Surgery Illustrated Surgical Atlas The artificial genitourinary sphincter
|
|
|
- Arron Park
- 6 years ago
- Views:
Transcription
1 BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas The artificial genitourinary sphincter John T. Stoffel and David M. Barrett Department of Urology, Lahey Clinic Medical Center, Burlington, USA Accepted for publication 2008 ILLUSTRATIONS by STEPHAN SPITZER, INTRODUCTION Since its introduction by Scott in 1973, the artificial genitourinary sphincter (AUS) has proven to be an effective treatment for refractory urinary incontinence [1]. Over the years, the original AUS 721 model had many revisions to the cuff, pump and reservoir components. The most current development, the narrow back-cuff AMS 800 (American Medical Systems, Minnetonka, MN, USA), has reported continence rates of 61 96% and with low morbidity [2,3]. In this article describing the implantation of the AMS 800 AUS, our goal is to outline proper patient selection, define current surgical technique, and identify troublesome postoperative care issues. PLANNING AND PREPARATION The checklist for the AMS 800 is: Before surgery Stable symptoms for >6 months; stress incontinence much greater than urge incontinence symptoms; Normal perineal/scrotal examination; Negative urine culture; Radiological or cystoscopic evidence of a patent urethra; Surgery Perioperative antibiotics (ampicillin/ gentamicin); AMS 800 components; Cuffs ( cm bulbar, 8 14 cm bladder neck); Control pump; Balloon reservoir (51 60, 61 70, 71 80, cmh 2 O); 644 JOURNAL COMPILATION 2008 BJU INTERNATIONAL 102, doi: /j x x
2 SURGERY ILLUSTRATED Tubing/AMS Quick Connectors/assembly tool; Water/contrast medium solution; 50 ml diatrizoate (Hypaque) + 60 ml water). PATIENT SELECTION The AMS 800 AUS is used primarily to treat symptomatic stress urinary incontinence in men, but the device can also be used to treat incontinence in women and children. All patients considering an AUS should have stable urinary symptoms for 6 months before implantation. Validated urinaryspecific quality-of-life questionnaires, e.g. the Incontinence Impact Questionnaire 7 and Urogenital Distress Inventory 6, can be helpful in determining both the type and severity of incontinence symptoms [4]. For patients with significant urge symptoms, multichannel fluoroscopic urodynamics are performed with an occluded urethra to evaluate detrusor overactivity and bladder compliance. Patients with studies showing uninhibited detrusor contractions, abnormal compliance (<20 ml/cmh 2 O), or grade >2 VUR are then treated with anticholinergics for 4 weeks and the studies repeated. AUS implantation is delayed in patients with continued abnormalities on urodynamic studies until the specific issues are addressed. Failure to treat refractory conditions might lead to lower patient satisfaction or upper urinary tract compromise. On physical examination, patients are evaluated for sufficient manual dexterity to activate the control pump. The perineal skin is examined for cellulitis, ulcers, or fungal infections. A urine culture is obtained for all patients before surgery, and those with positive samples are treated with antibiotics before surgery. All patients should also have cystoscopy or a urethrogram taken to document a urethra patent enough to accommodate a 16 F catheter or sound. PLANNING BEFORE SURGERY The most common indication for AUS implantation is urinary incontinence after prostatectomy. Bulbous urethral cuffs, usually of 4.5 cm, are generally used for this condition. A bladder neck cuff, 8 14 cm, is generally indicated for treating incontinence in men with congenital or acquired anatomical urethral abnormalities. Most patients having an AUS implanted will require a cmh 2 O reservoir, independent of cuff size or location. Patients with radiation damage or previous erosions might benefit from cmh 2 O reservoirs to minimize compression on damaged urethral tissues. PREPARATION/POSITIONING All patients receive broad-spectrum antibiotics, e.g. ampicillin and gentamicin, 1 h before surgical incision. During surgery, access to the operating room should be limited to essential personnel and throughtraffic strictly restricted. The patient is placed supine for a bladder neck cuff and in the dorsal lithotomy position for a perineal cuff. Perineal and scrotal skin is shaved with clippers after the patient is under anaesthesia. A meticulous 5-min sterile preparation with iodophors is then done and the patient draped with several layers such that only the lower abdomen, penis and scrotum are exposed. A perineal cuff also requires exposure to the perineum with care made to exclude the anus from the surgical field. A 12 F urethral catheter is sterilely placed after the patient is draped. During the procedure, the AMS sphincter components should be isolated from sharp surgical instruments and needles on a back table. These components should not be handled with gloves contaminated with blood or other body fluids. When clamping the AUS tubing, rubber-shod clamps should be used to prevent unrecognized tubing injury. JOURNAL COMPILATION 2008 BJU INTERNATIONAL 645
3 OPERATIVE TECHNIQUE BULBOUS URETHRAL CUFF IN MEN Figures 1 and 2 The bulbous urethra can be accessed via a midline perineal incision. The apex of incision should be located at the base of the scrotum and it is extended to 1 cm below the pubic symphysis. Retraction is established with a Richardson retractor cephalad and a Gelpi retractor caudad or with a Lone-Star (Cooper Surgical, Inc., Trumbull, CT, USA) self-retaining retractor system. Sharp dissection is used to expose the bulbocavernosus muscles over the bulbous urethra. 646 JOURNAL COMPILATION 2008 BJU INTERNATIONAL
4 SURGERY ILLUSTRATED JOURNAL COMPILATION 2008 BJU INTERNATIONAL 647
5 Figure 3 The bulbocavernosus muscles are divided sharply in the midline and retracted laterally. Blunt dissection is used to expose the tunica albuginea of the corpus cavernosum dorsally. A vein retractor can then be placed to gently retract the urethra medially to bluntly develop this plane between the corpus cavernosum and the dorsal urethral wall. Sharp dissection is used to dissect the dorsal urethra wall from the intracorporal septum. The urethra is at greatest risk for injury during this manoeuvre. 648 JOURNAL COMPILATION 2008 BJU INTERNATIONAL
6 SURGERY ILLUSTRATED Figure 4 A right-angle can be used to gently puncture the septum if visualization does not allow safe sharp dissection. A 5 mm Penrose retractor can then be passed under the urethra and used to elevate the urethra off the septum to facilitate better exposure for sharp dissection. If the urethra is violated during the dissection, abort the procedure and leave the catheter in place for 3 weeks. The AUS can be safely implanted 3 months after the injury. The dorsal urethral wall is usually dissected in a proximal direction off the corpus cavernosum. Success rates can be higher when the cuff is placed as proximal as possible on the exposed bulbous urethra. Once the dorsal urethral wall is dissected off the intracorporal septum for 2 cm, the urethral diameter is measured; most men will require a 4.5-cm cuff. The AMS 800 AUS components are then prepared at the back table. The surgeon or surgical technician usually changes gloves to avoid contamination before handling the components. The cuff, pump and reservoir are soaked in sterile water and purged of air. The tubing of each piece is clamped with a rubber-shod clamp near the end of the tubing to prevent air from re-entering the system. JOURNAL COMPILATION 2008 BJU INTERNATIONAL 649
