Open-Heart Surgery in Patients More than 65 Years Old
|
|
|
- Elvin Carr
- 5 years ago
- Views:
Transcription
1 Open-Heart Surgery in Patients More than 65 Years Old Donald A. Barnhorst, M.D., Emilio R. Giuliani, M.D., James R. Pluth, M.D., Gordon K. Danielson, M.D., Robert B. Wallace, M.D., and Dwight C. McGoon, M.D. ABSTRACT At the Mayo Clinic from 1968 to 1973, 305 open-heart operations were performed on patients more than 65 years old. The overall operative mortality rate was 15.7%. Of the various types of operations, aortic valve replacement was associated with a mortality of 10.6%; mitral valve replacement, 20.0%; multiple valve replacements, 42.4%; coronary artery grafting, 3.7%; coronary grafting plus valve replacement, 23.1%; and miscellaneous procedures, 8.3%. Advanced disease, inability to achieve good coronary perfusion during operation, intraoperative ventricular fibrillation, postoperative myocardial infarction, and low cardiac output were factors in mortality. Open-heart operations can be done in patients more than 65 years old with an acceptable operative mortality. A s results have progessively improved in open-heart surgery, the indications for operation have been extended further toward the extremes of age. Various authors [ 1-3, 8-10] have documented that cardiac procedures can be performed on older patients with an operative risk not too disparate from that of the general population. Likewise, satisfactory results can be obtained for sufficiently long periods to warrant these risks [l-3, 8, 91. We have attempted to identify the operative mortality for the commonly performed open-heart procedures in patients who are older than 65 years of age [5]. For this group, we have reviewed in addition multiple preoperative, operative, and postoperative factors in survivors and nonsurvivors in an attempt to identify remediable causes of death. Clinical Material and Methods A total of 305 open-heart operations were performed on 300 patients who were 66 years of age or older during the 5-year period from September, 1968, to August, One hundred eighty-five operations were done on men and 120 on women. Eighteen were done on patients in New York Heart Association Functional Class 11, 228 in Class 111 patients, and 59 on patients who were in Class IV at the time of operation. Some of the Class 111 patients From the Mayo Clinic and Mayo Foundation, Rochester, Minn. Presented at the Tenth Anniversary Meeting of The Society of Thoracic Suzgeons, Los Angeles, Calif., Jan , Address reprint requests to Dr. Barnhorst, Mayo Clinic, Rochester, Minn VOL. 18, NO. 1, JULY,
2 BARNHORST ET AL. had been in Class IV prior to operation but their conditions had improved with medical therapy. Of the 305 procedures, 214 involved patients who were between 66 and 70 years old, 74 were done on patients between 71 and 75 years, and 17 on patients between 76 and 80 years. Bypass techniques were reasonably uniform. A bubble oxygenator with mild hypothermia was used in all patients. For patients in whom the aortic root was opened, coronary perfusion was induced whenever possible. Mitral valve replacements were done either with the aorta cross-clamped or with induced electric fibrillation. Results Operative mortality varied considerably among the patients undergoing the various procedures (Table 1). Forty-eight patients died within the first postoperative month or while still in the hospital, for an overall operative mortality rate of 15.7a/,. Operative mortality was low for patients who underwent coronary artery bypass grafting. The only death was that of a 67- year-old woman who was discharged from the hospital after an uneventful postoperative course. She returned 1 week later with deep venous thrombophlebitis and died 2 days later from a massive embolus occluding both carotid arteries. The origin of the embolus was not determined at postmortem examination. Mortality for aortic valve replacement was similarly reasonable, although it was approximately twice that in our overall series of aortic valve replacement [6, 71. The mortality rate of ZOyo for isolated mitral valve replacement also was twice as high as in our earlier 10-year review of patients of all ages [12]. The category of multiple valve replacements includes all operative procedures involving the surgical correction of more than one valve. These patients had at least one valve replaced with a prosthesis, but some had a second or third valve abnormality treated with commissurotomy or valvuloplasty rather than valve replacement. Two patients who survived and 2 who died had undergone triple-valve replacement. The entire group of TABLE 1. RESULTS OF OPEN-HEART OPERATIONS IN PATIENTS MORE THAN 65 YEARS OLD-SEPTEMBER, 1968, TO AUGUST, 1973 No. of No. of Mortality Procedure Operations Deaths (%) Aortic valve replacement Mitral valve replacement Multiple valve replacements Coronary artery bypass grafting Coronary artery bypass grafting plus valve replacement Miscellaneous Total THE ANNALS OF THORACIC SURGERY
3 Open-Heart Surgeiy in Older Patients TABLE 2. CAUSES OF DEATH AFTER OPEN-HEART OPERATIONS IN 48 PATIENTS MORE THAN 65 YEARS OLD- SEPTEMBER, 1968, TO AUGUST, 1973 Cause of Death Myocardial infarction Low cardiac output syndrome Sepsis Ventricular arrhythmia Cerebrovascular accident Technical error Hemorrhage Pulmonary insufficiency Renal failure Hepatic failure Total No. of Patients patients with multiple valve problems had the highest mortality rate (42.4%)- The combination of valve replacement with coronary artery bypass grafting resulted in an overall mortality of 23.1 yo, with 2 deaths occurring among 9 patients who had aortic valve replacement and 1 death among 4 patients who had mitral valve replacement. In the miscellaneous group of operative procedures, 3 of the 12 patients underwent closure of an atrial septal defect; none of these patients died. The 1 death in the miscellaneous group resulted from persistently low cardiac output in a patient who had cardiac arrest in the operating room and who, after resuscitation, underwent ventricular septal myotomy and mitral valvuloplasty for idiopathic hypertrophic subaortic stenosis. Myocardial infarction and low cardiac output syndromes were the main causes of death among the 48 patients who died (Table 2). Sepsis accounted for 8 deaths, but several patients had sepsis as the last insult in an already difficult postoperative course. For each type of procedure, survivors and nonsurvivors were compared with respect to various factors. In patients who underwent aortic valve replacement, more deaths occurred in those who were in Functional Class IV (p < 0.05), in those who had had a significant period of hypotension prior to the induction of bypass (p > 0.05), and in those who had less than ideal coronary artery perfusion during bypass (p < 0.05) (Tables 3-5). Coronary perfusion was considered good if both right and left coronary arteries were perfused throughout most of the procedure at flows of at least 100 ml. per minute for the left coronary artery and at least 50 ml. per minute for the right coronary artery. Perfusion was also considered good if the right coronary artery was too small to cannulate but left coronary flow was good and the heart remained beating. Fair or poor coronary perfusion was defined as the inability to perfuse either of the coronary arteries or the ability to perfuse only the right coronary artery or both arteries only sporadically. VOI.. 18, NO. 1, JULY,
4 BARNHOKST ET AL. TABLE 3. PREOPERATIVE VARIABLES IN 143 SURVIVORS AND 17 NONSURVIVORS OF OPEN-HEART' OPERATIONS FOR AORTIC VALVE REPLACEMENT IN PATIENTS MORE THAN 65 YEARS OLD-SEPTEMBER, 1968, TO AUGUST, 1973 Survivors Nonsurvivors Variable (73 (%) Functional Class IV Congestive heart failure Atrial fibrillation Normal sinus rhythm Associated coronary disease Coronary angiography performed Primarily aortic stenosis Primarily aortic insufficiency Previous myocardial infarction The incidence of most postoperative complications was significantly higher among nonsurvivors than survivors, especially low cardiac output (p < 0.01) and myocardial infarction (p < 0.01). Coronary artery disease did not seem to significantly affect early survival after aortic valve replacement. Associated coronary artery disease was deemed present if the patient had documented angiographic evidence or electrocardiographic changes characteristic of previous myocardial infarction or if the operating surgeon found severe coronary disease at operation. By these criteria, the degree of involvement could not be compared accurately between survivors and nonsurvivors. Mean bypass time was longer in nonsurvivors, but this was largely due to prolonged bypass support in patients who did poorly after the first attempt to discontinue perfusion. Of patients undergoing mitral valve replacement, more nonsurvivors than survivors were in Functional Class IV (p < 0.05), had primarily mitral regurgitation (p > 0.05), had evidence of previous myocardial infarction (p < 0.01), and were in ventricular fibrillation during bypass (Tables 6-8). More nonsurvivors than survivors had postoperative complications. Especially lethal was acute myocardial infarction. No patient with primarily mitral TABLE 4. OPERATIVE VARIABLES IN 143 SURVIVORS AND 17 NONSURVIVORS OF OPEN-HEART OPERATIONS FOR AORTIC VALVE REPLACEMENT IN PATIENTS MORE THAN 65 YEARS OLD-SEPTEMBER, 1968, TO AUGUST, 1973 Variable Survivors Nonsurvivors Mean operating time 4.0 hr. 4.6 hr. Hypotension before bypass 5.6% 17.6y0 Mean bypass time 1.4 hr. 2.3 hr. Bypass rhythm Beating 55.9y0 47.1% Ventricular fibrillation 44.1 % 52.9y0 Coronary perfusion Good 90.1 yo 70.6% Fair to none 9.9% 29.4y0 84 THE ANNALS OF THORACIC SURGERY
5 Open-Heart Surgery in Older Patients TABLE 5. POSTOPERATIVE COMPLICATIONS IN 143 SURVIVORS AND 15 NONSURVIVORS OF OPEN-HEART OPERATIONS FOR AORTIC VALVE REPLACEMENT IN PATIENTS MORE THAN 65 YEARS OLD- SEPTEMBER, 1968, TO AUGUST, 1973 Complication D ysrhy thmia Low cardiac output Myocardial infarction Cerebrovascular Renal Pulmonary Sepsis Survivors Nonsurvivors (%) (%) stenosis died, indicating the better prognosis for patients with this lesion. The incidence of associated coronary artery disease, using the same criteria as for patients with aortic valve replacement, was the same in both survivors and those who died during or after mitral valve replacement. Similar variables were considered in the patients undergoing other procedures. In the group having multiple valve replacement, ventricular fibrillation during bypass was associated with a significantly higher mortality (p < 0.05) and postoperative complications were more numerous in nonsurvivors than in survivors. Low cardiac output was a particular problem, occurring in 26.30/, of survivors and in 92.3a/, of nonsurvivors. Comment The operative mortality was 10.6oj, for patients older than 65 years of age who underwent aortic valve replacement. A significant percentage of these patients had far-advanced disease, and this was a definite factor contributing to their deaths. Adequacy of intraoperative coronary perfusion in this age group also seemed to be a factor in operative survival. Mitral valve replacement was associated with twice the mortality rate TABLE 6. PREOPERATIVE VARIABLES IN 47 SURVIVORS AND 12 NONSURVIVORS OF OPEN-HEART OPERATIONS FOR MITRAL VALVE REPLACEMENT IN PATIENTS MORE THAN 65 YEARS OLD-SEPTEMBER, 1968, TO AUGUST, 1973 Survivors Nonsurvivors Variable (%) (%) Functional Class IV Primarily mitral stenosis Primarily mitral regurgitation Combined mitral stenosis & mitral regurgitation Atrial fibrillation Normal sinus rhythm Previous myocardial infarction Associated coronary disease Coronary angiography performed VOL. 18, NO. 1, JULY,
6 BARNHORST ET AL. TABLE 7. OPERATIVE VARIABLES IN 47 SURVIVORS AND 12 NONSURVIVORS OF OPEN-HEART OPERATIONS FOR MITRAL VALVE REPLACEMENT IN PATIENTS MORE THAN 65 YEARS OLD-SEPTEMBER, 1968, TO AUGUST, 1973 Variable Mean operating time Hypotension before bypass Mean bypass time Mean ischemia time Bypass rhythm Arrest & beating Arrest & ventricular fibrillation Ventricular fibrillation Hypotension after bypass RVY/LVP > 0.4 Survivors Nonsurvivors 3.7 hr. 3.8 hr. 6.5% 8.3% 1.1 hr. 1.5 hr min min /, 74.5% 2.1% 34.0% 48.7y0 8.3% 75.0y0 16.7% 41.7% 45.5y0 seen in the general population, probably because these patients had faradvanced disease and many had postmyocardial infarction mitral regurgitation. No patient with mitral stenosis alone died after mitral valve replacement. The data suggest a relationship between ventricular fibrillation during bypass and mortality, but there were too few patients to draw statistical conclusions. As with patients who had aortic valve replacement, the incidence of complications after mitral valve replacement was higher for patients who did not survive the operation. Survivors and nonsurvivors of each type of operation probably had equal incidences of coronary artery disease. Whether survivors and nonsurvivors had disease of equal severity could not be determined; however, the higher incidence of myocardial infarctions among nonsurvivors in all groups indicates that coronary artery disease was probably more severe in patients not surviving operation. The high mortality rate associated with multiple valve replacements is disappointing. Equal numbers of survivors and nonsurvivors were in Functional Class IV, but some indication of the severity of disease in these patients is that 47y0 of survivors and 430/, of nonsurvivors required inotropic or bypass support at the conclusion of the operation. Of statistical TABLE 8. POSTOPERATIVE COMPLICATIONS IN 47 SURVIVORS AND 12 NONSURVIVORS OF OPEN-HEART OPERATIONS FOR MITRAL VALVE REPLACEMENT IN PATIENTS MORE THAN 65 YEARS OLD- SEPTEMBER, 1968, TO AUGUST, 1973 Complication Dysrhy thmia Low cardiac output Myocardial infarction Cerebrovascular Renal Pulmonary Sepsis Survivors Nonsurvivors (%) (%) THE ANNALS OF THORACIC SURGERY
7 Open-Heart Surgery in Older Patients significance among the operative variables in these patients was the use of ventricular fibrillation during bypass in more of the nonsurviving patients. No conclusions can be drawn from our results in the group with combined valve replacement and coronary artery bypass grafting. The total mortality of 23.1y0 (22yo for aortic valve replacement and coronary artery bypass grafting and 25y0 for mitral valve replacement and coronary artery bypass grafting) did not lower the mortality of valve replacement alone. Comparing patients who had coronary grafts plus valve replacement with those who had valve replacement alone is difficult because of the incomplete assessment of coronary anatomy in many patients undergoing valve replacement alone. Two of the 3 deaths in the group with combined valve replacement and coronary artery bypass grafting were related to coronary artery disease, and this casts some doubt on the belief that the use of routine coronary arteriography and the grafting of significant coronary lesions will lower the mortality rate [9]. Our current practice is not to assess or to repair coronary arteries unless the patient has prominent symptoms of myocardial ischemia. The potential gain in early survival from grafting anatomically threatening coronary lesions may be counterbalanced by the increased mortality attendant on the combined procedure in patients older than 65 years of age. The role of prophylactic coronary artery bypass grafting in improving late operative results remains to be defined. Reduction of operative mortality for patients older than 65 years of age should result from earlier operation (that is, before Class IV status is reached), careful protection of the myocardium intraoperatively, and vigorous treatment of low cardiac output after operation. Myocardial protection includes good coronary perfusion, avoidance of ventricular fibrillation when possible, and moderate myocardial cooling when indicated. Although aortic valve replacement can be safely performed without coronary perfusion on many patients in the general population, good intraoperative coronary perfusion was associated with better operative survival in patients 66 years old or older. The potentially deleterious effects of ventricular fibrillation on subendocardial blood flow have been reported [4, 111. Significantly more nonsurvivors of multiple valve replacement operations were maintained in ventricular fibrillation during their operations. Similarly, more patients who died after mitral valve replacement were in ventricular fibrillation during operation, although the few patients involved did not permit statistical comparison. The high incidence of low cardiac output after these procedures may be related partly to subendocardial ischemia. These data suggest that avoiding intraoperative ventricular fibrillation and maintaining a beating heart, when possible, may improve operative results. References 1. Ahmad, A,, and Starr, A. J. 31:322, Valve replacement in geriatric patients. Br. Heart VOL. 18, NO. 1, JULY,
8 BARNHORST ET AL. 2. Ashor, G. W., Meyer, B. W., Lindesmith, G. G., Stiles, Q. R., Walker, G. H., and Tucker, B. L. Coronary artery disease: Surgery in 100 patients 65 years of age and older. Arch. Surg. 107:30, Austen, W. G., DeSanctis, R. W., Buckley, M. J., Mundth, E. D., and Scannell, J. G. Surgical management of aortic valve disease in the elderly. J.A.M.A. 211:624, Buckberg, G. D., Towers, B., Paglia, D. E., Mulder, D. G., and Maloney, J. V. Subendocardial ischemia after cardiopulmonary bypass. J. Thorac. Cardiovasc. Surg. 64:669, Carlson, R. G., Shafer, R. B., Eliot, R. S., Sellers, R. D., and Lillehei, C. W. Results of cardiac surgery in 273 older patients. Geriatrics 22:173, Danielson, G. K., Oxman, H. A., Connolly, D. C., Wallace, R. B., Pluth, J. R., and McGoon, D. C. Nine year experience with Starr-Edwards aortic valve replacement (abstract). Am. J. Cardiol. 31: 127, Duvoisin, G. E., and McGoon, D. C. Aortic valve replacement with a ballvalve prosthesis: Detailed analysis of early and late results. Arch. Surg. 99:684, Finegan, R. E., Gianelly, R. E., and Harrison, D. C. Aortic stenosis in the elderly: Relevance of age to diagnosis and treatment. N. Engl. J. Med. 281:1261, Guthrie, R. B., Spellberg, R. D., Benedict,.J. S., and Buhl, T. L. Openheart valve surgery in patients 65 and older. Arch. Surg. 105:42, Killen, D. A., and Collins, H. A. Open heart surgery beyond the sixth decade of life. South. Med. J. 65:397, Lufschanowski, R., and Leachman, R. D. Ventricular contraction-an important adjunct to sub-endocardial perfusion (editorial). Chest 63:653, Oxman, H. A., Connolly, D. C., McGoon, D. C., Wallace, R. B., Danielson, G. K., and Pluth, J. R. Ten year experience with isolated Starr-Edwards mitral valve replacement (abstract). Am. J. Cardiol. 29:284, Discussion DR. JACK J. GREENBERG (Miami Beach, Fla.): Dr. Barnhorst and his colleagues from the Mayo Clinic have again presented an excellent review of their experience, this time involving cardiac surgery in patients over 65 years old. This magic age was chosen by the authors, as well as our government friends, to indicate entrance into the elderly bracket. The authors set out to accomplish two goals: (1) to identify mortality statistics in the above-65 age group, and (2) to identify the factors that might be implicated as causes of mortality. The statistics they report indicate that operative mortality for valve and coronary artery surgery at the Mayo Clinic, although higher than that of their total population group, is certainly satisfactory. The 2074 mortality for mitral valve replacement reflects a significant number of patients whose operations were for coronary artery disease, and it is of note that in this above45 group, no patient who had had mitral valve replacement for rheumatic disease alone died. At the risk of being accused of presenting another paper, I w.ould like to discuss our experience in Miami with operations in the over-65 age group. I think our statistics are quite comparable with the Mayo Clinic s, and they support their finding that in patients over 65 the hospital mortality is very close to that of the general population below age 65. As in the authors series, we found that in aortic valve replacement for aortic stenosis there is a higher mortality among patients with aortic stenosis rather than aortic insufficiency. This is due to several factors, and it is in this group of patients that we attempt to keep a beating heart and concur with the authors 88 THE ANNALS OF THORACIC SURGERY
9 1 Open-Heart Surgery in Older Patients that avoidance of ventricular fibrillation in aortic valve replacement is important. The fact that mitral valve replacement in our series was done with elective ventricular fibrillation certainly does not indicate that myocardial protection cannot be given with ventricular fibrillation, however. In addition to identifying causes of mortality, it is most important to assess hemodynamic results in patients undergoing cardiac surgery. I think it must be recognized that hemodynamic factors improve less well in the older age group than in younger patients. The authors have admirably achieved their objectives, they have reported excellent operative statistics, and they have revealed areas of patient management that will aid all of us in dealing with the older cardiac patient. DR. GEORGE B. WISOFF (New Hyde Park, N.Y.): I would like to report on a few patients who haven t the air fare to make it from New York to Miami or the May.0 Clinic and just make a few comments about technique. We too believe that prolongation of useful life is a desirable goal in treatment of the elderly. In 44 patients with coronary disease who were over the age of 65 and were operated on, the preoperative and postoperative clinical and physiological status has been the same as in the younger group, except for more advanced symptomatic classification. Probably this was due to delayed physician referral. We analyzed the patients over the age of 70 and found that we had 24 more women than men. Again, aortic valve replacement was predominant. Hospital deaths in the over-70 group were similar to the experiences reported already. Altogether, within nearly two years we have lost 25% of these older patients. We believe technical factors are very important. Because of heavy calcification, we find that it is usually impossible to cannulate the coronary artery in the over-70 group, so we don t even try. The aorta closure usually requires buttressing sutures because of heavy calcification. I would question the authors about any of the technical factors that might be important in the management of this elderly group. DR. VIKING 0. BJORK (Stockholm, Sweden): I congratulate the authors on their excellent research results in older patients, which justify extension of the indications for operation in this group. In order to compare the hemodynamic effect of aortic valve replacement in two age groups-above and below 60 years-henze evaluated left ventricular pump function at rest and during exercise in 11 patients 60 to 68 years of age before and seven months after operation with the Bjiirk-Shiley tilting-disc valve. The left ventricular enddiastolic pressure, end-systolic pressure, and systolic stroke work were of equal magnitude and diminished to the same extent in both groups, indicating an adequate unloading of the left ventricle. Stroke work index was lower in the over-60 group, as was the change in stroke volume per unit change in left ventricular end-diastolic pressure. This indicates a higher degree of myocardial stiffness in the older patients but an equal improvement in left ventricular pump function in both groups followinq valve replacement. The 60- year-old myocardium begins to lose some of its ability to recover from prolonged overwork, but aortic valve replacement brings about an identical improvement in left ventricular pump function in both young and old patients. I think the observation of better results in patients not having ventricular fibrillation durilig operation is very interesting. We like to keep the heart pumping with coronary perfusion, and I also like the idea of including patients above 60 or 65 in the younger middle-age group. VOL. 18, NO. 1, JULY,
10 BARNHORST ET AL. DR. BARNHORST: I wish to thank the discussants for their comments. In reply to Dr. Greenberg s remarks about ventricular fibrillation, I share his view that in the relatively nonhypertrophied heart, ventricular fibrillation is likely not to cause any significant problems. I think that ample experimental data now available give reasonably conclusive evidence that it is the heavily hypertrophied heart in which prolonged electric fibrillation is harmful. I would also like to compliment both Dr. Greenberg and Dr. Wisoff far their excellent results. We found, in contrast to Dr. Wisoffs experience, that the majority of patients undergoing aortic valve replacement were able to have coronary artery perfusion without difficulty, and I still think it is preferable. We are able to keep a beating heart throughout the procedure, and even in those patients who fibrillate in spite of good coronary perfusion, we are able then to defibrillate the heart electrically and maintain a beating heart through the remainder of the procedure. We suspect this is helpful, although the evidence is not hard and fast. Dr. Wisoff, we also encountered more technical problems in elderly patients when closing the aortotomy. A particular problem in all these patients is the ventricular vent site, and we have learned to buttress that fairly carefully with Teflon-felt pledgets to ensure good closure and less tearing of the adjacent myocardium. I would like to compliment Professor Bjork on his excellent hemodynamic data. It is obviously important to have good objective information to warrant the increased risk in patients of this age group. 90 THE ANNALS OF THORACIC SURGERY
in Patients Having Aortic Valve Replacement John T. Santinga, M.D., Marvin M. Kirsh, M.D., Jairus D. Flora, Jr., Ph.D., and James F. Brymer, M.D.
 Factors Relating to Late Sudden Death in Patients Having Aortic Valve Replacement John T. Santinga, M.D., Marvin M. Kirsh, M.D., Jairus D. Flora, Jr., Ph.D., and James F. Brymer, M.D. ABSTRACT The preoperative
Factors Relating to Late Sudden Death in Patients Having Aortic Valve Replacement John T. Santinga, M.D., Marvin M. Kirsh, M.D., Jairus D. Flora, Jr., Ph.D., and James F. Brymer, M.D. ABSTRACT The preoperative
Idiopathic Hypertrophic Subaortic Stenosis and Mitral Stenosis
 CASE REPORTS Idiopathic Hypertrophic Subaortic Stenosis and Mitral Stenosis Martin J. Nathan, M.D., Roman W. DeSanctis, M.D., Mortimer J. Buckley, M.D., Charles A. Sanders, M.D., and W. Gerald Austen,
CASE REPORTS Idiopathic Hypertrophic Subaortic Stenosis and Mitral Stenosis Martin J. Nathan, M.D., Roman W. DeSanctis, M.D., Mortimer J. Buckley, M.D., Charles A. Sanders, M.D., and W. Gerald Austen,
Ostium primum defects with cleft mitral valve
 Thorax (1965), 20, 405. VIKING OLOV BJORK From the Department of Thoracic Surgery, University Hospital, Uppsala, Sweden Ostium primum defects are common; by 1955, 37 operated cases had been reported by
Thorax (1965), 20, 405. VIKING OLOV BJORK From the Department of Thoracic Surgery, University Hospital, Uppsala, Sweden Ostium primum defects are common; by 1955, 37 operated cases had been reported by
Mechanical Bleeding Complications During Heart Surgery
 Mechanical Bleeding Complications During Heart Surgery Arthur C. Beall, Jr., M.D., Kenneth L. Mattox, M.D., Mary Martin, R.N., C.C.P., Bonnie Cromack, C.C.P., and Gary Cornelius, C.C.P. * Potential for
Mechanical Bleeding Complications During Heart Surgery Arthur C. Beall, Jr., M.D., Kenneth L. Mattox, M.D., Mary Martin, R.N., C.C.P., Bonnie Cromack, C.C.P., and Gary Cornelius, C.C.P. * Potential for
and Coronary Artery Surgery George M. Callard, M.D., John B. Flege, Jr., M.D., and Joseph C. Todd, M.D.
 Combined Valvular and Coronary Artery Surgery George M. Callard, M.D., John B. Flege, Jr., M.D., and Joseph C. Todd, M.D. ABSTRACT Between July, 97, and March, 975,45 patients underwent combined valvular
Combined Valvular and Coronary Artery Surgery George M. Callard, M.D., John B. Flege, Jr., M.D., and Joseph C. Todd, M.D. ABSTRACT Between July, 97, and March, 975,45 patients underwent combined valvular
University of Florida Department of Surgery. CardioThoracic Surgery VA Learning Objectives
 University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014
 Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Ten-Year Follow-up in Aortic Valve Replacement Using the Bjork-Shiley Prosthesis
 Ten-Year Follow-up in Aortic Valve Replacement Using the Bjork-Shiley Prosthesis David Cheung, M.D., Robert J. Flemma, M.D., Donald C. Mullen, M.D., Denvard Lepley, Jr., M.D., Alfred J. Anderson, M.S.,
Ten-Year Follow-up in Aortic Valve Replacement Using the Bjork-Shiley Prosthesis David Cheung, M.D., Robert J. Flemma, M.D., Donald C. Mullen, M.D., Denvard Lepley, Jr., M.D., Alfred J. Anderson, M.S.,
Extreme pulmonary hypertension caused by mitral valve disease
 British Heart Journal, I975, 37, 74-78. Extreme pulmonary hypertension caused by mitral valve disease Natural history and results of surgery C. Ward and B. W. Hancock From the Cardio-Thoracic Unit, Northern
British Heart Journal, I975, 37, 74-78. Extreme pulmonary hypertension caused by mitral valve disease Natural history and results of surgery C. Ward and B. W. Hancock From the Cardio-Thoracic Unit, Northern
CASE REPORTS. Anomalous Origin of the Left Coronary Artery from the Pulmonary Artery
 CASE REPORTS Anomalous Origin of the Left Coronary Artery from the Pulmonary Artery Definitive Surgical Treatment by Saphenous Vein Interposition in a 17-Month-Old Child P. Venugopal, M.D., and S. Subramanian,
CASE REPORTS Anomalous Origin of the Left Coronary Artery from the Pulmonary Artery Definitive Surgical Treatment by Saphenous Vein Interposition in a 17-Month-Old Child P. Venugopal, M.D., and S. Subramanian,
Common Codes for ICD-10
 Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
EACTS Adult Cardiac Database
 EACTS Adult Cardiac Database Quality Improvement Programme List of changes to Version 2.0, 13 th Dec 2018, compared to version 1.0, 1 st May 2014. INTRODUCTORY NOTES This document s purpose is to list
EACTS Adult Cardiac Database Quality Improvement Programme List of changes to Version 2.0, 13 th Dec 2018, compared to version 1.0, 1 st May 2014. INTRODUCTORY NOTES This document s purpose is to list
Aortocoronary Bypass in the Treatment of Left Main Coronary Artery Stenosis
 Aortocoronary Bypass in the Treatment of Left Main Coronary Artery Stenosis W. C. Alford, Jr., M.D., I. J. Shaker, M.D., C. S. Thomas, Jr., M.D., W. S. Stoney, M.D., G. R. Burrus, M.D., and H. L. Page,
Aortocoronary Bypass in the Treatment of Left Main Coronary Artery Stenosis W. C. Alford, Jr., M.D., I. J. Shaker, M.D., C. S. Thomas, Jr., M.D., W. S. Stoney, M.D., G. R. Burrus, M.D., and H. L. Page,
Aortic Valve Surgery as an Emergency Procedure
 Aortic Valve Surgery as an Emergency Procedure By ADOLPH M. HUITER, JR., M.D., ROMAN W. DE SANCrIS, M.D., MARTIN J. NATHAN, M.D., MORTIMER J. BuCKLEY, M.D., ELDRED D. MUNDTH, M.D., WILLARD M. DAGGETT,
Aortic Valve Surgery as an Emergency Procedure By ADOLPH M. HUITER, JR., M.D., ROMAN W. DE SANCrIS, M.D., MARTIN J. NATHAN, M.D., MORTIMER J. BuCKLEY, M.D., ELDRED D. MUNDTH, M.D., WILLARD M. DAGGETT,
Emergency surgery in acute coronary syndrome
 Emergency surgery in acute coronary syndrome Teerawoot Jantarawan Division of Cardiothoracic Surgery, Department of Surgery, Faculty of Medicine Siriraj Hospital, Mahidol University, Bangkok, Thailand
Emergency surgery in acute coronary syndrome Teerawoot Jantarawan Division of Cardiothoracic Surgery, Department of Surgery, Faculty of Medicine Siriraj Hospital, Mahidol University, Bangkok, Thailand
Unusual Complications During Mitral Valve Replacement in the Presence of Calcification of the Annulus
 Unusual Complications During Mitral Valve Replacement in the Presence of Calcification of the Annulus Horace MacVaugh, 111, M.D., Claude R. Joyner, M.D., and Julian Johnson, M.D. ABSTRACT Replacement of
Unusual Complications During Mitral Valve Replacement in the Presence of Calcification of the Annulus Horace MacVaugh, 111, M.D., Claude R. Joyner, M.D., and Julian Johnson, M.D. ABSTRACT Replacement of
Index of subjects. effect on ventricular tachycardia 30 treatment with 101, 116 boosterpump 80 Brockenbrough phenomenon 55, 125
 145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
Results of Mitral Valve Replacement, with Special Reference to the Functional Tricuspid Insufficiency
 Results of Mitral Valve Replacement, with Special Reference to the Functional Tricuspid Insufficiency Ken-ichi ASANO, M.D., Masahiko WASHIO, M.D., and Shoji EGUCHI, M.D. SUMMARY (1) Surgical results of
Results of Mitral Valve Replacement, with Special Reference to the Functional Tricuspid Insufficiency Ken-ichi ASANO, M.D., Masahiko WASHIO, M.D., and Shoji EGUCHI, M.D. SUMMARY (1) Surgical results of
Kinsing Ko, Thom de Kroon, Najim Kaoui, Bart van Putte, Nabil Saouti. St. Antonius Hospital, Nieuwegein, The Netherlands
 Minimal Invasive Mitral Valve Surgery After Previous Sternotomy Without Aortic Clamping: Short- and Long Term Results of a Single Surgeon Single Institution Kinsing Ko, Thom de Kroon, Najim Kaoui, Bart
Minimal Invasive Mitral Valve Surgery After Previous Sternotomy Without Aortic Clamping: Short- and Long Term Results of a Single Surgeon Single Institution Kinsing Ko, Thom de Kroon, Najim Kaoui, Bart
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Clinical Applications of Femoral Vein-to-Artery Cannulation for Mechanical Cardiopulmonary Support and Bypass
 Clinical Applications of Femoral Vein-to-Artery Cannulation for Mechanical Cardiopulmonary Support and Bypass Robert L. Berger, M.D., Virender K. Saini, M.D., and Everett L. Dargan, M.D. ABSTRACT Femoral
Clinical Applications of Femoral Vein-to-Artery Cannulation for Mechanical Cardiopulmonary Support and Bypass Robert L. Berger, M.D., Virender K. Saini, M.D., and Everett L. Dargan, M.D. ABSTRACT Femoral
ADVANCED CARDIOVASCULAR IMAGING. Medical Knowledge. Goals and Objectives PF EF MF LF Aspirational
 Medical Knowledge Goals and Objectives PF EF MF LF Aspirational Know the basic principles of magnetic resonance imaging (MRI) including the role of the magnetic fields and gradient coil systems, generation
Medical Knowledge Goals and Objectives PF EF MF LF Aspirational Know the basic principles of magnetic resonance imaging (MRI) including the role of the magnetic fields and gradient coil systems, generation
PROGRESS IN CARDIOVASCULAR SURGERY. Congenital Mitral Stenosis and Mitral Insufficiency
 PROGRESS IN CARDIOVASCULAR SURGERY Congenital Mitral Stenosis and Mitral Insufficiency GEORGE W. B. STARKEY, M.D.* Boston, Massachusetts CONGENITAL MITRAL STENOSIS AND mitral insufficiency are rare, particularly
PROGRESS IN CARDIOVASCULAR SURGERY Congenital Mitral Stenosis and Mitral Insufficiency GEORGE W. B. STARKEY, M.D.* Boston, Massachusetts CONGENITAL MITRAL STENOSIS AND mitral insufficiency are rare, particularly
Late Results after Correction of Ventricular Septal Defect with Severe Pulmonary Hypertension
 Tohoku J. Exp. Med., 1994, 174, 41-48 Late Results after Correction of Ventricular Septal Defect with Severe Pulmonary Hypertension KIYOSHI HANEDA, NAOSHI SATO, TAKAO TOGO, MAKOTO MIURA, MASAKI RATA and
Tohoku J. Exp. Med., 1994, 174, 41-48 Late Results after Correction of Ventricular Septal Defect with Severe Pulmonary Hypertension KIYOSHI HANEDA, NAOSHI SATO, TAKAO TOGO, MAKOTO MIURA, MASAKI RATA and
Demonstration of Uneven. the infusion on myocardial temperature was insufficient
 Demonstration of Uneven in Patients with Coronary Lesions Rolf Ekroth, M.D., HAkan erggren, M.D., Goran Sudow, M.D., Josef Wojciechowski, M.D., o F. Zackrisson, M.D., and Goran William-Olsson, M.D. ASTRACT
Demonstration of Uneven in Patients with Coronary Lesions Rolf Ekroth, M.D., HAkan erggren, M.D., Goran Sudow, M.D., Josef Wojciechowski, M.D., o F. Zackrisson, M.D., and Goran William-Olsson, M.D. ASTRACT
Left Ventricular Wall Resection for Aneurysm and Akinesia due to Coronary Artery Disease: Fifty Consecutive Patients
 Left Ventricular Wall Resection for Aneurysm and Akinesia due to Coronary Artery Disease: Fifty Consecutive Patients Armand A. Lefemine, M.D., Rajagopalan Govindarajan, M.D., K. Ramaswamy, M.D., Harrison
Left Ventricular Wall Resection for Aneurysm and Akinesia due to Coronary Artery Disease: Fifty Consecutive Patients Armand A. Lefemine, M.D., Rajagopalan Govindarajan, M.D., K. Ramaswamy, M.D., Harrison
Assessing Cardiac Risk in Noncardiac Surgery. Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington
 Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
ATRIAL SEPTAL DEFECTS
 ORIGINAL STUDY Long-term follow-up of children after repair of atrial septal defects JAMES MANDELIK, MD; DOUGLAS S. MOODIE, MD; RICHARD STERBA, MD; DANIEL MURPHY, MD; ELIOT ROSENKRANZ, MD; SHARON MEDENDORP,
ORIGINAL STUDY Long-term follow-up of children after repair of atrial septal defects JAMES MANDELIK, MD; DOUGLAS S. MOODIE, MD; RICHARD STERBA, MD; DANIEL MURPHY, MD; ELIOT ROSENKRANZ, MD; SHARON MEDENDORP,
Management of Fusiform Ascending Aortic Aneurysms
 Management of Fusiform Ascending Aortic Aneurysms Stuart Houser, M.D., Jose Mijangos, M.D., Amarenda Sengupta, M.D., Lawrence Zaroff, M.D., Robert Weiner, M.D., and James A. DeWeese, M.D. ABSTRACT Thirteen
Management of Fusiform Ascending Aortic Aneurysms Stuart Houser, M.D., Jose Mijangos, M.D., Amarenda Sengupta, M.D., Lawrence Zaroff, M.D., Robert Weiner, M.D., and James A. DeWeese, M.D. ABSTRACT Thirteen
Mitral Valve Disease, When to Intervene
 Mitral Valve Disease, When to Intervene Swedish Heart and Vascular Institute Ming Zhang MD PhD Interventional Cardiology Structure Heart Disease Conflict of Interest None Current ACC/AHA guideline Stages
Mitral Valve Disease, When to Intervene Swedish Heart and Vascular Institute Ming Zhang MD PhD Interventional Cardiology Structure Heart Disease Conflict of Interest None Current ACC/AHA guideline Stages
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders
 C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
Coronary arteriography in complicated acute myocardial infarction; clinical and angiographic correlates
 Coronary arteriography in complicated acute myocardial ; clinical and angiographic correlates Luis M. de la Fuente, M.D. Buenos Aires, Argentina From January 1979 to June 30, 1979, we performed coronary
Coronary arteriography in complicated acute myocardial ; clinical and angiographic correlates Luis M. de la Fuente, M.D. Buenos Aires, Argentina From January 1979 to June 30, 1979, we performed coronary
Coronary Atherosclerosis in Valvular Heart Disease
 Coronary Atherosclerosis in Valvular Heart Disease Jerome Lacy, M.D., Robert Goodin, M.D., Daniel McMartin, M.D., Ronald Masden, M.D., and Nancy Flowers, M.D. ABSTRACT To evaluate the usefulness of routine
Coronary Atherosclerosis in Valvular Heart Disease Jerome Lacy, M.D., Robert Goodin, M.D., Daniel McMartin, M.D., Ronald Masden, M.D., and Nancy Flowers, M.D. ABSTRACT To evaluate the usefulness of routine
Intra-operative Echocardiography: When to Go Back on Pump
 Intra-operative Echocardiography: When to Go Back on Pump GREGORIO G. ROGELIO, MD., F.P.C.C. OUTLINE A. Indications for Intraoperative Echocardiography B. Role of Intraoperative Echocardiography C. Criteria
Intra-operative Echocardiography: When to Go Back on Pump GREGORIO G. ROGELIO, MD., F.P.C.C. OUTLINE A. Indications for Intraoperative Echocardiography B. Role of Intraoperative Echocardiography C. Criteria
Mitral incompetence after repair of ostium
 Thorax (1965), 20, 40. Mitral incompetence after repair of ostium primum septal defects A. R. C. DOBELL, D. R. MURPHY, G. M. KARN, AND A. MARTINEZ-CARO From the Department of Cardiovascular Surgery, the
Thorax (1965), 20, 40. Mitral incompetence after repair of ostium primum septal defects A. R. C. DOBELL, D. R. MURPHY, G. M. KARN, AND A. MARTINEZ-CARO From the Department of Cardiovascular Surgery, the
Late Recovery of Conduction following Surgically Induced Atrioventricular Block
 Late Recovery of Conduction following Surgically Induced Atrioventricular Block Thomas W. Smith, M.D., James C. McFarland, M.D., Mortimer J. Buckley, M.D., and W. Gerald Austen, M.D. U se of long-term
Late Recovery of Conduction following Surgically Induced Atrioventricular Block Thomas W. Smith, M.D., James C. McFarland, M.D., Mortimer J. Buckley, M.D., and W. Gerald Austen, M.D. U se of long-term
Bicuspid aortic root spared during ascending aorta surgery: an update of long-term results
 Short Communication Bicuspid aortic root spared during ascending aorta surgery: an update of long-term results Marco Russo, Guglielmo Saitto, Paolo Nardi, Fabio Bertoldo, Carlo Bassano, Antonio Scafuri,
Short Communication Bicuspid aortic root spared during ascending aorta surgery: an update of long-term results Marco Russo, Guglielmo Saitto, Paolo Nardi, Fabio Bertoldo, Carlo Bassano, Antonio Scafuri,
Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease
 Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease TIRONE E. DAVID, MD ; SEMIN THORAC CARDIOVASC SURG 19:116-120c 2007 ELSEVIER INC. PRESENTED BY INTERN 許士盟 Mitral valve
Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease TIRONE E. DAVID, MD ; SEMIN THORAC CARDIOVASC SURG 19:116-120c 2007 ELSEVIER INC. PRESENTED BY INTERN 許士盟 Mitral valve
SUPPLEMENTAL MATERIAL
 SUPPLEMENTAL MATERIAL Table S1: Number and percentage of patients by age category Distribution of age Age
SUPPLEMENTAL MATERIAL Table S1: Number and percentage of patients by age category Distribution of age Age
The operative mortality rate after redo valvular operations
 Clinical Outcomes of Redo Valvular Operations: A 20-Year Experience Naoto Fukunaga, MD, Yukikatsu Okada, MD, Yasunobu Konishi, MD, Takashi Murashita, MD, Mitsuru Yuzaki, MD, Yu Shomura, MD, Hiroshi Fujiwara,
Clinical Outcomes of Redo Valvular Operations: A 20-Year Experience Naoto Fukunaga, MD, Yukikatsu Okada, MD, Yasunobu Konishi, MD, Takashi Murashita, MD, Mitsuru Yuzaki, MD, Yu Shomura, MD, Hiroshi Fujiwara,
Cardiac anaesthesia. Simon May
 Cardiac anaesthesia Simon May Contents Cardiac: Principles of peri-operative management for cardiac surgery Cardiopulmonary bypass, cardioplegia and off pump cardiac surgery Cardiac disease and its implications
Cardiac anaesthesia Simon May Contents Cardiac: Principles of peri-operative management for cardiac surgery Cardiopulmonary bypass, cardioplegia and off pump cardiac surgery Cardiac disease and its implications
Long-term results (22 years) of the Ross Operation a single institutional experience
 Long-term results (22 years) of the Ross Operation a single institutional experience Authors: Costa FDA, Schnorr GM, Veloso M,Calixto A, Colatusso D, Balbi EM, Torres R, Ferreira ADA, Colatusso C Department
Long-term results (22 years) of the Ross Operation a single institutional experience Authors: Costa FDA, Schnorr GM, Veloso M,Calixto A, Colatusso D, Balbi EM, Torres R, Ferreira ADA, Colatusso C Department
Atrial fibrillation (AF) is associated with increased morbidity
 Ablation of Atrial Fibrillation with Concomitant Surgery Edward G. Soltesz, MD, MPH, and A. Marc Gillinov, MD Atrial fibrillation (AF) is associated with increased morbidity and mortality in coronary artery
Ablation of Atrial Fibrillation with Concomitant Surgery Edward G. Soltesz, MD, MPH, and A. Marc Gillinov, MD Atrial fibrillation (AF) is associated with increased morbidity and mortality in coronary artery
Emergency Intraoperative Echocardiography
 Emergency Intraoperative Echocardiography Justiaan Swanevelder Department of Anaesthesia, Glenfield Hospital University Hospitals of Leicester NHS Trust, UK Carl Gustav Jung (1875-1961) Your vision will
Emergency Intraoperative Echocardiography Justiaan Swanevelder Department of Anaesthesia, Glenfield Hospital University Hospitals of Leicester NHS Trust, UK Carl Gustav Jung (1875-1961) Your vision will
Quality ID #166 (NQF 0131): Coronary Artery Bypass Graft (CABG): Stroke- National Quality Strategy Domain: Effective Clinical Care
 Quality ID #166 (NQF 0131): Coronary Artery Bypass Graft (CABG): Stroke- National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Outcome
Quality ID #166 (NQF 0131): Coronary Artery Bypass Graft (CABG): Stroke- National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Outcome
Repair or Replacement
 Surgical intervention post MitraClip Device: Repair or Replacement Saudi Heart Association, February 21-24 Rüdiger Lange, MD, PhD Nicolo Piazza, MD, FRCPC, FESC German Heart Center, Munich, Germany Division
Surgical intervention post MitraClip Device: Repair or Replacement Saudi Heart Association, February 21-24 Rüdiger Lange, MD, PhD Nicolo Piazza, MD, FRCPC, FESC German Heart Center, Munich, Germany Division
Surgical Management of Ventricular Septa1 Defects and Mitral Regurgitation Complicating Acute Myocardial Infarction
 Surgical Management of Ventricular Septa1 Defects and Mitral Regurgitation Complicating Acute Myocardial Infarction Mortimer J. Huckley, M.D., Eldred D. Mundth, M.D., Willard M. Daggett, M.D., Herman K.
Surgical Management of Ventricular Septa1 Defects and Mitral Regurgitation Complicating Acute Myocardial Infarction Mortimer J. Huckley, M.D., Eldred D. Mundth, M.D., Willard M. Daggett, M.D., Herman K.
Right-Sided Bacterial Endocarditis
 New Concepts in the Treatment of the Uncontrollable Infection Agustin Arbulu, M.D., Ali Kafi, M.D., Norman W. Thorns, M.D., and Robert F. Wilson, M.D. ABSTRACT Our experience with 25 patients with right-sided
New Concepts in the Treatment of the Uncontrollable Infection Agustin Arbulu, M.D., Ali Kafi, M.D., Norman W. Thorns, M.D., and Robert F. Wilson, M.D. ABSTRACT Our experience with 25 patients with right-sided
Cardiovascular System Notes: Heart Disease & Disorders
 Cardiovascular System Notes: Heart Disease & Disorders Interesting Heart Facts The Electrocardiograph (ECG) was invented in 1902 by Willem Einthoven Dutch Physiologist. This test is still used to evaluate
Cardiovascular System Notes: Heart Disease & Disorders Interesting Heart Facts The Electrocardiograph (ECG) was invented in 1902 by Willem Einthoven Dutch Physiologist. This test is still used to evaluate
Journal of the American College of Cardiology Vol. 33, No. 6, by the American College of Cardiology ISSN /99/$20.
 Journal of the American College of Cardiology Vol. 33, No. 6, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00061-3 for Prediction
Journal of the American College of Cardiology Vol. 33, No. 6, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00061-3 for Prediction
Skin supplied by T1-4 (medial upper arm and neck) T5-9- epigastrium Visceral afferents from skin and heart are the same dorsal root ganglio
 Cardio 2 ECG... 3 Cardiac Remodelling... 11 Valvular Diseases... 13 Hypertension... 18 Aortic Coarctation... 24 Erythropoiesis... 27 Haemostasis... 30 Anaemia... 36 Atherosclerosis... 44 Angina... 48 Myocardial
Cardio 2 ECG... 3 Cardiac Remodelling... 11 Valvular Diseases... 13 Hypertension... 18 Aortic Coarctation... 24 Erythropoiesis... 27 Haemostasis... 30 Anaemia... 36 Atherosclerosis... 44 Angina... 48 Myocardial
Septal Myectomy, Papillary Muscle Resection, and Mitral Valve Replacement for Hypertrophic Obstructive Cardiomyopathy: A Case Report
 Case Report Septal Myectomy, Papillary Muscle Resection, and Mitral Valve Replacement for Hypertrophic Obstructive Cardiomyopathy: A Case Report Junichiro Takahashi, MD, 1 Yutaka Wakamatsu, MD, 1 Jun Okude,
Case Report Septal Myectomy, Papillary Muscle Resection, and Mitral Valve Replacement for Hypertrophic Obstructive Cardiomyopathy: A Case Report Junichiro Takahashi, MD, 1 Yutaka Wakamatsu, MD, 1 Jun Okude,
Each patient was weighed before operation. Other factors recorded, though not discussed in
 ) valve British Heart Journal, I972, 34, 227-23I. Transient systolic hypertension after aortic replacement M. J. McQueen, M.. Watson, and W. H. Bain From the Cardiac Surgical Unit, University Department
) valve British Heart Journal, I972, 34, 227-23I. Transient systolic hypertension after aortic replacement M. J. McQueen, M.. Watson, and W. H. Bain From the Cardiac Surgical Unit, University Department
Reversal of Advanced Left Ventricular Dysfunction Following Aortic Valve Replacement for Aortic Stenosis
 Reversal of Advanced Left Ventricular Dysfunction Following Aortic Valve Replacement for Aortic Stenosis Robert P. Croke, M.D., Roque Pifarre, M.D., Henry Sullivan, M.D., Rolf Gunnar, M.D., and Henry Loeb,
Reversal of Advanced Left Ventricular Dysfunction Following Aortic Valve Replacement for Aortic Stenosis Robert P. Croke, M.D., Roque Pifarre, M.D., Henry Sullivan, M.D., Rolf Gunnar, M.D., and Henry Loeb,
Does Patient-Prosthesis Mismatch Affect Long-term Results after Mitral Valve Replacement?
 Original Article Does Patient-Prosthesis Mismatch Affect Long-term Results after Mitral Valve Replacement? Hiroaki Sakamoto, MD, PhD, and Yasunori Watanabe, MD, PhD Background: Recently, some articles
Original Article Does Patient-Prosthesis Mismatch Affect Long-term Results after Mitral Valve Replacement? Hiroaki Sakamoto, MD, PhD, and Yasunori Watanabe, MD, PhD Background: Recently, some articles
Experience with counterpulsation in
 British Heart J7ournal, 1977, 39, 198-202 Experience with counterpulsation in cardiac surgical patients G. H. SMITH AND W. E. MORGAN From Sheffield Cardiothoracic Unit, Northern General Hospital, Sheffield
British Heart J7ournal, 1977, 39, 198-202 Experience with counterpulsation in cardiac surgical patients G. H. SMITH AND W. E. MORGAN From Sheffield Cardiothoracic Unit, Northern General Hospital, Sheffield
Although most patients with Ebstein s anomaly live
 Management of Neonatal Ebstein s Anomaly Christopher J. Knott-Craig, MD, FACS Although most patients with Ebstein s anomaly live through infancy, those who present clinically as neonates are a distinct
Management of Neonatal Ebstein s Anomaly Christopher J. Knott-Craig, MD, FACS Although most patients with Ebstein s anomaly live through infancy, those who present clinically as neonates are a distinct
Cardiovascular Disorders. Heart Disorders. Diagnostic Tests for CV Function. Bio 375. Pathophysiology
 Cardiovascular Disorders Bio 375 Pathophysiology Heart Disorders Heart disease is ranked as a major cause of death in the U.S. Common heart diseases include: Congenital heart defects Hypertensive heart
Cardiovascular Disorders Bio 375 Pathophysiology Heart Disorders Heart disease is ranked as a major cause of death in the U.S. Common heart diseases include: Congenital heart defects Hypertensive heart
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Pulmonary Valve Replacement
 Pulmonary Valve Replacement with Fascia Lata J. C. R. Lincoln, F.R.C.S., M. Geens, M.D., M. Schottenfeld, M.D., and D. N. Ross, F.R.C.S. ABSTRACT The purpose of this paper is to describe a technique of
Pulmonary Valve Replacement with Fascia Lata J. C. R. Lincoln, F.R.C.S., M. Geens, M.D., M. Schottenfeld, M.D., and D. N. Ross, F.R.C.S. ABSTRACT The purpose of this paper is to describe a technique of
CIPG Transcatheter Aortic Valve Replacement- When Is Less, More?
 CIPG 2013 Transcatheter Aortic Valve Replacement- When Is Less, More? James D. Rossen, M.D. Professor of Medicine and Neurosurgery Director, Cardiac Catheterization Laboratory and Interventional Cardiology
CIPG 2013 Transcatheter Aortic Valve Replacement- When Is Less, More? James D. Rossen, M.D. Professor of Medicine and Neurosurgery Director, Cardiac Catheterization Laboratory and Interventional Cardiology
Rationale for Prophylactic Support During Percutaneous Coronary Intervention
 Rationale for Prophylactic Support During Percutaneous Coronary Intervention Navin K. Kapur, MD, FACC, FSCAI Assistant Director, Interventional Cardiology Director, Interventional Research Laboratories
Rationale for Prophylactic Support During Percutaneous Coronary Intervention Navin K. Kapur, MD, FACC, FSCAI Assistant Director, Interventional Cardiology Director, Interventional Research Laboratories
Results of Reoperation
 Results of Reoperation for Recurrent Angina Pectoris William I. Norwood, M.D., Lawrence H. Cohn, M.D., and John J. Collins, Jr., M.D. ABSTRACT Although a coronary bypass operation improves the quality
Results of Reoperation for Recurrent Angina Pectoris William I. Norwood, M.D., Lawrence H. Cohn, M.D., and John J. Collins, Jr., M.D. ABSTRACT Although a coronary bypass operation improves the quality
TSDA Boot Camp September 13-16, Introduction to Aortic Valve Surgery. George L. Hicks, Jr., MD
 TSDA Boot Camp September 13-16, 2018 Introduction to Aortic Valve Surgery George L. Hicks, Jr., MD Aortic Valve Pathology and Treatment Valvular Aortic Stenosis in Adults Average Course (Post mortem data)
TSDA Boot Camp September 13-16, 2018 Introduction to Aortic Valve Surgery George L. Hicks, Jr., MD Aortic Valve Pathology and Treatment Valvular Aortic Stenosis in Adults Average Course (Post mortem data)
Introduction. Study Design. Background. Operative Procedure-I
 Risk Factors for Mortality After the Norwood Procedure Using Right Ventricle to Pulmonary Artery Shunt Ann Thorac Surg 2009;87:178 86 86 Addressor: R1 胡祐寧 2009/3/4 AM7:30 SICU 討論室 Introduction Hypoplastic
Risk Factors for Mortality After the Norwood Procedure Using Right Ventricle to Pulmonary Artery Shunt Ann Thorac Surg 2009;87:178 86 86 Addressor: R1 胡祐寧 2009/3/4 AM7:30 SICU 討論室 Introduction Hypoplastic
The incidence and risk factors of arrhythmias in the early period after cardiac surgery in pediatric patients
 The Turkish Journal of Pediatrics 2008; 50: 549-553 Original The incidence and risk factors of arrhythmias in the early period after cardiac surgery in pediatric patients Selman Vefa Yıldırım 1, Kürşad
The Turkish Journal of Pediatrics 2008; 50: 549-553 Original The incidence and risk factors of arrhythmias in the early period after cardiac surgery in pediatric patients Selman Vefa Yıldırım 1, Kürşad
Pulmonarv Arterv Plication: with Type I Trunms Arteriosus. A New S&gical Procedure for Small Infants
 Pulmonarv Arterv Plication: A New S&gical Procedure for Small Infants with Type I Trunms Arteriosus S. Bert Litwin, M.D., and David Z. Friedberg, M.D. ABSTRACT A new technique is reported for constriction
Pulmonarv Arterv Plication: A New S&gical Procedure for Small Infants with Type I Trunms Arteriosus S. Bert Litwin, M.D., and David Z. Friedberg, M.D. ABSTRACT A new technique is reported for constriction
Epicardial Pacemaker Implantation for Complete Heart Block
 for Complete Heart Block Donald G. Mulder, M.D., and C. Gordon Frank, M.D. S udden death or progressive cardiac failure threatens life in the patient with complete heart block. The slow heart rate and
for Complete Heart Block Donald G. Mulder, M.D., and C. Gordon Frank, M.D. S udden death or progressive cardiac failure threatens life in the patient with complete heart block. The slow heart rate and
Surgery and device intervention for the elderly with heart failure: assessing the need. Devices and Technology for heart failure in 2011
 Surgery and device intervention for the elderly with heart failure: assessing the need Devices and Technology for heart failure in 2011 Assessing cardiovascular function / prognosis (in the elderly): composite
Surgery and device intervention for the elderly with heart failure: assessing the need Devices and Technology for heart failure in 2011 Assessing cardiovascular function / prognosis (in the elderly): composite
16 YEAR RESULTS Carpentier-Edwards PERIMOUNT Mitral Pericardial Bioprosthesis, Model 6900
 CLINICAL COMMUNIQUé 6 YEAR RESULTS Carpentier-Edwards PERIMOUNT Mitral Pericardial Bioprosthesis, Model 69 The Carpentier-Edwards PERIMOUNT Mitral Pericardial Valve, Model 69, was introduced into clinical
CLINICAL COMMUNIQUé 6 YEAR RESULTS Carpentier-Edwards PERIMOUNT Mitral Pericardial Bioprosthesis, Model 69 The Carpentier-Edwards PERIMOUNT Mitral Pericardial Valve, Model 69, was introduced into clinical
Debridement-valvotomy for aortic stenosis
 Thorax (1967), 22, 314. Debridement-valvotomy for aortic stenosis in adults A follow-up of 76 patients P. J. HURLEY1, J. B. LOWE, AND B. G. BARRATT-BOYES From the Cardiothoracic Surgical Unit, Green Lane
Thorax (1967), 22, 314. Debridement-valvotomy for aortic stenosis in adults A follow-up of 76 patients P. J. HURLEY1, J. B. LOWE, AND B. G. BARRATT-BOYES From the Cardiothoracic Surgical Unit, Green Lane
Tricuspid Valve Repair for Ebstein's Anomaly
 Tricuspid Valve Repair for Ebstein's Anomaly Joseph A. Dearani, MD, and Gordon K. Danielson, MD E bstein's anomaly is a malformation of the tricuspid valve and right ventricle that is characterized by
Tricuspid Valve Repair for Ebstein's Anomaly Joseph A. Dearani, MD, and Gordon K. Danielson, MD E bstein's anomaly is a malformation of the tricuspid valve and right ventricle that is characterized by
Perioperative Management of DORV Case
 Perioperative Management of DORV Case James P. Spaeth, MD Department of Anesthesia Cincinnati Children s Hospital Medical Center University of Cincinnati Objectives: 1. Discuss considerations regarding
Perioperative Management of DORV Case James P. Spaeth, MD Department of Anesthesia Cincinnati Children s Hospital Medical Center University of Cincinnati Objectives: 1. Discuss considerations regarding
Rhythm Disorders 2017 TazKai LLC and NRSNG.com
 Rhythm Disorders 1. Outline the conduction system of the heart. 2. What do the different portions of the EKG represent? 3. Define the following terms: a. Automaticity b. Conductivity c. Excitability d.
Rhythm Disorders 1. Outline the conduction system of the heart. 2. What do the different portions of the EKG represent? 3. Define the following terms: a. Automaticity b. Conductivity c. Excitability d.
10/8/2018. Lecture 9. Cardiovascular Health. Lecture Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor
 Lecture 9 Cardiovascular Health 1 Lecture 9 1. Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor 1 The Heart Muscular Pump The Heart Receives blood low pressure then increases the pressure
Lecture 9 Cardiovascular Health 1 Lecture 9 1. Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor 1 The Heart Muscular Pump The Heart Receives blood low pressure then increases the pressure
The Heart & Pericardium Dr. Rakesh Kumar Verma Assistant Professor Department of Anatomy KGMU UP Lucknow
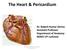 The Heart & Pericardium Dr. Rakesh Kumar Verma Assistant Professor Department of Anatomy KGMU UP Lucknow Fibrous skeleton Dense fibrous connective tissue forms a structural foundation around AV & arterial
The Heart & Pericardium Dr. Rakesh Kumar Verma Assistant Professor Department of Anatomy KGMU UP Lucknow Fibrous skeleton Dense fibrous connective tissue forms a structural foundation around AV & arterial
Pathophysiology: Left To Right Shunts
 Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
Adult Cardiac Surgery
 Adult Cardiac Surgery Mahmoud ABU-ABEELEH Associate Professor Department of Surgery Division of Cardiothoracic Surgery School of Medicine University Of Jordan Adult Cardiac Surgery: Ischemic Heart Disease
Adult Cardiac Surgery Mahmoud ABU-ABEELEH Associate Professor Department of Surgery Division of Cardiothoracic Surgery School of Medicine University Of Jordan Adult Cardiac Surgery: Ischemic Heart Disease
The Edge-to-Edge Technique f For Barlow's Disease
 The Edge-to-Edge Technique f For Barlow's Disease Ottavio Alfieri, Michele De Bonis, Elisabetta Lapenna, Francesco Maisano, Lucia Torracca, Giovanni La Canna. Department of Cardiac Surgery, San Raffaele
The Edge-to-Edge Technique f For Barlow's Disease Ottavio Alfieri, Michele De Bonis, Elisabetta Lapenna, Francesco Maisano, Lucia Torracca, Giovanni La Canna. Department of Cardiac Surgery, San Raffaele
CARDIOGENIC SHOCK. Antonio Pesenti. Università degli Studi di Milano Bicocca Azienda Ospedaliera San Gerardo Monza (MI)
 CARDIOGENIC SHOCK Antonio Pesenti Università degli Studi di Milano Bicocca Azienda Ospedaliera San Gerardo Monza (MI) Primary myocardial dysfunction resulting in the inability of the heart to mantain an
CARDIOGENIC SHOCK Antonio Pesenti Università degli Studi di Milano Bicocca Azienda Ospedaliera San Gerardo Monza (MI) Primary myocardial dysfunction resulting in the inability of the heart to mantain an
164 Ann Thorac Surg 45: , Feb Copyright by The Society of Thoracic Surgeons
 Heart Valve Replacement with the Bjork-Shiley Mbnostrut Valve: Early Results of a Multicenter Clinical Investigation Lars I. Thulin, M.D., William H. Bain, F.R.C.S., Hans H. Huysmans, M.D., Gerrit van
Heart Valve Replacement with the Bjork-Shiley Mbnostrut Valve: Early Results of a Multicenter Clinical Investigation Lars I. Thulin, M.D., William H. Bain, F.R.C.S., Hans H. Huysmans, M.D., Gerrit van
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
fascia latat The patients were aged 24 to 60 years (average age 45 6 years) and five were women. Thirteen had
 Aortic valve replacement with unsupported fascia latat Thorax (1973), 28, 603. KENNETH HEARN, JANE SOMERVILLE, RICHARD SUTTON, JOHN WRIGHT2, and DONALD ROSS National Heart Hospital and Institute of Cardiology,
Aortic valve replacement with unsupported fascia latat Thorax (1973), 28, 603. KENNETH HEARN, JANE SOMERVILLE, RICHARD SUTTON, JOHN WRIGHT2, and DONALD ROSS National Heart Hospital and Institute of Cardiology,
A DAYS CARDIOVASCULAR UNIT GUIDE DUE WEDNESDAY 4/12
 A DAYS CARDIOVASCULAR UNIT GUIDE DUE WEDNESDAY 4/12 MONDAY TUESDAY WEDNESDAY THURSDAY FRIDAY 3/20 - B 3/21 - A 3/22 - B 3/23 - A 3/24 - B 3/27 - A Dissection Ethics Debate 3/28 - B 3/29 - A Intro to Cardiovascular
A DAYS CARDIOVASCULAR UNIT GUIDE DUE WEDNESDAY 4/12 MONDAY TUESDAY WEDNESDAY THURSDAY FRIDAY 3/20 - B 3/21 - A 3/22 - B 3/23 - A 3/24 - B 3/27 - A Dissection Ethics Debate 3/28 - B 3/29 - A Intro to Cardiovascular
The 2014 Mayo Approach to the Management of HCM and Non-Compaction
 The 2014 Mayo Approach to the Management of HCM and Non-Compaction R A Nishimura MD MACC MACP Judd and Mary Morris Leighton Professor Mayo Clinic No disclosures or conflict of interest CP1288794-1 Let
The 2014 Mayo Approach to the Management of HCM and Non-Compaction R A Nishimura MD MACC MACP Judd and Mary Morris Leighton Professor Mayo Clinic No disclosures or conflict of interest CP1288794-1 Let
Understanding the Cardiopulmonary Bypass Machine and Its Tubing
 Understanding the Cardiopulmonary Bypass Machine and Its Tubing Robert S. Leckie, MD Division of Cardiac Anesthesia, Beth Israel Deaconess Medical Center ABL 1/09 Reservoir Bucket This is a cartoon of
Understanding the Cardiopulmonary Bypass Machine and Its Tubing Robert S. Leckie, MD Division of Cardiac Anesthesia, Beth Israel Deaconess Medical Center ABL 1/09 Reservoir Bucket This is a cartoon of
Cardiovascular System
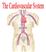 Cardiovascular System angio BELLWORK Day One: Define using technology hemo/hema cardio Medical Therapeutics Standards 11) Outline the gross normal structure and function of all body systems and summarize
Cardiovascular System angio BELLWORK Day One: Define using technology hemo/hema cardio Medical Therapeutics Standards 11) Outline the gross normal structure and function of all body systems and summarize
Debate in Management of native COA; Balloon Versus Surgery
 Debate in Management of native COA; Balloon Versus Surgery Dr. Amira Esmat, El Tantawy, MD Professor of Pediatrics Consultant Pediatric Cardiac Interventionist Faculty of Medicine Cairo University 23/2/2017
Debate in Management of native COA; Balloon Versus Surgery Dr. Amira Esmat, El Tantawy, MD Professor of Pediatrics Consultant Pediatric Cardiac Interventionist Faculty of Medicine Cairo University 23/2/2017
Presenter: Steven Brust, HCS-D, HCS-H Product Manager, Home Health Coding Center
 Presenter: Steven Brust, HCS-D, HCS-H Product Manager, Home Health Coding Center Pinpoint & properly assign the appropriate heart failure codes Left- vs. Right-sided Left ventricular failure (LVF) may
Presenter: Steven Brust, HCS-D, HCS-H Product Manager, Home Health Coding Center Pinpoint & properly assign the appropriate heart failure codes Left- vs. Right-sided Left ventricular failure (LVF) may
Following Mitral Valve Replacement
 Re air of a Subvalvular Le rt Ventricular Aneurysm Following Mitral Valve Replacement Darryl J. Sutorius, M.D., James A. Helmsworth, M.D., James A. Majeski, Ph.D., M.D., and Stephen F. Miller, M.D. ABSTRACT
Re air of a Subvalvular Le rt Ventricular Aneurysm Following Mitral Valve Replacement Darryl J. Sutorius, M.D., James A. Helmsworth, M.D., James A. Majeski, Ph.D., M.D., and Stephen F. Miller, M.D. ABSTRACT
Acute Aortic Regurgitation Secondary to Aortic Dissection
 Acute Aortic Regurgitation Secondary to Aortic Dissection Surgical Management Without Valve Replacement Hassan Najafi, M.D., William S. Dye, M.D., Hushang Javid, M.D., James A. Hunter, M.D., Marshall D.
Acute Aortic Regurgitation Secondary to Aortic Dissection Surgical Management Without Valve Replacement Hassan Najafi, M.D., William S. Dye, M.D., Hushang Javid, M.D., James A. Hunter, M.D., Marshall D.
(Ann Thorac Surg 2008;85:845 53)
 I Made Adi Parmana The utility of intraoperative TEE has become increasingly more evident as anesthesiologists, cardiologists, and surgeons continue to appreciate its potential application as an invaluable
I Made Adi Parmana The utility of intraoperative TEE has become increasingly more evident as anesthesiologists, cardiologists, and surgeons continue to appreciate its potential application as an invaluable
The strategy of sequential use of antegrade and. Can Retrograde Cardioplegia Alone Provide Adequate Protection for Cardiac Valve Surgery?
 Can Retrograde Cardioplegia Alone Provide Adequate Protection for Cardiac Valve Surgery?* Nirupama G. Talwalkar, MD, FCCP; Gerald M. Lawrie, MD, FCCP; Nan Earle, BS; and Michael E. DeBakey, MD, FCCP Background:
Can Retrograde Cardioplegia Alone Provide Adequate Protection for Cardiac Valve Surgery?* Nirupama G. Talwalkar, MD, FCCP; Gerald M. Lawrie, MD, FCCP; Nan Earle, BS; and Michael E. DeBakey, MD, FCCP Background:
Surgical AVR: Are there any contraindications? Pyowon Park Samsung Medical Center Seoul, Korea
 Surgical AVR: Are there any contraindications? Pyowon Park Samsung Medical Center Seoul, Korea Contents Decision making in surgical AVR in old age Clinical results of AVR with tissue valve Impact of 19mm
Surgical AVR: Are there any contraindications? Pyowon Park Samsung Medical Center Seoul, Korea Contents Decision making in surgical AVR in old age Clinical results of AVR with tissue valve Impact of 19mm
GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA
 GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA The newborn is not an adult, nor a child. In people of all ages, death can occur from a failure of breathing and / or circulation. The interventions required to aid
GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA The newborn is not an adult, nor a child. In people of all ages, death can occur from a failure of breathing and / or circulation. The interventions required to aid
Nothing to Disclose. Severe Pulmonary Hypertension
 Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
Pathophysiology: Left To Right Shunts
 Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adverse drug events, polypharmacy and perioperative considerations in elderly patients, 377 389 Age, and risk of postoperative urinary retention,
Note: Page numbers of article titles are in boldface type. A Adverse drug events, polypharmacy and perioperative considerations in elderly patients, 377 389 Age, and risk of postoperative urinary retention,
Index. interventional.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Alagille syndrome, pulmonary artery stenosis in, 143 145, 148 149 Amplatz devices for atrial septal defect closure, 42 46 for coronary
Index Note: Page numbers of article titles are in boldface type. A Alagille syndrome, pulmonary artery stenosis in, 143 145, 148 149 Amplatz devices for atrial septal defect closure, 42 46 for coronary
