Long-Term Results of Transcatheter Closure of Patent Ductus Arteriosus in Infants Using Amplatzer Duct Occluder
|
|
|
- Norman Andrews
- 5 years ago
- Views:
Transcription
1 Original Article Iran J Pediatr Aug 2013; Vol 23 (No 4), Pp: Long-Term Results of Transcatheter Closure of Patent Ductus Arteriosus in Infants Using Amplatzer Duct Occluder Mostafa Behjati-Ardakani* 1, MD; Mohammad-Amin Behjati-Ardakani 2 ; Seyed-Habibolla Hosseini 3, MD; Noormohammad Noori 4, MD 1. Yazd Cardiovascular Research Center, Shahid Sadoughi University of Medical sciences, Yazd, Iran 2. Baqiyatallah University of Medical Sciences, Tehran, Iran 3. Department of Anesthesiology, Shahid Sadoughi University of Medical Sciences, Yazd, Iran 4. Department of Pediatrics, Zahedan University of Medical Sciences, Zahedan, Iran Received: Nov 12, 2012; Accepted: Apr 09, 2013; First Online Available: May 27, 2013 Abstract Objective: Patent ductus arteriosus (PDA) is one of the most frequently seen congenital heart diseases. Its closure is recommended because of the risk of infective endocardis, as well as morbidity and mortality in the long. The aim of this study was to assess the long term results of the transcatheter closure of PDA in infants using amplatzer duct occlude (ADO). Methods: From May 2004 to September 2011, forty eight infants underwent transcatheter closure of PDA. A lateral or right anterior oblique view aortogram was done to locate PDA and to measure its size. Before discharge, repeat aortogram was performed to evaluate eventual residual shunt and to confirm the appropriate deployment of the ADO. Follow up evaluations were done with transthoracic echocardiography at discharge, 1 month, 6 months, 12 months and yearly thereafter. Findings: The mean age of patients at procedure was 9.18±2.32 (range 3 to 12) months, mean weight 6.73±1.16 (range 4.5 to 10.1) kg. The PDA occluded completely in 20 out of the 48 patients. Twenty four patients had trivial or mild shunt and two patients had moderate residual shunt which disappeared in one patient within 24 hours and other patient with moderate shunt in 1 month. One patient (age 8 months) had mild LPA stenosis. The device emobolization occurred in two patients, immediately after the procedure in one and during night in the other patient Conclusion: The long term results suggested that transcatheter closure of PDA using Amplatzer duct occluder is a safe and effective treatment in infants less than 1 year of age with minimal complications. Iranian Journal of Pediatrics, Volume 23 (Number 4), August 2013, Pages: Key Words: Patent Ductus Arteriosus; Transcatheter Closure; Congenital Heart Defect Introduction Patent ductus arteriosus (PDA) is the second most common form of congenital heart defects [1]. This accounts for approximately 5-10 percent of all congenital heart defects. In the modern era, the true incidence may be as high as 1 in 500 term newborns later in infancy, because many cases with silent PDA are discovered incidentally by echocardiography done for other purposes [2]. Since 1939, surgical correction has become a gold standard for the treatment of PDA [3]. * Corresponding Author; Address: Cardiovascular Research Center, Afshar Hospital, Jomhouri Boulevard, Yazd, Islamic Republic of Iran dr_behjati@yahoo.com 2013 by Pediatrics Center of Excellence, Children s Medical Center, Tehran University of Medical Sciences, All rights reserved.
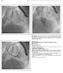
2 412 Long-Term Results of Transcatheter Closure of PDA in Infants Since the first description of transcatheter closure of PDA with an Ivalon plug by Porstmann et al [4] several other devices such as Duct-occluder device (coil) [5] and Amplatzer duct occluder (ADO) [6] have been developed. Immediate, short, and intermediate term results of transcatheter closure of PDA with ADO have been well documented [7-9]. The purpose of this study was to evaluate the results of long term follow up of transcatheter closure of PDA using ADO in infants. Subjects and Methods From May 2004 to September 2011, forty eight patients (19 boys and 39 girls) underwent transcatheter closure of PDA. Age at procedure ranged from 4 to 12 (mean 9.18±2.32) months. Median weight was 7 (range 4.5 to 10.1) kg. Infants selected for transcatheter closure had clinical and echocardiographic features of a moderate to large PDA and weighed 4.5 kg. The inclusion criteria were (1) patients aged less th an 12 months and (2) patients with a moderate to large isolated PDA. Exclusion criteria were (1) PDA associated with any other congenital heart disease which could be corrected surgically; (2) patients with significant cardiac and non-cardiac co-morbidities that could impact clinical outcome of duct closure as well as those with evidence of severe congestive heart failure; (3) PDA with severe pulmonary artery hypertension and rightto-left shunt; (4) patients with window-type PDA; (4) patients weighing <4.5 kg. These patients had one or more of the following: symptoms and signs of cardiac failure, pulmonary hypertension, failure to thrive, and recurrent pneumonia. All patients had signs of significant left to right shunting through PDA with left ventricular volume overload and left atrial enlargement on transthoracic echocardiography. Associated congenital cardiac anomalies observed included ventricular septal defect (2 patients), mild pulmonary stenosis (1 patient), double outlet right ventricle, pulmonary stenosis (1 patient) and atrial septal defect (1 patient). Two of the patients had a moderate residual shunt following surgical ligation. Device and procedure Informed written consent was obtained prior to procedure from the parents of all patients. Procedures were done under general anesthesia. Right and left cardiac catheterization was performed for hemodynamic assessment and shunt estimation. Prophylactic antibiotics with 30mg/kg cefazoline was administrated at beginning of the procedure and two subsequent doses 8 hours apart and 100IU/kg of sodium heparin was administrated to maintain activated clotting time more than 250 sec after catheterizing the femoral artery. A descending aortogram in right anterior oblique or lateral view was done with a 4 or 5 French pigtail catheter to define the morphology, the aortic ampulla, length of the duct, size of the duct at narrowest part and the center of the PDA (Fig. 1). Subsequently, a inch (0.8 mm) exchange wire was placed across the ductus from the pulmonary artery using a 4 or 5 French multipurpose catheter. Over the wire a 6 or 7 French long sheath (AGA Medical Corporation) was introduced from the right or left femoral vein through the ductus into the descending aorta. The ADO was chosen 1-2 mm larger than the narrowest part of the PDA. Under fluoroscopy guidance, the device was introduced into the delivery sheath and advanced into the descending aorta, where the retention disk was deployed. Then, the sheath and delivery cable were pulled back until extruded in descending Aorta against the aortic end of PDA, while a gentle tension was Fig. 1: Descending aortogram in lateral view showing medium sized patent ductus arteriosus
3 Behjati-Ardakani M, et al 413 Fig. 2: Descending aortogram in lateral view before release of the amplatzer duct occlude showing no residual shunt and appropriate deployment of device Fig. 3: Descending aortogram in lateral view after release of the amplatzer duct occlude showing complete occlusion and appropriate device position maintained on delivery cable. The introducing sheath was withdrawn into the pulmonary artery to deploy the conical part of the ADO. With the device still attached to the cable, descending aortogram was performed to confirm proper device position and exclude aortic obstruction or significant residual shunt (Fig. 2). The ADO was retracted into the delivery sheath if a significant shunt or aortic obstruction was detected. Once optimal position was confirmed, the device was released by counter-clockwise rotation of the delivery cable. Descending aortogram in lateral position before release of the device showed complete occlusion of PDA and appropriate device deployment (Fig. 2). A repeat angiogram was done 10 minutes after release to check for residual shunt or aortic obstruction. Fig. 3 shows descending aortogram in lateral view after release of the ADO showing complete occlusion and appropriate device position. All patients were discharged on the next day after the procedure and given no medication. All patients had complete transthoracic echocardiographic studies before discharge, at 1, 6, and 12 months and then yearly thereafter. Endocarditis prophylaxis was discontinued at the six month's follow up if the duct was completely occluded. Statistical analysis Results are expressed as mean±sd, percentage, median and range. The data were analyzed with statistical program SPSS version for Windows. Continuous variables with normal distribution are expressed as mean [± standard deviation (SD) ]. Continuous variables with inappropriate distribution are expressed as median. Findings The device was successfully deployed in 46 (95.8%) patients. Device embolization occurred in two (4%) patients. In one patient, distal embolization of device occurred immediately after the procedure. This device was successfully retrieved in catheterization laboratory and the patient underwent uneventful repeat device implanation for PDA occlusion. Another patient had a moderate shunt and device embolization in main PA and was referred for surgical removal and duct ligation. Demographic and catheterization data of the patients undergoing transcatheter closure of PDA are listed in Table 1. In five patients, the devices were too small to close the defect; therefore, larger ADOs were implanted. Angiography at the end of the procedure demonstrated complete occlusion in 20 (41.6%) patients and residual shunt in 27 patients. Among these twenty seven patients, twenty four had a trivial mesh leak shunt, one patient had
