Heart Overview. Chapter 18. Heart. Heart. Two Circuits. Organization of the Cardiovascular System. The Heart. Located directly behind sternum
|
|
|
- Mildred Fowler
- 5 years ago
- Views:
Transcription
1 Heart Overview Chapter 18 The Heart Heart anatomy Cardiac muscle cells Heart chambers, valves and vessels Conducting system EKG Cardiac cycle Contractile and pacemaker cells Cardiodynamics Cardiac disorders Organization of the Cardiovascular System Heart Pump of cardiovascular system Approximate size of clenched fist Made of cardiac muscle Beats ~100,000 times/day Pumps 8,000L of blood/day (how much do you have?) Top (base): ½ inch to left of midline Bottom (apex): 3 inches to the left of midline Rotated slightly so that right side faces anteriorly Figure 20 1 Heart Located directly behind sternum Between 2 pleural cavities in the mediastinum Figure 20 2a Two Circuits Pulmonary circuit: Carries blood to and from gas exchange surfaces of lungs Right heart Systemic circuit: Carries blood to and from the body Left heart Blood alternates between pulmonary circuit and systemic circuit (has to go through both, then starts over again) 1
2 Pericardium Pericardium a double-walled sac around the heart composed of: A superficial fibrous pericardium A deep two-layer serous pericardium Parietal pericardium (outter) lines the internal surface of the fibrous pericardium Visceral pericardium (inner) or epicardium lines the surface of the heart They are separated by the fluid-filled pericardial cavity filled with pericardial fluid Protects and anchors the heart Prevents overfilling of the heart with blood Allows for the heart to work in a relatively friction-free environment Pericardium Pericarditis: Complication of viral infections that causes infection of the pericardium Risk of cardiac tamponade The Heart Wall Epicardium: outer layer Myocardium: middle layer Endocardium: inner layer Figure 20 4 Heart Wall Epicardium Visceral pericardium, covers the heart Myocardium = muscular wall of the heart Concentric layers of cardiac muscle tissue Atrial myocardium wraps around great vessels 2 divisions of ventricular myocardium Superficial ventricular muscles: surround ventricles Deep ventricular muscles: spiral around and between ventricles Fibrous skeleton of the heart crisscrossing, interlacing layer of connective tissue Endocardium endothelial layer (tissue type?) Cardiac Muscle Cells Characteristics of Cardiac Muscle Cells Small with one, central nucleus Branching interconnections between cells Intercalated discs: interconnect cardiac muscle cells secured by desmosomes to convey force of contraction linked by gap junctions to propagate action potentials Figure
3 Cardiac Cells vs. Skeletal Fibers General Anatomy of the Heart Great veins and arteries at the base Pointed tip is apex Surrounded by pericardial sac Table 20-1 Figure 20 2c Specific Heart Anatomy 4 Chambers of the Heart Anterior View Posterior View Right atrium: collects blood from systemic circuit Right ventricle: pumps blood to pulmonary circuit Left atrium: collects blood from pulmonary circuit Left ventricle: pumps blood to systemic circuit Blood Vessels Arteries: carry blood away from heart Veins: carry blood to heart Capillaries: networks between arteries and veins Also called exchange vessels because only in capillaries exchange materials (dissolved gases, nutrients, wastes) between blood and tissues Heart Anatomy Overview 4 chambers (RA, RV, LA, LV) 4 valves 2 at entry to ventricles (from atria) 2 at exit from ventricles (to great vessels) None at entry to atria 4 major vessels at the base Superior vena cava (entry) Inferior vena cava (entry) Aorta (exit) Pulmonary trunk (exit) 4 Pulmonary veins (entry) = not major vessels 3
4 Movie Heart dividing lines Heart Anatomy Sulci Grooves in the heart that divide it contain blood vessels of cardiac muscle Coronary sulcus divides atria and ventricles Closer to base (top) than apex Anterior and posterior interventricular sulci separate left and right ventricles Chambers of the heart Right Atrium receives deoxygenated blood through vena cavae Left Atrium receives oxygenated blood through pulmonary veins Right Ventricle pumps blood to lungs through the pulmonary arteries Left Ventricle pumps blood into the systemic circuit through the aorta Atria Small, thin-walled Expandable outer auricles = flaps on anterior surface Fill with blood passively Separated by interatrial septum Connected to ventricles via atrioventricular valves Internally covered with pectinate (comb) muscles, ridges on anterior atrial wall and inner surfaces of right auricle Ventricles Right ventricle wall is thinner; LV develops 4-6 times more pressure than left ventricle Right ventricle is pouchshaped, left ventricle is round Similar internally, but right ventricle has moderator band How do volumes compare? Figure 20 7 Trabeculae Carneae Muscular ridges on internal surface of ventricles Includes moderator band (in RV): ridge contains part of conducting system coordinates contractions of cardiac muscle cells 4
5 The Heart Valves Four valves, all at same level in heart Fibrous skeleton: conective tissue Figure 20 6a Figure 20 8 Atrioventricular (AV) Valves Right AV valve (tricuspid): between RA and RV Left AV valve (bicuspid or mitral): between LA and LV Have 3 or 2 fibrous flaps, respectively Permit blood flow in 1 direction: atria to ventricles Free edges of flaps attach via chordae tendineae to papillary muscles of ventricle Blood pressure closes valve cusps during ventricular contraction muscles tense chordae tendineae, preventing valves from swinging into atria (opening backward) Atrioventricular Valve Function Figure 18.9 Semilunar Valves Semilunar Valve Function Pulmonary valve between RV and pulmonary trunk Aortic valve between LV and aorta Prevent backflow from great vessels (pulmonary trunk and aorta) into ventricles Have no muscular support Both have 3 crescent-shaped cusps, support like a tripod Figure
6 Movie Regurgitation Heart valves Failure of valves Causes backflow of blood into atria Can cause heart murmur Valvular Heart Disease (VHD) Genetic, or complication of carditis (inflammation of heart muscle) Rheumatic fever is a common cause Decreases valve function to point where adequate circulation is no longer possible Great Vessels - Veins Vena Cavae deliver systemic circulation to right atrium (oxy or deoxy?) Superior vena cava: receives blood from head, neck, upper limbs, and chest Inferior vena cava: receives blood from trunk, and viscera, lower limbs Right and left pulmonary veins return blood from lungs (oxy or deoxy?) Great Vessels - Arteries Aortareceives blood from LV (through which valve?) (oxy or deoxy?) Ascending aorta curve to form aortic arch sends off three branches and turns down to become descending aorta Pulmonary trunk splits into left and right pulmonary arteries to send blood from (chamber) through (valve) to lungs. (oxy or deoxy?) 6
7 Pulmonary Circuit To RA from superior and inferior vena cavae RA through open tricuspid valve to RV Conus arteriosus (superior right ventricle) through pulmonary valve to pulmonary trunk Pulmonary trunk divides into left and right pulmonary arteries, to right and left lungs, respectively Systemic Circuit Blood returns from lungs to left atrium through 2 left and 2 right pulmonary veins Left atrium to left ventricle through mitral valve Left ventricle through aortic SL valve into ascending aorta Ascending aorta turns (aortic arch) and becomes descending aorta Complete Pathway of Blood Through the Heart and Lungs Right atrium tricuspid valve right ventricle pulmonary semilunar valve pulmonary arteries lungs pulmonary veins left atrium bicuspid valve left ventricle aortic semilunar valve aorta systemic circulation vena cavae repeat Foramen Ovale Before birth, is an opening through interatrial septum Connects the 2 atria Seals off at birth, forming fossa ovalis Why connect the two atria? PFO can cause problems in adulthood but usually only with strenuous exercise or high altitude Aortic Sinuses Dilations at the base of ascending aorta Prevent aortic semilunar valve cusps from sticking to aorta when open Origin points of right and left coronary arteries Internal Heart Dividing Lines Septa Interatrial septum: separates atria Interventricular septum: separates ventricles 7
8 Coronary Circulation Coronary Circulation Coronary arteries Left and right Originate at aortic sinuses Elastic rebound forces blood through coronary arteries only between contractions Cardiac veins return blood to coronary sinus, opens into right atrium Figure 18.7a Coronary Arteries Right Coronary Artery. Supplies blood to: right atrium, portions of both ventricles, cells of sinoatrial (SA) and atrioventricular (AV) nodes Branches include marginal arteries (surface of right ventricle) posterior interventricular artery Left Coronary Artery. Supplies blood to: left ventricle, left atrium, interventricular septum Main branches: circumflex artery anterior interventricular artery Arterial Anastomoses Interconnect anterior and posterior interventricular arteries Stabilize blood supply to cardiac muscle by providing collateral circulation e.g. RCA meets with the circumflex artery (which is a branch of the LCA) 2 Types of Cardiac Muscle Cells Contractile cells: account for 99% of heart tissue activated by change in the membrane potential (just like skeletal muscle cells) produce contractions, generate force Conducting system: initiate and distribute electical activity consists of nodes and internodal pathways controls and coordinates heartbeat Action Potentials in Skeletal and Cardiac Muscle Figure
