Another look at human sperm morphology
|
|
|
- Winfred Hubbard
- 5 years ago
- Views:
Transcription
1 Human Reproduction, Vol.31, No.1 pp , 2016 Advanced Access publication on October 14, 2015 doi: /humrep/dev251 ORIGINAL ARTICLE Andrology Another look at human sperm morphology J. Auger 1,2, *, P. Jouannet 3, and F. Eustache 2,4 1 Service d Histologie-Embryologie, Biologie de la Reproduction/CECOS, Hôpitaux Universitaires Paris Centre, Site Port-Royal, 53, Avenue de l Observatoire, Paris, France 2 INSERM U1016, Equipe "Génomique, Epigénétique et Physiologie de la Reproduction", Institut Cochin, Université Paris Descartes, Paris, France 3 Université Paris Descartes, Paris, France 4 Service d Histologie-Embryologie, Cytogénétique, Biologie de la Reproduction/CECOS, Hôpitaux Universitaires Paris Seine-Saint-Denis, Site Jean Verdier, Bondy Cedex, France *Correspondence address. Tel: ; Fax: ; jacques.auger@aphp.fr Submitted on June 17, 2015; resubmitted on August 29, 2015; accepted on September 15, 2015 study question: Can a standardized assessment of abnormal human sperm morphology provide additional useful information by identifying men with more severe disturbances in different types of abnormalities? summaryanswer: Definition-based categorization of sperm head, midpiece and tail defects has shown how differently these abnormalities are distributed in fertile men and other groups of men, thus providing high and low thresholds, a starting point for diagnosis or research purposes. what is known already: Several recent studies have reported indisputable genetic origins for various sperm defects. A few studies have also identified associations between environmental factors and low percentages of morphologically normal spermatozoa. Nevertheless, with the exceptionofrare situations in which thevast majorityof spermatozoa have specific, easily characterized defects, such as globozoospermia, little attention has been paid to the description and precise quantification of human sperm abnormalities. The lack of standardization in the phenotyping of sperm morphological defects by conventional microscopy is a limiting factor for diagnosis and for intra- or inter-observer or centre consistency in studies investigating the causal factors and possible functional consequences of the abnormalities detected. There are currently no baseline data for abnormalities of sperm morphology based on a standardized classification, in the general population, among fertile or other groups of men. study design, size, duration: This study is based on detailed sperm abnormality datasets acquired by a standardized classification method, from several groups of men, over the same 5-year period. participants/materials, setting, methods: We studied cross-sectional data from fertile men (n ¼ 926), male partners from infertile couples (n ¼ 1747) and testicular cancer patients (n ¼ 239). We used a standardized classification to analyse Shorr-stained slides, taking into account all the abnormalities encountered. main results and the role of chance: Most sperm defects were significantly more frequent in infertile than in fertile men, with 20 30% of infertile men having frequencies of abnormalities above the 95th percentile in fertile men for 9 out of the 15 categories of abnormalities. Interestingly, several head abnormalities were significantly more frequent in patients with testicular cancer than in infertile men, highlighting the particular impact of this condition on sperm morphogenesis. We used the 95th percentile in fertile men as the lower threshold and the 99th percentile in infertile men as an extreme upper threshold, for the classification of morphological abnormality frequencies into three levels: low, intermediate and high. The assessment of several semen samples, with or without a genetic background, for abnormal sperm morphology, based on the percentage of normal spermatozoa, a teratozoospermia index, and the detailed profile of abnormalities categorized according to the three levels proposed, has highlighted the value of detailed phenotyping for diagnosis and research purposes. limitations, reasons for caution: The thresholds proposed for the various categories of sperm abnormality should be considered relative rather than absolute, owing to the known sampling error related to the limited number of spermatozoa assessed per sample, or when studying the general population or populations from regions other than Western Europe. The standardized assessment of abnormal sperm morphology requires time and experience. We therefore suggest that this assessment is carried out during a first andrological check-up or for epidemiological or research studies, rather than in the routine management of infertile couples for assisted reproductive technologies. wider implications of the findings: The study design used for the fertile group of men was similar to that previously used for the WHO reference values, providing a rationale for considering the 95th percentile in fertile men as the level below which abnormalities may be considered to occur at a frequency representing random background variations of a normal spermiogenesis process. The crude frequencies obtained, and the & The Author Published by Oxford University Press on behalf of the European Society of Human Reproduction and Embryology. All rights reserved. For Permissions, please journals.permissions@oup.com
2 Abnormal sperm morphology 11 three levels of abnormality frequency proposed for each standardized category of sperm defect, provide baseline data useful for diagnosis and a starting point for future studies aiming to identify associations with genetic or environmental factors. study funding/competing interest(s): Part of this study was supported by contract BMH4-CT from the European Union. The authors have no competing interests to declare. Key words: fertile men / human semen / infertility diagnosis / multiple anomalies index / reference values / sperm defects / standardization Introduction Spermmorphologyassessment, ona stained semen smear, revealsa plethora of morphological variations or abnormalities of the sperm head, midpiece and tail components. These abnormalities primarily reflect the complexity of terminal sperm differentiation following several biochemical and morphological changes (acrosome formation, flagellar development, chromatin condensation and major reorganization of the nucleus and cytoplasm) and the influence of multiple genetic or micro- or macroenvironmental factors modulating or disrupting this crucial stage in morphogenesis. Normal and abnormal sperm cells exhibit a number of features on stained smears studied by conventional microscopy. Various sperm morphology classifications have been proposed from the early 1950s (notably with the remarkable contribution of MacLeod and Gold, 1951) until the 1970s (reviewed in Mortimer and Menkveld, 2001) for categorizing spermatozoa according to these various aspects. Spermatozoa retrieved from the uterine cavity or in the vicinity of oocytes recovered from the female reproductive tract, and thus clearly with the potential to migrate in the female genital tract and to bind to oocytes, were found to be more homogeneous in appearance than those from a native semen sample. This observation helped to define the appearance of potentially fertilizing (morphologically normal) spermatozoa (Menkveld et al., 1990; Liu and Baker, 1992). With the development of assisted reproductive technologies (ART) from the 1980s onwards, initially through IVF and then with the development of ICSI in the 1990s, sperm morphology analysis became important for prognostic reasons, but was mostly restricted to assessments of the proportion of normal spermatozoa (Ombelet et al., 1997). The sperm morphology assessment carried out primarily in the context of ART is generally considered to constitute the cornerstone of such analyses in humans. These methods have been fully endorsed in the WHO laboratory manual for the examination and processing of human semen, as the reference method for assessing human sperm morphology (WHO5: World Health Organization, 2010). Several studies have identified genetic causes of various morphological abnormalities of spermatozoa, such as globozoospermia and macrocephalic sperm, when these abnormalities concern the vast majority of the sperm cells present (Guichaoua et al., 2009), and associations between genetic, lifestyle or environmental factors and abnormal sperm morphology have also been reported (Wyrobek et al., 1983; Buck Louis et al., 2014). However, the precise origins of many of the human sperm abnormalities observed are far from well understood, and the precise impact of these abnormalities on sperm fertility potential also remains unclear. As a consequence, it has recently been suggested that precise analyses of the number of sperm abnormalities by conventional microscopy would be a useful approach for diagnosis or research purposes (Menkveld, 2013; Mitchell et al., 2015). The WHO5 report (World Health Organization, 2010) has come to a similar conclusion, with its statement that categorizing all abnormal forms of spermatozoa may be of diagnostic or research benefit. WHO5 contains a rich iconography on morphological abnormalities of spermatozoa, with legends providing a simple conclusion: normal or abnormal spermatozoon, with comments in some cases, such as pyriform and amorphous head. This document does not propose clear definitions of the various abnormalities of human sperm cells, and the corresponding diagnostic or research benefits are neither demonstrated nor discussed. This limits the morphological evaluations of spermatozoa and comparisons of the results obtained by different observers or in different studies (Wang et al., 2014). We have previously reported and used a method for categorizing normal sperm morphology and the various sperm defects encountered (Auger, 2010), in line with contemporary knowledge of sperm assembly (Chemes and Rawe, 2003), the correspondence between the defects observed on conventional microscopy and transmission electron microscopy (Bisson and David, 1975), and the functional consequences of most of the defects categorized (Chemes and Alvarez Sedo, 2012). One of the principal advantages of such a standardized categorization is the provision of basic data about the distributions of various sperm defects. This study, based on our standardized method, was designed to establish reference ranges for morphological abnormalities of human spermatozoa, through the analysis of three large groups of men: fertile men, infertile men and men with testicular germ cell tumours (TGCTs). Thresholds for future clinical, epidemiological or basic studies are proposed and discussed. Materials and Methods Subjects studied Sperm morphology was assessed in three groups of men: a homogeneous group of fertile men and two different groups of men of unknown fertility status (male partners from infertile couples, referred to hereafter as infertile men for convenience, and men with testicular cancer). The fertile men were the male partners of pregnant women participating in a study investigating possible geographical differences in semen quality (Jørgensen et al., 2001). Each of the men provided a single semen sample. They were recruited from four different European cities in These men had a mean age of 31 years (interquartile range (IQR): years old) and their partners had become pregnant without the need for fertility treatment (e.g. stimulation of ovulation, ART). In the protocol of this international study, sperm morphology was analysed in a centralized manner, in our laboratory, to minimize the well-known wide variability in human morphology assessment by different observers and centres (Ombelet et al., 1998; Eustache and Auger, 2003). A first analysis focusing on geographical variation in sperm morphology and the influence of environmental and lifestyle factors has already been published (Auger et al., 2001), but the distributions of the various sperm abnormalities were not reported. In this study, only sperm morphology was assessed for couples for whom a pregnancy was achieved within 1 year (n ¼ 926), in accordance with the
