Current Indications for the Use of The Artificial Genitourinary Sphincter and Management of It s Complications
|
|
|
- Gyles Martin
- 5 years ago
- Views:
Transcription
1 Article TheScientificWorldJOURNAL (2004) 4 (S1), ISSN X; DOI /tsw Current Indications for the Use of The Artificial Genitourinary Sphincter and Management of It s Complications Daniel S. Elliott, M.D. and David M. Barrett, M.D. Mayo Clinic, Department of Urology, Rochester, MN s: Elliott.Daniel@mayo.edu Previously published in the Digital Urology Journal DOMAIN: urology, aging, medical care (men s health), surgery INTRODUCTION The first artificial urinary sphincter was implanted in 1972 and since then many advances in product design, improvements of surgical techniques, and proper patient selection have resulted in decreasing complication rates and improved patient satisfaction. 1 The currently used artificial sphincter (AUS) is the American Medical Systems (AMS) 800. This prosthesis consists of silicone components: (1) an elastic pressure-balloon reservoir; (2) a control pump; and (3) an inflatable occlusive urethral cuff. The balloon reservoir is manufactured to hold a volume of fluid which exerts a range of preset pressures (51-60, 61-70, 71-80, and 81-90cm water) that can be selected from based on the site of cuff placement and the clinical situation. The pump contains a unidirectional valve, a refill-delay resistor and a deactivation button. This assembly allows for complete control of cuff activation/deactivation by the patient and physician. In the activated mode, the urethral cuff is de-pressurized by squeezing the pump, thereby, forcing fluid from the cuff through the unidirectional valve into the balloon reservoir (Fig. 1). Following a delay period of three to five minutes, time allowed for voiding, fluid automatically flows back to repressurize the cuff. The AMS-800 can be non-surgically deactivated by pressing the deactivation button on the pump which prevents fluid in the balloon from returning to the cuff. Deactivation allows for healing to take place without compression on the urethra. Deactivation also facilitates catheterization, cystoscopy and transurethral resection, if necessary. Activation is accomplished by a sustained squeeze of the pump. INDICATIONS FOR AUS IMPLANTATION AND PATIENT SELECTION The candidate for AUS implantation is the patient with urinary incontinence due to sphincteric insufficiency, with normal detrusor function and bladder compliance. Recognizing that urinary incontinence may be the result of coexisting sphincteric incompetence and bladder compliance and contractility abnormalities, AUS implantation can be considered in these patients assuming that these coexisting abnormalities can be adequately managed. 114
2 FIGURE 1. Components and cycling of the AS-800 AUS; pressure on the pump transfers fluid out of the cuff to the reservoir, the cuff then refills passively. Patients with sphincteric incontinence from a variety of causes are appropriate candidates for AUS implantation. In our experience the most common etiologies for incontinence requiring AUS are following radical retropubic prostatectomy and transurethral resection of the prostate. 2 A minimum of six months is recommended between the time of prostatectomy and AUS implantation to allow time for continence to return. Sphincteric insufficiency may also develop following injury or radiation to the pelvis and spinal cord. Congenital disorders such as myelomeningocele can result in loss of sphincteric function. The bladder neck is the site of cuff placement in these patients. All women and children who are candidates for AUS implantation have cuffs placed on the bladder neck. The bladder neck is the optimal location for AUS implantation because of the thick muscular tissue and good blood supply in this area. However, following prostatectomy, the bladder neck tissue becomes scarred and fixed to the surrounding tissues, and, therefore, the bulbous urethra is the preferred site for cuff placement in this group of patients. PREOPERATIVE CONSIDERATIONS Preoperative evaluation should include urine analysis and culture to assure that the urine is sterile prior to AUS implantation. Upper tract abnormalities should be evaluated with excretory urogram and/or voiding cystourethrogram if warranted by the patients history. Repair of grade two, or greater, reflux should be repaired at or before the time of AUS implantation. Bladder augmentation may be required in patients with noncompliant, low capacity bladders to make them suitable candidates for AUS implantation. Urodynamic studies are recommended in specific patient situations, however it is not mandatory. If there are concerns about bladder dysfunction then either urodynamics, or preferably a videoeurodynamics is required. OPERATIVE TECHNIQUE 115
3 Patients are usually admitted the morning of surgery. Patients having bladder neck cuff placement are instructed to undergo a Fleets enema in the evening prior to surgery. At the time of surgery, infection precautions cannot be overemphasized. On the morning of surgery, females should have a standard vaginal douche preparation. Broad-spectrum intravenous antibiotics, most commonly vancomycin and gentamicin, are administered in the preoperative holding area. Antibiotic prophylaxis must include coverage for Staphylococcus epidermidis and Escherichia coli, as these organism are responsible up to 80% of genitourinary prosthetic infections. 3 In the operating room strict adherence to sterile techniques are essential to minimize potential infections. A complete ten-minute surgical scrub (abdomen, external genitalia and perineum with iodophors, is undertaken immediately following the surgical shaving. Draping should allow access to the lower abdomen and perineum. A 12-French Foley catheter is inserted in all males after preparation and draping. All operating room personnel should wear surgical hoods to limit contamination of the operative field, and traffic in and out of the operating room should be limited. 2 The prosthesis should be handled only when necessary and should be isolated away from tissue, blood, and sponge and towel fibers, which could cause malfunction of the device. FIGURE 2. The position of the bulbous urethral cuff, reservoir, and pump in the adult male. Bulbous Urethral Cuff in the Adult Male (Fig. 2) The patients are positioned in the dorsolithotomy position to expose the perineum. After hair removal, skin preparation and draping, a sterile 12-F Foley catheter is placed and the bladder is drained. A 4-5cm midline skin incision is made over the bulbous urethra (Fig. 3). Through the perineal incision, deeper tissues are divided and carried down until the bulbocavernosus muscle is identified. A plane is established between the bulbocavernosus muscle and the tunica albuginea of the corporal bodies circumferentially for a length of 1.5-2cm. At our institution, we preserve the bulbocavernosus muscle. Though the decision to place the cuff around the muscle is not shared by all, it is our feeling that the muscle will theoretically provide more bulk and potentially decrease the risk for atrophy and subsequent cuff erosion. This plane allows placement of the cuff around the muscular tissue, and not directly in contact with the urethral bulb, to reduce the risk of cuff erosion. Special care must be taken to avoid injury to the urethra at the 12 o'clock position where the dorsal urethra is attached to the intercorporal septum. If the urethral defect is large and/or the repair is questionable, the procedure should be abandoned 116
4 FIGURE 3. Site of perineal incision for placement of the bulbous urethral cuff. An incision 4-5 cm in length the median raphe along the scrotum. and a Foley catheter left in place. If the urethral injury is small, the defect can be closed with 4-0 or 5-0 absorbable suture and a different urethral segment is chosen for cuff placement. An unrecognized urethral injury can lead to early cuff erosion. Although cuffs of varying sizes are available, in our recent series 267 of 272 (98%) of our patients received a 4.5cm cuff around the bulbous urethra. 2 The cuff is passed tab-first behind the urethra (Fig. 4) in the direction that points toward the side of subsequent pump and reservoir placement, usually the side of hand dominance. Next, the cuff tubing is brought anteriorly and is passed through the opening in the tab, and the cuff is snapped into place using gentle opposing traction applied to the tab and tubing. The tubing now should be pointed toward the side where the reservoir will be inserted (Fig. 5). A rubber shod clamp closed to the first click is placed near the end of the tubing. FIGURE 4. Passing the cuff around the bulbous urethra. 117
5 FIGURE 5. Completion of cuff placement around the bulbous urethra and securing in place. FIGURE 6. Placement of balloon reservoir deep to the rectus muscle. Reservoir placement (Fig. 6) follows by making a 4-5cm transverse incision in the lower abdomen overlying the rectus sheath. The anterior rectus sheath is exposed and subsequently incised parallel to the fascia approximately 2cm. A pocket is bluntly created between the belly of the rectus muscle to allow for placement of the deflated balloon reservoir beneath the muscle in a preperitoneal location. The balloon reservoir is filled with 22cc and a shod clamp is placed near the end of the reservoir tubing, on the first click, to prevent fluid loss. It is our practice to fill the reservoir with iso-isomotic contrast medium. We feel this simplifies future diagnosis and management of patients who return in the future with recurrent urinary incontinence. 118
