Troponin I and risk stratification of patients with acute nonmassive pulmonary embolism
|
|
|
- Ruth Lane
- 6 years ago
- Views:
Transcription
1 Eur Respir J 2008; 31: DOI: / CopyrightßERS Journals Ltd 2008 Troponin I and risk stratification of patients with acute nonmassive pulmonary embolism D. Jiménez*, G. Díaz*, J. Molina*, D. Martí #, J. Del Rey ", S. García-Rull*, C. Escobar #, R. Vidal*, A. Sueiro* and R.D. Yusen + ABSTRACT: The assessment of risk and appropriate treatment of patients with acute pulmonary embolism (PE) remains a challenge. The prognostic performance of cardiac troponin I (ctni) in predicting 30-day all-cause mortality was prospectively assessed in consecutive haemodynamically stable patients with PE. The present study included 318 haemodynamically stable patients with PE. During the 30-day study period, 23 (7%) patients died. ctni was elevated (o0.1 ng?ml -1 ) in 102 (32%) patients. An age.65 yrs, systolic blood pressure,120 mmhg and severity of illness assessed using the PE severity index (PESI) were significantly associated with an increased risk for mortality, but no significant association was found between elevation of ctni and 30-day mortality in a logistic regression analysis. When only fatal PE was considered, multivariate analysis showed that severity of illness using the PESI and an elevated ctni (odds ratio 3.7, 95% confidence interval (CI) ) were associated with a significant increase in the risk for death. The negative predictive value (95% CI) of a negative ctni for mortality was 93 (90 97)%. In conclusion, in haemodynamically stable patients with acute pulmonary embolism, cardiac troponin I was not an independent predictor of 30-day all-cause mortality, although it did predict fatal pulmonary embolism. KEYWORDS: Prognosis, pulmonary embolism, troponin AFFILIATIONS Depts of *Respiratory, # Cardiology and, " Clinical Biochemistry, Ramón y Cajal Hospital, Madrid, Spain. + Divisions of Pulmonary and Critical Care Medicine and General Medical Sciences, Washington University School of Medicine, St Louis, MO, USA. CORRESPONDENCE D. Jiménez Castro Respiratory Dept Ramón y Cajal Hospital Madrid Spain Fax: djc_69_98@yahoo.com Received: August Accepted after revision: November Pulmonary embolism (PE) encompasses a wide spectrum of illnesses with diverse prognoses and management strategies [1]. Approximately 10% of patients with PE are critically ill and in cardiogenic shock. These patients warrant thrombolytic therapy unless contraindications preclude this management strategy [2]. At the other end of the spectrum are patients in whom PE has little impact on prognosis, with an average short-term mortality of,5% [3 6]. Although most of these patients remain hospitalised during initial therapy, some may be suitable for partial or complete outpatient management [7]. The risk stratification for patients with PE is important for two reasons. First, patients at high risk for complications could be treated more aggressively, i.e. with thrombolytic agents [8 10]. Secondly, patients estimated to be at low risk could be discharged early or managed entirely as outpatients, which could substantially reduce the use of healthcare resources. echocardiography has been proposed as the best established method for determining risk stratification and therapy [12]. Since echocardiography has some technical limitations, is expensive and not widely available in all medical centres, cardiac troponin testing may assist in determining the management of haemodynamically stable patients with acute PE. Although troponin elevation alone may not suffice to predict early death or major complications in patients with acute PE, prior studies suggest that normal troponin levels have a very high negative predictive value for mortality in patients with PE [13]. Thus, troponin may be potentially useful in identifying patients suitable for outpatient management. The present study was prospectively designed to assess the prognostic significance of elevated cardiac troponin I (ctni) in a cohort of haemodynamically stable patients with acute symptomatic PE. STATEMENT OF INTEREST None declared. Right ventricular dysfunction is a consequence of severe PE that is associated with poor prognosis and higher mortality rates in normotensive patients with acute PE [11]. To date, early detection of right ventricular dysfunction by bedside METHODS Study design In the prospective cohort study, consecutive eligible patients were approached for enrolment between January 1, 2003 and December 31, European Respiratory Journal Print ISSN Online ISSN c EUROPEAN RESPIRATORY JOURNAL VOLUME 31 NUMBER 4 847
2 RISK ASSESSMENT IN PULMONARY EMBOLISM D. JIMÉNEZ ET AL. Patients, setting and eligibility criteria Outpatients presenting with symptoms of acute PE at the Emergency Dept of Ramón y Cajal Hospital (Madrid, Spain) were screened (fig. 1). Eligible patients were required to have symptomatic PE confirmed by objective testing. Exclusion criteria were: haemodynamic instability at presentation (defined as having cardiogenic shock, systolic blood pressure,90 mmhg or the need for inotropic support despite blood pressure measurements); thrombolytic therapy indicated by decision of attending physician; and troponin levels not determined within 12 h of the diagnosis of PE. The study was approved by the Institutional Review Board of Ramón y Cajal Hospital. Diagnosis of PE A diagnosis of PE was suggested by: a high-probability ventilation perfusion scan according to the criteria of the prospective investigation of pulmonary embolism diagnosis [14]; an indeterminate ventilation perfusion lung scan and confirmed lower limb deep vein thrombosis on venous ultrasound [15]; or the finding of an intraluminal filling defect on PE protocol contrast enhance helical chest computed tomography [16]. ctni assay Blood samples were collected from an antecubital vein at the time of hospital admission. ctni levels were measured quantitatively using a microparticle enzyme immunoassay (Abbott Laboratories, Abbott Park, IL, USA). The analytical sensitivity for ctni is 0.08 ng?ml -1 and represents the lowest measurable concentration of ctni that can be distinguished from zero. Using this assay, ctni concentrations of o0.1 ng?ml -1 were regarded as indicating myocardial injury. The clinicians were unaware of the patients troponin levels throughout the hospital stay. Calculation of the prediction rule Using prospectively collected baseline data at the time of PE diagnosis, PE severity index (PESI) scores were retrospectively determined and each patient was classified into one of five PESI risk classes [17]. Anticoagulant therapy Patients were treated with therapeutic doses of parenteral anticoagulants while they were prescribed oral vitamin K antagonist therapy. After an initial overlap treatment period, patients were continued on dose-adjusted oral vitamin K antagonist therapy (acenocoumarol) with a target international normalised ratio (INR) of 2.5 (therapeutic range ). INR was usually monitored daily until the therapeutic range had been achieved, twice or three times weekly for the first few weeks and then once a week to once a month, depending on the stability of the results. Thrombolytic treatment and/or inotropic support were administered in patients with haemodynamic deterioration as deemed appropriate by the attending physician. Study end-points The primary end-point was all-cause mortality during the first 30 days of therapy. The secondary end-point was mortality due to PE during the same period of time. Mortality was assessed using patient or proxy interviews and/or hospital Patients with suspected PE n=1180 PE confirmed n=366 Patients included in study n=318 ctni-positive group n=102 PE excluded n=814 Patients excluded: haemodynamic instability # n=37 unavailable troponin measurement n=11 ctni-negative group n=216 FIGURE 1. Flow diagram of patients assessed for study eligibility. PE: pulmonary embolism; ctni: cardiac toponin I. # : defined as having cardiogenic shock, systolic blood pressure,90 mmhg or the need forinotropic support despite blood pressure measurements. chart review. Two independent experts adjudicated the cause of death as definite fatal PE or death from other causes. Statistical analysis Data are expressed as mean SD. All probability values are two-tailed and a p-value,0.05 was considered statistically significant. An unpaired t-test, Wilcoxon rank sum, Chisquared and Fisher s exact test were used when applicable. Logistic regression was used to examine the association between ctni testing and 30-day all-cause mortality, adjusting for other clinical predictors previously described in the literature. Only univariate predictor variables that were significantly associated with mortality (p,0.05) were added to the multivariate model. In order to assess the test and performance characteristics of the ctni-positive versus ctni-negative groups, the sensitivity, specificity, positive and negative predictive values and likelihood ratios for predicting all-cause mortality were estimated. All 95% confidence intervals (CIs) were computed from the binomial distribution. RESULTS A total of 366 consecutive patients with acute PE were screened. A total of 37 (10%) patients were excluded due to haemodynamic instability. Of the 329 stable patients, an additional 11 (3%) patients were excluded because troponin levels could not be determined within 12 h from the diagnosis of PE. All of the remaining eligible 318 patients (136 males and 182 females) who had a diagnosis of haemodynamically stable acute PE at the time of presentation to the emergency dept were enrolled (fig. 1). Of the 318 enrolled patients, 102 (32%) had elevated serum ctni levels (ctni-positive group) and the remaining 216 patients had normal serum ctni levels (ctni-negative group). 848 VOLUME 31 NUMBER 4 EUROPEAN RESPIRATORY JOURNAL
