We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
|
|
|
- Brendan Pitts
- 5 years ago
- Views:
Transcription
1 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4, , M Open access books available International authors and editors Downloads Our authors are among the 154 Countries delivered to TOP 1% most cited scientists 12.2% Contributors from top 500 universities Selection of our books indexed in the Book Citation Index in Web of Science Core Collection (BKCI) Interested in publishing with us? Contact book.department@intechopen.com Numbers displayed above are based on latest data collected. For more information visit
2 Provisional chapter A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) in Women Moreover, Its Reconstructive Surgery Abdel Karim M. El Hemaly, Laila A.E.S. Mousa, Ibrahim M. Kandil, Magdy S. Al Sayed, Mohammad Abdel Zaher, Magdi S.A. Soliman and Ahmad G. Serour Additional information is available at the end of the chapter 1. Introduction We put forward a new concept explaining the physiology of defecation and the anatomy of the internal anal sphincter (IAS). We explain the important role that the IAS plays in the control of defecation and fecal continence. Our aim is to explain the physiology of defection, factors that control fecal continence and causes of fecal incontinence in women together with the importance and the structure of the internal anal sphincter (IAS) and how it maintains fecal continence. The harmony between the central nervous system (CNS), the autonomic nervous system, the integrity of the anal sphincters and the muscles of the body are essential for keeping fecal continence. Traumatic injury can occur during childbirth affecting the anal sphincters and causing fecal incontinence (FI). Difficult vaginal deliveries can lead to more than one lesion at the same time. Simultaneous stress urinary incontinence (SUI), vaginal prolapse and fecal incontinence (FI) arise as a sequel to the cumulative trauma of recurrent frequent vaginal deliveries. We will describe a novel technique for the surgical repair of vaginal wall prolapse, SUI and fecal incontinence. Fecal Continence depends on a closed and empty anal canal, which in turn depends on four main factors: 2014 The Author(s). Licensee InTech. This chapter is distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
3 2 Fecal Incontinence 1. The integrity of the two anal sphincters: (the internal anal sphincter (IAS) and the external anal sphincter (EAS); both anal sphincters must be intact with healthy and strong walls. Intact healthy vascular and nerve supply are important factors for anal sphincter function. 2. An acquired high alpha-sympathetic tone at the IAS that keeps the anal canal closed and empty at all times until there is a desire and/ or a need to pass flatus &/ or stool and under suitable social circumstances. The high alpha-sympathetic tone is gained by learning and training in early childhood. 3. Healthy and strong pelvic floor muscles, including the levator ani, that maintain the angle between the rectum and the anal canal. 4. Synchronization and synergistic actions between the central nervous system (CNS), the autonomic nervous system, peripheral somatic nerves, the muscles and the anal sphincters. The closed and empty anal canal has a high anal pressure that is much higher than rectal pressure; rectal pressure reflects the abdominal pressure. We put forward a novel concept on the patho-physiology of defecation (1,2,3,4) (figure 1). Figure 1. Physiology of defecation Diagram that explains the steps that take place sequentially during defecation.
4 A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) in Women 3 2. Defecation in infancy and early childhood, before training Activation of stretch receptors in the rectum trigger impulses conveying rectal fullness which travel along the pelvic Parasympathetic (S2, 3 and 4) to the spinal cord sacral centers and lead to: 1. Reflex contraction of the rectal muscles. 2. Opening of the anal canal and relaxation of the external anal sphincter (EAS) allowing defection to occur. Mothers start to teach their children from the age of about two to three years how to control themselves and hold on until favorable social circumstances allow defecation. 3. Gaining control of defecation Gaining control is achieved by maintaining high alpha-sympathetic tone in the IAS keeping it contracted and the anal canal closed and empty at all times and until an appropriate place and time are available. On rectal distension, stretch receptors are stimulated. The sensation of rectal distension travels along the pelvic parasympathetic nerves to S 2, 3 and 4 to the sacral spinal cord centers. The ano-rectal junction contains specialized sensory end organs for tension, temperature, texture, touch and friction. Specialized afferent nerves sub serve these organized nerve endings. Controlled by the central nervous system (CNS), an intact sampling reflex allows the individual to choose whether to: a. Retain the rectal contents or, b. Discharge the contents whether flatus and/ or stool. Dependent on the available social circumstances, and once maturational control of continence has been achieved, if the woman chooses to retain rectal contents until a later time when social circumstances are more favourable, then she will: 1. Increase acquired high alpha-sympathetic tone at the IAS, ensuring its contraction and closure of the anal canal. 2. Augment the contraction of the EAS, which is a voluntary muscle, innervated with somatic nerve supply. 3. Increase the contraction of the levator ani muscles to exaggerate the angle between the rectum and anal canal. 4. Inhibit pelvic parasympathetic activity to the colon and the rectum preventing their muscular contractions. Discharge of the rectal contents occurs by relaxation of both anal sphincters (IAS & EAS) and the pelvic floor muscles, for a moment only to pass flatus, or for a longer time to release stool.
5 4 Fecal Incontinence When, an appropriate time and place are available and there is a desire to evacuate, under the control of the high CNS centers, through synergistic synchronized nervous actions between the autonomic, and the voluntary nervous systems, six neuromuscular actions will occur: 1. The woman will lower the acquired high alpha-sympathetic tone at the IAS relaxing it, opening the anal canal. 2. Through the voluntary NS, she will relax the pelvic floor muscles thus annulling the anorectal angle, to bring the anal canal and the rectum on one axis. She does so through relaxing the pelvic floor muscles. 3. Through the voluntary NS, she will also relax the EAS, which is a skeletal muscle innervated by the pudendal nerve. Then two synergistic synchronized actions between the voluntary and autonomic nervous system will occur. 4. The abdominal muscles and the diaphragm contract to increase the intra-abdominal pressure thus forcing the feces through the anal canal (The voluntary nervous system controls this action). 5. The smooth muscles of the distal colon and rectum contract; propelling the feces into the anal canal then to outside, (The autonomic nervous system does this action). 6. Subsequently, there will be sequential contractions of the three parts of the EAS: the deep, then the superficial then the subcutaneous parts that will squeeze the anal canal propelling any residual contents and emptying the anal canal completely. Fecal incontinence means involuntary escape of flatus, mucus and/ or stool. Fecal incontinence (FI) is one of the most distressing conditions, psychologically and socially, in any individual. It can lead to depression, social isolation, loss of self-esteem, loss of self-confidence and poor quality of life (QOL). Causes of FI include (5-17): a. Anal Sphincter damage: Traumatic injury to the anal sphincter, its nerve or blood supply, can lead to FI. Commonest causes are: 1. Childbirth trauma, 2. Trauma during and after surgery e.g. during performing surgical operation for piles; surgery for a pelvic or perineal tumor. 3. Traumatic injury caused by exposure to irradiation. 4. Damage of the nervous system. b. Pelvic floor dysfunction: 1. Rectocele, 2. Rectal prolapse, 3. Generalized weakness and sagging of the pelvic floor.
6 A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) in Women 5 c. Pelvic floor neuromuscular damage e.g. decreased perception of rectal sensations, decrease anal canal pressure, decreased squeeze pressure of the anal canal & impaired anal sensation. d. Constipation: Constipation is a common cause of fecal incontinence (it is similar to retention with overflow in urinary incontinence, UI). Constipation causes prolonged muscle and nerve stretching and leads to weakness of the intestinal muscles and nerves resulting in fecal incontinence. e. Diarrhea: Diarrhea, (similar to urge and urge incontinence in UI; overactive bladder in urinary incontinence) loose stool is more difficult to control than solid stool. Diarrhea can be: 1. Acute: e.g. G.I. infections, food poisoning. 2. Chronic: e.g. ulcerative colitis, Crohn s disease, diverticulitis or neoplasm; gastrectomy, vagotomy; malabsorption; thyrotoxicosis. When the cause of diarrhea is temporary such as G.I. infections or food reactions, incontinence tends to last for a short period. f. Nerve damage: damage to the autonomic, voluntary nervous systems or to the CNS can lead to FI. The sensation of rectal distension travels along the parasympathetic system to S 2, 3& 4. Damage to the sensory nerves &/or the motor nerves; or to the CNS can cause FI. If the damage affects the sensory nerves, detection of stool in the rectum is disabled, and one will not feel the need to defecate until it is too late. Causes of nerve damage include: 1. Childbirth trauma, 2. Long-term constipation, 3. Cerebral vascular accident, stroke, Neuropathy result of diseases such as diabetes mellitus, systemic lupus erthrymatosis (SLE) and disseminated sclerosis (DS). g. Loss of storage capacity of the rectum: Normally, the rectum stretches to hold stool until it is voluntarily discharged. However, rectal surgery, radiation treatment, and inflammatory bowel disease can cause scarring of the rectal wall. The rectal walls are unable to stretch as much and are unable to accommodate as much stool. Inflammatory bowel disease also can make rectal walls very irritated and thereby unable to keep stool h. Other causes: Fecal incontinence can have other causes including one or a combination of the following:
7 6 Fecal Incontinence 1. Congenital causes: In cases of imperforate anus, partial or complete lack of the sphincter mechanism (rare). 2. Patulous anus is associated with mental retardation. 3. Malabsorption conditions e.g. cystic fibrosis; drugs; and indigestible dietary fats that interfere with the intestinal absorption will lead to FI. 4. Lateral internal sphincterotomy (surgery for anal fissures); and surgery for high fistulain-ano. 5. Seizures and fits. 6. Perineal resection of the rectum for carcinoma. A major cause of fecal incontinence in young healthy women is anal sphincter damage during vaginal delivery, which occurs in as many as 18% in the USA. Studies from other countries indicate 5-20% of women report incontinence of stool 3-6 months after sphincter tear (EAS), and 29-53% of women report incontinence of flatus, despite having the tear repaired at delivery (5). Surgical repair of the torn EAS is by suturing end-to-end the torn edges of the EAS; or suturing after overlapping the torn edges. All published reports of the results of overlapping technique have shown significant improvements in symptoms of FI, with 60-80% achieving continence (6). It is also clear, however, that fecal control deteriorates over time with only 50% of the initial successful outcomes having improved continence at five years (7). Poor understanding of perineal anatomy and inadequate training in repair techniques are possible reasons for the high incidence of persistent symptoms (6,7). In addition, this can explain why repair of the EAS in cases of complete perineal tear whether by end-to-end or overlapping techniques does not lead to complete continence (7). The problem is that the role of the Internal Anal Sphincter (IAS) in defecation and FI is not quite clear. We will describe the IAS in a novel way and its important role in maintaining fecal continence and defecation (1, 2, 33), (figure 2). The IAS is a collagen-muscle tissue cylinder that surrounds the anal canal, and is in turn surrounded externally in its lower part by the EAS. Its nerve supply is from the alphasympathetic nerves coming through the thoracolumbar alpha-sympathetic nerves, from the hypogastric plexus (T10-L2). The collagen constitutes the firm frame (chassis) of the IAS, while the muscle is the mover of the sphincter in response to nerve stimulus. Its functions are: 1. On contraction, to keep the anal canal closed and empty with high anal pressure. 2. On relaxation, to open the anal canal to allow passage of flatus and/ or stool. An intact and strong IAS, through the acquired high alpha-sympathetic tone that maintains its contraction, keeps the anal canal closed and empty with high anal pressure, much higher than the rectal pressure.
8 A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) in Women 7 The IAS is in close relation to the posterior vaginal wall, which stretches very much during labor. Prolonged labor, difficult, multiple frequent labors cause overstretching of the posterior vaginal A wall, Novel leading Concept to flabbiness on the Patho-Physiology of the vagina with of Defecation subsequent and falling Fecal Incontinence down of the redundant (FI) vaginal in wall, women; posterior Moreover, vaginal its Reconstructive wall prolapse Surgery (rectocele). The redundancy of the vaginal wall is the result of rupture of its collagenous sheet (the vaginal firm frame). The rupture will affect and damage the intimately related IAS with subsequent FI. The rupture in the IAS affects the collagen layer (the collagen frame). Damage of the IAS causes dilation of the anal canal. Open and dilated anal canal with a lowered pressure allows the rectal contents to enter the open anal canal with subsequent fecal incontinence. Therefore, we can more correctly say that the first cause of FI is anal sphincter damage, with traumatic injury to one and/or both anal sphincters, IAS, EAS (figures: 3 to 15). A B (A)- Gray s Anatomy: Roger Warwick and Peter L. Williams (editors), 35th edition; Longman Group Ltd, 1973; anal musculature, Figure : The Colors anatomy by author. of the internal anal sphincter (IAS). The IAS, according to the new description, is a cylinder of collagen-muscle tissue that surrounds the anal canal. The external anal sphincter (EAS), with its three sections surrounds the IAS. (B)- Clinical Anatomy: A Revision and Applied Anatomy for Clinical Students, fifth edition, Harold Ellis (editor); Blackwell Scientific (A)- Gray s Publications, Anatomy: 1972; Roger 80. Warwick Colors by and author. Peter L. Williams (editors), 35th edition; Longman Group Ltd, 1973; anal musculature, Colors by author. Figure 2. (B)- The Clinical anatomy Anatomy: of the internal A Revision anal and sphincter Applied (IAS). Anatomy The IAS, for according Clinical Students, to the new fifth description, edition, Harold is a Ellis cylinder of collagen-muscle (editor); Blackwell tissue that Scientific surrounds Publications, the anal 1972; canal. 80. The Colors external by author. anal sphincter (EAS), with its three sections surrounds the IAS.
9 8 Fecal Incontinence Three dimension ultrasound (3DUS) images of the rectum and anal canal with torn IAS in patients with fecal incontinence (FI). FI is the main complaint in posterior vaginal wall prolapse (rectocele). Concomitant troubles, which commonly occur, are vaginal prolapse (anterior and posterior), stress urinary incontinence (SUI) and FI (1) (Figures: 13, 14 &15). The internal urethral sphincter (IUS) is in close contact to the anterior vaginal wall and will be involved in the childbirth trauma with subsequent SUI and anterior vaginal wall prolapse. Childbirth trauma is the major cause of damage, but aging, hormone deficiency (menopause) and degeneration from chronic and/or repeated infections causing collagen degeneration and A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) atrophy can add to the weakness of the internal urethral sphincter (IUS), IAS and the vagina. in women; Moreover, its Reconstructive Surgery Figure 3: Three dimension ultrasound (3DUS) images of the rectum and anal canal with torn IAS in patients with Figure 3. MRI images of a continent patient, (A), with an intact internal urethral sphincter (IUS), an intact IAS with a fecal incontinence (FI). closed and empty anal canal. In addition, the vagina is standing up and not prolapsed. In contrast, patient, (B) suffers from urinary incontinence, FI and vaginal prolapse as demonstrated by torn IUS, IAS and vagina.
