Traumatic injury to the anal sphincter sustained in a thirdor
|
|
|
- Lynne Parrish
- 6 years ago
- Views:
Transcription
1 Obstetric Anal Sphincter Injuries: A Survey of Clinical Practice Among Canadian Obstetricians Carolyn Best, BSc, MD, FRCSC, Harold P. Drutz, MD, FRCSC, May Alarab, MBChB, MRCOG, MRCPI, MSc Division of Urogynaecology and Reconstructive Pelvic Surgery, Department of Obstetrics and Gynaecology, Mount Sinai Hospital, University of Toronto, Toronto ON Abstract Objective: To describe the current practice, experience, and confidence of Canadian obstetricians in the management of obstetric anal sphincter injuries (OASIS) and to explore the need for national practice guidelines on this topic. Methods: We conducted a cross-sectional, Internet-based survey between December 2010 and March The survey was initially tested among a sample population and then distributed electronically to 665 Canadian obstetricians. Data were analyzed descriptively. The main outcome measures were the self-reported confidence and experience of Canadian obstetricians in OASIS management and the frequency of performing specific OASIS management steps. Results: The survey response rate was 28.7%. The majority of the respondents (95%) reported confidence in performing OASIS repairs. In the event of a perineal laceration, 47.9% of respondents routinely performed a rectal examination. Most OASIS repairs were performed in the delivery room (89.4%) under local anaesthesia (60.6%) when regional anaesthesia was not already present. If lacerated, the internal anal sphincter was repaired separately by 63.4% of respondents, and intraoperative antibiotics were ordered by 51.1% of respondents. Most (92%) reported the absence of a local protocol to guide OASIS repair. Conclusion: The confidence of Canadian obstetricians who participated in this survey in performing OASIS repairs was high. However, their experience in performing repairs and their use of management steps varied. The need for national guidelines and an increase in awareness is suggested. Résumé Objectif : Décrire les pratiques actuelles, l expérience et le degré de confiance des obstétriciens canadiens en ce qui a trait à la prise en charge des lésions obstétricales affectant le sphincter anal (OASIS), ainsi qu explorer la nécessité d élaborer des lignes directrices nationales à ce sujet. Key Words: Third-/fourth-degree tear, obstetric anal sphincter injury, practice survey Competing Interests: None declared. Received on December 6, 2011 Accepted on February 17, 2012 Méthodes : Nous avons mené un sondage transversal par Internet entre décembre 2010 et mars Le sondage a d abord été mis à l essai auprès d un échantillon populationnel, pour ensuite être distribué par voie électronique à 665 obstétriciens canadiens. Les données ont été analysées de façon descriptive. Les principaux critères d évaluation ont été la confiance et l expérience autosignalées par les obstétriciens canadiens en matière de prise en charge des OASIS, ainsi que la fréquence avec laquelle ils procédaient à des étapes particulières de la prise en charge des OASIS. Résultats : Le taux de réponse au sondage a été de 28,7 %. La majorité des répondants (95 %) ont signalé être confiants au moment de mener des interventions visant à réparer des OASIS. En présence d une lacération périnéale, 47,9 % des répondants procédaient systématiquement à la tenue d un examen rectal. La plupart des réparations d OASIS étaient menées dans la salle d accouchement (89,4 %) sous anesthésie locale (60,6 %), lorsqu une anesthésie régionale n avait pas déjà été mise en œuvre. Lorsqu il était lacéré, le sphincter anal interne a été réparé séparément par 63,4 % des répondants et l administration peropératoire d antibiotiques a été mise en œuvre par 51,1 % des répondants. La plupart des répondants (92 %) ont signalé l absence d un protocole local orientant la réparation des OASIS. Conclusion : La confiance des obstétriciens canadiens qui ont participé à ce sondage était élevée, en ce qui a trait à la tenue de réparations d OASIS. Toutefois, leur expérience en matière d exécution de ces réparations et leur utilisation des étapes de la prise en charge variaient. Nous suggérons la rédaction de lignes directrices nationales sur la prise en charge des OASIS et l intensification des efforts de sensibilisation à cette problématique. J Obstet Gynaecol Can 2012;34(8): INTRODUCTION Traumatic injury to the anal sphincter sustained in a thirdor fourth-degree laceration during vaginal delivery is the most common cause of anal incontinence in women of reproductive age. The main risk factors for obstetric anal sphincter injuries are primiparity, fetal macrosomia, midline episiotomy, prolonged second stage of labour, and forceps assisted delivery. 1 3 OASIS are recognized to occur in approximately 1% of vaginal deliveries, 4 with a reported incidence of 0.5% to 20%. 5 7 AUGUST JOGC AOÛT
2 Following conventional primary repair, the rate of persistent anal symptoms including incontinence has been reported to be as high as 59%, 7 12 with incontinence of flatus and fecal urgency being most common. The spectrum of distressing OASIS sequelae can also include incontinence of liquid or solid stool, passive soiling, perineal pain, dyspareunia, or leakage due to rectovaginal fistulae. Even though anal incontinence can severely compromise quality of life, social stigma and embarrassment may prevent many women from reporting symptoms to their physicians. Therefore, the true prevalence of anal symptoms following OASIS is unknown and is likely underestimated. Litigation related to OASIS and related consequences has increased worldwide over the last 10 years. 13 Missed diagnosis, lack of expertise, insufficient training, and inadequate surgical technique have all been suggested as possible reasons for the high rate of persistent symptoms after primary repair. 14 In an attempt to reduce morbidity and litigation, the Royal College of Obstetricians and Gynaecologists in the United Kingdom published clinical practice guidelines on the repair of third- and fourthdegree lacerations in Based on the available evidence at the time, the guidelines described the specific location, type of anaesthesia, method of repairing the sphincter, type of suture to be used, and perioperative medications that should be prescribed to provide optimal clinical results. The authors of the guidelines suggested that local protocols should be developed and implemented, both to aid in the complete documentation of the repair methods and to provide consistent care to women with sphincter injury. It has been suggested that primary sphincter repair immediately after delivery is more likely to be successful in the long term than a secondary repair performed remote from delivery. 15,16 Not only do obstetricians perform the majority of deliveries in Canada, but they are also the surgeons consulted when a significant laceration has occurred under the care of a midwife or family physician. The current practice among obstetricians in Canada in the repair of OASIS is unknown. It is suspected that without national guidelines or an established standard of care, the methods used across the country vary widely. Therefore, the specific aims of this study were threefold: ABBREVIATIONS EAS external anal sphincter IAS OASIS RCOG internal anal sphincter obstetric anal sphincter injuries Royal College of Obstetricians and Gynaecologists 1. to describe the current practice, experience, and confidence of Canadian obstetricians in the management of OASIS; 2. to determine whether local protocols on the repair of OASIS exist within Canada; and 3. to explore whether Canadian obstetricians would benefit from national practice guidelines on this topic. It is the intention of the authors to investigate Canadian practice, and also to stimulate discussion and heighten awareness of this important and under-recognized women s health issue. METHODS A cross-sectional survey designed to investigate OASIS management was distributed electronically to Canadian obstetrician gynaecologists in December The main outcomes were the self-reported confidence and experience of respondents who practised obstetrics in performing OASIS repairs and their frequency of performing specific management steps. Following an extensive review of the literature, a 25-item questionnaire was developed to encompass the important aspects of OASIS repair in evidence reported in current research and in the guidelines published by the RCOG in the United Kingdom. 4 The content validity of the questionnaire was reviewed by two experts on OASIS repair from the Division of Urogynaecology at Mount Sinai Hospital, Toronto, to confirm that the questions covered all relevant aspects of the topic. The questions were organized into four sections: 1. demographic data, 2. experience and training in OASIS repair, 3. management of OASIS repair, and 4. postoperative and postpartum care. The survey content and flow was then assessed by five practising obstetrician gynaecologists, and modifications were made according to their suggestions. The electronic format of the questionnaire was created with the use of FluidSurveys, an Internet-based survey vehicle. The online software allowed instant analysis and filtering of data as soon as the surveys were completed, and all data were stored within Canada. Reliability testing was then performed by administering the online version of the questionnaire to 40 staff physicians in the Department of Obstetrics and Gynaecology at Mount Sinai Hospital on two occasions, 748 AUGUST JOGC AOÛT 2012
