., B.Med.Sc., P.G.Dip.Surg.Anat., Ph.D., 2 Daniel Chubb, M.B.B.S., B.Med.Sc., 1 Rafael Acosta, M.D., E.B.O.P.R.A.S., 1 Birgitte J. Kiil, M.B.B.S., 3 Hanne Birke-Sorensen, M.D., 3 Damien Grinsell, M.B.B.S., F.R.A.C.S., 1 and Mark W. Ashton, M.B.B.S., M.D., F.R.A.C.S. 2 ABSTRACT Many techniques for flap monitoring following free tissue transfer have been described; however, there is little evidence that any of these techniques allow for greater rates of flap salvage over clinical monitoring alone. We sought to compare three established monitoring techniques across three experienced microsurgical centers in a comparable cohort of patients. A retrospective, matched cohort study of 398 consecutive free flaps in 347 patients undergoing autologous breast reconstruction was undertaken across three institutions during the same 3-year period, with a single form of postoperative monitoring used at each institution: clinical monitoring alone, the Cook-Swartz implantable Doppler probe, or microdialysis. Both objective and subjective measures of efficacy were assessed. Clinical monitoring alone, the implantable Doppler probe, and microdialysis showed statistically similar rates of flap salvage. False-negative rates were also statistically similar (only seen in the clinically monitored group). However, there was a statistically significant increase in false-positive alarms causing needless take-backs to theater in the microdialysis and implantable Doppler arms, p < This study did not find any technique superior to clinical monitoring alone. New monitoring technologies should be compared objectively with clinical monitoring as the current standard in postoperative flap monitoring. KEYWORDS: Breast reconstruction, deep inferior epigastric artery, DIEP flap, perforator flap, superficial inferior epigastric artery perforator flap, Cook probe 1 Department of Plastic Surgery, Uppsala University Hospital, Uppsala, Sweden; 2 Jack Brockhoff Reconstructive Plastic Surgery Research Unit, Department of Anatomy, University of Melbourne, Victoria, Australia; 3 Department of Plastic Surgery, Aarhus University Hospital, Aarhus, Denmark. Address for correspondence and reprint requests: Warren M. Rozen, M.B.B.S., B.Med.Sc., P.G.Dip.Surg.Anat., Ph.D., Jack Brockhoff Reconstructive Plastic Surgery Research Unit, Room E533, Department of Anatomy, University of Melbourne, Grattan St, Parkville, 3050, Victoria, Australia ( warrenrozen@hotmail.com). J Reconstr Microsurg 2010;26: Copyright # 2010 by Thieme Medical Publishers, Inc., 333 Seventh Avenue, New York, NY 10001, USA. Tel: +1(212) Received: December 10, Accepted after revision: January 21, Published online: March 10, DOI: ISSN X. 409
2 410 JOURNAL OF RECONSTRUCTIVE MICROSURGERY/VOLUME 26, NUMBER Microsurgical free tissue transfer is widely used internationally, and many authors now consider fasciocutaneous flaps such as the deep inferior epigastric artery flap to be the gold standard in breast reconstruction. Increased experience with these procedures and advances in preoperative planning have potentiated published flap loss rates of lower than 2%. 1 5 Preoperative assessment of flap vasculature has been shown to be useful in improving surgical outcomes and flap selection, 6 and the intraoperative evaluation of vascular pedicles has allowed for greater confidence in the viability of large free flaps. 7,8 Despite these advances, there is a low but significant risk with any such operation that arterial or venous compromise may occur, which will warrant a revision of the microsurgical anastomoses. With the potential for either flap salvage or flap loss, prompt and effective postoperative evaluation of flap viability is essential, and may potentiate early intervention. Whereas the no-reflow phenomenon will still mean that flaps are lost regardless of the microsurgeon s experience, optimal methods for postoperative monitoring of free flaps are being increasingly sought. A broad range of different technologies have been discussed for postoperative monitoring, but few studies use a relevant clinical outcome as the primary endpoint of the trial, and as such there is little evidence for any single technique. This is reflected in the wide variety of techniques currently used in this role: clinical monitoring alone, pulse oximetry, near infrared spectroscopy, perfusion photoplethysmography, surface temperature measurement, fluorometry, microdialysis, ultrasound, the hand-held Doppler probe, implanted (Cook-Swartz) Doppler probes, laser Doppler flowmetry, impedance plethysmography, confocal microscopy, nuclear medicine, subcutaneous ph measurement, hydrogen clearance, externalization of part of a buried flap, and white light spectrometry. Surveys of plastic surgical units across the United Kingdom showed that there is substantial variation in the methods, organization, and implementation of monitoring techniques following free tissue transfer The need for the earliest possible detection of free flap compromise has been widely shown to be an essential element in salvage, with the no-reflow phenomenon, first described in 1978, 12 showing that flap salvage was closely related to ischemic time. Recent publications confirm that flap survival is dependent on ischemic time, 3,13 16 reiterating the need for optimal methods for postoperative monitoring. Creech and Miller in outlined the essential criteria for free flap monitoring: Simple and harmless to the patient and flap; Rapid, repeatable, reliable, recordable, and rapidly responsive; Accurate and inexpensive; Objective and applicable to all kinds of flaps; and Equipped with simple displays that could alert relatively inexperienced personnel. Although operating techniques have changed since these criteria were first devised, they still aptly describe the issues that prospective monitoring techniques must address. As yet, there is no proven method that satisfies all of these criteria, and thus surgeons currently choose techniques based on cost, availability, and the method that satisfies their priorities in postoperative care. A recent single surgeon cohort study comparing the implantable Doppler probe with clinical assessment demonstrated an improvement in outcome measures with the implantable Doppler probe, 18 and we sought to further this analysis by comparing the use of three established monitoring techniques across three experienced microsurgical centers in a recent and comparable cohort of patients. Thus, this study, using the three different techniques (the implantable Cook-Swartz Doppler probe, microdialysis, and clinical monitoring alone) as the primary mode for postoperative monitoring, was designed. All these techniques have been previously shown to accurately predict the onset and existence of flap compromise. METHODS Study Design A retrospective, matched cohort study of 398 consecutive free flaps in 347 patients undergoing autologous breast reconstruction was undertaken across three institutions during the same 3-year period, with a single form of postoperative monitoring used at each institution. Only fasciocutaneous flaps (per the Mathes and Nahai classification 19 ) for breast reconstruction were included, all of which were suitable for monitoring with each of the techniques assessed. These comprised deep inferior epigastric artery perforator flaps (Types B and C fasciocutaneous flaps), superficial inferior epigastric artery flaps (Type A fasciocutaneous flaps), and superior gluteal artery perforator flaps (Type C fasciocutaneous flaps) (see Table 1). No buried flaps were included in the series. Of the 398 flaps monitored, 235 were monitored with clinical assessment only (Fig. 1), 121 were monitored with the Cook-Swartz implantable Doppler probe (Cook Medical, Cook Ireland Ltd, Limerick, Ireland) (Fig. 2), and 42 were monitored with microdialysis (CMA-Microdialysis AB, Solna, Sweden) (Fig. 3). Institutional ethical approval was obtained, with each patient consenting to the use of each monitoring technique.
3 POSTOPERATIVE MONITORING OF FREE FLAPS IN AUTOLOGOUS BREAST RECONSTRUCTION/WHITAKER ET AL 411 Table 1 Patient Demographics Comparing the Three Monitoring Technique Groups Patient Demographics Clinical Assessment Cook-Swartz Implantable Doppler Probe Microdialysis Number of patients Number of breast reconstructions Sex (% female) Number of DIEP flaps Number of SIEA flaps Number of SGAP flaps DIEP, deep inferior epigastric artery perforator; SGAP, superior gluteal artery perforator; SIEA, superficial inferior epigastric artery. Each monitoring technique was applied according to criteria dictated by the individual unit, with no required standard in technique. Clinical monitoring was achieved through the assessment of the color, temperature, tactility, capillary refill, bleeding, and appearance of the flap. The Cook-Swartz probe silicone cuff was applied to the venous pedicle following successful venous anastomosis (per manufacturer and literature specifications). Application was always distal to the anastomosis, and microclips were used for attachment. The probe was left in situ for at least 1 week during the monitoring period and then removed. Microdialysis probes were applied to varying regions of the flap based on surgeon preference, with lactate, glucose, glycerol, and pyruvate measured. A comparison between the three techniques for postoperative monitoring was performed. This included a comparison of demographic data, rates for return to theater (take-back rates), the salvage rates for those flaps returned to theater, and ultimate flap outcome in all cases. Of note, there were no logistical or other delays in returning to theater in any of the groups once the decision to return to theater had been made. Figure 1 Immediate postoperative photograph of a deep inferior epigastric artery perforator (DIEP) flap being monitored with clinical monitoring alone. Data Analysis The data were presented quantitatively, with all outcomes and the need to take-back recorded per flap, and the salvage rates recorded as the ultimate clinical outcome per flap. Each flap being monitored was recorded as either encountering a positive monitoring alarm or not encountering an alarm, with findings at theater noted Figure 2 Immediate postoperative photograph of a deep inferior epigastric artery perforator (DIEP) flap being monitored with the Cook-Swartz implantable Doppler probe. Figure 3 Photograph of a deep inferior epigastric artery perforator (DIEP) flap being monitored with microdialysis. The photograph is taken at the end of a reexploration performed on the third postoperative day based on microdialysis values.
