Leukocyte depletion has been implicated in attenuating
|
|
|
- Alexis Snow
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLES: CARDIOVASCULAR Leukocyte Depletion During Cardiac Operation: A New Approach Through the Venous Bypass Circuit Y. John Gu, MD, PhD, A. J. de Vries, MD, Paulien Vos, Piet W. Boonstra, MD, PhD, and Willem van Oeveren, PhD Departments of Cardiothoracic Surgery and Anaesthesiology, University Hospital Groningen, Groningen, the Netherlands Background. Leukocyte depletion recently has been introduced for cardiac surgical patients to attenuate leukocyte-mediated inflammation and organ reperfusion injury. We evaluated the feasibility of a new leukocyte depletion method in which systemic leukocyte depletion is achieved through the venous side of the cardiopulmonary bypass circuit under low blood flow. Methods. Forty cardiac surgical patients undergoing cardiopulmonary bypass were allocated randomly to a leukocyte depletion group and a control group. In the depletion group, leukocyte filtration was achieved with two filter sets located between the venous drainage and the venous reservoir. Leukocyte filtration was commenced after the start of rewarming but before the release of the aortic cross-clamp, and it was driven by a spare roller pump of the heart-lung machine. Results. All the episodes of filtration went smoothly within a period of 10 minutes and with a blood flow rate of 400 ml/min. The mean leukocyte removal rate calculated at the end of filtration was 69%. Circulating leukocytes were reduced by 38% in the depletion group compared with the control group at the moment of crossclamp release ( /L versus /L, p < 0.05). The postoperative inflammatory response also was reduced as indicated by less production of interleukin-8 (p < 0.05). Clinically, there was no significant difference between the two groups in postoperative PaO 2 or pulmonary hemodynamics. Conclusions. It is technically feasible to deplete circulating leukocytes through the venous side of the cardiopulmonary bypass circuit with a low blood flow rate. Future studies should focus on the duration and timing of leukocyte depletion to optimize the methodology of leukocyte depletion for cardiac surgical patients. (Ann Thorac Surg 1999;67:604 9) 1999 by The Society of Thoracic Surgeons Leukocyte depletion has been implicated in attenuating the leukocyte-mediated inflammatory response and organ injury in different experimental models of cardiac operations [1 3]. Clinically, at least three types of leukocyte-depleting techniques for cardiac surgical patients have been introduced since the early 1990s: an arterial line filter located on the arterial side of the extracorporeal circuit, a leukocyte-depleting filter for blood cardioplegia, and a transfusion filter for depleting leukocytes from the residual blood in the heart-lung machine at the end of cardiopulmonary bypass (CPB) [4 15]. For systemic leukocyte depletion from the CPB circuit, an arterial line leukocyte-depleting filter is used, usually from the initiation of CPB [6, 8, 11, 14]. The advantage of this method is the combination of the leukocytedepleting filter with the conventional arterial line filter. However, the filter is located on the arterial side of the circuit and thus is confronted with a high rate of blood flow, which may reduce its efficiency [3, 8]. We used a new clinical leukocyte depletion method in which systemic leukocyte depletion is achieved through the venous side of the CPB circuit. Using this approach, Accepted for publication July 13, Address reprint requests to Dr van Oeveren, Blood Interaction Research, Department of Cardiothoracic Surgery, University Hospital Groningen, Bloemsingel 10, 9712 KZ Groningen, the Netherlands. we started the process of leukocyte depletion during the middle period of CPB before the reperfusion phase and with a low rate of blood flow. We evaluated whether this method was technically feasible for depleting circulating leukocytes during CPB, and whether this temporary depletion method would affect patient outcome after cardiac operations. Patients and Methods Patients Forty patients undergoing coronary artery bypass grafting, heart valve replacement, or a combined procedure were included in this study. The patients were allocated randomly to a leukocyte depletion group and a control group. The study protocol was approved by the Medical Ethics Committee of the University Hospital in Groningen, The Netherlands, and informed consent was obtained from all the patients. Patients who had a history of allergy, infection, or preoperative pulmonary dysfunction were not included. The demographic data of the patients in both groups are listed in Table 1. Anesthesia Anesthesia was induced and maintained through the intravenous infusion of sufentanil citrate (1 to 3 g/kg) and midazolam (0.05 to 0.1 mg/kg). Muscle relaxation was 1999 by The Society of Thoracic Surgeons /99/$20.00 Published by Elsevier Science Inc PII S (99)
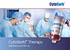
2 Ann Thorac Surg GU ET AL 1999;67:604 9 LEUKODEPLETION THROUGH A VENOUS CPB CIRCUIT 605 Table 1. Patient Demographic Information Characteristic Study Group a Leukodepletion Control p Value Age (y) Sex Male Female Height (cm) Weight (kg) Body surface area (m 2 ) CPB time (min) Cross-clamp time (min) a Values are means plus or minus standard deviation unless otherwise indicated. CPB cardiopulmonary bypass. achieved with pancuronium bromide (100 to 140 g/kg). Cefamandole (2 g) and dexamethasone (1 mg/kg) were administered after the induction of anesthesia. Anticoagulation was achieved through the intravenous administration of bovine lung heparin (300 IU/kg) about 5 minutes before the start of CPB. Cardiopulmonary Bypass The CPB circuit consisted of roller pumps (Stöckert Instrumentation, Munich, Germany) and a microporous polypropylene membrane oxygenator (CML Excel; Cobe Laboratories Inc, Lakewood, CO), and it was primed with 1,500 ml of Ringer s lactate solution plus 500 ml of 10% hydroxyethyl starch solution (Fresenius, Bad Homburg, Germany). Myocardial preservation during aortic crossclamping was achieved with 1LofSt. Thomas cardioplegia solution (4 C) infused into the aortic root. During CPB, moderate hypothermia was applied with a pump flow of 2.4 L min 1 m 2. Anticoagulation during CPB was monitored with the celite-activated clotting time (International Technidyne Co, Edison, NJ). After CPB, 3 mg/kg of protamine chloride was administered to neutralize the effect of heparin. Leukocyte Depletion Method Leukocyte depletion during CPB was achieved with the use of two Pall Duplex filter sets (J1647G; Pall Biomedical, Portsmouth, United Kingdom) equivalent to four transfusion leukocyte-depleting filters, as reported previously [13]. The filtration circuit was located between the venous drainage and the venous reservoir and was driven by a separate roller pump (Fig 1). Leukocyte depletion was performed during CPB after the start of rewarming but before the release of the aortic cross-clamp. For each filter set, 2,000 ml of the CPB perfusate was filtered at a flow rate of 400 ml/min. The total blood volume for filtration was 4,000 ml, and the entire filtration procedure was completed within 10 minutes. Efficiency of Leukocyte Removal by Filters At the end of each filtration period, blood samples were taken from the inlet and outlet of each filter set. Leukocytes, granulocytes, lymphocytes, and platelets were counted by an electronic cell counter (Cell-Dyn 610; Sequoia Turner, Mountain View, CA). The cell removal rate was calculated according the following fomula: (1 count outlet /count inlet ) 100. Efficiency of Leukocyte Removal in Patients Blood samples from patients were taken from the radial arterial catheter before operation, at several points during CPB, at the end of CPB, at the end of operation during skin closure, 1 hour and 3 hours after transfer to the intensive care unit, and at 6 am the next morning in the intensive care unit. Circulating leukocytes were counted by the Cell-Dyn electronic counter. Further, levels of inflammatory mediators were determined mainly during the postoperative course in 10 patients in each group. For these tests, leukocyte activation was indicated by elastase activity determined by an enzyme immunoassay (Kordia, Leiden, the Netherlands) and the soluble form of l- selectin (R & D Systems Europe, Abingdon, United Kingdom). Cytokine release was indicated by levels of interleukin-8 (Amersham International Inc, Buckinghamshire, United Kingdom). Clinically, pulmonary gas exchange function was determined by the partial arterial oxygen pressure (Pao 2 ) standardized at a 40% fraction of the inspired oxygen. Postoperative intubation time and blood loss were recorded from the intensive care data sheet. Length of stay in the intensive care unit and in the hospital were obtained from hospital registration records. Fig 1. Leukocyte depletion through the venous side of the cardiopulmonary bypass (CPB) circuit. The leukocyte-depleting filter is located between the venous drainage and the venous reservoir, with a side-line circuit driven by a separate roller pump with a low rate of blood flow.