7 Figures 5 and 6 The urethral cuff is passed tab first behind the dorsal urethra, toward the anticipated location of the control pump. The tubing is then fed through the tab and the tab is snapped closed over the ventrum of the urethra. The wound is then packed with moist sponges and covered with a sterile towel. Attention is next turned to the lower abdomen. A 5-cm transverse incision is made in the lower quadrant on the ipsilateral side of the urethral cuff tubing. The rectus fascia is exposed and incised for a 3-cm opening. The rectus abdominis muscles are separated and a pocket is then made beneath the muscle to accommodate the reservoir. The pocket is generally made in the direction of the space of Retzius. Failure to place the reservoir beneath the muscles will result in a palpable bulge from the inflated reservoir. Intraperitoneal reservoir placement might be necessary in thin patients. Interrupted 0 polydioxanone sutures are then pre-laced in the fascia. The reservoir is delivered into the pocket below the rectus muscles and the sutures are tied down, with care not to trap the reservoir tubing between the sutures and the fascia. The reservoir is then filled with 22 ml of the iso-osmotic Hypaque/water solution and the tubing re-clamped. 650 JOURNAL COMPILATION 2008 BJU INTERNATIONAL
8 SURGERY ILLUSTRATED JOURNAL COMPILATION 2008 BJU INTERNATIONAL 651
9 Figure 7 A subcutaneous tunnel is then created between the abdominal counter-incision and the hemiscrotum of the patient s dominant hand. Hegar dilators or a ring forceps can be used to create a subdartos scrotal pocket for the pump. The pocket should allow the pump to sit in the most dependant position in the scrotum, lateral to the testicle. The pump, positioned such that the control button is laterally orientated, is then delivered into the scrotal pocket with ring forceps. A Babcock clamp can be placed on the pump tubing in the scrotum to prevent migration after the pump is positioned. 652 JOURNAL COMPILATION 2008 BJU INTERNATIONAL
10 SURGERY ILLUSTRATED Figure 8 After positioning the pump, the urethral cuff tubing is delivered from the perineal incision to the abdominal counter-incision using a long Schnidt clamp or right-angle. The AMS 800 AUS has colour-coded tubing and similarly coloured tubes are connected with either 2 0 polypropylene suture or the AMS Quick Connect set. After the tubing connections are completed, all clamps are removed and the system is allowed to pressurize. The device is cycled twice to verify that all components are connected and functioning. The pump is then squeezed a final time and, after a s delay, the sphincter system is locked open by deploying the control button on the pump. Wounds are then irrigated and closed. The 12 F urethral catheter is left overnight. No further drains are used. a b JOURNAL COMPILATION 2008 BJU INTERNATIONAL 653
11 BLADDER NECK CUFF PLACEMENT Figures 9, 10 and 11 The bladder neck is approached through a midline incision on a patient placed supine. The rectus fascia is divided and the retroperitoneal space entered. In men, a plane is developed between the bladder neck and the rectum by first incising the endopelvic fascia laterally, elevating the urethra, and the carefully passing a right-angle between posterior urethral wall and the rectum. A 2- cm posterior dissection will allow adequate room for the bladder neck cuff. Rectal injury necessitates two-layer closure of the rectal wall violation and ending the case. Severe injuries (>2 cm) require omental interposition or diverting colostomy. POSTOPERATIVE CARE In our institution, patients are kept overnight for observation. On the first day after surgery the 12 F catheter is removed. With a properly placed, deactivated AUS, the patient should still have symptoms of stress urinary incontinence. If a patient has unexpected urinary retention or significant hesitancy after catheter removal, the 12 F catheter is carefully replaced and a voiding trial is attempted again in 24 h. Many voiding trial failures in a patient with a properly deactivated AUS necessitate a urodynamic evaluation and/or cuff replacement. All patients are discharged with acetaminophen and codeine for pain control. After catheter removal, no further antibiotics are given; routine wound care is used. Patients are instructed to avoid perineal pressure, e.g. bike riding, horseback riding, etc., and sexual activity is restricted during the 6-week recovery. Patients are also asked to gently push the pump to the most dependant part of the scrotum on a daily basis, to prevent pump migration. 654 JOURNAL COMPILATION 2008 BJU INTERNATIONAL
12 SURGERY ILLUSTRATED JOURNAL COMPILATION 2008 BJU INTERNATIONAL 655
13 656 JOURNAL COMPILATION 2008 BJU INTERNATIONAL
14 SURGERY ILLUSTRATED Figure 12 Patients return at 6 weeks after surgery for AUS activation. After the wounds are inspected, the patient is placed supine on the examination table. The AUS pump is isolated in the scrotum and squeezed until a gentle popping sensation confirms unlocking of the pump control pin. Fluid returning into the pump chamber further confirms successful activation. Patients are instructed to report dysuria, haematuria, or changes in voiding patterns. Any suspected UTI requires urine culture and a cystoscopy to exclude cuff erosion. Many patients with long-standing urinary incontinence might have some urinary frequency and urgency as the bladder begins to store larger volumes of urine. Timed voiding and fluid management usually resolves these symptoms but an anticholinergic can also be used. a b JOURNAL COMPILATION 2008 BJU INTERNATIONAL 657
15 FROM SURGEON TO SURGEON There are several challenges before and after surgery that a surgeon might encounter. The irradiated patient or with previous erosion: Patients with previous radiation therapy are at greater risk of urethral cuff erosion [5]. A lower pressure reservoir (51 60 cmh 2 O) can be used, or the cuff can be placed transcorporally [6] to minimize compressive trauma. The unstable bladder neck contracture: Bladder neck contractures are challenging. Some can be managed with a programme of transurethral radial incision followed by frequent balloon dilatation until the contracture stabilizes. Refractory contractures can benefit from placing a Urolume stent before the AUS [7]. Low compliance bladder: Urodynamics can be useful to identify patients with low bladder compliance. Patients not responding to anticholinergics will require either autoaugmentation or formal enterocystoplasty. Failure to improve bladder storage pressures before increasing the bladder outlet resistance will result in severe urge incontinence or upper tract damage. Unable to activate the pump: Occasionally, the pump control pin is locked in an open position and cannot be activated with gentle manipulation. There are several strategies to counter this problem. Pushing on the opposite side of the pump control button can occasionally force the pin into the open position and allow the pump chamber to fill. If this fails, bend the pump between the hands, using two thumbs to push the pin into the open position. A final attempt to activate the pump can be attempted under sedation or anaesthesia. Once the patient is asleep, the pump can be very vigorously squeezed without pain to the patient. Lacking success, the pump components should then be replaced. Persistent incontinence after AUS activation: this requires a methodical evaluation. Incontinence