4 414 Long-Term Results of Transcatheter Closure of PDA in Infants Table 1: Demographic and catheterization data of patients undergoing closure of PDA with amplatzer duct occlude Parameter Mean (Standard Deviation) Median Range Age (month) 9.1 (3.2) Weight (kg) 6.73 (1.16) Mean PAP (mmhg) (14.15) QP/Qs 2.75 (0.85) PDA size (mm) 5.7 (1.62) Amplatzer duct occlude (mm) 5.29 (1.55) Fluoroscopy Time (min) 6.23 (2.9) Procedure Time (min) (9.6) Follow-up (mo) 37.9 (23.36) PDA: Patent ductus arteriosus; PAP: Pulmonary Artery Pressure QP/QS: Pulmonary Blood Flow/ Systemic Blood Flow small and two patients moderate shunt. On the following day, trivial mesh leak shunt disappeared completely in all cases. In one patient, there was a moderate residual shunt immediately 24 hours after procedure and complete occlusion was achieved 1 month after the procedure. Also in one patient who had small residual shunt, complete closure occurred within 24 hours after the procedure Distal embolization of the device to main pulmonary occurred immediately after the procedure in one patient who had moderate residual shunt. This patient underwent surgical ligation after surgical removal of embolized device. Mild left pulmonary stenosis (gradient 20 mmhg) via encroachment of device was detected in 1 patient. There was no evidence of obstruction of descending aorta as confirmed by angiography and Doppler-color echocardiography. Thrombosis of right femoral artery or left femoral artery occurred in 6 and 2 patients respectively. Heparin infusion was used unsuccessfully in 3 patients. Streptokinase intravenous infusion (loading dos e IU/kg over one hour followed by IU/kg for six hours) produced a successful and complete turn of pulse without sequelae in two patients. One other patient underwent femoral artery thrombectomy. Mild inguinal hematoma occurred in two patients. One death (a 7-month old baby) occurred because of aspiration pneumonia five days after procedure. This patient had dextrocardia, large PDA, subsystemic PH, failure to thrive and congestive heart failure. Aspiration pneumonia occurred at home during bottle feeding. The patient was hospitalized, multiple antibiotics were administrated and finally the patient died the same day due to fulminant pulmonary infection and respiratory failure. Protrusion of ADO into descending aorta without obstruction occurred in 3 of 48 (6.25%) cases. Follow up for short (one day to 6 months), intermediate (6 months - 12 months) and long period (>1 year) showed no significant complications such as device embolization or malposition, hemolysis, thrombus formation, thromboembolism and infectious endocarditis. Congestive heart failure, failure to thrive and recurrent pulmonary infection were significantly improved. Discussion This study reports the result of long term (37.9±23.36 months, range 13.7 to 89.8 months) follow up in 46 infants who underwent transcatheter closure of PDA using Amplatzer duct occluder. Transcatheter closure of PDA is a wellestablished technique that has a low incidence of complication [10]. Transcatheter closure of PDA with ADO has significantly improved the outcomes of the percutaneous closure of medium and large sized ducts [11]. Several devices have been developed for PDA occlusion, currently, the only FDA-approved device for closure of PDA is the ADOI (AGA Medical Corporation, Gollden Valley, Minnesota, USA). In our study USA made (AGA medical corporation, Golden Valley, Minnesota, USA, n= 17) and China made (Starway Medical Supplies Ltd, n=31) forms of devices were used. The ADOI is a self-expanding conical device with a single retention skirt and composed of a nitinol wire mesh with polyester fabric sewn into
5 Behjati-Ardakani M, et al 415 the mesh to induce thrombosis; it received FDA approval in May 2003 [12]. The ADOI device has proved to be high effective in many reports [8,13,16]. The major favorable features are easy implantation, small delivery sheath (5-8 Fr), possibility of retrieval, ability of repositioning before release of device, low complication and high rate of occlusion [6,17,18]. Despite these advantages, transcatheter closure of PDA has rare complications, such as embolization, left pulmonary obstruction, descending aorta obstruction and femoral artery thrombosis (7,19,20]. Late complications are more rarely described and only late embolization of device and hemolysis are reported [21,22]. The result of our study of transcatheter PDA closure with ADO, with an occlusion rate of 95.7% at 24 hours, concur with results described in other reports [23,24]. Although many patients had a residual shunt at the end of the procedure, only one patient had moderate residual shunt after 24 hours. This patient was found to have complete occlusion at 1-month follow up. The phenomenon demon-strates the advantages of plug type design of the ADO for occlusion of PDAs. Faella and Hejazi [25] reported a large series of 360 patients with PDA occluded with the ADO. Closure was successful in all patients. Complication occurred in 6 patients: embolization 3, mild aortic obstruction due to large device in 1 patient and blood loss that required transfusion in 2 patients. Li JJ, et al [22] reported the successful use of the ADO to occlude PDA over a long-term follow up of five years. According to this study, late complication occurred in 5 patients consisting of hemolysis in 3 patients and loss of the femoral artery in 2 patients. In our study no late complications such as embolization, hemolysis, left pulmonary artery or aortic obstruction occurred. In our study, early device embolization occurred in one (2.1%) infant that required surgery. The reported rate of device embolization varies, between 0% to 3% [26-30]. One patient required blood transfusion because of significant blood loss during procedure. Rarely, a left pulmonary (LPA) obstruction occurs after transcatheter closure using ADO [12,25]. In current study, mild LPA obstruction (gradient <20 mmhg) occurred in one 8 months old patient. During follow up and with the patient's growth, pressure gradient gradually decreased and normalized 25 months after the procedure. However in our study no late major complication such as stenosis in either the LPA or descending thoracic aorta, hemolysis and endocarditis occurred. This study confirmed effectiveness of transcatheter closure of PDA using ADO both early and during intermediate and longterm follow up the same results were described by other authors [8,12,14,24,28,31]. A limitation of our study was its retrospective nature. Also, the learning curve for technique in the closure of PDA was not accounted for in the study. Conclusion Transcatheter closure of PDA with Amplatzer Duct Occluder in symptomatic infants is an effective and safe method for the treatment of medium to large PDA. The low incidence of complication and short hospital stay makes ADO ideal for transcatheter closure of medium to large PDA in infants. However, some complications including device embolization, left pulmonary stenosis and femoral artery thrombosis may have occurred in some cases. Acknowledgement: This study was supported by a grant from the Yazd cardiovascular research center. The authors wish to thank Dr MH Fallahzadeh for collecting data and statistical analysis. We also thank Sedigheh Bagheri and Aliakbar Ghafoori for preparation of the manuscript. Conflict of Interest: None References 1. Hammerman C. Patent ductus arteriosus. Clinical relevance of prostaglandins and prostaglandin inhibitors in PDA pathophysiology and treatment. Clin Perinatol 1995;22(2): Lloyd TR, Beekman RH 3rd. Clinically silent patent ductus arteriosus. Am Heart J 1994;127(6):
6 416 Long-Term Results of Transcatheter Closure of PDA in Infants 3. Mavroudis C, Backer CL, Gevitz M. Forty-six years of patent ductus arteriosus division at Children's Memorial Hospital of Chicago. Standards for comparison. Ann Surg 1994;220(3): Porstmann W, Wierny L, Warnke H. Closure of persistent ductus arteriosus without thoracotomy. Ger Med Mon 1967;12(6): Moore JW, Schneider DJ, Dimeglio D. The ductocclud device: design, clinical results, and future directions. J Interv Cardiol 2001;14(2): Masura J, Walsh KP, Thanopoulous B, et al. Catheter closure of moderate- to large-sized patent ductus arteriosus using the new Amplatzer duct occluder: immediate and short-term results. J Am Coll Cardiol 1998;31(4): Butera G, De Rosa G, Chessa M, et al. Transcatheter closure of persistent ductus arteriosus with the Amplatzer duct occluder in very young symptomatic children. Heart 2004;90(12): Wang JK, Wu MH, Lin MT, et al. Transcatheter closure of moderate-to-large patent ductus arteriosus in infants using Amplatzer duct occluder. Circ J 2010;74(2): Sivakumar K, Francis E, Krishnan P. Safety and feasibility of transcatheter closure of large patent ductus arteriosus measuring >or=4 mm in patients weighing <or=6 kg. J Interv Cardiol 2008;21(2): Fernández Ruiz A, del Cerro Marín MJ, Rubio Vidal D, et al. Transcatheter closure of patent ductus arteriosus using the Amplatzer duct occluder: initial results and mid-term follow-up. Rev Esp Cardiol 2002;55(10): Thanopoulos BD, Tsaousis GS, Djukic M, et al. Transcatheter closure of high pulmonary artery pressure persistent ductus arteriosus with the Amplatzer muscular ventricular septal defect occluder. Heart 