10 A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) in women; Moreover, its Reconstructive Surgery A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) in Women 9 A B DO Figure 4: MRI images of a continent patient, (A), with an intact internal urethral sphincter (IUS), an intact IAS Figure with a closed 4. MRI and images empty anal of a canal. patient In addition, who suffers the vagina from is SUI standing and FI. up The and IUS not prolapsed. is torn especially In contrast, in patient, its upper part with funneling (B) of suffers the bladder from urinary neck, incontinence, and torn IAS FI and with vaginal an open prolapse anal as canal. demonstrated by torn IUS, IAS and vagina. A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) in women; Moreover, its Reconstructive Surgery The patient previously had a classical repair so the vagina is not prolapsed. However, she suffers from combined SUI&FI. The anal canal is open and the IAS is torn Figure 5. Figure MRI images 5: MRI images of a patient of a patient who who suffers suffers from from SUI SUI and and FI. FI. The The IUS IUS is is torn torn especially in in its its upper upper part part with with funneling of the funneling bladder of neck, the bladder and torn neck, IAS and with torn an IAS open with anal open canal. canal. A B
11 is torn 10 Fecal Incontinence Figure 5: MRI images of a patient who suffers from SUI and FI. The IUS is torn especially in its upper part with funneling of the bladder neck, and torn IAS with an open anal canal. A B DO Intact IAS with an empty and closed anal canal. Prolapsed vagina Torn IAS with an open analcanal A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) in women; Moreover, its Reconstructive Surgery Figure Figure 6: MRI 6. MRI images images of a normal of a normal continent continent woman (A) woman with intact (A) with IUS, IAS intact with IUS, a closed IAS with empty a anal closed canal empty and anal canal and nor normal non-prolapsing vagina. vagina. Image Image (B) (B) is of is an of incontinent an incontinent patient patient with torn with IUS torn and torn IUS IAS and and torn prolapsed IAS and prolapsed vagina. vagina. A B Figure 7. Images with 3DUS of the rectum and anal canal in normal continent woman (B) with healthy, intact IAS and a closed empty anal canal. In contrast, in (A) the IAS is torn leading to a widely open anal canal in a patient with FI. Figure 7: Images with 3DUS of the rectum and anal canal in normal continent woman (B) with healthy, intact IAS and a closed empty anal canal. In contrast, in (A) the IAS is torn leading to a widely open anal canal in a patient with FI.
12 A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) in Women 11 A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) in women; Moreover, its Reconstructive Surgery Figure 8. An image with 3DUS of a patient with FI that shows torn IAS, and an open anal canal with a piece of stool in Figure 8: An image with 3DUS of a patient with FI that shows torn IAS, and an open anal canal with a piece of the anal canal. stool in the anal canal. Figure 9. Histopathology of a surgical specimen of the IAS stained with Masson trichrome acetate, showing a torn collagen sheet with relative healthy muscle bundles.
13 12 Fecal Incontinence A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) in women; Moreover, its Reconstructive Surgery A B Figure 10: Images with 3DUS of the rectum and anal canal in a normal continent woman (B) with a healthy, intact Figure 10. Images with 3DUS of the rectum and anal canal in a normal continent woman (B) with a healthy, intact IAS IAS and a closed empty anal canal. In contrast, in (A) the IAS is torn leading to a widely open anal canal in a and a closed empty anal canal. In contrast, in (A) the IAS is torn leading to a widely open anal canal in a patient with FI. patient with FI. Figure 11. Images with 3DUS of patients with FI. The IAS is torn and the anal canal is open. Figure 11: Images with 3DUS of patients with FI. The IAS is torn and the anal canal is open.
14 A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) in Women 13 A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) in women; Moreover, its Reconstructive Surgery A B C D Figure 12: Images with 3DUS of the rectum and anal canal in patients with FI. Images in C & D are of a complete perineal tear (fourth degree). The external anal sphincter is torn and appears as a horseshoe; in addition, the internal anal sphincter is torn as well. Images in A and B are of the internal anal sphincter, which is torn leading to an open dilated anal canal. The IAS in this image also appears like a horseshoe. Figure 12. Images with 3DUS of the rectum and anal canal in patients with FI. Images in C & D are of a complete perineal tear (fourth degree). The external anal sphincter is torn and appears as a horseshoe; in addition, the internal anal sphincter is torn as well. Images in A and B are of the internal anal sphincter, which is torn leading to an open dilated anal canal. The IAS in this image also appears like a horseshoe.
15 14 Fecal Incontinence Figure A Novel 13. images Concept of patients on the Patho-Physiology who suffer from pelvic of organ Defecation dysfunction and Fecal with SUI, Incontinence FI and vaginal (FI) prolapse simultaneously. The images show torn IUS and IAS. in women; Moreover, its Reconstructive Surgery A patient, who has SUI and FI, had 3DUS examination; the IUS is torn and the urethra is open. The IAS is torn and the anal canal is open and dilated. Figure 14: 3DUS images which show concomitant torn IUS and IAS in a patient who suffers pelvic floor Figure dysfunction 14. images which show concomitant torn IUS and IAS in a patient who suffers pelvic floor dysfunction
16 A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) in Women 15 A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) in women; Moreover, its Reconstructive Surgery A B C D E Figure 15: Surgical photos of a patient with anterior vaginal wall prolapse, posterior vaginal wall prolapse, SUI, Figure and FI. 15. The Surgical metal photos catheter of is a directed patient with forward anterior and vaginal upward wall (A), prolapse, which means posterior loss vaginal of posterior wall prolapse, urethro-vesical SUI, and FI. The angle. metal We catheter dissect the is directed IUS from forward the anterior and upward vaginal (A), wall which (B&C) means and loss mended of posterior the torn urethro-vesical IUS with simple angle. interrupted We dissect sutures the IUS (D&E). from the anterior vaginal wall (B&C) and mended the torn IUS with simple interrupted sutures (D&E). In addition, anal intercourse can cause traumatic damage of the IAS with subsequent FI (1, 2 & 3). 4. Diagnosis In addition to the clinical history and examination, imaging with three-dimension ultrasound (3DUS) and magnetic resonance (MRI) is an essential tool in the management of cases of FI. Typically, it shows an open anal canal with torn IAS. It may also reveal an open urethra and torn IUS with concomitant SUI and vaginal prolapse (figures: 3, 4, 5, 6, 7, 8, 10, 11, 12, 13 & 14). Histopathological examination of a torn piece of the IAS confirm that the rupture mainly affects the collagen frame of the IAS (figure 9).
17 16 Fecal Incontinence 5. Reconstructive surgery (figures: 15, 16, 17, 18 & 19) In conclusion, a major cause of FI in young patients is torn IAS. We have developed an operative procedure to expose and mend the torn edges of the IAS. Since there is usually concomitant vaginal prolapse and SUI, we try to correct these concurrently as part of this new operation. Urethro-Ano-Vaginoplasty Al Azhar repair operation A The Novel operation Concept consists the of Anterior Patho-Physiology and Posterior of sections. Defecation and Fecal Incontinence (FI) in women; Moreover, its Reconstructive Surgery In the Anterior section, we correct the SUI and the anterior vaginal wall descent through the following steps: (Figures: 15 & 16). Figure 16. After mending the IUS, we do overlapped the two vaginal flaps as seen in the photos. We bring the right vaginal flap underneath the left vaginal flap with this novel dragging suture as seen in (A) and (B), repeating it 4-6 times. Figure Then 16: After we suture mending the free the IUS, edge we of the do overlapped left vaginal the flap two as far vaginal laterally flaps in as the seen vagina the on photos. the right We as bring seen in the C& D. right Thus, vaginal we strengthen flap underneath the anterior the vaginal left vaginal wall and flap add with extra this strength novel dragging to the mended suture as IUS. seen in (A) and (B), repeating it 4-6 times. Then we suture the free edge of the left vaginal flap as far laterally in the vagina on the right as seen in C& We D. grasp Thus, the we cervix strengthen with the two anterior pairs vaginal of cervical wall and volsela. add extra We strength inject to the about mended IUS. ml. normal saline with adrenaline (2 per 200 thousand concentration}, beneath the vaginal wall to act as a hydro
18 A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) in Women 17 dissection and vasoconstrictor. This separates the anterior vaginal wall from the posterior wall of the IUS. We make a 2-4 cm transverse incision about three cm above the external cervical os. With a pair of dissecting scissors, we separate the anterior vaginal wall from the IUS. We cut the anterior vaginal wall longitudinally from the transverse cut all the way, down, to the submeatal sulcus, which correspond to the perineal membrane. We grasp each vaginal flap with three pairs of Kocher s forceps. The defect in the IUS will be apparent and on each side, we can clearly see two clear edges. One edge is of the anterior vaginal wall and the other is the torn posterior wall of the IUS. 1. Expose the IUS (we dissect the IUS clear from the anterior vaginal wall). 2. Mend the torn posterior wall of the IUS by several (6-8) simple interrupted sutures using number 0 polyglycan thread, sutures (figure 15). 3. Strengthen the anterior vaginal wall by overlapping the two vaginal flaps, using a novel dragging sutures, dragging the right vaginal flap underneath the left vaginal flap. Then we suture the free edge of the left vaginal flap as far lateral on the right side of the vagina. This strengthens the anterior vaginal wall and decreases its width, also adding extra support to the mended IUS, and preserving the body collagen. Posterior section (figures: 17, 18 & 19). Figure 17. Image A clearly shows the posterior vaginal wall even without straining. This is visible with posterior vaginal wall prolapse. Image (B) is 3DUS showing rectocele of the same patient who suffers FI.
19 18 Fecal Incontinence A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) in women; Moreover, its Reconstructive Surgery A B C D Figure 18. Surgical steps of posterior repair. We dissect the IAS from the posterior vaginal wall (A). We mend the sphincter (B&C), Figure 18: in addition, Surgical steps we of approximate posterior repair. the We two dissect levator the ani IAS muscles from the posterior by two stitches, vaginal wall but (A). we We do mend not tie the them till we finish overlapping sphincter (B&C), the posterior in addition, vaginal we approximate wall (D). the two levator ani muscles by two stitches, but we do not tie them till we finish overlapping the posterior vaginal wall (D). Figure 19. Images that show the steps taken to expose the torn IAS and mend it (A&B). We then overlapped the redundant posterior vaginal wall as is seen in (C). Next, we approximated the two levator ani muscles; and finally repaired the perineum as is seen in (D).
20 A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) in Women 19 We hydro dissect between the posterior vaginal wall, the anal canal and the rectum; and in the perineum as described for the anterior section. We make a V-shape incision at the line between the posterior vaginal wall and the perineal skin down to the perineum. Then we try to create a space between the posterior vaginal wall and the anal canal by sharp and blunt dissection. Next with a pair of dissecting scissors, we separate the posterior vaginal wall from the rectum and anal canal. Then we cut the posterior vaginal wall longitudinally in the midline to beyond the apex of the prolapse protrusion. We hold each vaginal flap with three pairs of Kocher s forceps. Two different edges can clearly be seen on each side, one is the vaginal edge, and the other is the anterior wall of the torn IAS. 1. We dissect the torn IAS clear from the posterior vaginal wall. 2. Mend the torn wall of the sphincter by serial interrupted simple sutures with number 0 polyglcan thread. 3. Approximate the two levator ani muscles. 4. Strengthen the posterior vaginal wall by overlapping the two vaginal flaps; thus, we also add extra support to the mended IAS and keeping the natural body collagen. 5. Repair the perineum. We put a Foley s catheter and vagina pack for 24 hours. List of abbreviations 3DUS: Three-Dimension Ultra Sound. CNS: Central Nervous System. EAS: External Anal Sphincter. EAS: External Anal Sphincter. EUS: External Urethral Sphincter. FI: Fecal Incontinence. GI: Gastro-Intestinal. IAS: Internal Anal Sphincter. IUS: Internal Urethral Sphincter MRI: Magnetic Resonance Imaging. NS: Nervous System. QOL: Quality Of Life. SUI: Stress Urinary Incontinence.
21 20 Fecal Incontinence T10-L2: Thoracic 10 to Lumbar two. UI: Urinary Incontinence. Author details Abdel Karim M. El Hemaly 1, Laila A.E.S. Mousa 1, Ibrahim M. Kandil 1, Magdy S. Al Sayed 2, Mohammad Abdel Zaher 1,3, Magdi S.A. Soliman 3 and Ahmad G. Serour 1 *Address all correspondence to: profakhemaly@hotmail.com 1 Al Azhar University, Cairo, Egypt 2 University Hospital, Salman Bin Abdul Aziz University, K.S.A., Egypt 3 Salman Bin Abdul Aziz University, K.S.A., Egypt References [1] Abdel Karim M El Hemaly, Laila A Mousa, Asim Kurjak, Ibrahim M Kandil, Ahmad G Serour. Pelvic Floor Dysfunction, the Role of Imaging and Reconstructive Surgery, Donald School Journal of Ultrasound in Obstetrics and Gynecology, DSJUOG, January-March 2013;7(1):86-97 [2] Abdel Karim M. El Hemaly*, Ibrahim M. Kandil, Asim Kurjak, Laila A. S. Mousa, Hossam H. Kamel, Ahmad G. Serour. Ultrasound Assessment of the Internal Anal Sphincter in Women with Fecal Incontinence and Posterior Vaginal Wall Prolapse (Rectocele). Donald School Journal of Ultrasound in Obstetrics and Gynecology, DSJUOG, vol. 5, No 4, ; October-December [3] Abdel Karim M. El Hemaly*, Laila A. S. Mousa Ibrahim M. Kandil, Fatma S. El Sokkary, Ahmad G. Serour, Hossam Hussein. Fecal Incontinence, A Novel Concept: The Role of the internal Anal sphincter (IAS) in defecation and fecal incontinence. Gynaecologia et Perinatologia, Vol19, No 2; April -June [4] Abdel Karim M. El Hemaly*, Laila A. S. Mousa Ibrahim M. Kandil, Fatma S. El Sokkary, Ahmad G. Serour, Hossam Hussein. Surgical Treatment of Stress Urinary Incontinence, Fecal Incontinence and Vaginal Prolapse by A Novel Operation "Urethro- Ano-Vaginoplasty" Gynaecologia et Perinatologia, Vol19, No 3; July- September [5] Pinta TM, Kylanpaa ML, Salmi TK, et al. Primary sphincter repair: Are the results of the operation good enough? Dis Colon Rectum 2004; 47:18-23.