due to urethral atrophy can be managed by reducing the size of urethral cuff, adding 5 10 ml more fluid to the reservoir, or placing a tandem cuff [8]. REFERENCES 1 Scott FB, Bradley WE, Timm GW. Treatment of urinary incontinence by implantable prosthetic sphincter. Urology 1973; 1: Hussain M, Greenwell TJ, Venn SN, Mundy AR. The current role of the artificial urinary sphincter for the treatment of urinary incontinence. J Urol 2005; 174: Elliott DS, Barrett DM. Mayo Clinic long term analysis of the functional durability of the AMS 800 artificial urinary sphincter: a review of 323 cases. J Urol 1998; 159: Uebersax JS, Wyman JF, Shumaker SA, McClish DK, Fantl JA. Short forms to assess life quality and symptom distress for urinary incontinence in women: the Incontinence Impact Questionnaire and the Urogenital Distress Inventory. Continence Program for Women Research Group. Neurourol Urodynam 1995; 14: Raj GV, Peterson AC, Webster GD. Outcomes following erosions of the artificial urinary sphincter. J Urol 2006; 175: Guralnick ML, Miller E, Toh KL, Webster GD. Transcorporal artificial cuff placement in cases requiring revision for erosion and urethral atrophy. J Urol 2002; 167: Elliott DS, Boone TB. Combined stent and artificial urinary sphincter for management of severe recurrent bladder neck contracture and stress incontinence after prostatectomy: a long-term evaluation. J Urol 2001; 165: DiMarco DS, Elliott DS. Tandem cuff artificial sphincter as a salvage procedure following failed primary sphincter placement for the treatment of postprostatectomy incontinence. J Urol 2003; 170: Correspondence: John T. Stoffel, Department of Urology, Lahey Clinic Medical Center, 41 Mall Road, Burlington, USA. John.T.Stoffel@lahey.org 658 JOURNAL COMPILATION 2008 BJU INTERNATIONAL
Current Indications for the Use of The Artificial Genitourinary Sphincter and Management of It s Complications
 Article TheScientificWorldJOURNAL (2004) 4 (S1), 114 127 ISSN 1537-744X; DOI 10.1100/tsw.2004.57 Current Indications for the Use of The Artificial Genitourinary Sphincter and Management of It s Complications
Article TheScientificWorldJOURNAL (2004) 4 (S1), 114 127 ISSN 1537-744X; DOI 10.1100/tsw.2004.57 Current Indications for the Use of The Artificial Genitourinary Sphincter and Management of It s Complications
Four-year follow-up on a Zephyr Surgical Implants 375 artificial urinary sphincter for male urinary incontinence from one urological centre in Poland
 320 O R I G I N A L P A P E R FUNCTIONAL UROLOGY Four-year follow-up on a Zephyr Surgical Implants 375 artificial urinary sphincter for male urinary incontinence from one urological centre in Poland Ireneusz
320 O R I G I N A L P A P E R FUNCTIONAL UROLOGY Four-year follow-up on a Zephyr Surgical Implants 375 artificial urinary sphincter for male urinary incontinence from one urological centre in Poland Ireneusz
Since the first published article, in 1974 by Scott et al on
 Perineal Approach for Artificial Urinary Sphincter Implantation Appears to Control Male Stress Incontinence Better Than the Transscrotal Approach Gerard D. Henry,* Stephen M. Graham, Mario A. Cleves, Caroline
Perineal Approach for Artificial Urinary Sphincter Implantation Appears to Control Male Stress Incontinence Better Than the Transscrotal Approach Gerard D. Henry,* Stephen M. Graham, Mario A. Cleves, Caroline
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Aus Artificial Uretheral Sphincter Port System
 NORFOLK VET PRODUCTS the AUS for the long-term relief of incontinence in dogs and cats making life easier for pets Speciality Medical Devices For The Veterinary Community the Aus Artificial Uretheral Sphincter
NORFOLK VET PRODUCTS the AUS for the long-term relief of incontinence in dogs and cats making life easier for pets Speciality Medical Devices For The Veterinary Community the Aus Artificial Uretheral Sphincter
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
AMS 800. Urinary Control System For Male Patients. Operating Room Manual
 AMS 800 Urinary Control System For Male Patients Operating Room Manual Table of Contents Introduction Overview... 1 Indications for Use... 1 Additional Information... 1 System Description... 1 System
AMS 800 Urinary Control System For Male Patients Operating Room Manual Table of Contents Introduction Overview... 1 Indications for Use... 1 Additional Information... 1 System Description... 1 System
Artificial urinary sphincter revision for urethral atrophy: comparing single cuff downsizing and tandem cuff placement
 ORIGINAL ARTICLE Vol. 43 (2): 264-270, March - April, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0240 Artificial urinary sphincter revision for urethral atrophy: comparing single cuff downsizing and tandem
ORIGINAL ARTICLE Vol. 43 (2): 264-270, March - April, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0240 Artificial urinary sphincter revision for urethral atrophy: comparing single cuff downsizing and tandem
West Yorkshire Major Trauma Network Clinical Guidelines 2015
 WYMTN: Pelvic fracture with urogenital trauma KEY RECOMMENDATIONS 1. During the initial exploratory survey / secondary survey, a. The external urethral meatus and the transurethral bladder catheter (if
WYMTN: Pelvic fracture with urogenital trauma KEY RECOMMENDATIONS 1. During the initial exploratory survey / secondary survey, a. The external urethral meatus and the transurethral bladder catheter (if
A New Artificial Urinary Sphincter with Conditional Occlusion for Stress Urinary Incontinence: Preliminary Clinical Results
 european urology xxx (2006) xxx xxx available at www.sciencedirect.com journal homepage: www.europeanurology.com Ageing Male A New Artificial Urinary Sphincter with Conditional Occlusion for Stress Urinary
european urology xxx (2006) xxx xxx available at www.sciencedirect.com journal homepage: www.europeanurology.com Ageing Male A New Artificial Urinary Sphincter with Conditional Occlusion for Stress Urinary
Surgery Illustrated Surgical Atlas Inguinal orchidectomy for testicular cancer
 Surgery Illustrated Focus on Details SURGERY ILLUSTRATED SURGICAL ATLASPIZZOCARO and GUARNERI PIZZOCARO and GUARNERI BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Inguinal orchidectomy for
Surgery Illustrated Focus on Details SURGERY ILLUSTRATED SURGICAL ATLASPIZZOCARO and GUARNERI PIZZOCARO and GUARNERI BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Inguinal orchidectomy for
MANUALFor Operating Room
 DOCUMENT OPERATING ROOM FOR MANUALFor Operating Room NOTE This document is a complementary checklist to the two training videos, which you can access and download from our website: ZSI 375 Training Video,
DOCUMENT OPERATING ROOM FOR MANUALFor Operating Room NOTE This document is a complementary checklist to the two training videos, which you can access and download from our website: ZSI 375 Training Video,
Cleveland Clinic Quarterly
 Cleveland Clinic Quarterly Volume 31 JULY 1964 No. 3 A MEDICAL SILASTIC PROSTHESIS FOR THE CONTROL OF URINARY INCONTINENCE IN THE MALE A Preliminary Report J A M E S K. W A T K I N S, M. D., * R A L P
Cleveland Clinic Quarterly Volume 31 JULY 1964 No. 3 A MEDICAL SILASTIC PROSTHESIS FOR THE CONTROL OF URINARY INCONTINENCE IN THE MALE A Preliminary Report J A M E S K. W A T K I N S, M. D., * R A L P
ZEPHYR SURGICAL IMPLANTS SÀRL
 For Operating Room NOTE This document is a complementary checklist to the two training videos, which you can be accessed and download from our website: ZSI 375 Training Video, ZSI 375 Functioning Protocol.
For Operating Room NOTE This document is a complementary checklist to the two training videos, which you can be accessed and download from our website: ZSI 375 Training Video, ZSI 375 Functioning Protocol.
Combination therapy for male erectile dysfunction and urinary incontinence
 sian J ndrol 2008; 10 (1): 149 154 DOI: 10.1111/j.1745-7262.2008.00364.x www.asiaandro.com. Clinical Experience. Combination therapy for male erectile dysfunction and urinary incontinence Helen Zafirakis
sian J ndrol 2008; 10 (1): 149 154 DOI: 10.1111/j.1745-7262.2008.00364.x www.asiaandro.com. Clinical Experience. Combination therapy for male erectile dysfunction and urinary incontinence Helen Zafirakis
Surgery Illustrated Surgical Atlas Millin Retropubic Prostatectomy
 BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Millin Retropubic Prostatectomy John M. Fitzpatrick Mater Misericordiae University Hospital Dublin & University College Dublin, Ireland Accepted
BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Millin Retropubic Prostatectomy John M. Fitzpatrick Mater Misericordiae University Hospital Dublin & University College Dublin, Ireland Accepted
THE ARTIFICIAL URINARY SPHINCTER:
 THE ARTIFICIAL URINARY SPHINCTER: A TREATMENT FOR POST- PROSTATECTOMY URINARY INCONTINENCE Andrew L. Siegel, M.D. Board-Certified Urologist and Urological Surgeon Director: Center for Continence Care An
THE ARTIFICIAL URINARY SPHINCTER: A TREATMENT FOR POST- PROSTATECTOMY URINARY INCONTINENCE Andrew L. Siegel, M.D. Board-Certified Urologist and Urological Surgeon Director: Center for Continence Care An
Loss of Bladder Control
 BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
Management of Post-Prostatectomy Urinary Incontinence and Sexual Dysfunction
 Management of Post-Prostatectomy Urinary Incontinence and Sexual Dysfunction Robert C. Eyre, MD, FACS Associate Clinical Professor of Surgery (Urology) Harvard Medical School Post-prostatectomy Incontinence
Management of Post-Prostatectomy Urinary Incontinence and Sexual Dysfunction Robert C. Eyre, MD, FACS Associate Clinical Professor of Surgery (Urology) Harvard Medical School Post-prostatectomy Incontinence
I-STOP TOMS Transobturator Male Sling
 I-STOP TOMS Transobturator Male Sling The CL Medical I-STOP TOMS sling for male stress urinary incontinence was developed in France where it is widely used and is the market leader. It is constructed with
I-STOP TOMS Transobturator Male Sling The CL Medical I-STOP TOMS sling for male stress urinary incontinence was developed in France where it is widely used and is the market leader. It is constructed with
PROBLEMS AND VARIATIONS THREE-COMPONENT INFLATABLE PENILE PROSTHESIS IN THE PLACEMENT OF THE. Troubleshooting for the Malfunctioning Prosthesis
 PROBLEMS AND VARIATIONS IN THE PLACEMENT OF THE 24 THREE-COMPONENT INFLATABLE PENILE PROSTHESIS Troubleshooting for the Malfunctioning Prosthesis Although there are ongoing changes in the design of penile
PROBLEMS AND VARIATIONS IN THE PLACEMENT OF THE 24 THREE-COMPONENT INFLATABLE PENILE PROSTHESIS Troubleshooting for the Malfunctioning Prosthesis Although there are ongoing changes in the design of penile
AMS 800. Operating Room Manual. Urinary Control System For Male, Female, and Pediatric Patients. English
 AMS 800 Urinary Control System For Male, Female, and Pediatric Patients Operating Room Manual English Table of Contents Contents Disclosures Indications For Use... 1 Contraindications... 1 Warnings...
AMS 800 Urinary Control System For Male, Female, and Pediatric Patients Operating Room Manual English Table of Contents Contents Disclosures Indications For Use... 1 Contraindications... 1 Warnings...
AMS Ambicor. Penile Prosthesis. Operating Room Manual. English
 AMS Ambicor Penile Prosthesis Operating Room Manual English This page intentionally left blank. Table of Contents General Information Detailed Device Description... 4 Device Characteristics... 4 Two-piece
AMS Ambicor Penile Prosthesis Operating Room Manual English This page intentionally left blank. Table of Contents General Information Detailed Device Description... 4 Device Characteristics... 4 Two-piece
Loss of Bladder Control
 BLADDER HEALTH Loss of Bladder Control SURGERY TO TREAT URINARY INCONTINENCE AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is Urinary Incontinence? Urinary incontinence
BLADDER HEALTH Loss of Bladder Control SURGERY TO TREAT URINARY INCONTINENCE AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is Urinary Incontinence? Urinary incontinence
Deirdre M. Bochove-Overgaauw* and Bart Ph. Schrier
 An Adjustable Sling for the Treatment of All Degrees of Male Stress Urinary Incontinence: Retrospective Evaluation of Efficacy and Complications After a Minimal Followup of 14 Months Deirdre M. Bochove-Overgaauw*
An Adjustable Sling for the Treatment of All Degrees of Male Stress Urinary Incontinence: Retrospective Evaluation of Efficacy and Complications After a Minimal Followup of 14 Months Deirdre M. Bochove-Overgaauw*
Transcorporal artificial urinary sphincter in radiated and non - radiated compromised urethra. Assessment with a minimum 2 year follow-up
 ORIGINAL ARTICLE Vol. 42 (3): 494-500, May - June, 2016 doi: 10.1590/S1677-5538.IBJU.2015.0329 Transcorporal artificial urinary sphincter in radiated and non - radiated compromised urethra. Assessment
ORIGINAL ARTICLE Vol. 42 (3): 494-500, May - June, 2016 doi: 10.1590/S1677-5538.IBJU.2015.0329 Transcorporal artificial urinary sphincter in radiated and non - radiated compromised urethra. Assessment
SURGERY FOR PEYRONIE S DISEASE. PEYRONIE S DISEASE WITHOUT IMPOTENCE Exposure and Mobilization of Dorsal Nerves and Vessels
 SURGERY FOR 25 PEYRONIE S DISEASE PEYRONIE S DISEASE WITHOUT Exposure and Mobilization of Dorsal Nerves and Vessels FIG. 25-1. Most surgeons use a degloving procedure via a circumferential skin incision
SURGERY FOR 25 PEYRONIE S DISEASE PEYRONIE S DISEASE WITHOUT Exposure and Mobilization of Dorsal Nerves and Vessels FIG. 25-1. Most surgeons use a degloving procedure via a circumferential skin incision
AMS 800. Urinary Control System. User s Guide. Table of Contents. The AMS 800 Urinary Control System...1. Using the AMS 800 Urinary Control System...
 AMS 800 Urinary Control System User s Guide Table of Contents The AMS 800 Urinary Control System...1 Using the AMS 800 Urinary Control System...2 Special precautions to take with your 800 before undergoing
AMS 800 Urinary Control System User s Guide Table of Contents The AMS 800 Urinary Control System...1 Using the AMS 800 Urinary Control System...2 Special precautions to take with your 800 before undergoing
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
AdVance Male Sling System
 AdVance Male Sling System Clinical study summary This document is a compilation and summary of several AdVance Male Sling System peer-reviewed journal articles. The information presented here is taken
AdVance Male Sling System Clinical study summary This document is a compilation and summary of several AdVance Male Sling System peer-reviewed journal articles. The information presented here is taken
Glossary of terms Urinary Incontinence
 Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
THE UROLOGY GROUP
 THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
Jennifer Locke UBC Department of Urologic Sciences Resident Year 3 October 12, Learning Objectives
 Artificial Urinary Sphincter after 40 Years of Use: Indications, Techniques and Outcomes Jennifer Locke UBC Department of Urologic Sciences Resident Year 3 October 12, 2016 Learning Objectives 1. Identify
Artificial Urinary Sphincter after 40 Years of Use: Indications, Techniques and Outcomes Jennifer Locke UBC Department of Urologic Sciences Resident Year 3 October 12, 2016 Learning Objectives 1. Identify
Blue Ridge Urogynecology
 Surgery for Stress Urinary Incontinence Surgery has proved to be a very effective treatment for stress incontinence. The best surgical procedures improve or cure the incontinence in 85 to 90 percent of
Surgery for Stress Urinary Incontinence Surgery has proved to be a very effective treatment for stress incontinence. The best surgical procedures improve or cure the incontinence in 85 to 90 percent of
Pelvic Injuries. Chapter 21
 Chapter 21 Introduction Injuries of the pelvis are an uncommon, but potentially lethal, battlefield injury. Blunt injuries may be associated with major hemorrhage and early mortality. Death within the
Chapter 21 Introduction Injuries of the pelvis are an uncommon, but potentially lethal, battlefield injury. Blunt injuries may be associated with major hemorrhage and early mortality. Death within the
University of Alberta Reconstructive Urology Fellowship
 FACULTY OF MEDICINE AND DENTISTRY DEPARTMENT OF SURGERY DIVISION OF UROLOGY Keith Rourke, MD, FRCSC Reconstructive Urology Professor Chair of Academic Urology Reconstructive Urology Fellowship Director
FACULTY OF MEDICINE AND DENTISTRY DEPARTMENT OF SURGERY DIVISION OF UROLOGY Keith Rourke, MD, FRCSC Reconstructive Urology Professor Chair of Academic Urology Reconstructive Urology Fellowship Director
Medical Review Criteria Invasive Treatment for Urinary Incontinence
 Medical Review Criteria Invasive Treatment for Urinary Incontinence Effective Date: December 21, 2016 Subject: Invasive Treatment for Urinary Incontinence Background: Urinary incontinence (the involuntary
Medical Review Criteria Invasive Treatment for Urinary Incontinence Effective Date: December 21, 2016 Subject: Invasive Treatment for Urinary Incontinence Background: Urinary incontinence (the involuntary
Canadian Undergraduate Urology Curriculum (CanUUC): Genitourinary Trauma. Last reviewed June 2014
 Canadian Undergraduate Urology Curriculum (CanUUC): Genitourinary Trauma Last reviewed June 2014 Session Objectives 1. Recognize hematuria as the cardinal symptom of urinary tract trauma. 1. Outline the
Canadian Undergraduate Urology Curriculum (CanUUC): Genitourinary Trauma Last reviewed June 2014 Session Objectives 1. Recognize hematuria as the cardinal symptom of urinary tract trauma. 1. Outline the
The impact of androgen deprivation on artificial urinary sphincter outcomes
 Original Article The impact of androgen deprivation on artificial urinary sphincter outcomes George C. Bailey 1, Brian J. Linder 1, Marcelino E. Rivera 1, Matthew J. Ziegelmann 1, Laureano J. Rangel 2,
Original Article The impact of androgen deprivation on artificial urinary sphincter outcomes George C. Bailey 1, Brian J. Linder 1, Marcelino E. Rivera 1, Matthew J. Ziegelmann 1, Laureano J. Rangel 2,
Desara TV and Desara Blue TV
 Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 9 Urinary Tract and Perineum Key Points 2 9.1 Urinary Bladder & Urinary Retention Acute retention of urine is an indication for emergency drainage of the bladder
Surgical Care at the District Hospital 1 9 Urinary Tract and Perineum Key Points 2 9.1 Urinary Bladder & Urinary Retention Acute retention of urine is an indication for emergency drainage of the bladder
SURGICAL PROCEDURE DESCRIPTIONS
 SURGICAL PROCEDURE DESCRIPTIONS GONADECTOMY: CASTRATION USING SCROTAL METHOD 1. The animal is anesthetized and placed in dorsal recumbency with the tail toward the surgeon. 2. The abdominal and scrotal
SURGICAL PROCEDURE DESCRIPTIONS GONADECTOMY: CASTRATION USING SCROTAL METHOD 1. The animal is anesthetized and placed in dorsal recumbency with the tail toward the surgeon. 2. The abdominal and scrotal
AMS 800 Urinary Control System ACTIVATING:
 AMS 800 Urinary Control System 1 ACTIVATING: Begin by stabilizing the control pump in the proper place by grasping the tubing above the control pump. Use your other hand to firmly squeeze the sides of
AMS 800 Urinary Control System 1 ACTIVATING: Begin by stabilizing the control pump in the proper place by grasping the tubing above the control pump. Use your other hand to firmly squeeze the sides of
Repair of Bulbar Urethra Using the Barbagli Technique
 22 Repair of Bulbar Urethra Using the Barbagli Technique G. Barbagli, M. Lazzeri 22.1 Introduction and Historical Background 182 22.2 Anatomical Remarks 182 22.3 Step-by-Step Surgical Details 183 22.3.1
22 Repair of Bulbar Urethra Using the Barbagli Technique G. Barbagli, M. Lazzeri 22.1 Introduction and Historical Background 182 22.2 Anatomical Remarks 182 22.3 Step-by-Step Surgical Details 183 22.3.1
Male urinary incontinence: Artificial sphincter
 GUIDELINES IN FOCUS Truzzi JC et al. Male urinary incontinence: Artificial sphincter Incontinência urinária masculina: Esfíncter artificial Authorship: Brazilian Society of Urology (SBU) Participants:
GUIDELINES IN FOCUS Truzzi JC et al. Male urinary incontinence: Artificial sphincter Incontinência urinária masculina: Esfíncter artificial Authorship: Brazilian Society of Urology (SBU) Participants:
Surgical Atlas Orthotopic ileal neobladder
 Surgery Illustrated ORTHOTOPIC ILEAL NEOBLADDER U.E. STUDER ET AL. Surgical Atlas Orthotopic ileal neobladder U.E. STUDER, C. VAROL and H. DANUSER University of Bern, Department of Urology, Bern, Switzerland
Surgery Illustrated ORTHOTOPIC ILEAL NEOBLADDER U.E. STUDER ET AL. Surgical Atlas Orthotopic ileal neobladder U.E. STUDER, C. VAROL and H. DANUSER University of Bern, Department of Urology, Bern, Switzerland
Surgical Atlas Anastomotic urethroplasty
 Surg Ill Article SURGERY ILLUSTRATED MUNDY Surgical Atlas Anastomotic urethroplasty ANTHONY R. MUNDY The Institute of Urology, London, UK ILLUSTRATIONS by STEPHAN SPITZER, www.spitzer-illustration.com
Surg Ill Article SURGERY ILLUSTRATED MUNDY Surgical Atlas Anastomotic urethroplasty ANTHONY R. MUNDY The Institute of Urology, London, UK ILLUSTRATIONS by STEPHAN SPITZER, www.spitzer-illustration.com
Surgical Atlas The posterior lumbotomy
 Original Article SURGERY ILLUSTRATED PANSADORO Surgical Atlas The posterior lumbotomy VITO PANSADORO Urology, Vincenzo Pansadoro Foundation, Rome, Italy ILLUSTRATIONS by STEPHAN SPITZER, www.spitzer-illustration.com
Original Article SURGERY ILLUSTRATED PANSADORO Surgical Atlas The posterior lumbotomy VITO PANSADORO Urology, Vincenzo Pansadoro Foundation, Rome, Italy ILLUSTRATIONS by STEPHAN SPITZER, www.spitzer-illustration.com
You have been booked for a. Flexible Cystoscopy. Under Local Anaesthetic
 You have been booked for a Flexible Cystoscopy Under Local Anaesthetic 1 WHAT IS A FLEXIBLE CYSTOSCOPY A flexible cystoscopy is a test to examine the uretha (waterpipe) and bladder using a thin, lighted
You have been booked for a Flexible Cystoscopy Under Local Anaesthetic 1 WHAT IS A FLEXIBLE CYSTOSCOPY A flexible cystoscopy is a test to examine the uretha (waterpipe) and bladder using a thin, lighted
Long-term results of the implantation of the AMS 800 artificial sphincter for post-prostatectomy incontinence: a single-center experience
 ORIGINAL ARTICLE Vol. 44 (1): 114-120, January - February, 2018 doi: 10.1590/S1677-5538.IBJU.2017.0165 Long-term results of the implantation of the AMS 800 artificial sphincter for post-prostatectomy incontinence:
ORIGINAL ARTICLE Vol. 44 (1): 114-120, January - February, 2018 doi: 10.1590/S1677-5538.IBJU.2017.0165 Long-term results of the implantation of the AMS 800 artificial sphincter for post-prostatectomy incontinence:
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA. A Minimally Invasive Innovative Treatment
 PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
What CPT and ICD-10-CM codes are reported?
 A patient is seen in the hospital s outpatient surgical area with a diagnosis of a displaced comminuted fracture of the lateral condyle, right elbow. An ORIF (open reduction) procedure was performed and
A patient is seen in the hospital s outpatient surgical area with a diagnosis of a displaced comminuted fracture of the lateral condyle, right elbow. An ORIF (open reduction) procedure was performed and
University of Alberta Reconstructive Urology Fellowship
 University of Alberta Reconstructive Urology Fellowship 1. Overview 2. Eligibility Requirements 3. Funding 4. Clinical Expectations 5. Academic Expectations 6. Objectives of Training 7. Teaching Methods
University of Alberta Reconstructive Urology Fellowship 1. Overview 2. Eligibility Requirements 3. Funding 4. Clinical Expectations 5. Academic Expectations 6. Objectives of Training 7. Teaching Methods
Instruction For Use for All Silicon Foley Catheter
 General Description: All Silicone Foley Catheter for single use is a thin, is a flexible tube passed through the urethra and into the bladder to drain urine. It is the most common type of indwelling urinary
General Description: All Silicone Foley Catheter for single use is a thin, is a flexible tube passed through the urethra and into the bladder to drain urine. It is the most common type of indwelling urinary
Urogynecology ICD-9 to ICD-10 Crosswalks
 1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
Introduction/Learning Objectives. Incontinence: Natural History. Course Outline 10/14/2016. Urinary Incontinence: Conservative Measures
 Management of Urinary Complications after Prostatectomy Course Faculty: Introduction/Learning Objectives Jaspreet S. Sandhu, MD Associate Attending Urologist Department of Surgery/Urology Memorial Sloan
Management of Urinary Complications after Prostatectomy Course Faculty: Introduction/Learning Objectives Jaspreet S. Sandhu, MD Associate Attending Urologist Department of Surgery/Urology Memorial Sloan
Management of Artificial Urinary Sphincter Dysfunction
 European Urology European Urology 46 (2004) 241 246 Management of Artificial Urinary Sphincter Dysfunction Frédéric Maillet, Jean-Marie Buzelin, Olivier Bouchot, Georges Karam * Clinique Urologique, CHU
European Urology European Urology 46 (2004) 241 246 Management of Artificial Urinary Sphincter Dysfunction Frédéric Maillet, Jean-Marie Buzelin, Olivier Bouchot, Georges Karam * Clinique Urologique, CHU
INSERTION OF AN ARTIFICIAL URINARY SPHINCTER IN MEN
 INSERTION OF AN ARTIFICIAL URINARY SPHINCTER IN MEN Procedure Specific Information What is the evidence base for this information? This publication includes advice from consensus panels, the British Association
INSERTION OF AN ARTIFICIAL URINARY SPHINCTER IN MEN Procedure Specific Information What is the evidence base for this information? This publication includes advice from consensus panels, the British Association
A.M.I. ATOMS System. Hydraulic system substitutes urinary sphincter function in incontinent males
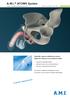 A.M.I. ATOMS System Product Group Urology Issue 11/2016 ATOMS = Adjustable TransObturator Male System Hydraulic system substitutes urinary sphincter function in incontinent males Long-term, adjustable
A.M.I. ATOMS System Product Group Urology Issue 11/2016 ATOMS = Adjustable TransObturator Male System Hydraulic system substitutes urinary sphincter function in incontinent males Long-term, adjustable
AMS 800 Urinary Control System
 AMS 800 Urinary Control System 1 DAILY USE: While the cuff is closed, urine stays inside the bladder. To urinate, open the cuff as follows: Feel for the control pump in your scrotum. Stabilize the control
AMS 800 Urinary Control System 1 DAILY USE: While the cuff is closed, urine stays inside the bladder. To urinate, open the cuff as follows: Feel for the control pump in your scrotum. Stabilize the control
The Surgical Learning Curve for Artificial Urinary Sphincter Procedures Compared to Typical Surgeon Experience
 EUROPEAN UROLOGY 60 (2011) 1285 1290 available at www.sciencedirect.com journal homepage: www.europeanurology.com Reconstructive Urology The Surgical Learning Curve for Artificial Urinary Sphincter Procedures
EUROPEAN UROLOGY 60 (2011) 1285 1290 available at www.sciencedirect.com journal homepage: www.europeanurology.com Reconstructive Urology The Surgical Learning Curve for Artificial Urinary Sphincter Procedures
LESSON ASSIGNMENT. Urinary System Diseases/Disorders. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 4 Urinary System Diseases/Disorders LESSON ASSIGNMENT Paragraphs 4-1 through 4-8. LESSON OBJECTIVES After completing this lesson, you should be able to: 4-1. Identify the purposes
LESSON ASSIGNMENT LESSON 4 Urinary System Diseases/Disorders LESSON ASSIGNMENT Paragraphs 4-1 through 4-8. LESSON OBJECTIVES After completing this lesson, you should be able to: 4-1. Identify the purposes
DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis.
 DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
THE BULKING AGENT WITH LONG-LASTING EFFECT!
 THE BULKING AGENT WITH LONG-LASTING EFFECT! Urogyn BV Transistorweg 5a 6534 AT Nijmegen The Netherlands t +31(0) 24 711 41 30 info@urogynbv.com www.urogynbv.com THE FIRST INJECTABLE IMPLANT THAT CAN COMPETE
THE BULKING AGENT WITH LONG-LASTING EFFECT! Urogyn BV Transistorweg 5a 6534 AT Nijmegen The Netherlands t +31(0) 24 711 41 30 info@urogynbv.com www.urogynbv.com THE FIRST INJECTABLE IMPLANT THAT CAN COMPETE
Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우
 Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우 Introduction Radical prostatectomy - treatment of choice for patients with localized prostate cancer. Urinary incontinence and/or
Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우 Introduction Radical prostatectomy - treatment of choice for patients with localized prostate cancer. Urinary incontinence and/or
Prevention of Surgical Injuries in Gynecology
 in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
SURGICAL MANAGEMENT OF POST-PROSTATECTOMY INCONTINENCE
 SURGICAL MANAGEMENT OF POST-PROSTATECTOMY INCONTINENCE Arthi Satyanarayan, Ryan Mooney, *Nirmish Singla Department of Urology, University of Texas Southwestern Medical Center, Dallas, Texas, USA *Correspondence
SURGICAL MANAGEMENT OF POST-PROSTATECTOMY INCONTINENCE Arthi Satyanarayan, Ryan Mooney, *Nirmish Singla Department of Urology, University of Texas Southwestern Medical Center, Dallas, Texas, USA *Correspondence
Desara and Desara Blue
 Desara and Desara Blue Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc.
Desara and Desara Blue Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc.
BULKAMID STANDARD OPERATING PROCEDURE
 BULKAMID STANDARD OPERATING PROCEDURE Contents 1 1 2 3-4 5-6 5-6 7 9-12 9 10 11 12 13 13 13 15 16 Products Bulkamid multiple use instruments Bulkamid single use instruments The Bulkamid system Pre-procedure
BULKAMID STANDARD OPERATING PROCEDURE Contents 1 1 2 3-4 5-6 5-6 7 9-12 9 10 11 12 13 13 13 15 16 Products Bulkamid multiple use instruments Bulkamid single use instruments The Bulkamid system Pre-procedure
A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience
 Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Management of LUTS after TURP and MIT
 Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Conclusions. Keywords
 Functional Urology Outcomes of single- vs double-cuff artificial urinary sphincter insertion in low- and high-risk profile male patients with severe stress urinary incontinence Sascha A. Ahyai*, Tim A.
Functional Urology Outcomes of single- vs double-cuff artificial urinary sphincter insertion in low- and high-risk profile male patients with severe stress urinary incontinence Sascha A. Ahyai*, Tim A.
Procedure Specific Information Sheet Open Radical Prostatectomy
 Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Center for Reconstructive Urethral Surgery Guido Barbagli Center for Reconstructive Urethral Surgery Arezzo - Italy
 Guido Barbagli Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it 23 rd ANNUAL EAU CONGRESS Sub-plenary Session on Male urinary incontinence 26 29 March 2008 Milan Italy Incontinence following
Guido Barbagli Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it 23 rd ANNUAL EAU CONGRESS Sub-plenary Session on Male urinary incontinence 26 29 March 2008 Milan Italy Incontinence following
Desara Blue OV D I. Sling for Female Stress Urinary Incontinence. Instructions For Use
 Desara Blue OV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc. 5171 Clareton
Desara Blue OV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc. 5171 Clareton
Female Epispadias Repair
 hoofdstuk 07 08-03-2001 15:25 Pagina 89 Female Epispadias Repair Female epispadias repair: a new 1-stage technique CHAPTER 7 Tom P.V.M de Jong, Pieter Dik and Aart J. Klijn Journal of Urology 2000, 164,
hoofdstuk 07 08-03-2001 15:25 Pagina 89 Female Epispadias Repair Female epispadias repair: a new 1-stage technique CHAPTER 7 Tom P.V.M de Jong, Pieter Dik and Aart J. Klijn Journal of Urology 2000, 164,
Allium Round Posterior Urethral Stent System (RPS) Instructions For Use
 Allium Round Posterior Urethral Stent System (RPS) Instructions For Use Manufactured by Allium Ltd. 2 Ha-Eshel St. Caesarea Industrial Park 38900 Israel Device Name: Allium Round Posterior Urethral Stent
Allium Round Posterior Urethral Stent System (RPS) Instructions For Use Manufactured by Allium Ltd. 2 Ha-Eshel St. Caesarea Industrial Park 38900 Israel Device Name: Allium Round Posterior Urethral Stent
Guido Barbagli. Center for Reconstructive ti Urethral lsurgery
 Guido Barbagli Center for Reconstructive ti Urethral lsurgery Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it Dedicated to Ruggero Lenzi, teacher and friend. His passing was a great
Guido Barbagli Center for Reconstructive ti Urethral lsurgery Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it Dedicated to Ruggero Lenzi, teacher and friend. His passing was a great
Center for Reconstructive Urology
 Center for Reconstructive Urology Urethral Reconstruction Post-Operative Instructions Following urethral reconstruction, your attention to proper post-operative follow-up will contribute to the success
Center for Reconstructive Urology Urethral Reconstruction Post-Operative Instructions Following urethral reconstruction, your attention to proper post-operative follow-up will contribute to the success
PERINEAL PROSTATECTOMY
 Abstract PERINEAL PROSTATECTOMY Pages with reference to book, From 204 To 206 Altaf Hussain Rathore ( Dept. of Surgery, Punjab Medical College, Faisalabad. ) A series of twenty-five medically high risk
Abstract PERINEAL PROSTATECTOMY Pages with reference to book, From 204 To 206 Altaf Hussain Rathore ( Dept. of Surgery, Punjab Medical College, Faisalabad. ) A series of twenty-five medically high risk
Urethrolysis; When, Why & How. M Karram Professor of Ob/Gyn & Urology University of Cincinnati
 Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
3. Urinary Catheters. Indications. Methods of Bladder Catheterization. Hashim Hashim
 3. Urinary Catheters Hashim Hashim Indications Urinary catheters are used to drain urine from the bladder. The main indications are: A. Diagnostic Measure post-void residual in the absence of ultrasound
3. Urinary Catheters Hashim Hashim Indications Urinary catheters are used to drain urine from the bladder. The main indications are: A. Diagnostic Measure post-void residual in the absence of ultrasound
A. Simonato, 1 M. Ennas, 1 A. Benelli, 1 A. Gregori, 2 F. Oneto, 1 E. Daglio, 1 P. Traverso, 1 and G. Carmignani 1. 1.
 Hindawi Publishing Corporation Advances in Urology Volume 2012, Article ID 481943, 6 pages doi:10.1155/2012/481943 Clinical Study Comparison between Two Different Two-Stage Transperineal Approaches to
Hindawi Publishing Corporation Advances in Urology Volume 2012, Article ID 481943, 6 pages doi:10.1155/2012/481943 Clinical Study Comparison between Two Different Two-Stage Transperineal Approaches to
Carpal Tunnel Release
 Carpal Tunnel Release Carpal tunnel syndrome is a condition in the hand and wrist caused by excessive pressure on the median nerve in the wrist. Compression of the nerve typically causes numbness and tingling
Carpal Tunnel Release Carpal tunnel syndrome is a condition in the hand and wrist caused by excessive pressure on the median nerve in the wrist. Compression of the nerve typically causes numbness and tingling
the liver and kidney function (both vital when dealing with anaesthetic drugs) and to rule out any unsuspected illnesses.
 Orchiectomy: Castration reduces overpopulation by inhibiting male fertility and decreases male aggressiveness, roaming, and undesirable urination behaviour. It helps prevent androgenrelated diseases, including
Orchiectomy: Castration reduces overpopulation by inhibiting male fertility and decreases male aggressiveness, roaming, and undesirable urination behaviour. It helps prevent androgenrelated diseases, including
Information for men considering a male sling procedure UHB is a no smoking Trust
 Information for men considering a male sling procedure UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Introduction
Information for men considering a male sling procedure UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Introduction
Dr. Syah Mirsya Warli, SpU Dr. Bungaran Sihombing,SpU Div. of Urology, Surgery Dept. Medical Faculty, University of Sumatera Utara
 Emergency Room Urology Dr. Syah Mirsya Warli, SpU Dr. Bungaran Sihombing,SpU Div. of Urology, Surgery Dept. Medical Faculty, University of Sumatera Utara Ref : Clinical Manual of Urology, (Philip M. Hanno
Emergency Room Urology Dr. Syah Mirsya Warli, SpU Dr. Bungaran Sihombing,SpU Div. of Urology, Surgery Dept. Medical Faculty, University of Sumatera Utara Ref : Clinical Manual of Urology, (Philip M. Hanno
SOP: Urinary Catheter in Dogs and Cats
 SOP: Urinary Catheter in Dogs and Cats These SOPs were developed by the Office of the University Veterinarian and reviewed by Virginia Tech IACUC to provide a reference and guidance to investigators during
SOP: Urinary Catheter in Dogs and Cats These SOPs were developed by the Office of the University Veterinarian and reviewed by Virginia Tech IACUC to provide a reference and guidance to investigators during
Bladder exstrophy and epispadias
 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Bladder exstrophy and epispadias This leaflet explains about bladder exstrophy and epispadias and what to expect
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Bladder exstrophy and epispadias This leaflet explains about bladder exstrophy and epispadias and what to expect
European Urology 47 (2005)
 European Urology European Urology 47 (2005) 209 213 The Comparison of Artificial Urinary Sphincter Implantation and Endourethral Macroplastique Injection for thetreatment of Postprostatectomy Incontinence
European Urology European Urology 47 (2005) 209 213 The Comparison of Artificial Urinary Sphincter Implantation and Endourethral Macroplastique Injection for thetreatment of Postprostatectomy Incontinence
TRANSURETHRAL RESECTION
 TRANSURETHRAL RESECTION OF THE PROSTATE GLAND 21 Prostatic sonographic studies of patients who have undergone a transurethral resection of the prostate gland reveal large volumes of residual prostate tissue
TRANSURETHRAL RESECTION OF THE PROSTATE GLAND 21 Prostatic sonographic studies of patients who have undergone a transurethral resection of the prostate gland reveal large volumes of residual prostate tissue
Before and After Your Surgery
 UW MEDICINE PATIENT EDUCATION Before and After Your Surgery Artificial urinary sphincter or male urethral sling surgery This handout explains how to prepare for and what to expect after artificial urinary
UW MEDICINE PATIENT EDUCATION Before and After Your Surgery Artificial urinary sphincter or male urethral sling surgery This handout explains how to prepare for and what to expect after artificial urinary
Pelvic Floor Muscle Exercises and Advice for Men
 Pelvic Floor Muscle Exercises and Advice for Men (formerly ACPWH) Useful resources Websites Pelvic Obstetric & Gynaecological Physiotherapy - pogp.csp.org.uk Bladder and Bowel Foundation - www.bladderandbowelfoundation.org
Pelvic Floor Muscle Exercises and Advice for Men (formerly ACPWH) Useful resources Websites Pelvic Obstetric & Gynaecological Physiotherapy - pogp.csp.org.uk Bladder and Bowel Foundation - www.bladderandbowelfoundation.org
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007 Hosted by: Australian Small Animal Veterinary Association (ASAVA) Australian Small Animal Veterinary Association (ASAVA)
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007 Hosted by: Australian Small Animal Veterinary Association (ASAVA) Australian Small Animal Veterinary Association (ASAVA)
A over-the-counter medical device that utilizes muscle stimulation for the treatment of stress, urge and mixed urinary incontinence.
 A over-the-counter medical device that utilizes muscle stimulation for the treatment of stress, urge and mixed urinary incontinence. An over-the-counter medical device that utilizes muscle stimulation
A over-the-counter medical device that utilizes muscle stimulation for the treatment of stress, urge and mixed urinary incontinence. An over-the-counter medical device that utilizes muscle stimulation
CAREFULLY READ ALL INSTRUCTIONS PRIOR TO USE
 CAREFULLY READ ALL INSTRUCTIONS PRIOR TO USE INDICATIONS FOR USE The LATERA Absorbable Nasal Implant is indicated for supporting upper and lower lateral nasal cartilage. CAUTION: Federal law restricts
CAREFULLY READ ALL INSTRUCTIONS PRIOR TO USE INDICATIONS FOR USE The LATERA Absorbable Nasal Implant is indicated for supporting upper and lower lateral nasal cartilage. CAUTION: Federal law restricts
Procedure: Chest Tube Placement (Tube Thoracostomy)
 Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