3 12 Auger et al. methodology used for the definition of the new WHO reference semen values (Cooper et al., 2010). The second population study consisted of male partners from infertile couples referred to the reproductive biology laboratory of Cochin Hospital Paris for routine semen analysis during the same time period. This group of 1747 men, for whom it was not possible to collect information about the duration of infertility of other clinical information in a systematic manner, was older than the fertile men (mean: 36.5; IQR: 32 40). The dataset consisted of the results of all consecutive routine semen analyses, with only the first semen analysis used in cases of repeated analyses for the same patient during the period. The third group of men consisted of patients referred to the reproductive biology laboratory of Cochin Hospital Paris by their urologist or oncologist, during the same time period, for semen cryopreservation before antineoplastic treatment for a TGCT. Semen was collected before orchidectomy (Petersen et al., 1999). These patients were younger than the men in the other two groups (mean: 29.2; IQR: 25 33). Pre-analytical steps in sperm morphology assessment All semen smears were prepared, fixed and stained according to the same standardized procedure. Briefly, smears were prepared from a 10 ml wellmixed drop of semen, which was allowed to dry in air, and then fixed by incubation for 1 h with a mixture of absolute ethanol (2/3) and acetic acid (1/3), before Shorr staining (World Health Organization, 1992) by an automated method (Sakura DRS601, Bayer Diagnostics, Puteaux, France) ensuring the homogeneous staining of different preparations. Methodology used for human sperm morphology classification The method used here for the assessment of human sperm morphology was essentially the original method of classification described by David et al. (1975) and then modified in the late 1990s to provide clear rules for the classification of normal and abnormal spermatozoa and for the categorization of the various sperm defects observed in stained smears through conventional microscopy (Auger et al., 2001). The various morphological categories are shown in Fig. 1, with a summary of the definitions in the figure legend. According to this method, morphologically normal spermatozoa are categorized on the basis of the same criteria proposed by WHO from the third edition of the manual to the recent WHO5 (World Health Organization, 1992, 2010, respectively). However, unlike the WHO5 guidelines, our classification considered all borderline aspects to be normal, as in previous classification systems (Freund, 1966; Eliasson, 1971) and as argued for in previous studies (Auger, 2010). Borderline aspects introduce marked uncertainty into classification systems and are a major component of the overall intra- and inter-observer variability in assessments without categorization rules. In the method used here, a reticle eyepiece with a micrometre was used whenever the observer had doubts about sperm size, in terms, for example, of the lengths of the major axis or the minor axis of the head, and decision-support criteria were defined for distinguishing borderline aspects of size and shape (see Supplementary data, Fig. S1). This method was initially developed for diagnostic purposes. It therefore categorizes the head, midpiece and principal piece defects most frequently observed in human sperm and known to correspond to particular aetiologies or ultrastructural alterations (Chemes and Rawe, 2003). The use of a multi-entry grid, accounting for all abnormalities and their combinations, without underestimating one abnormality with respect to the others (e.g. a sperm cell can have residual cytoplasm in excess as well as a bent tail), makes it possible to calculate an overall indicator of the level of teratozoospermia, the Multiple Anomalies Index (MAI), equal to the mean number of abnormalities per abnormal spermatozoon (Jouannet et al., 1988; World Health Organization, 2010). Our classification considers true excess residual cytoplasm (ERC), but not physiological cytoplasmic droplets (Cooper, 2005), as abnormal. Analytical procedure All stained smears were assigned to a pool of four experienced technicians who assessed them unaware of sample origins, by using the combination of a 100 oil-immersion bright-field objective and 10 eyepiece ( 1000 final magnification). Each of these technicians routinely assesses two to five stained smears daily, and their accuracy and reproducibility in assessments of human sperm morphology, based on the classification described here, are regularly proved to be consistent (an example for IQC is provided in Supplementary data, Table S1). Statistical methods For the three groups of men studied, only data from stained smears for which at least 100 spermatozoa could be classified were analysed. We also compared each abnormality category within each group of men, between men with and without normal sperm production and progressive motility, as defined in WHO5 (normozoospermic men: at least 39 million spermatozoa per ejaculate and at least 32% progressively motile sperm cells; World Health Organization, 2010). Age is not associated with sperm morphology, at least for the years age group (Schwartz et al., 1984). We also found no association between age and the extent of normal or abnormal morphology in the three groups of men studied (data not shown). We therefore did not adjust comparisons for age. All statistical comparisons between fertile men, infertile men and TGCT patients were performed with BMDP statistical software (Statistical Solutions, Cork, Ireland). The similarity of the mean values for the percentages of normal spermatozoa, all morphological defects and MAI values between the three groups was assessed by one-way analysis of variance (BMDP 7D subroutine), taking unequal variances into account (Brown Forsythe test) when necessary. When the null hypothesis was rejected, post hoc Tukey tests were used for pair-wise comparisons between groups of men. Crude datawere used to determine the distribution profiles for each morphological abnormality category, MAI and morphologically normal spermatozoa in the three groups of men studied. The curves best fitting each distribution profile were then constructed with the Fit-curve option of Sigmaplot software (Statistical Solutions). By analogy with the WHO reference thresholds for semen characteristics obtained for a similar population of fertile men (Cooper et al., 2010), we considered the 95th percentile for the various categories of abnormalities and MAI, and the 5th percentile for the percentage of normal spermatozoa in the fertile group as lower reference thresholds. Dichotomous categorization has been shown to be of little overall clinical relevance for semen variables (Björndahl, 2011). We therefore also used a second, experience-based, higher threshold, set at the 99th percentile for the population of infertile men, as an extreme level for the sperm abnormalities considered, potentially with a specific origin and possible pathological implications. We then defined three levels of sperm abnormalities on the basis of these two thresholds: a low level of abnormality (LLA), below the 95th percentile in fertile men; a high level of abnormality (HLA), above the 99th percentile in infertile men and an intermediate level of abnormality (ILA), between the 95th percentile in fertile men and the 99th percentile in infertile men. This ILA is probably nonrandom, particularly if it tends to increase towards extreme values. A preliminary validation of the utility of the three levels of abnormality proposed was made on a sample of six men, one of whom was fertile, the other five having specific teratozoospermia profiles with a known genetic background. Ethical approval The study was approved by the Cochin University Hospital for the three groups of French men studied and by all collaborating institutions for the fertile men from other European countries. Informed consent was obtained from all participants.
4 Abnormal sperm morphology 13 Figure 1 Standardized classification of normal and abnormal human sperm morphology. Morphologically normal spermatozoa are defined as in the 5th WHO manual (World Health Organization, 2010) except that all borderline aspects are considered normal (decision rules for borderline aspects are presented in Supplementary data, Figure S1); tapered head: increased major axis length and normal minor axis length; thin head: normal major axis length and decreased minor axis length; microcephalic: decreased major and minor axes lengths; macrocephalic: increased major and minor axes lengths; multiple heads: more than one head per sperm cell; abnormal post-acrosomal region: any type of outline and/or size and/or texture abnormality of the posterior part of the head; abnormal acrosomal region: any type of outline and/or size and/or texture abnormality of the anterior part of the head; abnormal (or excess) residual cytoplasm (or abnormal cytoplasmic remnant): residual cytoplasmic area. 30% of the head area, in any part of the sperm cell; thin midpiece: midpiece diameter, smaller than the principal piece diameter for. 40% of the whole midpiece length; bent/misaligned tail: may include neck anomalies, misalignment of the head major axis and midpiece axis or an acute angle ( 1208) between the head major axis and midpiece axis or an acute angle ( 1208) between the midpiece and the principal piece axes ; no tail: isolated head, no tail observed; short tail: a tail length (midpiece + principal piece) no more than five times the major axis length of the head; irregularly shaped tail: irregular or changing calibre along the tail; coiled tail: completely or partially coiled tail, with the coil close to or around the head (flat coiling or coiling atthe extremity of the tail reminiscent of hypo-osmotic coiling aspects should not be included in this category); multiple tails: more than one tail per sperm cell. Many of the spermatozoa presented more than one type of abnormality. The classification method encompasses all the abnormalities of each cell and the calculation of multiple anomalies index (MAI) (World Health Organization, 2010).
5 14 Auger et al. Results Fertile men Distributions of morphologically normal spermatozoa and of the various categories of sperm abnormality percentage and of MAI in the 926 fertile men are presented in Table I. The 5th percentile for the percentage of normal spermatozoa including all borderline aspects was 23% (95% CI, 20 26). Head abnormalities were more frequent than midpiece and principal piece defects. Texture or outline abnormalities of the acrosomal or post-acrosomal regions were markedly more frequent among head abnormalities than head size abnormalities. Bent and coiled tails were the most frequent flagellar abnormalities and were observed in most samples. In most fertile men, abnormal sperm cells generally had fewer than two associated abnormalities (95th percentile of MAI ¼ 1.92). Comparison of fertile men, infertile men and TGCT patients The distribution profiles of the percentages of normal spermatozoa, all morphological sperm abnormalities and MAI, in fertile men, infertile men and TGCT patients, are presented in Fig. 2. The distribution of the percentage of morphologically normal spermatozoa was essentially Gaussian in the three populations, but with a sharp shift towards lower values in infertile men and TGCT patients. More than 50% of TGCT patients and almost 40% of infertile men had a percentage of morphologically normal spermatozoa below the 5th percentile for fertile men. The frequency of each morphological abnormality was significantly higher in infertile men and TGCT patients than in fertile men. In the three groups of men studied, the distributions of the incidence of abnormal post-acrosomal regions, abnormal acrosomal regions, bent or misaligned midpieces, coiled tails and of the MAI were also almost Gaussian, but the curves were displaced to the right for infertile men and TGCT patients in comparison with the curve for fertile men. Other categories of sperm abnormalities followed an exponential decay distribution profile that was generally less steep in infertile men and TGCT patients than in fertile men. More than a quarter of TGCT patients had values above the 95th percentile for fertile men, for the categories microcephalic sperm cells, abnormal post-acrosomal and acrosomal regions, ERC and short tail. Similarly, more than a quarter of the male partners from infertile couples had a frequency of abnormalities greater than that of fertile men for the categories abnormal postacrosomal and acrosomal regions, thin midpiece, bent or misaligned midpiece and short tail. In addition, some sperm defects, microcephalic sperm cells, macrocephalic sperm cells, abnormal acrosomal regions and ERC, were significantly more frequent in TGCT patients than in infertile men. The MAI value was higher than the 95th percentile for fertile men in 47% of TGCT patients and in 28% of infertile men. Interestingly, in comparisons restricted to normozoospermic men, significant differences were still found between the three groups studied, for most of abnormality categories (Table II). The usefulness of the proposed three levels of abnormality The broad overlap between the distribution profiles of the various morphological abnormalities in fertile and infertile men precluded the Table I Distributions of morphologically normal spermatozoa (including borderline cells) and categories of spermatozoa with head, midpiece and principal piece abnormalities, in 926 fertile men. Distribution range (percentiles)... 1st 5th [95% CI] 10th 25th 50th 75th 90th 95th... Normal spermatozoa [20 26] Sperm defect categories * 99th 95th [95% CI] 90th 75th 50th 25th 10th 5th Tapered head 7 3 [2 4] Thin head [12 16] Microcephalic 11 7 [5 9] Macrocephalic 3 1 [0 2] Multiple heads 4 2 [1 3] Abnormal post-acrosomal region [39 45] Abnormal acrosomal region [57 63] Excess residual cytoplasm 8 4 [3 5] Thin midpiece Bent or misaligned tail [11 15] No tail 9 5 [4 6] Short tail 4 1 [0 2] Irregularly shaped tail 5 2 [1 3] Coiled tail [15 19] Multiple tails 3 1 [0 2] Multiple Anomalies Index (MAI) * See Fig. 1 for definitions.
6 Abnormal sperm morphology 15 Figure 2 Curves best fitting the distributions of the various sperm morphology characteristics assessed in fertile male partners of pregnant women (black line), male partners form infertile couples (blue line) and TGCT patients (red line). The vertical line represents the 95th percentile threshold in fertile men (5th percentile for the percentage of morphologically normal spermatozoa), and the percentages in blue and red represent the percentages for infertile men and TGCT patients, respectively, above the 95th percentile threshold (below the 5th percentile threshold for the percentage of normal spermatozoa). (A) Head abnormalities, (B) midpiece and principal piece abnormalities, (C) Multiple Anomalies Index (MAI) and normal spermatozoa.