2002;87(3): Pass RH, Hijazi Z, Hsu DT, et al. Multicenter USA Amplatzer patent ductus arteriosus occlusion device trial: initial and one-year results. J Am Coll Cardiol 2004;44(3): Wang JK, Wu MH, Hwang JJ, et al. Transcatheter closure of moderate to large patent ductus arteriosus with the Amplatzer duct occluder. Catheter Cardiovasc Interv 2007;69(4): Thanopoulos BV, Eleftherakis N, Tzannos K, et al. Further experience with catheter closure of patent ductus arteriosus using the new Amplatzer duct occluder in children. Am J Cardiol 2010;105(7): Choi DY, Kim NY, Jung MJ, et al. The results of transcatheter occlusion of patent ductus arteriosus: success rate and complications over 12 years in a single center. Korean Circ J 2010;40(5): Shabbir M, Akhtar K, Maadullah, et al. Transcatheter closure of large sized patent ductus arteriosus using the amplatzer duct occluder device. J Coll Physicians Surg Pak 2009;19(5): Al-Hamash SM, Wahab HA, Khalid ZH, et al. Transcatheter Closure of patent ductus arteriosus using Ado device: Retrospective study of 149 patients. Heart Views 2012;13(1): Fernández Ruiz A, del Cerro Marín MJ, Rubio Vidal D, et al. Transcatheter closure of patent ductus arteriosus using the Amplatzer duct occluder: initial results and mid-term follow-up. Rev Esp Cardiol 2002;55(10): Vavuranakis M, Tzannos KA, Thanopoulos BD, et al. Severe hemolysis complicating transcatheter occlusion of a patent ductus arteriosus: the importance of elimination of residual flow. Hellenic J Cardiol 2007;48(6): Galal MO. Advantages and disadvantages of coils for transcatheter closure of patent ductus arteriosus. J Interv Cardiol 2003;16(2): McMullan DM, Moulick A, Jonas RA. Late embolization of Amplatzer patent ductus arteriosus occlusion device with thoracic aorta embedment. Ann Thorac Surg 2007;83(3): Li JJ, Li YF, Zhang ZW, et al. A follow up study on transcatheter closure of patent ductus arteriosus with Amplatzer duct occluder in children. Zhonghua Er Ke Za Zhi 2005;43(8): Al-Motarreb A, Al-Hammadi1 M, Shamsan M, et al. Percutaneous transcatheter closure of patent ductus arteriosus using amplatzer duct occluder: First Yemeni experience. Chin Med J (Engl). 2001; 114(5): Masura J, Tittel P, Gavora P, et al. Long-term outcome of transcatheter patent ductus arteriosus closure using Amplatzer duct occluders. Am Heart J 2006;151(3):755.e7-755.e Faella HJ, Hijazi ZM. Closure of the patent ductus arteriosus with the amplatzer PDA device: immediate results of the international clinical trial. Catheter Cardiovasc Interv 2000;51(1): Al-Ata J, Arfi AM, Hussain A, et al. The efficacy and safety of the Amplatzer ductal occluder in young children and infants. Cardiol Young 2005; 15(3): Ali Khan MA, al Yousef S, Mullins CE, et al. Experience with 205 procedures of transcatheter closure of ductus arteriosus in 182 patients, with special reference to residual shunts and long-term follow-up. J Thorac Cardiovasc Surg 1992;104(6): Jang GY, Son CS, Lee JW, et al. Complications after transcatheter closure of patent ductus arteriosus. J Korean Med Sci 2007;22(3): Zhang Z, Qian M, Wang H, et al. Transcatheter closure in 354 pediatric cases of patent ductus arteriosus using five different devices. Chin Med J (Engl) 2001;114(5): Behjati-Ardakani M, Forouzannia SK, Dehghani M, et al. Transcatheter closure of patent ductus arterisus using the Amplatzer ductal occluder : early results and midterm follow-up. J Tehran Heart Cent 2008; 3(3): Parra-Bravo R, Cruz-Ramírez A, Rebolledo-Pineda V, et al. Transcatheter closure of patent ductus arteriosus using the amplatzer duct occluder in infants under 1 year of age. Rev Esp Cardiol 2009; 62(8):
Transcatheter closure of the patent ductus arteriosus using the new Amplatzer duct occluder: Initial clinical applications in children
 Transcatheter closure of the patent ductus arteriosus using the new Amplatzer duct occluder: Initial clinical applications in children Basil Thanopoulos, MD, PhD, a Nikolaos Eleftherakis, MD, a Konstantinos
Transcatheter closure of the patent ductus arteriosus using the new Amplatzer duct occluder: Initial clinical applications in children Basil Thanopoulos, MD, PhD, a Nikolaos Eleftherakis, MD, a Konstantinos
TRANSCATHETER CLOSURE OF PERSISTENT DUCTUS ARTERIOSUS USING THE AMPLATZER DUCT OCCLUDER IN INFANTS
 TRANSCATHETER CLOSURE OF PERSISTENT DUCTUS ARTERIOSUS USING THE AMPLATZER DUCT OCCLUDER IN INFANTS Al-Hakim FA 1, Harahsheh AS 2 & Hijazi IS 3 ABSTRACT Background: Despite technical improvements over the
TRANSCATHETER CLOSURE OF PERSISTENT DUCTUS ARTERIOSUS USING THE AMPLATZER DUCT OCCLUDER IN INFANTS Al-Hakim FA 1, Harahsheh AS 2 & Hijazi IS 3 ABSTRACT Background: Despite technical improvements over the
Initial Human Experience. Objectives: To evaluate the feasibility, safety, and efficacy of the Occlutech VR
 Catheterization and Cardiovascular Interventions 00:00 00 (2015) Original Studies The New Occlutech V R PDA Occluder: Initial Human Experience M. A. Elbashier Abdelbasit, 1 * MBBS, MD, Mazeni Alwi, 1 MBBS,
Catheterization and Cardiovascular Interventions 00:00 00 (2015) Original Studies The New Occlutech V R PDA Occluder: Initial Human Experience M. A. Elbashier Abdelbasit, 1 * MBBS, MD, Mazeni Alwi, 1 MBBS,
Paediatrica Indonesiana
 Paediatrica Indonesiana VOLUME 53 July NUMBER 4 Original Article Transcatheter vs. surgical closure of patent ductus arteriosus: outcomes and cost analysis Mulyadi M Djer, Mochammading, Mardjanis Said
Paediatrica Indonesiana VOLUME 53 July NUMBER 4 Original Article Transcatheter vs. surgical closure of patent ductus arteriosus: outcomes and cost analysis Mulyadi M Djer, Mochammading, Mardjanis Said
Original Policy Date
 MP 7.01.46 Transcatheter Closure of Patent Ductus Arteriosus Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return
MP 7.01.46 Transcatheter Closure of Patent Ductus Arteriosus Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return
IMAGES. in PAEDIATRIC CARDIOLOGY. Abstract
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2008 Apr-Jun; 10(2): 11 17. PMCID: PMC3232589 Transcatheter closure of symptomatic aortopulmonary window in an infant F Pillekamp, 1 T Hannes, 1
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2008 Apr-Jun; 10(2): 11 17. PMCID: PMC3232589 Transcatheter closure of symptomatic aortopulmonary window in an infant F Pillekamp, 1 T Hannes, 1
Transcatheter device occlusion of patent ductus arteriosus
 CONGENITAL HEART DISEASE The New Occlutech Duct Occluder: Immediate Results, Procedural Challenges, and Short-Term Follow-Up Vikram Kudumula, MRCPCH; Demetris Taliotis, MRCPCH; Christopher Duke, FRCP ABSTRACT:
CONGENITAL HEART DISEASE The New Occlutech Duct Occluder: Immediate Results, Procedural Challenges, and Short-Term Follow-Up Vikram Kudumula, MRCPCH; Demetris Taliotis, MRCPCH; Christopher Duke, FRCP ABSTRACT:
Transcatheter Closure of Patent Ductus Arteriosus Using ADO Device: Retrospective Study of 149 Patients
 Original Article Transcatheter Closure of Patent Ductus Arteriosus Using ADO Device: Retrospective Study of 149 Patients ABSTRACT Sadiq M. Al-Hamash, Hussein Abdul Wahab 1, Zayir H. Khalid 1, Isam V. Nasser
Original Article Transcatheter Closure of Patent Ductus Arteriosus Using ADO Device: Retrospective Study of 149 Patients ABSTRACT Sadiq M. Al-Hamash, Hussein Abdul Wahab 1, Zayir H. Khalid 1, Isam V. Nasser
Complications after Transcatheter Closure of Patent Ductus Arteriosus
 J Korean Med Sci 2007; 22: 484-90 ISSN 1011-8934 Copyright The Korean Academy of Medical Sciences Complications after Transcatheter Closure of Patent Ductus Arteriosus To evaluate the short- and mid-term
J Korean Med Sci 2007; 22: 484-90 ISSN 1011-8934 Copyright The Korean Academy of Medical Sciences Complications after Transcatheter Closure of Patent Ductus Arteriosus To evaluate the short- and mid-term
Patient guide: pfm Nit-Occlud PDA coil occlusion system. Catheter occlusion of. Patent Ductus Arteriosus. with the
 Patient guide: Catheter occlusion of Patent Ductus Arteriosus with the pfm Nit-Occlud PDA coil occlusion system pfm Produkte für die Medizin - AG Wankelstr. 60 D - 50996 Cologne Phone: +49 (0) 2236 96
Patient guide: Catheter occlusion of Patent Ductus Arteriosus with the pfm Nit-Occlud PDA coil occlusion system pfm Produkte für die Medizin - AG Wankelstr. 60 D - 50996 Cologne Phone: +49 (0) 2236 96
Type Size AP/PS RP/RS Qp/Qs. Ia Resistive <0.3 < Ib Resistive <0.3 < IIa Resistive <0.5 >2
 Transcatheter closure of VSD using Duct Occluder device Nguyen Lan Hieu, MD, PhD Hanoi Medical University Vietnam Heart Institute Anatomy of VSD 1. Perimembranous VSD: Aneurysm septal membranous(tv or
Transcatheter closure of VSD using Duct Occluder device Nguyen Lan Hieu, MD, PhD Hanoi Medical University Vietnam Heart Institute Anatomy of VSD 1. Perimembranous VSD: Aneurysm septal membranous(tv or
COMPLEMENTARY TECHNIQUES OF PERCUTANEOUS CLOSURE OF DUCTUS ARTERIOSUS USING DETACHABLE COOK COILS AND AMPLATZER DEVICES
 214 East African Medical Journal July 2013 East African Medical Journal Vol. 90 No. 7 July 2013 COMPLEMENTARY TECHNIQUES OF PERCUTANEOUS CLOSURE OF DUCTUS ARTERIOSUS USING DETACHABLE COOK COILS AND AMPLATZER
214 East African Medical Journal July 2013 East African Medical Journal Vol. 90 No. 7 July 2013 COMPLEMENTARY TECHNIQUES OF PERCUTANEOUS CLOSURE OF DUCTUS ARTERIOSUS USING DETACHABLE COOK COILS AND AMPLATZER
Evaluation of Gianturco Coils for Closure of Large (> 3.5 mm) Patent Ductus Arteriosus
 1856 JACC Vol. 30, No. 7 Evaluation of Gianturco Coils for Closure of Large (> 3.5 mm) Patent Ductus Arteriosus CARL Y. OWADA, MD, DAVID F. TEITEL, MD, PHILLIP MOORE, MD San Francisco, California Objectives.
