The microvascular anastomotic coupler for venous anastomoses in free flap breast reconstruction improves outcomes
|
|
|
- Alice Gray
- 6 years ago
- Views:
Transcription
1 Original Article The microvascular anastomotic coupler for venous anastomoses in free flap breast reconstruction improves outcomes Edmund Fitzgerald O Connor 1,2, Warren Matthew Rozen 2, Muhammad Chowdhry 2, Nakul Gamanlal Patel 2, Whitney T.H. Chow 1,2, Matthew Griffiths 1,2, Venkat V. Ramakrishnan 1,2 1 St Andrew s Anglia Ruskin (StAAR) Research Unit, 2 St Andrew s Centre for Plastic Surgery and Burns, Broomfield Hospital, Mid Essex Hospital Services NHS Trust, Chelmsford, Essex CM1 7ET, UK Correspondence to: Edmund Fitzgerald O Connor. St Andrew s Centre for Plastic Surgery and Burns, Room E322, Mayflower Ward, Level 3, Zone E, West Wing, Broomfield Hospital, Mid Essex Hospital Services NHS Trust, Chelmsford, Essex CM1 7ET, UK. edmundfitz@doctors.org.uk. Background: Venous couplers are ubiquitous around the world and are a useful tool for the reconstructive microsurgeon. A systematic review of coupler performance studies demonstrated a thrombosis rate range of 0% to 3%, whilst the average time of using the device is 5 minutes. There is sparse published data on cost analysis and the impact of operator experience on the anastomotic coupler device success. Improvements in outcomes other than time benefits have also not been shown. This study aims to address these deficiencies in the literature. Methods: A retrospective clinical study was undertaken, aiming to compare equivalent groups of patients that had free flap surgery with venous micro-anastomoses with those that had sutured anastomoses. The cohort comprised all patients undergoing microsurgical breast reconstruction at the St Andrew s Centre for Plastic Surgery & Burns from January 2009 to December Results: Between January 2010 to December 2014, 1,064 patients underwent 1,206 free flap breast reconstructions. The average age of patients was 50 years. Seventy percent of patients underwent mastectomy and immediate reconstruction during this period with the remaining 30% having a delayed reconstruction. The 1,206 free flaps comprised of 83 transverse myocutaneous gracilis (TMG) flaps, and 1,123 deep inferior epigastric artery perforator (DIEP) flaps. In total the coupler was used in 319 flaps, 26% of the cohort. There was a statistically significant clinical benefit in using the anastomotic coupler for venous anastomosis. Overall, the return to theatre rate was 12.69% whilst the overall flap loss rate was 0.75%. The overall coupler failure rate was significantly less at 1.4% whilst sutured vein failure rate was 3.57% (P=0.001). Conclusions: The anastomotic coupler for venous anastomosis in free flap surgery is associated with reduced operating times, reduced take-backs to theatre and cost benefits. This is the first study to demonstrate clear clinical benefits to anastomotic couplers, and suggests that these may be the gold standard for venous microanastomosis. With increasing experience with their use and technological advances, these outcomes may continue to improve. Keywords: Suture; vessel; rib; microsurgery; microvascular; free flap Submitted Apr 21, Accepted for publication May 22, doi: /j.issn X View this article at: Introduction Microvascular anastomotic techniques have evolved considerably since the first vessel anastomosis in Carrell sutured his anastomosis, and clinicians since then have proceeded to develop ways to build on this paradigm-changing achievement. Through new technology, techniques and treatments, we continue with the aim of improving the quality of care offered through microsurgical reconstructive techniques. Traditionally, vessel anastomosis utilized hand-tied monofilament microsutures, under microscope magnification. There have been developments in suture materials over time, and more recently, the use
2 Gland Surgery, Vol 5 No 2 April Figure 1 The coupling device is turned together to evert the vein wall edges ensuring intima to intima contact. Figure 2 Arterial anastomosis preformed in an end to end, interrupted sutured fashion. of microclips or vascular staples have become increasingly used. More popularised still are the use of coupling devices, which use a ring and hooks for microvascular anastomosis. Venous couplers were first described in 1962 by Nakayama, who used an interlocking metal ring with 12 pins to achieve a patent venous anastomosis (1). A reliable device was developed in Sweden in the early 1980 s known as the Unilink coupler and marketed by 3M (2). The technology has been since been refined further and is currently used across the world for microsurgical venous anastomosis as the microvascular anastomotic coupler system coupler system (Synovis Micro Companies Alliance, Birmingham, AL, USA). The venous coupler has been designed to provide intima to intima contact without intraluminal suture material which might act as a site for thrombus promotion. A systematic review of coupler performance studies demonstrated a thrombosis rate range of 0% to 3%, whilst the average time of using the device is 5 minutes (3). There is sparse published data on cost analysis and the impact of operator experience on the anastomotic coupler device success. Improvements in outcomes other than time benefits have also not been shown. This study aims to address these deficiencies in the literature. Methods A retrospective clinical study was undertaken, aiming to compare equivalent groups of patients that had free flap surgery with venous micro-anastomoses with those that had sutured anastomoses. The cohort comprised all patients undergoing microsurgical breast reconstruction at the St Andrew s Centre for Plastic Surgery & Burns from January 2009 to December Specific data from all microsurgical free tissue transfer operations were prospectively entered into a clinical database and collected. Key variables collected included patient demographics, operative time, coupler size, surgeon experience and complications. The surgeon level of experience was compared for consultant surgeon versus fellow/registrar; the recipient site was compared for the internal mammary versus the subscapular/ thoracodorsal axis; and the number of flaps was compared as to whether a case required a unilateral reconstruction, bilateral reconstructions, a bipedicled flap (two anastomoses in the chest) or stacked flaps (two flaps in series with one anastomosis in the chest). Venous anastomoses were undertaken with either a purely end to end, interrupted suturing technique, or the microvascular anastomotic coupling system (Synovis Micro Companies Alliance, Birmingham, AL, USA). Coupling technique comprised several key steps. Firstly, the use of a vessel sizer to determine the size of the coupler for any individual case, with the vessel end prepared and passed through the coupling ring. The vessel was fixed to the ring by everting the edges over sharp hooks. After each vessel end was prepared in this manner, the coupling device was turned to oppose the rings (Figure 1), and then detached from the ring to leave the completed anastomosis. All arterial anastomoses were performed in an end to end, interrupted sutured fashion (Figure 2). There were two main outcome measures investigated: anastomotic time and clinical anastomotic failures. Anastomotic time was recorded prospectively, and comprised the time from the end of vessel preparation until removal of vessel clamps. Clinical outcomes assessed were anastomotic failure, returns to theatre and overall flap failure. Statistical analysis was undertaken using SPSS (SPSS
3 90 Fitzgerald O Connor et al. Microvascular anastomotic coupler Table 1 Clinical outcomes for sutured versus coupled veins Variables Sutured vein revision (%) Coupled vein revision (%) Pearson s χ 2 Overall return to theatre (%) Reconstruction type Unilateral * Bilateral Unilateral bipedicle Unilateral stacked Total * Grade of surgeon Consultant * 0.46 Fellow/Registrar Total * 0.75 Anastomosis site Axilla Chest * 1.30 *, P Inc. IBM, Armok, NY, USA). A P value of 0.05 was used to represent statistical significance. Results Between January 2010 to December 2014, 1,064 patients underwent 1,206 free flap breast reconstructions. The average age of patients was 50 years. Seventy percent of patients underwent mastectomy and immediate reconstruction during this period with the remaining 30% having a delayed reconstruction. The 1,206 free flaps comprised of 83 transverse myocutaneous upper gracilis (TUG) flaps, and 1,123 deep inferior epigastric artery perforator (DIEP) flaps. In total the coupler was used in 319 flaps, 26% of the cohort. There was a statistically significant clinical benefit in using the anastomotic coupler for venous anastomosis (Table 1). Overall, the return to theatre rate was 12.69% whilst the overall flap loss rate was 0.75%. The overall coupler failure rate was significantly less at 1.4% whilst sutured vein failure rate was 3.57% (P=0.001). Of note, consultant surgeons had a lower coupler failure rate than more junior surgeons (fellows or registrars) at 0.57% versus 4.5% There was also a statistically significant time benefit in using the anastomotic coupler (Table 2). The average time to undertake a sutured vein anastomosis was 21 minutes whilst using the coupler device it was significantly less at 9.3 minutes (P=0.001). Fellows or Registrars took significantly less time to use the coupler at 15 minutes versus sutured vein at 35 minutes (P=0.001). When comparing different recipient sites, it took on average 4 more minutes to use a coupler in the axilla than a coupler in the internal mammary site, and 13 minutes more to suture at the internal mammary site as compared to using a coupler. Discussion Technology in free flap surgery has helped to transition what began as a high risk and significant undertaking in the early 1980 s to routine options in many reconstructive settings. Venous problems are more commonly seen in free flap surgery, and means to counter such problems are eagerly sought. Venous complications requiring a return to theatre and re-anastomosis in sutured anastomosis was 3.57% in our study, and this is commensurate with existing published data on venous complications (4). This contrasts to the venous thrombosis rate achieved with the coupler device of 1.44%, found to be significantly lower than the sutured cohort (P<0.01). Sutured repairs have an inherently higher risk for thrombosis, and are technique dependant on success. Suture material within the lumen, incompletely everted vessel edges and poor suture placement leading to leaks can all contribute to anastomotic failure (5). Blood flow modelling using computational fluid dynamics that assesses flow through a coupler anastomosis versus sutured, show a reduction in the key precursors to thrombin formation, changes in flow velocity profile and decreased wall shear stress (6).
4 Gland Surgery, Vol 5 No 2 April Table 2 Time for anastomosis Variables Patients Flaps Proportion (%) Artery (mins) Vein (mins) Coupler (mins) Student s t-test Reconstruction type Unilateral ** Bilateral * Unilateral bipedicle ** Unilateral stacked ** Total/Mean 1,064 1, ** Grade of surgeon Consultant ** Fellow/Registrar ** Recipient site Axilla ** Chest ** *, P 0.05; **, P Anastomosis time was significantly quicker with the coupler device. The average anastomosis time of 9 minutes is higher than some other large series in the published literature (3,7), however this was a statistically significant difference to sutured anastomosis, as mirrored in those other publications. Time is an important factor when considering the potential length of a complicated procedure, with increase operative time in microsurgical breast reconstruction associated with lower haemoglobin levels and an increase risk of postoperative complications (8). The cost savings alone are a significant consideration. Our unit began to routinely use the coupler system in late 2012, although the surgeons involved had all used the system in other hospitals. There was a significant difference in anastomosis times and failure rate in the coupler group when looking at surgeon seniority. Consultant surgeons took longer to use the coupler but had a significantly lower revision rate than fellows or registrars. Fellows and registrars took less time to use a coupler than sutured anastomosis but there was no significant difference in their anastomotic failure rates. This evidence points to a potential learning curve for the use of the coupler device, and that the time saving benefits must be tempered with the knowledge of potential increase in anastomosis revision rate in the hands of a more junior surgeon. This data reinforces the fact that with seniority and experience comes the insight and knowledge that microsurgery should never be rushed. Within a resource-constrained healthcare system, time is a significant cost factor to consider. The average time difference between sutured and coupler anastomosis was just over 11 minutes. Within our regional hospital system, the financial cost associated with running an operating theatre per hour has been calculated by the hospital as 14 GBP/min. Simplistically, this would indicate that couplers on average save 154. The current cost of the single use couplers excluding the initial investment in coupler set is This would indicate that it could be perceived as a cost neutral device. This assumption holds if the time saving allows further use of the fixed costs associated with running a theatre. Given that in our unit the senior author has routinely undertaken three DIEP reconstructions in one theatre in a single day, time saved can be realised as a net cost saving. Furthermore, if you extrapolate the reduction in return to theatre rates which are strongly associated with significant cost increase (9), the net saving for coupler use will increase further. While not a formal cost analysis, this data does point to couplers not being a cost strain. Coupler use has for the first time been demonstrated in a large cohort to be quicker not only in unilateral breast reconstruction but also in bilateral, bipedicled and stacked breast reconstruction cases. Couplers demonstrated over 12 minutes time saving in bilateral reconstructions, 14 minutes in bipedicled and 10 minutes in stacked flaps. There were no coupler failures in any of the bilateral, bipedicled or stacked flaps. In these operations which add an extra layer of complexity and time as compared to unilateral reconstructions, the added benefit of time saved and potential reduced risk of thrombosis are significant factors which
5 92 Fitzgerald O Connor et al. Microvascular anastomotic coupler may well influence a surgeon s decision to use couplers. The coupler is also recognised to reduce surgeon fatigue although this is difficult to quantify. In complex reconstructions the use of a coupler can dramatically reduce the complexity of required microsurgical demands. Multiple couplers can be used to extend vein grafts, in one case we have used five couplers in series to extend a vein graft. Anastomosis site was a different variable we chose to explore. The use of a coupler was associated with a significant reduction in anastomosis time in both sites the internal mammary system and the subscapular/thoracodorsal system. The time saving was greater using the coupler with the internal mammary artery and its perforators. It was also associated with a significant reduction in thrombosis rate at this site. When looking at the axilla there was a significant time saving but no difference in thrombosis rate. The coupler conveys time saving benefit irrespective of location of use, however in this cohort the thrombosis risk reduction benefit is only seen in its use on the anterior chest anastomosis location. The benefits to microvascular coupler anastomosis can be seen however there are some documented drawbacks. There is a learning curve to correct use of the system which surgeons used to hand sewn anastomosis will need to adjust to. There is the theoretical deskilling of the ability to perform a robust hand sewn venous anastomosis, although until the advent of a reliable arterial coupler this skill will always be used (3). Cost issues have previously been cited as a disadvantage to the use of the coupler system however our data suggests that at worst it s a cost neutral device and at best it can save a substantial cost in the prevention of reoperation and flap failure. Evolution in the coupler devices have continued over time, with a broader range of sizes available, improvements in the instrumentation for applying the vessels to the coupler device, and even couplers with in-built implantable Doppler probes for monitoring. With further technological advance, outcome measures may improve on current rates even further. Conclusions The anastomotic coupler for venous anastomosis in free flap surgery is associated with reduced operating times, reduced take-backs to theatre and cost benefits. This is the first study to demonstrate clear clinical benefits to anastomotic couplers, and suggests that these may be the gold standard for venous microanastomosis. With increasing experience with their use and technological advances, these outcomes may continue to improve. Acknowledgements None. Footnote Conflicts of Interest: The authors have no conflicts of interest to declare. References 1. Nakayama K, Tamiya T, Yamamoto K, et al. A simple new apparatus for small vessel anastomosisi (free autograft of the sigmoid included). Surgery 1962;52: Ostrup LT, Berggren A. The UNILINK instrument system for fast and safe microvascular anastomosis. Ann Plast Surg 1986;17: Ardehali B, Morritt AN, Jain A. Systematic review: anastomotic microvascular device. J Plast Reconstr Aesthet Surg 2014;67: Galanis C, Nguyen P, Koh J, et al. Microvascular lifeboats: a stepwise approach to intraoperative venous congestion in DIEP flap breast reconstruction. Plast Reconstr Surg 2014;134: Nahabedian MY, Momen B, Manson PN. Factors associated with anastomotic failure after microvascular reconstruction of the breast. Plast Reconstr Surg 2004;114: Wain RA, Whitty JP, Dalal MD, et al. Blood flow through sutured and coupled microvascular anastomoses: a comparative computational study. J Plast Reconstr Aesthet Surg 2014;67: Rozen WM, Whitaker IS, Acosta R. Venous coupler for free-flap anastomosis: outcomes of 1,000 cases. Anticancer Res 2010;30: Lymperopoulos NS, Sofos S, Constantinides J, et al. Blood loss and transfusion rates in DIEP flap breast reconstruction. Introducing a new predictor. J Plast Reconstr Aesthet Surg 2013;66: Paget JT, Young KC, Wilson SM. Accurately costing unilateral delayed DIEP flap breast reconstruction. J Plast Reconstr Aesthet Surg 2013;66: Cite this article as: Fitzgerald O Connor E, Rozen WM, Chowdhry M, Patel NG, Chow WT, Griffiths M, Ramakrishnan VV. The microvascular anastomotic coupler for venous anastomoses in free flap breast reconstruction improves outcomes.. doi: /j.issn X
The Synovis GEM COUPLER
 The Synovis GEM COUPLER e Synovis product portfolio includes Coupler, Flow Coupler and GeM MicroClip. ese products are used for joining small diameter vessels during autologous tissue breast reconstruction;
The Synovis GEM COUPLER e Synovis product portfolio includes Coupler, Flow Coupler and GeM MicroClip. ese products are used for joining small diameter vessels during autologous tissue breast reconstruction;
Samer Saour, Guido Libondi, Venkat Ramakrishnan. Introduction
 Original Article Microsurgical refinements with the use of internal mammary (IM) perforators as recipient vessels in transverse upper gracilis (TUG) autologous breast reconstruction Samer Saour, Guido
Original Article Microsurgical refinements with the use of internal mammary (IM) perforators as recipient vessels in transverse upper gracilis (TUG) autologous breast reconstruction Samer Saour, Guido
Increasing options in autologous microsurgical breast reconstruction: four free flaps for stacked bilateral breast reconstruction
 Case Report Increasing options in autologous microsurgical breast reconstruction: four free flaps for stacked bilateral breast reconstruction Warren Matthew Rozen 1,2, Nakul Gamanlal Patel 1, Venkat V.
Case Report Increasing options in autologous microsurgical breast reconstruction: four free flaps for stacked bilateral breast reconstruction Warren Matthew Rozen 1,2, Nakul Gamanlal Patel 1, Venkat V.
A multiple logistic regression analysis of complications following microsurgical breast reconstruction
 Original Article A multiple logistic regression analysis of complications following microsurgical breast reconstruction Samir Rao 1, Ellen C. Stolle 1, Sarah Sher 1, Chun-Wang Lin 1, Bahram Momen 2, Maurice
Original Article A multiple logistic regression analysis of complications following microsurgical breast reconstruction Samir Rao 1, Ellen C. Stolle 1, Sarah Sher 1, Chun-Wang Lin 1, Bahram Momen 2, Maurice
CLINICAL EXPERIENCE OF A MICROVASCULAR VENOUS COUPLER DEVICE IN FREE TISSUE TRANSFERS
 CLINICAL EXPERIENCE OF A MICROVASCULAR VENOUS COUPLER DEVICE IN FREE TISSUE TRANSFERS Kao-Ping Chang, Sin-Daw Lin, and Chung-Sheng Lai Faculty of Medicine, College of Medicine, Kaohsiung Medical University,
CLINICAL EXPERIENCE OF A MICROVASCULAR VENOUS COUPLER DEVICE IN FREE TISSUE TRANSFERS Kao-Ping Chang, Sin-Daw Lin, and Chung-Sheng Lai Faculty of Medicine, College of Medicine, Kaohsiung Medical University,
Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC
 Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study
 Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps
 Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Early Experience With Barbed Sutures for Abdominal Closure in Deep Inferior Epigastric Perforator Flap Breast Reconstruction
 Early Experience With Barbed Sutures for Abdominal Closure in Deep Inferior Epigastric Perforator Flap Breast Reconstruction Catherine de Blacam, MB, BCh, a Salih Colakoglu, MD, a Adeyiza O. Momoh, MD,
Early Experience With Barbed Sutures for Abdominal Closure in Deep Inferior Epigastric Perforator Flap Breast Reconstruction Catherine de Blacam, MB, BCh, a Salih Colakoglu, MD, a Adeyiza O. Momoh, MD,
Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps
 Original Article Breast Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps James L. Mayo, MD Robert J. Allen, MD, FACS Alireza Sadeghi, MD, FACS Background: In cases of bilateral breast
Original Article Breast Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps James L. Mayo, MD Robert J. Allen, MD, FACS Alireza Sadeghi, MD, FACS Background: In cases of bilateral breast
Few would deny that lower abdominal tissue BREAST. An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction.
 BREAST An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction Aldona J. Spiegel, M.D. Farah N. Khan, M.D. Houston, Texas Background: The deep inferior epigastric perforator (DIEP)
BREAST An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction Aldona J. Spiegel, M.D. Farah N. Khan, M.D. Houston, Texas Background: The deep inferior epigastric perforator (DIEP)
Breast Reconstruction: Current Strategies and Future Opportunities
 Breast Reconstruction: Current Strategies and Future Opportunities Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery
Breast Reconstruction: Current Strategies and Future Opportunities Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery
Breast Reconstruction Options
 Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction
 A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction In-Soo Baek 1, Jae-Pil You 1, Sung-Mi Rhee 1, Gil-Su Son 2, Deok-Woo Kim 1, Eun-Sang Dhong 1, Seung-Ha
A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction In-Soo Baek 1, Jae-Pil You 1, Sung-Mi Rhee 1, Gil-Su Son 2, Deok-Woo Kim 1, Eun-Sang Dhong 1, Seung-Ha
The venous anatomy of the abdominal wall for Deep Inferior Epigastric Artery (DIEP) flaps in breast reconstruction
 Original Article The venous anatomy of the abdominal wall for Deep Inferior Epigastric Artery (DIEP) flaps in breast reconstruction Warren M Rozen, Mark W Ashton The Taylor Lab, Room E533, Department of
Original Article The venous anatomy of the abdominal wall for Deep Inferior Epigastric Artery (DIEP) flaps in breast reconstruction Warren M Rozen, Mark W Ashton The Taylor Lab, Room E533, Department of
Breast Restoration Surgery After a mastectomy
 UW MEDICINE PATIENT EDUCATION Breast Restoration Surgery After a mastectomy This handout explains the most common procedures that are used at University of Washington Medical Center (UWMC) to restore a
UW MEDICINE PATIENT EDUCATION Breast Restoration Surgery After a mastectomy This handout explains the most common procedures that are used at University of Washington Medical Center (UWMC) to restore a
Annals of Medicine and Surgery
 Annals of Medicine and Surgery 4 (2015) 293e300 Contents lists available at ScienceDirect Annals of Medicine and Surgery journal homepage: www.annalsjournal.com Total rib -preservation technique of internal
Annals of Medicine and Surgery 4 (2015) 293e300 Contents lists available at ScienceDirect Annals of Medicine and Surgery journal homepage: www.annalsjournal.com Total rib -preservation technique of internal
Current Strategies in Breast Reconstruction
 Current Strategies in Breast Reconstruction Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery 12 th Annual School of
Current Strategies in Breast Reconstruction Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery 12 th Annual School of
Clinical Assessment Score for Monitoring Free Flaps in the Dark Skin
 Short Communication 18 Copyright University of Medicine, Tirana Clinical Assessment Score for Monitoring Free Flaps in the Dark Skin Bolaji Oyawale Mofikoya 1, Andrew Omotayo Ugburo 1, Orimisan M. Belie
Short Communication 18 Copyright University of Medicine, Tirana Clinical Assessment Score for Monitoring Free Flaps in the Dark Skin Bolaji Oyawale Mofikoya 1, Andrew Omotayo Ugburo 1, Orimisan M. Belie
JPRAS Open 3 (2015) 1e5. Contents lists available at ScienceDirect. JPRAS Open. journal homepage:
 JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
Immediate versus delayed free TRAM breast reconstruction: an analysis of perioperative factors and complications
 British Journal of Plastic Surgery (22), 55, l-6 9 22 The British Association of Plastic Surgeons doi:.54/bjps.22.3747 BRITISH JOURNAL OF / ~ ] PLASTIC SURGERY Immediate versus delayed free TRAM breast
British Journal of Plastic Surgery (22), 55, l-6 9 22 The British Association of Plastic Surgeons doi:.54/bjps.22.3747 BRITISH JOURNAL OF / ~ ] PLASTIC SURGERY Immediate versus delayed free TRAM breast
INTRODUCTION. Toshihiko Satake 1, Jun Sugawara 2, Kazunori Yasumura 1, Taro Mikami 2, Shinji Kobayashi 3, Jiro Maegawa 2. Idea and Innovation
 Mini-Flow-Through Deep Inferior Epigastric Perforator Flap for Breast Reconstruction with Preservation of Both Internal Mammary and Deep Inferior Epigastric Vessels Toshihiko Satake 1, Jun Sugawara 2,
Mini-Flow-Through Deep Inferior Epigastric Perforator Flap for Breast Reconstruction with Preservation of Both Internal Mammary and Deep Inferior Epigastric Vessels Toshihiko Satake 1, Jun Sugawara 2,
Evaluation of Tissue Blood Flow of the Gastric Tube after Vessel Anastomosis for Esophageal Reconstruction
 Kobe J. Med. Sci., Vol. 57, No. 3, pp. E87-E97, 2011 Evaluation of Tissue Blood Flow of the Gastric Tube after Vessel Anastomosis for Esophageal Reconstruction HITOSHI FUKUYAMA 1, HAJIME IKUTA 1, DAISUKE
Kobe J. Med. Sci., Vol. 57, No. 3, pp. E87-E97, 2011 Evaluation of Tissue Blood Flow of the Gastric Tube after Vessel Anastomosis for Esophageal Reconstruction HITOSHI FUKUYAMA 1, HAJIME IKUTA 1, DAISUKE
Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes
 DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
Medical Policy Original Effective Date: Revised Date: Page 1 of 8
 Page 1 of 8 Disclaimer Description Coverage Determination Refer to the member s specific benefit plan and Schedule of Benefits to determine coverage. This may not be a benefit on all plans, or the plan
Page 1 of 8 Disclaimer Description Coverage Determination Refer to the member s specific benefit plan and Schedule of Benefits to determine coverage. This may not be a benefit on all plans, or the plan
Intracranial-to-intracranial vascular anastomosis created using a microanastomotic device for the treatment of distal middle cerebral artery aneurysms
 J Neurosurg 97:486 491, 2002 Intracranial-to-intracranial vascular anastomosis created using a microanastomotic device for the treatment of distal middle cerebral artery aneurysms Technical note DAVID
J Neurosurg 97:486 491, 2002 Intracranial-to-intracranial vascular anastomosis created using a microanastomotic device for the treatment of distal middle cerebral artery aneurysms Technical note DAVID
Methods of autologous tissue breast reconstruction BREAST
 BREAST Comparison of Donor-Site Morbidity of SIEA, DIEP, and Muscle-Sparing TRAM Flaps for Breast Reconstruction Liza C. Wu, M.D. Anureet Bajaj, M.D. David W. Chang, M.D. Pierre M. Chevray, M.D., Ph.D.
BREAST Comparison of Donor-Site Morbidity of SIEA, DIEP, and Muscle-Sparing TRAM Flaps for Breast Reconstruction Liza C. Wu, M.D. Anureet Bajaj, M.D. David W. Chang, M.D. Pierre M. Chevray, M.D., Ph.D.
SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni
 SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni Icro Meattini, MD Radiation Oncology Department - University of Florence Azienda Ospedaliero Universitaria Careggi Firenze Breast
SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni Icro Meattini, MD Radiation Oncology Department - University of Florence Azienda Ospedaliero Universitaria Careggi Firenze Breast
Factors Associated with Anastomotic Failure after Microvascular Reconstruction of the Breast
 Factors Associated with Anastomotic Failure after Microvascular Reconstruction of the Breast Maurice Y. Nahabedian, M.D., Bahram Momen, Ph.D., and Paul N. Manson, M.D. Baltimore and College Park, Md. The
Factors Associated with Anastomotic Failure after Microvascular Reconstruction of the Breast Maurice Y. Nahabedian, M.D., Bahram Momen, Ph.D., and Paul N. Manson, M.D. Baltimore and College Park, Md. The
Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps
 BREAST SURGERY Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps Joshua L. Levine, MD,* Quintessa Miller, MD, Julie Vasile, MD,* Kamran Khoobehi,
BREAST SURGERY Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps Joshua L. Levine, MD,* Quintessa Miller, MD, Julie Vasile, MD,* Kamran Khoobehi,
Vessel Remodeling after Intima-to-Intima Contact Anastomosis
 Vessel Remodeling after Intima-to-Intima Contact Anastomosis Hyeonjung Yeo 1, Hyodong Kim 1, Daegu Son 2, Changbae Hong 3, Sun Young Kwon 4 1 Department of Plastic and Reconstructive Surgery, Daegu Fatima
Vessel Remodeling after Intima-to-Intima Contact Anastomosis Hyeonjung Yeo 1, Hyodong Kim 1, Daegu Son 2, Changbae Hong 3, Sun Young Kwon 4 1 Department of Plastic and Reconstructive Surgery, Daegu Fatima
Clinical Accuracy of Portrait 3D Surgical Simulation Platform in Breast Augmentation. Ryan K. Wong MD, David T Pointer BS, Kamran Khoobehi MD FACS
 Clinical Accuracy of Portrait 3D Surgical Simulation Platform in Breast Augmentation Ryan K. Wong MD, David T Pointer BS, Kamran Khoobehi MD FACS Division of Plastic, Reconstructive & Reconstructive Surgery,
Clinical Accuracy of Portrait 3D Surgical Simulation Platform in Breast Augmentation Ryan K. Wong MD, David T Pointer BS, Kamran Khoobehi MD FACS Division of Plastic, Reconstructive & Reconstructive Surgery,
ORIGINAL ARTICLE. The Implantable Cook-Swartz Doppler Probe. for postoperative monitoring in head and neck reconstruction.
 ORIGINAL ARTICLE The Implantable Cook-Swartz Doppler Probe for Postoperative Monitoring in Head and Neck Free Flap Reconstruction Jennifer P. Guillemaud, MD, BSc; Hadi Seikaly, MD, FRCSC; David Cote, MD,
ORIGINAL ARTICLE The Implantable Cook-Swartz Doppler Probe for Postoperative Monitoring in Head and Neck Free Flap Reconstruction Jennifer P. Guillemaud, MD, BSc; Hadi Seikaly, MD, FRCSC; David Cote, MD,
Intraoperative Fluorescence Imaging Systems
 Intraoperative Fluorescence Imaging Systems Policy Number: 10.01.530 Last Review: 01/2018 Origination: 01/2015 Next Review: 01/2019 Policy Intraoperative fluorescence imaging (SPY Imaging) to evaluate
Intraoperative Fluorescence Imaging Systems Policy Number: 10.01.530 Last Review: 01/2018 Origination: 01/2015 Next Review: 01/2019 Policy Intraoperative fluorescence imaging (SPY Imaging) to evaluate
Reconstruction with autologous tissue remains a
 Original Article Increased Flap Weight and Decreased Perforator Number Predict Fat Necrosis in DIEP Breast Reconstruction Carolyn L. Mulvey, BS* Carisa M. Cooney, MPH* Francis F. Daily, BS* Elizabeth Colantuoni,
Original Article Increased Flap Weight and Decreased Perforator Number Predict Fat Necrosis in DIEP Breast Reconstruction Carolyn L. Mulvey, BS* Carisa M. Cooney, MPH* Francis F. Daily, BS* Elizabeth Colantuoni,
The decision to repair a partial mastectomy CME. State of the Art and Science in Postmastectomy Breast Reconstruction.
 CME State of the Art and Science in Postmastectomy Breast Reconstruction Steven J. Kronowitz, M.D. Houston, Texas Learning Objectives: After reading this article, the participant should be able to: 1.
CME State of the Art and Science in Postmastectomy Breast Reconstruction Steven J. Kronowitz, M.D. Houston, Texas Learning Objectives: After reading this article, the participant should be able to: 1.
Breast reconstruction following mastectomy has
 Free full text on www.ijps.org Post-mastectomy breast reconstruction: Microsurgical methods Venkat Ramakrishnan, Makarand Tare St. Andrew s Centre for Burns and Plastic Surgery, BroomÞ eld Hospital, Chelmsford,
Free full text on www.ijps.org Post-mastectomy breast reconstruction: Microsurgical methods Venkat Ramakrishnan, Makarand Tare St. Andrew s Centre for Burns and Plastic Surgery, BroomÞ eld Hospital, Chelmsford,
Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps
 e50 Case Report THIEME Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps Shuhei Yoshida, MD 1 Isao Koshima, MD 1 Shogo Nagamatsu, MD 2 Kazunori Yokota, MD 2 Shuji Yamashita,
e50 Case Report THIEME Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps Shuhei Yoshida, MD 1 Isao Koshima, MD 1 Shogo Nagamatsu, MD 2 Kazunori Yokota, MD 2 Shuji Yamashita,
Thermal injury in TAPIA breast reconstruction Børsen-Koch, Mikkel; Gunnarsson, Gudjon L.; Sørensen, Jens Ahm; Thomsen, Jørn Bo
 Syddansk Universitet Thermal injury in TAPIA breast reconstruction Børsen-Koch, Mikkel; Gunnarsson, Gudjon L.; Sørensen, Jens Ahm; Thomsen, Jørn Bo Published in: Gland Surgery DOI: 10.21037/gs.2017.01.01
Syddansk Universitet Thermal injury in TAPIA breast reconstruction Børsen-Koch, Mikkel; Gunnarsson, Gudjon L.; Sørensen, Jens Ahm; Thomsen, Jørn Bo Published in: Gland Surgery DOI: 10.21037/gs.2017.01.01
Awareness and provision of reconstruction. Breast
 Original Article Breast Deep Inferior Epigastric Artery Perforator Flap Breast Reconstruction without Microsurgery Fellowship Training Hakan Orbay, MD, PhD* Brittany K. Busse, MD* Thomas R. Stevenson,
Original Article Breast Deep Inferior Epigastric Artery Perforator Flap Breast Reconstruction without Microsurgery Fellowship Training Hakan Orbay, MD, PhD* Brittany K. Busse, MD* Thomas R. Stevenson,
How many procedures to make a breast?
 British Journal of Plastic Surgery (00 ), 5, 7-3 9 00 The British Association of Plastic Surgeons doi: 0.05/bjps.000.3538 BRITISH JOURNAL OF PLASTIC SURGERY How many procedures to make a breast? A. D.
British Journal of Plastic Surgery (00 ), 5, 7-3 9 00 The British Association of Plastic Surgeons doi: 0.05/bjps.000.3538 BRITISH JOURNAL OF PLASTIC SURGERY How many procedures to make a breast? A. D.
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Fluorescence Angiography in Limb Salvage
 Fluorescence Angiography in Limb Salvage Ryan H. Fitzgerald, DPM, FACFAS Associate Professor of Surgery-University Of South Carolina School of Medicine, Greenville Etiology of Lower extremity wounds Neuropathy
Fluorescence Angiography in Limb Salvage Ryan H. Fitzgerald, DPM, FACFAS Associate Professor of Surgery-University Of South Carolina School of Medicine, Greenville Etiology of Lower extremity wounds Neuropathy
The Superficial Inferior Epigastric Artery (SIEA) Flap and Its Applications in Breast Reconstruction
 The Superficial Inferior Epigastric Artery (SIEA) Flap and Its Applications in Breast Reconstruction Zachary Menn and Aldona Spiegel Weill Cornell Medical College, The Methodist Hospital, Houston, Texas,
The Superficial Inferior Epigastric Artery (SIEA) Flap and Its Applications in Breast Reconstruction Zachary Menn and Aldona Spiegel Weill Cornell Medical College, The Methodist Hospital, Houston, Texas,
In the UK approximately 40,000
 The patient journey in DIEP flap breast reconstruction BY OLIVIER ALEXANDRE BRANFORD AND PAUL ANTHONY HARRIS In the UK approximately 40,000 women are diagnosed with breast cancer every year. About 40%
The patient journey in DIEP flap breast reconstruction BY OLIVIER ALEXANDRE BRANFORD AND PAUL ANTHONY HARRIS In the UK approximately 40,000 women are diagnosed with breast cancer every year. About 40%
Clinical applications for the internal mammary artery
 ORIGINAL ARTICLE The Internal Mammary Artery and Vein as Recipient Vessels for Microvascular Breast Reconstruction: Are We Burning a Future Bridge? Maurice Y. Nahabedian, MD, FACS Abstract: Clinical applications
ORIGINAL ARTICLE The Internal Mammary Artery and Vein as Recipient Vessels for Microvascular Breast Reconstruction: Are We Burning a Future Bridge? Maurice Y. Nahabedian, MD, FACS Abstract: Clinical applications
The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography
 BREAST The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography Corrine Wong, M.D. Purushottam Nagarkar, M.D. Sumeet Teotia, M.D. Nicholas
BREAST The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography Corrine Wong, M.D. Purushottam Nagarkar, M.D. Sumeet Teotia, M.D. Nicholas
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
Abdominal-based reconstruction is considered
 Original Article Salvage of Intraoperative Deep Inferior Epigastric Perforator Flap Venous Congestion with Augmentation of Venous Outflow: Flap Morbidity and Review of the Literature Oscar Ochoa, MD Steven
Original Article Salvage of Intraoperative Deep Inferior Epigastric Perforator Flap Venous Congestion with Augmentation of Venous Outflow: Flap Morbidity and Review of the Literature Oscar Ochoa, MD Steven
Citation for published version (APA): Benditte-Klepetko, H. C. (2014). Breast surgery: A problem of beauty or health?
 UvA-DARE (Digital Academic Repository) Breast surgery: A problem of beauty or health? Benditte-Klepetko, H.C. Link to publication Citation for published version (APA): Benditte-Klepetko, H. C. (2014).
UvA-DARE (Digital Academic Repository) Breast surgery: A problem of beauty or health? Benditte-Klepetko, H.C. Link to publication Citation for published version (APA): Benditte-Klepetko, H. C. (2014).
Advances and Innovations in Breast Reconstruction and Brest Surgery Presented by PCMC plastic surgeons
 Advances and Innovations in Breast Reconstruction and Brest Surgery Presented by PCMC plastic surgeons Options for reconstruction after mastectomy Implants Autologous tissue = from your own body: skin
Advances and Innovations in Breast Reconstruction and Brest Surgery Presented by PCMC plastic surgeons Options for reconstruction after mastectomy Implants Autologous tissue = from your own body: skin
Comparing the donor-site morbidity using DIEP, SIEA or MS-TRAM flaps for breast reconstructive surgery: A meta-analysis
 Journal of Plastic, Reconstructive & Aesthetic Surgery (2012) 65, 1474e1480 REVIEW Comparing the donor-site morbidity using DIEP, SIEA or MS-TRAM flaps for breast reconstructive surgery: A meta-analysis
Journal of Plastic, Reconstructive & Aesthetic Surgery (2012) 65, 1474e1480 REVIEW Comparing the donor-site morbidity using DIEP, SIEA or MS-TRAM flaps for breast reconstructive surgery: A meta-analysis
Intracranial vascular anastomosis using the microanastomotic system
 J Neurosurg 89:676 681, 1998 Intracranial vascular anastomosis using the microanastomotic system Technical note DAVID W. NEWELL, M.D., ANDREW T. DAILEY, M.D., AND STEPHEN L. SKIRBOLL, M.D. Department of
J Neurosurg 89:676 681, 1998 Intracranial vascular anastomosis using the microanastomotic system Technical note DAVID W. NEWELL, M.D., ANDREW T. DAILEY, M.D., AND STEPHEN L. SKIRBOLL, M.D. Department of
The dissection of the rectus abdominis myocutaneous flap with complete preservation of the anterior rectus sheath q
 The British Association of Plastic Surgeons (2003) 56, 395 400 The dissection of the rectus abdominis myocutaneous flap with complete preservation of the anterior rectus sheath q D. Erni*, Y.D. Harder
The British Association of Plastic Surgeons (2003) 56, 395 400 The dissection of the rectus abdominis myocutaneous flap with complete preservation of the anterior rectus sheath q D. Erni*, Y.D. Harder
Sweden 2 Jack Brockhoff Reconstructive Plastic Surgery Research Unit, Department
 A SINGLE CENTER COMPARISON OF ONE VERSUS TWO VENOUS ANASTOMOSES IN 564 CONSECUTIVE DIEP FLAPS: INVESTIGATING THE EFFECT ON VENOUS CONGESTION AND FLAP SURVIVAL MORTEZA ENAJAT, M.D., 1 WARREN M. ROZEN, M.B.B.S.,
A SINGLE CENTER COMPARISON OF ONE VERSUS TWO VENOUS ANASTOMOSES IN 564 CONSECUTIVE DIEP FLAPS: INVESTIGATING THE EFFECT ON VENOUS CONGESTION AND FLAP SURVIVAL MORTEZA ENAJAT, M.D., 1 WARREN M. ROZEN, M.B.B.S.,
Breast Reconstruction Surgery
 Breast Reconstruction Surgery I. Policy University Health Alliance (UHA) will reimburse for Breast Reconstruction Surgery when it is determined to be medically necessary and when it meets the medical criteria
Breast Reconstruction Surgery I. Policy University Health Alliance (UHA) will reimburse for Breast Reconstruction Surgery when it is determined to be medically necessary and when it meets the medical criteria
Breast Cancer Reconstruction
 Breast Cancer Jerome H. Liu, MD Tom S. Liu, MD Jerome H. Liu, MD Undergraduate: Brown University Medical School: University of California, Los Angeles Residency: UCLA Medical Center Fellowship:UCLA Medical
Breast Cancer Jerome H. Liu, MD Tom S. Liu, MD Jerome H. Liu, MD Undergraduate: Brown University Medical School: University of California, Los Angeles Residency: UCLA Medical Center Fellowship:UCLA Medical
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage
 Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
Hepatic Artery Reconstruction in Living Donor Liver Transplant Experience at King Hussein Medical Center
 Hepatic Artery Reconstruction in Living Donor Liver Transplant Experience at King Hussein Medical Center Khaldoun J. Haddadin MD FRCS (Eng)*, Nasser Q. Ahmad MD MRCSI*, Abdelhamid M. Aladwan MD ** ABSTRACT
Hepatic Artery Reconstruction in Living Donor Liver Transplant Experience at King Hussein Medical Center Khaldoun J. Haddadin MD FRCS (Eng)*, Nasser Q. Ahmad MD MRCSI*, Abdelhamid M. Aladwan MD ** ABSTRACT
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
Reconstruction of axillary scar contractures retrospective study of 124 cases over 25 years
 British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
Achieving ideal donor site aesthetics with autologous breast reconstruction
 Review Article Achieving ideal donor site aesthetics with autologous breast reconstruction Maurice Y. Nahabedian Department of Plastic Surgery, Georgetown University, Washington, DC 20007, USA Correspondence
Review Article Achieving ideal donor site aesthetics with autologous breast reconstruction Maurice Y. Nahabedian Department of Plastic Surgery, Georgetown University, Washington, DC 20007, USA Correspondence
Is Unilateral Implant or Autologous Breast Reconstruction Better in Obtaining Breast Symmetry?
 ORIGINAL ARTICLE Is Unilateral Implant or Autologous Breast Reconstruction Better in Obtaining Breast Symmetry? Oriana Cohen, MD, Kevin Small, MD, Christina Lee, BA, Oriana Petruolo, MD, Nolan Karp, MD,
ORIGINAL ARTICLE Is Unilateral Implant or Autologous Breast Reconstruction Better in Obtaining Breast Symmetry? Oriana Cohen, MD, Kevin Small, MD, Christina Lee, BA, Oriana Petruolo, MD, Nolan Karp, MD,
The Next Horizons in Reconstructive Microsurgery
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/the-next-horizonsreconstructive-microsurgery/7949/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/the-next-horizonsreconstructive-microsurgery/7949/
Figure 1. Anatomy of the breast
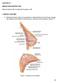 CHAPTER 12 BREAST RECONSTRUCTION Mihaela Rapolti, MD and Michelle Roughton, MD I. BREAST ANATOMY A. Mastering breast anatomy is essential for understanding how the breast changes with aging and principles
CHAPTER 12 BREAST RECONSTRUCTION Mihaela Rapolti, MD and Michelle Roughton, MD I. BREAST ANATOMY A. Mastering breast anatomy is essential for understanding how the breast changes with aging and principles
Anatomical study. Clinical study. R. Ogawa, H. Hyakusoku, M. Murakami, R. Aoki, K. Tanuma* and D. G. Pennington?
 British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
JMSCR Vol 07 Issue 01 Page January 2019
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v7i1.36 Original Article A Study on the
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v7i1.36 Original Article A Study on the
In a second stage or a second operation that tissue expander is removed through the same incision and the implant is placed within the chest pocket.
 Hello, I m Summer Hanson. I m an assistant professor in the Department of Plastics & Reconstructive Surgery at The University of Texas MD Anderson Cancer Center and today I m going to talk about the role
Hello, I m Summer Hanson. I m an assistant professor in the Department of Plastics & Reconstructive Surgery at The University of Texas MD Anderson Cancer Center and today I m going to talk about the role
Pocket Conversion Made Easy: A Simple Technique Using Alloderm to Convert Subglandular Breast Implants to the Dual-Plane Position
 Breast Surgery Pocket Conversion Made Easy: A Simple Technique Using Alloderm to Convert Subglandular Breast Implants to the Dual-Plane Position M. Mark Mofid, MD; and Navin K. Singh, MD Background: The
Breast Surgery Pocket Conversion Made Easy: A Simple Technique Using Alloderm to Convert Subglandular Breast Implants to the Dual-Plane Position M. Mark Mofid, MD; and Navin K. Singh, MD Background: The
Femoral reconstruction by single, folded or double free vascularised fibular grafts
 The British Association of Plastic Surgeons (2004) 57, 550 555 Femoral reconstruction by single, folded or double free vascularised fibular grafts K. Muramatsu*, K. Ihara, M. Shigetomi, S. Kawai Department
The British Association of Plastic Surgeons (2004) 57, 550 555 Femoral reconstruction by single, folded or double free vascularised fibular grafts K. Muramatsu*, K. Ihara, M. Shigetomi, S. Kawai Department
The most common type of breast reconstruction
 BREAST Breast Reconstruction with Perforator Flaps Jay W. Granzow, M.D., M.P.H. Joshua L. Levine, M.D. Ernest S. Chiu, M.D. Maria M. LoTempio, M.D. Robert J. Allen, M.D. New Orleans, La.; Charleston, S.C.;
BREAST Breast Reconstruction with Perforator Flaps Jay W. Granzow, M.D., M.P.H. Joshua L. Levine, M.D. Ernest S. Chiu, M.D. Maria M. LoTempio, M.D. Robert J. Allen, M.D. New Orleans, La.; Charleston, S.C.;
Peter McAllister, 1 Isabel Teo, 1 Kuen Chin, 1 Boikanyo Makubate, 2 and David Alexander Munnoch Introduction
 Hindawi Publishing Corporation Plastic Surgery International Volume 2016, Article ID 6085624, 9 pages http://dx.doi.org/10.1155/2016/6085624 Research Article Bilateral Breast Reconstruction with Abdominal
Hindawi Publishing Corporation Plastic Surgery International Volume 2016, Article ID 6085624, 9 pages http://dx.doi.org/10.1155/2016/6085624 Research Article Bilateral Breast Reconstruction with Abdominal
Current Approaches to Free Flap Monitoring
 CE 2.3 ANCC Contact Hours Current Approaches to Free Flap Monitoring Albert H. Chao, MD Susan Lamp, BSN, RN, CPSN Postoperative monitoring of free flaps remains an essential component of care in patients
CE 2.3 ANCC Contact Hours Current Approaches to Free Flap Monitoring Albert H. Chao, MD Susan Lamp, BSN, RN, CPSN Postoperative monitoring of free flaps remains an essential component of care in patients
ENHANCED RECOVERY CARE PROGRAMME FOR ABDOMINAL-BASED BREAST RECONSTRUCTIONS (MS-TRAM/DIEP)
 St Andrews Centre for Plastic Surgery ENHANCED RECOVERY CARE PROGRAMME FOR ABDOMINAL-BASED BREAST RECONSTRUCTIONS (MS-TRAM/DIEP) INTRODUCTION This leaflet aims to help you understand the Enhanced Recovery
St Andrews Centre for Plastic Surgery ENHANCED RECOVERY CARE PROGRAMME FOR ABDOMINAL-BASED BREAST RECONSTRUCTIONS (MS-TRAM/DIEP) INTRODUCTION This leaflet aims to help you understand the Enhanced Recovery
ABSTRACT. Sweden; 1 Department of Plastic Surgery, Uppsala University Hospital, Uppsala, 2 Jack Brockhoff Reconstructive Plastic Surgery Research
 Postoperative Monitoring of Free Flaps in Autologous Breast Reconstruction: A Multicenter Comparison of 398 Flaps Using Clinical Monitoring, Microdialysis, and the Implantable Doppler Probe Iain S. Whitaker,
Postoperative Monitoring of Free Flaps in Autologous Breast Reconstruction: A Multicenter Comparison of 398 Flaps Using Clinical Monitoring, Microdialysis, and the Implantable Doppler Probe Iain S. Whitaker,
Role of free tissue transfer in management of chronic venous ulcer
 Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Allograft Based Breast Reconstruction: Opportunity for a Second Look
 Allograft Based Breast Reconstruction: Opportunity for a Second Look Martin I. Newman, MD, FACS Director of Resident Education and Associate Program Director Department of Plastic and Reconstructive Surgery
Allograft Based Breast Reconstruction: Opportunity for a Second Look Martin I. Newman, MD, FACS Director of Resident Education and Associate Program Director Department of Plastic and Reconstructive Surgery
Reduction Mammaplasty and Mastopexy in Previously Irradiated Breasts
 Breast Surgery Reduction Mammaplasty and Mastopexy in Previously Irradiated Breasts Scott L. Spear, MD; Samir S. Rao, MD; Ketan M. Patel, MD; and Maurice Y. Nahabedian, MD The combination of lumpectomy
Breast Surgery Reduction Mammaplasty and Mastopexy in Previously Irradiated Breasts Scott L. Spear, MD; Samir S. Rao, MD; Ketan M. Patel, MD; and Maurice Y. Nahabedian, MD The combination of lumpectomy
Contralateral Prophylactic Mastectomy with Immediate Reconstruction: Added Benefits, Added Risks
 Contralateral Prophylactic Mastectomy with Immediate Reconstruction: Added Benefits, Added Risks Grant W. Carlson Wadley R. Glenn Professor of Surgery Divisions of Plastic Surgery & Surgical Oncology Emory
Contralateral Prophylactic Mastectomy with Immediate Reconstruction: Added Benefits, Added Risks Grant W. Carlson Wadley R. Glenn Professor of Surgery Divisions of Plastic Surgery & Surgical Oncology Emory
SCOPE OF PRACTICE PGY-6 PGY-7 PGY-8
 PGY-6 Round on all plastic surgery inpatients every day. Assess progress of patients and identify real or potential problems. Review patients progress with attending physicians daily and participate in
PGY-6 Round on all plastic surgery inpatients every day. Assess progress of patients and identify real or potential problems. Review patients progress with attending physicians daily and participate in
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
Breast reconstruction has an important role BREAST. A Two-Year Prospective Analysis of Trunk Function in TRAM Breast Reconstructions
 BREAST A Two-Year Prospective Analysis of Trunk Function in TRAM Breast Reconstructions Amy K. Alderman, M.D. William M. Kuzon, Jr., M.D., Ph.D. Edwin G. Wilkins, M.D. Ann Arbor, Mich. Background: Functional
BREAST A Two-Year Prospective Analysis of Trunk Function in TRAM Breast Reconstructions Amy K. Alderman, M.D. William M. Kuzon, Jr., M.D., Ph.D. Edwin G. Wilkins, M.D. Ann Arbor, Mich. Background: Functional
Breast Reconstruction in Women Under 30: A 10-Year Experience
 ORIGINAL ARTICLE Breast Reconstruction in Women Under 30: A 10-Year Experience Warren A. Ellsworth, MD,* Barbara L. Bass, MD, FACS, Roman J. Skoracki, MD, à and Lior Heller, MD* *Division of Plastic Surgery,
ORIGINAL ARTICLE Breast Reconstruction in Women Under 30: A 10-Year Experience Warren A. Ellsworth, MD,* Barbara L. Bass, MD, FACS, Roman J. Skoracki, MD, à and Lior Heller, MD* *Division of Plastic Surgery,
The London BreasT CenTre
 The London Breast Centre Contents Introduction 4 One-Stop Breast Care Clinic 5 Common breast problems 6 Hereditary breast cancer 8 Breast cancer and cancer screening 9 Breast diagnostic tests 10 Breast
The London Breast Centre Contents Introduction 4 One-Stop Breast Care Clinic 5 Common breast problems 6 Hereditary breast cancer 8 Breast cancer and cancer screening 9 Breast diagnostic tests 10 Breast
Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study
 Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study Raphael Sinna, MD, a Hassene Hajji, MD, b Quentin Qassemyar,
Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study Raphael Sinna, MD, a Hassene Hajji, MD, b Quentin Qassemyar,
Planning and optimising DIEP flaps with virtual surgery: the Navarra experience
 Journal of Plastic, Reconstructive & Aesthetic Surgery (2010) 63, 289e297 Planning and optimising DIEP flaps with virtual surgery: the Navarra experience Warren Matthew Rozen a, *, Emilio Garcia-Tutor
Journal of Plastic, Reconstructive & Aesthetic Surgery (2010) 63, 289e297 Planning and optimising DIEP flaps with virtual surgery: the Navarra experience Warren Matthew Rozen a, *, Emilio Garcia-Tutor
Issue Number: 0151 Date: 26/04/2018
 Bulletin Changes to CCSD Schedule of Procedures Issue Number: 0151 Date: 26/04/2018 The CCSD has reviewed requests to the CCSD Procedure Schedule for the month of April and has agreed on the following
Bulletin Changes to CCSD Schedule of Procedures Issue Number: 0151 Date: 26/04/2018 The CCSD has reviewed requests to the CCSD Procedure Schedule for the month of April and has agreed on the following
Endoscopic assisted harvest of the pedicled pectoralis major muscle flap
 British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
Sure closure skin stretching system, our clinical experience
 Free full text on www.ijps.org Original Article Sure closure skin stretching system, our clinical experience K. I. Subramania, S. Mohit, P. R. Sasidharan, M. K. Abraham, P. Arun, V. Kekatpure Department
Free full text on www.ijps.org Original Article Sure closure skin stretching system, our clinical experience K. I. Subramania, S. Mohit, P. R. Sasidharan, M. K. Abraham, P. Arun, V. Kekatpure Department
Nipple-Areolar Complex Reconstruction: A Review of the Literature and Introduction of the Rectangle-to-Cube Nipple Flap
 Nipple-Areolar Complex Reconstruction: A Review of the Literature and Introduction of the Rectangle-to-Cube Nipple Flap Joshua T. Henderson, BA, a ThomasJ.Lee,MD, b Andrew M. Swiergosz, BS, a Andrea R.
Nipple-Areolar Complex Reconstruction: A Review of the Literature and Introduction of the Rectangle-to-Cube Nipple Flap Joshua T. Henderson, BA, a ThomasJ.Lee,MD, b Andrew M. Swiergosz, BS, a Andrea R.
Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects
 Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects Joshua L. Levine, M.D., Nassif E. Soueid, M.D., and Robert J. Allen, M.D. New Orleans, La. Background: The use of lateral thoracic
Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects Joshua L. Levine, M.D., Nassif E. Soueid, M.D., and Robert J. Allen, M.D. New Orleans, La. Background: The use of lateral thoracic
Importance of the third arterial graft in multiple arterial grafting strategies
 Research Highlight Importance of the third arterial graft in multiple arterial grafting strategies David Glineur Department of Cardiovascular Surgery, Cliniques St Luc, Bouge and the Department of Cardiovascular
Research Highlight Importance of the third arterial graft in multiple arterial grafting strategies David Glineur Department of Cardiovascular Surgery, Cliniques St Luc, Bouge and the Department of Cardiovascular
The deep inferior epigastric perforator (DIEP) flap. Original Article Breast
 Original Article Breast Predictors of Reoperations in Deep Inferior Epigastric Perforator Flap Breast Reconstruction Dmytro Unukovych, MD, PhD Camilo Hernandez Gallego, MD Helena Aineskog, MD Andres Rodriguez-Lorenzo,
Original Article Breast Predictors of Reoperations in Deep Inferior Epigastric Perforator Flap Breast Reconstruction Dmytro Unukovych, MD, PhD Camilo Hernandez Gallego, MD Helena Aineskog, MD Andres Rodriguez-Lorenzo,
Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate surgical options
 A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate
A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate
CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion
 CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion Julien Pauchot, MD, PhD, a Emilie Ducroux, MD, b Grégoire Leclerc, MD, a Laurent Obert,
CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion Julien Pauchot, MD, PhD, a Emilie Ducroux, MD, b Grégoire Leclerc, MD, a Laurent Obert,
Procedure Information Guide
 Procedure Information Guide Breast reconstruction with abdominal tissue flap Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every
Procedure Information Guide Breast reconstruction with abdominal tissue flap Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every
Cost Analysis of 109 Microsurgical Reconstructions and Flap Monitoring with Microdialysis
 Cost Analysis of 109 Microsurgical Reconstructions and Flap Monitoring with Microdialysis Leena Setälä, M.D., Ph.D., 1 Heini Koskenvuori, M.Sc., 2 Daiva Gudaviciene, M.D., Ph.D., 3 Leena Berg, M.D., Ph.D.,
Cost Analysis of 109 Microsurgical Reconstructions and Flap Monitoring with Microdialysis Leena Setälä, M.D., Ph.D., 1 Heini Koskenvuori, M.Sc., 2 Daiva Gudaviciene, M.D., Ph.D., 3 Leena Berg, M.D., Ph.D.,
Distally based anterolateral thigh flap pedicled on the oblique branch of the lateral circumflex femoral artery
 Original Article Page 1 of 8 Distally based anterolateral thigh flap pedicled on the oblique branch of the lateral circumflex femoral artery Yuanbo Liu, Mengqing Zang, Shan Zhu, Bo Chen, Shanshan Li, Bingjian
Original Article Page 1 of 8 Distally based anterolateral thigh flap pedicled on the oblique branch of the lateral circumflex femoral artery Yuanbo Liu, Mengqing Zang, Shan Zhu, Bo Chen, Shanshan Li, Bingjian
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander.
 Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
B11 Breast Reconstruction with Abdominal Tissue Flap
 B11 Breast Reconstruction with Abdominal Tissue Flap Issued March 2011 You can get more information about this procedure from www.aboutmyhealth.org Tell us how useful you found this document at www.patientfeedback.org
B11 Breast Reconstruction with Abdominal Tissue Flap Issued March 2011 You can get more information about this procedure from www.aboutmyhealth.org Tell us how useful you found this document at www.patientfeedback.org
