TRENDS IN MAJOR RISK FACTORS FOR ANAL SPHINCTER LACERATIONS: A I 0-YEAR STUDY
|
|
|
- Drusilla Gregory
- 6 years ago
- Views:
Transcription
1 TRENDS IN MAJOR RISK FACTORS FOR ANAL SPHINCTER LACERATIONS: A I 0-YEAR STUDY N. L. McLeod, MD, FRCSC, I D. T. Gilmour, MD, FRCSC, 2 K. S. Joseph, MD, PhD, 3 S. A. Farrell, MD, FRCSC,4 E. R. Luther, MD, FRCSCs Department of Obstetrics and Gynaecology. Dalhousie University, Halifax NS 3Perinatal Epidemiology Research Unit: Department of Obstetrics and Gynaecology and Department of Pediatrics. Dalhousie University, Halifax NS Abstract Objectives: (I) To identify independent risk factors for anal sphincter laceration. (2) to determine the trend in rates of anal sphincter laceration over a 10-year period, and (3) to examine the impact of temporal trends in risk factors on anal sphincter laceration rates. Methods: Population-based data were obtained from the Nova Scotia Atlee Perinatal Database, on women who had a singleton vaginal live birth ~500 g for the years 1988 to Risk factors for anal sphincter laceration were identified using stepwise logistic regression. A multivariate model was used to study temporal changes in laceration rates after controlling for changes in parity, episiotomy rates. operative vaginal deliveries. birth weight. prolonged second stage of labour, and other determinants. Results: Nulliparity (relative risk [RR] :::: 6.97). occiput posterior position (RR :::: 2.44). non-vertex presentations (RR :::: 2.27), second stage ~ 120 min (RR range :::: ), delivery by an obstetrician (RR :::: 1.30), and birth weight ~3000 g (RR range :::: ) increased the risk of laceration. Instrument-assisted delivery involved risks that ranged from a 2-fold increase for a vacuum-assisted delivery (RR :::: 2.15) to a greater than 5-fold increase for a forceps delivery after an unsuccessful vacuum extraction (RR :::: 5.69). Episiotomy. particularly midline incisions. increased the risk of laceration (RR :::: 2.57). The risk of a sphincter lacera~ion increased 2-fold from 1988 to despite controlling for risk factors. Conclusions: Sufficient evidence exists about the risk factors for anal sphincter laceration to permit modification of management of labour and delivery to minimize the risk of anal sphincter laceration. Increased awareness of the clinical importance of recognition and repair of anal sphincter laceration may explain the rising incidence. Key Words Anal sphincter, laceration. risk factors, maternal and neonatal morbidity Competing interests: None declared. Received on August Revised and accepted on October Resume Objectifs : (I) Cerner les facteurs de risque independants de laceration du sphincter externe de I'anus; (2) determiner les tendances des taux de laceration du sphincter externe de I'anus sur une periode de loans; (3) examiner I'effet, sur les taux de laceration, de ces tendances temporelles quant aux facteurs de risque. Methodes : Des donnees stratifiees representatives ont ete recueillies aupres de la base de donnees perinatales ATLEE de la Nouvelle-Ecosse; elles portaient sur femmes ayant accouche d'un enfant unique et vivant de 500 g ou plus. par voie vaginale, de 1988 a On a identifie les facteurs de risque de laceration du sphincter externe de I'anus au moyen d'une analyse de regression sequentielle. Un modele a variables multiples a ete utilise pour etudier les changements temporels des taux de laceration apres avoir tenu compte des changements suivants : la parite, les taux d'episiotomie, les accouchements par voie vaginale avec chirurgie, Ie poids de naissance, un second stade du travail prolonge et certains aut res facteurs determinants. Resultats : Les facteurs suivants ont fait augmenter Ie risque de laceration: nulliparite (risque relatif [RR] :::: 6,97), presentation occipito-posterieure (RR :::: 2,44), presentations autres que du sommet (RR :::: 2.27), deuxieme stade ~ 120 min. (etendue du RR :::: de 1,47 a 2,02), accouchement en presence d'un obstetricien (RR :::: 1,30), poids de naissance 2: 3000 g (etendue du RR = de 1,43 a 6,63). Les accouchements OU I'utilisation d'instruments a ete necessaire comportaient des risques accrus allant du double, pour un accouchement par extraction sous vide (RR :::: 2,15), a plus du quintuple, pour un accouchement par application de forceps apres I'echec d'une extraction sous vide (RR = 5,69). L'episiotomie, surtout I'incision du plan median, a fait augmenter Ie risque de laceration (RR :::: 2.57). Le risque de laceration du sphincter externe a double de 1988 a 1997, et ce, en depit de la neutralisation de I'effet des facteurs de risque. Conclusions: Les donnees existantes sur les facteurs de risque de laceration du sphincter externe de I'anus sont suffisantes pour permettre la modification de la prise en charge du tra-. vail et de I'accouchement dans Ie but de minimiser Ie risque de laceration du sphincter externe de I'anus. 1/ se peut que I'augmentation graduelle de son incidence, que nous avons constatee, s'explique par une sensibilisation accrue a I'importance clinique de deceler et de reparer les lacerations du sphincter externe de I'anus. J Obstet Gynaecol Can 2003;25(7): JOGe JULY 2003
2 INTRODUCTION Obstetrical perineal trauma may lead to significant short- and long-term morbidities. 1 Clinically detected anal sphincter lacerations occur in 0.5% to 3.3% of vaginal deliveries. 1-7 Previous studies have identified nulliparity,3,5j-9 instrument-assisted vaginal delivery with either vacuum 10,11 or forceps,9,12-14 episiotomy,9,12-14 and increased birth weight3,5,6,9 as being significant risk factors for anal sphincter laceration. There have been limited or conflicting reports concerning other associated factors including epidural anaesthesia,5,7,9,10,12 duration of the second stage oflabour,7,15 and type of physician performing the delivery.12 These studies had small sample sizes5,7,12,16 and conflicting results concerning many of the risk factors. 5,12 The objectives of this study were to use the data from a large perinatal database to identify independent risk factors for anal sphincter laceration, determine the trend in rates of anal sphincter laceration over a 10-year period, and examine the impact of temporal trends in risk factors on anal sphincter laceration rates. METHODS We conducted a population-based retrospective cohort study over the 1 O-year period of 1988 to All singleton vaginal births resulting in a live neonate weighing ~500 g were included. Data were obtained from the Nova Scotia Arlee Perinatal Database, which contains information on maternal, labour and delivery, and neonatal characteristics for all births that occur in the province of Nova Scotia. Trained health-records personnel abstracted information from the database, and the data quality in the Nova Scotia Arlee Perinatal Database was assured by periodic data abstraction and validation studies to monitor data quality. 17 Third-degree lacerations were defined as those that extended partially or completely through the external anal sphincter. Fourth-degree lacerations were defined as those that extended through the rectal mucosa. Unless otherwise indicated, for this analysis, third- and fourth-degree lacerations were combined and referred to as anal sphincter laceration. For the purposes of this analysis, the criteria for fetal distress included one or more of: "fetal distress" documented in the chart by the attending physician; prolonged tachycardia, bradycardia, or fetal heart rate decelerations, which required interventions such as vacuum extraction or forceps delivery; and a scalp ph <7.2. The type of hospital was defined as: a tertiary care hospital, having obstetricians, pediatricians, and a level II neonatal intensive care unit (NICU); a regional hospital, having obstetricians and pediatricians, but no level II NICU; and a community hospital, having no obstetricians, pediatricians, or NICU. The second stage of labour was defined as the time from full cervical dilatation to delivery. Temporal trends in vaginal parity, episiotomy, spontaneous and operative vaginal deliveries, birth weight, and prolonged second stage were determined for the 10-year period. A single stepwise logistic regression was used to quantify the increased risk associated with individual factors while controlling for confounding variables. Relative risk (RR) and 95% confidence intervals (CI) were calculated, and a Pvalue of <0.05 was considered statistically significant. A multivariate model was used to examine temporal trends in anal sphincter laceration rates, after controlling for changes in relevant determinants. RESULTS During the 10-year study period, of