Evaluating the impact of radiation therapy on patient quality of life following primary artificial urinary sphincter placement
|
|
|
- Emery Lenard Newton
- 5 years ago
- Views:
Transcription
1 Original Article Evaluating the impact of radiation therapy on patient quality of life following primary artificial urinary sphincter placement Jason P. Joseph, Marcelino E. Rivera, Brian J. Linder, Boyd R. Viers, Daniel S. Elliott Department of Urology, Section of Pelvic and Reconstructive Surgery, Mayo Clinic, Rochester, MN, USA Contributions: (I) Conception and design: All authors; (II) Administrative support: All authors; (III) Provision of study materials or patients: DS Elliott; (IV) Collection and assembly of data: All authors; (V) Data analysis and interpretation: All authors; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Daniel S. Elliott, MD. Department of Urology, Section of Pelvic and Reconstructive Surgery, Mayo Clinic, 200 First Street SW, Rochester, MN 55905, USA. Background: The impact of prior radiation therapy on patient satisfaction following primary artificial urinary sphincter (AUS) placement is not well described, therefore our aim was to evaluate the effect of radiation on patient satisfaction among men undergoing primary AUS with and without a history of prior radiation. Methods: From , 1,082 men underwent primary AUS placement at our institution. Of these, 467 were alive, with an intact primary AUS and invited to participate in a mailed survey assessing AUS status, patient satisfaction, and urinary control. Clinical subjective outcomes were assessed via reported change in urinary control from pre-operative to post-aus placement. Results: In total, 229/467 (49%) of men with an intact primary AUS completed the survey, with a median follow-up of 8.4 years [interquartile range (IQR) ]. Of these, 64 men (28%) had a prior history of radiation therapy. Both men with and without history of radiation, reported a high likelihood of electing to have AUS surgery again, 87% vs. 91% respectively (P=0.87), and of recommending AUS surgery to a family member, 86% vs. 93% respectively (P=0.18). There were no significant differences between those with and without prior radiation with regard to rates of reported: substantial improvement in urinary control following surgery (72% vs. 78%, P=0.30), minimal bothersome leakage (57.1% vs. 66%, P=0.31), and pad use 1 pad/day (49% vs. 59%, P=0.06). Conclusions: In a large cohort of primary AUS implants with and without prior radiation therapy we noted a high-level of satisfaction and though many patients still utilized 1 or more pads/day with longterm follow-up. Importantly, there was no significant difference in quality of life (QoL) outcomes compared between those with and without prior radiation therapy. Keywords: Artificial urinary sphincter (AUS); incontinence; outcomes; radiation Submitted Oct 14, Accepted for publication Nov 23, doi: /tau View this article at: Introduction In the United States, the prevalence of urinary incontinence (UI) in men over 40 years of age is estimated at 45% and although definitions of incontinence vary, an increasing trend is seen with advancing age (1,2). UI can have a significant impact on mental health, in particular with regards to anxiety and depression, and has also been demonstrated to have a negative impact on health-related quality of life (QoL) (1). While there are multiple risk factors for UI, one of the most common iatrogenic causes is radical prostatectomy resulting in rates of stress UI estimated between 12 16% depending on surgical modality (3), with other iatrogenic causes including transurethral
2 2 Joseph et al. QoL, radiation therapy and AUS resection of the prostate and pelvic radiation therapy. Originally introduced in 1972 (4), the artificial urinary sphincter (AUS) is considered the preferred surgical therapy for moderate to severe stress UI. While the AUS has demonstrated acceptable intermediate to longterm durability with 5-year revision-free survival rates of 60 75% (5-8), the impact on urinary continence reported has varied considerably with rates of social continence, generally defined as 1 pad per day (PPD), ranging between % and dry rates reported between 4 86% (9). Likewise rates of patient satisfaction vary considerably, with reports ranging from 73% to 95% patient satisfaction (10-13). Notably, data regarding preoperative factors that predict patient satisfaction are sparse. Approximately 40% of men who undergo AUS placement after RP have received external beam radiation therapy (XRT) (14). Exposure to radiotherapy has been proposed as a risk factor for adverse AUS outcomes, though reports in the literature are conflicting (14-20). The impact of radiation therapy and AUS patient satisfaction and postoperative QoL has had minimal investigation, with no impact on long-term continence and patient satisfaction being reported in the one available report (19). Thus, we evaluated the impact of prior radiation therapy on patient satisfaction following primary AUS placement Methods After Institutional Review Board approval, we identified 1,082 male patients who underwent primary AUS implantation at Mayo Clinic (Rochester, MN, USA) from 1983 to 2011 by three surgeons (William Furlow, David Barrett and Daniel S. Elliott). After excluding patients that died during follow-up and/or underwent device revisions or explantations, we identified 467 primary AUS devices in-situ at the time of mailing. Patients were excluded from analysis if they underwent primary AUS implantation for neurogenic bladder dysfunction, were less than 18 years old, or declined research consent. All implanted devices were American Medical Systems 800 (AMS 800; American Medical Systems, Inc., Minnetonka, MN, USA). Patient clinical characteristics and details of the primary device placement were assessed. Given the retrospective study design, patients did not have standardized followup. Instead, following device placement, patients are evaluated 6 weeks post-operatively for device activation. Thereafter, patients are followed via office evaluation on an as needed basis, as determined by their continence or other device concerns. The Mayo Clinic AUS Registry monitors outcomes periodically by written patient correspondence and QoL questionnaires. Details regarding device survival were obtained from last office examination, operative reports, written or telephone correspondence. All patients who underwent AUS device implantation between 1983 and 2011 were invited to participate in a mail-in survey (Figure 1). The questionnaire administered assessed current device status and any previous explanations during patient follow-up. Patient satisfaction was measured utilizing questions adapted from previous studies focusing on AUS and QoL. Urinary continence parameters were also captured on the questionnaire adopted from the validated Expanded Prostate Cancer Index Composite urinary domain (EPIC-UD) (21). Patient reported change in urinary control from pre-operative to post-aus placement served as an indicator of overall AUS-QoL and satisfaction, and was assessed on a scale of 0 to 10. These answers were each multiplied by ten to convert to a scale, with 100 representing the highest rate of satisfaction/continence. An AUS-QoL score 70 was considered to be associated with patient satisfaction and was utilized to include the highest quartile of urinary control. Statistical analysis was performed using the SAS software package (SAS Institute, Inc.: Cary, NC, USA). Continuous features were summarized with medians and interquartile ranges (IQR); categorical features were summarized with frequency counts and percentages. After stratifying by overall, primary without radiation exposure and with radiation exposure, chi-square cross table analysis, and Spearman rank correlations, were used to investigate the relationship between overall satisfaction (defined by the AUS-related QoL score and likelihood to have AUS surgery again), as well as patient reported urinary continence outcomes. Survey outcomes were dichotomized to reflect the degree of satisfaction and urinary control. All statistical tests were 2-sided, with a P value <0.05 considered statistically significant. Results Of the 1,082 primary implantations during the study timeframe, 277 patients were deceased and 338 had undergone revision surgery prior to mailing. This left a total of 467 patients, living with their primary device-in situ. Of these patients, 64 patients with radiation and 165 patients without prior radiation therapy completed the survey, for a response rate of 229/467 (49%).