6 In most patients (82%) a 61-70cm water pressure balloon reservoir is used. 2 However, a lower pressure reservoir, usually a 51-60cm water pressure, is selected to minimize tissue ischemia in high risk patients such as those who have had radiation therapy or prior surgery. The fascial defect is closed with running absorbable suture after the inflated reservoir is properly positioned deep to the rectus muscle. On the ipsilateral side of the reservoir, a long clamp is passed over the pubis in the plane between Scarpa's fascia and the rectus fascia down to the perineal incision. The cuff tubing is gently grasped and guided up to the lower abdominal wound (Fig. 7). FIGURE 7. Positioning of cuff and reservoir tubing after placement of the balloon reservoir. To facilitate pump placement, an ipsilateral subcutaneous pouch is created superficial to Scarpa's fascia using Hegar dilators up to #15, just as is done during bladder neck cuff placement. The pouch extends down to the most dependent portion of the hemiscrotum. The pump is placed in the pouch with the deactivation button oriented laterally so that it is palpable against the skin. To prevent proximal migration of the pump during tubing connection, a Babcock clamp is loosely placed around the pump and scrotal skin. The appropriate tubing connections are now made. The cuff tubing is connected to the pump tubing with a right-angle connector to prevent kinking, and the reservoir tubing is connected to the pump tubing with a straight connector. Color-coded tubing has simplified this step. Tubing connections are either fastened with 2-0 prolene suture, or with the Quick-Connect set depending on the surgeon's preference. After the connections are completed, all clamps are removed from the tubing and the system is allowed to pressurize. Appropriate cycling of the device is demonstrated and then the sphincter is deactivated so that there is no urethral compression. Drains are not necessary nor recommended. The abdominal and perineal incisions are closed in layers with absorbable suture and then covered with sterile pressure(gentle) dressings. Bladder Neck Cuff in the Male Male patients undergoing bladder neck cuff placement are positioned supine with their legs abducted slightly. A rectal tube is placed to aid in the identification of the rectum during bladder neck dissection. A lower midline incision is made and carried down through the rectus and transversalis fascia. The peritoneum is not entered. The retropubic space is developed bluntly. A plane is developed superior to the 119
7 endopelvic fascia but distal to the posterior aspect of the bladder trigone where the ureters enter (Fig. 8,9). A plane is established between the bladder neck and proximal urethra anteriorly, and the rectum posteriorly. The width of this plane should be 2cm to accommodate the bladder neck cuff. An umbilical tape or Penrose drain is placed around the bladder neck. To identify injury to the bladder neck that may occurred during dissection, an antibiotic solution containing methylene blue is used to fill the bladder. Small tears can be closed with 3-0 or 4-0 absorbable suture. If a rectal injury is identified, the defect should be closed primarily and the sphincter implantation must be postponed. Using a calibrated measuring tape with the Foley catheter in place, the bladder neck is measured circumferentially (Fig. 10). In men the cuff size will range between 8-14cm. The Foley catheter should be removed if it is larger than 14-F. The cuff is passed posterior to the bladder neck towards the side of final pump and reservoir placement. The cuff is then snapped into place with the cuff tubing exiting laterally. The cuff tubing is then passed through the belly of the rectus muscle and the anterior rectus fascia approximately 4-5cm cephalad to the pubic symphysis on the side of future pump placement (Fig. 11). The end of the cuff tubing is clamped to the first click with a shodded clamp. FIGURE 8. Dissection around the bladder neck. FIGURE 9. Developing the plane superior to the endopelvic fascia but distal to the posterior aspect of the bladder trigone. 120
8 FIGURE 10. Location of components of the female AUS. FIGURE 11. Site of anterior vaginal wall incision for transvaginal AUS implantation. Balloon reservoir selection and placement follows cuff placement. The most commonly used balloon is the 61-70cm water pressure reservoir. The empty reservoir is placed in the prevesical space and the tubing is brought out through the rectus muscle and anterior fascia next to the cuff tubing (Fig. 11). Before the balloon is filled, the anterior abdominal fascia is closed in the midline with absorbable suture. The balloon is then filled with 22cc of iso-osmotic contrast medium, and the tubing is clamped at the first click with a shodded clamp. 121
9 Pump placement proceeds by creating a subcutaneous pocket in the lateral aspect of one hemiscrotum using Hegar dilators up to #15 (Fig. 11). The pump is placed in the dependent position of the scrotal pocket with the deactivation button positioned laterally for external access. Tubing connections between the pump and reservoir, and the pump and cuff are made using straight connectors tied with 2-0 prolene suture or fastened with a Quick-Connect set. The device is cycled (figure 12,13), then the cuff is deactivated. The surgical field is irrigated copiously with antibiotic solution, then the incision is closed in layers with absorbable suture. FIGURE 12. Dissection of vaginal wall off the bladder neck. AUS Implantation with a Penile Prosthesis Urinary incontinence and impotence often coexist after radical prostatectomy or radiation therapy. A penile prosthesis and AUS can be implanted simultaneously or in staged procedures at least two to three months apart. It is recommended that the AUS be implanted first if simultaneous procedures are undertaken. The procedure can be completed through a low transverse suprapubic incision if a multicomponent penile prosthesis is chosen. A midline perineal incision is also required if the sphincter cuff is to be placed on the bulbous urethra. The AUS components should be implanted, connected, cycled and deactivated prior to introducing the penile prosthesis. The individual reservoirs are placed under their respective rectus muscle. The pumps are placed in separate subcutaneous hemiscrotal pockets. Bladder Neck Cuff in the Female AUS implantation in females can be accomplished either through an abdominal or transvaginal approach. The decision to use the transvaginal approach is usually determined by the surgeon's experience with anatomy and techniques of transvaginal surgery. This review will focus on the transvaginal approach. The position of the AUS components are seen in figure
10 FIGURE 13. Cuff as it is passed behind the bladder neck transvaginally. Transvaginal Approach of Bladder Neck Cuff Placement Patients are positioned in the dorsal lithotomy position. A formal iodophor preparation of the vagina is completed. The lower abdomen and perineum are included in the surgical field. A sterile 16-F Foley catheter is inserted into the bladder per urethrum. The labia minora are retracted laterally using stay sutures, and a weighted speculum is placed in the vagina. A semicircular incision is made so that the apex of the incision is midway between the urethral meatus and the bladder neck (Fig. 11). The flap of vaginal wall is dissected free from the urethra with its base toward the bladder neck (Fig. 12). The retropubic space is entered with scissors pointing toward the ipsilateral shoulder on each side of the bladder neck. The endopelvic fascia is swepped laterally off the pubic bone. Using blunt dissection, the proximal urethra and bladder neck are mobilized off the underside of the pubis. After removal of the Foley catheter, the measuring tape is placed around the bladder neck. The appropriately sized cuff is then passed posteriorly towards the side of future pump and reservoir placement (Fig. 13). The cuff is snapped into place, and the cuff tubing should be exiting laterally (Fig. 14). Cystoscopy can be used at this point to check placement of the cuff so that the cuff is distal to the ureteral orifices. Following cuff placement, a transverse suprapubic incision is made, exposing the anterior abdominal fascia. A small midline incision is made through the fascia, thereby exposing the prevesical space. A 61-70cm water pressure balloon reservoir is placed through the fascial defect in the prevesical space. The reservoir tubing is brought through the rectus belly and fascia lateral to the midline on the side of future pump placement. The balloon is filled with 22cc of iso-osmotic contrast and a shodded clamp is placed at the end of the tubing to prevent fluid loss. The cuff tubing is transferred retropubically through the vaginal incision up into the abdominal incision. The cuff tubing should penetrate the rectus muscle and fascia near the reservoir tubing as previously illustrated (Fig. 10). Hegar dilators are used to create a subcutaneous pocket in the labia majora. The pump is placed into the most dependent portion of the pocket so that it can be easily accessed. Connections are then made between the pump and reservoir, and the pump and cuff tubing as previously described. The abdominal and vaginal incisions are closed in layers using absorbable suture. The Foley catheter is reinserted and an antibiotic-soaked pack is placed into the vagina. 123
