Factors Associated with Anastomotic Failure after Microvascular Reconstruction of the Breast
|
|
|
- Douglas Rafe Turner
- 5 years ago
- Views:
Transcription
1 Factors Associated with Anastomotic Failure after Microvascular Reconstruction of the Breast Maurice Y. Nahabedian, M.D., Bahram Momen, Ph.D., and Paul N. Manson, M.D. Baltimore and College Park, Md. The prevalence of anastomotic failure resulting in return to the operating room and flap necrosis after microvascular breast reconstruction ranges from 1 to 5 percent. The purpose of this study was to review a set of factors that may be associated with this occurrence. Microvascular reconstruction of the breast was performed in 198 women from January of 1998 to July of The mean age for all women was 47.7 years. There were 158 unilateral and 41 bilateral reconstructions, for a total of 240 flaps. The specific flaps included the free transverse rectus abdominis musculocutaneous flap (n 176), the deep inferior epigastric perforator flap (n 58), and the superior gluteal artery perforator flap (n 6). Upon recognition of anastomotic failure, women were immediately returned to the operating room. Factors that were considered relevant to anastomotic failure included the choice of recipient vessel, timing of reconstruction, previous chest wall radiation therapy, previous axillary lymph node dissection, tobacco use, diabetes mellitus, patient age, and hematoma. Patient follow-up ranged from 5 to 59 months. Descriptive statistics, Fisher s exact test, and exact logistic regression were used for analyses and to summarize data. Of the 240 flaps, return to the operating room was necessary for 20 (8.3 percent), total necrosis occurred in nine (3.8 percent), and the rate of flap salvage was 55 percent (11 of 20 flaps). Venous occlusion was responsible for 16 of the 20 returns and eight of the nine failures. Statistical analysis demonstrated that both return to the operating room and flap necrosis were significantly associated with venous occlusion, delayed reconstruction, and hematoma. Previous lymph node dissection and previous radiation therapy had only a weak association with return to the operating room. The results of this study demonstrate that venous occlusion is responsible for return to the operating room and flap necrosis in the majority of cases. Age, tobacco use, choice of recipient vessel, and diabetes mellitus were not associated with anastomotic failure. The significance of delayed reconstruction may be related to its frequent association with previous lymph node dissection and/or radiation therapy resulting in perivascular fibrosis. (Plast. Reconstr. Surg. 114: 74, 2004.) Microvascular reconstructions of the breast using free transverse rectus abdominis musculocutaneous (TRAM), deep inferior epigastric perforator (DIEP), and superior gluteal artery perforator (SGAP) flaps have been performed for nearly 15 years. 1 6 The advantages of these techniques are well described and include fewer abnormalities at the donor sites related to strength and contour, less fat necrosis, and improved symmetry Since inception, however, these techniques have been the topic of much discussion and controversy that has been primarily based on the complexity of these operations, risk of total flap failure, financial considerations, and patient satisfaction. 6,8,11 14 This controversy is heightened by the fact that pedicle flap counterparts, the pedicle TRAM flap and the latissimus dorsi flap, represent simpler methods of reconstruction with a decreased flap failure rate. The prevalence of anastomotic failure following microvascular breast reconstruction resulting in return to the operating room ranges from 5 to 10 percent and resulting in flap necrosis ranges from 1 to 5 percent. 6,8,15 The etiology of anastomotic failure is multifactorial and can be the result of preoperative, intraoperative, and postoperative factors that have been described previously. 16 Many factors can be optimized to improve anastomotic and flap success. These include patient selection, surgical technique, and postoperative hemodynamic monitoring. Some factors, however, cannot be completely optimized. These include From The Johns Hopkins University and the University of Maryland. Received for publication June 6, 2003; revised August 8, Presented at the 82nd Annual Meeting of the American Association of Plastic Surgeons, in Baltimore, Maryland, May 4 to 7, DOI: /01.PRS
2 Vol. 114, No. 1 / ANASTOMOTIC FAILURE 75 the effects of prior mastectomy and axillary lymph node dissection, prior chest wall radiation therapy, medical comorbidities, and advanced patient age. Thus, the purpose of this study was to evaluate a set of candidate factors and quantify those that associate significantly with anastomotic failure. Identification of these factors may improve outcomes following microvascular reconstruction of the breast. PATIENTS AND METHODS Patient Selection Microvascular reconstruction of the breast was performed in 198 women from January of 1998 to July of Standard indications included tobacco use, obesity, and averting a delay procedure. The authors indications also included preservation of abdominal strength, preservation of abdominal contour, minimizing the occurrence of fat necrosis, and the ability to reconstruct a breast of sufficient volume to minimize the need to perform additional operations for symmetry. During the initial evaluation, all patients were provided with the options of breast reconstruction using autologous tissue or implants. For women interested in autologous tissue, the abdomen was the primary donor site and the buttock was the secondary donor site. An assessment of the soft-tissue volume requirement of the breast was compared with the amount of soft tissue available in the abdominal area. In some situations, the abdomen was not a suitable donor site because of prior abdominal operations, morbid obesity, or inadequate volume. In these cases, the SGAP flap was considered as an alternative donor site. Operative Technique The salient features related to the harvest and elevation of the free TRAM, DIEP, and SGAP flaps have been previously described. 1,7,8,17,18 The selection of abdominal flaps, including the free TRAM and DIEP, was based on intraoperative assessment of the perforators. 8 When a large perforator was visualized (1.5 to 3 mm), a DIEP flap was performed and included from 1 to 3 perforators. In the absence of a dominant perforator or when perforator diameter was less than 1.5 mm, a muscle-sparing free TRAM (MS-1 or MS-2) was usually performed. The recipient vessels included the thoracodorsal or internal mammary artery and vein. For the initial 3 years of the study, the thoracodorsal vessels were used exclusively. Currently, the choice of recipient vessel is based on several factors primarily related to the timing of the reconstruction and the type of mastectomy performed. The thoracodorsal vessels are used for all unilateral or bilateral reconstructions following modified radical mastectomy in which the vessels are readily accessible. The internal mammary vessels are used for all delayed reconstructions as well as all unilateral and bilateral immediate reconstructions following sentinel lymph node biopsy or simple mastectomy. The benefit of this is to prevent perivascular and perilymphatic fibrosis in the axillary region and to minimize the incidence of lymphedema. In preparation for the microvascular anastomosis, 3000 to 5000 IU of heparin was administered intravenously, 5 minutes before division of the vascular pedicle. All anastomoses were performed by hand using 8-0 or 9-0 interrupted nylon sutures. The anastomotic coupler was not used in this series of reconstructions. The anastomotic technique was end to end for all flaps except one in which an end-to-side technique was used for an SGAP reconstruction. All operations for this analysis were performed by the primary author (Nahabedian) to minimize procedural variations. Postoperative Care and Monitoring Postoperative monitoring consisted of direct assessment of the flap every 15 minutes while in the recovery room, every hour for the first 24 hours, and every 2 hours for the next 48 hours. Women were usually discharged to home on the third postoperative day. The specific monitoring instruments included a handheld Doppler probe, assessment of surface temperature gradients, flap color, and capillary refill. The Doppler was used to assess arterial and venous flow. A biphasic signal was indicative of a patent artery and vein, whereas a monophasic signal was indicative of arterial or venous thrombosis. The implantable Doppler was not used in these reconstructions. Flaps demonstrating venous insufficiency were observed for signs of progression. Progressive venous insufficiency implies a gradual increase in congestion with a purplish discoloration indicative of venous occlusion. Nonprogressive venous insufficiency implies a mild and stable level of congestion that is indicative of patent but insufficient venous outflow. This form of venous insufficiency was managed with medic-
3 76 PLASTIC AND RECONSTRUCTIVE SURGERY, July 2004 inal leeches. The benefit of using leeches for venous congestion has been previously described. 19 The leeches were applied every 2 to 8 hours depending on the degree of venous insufficiency and continued for 2 to 4 days to allow venous collateralization to occur. Progressive venous insufficiency required reexploration. The decision to return to the operating room and explore the anastomosis was based on evidence or suspicion of vascular compromise. Venous occlusion manifested as a congested, tense, and warm flap with brisk and rapid capillary refill. Arterial occlusion manifested as a pale, cool flap with absent capillary refill. Salvage of the failing flap required prompt return to the operating room, usually within 30 to 60 minutes to minimize ischemic injury. An intravenous bolus of heparin, 3000 to 5000 IU (Wyeth-Ayerst, Philadelphia, Pa.), was administered. The anastomosis was evaluated both visually and with the hand-held Doppler probe. In case of venous thrombosis only, the vessel was divided at the site of the anastomosis. A Fogarty embolectomy catheter was passed proximally and distally to evacuate blood clot. When adequate venous flow was obtained, the vessel edges were débrided and anastomosed. When venous flow could not be achieved, it was assumed to be the result of thrombosis within the microvasculature of the flap. In these circumstances, a bolus of an intraarterial thrombolytic agent such as streptokinase (25,000 IU; AstraZeneca, Westborough, Mass.) or Retavase (10 units; Centocor, Malvern, Pa.) was administered. Absence of flow suggested irreversible thrombosis that required flap removal. Repair of the venous anastomosis with a vein graft or use of alternate recipient vessels was considered when there was insufficient length of the vascular pedicle. Statistical Analysis Descriptive statistics was used for data summarization. Statistical analyses were performed using the Fisher s exact test and exact logistic regression. 20 The FREQ and LOGISTIC procedures of the SAS System with the EXACT option were used. The EXACT option has been added to the LOGISTIC procedure of the SAS System version 8.1 for small and/or skewed data or for cases where the frequency of one or more cells is below 5 (the case in this study). No variable selection method can be used in combination with the EXACT option using this procedure, however. Therefore, we used the Fisher s exact test to first identify those explanatory variables which have pairwise significant associations with the response and then check the joint association of such explanatory variable with the response using the exact logistic regression. RESULTS The mean age for all women was 47.7 years (range, 25 to 75 years). Mean follow-up was 26 months (range, 5 to 56 months). The reconstruction was unilateral in 158 women and bilateral in 41 women, for a total of 240 flaps. The specific flaps used were the free TRAM (n 176), DIEP (n 58), and SGAP (n 6) flaps. Candidate factors to be associated with anastomotic failure are listed in Table I. The occurrence of each factor is based on the total number of flaps. Of the 240 flaps, return to the operating room was necessary for 20 (8.3 percent), total necrosis occurred in nine (3.8 percent), and the rate of flap salvage was 55 percent (11 of 20 flaps). Return to the operating room was necessary for 13 free TRAM, five DIEP, and two SGAP flaps. Total necrosis occurred in seven free TRAM flaps, one DIEP flap, and one SGAP flap. Circulatory abnormalities within the flap were recognized at a mean of 12 hours following the operation (range, 2 to 36 hours). Medicinal leeches were used on four flaps that demonstrated nonprogressive venous insufficiency. These leeches were used for 2 to 3 days. A blood transfusion was necessary in all women and included an autologous unit and 1 to 2 units of banked blood. The factors associated with return to the operating room were analyzed and listed in Table II. Venous occlusion was the primary reason for returning to the operating room in 16 of TABLE I Candidate Factors to Be Associated with Anastomotic Failure Factor No. of Flaps Percent Flaps Mean age, years 47.7 Immediate reconstruction Delayed reconstruction Thoracodorsal Internal mammary Previous axillary LND Previous chest wall XRT Tobacco use Diabetes mellitus 4 2 LND, lymph node dissection; XRT, radiation therapy.