the women in Nova Scotia who had a vaginal delivery of a liveborn singleton infant weighing ~500 g, 3244 (3.6%) were foufld to have an anal sphincter laceration. Women received episiotomies during 47.5% of the deliveries. Eighty-five percent of episiotomies were mediolateral incisions (n = 36792) and 15% (n = 6534) were midline. The maternal risk factors associated with anal sphincter laceration are presented in Table 1. Having no previous vaginal birth was the greatest risk of anal sphincter laceration (RR = 6.97, 95% CI = ). A prepregnancy maternal weight of <50 kg was associated with an increased risk oflaceration relative to a prepregnancy weight of 50 kg to 59 kg (RR = 1.34, 95% CI = ). Protective against anal sphincter laceration were both maternal age <25 years and a prepregnancy weight of ~60 kg, relative to maternal age of 25 to 29 years and a prepregnancy weight of 50 kg to 59 kg. The results of the analysis oflabour factors and risk of anal sphincter laceration are shown in Table 2. While a second stage duration ofless than 20 minutes was protective, a second stage of 120 minutes or longer was associated with an increased risk of sphincter laceration relative to a second-stage duration of 20 to 39 minutes. The risk increased for each hour beyond 2 houts. Fetal malposition at delivery and non-vertex presentation were each associated with a 2-fold increased risk oflaceration. Delivery by an obstetrician compared with delivery by a general practitioner (RR = 1.30, 95% CI = ) and the presence of fetal distress at the time of delivery (RR = 1.36,95% CI = ) both increased the risk of anal sphincter laceration. The use of epidural or spinal anaesthesia had a small protective effect. Table 3 illustrates delivery risk factors associated with anal sphincter laceration. All types of instrument-assisted vaginal delivery were associated with an increased risk of anal sphincter laceration compared to spontaneous vaginal delivery. Vacuum-assisted vaginal delivery was associated with a 2-fold increased risk (RR = 2.15, 95% CI = ). Forceps rotation also increased the risk (RR = 1.38,95% CI = ). With forceps-assisted vaginal deliveries, the risk increased with higher station at delivery (low forceps: RR = 3.53, 95% CI = ; mid-forceps: RR = 4.46, 95% CI = ). The highest risk of anal sphincter laceration from instrument-assisted vaginal deliveries was found for a forceps delivery following an unsuccessful JOGC JULY 2003
3 attempt at vacuum extraction (RR= 5.69, 95% CI = ). Episiotomy increased the risk, with midline incisions having more than twice the risk (RR = 2.57, 95% CI = ) of mediolateral incisions (RR = 1.14, 95% CI = ). Delivery in a tertiary-care hospital increased the risk of anal sphincter laceration (RR = 1.19,95% CI = ), when compared to a community hospital. Newborn risk factors are shown in Table 4. The risk of anal sphincter laceration increased progressively with increasing birth weight. Although delivery from 38 to 40 weeks was associated with increased risk of sphincter laceration relative to delivery at 37 weeks (38 weeks: RR = 1.48,95% CI = ; 39 weeks: RR = 1.43,95% CI 0= ; 40 weeks: RR 0= 1.35, 95% CI = ), delivery beyond 41 weeks' gestation was not associated with an increased risk. The temporal trend in anal sphincter laceration for the 1 O-year period is shown in Figure 1. Temporal trends in operative vaginal delivery, episiotomy, birth weight ;:::3000 g, and prolonged second stage are depicted in Figure 2. We observed an increase in the anal sphincter laceration rate from 2.8% (95% CI 0= ) in 1988 to 3.6% (95% CI = ) in 1997 (Pvalue for trend <0.001). This increase in laceration rates was confined to an increase in third-degree lacerations only; which increased from 2.1 % in 1988 to 3.1 % in The increase in laceration rates occurred despite a decrease in episiotomy rates from 66.7% (95% CI = ) in 1988 to 28.0% (95% CI = ) in 1997 (Pvalue for trend <0.001). The overall rate of instrument-assisted vaginal deliveries decreased over the 10-year study period. While the rate of forceps deliveries as a percentage of all vaginal deliveries decreased from 16.3% to 8.2%, vacuum-assisted deliveries increased from 0.3% to 4.6%. The proportion of singleton live births weighing ;:::3000 g increased from 82.8% to 83.4% over the 10-year study period. The percentage of women with a second stage longer than 2 hours increased over the study interval, from 11.3% in 1988 to 16.4% for vaginal deliveries of singletons in The proportion of women having had no previous vaginal birth did not change during the study period. After controlling for changes in all risk factors, we observed a 2-fold increase in anal sphincter laceration rates between 1988 and 1997 (P <0.001). DISCUSSION The large Nova Scotia Arlee Perinatal Database and the span of 10 years allowed a comprehensive evaluation of risk factors for anal sphincter laceration. The susceptibility to laceration in women undergoing their first vaginal delivery3,5,7-9 may be modifiable by massage,18 and is possibly due to differences in TABLE I MATERNAL RISK FACTORS ASSOCIATED WITH ANAL SPHINCTER LACERATION*t Risk Factor Crude RR (95% CI) Adjusted RR (95% CI) PValue Vaginal parity ( ) 6.97 ( ) <0.001 I 2.48 ( ) 2.23 ( ) < :: ( ) 0.47 ( ) 0.02 Maternal age (y) < ( ) 0.60 ( ) < ( ) 0.76 ( ) < ( ) ( ) ( ) 0.91 ( ) :: ( ) 0.84 ( ) 0.56 Prepregnancy weight (kg) < ( ) 1.34 ( ) < ( I) 0.89 ( ) ( ) 0.86 ( ) :: ( ) 0.75 ( ) <0.001 RR: relative risk; CI: confidence interval. 'Singleton vaginal delivery of liveborn 2::500 g. tanal sphincter lacerations included third- and fourth-degree lacerations. :J:Vaginal parity is defined as the number of prior vaginal deliveries. JOGC 2003
4 the elasticity and strength of connective tissue in the perineum. In our study population, all types of instrument-assisted vaginal delivery increased the risk of anal sphincter laceration compared to spontaneous vaginal delivery. Some authors 18 believe the placement of forceps on the fetal head, presumably increasing the presenting cranial diameter, predisposes to increased risk of perineal trauma when compared to vacuum delivery. Overall, there was a decrease in the number of instrument-assisted vaginal deliveries over the 10-year study period. While the rate of forceps delivery declined from 16.3% of all vaginal deliveries in 1988 to 8.2% in 1997, the rate of vacuum-assisted delivery increased 15-fold from 0.3% to 4.6% over the same time period. In this study, vacuum-assisted delivery carried approximately one-half the risk of anal sphincter laceration associated with mid-forceps delivery. The rate of episiotomy declined from 66.7% in 1988 to 28% in Previous work has demonstrated that episiotomy is highly associated with third- and fourth-degree obstetrical lacerations. 9,11-14 It should be anticipated that a significant decline in laceration rate would accompany such a change in episiotomy practice, yet this was not observed. Furthermore, 85% of the episiotomies in our study were by mediolateral incisions, and although our study and others 15,18 have demonstrated a risk oflaceration even with mediolateral incisions, this technique carries a lower risk than midline episiotomy. In this study, the risk of laceration increased progressively with increasing birth weight, in accordance with several previous studies. 3,5,6,9 With increasing fetal size, there is increasing risk of trauma to the mother. Ultrasound estimation of fetal weight may be helpful in counselling women about the route of delivery for macrosomic infants. In our study, increasing duration of the second stage of labour increased the rate of anal sphincter lacerations in our study population after the first 2 hours and there was a progressive TABLE 2 LABOUR RISK FACTORS ASSOCIATED WITH ANAL SPHINCTER LACERATION*t Risk Factor Crude RR (95% CI) Adjusted RR (95% CI) PValue Duration second stage (min) < ( ) 0.62 ( ) I ( ) 0.88 ( ) ( ) 1.09 ( ) ( ) 1.06 ( ) ( ) 1.47 ( ) < ( ) 1.79 ( ) < ( ) 2.02 ( ) <0.001 Position Occiput anterior Occiput posterior 3.30 ( ) 2.44 ( ) <0.001 Non-vertex 0.88 (Q ) 2.27 ( ) Type of physician General practitioner Obstetrician 3.10 ( ) 1.30 ( ) <0.001 Fetal distress No Yes 3.06 ( ) 1.36 ( ) <0.001 Labour augmentation No Yes 2.05 ( ) 0.91 ( ) 0.06 Epidural No Yes 3.28 ( ) 0.89 ( ) 0.03 RR: relative risk; CI: confidence interval. 'Singleton vaginal delivery of liveborn 2500 g. tanal sphincter laceration includes third- and fourth-degree lacerations. JOGC JULY 2003
