Review Article Selective Inguinal Lymphadenectomy in the Treatment of Invasive Squamous Cell Carcinoma of the Vulva
|
|
|
- Brook Farmer
- 5 years ago
- Views:
Transcription
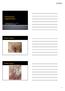
1 Hindawi Publishing Corporation International Journal of Surgical Oncology Volume 2011, Article ID , 6 pages doi: /2011/ Review Article Selective Inguinal Lymphadenectomy in the Treatment of Invasive Squamous Cell Carcinoma of the Vulva Christopher P. DeSimone, Jeffrey Elder, and John R. van Nagell Jr. Division of Gynecologic Oncology, Department of Obstetrics and Gynecology, The University of Kentucky Chandler Medical Center- Markey Cancer Center, 800 Rose Street, Lexington, KY , USA Correspondence should be addressed to Christopher P. DeSimone, cpdesi00@uky.edu Received 6 January 2011; Accepted 5 April 2011 Academic Editor: E. W. Martin Copyright 2011 Christopher P. DeSimone et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. En bloc radical vulvectomy with bilateral inguinofemoral lymphadenectomy has now been replaced by radical wide excision and selective inguinal lymphadenectomy based on the stage and location of invasive vulvar cancer. Early stage lateral cancers can be effectively treated by radical wide excision and ipsilateral superficial inguinal lymphadenectomy. Lymph node mapping using perilesional injection of radiocolloid and blue dye may identify sentinel lymph nodes which can be removed, thereby avoiding the morbidity of full inguinal lymphadenectomy in selected patients with early stage disease. 1. Introduction Although squamous cell carcinoma of the vulva is not common, it is occurring with increasing frequency in younger women, particularly in those exposed to human papilloma virus (HPV). With efforts at education, many patients are presenting with early stage disease which is amenable to surgery. This year, there will be approximately 3500 new casesofvulvarcancerintheunitedstates,representing5% of all gynecologic cancers [1]. The surgical management of this disease has evolved from en bloc resection of the entire vulva with bilateral superficial and deep inguinofemoral lymphadenectomy to a more conservative approach involving radical wide excision of the primary lesion and specific types of inguinal lymphadenectomy based on the stage and anatomic location of disease. 2. Anatomic Pathways of Spread and Staging The lymphatic drainage of the vulva has been studied extensively and described in numerous publications [2, 3]. Generally, lateralizing lesions (>1cm beyond the midline) drain to the ipsilateral superficial inguinal lymph nodes, whereas midline lesions can drain to either side (Figure 1). It is extremely rare for lateralizing vulvar cancers to spread to the contralateral inguinal lymph nodes if there is no evidence of ipsilateral lymph node metastases. Likewise, it is unusual for the deep inguinal nodes (below the cribriform fascia) to be involved in the absence of superficial inguinal lymph node spread. The current International Federation of Gynecology andobstetricsstagingsystemforvulvarcancerisnowbased on surgical findings as illustrated in Table 1 and reflects the extent and location of inguinal lymph node metastases. 3. Surgery of the Primary Vulvar Lesion The Basset-Way operation which was the standard of care in the operative management of patients with vulvar cancer included the en bloc resection of the primary lesion and surroundingvulvarskinaswellastheskinoverbothgroins (Figure 2(a)) [4]. Although this procedure was curative in the majority of cases, the wound defect was significant and incisional breakdown and lymphedema of both lower extremities were common. Currently, the surgical treatment of vulvar cancer involves radical wide excision of the primary lesion and inguinal lymphadenectomy through separate groin incisions (Figure 2(b)) [5]. Heaps and colleagues [6] reported that local control of vulvar cancers could be achieved in 100% of cases provided that a 1 cm margin of normal skin was included in the surgical specimen. These
2 2 International Journal of Surgical Oncology (a) (b) Figure 1: Lateral vulvar lesions >1 cm from the midline (a) spread initially to the ipsilateral superficial inguinal lymph nodes, whereas midline lesions can spread to both groins (b). (a) (b) Figure 2: The Bassett-Way operation includes en bloc radical resection of the primary lesion and surrounding vulvar skin as well as the skin over both groins (a). Radical wide excision of the vulvar cancer includes a margin of at least 1 cm of normal skin around the entire lesion. Inguinal lymphadenectomy is performed through separate groin incisions (b). observations were confirmed by De Hullu and coworkers [7] who reported that there was no local recurrence of T 1 or T 2 vulvar cancers when a margin of at least 8 mm normal skin was excised with the primary lesion. In contrast, patients with a margin of <8 mm had a local recurrence rate of 22%. At present, it is recommended that a margin of at least 1 cm of normal skin around the circumference of the primary vulvar lesion be included in the surgical specimen and that the underlying subcutaneous tissue be removed to the level of the perineal fascia. Inguinal lymphadenectomy is then performed through separate incisions. 4. Sentinel Lymphadenectomy Sentinel lymph node excision is now being recommended in selected patients with early stage squamous cell carcinoma as a means to avoid the operative morbidity associated with inguinofemoral lymphadenectomy [8 10]. It is estimated that only 25 30% of patients with early stage vulvar cancer have lymph node metastases, and complete inguinofemoral lymphadenectomy is associated with postoperative wound complications and lower extremity edema in 30 40% of patients [11]. Sentinel lymph node mapping using radiolabelled ultrafiltered sulfur colloid was initially reported as a method to identify regional lymph node metastases in breast cancer [12, 13] and cutaneous melanoma [4] andhas now been evaluated in patients with early stage vulvar cancer. Specifically, 1-2 mci of radiocolloid is injected intradermally around the lesion (Figure 3), and a hand held gamma detection device is used to identify the sentinel lymph node(s). Recently, lymphoscintigraphy has been combined with intraoperative perilesional injection of isosulfan blue as a method to identify sentinel nodes in the inguinal area. Localization of the sentinel node(s) is usually apparent 5 15 minutes after injection of blue dye and 30 minutes after injection of radiocolloid. Selman and colleagues [14] performed a systematic review of the accuracy of sentinel lymph node detection in identifying inguinal lymph node metastases in vulvar cancer and reported that the combination of 99 mtc radiocolloid and isosulfan blue dye successfully detected sentinel lymph nodes in 97% of cases. It also had a negative predictive value (NPV) of 99.1%. Further analysis has indicated that sentinel lymph node mapping is most accurate in patients with early stage lateral vulvar cancers [15]. A persisting concern about sentinel lymph node mapping in vulvar cancer is the frequency of groin recurrences in patients with negative sentinel lymph nodes. In a multiinstitutional observational study, Van Der Zee and coworkers
3 International Journal of Surgical Oncology 3 Table 1: FIGO staging of invasive cancer of the vulva. Stage I Tumor confined to the vulva Lesions 2cm in size confined to the vulva or IA perineum and with stromal invasion 1.0 mm, no nodal metastasis Lesions >2cm in size confined to the vulva or IB perineum with stromal invasion greater than 1.0 mm, no nodal metastasis Tumor of any size with extension to adjacent perineal Stage II structures (1/3 lower urethra, 1/3 lower vagina, anus), no nodal metastasis Tumor of any size with or without extension to adjacent Stage III perineal structures (1/3 lower urethra, 1/3 lower vagina, anus) with positive inguinofemoral lymph nodes IIIA With 1 lymph node metastasis ( 5mm), (i) With 2 or more lymph node metastases ( 5 mm), IIIB (ii) 3 or more lymph node metastases (<5 mm) IIIC With positive nodes with extracapsular spread Tumor invades other regional (2/3 upper urethra, 2/3 Stage IV upper vagina) or distant structures Tumor invades any of the following: (i) Upper urethra and/or vaginal mucosa, bladder IVA mucosa, rectal mucosa, or fixed to pelvic bone, (ii) Fixed or ulcerated inguinofemoral lymph nodes IVB Any distant metastasis including pelvic lymph nodes The depth of invasion is defined as the measurement of the tumor from the epithelial-stromal junction of the adjacent most superficial dermal papilla to the deepest point of invasion. Figure 3: Sentinel lymph node mapping. Sentinel lymph nodes are localized by perilesional injection of 99 mtc radiocolloid and isosulfan blue dye. [10] performed the sentinel node procedure in 623 groins of 403 assessable patients. Two hundred fifty-nine patients with unifocal vulvar cancers <4 cm diameter and negative sentinel nodes were followed without additional therapy for a median of 35 months. Six groin recurrences (2.3%) were observed, and the 3-year survival of these patients was 97%. Importantly, both short-term morbidity and long-term morbidity of patients having sentinel node excision were significantly reduced when compared to that of women undergoing complete inguinofemoral lymphadenectomy. These authors concluded that sentinel node dissection, performed by a quality-controlled multidisciplinary team, should be offered to selected patients with early stage vulvar cancer as a means to avoid the postoperative morbidity associated with inguinofemoral lymphadenectomy. There is a definite learning curve in the performance and interpretation of lymph node mapping, and it is recommended that a multidisciplinary group within each institution perform sentinel node mapping in at least cases before it becomes an accepted procedure [10, 16]. If sentinel lymph nodes cannot be identified by mapping or if there is uncertainty concerning interpretation of findings, a superficial inguinal lymphadenectomy should be performed. Patients with a positive sentinel node should undergo a full inguinofemoral lymphadenectomy followed by postoperative radiation therapy to the involved groin and pelvis. However, if the sentinel lymph nodes identified by mapping are histologically negative after review by an experienced multidisciplinary team, no further treatment is indicated. It should be emphasized that optimal candidates for sentinel lymph node mapping are patients who have lateral T 1 or T 2 unifocal vulvar cancers <4 cm diameter with nonpalpable groin nodes [10]. This procedure is less accurate in patients with midline vulvar lesions or those with advanced stage disease and clinically palpable inguinal nodes [17]. 5. Superficial Inguinal Lymphadenectomy Many surgeons concerned about the accuracy of sentinel lymph mapping have elected to perform superficial inguinal lymphadenectomy as the treatment of choice in patients with early stage vulvar cancer, believing that the superficial inguinal nodes are themselves sentinel nodes. Specifically, all inguinal lymph nodes above the cribriform fascia are removed en bloc (Figure 4). Approximately 8 10 lymph nodes are excised, and the saphenous vein is preserved in order to decrease the frequency of postoperative lower extremity lymphedema [18, 19]. Berman and coworkers [20] reported the outcomes of 50 patients with T 1 vulvar cancers <1 cm diameter with stromal invasion >5 mm who underwent radical wide excision and superficial inguinal lymphadenectomy. Women with positive superficial inguinal nodes underwent deep inguinal lymphadenectomy and radiation, whereas patients with negative superficial inguinal nodes received no further treatment. There were no isolated groin recurrences noted during a follow-up period of 36 months. Importantly, only 1 patient died of recurrent cancer, and wound complications were observed in only 12% of patients. These authors concluded that radical wide excision of the primary lesion and superficial inguinal lymphadenectomy was the treatment of choice for most women with early stage vulvar cancer and no evidence of enlarged inguinal lymph nodes on clinical examination. A persisting concern of this approach has been a significant but low incidence of groin recurrence in patients with negative superficial inguinal lymph nodes at the time of
4 4 International Journal of Surgical Oncology Figure 4: Radical wide excision and ipsilateral superficial inguinal lymphadenectomy is performed for lateral T 1 or T 2 vulvar cancers. All lymph nodes above the cribriform fascia are removed and the saphenous vein is preserved. Figure 5: Radical wide excision and bilateral inguinofemoral lymphadenectomy is performed for midline vulvar cancers. This illustration depicts the right superficial inguinal lymph nodes and the left deep femoral lymph nodes which are seen along the medial aspect of the fossa ovalis. lymphadenectomy. Two investigators have reported a 4 7% incidence of subsequent ipsilateral groin failure after negative primary superficial groin dissection [21, 22]. This is worrisome since the majority of patients with groin recurrence died of their disease. However, these studies were retrospective and in one series [21] the anatomic location of the primary vulvar lesion was not reported. In the most recent investigation [22], vulvar cancers that recurred in the groin after negative superficial inguinal lymphadenectomy were central periclitoral lesions and the number of lymph nodes removed was small ( 3 per groin). Therefore, these authors recommend superficial inguinal lymphadenectomy as the initial surgical approach in patients with lateral Stage I or Stage II vulvar cancers provided that an adequate number of superficial inguinal lymph nodes (8 10) are removed [22]. Currently, superficial inguinal lymphadenectomy should be considered only in patients with lateral T 1 and T 2 vulvar cancers having >1 mm stromal invasion and no clinical evidence of enlarged groin nodes. 6. Deep Inguinal Lymphadenectomy Anatomic studies have indicated that some superficial inguinal nodes may be located within the interstices of the cribriform fascia and could be missed by purely superficial inguinal lymphadenectomy [23]. Therefore, some surgeons choose to perform deep inguinal lymphadenectomy routinely at the time of superficial inguinal lymphadenectomy. The deep femoral lymph nodes are always located within the opening of the fossa ovalis medial to the femoral vein, and no lymph nodes are distal to the lower margin of the fossa ovalis or lateral to the femoral vein (Figure 5). For this reason, incision of the deep fascia of the adductor canal and dissection of the femoral vessels, sometimes performed as part of this procedure, are unnecessary. This is important since deep fascial incision and stripping of the femoral vessels is associated with postoperative wound breakdown, lymphocyst formation, and lower extremity edema in up to 40% of cases [11, 24]. At one time, patients with positive superficial or deep inguinal nodes were treated by pelvic lymphadenectomy. However, a prospective trial conducted by the Gynecologic Oncology Group showed that patients with inguinal lymph node metastasis at the time of groin dissection who were treated by postoperative inguinal and pelvic radiation had a significant survival advantage when compared to similar patients treated by pelvic lymphadenectomy [25]. Patients in the radiation therapy arm received Gy to the involved groin and pelvis, whereas patients randomized to pelvic lymphadenectomy underwent a standard extraperitoneal excision of the obturator, external iliac, internal iliac, and common iliac lymph nodes. This trial showed a statistically significant survival advantage to patients in the radiation therapy arm (68% versus 54% observed survival) on interim analysis [26]. Therefore, most vulvar cancer patients with positive superficial or deep inguinal lymph node metastases at the time of inguinal lymphadenectomy are treated now by postoperative radiation to the involved groin and pelvis. 7. Unilateral versus Bilateral Inguinal Lymphadenectomy Anatomic studies have confirmed that efferent lymphatics from the lateral vulva drain initially to the ipsilateral superficial inguinal lymph nodes [2, 27]. Likewise, lateral vulvar cancers (>1cm beyond the midline) do not spread to the contralateral inguinal lymph nodes without first involving the ipsilateral inguinal nodes [27, 28]. These anatomic observations have led to clinical trials evaluating the efficacy of radical wide excision and ipsilateral inguinal lymphadenectomy in the treatment of lateral vulvar cancers. DeSimone and coworkers [29], for example, treated 122 patients with lateral T 1 or T 2 vulvar cancers by radical vulvectomy (N = 60) or radical wide excision (N = 62) and bilateral inguinal lymphadenectomy. Twenty-six patients (21%) had ipsilateral inguinal lymph node metastases, but
5 International Journal of Surgical Oncology 5 there were no cases of spread to the contralateral inguinal lymph nodes. Patients with positive inguinal nodes were treated by postoperative radiation therapy to the involved groin and pelvis. All patients in the study were followed periodically by clinical examinations months (mean 59 months) after treatment. Eighteen patients (15%) developed recurrent vulvar cancer 13 to the ipsilateral vulvar skin, 2 to the ipsilateral groin, and 3 to the lung. There were no recurrences to the contralateral vulvar skin or groin. Likewise, there was no difference in the local recurrence rate of patients treated by radical vulvectomy versus those treated by radical wide excision. The 5-year disease-free survival was 98% for patients with T 1 lesions and 93% for patients with T 2 lesions. These authors concluded that women with lateral T 1 and T 2 vulvar cancers could be treated effectively by radical wide excision and ipsilateral inguinal lymphadenectomy. There is still some controversy concerning the performance of routine contralateral inguinofemoral lymphadenectomy in patients with lateral vulvar cancers and positive ipsilateral inguinal nodes. Isolated reports have indicated that contralateral inguinal lymph node metastases can occur in these patients. However, the frequency of contralateral spread in these patients is extremely low, and the risk of contralateral inguinal lymphadenectomy may outweigh its benefits, particularly if only a small number of ipsilateral nodes are positive. All vulvar cancers located within 1 cm of midline structures (clitoris, vagina, or anus) have the potential to spread to both groins, and should be treated by radical wide excision and bilateral inguinofemoral lymphadenectomy. 8. Summary The Bassett-Way operation, which emphasized en bloc resection of the vulva and both groins, has been replaced by radical wide excision and selective inguinal lymphadenectomy through separate groin incisions. The specific type of inguinal lymphadenectomy indicated depends on the stage and location of each cancer. Early stage lateral vulvar cancers can be treated safely by radical wide excision and ipsilateral superficial inguinal lymphadenectomy, whereas central vulvar cancers require bilateral inguinal lymphadenectomy. Deep inguinal lymphadenectomy, which involves surgical removal of the deep femoral nodes, is indicated in patients with centrally located early stage vulvar cancers, advanced stage vulvar cancers, and in patients with positive superficial inguinal lymph nodes. The deep femoral lymph nodes are always located medial to the femoral vein and can be removed without incising the deep fascia or dissecting the femoral vessels. Sentinel lymph node mapping should be offered to select patients with early stage lateral vulvar cancers as a means to avoid the postoperative morbidity associated with full inguinofemoral lymphadenectomy. References [1]A.Jemal,R.Siegel,E.Ward,Y.Hao,J.Xu,andM.J.Thun, Cancer statistics, 2009, CA: Cancer Journal for Clinicians,vol. 59, no. 4, pp , [2]A.A.PlentlandE.A.Friedman,Lymphatic System of the Female Genitalia: The Morphologic Basis of Oncologic Diagnosis and Therapy, Saunders, Philadelphia, Pa, USA, [3] D.C.Figge,H.K.Tamimi,andB.E.Greer, Lymphaticspread in carcinoma of the vulva, American Journal of Obstetrics and Gynecology, vol. 152, no. 4, pp , [4] S. Way, Carcinoma of the vulva, American Journal of Obstetrics and Gynecology, vol. 79, pp , [5] N.F.Hacker,R.S.Leuchter,J.S.Berek,T.W.Castaldo,andL. D. Lagasse, Radical vulvectomy and bilateral inguinal lymphadenectomy through separate groin incisions, Obstetrics and Gynecology, vol. 58, no. 5, pp , [6] J.M.Heaps,Y.S.Fu,F.J.Montz,N.F.Hacker,andJ.S.Berek, Surgical-pathologic variables predictive of local recurrence in squamous cell carcinoma of the vulva, Gynecologic Oncology, vol. 38, no. 3, pp , [7] J. A. De Hullu, H. Hollema, S. Lolkema et al., Vulvar carcinoma: the price of less radical surgery, Cancer, vol. 95, no. 11, pp , [8] J.A.DeHullu,H.Hollema,D.A.Piersetal., Sentinellymph node procedure is highly accurate squamous cell carcinoma of the vulva, Journal of Clinical Oncology, vol. 18, no. 15, pp , [9] R. G. Moore, K. Robison, A. K. Brown et al., Isolated sentinel lymph node dissection with conservative management in patients with squamous cell carcinoma of the vulva: a prospective trial, Gynecologic Oncology, vol. 109, no. 1, pp , [10] A. G. J. Van Der Zee, M. H. Oonk, J. A. De Hullu et al., Sentinel node dissection is safe in the treatment of early-stage vulvar cancer, Journal of Clinical Oncology, vol. 26, no. 6, pp , [11] K. N. Gaarenstroom, G. G. Kenter, J. B. Trimbos et al., Postoperative complications after vulvectomy and inguinofemoral lymphadenectomy using separate groin incisions, International Journal of Gynecological Cancer, vol. 13, no. 4, pp , [12] T. Kim, A. E. Giuliano, and G. H. Lyman, Lymphatic mapping and sentinel lymph node biopsy in early-stage breast carcinoma: a metaanalysis, Cancer, vol. 106, no. 1, pp. 4 16, [13] R. E. Mansel, L. Fallowfield, M. Kissin et al., Randomized multicenter trial of sentinel node biopsy versus standard axillary treatment in operable breast cancer: the ALMANAC trial, Journal of the National Cancer Institute, vol. 98, no. 9, pp , [14] T.J.Selman,D.M.Luesley,N.Acheson,K.S.Khan,andC.H. Mann, A systematic review of the accuracy of diagnostic tests for inguinal lymph node status in vulvar cancer, Gynecologic Oncology, vol. 99, no. 1, pp , [15] C. Louis-Sylvestre, E. Evangelista, F. Leonard, E. Itti, M. Meignan, and B. J. Paniel, Sentinel node localization should be interpreted with caution in midline vulvar cancer, Gynecologic Oncology, vol. 97, no. 1, pp , [16] C. F. Levenback, How safe is sentinel lymph node biopsy in patients with vulvar cancer? Journal of Clinical Oncology, vol. 26, no. 6, pp , [17] M. Frumovitz, P. T. Ramirez, G. Tortolero-Luna et al., Characteristics of recurrence in patients who underwent lymphatic mapping for vulvar cancer, Gynecologic Oncology, vol. 92, no. 1, pp , [18] S. C. Plaxe, P. S. Braly, and P. R. Dottino, A simplified approach to superficial inguinal dissection with sparing of the saphenous vein in patients with carcinoma of the vulva,
6 6 International Journal of Surgical Oncology Surgery Gynecology and Obstetrics, vol. 176, no. 3, pp , [19] S. H. Zhang, A. K. Sood, J. I. Sorosky, B. Anderson, and R. E. Buller, Preservation of the saphenous vein during inguinal lymphadenectomy decreases morbidity in patients with carcinoma of the vulva, Cancer, vol. 89, no. 7, pp , [20] M.L.Berman,J.T.Soper,W.T.Creasman,G.T.Olt,andP. J. SiSaia, Conservative surgical management of superficially invasive stage I vulvar carcinoma, Gynecologic Oncology, vol. 35, no. 3, pp , [21] M. E. Gordinier, A. Malpica, T. W. Burke et al., Groin recurrence in patients with vulvar cancer with negative nodes on superficial inguinal lymphadenectomy, Gynecologic Oncology, vol. 90, no. 3, pp , [22] T.O.Kirby,R.P.Rocconi,T.M.Numnumetal., Outcomes of stage I/II vulvar cancer patients after negative superficial inguinal lymphadenectomy, Gynecologic Oncology, vol.98, no. 2, pp , [23]C.N.Hudson,H.Shulver,andD.C.Lowe, Thesurgeryof inguino-femoral lymph nodes: is it adequate or excessive? International Journal of Gynecological Cancer,vol.14,no.5,pp , [24] N. Gould, S. Kamelle, T. Tillmanns et al., Predictors of complications after inguinal lymphadenectomy, Gynecologic Oncology, vol. 82, no. 2, pp , [25] F. B. Stehman, B. N. Bundy, G. Thomas et al., Groin dissection versus groin radiation in carcinoma of the vulva: a Gynecologic Oncology Group study, International Journal of Radiation Oncology Biology Physics, vol. 24, no. 2, pp , [26] C. Kunos, F. Simpkins, H. Gibbons, C. Tian, and H. Homesley, Radiation therapy compared with pelvic node resection for node-positive vulvar cancer: a randomized controlled trial, Obstetrics and Gynecology, vol. 114, no. 3, pp , [27] H. D. Homesley, B. N. Bundy, A. Sedlis et al., Assessment of current International Federation of Gynecology and Obstetrics staging of vulvar carcinoma relative to prognostic factors for survival (A Gynecologic Oncology Group Study), American Journal of Obstetrics and Gynecology, vol. 164, no. 4, pp , [28] S. J. Andrews, B. T. Williams, P. D. DePriest et al., Therapeutic implications of lymph nodal spread in lateral T 1 and T 2 squamous cell carcinoma of the vulva, Gynecologic Oncology, vol. 55, no. 1, pp , [29] C. P. DeSimone, J. S. Van Ness, A. L. Cooper et al., The treatment of lateral T1 and T2 squamous cell carcinomas of the vulva confined to the labium majus or minus, Gynecologic Oncology, vol. 104, no. 2, pp , 2007.
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER VULVAR
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER VULVAR Last Revision Date July 2015 1 Site Group: Gynecologic Cancer Vulvar Author: Dr. Stephane Laframboise 1. INTRODUCTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER VULVAR Last Revision Date July 2015 1 Site Group: Gynecologic Cancer Vulvar Author: Dr. Stephane Laframboise 1. INTRODUCTION
Proposed All Wales Vulval Cancer Guidelines. Dr Amanda Tristram
 Proposed All Wales Vulval Cancer Guidelines Dr Amanda Tristram Previous FIGO staging FIGO Stage Features TNM Ia Lesion confined to vulva with
Proposed All Wales Vulval Cancer Guidelines Dr Amanda Tristram Previous FIGO staging FIGO Stage Features TNM Ia Lesion confined to vulva with
Clinical Study Morbidity of Inguinofemoral Lymphadenectomy in Vulval Cancer
 The Scientific World Journal Volume 2012, Article ID 341253, 4 pages doi:10.1100/2012/341253 The cientificworldjournal Clinical Study Morbidity of Inguinofemoral Lymphadenectomy in Vulval Cancer A. A.
The Scientific World Journal Volume 2012, Article ID 341253, 4 pages doi:10.1100/2012/341253 The cientificworldjournal Clinical Study Morbidity of Inguinofemoral Lymphadenectomy in Vulval Cancer A. A.
Guideline for the Management of Vulval Cancer
 Version History Guideline for the Management of Vulval Cancer Version Date Brief Summary of Change Issued 2.0 20.02.08 Endorsed by the Governance Committee 2.1 19.11.10 Circulated at NSSG meeting 2.2 13.04.11
Version History Guideline for the Management of Vulval Cancer Version Date Brief Summary of Change Issued 2.0 20.02.08 Endorsed by the Governance Committee 2.1 19.11.10 Circulated at NSSG meeting 2.2 13.04.11
Vulvar Carcinoma. Definition: Cases should be classified as carsinoma of the vulva when the primary site growth is in the vulva Malignant melanoma sho
 Carcinoma Vulva & Vagina Subdivisi Onkologi Ginekologi Bagian Obgin FK USU Vulvar Carcinoma. Definition: Cases should be classified as carsinoma of the vulva when the primary site growth is in the vulva
Carcinoma Vulva & Vagina Subdivisi Onkologi Ginekologi Bagian Obgin FK USU Vulvar Carcinoma. Definition: Cases should be classified as carsinoma of the vulva when the primary site growth is in the vulva
SCAN Gynaecological Group. Clinical Management Protocols vulval cancer
 SE Scotland Cancer Network SCAN Gynaecological Group Clinical Management Protocols vulval cancer 2009 www.scan.scot.nhs.uk August 2001 updated annually, most recently INTRODUCTION The South East Scotland
SE Scotland Cancer Network SCAN Gynaecological Group Clinical Management Protocols vulval cancer 2009 www.scan.scot.nhs.uk August 2001 updated annually, most recently INTRODUCTION The South East Scotland
Staging and Treatment Update for Gynecologic Malignancies
 Staging and Treatment Update for Gynecologic Malignancies Bunja Rungruang, MD Medical College of Georgia No disclosures 4 th most common new cases of cancer in women 5 th and 6 th leading cancer deaths
Staging and Treatment Update for Gynecologic Malignancies Bunja Rungruang, MD Medical College of Georgia No disclosures 4 th most common new cases of cancer in women 5 th and 6 th leading cancer deaths
3/25/2019. J. Anthony Rakowski D.O., F.A.C.O.O.G. MSU SCS Board Review Coarse
 J. Anthony Rakowski D.O., F.A.C.O.O.G. MSU SCS Board Review Coarse 1 4 th most common GYN cancer 5% of malignancies of GYN type. 4850 new cases annually 1030 deaths Cigarette smoking Vulvar dystrophy (Lichen
J. Anthony Rakowski D.O., F.A.C.O.O.G. MSU SCS Board Review Coarse 1 4 th most common GYN cancer 5% of malignancies of GYN type. 4850 new cases annually 1030 deaths Cigarette smoking Vulvar dystrophy (Lichen
Clinical Pathological Conference. Malignant Melanoma of the Vulva
 Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
The International Federation of Gynecology and Obstetrics (FIGO) updated the staging
 Continuing Education Column Revised FIGO Staging System Hee Sug Ryu, MD Department of Obstetrics and Gynecology, Ajou University School of Medicine E - mail : hsryu@ajou.ac.kr J Korean Med Assoc 2010;
Continuing Education Column Revised FIGO Staging System Hee Sug Ryu, MD Department of Obstetrics and Gynecology, Ajou University School of Medicine E - mail : hsryu@ajou.ac.kr J Korean Med Assoc 2010;
Prognostic factors associated with local recurrence in squamous cell carcinoma of the vulva
 Original Article J Gynecol Oncol Vol. 24, No. 3:242-248 pissn 2005-0380 eissn 2005-0399 Prognostic factors associated with local recurrence in squamous cell carcinoma of the vulva Sara Iacoponi, Ignacio
Original Article J Gynecol Oncol Vol. 24, No. 3:242-248 pissn 2005-0380 eissn 2005-0399 Prognostic factors associated with local recurrence in squamous cell carcinoma of the vulva Sara Iacoponi, Ignacio
Type I. Type II. Excess estrogen Lynch Endometrioid adenocarcinoma PTEN. High grade More aggressive Serous, Clear Cell p53
 Type I Excess estrogen Lynch Endometrioid adenocarcinoma PTEN Type II High grade More aggressive Serous, Clear Cell p53 Stage I IA IB Stage II Stage III IIIA IIIB IIIC IIIC1 IIIC2 Stage IV IVA IVB nodes
Type I Excess estrogen Lynch Endometrioid adenocarcinoma PTEN Type II High grade More aggressive Serous, Clear Cell p53 Stage I IA IB Stage II Stage III IIIA IIIB IIIC IIIC1 IIIC2 Stage IV IVA IVB nodes
BREAST CANCER SURGERY. Dr. John H. Donohue
 Dr. John H. Donohue HISTORY References to breast surgery in ancient Egypt (ca 3000 BCE) Mastectomy described in numerous medieval texts Petit formulated organized approach in 18 th Century Improvements
Dr. John H. Donohue HISTORY References to breast surgery in ancient Egypt (ca 3000 BCE) Mastectomy described in numerous medieval texts Petit formulated organized approach in 18 th Century Improvements
Cervical Cancer: 2018 FIGO Staging
 Cervical Cancer: 2018 FIGO Staging Jonathan S. Berek, MD, MMS Laurie Kraus Lacob Professor Stanford University School of Medicine Director, Stanford Women s Cancer Center Senior Scientific Advisor, Stanford
Cervical Cancer: 2018 FIGO Staging Jonathan S. Berek, MD, MMS Laurie Kraus Lacob Professor Stanford University School of Medicine Director, Stanford Women s Cancer Center Senior Scientific Advisor, Stanford
Kentaro Tanaka, 1 Hiroki Mori, 1 Mutsumi Okazaki, 1 Aya Nishizawa, 2 and Hiroo Yokozeki Introduction. 2. Case Presentation
 Case Reports in Oncological Medicine Volume 2013, Article ID 259326, 4 pages http://dx.doi.org/10.1155/2013/259326 Case Report Long-Term Treatment Outcome after Only Popliteal Lymph Node Dissection for
Case Reports in Oncological Medicine Volume 2013, Article ID 259326, 4 pages http://dx.doi.org/10.1155/2013/259326 Case Report Long-Term Treatment Outcome after Only Popliteal Lymph Node Dissection for
Vulvar Cancer Surgical Treatment Complications Management; 5 Years Experience, SECI
 Med. J. Cairo Univ., Vol. 84, No. 2, March: 343-350, 2016 www.medicaljournalofcairouniversity.net Vulvar Cancer Surgical Treatment Complications Management; 5 Years Experience, SECI MAHMOUD H. ESHOIEBY,
Med. J. Cairo Univ., Vol. 84, No. 2, March: 343-350, 2016 www.medicaljournalofcairouniversity.net Vulvar Cancer Surgical Treatment Complications Management; 5 Years Experience, SECI MAHMOUD H. ESHOIEBY,
Invasive Cervical Cancer: Squamous Cell, Adenocarcinoma, Adenosquamous
 Note: If available, clinical trials should be considered as preferred treatment options for eligible patients (www.mdanderson.org/gynonctrials). Other co-morbidities are taken into consideration prior
Note: If available, clinical trials should be considered as preferred treatment options for eligible patients (www.mdanderson.org/gynonctrials). Other co-morbidities are taken into consideration prior
New NCCN Guidelines for Vulvar Cancer
 New NCCN Guidelines for Vulvar Cancer Benjamin E. Greer, MD Fred Hutchinson Cancer Research Center/ Seattle Cancer Care Alliance Vulvar Cancer Objectives: 1) Overview of vulvar carcinoma and FIGO staging.
New NCCN Guidelines for Vulvar Cancer Benjamin E. Greer, MD Fred Hutchinson Cancer Research Center/ Seattle Cancer Care Alliance Vulvar Cancer Objectives: 1) Overview of vulvar carcinoma and FIGO staging.
Vulva Cancer Histopathology Reporting Proforma
 Vulva Cancer Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given name(s) Ethnicity Unknown AboriginalTorres
Vulva Cancer Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given name(s) Ethnicity Unknown AboriginalTorres
Melanoma. Kaushik Mukherjee MD A. Scott Pearson MD
 Melanoma Kaushik Mukherjee MD A. Scott Pearson MD Disclosures You still have to study Not all inclusive No Western blots Extensive use of Google Image Search and Sabiston Melanoma Basics 8 th most common
Melanoma Kaushik Mukherjee MD A. Scott Pearson MD Disclosures You still have to study Not all inclusive No Western blots Extensive use of Google Image Search and Sabiston Melanoma Basics 8 th most common
Melanoma Quality Reporting
 Melanoma Quality Reporting September 1, 2013 December 31, 2016 Laurence McCahill, MD Surgical Oncologist Metro Health Surgical Oncology Metro Health Professional Building 2122 Health Drive SW Wyoming,
Melanoma Quality Reporting September 1, 2013 December 31, 2016 Laurence McCahill, MD Surgical Oncologist Metro Health Surgical Oncology Metro Health Professional Building 2122 Health Drive SW Wyoming,
Melanoma Surgery Update James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division
 Melanoma Surgery Update 2018 James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division Surgery for Melanoma Mainstay of treatment for potentially
Melanoma Surgery Update 2018 James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division Surgery for Melanoma Mainstay of treatment for potentially
Vaginal intraepithelial neoplasia
 Vaginal intraepithelial neoplasia The terminology and pathology of VAIN are analogous to those of CIN (VAIN I-III). The main difference is that vaginal epithelium does not normally have crypts, so the
Vaginal intraepithelial neoplasia The terminology and pathology of VAIN are analogous to those of CIN (VAIN I-III). The main difference is that vaginal epithelium does not normally have crypts, so the
CLINICAL PRACTICE GUID ELINES
 t SOGC CLINICAL PRACTICE GUID ELINES No. 2, May 1993 This has been provided by the Oncology Committee, Socieq of Obstetricians and Gynaecologists of Canada CURRENT CONCEPTS IN MANAGEMENT OF VULVAR CANCER
t SOGC CLINICAL PRACTICE GUID ELINES No. 2, May 1993 This has been provided by the Oncology Committee, Socieq of Obstetricians and Gynaecologists of Canada CURRENT CONCEPTS IN MANAGEMENT OF VULVAR CANCER
Cervical Cancer 3/25/2019. Abnormal vaginal bleeding
 Cervical Cancer Abnormal vaginal bleeding Postcoital, intermenstrual or postmenopausal Vaginal discharge Pelvic pain or pressure Asymptomatic In most patients who are not sexually active due to symptoms
Cervical Cancer Abnormal vaginal bleeding Postcoital, intermenstrual or postmenopausal Vaginal discharge Pelvic pain or pressure Asymptomatic In most patients who are not sexually active due to symptoms
Omitting Preoperative Lymphoscintigraphy Does Not Decrease Sentinel Lymph Node Detection Rate in Vulvar Cancer
 International Journal of Clinical Oncology and Cancer Research 2018; 3(3): 30-34 http://www.sciencepublishinggroup.com/j/ijcocr doi: 10.11648/j.ijcocr.20180303.13 ISSN: 2578-9503 (Print); ISSN: 2578-9511
International Journal of Clinical Oncology and Cancer Research 2018; 3(3): 30-34 http://www.sciencepublishinggroup.com/j/ijcocr doi: 10.11648/j.ijcocr.20180303.13 ISSN: 2578-9503 (Print); ISSN: 2578-9511
Radionuclide detection of sentinel lymph node
 Radionuclide detection of sentinel lymph node Sophia I. Koukouraki Assoc. Professor Department of Nuclear Medicine Medicine School, University of Crete 1 BACKGROUND The prognosis of malignant disease is
Radionuclide detection of sentinel lymph node Sophia I. Koukouraki Assoc. Professor Department of Nuclear Medicine Medicine School, University of Crete 1 BACKGROUND The prognosis of malignant disease is
Vulvar cancer: Know what to expect
 Vulvar cancer: Know what to expect For women with vulvar cancer What is the vulva? The vulva is the external (outside) part of the female genitals. The vulva includes the outer and inner lip, the clitoris,
Vulvar cancer: Know what to expect For women with vulvar cancer What is the vulva? The vulva is the external (outside) part of the female genitals. The vulva includes the outer and inner lip, the clitoris,
The Role of Radiation in the Management of Gynecologic Cancers. Scott Glaser, MD
 The Role of Radiation in the Management of Gynecologic Cancers Scott Glaser, MD Nothing to disclose DISCLOSURE Outline The role of radiation in: Endometrial Cancer Adjuvant Medically inoperable Cervical
The Role of Radiation in the Management of Gynecologic Cancers Scott Glaser, MD Nothing to disclose DISCLOSURE Outline The role of radiation in: Endometrial Cancer Adjuvant Medically inoperable Cervical
SLN Mapping in Cervical Cancer. Memorial Sloan Kettering Cancer Center New York, USA
 Lead Grou p Log SLN Mapping in Cervical Cancer Nadeem R. Abu-Rustum, M.D. Memorial Sloan Kettering Cancer Center New York, USA Conflict of Interest Disclosure Nadeem R. Abu-Rustum, M.D. I have no financial
Lead Grou p Log SLN Mapping in Cervical Cancer Nadeem R. Abu-Rustum, M.D. Memorial Sloan Kettering Cancer Center New York, USA Conflict of Interest Disclosure Nadeem R. Abu-Rustum, M.D. I have no financial
New diagnostic and therapeutic options in early-stage vulvar cancer Oonk, Maaike Henrike Marije
 University of Groningen New diagnostic and therapeutic options in early-stage vulvar cancer Oonk, Maaike Henrike Marije IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF)
University of Groningen New diagnostic and therapeutic options in early-stage vulvar cancer Oonk, Maaike Henrike Marije IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF)
ECC or Margins Positive?
 CLINICAL PRESENTATION This practice algorithm has been specifically developed for M. D. Anderson using a multidisciplinary approach and taking into consideration circumstances particular to M. D. Anderson,
CLINICAL PRESENTATION This practice algorithm has been specifically developed for M. D. Anderson using a multidisciplinary approach and taking into consideration circumstances particular to M. D. Anderson,
Sentinel Lymph Node Biopsy Is Valuable For All Cancer. Surgery Grand Rounds Debate October 6, 2008 Joel Baumgartner
 Sentinel Lymph Node Biopsy Is Valuable For All Cancer Surgery Grand Rounds Debate October 6, 2008 Joel Baumgartner History Lymphatics first described by Rasmus Bartholin in 1653 Rudolf Virchow postulated
Sentinel Lymph Node Biopsy Is Valuable For All Cancer Surgery Grand Rounds Debate October 6, 2008 Joel Baumgartner History Lymphatics first described by Rasmus Bartholin in 1653 Rudolf Virchow postulated
Cutaneous Melanoma: Epidemiology (USA) The Sentinel Node in Head and Neck Melanoma. Cutaneous Melanoma: Epidemiology (USA)
 The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
VULVAR CARCINOMA. Page 1 of 5
 VULVAR CARCINOMA EXAMPLE OF A VULVAR CARCINOMA USING PROPOSED TEMPLATE Case: Invasive squamous cell carcinoma arising in D-VIN Tumor in left labia major Left partial vaginectomy and sentinel lymph node
VULVAR CARCINOMA EXAMPLE OF A VULVAR CARCINOMA USING PROPOSED TEMPLATE Case: Invasive squamous cell carcinoma arising in D-VIN Tumor in left labia major Left partial vaginectomy and sentinel lymph node
Staging. Carcinoma confined to the corpus. Carcinoma confined to the endometrium. Less than ½ myometrial invasion. Greater than ½ myometrial invasion
 5 th of June 2009 Background Most common gynaecological carcinoma in developed countries Most cases are post-menopausal Increasing incidence in certain age groups Increasing death rates in the USA 5-year
5 th of June 2009 Background Most common gynaecological carcinoma in developed countries Most cases are post-menopausal Increasing incidence in certain age groups Increasing death rates in the USA 5-year
Clinical application of sartorius tendon transposition during radical vulvectomy: a case control study of 58 cases at a single institution
 Original Article J Gynecol Oncol pissn 2005-0380 eissn 2005-0399 Clinical application of sartorius tendon transposition during radical vulvectomy: a case control study of 58 cases at a single institution
Original Article J Gynecol Oncol pissn 2005-0380 eissn 2005-0399 Clinical application of sartorius tendon transposition during radical vulvectomy: a case control study of 58 cases at a single institution
Sentinel Lymph Node Biopsy for Breast Cancer
 Sentinel Lymph Node Biopsy for Breast Cancer Registrar Tutorial Adam Cichowitz Surgical Registrar The Royal Melbourne Hospital Sentinel Lymph Node Biopsy Axillary LN status important prognostic factor
Sentinel Lymph Node Biopsy for Breast Cancer Registrar Tutorial Adam Cichowitz Surgical Registrar The Royal Melbourne Hospital Sentinel Lymph Node Biopsy Axillary LN status important prognostic factor
Rebecca Vogel, PGY-4 March 5, 2012
 Rebecca Vogel, PGY-4 March 5, 2012 Historical Perspective Changes In The Staging System Studies That Started The Talk Where We Go From Here Cutaneous melanoma has become an increasingly growing problem,
Rebecca Vogel, PGY-4 March 5, 2012 Historical Perspective Changes In The Staging System Studies That Started The Talk Where We Go From Here Cutaneous melanoma has become an increasingly growing problem,
Chapter 8 Adenocarcinoma
 Page 80 Chapter 8 Adenocarcinoma Overview In Japan, the proportion of squamous cell carcinoma among all cervical cancers has been declining every year. In a recent survey, non-squamous cell carcinoma accounted
Page 80 Chapter 8 Adenocarcinoma Overview In Japan, the proportion of squamous cell carcinoma among all cervical cancers has been declining every year. In a recent survey, non-squamous cell carcinoma accounted
Staging Classifications and Clinical Practice Guidelines for Gynaecological Cancers
 Pages 10/10/06 10:29 Page i Staging Classifications and Clinical Practice Guidelines for Gynaecological Cancers Emeritus Editor: JL Benedet Editors: Sergio Pecorelli, Hextan YS Ngan and Neville F Hacker
Pages 10/10/06 10:29 Page i Staging Classifications and Clinical Practice Guidelines for Gynaecological Cancers Emeritus Editor: JL Benedet Editors: Sergio Pecorelli, Hextan YS Ngan and Neville F Hacker
Sentinel Lymph Node Biopsy in Other Tumours: Sentinel Lymph Node Biopsy in Other Tumours. Methodology. Results. Key Questions to Consider
 Sentinel Lymph Node Biopsy in Other Tumours Dr. Rona Cheifetz Surgical Oncology Update November 24, 2006 Sentinel Lymph Node Biopsy in Other Tumours: An Operation Looking for an Application Dr. Rona Cheifetz
Sentinel Lymph Node Biopsy in Other Tumours Dr. Rona Cheifetz Surgical Oncology Update November 24, 2006 Sentinel Lymph Node Biopsy in Other Tumours: An Operation Looking for an Application Dr. Rona Cheifetz
University of Groningen
 University of Groningen Patterns and frequency of s of squamous cell carcinoma of the vulva Woolderink, Jorien; de Bock, Gertruida H; de Hullu, Joanne A.; Davy, Margaret J.; van der Zee, Ate; Mourits,
University of Groningen Patterns and frequency of s of squamous cell carcinoma of the vulva Woolderink, Jorien; de Bock, Gertruida H; de Hullu, Joanne A.; Davy, Margaret J.; van der Zee, Ate; Mourits,
GUIDELINES ON PENILE CANCER
 GUIDELINES ON PENILE CANCER (Text updated March 2005) G. Pizzocaro (chairman), F. Algaba, S. Horenblas, H. van der Poel, E. Solsona, S. Tana, N. Watkin 58 Penile Cancer Eur Urol 2004;46(1);1-8 Introduction
GUIDELINES ON PENILE CANCER (Text updated March 2005) G. Pizzocaro (chairman), F. Algaba, S. Horenblas, H. van der Poel, E. Solsona, S. Tana, N. Watkin 58 Penile Cancer Eur Urol 2004;46(1);1-8 Introduction
Squamous vulval cancer an update
 DOI: 10.1111/tog.12059 The Obstetrician & Gynaecologist http://onlinetog.org 2013;15:227 31 Review Squamous vulval cancer an update Claire Bailey MRCOG, 1, * David Luesley MA MD FRCOG 2 1 Specialist Trainee,
DOI: 10.1111/tog.12059 The Obstetrician & Gynaecologist http://onlinetog.org 2013;15:227 31 Review Squamous vulval cancer an update Claire Bailey MRCOG, 1, * David Luesley MA MD FRCOG 2 1 Specialist Trainee,
Session Number: 1020 Session: Adenocarcinoma of the Cervix: Diagnostic Pitfalls and New Prognostic Implications. Andres A. Roma, MD Cleveland Clinic
 Session Number: 1020 Session: Adenocarcinoma of the Cervix: Diagnostic Pitfalls and New Prognostic Implications Andres A. Roma, MD Cleveland Clinic No Disclosures In the past 12 months, I have not had
Session Number: 1020 Session: Adenocarcinoma of the Cervix: Diagnostic Pitfalls and New Prognostic Implications Andres A. Roma, MD Cleveland Clinic No Disclosures In the past 12 months, I have not had
CPC on Cervical Pathology
 CPC on Cervical Pathology Dr. W.K. Ng Senior Medical Officer Department of Clinical Pathology Pamela Youde Nethersole Eastern Hospital Cervical Smear: High Grade SIL (CIN III) Cervical Smear: High Grade
CPC on Cervical Pathology Dr. W.K. Ng Senior Medical Officer Department of Clinical Pathology Pamela Youde Nethersole Eastern Hospital Cervical Smear: High Grade SIL (CIN III) Cervical Smear: High Grade
University of Kentucky. Markey Cancer Center
 University of Kentucky Markey Cancer Center Invasive Cancer of the Vagina and Urethra Fred Ueland, MD No matter what you accomplish in your life, the size of your funeral will still be determined by the
University of Kentucky Markey Cancer Center Invasive Cancer of the Vagina and Urethra Fred Ueland, MD No matter what you accomplish in your life, the size of your funeral will still be determined by the
SENTINEL NODES FOR EARLY VULVAL CANCER:
 SENTINEL NODES FOR EARLY VULVAL CANCER: FEASIBILITY AND SAFETY IN A LOW RESOURCE SETTING LINDA ROGERS RCOG Congress 2017 None Declaration of Interests Vulval Cancer Rare 4% of all gynaecological malignancies
SENTINEL NODES FOR EARLY VULVAL CANCER: FEASIBILITY AND SAFETY IN A LOW RESOURCE SETTING LINDA ROGERS RCOG Congress 2017 None Declaration of Interests Vulval Cancer Rare 4% of all gynaecological malignancies
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER CERVIX
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER CERVIX Site Group: Gynecology Cervix Author: Dr. Stephane Laframboise 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING AND
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER CERVIX Site Group: Gynecology Cervix Author: Dr. Stephane Laframboise 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING AND
Cervical cancer presentation
 Carcinoma of the cervix: Carcinoma of the cervix is the second commonest cancer among women worldwide, with only breast cancer occurring more commonly. Worldwide, cervical cancer accounts for about 500,000
Carcinoma of the cervix: Carcinoma of the cervix is the second commonest cancer among women worldwide, with only breast cancer occurring more commonly. Worldwide, cervical cancer accounts for about 500,000
Surgical Techniques for Vulvar Cancer
 Surgical Techniques for Vulvar Cancer 54 Neville F. Hacker, MD Penny Blomfield, MD Modern management of vulvar cancer requires an individualized approach, with each patient requiring an assessment of the
Surgical Techniques for Vulvar Cancer 54 Neville F. Hacker, MD Penny Blomfield, MD Modern management of vulvar cancer requires an individualized approach, with each patient requiring an assessment of the
C ORPUS UTERI C ARCINOMA STAGING FORM (Carcinosarcomas should be staged as carcinomas)
 CLINICAL C ORPUS UTERI C ARCINOMA STAGING FORM PATHOLOGIC Extent of disease before S TAGE C ATEGORY D EFINITIONS Extent of disease through any treatment completion of definitive surgery y clinical staging
CLINICAL C ORPUS UTERI C ARCINOMA STAGING FORM PATHOLOGIC Extent of disease before S TAGE C ATEGORY D EFINITIONS Extent of disease through any treatment completion of definitive surgery y clinical staging
ENDOMETRIAL CANCER. Endometrial cancer is a great concern in UPDATE. For personal use only. Copyright Dowden Health Media
 For mass reproduction, content licensing and permissions contact Dowden Health Media. UPDATE ENDOMETRIAL CANCER Are lymphadenectomy and external-beam radiotherapy valuable in women who have an endometrial
For mass reproduction, content licensing and permissions contact Dowden Health Media. UPDATE ENDOMETRIAL CANCER Are lymphadenectomy and external-beam radiotherapy valuable in women who have an endometrial
New Cancer Cases By Site Breast 28% Lung 14% Colo-Rectal 10% Uterus 6% Thyroid 5% Lymphoma 4% Ovary 3%
 Uterine Malignancy New Cancer Cases By Site 2010 Breast 28% Lung 14% Colo-Rectal 10% Uterus 6% Thyroid 5% Lymphoma 4% Ovary 3% Cancer Deaths By Site 2010 Lung 26% Breast 15% Colo-Rectal 9% Pancreas 7%
Uterine Malignancy New Cancer Cases By Site 2010 Breast 28% Lung 14% Colo-Rectal 10% Uterus 6% Thyroid 5% Lymphoma 4% Ovary 3% Cancer Deaths By Site 2010 Lung 26% Breast 15% Colo-Rectal 9% Pancreas 7%
Advances in Breast Surgery. Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015
 Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Best Practice & Research Clinical Obstetrics and Gynaecology
 YBEOG_proof April 0 / Best Practice & Research Clinical Obstetrics and Gynaecology xxx (0) e Contents lists available at ScienceDirect Best Practice & Research Clinical Obstetrics and Gynaecology journal
YBEOG_proof April 0 / Best Practice & Research Clinical Obstetrics and Gynaecology xxx (0) e Contents lists available at ScienceDirect Best Practice & Research Clinical Obstetrics and Gynaecology journal
of surgical management of early invasive cervical cancer chapter Diagnosis and staging Wertheim described the principles
 chapter 14. Surgical management of early invasive cervical cancer CHAPTER 1 Wertheim described the principles of surgical management of invasive cervical cancer more than 100 years ago in his treatise
chapter 14. Surgical management of early invasive cervical cancer CHAPTER 1 Wertheim described the principles of surgical management of invasive cervical cancer more than 100 years ago in his treatise
Vagina. 1. Introduction. 1.1 General Information and Aetiology
 Vagina 1. Introduction 1.1 General Information and Aetiology The vagina is part of internal female reproductive system. It is an elastic, muscular tube that connects the outside of the body to the cervix.
Vagina 1. Introduction 1.1 General Information and Aetiology The vagina is part of internal female reproductive system. It is an elastic, muscular tube that connects the outside of the body to the cervix.
Uterine Cervix. Protocol applies to all invasive carcinomas of the cervix.
 Uterine Cervix Protocol applies to all invasive carcinomas of the cervix. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition and FIGO 2001 Annual Report Procedures Cytology (No Accompanying
Uterine Cervix Protocol applies to all invasive carcinomas of the cervix. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition and FIGO 2001 Annual Report Procedures Cytology (No Accompanying
Gynecological Cancers in Primary Care
 Gynecological Cancers in Primary Care Nora M. Lersch MSN CRNP AOCNP Division of Gynecological Oncology Objectives Identify the incidence of ovarian, cervical, vulvar and endometrial cancer Identify common
Gynecological Cancers in Primary Care Nora M. Lersch MSN CRNP AOCNP Division of Gynecological Oncology Objectives Identify the incidence of ovarian, cervical, vulvar and endometrial cancer Identify common
Advances in Localized Breast Cancer
 Advances in Localized Breast Cancer Melissa Camp, MD, MPH and Fariba Asrari, MD June 18, 2018 Moderated by Elissa Bantug 1 Advances in Surgery for Breast Cancer Melissa Camp, MD June 18, 2018 2 Historical
Advances in Localized Breast Cancer Melissa Camp, MD, MPH and Fariba Asrari, MD June 18, 2018 Moderated by Elissa Bantug 1 Advances in Surgery for Breast Cancer Melissa Camp, MD June 18, 2018 2 Historical
Head & Neck Squamous Carcinoma: Artifacts, Challenges, and Controversies. Agenda
 Head & Neck Squamous Carcinoma: Artifacts, Challenges, and Controversies Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory Medicine University
Head & Neck Squamous Carcinoma: Artifacts, Challenges, and Controversies Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory Medicine University
Chapter 2: Initial treatment for endometrial cancer (including histologic variant type)
 Chapter 2: Initial treatment for endometrial cancer (including histologic variant type) CQ01 Which surgical techniques for hysterectomy are recommended for patients considered to be stage I preoperatively?
Chapter 2: Initial treatment for endometrial cancer (including histologic variant type) CQ01 Which surgical techniques for hysterectomy are recommended for patients considered to be stage I preoperatively?
An Unusual Case of Cervical Cancer with Inguinal Lymph Node Metastasis: A Case Report and Review of the Literature
 Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.9655003 Volume 1, Issue 1 Case Report An Unusual Case of Cervical Cancer with Inguinal Lymph Node Metastasis: A Case Report and Review
Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.9655003 Volume 1, Issue 1 Case Report An Unusual Case of Cervical Cancer with Inguinal Lymph Node Metastasis: A Case Report and Review
Position Statement on Management of the Axilla in Patients with Invasive Breast Cancer
 - Official Statement - Position Statement on Management of the Axilla in Patients with Invasive Breast Cancer Sentinel lymph node (SLN) biopsy has replaced axillary lymph node dissection (ALND) for the
- Official Statement - Position Statement on Management of the Axilla in Patients with Invasive Breast Cancer Sentinel lymph node (SLN) biopsy has replaced axillary lymph node dissection (ALND) for the
SPECT/CT Imaging of the Sentinel Lymph Node
 IAEA Regional Training Course on Hybrid Imaging SPECT/CT Imaging of the Sentinel Lymph Node Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa, Italy Vilnius,
IAEA Regional Training Course on Hybrid Imaging SPECT/CT Imaging of the Sentinel Lymph Node Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa, Italy Vilnius,
Protocol for the Examination of Specimens From Patients With Primary Carcinoma of the Vulva
 Protocol for the Examination of Specimens From Patients With Primary Carcinoma of the Vulva Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual,
Protocol for the Examination of Specimens From Patients With Primary Carcinoma of the Vulva Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual,
Japan Society of Gynecologic Oncology guidelines 2015 for the treatment of vulvar cancer and vaginal cancer
 Int J Clin Oncol (2018) 23:201 234 https://doi.org/10.1007/s10147-017-1193-z SPECIAL ARTICLE Japan Society of Gynecologic Oncology guidelines 2015 for the treatment of vulvar cancer and vaginal cancer
Int J Clin Oncol (2018) 23:201 234 https://doi.org/10.1007/s10147-017-1193-z SPECIAL ARTICLE Japan Society of Gynecologic Oncology guidelines 2015 for the treatment of vulvar cancer and vaginal cancer
Use of the dye guided sentinel lymph node biopsy method alone for breast cancer metastasis to avoid unnecessary axillary lymph node dissection
 456 Use of the dye guided sentinel lymph node biopsy method alone for breast cancer metastasis to avoid unnecessary axillary lymph node dissection TOMOKO TAKAMARU 1, GORO KUTOMI 1, FUKINO SATOMI 1, HIROAKI
456 Use of the dye guided sentinel lymph node biopsy method alone for breast cancer metastasis to avoid unnecessary axillary lymph node dissection TOMOKO TAKAMARU 1, GORO KUTOMI 1, FUKINO SATOMI 1, HIROAKI
North of Scotland Cancer Network Clinical Management Guideline for Carcinoma of the Uterine Cervix
 THIS DOCUMENT North of Scotland Cancer Network Carcinoma of the Uterine Cervix UNCONTROLLED WHEN PRINTED DOCUMENT CONTROL Prepared by A Kennedy/AG Macdonald/Others Approved by NOT APPROVED Issue date April
THIS DOCUMENT North of Scotland Cancer Network Carcinoma of the Uterine Cervix UNCONTROLLED WHEN PRINTED DOCUMENT CONTROL Prepared by A Kennedy/AG Macdonald/Others Approved by NOT APPROVED Issue date April
1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter.
 Skin Cancer follow up guidelines If NEW serious diagnosis given: 1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter. 2. Free prescription information details. 3.
Skin Cancer follow up guidelines If NEW serious diagnosis given: 1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter. 2. Free prescription information details. 3.
Vulvar Carcinoma Robert L. Coleman, MD Joseph T. Santoso, MD*
 Vulvar Carcinoma Robert L. Coleman, MD Joseph T. Santoso, MD* Address University of Texas, Southwestern Medical Center, Division of Gynecologic Oncology, 5323 Harry Hines Blvd., J7.124, Dallas, TX 75235-9032,
Vulvar Carcinoma Robert L. Coleman, MD Joseph T. Santoso, MD* Address University of Texas, Southwestern Medical Center, Division of Gynecologic Oncology, 5323 Harry Hines Blvd., J7.124, Dallas, TX 75235-9032,
Role and extension of lymph node dissection in kidney, bladder and prostate cancer. Omar Ghanem (PGY3 ) Moderator: Dr A. Noujem 30 th March 2017
 Role and extension of lymph node dissection in kidney, bladder and prostate cancer Omar Ghanem (PGY3 ) Moderator: Dr A. Noujem 30 th March 2017 Bladder Cancer LN dissection in Bladder cancer 25% of patients
Role and extension of lymph node dissection in kidney, bladder and prostate cancer Omar Ghanem (PGY3 ) Moderator: Dr A. Noujem 30 th March 2017 Bladder Cancer LN dissection in Bladder cancer 25% of patients
VULVAR CANCER GUIDELINES
 VULVAR ANER GUIDELINES www.esgo.org Broz_210x297_9_16_b.indd 1 13.09.16 21:48 The European Society of Gynaecological Oncology (ESGO) developed guidelines covering diagnosis and referral, preoperative investigations,
VULVAR ANER GUIDELINES www.esgo.org Broz_210x297_9_16_b.indd 1 13.09.16 21:48 The European Society of Gynaecological Oncology (ESGO) developed guidelines covering diagnosis and referral, preoperative investigations,
Janjira Petsuksiri, M.D
 GYN malignancies Janjira Petsuksiri, M.D Outlines Cervical cancer Endometrial cancer Ovarian cancer Vaginal cancer Vulva cancer 2 CA Cervix Epidemiology - Second most common female cancer Risk factors
GYN malignancies Janjira Petsuksiri, M.D Outlines Cervical cancer Endometrial cancer Ovarian cancer Vaginal cancer Vulva cancer 2 CA Cervix Epidemiology - Second most common female cancer Risk factors
Oral cancer: Prognosis & Treatment. Dr. Hani Al Sheikh Radhi
 Oral cancer: Prognosis & Treatment Dr. Hani Al Sheikh Radhi Prognostic factors in Oral caner TNM staging T stage N stage M stage Site Histological Factors Vascular & Perineural Invasion Surgical Margins
Oral cancer: Prognosis & Treatment Dr. Hani Al Sheikh Radhi Prognostic factors in Oral caner TNM staging T stage N stage M stage Site Histological Factors Vascular & Perineural Invasion Surgical Margins
Practice of Axilla Surgery
 Summer School of Breast Disease 2016 Practice of Axilla Surgery Axillary Lymph Node Dissection & Sentinel Lymph Node Biopsy 연세의대외과 박세호 Contents Anatomy of the axilla Axillary lymph node dissection (ALND)
Summer School of Breast Disease 2016 Practice of Axilla Surgery Axillary Lymph Node Dissection & Sentinel Lymph Node Biopsy 연세의대외과 박세호 Contents Anatomy of the axilla Axillary lymph node dissection (ALND)
MR Imaging of Carcinoma of the Vulva
 S. A. Aslam Sohaib 1,2 Polly S. Richards 1 Thomas Ind 2 Arjun R. Jeyarajah 3 John H. Shepherd 3 Ian J. Jacobs 3 Rodney H. Reznek 1 Received May 7, 2001; accepted after revision August 20, 2001. S. A. Sohaib
S. A. Aslam Sohaib 1,2 Polly S. Richards 1 Thomas Ind 2 Arjun R. Jeyarajah 3 John H. Shepherd 3 Ian J. Jacobs 3 Rodney H. Reznek 1 Received May 7, 2001; accepted after revision August 20, 2001. S. A. Sohaib
6. Cervical Lymph Nodes and Unknown Primary Tumors of the Head and Neck
 1 Terms of Use The cancer staging form is a specific document in the patient record; it is not a substitute for documentation of history, physical examination, and staging evaluation, or for documenting
1 Terms of Use The cancer staging form is a specific document in the patient record; it is not a substitute for documentation of history, physical examination, and staging evaluation, or for documenting
Coversheet for Network Site Specific Group Agreed Documentation
 Coversheet for Network Site Specific Group Agreed Documentation This sheet is to accompany all documentation agreed by Pan Birmingham Cancer Network Site Specific Groups. This will assist the Network Governance
Coversheet for Network Site Specific Group Agreed Documentation This sheet is to accompany all documentation agreed by Pan Birmingham Cancer Network Site Specific Groups. This will assist the Network Governance
Initial Experience with Videoscopic Inguinal Lymphadenectomy
 Ann Surg Oncol (2011) 18:977 982 DOI 10.1245/s10434-010-1490-5 ORIGINAL ARTICLE MELANOMAS Initial Experience with Videoscopic Inguinal Lymphadenectomy Keith A. Delman, MD 1,3,4, David A. Kooby, MD 1,3,
Ann Surg Oncol (2011) 18:977 982 DOI 10.1245/s10434-010-1490-5 ORIGINAL ARTICLE MELANOMAS Initial Experience with Videoscopic Inguinal Lymphadenectomy Keith A. Delman, MD 1,3,4, David A. Kooby, MD 1,3,
EGFR expression is associated with groin node metastases in vulvar cancer, but does not improve their prediction
 Gynecologic Oncology 104 (2007) 109 113 www.elsevier.com/locate/ygyno EGFR expression is associated with groin node metastases in vulvar cancer, but does not improve their prediction M.H.M. Oonk a, G.H.
Gynecologic Oncology 104 (2007) 109 113 www.elsevier.com/locate/ygyno EGFR expression is associated with groin node metastases in vulvar cancer, but does not improve their prediction M.H.M. Oonk a, G.H.
NEW SURGICAL APPROACHES TO MELANOMA THERAPY
 NEW SURGICAL APPROACHES TO MELANOMA THERAPY Melanoma 2003: New Insights Into Therapy & Treatment Douglas L. Fraker, M.D. University of Pennsylvania Surgical Treatment of Melanoma Primary resection margins
NEW SURGICAL APPROACHES TO MELANOMA THERAPY Melanoma 2003: New Insights Into Therapy & Treatment Douglas L. Fraker, M.D. University of Pennsylvania Surgical Treatment of Melanoma Primary resection margins
La Pianificazione e I Volumi di Trattamento
 TRATTAMENTI INTEGRATI NEL CARCINOMA DELLA VULVA La Pianificazione e I Volumi di Trattamento PAOLO MUTO Direttore UOC Radioterapia ISTITUTO NAZIONALE TUMORI IRCCS Fondazione Pascale di Napoli Minimize collateral
TRATTAMENTI INTEGRATI NEL CARCINOMA DELLA VULVA La Pianificazione e I Volumi di Trattamento PAOLO MUTO Direttore UOC Radioterapia ISTITUTO NAZIONALE TUMORI IRCCS Fondazione Pascale di Napoli Minimize collateral
Vulvar Cancer Pocket Guidelines
 Vulvar ancer Pocket Guidelines guidelines.esgo.org 2 POKET GUIDELINES VULVAR ANER based on ESGO Guidelines for the Management of Patients with Vulvar ancer Oonk, M. H. M., Planchamp, F., Baldwin, P., Bidzinski,
Vulvar ancer Pocket Guidelines guidelines.esgo.org 2 POKET GUIDELINES VULVAR ANER based on ESGO Guidelines for the Management of Patients with Vulvar ancer Oonk, M. H. M., Planchamp, F., Baldwin, P., Bidzinski,
International prospective validation trial of sentinel node biopsy in cervical cancer
 Cervix cancer committee International prospective validation trial of sentinel node biopsy in cervical cancer N Abu-Rustum, F Lécuru, P Mathevet, M Plante. F Bonnetain (Statistics) G Chatellier (Clinical
Cervix cancer committee International prospective validation trial of sentinel node biopsy in cervical cancer N Abu-Rustum, F Lécuru, P Mathevet, M Plante. F Bonnetain (Statistics) G Chatellier (Clinical
Review Article. Penile Carcinoma: Lessons Learned from Vulvar Carcinoma. Michelle J. Longpre,* Paul H. Lange, Janice S. Kwon* and Peter C.
 Review Article Penile Carcinoma: Lessons Learned from Vulvar Carcinoma Michelle J. Longpre,* Paul H. Lange, Janice S. Kwon* and Peter C. Black*, From the Department of Urologic Sciences, and the Department
Review Article Penile Carcinoma: Lessons Learned from Vulvar Carcinoma Michelle J. Longpre,* Paul H. Lange, Janice S. Kwon* and Peter C. Black*, From the Department of Urologic Sciences, and the Department
Debate Axillary dissection - con. Prof. Dr. Rodica Anghel Institute of Oncology Bucharest
 Debate Axillary dissection - con Prof. Dr. Rodica Anghel Institute of Oncology Bucharest Summer School of Oncology, third edition Updated Oncology 2015: State of the Art News & Challenging Topics Bucharest,
Debate Axillary dissection - con Prof. Dr. Rodica Anghel Institute of Oncology Bucharest Summer School of Oncology, third edition Updated Oncology 2015: State of the Art News & Challenging Topics Bucharest,
VULVAR CANCER SURGERY: WHY, WHEN AND HOW
 Giovanni Scambia Dipartimento per la Salute della Donna, della Vita Nascente, del Bambino e dell Adolescente Policlinico A.Gemelli Sede di Roma Università Cattolica del Sacro Cuore Centro di Ricerca e
Giovanni Scambia Dipartimento per la Salute della Donna, della Vita Nascente, del Bambino e dell Adolescente Policlinico A.Gemelli Sede di Roma Università Cattolica del Sacro Cuore Centro di Ricerca e
Update on Sentinel Node Biopsy in Endometrial Cancer: Feasibility, Technique, Impact
 Update on Sentinel Node Biopsy in Endometrial Cancer: Feasibility, Technique, Impact Bjørn Hagen, MD, PhD St Olavs Hospital Trondheim University Hospital Trondheim, Norway Endometrial Cancer (EC) The most
Update on Sentinel Node Biopsy in Endometrial Cancer: Feasibility, Technique, Impact Bjørn Hagen, MD, PhD St Olavs Hospital Trondheim University Hospital Trondheim, Norway Endometrial Cancer (EC) The most
North of Scotland Cancer Network Clinical Management Guideline for Endometrial Cancer
 THIS DOCUMENT North of Scotland Cancer Network Clinical Management Guideline for Endometrial Cancer Based on WOSCAN CMG with further extensive consultation within NOSCAN UNCONTROLLED WHEN PRINTED DOCUMENT
THIS DOCUMENT North of Scotland Cancer Network Clinical Management Guideline for Endometrial Cancer Based on WOSCAN CMG with further extensive consultation within NOSCAN UNCONTROLLED WHEN PRINTED DOCUMENT
Gynecologic Oncologist. Surgery Chemotherapy Radiation Therapy Hormonal Therapy Immunotherapy. Cervical cancer
 Gynecologic Oncology Pre invasive vulvar, vaginal, & cervical disease Vulvar Cervical Endometrial Uterine Sarcoma Fallopian Tube Ovarian GTD Gynecologic Oncologist Surgery Chemotherapy Radiation Therapy
Gynecologic Oncology Pre invasive vulvar, vaginal, & cervical disease Vulvar Cervical Endometrial Uterine Sarcoma Fallopian Tube Ovarian GTD Gynecologic Oncologist Surgery Chemotherapy Radiation Therapy
Intra-operative frozen section analysis of common iliac lymph nodes in patients with stage IB1 and IIA1 cervical cancer
 Arch Gynecol Obstet (2012) 285:811 816 DOI 10.1007/s00404-011-2038-z GYNECOLOGIC ONCOLOGY Intra-operative frozen section analysis of common iliac lymph nodes in patients with stage IB1 and IIA1 cervical
Arch Gynecol Obstet (2012) 285:811 816 DOI 10.1007/s00404-011-2038-z GYNECOLOGIC ONCOLOGY Intra-operative frozen section analysis of common iliac lymph nodes in patients with stage IB1 and IIA1 cervical
Index. Surg Oncol Clin N Am 14 (2005) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 14 (2005) 433 439 Index Note: Page numbers of article titles are in boldface type. A Abdominosacral resection, of recurrent rectal cancer, 202 215 Ablative techniques, image-guided,
Surg Oncol Clin N Am 14 (2005) 433 439 Index Note: Page numbers of article titles are in boldface type. A Abdominosacral resection, of recurrent rectal cancer, 202 215 Ablative techniques, image-guided,
Protocol for the Examination of Specimens from Patients with Carcinoma of the Vulva
 Protocol for the Examination of Specimens from Patients with Carcinoma of the Vulva Protocol applies to all invasive carcinomas of the vulva. Based on AJCC/UICC TNM, 7th edition, and FIGO 2008 Annual Report
Protocol for the Examination of Specimens from Patients with Carcinoma of the Vulva Protocol applies to all invasive carcinomas of the vulva. Based on AJCC/UICC TNM, 7th edition, and FIGO 2008 Annual Report
Risk assessment of lymph node metastasis before surgery in endometrial cancer: Do we need a clinical trial for low-risk patients?
 bs_bs_banner doi:10.1111/jog.12281 J. Obstet. Gynaecol. Res. Vol. 40, No. 2: 322 326, February 2014 Risk assessment of lymph node metastasis before surgery in endometrial cancer: Do we need a clinical
bs_bs_banner doi:10.1111/jog.12281 J. Obstet. Gynaecol. Res. Vol. 40, No. 2: 322 326, February 2014 Risk assessment of lymph node metastasis before surgery in endometrial cancer: Do we need a clinical
NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines ) Vulvar Cancer. (Squamous Cell Carcinoma) Version December 17, NCCN.
 NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines ) Vulvar Cancer (Squamous Cell Carcinoma) Version 2.2019 December 17, 2018 NCCN.org Continue *Wui-Jin Koh, MD/Chair Fred Hutchinson Cancer
NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines ) Vulvar Cancer (Squamous Cell Carcinoma) Version 2.2019 December 17, 2018 NCCN.org Continue *Wui-Jin Koh, MD/Chair Fred Hutchinson Cancer
Canadian Scientific Journal. Intraoperative color detection of lymph nodes metastases in thyroid cancer
 Canadian Scientific Journal 2 (2014) Contents lists available at Canadian Scientific Journal Canadian Scientific Journal journal homepage: Intraoperative color detection of lymph nodes metastases in thyroid
Canadian Scientific Journal 2 (2014) Contents lists available at Canadian Scientific Journal Canadian Scientific Journal journal homepage: Intraoperative color detection of lymph nodes metastases in thyroid