4 412 JOURNAL OF RECONSTRUCTIVE MICROSURGERY/VOLUME 26, NUMBER Figure 4 Flow chart for the recording of outcomes for each flap monitored, with each flap being recorded as either encountering a positive monitoring alarm or not encountering an alarm, with findings at theater noted, and ultimate outcomes recorded for each group. and recorded in a flow chart (Fig. 4). True-positives comprised flaps in which positive monitoring alarms were found to have true pedicle compromise, falsepositives comprised flaps in which positive monitoring alarms were found to have no pedicle compromise, truenegatives comprised flaps in which there were no alarms and flaps survived, and false-negatives comprised flaps in which there were no alarms but flaps ultimately failed. Outcome Measures The primary outcome measure in comparing techniques comprised objective assessments of monitoring efficacy, as previously outlined by Whitney et al and Lineaweaver. 20,21 Unlike other diagnostic tests, in which sensitivity and specificity are the most useful measures of efficacy, monitoring is time dependent, in that all monitoring tests will eventually show a positive result; however, it is the time course to this result that affects free flap outcomes. As such, the flap salvage rate for flaps returned to theater (with early intervention resulting in flap salvage) and the false-positive rate (the limitation of a given technique being unnecessary returns to theater) are the two most important measures of efficacy. Of note, these calculations are true measures of efficacy because they are independent of surgeon decision making. A secondary outcome measure comprised the false-negative rate, which although theoretically may be a measure of monitoring efficacy, is dependent on surgeon decision making because the decision to take a flap to theater for revision changes this measure (a failing flap could be categorized as either true-positive if taken back to theater or false-negative if not taken back). Decisions such as this should clearly not influence an objective measure of monitoring efficacy, and thus such cases are more accurately represented by reducing the flap salvage rate of the given monitoring technique. Finally, the qualitative (subjective) benefits of the use of each monitoring technique were evaluated. The flap salvage rate was calculated as a quotient of all flaps with true pedicle compromise that ultimately survived and all flaps with true pedicle compromise (all true-positives and all false-negatives). The falsepositive rate was calculated as a quotient of all flaps with positive monitoring alarms that were found to have no pedicle compromise (false-positives) and all flaps with no pedicle compromise (all false-positives and all truenegatives). The false-negative rate was calculated as a quotient of all flaps without monitoring alarms that were found to have pedicle compromise (false-negatives) and all flaps with pedicle compromise (all falsenegatives and all true-positives). Data for each monitoring group were analyzed for statistical significance performed using the Fisher exact test. Statistical significance was considered at p RESULTS The three groups analyzed were comparable in terms of patient cohort and operative technique (Table 1). Although there were differences between institutions in patient volume and experience with breast reconstruction, all institutions were experienced microsurgical centers with significant experience in a range of microsurgical procedures. There were 28 flaps in the series that required take-back to theater on the basis of positive monitoring
5 POSTOPERATIVE MONITORING OF FREE FLAPS IN AUTOLOGOUS BREAST RECONSTRUCTION/WHITAKER ET AL 413 Figure 5 Flow chart for the recording of outcomes for each flap monitored. CM, clinical monitoring; IDP, implantable Doppler probe; MD, microdialysis. test findings. Of the eight such cases that were monitored clinically (Fig. 5), two did not return to theater before there was evidence of flap necrosis (falsenegatives), whereas six returned for venous compromise and were all salvaged. Of the 11 cases monitored with the implantable Doppler probe, 8 were revised and salvaged, 2 were unsalvageable, and 1 was a false-positive monitoring alarm. Of the nine cases monitored with microdialysis, five were salvaged, one failed, and three were false-positive alarms, with only territorial issues identified. In terms of the primary outcome measure, there were statistically significant differences between the groups (Table 2). There was no significant difference in salvage rates between the three groups, with high salvage rates in all groups (range 75 to 83%, p ¼ 0.93). However, a significant difference was found between groups in terms of false-positive rates: with no falsepositives in the clinically monitored group (0%), 0.9% false-positives in the implantable Doppler group, and 8.1% false-positives in the microdialysis group (p < 0.001). In these cases, a patent flowing pedicle was identified upon return to the theater, but territorial congestion was noted. In terms of the secondary outcome measure, there was no statistically significant difference between groups for the false-negative rate (see Table 2). In the clinically monitored group, there were two false-negatives but no flaps that failed after reexploration; on the other hand, there were no false-negatives in the other two groups but there were failed flaps following reexploration. As mentioned, the decision to reexplore a flap is based upon individual surgeon preference, and is not a true test of the monitoring technique because a false-negative may be equivalent to a true-positive, unsalvageable flap, if the decision to reexplore is not made. The third outcome measure, the secondary measure of qualitative assessment in the use of these techni- Table 2 Primary Outcome Measures 1 and 2: Quantitative Assessment of the Efficacy of each Monitoring Technique by Primary Outcome Measure 1, Flap Salvage Rate, and False-Positive Rate, and Primary Outcome Measure 2, Timing of Flap Loss Flap Loss Rate after Attempted Salvage, and the Rate of Missed Flap Losses (the False-Negative Rate) Clinical Assessment Cook-Swartz Implantable Doppler Probe Microdialysis p Value Primary Outcome Measures Flap salvage rate (salvaged flaps/ compromised flaps) (n, %) False-positive rate (false-positives/ uncompromised flaps) (n, %) Secondary Outcome Measure False-negative rate (false-negatives/ compromised flaps) (n, %) 6/8 ¼ 75% 8/10 ¼ 80% 5/6 ¼ 83% /227 ¼ 0% 1/111 ¼ 0.9% 3/37 ¼ 8.1% < /8 ¼ 25% 0/10 ¼ 0% 0/6 ¼ 0% 0.11
6 414 JOURNAL OF RECONSTRUCTIVE MICROSURGERY/VOLUME 26, NUMBER ques, demonstrated each technique to have positive and negative attributes. The particular benefits of clinical monitoring are cost and the ability to readily distinguish territorial compromise, whereas the implantable Doppler probe and microdialysis improve patient comfort during assessment and provide an objective monitor. The implantable Doppler probe uniquely avoids any physiologic or sampling delay in diagnosis by providing an instantaneous measure of pedicle flow. DISCUSSION The results of this study demonstrate both the utility and pitfalls of each different monitoring technique in the postoperative monitoring of free flaps. This study demonstrated that the use of microdialysis and the implantable Doppler significantly increases the rate of unnecessary take-backs to theater (the false-positive rate) over the use of clinical monitoring alone. This is in the context of both the implantable Doppler probe and microdialysis not significantly improving the salvage rate of free flaps or false-negative rate (although falsenegatives were eliminated in these groups). Both benefits and pitfalls of each of the techniques evaluated were identified, and the evaluation of objective outcomes showed that neither adjunctive technique was superior to clinical monitoring alone. Implantable Doppler Probe The implantable Doppler probe manufactured by Cook has gained recent attention in the plastic surgery literature. 5,22 30 The first attempts to utilize an implantable Doppler probe for free flap monitoring was in 1984, by Parker et al, 29 and soon thereafter the Cook- Swartz probe was developed in 1988 specifically for use in free flap operations. 30 It was initially used on the arterial pedicle, but subsequent studies showed it to be more sensitive when placed on the venous anastomosis, particularly for the detection of venous thrombosis. 23 A study by Kind et al 27 of 135 free flap operations in 1998 showed that the Cook-Swartz probe produced a high false-positive rate (20% of positive results, with a 2.9% false-positive rate as calculated by our method) and no false-negative results. All of the 16 compromised flaps were salvaged. The use of the probe was well received by all junior and senior medical staff and nursing staff. Results similar to those of Kind et al were seen in a separate analysis of the Cook-Swartz arm of our study. 25 The Cook-Swartz probe does have a small false-positive rate, 25,27 and initial studies were associated with a low rate of probe malfunction, which was thought to be due to a learning curve for surgeons in applying the probe 23,29,30 (problems pertaining particularly to probe placement). Rosenberg et al 31 found a high false-positive rate of 88%, which was actually 37% as calculated by our method, but no other trial has replicated a false-positive rate as high as this. It is difficult to ascertain why this result was so much higher than other reported rates, but the learning curve could play a part because only 20 cases of implanted Doppler monitoring were presented. These results by Rosenberg et al also applied to a diverse range of flap types and recipient sites making interpretation difficult. A recent large cohort study demonstrated an improvement in flap salvage rate with the Cook-Swartz probe over clinical monitoring alone, and a meta-analysis of the literature confirmed the statistically significant benefit of the Cook-Swartz probe over clinical monitoring. 18 Microdialysis This technique was first described in the setting of free flap monitoring by Udesen et al, 32 who described the use of a double lumen catheter with a semipermeable membrane at the end. This catheter is placed within the flap to be monitored (see Fig. 3), and a small amount of fluid is pumped through the catheter. As this fluid passes through a semipermeable membrane, small molecules pass into the dialysate, which are then analyzed. The levels of certain metabolites within the transferred tissue are used to ascertain the metabolic state of that tissue. There are many molecules capable of being assessed with microdialysis, with typical metabolites comprising lactate, glucose, glycerol, and pyruvate Udesen et al used a similar catheter placed elsewhere in the body for a reference comparison, whereas some later studies have simply compared results with reference values or used increasing lactate:pyruvate ratios as a measure of ischemia. Authors have generally agreed that microdialysis provides a timely and sensitive indication of flap ischemia. Studies comparing different flaps and regions within flaps have shown significant differences in microdialysis results, 33 an illustration of the sensitivity of this technique. Sorensen 35 successfully used microdialysis in buried free jejunal transfers to identify early flap compromise, salvaging two such transfers. Jyränki et al 34 reported a case series of free flaps monitored with microdialysis, and reported two cases in which metabolic change occurred before clinical signs; however, both flaps were unsalvageable upon reexploration. The mechanisms of action of each technique assessed in this study may explain our findings. The implantable Doppler probe measures and records flow within the vascular pedicle, and is thus an immediate reflection of impaired flow. 23,28 This occurs before clinical signs of ischemia become evident, and possibly earlier than the measurable biochemical markers of ischemia change. Microdialysis requires the biochemical markers of ischemia to rise, and requires a time delay (albeit small) for collection, testing, and the representation of results in graphical form. Clinical assessment can