5 TABLE 3 DELIVERY RISK FACTORS ASSOCIATED WITH ANAL SPHINCTER LACERATION*t Risk Factor Crude RR (95% CI) Adjusted RR (95% CI) PValue Rotation No rotation Manual 3.88 ( ) 0.95 ( ) 0.64 Forceps 8.60 ( ) 1.38 (1.12-1,48) <0.001 Method of delivery Spontaneous Vacuum 5.11 ( ) 2.15 (I ) <0.001 Outlet forceps 8.62 ( ) 3.62 ( ) <0.001 Low mid-forceps 9.68 ( ) 3.53 ( ) <0.001 Mid-forceps ( ) 4.46 ( ) <0.001 Forceps after vacuum ( ) 5.69 ( I) <0.001 Episiotomy None Mediolateral 4.15 ( ) 1.14 ( ) 0.03 Midline 6.38 ( ) 2.57 ( ) <0.001 Type of hospital Community Regional 1.19 ( ) 0.89 ( ) 0.21 Tertiary 1.86 ( I) 1.19 ( ) 0.04 RR: relative risk; CI: confidence interval. 'Singleton vaginal delivery of liveborn ;::500 g. tanal sphincter laceration includes third- and fourth-degree lacerations. TABLE 4 NEWBORN RISK FACTORS ASSOCIATED WITH ANAL SPHINCTER LACERATION*t Risk Factor Crude RR (95% CI) Adjusted RR (95% CI) PValue Birth weight (g) < ( ) 0.52 ( ) ( ) 0.84 ( ) ( ) 1.43 ( ) < ( ) 2.00 ( ) < ( ) 2.95 ( ) < ( ) 3.51 ( ) <0.001 ;:: ( ) 6.63 ( ) <0.001 Gestational age (wk) < ( ) 0.88 ( ) ,47 ( ) 1,48 ( ) ( ) 1.43 ( ) ( ) 1.35 ( ) ( ) 1.30 ( ) ( ) 1.31 ( ) 0.07 ;:: ( ) 0.89 (0.54-1,46) 0.64 RR: relative risk; Ci: confidence interval. 'Singleton vaginal delivery of liveborn 2':500 g. tanal sphincter laceration includes third- and fourth-degree lacerations. JOGe JULY 2003
6 ... c:: II) u l- II) a ~ ~ Year ---- Anal sphincter laceration rate Figure I. Temporal trends in anal sphincter laceration rates ~ c:: II) u l- II) 50 a r ~----~~==~ 20 +~ _ ~~I 10~::~jl====~====='-~==~~::::=~,t::::!:===~-::::::::-:::::r o Year -+-- Birth weight> 3000 g Second stage> 120 min Episiotomy ~Forceps ~Vacuum Figure 2. Temporal trends in risk factors for anal sphincter lacerations. JOGe JULY 2003
7 increase in risk with every hour beyond 2 hours in the second stage. Other investigators 1 5 have not found duration of the second stage to be related to anal sphincter laceration, but some authors 7 have suggested a protective effect of maternal pushing for less than 30 minutes. Over the 10-year study period, the number of women who experienced a second stage longer than 2 hours increased from 11.3% in 1988 to 16.4% in Delivery by an obstetrician increased the risk of anal sphincter laceration. Since information on trainee supervision was not available within our data source, we could not ascertain whether this increased risk associated with obstetricians was due to the confounding effect of trainees. However, Combs et al 12 found no significant difference in third- or fourth-degree lacerations at instrument-assisted vaginal delivery, when delivery by residents was compared to delivery by faculty. In this large population of women, although the overall incidence of anal sphincter laceration was consistent with other reports in the literature,i-7 the incidence increased over the 10-year study period despite decreasing rates of episiotomy and instrument-assisted vaginal delivery, and constant rates of first vaginal delivery and birth weight ~3000 g. There was an increase in the rate of women experiencing a second stage longer than 2 hours. The multivariate model used in our analysis allowed us to control for these confounders, while examining the change in risk of anal sphincter laceration. Our observed 2-fold increase in the risk of sustaining an anal sphincter laceration over the study period (RR = 1.94,95% CI = ), was not explained by changes in duration oflabour or rates of any of the recognized risk factors. Other unrecognized factors or practices may therefore be important determinants of risk. Recognition of the importance of avoiding perineal trauma has grown over the last decade l4,19 and a clinical trial has assessed strategies to minimize this trauma. 20 Increased awareness among physicians of the potential implications of vaginal birth for urinary and anal incontinence, pelvic floor function, and perineal pain has prompted questions about the wisdom of attempting vaginal delivery when severe perineal or pelvic floor trauma is likely to occur,4,21,22 and probably a higher rate of recognition of perineal injury at the time of delivery. This phenomenon may have resulted in the higher rate of sphincter lacerations found in our study. The fact that the increase in anal sphincter laceration rates appears to be restricted to third-degree tears would tend to support this hypothesis. Requests by women for elective Caesarean delivery to protect the pelvic floor are increasing and greater numbers of physicians are complying with these requests. 23 While the risk factors identified in our study do not explain the increased rate of anal sphincter laceration observed over the study period, they do provide guidance to physicians and midwives. Prevention of sphincter lacerations and their subsequent morbidities requires the delivery attendant to identify the woman at risk, and modify management to optimize the birth outcome. Parity and birth weight are non-modifiable factors. Intervention may alter the duration of the second stage, and the use of episiotomy and instrument-assisted delivery are choices. Our data support the recommendation that episiotomy should be avoided whenever possible, and when absolutely necessary, a mediolateral technique should be used. Manual rotation (if required), careful selection of instrument for operative vaginal delivery, and optimal management of the second stage of labour may reduce the risk of anal sphincter laceration. Women with multiple risk factors for anal sphincter laceration should be counselled regarding the implications of such an injury, as well as the potential benefits and risks of choosing Caesarean delivery as an alternative. REFERENCES I. Sultan AH. Anal incontinence after childbirth [review]. Curr Opin Obstet Gynecol 1997;9:32H. 2. Haadem K, Ohrlander S, Lingman G. Long term ailments due to anal sphincter rupture caused by delivery: a hidden problem. Eur J Obstet Gynecol Reprod Bioi 1988;27: Sultan AH, Kamm MA, Hudson CN, Bartram CI. Third degree obstetric anal sphincter tears: risk factors and outcome of primary repair. BMJ 1994;308(6933): Tetzschner 1; Sorensen M, Lose G, Christiansen J. Anal and urinary incontinence in women with obstetric anal sphincter rupture. Br J Obstet Gynaecol 1996; I 03( I 0): I S. Poen AC, Felt-Bersma RJF, Dekker GA, Deville W, Cuesta MA, Muewissen SGM. Third degree obstetric perineal tears: risk factors and the preventive role of mediolateral episiotomy. Br J Obstet Gynaecol 1997; I 04(5):563~. 6. Buekens P. Lagasse R, Dramaix M,Woliast E. Episiotomy and third degree tears. Br J Obstet Gynaecol 1985;92: Samuelsson E, Ladfors L,Wennerholm UB, Gareberg B, Nyberg K, Hagberg H. Anal sphincter tears: prospective study of obstetric risk factors. Br J Obstet Gynaecol 2000; I 07: Sorensen M,TetzschnerTT. Rasmussen 00, Bjarnsen J, Christiansen J. Sphincter rupture in childbirth. Br J Surg 1993;80: Zetterstrom J, Lopez A, Anzen B, Norman M, Holmstrom B, Mellgren A. Anal sphincter tears at vaginal delivery: risk factors and clinical outcome of primary repair. Obstet Gynecol 1999;94:21~. 10. Robinson IN, Norwitz ER, Cohen AP. McElrath TF, Liberman ES. Epidural analgesia and third or fourth degree lacerations in nulliparas. Obstet Gynecol 1999;94: I I. Ezenagu LC, Kakarua R, Bofill JA. Sequential use of instruments at operative vaginal delivery: is it safe? Am J Obstet Gynecol 1999; 180: Combs CA, Robertson PA, Laros RK Jr. Risk factors for third-degree and fourth-degree perineal laceration in forceps and vacuum deliveries. Am J Obstet Gynecol 1990; 163( I Pt I): I OH. 13. Labrecque M, Baillargeon L, Dallaire M, Tremblay A, Pinault Jj, Gingras S. Association between median episiotomy and severe perineal lacerations in primiparous women. Can Med Assoc J 1997; 156:797~ Klein MC, Gauthier RJ, Robbins JM, Kaczorowski J,Jorgensen SH, Franco ED, et al. Relationship of episiotomy to perineal trauma and morbidity, sexual dysfunction, and pelvic floor relaxation. Am J Obstet Gynecol 1994; 171 : Bek K, Laurberg S. Intervention during labor: risk factors associated with complete tear of the anal sphincter. Acta Obstet Gynecol Scand 1992;71 :52H. 16. Haadem K, Dahlstrom JA, Ling L, Ohrlander S. Anal sphincter function after delivery rupture. Obstet Gynecol 1987;70:53~. JOGC JULY 2003
