Prognostic value of the ECG on admission in patients with acute major pulmonary embolism
|
|
|
- Anabel Morgan
- 5 years ago
- Views:
Transcription
1 Eur Respir J 2005; 25: DOI: / CopyrightßERS Journals Ltd 2005 Prognostic value of the ECG on admission in patients with acute major pulmonary embolism A. Geibel*, M. Zehender*, W. Kasper #, M. Olschewski ", C. Klima* and S.V. Konstantinides + ABSTRACT: A number of ECG abnormalities can be observed in the acute phase of pulmonary embolism (PE). Their prognostic value has not yet been systematically studied in large patient populations. In 508 patients with acute major PE derived from a large prospective registry, the current authors assessed, on admission, the impact of specific pathological ECG findings on early (30- day) mortality. Atrial arrhythmias, complete right bundle branch block, peripheral low voltage, pseudoinfarction pattern (Q waves) in leads III and avf, and ST segment changes (elevation or depression) over the left precordial leads, were all significantly more frequent in patients with a fatal outcome. Overall, 29% of the patients who exhibited at least one of these abnormalities on admission did not survive to hospital discharge, as opposed to only 11% of the patients without a pathological 12-lead ECG. Multivariate analysis revealed that the presence of at least one of the above ECG findings was, besides haemodynamic instability, syncope and pre-existing chronic pulmonary disease, a significant independent predictor of outcome. In conclusion, ECG may be a useful, simple, non-costly tool for initial risk stratification of patients with acute major pulmonary embolism. KEYWORDS: Mortality, prognosis, pulmonary arterial hypertension, pulmonary embolism, pulmonary embolism diagnosis AFFILIATIONS *Dept of Cardiology and Angiology, Albert Ludwigs University of Freiburg, and " Institute for Medical Biometry and Statistics, University of Freiburg, Freiburg, and # Dept of Internal Medicine, St. Josefs Hospital, Wiesbaden, and + Dept of Cardiology and Pulmonary Medicine, Georg August University of Goettingen, Goettingen, Germany. CORRESPONDENCE S.V. Konstantinides Georg August University of Goettingen Dept of Cardiology and Pulmonary Medicine Robert Koch Strasse 40 Goettingen D Germany Fax: skonstan@med. uni-goettingen.de Early identification of high-risk patients with acute pulmonary embolism (PE) remains a challenge in clinical practice [1]. It has been argued that development of right ventricular dysfunction as a result of acute pulmonary hypertension (PH) is a crucial pathophysiological event, which may initiate a vicious circle of progressive haemodynamic instability [2]. In accordance with this hypothesis, it is presently acknowledged that overt right ventricular failure with persistent arterial hypotension or shock predicts a particularly poor outcome and, thus, should set the indication for immediate thrombolytic, interventional or surgical treatment of PE [3, 4]. Furthermore, and importantly, a number of prospective [5 7] and retrospective [8] studies, as well as two large registries [1, 9], have demonstrated that echocardiographic diagnosis of right ventricular enlargement or hypokinesis [10] is associated with an increased risk of death or potentially life-threatening complications, even in the absence of arterial hypotension on admission. Accordingly, in a recent large randomised trial, echocardiographic parameters were used to randomise patients to early thrombolytic treatment or heparin alone [11]. However, availability of cardiac ultrasound on a round-the-clock basis may pose significant logistical problems in several hospitals, and echocardiography may be of poor quality in overweight or mechanically ventilated patients, or in those with chronic pulmonary disease. A number of studies suggest that cardiac biomarkers, and cardiac troponins and natriuretic peptides, may represent an important step towards reliable risk stratification of patients with PE [12]. More recently, it was reported that right ventricular enlargement based on reconstructed four-chamber views of the heart on chest computed tomography (CT; newer-generation, multidetector-row scanners) may also indicate potentially life-threatening PE [13]. However, while the prognostic value of novel laboratory markers and imaging modalities is being evaluated, it remains unknown whether triage of Received: October Accepted after revision: January European Respiratory Journal Print ISSN Online ISSN c EUROPEAN RESPIRATORY JOURNAL VOLUME 25 NUMBER 5 843
2 ECG IN MAJOR PULMONARY EMBOLISM A. GEIBEL ET AL. patients with acute PE could become faster and easier if it included a simple, ubiquitously available, generally comprehensible and non-costly baseline test, such as the 12-lead ECG. In fact, it has been known for many years that a number of (usually transient) ECG abnormalities can be observed in the acute phase of PE [14], and some [15, 16], although not all [17], earlier studies suggested that these abnormalities might be related to the severity of PE. Conversely, the implications of specific pathological ECG findings with regard to the clinical outcome, and particularly the risk of death during the inhospital phase, have not yet been systematically studied in a large population of consecutive patients with PE. In order to directly address this issue, the current authors analysed the data of a large prospective multicentre registry [1], investigating the prognostic value of specific ECG parameters on admission in 508 patients with acute major PE. METHODS Study protocol The rationale, study protocol and inclusion criteria of the Management Strategy and Prognosis in Pulmonary Embolism Registry have been described previously [1, 18]. Briefly, 204 participating centres throughout Germany prospectively registered a total of 1,001 consecutive patients in whom the diagnosis of major (i.e. submassive or massive) PE was made according to predefined criteria. The inclusion criteria of the registry consisted of the following findings signifying right ventricular dysfunction and/or PH caused by PE: 1) arterial hypotension (systolic blood pressure,90 mmhg or a pressure drop of o40 mmhg for.15 min, if not caused by new-onset arrhythmia, hypovolaemia, or sepsis); 2) cardiogenic shock (arterial hypotension as defined previously accompanied by clinical signs of organ perfusion and hypoxia); 3) circulatory collapse with need for cardiopulmonary resuscitation; 4) echocardiographic findings indicating right ventricular pressure overload and/or PH (right ventricular dilatation, paradoxical septal wall motion, loss of inspiratory collapse of the inferior vena cava, or tricuspid regurgitation jet velocity.2.8 m?s -1 or,2.5 m?s -1 in the absence of inspiratory collapse of the inferior vena cava) without evidence of mitral valve disease or left ventriclar dysfunction; and 5) diagnosis of precapillary PH (mean pulmonary artery pressure.20 mmhg in the presence of normal pulmonary artery occlusion pressures) by catheterisation of the right side of the heart. For inclusion in the registry, patients had to have clinical suspicion of PE [1] and fulfil at least one of the above criteria at presentation. Patients in whom PE was an accidental finding and not the primary clinical diagnosis on admission were excluded. Confirmation of venous thromboembolism by imaging studies (pulmonary angiography, ventilation perfusion lung scan, and leg ultrasound or phlebography) was recommended in agreement with guidelines existing at the time the registry was established [19, 20]. The steering committee of the registry did not dictate specific management strategies to the participating centres and physicians. The present study considered for statistical evaluation those registry patients who presented with acute symptom onset, i.e. those who were admitted to the hospital within 48 h after suffering symptoms related to PE, and who had a complete 12- lead ECG registration. Data acquisition Using a standardised questionnaire, complete information was obtained on: 1) the clinical symptoms and signs of the patients on admission; 2) the presence of underlying diseases or predisposing factors for venous thromboembolism; 3) the findings of all diagnostic procedures performed, including the original 12-lead ECG and the echocardiogram; 4) the treatment given to the patients (e.g. thrombolysis or heparin alone); and 5) the patients clinical course (duration of hospital stay, causes of death for patients who died during the first 30 days after admission, major bleeding or other cardiovascular complications, and clinically apparent recurrence of PE as diagnosed by the on-site clinical investigator). Original ECG tracings were sent to the coordinating centre (University of Freiburg, Freiburg, Germany) and analysed independently by two experienced cardiologists (A. Geibel and C. Klima) who were unaware of the patients history and outcome. The following ECG abnormalities were regarded as suggestive of right ventricular overload [15, 21] and evaluated with regard to their impact on in-hospital mortality: 1) sinus tachycardia (.100 beats?min -1 ) or bradycardia (,60 beats?min -1 ); 2) atrial arrhythmias; 3) atrioventricular conduction abnormalities; 4) abnormal axis pattern (S1Q3T3 pattern, i.e. S waves in lead I and Q waves in lead III with T-wave inversion in III); 5) shift in the transition zone (R5S) to V5 or further leftward; 6) complete or incomplete right bundle branch block (RBBB); 7) peripheral low voltage (in the limb leads); 8) pseudoinfarction pattern (prominent Q waves) in leads III and avf; 9) ST segment elevation o0.1 mv over the right (V2 V3) or the left (V4 V6) precordial leads; 10) ST segment depression o0.05 mv over the right or the left precordial leads; and 11) T-wave inversion over the right or the left precordial leads. Statistical analysis The prognostic relevance of ECG and other important baseline parameters with respect to in-hospital mortality was analysed univariately using Fisher s exact test. To additionally define the role of ECG and that of clinical and echocardiographic findings as determinants of outcome, a multiple logistical regression model was applied to the end point of overall mortality, taking into account those variables that reached a p- value,0.20 in the univariate comparison. The results of the logistical regression model are presented as estimated odds ratios with the corresponding 95% confidence intervals. All significance tests were two-sided. RESULTS Diagnosis, treatment and in-hospital clinical course In total, 508 patients were analysed, 294 females and 214 males, with a mean SD age of yrs (range yrs). As part of the diagnostic workup on admission, a high-probability lung scan was obtained in 270 patients (53%), and pulmonary angiography was performed in 84 patients (17%), confirming the presence of pulmonary thromboembolic obstruction in all cases. In addition, the diagnosis of deep venous thrombosis was established in 358 of the patients (70%) studied by vein sonography or phlebography. Overall, 469 study patients (92%) had confirmation of venous thromboembolism by at least one of these imaging studies. In the remaining patients, whose clinical and haemodynamic condition was considered 844 VOLUME 25 NUMBER 5 EUROPEAN RESPIRATORY JOURNAL