4 Vol. 114, No. 1 / ANASTOMOTIC FAILURE 77 TABLE II Factors Associated with Return to Operating Room TABLE III Factors Associated with Flap Failure Factor No. of Flaps Total Flaps Returned to OR (%) Total Flaps for Each Factor (%) Flaps Mean age, years 47.4 Immediate reconstruction Delayed reconstruction Thoracodorsal Internal mammary Previous axillary LND Previous chest wall XRT Tobacco use Diabetes mellitus Hematoma Arterial occlusion Venous occlusion OR, operating room; LND, lymph node dissection; XRT, radiation therapy. Factor No. of Flap Failures Percent of Failures Percent of Factor Flaps Mean age, years 46.3 Immediate reconstruction Delayed reconstruction Thoracodorsal Internal mammary Previous LND Previous XRT Tobacco use Diabetes mellitus Hematoma Arterial occlusion Venous occlusion LND, lymph node dissection; XRT, radiation therapy. the 20 flaps. Although the majority of women that required re-exploration had immediate reconstruction (65 percent versus 35 percent), the percentage, when evaluated for all women following delayed or immediate reconstruction, was higher for delayed reconstruction (20 percent versus 6 percent, respectively). Analysis of recipient vessels demonstrated that the thoracodorsal artery and vein required reexploration in the majority of cases (15 versus five). The percentage was higher, however, for the internal mammary (13 percent versus 7 percent) when the analysis included all women. Of the 20 women who required return to the operating room, the case of one woman was considered to be preventable and related to a technical factor and 19 were not. The technical factor included a bleeding venous branch resulting in a hematoma, venous thrombosis, and flap necrosis. There was no obvious etiology for the remaining 19 flaps. In these flaps, intraoperative evaluation of the thrombosed vessels demonstrated that all of the anastomoses were intact without evidence of an intimal flap or back-wall suture placement. Factors associated with flap failure were examined and are listed in Table III.. Of the total number of flap failures, five occurred following immediate and four following delayed reconstruction. When evaluated based on all women who had delayed reconstruction, however, there was a fivefold increase (11.4 percent versus 2.4 percent) in flap failure following delayed reconstruction. Venous occlusion appeared to be responsible for anastomotic failure in eight of the nine flap failures. Descriptive results of the analysis of the women who required re-exploration and who had flap failure are listed in Table IV. Statistical Analysis The results of the Fisher s exact test indicating the probability of the significance of the associations between the response and explanatory factors are shown in Table V. The Fisher s exact test indicated that return to the operating room associated significantly with venous occlusion (p 0.001), delayed reconstruction (p 0.01), and hematoma (p 0.001). Flap necrosis associated significantly with venous occlusion (p 0.01), delayed reconstruction (p 0.028), and hematoma (p 0.024). Previous lymph node dissection (p 0.06) and previous radiation therapy (p 0.06) approached significance in their associations with return to the operating room but not with flap necrosis. Age, tobacco use, choice of recipient vessel, and diabetes mellitus were not associated significantly with anastomotic or flap failure. For the majority of cases in this study, venous occlusion appeared to be responsible for returning to the operating room and flap necrosis. The results of the exact logistic regression including the return to the operating room as the response variable and venous occlusion, delayed reconstruction, hematoma, previous lymph node dissection, and previous radiation therapy as the explanatory variables that had pairwise significant associations with the return to the operating room based on the Fisher s exact test indicated a significant (p ) joint association. Venous occlusion and hematoma, however, were the only variables with
5 78 PLASTIC AND RECONSTRUCTIVE SURGERY, July 2004 TABLE IV Descriptive Results of Patients Who Had Flap Failure and Required Re-exploration Patient Flap Flap Outcome Age (yrs) Tobacco Diabetes Mellitus Timing of Reconstruction Occlusion Recipient Vessel Hematoma Previous ALND Previous XRT 1 Free TRAM Failure 58 No No Immediate Vein Thoracodorsal No No No 2 Free TRAM Failure 54 No No Delayed Vein Thoracodorsal No Yes No 3 Free TRAM Salvage 57 No No Delayed Vein Thoracodorsal No Yes Yes 4 Free TRAM Salvage 63 No No Immediate Artery Thoracodorsal Yes No No 5 Free TRAM Failure 32 No No Delayed Vein Thoracodorsal No Yes No 6 Free TRAM Salvage 37 Yes No Immediate Vein Thoracodorsal Yes No No 7 Free TRAM Salvage 53 No No Delayed Artery Thoracodorsal No Yes Yes 8 Free TRAM Failure 52 No No Immediate Vein Thoracodorsal No Yes No 9 DIEP Salvage 40 No No Immediate Vein Internal Mammary No Yes Yes 10 Free TRAM Failure 47 No No Delayed Vein Internal Mammary No Yes No 11 DIEP Failure 51 No No Immediate Vein Thoracodorsal Yes No Yes 12 Free TRAM Salvage 44 No No Immediate Artery Thoracodorsal No Yes No 13 DIEP Salvage 53 No No Immediate Vein Thoracodorsal Yes No No 14 DIEP Salvage 39 No No Immediate Vein Thoracodorsal No No No 15 Free TRAM Salvage 50 No No Immediate Vein Thoracodorsal Yes No No 16 SGAP Salvage 50 No No Delayed Vein Internal Mammary No No No 17 DIEP Salvage 35 No No Immediate Vein Thoracodorsal No No No 18 SGAP Failure 36 No No Immediate Vein Internal Mammary No No No 19 Free TRAM Failure 33 No No Immediate Artery Thoracodorsal No No No 20 Free TRAM Failure 54 No No Delayed Vein Internal Mammary Yes No Yes TRAM, transverse rectus abdominis musculocutaneous; DIEP, deep inferior epigastric perforator; SGAP, superior gluteal artery perforator; ALND, axillary lymph node dissection; XRT, radiation therapy. individual significant associations (p 0.001, and p 0.03) with the response in the presence of other variables. The results of the exact logistic regression model including flap necrosis as the response variable and venous occlusion, delayed reconstruction, and hematoma (the variables that had pairwise significant associations with the flap necrosis based on the Fisher s exact test) indicated that although the joint association of these variables was significant (p ), only venous occlusion had an individual significant (p 0.001) association with the response in the presence of the other two variables. DISCUSSION Flap failure following microvascular reconstruction of the breast is a devastating complication. The literature contains a plethora of information regarding techniques and outcomes after microvascular reconstruction 1 6 ; however, there is a paucity of information regarding mechanisms of flap failure. 15,16,18 Although factors that might increase the risk of anastomotic and flap failure have been identified, it remains unclear as to what factors differentiate between success and failure. Those factors that may increase the risk of failure can be divided into two groups: those that are within the control of the surgeon and those that are not. Factors that can be controlled by the surgeon are ultimately related to meticulous technique, knowledge of the relevant anatomy, and attention to detail. In 1994, Khouri stated, The difference between success and failure in free flap surgery rests upon a multitude of minute details. There is no cookbook or quick-fix recipe; the entire operation must be flawlessly executed with no room for TABLE V Probabilities of Significance of Associations between Factors Factor Return to Operating Room Flap Failure Age Tobacco use Diabetes mellitus Delayed reconstruction Thoracodorsal Internal mammary Previous LND Previous XRT Hematoma Venous occlusion LND, lymph node dissection; XRT, radiation therapy.