1856 JACC Vol. 30, No. 7 Evaluation of Gianturco Coils for Closure of Large (> 3.5 mm) Patent Ductus Arteriosus CARL Y. OWADA, MD, DAVID F. TEITEL, MD, PHILLIP MOORE, MD San Francisco, California Objectives.
Nit-Occlud. Coil System for PDA Closure IMPLANTATION POCKET GUIDE. Rx only CV / B. Braun Interventional Systems Inc.
 Refer to the Nit-Occlud PDA Instructions for Use for relevant warnings, precautions, complications and contraindications. This device has been designed for single use only. Nit-Occlud Coil System for PDA
Refer to the Nit-Occlud PDA Instructions for Use for relevant warnings, precautions, complications and contraindications. This device has been designed for single use only. Nit-Occlud Coil System for PDA
Journal of the American College of Cardiology Vol. 33, No. 5, by the American College of Cardiology ISSN /99/$20.
 Journal of the American College of Cardiology Vol. 33, No. 5, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00011-X Transcatheter
Journal of the American College of Cardiology Vol. 33, No. 5, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00011-X Transcatheter
Percutaneous VSD closure
 Percutaneous VSD closure Gianfranco Butera San Donato Milanese - Italy Patients selection Pts having hemodynamically significant VSD Left ventricular enlargement (left ventricular overload),defined as
Percutaneous VSD closure Gianfranco Butera San Donato Milanese - Italy Patients selection Pts having hemodynamically significant VSD Left ventricular enlargement (left ventricular overload),defined as
PDA Device Closure with and without Arterial Access
 Research Article imedpub Journals www.imedpub.com Interventional Cardiology Journal DOI: 10.21767/2471-8157.100061 Abstract PDA Device Closure with and without Arterial Access Background: PDA device closure
Research Article imedpub Journals www.imedpub.com Interventional Cardiology Journal DOI: 10.21767/2471-8157.100061 Abstract PDA Device Closure with and without Arterial Access Background: PDA device closure
Hybrid Muscular VSD Closure in Small Weight Children
 Hybrid Muscular VSD Closure in Small Weight Children Shakeel A Qureshi, on behalf of: John P. Cheatham, MD George H. Dunlap Endowed Chair in Interventional Cardiology Director Cardiac Catheterization &
Hybrid Muscular VSD Closure in Small Weight Children Shakeel A Qureshi, on behalf of: John P. Cheatham, MD George H. Dunlap Endowed Chair in Interventional Cardiology Director Cardiac Catheterization &
Case submission for CSI Asia-Pacific Case 2
 Case submission for CSI Asia-Pacific 2018- Case 2 Title Page Case category: Coarctation and ducts, valves Title: Simultaneous balloon aortic valvuloplasty with transcatheter closure of large hypertensive
Case submission for CSI Asia-Pacific 2018- Case 2 Title Page Case category: Coarctation and ducts, valves Title: Simultaneous balloon aortic valvuloplasty with transcatheter closure of large hypertensive
INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE. Krishna Kumar SevenHills Hospital, Mumbai, India
 INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE Krishna Kumar SevenHills Hospital, Mumbai, India Why talk about it? What is the big deal? Are we not stating the obvious?
INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE Krishna Kumar SevenHills Hospital, Mumbai, India Why talk about it? What is the big deal? Are we not stating the obvious?
Fabien Praz, Andreas Wahl, Sophie Beney, Stephan Windecker, Heinrich P. Mattle*, Bernhard Meier
 Procedural Outcome after Percutaneous Closure of Patent Foramen Ovale using the Amplatzer PFO Occluder Without Intra-Procedural Echocardiography in 1,000 Patients Fabien Praz, Andreas Wahl, Sophie Beney,
Procedural Outcome after Percutaneous Closure of Patent Foramen Ovale using the Amplatzer PFO Occluder Without Intra-Procedural Echocardiography in 1,000 Patients Fabien Praz, Andreas Wahl, Sophie Beney,
PDA: Closure Using Coils and Devices: Indications, Technique & Outcome
 PDA: Closure Using Coils and Devices: Indications, Technique & Outcome Daniel Levi, MD, FSCAI Associate Professor of Pediatrics UCLA Biomedical Engineering Mattel Children s Hospital at UCLA, Division
PDA: Closure Using Coils and Devices: Indications, Technique & Outcome Daniel Levi, MD, FSCAI Associate Professor of Pediatrics UCLA Biomedical Engineering Mattel Children s Hospital at UCLA, Division
Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder.
 Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder. First case with a novel delivery system. Werner Budts, Md, PhD, FESC Congenital and Structural Cardiology University
Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder. First case with a novel delivery system. Werner Budts, Md, PhD, FESC Congenital and Structural Cardiology University
Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin. Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong
 Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong Classification (by Kirklin) I. Subarterial (10%) Outlet, conal, supracristal,
Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong Classification (by Kirklin) I. Subarterial (10%) Outlet, conal, supracristal,
Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device
 273 Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device Amena Hussain MD, Muhamed Saric MD, Scott Bernstein MD, Douglas Holmes MD, Larry Chinitz MD NYU Langone Medical Center, United
273 Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device Amena Hussain MD, Muhamed Saric MD, Scott Bernstein MD, Douglas Holmes MD, Larry Chinitz MD NYU Langone Medical Center, United
A case report: Percutaneous transcatheter treatment of Lutembacher syndrome
 A case report: Percutaneous transcatheter treatment of Lutembacher syndrome Dr. Sainath Hegde* Dr. Tukaram Aute** *Registrar, Dept of Cardiology, M.G.M Hospital, Aurangabad. **Asst. Prof, Dept of Cardiology,
A case report: Percutaneous transcatheter treatment of Lutembacher syndrome Dr. Sainath Hegde* Dr. Tukaram Aute** *Registrar, Dept of Cardiology, M.G.M Hospital, Aurangabad. **Asst. Prof, Dept of Cardiology,
Pathophysiology: Left To Right Shunts
 Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
Reopening After Successful Coil Occlusion for Patent Ductus Arteriosus
 444 JACC Vol. 31, No. 2 PEDIATRIC CARDIOLOGY Reopening After Successful Coil Occlusion for Patent Ductus Arteriosus CURT J. DANIELS, MD, STEVEN C. CASSIDY, MD, FACC, DOUGLAS W. TESKE, MD, FACC, JOHN J.
444 JACC Vol. 31, No. 2 PEDIATRIC CARDIOLOGY Reopening After Successful Coil Occlusion for Patent Ductus Arteriosus CURT J. DANIELS, MD, STEVEN C. CASSIDY, MD, FACC, DOUGLAS W. TESKE, MD, FACC, JOHN J.