3 D. JIMÉNEZ ET AL. RISK ASSESSMENT IN PULMONARY EMBOLISM TABLE 1 Baseline characteristics of 318 consecutive patients with acute pulmonary embolism Group OR (95% CI) p-value ctni-positive ctni-negative Subjects n Clinical characteristics Age.65 yrs 86 (84) 154 (71) 2.2 ( ) 0.02 Male 44 (43) 92 (43) 1.0 ( ) 0.90 Risk factors for venous thromboembolism Cancer 18 (18) 30 (14) 1.3 ( ) 0.45 Surgery 10 (10) 17 (8) 1.5 ( ) 0.70 Immobility for o4 days 19 (19) 32 (15) 1.3 ( ) 0.46 Previous venous thromboembolism 12 (12) 25 (12) 1.0 ( ) 0.86 Comorbid diseases Chronic lung disease 14 (14) 39 (18) 0.7 ( ) 0.47 Congestive heart failure 19 (19) 26 (12) 1.7 ( ) 0.14 Clinical presentation at admission Syncope 34 (34) 25 (12) 3.8 ( ), Chest pain 43 (43) 127 (59) 0.5 ( ) 0.01 Dyspnoea 77 (77) 155 (72) 1.2 ( ) 0.42 Cardiac frequency o100 beats?min (50) 79 (37) 1.7 ( ) 0.04 PO2,60 mmhg 52 (52) 120 (56) 0.8 ( ) 0.59 Systolic blood pressure,120 mmhg 37 (36) 71 (33) 1.2 ( ) 0.69 ECG SI-QIII pattern 16 (16) 19 (9) 1.9 ( ) 0.09 Complete/incomplete right bundle branch block 23 (23) 24 (11) 2.3 ( ) Inverted T-waves in V 1 through V 3 18 (18) 25 (12) 1.6 ( ) 0.20 Data are presented as n (%), unless otherwise stated. OR: odds ratio; CI: confidence interval; PO2: partial pressure of oxygen. Patients in the ctni-positive group were significantly older when compared with patients in the ctni-negative group. Syncope on presentation was more frequent in the ctnipositive group, whereas chest pain was more frequent in the ctni-negative group (table 1). There was a significant association between elevated troponin levels and the presence of a right bundle branch block on the ECG (p50.008) and sinus tachycardia (p50.04). There was no association between Cumulative survival % Cumulative survival % Days Days FIGURE 2. Kaplan Meier 30-day all-cause mortality of cardiac troponin I (ctni)-positive (----) and -negative (?????) test groups. The numbers of patients at risk in the ctni-positive group were 102, 96, 95, 93, 93, 93 and 93, while in the ctninegative group they were 216, 216, 214, 211, 207, 205 and 202 for day 0, 5, 10, 15, 20, 25 and 30, respectively. FIGURE 3. Kaplan Meier 30-day pulmonary embolism-related mortality of cardiac troponin I (ctni)-positive (----) and -negative (?????) test groups. The numbers of patients at risk in the ctni-positive group were 102, 96, 95, 94, 94, 94 and 94, while in the ctni-negative group they were 216, 216, 215, 213, 213, 213 and 212 for day 0, 5, 10, 15, 20, 25 and 30, respectively. c EUROPEAN RESPIRATORY JOURNAL VOLUME 31 NUMBER 4 849
4 RISK ASSESSMENT IN PULMONARY EMBOLISM D. JIMÉNEZ ET AL. elevated troponin levels and the presence of an S1Q3T3 pattern or T-wave inversion on ECG. During the 1-month follow-up period, 23 (7%) patients died. In the ctni-positive group, 30-day all-cause mortality was 9% compared with 6% in the ctni-negative group (odds ratio (OR) 1.4, 95% CI ; p50.46). The ctni-positive group had a trend toward earlier death compared with the ctni-negative group (log rank p50.402; fig. 2). Mortality in the ctni-positive group was the result of thromboembolic disease (eight cases) and seizures (one case). Mortality in the ctni-negative group was the result of thromboembolic disease (four cases), heart failure (four cases), malignancy (two cases), infection (two cases), renal insufficiency (one case) and unspecified cause (one case). For 30-day PE-related mortality, survival was lower in the ctni-positive group compared with the ctni-negative group (log rank p50.008; fig. 3). Most (eight out of nine) of the early deaths (within 7 10 days after diagnosis) were due to complications of PE. Troponin test was positive in seven of the nine patients who died early. Four of the eight patients who died early from PE complications had the lowest positive troponin level. Univariate analysis of data from the 318 patients revealed that age.65 yrs, systolic blood pressure (SBP),120 mmhg and severity of illness assessed using the PESI were significantly associated with 30-day mortality (table 2). Upon multivariate analysis, patients with an SBP,120 mmhg (OR 4.0, 95% CI ; p50.003) and severity of illness (OR 7.8, 95% CI ; p50.05) were independently associated with an increased risk for 1-month mortality. When only fatal PE was considered, multivariate analysis showed that severity of illness using the PESI and an elevated ctni (OR 3.7, 95% CI ; p50.03) were associated with a significant increase in the risk for 30- day all-cause mortality. The negative predictive value of a negative ctni (,0.1 ng?ml -1 ) for 30-day all-cause mortality was 93% (95% CI 90 97%), while the negative likelihood ratio was 1.0% ( %). The negative predictive value of a negative ctni (,0.1 ng?ml -1 ) for 30-day PE-related mortality was 98% (96 100%), while the negative likelihood ratio was 0.5% ( %; table 3). DISCUSSION There are two principal conclusions that follow from the present results. First, an elevated ctni was associated with a 4.5-fold increased risk of fatal PE, but it did not appear to confer an increased risk of all-cause death. Secondly, although a low ctni level exhibited a very high negative predictive value with regard to prognosis, troponin by itself does not TABLE 2 Risk factors for 30-day all-cause mortality Nonsurvivors Survivors OR (95%CI) p-value Subjects n Clinical characteristics Age.65 yrs 22 (96) 218 (74) 7.8 ( ) 0.03 Male 10 (43) 126 (43) 1.0 ( ) 0.83 Risk factors for venous thromboembolism Cancer 6 (26) 42 (14) 2.1 ( ) 0.21 Surgery 1 (4) 26 (9) 0.5 ( ) 0.66 Immobility for o4 days 7 (30) 44 (15) 2.5 ( ) 0.11 Previous venous thromboembolism 2 (9) 35 (12) 0.7 ( ) 0.92 Underlying diseases Chronic lung disease 4 (17) 49 (17) 1.1 ( ) 0.77 Congestive heart failure 3 (13) 42 (14) 0.9 ( ) 0.86 Clinical presentation at admission Syncope 2 (9) 57 (19) 0.4 ( ) 0.36 Chest pain 9 (39) 161 (55) 0.5 ( ) 0.20 Dyspnoea 17 (74) 215 (73) 1.0 ( ) 0.89 Cardiac frequency o100 beats?min -1 9 (39) 120 (41) 0.9 ( ) 0.97 PO 2,60 mmhg 14 (61) 158 (54) 1.3 ( ) 0.66 Systolic blood pressure,120 mmhg 14 (61) 94 (32) 3.3 ( ) PESI high-risk strata # 22 (96) 196 (66) 11.1 ( ) Electrocardiogram SI-QIII pattern 0 (0) 35 (12) 0.16 Complete/incomplete right bundle branch block 1 (4) 46 (16) 0.2 (0 1.9) 0.21 Inverted T-waves in V 1 through V 3 3 (13) 40 (14) 1.0 ( ) 0.86 Laboratory findings ctni.0.1 ng?ml -1 9 (39) 93 (32) 1.4 ( ) 0.65 Data are presented as n (%), unless otherwise stated. OR: odds ratio; CI: confidence interval; PO2: partial pressure of oxygen; PESI: pulmonary embolism severity index; ctni: cardiac troponin I. # : strata defined in [17]. 850 VOLUME 31 NUMBER 4 EUROPEAN RESPIRATORY JOURNAL
5 D. JIMÉNEZ ET AL. RISK ASSESSMENT IN PULMONARY EMBOLISM TABLE 3 Risk factors for fatal pulmonary embolism (PE) during 30-days of follow-up Fatal PE Non-fatal PE OR (95% CI) p-value Subjects n Clinical characteristics Age.65 yrs 12 (100) 228 (74) 0.09 Male 5 (42) 131 (43) 0.9 ( ) 0.82 Risk factors for venous thromboembolism Cancer 4 (33) 44 (14) 3.0 ( ) 0.16 Surgery 1 (8) 26 (8) 1.0 ( ) 0.58 Immobility for o4 days 3 (25) 48 (16) 1.8 ( ) 0.67 Previous venous thromboembolism 2 (17) 35 (11) 1.5 ( ) 0.86 Underlying diseases Chronic lung disease 4 (33) 49 (16) 2.6 ( ) 0.25 Congestive heart failure 3 (25) 42 (14) 2.1 ( ) 0.52 Clinical presentation at admission Syncope 2 (17) 57 (19) 0.9 ( ) 0.84 Chest pain 6 (50) 164 (54) 0.9 ( ) 0.98 Dyspnoea 8 (67) 224 (73) 0.7 ( ) 0.89 Cardiac frequency o100 beats?min -1 5 (42) 124 (40) 1.0 ( ) 0.87 PO 2,60 mmhg 7 (58) 165 (54) 1.2 ( ) 0.98 Systolic blood pressure,120 mmhg 6 (50) 102 (33) 2.0 ( ) 0.36 PESI high-risk strata # 12 (100) 206 (67) 0.03 Electrocardiogram SI-QIII pattern 0 (0) 35 (11) 0.46 Complete/incomplete right bundle branch block 1 (8) 46 (15) 0.5 ( ) 0.79 Inverted T-waves in V 1 through V 3 1 (8) 42 (14) 0.6 ( ) 0.87 Laboratory findings, ctni.0.1 ng?ml -1 8 (67) 94 (31) 4.5 ( ) 0.02 Data are presented as n (%), unless otherwise stated. OR: odds ratio; CI: confidence interval; PO2: partial pressure of oxygen; PESI: PE severity index; ctni: cardiac troponin I. # : strata defined in [17]. appear to clinically significantly change the pre- to post-test probability (i.e. positive and negative likelihood ratios are not extreme) of risk of death or PE-related complications. PE encompasses a wide spectrum of presentations, prognoses and consequent management strategies [11]. A tool that accurately predicts adverse outcomes at the time of presentation could determine management and outcomes. ctni may have a role for risk stratification and prognostication in patients with acute PE. ctni may also serve as a surrogate for echocardiographic right ventricle dysfunction, and increased concentrations of cardiac troponins have been found to predict fatal outcome in patients with haemodynamically stable PE in other studies [18, 19]. The present study enrolled a large number of consecutive patients with haemodynamically stable acute PE. Elevated ctni plasma concentrations were found in 32% of the 318 investigated cases. This detection rate was similar to that of the study by KOSTRUBIEC et al. [20] and lies within the range of the results of other studies that have assessed the usefulness of troponin in patients with stable PE [18, 19]. In a study of 458 patients with submassive PE, the incidence of ctni.0.5 mg?l -1 was 13% [18]. The discrepancy between that study and the present findings is probably the result of differences in the cut-off value used to define an elevated cardiac troponin. Moreover, in the study by DOUKETIS et al. [18], patients were derived from a randomised controlled trial [21], which tends to exclude sicker patients. In another study of 106 patients with PE of unspecified severity, 41% had a ctni.0.07 mg?l -1 [19]. However, although patients included in that study were normotensive, they had been referred for echocardiographic assessment of right ventricular dysfunction, thus reflecting a group of PE patients of higher severity. A positive troponin test independently predicted fatal PE. The PE-related deaths mainly occurred within 1 week of diagnosis of PE. A positive troponin test did not predict all-cause mortality. Severity of illness, based on a validated clinical model (i.e. PESI), predicted both overall and specific PE mortality. The present authors, therefore, propose that an elevated ctni is a marker of decreased cardiorespiratory reserve in patients with PE, while the PESI also underscores the prognostic significance of other important clinical factors, such as age, cancer or previous lung or cardiac disease. The clinical benefit of cardiac troponins is foremost due to the high negative predictive value [13]. Troponin testing in normotensive patients with PE appears to be most relevant as a screening test for the identification of low-risk patients c EUROPEAN RESPIRATORY JOURNAL VOLUME 31 NUMBER 4 851