6 Vol. 114, No. 1 / ANASTOMOTIC FAILURE 79 error. 16 There are other factors, however, that cannot be controlled by the surgeon. These factors include patients age, previous radiation therapy, previous axillary lymph node dissection, delayed reconstruction, scar, postoperative hematoma, and the effects of diabetes mellitus and tobacco use. It was the purpose of this study to evaluate these factors and determine whether there was an association with anastomotic and flap failure. In selecting the factors associated with anastomotic failure for this study, it became evident that all were ultimately related to the quality of the recipient and donor vessels. Although the authors recognize that there is an association between obesity and flap failure, obesity was not included as a candidate factor in this study because obesity is related to patient selection rather than the quality of recipient vessels. Chang et al. 21 have demonstrated that flap failure is increased in obese and overweight women (p 0.05) when compared with normal weight women (3.2 percent versus 1.9 percent versus 0 percent, respectively). The factors that were selected for this analysis have all been previously analyzed, though usually one at a time. To the best of our knowledge, however, evaluation of all these factors and their impact on a specific endpoint (anastomotic and flap failure) has not been performed previously for microsurgical reconstruction of the breast. Review of previous studies has generated support and provided the basis for this study. Advanced patient age and its relationship to microvascular success have been evaluated in two recent studies. Lipa et al. 22 have demonstrated a flap failure rate of 1.7 percent (one of 58 women) following free TRAM reconstruction in women over 65 years of age. Girotto et al. 23 have demonstrated 100 percent flap survival following reconstruction in seven women with either a free TRAM or DIEP flap in women over 65 years of age. No additional morbidity was related to advanced patient age in these two studies. Serletti et al. 24 have demonstrated that it is the American Society of Anesthesiologists physical status of the patient and length of the operation that are the significant predictors of postoperative morbidity. The microangiopathic alterations associated with diabetes mellitus have been extensively studied in both experimental and clinical studies. Experimental studies using rats have demonstrated that the degree of intimal repair and endothelialization is lower in poorly controlled diabetics and can lead to anastomotic failure. 25 When glucose levels are well controlled, however, patency of the anastomosis is less affected. 26 Indeed, clinical studies have demonstrated that patients with diabetes mellitus are not at increased risk for flap failure, abnormal healing of the anastomosis, or intolerance to an ischemic challenge as long as normoglycemia is maintained. 27,28 Khouri et al., 15 in a prospective study of microvascular procedures that included breast reconstruction, reported no increase in anastomotic or flap failure in patients with diabetes mellitus, advanced age, or with a history of tobacco use. The vascular manifestations associated with tobacco use are well known Some of the alterations that can occur include decreased endothelial synthesis of nitric oxide that impairs endothelium-dependent vasodilation of arteries, development of atherosclerosis, and increased plasma fibrinogen levels that potentiate vascular thrombosis through platelet activation. 32,33 Clinical studies evaluating the effects of tobacco use on a microvascular anastomosis following free TRAM reconstruction have not demonstrated additional morbidity, however. Chang et al. 34 reported that the incidence of vessel thrombosis and flap loss was comparable to that observed in women who did not use tobacco. Padubidri et al. 35 have demonstrated that the incidence of total flap necrosis did not differ among smokers, exsmokers, and nonsmokers (2.6 percent versus 4.3 percent versus 1 percent, respectively). The authors did not distinguish between the free TRAM and the pedicle TRAM in their study. The effect of radiation on arteries and veins has been well documented. Perivascular fibrosis, endothelial damage, and microvascular occlusion can impair the quality of recipient vessels Recent studies have elucidated the anatomic and physiological changes on arteries and veins that are associated with radiation. Schultze-Mosgau et al. 39 demonstrated that the histological changes following radiation were dose-dependent. After a dose of 60 to 70 Gy, the histologic changes included intimal dehiscence, hyalinosis, and a decreased ratio of the media to total vessel area. These changes were observed in the artery but not in the vein. When no radiation was administered or when the radiation dose was 40 to 50 Gy, these changes were not observed. Beckman et al. 36 demonstrated that external beam radiation impaired endothelial-dependent vasodilation of
7 80 PLASTIC AND RECONSTRUCTIVE SURGERY, July 2004 arteries that might contribute to the development of arterial occlusive disease. The clinical significance of this phenomenon may be related to slow recovery from vasospasm that can lead to arterial thrombosis. The selection of recipient vessels for microvascular breast reconstruction has been well studied. The vessels that are most commonly used include the internal mammary and thoracodorsal artery and vein. Anatomical studies of the internal mammary vessels at the level of the fourth rib have demonstrated a diameter of 0.99 to 2.55 mm for the artery and 0.64 to 4.45 mm for the vein. 40,41 The diameter of the thoracodorsal vessels ranges from 1.5 to 3.0 mm for the artery and 2.5 to 4.5 mm for the vein. 41,42 Clark et al. 43 reported that the diameter of the internal mammary vein became unsuitable for microvascular anastomosis below the level of the fourth rib. Lorenzetti et al. 44,45 studied the blood flow rate of the inferior epigastric, internal mammary, and thoracodorsal arteries and demonstrated flow rates of 11 ml/minute (range, 5 to 17 ml/minute), 25 ml/minute (range, 15 to 35 ml/ minute), and 5 ml/minute (range, 2 to 8 ml/minute), respectively. The conclusions from this study were that either vessel was capable of adequate inflow to the flap and that blood flow in the flap was independent of the flow rate of the recipient artery. Clinical trials comparing the efficacy of the internal mammary and thoracodorsal vessels have been useful. In a recent prospective study of 100 patients, Moran et al. 46 reported that either vessel was suitable for microvascular anastomosis. However, the rate of conversion from the initial recipient vessel to an alternate vessel was 12.5 percent for the internal mammary and 7 percent for the thoracodorsal. Numerous studies have demonstrated that the success rates using the internal mammary or thoracodorsal vessels range from 95 to 99 percent. 8,47,48 The results of our study demonstrate that venous occlusion was responsible for return to the operating room and flap necrosis in the majority of cases. The two factors that were associated most significantly with both anastomotic and flap failure were delayed reconstruction and postoperative hematoma. A weak association was detected between return to the operating room with previous axillary lymph node dissection and previous radiation therapy. No association was detected between patient age, tobacco use, choice of recipient vessel, and diabetes mellitus. The importance of delayed reconstruction is most likely related to its frequent association with previous axillary lymph node dissection and/or radiation therapy resulting in perivascular fibrosis. This is more commonly observed with the thoracodorsal artery and vein. In fact, the results of this study have demonstrated that anastomotic and flap failure occurred most often in the delayed setting in which the thoracodorsal vessels were used. The significant associations between hematoma with anastomotic and flap failure were surprising. The most likely explanation may be that a hematoma compresses not only the vascular pedicle but also the flap itself, resulting in thrombosis of the microvasculature. The deleterious effect of a hematoma is exacerbated in the delayed setting because the flap is inset within a relatively confined space. We observed extensive thrombosis both in the vascular pedicle and in the flap itself with hematoma volumes ranging from 100 to 150 cc. Although the exact source of the hematoma was found in only one woman, a logical explanation is available. In the setting of venous thrombosis, the flap becomes hypertensive and the blood vessels that were previously coagulated begin to bleed resulting in a hematoma. Based on these results, our algorithm for microvascular breast reconstruction has been refined. Although advanced patient age, tobacco use, and diabetes mellitus do not appear to affect anastomotic and flap success, women are advised to stop smoking tobacco for 2 weeks before surgery and to maintain glycemic control. The timing of the reconstruction is an important aspect that can affect the quality of the recipient vessels. Although the selection of vessels did not influence the outcome of microvascular reconstruction in this study, we believe that this factor may affect anastomotic success in some cases. Early in our experience, the thoracodorsal artery and vein were used for all immediate and delayed reconstructions. In the delayed setting, in which a previous axillary lymph node dissection had been performed, perivascular fibrosis was found to occasionally compromise the quality of the recipient vessels. This was further aggravated in the presence of radiation therapy. Of the first three flap failures in this study, two followed delayed reconstruction in which an axillary lymph node dissection had been performed (Table IV). Our current vessel of choice for delayed reconstruc-
8 Vol. 114, No. 1 / ANASTOMOTIC FAILURE 81 tions is the internal mammary artery and vein because these vessels are of relatively large caliber, have excellent inflow and outflow, and tolerate radiation. In addition, obstruction of flow resulting from pedicle malposition has not been observed. Our algorithm for salvaging the flap following anastomotic failure has also been modified and refined. The decision to return to the operating room is based on evidence or suspicion of vascular compromise. Women are transported to the operating room usually within 30 minutes from the time of recognition. A heparin bolus is administered to prevent progression of the clot. The anastomosis and the chest wall are thoroughly inspected. When a hematoma is identified, hemostasis is obtained using clips or sutures. In only one of the six patients from this study with a postoperative hematoma was an active bleeding vessel found. Thrombosis of the artery and/or vein is managed by dividing the vessels at the anastomosis and inspecting the vessels for red or white clot representing blood or platelets, respectively. The technique of reestablishing flow is described in the Patients and Methods section. After restoration of flow, two new drains are placed along the axilla and the inferior border of the breast. Women are maintained on dextran 40 at 30 cc per hour. Heparin infusion is not maintained unless there is a problem with thrombosis intraoperatively. CONCLUSIONS The success of the anastomosis and survival of the flap seems to depend on two sets of factors. Factors that can be controlled by the surgeon are ultimately related to proper patient selection, knowledge of the relevant anatomy, an understanding of flap physiology, and meticulous technique. Factors that are outside the control of the surgeon include advanced age, comorbidities, prior axillary lymph node dissection, and prior radiation therapy. Recognition of these two variables facilitates understanding of the factors that constitute the difference between flap failure and flap success. Maurice Nahabedian, M.D. Johns Hopkins Hospital 601 North Caroline Street, 8152C Baltimore, Md mnahabed@jhmi.edu REFERENCES 1. Grotting, J. C., Urist, M. M., Maddox, W. A., and Vasconez, L. O. Conventional TRAM flap versus free microsurgical TRAM flap for immediate breast reconstruction. Plast. Reconstr. Surg. 83: 824, Allen, R. J., and Tucker, C. Superior gluteal artery perforator free flap for breast reconstruction. Plast. Reconstr. Surg. 95: 1207, Allen, R. J., and Treece, P. Deep inferior epigastric perforator flap for breast reconstruction. Ann. Plast. Surg. 32: 32, Koshima, I., and Soeda, S. Inferior epigastric artery skin flaps without rectus abdominis muscle. Br. J. Plast. Surg. 42: 645, Arnez, Z. M., Smith, R. W., Eder, E., Solinc, M., and Kersnic, M. Breast reconstruction by the free lower transverse rectus abdominis musculocutaneous flap. Br. J. Plast. Surg. 41: 500, Serletti, J. M., and Moran, S. L. Microvascular reconstruction of the breast. Semin. Surg. Oncol. 