3 A. GEIBEL ET AL. ECG IN MAJOR PULMONARY EMBOLISM too critical to permit transportation from the emergency room or intensive care unit, the diagnosis of acute (massive) PE was based on clinical probability combined with bedside transthoracic echocardiography, if the latter indicated PH and/or acute right ventricular pressure overload in the absence of left ventricular or mitral valve disease [1]. A complete echocardiographic examination was available in 348 patients (69%), and revealed the presence of right ventricular pressure overload and/or PH in 306 patients (88%). Furthermore, 133 patients (26%) underwent catheterisation of the right side of the heart, which disclosed the presence of precapillary PH in 88% of the cases. After diagnosis of major PE, 204 patients (40%) received thrombolytic treatment within the first 24 h. The remaining 304 patients initially underwent conventional heparin anticoagulation. Of these patients, 41 (13%) underwent thrombolytic treatment by the attending physicians later during the hospital stay (i.e. after the first 24 h). The mean duration of hospital stay after diagnosis of major PE was days. Overall 30-day mortality was 23%, and death was directly related to the pulmonary thromboembolic event in almost all cases (116 of 118 deaths; 98%). Recurrence of PE was reported in 79 patients (16%). Clinical, echocardiographic and ECG findings on admission: correlation with patient outcome The clinical characteristics of the patients at the time of diagnosis are summarised in table 1. The mean age of the patients who survived to hospital discharge was yrs compared with yrs in those who died (p50.002). There were no differences between survivors and nonsuvivors, with regard to the history of recent surgery or major trauma, previous venous thrombosis or PE, cancer, stroke or pregnancy. Conversely, arterial hypotension or shock, syncope, and history of chronic cardiac or pulmonary disease were all significantly associated with a higher death rate (table 1). TABLE 2 Relationship of ECG abnormalities on admission to the outcome of patients with acute pulmonary embolism Parameter Survivors Nonsurvivors p-value Subjects n Sinus tachycardia.100 beats?min (67) 87 (77) Atrial arrhythmia 46 (12) 29 (25) Abnormal axis pattern # 85 (22) 29 (25) 0.53 Shift in the transition zone to V5 138 (35) 51 (43) 0.13 Complete RBBB 51 (14) 33 (29),0.001 Incomplete RBBB 74 (19) 14 (12) 0.53 Peripheral low voltage 84 (22) 41 (35) Q in leads III and avf, but not in II 28 (7.2) 16 (14) ST elevation in leads I, II, V4 V6 22 (5.8) 18 (16) ST depression in leads I, II, V4 V6 142 (38) 56 (49) T-wave inversion in leads V2 V3 194 (50) 52 (44) 0.39 T-wave inversion in leads V4 V6 128 (34) 48 (42) 0.12 Data are presented as n (%), unless otherwise stated. RBBB: right bundle branch block. # : S1Q3T3. Dilatation of the right ventricle (i.e. right ventricle appearing larger than the left ventricle from the apical or subcostal view, or right ventricular end-diastolic diameter.30 mm from the parasternal view) was detected in 259 of the 348 patients (74%) who underwent echocardiography. In these patients 30-day mortality was 25% as opposed to 13% in those without a dilated right ventricle (p50.016). The 12-lead ECG also exhibited significant differences between survivors and the nonsurvivors during the first 30 days after admission. As shown in table 2, atrial arrhythmias (mostly atrial fibrillation or flutter), complete RBBB, peripheral low voltage, pseudoinfarction pattern (Q waves) in leads III and TABLE 1 Association between baseline clinical characteristics and 30-day mortality Clinical characteristics at diagnosis Survivors Nonsurvivors p-value Subjects n Age.65 yrs 193 (49) 71 (60) Females/males (ratio) 225/165 (1.4:1) 69/49 (1.4:1) 0.92 Syncope 140 (36) 66 (56),0.001 Arterial hypotension 226 (58) 101 (86), Recent major surgery # 55 (14) 15 (13) 0.76 Major trauma or fracture # 12 (3.1) 5 (4.2) 0.56 History of venous thrombosis 114 (29) 33 (28) 0.82 History of pulmonary embolism 49 (13) 13 (11) 0.75 History of cardiac disease 112 (29) 45 (38) 0.05 Chronic pulmonary disease 31 (8.0) 20 (17) Cancer 44 (11) 19 (16) 0.20 History of stroke 17 (4.4) 8 (6.8) 0.33 Gestation 12 (5.3) 1 (1.5) 0.31 Data are presented as n (%), unless otherwise stated. Arterial hypotension was defined as systolic blood pressure,90 mmhg, or a pressure drop of o40 mmhg for at least 15 min, if not caused by new-onset arrhythmia, hypovolaemia or sepsis. # : within 10 days. c EUROPEAN RESPIRATORY JOURNAL VOLUME 25 NUMBER 5 845
4 ECG IN MAJOR PULMONARY EMBOLISM A. GEIBEL ET AL. avf, and ST segment changes (elevation or depression) over the left precordial leads were all significantly more frequent in patients with a fatal outcome. Overall, 29% of the patients who exhibited at least one of these abnormalities on admission did not survive to hospital discharge, as opposed to only 11% of the patients without a pathological 12-lead ECG (p,0.001). This difference yielded a positive predictive value of 29% and a negative predictive value of 84% with respect to 30-day mortality. In addition, there appeared to be a tendency towards a correlation between a pathological ECG and the dysfunction (dilatation) of the right ventricle on the initial echocardiogram. Overall, 78% of the current patients who exhibited at least one of the ECG findings mentioned previously also had an abnormal echocardiogram, compared with 68% of those without a pathological ECG (p50.068). The calculated prognostic sensitivity and specificity, as well as the negative and positive predictive value, of each one of the ECG parameters, which were univariately associated with an adverse outcome (p,0.05), are displayed in table 3. When examined by multiple logistical regression analysis (data not shown), none of these ECG abnormalities (atrial arrhythmias, complete RBBB, peripheral low voltage, Q in leads III and avf but not in II, or ST elevation or depression in leads I, II, V4 6) was individually associated with a poor outcome after adjustment for the patients clinical symptoms and findings on admission, and for the presence of pre-existing pulmonary and cardiac disease. However, multivariate analysis (table 4) revealed that the presence of at least one of these findings was, besides haemodynamic instability, syncope and chronic pulmonary disease, a significant independent predictor of outcome. DISCUSSION Since the 1970s, a number of carefully designed cohort studies [22 25], registries [1, 9, 26] and prospective randomised therapeutic trials [27, 28] have substantially improved understanding of the clinical course and prognosis of acute PE. At present, more than 30 yrs after the experimental studies of MCINTYRE and SASAHARA [29, 30] on the haemodynamic response to pulmonary vascular obstruction, right ventricular dysfunction and failure is widely accepted to be the single most important determinant of outcome in the acute phase of venous thromboembolism. Accordingly, the prognostic value TABLE 3 Prognostic sensitivity, specificity, positive predictive value (PPV) and negative predictive value (NPV) of ECG findings with regard to 30-day mortality Parameter Sensitivity Specificity PPV NPV Atrial arrhythmia Complete RBBB Peripheral low voltage Q in leads III and avf, but not in II ST elevation I, II, V4 V ST depression I, II, V4 V Data are presented as %. RBBB: right bundle branch block. TABLE 4 Predictors of 30-day mortality in patients with acute major pulmonary embolism Clinical characteristics Odds ratio (95% CI) p-value Age.65 yrs 1.21 ( ) 0.39 Arterial hypotension 3.55 ( ),0.001 Syncope 1.63 ( ) Chronic pulmonary disease 2.11 ( ) Abnormal ECG # 2.56 ( ),0.001 CI: confidence interval. # : at least one of the following ECG findings on admission (also shown in table 3): atrial arrhythmia; complete right bundle branch block; peripheral low voltage; Q in leads III and avf, but not in II; ST elevation in leads I, II, V4 6; and ST depression in leads I, II, V4 6. of echocardiographic and, more recently, CT imaging in patients with suspected PE lies primarily in the detection of right ventricular dilatation and/or hypokinesis [10, 13, 31, 32]. However, it has never been directly tested in a large patient population whether risk assessment based on acute right heart strain might also be possible using a simple baseline test, such as the 12-lead ECG. This hypothesis appears to be supported by a number of earlier and more recent reports, which suggested that specific ECG changes may correlate with the severity of PE [15, 16, 33]. The present study was based on the population of a large prospective multicentre registry [1], which investigated management strategies and the prognosis of acute PE. As with a previous large thrombolysis trial, the current study focused on patients with submassive and massive PR, i.e. patients at a particularly high risk of death or major cardiovascular complications during the hospital stay [34]. However, rather than attempting to correlate the ECG abnormalities with angiographic, haemodynamic or scintigraphic findings indicating severe PE [15, 16, 33], the present study directly examined the prognostic relevance of the 12-lead ECG with regard to 30-day mortality. Univariate analysis of the large study population (n5508) suggested that a number of ECG changes on admission, including atrial arrhythmias, complete RBBB, peripheral low voltage, and ST segment changes (elevation or depression) over the left precordial leads, were significantly associated with an adverse clinical outcome. Thus, the ECG abnormalities that were reported in earlier studies [15, 35] to indicate severe PE also appeared to affect prognosis in the present study, although the current authors could not confirm the prognostic relevance of the anterior subepicardial ischaemic pattern indicated by T-wave inversion over leads V1 V4 [16]. In addition, there appeared to be a tendency towards a correlation between a pathological ECG (defined as at least one of the above abnormalities) and the echocardiographic detection of right ventricular dilatation, a reliable marker of overt or impending right ventricular failure and an established predictor of in-hospital outcome [5, 31]. When examined by multivariate analysis, none of the ECG abnormalities was individually associated with a poor outcome after adjustment for the patients clinical symptoms and findings on admission, and for the presence of pre-existing pulmonary and cardiac disease. However, multiple logistical 846 VOLUME 25 NUMBER 5 EUROPEAN RESPIRATORY JOURNAL