22 A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) in Women 21 [6] France-Borello Diane, Kathryn L.Burgio, Holly E. Richter, Hallina Zycnski, Mary Pat Fitzgerald, William Whitehead, Paul Fine, Ingrid Nygaard, Victoria L. Handa, Anthony G. Vesco, Anne M. Wiber and Morton B. Brown; PhD, for the Pelvic Floor Disorders, Network, Fecal and Urinary incontinence in primiparous women. Obstet & Gynecol 2006; 108(4): [7] Halverson AL, Hull TL. Long-term outcome of overlapping anal sphincter repair. Dis Colon Rectum 2002; 45: [8] Sultan AH, Thakar R. Lower genital tract and anal sphincter trauma. Best Pract Res Clin Obstet Gyecol 2002; 16: [9] Faltin DL, Boulvain M, Floris LA, et al. Diagnosis of anal sphincter tears to prevent fecal incontinence: a randomized controlled trial. Obstet Gynecol 2005;106(1): [10] Nichols CM, Ramakrishnan V, Gill EJ, et al. Anal incontinence in women with and those without pelvic floor disorders. Obstet Gynecol 2005; 106(6): [11] Dietz HP, Lanzarone V. Levator trauma after vaginal delivery. Obstet Gynecol 2005;106(4): [12] Jackson SL, Weber AM, Hull TL, et al. Fecal incontinence in women with urinary incontinence and pelvic organ prolapse. Obstet Gynecol 1997; 89(3): [13] Mimura T, Kaminishi M, Kamm MA. Diagnostic evaluation of patients with faecal incontinence at a specialist institution. Dig Surg 2004; 21(3): [14] Kruger JA, Heap SW, Murphy BA, et al. Pelvic floor function in nulliparous women using three-dimensional ultrasound and magnetic resonance imaging. Obstet Gynecol 2008;111(3): [15] Soligo M, Salvatore S, Milani R, et al. Double incontinence in urogynecologic practice: a new insight. Am J Obstet Gynecol 2003; 189(2): [16] Nichols CM, Gill EJ, Nguyen T, et al. Anal sphincter injury in women with pelvic floor disorders. Obstet Gynecol 2004; 104(4): [17] Chen GD, Hu SW, Chen YC, et al. Prevalence and correlations of anal incontinence and constipation in Taiwanese women. Neurourol Urodyn 2003; 22(7): [18] Gray s Anatomy: Roger Warwick and Peter L. Williams (editors), 35th edition; Longman Group Ltd, 1973; anal musculature, [19] Clinical Anatomy: A Revision and Applied Anatomy for Clinical Students, fifth edition, Harold Ellis (editor); Blackwell Scientific Publications, 1972; 80.
23
Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence
 Cronicon OPEN ACCESS GYNAECOLOGY Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence Abdel Karim M El Hemaly 1 * and Laila ASE Mousa 1 1 Professor of Obstetrics and gynaecology,
Cronicon OPEN ACCESS GYNAECOLOGY Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence Abdel Karim M El Hemaly 1 * and Laila ASE Mousa 1 1 Professor of Obstetrics and gynaecology,
Accidental Bowel Leakage (Fecal Incontinence)
 Accidental Bowel Leakage (Fecal Incontinence) What is Accidental Bowel Leakage (ABL)? Accidental bowel leakage is the inability to control solid or liquid stool. This is the inability to control gas and
Accidental Bowel Leakage (Fecal Incontinence) What is Accidental Bowel Leakage (ABL)? Accidental bowel leakage is the inability to control solid or liquid stool. This is the inability to control gas and
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
MCOMPASS ANAL MANOMETRY AN OVERVIEW
 MCOMPASS ANAL MANOMETRY AN OVERVIEW ANAL MANOMETRY MEASURES PRESSURE ALLOWS INTERPRITATION SENSATION RAIR RECTAL COMPLIANCE MOTIVATION OF THE PATIENT FUNCTION OF THE PUDENDAL NERVE WHEN TO USE ANAL MANOMETRY
MCOMPASS ANAL MANOMETRY AN OVERVIEW ANAL MANOMETRY MEASURES PRESSURE ALLOWS INTERPRITATION SENSATION RAIR RECTAL COMPLIANCE MOTIVATION OF THE PATIENT FUNCTION OF THE PUDENDAL NERVE WHEN TO USE ANAL MANOMETRY
MCOMPASS ANAL MANOMETRY AN OVERVIEW
 MCOMPASS ANAL MANOMETRY AN OVERVIEW ANAL MANOMETRY MEASURES PRESSURE ALLOWS INTERPRITATION SENSATION RAIR RECTAL COMPLIANCE MOTIVATION OF THE PATIENT FUNCTION OF THE PUDENDAL NERVE WHEN TO USE ANAL MANOMETRY
MCOMPASS ANAL MANOMETRY AN OVERVIEW ANAL MANOMETRY MEASURES PRESSURE ALLOWS INTERPRITATION SENSATION RAIR RECTAL COMPLIANCE MOTIVATION OF THE PATIENT FUNCTION OF THE PUDENDAL NERVE WHEN TO USE ANAL MANOMETRY
Postpartum Complications
 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May Dr. Annie Leong MBBS, FRANZCOG, CU
 EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May 2011 Dr. Annie Leong MBBS, FRANZCOG, CU Restore normal perineal anatomy Achieve good haemostasis Avoid infection and wound breakdown Avoid coital
EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May 2011 Dr. Annie Leong MBBS, FRANZCOG, CU Restore normal perineal anatomy Achieve good haemostasis Avoid infection and wound breakdown Avoid coital
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Physiologic Anatomy and Nervous Connections of the Bladder
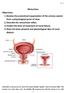 Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Surgical Management for Defecation Dysfunction
 Defecatory Dysfunction Surgical Management for Defecation Dysfunction JMAJ 46(9): 378 383, 2003 Tatsuo TERAMOTO Professor, 1st Department of Surgery, School of Medicine, Toho University Abstract: Typical
Defecatory Dysfunction Surgical Management for Defecation Dysfunction JMAJ 46(9): 378 383, 2003 Tatsuo TERAMOTO Professor, 1st Department of Surgery, School of Medicine, Toho University Abstract: Typical
2/5/2016. Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach
 Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Fecal Incontinence. Inability to retain feces or bowel movements, resulting in involuntary passage of feces or bowel movements
 Fecal Incontinence (Involuntary Passage of Feces or Bowel Movements) Basics OVERVIEW Inability to retain feces or bowel movements, resulting in involuntary passage of feces or bowel movements GENETICS
Fecal Incontinence (Involuntary Passage of Feces or Bowel Movements) Basics OVERVIEW Inability to retain feces or bowel movements, resulting in involuntary passage of feces or bowel movements GENETICS
Anorectal Diagnostic Overview
 Anorectal Diagnostic Overview 11-25-09 3.11.2010 2009 2010 Anorectal Manometry Overview Measurement of pressures and the annotation of rectal sensation throughout the rectum and anal canal to determine:
Anorectal Diagnostic Overview 11-25-09 3.11.2010 2009 2010 Anorectal Manometry Overview Measurement of pressures and the annotation of rectal sensation throughout the rectum and anal canal to determine:
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology
 Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives
 Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Anal Sphincter Injuries: Acute Management
 Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
17 th European congress of Physical Rehabilitation Medicine. 38th SIMFER congress
 17 th European congress of Physical Rehabilitation Medicine 38th SIMFER congress European Rehabilitation: Quality, Evidence, Efficacy and Effectiveness Venice, May 23 27 2010 THE PHYSIATRIST AND URO-GYNECOLOGICAL
17 th European congress of Physical Rehabilitation Medicine 38th SIMFER congress European Rehabilitation: Quality, Evidence, Efficacy and Effectiveness Venice, May 23 27 2010 THE PHYSIATRIST AND URO-GYNECOLOGICAL
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests. Amelyn R.
 Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
GI Physiology - Investigating and treating patients with pelvic floor dysfunction. Lynne Smith Department of GI Physiology NGH Sheffield
 GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
Pelvic Floor Ultrasound Imaging. Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague)
 Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Ultrasonic Assessment of the Internal Urethral Sphincter in Stress Urinary Incontinence
 ISPUB.COM The Internet Journal of Gynecology and Obstetrics Volume 2 Number 1 Ultrasonic Assessment of the Internal Urethral Sphincter in Stress Urinary Incontinence I Kandil, A El Hemaly, M Radwan Citation
ISPUB.COM The Internet Journal of Gynecology and Obstetrics Volume 2 Number 1 Ultrasonic Assessment of the Internal Urethral Sphincter in Stress Urinary Incontinence I Kandil, A El Hemaly, M Radwan Citation
Duc M. Vo, MD, FACS Northwest Surgical Specialists
 Duc M. Vo, MD, FACS Northwest Surgical Specialists Disclosures none Outline Definition Etiologies Exam findings Additional testing Medical management Surgical options What is fecal incontinence? Recurrent
Duc M. Vo, MD, FACS Northwest Surgical Specialists Disclosures none Outline Definition Etiologies Exam findings Additional testing Medical management Surgical options What is fecal incontinence? Recurrent
TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
Regulation of the Urinary Bladder Chapter 26
 Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
Vincent Letouzey, MD, PhD
 How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
CONSTIPATION. Atan Baas Sinuhaji
 CONSTIPATION Atan Baas Sinuhaji Sub Division of Pediatrics Gastroentero-Hepatolgy Department of ChildHealth,School of Medicine University of Sumatera Utara MEDAN DEFECATION REGULAR PATTERN CONSTIPATION
CONSTIPATION Atan Baas Sinuhaji Sub Division of Pediatrics Gastroentero-Hepatolgy Department of ChildHealth,School of Medicine University of Sumatera Utara MEDAN DEFECATION REGULAR PATTERN CONSTIPATION
Robotic Ventral Rectopexy
 Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Pelvic Floor Disorders. Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon
 Pelvic Floor Disorders Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon What is Pelvic Floor Disorder Surgical perspective symptoms of RED, FI or prolapse on the background
Pelvic Floor Disorders Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon What is Pelvic Floor Disorder Surgical perspective symptoms of RED, FI or prolapse on the background
Obstetric Anal Sphincter Injury. An update on best practices. Objectives
 Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
NEUROGENIC BLADDER. Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph
 NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
Childbirth Trauma & Its Complications 23/ Mr Stergios K. Doumouchtsis
 Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
High-field (3T) magnetic resonance defecography with functional assessment of the evacuation phase: A pictorial essay
 High-field (3T) magnetic resonance defecography with functional assessment of the evacuation phase: A pictorial essay Poster No.: C-430 Congress: ECR 2009 Type: Educational Exhibit Topic: Abdominal and
High-field (3T) magnetic resonance defecography with functional assessment of the evacuation phase: A pictorial essay Poster No.: C-430 Congress: ECR 2009 Type: Educational Exhibit Topic: Abdominal and
Prolapse & Urogynaecology. Hester Mannion and Fabi Sica
 Prolapse & Urogynaecology Hester Mannion and Fabi Sica Take home messages Prolapse and associated incontinence is very common It has a devastating effect on the QoL of the patient and their partner Strategies
Prolapse & Urogynaecology Hester Mannion and Fabi Sica Take home messages Prolapse and associated incontinence is very common It has a devastating effect on the QoL of the patient and their partner Strategies
Increased motor unit fibre density in the external
 Journal of Neurology, Neurosurgery, and Psychiatry, 1980, 43, 343-347 Increased motor unit fibre density in the external anal sphincter muscle in ano-rectal incontinence: a single fibre EMG study M E NEILL
Journal of Neurology, Neurosurgery, and Psychiatry, 1980, 43, 343-347 Increased motor unit fibre density in the external anal sphincter muscle in ano-rectal incontinence: a single fibre EMG study M E NEILL
Bowel dysfunctions following hysterectomy
 Bowel dysfunctions following hysterectomy Marco Scaglia Retrospective studies Retrospective studies 6% of patients developed new symptoms (Carlson 1994) Constipation is more common in women after hysterectomy
Bowel dysfunctions following hysterectomy Marco Scaglia Retrospective studies Retrospective studies 6% of patients developed new symptoms (Carlson 1994) Constipation is more common in women after hysterectomy
Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury. Original Policy Date
 MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases
 CASE REPORT Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases Vasant Kawade 1 and Abhijit Ambike 2 Professor and Head, Department of OBGY, B.K.L.Walawakarl Rural Medical
CASE REPORT Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases Vasant Kawade 1 and Abhijit Ambike 2 Professor and Head, Department of OBGY, B.K.L.Walawakarl Rural Medical
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
Summary. Neuro-urodynamics. The bladder cycle. and voiding. 14/12/2015. Neural control of the LUT Initial assessment Urodynamics
 Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Hemorrhoids. Carlos R. Alvarez-Allende PGY-III Colorectal Surgery
 Hemorrhoids Carlos R. Alvarez-Allende PGY-III Colorectal Surgery Overview Anatomy Classification Etiology Incidence Symptoms Differential Diagnosis Medical Management Surgical Management Anatomy Anal canal
Hemorrhoids Carlos R. Alvarez-Allende PGY-III Colorectal Surgery Overview Anatomy Classification Etiology Incidence Symptoms Differential Diagnosis Medical Management Surgical Management Anatomy Anal canal
8 A SIMPLE FISTULA REPAIR, STEP BY STEP
 8 A SIMPLE FISTULA REPAIR, STEP BY STEP The first step is to suture the labia to the thighs and cover the anus with a swab (Figure 31). Figure 31 The labia are sutured to the thighs and the anus is covered
8 A SIMPLE FISTULA REPAIR, STEP BY STEP The first step is to suture the labia to the thighs and cover the anus with a swab (Figure 31). Figure 31 The labia are sutured to the thighs and the anus is covered
ACG Clinical Guideline: Management of Benign Anorectal Disorders
 ACG Clinical Guideline: Management of Benign Anorectal Disorders Arnold Wald, MD, MACG 1, Adil E. Bharucha, MBBS, MD 2, Bard C. Cosman, MD, MPH, FASCRS 3 and William E. Whitehead, PhD, MACG 4 1 Division
ACG Clinical Guideline: Management of Benign Anorectal Disorders Arnold Wald, MD, MACG 1, Adil E. Bharucha, MBBS, MD 2, Bard C. Cosman, MD, MPH, FASCRS 3 and William E. Whitehead, PhD, MACG 4 1 Division
Objectives. Key Outlines:
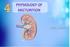 Objectives! Iden8fy and describe the Func8onal Anatomy of Urinary Bladder! Describe the mechanism of filling and emptying of the urinary bladder! Cystometrogram! Appreciate neurogenic control of the mechanism
Objectives! Iden8fy and describe the Func8onal Anatomy of Urinary Bladder! Describe the mechanism of filling and emptying of the urinary bladder! Cystometrogram! Appreciate neurogenic control of the mechanism
Appendix B Protocol for management of obstetric anal sphincter injury THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS
 Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Novel Options for the Management of Fecal Incontinence
 Novel Options for the Management of Fecal Incontinence Arnold Wald, MD, MACG University of Wisconsin School of Medicine and Public Health, Madison WI ANORECTAL CONTINENCE MECHANISMS Reservoir Elements
Novel Options for the Management of Fecal Incontinence Arnold Wald, MD, MACG University of Wisconsin School of Medicine and Public Health, Madison WI ANORECTAL CONTINENCE MECHANISMS Reservoir Elements
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Uterine prolapse & Fistulas. Raja Nursing Instructor RN, DCHN, Post RN. BSc.N
 Uterine prolapse & Fistulas Raja Nursing Instructor RN, DCHN, Post RN. BSc.N 31/03/2016 Objectives 1. Review the anatomy & physiology of female reproductive system 2. Discuss the causes, pathophysiology,
Uterine prolapse & Fistulas Raja Nursing Instructor RN, DCHN, Post RN. BSc.N 31/03/2016 Objectives 1. Review the anatomy & physiology of female reproductive system 2. Discuss the causes, pathophysiology,
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
5/29/2015. Objectives. Functions of the PFM. Various phases of PFM. Evaluation of the PFM
 The Physical Therapist s Approach to the Female Pelvic Floor Musculature Examination and Treatment. Presented By: Evelyne Burtis, DPT Objectives Core and pelvic floor muscles (PFM) Functions of the PFM
The Physical Therapist s Approach to the Female Pelvic Floor Musculature Examination and Treatment. Presented By: Evelyne Burtis, DPT Objectives Core and pelvic floor muscles (PFM) Functions of the PFM
Chapter 14 The Autonomic Nervous System Chapter Outline
 Chapter 14 The Autonomic Nervous System Chapter Outline Module 14.1 Overview of the Autonomic Nervous System (Figures 14.1 14.3) A. The autonomic nervous system (ANS) is the involuntary arm of the peripheral
Chapter 14 The Autonomic Nervous System Chapter Outline Module 14.1 Overview of the Autonomic Nervous System (Figures 14.1 14.3) A. The autonomic nervous system (ANS) is the involuntary arm of the peripheral
Guide to Pelvic Floor Multicompartment Scanning
 Guide to Pelvic Floor Multicompartment Scanning These guidelines have been prepared by Giulio A. Santoro, MD, PhD, Head Pelvic Floor Unit, Section of Anal Physiology and Ultrasound, Coloproctology Service,
Guide to Pelvic Floor Multicompartment Scanning These guidelines have been prepared by Giulio A. Santoro, MD, PhD, Head Pelvic Floor Unit, Section of Anal Physiology and Ultrasound, Coloproctology Service,
Human Anatomy rectum
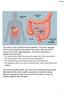 rectum The colon is also called the large intestine. The ileum (last part of the small intestine) connects to the cecum (first part of the colon) in the lower right abdomen. The rest of the colon is divided
rectum The colon is also called the large intestine. The ileum (last part of the small intestine) connects to the cecum (first part of the colon) in the lower right abdomen. The rest of the colon is divided
10/15/2012. Pelvic Pain and Dysfunction
 Pain and Holly Bommersbach PT, MPT Angela De La Cruz PT, MPT Pain which occurs in the perineal and/or anal areas Pain in the lower abdomen, low back and/or pelvic girdle Pain may often affect other areas,
Pain and Holly Bommersbach PT, MPT Angela De La Cruz PT, MPT Pain which occurs in the perineal and/or anal areas Pain in the lower abdomen, low back and/or pelvic girdle Pain may often affect other areas,
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Pelvic Floor Overactivity: Definition and Pathophysiology
 + Pelvic Floor Overactivity: Definition and Pathophysiology WS # 24 The Overactive Pelvic Floor Anna Padoa, MD Urogynecology and Pelvic Floor Service Assaf Harofeh Medical Center + Definition of overactive
+ Pelvic Floor Overactivity: Definition and Pathophysiology WS # 24 The Overactive Pelvic Floor Anna Padoa, MD Urogynecology and Pelvic Floor Service Assaf Harofeh Medical Center + Definition of overactive
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
A Nursing Assessment Tool for Adults With Fecal Incontinence
 Journal of Wound, Ostomy and Continence Nursing 2000, 279- A Nursing Assessment Tool for Adults With Fecal Incontinence Christine Norton, MA, RN, and Sonya Chelvanayagam, MSc, RN Abstract Fecal incontinence
Journal of Wound, Ostomy and Continence Nursing 2000, 279- A Nursing Assessment Tool for Adults With Fecal Incontinence Christine Norton, MA, RN, and Sonya Chelvanayagam, MSc, RN Abstract Fecal incontinence
Urodynamic and electrophysiological investigations in neuro-urology
 Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
Le fort s operation for prolapse uterus: A forgotten procedure
 2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
ParasymPathetic Nervous system. Done by : Zaid Al-Ghnaneem
 ParasymPathetic Nervous system Done by : Zaid Al-Ghnaneem In this lecture we are going to discuss Parasympathetic, in the last lecture we took sympathetic and one of the objectives of last lecture was
ParasymPathetic Nervous system Done by : Zaid Al-Ghnaneem In this lecture we are going to discuss Parasympathetic, in the last lecture we took sympathetic and one of the objectives of last lecture was
CHERRY BAKER AND TRACEY GJERTSEN BSC MCSP HCPC INTRODUCTION TO DIAMOND TRAINING REHAB AND PERFORMANCE FOR PELVIC POWER
 CHERRY BAKER AND TRACEY GJERTSEN BSC MCSP HCPC INTRODUCTION TO DIAMOND TRAINING REHAB AND PERFORMANCE FOR PELVIC POWER What is it? Where is it? Breathing Graded relaxation Incontinence Stress Incontinence
CHERRY BAKER AND TRACEY GJERTSEN BSC MCSP HCPC INTRODUCTION TO DIAMOND TRAINING REHAB AND PERFORMANCE FOR PELVIC POWER What is it? Where is it? Breathing Graded relaxation Incontinence Stress Incontinence
Pelvic organ prolapse. Information for patients Continence Service
 Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
Incontinence; Lets talk about it. Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery
 Incontinence; Lets talk about it Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery Select the most appropriate subtitle for this talk A: Bladders gone wild! B: There s no such thing
Incontinence; Lets talk about it Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery Select the most appropriate subtitle for this talk A: Bladders gone wild! B: There s no such thing
Technologies and architectures" Stimulator, electrodes, system flexibility, reliability, security, etc."
 March 2011 Introduction" Basic principle (Depolarization, hyper polarization, etc.." Stimulation types (Magnetic and electrical)" Main stimulation parameters (Current, voltage, etc )" Characteristics (Muscular
March 2011 Introduction" Basic principle (Depolarization, hyper polarization, etc.." Stimulation types (Magnetic and electrical)" Main stimulation parameters (Current, voltage, etc )" Characteristics (Muscular
Toning your pelvic floor WELCOME
 Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Pelvic Floor and More.. Urinary Continence. Urinary Incontinence. Normal Bladder Function
 Pelvic Floor and More.. Jo Pitts Women s and Men s Health Physiotherapist Milton Keynes University Hospital Women s and Men s Health Physiotherapy at MKUH Pregnancy-related back and pelvic girdle pain
Pelvic Floor and More.. Jo Pitts Women s and Men s Health Physiotherapist Milton Keynes University Hospital Women s and Men s Health Physiotherapy at MKUH Pregnancy-related back and pelvic girdle pain
Bard: Continence Therapy. Stress Urinary Incontinence. Regaining Control. Restoring Your Lifestyle.
 Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Urinary incontinence is a common problem and one that can be resolved by working
Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Urinary incontinence is a common problem and one that can be resolved by working
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 24 The Digestive System Introduction The purpose of this chapter is to Identify the anatomical components of the digestive system as well as their
Principles of Anatomy and Physiology 14 th Edition CHAPTER 24 The Digestive System Introduction The purpose of this chapter is to Identify the anatomical components of the digestive system as well as their
Use of gatekeeper in obese patients with fecal incontinence before bariatric surgery, is it improving the results?
 International Surgery Journal Ibrahim AAM. Int Surg J. 2017 Nov;4(11):3594-3598 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20174876
International Surgery Journal Ibrahim AAM. Int Surg J. 2017 Nov;4(11):3594-3598 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20174876
Faecal Incontinence: Assessment and Management
 Mrs PK; 56 yrs; Married; 2 children Faecal Incontinence: Assessment and Management Professor Marc A Gladman MBBS DFFP PhD MRCOG FRCS (UK) FRACS Professor of Colorectal Surgery >10 years of incontinence
Mrs PK; 56 yrs; Married; 2 children Faecal Incontinence: Assessment and Management Professor Marc A Gladman MBBS DFFP PhD MRCOG FRCS (UK) FRACS Professor of Colorectal Surgery >10 years of incontinence
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Lets talk about Faecal incontinence (FI) in Scleroderma
 Lets talk about Faecal incontinence (FI) in Scleroderma Dr. Shamaila Butt Gastroenterology Research Registrar GI Physiology unit University College Hospital London GI manifestations in Scleroderma Oesophagus
Lets talk about Faecal incontinence (FI) in Scleroderma Dr. Shamaila Butt Gastroenterology Research Registrar GI Physiology unit University College Hospital London GI manifestations in Scleroderma Oesophagus
Obstetric Anal Sphincter Injury- A guideline. Mr David Sim Ms Patricia McStay. Dr Martina Hogan Dept./Division Only: YES-IMWH Directorate Only: NO
 CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
The Egyptian Journal of Hospital Medicine (April 2018) Vol. 71 (3), Page
 The Egyptian Journal of Hospital Medicine (April 2018) Vol. 71 (3), Page 2742-2750 Role of dynamic MRI in assessment of Pelvic Floor Dysfunction in Females Nada Ahmed Hussein, Naglaa Hussein Shebrya, Nermeen
The Egyptian Journal of Hospital Medicine (April 2018) Vol. 71 (3), Page 2742-2750 Role of dynamic MRI in assessment of Pelvic Floor Dysfunction in Females Nada Ahmed Hussein, Naglaa Hussein Shebrya, Nermeen
ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION. Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital
 ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital Accidental Bowel Leakage What Gets the Woman into Your Office 67%
ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital Accidental Bowel Leakage What Gets the Woman into Your Office 67%
Postoperative Care for Pelvic Fistulae. Peter Jeppson, MD October 3, 2017
 Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Loss of Bladder Control
 BLADDER HEALTH Loss of Bladder Control SURGERY TO TREAT URINARY INCONTINENCE AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is Urinary Incontinence? Urinary incontinence
BLADDER HEALTH Loss of Bladder Control SURGERY TO TREAT URINARY INCONTINENCE AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is Urinary Incontinence? Urinary incontinence
ICD-10 Common Codes for Pelvic Rehab Providers
 ICD-10 Common Codes for Pelvic Rehab Providers With ICD-10 changes taking place in 2015, we thought it would be helpful to put together a bit of a cheat sheet for our pelvic health providers. Keep in mind
ICD-10 Common Codes for Pelvic Rehab Providers With ICD-10 changes taking place in 2015, we thought it would be helpful to put together a bit of a cheat sheet for our pelvic health providers. Keep in mind
3D Dynamic Ultrasound In Obstructed Defecation
 3D Dynamic Ultrasound In Obstructed Defecation By Ramy Salahudin Abdelkader Assist. Lecturer of General Surgery Cairo University Introduction Pelvic floor is complex system, with passive and active components
3D Dynamic Ultrasound In Obstructed Defecation By Ramy Salahudin Abdelkader Assist. Lecturer of General Surgery Cairo University Introduction Pelvic floor is complex system, with passive and active components
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 3. October 16, 2015
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 3 October 16, 2015 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) A. B. A B C. D. C D 2. Identify the structures. (2
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 3 October 16, 2015 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) A. B. A B C. D. C D 2. Identify the structures. (2
Autonomic Nervous System
 Autonomic Nervous System Autonomic nervous system organization Sympathetic Nervous System division of the autonomic nervous system that arouses the body, mobilizing its energy in stressful situations
Autonomic Nervous System Autonomic nervous system organization Sympathetic Nervous System division of the autonomic nervous system that arouses the body, mobilizing its energy in stressful situations
Neuropathic Bladder. Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014
 Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Dana Alrafaiah. - Amani Nofal. - Ahmad Alsalman. 1 P a g e
 - 2 - Dana Alrafaiah - Amani Nofal - Ahmad Alsalman 1 P a g e This lecture will discuss five topics as follows: 1- Arrangement of pelvic viscera. 2- Muscles of Pelvis. 3- Blood Supply of pelvis. 4- Nerve
- 2 - Dana Alrafaiah - Amani Nofal - Ahmad Alsalman 1 P a g e This lecture will discuss five topics as follows: 1- Arrangement of pelvic viscera. 2- Muscles of Pelvis. 3- Blood Supply of pelvis. 4- Nerve
Outpatient Rehabilitation Services
 Outpatient Rehabilitation Services Shapiro Building, 2nd Floor 330 Brookline Avenue Boston, MA 02215 (617) 754-9100 bidmc.org/pelvicfloorpt Outpatient Rehabilitation Services ALL ABOUT YOUR Pelvic Floor
Outpatient Rehabilitation Services Shapiro Building, 2nd Floor 330 Brookline Avenue Boston, MA 02215 (617) 754-9100 bidmc.org/pelvicfloorpt Outpatient Rehabilitation Services ALL ABOUT YOUR Pelvic Floor
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS
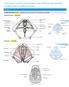 THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
Urinary incontinence. Urology Department. Patient Information Leaflet
 Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Surgical treatment of urinary stress incontinence with tension free vaginal tape
 Surgical treatment of urinary stress incontinence with tension free vaginal tape Gynaecology department 01935 384 385 yeovilhospital.nhs.uk Many surgical operations are available for the treatment of
Surgical treatment of urinary stress incontinence with tension free vaginal tape Gynaecology department 01935 384 385 yeovilhospital.nhs.uk Many surgical operations are available for the treatment of
Bowel Management for Children with Anorectal Malformations by Kathleen Guardino, RN, MSN
 Bowel Management for Children with Anorectal Malformations by Kathleen Guardino, RN, MSN Dr. Alberto Peña, Chief of Surgery at Schneider Children's Hospital created the posterior sagittal anorectoplasty
Bowel Management for Children with Anorectal Malformations by Kathleen Guardino, RN, MSN Dr. Alberto Peña, Chief of Surgery at Schneider Children's Hospital created the posterior sagittal anorectoplasty