19: 264, Nahabedian, M. Y., Dooley, W., Singh, N., and Manson, P. N. Contour abnormalities of the abdomen following breast reconstruction with abdominal flaps: The role of muscle preservation. Plast. Reconstr. Surg. 109: 91, Nahabedian, M. Y., Momen, B., Galdino, G., and Manson, P. N. Breast reconstruction with the free TRAM or DIEP flap: Patient selection, choice of flap, and outcome. Plast. Reconstr. Surg. 110: 466, Kroll, S. S., Schusterman, M. A., Reece, G. P., Miller, M. J., Robb, G., and Evans, G. R. Abdominal wall strength, bulging, and hernia after TRAM flap breast reconstruction. Plast. Reconstr. Surg. 96: 616, Blondeel, P. N., Arnstein, M., Verstraete, K., et al. Venous congestion and blood flow in free transverse rectus abdominis myocutaneous and deep inferior epigastric perforator flaps. Plast. Reconstr. Surg. 106: 1295, Kaplan, J. L., and Allen, R. J. Cost-based comparison between perforator flaps and TRAM flaps for breast reconstruction. Plast. Reconstr. Surg. 105: 943, Kroll, S. S., Reece, G. P., Miller, M. M., et al. Comparison of cost for DIEP and free TRAM flap breast reconstruction. Plast. Reconstr. Surg. 107: 1413, Kerrigan, C. L., and Collins, E. D. Are perforator flaps truly more cost effective than TRAM flaps: How good is the evidence? (Letter) Plast. Reconstr. Surg. 105: 943, Alderman, A. K., Wilkins, E. G., Lowery, J. C., Kim, M., and Davis, J. A. Determinants of patient satisfaction in postmastectomy breast reconstruction. Plast. Reconstr. Surg. 106: 769, Khouri, R. K., Cooley, B. C., Kunselman, A. R., et al. A prospective study of microvascular free-flap surgery and outcome. Plast. Reconstr. Surg. 102: 711, Khouri, R. K. Avoiding free flap failure. Clin. Plast. Surg. 19: 773, Blondeel, P. N. The sensate free superior gluteal artery perforator (SGAP) flap: A valuable alternative in autologous breast reconstruction. Br. J. Plast. Surg. 52: 185, Kroll, S. S., Schusterman, M. A., Reece, G. P., et al. Choice of flap and incidence of free flap success. Plast. Reconstr. Surg. 98: 459, Conforti, M. L., Connor, N. P., Heisey, D. M., and Hartig, G. K. Evaluation of performance characteristics of the medicinal leech (Hirudo medicinalis) for the treat-
9 82 PLASTIC AND RECONSTRUCTIVE SURGERY, July 2004 ment of venous congestion. Plast. Reconstr. Surg. 109: 228, Hosmer, D. W., Hosmer, T., Le Cessie, S., and Lemeshow, S. A comparison of goodness-of-fit tests for the logistic regression model. Stat. Med. 16: 965, Chang, D. W., Wang, B., Robb, G. L., et al. Effect of obesity on flap and donor-site complications in free transverse rectus abdominis myocutaneous flap breast reconstruction. Plast. Reconstr. Surg. 105: 1640, Lipa, J. A., Youssef, A. A., Kuerer, H. M., Robb, G. L., and Chang, D. W. Breast reconstruction in older women: Advantages of autogenous tissue. Plast. Reconstr. Surg. 111: 1110, Girotto, J. A., Schreiber, J., and Nahabedian, M. Y. Breast reconstruction in the elderly: Preserving excellent quality of life. Ann. Plast. Surg. 50: 572, Serletti, J. M., Higgins, J. P., Moran, S., and Orlando, G. S. Factors affecting outcome in free tissue transfer in the elderly. Plast. Reconstr. Surg. 106: 66, Barr, L. C., and Joyce, A. D. Microvascular anastomoses in diabetes: An experimental study. Br. J. Plast. Surg. 42: 50, Colen, L. B., Stevenson, A., Siderov, V., et al. Microvascular anastomotic thrombosis in experimental diabetes mellitus. Plast. Reconstr. Surg. 99: 156, Cooley, B. C., Hanel, D. P., Anderson, R. B., Foster, M. D., and Gould, J. S. The influence of diabetes on free flap transfer: I. Flap survival and microvascular healing. Ann. Plast. Surg. 29: 58, Cooley, B. C., Hanel, D. P., Lan, M., Li, X., and Gould, J. S. The influence of diabetes on free flap transfer: II. The effect of ischemia on flap survival. Ann. Plast. Surg. 29: 65, Fagerstrom, K. The epidemiology of smoking: Health consequences and benefits of cessation. Drugs 62: 1, Cole, C. W., Hill, G. B., and Farzad, E. Cigarette smoking and peripheral arterial occlusive disease. Surgery 114: 756, Powell, J. T. Vascular damage from smoking: Disease mechanism at the arterial wall. Vasc. Med. 3: 21, Blann, A. D., Kirkpatrick, U., Devine, C., Naser, S., and McCollum, C. N. The influence of acute smoking on leukocytes, platelets, and the endothelium. Atherosclerosis 141: 133, Hutchinson, S. Smoking as a risk factor for endothelial dysfunction. Can. J. Cardiol. 14: 20, Chang, D. W., Reece, G. P., Wang, B., et al. Effect of smoking on complication in patients undergoing free TRAM breast reconstruction. Plast. Reconstr. Surg. 105: 2374, Padubidri, A. N., Yetman, R., Browne, E., et al. Complications of postmastectomy breast reconstruction in smokers, ex-smokers, and nonsmokers. Plast. Reconstr. Surg. 107: 342, Beckman, J. A., Thakore, A., Kalinowski, B. H., Harris, J. R., and Creager, M. A. Radiation therapy impairs endothelium-dependent vasodilation in humans. J. Am. Coll. Cardiol. 37: 761, Bernstein, E. F., Sullivan, F. J., Mitchell, J. B., Salomon, G. D., and Glatstein, E. Biology of chronic radiation effect on tissues and wound healing. Clin. Plast. Surg. 20: 435, Drake, D. B., and Oishi, S. N. Wound healing considerations in chemotherapy and radiation therapy. Clin. Plast. Surg. 22: 31, Schultze-Mosgau, S., Grabenbauer, G. G., Wehrhan, F., et al. Histomorphological structural changes of head and neck blood vessels after pre- or postoperative radiotherapy (in German). Strahlenther. Onkol. 178: 299, Hefel, L., Schwabegger, A., Ninkovic, M., et al. Internal mammary vessels: Anatomical and clinical implications. Br. J. Plast. Surg. 48: 527, Feng, L. J. Recipient vessels in free-flap breast reconstruction: A study of the internal mammary and thoracodorsal vessels. Plast. Reconstr. Surg. 99: 405, Strauch, B., and Yu, H. L. Atlas of Microvascular Surgery: Anatomy and Operative Approaches, 1st Ed. New York: Thieme, Pp Clark, C. P., Rohrich, R. J., Copit, S., Pittman, C. E., and Robinson, J. An anatomic study of the internal mammary veins: Clinical implications for free tissue transfer breast reconstruction. Plast. Reconstr. Surg. 99: 400, Lorenzetti, F., Kuokkanen, H., von Smitten, K., and Asko- Seljavaara, S. Intraoperative evaluation of blood flow in the internal mammary or thoracodorsal artery as a recipient vessel for a free TRAM flap. Ann. Plast. Surg. 46: 590, Lorenzetti, F., Souminen, S., Tukiaanen, E., et al. Evaluation of blood flow in free microvascular flaps. J. Reconstr. Microsurg. 17: 163, Moran, S. L., Nava, G., Benham, A. H., and Serletti, J. M. An outcome analysis comparing the thoracodorsal and internal mammary vessels as recipient sites for microvascular breast reconstruction: A prospective study of 100 patients. Plast. Reconstr. Surg. 111: 1876, Dupin, C. L., Allen, R. J., Glass, C. A., and Bunch, R. The internal mammary artery and vein as a recipient site for free-flap breast reconstruction: A report of 110 consecutive cases. Plast. Reconstr. Surg. 98: 685, Robb, G. L. Thoracodorsal vessels as a recipient site. Clin. Plast. Surg. 25: 207, 1998.
A multiple logistic regression analysis of complications following microsurgical breast reconstruction
 Original Article A multiple logistic regression analysis of complications following microsurgical breast reconstruction Samir Rao 1, Ellen C. Stolle 1, Sarah Sher 1, Chun-Wang Lin 1, Bahram Momen 2, Maurice
Original Article A multiple logistic regression analysis of complications following microsurgical breast reconstruction Samir Rao 1, Ellen C. Stolle 1, Sarah Sher 1, Chun-Wang Lin 1, Bahram Momen 2, Maurice
Clinical applications for the internal mammary artery
 ORIGINAL ARTICLE The Internal Mammary Artery and Vein as Recipient Vessels for Microvascular Breast Reconstruction: Are We Burning a Future Bridge? Maurice Y. Nahabedian, MD, FACS Abstract: Clinical applications
ORIGINAL ARTICLE The Internal Mammary Artery and Vein as Recipient Vessels for Microvascular Breast Reconstruction: Are We Burning a Future Bridge? Maurice Y. Nahabedian, MD, FACS Abstract: Clinical applications
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps
 Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Few would deny that lower abdominal tissue BREAST. An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction.
 BREAST An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction Aldona J. Spiegel, M.D. Farah N. Khan, M.D. Houston, Texas Background: The deep inferior epigastric perforator (DIEP)
BREAST An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction Aldona J. Spiegel, M.D. Farah N. Khan, M.D. Houston, Texas Background: The deep inferior epigastric perforator (DIEP)
Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC
 Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Breast reconstruction has an important role BREAST. A Two-Year Prospective Analysis of Trunk Function in TRAM Breast Reconstructions
 BREAST A Two-Year Prospective Analysis of Trunk Function in TRAM Breast Reconstructions Amy K. Alderman, M.D. William M. Kuzon, Jr., M.D., Ph.D. Edwin G. Wilkins, M.D. Ann Arbor, Mich. Background: Functional
BREAST A Two-Year Prospective Analysis of Trunk Function in TRAM Breast Reconstructions Amy K. Alderman, M.D. William M. Kuzon, Jr., M.D., Ph.D. Edwin G. Wilkins, M.D. Ann Arbor, Mich. Background: Functional
Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps
 BREAST SURGERY Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps Joshua L. Levine, MD,* Quintessa Miller, MD, Julie Vasile, MD,* Kamran Khoobehi,
BREAST SURGERY Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps Joshua L. Levine, MD,* Quintessa Miller, MD, Julie Vasile, MD,* Kamran Khoobehi,
A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction
 A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction In-Soo Baek 1, Jae-Pil You 1, Sung-Mi Rhee 1, Gil-Su Son 2, Deok-Woo Kim 1, Eun-Sang Dhong 1, Seung-Ha
A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction In-Soo Baek 1, Jae-Pil You 1, Sung-Mi Rhee 1, Gil-Su Son 2, Deok-Woo Kim 1, Eun-Sang Dhong 1, Seung-Ha
Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps
 Original Article Breast Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps James L. Mayo, MD Robert J. Allen, MD, FACS Alireza Sadeghi, MD, FACS Background: In cases of bilateral breast
Original Article Breast Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps James L. Mayo, MD Robert J. Allen, MD, FACS Alireza Sadeghi, MD, FACS Background: In cases of bilateral breast
Methods of autologous tissue breast reconstruction BREAST
 BREAST Comparison of Donor-Site Morbidity of SIEA, DIEP, and Muscle-Sparing TRAM Flaps for Breast Reconstruction Liza C. Wu, M.D. Anureet Bajaj, M.D. David W. Chang, M.D. Pierre M. Chevray, M.D., Ph.D.