3 Translational Andrology and Urology, Figure 1 Artificial urinary sphincter quality of life survey. Clinical and demographic information for patients included in the study, stratified by prior pelvic radiation exposure are demonstrated in Table 1. Notably, men with prior radiation therapy were older (P=0.01) and more likely to have received androgen deprivation therapy (P<0.01). There was no significant difference between the cohorts in other clinical characteristics including body mass index (P=0.30) or coronary artery disease (P=0.56). For all responders, at a median follow-up was 8.4 years (IQR ), 73% reported an AUS-related QoL score 70/100, 90% would undergo surgery again, 56% wore 1 PPD, 82% reported leakage on a daily basis, and 64% reported minimal leakage-related bother. When stratified by exposure to prior radiation therapy (Table 2), there were no significant differences in patient reported AUSrelated satisfaction (P=0.29) or the rate of those using 1 pad (P=0.06) between cohorts. Specifically, there were equivalent rates of perceived satisfaction between those with and without prior radiation therapy including willingness to undergo AUS surgery again (87% vs. 91%, P=0.87) and likelihood to recommend AUS surgery to a friend or family member (86% vs. 93%, P=0.18). Likewise, there was
4 4 Joseph et al. QoL, radiation therapy and AUS Table 1 Clinical variables by primary AUS without and with pelvic radiation exposure. Clinical variable Without pelvic radiation (n=165) With pelvic radiation (n=64) Total (n=229) P value Age at surgery, years, median [IQR] 70 [64 73] 72 [67 77] 70 [65 75] 0.01 BMI, kg/m 2, median [IQR] 28 [26 30] 29 [27 33] 28 [26 31] 0.30 Diabetes mellitus, no. (%) 15 (9.1) 6 (9.4) 21 (9.2) 0.79 Current smoker, no. (%) 6 (3.6) 2 (3.1) 8 (3.5) 0.71 Former smoker, no. (%) 76 (46.1) 32 (50.0) 108 (47.2) 0.72 Coronary artery disease, no. (%) 24 (14.5) 13 (20.3) 37 (16.2) 0.56 Cerebral vascular disease, no. (%) 0 (0.0) 4 (6.3) 4 (1.7) <0.01 Myocardial infarction, no. (%) 9 (5.5) 3 (4.7) 12 (5.2) 0.64 COPD, no. (%) 10 (6.1) 9 (14.1) 19 (8.3) 0.11 TURP, no. (%) 17 (10.3) 5 (7.8) 22 (9.6) 0.41 Androgen deprivation therapy, no. (%) 5 (3.0) 16 (25.0) 21 (9.2) <0.01 Male urethral sling, no. (%) 4 (2.3) 4 (6.3) 8 (3.5) 0.15 Radical prostatectomy, no. (%) 140 (84.8) 50 (78.1) 190 (83.0) 0.47 equivalence in patient reported AUS QoL following device implantation 70% vs. 77% (P=0.29). Of note, the median follow-up for those with prior radiation exposure was shorter than for patients without prior radiation therapy (median 7.1 vs. 8.9 years; P<0.01). Discussion Here, in a large single institution series of primary AUS placements with a median of 8.4 years of follow-up, we found a high-rate of AUS-related QoL and satisfaction, acceptable urinary control, and no significant differences in functional outcomes among men with primary AUS placement without or with radiation exposure. Overall, 73% of men reported an AUS-related QoL score 70 (scale 0 100) and 90% would elect to undergo AUS surgery again. Importantly, our findings demonstrate modest rates of complete urinary control with extended follow-up including 56% of patients reporting 1 PPD (social continence) and 82% with leakage on a daily basis. These findings highlight the need for appropriate patient counseling and expectations regarding long-term AUS functional outcomes. There is limited data available in the literature regarding the impact of prior radiation therapy on QoL in patients undergoing AUS placement (19). In this series, Walsh et al. evaluated 98 patients, 22 having received radiation therapy, and 92% of patients without prior radiation therapy reported that they were very or somewhat satisfied with surgery versus 89% in irradiated patients (P value listed as not significant, no value provided) (19). However, they did report a significant difference between those with and without radiation regarding rates of infection and erosion, urethral atrophy and resolution of incontinence after AUS placement (P<0.05). Likewise, irradiated patients had significantly higher rates of patients with little to no improvement and fewer patients being completely dry. At a mean follow-up of 46 months they concluded that AUS placement in an irradiated patient did not affect long-term continence or overall satisfaction. Our findings augment the existing literature in a larger cohort, with longer follow-up. We note similar results regarding patients satisfaction, specifically, there were equivalent rates of perceived satisfaction between those with and without prior radiation therapy including willingness to undergo AUS surgery again (87% vs. 91%) and likelihood to recommend AUS surgery to a friend or family member (86% vs. 93%). We noted no significant difference between these groups likewise with regards to continence with 56% of patients reporting 1 PPD, 82% leakage on a daily basis, and 36% significant leakage-related bother. Differences between our results and those previously published may be secondary to disparate populations, sample size, surgical technique and the longer follow-up available in our cohort (median 100 months, as compared to 46 months).
5 Translational Andrology and Urology, Table 2 Clinical variables for quality of life questions by type of exposure Clinical variable Without XRT (n=165) With XRT (n=64) Total (n=229) P value Would undergo AUS surgery again, no. (%) 0.87 Very likely 132 (80.0) 52 (81.3) 184 (80.3) Likely 17 (10.3) 4 (6.3) 21 (9.2) Neutral 10 (6.0) 2 (3.1) 12 (5.2) Unlikely 1 (0.6) 3 (4.7) 4 (1.7) Very unlikely 3 (1.8) 3 (4.7) 6 (2.6) Would recommend AUS to friend/family member with similar problem, no. (%) 0.18 Very likely 127 (77.0) 45 (70.3) 172 (75.1) Likely 25 (15.2) 10 (15.6) 35 (15.3) Neutral 9 (5.5) 2 (3.1) 11 (4.8) Unlikely 1 (0.6) 3 (4.7) 4 (1.7) Very unlikely 2 (1.2) 4 (6.3) 6 (2.6) In continence now relative to before surgery, no. (%) (much worse now) 5 (3.0) 3 (4.7) 8 (3.5) 10 1 (0.6) 2 (3.1) 3 (1.3) 20 4 (2.4) 2 (3.1) 6 (2.6) 30 4 (2.4) 5 (7.1) 9 (3.9) 40 5 (3.0) 3 (4.7) 8 (3.5) (9.7) 3 (4.7) 19 (8.3) 60 5 (3.0) 2 (3.1) 7 (3.1) 70 8 (4.8) 6 (9.5) 14 (6.1) (24.2) 12 (19.0) 52 (22.7) (20.0) 6 (9.1) 39 (17.0) 100 (much better now) 43 (26.1) 19 (29.7) 62 (27.1) Urine leakage in last 4 weeks, no. (%) 0.95 More than once/day 104 (63.0) 41 (64.1) 145 (63.3) About once/day 29 (17.7) 10 (15.6) 39 (17.0) More than once/week 9 (5.5) 4 (6.3) 13 (5.7) Once/week 8 (4.9) 1 (1.6) 9 (3.9) Rarely/never 13 (7.9) 7 (11.0) 20 (8.7) Degree of urinary control, no. (%) 0.81 No control 11 (6.7) 5 (7.1) 16 (7.0) Frequent dribbling 63 (38.2) 22 (34.4) 85 (37.1) Occasional dribbling 76 (46.1) 30 (46.9) 106 (46.1) Total control 14 (8.5) 6 (9.4) 20 (8.7) Table 2 (continued)
6 6 Joseph et al. QoL, radiation therapy and AUS Table 2 (continued) Clinical variable Without XRT (n=165) With XRT (n=64) Total (n=229) P value Pads/day in last 4 weeks, no. (%) (15.8) 2 (3.1) 28 (12.2) 1 70 (42.4) 29 (45.3) 99 (43.2) 2 40 (24.2) 19 (29.7) 59 (25.8) 3 28 (17.0) 13 (20.3) 41 (18.0) Perceived bother from leakage, no. (%) 0.31 None 18 (11.0) 6 (9.4) 24 (10.5) Very small 42 (25.5) 17 (26.6) 59 (25.8) Small 48 (29.1) 13 (20.3) 61 (26.6) Moderate 42 (25.2) 16 (25.0) 58 (25.3) Large 14 (8.5) 11 (17.2) 25 (11.0) AUS, artificial urinary sphincter; XRT, radiation therapy. We recognize that our study is limited by its retrospective design, and as such, we were unable to objectively assess the degree of preoperative UI. Moreover, due to the inclusion of only primary implants and use of a survey there is the potential for selection bias. Furthermore, our survey response rate was 49% among those alive, which may introduce a response bias. Further investigations utilizing a standardized, validated patient follow-up are needed to further validate our data. Conclusions In a large cohort of primary AUS implants, we noted a high-level of satisfaction and modest urinary control at a median follow-up of over 8 years. Importantly, we found no differences in QoL outcomes in among patients with versus without prior radiation therapy among those with the primary device in place. This information can be used when counselling potential AUS patients