LAPAROSCOPIC PARAVAGINAL REPAIR PLUS BURCH COLPOSUSPENSION: REVIEW AND DESCRIPTIVE TECHNIQUE
|
|
|
- Jerome Cain
- 5 years ago
- Views:
Transcription
1 ELSEVIER LAPAROSCOPIC PARAVAGINAL REPAIR PLUS BURCH COLPOSUSPENSION: REVIEW AND DESCRIPTIVE TECHNIQUE JOHN R. MIKLOS AND NEERAj KOHL! ABSTRACT The objective of this article was to review the available literature on laparoscopic Burch urethropexy cure rates and describe the authors' laparoscopic technique and experience with Burch urethropexy and paravaginal repair. A MEDLINE search (1991 to 1999) was performed for articles describing the laparoscopic Burch urethropexy using suture to elevate and stabilize the paraurethral tissue. Also a retrospective chart review of the authors' 171 consecutive patients between January 1997 and December 1999 was done. The laparoscopic Burch urethropexy and paravaginal repair is described using an open laparoscopic technique with 3 accessory ports for access. A transperitoneal approach is taken to gain access to the space of Retzius. The anterior vaginal wall and its paravaginal defects, if present, are identified. Nonabsorbable sutures are placed in a conventional fashion. The paravaginal repair is used for support of the anterior vaginal wall proximal to the urethral vesical junction and the Burch urethropexy distal to the vesical neck. An average of 6 sutures are used for the paravaginal repair and 4 sutures for the Burch urethropexy. Cystoscopy is performed to ensure no breech of lower urinary tract integrity. In all, 20 articles describing a laparoscopic Burch urethropexy and postoperative cure rate were identified. Cure rates ranged from 69% to 100%. A review of our experience revealed 130 of 171 patients had a Burch urethropexy and paravaginal repair, 23 of 171 patients a Burch urethropexy alone, and 18 of 171 patients a paravaginal repair alone. Of the authors' 171 patients, 4 (2.3%) had injury to the lower urinary tract during laparoscopic Burch urethropexy or paravaginal repair. All 4 injuries were cystotomies, 2 in patients with previous open retropubic urethropexies. No ureteral ligations or intravesical placement of suture was diagnosed. Other surgical parameters for the laparoscopic Burch uethropexy and paravaginal repair include an estimated blood loss of 50 ml, average hospital stay of less than 23 hours, and an average operative time of 70 minutes. All patients had their surgery completed via laparoscopy. The literature review and our personal experience suggests that the laparoscopic Burch urethropexy and paravaginal repair are safe and effective alternatives to traditional laparotomy for the treatment of genuine anatomic stress urine incontinence and cystourethrocele resulting from lateral vaginal wall defects. UROLOGY 56 (SuppI6A): 64-69, 2000, Elsevier Science Inc. S ince the introduction of the retropubic urethral suspension in 1910, over 100 different surgical techniques for the treatment of genuine stress urinary incontinence (GSUI) have been described.1 Many have been modifications of original procedures in an attempt to improve clinical outcome, From Urogynecology and Reconstructive Pelvic Surgery, Northside Hospital, Atlanta, Georgia, USA, Medical College of Georgia, Augusta, Georgia, USA (J.R.M.), and Urogynecology and Reconstructive Pelvic Surgery, Mount Auburn Hospital, Harvard University, Boston, Massachusetts, USA (N.K.) Reprint requests:]ohn R. Miklos, MD, 3400 C Old Milton Parkway, Suite 330, Alpharetta (Atlanta), GA j ohnrmiklos@yahoo.com (Q 2000, ElSEVIER SCIENCE INC. 64 ALL RIGHTS RESERVED shorten operative time, and reduce surgical morbidity. Despite the number of surgical procedures developed each year, the Burch colposuspension and pubovaginal sling operations have remained the mainstay of surgical correction for GSUI because of their high long-term cure rates. However, these procedures do not address the concurrent anterior vaginal wall prolapse often associated with GSUI secondary to urethral hypermobility. We present a laparoscopic approach to anterior vaginal wall reconstruction using the paravaginal repair and Burch colposuspension for treatment of cystocele and stress urinary incontinence, respectively, resulting from lateral vaginal wall support defects /00/$20.00 PII (00)
2 Emphasizing the principles of minimally invasive surgery, the laparoscopic approach has been successfully adopted for many procedures that previously relied on an abdominal or transvaginal route. First described in 1991, the laparoscopic retropubic colposuspension has rapidly gained popularity because of its many reported advantages, including improved visualization, shorter hospital stay, faster recovery, and decreased blood loss.2 OPERATIVE INDICATIONS Laparoscopy should be considered only as a mode of abdominal access and not a change in the operative technique. Ideally the indications for a laparoscopic approach to retropubic colposuspension should be the same as an open (laparotomy) approach. This would include patients with GSUI and urethral hypennobility. The authors believe the laparoscopic Burch colposuspension can be substituted for an open Burch colposuspension in the majority of cases. Factors that might influence this decision include any history of previous pelvic or anti-incontinence surgery, the patient's age and weight, the need for concomitant surgery, contraindications to general anesthesia, and the surgeon's experience. The surgeon's decision to proceed with a laparoscopic approach should be based on an objective clinical assessment of the patient as well as the surgeon's own surgical skills. If the patient demonstrates a cystocele secondary to a paravaginal defect diagnosed either pre- or intraoperatively, a paravaginal defect repair should be perfonned before the colposuspension. This approach combines the paravaginal repair with Burch colposuspension for treatment of anterior vaginal prolapse secondary to paravaginal defects and stress urine incontinence secondary to urethral hypermobility.3 PREOPERATIVE CONSIDERATIONS We recommend that all patients have a modified bowel preparation consisting of a full liquid diet 48 hours before scheduled surgery and a clear liquid diet and one bottle of magnesium citrate 24 hours before surgery. This regimen appears to improve visualization of the operative field by bowel decompression and reduces that chance of contamination in case of accidental bowel injury. A single dose of prophylactic intravenous antibiotics is administered 30 minutes before surgery. Antiembolic compression stockings are routinely used. The patient