Despite the growing body of medical
|
|
|
- Virgil Lionel Lang
- 5 years ago
- Views:
Transcription
1 SURGICAL TECHNIQUES BY VINCENT R. LUCENTE, MD, MBA, AND MILES MURPHY, MD Laparoscopic Burch colposuspension for stress urinary incontinence: When, how, and why? Female SUI is a common condition without a clear-cut surgical solution. Here, the authors offer step-by-step guidance on a laparoscopic technique to effectively treat this growing problem. Despite the growing body of medical knowledge on stress urinary incontinence (SUI), controversies over its management remain. SUI is the most common type of incontinence and occurs almost exclusively in females. A recent survey by the National Association for Continence revealed that SUI affects approximately 16.5 million women in the United States. 1 Nearly two thirds of these women are under 50 years of age. KEY POINTS Laparoscopic Burch colposuspension provides high long-term success rates, reduced morbidity, and accelerated convalescence. A growing number of studies have shown the laparoscopic Burch to have results similar to traditional laparotomy when conventional surgical techniques and suture materials are used. When we limit the discussion to 2 comparable techniques a laparoscopic versus open 2-suture procedure there is moderately strong evidence that the laparoscopic approach maintains efficacy while modestly reducing morbidity. The selection of suture material and the total number and placement of sutures are crucial to the long-term cure rate. Still, there is no surgical procedure of choice for women with this condition. In fact, a recent systematic review of the literature by Black and Downs could not determine the best procedure based on scientific clinical evidence. 2 Among the large number of surgical options for SUI treatment is bladder-neck suspension via a laparoscopic Burch colposuspension. When it is properly executed, this procedure offers high long-term success rates, reduced morbidity, and accelerated convalescence. In this article, we describe how to perform the laparoscopic Burch procedure (reviewing both conventional suturing techniques and the Tanagho modification) 3 and discuss when to consider a laparoscopic approach. In addition, we explain why the procedure should be part of your surgical options for female SUI. Dr. Lucente is medical director of the Institute for Female Pelvic Medicine and Reconstructive Surgery in Allentown, Pa, and associate professor of clinical OBG, Pennsylvania State University College of Medicine, Hershey, Pa. Dr. Murphy is clinical instructor in the division of female pelvic medicine and reconstructive surgery, University of Louisville, Louisville, Ky. 20 OBG MANAGEMENT February 2003
2 Laparoscopic Burch colposuspension for stress urinary incontinence Retropubic versus transvaginal suspensions ith so many surgeries to choose from, Wdetermining which procedure would be best for a woman with genuine stress urinary incontinence is a challenge. In 1997, the American Urological Association published a report designed to offer some guidance. An 8-member panel reviewed data from 282 articles, all of which followed patients for a minimum of 12 months for short-term cure/dry results, and 48 months for long-term results. The Report on the Surgical Management of Female Stress Urinary Incontinence based on expert opinion and evidence from the literature (as determined by probability estimates) stated that retropubic suspensions and slings are the most efficacious procedures for long-term success. Still, the panel noted that these interventions are associated with slightly higher complication rates including an increased incidence of voiding dysfunction and longer convalescence than other SUI procedures. For patients willing to accept these complication rates for the sake of improved long-term success, the panel concluded, retropubic suspension and slings are appropriate. However, for patients valuing a decreased hospital stay, reduced morbidity, and an earlier return to normal activity, transvaginal suspensions the only minimally invasive option widely offered at that time were the better option. 4 The Burch procedure n the classic Burch colposuspension, a Iphysician places 2 bilateral nonabsorbable sutures through the pubocervical fascia 1 at the level of the midurethra, the other at the urethrovesical junction (UVJ) and fixes them to Cooper s ligament. But since 1991, when Vancaille and Schuessler introduced a laparoscopic approach to a retropubic colposuspension (MMK technique), 5 a growing number of studies have shown the laparoscopic Burch to have results similar to traditional laparotomy when conventional surgical techniques and suture materials are used A number of reports have also described modifications or alternatives to the classic laparoscopic Burch These variations Retropubic suspensions and slings are associated with slightly higher complication rates than other SUI procedures. which use stapling devices, mesh placement, bone anchors, and even fibrin glue avoid laparoscopic suturing, thereby reducing the surgical complexity and shortening the learning curve. They also may lower the cost per procedure by decreasing time in the operating room Still, an experienced laparoscopist who has mastered endoscopic suturing can perform a laparoscopic Burch using standard suturing in a time frame comparable to that of one of the modifications. 33 As far as outcomes go, it is the selection of suture material, the total number of sutures used, and their proper placement that are crucial to an optimal long-term cure rate regardless of the surgical access to the space of Retzius In fact, if a surgeon laparoscopically employs the identical operative technique, suture for suture, that he or she would use via laparotomy, there is no biological reason why the continence cure rates would be any different. When? Burch procedure versus the TVT sling everal studies have demonstrated that for Spatients with intrinsic sphincter deficiency (ISD) the Burch colposuspension cure/dry rate is less than that of a standard sling procedure. 37 We therefore obtain urodynamic studies on all patients presenting with SUI who we feel are at risk for ISD (TABLE). For patients with ISD and urethral hypermobility, we recommend the minimally invasive pubo- February 2003 OBG MANAGEMENT 23
3 Laparoscopic Burch colposuspension for stress urinary incontinence TABLE Patients at risk for intrinsic sphincter deficiency Age > 60 years History of prior incontinence surgery History of pelvic radiation Positive standing stress test without hypermobility Positive standing stress test with an empty bladder Leakage much greater than stress load Decreased tactile resistance when placing a cotton swab transurethrally vaginal sling tension-free vaginal tape (TVT) procedure. In the absence of urethral hypermobility, we first utilize periurethral bulking agents to correct the ISD. If this is not successful, we proceed with urethrolysis and a traditional sling procedure. For women who have concomitant pelvicsupport defects such as uterine prolapse, vaginal vault inversion, or lateral cystoceles, we routinely perform laparoscopic reconstructive surgery, including the laparoscopic Burch for correction of the SUI. Still, the difficult question remains: Which minimally invasive procedure a laparoscopic Burch or a TVT is preferable for the patient with genuine SUI without ISD or any additional pelvic-support defects aside from urethral hypermobility? Only a few studies comparing the clinical outcomes of the TVT and laparoscopic Burch procedures have reported preliminary findings. One retrospective study of 74 women followed for at least 1 year demonstrated an overall objective cure rate of 88% for the laparoscopic Burch versus 92% for the TVT procedure. 