who have undergone previous XRT. Acknowledgements None. Footnote Conflicts of Interest: The authors have no conflicts of interest to declare. Ethical Statement: The study was approved by Mayo Clinic Institutional Review Board (No ). References 1. Coyne KS, Kvasz M, Ireland AM, et al. Urinary incontinence and its relationship to mental health and health-related quality of life in men and women in Sweden, the United Kingdom, and the United States. Eur Urol 2012;61: Markland AD, Goode PS, Redden DT, et al. Prevalence of urinary incontinence in men: results from the national health and nutrition examination survey. J Urol 2010;184: Hu JC, Gu X, Lipsitz SR, et al. Comparative effectiveness of minimally invasive vs open radical prostatectomy. JAMA 2009;302: Scott FB, Bradley WE, Timm GW. Treatment of urinary incontinence by an implantable prosthetic urinary sphincter. J Urol 1974;112: Kim SP, Sarmast Z, Daignault S, et al. Long-term durability and functional outcomes among patients with artificial urinary sphincters: a 10-year retrospective review from the University of Michigan. J Urol 2008;179: Lai HH, Hsu EI, Teh BS, et al. 13 years of experience with artificial urinary sphincter implantation at Baylor College of Medicine. J Urol 2007;177: Linder BJ, de Cogain M, Elliott DS. Long-term device outcomes of artificial urinary sphincter reimplantation
7 Translational Andrology and Urology, following prior explantation for erosion or infection. J Urol 2014;191: Linder BJ, Rivera ME, Ziegelmann MJ, et al. Longterm Outcomes Following Artificial Urinary Sphincter Placement: An Analysis of 1082 Cases at Mayo Clinic. Urology 2015;86: Van der Aa F, Drake MJ, Kasyan GR, et al. The artificial urinary sphincter after a quarter of a century: a critical systematic review of its use in male non-neurogenic incontinence. Eur Urol 2013;63: Litwiller SE, Kim KB, Fone PD, et al. Post-prostatectomy incontinence and the artificial urinary sphincter: a longterm study of patient satisfaction and criteria for success. J Urol 1996;156: Haab F, Trockman BA, Zimmern PE, et al. Quality of life and continence assessment of the artificial urinary sphincter in men with minimum 3.5 years of followup. J Urol 1997;158: Gousse AE, Madjar S, Lambert MM, et al. Artificial urinary sphincter for post-radical prostatectomy urinary incontinence: long-term subjective results. J Urol 2001;166: Montague DK, Angermeier KW, Paolone DR. Long-term continence and patient satisfaction after artificial sphincter implantation for urinary incontinence after prostatectomy. J Urol 2001;166: Rivera ME, Linder BJ, Ziegelmann MJ, et al. The Impact of Prior Radiation Therapy on Artificial Urinary Sphincter Device Survival. J Urol 2016;195: Aaronson DS, Elliott SP, McAninch JW. Transcorporal artificial urinary sphincter placement for incontinence in high-risk patients after treatment of prostate cancer. Urology 2008;72: Bates AS, Martin RM, Terry TR. Complications following artificial urinary sphincter placement after radical prostatectomy and radiotherapy: a meta-analysis. BJU Int 2015;116: Wang Y, Hadley HR. Experiences with the artificial urinary sphincter in the irradiated patient. J Urol 1992;147: Pérez LM, Webster GD. Successful outcome of artificial urinary sphincters in men with post-prostatectomy urinary incontinence despite adverse implantation features. J Urol 1992;148: Walsh IK, Williams SG, Mahendra V, et al. Artificial urinary sphincter implantation in the irradiated patient: safety, efficacy and satisfaction. BJU Int 2002;89: Gundian JC, Barrett DM, Parulkar BG. Mayo Clinic experience with use of the AMS800 artificial urinary sphincter for urinary incontinence following radical prostatectomy. J Urol 1989;142: Bukavina L, Chaparala H, Kartha G, et al. Public Restroom Habits in Patients After Artificial Urinary Sphincter Implantation. Urology 2015;86: Cite this article as: Joseph JP, Rivera ME, Linder BJ, Viers BR, Elliott DS. Evaluating the impact of radiation therapy on patient quality of life following primary artificial urinary sphincter placement.. doi: / tau
Artificial urinary sphincter revision for urethral atrophy: comparing single cuff downsizing and tandem cuff placement
 ORIGINAL ARTICLE Vol. 43 (2): 264-270, March - April, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0240 Artificial urinary sphincter revision for urethral atrophy: comparing single cuff downsizing and tandem
ORIGINAL ARTICLE Vol. 43 (2): 264-270, March - April, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0240 Artificial urinary sphincter revision for urethral atrophy: comparing single cuff downsizing and tandem
The impact of androgen deprivation on artificial urinary sphincter outcomes
 Original Article The impact of androgen deprivation on artificial urinary sphincter outcomes George C. Bailey 1, Brian J. Linder 1, Marcelino E. Rivera 1, Matthew J. Ziegelmann 1, Laureano J. Rangel 2,
Original Article The impact of androgen deprivation on artificial urinary sphincter outcomes George C. Bailey 1, Brian J. Linder 1, Marcelino E. Rivera 1, Matthew J. Ziegelmann 1, Laureano J. Rangel 2,
Four-year follow-up on a Zephyr Surgical Implants 375 artificial urinary sphincter for male urinary incontinence from one urological centre in Poland
 320 O R I G I N A L P A P E R FUNCTIONAL UROLOGY Four-year follow-up on a Zephyr Surgical Implants 375 artificial urinary sphincter for male urinary incontinence from one urological centre in Poland Ireneusz
320 O R I G I N A L P A P E R FUNCTIONAL UROLOGY Four-year follow-up on a Zephyr Surgical Implants 375 artificial urinary sphincter for male urinary incontinence from one urological centre in Poland Ireneusz
Since the first published article, in 1974 by Scott et al on
 Perineal Approach for Artificial Urinary Sphincter Implantation Appears to Control Male Stress Incontinence Better Than the Transscrotal Approach Gerard D. Henry,* Stephen M. Graham, Mario A. Cleves, Caroline
Perineal Approach for Artificial Urinary Sphincter Implantation Appears to Control Male Stress Incontinence Better Than the Transscrotal Approach Gerard D. Henry,* Stephen M. Graham, Mario A. Cleves, Caroline
The Surgical Learning Curve for Artificial Urinary Sphincter Procedures Compared to Typical Surgeon Experience
 EUROPEAN UROLOGY 60 (2011) 1285 1290 available at www.sciencedirect.com journal homepage: www.europeanurology.com Reconstructive Urology The Surgical Learning Curve for Artificial Urinary Sphincter Procedures
EUROPEAN UROLOGY 60 (2011) 1285 1290 available at www.sciencedirect.com journal homepage: www.europeanurology.com Reconstructive Urology The Surgical Learning Curve for Artificial Urinary Sphincter Procedures
Long-term results of the implantation of the AMS 800 artificial sphincter for post-prostatectomy incontinence: a single-center experience
 ORIGINAL ARTICLE Vol. 44 (1): 114-120, January - February, 2018 doi: 10.1590/S1677-5538.IBJU.2017.0165 Long-term results of the implantation of the AMS 800 artificial sphincter for post-prostatectomy incontinence:
ORIGINAL ARTICLE Vol. 44 (1): 114-120, January - February, 2018 doi: 10.1590/S1677-5538.IBJU.2017.0165 Long-term results of the implantation of the AMS 800 artificial sphincter for post-prostatectomy incontinence:
Transcorporal artificial urinary sphincter in radiated and non - radiated compromised urethra. Assessment with a minimum 2 year follow-up
 ORIGINAL ARTICLE Vol. 42 (3): 494-500, May - June, 2016 doi: 10.1590/S1677-5538.IBJU.2015.0329 Transcorporal artificial urinary sphincter in radiated and non - radiated compromised urethra. Assessment
ORIGINAL ARTICLE Vol. 42 (3): 494-500, May - June, 2016 doi: 10.1590/S1677-5538.IBJU.2015.0329 Transcorporal artificial urinary sphincter in radiated and non - radiated compromised urethra. Assessment
Conclusions. Keywords
 Functional Urology Outcomes of single- vs double-cuff artificial urinary sphincter insertion in low- and high-risk profile male patients with severe stress urinary incontinence Sascha A. Ahyai*, Tim A.
Functional Urology Outcomes of single- vs double-cuff artificial urinary sphincter insertion in low- and high-risk profile male patients with severe stress urinary incontinence Sascha A. Ahyai*, Tim A.
AdVance Male Sling System
 AdVance Male Sling System Clinical study summary This document is a compilation and summary of several AdVance Male Sling System peer-reviewed journal articles. The information presented here is taken
AdVance Male Sling System Clinical study summary This document is a compilation and summary of several AdVance Male Sling System peer-reviewed journal articles. The information presented here is taken
Long-term functional outcomes after artificial urinary sphincter implantation in men with stress urinary. incontinence
 Long-term functional outcomes after artificial urinary sphincter implantation in men with stress urinary incontinence Priscilla Léon, Emmanuel Chartier-Kastler, Morgan Rouprêt, Vanina Ambrogi, Pierre Mozer,
Long-term functional outcomes after artificial urinary sphincter implantation in men with stress urinary incontinence Priscilla Léon, Emmanuel Chartier-Kastler, Morgan Rouprêt, Vanina Ambrogi, Pierre Mozer,
Describing the learning curve for bulbar urethroplasty
 Original Article Describing the learning curve for bulbar urethroplasty Marco Spilotros, Sachin Malde, Tamsin J. Greenwell Department of Urology, University College London Hospital, London, UK Contributions:
Original Article Describing the learning curve for bulbar urethroplasty Marco Spilotros, Sachin Malde, Tamsin J. Greenwell Department of Urology, University College London Hospital, London, UK Contributions:
Managing urinary morbidity after brachytherapy. Kieran O Flynn Department of Urology, Salford Royal Foundation Trust, Manchester
 Managing urinary morbidity after brachytherapy Kieran O Flynn Department of Urology, Salford Royal Foundation Trust, Manchester Themes Can we predict urinary morbidity? Prevention of urinary morbidity
Managing urinary morbidity after brachytherapy Kieran O Flynn Department of Urology, Salford Royal Foundation Trust, Manchester Themes Can we predict urinary morbidity? Prevention of urinary morbidity
Life after prostate cancer End your frustration. Restore your normalcy. Renew your confidence. Take the next step
 Take the next step Visit EDCure.org to: Take the online ED quiz and get your customized treatment results Find an ED specialist in your area Register for free educational seminars to learn more about treatment
Take the next step Visit EDCure.org to: Take the online ED quiz and get your customized treatment results Find an ED specialist in your area Register for free educational seminars to learn more about treatment
Department of Urology, Cochin hospital Paris Descartes University
 Technical advances in the treatment of localized prostate cancer Pr Michaël Peyromaure Department of Urology, Cochin hospital Paris Descartes University Introduction Curative treatments of localized prostate
Technical advances in the treatment of localized prostate cancer Pr Michaël Peyromaure Department of Urology, Cochin hospital Paris Descartes University Introduction Curative treatments of localized prostate
Urethral catheter removal 3 days after radical retropubic prostatectomy is feasible and desirable
 Urethral catheter 3 days after radical retropubic prostatectomy is feasible and desirable (2002) 5, 291 295 ß 2002 Nature Publishing Group All rights reserved 1365 7852/02 $25.00 www.nature.com/pcan JM
Urethral catheter 3 days after radical retropubic prostatectomy is feasible and desirable (2002) 5, 291 295 ß 2002 Nature Publishing Group All rights reserved 1365 7852/02 $25.00 www.nature.com/pcan JM
Department of Urology, University Hospital Ulm, Prittwitzstrasse 43, D Ulm, Germany
 International Scholarly Research Network ISRN Urology Volume 2012, Article ID 304205, 5 pages doi:10.5402/2012/304205 Clinical Study The Retrourethral Transobturator Sling Suspension in the Treatment of
International Scholarly Research Network ISRN Urology Volume 2012, Article ID 304205, 5 pages doi:10.5402/2012/304205 Clinical Study The Retrourethral Transobturator Sling Suspension in the Treatment of
Life after prostate cancer. End your frustration. Restore your normalcy. Renew your confidence. Erectile dysfunction and male incontinence
 Life after prostate cancer End your frustration. Restore your normalcy. Renew your confidence. Erectile dysfunction and male incontinence Welcome This brochure is designed to help you learn more about
Life after prostate cancer End your frustration. Restore your normalcy. Renew your confidence. Erectile dysfunction and male incontinence Welcome This brochure is designed to help you learn more about
Fan Zhang 1,2 and Limin Liao 1,2*
 Zhang and Liao BMC Urology (018) 18:3 DOI 10.1186/s1894-018-0314-y RESEARCH ARTICLE Artificial urinary sphincter implantation: an important component of complex surgery for urinary tract reconstruction
Zhang and Liao BMC Urology (018) 18:3 DOI 10.1186/s1894-018-0314-y RESEARCH ARTICLE Artificial urinary sphincter implantation: an important component of complex surgery for urinary tract reconstruction
Deirdre M. Bochove-Overgaauw* and Bart Ph. Schrier
 An Adjustable Sling for the Treatment of All Degrees of Male Stress Urinary Incontinence: Retrospective Evaluation of Efficacy and Complications After a Minimal Followup of 14 Months Deirdre M. Bochove-Overgaauw*
An Adjustable Sling for the Treatment of All Degrees of Male Stress Urinary Incontinence: Retrospective Evaluation of Efficacy and Complications After a Minimal Followup of 14 Months Deirdre M. Bochove-Overgaauw*
Outcome and complications of adjustable continence therapy (ProACT ) after radical prostatectomy: 10 years experience in 143 patients
 Received: 16 August 2017 Accepted: 13 November 2017 DOI: 10.1002/nau.23463 ORIGINAL CLINICAL ARTICLE Outcome and complications of adjustable continence therapy (ProACT ) after radical prostatectomy: 10
Received: 16 August 2017 Accepted: 13 November 2017 DOI: 10.1002/nau.23463 ORIGINAL CLINICAL ARTICLE Outcome and complications of adjustable continence therapy (ProACT ) after radical prostatectomy: 10
Presentation, management, and outcomes of complications following prostate cancer therapy
 Original Article Presentation, management, and outcomes of complications following prostate cancer therapy Uwais B. Zaid, Jack W. McAninch, Allison S. Glass, Nadya M. Cinman, Benjamin N. Breyer Department
Original Article Presentation, management, and outcomes of complications following prostate cancer therapy Uwais B. Zaid, Jack W. McAninch, Allison S. Glass, Nadya M. Cinman, Benjamin N. Breyer Department
Fix your incontinence Find your happiness. Restore your normalcy. Renew your confidence. Male stress urinary incontinence
 Fix your incontinence Find your happiness. Restore your normalcy. Renew your confidence. Male stress urinary incontinence Understanding your condition What is incontinence? Incontinence is defined as any
Fix your incontinence Find your happiness. Restore your normalcy. Renew your confidence. Male stress urinary incontinence Understanding your condition What is incontinence? Incontinence is defined as any
Jaspreet S. Sandhu,*,, Geoffrey T. Gotto,*, Luis A. Herran, Peter T. Scardino, James A. Eastham and Farhang Rabbani
 Age, Obesity, Medical Comorbidities and Surgical Technique are Predictive of Symptomatic Anastomotic Strictures After Contemporary Radical Prostatectomy Jaspreet S. Sandhu,*,, Geoffrey T. Gotto,*, Luis
Age, Obesity, Medical Comorbidities and Surgical Technique are Predictive of Symptomatic Anastomotic Strictures After Contemporary Radical Prostatectomy Jaspreet S. Sandhu,*,, Geoffrey T. Gotto,*, Luis
Jennifer Locke UBC Department of Urologic Sciences Resident Year 3 October 12, Learning Objectives
 Artificial Urinary Sphincter after 40 Years of Use: Indications, Techniques and Outcomes Jennifer Locke UBC Department of Urologic Sciences Resident Year 3 October 12, 2016 Learning Objectives 1. Identify
Artificial Urinary Sphincter after 40 Years of Use: Indications, Techniques and Outcomes Jennifer Locke UBC Department of Urologic Sciences Resident Year 3 October 12, 2016 Learning Objectives 1. Identify
I-STOP TOMS Transobturator Male Sling
 I-STOP TOMS Transobturator Male Sling The CL Medical I-STOP TOMS sling for male stress urinary incontinence was developed in France where it is widely used and is the market leader. It is constructed with
I-STOP TOMS Transobturator Male Sling The CL Medical I-STOP TOMS sling for male stress urinary incontinence was developed in France where it is widely used and is the market leader. It is constructed with
Management of Post-Prostatectomy Urinary Incontinence and Sexual Dysfunction
 Management of Post-Prostatectomy Urinary Incontinence and Sexual Dysfunction Robert C. Eyre, MD, FACS Associate Clinical Professor of Surgery (Urology) Harvard Medical School Post-prostatectomy Incontinence
Management of Post-Prostatectomy Urinary Incontinence and Sexual Dysfunction Robert C. Eyre, MD, FACS Associate Clinical Professor of Surgery (Urology) Harvard Medical School Post-prostatectomy Incontinence
Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer
 Original Article Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer Sunai Leewansangtong, Suchai Soontrapa, Chaiyong Nualyong, Sittiporn Srinualnad, Tawatchai Taweemonkongsap and Teerapon
Original Article Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer Sunai Leewansangtong, Suchai Soontrapa, Chaiyong Nualyong, Sittiporn Srinualnad, Tawatchai Taweemonkongsap and Teerapon
10th anniversary of 1st validated CaPspecific
 Quality of Life after Treatment of Localised Prostate Cancer Dr Jeremy Grummet Clinical Uro-Oncology Fellow May 28, 2008 1 Why? This is important May be viewed as soft science Until we know which treatment
Quality of Life after Treatment of Localised Prostate Cancer Dr Jeremy Grummet Clinical Uro-Oncology Fellow May 28, 2008 1 Why? This is important May be viewed as soft science Until we know which treatment
Artificial urinary sphincter for urinary incontinence after radical prostatectomy: a historical cohort from 2004 to 2015
 ORIGINAL ARTICLE Vol. 43 (1): 150-154, January - February, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0244 Artificial urinary sphincter for urinary incontinence after radical prostatectomy: a historical cohort
ORIGINAL ARTICLE Vol. 43 (1): 150-154, January - February, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0244 Artificial urinary sphincter for urinary incontinence after radical prostatectomy: a historical cohort
SURGICAL MANAGEMENT OF POST-PROSTATECTOMY INCONTINENCE
 SURGICAL MANAGEMENT OF POST-PROSTATECTOMY INCONTINENCE Arthi Satyanarayan, Ryan Mooney, *Nirmish Singla Department of Urology, University of Texas Southwestern Medical Center, Dallas, Texas, USA *Correspondence
SURGICAL MANAGEMENT OF POST-PROSTATECTOMY INCONTINENCE Arthi Satyanarayan, Ryan Mooney, *Nirmish Singla Department of Urology, University of Texas Southwestern Medical Center, Dallas, Texas, USA *Correspondence
2/14/09. Why Discuss this topic? Managing Local Recurrences after Radiation Failure. PROSTATE CANCER Second Treatment
 Why Discuss this topic? Mack Roach III, MD Professor and Chair Radiation Oncology UCSF Managing Local Recurrences after Radiation Failure 1. ~15 to 75% of CaP pts recur after definitive RT. 2. Heterogeneous
Why Discuss this topic? Mack Roach III, MD Professor and Chair Radiation Oncology UCSF Managing Local Recurrences after Radiation Failure 1. ~15 to 75% of CaP pts recur after definitive RT. 2. Heterogeneous
Urinary Adverse Events after Radiation Therapy for Prostate Cancer
 Urinary Adverse Events after Radiation Therapy for Prostate Cancer Sexual Medicine Society of North America Scottsdale, Arizona 2016 Jaspreet S. Sandhu, MD Department of Surgery/Urology Memorial Sloan
Urinary Adverse Events after Radiation Therapy for Prostate Cancer Sexual Medicine Society of North America Scottsdale, Arizona 2016 Jaspreet S. Sandhu, MD Department of Surgery/Urology Memorial Sloan
Research Article Urinary Catheterization May Not Adversely Impact Quality of Life in Multiple Sclerosis Patients
 ISRN Neurology, Article ID 167030, 4 pages http://dx.doi.org/10.1155/2014/167030 Research Article Urinary Catheterization May Not Adversely Impact Quality of Life in Multiple Sclerosis Patients Rebecca
ISRN Neurology, Article ID 167030, 4 pages http://dx.doi.org/10.1155/2014/167030 Research Article Urinary Catheterization May Not Adversely Impact Quality of Life in Multiple Sclerosis Patients Rebecca
Understanding your treatment options for male stress urinary incontinence and erectile dysfunction
 Understanding your treatment options for male stress urinary incontinence and erectile dysfunction Male Stress Urinary Incontinence and Erectile Dysfunction What causes male stress urinary incontinence
Understanding your treatment options for male stress urinary incontinence and erectile dysfunction Male Stress Urinary Incontinence and Erectile Dysfunction What causes male stress urinary incontinence
Introduction. Keywords Male urinary incontinence Artificial urinary sphincter Compressive adjustable slings
 https://doi.org/10.1007/s00345-018-2523-0 ORIGINAL ARTICLE Comparison of adjustable male slings and artificial urinary sphincter in the treatment of male urinary incontinence: a retrospective analysis
https://doi.org/10.1007/s00345-018-2523-0 ORIGINAL ARTICLE Comparison of adjustable male slings and artificial urinary sphincter in the treatment of male urinary incontinence: a retrospective analysis
Comparison of bone-anchored male sling and collagen implant for the treatment of male incontinence
 Blackwell Publishing AsiaMelbourne, AustraliaIJUInternational Journal of Urology0919-81722006 Blackwell Publishing Asia Pty Ltd???2006130012071211Original ArticleComparison of male sling and collagen implant
Blackwell Publishing AsiaMelbourne, AustraliaIJUInternational Journal of Urology0919-81722006 Blackwell Publishing Asia Pty Ltd???2006130012071211Original ArticleComparison of male sling and collagen implant
Male urinary incontinence: Artificial sphincter
 GUIDELINES IN FOCUS Truzzi JC et al. Male urinary incontinence: Artificial sphincter Incontinência urinária masculina: Esfíncter artificial Authorship: Brazilian Society of Urology (SBU) Participants:
GUIDELINES IN FOCUS Truzzi JC et al. Male urinary incontinence: Artificial sphincter Incontinência urinária masculina: Esfíncter artificial Authorship: Brazilian Society of Urology (SBU) Participants:
Management of Artificial Urinary Sphincter Dysfunction
 European Urology European Urology 46 (2004) 241 246 Management of Artificial Urinary Sphincter Dysfunction Frédéric Maillet, Jean-Marie Buzelin, Olivier Bouchot, Georges Karam * Clinique Urologique, CHU
European Urology European Urology 46 (2004) 241 246 Management of Artificial Urinary Sphincter Dysfunction Frédéric Maillet, Jean-Marie Buzelin, Olivier Bouchot, Georges Karam * Clinique Urologique, CHU
A.M.I. ATOMS System. Hydraulic system substitutes urinary sphincter function in incontinent males
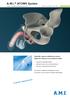 A.M.I. ATOMS System Product Group Urology Issue 11/2016 ATOMS = Adjustable TransObturator Male System Hydraulic system substitutes urinary sphincter function in incontinent males Long-term, adjustable
A.M.I. ATOMS System Product Group Urology Issue 11/2016 ATOMS = Adjustable TransObturator Male System Hydraulic system substitutes urinary sphincter function in incontinent males Long-term, adjustable
Prostate Cancer Case Study 1. Medical Student Case-Based Learning
 Prostate Cancer Case Study 1 Medical Student Case-Based Learning The Case of Mr. Powers Prostatic Nodule The effervescent Mr. Powers is found by his primary care provider to have a prostatic nodule. You
Prostate Cancer Case Study 1 Medical Student Case-Based Learning The Case of Mr. Powers Prostatic Nodule The effervescent Mr. Powers is found by his primary care provider to have a prostatic nodule. You
Elsevier Editorial System(tm) for European Urology Manuscript Draft
 Elsevier Editorial System(tm) for European Urology Manuscript Draft Manuscript Number: EURUROL-D-13-00306 Title: Post-Prostatectomy Incontinence and Pelvic Floor Muscle Training: A Defining Problem Article
Elsevier Editorial System(tm) for European Urology Manuscript Draft Manuscript Number: EURUROL-D-13-00306 Title: Post-Prostatectomy Incontinence and Pelvic Floor Muscle Training: A Defining Problem Article
Comiter CV (2002). "The male sling for stress urinary incontinence: a prospective study." J Urol 167(2 Pt 1):
 Bacon, C. G., E. Giovannucci, et al. (2002). "The association of treatment-related symptoms with qualityof-life outcomes for localized prostate carcinoma patients." Cancer 94(3): 862-71. BACKGROUND: Most
Bacon, C. G., E. Giovannucci, et al. (2002). "The association of treatment-related symptoms with qualityof-life outcomes for localized prostate carcinoma patients." Cancer 94(3): 862-71. BACKGROUND: Most
MATERIALS AND METHODS
 Primary Triple Androgen Blockade (TAB) followed by Finasteride Maintenance (FM) for clinically localized prostate cancer (CL-PC): Long term follow-up and quality of life (QOL) SJ Tucker, JN Roundy, RL
Primary Triple Androgen Blockade (TAB) followed by Finasteride Maintenance (FM) for clinically localized prostate cancer (CL-PC): Long term follow-up and quality of life (QOL) SJ Tucker, JN Roundy, RL
Point/Counterpoint: Quality of Life Considerations for Patients with Muscle Invasive Bladder Cancer Pro Trimodality Therapy
 Point/Counterpoint: Quality of Life Considerations for Patients with Muscle Invasive Bladder Cancer Pro Trimodality Therapy Kimberley S. Mak, MD, MPH Assistant Professor Boston Medical Center Boston University
Point/Counterpoint: Quality of Life Considerations for Patients with Muscle Invasive Bladder Cancer Pro Trimodality Therapy Kimberley S. Mak, MD, MPH Assistant Professor Boston Medical Center Boston University
A Simplified Urinary Incontinence Score for the Evaluation of Treatment Outcomes
 Neurourology and Urodynamics 19:127 135 (2000) A Simplified Urinary Incontinence Score for the Evaluation of Treatment Outcomes Asnat Groutz, Jerry G. Blaivas,* and Jarrod E. Rosenthal Weill Medical College,
Neurourology and Urodynamics 19:127 135 (2000) A Simplified Urinary Incontinence Score for the Evaluation of Treatment Outcomes Asnat Groutz, Jerry G. Blaivas,* and Jarrod E. Rosenthal Weill Medical College,
Sacral neuromodulation (SNM), using permanent foramen S3 electrode, Early versus late treatment of voiding dysfunction with pelvic neuromodulation
 ORIGINAL RESEARCH Early versus late treatment of voiding dysfunction with pelvic neuromodulation Magdy M. Hassouna, MD, PhD; Mohamed S. Elkelini, MD See related article on page 111 Abstract Introduction:
ORIGINAL RESEARCH Early versus late treatment of voiding dysfunction with pelvic neuromodulation Magdy M. Hassouna, MD, PhD; Mohamed S. Elkelini, MD See related article on page 111 Abstract Introduction:
Original Policy Date
 MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
Short-term evaluation of the adjustable bulbourethral male sling for post-prostatectomy urinary incontinence
 Received: 26 September 2017 Revised: 9 March 2018 Accepted: 23 April 2018 DOI: 10.1111/luts.12227 ORIGINAL ARTICLE Short-term evaluation of the adjustable bulbourethral male sling for post-prostatectomy
Received: 26 September 2017 Revised: 9 March 2018 Accepted: 23 April 2018 DOI: 10.1111/luts.12227 ORIGINAL ARTICLE Short-term evaluation of the adjustable bulbourethral male sling for post-prostatectomy
VOIDING DYSFUNCTION IN ELDERLY MALE CURRENT STATUS
 VOIDING DYSFUNCTION IN ELDERLY MALE CURRENT STATUS DR. FRANCIS LEE Voiding dysfunction Storage Emptying Common voiding dysfunction in elderly male Emptying BPH Storage Incontinence Overactive bladder Post-prostatectomy
VOIDING DYSFUNCTION IN ELDERLY MALE CURRENT STATUS DR. FRANCIS LEE Voiding dysfunction Storage Emptying Common voiding dysfunction in elderly male Emptying BPH Storage Incontinence Overactive bladder Post-prostatectomy
A New Artificial Urinary Sphincter with Conditional Occlusion for Stress Urinary Incontinence: Preliminary Clinical Results
 european urology xxx (2006) xxx xxx available at www.sciencedirect.com journal homepage: www.europeanurology.com Ageing Male A New Artificial Urinary Sphincter with Conditional Occlusion for Stress Urinary
european urology xxx (2006) xxx xxx available at www.sciencedirect.com journal homepage: www.europeanurology.com Ageing Male A New Artificial Urinary Sphincter with Conditional Occlusion for Stress Urinary
2017 American Medical Association. All rights reserved.
 Supplementary Online Content Borocas DA, Alvarez J, Resnick MJ, et al. Association between radiation therapy, surgery, or observation for localized prostate cancer and patient-reported outcomes after 3
Supplementary Online Content Borocas DA, Alvarez J, Resnick MJ, et al. Association between radiation therapy, surgery, or observation for localized prostate cancer and patient-reported outcomes after 3
Prostate Cancer: 2010 Guidelines Update
 Prostate Cancer: 2010 Guidelines Update James L. Mohler, MD Chair, NCCN Prostate Cancer Panel Associate Director for Translational Research, Professor and Chair, Department of Urology, Roswell Park Cancer
Prostate Cancer: 2010 Guidelines Update James L. Mohler, MD Chair, NCCN Prostate Cancer Panel Associate Director for Translational Research, Professor and Chair, Department of Urology, Roswell Park Cancer
Laparoscopic Surgery. The Da Vinci Robot. Limits of Laparoscopy. What Robotics Offers. Robotic Urologic Surgery: A New Era in Patient Care
 Laparoscopic Surgery Robotic Urologic Surgery: A New Era in Patient Care Laparoscopic technique was introduced in urologic surgery in the 1990s Benefits: Improved recovery time, decreased morbidity Matthew
Laparoscopic Surgery Robotic Urologic Surgery: A New Era in Patient Care Laparoscopic technique was introduced in urologic surgery in the 1990s Benefits: Improved recovery time, decreased morbidity Matthew
Detrusor underactivity is prevalent after radical prostatectomy: a urodynamic study including risk factors
 original research Detrusor underactivity is prevalent after radical prostatectomy: a urodynamic study including risk factors Doreen E. Chung, MD, FRCSC; * Benjamin Dillon, MD; Jordan Kurta, MD; Alexandra
original research Detrusor underactivity is prevalent after radical prostatectomy: a urodynamic study including risk factors Doreen E. Chung, MD, FRCSC; * Benjamin Dillon, MD; Jordan Kurta, MD; Alexandra
6 Page Male Incontinence Booklet 10/09/ :44 Page 1. The Natural Non-Surgical Option for Male Urinary Incontinence
 6 Page Male Incontinence Booklet /9/ :44 Page The Natural Non-Surgical Option for Male Urinary Incontinence 6 Page Male Incontinence Booklet /9/ :44 Page Stress Urinary Incontinence - A Stressful Prospect
6 Page Male Incontinence Booklet /9/ :44 Page The Natural Non-Surgical Option for Male Urinary Incontinence 6 Page Male Incontinence Booklet /9/ :44 Page Stress Urinary Incontinence - A Stressful Prospect
European Urology 47 (2005)
 European Urology European Urology 47 (2005) 209 213 The Comparison of Artificial Urinary Sphincter Implantation and Endourethral Macroplastique Injection for thetreatment of Postprostatectomy Incontinence
European Urology European Urology 47 (2005) 209 213 The Comparison of Artificial Urinary Sphincter Implantation and Endourethral Macroplastique Injection for thetreatment of Postprostatectomy Incontinence
Periurethral constrictor: late results of the treatment of post prostatectomy urinary incontinence
 Clinical Urology International Braz J Urol Vol 37 (4): 483-487, July - August, 2011 Periurethral constrictor: late results of the treatment of post prostatectomy urinary incontinence Roberto S. Lima, Evandilson
Clinical Urology International Braz J Urol Vol 37 (4): 483-487, July - August, 2011 Periurethral constrictor: late results of the treatment of post prostatectomy urinary incontinence Roberto S. Lima, Evandilson
Inception Cohort. Center for Evidence-Based Medicine, Oxford VIP-- Inception Cohort (2008) Nov Dec
 VIP-- Inception Cohort (28) Robotic Prostatectomy: Oncological and Functional Outcomes after 4 cases The Donald Smith Lecture Nov 2- Dec 28---- ----42 patients Patient 1 to patient 38 PSA follow-up -------3481
VIP-- Inception Cohort (28) Robotic Prostatectomy: Oncological and Functional Outcomes after 4 cases The Donald Smith Lecture Nov 2- Dec 28---- ----42 patients Patient 1 to patient 38 PSA follow-up -------3481
Quality of Life After Modern Treatment Options for Prostate Cancer Ronald Chen, MD, MPH
 Quality of Life After Modern Treatment Options I will be presenting some recently published data on the quality of life after modern treatment options for prostate cancer. My name is Dr. Ronald Chen. I'm
Quality of Life After Modern Treatment Options I will be presenting some recently published data on the quality of life after modern treatment options for prostate cancer. My name is Dr. Ronald Chen. I'm
Stereotactic Ablative Radiotherapy for Prostate Cancer
 Stereotactic Ablative Radiotherapy for Prostate Cancer Laurie Cuttino, MD Associate Professor of Radiation Oncology VCU Massey Cancer Center Director of Radiation Oncology Sarah Cannon Cancer Center at
Stereotactic Ablative Radiotherapy for Prostate Cancer Laurie Cuttino, MD Associate Professor of Radiation Oncology VCU Massey Cancer Center Director of Radiation Oncology Sarah Cannon Cancer Center at
Information for men considering a male sling procedure UHB is a no smoking Trust
 Information for men considering a male sling procedure UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Introduction
Information for men considering a male sling procedure UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Introduction
ORIGINAL ARTICLE ABSTRACT ARTICLE INFO
 ORIGINAL ARTICLE Vol. 44 (6): 1215-1223, November - December, 2018 doi: 10.1590/S1677-5538.IBJU.2018.0128 Artificial sphincter BR - SL - AS 904 in the treatment of urinary incontinence after radical prostatectomy:
ORIGINAL ARTICLE Vol. 44 (6): 1215-1223, November - December, 2018 doi: 10.1590/S1677-5538.IBJU.2018.0128 Artificial sphincter BR - SL - AS 904 in the treatment of urinary incontinence after radical prostatectomy:
The role of synthetic slings in male stress incontinence
 Arab Journal of Urology (2011) 9, 129 134 Arab Journal of Urology (Official Journal of the Arab Association of Urology) www.sciencedirect.com URODYNAMICS/FEMALE UROLOGY ORIGINAL ARTICLE The role of synthetic
Arab Journal of Urology (2011) 9, 129 134 Arab Journal of Urology (Official Journal of the Arab Association of Urology) www.sciencedirect.com URODYNAMICS/FEMALE UROLOGY ORIGINAL ARTICLE The role of synthetic
Does RT favor RP in long term Quality of Life? Juanita Crook MD FRCPC Professor of Radiation Oncology University of British Columbia
 Does RT favor RP in long term Quality of Life? Juanita Crook MD FRCPC Professor of Radiation Oncology University of British Columbia Disclosures Advisory Board/honoraria: Varian Advisory Board: Breast
Does RT favor RP in long term Quality of Life? Juanita Crook MD FRCPC Professor of Radiation Oncology University of British Columbia Disclosures Advisory Board/honoraria: Varian Advisory Board: Breast
UI α (n=150) Mean (SD) or N (%)
 Supplementary Table 1: Descriptive characteristics of male LURN participants Overall (n=477) UI α (n=150) PVD β (n=211) non-ui γ (n=116) * Age 60.9 (13.3) 63.5 (11.5) 57.9 (14.1) 63.1 (12.8) 0.001 Race
Supplementary Table 1: Descriptive characteristics of male LURN participants Overall (n=477) UI α (n=150) PVD β (n=211) non-ui γ (n=116) * Age 60.9 (13.3) 63.5 (11.5) 57.9 (14.1) 63.1 (12.8) 0.001 Race
EUROPEAN UROLOGY 56 (2009)
 EUROPEAN UROLOGY 56 (2009) 923 927 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Incontinence Editorial by Drogo K. Montague on pp. 934 935 of this issue
EUROPEAN UROLOGY 56 (2009) 923 927 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Incontinence Editorial by Drogo K. Montague on pp. 934 935 of this issue
Satisfaction and Regret after Open Retropubic or Robot- Assisted Laparoscopic Radical Prostatectomy
 european urology 54 (2008) 785 793 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer Satisfaction and Regret after Open Retropubic or Robot- Assisted Laparoscopic
european urology 54 (2008) 785 793 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer Satisfaction and Regret after Open Retropubic or Robot- Assisted Laparoscopic
Authors KC Cheng, LF Lee, KW Wong, HC Chan, CL Cho, H Chau, KM Lam, HS So. Division of Urology, Department of Surgery, United Christian Hospital
 Efficacy of Routine Screening of Urine Culture before Transurethral Prostatectomy on the Improvement of the Post Operative Outcome - a Single Centre Experience Authors KC Cheng, LF Lee, KW Wong, HC Chan,
Efficacy of Routine Screening of Urine Culture before Transurethral Prostatectomy on the Improvement of the Post Operative Outcome - a Single Centre Experience Authors KC Cheng, LF Lee, KW Wong, HC Chan,
When PSA fails. Urology Grand Rounds Alexandra Perks. Rising PSA after Radical Prostatectomy
 When PSA fails Urology Grand Rounds Alexandra Perks Rising PSA after Radical Prostatectomy Issues Natural History Local vs Metastatic Treatment options 1 10 000 men / year in Canada 4000 RRP 15-year PSA
When PSA fails Urology Grand Rounds Alexandra Perks Rising PSA after Radical Prostatectomy Issues Natural History Local vs Metastatic Treatment options 1 10 000 men / year in Canada 4000 RRP 15-year PSA
MARK S. SHIMKO, M.D. Chesapeake Urology Associates, LLC
 MARK S. SHIMKO, M.D. Chesapeake Urology Associates, LLC 1342 S. Division Street, Unit 401 Salisbury, MD 21804 410-546-2133 314 Franklin Avenue, Suite 302 Berlin, MD 21811 410-641-3735 1340 Middleford Road,
MARK S. SHIMKO, M.D. Chesapeake Urology Associates, LLC 1342 S. Division Street, Unit 401 Salisbury, MD 21804 410-546-2133 314 Franklin Avenue, Suite 302 Berlin, MD 21811 410-641-3735 1340 Middleford Road,
Preoperative Gleason score, percent of positive prostate biopsies and PSA in predicting biochemical recurrence after radical prostatectomy
 JBUON 2013; 18(4): 954-960 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Gleason score, percent of positive prostate and PSA in predicting biochemical
JBUON 2013; 18(4): 954-960 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Gleason score, percent of positive prostate and PSA in predicting biochemical
EAU GUIDELINES POCKET EDITION 3
 EAU GUIDELINES POCKET EDITION 3 CONTENTS: BENIGN PROSTATIC HYPERPLASIA URINARY INCONTINENCE UROLITHIASIS 2 3 EAU POCKET GUIDELINES POCKET EDITION 3 This is one of a series of convenient pocket size books
EAU GUIDELINES POCKET EDITION 3 CONTENTS: BENIGN PROSTATIC HYPERPLASIA URINARY INCONTINENCE UROLITHIASIS 2 3 EAU POCKET GUIDELINES POCKET EDITION 3 This is one of a series of convenient pocket size books
How to select the right patient for the right treatment: What role does sexuality play in Pca treatment?
 How to select the right patient for the right treatment: What role does sexuality play in Pca treatment? Andrea Salonia, MD, PhD, FECSM Università Vita-Salute San Raffaele Director, URI-Urological Research
How to select the right patient for the right treatment: What role does sexuality play in Pca treatment? Andrea Salonia, MD, PhD, FECSM Università Vita-Salute San Raffaele Director, URI-Urological Research
Suburethral sling at the time of radical prostatectomy in patients at high risk of postoperative incontinence
 Original Article IMMEDIATE SLING DURING RP IN HIGH-RISK PATIENTS WESTNEY et al. Suburethral sling at the time of radical prostatectomy in patients at high risk of postoperative incontinence O. LENAINE
Original Article IMMEDIATE SLING DURING RP IN HIGH-RISK PATIENTS WESTNEY et al. Suburethral sling at the time of radical prostatectomy in patients at high risk of postoperative incontinence O. LENAINE
University of Alberta Reconstructive Urology Fellowship
 FACULTY OF MEDICINE AND DENTISTRY DEPARTMENT OF SURGERY DIVISION OF UROLOGY Keith Rourke, MD, FRCSC Reconstructive Urology Professor Chair of Academic Urology Reconstructive Urology Fellowship Director
FACULTY OF MEDICINE AND DENTISTRY DEPARTMENT OF SURGERY DIVISION OF UROLOGY Keith Rourke, MD, FRCSC Reconstructive Urology Professor Chair of Academic Urology Reconstructive Urology Fellowship Director
A comparison of preliminary oncologic outcome and postoperative complications between patients undergoing either open or robotic radical cystectomy
 ORIGINAL ARTICLE Vol. 42 (4): 663-670, July - August, 2016 doi: 10.1590/S1677-5538.IBJU.2015.0393 A comparison of preliminary oncologic outcome and postoperative complications between patients undergoing
ORIGINAL ARTICLE Vol. 42 (4): 663-670, July - August, 2016 doi: 10.1590/S1677-5538.IBJU.2015.0393 A comparison of preliminary oncologic outcome and postoperative complications between patients undergoing
Role of androgens for urethral homeostasis
 Original Article Role of androgens for urethral homeostasis Matthias D. Hofer 1, Allen F. Morey 2 1 Department of Urology, Northwestern University, Chicago, IL, USA; 2 Department of Urology, UT Southwestern,
Original Article Role of androgens for urethral homeostasis Matthias D. Hofer 1, Allen F. Morey 2 1 Department of Urology, Northwestern University, Chicago, IL, USA; 2 Department of Urology, UT Southwestern,
Tomonori Yamanishi,* Tomoya Mizuno, Miho Watanabe, Mikihiko Honda and Ken-Ichiro Yoshida
 Randomized, Placebo Controlled Study of Electrical Stimulation With Pelvic Floor Muscle Training for Severe Urinary Incontinence After Radical Prostatectomy Tomonori Yamanishi,* Tomoya Mizuno, Miho Watanabe,
Randomized, Placebo Controlled Study of Electrical Stimulation With Pelvic Floor Muscle Training for Severe Urinary Incontinence After Radical Prostatectomy Tomonori Yamanishi,* Tomoya Mizuno, Miho Watanabe,
NIH Public Access Author Manuscript World J Urol. Author manuscript; available in PMC 2012 February 1.
 NIH Public Access Author Manuscript Published in final edited form as: World J Urol. 2011 February ; 29(1): 11 14. doi:10.1007/s00345-010-0625-4. Significance of preoperative PSA velocity in men with low
NIH Public Access Author Manuscript Published in final edited form as: World J Urol. 2011 February ; 29(1): 11 14. doi:10.1007/s00345-010-0625-4. Significance of preoperative PSA velocity in men with low
Erectile Dysfunction (ED) after Radiotherapy (RT) for Prostate Cancer. William M. Mendenhall, MD
 Erectile Dysfunction (ED) after Radiotherapy (RT) for Prostate Cancer William M. Mendenhall, MD Meta-Analysis of Probability of Maintaining Erectile Function after Treatment of Localized Cancer Treatment
Erectile Dysfunction (ED) after Radiotherapy (RT) for Prostate Cancer William M. Mendenhall, MD Meta-Analysis of Probability of Maintaining Erectile Function after Treatment of Localized Cancer Treatment
Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP)
 JRural Med 2007 ; 2 : 93 97 Original article Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP) Shuzo Hamamoto 1,TakehikoOkamura 1,HideyukiKamisawa 1,KentaroMizuno 1,
JRural Med 2007 ; 2 : 93 97 Original article Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP) Shuzo Hamamoto 1,TakehikoOkamura 1,HideyukiKamisawa 1,KentaroMizuno 1,
1. Introduction. 2. Methods. high-risk NMIBC in men with and without a prior history of RT for PC.
 ISRN Urology Volume 2013, Article ID 405064, 5 pages http://dx.doi.org/10.1155/2013/405064 Research Article Radical Cystectomy after BCG Immunotherapy for High-Risk Nonmuscle-Invasive Bladder Cancer in
ISRN Urology Volume 2013, Article ID 405064, 5 pages http://dx.doi.org/10.1155/2013/405064 Research Article Radical Cystectomy after BCG Immunotherapy for High-Risk Nonmuscle-Invasive Bladder Cancer in
Anatomical and Functional Results of Pelvic Organ Prolapse Mesh Repair: A Prospective Study of 105 Cases
 International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
Survivorship Beyond Convalescence: 48-Month Quality-of-Life Outcomes After Treatment for Localized Prostate Cancer
 BRIEF COMMUNICATION Survivorship Beyond Convalescence: 48-Month Quality-of-Life Outcomes After Treatment for Localized Prostate Cancer John L. Gore, Lorna Kwan, Steve P. Lee, Robert E. Reiter, Mark S.
BRIEF COMMUNICATION Survivorship Beyond Convalescence: 48-Month Quality-of-Life Outcomes After Treatment for Localized Prostate Cancer John L. Gore, Lorna Kwan, Steve P. Lee, Robert E. Reiter, Mark S.
Prostate Cancer Treatment Decision Information Background
 Prostate Cancer Treatment Decision Information Background A group of Radiotherapy Clinics of Georgia (RCOG) prostate cancer (PCa) patients developed this web site, in part, based on a slide presentation
Prostate Cancer Treatment Decision Information Background A group of Radiotherapy Clinics of Georgia (RCOG) prostate cancer (PCa) patients developed this web site, in part, based on a slide presentation
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/28958 holds various files of this Leiden University dissertation Author: Keurentjes, Johan Christiaan Title: Predictors of clinical outcome in total hip
Cover Page The handle http://hdl.handle.net/1887/28958 holds various files of this Leiden University dissertation Author: Keurentjes, Johan Christiaan Title: Predictors of clinical outcome in total hip
Evaluation of Sexual Dysfunction in Lower Urinary Tract Symptoms/Benign Prostatic Hyperplasia Patients
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/10 Evaluation of Sexual Dysfunction in Lower Urinary Tract Symptoms/Benign Prostatic Hyperplasia Patients N. Narayanamoorthy,
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/10 Evaluation of Sexual Dysfunction in Lower Urinary Tract Symptoms/Benign Prostatic Hyperplasia Patients N. Narayanamoorthy,
Management of the devastated posterior urethra and bladder neck: refractory incontinence and stenosis
 Review Article Management of the devastated posterior urethra and bladder neck: refractory incontinence and stenosis Kirk M. Anderson, Ty T. Higuchi, Brian J. Flynn Division of Urology, University of Colorado
Review Article Management of the devastated posterior urethra and bladder neck: refractory incontinence and stenosis Kirk M. Anderson, Ty T. Higuchi, Brian J. Flynn Division of Urology, University of Colorado
Policy #: 370 Latest Review Date: December 2013
 Name of Policy: Nerve Graft in Association with Radical Prostatectomy Policy #: 370 Latest Review Date: December 2013 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits
Name of Policy: Nerve Graft in Association with Radical Prostatectomy Policy #: 370 Latest Review Date: December 2013 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits
Posterior Rhabdosphincter Reconstruction During Robotic Assisted Radical Prostatectomy: Results From a Phase II Randomized Clinical Trial
 Posterior Rhabdosphincter Reconstruction During Robotic Assisted Radical Prostatectomy: Results From a Phase II Randomized Clinical Trial Douglas E. Sutherland, Brian Linder, Anna M. Guzman, Mark Hong,
Posterior Rhabdosphincter Reconstruction During Robotic Assisted Radical Prostatectomy: Results From a Phase II Randomized Clinical Trial Douglas E. Sutherland, Brian Linder, Anna M. Guzman, Mark Hong,
Survival outcomes for men in rural and remote NSW. Trend in prostate cancer incidence and mortality rates in Australia. The prostate cancer conundrum
 7/8/20 7/8/20 Using PROMS to better understand prostate cancer outcomes: The NSW Prostate Cancer Care and Outcomes Study David Smith Research Fellow Cancer Research Division Monash Uni, 26 th June 20 Survival
7/8/20 7/8/20 Using PROMS to better understand prostate cancer outcomes: The NSW Prostate Cancer Care and Outcomes Study David Smith Research Fellow Cancer Research Division Monash Uni, 26 th June 20 Survival
Hong Kong College of Surgical Nursing
 Hong Kong College of Surgical Nursing Higher Surgical Nursing Training: Part B Specialty - Urological Nursing Curriculum TABLE OF CONTENTS No. Contents Page. Introduction. Aims. Learning Objectives 4.
Hong Kong College of Surgical Nursing Higher Surgical Nursing Training: Part B Specialty - Urological Nursing Curriculum TABLE OF CONTENTS No. Contents Page. Introduction. Aims. Learning Objectives 4.
Management of Voiding Dysfunction after Prostate Radiotherapy
 Management of Voiding Dysfunction after Prostate Radiotherapy Up to Date Symposium on Uro-Oncology December 7, 2012 Belo Horizonte, Brazil Jaspreet S. Sandhu, MD Department of Surgery/Urology Memorial
Management of Voiding Dysfunction after Prostate Radiotherapy Up to Date Symposium on Uro-Oncology December 7, 2012 Belo Horizonte, Brazil Jaspreet S. Sandhu, MD Department of Surgery/Urology Memorial
Policy #: 213 Latest Review Date: September 2012
 Name of Policy: Temporary Prostatic Stent Policy #: 213 Latest Review Date: September 2012 Category: Medicine Policy Grade: Active Policy but no longer scheduled for regular literature reviews and updates.
Name of Policy: Temporary Prostatic Stent Policy #: 213 Latest Review Date: September 2012 Category: Medicine Policy Grade: Active Policy but no longer scheduled for regular literature reviews and updates.
PRE-OPERATIVE URODYNAMIC
 PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
Urinary Incontinence. Vibhash Mishra Consultant Urological Surgeon Royal Free Hospital
 Urinary Incontinence Vibhash Mishra Consultant Urological Surgeon Royal Free Hospital Affects women of all ages Impacts physical, psychological & social wellbeing Impact on families & carers Costs the
Urinary Incontinence Vibhash Mishra Consultant Urological Surgeon Royal Free Hospital Affects women of all ages Impacts physical, psychological & social wellbeing Impact on families & carers Costs the
Subject Index. Androgen antiandrogen therapy, see Hormone ablation therapy, prostate cancer synthesis and metabolism 49
 OOOOOOOOOOOOOOOOOOOOOOOOOOOOOO Subject Index Androgen antiandrogen therapy, see Hormone ablation therapy, synthesis and metabolism 49 Bacillus Calmette-Guérin adjunct therapy with transurethral resection
OOOOOOOOOOOOOOOOOOOOOOOOOOOOOO Subject Index Androgen antiandrogen therapy, see Hormone ablation therapy, synthesis and metabolism 49 Bacillus Calmette-Guérin adjunct therapy with transurethral resection
Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study
 Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study Yvonne KY CHENG MBChB, MRCOG William WK TO MBBS, M Phil, FRCOG, FHKAM (O&G) HX
Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study Yvonne KY CHENG MBChB, MRCOG William WK TO MBBS, M Phil, FRCOG, FHKAM (O&G) HX
Facing Prostate Cancer Surgery? Learn about minimally invasive da Vinci Surgery
 Facing Prostate Cancer Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Prostate Cancer Your prostate is a walnut-sized gland that is part of the male reproductive system. The prostate
Facing Prostate Cancer Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Prostate Cancer Your prostate is a walnut-sized gland that is part of the male reproductive system. The prostate