11 FIGURE 14. Completed cuff placement. Bladder Neck Cuff Placement in Children Children who are candidates for AUS implantation are frequently myelodysplastic with urinary incontinence secondary to sphincteric insufficiency and a neurogenic bladder. Many of these children will require intermittent self-catheterization after AUS implantation. They, therefore, should prior to surgery understand the potential outcomes and be able to demonstrate manual dexterity as well as compliance with medical recommendations. The bladder neck is the only site of cuff implantation in children, both male and female. The preoperative and intraoperative technique follows the same guidelines as for adults with bladder neck cuff placement. The children are positioned supine with knees bent. A lower midline abdominal incision is made and the prevesical space is developed while remaining extraperitoneal. Meticulous dissection must be carried out as the urethral and vaginal tissues are fragile. The plane between the bladder neck and rectum or bladder neck and vagina, respectively, is developed. An anterior midline cystotomy may facilitate dissection. Cuff size in children is usually 6-8cm. A 61-70cm water pressure balloon is used. As with adults, the reservoir is placed in the prevesical space and the pump is placed in either the labia majora or scrotum. To accommodate growth, the pump tubing may need to be lengthened with time. Regular examinations, including voiding cystourethrogram and urodynamic studies, should be completed to avoid upper tract damage. AUS Implantation During Bladder Reconstruction When sphincteric incompetence accompanies detrusor hyperreflexia and low compliance, augmentation cystoplasty combined with AUS implantation can result in continence with a decreased risk of upper tract deterioration. The augmentation cystoplasty is performed first, and then the AUS is implanted (Fig. 15). Cuff placement around the bladder neck follows the same technique as previously described. 124
12 FIGURE 15. Augmentation cystoplasty with simultaneous AUS implantation; bladder open to show ureteroneocystotomy. POSTOPERATIVE CONSIDERATIONS Hospital stay after AUS implantation using a bulbous urethral cuff is usually one day with the occasional patient remaining in the hospital for two days. Bladder neck cuff placement requires 4-5 days. Oral pain medication is usually adequate for analgesia. Ice packs applied to the labia or scrotum for hours postoperatively reduces swelling around the pump. Broad spectrum intravenous antibiotics (vancomycin and gentamicin) are continued throughout the hospitalization. Oral antibiotics (usually a cephalosporin) are continued for 2 weeks following discharge. Patients may shower daily and take a bath 5 days after surgery. The Foley catheter is removed the morning after surgery and most patients will be able to urinate. If patients are unable to void, intermittent self-catheterization is begun with a small caliber urethral catheter until spontaneous voiding returns. Prolonged catheterization after AUS implantation should be discouraged due to increased risk of cuff erosion. Some patients will report a transient improvement in urinary control in the immediate postoperative period due to increased resistance from edema near the cuff site. Incontinence is expected during the deactivation period, and, therefore, some form of protection should be worn until sphincter activation. Patients should be instructed to gently pull down their pump once each day to prevent upward migration during the capsule-forming period. Ambulation is encouraged postoperatively. Patients are cautioned to avoid excessive compression of the perineum and lower abdomen. Heavy lifting and straining is restricted for at least 6 weeks. Patients with bulbourethral cuffs are permanently restricted from riding a bicycle and horseback riding. Sexual activity should be avoided until sphincter activation. Patients should wear a Medic Alert bracelet to notify medical personnel of the presence of the AUS and the necessity for cuff deactivation prior to Foley catheter placement. 125
13 AUS ACTIVATION Cuff activation takes place 4-6 weeks following implantation. By this time, scrotal or labial swelling and tenderness has subsided, and incisions are well healed. Successful activation and cuff filling can be confirmed with pre and post-activation radiographs. Patients are given another demonstration of how to cycle the sphincter, and are required to demonstrate, independently, how to compress the pump, open the cuff and void. Patients who were dry at night prior to sphincter implantation do not require cuff activation for continence while sleeping. These patients can be instructed in cuff deactivation at night. Deactivation has the benefit of reducing the risk of tissue ischemia, urethral atrophy and urethral cuff erosion 5. If patients are unable to empty their bladder, they are instructed to practice self-intermittent catheterization (SIC) with the cuff deflated during catheterization. Immediate Postoperative Complications Urinary retention may occur in the immediate postoperative period due to urethral edema. The sphincter pump should be checked to confirm that it is in the open position. Most patients will begin voiding after a brief period of intermittent catheterization with a small caliber (10-12F) catheter. If prolonged SIC is required, the cuff should be in the deflated position prior to catheterization. Urinary retention after cuff activation should signal the possibility of stricture disease or bladder neck contracture. Urethral instrumentation should always be performed with the cuff deactivated and with the smallest size cystoscope possible. If prolonged bladder drainage is necessary, a suprapubic tube should be inserted to avoid urethral cuff erosion. Hematoma is the most common minor complication of AUS implantation. Labial or scrotal hematomas can displace the pump and make external manipulation difficult. Most hematomas will resolve spontaneously. Rarely, a large hematoma will require evacuation. Long Term Complications Persistent or recurrent urinary incontinence is most commonly due to mechanical failure, tissue atrophy or cuff erosion. Inflate-deflate radiographs can evaluate the hydraulic function of the AUS. If the radiopaque fluid is not in the system, then a leak has developed. Surgical exploration and close inspection is required to identify the site of leakage. The most common site of leakage is the lower surface of the cuff. 2 Once the site of leakage has been identified, the individual components can be replaced. If there is fluid present and there is no filling of the cuff during cycling, there is obstruction to flow such as occurs with a tubing kink (a rare occurrence following the availability of kinkless tubing) or foreign body (including air lock) plugging the tubing. Again, surgical exploration is required to identify the location of obstruction. If normal cuff deflation and inflation is present, a urethrogram followed by urethroscopy will exclude cuff erosion. If the onset of the incontinence is insidious, one should suspect cuff-compression tissue atrophy. Urodynamic evaluation with leak point pressure measurement and cystoscopy will reveal poor urethral occlusion when tissue atrophy is present. One of three methods are theoretically available to treat recurrent incontinence due to tissue atrophy: (1) increase the pressure of the balloon reservoir, (2) reduce cuff size by 0.5cm increments, and (3) place a tandem cuff distal to the original cuff in patients with a bulbourethral cuff. In patients with a bladder neck cuff, the reservoir is easier to access than the cuff and therefore the balloon reservoir pressure can be increased. However, in patients with bulbar urethral cuffs, it is never our practice to either increase balloon pressure reservoir or decrease cuff size. It is our feeling that these two procedures will only lead to further worsening of the urethral atrophy and resultant incontinence and possible erosion. Therefore, we managed recurrent incontinence secondary to urethral atrophy with the placement of a tandem cuff