38 There were no significant differences in time to resumption of normal voiding or in irritative symptoms such as frequency, urgency, and urge incontinence. The TVT group, however, was noted to have a shorter operative time and hospital stay. Another study reported a higher cure or improvement rate (94%) among patients undergoing the laparoscopic Burch than the TVT (82%). Postoperative voiding difficulty was also significantly less in the laparoscopic group (0% versus 18%). 39 Although these early studies suggest that laparoscopic Burch and TVT are comparable, we anxiously await the results of welldesigned, prospective, randomized clinical trials currently under way. One recent report (level I evidence) has demonstrated that the open Burch and the TVT procedure have equivalent results. 40 How? The laparoscopic Burch technique Preparing the patient. As always, obtain informed consent prior to the procedure. Beyond the usual surgical risks of blood loss, infection, surgical injury, failure rate, and thromboembolic complications, patients also face potential postoperative voiding dysfunction, as mentioned earlier, as well as de novo detrusor instability. Also inform your patients of the possible conversion to laparotomy. Administer a single intravenous dose of an appropriate broad-spectrum antibiotic no more than 1 hour prior to surgery. For patients undergoing additional laparoscopic reconstructive surgery, we recommend a modified bowel preparation to improve visualization by decompressing the sigmoid colon. Administer general anesthesia and place the patient in a dorsal lithotomy position with both arms tucked. Support the patient s lower extremities with Allen Universal Stirrups (Allen Medical Systems, Mayfield, Ohio) and avoid excessive flexion of the knees or hips. Insert a 16F 3-way Foley catheter into the bladder this allows intermittent bladder fill- 24 OBG MANAGEMENT February 2003
4 ing during the procedure and inflate the bulb to 10 cc to facilitate identification of the UVJ throughout surgery. Entering the space of Retzius. We routinely perform operative laparoscopy after Veress needle insertion and insufflation through an umbilical incision. (Use open laparoscopy for patients with prior abdominal surgery and paraumbilical scarring.) Under direct visualization, place 2 additional accessory 10-mm trocars in the lower quadrants, just lateral to the inferior epigastric arteries. Brief insufflation to greater than 20 mm Hg intra-abdominal pressure facilitates safe entry for these secondary trocars. Although you may opt for smaller trocars, the 10-mm size allows unhindered passage of suture, thus providing more options for maximizing favorable ergonomics with future suture placement. Although a preperitoneal, or extraperitoneal, approach has been described, we favor a transperitoneal entrance into the space of Retzius. The extraperitoneal approach allows With experience, a transperitoneal approach into the space of Retzius will not prolong operative time. the use of regional anesthesia, avoids intraabdominal adhesions, and eliminates the associated risks of peritoneal entry. 31 The disadvantages, however, are significant, including failure to enter the retropubic space secondary to abdominal wall scarring, the inability to perform concomitant vault suspension, and the cost of commercially available dissecting balloons. With experience, a transperitoneal approach will not prolong operative time. Approaching the bladder. Distend the bladder in a retrograde fashion with 300 ml to
5 Laparoscopic Burch colposuspension for stress urinary incontinence FIGURE 1 FIGURE 2 Pictured is the distended bladder, forceps (right) at the bladder margin, endoshears (left) at level of incision, and urachus. Create a transverse incision using monopolar scissors. Note the loose areolar tissue of prevesicle space. FIGURE 3 FIGURE 4 Locate the pubic symphysis and ramus using the pelvic brim as a landmark. Apply medial traction to the bladder as the paravesical space is developed down to the level of pubocervical fascia. Note Cooper s ligament, seen anteriorly. FIGURE 5 FIGURE 6 Gently remove the overlying periurethral and perivesical fat to expose white pubocervical fascia. Apply counter traction on the suture from the first pass to facilitate better tissue purchase on the second pass of the helical suture. 26 OBG MANAGEMENT February 2003
6 Laparoscopic Burch colposuspension for stress urinary incontinence FIGURE 7 FIGURE 8 Place the needle through Cooper s ligament. Pass the second needle at a deeper depth through Cooper s ligament to encircle fibers within the suture. This will minimize the risk of pull out. FIGURE 9 FIGURE 10 Place both sutures before extracorporeal tying. Suture tension should create only a small knuckle of pubocervical fascia, approximating obturator fascia laterally. FIGURE 11 FIGURE 12 Both sides completed. Close the retropubic space. February 2003 OBG MANAGEMENT 29
7 Laparoscopic Burch colposuspension for stress urinary incontinence 400 ml of normal saline. This allows identification of the superior margin of the bladder dome and provides mass traction posteriorly. Use the urachus to identify the midline; then, grasp the anterior abdominal wall peritoneum and apply downward traction (FIG- URE 1). Next, create a transverse incision 3 cm to 4 cm above the bladder reflection, using monopolar endoscopic scissors on a 70-watt pure-cut setting (FIGURE 2). The incision should be within the obliterated umbilical ligaments, but can be extended slightly beyond for patients undergoing a combined laparoscopic Burch-paravaginal repair. 41 Using a combination of blunt and electrocautery dissection, you then can easily dissect the loose areolar tissue of the prevesicle space down to the level of the pubic symphysis and ramus (FIGURE 3). As the paravesical space is further developed, the pubocervical fascia will become exposed at the level of the UVJ. You must carefully protect the urethra, avoiding aggressive midline dissection as well as the obturator neurovascular bundle laterally. Medial traction on the bladder, perpendicular to the slope of the pubic ramus, encourages identification of the proper surgical plane. Use electrocautery to maintain meticulous hemostasis at all times. Identify Cooper s ligament, and bluntly dissect away any obstructing fat or areolar tissue (FIGURE 4). To encourage scarification, gently remove excessive overlying periurethral and perivesical fat from pubocervical fascia at the level of the bladder neck, while avoiding any dissection within 1 cm lateral to the urethra (FIGURE 5). Placing the sutures. Using an extra-long (36-in), doubled-armed, nonabsorbable suture on an SH needle, place the sutures in the consistent sequence outlined below (note that sturdy needle drivers will facilitate secure needle placement): First, introduce a needle from the contralateral port and pass it through the pubocervical fascia at the level of the midurethra, using 32 OBG MANAGEMENT February 2003