3 606 GU ET AL Ann Thorac Surg LEUKODEPLETION THROUGH A VENOUS CPB CIRCUIT 1999;67:604 9 Table 2. Rate of Cell Removal by Leukocyte-depleting Filters a Type of Cell No. of Filtration Inlet ( 10 9 /L) Cell Count Outlet ( 10 9 /L) Removal (%) Leukocytes First set ( ) 1.5 ( ) 68.1 ( ) Second set ( ) 1.5 ( ) 69.6 ( ) Average ( ) 1.5 ( ) 68.8 ( ) Granulocytes First set ( ) 1.0 ( ) 73.5 ( ) Second set ( ) 1.0 ( ) 76.0 ( ) Average ( ) 1.0 ( ) 74.7 ( ) Lymphocytes First set ( ) 0.5 ( ) 45.0 (0 85.7) Second set ( ) 0.5 ( ) 49.4 (0 85.7) Average ( ) 0.5 ( ) 47.1 (0 85.7) Platelets First set (59 182) 72 (4 168) 33.7 (0 94.0) Second set (33 178) 74 (27 158) 22.3 (0 40.4) Average (33 182) 73 (4 168) 28.2 (0 94.0) a Blood samples were taken from both the inlet and the outlet of each filter set after the filtration of 2,000 ml of blood during cardiopulmonary bypass. Data are means with range in parentheses. Statistics Data for cell counts are expressed as means with the minimal and maximal counts in parentheses except where otherwise indicated. Data for the inflammatory markers and the postoperative observations are expressed as means plus or minus standard deviation. The Student s t-test or the Mann-Whitney U test was used for comparing differences between the two groups. A p value of less than 0.05 was considered statistically significant. Fig 2. The leukocyte removal rate (efficiency) is similar between the first and second filter sets in individual patients undergoing leukocyte depletion, suggesting that the efficiency of leukocyte depletion during cardiopulmonary bypass is patient-related rather than filter-related. in both the depletion and control groups (Fig 4). After filtration, the count was significantly lower in the depletion group than in the control group at the moment of aortic cross-clamp release ( /L versus /L, p 0.05), reflecting a 38% reduction in circulating leukocytes. After release of the cross-clamp during the reperfusion period, the leukocyte count increased quickly to /L in the depletion group, which Results Leukocyte Removal by Filters The mean overall leukocyte removal rate was 69% as evaluated at the end of filtration (Table 2). Equivalent granulocye, lymphocyte, and platelet removal rates were 75%, 47%, and 28%, respectively. A large variation in the leukocyte removal rate was observed between patients. However, for any one patient, the leukocyte removal rate for the first filter set was similar to the removal rate for the second filter set (r 0.918, p 0.01) (Fig 2). The leukocyte removal rate was positively correlated with the nasopharyngeal temperature during CPB as recorded before the start of filtration (r 0.498, p 0.05) (Fig 3). In addition, the leukocyte removal rate was negatively correlated with the aortic cross-clamp time (r 0.505, p 0.05), but was not correlated with the preoperative soluble l-selectin level (r 0.356) or with the prefiltration systemic leukocyte count (r 0.089). Leukocyte Depletion in Patients Before CPB and before the start of leukocyte filtration during CPB, the circulating leukocyte count was similar Fig 3. Relation between the leukocyte removal rate (data drawn from the first filter set) and the nasopharyngeal temperature recorded before filtration in the 20 patients who underwent leukocyte depletion. A low temperature tended to reduce the efficiency of leukocyte depletion during cardiopulmonary bypass.
4 Ann Thorac Surg GU ET AL 1999;67:604 9 LEUKODEPLETION THROUGH A VENOUS CPB CIRCUIT 607 Table 4. Postoperative Observations a Observation Study Group Leukodepletion Control p Value Pao 2 on arrival in ICU (kpa) Pao 2 at extubation (kpa) Intubation time (h) Urine output (ml/24 h) 2, , Blood loss (ml/24 h) ICU stay (d) Hospital stay (d) a Values are means plus or minus standard deviation. Fig 4. Circulating leukocyte count during cardiopulmonary bypass (CPB) and during the postoperative period in the intensive care unit (ICU) in the leukocyte depletion group and the control group. Data are expressed as means plus or minus the standard error of the mean. The arrow indicates the start of 10 minutes of filtration. T1 before CPB; T2 before filtration; T3 end of filtration; T4 aortic cross-clamp release; T5 5 minutes after clamp release; T6 end of CPB; T7 end of operation; T8 1 hour in ICU; T9 3 hours in ICU; T10 next morning in ICU. *p 0.05 between the two groups. was similar to the count of /L in the control group. Leukocytosis developed in both groups during the postoperative period and lasted until the next morning. Inflammatory Mediators The concentration of interleukin-8 was very low in both the depletion and control groups before CPB. It increased in both groups during CPB and postoperatively in the intensive care unit, but was significantly lower in the depletion group than in the control group ( p 0.05) (Table 3). The level of leukocyte elastase was slightly lower in the depletion group than in the control group during and after CPB. The soluble form of l-selectin was decreased in both groups during and after CPB; there was no significant difference between the two groups. Clinical Observations On arrival in the intensive care unit, the Pao 2 was at 40%, Fio 2 was kilopascal in the depletion group and ICU intensive care unit; kilopascal in the control group; there was no statistical difference between the two groups. In addition, the Pao 2 was similar between the two groups after extubation. Further, there was no statistical difference between the two groups with regard to the intubation time, urine output, blood loss, or intensive care unit or hospital stay (Table 4). Comment kpa kilopascal. Leukocyte depletion is a relatively new technique for attenuating the unwanted inflammatory response in cardiac surgical patients [16 18]. As a systemic approach that targets the circulating leukocytes, the arterial line filter is the only practical method available. Although several studies have suggested that this filter is associated with a reduction in circulating leukocytes [6, 11, 14], it faces a very high rate of blood flow during perfusion. Our current study demonstrated that 10 minutes of leukocyte depletion under a low rate of blood flow, achieved with a duplex filter set located on the venous side of the CPB circuit, resulted in a 38% reduction in circulating leukocytes at the moment of aortic crossclamp release compared with control. It proved technically feasible to locate a leukocyte removal filter between the venous drainage and the venous reservoir. For adequate bodily perfusion during CPB for adult Table 3. Levels of Inflammatory Mediators Before and After Operation a Inflammatory Mediator Before CPB End of CPB 1 Hour in ICU 3 Hours in ICU POD 1 Interleukin-8 (pg/ml) Depletion b Control Elastase (ng/ml) Depletion Control Soluble l-selectin (ng/ml) Depletion Control a Values are means plus or minus standard deviation; b p 0.05 compared with control. CPB cardiopulmonary bypass; ICU intensive care unit; POD postoperative day.
5 608 GU ET AL Ann Thorac Surg LEUKODEPLETION THROUGH A VENOUS CPB CIRCUIT 1999;67:604 9 patients, a high rate of blood flow (as high as 4,000 ml/min or more) is required on the arterial side of the CPB circuit. Although the arterial line leukocytedepleting filter is designed to accommodate such a high rate of flow, it has been described as relatively inefficient at the beginning of CPB [3]. Using the current method through the venous side of the CPB circuit, the rate of blood flow for leukocyte depletion can be reduced considerably. It is conceivable that a high rate of blood flow exerts a greater hemodynamic force that is likely to propel leukocytes through the filter, whereas a lower rate of blood flow allows a longer contact time between the leukocytes and the filter medium, a mechanism that is known to promote leukocyte adhesion to the filter medium [19]. In this study, the mean leukocyte removal rate was 69% as calculated across the filter at the end of filtration. This filter efficiency was lower than expected; we previously obtained a much higher filter efficiency by filtering the residual blood in the heart-lung machine using a similar rate of blood flow [13]. However, a major difference between the two studies was the method of blood sampling used. In the previous study, a blood sample was taken at the end of filtration from a retention bag containing a mixture of all the filtered blood. The result reflected the average efficiency over the entire period of filtration. In the current study, however, the blood sample was taken at the end of filtration from the outlet of the filtration circuit. This represents the lowest removal rate, because it is known that filtration efficiency can decrease as the volume of blood filtered increases. Therefore, the overall leukocyte removal rate would be higher than estimated. In this study, an interesting phenomenon was noted with regard to the efficiency of leukocyte filters during CPB. Although the leukocyte removal rates were variable between patients, in any individual patient, the leukocyte removal rate of the first filter set bore a close relation to that of the second filter set (Fig 2). This suggests that patient-related factors, rather than varying capacity of the filters, may influence the efficiency of leukocyte depletion during CPB. Several possible factors were investigated. First, temperature may influence leukocyte depletion during CPB, because temperature is known to influence leukocyte adhesion [20, 21]. In this study, a positive correlation was found between the nasopharyngeal temperature before the start of filtration and the efficiency of leukocyte removal, suggesting that hypothermia tends to reduce the efficiency of leukocyte depletion during CPB. Second, medication given before operation may affect leukocyte adhesion (eg, the use of the cyclooxygenase inhibitor, aspirin). However, we could not find a relation between the efficiency of leukocyte depletion and the preoperative use of aspirin or the preoperative concentration of the leukocyte activation marker, soluble l-selectin. Finally, the systemic leukocyte count before filtration seems less likely to play a role in the efficiency of leukocyte removal, because no relation was found between these two variables. Clinically, this temporary filtration protocol did not improve lung function, although a reduced interleukin-8 concentration was observed in patients who underwent leukocyte depletion. The timing of leukocyte filtration in this study may have influenced the overall outcome of systemic leukocyte depletion. Initiating leukocyte