5 A. GEIBEL ET AL. ECG IN MAJOR PULMONARY EMBOLISM regression revealed that the presence of at least one of these findings was, besides haemodynamic instability, syncope and chronic pulmonary disease, a significant independent predictor of early death. The physiological basis for the ECG findings associated with PE still remains difficult to define. Although it was suggested as early as 1938 that the ECG might reflect the development of right ventricular distention [14], this association now seems to be much more complex than initially thought. In particular, the appearance and the temporal pattern of ECG changes did not reliably correlate with the appearance and resolution of PH or of echocardiographically diagnosed right ventricular enlargement in subsequent reports [16, 17] and in the present study. Furthermore, although it is appealing to assume that the ECG findings in PE are the result of myocardial ischaemia and/or right ventricular wall stress, studies using scintigraphic and enzymatic (creatine kinase) assessment have not been able to demonstrate evidence of ischaemia in patients with T-wave changes over the anterior precordial leads [13]. In conclusion, in a large population of 508 patients with acute major pulmonary embolism, the present study demonstrated that the presence of at least one prespecified ECG abnormality on admission was, apart from the clinical findings at presentation, a predictor of outcome in the acute phase. Thus, the present results support the notion that the ECG may be useful as a simple, non-costly initial tool for assessing the patients prognosis and for guiding further diagnostic work-up and therapeutic decisions in clinical practice. This aspect may also have to be considered when designing future studies to evaluate the prognostic value and, particularly, the therapeutic implications of novel laboratory markers and/or radiological modalities in patients with acute major pulmonary embolism. REFERENCES 1 Kasper W, Konstantinides S, Geibel A, et al. Management strategies and determinants of outcome in acute major pulmonary embolism: results of a multicenter registry. J Am Coll Cardiol 1997; 30: Lualdi JC, Goldhaber SZ. Right ventricular dysfunction after acute pulmonary embolism: pathophysiologic factors, detection, and therapeutic implications. Am Heart J 1995; 130: Cannon CP, Goldhaber SZ. Cardiovascular risk stratification of pulmonary embolism. Am J Cardiol 1996; 78: Wood KE. The presence of shock defines the threshold to initiate thrombolytic therapy in patients with pulmonary embolism. Intensive Care Med 2002; 28: Kasper W, Konstantinides S, Geibel A, Tiede N, Krause T, Just H. Prognostic significance of right ventricular afterload stress detected by echocardiography in patients with clinically suspected pulmonary embolism. Heart 1997; 77: Ribeiro A, Lindmarker P, Juhlin-Dannfelt A, Johnsson H, Jorfeldt L. Echocardiography Doppler in pulmonary embolism: right ventricular dysfunction as a predictor of mortality rate. Am Heart J 1997; 134: Grifoni S, Olivotto I, Cecchini P, et al. Short-term clinical outcome of patients with acute pulmonary embolism, normal blood pressure, and echocardiographic right ventricular dysfunction. Circulation 2000; 101: Vieillard-Baron A, Page B, Augarde R, et al. Acute cor pulmonale in massive pulmonary embolism: incidence, echocardiographic pattern, clinical implications and recovery rate. Intensive Care Med 2001; 27: Goldhaber SZ, Visani L, De Rosa M. Acute pulmonary embolism: clinical outcomes in the International Cooperative Pulmonary Embolism Registry (ICOPER). Lancet 1999; 353: Goldhaber SZ. Echocardiography in the management of pulmonary embolism. Ann Intern Med 2002; 136: Konstantinides S, Geibel A, Heusel G, Heinrich F, Kasper W. Heparin plus alteplase compared with heparin alone in patients with submassive pulmonary embolism. N Engl J Med 2002; 347: Kucher N, Goldhaber SZ. Cardiac biomarkers for risk stratification of patients with acute pulmonary embolism. Circulation 2003; 108: Schoepf UJ, Kucher N, Kipfmueller F, Quiroz R, Costello P, Goldhaber SZ. Right ventricular enlargement on chest computed tomography: a predictor of early death in acute pulmonary embolism. Circulation 2004; 110: Wood KE. Major pulmonary embolism: review of a pathophysiologic approach to the golden hour of hemodynamically significant pulmonary embolism. Chest 2002; 121: Stein PD, Dalen JE, McIntyre KM, Sasahara AA, Wenger NK, Willis PW 3rd. The electrocardiogram in acute pulmonary embolism. Prog Cardiovasc Dis 1975; 17: Ferrari E, Imbert A, Chevalier T, Mihoubi A, Morand P, Baudouy M. The ECG in pulmonary embolism. Predictive value of negative T waves in precordial leads - 80 case reports. Chest 1997; 111: Sreeram N, Cheriex EC, Smeets JL, Gorgels AP, Wellens HJ. Value of the 12-lead electrocardiogram at hospital admission in the diagnosis of pulmonary embolism. Am J Cardiol 1994; 73: Konstantinides S, Geibel A, Olschewski M, et al. Association between thrombolytic treatment and the prognosis of hemodynamically stable patients with major pulmonary embolism: results of a multicenter registry. Circulation 1997; 96: Suspected acute pulmonary embolism: a practical approach. British Thoracic Society, Standards of Care Committee. Thorax 1997; 52: Suppl. 4, S1 S Opinions regarding the diagnosis and management of venous thromboembolic disease. ACCP Consensus Committee on Pulmonary Embolism. Chest 1996; 109: Miniati M, Prediletto R, Formichi B, et al. Accuracy of clinical assessment in the diagnosis of pulmonary embolism. Am J Respir Crit Care Med 1999; 159: Alpert JS, Smith R, Carlson J, Ockene IS, Dexter L, Dalen JE. Mortality in patients treated for pulmonary embolism. JAMA 1976; 236: Hall RJ, Sutton GC, Kerr IH. Long-term prognosis of treated acute massive pulmonary embolism. Br Heart J 1977; 39: c EUROPEAN RESPIRATORY JOURNAL VOLUME 25 NUMBER 5 847
6 ECG IN MAJOR PULMONARY EMBOLISM A. GEIBEL ET AL. 24 Optimum duration of anticoagulation for deep-vein thrombosis and pulmonary embolism. Research Committee of the British Thoracic Society. Lancet 1992; 340: Carson JL, Kelley MA, Duff A, et al. The clinical course of pulmonary embolism. N Engl J Med 1992; 326: Hamel E, Pacouret G, Vincentelli D, et al. Thrombolysis or heparin therapy in massive pulmonary embolism with right ventricular dilation: results from a 128-patient monocenter registry. Chest 2001; 120: The urokinase pulmonary embolism trial. A national cooperative study. Circulation 1973; 47: Suppl. 2, II1 II Goldhaber SZ, Haire WD, Feldstein ML, et al. Alteplase versus heparin in acute pulmonary embolism: randomised trial assessing right-ventricular function and pulmonary perfusion. Lancet 1993; 341: McIntyre KM, Sasahara AA. Hemodynamic and ventricular responses to pulmonary embolism. Prog Cardiovasc Dis 1974; 17: McIntyre KM, Sasahara AA. Determinants of right ventricular function and hemodynamics after pulmonary embolism. Chest 1974; 65: Kasper W, Meinertz T, Henkel B, et al. Echocardiographic findings in patients with proved pulmonary embolism. Am Heart J 1986; 112: Konstantinides S, Geibel A, Kasper W. Role of cardiac ultrasound in the detection of pulmonary embolism. Semin Resp Crit Care Med 1996; 17: Daniel KR, Courtney DM, Kline JA. Assessment of cardiac stress from massive pulmonary embolism with 12-lead ECG. Chest 2001; 120: Konstantinides S. Thrombolysis in submassive pulmonary embolism? Yes. J Thromb Haemost 2003; 1: Miller GA, Sutton GC. Acute massive pulmonary embolism. Clinical and haemodynamic findings in 23 patients studied by cardiac catheterization and pulmonary arteriography. Br Heart J 1970; 32: VOLUME 25 NUMBER 5 EUROPEAN RESPIRATORY JOURNAL
ORIGINAL INVESTIGATION
 ORIGINAL INVESTIGATION Prognostic Role of Echocardiography Among Patients With Acute Pulmonary Embolism and a Systolic Arterial Pressure of 90 mm Hg or Higher Nils Kucher, MD; Elisa Rossi, BS; Marisa De
ORIGINAL INVESTIGATION Prognostic Role of Echocardiography Among Patients With Acute Pulmonary Embolism and a Systolic Arterial Pressure of 90 mm Hg or Higher Nils Kucher, MD; Elisa Rossi, BS; Marisa De
Despite important advances in diagnosis and treatment,
 Importance of Cardiac Troponins I and T in Risk Stratification of Patients With Acute Pulmonary Embolism Stavros Konstantinides, MD; Annette Geibel, MD; Manfred Olschewski, PhD; Wolfgang Kasper, MD; Nadine
Importance of Cardiac Troponins I and T in Risk Stratification of Patients With Acute Pulmonary Embolism Stavros Konstantinides, MD; Annette Geibel, MD; Manfred Olschewski, PhD; Wolfgang Kasper, MD; Nadine
Chapter 1. Introduction
 Chapter 1 Introduction Introduction 9 Even though the first reports on venous thromboembolism date back to the 13 th century and the mechanism of acute pulmonary embolism (PE) was unraveled almost 150
Chapter 1 Introduction Introduction 9 Even though the first reports on venous thromboembolism date back to the 13 th century and the mechanism of acute pulmonary embolism (PE) was unraveled almost 150
DIAGNOSTIC evaluation for acute pulmonary
 994 2-D ECHO Jackson et al. ECHOCARDIOGRAPHY FOR PULMONARY EMBOLISM Prospective Evaluation of Two-dimensional Transthoracic Echocardiography in Emergency Department Patients with Suspected Pulmonary Embolism
994 2-D ECHO Jackson et al. ECHOCARDIOGRAPHY FOR PULMONARY EMBOLISM Prospective Evaluation of Two-dimensional Transthoracic Echocardiography in Emergency Department Patients with Suspected Pulmonary Embolism
S (18) doi: /j.ajem Reference: YAJEM 57346
 Accepted Manuscript A portrait of patients who die in-hospital from acute pulmonary embolism Hesham R. Omar, Mehdi Mirsaeidi, Bishoy Abraham, Garett Enten, Devanand Mangar, Enrico M. Camporesi PII: S0735-6757(18)30172-4
Accepted Manuscript A portrait of patients who die in-hospital from acute pulmonary embolism Hesham R. Omar, Mehdi Mirsaeidi, Bishoy Abraham, Garett Enten, Devanand Mangar, Enrico M. Camporesi PII: S0735-6757(18)30172-4
Troponin I and risk stratification of patients with acute nonmassive pulmonary embolism
 Eur Respir J 2008; 31: 847 853 DOI: 10.1183/09031936.00113307 CopyrightßERS Journals Ltd 2008 Troponin I and risk stratification of patients with acute nonmassive pulmonary embolism D. Jiménez*, G. Díaz*,
Eur Respir J 2008; 31: 847 853 DOI: 10.1183/09031936.00113307 CopyrightßERS Journals Ltd 2008 Troponin I and risk stratification of patients with acute nonmassive pulmonary embolism D. Jiménez*, G. Díaz*,
Pulmonary hypertension (PH) and right ventricular (RV)
 Pulmonary Embolism One-Year Follow-Up With Echocardiography Doppler and Five-Year Survival Analysis Ary Ribeiro, MD; Per Lindmarker, MD; Hans Johnsson, MD, PhD; Anders Juhlin-Dannfelt, MD, PhD; Lennart
Pulmonary Embolism One-Year Follow-Up With Echocardiography Doppler and Five-Year Survival Analysis Ary Ribeiro, MD; Per Lindmarker, MD; Hans Johnsson, MD, PhD; Anders Juhlin-Dannfelt, MD, PhD; Lennart
Cardiovascular Images
 Cardiovascular Images Pulmonary Embolism Diagnosed From Right Heart Changes Seen After Exercise Stress Echocardiography Brian C. Case, MD; Micheas Zemedkun, MD; Amarin Sangkharat, MD; Allen J. Taylor,
Cardiovascular Images Pulmonary Embolism Diagnosed From Right Heart Changes Seen After Exercise Stress Echocardiography Brian C. Case, MD; Micheas Zemedkun, MD; Amarin Sangkharat, MD; Allen J. Taylor,
ORIGINAL INVESTIGATION. Thrombolysis vs Heparin in the Treatment of Pulmonary Embolism
 Thrombolysis vs Heparin in the Treatment of Pulmonary Embolism A Clinical Outcome Based Meta-analysis ORIGINAL INVESTIGATION Giancarlo Agnelli, MD; Cecilia Becattini, MD; Timo Kirschstein, MD Background:
Thrombolysis vs Heparin in the Treatment of Pulmonary Embolism A Clinical Outcome Based Meta-analysis ORIGINAL INVESTIGATION Giancarlo Agnelli, MD; Cecilia Becattini, MD; Timo Kirschstein, MD Background:
Should thrombolysis have a greater role in the management of pulmonary embolism?