8 17. Dodds LA, Smith L. Nova Scotia Atlee Perinatal Database: chart review. Halifax (NS): Reproductive Care Program of Nova Scotia; Eason E, Labrecque M, Wells G, Feldman P. Preventing perineal trauma during childbirth: a systematic review. Obstet Gynecol 2000;95: Logue M. Putting research into practice: perineal management during delivery. In: Robinson S, Thomson AM, editors. Midwives, research and childbirth. 2nd ed. London: Chapman and Hall; p House MJ, Cario G,Jones MH. Episiotomy and the perineum: a random controlled trial. J Obstet Gynecol 1986;7: I 07-1 O. 21. Farrell SA, Allen VM, Baskett TF. Parturition and urinary incontinence in primiparous women. Obstet Gynecol 200 I ;97: Farrell SA, Allen VM, Baskett TF. Anal incontinence in priparas. J Soc Obstet Gynaecol Can 200 I ;23: Sultan AH, Stanton SL. Preserving the pelvic floor and perineum during childbirth-elective Caesarean section? Br J Obstet Gynaecol 1996;103: The Use of Fetal Doppler in Obstetrics Programmes in 2003 Ma;llu1lallCt! of Certificatiotl Program of th Royal o//' of Physicilms and urgeon,s of,uuja. UpCOMING progbammes Toronto Sep mber Vantouv r <ktobef 24 & 25 Toronto 0\1 mber 14 & 15 Don't miss thi valuable self-directed learning module on The Use of F tal Doppler in Obstetrics. Supported by an un tricted u donaj grant from For mont orma ow qc.org or CX)II Ihe SOGC at (613) ext 248 JOGe
Anal incontinence after childbirth is more common than was previously believed. Anal incontinence after childbirth. Methods
 Anal incontinence after childbirth Research Recherche From *the Department of Obstetrics and Gynecology, University of Ottawa, Ottawa, Ont.; the Departments of Family Medicine and Social and Preventive
Anal incontinence after childbirth Research Recherche From *the Department of Obstetrics and Gynecology, University of Ottawa, Ottawa, Ont.; the Departments of Family Medicine and Social and Preventive
Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study
 ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
Anal Sphincter Injuries: Acute Management
 Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Prevalence and Risk Factors for Urinary and Fecal Incontinence Four Months After Vaginal Delivery
 WOMEN'S HEALTH WOMEN'S HEALTH Prevalence and Risk Factors for Urinary and Fecal Incontinence Four Months After Vaginal Delivery Sandra A. Baydock, MD, 1 Catherine Flood, MD, 1 Jane A. Schulz, MD, 1 Dianna
WOMEN'S HEALTH WOMEN'S HEALTH Prevalence and Risk Factors for Urinary and Fecal Incontinence Four Months After Vaginal Delivery Sandra A. Baydock, MD, 1 Catherine Flood, MD, 1 Jane A. Schulz, MD, 1 Dianna
Appendix B Protocol for management of obstetric anal sphincter injury THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS
 Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Midline episiotomy and anal incontinence: retrospective cohort study
 Obstetrics and Gynecology Epidemiology Center, Brigham and Women s Hospital, Harvard Medical School, 221 Longwood Avenue, Boston, MA 02115, Lisa B Signorello study coordinator Bernard L Harlow associate
Obstetrics and Gynecology Epidemiology Center, Brigham and Women s Hospital, Harvard Medical School, 221 Longwood Avenue, Boston, MA 02115, Lisa B Signorello study coordinator Bernard L Harlow associate
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION
 OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
Impact of Delivery Types on Women s Postpartum Sexual Health
 Reproduction & Contraception (2003) 14 (4):237~242 Impact of Delivery Types on Women s Postpartum Sexual Health Huan-ying WANG 1, Xiao-yang XU 2, Zhen-wei YAO 1, Qin ZHOU 1 Key words: postpartum; sexual
Reproduction & Contraception (2003) 14 (4):237~242 Impact of Delivery Types on Women s Postpartum Sexual Health Huan-ying WANG 1, Xiao-yang XU 2, Zhen-wei YAO 1, Qin ZHOU 1 Key words: postpartum; sexual
Obstetric Anal Sphincter Injury- A guideline. Mr David Sim Ms Patricia McStay. Dr Martina Hogan Dept./Division Only: YES-IMWH Directorate Only: NO
 CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS
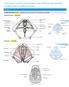 THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem
 Eur. J. Obstet. Gynecol. Reprod. Biol., 27 (1988) 27-32 Elsevier 27 EJO 00556 Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem Knut Haadem, Sten Ohrlander and G6ran
Eur. J. Obstet. Gynecol. Reprod. Biol., 27 (1988) 27-32 Elsevier 27 EJO 00556 Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem Knut Haadem, Sten Ohrlander and G6ran
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital
 Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
Postpartum Complications
 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
Faecal incontinence after childbirth
 Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
Vincent Letouzey, MD, PhD
 How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
Obstetric Anal Sphincter Injury. An update on best practices. Objectives
 Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
In healthy young women, anal sphincter tear at
 Risk Factors for Anal Sphincter Tear During Vaginal Delivery Mary P. FitzGerald, MD, Anne M. Weber, MD, MS, Nancy Howden, MD, MS, Geoffrey W. Cundiff, MD, and Mort B. Brown, PhD, for the Pelvic Floor Disorders
Risk Factors for Anal Sphincter Tear During Vaginal Delivery Mary P. FitzGerald, MD, Anne M. Weber, MD, MS, Nancy Howden, MD, MS, Geoffrey W. Cundiff, MD, and Mort B. Brown, PhD, for the Pelvic Floor Disorders
Childbirth Trauma & Its Complications 23/ Mr Stergios K. Doumouchtsis
 Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Occult anal sphincter injuries myth or reality?
 DOI: 10.1111/j.1471-0528.2006.00799.x www.blackwellpublishing.com/bjog Intrapartum care Occult anal sphincter injuries myth or reality? Vasanth Andrews, a Abdul H Sultan, a Ranee Thakar, a Peter W Jones
DOI: 10.1111/j.1471-0528.2006.00799.x www.blackwellpublishing.com/bjog Intrapartum care Occult anal sphincter injuries myth or reality? Vasanth Andrews, a Abdul H Sultan, a Ranee Thakar, a Peter W Jones
How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial
 DOI: 10.1111/j.1471-0528.2006.00806.x www.blackwellpublishing.com/bjog Intrapartum care How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial Abimbola
DOI: 10.1111/j.1471-0528.2006.00806.x www.blackwellpublishing.com/bjog Intrapartum care How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial Abimbola
Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship?
 DOI 10.1007/s00192-007-0431-8 ORIGINAL ARTICLE Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship? Inka Scheer & Vasanth Andrews & Ranee Thakar & Abdul H. Sultan
DOI 10.1007/s00192-007-0431-8 ORIGINAL ARTICLE Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship? Inka Scheer & Vasanth Andrews & Ranee Thakar & Abdul H. Sultan
Repair of vaginal tears and episiotomy guidelines
 Repair of vaginal tears and episiotomy guidelines Purpose These guidelines assist practitioners in the repair of vaginal and perineal tears including the reasons for, and the techniques of performing an
Repair of vaginal tears and episiotomy guidelines Purpose These guidelines assist practitioners in the repair of vaginal and perineal tears including the reasons for, and the techniques of performing an
The Perineal Clinic: - the management of women following OASI
 The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
2/25/2013. Speaker Disclosure. Learning Objectives. Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth
 Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
Clinical Guideline for: The Management of Perineal Trauma following Childbirth
 For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author s Line Manager: Supported
For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author s Line Manager: Supported
Natural progression of anal incontinence after childbirth
 Int Urogynecol J (2009) 20:1029 1035 DOI 10.1007/s00192-009-0901-2 ORIGINAL ARTICLE Natural progression of anal incontinence after childbirth Johan Nordenstam & Daniel Altman & Sophia Brismar & Jan Zetterström
Int Urogynecol J (2009) 20:1029 1035 DOI 10.1007/s00192-009-0901-2 ORIGINAL ARTICLE Natural progression of anal incontinence after childbirth Johan Nordenstam & Daniel Altman & Sophia Brismar & Jan Zetterström
Perineal Tears. Obstetrics & Gynaecology Women & Children s Group
 Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Obstetrical Anal Sphincter Injuries (OASIS): Prevention, Recognition, and Repair
 SOGC CLINICAL PRACTICE GUIDELINE No. 330, December 2015 Obstetrical Anal Sphincter Injuries (OASIS): Prevention, Recognition, and Repair This clinical practice guideline has been prepared by the Urogynaecology
SOGC CLINICAL PRACTICE GUIDELINE No. 330, December 2015 Obstetrical Anal Sphincter Injuries (OASIS): Prevention, Recognition, and Repair This clinical practice guideline has been prepared by the Urogynaecology
Vaginal Parity and Pelvic Organ Prolapse
 The Journal of Reproductive Medicine Vaginal Parity and Pelvic Organ Prolapse Lieschen H. Quiroz, M.D., Alvaro Muñoz, Ph.D., Stuart H. Shippey, M.D., Robert E. Gutman, M.D., and Victoria L. Handa, M.D.