depletion before the release of the aortic cross-clamp is theoretically attractive for reducing leukocyte-mediated lung injury during the reperfusion period. However, this attempt is counteracted by concomitant rewarming of the systemic blood, which is known to contribute to systemic leukocytosis. Further, the duration of leukocyte depletion must be considered. The 10-minute filtration protocol used in the current study was chosen based on calculations of filter efficiency from our previous study [13]. A protocol of such short duration apparently is insufficient for targeting the circulating leukocytes during rewarming. However, a longer period of filtration may deplete sufficient leukocytes but be complicated by the potential release of elastase from trapped leukocytes [8]. One possible disadvantage of this method is that a separate filter circuit with a roller pump is required to allow low-flow filtration. However, this is not a practical problem, because most heart-lung machines contain at least one spare pump head and most perfusionists are familiar with the installation of and perfusion with a parallel circuit (eg, a hemofiltration circuit). This method may have an advantage in that the filter and its circuit, like the hemofiltration circuit, can be installed by the perfusionist at any time during CPB without the preinstallation required by the custom packs. We conclude that it is technically feasible to install a leukocyte filter device on the venous side of the CPB circuit that is driven by a separate roller pump using a low rate of blood flow. Ten minutes of leukocyte depletion before the reperfusion phase using this method achieved a 38% reduction in circulating leukocytes. Postoperatively, this temporary leukocyte depletion method resulted in a reduction in interleukin-8 production but not an improvement in lung function. This study poses additional questions about systemic leukocyte depletion during CPB, such as the optimal duration and timing of leukocyte depletion, that need to be explored further to optimize the overall methodology of leukocyte depletion for cardiac surgical patients. We acknowledge the technical support and sponsorship provided by Pall Biomedical UK, and the cooperation of the perfusion staff of the University Hospital in Groningen. References 1. Breda MA, Drinkwater DC, Laks H, et al. Prevention of reperfusion injury in the neonatal heart with leukocytedepleted blood. J Thorac Cardiovasc Surg 1989;97: Bando K, Pillai R, Cameron DE, et al. Leukocyte depletion ameliorates free radical-mediated lung injury after cardiopulmonary bypass. J Thorac Cardiovasc Surg 1990;99: Bolling KS, Halldorsson A, Allen BS, et al. Prevention of the hypoxic reoxygenation injury with the use of a leukocytedepleting filter. J Thorac Cardiovasc Surg 1997;113: Gu YJ, Obster R, Gallandat Huet RCG, Eijgelaar A, van Oeveren W. Leukocyte depletion reduces the postoperative
6 Ann Thorac Surg GU ET AL 1999;67:604 9 LEUKODEPLETION THROUGH A VENOUS CPB CIRCUIT 609 inflammatory response in patients following open-heart surgery. Intensive Care Med 1992;18:(Suppl 1):S Pearl JM, Drinkwater DC, Laks H, Capouya ER, Gates RN. Leukocyte-depleted reperfusion of transplanted human hearts: a randomized, double-blind clinical trial. J Heart Lung Transplant 1992;11: Palanzo DA, Manley NJ, Montesano RM, Yeisley GL, Gordon D. Clinical evaluation of the LeukoGuard (LG-6) arterial line filter for routine open-heart surgery. Perfusion 1993;8: Sawa Y, Matsuda H, Shimazaki Y, et al. Evaluation of leukocyte-depleted terminal blood cardioplegic solution in patients undergoing elective and emergency coronary artery bypass grafting. J Thorac Cardiovasc Surg 1994;108: Mihaljevic T, Tönz M, von Segesser LK, et al. The influence of leukocyte filtration during cardiopulmonary bypass on postoperative lung function. A clinical study. J Thorac Cardiovasc Surg 1995;109: De Vries AJ, Gu YJ, Boonstra PW, van Oeveren W. Transfusion of leucocyte-depleted heart-lung machine blood improves lung function following cardiopulmonary bypass. Br J Anaesth 1995;74(Suppl): Hachida M, Hanayama N, Okamura T, et al. The role of leukocyte depletion in reducing injury to myocardium and lung during cardiopulmonary bypass. ASAIO J 1995;41: M Johnson D, Thomson D, Mycyk T, Burbridge B, Mayers I. Depletion of neutrophils by filter during aortocoronary bypass surgery transiently improves postoperative cardiorespiratory status. Chest 1995;107: Gu YJ, de Vries AJ, Boonstra PW, van Oeveren W. Clinical performance of a high-efficiency rapid flow leucocyte removal filter for leucocyte depletion of heparinized cardiopulmonary bypass perfusate. Perfusion 1995;10: Gu YJ, de Vries AJ, Boonstra PW, van Oeveren W. Leukocyte depletion results in improved lung function and reduced inflammatory response after cardiac surgery. J Thorac Cardiovasc Surg 1996;112: Thurlow PJ, Doolan L, Sharp R, Sullivan M, Smith B, Andersen LW. Laboratory studies of the effect of Pall extracorporeal leucocyte filters LG6 and AV6 on patients undergoing coronary bypass grafts. Perfusion 1996;11: Allen BS, Rahman S, Ilbawi MN, et al. Detrimental effects of cardiopulmonary bypass in cyanotic infants: preventing the reoxygenation injury. Ann Thorac Surg 1997;64: Silvey G, Ammar T, Reich DL, Vele-Cantos F, Joffe D, Ergin AM. Cardiopulmonary bypass for adult patients: a survey of equipment and techniques. J Cardiothorac Vasc Anesth 1995;9: Allen S, Lloyd G, Butz H. Leucocytes and the systemic inflammatory response. J Anästh Intens 1996;5:S Allen SM. Leucocyte depletion in cardiothoracic surgery. Perfusion 1996;11: Steneker I, van Luyn MJA, van Wachem PB, Biewenga J. Electron microscopic examination of white cell-reduction by four different filters. Transfusion 1992;32: Menasché P, Peynet J, Haeffner-Cavaillon N, et al. Influence of temperature on neutrophil trafficing during clinical cardiopulmonary bypass. Circulation 1995;92(Suppl 2): Le Deist F, Menasché P, Kucharski C, Bel A, Piwanica A, Bloch G. Hypothermia during cardiopulmonary bypass delays but does not prevent neutrophil-endothelial cell adhesion. A clinical study. Circulation 1995;92(Suppl 2):354 8.
Reduction of the Inflammatory Response in Patients Undergoing Minimally Invasive Coronary Artery Bypass Grafting. Patients and Methods Patients
 Reduction of the Inflammatory Response in Patients Undergoing Minimally Invasive Coronary Artery Bypass Grafting Y. John Gu, MD, PhD, Massimo A. Mariani, MD, PhD, Willem van Oeveren, PhD, Jan G. Grandjean,
Reduction of the Inflammatory Response in Patients Undergoing Minimally Invasive Coronary Artery Bypass Grafting Y. John Gu, MD, PhD, Massimo A. Mariani, MD, PhD, Willem van Oeveren, PhD, Jan G. Grandjean,
Leukocyte Depletion in Cardiac Surgery and Cardiology
 Leukocyte Depletion in Cardiac Surgery and Cardiology Leukocyte Depletion in Cardiac Surgery and Cardiology Editors Georg Matheis Frankfurt Anton Moritz Frankfurt Martin Scholz Frankfurt 32 figures and
Leukocyte Depletion in Cardiac Surgery and Cardiology Leukocyte Depletion in Cardiac Surgery and Cardiology Editors Georg Matheis Frankfurt Anton Moritz Frankfurt Martin Scholz Frankfurt 32 figures and
Conventional CABG Or On Pump Beating Heart: A Difference In Myocardial Injury?
 Conventional CABG Or On Pump Beating Heart: A Difference In Myocardial Injury? Kornelis J. Koopmans Medical Center Leeuwarden Leeuwarden, The Netherlands I have no disclosures Disclosures Different techniques
Conventional CABG Or On Pump Beating Heart: A Difference In Myocardial Injury? Kornelis J. Koopmans Medical Center Leeuwarden Leeuwarden, The Netherlands I have no disclosures Disclosures Different techniques
Cardiopulmonary bypass (CPB) is associated with the development of
 Activation of neutrophils and monocytes by a leukocytedepleting filter used throughout cardiopulmonary bypass Minna Ilmakunnas, MD a,b Eero J. Pesonen, MD, PhD b Jouni Ahonen, MD, PhD b Juhani Rämö, MD,
Activation of neutrophils and monocytes by a leukocytedepleting filter used throughout cardiopulmonary bypass Minna Ilmakunnas, MD a,b Eero J. Pesonen, MD, PhD b Jouni Ahonen, MD, PhD b Juhani Rämö, MD,
The systemic inflammatory response that occurs to a
 Inflammatory Mediators in Adults Undergoing Cardiopulmonary Bypass: Comparison of Centrifugal and Roller Pumps Saeed Ashraf, FRCS(C/Th), John Butler, FRCS(I), Yi Tian, MCh, Dahlia Cowan, BSc, Simon Lintin,
Inflammatory Mediators in Adults Undergoing Cardiopulmonary Bypass: Comparison of Centrifugal and Roller Pumps Saeed Ashraf, FRCS(C/Th), John Butler, FRCS(I), Yi Tian, MCh, Dahlia Cowan, BSc, Simon Lintin,
Total Leukocyte Control for Elective Coronary Bypass Surgery Does Not Improve Short-Term Outcome
 Total Leukocyte Control for Elective Coronary Bypass Surgery Does Not Improve Short-Term Outcome Robert F. Salamonsen, MD, James Anderson, CCP, Michael Anderson, FJFICM, Michael Bailey, MS, Geoff Magrin,
Total Leukocyte Control for Elective Coronary Bypass Surgery Does Not Improve Short-Term Outcome Robert F. Salamonsen, MD, James Anderson, CCP, Michael Anderson, FJFICM, Michael Bailey, MS, Geoff Magrin,
ECMO vs. CPB for Intraoperative Support: How do you Choose?
 ECMO vs. CPB for Intraoperative Support: How do you Choose? Shaf Keshavjee MD MSc FRCSC FACS Director, Toronto Lung Transplant Program Surgeon-in-Chief, University Health Network James Wallace McCutcheon
ECMO vs. CPB for Intraoperative Support: How do you Choose? Shaf Keshavjee MD MSc FRCSC FACS Director, Toronto Lung Transplant Program Surgeon-in-Chief, University Health Network James Wallace McCutcheon
CCAS CPB Workshop Curriculum Outline Perfusion: What you might not know
 CCAS CPB Workshop Curriculum Outline Perfusion: What you might not know Scott Lawson, CCP Carrie Striker, CCP Disclosure: Nothing to disclose Objectives: * Demonstrate how the cardiopulmonary bypass machine
CCAS CPB Workshop Curriculum Outline Perfusion: What you might not know Scott Lawson, CCP Carrie Striker, CCP Disclosure: Nothing to disclose Objectives: * Demonstrate how the cardiopulmonary bypass machine
Going on Bypass. What happens before, during and after CPB. Perfusion Dept. Royal Children s Hospital Melbourne, Australia
 Going on Bypass What happens before, during and after CPB. Perfusion Dept. Royal Children s Hospital Melbourne, Australia Circulation Brain Liver Kidneys Viscera Muscle Skin IVC, SVC Pump Lungs R.A. L.V.
Going on Bypass What happens before, during and after CPB. Perfusion Dept. Royal Children s Hospital Melbourne, Australia Circulation Brain Liver Kidneys Viscera Muscle Skin IVC, SVC Pump Lungs R.A. L.V.