7 16 Auger et al. Figure 2 Continued.
8 Abnormal sperm morphology 17 Figure 2 Continued. definition of a single meaningful threshold for each abnormality category. We found that the experience-based threshold chosen for the definition of the HLA category (the 99th percentile in the population of infertile men) differed considerably between abnormalities. For example, it was 95% for abnormal acrosomal regions, but only 5% for macrocephalic spermatozoa and 4% for a thin midpiece (Table III). Similarly, the threshold defining LLA (the 95th percentile for the population of fertile men) was 3% for seven morphological abnormalities (tapered head, macrocephalic sperm, multiple heads, thin midpiece, short tail, irregularly shaped tail and multiple tails), but as high as 60% for abnormal acrosomal regions (Table III). Figure 3 illustrates the possible relevance of the three levels of abnormality proposed for diagnosis or research purposes. It shows the sperm morphology profiles for six men, one of whom was fertile, the other five being infertile with several types of characterized teratozoospermia of known genetic origin. The graphical representation of the abnormal morphology profile shows both the exact level of each category of abnormality and the relative level according to the defined three-level/colour ranges of abnormalities taken from the thresholds defined in the distributions in large groups of fertile and infertile men. This figure demonstrates that, in such clinical situations, the simple recording of the percentage of normal spermatozoa or the determination of MAI is not informative for diagnosis (see Fig 3A, B and D). In contrast, the different categories of abnormality level low (LLA), high (HLA) or intermediate (ILA) based on the frequencies determined according to our standardized definitions for each category of abnormality, provided a clear picture of the morphological background noise (LLA for all abnormalities) characteristic of fertile men, or of the combination of high levels of head or midpiece or principal piece defects characterizing particular pathological morphologies. Examples C and D refer to well-known genetic monomorphic syndromes (note the normal MAI) that are easily discernible. Examples E and F show more complex profiles (several yellow and red categories and a high MAI) that deserve investigations. A recent study has shown the genetic origin of the combination of the various tail defects; here we show that noticeable levels of defects of the head or midpiece compartment may be associated with tail defects suggesting a possible different genetic origin. In addition, examples in Fig. 3 show that: (i) a relatively high percentage of certain abnormalities may correspond to LLA and therefore has little meaning as for the abnormality Abnormal postacrosomal region ( 25 30%, see A, D, B); (ii) a relatively low percentage of certain abnormalities may correspond to HLA and therefore has an important meaning, for example Thin midpiece or Irregular tail (B, for both) and (iii) some semen samples may have a rate of morphologically normal spermatozoa in the normal limits but may have a HLA for some categories of anomalies (D and B). These examples provide an indication of the potential usefulness of this approach for future studies aiming to identify similar or new specific profiles related to genetic or environmental factors. Discussion This study is the first to report the distribution of various head, midpiece and principal piece defects encountered in human spermatozoa in large groups of fertile men, infertile men and patients with a testicular cancer, through the use of a standardized classification method. For all the characteristics studied, the distributions observed for infertile men and TGCT patients deviated from that for fertile men, with several abnormality categories even displaying significantly higher frequencies in TGCT patients than in infertile men. Information obtained from a standardized detailed sperm morphology assessment The incidence of tapered heads was low in all three groups and lower than published values (Andrade-Rocha, 2007), possibly due to the lack of a precise definition of tapered heads in other studies (thin heads or amorphous head shapes may have been included). Thin heads (normal sperm head length but narrower width) have rarely been described, probably owing to confusion with tapered heads. Thin heads were more frequently observed in infertile patients and men with TGCT and may reflect abnormal nuclear morphogenesis (Auger et al., 1990) and fragmented DNA (Gandini et al., 2000). The relatively high incidence of this abnormality in fertile men is probably dependent on complex, multiple, environmental factors rather than genetic determinants. A high incidence of thin heads has been reported in varicocele (Prasivoravong et al., 2014) and experimental cryptorchidism (Mieusset et al., 1987).
9 18 Auger et al. Table II Comparison of men with a normal total sperm count and motility according to World Health Organization (2010) criteria, for the various standardized sperm morphological categories. Fertile men Infertile men TGCT patients F-Value P-Value n n n Normal spermatozoa * *, ** 291, (41 62) 37 (24 48) 28 (20 38) Tapered head * * 18, (0 1) 0(0 1) 1(0 2) Thin head * * 55, (1 7) 5 (2 10) 7 (3 11) Microcephalic * *, ** 89, (1 3) 3 (1 6) 6 (2 13) Macrocephalic *, ** 8, (0 0) 0(0 0) 0(0 1) Multiple heads * , (0 1) 0(0 1) 0(0 1) Abnormal post-acrosomal region * * 115, (12 28) 28 (17 40) 29 (20 41) Abnormal acrosomal region * *, ** 165, (22 41) 40 (29 54) 56 (43 67) Excess residual cytoplasm * *, ** 105, (0 1) 1(0 3) 3(1 5) Thin midpiece * * 31, (0 0) 0(0 0) 0(0 0) Bent or misaligned tail * *, ** 140, (3 8) 8 (6 12) 6 (4 11) No tail NS 1 (0 2) 1(0 2) 1 (0 2) Short tail * * 68, (0 0) 0(0 1) 0(0 2) Irregularly shaped tail * * 51, (0 1) 0(0 2) 0(0 1) Coiled tail * * 21, (3 8) 7 (4 11) 6 (3 11) Multiple tails * * 32, (0 1) 0(0 1) 0(0 1) Multiple Anomalies Index (MAI) * *, ** 127, ( ) 1.71 ( ) 1.78 (1.62 2) Mean + SD. Median (IQ range). For each morphological category, differences between the three groups of men were investigated by one-way analysis of variance taking unequal variances into account (Brown Forsythe test). For pair-wise comparisons, post hoc Tukey tests were carried out, with: *P,0.01 in comparisons with fertile men, **P,0.01 in comparisons with infertile men For both situations, it was found to decrease a few months after exposure. Microcephalic spermatozoa which have an immature chromatin (Karaca et al., 2014), a high level of DNA fragmentation (Tang et al., 2010) and even abnormal nuclear protein profiles (Blanchard et al., 1990) were two to three times more frequent in infertile than in fertile men, as previously reported (Kalahanis et al., 2002). This frequency was also higher in TGCT patients than in infertile men. The incidence of macrocephalic sperm cells was low in all three groups as reported in infertile men in a study based on the same classification (Guichaoua et al., 2009). In this series, the maximal incidence was 12%. Higher frequencies are rarely observed and such cases result from specific gene deficiencies (Achard et al., 2007). Abnormalities of the acrosomal and post-acrosomal regions were more frequent in infertile than in fertile men. The frequency of abnormal acrosomal region was higher in TGCT patients than in infertile men suggesting an additional role of TGCT-related causal factors. The broad distributions of acrosomal and post-acrosomal abnormalities whose definitions include size or form or texture defects may reflect various aspects of sperm head morphogenesis possibly due to multiple micro-environmental and genetic factors. The incidence of true ERC, not including physiological cytoplasmic droplets (Cooper, 2005), was very low in fertile men and between the 75th and 95th percentile values of fertile men in unselected infertile men. It was more homogeneously distributed in TGCT patients with a higher mean value close to the 95th percentile for fertile men and higher than in infertile men. TGCT may affect spermiogenesis, and this high frequency may reflect Sertoli cell dysfunction in these patients
10 Abnormal sperm morphology 19 Table III Low, intermediate and high levels abnormalities (LLA, ILA and HLA, respectively) for each sperm abnormality category based on the distributions in 926 male partners of pregnant women (F) and 1747 male partners from infertile couples (I). Morphology characteristic Level of abnormality... LLA ( 95th ILA (>95th percentile F; 99th HLA (>99th percentile I) percentile F) percentile I) (max value) *... Tapered head (50) Thin head (68) Microcephalic (72) Macrocephalic (12) Multiple heads (33) Abnormal post-acrosomal region (95) Abnormal acrosomal region (99) Excess residual cytoplasm (44) Thin midpiece (17) Bent or misaligned midpiece (36) No tail (31) Short tail (57) Irregularly shaped tail (34) Coiled tail (71) Multiple tails (8) * Maximum values observed in this series. (Russell et al., 1989). However, it remains unclear whether and how this disease interferes with sperm morphogenesis. Most infertile men had an incidence of ERC below 20%. Only a few cases had a markedly higher frequency of ERC, from 30 to 44%, probably corresponding to a highly specific context or causal factor. In these extreme cases, the high incidence of ERC may jeopardise fertilizing potential due to the ability of sperm with ERC to generate high levels of ROS (Rengan et al., 2012). A bent midpiece showed a higher incidence than other midpiece and principal piece abnormalities (95th percentile value of 13% for fertile men). This may partly reflect the inclusion in the same category of midpieces bent at the neck or principal pieces and misalignments, and it may hide more subtle differences between the groups of men studied. In a study based on the same approach, the incidence of bent midpiece was increased during and decreased after experimental cryptorchidism (Mieusset et al., 1987). With the exception of an absent tail, the incidence of principal piece abnormalities was higher in infertile men and TGCT patients than in fertile men. Detailed high-magnification examination, by light microscopy, of flagellar morphology on semen smears obtained and stained according to a rigorous procedure (World Health Organization, 2010) can be used to detect pathological or genetic conditions when a certain category of tail abnormality is present at high frequency by the approach described here (Mitchell et al., 2015), or by the detection of associations of various tail abnormalities at high levels. For example, an abnormal frequency of thick or irregular tails of normal length, as observed by light microscopy, has led to the description of a new type of sliding spermatozoa, characterized by periaxonemal defects at the TEM level (Feneux et al., 1985). Men with sperm cells presenting a combination of five morphological defects of the sperm tail, as categorized in our study, were found to have mutations of DNAH1 encoding an inner arm heavy chain dynein (Ben khelifa et al., 2014). According to our definition, coiled tails category includes coiling with the head inside or outside the coils, two forms of coiling with different origins (Yeung et al., 2009). The incidence of all coiled tails in the infertile population, with a mean value of 10%, was similar to that reported by Yeung et al. (3% head-in-coil and 8% other coiled sperm) for a comparable population and higher than in the fertile men studied (mean ¼ 6.5%). The percentage of men with more than 20% of spermatozoa with coiled tails was 10% for infertile men and 11% for TGCT patients, an incidence similar to that reported by Yeung and co-workers. This abnormality is positively associated with heavy smoking, and may fluctuate with levels of neutral a-glucosidase, suggesting the negative influence of a deleterious epididymal environment (Yeung et al., 2009). The incidence of multiple tails was very low in all three populations, typically below 1%, the maximum incidence in this series being 8%. A higher incidence, which may affect the vast majority of the spermatozoa, is rare and associated with macrocephalic heads in the macrocephalic sperm syndrome caused by homozygous mutations of the aurora kinase C gene (Dieterich et al., 2007). Clinical relevance of a standardized and detailed assessment of normal and abnormal sperm morphology The 5th percentile value of normal spermatozoa in our population of fertile men, taken as the reference threshold, as in WHO5, was 23%. The similarity in the groups of fertile men studied here and in the study by Cooper et al. (2010) made it possible to compare our 23% threshold with the 4% threshold obtained using the WHO5 criteria that consider all
11 20 Auger et al. Figure 3 Examples of six profiles of morphological sperm abnormalities with the corresponding percentage of normal spermatozoa and MAI, based on the standardized classification, with a representation of low (green), intermediate (yellow) and high (red) levels of abnormality, based on the distributions in fertile and infertile men (see Statistical methods). (A) A fertile man with low levels of abnormality; (B) an infertile patient with a normal frequency of normal spermatozoa and MAI despite an abnormally high level of double-headed spermatozoa; (C) an infertile patient with a globozoospermia-like profile (Guichaoua et al., 2009) and no normal sperm cell, and a relatively low MAI due principally to very high levels of microcephalic sperm cells, essentially combined with an abnormal acrosomal region; (D) an infertile patient with fibrous sheath dysplasia (Chemes et al., 1987), despite normal levels for the percentage of normal spermatozoa and MAI; (E) an infertile patient with high levels of multiple morphological abnormalities of the flagella (Ben Khelifa et al., 2014) and an exceptionally high level of thin midpieces, resulting in low numbers of normal spermatozoa and a high MAI; (F) an infertile patient with MMAF together with high levels of thin and microcephalic heads resulting in a very high MAI. ERC, excess residual cytoplasm; DFS, dysplasia of the fibrous sheath; MMAF, multiple morphological abnormalities of the flagella.