3 Obstetric Anal Sphincter Injuries: A Survey of Clinical Practice Among Canadian Obstetricians two months apart. The survey results were found to be similar and reproducible based on the responses collected from the two time points. After approval of the survey validation process was obtained from the Council of the SOGC, a cover letter describing the nature and purpose of the study and a link to the online survey was sent via to the 665 SOGC members who had previously given permission to receive electronic research surveys. Consent was implied by completion of the survey. A reminder to complete the survey was ed in January 2011, and responses were accepted until the end of March All responses were confidential. The data were analyzed descriptively. Ethics approval for the study was obtained from the Research Ethics Board at Mount Sinai Hospital in Toronto, Ontario. RESULTS A total of 191 responses were received, a response rate of 28.7%. The first question of the survey identified those currently practising obstetrics versus those currently practising only gynaecology. The remaining questions on OASIS practice were answered only by the 142 (73.9%) who currently practise obstetrics. The demographic data collected from the respondents is summarized in Table 1. When asked to estimate the number of repairs performed in the preceding year, 60.5% of respondents indicated that they had repaired fewer than 10 third-degree lacerations, and 76.8% repaired fewer than five fourth-degree lacerations (Table 2). Confidence in the identification of OASIS following delivery was reported to be high, with 78.2% indicating that they were very confident and the remainder confident. Rates of confidence in performing laceration repairs were slightly lower but still high, with 95% reporting that they were either very confident or confident, and just 4.9% choosing either not very confident or not at all confident (Table 3). There was no statistically significant correlation between years in practice and confidence in performing OASIS repairs. When asked about training, 11.9% felt that their residency training had not adequately prepared them to perform OASIS repairs in practice. In the event of an apparent second-degree perineal laceration after a vaginal delivery, 52.1% of obstetricians completing the survey did not routinely perform a rectal examination to assess the integrity of the anal sphincter. The majority of OASIS repairs were performed in the delivery room (89.4%) as opposed to the operating room. Table 1. Characteristics of survey respondents currently practising obstetrics Respondents Characteristic n/n (%) Year residency training completed 2001 to /142 (42.9) 1991 to /142 (26.1) 1981 to /142 (19.0) 1980 or earlier 17/142 (12.0) Location of residency training Within Canada 131/140 (93.6) Outside Canada 9/140 (6.4) Type of practice University teaching hospital 65/138 (47.1) Community hospital 73/138 (52.9) Level of obstetrical/neonatal unit Level 1 13/141 (9.2) Level 2 76/141 (53.9) Level 3 52/141 (36.9) Province of current practice Alberta 16/142 (11.3) British Columbia 15/142 (10.6) Manitoba 3/142 (2.1) New Brunswick 1/142 (0.7) Newfoundland 3/142 (2.1) Nova Scotia 11/142 (7.7) Ontario 57/142 (40.1) Quebec 31/142 (21.8) Saskatchewan 5/142 (3.5) For a patient who did not receive regional anaesthesia during delivery, 60.6% of respondents indicated that they would perform a third- or fourth-degree laceration repair under local anaesthetic. If laceration was complete, 69.5% of respondents performed an end-to-end repair of the EAS, and 63.4% responded that they would repair the internal anal sphincter separately. Most reported using delayed-absorbable (braided or monofilament) suture to repair the EAS (90.1%); chromic or plain catgut was used by 7.0%, and permanent suture was used by 0.7%. Ninety-two percent of respondents were not aware of a protocol to guide OASIS repair at their hospital, and 51.1% routinely ordered intraoperative prophylactic antibiotics during repair. The responses on OASIS management are summarized in Table 4. During postpartum care for a woman who has sustained OASIS, 97.2% of the survey respondents routinely ordered laxatives or stool softeners, and 28.9% ordered a AUGUST JOGC AOÛT
4 Table 2. Self-estimated number of third- and fourth-degree laceration repairs performed by survey respondents in the last year Number of repairs performed (N = 142), n (%) Type of laceration < 5 5 to to 15 > 15 Third-degree 29 (20.4) 57 (40.1) 29 (20.4) 28 (19.0) Fourth-degree 109 (76.8) 27 (18.3) 7 (4.9) 0 (0) Table 3. Self-reported degree of confidence among survey respondents in identifying and repairing OASIS Degree of confidence (N = 142), n (%) Task Very confident Confident Not so confident Not at all confident Identifying OASIS 111 (78.2) 31 (21.8) 0 (0) 0 (0) Repairing OASIS 78 (54.9) 57 (40.1) 6 (4.2) 1 (0.7) course of postoperative antibiotics. Eighty-four percent of respondents indicated that they routinely arranged followup for women after OASIS, with 91.4 % suggesting they see an obstetrician. When asked to whom they would refer a patient who presented with fecal incontinence at six months postpartum after OASIS, the responses were variable, with 20.4% choosing a general surgeon, 42.9% a colorectal surgeon, 29.6% a urogynaecologist, and 7.0% other. The majority of those choosing other for referral for fecal incontinence postpartum suggested that they would send the patient to a physiotherapist. The majority (95.7%) of Canadian obstetricians who completed the survey felt that evidence-based guidelines on the repair of obstetrical anal sphincter injuries would be helpful in their practice. DISCUSSION Following vaginal delivery, women are at risk of developing anal symptoms, particularly if there is an anatomic disruption of the external or internal anal sphincters. Despite recognition and repair of such disruption, the reported incidence of anal incontinence and related symptoms after sphincter laceration is high. 3,7 12 Primary repair after delivery is the repair most likely to preserve long-term continence. 15,16 Therefore, as the surgeons attending delivery and those responsible for the majority of repairs, obstetricians play a pivotal role in providing the best clinical results when an anal sphincter injury has occurred. The goal of this study was to investigate and describe the current practice in OASIS management among obstetricians in Canada and to explore whether national guidelines are needed to establish a standard of care. A critical step in the repair of OASIS is recognition of the injury when it has occurred. It is obviously impossible to provide a high-quality repair to an undetected laceration, and an undiagnosed injury is almost certain to result in some degree of incontinence. Studies indicate that heightened awareness of OASIS and training in its identification may be associated with an increase in OASIS detection; in one centre, when an experienced research fellow attended all deliveries with an apparent second-degree perineal laceration, the reported incidence of OASIS doubled from 7.5% to 15% because many tears were upstaged to third- or fourth-degree lacerations. 17 In another study, 87% of midwives and 28% of obstetricians failed to correctly identify the extent of sphincter injury after careful independent examination, and endoanal ultrasound performed immediately after delivery was not more likely to detect OASIS than a thorough physical examination alone. 18 As a result of these findings, the RCOG guidelines state that all women having a vaginal delivery with evidence of genital tract trauma should be systematically examined to assess the severity of the damage prior to suturing. 4 Canadian obstetricians reported confidence in identifying OASIS, but only 47.9% routinely performed a rectal examination in the event of an apparent seconddegree laceration. This response may be one of the most important findings in this study, because it suggests the possibility of under-detection of OASIS without complete anal sphincter assessment in many cases. Further study involving standardized clinical examination with digital rectal examination following perineal laceration is required in order to quantify the incidence and detection rate of OASIS in Canada. 750 AUGUST JOGC AOÛT 2012
5 Obstetric Anal Sphincter Injuries: A Survey of Clinical Practice Among Canadian Obstetricians Table 4. Survey responses on intraoperative and postoperative OASIS management Number of responses Survey question n/n (%) Local protocol to guide OASIS management? No 130/141 (92.2) Yes 11/141 (7.8) Routine rectal examination after perineal laceration? Yes 68/142 (47.9) No 74/142 (52.1) Location of repair? Delivery room 127/142 (89.4) Operating room 15/142 (10.6) Anaesthesia for repair after no regional anaesthesia for delivery? Local 86/142 (60.6) Regional 48/142 (33.8) General 8/142 (5.6) Type of repair of external anal sphincter? End-to-end 98/141 (69.5) Overlapping 43/141 (30.5) Routine repair of internal anal sphincter? Yes 90/142 (63.4) No 52/142 (36.6) Routine intraoperative antibiotic prophylaxis? Yes 72/141 (51.1) No 69/141 (48.9) Routine postoperative antibiotics? Yes 41/142 (28.9) No 101/142 (71.1) Routine postoperative laxative/stool softener? Yes 138/142 (97.2) No 4/142 (2.8) Routine postoperative follow-up arranged? Yes 119/141 (84.4) No 22/141 (15.6) Only a few elements of OASIS care have been investigated in randomized trials. Based on expert opinion, the RCOG recommends that third- and fourth-degree tears be repaired in the operating room under regional anaesthesia to provide complete visualization of retracted sphincter muscles and to allow approximation with minimal tension. 4 The majority of OASIS repairs in Canada appear to be performed in the delivery room (89.4%), with local anaesthesia provided (60.6% of the time) only to women who delivered without regional anaesthesia. This result likely represents a practical element of care on a busy unit, with the operating room reserved for operative deliveries and complications other than perineal lacerations. Without further study, it is difficult to quantify the potential impact of additional anaesthesia, lighting, and instruments on the quality of OASIS repair. It makes intuitive sense for centres to consider such operative conditions in the event of a higher degree or more complex tear in which tissue identification can be challenging. Complete lacerations of the EAS have traditionally been repaired in an end-to end (approximation) fashion by obstetricians, while colorectal surgeons often perform an overlapping sphincteroplasty. Sultan et al. demonstrated that anal incontinence following OASIS was significantly AUGUST JOGC AOÛT