9 Cardiac activity contractile cells Resting Potentials Ventricular cells -90 mv. Threshold = -75mV Atrial cells: -80 mv Signal to depolarize comes from: Conducting system Adjacent myocytes (via gap junctions) Threshold is usually reached in the latter manner in a portion of membrane near intercalated discs Then Cardiac Action Potential 1. Rapid depolarization: voltage-regulated sodium channels (fast channels) open 2. Plateau: At ~+30mV sodium channels close and inactivate, but no net loss of positive ions occurs because voltage-regulated calcium channels (slow channels) open and calcium ion entry roughly balances Na + ion loss Holds membrane at 0 mv plateau for ~175msec 3. Repolarization: slow calcium channels close slow potassium channels open rapid repolarization restores resting potential The Refractory Periods Absolute refractory period: long cardiac muscle cells cannot respond Relative refractory period: short response depends on degree of stimulus Length of cardiac action potential in ventricular cell is msecs 30 times longer than skeletal muscle fiber long refractory period prevents summation and tetany Calcium and Contraction Contraction of a cardiac muscle cell is produced by an increase in calcium ion concentration around myofibrils 20% of calcium ions required for a contraction enter cell membrane through slow channels during plateau phase This extracellular Ca 2+ triggers release of calcium ion reserves from sarcoplasmic reticulum (80%) This is why heart is so sensitive to blood calcium Pacemaker potentials Pacemaker cells At special site in the heart, cells have unstable resting potential These pacemaker cells depolarize spontaneously to initiate heartbeat = automaticity The SA and AV nodes have the greatest concentrations of autorhythmic cells Spontaneous electrical activity caused by special channels: Na + channels slowly open, allowing Na + in K + channels close Ca 2+ channels open to start, sustain AP No fast Na + channels at all! 9
10 The Cardiac Cycle The Heartbeat A single contraction of the heart Lasts about 370msec (cf. neurons?) The entire heart contracts in series: first the atria then the ventricles Figure The Cardiac Cycle Period from the start of one heartbeat to the start of the next Includes: 370msec for heart contraction A ~400msec delay Begins with action potential at SA node Transmitted through conducting system Produces action potentials in cardiac muscle cells (contractile cells) force The Conducting System A system of specialized cardiac muscle cells that initiates and distributes electrical impulses that stimulate contraction Cells display automaticity: contract automatically (without need for any external stimulation from nerves or other muscles SA and AV nodes are the pacesetters The Conducting System Sinoatrial (SA) Node In posterior wall of right atrium Contains pacemaker cells Connected to AV node by internodal pathways Begins atrial activation (Step 1) Figure
11 Atrioventricular (AV) Node In floor of right atrium Receives impulse from SA 50msec (Step 2) Takes ~100msec for impulse to travel through the AV node, delays impulse (Step 3) Atrial contraction begins (@150 msec) Delay limits maximum HR to ~230bpm Pacemaker potential An unstable resting potential of conducting cells in SA and AV node that gradually depolarizes toward threshold SA node depolarizes faster ( APs/min) than AV node (40-60 per minute) and so SA fires first, establishing heart rate (hence we call these the pacemaker cells) Why is your resting heart rate not bpm? Conducting Cells Interconnect SA and AV nodes Distribute stimulus through myocardium In the atrium, called internodal pathways In the ventricles: AV bundle and bundle branches The AV Bundle (bundle of His) Only electrical connection between A and V Travels in the septum Carries impulse to left and right bundle branches, which conduct to Purkinje fibers at 175 msec (Step 4), and to the moderator band, which conducts to papillary muscles The Purkinje Fibers Distribute impulse through ventricles (Step 5) to contractile cells Trigger ventricular contraction to begin (@ 225msec) after atrial contraction is completed Impulse Conduction through the Heart Figure
12 Abnormal Pacemaker Function Bradycardia: abnormally slow heart rate Tachycardia: abnormally fast heart rate Ectopic Pacemaker Abnormal cells generate high rate of action potentials Bypass conducting system Disrupt ventricular contractions Heart Excitation Related to ECG SA node generates impulse; Impulse delayed Impulse passes to Ventricular excitation atrial excitation begins at AV node heart apex; ventricular complete excitation begins SA node AV node Bundle Purkinje branches fibers Figure Electrocardiogram (ECG) ECG Electrical events in the cardiac cycle can be recorded at the surface of the body using an electrocardiogram (ECG) Abnormal patterns diagnose cardiac arrhythmias, (abnormal patterns of cardiac electrical activity) due to damage or disease Figure 20 14b Features of an ECG P wave: SA node and atria depolarize (begin contraction ~25msec after P wave starts) QRS complex: ventricles depolarize (begin contracting just after R peak) T wave: ventricles repolarize Time Intervals P R interval: from start of atrial depolarization to start of QRS complex Q T interval: from ventricular depolarization to ventricular repolarization 12
13 EKG problems Large QRS caused by hypertrophy Small QRS reduced heart muscle mass Small T low energy reserves, ischemia Long P-R interval damage to conducting pathways Long Q-T interval conduction problems, myocardial damage, ischemia, congenital defect The Cardiac Cycle The period between the start of one heartbeat and the beginning of the next Includes both contraction and relaxation Each chamber undergoes: systole(contraction) pressure rises diastole(relaxation) pressure falls Blood flows from high to low pressure, controlled by timing of contractions and directed by one-way valves Phases of the Cardiac Cycle 1. Atrial systole 2. Atrial diastole 3. Ventricular systole 4. Ventricular diastole Cardiac Cycle and Heart Rate At 75 beats per minute, each cardiac cycle lasts about 800 msecs When heart rate increases all phases of cardiac cycle shorten, but particularly ventricular diastole (less time spent resting) Figure
14 Pressure and Volume in the Cardiac Cycle 8 Steps in the Cardiac Cycle Begin: all relaxed, ventricles 70% filled 1. Atrial systole begins atrial contraction begins rising pressure forces open right and left AV valves no venous flow into atria but little backflow either 2. Atria eject blood into ventricles: filling ventricles (topping them off) 3. Atrial systole ends (100msec): ventricles contain maximum volume = end-diastolic volume (EDV) which is normally about 130ml Figure Steps in the Cardiac Cycle 4. Ventricular systole begins: AV valves close as P vent quickly exceeds P atria pressure in ventricles continues to rise All valves closed: isovolumetric ventricular contraction 5. Ventricular ejection: When pressure in ventricles exceeds arterial pressure in great vessels, semilunar valves forced open blood flows into pulmonary and aortic trunks (isotonic contraction) Stroke volume (SV) = 80ml. Percent of enddiastolic volume that is ejected = ejection fraction around 60% 8 Steps in the Cardiac Cycle 6. Ventricular pressure falls near end of systole: backflow from vessel trunks closes semilunar valves ventricles contain end-systolic volume (ESV), about 40% of end-diastolic volume or 50ml Aortic elastic recoil causes dicrotic notch (double beat). ESV = 50ml or 40% 7. Ventricular diastole (starts at 370msec): ventricular pressure is still higher than atrial pressure all heart valves are closed ventricles relax (isovolumetric relaxation) Lasts for remaining 430msec of cycle plus 100msec of the next cycle 8 Steps in the Cardiac Cycle 8. Falling ventricular pressure drops below atrial pressure: forces AV valves open passive atrial filling (continuous during atrial diastole) passive ventricular filling (to 70% full) cardiac cycle ends Repeat Movie Cardiac cycle Note that: AV valves close early (step 3), open late (step 8) SL valves open and close in between (step 5 open, step 6 closed) 14
15 Heart Failure Lack of adequate blood flow to peripheral tissues and organs due to inadequate cardiovascular output (usually due to ventricular damage) Atrial damage can be inconsequential, or problematic depending on what is damaged. Auscultation - Heart Sounds lub-dup S 1 : loud sounds produced by AV valves closing, signifies beginning of systole S 2 : loud sounds produced by semilunar valves closing at the beginning of ventricular diastole Sounds are actually produced by blood changing flow patterns Aerobic Energy of Heart From mitochondrial breakdown of fatty acids and glucose (lots of mitochondria in cardiac myocytes) Oxygen from circulating hemoglobin Cardiac muscles store oxygen in myoglobin Important Cardiodynamics Terms End-diastolic volume (EDV) Max filling after atrial systole (usually about 130ml) End-systolic volume (ESV) Residual volume after ventricular systole (usually about 50ml) Stroke volume (SV): SV = EDV - ESV Volume (ml) of blood ejected per beat Stroke Volume Figure