is intubated, given general anesthesia, and placed in a dorsal lithotomy position with both arms tucked to her side. A 16F 3-way Foley catheter with a 5-mL balloon tip is inserted into the bladder and attached to continuous drainage. UROLOGY.56 (Supplement 6A), Decemb'T 2000 Superficial epigastric artery Superficial circumflex Iliac artery Femoral ertery FIGURE I. Abdominal port placement: used for combined Burch procedure and paravaginal repair. (@ 2000 by Miklos and Kohli.) SURGICAL TECHNIQUE LAPAROSCOPIC PARAVAGINAL REPAIR We routinely perform open laparoscopy at the inferior margin of the umbilicus. A 10-mm access port is used at this site to introduce the laparoscope. The abdomen is insufflated with CO2 to IS mm Hg intra-abdominal pressure. Three additional ports are placed under direct vision (Fig. 1). The choice of the individual port size depends on what concomitant surgery is planned for that patient. The bladder is filled in a retrograde fashion with 200 to 300 ml normal saline, allowing identification of the superior border of the bladder edge. Entrance into the space of Retzius is accomplished by a transperitoneal approach using a harmonic scalpel. The incision is made approximately 3 cm above the bladder reflection, beginning along the medial border of the right obliterated umbilicalligament. Immediate identification of loose areolar tissue at the point of incision confirms a proper plane of dissection. After the space of Retzius has been entered and the pubic ramus visualized, the bladder is drained to prevent injury. The retropubic space is developed by separating the loose areolar and fatty layers using blunt dissection. Blunt dissection is continued until the retropubic anatomy is visualized. The pubic symphysis and bladder neck are identified in the midline and the obturator neurovascular bundle, Cooper's ligament, and the arcus tendinous fascia pelvis are visualized bilaterally along the pelvic sidewall (Fig. 2). The anterior vaginal wall and its point of lateral attachment from its origin at the pubic symphysis to its insertion at the ischial spine is identified. If paravaginal wall defects are present, the lateral margins of the pubocer- 65
3 Urethra FIGURE 2. Space of Retzius: normal anatomy by Miklos and Kohli.) FIGURE 4. Paravaginal repair: reapproximation of vaginal wall to the obturator internus at the arcus tendineus fascia pelvis. (( by Mixlos and Kohli.) is begun by inserting the surgeon's nondominant hand into the vagina to elevate the anterior vaginal wall and the pubocervical fascia to their normal attachment along the arcus tendineus fascia pelvis. A 2-0 nonabsorbable suture with attached needle are introduced through the -mm port, and the needle is grasped using a laparoscopic needle,. driver. The first suture is placed near the apex of the L I.vagina through the paravesical portion of the evaot ani pubocervical fascia. The needle is then passed through the ipsilateral obturator intemus muscle and fascia around the arcus tendineus fascia at its origin 1 to 2 cm distal to the ischial spine. The suture is secured using an extracorporeal knot-tying technique. Good tissue approximation is accomplished without a suture bridge. Sutures are FIGURE 3. Paravaginal defects: lateral vaginal wall placed sequentially along the paravaginal defects defects result in a cystourethrocele as seen from the space of Retzius. (@ 2000 by Miklos and Kohli.) distal to the urethrovesical junction. The surgical procedure is repeated on the patient's opposite side if bilateral defects are present. Upon completion of the bilateral paravaginal repair, the Burch colpo- suspension is performed. By performing the para- vaginal defect repair first, normal anatomic sup- port of the anterior vaginal segment is recreated, reducing the chance of overelevation of the para- urethral Burch sutures and subsequent voiding dysfunction. vical fascia will be detached from the pelvic sidewall at the arcus tendinous fascia pelvis (white line). The lateral margins of the detached pubocervical fascia and the broken edge of the white line can usually be clearly visualized confirming the paravaginal defect. Unilateral or bilateral defects may be present (Fig. 3). We recommend completion of the laparoscopic paravaginal repair before the colposuspension. After identification of the defect, the combined repair from the ischial spine toward the urethrovesical junction. Usually, a series of 2 to 4 sutures is placed between the ischial spine and a point 1 to 2 cm proximal to the urethrovesical junction (Fig. 4). The laparoscopic colposuspension is performed 66 UROLOGY 56 (Supplement 6A). December 2000
4 furosemide intravenously, and a 70-degree cystoscope is used to visualize the bladder lumen, assess for unintentional stitch penetration, and confirm bilateral ureteral patency. After cystoscopy, attention is returned to laparoscopy. We recommend routine closure of the anterior peritoneal defect using a multifire hernia stapler. All ancillary trocar sheaths are removed under direct vision to ensure hemostasis and exclude iatrogenic bowel herniation. Excess gas is expelled and fascial defects of 10 mm or more are closed using delayed absorbable suture. Postoperative bladder drainage and voiding trials are accomplished using either a transurethral catheter, suprapubic tube, or intermittent selfcatheterization. C Mikk>slKohli FIGURE 5. Paravaginal repair plus Burch urethropexy. (@ 2000 by Miklos and Kohli.) LAPAROSCOPIC BURCH COLPOSUSPENSION This laparoscopic technique parallels our open technique and has previously been described.4 The laparoscopic colposuspension is performed using nonabsorbable No. 0 sutures; we routinely use polytrifluoroethlyene. The surgeon's nondominant hand is placed in the vagina and a finger is used to elevate the vagina. The endopelvic fascia on both sides of the bladder neck and midurethra is exposed using an endoscopic blunt dissector. The first suture is placed 2 cm lateral to the urethra at the level of the midurethra. A figure of 8 suture, incorporating the entire thickness of the anterior vaginal wall excluding the epithelium, is taken, and the suture is then passed through the ipsilateral Cooper's ligament. With an assistant's fingers in the vagina to elevate the anterior vaginal wall toward Cooper's ligament, the suture is tied down with a series of extracorporeal knots using an endoscopic knot pusher. An additional suture is then placed in a similar fashion at the level of the urethrovesical junction, approximately 2 cm lateral to the bladder edge on the same side. The