Atrial Septal Defect Closure. Stephen Brecker Director, Cardiac Catheterisation Labs
 Stephen Brecker Director, Cardiac Catheterisation Labs ADVANCED ANGIOPLASTY Incorporating The Left Main 5 Plus Course Conflicts of Interest The following companies have supported educational courses held
Stephen Brecker Director, Cardiac Catheterisation Labs ADVANCED ANGIOPLASTY Incorporating The Left Main 5 Plus Course Conflicts of Interest The following companies have supported educational courses held
Jian Fang 1, Shaobo Xie 2, Lunchao Ma 2, Chao Yang 2. Original Article
 Original Article Anatomic and surgical factors affecting the switch from minimally invasive transthoracic occlusion to open surgery during ventricular septal defect repair Jian Fang 1, Shaobo Xie 2, Lunchao
Original Article Anatomic and surgical factors affecting the switch from minimally invasive transthoracic occlusion to open surgery during ventricular septal defect repair Jian Fang 1, Shaobo Xie 2, Lunchao
5.8 Congenital Heart Disease
 5.8 Congenital Heart Disease Congenital heart diseases (CHD) refer to structural or functional heart diseases, which are present at birth. Some of these lesions may be discovered later. prevalence of Chd
5.8 Congenital Heart Disease Congenital heart diseases (CHD) refer to structural or functional heart diseases, which are present at birth. Some of these lesions may be discovered later. prevalence of Chd
Transcatheter closure of right coronary artery fistula to the right ventricle
 Case Report Transcatheter closure of right coronary artery fistula to the right ventricle Abstract Coronary artery fistula (CAF) is an uncommon anomaly usually congenital but can be acquired. Although,
Case Report Transcatheter closure of right coronary artery fistula to the right ventricle Abstract Coronary artery fistula (CAF) is an uncommon anomaly usually congenital but can be acquired. Although,
Trans catheter closure of large ductus arteriosus in patients with severe pulmonary hypertension: safety and efficacy of test occlusion
 Trans catheter closure of large ductus arteriosus in patients with severe pulmonary hypertension: safety and efficacy of test occlusion Sulafa KM Ali, FRCPCH, FACC Sudan Heart Institute, Department of
Trans catheter closure of large ductus arteriosus in patients with severe pulmonary hypertension: safety and efficacy of test occlusion Sulafa KM Ali, FRCPCH, FACC Sudan Heart Institute, Department of
Follow-up after VSD closure- what to look for?
 The 3rd Congress of Congenital heart disease Ventricular Septal Defect from A-Z January 9-11. 2013, Ho Chi Minh City, Vietnam Follow-up after VSD closure- what to look for? Nina Wunderlich University Hospital
The 3rd Congress of Congenital heart disease Ventricular Septal Defect from A-Z January 9-11. 2013, Ho Chi Minh City, Vietnam Follow-up after VSD closure- what to look for? Nina Wunderlich University Hospital
Transcatheter Closure of Atrial Septal Defects in a Center With Limited Resources: Outcomes and Short Term Follow-Up
 Iran J Pediatr. 2015 December; 25(6): e3906. Published online 2015 December 23. doi: 10.5812/ijp.3906 Research Article Transcatheter Closure of Atrial Septal Defects in a Center With Limited Resources:
Iran J Pediatr. 2015 December; 25(6): e3906. Published online 2015 December 23. doi: 10.5812/ijp.3906 Research Article Transcatheter Closure of Atrial Septal Defects in a Center With Limited Resources:
Efficacy and Safety of Using Amplatzer Ductal Occluder for Transcatheter Closure of Perimembranous Ventricular Septal Defect in Pediatrics
 Iran J Pediatr. 2015 April; 25(2):e386. Published online 2015 April 18. DOI: 10.5812/ijp.386 Research Article Efficacy and Safety of Using Amplatzer Ductal Occluder for Transcatheter Closure of Perimembranous
Iran J Pediatr. 2015 April; 25(2):e386. Published online 2015 April 18. DOI: 10.5812/ijp.386 Research Article Efficacy and Safety of Using Amplatzer Ductal Occluder for Transcatheter Closure of Perimembranous
1. Definition/Overview
 VCAwestlaspecialty.com VCA West Los Angeles recently performed closure of a patent ductus arteriosus via percutaneous transarterial embolization with an Amplatz canine ductal occluder on a female, four-month-old
VCAwestlaspecialty.com VCA West Los Angeles recently performed closure of a patent ductus arteriosus via percutaneous transarterial embolization with an Amplatz canine ductal occluder on a female, four-month-old
Percutaneous Coronary Intervention and Pulmonary Balloon Valvuloplasty in a Patient With Severe Valvular Pulmonary Stenosis
 Case Report Percutaneous Coronary Intervention and Pulmonary Balloon Valvuloplasty in a 56-Year-Old Woman With Severe Valvular Pulmonary Stenosis: A Case Report Ata Firouzi 1, MD; Omid Shafe* 1, MD; Farzad
Case Report Percutaneous Coronary Intervention and Pulmonary Balloon Valvuloplasty in a 56-Year-Old Woman With Severe Valvular Pulmonary Stenosis: A Case Report Ata Firouzi 1, MD; Omid Shafe* 1, MD; Farzad
For Personal Use. Copyright HMP 2013
 Case Report J INVASIVE CARDIOL 2013;25(2):E42-E44 Percutaneous Closure of Iatrogenic Ventricular Septal Defect Following Surgical Aortic Valve Replacement Using Two Different Approaches Takashi Matsumoto,
Case Report J INVASIVE CARDIOL 2013;25(2):E42-E44 Percutaneous Closure of Iatrogenic Ventricular Septal Defect Following Surgical Aortic Valve Replacement Using Two Different Approaches Takashi Matsumoto,
Congenital heart disease. By Dr Saima Ali Professor of pediatrics
 Congenital heart disease By Dr Saima Ali Professor of pediatrics What is the most striking clinical finding in this child? Learning objectives By the end of this lecture, final year student should be able
Congenital heart disease By Dr Saima Ali Professor of pediatrics What is the most striking clinical finding in this child? Learning objectives By the end of this lecture, final year student should be able
Pathophysiology: Left To Right Shunts
 Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
CONGENITAL HEART DEFECTS IN ADULTS
 CONGENITAL HEART DEFECTS IN ADULTS THE ROLE OF CATHETER INTERVENTIONS Mario Carminati CONGENITAL HEART DEFECTS IN ADULTS CHD in natural history CHD with post-surgical sequelae PULMONARY VALVE STENOSIS
CONGENITAL HEART DEFECTS IN ADULTS THE ROLE OF CATHETER INTERVENTIONS Mario Carminati CONGENITAL HEART DEFECTS IN ADULTS CHD in natural history CHD with post-surgical sequelae PULMONARY VALVE STENOSIS
AMPLATZER Septal Occluder Structural Heart Therapy. Over 15 years of. Demonstrated. Clinical Experience. We ll show you our data. Ask to see theirs.
 AMPLATZER Septal Occluder Structural Heart Therapy Over 15 years of Demonstrated Clinical Experience We ll show you our data. Ask to see theirs. Leading the Standard of Care 1,2 The AMPLATZER Septal Occluder
AMPLATZER Septal Occluder Structural Heart Therapy Over 15 years of Demonstrated Clinical Experience We ll show you our data. Ask to see theirs. Leading the Standard of Care 1,2 The AMPLATZER Septal Occluder
Transcatheter Closure of Atrial Septal Defect with Amplatzer Device in Children and Adolescents: Short and Midterm results; an Iranian Experience
 Original Article Iran J Pediatr Jun 2011; Vol 21 (No 2), Pp: 166-172 Transcatheter Closure of Atrial Septal Defect with Amplatzer Device in Children and Adolescents: Short and Midterm results; an Iranian
Original Article Iran J Pediatr Jun 2011; Vol 21 (No 2), Pp: 166-172 Transcatheter Closure of Atrial Septal Defect with Amplatzer Device in Children and Adolescents: Short and Midterm results; an Iranian
Muscular VSD Occluder
 Muscular VSD Occluder Instructions for Use Device Description The AMPLATZER Muscular VSD Occluder is a self-expanding, double-disc device made from a nitinol wire mesh. The 2 discs are linked together
Muscular VSD Occluder Instructions for Use Device Description The AMPLATZER Muscular VSD Occluder is a self-expanding, double-disc device made from a nitinol wire mesh. The 2 discs are linked together
IMAGES. in PAEDIATRIC CARDIOLOGY
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2005 Jan-Mar; 7(1): 12 17. PMCID: PMC3232568 Stent implantation for coarctation facilitated by the anterograde trans-septal approach N Sreeram and
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2005 Jan-Mar; 7(1): 12 17. PMCID: PMC3232568 Stent implantation for coarctation facilitated by the anterograde trans-septal approach N Sreeram and
Treatment of Inter-MitraClip Regurgitation Due to Posterior Leaflet Cleft by Use of The Amplatzer Vascular Plug II device
 Volume 1, Issue 3 Case Report ISSN: 2572-9292 Treatment of Inter-MitraClip Regurgitation Due to Posterior Leaflet Cleft by Use of The Amplatzer Vascular Plug II device Neha M. Mantri, Gagan D. Singh, Thomas
Volume 1, Issue 3 Case Report ISSN: 2572-9292 Treatment of Inter-MitraClip Regurgitation Due to Posterior Leaflet Cleft by Use of The Amplatzer Vascular Plug II device Neha M. Mantri, Gagan D. Singh, Thomas
Percutaneous Device Closure of Congenital VSDs Current techniques and results for treating ventricular septal defects.
 Percutaneous Device Closure of Congenital VSDs Current techniques and results for treating ventricular septal defects. BY KARIM A. DIAB, MD; QI-LING CAO, MD; AND ZIYAD M. HIJAZI, MD, MPH During the past
Percutaneous Device Closure of Congenital VSDs Current techniques and results for treating ventricular septal defects. BY KARIM A. DIAB, MD; QI-LING CAO, MD; AND ZIYAD M. HIJAZI, MD, MPH During the past
Transcatheter Closure of Atrial Septal Defects with Superior-anterior Rim Deficiency Using Amplatzer Septal Occluder
 ORIGINAL ARTICLE Transcatheter Closure of Atrial Septal Defects with Superior-anterior Rim Deficiency Using Amplatzer Septal Occluder Chien-Fu Huang, 1 Chih-Yuan Fang, 2 Sheung-Fat Ko, 3 Shao-Ju Chien,
ORIGINAL ARTICLE Transcatheter Closure of Atrial Septal Defects with Superior-anterior Rim Deficiency Using Amplatzer Septal Occluder Chien-Fu Huang, 1 Chih-Yuan Fang, 2 Sheung-Fat Ko, 3 Shao-Ju Chien,
CARDIAC INTERVENTIONS IN PEDIATRIC CARDIOLOGY: THE FUTURE
 CARDIAC INTERVENTIONS IN PEDIATRIC CARDIOLOGY: THE FUTURE Vikas Kohli From the: Senior Consultant Pediatric Cardiology, Apollo Centre of Advance Pediatrics, Indraprastha Apollo Hospitals, New Delhi-110044.