7 POSTOPERATIVE MONITORING OF FREE FLAPS IN AUTOLOGOUS BREAST RECONSTRUCTION/WHITAKER ET AL 415 demonstrate early changes in perfusion that may reflect flap ischemia; however, this occurs some time after flow is noted to be reduced on Cook-Swartz Doppler monitoring. 23 As such, there are intuitive benefits of the implantable Doppler probe over microdialysis, broadly categorized as physiologic error and sampling error. Physiologically, the Doppler probe can identify impaired pedicle flow substantially earlier in the course of venous compromise than the measurable effects of tissue necrosis as with microdialysis. In terms of sampling error, the implanted Doppler probe provides a continuous measurement of pedicle flow (although in practice it is often tested intermittently), compared with the static evaluation with clinical assessment (as it is usually performed) and microdialysis, at given points in time. This error is compounded with microdialysis because there is an analysis period even after the sample has been collected. These factors are all contributors to a reduction in the time to detection of flap ischemia, extending the time between ischemic onset and reexploration, which is known to be a key factor in the salvage rate for free flaps. 3,12 16 Although we have assessed these techniques on objective clinical criteria, in which we have explained the benefit of flap salvage rate and false-positive rate as the most objective, monitoring methods are not necessarily to be judged on a single set of clinical criteria alone. Other factors, such as ease of use, patient comfort, and cost come into play. In addition, the ability of clinical monitoring to distinguish between territorial compromise and obstructive compromise is a key factor in minimizing false-positives, and selecting those cases for which any intervention is appropriate. The current trial does not identify either adjunctive method as producing a better clinical outcome when compared with subjective clinical monitoring alone. In fact, comparisons of large studies using different monitoring techniques have revealed similar flap success rates (98 to 99%) and salvage rates (up to 80%), regardless of the monitoring system used. 1 5 In our study, we compared the techniques as stand-alone measures; however, an additional use for objective monitoring techniques is as an adjunct to clinical monitoring, providing added reassurance to clinical assessment and potentially improving outcome measures. When used as stand-alone measures, the implantable Doppler probe and microdialysis are capable of being used without the need to wake the patient, and thus avoid the sleep deprivation of half-hourly flap observations. A unique group of microvascular transfers are more difficult to assess and thus have lower salvage rates. 3 This group of buried free flaps cannot be easily monitored clinically, and several authors have advocated the use of adjunctive monitoring techniques in such flaps. 1 It is in this group that the results of this study and those of the future studies on advanced monitoring techniques will become particularly applicable. CONCLUSION Many objective and subjective techniques for flap monitoring have been described to monitor free tissue transfers, 36 and despite significant research efforts, there has been little evidence that any of these techniques allow for greater rates of flap salvage over clinical monitoring alone. This study has shown that in the participating three international units, clinical monitoring alone, the Cook-Swartz implantable Doppler probe, and microdialysis showed statistically similar rates of flap salvage and false-negative rates (only seen in the clinical group). However, there was a statistically significant increase in false-positive alarms causing needless take-backs to theater in the microdialysis and implantable Doppler arms, p < This study, thus, did not show any technique to be better than clinical monitoring alone. Future monitoring studies with clinically relevant results are advised, rather than just the publication of uncontrolled data with a single method. REFERENCES 1. Disa JJ, Cordeiro PG, Hidalgo DA. Efficacy of conventional monitoring techniques in free tissue transfer: an 11-year experience in 750 consecutive cases. Plast Reconstr Surg 1999;104: Gill PS, Hunt JP, Guerra AB, et al. A 10-year retrospective review of 758 DIEP flaps for breast reconstruction. Plast Reconstr Surg 2004;113: Bui DT, Cordeiro PG, Hu QY, Disa JJ, Pusic A, Mehrara BJ. Free flap reexploration: indications, treatment, and outcomes in 1193 free flaps. Plast Reconstr Surg 2007;119: Heller L, Levin LS, Klitzman B. Laser Doppler flowmeter monitoring of free-tissue transfers: blood flow in normal and complicated cases. Plast Reconstr Surg 2001;107: de la Torre J, Hedden W, Grant JH III, Gardner PM, Fix RJ, Vásconez LO. Retrospective review of the internal Doppler probe for intra- and postoperative microvascular surveillance. J Reconstr Microsurg 2003;19: Rozen WM, Ashton MW, Stella DL, Phillips TJ, Taylor GI. The accuracy of computed tomographic angiography for mapping the perforators of the DIEA: a cadaveric study. Plast Reconstr Surg 2008;122: Holm C, Mayr M, Höfter E, Raab N, Ninkovic M. Interindividual variability of the SIEA Angiosome: effects on operative strategies in breast reconstruction. Plast Reconstr Surg 2008;122: Holm C, Mayr M, Höfter E, Ninkovic M. The versatility of the SIEA flap: a clinical assessment of the vascular territory of the superficial epigastric inferior artery. J Plast Reconstr Aesthet Surg 2007;60: Whitaker IS, Gulati V, Ross GL, Menon A, Ong TK. Variations in the postoperative management of free tissue
8 416 JOURNAL OF RECONSTRUCTIVE MICROSURGERY/VOLUME 26, NUMBER transfers to the head and neck in the United Kingdom. Br J Oral Maxillofac Surg 2007;45: Whitaker IS, Oliver DW, Ganchi PA. Postoperative monitoring of microvascular tissue transfers: current practice in the United Kingdom and Ireland. Plast Reconstr Surg 2003;111: Jallali N, Ridha H, Butler PE. Postoperative monitoring of free flaps in UK plastic surgery units. Microsurgery 2005;25: May JW Jr, Chait LA, O Brien BM, Hurley JV. The noreflow phenomenon in experimental free flaps. Plast Reconstr Surg 1978;61: Smit JM, Zeebregts CJ, Acosta R. Timing of presentation of the first signs of vascular compromise dictates the salvage outcome of free flap transfers. Plast Reconstr Surg 2008;122: Smit JM, Acosta R, Zeebregts CJ, Liss AG, Anniko M, Hartman EH. Early reintervention of compromised free flaps improves success rate. Microsurgery 2007;27: Hofer SO, Damen TH, Mureau MA, Rakhorst HA, Roche NA. A critical review of perioperative complications in 175 free deep inferior epigastric perforator flap breast reconstructions. Ann Plast Surg 2007;59: Chen KT, Mardini S, Chuang DC, et al. Timing of presentation of the first signs of vascular compromise dictates the salvage outcome of free flap transfers. Plast Reconstr Surg 2007;120: Creech B, Miller S. Evaluation of circulation in skin flaps. In: Grabb WC, Myers MB, eds. Skin Flaps. Boston, MA: Little Brown; 1975: Rozen WM, Chubb D, Whitaker IS, Acosta R. The efficacy of postoperative monitoring: a single surgeon comparison of clinical monitoring and the implantable Doppler probe in 547 consecutive free flaps. Microsurgery 2009;30: Mathes SJ, Nahai F. Flap selection. Fascia/fasciocutaneous vascular classification. In: Reconstructive Surgery Principles, Anatomy and Technique. Vol. 1. New York: Churchill Livingstone; 1997: Whitney TM, Lineaweaver WC, Billys JB, et al. Improved salvage of complicated microvascular transplants monitored with quantitative fluorometry. Plast Reconstr Surg 1992;90: Lineaweaver WC. The implantable Doppler probe. Plast Reconstr Surg 1988;82: Whitaker IS, Smit JM, Acosta R. A simple method of implantable Doppler cuff attachment: experience in 150 DIEP breast reconstructions. J Plast Reconstr Aesthet Surg 2008;61: Swartz WM, Izquierdo R, Miller MJ. Implantable venous Doppler microvascular monitoring: laboratory investigation and clinical results. Plast Reconstr Surg 1994;93: Solomon GA, Yaremchuk MJ, Manson PN. Doppler ultrasound surface monitoring of both arterial and venous flow in clinical free tissue transfers. J Reconstr Microsurg 1986;3: Smit JM, Whitaker IS, Liss AG, Audolfsson T, Kildal M, Acosta R. Post operative monitoring of microvascular breast reconstructions using the implantable Cook-Swartz doppler system: a study of 145 probes & technical discussion. J Plast Reconstr Aesthet Surg 2008;62: Pryor SG, Moore EJ, Kasperbauer JL. Implantable Doppler flow system: experience with 24 microvascular free-flap operations. Otolaryngol Head Neck Surg 2006;135: Kind GM, Buntic RF, Buncke GM, Cooper TM, Siko PP, Buncke HJ Jr. The effect of an implantable Doppler probe on the salvage of microvascular tissue transplants. Plast Reconstr Surg 1998;101: ; discussion Oliver DW, Whitaker IS, Giele H, Critchley P, Cassell O. The Cook-Swartz venous Doppler probe for the postoperative monitoring of free tissue transfers in the United Kingdom: a preliminary report. Br J Plast Surg 2005;58: Parker PM, Fischer JC, Shaw WW. Implantable pulsed Doppler cuff for long-term monitoring of free flaps: a preliminary study. Microsurgery 1984;5: Swartz WM, Jones NF, Cherup L, Klein A. Direct monitoring of microvascular anastomoses with the 20-MHz ultrasonic Doppler probe: an experimental and clinical study. Plast Reconstr Surg 1988;81: Rosenberg JJ, Fornage BD, Chevray PM. Monitoring buried free flaps: limitations of the implantable Doppler and use of color duplex sonography as a confirmatory test. Plast Reconstr Surg 2006;118: ; discussion Udesen A, Løntoft E, Kristensen SR. Monitoring of free TRAM flaps with microdialysis. J Reconstr Microsurg 2000; 16: Edsander-Nord A, Röjdmark J, Wickman M. Metabolism in pedicled and free TRAM flaps: a comparison using the microdialysis technique. Plast Reconstr Surg 2002;109: Jyränki J, Suominen S, Vuola J, Bäck L. Microdialysis in clinical practice: monitoring intraoral free flaps. Ann Plast Surg 2006;56: Sorensen HB. Free jejunal flaps can be monitored by use of microdialysis. J Reconstr Microsurg 2008;24: Whitaker IS, Karoo ROS, Oliver DW, Ganchi PA, Gulati V, Malata CM. Current techniques in the post-operative monitoring of microvascular free-tissue transfers. Eur J Plast Surg 2005;27:
ORIGINAL ARTICLE. The Implantable Cook-Swartz Doppler Probe. for postoperative monitoring in head and neck reconstruction.
