Defensin deficiency, intestinal microbes, and the clinical phenotypes of Crohn s disease
|
|
|
- Melanie Green
- 5 years ago
- Views:
Transcription
1 Defensin deficiency, intestinal microbes, and the clinical phenotypes of Crohn s disease Jan Wehkamp,*,1 Michael Schmid, Klaus Fellermann, and Eduard F. Stange *Department of Microbiology and Immunology, University of California, Davis; and Department of Internal Medicine I, Robert Bosch Hospital and Dr. Margarete Fischer Bosch Institute, Stuttgart, Germany Abstract: Crohn s disease is a chronic, inflammatory disease of the intestinal mucosa. Although intestinal bacteria are implicated in disease pathogenesis, the etiology is still unclear. The main location of disease is the small intestine (ileum) and the colon. Ileal disease has been linked to a mutation in the NOD2 gene. Defensins are antimicrobial peptides and in the ileum, are mainly expressed in Paneth cells, epithelial cells that also express NOD2. In the colon, defensins are expressed by enterocytes or metaplastic Paneth cells. Crohn s disease patients with ileal involvement, compared with controls or Crohn s patients without ileal involvement, have diminished expression of ileal Paneth cell defensins. This decrease is even more pronounced in Crohn s patients displaying a NOD2 mutation. In contrast, Crohn s disease of the colon is characterized by an impaired induction of -defensins in enterocytes. The colonic expression of the constitutive -defensin 1 is also decreased in the inflamed colonic mucosa, but this decrease is less specific to Crohn s disease, as it can also be found in ulcerative colitis patients. In conclusion, the regional localizations of Crohn s disease, ileal or colonic disease, can be linked to different defensin profiles. Crohn s disease of the ileum is associated with diminished defensin expression in Paneth cells. Crohn s disease of the colon is associated with diminished -defensin expression in enterocytes. Thus, it can be speculated that decreased defensin levels lead to a weakened intestinal barrier function to intestinal microbes and might be crucial in the pathophysiology of Crohn s disease. J. Leukoc. Biol. 77: ; Key Words: NOD2 Paneth cells probiotic bacteria E. coli Nissle 1917 Crohn s disease INTRODUCTION Crohn s disease is a chronic disease of the intestine characterized by a transmural inflammation of the gut. Although the distal ileum is affected in 70% of patients, the disease can be located anywhere from the oral cavity to the rectum. By comparison, ulcerative colitis, which is also a chronic disease of the intestine, is restricted to the colon, and the inflammation is limited to the mucosa. Both diseases constitute the two major chronic inflammatory bowel diseases (IBDs) affecting one in 500 individuals. The principle treatment for both diseases is a suppression of the inflammatory process. Because of substantial side-effects and uncontrolled relapses, this therapy remains far from satisfactory for patients and physicians. The etiology of Crohn s disease and ulcerative colitis is still enigmatic. There is convincing evidence that the development of Crohn s disease is associated with good hygiene standards. In developing countries, infectious intestinal diseases are extremely common, and yet, idiopathic IBDs, especially Crohn s disease, practically do not exist. We have recently discussed the idea of an association of Crohn s disease with the more pathogen-free living conditions in the Western world [1]. The first occurrence of Crohn s disease often starts after a bacterial infection [2]. The classical interpretation of this infectiontriggered beginning of this chronic inflammatory disease is a loss of mucosal tolerance toward the bacteria responsible for the inflammatory process. According to our hypothesis, the host with IBD may be more likely to contract an intestinal infection because of a defective mucosal barrier. These epidemiological factors have to be seen with the understanding of a certain genetic background, rendering the host susceptible to infections. The recent finding that approximately one-third of Crohn s disease patients have a loss of function mutation in the NOD2 gene represents a major advance [3 6]. NOD2 is a general sensor of peptidoglycan through muramyl dipeptide detection [7]. Initially fitting well with the more common understanding of the disease, the pathophysiology of NOD2 in Crohn s disease was proposed to link to immunological dysregulation in monocytes [8]. Alternatively, intestinal epithelial cells and Paneth cells [9 11], which have also been demonstrated to express NOD2, might be compromised in their antibacterial response. It has been shown recently that intestinal epithelial cells transfected with mutated NOD2 are not able to respond appropriately to an in vitro challenge with Salmonella [12]. It is interesting that a mutation in the NOD2 gene, especially SNP13, is associated with ileal localization of disease [13]. As compared with monocytes, which are widely distributed, Pan- 1 Correspondence: Department of Microbiology and Immunology, University of California, Davis, 1 Shield Avenue, Tupper Hall 3146, Davis, CA jwehkamp@ucdavis.edu Received September 22, 2004; revised October 28, 2004; accepted December 3, 2004; doi: /jlb Journal of Leukocyte Biology Volume 77, April /05/ Society for Leukocyte Biology
2 eth cells and their main effector molecules [human defensin 5 (HD5) and HD6] are normally restricted to the small intestine, which fits the phenotype of ileal affection in Crohn s disease. We and a growing number of others favor the hypothesis of a primary defect in the defensin-mediated antibacterial mucosal barrier, which is outlined and updated [1, 14] in this article. A simplified illustration of this concept is shown in Figure 1. A new and fascinating aspect of the recent data about defensin profiles in Crohn s disease is the association of diminished defensin expression or lack of defensin induction to the main clinical phenotypes, ileal and colonic Crohn s disease. As discussed in this article, ileal disease is associated with a diminished expression of the main ileal antibiotic effector molecules (HD5 and HD6). Conversely, Crohn s colitis is associated with a lack of -defensin induction. In this review, we will discuss known and recent findings, which are consistent with our general hypotheses of Crohn s disease as a defensin deficiency syndrome [1, 14]. PATHOPHYSIOLOGY: THE ROLE OF LUMINAL AND MUCOSAL BACTERIA For many years, there has been an ongoing discussion that IBDs are caused by a specific, hitherto unrecognized infection. The potential role of several pathogenic microbes, such as mycobacterium, listeria, and rubiella (measle) infection and saccharomyces, has been discussed recently [1]. The multitude of identified mucosal pathogens or antibodies does not seem to be restricted to a single microorganism and suggests that the mucosa in Crohn s disease is more susceptible in general to harbor commensal as well as potentially pathogenic bacteria. It is expected that research has focused initially on pathogenic bacteria in Crohn s disease, but what about nonpathogenic bacteria, which are part of the bacterial flora? Does the flora change in Crohn s disease? Does the ileum as the main location of the disease, which usually does not harbor many bacteria, or the colon mucosa contain more bacteria in Crohn s disease? First, there is a tremendous increase in the mucosal-associated bacterial counts in the neoterminal ileum after ileocecal resection for Crohn s disease, and this colonization may be related to postoperative relapse [16]. As discussed recently [1], different groups, mainly from France and Germany, have demonstrated convincingly that the mucosa in IBD is characterized by adherent and sometimes invading Escherichia coli strains from the lumen [17, 18]. In contrast, normal mucosa is virtually sterile when washed a few times in saline. Although the causal link has not yet been proven, a breakdown in the expression or function of the antimicrobial mucosal barrier may well explain these findings, which have been reviewed recently by Linskens et al. [19]. An interesting study from the group in France, Darfeuille-Michaud and colleagues [20], described adherent, invasive E. coli strains specifically in the ileal mucosa of Crohn s disease patients but not in ulcerative colitis. Another recent study has found increased levels of adherent E. coli in Crohn s disease colonic mucosa as well as in colon cancer [21]. All of these findings fit well with the hypothesis of a break-in mucosal tolerance toward various luminal bacteria in IBDs [22]. To summarize, these findings indicate that Crohn s mucosa may often be the target of various infections, but the proof that the disease is caused by these agents is missing. In addition, the immune response in the gut mucosa is not specific for any of these suspicious agents but rather, general response to a multitude of organisms. Rather, it is conceivable that there may be a primary defect in the peptide barrier of intestinal antibiotic defensins, which protect the normal mucosa extremely efficiently against adherent or invasive microbes. Rather than a specific infection, the commensal flora itself may cause inflammation in the absence of an adequate epithelial barrier function. Thus, not infection but rather the imbalance between the commensal flora and the host s epithelium may be crucial to Crohn s disease pathogenesis. We believe that a thorough understanding of these functionally relevant peptides is crucial for the understanding of mucosal biology, and an impaired balance of these effector molecules might explain many aspects of pathogenesis in IBDs. DEFENSIN EXPRESSION AND REGULATION IN THE INTESTINAL TRACT Fig. 1. Simplified model of the normal reaction (upper) in the healthy intestine (modified figure from Huttner and Bevins [15]), as well as the defective antimicrobial barrier in the intestine of Crohn s disease patients. In the healthy gut, the microbes cannot invade the mucosa because of an effective antimicrobial barrier (defensins). In Crohn s disease (lower), especially in patients with ileal affection, this antimicrobial barrier is disturbed, and bacteria can invade the mucosa. According to this hypothesis, a bacterial invasion as a result of a defensin deficiency is the primary reason for the secondary inflammation. Many important studies in the field of defensins have focused on the human and nonvertebrate skin as another barrier of the body exposed to a multitude of bacteria. These studies resulted in the isolation of various peptides exhibiting potent antibiotic activity toward gram-positive and -negative bacteria, as well as enveloped viruses and fungi [23 25]. A similar system of antibiotic peptides is apparently synthesized and secreted by the intestinal mucosa as part of innate immunity but has received little attention, at least in the field of clinical gastroenterology. With more knowledge about defensins in the gas- Wehkamp et al. Defensin deficiency and Crohn s disease 461
