Michael Paddock 1*, Nicola Robson Academic Unit of Radiology, University of Sheffield, Royal Hallamshire Hospital, Sheffield, United Kingdom
|
|
|
- Elisabeth Watson
- 5 years ago
- Views:
Transcription
1 The curious case of the disappearing IVC: A case report and review of the aetiology of Inferior Vena Michael Paddock 1*, Nicola Robson 2 1. Academic Unit of Radiology, University of Sheffield, Royal Hallamshire Hospital, Sheffield, United Kingdom 2. Department of Radiology, Poole Hospital NHS Foundation Trust, Poole, Dorset, United Kingdom * Correspondence: Dr Michael Paddock, Academic Unit of Radiology, University of Sheffield, Floor C, Royal Hallamshire Hospital, Glossop Road, Sheffield, S10 2JF, United Kingdom ( michael.paddock@doctors.org.uk) :: DOI: /jrcr.v8i ABSTRACT We report the case of a previously well 18-year-old male who presented to the Emergency Department with lower limb pain. An ultrasound demonstrated extensive left sided deep vein thrombosis and computed tomography demonstrated inferior vena cava agenesis, leading to the diagnosis of inferior vena cava agenesis associated deep vein thrombosis. The aetiology of inferior vena cava agenesis is explored in depth. CASE REPORT CASE REPORT An 18-year-old man presented to the Emergency Department (ED) complaining of a swollen, painful left knee after sustaining a 'twisting' injury of the left lower limb. The symptoms worsened on repeated activity. Past history is relevant for mild learning difficulties and operations for a 'blocked bowel' when he was younger, for which the patient and his mother were unable to elaborate. However, later review of the medical notes revealed an episode of abdominal distension, grunting and acidosis on day 4 of life after a full term birth. An unsuccessful anal dilation and bowel decompression preceded the formation of a descending loop colostomy. This was reversed at 16 months but an anastomotic leak gave rise to peritonitis necessitating a further defunctioning colostomy, eventually closed at 4 years of age. Additionally, he had a pyloromyotomy for pyloric stenosis at 2 months of age. There was no history of risk factors for venous thromboembolism (VTE) or deep vein thrombosis (DVT) and no family history of VTE or clotting diatheses. He denied smoking, taking alcohol or illegal drugs, and was otherwise well. Initial examination revealed normal vital signs and significant swelling to the left calf and the posterior aspect of the left thigh with no associated superficial venous swelling, effusion or instability of the left knee. Peripheral pulses were palpable but left foot capillary refill time was prolonged at 3 to 4 seconds and the limb was cool to the touch. Neurological examination was normal. Abdominal examination revealed numerous well-healed surgical scars in a soft, non-tender abdomen with normal bowel sounds and no inguinal lymphadenopathy. Blood tests revealed a neutrophilic leucocytosis and a significantly elevated d-dimer level (1850 ng/ml, NR ng/ml). Platelet count, international normalised ratio, prothrombin time, activated partial thromboplastin time, urea, electrolytes, liver function tests and bone profile were all within the normal range. An urgent ultrasound (US) of the left leg was performed where compression venography revealed evidence of extensive DVT. Incompletely occluding thrombus was seen in the left external iliac, common femoral vein and superficial femoral vein with some venous flow in the popliteal vein. The left common iliac vein was poorly visualised but contained 38
2 thrombus (Fig. 1). The posterior tibial and peroneal veins appeared clear. The inferior vena cava (IVC), although not well seen, had detectable venous flow in its distal portion. A chest radiograph (Fig. 2) demonstrated a normal heart size and no lung lesions with the caveat that a pulmonary embolus (PE) could not be excluded on the basis of these findings. He was managed with elevation of the limb and anticoagulation with a low molecular weight heparin. He was not DVT thrombolysed given that distal neurovascular status was intact. A CT (computed tomography) scan was organised and demonstrated that the intra-abdominal IVC was smaller (Fig. 3) than usual, and numerous venous collaterals in the abdomen and pelvis were visualised. The two common iliac veins contained thrombus and formed a small right-sided IVC. The right-sided iliac vein crossed the midline dividing and draining deep structures with collaterals noted between the psoas and iliacus muscle. A large collateral vein with thrombus extended from this iliac vessel in the pelvis, to drain the right kidney (Fig. 4), connecting into the IVC that directly drained the left kidney. On the left, a prominent gonadal vein was seen to connect to a lumbar vein forming a focal bulbous region with a vein passing from here, anterior to the aorta, to the suprarenal portion of the IVC, also draining the left kidney (Fig. 5). Collaterals with thrombus were demonstrated draining into this bulbous left sided vein in a similar manner to that which a congenital left sided IVC would, however their multiple nature and more lateral lie was noted (Fig. 6). Additionally, they arose from a small vein which appeared to connect directly to the left external iliac system and were therefore considered less likely to represent a double IVC anomaly, as opposed to the opening up of venous channels due to previous thrombosis: either is possible. Due to poor opacification it was difficult to follow the extent of clot, but there was suspicion of IVC thrombus in its infrarenal portion. Of note, a bony sacral defect was also demonstrated (Fig. 7). The haematology team recommended a thrombophilia screen and immediate commencement of vitamin K antagonist therapy, initially for 6 months, with further review as an outpatient. The patient was made aware that he may have to continue lifelong anticoagulation and was discharged home. The outpatient haematology review revealed no evidence of inherited thrombophilia; a weakly positive lupus anticoagulant result in isolation was not thought to be of clinical significance. The patient received 6 months of oral anticoagulation therapy in total and was subsequently discharged from follow up. DISCUSSION Aetiology Anomalies of the IVC are estimated in 0.5% of the general population [1]. DVT is associated with high morbidity and mortality and has an estimated prevalence rate of 1 per 1000 [2]. A lower prevalence rate exists in younger patient groups with an incidence as low as 1 per [3]. The aetiology of DVT is associated with congenital risk factors (thrombophilias, autoimmune conditions) and acquired risk factors (oral contraceptive use, prolonged immobilisation, neoplastic disease): one or more of these risk factors may be found in up to 80% of patients with confirmed DVT [4]. IVC anomalies may be found in up to 5% of this younger patient population with confirmed DVT [5-7], which is greater than the expected rate: up to 5% observed versus 0.5% expected [1]. There is no firm consensus of the etiology of IVC agenesis (IVCA) with the literature presenting two schools of thought: congenital absence [3, 4] or early IVC thrombosis in the perinatal period [8, 9]. Congenital IVCA suggests defective embryonic development of all 3 renal IVC segments (infra-, renal and supra-) at week six to eight of gestation [4, 10], resulting in progressive segmental hypoplasia of the renal IVC [11]. Recent literature has demonstrated a link between confirmed perinatal IVC thrombosis and infrarenal IVC absence suggesting that thrombosis of the IVC leads to subsequent hypoplasia and 'absence' of the IVC [8, 9]. The CT images of our patient confirmed a rudimentary IVC, with no definable infrarenal IVC. The bulbous vein described is rather like a left IVC and has the usual connections to the right IVC. One could postulate that the left para-aortic collateral, which is single at the bifurcation, could be a small left IVC which thrombosed at some stage and may represent a possible hypoplastic remnant that may have recannulated, or, that it may represent a true congenital double IVC with a small left sided vessel, possibly associated with partial sacral agenesis (Fig. 7). There is one case report that describes sacral agenesis with an anomalous inferior and superior vena cava in conjunction with Goldenhar (oculoauriculovertebral) syndrome [12]. IVC anomalies may present with non-specific, vague symptoms, such as lower back [5, 10] or abdominal pain [3, 5], or may be typically asymptomatic [4]. The expected rate described above may also be an underestimation given the asymptomology as it may only be discovered as an incidental finding on imaging or at surgery. IVC abnormalities have been associated with other congenital abnormalities, mainly in those organs (spleen, liver, heart and lung) whose embryological development occurs at the same time of the IVC [4, 13]. Additionally, patients without associated congenital anomalies are typically asymptomatic [4]. A Brazilian case report has highlighted a potential association between partial IVCA and congenital abnormalities of the gut [14]. Our patient presented with features consistent with bowel obstruction in the neonatal period, the cause of which was speculated to include a congenital aetiology. In the absence of other risk factors, extensive intra-abdominal surgery in our patient's infancy may have been a risk factor for IVCA, subsequently leading to inferior vena cava agenesis associated deep vein thrombosis (IVCA-aDVT). It currently remains unknown whether catheter related procedures in the neonatal period carry a similar risk of thrombosis and further review of the medical notes did not allude to these procedures being performed. 39
3 IVCA-aDVT has been described as a separate clinical entity in the literature [1, 5, 6, 15]. A retrospective analysis indicated that the incidence of IVCA-aDVT was greater in males: in a review of 72 documented cases, nearly 82% of IVCA-aDVT patients were male [5]. Affected patients are typically in their second to fourth decade of life [16] and a prospective study stated that occurrence of DVT affected those aged less than 30 years [11]. Iqbal et al, hypothesises that inadequate flow in collateral vessels results in chronic venous hypertension and venous stasis, promoting the formation of further venous collaterals which may 'precipitate thrombosis' [3]. Lambert et al, proposes that the inability of the venous collateral system to cope with the demands of increasing blood flow, results in venous stasis and a subsequent propensity for clotting, resulting in the formation of DVT [5]. It has been demonstrated in the literature that IVCA is an independent risk factor for DVT by this proposed mechanism [6, 8, 17] resulting from subsequent changes in 'venous flow velocity' [1]. Our patient may have become symptomatic when the collateral venous system was unable to maintain venous homeostasis, possibly secondary to blockage from new clot formation from resultant vessel endothelial instability, or changes in venous flow velocity following the twisting injury at the knee. Concurrent PE is not a frequent finding with IVCA-aDVT given that a true IVC does not exist. Any emboli would have to travel through the collateral networks or the azygos/hemiazygos system to reach the pulmonary circulation [5], explaining the low frequency of lung involvement. However, one case report has highlighted this mechanism as a rare cause for PE [4]. Moreover, a prophylactic IVC filter would not be recommended given the low instance of PE in these patients. Imaging findings US, CT and Magnetic Resonance Imaging (MRI) have supplanted direct contrast venography of the IVC for diagnosis. US is a relatively good and cheap first line method for assessment of the IVC, however it is operator dependent and is limited by body habitus and bowel gas. In this case, visualisation was poor and the small infrarenal IVC could not be demonstrated on US: CT or MRI better assess anomalies of the IVC for this reason. CT confers the added advantage of demonstrating additional pathology such as pelvic masses and collateral circulation. However, CT imaging does 'not contribute to diagnosing IVCA if it is not specifically sought' [5]. Multiplanar reconstruction allows for excellent imaging on the whole but the poor opacification in this patient limited this technique. In retrospect, a pedal vein injection of contrast may have improved visualisation. MRI is replacing CT as the choice of imaging modality and is thought to be more accurate in detecting thrombosis and IVC anomalies [18]. as part of a clinical syndrome or other congenital abnormalities, or an adult presenting with recurrent DVT. Treatment and prognosis Prolonged vitamin K antagonist therapy appears to be the mainstay of management with outpatient haematology input to monitor progress and manage the risks of long-term anticoagulation therapy. Thrombophilia and/or autoimmune screening should be performed to exclude an underlying clinical condition or syndrome with prothrombotic tendencies. Elastic stocking and leg elevation are useful anti-vte measures in addition to limiting further acquired thrombotic risk factors. Treatment with low molecular weight heparin may be used as a safe alternative in patients with contraindications for long-term oral anticoagulation therapy [7]. Catheter directed thrombolytic therapy, although sometimes used in young patients, is problematic in those with abnormal anatomy. Surgical management is rarely indicated but should be considered if there is coexisting vascular impairment and depending on the extent of the DVT. Zhou et al, describe successful polytetrafluoroethylene graft placement in a symptomatic patient with infrarenal IVC absence and collateral formation resulting in pelvic congestion and lower extremity swelling. The graft connected the common femoral vein to the suprarenal IVC [19]. However, there is currently no evidence based best practice guidance regarding the long-term management of IVCA-aDVT, rather, current accepted DVT management as applied to IVCA-aDVT. Patients with IVCA are at risk of long-standing asymptomatic clot formation and accumulation with a resultant high risk of DVT and recurrence. Early identification of these patients may allow for earlier intervention such that later risk in adulthood is reduced, however, there currently exists no data regarding long-term morbidity and mortality [9]. Differential diagnoses The differential diagnosis as discussed above would lie mainly between a congenital absence of the infrarenal IVC or IVC thrombosis in the perinatal period. It is possible that a small left IVC was thrombosed and became recannulated or that the patient may have had a double IVC with a small left sided vessel. The IVC embryogenesis involves anastomoses between three paired embryonic veins. This is a complex process and anomalies are numerous. Thrombosis in the perinatal period could lead to persistence of channels that would otherwise have regressed. Various anomalies and illustrations of these are described in Tables 2 and 3. TEACHING POINT Imaging the IVC may not always be able to delineate the true of aetiology of IVCA in patients. However, imaging should be interpreted in the context of the history and clinical presentation, which may give credence to one of the proposed aetiologies presented above. This may have ramifications for long-term patient management, for example, in a young child A young male presenting with a more proximal deep vein thrombosis in the absence of acquired venous thromboembolism risk factors should raise the suspicion of inferior vena cava agenesis and warrant further investigation. 40
4 REFERENCES 1. Chee YL, Culligan DJ, Watson HG. Inferior vena cava malformation as a risk factor for deep venous thrombosis in the young. British journal of haematology Sep;114(4): PMID: Lin HJ, Owens TR, Sinow RM, Fu PC, Jr., DeVito A, Beall MH, et al. Anomalous inferior and superior venae cavae with oculoauriculovertebral defect: review of Goldenhar complex and malformations of left-right asymmetry. American journal of medical genetics Jan 6;75(1): PMID: Konopka CL, Salame M, Padulla GA, Muradás RR, Batistella JC. Agenesis of inferior vena cava associated with deep venous thrombosis. Jornal Vascular Brasileiro September 2010;9(3). 13. Obernosterer A, Aschauer M, Schnedl W, Lipp RW. Anomalies of the inferior vena cava in patients with iliac venous thrombosis. Annals of internal medicine Jan 1;136(1): PMID: Iqbal J, Nagaraju E. Congenital absence of inferior vena cava and thrombosis: a case report. Journal of medical case reports. 2008;2:46. PMID: Sandercoe GD, Brooke-Cowden GL. Developmental anomaly of the inferior vena cava. ANZ journal of surgery May;73(5): PMID: Cho BC, Choi HJ, Kang SM, Chang J, Lee SM, Yang DG, et al. Congenital absence of inferior vena cava as a rare cause of pulmonary thromboembolism. Yonsei medical journal Oct 31;45(5): PMID: Lambert M, Marboeuf P, Midulla M, Trillot N, Beregi JP, Mounier-Vehier C, et al. Inferior vena cava agenesis and deep vein thrombosis: 10 patients and review of the literature. Vascular medicine Dec;15(6): PMID: Ruggeri M, Tosetto A, Castaman G, Rodeghiero F. Congenital absence of the inferior vena cava: a rare risk factor for idiopathic deep-vein thrombosis. Lancet Feb 10;357(9254):441. PMID: Vasco PG, Lopez AR, Pineiro ML, Rivera JI. Deep venous thrombosis caused by congenital inferior vena cava agenesis and heterozygous factor V Leiden mutation - a case report. The International journal of angiology : official publication of the International College of Angiology, Inc Fall;18(3): PMID: Felicio ML, Martins AS, Andrade RR, Silva MA. Partial absence of the inferior vena cava associated with bowel malformation. Revista brasileira de cirurgia cardiovascular : orgao oficial da Sociedade Brasileira de Cirurgia Cardiovascular Jul-Sep;22(3): PMID: Gayer G, Luboshitz J, Hertz M, Zissin R, Thaler M, Lubetsky A, et al. Congenital anomalies of the inferior vena cava revealed on CT in patients with deep vein thrombosis. AJR American journal of roentgenology Mar;180(3): PMID: Onzi RR, Costa LF, Angnes RF, Domingues LA, Moraes P, Scaffaro LA, et al. Inferior vena cava malformation and deep venous thrombosis: a risk factor of venous thrombosis in the young. Jornal Vascular Brasileiro. 2007;6(2). 18. McAree BJ, O'Donnell ME, Boyd C, Spence RA, Lee B, Soong CV. Inferior vena cava thrombosis in young adults--a review of two cases. The Ulster medical journal May;78(2): PMID: Ramanathan T, Hughes TM, Richardson AJ. Perinatal inferior vena cava thrombosis and absence of the infrarenal inferior vena cava. Journal of vascular surgery May;33(5): PMID: Alicioglu B, Kaplan M, Ege T. Absence of infrarenal inferior vena cava is not a congenital abnormality. Bratislavske lekarske listy. 2009;110(5): PMID: Zhou W, Rosenberg W, Lumsden A, Li J. Successful surgical management of pelvic congestion and lower extremity swelling owing to absence of infrarenal inferior vena cava. Vascular Nov-Dec;13(6): PMID: Bass, J.E, et al. Spectrum of congenital anomalies of the inferior vena cava: cross-sectional imaging findings. Radiographics. 2000;20(3): PMID: Yigit H, Yagmurlu B, Yigit N, Fitoz S, Kosar P. Low back pain as the initial symptom of inferior vena cava agenesis. AJNR American journal of neuroradiology Mar;27(3): PMID: Garcia-Fuster MJ, Forner MJ, Flor-Lorente B, Soler J, Campos S. Anomalias de la vena cava y trombosis venosa profunda. Revista espanola de cardiologia Feb;59(2): PMID:
5 FIGURES Figure 1: 18-year-old male with extensive DVT and infrarenal IVC agenesis. FINDINGS: Sagittal ultrasound image shows thrombus in the left common iliac vein (green arrow) with good blood flow in the artery overlying. TECHNIQUE: Ultrasonography was performed using a Philips IU22 (Philips Healthcare UK) ultrasound machine with linear array and curvilinear 5-2 megahertz (MHz) probes. Figure 2: 18-year-old male with extensive DVT and infrarenal IVC agenesis. FINDINGS: Normal posterior-anterior chest radiograph appearances. Figure 3: 18-year-old male with extensive DVT and infrarenal IVC agenesis. FINDINGS: Venous phase axial (a) and coronal (b) enhanced computed tomography of the abdomen demonstrating the small right sided suprarenal IVC cava (white arrows; solid white arrow in magnification (b)). TECHNIQUE: The patient was imaged on a Siemens Sensation 16 CT Scanner (Siemens Medical, Forchheim Germany) scanned helically with axial reconstruction at 1.5mms, matrix size 512x512, with 120kVp and modulated mas varying from 70 to 205. An initial scan was acquired after administration of non ionic Iopamidol (Niopam 300mg Iodine/ml Bracco UK Limited) IV Contrast triggered from the aorta with 25 second delayed imaging performed from pelvis to lung apices with a second study of the pelvis visually triggered over the IVC as initial opacification of pelvic veins was poor. A pump injection was used with a speed of 4 mls/sec. The legs were not imaged as ultrasound had provided diagnostic information regarding the presence of thrombus on the left side. 42
6 Figure 4: 18-year-old male with extensive DVT and infrarenal IVC agenesis. FINDINGS: Coronal views of the abdomen at different levels (a posterior to b) demonstrating a large collateral vessel (white arrows; hollow white arrow in magnification (a)) containing thrombus, draining the right kidney. TECHNIQUE: The patient was imaged on a Siemens Sensation 16 CT Scanner (Siemens Medical, Forchheim Germany) scanned helically with axial reconstruction at 1.5mms, matrix size 512x512, with 120kVp and modulated mas varying from 70 to 205. An initial scan was acquired after administration of non ionic Iopamidol (Niopam 300mg Iodine/ml Bracco UK Limited) IV Contrast triggered from the aorta with 25 second delayed imaging performed from pelvis to lung apices with a second study of the pelvis visually triggered over the IVC as initial opacification of pelvic veins was poor. A pump injection was used with a speed of 4 mls/sec. The legs were not imaged as ultrasound had provided diagnostic information regarding the presence of thrombus on the left side. Figure 5: 18-year-old male with extensive DVT and infrarenal IVC agenesis. FINDINGS: Computed tomography axial scan (a) of the abdomen showing a lumbar vein (blue arrow in main image (a); solid blue arrow in magnification (a)) forming bulbous left 'inferior vena cava' (white arrow in main image; solid white arrow in magnification (a)). Coronal image (b) demonstrating a left gonadal vein (blue arrow in main image (b); solid blue arrow in magnification (b)) with left sided collaterals (orange arrow in main image (b); solid orange arrow in magnification (b)) draining into the bulbous left 'inferior vena cava' which crosses the aorta to join the suprarenal portion of the right sided inferior vena cava (white arrow in main image (b); solid white arrow in magnification (b)). TECHNIQUE: The patient was imaged on a Siemens Sensation 16 CT Scanner (Siemens Medical, Forchheim Germany) scanned helically with axial reconstruction at 1.5mms, matrix size 512x512, with 120kVp and modulated mas varying from 70 to 205. An initial scan was acquired after administration of non ionic Iopamidol (Niopam 300mg Iodine/ml Bracco UK Limited) IV Contrast triggered from the aorta with 25 second delayed imaging performed from pelvis to lung apices with a second study of the pelvis visually triggered over the IVC as initial opacification of pelvic veins was poor. A pump injection was used with a speed of 4 mls/sec. The legs were not imaged as ultrasound had provided diagnostic information regarding the presence of thrombus on the left side. 43
7 Figure 6: 18-year-old male with extensive DVT and infrarenal IVC agenesis. FINDINGS: Computed tomography axial scan of the abdomen demonstrating the right sided inferior vena cava (white arrow; solid white arrow in magnification) and left sided collaterals containing thrombus (blue arrow; blue solid arrow in magnification). TECHNIQUE: The patient was imaged on a Siemens Sensation 16 CT Scanner (Siemens Medical, Forchheim Germany) scanned helically with axial reconstruction at 1.5mms, matrix size 512x512, with 120kVp and modulated mas varying from 70 to 205. An initial scan was acquired after administration of non ionic Iopamidol (Niopam 300mg Iodine/ml Bracco UK Limited) IV Contrast triggered from the aorta with 25 second delayed imaging performed from pelvis to lung apices with a second study of the pelvis visually triggered over the IVC as initial opacification of pelvic veins was poor. A pump injection was used with a speed of 4 mls/sec. The legs were not imaged as ultrasound had provided diagnostic information regarding the presence of thrombus on the left side. Figure 7: 18-year-old male with extensive DVT and infrarenal IVC agenesis. FINDINGS: A three-dimensional volumetric reconstruction demonstrating the left sided sacral bony defect (white arrow). TECHNIQUE: The patient was imaged on a Siemens Sensation 16 CT Scanner (Siemens Medical, Forchheim Germany) scanned helically with axial reconstruction at 1.5mms, matrix size 512x512, with 120kVp and modulated mas varying from 70 to 205. An initial scan was acquired after administration of non ionic Iopamidol (Niopam 300mg Iodine/ml Bracco UK Limited) IV Contrast triggered from the aorta with 25 second delayed imaging performed from pelvis to lung apices with a second study of the pelvis visually triggered over the IVC as initial opacification of pelvic veins was poor. A pump injection was used with a speed of 4 mls/sec. The legs were not imaged as ultrasound had provided diagnostic information regarding the presence of thrombus on the left side. 44
8 Aetiology Inferior vena cava agenesis associated deep vein thrombosis; may present as part of a clinical syndrome with congenital abnormalities Incidence Inferior vena cava anomalies may be found in up to 5% of younger patients with confirmed DVT (5% observed vs. 0.5% expected) Gender ratio Male:female = 4:1 Age predilection Risk factors Treatment Prognosis Findings on imaging Second to fourth decade of life Inferior vena cava agenesis, venous collateral formation Accepted DVT management; exclude thrombophilia Good, as responds to management; risk of recurrence in prothrombotic state Hypoplastic remnants or complete absence of the infrarenal IVC; venous collateral formation; venous thrombus. Operator dependant views of IVC on US; CT or MRI better assess IVC anomalies and extent of venous thrombus Table 1: Summary table for inferior vena cava agenesis associated deep vein thrombosis. Diagnosis Left IVC Double IVC Absence of infrarenal IVC Retro aortic and circumaortic left renal vein Azygos or hemiazygos continuation of IVC Retrocaval ureter Cause of anomaly & incidence in population Persistence of the left supracardinal vein and regression of the right supracardinal vein % Persistence of both supracardinal veins. 1 3% Intrauterine or perinatal thrombosis of the IVC. Very rare. Persistence of the posterior supracardinal-supracardinal anastomosis with ventral arch regression % Failure of the right subcardinal-hepatic vein anastomosis to form with atrophy of right subcardinal vein. 0.6% Infrarenal IVC develops from the right posterior cardinal vein that lies anterior and lateral to the ureter. Differential diagnosis Left para-aortic lymphadenopathy. Left para-aortic lymphadenopathy. Enlarged collateral vessels simulate a paraspinal mass. Left para-aortic lymphadenopathy. CT & MRI findings Contrast enhanced CT or MRI demonstrates an isolated left IVC that joins the left renal vein and crosses anterior to the aorta to join the normal right IVC. Imaging as for the left IVC but occasionally the left IVC crosses at a level below the renal vein: there can be a difference in size between the 2 IVCs. Associated anomalies seen on imaging include right double IVC with retro-aortic right renal vein and double IVC with hemiazygos continuation on the left. Contrast enhanced CT/MRI demonstrate absence of the infrarenal IVC with prominent ascending lumbar veins that drain into the azygos-hemiazygos system. Contrast enhanced CT/MRI demonstrate a single left renal vein which passes behind the aorta to join the right sided IVC or circumaortic venous ring with one vein coursing anterior and the other posterior to the aorta. Contrast enhanced CT/MRI demonstrates azygos vein continuation of the infrarenal IVC, and, if left IVC, as hemiazygos vein. The renal segment receives blood from both kidneys and passes posterior to the crura to enter the thorax as the azygos vein that joins the SVC in the normal place. The hepatic segment drains directly into the right atrium. Contrast enhanced CT/MRI demonstrates part of the right ureter trapped posterior and medial to the IVC. Significant compression could result in hydronephrosis. Table 2: Summary table for variants and anomalies of the IVC with corresponding imaging appearances on CT/MRI. 45
9 Table 3: Summary table with illustrations of variants and anomalies of the IVC (Adapted from Radiographics 2000;20: [20].) 46
10 ABBREVIATIONS CT = computed tomography DVT = deep vein thrombosis ED = Emergency Department IVC = inferior vena cava IVCA = inferior vena cava agenesis IVCA-aDVT = inferior vena cava agenesis associated deep vein thrombosis MRI = magnetic resonance imaging NR = normal range PE = pulmonary embolus US = ultrasound VTE = venous thromboembolism KEYWORDS Inferior vena cava agenesis; deep vein thrombosis; inferior vena cava agenesis associated deep vein thrombosis; inferior vena cava anomalies; venous thromboembolism; IVC ACKNOWLEDGMENTS We would like to thank Dr Daven Amin for his help in obtaining follow up information on the patient, Mrs Kate Crehan for providing the illustrations and Ms Sarah Daniels for her insight. Online access This publication is online available at: Peer discussion Discuss this manuscript in our protected discussion forum at: Interactivity This publication is available as an interactive article with scroll, window/level, magnify and more features. Available online at Published by EduRad 47
Absence of infra-renal segment of inferior vena cava with anomalous right renal vein
 Absence of infra-renal segment of inferior vena cava with anomalous right renal vein Authors: VS Ajay-Chandrasekar, V Kaliyaperumal & D Alfred Location: Aintree University Hospitals NHS trust, Liverpool,
Absence of infra-renal segment of inferior vena cava with anomalous right renal vein Authors: VS Ajay-Chandrasekar, V Kaliyaperumal & D Alfred Location: Aintree University Hospitals NHS trust, Liverpool,
Popliteal vein aneurysm presenting as recurrent pulmonary embolism
 vein aneurysm presenting as recurrent pulmonary embolism Joel Lim 1*, Martin Marshall 2 1. Department of Clinical Services, Royal Perth Hospital, Perth, Australia 2. Department of Diagnostic and Radiology,
vein aneurysm presenting as recurrent pulmonary embolism Joel Lim 1*, Martin Marshall 2 1. Department of Clinical Services, Royal Perth Hospital, Perth, Australia 2. Department of Diagnostic and Radiology,
Sakshi Bami, 1 Yarelis Vazquez, 2 Valeriy Chorny, 1 Rachelle Goldfisher, 2 and John Amodio Introduction. 2. Case Report
 Case Reports in Pediatrics Volume 2015, Article ID 864047, 5 pages http://dx.doi.org/10.1155/2015/864047 Case Report Deep Venous Thrombosis of the Leg, Associated with Agenesis of the Infrarenal Inferior
Case Reports in Pediatrics Volume 2015, Article ID 864047, 5 pages http://dx.doi.org/10.1155/2015/864047 Case Report Deep Venous Thrombosis of the Leg, Associated with Agenesis of the Infrarenal Inferior
Journal of Radiology Case Reports
 Dysgenesis of the inferior vena cava associated with deep venous thrombosis and a partial Protein C deficiency Howard Tribe *1, Rudi Borgstein 1 1. Department of Radiology, North Middlesex Hospital, London,
Dysgenesis of the inferior vena cava associated with deep venous thrombosis and a partial Protein C deficiency Howard Tribe *1, Rudi Borgstein 1 1. Department of Radiology, North Middlesex Hospital, London,
Circumcaval Ureter: Embryology
 european urology supplements 5 (2006) 444 448 available at www.sciencedirect.com journal homepage: www.europeanurology.com Circumcaval Ureter: Embryology Arianna Lesma *, Aldo Bocciardi, Patrizio Rigatti
european urology supplements 5 (2006) 444 448 available at www.sciencedirect.com journal homepage: www.europeanurology.com Circumcaval Ureter: Embryology Arianna Lesma *, Aldo Bocciardi, Patrizio Rigatti
CT Evaluation of Anomalies of the Inferior Vena Cava and Left Renal Vein
 CT Evaluation of Anomalies of the Inferior Vena Cava and Left Renal Vein STUART A. ROYAL1 AND PETER W. CALLEN1 Two patients with duplication of the inferior vena cava and two patients with a retroaortlc
CT Evaluation of Anomalies of the Inferior Vena Cava and Left Renal Vein STUART A. ROYAL1 AND PETER W. CALLEN1 Two patients with duplication of the inferior vena cava and two patients with a retroaortlc
Anomalies of the inferior vena cava
 Anomalies of the inferior vena cava Joseph M. Giordano, M.D., and Hugh H. Trout III, M.D., Washington, D.C. The inferior vena cava is formed by a complex process of embryogenesis during the sixth to tenth
Anomalies of the inferior vena cava Joseph M. Giordano, M.D., and Hugh H. Trout III, M.D., Washington, D.C. The inferior vena cava is formed by a complex process of embryogenesis during the sixth to tenth
CASE REPORT CECT EVALUATION OF AN ISOLATED LONG SEGMENT IVC THROMBUS IN A PATIENT WITH ACUTE ON CHRONIC PANCREATITIS: A CASE REPORT
 CECT EVALUATION OF AN ISOLATED LONG SEGMENT IVC THROMBUS IN A PATIENT WITH ACUTE ON CHRONIC PANCREATITIS: A Pronami Borah 1, Biswajit Borah 2, Kangkana Mahanta 3, Rudra K. Gogoi 4 HOW TO CITE THIS ARTICLE:
CECT EVALUATION OF AN ISOLATED LONG SEGMENT IVC THROMBUS IN A PATIENT WITH ACUTE ON CHRONIC PANCREATITIS: A Pronami Borah 1, Biswajit Borah 2, Kangkana Mahanta 3, Rudra K. Gogoi 4 HOW TO CITE THIS ARTICLE:
K. Hoffmann 1, A. Piekarek 2, J. Bieda 2, K. Karmelita-Katulska 2, 3, D. Gawrysiak 1, W. Bryl 1 INTRODUCTION C A S E R E P O R T
 C A S E R E P O R T Folia Morphol. Vol. 74, No. 1, pp. 122 126 DOI: 10.5603/FM.2015.0017 Copyright 2015 Via Medica ISSN 0015 5659 www.fm.viamedica.pl Absence of the suprarenal segment of the inferior vena
C A S E R E P O R T Folia Morphol. Vol. 74, No. 1, pp. 122 126 DOI: 10.5603/FM.2015.0017 Copyright 2015 Via Medica ISSN 0015 5659 www.fm.viamedica.pl Absence of the suprarenal segment of the inferior vena
Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism
 Agency for Healthcare Research and Quality Evidence Report/Technology Assessment Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism Summary Number 68 Overview Venous thromboembolism
Agency for Healthcare Research and Quality Evidence Report/Technology Assessment Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism Summary Number 68 Overview Venous thromboembolism
Congenital Absence of IVC with Azygous Continuation
 Congenital Absence of IVC with Azygous Continuation M. J. Rauf ( Departments of Radiology, Liaquat National Postgraduate Medical Center, Karachi. ) K. R. Makhdoomi ( Departments of Vascular Surgery, Liaquat
Congenital Absence of IVC with Azygous Continuation M. J. Rauf ( Departments of Radiology, Liaquat National Postgraduate Medical Center, Karachi. ) K. R. Makhdoomi ( Departments of Vascular Surgery, Liaquat
Deep Vein Thrombosis and Pulmonary Embolism: Patient Information
 Deep Vein Thrombosis and Pulmonary Embolism: Patient Information A Deep Vein Thrombosis (DVT) and a Pulmonary Embolism (PE) are both disorders of unwanted blood clotting. Unwanted blood clots can occur
Deep Vein Thrombosis and Pulmonary Embolism: Patient Information A Deep Vein Thrombosis (DVT) and a Pulmonary Embolism (PE) are both disorders of unwanted blood clotting. Unwanted blood clots can occur
VESSELS: GROSS ANATOMY
 ACTIVITY 10: VESSELS AND CIRCULATION OBJECTIVES: 1) How to get ready: Read Chapter 23, McKinley et al., Human Anatomy, 4e. All text references are for this textbook. 2) Observe and sketch histology slide
ACTIVITY 10: VESSELS AND CIRCULATION OBJECTIVES: 1) How to get ready: Read Chapter 23, McKinley et al., Human Anatomy, 4e. All text references are for this textbook. 2) Observe and sketch histology slide
Venous thrombosis is common and often occurs spontaneously, but it also frequently accompanies medical and surgical conditions, both in the community
 Venous Thrombosis Venous Thrombosis It occurs mainly in the deep veins of the leg (deep vein thrombosis, DVT), from which parts of the clot frequently embolize to the lungs (pulmonary embolism, PE). Fewer
Venous Thrombosis Venous Thrombosis It occurs mainly in the deep veins of the leg (deep vein thrombosis, DVT), from which parts of the clot frequently embolize to the lungs (pulmonary embolism, PE). Fewer
CURRENT & FUTURE THERAPEUTIC MANAGEMENT OF VENOUS THROMBOEMBOLISM. Gordon Lowe Professor of Vascular Medicine University of Glasgow
 CURRENT & FUTURE THERAPEUTIC MANAGEMENT OF VENOUS THROMBOEMBOLISM Gordon Lowe Professor of Vascular Medicine University of Glasgow VENOUS THROMBOEMBOLISM Common cause of death and disability 50% hospital-acquired
CURRENT & FUTURE THERAPEUTIC MANAGEMENT OF VENOUS THROMBOEMBOLISM Gordon Lowe Professor of Vascular Medicine University of Glasgow VENOUS THROMBOEMBOLISM Common cause of death and disability 50% hospital-acquired
Posterior Rectus Sheath Hernia Causing Intermittent Small Bowel Obstruction
 Posterior Rectus Sheath Hernia Causing Intermittent Small Bowel Obstruction Scott Lenobel 1*, Robert Lenobel 2, Joseph Yu 1 1. Department of Radiology, The Ohio State University Wexner Medical Center,
Posterior Rectus Sheath Hernia Causing Intermittent Small Bowel Obstruction Scott Lenobel 1*, Robert Lenobel 2, Joseph Yu 1 1. Department of Radiology, The Ohio State University Wexner Medical Center,
YOU MUST BRING GLOVES FOR THIS ACTIVITY
 ACTIVITY 10: VESSELS AND CIRCULATION OBJECTIVES: 1) How to get ready: Read Chapter 23, McKinley et al., Human Anatomy, 5e. All text references are for this textbook. 2) Observe and sketch histology slide
ACTIVITY 10: VESSELS AND CIRCULATION OBJECTIVES: 1) How to get ready: Read Chapter 23, McKinley et al., Human Anatomy, 5e. All text references are for this textbook. 2) Observe and sketch histology slide
DOPPLER ULTRASOUND OF DEEP VENOUS THROMBOSIS
 TOKUDA HOSPITAL SOFIA DOPPLER ULTRASOUND OF DEEP VENOUS THROMBOSIS MILENA STANEVA, MD, PhD Department of vascular surgery and angiology Venous thromboembolic disease continues to cause significant morbidity
TOKUDA HOSPITAL SOFIA DOPPLER ULTRASOUND OF DEEP VENOUS THROMBOSIS MILENA STANEVA, MD, PhD Department of vascular surgery and angiology Venous thromboembolic disease continues to cause significant morbidity
DVT - initial management NSCCG
 Background information Information resources for patients and carers Updates to this care map Synonyms Below knee DVT and bleeding risks Patient with confirmed DVT Scan confirms superficial thrombophlebitis
Background information Information resources for patients and carers Updates to this care map Synonyms Below knee DVT and bleeding risks Patient with confirmed DVT Scan confirms superficial thrombophlebitis
The Cardiovascular System (Part II)
 The Cardiovascular System (Part II) 黃敏銓 mchuang@ntu.edu.tw 解剖學暨細胞生物學研究所 1 Development of veins Three paired veins drain into the tubular heart of a 4-week embryo Vitelline veins: poorly oxygenated blood
The Cardiovascular System (Part II) 黃敏銓 mchuang@ntu.edu.tw 解剖學暨細胞生物學研究所 1 Development of veins Three paired veins drain into the tubular heart of a 4-week embryo Vitelline veins: poorly oxygenated blood
3 Circulatory Pathways
 40 Chapter 3 Circulatory Pathways Systemic Arteries -Arteries carry blood away from the heart to the various organs of the body. -The aorta is the longest artery in the body; it branches to give rise to
40 Chapter 3 Circulatory Pathways Systemic Arteries -Arteries carry blood away from the heart to the various organs of the body. -The aorta is the longest artery in the body; it branches to give rise to
General Imaging. Imaging modalities. Incremental CT. Multislice CT Multislice CT [ MDCT ]
![General Imaging. Imaging modalities. Incremental CT. Multislice CT Multislice CT [ MDCT ] General Imaging. Imaging modalities. Incremental CT. Multislice CT Multislice CT [ MDCT ]](/thumbs/76/74079340.jpg) General Imaging Imaging modalities Conventional X-rays Ultrasonography [ US ] Computed tomography [ CT ] Radionuclide imaging Magnetic resonance imaging [ MRI ] Angiography conventional, CT,MRI Interventional
General Imaging Imaging modalities Conventional X-rays Ultrasonography [ US ] Computed tomography [ CT ] Radionuclide imaging Magnetic resonance imaging [ MRI ] Angiography conventional, CT,MRI Interventional
Mabel Labrada, MD Miami VA Medical Center
 Mabel Labrada, MD Miami VA Medical Center *1-Treatment for acute DVT with underlying malignancy is for 3 months. *2-Treatment of provoked acute proximal DVT can be stopped after 3months of treatment and
Mabel Labrada, MD Miami VA Medical Center *1-Treatment for acute DVT with underlying malignancy is for 3 months. *2-Treatment of provoked acute proximal DVT can be stopped after 3months of treatment and
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/19768 holds various files of this Leiden University dissertation. Author: Langevelde, Kirsten van Title: Are pulmonary embolism and deep-vein thrombosis
Cover Page The handle http://hdl.handle.net/1887/19768 holds various files of this Leiden University dissertation. Author: Langevelde, Kirsten van Title: Are pulmonary embolism and deep-vein thrombosis
Deep Vein Thrombosis
 Deep Vein Thrombosis Introduction Deep vein thrombosis (DVT) is a blood clot in a vein. This condition can affect men and women of any age and race. DVT is a potentially serious condition. If not treated,
Deep Vein Thrombosis Introduction Deep vein thrombosis (DVT) is a blood clot in a vein. This condition can affect men and women of any age and race. DVT is a potentially serious condition. If not treated,
Interrupted Inferior Vena Cava and Left-Sided Subrenal Inferior Vena Cava
 Case Report Interrupted Inferior Vena Cava and Left-Sided Subrenal Inferior Vena Cava Prenatal Diagnosis S. Boopathy Vijayaraghavan, MD, DMRD, Vaijayanthi Raja, MBBS, DGO, T. V. Chitra, MD, DGO A n interrupted
Case Report Interrupted Inferior Vena Cava and Left-Sided Subrenal Inferior Vena Cava Prenatal Diagnosis S. Boopathy Vijayaraghavan, MD, DMRD, Vaijayanthi Raja, MBBS, DGO, T. V. Chitra, MD, DGO A n interrupted
The posterior abdominal wall. Prof. Oluwadiya KS
 The posterior abdominal wall Prof. Oluwadiya KS www.oluwadiya.sitesled.com Posterior Abdominal Wall Lumbar vertebrae and discs. Muscles opsoas, quadratus lumborum, iliacus, transverse, abdominal wall
The posterior abdominal wall Prof. Oluwadiya KS www.oluwadiya.sitesled.com Posterior Abdominal Wall Lumbar vertebrae and discs. Muscles opsoas, quadratus lumborum, iliacus, transverse, abdominal wall
Communicating Vein between the Left Renal Vein and Left Ascending Lumber Vein: Incidence and Significance on Abdominal CT
 YAO ET AL ORIGINAL ARTICLE Radiation Medicine: Vol. 21 No. 6, 252 257 p.p., 2003 Communicating Vein between the Left Renal Vein and Left Ascending Lumber Vein: Incidence and Significance on Abdominal CT
YAO ET AL ORIGINAL ARTICLE Radiation Medicine: Vol. 21 No. 6, 252 257 p.p., 2003 Communicating Vein between the Left Renal Vein and Left Ascending Lumber Vein: Incidence and Significance on Abdominal CT
Artery 1 Head and Thoracic Arteries. Arrange the parts in the order blood flows through them.
 Artery 1 Head and Thoracic Arteries 1. Given the following parts of the aorta: 1. abdominal aorta 2. aortic arch 3. ascending aorta 4. thoracic aorta Arrange the parts in the order blood flows through
Artery 1 Head and Thoracic Arteries 1. Given the following parts of the aorta: 1. abdominal aorta 2. aortic arch 3. ascending aorta 4. thoracic aorta Arrange the parts in the order blood flows through
A rare case of May-Thurner-like syndrome in an elderly lady
 CASE REPORT A rare case of May-Thurner-like syndrome in an elderly lady Chris Pui Yan Yee 1, Kapil Sahnan 2, Robert Hywel Thomas 1, Kaji Sritharan 1 1. Department of Vascular Surgery, St Mary's Hospital,
CASE REPORT A rare case of May-Thurner-like syndrome in an elderly lady Chris Pui Yan Yee 1, Kapil Sahnan 2, Robert Hywel Thomas 1, Kaji Sritharan 1 1. Department of Vascular Surgery, St Mary's Hospital,
Obliterative hepatocavopathy ultrasound and cavography findings
 doi:10.2478/v10019-008-0020-6 case report Obliterative hepatocavopathy ultrasound and cavography findings Ramazan Kutlu Department of Radiology, Inonu University School of Medicine, Malatya, Turkey ackgound.
doi:10.2478/v10019-008-0020-6 case report Obliterative hepatocavopathy ultrasound and cavography findings Ramazan Kutlu Department of Radiology, Inonu University School of Medicine, Malatya, Turkey ackgound.
CT presentations of anatomic variants in superior vena cava system
 CT presentations of anatomic variants in superior vena cava system Poster No.: C-1896 Congress: ECR 2016 Type: Educational Exhibit Authors: N. Janeski, I. Blazic, A. Cvijovic ; Zemun/RS, Belgrade/RS Keywords:
CT presentations of anatomic variants in superior vena cava system Poster No.: C-1896 Congress: ECR 2016 Type: Educational Exhibit Authors: N. Janeski, I. Blazic, A. Cvijovic ; Zemun/RS, Belgrade/RS Keywords:
Case Report Idiopathic Thrombosis of the Inferior Vena Cava and Bilateral Femoral Veins in an Otherwise Healthy Male Soldier
 Case Reports in Medicine Volume 2013, Article ID 246201, 4 pages http://dx.doi.org/10.1155/2013/246201 Case Report Idiopathic Thrombosis of the Inferior Vena Cava and Bilateral Femoral Veins in an Otherwise
Case Reports in Medicine Volume 2013, Article ID 246201, 4 pages http://dx.doi.org/10.1155/2013/246201 Case Report Idiopathic Thrombosis of the Inferior Vena Cava and Bilateral Femoral Veins in an Otherwise
A A U
 PVD Venous AUC Rating Sheet 2nd Round 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 Median I NI MADM Rating Agree Disagree Upper Extremity Venous Evaluation Table 1. Venous Duplex of the Upper Extremities for Patency
PVD Venous AUC Rating Sheet 2nd Round 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 Median I NI MADM Rating Agree Disagree Upper Extremity Venous Evaluation Table 1. Venous Duplex of the Upper Extremities for Patency
Lab CT scan. Murad Kharabsheh Yaman Alali
 Lab CT scan Murad Kharabsheh Yaman Alali Some rules to read The CT Scan : 1. Remember that it s a transverse section across the body and we are looking at the inferior part of the section (not the superior),
Lab CT scan Murad Kharabsheh Yaman Alali Some rules to read The CT Scan : 1. Remember that it s a transverse section across the body and we are looking at the inferior part of the section (not the superior),
Management of the persistent sciatic artery with coexistent aortoiliac aneurysms; endovascular and open techniques.
 ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 14 Number 2 Management of the persistent sciatic artery with coexistent aortoiliac aneurysms; endovascular and open A Rodriguez-Rivera,
ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 14 Number 2 Management of the persistent sciatic artery with coexistent aortoiliac aneurysms; endovascular and open A Rodriguez-Rivera,
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/19768 holds various files of this Leiden University dissertation. Author: Langevelde, Kirsten van Title: Are pulmonary embolism and deep-vein thrombosis
Cover Page The handle http://hdl.handle.net/1887/19768 holds various files of this Leiden University dissertation. Author: Langevelde, Kirsten van Title: Are pulmonary embolism and deep-vein thrombosis
Deep Vein Thrombosis
 Deep Vein Thrombosis from NHS (UK) guidelines Introduction Deep vein thrombosis (DVT) is a blood clot in one of the deep veins in the body. Blood clots that develop in a vein are also known as venous thrombosis.
Deep Vein Thrombosis from NHS (UK) guidelines Introduction Deep vein thrombosis (DVT) is a blood clot in one of the deep veins in the body. Blood clots that develop in a vein are also known as venous thrombosis.
Starting with deep venous treatment
 Starting with deep venous treatment Carsten Arnoldussen, MD Interventional Radiologist Maastricht University Medical Centre, Maastricht VieCuri Medical Centre, Venlo The Netherlands Background Maastricht
Starting with deep venous treatment Carsten Arnoldussen, MD Interventional Radiologist Maastricht University Medical Centre, Maastricht VieCuri Medical Centre, Venlo The Netherlands Background Maastricht
Management of an Unusual Iliac Fossa Venous Plexus
 Management of an Unusual Iliac Fossa Venous Plexus Irwin M Best, Emory University Journal Title: Case Reports in Vascular Medicine Volume: Volume 2011, Number 2011 Publisher: 2011-11-22, Pages 1-4 Type
Management of an Unusual Iliac Fossa Venous Plexus Irwin M Best, Emory University Journal Title: Case Reports in Vascular Medicine Volume: Volume 2011, Number 2011 Publisher: 2011-11-22, Pages 1-4 Type
The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3-
 1 2 The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3- Vitelline vein from yolk sac 3 However!!!!! The left
1 2 The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3- Vitelline vein from yolk sac 3 However!!!!! The left
Pulmonary Emboli without Leg Symptoms, May-Thurner syndrome. Case Report and Review
 ISPUB.COM The Internet Journal of Internal Medicine Volume 9 Number 2 Pulmonary Emboli without Leg Symptoms, May-Thurner syndrome. Case Report and Review A Hamo, M Alyaseen, F Alkhankan, T Gress Citation
ISPUB.COM The Internet Journal of Internal Medicine Volume 9 Number 2 Pulmonary Emboli without Leg Symptoms, May-Thurner syndrome. Case Report and Review A Hamo, M Alyaseen, F Alkhankan, T Gress Citation
Pulmonary Embolism. Thoracic radiologist Helena Lauri
 Pulmonary Embolism Thoracic radiologist Helena Lauri 8.5.2017 Statistics 1-2 out of 1000 adults annually are diagnosed with deep vein thrombosis (DVT) and/or pulmonary embolism (PE) About half of patients
Pulmonary Embolism Thoracic radiologist Helena Lauri 8.5.2017 Statistics 1-2 out of 1000 adults annually are diagnosed with deep vein thrombosis (DVT) and/or pulmonary embolism (PE) About half of patients
Pulmonary Embolism. Medicine for Managers. Dr Paul Lambden BSc MB BS BDS FDSRCSEng MRCS LRCP DRCOG MHSM FRSH
 nhsmanagers.net Briefing 26 June 2016 Medicine for Managers Dr Paul Lambden BSc MB BS BDS FDSRCSEng MRCS LRCP DRCOG MHSM FRSH Pulmonary Embolism Pulmonary embolism is a potentially life-threatening disorder
nhsmanagers.net Briefing 26 June 2016 Medicine for Managers Dr Paul Lambden BSc MB BS BDS FDSRCSEng MRCS LRCP DRCOG MHSM FRSH Pulmonary Embolism Pulmonary embolism is a potentially life-threatening disorder
A rare bilateral varaiation in renal vascular pedicle
 Case Report: A rare bilateral varaiation in renal vascular pedicle *Anshu Mishra, *Parmatma Prasad Mishra, **Gyan Prakash Mishra *Department of Anatomy, Integral Institute of Medical Sciences and Research,
Case Report: A rare bilateral varaiation in renal vascular pedicle *Anshu Mishra, *Parmatma Prasad Mishra, **Gyan Prakash Mishra *Department of Anatomy, Integral Institute of Medical Sciences and Research,
Anticoagulation Forum: Management of Tiny Clots
 Anticoagulation Forum: Management of Tiny Clots Casey O Connell, MD FACP Associate Professor Jane Anne Nohl Division of Hematology Keck School of Medicine USC DISCLOSURES None 4/11/2017 Objectives Define
Anticoagulation Forum: Management of Tiny Clots Casey O Connell, MD FACP Associate Professor Jane Anne Nohl Division of Hematology Keck School of Medicine USC DISCLOSURES None 4/11/2017 Objectives Define
Deep vein thrombosis (DVT) and pulmonary embolism (PE) advice for ophthalmic surgery patients
 Deep vein thrombosis (DVT) and pulmonary embolism (PE) advice for ophthalmic surgery patients What is a deep vein thrombosis (DVT)? A DVT is a blood clot that forms within a vein deep in the leg but can
Deep vein thrombosis (DVT) and pulmonary embolism (PE) advice for ophthalmic surgery patients What is a deep vein thrombosis (DVT)? A DVT is a blood clot that forms within a vein deep in the leg but can
STUDY OF AZYGOS SYSTEM AND ITS VARIATIONS B. Vijaya Nirmala 1, Teresa Rani S 2
 STUDY OF AZYGOS SYSTEM AND ITS VARIATIONS B. Vijaya Nirmala 1, Teresa Rani S 2 HOW TO CITE THIS ARTICLE: B. Vijaya Nirmala, Teresa Rani S. Study of Azygos System and its Variations. Journal of Evolution
STUDY OF AZYGOS SYSTEM AND ITS VARIATIONS B. Vijaya Nirmala 1, Teresa Rani S 2 HOW TO CITE THIS ARTICLE: B. Vijaya Nirmala, Teresa Rani S. Study of Azygos System and its Variations. Journal of Evolution
Renal vascular evaluation with 64 Multislice Computerized Tomography Daniela Stoisa, Fabrizzio E. Galiano, Andrés Quaranta, Roberto L.
 Renal vascular evaluation with 64 Multislice Computerized Tomography Daniela Stoisa, Fabrizzio E. Galiano, Andrés Quaranta, Roberto L. Villavicencio Footnote Diagnóstico Médico Oroño. Bv. Oroño 1515. 2000.
Renal vascular evaluation with 64 Multislice Computerized Tomography Daniela Stoisa, Fabrizzio E. Galiano, Andrés Quaranta, Roberto L. Villavicencio Footnote Diagnóstico Médico Oroño. Bv. Oroño 1515. 2000.
Guidelines, Policies and Statements D20 Statement on Peripheral Venous Ultrasound
 Guidelines, Policies and Statements D20 Statement on Peripheral Venous Ultrasound Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
Guidelines, Policies and Statements D20 Statement on Peripheral Venous Ultrasound Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
Disclosures. DVT: Diagnosis and Treatment. Questions To Ask. Dr. Susanna Shin - DVT: Diagnosis and Treatment. Acute Venous Thromboembolism (VTE) None
 Disclosures DVT: Diagnosis and Treatment None Susanna Shin, MD, FACS Assistant Professor University of Washington Acute Venous Thromboembolism (VTE) Deep Venous Thrombosis (DVT) Pulmonary Embolism (PE)
Disclosures DVT: Diagnosis and Treatment None Susanna Shin, MD, FACS Assistant Professor University of Washington Acute Venous Thromboembolism (VTE) Deep Venous Thrombosis (DVT) Pulmonary Embolism (PE)
Inferior Vena Cava Filter for DVT
 Inferior Vena Cava Filter for DVT Deep Vein Thrombosis A deep vein thrombosis (DVT) is a blood clot that forms in a deep vein. This is a serious condition that occurs more often than you might think. If
Inferior Vena Cava Filter for DVT Deep Vein Thrombosis A deep vein thrombosis (DVT) is a blood clot that forms in a deep vein. This is a serious condition that occurs more often than you might think. If
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Risk factors for DVT. Venous thrombosis & pulmonary embolism. Anticoagulation (cont d) Diagnosis 1/5/2018. Ahmed Mahmoud, MD
 Risk factors for DVT Venous thrombosis & pulmonary embolism Ahmed Mahmoud, MD Surgery ; post op especially for long cases, pelvic operations (THR), Trauma ; long bone fractures, pelvic fractures (posterior
Risk factors for DVT Venous thrombosis & pulmonary embolism Ahmed Mahmoud, MD Surgery ; post op especially for long cases, pelvic operations (THR), Trauma ; long bone fractures, pelvic fractures (posterior
Venous thrombosis & pulmonary embolism. Ahmed Mahmoud, MD
 Venous thrombosis & pulmonary embolism Ahmed Mahmoud, MD Risk factors for DVT Surgery ; post op especially for long cases, pelvic operations (THR), Trauma ; long bone fractures, pelvic fractures (posterior
Venous thrombosis & pulmonary embolism Ahmed Mahmoud, MD Risk factors for DVT Surgery ; post op especially for long cases, pelvic operations (THR), Trauma ; long bone fractures, pelvic fractures (posterior
Pulmonary Thromboembolism
 Pulmonary Thromboembolism James Allen, MD Epidemiology of Pulmonary Embolism 1,500,000 new cases per year in the United States Often asymptomatic 300,000 deaths per year DVT or PE present in 10% of ICU
Pulmonary Thromboembolism James Allen, MD Epidemiology of Pulmonary Embolism 1,500,000 new cases per year in the United States Often asymptomatic 300,000 deaths per year DVT or PE present in 10% of ICU
HUMAN HEART. Learn the following structures on the heart models.
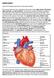 HUMAN HEART Learn the following structures on the heart models. The human heart has four chambers that consist of the right atrium, left atrium, right ventricle, and left ventricle. The atria are smaller
HUMAN HEART Learn the following structures on the heart models. The human heart has four chambers that consist of the right atrium, left atrium, right ventricle, and left ventricle. The atria are smaller
Chest and cardiovascular
 Module 1 Chest and cardiovascular A. Doss and M. J. Bull 1. Regarding the imaging modalities of the chest: High resolution computed tomography (HRCT) uses a slice thickness of 4 6 mm to identify mass lesions
Module 1 Chest and cardiovascular A. Doss and M. J. Bull 1. Regarding the imaging modalities of the chest: High resolution computed tomography (HRCT) uses a slice thickness of 4 6 mm to identify mass lesions
Interventional Treatment VTE: Radiologic Approach
 Interventional Treatment VTE: Radiologic Approach Hae Giu Lee, MD Professor, Dept of Radiology Seoul St. Mary s Hospital The Catholic University of Korea Introduction Incidence High incidence: 250,000-1,000,000/year
Interventional Treatment VTE: Radiologic Approach Hae Giu Lee, MD Professor, Dept of Radiology Seoul St. Mary s Hospital The Catholic University of Korea Introduction Incidence High incidence: 250,000-1,000,000/year
Prevention and management of deep venous thrombosis (DVT) John Fletcher Wound Care Association of New South Wales
 Prevention and management of deep venous thrombosis (DVT) John Fletcher Wound Care Association of New South Wales Merimbula, 6 th November 2010 University of Sydney Department of Surgery Westmead Hospital
Prevention and management of deep venous thrombosis (DVT) John Fletcher Wound Care Association of New South Wales Merimbula, 6 th November 2010 University of Sydney Department of Surgery Westmead Hospital
Supplementary Online Content
 Supplementary Online Content Smith D, Chudgar A, Daly B, Cooper M. Evaluation of potential renal transplant recipients with computed tomography angiography. Arch Intern Med. doi: 10.1001/archsurg.2012.1466.
Supplementary Online Content Smith D, Chudgar A, Daly B, Cooper M. Evaluation of potential renal transplant recipients with computed tomography angiography. Arch Intern Med. doi: 10.1001/archsurg.2012.1466.
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Bilateral Accessory Renal Arteries, Additional Right Renal Vein and Retroaortic Left Renal Vein- A Case Report
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Bilateral Accessory Renal Arteries, Additional Right Renal Vein and Retroaortic Left Renal Vein- A Case Report
Dr. Riaz JanMohamed Consultant Haematologist The Hillingdon Hospital Foundation Trust
 MANAGEMENT OF PATIENTS WITH DEEP VEIN THROMBOSIS (DVT) IN THE COMMUNITY SETTING & ANTICOAGULATION CLINICS THE PAST, PRESENT AND THE FUTURE Dr. Riaz JanMohamed Consultant Haematologist The Hillingdon Hospital
MANAGEMENT OF PATIENTS WITH DEEP VEIN THROMBOSIS (DVT) IN THE COMMUNITY SETTING & ANTICOAGULATION CLINICS THE PAST, PRESENT AND THE FUTURE Dr. Riaz JanMohamed Consultant Haematologist The Hillingdon Hospital
CARDIOVASCULAR DANIL HAMMOUDI.MD
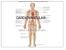 CARDIOVASCULAR DANIL HAMMOUDI.MD 18 Systemic Circulation Figure 19.19 Pulmonary Circulation Figure 19.18b 1. Thyroid gland 2. Trachea 3. Brachiocephalic 4. Common carotid 5. Internal jugular 6. Superior
CARDIOVASCULAR DANIL HAMMOUDI.MD 18 Systemic Circulation Figure 19.19 Pulmonary Circulation Figure 19.18b 1. Thyroid gland 2. Trachea 3. Brachiocephalic 4. Common carotid 5. Internal jugular 6. Superior
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS
 VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
in PAEDIATRIC CARDIOLOGY
 IMAGES in PAEDIATRIC CARDIOLOGY Morrison ML, 1 Sands AJ, 1 Paterson A. 2 Primitive hepatic venous plexus in a child with scimitar syndrome and pulmonary 1 Department of Paediatric Cardiology, Royal Belfast
IMAGES in PAEDIATRIC CARDIOLOGY Morrison ML, 1 Sands AJ, 1 Paterson A. 2 Primitive hepatic venous plexus in a child with scimitar syndrome and pulmonary 1 Department of Paediatric Cardiology, Royal Belfast
Case 47 Clinical Presentation
 93 Case 47 C Clinical Presentation 45-year-old man presents with chest pain and new onset of a murmur. Echocardiography shows severe aortic insufficiency. 94 RadCases Cardiac Imaging Imaging Findings C
93 Case 47 C Clinical Presentation 45-year-old man presents with chest pain and new onset of a murmur. Echocardiography shows severe aortic insufficiency. 94 RadCases Cardiac Imaging Imaging Findings C
Pulmonary Embolism. Pulmonary Embolism. Pulmonary Embolism. PE - Clinical
 Pulmonary embolus - a practical approach to investigation and treatment Sam Janes Wellcome Senior Fellow and Respiratory Physician, University College London Background Diagnosis Treatment Common: 50 cases
Pulmonary embolus - a practical approach to investigation and treatment Sam Janes Wellcome Senior Fellow and Respiratory Physician, University College London Background Diagnosis Treatment Common: 50 cases
ACR Appropriateness Criteria Suspected Lower Extremity Deep Vein Thrombosis EVIDENCE TABLE
 . Fowkes FJ, Price JF, Fowkes FG. Incidence of diagnosed deep vein thrombosis in the general population: systematic review. Eur J Vasc Endovasc Surg 003; 5():-5.. Hamper UM, DeJong MR, Scoutt LM. Ultrasound
. Fowkes FJ, Price JF, Fowkes FG. Incidence of diagnosed deep vein thrombosis in the general population: systematic review. Eur J Vasc Endovasc Surg 003; 5():-5.. Hamper UM, DeJong MR, Scoutt LM. Ultrasound
PULMONARY VENOLOBAR SYNDROME. Dr.C.Anandhi DNB Resident, Southern Railway Headquarters Hospital.
 PULMONARY VENOLOBAR SYNDROME Dr.C.Anandhi DNB Resident, Southern Railway Headquarters Hospital. Presenting complaint: 10 yrs old girl with recurrent episodes of lower respiratory tract infection from infancy.
PULMONARY VENOLOBAR SYNDROME Dr.C.Anandhi DNB Resident, Southern Railway Headquarters Hospital. Presenting complaint: 10 yrs old girl with recurrent episodes of lower respiratory tract infection from infancy.
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/19768 holds various files of this Leiden University dissertation. Author: Langevelde, Kirsten van Title: Are pulmonary embolism and deep-vein thrombosis
Cover Page The handle http://hdl.handle.net/1887/19768 holds various files of this Leiden University dissertation. Author: Langevelde, Kirsten van Title: Are pulmonary embolism and deep-vein thrombosis
Inferior vena cava: review of anatomic variants and pathologic processes.
 Inferior vena cava: review of anatomic variants and pathologic processes. Poster No.: C-0058 Congress: ECR 2016 Type: Educational Exhibit Authors: J. Galvan Fernandez, I. Jimenez Cuenca, S. Perez, J. C.
Inferior vena cava: review of anatomic variants and pathologic processes. Poster No.: C-0058 Congress: ECR 2016 Type: Educational Exhibit Authors: J. Galvan Fernandez, I. Jimenez Cuenca, S. Perez, J. C.
Proper Diagnosis of Venous Thromboembolism (VTE)
 Proper Diagnosis of Venous Thromboembolism (VTE) Whal Lee, M.D. Seoul National University Hospital Department of Radiology 2 nd EFORT Asia Symposium, 3 rd November 2010, Taipei DVT - Risk Factors Previous
Proper Diagnosis of Venous Thromboembolism (VTE) Whal Lee, M.D. Seoul National University Hospital Department of Radiology 2 nd EFORT Asia Symposium, 3 rd November 2010, Taipei DVT - Risk Factors Previous
CT abdomen and pelvis
 CT abdomen and pelvis General indications: Assessment of vague abdominal symptoms (pain, colics,distenstion,...) Varifecation of a lesion discovered by other diagnostic modalities as US, barium,ivp, Staging
CT abdomen and pelvis General indications: Assessment of vague abdominal symptoms (pain, colics,distenstion,...) Varifecation of a lesion discovered by other diagnostic modalities as US, barium,ivp, Staging
Nutcracker Syndrome. Dr Heena Kithany Specialty Registrar Dorset County Hospitals NHS Trust
 Nutcracker Syndrome Dr Heena Kithany Specialty Registrar Dorset County Hospitals NHS Trust Case 1: JB Referred at 17.9yrs with intermittent abdominal pain and few episodes of painless frank haematuria
Nutcracker Syndrome Dr Heena Kithany Specialty Registrar Dorset County Hospitals NHS Trust Case 1: JB Referred at 17.9yrs with intermittent abdominal pain and few episodes of painless frank haematuria
NOTE: Deep Vein Thrombosis (DVT) Risk Factors
 Deep Vein Thrombosis (DVT) Deep Vein Thrombosis (DVT) is the formation of a blood clot, known as a thrombus, in the deep leg vein. It is a very serious condition that can cause permanent damage to the
Deep Vein Thrombosis (DVT) Deep Vein Thrombosis (DVT) is the formation of a blood clot, known as a thrombus, in the deep leg vein. It is a very serious condition that can cause permanent damage to the
Carry this card with you at all times. Show this card to any medical professional treating you. Patient Implant Card. Option ELITE Vena Cava Filter.
 Patient Guide A Safe Option for a Healthier You! P/N: P-2017-0175-00 Rev B 1. Static magnetic field of 3 Tesla or less. 2. Spatial gradient magnetic field of 720 Gauss/cm or less. 3. Maximum whole body
Patient Guide A Safe Option for a Healthier You! P/N: P-2017-0175-00 Rev B 1. Static magnetic field of 3 Tesla or less. 2. Spatial gradient magnetic field of 720 Gauss/cm or less. 3. Maximum whole body
Prof. Nabil CHAKFE et coll.
 Prof. Nabil CHAKFE et coll. For the Department of Vascular Surgery and Kidney Transplantation University Hospital of Strasbourg, FRANCE Popliteal artery entrapment: misdiagnosed Epidemiology Prevalence:
Prof. Nabil CHAKFE et coll. For the Department of Vascular Surgery and Kidney Transplantation University Hospital of Strasbourg, FRANCE Popliteal artery entrapment: misdiagnosed Epidemiology Prevalence:
Meissner MH, Gloviczki P, Comerota AJ, Dalsing MC, Eklof BG, Gillespie DL, et al. J Vasc Surg. 2012;55:
 Early thrombus removal strategies for acute deep venous thrombosis: Clinical Practice Guidelines of the Society for Vascular Surgery and the American Venous Forum Meissner MH, Gloviczki P, Comerota AJ,
Early thrombus removal strategies for acute deep venous thrombosis: Clinical Practice Guidelines of the Society for Vascular Surgery and the American Venous Forum Meissner MH, Gloviczki P, Comerota AJ,
Suspected Deep Vein Thrombosis (DVT) Pathway for Non Pregnant patients Updated November 2016, with new D-dimer reference range
 Suspected Deep Vein Thrombosis (DVT) Pathway for Non Pregnant patients Updated November 2016, with new D-dimer reference range Suspect a DVT? Complete a Two-level DVT Wells score on ICE system (see page
Suspected Deep Vein Thrombosis (DVT) Pathway for Non Pregnant patients Updated November 2016, with new D-dimer reference range Suspect a DVT? Complete a Two-level DVT Wells score on ICE system (see page
Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship
 Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship CLINICAL PROBLEMS IN VASCULAR SURGERY 1. ABDOMINAL AORTIC ANEURYSM A 70 year old man presents in the emergency department with
Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship CLINICAL PROBLEMS IN VASCULAR SURGERY 1. ABDOMINAL AORTIC ANEURYSM A 70 year old man presents in the emergency department with
POINT OF CARE ULTRASOUND - Venous US for DVT
 POINT OF CARE ULTRASOUND - Venous US for DVT The diagnosis of deep venous thrombosis (DVT) using ultrasound in the emergency department. DVT US is easy to perform and can be usually be completed in less
POINT OF CARE ULTRASOUND - Venous US for DVT The diagnosis of deep venous thrombosis (DVT) using ultrasound in the emergency department. DVT US is easy to perform and can be usually be completed in less
COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP)
 The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 16 December 1999 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE FOR GUIDANCE ON CLINICAL
The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 16 December 1999 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE FOR GUIDANCE ON CLINICAL
Guidelines, Policies and Statements D5 Statement on Abdominal Scanning
 Guidelines, Policies and Statements D5 Statement on Abdominal Scanning Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
Guidelines, Policies and Statements D5 Statement on Abdominal Scanning Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
PREVENTION AND TREATMENT OF VENOUS THROMBOEMBOLISM
 PREVENTION AND TREATMENT OF VENOUS THROMBOEMBOLISM International Consensus Statement 2013 Guidelines According to Scientific Evidence Developed under the auspices of the: Cardiovascular Disease Educational
PREVENTION AND TREATMENT OF VENOUS THROMBOEMBOLISM International Consensus Statement 2013 Guidelines According to Scientific Evidence Developed under the auspices of the: Cardiovascular Disease Educational
THE popliteal artery is the second most common site of aneurysm. The
 POPLITEAL ANEURYSM Treatment by Vein Graft: Case Report A. W. HUMPHRIES, M.D. Department of Orthopedic Surgery F. A. LeFEVRE, M.D. and V. G. dewolfe, M.D. Department of Cardiovascular Disease THE popliteal
POPLITEAL ANEURYSM Treatment by Vein Graft: Case Report A. W. HUMPHRIES, M.D. Department of Orthopedic Surgery F. A. LeFEVRE, M.D. and V. G. dewolfe, M.D. Department of Cardiovascular Disease THE popliteal
Diagnostic Imaging
 www.fisiokinesiterapia.biz Diagnostic Imaging Diagnostic Imaging is no longer limited to radiography. Major technological advancements have lead to the use of new and improved imaging technologies. The
www.fisiokinesiterapia.biz Diagnostic Imaging Diagnostic Imaging is no longer limited to radiography. Major technological advancements have lead to the use of new and improved imaging technologies. The
Computed tomography manifestations of common inferior vena cava dysplasia and its clinical significance
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 5: 631-635, 2013 Computed tomography manifestations of common inferior vena cava dysplasia and its clinical significance ZHEN-YU QIAN 1*, MING-FENG YANG 2*, KE-QIANG
EXPERIMENTAL AND THERAPEUTIC MEDICINE 5: 631-635, 2013 Computed tomography manifestations of common inferior vena cava dysplasia and its clinical significance ZHEN-YU QIAN 1*, MING-FENG YANG 2*, KE-QIANG
Percutaneously Inserted AngioVac Suction Thrombectomy for the Treatment of Filter-Related. Iliocaval Thrombosis
 Percutaneously Inserted AngioVac Suction Thrombectomy for the Treatment of Filter-Related Iliocaval Thrombosis Faiz D. Francis, DO; Gianvito Salerno, MD; Sabbah D. Butty, MD Abstract In the setting of
Percutaneously Inserted AngioVac Suction Thrombectomy for the Treatment of Filter-Related Iliocaval Thrombosis Faiz D. Francis, DO; Gianvito Salerno, MD; Sabbah D. Butty, MD Abstract In the setting of
DVT and Pulmonary Embolus. Dr Piers Blombery BSc(Biomed), MBBS (Hons), FRACP, FRCPA Consultant Haematologist Peter MacCallum Cancer Centre
 DVT and Pulmonary Embolus Dr Piers Blombery BSc(Biomed), MBBS (Hons), FRACP, FRCPA Consultant Haematologist Peter MacCallum Cancer Centre Overview Structure of deep and superficial venous system of upper
DVT and Pulmonary Embolus Dr Piers Blombery BSc(Biomed), MBBS (Hons), FRACP, FRCPA Consultant Haematologist Peter MacCallum Cancer Centre Overview Structure of deep and superficial venous system of upper
Discussion Leader: Doug Bias, M.D.
 In low-risk patients with isolated calf DVT (IDDVT), what is the morbidity risk of treating with repeat ultrasound/observation versus anticoagulation? Discussion Leader: Doug Bias, M.D. Clinical Scenario:
In low-risk patients with isolated calf DVT (IDDVT), what is the morbidity risk of treating with repeat ultrasound/observation versus anticoagulation? Discussion Leader: Doug Bias, M.D. Clinical Scenario:
DEEP VEIN THROMBOSIS (DVT): TREATMENT
 DEEP VEIN THROMBOSIS (DVT): TREATMENT OBJECTIVE: To provide an evidence-based approach to treatment of patients presenting with deep vein thrombosis (DVT). BACKGROUND: An estimated 45,000 patients in Canada
DEEP VEIN THROMBOSIS (DVT): TREATMENT OBJECTIVE: To provide an evidence-based approach to treatment of patients presenting with deep vein thrombosis (DVT). BACKGROUND: An estimated 45,000 patients in Canada
Lung sequestration and Scimitar syndrome
 Lung sequestration and Scimitar syndrome Imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Rotterdam, The Netherlands Pulmonary sequestration Pulmonary sequestration (PS)
Lung sequestration and Scimitar syndrome Imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Rotterdam, The Netherlands Pulmonary sequestration Pulmonary sequestration (PS)
Stent-assisted coil embolization of a wide-necked renal artery aneurysm
 Stent-assisted coil embolization of a wide-necked renal artery aneurysm Bjoern Kitzing 1*, John Vedelago 1, Nick Bajic 1, Grace Lai 1, Richard Waugh 1 1. Department of Radiology, Royal Prince Alfred Hospital,
Stent-assisted coil embolization of a wide-necked renal artery aneurysm Bjoern Kitzing 1*, John Vedelago 1, Nick Bajic 1, Grace Lai 1, Richard Waugh 1 1. Department of Radiology, Royal Prince Alfred Hospital,
CHAPTER 2 VENOUS THROMBOEMBOLISM
 CHAPTER 2 VENOUS THROMBOEMBOLISM Objectives Venous Thromboembolism (VTE) Prevalence Patho-physiology Risk Factors Diagnosis Pulmonary Embolism (PE) Management of DVT/PE Prevention VTE Patho-physiology
CHAPTER 2 VENOUS THROMBOEMBOLISM Objectives Venous Thromboembolism (VTE) Prevalence Patho-physiology Risk Factors Diagnosis Pulmonary Embolism (PE) Management of DVT/PE Prevention VTE Patho-physiology
What is the real place of venous echo Doppler in aircrew member flying rehabilitation after a thromboembolism event?
 89 th ASMA ANNUAL SCIENTIFIC MEETING DALLAS- May 6-10, 2018 What is the real place of venous echo Doppler in aircrew member flying rehabilitation after a thromboembolism event? S BISCONTE (1), V MARICOURT
89 th ASMA ANNUAL SCIENTIFIC MEETING DALLAS- May 6-10, 2018 What is the real place of venous echo Doppler in aircrew member flying rehabilitation after a thromboembolism event? S BISCONTE (1), V MARICOURT
Abdominal Exam: The examination of the abdomen used by physicians to detect an abdominal aortic aneurysm.
 Glossary of Terms Abdominal Exam: The examination of the abdomen used by physicians to detect an abdominal aortic aneurysm. Angiogram: A diagnostic test requiring the insertion of a catheter into an artery
Glossary of Terms Abdominal Exam: The examination of the abdomen used by physicians to detect an abdominal aortic aneurysm. Angiogram: A diagnostic test requiring the insertion of a catheter into an artery
Anomalies of the inferior vena cava in patients with deep venous thrombosis. Pictorial essay.
 Pictorial essay Medical Ultrasonography 2012, Vol. 14, no. 1, 53-59 Anomalies of the inferior vena cava in patients with deep venous thrombosis. Pictorial essay. Sorin Pop 1, Iulianu Opincaru 2 1 1 st
Pictorial essay Medical Ultrasonography 2012, Vol. 14, no. 1, 53-59 Anomalies of the inferior vena cava in patients with deep venous thrombosis. Pictorial essay. Sorin Pop 1, Iulianu Opincaru 2 1 1 st
How long to continue anticoagulation after DVT?
 How long to continue anticoagulation after DVT? Dr. Nihar Ranjan Pradhan M.S., DNB (Vascular Surgery), FVES(UK) Consultant Vascular Surgeon Apollo Hospital, Jubilee Hills, Hyderabad (Formerly Faculty in
How long to continue anticoagulation after DVT? Dr. Nihar Ranjan Pradhan M.S., DNB (Vascular Surgery), FVES(UK) Consultant Vascular Surgeon Apollo Hospital, Jubilee Hills, Hyderabad (Formerly Faculty in
IVC FILTERS: A CASE REPORT REVIEWING THE INDICATIONS FOR PLACEMENT, RETRIEVAL AND ANTICOAGULATION
 IVC FILTERS: A CASE REPORT REVIEWING THE INDICATIONS FOR PLACEMENT, RETRIEVAL AND ANTICOAGULATION Resident(s): George Athanasatos Attending(s): Daniel Golwyn Program/Dept: Interventional Radiology CHIEF
IVC FILTERS: A CASE REPORT REVIEWING THE INDICATIONS FOR PLACEMENT, RETRIEVAL AND ANTICOAGULATION Resident(s): George Athanasatos Attending(s): Daniel Golwyn Program/Dept: Interventional Radiology CHIEF