Transfusion and Blood Conservation
 Transfusion and Blood Conservation Kenneth G. Shann, CCP Assistant Director, Perfusion Services Senior Advisor, Performance Improvement Department of Cardiovascular and Thoracic Surgery Montefiore Medical
Transfusion and Blood Conservation Kenneth G. Shann, CCP Assistant Director, Perfusion Services Senior Advisor, Performance Improvement Department of Cardiovascular and Thoracic Surgery Montefiore Medical
Intraoperative application of Cytosorb in cardiac surgery
 Intraoperative application of Cytosorb in cardiac surgery Dr. Carolyn Weber Heart Center of the University of Cologne Dept. of Cardiothoracic Surgery Cologne, Germany SIRS & Cardiopulmonary Bypass (CPB)
Intraoperative application of Cytosorb in cardiac surgery Dr. Carolyn Weber Heart Center of the University of Cologne Dept. of Cardiothoracic Surgery Cologne, Germany SIRS & Cardiopulmonary Bypass (CPB)
The Efficacy of Low Prime Volume Completely Closed Cardiopulmonary Bypass in Coronary Artery Revascularization
 Original Article The Efficacy of Low Prime Volume Completely Closed Cardiopulmonary Bypass in Coronary Artery Revascularization Hideaki Takai, MD, Kiyoyuki Eishi, MD, Shiro Yamachika, MD, Shiro Hazama,
Original Article The Efficacy of Low Prime Volume Completely Closed Cardiopulmonary Bypass in Coronary Artery Revascularization Hideaki Takai, MD, Kiyoyuki Eishi, MD, Shiro Yamachika, MD, Shiro Hazama,
LEUKOCYTE DEPLETION RESULTS IN IMPROVED LUNG FUNCTION AND REDUCED INFLAMMATORY RESPONSE AFTER CARDIAC SURGERY
 LEUKOCYTE DEPLETION RESULTS IN IMPROVED LUNG FUNCTION AND REDUCED INFLAMMATORY RESPONSE AFTER CARDIAC SURGERY Y. J. Gu, MD, PhD ~ A. J. devries, MD b P. W. Boonstra, MD, PhD a W. van Oeveren, PhD a Leukocyte
LEUKOCYTE DEPLETION RESULTS IN IMPROVED LUNG FUNCTION AND REDUCED INFLAMMATORY RESPONSE AFTER CARDIAC SURGERY Y. J. Gu, MD, PhD ~ A. J. devries, MD b P. W. Boonstra, MD, PhD a W. van Oeveren, PhD a Leukocyte
Intra-operative Effects of Cardiac Surgery Influence on Post-operative care. Richard A Perryman
 Intra-operative Effects of Cardiac Surgery Influence on Post-operative care Richard A Perryman Intra-operative Effects of Cardiac Surgery Cardiopulmonary Bypass Hypothermia Cannulation events Myocardial
Intra-operative Effects of Cardiac Surgery Influence on Post-operative care Richard A Perryman Intra-operative Effects of Cardiac Surgery Cardiopulmonary Bypass Hypothermia Cannulation events Myocardial
Recent experimental studies have documented that 1
 Detrimental Effects of Cardiopulmonary Bypass in Cyanotic Infants: Preventing the Reoxygenation Injury Bradley S. Allen, MD, Shaikh Rahman, MS, Michel N. Ilbawi, MD, Michael Kronon, MD, Kirk S. Bolling,
Detrimental Effects of Cardiopulmonary Bypass in Cyanotic Infants: Preventing the Reoxygenation Injury Bradley S. Allen, MD, Shaikh Rahman, MS, Michel N. Ilbawi, MD, Michael Kronon, MD, Kirk S. Bolling,
Department of Anaesthesiology, Erasmus University Medical Center, Rotterdam, The Netherlands
 Intravenous device feasible for controlled cooling and rewarming of individuals with abnormal body core temperature A. Struijs 1, F. De Ruiter 1, A. Weijerse 1, J. Klein 2, A.J.J.C. Bogers 1 1 Department
Intravenous device feasible for controlled cooling and rewarming of individuals with abnormal body core temperature A. Struijs 1, F. De Ruiter 1, A. Weijerse 1, J. Klein 2, A.J.J.C. Bogers 1 1 Department
University of Groningen. Impaired Organ Perfusion Morariu, Aurora
 University of Groningen Impaired Organ Perfusion Morariu, Aurora IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Impaired Organ Perfusion Morariu, Aurora IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Understanding the Cardiopulmonary Bypass Machine and Its Tubing
 Understanding the Cardiopulmonary Bypass Machine and Its Tubing Robert S. Leckie, MD Division of Cardiac Anesthesia, Beth Israel Deaconess Medical Center ABL 1/09 Reservoir Bucket This is a cartoon of
Understanding the Cardiopulmonary Bypass Machine and Its Tubing Robert S. Leckie, MD Division of Cardiac Anesthesia, Beth Israel Deaconess Medical Center ABL 1/09 Reservoir Bucket This is a cartoon of
August, 2015 STATE MEDICAL FACULTY OF WEST BENGAL. Preliminary Examinations for Diploma in Perfusion Technology : DPfT. Paper I ANATOMY & PHYSIOLOGY
 August, 2015 STATE MEDICAL FACULTY OF WEST BENGAL Paper I ANATOMY & PHYSIOLOGY Time 3 hours Full Marks 80 Group A Q-1) Write the correct Answer: 10x1 = 10 i) The posterior descending artery is branch of
August, 2015 STATE MEDICAL FACULTY OF WEST BENGAL Paper I ANATOMY & PHYSIOLOGY Time 3 hours Full Marks 80 Group A Q-1) Write the correct Answer: 10x1 = 10 i) The posterior descending artery is branch of
CytoSorb Therapy. Indications and Set-up
 CytoSorb Therapy Indications and Set-up CytoSorb therapy REGAIN CONTROL The statements in this document do not constitute diagnostic or therapeutic recommendations. It is a best practice collection, based
CytoSorb Therapy Indications and Set-up CytoSorb therapy REGAIN CONTROL The statements in this document do not constitute diagnostic or therapeutic recommendations. It is a best practice collection, based
Clinical Evaluation of the Accuracy and Precision of the CDI 500 In-line Blood Gas Monitor With and Without Gas Calibration
 The Journal of ExtraCorporeal Technology Original Articles Clinical Evaluation of the Accuracy and Precision of the CDI 500 In-line Blood Gas Monitor With and Without Gas Calibration Anne Louise Bellaiche,
The Journal of ExtraCorporeal Technology Original Articles Clinical Evaluation of the Accuracy and Precision of the CDI 500 In-line Blood Gas Monitor With and Without Gas Calibration Anne Louise Bellaiche,
Parwis Massoudy, MD; Stefan Zahler, PhD; Bernhard F. Becker, MD, PhD; Siegmund L. Braun, MD; Andreas Barankay, MD; and Hans Meisner, MD
 Evidence for Inflammatory Responses of the Lungs During Coronary Artery Bypass Grafting With Cardiopulmonary Bypass* Parwis Massoudy, MD; Stefan Zahler, PhD; Bernhard F. Becker, MD, PhD; Siegmund L. Braun,
Evidence for Inflammatory Responses of the Lungs During Coronary Artery Bypass Grafting With Cardiopulmonary Bypass* Parwis Massoudy, MD; Stefan Zahler, PhD; Bernhard F. Becker, MD, PhD; Siegmund L. Braun,
Does ambroxol confer a protective effect on the lungs in patients undergoing cardiac surgery or having lung resection?
 Interactive CardioVascular and Thoracic Surgery 18 (2014) 830 834 doi:10.1093/icvts/ivu061 Advance Access publication 12 March 2014 BEST EVIDENCE TOPIC THORACIC Does ambroxol confer a protective effect
Interactive CardioVascular and Thoracic Surgery 18 (2014) 830 834 doi:10.1093/icvts/ivu061 Advance Access publication 12 March 2014 BEST EVIDENCE TOPIC THORACIC Does ambroxol confer a protective effect
OPCAB IS NOT BETTER THAN CONVENTIONAL CABG
 OPCAB IS NOT BETTER THAN CONVENTIONAL CABG Harold L. Lazar, M.D. Harold L. Lazar, M.D. Professor of Cardiothoracic Surgery Boston Medical Center and the Boston University School of Medicine Boston, MA
OPCAB IS NOT BETTER THAN CONVENTIONAL CABG Harold L. Lazar, M.D. Harold L. Lazar, M.D. Professor of Cardiothoracic Surgery Boston Medical Center and the Boston University School of Medicine Boston, MA
Erik J. Fransen, MSc, PhD; Jart H. C. Diris, MSc; Jos G. Maessen, MD, PhD; Wim Th. Hermens, PhD; Marja P. van Dieijen-Visser, MD, PhD
 Evaluation of New Cardiac Markers for Ruling Out Myocardial Infarction After Coronary Artery Bypass Grafting* Erik J. Fransen, MSc, PhD; Jart H. C. Diris, MSc; Jos G. Maessen, MD, PhD; Wim Th. Hermens,
Evaluation of New Cardiac Markers for Ruling Out Myocardial Infarction After Coronary Artery Bypass Grafting* Erik J. Fransen, MSc, PhD; Jart H. C. Diris, MSc; Jos G. Maessen, MD, PhD; Wim Th. Hermens,
Cardiac anaesthesia. Simon May
 Cardiac anaesthesia Simon May Contents Cardiac: Principles of peri-operative management for cardiac surgery Cardiopulmonary bypass, cardioplegia and off pump cardiac surgery Cardiac disease and its implications
Cardiac anaesthesia Simon May Contents Cardiac: Principles of peri-operative management for cardiac surgery Cardiopulmonary bypass, cardioplegia and off pump cardiac surgery Cardiac disease and its implications
Evidence of Systemic Cytokine Release in Patients Undergoing Cardiopulmonary Bypass
 The Journal of The American Society of Extra-Corporeal Technology Evidence of Systemic Cytokine Release in Patients Undergoing Cardiopulmonary Bypass Jeffrey Halter, MD; Jay Steinberg, DO; Gregory Fink,
The Journal of The American Society of Extra-Corporeal Technology Evidence of Systemic Cytokine Release in Patients Undergoing Cardiopulmonary Bypass Jeffrey Halter, MD; Jay Steinberg, DO; Gregory Fink,
Retransfusion of Suctioned Blood During Cardiopulmonary Bypass Impairs Hemostasis
 Retransfusion of Suctioned Blood During Cardiopulmonary Bypass Impairs Hemostasis Jacob de Haan, Msc, Piet W. Boonstra, MD, PhD, Stefan H. J. Monnink, MD, Tjark Ebels, MD, PhD, and Willem van Oeveren,
Retransfusion of Suctioned Blood During Cardiopulmonary Bypass Impairs Hemostasis Jacob de Haan, Msc, Piet W. Boonstra, MD, PhD, Stefan H. J. Monnink, MD, Tjark Ebels, MD, PhD, and Willem van Oeveren,
Journal of the American College of Cardiology Vol. 33, No. 6, by the American College of Cardiology ISSN /99/$20.
 Journal of the American College of Cardiology Vol. 33, No. 6, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00061-3 for Prediction
Journal of the American College of Cardiology Vol. 33, No. 6, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00061-3 for Prediction
Optimizing Blood ManagementTM
 Optimizing Blood ManagementTM A Multi-Strategy Approach to Controlling Inflammatory Response Terumo Introduces the Optimizing Blood Management Relationship Browser. For the full interactive experience,
Optimizing Blood ManagementTM A Multi-Strategy Approach to Controlling Inflammatory Response Terumo Introduces the Optimizing Blood Management Relationship Browser. For the full interactive experience,
Cardiothoracic Fellow Expectations Division of Cardiac Anesthesia, Beth Israel Deaconess Medical Center
 The fellowship in Cardiothoracic Anesthesia at the Beth Israel Deaconess Medical Center is intended to provide the foundation for a career as either an academic cardiothoracic anesthesiologist or clinical
The fellowship in Cardiothoracic Anesthesia at the Beth Israel Deaconess Medical Center is intended to provide the foundation for a career as either an academic cardiothoracic anesthesiologist or clinical
Cardioplegia Circuit Products { CARDIOPLEGIA ADAPTERS}
 Cardioplegia Circuit Products { CARDIOPLEGIA ADAPTERS} Cardioplegia adapters are designed to permit customization of the cardioplegia circuit. Medtronic adapters can be used to connect multiple cardioplegia
Cardioplegia Circuit Products { CARDIOPLEGIA ADAPTERS} Cardioplegia adapters are designed to permit customization of the cardioplegia circuit. Medtronic adapters can be used to connect multiple cardioplegia
OPCABG for Full Myocardial Revascularisation How we do it
 OPCABG for Full Myocardial Revascularisation How we do it 28 th SHA Conferance Dr.Farouk Oueida Head of Cardiac Surgery Dept. SBCC-Dammam KSA The Less Invasive CABG Full Revascularisation Full Sternotomy
OPCABG for Full Myocardial Revascularisation How we do it 28 th SHA Conferance Dr.Farouk Oueida Head of Cardiac Surgery Dept. SBCC-Dammam KSA The Less Invasive CABG Full Revascularisation Full Sternotomy
Case scenario V AV ECMO. Dr Pranay Oza
 Case scenario V AV ECMO Dr Pranay Oza Case Summary 53 y/m, k/c/o MVP with myxomatous mitral valve with severe Mitral regurgitation underwent Mitral valve replacement with mini thoracotomy Pump time nearly
Case scenario V AV ECMO Dr Pranay Oza Case Summary 53 y/m, k/c/o MVP with myxomatous mitral valve with severe Mitral regurgitation underwent Mitral valve replacement with mini thoracotomy Pump time nearly
Perioperative Management of DORV Case
 Perioperative Management of DORV Case James P. Spaeth, MD Department of Anesthesia Cincinnati Children s Hospital Medical Center University of Cincinnati Objectives: 1. Discuss considerations regarding
Perioperative Management of DORV Case James P. Spaeth, MD Department of Anesthesia Cincinnati Children s Hospital Medical Center University of Cincinnati Objectives: 1. Discuss considerations regarding
Absolute Cerebral Oximeters for Cardiovascular Surgical Cases
 Absolute Cerebral Oximeters for Cardiovascular Surgical Cases Mary E. Arthur, MD, Associate Professor, Anesthesiology and Perioperative Medicine Medical College of Georgia at Georgia Regents University
Absolute Cerebral Oximeters for Cardiovascular Surgical Cases Mary E. Arthur, MD, Associate Professor, Anesthesiology and Perioperative Medicine Medical College of Georgia at Georgia Regents University
Minimally Invasive Aortic Surgery With Emphasis On Technical Aspects, Extracorporeal Circulation Management And Cardioplegic Techniques
 Minimally Invasive Aortic Surgery With Emphasis On Technical Aspects, Extracorporeal Circulation Management And Cardioplegic Techniques Konstadinos A Plestis, MD System Chief of Cardiothoracic and Vascular
Minimally Invasive Aortic Surgery With Emphasis On Technical Aspects, Extracorporeal Circulation Management And Cardioplegic Techniques Konstadinos A Plestis, MD System Chief of Cardiothoracic and Vascular
IMPROVE PATIENT OUTCOMES AND SAFETY IN ADULT CARDIAC SURGERY.
 Clinical Evidence Guide IMPROVE PATIENT OUTCOMES AND SAFETY IN ADULT CARDIAC SURGERY. With the INVOS cerebral/somatic oximeter An examination of controlled studies reveals that responding to cerebral desaturation
Clinical Evidence Guide IMPROVE PATIENT OUTCOMES AND SAFETY IN ADULT CARDIAC SURGERY. With the INVOS cerebral/somatic oximeter An examination of controlled studies reveals that responding to cerebral desaturation
University of Groningen. Acute kidney injury after cardiac surgery Loef, Berthus Gerard
 University of Groningen Acute kidney injury after cardiac surgery Loef, Berthus Gerard IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it.
University of Groningen Acute kidney injury after cardiac surgery Loef, Berthus Gerard IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it.
CLOTTING AND FIBRINOLYTIC DISTURBANCE DURING LUNG TRANSPLANTATION: EFFECT OF LOW-DOSE APROTININ
 CLOTTING AND FIBRINOLYTIC DISTURBANCE DURING LUNG TRANSPLANTATION: EFFECT OF LOW-DOSE APROTININ Y. J. Gu, MD, PhD J. de Haan, PhD U. P. M. Brenken, MD, PhD W. J. de Boer, MD Jm. Prop, MD, PhD W. van Oeveren,
CLOTTING AND FIBRINOLYTIC DISTURBANCE DURING LUNG TRANSPLANTATION: EFFECT OF LOW-DOSE APROTININ Y. J. Gu, MD, PhD J. de Haan, PhD U. P. M. Brenken, MD, PhD W. J. de Boer, MD Jm. Prop, MD, PhD W. van Oeveren,
Veno-Venous ECMO Support. Chris Cropsey, MD Sept. 21, 2015
 Veno-Venous ECMO Support Chris Cropsey, MD Sept. 21, 2015 Objectives List indications and contraindications for ECMO Describe hemodynamics and oxygenation on ECMO Discuss evidence for ECMO outcomes Identify
Veno-Venous ECMO Support Chris Cropsey, MD Sept. 21, 2015 Objectives List indications and contraindications for ECMO Describe hemodynamics and oxygenation on ECMO Discuss evidence for ECMO outcomes Identify
Navigating the Dichotomies Between Literature and Your Clinical Practice
 Navigating the Dichotomies Between Literature and Your Clinical Practice Robert Groom, CCP, FPP Cardiovascular Institute at Maine Medical Center Disclosures No relevant conflicts related to this presentation
Navigating the Dichotomies Between Literature and Your Clinical Practice Robert Groom, CCP, FPP Cardiovascular Institute at Maine Medical Center Disclosures No relevant conflicts related to this presentation
University of Bristol - Explore Bristol Research
 Rogers, C., Capoun, R., Scott, L., Taylor, J., Angelini, G., Narayan, P.,... Ascione, R. (2017). Shortening cardioplegic arrest time in patients undergoing combined coronary and valve surgery: results
Rogers, C., Capoun, R., Scott, L., Taylor, J., Angelini, G., Narayan, P.,... Ascione, R. (2017). Shortening cardioplegic arrest time in patients undergoing combined coronary and valve surgery: results
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation, radiofrequency, anesthetic considerations for, 479 489 Acute aortic syndrome, thoracic endovascular repair of, 457 462 aortic
Index Note: Page numbers of article titles are in boldface type. A Ablation, radiofrequency, anesthetic considerations for, 479 489 Acute aortic syndrome, thoracic endovascular repair of, 457 462 aortic
The increasing use of normothermic cardiopulmonary
 A Prospective, Randomized Study of Cardiopulmonary Bypass Temperature and Blood Transfusion Paul E. Stensrud, MD, Gregory A. Nuttall, MD, Maria A. de Castro, MD, Martin D. Abel, MD, Mark H. Ereth, MD,
A Prospective, Randomized Study of Cardiopulmonary Bypass Temperature and Blood Transfusion Paul E. Stensrud, MD, Gregory A. Nuttall, MD, Maria A. de Castro, MD, Martin D. Abel, MD, Mark H. Ereth, MD,
Blood Management of the Cardiac Patient in the Postoperative Period
 Blood Management of the Cardiac Patient in the Postoperative Period Al Stammers, MSA, CCP, Eric Tesdahl, PhD Andy Stasko MS, CCP, RRT, Linda Mongero, BS, CCP, Sam Weinstein, MD, MBA Goal To examine the
Blood Management of the Cardiac Patient in the Postoperative Period Al Stammers, MSA, CCP, Eric Tesdahl, PhD Andy Stasko MS, CCP, RRT, Linda Mongero, BS, CCP, Sam Weinstein, MD, MBA Goal To examine the
Leukodepletion Reduces Renal Injury in Coronary Revascularization: A Prospective Randomized Study
 Leukodepletion Reduces Renal Injury in Coronary Revascularization: A Prospective Randomized Study Augustine T. M. Tang, FRCSEd, DM, Christos Alexiou, FRCS, Jeff Hsu, Stuart V. Sheppard, PhD, Marcus P.
Leukodepletion Reduces Renal Injury in Coronary Revascularization: A Prospective Randomized Study Augustine T. M. Tang, FRCSEd, DM, Christos Alexiou, FRCS, Jeff Hsu, Stuart V. Sheppard, PhD, Marcus P.
Goal Directed Perfusion: theory, clinical results, and key rules
 Goal Directed Perfusion: theory, clinical results, and key rules M. Ranucci Director of Clinical Research Dept of Cardiothoracic and Vascular Anesthesia and Intensive Care IRCCS Policlinico S.Donato Ranuuci,
Goal Directed Perfusion: theory, clinical results, and key rules M. Ranucci Director of Clinical Research Dept of Cardiothoracic and Vascular Anesthesia and Intensive Care IRCCS Policlinico S.Donato Ranuuci,
Supplementary Online Content
 1 Supplementary Online Content Leme AC, Hajjar LA, Volpe MS, et al. Effect of intensive vs moderate alveolar recruitment strategies added to lung-protective ventilation on postoperative pulmonary complications:
1 Supplementary Online Content Leme AC, Hajjar LA, Volpe MS, et al. Effect of intensive vs moderate alveolar recruitment strategies added to lung-protective ventilation on postoperative pulmonary complications:
University of Florida Department of Surgery. CardioThoracic Surgery VA Learning Objectives
 University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
Cardiopulmonary bypass (CPB) is associated with a
 Biocompatibility of Silicone-Coated Oxygenator in Cardiopulmonary Bypass Akira Shimamoto, MD, Shinji Kanemitsu, MD, Kazuya Fujinaga, MD, Motoshi Takao, MD, PhD, Koji Onoda, MD, PhD, Takatsugu Shimono,
Biocompatibility of Silicone-Coated Oxygenator in Cardiopulmonary Bypass Akira Shimamoto, MD, Shinji Kanemitsu, MD, Kazuya Fujinaga, MD, Motoshi Takao, MD, PhD, Koji Onoda, MD, PhD, Takatsugu Shimono,
Demonstration of Uneven. the infusion on myocardial temperature was insufficient
 Demonstration of Uneven in Patients with Coronary Lesions Rolf Ekroth, M.D., HAkan erggren, M.D., Goran Sudow, M.D., Josef Wojciechowski, M.D., o F. Zackrisson, M.D., and Goran William-Olsson, M.D. ASTRACT
Demonstration of Uneven in Patients with Coronary Lesions Rolf Ekroth, M.D., HAkan erggren, M.D., Goran Sudow, M.D., Josef Wojciechowski, M.D., o F. Zackrisson, M.D., and Goran William-Olsson, M.D. ASTRACT
Incidence and pattern of Thrombocytopenia in cardiac surgery patients
 1019 ORIGINAL ARTICLE Incidence and pattern of Thrombocytopenia in cardiac surgery patients Mohammad Hamid, Mohammad Irfan Akhtar, Hamid Iqil Naqvi, Khalid Ahsan Abstract Objective: To observe the incidence
1019 ORIGINAL ARTICLE Incidence and pattern of Thrombocytopenia in cardiac surgery patients Mohammad Hamid, Mohammad Irfan Akhtar, Hamid Iqil Naqvi, Khalid Ahsan Abstract Objective: To observe the incidence
Effect of Leukocyte Depletion on Endothelial Cell Activation and Transendothelial Migration of Leukocytes During Cardiopulmonary Bypass
 Effect of Leukocyte Depletion on Endothelial Cell Activation and Transendothelial Migration of Leukocytes During Cardiopulmonary Bypass Ying-Fu Chen, MD, PhD, Wen-Chan Tsai, MD, Ching-Cheng Lin, MD, Li-Yu
Effect of Leukocyte Depletion on Endothelial Cell Activation and Transendothelial Migration of Leukocytes During Cardiopulmonary Bypass Ying-Fu Chen, MD, PhD, Wen-Chan Tsai, MD, Ching-Cheng Lin, MD, Li-Yu
Are Circulating Adhesion Molecules Specifically Changed in Cardiac Surgical Patients?
 ORIGINAL ARTICLES: CARDIOVASCULAR Are Circulating Adhesion Molecules Specifically Changed in Cardiac Surgical Patients? Joachim Boldt, MD, Bernd Kumle, MD, Michael Papsdorf, and Gunter Hempelmann, MD Department
ORIGINAL ARTICLES: CARDIOVASCULAR Are Circulating Adhesion Molecules Specifically Changed in Cardiac Surgical Patients? Joachim Boldt, MD, Bernd Kumle, MD, Michael Papsdorf, and Gunter Hempelmann, MD Department
Goals and Objectives. Assessment Methods/Tools
 CA-2 CARDIOTHORACIC ANESTHESIA ROTATION Medical Center Fairview (UMMC) Rotation Site Director: Drs. Ioanna Apostolidou & Douglas Koehntop Rotation Duration: 6 weeks Introduction: The overall goal of the
CA-2 CARDIOTHORACIC ANESTHESIA ROTATION Medical Center Fairview (UMMC) Rotation Site Director: Drs. Ioanna Apostolidou & Douglas Koehntop Rotation Duration: 6 weeks Introduction: The overall goal of the
Cardiopulmonary Bypass for Thoracic Aortic Aneurysm: A Report on 488 Cases
 The Journal of The American Society of Extra-Corporeal Technology Cardiopulmonary Bypass for Thoracic Aortic Aneurysm: A Report on 488 Cases Yulong Guan, MD; Jing Yang, MD; Caihong Wan, MD; Meiling He;
The Journal of The American Society of Extra-Corporeal Technology Cardiopulmonary Bypass for Thoracic Aortic Aneurysm: A Report on 488 Cases Yulong Guan, MD; Jing Yang, MD; Caihong Wan, MD; Meiling He;
Comparison of Tranexamic Acid and Aminocaproic Acid in Coronary Bypass Surgery
 Butler Journal of Undergraduate Research Volume 2 Article 24 2016 Comparison of Tranexamic Acid and Aminocaproic Acid in Coronary Bypass Surgery Lisa K. LeCleir Butler University, lisa.lecleir@gmail.com
Butler Journal of Undergraduate Research Volume 2 Article 24 2016 Comparison of Tranexamic Acid and Aminocaproic Acid in Coronary Bypass Surgery Lisa K. LeCleir Butler University, lisa.lecleir@gmail.com
Solution for cardiac perfusion in viaflex plastic container
 CARDIOPLEGIA SOLUTION A Solution for cardiac perfusion in viaflex plastic container DESCRIPTION Cardioplegia Solution A is a sterile, non-pyrogenic solution in a Viaflex bag. It is used to induce cardiac
CARDIOPLEGIA SOLUTION A Solution for cardiac perfusion in viaflex plastic container DESCRIPTION Cardioplegia Solution A is a sterile, non-pyrogenic solution in a Viaflex bag. It is used to induce cardiac
Interventions designed to improve intensive care unit
 Readmission to the Intensive Care Unit After Fast- Track Cardiac Surgery: Risk Factors and Outcomes Alexander Kogan, MD, Jonathan Cohen, MD, Ehud Raanani, MD, Gideon Sahar, MD, Boris Orlov, MD, Pierre
Readmission to the Intensive Care Unit After Fast- Track Cardiac Surgery: Risk Factors and Outcomes Alexander Kogan, MD, Jonathan Cohen, MD, Ehud Raanani, MD, Gideon Sahar, MD, Boris Orlov, MD, Pierre
Coronary Artery Bypass Graft: Monitoring Patients and Detecting Complications
 Coronary Artery Bypass Graft: Monitoring Patients and Detecting Complications Madhav Swaminathan, MD, FASE Professor of Anesthesiology Division of Cardiothoracic Anesthesia & Critical Care Duke University
Coronary Artery Bypass Graft: Monitoring Patients and Detecting Complications Madhav Swaminathan, MD, FASE Professor of Anesthesiology Division of Cardiothoracic Anesthesia & Critical Care Duke University
Perioperative Management of TAPVC
 Perioperative Management of TAPVC Professor Andrew Wolf Rush University Medical Center,Chicago USA Bristol Royal Children s Hospital UK I have no financial disclosures relevant to this presentation TAPVC
Perioperative Management of TAPVC Professor Andrew Wolf Rush University Medical Center,Chicago USA Bristol Royal Children s Hospital UK I have no financial disclosures relevant to this presentation TAPVC
Transfusion & Mortality. Philippe Van der Linden MD, PhD
 Transfusion & Mortality Philippe Van der Linden MD, PhD Conflict of Interest Disclosure In the past 5 years, I have received honoraria or travel support for consulting or lecturing from the following companies:
Transfusion & Mortality Philippe Van der Linden MD, PhD Conflict of Interest Disclosure In the past 5 years, I have received honoraria or travel support for consulting or lecturing from the following companies:
Effects of Prostacyclin Infusion on Platelet Activation and Postoperative Blood Loss in Coronary Bypass
 Effects of Prostacyclin Infusion on Platelet Activation and Postoperative Blood Loss in Coronary Bypass Claes Aren, M.D., Kurt Feddersen, M.D., and Kjell Ridegran, M.D. ABSTRACT The effects of infusion
Effects of Prostacyclin Infusion on Platelet Activation and Postoperative Blood Loss in Coronary Bypass Claes Aren, M.D., Kurt Feddersen, M.D., and Kjell Ridegran, M.D. ABSTRACT The effects of infusion
Congenital heart operations place extreme demands
 Assisted Venous Drainage Cardiopulmonary Bypass in Congenital Heart Surgery Jorge W. Ojito, CCP, Robert L. Hannan, MD, Kagami Miyaji, MD, Jeffrey A. White, MS, Todd W. McConaghey, CCP, Jeffrey P. Jacobs,
Assisted Venous Drainage Cardiopulmonary Bypass in Congenital Heart Surgery Jorge W. Ojito, CCP, Robert L. Hannan, MD, Kagami Miyaji, MD, Jeffrey A. White, MS, Todd W. McConaghey, CCP, Jeffrey P. Jacobs,
Heart transplantation is the gold standard treatment for
 Organ Care System for Heart Procurement and Strategies to Reduce Primary Graft Failure After Heart Transplant Masaki Tsukashita, MD, PhD, and Yoshifumi Naka, MD, PhD Primary graft failure is a rare, but
Organ Care System for Heart Procurement and Strategies to Reduce Primary Graft Failure After Heart Transplant Masaki Tsukashita, MD, PhD, and Yoshifumi Naka, MD, PhD Primary graft failure is a rare, but
Expanding Horizons: AngioVac Suction Thrombectomy at UTHealth
 Expanding Horizons: AngioVac Suction Thrombectomy at UTHealth Naveed Saqib, MD Assistant Professor Department of Cardiothoracic and Vascular Surgery McGovern Medical School The University of Texas Science
Expanding Horizons: AngioVac Suction Thrombectomy at UTHealth Naveed Saqib, MD Assistant Professor Department of Cardiothoracic and Vascular Surgery McGovern Medical School The University of Texas Science
Patient. Venous reservoir. Hemofilter. Heat exchanger. Pump mode. Oxygenator. CHAPTER II - Extracorporeal Circulation (ECC)
 CHAPTER II - Extracorporeal Circulation (ECC) ECC is a complex method that allows substitution, for a certain period of time,of heart and lung functions: circulation, gas exchange, acid-base balance, regulation
CHAPTER II - Extracorporeal Circulation (ECC) ECC is a complex method that allows substitution, for a certain period of time,of heart and lung functions: circulation, gas exchange, acid-base balance, regulation
Is the patient at risk for blood loss of 1000 mls? Avoid these Guidelines. Avoid these Guidelines. Yes. Yes. Yes. Yes. Yes
 Clinical Guidelines Acute rmovolemic Hemodilution Guidelines for Cardiac Surgery Department of Anesthesiology and Perioperative Medicine Date: 12-30-2012 Is the patient at risk for blood loss of 1000 mls?
Clinical Guidelines Acute rmovolemic Hemodilution Guidelines for Cardiac Surgery Department of Anesthesiology and Perioperative Medicine Date: 12-30-2012 Is the patient at risk for blood loss of 1000 mls?
Cardiopulmonary Bypass in Cyanotic Patients. A Review of the Problems and Suggested Strategies
 Cardiopulmonary Bypass in Cyanotic Patients A Review of the Problems and Suggested Strategies Extra-ordinary Problems Encountered During C.P.B. for Cyanotic Heart Disease 1. Extra Dilutional Requirements
Cardiopulmonary Bypass in Cyanotic Patients A Review of the Problems and Suggested Strategies Extra-ordinary Problems Encountered During C.P.B. for Cyanotic Heart Disease 1. Extra Dilutional Requirements
University of Groningen. The role of cell savers and filters in cardiac surgery Vermeijden, Jan Wytze
 University of Groningen The role of cell savers and filters in cardiac surgery Vermeijden, Jan Wytze IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
University of Groningen The role of cell savers and filters in cardiac surgery Vermeijden, Jan Wytze IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
Interesting Cases - A Case Report: Renal Cell Carcinoma With Tumor Mass In IVC And Heart. O Wenker, L Chaloupka, R Joswiak, D Thakar, C Wood, G Walsh
 ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 3 Number 2 Interesting Cases - A Case Report: Renal Cell Carcinoma With Tumor Mass In IVC And Heart O Wenker, L Chaloupka, R
ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 3 Number 2 Interesting Cases - A Case Report: Renal Cell Carcinoma With Tumor Mass In IVC And Heart O Wenker, L Chaloupka, R
Efficacy of Ultrafiltration in Removing Inflammatory Mediators During Pediatric Cardiac Operations
 Efficacy of Ultrafiltration in Removing Inflammatory Mediators During Pediatric Cardiac perations Ming-Jiuh Wang, MD, Ing-Sh Chiu, MD, PhD, Chao-Ming Hsu, MD, Chao-Min Wang, MD, Pei-Lin Lin, MD, Chung-I
Efficacy of Ultrafiltration in Removing Inflammatory Mediators During Pediatric Cardiac perations Ming-Jiuh Wang, MD, Ing-Sh Chiu, MD, PhD, Chao-Ming Hsu, MD, Chao-Min Wang, MD, Pei-Lin Lin, MD, Chung-I
Shervin Ziabakhsh Tabary., Asian Journal of Pharmaceutical Technology & Innovation, 02 (05); 2014; 01-08
 Shervin Ziabakhsh Tabary., Asian Journal of Pharmaceutical Technology & Innovation, 02 (05); 2014; 01-08 Asian Journal of Pharmaceutical Technology & Innovation ISSN: 2347-8810 Received on: 18-02-2014
Shervin Ziabakhsh Tabary., Asian Journal of Pharmaceutical Technology & Innovation, 02 (05); 2014; 01-08 Asian Journal of Pharmaceutical Technology & Innovation ISSN: 2347-8810 Received on: 18-02-2014
Jennifer A. Brown The Cleveland Clinic School of Perfusion Cleveland, Ohio
 Biventricular Heart Failure Advanced Treatment Options at The Cleveland Clinic Jennifer A. Brown The Cleveland Clinic School of Perfusion Cleveland, Ohio I have no disclosures. Examine respiratory and
Biventricular Heart Failure Advanced Treatment Options at The Cleveland Clinic Jennifer A. Brown The Cleveland Clinic School of Perfusion Cleveland, Ohio I have no disclosures. Examine respiratory and
Clinical Performance of Microporous Polypropylene Hollow-Fiber Oxygenator
 Clinical Performance of Microporous Polypropylene Hollow-Fiber Oxygenator Kozo Suma, M.D., Takayuki Tsuji, M.D., Yasuo Takeuchi, M.D., Kenji Inoue, M.D., Kenji Shiroma, M.D., Tetsuo Yoshikawa, M.D., and
Clinical Performance of Microporous Polypropylene Hollow-Fiber Oxygenator Kozo Suma, M.D., Takayuki Tsuji, M.D., Yasuo Takeuchi, M.D., Kenji Inoue, M.D., Kenji Shiroma, M.D., Tetsuo Yoshikawa, M.D., and
Effect of Sodium Nitroprusside during the Payback Period of Cardiopulmonary Bypass on the Incidence of Postoperative Arrhythmias
 Effect of Sodium Nitroprusside during the Payback Period of Cardiopulmonary Bypass on the Incidence of Postoperative Arrhythmias Kit V. Arom, M.D., David M. Angaran, M.S., William G. Lindsay, M.D., William
Effect of Sodium Nitroprusside during the Payback Period of Cardiopulmonary Bypass on the Incidence of Postoperative Arrhythmias Kit V. Arom, M.D., David M. Angaran, M.S., William G. Lindsay, M.D., William
ECMO & Renal Failure Epidemeology Renal failure & effect on out come
 ECMO Induced Renal Issues Transient renal dysfunction Improvement in renal function ECMO & Renal Failure Epidemeology Renal failure & effect on out come With or Without RRT Renal replacement Therapy Utilizes
ECMO Induced Renal Issues Transient renal dysfunction Improvement in renal function ECMO & Renal Failure Epidemeology Renal failure & effect on out come With or Without RRT Renal replacement Therapy Utilizes
C-reactive protein (CRP), the prototypical acute-phase
 Increased Preoperative C-Reactive Protein Plasma Levels as a Risk Factor for Postoperative Infections Erik J. Fransen, MSc, Jos G. Maessen, MD, PhD, Theodoor W. O. Elenbaas, MD, Egidius E. H. L. van Aarnhem,
Increased Preoperative C-Reactive Protein Plasma Levels as a Risk Factor for Postoperative Infections Erik J. Fransen, MSc, Jos G. Maessen, MD, PhD, Theodoor W. O. Elenbaas, MD, Egidius E. H. L. van Aarnhem,
Repair of Complete Atrioventricular Septal Defects Single Patch Technique
 Repair of Complete Atrioventricular Septal Defects Single Patch Technique Fred A. Crawford, Jr., MD The first repair of a complete atrioventricular septal defect was performed in 1954 by Lillehei using
Repair of Complete Atrioventricular Septal Defects Single Patch Technique Fred A. Crawford, Jr., MD The first repair of a complete atrioventricular septal defect was performed in 1954 by Lillehei using
The Effects of Cardiopulmonary Bypass with Hollow Fiber Membrane Oxygenator on Blood Clotting Measured by Thromboelastography
 Physiol. Res. 51: 145-150, 2002 The Effects of Cardiopulmonary Bypass with Hollow Fiber Membrane Oxygenator on Blood Clotting Measured by Thromboelastography M. HORÁČEK, K. CVACHOVEC Department of Anesthesiology
Physiol. Res. 51: 145-150, 2002 The Effects of Cardiopulmonary Bypass with Hollow Fiber Membrane Oxygenator on Blood Clotting Measured by Thromboelastography M. HORÁČEK, K. CVACHOVEC Department of Anesthesiology
The control patients had at least the combination of cardiovascular failure necessitating vasoactive
 ELECTRONIC SUPPLEMENTARY MATERIAL Material and methods Patients The control patients had at least the combination of cardiovascular failure necessitating vasoactive medication, respiratory failure necessitating
ELECTRONIC SUPPLEMENTARY MATERIAL Material and methods Patients The control patients had at least the combination of cardiovascular failure necessitating vasoactive medication, respiratory failure necessitating
EXTRA CORPOREAL MEMBRANE OXYGENATION
 EXTRA CORPOREAL MEMBRANE OXYGENATION Basic Overview and Case Study Bob Hayes, Chief Perfusionist Enloe Medical Center Jenny Humphries, RN, BSN, MBA, CFRN Chief Flight Nurse, Enloe FlightCare Normal Cardiopulmonary
EXTRA CORPOREAL MEMBRANE OXYGENATION Basic Overview and Case Study Bob Hayes, Chief Perfusionist Enloe Medical Center Jenny Humphries, RN, BSN, MBA, CFRN Chief Flight Nurse, Enloe FlightCare Normal Cardiopulmonary
Retrograde Autologous Priming: Is It Useful in Elective On-Pump Coronary Artery Bypass Surgery?
 Retrograde Autologous Priming: Is It Useful in Elective On-Pump Coronary Artery Bypass Surgery? Gregory P. Eising, MD, Martin Pfauder, Markus Niemeyer, Peter Tassani, MD, Hubert Schad, MD, Robert Bauernschmitt,
Retrograde Autologous Priming: Is It Useful in Elective On-Pump Coronary Artery Bypass Surgery? Gregory P. Eising, MD, Martin Pfauder, Markus Niemeyer, Peter Tassani, MD, Hubert Schad, MD, Robert Bauernschmitt,
Contemporary practice of cardiac surgery encounters
 Effects of Combined Conventional and Modified Ultrafiltration in Adult Patients Ugursay Kiziltepe, MD, Adnan Uysalel, MD, Tumer Corapcioglu, MD, Klara Dalva, MD, Hamdi Akan, MD, and Hakki Akalin, MD Department
Effects of Combined Conventional and Modified Ultrafiltration in Adult Patients Ugursay Kiziltepe, MD, Adnan Uysalel, MD, Tumer Corapcioglu, MD, Klara Dalva, MD, Hamdi Akan, MD, and Hakki Akalin, MD Department
A Single-Center Analysis of Methylprednisolone Use during Pediatric Cardiopulmonary Bypass
 The Journal of ExtraCorporeal Technology Original Articles A Single-Center Analysis of Methylprednisolone Use during Pediatric Cardiopulmonary Bypass Molly Dreher, MA; Andrew C. Glatz, MD, MSCE; Andrea
The Journal of ExtraCorporeal Technology Original Articles A Single-Center Analysis of Methylprednisolone Use during Pediatric Cardiopulmonary Bypass Molly Dreher, MA; Andrew C. Glatz, MD, MSCE; Andrea
ADULT OXYGENATORS CATALOGUE
 ADULT OXYGENATORS CATALOGUE A solution for every need Clinical flexibility Optimized priming High performance gas exchange Low contact surface Low GME activity Easy to set up and debubbling The path of
ADULT OXYGENATORS CATALOGUE A solution for every need Clinical flexibility Optimized priming High performance gas exchange Low contact surface Low GME activity Easy to set up and debubbling The path of
Immediate pulmonary dysfunction in ischemic heart disease patients undergoing off-pump versus on-pump CABG
 Available online at www.sciencedirect.com ScienceDirect Journal of the Egyptian Society of Cardio-Thoracic Surgery 24 (2016) 15e20 http://www.journals.elsevier.com/journal-of-the-egyptian-society-of-cardio-thoracic-surgery/
Available online at www.sciencedirect.com ScienceDirect Journal of the Egyptian Society of Cardio-Thoracic Surgery 24 (2016) 15e20 http://www.journals.elsevier.com/journal-of-the-egyptian-society-of-cardio-thoracic-surgery/
Materials and Methods
 Anesthesiology 2003; 99:42 7 2003 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Large-dose Hydroxyethyl Starch 130/0.4 Does Not Increase Blood Loss and Transfusion Requirements
Anesthesiology 2003; 99:42 7 2003 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Large-dose Hydroxyethyl Starch 130/0.4 Does Not Increase Blood Loss and Transfusion Requirements
Technique for Routine Use of Heparin Bonded Circuits with a Reduced Anticoagulation Protocol
 Original Article Technique for Routine Use of Heparin Bonded Circuits with a Reduced Anticoagulation Protocol Paul J. O Gara, BS, CCP; Patrick R. Treanor, CCP; Kevin J. Lilly, CCP; Richard F. Crowley,
Original Article Technique for Routine Use of Heparin Bonded Circuits with a Reduced Anticoagulation Protocol Paul J. O Gara, BS, CCP; Patrick R. Treanor, CCP; Kevin J. Lilly, CCP; Richard F. Crowley,
33rd International Meeting of the German Society for Cardiovascular Engineering. May 20 22, 2004 Celle, Germany
 33rd International Meeting of the German Society for Cardiovascular Engineering May 20 22, 2004 Celle, Germany The Journal of The American Society of Extra-Corporeal Technology Abstracts OXYGENATOR TYPE
33rd International Meeting of the German Society for Cardiovascular Engineering May 20 22, 2004 Celle, Germany The Journal of The American Society of Extra-Corporeal Technology Abstracts OXYGENATOR TYPE
How can ROTEM testing help you in cardiac surgery?
 How can ROTEM testing help you in cardiac surgery? Complicated bleeding situations can appear intra and post operatively. They can be life-threatening and always require immediate action. A fast differential
How can ROTEM testing help you in cardiac surgery? Complicated bleeding situations can appear intra and post operatively. They can be life-threatening and always require immediate action. A fast differential
Measure #164 (NQF 0129): Coronary Artery Bypass Graft (CABG): Prolonged Intubation National Quality Strategy Domain: Effective Clinical Care
 Measure #164 (NQF 0129): Coronary Artery Bypass Graft (CABG): Prolonged Intubation National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY DESCRIPTION:
Measure #164 (NQF 0129): Coronary Artery Bypass Graft (CABG): Prolonged Intubation National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY DESCRIPTION:
Index. Note: Page numbers of article titles are in boldface type
 Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Acute Kidney Injury after Cardiac Surgery: Incidence, Risk Factors and Prevention
 Acute Kidney Injury after Cardiac Surgery: Incidence, Risk Factors and Prevention Hong Liu, MD Professor of Clinical Anesthesiology Department of Anesthesiology and Pain Medicine University of California
Acute Kidney Injury after Cardiac Surgery: Incidence, Risk Factors and Prevention Hong Liu, MD Professor of Clinical Anesthesiology Department of Anesthesiology and Pain Medicine University of California
THE EFFECT OF POSITIVE PRESSURE VENTILATORY PATTERNS ON POST-BYPASS LUNG FUNCTIONS
 THE EFFECT OF POSITIVE PRESSURE VENTILATORY PATTERNS ON POST-BYPASS LUNG FUNCTIONS MOHAMED ESSAM A-MEGUID *, EMAD EL-DIN MANSOUR * AND KHALED M. ABDULLAH ** Abstract Background: This study aimed at evaluating
THE EFFECT OF POSITIVE PRESSURE VENTILATORY PATTERNS ON POST-BYPASS LUNG FUNCTIONS MOHAMED ESSAM A-MEGUID *, EMAD EL-DIN MANSOUR * AND KHALED M. ABDULLAH ** Abstract Background: This study aimed at evaluating
Cardiac surgery is associated with a high incidence of
 Retrograde Autologous Priming of the Cardiopulmonary Bypass Circuit Reduces Blood Transfusion After Coronary Artery Surgery Subramaniam Balachandran, FRCA, Michael H. Cross, FRCA, Sivagnanam Karthikeyan,
Retrograde Autologous Priming of the Cardiopulmonary Bypass Circuit Reduces Blood Transfusion After Coronary Artery Surgery Subramaniam Balachandran, FRCA, Michael H. Cross, FRCA, Sivagnanam Karthikeyan,
ANESTHESIA AND CARDIOPULMONARY BYPASS FOR CONGENITAL HEART SURGERY
 ANESTHESIA AND CARDIOPULMONARY BYPASS FOR CONGENITAL HEART SURGERY Chawki F. elzein * Normal Cardio-Respiratory Physiology In Neonates And Infants The neonate has a limited respiratory reserve and is prone
ANESTHESIA AND CARDIOPULMONARY BYPASS FOR CONGENITAL HEART SURGERY Chawki F. elzein * Normal Cardio-Respiratory Physiology In Neonates And Infants The neonate has a limited respiratory reserve and is prone
Annals of Cardiac Anaesthesia 2005; 8: Shinde et al. Blood Lactate Levels during CPB 39
 Annals of Cardiac Anaesthesia 2005; 8: 39 44 Shinde et al. Blood Lactate Levels during CPB 39 Blood Lactate Levels During Cardiopulmonary Bypass for Valvular Heart Surgery ORIGINAL ARTICLES Santosh B Shinde,
Annals of Cardiac Anaesthesia 2005; 8: 39 44 Shinde et al. Blood Lactate Levels during CPB 39 Blood Lactate Levels During Cardiopulmonary Bypass for Valvular Heart Surgery ORIGINAL ARTICLES Santosh B Shinde,