3 trointestinal tract, especially over the past 5 years, we also begin to better appreciate the enormous complexity of expression and regulation of these peptides. Six -defensins and four epithelial -defensins have been identified in the different parts of human intestinal mucosa so far. The -defensins comprise of human neutrophil peptides 1 4, produced by granulocytes, and HD5 and HD6, synthesized in Paneth cells [26]. REGULATION OF -DEFENSINS The -defensins are of epithelial origin and abundant in skin, urogenital tract, intestine, and lung [27]. Defensins can be divided into constitutive forms, e.g., human -defensin 1 (HBD-1) with its widespread, stable distribution [28], and inducible peptides such as HBD-2 [23]. The mechanisms of activation are still under investigation and are complex. Induction by cytokines, such as interleukin (IL)-1 and tumor necrosis factor (TNF- ), has been shown in addition to a direct response to bacterial components, such as lipopolysaccharides (LPS) and lipoproteins [29, 30]. Possible signaling pathways involve Toll like receptors (TLRs), especially TLR2 and TLR4 [31, 32], but more work has to be done in various intestinal epithelial cells, which express various pattern recognition receptors recognizing microbial pathogen-associated molecular patterns as nonself to rapidly initiate innate immune responses of survival and to activate defense strategies against luminal pathogens [33, 34]. This system of several functional TLRs appears to be a key regulator of the innate response system. Different TLRs are responding to different pathogens and bacterial components, including among others, LPS and flagellin. In the context of pathogen recognition receptors, NOD2/CARD15 is an intracellular receptor for a peptidoglycan that induces nuclear factor (NF)- B [35], which in turn is known to trigger HBD-2 transcription. In colonic epithelial cells in vitro, a recent study has shown a specific NF- B- and activated protein 1 (AP1)- dependent induction of HBD-2 by probiotic bacteria such as E. coli Nissle 1917 and Lactobacilli [36]. In the same study, normal LPS, probiotic E. coli Nissle LPS, as well as 50 other E. coli strains tested did not induce HBD-2 [36]. The induction of HBD-2 by LPS has been described for the airway epithelia [30] and by indirect IL-1 signaling in skin [37]. The lack of response to LPS in the colon is consistent with the lack of HBD-2 expression in the uninflamed state [38, 39]. Although in vitro studies of HBD-2 suggest an activation by inflammatory agents or inflammation itself [37, 40, 41], the induction of HBD-2 does not necessarily correlate with proinflammatory cytokines such as IL-8 or TNF- in vivo [38]. Consistent with these findings in the colon, the upregulation of HBD-2 in gastritis was restricted to that triggered by Helicobacter pylori infection [42]. Future studies will hopefully be able to address these complicated interactions and their regulation in vivo. PANETH CELL DEFENSINS An illustration and hemotoxilin and eosin (HE) staining of Paneth cells in the small intestine are given in Figure 2. HD5 is released as a propeptide from Paneth cells and at least in man, is activated by trypsin in the lumen of the intestinal crypts [44]. The functional significance in bacterial infection has recently been shown in HD5 transgenic mice, which are protected from lethal Salmonella infection [45]. Conversely, matrilysin, which is the relevant protease in mice, may be knocked out genetically, and these deficient mice fail to process defensins efficiently, exhibiting higher bacterial counts and developing intestinal inflammation [46]. Little is known about the regulation of Paneth cell -defensins. No obvious NF- B binding sites have been described [26], but because of the lack of an appropriate human cell culture model for Paneth cells, it is hard to study directly the regulation of human Paneth cell defensins. In mice, it has been shown that TLR9 is involved in Paneth cell degranulation [47]. It has been shown in mice that bacteria such as Salmonella are able to downregulate Paneth cell defensin expression [48]. Mice Paneth cell defensins contribute to 70% of total ileal antimicrobial activity, and these ileal peptides are released after stimulation with LPS and other bacterial products [43]. In this context, it might be important to mark the different milieu of colonic and ileal bacterial flora: In the small intestine, where nutrient absorption occurs, the bacterial counts are much lower as compared with the colon, where bacteria are a significant proportion of the luminal content. DEFENSINS AND LOCALIZATION OF CROHN S DISEASE: COLONIC EXPRESSION OF DEFENSINS IN CROHN S COLITIS Some antibacterial factors such as defensins appear to be induced in Crohn s diseae and ulcerative colitis. Human neutrophil peptides 1 3 as well as lysozyme are expressed in surface enterocytes of mucosa with active IBD but not in Fig. 2. HE staining (A) as well as schematic demonstration (B) of the small intestine. Paneth cells are expressed at the base of the crypts. Paneth cells are the only source of -defensins HD5 and HD6, which are the major antibacterial factors in the ileum. In mice, Paneth cell defensins contribute to 70% of antibiotic activity [43]. (Figures as published with the permission of Nature Immunology.) 462 Journal of Leukocyte Biology Volume 77, April
4 controls [49]. HD5 is stored in a precursor form in normal Paneth cells and is also expressed by metaplastic colonic Paneth cells [50, 51]. The -defensins show a conspicuous difference between Crohn s disease and ulcerative colitis in the colon. It has been suggested that HBD-1 is constitutively expressed in the intestinal epithelium [40, 52], and qualitative investigations indeed showed constitutive expression in normal tissue and IBD mucosa [41]. With the quantitative approach, a paradoxical decrease of HBD-1 was found in inflamed mucosa of Crohn s disease and ulcerative colitis, respectively [38]. Unpublished data from our group also suggest a colonic decrease of HBD-1 in case of patients with a NOD2 mutation, but the mechanism and biological relevance of this observation are still unclear. This decrease of HBD-1, in the case of NOD2 mutation, is comparable with the published decrease in inflamed tissue [38], which could be confirmed in an independent group. However, it remains to be shown that such a decrease in mrna levels actually translates into the protein level and more importantly, in a diminished mucosal antibacterial activity. The inducible HBD-2, which has been described originally in the skin [23], is also expressed in the colon during inflammation [40], particularly in ulcerative colitis [41]. It has now been shown by various independent groups that HBD-2 is highly induced in inflamed mucosa of ulcerative colitis patients. As compared with ulcerative colitis, this induction is diminished in Crohn s disease [38, 39, 41]. Most likely, there is a lack of -defensin induction in Crohn s disease contributing to a defective antimicrobial barrier, or alternatively, there is an excessive induction in ulcerative colitis. The third defensin studied was HBD-3, which was reported by Harder et al. [24] as a novel, inducible -defensin in skin. Recently, we described HBD-3 in the human colon. Although HBD-3 was also slightly induced in inflamed Crohn s mucosa, its expression was preferentially enhanced in inflamed and noninflamed ulcerative colitis [38]. More recently, Fahlgren and colleagues [53] from Sweden confirmed and significantly extended these studies. In the colon and in the ileum, HBD-3 and -4 could only be found in inflamed ulcerative colitis. In Crohn s colitis as well as Crohn s ileitis, the expression of both inducible peptides was diminished or deficient. Furthermore, enterocytes were identified as the source of HBD-3 and -4 expression by in situ hybridization [53]. It is interesting that different inducible -defensins follow the same pattern, and further studies have to answer the question of the mechanism as well as the functional consequences. A deficiency in the antimicrobial defense systems of defensins may be a reasonable and plausible explanation for the break of the antibacterial barrier function in IBDs. ILEAL EXPRESSION OF DEFENSINS IN CROHN S ILEITIS According to unpublished data, HBD-1 shows a stable ileal expression, which remains unchanged in the case of disease, suggesting that this peptide does not play an important role in case of ileitis. A recent study showed a decreased ileal Paneth cell HD5 and HD6 expression in patients with ileal disease as compared with controls and colonic-nonileal Crohn s disease. This difference was even more pronounced in patients with a NOD2 mutation, but it is important to point out that the NOD2 wild-type patients already have decreased levels of Paneth cell defensins [54]. The functional significance of HD5 [45] as well as the fact that mouse Paneth cell defensins contribute to 70% of the antibiotic activity in the ileum [43] illustrate the potential importance of these findings. We could extend these studies recently in surgical specimens from patients from the Cleveland Clinic Foundation (OH). Again, HD5 and HD6 were significantly reduced in Crohn s ileitis. The Western blot for HD5 showed the same decrease on the protein level (J. Wehkamp et al., manuscript in preparation). In contrast, other Paneth cell products were unaffected in the same patients, suggesting that the number of Paneth cells is unchanged. CONSEQUENCES FOR THERAPY: THE ROLE OF ANTIBIOTICS AND PROBIOTICS A primary lack in the antimicrobial mucosal barrier in Crohn s disease would drastically change therapeutic concepts. If a deficiency of these endogenous antibiotics triggered relapse, it would be expected that exogenous antibiotics were an efficacious treatment option. Indeed, antibiotics appear to be effective in Crohn s disease and similarly, probiotics, such as E. coli Nissle 1917 in ulcerative colitis [1, 55 59]. It is conceivable that the effect of probiotic bacteria is partly a result of the induction of -defensins, as demonstrated in vitro. In contrast to more then 50 tested E. coli, the probiotic strain E. coli Nissle 1917 and other known probiotic strains such as Lactobacilli and Pedicoccus potently up-regulated HBD-2 expression in intestinal epithelial cells [36]. The induction of HBD-2 is dependent on NF- kb and AP1 activation [36], which is consistent with induction of IL-8 as described recently [60, 61]. This induction of antimicrobial peptides by probiotic bacteria has recently been demonstrated in bees [62], and the same observation in different species suggests a broad and conserved mechanism, which underlines the potential importance of this finding. CONCLUDING REMARKS It is remarkable that the main clinical phenotypes, ileal and colonic Crohn s disease, can be linked to a characteristic lowered defensin profile. Ileal Crohn s disease is associated with a lack of ileal Paneth cell defensins, which are characteristic of the small intestine. Conversely, colonic Crohn s disease is associated with a lack of -defensin induction, which cannot be found in the normal colon. As colon and ileum drastically contrast in the number of Paneth cell defensins, the present hypothesis appears to provide a plausible explanation for disease localization. As compared with other inflammatory cells, which are widely distributed, Paneth cells and their effector molecules (HD5 and HD6) are expressed almost exclusively in the small intestine. So it can be concluded that the small intestine as the site of crime with severe inflammation shows an impaired expression of these antibiotic effector molecules. At the same time, it harbors adherent bacteria on the Wehkamp et al. Defensin deficiency and Crohn s disease 463
5 surface as well as increased bacterial counts in the lumen. The multitude of defensins, of which many might still be unknown, other antibiotic peptides, and related transcription factors or transporters leaves enough room for clinical diversity among patients. It should also be determined whether differential expression or mutations in other pattern recognition receptors [63 65] translate into an altered expression of defensins. This understanding of the disease would also drastically change the understanding of therapy. New strategies would try to strengthen the barrier function and protective innate immunity rather than only suppressing the inflammatory secondary response. E. coli Nissle 1917 in addition to Lactobacilli and other known probiotics or even helminths may have the common feature of inducing the antimicrobial peptides, which might be an important feature to help the mucosa to prevent bacterial invasion [36]. ACKNOWLEDGEMENTS The work was generously supported by the Robert Bosch Foundation, Stuttgart, Germany. Helpful discussions and joint investigations with C. Bevins, J. M. Schröder, and J. Harder are gratefully acknowledged. REFERENCES 1. Fellermann, K., Wehkamp, J., Herrlinger, K. R., Stange, E. F. (2003) Crohn s disease: a defensin deficiency syndrome? Eur. J. Gastroenterol. Hepatol. 15, Stallmach, A., Carstens, O. (2002) Role of infections in the manifestation or reactivation of inflammatory bowel diseases. Inflamm. Bowel. Dis. 8, Hugot, J-P., Chamaillard, C., Zouali, H., Lesage, S., Cezard, J-P., Belaiche, J., Almer, S., Tysk, C., O Morain, C. A., Gassull, M., Binder, V., Finkel, Y., Cortot, A., Modigliani, R., Laurent-Puig, P., Gower-Rousseau, C., Macry, J., Colombel, J-F., Sahbatou, M., Thomas, G. (2001) Association of NOD2 leucine-rich repeat variants with susceptibility to Crohn s disease. Nature 411, Hampe, J., Cuthbert, A., Croucher, P. J., Mirza, M. M., Mascheretti, S., Fisher, S., Frenzel, H., King, K., Hasselmeyer, A., MacPherson, A. J., Bridger, S., van Deventer, S., Forbes, A., Nikolaus, S., Lennard-Jones, J. E., Foelsch, U. R., Krawczak, M., Lewis, C., Schreiber, S., Mathew, C. G. (2001) Association between insertion mutation in NOD2 gene and Crohn s disease in German and British populations. Lancet 357, Ogura, Y., Bonen, D. K., Inohara, N., Nicolae, D. L., Chen, F. F., Ramos, R., Britton, H., Moran, T., Karalluskas, R., Duerr, R. H., Achkar, J-P., Brant, S. R., Bayless, T. M., Kirschner, B. S., Hanauer, S. B., Nunez, G., Cho, J. H. (2001) A frameshift mutation in NOD2 associated with susceptibility to Crohn s disease. Nature 411, Bonen, D. K., Cho, J. H. (2003) The genetics of inflammatory bowel disease. Gastroenterology 124, Girardin, S. E. (2003) NOD2 is a general sensor of peptidoglycan through muramyl dipeptide (MDP) detection. J. Biol. Chem. 278, Ogura, Y., Inohara, N., Benito, A., Chen, F. F., Yamaoka, S., Nunez, G. (2001) NOD2, a Nod1/Apaf-1 family member that is restricted to monocytes and activates NF- B. J. Biol. Chem. 276, Ogura, Y., Lala, S., Xin, W., Smith, E., Dowds, T. A., Chen, F. F., Zimmermann, E., Tretiakova, M., Cho, J. H., Hart, J., Greenson, J. K., Keshav, S., Nunez, G. (2003) Expression of NOD2 in Paneth cells: a possible link to Crohn s ileitis. Gut 52, Lala, S., Ogura, Y., Osborne, C., Hor, S. Y., Bromfield, A., Davies, S., Ogunbiyi, O., Nunez, G., Keshav, S. (2003) Crohn s disease and the NOD2 gene: a role for Paneth cells. Gastroenterology 125, Rosenstiel, P., Fantini, M., Brautigam, K., Kuhbacher, T., Waetzig, G. H., Seegert, D., Schreiber, S. (2003) TNF- and IFN- regulate the expression of the NOD2 (CARD15) gene in human intestinal epithelial cells. Gastroenterology 124, Hisamatsu, T., Suzuki, M., Reinecker, H. C., Nadeau, W. J., McCormick, B. A., Podolsky, D. K. (2003) CARD15/NOD2 functions as an antibacterial factor in human intestinal epithelial cells. Gastroenterology 124, Cuthbert, A. P., Fisher, S. A., Mirza, M. M., King, K., Hampe, J., Croucher, P. J., Mascheretti, S., Sanderson, J., Forbes, A., Mansfield, J., Schreiber, S., Lewis, C. M., Mathew, C. G. (2002) The contribution of NOD2 gene mutations to the risk and site of disease in inflammatory bowel disease. Gastroenterology 122, Schmid, M., Fellermann, K., Wehkamp, J., Herrlinger, K., Stange, E. F. (2004) The role of defensins in the pathogenesis of chronic-inflammatory bowel disease. Z. Gastroenterol. 42, Huttner, K. M., Bevins, C. L. (1999) Antimicrobial peptides as mediators of epithelial host defense. Pediatr. Res. 45, Neut, C., Bulois, P., Desreumaux, P., Membre, J. M., Lederman, E., Gambiez, L., Cortot, A., Quandalle, P., van Kruiningen, H., Colombel, J. F. (2002) Changes in the bacterial flora of the neoterminal ileum after ileocolonic resection for Crohn s disease. Am. J. Gastroenterol. 97, Darfeuille-Michaud, A., Neut, C., Barnich, N., Lederman, E., di Martino, P., Desreumaux, P., Gambiez, L., Joly, B., Cortot, A., Colombel, J-F. (1998) Presence of adherent Escherichia coli strains in ileal mucosa of patients with Crohn s disease. Gastroenterology 115, Swidsinski, A., Ladhoff, A., Pernthaler, A., Swidsinski, S., Loening- Baucke, V., Ortner, M., Weber, J., Hoffmann, U., Schreiber, S., Dietel, M., Lochs, H. (2002) Mucosal flora in inflammatory bowel disease. Gastroenterology 122, Linskens, R. K., Huijsdens, X. W., Savelkoul, P. H., Vandenbroucke- Grauls, C. M., Meuwissen, S. G. (2001) The bacterial flora in inflammatory bowel disease: current insights in pathogenesis and the influence of antibiotics and probiotics. Scand. J. Gastroenterol. Suppl. 234, Darfeuille-Michaud, A., Boudeau, J., Bulois, P., Neut, C., Glasser, A. L., Barnich, N., Bringer, M. A., Swidsinski, A., Beaugerie, L., Colombel, J. F. (2004) High prevalence of adherent-invasive Escherichia coli associated with ileal mucosa in Crohn s disease. Gastroenterology 127, Martin, H. M., Campbell, B. J., Hart, C. A., Mpofu, C., Nayar, M., Singh, R., Englyst, H., Williams, H. F., Rhodes, J. M. (2004) Enhanced Escherichia coli adherence and invasion in Crohn s disease and colon cancer. Gastroenterology 127, Duchmann, R., May, E., Heike, M., Knolle, P., Neurath, M., Meyer zum Büschenfelde, K-H. (1999) T cell specifity and cross reactivity towards enterobacteria, Bacteroides, Bifidobacterium, and antigens from resident intestinal flora in humans. Gut 44, Harder, J., Bartels, J., Christophers, E., Schröder, J. M. (1997) A peptide antibiotic from human skin. Nature 387, Harder, J., Bartels, J., Christophers, E., Schröder, J. M. (2001) Isolation and characterization of human -defensin-3, a novel human inducible peptide antibiotic. J. Biol. Chem. 276, Zasloff, M. (1992) Antibiotic peptides as mediators of innate immunity. Curr. Opin. Immunol. 4, Jones, D. E., Bevins, C. L. (1992) Paneth cells of the human small intestine express an antimicrobial peptide gene. J. Biol. Chem. 267, Ganz, T. (2003) Defensins: antimicrobial peptides of innate immunity. Nat. Rev. Immunol. 3, Zhao, C., Wang, I., Lehrer, R. I. (1996) Widespread expression of -defensin hbd-1 in human secretory glands and epithelial cells. FEBS Lett. 396, Becker, M. N., Diamond, G., Verghese, M. W., Randell, S. H. (2000) CD14-dependent lipopolysaccharide-induced -defensin-2 expression in human tracheobronchial epithelium. J. Biol. Chem. 275, Diamond, G., Russell, J. P., Bevins, C. L. (1996) Inducible expression of an antibiotic peptide gene in lipopolysaccharide-challenged tracheal epithelial cells. Proc. Natl. Acad. Sci. USA 93, Wang, X., Zhang, Z., Louboutin, J. P., Moser, C., Weiner, D. J., Wilson, J. M. (2003) Airway epithelia regulate expression of human -defensin 2 through Toll-like receptor 2. FASEB J. 17, Biragyn, A., Ruffini, P. A., Leifer, C. A., Klyushnenkova, E., Shakhov, A., Chertov, O., Shirakawa, A. K., Farber, J. M., Segal, D. M., Oppenheim, J. J., Kwak, L. W. (2002) Toll-like receptor 4-dependent activation of dendritic cells by -defensin 2. Science 298, Otte, J. M., Kiehne, K., Herzig, K. H. (2003) Antimicrobial peptides in innate immunity of the human intestine. J. Gastroenterol. 38, Cario, E., Gerken, G., Podolsky, D. K. (2002) For whom the bell tolls! innate defense mechanisms and survival strategies of the intestinal epithelium against lumenal pathogens. Z. Gastroenterol. 40, Journal of Leukocyte Biology Volume 77, April
6 35. Ogura, Y., Bonen, D. K., Inohara, N., Nicolae, D. L., Chen, F. F., Ramos, R., Britton, H., Moran, T., Karalluskas, R., Duerr, R. H., Achkar, J-P., Brant, S. R., Bayless, T. M., Kirschner, B. S., Hanauer, S. B., Nunez, G., Cho, J. H. (2001) A frameshift mutation in NOD2 associated with susceptibility to Crohn s diease. Nature 411, Wehkamp, J., Harder, J., Wehkamp, K., Wehkamp v.meissner, B., Schlee, M., Enders, C., Sonnenborn, U., Nuding, S., Fellermann, K., Schroeder, J. M., Stange, E. F. (2004) NF- B and AP-1 mediated induction of human defensin-2 in intestinal epithelial cells by E. coli Nissle 1917: a novel effect of a probiotic bacterium. Infect. Immun. 72, Liu, L., Roberts, A. A., Ganz, T. (2003) By IL-1 signaling, monocytederived cells dramatically enhance the epidermal antimicrobial response to lipopolysaccharide. J. Immunol. 170, Wehkamp, J., Harder, J., Weichenthal, M., Mueller, O., Herrlinger, K. R., Fellermann, K., Schroeder, J. M., Stange, E. F. (2003) Inducible and constitutive -defensins are differentially expressed in Crohn s disease and ulcerative colitis. Inflamm. Bowel. Dis. 9, Fahlgren, A., Hammarstrom, S., Danielsson, A., Hammarstrom, M. L. (2003) Increased expression of antimicrobial peptides and lysozyme in colonic epithelial cells of patients with ulcerative colitis. Clin. Exp. Immunol. 131, O Neil, D. A., Porter, E. M., Elewaut, D., Anderson, G. M., Eckmann, L., Ganz, T., Kagnoff, M. F. (1999) Expression and regulation of the human -defensins hbd-1 and hbd-2 in intestinal epithelium. J. Immunol. 163, Wehkamp, J., Fellermann, K., Herrlinger, K. R., Baxmann, S., Schmidt, K., Schwind, B., Duchrow, M., Wohlschlager, C., Feller, A. C., Stange, E. F. (2002) Human -defensin 2 but not -defensin 1 is expressed preferentially in colonic mucosa of inflammatory bowel disease. Eur. J. Gastroenterol. Hepatol. 14, Wehkamp, J., Schmidt, K., Herrlinger, K. R., Baxmann, S., Behling, S., Wohlschlager, C., Feller, A. C., Stange, E. F., Fellermann, K. (2003) Defensin pattern in chronic gastritis: HBD-2 is differentially expressed with respect to Helicobacter pylori status. J. Clin. Pathol. 