8 your index finger for transvaginal guidance. If you think the tissue bite will not purchase nearly the entire thickness of the anterior vaginal wall, place a second helical throw (FIGURE 6). Next, bring the suture up through Cooper s ligament and store it by hooking the anterior wall peritoneum (FIGURE 7). Bring up the second arm (needle) of the suture through Cooper s ligament, but at a different depth than the first pass so ligament fibers are truly encircled by the suture (FIGURE 8). Retrieve both needles, bringing them out through the same port, but do not yet tie the suture. Introduce the second suture through the ipsilateral port and place it in the same fashion at the level of the UVJ. Again, use helical throws as necessary. Once both sutures have been placed, tie them extracorporeally in sequence using a closed-loop knot pusher. (Waiting until both sutures are placed before tying allows exposure for easy placement of the second suture [FIGURE 9].) The appropriate tension should create a small, localized knuckle of pubocervical fascia that approximates laterally to the obturator internus fascia (FIGURE 10). Repeat this procedure in the same sequence on the opposite side of the pelvis (FIGURE 11), then close the retropubic space using a running continuous 2-0 suture reapproximating the peritoneum (FIGURE 12). Close the laparoscopic ports at the fascia level using a Veress needle threaded with a 0-Vicryl. Both ends of the suture are passed on either side of the fascial incision. Using a contralateral grasping forceps, the suture end is freed from the Veress needle, then retrieved using an ipsilateral forceps. This port closure technique is easy to perform as well as cost- effective. Postoperative care. Place a suprapubic catheter with a 2-way stop clock; this makes postoperative voiding trials easier for both patients and nursing staff. Most patients will be discharged the day after surgery. If the patient still has an elevated postvoid residual, she ll likely find going home with the suprapubic catheter more acceptable than intermittent self-catheterization or an indwelling Foley running to a leg bag. For postoperative discomfort, acetaminophen and nonsteroidal anti-inflammatory preparations are generally sufficient. Patients can resume normal living activities within days, but should be cautioned to delay strenuous work or exercise for at least 8 weeks. Why? A look at the evidence he learning curve for laparoscopic Burch Tis steep and somewhat long approximately 20 cases. The real question, therefore, is whether the benefits justify the time needed to master this procedure. In other words, is there clinical evidence that, once the plateau of this curve has been reached, we can reduce patient morbidity while maintaining efficacy compared to the traditional open technique? If not, there s little reason for surgeons to learn the technique. If there is, however, more physicians should include the laparoscopic Burch in their surgical arsenal. The real question is whether the benefits of the laparoscopic Burch justify the time needed to master the procedure. When we limit the discussion to 2 comparable techniques, a laparoscopic versus open 2-suture procedure, there is moderately strong evidence that the laparoscopic approach maintains efficacy while modestly reducing morbidity. 42 The strength of this evidence is established in 6 studies, including 3 randomized trials (level I evidence). 8,18,23,24,43,44 Currently, data are insufficient regarding a laparoscopic approach to make concomitant site-specific defect repairs However, if the procedures are performed in the same fashion, suture for suture, as their abdominal February 2003 OBG MANAGEMENT 33
9 Laparoscopic Burch colposuspension for stress urinary incontinence counterparts, we should expect to see, as we have with the laparoscopic Burch, similar efficacy rates between the laparoscopic and open approaches. So, in closing, we encourage our colleagues to reignite their interest in learning laparoscopic reconstructive surgery and recommit to reaching that learning curve plateau. Why? We owe it to our patients. REFERENCES 1. National Association for Incontinence Quarterly Report. Summer 2002, Vol 20 No Black NA, Down SH. The effectiveness of surgery for stress incontinence in women: A systematic review. Br J Urol. 1996;78: Tanagho E. Colpocystourethropexy: The way we do it. J Urol. 1976;116: Leach, GE, Dinochowski RR, Appell RA, et al. Female stress urinary incontinence clinical guidelines panel: Report on the surgical management of female stress urinary incontinence. Baltimore, Md: American Urological Association, Inc.; Vancaille TG, Schuessler W. Laparoscopic bladder neck suspension. J Laparoendosc Surg. 1991;1: Albala DM, Schuessler WW, Vancaillie TG. Laparoscopic bladder suspension for the treatment of stress incontinence. Semin Urol. 1992;10: Burton G. A randomized comparison of laparoscopic and open colposuspension [abstract]. Neurourol Urodyn. 1993;16: Polascik TJ, Moore RG, Roseberg MT, Kavoussi LR. Comparison of laparoscopic and open retropubic colposuspension for treatment of stress urinary incontinence. Urology. 1995;45: Liu CY. Laparoscopic treatment of genuine urinary stress incontinence. Clin Obstet Gynecol. 1994;8: Gunn GC, Cooper RP, Gordon NS, Gragnon L. Use of a new device for endoscopic suturing in the laparoscopic Burch procedure. J Am Assoc Gynecol Laparosc. 1994;2: Nezhat CH, Nezhat F, Nezhat CR, et al. Laparoscopic retropubic cystocolposuspension. J Am Assoc Gynecol Laparosc. 1994;1: Lyons TL, Winer WK. Clinical outcomes with laparoscopic approaches and open Burch procedures for urinary stress incontinence. J Am Assoc Gynecol Laparosc. 1995;2: McDougal EM, Klutke CG, Cornell T. Comparison of transvaginal versus laparoscopic bladder neck suspension for stress urinary incontinence. Adult Urol. 1995;45: Ross JW. Laparoscopic Burch repair compared to laparotomy Burch for cure of urinary stress incontinence. Int Urogynecol. 1995;6: Langebrekke A, Dahlstrom B, Eraker R, Urnes A. The laparoscopic Burch procedure: a preliminary report. Acta Obstet Gynecol Scand. 1995;74: Radomski SB, Herschorn S. Laparoscopic Burch bladder neck suspension: early results. J Urol. 1996;155: Ross JW. Two techniques of laparoscopic Burch repair for stress incontinence: a prospective randomized study. J Am Assoc Gynecol Laparoscopists. 1996;3: Lam AM, Jenkins GJ, Hyslop RS. Laparoscopic results. Med J Aust. 1995;162: Su TH, Wang KG, Hsu CY, Wei H, Hong BK. Prospective comparison of laparoscopic and traditional colposuspensions in the treatment of genuine stress incontinence. Acta Obstet Gynecol. 1997;76: Papasakelariou C, Papasakelariou B. Laparoscopic bladder neck suspension. J Am Assoc Gynecol Laparosc. 1997;4: Lobel RW, Davis GD. Long-term results of laparoscopic Burch colposuspension. J Am Assoc Gynecol Laparosc. 1997;4: Ross JW. Multichannel urodynamic evaluation of laparoscopic Burch colposuspension for genuine stress incontinence. Obstet Gynecol. 1998;91: Miannay E, Cosson M, Querleu D, et al. [Comparison of laparoscopic and laparotomy colposuspension in the treatment of urinary stress incontinence. Comparative study of 72 matched cases][french]. Contracept Fertil Sex. 1998;26: Saidi MH, Gallagher MS, Skop IP, et al. Extrperitoneal laparoscopic colposuspension: short-term cure rate, complications and duration of hospital stay in comparison with Burch colposuspension. Obstet Gynecol. 1998;92: Henley C. The Henley staple-suture technique for laparoscopic Burch colposuspension. J Am Assoc Gynecol Laparosc. 1995;2: Das S, Palmer JK. Laparoscopic colposuspension. J Urol. 1995;154: Ou CS, Presthus J, Beadle E. Laparoscopic bladder neck suspension using hernia mesh and surgical staples. J Laparoendosc Surg. 1993;3: Kiilholma P, Haarala M, Polvi II, Makinen J, Chancellor MB. Sutureless colposuspension with fibrin sealant. Tech Urol. 1995;1: Lose G. Laparoscopic Burch colposuspension. Acta Obstet Gynecol Scand Suppl. 1998;168: Miannay E, Cosson M, Lanvin D, et al. Comparison of open retropubic and laparoscopic colposuspension for treatment of stress urinary incontinence. Eur J Obstet Gynecol Reprod Biol. 1998;79: Saidi MH, Sadler RK, Saidi JA. Extraperitoneal laparoscopic colposuspension for genuine urinary stress incontinence. J Am Assoc Gynecol Laparosc. 1998;9: Ou CS, Rowbotham R. Five-year follow-up of a laparoscopic bladder neck suspension using synthetic mesh and surgical staples. J Laparoendosc Adv Surg Techn A. 1999;9: Zullo F, Morelli M, Russo T, et al. Two techniques of laparoscopic retropubic urethropexy. J Am Assoc Gynecol Laparosc. 2001;12: Langer R, Lipshitz Y, Halperin R, et al. Long-term (10-15 years) follow-up after Burch colposuspension for urinary stress incontinence. Int Urogynecol J. 2001; 12: Herbertsson G, Iosif CS. Surgical results and urodynamic studies 10 years after retropubic colpurethropexy. Acta Obstet Gynecol Scand. 1993;72: Parasio M, Falcone T, Walters M. Laparoscopic surgery for genuine stress incontinence. Int Urogynecol J. 1999;10: Horbach NS. Suburethral sling procedures. Urogynecology and Urodynamics: Theory and Practice. 4th ed. Baltimore, Md: Williams and Wilkins; 1996: Vassallo B, Murphy M, Lucente V, Karram M. TVT versus Laparoscopic Burch: a retrospective review at 1-4 years. 27th Scientific Meeting of the Society of Gynecologic Surgeons. March 5-7, Fotte A. Which is the best minimally invasive procedure? TVT versus laparoscopic colposuspension. Presented at the 31st annual meeting of the International Continence Society; September 18-21, 2001; Seoul, Korea. 40. Ward KL, Hilton P. Prospective multicentre randomized trial of tension-free vaginal tape and colposuspension as primary treatment for stress incontinence. BMJ. 2002;326: Miklos J, Kohli N. Laparoscopic paravaginal repair plus Burch colposuspension: review and descriptive technique. Urology. 2000;56: Walter A. Laparoscopic repairs for stress urinary incontinence and pelvic organ prolapse: show me the evidence. Presented at the annual meeting of the American Urogynecologic Society; 2002; San Diego, Calif. 43. Summitt RL, Lucente V, Karram MM, Shull BL, Bent AE. Randomized comparison of laparoscopic and transabdominal Burch urethropexy for the treatment of genuine stress incontinence. Obstet Gynecol. 2000;95:(suppl): Fatthy H, El Hao M, Samaha I, Abdallah K. Modified Burch colposuspension: laparoscopy versus laparotomy. J Am Assoc Gynecol Laparosc. 2001;8: Ross JW. Techniques of laparoscopic repair for total vault eversion after hysterectomy. J Am Assoc Gynecol Laparosc. 1997;4: Ross JW. Laparoscopic approach for severe pelvic vault prolapse. J Am Assoc Gynecol Laparosc. 1996;3(suppl): Lyons TL,Winer WK. Laparoscopic rectocele repair using polyglactin mesh. J Am Assoc Gynecol Laparosc. 1997;4: Ostrzenski A. Laparoscopic colposuspension for total vaginal prolapse. Int J Gynaecol Obstet. 1996;55: Carter JE, Winter M, Mendehlsohn S, Saye W, Richardson AC. Vaginal vault suspension and enterocele repair by Richardson-Saye laparoscopic technique: description of training technique and results. JSLS. 2001;5: Cosson M, Rajabally R, Bogaert E, Querleu D, Crepin G. Laparoscopic sacrocolpopexy, hysterectomy and Burch colposuspension: feasibility and short-term complications of 77 procedures. JSLS. 2002;6: Miklos JR, Moore RD, Kohli N. Laparoscopic surgery for pelvic support defects. Curr Opin Obstet Gynecol. 2002;14: Dr. Lucente is a consultant for GyneCare. Dr. Murphy reports no financial relationship with any companies whose products are mentioned in this article. 34 OBG MANAGEMENT February 2003
Paravaginal Repair: A Laparoscopic Approach
 44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
LAPAROSCOPIC PARAVAGINAL REPAIR PLUS BURCH COLPOSUSPENSION: REVIEW AND DESCRIPTIVE TECHNIQUE
 ELSEVIER LAPAROSCOPIC PARAVAGINAL REPAIR PLUS BURCH COLPOSUSPENSION: REVIEW AND DESCRIPTIVE TECHNIQUE JOHN R. MIKLOS AND NEERAj KOHL! ABSTRACT The objective of this article was to review the available
ELSEVIER LAPAROSCOPIC PARAVAGINAL REPAIR PLUS BURCH COLPOSUSPENSION: REVIEW AND DESCRIPTIVE TECHNIQUE JOHN R. MIKLOS AND NEERAj KOHL! ABSTRACT The objective of this article was to review the available
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience
 Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Urethrolysis; When, Why & How. M Karram Professor of Ob/Gyn & Urology University of Cincinnati
 Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Operative Approach to Stress Incontinence. Goals of presentation. Preoperative evaluation: Urodynamic Testing? Michelle Y. Morrill, M.D.
 Operative Approach to Stress Incontinence Goals of presentation Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Review preoperative care & evaluation
Operative Approach to Stress Incontinence Goals of presentation Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Review preoperative care & evaluation
REPAIR OF LARGE CYSTOCELE
 REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
Maud Ankardal, a Anne Ekerydh, b Kristina Crafoord, c Ian Milsom, a Jan-Henrik Stjerndahl, a Marie Ellström Engh a
 BJOG: an International Journal of Obstetrics and Gynaecology September 2004, Vol. 111, pp. 974 981 DOI: 10.1111/j.1471-0528.2004.00220.x A randomised trial comparing open Burch colposuspension using sutures
BJOG: an International Journal of Obstetrics and Gynaecology September 2004, Vol. 111, pp. 974 981 DOI: 10.1111/j.1471-0528.2004.00220.x A randomised trial comparing open Burch colposuspension using sutures
Blue Ridge Urogynecology
 Surgery for Stress Urinary Incontinence Surgery has proved to be a very effective treatment for stress incontinence. The best surgical procedures improve or cure the incontinence in 85 to 90 percent of
Surgery for Stress Urinary Incontinence Surgery has proved to be a very effective treatment for stress incontinence. The best surgical procedures improve or cure the incontinence in 85 to 90 percent of
Effect of Anesthesia on Voiding Function After Tension-Free Vaginal Tape Procedure
 Effect of Anesthesia on Voiding Function After Tension-Free Vaginal Tape Procedure M. Murphy, MD, M. H. Heit, MD, MSPH, L. Fouts, MD, C. A. Graham, MD, L. Blackwell, RN, and P. J. Culligan, MD OBJECTIVE:
Effect of Anesthesia on Voiding Function After Tension-Free Vaginal Tape Procedure M. Murphy, MD, M. H. Heit, MD, MSPH, L. Fouts, MD, C. A. Graham, MD, L. Blackwell, RN, and P. J. Culligan, MD OBJECTIVE:
PUBOVAGINAL SLING IN THE TREATMENT OF STRESS URINARY INCONTINENCE FOR URETHRAL HYPERMOBILITY AND INTRINSIC SPHINCTERIC DEFICIENCY
 Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology PUBOVAGINAL SLING IN SUI Vol. 29 (6): 540-544, November - December, 2003 PUBOVAGINAL SLING IN THE TREATMENT
Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology PUBOVAGINAL SLING IN SUI Vol. 29 (6): 540-544, November - December, 2003 PUBOVAGINAL SLING IN THE TREATMENT
Sep \8958 Appell Dmochowski.ppt LMF 1
 Surgical Outcomes (How did we get ourselves into this mess?) Roger R. Dmochowski, MD, FACS Department of Urologic Surgery Vanderbilt University School of Medicine Nashville, Tennessee Considerations Evaluation
Surgical Outcomes (How did we get ourselves into this mess?) Roger R. Dmochowski, MD, FACS Department of Urologic Surgery Vanderbilt University School of Medicine Nashville, Tennessee Considerations Evaluation
2 Oulu University Hospital, Oulu, 5 Tampere University Hospital, Tampere,
 Acta Obstet Gynecol Scand 2003: 82: 665--671 Copyright # Acta Obstet Gynecol Scand 2003 Printed in Denmark. All rights reserved Acta Obstetricia et Gynecologica Scandinavica ISSN 0001-6349 ORIGINAL ARTICLE
Acta Obstet Gynecol Scand 2003: 82: 665--671 Copyright # Acta Obstet Gynecol Scand 2003 Printed in Denmark. All rights reserved Acta Obstetricia et Gynecologica Scandinavica ISSN 0001-6349 ORIGINAL ARTICLE
Medical Policy Title: Radiofrequency ARBenefits Approval: 10/19/2011
 Medical Policy Title: Radiofrequency ARBenefits Approval: 10/19/2011 Treatment, Urinary Stress Incontinence, Transurethral Effective Date: 01/01/2012 Document: ARB0359 Revision Date: Code(s): 53860 Transurethral
Medical Policy Title: Radiofrequency ARBenefits Approval: 10/19/2011 Treatment, Urinary Stress Incontinence, Transurethral Effective Date: 01/01/2012 Document: ARB0359 Revision Date: Code(s): 53860 Transurethral
Tension-Free Vaginal Tape versus Laparoscopic Bladder Neck Suspension for Stress Urinary Incontinence. Ching-Chung Liang, MD; Yung-Kuei Soong, MD
 Original Article 360 Tension-Free Vaginal Tape versus Laparoscopic Bladder Neck Suspension for Stress Urinary Incontinence Ching-Chung Liang, MD; Yung-Kuei Soong, MD Results: Background: Owing to their
Original Article 360 Tension-Free Vaginal Tape versus Laparoscopic Bladder Neck Suspension for Stress Urinary Incontinence Ching-Chung Liang, MD; Yung-Kuei Soong, MD Results: Background: Owing to their
Is the role of Burch colposuspension fading away in this epoch for treating female urinary incontinence?
 Int Urogynecol J (2007) 18:937 942 DOI 10.1007/s00192-006-0264-x ORIGINAL ARTICLE Is the role of Burch colposuspension fading away in this epoch for treating female urinary incontinence? SooCheen Ng &
Int Urogynecol J (2007) 18:937 942 DOI 10.1007/s00192-006-0264-x ORIGINAL ARTICLE Is the role of Burch colposuspension fading away in this epoch for treating female urinary incontinence? SooCheen Ng &
Desara and Desara Blue
 Desara and Desara Blue Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc.
Desara and Desara Blue Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc.
Female Urology. The Results of Grade IV Cystocele Repair Using Mesh. Introduction ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M
 Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
Desara Blue OV D I. Sling for Female Stress Urinary Incontinence. Instructions For Use
 Desara Blue OV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc. 5171 Clareton
Desara Blue OV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc. 5171 Clareton
Burch Colposuspension and Tension-Free Vaginal Tape in the Management of Stress Urinary Incontinence in Women
 European Urology European Urology 41 2002) 469±473 Colposuspension and Tension-Free Vaginal Tape in the Management of Stress Urinary Incontinence in Women A. Liapis *, P. Bakas, G. Creatsas 2nd Department
European Urology European Urology 41 2002) 469±473 Colposuspension and Tension-Free Vaginal Tape in the Management of Stress Urinary Incontinence in Women A. Liapis *, P. Bakas, G. Creatsas 2nd Department
When the suburethral sling was first
 SURGICAL TECHNIQUES BY CHERYL IGLESIA, MD, AND MARIA PETTIT CANTER, MD Treating stress urinary incontinence with suburethral slings Recent modifications to suburethral sling procedures have brought them
SURGICAL TECHNIQUES BY CHERYL IGLESIA, MD, AND MARIA PETTIT CANTER, MD Treating stress urinary incontinence with suburethral slings Recent modifications to suburethral sling procedures have brought them
q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE
 493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation in uterine leiomyoma management, 719 723 Adnexal masses diagnosis of, 664 667 imaging in, 664 665 laboratory studies in, 665
Index Note: Page numbers of article titles are in boldface type. A Ablation in uterine leiomyoma management, 719 723 Adnexal masses diagnosis of, 664 667 imaging in, 664 665 laboratory studies in, 665
Laparoscopic surgery for pelvic support defects
 ~ Laparoscopic surgery for pelvic support defects John R. Miklosa, Robert D. Mooreb and Neeraj Kohlia Reconstructive pelvic surgery for the treatment of vaginal prolapse continues to evolve as surgeons
~ Laparoscopic surgery for pelvic support defects John R. Miklosa, Robert D. Mooreb and Neeraj Kohlia Reconstructive pelvic surgery for the treatment of vaginal prolapse continues to evolve as surgeons
Desara TV and Desara Blue TV
 Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
Sarah A. Huber, 1 LaChanda Dunlap-Wright, 2 John R. Miklos, 1 and Robert D. Moore Introduction
 Case Reports in Urology Volume 2016, Article ID 6180756, 5 pages http://dx.doi.org/10.1155/2016/6180756 Case Report Concomitant Laparoscopic Burch Urethropexy and Combined Vaginal-Laparoscopic Mesh Sling
Case Reports in Urology Volume 2016, Article ID 6180756, 5 pages http://dx.doi.org/10.1155/2016/6180756 Case Report Concomitant Laparoscopic Burch Urethropexy and Combined Vaginal-Laparoscopic Mesh Sling
Comparison of Laparoscopic Burch and Tension-Free Vaginal Tape in Treating Stress Urinary Incontinence in Obese Patients
 SCIENTIFIC PAPER Comparison of Laparoscopic Burch and Tension-Free Vaginal Tape in Treating Stress Urinary Incontinence in Obese Patients Maurice K. Chung, RPh, MD, Rosemary P. Chung, BSN, PA-C ABSTRACT
SCIENTIFIC PAPER Comparison of Laparoscopic Burch and Tension-Free Vaginal Tape in Treating Stress Urinary Incontinence in Obese Patients Maurice K. Chung, RPh, MD, Rosemary P. Chung, BSN, PA-C ABSTRACT
Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study
 Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study Yvonne KY CHENG MBChB, MRCOG William WK TO MBBS, M Phil, FRCOG, FHKAM (O&G) HX
Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study Yvonne KY CHENG MBChB, MRCOG William WK TO MBBS, M Phil, FRCOG, FHKAM (O&G) HX
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence
 A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
Treatment Outcomes of Tension-free Vaginal Tape Insertion
 Are the Treatment Outcomes of Tension-free Vaginal Tape Insertion the Same for Patients with Stress Urinary Incontinence with or without Intrinsic Sphincter Deficiency? A Retrospective Study in Hong Kong
Are the Treatment Outcomes of Tension-free Vaginal Tape Insertion the Same for Patients with Stress Urinary Incontinence with or without Intrinsic Sphincter Deficiency? A Retrospective Study in Hong Kong
New Insights in the Surgical Management of Stress Urinary Incontinence in Women
 New Insights in the Surgical Management of Stress Urinary Incontinence in Women Gabriel Gillon MD Dept. of Urology Rabin Med. Cent. /Beilinson Incontinence and LUTS 25/6/2009 Symposium Ramat Aviv New Insights
New Insights in the Surgical Management of Stress Urinary Incontinence in Women Gabriel Gillon MD Dept. of Urology Rabin Med. Cent. /Beilinson Incontinence and LUTS 25/6/2009 Symposium Ramat Aviv New Insights
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
Imaging of Pelvic Floor Weakness. Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne
 Imaging of Pelvic Floor Weakness Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne Outline Overview and Epidemiology Risk Factors, Causes and Results Review of Relevant
Imaging of Pelvic Floor Weakness Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne Outline Overview and Epidemiology Risk Factors, Causes and Results Review of Relevant
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
SAFYRE TM : A READJUSTABLE MINIMALLY INVASIVE SLING FOR FEMALE URINARY STRESS INCONTINENCE
 Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology SAFYRE TM - SLING FOR FEMALE SUI Vol. 29 (4): 353-359, July - August, 2003 SAFYRE TM : A READJUSTABLE
Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology SAFYRE TM - SLING FOR FEMALE SUI Vol. 29 (4): 353-359, July - August, 2003 SAFYRE TM : A READJUSTABLE
Resolution of urge urinary incontinence with midurethral sling surgery in patients with mixed incontinence and low-pressure urethra
 Gynecol Surg (2012) 9:427 432 DOI 10.1007/s10397-012-0735-7 ORIGINAL ARTICLE Resolution of urge urinary incontinence with midurethral sling surgery in patients with mixed incontinence and low-pressure
Gynecol Surg (2012) 9:427 432 DOI 10.1007/s10397-012-0735-7 ORIGINAL ARTICLE Resolution of urge urinary incontinence with midurethral sling surgery in patients with mixed incontinence and low-pressure
A SIMPLE SURGICAL TECHNIQUE TO MINIMIZE POSTOPERATIVE URINARY RETENTION WITH A PUBOVAGINAL SLING
 Urological Neurology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 27 (3): 275-280, May - June, 2001 A SIMPLE SURGICAL TECHNIQUE TO MINIMIZE POSTOPERATIVE URINARY
Urological Neurology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 27 (3): 275-280, May - June, 2001 A SIMPLE SURGICAL TECHNIQUE TO MINIMIZE POSTOPERATIVE URINARY
Prolapse & Stress Incontinence
 Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
Tension-free Vaginal Tape for Urodynamic Stress Incontinence
 Long-term Results of Tension-free Vaginal Tape Insertion for Urodynamic Stress Incontinence in Chinese Women at Eight-year Follow-up: a Prospective Study YM CHAN MBBS, MRCOG, FHKAM (O&G), DCG, DCH, DFM,
Long-term Results of Tension-free Vaginal Tape Insertion for Urodynamic Stress Incontinence in Chinese Women at Eight-year Follow-up: a Prospective Study YM CHAN MBBS, MRCOG, FHKAM (O&G), DCG, DCH, DFM,
A New Technique for Performing a Laparoscopic Hysterectomy Using Microlaparoscopy: Microlaparoscopic Assisted Vaginal Hysterectomy (mlavh)
 A New Technique for Performing a Laparoscopic Hysterectomy Using Microlaparoscopy: Microlaparoscopic Assisted Vaginal Hysterectomy (mlavh) ABSTRACT In an effort to further decrease patient postoperative
A New Technique for Performing a Laparoscopic Hysterectomy Using Microlaparoscopy: Microlaparoscopic Assisted Vaginal Hysterectomy (mlavh) ABSTRACT In an effort to further decrease patient postoperative
Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse
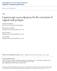 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2004 Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse Chandru P. Sundaram Indiana University
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2004 Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse Chandru P. Sundaram Indiana University
Management of recurrent stress urinary incontinence and urinary retention following midurethral sling insertion in women
 UROLOGY doi 10.1308/003588412X13373405385610 Management of recurrent stress urinary incontinence and urinary retention following midurethral sling H Hashim 1, TR Terry 2 1 North Bristol NHS Trust, UK 2
UROLOGY doi 10.1308/003588412X13373405385610 Management of recurrent stress urinary incontinence and urinary retention following midurethral sling H Hashim 1, TR Terry 2 1 North Bristol NHS Trust, UK 2
Current trend in anti-incontinence surgery
 Current trend in anti-incontinence surgery 吳銘斌醫師 (Ming-Ping Wu, M.D., Ph.D.) 奇美醫院婦產部婦女泌尿暨骨盆醫學科主任台北醫學大學醫學院婦產學科副教授成功大學醫學院臨床醫學所博士 Anti-incontinence surgery Bladder buttress operation: Kelly plication Needle
Current trend in anti-incontinence surgery 吳銘斌醫師 (Ming-Ping Wu, M.D., Ph.D.) 奇美醫院婦產部婦女泌尿暨骨盆醫學科主任台北醫學大學醫學院婦產學科副教授成功大學醫學院臨床醫學所博士 Anti-incontinence surgery Bladder buttress operation: Kelly plication Needle
Pathophysiological Rationale for Surgical Treatments of Stress Urinary Incontinence
 Pathophysiological Rationale for Surgical Treatments of Stress Urinary Incontinence Urology Grand Rounds April 6, 2005 Herman Christopher Kwan R4 A familiar case? 62 year old female initial presentation
Pathophysiological Rationale for Surgical Treatments of Stress Urinary Incontinence Urology Grand Rounds April 6, 2005 Herman Christopher Kwan R4 A familiar case? 62 year old female initial presentation
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
INJ. Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple Sutures: Surgical Technique and Results.
 Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
Int Urogynecol J (2010) 21: DOI /s ORIGINAL ARTICLE Experience with TVT-SECUR sling for stress urinary incontinence: a 1
 Int Urogynecol J (2010) 21:767 772 DOI 10.1007/s00192-010-1114-4 ORIGINAL ARTICLE Experience with TVT-SECUR sling for stress urinary incontinence: a 141-case analysis Salil Khandwala & Chaandini Jayachandran
Int Urogynecol J (2010) 21:767 772 DOI 10.1007/s00192-010-1114-4 ORIGINAL ARTICLE Experience with TVT-SECUR sling for stress urinary incontinence: a 141-case analysis Salil Khandwala & Chaandini Jayachandran
Medical Review Criteria Invasive Treatment for Urinary Incontinence
 Medical Review Criteria Invasive Treatment for Urinary Incontinence Effective Date: December 21, 2016 Subject: Invasive Treatment for Urinary Incontinence Background: Urinary incontinence (the involuntary
Medical Review Criteria Invasive Treatment for Urinary Incontinence Effective Date: December 21, 2016 Subject: Invasive Treatment for Urinary Incontinence Background: Urinary incontinence (the involuntary
Transvaginal and Transurethral Radiofrequency Tissue Remodeling for Urinary Stress Incontinence
 Transvaginal and Transurethral Radiofrequency Tissue Remodeling for Urinary Stress Incontinence Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary,
Transvaginal and Transurethral Radiofrequency Tissue Remodeling for Urinary Stress Incontinence Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary,
What you should know about your diagnosis of incontinence
 What you should know about your diagnosis of incontinence What is Stress Urinary Incontinence? WHAT IS NORMAL URINARY FUNCTION? Urine is a normal waste product of the body that is manufactured by the kidneys
What you should know about your diagnosis of incontinence What is Stress Urinary Incontinence? WHAT IS NORMAL URINARY FUNCTION? Urine is a normal waste product of the body that is manufactured by the kidneys
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
Surgery for stress incontinence:
 Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
Laparoscopic retropubic urethropexy Hannah S L, Chin A
 Laparoscopic retropubic urethropexy Hannah S L, Chin A Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion on NHS EED. Each abstract contains a brief
Laparoscopic retropubic urethropexy Hannah S L, Chin A Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion on NHS EED. Each abstract contains a brief
As more patients express reservations
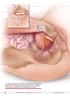 The autologous pubovaginal sling supports the proximal urethra and bladder neck to achieve continence by providing a direct compressive force on the urethra and bladder outlet, or by reestablishing a reinforcing
The autologous pubovaginal sling supports the proximal urethra and bladder neck to achieve continence by providing a direct compressive force on the urethra and bladder outlet, or by reestablishing a reinforcing
Risk Factors of Voiding Dysfunction and Patient Satisfaction After Tension-free Vaginal Tape Procedure
 J Korean Med Sci 2005; 20: 1006-10 ISSN 1011-8934 Copyright The Korean Academy of Medical Sciences Risk Factors of Voiding Dysfunction and Patient Satisfaction After Tension-free Vaginal Tape Procedure
J Korean Med Sci 2005; 20: 1006-10 ISSN 1011-8934 Copyright The Korean Academy of Medical Sciences Risk Factors of Voiding Dysfunction and Patient Satisfaction After Tension-free Vaginal Tape Procedure
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Current status in pelvic organ prolapse surgery: an evidence based review
 Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Trans-Obturator Tape Operation Using MONARC Technique (Outside-In Technique) --- Revisited Objective and Subjective Assessment
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 8 Ver. I (August. 2016), PP 58-68 www.iosrjournals.org Trans-Obturator Tape Operation Using
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 8 Ver. I (August. 2016), PP 58-68 www.iosrjournals.org Trans-Obturator Tape Operation Using
SURGICAL. How to manage the cuff at vaginal hysterectomy. For personal use only. Copyright Dowden Health Media TECHNIQUES
 For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
30/06/2014. Gynaecological Surgery. Mr Alfred Cutner, Consultant Gynaecologist, University College Hospital, London WHAT IS LAPAROSCOPIC SURGERY?
 Gynaecological Surgery Mr Alfred Cutner, Consultant Gynaecologist, University College Hospital, London Laparoscopic surgery techniques Common complications of laparoscopic surgery Intra-operative injuries:
Gynaecological Surgery Mr Alfred Cutner, Consultant Gynaecologist, University College Hospital, London Laparoscopic surgery techniques Common complications of laparoscopic surgery Intra-operative injuries:
Stress Urinary Incontinence in Women. What YOU can do about it...
 Stress Urinary Incontinence in Women What YOU can do about it... www.gynecare.com Stress Urinary Incontinence in Women: It's Common. It's Treatable. Would it surprise you... To learn that more than 13
Stress Urinary Incontinence in Women What YOU can do about it... www.gynecare.com Stress Urinary Incontinence in Women: It's Common. It's Treatable. Would it surprise you... To learn that more than 13
Clinical Study Initial Experience with Robotic Retropubic Urethropexy Compared to Open Retropubic Urethropexy
 Obstetrics and Gynecology International Volume 2013, Article ID 315680, 5 pages http://dx.doi.org/10.1155/2013/315680 Clinical Study Initial Experience with Retropubic Urethropexy Compared to Open Retropubic
Obstetrics and Gynecology International Volume 2013, Article ID 315680, 5 pages http://dx.doi.org/10.1155/2013/315680 Clinical Study Initial Experience with Retropubic Urethropexy Compared to Open Retropubic
Robot Assisted Rectopexy
 1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation
 Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
A Simplified Urinary Incontinence Score for the Evaluation of Treatment Outcomes
 Neurourology and Urodynamics 19:127 135 (2000) A Simplified Urinary Incontinence Score for the Evaluation of Treatment Outcomes Asnat Groutz, Jerry G. Blaivas,* and Jarrod E. Rosenthal Weill Medical College,
Neurourology and Urodynamics 19:127 135 (2000) A Simplified Urinary Incontinence Score for the Evaluation of Treatment Outcomes Asnat Groutz, Jerry G. Blaivas,* and Jarrod E. Rosenthal Weill Medical College,
Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566
 Single-incision short sling mesh insertion for stress urinary incontinence in women Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566 Your responsibility This guidance
Single-incision short sling mesh insertion for stress urinary incontinence in women Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566 Your responsibility This guidance
Urinary incontinence and prolapse are common,
 Advances In Urogynecology Series Nonsurgical and Minimally Invasive Outpatient Treatments for Stress Urinary Incontinence and Pelvic Organ Prolapse Jyot Saini, MD; Neeraj Kohli, MD, MBA; John R. Miklos,
Advances In Urogynecology Series Nonsurgical and Minimally Invasive Outpatient Treatments for Stress Urinary Incontinence and Pelvic Organ Prolapse Jyot Saini, MD; Neeraj Kohli, MD, MBA; John R. Miklos,
How to Achieve Long-Term Success in the Treatment of Female Urinary Stress Incontinence? Novel Modification on Vaginal Sling
 www.kjurology.org DOI:10.4111/kju.2011.52.3.184 Voiding Dysfunction How to Achieve Long-Term Success in the Treatment of Female Urinary Stress Incontinence? Novel Modification on Vaginal Sling Mahmoud
www.kjurology.org DOI:10.4111/kju.2011.52.3.184 Voiding Dysfunction How to Achieve Long-Term Success in the Treatment of Female Urinary Stress Incontinence? Novel Modification on Vaginal Sling Mahmoud
Long-Term Outcome of the Tension-Free Vaginal Tape Procedure in Female Urinary Incontinence: A 6-Year Follow-Up
 www.kjurology.org DOI:10.4111/kju.2010.51.6.409 Voiding Dysfunction Long-Term Outcome of the Tension-Free Vaginal Tape Procedure in Female Urinary Incontinence: A 6-Year Follow-Up Jun Hyung Lee, Min Chul
www.kjurology.org DOI:10.4111/kju.2010.51.6.409 Voiding Dysfunction Long-Term Outcome of the Tension-Free Vaginal Tape Procedure in Female Urinary Incontinence: A 6-Year Follow-Up Jun Hyung Lee, Min Chul
Prevention of Surgical Injuries in Gynecology
 in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Innovations in mesh kit technology for vaginal wall prolapse
 Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Repeat midurethral sling treatment for prior midurethral sling failure
 Gynecol Surg (2012) 9:17 21 DOI 10.1007/s10397-011-0675-7 REVIEW ARTICLE Repeat midurethral sling treatment for prior midurethral sling failure Chi-Feng Su & Kwong-Pang Tsui & Horng-Jyh Tsai & Gin-Den
Gynecol Surg (2012) 9:17 21 DOI 10.1007/s10397-011-0675-7 REVIEW ARTICLE Repeat midurethral sling treatment for prior midurethral sling failure Chi-Feng Su & Kwong-Pang Tsui & Horng-Jyh Tsai & Gin-Den
Brief involuntary urine loss associated with an increase in abdominal pressure. Pathophysiology of Stress Urinary Incontinence Edward J.
 TREATMENT OF SUI Pathophysiology of Stress Urinary Incontinence Edward J. McGuire, MD Department of Urology, University of Michigan Medical Center, Ann Arbor, MI All cases of stress urinary incontinence
TREATMENT OF SUI Pathophysiology of Stress Urinary Incontinence Edward J. McGuire, MD Department of Urology, University of Michigan Medical Center, Ann Arbor, MI All cases of stress urinary incontinence
ABSTRACT R.D. MOORE, D.O., F.A.C.O.G., F.A.C.S. DIRECTOR, ADVANCED PELVIC SURGERY DIRECTOR, UROGYNECOLOGY ATLANTA UROGYNECOLOGY ASSOCIATES ATLANTA, GA
 Single-Center Retrospective Study of the Technique, Safety, and 12-Month Efficacy of the MiniArc Single-Incision Sling: A New Minimally Invasive Procedure for Treatment of Female SUI R.D. MOORE, D.O.,
Single-Center Retrospective Study of the Technique, Safety, and 12-Month Efficacy of the MiniArc Single-Incision Sling: A New Minimally Invasive Procedure for Treatment of Female SUI R.D. MOORE, D.O.,
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time
 EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
One Slim Needle One Incision. One Simple Solution for Stress Urinary Incontinence. The Difference is in the Data
 CONTINENCE SOLUTIONS One Slim Needle One Incision ordering information Description US International Order Number Order Number One Simple Solution for Stress Urinary Incontinence MiniArc Single-Incision
CONTINENCE SOLUTIONS One Slim Needle One Incision ordering information Description US International Order Number Order Number One Simple Solution for Stress Urinary Incontinence MiniArc Single-Incision
Clinical Study Cough Test during Tension-Free Vaginal Tape Procedure in Preventing Postoperative Urinary Retention
 Advances in Urology Volume 2013, Article ID 797854, 4 pages http://dx.doi.org/10.1155/2013/797854 Clinical Study Cough Test during Tension-Free Vaginal Tape Procedure in Preventing Postoperative Urinary
Advances in Urology Volume 2013, Article ID 797854, 4 pages http://dx.doi.org/10.1155/2013/797854 Clinical Study Cough Test during Tension-Free Vaginal Tape Procedure in Preventing Postoperative Urinary
Loss of Bladder Control
 BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
Urethral pressure measurement in stress incontinence: does it help?
 Int Urol Nephrol (2009) 41:491 495 DOI 10.1007/s11255-008-9506-9 UROLOGY - ORIGINAL PAPER Urethral pressure measurement in stress incontinence: does it help? Bassem S. Wadie Æ Ahmed S. El-Hefnawy Received:
Int Urol Nephrol (2009) 41:491 495 DOI 10.1007/s11255-008-9506-9 UROLOGY - ORIGINAL PAPER Urethral pressure measurement in stress incontinence: does it help? Bassem S. Wadie Æ Ahmed S. El-Hefnawy Received:
Bard: Continence Therapy. Stress Urinary Incontinence. Regaining Control. Restoring Your Lifestyle.
 Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Urinary incontinence is a common problem and one that can be resolved by working
Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Urinary incontinence is a common problem and one that can be resolved by working
1) What conditions is vaginal mesh used to commonly treat? Vaginal mesh is used to treat two different health issues in women:
 Vaginal Mesh Frequently Asked Questions 1) What conditions is vaginal mesh used to commonly treat? Vaginal mesh is used to treat two different health issues in women: a) stress urinary incontinence (SUI)
Vaginal Mesh Frequently Asked Questions 1) What conditions is vaginal mesh used to commonly treat? Vaginal mesh is used to treat two different health issues in women: a) stress urinary incontinence (SUI)
FEMALE URINARY INCONTINENCE: WHAT IT IS AND WHAT YOU CAN DO ABOUT IT
 URO-GYNECOLOGY PATIIENT IINFORMATIION SHEET FEMALE URINARY INCONTINENCE: WHAT IT IS AND WHAT YOU CAN DO ABOUT IT What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for
URO-GYNECOLOGY PATIIENT IINFORMATIION SHEET FEMALE URINARY INCONTINENCE: WHAT IT IS AND WHAT YOU CAN DO ABOUT IT What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for
I-STOP TOMS Transobturator Male Sling
 I-STOP TOMS Transobturator Male Sling The CL Medical I-STOP TOMS sling for male stress urinary incontinence was developed in France where it is widely used and is the market leader. It is constructed with
I-STOP TOMS Transobturator Male Sling The CL Medical I-STOP TOMS sling for male stress urinary incontinence was developed in France where it is widely used and is the market leader. It is constructed with
Treatment of Female Stress Urinary Incontinence by Trans-Obturaror Tension-Free Vaginal Tape (TVT-O): A Prospecive Controlled Study
 Med. J. Cairo Univ., Vol. 79, No. 1, June: 267-272, 2011 www.medicaljournalofcairouniversity.com Treatment of Female Stress Urinary Incontinence by Trans-Obturaror Tension-Free Vaginal Tape (TVT-O): A
Med. J. Cairo Univ., Vol. 79, No. 1, June: 267-272, 2011 www.medicaljournalofcairouniversity.com Treatment of Female Stress Urinary Incontinence by Trans-Obturaror Tension-Free Vaginal Tape (TVT-O): A
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
Nine-year experience in sub-urethral prosthesis for the treatment of female stress urinary incontinence
 Nine-year experience in sub-urethral prosthesis for the treatment of female stress urinary incontinence Adrian Haşegan Department of Urology, Emergency County Hospital Sibiu, Faculty of Medicine Abstract
Nine-year experience in sub-urethral prosthesis for the treatment of female stress urinary incontinence Adrian Haşegan Department of Urology, Emergency County Hospital Sibiu, Faculty of Medicine Abstract
LAPAROSCOPIC BURCH COLPOSUSPENSION
 ,,,,,, GYNAECOLOGY,,,,,, LAPAROSCOPIC BURCH COLPOSUSPENSION Catherine Allaire, MD CM, FRCSC, Clinical Instructor, Department of Obstetrics and G ynae co logy, University of British Columbia ABSTRACT Objective:
,,,,,, GYNAECOLOGY,,,,,, LAPAROSCOPIC BURCH COLPOSUSPENSION Catherine Allaire, MD CM, FRCSC, Clinical Instructor, Department of Obstetrics and G ynae co logy, University of British Columbia ABSTRACT Objective:
Step by step High uterosacral vaginal vault suspension to repair enterocele and apical prolapse
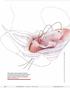 When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
UroToday International Journal. Volume 4 - February 2011
 UroToday International Journal Scott Serels, 1 Sandy B Nosseir, 2 Lawrence R Lind, 2 Harvey A Winkler 2 1 Bladder Control Center of Norwalk and Section of Urogynecology, Norwalk Hospital, Norwalk, CT,
UroToday International Journal Scott Serels, 1 Sandy B Nosseir, 2 Lawrence R Lind, 2 Harvey A Winkler 2 1 Bladder Control Center of Norwalk and Section of Urogynecology, Norwalk Hospital, Norwalk, CT,
Site-specific fascial defects in the diagnosis and surgical management of enterocele
 Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
RETROPUBIC SLING PLACEMENT: ISSUES TO CONSIDER
 RETROPUBIC SLING PLACEMENT: ISSUES TO CONSIDER Una Lee MD, FPMRS and Jane Miller MD, FPMRS Patient care and counseling Patient selection Patient expectations/goals Informed consent and conversation about
RETROPUBIC SLING PLACEMENT: ISSUES TO CONSIDER Una Lee MD, FPMRS and Jane Miller MD, FPMRS Patient care and counseling Patient selection Patient expectations/goals Informed consent and conversation about
Robot-Assisted Gynecologic Surgery. Gynecologic Surgery
 Robot-Assisted Gynecologic Surgery Alison F. Jacoby, MD Department of Obstetrics, Gynecology and Reproductive Sciences University of California, San Francisco Robot-Assisted Gynecologic Surgery Clinical
Robot-Assisted Gynecologic Surgery Alison F. Jacoby, MD Department of Obstetrics, Gynecology and Reproductive Sciences University of California, San Francisco Robot-Assisted Gynecologic Surgery Clinical
Anatomical and Functional Results of Pelvic Organ Prolapse Mesh Repair: A Prospective Study of 105 Cases
 International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
Stress Urinary Incontinence Surgery with Mini Sling Just-Swing System: Our Office Experience
 Journal of Women s Health and Gynecology Review Stress Urinary Incontinence Surgery with Mini Sling Just-Swing System: Our Office Experience Ana Ribeiro *, Maria Boia, Ana Cláudia Santos, Isabel Ferreira,
Journal of Women s Health and Gynecology Review Stress Urinary Incontinence Surgery with Mini Sling Just-Swing System: Our Office Experience Ana Ribeiro *, Maria Boia, Ana Cláudia Santos, Isabel Ferreira,