CARDIAC INTERVENTIONS IN PEDIATRIC CARDIOLOGY: THE FUTURE Vikas Kohli From the: Senior Consultant Pediatric Cardiology, Apollo Centre of Advance Pediatrics, Indraprastha Apollo Hospitals, New Delhi-110044.
Perimembranous ventricular septal defects (pmvsds) are
 Transcatheter Closure of Congenital Perimembranous Ventricular Septal Defect in Children Using Symmetric Occluders: An 8-Year Multiinstitutional Experience Lei Wang, MD, PhD,* Sancheng Cao, MD, Jun Li,
Transcatheter Closure of Congenital Perimembranous Ventricular Septal Defect in Children Using Symmetric Occluders: An 8-Year Multiinstitutional Experience Lei Wang, MD, PhD,* Sancheng Cao, MD, Jun Li,
Original Article Atrial Septal Defect (ASD) Pak Armed Forces Med J 2014; 64 (2):
 Original Article Atrial Septal Defect (ASD) Pak Armed Forces Med J 2014; 64 (2): 355-59 TRANSCATHETER DEVICE CLOSURE OF SECUNDUM ATRIAL SEPTAL DEFECT (ASD) IN YOUNG CHILDREN Nadeem Sadiq, Maad Ullah, Mehboob
Original Article Atrial Septal Defect (ASD) Pak Armed Forces Med J 2014; 64 (2): 355-59 TRANSCATHETER DEVICE CLOSURE OF SECUNDUM ATRIAL SEPTAL DEFECT (ASD) IN YOUNG CHILDREN Nadeem Sadiq, Maad Ullah, Mehboob
An aortic pseudoaneurysm (PSA) can occur
 Percutaneous Transcatheter Closure of a Large Pseudoaneurysm Arising From Anastomosis of a Surgical Graft With an Amplatzer Vascular Plug 4 Mark J. Russo, MD 1 ; Ross Milner, MD 2 ; Atman P. Shah, MD 2
Percutaneous Transcatheter Closure of a Large Pseudoaneurysm Arising From Anastomosis of a Surgical Graft With an Amplatzer Vascular Plug 4 Mark J. Russo, MD 1 ; Ross Milner, MD 2 ; Atman P. Shah, MD 2
Inadvertent ligation of the left pulmonary artery during intended ductal ligation
 DOI 10.1186/s13104-015-1467-3 CASE REPORT Open Access Inadvertent ligation of the left pulmonary artery during intended ductal ligation Endale Tefera 1*, Ramon Bermudez Cañete 2 and Carin van Doorn 3 Abstract
DOI 10.1186/s13104-015-1467-3 CASE REPORT Open Access Inadvertent ligation of the left pulmonary artery during intended ductal ligation Endale Tefera 1*, Ramon Bermudez Cañete 2 and Carin van Doorn 3 Abstract
Stent implantation into the patent ductus arteriosus in cyanotic congenital heart disease with duct-dependent or diminished pulmonary circulation
 The Turkish Journal of Pediatrics 2007; 49: 413-417 Original Stent implantation into the patent ductus arteriosus in cyanotic congenital heart disease with duct-dependent or diminished pulmonary circulation
The Turkish Journal of Pediatrics 2007; 49: 413-417 Original Stent implantation into the patent ductus arteriosus in cyanotic congenital heart disease with duct-dependent or diminished pulmonary circulation
Index. cardiology.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACHD. See Adult congenital heart disease (ACHD) Adult congenital heart disease (ACHD), 503 512 across life span prevalence of, 504 506
Index Note: Page numbers of article titles are in boldface type. A ACHD. See Adult congenital heart disease (ACHD) Adult congenital heart disease (ACHD), 503 512 across life span prevalence of, 504 506
ΔΙΑΧΕΙΡΙΣΗ ΑΣΘΕΝΩΝ ΜΕ ΜΕΣΟΚΟΛΠΙΚΗ ΕΠΙΚΟΙΝΩΝΙΑ ΖΑΧΑΡΑΚΗ ΑΓΓΕΛΙΚΗ ΚΑΡΔΙΟΛΟΓΟΣ ΗΡΑΚΛΕΙΟ - ΚΡΗΤΗ
 ΔΙΑΧΕΙΡΙΣΗ ΑΣΘΕΝΩΝ ΜΕ ΜΕΣΟΚΟΛΠΙΚΗ ΕΠΙΚΟΙΝΩΝΙΑ ΖΑΧΑΡΑΚΗ ΑΓΓΕΛΙΚΗ ΚΑΡΔΙΟΛΟΓΟΣ ΗΡΑΚΛΕΙΟ - ΚΡΗΤΗ European Accreditation in TTE, TEE and CHD Echocardiography NOTHING TO DECLARE ATRIAL SEPTAL DEFECT TYPES SECUNDUM
ΔΙΑΧΕΙΡΙΣΗ ΑΣΘΕΝΩΝ ΜΕ ΜΕΣΟΚΟΛΠΙΚΗ ΕΠΙΚΟΙΝΩΝΙΑ ΖΑΧΑΡΑΚΗ ΑΓΓΕΛΙΚΗ ΚΑΡΔΙΟΛΟΓΟΣ ΗΡΑΚΛΕΙΟ - ΚΡΗΤΗ European Accreditation in TTE, TEE and CHD Echocardiography NOTHING TO DECLARE ATRIAL SEPTAL DEFECT TYPES SECUNDUM
CoA Stenting Alexandria Experience
 CoA Stenting Alexandria Experience By Hani Mahmoud Adel, M.D Alexandria University 2/27/2017 CE 2017 Cairo 1 Coarctation of the aorta is the eighth most common form of congenital heart disease & accounts
CoA Stenting Alexandria Experience By Hani Mahmoud Adel, M.D Alexandria University 2/27/2017 CE 2017 Cairo 1 Coarctation of the aorta is the eighth most common form of congenital heart disease & accounts
Incidental Discovery of a Patent Ductus Arteriosus in Adults
 BRIEF REPORT Incidental Discovery of a Patent Ductus Arteriosus in Adults Harvey D. Cassidy, MD, Lynsey A. Cassidy, MD, and Joseph L. Blackshear, MD Patent ductus arteriosus (PDA) is an uncommon clinical
BRIEF REPORT Incidental Discovery of a Patent Ductus Arteriosus in Adults Harvey D. Cassidy, MD, Lynsey A. Cassidy, MD, and Joseph L. Blackshear, MD Patent ductus arteriosus (PDA) is an uncommon clinical
Originally Posted: November 15, 2014 BRUIT IN THE GROIN
 Originally Posted: November 15, 2014 BRUIT IN THE GROIN Resident(s): Donald ML Tse, MD Attending(s): KT Tan, MD Program/Dept(s): University Health Network/Mount Sinai Hospital, Toronto, ON, Canada CHIEF
Originally Posted: November 15, 2014 BRUIT IN THE GROIN Resident(s): Donald ML Tse, MD Attending(s): KT Tan, MD Program/Dept(s): University Health Network/Mount Sinai Hospital, Toronto, ON, Canada CHIEF
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
For Personal Use. Copyright HMP 2013
 Case Report With Brief Review J INVASIVE CARDIOL 2013;25(4):E78-E80 Percutaneous Transjugular Device Closure of Postoperative Residual Atrial Septal Defect Saktheeswaran Mahesh Kumar, MD, DM, Sasidharan
Case Report With Brief Review J INVASIVE CARDIOL 2013;25(4):E78-E80 Percutaneous Transjugular Device Closure of Postoperative Residual Atrial Septal Defect Saktheeswaran Mahesh Kumar, MD, DM, Sasidharan
6). However, for cases in which an ASO cannot
 Hiroshima J. Med. Sci. Vol. 64, No. 1 2, 1~7, June, 1 HIJM 64 1 1 A Logical Method of Selecting an Approach for Amplatzer Septal Occluder Implantation: Using Transesophageal Echocardiography to Reduce
Hiroshima J. Med. Sci. Vol. 64, No. 1 2, 1~7, June, 1 HIJM 64 1 1 A Logical Method of Selecting an Approach for Amplatzer Septal Occluder Implantation: Using Transesophageal Echocardiography to Reduce
Pattern of Congenital Heart Disease A Hospital-Based Study *Sadiq Mohammed Al-Hamash MBChB, FICMS
 Pattern of Congenital Heart Disease A Hospital-Based Study *Sadiq Mohammed Al-Hamash MBChB, FICMS ABSTRACT Background: The congenital heart disease occurs in 0,8% of live births and they have a wide spectrum
Pattern of Congenital Heart Disease A Hospital-Based Study *Sadiq Mohammed Al-Hamash MBChB, FICMS ABSTRACT Background: The congenital heart disease occurs in 0,8% of live births and they have a wide spectrum
Transcatheter Closure of Atrial Septal Defect with Amplatzer Septal Occluder in Adults: Immediate, Short, and Intermediate-Term Results
 TEHRAN HEART CENTER Original Article Transcatheter Closure of Atrial Septal Defect with Amplatzer Septal Occluder in Adults: Immediate, Short, and Intermediate-Term Results Mostafa Behjati, MD *, Mansour
TEHRAN HEART CENTER Original Article Transcatheter Closure of Atrial Septal Defect with Amplatzer Septal Occluder in Adults: Immediate, Short, and Intermediate-Term Results Mostafa Behjati, MD *, Mansour