The Journal of Reproductive Medicine Vaginal Parity and Pelvic Organ Prolapse Lieschen H. Quiroz, M.D., Alvaro Muñoz, Ph.D., Stuart H. Shippey, M.D., Robert E. Gutman, M.D., and Victoria L. Handa, M.D.
Episiotomy and obstetric outcomes among women living with type 3 female genital mutilation: a secondary analysis
 Rodriguez et al. Reproductive Health (2016) 13:131 DOI 10.1186/s12978-016-0242-9 RESEARCH Open Access Episiotomy and obstetric outcomes among women living with type 3 female genital mutilation: a secondary
Rodriguez et al. Reproductive Health (2016) 13:131 DOI 10.1186/s12978-016-0242-9 RESEARCH Open Access Episiotomy and obstetric outcomes among women living with type 3 female genital mutilation: a secondary
The improvements in maternal mortality seen in the
 WOMEN'S HEALTH Female Education and Maternal Mortality: A Worldwide Survey Chryssa McAlister, BSc, 1 Thomas F. Baskett, MB, FRCSC 2 1 Faculty of Medicine, Dalhousie University, Halifax NS 2 Department
WOMEN'S HEALTH Female Education and Maternal Mortality: A Worldwide Survey Chryssa McAlister, BSc, 1 Thomas F. Baskett, MB, FRCSC 2 1 Faculty of Medicine, Dalhousie University, Halifax NS 2 Department
Circumcision bleeding complications: Neonatal intensive care infants compared to. those in the normal newborn nursery
 Circumcision bleeding complications: Neonatal intensive care infants compared to those in the normal newborn nursery Abigail R. Litwiller MD 1, David M. Haas MD, MS 2 1 Department of OB/GYN, University
Circumcision bleeding complications: Neonatal intensive care infants compared to those in the normal newborn nursery Abigail R. Litwiller MD 1, David M. Haas MD, MS 2 1 Department of OB/GYN, University
Third & Fourth Degree Tears guideline (GL926)
 Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
AL-AZHAR ASSIUT MEDICAL JOURNAL
 TOPICAL LIDOCAINE-PRILOCAINE CREAM (EMLA) VERSUS MEPIVACAINE INFILTRATION FOR REDUCING PAIN DURING REPAIR OF MEDIOLATERAL EPISIOTOMY AFTER SPONTANEOUS VAGINAL DELIVERY Hossam M Abdelnaby and Ahmed Mahmoud
TOPICAL LIDOCAINE-PRILOCAINE CREAM (EMLA) VERSUS MEPIVACAINE INFILTRATION FOR REDUCING PAIN DURING REPAIR OF MEDIOLATERAL EPISIOTOMY AFTER SPONTANEOUS VAGINAL DELIVERY Hossam M Abdelnaby and Ahmed Mahmoud
FACTORS ASSOCIATED WITH URINARY STRESS INCONTINENCE IN PRIMIPARAS
 P.L. Chou, et al ORIGINAL ARTICLE FACTORS ASSOCIATED WITH URINARY STRESS INCONTINENCE IN PRIMIPARAS Pei-Ling Chou, Fang-Ping Chen*, Li-Fen Teng Department of Obstetrics and Gynecology, Keelung Chang Gung
P.L. Chou, et al ORIGINAL ARTICLE FACTORS ASSOCIATED WITH URINARY STRESS INCONTINENCE IN PRIMIPARAS Pei-Ling Chou, Fang-Ping Chen*, Li-Fen Teng Department of Obstetrics and Gynecology, Keelung Chang Gung
(UI Urine incontinence)! " # $% &'! ( ) * " " +, -. &/ !!" # $%& /'0 = ='' &!( )'*(" &%: "## $ "% % &' ( )* .!
 39/0/5: 39//8:! "#/7 / 6 4 3!!" # $%& /'0 -. (SI Stress incontinence) '' &!( )'*("&%!%!" #$ :!*8>4 &'!% = / ;
39/0/5: 39//8:! "#/7 / 6 4 3!!" # $%& /'0 -. (SI Stress incontinence) '' &!( )'*("&%!%!" #$ :!*8>4 &'!% = / ;
Pregnancy and childbirth: the effects on pelvic floor muscles
 Page 1 of 9 Pregnancy and childbirth: the effects on pelvic floor muscles 26 February, 2009 Stress incontinence can follow childbirth as pelvic floor muscles are damaged AUTHOR Julia Herbert, MSc, MCSP,
Page 1 of 9 Pregnancy and childbirth: the effects on pelvic floor muscles 26 February, 2009 Stress incontinence can follow childbirth as pelvic floor muscles are damaged AUTHOR Julia Herbert, MSc, MCSP,
Maternity Information Leaflet. Care of the Perineum (including Pelvic Floor Exercises) Version 2
 Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Risk factors and management of obstetric perineal injury
 Risk factors and management of obstetric perineal injury Ruwan J Fernando Abstract Perineal injury sustained during childbirth is a major aetiological factor in the development of perineal pain, sexual
Risk factors and management of obstetric perineal injury Ruwan J Fernando Abstract Perineal injury sustained during childbirth is a major aetiological factor in the development of perineal pain, sexual
List of performance and attendance at practical training in Obstetrics, Gynaecology and Reproduction
 List of performance and attendance at practical training in Obstetrics, Gynaecology and Reproduction Academic year: 0/ Name and surname: Explanation of proficiency levels of the required skills and/or
List of performance and attendance at practical training in Obstetrics, Gynaecology and Reproduction Academic year: 0/ Name and surname: Explanation of proficiency levels of the required skills and/or
AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA
 AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA NEED FOR A WORKING GROUP ON CHILDBIRTH TRAUMA A: Background
AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA NEED FOR A WORKING GROUP ON CHILDBIRTH TRAUMA A: Background
NEW POSTNATAL URINARY INCONTINENCE : OBSTETRIC AND OTHER RISK FACTORS IN PRIMIPARAE. New postnatal urinary incontinence in primiparae
 Author Posting. The Authors 2006. This is the author s version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in BJOG, 113(2):208-17. doi:10.1111/j.1471-0528.2005.00840.x
Author Posting. The Authors 2006. This is the author s version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in BJOG, 113(2):208-17. doi:10.1111/j.1471-0528.2005.00840.x
= 0.002) 117 #!. 12, : = 0.45; P
 Background: Psychosocial factors governing the use of postoperative, intravenous patient-controlled analgesia (PCA) have received little attention in spite of the fact that PCA is the most common modality
Background: Psychosocial factors governing the use of postoperative, intravenous patient-controlled analgesia (PCA) have received little attention in spite of the fact that PCA is the most common modality
Does delayed child-bearing increase the risk of levator injury in labour?