procedure is repeated on the opposite side. Excessive tension on the vaginal wall should be avoided when tying down the sutures. We routinely leave a suture bridge of approximately of 2 to 3 cm (Fig. 5). Upon completion of the paravaginal repair and Burch urethropexy, the intra-abdominal pressure is reduced to 10 to mm Hg, and the retropubic space is inspected for hemostasis. Cystoscopy is performed to rule out urinary tract injury. The patient is given 5 ml of indigo carmine and 10 ml CLINICAL RESULTS Since Vancaillie and Schuessler2 published the first laparoscopic colposuspension case series in 1991, many other investigators have reported their experience. Review of the literature reveals a lack of uniformity in surgical technique and surgical materials used for colposuspension. This lack of standardization is also noted with the conventional open (laparotomy) technique. Because of this lack of standardization and the steep learning curve associated with laparoscopic suturing, surgeons have attempted to develop faster and easier ways of performing a laparoscopic Burch colposuspension. These modifications have included the use of stapling devices,s bone anchors,6 synthetic mesh,7 and fibrin glue.8 However, we believe the laparoscopic approach should be identical with the open technique to allow comparative studies. There are several reported laparoscopic Burch colposuspension case series that have used conventional surgical technique and suture materials. Published cure rates range from 69% to 100 ;(" with the majority of the studies reporting cure rates greater than 80% (Table Although there have been no studies regarding the long-term results of the laparoscopic paravaginal plus colposuspension procedure, one would assume that there is a higher cure rate for the paravaginal plus Burch colposuspension (8 to sutures) compared with the Burch colposuspension only (4 sutures) for the treatment of stress urinary incontinence, because more sutures results in a greater distribution of force to the pelvic floor during episodes of increased abdominal pressure. Most authors have reported decreased blood loss, shortened hospitalization, and decreased postoperative pain and recovery time. Our experience of 171 laparoscopic paravaginal repair and Burch urethropexy procedures has seen an average operative time of 70 minutes, hospital stays of less than 23 hours, estimated blood loss of less than 50 IJROLOGY 56 (Supplement 6A), December
5 TABLE I. Author (year) Review of laparoscopic Burch urethrocystopexy conventional suturing technique No. of Patients AIbalaeta/(1992)1O 10 Burton (1993)11 30 Polasciketa/(1994) Liu (1994) Gunneta/(1994)14 15 Nezhat et a/ (1994)15 62 Lyons (1995)16 10 McDougal et a/ (1995)17 10 Ross (1995)18 32 Langebrekke et a/ (1995)19 8 Radomski et a/ (1995)20 34 Ross (1996)21 35 Cooper et a/ (1996) Lam et a/ (1997) Su et a/ (1997)24 46 Papasakelariou and Papasakelariou25 32 Lobel and Davis (1997)26 35 Ross (1998)27 48 Miannay et a/ (1998)28 36 Saidi et a/ (1998)29 70.Some or all urethrocyslopmes performed using only one suture on each side Follow-up (mo) > Objective Data Cure Rate (%) * 78* * 91 69* ml, and an overall lower urinary tract injury rate of less than 3 ;c, without an incidence of ureteral compromise. Although some have reported subsequent laparotomy to repair the cystotomy, in all cases we have been able to repair the bladder laparoscopically. This is performed using a delayed absorbable suture in an interrupted single-layer fashion. Because all cystotomies were found in the dome of the bladder, prolonged bladder catheterization was not necessary. The Foley catheter was removed when the patient could empty 80 ;c, of her total bladder volume. Early recognition of bladder injury and proficiency in laparoscopic suturing techniques are critical elements in this approach. Reports suggest this complication depends on the learning curve and declines with increasing surgical experience.16 CONCLUSION Despite its recent introduction and lack of longterm data, the laparoscopic Burch colposuspension has become popular for treatment of urinary stress incontinence. Although initial data suggest this technique is a safe and effective alternative to traditionallaparotomy, surgeons should approach it with caution. Laparoscopic suturing and a thorough knowledge of anatomy are essential if we are to have long-term outcome data equivalent to the traditional open technique. Future prospective randomized clinical trials may establish the laparoscopic approach as a minimally invasive method for successful long-term treatment of genuine an- 68 atomic stress urinary incontinence as well as anterior vaginal segment prolapse. REFERENCES 1. Goebell R: Zur operativen beseillgung der angeharenen incontinence vesicae. Incontinentia Vesicae Gynakol Urol 2: , Vancaille TG, and Schussler W: Laparosocpic bladderneck suspension.] Laparoendosc Surg 1: , Miklos]R, and Kohli N: "Paravaginal Plus" Burch procedure: a laparoscopic approach. ] Pelvic Surg 4: , Kohli N, and Miklos]R: Laparoscopic Burch colposuspension: a modem approach. Contemp abstet Gynecol 42: 36-55, Henley C: The Henley staple-suture technique for laparoscopic Burch colposuspension. ] Am Assoc Gynecol Laparoscopists 2: , Das S, and Palmer ]K: Laparoscopic colpo-suspension. ] Uro1154: , au CS, Presthus], and Beadle E: Laparoscopic bladder neck suspension using hernia mesh and surgical staples. ] Laparoendosc Surg 3: , Kiilholma P, Haarala M, Polvi H, Makinen], and Chancellor MB: Sutureless colposuspension with fibrin sealant. Tech Uroll: 81-3, Albala DM, Schuessler WW, and Vancaillie TG: Laparoscopic bladder suspension for the treatment of stress incontinence. Semin Uroll0: , Burton G: A randomized comparison of laparoscopic and open colposuspension (abstract). Neurourol Urodyn 16: , Polascik T], Moore RG, Rosenberg MT, and Kavoussi LR: Comparison of laparoscopic and open retropubic colposuspension for treatment of stress urinary incontinence. Urology45: , Liu CY: Laparoscopic treatment of genuine urinary stress incontinence. Clin abstet Gynecol8: , UROLOGY 56 (Supplement 6A), December 2000