6 RISK ASSESSMENT IN PULMONARY EMBOLISM D. JIMÉNEZ ET AL. suitable for outpatient management. The present results indicate that troponin testing does not identify patients with stable PE who are at very low risk of fatal medical outcomes. This result could be explained as a consequence of a lower performance of the troponin testing in the present series with respect to previously published studies [19, 22 24]. Since the negative likelihood ratio was not extreme, the present results may also warrant the need to combine troponin measurement with other tools (e.g. clinical prognostic scores, echocardiography) in order to identify low-risk patients for out-ofhospital treatment of acute PE [25]. There are several limitations to the present study that should be acknowledged. First, it has been recommended that a second biomarker test should be obtained 6 12 h after an initially negative test in a PE patient with a symptom duration of,6 h [26]. It is, however, questionable whether repeated troponin measurements represent a practical and economic approach for optimising risk stratification of PE. Secondly, coronary artery disease-related positive ctni was excluded based on ECGs and clinical evolution of the patients. Thus, it cannot be excluded that significant coronary artery stenosis or even acute coronary syndrome may have been present in some of the study patients, limiting the specificity of troponin measurements. However, the study protocol required confirmation of PE in all cases. Therefore, additional diagnostic workup in order to exclude concomitant coronary artery disease was not deemed appropriate. Finally, it has been shown that the use of troponin measurement and echocardiography in combination can identify patients at high risk for death after PE [27, 28]. However, as echocardiography was not a protocol requirement in the present study, those results could not be confirmed. In conclusion, the present results support the value of cardiac troponin I for the prediction of 30-day pulmonary embolismrelated mortality but not all-cause mortality, in a large series of stable patients presenting to the emergency dept with acute pulmonary embolism. ACKNOWLEDGEMENTS The authors would like to thank D. Aujesky (Dept of Internal Medicine, University of Lausanne, Lausanne, Switzerland), J.L. Lobo (Respiratory Dept, Txagorritxu Hospital, Vitoria, Spain) and M. Monreal (Medicine Dept, Germans Trias i Pujol Hospital, Barcelona, Spain) for their helpful comments on earlier versions of this manuscript. REFERENCES 1 Goldhaber SZ. Cardiac biomarkers in pulmonary embolism. Chest 2003; 123: Büller H, Agnellli G, Hull RD, Hyers TM, Prins MH, Raskob GE. Antithrombotic therapy for venous thromboembolic disease: the Seventh ACCP Conference on Antithrombotic and Thrombolytic Therapy. Chest 2004; 126: Suppl. 3, 401S 428S. 3 Goldhaber SZ, Visani L, De Rosa M. Acute pulmonary embolism: clinical outcomes in the International Cooperative Pulmonary Embolism Registry (ICOPER). Lancet 1999; 353: Grifoni S, Olivotto I, Cecchini P, et al. Short-term clinical outcome of patients with acute pulmonary embolism, normal blood pressure, and echocardiographic right ventricular dysfunction. Circulation 2000; 101: Kreit JW. The impact of right ventricular dysfunction on the prognosis and therapy of normotensive patients with pulmonary embolism. Chest 2004; 125: Ribeiro A, Lindmarker P, Juhlin-Dannfelt A, Johnsson H, Jorfeldt L. Echocardiography Doppler in pulmonary embolism: right ventricular dysfunction as a predictor of mortality rate. Am Heart J 1997; 134: British Thoracic Society Standards of Care Committee Pulmonary Embolism Guideline Development Group. British Thoracic Society guidelines for the management of suspected acute pulmonary embolism. Thorax 2003; 58: Konstantinides S, Geibel A, Heusel G, Heinrich F, Kasper W. Management Strategies and Prognosis of Pulmonary Embolism-3 Trial Investigators. Heparin plus alteplase compared with heparin alone in patients with submassive pulmonary embolism. N Engl J Med 2002; 347: Hamel E, Pacouret G, Vincentelli D, et al. Thrombolysis or heparin therapy in massive pulmonary embolism with right ventricular dilation: results from a 128-patient monocenter registry. Chest 2001; 120: Goldhaber SZ, Haire WD, Feldstein ML, et al. Alteplase versus heparin in acute pulmonary embolism: randomised trial assesing right-ventricular function and pulmonary perfusion. Lancet 1993; 341: Kasper W, Konstantinides S, Geibel A, Tiede N, Krause T, Just H. Prognostic significance of right ventricular afterload stress detected by echocardiography in patients with clinically suspected pulmonary embolism. Heart 1997; 77: ten Wolde M, Söhne M, Quak E, Mac Gillavry MR, Büller HR. Prognostic value of echocardiographically assessed right ventricular dysfunction in patients with pulmonary embolism. Arch Intern Med 2004; 164: Konstantinides S. Pulmonary embolism: impact of right ventricular dysfunction. Curr Opin Cardiol 2005; 20: Value of the ventilation/perfusion scan in acute pulmonary embolism. Results of the prospective investigation of the pulmonary embolism diagnosis (PIOPED). The PIOPED investigators. JAMA 1990; 263: Turkstra F, Kuijer PM, van Beek EJ, Brandjes DP, ten Cate JW, Büller HR. Diagnostic utility of ultrasonography of leg veins in patients suspected of having pulmonary embolism. Ann Intern Med 1997; 126: Remy-Jardin M, Remy J, Wattinne L, Giraud F. Central pulmonary thromboembolism: diagnosis with spiral volumetric CT with the single-breath-hold-technique comparison with pulmonary angiography. Radiology 1992; 185: Aujesky D, Obrosky DS, Stone RA, et al. Derivation and validation of a prognostic model for pulmonary embolism. Am J Respir Crit Care Med 2005; 172: Douketis JD, Leeuwenkamp O, Grobara P, et al. The incidence and prognostic significance of elevated cardiac troponins in patients with submassive pulmonary embolism. J Thromb Haemost 2005; 3: VOLUME 31 NUMBER 4 EUROPEAN RESPIRATORY JOURNAL
7 D. JIMÉNEZ ET AL. RISK ASSESSMENT IN PULMONARY EMBOLISM 19 Pruszczyk P, Bochowicz A, Torbicki A, et al. Cardiac troponin T monitoring identifies high-risk group of normotensive patients with acute pulmonary embolism. Chest 2003; 123: Kostrubiec M, Pruszczyk, P, Bochowicz A, et al. Biomarkerbased risk assessment model in acute pulmonary embolism. Eur Heart J 2005; 26: Büller HR, Davidson BL, Decousus H, et al. Subcutaneous fondaparinux versus intravenous unfractionated heparin in the initial treatment of pulmonary embolism. N Engl J Med 2003; 349: Giannitsis E, Müller-Bardorff M, Kurowski V, et al. Independent prognostic value of cardiac troponin T in patients with confirmed pulmonary embolism. Circulation 2000; 102: Janata K, Holzer M, Laggner AN, Müllner M. Cardiac troponin T in the severity assessment of patients with pulmonary embolism: cohort study. BMJ 2003; 326: Konstantinides S, Geibel A, Olschewski M, et al. Importance of cardiac troponins I and T in risk stratification of patients with acute pulmonary embolism. Circulation 2002; 106: Jiménez D, Yusen RD, Otero R, et al. Prognostic models for selecting patients with acute pulmonary embolism for initial outpatient therapy. Chest 2007; 132: Kucher N, Printzen G, Goldhaber SZ. Prognostic role of brain natriuretic peptide in acute pulmonary embolism. Circulation 2003; 107: Scridon T, Scridon C, Skali H, Alvarez A, Goldhaber SZ, Solomon SD. Prognostic significance of troponin elevation and right ventricular enlargement in acute pulmonary embolism. Am J Cardiol 2005; 96: Binder L, Pieske B, Olschewski M, et al. N-terminal probrain natriuretic peptide or troponin testing followed by echocardiography for risk stratification of acute pulmonary embolism. Circulation 2005; 112: EUROPEAN RESPIRATORY JOURNAL VOLUME 31 NUMBER 4 853
Venous thromboembolism (VTE) is a common. Changes in PESI scores predict mortality in intermediate-risk patients with acute pulmonary embolism
 Eur Respir J 2013; 41: 354 359 DOI: 10.1183/09031936.00225011 CopyrightßERS 2013 Changes in PESI scores predict mortality in intermediate-risk patients with acute pulmonary embolism Lisa Moores*, Celia
Eur Respir J 2013; 41: 354 359 DOI: 10.1183/09031936.00225011 CopyrightßERS 2013 Changes in PESI scores predict mortality in intermediate-risk patients with acute pulmonary embolism Lisa Moores*, Celia
The shock index and the simplified PESI for identification of low-risk patients with acute pulmonary embolism
 Eur Respir J 211; 37: 762 766 DOI: 1.1183/931936.711 CopyrightßERS 211 The shock index and the simplified PESI for identification of low-risk patients with acute pulmonary embolism A. Sam*, D. Sánchez*,
Eur Respir J 211; 37: 762 766 DOI: 1.1183/931936.711 CopyrightßERS 211 The shock index and the simplified PESI for identification of low-risk patients with acute pulmonary embolism A. Sam*, D. Sánchez*,
ORIGINAL INVESTIGATION
 ORIGINAL INVESTIGATION Prognostic Role of Echocardiography Among Patients With Acute Pulmonary Embolism and a Systolic Arterial Pressure of 90 mm Hg or Higher Nils Kucher, MD; Elisa Rossi, BS; Marisa De
ORIGINAL INVESTIGATION Prognostic Role of Echocardiography Among Patients With Acute Pulmonary Embolism and a Systolic Arterial Pressure of 90 mm Hg or Higher Nils Kucher, MD; Elisa Rossi, BS; Marisa De
RISK STRATIFICATION OF PATIENTS WITH ACUTE SYMPTOMATIC PULMONARY EMBOLISM. David Jiménez, MD, PhD, FCCP Ramón y Cajal Hospital, IRYCIS Madrid, Spain
 RISK STRATIFICATION OF PATIENTS WITH ACUTE SYMPTOMATIC PULMONARY EMBOLISM David Jiménez, MD, PhD, FCCP Ramón y Cajal Hospital, IRYCIS Madrid, Spain Potential Conflicts of Interest Financial conflicts of
RISK STRATIFICATION OF PATIENTS WITH ACUTE SYMPTOMATIC PULMONARY EMBOLISM David Jiménez, MD, PhD, FCCP Ramón y Cajal Hospital, IRYCIS Madrid, Spain Potential Conflicts of Interest Financial conflicts of
Prognostic value of the ECG on admission in patients with acute major pulmonary embolism
 Eur Respir J 2005; 25: 843 848 DOI: 10.1183/09031936.05.00119704 CopyrightßERS Journals Ltd 2005 Prognostic value of the ECG on admission in patients with acute major pulmonary embolism A. Geibel*, M.
Eur Respir J 2005; 25: 843 848 DOI: 10.1183/09031936.05.00119704 CopyrightßERS Journals Ltd 2005 Prognostic value of the ECG on admission in patients with acute major pulmonary embolism A. Geibel*, M.
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/21764 holds various files of this Leiden University dissertation. Author: Mos, Inge Christina Maria Title: A more granular view on pulmonary embolism Issue
Cover Page The handle http://hdl.handle.net/1887/21764 holds various files of this Leiden University dissertation. Author: Mos, Inge Christina Maria Title: A more granular view on pulmonary embolism Issue
Chapter 1. Introduction
 Chapter 1 Introduction Introduction 9 Even though the first reports on venous thromboembolism date back to the 13 th century and the mechanism of acute pulmonary embolism (PE) was unraveled almost 150
Chapter 1 Introduction Introduction 9 Even though the first reports on venous thromboembolism date back to the 13 th century and the mechanism of acute pulmonary embolism (PE) was unraveled almost 150
Troponin-Based Risk Stratification of Patients With Acute Nonmassive Pulmonary Embolism. Systematic Review and Metaanalysis
 CHEST Troponin-Based Risk Stratification of Patients With Acute Nonmassive Pulmonary Embolism Systematic Review and Metaanalysis David Jiménez, MD; Fernando Uresandi, MD; Remedios Otero, MD; José Luis
CHEST Troponin-Based Risk Stratification of Patients With Acute Nonmassive Pulmonary Embolism Systematic Review and Metaanalysis David Jiménez, MD; Fernando Uresandi, MD; Remedios Otero, MD; José Luis
DECLARATION OF CONFLICT OF INTEREST
 DECLARATION OF CONFLICT OF INTEREST IDENTIFYING LOW-RISK PULMONARY EMBOLISM CLINICAL SCORES David Jiménez, MD, PhD Respiratory Department Ramón y Cajal Hospital Madrid, Spain Potential Conflicts of Interest
DECLARATION OF CONFLICT OF INTEREST IDENTIFYING LOW-RISK PULMONARY EMBOLISM CLINICAL SCORES David Jiménez, MD, PhD Respiratory Department Ramón y Cajal Hospital Madrid, Spain Potential Conflicts of Interest
Should thrombolysis have a greater role in the management of pulmonary embolism?
 ORIGINAL PAPERS Clinical Medicine 2009, Vol 9, No 5: 431 5 Should thrombolysis have a greater role in the management of pulmonary embolism? Peter O Jenkins, Javed Sultanzadeh, Manasi Bhagwat and Paul F
ORIGINAL PAPERS Clinical Medicine 2009, Vol 9, No 5: 431 5 Should thrombolysis have a greater role in the management of pulmonary embolism? Peter O Jenkins, Javed Sultanzadeh, Manasi Bhagwat and Paul F
Supplementary Online Content
 Supplementary Online Content Mismetti P, Laporte S, Pellerin O, Ennezat P-V, Couturaud F, Elias A, et al. Effect of a retrievable inferior vena cava filter plus anticoagulation vs anticoagulation alone
Supplementary Online Content Mismetti P, Laporte S, Pellerin O, Ennezat P-V, Couturaud F, Elias A, et al. Effect of a retrievable inferior vena cava filter plus anticoagulation vs anticoagulation alone
Biomarker-based risk assessment model in acute pulmonary embolism
 European Heart Journal (2005) 26, 2166 2172 doi:10.1093/eurheartj/ehi336 Clinical research Biomarker-based risk assessment model in acute pulmonary embolism Maciej Kostrubiec 1, Piotr Pruszczyk 1 *, Anna
European Heart Journal (2005) 26, 2166 2172 doi:10.1093/eurheartj/ehi336 Clinical research Biomarker-based risk assessment model in acute pulmonary embolism Maciej Kostrubiec 1, Piotr Pruszczyk 1 *, Anna
The Pulmonary Embolism Severity Index in Predicting the Prognosis of Patients With Pulmonary Embolism
 ORIGINAL ARTICLE DOI: 10.3904/kjim.2009.24.2.123 The Pulmonary Embolism Severity Index in Predicting the Prognosis of Patients With Pulmonary Embolism Won-Ho Choi 1, Sung Uk Kwon 1,2, Yoon Jung Jwa 1,
ORIGINAL ARTICLE DOI: 10.3904/kjim.2009.24.2.123 The Pulmonary Embolism Severity Index in Predicting the Prognosis of Patients With Pulmonary Embolism Won-Ho Choi 1, Sung Uk Kwon 1,2, Yoon Jung Jwa 1,
ORIGINAL INVESTIGATION. Thrombolytic Therapy and Mortality in Patients With Acute Pulmonary Embolism
 ORIGINAL INVESTIGATION Thrombolytic Therapy and in Patients With Acute Pulmonary Embolism Said A. Ibrahim, MD, MPH; Roslyn A. Stone, PhD; D. Scott Obrosky, MSc; Ming Geng, MSc; Michael J. Fine, MD, MSc;
ORIGINAL INVESTIGATION Thrombolytic Therapy and in Patients With Acute Pulmonary Embolism Said A. Ibrahim, MD, MPH; Roslyn A. Stone, PhD; D. Scott Obrosky, MSc; Ming Geng, MSc; Michael J. Fine, MD, MSc;
Cardiac troponin I for predicting right ventricular dysfunction and intermediate risk in patients with normotensive pulmonary embolism
 Neth Heart J (2015) 23:55 61 DOI 10.1007/s12471-014-0628-7 ORIGINAL ARTICLE: SHORT COMMUNICATION Cardiac troponin I for predicting right ventricular dysfunction and intermediate risk in patients with normotensive
Neth Heart J (2015) 23:55 61 DOI 10.1007/s12471-014-0628-7 ORIGINAL ARTICLE: SHORT COMMUNICATION Cardiac troponin I for predicting right ventricular dysfunction and intermediate risk in patients with normotensive
PULMONARY EMBOLISM (PE): DIAGNOSIS AND TREATMENT
 PULMONARY EMBOLISM (PE): DIAGNOSIS AND TREATMENT OBJECTIVE: To provide a diagnostic algorithm and treatment options for patients with acute pulmonary embolism (PE). BACKGROUND: Venous thromboembolism (VTE)
PULMONARY EMBOLISM (PE): DIAGNOSIS AND TREATMENT OBJECTIVE: To provide a diagnostic algorithm and treatment options for patients with acute pulmonary embolism (PE). BACKGROUND: Venous thromboembolism (VTE)
Open Access Original Article
 Open Access Original Article Prognostic role of simplified Pulmonary Embolism Severity Index and the European Society of Cardiology Prognostic Model in short- and long-term risk stratification in pulmonary
Open Access Original Article Prognostic role of simplified Pulmonary Embolism Severity Index and the European Society of Cardiology Prognostic Model in short- and long-term risk stratification in pulmonary
DIAGNOSTIC evaluation for acute pulmonary
 994 2-D ECHO Jackson et al. ECHOCARDIOGRAPHY FOR PULMONARY EMBOLISM Prospective Evaluation of Two-dimensional Transthoracic Echocardiography in Emergency Department Patients with Suspected Pulmonary Embolism
994 2-D ECHO Jackson et al. ECHOCARDIOGRAPHY FOR PULMONARY EMBOLISM Prospective Evaluation of Two-dimensional Transthoracic Echocardiography in Emergency Department Patients with Suspected Pulmonary Embolism
Ryan Walsh, MD Department of Emergency Medicine Madigan Army Medical Center
 Ryan Walsh, MD Department of Emergency Medicine Madigan Army Medical Center The opinions expressed herein are solely those of the author and do not represent the official views of the Department of Defense
Ryan Walsh, MD Department of Emergency Medicine Madigan Army Medical Center The opinions expressed herein are solely those of the author and do not represent the official views of the Department of Defense
Despite important advances in diagnosis and treatment,
 Importance of Cardiac Troponins I and T in Risk Stratification of Patients With Acute Pulmonary Embolism Stavros Konstantinides, MD; Annette Geibel, MD; Manfred Olschewski, PhD; Wolfgang Kasper, MD; Nadine
Importance of Cardiac Troponins I and T in Risk Stratification of Patients With Acute Pulmonary Embolism Stavros Konstantinides, MD; Annette Geibel, MD; Manfred Olschewski, PhD; Wolfgang Kasper, MD; Nadine
ORIGINAL INVESTIGATION. Thrombolysis vs Heparin in the Treatment of Pulmonary Embolism
 Thrombolysis vs Heparin in the Treatment of Pulmonary Embolism A Clinical Outcome Based Meta-analysis ORIGINAL INVESTIGATION Giancarlo Agnelli, MD; Cecilia Becattini, MD; Timo Kirschstein, MD Background:
Thrombolysis vs Heparin in the Treatment of Pulmonary Embolism A Clinical Outcome Based Meta-analysis ORIGINAL INVESTIGATION Giancarlo Agnelli, MD; Cecilia Becattini, MD; Timo Kirschstein, MD Background:
S (18) doi: /j.ajem Reference: YAJEM 57346
 Accepted Manuscript A portrait of patients who die in-hospital from acute pulmonary embolism Hesham R. Omar, Mehdi Mirsaeidi, Bishoy Abraham, Garett Enten, Devanand Mangar, Enrico M. Camporesi PII: S0735-6757(18)30172-4
Accepted Manuscript A portrait of patients who die in-hospital from acute pulmonary embolism Hesham R. Omar, Mehdi Mirsaeidi, Bishoy Abraham, Garett Enten, Devanand Mangar, Enrico M. Camporesi PII: S0735-6757(18)30172-4
Epidemiology. Update on Pulmonary Embolism. Keys to PE Management 5/5/2014. Diagnosis. Risk stratification. Treatment
 Update on Pulmonary Embolism Steven M. Dean, DO, FACP, RPVI Program Director- Vascular Medicine Associate Professor of Internal Medicine Division of Cardiovascular Medicine The Ohio State University Keys
Update on Pulmonary Embolism Steven M. Dean, DO, FACP, RPVI Program Director- Vascular Medicine Associate Professor of Internal Medicine Division of Cardiovascular Medicine The Ohio State University Keys
Acute pulmonary embolism: risk stratification in the emergency department
 Intern Emerg Med (2007) 2:119 129 DOI 10.1007/s11739-007-0033-y 119 REVIEW C. Becattini G. Agnelli Acute pulmonary embolism: risk stratification in the emergency department Received: 16 October 2006 /
Intern Emerg Med (2007) 2:119 129 DOI 10.1007/s11739-007-0033-y 119 REVIEW C. Becattini G. Agnelli Acute pulmonary embolism: risk stratification in the emergency department Received: 16 October 2006 /
Management of Acute Pulmonary Embolism. Judith Hurdman Consultant Respiratory Physician
 Management of Acute Pulmonary Embolism Judith Hurdman Consultant Respiratory Physician Judith.hurdman@sth.nhs.uk Overview Risk Stratification Who can be managed as an outpatient? To thrombolyse or not
Management of Acute Pulmonary Embolism Judith Hurdman Consultant Respiratory Physician Judith.hurdman@sth.nhs.uk Overview Risk Stratification Who can be managed as an outpatient? To thrombolyse or not
The effects of cause of death classification on prognostic assessment of patients with pulmonary embolism
 Journal of Thrombosis and Haemostasis, 9: 2201 2207 DOI: 10.1111/j.1538-7836.2011.04490.x ORIGINAL ARTICLE The effects of cause of death classification on prognostic assessment of patients with pulmonary
Journal of Thrombosis and Haemostasis, 9: 2201 2207 DOI: 10.1111/j.1538-7836.2011.04490.x ORIGINAL ARTICLE The effects of cause of death classification on prognostic assessment of patients with pulmonary
Acute pulmonary embolism: mortality prediction by the 2014 European Society of Cardiology risk stratification model
 ERJ Express. Published on May 12, 2016 as doi: 10.1183/13993003.00024-2016 ORIGINAL ARTICLE IN PRESS CORRECTED PROOF Acute pulmonary embolism: mortality prediction by the 2014 European Society of Cardiology
ERJ Express. Published on May 12, 2016 as doi: 10.1183/13993003.00024-2016 ORIGINAL ARTICLE IN PRESS CORRECTED PROOF Acute pulmonary embolism: mortality prediction by the 2014 European Society of Cardiology
Is it safe to manage pulmonary embolism in Primary Care? Roopen Arya King s College Hospital
 Is it safe to manage pulmonary embolism in Primary Care? Roopen Arya King s College Hospital A few definitions Safe Avoid death, recurrent thrombosis, bleeding Manage Diagnosis + treatment Pulmonary embolism
Is it safe to manage pulmonary embolism in Primary Care? Roopen Arya King s College Hospital A few definitions Safe Avoid death, recurrent thrombosis, bleeding Manage Diagnosis + treatment Pulmonary embolism
Modified Bova score for risk stratification and short-term outcome in acute pulmonary embolism
 ORIGINAL ARTICLE Modified Bova score for risk stratification and short-term outcome in acute pulmonary embolism K. Keller 1,2, J. Beule 3, J.O. Balzer 4,5 *, W. Dippold 3 * *Both authors are co-shared
ORIGINAL ARTICLE Modified Bova score for risk stratification and short-term outcome in acute pulmonary embolism K. Keller 1,2, J. Beule 3, J.O. Balzer 4,5 *, W. Dippold 3 * *Both authors are co-shared
Pulmonary embolism (PE)-associated
 Hellenic J Cardiol 2010; 51: 437-450 Review Article Management of Acute Pulmonary Embolism: A Contemporary, Risk-Tailored Approach Ge o r g i o s K. Ch a l i k i a s, Dimitrios N. Tz i a k a s, Dimitrios
Hellenic J Cardiol 2010; 51: 437-450 Review Article Management of Acute Pulmonary Embolism: A Contemporary, Risk-Tailored Approach Ge o r g i o s K. Ch a l i k i a s, Dimitrios N. Tz i a k a s, Dimitrios
Diagnosis and initial treatment of patients with suspected pulmonary thromboembolism
 Diagnosis and initial treatment of patients with suspected pulmonary thromboembolism Pulmonary thromboembolism (PTE) remains a frequently occurring diagnostic problem, with an incidence of approximately
Diagnosis and initial treatment of patients with suspected pulmonary thromboembolism Pulmonary thromboembolism (PTE) remains a frequently occurring diagnostic problem, with an incidence of approximately
A 50-year-old woman with syncope
 Hira Shahzad 1, Ali Bin Sarwar Zubairi 2 1 Medical College, Aga Khan University Hospital, Karachi 2 Department of Medicine, Aga Khan University Hospital, Karachi, Pakistan Ali Bin Sarwar Zubairi Associate
Hira Shahzad 1, Ali Bin Sarwar Zubairi 2 1 Medical College, Aga Khan University Hospital, Karachi 2 Department of Medicine, Aga Khan University Hospital, Karachi, Pakistan Ali Bin Sarwar Zubairi Associate
Identification of intermediate-risk patients with acute symptomatic pulmonary embolism
 ORIGINAL ARTICLE PULMONARY VASCULAR DISEASES Identification of intermediate-risk patients with acute symptomatic pulmonary embolism Carlo Bova 1, Olivier Sanchez 2,3, Paolo Prandoni 4, Mareike Lankeit
ORIGINAL ARTICLE PULMONARY VASCULAR DISEASES Identification of intermediate-risk patients with acute symptomatic pulmonary embolism Carlo Bova 1, Olivier Sanchez 2,3, Paolo Prandoni 4, Mareike Lankeit
Pulmonary Embolism Newer Concepts and Role of Thrombolysis
 CHAPTER 69 Pulmonary Embolism Newer Concepts and Role of Thrombolysis J. P. S. Sawhney, A. Bakhshi, B. Kandpal Introduction Pulmonary embolism (PE) is a common cardiovascular and cardiopulmonary illness
CHAPTER 69 Pulmonary Embolism Newer Concepts and Role of Thrombolysis J. P. S. Sawhney, A. Bakhshi, B. Kandpal Introduction Pulmonary embolism (PE) is a common cardiovascular and cardiopulmonary illness
Disclosures. Objectives
 BRIGHAM AND WOMEN S HOSPITAL Treatment of Massive and Submassive Pulmonary Embolism Gregory Piazza, MD, MS Assistant Professor of Medicine Harvard Medical School Staff Physician, Cardiovascular Division
BRIGHAM AND WOMEN S HOSPITAL Treatment of Massive and Submassive Pulmonary Embolism Gregory Piazza, MD, MS Assistant Professor of Medicine Harvard Medical School Staff Physician, Cardiovascular Division
Management of Massive and Sub-Massive Pulmonary Embolism
 Management of Massive and Sub-Massive Pulmonary Embolism M. Montero-Baker, MD L Leon Jr., MD, RVT, FACS Tucson Medical Center Vascular and Endovascular Surgery Section CASE PRESENTATION 54 YEAR- OLD CAUCASIAN
Management of Massive and Sub-Massive Pulmonary Embolism M. Montero-Baker, MD L Leon Jr., MD, RVT, FACS Tucson Medical Center Vascular and Endovascular Surgery Section CASE PRESENTATION 54 YEAR- OLD CAUCASIAN
Impaired renal function predicts short term prognosis in patients with acute pulmonary embolism
 Impaired renal function predicts short term prognosis in patients with acute pulmonary embolism Kostrubiec Maciej, Łabyk Andrzej, Pedowska-Włoszek Jusyna, Pacho Szymon, Jankowski Krzysztof, Koczaj-Bremer
Impaired renal function predicts short term prognosis in patients with acute pulmonary embolism Kostrubiec Maciej, Łabyk Andrzej, Pedowska-Włoszek Jusyna, Pacho Szymon, Jankowski Krzysztof, Koczaj-Bremer
Management of Intermediate-Risk Pulmonary Embolism
 Management of Intermediate-Risk Pulmonary Embolism Stavros V. Konstantinides, MD, PhD, FESC Professor, Clinical Trials in Antithrombotic Therapy Center for Thrombosis und Hemostasis, University of Mainz,
Management of Intermediate-Risk Pulmonary Embolism Stavros V. Konstantinides, MD, PhD, FESC Professor, Clinical Trials in Antithrombotic Therapy Center for Thrombosis und Hemostasis, University of Mainz,
PULMONARY EMBOLISM -CASE REPORT-
 University Goce Delcev, Faculty of Medical sciences, Stip University Clinic of Cardiology, Skopje R. Of Macedonia PULMONARY EMBOLISM -CASE REPORT- Gordana Kamceva MD mr.sci Acknowledgment Marija Vavlukis
University Goce Delcev, Faculty of Medical sciences, Stip University Clinic of Cardiology, Skopje R. Of Macedonia PULMONARY EMBOLISM -CASE REPORT- Gordana Kamceva MD mr.sci Acknowledgment Marija Vavlukis
Acute pulmonary embolism has a wide spectrum of. Prognostic Value of Troponins in Acute Pulmonary Embolism A Meta-Analysis
 Prognostic Value of Troponins in Acute Pulmonary Embolism A Meta-Analysis Cecilia Becattini, MD; Maria Cristina Vedovati, MD; Giancarlo Agnelli, MD Background Whether elevated serum troponin levels identify
Prognostic Value of Troponins in Acute Pulmonary Embolism A Meta-Analysis Cecilia Becattini, MD; Maria Cristina Vedovati, MD; Giancarlo Agnelli, MD Background Whether elevated serum troponin levels identify
Timing of NT-pro-BNP sampling for predicting adverse outcome after acute pulmonary embolism
 7 Frederikus A. Klok Noortje van der Bijl Inge C.M. Mos Albert de Roos Lucia J. M. Kroft Menno V. Huisman Timing of NT-pro-BNP sampling for predicting adverse outcome after acute pulmonary embolism Letter
7 Frederikus A. Klok Noortje van der Bijl Inge C.M. Mos Albert de Roos Lucia J. M. Kroft Menno V. Huisman Timing of NT-pro-BNP sampling for predicting adverse outcome after acute pulmonary embolism Letter
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/40114 holds various files of this Leiden University dissertation Author: Exter, Paul L. den Title: Diagnosis, management and prognosis of symptomatic and
Cover Page The handle http://hdl.handle.net/1887/40114 holds various files of this Leiden University dissertation Author: Exter, Paul L. den Title: Diagnosis, management and prognosis of symptomatic and
PREVENTION AND TREATMENT OF VENOUS THROMBOEMBOLISM
 PREVENTION AND TREATMENT OF VENOUS THROMBOEMBOLISM International Consensus Statement 2013 Guidelines According to Scientific Evidence Developed under the auspices of the: Cardiovascular Disease Educational
PREVENTION AND TREATMENT OF VENOUS THROMBOEMBOLISM International Consensus Statement 2013 Guidelines According to Scientific Evidence Developed under the auspices of the: Cardiovascular Disease Educational
Epidemiology of Pulmonary Embolism (PE)
 Why Treat Submassive PE Abstract: Massive Pulmonary Embolism (PE) requires immediate lifesaving intervention for the patient. For the submassive PE patient, characterized by presence of right ventricular
Why Treat Submassive PE Abstract: Massive Pulmonary Embolism (PE) requires immediate lifesaving intervention for the patient. For the submassive PE patient, characterized by presence of right ventricular
Pulmonary embolism: Acute management. Cecilia Becattini University of Perugia, Italy
 Pulmonary embolism: Acute management Cecilia Becattini University of Perugia, Italy Acute pulmonary embolism: Acute management Diagnosis Risk stratification Treatment Non-high risk PE: diagnosis 3-mo VTE
Pulmonary embolism: Acute management Cecilia Becattini University of Perugia, Italy Acute pulmonary embolism: Acute management Diagnosis Risk stratification Treatment Non-high risk PE: diagnosis 3-mo VTE
Massive and Submassive Pulmonary Embolism: 2017 Update and Future Directions
 Massive and Submassive Pulmonary Embolism: 2017 Update and Future Directions Kush R Desai, MD Assistant Professor of Radiology Northwestern University Feinberg School of Medicine Chicago, IL Disclosures
Massive and Submassive Pulmonary Embolism: 2017 Update and Future Directions Kush R Desai, MD Assistant Professor of Radiology Northwestern University Feinberg School of Medicine Chicago, IL Disclosures
Guideline for Thrombolysis Therapy in Pulmonary Embolism
 Guideline for Thrombolysis Therapy in Pulmonary Embolism Dr Jane Strong Consultant Haematologist Trust ref: B24/2016 1. Introduction / Scope All Patients with pulmonary embolism (PE) require rapid risk
Guideline for Thrombolysis Therapy in Pulmonary Embolism Dr Jane Strong Consultant Haematologist Trust ref: B24/2016 1. Introduction / Scope All Patients with pulmonary embolism (PE) require rapid risk
CARDIAC PROBLEMS IN PREGNANCY
 CARDIAC PROBLEMS IN PREGNANCY LAS VEGAS, NEVADA, USA 27 February 1 March 2016 SUCCESSFUL TREATMENT WITH RECOMBINANT TISSUE PLASMINOGEN ACTIVATOR OF MASSIVE PULMONARY EMBOLISM IN THE 16 TH WEEK OF PREGNANCY
CARDIAC PROBLEMS IN PREGNANCY LAS VEGAS, NEVADA, USA 27 February 1 March 2016 SUCCESSFUL TREATMENT WITH RECOMBINANT TISSUE PLASMINOGEN ACTIVATOR OF MASSIVE PULMONARY EMBOLISM IN THE 16 TH WEEK OF PREGNANCY
N-terminal pro-brain natriuretic peptide in patients with acute pulmonary embolism
 Eur Respir J 23; 22: 649 653 DOI: 1.1183/931936.3.2333 Printed in UK all rights reserved Copyright #ERS Journals Ltd 23 European Respiratory Journal ISSN 93-1936 N-terminal pro-brain natriuretic peptide
Eur Respir J 23; 22: 649 653 DOI: 1.1183/931936.3.2333 Printed in UK all rights reserved Copyright #ERS Journals Ltd 23 European Respiratory Journal ISSN 93-1936 N-terminal pro-brain natriuretic peptide
Acute and long-term treatment of PE. Cecilia Becattini University of Perugia
 Acute and long-term treatment of PE Cecilia Becattini University of Perugia Acute and long-term treatment of VTE What is the optimal acute phase treatment for the patient? Intravenous thrombolysis One
Acute and long-term treatment of PE Cecilia Becattini University of Perugia Acute and long-term treatment of VTE What is the optimal acute phase treatment for the patient? Intravenous thrombolysis One
VTE & Medical Patients: Case Scenario
 The Saudi Association for Venous Thromboembolism SAVTE The 2 nd SAVTE Symposium 1-3 May, 2012 Casablanca, Morocco VTE & Medical Patients: Case Scenario Majdy Idrees Riyadh, Saudi Arabia Majdy M Idrees,
The Saudi Association for Venous Thromboembolism SAVTE The 2 nd SAVTE Symposium 1-3 May, 2012 Casablanca, Morocco VTE & Medical Patients: Case Scenario Majdy Idrees Riyadh, Saudi Arabia Majdy M Idrees,
Updates in venous thromboembolism. Cecilia Becattini University of Perugia
 Updates in venous thromboembolism Cecilia Becattini University of Perugia News for VTE Diagnosis Treatment the acute phase the agents Pulmonary embolism: diagnosis Vein ultrasonography Meta-analysis 15
Updates in venous thromboembolism Cecilia Becattini University of Perugia News for VTE Diagnosis Treatment the acute phase the agents Pulmonary embolism: diagnosis Vein ultrasonography Meta-analysis 15
Chapter 6. F.A. Klok, N. van der Bijl, J. Eikenboom, C.J. van Rooden, A. de Roos, L.J.M. Kroft and M.V. Huisman. Equally contributed
 Chapter 6 Comparison of CT assessed right ventricular size and cardiac biomarkers for predicting short term clinical outcome in normotensive patients suspected for having acute pulmonary embolism F.A.
Chapter 6 Comparison of CT assessed right ventricular size and cardiac biomarkers for predicting short term clinical outcome in normotensive patients suspected for having acute pulmonary embolism F.A.
Assessment of severity and prognosis in patients with pulmonary embolism attending to clot load score on MDCT pulmonary angiography
 Assessment of severity and prognosis in patients with pulmonary embolism attending to clot load score on MDCT pulmonary angiography Award: Certificate of Merit Poster No.: C-0890 Congress: ECR 2018 Type:
Assessment of severity and prognosis in patients with pulmonary embolism attending to clot load score on MDCT pulmonary angiography Award: Certificate of Merit Poster No.: C-0890 Congress: ECR 2018 Type:
Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine
 Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine Venous thromboembolism: pulmonary embolism (PE) deep vein thrombosis (DVT) 1% of all patients admitted to hospital 5% of in-hospital mortality
Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine Venous thromboembolism: pulmonary embolism (PE) deep vein thrombosis (DVT) 1% of all patients admitted to hospital 5% of in-hospital mortality
The clinical presentation of acute pulmonary embolism ranges
 The new england journal of medicine review article Current Concepts Acute Pulmonary Embolism Giancarlo Agnelli, M.D., and Cecilia Becattini, M.D., Ph.D. From the Internal and Cardiovascular Medicine and
The new england journal of medicine review article Current Concepts Acute Pulmonary Embolism Giancarlo Agnelli, M.D., and Cecilia Becattini, M.D., Ph.D. From the Internal and Cardiovascular Medicine and
Out of hospital treatment of pulmonary embolism: guidance through risk assessment. Mariëtte Jacqueline Agterof
 Out of hospital treatment of pulmonary embolism: guidance through risk assessment Mariëtte Jacqueline Agterof ISBN: 978-90-393-5543-5 Cover design: Francien Frommé www.grootzus.nl Layout: Ipskamp Drukkers
Out of hospital treatment of pulmonary embolism: guidance through risk assessment Mariëtte Jacqueline Agterof ISBN: 978-90-393-5543-5 Cover design: Francien Frommé www.grootzus.nl Layout: Ipskamp Drukkers
Right ventricular (RV) dysfunction is a frequent consequence
 Independent Prognostic Value of Cardiac Troponin T in Patients With Confirmed Pulmonary Embolism Evangelos Giannitsis, MD; Margit Müller-Bardorff, MD; Volkhard Kurowski, MD; Britta Weidtmann, MD; Uwe Wiegand,
Independent Prognostic Value of Cardiac Troponin T in Patients With Confirmed Pulmonary Embolism Evangelos Giannitsis, MD; Margit Müller-Bardorff, MD; Volkhard Kurowski, MD; Britta Weidtmann, MD; Uwe Wiegand,
Age-adjusted hstnt cut-off value for risk stratification of pulmonary embolism
 ERJ Express. Published on January 22, 2015 as doi: 10.1183/09031936.00174514 ORIGINAL ARTICLE IN PRESS CORRECTED PROOF Age-adjusted hstnt for risk stratification of pulmonary embolism Anja Kaeberich 1,
ERJ Express. Published on January 22, 2015 as doi: 10.1183/09031936.00174514 ORIGINAL ARTICLE IN PRESS CORRECTED PROOF Age-adjusted hstnt for risk stratification of pulmonary embolism Anja Kaeberich 1,
M ortality from pulmonary embolic disease has
 123 ORIGINAL ARTICLE Outpatient diagnosis of pulmonary embolism: the MIOPED (Manchester Investigation Of Pulmonary Embolism Diagnosis) study K Hogg, D Dawson, K Mackway-Jones... See end of article for
123 ORIGINAL ARTICLE Outpatient diagnosis of pulmonary embolism: the MIOPED (Manchester Investigation Of Pulmonary Embolism Diagnosis) study K Hogg, D Dawson, K Mackway-Jones... See end of article for
Acute and long-term treatment of VTE. Cecilia Becattini University of Perugia
 Acute and long-term treatment of VTE Cecilia Becattini University of Perugia Acute and long-term treatment of VTE The goals The acute PE phase After the acute phase Treatment for VTE Goals of acute treatment
Acute and long-term treatment of VTE Cecilia Becattini University of Perugia Acute and long-term treatment of VTE The goals The acute PE phase After the acute phase Treatment for VTE Goals of acute treatment
Optimal Management of Intermediate-Risk Pulmonary Embolism
 Optimal Management of Intermediate-Risk Pulmonary Embolism Stavros V. Konstantinides, MD, PhD, FESC Professor, Clinical Trials in Antithrombotic Therapy Center for Thrombosis und Hemostasis, University
Optimal Management of Intermediate-Risk Pulmonary Embolism Stavros V. Konstantinides, MD, PhD, FESC Professor, Clinical Trials in Antithrombotic Therapy Center for Thrombosis und Hemostasis, University
European Heart Journal
 European Heart Journal Prognostic value of right ventricular dysfunction in patients with haemodynamically stable pulmonary embolism: a systematic review Olivier Sanchez, Ludovic Trinquart, Isabelle Colombet,
European Heart Journal Prognostic value of right ventricular dysfunction in patients with haemodynamically stable pulmonary embolism: a systematic review Olivier Sanchez, Ludovic Trinquart, Isabelle Colombet,
Cardiovascular Images
 Cardiovascular Images Pulmonary Embolism Diagnosed From Right Heart Changes Seen After Exercise Stress Echocardiography Brian C. Case, MD; Micheas Zemedkun, MD; Amarin Sangkharat, MD; Allen J. Taylor,
Cardiovascular Images Pulmonary Embolism Diagnosed From Right Heart Changes Seen After Exercise Stress Echocardiography Brian C. Case, MD; Micheas Zemedkun, MD; Amarin Sangkharat, MD; Allen J. Taylor,
Early Transoesophageal Echocardiography (TOE) in Cardiac Arrest: A Case Study
 Case reports Early Transoesophageal Echocardiography (TOE) in Cardiac Arrest: A Case Study N. SIMPSON, N. ORFORD Intensive Care Unit, The Geelong Hospital, Geelong, VICTORIA ABSTRACT We describe a case
Case reports Early Transoesophageal Echocardiography (TOE) in Cardiac Arrest: A Case Study N. SIMPSON, N. ORFORD Intensive Care Unit, The Geelong Hospital, Geelong, VICTORIA ABSTRACT We describe a case
Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism A pulmonary embolism (PE) is
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism A pulmonary embolism (PE) is
Computed tomography pulmonary angiogram as a result of medical emergency team calls: a 5-year retrospective audit
 Computed tomography pulmonary angiogram as a result of medical emergency team calls: a 5-year retrospective audit Manisa Ghani and Antony Tobin Pulmonary embolism (PE) is a cardiovascular emergency with
Computed tomography pulmonary angiogram as a result of medical emergency team calls: a 5-year retrospective audit Manisa Ghani and Antony Tobin Pulmonary embolism (PE) is a cardiovascular emergency with
The Prognostic Value of Undetectable Highly Sensitive Cardiac Troponin I in Patients With Acute Pulmonary Embolism
 [ Original Research Pulmonary Vascular Disease ] The Prognostic Value of Undetectable Highly Sensitive Cardiac Troponin I in Patients With Acute Pulmonary Embolism Emad U. Hakemi, MD ; Tareq Alyousef,
[ Original Research Pulmonary Vascular Disease ] The Prognostic Value of Undetectable Highly Sensitive Cardiac Troponin I in Patients With Acute Pulmonary Embolism Emad U. Hakemi, MD ; Tareq Alyousef,
PE is a difficult diagnosis that may be missed because of non-specific clinical presentation.
 Pulmonary embolism (PE) is a relatively common cardiovascular emergency. By occluding the pulmonary arterial bed it may lead to acute life-threatening (3% early mortality rate), but potentially reversible
Pulmonary embolism (PE) is a relatively common cardiovascular emergency. By occluding the pulmonary arterial bed it may lead to acute life-threatening (3% early mortality rate), but potentially reversible
CURRENT & FUTURE THERAPEUTIC MANAGEMENT OF VENOUS THROMBOEMBOLISM. Gordon Lowe Professor of Vascular Medicine University of Glasgow
 CURRENT & FUTURE THERAPEUTIC MANAGEMENT OF VENOUS THROMBOEMBOLISM Gordon Lowe Professor of Vascular Medicine University of Glasgow VENOUS THROMBOEMBOLISM Common cause of death and disability 50% hospital-acquired
CURRENT & FUTURE THERAPEUTIC MANAGEMENT OF VENOUS THROMBOEMBOLISM Gordon Lowe Professor of Vascular Medicine University of Glasgow VENOUS THROMBOEMBOLISM Common cause of death and disability 50% hospital-acquired
Treatment of venous thromboembolism: focus on patient characteristics and bleeding complications Brekelmans, M.P.A.
 UvA-DARE (Digital Academic Repository) Treatment of venous thromboembolism: focus on patient characteristics and bleeding complications Brekelmans, M.P.A. Link to publication Citation for published version
UvA-DARE (Digital Academic Repository) Treatment of venous thromboembolism: focus on patient characteristics and bleeding complications Brekelmans, M.P.A. Link to publication Citation for published version
Brain-Type Natriuretic Peptide Levels in the Prediction of Adverse Outcome in Patients with Pulmonary Embolism A Systematic Review and Meta-analysis
 Brain-Type Natriuretic Peptide Levels in the Prediction of Adverse Outcome in Patients with Pulmonary Embolism A Systematic Review and Meta-analysis Frederikus A. Klok 1 *, Inge C. M. Mos 1 *, and Menno
Brain-Type Natriuretic Peptide Levels in the Prediction of Adverse Outcome in Patients with Pulmonary Embolism A Systematic Review and Meta-analysis Frederikus A. Klok 1 *, Inge C. M. Mos 1 *, and Menno
Clinical Guide - Suspected PE (Reviewed 2006)
 Clinical Guide - Suspected (Reviewed 2006) Principal Developer: B. Geerts Secondary Developers: C. Demers, C. Kearon Background Investigation of patients with suspected pulmonary emboli () remains problematic
Clinical Guide - Suspected (Reviewed 2006) Principal Developer: B. Geerts Secondary Developers: C. Demers, C. Kearon Background Investigation of patients with suspected pulmonary emboli () remains problematic
Venous Thrombosis. Magnitude of the Problem. DVT 2 Million PE 600,000. Death 60,000. Estimated Cost of VTE Care $1.5 Billion/year.
 Venous Thrombosis Magnitude of the Problem DVT 2 Million Postthrombotic Syndrome 800,000 PE 600,000 Death 60,000 Silent PE 1 Million Pulmonary Hypertension 30,000 Estimated Cost of VTE Care $1.5 Billion/year
Venous Thrombosis Magnitude of the Problem DVT 2 Million Postthrombotic Syndrome 800,000 PE 600,000 Death 60,000 Silent PE 1 Million Pulmonary Hypertension 30,000 Estimated Cost of VTE Care $1.5 Billion/year
Innovative Endovascular Approach to Pulmonary Embolism by Ultrasound Enhanced Thrombolysis. Prof. Ralf R.Kolvenbach MD,PhD,FEBVS
 Innovative Endovascular Approach to Pulmonary Embolism by Ultrasound Enhanced Thrombolysis Prof. Ralf R.Kolvenbach MD,PhD,FEBVS Conflict of Interest BTG Standard PE therapy ANTICOAGULATION (AC) HEPARIN
Innovative Endovascular Approach to Pulmonary Embolism by Ultrasound Enhanced Thrombolysis Prof. Ralf R.Kolvenbach MD,PhD,FEBVS Conflict of Interest BTG Standard PE therapy ANTICOAGULATION (AC) HEPARIN
What is New in Acute Pulmonary Embolism? Interventional Treatment. Prof. Nils Kucher University Hospital Bern Switzerland
 What is New in Acute Pulmonary Embolism? Interventional Treatment Prof. Nils Kucher University Hospital Bern Switzerland nils.kucher@insel.ch Disclosure of Interest Dr. Kucher received research grants
What is New in Acute Pulmonary Embolism? Interventional Treatment Prof. Nils Kucher University Hospital Bern Switzerland nils.kucher@insel.ch Disclosure of Interest Dr. Kucher received research grants
Systemic Fibrinolytic Therapy in the Presence of Absolute Contraindication; a Case Series
 Emergency. 2018; 6 (1): e25 CASE REPORT Systemic Fibrinolytic Therapy in the Presence of Absolute Contraindication; a Case Series Mahdi Pishgahi 1, Toktam Alirezaei 1, Behzad Hajimoradi 1, S. Mojtaba Nekooghadam
Emergency. 2018; 6 (1): e25 CASE REPORT Systemic Fibrinolytic Therapy in the Presence of Absolute Contraindication; a Case Series Mahdi Pishgahi 1, Toktam Alirezaei 1, Behzad Hajimoradi 1, S. Mojtaba Nekooghadam
4/18/2018. Objectives. Background. 1) Compare and contrast the various validated tools for the identification of patients with pulmonary embolism
 Pulmonary Embolism: Assessment, risk-stratification, and treatment plan for the outpatient management of low-risk patients Presentation by Joshua T. Wood, PharmD/PGY-1 Resident Providence St. Patrick Hospital;
Pulmonary Embolism: Assessment, risk-stratification, and treatment plan for the outpatient management of low-risk patients Presentation by Joshua T. Wood, PharmD/PGY-1 Resident Providence St. Patrick Hospital;
Diagnostic approach to pulmonary embolism and lessons from a busy acute assessment unit in the UK
 Diagnostic approach to pulmonary embolism and lessons from a busy acute assessment unit in the UK The diagnosis of pulmonary embolism (PE) can be very elusive and, if missed, mayhave fatal consequences.
Diagnostic approach to pulmonary embolism and lessons from a busy acute assessment unit in the UK The diagnosis of pulmonary embolism (PE) can be very elusive and, if missed, mayhave fatal consequences.
Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism
 Agency for Healthcare Research and Quality Evidence Report/Technology Assessment Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism Summary Number 68 Overview Venous thromboembolism
Agency for Healthcare Research and Quality Evidence Report/Technology Assessment Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism Summary Number 68 Overview Venous thromboembolism
Single-Center, Retrospective, Observational Analysis of Patients with Submassive Pulmonary Embolism (PE) Receiving Catheter- Directed Thrombolysis
 Single-Center, Retrospective, Observational Analysis of Patients with Submassive Pulmonary Embolism (PE) Receiving Catheter- Directed Thrombolysis John A. Phillips, M.D. OhioHealth Heart and Vascular Physicians
Single-Center, Retrospective, Observational Analysis of Patients with Submassive Pulmonary Embolism (PE) Receiving Catheter- Directed Thrombolysis John A. Phillips, M.D. OhioHealth Heart and Vascular Physicians
COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP)
 The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 16 December 1999 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE FOR GUIDANCE ON CLINICAL
The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 16 December 1999 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE FOR GUIDANCE ON CLINICAL
Acute Pulmonary Embolism and Deep Vein Thrombosis. Barbara LeVarge MD Beth Israel Deaconess Medical Center Pulmonary Hypertension Center COPYRIGHT
 Acute Pulmonary Embolism and Deep Vein Thrombosis Barbara LeVarge MD Beth Israel Deaconess Medical Center Pulmonary Hypertension Center Acute PE and DVT No disclosures. Acute PE and DVT Learning objectives
Acute Pulmonary Embolism and Deep Vein Thrombosis Barbara LeVarge MD Beth Israel Deaconess Medical Center Pulmonary Hypertension Center Acute PE and DVT No disclosures. Acute PE and DVT Learning objectives
Plasma MR-proADM is superior to NTproBNP for all-cause short term mortality prediction in acute pulmonary embolism.
 J. Pedowska-Wloszek, M. Kostrubiec, A. Labyk, S. Pacho, O. Dzikowska-Diduch, P. Bienias, B. Lichodziejewska, P. Palczewski, M. Ciurzynski, P. Pruszczyk Plasma MR-proADM is superior to NTproBNP for all-cause
J. Pedowska-Wloszek, M. Kostrubiec, A. Labyk, S. Pacho, O. Dzikowska-Diduch, P. Bienias, B. Lichodziejewska, P. Palczewski, M. Ciurzynski, P. Pruszczyk Plasma MR-proADM is superior to NTproBNP for all-cause
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/40114 holds various files of this Leiden University dissertation Author: Exter, Paul L. den Title: Diagnosis, management and prognosis of symptomatic and
Cover Page The handle http://hdl.handle.net/1887/40114 holds various files of this Leiden University dissertation Author: Exter, Paul L. den Title: Diagnosis, management and prognosis of symptomatic and
Screening for CETPH after acute pulmonary embolism: is it needed? Menno V. Huisman Department of Vascular Medicine LUMC Leiden
 Screening for CETPH after acute pulmonary embolism: is it needed? Menno V. Huisman Department of Vascular Medicine LUMC Leiden m.v.huisman@lumc.nl Background CETPH Chronic Thrombo Embolic Pulmonary Hypertension
Screening for CETPH after acute pulmonary embolism: is it needed? Menno V. Huisman Department of Vascular Medicine LUMC Leiden m.v.huisman@lumc.nl Background CETPH Chronic Thrombo Embolic Pulmonary Hypertension
DEEP VEIN THROMBOSIS (DVT): TREATMENT
 DEEP VEIN THROMBOSIS (DVT): TREATMENT OBJECTIVE: To provide an evidence-based approach to treatment of patients presenting with deep vein thrombosis (DVT). BACKGROUND: An estimated 45,000 patients in Canada
DEEP VEIN THROMBOSIS (DVT): TREATMENT OBJECTIVE: To provide an evidence-based approach to treatment of patients presenting with deep vein thrombosis (DVT). BACKGROUND: An estimated 45,000 patients in Canada
Clinically Suspected Acute Recurrent Pulmonary Embolism: A Diagnostic Challenge
 7 Clinically Suspected Acute Recurrent Pulmonary Embolism: A Diagnostic Challenge M. Nijkeuter, H. Kwakkel- van Erp, M. Sohne, L.W. Tick, M.J.H.A. Kruip, E.F. Ullmann, M.H.H Kramer, H.R. Büller, M.H. Prins,
7 Clinically Suspected Acute Recurrent Pulmonary Embolism: A Diagnostic Challenge M. Nijkeuter, H. Kwakkel- van Erp, M. Sohne, L.W. Tick, M.J.H.A. Kruip, E.F. Ullmann, M.H.H Kramer, H.R. Büller, M.H. Prins,
SAFETY OF A PULMONARY EMBOLISM AMBULATORY TREATMENT PROGRAM
 SAFETY OF A PULMONARY EMBOLISM AMBULATORY TREATMENT PROGRAM Mahir M. Hamad 1, MD, FRCP, Elrasheed A. Ellidir 1, MD, MRCP, Charlotte Routh 1, MD, MRCP, Siraj O. Wali 2, FACP, FCCP, and Vincent M. Connolly
SAFETY OF A PULMONARY EMBOLISM AMBULATORY TREATMENT PROGRAM Mahir M. Hamad 1, MD, FRCP, Elrasheed A. Ellidir 1, MD, MRCP, Charlotte Routh 1, MD, MRCP, Siraj O. Wali 2, FACP, FCCP, and Vincent M. Connolly
Postoperative Acute Pulmonary Embolism: A Case Report. S Mishra, P Kundra, B Hemavathi, A Badhe, M Ravishankar
 ISPUB.COM The Internet Journal of Anesthesiology Volume 13 Number 2 S Mishra, P Kundra, B Hemavathi, A Badhe, M Ravishankar Citation S Mishra, P Kundra, B Hemavathi, A Badhe, M Ravishankar.. The Internet
ISPUB.COM The Internet Journal of Anesthesiology Volume 13 Number 2 S Mishra, P Kundra, B Hemavathi, A Badhe, M Ravishankar Citation S Mishra, P Kundra, B Hemavathi, A Badhe, M Ravishankar.. The Internet
Usefulness of Clinical Pre-test Scores for a Correct Diagnostic Pathway in Patients with Suspected Pulmonary Embolism in Emergency Room
 Send Orders for Reprints to reprints@benthamscience.net The Open Emergency Medicine Journal, 2013, 5, (Suppl 1: M-4) 19-24 19 Open Access Usefulness of Clinical Pre-test Scores for a Correct Diagnostic
Send Orders for Reprints to reprints@benthamscience.net The Open Emergency Medicine Journal, 2013, 5, (Suppl 1: M-4) 19-24 19 Open Access Usefulness of Clinical Pre-test Scores for a Correct Diagnostic
Results from RE-COVER RE-COVER II RE-MEDY RE-SONATE EXECUTIVE SUMMARY
 Assessment of the safety and efficacy of dabigatran etexilate (Pradaxa ) in the treatment of deep vein thrombosis (DVT) and pulmonary embolism (PE) and the prevention of recurrent DVT and PE Results from
Assessment of the safety and efficacy of dabigatran etexilate (Pradaxa ) in the treatment of deep vein thrombosis (DVT) and pulmonary embolism (PE) and the prevention of recurrent DVT and PE Results from
The diagnosis and prognosis of venous thromboembolism : variations on a theme Gibson, N.S.
 UvA-DARE (Digital Academic Repository) The diagnosis and prognosis of venous thromboembolism : variations on a theme Gibson, N.S. Link to publication Citation for published version (APA): Gibson, N. S.
UvA-DARE (Digital Academic Repository) The diagnosis and prognosis of venous thromboembolism : variations on a theme Gibson, N.S. Link to publication Citation for published version (APA): Gibson, N. S.
Challenges in the management of acute pulmonary embolism
 Challenges in the management of acute pulmonary embolism Case: A pregnant woman presenting with clinical suspicion of acute venous thromboembolism: Appropriate diagnostic and therapeutic strategy in pregnancy.
Challenges in the management of acute pulmonary embolism Case: A pregnant woman presenting with clinical suspicion of acute venous thromboembolism: Appropriate diagnostic and therapeutic strategy in pregnancy.
Venous thromboembolic diseases: diagnosis, management and thrombophilia testing (2012) NICE guideline CG144
 Venous thromboembolic diseases: diagnosis, management and thrombophilia testing (2012) NICE guideline CG144 Appendix A: Summary of new evidence from Summary of evidence from previous year Diagnosis Diagnostic
Venous thromboembolic diseases: diagnosis, management and thrombophilia testing (2012) NICE guideline CG144 Appendix A: Summary of new evidence from Summary of evidence from previous year Diagnosis Diagnostic
DVT PROPHYLAXIS IN HOSPITALIZED MEDICAL PATIENTS SAURABH MAJI SR (PULMONARY,MEDICINE)
 DVT PROPHYLAXIS IN HOSPITALIZED MEDICAL PATIENTS SAURABH MAJI SR (PULMONARY,MEDICINE) Introduction VTE (DVT/PE) is an important complication in hospitalized patients Hospitalization for acute medical illness
DVT PROPHYLAXIS IN HOSPITALIZED MEDICAL PATIENTS SAURABH MAJI SR (PULMONARY,MEDICINE) Introduction VTE (DVT/PE) is an important complication in hospitalized patients Hospitalization for acute medical illness
VTE General Background
 VTE General Background VTE incidence is about 1:1000 persons annually >250,000 admissions for VTE annually >100,000 people die of PE annually >90% of PE s arise from lower limb DVT 50% of DVT at diagnosis
VTE General Background VTE incidence is about 1:1000 persons annually >250,000 admissions for VTE annually >100,000 people die of PE annually >90% of PE s arise from lower limb DVT 50% of DVT at diagnosis
Electrocardiographic findings in pulmonary embolism
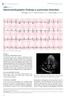 Singapore Med J 2015; 56(10): 533-537 doi: 10.11622/smedj.2015147 Electrocardiography Series CMEArticle Electrocardiographic findings in pulmonary embolism Elaine Boey1, MBBS, MRCP, Swee-Guan Teo2, MRCP,
Singapore Med J 2015; 56(10): 533-537 doi: 10.11622/smedj.2015147 Electrocardiography Series CMEArticle Electrocardiographic findings in pulmonary embolism Elaine Boey1, MBBS, MRCP, Swee-Guan Teo2, MRCP,
Handbook for Venous Thromboembolism
 Handbook for Venous Thromboembolism Gregory Piazza Benjamin Hohlfelder Samuel Z. Goldhaber Handbook for Venous Thromboembolism Gregory Piazza Cardiovascular Division Harvard Medical School Brigham and
Handbook for Venous Thromboembolism Gregory Piazza Benjamin Hohlfelder Samuel Z. Goldhaber Handbook for Venous Thromboembolism Gregory Piazza Cardiovascular Division Harvard Medical School Brigham and