6 associated with an EAS defect on endoanal ultrasound in the postpartum period. Such a defect was found in significantly more women following OASIS repair (85%) than in those who had not sustained a sphincter injury (33%). 3 In 1999, this group was the first to suggest the use of an overlapping technique for OASIS repair along with separate careful suturing of the IAS, aimed to improve postpartum outcomes. In a small retrospective study of 32 women receiving overlapping sphincteroplasty with delayed absorbable suture, only two had incontinence of flatus and none had fecal incontinence five months after delivery. 19 Six randomized trials have since been conducted comparing end-to-end and overlapping sphincter repairs following OASIS A Cochrane Review and meta-analysis of three of these trials found no statistically significant difference between the two techniques in overall perineal pain, dyspareunia, incontinence of flatus, fecal incontinence, or quality of life at 12 months postpartum. 26 There was, however, a significantly lower risk of fecal urgency and deterioration of anal symptoms over 12 months with the overlapping technique. The significant findings in favour of overlapping repair came mostly from the study by Fernando et al., 22 in which all repairs were conducted by two surgeons equally experienced in both methods. Because of the limitations and heterogeneity of the studies, one technique could not ultimately be recommended over the other. A recently published randomized trial by Farrell et al. 25 strove to overcome the limitations of the previous trials by including only primiparous women with complete EAS injury, with a more common primary outcome of incontinence of flatus. At six months, the rates of incontinence of flatus (61% vs. 39%) and fecal incontinence (15% vs. 8%) were higher among those who underwent overlapping repair than those who had endto-end repair. The authors proposed that the additional dissection required to perform the overlapping repair may cause enough denervation and scarring to compromise EAS function. In contrast to the study of Fernando et al., 22 79% of the surgeons in the study by Farrell et al. 25 had performed fewer than 10 overlapping repairs prior to the study, but the experience of the surgeon was not found to correlate with clinical outcomes. In the current Canadian survey, 69.5% of respondents indicated that they routinely perform an end-to-end approximation of the EAS following laceration. Although those experienced in the overlapping technique may not change their practice from the results of this recent trial alone, obstetricians who are mainly proficient in the end-to-end technique can be assured that they are likely providing patients a good quality repair. Surgeons repairing OASIS should choose the method of repair with which they are most comfortable and in which they are most experienced. The IAS plays an important role in anal continence by providing resting anal sphincter tone. 27 Disruption of the IAS can lead to passive soiling with liquid stool. The IAS often retracts and can be difficult to find following laceration, but a persistent IAS defect following OASIS repair has been found to be associated with higher rates of fecal incontinence. 9,11,28,29 Farrell et al. found higher rates of anal incontinence (of both flatus and feces) when defects in both the EAS and IAS were found on ultrasound than when there was a defect in the EAS alone. 25 Only 36.6% of Canadian obstetricians who participated in the survey repaired a lacerated IAS separately. This may indicate the need for additional training in IAS laceration identification and repair. The majority of survey respondents indicated that they use delayed absorbable suture to repair the EAS, in the form of either a monofilament such as polydiaxanone or a braided suture such as polyglactin. All of the randomized trials comparing sphincter repair techniques used these delayed absorbable suture materials A randomized trial comparing 3 0 polydiaxanone and 2 0 polyglactin for EAS repair reported no significant difference in perineal pain, anal incontinence, or suture migration at 12 months, 21 and thus the RCOG recommends the use of either suture type. 4 Only 7.0% of Canadian obstetricians reported using chromic or plain catgut suture for sphincter laceration repair. Because of its considerably shorter halflife, catgut is less likely to provide a repair strong enough to allow for optimal healing of the sphincter. Data from randomized trials have favoured the use of more delayed absorbable suture over chromic or plain catgut for seconddegree laceration and episiotomy repairs, with less perineal pain postpartum. 30 To reduce the likelihood of wound and sphincter repair dehiscence, it has been recommended that laxatives be prescribed to women following OASIS. 4 A single randomized trial comparing the use of laxatives with the use of a constipating agent after OASIS repair found that patients who took laxatives had a significantly earlier and less painful first bowel movement and earlier discharge from hospital, but no difference in sphincter continence or anal symptoms was found. 31 Consistent with the intuitive sense of this recommendation and the evidence, 97.2% of Canadian obstetricians routinely prescribe laxatives after OASIS repair. A course of broadspectrum antibiotic prophylaxis during and after OASIS repair has been recommended to reduce the risk of wound breakdown due to infection. 4 A randomized trial comparing a single prophylactic intravenous dose of a 752 AUGUST JOGC AOÛT 2012
7 Obstetric Anal Sphincter Injuries: A Survey of Clinical Practice Among Canadian Obstetricians second-generation cephalosporin during repair of OASIS with placebo showed a significantly lower rate of perineal complication at two weeks postpartum for the women who received the antibiotics. 32 We found that only one half of responding Canadian obstetricians provide antibiotics during OASIS repair, and just 28.9% routinely prescribe them postoperatively. Adequate surgical training, competence, and experience are critical elements in providing high quality outcomes following any type of surgical procedure. Perineal laceration repairs are one of the most basic and common surgical procedures performed by obstetricians. When an anal sphincter laceration has occurred along with a perineal tear, an attempt at sphincter repair by an inexperienced clinician can increase the risk of persistent anal symptoms and incontinence. A survey of clinical practice and experience in OASIS in the United Kingdom found that 64% of both obstetricians and trainees reported either a lack of or unsatisfactory training in performing OASIS repairs. 14 In our study, just 11.9% of Canadian obstetricians completing the survey felt that their residency training was inadequate in preparing them to manage OASIS in practice. Obstetricians also reported high rates of confidence in actually performing the repairs, with 95% claiming to be either very confident or confident. Although these figures may be reassuring in light of the previous United Kingdom survey results, it is unclear whether or not such responses are over-confident without knowing the true incidence of OASIS or the Canadian-specific risk of postoperative anal symptoms. Regardless of their surgical confidence, obstetricians perform few OASIS repairs each year, and this may provide even fewer opportunities for hands-on experience for residents in teaching centres. The majority of respondents (60.5%) estimated that they perform fewer than 10 third-degree repairs, and 76.8% perform fewer than five fourth-degree laceration repairs per year. Medico-legal action related to OASIS has declined in the United Kingdom since the publication of clinical practice guidelines and the creation of specialized multidisciplinary perineal clinics designed to provide standardized followup and care to women after sphincter repair. 4 The RCOG recommends that centres develop protocols in OASIS management, documentation, and follow-up, specifying that all women should be offered physiotherapy and evaluation by an obstetrician gynaecologist at six to 12 weeks postpartum. 4 Ninety-two percent of Canadian obstetricians responded that they currently do not have a protocol on OASIS management at their hospital. Although the majority (91.4%) felt that patients should be seen by an obstetrician following OASIS, 8.6% felt that follow-up with the patient s family doctor was adequate. When asked to whom they would refer a patient with fecal incontinence six months after OASIS, responses varied and included a colorectal or general surgeon, a urogynaecologist, and a physiotherapist. The frequency of litigation related to OASIS in Canada is not clear, as this information is not publicly available. However, because of national differences in medical education, health care systems, resource allocation, and medico-legal cultures, it is conceivable that guidelines and protocols specific to Canadian practice may be necessary. Indeed, 95.7% of survey respondents indicated that national guidelines on OASIS would be useful in their practice. Clear and graded recommendations based on the available evidence would help to ensure consistent care and follow-up for patients who sustain a sphincter injury; especially since women who are symptomatic postpartum may not feel comfortable volunteering their distress. Limitations of this study include the response rate of 28.7%, with the responses possibly not being representative of the opinions of Canadian obstetricians as a whole. A higher rate of response (56%) was obtained in a similar survey conducted by mail in the United Kingdom. The electronic format limited distribution to SOGC members with access. Although all Canadian provinces were represented in the sample of respondents, the survey was provided in English only and was not translated into French. Surveys were distributed only to SOGC members who had previously consented to receive research surveys. This population could have provided an inherent selection bias, because those willing to participate in surveys may have more interest in research and more knowledge of clinical evidence in obstetrics. Criticisms from respondents included the fact that third- and fourth-degree lacerations were grouped together for most questions on management, but that they managed repair of these two types of lacerations differently. Previously published reports and guidelines, however, do not separate third- and fourthdegree lacerations, as both are considered significant risk factors for anal incontinence and it has been assumed they should be managed in a similar fashion. CONCLUSION Although they do not perform many repairs of OASIS per year, Canadian obstetricians who responded to the current survey reported that they were confident in identifying and repairing sphincter lacerations. Overall, many aspects of the management of OASIS by Canadian obstetricians are consistent with what is suggested by the available evidence, AUGUST JOGC AOÛT
8 but numerous recommendation made by the RCOG in the United Kingdom are not being followed. Further study of the incidence of OASIS and the prevalence of long-term anal symptoms in Canada is needed to provide context for the findings of this study. A need for Canadian clinical practice guidelines and protocols in OASIS management is suggested. ACKNOWLEDGEMENTS The authors would like to thank the obstetricians and gynaecologists at Mount Sinai Hospital in Toronto for their assistance in the testing and validation of the survey, and the Society of Obstetricians and Gynaecologists of Canada for providing the opportunity to distribute the survey electronically. REFERENCES 1. Dahl C, Kjolhede P. Obstetric anal sphincter rupture in older primiparous women: a case control study. Acta Obstet Gynecol Scand 2006;85: Raisanen S, Vehvilainen-Julkunen K, Gissler M, Heinonen S. The increased incidence of obstetrical anal sphincter rupture an emerging trend in Finland. Prev Med 2009;49: Sultan AH, Kamm MA, Hudson CN, Bartram CI. Third degree obstetric anal sphincter tears: risk factors and outcome of primary repair. BMJ 1994;308: Fernando RJ, Williams AA, Adams EJ. The management of third and fourth degree perineal tears. Green Top Guideline No. 29. London: Royal College of Obstetricians and Gynaecologists; March Crawford LA, Quint EH, Pearl M, DeLancey JOL. Incontinence following rupture of the anal sphincter during delivery. Obstet Gynecol 1993;82: Handa VL, Danielsen BH, Gilbert WM. Obstetric anal sphincter lacerations. Obstet Gynecol 2001;98: Walsh CJ, Mooney EF, Upton GJ, Motson RW. Incidence of third-degree perineal tears in labour and outcome after primary repair. Br J Surg 1996;83: Sultan AH, Thakar R. Lower genital tract and anal sphincter trauma. Best Pract Res Clin Obstet Gynaecol 2002;16: Goeffeng AR, Andersch B, Andersson M, Berndtsson I. Objective methods cannot predict anal incontinence after primary repair of extensive anal tears. Acta Obstet Gynecol Scand 1998;77: Haadem K, Dahlstrom JA, Lingman G. Anal sphincter function after delivery: a prospective study in women with sphincter rupture and controls. Eur J Obstet Gynecol Reprod Biol 1990;35: Poen AC, Felt-Bersma RJF, Strijers RL, Dekker GA, Cuesta MA, Meuwissen SG. Third degree obstetric perineal tear: long term clinical and functional results after primary repair. Br J Surg 1998;85: Nazir M, Carlsen E, Jacobsen AF, Nesheim BI. Is there any correlation between objective anal testing, rupture grade and bowel symptoms after primary repair of obstetric anal sphincter injury? Dis Colon Rectum 2002;45: Sultan AH. Obstetric perineal injury and anal incontinence. Clin Risk 1999;5(5): Fernando RJ, Sultan AH, Radley S, Jones PW, Johanson RB. Management of obstetric anal sphincter injury: a systematic review & national practice survey. BMC Health Serv Res 2002;2: Dudding TC, Vaizey CJ, Kamm MA. Obstetric anal sphincter injury. Incidence, risk factors and management. Ann Surg 2008:247; Johnson E, Carlsen E, Steen TB, Backer Hjorthaug JO, Tandberg Eriksen M, Johannessen H. Short and long term results of secondary anterior sphincteroplasty in 33 patients with obstetric injury. Acta Obstet Gynecol Scand 2010;89: Groom KM, Paterson-Brown S. Can we improve on the diagnosis of third degree tears? Eur J Obstet Gynecol Reprod Biol 2002;101: Andrews V, Thakar R, Sultan AH, Jones PW. Occult anal sphincter injuries myth or reality? BJOG 2006;113: Sultan AH, Monga AK, Kumar D, Stanton SL. Primary repair of obstetrical anal sphincter rupture using the overlap technique. Br J Obstet Gynaecol 1999;106: Fitzpatrick M, Behan M, O Connell PR, O Herlihy C. A randomized clinical trial comparing primary overlap with approximation repair of third degree obstetric tears. Am J Obstet Gynecol 2000;183: Williams A, Adams EJ, Tincello DG, Alfirevic Z, Walkinshaw SA, Richmond DH. How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial. BJOG 2006;113: Fernando RJ, Sultan AH, Kettle C, Radley S, Jones P, O Brien PMS. Repair techniques for obstetric anal sphincter injuries. A randomized controlled trial. Obstet Gynecol 2006;107: Garcia V, Rogers RG, Kim SS, Hall RJ, Kammerer-Doak DN. Primary repair of obstetric anal sphincter laceration: a randomized trial of two surgical techniques. Am J Obstet Gynecol 2005;192: Rygh AB, Korner H. The overlap technique versus end-to-end approximation technique for the primary repair of obstetric anal sphincter rupture: a randomized controlled study. Acta Obstet Gynecol Scand 2010;89: Farrell SA, Gilmour D, Turnbull GK, Schmidt MH, Baskett TF, Flowerdew G, et al. Overlapping compared with end-to-end repair of third and fourth degree obstetric anal sphincter tears. A randomized controlled trial. Obstet Gynecol 2010;116: Fernando R, Sultan AH, Kettle C, Thakar R, Radley S. Methods of repair of obstetric anal sphincter injury. Cochrane Database Syst Rev 2006, Issue 3. Art. No.:CD Sangwan YP, Solla JA. Internal anal sphincter: advances and insights. Dis Colon Rectum 1998; 41: de Leeuw JW, Srujik PC, Vierhout ME, Wallenburg HC. Risk factors for third degree perineal ruptures during delivery. BJOG 2001;108: Mahoney R, Behan M, Daly L, Kirwan C, O Herlihy C, O Connell R. Internal anal sphincter defect influences continence outcome following obstetric anal sphincter injury. Am J Obstet Gynecol 2007:196(3):217.e1 e Kettle C, Dowswell T, Ismail KMK. Absorbable suture materials for primary repair of episiotomy and second degree tears. Cochrane Database Syst Rev 2010, Issue 6. Art. No.:CD Mahony R, Behan M, O Herlihy C, O Connell PR. Randomized clinical trial of bowel confinement vs. laxative use after primary repair of a third degree obstetric anal sphincter tear. Dis Colon Rectum 2004;47: Duggal N, Mercado C, Daniels K, Bujor A, Caugey AB, El-Sayed YY. Antibiotic prophylaxis for prevention of postpartum perineal wound complications. Obstet Gynecol 2008;111: AUGUST JOGC AOÛT 2012
Anal Sphincter Injuries: Acute Management
 Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Obstetric Anal Sphincter Injury. An update on best practices. Objectives
 Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Royal College of Obstetricians and Gynaecologists
 Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Appendix B Protocol for management of obstetric anal sphincter injury THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS
 Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Title: A modified surgical approach to women with obstetric anal sphincter tears
 Reviewer's report Title: A modified surgical approach to women with obstetric anal sphincter tears Version: 3 Date: 27 January 2010 Reviewer: Stig S Norderval Reviewer's report: Review on manuscript entitled:
Reviewer's report Title: A modified surgical approach to women with obstetric anal sphincter tears Version: 3 Date: 27 January 2010 Reviewer: Stig S Norderval Reviewer's report: Review on manuscript entitled:
Occult anal sphincter injuries myth or reality?
 DOI: 10.1111/j.1471-0528.2006.00799.x www.blackwellpublishing.com/bjog Intrapartum care Occult anal sphincter injuries myth or reality? Vasanth Andrews, a Abdul H Sultan, a Ranee Thakar, a Peter W Jones
DOI: 10.1111/j.1471-0528.2006.00799.x www.blackwellpublishing.com/bjog Intrapartum care Occult anal sphincter injuries myth or reality? Vasanth Andrews, a Abdul H Sultan, a Ranee Thakar, a Peter W Jones
How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial
 DOI: 10.1111/j.1471-0528.2006.00806.x www.blackwellpublishing.com/bjog Intrapartum care How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial Abimbola
DOI: 10.1111/j.1471-0528.2006.00806.x www.blackwellpublishing.com/bjog Intrapartum care How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial Abimbola
EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May Dr. Annie Leong MBBS, FRANZCOG, CU
 EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May 2011 Dr. Annie Leong MBBS, FRANZCOG, CU Restore normal perineal anatomy Achieve good haemostasis Avoid infection and wound breakdown Avoid coital
EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May 2011 Dr. Annie Leong MBBS, FRANZCOG, CU Restore normal perineal anatomy Achieve good haemostasis Avoid infection and wound breakdown Avoid coital
Obstetric Anal Sphincter Injury- A guideline. Mr David Sim Ms Patricia McStay. Dr Martina Hogan Dept./Division Only: YES-IMWH Directorate Only: NO
 CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases
 CASE REPORT Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases Vasant Kawade 1 and Abhijit Ambike 2 Professor and Head, Department of OBGY, B.K.L.Walawakarl Rural Medical
CASE REPORT Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases Vasant Kawade 1 and Abhijit Ambike 2 Professor and Head, Department of OBGY, B.K.L.Walawakarl Rural Medical
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION
 OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
Clinical Guideline for: The Management of Perineal Trauma following Childbirth
 For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author s Line Manager: Supported
For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author s Line Manager: Supported
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital
 Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
Immediate or delayed repair of obstetric anal sphincter tears a randomised controlled trial*
 DOI: 10.1111/j.1471-0528.2008.01726.x www.blackwellpublishing.com/bjog General obstetrics Immediate or delayed repair of obstetric anal sphincter tears a randomised controlled trial* J Nordenstam, a,b
DOI: 10.1111/j.1471-0528.2008.01726.x www.blackwellpublishing.com/bjog General obstetrics Immediate or delayed repair of obstetric anal sphincter tears a randomised controlled trial* J Nordenstam, a,b
Risk factors and management of obstetric perineal injury
 Risk factors and management of obstetric perineal injury Ruwan J Fernando Abstract Perineal injury sustained during childbirth is a major aetiological factor in the development of perineal pain, sexual
Risk factors and management of obstetric perineal injury Ruwan J Fernando Abstract Perineal injury sustained during childbirth is a major aetiological factor in the development of perineal pain, sexual
Postpartum Complications
 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
Vincent Letouzey, MD, PhD
 How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
The Perineal Clinic: - the management of women following OASI
 The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
Obstetric anal sphincter injury is the most common
 Repair Techniques for Obstetric Anal Sphincter Injuries A Randomized Controlled Trial Ruwan J. Fernando, MD, MRCOG, Abdul H. Sultan, MD, FRCOG, Christine Kettle, PhD, Simon Radley, MD, FRCS, Peter Jones,
Repair Techniques for Obstetric Anal Sphincter Injuries A Randomized Controlled Trial Ruwan J. Fernando, MD, MRCOG, Abdul H. Sultan, MD, FRCOG, Christine Kettle, PhD, Simon Radley, MD, FRCS, Peter Jones,
Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study
 ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
Hands-on Workshop. Cape Town, South Africa 3 August Chairpersons
 Hands-on Workshop www.perineum.net Cape Town, South Africa 3 August 2016 Chairpersons Mr Abdul H Sultan, MB.ChB (Natal), MD, FRCOG Consultant Obstetrician & Urogynaecologist Miss Ranee Thakar, MB.BS, MD,
Hands-on Workshop www.perineum.net Cape Town, South Africa 3 August 2016 Chairpersons Mr Abdul H Sultan, MB.ChB (Natal), MD, FRCOG Consultant Obstetrician & Urogynaecologist Miss Ranee Thakar, MB.BS, MD,
Third & Fourth Degree Tears guideline (GL926)
 Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
Anal incontinence after childbirth is more common than was previously believed. Anal incontinence after childbirth. Methods
 Anal incontinence after childbirth Research Recherche From *the Department of Obstetrics and Gynecology, University of Ottawa, Ottawa, Ont.; the Departments of Family Medicine and Social and Preventive
Anal incontinence after childbirth Research Recherche From *the Department of Obstetrics and Gynecology, University of Ottawa, Ottawa, Ont.; the Departments of Family Medicine and Social and Preventive
2/5/2016. Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach
 Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Childbirth Trauma & Its Complications 23/ Mr Stergios K. Doumouchtsis
 Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Teaching Pelvic Examinations Under Anaesthesia: What Do Women Think?
 EDUCATION Teaching Pelvic Examinations Under Anaesthesia: What Do Women Think? Sara Wainberg, MD, 1 Heather Wrigley, MD, 1 Justine Fair, BSc, 2 Sue Ross, PhD 1,3,4 1 Department of Family Medicine, Faculty
EDUCATION Teaching Pelvic Examinations Under Anaesthesia: What Do Women Think? Sara Wainberg, MD, 1 Heather Wrigley, MD, 1 Justine Fair, BSc, 2 Sue Ross, PhD 1,3,4 1 Department of Family Medicine, Faculty
Postoperative Care for Pelvic Fistulae. Peter Jeppson, MD October 3, 2017
 Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Effect of subsequent vaginal delivery on bowel symptoms and anorectal function in women who sustained a previous obstetric anal sphincter injury
 International Urogynecology Journal (2018) 29:1579 1588 https://doi.org/10.1007/s00192-018-3601-y ORIGINAL ARTICLE Effect of subsequent vaginal delivery on bowel symptoms and anorectal function in women
International Urogynecology Journal (2018) 29:1579 1588 https://doi.org/10.1007/s00192-018-3601-y ORIGINAL ARTICLE Effect of subsequent vaginal delivery on bowel symptoms and anorectal function in women
Repair of vaginal tears and episiotomy guidelines
 Repair of vaginal tears and episiotomy guidelines Purpose These guidelines assist practitioners in the repair of vaginal and perineal tears including the reasons for, and the techniques of performing an
Repair of vaginal tears and episiotomy guidelines Purpose These guidelines assist practitioners in the repair of vaginal and perineal tears including the reasons for, and the techniques of performing an
anal incontinence; endoanal ultrasonography; grading systems; obstetric sphincter tears; three-dimensional
 Ultrasound Obstet Gynecol 2012; 40: 207 214 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.10154 Incontinence after primary repair of obstetric anal sphincter tears
Ultrasound Obstet Gynecol 2012; 40: 207 214 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.10154 Incontinence after primary repair of obstetric anal sphincter tears
AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA
 AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA NEED FOR A WORKING GROUP ON CHILDBIRTH TRAUMA A: Background
AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA NEED FOR A WORKING GROUP ON CHILDBIRTH TRAUMA A: Background
Results of a national needs. assessment for continuing medical education of family
 ORIGINAL ARTICLE Results of a national needs assessment for continuing medical education of family physicians related to erectile dysfunction and/or male sexual dysfunction Richard A Ward MD CCFP FCFP
ORIGINAL ARTICLE Results of a national needs assessment for continuing medical education of family physicians related to erectile dysfunction and/or male sexual dysfunction Richard A Ward MD CCFP FCFP
Guideline for Management and Repair of Perineal Trauma
 Guideline for Management and Repair of Perineal Trauma Author: Labour Ward Forum Specialty: Maternity Date Approved: September 2014 Approved by: W&CH Clinical Governance Committee Date for Review: August
Guideline for Management and Repair of Perineal Trauma Author: Labour Ward Forum Specialty: Maternity Date Approved: September 2014 Approved by: W&CH Clinical Governance Committee Date for Review: August
Obstetrical Anal Sphincter Injuries (OASIS): Prevention, Recognition, and Repair
 SOGC CLINICAL PRACTICE GUIDELINE No. 330, December 2015 Obstetrical Anal Sphincter Injuries (OASIS): Prevention, Recognition, and Repair This clinical practice guideline has been prepared by the Urogynaecology
SOGC CLINICAL PRACTICE GUIDELINE No. 330, December 2015 Obstetrical Anal Sphincter Injuries (OASIS): Prevention, Recognition, and Repair This clinical practice guideline has been prepared by the Urogynaecology
Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem
 Eur. J. Obstet. Gynecol. Reprod. Biol., 27 (1988) 27-32 Elsevier 27 EJO 00556 Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem Knut Haadem, Sten Ohrlander and G6ran
Eur. J. Obstet. Gynecol. Reprod. Biol., 27 (1988) 27-32 Elsevier 27 EJO 00556 Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem Knut Haadem, Sten Ohrlander and G6ran
PERINEAL REPAIR: COMPARISON OF SUTURE MATERIALS AND SUTURING TECHNIQUES
 ORIGINAL ARTICLE PERINEAL REPAIR: COMPARISON OF SUTURE MATERIALS AND SUTURING TECHNIQUES FOUZIA PERVEEN, TEHMINA SHABBIR ABSTRACT Objective Study design Place & Duration of study To compare the outcome
ORIGINAL ARTICLE PERINEAL REPAIR: COMPARISON OF SUTURE MATERIALS AND SUTURING TECHNIQUES FOUZIA PERVEEN, TEHMINA SHABBIR ABSTRACT Objective Study design Place & Duration of study To compare the outcome
Faecal incontinence after childbirth
 Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
Managing Expectations of Surgical Training: A National Perspective on Gynaecologic Endoscopy Practice
 EDUCATION Managing Expectations of Surgical Training: A National Perspective on Gynaecologic Endoscopy Practice Kristina Arendas, MD, FRCSC, Glenn D. Posner, MDCM, MEd, FRCSC, Sukhbir S. Singh, MD, FRCSC
EDUCATION Managing Expectations of Surgical Training: A National Perspective on Gynaecologic Endoscopy Practice Kristina Arendas, MD, FRCSC, Glenn D. Posner, MDCM, MEd, FRCSC, Sukhbir S. Singh, MD, FRCSC
Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship?
 DOI 10.1007/s00192-007-0431-8 ORIGINAL ARTICLE Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship? Inka Scheer & Vasanth Andrews & Ranee Thakar & Abdul H. Sultan
DOI 10.1007/s00192-007-0431-8 ORIGINAL ARTICLE Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship? Inka Scheer & Vasanth Andrews & Ranee Thakar & Abdul H. Sultan
Natural progression of anal incontinence after childbirth
 Int Urogynecol J (2009) 20:1029 1035 DOI 10.1007/s00192-009-0901-2 ORIGINAL ARTICLE Natural progression of anal incontinence after childbirth Johan Nordenstam & Daniel Altman & Sophia Brismar & Jan Zetterström
Int Urogynecol J (2009) 20:1029 1035 DOI 10.1007/s00192-009-0901-2 ORIGINAL ARTICLE Natural progression of anal incontinence after childbirth Johan Nordenstam & Daniel Altman & Sophia Brismar & Jan Zetterström
Corneal transplant (CT) surgery remains the most common
 Efficacy of Routine Notification and Request on reducing corneal transplantation wait times in Canada Mahta Rasouli,* MD; Valerie B. Caraiscos, MD, PhD; Allan R. Slomovic, MA, MD, FRCSC ABSTRACT RÉSUMÉ
Efficacy of Routine Notification and Request on reducing corneal transplantation wait times in Canada Mahta Rasouli,* MD; Valerie B. Caraiscos, MD, PhD; Allan R. Slomovic, MA, MD, FRCSC ABSTRACT RÉSUMÉ
Retrospective Review of Predisposing Factors and Surgical Outcomes in Obstetric Fistula Patients at a Single Teaching Hospital in Western Kenya
 GYNAEcOLOGY Retrospective Review of Predisposing Factors and Surgical Outcomes in Obstetric Fistula Patients at a Single Teaching Hospital in Western Kenya Erin McFadden, MD, 1 Sarah Jane Taleski, MHSc,
GYNAEcOLOGY Retrospective Review of Predisposing Factors and Surgical Outcomes in Obstetric Fistula Patients at a Single Teaching Hospital in Western Kenya Erin McFadden, MD, 1 Sarah Jane Taleski, MHSc,
Physiotherapists in Canada, 2011 National and Jurisdictional Highlights
 pic pic pic Physiotherapists in Canada, 2011 National and Jurisdictional Highlights Spending and Health Workforce Our Vision Better data. Better decisions. Healthier Canadians. Our Mandate To lead the
pic pic pic Physiotherapists in Canada, 2011 National and Jurisdictional Highlights Spending and Health Workforce Our Vision Better data. Better decisions. Healthier Canadians. Our Mandate To lead the
TRENDS IN MAJOR RISK FACTORS FOR ANAL SPHINCTER LACERATIONS: A I 0-YEAR STUDY
 TRENDS IN MAJOR RISK FACTORS FOR ANAL SPHINCTER LACERATIONS: A I 0-YEAR STUDY N. L. McLeod, MD, FRCSC, I D. T. Gilmour, MD, FRCSC, 2 K. S. Joseph, MD, PhD, 3 S. A. Farrell, MD, FRCSC,4 E. R. Luther, MD,
TRENDS IN MAJOR RISK FACTORS FOR ANAL SPHINCTER LACERATIONS: A I 0-YEAR STUDY N. L. McLeod, MD, FRCSC, I D. T. Gilmour, MD, FRCSC, 2 K. S. Joseph, MD, PhD, 3 S. A. Farrell, MD, FRCSC,4 E. R. Luther, MD,
Colposcopic Episodes of Care: Referral, Treatment, Follow-Up, and Exit Patterns of Care for Women With Abnormal Pap Smears
 GYNAECOLOGY Colposcopic Episodes of Care: Referral, Treatment, Follow-Up, and Exit Patterns of Care for Women With Abnormal Pap Smears Rachel Kupets, MD, 1 Yan Lu, MSc, 2 Danielle Vicus, MD, 1 Lawrence
GYNAECOLOGY Colposcopic Episodes of Care: Referral, Treatment, Follow-Up, and Exit Patterns of Care for Women With Abnormal Pap Smears Rachel Kupets, MD, 1 Yan Lu, MSc, 2 Danielle Vicus, MD, 1 Lawrence
SUTURING AN EPISIOTOMY/GENITAL LACERATION
 WOMEN AND NEWBORN HEALTH SERVICE CLINICAL GUIDELINES SECTION B : GUIDELINES RELEVANT TO OBSTETRICS AND MIDWIFERY 5 INTRAPARTUM CARE 5.15 PERINEAL REPAIR Authorised by: OGCCU 5.15.1 SUTURING AN EPISIOTOMY/GENITAL
WOMEN AND NEWBORN HEALTH SERVICE CLINICAL GUIDELINES SECTION B : GUIDELINES RELEVANT TO OBSTETRICS AND MIDWIFERY 5 INTRAPARTUM CARE 5.15 PERINEAL REPAIR Authorised by: OGCCU 5.15.1 SUTURING AN EPISIOTOMY/GENITAL
Fertility Treatment Decision-Making: The Effect of Insurance Coverage for Fertility Medications
 GYNAECOLOGY Fertility Treatment Decision-Making: The Effect of Insurance Coverage for Fertility Medications Claire Ann Jones, MD, 1 Laura Gra, hd, 2 Kimberl Liu, MD, FRCSC, MSL 1,3 1 Department of Obstetrics
GYNAECOLOGY Fertility Treatment Decision-Making: The Effect of Insurance Coverage for Fertility Medications Claire Ann Jones, MD, 1 Laura Gra, hd, 2 Kimberl Liu, MD, FRCSC, MSL 1,3 1 Department of Obstetrics
Perineal Tears. Obstetrics & Gynaecology Women & Children s Group
 Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS
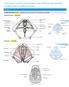 THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION. Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital
 ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital Accidental Bowel Leakage What Gets the Woman into Your Office 67%
ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital Accidental Bowel Leakage What Gets the Woman into Your Office 67%
Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF)
 Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF) Blair B. Washington MD, MHA Urogynecology & Reconstructive Pelvic Surgery Virginia Mason Medical Center Disclosures
Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF) Blair B. Washington MD, MHA Urogynecology & Reconstructive Pelvic Surgery Virginia Mason Medical Center Disclosures
for a review under the Accident Compensation Act
 FairWay Resolution Limited Tā te Hinengaro Tōkeke Whakatau Review numbers: Application by for a review under the Accident Compensation Act Held at Date of hearing 2 November 2016, adjourned part-heard;
FairWay Resolution Limited Tā te Hinengaro Tōkeke Whakatau Review numbers: Application by for a review under the Accident Compensation Act Held at Date of hearing 2 November 2016, adjourned part-heard;
Obstetric and Gynecologic Resident Ultrasound Education Project
 ORIGINAL RESEARCH Obstetric and Gynecologic Resident Ultrasound Education Project Is the Current Level of Gynecologic Ultrasound Training in Canada Meeting the Needs of Residents and Faculty? Jessica Green,
ORIGINAL RESEARCH Obstetric and Gynecologic Resident Ultrasound Education Project Is the Current Level of Gynecologic Ultrasound Training in Canada Meeting the Needs of Residents and Faculty? Jessica Green,
A retrospective postal survey of women s experiences of physiotherapy management following a third- or fourth-degree perineal tear
 Journal of the Association of Chartered Physiotherapists in Women s Health, Spring 2008, 102, 25 35 CLINICAL PAPER A retrospective postal survey of women s experiences of physiotherapy management following
Journal of the Association of Chartered Physiotherapists in Women s Health, Spring 2008, 102, 25 35 CLINICAL PAPER A retrospective postal survey of women s experiences of physiotherapy management following
Surgical management of stress urinary incontinence in Scotland and Wales: A questionnaire study
 International Journal of Surgery (2007) 5, 162e166 www.theijs.com Surgical management of stress urinary incontinence in Scotland and Wales: A questionnaire study Min Yu Lim a, *, Mahesh Perera b, Ian Ramsay
International Journal of Surgery (2007) 5, 162e166 www.theijs.com Surgical management of stress urinary incontinence in Scotland and Wales: A questionnaire study Min Yu Lim a, *, Mahesh Perera b, Ian Ramsay
General Anesthesia Gender patterns amongst Canadian anesthesiologists
 437 General Anesthesia Gender patterns amongst Canadian anesthesiologists [La proportion hommes-femmes chez les anesthésiologistes canadiens] Mark Otto Baerlocher MD,* Rumana Hussain BSc, John Bradley
437 General Anesthesia Gender patterns amongst Canadian anesthesiologists [La proportion hommes-femmes chez les anesthésiologistes canadiens] Mark Otto Baerlocher MD,* Rumana Hussain BSc, John Bradley
2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL)
 E10d 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No.
E10d 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No.
Perineal and Anal Sphincter Trauma
 Perineal and Anal Sphincter Trauma Abdul H. Sultan, Ranee Thakar and Dee E. Fenner (Eds) Perineal and Anal Sphincter Trauma Diagnosis and Clinical Management Abdul H. Sultan, MB ChB, MD, FRCOG Consultant
Perineal and Anal Sphincter Trauma Abdul H. Sultan, Ranee Thakar and Dee E. Fenner (Eds) Perineal and Anal Sphincter Trauma Diagnosis and Clinical Management Abdul H. Sultan, MB ChB, MD, FRCOG Consultant
Informing a research agenda for the Canadian chiropractic profession
 Commentary Informing a research agenda for the Canadian chiropractic profession Simon D French, PhD, MPH, BAppSc(Chiro)¹,2 Ronda Parkes, BFA 3 Paul Bruno, BHK, DC, PhD 4 Steven Passmore, Hons BKin, MS,
Commentary Informing a research agenda for the Canadian chiropractic profession Simon D French, PhD, MPH, BAppSc(Chiro)¹,2 Ronda Parkes, BFA 3 Paul Bruno, BHK, DC, PhD 4 Steven Passmore, Hons BKin, MS,
Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England,
 DOI: 10.1111/1471-0528.12076 www.bjog.org Urogynaecology Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England, 2002 2008 A Pradhan, a DG Tincello, b R Kearney a a Department
DOI: 10.1111/1471-0528.12076 www.bjog.org Urogynaecology Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England, 2002 2008 A Pradhan, a DG Tincello, b R Kearney a a Department
Guidelines on the Management of Complications related to Female Genital Mutilation
 Guidelines on the Management of Complications related to Female Genital Mutilation Scoping Survey Instructions The following is a list of 33 potential questions which could guide the evidence retrieval
Guidelines on the Management of Complications related to Female Genital Mutilation Scoping Survey Instructions The following is a list of 33 potential questions which could guide the evidence retrieval
Minimally Invasive Hysterectomies: A Survey of Current Practices. amongst members of the International Society for Gynaecologic Endoscopy
 Minimally Invasive Hysterectomies: A Survey of Current Practices amongst members of the International Society for Gynaecologic Endoscopy Abstract Study Objective This study aimed to explore the current
Minimally Invasive Hysterectomies: A Survey of Current Practices amongst members of the International Society for Gynaecologic Endoscopy Abstract Study Objective This study aimed to explore the current
Prevalence and Risk Factors for Urinary and Fecal Incontinence Four Months After Vaginal Delivery
 WOMEN'S HEALTH WOMEN'S HEALTH Prevalence and Risk Factors for Urinary and Fecal Incontinence Four Months After Vaginal Delivery Sandra A. Baydock, MD, 1 Catherine Flood, MD, 1 Jane A. Schulz, MD, 1 Dianna
WOMEN'S HEALTH WOMEN'S HEALTH Prevalence and Risk Factors for Urinary and Fecal Incontinence Four Months After Vaginal Delivery Sandra A. Baydock, MD, 1 Catherine Flood, MD, 1 Jane A. Schulz, MD, 1 Dianna
Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan
 Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Stapled transanal rectal resection for obstructed defaecation syndrome
 Stapled transanal rectal resection for obstructed Issued: June 2010 www.nice.org.uk/ipg351 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Stapled transanal rectal resection for obstructed Issued: June 2010 www.nice.org.uk/ipg351 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Obstetric anal sphincter injuries: Incidence, risk factors, consequences and prevention
 Obstetric anal sphincter injuries: Incidence, risk factors, consequences and prevention Katariina Laine, MD PhD thesis 2013 Katariina Laine, MD Department of Obstetrics Oslo University Hospital, Ullevål
Obstetric anal sphincter injuries: Incidence, risk factors, consequences and prevention Katariina Laine, MD PhD thesis 2013 Katariina Laine, MD Department of Obstetrics Oslo University Hospital, Ullevål
In healthy young women, anal sphincter tear at
 Risk Factors for Anal Sphincter Tear During Vaginal Delivery Mary P. FitzGerald, MD, Anne M. Weber, MD, MS, Nancy Howden, MD, MS, Geoffrey W. Cundiff, MD, and Mort B. Brown, PhD, for the Pelvic Floor Disorders
Risk Factors for Anal Sphincter Tear During Vaginal Delivery Mary P. FitzGerald, MD, Anne M. Weber, MD, MS, Nancy Howden, MD, MS, Geoffrey W. Cundiff, MD, and Mort B. Brown, PhD, for the Pelvic Floor Disorders
The circumferential obstetric fistula: characteristics, management and outcomes
 DOI: 10.1111/j.1471-0528.2007.01329.x www.blackwellpublishing.com/bjog Short communication The circumferential obstetric fistula: characteristics, management and outcomes A Browning Barhirdar Hamlin Fistula
DOI: 10.1111/j.1471-0528.2007.01329.x www.blackwellpublishing.com/bjog Short communication The circumferential obstetric fistula: characteristics, management and outcomes A Browning Barhirdar Hamlin Fistula
Impact of Patient Education on Knowledge of Influenza and Vaccine Recommendations Among Pregnant Women
 OBSTETRICS OBSTETRICS Impact of Patient Education on Knowledge of Influenza and Vaccine Recommendations Among Pregnant Women Mark H. Yudin, MD, MSc, 1 Maryam Salripour, BSc, CIC, MPH, 2 Michael D. Sgro,
OBSTETRICS OBSTETRICS Impact of Patient Education on Knowledge of Influenza and Vaccine Recommendations Among Pregnant Women Mark H. Yudin, MD, MSc, 1 Maryam Salripour, BSc, CIC, MPH, 2 Michael D. Sgro,
2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL)
 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service
2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service
Care of your Perineum following 3 rd and 4 th degree tears
 Maternity Services Care of your Perineum following 3 rd and 4 th degree tears Introduction This leaflet aims to give you information about the repair and aftercare of the third or fourth degree tear you
Maternity Services Care of your Perineum following 3 rd and 4 th degree tears Introduction This leaflet aims to give you information about the repair and aftercare of the third or fourth degree tear you
Do Unsutured Second-Degree Perineal Lacerations Affect Postpartum Functional Outcomes?
 Do Unsutured Second-Degree Perineal Lacerations Affect Postpartum Functional Outcomes? Lawrence M. Leeman, MD, Rebecca G. Rogers, MD, Betsy Greulich, CNM, and Leah L. Albers, DrPH Background: To compare
Do Unsutured Second-Degree Perineal Lacerations Affect Postpartum Functional Outcomes? Lawrence M. Leeman, MD, Rebecca G. Rogers, MD, Betsy Greulich, CNM, and Leah L. Albers, DrPH Background: To compare
WHAT IS LARS? LOW ANTERIOR RESECTIONSYNDROME. Sophie Pilkington. Colorectal Surgeon University Hospital Southampton
 WHAT IS LARS? LOW ANTERIOR RESECTIONSYNDROME Sophie Pilkington Colorectal Surgeon University Hospital Southampton INTRODUCTION UK Bowel cancer 2013 41,100 new cases INTRODUCTION UK Bowel cancer 2013 41,100
WHAT IS LARS? LOW ANTERIOR RESECTIONSYNDROME Sophie Pilkington Colorectal Surgeon University Hospital Southampton INTRODUCTION UK Bowel cancer 2013 41,100 new cases INTRODUCTION UK Bowel cancer 2013 41,100
Rectal analgesia for the relief of perineal pain after childbirth: a randomised controlled trial of diclofenac suppositories
 BJOG: an International Journal of Obstetrics and Gynaecology October 2004, Vol. 111, pp. 1059 1064 DOI: 10.1111/j.1471-0528.2004.00156.x Rectal analgesia for the relief of perineal pain after childbirth:
BJOG: an International Journal of Obstetrics and Gynaecology October 2004, Vol. 111, pp. 1059 1064 DOI: 10.1111/j.1471-0528.2004.00156.x Rectal analgesia for the relief of perineal pain after childbirth:
Does Laparoscopy Safely Improve Technicity for Complex Hysterectomy Cases?