Perventricular Closure of Muscular VSD s
 Perventricular Closure of Muscular VSD s Dr Damien Kenny, MB, MD Assistant Professor of Pediatrics Director of the Cardiac Catheterization Hybrid Suite Co-Director of the Rush Adult Congenital Heart Disease
Perventricular Closure of Muscular VSD s Dr Damien Kenny, MB, MD Assistant Professor of Pediatrics Director of the Cardiac Catheterization Hybrid Suite Co-Director of the Rush Adult Congenital Heart Disease
Anatomy & Physiology
 1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
First Transfemoral Aortic Valve Implantation In Bulgaria - Crossing The Valve With The Device Is Not Always
 ISPUB.COM The Internet Journal of Cardiology Volume 9 Number 2 First Transfemoral Aortic Valve Implantation In Bulgaria - Crossing The Valve With The Device Is Not T D, J P. Citation T D, J P.. First Transfemoral
ISPUB.COM The Internet Journal of Cardiology Volume 9 Number 2 First Transfemoral Aortic Valve Implantation In Bulgaria - Crossing The Valve With The Device Is Not T D, J P. Citation T D, J P.. First Transfemoral
Uptofate Study Summary
 CONGENITAL HEART DISEASE Uptofate Study Summary Acyanotic Atrial septal defect Ventricular septal defect Patent foramen ovale Patent ductus arteriosus Aortic coartation Pulmonary stenosis Cyanotic Tetralogy
CONGENITAL HEART DISEASE Uptofate Study Summary Acyanotic Atrial septal defect Ventricular septal defect Patent foramen ovale Patent ductus arteriosus Aortic coartation Pulmonary stenosis Cyanotic Tetralogy
Outcomes Associated with the Off-label Use of Medical Devices in Congenital Heart Disease at a Single Institute
 Original Article Print ISSN 1738-5520 On-line ISSN 1738-5555 Korean Circulation Journal Outcomes Associated with the Off-label Use of Medical Devices in Congenital Heart Disease at a Single Institute Young
Original Article Print ISSN 1738-5520 On-line ISSN 1738-5555 Korean Circulation Journal Outcomes Associated with the Off-label Use of Medical Devices in Congenital Heart Disease at a Single Institute Young
TCTAP C-217 Bilateral Pulmonary Arterio Venus Fistula Managed by Vascular Plugs and Coil Manotosh Panja 1 1 BelleVue Clinic, India
 S450 JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY, VOL. 65, NO. 17, SUPPL S, 2015 Case Summary. Aneurysm at LVOT is a rare complication after Bentall operation and the aneurysm may increase in size. In
S450 JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY, VOL. 65, NO. 17, SUPPL S, 2015 Case Summary. Aneurysm at LVOT is a rare complication after Bentall operation and the aneurysm may increase in size. In
AMPLATZER Septal Occluder
 AMPLATZER Septal Occluder A Patient s Guide to the Non-Surgical Closure of the Atrial Septal Defect Using the AMPLATZER Septal Occluder System leadership through innovation TM AGA Medical Corporation 5050
AMPLATZER Septal Occluder A Patient s Guide to the Non-Surgical Closure of the Atrial Septal Defect Using the AMPLATZER Septal Occluder System leadership through innovation TM AGA Medical Corporation 5050
Case 47 Clinical Presentation
 93 Case 47 C Clinical Presentation 45-year-old man presents with chest pain and new onset of a murmur. Echocardiography shows severe aortic insufficiency. 94 RadCases Cardiac Imaging Imaging Findings C
93 Case 47 C Clinical Presentation 45-year-old man presents with chest pain and new onset of a murmur. Echocardiography shows severe aortic insufficiency. 94 RadCases Cardiac Imaging Imaging Findings C
Transcatheter closure of atrial septal defects with transthoracic echocardiography
 Cardiology in the Young (2011), 21, 204 208 doi:10.1017/s1047951110001782 r Cambridge University Press, 2010 Original Article Transcatheter closure of atrial septal defects with transthoracic echocardiography
Cardiology in the Young (2011), 21, 204 208 doi:10.1017/s1047951110001782 r Cambridge University Press, 2010 Original Article Transcatheter closure of atrial septal defects with transthoracic echocardiography
Perventricular Closure of Muscular VSD
 Perventricular Closure of Muscular VSD John P. Cheatham, MD, MSCAI George H. Dunlap Endowed Chair in Interventional Cardiology Co-Director, The Heart Center, Nationwide Children s Hospital Professor, Pediatrics
Perventricular Closure of Muscular VSD John P. Cheatham, MD, MSCAI George H. Dunlap Endowed Chair in Interventional Cardiology Co-Director, The Heart Center, Nationwide Children s Hospital Professor, Pediatrics
Device closure of congenital ventricular septal defects with Amplatzer devices: first experiences in Turkey
 The Turkish Journal of Pediatrics 2008; 50: 106-113 Original Device closure of congenital ventricular septal defects with Amplatzer devices: first experiences in Turkey Alpay Çeliker, Süheyla Özkutlu,
The Turkish Journal of Pediatrics 2008; 50: 106-113 Original Device closure of congenital ventricular septal defects with Amplatzer devices: first experiences in Turkey Alpay Çeliker, Süheyla Özkutlu,
AORTIC COARCTATION. Synonyms: - Coarctation of the aorta
 AORTIC COARCTATION Synonyms: - Coarctation of the aorta Definition: Aortic coarctation is a congenital narrowing of the aorta, usually located after the left subclavian artery, near the ductus or the ligamentum
AORTIC COARCTATION Synonyms: - Coarctation of the aorta Definition: Aortic coarctation is a congenital narrowing of the aorta, usually located after the left subclavian artery, near the ductus or the ligamentum
Transcatheter Closure of Fenestration with Detachable Coils After the Fontan Operation
 J Korean Med Sci 2006; 21: 859-64 ISSN 1011-8934 Copyright The Korean Academy of Medical Sciences Transcatheter Closure of Fenestration with Detachable Coils After the Fontan Operation We report our experience
J Korean Med Sci 2006; 21: 859-64 ISSN 1011-8934 Copyright The Korean Academy of Medical Sciences Transcatheter Closure of Fenestration with Detachable Coils After the Fontan Operation We report our experience
IMAGES. in PAEDIATRIC CARDIOLOGY
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2006 Jul-Sep; 8(3): 1 6. PMCID: PMC3232564 A large, single pulmonary arteriovenous fistula presenting hours after birth AH McBrien, 1 AJ Sands,
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2006 Jul-Sep; 8(3): 1 6. PMCID: PMC3232564 A large, single pulmonary arteriovenous fistula presenting hours after birth AH McBrien, 1 AJ Sands,
2) VSD & PDA - Dr. Aso
 2) VSD & PDA - Dr. Aso Ventricular Septal Defect (VSD) Most common cardiac malformation 25-30 % Types of VSD: According to position perimembranous, inlet, muscular. According to size small, medium, large.
2) VSD & PDA - Dr. Aso Ventricular Septal Defect (VSD) Most common cardiac malformation 25-30 % Types of VSD: According to position perimembranous, inlet, muscular. According to size small, medium, large.