14 Cuff erosion is a serious complication requiring cuff removal. Cuff erosion can present with pain, swelling, recurrent incontinence, infection, retention, and bloody urethral discharge. Erosion that presents in the immediate postoperative period is due to an unrecognized iatrogenic urethral injury at the time of surgery. Cystourethroscopy confirms the clinical suspicion. In the absence of infection, the cuff is removed and a stainless steel plug is placed in the cuff tubing. After adequate healing, a new cuff can be inserted. If infection is present, the entire device must be removed. After erosion is identified and the cuff has been removed, a silicone catheter should be left in place for 3-6 weeks to allow for urethral healing. Prosthetic infections can present at anytime but usually will occur within the first 1-2 postoperative months. 2 Following a sufficient recovery time, reoperation and re-implantion of the AUS is encouraged. The surgeon should be aware that this may be a difficult procedure given the degree of reactionary tissue surrounding the bulbar urethra. Currently, we are frequently resorting to transcorporal placement of the cuff to minimize the risk of urethral injury and subsequent erosion.7 At this point in time, we are very encourage with this approach. CONCLUSION The AUS remains the gold standard for the treatment of stress urinary incontinence in men. Its indications and use in children and woman has decreased over the years secondary to the introduction of better alternatives in these patient populations. It is critical for the urologist implanting the AUS to have a very good working knowledge of the AUS to prevent needless complications and to insure the highest degree of success possible. REFERENCES 1. Light, J.K., Implantation of the AS 800 Artificial Urinary Sphincter, Problems in Urology, Vol. 7, Number 3, p , Elliott, D.S., Barrett, D.M., The Mayo Clinic Long Term Analysis of the Functional Durability of the AMS 800 Artificial Urinary Sphincter: A Review of 323 Cases. Accepted for publication August 1997, J. of Urology. 3. Blum, M.D. Infections of genitourinary prostheses. Infect Dis Clin North Am 1989; 3: Carson, C.C. III. Infections in genitourinary prostheses. Urol Clin North Am 1989; 16: Elliott DS, Barrett DM, Gohma M, Boone TB: Does Nocturnal Deactivation of the Artificial Urinary Sphincter Lessen the Risk for Urethral Atrophy? Urology, 57 (6) , June DiMarco DS, Elliott DS: Tandem cuff artificial urinary sphincter as a salvage procedure following failed primary sphincter placement for the treatment of post-prostatectomy incontinence. J. Urol, , September Guralnick ML, Miller E, Toh KL, Webster GD: Transcorporal artificial urinary sphincter cuff placement in cases requiring revision for erosion and urethral atrophy. : J Urol May;167(5): This article should be referenced as follows: Elliott, D.S. and Barrett, D.M. (2004) The artificial genitourinary sphincter. TheScientificWorldJOURNAL 4 (S1), Handling Editor: Anthony Atala, Principle Editor for Urology a domain of TheScientificWorldJOURNAL. 127
15 MEDIATORS of INFLAMMATION The Scientific World Journal Gastroenterology Research and Practice Journal of Diabetes Research International Journal of Journal of Endocrinology Immunology Research Disease Markers Submit your manuscripts at BioMed Research International PPAR Research Journal of Obesity Journal of Ophthalmology Evidence-Based Complementary and Alternative Medicine Stem Cells International Journal of Oncology Parkinson s Disease Computational and Mathematical Methods in Medicine AIDS Behavioural Neurology Research and Treatment Oxidative Medicine and Cellular Longevity
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Surgery Illustrated Surgical Atlas The artificial genitourinary sphincter
 BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas The artificial genitourinary sphincter John T. Stoffel and David M. Barrett Department of Urology, Lahey Clinic Medical Center, Burlington, USA
BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas The artificial genitourinary sphincter John T. Stoffel and David M. Barrett Department of Urology, Lahey Clinic Medical Center, Burlington, USA
Cleveland Clinic Quarterly
 Cleveland Clinic Quarterly Volume 31 JULY 1964 No. 3 A MEDICAL SILASTIC PROSTHESIS FOR THE CONTROL OF URINARY INCONTINENCE IN THE MALE A Preliminary Report J A M E S K. W A T K I N S, M. D., * R A L P
Cleveland Clinic Quarterly Volume 31 JULY 1964 No. 3 A MEDICAL SILASTIC PROSTHESIS FOR THE CONTROL OF URINARY INCONTINENCE IN THE MALE A Preliminary Report J A M E S K. W A T K I N S, M. D., * R A L P
Aus Artificial Uretheral Sphincter Port System
 NORFOLK VET PRODUCTS the AUS for the long-term relief of incontinence in dogs and cats making life easier for pets Speciality Medical Devices For The Veterinary Community the Aus Artificial Uretheral Sphincter
NORFOLK VET PRODUCTS the AUS for the long-term relief of incontinence in dogs and cats making life easier for pets Speciality Medical Devices For The Veterinary Community the Aus Artificial Uretheral Sphincter
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
REPAIR OF LARGE CYSTOCELE
 REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
THE ARTIFICIAL URINARY SPHINCTER:
 THE ARTIFICIAL URINARY SPHINCTER: A TREATMENT FOR POST- PROSTATECTOMY URINARY INCONTINENCE Andrew L. Siegel, M.D. Board-Certified Urologist and Urological Surgeon Director: Center for Continence Care An
THE ARTIFICIAL URINARY SPHINCTER: A TREATMENT FOR POST- PROSTATECTOMY URINARY INCONTINENCE Andrew L. Siegel, M.D. Board-Certified Urologist and Urological Surgeon Director: Center for Continence Care An
MANUALFor Operating Room
 DOCUMENT OPERATING ROOM FOR MANUALFor Operating Room NOTE This document is a complementary checklist to the two training videos, which you can access and download from our website: ZSI 375 Training Video,
DOCUMENT OPERATING ROOM FOR MANUALFor Operating Room NOTE This document is a complementary checklist to the two training videos, which you can access and download from our website: ZSI 375 Training Video,
ZEPHYR SURGICAL IMPLANTS SÀRL
 For Operating Room NOTE This document is a complementary checklist to the two training videos, which you can be accessed and download from our website: ZSI 375 Training Video, ZSI 375 Functioning Protocol.
For Operating Room NOTE This document is a complementary checklist to the two training videos, which you can be accessed and download from our website: ZSI 375 Training Video, ZSI 375 Functioning Protocol.
TRANSURETHRAL RESECTION
 TRANSURETHRAL RESECTION OF THE PROSTATE GLAND 21 Prostatic sonographic studies of patients who have undergone a transurethral resection of the prostate gland reveal large volumes of residual prostate tissue
TRANSURETHRAL RESECTION OF THE PROSTATE GLAND 21 Prostatic sonographic studies of patients who have undergone a transurethral resection of the prostate gland reveal large volumes of residual prostate tissue
PROBLEMS AND VARIATIONS THREE-COMPONENT INFLATABLE PENILE PROSTHESIS IN THE PLACEMENT OF THE. Troubleshooting for the Malfunctioning Prosthesis
 PROBLEMS AND VARIATIONS IN THE PLACEMENT OF THE 24 THREE-COMPONENT INFLATABLE PENILE PROSTHESIS Troubleshooting for the Malfunctioning Prosthesis Although there are ongoing changes in the design of penile
PROBLEMS AND VARIATIONS IN THE PLACEMENT OF THE 24 THREE-COMPONENT INFLATABLE PENILE PROSTHESIS Troubleshooting for the Malfunctioning Prosthesis Although there are ongoing changes in the design of penile
AMS Ambicor. Penile Prosthesis. Operating Room Manual. English
 AMS Ambicor Penile Prosthesis Operating Room Manual English This page intentionally left blank. Table of Contents General Information Detailed Device Description... 4 Device Characteristics... 4 Two-piece
AMS Ambicor Penile Prosthesis Operating Room Manual English This page intentionally left blank. Table of Contents General Information Detailed Device Description... 4 Device Characteristics... 4 Two-piece
West Yorkshire Major Trauma Network Clinical Guidelines 2015
 WYMTN: Pelvic fracture with urogenital trauma KEY RECOMMENDATIONS 1. During the initial exploratory survey / secondary survey, a. The external urethral meatus and the transurethral bladder catheter (if
WYMTN: Pelvic fracture with urogenital trauma KEY RECOMMENDATIONS 1. During the initial exploratory survey / secondary survey, a. The external urethral meatus and the transurethral bladder catheter (if
Management of Post-Prostatectomy Urinary Incontinence and Sexual Dysfunction
 Management of Post-Prostatectomy Urinary Incontinence and Sexual Dysfunction Robert C. Eyre, MD, FACS Associate Clinical Professor of Surgery (Urology) Harvard Medical School Post-prostatectomy Incontinence
Management of Post-Prostatectomy Urinary Incontinence and Sexual Dysfunction Robert C. Eyre, MD, FACS Associate Clinical Professor of Surgery (Urology) Harvard Medical School Post-prostatectomy Incontinence
Blue Ridge Urogynecology
 Surgery for Stress Urinary Incontinence Surgery has proved to be a very effective treatment for stress incontinence. The best surgical procedures improve or cure the incontinence in 85 to 90 percent of
Surgery for Stress Urinary Incontinence Surgery has proved to be a very effective treatment for stress incontinence. The best surgical procedures improve or cure the incontinence in 85 to 90 percent of
Desara TV and Desara Blue TV
 Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
The number following the procedure code is the TRICARE payment group. KIDNEY
 TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis.
 DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
AMS 800 Urinary Control System ACTIVATING:
 AMS 800 Urinary Control System 1 ACTIVATING: Begin by stabilizing the control pump in the proper place by grasping the tubing above the control pump. Use your other hand to firmly squeeze the sides of
AMS 800 Urinary Control System 1 ACTIVATING: Begin by stabilizing the control pump in the proper place by grasping the tubing above the control pump. Use your other hand to firmly squeeze the sides of
Instruction For Use for All Silicon Foley Catheter
 General Description: All Silicone Foley Catheter for single use is a thin, is a flexible tube passed through the urethra and into the bladder to drain urine. It is the most common type of indwelling urinary
General Description: All Silicone Foley Catheter for single use is a thin, is a flexible tube passed through the urethra and into the bladder to drain urine. It is the most common type of indwelling urinary
Female Epispadias Repair
 hoofdstuk 07 08-03-2001 15:25 Pagina 89 Female Epispadias Repair Female epispadias repair: a new 1-stage technique CHAPTER 7 Tom P.V.M de Jong, Pieter Dik and Aart J. Klijn Journal of Urology 2000, 164,
hoofdstuk 07 08-03-2001 15:25 Pagina 89 Female Epispadias Repair Female epispadias repair: a new 1-stage technique CHAPTER 7 Tom P.V.M de Jong, Pieter Dik and Aart J. Klijn Journal of Urology 2000, 164,
AMS 800. Operating Room Manual. Urinary Control System For Male, Female, and Pediatric Patients. English
 AMS 800 Urinary Control System For Male, Female, and Pediatric Patients Operating Room Manual English Table of Contents Contents Disclosures Indications For Use... 1 Contraindications... 1 Warnings...
AMS 800 Urinary Control System For Male, Female, and Pediatric Patients Operating Room Manual English Table of Contents Contents Disclosures Indications For Use... 1 Contraindications... 1 Warnings...
AMS 800. Urinary Control System For Male Patients. Operating Room Manual
 AMS 800 Urinary Control System For Male Patients Operating Room Manual Table of Contents Introduction Overview... 1 Indications for Use... 1 Additional Information... 1 System Description... 1 System
AMS 800 Urinary Control System For Male Patients Operating Room Manual Table of Contents Introduction Overview... 1 Indications for Use... 1 Additional Information... 1 System Description... 1 System
AMS 800. Urinary Control System. User s Guide. Table of Contents. The AMS 800 Urinary Control System...1. Using the AMS 800 Urinary Control System...
 AMS 800 Urinary Control System User s Guide Table of Contents The AMS 800 Urinary Control System...1 Using the AMS 800 Urinary Control System...2 Special precautions to take with your 800 before undergoing
AMS 800 Urinary Control System User s Guide Table of Contents The AMS 800 Urinary Control System...1 Using the AMS 800 Urinary Control System...2 Special precautions to take with your 800 before undergoing
Penile implants What to expect and how to prepare
 Penile implants What to expect and how to prepare Penile implants can restore erectile function. Explore your choices and find out what to expect from this procedure. Penile implants are artificial devices
Penile implants What to expect and how to prepare Penile implants can restore erectile function. Explore your choices and find out what to expect from this procedure. Penile implants are artificial devices
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
LESSON ASSIGNMENT. Urinary System Diseases/Disorders. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 4 Urinary System Diseases/Disorders LESSON ASSIGNMENT Paragraphs 4-1 through 4-8. LESSON OBJECTIVES After completing this lesson, you should be able to: 4-1. Identify the purposes
LESSON ASSIGNMENT LESSON 4 Urinary System Diseases/Disorders LESSON ASSIGNMENT Paragraphs 4-1 through 4-8. LESSON OBJECTIVES After completing this lesson, you should be able to: 4-1. Identify the purposes
THE operation of reimplantation of the ureter into the bladder has undergone
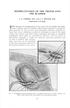 REIMPLANTATION OF THE URETER INTO THE BLADDER J. G. WARDEN, M.D., and C. C. HIGGINS, M.D. Department of Urology THE operation of reimplantation of the ureter into the bladder has undergone a stormy course
REIMPLANTATION OF THE URETER INTO THE BLADDER J. G. WARDEN, M.D., and C. C. HIGGINS, M.D. Department of Urology THE operation of reimplantation of the ureter into the bladder has undergone a stormy course
Desara and Desara Blue
 Desara and Desara Blue Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc.
Desara and Desara Blue Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc.
SOP: Urinary Catheter in Dogs and Cats
 SOP: Urinary Catheter in Dogs and Cats These SOPs were developed by the Office of the University Veterinarian and reviewed by Virginia Tech IACUC to provide a reference and guidance to investigators during
SOP: Urinary Catheter in Dogs and Cats These SOPs were developed by the Office of the University Veterinarian and reviewed by Virginia Tech IACUC to provide a reference and guidance to investigators during
Sara Schaenzer Grand Rounds January 24 th, 2018
 Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience
 Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Canadian Undergraduate Urology Curriculum (CanUUC): Genitourinary Trauma. Last reviewed June 2014
 Canadian Undergraduate Urology Curriculum (CanUUC): Genitourinary Trauma Last reviewed June 2014 Session Objectives 1. Recognize hematuria as the cardinal symptom of urinary tract trauma. 1. Outline the
Canadian Undergraduate Urology Curriculum (CanUUC): Genitourinary Trauma Last reviewed June 2014 Session Objectives 1. Recognize hematuria as the cardinal symptom of urinary tract trauma. 1. Outline the
Use of the Silastic Sheath in Bladder Neck Reconstruction
 Article TheScientificWorldJOURNAL (2004) 4 (S1), 103 107 ISSN 1537-744X; DOI 10.1100/tsw.2004.54 Use of the Silastic Sheath in Bladder Neck Reconstruction D.A. Diamond, M.D. 1, G.F. Quimby, M.D. 2, R.C.
Article TheScientificWorldJOURNAL (2004) 4 (S1), 103 107 ISSN 1537-744X; DOI 10.1100/tsw.2004.54 Use of the Silastic Sheath in Bladder Neck Reconstruction D.A. Diamond, M.D. 1, G.F. Quimby, M.D. 2, R.C.