BREAST Comparison of Donor-Site Morbidity of SIEA, DIEP, and Muscle-Sparing TRAM Flaps for Breast Reconstruction Liza C. Wu, M.D. Anureet Bajaj, M.D. David W. Chang, M.D. Pierre M. Chevray, M.D., Ph.D.
Reconstruction with autologous tissue remains a
 Original Article Increased Flap Weight and Decreased Perforator Number Predict Fat Necrosis in DIEP Breast Reconstruction Carolyn L. Mulvey, BS* Carisa M. Cooney, MPH* Francis F. Daily, BS* Elizabeth Colantuoni,
Original Article Increased Flap Weight and Decreased Perforator Number Predict Fat Necrosis in DIEP Breast Reconstruction Carolyn L. Mulvey, BS* Carisa M. Cooney, MPH* Francis F. Daily, BS* Elizabeth Colantuoni,
Breast Reconstruction Options
 Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
Breast Restoration Surgery After a mastectomy
 UW MEDICINE PATIENT EDUCATION Breast Restoration Surgery After a mastectomy This handout explains the most common procedures that are used at University of Washington Medical Center (UWMC) to restore a
UW MEDICINE PATIENT EDUCATION Breast Restoration Surgery After a mastectomy This handout explains the most common procedures that are used at University of Washington Medical Center (UWMC) to restore a
Immediate versus delayed free TRAM breast reconstruction: an analysis of perioperative factors and complications
 British Journal of Plastic Surgery (22), 55, l-6 9 22 The British Association of Plastic Surgeons doi:.54/bjps.22.3747 BRITISH JOURNAL OF / ~ ] PLASTIC SURGERY Immediate versus delayed free TRAM breast
British Journal of Plastic Surgery (22), 55, l-6 9 22 The British Association of Plastic Surgeons doi:.54/bjps.22.3747 BRITISH JOURNAL OF / ~ ] PLASTIC SURGERY Immediate versus delayed free TRAM breast
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study
 Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
JPRAS Open 3 (2015) 1e5. Contents lists available at ScienceDirect. JPRAS Open. journal homepage:
 JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate surgical options
 A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate
A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate
Breast Reconstruction
 Steven E. Copit, M.D. Chief- Division of Plastic Surgery Thomas Jefferson University Hospital Philadelphia, PA analysis of The Defect Skin Breast Volume Nipple Areola Complex analysis of The Defect the
Steven E. Copit, M.D. Chief- Division of Plastic Surgery Thomas Jefferson University Hospital Philadelphia, PA analysis of The Defect Skin Breast Volume Nipple Areola Complex analysis of The Defect the
Breast Reconstruction: Current Strategies and Future Opportunities
 Breast Reconstruction: Current Strategies and Future Opportunities Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery
Breast Reconstruction: Current Strategies and Future Opportunities Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery
The most common type of breast reconstruction
 BREAST Breast Reconstruction with Perforator Flaps Jay W. Granzow, M.D., M.P.H. Joshua L. Levine, M.D. Ernest S. Chiu, M.D. Maria M. LoTempio, M.D. Robert J. Allen, M.D. New Orleans, La.; Charleston, S.C.;
BREAST Breast Reconstruction with Perforator Flaps Jay W. Granzow, M.D., M.P.H. Joshua L. Levine, M.D. Ernest S. Chiu, M.D. Maria M. LoTempio, M.D. Robert J. Allen, M.D. New Orleans, La.; Charleston, S.C.;
The dissection of the rectus abdominis myocutaneous flap with complete preservation of the anterior rectus sheath q
 The British Association of Plastic Surgeons (2003) 56, 395 400 The dissection of the rectus abdominis myocutaneous flap with complete preservation of the anterior rectus sheath q D. Erni*, Y.D. Harder
The British Association of Plastic Surgeons (2003) 56, 395 400 The dissection of the rectus abdominis myocutaneous flap with complete preservation of the anterior rectus sheath q D. Erni*, Y.D. Harder
Samer Saour, Guido Libondi, Venkat Ramakrishnan. Introduction
 Original Article Microsurgical refinements with the use of internal mammary (IM) perforators as recipient vessels in transverse upper gracilis (TUG) autologous breast reconstruction Samer Saour, Guido
Original Article Microsurgical refinements with the use of internal mammary (IM) perforators as recipient vessels in transverse upper gracilis (TUG) autologous breast reconstruction Samer Saour, Guido
Current Strategies in Breast Reconstruction
 Current Strategies in Breast Reconstruction Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery 12 th Annual School of
Current Strategies in Breast Reconstruction Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery 12 th Annual School of
Update on Breast Reconstruction Using Free TRAM, DIEP, and SIEA Flaps
 Update on Breast Reconstruction Using Free TRAM, DIEP, and SIEA Flaps Pierre M. Chevray, M.D., Ph.D. 1 ABSTRACT Breast reconstruction using autologous tissue is commonly accomplished using the transverse
Update on Breast Reconstruction Using Free TRAM, DIEP, and SIEA Flaps Pierre M. Chevray, M.D., Ph.D. 1 ABSTRACT Breast reconstruction using autologous tissue is commonly accomplished using the transverse
Breast Reconstruction Surgery
 Breast Reconstruction Surgery I. Policy University Health Alliance (UHA) will reimburse for Breast Reconstruction Surgery when it is determined to be medically necessary and when it meets the medical criteria
Breast Reconstruction Surgery I. Policy University Health Alliance (UHA) will reimburse for Breast Reconstruction Surgery when it is determined to be medically necessary and when it meets the medical criteria
Interesting Case Series. Scalp Reconstruction With Free Latissimus Dorsi Muscle
 Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
The progress in microsurgical procedures has led
 Original Article Breast reconstruction with free anterolateral thigh flap Ranjit Raje, Ramesh Chepauk, Kanti Shetty, Rajendra Prasad J. S. Plastic & Reconstructive Services, Department of Surgical Oncology,
Original Article Breast reconstruction with free anterolateral thigh flap Ranjit Raje, Ramesh Chepauk, Kanti Shetty, Rajendra Prasad J. S. Plastic & Reconstructive Services, Department of Surgical Oncology,
INTRODUCTION. Toshihiko Satake 1, Jun Sugawara 2, Kazunori Yasumura 1, Taro Mikami 2, Shinji Kobayashi 3, Jiro Maegawa 2. Idea and Innovation
 Mini-Flow-Through Deep Inferior Epigastric Perforator Flap for Breast Reconstruction with Preservation of Both Internal Mammary and Deep Inferior Epigastric Vessels Toshihiko Satake 1, Jun Sugawara 2,
Mini-Flow-Through Deep Inferior Epigastric Perforator Flap for Breast Reconstruction with Preservation of Both Internal Mammary and Deep Inferior Epigastric Vessels Toshihiko Satake 1, Jun Sugawara 2,
The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography
 BREAST The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography Corrine Wong, M.D. Purushottam Nagarkar, M.D. Sumeet Teotia, M.D. Nicholas
BREAST The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography Corrine Wong, M.D. Purushottam Nagarkar, M.D. Sumeet Teotia, M.D. Nicholas
Advances in Localized Breast Cancer
 Advances in Localized Breast Cancer Melissa Camp, MD, MPH and Fariba Asrari, MD June 18, 2018 Moderated by Elissa Bantug 1 Advances in Surgery for Breast Cancer Melissa Camp, MD June 18, 2018 2 Historical
Advances in Localized Breast Cancer Melissa Camp, MD, MPH and Fariba Asrari, MD June 18, 2018 Moderated by Elissa Bantug 1 Advances in Surgery for Breast Cancer Melissa Camp, MD June 18, 2018 2 Historical
Prophylactic Mastectomy & Reconstructive Implications
 Prophylactic Mastectomy & Reconstructive Implications Minas T Chrysopoulo, MD PRMA Center For Advanced Breast Reconstruction Prophylactic Mastectomy Surgical removal of one or both breasts to reduce the
Prophylactic Mastectomy & Reconstructive Implications Minas T Chrysopoulo, MD PRMA Center For Advanced Breast Reconstruction Prophylactic Mastectomy Surgical removal of one or both breasts to reduce the
Advances in Breast Surgery. Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015
 Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Advances and Surgical Decision-Making for Breast Reconstruction
 893 Advances and Surgical Decision-Making for Breast Reconstruction Steven J. Kronowitz, MD 1 Henry M. Kuerer, MD, PhD 2 1 Department of Plastic and Reconstructive Surgery, The University of Texas M. D.
893 Advances and Surgical Decision-Making for Breast Reconstruction Steven J. Kronowitz, MD 1 Henry M. Kuerer, MD, PhD 2 1 Department of Plastic and Reconstructive Surgery, The University of Texas M. D.
Breast reconstruction following mastectomy has
 Free full text on www.ijps.org Post-mastectomy breast reconstruction: Microsurgical methods Venkat Ramakrishnan, Makarand Tare St. Andrew s Centre for Burns and Plastic Surgery, BroomÞ eld Hospital, Chelmsford,
Free full text on www.ijps.org Post-mastectomy breast reconstruction: Microsurgical methods Venkat Ramakrishnan, Makarand Tare St. Andrew s Centre for Burns and Plastic Surgery, BroomÞ eld Hospital, Chelmsford,
breast reconstruction
 2.0 ANCC CONTACT HOURS Autologous microvascular breast reconstruction Postoperative strategies to improve outcomes By Maurice Y. Nahabedian, MD, FACS, and Anissa G. Nahabedian, BSN, RN BREAST RECONSTRUCTION
2.0 ANCC CONTACT HOURS Autologous microvascular breast reconstruction Postoperative strategies to improve outcomes By Maurice Y. Nahabedian, MD, FACS, and Anissa G. Nahabedian, BSN, RN BREAST RECONSTRUCTION
Breast Reconstruction in Women Under 30: A 10-Year Experience
 ORIGINAL ARTICLE Breast Reconstruction in Women Under 30: A 10-Year Experience Warren A. Ellsworth, MD,* Barbara L. Bass, MD, FACS, Roman J. Skoracki, MD, à and Lior Heller, MD* *Division of Plastic Surgery,
ORIGINAL ARTICLE Breast Reconstruction in Women Under 30: A 10-Year Experience Warren A. Ellsworth, MD,* Barbara L. Bass, MD, FACS, Roman J. Skoracki, MD, à and Lior Heller, MD* *Division of Plastic Surgery,
The decision to repair a partial mastectomy CME. State of the Art and Science in Postmastectomy Breast Reconstruction.