16 Important Cardiodynamics Terms Ejection fraction: the percentage of EDV represented by SV Cardiac output (CO): the volume pumped by each ventricle in 1 minute (equals how much blood gets to the tissues every minute) CO = HR (in bpm) x SV What is CO for a HR of 80bpm and a SV of 80ml/beat? Adjusting CO to Conditions Cardiac output: Can be adjusted by changes in heart rate or stroke volume Stroke volume can be increased 2x: adjusted by changing EDV or ESV Heart rate can be increased 2.5: adjusted by autonomic nervous system or hormones (How?) Factors Affecting Stroke Volume Changes in EDV or ESV Slow heartbeat and exercise increase venous return to the heart, increasing SV Blood loss and extremely rapid heartbeat decrease SV EDV affected by: filling time (duration of ventricular diastole) rate of venous return (rate of blood flow during ventricular diastole) ESV affected by: Preload: degree of ventricular stretching during diastole due to amount of blood (increased by greater venous return) Contractility: force produced during contraction, at a given preload Afterload: tension the ventricle must produce to open the semilunar valve and eject blood to the great vessels Preload and Afterload EDV and Stroke Volume At rest: EDV is low myocardium stretches little (low preload) stroke volume is low, ESV is high (lots left) With exercise: EDV increases (increased venous return) myocardium stretches more stroke volume increases, ESV decreases Figure
17 The Frank Starling Principle Preload, or degree of stretch, of cardiac muscle cells before they contract is the critical factor controlling stroke volume As EDV increases, stroke volume increases (and vice versa) Basically, if there is a lot of blood in the ventricles (increased venous return), stretching causes them to pump more blood out. More in more out Keeps the two sides of the heart in balance ESV and Stroke Volume Contractility Is affected by: Sympathetic activation NE released by postganglionic fibers of cardiac nerves E and NE released by adrenal medullae cause ventricles to contract with more force increases ejection fraction and decreases ESV Parasympathetic activity acetylcholine released by vagus nerves reduces force of cardiac contractions Hormones Drugs mimic hormone actions: stimulate or block beta 1 receptors (beta-blockers) affect calcium ions e.g., calcium channel blockers (negative inotropic effects) decrease contractility ESV and Stroke Volume Afterload As afterload increases, takes longer before SL valves open and thus less blood will be ejected: ESV increases and stroke volume decreases Increased by any factor that restricts arterial blood flow (like atherosclerosis) Extremely high afterload can cause heart failure Heart Rate Control Factors 1. Autonomic nervous system: sympathetic and parasympathetic Note: we just saw how the autonomic NS can affect contractility, which affects stroke volume 2. Circulating hormones (thyroxine, E and NE in blood all increase HR) 3. Venous return and stretch receptors Autonomic NS Innervation Heart is stimulated by the sympathetic cardioacceleratory center Heart is inhibited by the parasympathetic cardioinhibitory center Figure (Navigator) Autonomic Innervation Vagus nerves (X) carry parasympathetic preganglionic fibers to small ganglia in cardiac plexus SA and AV nodes Sympathetic postganglionic fibers cardiac plexus SA and AV nodes Autonomic tone: dual innervation maintains resting tone by releasing ACh and NE (which dominates?) fine adjustments meet needs of other systems 17
18 Cardiac reflexes Cardiac centers in medulla monitor: baroreceptors (blood pressure) chemoreceptors (arterial oxygen and carbon dioxide levels) Cardiac centers adjust cardiac activity via sympathetic (NE increases HR) and parasympathetic (ACh decreases HR) activity Atrial (Bainbridge) Reflex Sympathetic reflex initiated in response to increased venous return (remember that increased venous return also caused increased stroke volume, called?) Stretch receptors in right atrium trigger increase in heart rate through increased sympathetic activity to pump out the excess blood and decrease venous pressure Autonomic NS Regulation of Pacemaker Cells in SA, AV Nodes Membrane potential of pacemaker cells is less negative than other cardiac cells (-60mv) Sympathetic and parasympathetic stimulation are both greatest at SA node (heart rate) Rate of spontaneous depolarization depends on: resting membrane potential (where you start) ACh (para NS) opens K+ channels. Result? NE binds to Beta adrenergic receptors, opens sodium-calcium ion channels. Result? Autonomic Pacemaker Regulation Figure KEY CONCEPT Cardiac output: the amount of blood pumped by the left ventricle each minute adjusted by the ANS in response to: circulating hormones changes in blood volume alterations in venous return Most healthy people can increase cardiac output by % = cardiac reserve Summary Heart anatomy Cardiac muscle cells Heart chambers, valves and vessels Conducting system EKG Cardiac cycle Contractile and pacemaker cells Cardiodynamics 18
19 Heart Failure Inadequate cardiac output to meet demand Due to left ventricular insufficiency If LV not pumping enough, blood backs up in the pulmonary circulation. Elevated pressures cause increased loss of plasma to interstitial fluid of lungs = CHF (congestive heart failure). If severe, can cause pulmonary edema (fluid fills air spaces) Treatment? Digoxin positive inotrope to increase contraction force. Blood pressure reducers: diuretics, vasodilators, spirinolactone (ald antagonist) Cardiomyopathy Cardiac muscle degeneration and fibrosis Can lead to heat failure Hypertrophic cardiomyopathy ; thickened left ventricular walls Heart Block Damage to conduction pathways Often show abnormal ECG Escape when condicting pathways damaged, ventricles can escape control of SA or AV node usually by autorhythmicity of Purkinje fibers. Ventricles continue to beat but only at 40-50bpm (which the intrinsic rate of the Purkinje fibers) Tachycardias Atrial fibrillation: atrial depolarization occurs so fast that the atrium appears to quiver. Ventricles cannot follow this rate Not usually life threatening because of escape Ventricular arrhythmias Ventricular tachycardia (V-tach) Ventricular fibrilation (V-fib) = cardiac arrest No rhythm. Defibrillator can restore by unifying cell activity Cardiac technologies Pacemakers: treat chronic bradycardia due to conduction deficits, etc. External defibrillators (clear!): can rescue from cardiac arrest Implantable defibrillators: for people with chronic heart conditions (often congenital) LVAD: Left ventricular assist device Implantable pump in parallel with the left ventricle for those with LV insufficiency Boosts cardiac output by allowing some blood to bypass the left ventricle and enter the aorta at sufficient pressure Examining the heart Coronary angiogram: catheter is threaded up through femoral artery into aortic sinus. Dye released that can be seen on a series of high speed X-rays Echocardiogram: heart ultrasound 19
20 Ionic imbalances Potassium Hyperkalemia decreases K+ gradient, inhibits repolarization Hypokalemia- increases K+ gradient, causes hyperpolarization of resting membranes Calcium Hypercalcemia: cardiac muscle cells become very excitable Hypocalcemia Coronary artery disease Can cause coronary ischemia (reduced blood flow) to heart Atherosclerosis: plaques caused by fatty deposits in vessels cause narrowing of artery Angina pectoris: pain associated with heart ischemia Treatments: Vasodilators (nitroglycerin) Beta blockers (propanolol) Calcium channel blockers Balloon angiplasty with stents recently shown to be no better at preventing death from a second heart attack than drugs alone Coronary artery bypass leg vein grafts MIs Myocardial infarction blockage in coronary circulation causes cells to die Most due to CAD, usually thromboses Blood tests for markers of anerobic metabolism, like lactate dehydrogenase, can indicate a heat attack About 25% die before receiving any medical attention About 50% die within the first year Women have fewer MIs but their mortality rate is higher. Recent evidence indicates that men and women have different kinds of CAD 20
The Heart. C h a p t e r. PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris
 C h a p t e r 20 The Heart PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin Cummings Introduction
C h a p t e r 20 The Heart PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin Cummings Introduction
Approximately the size of your fist Location. Pericardial physiology
 Heart Anatomy Approximately the size of your fist Location Superior surface of diaphragm Left of the midline Anterior to the vertebral column, posterior to the sternum Wednesday, March 28, 2012 Muscle
Heart Anatomy Approximately the size of your fist Location Superior surface of diaphragm Left of the midline Anterior to the vertebral column, posterior to the sternum Wednesday, March 28, 2012 Muscle
Chapter 18 - Heart. I. Heart Anatomy: size of your fist; located in mediastinum (medial cavity)
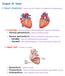 Chapter 18 - Heart I. Heart Anatomy: size of your fist; located in mediastinum (medial cavity) A. Coverings: heart enclosed in double walled sac called the pericardium 1. Fibrous pericardium: dense connective
Chapter 18 - Heart I. Heart Anatomy: size of your fist; located in mediastinum (medial cavity) A. Coverings: heart enclosed in double walled sac called the pericardium 1. Fibrous pericardium: dense connective
Chapter 20: Cardiovascular System: The Heart
 Chapter 20: Cardiovascular System: The Heart I. Functions of the Heart A. List and describe the four functions of the heart: 1. 2. 3. 4. II. Size, Shape, and Location of the Heart A. Size and Shape 1.
Chapter 20: Cardiovascular System: The Heart I. Functions of the Heart A. List and describe the four functions of the heart: 1. 2. 3. 4. II. Size, Shape, and Location of the Heart A. Size and Shape 1.
Cardiovascular System
 Cardiovascular System The Heart Cardiovascular System The Heart Overview What does the heart do? By timed muscular contractions creates pressure gradients blood moves then from high pressure to low pressure
Cardiovascular System The Heart Cardiovascular System The Heart Overview What does the heart do? By timed muscular contractions creates pressure gradients blood moves then from high pressure to low pressure
THE CARDIOVASCULAR SYSTEM. Heart 2
 THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
Ch 19: Cardiovascular System - The Heart -
 Ch 19: Cardiovascular System - The Heart - Give a detailed description of the superficial and internal anatomy of the heart, including the pericardium, the myocardium, and the cardiac muscle. Trace the
Ch 19: Cardiovascular System - The Heart - Give a detailed description of the superficial and internal anatomy of the heart, including the pericardium, the myocardium, and the cardiac muscle. Trace the
The Heart. The Heart A muscular double pump. The Pulmonary and Systemic Circuits
 C H A P T E R 19 The Heart The Heart A muscular double pump circuit takes blood to and from the lungs Systemic circuit vessels transport blood to and from body tissues Atria receive blood from the pulmonary
C H A P T E R 19 The Heart The Heart A muscular double pump circuit takes blood to and from the lungs Systemic circuit vessels transport blood to and from body tissues Atria receive blood from the pulmonary
11/10/2014. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
The Heart. PowerPoint Lecture Presentations prepared by Jason LaPres. Lone Star College North Harris Pearson Education, Inc.
 20 The Heart PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris An Introduction to the Cardiovascular System Learning Outcomes Describe the superficial anatomy of
20 The Heart PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris An Introduction to the Cardiovascular System Learning Outcomes Describe the superficial anatomy of
The Cardiovascular System: The Heart
 PowerPoint Lecture Slides prepared by Meg Flemming Austin Community College C H A P T E R 12 The Cardiovascular System: The Heart Chapter 12 Learning Outcomes 12-1 12-2 Describe the anatomy of the heart,
PowerPoint Lecture Slides prepared by Meg Flemming Austin Community College C H A P T E R 12 The Cardiovascular System: The Heart Chapter 12 Learning Outcomes 12-1 12-2 Describe the anatomy of the heart,
Chapter 13 The Cardiovascular System: Cardiac Function
 Chapter 13 The Cardiovascular System: Cardiac Function Overview of the Cardiovascular System The Path of Blood Flow through the Heart and Vasculature Anatomy of the Heart Electrical Activity of the Heart
Chapter 13 The Cardiovascular System: Cardiac Function Overview of the Cardiovascular System The Path of Blood Flow through the Heart and Vasculature Anatomy of the Heart Electrical Activity of the Heart
The Heart. Size, Form, and Location of the Heart. 1. Blunt, rounded point; most inferior part of the heart.
 12 The Heart FOCUS: The heart is composed of cardiac muscle cells, which are elongated, branching cells that appear striated. Cardiac muscle cells behave as a single electrical unit, and the highly coordinated
12 The Heart FOCUS: The heart is composed of cardiac muscle cells, which are elongated, branching cells that appear striated. Cardiac muscle cells behave as a single electrical unit, and the highly coordinated
10/23/2017. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
2. right heart = pulmonary pump takes blood to lungs to pick up oxygen and get rid of carbon dioxide
 A. location in thorax, in inferior mediastinum posterior to sternum medial to lungs superior to diaphragm anterior to vertebrae orientation - oblique apex points down and to the left 2/3 of mass on left
A. location in thorax, in inferior mediastinum posterior to sternum medial to lungs superior to diaphragm anterior to vertebrae orientation - oblique apex points down and to the left 2/3 of mass on left
THE HEART. A. The Pericardium - a double sac of serous membrane surrounding the heart
 THE HEART I. Size and Location: A. Fist-size weighing less than a pound (250 to 350 grams). B. Located in the mediastinum between the 2 nd rib and the 5 th intercostal space. 1. Tipped to the left, resting
THE HEART I. Size and Location: A. Fist-size weighing less than a pound (250 to 350 grams). B. Located in the mediastinum between the 2 nd rib and the 5 th intercostal space. 1. Tipped to the left, resting
Human Anatomy, First Edition
 Human Anatomy, First Edition McKinley & O'Loughlin Chapter 22 : Heart 1 Functions of the Heart Center of the cardiovascular system, the heart. Connects to blood vessels that transport blood between the
Human Anatomy, First Edition McKinley & O'Loughlin Chapter 22 : Heart 1 Functions of the Heart Center of the cardiovascular system, the heart. Connects to blood vessels that transport blood between the
- what other structures, besides the heart, does the mediastinum contain?
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) An Introduction to the Cardiovascular System - read the paragraphs under this heading on page 580 The Heart is a Four Chambered Organ describe
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) An Introduction to the Cardiovascular System - read the paragraphs under this heading on page 580 The Heart is a Four Chambered Organ describe
Collin County Community College. ! BIOL Anatomy & Physiology! WEEK 5. The Heart
 Collin County Community College! BIOL. 2402 Anatomy & Physiology! WEEK 5 The Heart 1 (1578-1657) A groundbreaking work in the history of medicine, English physician William Harvey s Anatomical Essay on
Collin County Community College! BIOL. 2402 Anatomy & Physiology! WEEK 5 The Heart 1 (1578-1657) A groundbreaking work in the history of medicine, English physician William Harvey s Anatomical Essay on
Anatomy of the Heart. Figure 20 2c
 Anatomy of the Heart Figure 20 2c Pericardium & Myocardium Remember, the heart sits in it s own cavity, known as the mediastinum. The heart is surrounded by the Pericardium, a double lining of the pericardial
Anatomy of the Heart Figure 20 2c Pericardium & Myocardium Remember, the heart sits in it s own cavity, known as the mediastinum. The heart is surrounded by the Pericardium, a double lining of the pericardial
the Cardiovascular System I
 the Cardiovascular System I By: Dr. Nabil A Khouri MD, MsC, Ph.D MEDIASTINUM 1. Superior Mediastinum 2. inferior Mediastinum Anterior mediastinum. Middle mediastinum. Posterior mediastinum Anatomy of
the Cardiovascular System I By: Dr. Nabil A Khouri MD, MsC, Ph.D MEDIASTINUM 1. Superior Mediastinum 2. inferior Mediastinum Anterior mediastinum. Middle mediastinum. Posterior mediastinum Anatomy of
The Cardiovascular System: The Heart: Part A
 PowerPoint Lecture Slides prepared by Janice Meeking, Mount Royal College CHAPTER 18 The Cardiovascular System: The Heart: Part A Heart Anatomy Approximately the size of a fist Location In the mediastinum
PowerPoint Lecture Slides prepared by Janice Meeking, Mount Royal College CHAPTER 18 The Cardiovascular System: The Heart: Part A Heart Anatomy Approximately the size of a fist Location In the mediastinum
Functions of the Heart
 Cardiovascular System The Heart What is the Cardiovascular System? Blood circulated in Arteries, veins, and capillaries by the Pumping action of the heart Functions of the Heart Generating blood pressure
Cardiovascular System The Heart What is the Cardiovascular System? Blood circulated in Arteries, veins, and capillaries by the Pumping action of the heart Functions of the Heart Generating blood pressure
The Heart. PowerPoint Lecture Presentations prepared by Jason LaPres
 20 The Heart PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris NOTE: Presentations extensively modi6ied for use in MCB 244 & 246 at the University of Illinois by
20 The Heart PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris NOTE: Presentations extensively modi6ied for use in MCB 244 & 246 at the University of Illinois by
The Cardiovascular System Part I: Heart Outline of class lecture After studying part I of this chapter you should be able to:
 The Cardiovascular System Part I: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Describe the functions of the heart 2. Describe the location of the heart,
The Cardiovascular System Part I: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Describe the functions of the heart 2. Describe the location of the heart,
*Generating blood pressure *Routing blood: separates. *Ensuring one-way blood. *Regulating blood supply *Changes in contraction
 *Generating blood pressure *Routing blood: separates pulmonary and systemic circulations *Ensuring one-way blood flow: valves *Regulating blood supply *Changes in contraction rate and force match blood
*Generating blood pressure *Routing blood: separates pulmonary and systemic circulations *Ensuring one-way blood flow: valves *Regulating blood supply *Changes in contraction rate and force match blood
Chapter 20 (1) The Heart
 Chapter 20 (1) The Heart Learning Objectives Describe the location and structure of the heart Describe the path of a drop of blood from the superior vena cava or inferior vena cava through the heart out
Chapter 20 (1) The Heart Learning Objectives Describe the location and structure of the heart Describe the path of a drop of blood from the superior vena cava or inferior vena cava through the heart out
THE CARDIOVASCULAR SYSTEM. Part 1
 THE CARDIOVASCULAR SYSTEM Part 1 CARDIOVASCULAR SYSTEM Blood Heart Blood vessels What is the function of this system? What other systems does it affect? CARDIOVASCULAR SYSTEM Functions Transport gases,
THE CARDIOVASCULAR SYSTEM Part 1 CARDIOVASCULAR SYSTEM Blood Heart Blood vessels What is the function of this system? What other systems does it affect? CARDIOVASCULAR SYSTEM Functions Transport gases,
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 20 The Cardiovascular System: The Heart Introduction The purpose of the chapter is to: 1. Learn about the components of the cardiovascular system
Principles of Anatomy and Physiology 14 th Edition CHAPTER 20 The Cardiovascular System: The Heart Introduction The purpose of the chapter is to: 1. Learn about the components of the cardiovascular system
Cardiovascular system
 BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
The HEART. What is it???? Pericardium. Heart Facts. This muscle never stops working It works when you are asleep
 This muscle never stops working It works when you are asleep The HEART It works when you eat It really works when you exercise. What is it???? Located between the lungs in the mid thoracic region Apex
This muscle never stops working It works when you are asleep The HEART It works when you eat It really works when you exercise. What is it???? Located between the lungs in the mid thoracic region Apex
10. Thick deposits of lipids on the walls of blood vessels, called, can lead to serious circulatory issues. A. aneurysm B. atherosclerosis C.
 Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Blood must move! 4/15/2014. Heart Basics
 What is the CARDIOVASCULAR system? The cardiovascular system carries blood and dissolved substances to and from different places in the body. The Heart has the job of pumping these things around the body.
What is the CARDIOVASCULAR system? The cardiovascular system carries blood and dissolved substances to and from different places in the body. The Heart has the job of pumping these things around the body.
Heart Anatomy. 7/5/02 Stephen G Davenport 1
 Heart Anatomy Copyright 1999, Stephen G. Davenport, No part of this publication may be reproduced, stored in a retrieval system, or transmitted, in any form without prior written permission. 7/5/02 Stephen
Heart Anatomy Copyright 1999, Stephen G. Davenport, No part of this publication may be reproduced, stored in a retrieval system, or transmitted, in any form without prior written permission. 7/5/02 Stephen
Circulation. Circulation = is a process used for the transport of oxygen, carbon! dioxide, nutrients and wastes through-out the body
 Circulation Circulation = is a process used for the transport of oxygen, carbon! dioxide, nutrients and wastes through-out the body Heart = muscular organ about the size of your fist which pumps blood.
Circulation Circulation = is a process used for the transport of oxygen, carbon! dioxide, nutrients and wastes through-out the body Heart = muscular organ about the size of your fist which pumps blood.
Chapter 20 THE CARDIOVASCULAR SYSTEM: THE HEART
 Chapter 20 THE CARDIOVASCULAR SYSTEM: THE HEART INTRODUCTION A. The cardiovascular system consists of the blood, heart, and blood vessels. B. The heart is the pump that circulates the blood through an
Chapter 20 THE CARDIOVASCULAR SYSTEM: THE HEART INTRODUCTION A. The cardiovascular system consists of the blood, heart, and blood vessels. B. The heart is the pump that circulates the blood through an
The Cardiovascular System
 Chapter 18 Part A The Cardiovascular System 1/19/16 1 Annie Leibovitz/Contact Press Images Similarities of Cardiac and Skeletal Muscle RMP Ion concentration Deploarization Action Potential Repolarization
Chapter 18 Part A The Cardiovascular System 1/19/16 1 Annie Leibovitz/Contact Press Images Similarities of Cardiac and Skeletal Muscle RMP Ion concentration Deploarization Action Potential Repolarization
Chapter 14. The Cardiovascular System
 Chapter 14 The Cardiovascular System Introduction Cardiovascular system - heart, blood and blood vessels Cardiac muscle makes up bulk of heart provides force to pump blood Function - transports blood 2
Chapter 14 The Cardiovascular System Introduction Cardiovascular system - heart, blood and blood vessels Cardiac muscle makes up bulk of heart provides force to pump blood Function - transports blood 2
INTRODUCTORY REMARKS:
 INTRODUCTORY REMARKS: The circulatory system provides a way for the blood to be transported throughout the body. This provides nutrients to the cells and allows wastes to be removed. Open vs. Closed Circulatory
INTRODUCTORY REMARKS: The circulatory system provides a way for the blood to be transported throughout the body. This provides nutrients to the cells and allows wastes to be removed. Open vs. Closed Circulatory
The Cardiovascular System. Chapter 15. Cardiovascular System FYI. Cardiology Closed systemof the heart & blood vessels. Functions
 Chapter 15 Cardiovascular System FYI The heart pumps 7,000 liters (4000 gallons) of blood through the body each day The heart contracts 2.5 billion times in an avg. lifetime The heart & all blood vessels
Chapter 15 Cardiovascular System FYI The heart pumps 7,000 liters (4000 gallons) of blood through the body each day The heart contracts 2.5 billion times in an avg. lifetime The heart & all blood vessels
The Circulatory System. The Heart, Blood Vessels, Blood Types
 The Circulatory System The Heart, Blood Vessels, Blood Types The Closed Circulatory System Humans have a closed circulatory system, typical of all vertebrates, in which blood is confined to vessels and
The Circulatory System The Heart, Blood Vessels, Blood Types The Closed Circulatory System Humans have a closed circulatory system, typical of all vertebrates, in which blood is confined to vessels and
The Cardiovascular System
 The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System. anatom.ua 1
 The Cardiovascular System anatom.ua 1 The Closed Circulatory System Humans have a closed circulatory system, typical of all vertebrates, in which blood is confined to vessels and is distinct from the interstitial
The Cardiovascular System anatom.ua 1 The Closed Circulatory System Humans have a closed circulatory system, typical of all vertebrates, in which blood is confined to vessels and is distinct from the interstitial
The Heart. Happy Friday! #takeoutyournotes #testnotgradedyet
 The Heart Happy Friday! #takeoutyournotes #testnotgradedyet Introduction Cardiovascular system distributes blood Pump (heart) Distribution areas (capillaries) Heart has 4 compartments 2 receive blood (atria)
The Heart Happy Friday! #takeoutyournotes #testnotgradedyet Introduction Cardiovascular system distributes blood Pump (heart) Distribution areas (capillaries) Heart has 4 compartments 2 receive blood (atria)
4. The two inferior chambers of the heart are known as the atria. the superior and inferior vena cava, which empty into the left atrium.
 Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
CV Anatomy Quiz. Dr Ella Kim Dr Pip Green
 CV Anatomy Quiz Dr Ella Kim Dr Pip Green Q1 The location of the heart is correctly described as A) lateral to the lungs. B) medial to the sternum. C) superior to the diaphragm. D) posterior to the spinal
CV Anatomy Quiz Dr Ella Kim Dr Pip Green Q1 The location of the heart is correctly described as A) lateral to the lungs. B) medial to the sternum. C) superior to the diaphragm. D) posterior to the spinal
BIOL 4350 Cardiovascular Physiology Dr. Hamilton. Using the figure above, match the following: 1. Purkinje fibers. 2. SA node. 3. AV node.
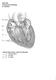 BIOL 4350 Cardiovascular Physiology Dr. Hamilton Using the figure above, match the following: 1. Purkinje fibers. 2. SA node. 3. AV node. 1 Using the figure above, match the following: 4. Atrial depolarization.
BIOL 4350 Cardiovascular Physiology Dr. Hamilton Using the figure above, match the following: 1. Purkinje fibers. 2. SA node. 3. AV node. 1 Using the figure above, match the following: 4. Atrial depolarization.
The Cardiovascular System
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Cardiovascular System 11 PART A The Cardiovascular System A closed system of the heart and blood
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Cardiovascular System 11 PART A The Cardiovascular System A closed system of the heart and blood
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies
 Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 27 The Cardiovascular System Lesson 1: Overview of the Cardiovascular System Lesson Objectives Upon
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 27 The Cardiovascular System Lesson 1: Overview of the Cardiovascular System Lesson Objectives Upon
BIOLOGY 2060 LECTURE NOTES ANATOMY & PHYSIOLOGY II (A. IMHOLTZ) HEART P1 OF 5
 BIOLOGY 2060 LECTURE NOTES ANATOMY & PHYSIOLOGY II (A. IMHOLTZ) HEART P1 OF 5 1. Heart Functions a. Generates pressure that propels blood thru blood vessels. (Tissue perfusion.) b. Separates oxygenated
BIOLOGY 2060 LECTURE NOTES ANATOMY & PHYSIOLOGY II (A. IMHOLTZ) HEART P1 OF 5 1. Heart Functions a. Generates pressure that propels blood thru blood vessels. (Tissue perfusion.) b. Separates oxygenated
Lab Activity 23. Cardiac Anatomy. Portland Community College BI 232
 Lab Activity 23 Cardiac Anatomy Portland Community College BI 232 Cardiac Muscle Histology Branching cells Intercalated disc: contains many gap junctions connecting the adjacent cell cytoplasm, creates
Lab Activity 23 Cardiac Anatomy Portland Community College BI 232 Cardiac Muscle Histology Branching cells Intercalated disc: contains many gap junctions connecting the adjacent cell cytoplasm, creates
QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY]
![QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY] QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY]](/thumbs/96/126998162.jpg) QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY] Learning Objectives: Describe the ionic basis of action potentials in cardiac contractile and autorhythmic cells Explain the relationship
QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY] Learning Objectives: Describe the ionic basis of action potentials in cardiac contractile and autorhythmic cells Explain the relationship
The Cardiovascular System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 11 The Cardiovascular System Slides 11.1 11.19 Lecture Slides in PowerPoint by Jerry L. Cook The Cardiovascular System
Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 11 The Cardiovascular System Slides 11.1 11.19 Lecture Slides in PowerPoint by Jerry L. Cook The Cardiovascular System
Figure ) The specific chamber of the heart that is indicated by letter A is called the. Diff: 1 Page Ref: 364
 Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 11 The Cardiovascular System Short Answer Figure 11.1 Using Figure 11.1, identify the following: 1) The Purkinje fibers are indicated by label.
Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 11 The Cardiovascular System Short Answer Figure 11.1 Using Figure 11.1, identify the following: 1) The Purkinje fibers are indicated by label.
Chapter 20! The Heart!
 Chapter 20! The Heart! SECTION 20-1! The heart is a four-chambered organ, supplied by the coronary circulation, that pumps oxygen-poor blood to the lungs and oxygen-rich blood to the rest of the body!
Chapter 20! The Heart! SECTION 20-1! The heart is a four-chambered organ, supplied by the coronary circulation, that pumps oxygen-poor blood to the lungs and oxygen-rich blood to the rest of the body!
Heart. Structure Physiology of blood pressure and heartbeat
 Heart Structure Physiology of blood pressure and heartbeat Location and Anatomy Location and Anatomy Pericardial cavity: surrounds, isolates, and anchors heart Parietal pericardium lined with serous membrane
Heart Structure Physiology of blood pressure and heartbeat Location and Anatomy Location and Anatomy Pericardial cavity: surrounds, isolates, and anchors heart Parietal pericardium lined with serous membrane
37 1 The Circulatory System
 H T H E E A R T 37 1 The Circulatory System The circulatory system and respiratory system work together to supply cells with the nutrients and oxygen they need to stay alive. a) The respiratory system:
H T H E E A R T 37 1 The Circulatory System The circulatory system and respiratory system work together to supply cells with the nutrients and oxygen they need to stay alive. a) The respiratory system:
Electrical Conduction
 Sinoatrial (SA) node Electrical Conduction Sets the pace of the heartbeat at 70 bpm AV node (50 bpm) and Purkinje fibers (25 40 bpm) can act as pacemakers under some conditions Internodal pathway from
Sinoatrial (SA) node Electrical Conduction Sets the pace of the heartbeat at 70 bpm AV node (50 bpm) and Purkinje fibers (25 40 bpm) can act as pacemakers under some conditions Internodal pathway from
IP: Regulation of Cardiac Output
 ANP 1105D Winter 2013 Assignment 9: The Heart, part 2: Chap... Assignment 9: The Heart, part 2: Chapter 18 Signed in as Alex Sokolowski Help Close Resources Due: 11:59pm on Monday, March 25, 2013 Note:
ANP 1105D Winter 2013 Assignment 9: The Heart, part 2: Chap... Assignment 9: The Heart, part 2: Chapter 18 Signed in as Alex Sokolowski Help Close Resources Due: 11:59pm on Monday, March 25, 2013 Note:
CARDIOVASCULAR SYSTEM
 CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
The Cardiovascular System
 The Cardiovascular System The Manila Times College of Subic Prepared by: Stevens B. Badar, RN, MANc THE HEART Anatomy of the Heart Location and Size approx. the size of a person s fist, hollow and cone-shaped,
The Cardiovascular System The Manila Times College of Subic Prepared by: Stevens B. Badar, RN, MANc THE HEART Anatomy of the Heart Location and Size approx. the size of a person s fist, hollow and cone-shaped,
The Cardiovascular System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Slides 11.1 11.19 Seventh Edition Chapter 11 The Cardiovascular System Functions of the Cardiovascular system Function of the heart: to pump blood
Essentials of Human Anatomy & Physiology Elaine N. Marieb Slides 11.1 11.19 Seventh Edition Chapter 11 The Cardiovascular System Functions of the Cardiovascular system Function of the heart: to pump blood
Cardiovascular System
 Cardiovascular System Purpose Transport oxygen and nutrients Take waste products away from tissues & organs Things we learned Blood pressure: the force of blood pushing against the walls of blood vessels
Cardiovascular System Purpose Transport oxygen and nutrients Take waste products away from tissues & organs Things we learned Blood pressure: the force of blood pushing against the walls of blood vessels
Unit 6: Circulatory System. 6.2 Heart
 Unit 6: Circulatory System 6.2 Heart Functions of Circulatory System 1. The heart is the pump necessary to circulate blood to all parts of the body 2. Arteries, veins and capillaries are the structures
Unit 6: Circulatory System 6.2 Heart Functions of Circulatory System 1. The heart is the pump necessary to circulate blood to all parts of the body 2. Arteries, veins and capillaries are the structures
BIOLOGY 2060 LECTURE NOTES ANATOMY & PHYSIOLOGY II (A. IMHOLTZ) HEART P1 OF 7
 BIOLOGY 2060 LECTURE NOTES ANATOMY & PHYSIOLOGY II (A. IMHOLTZ) HEART P1 OF 7 1. Heart a. Generates the pressure that propels blood thru blood vessels. b. Separates oxygenated and deoxygenated blood separate.
BIOLOGY 2060 LECTURE NOTES ANATOMY & PHYSIOLOGY II (A. IMHOLTZ) HEART P1 OF 7 1. Heart a. Generates the pressure that propels blood thru blood vessels. b. Separates oxygenated and deoxygenated blood separate.
Cardiovascular System Notes: Heart Disease & Disorders
 Cardiovascular System Notes: Heart Disease & Disorders Interesting Heart Facts The Electrocardiograph (ECG) was invented in 1902 by Willem Einthoven Dutch Physiologist. This test is still used to evaluate
Cardiovascular System Notes: Heart Disease & Disorders Interesting Heart Facts The Electrocardiograph (ECG) was invented in 1902 by Willem Einthoven Dutch Physiologist. This test is still used to evaluate
Cardiovascular Anatomy Dr. Gary Mumaugh
 Cardiovascular Anatomy Dr. Gary Mumaugh Location of Heart Approximately the size of your fist Location o Superior surface of diaphragm o Left of the midline in mediastinum o Anterior to the vertebral column,
Cardiovascular Anatomy Dr. Gary Mumaugh Location of Heart Approximately the size of your fist Location o Superior surface of diaphragm o Left of the midline in mediastinum o Anterior to the vertebral column,
Cardiac physiology. b. myocardium -- cardiac muscle and fibrous skeleton of heart
 I. Heart anatomy -- general gross. A. Size/orientation - base/apex B. Coverings D. Chambers 1. parietal pericardium 2. visceral pericardium 3. Layers of heart wall a. epicardium Cardiac physiology b. myocardium
I. Heart anatomy -- general gross. A. Size/orientation - base/apex B. Coverings D. Chambers 1. parietal pericardium 2. visceral pericardium 3. Layers of heart wall a. epicardium Cardiac physiology b. myocardium
THE HEART Dr. Ali Ebneshahidi
 THE HEART Dr. Ali Ebneshahidi Functions is of the heart & blood vessels 1. The heart is an essential pumping organ in the cardiovascular system where the right heart pumps deoxygenated blood (returned
THE HEART Dr. Ali Ebneshahidi Functions is of the heart & blood vessels 1. The heart is an essential pumping organ in the cardiovascular system where the right heart pumps deoxygenated blood (returned
Circulatory system. Terminology. Ventricles and resistance. Pressure gradients move blood through the heart and vessels.
 Circulatory system Pressure gradients move blood through the heart and vessels. Pulmonary circulation vs. systemic circulation (to pulmonary circuit) liver head and arms heart aorta diaphragm (from pulmonary
Circulatory system Pressure gradients move blood through the heart and vessels. Pulmonary circulation vs. systemic circulation (to pulmonary circuit) liver head and arms heart aorta diaphragm (from pulmonary
Cardiovascular System: The Heart
 Cardiovascular System: The Heart I. Anatomy of the Heart (See lab handout for terms list) A. Describe the size, shape and location of the heart B. Describe the structure and function of the pericardium
Cardiovascular System: The Heart I. Anatomy of the Heart (See lab handout for terms list) A. Describe the size, shape and location of the heart B. Describe the structure and function of the pericardium
Cardiovascular System Notes: Physiology of the Heart
 Cardiovascular System Notes: Physiology of the Heart Interesting Heart Fact Capillaries are so small it takes ten of them to equal the thickness of a human hair. Review What are the 3 parts of the cardiovascular
Cardiovascular System Notes: Physiology of the Heart Interesting Heart Fact Capillaries are so small it takes ten of them to equal the thickness of a human hair. Review What are the 3 parts of the cardiovascular
LECTURE 5. Anatomy of the heart
 LECTURE 5. Anatomy of the heart Main components of the CVS: Heart Blood circulatory system arterial compartment haemomicrocirculatory (=microvascular) compartment venous compartment Lymphatic circulatory
LECTURE 5. Anatomy of the heart Main components of the CVS: Heart Blood circulatory system arterial compartment haemomicrocirculatory (=microvascular) compartment venous compartment Lymphatic circulatory
The Cardiovascular System (Heart)
 The Cardiovascular System The Cardiovascular System (Heart) A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function
The Cardiovascular System The Cardiovascular System (Heart) A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function
human anatomy 2016 lecture thirteen Dr meethak ali ahmed neurosurgeon
 Heart The heart is a hollow muscular organ that is somewhat pyramid shaped and lies within the pericardium in the mediastinum. It is connected at its base to the great blood vessels but otherwise lies
Heart The heart is a hollow muscular organ that is somewhat pyramid shaped and lies within the pericardium in the mediastinum. It is connected at its base to the great blood vessels but otherwise lies
Principles of Biomedical Systems & Devices. Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont
 Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Using Figure 14.1, match the following: 1) Myelin sheath. 1) 2) Cell body of ANS preganglionic neuron. 2)
 Practice Exam 1 AP 2 chapters 14 and 18 Name MATCHING: Match labeled areas with the appropriate terminology from the list below. Figure 14.1 Using Figure 14.1, match the following: 1) Myelin sheath. 1)
Practice Exam 1 AP 2 chapters 14 and 18 Name MATCHING: Match labeled areas with the appropriate terminology from the list below. Figure 14.1 Using Figure 14.1, match the following: 1) Myelin sheath. 1)
BIO 136 Human Anatomy & Physiology For Non-Majors 11:39 am, Mar 08, 2006
 Jim Swan 1 These slides are from class presentations, reformatted for static viewing. The content contained in these pages is also in the Class Notes pages in a narrative format. Best screen resolution
Jim Swan 1 These slides are from class presentations, reformatted for static viewing. The content contained in these pages is also in the Class Notes pages in a narrative format. Best screen resolution
8:49 am, Jan 28, 2008
 Jim Swan 1 These slides are from class presentations, reformatted for static viewing. The content contained in these pages is also in the Class Notes pages in a narrative format. Best screen resolution
Jim Swan 1 These slides are from class presentations, reformatted for static viewing. The content contained in these pages is also in the Class Notes pages in a narrative format. Best screen resolution
The Heart and Heart Disease
 The Heart and Heart Disease Illustration of the heart by Leonardo DaVinci heart-surgeon.com/ history.html 2/14/2010 1 I. Location, Size and Position of the Heart A. Triangular organ located 1. of mass
The Heart and Heart Disease Illustration of the heart by Leonardo DaVinci heart-surgeon.com/ history.html 2/14/2010 1 I. Location, Size and Position of the Heart A. Triangular organ located 1. of mass
Part 1. Copyright 2011 Pearson Education, Inc. Figure Copyright 2011 Pearson Education, Inc.
 PowerPoint Lecture Slides prepared by Leslie Hendon University of Alabama, Birmingham C H A P T E R The Heart 19 Part 1 The Heart A muscular double pump circuit vessels transport blood to and from the
PowerPoint Lecture Slides prepared by Leslie Hendon University of Alabama, Birmingham C H A P T E R The Heart 19 Part 1 The Heart A muscular double pump circuit vessels transport blood to and from the
The cardiovascular system is composed of the heart and blood vessels that carry blood to and from the body s organs. There are 2 major circuits:
 1 The cardiovascular system is composed of the heart and blood vessels that carry blood to and from the body s organs. There are 2 major circuits: pulmonary and systemic. The pulmonary goes out to the
1 The cardiovascular system is composed of the heart and blood vessels that carry blood to and from the body s organs. There are 2 major circuits: pulmonary and systemic. The pulmonary goes out to the
Chapter 20 (2) The Heart
 Chapter 20 (2) The Heart ----------------------------------------------------------------------------------------------------------------------------------------- Describe the component and function of
Chapter 20 (2) The Heart ----------------------------------------------------------------------------------------------------------------------------------------- Describe the component and function of
CIRCULATORY SYSTEM BLOOD VESSELS
 Name: Block: CIRCULATORY SYSTEM Multicellular organisms (above the level of roundworms) rely on a circulatory system to bring nutrients to, and take wastes away from, cells. In higher organisms such as
Name: Block: CIRCULATORY SYSTEM Multicellular organisms (above the level of roundworms) rely on a circulatory system to bring nutrients to, and take wastes away from, cells. In higher organisms such as
Chapter 20b Cardiac Physiology
 Chapter 20b Cardiac Physiology Heart Valve Mechanics The heart valve openand close because of pressure gradients. When pressure on one side is greater than the other, it pushes the valve open. For example,
Chapter 20b Cardiac Physiology Heart Valve Mechanics The heart valve openand close because of pressure gradients. When pressure on one side is greater than the other, it pushes the valve open. For example,
Anatomy Review: The Heart Graphics are used with permission of A.D.A.M. Software, Inc. and Benjamin/Cummings Publishing Co.
 Anatomy Review: The Heart Graphics are used with permission of A.D.A.M. Software, Inc. and Benjamin/Cummings Publishing Co. Anatomy Views Label the diagrams of the heart below: Interactive Physiology Study
Anatomy Review: The Heart Graphics are used with permission of A.D.A.M. Software, Inc. and Benjamin/Cummings Publishing Co. Anatomy Views Label the diagrams of the heart below: Interactive Physiology Study
The Cardiovascular System
 11 PART A The Cardiovascular System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Cardiovascular
11 PART A The Cardiovascular System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Cardiovascular
Practice Exercises for the Cardiovascular System
 Practice Exercises for the Cardiovascular System On the diagram below, color the oxygen-rich blood red and the oxygen-poor blood blue. Label the parts: Continued on the next page... Label the parts on
Practice Exercises for the Cardiovascular System On the diagram below, color the oxygen-rich blood red and the oxygen-poor blood blue. Label the parts: Continued on the next page... Label the parts on
IB TOPIC 6.2 THE BLOOD SYSTEM
 IB TOPIC 6.2 THE BLOOD SYSTEM THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
IB TOPIC 6.2 THE BLOOD SYSTEM THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
Cardiovascular System
 Cardiovascular System I. Structure of the Heart A. Average adult heart is 14 cm long and 9 cm wide. B. Lies in the mediastinum. C. Enclosed in the pericardium. 1. Fibrous pericardium- Outer, tough connective
Cardiovascular System I. Structure of the Heart A. Average adult heart is 14 cm long and 9 cm wide. B. Lies in the mediastinum. C. Enclosed in the pericardium. 1. Fibrous pericardium- Outer, tough connective
Chapter 14. Circulatory System Images. VT-122 Anatomy & Physiology II
 Chapter 14 Circulatory System Images VT-122 Anatomy & Physiology II The mediastinum Dog heart Dog heart Cat heart Dog heart ultrasound Can see pericardium as distinct bright line Pericardial effusion Fluid
Chapter 14 Circulatory System Images VT-122 Anatomy & Physiology II The mediastinum Dog heart Dog heart Cat heart Dog heart ultrasound Can see pericardium as distinct bright line Pericardial effusion Fluid
AP2 Lab 3 Coronary Vessels, Valves, Sounds, and Dissection
 AP2 Lab 3 Coronary Vessels, Valves, Sounds, and Dissection Project 1 - BLOOD Supply to the Myocardium (Figs. 18.5 &18.10) The myocardium is not nourished by the blood while it is being pumped through the
AP2 Lab 3 Coronary Vessels, Valves, Sounds, and Dissection Project 1 - BLOOD Supply to the Myocardium (Figs. 18.5 &18.10) The myocardium is not nourished by the blood while it is being pumped through the
Anatomy of the Heart
 Biology 212: Anatomy and Physiology II Anatomy of the Heart References: Saladin, KS: Anatomy and Physiology, The Unity of Form and Function 8 th (2018). Required reading before beginning this lab: Chapter
Biology 212: Anatomy and Physiology II Anatomy of the Heart References: Saladin, KS: Anatomy and Physiology, The Unity of Form and Function 8 th (2018). Required reading before beginning this lab: Chapter
Introduction. Circulation
 Introduction Circulation 1- Systemic (general) circulation 2- Pulmonary circulation carries oxygenated blood to all parts of the body carries deoxygenated blood to the lungs From Lt. ventricle aorta From
Introduction Circulation 1- Systemic (general) circulation 2- Pulmonary circulation carries oxygenated blood to all parts of the body carries deoxygenated blood to the lungs From Lt. ventricle aorta From
d) Cardiovascular System Higher Human Biology
 d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
Approximately the size of your fist Location Superior surface of diaphragm Left of the midline in mediastinum Anterior to the vertebral column,
 Dr. Gary Mumaugh Approximately the size of your fist Location Superior surface of diaphragm Left of the midline in mediastinum Anterior to the vertebral column, posterior to the sternum Posteriorly the
Dr. Gary Mumaugh Approximately the size of your fist Location Superior surface of diaphragm Left of the midline in mediastinum Anterior to the vertebral column, posterior to the sternum Posteriorly the
THE HEART OBJECTIVES: LOCATION OF THE HEART IN THE THORACIC CAVITY CARDIOVASCULAR SYSTEM
 BIOLOGY II CARDIOVASCULAR SYSTEM ACTIVITY #3 NAME DATE HOUR THE HEART OBJECTIVES: Describe the anatomy of the heart and identify and give the functions of all parts. (pp. 356 363) Trace the flow of blood
BIOLOGY II CARDIOVASCULAR SYSTEM ACTIVITY #3 NAME DATE HOUR THE HEART OBJECTIVES: Describe the anatomy of the heart and identify and give the functions of all parts. (pp. 356 363) Trace the flow of blood
Blood Functions. Blood and the Cardiovascular System. Blood. Plasma. Erythrocytes (RBCs) Erythrocytes (RBCs) 4/7/2017
 Blood Functions Blood and the Cardiovascular System Distribution Delivery of oxygen and nutrients to all body cells; Transport of wastes to lungs and excretory organs; Transport of hormones Regulation
Blood Functions Blood and the Cardiovascular System Distribution Delivery of oxygen and nutrients to all body cells; Transport of wastes to lungs and excretory organs; Transport of hormones Regulation
Cardiovascular Physiology. Heart Physiology. Introduction. The heart. Electrophysiology of the heart
 Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