Paediatrics Revision Session Cardiology. Emma Walker 7 th May 2016
 Paediatrics Revision Session Cardiology Emma Walker 7 th May 2016 Cardiovascular Examination! General:! Make it fun!! Change how you act depending on their age! Introduction! Introduce yourself & check
Paediatrics Revision Session Cardiology Emma Walker 7 th May 2016 Cardiovascular Examination! General:! Make it fun!! Change how you act depending on their age! Introduction! Introduce yourself & check
Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism A pulmonary embolism (PE) is
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism A pulmonary embolism (PE) is
Transcatheter closure of ventricular septal defects with nitinol wire occluders of type patent ductus arteriosus
 Pediatric cardiology Transcatheter closure of ventricular septal defects with nitinol wire occluders of type patent ductus arteriosus Arkadiusz Wierzyk 1, Małgorzata Szkutnik 1, Roland Fiszer 1, Paweł
Pediatric cardiology Transcatheter closure of ventricular septal defects with nitinol wire occluders of type patent ductus arteriosus Arkadiusz Wierzyk 1, Małgorzata Szkutnik 1, Roland Fiszer 1, Paweł
Transcatheter closure of patent foramen ovale using the internal jugular venous approach
 New methods in diagnosis and therapy Transcatheter closure of patent foramen ovale using the internal jugular venous approach Przemysław Węglarz 1,2, Ewa Konarska-Kuszewska 2, Tadeusz Zębik 2, Piotr Kuszewski
New methods in diagnosis and therapy Transcatheter closure of patent foramen ovale using the internal jugular venous approach Przemysław Węglarz 1,2, Ewa Konarska-Kuszewska 2, Tadeusz Zębik 2, Piotr Kuszewski
Secundum atrial septal defect (ASD) is a common congenital heart disease and
 Device closure of atrial septal defects with the Amplatzer septal occluder: Safety and outcome in infants Karim A. Diab, MD, a Qi-Ling Cao, MD, a Emile A. Bacha, MD, b and Ziyad M. Hijazi, MD, MPH a Objective:
Device closure of atrial septal defects with the Amplatzer septal occluder: Safety and outcome in infants Karim A. Diab, MD, a Qi-Ling Cao, MD, a Emile A. Bacha, MD, b and Ziyad M. Hijazi, MD, MPH a Objective:
Successful Percutaneous Closure of Mitral Bioprosthetic Paravalvular Leak Using Figulla ASD Occluder
 Hans R. Figulla, M.D., PhD ; Ali Hamadanchi, M.D. Medicine, Pneumology Universitity Hospital, Jena, Germany Successful Percutaneous Closure of Mitral Bioprosthetic Paravalvular Leak Using Figulla ASD Occluder
Hans R. Figulla, M.D., PhD ; Ali Hamadanchi, M.D. Medicine, Pneumology Universitity Hospital, Jena, Germany Successful Percutaneous Closure of Mitral Bioprosthetic Paravalvular Leak Using Figulla ASD Occluder
Risk Factors and Outcomes of Post-Procedure Heart Blocks After Transcatheter Device Closure of Perimembranous Ventricular Septal Defect
 JACC: CARDIOVASCULAR INTERVENTIONS VOL. 5, NO. 4, 2012 2012 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION ISSN 1936-8798/$36.00 PUBLISHED BY ELSEVIER INC. DOI: 10.1016/j.jcin.2012.01.015 Risk Factors
JACC: CARDIOVASCULAR INTERVENTIONS VOL. 5, NO. 4, 2012 2012 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION ISSN 1936-8798/$36.00 PUBLISHED BY ELSEVIER INC. DOI: 10.1016/j.jcin.2012.01.015 Risk Factors
Devices to Protect Against Stroke in Atrial Fibrillation
 Devices to Protect Against Stroke in Atrial Fibrillation Jonathan C. Hsu, MD, MAS Associate Clinical Professor Division of Cardiology, Section of Cardiac Electrophysiology June 2, 2018 Disclosures Honoraria
Devices to Protect Against Stroke in Atrial Fibrillation Jonathan C. Hsu, MD, MAS Associate Clinical Professor Division of Cardiology, Section of Cardiac Electrophysiology June 2, 2018 Disclosures Honoraria
Development of catheter-based treatment of patent ductus arteriosus: A medium-sized centre experience
 Archives of Cardiovascular Disease (2009) 102, 111 118 CLINICAL RESEARCH Development of catheter-based treatment of patent ductus arteriosus: A medium-sized centre experience Fermeture percutanée du canal
Archives of Cardiovascular Disease (2009) 102, 111 118 CLINICAL RESEARCH Development of catheter-based treatment of patent ductus arteriosus: A medium-sized centre experience Fermeture percutanée du canal
Pediatric Echocardiography Examination Content Outline
 Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Screening for Critical Congenital Heart Disease
 Screening for Critical Congenital Heart Disease Caroline K. Lee, MD Pediatric Cardiology Disclosures I have no relevant financial relationships or conflicts of interest 1 Most Common Birth Defect Most
Screening for Critical Congenital Heart Disease Caroline K. Lee, MD Pediatric Cardiology Disclosures I have no relevant financial relationships or conflicts of interest 1 Most Common Birth Defect Most
Debate: Should Ductal Stent Implantation be Considered for All Newborn Infants with Reduced Pulmonary Blood Flow?_Pros
 Debate: Should Ductal Stent Implantation be Considered for All Newborn Infants with Reduced Pulmonary Blood Flow?_Pros Mazeni Alwi Institut Jantung Negara Kuala Lumpur, Malaysia 5 th Asia Pacific Congenital
Debate: Should Ductal Stent Implantation be Considered for All Newborn Infants with Reduced Pulmonary Blood Flow?_Pros Mazeni Alwi Institut Jantung Negara Kuala Lumpur, Malaysia 5 th Asia Pacific Congenital
Balloon Catheter Test in Patients with Atrial Septal Defect and Patent Ductus Arteriosus
 Balloon Catheter Test in Patients with Atrial Septal Defect and Patent Ductus Arteriosus Takeo SAKURAI, M.D., Hideaki HOSHINO, M.D., Yoshio SUZUKI, M.D., Hideki YOKOI, M.D., Kozo SAKANAKA, M.D., Katsumi
Balloon Catheter Test in Patients with Atrial Septal Defect and Patent Ductus Arteriosus Takeo SAKURAI, M.D., Hideaki HOSHINO, M.D., Yoshio SUZUKI, M.D., Hideki YOKOI, M.D., Kozo SAKANAKA, M.D., Katsumi
Transcatheter Closure of Secundum Atrial Septal Defects in the Elderly
 REVIEW DOI 10.4070 / kcj.2009.39.2.47 Print ISSN 1738-5520 / On-line ISSN 1738-5555 Copyright c 2009 The Korean Society of Cardiology Transcatheter Closure of Secundum Atrial Septal Defects in the Elderly
REVIEW DOI 10.4070 / kcj.2009.39.2.47 Print ISSN 1738-5520 / On-line ISSN 1738-5555 Copyright c 2009 The Korean Society of Cardiology Transcatheter Closure of Secundum Atrial Septal Defects in the Elderly
Reliability of Echocardiography Measurement of Patent Ductus Arteriosus Minimum Diameter: A Meta-analysis
 International Journal of Cardiovascular and Cerebrovascular Disease 4(): 15-19, 016 DOI: 10.13189/ijccd.016.04001 http://www.hrpub.org Reliability of Echocardiography Measurement of Patent Ductus Arteriosus
International Journal of Cardiovascular and Cerebrovascular Disease 4(): 15-19, 016 DOI: 10.13189/ijccd.016.04001 http://www.hrpub.org Reliability of Echocardiography Measurement of Patent Ductus Arteriosus
Διαδερμική θεραπεία των παραβαλβιδικών διαφυγών Σ.Ράμμος
 ΔΜΙΝΑΡΙΟ ΔΠΙΣΗΜΟΝΙΚΩΝ ΔΝΩΔΩΝ ΔΛΛΗΝΙΚΟΤ ΚΟΛΛΔΓΙΟΤ ΚΑΡ ΙΟΛΟΓΙΑ 2-4.10.2015 Δπιζηημονική Ένωζη Δπεμβαηικής Καρδιολογίας Βαλβιδοπάθειες, Γιαδερμικές παρεμβάζεις Διαδερμική θεραπεία των παραβαλβιδικών διαφυγών
ΔΜΙΝΑΡΙΟ ΔΠΙΣΗΜΟΝΙΚΩΝ ΔΝΩΔΩΝ ΔΛΛΗΝΙΚΟΤ ΚΟΛΛΔΓΙΟΤ ΚΑΡ ΙΟΛΟΓΙΑ 2-4.10.2015 Δπιζηημονική Ένωζη Δπεμβαηικής Καρδιολογίας Βαλβιδοπάθειες, Γιαδερμικές παρεμβάζεις Διαδερμική θεραπεία των παραβαλβιδικών διαφυγών
Percutaneous closure of large VSD using a home-made fenestrated atrial septal occluder in 18-year-old with pulmonary hypertension
 Kamali et al. BMC Cardiovascular Disorders 2014, 14:74 CASE REPORT Percutaneous closure of large VSD using a home-made fenestrated atrial septal occluder in 18-year-old with pulmonary hypertension Hacer
Kamali et al. BMC Cardiovascular Disorders 2014, 14:74 CASE REPORT Percutaneous closure of large VSD using a home-made fenestrated atrial septal occluder in 18-year-old with pulmonary hypertension Hacer
PATENT DUCTUS ARTERIOSUS (PDA)
 PATENT DUCTUS ARTERIOSUS (PDA) It is a channel that connect the pulmonary artery with the descending aorta (isthumus part). It results from the persistence of patency of the fetal ductus arteriosus after
PATENT DUCTUS ARTERIOSUS (PDA) It is a channel that connect the pulmonary artery with the descending aorta (isthumus part). It results from the persistence of patency of the fetal ductus arteriosus after
The 1st transvascular patent ductus arteriosus
 J Vet Intern Med 2012;26:85 92 Occlusion Devices and Approaches in Canine Patent Ductus Arteriosus: Comparison of Outcomes M. K. Singh, M. D. Kittleson, P. H. Kass, and L. G. Griffiths Background: A comparison
J Vet Intern Med 2012;26:85 92 Occlusion Devices and Approaches in Canine Patent Ductus Arteriosus: Comparison of Outcomes M. K. Singh, M. D. Kittleson, P. H. Kass, and L. G. Griffiths Background: A comparison