6 14. Gunn GC, Cooper RP, Gordon NS, and Gragnon L: Use of a new device for endoscopic suturing in the laparoscopic Burch procedure. J Am Assoc Gynecol Laparoscopists 2: 65-70, Nezhat CH, Nezhat F, Nezhat CR, et al: Laparoscopic retropubic cystocolposuspension. ] Am Assoc Gynecol Laparoscopists 1: , Lyons TL, and Winer WK: Clinical outcomes with laparoscopic approaches and open Burch procedures for urinary stress incontinence. J Am Assoc Gynecol Laparoscopists 2: , McDougal EM, Klutke CG, and Cornell T: Comparison of transvaginal versus laparoscopic bladder neck suspension for stress urinary incontinence. Adult Urol 45: , Ross]W: Laparoscopic Burch repair compared to laparotomy Burch for cure of urinary stress incontinence. lnt Urogynecol6: , Langebrekke A, Dahlstrom B, Eraker R, and Urnes A: The laparoscopic Burch procedure: a preliminary report. Acta Obstet Gynecol Scand 74: , Radomski SB, and Herschorn S: Laparoscopic Burch bladder neck suspension: early results.] Uro1155: , RossJW: Two techniques oflaparoscopic Burch repair for stress incontinence: a prospective randomized study.] Am Assoc Gynecol Laparoscopists 3: , Cooper MJ, Cario G, Lam A, and Carolton M: A review of results in a series of 113 laparoscopic colposuspensions. Aust N ZJ Obstet Gynaecol36: 44-49, Lam AM, Jenkins GJ, and Hyslop RS: Laparoscopic Burch colposuspension for stress incontinence: preliminary results. MedJ Aust 162: 18-22, Su TH, Wang KG, Hsu CY, Wei H, and Hong BK: Prospective comparison of laparoscopic and traditional colposuspensions in the treatment of genuine stress incontinence. Acta Obstet Gynecol76: , Papasakelariou C, and Papasakelariou B: Laparoscopic bladder neck suspension. J Am Assoc Gynecol Laparoscopists 4: , Lobel RW, and Davis GD: Long-term results of laparoscopic Burch colposuspension. J Am Assoc Gyencol Laparoscopists 4: , RossJW: Multichannel urodynamic evaluation of lap a- roscopic Burch colposuspension for genuine stress incontinence. Obstet Gynecol91: 55-59, Miannay E, Casson M, Querleu D, and Crepin G: Comparison etre la colposuspension par coelioscopie et laprotomi dans Ie traitement de l'incontinence urinaire d'effort. Etude comparative a partir de 72 cas apparies. Contracept Fertil Sex 26: , Saidi MH, Gallagher MS, Skop IP, et al: Extraperitoneal laparoscopic colposuspension: short-term cure rate, complications and duration of hospital stay comparison with Burch colposuspension. Obstet Gynecol92: , UROLOGY 56 (Supplement 6A), December
Paravaginal Repair: A Laparoscopic Approach
 44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
Despite the growing body of medical
 SURGICAL TECHNIQUES BY VINCENT R. LUCENTE, MD, MBA, AND MILES MURPHY, MD Laparoscopic Burch colposuspension for stress urinary incontinence: When, how, and why? Female SUI is a common condition without
SURGICAL TECHNIQUES BY VINCENT R. LUCENTE, MD, MBA, AND MILES MURPHY, MD Laparoscopic Burch colposuspension for stress urinary incontinence: When, how, and why? Female SUI is a common condition without
A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience
 Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Laparoscopic surgery for pelvic support defects
 ~ Laparoscopic surgery for pelvic support defects John R. Miklosa, Robert D. Mooreb and Neeraj Kohlia Reconstructive pelvic surgery for the treatment of vaginal prolapse continues to evolve as surgeons
~ Laparoscopic surgery for pelvic support defects John R. Miklosa, Robert D. Mooreb and Neeraj Kohlia Reconstructive pelvic surgery for the treatment of vaginal prolapse continues to evolve as surgeons
Blue Ridge Urogynecology
 Surgery for Stress Urinary Incontinence Surgery has proved to be a very effective treatment for stress incontinence. The best surgical procedures improve or cure the incontinence in 85 to 90 percent of
Surgery for Stress Urinary Incontinence Surgery has proved to be a very effective treatment for stress incontinence. The best surgical procedures improve or cure the incontinence in 85 to 90 percent of
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Desara and Desara Blue
 Desara and Desara Blue Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc.
Desara and Desara Blue Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc.
REPAIR OF LARGE CYSTOCELE
 REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
Desara TV and Desara Blue TV
 Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
Desara Blue OV D I. Sling for Female Stress Urinary Incontinence. Instructions For Use
 Desara Blue OV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc. 5171 Clareton
Desara Blue OV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc. 5171 Clareton
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
Burch Colposuspension and Tension-Free Vaginal Tape in the Management of Stress Urinary Incontinence in Women
 European Urology European Urology 41 2002) 469±473 Colposuspension and Tension-Free Vaginal Tape in the Management of Stress Urinary Incontinence in Women A. Liapis *, P. Bakas, G. Creatsas 2nd Department
European Urology European Urology 41 2002) 469±473 Colposuspension and Tension-Free Vaginal Tape in the Management of Stress Urinary Incontinence in Women A. Liapis *, P. Bakas, G. Creatsas 2nd Department
Medical Policy Title: Radiofrequency ARBenefits Approval: 10/19/2011
 Medical Policy Title: Radiofrequency ARBenefits Approval: 10/19/2011 Treatment, Urinary Stress Incontinence, Transurethral Effective Date: 01/01/2012 Document: ARB0359 Revision Date: Code(s): 53860 Transurethral
Medical Policy Title: Radiofrequency ARBenefits Approval: 10/19/2011 Treatment, Urinary Stress Incontinence, Transurethral Effective Date: 01/01/2012 Document: ARB0359 Revision Date: Code(s): 53860 Transurethral
Female Urology. The Results of Grade IV Cystocele Repair Using Mesh. Introduction ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M
 Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
2 Oulu University Hospital, Oulu, 5 Tampere University Hospital, Tampere,
 Acta Obstet Gynecol Scand 2003: 82: 665--671 Copyright # Acta Obstet Gynecol Scand 2003 Printed in Denmark. All rights reserved Acta Obstetricia et Gynecologica Scandinavica ISSN 0001-6349 ORIGINAL ARTICLE
Acta Obstet Gynecol Scand 2003: 82: 665--671 Copyright # Acta Obstet Gynecol Scand 2003 Printed in Denmark. All rights reserved Acta Obstetricia et Gynecologica Scandinavica ISSN 0001-6349 ORIGINAL ARTICLE
Urethrolysis; When, Why & How. M Karram Professor of Ob/Gyn & Urology University of Cincinnati
 Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Prevention of Surgical Injuries in Gynecology
 in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
Clinical Study Initial Experience with Robotic Retropubic Urethropexy Compared to Open Retropubic Urethropexy
 Obstetrics and Gynecology International Volume 2013, Article ID 315680, 5 pages http://dx.doi.org/10.1155/2013/315680 Clinical Study Initial Experience with Retropubic Urethropexy Compared to Open Retropubic
Obstetrics and Gynecology International Volume 2013, Article ID 315680, 5 pages http://dx.doi.org/10.1155/2013/315680 Clinical Study Initial Experience with Retropubic Urethropexy Compared to Open Retropubic
A New Technique for Performing a Laparoscopic Hysterectomy Using Microlaparoscopy: Microlaparoscopic Assisted Vaginal Hysterectomy (mlavh)
 A New Technique for Performing a Laparoscopic Hysterectomy Using Microlaparoscopy: Microlaparoscopic Assisted Vaginal Hysterectomy (mlavh) ABSTRACT In an effort to further decrease patient postoperative
A New Technique for Performing a Laparoscopic Hysterectomy Using Microlaparoscopy: Microlaparoscopic Assisted Vaginal Hysterectomy (mlavh) ABSTRACT In an effort to further decrease patient postoperative
Sarah A. Huber, 1 LaChanda Dunlap-Wright, 2 John R. Miklos, 1 and Robert D. Moore Introduction
 Case Reports in Urology Volume 2016, Article ID 6180756, 5 pages http://dx.doi.org/10.1155/2016/6180756 Case Report Concomitant Laparoscopic Burch Urethropexy and Combined Vaginal-Laparoscopic Mesh Sling
Case Reports in Urology Volume 2016, Article ID 6180756, 5 pages http://dx.doi.org/10.1155/2016/6180756 Case Report Concomitant Laparoscopic Burch Urethropexy and Combined Vaginal-Laparoscopic Mesh Sling
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Urinary Bladder. Prof. Imran Qureshi
 Urinary Bladder Prof. Imran Qureshi Urinary Bladder It develops from the upper end of the urogenital sinus, which is continuous with the allantois. The allantois degenerates and forms a fibrous cord in
Urinary Bladder Prof. Imran Qureshi Urinary Bladder It develops from the upper end of the urogenital sinus, which is continuous with the allantois. The allantois degenerates and forms a fibrous cord in
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC BURCH COLPOSUSPENSION
 ,,,,,, GYNAECOLOGY,,,,,, LAPAROSCOPIC BURCH COLPOSUSPENSION Catherine Allaire, MD CM, FRCSC, Clinical Instructor, Department of Obstetrics and G ynae co logy, University of British Columbia ABSTRACT Objective:
,,,,,, GYNAECOLOGY,,,,,, LAPAROSCOPIC BURCH COLPOSUSPENSION Catherine Allaire, MD CM, FRCSC, Clinical Instructor, Department of Obstetrics and G ynae co logy, University of British Columbia ABSTRACT Objective:
Tension-Free Vaginal Tape versus Laparoscopic Bladder Neck Suspension for Stress Urinary Incontinence. Ching-Chung Liang, MD; Yung-Kuei Soong, MD
 Original Article 360 Tension-Free Vaginal Tape versus Laparoscopic Bladder Neck Suspension for Stress Urinary Incontinence Ching-Chung Liang, MD; Yung-Kuei Soong, MD Results: Background: Owing to their
Original Article 360 Tension-Free Vaginal Tape versus Laparoscopic Bladder Neck Suspension for Stress Urinary Incontinence Ching-Chung Liang, MD; Yung-Kuei Soong, MD Results: Background: Owing to their
Medical Review Criteria Invasive Treatment for Urinary Incontinence
 Medical Review Criteria Invasive Treatment for Urinary Incontinence Effective Date: December 21, 2016 Subject: Invasive Treatment for Urinary Incontinence Background: Urinary incontinence (the involuntary
Medical Review Criteria Invasive Treatment for Urinary Incontinence Effective Date: December 21, 2016 Subject: Invasive Treatment for Urinary Incontinence Background: Urinary incontinence (the involuntary
Objectives. Pelvic Anatomy: Staying Out of Trouble. Disclosures. Anatomy 101. Anterior Abdominal Wall. Arcuate Line. Abheha Satkunaratnam MD, FRCS(C)
 Objectives Pelvic Anatomy: Staying Out of Trouble Abheha Satkunaratnam MD, FRCS(C) To focus on key anatomy for the gynaecologic surgeon advancing their minimally invasive gynaecologic skills To provide
Objectives Pelvic Anatomy: Staying Out of Trouble Abheha Satkunaratnam MD, FRCS(C) To focus on key anatomy for the gynaecologic surgeon advancing their minimally invasive gynaecologic skills To provide
Maud Ankardal, a Anne Ekerydh, b Kristina Crafoord, c Ian Milsom, a Jan-Henrik Stjerndahl, a Marie Ellström Engh a
 BJOG: an International Journal of Obstetrics and Gynaecology September 2004, Vol. 111, pp. 974 981 DOI: 10.1111/j.1471-0528.2004.00220.x A randomised trial comparing open Burch colposuspension using sutures
BJOG: an International Journal of Obstetrics and Gynaecology September 2004, Vol. 111, pp. 974 981 DOI: 10.1111/j.1471-0528.2004.00220.x A randomised trial comparing open Burch colposuspension using sutures
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
ig. 2. The organs and their outlet tubes.
 Fig. 1. Birth-related laxity. The diagram shows the baby s head severely stretching ligaments and other tissues in and outside the vagina. This may cause various degrees of looseness, prolapse of the bladder
Fig. 1. Birth-related laxity. The diagram shows the baby s head severely stretching ligaments and other tissues in and outside the vagina. This may cause various degrees of looseness, prolapse of the bladder
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
SURGICAL. How to manage the cuff at vaginal hysterectomy. For personal use only. Copyright Dowden Health Media TECHNIQUES
 For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
Imaging of Pelvic Floor Weakness. Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne
 Imaging of Pelvic Floor Weakness Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne Outline Overview and Epidemiology Risk Factors, Causes and Results Review of Relevant
Imaging of Pelvic Floor Weakness Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne Outline Overview and Epidemiology Risk Factors, Causes and Results Review of Relevant
Surgical management of the undescended testis is performed
 Undescended Testes/Orchiopexy James C.Y. Dunn, MD, PhD, 1 Akemi L. Kawaguchi, MD, 2 and Eric W. Fonkalsrud, MD 1 Surgical management of the undescended testis is performed to prevent the potential complications
Undescended Testes/Orchiopexy James C.Y. Dunn, MD, PhD, 1 Akemi L. Kawaguchi, MD, 2 and Eric W. Fonkalsrud, MD 1 Surgical management of the undescended testis is performed to prevent the potential complications
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
A SIMPLE SURGICAL TECHNIQUE TO MINIMIZE POSTOPERATIVE URINARY RETENTION WITH A PUBOVAGINAL SLING
 Urological Neurology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 27 (3): 275-280, May - June, 2001 A SIMPLE SURGICAL TECHNIQUE TO MINIMIZE POSTOPERATIVE URINARY
Urological Neurology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 27 (3): 275-280, May - June, 2001 A SIMPLE SURGICAL TECHNIQUE TO MINIMIZE POSTOPERATIVE URINARY
NOTES FROM GUTMAN LECTURE 10/26 Use this outline to study from. As you go through Gutman s lecture, fill in the topics.