 GYNAECOLOGY Does Laparoscopy Safely Improve Technicity for Complex Hysterectomy Cases? Amanda Grant-Orser, BSc, 1 Ramadan El Sugy, MD, 1,2 Sukhbir S. Singh, MD, FRCSC 1,2,3 1 Department of Obstetrics and
GYNAECOLOGY Does Laparoscopy Safely Improve Technicity for Complex Hysterectomy Cases? Amanda Grant-Orser, BSc, 1 Ramadan El Sugy, MD, 1,2 Sukhbir S. Singh, MD, FRCSC 1,2,3 1 Department of Obstetrics and
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 3, Issue 3 2013 Article 5 Closed Versus Open Lateral Internal Sphincterotomy Technique in Treatment of Anal Fissure Seyed Reza Mousavi Jr Shohada Medical Center,
World Journal of Colorectal Surgery Volume 3, Issue 3 2013 Article 5 Closed Versus Open Lateral Internal Sphincterotomy Technique in Treatment of Anal Fissure Seyed Reza Mousavi Jr Shohada Medical Center,
Midline episiotomy and anal incontinence: retrospective cohort study
 Obstetrics and Gynecology Epidemiology Center, Brigham and Women s Hospital, Harvard Medical School, 221 Longwood Avenue, Boston, MA 02115, Lisa B Signorello study coordinator Bernard L Harlow associate
Obstetrics and Gynecology Epidemiology Center, Brigham and Women s Hospital, Harvard Medical School, 221 Longwood Avenue, Boston, MA 02115, Lisa B Signorello study coordinator Bernard L Harlow associate
2/25/2013. Speaker Disclosure. Learning Objectives. Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth
 Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
Impact of Delivery Types on Women s Postpartum Sexual Health
 Reproduction & Contraception (2003) 14 (4):237~242 Impact of Delivery Types on Women s Postpartum Sexual Health Huan-ying WANG 1, Xiao-yang XU 2, Zhen-wei YAO 1, Qin ZHOU 1 Key words: postpartum; sexual
Reproduction & Contraception (2003) 14 (4):237~242 Impact of Delivery Types on Women s Postpartum Sexual Health Huan-ying WANG 1, Xiao-yang XU 2, Zhen-wei YAO 1, Qin ZHOU 1 Key words: postpartum; sexual
Faecal Incontinence: Assessment and Management
 Mrs PK; 56 yrs; Married; 2 children Faecal Incontinence: Assessment and Management Professor Marc A Gladman MBBS DFFP PhD MRCOG FRCS (UK) FRACS Professor of Colorectal Surgery >10 years of incontinence
Mrs PK; 56 yrs; Married; 2 children Faecal Incontinence: Assessment and Management Professor Marc A Gladman MBBS DFFP PhD MRCOG FRCS (UK) FRACS Professor of Colorectal Surgery >10 years of incontinence
A National Survey of Endoscopic Practice Among Gynaecologists in Canada
 A National Survey of Endoscopic Practice Among Gynaecologists in Canada Innie Chen, MD, 1 Krisztina I. Bajzak, MD, FRCPC, 2 Yanfang Guo, MB, MSc, 3 Sukhbir S. Singh, MD, FRCSC 4 1 Department of Obstetrics
A National Survey of Endoscopic Practice Among Gynaecologists in Canada Innie Chen, MD, 1 Krisztina I. Bajzak, MD, FRCPC, 2 Yanfang Guo, MB, MSc, 3 Sukhbir S. Singh, MD, FRCSC 4 1 Department of Obstetrics
Post operative voiding dysfunction and the Value of Urodynamics. Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist
 Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Sphincter exercises for people with bowel control problems. Information for patients. Physiotherapy Department
 Sphincter exercises for people with bowel control problems Information for patients Physiotherapy Department 01625 661481 @EastCheshireNHS Leaflet Ref: 11229 Published: June 18 Review: 31/0/5/2021 Page
Sphincter exercises for people with bowel control problems Information for patients Physiotherapy Department 01625 661481 @EastCheshireNHS Leaflet Ref: 11229 Published: June 18 Review: 31/0/5/2021 Page
Discharge information for patients Fistula plug for anal fistula
 Discharge information for patients Fistula plug for anal fistula Clinical Sciences Building Colorectal Surgery 0161 206 1249 All Rights Reserved 2017. Document for issue as handout.. What is an anal fistula?
Discharge information for patients Fistula plug for anal fistula Clinical Sciences Building Colorectal Surgery 0161 206 1249 All Rights Reserved 2017. Document for issue as handout.. What is an anal fistula?
Tertiary, regional and local pelvic floor service providers: the future. model? Andrew Williams
 Tertiary, regional and local pelvic floor service providers: the future Andrew Williams model? Pelvic Floor Unit Guy s and St Thomas NHS Foundation Trust Background 23% women suffer at least one pelvic
Tertiary, regional and local pelvic floor service providers: the future Andrew Williams model? Pelvic Floor Unit Guy s and St Thomas NHS Foundation Trust Background 23% women suffer at least one pelvic
ABSTRACT. KEY WORDS antibiotics; prophylaxis; hysterectomy
 Infectious Diseases in Obstetrics and Gynecology 8:230-234 (2000) (C) 2000 Wiley-Liss, Inc. Wound Infection in Gynecologic Surgery Aparna A. Kamat,* Leo Brancazio, and Mark Gibson Department of Obstetrics
Infectious Diseases in Obstetrics and Gynecology 8:230-234 (2000) (C) 2000 Wiley-Liss, Inc. Wound Infection in Gynecologic Surgery Aparna A. Kamat,* Leo Brancazio, and Mark Gibson Department of Obstetrics
A scoring system for the assessment of bowel and lower urinary tract symptoms in women
 BJOG: an International Journal of Obstetrics and Gynaecology April 2002, Vol. 109, pp. 424 430 A scoring system for the assessment of bowel and lower urinary tract symptoms in women L. Hiller a, H.D. Bradshaw
BJOG: an International Journal of Obstetrics and Gynaecology April 2002, Vol. 109, pp. 424 430 A scoring system for the assessment of bowel and lower urinary tract symptoms in women L. Hiller a, H.D. Bradshaw
Clinical Curriculum: Urogynecology
 Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Respirology manpower in Canada A report for the Canadian Thoracic Society Education Committee
 ORIGINAL ARTICLE Respirology manpower in Canada A report for the Canadian Thoracic Society Education Committee Donald W Cockcroft MD FRCPC 1, David Wensley MD FRCPC 2 1 Department of Medicine, Division
ORIGINAL ARTICLE Respirology manpower in Canada A report for the Canadian Thoracic Society Education Committee Donald W Cockcroft MD FRCPC 1, David Wensley MD FRCPC 2 1 Department of Medicine, Division
period, cesarean delivery is thought to protect against anal incontinence, 3 albeit incompletely. In this study, we investigated anal incontinence
 Obstetrical anal sphincter laceration and anal incontinence 5-10 years after childbirth Emily C. Evers, MPH; Joan L. Blomquist, MD; Kelly C. McDermott, BS; Victoria L. Handa, MD, MHS OBJECTIVE: The purpose
Obstetrical anal sphincter laceration and anal incontinence 5-10 years after childbirth Emily C. Evers, MPH; Joan L. Blomquist, MD; Kelly C. McDermott, BS; Victoria L. Handa, MD, MHS OBJECTIVE: The purpose
PARTICULARS, SCHEDULE 2- THE SERVICES, A- SERVICE SPECIFICATIONS. A08/S/d Colorectal: Faecal Incontinence (Adult)
 A08/S/d 2013/14 NHS STANDARD CONTRACT FOR COLORECTAL: FAECAL INCONTINENCE (ADULT) PARTICULARS, SCHEDULE 2- THE SERVICES, A- SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider
A08/S/d 2013/14 NHS STANDARD CONTRACT FOR COLORECTAL: FAECAL INCONTINENCE (ADULT) PARTICULARS, SCHEDULE 2- THE SERVICES, A- SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider
Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566
 Single-incision short sling mesh insertion for stress urinary incontinence in women Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566 Your responsibility This guidance
Single-incision short sling mesh insertion for stress urinary incontinence in women Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566 Your responsibility This guidance
Faecal incontinence persisting after childbirth: a 12 year longitudinal
 Author Posting. The Authors 2013. This is the authors version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in British Journal of Obstetrics
Author Posting. The Authors 2013. This is the authors version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in British Journal of Obstetrics
University of Bristol - Explore Bristol Research
 O'brien, S., Dua, A., & Vij, M. (2016). Practices in pelvic organ prolapse operations among surgeons: an international survey identifying needs for further research. International Urogynecology Journal,
O'brien, S., Dua, A., & Vij, M. (2016). Practices in pelvic organ prolapse operations among surgeons: an international survey identifying needs for further research. International Urogynecology Journal,
Motility Disorders. Pelvic Floor. Colorectal Center for Functional Bowel Disorders (N = 701) January 2010 November 2011
 Motility Disorders Pelvic Floor Colorectal Center for Functional Bowel Disorders (N = 71) January 21 November 211 New Patients 35 3 25 2 15 1 5 Constipation Fecal Incontinence Rectal Prolapse Digestive-Genital
Motility Disorders Pelvic Floor Colorectal Center for Functional Bowel Disorders (N = 71) January 21 November 211 New Patients 35 3 25 2 15 1 5 Constipation Fecal Incontinence Rectal Prolapse Digestive-Genital
Nutrition Education for Women With Newly Diagnosed Gestational Diabetes Mellitus: Small-group vs. Individual Counselling
 nutrition education for women with gdm Nutrition Education for Women With Newly Diagnosed Gestational Diabetes Mellitus: Small-group vs. Individual Counselling Ann Murphy RD BAA, Anne Guilar RD BASc, Diane
nutrition education for women with gdm Nutrition Education for Women With Newly Diagnosed Gestational Diabetes Mellitus: Small-group vs. Individual Counselling Ann Murphy RD BAA, Anne Guilar RD BASc, Diane
K. Jundt 1, I. scheer 2, v. von Bodungen 1, F. Krumbachner 1, K. Friese 1, U. M. Peschers 3
 362 EU Ro PE an JoUR nal of MED I cal RE search Eur J Med Res (2010) 15: 362-366 I. Holzapfel Publishers 2010 WHat HaRM DoEs a second DElIvERy to the PElvIc FlooR? K. Jundt 1, I. scheer 2, v. von Bodungen
362 EU Ro PE an JoUR nal of MED I cal RE search Eur J Med Res (2010) 15: 362-366 I. Holzapfel Publishers 2010 WHat HaRM DoEs a second DElIvERy to the PElvIc FlooR? K. Jundt 1, I. scheer 2, v. von Bodungen