 CME State of the Art and Science in Postmastectomy Breast Reconstruction Steven J. Kronowitz, M.D. Houston, Texas Learning Objectives: After reading this article, the participant should be able to: 1.
CME State of the Art and Science in Postmastectomy Breast Reconstruction Steven J. Kronowitz, M.D. Houston, Texas Learning Objectives: After reading this article, the participant should be able to: 1.
Citation for published version (APA): Benditte-Klepetko, H. C. (2014). Breast surgery: A problem of beauty or health?
 UvA-DARE (Digital Academic Repository) Breast surgery: A problem of beauty or health? Benditte-Klepetko, H.C. Link to publication Citation for published version (APA): Benditte-Klepetko, H. C. (2014).
UvA-DARE (Digital Academic Repository) Breast surgery: A problem of beauty or health? Benditte-Klepetko, H.C. Link to publication Citation for published version (APA): Benditte-Klepetko, H. C. (2014).
Medical Journal of the Volume 20 Islamic Republic of Iran Number 3 Fall 1385 November Original Articles
 Medical Journal of the Volume 0 Islamic Republic of Iran Number 3 Fall 38 November 00 Original Articles ANATOMY OF THE SUPERFICIAL INFERIOR EPIGASTRIC ARTERY FLAP MAHDI FATHI, M.D., EBRAHIM HATAMIPOUR,
Medical Journal of the Volume 0 Islamic Republic of Iran Number 3 Fall 38 November 00 Original Articles ANATOMY OF THE SUPERFICIAL INFERIOR EPIGASTRIC ARTERY FLAP MAHDI FATHI, M.D., EBRAHIM HATAMIPOUR,
How many procedures to make a breast?
 British Journal of Plastic Surgery (00 ), 5, 7-3 9 00 The British Association of Plastic Surgeons doi: 0.05/bjps.000.3538 BRITISH JOURNAL OF PLASTIC SURGERY How many procedures to make a breast? A. D.
British Journal of Plastic Surgery (00 ), 5, 7-3 9 00 The British Association of Plastic Surgeons doi: 0.05/bjps.000.3538 BRITISH JOURNAL OF PLASTIC SURGERY How many procedures to make a breast? A. D.
Updates in Breast Care. Truth or Hype. History of Breast Cancer Surgery. Dr Karen Barbosa 5/3/2017 4/20/2017
 Updates in Breast Care Dr Karen Barbosa 4/20/2017 Truth or Hype Princess Bust Developer Sears, Roebuck and Co. 1897 Promised to make the breast round, firm and beautiful History of Breast Cancer Surgery
Updates in Breast Care Dr Karen Barbosa 4/20/2017 Truth or Hype Princess Bust Developer Sears, Roebuck and Co. 1897 Promised to make the breast round, firm and beautiful History of Breast Cancer Surgery
SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni
 SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni Icro Meattini, MD Radiation Oncology Department - University of Florence Azienda Ospedaliero Universitaria Careggi Firenze Breast
SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni Icro Meattini, MD Radiation Oncology Department - University of Florence Azienda Ospedaliero Universitaria Careggi Firenze Breast
Flaps vs Grafts. Ronen Avram, MD MSc FRCSC
 Flaps vs Grafts Ronen Avram, MD MSc FRCSC POS Keratoacanthoma is not a malignant tumor! Methods of Reconstruction Reconstructive Ladder Primary closure Primary Delayed Secondary Intention Skin Graft Pedicled
Flaps vs Grafts Ronen Avram, MD MSc FRCSC POS Keratoacanthoma is not a malignant tumor! Methods of Reconstruction Reconstructive Ladder Primary closure Primary Delayed Secondary Intention Skin Graft Pedicled
Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes
 DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
The free thoracodorsal artery perforator flap in head and neck reconstruction
 European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 167 171 Available online at www.sciencedirect.com TECHNICAL NOTE The free thoracodorsal artery perforator flap in head and neck
European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 167 171 Available online at www.sciencedirect.com TECHNICAL NOTE The free thoracodorsal artery perforator flap in head and neck
Michael A. Howard a, Babak Mehrara b, * REVIEW. Introduction
 International Journal of Surgery (2005) 3, 53e60 www.int-journal-surgery.com REVIEW Emerging trends in microsurgical breast reconstruction: Deep inferior epigastric artery perforator (DIEP) and the superior
International Journal of Surgery (2005) 3, 53e60 www.int-journal-surgery.com REVIEW Emerging trends in microsurgical breast reconstruction: Deep inferior epigastric artery perforator (DIEP) and the superior
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer. Oncoplastic and Reconstructive Surgery
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Oncoplastic and Reconstructive Surgery Plastic-reconstructive aspects after mastectomy Versions 2002 2017: Audretsch / Bauerfeind
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Oncoplastic and Reconstructive Surgery Plastic-reconstructive aspects after mastectomy Versions 2002 2017: Audretsch / Bauerfeind
The use of postmastectomy radiation therapy (PMRT) to prevent
 NORTHEASTERN SOCIETY OF PLASTIC SURGEONS Postmastectomy Radiation Therapy and Breast An Analysis of Complications and Patient Satisfaction Bernard T. Lee, MD,* Tolulope A. Adesiyun, BS,* Salih Colakoglu,
NORTHEASTERN SOCIETY OF PLASTIC SURGEONS Postmastectomy Radiation Therapy and Breast An Analysis of Complications and Patient Satisfaction Bernard T. Lee, MD,* Tolulope A. Adesiyun, BS,* Salih Colakoglu,
INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP
 INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify
INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify
B11 Breast Reconstruction with Abdominal Tissue Flap
 B11 Breast Reconstruction with Abdominal Tissue Flap Issued March 2011 You can get more information about this procedure from www.aboutmyhealth.org Tell us how useful you found this document at www.patientfeedback.org
B11 Breast Reconstruction with Abdominal Tissue Flap Issued March 2011 You can get more information about this procedure from www.aboutmyhealth.org Tell us how useful you found this document at www.patientfeedback.org
Microvascular free tissue transfer is a standard
 ORIGINAL ARTICLE INTERNAL MAMMARY ARTERY AND VEIN: RECIPIENT VESSELS FOR FREE TISSUE TRANSFER TO THE HEAD AND NECK IN THE VESSEL-DEPLETED NECK Mark L. Urken, MD, 1 Kevin M. Higgins, MD, 2 Bryant Lee, MD,
ORIGINAL ARTICLE INTERNAL MAMMARY ARTERY AND VEIN: RECIPIENT VESSELS FOR FREE TISSUE TRANSFER TO THE HEAD AND NECK IN THE VESSEL-DEPLETED NECK Mark L. Urken, MD, 1 Kevin M. Higgins, MD, 2 Bryant Lee, MD,
Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps
 e50 Case Report THIEME Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps Shuhei Yoshida, MD 1 Isao Koshima, MD 1 Shogo Nagamatsu, MD 2 Kazunori Yokota, MD 2 Shuji Yamashita,
e50 Case Report THIEME Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps Shuhei Yoshida, MD 1 Isao Koshima, MD 1 Shogo Nagamatsu, MD 2 Kazunori Yokota, MD 2 Shuji Yamashita,
Anterolateral Thigh Flap for Postmastectomy Breast Reconstruction
 Anterolateral Thigh Flap for Postmastectomy Breast Reconstruction Fu-chan Wei, M.D., Sinikka Suominen, M.D., Ph.D., Ming-huei Cheng, M.D., Naci Celik, M.D., and Yung-lung Lai, M.D. Taipei, Taiwan Most
Anterolateral Thigh Flap for Postmastectomy Breast Reconstruction Fu-chan Wei, M.D., Sinikka Suominen, M.D., Ph.D., Ming-huei Cheng, M.D., Naci Celik, M.D., and Yung-lung Lai, M.D. Taipei, Taiwan Most
Breast Reconstruction. Westmead Breast Cancer Institute
 Breast Reconstruction Westmead Breast Cancer Institute What is breast reconstruction? Breast reconstruction is a surgical procedure that creates a shape on the chest wall following a mastectomy. Occasionally,
Breast Reconstruction Westmead Breast Cancer Institute What is breast reconstruction? Breast reconstruction is a surgical procedure that creates a shape on the chest wall following a mastectomy. Occasionally,
Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects
 Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects Joshua L. Levine, M.D., Nassif E. Soueid, M.D., and Robert J. Allen, M.D. New Orleans, La. Background: The use of lateral thoracic
Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects Joshua L. Levine, M.D., Nassif E. Soueid, M.D., and Robert J. Allen, M.D. New Orleans, La. Background: The use of lateral thoracic
In the UK approximately 40,000
 The patient journey in DIEP flap breast reconstruction BY OLIVIER ALEXANDRE BRANFORD AND PAUL ANTHONY HARRIS In the UK approximately 40,000 women are diagnosed with breast cancer every year. About 40%
The patient journey in DIEP flap breast reconstruction BY OLIVIER ALEXANDRE BRANFORD AND PAUL ANTHONY HARRIS In the UK approximately 40,000 women are diagnosed with breast cancer every year. About 40%
Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION
 Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION BREAST RECONSTRUCTION: A WOMAN S DECISION Options and Information Our approach to breast reconstruction entails a very
Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION BREAST RECONSTRUCTION: A WOMAN S DECISION Options and Information Our approach to breast reconstruction entails a very
BREAST RECONSTRUCTION POST MASTECTOMY
 UnitedHealthcare Commercial Coverage Determination Guideline BREAST RECONSTRUCTION POST MASTECTOMY Guideline Number: SUR057 Effective Date: January 1, 2019 Table of Contents Page INSTRUCTIONS FOR USE...