 NOTES FROM GUTMAN LECTURE 10/26 Use this outline to study from. As you go through Gutman s lecture, fill in the topics. Anatomy above the arcuate line Skin Camper s fascia Scarpa s fascia External oblique
NOTES FROM GUTMAN LECTURE 10/26 Use this outline to study from. As you go through Gutman s lecture, fill in the topics. Anatomy above the arcuate line Skin Camper s fascia Scarpa s fascia External oblique
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Laparoscopic retropubic urethropexy Hannah S L, Chin A
 Laparoscopic retropubic urethropexy Hannah S L, Chin A Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion on NHS EED. Each abstract contains a brief
Laparoscopic retropubic urethropexy Hannah S L, Chin A Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion on NHS EED. Each abstract contains a brief
Tension-free Vaginal Tape for Urodynamic Stress Incontinence
 Long-term Results of Tension-free Vaginal Tape Insertion for Urodynamic Stress Incontinence in Chinese Women at Eight-year Follow-up: a Prospective Study YM CHAN MBBS, MRCOG, FHKAM (O&G), DCG, DCH, DFM,
Long-term Results of Tension-free Vaginal Tape Insertion for Urodynamic Stress Incontinence in Chinese Women at Eight-year Follow-up: a Prospective Study YM CHAN MBBS, MRCOG, FHKAM (O&G), DCG, DCH, DFM,
Site-specific fascial defects in the diagnosis and surgical management of enterocele
 Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
Robot Assisted Rectopexy
 1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
Female Epispadias Repair
 hoofdstuk 07 08-03-2001 15:25 Pagina 89 Female Epispadias Repair Female epispadias repair: a new 1-stage technique CHAPTER 7 Tom P.V.M de Jong, Pieter Dik and Aart J. Klijn Journal of Urology 2000, 164,
hoofdstuk 07 08-03-2001 15:25 Pagina 89 Female Epispadias Repair Female epispadias repair: a new 1-stage technique CHAPTER 7 Tom P.V.M de Jong, Pieter Dik and Aart J. Klijn Journal of Urology 2000, 164,
West Yorkshire Major Trauma Network Clinical Guidelines 2015
 WYMTN: Pelvic fracture with urogenital trauma KEY RECOMMENDATIONS 1. During the initial exploratory survey / secondary survey, a. The external urethral meatus and the transurethral bladder catheter (if
WYMTN: Pelvic fracture with urogenital trauma KEY RECOMMENDATIONS 1. During the initial exploratory survey / secondary survey, a. The external urethral meatus and the transurethral bladder catheter (if
PUBOVAGINAL SLING IN THE TREATMENT OF STRESS URINARY INCONTINENCE FOR URETHRAL HYPERMOBILITY AND INTRINSIC SPHINCTERIC DEFICIENCY
 Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology PUBOVAGINAL SLING IN SUI Vol. 29 (6): 540-544, November - December, 2003 PUBOVAGINAL SLING IN THE TREATMENT
Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology PUBOVAGINAL SLING IN SUI Vol. 29 (6): 540-544, November - December, 2003 PUBOVAGINAL SLING IN THE TREATMENT
When the suburethral sling was first
 SURGICAL TECHNIQUES BY CHERYL IGLESIA, MD, AND MARIA PETTIT CANTER, MD Treating stress urinary incontinence with suburethral slings Recent modifications to suburethral sling procedures have brought them
SURGICAL TECHNIQUES BY CHERYL IGLESIA, MD, AND MARIA PETTIT CANTER, MD Treating stress urinary incontinence with suburethral slings Recent modifications to suburethral sling procedures have brought them
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Current trend in anti-incontinence surgery
 Current trend in anti-incontinence surgery 吳銘斌醫師 (Ming-Ping Wu, M.D., Ph.D.) 奇美醫院婦產部婦女泌尿暨骨盆醫學科主任台北醫學大學醫學院婦產學科副教授成功大學醫學院臨床醫學所博士 Anti-incontinence surgery Bladder buttress operation: Kelly plication Needle
Current trend in anti-incontinence surgery 吳銘斌醫師 (Ming-Ping Wu, M.D., Ph.D.) 奇美醫院婦產部婦女泌尿暨骨盆醫學科主任台北醫學大學醫學院婦產學科副教授成功大學醫學院臨床醫學所博士 Anti-incontinence surgery Bladder buttress operation: Kelly plication Needle
Inferior Pelvic Border
 Pelvis + Perineum Pelvic Cavity Enclosed by bony, ligamentous and muscular wall Contains the urinary bladder, ureters, pelvic genital organs, rectum, blood vessels, lymphatics and nerves Pelvic inlet (superior
Pelvis + Perineum Pelvic Cavity Enclosed by bony, ligamentous and muscular wall Contains the urinary bladder, ureters, pelvic genital organs, rectum, blood vessels, lymphatics and nerves Pelvic inlet (superior
Cleveland Clinic Quarterly
 Cleveland Clinic Quarterly Volume 31 JULY 1964 No. 3 A MEDICAL SILASTIC PROSTHESIS FOR THE CONTROL OF URINARY INCONTINENCE IN THE MALE A Preliminary Report J A M E S K. W A T K I N S, M. D., * R A L P
Cleveland Clinic Quarterly Volume 31 JULY 1964 No. 3 A MEDICAL SILASTIC PROSTHESIS FOR THE CONTROL OF URINARY INCONTINENCE IN THE MALE A Preliminary Report J A M E S K. W A T K I N S, M. D., * R A L P
INJ. Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple Sutures: Surgical Technique and Results.
 Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
DISMEMBERED LAPAROSCOPIC PYELOPLASTY WITH ANTEGRADE PLACEMENT OF URETERAL STENT: SIMPLIFICATION OF THE TECHNIQUE
 Surgical Technique International Braz J Urol Official Journal of the Brazilian Society of Urology Vol. 28 (5): 439-445, September - October, 2002 DISMEMBERED LAPAROSCOPIC PYELOPLASTY WITH ANTEGRADE PLACEMENT
Surgical Technique International Braz J Urol Official Journal of the Brazilian Society of Urology Vol. 28 (5): 439-445, September - October, 2002 DISMEMBERED LAPAROSCOPIC PYELOPLASTY WITH ANTEGRADE PLACEMENT
Procedure related complications and how to prevent them
 Procedure related complications and how to prevent them Rama Jayanthi, M.D. Section of Urology Nationwide Children s Hospital The Ohio State University Retroperitoneoscopic surgery Inadvertent peritoneal
Procedure related complications and how to prevent them Rama Jayanthi, M.D. Section of Urology Nationwide Children s Hospital The Ohio State University Retroperitoneoscopic surgery Inadvertent peritoneal
Robotic distal ureterectomy with psoas hitch and ureteroneocystostomy: Surgical technique and outcomes
 Asian Journal of Urology (2015) 2, 123e127 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur CASE REPORT Robotic distal with psoas hitch and
Asian Journal of Urology (2015) 2, 123e127 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur CASE REPORT Robotic distal with psoas hitch and
New Insights in the Surgical Management of Stress Urinary Incontinence in Women
 New Insights in the Surgical Management of Stress Urinary Incontinence in Women Gabriel Gillon MD Dept. of Urology Rabin Med. Cent. /Beilinson Incontinence and LUTS 25/6/2009 Symposium Ramat Aviv New Insights
New Insights in the Surgical Management of Stress Urinary Incontinence in Women Gabriel Gillon MD Dept. of Urology Rabin Med. Cent. /Beilinson Incontinence and LUTS 25/6/2009 Symposium Ramat Aviv New Insights
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications
 Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
What CPT and ICD-10-CM codes are reported?