12 Abnormal sperm morphology 21 borderline aspects to be abnormal. The marked difference between these two values could correspond primarily to the inclusion or exclusion of the borderline aspects in the normal sperm categorization (Eliasson, 2010; Handelsman and Cooper, 2010). The use of a set of criteria for borderline aspects (Rothmann et al., 2013) could be useful in answering the question of whether the borderline aspects per se matter or not. A recent epidemiological study (Buck Louis et al., 2014) showed that normal sperm morphology, whether according to the traditional WHO approach (including borderline forms) or to the strict criteria (excluding borderline forms, as in WHO5), displays a similar level of association with time to pregnancy. However, a possible bias in this study cannot be ruled out, because a given laboratory does not generally use both approaches during routine semen analysis. Using the 5th percentile value of normal spermatozoa in fertile men as a threshold, more than one-third of unselected infertile men and half of TGCT patients were below this threshold. No such discrimination was reported when using the strict criteria classification, for comparisons of fertile men and selected infertile men (Guzick et al., 2001) or with use of the reported 4% threshold for morphologically normal sperm cells according to the pregnancy rate in IUI (Deveneau et al., 2014). The incidence of various sperm abnormalities or the resulting MAI may be associated with the probability of pregnancy (Jouannet et al., 1988; Slama et al., 2002; Buck-Louis et al., 2014). However, this does not imply that a single category of abnormalities considered independently of other co-variables could serve as a powerful fertility prognostic tool. Thus, none of the abnormality categories studied can be used in isolation, to discriminate, with high specificity and sensitivity, between the male partners of pregnant women, and infertile men or testicular cancer patients, as previously reported for other semen characteristics (Ombelet et al., 1997; Björndahl, 2011). However, high frequencies of some crucial categories of abnormalities may reflect overall changes to the spermiogenic process, with functional consequences resulting in a lower probability of natural conception within a short period of time (Jouannet et al., 1988), or a lower rate of fertilization (Jeulin et al., 1986). This should be borne in mind in the management of infertile couples. Is it reasonable to determine the profile of all morphological abnormalities systematically in ART? Indeed, the standardized assessment of sperm abnormalities requires attention to detail, rather than a simple dichotomous classification of normal and abnormal spermatozoa. Training and quality control are required (Eustache and Auger, 2003). In our experience, acceptable levels of variability can be achieved after an initial period of theoretical and practical training no longer than that for the evaluation of sperm motility. Quality controls (e.g. in Supplementary data, Figure S1) indicate non-critical variations provided that regular quality controls ensure the maintenance of competence (the episodic discrepancies observed are no greater for the assessment of sperm defects than for normal sperm assessments). A detailed standardized assessment of morphology abnormalities could be recommended for the first andrology check-up for infertile couples, regardless of whether ART is to be carried out. It may be useful if carried out in addition to an andrological check-up in which medical history, lifestyle factors and work environment are considered. In contrast, owing to the known stability of sperm morphological features, a detailed morphological assessment is not required in the subsequent follow-up or during ART. However, if a factor (fever, medication, temporary exposure to toxicants etc.) is thought to have influenced the sperm morphological profile, a repeat assessment should be considered. Towards a new quantification of sperm abnormalities for clinical and research purposes We propose three levels of defects based on the percentiles for fertile and infertile men: a low level 95th percentile for fertile men; an intermediate level.95th percentile for fertile men and,99th percentile for infertile men and a high level 99th percentile for infertile men. This three-level stratification of morphological abnormalities is potentially useful for studies considering genetic determinants or the role of environmental factors capable of disrupting sperm morphogenesis, as illustrated in Fig. 3. The low level of abnormality essentially corresponds to non-specific background noise. In contrast, the HLA, which excludes most fertile men and corresponds to extreme values in the infertile population, may be considered a biomarker of a causal genetic or environmental factor requiring investigation. Despite, the large overlap between fertile and infertile men with intermediate levels of abnormality, the intermediate category should not be considered as a random signal in any of the male populations studied (see Fig. 3E and F). The potential of a standardized assessment of sperm defects for epidemiological, genetic and basic studies A few studies have reported associations between the extent of various sperm defects and pathological conditions, such as varicocele or cryptorchidism (Auger et al., 2001; Andrade-Rocha, 2007; Cakan et al., 2008), environmental or occupational exposures (Bigelow et al., 1998; Gebreegziabher et al., 2004; Hansen et al., 2010). However, the imprecise definition of sperm defects in most of these studies constitutes a confounding factor. An interesting alternative approach for basic or epidemiological studies is the combination of light microscopy with computer vision, which is highly accurate and precise, provided that preanalytical and analytical set-ups are optimized (Bellastella et al., 2010). Several reports have demonstrated the relevance of this approach for such studies (Schrader et al., 1990; Fenster et al., 1997). The measurement of various morphometric features of all sperm cells and the visual estimation of well-characterized abnormalities may be complementary approaches as recently reported (Buck Louis et al., 2014). However, it should be pointed out that computer vision is mainly applied for the measurement of a set of features mainly of the sperm head compartment, and not the midpiece and principal piece. In contrast, the visual approach, although not allowing precise and reproducible measurements of the various sperm compartments, is more appropriate than computer vision for pattern recognition of an entire sperm cell. Overall, the choice of the method used depends on the laboratory equipment (only a minority of reproductive laboratories have analytical cytometry facilities) and of the aims of the study (Auger, 2010, for a detailed comparison of the advantages and limits of visual and computer-aided approaches). Only rare morphological syndromes such as globozoospermia, macrocephalia, decapitated sperm syndrome and fibrous sheath dysplasia have been described in men consulting for infertility, and several causal mutations have been identified (Coutton et al., 2015). However, these mutations do not account for all cases and the variability of clinical forms observed suggests that other mutations or other genes may be involved. Partial forms of these syndromes in which apparently normal spermatozoa coexist with those of the morphological type of interest are less rarely
Importance of Papanicolaou Staining for Sperm Morphologic Analysis Comparison With an Automated Sperm Quality Analyzer
 Anatomic Pathology / Pap Staining for Sperm Morphologic Analysis Importance of Papanicolaou Staining for Sperm Morphologic Analysis Comparison With an Automated Sperm Quality Analyzer Smita Singh, MD,
Anatomic Pathology / Pap Staining for Sperm Morphologic Analysis Importance of Papanicolaou Staining for Sperm Morphologic Analysis Comparison With an Automated Sperm Quality Analyzer Smita Singh, MD,
The new 5 th WHO manual semen parameter reference values do they help or hinder?
 The new 5 th WHO manual semen parameter reference values do they help or hinder? Roelof Menkveld, PhD Andrology Laboratory, Department of Obstetrics and Gynaecology, Tygerberg Academic Hospital and University
The new 5 th WHO manual semen parameter reference values do they help or hinder? Roelof Menkveld, PhD Andrology Laboratory, Department of Obstetrics and Gynaecology, Tygerberg Academic Hospital and University
Computer Assisted Semen Analysis. M i r a S p e r m A n a l y z e r
 Computer Assisted Semen Analysis M i r a 9 S p e r m A n a l y z e r CASA Mira9 Sperm Analyzer Mira9 (CASA) Specifications System Components 1. PC include Mira9 CASA software. 2. Mira9 special slide. 3.
Computer Assisted Semen Analysis M i r a 9 S p e r m A n a l y z e r CASA Mira9 Sperm Analyzer Mira9 (CASA) Specifications System Components 1. PC include Mira9 CASA software. 2. Mira9 special slide. 3.
Testosterone Therapy-Male Infertility
 Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Microscope Requirements
 SEMEN EVALUATION EQUIPMENT Microscope Requirements Good quality lenses Phase-contrast preferred for % progressive motility evaluations Objectives 10X, 20X*, 40X*, 100X, minimum Heated stage preferred *Preferably
SEMEN EVALUATION EQUIPMENT Microscope Requirements Good quality lenses Phase-contrast preferred for % progressive motility evaluations Objectives 10X, 20X*, 40X*, 100X, minimum Heated stage preferred *Preferably
Characterization of Human Sperm Components for an Accu. an Accurate Morphological Analysis. Violeta Chang. June, 2014
 Characterization of Human Sperm Components for an Accurate Morphological Analysis Department of Computer Science University of Chile June, 2014 Outline 1 Introduction The Basic Problem That We Studied
Characterization of Human Sperm Components for an Accurate Morphological Analysis Department of Computer Science University of Chile June, 2014 Outline 1 Introduction The Basic Problem That We Studied
DNA FRAGMENTATION INDEX (DFI) OF HUMAN SEMEN BY MODIFIED ANILINE BLUE METHOD
 DNA FRAGMENTATION INDEX (DFI) OF HUMAN SEMEN BY MODIFIED ANILINE BLUE METHOD *Patil P., Bambulkar S., Ajgaonkar S., Patil R., Patil A. and Nikam V. Department of Anatomy, D Y Patil Medical College and
DNA FRAGMENTATION INDEX (DFI) OF HUMAN SEMEN BY MODIFIED ANILINE BLUE METHOD *Patil P., Bambulkar S., Ajgaonkar S., Patil R., Patil A. and Nikam V. Department of Anatomy, D Y Patil Medical College and
Time to pregnancy and semen parameters: a cross-sectional study among fertile couples from four European cities
 Human Reproduction Vol.17, No.2 pp. 503 515, 2002 Time to pregnancy and semen parameters: a cross-sectional study among fertile couples from four European cities R.Slama 1,11, F.Eustache 2, B.Ducot 1,
Human Reproduction Vol.17, No.2 pp. 503 515, 2002 Time to pregnancy and semen parameters: a cross-sectional study among fertile couples from four European cities R.Slama 1,11, F.Eustache 2, B.Ducot 1,
Soft Computing for Human Spermatozoa Morphology
 Soft Computing for Human Spermatozoa Morphology Jia Lu Computer Science and Information System, University of Phoenix, U.S.A 5050 NW 125 Avenue, Coral Spring, FL 33076, USA Yunxia Hu Department of Health
Soft Computing for Human Spermatozoa Morphology Jia Lu Computer Science and Information System, University of Phoenix, U.S.A 5050 NW 125 Avenue, Coral Spring, FL 33076, USA Yunxia Hu Department of Health
Information Sheet. Male Infertility
 Infertility National Public Awareness Campaign Information Sheet Male Infertility In approximately half of couples complaining of infertility part of the problem lies with the male. Male infertility has
Infertility National Public Awareness Campaign Information Sheet Male Infertility In approximately half of couples complaining of infertility part of the problem lies with the male. Male infertility has
Animal Science 434. Sperm Head. Sperm From Different Species. Sperm Structure. Epididymis, Ejaculation and Semen. Head Acrosome Neck Middle Piece
 Sperm Structure Head Acrosome Neck Middle Piece Animal Science 434 Annulus Principal Piece Epididymis, Ejaculation and Semen End Piece Sperm From Different Species Sperm Head (Equatorial Segment) Nucleus
Sperm Structure Head Acrosome Neck Middle Piece Animal Science 434 Annulus Principal Piece Epididymis, Ejaculation and Semen End Piece Sperm From Different Species Sperm Head (Equatorial Segment) Nucleus
Optimize your success
 ANDROLOGY BY ORIGIO Optimize your success by selecting the highest quality sperm QUALITY CONTROL OOCYTE RETRIEVAL ANDROLOGY & IUI FERTILIZATION CULTURE PGD & PGS CRYOPRESERVATION EMBRYO TRANSFER The importance
ANDROLOGY BY ORIGIO Optimize your success by selecting the highest quality sperm QUALITY CONTROL OOCYTE RETRIEVAL ANDROLOGY & IUI FERTILIZATION CULTURE PGD & PGS CRYOPRESERVATION EMBRYO TRANSFER The importance
Computer-aided evaluation of assessment of grade a spermatozoa by experienced technicians
 Computer-aided evaluation of assessment of grade a spermatozoa by experienced technicians Trevor G. Cooper, Ph.D., and Ching-Hei Yeung, Ph.D. Institute of Reproductive Medicine of the University of Münster,
Computer-aided evaluation of assessment of grade a spermatozoa by experienced technicians Trevor G. Cooper, Ph.D., and Ching-Hei Yeung, Ph.D. Institute of Reproductive Medicine of the University of Münster,
To General Embryology Dr: Azza Zaki
 Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Semen analysis report. 2nd symposium of Croatian Society of Clinical Embryologist and Andrology Workshop, Opatija, November, 2014
 Semen analysis report 2nd symposium of Croatian Society of Clinical Embryologist and Andrology Workshop, Opatija, 28-30 November, 2014 No single test or sperm parameter was found to be absolute in its
Semen analysis report 2nd symposium of Croatian Society of Clinical Embryologist and Andrology Workshop, Opatija, 28-30 November, 2014 No single test or sperm parameter was found to be absolute in its
By Dr.Burde Kaustubh Girish DNB Narayana Hrudayalaya
 By Dr.Burde Kaustubh Girish DNB Narayana Hrudayalaya The DNA is packed in sperm in a volume that is less than 10% somatic cell nucleus During spermatogenesis, DNA is initially packaged by histones Following
By Dr.Burde Kaustubh Girish DNB Narayana Hrudayalaya The DNA is packed in sperm in a volume that is less than 10% somatic cell nucleus During spermatogenesis, DNA is initially packaged by histones Following
Seminal fluid analysis
 What is semen? Semen is the fluid formed at ejaculation. Made of secretions of all the accessory glands of the male genital tract and testicular sperm component Semen quality is maintained by all the accessory
What is semen? Semen is the fluid formed at ejaculation. Made of secretions of all the accessory glands of the male genital tract and testicular sperm component Semen quality is maintained by all the accessory
ICSI FROM FRESH TESE IN ABSOLUTE ASTHENOZOOSPERMIA: AN OPTION OR SOLUTION?
 ICSI FROM FRESH TESE IN ABSOLUTE ASTHENOZOOSPERMIA: AN OPTION OR SOLUTION? Mirco Castiglioni 1 Benedetta Scarselli 2 Valentina Zambelli 2 Giovanni M. Colpi 1 1) Andrological Urology & IVF Unit (Director:
ICSI FROM FRESH TESE IN ABSOLUTE ASTHENOZOOSPERMIA: AN OPTION OR SOLUTION? Mirco Castiglioni 1 Benedetta Scarselli 2 Valentina Zambelli 2 Giovanni M. Colpi 1 1) Andrological Urology & IVF Unit (Director:
FACT SHEET. Failure of Ovulation Blocked or Damaged Fallopian TubesHostile Cervical Mucus Endometriosis Fibroids
 FACT SHEET Overview of infertility If getting pregnant has been a challenge for you and your partner, you're not alone. Ten to 15 percent of couples in the Lithuania are infertile. Infertility is defined
FACT SHEET Overview of infertility If getting pregnant has been a challenge for you and your partner, you're not alone. Ten to 15 percent of couples in the Lithuania are infertile. Infertility is defined
Influence of Oxidative Stress on Functional Integrity of Human Spermatozoal Membrane.
 The Journal of Obstetrics and Gynecology of India, March / April 2011 pg 195-199 Original Article Influence of Oxidative Stress on Functional Integrity of Human Spermatozoal Membrane. Chaudhari Ajay 1,
The Journal of Obstetrics and Gynecology of India, March / April 2011 pg 195-199 Original Article Influence of Oxidative Stress on Functional Integrity of Human Spermatozoal Membrane. Chaudhari Ajay 1,
Elena Moretti, Ph.D., Nicola Antonio Pascarelli, Ph.D., Maria Grazia Federico, Ph.D., Tommaso Renieri, Ph.D., and Giulia Collodel, Ph.D.
 CASE REPORT Abnormal elongation of midpiece, absence of axoneme and outer dense fibers at principal piece level, supernumerary microtubules: a sperm defect of possible genetic origin? Elena Moretti, Ph.D.,
CASE REPORT Abnormal elongation of midpiece, absence of axoneme and outer dense fibers at principal piece level, supernumerary microtubules: a sperm defect of possible genetic origin? Elena Moretti, Ph.D.,
Sergey I. Moskovtsev and Clifford L. Librach
 Chapter 2 Methods of Sperm Vitality Assessment Sergey I. Moskovtsev and Clifford L. Librach Abstract Sperm vitality is a re fl ection of the proportion of live, membrane-intact spermatozoa determined by
Chapter 2 Methods of Sperm Vitality Assessment Sergey I. Moskovtsev and Clifford L. Librach Abstract Sperm vitality is a re fl ection of the proportion of live, membrane-intact spermatozoa determined by
Determination of the ultrastructural pathology of human sperm by atomic force microscopy
 FERTILITY AND STERILITY VOL. 75, NO. 5, MAY 2001 Copyright 2001 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Determination of the ultrastructural
FERTILITY AND STERILITY VOL. 75, NO. 5, MAY 2001 Copyright 2001 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Determination of the ultrastructural
Rodriguez The Semen Analysis
 RODRIGUEZ 2016 Rodriguez 2016 The Semen Analysis DISCLOSURE "Yo divulgo que no tengo relación financiera con intereses comerciales". RODRIGUEZ 2016 Question1 Fill the Blanks with the Correct Statement
RODRIGUEZ 2016 Rodriguez 2016 The Semen Analysis DISCLOSURE "Yo divulgo que no tengo relación financiera con intereses comerciales". RODRIGUEZ 2016 Question1 Fill the Blanks with the Correct Statement
Lack of a head in human spermatozoa from sterile patients: a syndrome associated with impaired fertilization*
 FERTILITY AND STERILITY Copyright 1987 The American Fertility Society Printed in U.8A. Lack of a head in human spermatozoa from sterile patients: a syndrome associated with impaired fertilization* Hector
FERTILITY AND STERILITY Copyright 1987 The American Fertility Society Printed in U.8A. Lack of a head in human spermatozoa from sterile patients: a syndrome associated with impaired fertilization* Hector
The spermatogenesis CHARACTERISTICS OF THE SPERMATOZOON 26/04/2017. Reproductive Biotechnologies Andrology I. Prof. Alberto Contri
 Reproductive Biotechnologies Andrology I The spermatogenesis Prof. Alberto Contri CHARACTERISTICS OF THE SPERMATOZOON 1) Aploid cell with high condensed DNA 2) Forward motility - flagellum 3) Enzymes for
Reproductive Biotechnologies Andrology I The spermatogenesis Prof. Alberto Contri CHARACTERISTICS OF THE SPERMATOZOON 1) Aploid cell with high condensed DNA 2) Forward motility - flagellum 3) Enzymes for
Case Report Successful Pregnancy in a Couple with Severe Male Factor Infertility after Selection of Sperm with Cytoplasmic Droplets
 Case Reports in Obstetrics and Gynecology Volume 2015, Article ID 276931, 4 pages http://dx.doi.org/10.1155/2015/276931 Case Report Successful Pregnancy in a Couple with Severe Male Factor Infertility
Case Reports in Obstetrics and Gynecology Volume 2015, Article ID 276931, 4 pages http://dx.doi.org/10.1155/2015/276931 Case Report Successful Pregnancy in a Couple with Severe Male Factor Infertility
East and North Hertfordshire CCG. Fertility treatment and referral criteria for tertiary level assisted conception
 East and North Hertfordshire CCG Fertility treatment and referral criteria for tertiary level assisted conception December 2015 1 1. Introduction This policy sets out the entitlement and service that will
East and North Hertfordshire CCG Fertility treatment and referral criteria for tertiary level assisted conception December 2015 1 1. Introduction This policy sets out the entitlement and service that will
TECHNICAL GUIDANCE FOR THE ACCREDITATION OF ANDROLOGY LABORATORIES
 TECHNICAL GUIDANCE FOR THE ACCREDITATION OF ANDROLOGY LABORATORIES Approved By: Chief Executive Officer: Ron Josias Accreditation Executive: Mpho Phaloane Revised By: Medical Specialist Technical Committee
TECHNICAL GUIDANCE FOR THE ACCREDITATION OF ANDROLOGY LABORATORIES Approved By: Chief Executive Officer: Ron Josias Accreditation Executive: Mpho Phaloane Revised By: Medical Specialist Technical Committee
ESHRE Monographs: Manual on Basic Semen Analysis pp , Sperm morphology
 ESHRE Monographs: Manual on Basic Semen Analysis pp. 13 17, 2002 5. Sperm morphology Principles The morphology seen with the microscope is not the true morphology of a living spermatozoon, but an image
ESHRE Monographs: Manual on Basic Semen Analysis pp. 13 17, 2002 5. Sperm morphology Principles The morphology seen with the microscope is not the true morphology of a living spermatozoon, but an image
Seminal leukocytes and clinical outcomes with donor sperm insemination
 Seminal leukocytes and clinical outcomes with donor sperm insemination Virginie Barraud-Lange, M.D., Ph.D., a,b Jean-Christophe Pont, Pharm.D., a Khaled Pocate, M.D., a Jean Marie Kunstmann, M.D., a Celine
Seminal leukocytes and clinical outcomes with donor sperm insemination Virginie Barraud-Lange, M.D., Ph.D., a,b Jean-Christophe Pont, Pharm.D., a Khaled Pocate, M.D., a Jean Marie Kunstmann, M.D., a Celine
Clinical evaluation of infertility
 Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
The use of assisted reproductive technology before male factor infertility evaluation
 Original Article The use of assisted reproductive technology before male factor infertility evaluation Madhur Nayan 1, Nahid Punjani 2, Ethan Grober 1, Kirk Lo 1,3,4, Keith Jarvi 1,3,4 1 Division of Urology,
Original Article The use of assisted reproductive technology before male factor infertility evaluation Madhur Nayan 1, Nahid Punjani 2, Ethan Grober 1, Kirk Lo 1,3,4, Keith Jarvi 1,3,4 1 Division of Urology,
Sperm nuclear chromatin normality: relationship with sperm morphology, sperm-zona pellucida binding, and fertilization rates in vitro*
 FERTILITY AND STERILITY Copyright Q 1992 The American Fertility Society Vol. 58, No.6, December 1992 Printed on acid-free paper in U.S.A. Sperm nuclear chromatin normality: relationship with sperm morphology,
FERTILITY AND STERILITY Copyright Q 1992 The American Fertility Society Vol. 58, No.6, December 1992 Printed on acid-free paper in U.S.A. Sperm nuclear chromatin normality: relationship with sperm morphology,
An ultrastructural and immunocytochemical study of a rare genetic sperm tail defect that causes infertility in humans
 FERTILITY AND STERILITY VOL. 82, NO. 2, AUGUST 2004 Copyright 2004 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A. An ultrastructural and immunocytochemical
FERTILITY AND STERILITY VOL. 82, NO. 2, AUGUST 2004 Copyright 2004 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A. An ultrastructural and immunocytochemical
ANDROVISION - MORE THAN CASA
 ANDROVISION - MORE THAN CASA AndroVision CASA system with Zeiss AxioScope optics and automated ScanStage Computerized semen analysis AndroVision is a highly precise CASA* system for standardised, interactive
ANDROVISION - MORE THAN CASA AndroVision CASA system with Zeiss AxioScope optics and automated ScanStage Computerized semen analysis AndroVision is a highly precise CASA* system for standardised, interactive
Andrology Services at HA Past, Present and Future. W.S.B. Yeung Department of Obstetrics and Gynaecology The University of Hong Kong
 Andrology Services at HA Past, Present and Future W.S.B. Yeung Department of Obstetrics and Gynaecology The University of Hong Kong Content How is semen analysis done? Is it useful? Past Present Future
Andrology Services at HA Past, Present and Future W.S.B. Yeung Department of Obstetrics and Gynaecology The University of Hong Kong Content How is semen analysis done? Is it useful? Past Present Future
Fertility Services Commissioning Policy
 Fertility Services Commissioning Policy NEE CCG Policy Reference: Where patients have commenced treatment in any cycle prior to this version becoming effective, they are subject to the eligibility criteria
Fertility Services Commissioning Policy NEE CCG Policy Reference: Where patients have commenced treatment in any cycle prior to this version becoming effective, they are subject to the eligibility criteria
PROCEDURES LAPAROSCOPY
 PROCEDURES - Further infertility work-up if indicated (ultrasound examination / semen decontamination etc.) - Office Hysteroscopy where indicated - Laparoscopic and /or hysteroscopic surgery where indicated
PROCEDURES - Further infertility work-up if indicated (ultrasound examination / semen decontamination etc.) - Office Hysteroscopy where indicated - Laparoscopic and /or hysteroscopic surgery where indicated
Male Fertility: Your Questions Answered
 Male Fertility: Your Questions Answered Michael S. Neal Scientific Director, ONE Fertility, 3210 Harvester Rd. Burlington, Ontario www.onefertility.com mneal@onefertility.com Outline Assisted Conception
Male Fertility: Your Questions Answered Michael S. Neal Scientific Director, ONE Fertility, 3210 Harvester Rd. Burlington, Ontario www.onefertility.com mneal@onefertility.com Outline Assisted Conception
Assessing human sperm morphology: top models, underdogs or biometrics?
 36 Perspectives : top models, underdogs or biometrics? Asian Journal of Andrology (2010) 12: 36 46 2010 AJA, SIMM & SJTU All rights reserved 1008-682X/09 $ 32.00 www.nature.com/aja Service d Histologie-Embryologie,
36 Perspectives : top models, underdogs or biometrics? Asian Journal of Andrology (2010) 12: 36 46 2010 AJA, SIMM & SJTU All rights reserved 1008-682X/09 $ 32.00 www.nature.com/aja Service d Histologie-Embryologie,
WHY INVESTIGATE FOR INFERTILITY
 WHY INVESTIGATE FOR INFERTILITY Intrauterine Insemination 1 About this booklet This series of booklets has been developed and written with the support of leading fertility clinics across Australia, and
WHY INVESTIGATE FOR INFERTILITY Intrauterine Insemination 1 About this booklet This series of booklets has been developed and written with the support of leading fertility clinics across Australia, and
Fertility treatment and referral criteria for tertiary level assisted conception
 Fertility treatment and referral criteria for tertiary level assisted conception Version Number Name of Originator/Author Cross Reference V2 East of England Consortium Commissioning Policy for Fertility
Fertility treatment and referral criteria for tertiary level assisted conception Version Number Name of Originator/Author Cross Reference V2 East of England Consortium Commissioning Policy for Fertility
SpermComet DNA Test your results and what they mean
 SpermComet DNA Test your results and what they mean Sperm DNA damage and why it is important for your fertility. You and your partner are each going to give some of your DNA to your baby, so the health
SpermComet DNA Test your results and what they mean Sperm DNA damage and why it is important for your fertility. You and your partner are each going to give some of your DNA to your baby, so the health
Computerized semen analysis. Product features. Basic system
 AndroVision - more than CASA AndroVision CASA system with Zeiss AxioScope optics and automated ScanStage Computerized semen analysis AndroVision is a highly precise CASA* system for standardised, interactive
AndroVision - more than CASA AndroVision CASA system with Zeiss AxioScope optics and automated ScanStage Computerized semen analysis AndroVision is a highly precise CASA* system for standardised, interactive
CM-B 2008: Semen Analysis INTRODUCTION ANATOMY AND PHYSIOLOGY
 INTRODUCTION Semen analysis is a laboratory test that is primarily used for evaluating fertility potential and for assessing success following a vasectomy procedure. The composition of semen, also known
INTRODUCTION Semen analysis is a laboratory test that is primarily used for evaluating fertility potential and for assessing success following a vasectomy procedure. The composition of semen, also known
Novel Technologies for Selecting the Best Sperm for IVF and ICSI
 Novel Technologies for Selecting the Best Sperm for IVF and ICSI Denny Sakkas, Ph.D. Scientific Director, Boston IVF Waltham, MA, USA Testing The Sperm Population NOW Sperm DNA testing Although we are
Novel Technologies for Selecting the Best Sperm for IVF and ICSI Denny Sakkas, Ph.D. Scientific Director, Boston IVF Waltham, MA, USA Testing The Sperm Population NOW Sperm DNA testing Although we are
FERTILITY & TCM. On line course provided by. Taught by Clara Cohen
 FERTILITY & TCM On line course provided by Taught by Clara Cohen FERTILITY & TCM FERTILITY AND TCM THE PRACTITIONER S ROLE CAUSES OF INFERTILITY RISK FACTORS OBJECTIVES UNDERSTANDING TESTS Conception in
FERTILITY & TCM On line course provided by Taught by Clara Cohen FERTILITY & TCM FERTILITY AND TCM THE PRACTITIONER S ROLE CAUSES OF INFERTILITY RISK FACTORS OBJECTIVES UNDERSTANDING TESTS Conception in
Sperm nuclear vacuoles, as assessed by motile sperm organellar morphological examination, are mostly of acrosomal origin
 Reproductive BioMedicine Online (2010) 20, 132 137 www.sciencedirect.com www.rbmonline.com ARTICLE Sperm nuclear vacuoles, as assessed by motile sperm organellar morphological examination, are mostly of
Reproductive BioMedicine Online (2010) 20, 132 137 www.sciencedirect.com www.rbmonline.com ARTICLE Sperm nuclear vacuoles, as assessed by motile sperm organellar morphological examination, are mostly of
Male Infertility Research
 Male Infertility Research Quantitative evaluation of spermatozoa ultrastructure after acupuncture treatment for idiopathic male infertility. Effect of Acupuncture on Sperm Parameters of Males Suffering
Male Infertility Research Quantitative evaluation of spermatozoa ultrastructure after acupuncture treatment for idiopathic male infertility. Effect of Acupuncture on Sperm Parameters of Males Suffering
Fertilization depends on mechanisms that help sperm meet eggs of the same species.
 Fertilization depends on mechanisms that help sperm meet eggs of the same species. www.uchsc.edu/ltc/fertilization.html Fertilization union of sperm and egg Is a chain of events. Interruption of any step
Fertilization depends on mechanisms that help sperm meet eggs of the same species. www.uchsc.edu/ltc/fertilization.html Fertilization union of sperm and egg Is a chain of events. Interruption of any step
Assessment of Fertility Status in the Male Sumatran Rhino at the Sumateran Rhino Sanctuary, Way Kambas National Park, Lampung
 HAYATI Journal of Biosciences, March 2008, p 39-44 ISSN: 1978-3019 Vol. 15, No. 1 Assessment of Fertility Status in the Male Sumatran Rhino at the Sumateran Rhino Sanctuary, Way Kambas National Park, Lampung
HAYATI Journal of Biosciences, March 2008, p 39-44 ISSN: 1978-3019 Vol. 15, No. 1 Assessment of Fertility Status in the Male Sumatran Rhino at the Sumateran Rhino Sanctuary, Way Kambas National Park, Lampung
Sperm gamete screening
 Sperm gamete screening Juan G. Alvarez, M.D, Ph.D Instituto Marquès, Barcelona Harvard Medical School, Boston Sperm screening Standard semen analysis Sperm capacitation Oocyte activating factor (PLC zeta
Sperm gamete screening Juan G. Alvarez, M.D, Ph.D Instituto Marquès, Barcelona Harvard Medical School, Boston Sperm screening Standard semen analysis Sperm capacitation Oocyte activating factor (PLC zeta
International Journal of Current Research and Academic Review ISSN: Volume 2 Number 12 (December-2014) pp
 International Journal of Current Research and Academic Review ISSN: 2347-3215 Volume 2 Number 12 (December-2014) pp. 47-63 www.ijcrar.com A Study of Hypo Osmotic Swelling Test in Human Spermatozoa R.Jothipriya*,
International Journal of Current Research and Academic Review ISSN: 2347-3215 Volume 2 Number 12 (December-2014) pp. 47-63 www.ijcrar.com A Study of Hypo Osmotic Swelling Test in Human Spermatozoa R.Jothipriya*,
Effect of method and clinician on stallion sperm morphology evaluation
 Available online at www.sciencedirect.com Theriogenology 76 (2011) 745 750 www.theriojournal.com Effect of method and clinician on stallion sperm morphology evaluation Leonardo F.C. Brito,1, Lauren M.
Available online at www.sciencedirect.com Theriogenology 76 (2011) 745 750 www.theriojournal.com Effect of method and clinician on stallion sperm morphology evaluation Leonardo F.C. Brito,1, Lauren M.
Information Booklet. Exploring the causes of infertility and treatment options.
 Information Booklet Exploring the causes of infertility and treatment options www.ptafertility.co.za info@ptafertility.co.za +27 12 998 8854 Faith is taking the first step even if you don t see the whole
Information Booklet Exploring the causes of infertility and treatment options www.ptafertility.co.za info@ptafertility.co.za +27 12 998 8854 Faith is taking the first step even if you don t see the whole
A Peculiar Type of Spermateleosis in the Spider Beetle Ptinus hirtellus Sturm
 76 Cytologia 24 A Peculiar Type of Spermateleosis in the Spider Beetle Ptinus hirtellus Sturm Joseph Jacob1 Institute of Animal Genetics, University of Edinburgh, Edinburgh 9, Scotland Received September
76 Cytologia 24 A Peculiar Type of Spermateleosis in the Spider Beetle Ptinus hirtellus Sturm Joseph Jacob1 Institute of Animal Genetics, University of Edinburgh, Edinburgh 9, Scotland Received September
Men: Do You Really Want to Be Dads?
 Men: Do You Really Want to Be Dads? This newsletter is directed to the husbands or male partners of women who are trying to conceive using assisted reproductive medicine. I direct this to you men because
Men: Do You Really Want to Be Dads? This newsletter is directed to the husbands or male partners of women who are trying to conceive using assisted reproductive medicine. I direct this to you men because
Spermatozoa motility in reverse gear? An observation of backward-moving human spermatozoa.
 Spermatozoa motility in reverse gear? An observation of backward-moving human spermatozoa. Correspondence sranjanivenkadesan@gmail.com Disciplines Medical Sciences Keywords Spermatozoa, Motility Humans
Spermatozoa motility in reverse gear? An observation of backward-moving human spermatozoa. Correspondence sranjanivenkadesan@gmail.com Disciplines Medical Sciences Keywords Spermatozoa, Motility Humans
Fertility treatment in trends and figures
 Fertility treatment in 2010 trends and figures Contents Page No: Foreword by the Chair of the HFEA 3 Summary 4 Section 1: Overview How many fertility clinics were there in the UK in 2010? 6 How many women
Fertility treatment in 2010 trends and figures Contents Page No: Foreword by the Chair of the HFEA 3 Summary 4 Section 1: Overview How many fertility clinics were there in the UK in 2010? 6 How many women
Biology of fertility control. Higher Human Biology
 Biology of fertility control Higher Human Biology Learning Intention Compare fertile periods in females and males What is infertility? Infertility is the inability of a sexually active, non-contracepting
Biology of fertility control Higher Human Biology Learning Intention Compare fertile periods in females and males What is infertility? Infertility is the inability of a sexually active, non-contracepting
Infertility F REQUENTLY A SKED Q UESTIONS. Q: Is infertility a common problem?
 Infertility (female factors). In another one third of cases, infertility is due to the man (male factors). The remaining cases are caused by a mixture of male and female factors or by unknown factors.
Infertility (female factors). In another one third of cases, infertility is due to the man (male factors). The remaining cases are caused by a mixture of male and female factors or by unknown factors.
VideoTesT-Sperm 2.1 VideoTesT-Sperm 2.1 Motility Morphology Motility Standard Method Morphology Standard Method Database
 VideoTesT-Sperm 2.1 CASA is designed to equip the workplace of specialists dealing with sperm analysis. The analyzer enables experts to count the amount of spermatozoa and to estimate their motility parameters
VideoTesT-Sperm 2.1 CASA is designed to equip the workplace of specialists dealing with sperm analysis. The analyzer enables experts to count the amount of spermatozoa and to estimate their motility parameters
Fertility of ejaculated and testicular megalohead spermatozoa with intracytoplasmic sperm injection
 Human Reproduction vol.14 no.3 pp.726 730, 1999 Fertility of ejaculated and testicular megalohead spermatozoa with intracytoplasmic sperm injection S.Kahraman 1,4, C.Akarsu 1, G.Cengiz 1, K.Dirican 1,
Human Reproduction vol.14 no.3 pp.726 730, 1999 Fertility of ejaculated and testicular megalohead spermatozoa with intracytoplasmic sperm injection S.Kahraman 1,4, C.Akarsu 1, G.Cengiz 1, K.Dirican 1,
**Florida licensees, please note: This exercise will appear in CE Broker under the specialty of Andrology.
 EDUCATIONAL COMMENTARY SEMEN ANALYSIS AND FERTILITY Commentary provided by: Henry C. Lee, CLS, MASCP, CPHQ Laboratory Manager Arrowhead Regional Medical Center Colton, CA Educational commentary is provided
EDUCATIONAL COMMENTARY SEMEN ANALYSIS AND FERTILITY Commentary provided by: Henry C. Lee, CLS, MASCP, CPHQ Laboratory Manager Arrowhead Regional Medical Center Colton, CA Educational commentary is provided
Semen. Dr. Mohamed Saad Daoud
 Semen Dr. Mohamed Saad Daoud 1 Reference Books: Urinanalysis and body fluids (Susan King Strasinger- Marjorie Schaub De Lorenzo) Fifth edition Dr. Mohamed Saad Daoud 2 Diagram of the male genitalia Dr.
Semen Dr. Mohamed Saad Daoud 1 Reference Books: Urinanalysis and body fluids (Susan King Strasinger- Marjorie Schaub De Lorenzo) Fifth edition Dr. Mohamed Saad Daoud 2 Diagram of the male genitalia Dr.
Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia
 Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia Thomas A. Masterson; Aubrey B. Greer; Ranjith Ramasamy University of Miami, Miami, FL, United
Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia Thomas A. Masterson; Aubrey B. Greer; Ranjith Ramasamy University of Miami, Miami, FL, United
5 15/3/2012. Malik Al-Momani
 5 15/3/2012 Malik Al-Momani بسم هللا الرحمن الرحيم Spermatogenesis Note : Please refer to slides so see photos. Quick Revision : - Testis is divided by septum into testicular lobules, inside the lobules
5 15/3/2012 Malik Al-Momani بسم هللا الرحمن الرحيم Spermatogenesis Note : Please refer to slides so see photos. Quick Revision : - Testis is divided by septum into testicular lobules, inside the lobules
Bank your future: Insemination and semen cryopreservation. Disclosure. Lecture objectives
 Bank your future: Insemination and semen cryopreservation Roelof Menkveld, PhD Andrology Laboratory, Department of Obstetrics and Gynaecology, Tygerberg Academic Hospital and University of Stellenbosch.
Bank your future: Insemination and semen cryopreservation Roelof Menkveld, PhD Andrology Laboratory, Department of Obstetrics and Gynaecology, Tygerberg Academic Hospital and University of Stellenbosch.
NICE fertility guidelines. Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic
 NICE fertility guidelines Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic About the LWC 4 centres around the UK London Cardiff Swansea Darlington The largest sperm bank in
NICE fertility guidelines Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic About the LWC 4 centres around the UK London Cardiff Swansea Darlington The largest sperm bank in
Abnormalities of Spermatogenesis
 Abnormalities of Spermatogenesis Male Factor 40% of the cause for infertility Sperm is constantly produced by the germinal epithelium of the testicle Sperm generation time 73 days Sperm production is thermoregulated
Abnormalities of Spermatogenesis Male Factor 40% of the cause for infertility Sperm is constantly produced by the germinal epithelium of the testicle Sperm generation time 73 days Sperm production is thermoregulated
Infertility treatment
 In the name of God Infertility treatment Treatment options The optimal treatment is one that provide an acceptable success rate, has minimal risk and is costeffective. The treatment options are: 1- Ovulation
In the name of God Infertility treatment Treatment options The optimal treatment is one that provide an acceptable success rate, has minimal risk and is costeffective. The treatment options are: 1- Ovulation
A. Macroscopic and Physical tests:- 1. Volume 2. Colour 3. Consistency and cloudiness 4. Osmotic pressure 5. Specific Gravity 6. Electro Conductivity
 EXAMINATION AND EVALUATION OF SEMEN. Evaluation of Semen. A. Macroscopic and Physical tests:- 1. Volume 2. Colour 3. Consistency and cloudiness 4. Osmotic pressure 5. Specific Gravity 6. Electro Conductivity
EXAMINATION AND EVALUATION OF SEMEN. Evaluation of Semen. A. Macroscopic and Physical tests:- 1. Volume 2. Colour 3. Consistency and cloudiness 4. Osmotic pressure 5. Specific Gravity 6. Electro Conductivity
Ultrastructural findings in semen samples of infertile men infected with Chlamydia trachomatis and mycoplasmas
 IMAGES IN REPRODUCTIVE MEDICINE Ultrastructural findings in semen samples of infertile men infected with Chlamydia trachomatis and mycoplasmas Guadalupe Gallegos-Avila, M.D., a Marta Ortega-Martınez, Ph.D.,
IMAGES IN REPRODUCTIVE MEDICINE Ultrastructural findings in semen samples of infertile men infected with Chlamydia trachomatis and mycoplasmas Guadalupe Gallegos-Avila, M.D., a Marta Ortega-Martınez, Ph.D.,
INTRACYTOPLASMIC SPERM INJECTION
 1 Background... 2 2 Male Factor Infertility... 2 3 ICSI... 3 4 Surgical sperm aspiration... 4 5 What is the chance of success?... 6 6 What are the risks?... 7 M Rajkhowa, October 2004 Authorised by V Kay
1 Background... 2 2 Male Factor Infertility... 2 3 ICSI... 3 4 Surgical sperm aspiration... 4 5 What is the chance of success?... 6 6 What are the risks?... 7 M Rajkhowa, October 2004 Authorised by V Kay
Defective sperm zona pellucida interaction: a major cause of failure of fertilization in clinical in-vitro fertilization
 Human Reproduction vol.15 no.3 pp.702 708, 2000 Defective sperm zona pellucida interaction: a major cause of failure of fertilization in clinical in-vitro fertilization D.Y.Liu 1 and H.W.G.Baker However,
Human Reproduction vol.15 no.3 pp.702 708, 2000 Defective sperm zona pellucida interaction: a major cause of failure of fertilization in clinical in-vitro fertilization D.Y.Liu 1 and H.W.G.Baker However,
Male infertility too often ignored & forgotten
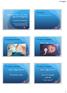 Male infertility too often ignored & forgotten The journey 1. of the men A review of the guidelines Joo Teoh FRANZCOG MRCP(Ire) MRCOG MBBCh MSc(Lon) MD(Glasgow) SubspecialtyRepromed(UK) Consultant Obstetrician
Male infertility too often ignored & forgotten The journey 1. of the men A review of the guidelines Joo Teoh FRANZCOG MRCP(Ire) MRCOG MBBCh MSc(Lon) MD(Glasgow) SubspecialtyRepromed(UK) Consultant Obstetrician
Access to IVF. Help us decide Discussion paper. South Central Specialised Commissioning Group C - 1
 Access to IVF Help us decide Discussion paper South Central Specialised Commissioning Group 1 C - 1 Access to IVF treatment Contents 1. Background 3 2. Developing a single policy for NHS South Central..4
Access to IVF Help us decide Discussion paper South Central Specialised Commissioning Group 1 C - 1 Access to IVF treatment Contents 1. Background 3 2. Developing a single policy for NHS South Central..4
Fertility Services Commissioning Policy
 Fertility Services Commissioning Policy Author: Commissioning Team Version No: Two Policy Effective From: 29 September 2016 Review Date: September 2017 Policy Amendment: 02 August 2017 Document Reader
Fertility Services Commissioning Policy Author: Commissioning Team Version No: Two Policy Effective From: 29 September 2016 Review Date: September 2017 Policy Amendment: 02 August 2017 Document Reader
Lecture Outline. Biost 517 Applied Biostatistics I. Purpose of Descriptive Statistics. Purpose of Descriptive Statistics
 Biost 517 Applied Biostatistics I Scott S. Emerson, M.D., Ph.D. Professor of Biostatistics University of Washington Lecture 3: Overview of Descriptive Statistics October 3, 2005 Lecture Outline Purpose
Biost 517 Applied Biostatistics I Scott S. Emerson, M.D., Ph.D. Professor of Biostatistics University of Washington Lecture 3: Overview of Descriptive Statistics October 3, 2005 Lecture Outline Purpose
Male Factor Infertility
 Male Factor Infertility Simplified Evaluaon and Treatment* ^ * In 20 minutes or less In 20 slides ^ 5 minute office visit ALWAYS EVALUATE THE MALE & THE FEMALE Why 1. To help the coupleachieve a pregnancy
Male Factor Infertility Simplified Evaluaon and Treatment* ^ * In 20 minutes or less In 20 slides ^ 5 minute office visit ALWAYS EVALUATE THE MALE & THE FEMALE Why 1. To help the coupleachieve a pregnancy
The Comet and TUNEL Assays
 Sperm DNA: organization, protection and vulnerability from basic science to clinical application Methods to assess the status of the sperm DNA: The Comet and TUNEL Assays Lars Björndahl Centre for Andrology
Sperm DNA: organization, protection and vulnerability from basic science to clinical application Methods to assess the status of the sperm DNA: The Comet and TUNEL Assays Lars Björndahl Centre for Andrology
Adoption and Foster Care
 GLOSSARY Family building via Adoption and Foster Care October 2018 www.familyequality.org/resources A Anonymous Donor: A person who donated sperm or eggs with the intention of never meeting resulting children.
GLOSSARY Family building via Adoption and Foster Care October 2018 www.familyequality.org/resources A Anonymous Donor: A person who donated sperm or eggs with the intention of never meeting resulting children.
Sperm morphologic features as a prognostic factor in in vitro fertilization
 FERTILITY AND STERILITY Copyright c 1986 The American Fertility Society Printed in U.SA. Sperm morphologic features as a prognostic factor in in vitro fertilization Thinus F. Kruger, M.D.*t Roelof Menkveld,
FERTILITY AND STERILITY Copyright c 1986 The American Fertility Society Printed in U.SA. Sperm morphologic features as a prognostic factor in in vitro fertilization Thinus F. Kruger, M.D.*t Roelof Menkveld,
OUTCOME OF TREATMENT FOR OAT SYNDROME BY INTRACYTOPLASMIC SPERM INJECTION AT THE ART CENTER
 OUTCOME OF TREATMENT FOR OAT SYNDROME BY INTRACYTOPLASMIC SPERM INJECTION AT THE ART CENTER Ho Sy Hung, Trinh Thi Thuy Hanoi Medical University, Thaibinh Medical University INTRODUCTION Infertility rate
OUTCOME OF TREATMENT FOR OAT SYNDROME BY INTRACYTOPLASMIC SPERM INJECTION AT THE ART CENTER Ho Sy Hung, Trinh Thi Thuy Hanoi Medical University, Thaibinh Medical University INTRODUCTION Infertility rate
Guidelines on safer conception in fertile HIV infected individuals
 Guidelines on safer conception in fertile HIV infected individuals couples Vivian Black Co-authors: L-G Bekker, H Rees, S Black, D Cooper, S Mall, C Mnyami, F Conradie, I Mahabeer, L Gilbert, S Schwartz,
Guidelines on safer conception in fertile HIV infected individuals couples Vivian Black Co-authors: L-G Bekker, H Rees, S Black, D Cooper, S Mall, C Mnyami, F Conradie, I Mahabeer, L Gilbert, S Schwartz,
and W. Singleton, Department of Animal Science, Purdue University.
 Introduction Determining the initial quality of a boar ejaculate is the first step in semen processing and should ensure that prior to further processing, a high quality artificial insemination dose of
Introduction Determining the initial quality of a boar ejaculate is the first step in semen processing and should ensure that prior to further processing, a high quality artificial insemination dose of
micromanipulation by vitrolife A complete solution for ICSI procedures.
 micromanipulation by vitrolife A complete solution for ICSI procedures. 1 tested, tried and trusted Vitrolife micromanipulation products have been used from the beginning. Used worldwide Vitrolife is the
micromanipulation by vitrolife A complete solution for ICSI procedures. 1 tested, tried and trusted Vitrolife micromanipulation products have been used from the beginning. Used worldwide Vitrolife is the
Results and Discussion
 The AMH and Inhibin B in serum and follicular fluid was a very good predictive marker for assessment of oocyte quantity but did not correlate with the maturity of the oocyte or fertilization or reproductive
The AMH and Inhibin B in serum and follicular fluid was a very good predictive marker for assessment of oocyte quantity but did not correlate with the maturity of the oocyte or fertilization or reproductive
Fertility Desires/Management of Serodiscordant HIV + Couples
 Fertility Desires/Management of Serodiscordant HIV + Couples William R. Short, MD, MPH Assistant Professor of Medicine Division Of Infectious Diseases Jefferson Medical College of Thomas Jefferson University
Fertility Desires/Management of Serodiscordant HIV + Couples William R. Short, MD, MPH Assistant Professor of Medicine Division Of Infectious Diseases Jefferson Medical College of Thomas Jefferson University
INVESTIGATING FIT WITH THE RASCH MODEL. Benjamin Wright and Ronald Mead (1979?) Most disturbances in the measurement process can be considered a form
 INVESTIGATING FIT WITH THE RASCH MODEL Benjamin Wright and Ronald Mead (1979?) Most disturbances in the measurement process can be considered a form of multidimensionality. The settings in which measurement
INVESTIGATING FIT WITH THE RASCH MODEL Benjamin Wright and Ronald Mead (1979?) Most disturbances in the measurement process can be considered a form of multidimensionality. The settings in which measurement
Fertility Services Commissioning Policy
 Fertility Services Commissioning Policy NEE CCG Policy Reference: NEE/CCG/2015/057 Where patients have commenced treatment in any cycle prior to this version becoming effective, they are subject to the
Fertility Services Commissioning Policy NEE CCG Policy Reference: NEE/CCG/2015/057 Where patients have commenced treatment in any cycle prior to this version becoming effective, they are subject to the
InterMedics Training Academy (ITA) Embryology Training and Lab Management
 InterMedics Training Academy (ITA) Embryology Training and Lab Management InterMedics is at the forefront of IVF service delivery in India and has recently opened its own training facility in Mumbai. Optimal
InterMedics Training Academy (ITA) Embryology Training and Lab Management InterMedics is at the forefront of IVF service delivery in India and has recently opened its own training facility in Mumbai. Optimal
Differences in Human Spermatozoa
 Differences in Human Spermatozoa Landrum B. Shettles, M.D. RECENT OBSERVATIONS show that thin, dried, unstained smears of human spermatozoa viewed through the dry objectives of the phase-contrast microscope
Differences in Human Spermatozoa Landrum B. Shettles, M.D. RECENT OBSERVATIONS show that thin, dried, unstained smears of human spermatozoa viewed through the dry objectives of the phase-contrast microscope
Quality control workshops in standardization of sperm concentration and motility assessment in multicentre studies
 international journal of andrology, 28:144 149 (5) doi:.1111/j.1365-265.5.518.x Quality control workshops in standardization of sperm concentration and motility assessment in multicentre studies GUNNAR
international journal of andrology, 28:144 149 (5) doi:.1111/j.1365-265.5.518.x Quality control workshops in standardization of sperm concentration and motility assessment in multicentre studies GUNNAR
The sperm HBA that has been developed as a commercial diagnostic kit for assessing sperm. Proceedings of Singapore Healthcare Volume 22 Number
 original article Relationship between Sperm Hyaluronan-binding Assay (HBA) Scores on Embryo Development, Fertilisation, and Pregnancy Rate in Patients Undergoing Intra-cytoplasmic Sperm Injection (ICSI)
original article Relationship between Sperm Hyaluronan-binding Assay (HBA) Scores on Embryo Development, Fertilisation, and Pregnancy Rate in Patients Undergoing Intra-cytoplasmic Sperm Injection (ICSI)
Clinical Policy Committee
 Northern, Eastern and Western Devon Clinical Commissioning Group South Devon and Torbay Clinical Commissioning Group Clinical Policy Committee Commissioning policy: Assisted Conception Fertility treatments
Northern, Eastern and Western Devon Clinical Commissioning Group South Devon and Torbay Clinical Commissioning Group Clinical Policy Committee Commissioning policy: Assisted Conception Fertility treatments
Male Reproductive System
 Male Reproductive System Constitution of male reproductive system Genital gland ----testis Genital ducts epididymis / ductus deferens / urinary duct Accessory sex glands Penis prostate gland Seminal vesicle
Male Reproductive System Constitution of male reproductive system Genital gland ----testis Genital ducts epididymis / ductus deferens / urinary duct Accessory sex glands Penis prostate gland Seminal vesicle