 Australian and New Zealand Journal of Obstetrics and Gynaecology 2007; 47: 491 495 Blackwell Publishing Asia Original Article Delayed child-bearing and levator injury Does delayed child-bearing increase
Australian and New Zealand Journal of Obstetrics and Gynaecology 2007; 47: 491 495 Blackwell Publishing Asia Original Article Delayed child-bearing and levator injury Does delayed child-bearing increase
Royal College of Obstetricians and Gynaecologists
 Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Obstetric anal sphincter injuries: Incidence, risk factors, consequences and prevention
 Obstetric anal sphincter injuries: Incidence, risk factors, consequences and prevention Katariina Laine, MD PhD thesis 2013 Katariina Laine, MD Department of Obstetrics Oslo University Hospital, Ullevål
Obstetric anal sphincter injuries: Incidence, risk factors, consequences and prevention Katariina Laine, MD PhD thesis 2013 Katariina Laine, MD Department of Obstetrics Oslo University Hospital, Ullevål
Traumatic injury to the anal sphincter sustained in a thirdor
 Obstetric Anal Sphincter Injuries: A Survey of Clinical Practice Among Canadian Obstetricians Carolyn Best, BSc, MD, FRCSC, Harold P. Drutz, MD, FRCSC, May Alarab, MBChB, MRCOG, MRCPI, MSc Division of
Obstetric Anal Sphincter Injuries: A Survey of Clinical Practice Among Canadian Obstetricians Carolyn Best, BSc, MD, FRCSC, Harold P. Drutz, MD, FRCSC, May Alarab, MBChB, MRCOG, MRCPI, MSc Division of
Guideline for Management and Repair of Perineal Trauma
 Guideline for Management and Repair of Perineal Trauma Author: Labour Ward Forum Specialty: Maternity Date Approved: September 2014 Approved by: W&CH Clinical Governance Committee Date for Review: August
Guideline for Management and Repair of Perineal Trauma Author: Labour Ward Forum Specialty: Maternity Date Approved: September 2014 Approved by: W&CH Clinical Governance Committee Date for Review: August
Obstetric anal sphincter injury is the most common
 Repair Techniques for Obstetric Anal Sphincter Injuries A Randomized Controlled Trial Ruwan J. Fernando, MD, MRCOG, Abdul H. Sultan, MD, FRCOG, Christine Kettle, PhD, Simon Radley, MD, FRCS, Peter Jones,
Repair Techniques for Obstetric Anal Sphincter Injuries A Randomized Controlled Trial Ruwan J. Fernando, MD, MRCOG, Abdul H. Sultan, MD, FRCOG, Christine Kettle, PhD, Simon Radley, MD, FRCS, Peter Jones,
Title: A modified surgical approach to women with obstetric anal sphincter tears
 Reviewer's report Title: A modified surgical approach to women with obstetric anal sphincter tears Version: 3 Date: 27 January 2010 Reviewer: Stig S Norderval Reviewer's report: Review on manuscript entitled:
Reviewer's report Title: A modified surgical approach to women with obstetric anal sphincter tears Version: 3 Date: 27 January 2010 Reviewer: Stig S Norderval Reviewer's report: Review on manuscript entitled:
Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases
 CASE REPORT Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases Vasant Kawade 1 and Abhijit Ambike 2 Professor and Head, Department of OBGY, B.K.L.Walawakarl Rural Medical
CASE REPORT Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases Vasant Kawade 1 and Abhijit Ambike 2 Professor and Head, Department of OBGY, B.K.L.Walawakarl Rural Medical
K. Jundt 1, I. scheer 2, v. von Bodungen 1, F. Krumbachner 1, K. Friese 1, U. M. Peschers 3
 362 EU Ro PE an JoUR nal of MED I cal RE search Eur J Med Res (2010) 15: 362-366 I. Holzapfel Publishers 2010 WHat HaRM DoEs a second DElIvERy to the PElvIc FlooR? K. Jundt 1, I. scheer 2, v. von Bodungen
362 EU Ro PE an JoUR nal of MED I cal RE search Eur J Med Res (2010) 15: 362-366 I. Holzapfel Publishers 2010 WHat HaRM DoEs a second DElIvERy to the PElvIc FlooR? K. Jundt 1, I. scheer 2, v. von Bodungen
Among parous women, cesarean birth reduces the
 Pelvic Floor Disorders After Vaginal Birth Effect of Episiotomy, Perineal Laceration, and Operative Birth Victoria L. Handa, MD, MHS, Joan L. Blomquist, MD, Kelly C. McDermott, BS, Sarah Friedman, MD,
Pelvic Floor Disorders After Vaginal Birth Effect of Episiotomy, Perineal Laceration, and Operative Birth Victoria L. Handa, MD, MHS, Joan L. Blomquist, MD, Kelly C. McDermott, BS, Sarah Friedman, MD,
Retrospective Review of Predisposing Factors and Surgical Outcomes in Obstetric Fistula Patients at a Single Teaching Hospital in Western Kenya
 GYNAEcOLOGY Retrospective Review of Predisposing Factors and Surgical Outcomes in Obstetric Fistula Patients at a Single Teaching Hospital in Western Kenya Erin McFadden, MD, 1 Sarah Jane Taleski, MHSc,
GYNAEcOLOGY Retrospective Review of Predisposing Factors and Surgical Outcomes in Obstetric Fistula Patients at a Single Teaching Hospital in Western Kenya Erin McFadden, MD, 1 Sarah Jane Taleski, MHSc,
Diagnosis of gestational diabetes mellitus: comparison between National Diabetes Data Group and Carpenter Coustan criteria
 Asian Biomedicine Vol. 8 No. 4 August 2014; 505-509 Brief communication (Original) DOI: 10.5372/1905-7415.0804.320 Diagnosis of gestational diabetes mellitus: comparison between National Diabetes Data
Asian Biomedicine Vol. 8 No. 4 August 2014; 505-509 Brief communication (Original) DOI: 10.5372/1905-7415.0804.320 Diagnosis of gestational diabetes mellitus: comparison between National Diabetes Data
Immediate or delayed repair of obstetric anal sphincter tears a randomised controlled trial*
 DOI: 10.1111/j.1471-0528.2008.01726.x www.blackwellpublishing.com/bjog General obstetrics Immediate or delayed repair of obstetric anal sphincter tears a randomised controlled trial* J Nordenstam, a,b
DOI: 10.1111/j.1471-0528.2008.01726.x www.blackwellpublishing.com/bjog General obstetrics Immediate or delayed repair of obstetric anal sphincter tears a randomised controlled trial* J Nordenstam, a,b
Severity of Hypoxic Ischaemic Encephalopathy in Neonates with Birth Asphyxia
 Journal of Rawalpindi Medical College (JRMC); 2007; (): 8-22 Severity of Hypoxic Ischaemic Encephalopathy in Neonates with Birth Asphyxia Rubina Zulfiqar, Samiya Naeemullah Department of Paediatrics, Holy
Journal of Rawalpindi Medical College (JRMC); 2007; (): 8-22 Severity of Hypoxic Ischaemic Encephalopathy in Neonates with Birth Asphyxia Rubina Zulfiqar, Samiya Naeemullah Department of Paediatrics, Holy
RANZCOG Advanced Training Modules
 RANZCOG Advanced Training Modules Generalist Obstetrics ATM and Generalist Gynaecology ATM The Generalist ATMs in each of Obstetrics and Gynaecology provide a framework for trainees to consolidate and
RANZCOG Advanced Training Modules Generalist Obstetrics ATM and Generalist Gynaecology ATM The Generalist ATMs in each of Obstetrics and Gynaecology provide a framework for trainees to consolidate and
FACT SHEET 1. Breastfeeding in Ontario Notable Trends within the Province
 Breastfeeding in Ontario Notable Trends within the Province In order to gain a greater understanding of breastfeeding in Ontario, breastfeeding data was retrieved from the Better Outcomes Registry and
Breastfeeding in Ontario Notable Trends within the Province In order to gain a greater understanding of breastfeeding in Ontario, breastfeeding data was retrieved from the Better Outcomes Registry and
Labor & Delivery Management for Women Living with HIV. Pooja Mittal, DO Lisa Rahangdale, MD
 Labor & Delivery Management for Women Living with HIV Pooja Mittal, DO Lisa Rahangdale, MD Statistics for Perinatally Acquired HIV Timing of Perinatal HIV Transmission Most transmission occurs close to
Labor & Delivery Management for Women Living with HIV Pooja Mittal, DO Lisa Rahangdale, MD Statistics for Perinatally Acquired HIV Timing of Perinatal HIV Transmission Most transmission occurs close to
anal incontinence; endoanal ultrasonography; grading systems; obstetric sphincter tears; three-dimensional
 Ultrasound Obstet Gynecol 2012; 40: 207 214 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.10154 Incontinence after primary repair of obstetric anal sphincter tears
Ultrasound Obstet Gynecol 2012; 40: 207 214 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.10154 Incontinence after primary repair of obstetric anal sphincter tears
Operative Vaginal Delivery and Pelvic Floor Trauma. Anna Padoa, MD Urogynecology Service Dept of Ob & Gyn Assaf Harofe Medical Center
 + Operative Vaginal Delivery and Pelvic Floor Trauma Anna Padoa, MD Urogynecology Service Dept of Ob & Gyn Assaf Harofe Medical Center + Vaginal birth and the pelvic floor Mechanisms of injury Damage to
+ Operative Vaginal Delivery and Pelvic Floor Trauma Anna Padoa, MD Urogynecology Service Dept of Ob & Gyn Assaf Harofe Medical Center + Vaginal birth and the pelvic floor Mechanisms of injury Damage to
Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or???
 Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or??? Dr Barry O Reilly Head of department of Urogynaecology Cork University Maternity Hospital Ireland
Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or??? Dr Barry O Reilly Head of department of Urogynaecology Cork University Maternity Hospital Ireland
UNDERSTANDING EPISIOTOMY C-SECTION AND RECTOCELE. Our suture portfolio meets all your procedural needs
 UNDERSTANDING EPISIOTOMY C-SECTION AND RECTOCELE Our suture portfolio meets all your procedural needs GYNECOLOGY Episiotomy A surgically planned incision on the perineum and the posterior vaginal wall,
UNDERSTANDING EPISIOTOMY C-SECTION AND RECTOCELE Our suture portfolio meets all your procedural needs GYNECOLOGY Episiotomy A surgically planned incision on the perineum and the posterior vaginal wall,
Birth trauma: short and long term effects of forceps delivery compared with spontaneous delivery on various pelvic floor parameters
 British Journal of Obstetrics and Gynaecology November 2000, Vol107, pp. 1360-1365 Birth trauma: short and long term effects of forceps delivery compared with spontaneous delivery on various pelvic floor
British Journal of Obstetrics and Gynaecology November 2000, Vol107, pp. 1360-1365 Birth trauma: short and long term effects of forceps delivery compared with spontaneous delivery on various pelvic floor
Chronic pain after childbirth. Petter Kainu Split
 Chronic pain after childbirth Petter Kainu Split 9.5.13 Backround: 128 milj. births per year world wide 18.5 milj. caesarean sections (WHO 2008) 234 milj. surgical operations per year (WHO 2004) Chronic
Chronic pain after childbirth Petter Kainu Split 9.5.13 Backround: 128 milj. births per year world wide 18.5 milj. caesarean sections (WHO 2008) 234 milj. surgical operations per year (WHO 2004) Chronic
POSTGRADUATE TRAINING AND ASSESSMENT IN OBSTETRICS AND GYNAECOLOGY LOG BOOK
 POSTGRADUATE TRAINING AND ASSESSMENT IN OBSTETRICS AND GYNAECOLOGY LOG BOOK Approved by The UEMS Section of Obstetrics and Gynaecology and The European Board and College of Obstetrics and Gynaecology (EBCOG)
POSTGRADUATE TRAINING AND ASSESSMENT IN OBSTETRICS AND GYNAECOLOGY LOG BOOK Approved by The UEMS Section of Obstetrics and Gynaecology and The European Board and College of Obstetrics and Gynaecology (EBCOG)
Pregnancy and HIV Reviewing the Vertical Transmission Risks 2015 OCN Education Day V Logan Kennedy RN, MN Research Associate and Clinical Nursing
 Pregnancy and HIV Reviewing the Vertical Transmission Risks 2015 OCN Education Day V Logan Kennedy RN, MN Research Associate and Clinical Nursing Specialist Women s College Research Institute, Women s
Pregnancy and HIV Reviewing the Vertical Transmission Risks 2015 OCN Education Day V Logan Kennedy RN, MN Research Associate and Clinical Nursing Specialist Women s College Research Institute, Women s
2/5/2016. Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach
 Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Birth Trauma. H. P. Dietz. University of Sydney, Nepean Campus. Penrith, Australia
 Birth Trauma H. P. Dietz University of Sydney, Nepean Campus Penrith, Australia Procedures in US (2010): 1.6 Prolapse Urinary Incontinence Fecal Incontinence Prolapse 200.000 Urinary Incontinence 120.000
Birth Trauma H. P. Dietz University of Sydney, Nepean Campus Penrith, Australia Procedures in US (2010): 1.6 Prolapse Urinary Incontinence Fecal Incontinence Prolapse 200.000 Urinary Incontinence 120.000
Acupuncture during pregnancy Research
 Acupuncture during pregnancy Research The information in this handout has been arranged into the following simplified pregnancy categories: Page 2 - Nausea and vomiting Page 3 - Mental health Page 4 -
Acupuncture during pregnancy Research The information in this handout has been arranged into the following simplified pregnancy categories: Page 2 - Nausea and vomiting Page 3 - Mental health Page 4 -
CONTINENCE PESSARIES IN THE MANAGEMENT OF URINARY INCONTINENCE IN WOMEN
 CONTINENCE PESSARIES IN THE MANAGEMENT OF URINARY INCONTINENCE IN WOMEN Scott A. Farrell, MD, FRCSC, Baljit Singh, MD, FRCSC, Lateefa Aldakhil, MD, FRCSC Department of Obstetrics and Gynaecology, Dalhousie
CONTINENCE PESSARIES IN THE MANAGEMENT OF URINARY INCONTINENCE IN WOMEN Scott A. Farrell, MD, FRCSC, Baljit Singh, MD, FRCSC, Lateefa Aldakhil, MD, FRCSC Department of Obstetrics and Gynaecology, Dalhousie
ENTRY INTO SPECIALTY TRAINING USING THE CESR (CP) ROUTE DETAILS OF PREVIOUS POSTS IN OBSTETRICS & GYNAECOLOGY PRIOR TO APPOINTMENT TO NTN
 ENTRY INTO SPECIALTY TRAINING USING THE CESR (CP) ROUTE DETAILS OF PREVIOUS POSTS IN OBSTETRICS & GYNAECOLOGY PRIOR TO APPOINTMENT TO NTN PERSONAL DETAILS Trainee name Surname Forename(s) NTN Details NTN
ENTRY INTO SPECIALTY TRAINING USING THE CESR (CP) ROUTE DETAILS OF PREVIOUS POSTS IN OBSTETRICS & GYNAECOLOGY PRIOR TO APPOINTMENT TO NTN PERSONAL DETAILS Trainee name Surname Forename(s) NTN Details NTN
Risk factors for monozygotic twinning in IVF: a multicenter, cohort study
 Risk factors for monozygotic twinning in IVF: a multicenter, cohort study New England Fertility Society May 6 th, 2017. Denis A. Vaughan Nothing to disclose Disclosures Objectives Background on monozygotic
Risk factors for monozygotic twinning in IVF: a multicenter, cohort study New England Fertility Society May 6 th, 2017. Denis A. Vaughan Nothing to disclose Disclosures Objectives Background on monozygotic
Bladder care postpartum including bladder care for women with epidural analgesia (GL792)
 Bladder care postpartum including bladder care for women with epidural analgesia (GL792) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children's Services Clinical Governance Committee
Bladder care postpartum including bladder care for women with epidural analgesia (GL792) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children's Services Clinical Governance Committee
SUTURING AN EPISIOTOMY/GENITAL LACERATION
 WOMEN AND NEWBORN HEALTH SERVICE CLINICAL GUIDELINES SECTION B : GUIDELINES RELEVANT TO OBSTETRICS AND MIDWIFERY 5 INTRAPARTUM CARE 5.15 PERINEAL REPAIR Authorised by: OGCCU 5.15.1 SUTURING AN EPISIOTOMY/GENITAL
WOMEN AND NEWBORN HEALTH SERVICE CLINICAL GUIDELINES SECTION B : GUIDELINES RELEVANT TO OBSTETRICS AND MIDWIFERY 5 INTRAPARTUM CARE 5.15 PERINEAL REPAIR Authorised by: OGCCU 5.15.1 SUTURING AN EPISIOTOMY/GENITAL
Lindsey Tingen, MD Department of Obstetrics and Gynecology, Greenville Health System Greenville, SC
 Postpartum IUD Insertion: Continued Usage at Six Months Based on Expulsion and Removal Rates at Greenville Memorial Hospital in the First Year After Adoption of the Practice Lindsey Tingen, MD Department
Postpartum IUD Insertion: Continued Usage at Six Months Based on Expulsion and Removal Rates at Greenville Memorial Hospital in the First Year After Adoption of the Practice Lindsey Tingen, MD Department
The Pelvic Floor: Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology
 The Pelvic Floor: What She Can Expect After Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology Objectives Understand risk factors and treatment
The Pelvic Floor: What She Can Expect After Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology Objectives Understand risk factors and treatment
Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England,
 DOI: 10.1111/1471-0528.12076 www.bjog.org Urogynaecology Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England, 2002 2008 A Pradhan, a DG Tincello, b R Kearney a a Department
DOI: 10.1111/1471-0528.12076 www.bjog.org Urogynaecology Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England, 2002 2008 A Pradhan, a DG Tincello, b R Kearney a a Department
Title: Epidural Analgesia for Pain Management in Labour. Date: May 03, 2007
 Title: Epidural Analgesia for Pain Management in Labour Date: May 03, 2007 Context and policy issues: Balancing pain control with unwanted maternal and neonatal effects remains a hotly debated topic for
Title: Epidural Analgesia for Pain Management in Labour Date: May 03, 2007 Context and policy issues: Balancing pain control with unwanted maternal and neonatal effects remains a hotly debated topic for
Fertility Treatment Decision-Making: The Effect of Insurance Coverage for Fertility Medications
 GYNAECOLOGY Fertility Treatment Decision-Making: The Effect of Insurance Coverage for Fertility Medications Claire Ann Jones, MD, 1 Laura Gra, hd, 2 Kimberl Liu, MD, FRCSC, MSL 1,3 1 Department of Obstetrics
GYNAECOLOGY Fertility Treatment Decision-Making: The Effect of Insurance Coverage for Fertility Medications Claire Ann Jones, MD, 1 Laura Gra, hd, 2 Kimberl Liu, MD, FRCSC, MSL 1,3 1 Department of Obstetrics
for a review under the Accident Compensation Act
 FairWay Resolution Limited Tā te Hinengaro Tōkeke Whakatau Review numbers: Application by for a review under the Accident Compensation Act Held at Date of hearing 2 November 2016, adjourned part-heard;
FairWay Resolution Limited Tā te Hinengaro Tōkeke Whakatau Review numbers: Application by for a review under the Accident Compensation Act Held at Date of hearing 2 November 2016, adjourned part-heard;
PERINEAL REPAIR: COMPARISON OF SUTURE MATERIALS AND SUTURING TECHNIQUES
 ORIGINAL ARTICLE PERINEAL REPAIR: COMPARISON OF SUTURE MATERIALS AND SUTURING TECHNIQUES FOUZIA PERVEEN, TEHMINA SHABBIR ABSTRACT Objective Study design Place & Duration of study To compare the outcome
ORIGINAL ARTICLE PERINEAL REPAIR: COMPARISON OF SUTURE MATERIALS AND SUTURING TECHNIQUES FOUZIA PERVEEN, TEHMINA SHABBIR ABSTRACT Objective Study design Place & Duration of study To compare the outcome
Urinary Incontinence after Vaginal Delivery or Cesarean Section
 The new england journal of medicine original article Urinary after Vaginal Delivery or Cesarean Section Guri Rortveit, M.D., Anne Kjersti Daltveit, Ph.D., Yngvild S. Hannestad, M.D., and Steinar Hunskaar,
The new england journal of medicine original article Urinary after Vaginal Delivery or Cesarean Section Guri Rortveit, M.D., Anne Kjersti Daltveit, Ph.D., Yngvild S. Hannestad, M.D., and Steinar Hunskaar,
period, cesarean delivery is thought to protect against anal incontinence, 3 albeit incompletely. In this study, we investigated anal incontinence
 Obstetrical anal sphincter laceration and anal incontinence 5-10 years after childbirth Emily C. Evers, MPH; Joan L. Blomquist, MD; Kelly C. McDermott, BS; Victoria L. Handa, MD, MHS OBJECTIVE: The purpose
Obstetrical anal sphincter laceration and anal incontinence 5-10 years after childbirth Emily C. Evers, MPH; Joan L. Blomquist, MD; Kelly C. McDermott, BS; Victoria L. Handa, MD, MHS OBJECTIVE: The purpose
A Population-Based Study of Pregnancy and Delivery Characteristics Among Women with Vulvodynia
 Pain Ther (2012) 1:2 DOI 10.1007/s40122-012-0002-7 ORIGINAL RESEARCH A Population-Based Study of Pregnancy and Delivery Characteristics Among Women with Vulvodynia Ruby H. N. Nguyen Elizabeth G. Stewart
Pain Ther (2012) 1:2 DOI 10.1007/s40122-012-0002-7 ORIGINAL RESEARCH A Population-Based Study of Pregnancy and Delivery Characteristics Among Women with Vulvodynia Ruby H. N. Nguyen Elizabeth G. Stewart
INTERNATIONAL JOURNAL OF WOMEN'S HEALTH AND REPRODUCTION SCIENCES
 Original Article INTERNATIONAL JOURNAL OF WOMEN'S HEALTH AND REPRODUCTION SCIENCES http://www.ijwhr.net Urinary Incontinence During Pregnancy and Postpartum Incidence, Severity and Risk Factors in Alzahra
Original Article INTERNATIONAL JOURNAL OF WOMEN'S HEALTH AND REPRODUCTION SCIENCES http://www.ijwhr.net Urinary Incontinence During Pregnancy and Postpartum Incidence, Severity and Risk Factors in Alzahra
Childbirth and prolapse: long-term associations with the symptoms and objective measurement of pelvic organ prolapse
 DOI: 10.1111/1471-0528.12075 www.bjog.org Epidemiology Childbirth and prolapse: long-term associations with the symptoms and objective measurement of pelvic organ prolapse C Glazener, a A Elders, a C MacArthur,
DOI: 10.1111/1471-0528.12075 www.bjog.org Epidemiology Childbirth and prolapse: long-term associations with the symptoms and objective measurement of pelvic organ prolapse C Glazener, a A Elders, a C MacArthur,
Overview. In Vitro Fertilization: a Success Story
 Does IVF cause adverse perinatal outcomes? Paolo Rinaudo *, MD PhD Rebecca A. Jackson %, MD Departments of Ob/Gyn & *Center for Reproductive Sciences & % Epi/Biostats University of California, San Francisco
Does IVF cause adverse perinatal outcomes? Paolo Rinaudo *, MD PhD Rebecca A. Jackson %, MD Departments of Ob/Gyn & *Center for Reproductive Sciences & % Epi/Biostats University of California, San Francisco
It is well established that the development of
 Obstetrics Risk Estimation of Metabolic Syndrome at One and Three Years After a Pregnancy Complicated by Graeme N. Smith, MD, PhD, 1,2 Jessica Pudwell, MPH, 1,2 Mark Walker, MD, MSc, 3 Shi-Wu Wen, MB,
Obstetrics Risk Estimation of Metabolic Syndrome at One and Three Years After a Pregnancy Complicated by Graeme N. Smith, MD, PhD, 1,2 Jessica Pudwell, MPH, 1,2 Mark Walker, MD, MSc, 3 Shi-Wu Wen, MB,
EPIDURAL ANALGESIA FOR THE SURGICAL INDUCTION OF LABOUR
 Br. J. Anaesth. (1974), 46, 747 EPIDURAL ANALGESIA FOR THE SURGICAL INDUCTION OF LABOUR N. G. CASEBY SUMMARY Surgical induction of labour was performed on 80 patients under epidural analgesia and on 73
Br. J. Anaesth. (1974), 46, 747 EPIDURAL ANALGESIA FOR THE SURGICAL INDUCTION OF LABOUR N. G. CASEBY SUMMARY Surgical induction of labour was performed on 80 patients under epidural analgesia and on 73
Post operative voiding dysfunction and the Value of Urodynamics. Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist
 Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF)
 Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF) Blair B. Washington MD, MHA Urogynecology & Reconstructive Pelvic Surgery Virginia Mason Medical Center Disclosures
Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF) Blair B. Washington MD, MHA Urogynecology & Reconstructive Pelvic Surgery Virginia Mason Medical Center Disclosures
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
Gestational Diabetes. Gestational Diabetes:
 Gestational Diabetes Detection and Management Steven Gabbe, MD The Ohio State University Medical Center Gestational Diabetes: Detection and Management Learning Objectives: At the conclusion of this presentation,
Gestational Diabetes Detection and Management Steven Gabbe, MD The Ohio State University Medical Center Gestational Diabetes: Detection and Management Learning Objectives: At the conclusion of this presentation,
Maternal And Fetal Outcome In Pregnancies Complicated With Maternal Cardiac Diseases: Experience At A Tertiary Care Hospital
 ISPUB.COM The Internet Journal of Gynecology and Obstetrics Volume 19 Number 1 Maternal And Fetal Outcome In Pregnancies Complicated With Maternal Cardiac Diseases: Experience At A Tertiary Care Hospital
ISPUB.COM The Internet Journal of Gynecology and Obstetrics Volume 19 Number 1 Maternal And Fetal Outcome In Pregnancies Complicated With Maternal Cardiac Diseases: Experience At A Tertiary Care Hospital
Labour Epidurals and Maternal Pyrexia
 Labour Epidurals and Maternal Pyrexia Katherine W. Arendt, MD Associate Professor of Anesthesiology Mayo Clinic, Rochester, Minnesota Obstetric Anaesthetists Association November 2, 2015 2013 MFMER slide-1
Labour Epidurals and Maternal Pyrexia Katherine W. Arendt, MD Associate Professor of Anesthesiology Mayo Clinic, Rochester, Minnesota Obstetric Anaesthetists Association November 2, 2015 2013 MFMER slide-1
HbA1c level in last trimester pregnancy in predicting macrosomia and hypoglycemia in neonate
 International Journal of Contemporary Pediatrics Subash S et al. Int J Contemp Pediatr. 2016 Nov;3(4):1334-1338 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article DOI:
International Journal of Contemporary Pediatrics Subash S et al. Int J Contemp Pediatr. 2016 Nov;3(4):1334-1338 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article DOI:
