How and why to take a Martius labial interposition flap in female urology
|
|
|
- Molly Jackson
- 5 years ago
- Views:
Transcription
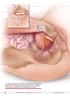
1 Review Article How and why to take a Martius labial interposition flap in female urology Ailsa Wilson 1, Samantha Pillay 1, Tamsin Greenwell 2 1 Continence Matters, Calvary North Adelaide Hospital, Adelaide, South Australia, Australia; 2 University College London Hospital, London W1G 9PH, UK Contributions: (I) Conception and design: A Wilson, T Greenwell; (II) Administrative support: None; (III) Provision of study materials or patients: None; (IV) Collection and assembly of data: None; (V) Data analysis and interpretation: None; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Ailsa Wilson. Continence Matters, Calvary North Adelaide Hospital, Adelaide, South Australia, Australia. info@continencematters.com; Tamsin Greenwell. Department of Urology, University College London Hospital at Westmoreland Street, London, W1G 9PH, UK. Tamsin.greenwell@uclh.nhs.uk. Abstract: The Martius modified labial fat pad flap at nearly 90 years old is still very much part of the modern vaginal surgeon s armamentarium. Here we describe this straightforward and adaptable technique, the avoidance of pitfalls, its advantages and uses in vaginal surgery, and outcomes both short and long term. Specifically patient reported outcomes related to scar perception and sexual function are explored. Keywords: Martius flap; vaginal mesh; urethral diverticulum; fistula; reconstructive urology Submitted Dec 12, Accepted for publication Mar 26, doi: /tau View this article at: Introduction The Martius modified labial fat pad flap (MMLFPF, referred to commonly as the Martius flap) remains the simplest and most versatile interposition tissue for complex vaginal surgery. In 1928 Martius described a labial flap of bulbocavernosus muscle for urethrovaginal fistula repair (1), which was later modified multiple times, and in modern usage generally refers to a labium majora fat pad flap without muscle (2). For urological indications following vaginal procedures where tissue integrity is a concern, it is placed between the periurethral or perivesical fascia and anterior vaginal wall closure. Whether operating in large academic groups or those for whom such cases arise only sporadically in their practice, all surgeons who wish to maximize success at first procedure will find it an extremely useful tool. Here we describe flap harvest and placement and the justification for its use. Technique After completion of the main vaginal procedure a swab is placed in the vagina and any vaginal retractor used is either removed or manipulated to permit easy access to the labia majora. The most dependent edge of the labia majora is marked and incised from level with the mons pubis posteriorly (Figure 1), extending if more length is required, to expose the bright yellow fibrofatty pad (Figure 2). There is a natural tissue plane around the pad where medial (Figure 3) and lateral (Figure 4) dissection can be facilitated by spreading with curved scissors and diathermy, ensuring that posteriorly the lateral attachment through which the blood supply from a branch of the internal pudendal is maintained. Posterior dissection is then performed (Figure 5) and the fat pad freed for the length required to transpose into the vagina and cover the area of surgery in a tension free manner, anything from 8 15 cm in general. Care should be taken to stay lateral to the bulbocavernosus and ischiocavernosus muscles. Too medial a dissection includes these structures and results in significant bleeding. Too superficial a dissection risks scar deformity. Superiorly the external pudendal artery and inferiorly the
2 S82 Wilson et al. How and why to take a Martius labial interposition flap in female urology Figure 1 Martius labial interposition flap planned labial skin incision. Figure 4 Mobilisation of lateral aspect of flap. Figure 2 Labial dissection to identify the golden fibrofatty pad. Figure 5 Posterior mobilisation of flap. Figure 3 Mobilisation of medial aspect of flap. internal pudendal artery supply are reasonably predictable and form a plexus within the flap. Once the desired length is achieved the flap is divided, most commonly at its superior margin (Figure 6) with a Roberts or right-angled clamp for pedicle control, followed by division and suture ligation with 3/0 or 2/0-vicryl, (Figure 7), leaving a broad vascular inferior base to the flap that is practical for most purposes. A tunnel connecting the pedicle base to the vaginal wound is formed by blunt dissection with fingers and Roberts clamp and then widened to admit at least two fingers (to alleviate compression on pedicle blood supply) (Figure 8). the flap is transferred gently through using a Satinsky clamp, which is the perfect configuration for this manoeuvre
3 Translational Andrology and Urology, Vol 6, Suppl 2 July 2017 S83 Figure 8 Formation of the lateral vaginal tunnel. Figure 6 Clamping of the superior pedicle. Figure 7 Martius flap after division of superior pedicle. Figure 9 Transfer of Martius flap to vagina with Satinsky clamp. (Figures 9,10). The flap is positioned over the operative field requiring reinforcement and sutured to the peri-vaginal fascia without tension with 2-0 or 3-0 interrupted absorbable sutures to prevent migration (Figure 11). Peri-urethral tissue may be used to suture the flap but is weaker and more liable to tear. Excess flap length should be trimmed as the benefit of the flap does not depend on a having a large mass of tissue. If additional tissue is required to support a large surgical field, bilateral flaps can be used. In the extremely uncommon event of insufficient vaginal skin or severe stenosis the flap can be pre-planned to include a full-thickness island of hairless skin from the medial labia majora surface (3). The vaginal wound is closed as usual, and labial wound closed in layers with absorbable suture over a small suction drain (such as a Minivac) and a pressure dressing is applied
4 S84 Wilson et al. How and why to take a Martius labial interposition flap in female urology Figure 12 Donor site appearance at end of surgery. Figure 10 Martius flap fully transferred to wound. Figure 11 Martius flap sutured over vaginal surgery site. (such as Opsite spray to skin, gauze and foam tape on tension) (Figure 12). It is important to cover the fat pad completely during closure an exposed fat pad tends to be associated with a dragging sensation radiating from the labia to the vagina. The drain and pressure dressing are removed at hours and other post-operative care determined by the primary procedure. Uses Tissue interposition can alleviate the surgical dilemmas of overlapping suture lines and poor quality tissue, create a layered closure in tissue where there may not be layers to close, and encourage neovascularity thereby improving healing and cure rates. Labial fat makes an excellent interposition tissue for the following reasons: (I) The fibrous component makes it a strong flap despite its adiposity; (II) It has 2 pedicles and will survive on either, giving positional flexibility for multiple vaginal applications and defect locations; (III) It is conveniently located in the same surgical field as vaginal surgery, unlike alternative flaps such as peritoneum, gracilis, or omentum; (IV) It is not bulky and can be tailored in-situ without compromise; (V) It is surprisingly cosmetic as the superficial labial fat is not disturbed and the labial incision quickly becomes inconspicuous (Figure 13); The main urological indications for the MMLFPF are (I) To improve healing and reduce fistulae or recurrence in urethral diverticulectomy (4,5), urethral mesh excision (4,6), vaginal repair of urethrovaginal (6) and vesicovaginal fistulae (6-8), and bladder neck closure for urethral erosion (9); (II) To prevent recurrent scarring of the urethra following urethrolysis or urethral stricture repair (7,10,11); (III) Protection of the fragile urethra and vagina from stress incontinence surgery complications (12);
5 Translational Andrology and Urology, Vol 6, Suppl 2 July 2017 S85 Figure 13 Appearance 6 weeks following right MFP harvest. tensioning a sling may however be more difficult to gauge over a Martius flap. Operative scenarios particularly deserving of interposition are fibrotic, scarred or previously irradiated tissue, tenuous periurethral fascia and revision surgery (13). Especially complex are those with failed prior diverticulectomy, mesh excision or fistula repair attempts (13). Reoperation for failure or complications can be tremendously debilitating with longterm adverse sequelae and medicolegal implications (14). Potential uses of the Martius flap are not limited to those described. Extended applications that have been more recently reported include: (I) Salvage of vaginally eroded synthetic mesh (midurethral sling or pelvic organ prolapse kit) by covering with a Martius flap (preserving tape function in preference to excising the eroded segment) (15,16); (II) Neovagina formation using a further alliteration of the Martius flap (17); (III) Transvaginal repair of the particularly challenging neobladder-vaginal fistula after radical cystectomy and orthotopic diversion (18,19); (IV) Paediatric vaginal reconstruction (after pretreatment with topical oestrogen)(20). Outcomes The relative rarity of female urethral reconstruction in developed countries (for example the small numbers of cases per year in even the quaternary referral centres publishing results) means an absence of large case control series or trials. Worldwide, vesicovaginal fistula repair would seem by numbers to be the most commonly occurring scenario where a MMLFPF could be of assistance, birth trauma being the commonest cause, with estimates of between one to two million women worldwide suffering from obstetric fistula (13,21,22). Another is reconstruction after vaginal trauma resulting from a particularly horrific rise in sexual torture in war ravaged areas like the Congo (23,24). The question has been raised regarding the necessity of using interposition tissue in obstetric vaginal fistulae and there is a trend in this indication to limit flap use to only the most complex cases (25). Browning s series of 440 obstetric VVF repairs (26) proposed that its use in this scenario be abandoned because of complications and lack of benefit (7) with a higher rate of postoperative incontinence in those with Martius flap interposition (44.9% vs %). As discussed previously (4) the poorer continence outcomes may have been confounded by indication as stratified analyses suggest those fistulae repaired with a Martius flap may have been more complex (more difficult to repair and have known higher rates of incontinence). A second series of 81 genitourinary fistulae operated on by a single surgeon (27) of which 28 (34.6%) received a MMLFPF, found the addition of a flap made no difference in the overall closure rate (85.7% vs. 79.2%, P=0.347) nor the closure of fistula with continence (60.7% vs. 67.9%, P=0.260). This small unrandomized series suggests in women where the fistula characteristics are thought to be poor enough to warrant interposition tissue, that its use yields surgical outcomes equivalent to those in milder cases not needing interposition. By way of western case series contrast, DeLancey and McGuire series of 37 repairs of complex fistulae using MMLFPF in 35 patients yielded an overall cure of 86.5% (8). The MMLFPF harvest carries little morbidity, takes little additional surgical time, improves healing, definitely does not worsen and does improve surgical outcomes in difficult cases. Good technique minimizes flap bulk and retraction from excessive tension, pedicle dissection or an inadequate tunnel. Rare reported complications include vaginal prominence of a bulky flap presenting as a vaginal mass (28). In terms of complications, Kasyan et al. (29) reported the highest rate (harvest site bleeding 19%, haematoma 5%, labial incision lymphorrhoea 13.5%, wound infection 5.4%) in their series of 37 patients. Long term patient reported outcomes were based on the 24 women
6 S86 Wilson et al. How and why to take a Martius labial interposition flap in female urology contactable for follow up, of whom 4 reported cosmetic problems and two reported intermittent mild pain. Lee et al. s (30) more recent prospective series of 122 patients undergoing MMLFPF surgery with a mean follow up of 85 months (6-202 months) recorded no perioperative complications, and low rates of long term complications of pain in 5%, numbness in 14% and labial distortion in 7%, which we feel is a more representative of general outcomes in experienced hands. Among sexually active patients, equivocal sexual function outcomes were recorded across different surgical indications, although it is difficult to control for other factors such as primary vaginal surgery indication, age, health status when assessing sexual function outcomes. Our previously reported series (4) found minimal morbidity with only 2 haematomas, 1 labial wound infection and very good cosmesis with 79% of patients rating the final cosmetic appearance as good or excellent and only 1 (0.6 %) rating it as unsatisfactory. Stress incontinence resulting from the vaginal surgery or pre-existing urethral incompetence may persist, and although a Martius flap may provide some minor degree of urethral support and facilitate reestablishment of continence (25), total reliance on it as a sling can lead to disappointment (13,25). Stress incontinence can be addressed concomitantly or preferably at a later surgery, depending on the patient scenario (25). Petrou s small series of 8 was the first to examine patient self-perception at the Martius harvest site (31). Although 62% reported numbness at the harvest site and 3 reported lingering pain a year after surgery, only 1 reported interference with sexual relations and it was not associated with perceived cosmetic disfigurement. Elkins (32) reported a 25% incidence of dyspareunia over the Martius flap harvest site in the vagina in 35 women following vesicovaginal and rectovaginal fistula repair. Female sexual dysfunction following vaginal surgery in general is underreported. The primary pathology or vaginal procedure are most likely the cause of the sexual dysfunction (33) and it is feasible that the addition of the Martius flap might help with alleviating adverse effects on sexual function. The potential for Martius flap associated side effects such as asymmetry, wound pain and dyspareunia, although extremely low, should be a point made in preoperative counselling. Body image distress sufficient to warrant further surgery is extremely rare; injectable bulking agents could be used in rare cases of significant labial asymmetry (34). Regarding labial sensation, a technique described by Deng et al of insitu flap harvest approaching from the vaginal wound without a separate labial incision may allow preservation of sensation although it will limit the amount of tissue that can be harvested (35). Conclusions For surgeons operating in developed countries, the Martius modified labial fat pad flap is a valuable tool in vaginal reconstruction with increasingly novel applications. The rate of complications and cosmetic dissatisfaction is low and outweighs the trouble of a failed operation. Randomised studies are welcomed in areas where flap use is declining. Acknowledgements None. Footnote Conflicts of Interest: The authors have no conflicts of interest to declare. References 1. Martius H. Die operative Wiederhellstellung der volkommen fehlenden Harnhohare unde des Sclessmuskels derselben. Zentralbl Gynakol 1928;52: SajjadiSG, Hortváth ÖP, Kalmár K. Martius flap: historical and anatomical considerations. Eur J Plast Surg 2012;35: Carr LK, Webster GD. Full-thickness cutaneous martius flaps: a useful technique in female reconstructive urology. Urology 1996;48: Malde S, Spilotros M, Wilson A, et al. The uses and outcomes of the Martius fat pad in female urology. World J Urol 2017;35: Nickles SW, Ikwuezunma G, MacLachlan L, et al. Simple vs complex urethral diverticulum: presentation and outcomes. Urology 2014;84: Blaivas JG, Mekel G. Management of urinary fistulas due to midurethral sling surgery. J Urol 2014;192: Lee D, Dillon BE, Zimmern PE. Long-term morbidity of Martius labial fat pad graft in vaginal reconstruction surgery. Urology 2013;82: Elkins TE, DeLancey JO, McGuire EJ. The use of modified Martius graft as an adjunctive technique in vesicovaginal and rectovaginal fistula repair. Obstet Gynecol 1990;75: Willis H, Safiano NA, Lloyd LK. Comparison of
7 Translational Andrology and Urology, Vol 6, Suppl 2 July 2017 S87 transvaginal and retropubic bladder neck closure with suprapubic catheter in women. J Urol 2015;193: Blaivas JG, Santos JA, Tsui JF, et al. Management of urethral stricture in women. J Urol 2012;188: Carey JM, Chon JK, Leach GE. Urethrolysis with Martius labial fat pad graft for iatrogenic bladder outlet obstruction. Urology 2003;61: Matte A, Delorme E. The Martius flap in stress urinary incontinence treated by suburethral sling. Prog Urol 2012;22: Abrams P, De Ridder D, De Vries C, et al. Obstetric fistula in the developing world. An International Consultation on Vesicovaginal Fistula. Marrakech, Morocco 2010 Oct Hansen BL, Dunn GE, Norton P, et al. Long-term followup of treatment for synthetic mesh complications. Female Pelvic Med Reconstr Surg 2014;20: Mortimer A, Khunda A, Ballard P. Martius graft for TOT extrusion: a case series. Int Urogynecol J 2016;27: Al-Badr A. Martius graft for management of exposed vaginal prolapse mesh. J Minim Invasive Gynecol 2013;20: Green AE, Escobar PF, Neubaurer N, et al. The martius flap neovagina revisited. Int J Gynecol Cancer 2005;15: Carmel ME, Goldman HB, Moore CK, et al. Transvaginal neobladder vaginal fistula repair after radical cystectomy with orthotopic urinary diversion in women. Neurourol Urodyn 2016;35: Tunuguntla HS, Manoharan M, Gousse AE. Management of neobladder-vaginal fistula and stress incontinence following radical cystectomy in women: a review. World J Urol 2005;23: Baskin D, Tatlidede S, Karşidağ SH. Martius repair in urethrovaginal defects. J Pediatr Surg 2005;40: Adler AJ, Ronsmans C, Calvert C, et al. Estimating the prevalence of obstetric fistula: a systematic review and meta-analysis. BMC Pregnancy Childbirth ;13: De Ridder D. An update on surgery for vesicovaginal and urethrovaginal fistulae. Curr Opin Urol 2011;21: Dossa NI, Zunzunegui MV, Hatem M, et al. Fistula and other adverse reproductive health outcomes among women victims of conflict-related sexual violence: a populationbased cross-sectional study. Birth 2014;41: Baelani I, Dünser MW. Facing medical care problems of victims of sexual violence in Goma/Eastern Democratic Republic of the Congo. Confl Health 2011;5: Ruminjo JK, Frajzyngier V, Bashir Abdullahi M, et al. Clinical procedures and practices used in the perioperative treatment of female genital fistula during a prospective cohort study. BMC Pregnancy Childbirth 2014;14: Browning A. Lack of value of the Martius fibrofatty graft in obstetric fistula repair. International Journal of Gynaecology & Obstetrics 2006;93: Tebeu PM, Fokom-Domgue J, Kengne Fosso G, et al. Comparative study of the outcome of surgical management of vesico-vaginal fistulas with and without interposition of the Martius graft: A Cameroonian experience. Prog Urol 2015;25: Kobashi KC, Mee SL, Leach GE. Vaginal Herniation of a Martius Fat Pad Graft Presenting as a Vaginal Mass. Infect Urol. 2000; Kasyan G, Tupikina N, Pushkar D. Use of Martius flap in the complex female urethral surgery. Cent European J Urol 2014;67: Lee, Dillon BE, Zimmern PE. Long-term morbidity of Martius labial fat pad graft in vaginal reconstruction surgery. Urology 2013;82: Petrou SP, Joyce J, Parra RO. Martius flap harvest site: patient self-perception. J Urol 2002;167: Elkins TE, DeLancey JO, McGuire EJ: The use of modified Martius graft as an adjunctive technique in vesicovaginal and rectovaginal fistula repair. Obstet Gynecol 1990, 75: Tunuguntla HS, Gousse AE. Female sexual dysfunction following vaginal surgery: a review. J Urol 2006;175: Fasola E, Gazzola R. Labia Majora Augmentation with Hyaluronic Acid Filler: Technique and Results. Aesthet Surg J 2016;36: Deng D, Rutman M, Rodriguez L, et al. The in situ Martius flap, description of a new technique. Nondiscussion Poster 330, International Continence Society, Montreal, Cite this article as: Wilson A, Pillay S, Greenwell T. How and why to take a Martius labial interposition flap in female urology.. doi: / tau
Use of Martius flap in the complex female urethral surgery
 202 Central European Journal of Urology original PAPEr TRAUMA AND RECONSTRUCTIVE UROLOGY Use of Martius flap in the complex female surgery George Kasyan, Nataliya Tupikina, Dmitry Pushkar Urology Department
202 Central European Journal of Urology original PAPEr TRAUMA AND RECONSTRUCTIVE UROLOGY Use of Martius flap in the complex female surgery George Kasyan, Nataliya Tupikina, Dmitry Pushkar Urology Department
Urethrolysis; When, Why & How. M Karram Professor of Ob/Gyn & Urology University of Cincinnati
 Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566
 Single-incision short sling mesh insertion for stress urinary incontinence in women Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566 Your responsibility This guidance
Single-incision short sling mesh insertion for stress urinary incontinence in women Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566 Your responsibility This guidance
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
Describing the learning curve for bulbar urethroplasty
 Original Article Describing the learning curve for bulbar urethroplasty Marco Spilotros, Sachin Malde, Tamsin J. Greenwell Department of Urology, University College London Hospital, London, UK Contributions:
Original Article Describing the learning curve for bulbar urethroplasty Marco Spilotros, Sachin Malde, Tamsin J. Greenwell Department of Urology, University College London Hospital, London, UK Contributions:
Management of Urethrovaginal Fistulas
 european urology 50 (2006) 1000 1005 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Management of Urethrovaginal Fistulas Dmitri Y. Pushkar *, Vladimir V.
european urology 50 (2006) 1000 1005 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Management of Urethrovaginal Fistulas Dmitri Y. Pushkar *, Vladimir V.
REPAIR OF LARGE CYSTOCELE
 REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
Pan African Urological Surgeons Association. African Journal of Urology.
 African Journal of Urology (2012) 18, 175 179 Pan African Urological Surgeons Association African Journal of Urology www.ees.elsevier.com/afju www.sciencedirect.com Martius flap and anterior vaginal wall
African Journal of Urology (2012) 18, 175 179 Pan African Urological Surgeons Association African Journal of Urology www.ees.elsevier.com/afju www.sciencedirect.com Martius flap and anterior vaginal wall
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
Post-Traumatic Female Urethral Reconstruction
 Post-Traumatic Female Urethral Reconstruction Jerry G. Blaivas, MD, and Rajveer S. Purohit, MD, MPH Corresponding author Jerry G. Blaivas, MD The New York Presbyterian Hospital, Weill Cornell Medical Center,
Post-Traumatic Female Urethral Reconstruction Jerry G. Blaivas, MD, and Rajveer S. Purohit, MD, MPH Corresponding author Jerry G. Blaivas, MD The New York Presbyterian Hospital, Weill Cornell Medical Center,
The circumferential obstetric fistula: characteristics, management and outcomes
 DOI: 10.1111/j.1471-0528.2007.01329.x www.blackwellpublishing.com/bjog Short communication The circumferential obstetric fistula: characteristics, management and outcomes A Browning Barhirdar Hamlin Fistula
DOI: 10.1111/j.1471-0528.2007.01329.x www.blackwellpublishing.com/bjog Short communication The circumferential obstetric fistula: characteristics, management and outcomes A Browning Barhirdar Hamlin Fistula
Risk Factors for De Novo Mixed Urinary Incontinence and Stress Urinary Incontinence Following Surgical Removal of a Urethral Diverticulum
 LUTS (2013) 5, 154 158 ORIGINAL ARTICLE Risk Factors for De Novo Mixed Urinary Incontinence and Stress Urinary Incontinence Following Surgical Removal of a Urethral Diverticulum JaeHeonKIM, 1 Kwang Woo
LUTS (2013) 5, 154 158 ORIGINAL ARTICLE Risk Factors for De Novo Mixed Urinary Incontinence and Stress Urinary Incontinence Following Surgical Removal of a Urethral Diverticulum JaeHeonKIM, 1 Kwang Woo
JPRAS Open 3 (2015) 1e5. Contents lists available at ScienceDirect. JPRAS Open. journal homepage:
 JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
A New Dimension in Vesicovaginal Fistula Management: An 8-year Experience at Ramathibodi Hospital
 Original Article A New Dimension in Vesicovaginal Fistula Management: An 8-year Experience at Ramathibodi Hospital Wachira Kochakarn and Wipaporn Pummangura, 1 Division of Urology, Department of Surgery,
Original Article A New Dimension in Vesicovaginal Fistula Management: An 8-year Experience at Ramathibodi Hospital Wachira Kochakarn and Wipaporn Pummangura, 1 Division of Urology, Department of Surgery,
Postoperative Care for Pelvic Fistulae. Peter Jeppson, MD October 3, 2017
 Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
University of Alberta Reconstructive Urology Fellowship
 FACULTY OF MEDICINE AND DENTISTRY DEPARTMENT OF SURGERY DIVISION OF UROLOGY Keith Rourke, MD, FRCSC Reconstructive Urology Professor Chair of Academic Urology Reconstructive Urology Fellowship Director
FACULTY OF MEDICINE AND DENTISTRY DEPARTMENT OF SURGERY DIVISION OF UROLOGY Keith Rourke, MD, FRCSC Reconstructive Urology Professor Chair of Academic Urology Reconstructive Urology Fellowship Director
Kuwabara, Kaoru; Nonaka, Takashi; H. Citation Journal of Clinical Urology, 7(5),
 NAOSITE: Nagasaki University's Ac Title Author(s) Gluteal-fold adipofascial perforato fistula reconstruction Fujioka, Masaki; Hayashida, Kenji; Kuwabara, Kaoru; Nonaka, Takashi; H Citation Journal of Clinical
NAOSITE: Nagasaki University's Ac Title Author(s) Gluteal-fold adipofascial perforato fistula reconstruction Fujioka, Masaki; Hayashida, Kenji; Kuwabara, Kaoru; Nonaka, Takashi; H Citation Journal of Clinical
THE USE OF DEEPITHELIALIZATION
 THE USE OF DEEPITHELIALIZATION IN URETHROPLASTY - Deepithelialization Stratum corneum - Epidermis Papillary dermis Reticular dermis Skin Healing in any reconstructive surgery depends on not only the intact
THE USE OF DEEPITHELIALIZATION IN URETHROPLASTY - Deepithelialization Stratum corneum - Epidermis Papillary dermis Reticular dermis Skin Healing in any reconstructive surgery depends on not only the intact
Case Based Urology Learning Program
 Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 19 CBULP 2011 044 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 19 CBULP 2011 044 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Le fort s operation for prolapse uterus: A forgotten procedure
 2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
Operative Approach to Stress Incontinence. Goals of presentation. Preoperative evaluation: Urodynamic Testing? Michelle Y. Morrill, M.D.
 Operative Approach to Stress Incontinence Goals of presentation Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Review preoperative care & evaluation
Operative Approach to Stress Incontinence Goals of presentation Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Review preoperative care & evaluation
The incidence of mesh extrusion after vaginal incontinence and pelvic floor prolapse surgery
 ORIGINAL ARTICLE The incidence of mesh extrusion after vaginal incontinence and pelvic floor prolapse surgery Seth Cohen, Elizabeth Kavaler Department of Urology, Lenox Hill Hospital, USA Correspondence:
ORIGINAL ARTICLE The incidence of mesh extrusion after vaginal incontinence and pelvic floor prolapse surgery Seth Cohen, Elizabeth Kavaler Department of Urology, Lenox Hill Hospital, USA Correspondence:
Anatomical and Functional Results of Pelvic Organ Prolapse Mesh Repair: A Prospective Study of 105 Cases
 International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
Role of free tissue transfer in management of chronic venous ulcer
 Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Blue Ridge Urogynecology
 Surgery for Stress Urinary Incontinence Surgery has proved to be a very effective treatment for stress incontinence. The best surgical procedures improve or cure the incontinence in 85 to 90 percent of
Surgery for Stress Urinary Incontinence Surgery has proved to be a very effective treatment for stress incontinence. The best surgical procedures improve or cure the incontinence in 85 to 90 percent of
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology
 Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Desara TV and Desara Blue TV
 Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
Buccal mucosa urethroplasty in a reoperative and reconstructive challenge hypospadias: a case report Hayrettin Ozturk
 1 Ped Urol Case Rep 2014;1(1):1-5 http://www.pediatricurologycasereports.com ISSN:2148-2969 DOI: 10.14534/PUCR.201412511 Buccal mucosa urethroplasty in a reoperative and reconstructive challenge hypospadias:
1 Ped Urol Case Rep 2014;1(1):1-5 http://www.pediatricurologycasereports.com ISSN:2148-2969 DOI: 10.14534/PUCR.201412511 Buccal mucosa urethroplasty in a reoperative and reconstructive challenge hypospadias:
11 th Dynasty- Egyptian mummies : Queen Henhenit circa 2050 BC wife of King Mentuhotep II VVF 550 BC- Ancient Egyptian documents (papyri)
 February 2019 11 th Dynasty- Egyptian mummies : Queen Henhenit circa 2050 BC wife of King Mentuhotep II VVF 550 BC- Ancient Egyptian documents (papyri) Prescription for a woman whose urine is in an irksome
February 2019 11 th Dynasty- Egyptian mummies : Queen Henhenit circa 2050 BC wife of King Mentuhotep II VVF 550 BC- Ancient Egyptian documents (papyri) Prescription for a woman whose urine is in an irksome
Obstetric Anal Sphincter Injury. An update on best practices. Objectives
 Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
8 A SIMPLE FISTULA REPAIR, STEP BY STEP
 8 A SIMPLE FISTULA REPAIR, STEP BY STEP The first step is to suture the labia to the thighs and cover the anus with a swab (Figure 31). Figure 31 The labia are sutured to the thighs and the anus is covered
8 A SIMPLE FISTULA REPAIR, STEP BY STEP The first step is to suture the labia to the thighs and cover the anus with a swab (Figure 31). Figure 31 The labia are sutured to the thighs and the anus is covered
Desara and Desara Blue
 Desara and Desara Blue Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc.
Desara and Desara Blue Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc.
Desara Blue OV D I. Sling for Female Stress Urinary Incontinence. Instructions For Use
 Desara Blue OV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc. 5171 Clareton
Desara Blue OV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc. 5171 Clareton
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Treatment Outcomes of Tension-free Vaginal Tape Insertion
 Are the Treatment Outcomes of Tension-free Vaginal Tape Insertion the Same for Patients with Stress Urinary Incontinence with or without Intrinsic Sphincter Deficiency? A Retrospective Study in Hong Kong
Are the Treatment Outcomes of Tension-free Vaginal Tape Insertion the Same for Patients with Stress Urinary Incontinence with or without Intrinsic Sphincter Deficiency? A Retrospective Study in Hong Kong
Repair of Bulbar Urethra Using the Barbagli Technique
 22 Repair of Bulbar Urethra Using the Barbagli Technique G. Barbagli, M. Lazzeri 22.1 Introduction and Historical Background 182 22.2 Anatomical Remarks 182 22.3 Step-by-Step Surgical Details 183 22.3.1
22 Repair of Bulbar Urethra Using the Barbagli Technique G. Barbagli, M. Lazzeri 22.1 Introduction and Historical Background 182 22.2 Anatomical Remarks 182 22.3 Step-by-Step Surgical Details 183 22.3.1
Endoscopic assisted harvest of the pedicled pectoralis major muscle flap
 British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
Management of Radiation-Induced Vesicovaginal Fistula
 european urology 55 (2009) 131 138 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Management of Radiation-Induced Vesicovaginal Fistula Dmitri Y. Pushkar
european urology 55 (2009) 131 138 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Management of Radiation-Induced Vesicovaginal Fistula Dmitri Y. Pushkar
I-STOP TOMS Transobturator Male Sling
 I-STOP TOMS Transobturator Male Sling The CL Medical I-STOP TOMS sling for male stress urinary incontinence was developed in France where it is widely used and is the market leader. It is constructed with
I-STOP TOMS Transobturator Male Sling The CL Medical I-STOP TOMS sling for male stress urinary incontinence was developed in France where it is widely used and is the market leader. It is constructed with
Urethral Diverticula, Urethro-Vaginal Fistulae, Vesico-Vaginal Fistulae
 EAU Update Series 1 (2003) 178 185 Urethral Diverticula, Urethro-Vaginal Fistulae, Vesico-Vaginal Fistulae C.R. Chapple * Royal Hallamshire Hospital, Sheffield Teaching Hospitals NHS Trust, Glossop Road,
EAU Update Series 1 (2003) 178 185 Urethral Diverticula, Urethro-Vaginal Fistulae, Vesico-Vaginal Fistulae C.R. Chapple * Royal Hallamshire Hospital, Sheffield Teaching Hospitals NHS Trust, Glossop Road,
Childbirth Trauma & Its Complications 23/ Mr Stergios K. Doumouchtsis
 Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Current Role of Urethrolysis and Partial Excision in Patients Seeking Revision of Anti-Incontinence Sling
 ORIGINAL ARTICLE Current Role of Urethrolysis and Partial Excision in Patients Seeking Revision of Anti-Incontinence Sling Alice Drain, MD,* Ekene Enemchukwu, MD, MPH, Nihar Shah, BA,* Raveen Syan, MD,*
ORIGINAL ARTICLE Current Role of Urethrolysis and Partial Excision in Patients Seeking Revision of Anti-Incontinence Sling Alice Drain, MD,* Ekene Enemchukwu, MD, MPH, Nihar Shah, BA,* Raveen Syan, MD,*
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
INTEGRATING COSMETIC-PLASTIC GYNECOLOGY
 INTEGRATING COSMETIC-PLASTIC GYNECOLOGY into CLINICAL PRACTICE: A SURGICAL WORKSHOP (New and Old Procedures, Videos, Dry & Wet Laboratories, and Didactic Lectures) WORKSHOP OVERVIEW Workshop Description
INTEGRATING COSMETIC-PLASTIC GYNECOLOGY into CLINICAL PRACTICE: A SURGICAL WORKSHOP (New and Old Procedures, Videos, Dry & Wet Laboratories, and Didactic Lectures) WORKSHOP OVERVIEW Workshop Description
We welcome comments and corrections which will be used to improve the system annually.
 ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
Female Epispadias Repair
 hoofdstuk 07 08-03-2001 15:25 Pagina 89 Female Epispadias Repair Female epispadias repair: a new 1-stage technique CHAPTER 7 Tom P.V.M de Jong, Pieter Dik and Aart J. Klijn Journal of Urology 2000, 164,
hoofdstuk 07 08-03-2001 15:25 Pagina 89 Female Epispadias Repair Female epispadias repair: a new 1-stage technique CHAPTER 7 Tom P.V.M de Jong, Pieter Dik and Aart J. Klijn Journal of Urology 2000, 164,
Free Flap Phalloplasty For Female To Male Gender Dysphoria
 SURGICAL TECHNIQUES Free Flap Phalloplasty For Female To Male Gender Dysphoria Giulio Garaffa, MD, PhD, FECSM, FRCS (Eng), David J. Ralph, BSc, MS, FRCS (Urol) St Peter s Andrology and the Institute of
SURGICAL TECHNIQUES Free Flap Phalloplasty For Female To Male Gender Dysphoria Giulio Garaffa, MD, PhD, FECSM, FRCS (Eng), David J. Ralph, BSc, MS, FRCS (Urol) St Peter s Andrology and the Institute of
Quality care in vesico-vaginal obstetric fistula: case series report from the regional hospital of Maroua-Cameroon
 Provisional PDF Published 27 April 2010 Case report, Volume 5, issue 6, 2010 Quality care in vesico-vaginal obstetric fistula: case series report from the regional hospital of Maroua-Cameroon Pierre Marie
Provisional PDF Published 27 April 2010 Case report, Volume 5, issue 6, 2010 Quality care in vesico-vaginal obstetric fistula: case series report from the regional hospital of Maroua-Cameroon Pierre Marie
Surgery of urogenital trauma in condition of war or precarity
 Surgery of urogenital trauma in condition of war or precarity C. H. Rochat Multi-disciplinary Center for Robotic Surgery, Geneva (www.beaulieu.ch) Geneva Foundation for Medical Education and Research (www.gfmer.ch)
Surgery of urogenital trauma in condition of war or precarity C. H. Rochat Multi-disciplinary Center for Robotic Surgery, Geneva (www.beaulieu.ch) Geneva Foundation for Medical Education and Research (www.gfmer.ch)
As more patients express reservations
 The autologous pubovaginal sling supports the proximal urethra and bladder neck to achieve continence by providing a direct compressive force on the urethra and bladder outlet, or by reestablishing a reinforcing
The autologous pubovaginal sling supports the proximal urethra and bladder neck to achieve continence by providing a direct compressive force on the urethra and bladder outlet, or by reestablishing a reinforcing
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Reconstructive Surgery
 Urology Journal UNRC/IUA Vol. 2, No. 4, 206-210 Autumn 2005 Printed in IRAN Reconstructive Surgery Abdorasol Mehrsai, 1 Hooman Djaladat, 2 * Alireza Sina, 1 Sepehr Salem, 1 Gholamreza Pourmand 1 1Department
Urology Journal UNRC/IUA Vol. 2, No. 4, 206-210 Autumn 2005 Printed in IRAN Reconstructive Surgery Abdorasol Mehrsai, 1 Hooman Djaladat, 2 * Alireza Sina, 1 Sepehr Salem, 1 Gholamreza Pourmand 1 1Department
Center for Reconstructive Urethral Surgery Guido Barbagli Center for Reconstructive Urethral Surgery Arezzo - Italy
 Guido Barbagli Arezzo - Italy E-mail: info@urethralcenter.it Website: www.urethralcenter.it SHANGHAI February 6 8, 2009 Prof. Qiang FU Professor FU day Professor FU and night Anterior urethroplasty using
Guido Barbagli Arezzo - Italy E-mail: info@urethralcenter.it Website: www.urethralcenter.it SHANGHAI February 6 8, 2009 Prof. Qiang FU Professor FU day Professor FU and night Anterior urethroplasty using
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
Combined tongue flap and V Y advancement flap for lower lip defects
 British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
The Case FOR Oncoplastic Surgery in Small Breasts. Barbara L. Smith, MD, PhD Massachusetts General Hospital Harvard Medical School Boston, MA USA
 The Case FOR Oncoplastic Surgery in Small Breasts Barbara L. Smith, MD, PhD Massachusetts General Hospital Harvard Medical School Boston, MA USA Changing issues in breast cancer management Early detection
The Case FOR Oncoplastic Surgery in Small Breasts Barbara L. Smith, MD, PhD Massachusetts General Hospital Harvard Medical School Boston, MA USA Changing issues in breast cancer management Early detection
Vaginoplasty using amnion graft along with a fourchette flap
 J Obstet Gynecol India Vol. 59, No. 4 : July/August 2009 pg 344-348 Original Article Vaginoplasty using amnion graft along with a fourchette flap Manhas Kamlesh 1, Manhas Amit 2 1 Prof & Head, 2 Resident,
J Obstet Gynecol India Vol. 59, No. 4 : July/August 2009 pg 344-348 Original Article Vaginoplasty using amnion graft along with a fourchette flap Manhas Kamlesh 1, Manhas Amit 2 1 Prof & Head, 2 Resident,
Sep \8958 Appell Dmochowski.ppt LMF 1
 Surgical Outcomes (How did we get ourselves into this mess?) Roger R. Dmochowski, MD, FACS Department of Urologic Surgery Vanderbilt University School of Medicine Nashville, Tennessee Considerations Evaluation
Surgical Outcomes (How did we get ourselves into this mess?) Roger R. Dmochowski, MD, FACS Department of Urologic Surgery Vanderbilt University School of Medicine Nashville, Tennessee Considerations Evaluation
Bladder replacement in men and women: when and when not? Outline. Continent Diversion History
 1 Bladder replacement in men and women: when and when not? Eila C. Skinner, MD Professor of Clinical Urology Keck USC School of Medicine Outline 1) Selection criteria for orthotopic diversion: Tumor-related
1 Bladder replacement in men and women: when and when not? Eila C. Skinner, MD Professor of Clinical Urology Keck USC School of Medicine Outline 1) Selection criteria for orthotopic diversion: Tumor-related
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence
 A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY)
 MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY) Physician Name: Your home for healthcare Female Pelvic Medicine and Reconstructive
MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY) Physician Name: Your home for healthcare Female Pelvic Medicine and Reconstructive
Pelvic Floor Ultrasound Imaging. Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague)
 Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
University of Alberta Reconstructive Urology Fellowship
 University of Alberta Reconstructive Urology Fellowship 1. Overview 2. Eligibility Requirements 3. Funding 4. Clinical Expectations 5. Academic Expectations 6. Objectives of Training 7. Teaching Methods
University of Alberta Reconstructive Urology Fellowship 1. Overview 2. Eligibility Requirements 3. Funding 4. Clinical Expectations 5. Academic Expectations 6. Objectives of Training 7. Teaching Methods
A SIMPLE SURGICAL TECHNIQUE TO MINIMIZE POSTOPERATIVE URINARY RETENTION WITH A PUBOVAGINAL SLING
 Urological Neurology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 27 (3): 275-280, May - June, 2001 A SIMPLE SURGICAL TECHNIQUE TO MINIMIZE POSTOPERATIVE URINARY
Urological Neurology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 27 (3): 275-280, May - June, 2001 A SIMPLE SURGICAL TECHNIQUE TO MINIMIZE POSTOPERATIVE URINARY
q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE
 493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
Surgical treatment of urinary stress incontinence with tension free vaginal tape
 Surgical treatment of urinary stress incontinence with tension free vaginal tape Gynaecology department 01935 384 385 yeovilhospital.nhs.uk Many surgical operations are available for the treatment of
Surgical treatment of urinary stress incontinence with tension free vaginal tape Gynaecology department 01935 384 385 yeovilhospital.nhs.uk Many surgical operations are available for the treatment of
Outcomes of Surgery of Female Urethral Diverticula Classified Using Magnetic Resonance Imaging
 european urology 51 (2007) 1664 1670 available at www.sciencedirect.com journal homepage: www.europeanurology.com Female Urology Incontinence Outcomes of Surgery of Female Urethral Diverticula Classified
european urology 51 (2007) 1664 1670 available at www.sciencedirect.com journal homepage: www.europeanurology.com Female Urology Incontinence Outcomes of Surgery of Female Urethral Diverticula Classified
Management of recurrent stress urinary incontinence and urinary retention following midurethral sling insertion in women
 UROLOGY doi 10.1308/003588412X13373405385610 Management of recurrent stress urinary incontinence and urinary retention following midurethral sling H Hashim 1, TR Terry 2 1 North Bristol NHS Trust, UK 2
UROLOGY doi 10.1308/003588412X13373405385610 Management of recurrent stress urinary incontinence and urinary retention following midurethral sling H Hashim 1, TR Terry 2 1 North Bristol NHS Trust, UK 2
Recent advances have improved the
 SURGICAL TECHNIQUES BY NEERAJ KOHLI, MD, MBA, and JOHN R. MIKLOS, MD Meeting the challenge of vesicovaginal fistula repair: Conservative and surgical measures A number of simple adjustments to technique
SURGICAL TECHNIQUES BY NEERAJ KOHLI, MD, MBA, and JOHN R. MIKLOS, MD Meeting the challenge of vesicovaginal fistula repair: Conservative and surgical measures A number of simple adjustments to technique
EUROPEAN UROLOGY 56 (2009)
 EUROPEAN UROLOGY 56 (2009) 193 200 available at www.sciencedirect.com journal homepage: www.europeanurology.com Female Urology Incontinence Transpubic Access Using Pedicle Tubularized Labial Urethroplasty
EUROPEAN UROLOGY 56 (2009) 193 200 available at www.sciencedirect.com journal homepage: www.europeanurology.com Female Urology Incontinence Transpubic Access Using Pedicle Tubularized Labial Urethroplasty
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY PARAMEDIAN FOREHEAD FLAP NASAL RECONSTRUCTION SURGICAL TECHNIQUE Brian Cervenka, Travis Tollefson, Patrik Pipkorn The paramedian forehead
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY PARAMEDIAN FOREHEAD FLAP NASAL RECONSTRUCTION SURGICAL TECHNIQUE Brian Cervenka, Travis Tollefson, Patrik Pipkorn The paramedian forehead
Clitorolabial Reconstruction in Circumcised Females with Clitoral Inclusion Cyst
 JKAU: Med. Sci., Vol. 16 No. 4, pp: 61-73 (2009 A.D. / 1430 A.H.) DOI: 10.4197/Med. 16-4.5 Clitorolabial Reconstruction in Circumcised Females with Clitoral Inclusion Cyst Yasir S. Jamal, FRCS(I), FICS
JKAU: Med. Sci., Vol. 16 No. 4, pp: 61-73 (2009 A.D. / 1430 A.H.) DOI: 10.4197/Med. 16-4.5 Clitorolabial Reconstruction in Circumcised Females with Clitoral Inclusion Cyst Yasir S. Jamal, FRCS(I), FICS