AMS 800 Urinary Control System
 AMS 800 Urinary Control System 1 DAILY USE: While the cuff is closed, urine stays inside the bladder. To urinate, open the cuff as follows: Feel for the control pump in your scrotum. Stabilize the control
AMS 800 Urinary Control System 1 DAILY USE: While the cuff is closed, urine stays inside the bladder. To urinate, open the cuff as follows: Feel for the control pump in your scrotum. Stabilize the control
Artificial urinary sphincter revision for urethral atrophy: comparing single cuff downsizing and tandem cuff placement
 ORIGINAL ARTICLE Vol. 43 (2): 264-270, March - April, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0240 Artificial urinary sphincter revision for urethral atrophy: comparing single cuff downsizing and tandem
ORIGINAL ARTICLE Vol. 43 (2): 264-270, March - April, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0240 Artificial urinary sphincter revision for urethral atrophy: comparing single cuff downsizing and tandem
Repair of Bulbar Urethra Using the Barbagli Technique
 22 Repair of Bulbar Urethra Using the Barbagli Technique G. Barbagli, M. Lazzeri 22.1 Introduction and Historical Background 182 22.2 Anatomical Remarks 182 22.3 Step-by-Step Surgical Details 183 22.3.1
22 Repair of Bulbar Urethra Using the Barbagli Technique G. Barbagli, M. Lazzeri 22.1 Introduction and Historical Background 182 22.2 Anatomical Remarks 182 22.3 Step-by-Step Surgical Details 183 22.3.1
Information for men considering a male sling procedure UHB is a no smoking Trust
 Information for men considering a male sling procedure UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Introduction
Information for men considering a male sling procedure UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Introduction
Since the first published article, in 1974 by Scott et al on
 Perineal Approach for Artificial Urinary Sphincter Implantation Appears to Control Male Stress Incontinence Better Than the Transscrotal Approach Gerard D. Henry,* Stephen M. Graham, Mario A. Cleves, Caroline
Perineal Approach for Artificial Urinary Sphincter Implantation Appears to Control Male Stress Incontinence Better Than the Transscrotal Approach Gerard D. Henry,* Stephen M. Graham, Mario A. Cleves, Caroline
Medical Review Criteria Invasive Treatment for Urinary Incontinence
 Medical Review Criteria Invasive Treatment for Urinary Incontinence Effective Date: December 21, 2016 Subject: Invasive Treatment for Urinary Incontinence Background: Urinary incontinence (the involuntary
Medical Review Criteria Invasive Treatment for Urinary Incontinence Effective Date: December 21, 2016 Subject: Invasive Treatment for Urinary Incontinence Background: Urinary incontinence (the involuntary
Desara Blue OV D I. Sling for Female Stress Urinary Incontinence. Instructions For Use
 Desara Blue OV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc. 5171 Clareton
Desara Blue OV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc. 5171 Clareton
Glossary of terms Urinary Incontinence
 Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Loss of Bladder Control
 BLADDER HEALTH Loss of Bladder Control SURGERY TO TREAT URINARY INCONTINENCE AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is Urinary Incontinence? Urinary incontinence
BLADDER HEALTH Loss of Bladder Control SURGERY TO TREAT URINARY INCONTINENCE AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is Urinary Incontinence? Urinary incontinence
Urethral Injuries: Realignment vs. Delayed Reconstruction
 Urethral Injuries: Realignment vs. Delayed Reconstruction E. Charles Osterberg, MD Assistant Professor of Surgery (Urology) Dell Medical School Chief of Urology and Genitourinary Reconstruction None Disclosures
Urethral Injuries: Realignment vs. Delayed Reconstruction E. Charles Osterberg, MD Assistant Professor of Surgery (Urology) Dell Medical School Chief of Urology and Genitourinary Reconstruction None Disclosures
THE UROLOGY GROUP
 THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
Dr. Aso Urinary Symptoms
 Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
SURGERY FOR PEYRONIE S DISEASE. PEYRONIE S DISEASE WITHOUT IMPOTENCE Exposure and Mobilization of Dorsal Nerves and Vessels
 SURGERY FOR 25 PEYRONIE S DISEASE PEYRONIE S DISEASE WITHOUT Exposure and Mobilization of Dorsal Nerves and Vessels FIG. 25-1. Most surgeons use a degloving procedure via a circumferential skin incision
SURGERY FOR 25 PEYRONIE S DISEASE PEYRONIE S DISEASE WITHOUT Exposure and Mobilization of Dorsal Nerves and Vessels FIG. 25-1. Most surgeons use a degloving procedure via a circumferential skin incision
Renal Trauma: Management Options
 Renal Trauma: Management Options Immediate surgical repair Nephrectomy Conservative management Alonso RC et al. Kidney in Danger: CT Findings of Blunt and Penetrating Renal Trauma. RadioGraphics 2009;
Renal Trauma: Management Options Immediate surgical repair Nephrectomy Conservative management Alonso RC et al. Kidney in Danger: CT Findings of Blunt and Penetrating Renal Trauma. RadioGraphics 2009;
Male urinary incontinence: Artificial sphincter
 GUIDELINES IN FOCUS Truzzi JC et al. Male urinary incontinence: Artificial sphincter Incontinência urinária masculina: Esfíncter artificial Authorship: Brazilian Society of Urology (SBU) Participants:
GUIDELINES IN FOCUS Truzzi JC et al. Male urinary incontinence: Artificial sphincter Incontinência urinária masculina: Esfíncter artificial Authorship: Brazilian Society of Urology (SBU) Participants:
Radical Cystectomy A Patient s Guide
 Radical Cystectomy A Patient s Guide Introduction The urinary system, which includes the bladder, urethra, ureters, and kidneys, helps maintain stable chemical conditions in the body, stores, and eliminates
Radical Cystectomy A Patient s Guide Introduction The urinary system, which includes the bladder, urethra, ureters, and kidneys, helps maintain stable chemical conditions in the body, stores, and eliminates
3. Urinary Catheters. Indications. Methods of Bladder Catheterization. Hashim Hashim
 3. Urinary Catheters Hashim Hashim Indications Urinary catheters are used to drain urine from the bladder. The main indications are: A. Diagnostic Measure post-void residual in the absence of ultrasound
3. Urinary Catheters Hashim Hashim Indications Urinary catheters are used to drain urine from the bladder. The main indications are: A. Diagnostic Measure post-void residual in the absence of ultrasound
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Jennifer Locke UBC Department of Urologic Sciences Resident Year 3 October 12, Learning Objectives
 Artificial Urinary Sphincter after 40 Years of Use: Indications, Techniques and Outcomes Jennifer Locke UBC Department of Urologic Sciences Resident Year 3 October 12, 2016 Learning Objectives 1. Identify
Artificial Urinary Sphincter after 40 Years of Use: Indications, Techniques and Outcomes Jennifer Locke UBC Department of Urologic Sciences Resident Year 3 October 12, 2016 Learning Objectives 1. Identify
Loss of Bladder Control
 BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
Combination therapy for male erectile dysfunction and urinary incontinence
 sian J ndrol 2008; 10 (1): 149 154 DOI: 10.1111/j.1745-7262.2008.00364.x www.asiaandro.com. Clinical Experience. Combination therapy for male erectile dysfunction and urinary incontinence Helen Zafirakis
sian J ndrol 2008; 10 (1): 149 154 DOI: 10.1111/j.1745-7262.2008.00364.x www.asiaandro.com. Clinical Experience. Combination therapy for male erectile dysfunction and urinary incontinence Helen Zafirakis
Managing your suprapubic catheter
 Managing your suprapubic catheter What you need to know The information contained in this booklet is intended to assist you in understanding your proposed surgery. Not all of the content will apply to
Managing your suprapubic catheter What you need to know The information contained in this booklet is intended to assist you in understanding your proposed surgery. Not all of the content will apply to
Center for Reconstructive Urology
 Center for Reconstructive Urology Urethral Reconstruction Post-Operative Instructions Following urethral reconstruction, your attention to proper post-operative follow-up will contribute to the success
Center for Reconstructive Urology Urethral Reconstruction Post-Operative Instructions Following urethral reconstruction, your attention to proper post-operative follow-up will contribute to the success
Managing your bladder with a Supra-pubic catheter at home
 Managing your bladder with a Supra-pubic catheter at home Providing a range of NHS services in Gateshead, South Tyneside and Sunderland. Managing your bladder with a Supra-pubic catheter at home The purpose
Managing your bladder with a Supra-pubic catheter at home Providing a range of NHS services in Gateshead, South Tyneside and Sunderland. Managing your bladder with a Supra-pubic catheter at home The purpose
Victoria Frohna s mold story
 Victoria Frohna s mold story January 2000 Discussion of the Artificial Urinary Sphincter (AUS) Dr. Charles Jennings Dr. Charles Jennings is a Diplomat with the American Board of Urology; a Member of the
Victoria Frohna s mold story January 2000 Discussion of the Artificial Urinary Sphincter (AUS) Dr. Charles Jennings Dr. Charles Jennings is a Diplomat with the American Board of Urology; a Member of the
Lee Jackson, M.D. Post-Operation Information and Instructions
 Post-Operation Information and Instructions While a robotic prostatectomy is performed routinely, it is still a relatively major surgery that will take some time and effort to recover from. The following
Post-Operation Information and Instructions While a robotic prostatectomy is performed routinely, it is still a relatively major surgery that will take some time and effort to recover from. The following
Surgical treatment of urinary stress incontinence with tension free vaginal tape
 Surgical treatment of urinary stress incontinence with tension free vaginal tape Gynaecology department 01935 384 385 yeovilhospital.nhs.uk Many surgical operations are available for the treatment of
Surgical treatment of urinary stress incontinence with tension free vaginal tape Gynaecology department 01935 384 385 yeovilhospital.nhs.uk Many surgical operations are available for the treatment of
Dr. Syah Mirsya Warli, SpU Dr. Bungaran Sihombing,SpU Div. of Urology, Surgery Dept. Medical Faculty, University of Sumatera Utara
 Emergency Room Urology Dr. Syah Mirsya Warli, SpU Dr. Bungaran Sihombing,SpU Div. of Urology, Surgery Dept. Medical Faculty, University of Sumatera Utara Ref : Clinical Manual of Urology, (Philip M. Hanno
Emergency Room Urology Dr. Syah Mirsya Warli, SpU Dr. Bungaran Sihombing,SpU Div. of Urology, Surgery Dept. Medical Faculty, University of Sumatera Utara Ref : Clinical Manual of Urology, (Philip M. Hanno
In some cases, a medical evaluation may be needed, to be performed by your primary care physician about 2-4 weeks prior to surgery.