 ORIGINAL PAPERS Clinical Medicine 2009, Vol 9, No 5: 431 5 Should thrombolysis have a greater role in the management of pulmonary embolism? Peter O Jenkins, Javed Sultanzadeh, Manasi Bhagwat and Paul F
ORIGINAL PAPERS Clinical Medicine 2009, Vol 9, No 5: 431 5 Should thrombolysis have a greater role in the management of pulmonary embolism? Peter O Jenkins, Javed Sultanzadeh, Manasi Bhagwat and Paul F
PREVENTION AND TREATMENT OF VENOUS THROMBOEMBOLISM
 PREVENTION AND TREATMENT OF VENOUS THROMBOEMBOLISM International Consensus Statement 2013 Guidelines According to Scientific Evidence Developed under the auspices of the: Cardiovascular Disease Educational
PREVENTION AND TREATMENT OF VENOUS THROMBOEMBOLISM International Consensus Statement 2013 Guidelines According to Scientific Evidence Developed under the auspices of the: Cardiovascular Disease Educational
CARDIAC PROBLEMS IN PREGNANCY
 CARDIAC PROBLEMS IN PREGNANCY LAS VEGAS, NEVADA, USA 27 February 1 March 2016 SUCCESSFUL TREATMENT WITH RECOMBINANT TISSUE PLASMINOGEN ACTIVATOR OF MASSIVE PULMONARY EMBOLISM IN THE 16 TH WEEK OF PREGNANCY
CARDIAC PROBLEMS IN PREGNANCY LAS VEGAS, NEVADA, USA 27 February 1 March 2016 SUCCESSFUL TREATMENT WITH RECOMBINANT TISSUE PLASMINOGEN ACTIVATOR OF MASSIVE PULMONARY EMBOLISM IN THE 16 TH WEEK OF PREGNANCY
Disclosures. Objectives
 BRIGHAM AND WOMEN S HOSPITAL Treatment of Massive and Submassive Pulmonary Embolism Gregory Piazza, MD, MS Assistant Professor of Medicine Harvard Medical School Staff Physician, Cardiovascular Division
BRIGHAM AND WOMEN S HOSPITAL Treatment of Massive and Submassive Pulmonary Embolism Gregory Piazza, MD, MS Assistant Professor of Medicine Harvard Medical School Staff Physician, Cardiovascular Division
Epidemiology. Update on Pulmonary Embolism. Keys to PE Management 5/5/2014. Diagnosis. Risk stratification. Treatment
 Update on Pulmonary Embolism Steven M. Dean, DO, FACP, RPVI Program Director- Vascular Medicine Associate Professor of Internal Medicine Division of Cardiovascular Medicine The Ohio State University Keys
Update on Pulmonary Embolism Steven M. Dean, DO, FACP, RPVI Program Director- Vascular Medicine Associate Professor of Internal Medicine Division of Cardiovascular Medicine The Ohio State University Keys
Epidemiology of Pulmonary Embolism (PE)
 Why Treat Submassive PE Abstract: Massive Pulmonary Embolism (PE) requires immediate lifesaving intervention for the patient. For the submassive PE patient, characterized by presence of right ventricular
Why Treat Submassive PE Abstract: Massive Pulmonary Embolism (PE) requires immediate lifesaving intervention for the patient. For the submassive PE patient, characterized by presence of right ventricular
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/21764 holds various files of this Leiden University dissertation. Author: Mos, Inge Christina Maria Title: A more granular view on pulmonary embolism Issue
Cover Page The handle http://hdl.handle.net/1887/21764 holds various files of this Leiden University dissertation. Author: Mos, Inge Christina Maria Title: A more granular view on pulmonary embolism Issue
Innovative Endovascular Approach to Pulmonary Embolism by Ultrasound Enhanced Thrombolysis. Prof. Ralf R.Kolvenbach MD,PhD,FEBVS
 Innovative Endovascular Approach to Pulmonary Embolism by Ultrasound Enhanced Thrombolysis Prof. Ralf R.Kolvenbach MD,PhD,FEBVS Catheter-based thrombolysis Local administration of lytic agent Higher local
Innovative Endovascular Approach to Pulmonary Embolism by Ultrasound Enhanced Thrombolysis Prof. Ralf R.Kolvenbach MD,PhD,FEBVS Catheter-based thrombolysis Local administration of lytic agent Higher local
PULMONARY EMBOLISM (PE): DIAGNOSIS AND TREATMENT
 PULMONARY EMBOLISM (PE): DIAGNOSIS AND TREATMENT OBJECTIVE: To provide a diagnostic algorithm and treatment options for patients with acute pulmonary embolism (PE). BACKGROUND: Venous thromboembolism (VTE)
PULMONARY EMBOLISM (PE): DIAGNOSIS AND TREATMENT OBJECTIVE: To provide a diagnostic algorithm and treatment options for patients with acute pulmonary embolism (PE). BACKGROUND: Venous thromboembolism (VTE)
Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine
 Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine Venous thromboembolism: pulmonary embolism (PE) deep vein thrombosis (DVT) 1% of all patients admitted to hospital 5% of in-hospital mortality
Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine Venous thromboembolism: pulmonary embolism (PE) deep vein thrombosis (DVT) 1% of all patients admitted to hospital 5% of in-hospital mortality
RISK STRATIFICATION OF PATIENTS WITH ACUTE SYMPTOMATIC PULMONARY EMBOLISM. David Jiménez, MD, PhD, FCCP Ramón y Cajal Hospital, IRYCIS Madrid, Spain
 RISK STRATIFICATION OF PATIENTS WITH ACUTE SYMPTOMATIC PULMONARY EMBOLISM David Jiménez, MD, PhD, FCCP Ramón y Cajal Hospital, IRYCIS Madrid, Spain Potential Conflicts of Interest Financial conflicts of
RISK STRATIFICATION OF PATIENTS WITH ACUTE SYMPTOMATIC PULMONARY EMBOLISM David Jiménez, MD, PhD, FCCP Ramón y Cajal Hospital, IRYCIS Madrid, Spain Potential Conflicts of Interest Financial conflicts of
Innovative Endovascular Approach to Pulmonary Embolism by Ultrasound Enhanced Thrombolysis. Prof. Ralf R.Kolvenbach MD,PhD,FEBVS
 Innovative Endovascular Approach to Pulmonary Embolism by Ultrasound Enhanced Thrombolysis Prof. Ralf R.Kolvenbach MD,PhD,FEBVS Conflict of Interest BTG Standard PE therapy ANTICOAGULATION (AC) HEPARIN
Innovative Endovascular Approach to Pulmonary Embolism by Ultrasound Enhanced Thrombolysis Prof. Ralf R.Kolvenbach MD,PhD,FEBVS Conflict of Interest BTG Standard PE therapy ANTICOAGULATION (AC) HEPARIN
Acute pulmonary embolism: risk stratification in the emergency department
 Intern Emerg Med (2007) 2:119 129 DOI 10.1007/s11739-007-0033-y 119 REVIEW C. Becattini G. Agnelli Acute pulmonary embolism: risk stratification in the emergency department Received: 16 October 2006 /
Intern Emerg Med (2007) 2:119 129 DOI 10.1007/s11739-007-0033-y 119 REVIEW C. Becattini G. Agnelli Acute pulmonary embolism: risk stratification in the emergency department Received: 16 October 2006 /
Diagnosis and initial treatment of patients with suspected pulmonary thromboembolism
 Diagnosis and initial treatment of patients with suspected pulmonary thromboembolism Pulmonary thromboembolism (PTE) remains a frequently occurring diagnostic problem, with an incidence of approximately
Diagnosis and initial treatment of patients with suspected pulmonary thromboembolism Pulmonary thromboembolism (PTE) remains a frequently occurring diagnostic problem, with an incidence of approximately
A cute pulmonary embolism (APE) is a common disease
 956 PULMONARY VASCULATURE Computed tomographic pulmonary angiography and prognostic significance in patients with acute pulmonary embolism A Ghuysen, B Ghaye, V Willems, B Lambermont, P Gerard, R F Dondelinger,
956 PULMONARY VASCULATURE Computed tomographic pulmonary angiography and prognostic significance in patients with acute pulmonary embolism A Ghuysen, B Ghaye, V Willems, B Lambermont, P Gerard, R F Dondelinger,
Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism A pulmonary embolism (PE) is
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism A pulmonary embolism (PE) is
Management of Acute Pulmonary Embolism. Judith Hurdman Consultant Respiratory Physician
 Management of Acute Pulmonary Embolism Judith Hurdman Consultant Respiratory Physician Judith.hurdman@sth.nhs.uk Overview Risk Stratification Who can be managed as an outpatient? To thrombolyse or not
Management of Acute Pulmonary Embolism Judith Hurdman Consultant Respiratory Physician Judith.hurdman@sth.nhs.uk Overview Risk Stratification Who can be managed as an outpatient? To thrombolyse or not
VTE & Medical Patients: Case Scenario
 The Saudi Association for Venous Thromboembolism SAVTE The 2 nd SAVTE Symposium 1-3 May, 2012 Casablanca, Morocco VTE & Medical Patients: Case Scenario Majdy Idrees Riyadh, Saudi Arabia Majdy M Idrees,
The Saudi Association for Venous Thromboembolism SAVTE The 2 nd SAVTE Symposium 1-3 May, 2012 Casablanca, Morocco VTE & Medical Patients: Case Scenario Majdy Idrees Riyadh, Saudi Arabia Majdy M Idrees,
Massive and Submassive Pulmonary Embolism: 2017 Update and Future Directions
 Massive and Submassive Pulmonary Embolism: 2017 Update and Future Directions Kush R Desai, MD Assistant Professor of Radiology Northwestern University Feinberg School of Medicine Chicago, IL Disclosures
Massive and Submassive Pulmonary Embolism: 2017 Update and Future Directions Kush R Desai, MD Assistant Professor of Radiology Northwestern University Feinberg School of Medicine Chicago, IL Disclosures
Cardiac troponin I for predicting right ventricular dysfunction and intermediate risk in patients with normotensive pulmonary embolism
 Neth Heart J (2015) 23:55 61 DOI 10.1007/s12471-014-0628-7 ORIGINAL ARTICLE: SHORT COMMUNICATION Cardiac troponin I for predicting right ventricular dysfunction and intermediate risk in patients with normotensive
Neth Heart J (2015) 23:55 61 DOI 10.1007/s12471-014-0628-7 ORIGINAL ARTICLE: SHORT COMMUNICATION Cardiac troponin I for predicting right ventricular dysfunction and intermediate risk in patients with normotensive
Echocardiography as a diagnostic and management tool in medical emergencies
 Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Electrocardiographic findings in pulmonary embolism
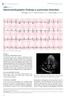 Singapore Med J 2015; 56(10): 533-537 doi: 10.11622/smedj.2015147 Electrocardiography Series CMEArticle Electrocardiographic findings in pulmonary embolism Elaine Boey1, MBBS, MRCP, Swee-Guan Teo2, MRCP,
Singapore Med J 2015; 56(10): 533-537 doi: 10.11622/smedj.2015147 Electrocardiography Series CMEArticle Electrocardiographic findings in pulmonary embolism Elaine Boey1, MBBS, MRCP, Swee-Guan Teo2, MRCP,
Submassive pulmonary embolism (PE) manifests a. Assessment of Cardiac Stress From Massive Pulmonary Embolism With 12-Lead ECG*
 Assessment of Cardiac Stress From Massive Pulmonary Embolism With 12-Lead ECG* Kurt R. Daniel, DO ; D. Mark Courtney, MD; and Jeffrey A. Kline, MD Background: Massive pulmonary embolism (PE) that causes
Assessment of Cardiac Stress From Massive Pulmonary Embolism With 12-Lead ECG* Kurt R. Daniel, DO ; D. Mark Courtney, MD; and Jeffrey A. Kline, MD Background: Massive pulmonary embolism (PE) that causes
Single-Center, Retrospective, Observational Analysis of Patients with Submassive Pulmonary Embolism (PE) Receiving Catheter- Directed Thrombolysis
 Single-Center, Retrospective, Observational Analysis of Patients with Submassive Pulmonary Embolism (PE) Receiving Catheter- Directed Thrombolysis John A. Phillips, M.D. OhioHealth Heart and Vascular Physicians
Single-Center, Retrospective, Observational Analysis of Patients with Submassive Pulmonary Embolism (PE) Receiving Catheter- Directed Thrombolysis John A. Phillips, M.D. OhioHealth Heart and Vascular Physicians
Venous Thrombosis. Magnitude of the Problem. DVT 2 Million PE 600,000. Death 60,000. Estimated Cost of VTE Care $1.5 Billion/year.
 Venous Thrombosis Magnitude of the Problem DVT 2 Million Postthrombotic Syndrome 800,000 PE 600,000 Death 60,000 Silent PE 1 Million Pulmonary Hypertension 30,000 Estimated Cost of VTE Care $1.5 Billion/year
Venous Thrombosis Magnitude of the Problem DVT 2 Million Postthrombotic Syndrome 800,000 PE 600,000 Death 60,000 Silent PE 1 Million Pulmonary Hypertension 30,000 Estimated Cost of VTE Care $1.5 Billion/year
Pulmonary embolism: Acute management. Cecilia Becattini University of Perugia, Italy
 Pulmonary embolism: Acute management Cecilia Becattini University of Perugia, Italy Acute pulmonary embolism: Acute management Diagnosis Risk stratification Treatment Non-high risk PE: diagnosis 3-mo VTE
Pulmonary embolism: Acute management Cecilia Becattini University of Perugia, Italy Acute pulmonary embolism: Acute management Diagnosis Risk stratification Treatment Non-high risk PE: diagnosis 3-mo VTE
Right ventricular (RV) dysfunction is a frequent consequence
 Independent Prognostic Value of Cardiac Troponin T in Patients With Confirmed Pulmonary Embolism Evangelos Giannitsis, MD; Margit Müller-Bardorff, MD; Volkhard Kurowski, MD; Britta Weidtmann, MD; Uwe Wiegand,
Independent Prognostic Value of Cardiac Troponin T in Patients With Confirmed Pulmonary Embolism Evangelos Giannitsis, MD; Margit Müller-Bardorff, MD; Volkhard Kurowski, MD; Britta Weidtmann, MD; Uwe Wiegand,
Management of Massive and Sub-Massive Pulmonary Embolism
 Management of Massive and Sub-Massive Pulmonary Embolism M. Montero-Baker, MD L Leon Jr., MD, RVT, FACS Tucson Medical Center Vascular and Endovascular Surgery Section CASE PRESENTATION 54 YEAR- OLD CAUCASIAN
Management of Massive and Sub-Massive Pulmonary Embolism M. Montero-Baker, MD L Leon Jr., MD, RVT, FACS Tucson Medical Center Vascular and Endovascular Surgery Section CASE PRESENTATION 54 YEAR- OLD CAUCASIAN
Case Report Free Floating Right Heart Thrombus Associated with Acute Pulmonary Embolism: An Unsettled Therapeutic Difficulty
 Case Reports in Cardiology Volume 2015, Article ID 364780, 4 pages http://dx.doi.org/10.1155/2015/364780 Case Report Free Floating Right Heart Thrombus Associated with Acute Pulmonary Embolism: An Unsettled
Case Reports in Cardiology Volume 2015, Article ID 364780, 4 pages http://dx.doi.org/10.1155/2015/364780 Case Report Free Floating Right Heart Thrombus Associated with Acute Pulmonary Embolism: An Unsettled
Guideline for Thrombolysis Therapy in Pulmonary Embolism
 Guideline for Thrombolysis Therapy in Pulmonary Embolism Dr Jane Strong Consultant Haematologist Trust ref: B24/2016 1. Introduction / Scope All Patients with pulmonary embolism (PE) require rapid risk
Guideline for Thrombolysis Therapy in Pulmonary Embolism Dr Jane Strong Consultant Haematologist Trust ref: B24/2016 1. Introduction / Scope All Patients with pulmonary embolism (PE) require rapid risk
ORIGINAL ARTICLE. Department of Internal Medicine and Cardiology, The Medical University of Warsaw, Poland
 ORIGINAL ARTICLE Cardiology Journal 2010, Vol. 17, No. 1, pp. 1 XXX Copyright 2009 Via Medica ISSN 1897 5593 Signs of myocardial ischemia on electrocardiogram correlate with elevated plasma cardiac troponin
ORIGINAL ARTICLE Cardiology Journal 2010, Vol. 17, No. 1, pp. 1 XXX Copyright 2009 Via Medica ISSN 1897 5593 Signs of myocardial ischemia on electrocardiogram correlate with elevated plasma cardiac troponin
PULMONARY EMBOLISM -CASE REPORT-
 University Goce Delcev, Faculty of Medical sciences, Stip University Clinic of Cardiology, Skopje R. Of Macedonia PULMONARY EMBOLISM -CASE REPORT- Gordana Kamceva MD mr.sci Acknowledgment Marija Vavlukis
University Goce Delcev, Faculty of Medical sciences, Stip University Clinic of Cardiology, Skopje R. Of Macedonia PULMONARY EMBOLISM -CASE REPORT- Gordana Kamceva MD mr.sci Acknowledgment Marija Vavlukis
Original Article Acute pulmonary embolism with electrocardiagraphic changes mimicking acute coronary syndrome: a case report and literature review
 Int J Clin Exp Med 2015;8(7):11038-11042 www.ijcem.com /ISSN:1940-5901/IJCEM0009683 Original Article Acute pulmonary embolism with electrocardiagraphic changes mimicking acute coronary syndrome: a case
Int J Clin Exp Med 2015;8(7):11038-11042 www.ijcem.com /ISSN:1940-5901/IJCEM0009683 Original Article Acute pulmonary embolism with electrocardiagraphic changes mimicking acute coronary syndrome: a case
Systemic or local thrombolysis in high-risk pulmonary embolism
 original article Cardiology Journal 2015, Vol. 22, No. 4, 467 474 DOI: 10.5603/CJ.a2014.0103 Copyright 2015 Via Medica ISSN 1897 5593 Systemic or local thrombolysis in high-risk pulmonary embolism Liviu
original article Cardiology Journal 2015, Vol. 22, No. 4, 467 474 DOI: 10.5603/CJ.a2014.0103 Copyright 2015 Via Medica ISSN 1897 5593 Systemic or local thrombolysis in high-risk pulmonary embolism Liviu
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
A 50-year-old woman with syncope
 Hira Shahzad 1, Ali Bin Sarwar Zubairi 2 1 Medical College, Aga Khan University Hospital, Karachi 2 Department of Medicine, Aga Khan University Hospital, Karachi, Pakistan Ali Bin Sarwar Zubairi Associate
Hira Shahzad 1, Ali Bin Sarwar Zubairi 2 1 Medical College, Aga Khan University Hospital, Karachi 2 Department of Medicine, Aga Khan University Hospital, Karachi, Pakistan Ali Bin Sarwar Zubairi Associate
Thrombolysis in PE. Outline. Disclosure. Overview on Pulmonary Embolism. Hot Topics in Emergency Medicine 2012 Midyear Clinical Meeting
 Disclosure Thrombolysis in PE Daniel P. Hays, PharmD, BCPS, FASHP reports no relevant financial relationships. Daniel P. Hays, PharmD, BCPS, FASHP Outline 55 YOF presents to ED with SOB PMH of DVT + noncompliance
Disclosure Thrombolysis in PE Daniel P. Hays, PharmD, BCPS, FASHP reports no relevant financial relationships. Daniel P. Hays, PharmD, BCPS, FASHP Outline 55 YOF presents to ED with SOB PMH of DVT + noncompliance
Early Transoesophageal Echocardiography (TOE) in Cardiac Arrest: A Case Study
 Case reports Early Transoesophageal Echocardiography (TOE) in Cardiac Arrest: A Case Study N. SIMPSON, N. ORFORD Intensive Care Unit, The Geelong Hospital, Geelong, VICTORIA ABSTRACT We describe a case
Case reports Early Transoesophageal Echocardiography (TOE) in Cardiac Arrest: A Case Study N. SIMPSON, N. ORFORD Intensive Care Unit, The Geelong Hospital, Geelong, VICTORIA ABSTRACT We describe a case
ORIGINAL INVESTIGATION. Thrombolytic Therapy and Mortality in Patients With Acute Pulmonary Embolism
 ORIGINAL INVESTIGATION Thrombolytic Therapy and in Patients With Acute Pulmonary Embolism Said A. Ibrahim, MD, MPH; Roslyn A. Stone, PhD; D. Scott Obrosky, MSc; Ming Geng, MSc; Michael J. Fine, MD, MSc;
ORIGINAL INVESTIGATION Thrombolytic Therapy and in Patients With Acute Pulmonary Embolism Said A. Ibrahim, MD, MPH; Roslyn A. Stone, PhD; D. Scott Obrosky, MSc; Ming Geng, MSc; Michael J. Fine, MD, MSc;
Use of EKOS Catheter in the management of Venous Mr. Manoj Niverthi, Mr. Sarang Pujari, and Ms. Nupur Dandavate, The GTF Group
 Use of EKOS Catheter in the management of Venous Thromboembolism @ Mr. Manoj Niverthi, Mr. Sarang Pujari, and Ms. Nupur Dandavate, The GTF Group Introduction Georgia Thrombosis Forum (GTF, www.gtfonline.net)
Use of EKOS Catheter in the management of Venous Thromboembolism @ Mr. Manoj Niverthi, Mr. Sarang Pujari, and Ms. Nupur Dandavate, The GTF Group Introduction Georgia Thrombosis Forum (GTF, www.gtfonline.net)
Systemic Fibrinolytic Therapy in the Presence of Absolute Contraindication; a Case Series
 Emergency. 2018; 6 (1): e25 CASE REPORT Systemic Fibrinolytic Therapy in the Presence of Absolute Contraindication; a Case Series Mahdi Pishgahi 1, Toktam Alirezaei 1, Behzad Hajimoradi 1, S. Mojtaba Nekooghadam
Emergency. 2018; 6 (1): e25 CASE REPORT Systemic Fibrinolytic Therapy in the Presence of Absolute Contraindication; a Case Series Mahdi Pishgahi 1, Toktam Alirezaei 1, Behzad Hajimoradi 1, S. Mojtaba Nekooghadam
ACUTE PULMONARY EMBOLISM MIMICS ACUTE CORONARY SYNDROME IN OLDER PATIENT
 CASE REPORT ACUTE PULMONARY EMBOLISM MIMICS ACUTE CORONARY SYNDROME IN OLDER PATIENT Chun-Chieh Liu 1,2 *, Ta-Chuan Hung 1,2, Charles Jia-Yin Hou 1,2, Cheng-Ho Tsai 1,2,3 1 Cardiovascular Medicine, Department
CASE REPORT ACUTE PULMONARY EMBOLISM MIMICS ACUTE CORONARY SYNDROME IN OLDER PATIENT Chun-Chieh Liu 1,2 *, Ta-Chuan Hung 1,2, Charles Jia-Yin Hou 1,2, Cheng-Ho Tsai 1,2,3 1 Cardiovascular Medicine, Department
Ryan Walsh, MD Department of Emergency Medicine Madigan Army Medical Center
 Ryan Walsh, MD Department of Emergency Medicine Madigan Army Medical Center The opinions expressed herein are solely those of the author and do not represent the official views of the Department of Defense
Ryan Walsh, MD Department of Emergency Medicine Madigan Army Medical Center The opinions expressed herein are solely those of the author and do not represent the official views of the Department of Defense
Acute pulmonary thromboembolism (PE) is a common,
 Role of Echocardiography in the Diagnosis and Treatment of Acute Pulmonary Thromboembolism David Leibowitz, MD, Jerusalem, Israel The diagnosis and treatment of acute pulmonary thromboembolism (PE) remains
Role of Echocardiography in the Diagnosis and Treatment of Acute Pulmonary Thromboembolism David Leibowitz, MD, Jerusalem, Israel The diagnosis and treatment of acute pulmonary thromboembolism (PE) remains
Cardiovascular emergencies. 05/March/2014 László Rudas Szeged
 Cardiovascular emergencies 05/March/2014 László Rudas Szeged Acute chest pain Acute heart failure Sudden cardiac death Acute chest pain What is the etiology? Chest pain signals emergency: - ACS - Pulmonary
Cardiovascular emergencies 05/March/2014 László Rudas Szeged Acute chest pain Acute heart failure Sudden cardiac death Acute chest pain What is the etiology? Chest pain signals emergency: - ACS - Pulmonary
Case Report Respirophasic Variations in the QRS Complex and Echocardiographic Equivalent in Pulmonary Embolism
 www.ipej.org 313 Case Report Respirophasic Variations in the QRS Complex and Echocardiographic Equivalent in Pulmonary Embolism Eftychios Siniorakis, MD, Spyridon Arvanitakis, BM, Dimitris Barlagiannis,
www.ipej.org 313 Case Report Respirophasic Variations in the QRS Complex and Echocardiographic Equivalent in Pulmonary Embolism Eftychios Siniorakis, MD, Spyridon Arvanitakis, BM, Dimitris Barlagiannis,
ECG Workshop. Nezar Amir
 ECG Workshop Nezar Amir Myocardial Ischemia ECG Infarct ECG in STEMI is dynamic & evolving Common causes of ST shift Infarct Localisation Left main artery occlusion: o diffuse ST-depression with ST elevation
ECG Workshop Nezar Amir Myocardial Ischemia ECG Infarct ECG in STEMI is dynamic & evolving Common causes of ST shift Infarct Localisation Left main artery occlusion: o diffuse ST-depression with ST elevation
Index. K Knobology, TTE artifact, image resolution, ultrasound, 14
 A Acute aortic regurgitation (AR), 124 128 Acute aortic syndrome (AAS) classic aortic dissection diagnosis, 251 263 evolutive patterns, 253 255 pathology, 250 251 classifications, 247 248 incomplete aortic
A Acute aortic regurgitation (AR), 124 128 Acute aortic syndrome (AAS) classic aortic dissection diagnosis, 251 263 evolutive patterns, 253 255 pathology, 250 251 classifications, 247 248 incomplete aortic
PE is a difficult diagnosis that may be missed because of non-specific clinical presentation.
 Pulmonary embolism (PE) is a relatively common cardiovascular emergency. By occluding the pulmonary arterial bed it may lead to acute life-threatening (3% early mortality rate), but potentially reversible
Pulmonary embolism (PE) is a relatively common cardiovascular emergency. By occluding the pulmonary arterial bed it may lead to acute life-threatening (3% early mortality rate), but potentially reversible
Emergency department bedside echocardiography diagnosis of massive pulmonary embolism with direct visualization of thrombus in the pulmonary artery
 Crit Ultrasound J (2011) 3:155 160 DOI 10.1007/s13089-011-0081-4 CASE REPORT Emergency department bedside echocardiography diagnosis of massive pulmonary embolism with direct visualization of thrombus
Crit Ultrasound J (2011) 3:155 160 DOI 10.1007/s13089-011-0081-4 CASE REPORT Emergency department bedside echocardiography diagnosis of massive pulmonary embolism with direct visualization of thrombus
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Other 12-Lead ECG Findings
 Other 12-Lead ECG Findings Left Atrial Enlargement Left atrial enlargement is illustrated by increased P wave duration in lead II, top ECG, and by the prominent negative P terminal force in lead V1, bottom
Other 12-Lead ECG Findings Left Atrial Enlargement Left atrial enlargement is illustrated by increased P wave duration in lead II, top ECG, and by the prominent negative P terminal force in lead V1, bottom
Timing of NT-pro-BNP sampling for predicting adverse outcome after acute pulmonary embolism
 7 Frederikus A. Klok Noortje van der Bijl Inge C.M. Mos Albert de Roos Lucia J. M. Kroft Menno V. Huisman Timing of NT-pro-BNP sampling for predicting adverse outcome after acute pulmonary embolism Letter
7 Frederikus A. Klok Noortje van der Bijl Inge C.M. Mos Albert de Roos Lucia J. M. Kroft Menno V. Huisman Timing of NT-pro-BNP sampling for predicting adverse outcome after acute pulmonary embolism Letter
Cardiorespiratory efficacy of thrombolytic therapy in acute massive pulmonary embolism: identification of predictive factors
 Eur Respir J 1999; 13: 610±615 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 0903-1936 Cardiorespiratory efficacy of thrombolytic therapy in acute
Eur Respir J 1999; 13: 610±615 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 0903-1936 Cardiorespiratory efficacy of thrombolytic therapy in acute
Prediction of the Site of Coronary Artery Lesion in Acute Inferior Myocardial Infarction with Right Sided Precordial Lead (V4r)
 Prediction of the Site of Coronary Artery Lesion in Acute Inferior Myocardial Infarction with Right Sided Precordial Lead (V4r) MS Alam, M Ullah, SU Ulabbi, MM Haque, R Uddin, MS Mamun, AAS Majumder National
Prediction of the Site of Coronary Artery Lesion in Acute Inferior Myocardial Infarction with Right Sided Precordial Lead (V4r) MS Alam, M Ullah, SU Ulabbi, MM Haque, R Uddin, MS Mamun, AAS Majumder National
Postoperative Acute Pulmonary Embolism: A Case Report. S Mishra, P Kundra, B Hemavathi, A Badhe, M Ravishankar
 ISPUB.COM The Internet Journal of Anesthesiology Volume 13 Number 2 S Mishra, P Kundra, B Hemavathi, A Badhe, M Ravishankar Citation S Mishra, P Kundra, B Hemavathi, A Badhe, M Ravishankar.. The Internet
ISPUB.COM The Internet Journal of Anesthesiology Volume 13 Number 2 S Mishra, P Kundra, B Hemavathi, A Badhe, M Ravishankar Citation S Mishra, P Kundra, B Hemavathi, A Badhe, M Ravishankar.. The Internet
TWO ELDERLY PATIENTS WITH DYSPNOEA : DIAGNOSIS AND MANAGEMENT
 W K Chan et al Two Elderly Patients with Dyspnoea TWO ELDERLY PATIENTS WITH DYSPNOEA : DIAGNOSIS AND MANAGEMENT Wai-kwong Chan, FRCP(Edin) Consultant Tsan-fai Chan, MRCP(UK) Medical Officer Chiu-sun Yue,
W K Chan et al Two Elderly Patients with Dyspnoea TWO ELDERLY PATIENTS WITH DYSPNOEA : DIAGNOSIS AND MANAGEMENT Wai-kwong Chan, FRCP(Edin) Consultant Tsan-fai Chan, MRCP(UK) Medical Officer Chiu-sun Yue,
Supplementary material 1. Definitions of study endpoints (extracted from the Endpoint Validation Committee Charter) 1.
 Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
Is Thrombolysis Only for a Crisis?
 Is Thrombolysis Only for a Crisis? December 19, 2017 Is Thrombolysis Only for a Crisis? Indications for Thrombolytic Therapy in Patients with Acute Pulmonary Embolism Case Scenario A 28 year old woman
Is Thrombolysis Only for a Crisis? December 19, 2017 Is Thrombolysis Only for a Crisis? Indications for Thrombolytic Therapy in Patients with Acute Pulmonary Embolism Case Scenario A 28 year old woman
International Journal of Current Research and Academic Review ISSN: Volume 3 Number 1 (January-2015) pp
 International Journal of Current Research and Academic Review ISSN: 2347-3215 Volume 3 Number 1 (January-2015) pp. 305-314 www.ijcrar.com The correlation of severity of pulmonary embolism in CT Angiography
International Journal of Current Research and Academic Review ISSN: 2347-3215 Volume 3 Number 1 (January-2015) pp. 305-314 www.ijcrar.com The correlation of severity of pulmonary embolism in CT Angiography
Assessment of severity and prognosis in patients with pulmonary embolism attending to clot load score on MDCT pulmonary angiography
 Assessment of severity and prognosis in patients with pulmonary embolism attending to clot load score on MDCT pulmonary angiography Award: Certificate of Merit Poster No.: C-0890 Congress: ECR 2018 Type:
Assessment of severity and prognosis in patients with pulmonary embolism attending to clot load score on MDCT pulmonary angiography Award: Certificate of Merit Poster No.: C-0890 Congress: ECR 2018 Type:
Heart Health ESC Guidelines on the diagnosis and management of acute pulmonary embolism
 Heart Health Open Access Received: Oct 22, 2014 Accepted: Dec 01, 2014 Published: Dec 05, 2014 http://dx.doi.org/10.14437/hhoa-1-105 Review Jiri Widimsky, Heart Health Open Access 2014, 1:1 2014 ESC Guidelines
Heart Health Open Access Received: Oct 22, 2014 Accepted: Dec 01, 2014 Published: Dec 05, 2014 http://dx.doi.org/10.14437/hhoa-1-105 Review Jiri Widimsky, Heart Health Open Access 2014, 1:1 2014 ESC Guidelines
Echocardiographic Cardiovascular Risk Stratification: Beyond Ejection Fraction
 Echocardiographic Cardiovascular Risk Stratification: Beyond Ejection Fraction October 4, 2014 James S. Lee, M.D., F.A.C.C. Associates in Cardiology, P.A. Silver Spring, M.D. Disclosures Financial none
Echocardiographic Cardiovascular Risk Stratification: Beyond Ejection Fraction October 4, 2014 James S. Lee, M.D., F.A.C.C. Associates in Cardiology, P.A. Silver Spring, M.D. Disclosures Financial none
Effectiveness and cost-effectiveness of thrombolysis in submassive pulmonary embolism Perlroth D J, Sanders G D, Gould M K
 Effectiveness and cost-effectiveness of thrombolysis in submassive pulmonary embolism Perlroth D J, Sanders G D, Gould M K Record Status This is a critical abstract of an economic evaluation that meets
Effectiveness and cost-effectiveness of thrombolysis in submassive pulmonary embolism Perlroth D J, Sanders G D, Gould M K Record Status This is a critical abstract of an economic evaluation that meets
Acute pulmonary embolism: mortality prediction by the 2014 European Society of Cardiology risk stratification model
 ERJ Express. Published on May 12, 2016 as doi: 10.1183/13993003.00024-2016 ORIGINAL ARTICLE IN PRESS CORRECTED PROOF Acute pulmonary embolism: mortality prediction by the 2014 European Society of Cardiology
ERJ Express. Published on May 12, 2016 as doi: 10.1183/13993003.00024-2016 ORIGINAL ARTICLE IN PRESS CORRECTED PROOF Acute pulmonary embolism: mortality prediction by the 2014 European Society of Cardiology
DECLARATION OF CONFLICT OF INTEREST
 DECLARATION OF CONFLICT OF INTEREST IDENTIFYING LOW-RISK PULMONARY EMBOLISM CLINICAL SCORES David Jiménez, MD, PhD Respiratory Department Ramón y Cajal Hospital Madrid, Spain Potential Conflicts of Interest
DECLARATION OF CONFLICT OF INTEREST IDENTIFYING LOW-RISK PULMONARY EMBOLISM CLINICAL SCORES David Jiménez, MD, PhD Respiratory Department Ramón y Cajal Hospital Madrid, Spain Potential Conflicts of Interest
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/40114 holds various files of this Leiden University dissertation Author: Exter, Paul L. den Title: Diagnosis, management and prognosis of symptomatic and
Cover Page The handle http://hdl.handle.net/1887/40114 holds various files of this Leiden University dissertation Author: Exter, Paul L. den Title: Diagnosis, management and prognosis of symptomatic and
Management of Intermediate-Risk Pulmonary Embolism
 Management of Intermediate-Risk Pulmonary Embolism Stavros V. Konstantinides, MD, PhD, FESC Professor, Clinical Trials in Antithrombotic Therapy Center for Thrombosis und Hemostasis, University of Mainz,
Management of Intermediate-Risk Pulmonary Embolism Stavros V. Konstantinides, MD, PhD, FESC Professor, Clinical Trials in Antithrombotic Therapy Center for Thrombosis und Hemostasis, University of Mainz,
N-terminal pro-brain natriuretic peptide in patients with acute pulmonary embolism
 Eur Respir J 23; 22: 649 653 DOI: 1.1183/931936.3.2333 Printed in UK all rights reserved Copyright #ERS Journals Ltd 23 European Respiratory Journal ISSN 93-1936 N-terminal pro-brain natriuretic peptide
Eur Respir J 23; 22: 649 653 DOI: 1.1183/931936.3.2333 Printed in UK all rights reserved Copyright #ERS Journals Ltd 23 European Respiratory Journal ISSN 93-1936 N-terminal pro-brain natriuretic peptide
Emergency Pulmonary Embolectomy after Failed Thrombolysis in a Community Hospital: A Choice of Institutional Preference?
 ISPUB.COM The Internet Journal of Emergency Medicine Volume 5 Number 1 Emergency Pulmonary Embolectomy after Failed Thrombolysis in a Community Hospital: A Choice of F Vandy, G Fromm, P Guentert, W Halloran,
ISPUB.COM The Internet Journal of Emergency Medicine Volume 5 Number 1 Emergency Pulmonary Embolectomy after Failed Thrombolysis in a Community Hospital: A Choice of F Vandy, G Fromm, P Guentert, W Halloran,
What is New in Acute Pulmonary Embolism? Interventional Treatment. Prof. Nils Kucher University Hospital Bern Switzerland
 What is New in Acute Pulmonary Embolism? Interventional Treatment Prof. Nils Kucher University Hospital Bern Switzerland nils.kucher@insel.ch Disclosure of Interest Dr. Kucher received research grants
What is New in Acute Pulmonary Embolism? Interventional Treatment Prof. Nils Kucher University Hospital Bern Switzerland nils.kucher@insel.ch Disclosure of Interest Dr. Kucher received research grants
Real life management of CTEPH: patient case
 2 nd International Congress on cardiovascular imaging in clinical practice k Real life management of CTEPH: patient case Anastasia Anthi Pulmonary Hypertension Clinic, Attikon University Hospital, Athens
2 nd International Congress on cardiovascular imaging in clinical practice k Real life management of CTEPH: patient case Anastasia Anthi Pulmonary Hypertension Clinic, Attikon University Hospital, Athens
Plasma MR-proADM is superior to NTproBNP for all-cause short term mortality prediction in acute pulmonary embolism.
