of Ventricular Tachycardia
|
|
|
- Gwendolyn Franklin
- 5 years ago
- Views:
Transcription
1 3103 Value of Physical Signs in the Diagnosis of Ventricular Tachycardia Clifford J. Garratt, DM; Michael J. Griffith, MD; Glenn Young, MB; Nicholas Curzen, MB; Stephen Brecker, MD; Anthony F. Rickards, MD; A. John Camm, MD Background Although the use of physical signs for the diagnosis of ventricular tachycardia (VT) was described in the early 1900s, their value in this role has never been systematically assessed. Methods and Results Using a blinded, randomized protocol, we examined the ability of 26 clinicians to detect ventriculoatrial (VA) dissociation during cardiac pacing in 21 patients with both atrial and ventricular pacing wires in situ after successful ablation of accessory pathways. In protocol 1 (10 patients), pacing was randomized to either ventricular pacing alone (simulating VT) or to atrioventricular sequential pacing (simulating supraventricular tachycardia or VT with intact VA conduction) at rates of 150 or 180 beats per minute. Each patient was examined by four clinicians blinded to the pacing mode. Clinicians were asked to make a diagnosis of "VA association" or "VA dissociation" after examining the patient for variability of the arterial pulse, jugular venous pulse (JVP), and first heart sound. In protocol 2 (11 patients), randomiza- Although the use of physical signs to identify ventriculoatrial (VA) dissociation during tachycardia (and therefore make a diagnosis of ventricular tachycardia) has been demonstrated since the early part of this century,1 the reliability of these signs has never been systematically assessed. To a large extent, this may reflect the rise of interest in the ECG that occurred after its introduction into widespread clinical use at this time. Nevertheless, despite the subsequent development and evaluation of a large number of ECG "rules" for the diagnosis of ventricular tachycardia (VT),2-5 the diagnosis continues to provide considerable difficulty in the setting of the emergency room, not infrequently with fatal or near-fatal results.6-8 The lack of a formal assessment of physical signs in this role may also be related to a specific difficulty in blinding clinicians to other clues to the diagnosis of a spontaneous tachycardia such as age of the patient or the presence of clinical evidence of structural heart disease. We sought to assess the value of physical signs in the diagnosis of VT using a blinded, randomized protocol in which ventricular and supraventricular tachycardias were simulated using ventricular and atrioventricular (AV) sequential pacing, respectively. Received June 1, 1994; revision accepted July 2, From the Academic Department of Cardiology, Glenfield Hospital, Groby Road, Leicester, England (C.J.G.); Royal Brompton National Heart and Lung Hospital, London (G.Y., S.J.B., N.C., A.F.R.); St George's Hospital Medical School, London (A.J.C.); and Freeman Hospital, Newcastle, England (M.J.G.). Correspondence to Dr Garratt, Academic Department of Cardiology, Glenfield Hospital, Groby Rd, Leicester LE3 9QP, UK American Heart Association, Inc. tion of pacing mode was performed between examination of each of the three physical signs so that the value of each sign was assessed individually. In protocol 1, a diagnosis of VA dissociation (VT) was made in 21 of 40 observations, with a specificity of 75%, sensitivity of 70%, and a positive predictive value (PPV) of 71%. In protocol 2, from a total of 132 observations (44 for each sign), the sensitivity, specificity, and PPV for a diagnosis of VT were as follows: arterial pulse, 61%, 71%, 70%; JVP, 96%, 75%, 82%; and first heart sound, 58%, 100%, 100%. Conclusions It is concluded that, in patients with a regular tachycardia of uncertain origin, clinically detectable variations in the first heart sound and JVP are highly specific and sensitive indicators, respectively, of a diagnosis of VT. Assessment of the arterial pulse is of little value in this role. (Circulation. 1994;90: ) Key Words * pacing * tachycardia * diagnosis Methods Patient and Clinician Selection All patients on the cardiology wards with temporary atrial and ventricular pacing wires inserted for clinical reasons were asked if they would participate in the study. Approval for the study was given by the local ethics committee, and informed consent was obtained from all patients. Twenty-one patients were included in the study (10 in protocol 1, 11 in protocol 2). Nineteen had temporary pacing wires inserted for repeat electrophysiological testing after catheter ablation of accessory pathways. None of these patients had clinical or echocardiographic evidence of structural heart disease, and mean age was 37 years. One 62-year-old patient had dilated cardiomyopathy, and one 65-year-old patient had complete heart block and an otherwise normal heart. Temporary pacing electrodes (6F bipolar right ventricular lead, SF bipolar "J" right atrial lead) had been inserted via the right or left subclavian venous route, as is our usual clinical practice. Patients who had given consent to the study underwent ventricular pacing at three rates (120, 150, and 180 beats per minute [bpm]) for 3 minutes at each rate while an electrogram was recorded from the atrial lead (Fig 1). Five patients were excluded from further study because intact VA conduction was evident (from the atrial electrogram) at these rates. Three patients were excluded because of discomfort during pacing at the higher rates. Clinicians were recruited for the study if they had regular contact with medical patients in an acute setting (emergency room or hospital ward) and were in the vicinity of the cardiology ward at the time that a patient was being studied. No clinicians refused to take part in the study. Patients were randomized to ventricular pacing or AV sequential pacing and to one of two rates (150 or 180 bpm).
2 3104 Circulation Vol 90, No 6 December 1994 V6 HRA r vp o F +0 ARP ABP V6 Ventricular AV Sequential Pacing Pacing FIG 1. Recording of atrial electrogram (HRA), jugular venous pressure (JVP), and arterial blood pressure (ABP) during ventricular and atrioventricular (AV) sequential pacing at a rate of 150 beats per minute. Venous and arterial pressure recording was not part of the study protocol but is shown here (in a patient with venous and arterial cannulas already in situ) for illustrative purposes. Variability of venous and arterial pressure waveforms can be seen during ventricular pacing. AV sequential pacing was performed with a paced AV delay that was programmed so that the VA/AV ratio remained constant at each rate, that is, 200 milliseconds at 150 bpm and 150 milliseconds at 180 bpm. Pacing was performed with the patient in bed and sitting at 45 degrees to the horizontal. After a 3-minute stabilization period of pacing, a clinician (blinded to the pacing mode) was asked to make a diagnosis of VA association or dissociation after examining the patient for variability of arterial pulse amplitude (at the radial and/or carotid artery), jugular venous pulse amplitude, and loudness of the first heart sound. No specific time limit was imposed for the examination and no specific sequence of examination was suggested, in an attempt to reproduce the usual clinical situation. The clinician was made aware that the pacing mode would remain unchanged throughout the examination. The true pacing mode was revealed to the clinician after his or her examination and declared diagnosis. Each patient was examined by four clinicians, with a 5-minute rest period (pacing stopped) between each examination. Pacing mode was rerandomized to AV or ventricular pacing at the initially selected rate before examination by each clinician. In this protocol, pacing mode was rerandomized to AV or ventricular pacing between examination of each of the three signs to assess the value of each sign individually. Pacing rate was randomized to one of three rates initially (120, 150, or 180 bpm), but thereafter the rate was left unchanged for each individual patient. AV sequential pacing was performed with a paced AV delay that was programmed so that the VA/AV ratio was constant at each rate, that is, 250 milliseconds at 120 bpm, 200 milliseconds at 150 bpm, and 150 milliseconds at 180 bpm. The clinician was made aware of the possibility of a change in pacing mode between examination of each of the signs. The patient's neck was covered during examination of the arterial pulse and first heart sound. As with protocol 1, each patient was examined by four clinicians, with a 5-minute rest period between each clinician. No patient was included in both protocols 1 and 2. Analysis of Results The sensitivity of the physical signs to detect VA dissociation was defined as true positives (correct diagnoses of VT) divided by the sum of true positives and false negatives (incorrect diagnoses of VA association). Specificity was defined as true negatives (correct diagnoses of VA association) divided by the sum of true negatives and false positives (incorrect diagnoses of VT). Positive predictive value refers to the study population (50% VT, 50% AV association) and was defined as true positives divided by the sum of true positives and false positives. Results Clinician Characteristics Twenty-six clinicians took part in the study: one attending physician, 2 senior cardiology fellows, 7 junior cardiology fellows, 8 senior residents, and 8 junior residents. All clinicians had some experience of assessment of physical signs in the setting of clinical cardiology (range, 3 months to 8 years), but only 2 claimed to have any experience of the use of physical signs as a means of arrhythmia diagnosis. Eleven clinicians examined only 1 patient, 3 examined 2 patients, 4 examined 5 patients, and 6 examined 6 patients. The great majority of clinicians took less than 5 minutes for the examination, and none took longer than 8 minutes. Value of Physical Signs to Diagnose VT A total of 40 observations were made in protocol 1 (10 patients each examined by 4 clinicians). A diagnosis of "VT" was made in 21 of the 40 observations, with a sensitivity of 75% (with 15 true positives from 20 observations during VA dissociation), specificity of 70% (with 6 false positives from 20 observations during VA association), and positive predictive value of 71% for this diagnosis in the study population. A total of 132 observations were made in protocol 2. Eleven patients were each examined by 4 clinicians, resulting in 44 observations for each of the three physical signs. The sensitivity, specificity, and positive predictive value of the individual signs for a diagnosis of VT were as follows: arterial pulse, 61%, 71%, 70%; jugular venous pressure, 96%, 75%, 82%; and first heart sound, 58%, 100%, 100%. A clinically detectable variation in the first heart sound was absolutely specific for a diagnosis of VT, with no false positives (from a total of 20 observations during VA association) and 14 true positives (from 24 observations during VA dissociation). The relatively poor predictive value of the clinical signs when assessed together (protocol 1) compared with examination of the first heart sound alone (protocol 2) may have been due to relative neglect of the findings of auscultation in favor of those of the arterial and venous pulse when all the signs are considered together (Table 1). The arterial pulse was found to be of little value in the diagnosis of VT both in terms of specificity and sensitivity. Although variability of the venous pulse was highly sensitive for a diagnosis of VT (with 23 true positives from 24 observations during VA dissociation), this sign was only 75% specific (5 false positives from a total of 20 observations during VA association).
3 Garratt et al Physical Signs and Ventricular Tachycardia 3105 TABLE 1. Value of Physical Signs in the Diagnosis of Ventricular Tachycardia All signs together Arterial pulse JVP First heart sound PPV indicates positive predictive value; JVP, jugular venous pulse. Effect of Tachycardia Rate on Ability to Diagnose VT The effect of tachycardia rate on the value of clinical signs to diagnose VT is described in Table 2. In protocol 1, 6 patients were examined at 150 bpm (total of 24 observations) and 4 were examined at 180 bpm (total of 16 observations). In protocol 2, 4 patients were examined at 120 bpm (16 observations for each sign), 4 at 150 bpm (16 observations for each sign), and 3 at 180 bpm (12 observations for each sign). When all the signs were assessed together (protocol 1), tachycardia rate had no detectable effect on the usefulness of the signs. Similarly, there was no clear relation between heart rate and the value of the arterial pulse when this sign was assessed separately (protocol 2). The absolute specificity of a variable first heart sound for a diagnosis of VT was, of course, independent of heart rate. The sensitivity of this latter sign, however, showed a direct relation with heart rate, so that at a rate of 180 bpm the sensitivity was 75%, compared with 50% for 150 bpm TABLE 2. Effect of Heart Rate on Ability to Diagnose Ventricular Tachycardia From Physical Signs (all signs) 150 bpm bpm Arterial pulse 120 bpm bpm bpm Jugular venous pulse 120 bpm bpm bpm First heart sound 120 bpm bpm bpm PPV indicates minute. positive predictive value; bpm, beats per 120 bpm [3v_ vi i;v V1a vi 150 bpm 180 bpm FIG 2. Effect of ventricular pacing rate on jugular venous pressure (JVP). Cannon A waves are more prominent during ventricular pacing at faster rates (bpm indicates beats per minute). and 27% for 120 bpm. The specificity and sensitivity of the venous pulse also increased at the higher heart rate (Fig 2), with both values reaching 100% at 180 bpm, although only 12 observations were made for each sign at this rate (8 observations of VA dissociation and 4 of VA association, all correctly diagnosed). Effect of 'Learning' on the Value of Clinical Signs Twenty-one clinicians took part in protocol 1. Eleven of these examined only 1 patient. Five clinicians saw 2 patients, 3 saw 3 patients, and 2 saw 5 patients. When assessment of the value of the physical signs is based only on the first patient examined by any clinician in protocol 1, the specificity and positive predictive value of all the signs together for a diagnosis of VT fall to 54% and 58%, respectively (Table 3). This suggests that the TABLE 3. Value of Physical Signs in the Diagnosis of Ventricular Tachycardia* All signs Arterial pulse JVP First heart sound PPV indicates positive predictive value; JVP, jugular venous pulse. *First patient examined by any particular clinician only.
4 3106 Circulation Vol 90, No 6 December 1994 ability to detect VA dissociation during tachycardia from the three physical signs together may be particularly poor in the absence of previous experience of assessment of these signs during tachycardia, possibly because of inappropriate attention to the arterial pulse (see below). Because the true pacing mode was revealed to the clinicians after the study of each patient, this may have led to a degree of "learning" in terms of the relative usefulness of the individual signs for making a diagnosis of VT. Twenty-one clinicians took part in protocol 2. Ten of these examined only 1 patient. Six clinicians saw 2 patients, 2 saw 3 patients, 1 saw 5 patients, and 2 saw 6 patients. When assessment of the value of the physical signs was based only on the first patient examined by any clinician in protocol 2, it can be seen that there was a small fall in the sensitivity of the first heart sound and venous pressure as a test for VT, but specificity and positive predictive value were well maintained for both signs. These results suggest that, even in the absence of previous specific experience, these particular physical signs are very useful in the diagnosis of VA dissociation during tachycardia. Discussion Sir James MacKensie' recorded the occurrence of slow independent jugular venous pulsations during presumed VT as long ago as Gallavardin9 recognized the clinical value of this observation and stated that if inspection of the jugular veins showed a recurring impulse occurring at a rate at about half that of the arterial rate, a diagnosis could be made of VT with conservation of the normal atrial rhythm. Other physical signs of mechanical AV dissociation were described by Levine10 (variability of intensity of the first heart sound during tachycardia) and by Wilson and coworkers11 (variability of arterial blood pressure). More recently, Schrire and Vogelpoel12 examined the value of combined ECG, phonocardiographic, and jugular venous pulse recordings in 9 cases of proven VT, the definitive diagnosis having been made using esophageal recordings of atrial activity. Eight of the 9 cases demonstrated both changing intensity of the first heart sound and independent slow jugular venous pulsations ("Cannon" A waves). In the remaining patient, coexistent atrial fibrillation was demonstrated. Although not tested in any controlled manner, the authors of this report were clearly of the opinion that these features of VT were detectable clinically, that is, without the use of phonocardiographic and jugular venous pulse recordings. Interest in the clinical signs of mechanical AV dissociation waned, however, with the recognition of cases of VT with 1:1 retrograde conduction to the atria13"14 and the development of ECG "rules" for the diagnosis of VT. The current study is the first to have analyzed systematically the value of physical signs in the diagnosis of VT. It has shown that clinically detectable variations in the first heart sound and jugular venous pressure are highly specific and sensitive indicators, respectively, of a diagnosis of VA dissociation during tachycardia. The arterial pulse is of little value in this role. These signs are particularly useful at rapid ventricular rates and can be interpreted successfully by nonspecialists in arrhythmia management. The use of pacing techniques to simulate tachycardias rather than the use of spontaneously occurring arrhythmias in the study allowed a blinded, randomized design that otherwise would not have been possible. As a direct consequence of the study design, the great majority of patients enrolled had structurally normal hearts, in contrast to patients presenting with spontaneous wide-complex regular tachycardias, who may have a number of structural myocardial abnormalities. The signs of mechanical AV dissociation during VT are dependent primarily on the presence of atrial contraction and will not be seen if the atrium is fibrillating or if there is another cause of atrial inactivity (electrical or mechanical). The coexistence of atrial fibrillation with VT in some patients is likely to result in a reduction of the sensitivity of physical signs for the diagnosis of VT in clinical practice. The presence of significant tricuspid incompetence (due to primary valve disease or secondary to right ventricular dilation) and the occurrence of VT with intact retrograde conduction are other potential causes of a decrease in sensitivity of the physical signs in clinical practice. In contrast, it is very unlikely that the specificity of the physical signs of mechanical VA dissociation would be reduced by the presence of structural heart disease. Although it is possible that variability of arterial pulse amplitude may be simulated by pulsus alternans associated with abnormal left ventricular function, it is difficult to conceive of a structural or functional anomaly that could mimic the slow, independent jugular venous pulsations or variability of the first heart sound associated with mechanical VA dissociation. VT is not the only cause of VA dissociation during wide-complex tachycardia. AV nodal reentrant tachycardia may be conducted with aberration to the ventricles (producing a regular wide-complex tachycardia) and with retrograde block to the atria. This cause of VA dissociation is so rare, however, that it continues to be the subject of case reports 20 years after its initial recognition.15'6 As a consequence, its relevance to the specificity of physical signs for identifying VT is likely to be minimal. By design, none of the patients included in this study suffered hemodynamic compromise during pacing-simulated tachycardia. The relevance of the findings of the study to very fast and hemodynamically unstable arrhythmias is not known. However, as the value of a clinical means of tachycardia diagnosis applies principally to hemodynamically stable arrhythmias that do not require immediate cardioversion, we do not consider this a major limitation. Most clinicians currently rely on patient history and specific ECG features to make a diagnosis of VT. Among patients referred for electrophysiological evaluation of broad-complex tachycardia, a history of previous myocardial infarction is known to have a very high predictive value for a diagnosis of VT. However, as pointed out by Tchou and coworkers,17 this patient group is already highly selected and is likely to differ from that presenting acutely to the emergency room. Patients with nonischemic cardiomyopathy (who may have VT in the absence of previous infarction) or atrial flutter in the setting of coronary disease (who may have supraventricular tachycardia after infarction) are often not referred for electrophysiological investigation. As a consequence, the true predictive value of the patient
5 Garratt et al Physical Signs and Ventricular Tachycardia 3107 history in the setting of the emergency room may be considerably less. Similarly, the sensitivity and specificity of the standard ECG criteria for the diagnosis of VT are suboptimal, with leads V1 and V6 frequently showing discordant morphology patterns that suggest different diagnoses.18 The most recent "rules" are those of Brugada and coworkers,18 who have devised a stepwise ECG approach based on the presence and width of an RS complex in the precordial leads during tachycardia, VA dissociation inferred from P-wave activity, and specific QRS patterns in V1 and V6. Although VA dissociation inferred from the ECG was 100% specific for VT, it could only be detected in 21% of VT episodes. Nevertheless, using their stepwise approach, these workers achieved very high sensitivity (99%) and specificity (96%) for a diagnosis of VT. It should be noted, however, that these results refer to ECG of patients not taking antiarrhythmic drug therapy: Specificity is very likely to fall if the patients are taking agents of antiarrhythmic class 1 or 3 at the time of presentation.19,20 In addition, these figures refer to ECG interpretation (including specific patterns in V1 and V6) by arrhythmia specialists at a time remote from patient presentation. Numerous publications have established the much poorer performance of nonspecialists at the time of first presentation of the arrhythmia.6-8 The current study was not designed to compare the value of physical signs with that of the patient history or ECG (or any other means of diagnosis) for the identification of VT. Nevertheless, the very high positive predictive value of a variable first heart sound (and of Cannon A waves during tachycardias with rates of 180 bpm) is likely to compare favorably with the patient history, the ECG, or the combination of the two in the diagnosis of VT Ṫhe findings of this study support those of Gallavardin9 (1920) and Levine10 (1927) and suggest that examination of the venous pressure waveform and first heart sound during tachycardia is of considerable value in the differential diagnosis of a broad-complex regular tachycardia. Direct comparison with other diagnostic methods in the clinical setting is warranted. References 1. MacKensie J. The Diseases of the Heart. Oxford, England: Oxford University Press; Pick A, Langendorf R. Differentiation of supraventricular and ventricular tachycardia. Prog Cardiovasc Dis. 1960;2: Sandler IA, Marriot H. The differential morphology of anomalous ventricular complexes of RBBB type in lead V,: ectopy versus aberration. Circulation. 1965;31: Wellens HJJ, Bar FW, Lie KI. The value of the electrocardiogram in the differential diagnosis of a tachycardia with a widened QRS complex. Am J Med. 1978;64: Kindwall KE, Brown J, Josephson ME. Electrocardiographic criteria for ventricular tachycardia in wide complex left bundle branch block morphology tachycardias. Am J CardioL 1988;61: Dancy M, Camm AJ, Ward DE. Misdiagnosis of chronic recurrent ventricular tachycardia. Lancet. 1985;254: Stewart RB, Bardy GH, Greene HL. Wide-complex tachycardia: misdiagnosis and outcome after emergent therapy. Ann Intern Med. 1986;104: Rankin AC, Rae AP, Cobbe SM. Misuse of intravenous verapamil in patients with ventricular tachycardia. Lancet. 1987;1: Gallavardin L. Tachycardie paroxystique ventriculaire. Arch Mal Coeur. 1920;13: Levine SA. Clinical recognition of paroxysmal ventricular tachycardia. Am Heart J. 1927;3: Wilson WS, Judge RD, Siegel JH. A simple diagnostic sign in ventricular tachycardia. N Engl J Med. 1964;270: Schrire V, Vogelpoel L. The clinical and electrocardiographic differentiation of supraventricular and ventricular tachycardias with regular rhythm. Am Heart J. 1955;49: Kistin AD. Retrograde conduction to the atria in ventricular tachycardia. Circulation. 1964;24: Massumi RA, Tawakkol AA, Kistin AD. Reevaluation of electrocardiographic and bedside criteria for diagnosis of ventricular tachycardia. Circulation. 1967;36: Wellens HJJ, Wesdorp JC, Duren DR, Lie KI. Second degree block during reciprocal atrioventricular nodal reentrant tachycardia. Circulation. 1976;53: Shimizu A, Ohe T, Takaki H, Kamakura S, Matsuhisa M, Sato I, Shimomura K. Narrow QRS complex tachycardia with atrioventricular dissociation. PACE Pacing Clin Electrophysiol. 1988;11: Tchou P, Young P, Mahmud R, Denker S, Jazayeri M, Akhtar M. Useful clinical criteria in the diagnosis of ventricular tachycardia. Am J Med. 1988;84: Brugada P, Brugada J, Mont L, Smeets J, Andries EW. A new approach to the differential diagnosis of a regular tachycardia with a wide QRS complex. Circulation. 1991;83: Camm AJ, Garratt CJ. Adenosine and supraventricular tachycardia. N EnglJ Med. 1991;325: Pollak A, Falk RH. New criteria for the diagnosis of regular, wide-complex tachycardias. Circulation. 1992;85: Letter.
Supraventricular Tachycardia (SVT)
 Supraventricular Tachycardia (SVT) Daniel Frisch, MD Cardiology Division, Electrophysiology Section Thomas Jefferson University Hospital daniel.frisch@jefferson.edu Short RP Are these the Mid same RP tachycardias?
Supraventricular Tachycardia (SVT) Daniel Frisch, MD Cardiology Division, Electrophysiology Section Thomas Jefferson University Hospital daniel.frisch@jefferson.edu Short RP Are these the Mid same RP tachycardias?
Differentiation of Ventricular Tachycardia from Junctional Tachycardia with Aberrant Conduction
 Differentiation of Ventricular Tachycardia from Junctional Tachycardia with Aberrant Conduction The Use of Competitive Atrial Pacing By ROBERT M. EASLEY, JR., M.D., AND SIDNEY GOLDSTEIN, M.D. SUMMARY A
Differentiation of Ventricular Tachycardia from Junctional Tachycardia with Aberrant Conduction The Use of Competitive Atrial Pacing By ROBERT M. EASLEY, JR., M.D., AND SIDNEY GOLDSTEIN, M.D. SUMMARY A
Atrioventricular (AV) Nodal Reentry Associated with 2:1 Infra-His Conduction Block during Tachycardia in a Patient with AV Nodal Triple Pathways
 Atrioventricular (AV) Nodal Reentry Associated with 2:1 Infra-His Conduction Block during Tachycardia in a Patient with AV Nodal Triple Pathways Haruhiko ABE, M.D., Takashi OHKITA, M.D., Masasuke FUJITA,
Atrioventricular (AV) Nodal Reentry Associated with 2:1 Infra-His Conduction Block during Tachycardia in a Patient with AV Nodal Triple Pathways Haruhiko ABE, M.D., Takashi OHKITA, M.D., Masasuke FUJITA,
Clinical Investigations
 Clinical Investigations The Lewis Lead for Detection of Ventriculoatrial Conduction Type Martin Huemer, MD; Henning Meloh, Philipp Attanasio, MD; Alexander Wutzler, MD; Abdul S. Parwani, MD; Hisao Matsuda,
Clinical Investigations The Lewis Lead for Detection of Ventriculoatrial Conduction Type Martin Huemer, MD; Henning Meloh, Philipp Attanasio, MD; Alexander Wutzler, MD; Abdul S. Parwani, MD; Hisao Matsuda,
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material
 1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
Sustained tachycardia with wide QRS
 Sustained tachycardia with wide QRS Courtesy from Prof. Antonio Américo Friedmann. Electrocardiology Service of University of Faculty of São Paulo. Opinions from colleagues Greetings to everyone, In a
Sustained tachycardia with wide QRS Courtesy from Prof. Antonio Américo Friedmann. Electrocardiology Service of University of Faculty of São Paulo. Opinions from colleagues Greetings to everyone, In a
Chapter 16: Arrhythmias and Conduction Disturbances
 Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
VENTRICULAR TACHYCARDIA WITH HEMODYNAMIC INSTABILITY REFRACTORY TO CARDIOVERSION: A CASE REPORT
 VENTRCULAR TACHYCARDA WTH HEMODYNAMC NSTABLTY REFRACTORY TO CARDOVERSON: A CASE REPORT Chun-Jen Chou, 1 Chee-Siong Lee, 2,3 and Wen-Ter Lai 2,3 1 Department of Emergency Medicine, Kaohsiung Municipal Hsiao-Kang
VENTRCULAR TACHYCARDA WTH HEMODYNAMC NSTABLTY REFRACTORY TO CARDOVERSON: A CASE REPORT Chun-Jen Chou, 1 Chee-Siong Lee, 2,3 and Wen-Ter Lai 2,3 1 Department of Emergency Medicine, Kaohsiung Municipal Hsiao-Kang
Supraventricular Tachycardia (SVT)
 Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
WPW syndrome and AVRT
 WPW syndrome and AVRT Myung-Yong Lee, MD, PhD Division of Cardiology Department of Internal Medicine School of Medicine Dankook University, Cheonan, Korea Supraventricular tachycardia (SVT) Paroxysmal
WPW syndrome and AVRT Myung-Yong Lee, MD, PhD Division of Cardiology Department of Internal Medicine School of Medicine Dankook University, Cheonan, Korea Supraventricular tachycardia (SVT) Paroxysmal
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology
 EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence
 www.ipej.org 125 Case Report A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence Miguel A. Arias MD, PhD; Eduardo Castellanos MD, PhD; Alberto Puchol MD;
www.ipej.org 125 Case Report A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence Miguel A. Arias MD, PhD; Eduardo Castellanos MD, PhD; Alberto Puchol MD;
Paroxysmal Supraventricular Tachycardia PSVT.
 Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Case Report Wide-QRS Tachycardia Inducible by Both Atrial and Ventricular Pacing
 Hellenic J Cardiol 2008; 49: 446-450 Case Report Wide-QRS Tachycardia Inducible by Both Atrial and Ventricular Pacing ELEFTHERIOS GIAZITZOGLOU, DEMOSTHENES G. KATRITSIS Department of Cardiology, Athens
Hellenic J Cardiol 2008; 49: 446-450 Case Report Wide-QRS Tachycardia Inducible by Both Atrial and Ventricular Pacing ELEFTHERIOS GIAZITZOGLOU, DEMOSTHENES G. KATRITSIS Department of Cardiology, Athens
When confronted with a tachycardia
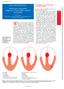 Heart 2001;86:579 585 ELECTROPHYSOLOGY Ventricular tachycardia: diagnosis of broad QRS complex tachycardia Hein JJ Wellens nteruniversity Cardiology nstitute of the Netherlands (CN), Utrecht, The Netherlands
Heart 2001;86:579 585 ELECTROPHYSOLOGY Ventricular tachycardia: diagnosis of broad QRS complex tachycardia Hein JJ Wellens nteruniversity Cardiology nstitute of the Netherlands (CN), Utrecht, The Netherlands
The Efficient and Smart Methods for Diagnosis of SVT 대구파티마병원순환기내과정병천
 The Efficient and Smart Methods for Diagnosis of SVT 대구파티마병원순환기내과정병천 Differentiation Supraventricular Origin from Ventricular Origin on ECG. QRS-Complex Width. 1. Narrow QRS-Complex Tachycardia (
The Efficient and Smart Methods for Diagnosis of SVT 대구파티마병원순환기내과정병천 Differentiation Supraventricular Origin from Ventricular Origin on ECG. QRS-Complex Width. 1. Narrow QRS-Complex Tachycardia (
Basic Electrophysiology Protocols
 Indian Journal of Cardiology ISSN-0972-1622 2012 by the Indian Society of Cardiology Vol. 15, (3-4), 27-37 [ 27 Review Article Shomu Bohora Assistant Professor, Deptt. of Cardiology, U.N. Mehta Institute
Indian Journal of Cardiology ISSN-0972-1622 2012 by the Indian Society of Cardiology Vol. 15, (3-4), 27-37 [ 27 Review Article Shomu Bohora Assistant Professor, Deptt. of Cardiology, U.N. Mehta Institute
II V 1 HRA 3 4 HB 5 6 HB 3 4 HB 1 2 CS 7 8 CS 5 6 CS 3 4 CS 1 2 ABL 3 4 ABL 1 2 RVA 3 4. T. Suga et al.
 Table 1. The distance between the positions of the catheter tip Patient Location Before elimination of After elimination of Number of the the accessory pathway the accessory pathway accessory pathway RAO
Table 1. The distance between the positions of the catheter tip Patient Location Before elimination of After elimination of Number of the the accessory pathway the accessory pathway accessory pathway RAO
The most common. hospitalized patients. hypotension due to. filling time Rate control in ICU patients may be difficult as many drugs cause hypotension
 Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
ECG QUIZ Luc DE ROY Brussels Belgium Disclosure in relation to this topic: none
 ECG QUIZ Luc DE ROY Brussels Belgium Disclosure in relation to this topic: none TEST EXAMPLE What is the colour of this rectangle? 1. Blue? 2. Red? 3. Purple? 4. Green? 5. Yellow? 6. 1 and 3? 7. Any of
ECG QUIZ Luc DE ROY Brussels Belgium Disclosure in relation to this topic: none TEST EXAMPLE What is the colour of this rectangle? 1. Blue? 2. Red? 3. Purple? 4. Green? 5. Yellow? 6. 1 and 3? 7. Any of
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
ECGs on the acute admission ward. - Cardiology Update -
 ECGs on the acute admission ward - Cardiology Update - Dr Simon Fynn Consultant Cardiologist Papworth Hospital, Cambridge RCP London Oct 2017 ECG 1 1. AF with BBB 2. Pre-excited AF 3. SVT with BBB 4.
ECGs on the acute admission ward - Cardiology Update - Dr Simon Fynn Consultant Cardiologist Papworth Hospital, Cambridge RCP London Oct 2017 ECG 1 1. AF with BBB 2. Pre-excited AF 3. SVT with BBB 4.
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment
 Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
CATHETER ABLATION FOR TACHYCARDIAS
 190 CATHETER ABLATION FOR TACHYCARDIAS MASOOD AKHTAR, M.D. T ACHY ARRHYTHMIAS constitute a major cause of mortality and morbidity. The most serious manifestation of cardiac arrhythmia is sudden cardiac
190 CATHETER ABLATION FOR TACHYCARDIAS MASOOD AKHTAR, M.D. T ACHY ARRHYTHMIAS constitute a major cause of mortality and morbidity. The most serious manifestation of cardiac arrhythmia is sudden cardiac
In certain cases of supraventricular
 Case Report Hellenic J Cardiol 2013; 54: 469-473 A Tachycardia with Varying QRS Morphology and RP Intervals: Differential Diagnosis and Therapy Socrates Korovesis, Eleftherios Giazitzoglou, Demosthenes
Case Report Hellenic J Cardiol 2013; 54: 469-473 A Tachycardia with Varying QRS Morphology and RP Intervals: Differential Diagnosis and Therapy Socrates Korovesis, Eleftherios Giazitzoglou, Demosthenes
Role of echocardiography in differential diagnosis of broad complex tachycardia
 Br Heart J 1985; 54: 166-72 Role of echocardiography in differential diagnosis of broad complex tachycardia CHRISTOPHER WREN, RONALD W F CAMPBELL, STEWART HUNTER From he Freeman Hospital, Newcasde upon
Br Heart J 1985; 54: 166-72 Role of echocardiography in differential diagnosis of broad complex tachycardia CHRISTOPHER WREN, RONALD W F CAMPBELL, STEWART HUNTER From he Freeman Hospital, Newcasde upon
a lecture series by SWESEMJR
 Arrhythmias Automaticity- the ability to depolarize spontaneously. Pacemakers: Sinoatrial node: 70 bpm AV-nodal area: 40 bpm His-Purkinje: 20-40 bpm it Mechanisms of arrhythmias 1. Increased automaticity
Arrhythmias Automaticity- the ability to depolarize spontaneously. Pacemakers: Sinoatrial node: 70 bpm AV-nodal area: 40 bpm His-Purkinje: 20-40 bpm it Mechanisms of arrhythmias 1. Increased automaticity
Transcoronary Chemical Ablation of Atrioventricular Conduction
 757 Transcoronary Chemical Ablation of Atrioventricular Conduction Pedro Brugada, MD, Hans de Swart, MD, Joep Smeets, MD, and Hein J.J. Wellens, MD In seven patients with symptomatic atrial fibrillation
757 Transcoronary Chemical Ablation of Atrioventricular Conduction Pedro Brugada, MD, Hans de Swart, MD, Joep Smeets, MD, and Hein J.J. Wellens, MD In seven patients with symptomatic atrial fibrillation
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
Declaration of conflict of interest NONE
 Declaration of conflict of interest NONE Transatlantic Electrophysiology Lessons for and from Iberoamerica European Society of Cardiology Mexican Society of Cardiology Wolff-Parkinson-White Syndrome in
Declaration of conflict of interest NONE Transatlantic Electrophysiology Lessons for and from Iberoamerica European Society of Cardiology Mexican Society of Cardiology Wolff-Parkinson-White Syndrome in
EKG Competency for Agency
 EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
Successful treatment of tachycardia-induced cardiomyopathy secondary to dual atrioventricular nodal nonreentrant tachycardia using cryoablation
 Successful treatment of tachycardia-induced cardiomyopathy secondary to dual atrioventricular nodal nonreentrant tachycardia using cryoablation Harold Rivner, MD, * Chris Healy, MD, Raul D. Mitrani, MD,
Successful treatment of tachycardia-induced cardiomyopathy secondary to dual atrioventricular nodal nonreentrant tachycardia using cryoablation Harold Rivner, MD, * Chris Healy, MD, Raul D. Mitrani, MD,
ECG ABNORMALITIES D R. T AM A R A AL Q U D AH
 ECG ABNORMALITIES D R. T AM A R A AL Q U D AH When we interpret an ECG we compare it instantaneously with the normal ECG and normal variants stored in our memory; these memories are stored visually in
ECG ABNORMALITIES D R. T AM A R A AL Q U D AH When we interpret an ECG we compare it instantaneously with the normal ECG and normal variants stored in our memory; these memories are stored visually in
were inserted into the right femoral vein and positioned system and intracardiac recordings were displayed
 CASE REPORTS Termination of Ventricular Tachycardia by Carotid Sinus Massage DAVID S. HESS, M.D., TIMOTHY HANLON, M.D., MELVIN SCHEINMAN, M.D., ROGER BUDGE, M.D., AND JAWAHAR DESAI, M.D. SUMMARY Intracardiac
CASE REPORTS Termination of Ventricular Tachycardia by Carotid Sinus Massage DAVID S. HESS, M.D., TIMOTHY HANLON, M.D., MELVIN SCHEINMAN, M.D., ROGER BUDGE, M.D., AND JAWAHAR DESAI, M.D. SUMMARY Intracardiac
Ventricular tachycardia Ventricular fibrillation and ICD
 EKG Conference Ventricular tachycardia Ventricular fibrillation and ICD Samsung Medical Center CCU D.I. Hur Ji Won 2006.05.20 Ventricular tachyarrhythmia ventricular tachycardia ventricular fibrillation
EKG Conference Ventricular tachycardia Ventricular fibrillation and ICD Samsung Medical Center CCU D.I. Hur Ji Won 2006.05.20 Ventricular tachyarrhythmia ventricular tachycardia ventricular fibrillation
Concise Review for Primary-Care Physicians
 Concise Review for Primary-Care Physicians Narrow QRS Complex Tachycardias STEPHEN J. PIEPER, M.D., AND MARSHALL S. STANTON, M.D. Regular narrow QRS complex tachycardias are a common problem encountered
Concise Review for Primary-Care Physicians Narrow QRS Complex Tachycardias STEPHEN J. PIEPER, M.D., AND MARSHALL S. STANTON, M.D. Regular narrow QRS complex tachycardias are a common problem encountered
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Pre-excited tachycardia: Atrial tachycardia with a bystander left lateral accessory pathway
 Pre-excited tachycardia: Atrial tachycardia with a bystander left lateral accessory pathway Jeffrey Munro, DO, Win-Kuang Shen, MD, FHRS, Komandoor Srivathsan, MD From the Department of Cardiovascular Disease,
Pre-excited tachycardia: Atrial tachycardia with a bystander left lateral accessory pathway Jeffrey Munro, DO, Win-Kuang Shen, MD, FHRS, Komandoor Srivathsan, MD From the Department of Cardiovascular Disease,
Ventriculoatrial Block During a Narrow-QRS Tachycardia: What Is the Tachycardia Mechanism? IV
 174 ARRHYTHMIA OF THE MONTH Section Editor: Fred Morady, M.D. Ventriculoatrial Block During a Narrow-QRS Tachycardia: What Is the Tachycardia Mechanism? IV FRED MORADY, M.D. From the Cardiology Division,
174 ARRHYTHMIA OF THE MONTH Section Editor: Fred Morady, M.D. Ventriculoatrial Block During a Narrow-QRS Tachycardia: What Is the Tachycardia Mechanism? IV FRED MORADY, M.D. From the Cardiology Division,
Dos and Don t in Cardiac Arrhythmia. Case 1 -ECG. Case 1. Management. Emergency Admissions. Reduction of TE risk -CHADS 2 score. Hospital Admissions
 Emergency Admissions Dos and Don t in Cardiac Arrhythmia Tom Wong, MD, FESC Consultant Cardiologist, Honorary Senior Lecturer Royal Brompton & Harefield Hospitals National Heart and Lung Institute, Imperial
Emergency Admissions Dos and Don t in Cardiac Arrhythmia Tom Wong, MD, FESC Consultant Cardiologist, Honorary Senior Lecturer Royal Brompton & Harefield Hospitals National Heart and Lung Institute, Imperial
Journal of the American College of Cardiology Vol. 36, No. 2, by the American College of Cardiology ISSN /00/$20.
 Journal of the American College of Cardiology Vol. 36, No. 2, 2000 2000 by the American College of Cardiology ISSN 0735-1097/00/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)00770-1 Diagnostic
Journal of the American College of Cardiology Vol. 36, No. 2, 2000 2000 by the American College of Cardiology ISSN 0735-1097/00/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)00770-1 Diagnostic
ARTICLE. Supraventricular Tachycardia in Infancy. Catherine D. DeAngelis, MD. In most infants, SVT is due to an accessory atrioventricular
 Supraventricular Tachycardia in Infancy Evaluation, Management, and Follow-up Susan P. Etheridge, MD; Victoria E. Judd, MD ARTICLE Background: Supraventricular tachycardia (SVT) occurs frequently in infancy.
Supraventricular Tachycardia in Infancy Evaluation, Management, and Follow-up Susan P. Etheridge, MD; Victoria E. Judd, MD ARTICLE Background: Supraventricular tachycardia (SVT) occurs frequently in infancy.
Circulation: Arrhythmia and Electrophysiology CHALLENGE OF THE WEEK
 A 14-year-old girl with Wolff-Parkinson-White syndrome and recurrent paroxysmal palpitations due to atrioventricular reentry tachycardia had undergone two prior failed left lateral accessory pathway ablations
A 14-year-old girl with Wolff-Parkinson-White syndrome and recurrent paroxysmal palpitations due to atrioventricular reentry tachycardia had undergone two prior failed left lateral accessory pathway ablations
ECG Basics Sonia Samtani 7/2017 UCI Resident Lecture Series
 ECG Basics Sonia Samtani 7/2017 UCI Resident Lecture Series Agenda I. Introduction II.The Conduction System III.ECG Basics IV.Cardiac Emergencies V.Summary The Conduction System Lead Placement avf Precordial
ECG Basics Sonia Samtani 7/2017 UCI Resident Lecture Series Agenda I. Introduction II.The Conduction System III.ECG Basics IV.Cardiac Emergencies V.Summary The Conduction System Lead Placement avf Precordial
Case 1 Left Atrial Tachycardia
 Case 1 Left Atrial Tachycardia A 16 years old woman was referred to our institution because of recurrent episodes of palpitations and dizziness despite previous ablation procedure( 13 years ago) of postero-septal
Case 1 Left Atrial Tachycardia A 16 years old woman was referred to our institution because of recurrent episodes of palpitations and dizziness despite previous ablation procedure( 13 years ago) of postero-septal
TACHYARRHYTHMIAs. Pawel Balsam, MD, PhD
 TACHYARRHYTHMIAs Pawel Balsam, MD, PhD SupraVentricular Tachycardia Atrial Extra Systole Sinus Tachycardia Focal A. Tachycardia AVRT AVNRT Atrial Flutter Atrial Fibrillation Ventricular Tachycardia Ventricular
TACHYARRHYTHMIAs Pawel Balsam, MD, PhD SupraVentricular Tachycardia Atrial Extra Systole Sinus Tachycardia Focal A. Tachycardia AVRT AVNRT Atrial Flutter Atrial Fibrillation Ventricular Tachycardia Ventricular
EKG Abnormalities. Adapted from:
 EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
Step by step approach to EKG rhythm interpretation:
 Sinus Rhythms Normal sinus arrhythmia Small, slow variation of the R-R interval i.e. variation of the normal sinus heart rate with respiration, etc. Sinus Tachycardia Defined as sinus rhythm with a rate
Sinus Rhythms Normal sinus arrhythmia Small, slow variation of the R-R interval i.e. variation of the normal sinus heart rate with respiration, etc. Sinus Tachycardia Defined as sinus rhythm with a rate
UNDERSTANDING YOUR ECG: A REVIEW
 UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
Electrocardiography for Healthcare Professionals
 Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 10: Pacemaker Rhythms and Bundle Branch Block Learning Outcomes 10.1 Describe the various pacemaker rhythms. 10.2
Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 10: Pacemaker Rhythms and Bundle Branch Block Learning Outcomes 10.1 Describe the various pacemaker rhythms. 10.2
Figure 2. Normal ECG tracing. Table 1.
 Figure 2. Normal ECG tracing that navigates through the left ventricle. Following these bundle branches the impulse finally passes to the terminal points called Purkinje fibers. These Purkinje fibers are
Figure 2. Normal ECG tracing that navigates through the left ventricle. Following these bundle branches the impulse finally passes to the terminal points called Purkinje fibers. These Purkinje fibers are
Clinical Cardiac Electrophysiology
 Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
PARA-HISSIAN CONCEALED ACCESSORY PATHWAY
 PARA-HISSIAN CONCEALED ACCESSORY PATHWAY Anamnestic Findings 41 y.o. man with normal cardiac findings on echocardiography, suffering for paroxysmal supra-ventricular tachycardia since 1982 with rapid onset
PARA-HISSIAN CONCEALED ACCESSORY PATHWAY Anamnestic Findings 41 y.o. man with normal cardiac findings on echocardiography, suffering for paroxysmal supra-ventricular tachycardia since 1982 with rapid onset
Arrhythmias and Heart Failure Dr Chris Lang Consultant Cardiologist and Electrophysiologist Royal Infirmary of Edinburgh
 Arrhythmias and Heart Failure Dr Chris Lang Consultant Cardiologist and Electrophysiologist Royal Infirmary of Edinburgh Arrhythmias and Heart Failure Ventricular Supraventricular VT/VF Primary prevention
Arrhythmias and Heart Failure Dr Chris Lang Consultant Cardiologist and Electrophysiologist Royal Infirmary of Edinburgh Arrhythmias and Heart Failure Ventricular Supraventricular VT/VF Primary prevention
Looks Like VT But Isn't - Successful Ablation Of A Left Free Wall Accessory Pathway With Mahaim-like Properties
 www.ipej.org 112 Case Report Looks Like VT But Isn't - Successful Ablation Of A Left Free Wall Accessory Pathway With Mahaim-like Properties Faizel Osman MD MRCP 1, Peter J Stafford BSc MD FRCP 2, G Andre
www.ipej.org 112 Case Report Looks Like VT But Isn't - Successful Ablation Of A Left Free Wall Accessory Pathway With Mahaim-like Properties Faizel Osman MD MRCP 1, Peter J Stafford BSc MD FRCP 2, G Andre
Pediatrics ECG Monitoring. Pediatric Intensive Care Unit Emergency Division
 Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Case-Based Practical ECG Interpretation for the Generalist
 Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Concealed Accessory Pathway in Late Presentation Wolff-Parkinson-White Syndrome
 CASE REPORT Concealed Accessory Pathway in Late Presentation Wolff-Parkinson-White Syndrome Stephanie Rose1, Richard Armstrong2, David Moore2 Third year medicine, Trinity College Dublin Department of Cardiology,
CASE REPORT Concealed Accessory Pathway in Late Presentation Wolff-Parkinson-White Syndrome Stephanie Rose1, Richard Armstrong2, David Moore2 Third year medicine, Trinity College Dublin Department of Cardiology,
Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC
 Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC Professor of Medicine Director of Cardiac Electrophysiology Temple University Health System Plumbing Electrical System Bradyarrhythmias Sinus Node
Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC Professor of Medicine Director of Cardiac Electrophysiology Temple University Health System Plumbing Electrical System Bradyarrhythmias Sinus Node
AV Nodal Reentrant Tachycardia with Mahaim Fiber Conduction
 AV Nodal Reentrant Tachycardia with Mahaim Fiber Conduction Chikayoshi KOMATSU, M.D., Katsuro ITO, M.D., Takanari ISHINAGA, M.D., Yasutaka TOKUHISA, M.D., Takashi TANOIRI, M.D., Hiroshi MAKINO, M.D., Jun
AV Nodal Reentrant Tachycardia with Mahaim Fiber Conduction Chikayoshi KOMATSU, M.D., Katsuro ITO, M.D., Takanari ISHINAGA, M.D., Yasutaka TOKUHISA, M.D., Takashi TANOIRI, M.D., Hiroshi MAKINO, M.D., Jun
Atrial fibrillation (AF) is the most common sustained
 Effect of Atrial Fibrillation and an Irregular Ventricular Response on Sympathetic Nerve Activity in Human Subjects Stephen L. Wasmund, PhD; Jian-Ming Li, MD, PhD; Richard L. Page, MD; Jose A. Joglar,
Effect of Atrial Fibrillation and an Irregular Ventricular Response on Sympathetic Nerve Activity in Human Subjects Stephen L. Wasmund, PhD; Jian-Ming Li, MD, PhD; Richard L. Page, MD; Jose A. Joglar,
SPLITTING OF HEART SOUNDS FROM VENTRICULAR
 Brit. Heart J., 1965, 27, 691. SPLITTING OF HEART SOUNDS FROM VENTRICULAR ASYNCHRONY IN BUNDLE-BRANCH BLOCK, VENTRICULAR ECTOPIC BEATS, AND ARTIFICIAL PACING* BY EDGAR HABER AND AUBREY LEATHAM From the
Brit. Heart J., 1965, 27, 691. SPLITTING OF HEART SOUNDS FROM VENTRICULAR ASYNCHRONY IN BUNDLE-BRANCH BLOCK, VENTRICULAR ECTOPIC BEATS, AND ARTIFICIAL PACING* BY EDGAR HABER AND AUBREY LEATHAM From the
Radiofrequency Catheter Ablation in a Patient with Tachycardiomyopathy due to Incessant Fascicular Tachycardia
 증례 Korean Circulation J 2004;34(11):1107-1112 Radiofrequency Catheter Ablation in a Patient with Tachycardiomyopathy due to Incessant Fascicular Tachycardia Hyung-Wook Park, MD, Young-Joon Hong, MD, Ju-Han
증례 Korean Circulation J 2004;34(11):1107-1112 Radiofrequency Catheter Ablation in a Patient with Tachycardiomyopathy due to Incessant Fascicular Tachycardia Hyung-Wook Park, MD, Young-Joon Hong, MD, Ju-Han
Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
 Journal of Geriatric Cardiology (2018) 15: 193 198 2018 JGC All rights reserved; www.jgc301.com Case Report Open Access Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
Journal of Geriatric Cardiology (2018) 15: 193 198 2018 JGC All rights reserved; www.jgc301.com Case Report Open Access Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE. Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology
 PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology Medical University of Łódź The heart is made up of four chambers Left Atrium Right Atrium Left Ventricle
PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology Medical University of Łódź The heart is made up of four chambers Left Atrium Right Atrium Left Ventricle
Use of Catheter Ablation in the Treatment of Ventricular Tachycardia Triggered by Premature Ventricular Contraction
 J Arrhythmia Vol 22 No 3 2006 Case Report Use of Catheter Ablation in the Treatment of Ventricular Tachycardia Triggered by Premature Ventricular Contraction sao Kato MD, Toru wa MD, Yasushi Suzuki MD,
J Arrhythmia Vol 22 No 3 2006 Case Report Use of Catheter Ablation in the Treatment of Ventricular Tachycardia Triggered by Premature Ventricular Contraction sao Kato MD, Toru wa MD, Yasushi Suzuki MD,
PEDIATRIC SVT MANAGEMENT
 PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
file://c:\documents and Settings\admin\My Documents\CV\92.htm
 Page 1 of 5 Amir Farjam Fazelifar, M.D. Assistant Professor of Cardiac Electrophysiology Academic Address: Shaheed Rajaei Cardiovascular, Medical & Research Center, Vali- Asr Avenue Tehran- Iran Tel /
Page 1 of 5 Amir Farjam Fazelifar, M.D. Assistant Professor of Cardiac Electrophysiology Academic Address: Shaheed Rajaei Cardiovascular, Medical & Research Center, Vali- Asr Avenue Tehran- Iran Tel /
Please check your answers with correct statements in answer pages after the ECG cases.
 ECG Cases ECG Case 1 Springer International Publishing AG, part of Springer Nature 2018 S. Okutucu, A. Oto, Interpreting ECGs in Clinical Practice, In Clinical Practice, https://doi.org/10.1007/978-3-319-90557-0
ECG Cases ECG Case 1 Springer International Publishing AG, part of Springer Nature 2018 S. Okutucu, A. Oto, Interpreting ECGs in Clinical Practice, In Clinical Practice, https://doi.org/10.1007/978-3-319-90557-0
FLB s What Are Those Funny-Looking Beats?
 FLB s What Are Those Funny-Looking Beats? Reading Assignment (pages 27-45 in Outline ) The 5-Step Method ECG #: Mearurements: Rhythm (s): Conduction: Waveform: Interpretation: A= V= PR= QRS= QT= Axis=
FLB s What Are Those Funny-Looking Beats? Reading Assignment (pages 27-45 in Outline ) The 5-Step Method ECG #: Mearurements: Rhythm (s): Conduction: Waveform: Interpretation: A= V= PR= QRS= QT= Axis=
Cardiac rhythm detailed monitoring by an implanted pacemaker: The iecg solution
 Cardiac rhythm detailed monitoring by an implanted pacemaker: The iecg solution Francesco Zanon, MD, FESC, FHRS Arrhythmia and Electrophysiology Unit, Cardiology Dept. Santa Maria della Misericordia General
Cardiac rhythm detailed monitoring by an implanted pacemaker: The iecg solution Francesco Zanon, MD, FESC, FHRS Arrhythmia and Electrophysiology Unit, Cardiology Dept. Santa Maria della Misericordia General
Bradydysrhythmias and Atrioventricular Conduction Blocks
 Emerg Med Clin N Am 24 (2006) 1 9 Bradydysrhythmias and Atrioventricular Conduction Blocks Jacob W. Ufberg, MD*, Jennifer S. Clark, MD Department of Emergency Medicine, Temple University School of Medicine,
Emerg Med Clin N Am 24 (2006) 1 9 Bradydysrhythmias and Atrioventricular Conduction Blocks Jacob W. Ufberg, MD*, Jennifer S. Clark, MD Department of Emergency Medicine, Temple University School of Medicine,
BSH Heart Failure Nurse and Healthcare Professional Study Day 2017
 BSH Heart Failure Nurse and Healthcare Professional Study Day 2017 Presentation title: Malignant Arrhythmias Speaker: Derek Connelly Conflicts of interest: Speakers fees / advisory boards: Boehringer Ingelheim,
BSH Heart Failure Nurse and Healthcare Professional Study Day 2017 Presentation title: Malignant Arrhythmias Speaker: Derek Connelly Conflicts of interest: Speakers fees / advisory boards: Boehringer Ingelheim,
Diploma in Electrocardiography
 The Society for Cardiological Science and Technology Diploma in Electrocardiography The Society makes this award to candidates who can demonstrate the ability to accurately record a resting 12-lead electrocardiogram
The Society for Cardiological Science and Technology Diploma in Electrocardiography The Society makes this award to candidates who can demonstrate the ability to accurately record a resting 12-lead electrocardiogram
Determination of Inadvertent Atrial Capture During Para-Hisian Pacing
 Determination of Inadvertent Atrial Capture During Para-Hisian Pacing Manoj Obeyesekere, MBBS; Peter Leong-Sit, MD; Allan Skanes, MD; Andrew Krahn, MD; Raymond Yee, MD; Lorne J. Gula, MD; Matthew Bennett,
Determination of Inadvertent Atrial Capture During Para-Hisian Pacing Manoj Obeyesekere, MBBS; Peter Leong-Sit, MD; Allan Skanes, MD; Andrew Krahn, MD; Raymond Yee, MD; Lorne J. Gula, MD; Matthew Bennett,
Case Report Simultaneous Accessory Pathway and AV Node Mechanical Block
 185 Case Report Simultaneous Accessory Pathway and AV Node Mechanical Block Daniel Garofalo, MD, FRACP, Alfonso Gomez Gallanti, MD, David Filgueiras Rama, MD, Rafael Peinado Peinado, PhD, FESC Unidad de
185 Case Report Simultaneous Accessory Pathway and AV Node Mechanical Block Daniel Garofalo, MD, FRACP, Alfonso Gomez Gallanti, MD, David Filgueiras Rama, MD, Rafael Peinado Peinado, PhD, FESC Unidad de
Uncommon forms of AV reentry: atrio and fasciculo-ventricular fibers, slow conducting fibers. Jesus Almendral, Madrid, Spain
 Uncommon forms of AV reentry: atrio and fasciculo-ventricular fibers, slow conducting fibers Jesus Almendral, Madrid, Spain Common forms of AV reentry Accessory pathways: Upper insertion: atrium Lower
Uncommon forms of AV reentry: atrio and fasciculo-ventricular fibers, slow conducting fibers Jesus Almendral, Madrid, Spain Common forms of AV reentry Accessory pathways: Upper insertion: atrium Lower
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD
 Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
Wolff-Parkinson-White Syndrome
 Wolff-Parkinson-White Syndrome www.consultant360.com /articles/wolff-parkinson-white-syndrome A 37-year-old woman presented to the office with intermittent dizziness, palpitations, and multiple syncopal
Wolff-Parkinson-White Syndrome www.consultant360.com /articles/wolff-parkinson-white-syndrome A 37-year-old woman presented to the office with intermittent dizziness, palpitations, and multiple syncopal
Cardiac Cycle. Each heartbeat is called a cardiac cycle. First the two atria contract at the same time.
 The Heartbeat Cardiac Cycle Each heartbeat is called a cardiac cycle. First the two atria contract at the same time. Next the two ventricles contract at the same time. Then all the chambers relax. http://www.youtube.com/watch?v=frd3k6lkhws
The Heartbeat Cardiac Cycle Each heartbeat is called a cardiac cycle. First the two atria contract at the same time. Next the two ventricles contract at the same time. Then all the chambers relax. http://www.youtube.com/watch?v=frd3k6lkhws
National Coverage Determination (NCD) for Cardiac Pacemakers (20.8)
 Page 1 of 12 Centers for Medicare & Medicaid Services National Coverage Determination (NCD) for Cardiac Pacemakers (20.8) Tracking Information Publication Number 100-3 Manual Section Number 20.8 Manual
Page 1 of 12 Centers for Medicare & Medicaid Services National Coverage Determination (NCD) for Cardiac Pacemakers (20.8) Tracking Information Publication Number 100-3 Manual Section Number 20.8 Manual
COMPLEX CASE STUDY INNOVATIVE COLLECTIONS. Case presentation
 The Journal of Innovations in Cardiac Rhythm Management, 3 (2012), 939 943 INNOVATIVE COLLECTIONS COMPLEX CASE STUDY Subtle Changes in Electrogram Morphology During Para-Hisian Pacing Performed on IV Adenosine:
The Journal of Innovations in Cardiac Rhythm Management, 3 (2012), 939 943 INNOVATIVE COLLECTIONS COMPLEX CASE STUDY Subtle Changes in Electrogram Morphology During Para-Hisian Pacing Performed on IV Adenosine:
Case Report Mahaim Fiber Accelerated Automaticity and Clues to a Mahaim Fiber Being Morphologically an Ectopic or a Split AV Node
 www.ipej.org 62 Case Report Mahaim Fiber Accelerated Automaticity and Clues to a Mahaim Fiber Being Morphologically an Ectopic or a Split AV Node Shomu Bohora, Narayanan Namboodiri, Santosh Dora, VK Ajit
www.ipej.org 62 Case Report Mahaim Fiber Accelerated Automaticity and Clues to a Mahaim Fiber Being Morphologically an Ectopic or a Split AV Node Shomu Bohora, Narayanan Namboodiri, Santosh Dora, VK Ajit
CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint
 CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Clinical Cardiac Electrophysiology MOC exam blueprint Based on feedback
CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Clinical Cardiac Electrophysiology MOC exam blueprint Based on feedback
Interactive Simulator for Evaluating the Detection Algorithms of Implantable Defibrillators
 22 March 2002 Interactive Simulator for Evaluating the Detection Algorithms of Implantable Defibrillators F. HINTRINGER, O. PACHINGER Division of Cardiology, Department for Internal Medicine, University
22 March 2002 Interactive Simulator for Evaluating the Detection Algorithms of Implantable Defibrillators F. HINTRINGER, O. PACHINGER Division of Cardiology, Department for Internal Medicine, University
AF Today: W. For the majority of patients with atrial. are the Options? Chris Case
 AF Today: W hat are the Options? Management strategies for patients with atrial fibrillation should depend on the individual patient. Treatment with medications seems adequate for most patients with atrial
AF Today: W hat are the Options? Management strategies for patients with atrial fibrillation should depend on the individual patient. Treatment with medications seems adequate for most patients with atrial
Unusual Tachycardia Association In A patient Without Structural Heart Disease
 www.ipej.org 233 Case Report Unusual Tachycardia Association In A patient Without Structural Heart Disease Eduardo Arana-Rueda, Alonso Pedrote, Lorena Garcia-Riesco, Manuel Frutos-Lopez, Juan A. Sanchez-Brotons
www.ipej.org 233 Case Report Unusual Tachycardia Association In A patient Without Structural Heart Disease Eduardo Arana-Rueda, Alonso Pedrote, Lorena Garcia-Riesco, Manuel Frutos-Lopez, Juan A. Sanchez-Brotons
Differentiating Junctional Tachycardia and Atrioventricular Node Re-Entry Tachycardia Based on Response to Atrial Extrastimulus Pacing
 Journal of the American College of Cardiology Vol. 52, No. 21, 2008 2008 by the American College of Cardiology Foundation ISSN 0735-1097/08/$34.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.08.030
Journal of the American College of Cardiology Vol. 52, No. 21, 2008 2008 by the American College of Cardiology Foundation ISSN 0735-1097/08/$34.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.08.030
Clinical Results with the Dual-Chamber Cardioverter Defibrillator Phylax AV - Efficacy of the SMART I Discrimination Algorithm
 April 2000 107 Clinical Results with the Dual-Chamber Cardioverter Defibrillator Phylax AV - Efficacy of the SMART I Discrimination Algorithm B. MERKELY Semmelweis University, Dept. of Cardiovascular Surgery,
April 2000 107 Clinical Results with the Dual-Chamber Cardioverter Defibrillator Phylax AV - Efficacy of the SMART I Discrimination Algorithm B. MERKELY Semmelweis University, Dept. of Cardiovascular Surgery,
Arrhythmic Complications of MI. Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine
 Arrhythmic Complications of MI Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine Objectives Brief overview -Pathophysiology of Arrhythmia ECG review of typical
Arrhythmic Complications of MI Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine Objectives Brief overview -Pathophysiology of Arrhythmia ECG review of typical
Paramedic Rounds. Tachyarrhythmia's. Sean Sutton Dallas Wood
 Paramedic Rounds Tachyarrhythmia's Sean Sutton Dallas Wood Objectives At the end of this session, the paramedic will be able to: State the key components of the cardiac conduction pathway, along with the
Paramedic Rounds Tachyarrhythmia's Sean Sutton Dallas Wood Objectives At the end of this session, the paramedic will be able to: State the key components of the cardiac conduction pathway, along with the
Huseng Vefali MD St. Luke s University Health Network Department of Cardiology
 Huseng Vefali MD St. Luke s University Health Network Department of Cardiology Learning Objectives Establish Consistent Approach to Interpreting ECGs Review Essential Cases for Paramedics and first responders
Huseng Vefali MD St. Luke s University Health Network Department of Cardiology Learning Objectives Establish Consistent Approach to Interpreting ECGs Review Essential Cases for Paramedics and first responders
dissociation and QRS morphology identical to
 Heart 1996;76:541-547 541 CSE STUDY Department of Cardiology, cademic Hospital, Maastricht, The Netherlands G Oreto J L R M Smeets L-M Rodriguez C Timmermans H J J Wellens Correspondence to: Dr G Oreto,
Heart 1996;76:541-547 541 CSE STUDY Department of Cardiology, cademic Hospital, Maastricht, The Netherlands G Oreto J L R M Smeets L-M Rodriguez C Timmermans H J J Wellens Correspondence to: Dr G Oreto,
Cardiac Arrhythmias. Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company
 Cardiac Arrhythmias Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company The Cardiovascular System Three primary functions Transport of oxygen, nutrients, and hormones to
Cardiac Arrhythmias Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company The Cardiovascular System Three primary functions Transport of oxygen, nutrients, and hormones to
Prediction of Life-Threatening Arrhythmia in Patients after Myocardial Infarction by Late Potentials, Ejection Fraction and Holter Monitoring
 Prediction of Life-Threatening Arrhythmia in Patients after Myocardial Infarction by Late Potentials, Ejection Fraction and Holter Monitoring Yu-Zhen ZHANG, M.D.,* Shi-Wen WANG, M.D.,* Da-Yi Hu, M.D.,**
Prediction of Life-Threatening Arrhythmia in Patients after Myocardial Infarction by Late Potentials, Ejection Fraction and Holter Monitoring Yu-Zhen ZHANG, M.D.,* Shi-Wen WANG, M.D.,* Da-Yi Hu, M.D.,**
ECG pre-reading manual. Created for the North West Regional EMET training program
 ECG pre-reading manual Created for the North West Regional EMET training program Author:- Dr Juan Carlos Ascencio-Lane juan.ascencio-lane@ths.tas.gov.au 1 Disclaimer This handbook has been created for
ECG pre-reading manual Created for the North West Regional EMET training program Author:- Dr Juan Carlos Ascencio-Lane juan.ascencio-lane@ths.tas.gov.au 1 Disclaimer This handbook has been created for
REtrive. REpeat. RElearn Design by. Test-Enhanced Learning based ECG practice E-book
 Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning based ECG practice E-book REtrive REpeat RElearn Design by S I T T I N U N T H A N G J U I P E E R I Y A W A
Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning based ECG practice E-book REtrive REpeat RElearn Design by S I T T I N U N T H A N G J U I P E E R I Y A W A
Title. CitationJournal of Electrocardiology, 39(4): Issue Date Doc URL. Type. File Information. coronary sinus ostium
 Title Nonreentrant atrioventricular nodal tachycardia due coronary sinus ostium Author(s)Yokoshiki, Hisashi; Sasaki, Koji; Shimokawa, Junichi CitationJournal of Electrocardiology, 39(4): 395-399 Issue
Title Nonreentrant atrioventricular nodal tachycardia due coronary sinus ostium Author(s)Yokoshiki, Hisashi; Sasaki, Koji; Shimokawa, Junichi CitationJournal of Electrocardiology, 39(4): 395-399 Issue
Clinical Policy: Holter Monitors Reference Number: CP.MP.113
 Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