 Robotic Assisted Laparoscopic Prostatectomy Information Sheet Preoperative Events: You will have a consultation appointment with one of the robotic surgeons. We will try to schedule this within a month
Robotic Assisted Laparoscopic Prostatectomy Information Sheet Preoperative Events: You will have a consultation appointment with one of the robotic surgeons. We will try to schedule this within a month
INFORMED CONSENT FOR INSERTION OF PENILE PROSTHESIS
 INFORMED CONSENT FOR INSERTION OF PENILE PROSTHESIS 1) I hereby request and authorize Dr. Harold M. Reed assisted by his designated urological associates and surgical technicians, to perform the urological
INFORMED CONSENT FOR INSERTION OF PENILE PROSTHESIS 1) I hereby request and authorize Dr. Harold M. Reed assisted by his designated urological associates and surgical technicians, to perform the urological
SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER
 SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER CHARLES C. HIGGINS, M.D. W. JAMES GARDNER, M.D. WM. A. NOSIK, M.D. The treatment of "cord bladder", a disturbance of bladder function from disease
SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER CHARLES C. HIGGINS, M.D. W. JAMES GARDNER, M.D. WM. A. NOSIK, M.D. The treatment of "cord bladder", a disturbance of bladder function from disease
I-STOP TOMS Transobturator Male Sling
 I-STOP TOMS Transobturator Male Sling The CL Medical I-STOP TOMS sling for male stress urinary incontinence was developed in France where it is widely used and is the market leader. It is constructed with
I-STOP TOMS Transobturator Male Sling The CL Medical I-STOP TOMS sling for male stress urinary incontinence was developed in France where it is widely used and is the market leader. It is constructed with
Four-year follow-up on a Zephyr Surgical Implants 375 artificial urinary sphincter for male urinary incontinence from one urological centre in Poland
 320 O R I G I N A L P A P E R FUNCTIONAL UROLOGY Four-year follow-up on a Zephyr Surgical Implants 375 artificial urinary sphincter for male urinary incontinence from one urological centre in Poland Ireneusz
320 O R I G I N A L P A P E R FUNCTIONAL UROLOGY Four-year follow-up on a Zephyr Surgical Implants 375 artificial urinary sphincter for male urinary incontinence from one urological centre in Poland Ireneusz
Deirdre M. Bochove-Overgaauw* and Bart Ph. Schrier
 An Adjustable Sling for the Treatment of All Degrees of Male Stress Urinary Incontinence: Retrospective Evaluation of Efficacy and Complications After a Minimal Followup of 14 Months Deirdre M. Bochove-Overgaauw*
An Adjustable Sling for the Treatment of All Degrees of Male Stress Urinary Incontinence: Retrospective Evaluation of Efficacy and Complications After a Minimal Followup of 14 Months Deirdre M. Bochove-Overgaauw*
Rama Nada. - Ensherah Mokheemer. - Ahmed salman. 1 P a g e
 - 5 - Rama Nada - Ensherah Mokheemer - Ahmed salman 1 P a g e We will continue talking about the urinary bladder The ligaments of the bladder: 1-Median umbilical ligament: Continuous with apex of the bladder
- 5 - Rama Nada - Ensherah Mokheemer - Ahmed salman 1 P a g e We will continue talking about the urinary bladder The ligaments of the bladder: 1-Median umbilical ligament: Continuous with apex of the bladder
Bard: Continence Therapy. Stress Urinary Incontinence. Regaining Control. Restoring Your Lifestyle.
 Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Urinary incontinence is a common problem and one that can be resolved by working
Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Urinary incontinence is a common problem and one that can be resolved by working
BULKAMID STANDARD OPERATING PROCEDURE
 BULKAMID STANDARD OPERATING PROCEDURE Contents 1 1 2 3-4 5-6 5-6 7 9-12 9 10 11 12 13 13 13 15 16 Products Bulkamid multiple use instruments Bulkamid single use instruments The Bulkamid system Pre-procedure
BULKAMID STANDARD OPERATING PROCEDURE Contents 1 1 2 3-4 5-6 5-6 7 9-12 9 10 11 12 13 13 13 15 16 Products Bulkamid multiple use instruments Bulkamid single use instruments The Bulkamid system Pre-procedure
Urinary Bladder. Prof. Imran Qureshi
 Urinary Bladder Prof. Imran Qureshi Urinary Bladder It develops from the upper end of the urogenital sinus, which is continuous with the allantois. The allantois degenerates and forms a fibrous cord in
Urinary Bladder Prof. Imran Qureshi Urinary Bladder It develops from the upper end of the urogenital sinus, which is continuous with the allantois. The allantois degenerates and forms a fibrous cord in
What CPT and ICD-10-CM codes are reported?
 A patient is seen in the hospital s outpatient surgical area with a diagnosis of a displaced comminuted fracture of the lateral condyle, right elbow. An ORIF (open reduction) procedure was performed and
A patient is seen in the hospital s outpatient surgical area with a diagnosis of a displaced comminuted fracture of the lateral condyle, right elbow. An ORIF (open reduction) procedure was performed and
Procedure Specific Information Sheet Open Radical Prostatectomy
 Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence
 A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
5 DIAGNOSIS. History taking
 5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
MP A Prospective Evaluation of the Catheter Science M3 Mini Catheter for Patients with Prostatic Obstruction. Gaines W. Hammond Jr.
 MP73-06 - A Prospective Evaluation of the Catheter Science M3 Mini Catheter for Patients with Prostatic Obstruction Gaines W. Hammond Jr. MD FACS M3 Mini Catheter M3 Segmented M3 Plus Dynamic Wings M3
MP73-06 - A Prospective Evaluation of the Catheter Science M3 Mini Catheter for Patients with Prostatic Obstruction Gaines W. Hammond Jr. MD FACS M3 Mini Catheter M3 Segmented M3 Plus Dynamic Wings M3
q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE
 493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
SUPRA PUBIC CATHETER(SPC)
 Suprapubic versus urethral catheter? When a long-term catheter to drain the bladder is advised, it can be placed in the urethra (water pipe) or suprapubically (directly into the bladder through the skin
Suprapubic versus urethral catheter? When a long-term catheter to drain the bladder is advised, it can be placed in the urethra (water pipe) or suprapubically (directly into the bladder through the skin
6 THE OPERATIONS BASIC PRINCIPLES
 6 THE OPERATIONS BASIC PRINCIPLES Basic principles are described here; strategies for specific situations are discussed in later sections. The basic principles in the repair of a fistula are: adequate
6 THE OPERATIONS BASIC PRINCIPLES Basic principles are described here; strategies for specific situations are discussed in later sections. The basic principles in the repair of a fistula are: adequate
Renal Pelvis Squamous Cell Carcinoma and Renal Cell Carcinoma in a Tuberculous Kidney
 Case Study TheScientificWorldJOURNAL (2004) 4, 965 968 ISSN 1537-744X; DOI 10.1100/tsw.2004.196 Renal Pelvis Squamous Cell Carcinoma and Renal Cell Carcinoma in a Tuberculous Kidney M. Al-Assiri 1, M.F.
