Studies of the Pituitary-Leydig Cell Axis
|
|
|
- Rosalyn Austin
- 6 years ago
- Views:
Transcription
1 Studies of the Pituitary-Leydig Cell Axis in Young Men with Hypogonadotropic Hypogonadism and Hyposmia: Comparison with Normal Men, Prepuberal Boys, and Hypopituitary Patients C. WAYNE BARDIN, GRIFF T. Ross, ARLEEN B. RPIaND, CHAUURS M. CARGILLE, and MORTIMER B. LIPsETr From the Endocrinology Branch, National Cancer Institute, National Institutes of Health, Bethesda, Maryland A B S T R A C T Pituitary and gonadal function was studied in seven chromatin-negative men, ages yr, with retarded sexual and somatic development, skeletal anomalies, and hyposnmia. These hyposmic patients were compared with normal men, prepuberal boys and hypogonadal patients with hypopituitarism. The urinary follicle-stimulating hormone (FSH) and luteinizing hormone (LH) levels of hyposmic subjects were the same as those of normal boys and hypopituitary patients but significantly lower than those of normal men. Clomiphene citrate did not cause an increase in plasma FSH and LH levels in either hypogonadal group as it does in normal men. In contrast to hypopituitary patients, thyroid and adrenocortical function and release of growth hormone in the hyposmic subjects were normal. The plasma testosterone levels were equally low in prepuberal, hypopituitary, and hyposmic patients but were increased to a greater extent by human chorionic gonadotropin (HCG) treatment in prepuberal and hypopituitary subjects than in the hyposmic patients. Prolonged treatment with HCG has failed to return plasma testosterone levels to normal in two hyposmic patients. These observations suggest that there are defects of both pituitary and Leydig cell function in men with the syndrome of hypogonadism, skeletal anomalies, and hyposmia. They have impaired secretion of FSH and LH and a Leydig cell insensitivity to gonadotropin. A preliminary report of this work was presented at the combined meeting of The American Society for Clinical Investigation and The American Federation for Clinical Research, 5 May Dr. Rifkind's present address is The Rockefeller Uniiversity, New York Received for publication 25 March The Journal of Clinical Investigation Volume INTRODUCTION Defective olfaction has been noted in patients with hypogonadotropic hypogonadism for many years. This association has been reported in individual patients (1) and in members of several kindreds (2-4). Despite the early recognition of patients with these signs, only with the recent development of precise methods for estimation of plasma androgens and gonadotropins have studies of the pituitary-leydig cell axis of these patients been possible. To better understand this type of hypogonadism, the dynamics of gonadotropin and testosterone secretion were studied in seven males with hypogonadotropic hypogonadism and hyposmia. Comparable studies were carried out in normal men and in two other groups of hypogonadal subjects: "normal" prepuberal boys and patients with hypopituitarism. METHODS Methods were as follows: total urinary gonadotropins (5); urinary 17-hydroxysteroids (6); plasma cortisol (7); plasma leutinizing hormone (LH) (8); plasma follicle-stimulating hormone (FSH) (9); plasma growth hormone (10); and plasma testosterone (11). Urinary FSH and LH excretion were measured in normal men and children by bioassay (12, 13) of extracts of large pools of urine (14). Since we showed subsequently that LH and FSH activity in urine extracts could be estimated by radioimmunoassay (9, 15) on aliquots of a single 24 hr collection, we measured the urinary LH and FSH excretion of hypopituitary and hyposmic patients by radioimmunoassay. The sensitivity of LH and FSH radioimmunoassays are 6 and 4 in miu/ml respectively.' As a consequence, potency 'Plasma and urinary LH and FSH levels are expressed in terms of milliinternational Units of the Second International Reference Preparation of human menopausal gonadotropin (IRP 2 HMG). For plasma values, 1 IU of IRP 2 HMG is equivalent to 50 and 21,Ag of LER 907, for FSH and LH respectively.
2 estimates at low levels of LH and FSH in plasma are not reliable. In plasma a 20% difference is needed to distinguish (P < 0.05) two values (LH or FSH) from one another. Mean plasma FSH concentrations in samples from 30 normal men were 9.6 miu/ml with 95% confidence limits of miu/ml. Mean LH concentrations in samples from 27 of them was 17.8 miu/ml with 95% confidence limits of miu/ml. Tests of hypothalamic-pituitary and testicular function were performed as follows: a bacterial pyrogen' was given intravenously at 0.6 Ag/kg and blood obtained at 0, 1, 2, and 4 hr. A normal response is defined as a doubling of plasma cortisol concentrations and an increase of plasma growth hormone to greater than 10 mug/ml (16). Arginine' (500 mg/kg) was infused for 0.5 hr and plasma obtained at 30-min intervals for 1.5 hr after the end of the infusion. In normal subjects plasma immunoreactive growth hormone levels increased to 10 mig/ml or more (17). Insulin, 0.1 U/kg intravenously in normal subjects, increased plasma growth hormone to at least 10 mug/ml when the blood sugar decreased 50%o. Clomiphene citrate was given by mouth 200 mg daily for 6 days and induced mean increases of 160 and 130%o in plasma LH and FSH levels respectively in normal men (18, 19). Human chorionic gonadotrophin (HCG), (APL, Ayerst Laboratories, New York), 4000 U intramuscularly daily for 4 days, caused at least a 100% increase in plasma testosterone levels in normal men (20). Metyrapone, 750 mg every 4 hr, caused a doubling of urinary 17-hydroxycorticoids in normal subjects. Except for the last, these tests have been standardized in this laboratory in normal men, ages yr. Hyposmic patients. Seven male subjects, ages yr, with hyposmia and hypogonadism were studied. They were referred to our clinic because of retarded sexual development and a eunuchoidal habitus. All had clinically evident hyposmia, and there was difficulty with recognition of a variety of substances such as coffee, wintergreen, and cloves. Two subjects had nerve deafness, and one of them was color-blind. The karyotype was 46, XY and the nuclear sex was chromatin negative in all seven subjects. Short fourth metacarpals were present by X-ray examination in four patients. The testes were either high in the inguinal canal or within the abdomen in four of the patients. Testicular biopsy was performed in all patients. The hyposmic patients had no family history of hypogonadism, and from a total of 15 siblings (10 sisters, five brothers), six women and two men were fertile. Pertinent clinical and laboratory features of each case are given in the Appendix and in Table I. Hypopituitary patients. Eight patients (ages 6-47) with presenting complaints of growth failure, hypogonadism, or suspected pituitary tumor were referred to the Endocrinology Clinic. Each was clinically hypogonadal, had low urinary gonadotropin titers, and either low basal levels or defective release of at least one other pituitary hormone (Table II). Studies of gonadal function were performed when the patients were receiving necessary adrenal or thyroid replacement therapy. "Normal" boys. Five prepubertal boys were evaluated because of short stature or cryptorchidism. Anterior pituitary function was normal, and the hypogonadism was judged to be compatible with the prepubertal state. Although these boys 'Piromen, purified Pseudomonas polysaccharide pyrogen, Travenol Laboratories, Morton Grove, Ill. 3Bulk 1, arginine-hcl from Schwarz Bio Research, Inc., was prepared in concentrations of 12.5 g/100 ml of hypotonic Ringers solution. are not representative of the normal population, they have been included for comparison with the other hypogonadal groups. Pertinent clinical and laboratory findings are presented in Table III. RESULTS Studies of gonadotropin secretion. Urinary LH and FSH excretions in hyposmic patients (LH, , SE; FSH, 1.5 ±0.39 IU/liter) were significantly less (P < 0.01) than those of normal men (LH, ; FSH, IU/liter) (Fig. 1). The gonadotropin concentrations in urine of normal children (LH, ; FSH, 2.2 ±0.4 IU/liter) and hypopituitary patients (LH, ; FSH, IU/liter) were the same as those of the hyposmic patients. No single estimation of urinary LH or FSH from any of these three groups of hypogonadal subjects was in the range of eugonadal adult men. Plasma LH and FSH concentrations for hyposmic and hypopituitary patients ranged from below the sensitivity of the assays into the normal range (Tables I and II). It is thus apparent that with the techniques employed in this study, the hypogonadal groups were distinguished from normal men by specific urinary rather than plasma gonadotropin assays. When clomiphene citrate was given to these patients, plasma LH increased in only one hyposmic and one hypopituitary subject (Figs. 2 and 3), and these increases were less than normal. Plasma FSH was not increased by clomiphene in either group (Figs. 2 and 3). Therefore, adult men were distinguished from the hypogonadal subjects by the response of plasma gonadotropins to clomiphene. Studies of plasma testosterone. In normal men plasma testosterone levels range from 0.4 to 1.0.ug/100 ml mean ( SE, l&g/100 ml) and increase 100% during HCG administration. In Fig. 4 the response of plasma testosterone to HCG in hyposmic subjects is compared with that of normal men. In six of the seven hyposmic subjects the plasma testosterone levels ranged between 0.02 and 0.04 Ag/100 ml and increased only slightly with HCG (Fig. 4). In one hyposmic patient (No. 4) the control plasma testosterone level was 0.2 ug/100 ml and increased to control normal with HCG. This patient was the only one whose LH level increased slightly in response to clomiphene (see Appendix, patient No. 4). Although testosterone response to HCG in hyposmic patients was significantly less than normal, it seemed pertinent to compare the HCG responsiveness in these subjects with that of other hypogonadotropic patients (Figs. 5 and 6). "Normal" boys had control plasma testosterone levels comparable to those of the hyposmic subjects and in the range for prepuberal boys reported by others (21). The mean increase of plasma testosterone during HCG administration was significantly greater (P < 0.05) in normal boys (0.33 ±0.04 [SE] Ag/100 ml) Hypogonadotropic Hypogonadism 2047
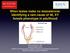
3 TABLE I Clinical and Laboratory Features of Patients with Urinary Bone Total urinary No. Patient Age Age Height Span Bony anomalies conadotropins LH FSH yr yr cm cm MU/day* IU/liter IU/liter 1 J. S <10 (1) - 2 D. F Short 4th metacarpals <10 (3) 1.2 ± Spina bifida >10 < 50 (1) Hypoplasia 1st rib 3 H. C Short 4th metacarpals <10 (3) ±0.1 4 P. H Short 4th and 5th <10 (4) metacarpals >10 < 50 (2) 5 N. XV Short 4th metacarpals <10 (1) 1.2 ± ±0.1 6 R. S Fibrous dysplasia of <10 (3) sphenoid >10 < 50 (1) 0.18 ± H. R Osteoporesis <10 (16) _ - > 10 < 50 (6) Normal men ± ±1.0 LH, leuteinizing hormone; FSH, follicle-stimulating hormone; arginine tolerance test; PBI, protein-bound iodine test. * Number of days at this level. t These patients had a normal response to metyrapone. Normal response given in Methods. and in hypopituitary patients (0.40 ±0.16)' than in hyposmic subjects (0.09 ±0.04) (Fig. 5). Even though the hyposmic patients were similar to normal boys with respect to gonadotropin excretion and other tests of pituitary function, their Leydig cells were relatively insensitive to acute HCG administration. Six hyposmic patients were treated with HCG ( ,000 IU/wk) for 3-8 months (See Appendix). Patient Nos. 2 and 5 had no objective clinical response to prolonged HCG treatment, and in patient No. 5 the plasma testosterone level rose to only 0.23 Ag/100 ml after 5 months of therapy.! Patient Nos. 3 and 6 had minimal clinical responses to long term HCG, and plasma testosterone levels increased to Ag/100 ml in patient No. 6 during this therapy. Patient Nos. 1 and 7 had good clinical responses to HCG treatment on more than one occasion, but plasma testosterone levels are not available. Histopathological studies. Histologic features of the testes of the hyposmic patients were similar to those of prepubertal boys. In five patients histological examination C, control; P, Piromen test; ITT, insulin tolerance test; ATT, revealed small seminiferous tubules which were lined by Sertoli cells and spermatogonia. In patient No. 5 there were a few primary spermatocytes. In patient No. 3 7 Z 6 zwe 0 5 W -J T- i LH ' Since the variances of the two groups were different a logarithmic transformation was employed to reduce variance and permit statistical evaluation of the means. Plasma testosterone levels after long-term HCG were determined by Dr. Marvin Kirschner Bardin, Ross, Rifkind, Cargille, and Lipsett MEN CHILDREN HYPOPITUITARY HYPOSMIC FIGURE 1 Urinary leuteinizing hormone (LH) and folliclestimulating hormone (FSH) levels in normal men and three groups of hypogonadal suspects. Mean +2 SE. The values for normal men and children have been reported previously (14).
4 Hypogonadotropic Hypogonadism and Hyposmnia Plasma LH Plasma FSH Plasma test- Plasma osterone Plasma growth hormone cortisol Clomi- Clomi- C phene C phene C HCG C P ITT ATT C P PBI miuimi miuimi pg/100 ml mpg/ml pug/100 ml Ag/ 100 ml 14 X t <6 < <6 <6 <6 < t < : spermatogenesis was more advanced with normal numbers of spermatocytes and rare spermatozoa. In all patients Leydig cells were either rare and poorly developed or unidentifiable. A typical biopsy specimen is shown in Fig. 7. DISCUSSION According to De Morsier defective olfaction accompanying hypogonadism was noted as early as 1850 (22). In 1944 Kallman and associates (2) reviewed the earlier reports of this association and emphasized its hereditary aspects by describing three involved kindreds. Some of the patients described by these investigators had color blindness, synkinesia, mental retardation, and nerve deafness in addition to anosmia and hypogonadism. In recent years additional kindreds and individual patients with hypogonadism and defective olfaction have been reported (1, 3, 4). In the present series, no family history of hypogonadism could be elicited, but a high incidence of extragenital and extragonadal anomalies were noted. All our patients had hyposmia (rather than anosmia) as did the members of the family described by Henkin (23). In addition to this sensory defect, color blindness and nerve deafness were present in two. Four patients had undescended testes, and four had short fourth metacarpals. In addition to the hyposmic patients described above there are several syndromes-in which secondary hypogonadism may occur in association with a variety of neurological and somatic abnormalities. In the Laurence- Moon Biedl syndrome, mental retardation, retinitis pigmentosa, and many other anomalies occur in a familial pattern with hypogonadotropic hypogonadism (24, 25) E E 20 Ic PLASMA LH PLASMA FSH I I CLOMIPHENE TREATMENT (Days) FIGURE 2 The plasma levels of LH and FSH in hyposmic patients before and during administration of clomiphene. The range of the responses in normal men are given by the shaded areas. Hypogonadotropic Hypogonadism 2049
5 TABLE I I Clinicalfand Laboratory Features Total urinary No. Patient Age Diagnosis Clinical features gonadotropins LH Urinary FSH MAU/day* lu/liter IU/liter 8 R.L. 6 Histiocytosis-X 9 L. D. 14 Idiopathic hypopituitarism 10 R. P. 15 Idiopathic hypopituitarism 11 R. K. 16 Chraniopharangioma 12 IR. M. 16 Idiopathic hypopituitarism 13 C. A. 23 Suprasellar tumor 14 L. V. 46 Pituitary tumor 15 J. M. 47 Pituitary tumor Diabetes insipidus Growth failure Short stature Short stature Diabetes insipidus Short stature Short stature Short stature Hypogonadism Hypogonadism Visual field defect Hypogonadism <10 (4) >10 < 50 (2) <10 (5) >10 < 50 (1) <10 (3) >10 < 50 (1) >50 < 200(1) <10 (4) >10 <50 (8) >50 <200(1) <10 (2) <10 (3) >10 < 50 (1) <10 (1) >10 < 50 (8) >50 < 200(3) >10<50 (4) >50 < 200(3) ± ± ± ± ± ±0.03 C, control; HCG, human chorionic gonadotrophin; P, Piromen test; ITT, insulin tolerance test; ATT, orginine tolerance test; PBI, protein-bound iodine test. * Number of days assayed at this level. t Normal response to metyrapone. Similarly, familial cerebellar ataxia has been associated with nerve deafness and secondary hypogonadism (26, 27). Although not described as part of cerebellar ataxia or the Laurence-Moon-Biedl syndrome, short fourth metacarpals were present in the X-rays of such patients (24, 27). Hypogonadotropic hypogonadism has also been associated with other familial diseases such as diabetes mellitus and hyperlipemia (28). Even though patients with gynecomastia, hypoandrogenization, and low gonadotropin excretion may have a primary defect of gonadotropin production, increased blood estrogens could also produce these same clinical and laboratory findings (29); a clomiphene stimulation test should be useful in this distinction. To further add to the heterogeneity of these syndromes, primary hypogonadism has also been described in patients with Laurence-Moon-.Biedl syndrome (29) and familial ataxia (30). Kallman et al. (2) felt that the most reasonable genetic explanation for the association of gonadal and other developmental defects in eunuchoidal patients was breakage and partial translocation of the X chromosome 2050 Bardin, Ross, Rifkind, Cargille, and Lipsett not determinable by morphological examination. Such a defect could affect not only the genes carried on the X chromosome but also genes controlling sex- via the auto- E PLASMA H-I PLASMA FSH 30 E j CLOMIPHENE TREATMENT (Days) FIGuRE 3 The plasma levels of LH and FSH in hypopituitary patients before and during clomiphene administration. The range of the responses in normal men are given by the shaded areas.
6 of Hypopituitary Patients Plasma LH Plasma FSH Plasma test- Plasma osteron Plasma growth hormone cortisol Clomi- Clomi- C phene C phene C HCG C P ITT ATT C P PBI miu/ml miu/ml Ag/100 ml mgg/ml Ug/10O ml AgI 100 ml - < < <6 <6 7 < <11 < <1 < 1 3 8t somes. While this theory is applicable to many of the pedigrees of hypogonadism with defective olfaction and probably to the Laurence-Moon-Biedl syndrome, it may also explain cases such as these accumulated in the present report. Rigorous examination of this postulate in our patients is not possible, since other members of the kinships are not affected. However, it is noteworthy that chromosome number and morphology were normal in our subjects. Although this has been noted by others, our studies emphasize that sporadic cases of hypogonadism associated with hyposmia and somatic anomalies can occur in the absence of a family history. Gonadotropin excretion. The onset of puberty is marked by an increase in gonadotropin and gonadal steroid secretion with subsequent development of secondary sexual characteristics. Therefore the clinical diagnosis of hypogonadotropic hypogonadism cannot be made until after the expected age of puberty, since children are by definition hypogonadal and hypogonadotropic. Although boys may undergo normal secondary sexual development after age 20, clinical and laboratory features associated with hypogonadism may be noted by age 17, if puberty does not occur (31, 32). These features include eunuchoidal body proportions, delayed bone age, small soft testes, and decreased development of androgen-dependent tissues and organs. In addition to these signs which are attributed to hypogonadotropism per se, our patients had hyposmia, bony anomalies, and cryptorchidism. These latter features make possible a presumptive diagnosis of hypogonadotropic hypogonadism even before the expected age of puberty. Despite the clinical usefulness of the total gonadotropin assay it is inadequate for easy quantification at low levels. Recently the LH and FSH excretion of children has been determined by both bioassay and radioimmunoassay. These two assays gave comparable results and indicated that the concentrations of LH and FSH in the urine of normal children is one-tenth and one-half as much as that in normal adult males, respectively (9, 14, 15). From our limited experience with hypogonadal subjects we would conclude that the urinary concentration of LH and FSH in some hypopituitary and hyposmic patients may be the same as those of normal children. Furthermore it is apparent that the hyposmic pa- Hypogonadotropic Hypogonadism 2051
7 TABLE III Clinical and Laboratory Features of "Normal" Boys Plasma testosterone Bone Total gonado- No. Patient Age age Height Weight tropins Control HCG Clinical features yr yr cm kg MU/24 hr pg/100 ml j.g/1oo ml 16 J. T <10(1)* Turner's phenotype (short stature, web neck) 17 K. P <10(3) Hypotonia >10(1) Mental retardation Cryptorchidism 18 R. N <10(4) Short stature 19 D. D <10(1) Short stature 20 G. V. W <10(6) Small right inguinal testis >10(4) * Numbers of days assayed at this level. tients cannot be distinguished from boys with delayed puberty on the basis of gonadotropin excretion. Clomiphene citrate, an analogue of the nonsteroidal estrogen chlorotrianisene, increases LH and FSH secretion in normal but not in hypopituitary men (18, 19). 2.or i E zl 1.2 Lfi z 0 a:.0 U) 0 U) Li H 0.8 < 0.6 0i 0. 4 Ȯ2 It was therefore pertinent to investigate the effect of clomiphene on the plasma gonadotropin levels of the boys with hyposmia and hypogonadism. In five patients with low plasma testosterone levels increases of plasma LH and FSH were not observed, whereas patient No. 4 (plasma testosterone, 0.2,g/100 ml) had a definite increase of plasma LH during clomiphene. These observations are in keeping with one theory proposed for clomiphene action which states that an antiestrogen (or antiandrogen) increases gonadotropin secretion by interrupting the negative feedback of gonadal steroids on the central nervous system. Since the hyposmic subjects E ~0. 0.6_ 0.5_ w o / z / Z / / 00.3 / w / -// E-/ / 40.2 / ' - X ~~/ //'- o HCG TREATMENT- DAYS FIGURE 4 Plasma testosterone levels in hyposmic patients (solid lines) before and after human chorionic gonadotropin (HCG) administration. The range in normal men is given by the shaded area Bardin, Ross, Rifkind, Cargille, and Lipsett HCG TREATMENT - DAYS FIGURE 5 Plasma testosterone levels in hyposmic patients (solid lines) and "normal" boys (hashed lines) before and after HCG administration.
8 1.5 QE 0 tj C, 0.6 z w en 0 w en -J a. ^7 r l 3 ~~~T ///,_ ~~~~// i_ a// /s go //// I Act,/"'s~~~~~~~,. F / 2 HCG TREATMENT - DAYS 4 FIGURE 6 Plasma testosterone levels in hyposmic (solid lines) and hypopituitary patients (hashed lines) before and after HCG administration. have not developed the normal negative feedback system, the low testosterone level fails to elicit an appropriate increase in plasma gonadotropins, and further interruption of androgen action on the brain by clomiphene does not facilitate LH and FSH secretion. The hyposmic patients we have described have hypogonadotropism without any other detectable anterior pituitary hormonal deficiency. Whether the gonadotropin deficit is the result of an isolated pituitary abnormality or a defect in the central nervous system is not known with certainty. There is no direct evidence to suggest that an intrinsic abnormality of the gonadotropinproducing cell of the pituitary is responsible for the hypogonadotropism. Alternatively, the association of abnormalities in the central nervous system and hypogonadotropism suggests that they could be causally related. In this regard hypoplasia of the hypothalamus and mammillary bodies has been reported in several autopsied cases (33), but in these patients other parameters of pituitary function were not carefully assessed. Furthermore, the association of hypogonadotropism with hyposmia is even more intriguing since olfaction is necessary for sexual attraction and arousal in many species. The olfactory apparatus is phylogenetically part of the rhinencephalon, and the amygdaloid nuclei in this portion of the brain may be important for controlling the onset of puberty (34, 35). Thus a diffuse abnormality of rhinencephalic function could relate hyposmia and hypogonadotropism. However, the occurrence of hypogonadotropic hypogonadism alone and in association with a variety of other neurological defects indicates that the gonadotropin deficiency may occur independent of the hyposmia. Thus it would appear that an exact neuroanatomical correlation between an affected area of the brain and hypogonadotropism has not been established. Testosterone secretion. During fetal life the testes secrete an androgen which is responsible for development of the external genitalia of the male. The presence of a normal phallus and scrotum in each of the hyposmic boys suggests that the gonad was active during fetal life. During the 1st yr of life the Leydig cells which are present at birth in the normal testes regress and are not usually recognizable histologically again until the time of puberty. The testes of patients with hypopituitarism and of the hyposmic boys were morphologically similar to those of the child, since Leydig cells were identified with difficulty. Reduced or "absent" Laydig cells is a common finding in patients with hypogonadotropic hypogonadism (31). HCG has been used for many years as a test of Leydig cell function and for the treatment of secondary hypogonadism in man. Its efficacy is due to its ability to stimulate testosterone production (20). Several investigators have also shown that HCG can increase testosterone excretion in children (36-38). Stuiver, Thijssen, and Van der Molen (39) demonstrated a uniform increase in the plasma testosterone of boys (age yr) with "delayed puberty," but there was a more variable response in hypopituitary patients. While it is impossible to compare quantitative results from two laboratories, it is noteworthy that these results are qualitatively similar to those obtained in our normal and hypopituitary patients. In the present study the response of the Leydig cells of three groups of hypogonadotropic subjects were compared. As a group the hyposmic boys were less responsive to 4 days of HCG than were the normal boys and hypopituitary patients. Kallman et al (2) indicated that three of their patients with hypogonadism and anosmia failed to respond clinically to HCG administration, and there is brief mention of similar observations by several other investigators (1, 40, 41), including a patient with Laurence-Moon-Biedl syndrome (24). Some of these reports are difficult to evaluate since no data are available to indicate that the gonadotropins administered produced a response in normal subjects. By contrast, Wieland, Folk, Taylor, and Hamwi (42) demonstrated, Hypogonadotropic Hypogonadism 2053
9 ~~* Ail * v*@*** of * * ^~~.7Di Ȧ _ s<*,, 3. RI U *.~~~~~~7<o > A v. < ' TV i', n* '-5 r _ 0 ~ Nr4:*'i~ ~ ~ ~ ~ J *>*~~~~~ \ * $ * *W7 *<>>.tt*',.* J U * <+^;^-^ ft.: *+i kb i r FIGURE 7 a Photomicrograph of normal testis from normal 28 yr old man H and E, X 150. b Photomicrograph of testis from a patient (No. 5) with hypogonadotrophic hypogonadism and hyposmia. Note spermatogenic arrest and absence of Leydig cells. H and E, X 150. by urinary testosterone excretion, that a patient with hypogonadism and gynecomastia responded less well to HCG than did two controls. In the present report the comparative studies of the plasma testosterone response to HCG provides the first quantitative evidence that the Leydig cells of hypogonadal boys with hyposmia are relatively insensitive to gonadotropins. The data available suggest that unresponsiveness of the Leydig cells in these patients is not a function of hypogonadotropism per se, since children and hypopituitary patients with similar gonadotropin levels showed a better response to HCG. Furthermore, some hyposmic patients failed to respond either clinically or with a normal testosterone increment to prolonged HCG administration. These observations are particularly significant since HCG treatment of prepuberal boys for 15 days increased plasma testosterone levels into the range of normal adult men (38). It would thus appear that the Leydig cell insensitivity represents a heretofore unemphasized gonadal abnormality in patients with hyposmia and hypogonadism. These patients may therefore have defects of both ends of the pituitary-leydig cell axis manifested by hypogonadotropism and gonadotropin unresponsiveness. APPENDIX Patients with hyposmia and hypogonadism Patient 1. J. S. had undescended testes at birth. He received injections of HCG at age 3 and 9 yr, and his left 2054 Bardin, Ross, Rifkind, Cargille, and Lipsett testes descended. At age 15 yr he was again treated by his referring physician with HCG, 1500 IU three times weekly for 4 months. During this period of treatment he developed axillary, pubic, and facial hair and noted an increase in phallic size. Patient 2. D. F. contracted chicken pox, bilateral otitis media, and pneumonia at 6 months of age. At 1 yr he was noted to be deaf. Between the ages of 9 and 11 yr he received several long courses of HCG for bilateral cryptorchidism. The testes did not descend, and axillary and pubic hair did not develop during HCG therapy. A right inguinal herniorrhaphy was performed at age 12 yr. At 14 yr he was referred to us. He had nerve deafness, color blindness, left amblyopia exanopsia with heterochromia of irides, and decreased vision in the left eye. His penis was infantile, and there was no palpable prostate. The small right testis (1 X 1.5 cm) was high in the inguinal canal, but the left testis was not palpable. Treatment with fluoxymestrone, 5 mg/day, caused secondary sexual development. Patient 3. H. C. was rejected by the army at age 18 because of failure to develop. The patient's father, however, had not undergone puberty until age 20 yr. He was referred to our service at age 20 at which time his penis and testes were infantile and the prostate was not palpable. After the studies were completed the patient received fluoxymestrone, 5 mg/day, with adequate virilization. PatieOt 4. PH was thought to have delayed sexual development at age 18 yr. Although he had erections, there were no ejaculations. At age 19 yr he was referred to our service. He had an infantile penis and no palpable prostate. Testes measured 1 X 1.5 cm. 1 yr after the tests were performed plasma testosterone was 0.04,ug/100 ml, and he coml)lained of decreased libido. Fluoxymestrone, 5 mg/day, caused adequate secondary sexual development and galactorrhea.
10 Patient 5. N. W. did not walk until age 18 months and at 3 yr was noted to be deaf. At age 22 he was referred to us because of sexual immaturity. He had nerve deafness and hyporeflexia. His penis (5 cm) and testes (1 X 2 cm) were infantile, and there was no palpable prostatic tissue. After studies he was treated with HCG, 1000 IU three times weekly for 3 months followed by 4000 IU three times weekly for 2 months without detectable change in phallic or prostatic size. The plasma testosterone level after the second course of HCG was 0.23,ug/100 ml. The patient was then treated with fluoxymestrone and underwent secondary sexual development. Patient 6. R. S. was treated with HCG at age 9 yr for bilateral inguinal testes. During this therapy he noted growth of facial, axillary, and pubic hair which stopped when the HCG was discontinued. He subsequently had erections but no ejaculations. At age 23 he was referred to our service. His penis was 5 cm and scrotal testes were 1 X 0.8 X 0.5 cm. No prostate tissue was palpable. The patient was then treated with HCG, 1000 IU twice weekly for 8 months. On this medication he noted gynecomastia, a slight increase in facial hair, and more frequent erections, but there were no ejaculations and no increase in prostate size. Plasma testosterone after 8 months of HCG therapy was /lg/100 ml. Patient 7. H. R. was given a series of HCG injections for bilateral cryptorchidism at age 14 yr. On this medication the left testis descended into the scrotum, and there was an increase in stature (3 inches) and slight growth of both pubic hair and penis. Thereafter the patient did not undergo puberty, and there was no increase in height. At age 21 yr he was referred to us. He had an infantile penis and testes and a small prostate. The right testis was high in the inguinal canal. HCG administration resulted in further growth of pubic hair, and penis and prostate increased in size. At age 22 after a right orchiopexy, fluoxymestrone (5 mg/day) was begun, and secondary sexual development continued. At 27 yr of age fluoxymestrone was discontinued for 2 months, and the studies in Table I were performed. ACKNOWLEDGMENTS We wish to thank the following physicians for referring the hyposmic patients to our service: R. J. Meyer, T. Ham, I. M. Goldstein, R. H. Nestmann, J. J. Canary, R. R. Pittman, and J. Sode. We gratefully acknowledge the technical assistance of Amel French, Phil Rayford, and Jane Smith. We also thank Dr. Ralph Powell for preparing the photomicrographs. REFERENCES 1. Pozanski, W. J., J. Bennett, and J. B. R. McKendry Urinary steroid pattern in male hypogonadotropic hypogonadism. Can. Med. Ass. J. 96: Kallmann, F., W. A. Schonfeld, and S. E. Barrera The genetic aspects of primary eunuchoidism. Amer. J. Ment. Defic. 48: Nowakowski, H., and W. Lenz Genetic aspects in male hypogonadism. Recent Progr. Hormone Res. 17: Sparkes, R. S., R. W. Simpson, and C. A. Paulsen Familial hypogonadotropic hypogonadism with anosmia. Arch Int. Med. 121: Klinefelter, H. F., F. Albright, and G. C. Griswold Experience with quantitative test for normal or decreased amounts of follicle stimulating hormone in urine in endocrinotogical diagnosis. J. Clin. Endocrinol. Metab. 3: Wilson, H., and M. B. Lipsett Use of periodate oxidation in the clinical analysis of urine corticoids. Anal. Biochem. 5: Spencer-Peet, J., J. R. Daly, and V. Smith A simple method for improving the specificity of the fluorometric determination of adrenal corticosteroids in human plasma. J. Endocrinol. 31: Odell, W. D., G. T. Ross, and P. L. Rayford Radioimmunoassay for luteinizing hormone in human plasma or serum: physiological studies. J. Clin. Invest. 46: Cargille, C. M., D. Rodbard, and G. T. Ross Radioimmunoassay of human follicle stimulating hormone: bias due to antisera. J. Clin. Endocrinol. Metab. 28: Glick, S. M., J. Roth, R. S. Yalow, and S. A. Berson Immunoassay of human growth hormone in plasma. Nature (London). 199: Bardin, C. W., and M. B. Lipsett Estimation of testosterone and androstenedione in human peripheral plasma. Steroids. 9: Steelman, S. L., and F. M. Pohley Assay of the follicle stimulating hormone based on the augmentation with human chorionic gonadotropin. Endocrinology. 53: McArthur, J. W The identification of pituitary interstitial cell stimulating hormone in human urine. Endocrinology. 50: Rifkind, A. B., H. E. Kulin, and G. T. Ross Follicle-stimulating hormone (FSH) and luteinizing hormone (LH) in the urine of prepubertal children. J. Clin. Invest. 46: Kulin, H. E., A. B. Rifkind, and G. T. Ross Human luteinizing hormone (LH) activity in processed and unprocessed urine measured by radioimmunoassay and bioassay. J. Clin. Endocrinol. Metab. 28: Kohler, P. O., B. W. O'Malley, P. L. Rayford, M. B. Lipsett, and W. D. Odell Effect of pyrogen on blood levels of pituitary trophic hormones. Observations of the usefulness of the growth hormone response in the detection of pituitary disease. J. Clin. Endocrinol. Metab. 27: Hembree, W. C., and G. T. Ross Arginine infusion and growth hormone secretion. Lancet. 1: Bardin, C. W., G. T. Ross, and M. B. Lipsett Site of action of clomiphene citrate in men: a study of the pituitary-leydig cell axis. J. Clin. Endocrinol. Metab. 27: Cargille, C. M., G. T. Ross, and C. W. Bardin Clomiphene and gonadotrophin in men. Lancet. 2: Lipsett, M. B., H. Wilson, M. A. Kirschner, S. G. Korenman, L. M. Fishman, G. A. Sarfaty, and C. W. Bardin Studies on Leydig cell physiology and pathology: secretion and metabolism of testosterone. Recent. Progr. Hormone. Res. 22: Frasier, S. D., and R. Horton Androgens in the peripheral plasma of prepubertal children and adults. Steroids. 8: De Morsier, G Etudes sur les dysraphies cranioencephaliques. Schweiz. Arch. Neurol. Psychiat. 74: Henkin, R. I Hypogonadism associated with familial hyposmia. Clin. Res. 13: 244. (Abstr.) Hypogonadotropic Hypogonadism 2055
11 24. Warkany, J., G. S. Frauenberger, and A. G. Mitchell Heredofamilial deviations. I. The Lawrence-Moon Biedl Syndrome. Amer. J. Dis. Child. 53: Roth, A. A Familial eunuchoidism: The Lawremce- Moon Biedl syndrome. J. Urol. 57: Volpe, R., W. S. Metzler, and M. W. Johnston Familial hypogonadotrophic eunuchoidism with cerebellar ataxia. J. Clin. Endocrinol. Metab. 23: Matthews, W. B., and A. T. Rundle Familial cerebellar ataxia and hypogonadism. Brain. 87: Lynch, H. T., A. R. Kaplan, M. J. Henn, and A. J. Krush Familial coexistence of diabetes mellitus, hyperlipemia, short stature and hypogonadism. Amer. J. Med. Sci. 252: Rosewater, S., G. Gwinup, and G. J. Hamwi Familial gynecomastia. Ann. Int. Med. 63: Hecht, A., and H. Ruskin Seminiferous tubule dysgenesis (Klinefelter's syndrome) associated with familial cerebellar ataxia. J. Clin. Endocrinol. Metab. 20: Albert, A Male hypogonadism. IV. The testis in prepubertal or pubertal gonadotropic failure. Mayo Clin. Proc. 29: Brasel, J. A., J. C. Wright, L. Wilkins, and R. M. Blizzard An evaluation of seventy-five patients with hypopituitarism beginning in childhood. Amer. J. Med. 38: Gauthier, G La dysplasie olfacto-genitale (Agenesie des lobes olfactifs avec absence de developpement gonadique 'a la puberte). Acta Neuroveg. 21: Elwers, M., and V. Critchlow Precocious ovarian stimulation following hypothalamic and amygdaloid lesions in rats. Amer. J. Physiol. 198: Elwers, M., and V. Critchlow Precocious ovarian stimulation following interruption of stria terminalis. A4mer. J. Physiol. 201: Knorr, D Testosterone excretion in boys treated with HCG for cryptorchidism. In Testosterone. J. Tamm, editor. George Thieme Verlag KG, Stuttgart. 1st edition Horton, R., F. Gaford, and S. D. Frasier Plasma androgens in childhood and puberty. Clin. Res. 17: 106. (Abstr.) 38. Saez, J. M., and J. Bertrand Studies on testicular function in children: plasma concentrations of testosterone, dehydroepiandrosterone and its sulfate before and after stimulation with human chorionic gonadotrophin. Steroids. 12: Stuiver, P. C., J. H. H. Thijssen, and H. J. Van der Molen Plasma testosterone, urinary excretion of 17 ketosteroid fractions and urinary total 17 ketosteroids before, during and after stimulation with HCG in patients with deficient testicular function. In Androgen in Normal and Pathological Conditions. A. Vermeulen, editor. Excerpta Medica Foundation, Amsterdam. International Congress Series. 101: Hurxthal, L. M Sublingual use of testosterone in 7 cases of hypogonadism: report of 3 congenital eunuchoids occurring in one family. J. Clin. Endocrinol. Metab. 3: Muller, P Die olfacto-genitale dysplasie. Gynaecologia. 158: Wieland, R. G., R. L. Folk, J. N. Taylor, and G. J. Hamwi Studies of male hypogonadism. I. Androgen metabolism in a male with gynecomastia and galactorrhea. J. Clin. Endocrinol. Metab. 27: Bardin, Ross, Rifkind, Cargille, and Lipsett
Urinary Testosterone Response to Human Chorionic Gonadotropin
 Urinary Testosterone Response to Human Chorionic Gonadotropin Evaluation of Male Patients with Hypogonadotropic Hypogonadism BRUCE L. FARISS, M.D.,* GERARD M. CERCHIO, M.D.,t and VINCENT C. D1 RAIMONDO,
Urinary Testosterone Response to Human Chorionic Gonadotropin Evaluation of Male Patients with Hypogonadotropic Hypogonadism BRUCE L. FARISS, M.D.,* GERARD M. CERCHIO, M.D.,t and VINCENT C. D1 RAIMONDO,
and Luteinizing Hormone as Measured by Radioimmunoassay Correlated with Sexual Development in Hypopituitary Subjects
 Serum Follicular - Stimulating Hormone and Luteinizing Hormone as Measured by Radioimmunoassay Correlated with Sexual Development in Hypopituitary Subjects ROBERT PENNY, THOMAS P. FOLEY, JR., and ROBERT
Serum Follicular - Stimulating Hormone and Luteinizing Hormone as Measured by Radioimmunoassay Correlated with Sexual Development in Hypopituitary Subjects ROBERT PENNY, THOMAS P. FOLEY, JR., and ROBERT
Correlation of Serum Follicular Stimulating Hormone
 Correlation of Serum Follicular Stimulating Hormone (FSH) and Luteinizing Hornone (LH) as Measured by Radioimmunoassay in Disorders of Sexual Development ROBERT PENNY, HARVEY J. GUYDA, ALIcE BAGHDASSARIAN,
Correlation of Serum Follicular Stimulating Hormone (FSH) and Luteinizing Hornone (LH) as Measured by Radioimmunoassay in Disorders of Sexual Development ROBERT PENNY, HARVEY J. GUYDA, ALIcE BAGHDASSARIAN,
TESTOSTERONE DEFINITION
 DEFINITION A hormone that is a hydroxyl steroid ketone (C19H28O2) produced especially by the testes or made synthetically and that is responsible for inducing and maintaining male secondary sex characteristics.
DEFINITION A hormone that is a hydroxyl steroid ketone (C19H28O2) produced especially by the testes or made synthetically and that is responsible for inducing and maintaining male secondary sex characteristics.
Follicle-Stimulating Hormone (FSH) and Luteinzing
 The Journal of Clinical Invest'gaio* Vol. 46, No. 12, 1967 Follicle-Stimulating Hormone (FSH) and Luteinzing Hormone (LH) in the Urine of Prepubertal Children * ARLEEN B. RIFKIND, HOWARD E. KULIN, AND
The Journal of Clinical Invest'gaio* Vol. 46, No. 12, 1967 Follicle-Stimulating Hormone (FSH) and Luteinzing Hormone (LH) in the Urine of Prepubertal Children * ARLEEN B. RIFKIND, HOWARD E. KULIN, AND
Index. urologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Acquired hypogonadism, prevalence of, 165 167 primary, 165 secondary, 167 Adipose tissue, as an organ, 240 241 Adrenal hyperplasia, congenital,
Note: Page numbers of article titles are in boldface type. A Acquired hypogonadism, prevalence of, 165 167 primary, 165 secondary, 167 Adipose tissue, as an organ, 240 241 Adrenal hyperplasia, congenital,
Clinical evaluation of infertility
 Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Yutaka; SAKAMOTO, Hiromi. Citation 泌尿器科紀要 (1986), 32(10):
 Title46XX male; report of case OKUYAMA, Akihiko; KONDO, Nobuyuki; Author(s) NAKAMURA, Masahiro; SONODA, Takao; Yutaka; SAKAMOTO, Hiromi Citation 泌尿器科紀要 (1986), 32(10): 1539-1542 Issue Date 1986-10 URL
Title46XX male; report of case OKUYAMA, Akihiko; KONDO, Nobuyuki; Author(s) NAKAMURA, Masahiro; SONODA, Takao; Yutaka; SAKAMOTO, Hiromi Citation 泌尿器科紀要 (1986), 32(10): 1539-1542 Issue Date 1986-10 URL
Reproductive FSH. Analyte Information
 Reproductive FSH Analyte Information 1 Follicle-stimulating hormone Introduction Follicle-stimulating hormone (FSH, also known as follitropin) is a glycoprotein hormone secreted by the anterior pituitary
Reproductive FSH Analyte Information 1 Follicle-stimulating hormone Introduction Follicle-stimulating hormone (FSH, also known as follitropin) is a glycoprotein hormone secreted by the anterior pituitary
DISORDERS OF MALE GENITALS
 Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 9. Testicular disorders/disorders of male genitals. Horm Res 2007;68(suppl 2):63 66 ESPE Code Diagnosis OMIM ICD10
Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 9. Testicular disorders/disorders of male genitals. Horm Res 2007;68(suppl 2):63 66 ESPE Code Diagnosis OMIM ICD10
The Effect of Clomiphene Citrate Male Infertility
 The Effect of Clomiphene Citrate Male Infertility. tn RAYMOND C. MELLINGER, M.D., and ROBERT J. THOMPSON, M.D. CLOMIPHENE CITRATE, an analog of the nonsteroidal estrogen TACE,* has proved effective in
The Effect of Clomiphene Citrate Male Infertility. tn RAYMOND C. MELLINGER, M.D., and ROBERT J. THOMPSON, M.D. CLOMIPHENE CITRATE, an analog of the nonsteroidal estrogen TACE,* has proved effective in
THE STIMULATION AND PROLONGED MAINTENANCE OF SPERMATOGENESIS BY HUMAN PITUITARY GONADOTROPHINS IN A PATIENT WITH HYPOGONADOTROPHIC HYPOGONADISM
 THE STIMULATION AND PROLONGED MAINTENANCE OF SPERMATOGENESIS BY HUMAN PITUITARY GONADOTROPHINS IN A PATIENT WITH HYPOGONADOTROPHIC HYPOGONADISM F. I. R. MARTIN Endocrine Clinic, Boyal Melbourne Hospital,
THE STIMULATION AND PROLONGED MAINTENANCE OF SPERMATOGENESIS BY HUMAN PITUITARY GONADOTROPHINS IN A PATIENT WITH HYPOGONADOTROPHIC HYPOGONADISM F. I. R. MARTIN Endocrine Clinic, Boyal Melbourne Hospital,
Male Hypogonadism Associated with Elevated LH, Normal FSH and Low Testosterone Possibly Due to an Abnormal LH Molecule
 INTERNATIONAL JOURNAL OF ANDROLOGY 2 (1979) 482-488 Andrology Center, Department of Modical Fathology, Catania Medical School, University of Catania, Catania, Italy. Male Hypogonadism Associated with Elevated
INTERNATIONAL JOURNAL OF ANDROLOGY 2 (1979) 482-488 Andrology Center, Department of Modical Fathology, Catania Medical School, University of Catania, Catania, Italy. Male Hypogonadism Associated with Elevated
Hypothalamus & Pituitary Gland
 Hypothalamus & Pituitary Gland Hypothalamus and Pituitary Gland The hypothalamus and pituitary gland form a unit that exerts control over the function of several endocrine glands (thyroid, adrenals, and
Hypothalamus & Pituitary Gland Hypothalamus and Pituitary Gland The hypothalamus and pituitary gland form a unit that exerts control over the function of several endocrine glands (thyroid, adrenals, and
Recently we had the opportunity of examining a young man with bilateral atrophy of the testes, whose case history may serve to point out the dangers
 From the 2. Medical Clinic, University of Hamburg, Germany (Professor Dr. A. Jores) BILATERAL TESTICULAR ATROPHY AS A RESULT OF SCROTAL HEMATOMA IN THE NEWBORN By Henryk Nowakowski Recently we had the
From the 2. Medical Clinic, University of Hamburg, Germany (Professor Dr. A. Jores) BILATERAL TESTICULAR ATROPHY AS A RESULT OF SCROTAL HEMATOMA IN THE NEWBORN By Henryk Nowakowski Recently we had the
Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature
 REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
OBJECTIVES. Rebecca McEachern, MD. Puberty: Too early, Too Late or Just Right? Special Acknowledgements. Maryann Johnson M.Ed.
 1 Puberty: Too early, Too Late or Just Right? Maryann Johnson M.Ed., BSN, RN Special Acknowledgements Rebecca McEachern, MD OBJECTIVES Illustrate basic endocrine system and hormonal pathways Define the
1 Puberty: Too early, Too Late or Just Right? Maryann Johnson M.Ed., BSN, RN Special Acknowledgements Rebecca McEachern, MD OBJECTIVES Illustrate basic endocrine system and hormonal pathways Define the
- production of two types of gametes -- fused at fertilization to form zygote
 Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Why is my body not changing? Conflicts of interest. Overview 11/9/2015. None
 Why is my body not changing? Murthy Korada Pediatrician, Pediatric Endocrinologist Ridge Meadows Hospital Surrey Memorial Hospital None Conflicts of interest Overview Overview of normal pubertal timing
Why is my body not changing? Murthy Korada Pediatrician, Pediatric Endocrinologist Ridge Meadows Hospital Surrey Memorial Hospital None Conflicts of interest Overview Overview of normal pubertal timing
Hypogonadotropic Hypogonadism
 Pituitary-Testicular Responsiveness in Male Hypogonadotropic Hypogonadism RICHARD L. WINSTIN and RIicIARD. Rnr From the Clinical Investigation Center, Naval Hospital, Oakland, the Department of Medicine,
Pituitary-Testicular Responsiveness in Male Hypogonadotropic Hypogonadism RICHARD L. WINSTIN and RIicIARD. Rnr From the Clinical Investigation Center, Naval Hospital, Oakland, the Department of Medicine,
Outline. Male Reproductive System Testes and Sperm Hormonal Regulation
 Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Report of 3 cases. 1969). Isolated deficiency of pituitary gonadotrophin secretion is uncommon,
 The Medical Unit, The Princess Margaret Hospital, Christchurch, New Zealand PITUITARY AND GONADAL FUNCTION IN HYPOGONADOTROPHIC HYPOGONADISM Report of 3 cases By E. A. Espiner and R. A. Donald ABSTRACT
The Medical Unit, The Princess Margaret Hospital, Christchurch, New Zealand PITUITARY AND GONADAL FUNCTION IN HYPOGONADOTROPHIC HYPOGONADISM Report of 3 cases By E. A. Espiner and R. A. Donald ABSTRACT
Action of reproductive hormones through the life span 9/22/99
 Action of reproductive hormones through the life span Do reproductive hormones affect the life span? One hypothesis about the rate of aging asserts that there is selective pressure for either high rate
Action of reproductive hormones through the life span Do reproductive hormones affect the life span? One hypothesis about the rate of aging asserts that there is selective pressure for either high rate
Unit 15 ~ Learning Guide
 Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Treatment of Oligospermia with Large Doses of Human Chorionic Gonadotropin
 Treatment of Oligospermia with Large Doses of Human Chorionic Gonadotropin A Preliminary Report S. J. GLASS, M.D., and H. M. HOLLAND, M.D. BEFORE discussing gonadotropic therapy of oligospermia, it is
Treatment of Oligospermia with Large Doses of Human Chorionic Gonadotropin A Preliminary Report S. J. GLASS, M.D., and H. M. HOLLAND, M.D. BEFORE discussing gonadotropic therapy of oligospermia, it is
3 year old boy with puberty. Katie Stanley, MD August 1, 2013
 3 year old boy with puberty Katie Stanley, MD August 1, 2013 Initial presentation 3 and 11/12 year old boy with signs of puberty Presented to outside endocrinologist in 2002 with: Pubic hair since 2.5
3 year old boy with puberty Katie Stanley, MD August 1, 2013 Initial presentation 3 and 11/12 year old boy with signs of puberty Presented to outside endocrinologist in 2002 with: Pubic hair since 2.5
When testes make no testosterone: Identifying a rare cause of 46, XY female phenotype in adulthood
 When testes make no testosterone: Identifying a rare cause of 46, XY female phenotype in adulthood Gardner DG, Shoback D. Greenspan's Basic & Clinical Endocrinology, 10e; 2017 Sira Korpaisarn, MD Endocrinology
When testes make no testosterone: Identifying a rare cause of 46, XY female phenotype in adulthood Gardner DG, Shoback D. Greenspan's Basic & Clinical Endocrinology, 10e; 2017 Sira Korpaisarn, MD Endocrinology
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization
 Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
Aromatase Inhibitors in Male Infertility:
 Aromatase Inhibitors in Male Infertility: The hype of hypogonadism? BEATRIZ UGALDE, PHARM.D. H-E-B/UNIVERSITY OF TEXAS COMMUNITY PHARMACY PGY1 03 NOVEMBER 2017 PHARMACOTHERAPY ROUNDS Disclosures No conflicts
Aromatase Inhibitors in Male Infertility: The hype of hypogonadism? BEATRIZ UGALDE, PHARM.D. H-E-B/UNIVERSITY OF TEXAS COMMUNITY PHARMACY PGY1 03 NOVEMBER 2017 PHARMACOTHERAPY ROUNDS Disclosures No conflicts
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on the Approach to Pediatric Anemia and Pallor. These podcasts are designed to give medical students an overview of key
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on the Approach to Pediatric Anemia and Pallor. These podcasts are designed to give medical students an overview of key
Testosterone Treatment: Myths Vs Reality. Fadi Al-Khayer, M.D, F.A.C.E
 Testosterone Treatment: Myths Vs Reality Fadi Al-Khayer, M.D, F.A.C.E The Biological Functions of Testosterone in Men Testosterone is essential to the musculoskeletal and metabolic systems throughout a
Testosterone Treatment: Myths Vs Reality Fadi Al-Khayer, M.D, F.A.C.E The Biological Functions of Testosterone in Men Testosterone is essential to the musculoskeletal and metabolic systems throughout a
IN SUMMARY HST 071 NORMAL & ABNORMAL SEXUAL DIFFERENTIATION Fetal Sex Differentiation Postnatal Diagnosis and Management of Intersex Abnormalities
 Harvard-MIT Division of Health Sciences and Technology HST.071: Human Reproductive Biology Course Director: Professor Henry Klapholz IN SUMMARY HST 071 Title: Fetal Sex Differentiation Postnatal Diagnosis
Harvard-MIT Division of Health Sciences and Technology HST.071: Human Reproductive Biology Course Director: Professor Henry Klapholz IN SUMMARY HST 071 Title: Fetal Sex Differentiation Postnatal Diagnosis
Growth hormone therapy in a girl with Turner syndrome showing a large increase over the initially predicted ht of 4 5
 Disorders of Growth and Puberty: How to Recognize the Normal Variants vs Patients Who Need to be Evaluated Paul Kaplowitz, M.D Pediatric Endocrinology. VCU School of Medicine Interpretation of Growth Charts
Disorders of Growth and Puberty: How to Recognize the Normal Variants vs Patients Who Need to be Evaluated Paul Kaplowitz, M.D Pediatric Endocrinology. VCU School of Medicine Interpretation of Growth Charts
Chapter 28: REPRODUCTIVE SYSTEM: MALE
 Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
FLASH CARDS. Kalat s Book Chapter 11 Alphabetical
 FLASH CARDS www.biologicalpsych.com Kalat s Book Chapter 11 Alphabetical alpha-fetoprotein alpha-fetoprotein Alpha-Fetal Protein (AFP) or alpha-1- fetoprotein. During a prenatal sensitive period, estradiol
FLASH CARDS www.biologicalpsych.com Kalat s Book Chapter 11 Alphabetical alpha-fetoprotein alpha-fetoprotein Alpha-Fetal Protein (AFP) or alpha-1- fetoprotein. During a prenatal sensitive period, estradiol
15) Presenting Problems in Reproductive Disease Dr. Taha
 Testicular & Breast Disorders in Male Hypogonadism Hypogonadism can refer to either: 15) Presenting Problems in Reproductive Disease Dr. Taha 1. The failure of the testes to produce adequate testosterone
Testicular & Breast Disorders in Male Hypogonadism Hypogonadism can refer to either: 15) Presenting Problems in Reproductive Disease Dr. Taha 1. The failure of the testes to produce adequate testosterone
Reproductive physiology. About this Chapter. Case introduction. The brain directs reproduction 2010/6/29. The Male Reproductive System
 Section Ⅻ Reproductive physiology Ming-jie Wang E-Mail: mjwang@shmu.edu.cn About this Chapter The reproductive organs and how they work the major endocrine functions of sexual glands actions of sex hormones
Section Ⅻ Reproductive physiology Ming-jie Wang E-Mail: mjwang@shmu.edu.cn About this Chapter The reproductive organs and how they work the major endocrine functions of sexual glands actions of sex hormones
GONADAL FUNCTION: An Overview
 GONADAL FUNCTION: An Overview University of PNG School of Medicine & Health Sciences Division of Basic Medical Sciences Clinical Biochemistry BMLS III & BDS IV VJ Temple 1 What are the Steroid hormones?
GONADAL FUNCTION: An Overview University of PNG School of Medicine & Health Sciences Division of Basic Medical Sciences Clinical Biochemistry BMLS III & BDS IV VJ Temple 1 What are the Steroid hormones?
Sexual Development. 6 Stages of Development
 6 Sexual Development 6 Stages of Development Development passes through distinct stages, the first of which is fertilization, when one sperm enters one ovum. To enter an ovum, a sperm must undergo the
6 Sexual Development 6 Stages of Development Development passes through distinct stages, the first of which is fertilization, when one sperm enters one ovum. To enter an ovum, a sperm must undergo the
Laura Stewart, MD, FRCPC Clinical Associate Professor Division of Pediatric Endocrinology University of British Columbia
 Precocious Puberty Laura Stewart, MD, FRCPC Clinical Associate Professor Division of Pediatric Endocrinology University of British Columbia Faculty Disclosure Faculty: Laura Stewart No relationships with
Precocious Puberty Laura Stewart, MD, FRCPC Clinical Associate Professor Division of Pediatric Endocrinology University of British Columbia Faculty Disclosure Faculty: Laura Stewart No relationships with
Chapter 14 Reproduction Review Assignment
 Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Male Reproduction Organs. 1. Testes 2. Epididymis 3. Vas deferens 4. Urethra 5. Penis 6. Prostate 7. Seminal vesicles 8. Bulbourethral glands
 Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Sexual dysfunction of chronic kidney disease. Razieh salehian.md psychiatrist
 Sexual dysfunction of chronic kidney disease Razieh salehian.md psychiatrist Disturbances in sexual function are a common feature of chronic renal failure. Sexual dysfunction is inversely associated with
Sexual dysfunction of chronic kidney disease Razieh salehian.md psychiatrist Disturbances in sexual function are a common feature of chronic renal failure. Sexual dysfunction is inversely associated with
EAU GUIDELINES ON MALE HYPOGONADISM
 EAU GUIDELINES ON MALE HYPOGONADISM (Limited text update March 2017) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch Introduction Male hypogonadism is a clinical syndrome caused by androgen
EAU GUIDELINES ON MALE HYPOGONADISM (Limited text update March 2017) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch Introduction Male hypogonadism is a clinical syndrome caused by androgen
Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems
 CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems 3. Male Reproductive anatomy and physiology. Testes = paired
CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems 3. Male Reproductive anatomy and physiology. Testes = paired
Variable X-linked recessive hypopituitarism with evidence of gonadotropin deficiency in two pre-pubertal males
 Clinical Genetics 1977: 11: 249-254 Variable X-linked recessive hypopituitarism with evidence of gonadotropin deficiency in two pre-pubertal males W. B. ZIPF, R. P. KELCH AND G. E. BACON C. S. Mott Childrens
Clinical Genetics 1977: 11: 249-254 Variable X-linked recessive hypopituitarism with evidence of gonadotropin deficiency in two pre-pubertal males W. B. ZIPF, R. P. KELCH AND G. E. BACON C. S. Mott Childrens
Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor)
 Indifferent ducts of embryo Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Y chromosome present Y chromosome absent Phenotypic sex is depends on development of external
Indifferent ducts of embryo Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Y chromosome present Y chromosome absent Phenotypic sex is depends on development of external
Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor)
 Indifferent ducts of embryo Y chromosome present Y chromosome absent Male Female penis ovary uterus vagina testis Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Phenotypic
Indifferent ducts of embryo Y chromosome present Y chromosome absent Male Female penis ovary uterus vagina testis Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Phenotypic
GUIDELINES ON MALE HYPOGONADISM
 GUIDELINES ON MALE HYPOGONADISM (Text update March 2015) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch, M. Punab Introduction Male hypogonadism is a clinical syndrome caused by androgen
GUIDELINES ON MALE HYPOGONADISM (Text update March 2015) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch, M. Punab Introduction Male hypogonadism is a clinical syndrome caused by androgen
Pulsatile gonadotrophin releasing hormone versus gonadotrophin treatment of hypothalamic hypogonadism in males
 Human Reproduction vol.8 Suppl.2 pp. 175-179, 1993 Pulsatile gonadotrophin releasing hormone versus gonadotrophin treatment of hypothalamic hypogonadism in males Jochen Schopohl Medizinische Klinik, Klinikum
Human Reproduction vol.8 Suppl.2 pp. 175-179, 1993 Pulsatile gonadotrophin releasing hormone versus gonadotrophin treatment of hypothalamic hypogonadism in males Jochen Schopohl Medizinische Klinik, Klinikum
Leydig cell hypofunction resulting in male pseudohermaphroditism*
 FERmlTY AND STERILlTY Copyright" 1982 The American Fertility Society Vol. 37, No.6, May 1982 Printed in U.S.A. Leydig cell hypofunction resulting in male pseudohermaphroditism* Peter A. Lee, M.D., Ph.D.t+1I
FERmlTY AND STERILlTY Copyright" 1982 The American Fertility Society Vol. 37, No.6, May 1982 Printed in U.S.A. Leydig cell hypofunction resulting in male pseudohermaphroditism* Peter A. Lee, M.D., Ph.D.t+1I
Male Reproductive System
 21-1 21-2 Reproductive System Male Reproductive System Genital Tract In males the testes, held outside the body in the scrotum (optimum temp of about 35 0 C), produce sperm. Sperm mature in coiled tubes
21-1 21-2 Reproductive System Male Reproductive System Genital Tract In males the testes, held outside the body in the scrotum (optimum temp of about 35 0 C), produce sperm. Sperm mature in coiled tubes
HCG (human chorionic gonadotropin); Novarel Pregnyl (chorionic gonadotropin); Ovidrel (choriogonadotropin alfa)
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.08.09 Subject: HCG Page: 1 of 5 Last Review Date: June 19, 2015 HCG Powder, Novarel, Pregnyl, Ovidrel
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.08.09 Subject: HCG Page: 1 of 5 Last Review Date: June 19, 2015 HCG Powder, Novarel, Pregnyl, Ovidrel
Chapter 22 The Reproductive System (I)
 Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
Laboratory Investigation of Male Gonadal Function. Dr N Oosthuizen Dept of Chemical Pathology UP 2010
 Laboratory Investigation of Male Gonadal Function Dr N Oosthuizen Dept of Chemical Pathology UP 2010 1 Figure 1. Hypothalamic-pituitary pituitary-testicular testicular axis 2 Testosterone (T) measurement
Laboratory Investigation of Male Gonadal Function Dr N Oosthuizen Dept of Chemical Pathology UP 2010 1 Figure 1. Hypothalamic-pituitary pituitary-testicular testicular axis 2 Testosterone (T) measurement
EAU GUIDELINES ON MALE HYPOGONADISM
 EAU GUIDELINES ON MALE HYPOGONADISM (Text update March 2015) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch, M. Punab Introduction Male hypogonadism is a clinical syndrome caused by
EAU GUIDELINES ON MALE HYPOGONADISM (Text update March 2015) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch, M. Punab Introduction Male hypogonadism is a clinical syndrome caused by
Hormonal factors associated with hypogonadismand infertility in males - chromosomal abnormality
 OSR Journal of Dental and Medical Sciences (OSR-JDMS) e-ssn: 2279-0853, p-ssn: 2279-0861. Volume 10, ssue 1 (Sep.- Oct. 2013), PP 71-75 Hormonal factors associated with hypogonadismand infertility in males
OSR Journal of Dental and Medical Sciences (OSR-JDMS) e-ssn: 2279-0853, p-ssn: 2279-0861. Volume 10, ssue 1 (Sep.- Oct. 2013), PP 71-75 Hormonal factors associated with hypogonadismand infertility in males
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Puberty and Pubertal Disorders Part 2: Precocious Puberty. These podcasts are designed to give medical students an overview
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Puberty and Pubertal Disorders Part 2: Precocious Puberty. These podcasts are designed to give medical students an overview
Chapter 14 The Reproductive System
 Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Isolated growth hormone deficiency
 Archives of Disease in Childhood, 1974, 49, 55. Isolated growth hormone deficiency Two families with autosomal dominant inheritance E. M. E. POSKITT and P. H. W. RAYNER From the Institute of Child Health,
Archives of Disease in Childhood, 1974, 49, 55. Isolated growth hormone deficiency Two families with autosomal dominant inheritance E. M. E. POSKITT and P. H. W. RAYNER From the Institute of Child Health,
Testosterone Therapy in Men with Hypogonadism
 Testosterone Therapy in Men with Hypogonadism (Endocrine Society 2018 Guideline) Ngwe Yin, MD Assistant Clinical Professor of Medicine, UCSF Fresno Medical Education Program Disclosures None Objective
Testosterone Therapy in Men with Hypogonadism (Endocrine Society 2018 Guideline) Ngwe Yin, MD Assistant Clinical Professor of Medicine, UCSF Fresno Medical Education Program Disclosures None Objective
Reproductive System Purpose General Structures Male Structures Functions Female Anatomy Structures Functions Clinical Applications
 The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
LH and FSH. Women. Men. Increased LH. Decreased LH. By Ronald Steriti, ND, PhD 2011
 LH and FSH By Ronald Steriti, ND, PhD 2011 Luteinizing hormone (LH) and follicle-stimulating hormone (FSH) are gonadotropins that stimulate the gonads - the testes in males, and the ovaries in females.
LH and FSH By Ronald Steriti, ND, PhD 2011 Luteinizing hormone (LH) and follicle-stimulating hormone (FSH) are gonadotropins that stimulate the gonads - the testes in males, and the ovaries in females.
10.7 The Reproductive Hormones
 10.7 The Reproductive Hormones December 10, 2013. Website survey?? QUESTION: Who is more complicated: men or women? The Female Reproductive System ovaries: produce gametes (eggs) produce estrogen (steroid
10.7 The Reproductive Hormones December 10, 2013. Website survey?? QUESTION: Who is more complicated: men or women? The Female Reproductive System ovaries: produce gametes (eggs) produce estrogen (steroid
A COMPARATIVE STUDY OF GERM CELL KINETICS IN THE TESTES OF CHILDREN WITH UNILATERAL CRYPTORCHIDISM: A PRELIMINARY REPORT*
 FERTILITY AND STERILITY Copyright 1970 by the Williams & Wilkins Co. Vol. 21, No. 11, November 1970 Printed in U.S.A. A COMPARATIVE STUDY OF GERM CELL KINETICS IN THE TESTES OF CHILDREN WITH UNILATERAL
FERTILITY AND STERILITY Copyright 1970 by the Williams & Wilkins Co. Vol. 21, No. 11, November 1970 Printed in U.S.A. A COMPARATIVE STUDY OF GERM CELL KINETICS IN THE TESTES OF CHILDREN WITH UNILATERAL
The Usefulness of GnRH and hcg Testing for the Differential Diagnosis of Delayed Puberty and Hypogonadotropic Hypogonadism in Prepubertal Boys
 The Usefulness of GnRH and hcg Testing for the Differential Diagnosis of Delayed Puberty and Hypogonadotropic Hypogonadism in Prepubertal Boys Naoko SATO 1), Noriyuki KATSUMATA 1), Reiko HORIKAWA 2) and
The Usefulness of GnRH and hcg Testing for the Differential Diagnosis of Delayed Puberty and Hypogonadotropic Hypogonadism in Prepubertal Boys Naoko SATO 1), Noriyuki KATSUMATA 1), Reiko HORIKAWA 2) and
Low Testosterone Consultation Information
 T Low Testosterone Consultation Information www.urologyaustin.com Andropause or Male Menopause This syndrome has been nicknamed ADAM, which stands for androgen deficiency of the aging male. It differs
T Low Testosterone Consultation Information www.urologyaustin.com Andropause or Male Menopause This syndrome has been nicknamed ADAM, which stands for androgen deficiency of the aging male. It differs
DAX1, testes development role 7, 8 DFFRY, spermatogenesis role 49 DMRT genes, male sex differentiation role 15
 Subject Index N-Acetylcysteine, sperm quality effects 71 Ambiguous genitalia, origins 1, 2 Anti-Müllerian hormone function 13 receptors 13 Sertoli cell secretion 10, 38 Apoptosis assays in testes 73, 74
Subject Index N-Acetylcysteine, sperm quality effects 71 Ambiguous genitalia, origins 1, 2 Anti-Müllerian hormone function 13 receptors 13 Sertoli cell secretion 10, 38 Apoptosis assays in testes 73, 74
Clinical Guideline ADRENARCHE MANAGEMENT OF CHILDREN PRESENTING WITH SIGNS OF EARLY ONSET PUBIC HAIR/BODY ODOUR/ACNE
 Clinical Guideline ADRENARCHE MANAGEMENT OF CHILDREN PRESENTING WITH SIGNS OF EARLY ONSET PUBIC HAIR/BODY ODOUR/ACNE Includes guidance for the distinction between adrenarche, precocious puberty and other
Clinical Guideline ADRENARCHE MANAGEMENT OF CHILDREN PRESENTING WITH SIGNS OF EARLY ONSET PUBIC HAIR/BODY ODOUR/ACNE Includes guidance for the distinction between adrenarche, precocious puberty and other
Carolyn Pheteplace. Department of Obstetrics and Gynecology,
 Department of Obstetrics and Gynecology, Harvard Medical School, and Department of Surgery, Peter Bent Brigham Hospital. Boston, Massachusetts, U. S. A. FOLLICLESTIMULATING HORMONE AND LUTEINIZING HORMONE
Department of Obstetrics and Gynecology, Harvard Medical School, and Department of Surgery, Peter Bent Brigham Hospital. Boston, Massachusetts, U. S. A. FOLLICLESTIMULATING HORMONE AND LUTEINIZING HORMONE
The Journal of Veterinary Medical Science
 Advance Publication The Journal of Veterinary Medical Science Accepted Date: 1 Jun 01 J-STAGE Advance Published Date: Jun 01 Theriogenology (Note) Therapeutic effects of oral clomiphene citrate in dogs
Advance Publication The Journal of Veterinary Medical Science Accepted Date: 1 Jun 01 J-STAGE Advance Published Date: Jun 01 Theriogenology (Note) Therapeutic effects of oral clomiphene citrate in dogs
SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY
 1 SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL SEMINAR: SEX HORMONES PART 1 An Overview What are steroid hormones? Steroid
1 SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL SEMINAR: SEX HORMONES PART 1 An Overview What are steroid hormones? Steroid
ANDROGEN DEFICIENCY/MALE HYPOGONADISM
 ANDROGEN DEFICIENCY/MALE HYPOGONADISM 1. Medical Condition Hypogonadism in men is a clinical syndrome that results from failure of the testes to produce physiological levels of testosterone (androgen deficiency)
ANDROGEN DEFICIENCY/MALE HYPOGONADISM 1. Medical Condition Hypogonadism in men is a clinical syndrome that results from failure of the testes to produce physiological levels of testosterone (androgen deficiency)
Male History, Clinical Examination and Testing
 Male History, Clinical Examination and Testing Dirk Vanderschueren, MD, PhD Case Jan is 29 years old and consults for 1 year primary subfertility partner 28 years old and normal gynaecological investigation
Male History, Clinical Examination and Testing Dirk Vanderschueren, MD, PhD Case Jan is 29 years old and consults for 1 year primary subfertility partner 28 years old and normal gynaecological investigation
Paul Hofman. Professor. Paediatrician Endocrinologist Liggins Institute, The University of Auckland, Starship Children Hospital, Auckland
 Professor Paul Hofman Paediatrician Endocrinologist Liggins Institute, The University of Auckland, Starship Children Hospital, Auckland 14:00-14:55 WS #108: Common pubertal variants how to distinguish
Professor Paul Hofman Paediatrician Endocrinologist Liggins Institute, The University of Auckland, Starship Children Hospital, Auckland 14:00-14:55 WS #108: Common pubertal variants how to distinguish
Reproductive Endocrinology. Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007
 Reproductive Endocrinology Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007 isabelss@hkucc.hku.hk A 3-hormone chain of command controls reproduction with
Reproductive Endocrinology Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007 isabelss@hkucc.hku.hk A 3-hormone chain of command controls reproduction with
LIE ASSAY OF GONADOTROPIN in human blood is one of the most important
 Changes in Human Serum FSH Levels During the Normal Menstrual Cycle MASAO IGARASHI, M.D., JUNJI KAMIOKA, M.D., YOICHI EHARA, M.D., and SEIICHI MATSUMOTO, M.D. LIE ASSAY OF GONADOTROPIN in human blood is
Changes in Human Serum FSH Levels During the Normal Menstrual Cycle MASAO IGARASHI, M.D., JUNJI KAMIOKA, M.D., YOICHI EHARA, M.D., and SEIICHI MATSUMOTO, M.D. LIE ASSAY OF GONADOTROPIN in human blood is
Study Guide Answer Key Reproductive System
 Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Isolated follicle-stimulating hormone deficiency in men: successful long-term gonadotropin therapy*
 FERTILITY AND STERILITY Copyright c 1984 The American Fertility Society Printed in U.SA. Isolated follicle-stimulating hormone deficiency in men: successful long-term gonadotropin therapy* Ahmed A.-K.
FERTILITY AND STERILITY Copyright c 1984 The American Fertility Society Printed in U.SA. Isolated follicle-stimulating hormone deficiency in men: successful long-term gonadotropin therapy* Ahmed A.-K.
REPRODUCCIÓN. La idea fija. Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
Puberty and Pubertal Disorders Part 3: Delayed Puberty
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Puberty and Pubertal Disorders Part 3: Delayed Puberty These podcasts are designed to give medical students an overview
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Puberty and Pubertal Disorders Part 3: Delayed Puberty These podcasts are designed to give medical students an overview
Reproductive physiology
 Reproductive physiology Sex hormones: Androgens Estrogens Gestagens Learning objectives 86 (also 90) Sex Genetic sex Gonadal sex Phenotypic sex XY - XX chromosomes testes - ovaries external features Tha
Reproductive physiology Sex hormones: Androgens Estrogens Gestagens Learning objectives 86 (also 90) Sex Genetic sex Gonadal sex Phenotypic sex XY - XX chromosomes testes - ovaries external features Tha
Treatment of Defective Spermatogenesis tvith Human Gonadotropins
 Treatment of Defective Spermatogenesis tvith Human Gonadotropins W. Z. POLISHUK, M.D., Z. PALTI, M.D., and A. LAUFER, M.D. TREATMENT of male sterility due to defective spermatogenesis is not satisfactory.
Treatment of Defective Spermatogenesis tvith Human Gonadotropins W. Z. POLISHUK, M.D., Z. PALTI, M.D., and A. LAUFER, M.D. TREATMENT of male sterility due to defective spermatogenesis is not satisfactory.
Ch 20: Reproduction. Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition
 Ch 20: Reproduction Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition SLOs Contrast mitosis/meiosis, haploid/diploid, autosomes/sex chromosomes. Outline the hormonal
Ch 20: Reproduction Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition SLOs Contrast mitosis/meiosis, haploid/diploid, autosomes/sex chromosomes. Outline the hormonal
Familial Gynecomastia with Increased Extraglandular Aromatization of Plasma Carbonl9-Steroids
 Familial Gynecomastia with Increased Extraglandular Aromatization of Plasma Carbonl9-Steroids G. D. Berkovitz, A. Guerami, T. R. Brown, P. C. MacDonald, and C. J. Migeon Division ofpediatric Endocrinology,
Familial Gynecomastia with Increased Extraglandular Aromatization of Plasma Carbonl9-Steroids G. D. Berkovitz, A. Guerami, T. R. Brown, P. C. MacDonald, and C. J. Migeon Division ofpediatric Endocrinology,
Hormones of brain-testicular axis
 (Hormone Function) Hormones of brain-testicular axis anterior pituitary drives changes during puberty controlled by GnRH from hypothalamus begins to secrete FSH, LH LH targets interstitial endocrinocytes
(Hormone Function) Hormones of brain-testicular axis anterior pituitary drives changes during puberty controlled by GnRH from hypothalamus begins to secrete FSH, LH LH targets interstitial endocrinocytes
Genetics of Hypogonadism. François Pralong Division of Endocrinology Lausanne University Hospital
 Genetics of Hypogonadism François Pralong Division of Endocrinology Lausanne University Hospital The Gonadotrope Axis GnRH LH FSH Sexsteroids(-) Inhibin/follistatin (+) Activin (+) Single Gene Mutations
Genetics of Hypogonadism François Pralong Division of Endocrinology Lausanne University Hospital The Gonadotrope Axis GnRH LH FSH Sexsteroids(-) Inhibin/follistatin (+) Activin (+) Single Gene Mutations
DEVELOPMENT (DSD) 1 4 DISORDERS OF SEX
 Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 4. Disorders of sex development (DSD). Horm Res 2007;68(suppl 2):21 24 ESPE Code Diagnosis OMIM ICD 10 4 DISORDERS
Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 4. Disorders of sex development (DSD). Horm Res 2007;68(suppl 2):21 24 ESPE Code Diagnosis OMIM ICD 10 4 DISORDERS
Androgen deficiency. Dr Rakesh Iyer Staff Specialist in Endocrinology Calvary hospital
 Androgen deficiency Dr Rakesh Iyer Staff Specialist in Endocrinology Calvary hospital Outline Pathological androgen deficiency - Background, causes, interpretation - Indications for treatment Androgen
Androgen deficiency Dr Rakesh Iyer Staff Specialist in Endocrinology Calvary hospital Outline Pathological androgen deficiency - Background, causes, interpretation - Indications for treatment Androgen
Let s Talk About Hormones!
 Let s Talk About Hormones! This lesson was created by Serena Reves and Nichelle Penney, with materials from the BCTF and The Pride Education Network. Hormones are responsible for the regulation of many
Let s Talk About Hormones! This lesson was created by Serena Reves and Nichelle Penney, with materials from the BCTF and The Pride Education Network. Hormones are responsible for the regulation of many
to ensure the. Sexual reproduction requires the (from the mother) by a (from the father). Fertilization is the fusion of.
 The Reproductive System Fill-In Notes Purpose of life: to ensure the. Stages of Human Development Sexual reproduction requires the (from the mother) by a (from the father). Fertilization is the fusion
The Reproductive System Fill-In Notes Purpose of life: to ensure the. Stages of Human Development Sexual reproduction requires the (from the mother) by a (from the father). Fertilization is the fusion
GUIDELINES ON. Introduction. G.R. Dohle, S. Arver, C. Bettocchi, S. Kliesch, M. Punab, W. de Ronde
 GUIDELINES ON Male Hypogonadism G.R. Dohle, S. Arver,. Bettocchi, S. Kliesch, M. Punab, W. de Ronde Introduction Male hypogonadism is a clinical syndrome caused by androgen deficiency. It may adversely
GUIDELINES ON Male Hypogonadism G.R. Dohle, S. Arver,. Bettocchi, S. Kliesch, M. Punab, W. de Ronde Introduction Male hypogonadism is a clinical syndrome caused by androgen deficiency. It may adversely
SISTEMA REPRODUCTOR (LA IDEA FIJA) Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
Reproductive Hormones
 Reproductive Hormones Male gonads: testes produce male sex cells! sperm Female gonads: ovaries produce female sex cells! ovum The union of male and female sex cells during fertilization produces a zygote
Reproductive Hormones Male gonads: testes produce male sex cells! sperm Female gonads: ovaries produce female sex cells! ovum The union of male and female sex cells during fertilization produces a zygote
FIGURE The tunica albuginea is a connective tissue capsule forming the outer part of each testis.
 Testicular Histology (see p. 1034 in text) FIGURE 28.3 1. The tunica albuginea is a connective tissue capsule forming the outer part of each testis. 2. Septa are extensions of the tunica albuginea that
Testicular Histology (see p. 1034 in text) FIGURE 28.3 1. The tunica albuginea is a connective tissue capsule forming the outer part of each testis. 2. Septa are extensions of the tunica albuginea that
The Reproductive System
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
Reproduction. AMH Anti-Müllerian Hormone. Analyte Information
 Reproduction AMH Anti-Müllerian Hormone Analyte Information - 1-2011-01-11 AMH Anti-Müllerian Hormone Introduction Anti-Müllerian Hormone (AMH) is a glycoprotein dimer composed of two 72 kda monomers 1.
Reproduction AMH Anti-Müllerian Hormone Analyte Information - 1-2011-01-11 AMH Anti-Müllerian Hormone Introduction Anti-Müllerian Hormone (AMH) is a glycoprotein dimer composed of two 72 kda monomers 1.
Analysis of the Sex-determining Region of the Y Chromosome (SRY) in a Case of 46, XX True Hermaphrodite
 Clin Pediatr Endocrinol 1994; 3(2): 91-95 Copyright (C) 1994 by The Japanese Society for Pediatric Endocrinology Analysis of the Sex-determining Region of the Y Chromosome (SRY) in a Case of 46, XX True
Clin Pediatr Endocrinol 1994; 3(2): 91-95 Copyright (C) 1994 by The Japanese Society for Pediatric Endocrinology Analysis of the Sex-determining Region of the Y Chromosome (SRY) in a Case of 46, XX True
2.0 Synopsis. Lupron Depot M Clinical Study Report R&D/09/093. (For National Authority Use Only) to Part of Dossier: Name of Study Drug:
 2.0 Synopsis Abbott Laboratories Individual Study Table Referring to Part of Dossier: Name of Study Drug: Volume: Abbott-43818 (ABT-818) leuprolide acetate for depot suspension (Lupron Depot ) Name of
2.0 Synopsis Abbott Laboratories Individual Study Table Referring to Part of Dossier: Name of Study Drug: Volume: Abbott-43818 (ABT-818) leuprolide acetate for depot suspension (Lupron Depot ) Name of
Select patients with hypogonadotropic hypogonadism may respond to treatment with clomiphene citrate
 Select patients with hypogonadotropic hypogonadism may respond to treatment with clomiphene citrate Scott J. Whitten, M.D., a Ajay K. Nangia, M.D., c and Peter N. Kolettis, M.D. b a Division of Reproductive
Select patients with hypogonadotropic hypogonadism may respond to treatment with clomiphene citrate Scott J. Whitten, M.D., a Ajay K. Nangia, M.D., c and Peter N. Kolettis, M.D. b a Division of Reproductive