UnitedHealthcare Commercial Coverage Determination Guideline BREAST RECONSTRUCTION POST MASTECTOMY Guideline Number: SUR057 Effective Date: January 1, 2019 Table of Contents Page INSTRUCTIONS FOR USE...
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
National Mastectomy & Breast Reconstruction Audit Datasheet - Mastectomy +/- Immediate Reconstruction
 Patient Registration data Surname Forename NHS/Private Hospital Number Date of birth Postcode Ethnicity Patient-reported outcomes consent Has this patient consented to being sent outcome questionnaires?
Patient Registration data Surname Forename NHS/Private Hospital Number Date of birth Postcode Ethnicity Patient-reported outcomes consent Has this patient consented to being sent outcome questionnaires?
BREAST RECONSTRUCTION POST MASTECTOMY
 UnitedHealthcare Commercial Coverage Determination Guideline BREAST RECONSTRUCTION POST MASTECTOMY Guideline Number: SUR057 Effective Date: February 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...
UnitedHealthcare Commercial Coverage Determination Guideline BREAST RECONSTRUCTION POST MASTECTOMY Guideline Number: SUR057 Effective Date: February 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...
Exercise & Breast Cancer Recovery
 Exercise & Breast Cancer Recovery LEARNING OBJECTIVES Demonstrate an understanding of the diagnosis and treatment of breast cancer Demonstrate an understanding of how breast cancer surgery and treatment
Exercise & Breast Cancer Recovery LEARNING OBJECTIVES Demonstrate an understanding of the diagnosis and treatment of breast cancer Demonstrate an understanding of how breast cancer surgery and treatment
Procedure Information Guide
 Procedure Information Guide Breast reconstruction with abdominal tissue flap Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every
Procedure Information Guide Breast reconstruction with abdominal tissue flap Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every
Challenging a Traditional Paradigm: 12-Year Experience with Autologous Free Flap Breast Reconstruction for Inflammatory Breast Cancer
 BREAST Challenging a Traditional Paradigm: 12-Year Experience with Autologous Free Flap Breast Reconstruction for Inflammatory Breast Cancer Edward I. Chang, M.D. Eric I. Chang, M.D. Ran Ito, M.D., Ph.D.
BREAST Challenging a Traditional Paradigm: 12-Year Experience with Autologous Free Flap Breast Reconstruction for Inflammatory Breast Cancer Edward I. Chang, M.D. Eric I. Chang, M.D. Ran Ito, M.D., Ph.D.
Supplementary Online Content
 Supplementary Online Content Abt NB, Flores JM, Baltodano PA, et al. Neoadjuvant chemotherapy and short-term in patients undergoing mastectomy with and without breast reconstruction. JAMA Surg. Published
Supplementary Online Content Abt NB, Flores JM, Baltodano PA, et al. Neoadjuvant chemotherapy and short-term in patients undergoing mastectomy with and without breast reconstruction. JAMA Surg. Published
PUT YOUR BEST FOOT FORWARD
 PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
Since originally described by Hartrampf et al. BREAST
 BREAST Assessment of Zonal Perfusion Using Intraoperative Angiography during Abdominal Flap Breast Reconstruction Albert Losken, M.D. Michael R. Zenn, M.D. Josh A. Hammel, M.D. Mark W. Walsh, M.D. Grant
BREAST Assessment of Zonal Perfusion Using Intraoperative Angiography during Abdominal Flap Breast Reconstruction Albert Losken, M.D. Michael R. Zenn, M.D. Josh A. Hammel, M.D. Mark W. Walsh, M.D. Grant
Abdominal-based reconstruction is considered
 Original Article Salvage of Intraoperative Deep Inferior Epigastric Perforator Flap Venous Congestion with Augmentation of Venous Outflow: Flap Morbidity and Review of the Literature Oscar Ochoa, MD Steven
Original Article Salvage of Intraoperative Deep Inferior Epigastric Perforator Flap Venous Congestion with Augmentation of Venous Outflow: Flap Morbidity and Review of the Literature Oscar Ochoa, MD Steven
Do Preexisting Abdominal Scars Threaten Wound Healing in Abdominoplasty?
 Do Preexisting Abdominal Scars Threaten Wound Healing in Abdominoplasty? Michele A. Shermak, MD, Jessie Mallalieu, PA-C, and David Chang, PhD, MPH, MBA The Johns Hopkins Medical Institutions, Division
Do Preexisting Abdominal Scars Threaten Wound Healing in Abdominoplasty? Michele A. Shermak, MD, Jessie Mallalieu, PA-C, and David Chang, PhD, MPH, MBA The Johns Hopkins Medical Institutions, Division
Case Study. TRAM Flap Reconstruction with an Associated Complication. Repair using DermaMatrix Acellular Dermis.
 Case Study TRAM Flap Reconstruction with an Associated Complication. Repair using DermaMatrix Acellular Dermis. TRAM Flap Reconstruction with an Associated Complication Challenge Insulin-dependent diabetes
Case Study TRAM Flap Reconstruction with an Associated Complication. Repair using DermaMatrix Acellular Dermis. TRAM Flap Reconstruction with an Associated Complication Challenge Insulin-dependent diabetes
Figure 1. Anatomy of the breast
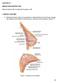 CHAPTER 12 BREAST RECONSTRUCTION Mihaela Rapolti, MD and Michelle Roughton, MD I. BREAST ANATOMY A. Mastering breast anatomy is essential for understanding how the breast changes with aging and principles
CHAPTER 12 BREAST RECONSTRUCTION Mihaela Rapolti, MD and Michelle Roughton, MD I. BREAST ANATOMY A. Mastering breast anatomy is essential for understanding how the breast changes with aging and principles
Latissimus Dorsi Myocutaneous Flap for Breast Reconstruction: Bad Rap or Good Flap?
 Latissimus Dorsi Myocutaneous Flap for Breast Reconstruction: Bad Rap or Good Flap? Galen Perdikis, MD, Stephanie Koonce, MD, George Collis, MD, and Dustin Eck, MD Mayo Clinic, Jacksonville, FL Correspondence:
Latissimus Dorsi Myocutaneous Flap for Breast Reconstruction: Bad Rap or Good Flap? Galen Perdikis, MD, Stephanie Koonce, MD, George Collis, MD, and Dustin Eck, MD Mayo Clinic, Jacksonville, FL Correspondence:
Goals of Care. Restore shape and function after cancer
 Goals of Care Restore shape and function after cancer Aid in physiological and psychological benefit Relationship with significant other Self esteem and positive body image Feeling of a whole body Avoid
Goals of Care Restore shape and function after cancer Aid in physiological and psychological benefit Relationship with significant other Self esteem and positive body image Feeling of a whole body Avoid
Anterograde Intra-Arterial Urokinase Injection for Salvaging Fibular Free Flap
 Anterograde Intra-Arterial Urokinase Injection for Salvaging Fibular Free Flap Dae-Sung Lee, Sun-Il Jung, Deok-Woo Kim, Eun-Sang Dhong Department of Plastic and Reconstructive Surgery, Korea University
Anterograde Intra-Arterial Urokinase Injection for Salvaging Fibular Free Flap Dae-Sung Lee, Sun-Il Jung, Deok-Woo Kim, Eun-Sang Dhong Department of Plastic and Reconstructive Surgery, Korea University
Is Unilateral Implant or Autologous Breast Reconstruction Better in Obtaining Breast Symmetry?