 A patient is seen in the hospital s outpatient surgical area with a diagnosis of a displaced comminuted fracture of the lateral condyle, right elbow. An ORIF (open reduction) procedure was performed and
A patient is seen in the hospital s outpatient surgical area with a diagnosis of a displaced comminuted fracture of the lateral condyle, right elbow. An ORIF (open reduction) procedure was performed and
Transvaginal and Transurethral Radiofrequency Tissue Remodeling for Urinary Stress Incontinence
 Transvaginal and Transurethral Radiofrequency Tissue Remodeling for Urinary Stress Incontinence Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary,
Transvaginal and Transurethral Radiofrequency Tissue Remodeling for Urinary Stress Incontinence Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary,
Innovations in mesh kit technology for vaginal wall prolapse
 Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Postoperative Care for Pelvic Fistulae. Peter Jeppson, MD October 3, 2017
 Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Step by step High uterosacral vaginal vault suspension to repair enterocele and apical prolapse
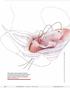 When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation in uterine leiomyoma management, 719 723 Adnexal masses diagnosis of, 664 667 imaging in, 664 665 laboratory studies in, 665
Index Note: Page numbers of article titles are in boldface type. A Ablation in uterine leiomyoma management, 719 723 Adnexal masses diagnosis of, 664 667 imaging in, 664 665 laboratory studies in, 665
q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE
 493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
Perhaps the most controversial of new laparoscopic operations is the repair of the inguinal hernia. The
 JOURNAL OF LAPAROENDOSCOPIC SURGERY Volume 2, Number 6, 1992 Mary Ann Liebert, Inc., Publishers Extraperitoneal Endoscopie Inguinal Hernia Repair GEORGE S. FERZLI, M.D., F.A.C.S., AZIZ MASSAD, M.D., and
JOURNAL OF LAPAROENDOSCOPIC SURGERY Volume 2, Number 6, 1992 Mary Ann Liebert, Inc., Publishers Extraperitoneal Endoscopie Inguinal Hernia Repair GEORGE S. FERZLI, M.D., F.A.C.S., AZIZ MASSAD, M.D., and
Lecture 56 Kidney and Urinary System
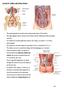 Lecture 56 Kidney and Urinary System The adrenal glands are located on the superomedial aspect of the kidney The right diagram shows a picture of the kidney with the abdominal walls and organs removed
Lecture 56 Kidney and Urinary System The adrenal glands are located on the superomedial aspect of the kidney The right diagram shows a picture of the kidney with the abdominal walls and organs removed
Recent advances have improved the
 SURGICAL TECHNIQUES BY NEERAJ KOHLI, MD, MBA, and JOHN R. MIKLOS, MD Meeting the challenge of vesicovaginal fistula repair: Conservative and surgical measures A number of simple adjustments to technique
SURGICAL TECHNIQUES BY NEERAJ KOHLI, MD, MBA, and JOHN R. MIKLOS, MD Meeting the challenge of vesicovaginal fistula repair: Conservative and surgical measures A number of simple adjustments to technique
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
The use of intraoperative cystoscopy in major vaginal and urogynecologic surgeries
 The use of intraoperative cystoscopy in major vaginal and urogynecologic surgeries Christina H. Kwon, MD, Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, and Peter K. Sand, MD Evanston, Ill OBJECTIVE: Our
The use of intraoperative cystoscopy in major vaginal and urogynecologic surgeries Christina H. Kwon, MD, Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, and Peter K. Sand, MD Evanston, Ill OBJECTIVE: Our
da Vinci Prostatectomy
 da Vinci Prostatectomy Justin T. Lee MD Director of Robotic Surgery Urology Associates of North Texas (UANT) USMD Prostate Cancer Center (www.usmdpcc.com) Prostate Cancer Facts Prostate cancer Leading
da Vinci Prostatectomy Justin T. Lee MD Director of Robotic Surgery Urology Associates of North Texas (UANT) USMD Prostate Cancer Center (www.usmdpcc.com) Prostate Cancer Facts Prostate cancer Leading
Surgery for stress incontinence:
 Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
Prolapse & Stress Incontinence
 Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
Sara Schaenzer Grand Rounds January 24 th, 2018
 Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
ABSITE Review: Hernias
 ABSITE Review: Inguinal and Femoral Hernias Sybile Val M.D. SUNY Downstate Medical Center Department of Surgery June 27, 2008 Objectives www.downstatesurgery.org Correctly identify anatomical landmarks
ABSITE Review: Inguinal and Femoral Hernias Sybile Val M.D. SUNY Downstate Medical Center Department of Surgery June 27, 2008 Objectives www.downstatesurgery.org Correctly identify anatomical landmarks
Peritoneal Dialysis Catheter Placement. Peritoneal Dialysis Catheter Placement. Peritoneal Dialysis Catheter Placement
 ASDIN Advanced Techniques Pre-course Feb. 24, 2012 New Orleans, La Randall L. Rasmussen, MD Special thank you to Drs. Rajeev Narayan, San Antonio, Tx and Hemant Dhingra, Fresno Ca for lending me slides
ASDIN Advanced Techniques Pre-course Feb. 24, 2012 New Orleans, La Randall L. Rasmussen, MD Special thank you to Drs. Rajeev Narayan, San Antonio, Tx and Hemant Dhingra, Fresno Ca for lending me slides
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology
 Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
What you should know about your diagnosis of incontinence
 What you should know about your diagnosis of incontinence What is Stress Urinary Incontinence? WHAT IS NORMAL URINARY FUNCTION? Urine is a normal waste product of the body that is manufactured by the kidneys
What you should know about your diagnosis of incontinence What is Stress Urinary Incontinence? WHAT IS NORMAL URINARY FUNCTION? Urine is a normal waste product of the body that is manufactured by the kidneys
Operative Approach to Stress Incontinence. Goals of presentation. Preoperative evaluation: Urodynamic Testing? Michelle Y. Morrill, M.D.
 Operative Approach to Stress Incontinence Goals of presentation Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Review preoperative care & evaluation
Operative Approach to Stress Incontinence Goals of presentation Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Review preoperative care & evaluation
Comparison of Laparoscopic Burch and Tension-Free Vaginal Tape in Treating Stress Urinary Incontinence in Obese Patients
 SCIENTIFIC PAPER Comparison of Laparoscopic Burch and Tension-Free Vaginal Tape in Treating Stress Urinary Incontinence in Obese Patients Maurice K. Chung, RPh, MD, Rosemary P. Chung, BSN, PA-C ABSTRACT
SCIENTIFIC PAPER Comparison of Laparoscopic Burch and Tension-Free Vaginal Tape in Treating Stress Urinary Incontinence in Obese Patients Maurice K. Chung, RPh, MD, Rosemary P. Chung, BSN, PA-C ABSTRACT
Brief involuntary urine loss associated with an increase in abdominal pressure. Pathophysiology of Stress Urinary Incontinence Edward J.
 TREATMENT OF SUI Pathophysiology of Stress Urinary Incontinence Edward J. McGuire, MD Department of Urology, University of Michigan Medical Center, Ann Arbor, MI All cases of stress urinary incontinence
TREATMENT OF SUI Pathophysiology of Stress Urinary Incontinence Edward J. McGuire, MD Department of Urology, University of Michigan Medical Center, Ann Arbor, MI All cases of stress urinary incontinence
Anterior vaginal wall prolapse occurs commonly
 Anterior vaginal wall prolapse: Innovative surgical approaches MARK D. WALTERS, MD, AND MARIE FIDELA R. PARAISO, MD Anterior vaginal wall prolapse occurs commonly and may coexist with disorders of micturition.
Anterior vaginal wall prolapse: Innovative surgical approaches MARK D. WALTERS, MD, AND MARIE FIDELA R. PARAISO, MD Anterior vaginal wall prolapse occurs commonly and may coexist with disorders of micturition.
Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study
 Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study Yvonne KY CHENG MBChB, MRCOG William WK TO MBBS, M Phil, FRCOG, FHKAM (O&G) HX
Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study Yvonne KY CHENG MBChB, MRCOG William WK TO MBBS, M Phil, FRCOG, FHKAM (O&G) HX
CHAU KHAC TU M.D., Ph.D.
 CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
8 A SIMPLE FISTULA REPAIR, STEP BY STEP
 8 A SIMPLE FISTULA REPAIR, STEP BY STEP The first step is to suture the labia to the thighs and cover the anus with a swab (Figure 31). Figure 31 The labia are sutured to the thighs and the anus is covered
8 A SIMPLE FISTULA REPAIR, STEP BY STEP The first step is to suture the labia to the thighs and cover the anus with a swab (Figure 31). Figure 31 The labia are sutured to the thighs and the anus is covered
Aus Artificial Uretheral Sphincter Port System
 NORFOLK VET PRODUCTS the AUS for the long-term relief of incontinence in dogs and cats making life easier for pets Speciality Medical Devices For The Veterinary Community the Aus Artificial Uretheral Sphincter
NORFOLK VET PRODUCTS the AUS for the long-term relief of incontinence in dogs and cats making life easier for pets Speciality Medical Devices For The Veterinary Community the Aus Artificial Uretheral Sphincter
Inguinal and Femoral Hernias. August 10, 2016 Basic Science Lecture Department of Surgery University of Tennessee Health Science Center
 Inguinal and Femoral Hernias August 10, 2016 Basic Science Lecture Department of Surgery University of Tennessee Health Science Center Background Approximately 20 million groin hernias are repaired each
Inguinal and Femoral Hernias August 10, 2016 Basic Science Lecture Department of Surgery University of Tennessee Health Science Center Background Approximately 20 million groin hernias are repaired each
This presentation will discuss the anatomy of the anterior abdominal wall as it pertains to gynaecological and obstetric surgery.
 This presentation will discuss the anatomy of the anterior abdominal wall as it pertains to gynaecological and obstetric surgery. 1 The border of the anterior abdominal wall is defined superiorly by the
This presentation will discuss the anatomy of the anterior abdominal wall as it pertains to gynaecological and obstetric surgery. 1 The border of the anterior abdominal wall is defined superiorly by the
Citation Acta medica Nagasakiensia. 1963, 8(
 NAOSITE: Nagasaki University's Ac Title Radical Operation For Prostatic Car Author(s) Kondoh, Atushi Citation Acta medica Nagasakiensia. 1963, 8( Issue Date 1963-12-25 URL http://hdl.handle.net/10069/15473
NAOSITE: Nagasaki University's Ac Title Radical Operation For Prostatic Car Author(s) Kondoh, Atushi Citation Acta medica Nagasakiensia. 1963, 8( Issue Date 1963-12-25 URL http://hdl.handle.net/10069/15473
KEYWORDS: cystocele; laparoscopic Burch colposuspension; ultrasound cystourethrography; urodynamic stress incontinence; voiding function
 Ultrasound Obstet Gynecol 2005; 25: 289 295 Published online in Wiley InterScience (www.interscience.wiley.com). DOI: 10.1002/uog.1838 Dynamic morphological changes in the anterior vaginal wall before
Ultrasound Obstet Gynecol 2005; 25: 289 295 Published online in Wiley InterScience (www.interscience.wiley.com). DOI: 10.1002/uog.1838 Dynamic morphological changes in the anterior vaginal wall before
T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks
 T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks R Botchorishvili, A Wattiez, G Mage, M Canis, B Rabischong, K Jardon, C Rivoire,
T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks R Botchorishvili, A Wattiez, G Mage, M Canis, B Rabischong, K Jardon, C Rivoire,
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence
 A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
How to Achieve Long-Term Success in the Treatment of Female Urinary Stress Incontinence? Novel Modification on Vaginal Sling
 www.kjurology.org DOI:10.4111/kju.2011.52.3.184 Voiding Dysfunction How to Achieve Long-Term Success in the Treatment of Female Urinary Stress Incontinence? Novel Modification on Vaginal Sling Mahmoud
www.kjurology.org DOI:10.4111/kju.2011.52.3.184 Voiding Dysfunction How to Achieve Long-Term Success in the Treatment of Female Urinary Stress Incontinence? Novel Modification on Vaginal Sling Mahmoud
Case Report. XCM Biologic Tissue Matrix. Components separation using sandwich technique for reconstruction of abdominal wall defect.
 Case Report XCM Biologic Tissue Matrix. Components separation using sandwich technique for reconstruction of abdominal wall defect. XCM Biologic Tissue Matrix. Components separation using sandwich technique
Case Report XCM Biologic Tissue Matrix. Components separation using sandwich technique for reconstruction of abdominal wall defect. XCM Biologic Tissue Matrix. Components separation using sandwich technique
One Slim Needle One Incision. One Simple Solution for Stress Urinary Incontinence. The Difference is in the Data
 CONTINENCE SOLUTIONS One Slim Needle One Incision ordering information Description US International Order Number Order Number One Simple Solution for Stress Urinary Incontinence MiniArc Single-Incision
CONTINENCE SOLUTIONS One Slim Needle One Incision ordering information Description US International Order Number Order Number One Simple Solution for Stress Urinary Incontinence MiniArc Single-Incision
SAFYRE TM : A READJUSTABLE MINIMALLY INVASIVE SLING FOR FEMALE URINARY STRESS INCONTINENCE
 Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology SAFYRE TM - SLING FOR FEMALE SUI Vol. 29 (4): 353-359, July - August, 2003 SAFYRE TM : A READJUSTABLE
Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology SAFYRE TM - SLING FOR FEMALE SUI Vol. 29 (4): 353-359, July - August, 2003 SAFYRE TM : A READJUSTABLE
Loss of Bladder Control
 BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
Polypropylene Mesh in Stress Urinary Incontinence. Liqaa R Al-Khuzaee, FICOG
 Iraqi JMS Published by Al-Nahrain College of Medicine ISSN 1681-6579 Email: Iraqi_jms_alnahrain@yahoo.com http://www. colmed-nahrain.edu.iq/ Polypropylene Mesh in Stress Urinary Incontinence Liqaa R Al-Khuzaee,
Iraqi JMS Published by Al-Nahrain College of Medicine ISSN 1681-6579 Email: Iraqi_jms_alnahrain@yahoo.com http://www. colmed-nahrain.edu.iq/ Polypropylene Mesh in Stress Urinary Incontinence Liqaa R Al-Khuzaee,