56, Ayabe, T., Satchell, D. P., Wilson, C. L., Parks, W. C., Selsted, M. E., Ouellette, A. J. (2000) Secretion of microbicidal -defensins by intestinal Paneth cell response to bacteria. Nat. Immunol. 8, Ghosh, D., Porter, E., Shen, B., Lee, S. K., Wilk, D., Drazba, J., Yadav, S. P., Crabb, J. W., Ganz, T., Bevins, C. L. (2002) Paneth cell trypsin is the processing enzyme for human defensin-5. Nat. Immunol. 3, Salzman, N. H., Ghosh, D., Huttner, K. M., Paterson, Y., Bevins, C. L. (2003) Protection against enteric salmonellosis in transgenic mice expressing a human intestinal defensin. Nature 422, Wilson, C. L., Ouellette, A. J., Satchell, D. P., Ayabe, T., Lopez-Boado, Y. S., Stratman, J. L., Hultgren, S. J., Matrisian, L. M., Parks, W. C. (1999) Regulation of intestinal -defensin activation by the metalloproteinase matrilysin in innate host defense. Science 286, Rumio, C., Besusso, D., Palazzo, M., Selleri, S., Sfondrini, L., Dubini, F., Menard, S., Balsari, A. (2004) Degranulation of Paneth cells via Toll-like receptor 9. Am. J. Pathol. 165, Salzman, N. H., Chou, M. M., de Jong, H., Liu, L., Porter, E. M., Paterson, Y. (2003) Enteric salmonella infection inhibits Paneth cell antimicrobial peptide expression. Infect. Immun. 71, Cunliffe, R. N., Kamal, M., Rose, F. R., James, P. D., Mahida, Y. R. (2002) Expression of antimicrobial neutrophil defensins in epithelial cells of active inflammatory bowel disease mucosa. J. Clin. Pathol. 55, Cunliffe, R. N., Rose, F. R., Keyte, J., Abberley, L., Chan, W. C., Mahida, Y. R. (2001) Human defensin 5 is stored in precursor form in normal Paneth cells and is expressed by some viloous epithelial cells and by metaplastic Paneth cells in the colon in inflammatory bowel disease. Gut 48, Wehkamp, J., Schwind, B., Herrlinger, K. R., Baxmann, S., Schmidt, K., Duchrow, M., Wohlschlager, C., Feller, A. C., Stange, E. F., Fellermann, K. (2002) Innate immunity and colonic inflammation: enhanced expression of epithelial -defensins. Dig. Dis. Sci. 47, Tollin, M., Bergman, P., Svenberg, T., Jornvall, H., Gudmundsson, G. H., Agerberth, B. (2003) Antimicrobial peptides in the first line defence of human colon mucosa. Peptides 24, Fahlgren, A., Hammarstrom, S., Danielsson, A., Hammarstrom, M. L. (2004) -Defensin-3 and -4 in intestinal epithelial cells display increased mrna expression in ulcerative colitis. Clin. Exp. Immunol. 137, Wehkamp, J., Harder, J., Weichenthal, M., Schwab, M., Schaeffeler, E., Schlee, M., Stallmach, A., Noack, F., Fritz, P., Schroder, J. M., Bevins, C. L., Fellermann, K., Stange, E. F. (2004) NOD2 (CARD15) mutations in Crohn s disease are associated with diminished mucosal -defensin expression. Gut 53, Sartor, R. B. (1997) Review article: role of the enteric microflora in the pathogenesis of intestinal inflammation and arthritis. Aliment. Pharmacol. Ther. 11 (Suppl. 3), Schultz, M., Scholmerich, J., Rath, H. C. (2003) Rationale for probiotic and antibiotic treatment strategies in inflammatory bowel diseases. Dig. Dis. 21, Kruis, W., Schutz, E., Fric, P., Fixa, B., Judmaier, G., Stolte, M. (1997) Double-blind comparison of an oral Escherichia coli preparation and mesalazine in maintaining remission of ulcerative colitis. Aliment. Pharmacol. Ther. 11, Rembacken, B. J., Snelling, A. M., Hawkey, P. M., Chalmers, D. M., Axon, A. T. (1999) Non-pathogenic Escherichia coli versus mesalazine for the treatment of ulcerative colitis: a randomized trial. Lancet 354, Kruis, W., Fric, P., Stolte, M. (2001) Maintenance of remission in ulcerative colitis is equally effective with Echerichia coli 1917 and with standard mesalamine. Gastroenterology 120, A Lammers, K. M., Helwig, U., Swennen, E., Rizzello, F., Venturi, A., Caramelli, E., Kamm, M. A., Brigidi, P., Gionchetti, P., Campieri, M. (2002) Effect of probiotic strains on interleukin 8 production by HT29/ 19A cells. Am. J. Gastroenterol. 97, Otte, J. M., Podolsky, D. K. (2004) Functional modulation of enterocytes by gram-positive and gram-negative microorganisms. Am. J. Physiol. Gastrointest. Liver Physiol. 286, G613 G Evans, J. D., Lopez, D. L. (2004) Bacterial probiotics induce an immune response in the honey bee (Hymenoptera: Apidae). J. Econ. Entomol. 97, Cario, E., Podolsky, D. K. (2000) Differential alteration in intestinal epithelial cell expression of Toll-like receptor 3 (TLR3) and TLR4 in inflammatory bowel disease. Infect. Immun. 68, Franchimont, D., Vermeire, S., El Housni, H., Pierik, M., Van Steen, K., Gustot, T., Quertinmont, E., Abramowicz, M., Van Gossum, A., Deviere, J., Rutgeerts, P. (2004) Deficient host-bacteria interactions in inflammatory bowel disease? The Toll-like receptor (TLR)-4 Asp299 gly polymorphism is associated with Crohn s disease and ulcerative colitis. Gut 53, Torok, H. P., Glas, J., Tonenchi, L., Mussack, T., Folwaczny, C. (2004) Polymorphisms of the lipopolysaccharide-signaling complex in inflammatory bowel disease: association of a mutation in the Toll-like receptor 4 gene with ulcerative colitis. Clin. Immunol. 112, Wehkamp et al. Defensin deficiency and Crohn s disease 465
They all do it! What?
 They all do it! What? Defensins: the endogenous antibiotics of body surfaces Wehkamp J et al. (2005) Mechanisms of Disease: defensins in gastrointestinal diseases Nat Clin Pract Gastroenterol Hepatol 2:
They all do it! What? Defensins: the endogenous antibiotics of body surfaces Wehkamp J et al. (2005) Mechanisms of Disease: defensins in gastrointestinal diseases Nat Clin Pract Gastroenterol Hepatol 2:
Probiotic bacteria: mechanisms of action?
 Probiotic bacteria: mechanisms of action? Probiotic derived antibacterial substances (microcins) Competitive inhibition of pathogens Modulation of inflammatory responses: Increasing antiinflammatory cytokine
Probiotic bacteria: mechanisms of action? Probiotic derived antibacterial substances (microcins) Competitive inhibition of pathogens Modulation of inflammatory responses: Increasing antiinflammatory cytokine
Why does Crohn's disease usually occur in terminal ileum?
 Journal of Crohn's and Colitis (2008) 2, 352 356 available at www.sciencedirect.com VIEWPOINT Why does Crohn's disease usually occur in terminal ileum? Renzo Caprilli University of Rome La Sapienza, Via
Journal of Crohn's and Colitis (2008) 2, 352 356 available at www.sciencedirect.com VIEWPOINT Why does Crohn's disease usually occur in terminal ileum? Renzo Caprilli University of Rome La Sapienza, Via
Gut Microbiota and IBD. Vahedi. H M.D Associate Professor of Medicine DDRI
 Gut Microbiota and IBD Vahedi. H M.D Associate Professor of Medicine DDRI 1393.3.1 2 GUT MICROBIOTA 100 Trillion Microbes - 10 times more than cells in our body Collective weight of about 1kg in human
Gut Microbiota and IBD Vahedi. H M.D Associate Professor of Medicine DDRI 1393.3.1 2 GUT MICROBIOTA 100 Trillion Microbes - 10 times more than cells in our body Collective weight of about 1kg in human
Escherichia coli Nissle 1917
 Immunoregulation in Inflammatory Bowel Diseases New therapeutic approaches Probiotics Escherichia coli Nissle 1917 Andreas Sturm Medizinische Klinik m.s. Hepatologie, Gastroenterologie, Endokrinologie
Immunoregulation in Inflammatory Bowel Diseases New therapeutic approaches Probiotics Escherichia coli Nissle 1917 Andreas Sturm Medizinische Klinik m.s. Hepatologie, Gastroenterologie, Endokrinologie
Genetics. Environment. You Are Only 10% Human. Pathogenesis of IBD. Advances in the Pathogenesis of IBD: Genetics Leads to Function IBD
 Advances in the Pathogenesis of IBD: Genetics Leads to Function Pathogenesis of IBD Environmental Factors Microbes Scott Plevy, MD Associate Professor of Medicine, Microbiology & Immunology UNC School
Advances in the Pathogenesis of IBD: Genetics Leads to Function Pathogenesis of IBD Environmental Factors Microbes Scott Plevy, MD Associate Professor of Medicine, Microbiology & Immunology UNC School
Innate immune regulation of T-helper (Th) cell homeostasis in the intestine
 Innate immune regulation of T-helper (Th) cell homeostasis in the intestine Masayuki Fukata, MD, Ph.D. Research Scientist II Division of Gastroenterology, Department of Medicine, F. Widjaja Foundation,
Innate immune regulation of T-helper (Th) cell homeostasis in the intestine Masayuki Fukata, MD, Ph.D. Research Scientist II Division of Gastroenterology, Department of Medicine, F. Widjaja Foundation,
Inflammatory bowel disease (IBD)
 The Journal of Immunology The Paneth Cell -Defensin Deficiency of Ileal Crohn s Disease Is Linked to Wnt/Tcf-4 1 Jan Wehkamp, 2 * Guoxing Wang,* Irmgard Kübler,* Sabine Nuding,* Alex Gregorieff, Anke Schnabel,*
The Journal of Immunology The Paneth Cell -Defensin Deficiency of Ileal Crohn s Disease Is Linked to Wnt/Tcf-4 1 Jan Wehkamp, 2 * Guoxing Wang,* Irmgard Kübler,* Sabine Nuding,* Alex Gregorieff, Anke Schnabel,*
The enteric microbiota: Implications for IBD. Eugene B. Chang, M.D. University of Chicago
 The enteric microbiota: Implications for IBD Eugene B. Chang, M.D. University of Chicago On a per cell basis, humans are mostly prokaryote 100 90 80 70 60 50 40 30 20 10 0 EuK ProK The microbial flora
The enteric microbiota: Implications for IBD Eugene B. Chang, M.D. University of Chicago On a per cell basis, humans are mostly prokaryote 100 90 80 70 60 50 40 30 20 10 0 EuK ProK The microbial flora
Faecalibacterium prausnitzii
 Faecalibacterium prausnitzii is an anti-inflammatory commensal bacterium identified by gut microbiota analysis of Crohn disease patients PNAS 105(43): 16731-16736, 2008. Speaker: Ming-Cheng Chen Advisor:
Faecalibacterium prausnitzii is an anti-inflammatory commensal bacterium identified by gut microbiota analysis of Crohn disease patients PNAS 105(43): 16731-16736, 2008. Speaker: Ming-Cheng Chen Advisor:
The cause of ulcerative colitis (UC) and Crohn s disease
 GASTROENTEROLOGY 2003;124:1767 1773 Inflammatory Bowel Disease in a Swedish Twin Cohort: A Long- Term Follow-up of Concordance and Clinical Characteristics JONAS HALFVARSON,* LENNART BODIN, CURT TYSK,*
GASTROENTEROLOGY 2003;124:1767 1773 Inflammatory Bowel Disease in a Swedish Twin Cohort: A Long- Term Follow-up of Concordance and Clinical Characteristics JONAS HALFVARSON,* LENNART BODIN, CURT TYSK,*
April 2003 EDITORIALS 1145
 April 2003 EDITORIALS 1145 experience in 500 patients (abstr). Gastroenterology 2003 (in press). 11. Sands B, Van Deventer S, Bernstein C, Kamm M, Rachmilewicz D, Chey W, Lashner B, Wolf D, Blank M, Wild
April 2003 EDITORIALS 1145 experience in 500 patients (abstr). Gastroenterology 2003 (in press). 11. Sands B, Van Deventer S, Bernstein C, Kamm M, Rachmilewicz D, Chey W, Lashner B, Wolf D, Blank M, Wild
Commensal Bacteria, Toll-like Receptors and Intestinal Injury. Journal Club December 16, 2004
 Commensal Bacteria, Toll-like Receptors and Intestinal Injury Journal Club December 16, 2004 Gut-Commensal Interactions Nutrient metabolism Tissue development Resistance to colonization with pathogens
Commensal Bacteria, Toll-like Receptors and Intestinal Injury Journal Club December 16, 2004 Gut-Commensal Interactions Nutrient metabolism Tissue development Resistance to colonization with pathogens
Studies on probiotics effects on innate immune functions in the gastrointestinal tract of broiler chicks (SUMMARY)
 Doctoral Thesis Studies on probiotics effects on innate immune functions in the gastrointestinal tract of broiler chicks (SUMMARY) ELSAYED SEDDEK IBRAHEM MOHAMMED Department of Bioresource Science Graduate
Doctoral Thesis Studies on probiotics effects on innate immune functions in the gastrointestinal tract of broiler chicks (SUMMARY) ELSAYED SEDDEK IBRAHEM MOHAMMED Department of Bioresource Science Graduate
Genetics of Pediatric Inflammatory Bowel Disease
 Genetics of Pediatric Inflammatory Bowel Disease Judith Kelsen MD Assistant Professor of Pediatrics Division of Gastroenterology, Hepatology, and Nutrition IBD Education Day 2/9/2014 Objectives Brief overview
Genetics of Pediatric Inflammatory Bowel Disease Judith Kelsen MD Assistant Professor of Pediatrics Division of Gastroenterology, Hepatology, and Nutrition IBD Education Day 2/9/2014 Objectives Brief overview
the intestinal barrier
 intestinal defensins/antimicrobial peptides the intestinal barrier Jan Wehkamp, Stuttgart, tt t Germany Dr. Margarete Fischer Bosch Institute of Clinical Pharmacology, Stuttgart, Germany Medicine I Robert
intestinal defensins/antimicrobial peptides the intestinal barrier Jan Wehkamp, Stuttgart, tt t Germany Dr. Margarete Fischer Bosch Institute of Clinical Pharmacology, Stuttgart, Germany Medicine I Robert
Necrotizing Enterocolitis: The Role of the Immune System
 Necrotizing Enterocolitis: The Role of the Immune System Patricia Denning, M.D. Associate Professor in Pediatrics Division of Neonatology Emory University School of Medicine What is NEC? What is NEC? Necrotizing
Necrotizing Enterocolitis: The Role of the Immune System Patricia Denning, M.D. Associate Professor in Pediatrics Division of Neonatology Emory University School of Medicine What is NEC? What is NEC? Necrotizing
Running head: CHRON'S DISEASE GENE-ENVIRONMENTAL INTERACTION 1
 Running head: CHRON'S DISEASE GENE-ENVIRONMENTAL INTERACTION 1 A review of Crohn's Disease Gene-Environmental Interaction A study of gene-environment interaction between genetic susceptibility variants
Running head: CHRON'S DISEASE GENE-ENVIRONMENTAL INTERACTION 1 A review of Crohn's Disease Gene-Environmental Interaction A study of gene-environment interaction between genetic susceptibility variants
Chapter 3 The Induced Responses of Innate Immunity
 Chapter 3 The Induced Responses of Innate Immunity Pattern recognition by cells of the innate immune system Pattern recognition by cells of the innate immune system 4 main pattern recognition receptors
Chapter 3 The Induced Responses of Innate Immunity Pattern recognition by cells of the innate immune system Pattern recognition by cells of the innate immune system 4 main pattern recognition receptors
The effect of probiotics on animal health: a focus on host s natural intestinal defenses
 The effect of probiotics on animal health: a focus on host s natural intestinal defenses Guillaume Tabouret Animal Health Dept. Joint Unit 1225 Host Pathogens Interactions History of probiotics and definition
The effect of probiotics on animal health: a focus on host s natural intestinal defenses Guillaume Tabouret Animal Health Dept. Joint Unit 1225 Host Pathogens Interactions History of probiotics and definition
Alterations of the CARD15/NOD2 Gene and the Impact on Management and Treatment of Crohn s Disease Patients
 Review Article Dig Dis 2003;21:339 345 DOI: 10.1159/000075357 Alterations of the CARD15/NOD2 Gene and the Impact on Management and Treatment of Crohn s Disease Patients Helga-Paula Török a,b Jürgen Glas
Review Article Dig Dis 2003;21:339 345 DOI: 10.1159/000075357 Alterations of the CARD15/NOD2 Gene and the Impact on Management and Treatment of Crohn s Disease Patients Helga-Paula Török a,b Jürgen Glas
Dysbiosis & Inflammation
 MASTERING THE MICROBIOME: Dysbiosis & Inflammation 2017 Tom Fabian, PhD It is reasonable to propose that the composition of the microbiome and its activities are involved in most, if not all, of the biological
MASTERING THE MICROBIOME: Dysbiosis & Inflammation 2017 Tom Fabian, PhD It is reasonable to propose that the composition of the microbiome and its activities are involved in most, if not all, of the biological
Innate immunity. Abul K. Abbas University of California San Francisco. FOCiS
 1 Innate immunity Abul K. Abbas University of California San Francisco FOCiS 2 Lecture outline Components of innate immunity Recognition of microbes and dead cells Toll Like Receptors NOD Like Receptors/Inflammasome
1 Innate immunity Abul K. Abbas University of California San Francisco FOCiS 2 Lecture outline Components of innate immunity Recognition of microbes and dead cells Toll Like Receptors NOD Like Receptors/Inflammasome
C Gasche, P Grundtner
 162 Recent advances in clinical practice GENOTYPES AND PHENOTYPES IN CROHN S DISEASE: DO THEY HELP IN CLINICAL MANAGEMENT? c CROHN S See end of article for authors affiliations Correspondence to: Professor
162 Recent advances in clinical practice GENOTYPES AND PHENOTYPES IN CROHN S DISEASE: DO THEY HELP IN CLINICAL MANAGEMENT? c CROHN S See end of article for authors affiliations Correspondence to: Professor
Innate Immunity. Chapter 3. Connection Between Innate and Adaptive Immunity. Know Differences and Provide Examples. Antimicrobial peptide psoriasin
 Chapter Know Differences and Provide Examples Innate Immunity kin and Epithelial Barriers Antimicrobial peptide psoriasin -Activity against Gram (-) E. coli Connection Between Innate and Adaptive Immunity
Chapter Know Differences and Provide Examples Innate Immunity kin and Epithelial Barriers Antimicrobial peptide psoriasin -Activity against Gram (-) E. coli Connection Between Innate and Adaptive Immunity
Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases. Abul K. Abbas UCSF
 Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases Abul K. Abbas UCSF Balancing lymphocyte activation and control Activation Effector T cells Tolerance Regulatory T cells
Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases Abul K. Abbas UCSF Balancing lymphocyte activation and control Activation Effector T cells Tolerance Regulatory T cells
A Case of Inflammatory Bowel Disease
 A Case of Inflammatory Bowel Disease Dr Barrie Rathbone www.le.ac.uk 26 year old Polish woman Admitted as emergency under surgeons RUQ and RIF pain Abdominal pain had occurred intermittently for a few
A Case of Inflammatory Bowel Disease Dr Barrie Rathbone www.le.ac.uk 26 year old Polish woman Admitted as emergency under surgeons RUQ and RIF pain Abdominal pain had occurred intermittently for a few
Intestinal Microbiota in Health and Disease
 Intestinal Microbiota in Health and Disease February 27, 2015 Master s Course in Gastroenterology Prof. Kathy McCoy 1 Overview Overview of Gut Microbiota Microbiota in Health Microbiota in Disease 2 Gut
Intestinal Microbiota in Health and Disease February 27, 2015 Master s Course in Gastroenterology Prof. Kathy McCoy 1 Overview Overview of Gut Microbiota Microbiota in Health Microbiota in Disease 2 Gut
The fundamental basis of inflammatory bowel disease
 Science in medicine The fundamental basis of inflammatory bowel disease Warren Strober, Ivan Fuss, and Peter Mannon Mucosal Immunity Section, Laboratory of Host Defenses, National Institute of Allergy
Science in medicine The fundamental basis of inflammatory bowel disease Warren Strober, Ivan Fuss, and Peter Mannon Mucosal Immunity Section, Laboratory of Host Defenses, National Institute of Allergy
2. Innate immunity 2013
 1 Innate Immune Responses 3 Innate immunity Abul K. Abbas University of California San Francisco The initial responses to: 1. Microbes: essential early mechanisms to prevent, control, or eliminate infection;
1 Innate Immune Responses 3 Innate immunity Abul K. Abbas University of California San Francisco The initial responses to: 1. Microbes: essential early mechanisms to prevent, control, or eliminate infection;
Understanding clinical aspects of Crohn s disease and ulcerative colitis: Implications for the basic scientist
 Understanding clinical aspects of Crohn s disease and ulcerative colitis: Implications for the basic scientist Scott Plevy, MD Associate Professor of Medicine, Microbiology & Immunology UNC School of Medicine
Understanding clinical aspects of Crohn s disease and ulcerative colitis: Implications for the basic scientist Scott Plevy, MD Associate Professor of Medicine, Microbiology & Immunology UNC School of Medicine
Innate Immunity. Connection Between Innate and Adaptive Immunity. Know Differences and Provide Examples Chapter 3. Antimicrobial peptide psoriasin
 Know Differences and Provide Examples Chapter * Innate Immunity * kin and Epithelial Barriers * Antimicrobial peptide psoriasin -Activity against Gram (-) E. coli Connection Between Innate and Adaptive
Know Differences and Provide Examples Chapter * Innate Immunity * kin and Epithelial Barriers * Antimicrobial peptide psoriasin -Activity against Gram (-) E. coli Connection Between Innate and Adaptive
CARD15 and Crohn s Disease: Healthy Homozygous Carriers of the 3020insC Frameshift Mutation
 THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 98, No. 3, 2003 2003 by Am. Coll. of Gastroenterology ISSN 0002-9270/03/$30.00 Published by Elsevier Science Inc. doi:10.1016/s0002-9270(02)06009-4 CARD15
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 98, No. 3, 2003 2003 by Am. Coll. of Gastroenterology ISSN 0002-9270/03/$30.00 Published by Elsevier Science Inc. doi:10.1016/s0002-9270(02)06009-4 CARD15
Genetic and Environmental Risks for IBD
 Genetic and Environmental Risks for IBD CCFA April 26, 2014 Presented by: Name goes here April 30, 2014 TheoTheodore 1 Genetic and Environmental Risks for IBD Theodore M. Bayless, M.D. Director Emeritus
Genetic and Environmental Risks for IBD CCFA April 26, 2014 Presented by: Name goes here April 30, 2014 TheoTheodore 1 Genetic and Environmental Risks for IBD Theodore M. Bayless, M.D. Director Emeritus
Lavanya Nutankalva,MD Consultant: Infectious Diseases
 Lavanya Nutankalva,MD Consultant: Infectious Diseases Introduction The word Probiotic was derived from the Greek phrase meaning for life." was first coined in the 1960s by Lilly and Stillwell. Probiotics
Lavanya Nutankalva,MD Consultant: Infectious Diseases Introduction The word Probiotic was derived from the Greek phrase meaning for life." was first coined in the 1960s by Lilly and Stillwell. Probiotics
Date of preparation: 06/ IBD/
 Mechanisms Mechanisms of of Disease Disease: The The Science of of IBD IBD 64002 Date of preparation: 06/11 2013 IBD/2013-11-01 Table of Contents IBD Background and Disease Management Etiology and Pathophysiology
Mechanisms Mechanisms of of Disease Disease: The The Science of of IBD IBD 64002 Date of preparation: 06/11 2013 IBD/2013-11-01 Table of Contents IBD Background and Disease Management Etiology and Pathophysiology
Overview of the immune system
 Overview of the immune system Immune system Innate (nonspecific) 1 st line of defense Adaptive (specific) 2 nd line of defense Cellular components Humoral components Cellular components Humoral components
Overview of the immune system Immune system Innate (nonspecific) 1 st line of defense Adaptive (specific) 2 nd line of defense Cellular components Humoral components Cellular components Humoral components
Paneth cells: leukocyte-like mediators of innate immunity in the intestine
 Paneth cells: leukocyte-like mediators of innate immunity in the intestine Satish Keshav 1 Department of Medicine, Centre for Gastroenterology, Royal Free and University College Medical School, UCL, London,
Paneth cells: leukocyte-like mediators of innate immunity in the intestine Satish Keshav 1 Department of Medicine, Centre for Gastroenterology, Royal Free and University College Medical School, UCL, London,
Periodontal status of patients with Crohn s Disease
 Page 1 of 5 ISSN 1612-7749 Quintessence International Publishing Group» Home» Issues» Issue 1 / 1999 [1-8]» Issue 2 / 1999 [9-19]» Issue 3 / 1999 [20-23]» Issue 4 / 1999 [24-27]» Issue 1 / 2000 [28-35]»
Page 1 of 5 ISSN 1612-7749 Quintessence International Publishing Group» Home» Issues» Issue 1 / 1999 [1-8]» Issue 2 / 1999 [9-19]» Issue 3 / 1999 [20-23]» Issue 4 / 1999 [24-27]» Issue 1 / 2000 [28-35]»
محاضرة مناعت مدرس المادة :ا.م. هدى عبدالهادي علي النصراوي Immunity to Infectious Diseases
 محاضرة مناعت مدرس المادة :ا.م. هدى عبدالهادي علي النصراوي Immunity to Infectious Diseases Immunity to infection depends on a combination of innate mechanisms (phagocytosis, complement, etc.) and antigen
محاضرة مناعت مدرس المادة :ا.م. هدى عبدالهادي علي النصراوي Immunity to Infectious Diseases Immunity to infection depends on a combination of innate mechanisms (phagocytosis, complement, etc.) and antigen
Innate Immunity. Natural or native immunity
 Innate Immunity 1 Innate Immunity Natural or native immunity 2 When microbes enter in the body 3 Secondly, it also stimulates the adaptive immune system 4 Immunologic memory 5 Components of Innate Immunity
Innate Immunity 1 Innate Immunity Natural or native immunity 2 When microbes enter in the body 3 Secondly, it also stimulates the adaptive immune system 4 Immunologic memory 5 Components of Innate Immunity
Innate immunity as a therapeutic target in IBD. Elke Cario Division of Gastroenterology & Hepatology University Hospital of Essen Essen, Germany
 Innate immunity as a therapeutic target in IBD Elke Cario Division of Gastroenterology & Hepatology University Hospital of Essen Essen, Germany The intestinal mucosa must rapidly recognize luminal pathogens
Innate immunity as a therapeutic target in IBD Elke Cario Division of Gastroenterology & Hepatology University Hospital of Essen Essen, Germany The intestinal mucosa must rapidly recognize luminal pathogens
Animal Models to Understand Immunity
 Animal Models to Understand Immunity Hussein El Saghire hesaghir@sckcen.be Innate Adaptive immunity Immunity MAPK and NF-kB TLR pathways receptors Fast Slow Non-specific Specific NOD-like receptors T-cell
Animal Models to Understand Immunity Hussein El Saghire hesaghir@sckcen.be Innate Adaptive immunity Immunity MAPK and NF-kB TLR pathways receptors Fast Slow Non-specific Specific NOD-like receptors T-cell
A large body of evidence from both animal models and
 405 INFLAMMATION AND INFLAMMATORY BOWEL DISEASE Ineffectiveness of probiotics in preventing after curative resection for Crohn s disease: a randomised controlled trial with Lactobacillus GG C Prantera,
405 INFLAMMATION AND INFLAMMATORY BOWEL DISEASE Ineffectiveness of probiotics in preventing after curative resection for Crohn s disease: a randomised controlled trial with Lactobacillus GG C Prantera,
2 االستاذ المساعد الدكتور خالد ياسين الزاملي \ مناعة \ المرحلة الثانية \ التحليالت المرضية \
 Innate Immunity Innate immunity: is the resistance that an individual possesses by birth. Innate immunity may be classified as (a) individual immunity (b) racial immunity (c) species immunity. Factors
Innate Immunity Innate immunity: is the resistance that an individual possesses by birth. Innate immunity may be classified as (a) individual immunity (b) racial immunity (c) species immunity. Factors
Innate Immunity. Natural or native immunity
 Innate Immunity 1 Innate Immunity Natural or native immunity 2 When microbes enter in the body 3 Secondly, it also stimulates the adaptive immune system 4 Immunologic memory 5 Components of Innate Immunity
Innate Immunity 1 Innate Immunity Natural or native immunity 2 When microbes enter in the body 3 Secondly, it also stimulates the adaptive immune system 4 Immunologic memory 5 Components of Innate Immunity
ESPEN Congress Vienna Networking with your microbiota Specific evidence-based indications. H. Lochs (Germany)
 ESPEN Congress Vienna 2009 Networking with your microbiota Specific evidence-based indications H. Lochs (Germany) Probiotics Evidence based indications H. Lochs Medizinische Klinik mit Schwerpunkt Gastroenterologie,
ESPEN Congress Vienna 2009 Networking with your microbiota Specific evidence-based indications H. Lochs (Germany) Probiotics Evidence based indications H. Lochs Medizinische Klinik mit Schwerpunkt Gastroenterologie,
Humoral Immune Response And Luminal Microorganisms In Patients With Indeterminate Colitis
 ISPUB.COM The Internet Journal of Gastroenterology Volume 9 Number 1 Humoral Immune Response And Luminal Microorganisms In Patients With Indeterminate Colitis B Mahdi, W Salih, B Kadum, R Hasan, M Ameen
ISPUB.COM The Internet Journal of Gastroenterology Volume 9 Number 1 Humoral Immune Response And Luminal Microorganisms In Patients With Indeterminate Colitis B Mahdi, W Salih, B Kadum, R Hasan, M Ameen
D2 inhibits TLR2- initiated 12p40 transcription (-) TLR2 PGN MDP. MyD88 IRAK ECSIT TRAF6 NIK. Smallest unit of PGN muramyl dipeptide IKK.
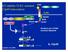 D2 inhibits TLR2- initiated 12p40 transcription CARD CARD NOD2 LRR RICK/Rip2 NIK MDP TRAF6 PGN TLR2 MyD88 IRAK ECSIT (-) IKK Smallest unit of PGN muramyl dipeptide IκB NF-κB atanabe et al, 2004 NF-κB IL-12p40
D2 inhibits TLR2- initiated 12p40 transcription CARD CARD NOD2 LRR RICK/Rip2 NIK MDP TRAF6 PGN TLR2 MyD88 IRAK ECSIT (-) IKK Smallest unit of PGN muramyl dipeptide IκB NF-κB atanabe et al, 2004 NF-κB IL-12p40
Signal Transduction in Inflammatory Bowel Disease
 E v e n t s 0 6 4 Signal Transduction in Inflammatory Bowel Disease 0 1 2 3 4 1 0 1 0 1 0 1 0 1 0 F L 2 - H e ig h t Vineeta Khare Ph.D Overview Inflammatory Bowel Diseases 1. Epidemiology, Symptoms and
E v e n t s 0 6 4 Signal Transduction in Inflammatory Bowel Disease 0 1 2 3 4 1 0 1 0 1 0 1 0 1 0 F L 2 - H e ig h t Vineeta Khare Ph.D Overview Inflammatory Bowel Diseases 1. Epidemiology, Symptoms and
Inflammatory Bowel Disease A model for translational medicine. D P Jewell Professor Emeritus of Gastroenterology University of Oxford
 Inflammatory Bowel Disease A model for translational medicine D P Jewell Professor Emeritus of Gastroenterology University of Oxford Samuel Wilks 1859, Pathological Treatises of Guy s Hospital The London
Inflammatory Bowel Disease A model for translational medicine D P Jewell Professor Emeritus of Gastroenterology University of Oxford Samuel Wilks 1859, Pathological Treatises of Guy s Hospital The London
Genetic basis for increased intestinal permeability in families with Crohn s disease: Role of CARD insC mutation?
 Gut Online First, published on July 29, 2005 as 10.1136/gut.2005.065557 1 Genetic basis for increased intestinal permeability in families with Crohn s disease: Role of CARD15 3020insC mutation? Sabine
Gut Online First, published on July 29, 2005 as 10.1136/gut.2005.065557 1 Genetic basis for increased intestinal permeability in families with Crohn s disease: Role of CARD15 3020insC mutation? Sabine
Title: Toll like receptor four (tlrfour) polymorphisms in tunisians patients with crohn's disease: genotype-phenotype correlation
 Author's response to reviews Title: Toll like receptor four (tlrfour) polymorphisms in tunisians patients with crohn's disease: genotype-phenotype correlation Authors: Lilia Zouiten (w.mekki@laposte.net)
Author's response to reviews Title: Toll like receptor four (tlrfour) polymorphisms in tunisians patients with crohn's disease: genotype-phenotype correlation Authors: Lilia Zouiten (w.mekki@laposte.net)
Azienda Ospedaliera S. Camillo Forlanini. Unità Operativa di Gastroenterologia. Moscow June Cosimo Prantera
 / Azienda Ospedaliera S. Camillo Forlanini Unità Operativa di Gastroenterologia Moscow June 2006 Cosimo Prantera ANTIBIOTICS AND BACTERIAL SPECIES Metronidazole Bacteroides - Clostridia Ciprofloxacin Escherichia
/ Azienda Ospedaliera S. Camillo Forlanini Unità Operativa di Gastroenterologia Moscow June 2006 Cosimo Prantera ANTIBIOTICS AND BACTERIAL SPECIES Metronidazole Bacteroides - Clostridia Ciprofloxacin Escherichia
T he integrity of gut barrier function in patients with
 342 INFLAMMATORY BOWEL DISEASE Genetic basis for increased intestinal permeability in families with Crohn s disease: role of CARD15 3020insC mutation? S Buhner, C Buning, J Genschel, K Kling, D Herrmann,
342 INFLAMMATORY BOWEL DISEASE Genetic basis for increased intestinal permeability in families with Crohn s disease: role of CARD15 3020insC mutation? S Buhner, C Buning, J Genschel, K Kling, D Herrmann,
Inflammatory Bowel Diseases (IBD) Clinical aspects Nitsan Maharshak M.D., IBD Center, Department of Gastroenterology and Liver Diseases Tel Aviv Soura
 Inflammatory Bowel Diseases (IBD) Clinical aspects Nitsan Maharshak M.D., IBD Center, Department of Gastroenterology and Liver Diseases Tel Aviv Sourasky Medical Center Tel Aviv, Israel IBD- clinical features
Inflammatory Bowel Diseases (IBD) Clinical aspects Nitsan Maharshak M.D., IBD Center, Department of Gastroenterology and Liver Diseases Tel Aviv Sourasky Medical Center Tel Aviv, Israel IBD- clinical features
Understanding probiotics and health
 Understanding probiotics and health Gemma Laws MSc Student Microbiology and Immunology Department The gut microbiota The name given to the total microbial population living in our intestine Bacteria, fungi,
Understanding probiotics and health Gemma Laws MSc Student Microbiology and Immunology Department The gut microbiota The name given to the total microbial population living in our intestine Bacteria, fungi,
CARD15 Gene Mutations and Risk for Early Surgery in Pediatric-Onset Crohn s Disease
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2004;2:1003 1009 CARD15 Gene Mutations and Risk for Early Surgery in Pediatric-Onset Crohn s Disease SUBRA KUGATHASAN,* NICOLE COLLINS,* KAREN MARESSO, RAYMOND
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2004;2:1003 1009 CARD15 Gene Mutations and Risk for Early Surgery in Pediatric-Onset Crohn s Disease SUBRA KUGATHASAN,* NICOLE COLLINS,* KAREN MARESSO, RAYMOND
Epithelial Cells and Their Neighbors. IV. Bacterial contributions to intestinal epithelial barrier integrity
 Epithelial Cells and Their Neighbors. IV. Bacterial contributions to intestinal epithelial barrier integrity Anisa S. Ismail and Lora V. Hooper Am J Physiol Gastrointest Liver Physiol 289:779-784, 2005.
Epithelial Cells and Their Neighbors. IV. Bacterial contributions to intestinal epithelial barrier integrity Anisa S. Ismail and Lora V. Hooper Am J Physiol Gastrointest Liver Physiol 289:779-784, 2005.
Accepted Manuscript. Innate immune cells regulate oncoimmunity and cancer development. Ai-Ping Bai, Yuan Guo
 Accepted Manuscript Innate immune cells regulate oncoimmunity and cancer development Ai-Ping Bai, Yuan Guo PII: S0016-5085(18)34974-6 DOI: 10.1053/j.gastro.2018.08.057 Reference: YGAST 62119 To appear
Accepted Manuscript Innate immune cells regulate oncoimmunity and cancer development Ai-Ping Bai, Yuan Guo PII: S0016-5085(18)34974-6 DOI: 10.1053/j.gastro.2018.08.057 Reference: YGAST 62119 To appear
Microbiome GI Disorders
 Microbiome GI Disorders Prof. Ram Dickman Neurogastroenterology Unit Rabin Medical Center Israel 1 Key Points Our gut microbiota Were to find them? Symbiosis or Why do we need them? Dysbiosis or when things
Microbiome GI Disorders Prof. Ram Dickman Neurogastroenterology Unit Rabin Medical Center Israel 1 Key Points Our gut microbiota Were to find them? Symbiosis or Why do we need them? Dysbiosis or when things
TD-BF01: Innate immunity to microorganisms
 TD-BF01: Innate immunity to microorganisms I. Toll receptors (adapted from Takeuchi, O. et al. (1999) Immunity 11:443; Kawai, T. et al. (1999) Immunity 11:115; Hemmi, H. et al. (2000) Nature 408:740; Muzio,
TD-BF01: Innate immunity to microorganisms I. Toll receptors (adapted from Takeuchi, O. et al. (1999) Immunity 11:443; Kawai, T. et al. (1999) Immunity 11:115; Hemmi, H. et al. (2000) Nature 408:740; Muzio,
The Innate Immune Response
 The Innate Immune Response FUNCTIONS OF THE IMMUNE SYSTEM: Recognize, destroy and clear a diversity of pathogens. Initiate tissue and wound healing processes. Recognize and clear damaged self components.
The Innate Immune Response FUNCTIONS OF THE IMMUNE SYSTEM: Recognize, destroy and clear a diversity of pathogens. Initiate tissue and wound healing processes. Recognize and clear damaged self components.
Differential responses of human colonic ILCs to gut commensal bacteria altered during HIV infection
 Differential responses of human colonic ILCs to gut commensal bacteria altered during HIV infection Moriah J. Castleman, Ph.D. Laboratory of Dr. Cara Wilson University of Colorado Anschutz Medical Campus
Differential responses of human colonic ILCs to gut commensal bacteria altered during HIV infection Moriah J. Castleman, Ph.D. Laboratory of Dr. Cara Wilson University of Colorado Anschutz Medical Campus
INFLAMMASOME IN INTESTINAL INFLAMMATION AND CANCER. Laura Stronati ENEA - Roma
 INFLAMMASOME IN INTESTINAL INFLAMMATION AND CANCER Laura Stronati ENEA - Roma Inflammasome: definition, components and activation TLRs NODs RLRs CLRs PRRs LPS, Flagellin, DNA, RNA, etc) PAMPs DAMPs ATP,
INFLAMMASOME IN INTESTINAL INFLAMMATION AND CANCER Laura Stronati ENEA - Roma Inflammasome: definition, components and activation TLRs NODs RLRs CLRs PRRs LPS, Flagellin, DNA, RNA, etc) PAMPs DAMPs ATP,
Components of the innate immune system
 Components of the innate immune system Before our discussion about innate immunity Differences between innate and adaptive systems: Innate immune system = natural = native -Germline: prepared before exposure
Components of the innate immune system Before our discussion about innate immunity Differences between innate and adaptive systems: Innate immune system = natural = native -Germline: prepared before exposure
Innate Immunity & Inflammation
 Innate Immunity & Inflammation The innate immune system is an evolutionally conserved mechanism that provides an early and effective response against invading microbial pathogens. It relies on a limited
Innate Immunity & Inflammation The innate immune system is an evolutionally conserved mechanism that provides an early and effective response against invading microbial pathogens. It relies on a limited
Pathogenicity of Infectious Diseases
 Pathogenicity of Infectious Diseases Pathogenicity of Infectious Diseases HOST DISEASE TRIAD PATHOGEN ENVIRONMENT OTHER MICROBES Microbial Interactions KOCH'S POSTULATES Four criteria that were established
Pathogenicity of Infectious Diseases Pathogenicity of Infectious Diseases HOST DISEASE TRIAD PATHOGEN ENVIRONMENT OTHER MICROBES Microbial Interactions KOCH'S POSTULATES Four criteria that were established
Cutaneous Immunology: Innate Immune Responses. Skin Biology Lecture Series
 Cutaneous Immunology: Innate Immune Responses Skin Biology Lecture Series The Immune Response: Innate and Adaptive Components Source: Wolff, Goldsmith, Katz, Gilchrest, Paller, Leffell. Fitzpatrick s Dermatology
Cutaneous Immunology: Innate Immune Responses Skin Biology Lecture Series The Immune Response: Innate and Adaptive Components Source: Wolff, Goldsmith, Katz, Gilchrest, Paller, Leffell. Fitzpatrick s Dermatology
Bruce A. Beutler and Jules A. Hoffmann. Ralph M. Steinman
 PRESS RELEASE 20-0-03 The Nobel Assembly at Karolinska Institutet has today decided that The 20 Nobel Prize in Physiology or Medicine shall be divided, with one half jointly to Bruce A. Beutler and Jules
PRESS RELEASE 20-0-03 The Nobel Assembly at Karolinska Institutet has today decided that The 20 Nobel Prize in Physiology or Medicine shall be divided, with one half jointly to Bruce A. Beutler and Jules
ORIGINAL COMMUNICATION Interactions between the microbiota and the intestinal mucosa
 (2002) 56, Suppl 3, S60 S64 ß 2002 Nature Publishing Group All rights reserved 0954 3007/02 $25.00 www.nature.com/ejcn ORIGINAL COMMUNICATION Interactions between the microbiota and the intestinal mucosa
(2002) 56, Suppl 3, S60 S64 ß 2002 Nature Publishing Group All rights reserved 0954 3007/02 $25.00 www.nature.com/ejcn ORIGINAL COMMUNICATION Interactions between the microbiota and the intestinal mucosa
17 th International Conference of the Inflammation Research Association: Wednesday AM (Day 4) September 9-13, 2012
 17 th International Conference of the Inflammation Research Association: Wednesday AM (Day 4) September 9-13, 2012 The Sagamore Resort, Bolton Landing, NY, USA The following report includes highlights
17 th International Conference of the Inflammation Research Association: Wednesday AM (Day 4) September 9-13, 2012 The Sagamore Resort, Bolton Landing, NY, USA The following report includes highlights
NOD2 Activation promotes anti-inflammatory activity of human Umbilical cord blood MSCs against Inflammatory bowel disease
 NOD2 Activation promotes anti-inflammatory activity of human Umbilical cord blood MSCs against Inflammatory bowel disease Prof. Kyung-Sun Kang, DVM, PhD. Adult Stem Cell Research Center Seoul National
NOD2 Activation promotes anti-inflammatory activity of human Umbilical cord blood MSCs against Inflammatory bowel disease Prof. Kyung-Sun Kang, DVM, PhD. Adult Stem Cell Research Center Seoul National
Efficacy of Lactobacillus GG in maintaining remission of ulcerative colitis
 Alimentary Pharmacology & Therapeutics Efficacy of Lactobacillus GG in maintaining remission of ulcerative colitis M.A.ZOCCO,L.ZILERIDALVERME,F.CREMONINI,A.C.PISCAGLIA,E.C.NISTA,M.CANDELLI, M. NOVI, D.
Alimentary Pharmacology & Therapeutics Efficacy of Lactobacillus GG in maintaining remission of ulcerative colitis M.A.ZOCCO,L.ZILERIDALVERME,F.CREMONINI,A.C.PISCAGLIA,E.C.NISTA,M.CANDELLI, M. NOVI, D.
INTRODUCING YOUR GUT BACTERIA
 INTRODUCING YOUR GUT BACTERIA Microflora Intestinal flora 1.5 kg We would die with 5 years of birth if we did not have them as we would not develop a proper immune system 1000 species and 5000 strains
INTRODUCING YOUR GUT BACTERIA Microflora Intestinal flora 1.5 kg We would die with 5 years of birth if we did not have them as we would not develop a proper immune system 1000 species and 5000 strains
modulates cytokine expression in Caco-2 cells infected with Crohn's disease-associated E. coli LF82
 AEM Accepts, published online ahead of print on 11 February 2011 Appl. Environ. Microbiol. doi:10.1128/aem.01601-10 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions.
AEM Accepts, published online ahead of print on 11 February 2011 Appl. Environ. Microbiol. doi:10.1128/aem.01601-10 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions.
EXOGENOUS and ENDOGENOUS DANGER SIGNALS in INFLAMMATORY BOWEL DISEASE
 EXOGENOUS and ENDOGENOUS DANGER SIGNALS in INFLAMMATORY BOWEL DISEASE by Shaival H. Davé B.A. in Molecular & Cell Biology: Biochemistry & Molecular Biology University of California at Berkeley, 1998 Submitted
EXOGENOUS and ENDOGENOUS DANGER SIGNALS in INFLAMMATORY BOWEL DISEASE by Shaival H. Davé B.A. in Molecular & Cell Biology: Biochemistry & Molecular Biology University of California at Berkeley, 1998 Submitted
Gut Lung Axis Implication of the Gut Microbiota beyond its niche
 Gut Lung Axis Implication of the Gut Microbiota beyond its niche Reema Subramanian PhD Candidate (4 th year) Supervisor: Prof. Margaret Ip Department of Microbiology, CUHK Joint Graduate Student Seminar
Gut Lung Axis Implication of the Gut Microbiota beyond its niche Reema Subramanian PhD Candidate (4 th year) Supervisor: Prof. Margaret Ip Department of Microbiology, CUHK Joint Graduate Student Seminar
Microbiology - Problem Drill 21: Microbial Diseases of the Digestive System
 Microbiology - Problem Drill 21: Microbial Diseases of the Digestive System No. 1 of 10 1. Which of the following organs is not part of the gastrointestinal tract (GI)? (A) Esophagus (B) Small intestine
Microbiology - Problem Drill 21: Microbial Diseases of the Digestive System No. 1 of 10 1. Which of the following organs is not part of the gastrointestinal tract (GI)? (A) Esophagus (B) Small intestine
Probiotics in the ICU. Who could benefit? Nadia J van Rensburg RD(SA) Groote Schuur Hospital, Cape Town
 Probiotics in the ICU. Who could benefit? Nadia J van Rensburg RD(SA) Groote Schuur Hospital, Cape Town Outline Introduction: a brief overview Probiotics: Current guidelines Reviews and Meta-analyses IBD
Probiotics in the ICU. Who could benefit? Nadia J van Rensburg RD(SA) Groote Schuur Hospital, Cape Town Outline Introduction: a brief overview Probiotics: Current guidelines Reviews and Meta-analyses IBD
The Nobel Prize in Physiology or Medicine for 2005
 The Nobel Prize in Physiology or Medicine for 2005 jointly to Barry J. Marshall and J. Robin Warren for their discovery of "the bacterium Helicobacter pylori and its role in gastritis and peptic ulcer
The Nobel Prize in Physiology or Medicine for 2005 jointly to Barry J. Marshall and J. Robin Warren for their discovery of "the bacterium Helicobacter pylori and its role in gastritis and peptic ulcer
ABIMMUNE Repurposing disused antibiotics with immune modulators as antimicrobial strategy for respiratory tract infections
 ABIMMUNE Repurposing disused antibiotics with immune modulators as antimicrobial strategy for respiratory tract infections Jean-Claude Sirard Christophe Carnoy Fiordiligie Casilag Delphine Cayet The partners
ABIMMUNE Repurposing disused antibiotics with immune modulators as antimicrobial strategy for respiratory tract infections Jean-Claude Sirard Christophe Carnoy Fiordiligie Casilag Delphine Cayet The partners
Exosomes as a. Novel Therapeutic Approach to Gastrointestinal Diseases Rebecca Murray APRN, FNP, CDE
 Exosomes as a Novel Therapeutic Approach to Gastrointestinal Diseases Rebecca Murray APRN, FNP, CDE Endocrine Nurse Practitioner Institute for Hormonal Balance Orlando, FL Medical Director Ward-Murray
Exosomes as a Novel Therapeutic Approach to Gastrointestinal Diseases Rebecca Murray APRN, FNP, CDE Endocrine Nurse Practitioner Institute for Hormonal Balance Orlando, FL Medical Director Ward-Murray
Environmental factors affecting IBD Have we made progress? Peter Laszlo Lakatos 1st Department of Medicine Semmelweis University Budapest Hungary
 Environmental factors affecting IBD Have we made progress? Peter Laszlo Lakatos 1st Department of Medicine Semmelweis University Budapest Hungary Environmental factors in IBD Are associated with disease
Environmental factors affecting IBD Have we made progress? Peter Laszlo Lakatos 1st Department of Medicine Semmelweis University Budapest Hungary Environmental factors in IBD Are associated with disease
Fructo-oligosaccharides in Crohn s disease: a prospective randomised double blind controlled trial
 Fructo-oligosaccharides in Crohn s disease: a prospective randomised double blind controlled trial Principal investigator: Dr James Lindsay St Bartholomew's Hospital and The Royal London Hospital Queen
Fructo-oligosaccharides in Crohn s disease: a prospective randomised double blind controlled trial Principal investigator: Dr James Lindsay St Bartholomew's Hospital and The Royal London Hospital Queen
Sarkis K Mazmanian, California Institute of Technology
 Sarkis K Mazmanian, California Institute of Technology The human microbiota The human gut harbors 10 11-10 12 bacteria per gram colonic content (>10 14 total bacteria) Total bacteria outnumber human cells
Sarkis K Mazmanian, California Institute of Technology The human microbiota The human gut harbors 10 11-10 12 bacteria per gram colonic content (>10 14 total bacteria) Total bacteria outnumber human cells
Innate Immunity. Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 2 August 2016
 Innate Immunity Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 2 August 2016 Objectives: Explain how innate immune system recognizes foreign substances
Innate Immunity Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 2 August 2016 Objectives: Explain how innate immune system recognizes foreign substances
Medical Virology Immunology. Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University
 Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
IL-12 family members in experimental colitis. Markus F. Neurath I. Medical Clinic Johannes Gutenberg-University Mainz, Germany
 IL-12 family members in experimental colitis Markus F. Neurath I. Medical Clinic Johannes Gutenberg-University Mainz, Germany IBD - Pathogenesis Genetic Predisposition Bacterial Antigens Activation of
IL-12 family members in experimental colitis Markus F. Neurath I. Medical Clinic Johannes Gutenberg-University Mainz, Germany IBD - Pathogenesis Genetic Predisposition Bacterial Antigens Activation of
PBS Class #2 Introduction to the Immune System part II Suggested reading: Abbas, pgs , 27-30
 PBS 803 - Class #2 Introduction to the Immune System part II Suggested reading: Abbas, pgs. 15-25, 27-30 Learning Objectives Compare and contrast the maturation of B and T lymphocytes Compare and contrast
PBS 803 - Class #2 Introduction to the Immune System part II Suggested reading: Abbas, pgs. 15-25, 27-30 Learning Objectives Compare and contrast the maturation of B and T lymphocytes Compare and contrast
Toll-like Receptors (TLRs): Biology, Pathology and Therapeutics
 Toll-like Receptors (TLRs): Biology, Pathology and Therapeutics Dr Sarah Sasson SydPATH Registrar 23 rd June 2014 TLRs: Introduction Discovered in 1990s Recognise conserved structures in pathogens Rely
Toll-like Receptors (TLRs): Biology, Pathology and Therapeutics Dr Sarah Sasson SydPATH Registrar 23 rd June 2014 TLRs: Introduction Discovered in 1990s Recognise conserved structures in pathogens Rely
The role of gut microbiome in IBS
 The role of gut microbiome in IBS Chung Owyang, MD H. Marvin Pollard Professor of Internal Medicine Professor of Molecular and Integrative Physiology Chief, Division of Gastroenterology Director, Pollard
The role of gut microbiome in IBS Chung Owyang, MD H. Marvin Pollard Professor of Internal Medicine Professor of Molecular and Integrative Physiology Chief, Division of Gastroenterology Director, Pollard
Felix Yarovinsky. Department of Immunology, UT Southwestern Medical Center. Innate immune defense to Toxoplasma gondii
 Felix Yarovinsky Department of Immunology, UT Southwestern Medical Center Innate immune defense to Toxoplasma gondii Pathogen recognition by innate immune cells Pathogen Parasites Viruses Bacteria Initiator
Felix Yarovinsky Department of Immunology, UT Southwestern Medical Center Innate immune defense to Toxoplasma gondii Pathogen recognition by innate immune cells Pathogen Parasites Viruses Bacteria Initiator
Homeopathic Products. Evidence??
 Homeopathic Products Principle of analogy or Law of Similars Small or infinitesimal doses (3X-30C) Avogadro s number=6x10 23 = ~23X Succussion and potentization (see http://www.boiron.com/en/htm/02_medi_hom
Homeopathic Products Principle of analogy or Law of Similars Small or infinitesimal doses (3X-30C) Avogadro s number=6x10 23 = ~23X Succussion and potentization (see http://www.boiron.com/en/htm/02_medi_hom
Crypt abscess-associated microbiota in inflammatory bowel disease and acute self-limited colitis
 Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v16.i5.583 World J Gastroenterol 2010 February 7; 16(5): 583-587 ISSN 1007-9327 (print) 2010 Baishideng. All rights
Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v16.i5.583 World J Gastroenterol 2010 February 7; 16(5): 583-587 ISSN 1007-9327 (print) 2010 Baishideng. All rights
C rohn s disease (CD) is a chronic idiopathic inflammatory
 223 INFLAMMATORY BOWEL DISEASE Epithelioid granulomas, pattern recognition receptors, and phenotypes of Crohn s disease M Pierik, G De Hertogh, S Vermeire, G Van Assche, P Van Eyken, S Joossens, G Claessens,
223 INFLAMMATORY BOWEL DISEASE Epithelioid granulomas, pattern recognition receptors, and phenotypes of Crohn s disease M Pierik, G De Hertogh, S Vermeire, G Van Assche, P Van Eyken, S Joossens, G Claessens,
Combined azithromycin and metronidazole therapy is effective in inducing remission in pediatric Crohn's disease
 Journal of Crohn's and Colitis (2011) 5, 222 226 available at www.sciencedirect.com Combined azithromycin and metronidazole therapy is effective in inducing remission in pediatric Crohn's disease Arie
Journal of Crohn's and Colitis (2011) 5, 222 226 available at www.sciencedirect.com Combined azithromycin and metronidazole therapy is effective in inducing remission in pediatric Crohn's disease Arie
Myalgic encephalomyelitis: A highly prevalent debilitating disease
 Myalgic encephalomyelitis: A highly prevalent debilitating disease Persistent, debilitating fatigue associated with numerous physical and neurocognitive symptoms Disease severity can range from moderate
Myalgic encephalomyelitis: A highly prevalent debilitating disease Persistent, debilitating fatigue associated with numerous physical and neurocognitive symptoms Disease severity can range from moderate
Bacterial Diseases IMMUNITY TO BACTERIAL INFECTIONS. Gram Positive Bacteria. Gram Negative Bacteria. Many Infectious agents and many diseases
 IMMUNITY TO BACTERIAL INFECTIONS Chapter 18 Bacterial Diseases Many Infectious agents and many diseases Bacteria can Infect any part of the body Cause disease due to Growth of the microbe in a tissue Produce
IMMUNITY TO BACTERIAL INFECTIONS Chapter 18 Bacterial Diseases Many Infectious agents and many diseases Bacteria can Infect any part of the body Cause disease due to Growth of the microbe in a tissue Produce
Lecture on Innate Immunity and Inflammation
 Lecture on Innate Immunity and Inflammation Evolutionary View Epithelial barriers to infection Four main types of innate recognition molecules:tlrs, CLRs, NLRs, RLRs NF-κB, the master transcriptional regulator
Lecture on Innate Immunity and Inflammation Evolutionary View Epithelial barriers to infection Four main types of innate recognition molecules:tlrs, CLRs, NLRs, RLRs NF-κB, the master transcriptional regulator