2. List the 8 pelvic spaces: list one procedure or dissection which involves entering that space.
 Name: Anatomy Quiz: Pre / Post 1. In making a pfannensteil incision you would traverse through the following layers: a) Skin, Camper s fascia, Scarpa s fascia, external oblique aponeurosis, internal oblique
Name: Anatomy Quiz: Pre / Post 1. In making a pfannensteil incision you would traverse through the following layers: a) Skin, Camper s fascia, Scarpa s fascia, external oblique aponeurosis, internal oblique
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY NASOLABIAL FLAP FOR ORAL CAVITY RECONSTRUCTION Harry Wright, Scott Stephan, James Netterville Designed as a true myocutaneous flap pedicled
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY NASOLABIAL FLAP FOR ORAL CAVITY RECONSTRUCTION Harry Wright, Scott Stephan, James Netterville Designed as a true myocutaneous flap pedicled
Gökmen Sukgen, 1 Esra SaygJlJ YJlmaz, 2 and Eralp BaGer Introduction. 2. Case Presentation
 Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Alexander C Vlantis. Selective Neck Dissection 33
 05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
PUBOVAGINAL SLING IN THE TREATMENT OF STRESS URINARY INCONTINENCE FOR URETHRAL HYPERMOBILITY AND INTRINSIC SPHINCTERIC DEFICIENCY
 Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology PUBOVAGINAL SLING IN SUI Vol. 29 (6): 540-544, November - December, 2003 PUBOVAGINAL SLING IN THE TREATMENT
Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology PUBOVAGINAL SLING IN SUI Vol. 29 (6): 540-544, November - December, 2003 PUBOVAGINAL SLING IN THE TREATMENT
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY RECTUS ABDOMINIS FLAP FOR HEAD & NECK RECONSTRUCTION Patrik Pipkorn, Brian Nussenbaum The rectus abdominis flap is based on the deep inferior
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY RECTUS ABDOMINIS FLAP FOR HEAD & NECK RECONSTRUCTION Patrik Pipkorn, Brian Nussenbaum The rectus abdominis flap is based on the deep inferior
Introduction to GYN Specialties
 Outline Introduction to GYN Specialties Gynecologic Oncology* Female Pelvic Medicine and Reconstructive Surgery* Reproductive Endocrinology and Infertility* Pediatric and Adolescent Gynecology** Family
Outline Introduction to GYN Specialties Gynecologic Oncology* Female Pelvic Medicine and Reconstructive Surgery* Reproductive Endocrinology and Infertility* Pediatric and Adolescent Gynecology** Family
Atlas of Urologic Surgery
 Atlas of Urologic Surgery Hinman, F ISBN-13: 9781416042105 Table of Contents Section I: Surgical Basics Chapter 1 Surgical Basics Section II: The Urologist at Work Chapter 2 Basic Surgical Techniques Chapter
Atlas of Urologic Surgery Hinman, F ISBN-13: 9781416042105 Table of Contents Section I: Surgical Basics Chapter 1 Surgical Basics Section II: The Urologist at Work Chapter 2 Basic Surgical Techniques Chapter
Modern methods of imaging in urogynecology when do we really need them?
 Archives of Perinatal Medicine 23(2), 77 81, 2017 ORIGINAL PAPER Modern methods of imaging in urogynecology when do we really need them? GRZEGORZ SURKONT, EDYTA WLAŹLAK Abstract Imaging is more often used
Archives of Perinatal Medicine 23(2), 77 81, 2017 ORIGINAL PAPER Modern methods of imaging in urogynecology when do we really need them? GRZEGORZ SURKONT, EDYTA WLAŹLAK Abstract Imaging is more often used
Prevention of Surgical Injuries in Gynecology
 in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases
 J Oral Maxillofac Surg 58:1104-1108, 2000 Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases Yadranko Ducic, MD, FRCS (C),* and Mark Burye, DDS Purpose: This article describes
J Oral Maxillofac Surg 58:1104-1108, 2000 Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases Yadranko Ducic, MD, FRCS (C),* and Mark Burye, DDS Purpose: This article describes
Research Article Transvesicoscopic Repair of Vesicovaginal Fistula
 Diagnostic and Therapeutic Endoscopy Volume 2010, Article ID 760348, 4 pages doi:10.1155/2010/760348 Research Article Transvesicoscopic Repair of Vesicovaginal Fistula R. B. Nerli and Mallikarjun Reddy
Diagnostic and Therapeutic Endoscopy Volume 2010, Article ID 760348, 4 pages doi:10.1155/2010/760348 Research Article Transvesicoscopic Repair of Vesicovaginal Fistula R. B. Nerli and Mallikarjun Reddy
6 THE OPERATIONS BASIC PRINCIPLES
 6 THE OPERATIONS BASIC PRINCIPLES Basic principles are described here; strategies for specific situations are discussed in later sections. The basic principles in the repair of a fistula are: adequate
6 THE OPERATIONS BASIC PRINCIPLES Basic principles are described here; strategies for specific situations are discussed in later sections. The basic principles in the repair of a fistula are: adequate
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Sara Schaenzer Grand Rounds January 24 th, 2018
 Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Marietta Mahendeka, M.D. Obstetrician and Gynaecologist Bugando Medical Centre Tanzania. Tutor: Dr Luc de Bernis, WHO
 A COMPARATIVE STUDY OF THE MANAGEMENT OF VESICO AND/OR RECTO-VAGINAL FISTULAE AT BUGANDO MEDICAL CENTRE, MWANZA, TANZANIA, EAST AFRICA: A RETROSPECTIVE STUDY Marietta Mahendeka, M.D. Obstetrician and Gynaecologist
A COMPARATIVE STUDY OF THE MANAGEMENT OF VESICO AND/OR RECTO-VAGINAL FISTULAE AT BUGANDO MEDICAL CENTRE, MWANZA, TANZANIA, EAST AFRICA: A RETROSPECTIVE STUDY Marietta Mahendeka, M.D. Obstetrician and Gynaecologist
Infracoccygeal sacropexy using mesh for uterine prolapse repair
 Infracoccygeal sacropexy using mesh for uterine Issued: January 2009 www.nice.org.uk/ipg280 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Infracoccygeal sacropexy using mesh for uterine Issued: January 2009 www.nice.org.uk/ipg280 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Posterior Deep Endometriosis. What is the best approach? Posterior Deep Endometriosis. Should we perform a routine excision of the vagina??
 Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst Polyclinique Hotel Dieu CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix -Rectum
Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst Polyclinique Hotel Dieu CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix -Rectum
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation in uterine leiomyoma management, 719 723 Adnexal masses diagnosis of, 664 667 imaging in, 664 665 laboratory studies in, 665
Index Note: Page numbers of article titles are in boldface type. A Ablation in uterine leiomyoma management, 719 723 Adnexal masses diagnosis of, 664 667 imaging in, 664 665 laboratory studies in, 665
Female Urology. The Results of Grade IV Cystocele Repair Using Mesh. Introduction ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M
 Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
Urinary and faecal incontinence following delayed primary repair of obstetric genital fistula
 BJOG: an International Journal of Obstetrics and Gynaecology July 2002, Vol. 109, pp. 828 832 Urinary and faecal incontinence following delayed primary repair of obstetric genital fistula Christine Murray,
BJOG: an International Journal of Obstetrics and Gynaecology July 2002, Vol. 109, pp. 828 832 Urinary and faecal incontinence following delayed primary repair of obstetric genital fistula Christine Murray,
Daniel K Roberts MD, PhD 2014 Annual Clinical Update
 Daniel K Roberts MD, PhD 2014 Annual Clinical Update Kevin E Miller, MD Division of Female Pelvic Medicine and Reconstructive Surgery Dept. of OBGYN University of Kansas School of Medicine- Wichita at
Daniel K Roberts MD, PhD 2014 Annual Clinical Update Kevin E Miller, MD Division of Female Pelvic Medicine and Reconstructive Surgery Dept. of OBGYN University of Kansas School of Medicine- Wichita at
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander.
 Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