 J. Pedowska-Wloszek, M. Kostrubiec, A. Labyk, S. Pacho, O. Dzikowska-Diduch, P. Bienias, B. Lichodziejewska, P. Palczewski, M. Ciurzynski, P. Pruszczyk Plasma MR-proADM is superior to NTproBNP for all-cause
J. Pedowska-Wloszek, M. Kostrubiec, A. Labyk, S. Pacho, O. Dzikowska-Diduch, P. Bienias, B. Lichodziejewska, P. Palczewski, M. Ciurzynski, P. Pruszczyk Plasma MR-proADM is superior to NTproBNP for all-cause
Right ECG. Contents. RAE vs. P Pulmonale: Are they the same? 12 Lead ECGs of Patient with COPD Exacerbation Before and After Treatment
 Contents Right ECG Wang, Tzong-Luen MD, PhD, JM, FESC, FACC, FCAPSC Professor, Medical College, Fu-Jen Catholic University Chief, ED, Shin-Kong Wu Ho-Su Memorial Hospital CEO, National Resuscitation Council,
Contents Right ECG Wang, Tzong-Luen MD, PhD, JM, FESC, FACC, FCAPSC Professor, Medical College, Fu-Jen Catholic University Chief, ED, Shin-Kong Wu Ho-Su Memorial Hospital CEO, National Resuscitation Council,
Critical Review Form Therapy
 Critical Review Form Therapy Alteplase versus heparin in acute pulmonary embolism: randomised trial assessing right-ventricular function and pulmonary perfusion Lancet 1993; 341:501-511 Objective: To determine
Critical Review Form Therapy Alteplase versus heparin in acute pulmonary embolism: randomised trial assessing right-ventricular function and pulmonary perfusion Lancet 1993; 341:501-511 Objective: To determine
Acute and long-term treatment of VTE. Cecilia Becattini University of Perugia
 Acute and long-term treatment of VTE Cecilia Becattini University of Perugia Acute and long-term treatment of VTE The goals The acute PE phase After the acute phase Treatment for VTE Goals of acute treatment
Acute and long-term treatment of VTE Cecilia Becattini University of Perugia Acute and long-term treatment of VTE The goals The acute PE phase After the acute phase Treatment for VTE Goals of acute treatment
ECG ABNORMALITIES D R. T AM A R A AL Q U D AH
 ECG ABNORMALITIES D R. T AM A R A AL Q U D AH When we interpret an ECG we compare it instantaneously with the normal ECG and normal variants stored in our memory; these memories are stored visually in
ECG ABNORMALITIES D R. T AM A R A AL Q U D AH When we interpret an ECG we compare it instantaneously with the normal ECG and normal variants stored in our memory; these memories are stored visually in
Assessing the Impact on the Right Ventricle
 Advances in Tricuspid Regurgitation Congress of the European Society of Cardiology (ESC) Munich, August 25-29, 2012 Assessing the Impact on the Right Ventricle Stephan Rosenkranz, MD Clinic III for Internal
Advances in Tricuspid Regurgitation Congress of the European Society of Cardiology (ESC) Munich, August 25-29, 2012 Assessing the Impact on the Right Ventricle Stephan Rosenkranz, MD Clinic III for Internal
Adel Hasanin Ahmed 1
 Adel Hasanin Ahmed 1 PERICARDIAL DISEASE The pericardial effusion ends anteriorly to the descending aorta and is best visualised in the PLAX. PSAX is actually very useful sometimes for looking at posterior
Adel Hasanin Ahmed 1 PERICARDIAL DISEASE The pericardial effusion ends anteriorly to the descending aorta and is best visualised in the PLAX. PSAX is actually very useful sometimes for looking at posterior
Sachin Kumar Amruthlal Jain, 1 Brijesh Patel, 2 Wadie David, 2 Ayad Jazrawi, 1 and Patrick Alexander Introduction
 Hindawi Publishing Corporation Case Reports in Medicine Volume 2014, Article ID 297951, 8 pages http://dx.doi.org/10.1155/2014/297951 Case Report Unloading of Right Ventricle and Clinical Improvement after
Hindawi Publishing Corporation Case Reports in Medicine Volume 2014, Article ID 297951, 8 pages http://dx.doi.org/10.1155/2014/297951 Case Report Unloading of Right Ventricle and Clinical Improvement after
Case Report Sinus Venosus Atrial Septal Defect as a Cause of Palpitations and Dyspnea in an Adult: A Diagnostic Imaging Challenge
 Case Reports in Medicine Volume 2015, Article ID 128462, 4 pages http://dx.doi.org/10.1155/2015/128462 Case Report Sinus Venosus Atrial Septal Defect as a Cause of Palpitations and Dyspnea in an Adult:
Case Reports in Medicine Volume 2015, Article ID 128462, 4 pages http://dx.doi.org/10.1155/2015/128462 Case Report Sinus Venosus Atrial Septal Defect as a Cause of Palpitations and Dyspnea in an Adult:
Significance of ST-segment deviation in patients with acute pulmonary embolism and negative T waves
 Powered by TCPDF (www.tcpdf.org) This is a provisional PDF only. Copyedited and fully formatted version will be made available soon. ONLINE FIRST ISSN: 1897-5593 e-issn: 1898-018X Significance of ST-segment
Powered by TCPDF (www.tcpdf.org) This is a provisional PDF only. Copyedited and fully formatted version will be made available soon. ONLINE FIRST ISSN: 1897-5593 e-issn: 1898-018X Significance of ST-segment
Management of Acute Pulmonary Embolism: Anticipating and Responding to Complexity Ahmed Zaky, M.D., M.P.H. University of Alabama, Birmingham, AL
 Session: L213 Session: L403 Management of Acute Pulmonary Embolism: Anticipating and Responding to Complexity Ahmed Zaky, M.D., M.P.H. University of Alabama, Birmingham, AL Disclosures: This presenter
Session: L213 Session: L403 Management of Acute Pulmonary Embolism: Anticipating and Responding to Complexity Ahmed Zaky, M.D., M.P.H. University of Alabama, Birmingham, AL Disclosures: This presenter
Updates in venous thromboembolism. Cecilia Becattini University of Perugia
 Updates in venous thromboembolism Cecilia Becattini University of Perugia News for VTE Diagnosis Treatment the acute phase the agents Pulmonary embolism: diagnosis Vein ultrasonography Meta-analysis 15
Updates in venous thromboembolism Cecilia Becattini University of Perugia News for VTE Diagnosis Treatment the acute phase the agents Pulmonary embolism: diagnosis Vein ultrasonography Meta-analysis 15
TAMPONADE CARDIAQUE. Dr Cédrick Zaouter TUSAR 15 décembre 2015
 TAMPONADE CARDIAQUE Dr Cédrick Zaouter TUSAR 15 décembre 2015 OUTLINE History Incidence Definition Pathophysiology Aetiologies Investigations - Echocardiography Treatment of cardiac tamponade Pericardial
TAMPONADE CARDIAQUE Dr Cédrick Zaouter TUSAR 15 décembre 2015 OUTLINE History Incidence Definition Pathophysiology Aetiologies Investigations - Echocardiography Treatment of cardiac tamponade Pericardial
Masqueraders of STEMI
 Masqueraders of STEMI Steven M. Costa, M.D. Assistant Professor Department of Medicine Division of Cardiology Scott & White Memorial Hospital and Clinic Texas A&M University Health Science Center Disclosures
Masqueraders of STEMI Steven M. Costa, M.D. Assistant Professor Department of Medicine Division of Cardiology Scott & White Memorial Hospital and Clinic Texas A&M University Health Science Center Disclosures
Left atrial function. Aliakbar Arvandi MD
 In the clinic Left atrial function Abstract The left atrium (LA) is a left posterior cardiac chamber which is located adjacent to the esophagus. It is separated from the right atrium by the inter-atrial
In the clinic Left atrial function Abstract The left atrium (LA) is a left posterior cardiac chamber which is located adjacent to the esophagus. It is separated from the right atrium by the inter-atrial
Das recht Ventrikel ist auch noch da! RV function The RV operates as. Physiology Not very sensitive to preload Good compliance of the free wall
 Das recht Ventrikel ist auch noch da! I.Michaux Intensive Care Medicine University Hospital CHU UCL Namur Mont-Godinne Belgium RV function The RV operates as a low pressure, volume pump, moving the blood
Das recht Ventrikel ist auch noch da! I.Michaux Intensive Care Medicine University Hospital CHU UCL Namur Mont-Godinne Belgium RV function The RV operates as a low pressure, volume pump, moving the blood
Myocardial contusion injury (MCI) may occur as a rare
 Cardiovascular Images Myocardial Contusion in an 8-Year-Old Boy A Kick to the Heart Danielle M. Moyé, MD; Adrian K. Dyer, MD; Poonam P. Thankavel, MD Myocardial contusion injury (MCI) may occur as a rare
Cardiovascular Images Myocardial Contusion in an 8-Year-Old Boy A Kick to the Heart Danielle M. Moyé, MD; Adrian K. Dyer, MD; Poonam P. Thankavel, MD Myocardial contusion injury (MCI) may occur as a rare
The shock index and the simplified PESI for identification of low-risk patients with acute pulmonary embolism
 Eur Respir J 211; 37: 762 766 DOI: 1.1183/931936.711 CopyrightßERS 211 The shock index and the simplified PESI for identification of low-risk patients with acute pulmonary embolism A. Sam*, D. Sánchez*,
Eur Respir J 211; 37: 762 766 DOI: 1.1183/931936.711 CopyrightßERS 211 The shock index and the simplified PESI for identification of low-risk patients with acute pulmonary embolism A. Sam*, D. Sánchez*,