 ORIGINAL ARTICLE The Implantable Cook-Swartz Doppler Probe for Postoperative Monitoring in Head and Neck Free Flap Reconstruction Jennifer P. Guillemaud, MD, BSc; Hadi Seikaly, MD, FRCSC; David Cote, MD,
ORIGINAL ARTICLE The Implantable Cook-Swartz Doppler Probe for Postoperative Monitoring in Head and Neck Free Flap Reconstruction Jennifer P. Guillemaud, MD, BSc; Hadi Seikaly, MD, FRCSC; David Cote, MD,
Clinical Assessment Score for Monitoring Free Flaps in the Dark Skin
 Short Communication 18 Copyright University of Medicine, Tirana Clinical Assessment Score for Monitoring Free Flaps in the Dark Skin Bolaji Oyawale Mofikoya 1, Andrew Omotayo Ugburo 1, Orimisan M. Belie
Short Communication 18 Copyright University of Medicine, Tirana Clinical Assessment Score for Monitoring Free Flaps in the Dark Skin Bolaji Oyawale Mofikoya 1, Andrew Omotayo Ugburo 1, Orimisan M. Belie
The Use of Visible Light Spectroscopy to Measure Tissue Oxygenation in Free Flap Reconstruction
 The Use of Visible Light Spectroscopy to Measure Tissue Oxygenation in Free Flap Reconstruction Agustin Cornejo, M.D., 1,2 Thomas Rodriguez, M.S., 1,2 Megan Steigelman, M.D., 2 Stacy Stephenson, M.D.,
The Use of Visible Light Spectroscopy to Measure Tissue Oxygenation in Free Flap Reconstruction Agustin Cornejo, M.D., 1,2 Thomas Rodriguez, M.S., 1,2 Megan Steigelman, M.D., 2 Stacy Stephenson, M.D.,
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study
 Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
A multiple logistic regression analysis of complications following microsurgical breast reconstruction
 Original Article A multiple logistic regression analysis of complications following microsurgical breast reconstruction Samir Rao 1, Ellen C. Stolle 1, Sarah Sher 1, Chun-Wang Lin 1, Bahram Momen 2, Maurice
Original Article A multiple logistic regression analysis of complications following microsurgical breast reconstruction Samir Rao 1, Ellen C. Stolle 1, Sarah Sher 1, Chun-Wang Lin 1, Bahram Momen 2, Maurice
Sweden 2 Jack Brockhoff Reconstructive Plastic Surgery Research Unit, Department
 A SINGLE CENTER COMPARISON OF ONE VERSUS TWO VENOUS ANASTOMOSES IN 564 CONSECUTIVE DIEP FLAPS: INVESTIGATING THE EFFECT ON VENOUS CONGESTION AND FLAP SURVIVAL MORTEZA ENAJAT, M.D., 1 WARREN M. ROZEN, M.B.B.S.,
A SINGLE CENTER COMPARISON OF ONE VERSUS TWO VENOUS ANASTOMOSES IN 564 CONSECUTIVE DIEP FLAPS: INVESTIGATING THE EFFECT ON VENOUS CONGESTION AND FLAP SURVIVAL MORTEZA ENAJAT, M.D., 1 WARREN M. ROZEN, M.B.B.S.,
Cost Analysis of 109 Microsurgical Reconstructions and Flap Monitoring with Microdialysis
 Cost Analysis of 109 Microsurgical Reconstructions and Flap Monitoring with Microdialysis Leena Setälä, M.D., Ph.D., 1 Heini Koskenvuori, M.Sc., 2 Daiva Gudaviciene, M.D., Ph.D., 3 Leena Berg, M.D., Ph.D.,
Cost Analysis of 109 Microsurgical Reconstructions and Flap Monitoring with Microdialysis Leena Setälä, M.D., Ph.D., 1 Heini Koskenvuori, M.Sc., 2 Daiva Gudaviciene, M.D., Ph.D., 3 Leena Berg, M.D., Ph.D.,
The venous anatomy of the abdominal wall for Deep Inferior Epigastric Artery (DIEP) flaps in breast reconstruction
 Original Article The venous anatomy of the abdominal wall for Deep Inferior Epigastric Artery (DIEP) flaps in breast reconstruction Warren M Rozen, Mark W Ashton The Taylor Lab, Room E533, Department of
Original Article The venous anatomy of the abdominal wall for Deep Inferior Epigastric Artery (DIEP) flaps in breast reconstruction Warren M Rozen, Mark W Ashton The Taylor Lab, Room E533, Department of
Planning and optimising DIEP flaps with virtual surgery: the Navarra experience
 Journal of Plastic, Reconstructive & Aesthetic Surgery (2010) 63, 289e297 Planning and optimising DIEP flaps with virtual surgery: the Navarra experience Warren Matthew Rozen a, *, Emilio Garcia-Tutor
Journal of Plastic, Reconstructive & Aesthetic Surgery (2010) 63, 289e297 Planning and optimising DIEP flaps with virtual surgery: the Navarra experience Warren Matthew Rozen a, *, Emilio Garcia-Tutor
Microvascular free flap reconstruction is a versatile option for coverage
 Original article Postoperative monitoring of free flap reconstruction: A comparison of external ultrasonography and the implantable probe Rayaad C Hosein MD, Agustin Cornejo MD, Howard T Wang MD RC Hosein,
Original article Postoperative monitoring of free flap reconstruction: A comparison of external ultrasonography and the implantable probe Rayaad C Hosein MD, Agustin Cornejo MD, Howard T Wang MD RC Hosein,
Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps
 e50 Case Report THIEME Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps Shuhei Yoshida, MD 1 Isao Koshima, MD 1 Shogo Nagamatsu, MD 2 Kazunori Yokota, MD 2 Shuji Yamashita,
e50 Case Report THIEME Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps Shuhei Yoshida, MD 1 Isao Koshima, MD 1 Shogo Nagamatsu, MD 2 Kazunori Yokota, MD 2 Shuji Yamashita,
Current Approaches to Free Flap Monitoring
 CE 2.3 ANCC Contact Hours Current Approaches to Free Flap Monitoring Albert H. Chao, MD Susan Lamp, BSN, RN, CPSN Postoperative monitoring of free flaps remains an essential component of care in patients
CE 2.3 ANCC Contact Hours Current Approaches to Free Flap Monitoring Albert H. Chao, MD Susan Lamp, BSN, RN, CPSN Postoperative monitoring of free flaps remains an essential component of care in patients
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps
 Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Increasing options in autologous microsurgical breast reconstruction: four free flaps for stacked bilateral breast reconstruction
 Case Report Increasing options in autologous microsurgical breast reconstruction: four free flaps for stacked bilateral breast reconstruction Warren Matthew Rozen 1,2, Nakul Gamanlal Patel 1, Venkat V.
Case Report Increasing options in autologous microsurgical breast reconstruction: four free flaps for stacked bilateral breast reconstruction Warren Matthew Rozen 1,2, Nakul Gamanlal Patel 1, Venkat V.
Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study
 Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study Raphael Sinna, MD, a Hassene Hajji, MD, b Quentin Qassemyar,
Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study Raphael Sinna, MD, a Hassene Hajji, MD, b Quentin Qassemyar,
Few would deny that lower abdominal tissue BREAST. An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction.
 BREAST An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction Aldona J. Spiegel, M.D. Farah N. Khan, M.D. Houston, Texas Background: The deep inferior epigastric perforator (DIEP)
BREAST An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction Aldona J. Spiegel, M.D. Farah N. Khan, M.D. Houston, Texas Background: The deep inferior epigastric perforator (DIEP)
The Superficial Inferior Epigastric Artery Flap and its Relevant Vascular Anatomy in Korean Women
 The Superficial Inferior Epigastric Artery Flap and its Relevant Vascular Anatomy in Korean Women Original Article Byung Jun Kim, Jun Ho Choi, Tae Hoon Kim, Ung Sik Jin, Kyung Won Minn, Hak Chang Department
The Superficial Inferior Epigastric Artery Flap and its Relevant Vascular Anatomy in Korean Women Original Article Byung Jun Kim, Jun Ho Choi, Tae Hoon Kim, Ung Sik Jin, Kyung Won Minn, Hak Chang Department
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
Since originally described by Hartrampf et al. BREAST
 BREAST Assessment of Zonal Perfusion Using Intraoperative Angiography during Abdominal Flap Breast Reconstruction Albert Losken, M.D. Michael R. Zenn, M.D. Josh A. Hammel, M.D. Mark W. Walsh, M.D. Grant
BREAST Assessment of Zonal Perfusion Using Intraoperative Angiography during Abdominal Flap Breast Reconstruction Albert Losken, M.D. Michael R. Zenn, M.D. Josh A. Hammel, M.D. Mark W. Walsh, M.D. Grant
The microvascular anastomotic coupler for venous anastomoses in free flap breast reconstruction improves outcomes
 Original Article The microvascular anastomotic coupler for venous anastomoses in free flap breast reconstruction improves outcomes Edmund Fitzgerald O Connor 1,2, Warren Matthew Rozen 2, Muhammad Chowdhry
Original Article The microvascular anastomotic coupler for venous anastomoses in free flap breast reconstruction improves outcomes Edmund Fitzgerald O Connor 1,2, Warren Matthew Rozen 2, Muhammad Chowdhry
Intraoperative Fluorescence Imaging Systems
 Intraoperative Fluorescence Imaging Systems Policy Number: 10.01.530 Last Review: 01/2018 Origination: 01/2015 Next Review: 01/2019 Policy Intraoperative fluorescence imaging (SPY Imaging) to evaluate
Intraoperative Fluorescence Imaging Systems Policy Number: 10.01.530 Last Review: 01/2018 Origination: 01/2015 Next Review: 01/2019 Policy Intraoperative fluorescence imaging (SPY Imaging) to evaluate
Developing preoperative planning of DIEP flaps with multislice-ct angiography
 Developing preoperative planning of DIEP flaps with multislice-ct angiography Poster No.: C-1030 Congress: ECR 2013 Type: Scientific Exhibit Authors: M. Casares Santiago, L. Gijón de la Santa, E. García
Developing preoperative planning of DIEP flaps with multislice-ct angiography Poster No.: C-1030 Congress: ECR 2013 Type: Scientific Exhibit Authors: M. Casares Santiago, L. Gijón de la Santa, E. García
Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes
 DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC
 Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Early Experience With Barbed Sutures for Abdominal Closure in Deep Inferior Epigastric Perforator Flap Breast Reconstruction
 Early Experience With Barbed Sutures for Abdominal Closure in Deep Inferior Epigastric Perforator Flap Breast Reconstruction Catherine de Blacam, MB, BCh, a Salih Colakoglu, MD, a Adeyiza O. Momoh, MD,
Early Experience With Barbed Sutures for Abdominal Closure in Deep Inferior Epigastric Perforator Flap Breast Reconstruction Catherine de Blacam, MB, BCh, a Salih Colakoglu, MD, a Adeyiza O. Momoh, MD,
Methods of autologous tissue breast reconstruction BREAST
 BREAST Comparison of Donor-Site Morbidity of SIEA, DIEP, and Muscle-Sparing TRAM Flaps for Breast Reconstruction Liza C. Wu, M.D. Anureet Bajaj, M.D. David W. Chang, M.D. Pierre M. Chevray, M.D., Ph.D.
BREAST Comparison of Donor-Site Morbidity of SIEA, DIEP, and Muscle-Sparing TRAM Flaps for Breast Reconstruction Liza C. Wu, M.D. Anureet Bajaj, M.D. David W. Chang, M.D. Pierre M. Chevray, M.D., Ph.D.
The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography
 BREAST The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography Corrine Wong, M.D. Purushottam Nagarkar, M.D. Sumeet Teotia, M.D. Nicholas
BREAST The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography Corrine Wong, M.D. Purushottam Nagarkar, M.D. Sumeet Teotia, M.D. Nicholas
The deep inferior epigastric perforator (DIEP) flap. Original Article Breast
 Original Article Breast Predictors of Reoperations in Deep Inferior Epigastric Perforator Flap Breast Reconstruction Dmytro Unukovych, MD, PhD Camilo Hernandez Gallego, MD Helena Aineskog, MD Andres Rodriguez-Lorenzo,
Original Article Breast Predictors of Reoperations in Deep Inferior Epigastric Perforator Flap Breast Reconstruction Dmytro Unukovych, MD, PhD Camilo Hernandez Gallego, MD Helena Aineskog, MD Andres Rodriguez-Lorenzo,
The Synovis GEM COUPLER
 The Synovis GEM COUPLER e Synovis product portfolio includes Coupler, Flow Coupler and GeM MicroClip. ese products are used for joining small diameter vessels during autologous tissue breast reconstruction;
The Synovis GEM COUPLER e Synovis product portfolio includes Coupler, Flow Coupler and GeM MicroClip. ese products are used for joining small diameter vessels during autologous tissue breast reconstruction;
Breast Reconstruction: Current Strategies and Future Opportunities
 Breast Reconstruction: Current Strategies and Future Opportunities Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery
Breast Reconstruction: Current Strategies and Future Opportunities Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery
Alexis Laungani MD, Erik L Ritman MD PhD, Nirusha Lachman PhD, Jodie Christner PhD, Andrew Vercnocke Medical Imaging Analyst, Steven Jorgensen
 Alexis Laungani MD, Erik L Ritman MD PhD, Nirusha Lachman PhD, Jodie Christner PhD, Andrew Vercnocke Medical Imaging Analyst, Steven Jorgensen Engineer, Jill Anderson Research Technologist, Terry Regnier
Alexis Laungani MD, Erik L Ritman MD PhD, Nirusha Lachman PhD, Jodie Christner PhD, Andrew Vercnocke Medical Imaging Analyst, Steven Jorgensen Engineer, Jill Anderson Research Technologist, Terry Regnier
Anatomical relationship between arteries and veins in the paraumbilical region q
 The British Association of Plastic Surgeons (2003) 56, 552 556 Anatomical relationship between arteries and veins in the paraumbilical region q N. Imanishi a, *, H. Nakajima b, T. Minabe c, H. Chang d,
The British Association of Plastic Surgeons (2003) 56, 552 556 Anatomical relationship between arteries and veins in the paraumbilical region q N. Imanishi a, *, H. Nakajima b, T. Minabe c, H. Chang d,
Medical Journal of the Volume 20 Islamic Republic of Iran Number 3 Fall 1385 November Original Articles
 Medical Journal of the Volume 0 Islamic Republic of Iran Number 3 Fall 38 November 00 Original Articles ANATOMY OF THE SUPERFICIAL INFERIOR EPIGASTRIC ARTERY FLAP MAHDI FATHI, M.D., EBRAHIM HATAMIPOUR,
Medical Journal of the Volume 0 Islamic Republic of Iran Number 3 Fall 38 November 00 Original Articles ANATOMY OF THE SUPERFICIAL INFERIOR EPIGASTRIC ARTERY FLAP MAHDI FATHI, M.D., EBRAHIM HATAMIPOUR,
Quantitative assessment of partial vascular occlusions in a swine pedicle flap model using spatial frequency domain imaging
 Quantitative assessment of partial vascular occlusions in a swine pedicle flap model using spatial frequency domain imaging Adrien Ponticorvo, 1 Eren Taydas, 1 Amaan Mazhar, 2 Thomas Scholz, 3 Hak-Su Kim,
Quantitative assessment of partial vascular occlusions in a swine pedicle flap model using spatial frequency domain imaging Adrien Ponticorvo, 1 Eren Taydas, 1 Amaan Mazhar, 2 Thomas Scholz, 3 Hak-Su Kim,
JPRAS Open 3 (2015) 1e5. Contents lists available at ScienceDirect. JPRAS Open. journal homepage:
 JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
Plastic surgery of the breast includes; augmentation, reduction, Plastic Surgery of the Breast. Abstract. Continuing Education Column
 Plastic Surgery of the Breast Keuk Shun Shin, M.D. Keuk SHUN SHIN s Asthetic Plastic Surgery E mail: drsks@drsks.co.kr Abstract Plastic surgery of the breast includes; augmentation, reduction, reconstruction
Plastic Surgery of the Breast Keuk Shun Shin, M.D. Keuk SHUN SHIN s Asthetic Plastic Surgery E mail: drsks@drsks.co.kr Abstract Plastic surgery of the breast includes; augmentation, reduction, reconstruction
A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction
 A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction In-Soo Baek 1, Jae-Pil You 1, Sung-Mi Rhee 1, Gil-Su Son 2, Deok-Woo Kim 1, Eun-Sang Dhong 1, Seung-Ha
A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction In-Soo Baek 1, Jae-Pil You 1, Sung-Mi Rhee 1, Gil-Su Son 2, Deok-Woo Kim 1, Eun-Sang Dhong 1, Seung-Ha
Evaluation of dynamic infrared thermography as an alternative to CT angiography for perforator mapping in breast reconstruction: a clinical study
 Weum et al. BMC Medical Imaging (2016) 16:43 DOI 10.1186/s12880-016-0144-x RESEARCH ARTICLE Open Access Evaluation of dynamic infrared thermography as an alternative to CT angiography for perforator mapping
Weum et al. BMC Medical Imaging (2016) 16:43 DOI 10.1186/s12880-016-0144-x RESEARCH ARTICLE Open Access Evaluation of dynamic infrared thermography as an alternative to CT angiography for perforator mapping
Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect of Upper and Middle Third Leg
 Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Reconstruction with autologous tissue remains a
 Original Article Increased Flap Weight and Decreased Perforator Number Predict Fat Necrosis in DIEP Breast Reconstruction Carolyn L. Mulvey, BS* Carisa M. Cooney, MPH* Francis F. Daily, BS* Elizabeth Colantuoni,
Original Article Increased Flap Weight and Decreased Perforator Number Predict Fat Necrosis in DIEP Breast Reconstruction Carolyn L. Mulvey, BS* Carisa M. Cooney, MPH* Francis F. Daily, BS* Elizabeth Colantuoni,
Breast Reconstruction Options
 Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
Current Strategies in Breast Reconstruction
 Current Strategies in Breast Reconstruction Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery 12 th Annual School of
Current Strategies in Breast Reconstruction Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery 12 th Annual School of
Evaluation of Tissue Blood Flow of the Gastric Tube after Vessel Anastomosis for Esophageal Reconstruction
 Kobe J. Med. Sci., Vol. 57, No. 3, pp. E87-E97, 2011 Evaluation of Tissue Blood Flow of the Gastric Tube after Vessel Anastomosis for Esophageal Reconstruction HITOSHI FUKUYAMA 1, HAJIME IKUTA 1, DAISUKE
Kobe J. Med. Sci., Vol. 57, No. 3, pp. E87-E97, 2011 Evaluation of Tissue Blood Flow of the Gastric Tube after Vessel Anastomosis for Esophageal Reconstruction HITOSHI FUKUYAMA 1, HAJIME IKUTA 1, DAISUKE
PUT YOUR BEST FOOT FORWARD
 PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
Fluorescence Angiography in Limb Salvage
 Fluorescence Angiography in Limb Salvage Ryan H. Fitzgerald, DPM, FACFAS Associate Professor of Surgery-University Of South Carolina School of Medicine, Greenville Etiology of Lower extremity wounds Neuropathy
Fluorescence Angiography in Limb Salvage Ryan H. Fitzgerald, DPM, FACFAS Associate Professor of Surgery-University Of South Carolina School of Medicine, Greenville Etiology of Lower extremity wounds Neuropathy
CT-guided deep inferior epigastric perforator (DIEP) flap localization: a road-map for the onco-plastic surgeon
 CT-guided deep inferior epigastric perforator (DIEP) flap localization: a road-map for the onco-plastic surgeon Poster No.: C-1261 Congress: ECR 2014 Type: Scientific Exhibit Authors: F. Fiocchi, C. Sala,
CT-guided deep inferior epigastric perforator (DIEP) flap localization: a road-map for the onco-plastic surgeon Poster No.: C-1261 Congress: ECR 2014 Type: Scientific Exhibit Authors: F. Fiocchi, C. Sala,
INTRODUCTION. Toshihiko Satake 1, Jun Sugawara 2, Kazunori Yasumura 1, Taro Mikami 2, Shinji Kobayashi 3, Jiro Maegawa 2. Idea and Innovation
 Mini-Flow-Through Deep Inferior Epigastric Perforator Flap for Breast Reconstruction with Preservation of Both Internal Mammary and Deep Inferior Epigastric Vessels Toshihiko Satake 1, Jun Sugawara 2,
Mini-Flow-Through Deep Inferior Epigastric Perforator Flap for Breast Reconstruction with Preservation of Both Internal Mammary and Deep Inferior Epigastric Vessels Toshihiko Satake 1, Jun Sugawara 2,
Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps
 BREAST SURGERY Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps Joshua L. Levine, MD,* Quintessa Miller, MD, Julie Vasile, MD,* Kamran Khoobehi,
BREAST SURGERY Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps Joshua L. Levine, MD,* Quintessa Miller, MD, Julie Vasile, MD,* Kamran Khoobehi,
The earlier clinic experience of the reverse-flow anterolateral thigh island flap
 British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
Deep inferior epigastric perforator (DIEP) flaps for breast reconstruction: Preoperative imaging - experience on 18 consecutive patients
 Deep inferior epigastric perforator (DIEP) flaps for breast reconstruction: Preoperative imaging - experience on 18 consecutive patients Award: Magna Cum Laude Poster No.: C-809 Congress: ECR 2009 Type:
Deep inferior epigastric perforator (DIEP) flaps for breast reconstruction: Preoperative imaging - experience on 18 consecutive patients Award: Magna Cum Laude Poster No.: C-809 Congress: ECR 2009 Type:
Comparing the donor-site morbidity using DIEP, SIEA or MS-TRAM flaps for breast reconstructive surgery: A meta-analysis
 Journal of Plastic, Reconstructive & Aesthetic Surgery (2012) 65, 1474e1480 REVIEW Comparing the donor-site morbidity using DIEP, SIEA or MS-TRAM flaps for breast reconstructive surgery: A meta-analysis
Journal of Plastic, Reconstructive & Aesthetic Surgery (2012) 65, 1474e1480 REVIEW Comparing the donor-site morbidity using DIEP, SIEA or MS-TRAM flaps for breast reconstructive surgery: A meta-analysis
The Superficial Inferior Epigastric Artery (SIEA) Flap and Its Applications in Breast Reconstruction
 The Superficial Inferior Epigastric Artery (SIEA) Flap and Its Applications in Breast Reconstruction Zachary Menn and Aldona Spiegel Weill Cornell Medical College, The Methodist Hospital, Houston, Texas,
The Superficial Inferior Epigastric Artery (SIEA) Flap and Its Applications in Breast Reconstruction Zachary Menn and Aldona Spiegel Weill Cornell Medical College, The Methodist Hospital, Houston, Texas,
Deposited on: 13 December 2010
 Ng, Z.Y., Fogg, Q., and Shoaib, T. (2010) Where to find facial artery perforators: a reference point. Journal of Plastic, Reconstructive & Aesthetic Surgery, 63 (12). pp. 2046-2051. ISSN 1748-6815. http://eprints.gla.ac.uk/45921/
Ng, Z.Y., Fogg, Q., and Shoaib, T. (2010) Where to find facial artery perforators: a reference point. Journal of Plastic, Reconstructive & Aesthetic Surgery, 63 (12). pp. 2046-2051. ISSN 1748-6815. http://eprints.gla.ac.uk/45921/
Anatomical study. Clinical study. R. Ogawa, H. Hyakusoku, M. Murakami, R. Aoki, K. Tanuma* and D. G. Pennington?
 British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps
 Original Article Breast Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps James L. Mayo, MD Robert J. Allen, MD, FACS Alireza Sadeghi, MD, FACS Background: In cases of bilateral breast
Original Article Breast Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps James L. Mayo, MD Robert J. Allen, MD, FACS Alireza Sadeghi, MD, FACS Background: In cases of bilateral breast
Tor Chiu. Deep Inferior Epigastric Artery Perforator Flap 161
 18 Deep Inferior Epigastric Artery Perforator Flap Tor Chiu Deep Inferior Epigastric Artery Perforator Flap 161 Deep Inferior Epigastric Artery Perforator Flap FLAP TERRITORY The deep inferior epigastric
18 Deep Inferior Epigastric Artery Perforator Flap Tor Chiu Deep Inferior Epigastric Artery Perforator Flap 161 Deep Inferior Epigastric Artery Perforator Flap FLAP TERRITORY The deep inferior epigastric
The use of postmastectomy radiation therapy (PMRT) to prevent
 NORTHEASTERN SOCIETY OF PLASTIC SURGEONS Postmastectomy Radiation Therapy and Breast An Analysis of Complications and Patient Satisfaction Bernard T. Lee, MD,* Tolulope A. Adesiyun, BS,* Salih Colakoglu,
NORTHEASTERN SOCIETY OF PLASTIC SURGEONS Postmastectomy Radiation Therapy and Breast An Analysis of Complications and Patient Satisfaction Bernard T. Lee, MD,* Tolulope A. Adesiyun, BS,* Salih Colakoglu,
A Study of Internal Thoracic Arteriovenous Principal Perforators by Using Multi-detector Row Computed Tomography Angiography
 A Study of Internal Thoracic Arteriovenous Principal Perforators by Using Multi-detector Row Computed Tomography Angiography Ko Okumura, MD, a,b Kazunobu Hashikawa, MD, PhD, a Shunsuke Sakakibara, MD,
A Study of Internal Thoracic Arteriovenous Principal Perforators by Using Multi-detector Row Computed Tomography Angiography Ko Okumura, MD, a,b Kazunobu Hashikawa, MD, PhD, a Shunsuke Sakakibara, MD,
Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION
 Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION BREAST RECONSTRUCTION: A WOMAN S DECISION Options and Information Our approach to breast reconstruction entails a very
Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION BREAST RECONSTRUCTION: A WOMAN S DECISION Options and Information Our approach to breast reconstruction entails a very
Monitoring of partial and full venous outflow obstruction in a porcine flap model using laser. speckle contrast imaging
 Monitoring of partial and full venous outflow obstruction in a porcine flap model using laser speckle contrast imaging Johan Zotterman, Max Bergkvist, Fredrik Iredahl, Erik Tesselaar and Simon Farnebo
Monitoring of partial and full venous outflow obstruction in a porcine flap model using laser speckle contrast imaging Johan Zotterman, Max Bergkvist, Fredrik Iredahl, Erik Tesselaar and Simon Farnebo
Prophylactic Mastectomy & Reconstructive Implications
 Prophylactic Mastectomy & Reconstructive Implications Minas T Chrysopoulo, MD PRMA Center For Advanced Breast Reconstruction Prophylactic Mastectomy Surgical removal of one or both breasts to reduce the
Prophylactic Mastectomy & Reconstructive Implications Minas T Chrysopoulo, MD PRMA Center For Advanced Breast Reconstruction Prophylactic Mastectomy Surgical removal of one or both breasts to reduce the
Thermal injury in TAPIA breast reconstruction Børsen-Koch, Mikkel; Gunnarsson, Gudjon L.; Sørensen, Jens Ahm; Thomsen, Jørn Bo
 Syddansk Universitet Thermal injury in TAPIA breast reconstruction Børsen-Koch, Mikkel; Gunnarsson, Gudjon L.; Sørensen, Jens Ahm; Thomsen, Jørn Bo Published in: Gland Surgery DOI: 10.21037/gs.2017.01.01
Syddansk Universitet Thermal injury in TAPIA breast reconstruction Børsen-Koch, Mikkel; Gunnarsson, Gudjon L.; Sørensen, Jens Ahm; Thomsen, Jørn Bo Published in: Gland Surgery DOI: 10.21037/gs.2017.01.01
The gluteal perforator-based flap in repair of pressure sores
 The British Association of Plastic Surgeons (2004) 57, 342 347 CASE REPORTS The gluteal perforator-based flap in repair of pressure sores Çilingir Meltem*, Çelik Esra, Fındık Hasan, Duman Ali Department
The British Association of Plastic Surgeons (2004) 57, 342 347 CASE REPORTS The gluteal perforator-based flap in repair of pressure sores Çilingir Meltem*, Çelik Esra, Fındık Hasan, Duman Ali Department
Breast cancer is the most common malignancy BREAST
 BREAST Intraoperative Perfusion Mapping with Laser-Assisted Indocyanine Green Imaging Can Predict and Prevent Complications in Immediate Breast Reconstruction Ewa Komorowska-Timek, M.D. Geoffrey C. Gurtner,
BREAST Intraoperative Perfusion Mapping with Laser-Assisted Indocyanine Green Imaging Can Predict and Prevent Complications in Immediate Breast Reconstruction Ewa Komorowska-Timek, M.D. Geoffrey C. Gurtner,
Buried Flap Reconstruction after Nipple-Sparing Mastectomy: Advancing toward Single-Stage Breast Reconstruction
 BREAST Buried Flap Reconstruction after Nipple-Sparing Mastectomy: Advancing toward Single-Stage Breast Reconstruction Steven M. Levine, M.D. Chelsea Snider, M.D. Grace Gerald, B.S. Neil Tanna, M.D. P.
BREAST Buried Flap Reconstruction after Nipple-Sparing Mastectomy: Advancing toward Single-Stage Breast Reconstruction Steven M. Levine, M.D. Chelsea Snider, M.D. Grace Gerald, B.S. Neil Tanna, M.D. P.
Clinical Accuracy of Portrait 3D Surgical Simulation Platform in Breast Augmentation. Ryan K. Wong MD, David T Pointer BS, Kamran Khoobehi MD FACS
 Clinical Accuracy of Portrait 3D Surgical Simulation Platform in Breast Augmentation Ryan K. Wong MD, David T Pointer BS, Kamran Khoobehi MD FACS Division of Plastic, Reconstructive & Reconstructive Surgery,
Clinical Accuracy of Portrait 3D Surgical Simulation Platform in Breast Augmentation Ryan K. Wong MD, David T Pointer BS, Kamran Khoobehi MD FACS Division of Plastic, Reconstructive & Reconstructive Surgery,
Breast reconstruction has an important role BREAST. A Two-Year Prospective Analysis of Trunk Function in TRAM Breast Reconstructions
 BREAST A Two-Year Prospective Analysis of Trunk Function in TRAM Breast Reconstructions Amy K. Alderman, M.D. William M. Kuzon, Jr., M.D., Ph.D. Edwin G. Wilkins, M.D. Ann Arbor, Mich. Background: Functional
BREAST A Two-Year Prospective Analysis of Trunk Function in TRAM Breast Reconstructions Amy K. Alderman, M.D. William M. Kuzon, Jr., M.D., Ph.D. Edwin G. Wilkins, M.D. Ann Arbor, Mich. Background: Functional
Role of free tissue transfer in management of chronic venous ulcer
 Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Awareness and provision of reconstruction. Breast
 Original Article Breast Deep Inferior Epigastric Artery Perforator Flap Breast Reconstruction without Microsurgery Fellowship Training Hakan Orbay, MD, PhD* Brittany K. Busse, MD* Thomas R. Stevenson,
Original Article Breast Deep Inferior Epigastric Artery Perforator Flap Breast Reconstruction without Microsurgery Fellowship Training Hakan Orbay, MD, PhD* Brittany K. Busse, MD* Thomas R. Stevenson,
Citation for published version (APA): Benditte-Klepetko, H. C. (2014). Breast surgery: A problem of beauty or health?
 UvA-DARE (Digital Academic Repository) Breast surgery: A problem of beauty or health? Benditte-Klepetko, H.C. Link to publication Citation for published version (APA): Benditte-Klepetko, H. C. (2014).
UvA-DARE (Digital Academic Repository) Breast surgery: A problem of beauty or health? Benditte-Klepetko, H.C. Link to publication Citation for published version (APA): Benditte-Klepetko, H. C. (2014).
Medical Policy Original Effective Date: Revised Date: Page 1 of 8
 Page 1 of 8 Disclaimer Description Coverage Determination Refer to the member s specific benefit plan and Schedule of Benefits to determine coverage. This may not be a benefit on all plans, or the plan
Page 1 of 8 Disclaimer Description Coverage Determination Refer to the member s specific benefit plan and Schedule of Benefits to determine coverage. This may not be a benefit on all plans, or the plan
Latissimus Dorsi Myocutaneous Flap for Breast Reconstruction: Bad Rap or Good Flap?
 Latissimus Dorsi Myocutaneous Flap for Breast Reconstruction: Bad Rap or Good Flap? Galen Perdikis, MD, Stephanie Koonce, MD, George Collis, MD, and Dustin Eck, MD Mayo Clinic, Jacksonville, FL Correspondence:
Latissimus Dorsi Myocutaneous Flap for Breast Reconstruction: Bad Rap or Good Flap? Galen Perdikis, MD, Stephanie Koonce, MD, George Collis, MD, and Dustin Eck, MD Mayo Clinic, Jacksonville, FL Correspondence:
Breast Reconstruction in Women Under 30: A 10-Year Experience
 ORIGINAL ARTICLE Breast Reconstruction in Women Under 30: A 10-Year Experience Warren A. Ellsworth, MD,* Barbara L. Bass, MD, FACS, Roman J. Skoracki, MD, à and Lior Heller, MD* *Division of Plastic Surgery,
ORIGINAL ARTICLE Breast Reconstruction in Women Under 30: A 10-Year Experience Warren A. Ellsworth, MD,* Barbara L. Bass, MD, FACS, Roman J. Skoracki, MD, à and Lior Heller, MD* *Division of Plastic Surgery,
UC SF. Disclosures. Vascular Assessment of the Diabetic Foot. What are the best predictors of wound healing? None. Non-Invasive Vascular Studies
 Disclosures Vascular Assessment of the Diabetic Foot What are the best predictors of wound healing? None Shant Vartanian MD Assistant Professor of Vascular Surgery UCSF Vascular Symposium April 20, 2013
Disclosures Vascular Assessment of the Diabetic Foot What are the best predictors of wound healing? None Shant Vartanian MD Assistant Professor of Vascular Surgery UCSF Vascular Symposium April 20, 2013
The gastrocnemius with soleus bi-muscle flap
 The British Association of Plastic Surgeons (2004) 57, 77 82 The gastrocnemius with soleus bi-muscle flap Ikuo Hyodo a, *, Bin Nakayama b, Mitsuru Takahashi c, Kazuhiro Toriyama d, Yuzuru Kamei d, Shuhei
The British Association of Plastic Surgeons (2004) 57, 77 82 The gastrocnemius with soleus bi-muscle flap Ikuo Hyodo a, *, Bin Nakayama b, Mitsuru Takahashi c, Kazuhiro Toriyama d, Yuzuru Kamei d, Shuhei
Peter McAllister, 1 Isabel Teo, 1 Kuen Chin, 1 Boikanyo Makubate, 2 and David Alexander Munnoch Introduction
 Hindawi Publishing Corporation Plastic Surgery International Volume 2016, Article ID 6085624, 9 pages http://dx.doi.org/10.1155/2016/6085624 Research Article Bilateral Breast Reconstruction with Abdominal
Hindawi Publishing Corporation Plastic Surgery International Volume 2016, Article ID 6085624, 9 pages http://dx.doi.org/10.1155/2016/6085624 Research Article Bilateral Breast Reconstruction with Abdominal
Experimental. Vascular Occlusion in a Porcine Flap Model: Effects on Blood Cell Concentration and Oxygenation.
 Experimental Vascular Occlusion in a Porcine Flap Model: Effects on Blood Cell Concentration and Oxygenation Max Bergkvist, MD* Johan Zötterman, MD* Joakim Henricson, PhD Fredrik Iredahl, MD, PhD Erik
Experimental Vascular Occlusion in a Porcine Flap Model: Effects on Blood Cell Concentration and Oxygenation Max Bergkvist, MD* Johan Zötterman, MD* Joakim Henricson, PhD Fredrik Iredahl, MD, PhD Erik
Viability of five different pre- and intraoperative imaging methods for autologous breast reconstruction
 Eur Surg DOI 10.1007/s10353-016-0449-6 Viability of five different pre- and intraoperative imaging methods for autologous breast reconstruction. F. Schrögendorfer S. Nickl M. eck D. B. Lumenta C. Loewe
Eur Surg DOI 10.1007/s10353-016-0449-6 Viability of five different pre- and intraoperative imaging methods for autologous breast reconstruction. F. Schrögendorfer S. Nickl M. eck D. B. Lumenta C. Loewe
Updates in Breast Care. Truth or Hype. History of Breast Cancer Surgery. Dr Karen Barbosa 5/3/2017 4/20/2017
 Updates in Breast Care Dr Karen Barbosa 4/20/2017 Truth or Hype Princess Bust Developer Sears, Roebuck and Co. 1897 Promised to make the breast round, firm and beautiful History of Breast Cancer Surgery
Updates in Breast Care Dr Karen Barbosa 4/20/2017 Truth or Hype Princess Bust Developer Sears, Roebuck and Co. 1897 Promised to make the breast round, firm and beautiful History of Breast Cancer Surgery
ORIGINAL ARTICLE DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS
 DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS Peddi Manjunath 1, Ramesha K.T 2, Smitha S Segu 3, Jainath 4, Shankarappa M 5 HOW TO CITE THIS ARTICLE: Peddi Manjunath, Ramesha KT, Smitha
DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS Peddi Manjunath 1, Ramesha K.T 2, Smitha S Segu 3, Jainath 4, Shankarappa M 5 HOW TO CITE THIS ARTICLE: Peddi Manjunath, Ramesha KT, Smitha
Factors Associated with Anastomotic Failure after Microvascular Reconstruction of the Breast
 Factors Associated with Anastomotic Failure after Microvascular Reconstruction of the Breast Maurice Y. Nahabedian, M.D., Bahram Momen, Ph.D., and Paul N. Manson, M.D. Baltimore and College Park, Md. The
Factors Associated with Anastomotic Failure after Microvascular Reconstruction of the Breast Maurice Y. Nahabedian, M.D., Bahram Momen, Ph.D., and Paul N. Manson, M.D. Baltimore and College Park, Md. The
Quantitative analysis of hemodynamics of congested island flaps under leech therapy
 213 ORIGINAL Quantitative analysis of hemodynamics of congested island flaps under leech therapy Keisuke Kashiwagi, Ichiro Hashimoto, Yoshiro Abe, Kunio Kotsu, Masahiro Yamano, and Hideki Nakanishi Department
213 ORIGINAL Quantitative analysis of hemodynamics of congested island flaps under leech therapy Keisuke Kashiwagi, Ichiro Hashimoto, Yoshiro Abe, Kunio Kotsu, Masahiro Yamano, and Hideki Nakanishi Department
Variation of Superficial Palmar Arch: A Case Report
 Article ID: WMC003387 ISSN 2046-1690 Variation of Superficial Palmar Arch: A Case Report Corresponding Author: Dr. Liju S Mathew, Demonstrator, Anatomy, Gulf Medical University, 4184 - United Arab Emirates
Article ID: WMC003387 ISSN 2046-1690 Variation of Superficial Palmar Arch: A Case Report Corresponding Author: Dr. Liju S Mathew, Demonstrator, Anatomy, Gulf Medical University, 4184 - United Arab Emirates
RECONSTRUCTION OF SCALP DEFECTS: AN INSTITUTIONAL EXPERIENCE Sathyanarayana B. C 1, Somashekar Srinivas 2
 RECONSTRUCTION OF SCALP DEFECTS: AN INSTITUTIONAL EXPERIENCE Sathyanarayana B. C 1, Somashekar Srinivas 2 HOW TO CITE THIS ARTICLE: Sathyanarayana B. C, Somashekar Srinivas. Reconstruction of Scalp Defects:
RECONSTRUCTION OF SCALP DEFECTS: AN INSTITUTIONAL EXPERIENCE Sathyanarayana B. C 1, Somashekar Srinivas 2 HOW TO CITE THIS ARTICLE: Sathyanarayana B. C, Somashekar Srinivas. Reconstruction of Scalp Defects:
Endovascular treatment of popliteal artery aneurysm: preliminary results
 Endovascular treatment of popliteal artery aneurysm: preliminary results Poster No.: C-0483 Congress: ECR 2012 Type: Scientific Paper Authors: G. Guzzardi, R. Fossaceca, P. Cerini, C. Stanca, I. Di Gesù,
Endovascular treatment of popliteal artery aneurysm: preliminary results Poster No.: C-0483 Congress: ECR 2012 Type: Scientific Paper Authors: G. Guzzardi, R. Fossaceca, P. Cerini, C. Stanca, I. Di Gesù,
T. Rapis, S.N. Zanakis, I.F. Letsa, A.P. Karamanos CLINICAL CASE. Summary. Introduction
 Journal of BUON 8: 397-401, 2003 2003 Zerbinis Medical Publications. Printed in Greece CLINICAL CASE Basal cell carcinoma of the posterior neck, reconstructed with lower trapezius island musculocutaneous
Journal of BUON 8: 397-401, 2003 2003 Zerbinis Medical Publications. Printed in Greece CLINICAL CASE Basal cell carcinoma of the posterior neck, reconstructed with lower trapezius island musculocutaneous
Samer Saour, Guido Libondi, Venkat Ramakrishnan. Introduction
 Original Article Microsurgical refinements with the use of internal mammary (IM) perforators as recipient vessels in transverse upper gracilis (TUG) autologous breast reconstruction Samer Saour, Guido
Original Article Microsurgical refinements with the use of internal mammary (IM) perforators as recipient vessels in transverse upper gracilis (TUG) autologous breast reconstruction Samer Saour, Guido
Interesting Case Series. Reconstruction of Dorsal Wrist Defects
 Interesting Case Series Reconstruction of Dorsal Wrist Defects Maelee Yang, BS, and Joseph Meyerson, MD The Ohio State University Wexner Medical Center, Columbus Correspondence: maelee.yang@osumc.edu Keywords:
Interesting Case Series Reconstruction of Dorsal Wrist Defects Maelee Yang, BS, and Joseph Meyerson, MD The Ohio State University Wexner Medical Center, Columbus Correspondence: maelee.yang@osumc.edu Keywords:
DO NOT DUPLICATE. Negative pressure wound therapy (NPWT) has revolutionized the
 Original research WOUNDS 2013;25(4):89 93 From the Aesthetic and Plastic Surgery Institute, University of California Irvine, Orange, CA and Long Beach Memorial Medical Center, Long Beach, CA Address correspondence
Original research WOUNDS 2013;25(4):89 93 From the Aesthetic and Plastic Surgery Institute, University of California Irvine, Orange, CA and Long Beach Memorial Medical Center, Long Beach, CA Address correspondence
Increase of Visible Veins After Breast Augmentation. Yuri Andonakis, MD,* and Berend van der Lei, MD, PhD*
 BREAST SURGERY A Retrospective Analysis of 78 Consecutive Breast Augmentation Patients Yuri Andonakis, MD,* and Berend van der Lei, MD, PhD* Abstract: A retrospective study was undertaken to determine
BREAST SURGERY A Retrospective Analysis of 78 Consecutive Breast Augmentation Patients Yuri Andonakis, MD,* and Berend van der Lei, MD, PhD* Abstract: A retrospective study was undertaken to determine
Failure by congestion of pedicled and free flaps for reconstruction of lower limbs after trauma: the role of negative-pressure wound therapy
 J Orthopaed Traumatol (2013) 14:213 217 DOI 10.1007/s10195-013-0236-0 BRIEF COMMUNICATION Failure by congestion of pedicled and free flaps for reconstruction of lower limbs after trauma: the role of negative-pressure
J Orthopaed Traumatol (2013) 14:213 217 DOI 10.1007/s10195-013-0236-0 BRIEF COMMUNICATION Failure by congestion of pedicled and free flaps for reconstruction of lower limbs after trauma: the role of negative-pressure
The FLARE intraoperative near-infrared fluorescence imaging system: a first-inhuman clinical trial in perforator flap breast reconstruction
 Chapter 10 The FLARE intraoperative near-infrared fluorescence imaging system: a first-inhuman clinical trial in perforator flap breast reconstruction Lee BT, Hutteman M, Gioux S, Stockdale A, Lin SJ,
Chapter 10 The FLARE intraoperative near-infrared fluorescence imaging system: a first-inhuman clinical trial in perforator flap breast reconstruction Lee BT, Hutteman M, Gioux S, Stockdale A, Lin SJ,
Figure 1. Anatomy of the breast
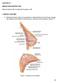 CHAPTER 12 BREAST RECONSTRUCTION Mihaela Rapolti, MD and Michelle Roughton, MD I. BREAST ANATOMY A. Mastering breast anatomy is essential for understanding how the breast changes with aging and principles
CHAPTER 12 BREAST RECONSTRUCTION Mihaela Rapolti, MD and Michelle Roughton, MD I. BREAST ANATOMY A. Mastering breast anatomy is essential for understanding how the breast changes with aging and principles
B11 Breast Reconstruction with Abdominal Tissue Flap
 B11 Breast Reconstruction with Abdominal Tissue Flap Issued March 2011 You can get more information about this procedure from www.aboutmyhealth.org Tell us how useful you found this document at www.patientfeedback.org
B11 Breast Reconstruction with Abdominal Tissue Flap Issued March 2011 You can get more information about this procedure from www.aboutmyhealth.org Tell us how useful you found this document at www.patientfeedback.org
The Influence of Pfannenstiel Incision Scarring on Deep Inferior Epigastric Perforator
 The Influence of Pfannenstiel Incision Scarring on Deep Inferior Epigastric Perforator Young Jin Park, Eun Key Kim, Ji Young Yun, Jin Sup Eom, Taik Jong Lee Department of Plastic Surgery, Asan Medical
The Influence of Pfannenstiel Incision Scarring on Deep Inferior Epigastric Perforator Young Jin Park, Eun Key Kim, Ji Young Yun, Jin Sup Eom, Taik Jong Lee Department of Plastic Surgery, Asan Medical
Extended double pedicle free tensor
 e141 Case Report Extended double pedicle free tensor fascia latae myocutaneous flap for abdominal wall reconstruction Dorai A A, Halim A S ABSTRACT Extensive full thickness anterior abdominal wall defects
e141 Case Report Extended double pedicle free tensor fascia latae myocutaneous flap for abdominal wall reconstruction Dorai A A, Halim A S ABSTRACT Extensive full thickness anterior abdominal wall defects
Microvascular Free Flaps: Experience in Kwong Wah Hospital
 VOL. VOL.NO. NO. MAYNOVEMBER Microvascular Free Flaps: Experience in Kwong Wah Hospital Dr. Chiu-ming Ho, Dr. Vana SH Chan, Dr. Ming-shiaw Cheng, Dr. Wing-yung Cheung Division of Plastic Surgery, Department
VOL. VOL.NO. NO. MAYNOVEMBER Microvascular Free Flaps: Experience in Kwong Wah Hospital Dr. Chiu-ming Ho, Dr. Vana SH Chan, Dr. Ming-shiaw Cheng, Dr. Wing-yung Cheung Division of Plastic Surgery, Department
Update on Breast Reconstruction Using Free TRAM, DIEP, and SIEA Flaps
 Update on Breast Reconstruction Using Free TRAM, DIEP, and SIEA Flaps Pierre M. Chevray, M.D., Ph.D. 1 ABSTRACT Breast reconstruction using autologous tissue is commonly accomplished using the transverse
Update on Breast Reconstruction Using Free TRAM, DIEP, and SIEA Flaps Pierre M. Chevray, M.D., Ph.D. 1 ABSTRACT Breast reconstruction using autologous tissue is commonly accomplished using the transverse
SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni
 SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni Icro Meattini, MD Radiation Oncology Department - University of Florence Azienda Ospedaliero Universitaria Careggi Firenze Breast
SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni Icro Meattini, MD Radiation Oncology Department - University of Florence Azienda Ospedaliero Universitaria Careggi Firenze Breast
Scientific Paper. Page 1 of 39
 Abdominal wall vascularisation mapping in microsurgeons preoperative planning: a retrospective study on 174 CT angiographies. DIEA, SIEA and SICA prevalence, caliber and branching pattern Poster No.: B-686
Abdominal wall vascularisation mapping in microsurgeons preoperative planning: a retrospective study on 174 CT angiographies. DIEA, SIEA and SICA prevalence, caliber and branching pattern Poster No.: B-686