 ORIGINAL ARTICLE Is Unilateral Implant or Autologous Breast Reconstruction Better in Obtaining Breast Symmetry? Oriana Cohen, MD, Kevin Small, MD, Christina Lee, BA, Oriana Petruolo, MD, Nolan Karp, MD,
ORIGINAL ARTICLE Is Unilateral Implant or Autologous Breast Reconstruction Better in Obtaining Breast Symmetry? Oriana Cohen, MD, Kevin Small, MD, Christina Lee, BA, Oriana Petruolo, MD, Nolan Karp, MD,
Risk factors for the initiation and aggravation of lymphoedema after axillary lymph node dissection for breast cancer
 HEALTH SERVICES RESEARCH FUND Risk factors for the initiation and aggravation of lymphoedema after axillary lymph node dissection for breast cancer Key Messages 1. Previous inflammation or infection of
HEALTH SERVICES RESEARCH FUND Risk factors for the initiation and aggravation of lymphoedema after axillary lymph node dissection for breast cancer Key Messages 1. Previous inflammation or infection of
Medical Policy Original Effective Date: Revised Date: Page 1 of 8
 Page 1 of 8 Disclaimer Description Coverage Determination Refer to the member s specific benefit plan and Schedule of Benefits to determine coverage. This may not be a benefit on all plans, or the plan
Page 1 of 8 Disclaimer Description Coverage Determination Refer to the member s specific benefit plan and Schedule of Benefits to determine coverage. This may not be a benefit on all plans, or the plan
Comparing the donor-site morbidity using DIEP, SIEA or MS-TRAM flaps for breast reconstructive surgery: A meta-analysis
 Journal of Plastic, Reconstructive & Aesthetic Surgery (2012) 65, 1474e1480 REVIEW Comparing the donor-site morbidity using DIEP, SIEA or MS-TRAM flaps for breast reconstructive surgery: A meta-analysis
Journal of Plastic, Reconstructive & Aesthetic Surgery (2012) 65, 1474e1480 REVIEW Comparing the donor-site morbidity using DIEP, SIEA or MS-TRAM flaps for breast reconstructive surgery: A meta-analysis
The microvascular anastomotic coupler for venous anastomoses in free flap breast reconstruction improves outcomes
 Original Article The microvascular anastomotic coupler for venous anastomoses in free flap breast reconstruction improves outcomes Edmund Fitzgerald O Connor 1,2, Warren Matthew Rozen 2, Muhammad Chowdhry
Original Article The microvascular anastomotic coupler for venous anastomoses in free flap breast reconstruction improves outcomes Edmund Fitzgerald O Connor 1,2, Warren Matthew Rozen 2, Muhammad Chowdhry
Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study
 Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study Raphael Sinna, MD, a Hassene Hajji, MD, b Quentin Qassemyar,
Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study Raphael Sinna, MD, a Hassene Hajji, MD, b Quentin Qassemyar,
In autogenous breast reconstruction, traditional SPECIAL TOPIC
 SPECIAL TOPIC Wall following Free TRAM or DIEP Flap Reconstruction: A Meta-Analysis and Critical Review Li-Xing Man, M.D., M.Sc. Jesse C. Selber, M.D., M.P.H. Joseph M. Serletti, M.D. Pittsburgh and Philadelphia,
SPECIAL TOPIC Wall following Free TRAM or DIEP Flap Reconstruction: A Meta-Analysis and Critical Review Li-Xing Man, M.D., M.Sc. Jesse C. Selber, M.D., M.P.H. Joseph M. Serletti, M.D. Pittsburgh and Philadelphia,
4/30/2010. Options for abdominal wall reconstruction. Scott L. Hansen, MD
 Components Separation Scott L. Hansen, MD University of California, San Francisco Chief, Plastic and Reconstructive Surgery San Francisco General Hospital Overview Options for abdominal wall reconstruction
Components Separation Scott L. Hansen, MD University of California, San Francisco Chief, Plastic and Reconstructive Surgery San Francisco General Hospital Overview Options for abdominal wall reconstruction
Fluorescence Angiography in Limb Salvage
 Fluorescence Angiography in Limb Salvage Ryan H. Fitzgerald, DPM, FACFAS Associate Professor of Surgery-University Of South Carolina School of Medicine, Greenville Etiology of Lower extremity wounds Neuropathy
Fluorescence Angiography in Limb Salvage Ryan H. Fitzgerald, DPM, FACFAS Associate Professor of Surgery-University Of South Carolina School of Medicine, Greenville Etiology of Lower extremity wounds Neuropathy
Microvascular Free Flaps: Experience in Kwong Wah Hospital
 VOL. VOL.NO. NO. MAYNOVEMBER Microvascular Free Flaps: Experience in Kwong Wah Hospital Dr. Chiu-ming Ho, Dr. Vana SH Chan, Dr. Ming-shiaw Cheng, Dr. Wing-yung Cheung Division of Plastic Surgery, Department
VOL. VOL.NO. NO. MAYNOVEMBER Microvascular Free Flaps: Experience in Kwong Wah Hospital Dr. Chiu-ming Ho, Dr. Vana SH Chan, Dr. Ming-shiaw Cheng, Dr. Wing-yung Cheung Division of Plastic Surgery, Department
Abdominal perforator vs. muscle sparing flaps for breast reconstruction
 Review Article Abdominal perforator vs. muscle sparing flaps for breast reconstruction Paris D. Butler, Liza C. Wu Division of Plastic Surgery, Department of Surgery, University of Pennsylvania Health
Review Article Abdominal perforator vs. muscle sparing flaps for breast reconstruction Paris D. Butler, Liza C. Wu Division of Plastic Surgery, Department of Surgery, University of Pennsylvania Health
The lumbar artery perforator based island flap: anatomical study and case reports
 British Journal of Plastic Surgery (1999), 52, 541 546 1999 The British Association of Plastic Surgeons The lumbar artery perforator based island flap: anatomical study and case reports H. Kato*, M. Hasegawa,
British Journal of Plastic Surgery (1999), 52, 541 546 1999 The British Association of Plastic Surgeons The lumbar artery perforator based island flap: anatomical study and case reports H. Kato*, M. Hasegawa,
BREAST RECONSTRUCTION/REMOVAL AND REPLACEMENT OF IMPLANTS
 Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent upon
Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent upon
Increasing options in autologous microsurgical breast reconstruction: four free flaps for stacked bilateral breast reconstruction
 Case Report Increasing options in autologous microsurgical breast reconstruction: four free flaps for stacked bilateral breast reconstruction Warren Matthew Rozen 1,2, Nakul Gamanlal Patel 1, Venkat V.
Case Report Increasing options in autologous microsurgical breast reconstruction: four free flaps for stacked bilateral breast reconstruction Warren Matthew Rozen 1,2, Nakul Gamanlal Patel 1, Venkat V.
In a second stage or a second operation that tissue expander is removed through the same incision and the implant is placed within the chest pocket.
 Hello, I m Summer Hanson. I m an assistant professor in the Department of Plastics & Reconstructive Surgery at The University of Texas MD Anderson Cancer Center and today I m going to talk about the role
Hello, I m Summer Hanson. I m an assistant professor in the Department of Plastics & Reconstructive Surgery at The University of Texas MD Anderson Cancer Center and today I m going to talk about the role
The Superficial Inferior Epigastric Artery (SIEA) Flap and Its Applications in Breast Reconstruction
 The Superficial Inferior Epigastric Artery (SIEA) Flap and Its Applications in Breast Reconstruction Zachary Menn and Aldona Spiegel Weill Cornell Medical College, The Methodist Hospital, Houston, Texas,
The Superficial Inferior Epigastric Artery (SIEA) Flap and Its Applications in Breast Reconstruction Zachary Menn and Aldona Spiegel Weill Cornell Medical College, The Methodist Hospital, Houston, Texas,
Achieving ideal donor site aesthetics with autologous breast reconstruction
 Review Article Achieving ideal donor site aesthetics with autologous breast reconstruction Maurice Y. Nahabedian Department of Plastic Surgery, Georgetown University, Washington, DC 20007, USA Correspondence
Review Article Achieving ideal donor site aesthetics with autologous breast reconstruction Maurice Y. Nahabedian Department of Plastic Surgery, Georgetown University, Washington, DC 20007, USA Correspondence
Annals of Medicine and Surgery
 Annals of Medicine and Surgery 4 (2015) 293e300 Contents lists available at ScienceDirect Annals of Medicine and Surgery journal homepage: www.annalsjournal.com Total rib -preservation technique of internal
Annals of Medicine and Surgery 4 (2015) 293e300 Contents lists available at ScienceDirect Annals of Medicine and Surgery journal homepage: www.annalsjournal.com Total rib -preservation technique of internal
The success of breast conservation protocols BREAST. Implant Reconstruction in Breast Cancer Patients Treated with Radiation Therapy
 BREAST Implant Reconstruction in Breast Cancer Patients Treated with Radiation Therapy Jeffrey A. Ascherman, M.D. Matthew M. Hanasono, M.D. Martin I. Newman, M.D. Duncan B. Hughes, M.D. New York, N.Y.
BREAST Implant Reconstruction in Breast Cancer Patients Treated with Radiation Therapy Jeffrey A. Ascherman, M.D. Matthew M. Hanasono, M.D. Martin I. Newman, M.D. Duncan B. Hughes, M.D. New York, N.Y.
Microsurgical Breast Reconstruction in Thin Patients: The Impact of Low Body Mass Indices
 20 Original Article Microsurgical Breast Reconstruction in Thin Patients: The Impact of Low Body Mass Indices Katie E. Weichman, MD 1 Neil Tanna, MD, MBA 1 P. Niclas Broer, MD 1 Stelios Wilson, MD 1 Hamdan
20 Original Article Microsurgical Breast Reconstruction in Thin Patients: The Impact of Low Body Mass Indices Katie E. Weichman, MD 1 Neil Tanna, MD, MBA 1 P. Niclas Broer, MD 1 Stelios Wilson, MD 1 Hamdan
Autogenous Tissue Breast Reconstruction in the Silicone-Intolerant Patient
 440 Autogenous Tissue Breast Reconstruction in the Silicone-Intolerant Patient Lu-Jean Feng, M.D.,* Kate Mauceri, R.N.,* and Bruce E. Berger, M.D.t Background. Concerns regarding the safety of silicone
440 Autogenous Tissue Breast Reconstruction in the Silicone-Intolerant Patient Lu-Jean Feng, M.D.,* Kate Mauceri, R.N.,* and Bruce E. Berger, M.D.t Background. Concerns regarding the safety of silicone
Role of heparin in microvascular free flap surgery in head and neck reconstruction
 International Surgery Journal Agrawal G et al. Int Surg J. 2015 Nov;2(4):534-538 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20151075
International Surgery Journal Agrawal G et al. Int Surg J. 2015 Nov;2(4):534-538 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20151075
Breast Reconstruction: Patient Information Document
 breastreconstructioncanada.ca Breast Reconstruction: Patient Information Document By Dr. Nicolas Guay Dr. Haemi Lee STANDARDIZED BREAST RECONSTRUCTION PATIENT INFORMATION TABLE OF CONTENTS Glossary...
breastreconstructioncanada.ca Breast Reconstruction: Patient Information Document By Dr. Nicolas Guay Dr. Haemi Lee STANDARDIZED BREAST RECONSTRUCTION PATIENT INFORMATION TABLE OF CONTENTS Glossary...
Peter McAllister, 1 Isabel Teo, 1 Kuen Chin, 1 Boikanyo Makubate, 2 and David Alexander Munnoch Introduction
 Hindawi Publishing Corporation Plastic Surgery International Volume 2016, Article ID 6085624, 9 pages http://dx.doi.org/10.1155/2016/6085624 Research Article Bilateral Breast Reconstruction with Abdominal
Hindawi Publishing Corporation Plastic Surgery International Volume 2016, Article ID 6085624, 9 pages http://dx.doi.org/10.1155/2016/6085624 Research Article Bilateral Breast Reconstruction with Abdominal
Breast Cancer Reconstruction
 Breast Cancer Jerome H. Liu, MD Tom S. Liu, MD Jerome H. Liu, MD Undergraduate: Brown University Medical School: University of California, Los Angeles Residency: UCLA Medical Center Fellowship:UCLA Medical
Breast Cancer Jerome H. Liu, MD Tom S. Liu, MD Jerome H. Liu, MD Undergraduate: Brown University Medical School: University of California, Los Angeles Residency: UCLA Medical Center Fellowship:UCLA Medical
CLINICAL EXPERIENCE OF A MICROVASCULAR VENOUS COUPLER DEVICE IN FREE TISSUE TRANSFERS
 CLINICAL EXPERIENCE OF A MICROVASCULAR VENOUS COUPLER DEVICE IN FREE TISSUE TRANSFERS Kao-Ping Chang, Sin-Daw Lin, and Chung-Sheng Lai Faculty of Medicine, College of Medicine, Kaohsiung Medical University,
CLINICAL EXPERIENCE OF A MICROVASCULAR VENOUS COUPLER DEVICE IN FREE TISSUE TRANSFERS Kao-Ping Chang, Sin-Daw Lin, and Chung-Sheng Lai Faculty of Medicine, College of Medicine, Kaohsiung Medical University,