Case Study TheScientificWorldJOURNAL (2004) 4, 965 968 ISSN 1537-744X; DOI 10.1100/tsw.2004.196 Renal Pelvis Squamous Cell Carcinoma and Renal Cell Carcinoma in a Tuberculous Kidney M. Al-Assiri 1, M.F.
Urethrolysis; When, Why & How. M Karram Professor of Ob/Gyn & Urology University of Cincinnati
 Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Kelly procedure. How does the urinary system work? What is a Kelly procedure and why does my child need one?
 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Kelly procedure This information sheet from Great Ormond Street Hospital (GOSH) explains the Kelly procedure used
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Kelly procedure This information sheet from Great Ormond Street Hospital (GOSH) explains the Kelly procedure used
Colposuspension operation
 Colposuspension operation This information explains: Overview... 1 Your admission date... 1 The operation... 2 The anaesthetic... 2 After the operation... 3 Problems... 3 Going home... 4 Getting back to
Colposuspension operation This information explains: Overview... 1 Your admission date... 1 The operation... 2 The anaesthetic... 2 After the operation... 3 Problems... 3 Going home... 4 Getting back to
Before and After Your Surgery
 UW MEDICINE PATIENT EDUCATION Before and After Your Surgery Artificial urinary sphincter or male urethral sling surgery This handout explains how to prepare for and what to expect after artificial urinary
UW MEDICINE PATIENT EDUCATION Before and After Your Surgery Artificial urinary sphincter or male urethral sling surgery This handout explains how to prepare for and what to expect after artificial urinary
Pelvic Injuries. Chapter 21
 Chapter 21 Introduction Injuries of the pelvis are an uncommon, but potentially lethal, battlefield injury. Blunt injuries may be associated with major hemorrhage and early mortality. Death within the
Chapter 21 Introduction Injuries of the pelvis are an uncommon, but potentially lethal, battlefield injury. Blunt injuries may be associated with major hemorrhage and early mortality. Death within the
Center for Reconstructive Urethral Surgery Guido Barbagli Center for Reconstructive Urethral Surgery Arezzo - Italy
 Guido Barbagli Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it 23 rd ANNUAL EAU CONGRESS Sub-plenary Session on Male urinary incontinence 26 29 March 2008 Milan Italy Incontinence following
Guido Barbagli Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it 23 rd ANNUAL EAU CONGRESS Sub-plenary Session on Male urinary incontinence 26 29 March 2008 Milan Italy Incontinence following
LDR prostate brachytherapy
 LDR prostate brachytherapy Introduction Low dose rate (LDR) prostate brachytherapy is a modern, effective minimally invasive treatment appropriate for many men with early prostate cancer. I perform this
LDR prostate brachytherapy Introduction Low dose rate (LDR) prostate brachytherapy is a modern, effective minimally invasive treatment appropriate for many men with early prostate cancer. I perform this
RADICAL PROSTATECTOMY
 Tennyson Centre Suite 19 520 South Road Kurralta Park SA 5037 P 08 8292 2399 F 08 8292 2388 admin@urologicalsolutions.com.au www.urologicalsolutions.com.au Darwin Private Hospital Suite 5 Rocklands Drive
Tennyson Centre Suite 19 520 South Road Kurralta Park SA 5037 P 08 8292 2399 F 08 8292 2388 admin@urologicalsolutions.com.au www.urologicalsolutions.com.au Darwin Private Hospital Suite 5 Rocklands Drive
Information for Patients. Urinary Incontinence. English
 Information for Patients Urinary Incontinence English Table of contents What is urinary incontinence?... 3 Causes of urinary incontinence... 3 Types of urinary incontinence... 3 Stress urinary incontinence...
Information for Patients Urinary Incontinence English Table of contents What is urinary incontinence?... 3 Causes of urinary incontinence... 3 Types of urinary incontinence... 3 Stress urinary incontinence...
limbsandthings.com Advanced Catheterisation Trainer User Guide For more skills training products visit Limbs & Things Ltd.
 Advanced Catheterisation Trainer Product No: 60150 User Guide For more skills training products visit limbsandthings.com Limbs & Things Ltd. Sussex Street, St Philips Bristol, BS2 0RA, UK sales@limbsandthings.com
Advanced Catheterisation Trainer Product No: 60150 User Guide For more skills training products visit limbsandthings.com Limbs & Things Ltd. Sussex Street, St Philips Bristol, BS2 0RA, UK sales@limbsandthings.com
Guido Barbagli. Center for Reconstructive ti Urethral lsurgery
 Guido Barbagli Center for Reconstructive ti Urethral lsurgery Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it Dedicated to Ruggero Lenzi, teacher and friend. His passing was a great
Guido Barbagli Center for Reconstructive ti Urethral lsurgery Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it Dedicated to Ruggero Lenzi, teacher and friend. His passing was a great
Inferior Pelvic Border
 Pelvis + Perineum Pelvic Cavity Enclosed by bony, ligamentous and muscular wall Contains the urinary bladder, ureters, pelvic genital organs, rectum, blood vessels, lymphatics and nerves Pelvic inlet (superior
Pelvis + Perineum Pelvic Cavity Enclosed by bony, ligamentous and muscular wall Contains the urinary bladder, ureters, pelvic genital organs, rectum, blood vessels, lymphatics and nerves Pelvic inlet (superior
Guido Barbagli. Center for Reconstructive ti Urethral lsurgery
 Guido Barbagli Center for Reconstructive ti Urethral lsurgery Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it 10 th Mediterranean Congress of Urology 10 and 8 th Congress of Pan African
Guido Barbagli Center for Reconstructive ti Urethral lsurgery Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it 10 th Mediterranean Congress of Urology 10 and 8 th Congress of Pan African
Citation Acta medica Nagasakiensia. 1963, 8(
 NAOSITE: Nagasaki University's Ac Title Radical Operation For Prostatic Car Author(s) Kondoh, Atushi Citation Acta medica Nagasakiensia. 1963, 8( Issue Date 1963-12-25 URL http://hdl.handle.net/10069/15473
NAOSITE: Nagasaki University's Ac Title Radical Operation For Prostatic Car Author(s) Kondoh, Atushi Citation Acta medica Nagasakiensia. 1963, 8( Issue Date 1963-12-25 URL http://hdl.handle.net/10069/15473
Uroradiology For Medical Students
 Uroradiology For Medical Students Lesson 4: Cystography & Urethrography - Part 2 American Urological Association Review Cystography is useful in evaluating the bladder, the urethra and the competence of
Uroradiology For Medical Students Lesson 4: Cystography & Urethrography - Part 2 American Urological Association Review Cystography is useful in evaluating the bladder, the urethra and the competence of
Indwelling Urinary Catheter Template for Care Plan Development Problem No: be a last resort when all suprapubic catheter in CAUTI
 Indwelling Urinary Catheter Template for Care Plan Development Problem No: Name: DOB Address: Indwelling Urinary Catheter (Urethral/ Suprapubic) Date Assessed Need GOAL INTERVENTION Evaluation of intervention/
Indwelling Urinary Catheter Template for Care Plan Development Problem No: Name: DOB Address: Indwelling Urinary Catheter (Urethral/ Suprapubic) Date Assessed Need GOAL INTERVENTION Evaluation of intervention/
Bladder Trauma Data Collection Sheet
 Bladder Trauma Data Collection Sheet If there was no traumatic injury with PENETRATION of the bladder DO NOT proceed Date of injury: / / Time of injury: Date of hospital arrival: / / Time of hospital arrival:
Bladder Trauma Data Collection Sheet If there was no traumatic injury with PENETRATION of the bladder DO NOT proceed Date of injury: / / Time of injury: Date of hospital arrival: / / Time of hospital arrival:
