Middle Lobe Torsion after Unilateral Lung Transplant
|
|
|
- Agnes Walton
- 5 years ago
- Views:
Transcription
1 Middle Lobe Torsion after Unilateral Lung Transplant Chad S Cox 1, Summer J Decker 1, Mark Rolfe 2, Todd R Hazelton 1, Carlos A Rojas 1* 1. Department of Radiology, University of South Florida Morsani College of Medicine, Tampa, USA 2. Department of Pulmonology and Critical Care, Tampa General Hospital, Tampa, USA * Correspondence: Carlos A. Rojas, Department of Radiology, USF Health, 2 Tampa General Circle, STC 7031, Tampa, Florida 33606, USA ( crojas@health.usf.edu) :: DOI: /jrcr.v10i ABSTRACT Lobar torsion is well documented after pneumonectomy, but is very rare after lung transplant. To the best of our knowledge, this is the twelfth reported case of lobar torsion after lung transplant. In our case, bronchoscopies and chest radiographs were inconclusive; however, CT scan clearly demonstrated findings consistent with right middle lobe torsion. We review the literature and discuss the epidemiology, clinical presentation, imaging features, and treatment considerations for this condition. We also propose that if a clinical picture could be secondary to torsion and bronchoscopies and chest x ray are inconclusive that a CT scan should be obtained as soon as possible since early recognition increases the likelihood of being able to successfully detorse the lung and avoid lobectomy. CASE REPORT The patient is a 72 year old male with a history of endstage pulmonary fibrosis with progressive deterioration of his clinical status and increasing daily requirements for oxygen presented for bilateral lung transplant. The implantation of the right lung was very difficult due to the large size of the donor lung and deep cavity of the recipient s right chest. Additionally, patient s left pleural space was much smaller and the heart was deviated to the left making it technically difficult to transplant his left lung because it would require another run of cardiopulmonary bypass which potentially could compromise the function of the right lung and patient outcome. Hence only a right lung transplant was performed to minimize complications. After the procedure the patient was transported from the operating room to the intensive care unit on mechanical ventilation. Oxygen saturation remained 100% during transfer and there were no immediate post-operative complications. Shortly after arriving to the intensive care unit the patient began having CASE REPORT episodes of hypotension. Vasopressors were being administered to maintain mean arterial pressure above 65 mmhg. An arterial blood gas was obtained and revealed proper oxygenation. A bronchoscopy was performed which revealed a normal anastomosis. A chest radiograph was obtained after the procedure which demonstrated right lower lung base peripheral opacity (Figure 1). Patient s pulmonary arterial pressure was elevated at mmhg. The morning after the procedure the patient was no longer sedated and was being weaned off of vasopressors. Then his oxygen saturation dropped to 78% with thick bloody secretions noted in the endotracheal tube. A repeat bronchoscopy revealed a normal anastomosis and a large left mucous plug, but no conclusive evidence for why the patient was not improving. Clinically, the patient was anxious and this was thought to be contributing the patient s desaturation. A few hours later the patient was still desaturating with minimal exertion. Venous oxygen saturation was noted to be approximately 40%. He had leukocytosis of 19,000, and he was on antibiotics. The patient was tachypneic with a 15
2 respiratory rate of 35 breaths per minute. Patient was resedated, was diuresed as blood pressure allowed, and continued on aggressive pulmonary hygiene with nebulizers. A repeat chest radiograph was obtained and revealed persistent right lower lung base consolidation. On postoperative day two, the patient failed weaning of vasopressors and was given albumin for his labile blood pressure. Patient s mean pulmonary arterial pressures were still elevated. Patient was on 5 parts per million of nitric oxide and was started on 10mg sildenafil TID for pulmonary hypertension. On post-operative day two, the patient was no longer experiencing desaturations but remained on nitric oxide, vasopressors, and mechanical ventilation. On post-operative day three the patient started having repeat instances of desaturations with continued labile blood pressures. The patient s pulmonary arterial pressures were still elevated and were now above 40 with an increasing oxygen requirement on 50% FIO2. A repeat bronchoscopy was performed which demonstrated tapering of the distal airways with bilateral huge mucous plugs. The patient was continued on conservative management. On post-operative day four, a chest radiograph once again revealed persistent consolidation of the right lower lung zone. Computed Tomography (CT) was obtained which revealed abnormal posterior displacement of the right middle lobe with anterior displacement of the right lower lobe. There was curvilinear bronchovascular structures and tapering of the right middle lobe bronchus compatible with right middle lobe torsion. The patient was taken to the operating room and right middle lobe torsion was confirmed. A right middle lobe pneumonectomy was performed. Three weeks after the procedure the patient is still alive in the hospital and has required mechanical ventilation but is clinically improving. DISCUSSION Etiology & Demographics: Simply stated, lung torsion occurs when a lung lobe is able to twist around its pedicle. Lung torsion is a very rare entity with most cases being documented after lobectomy with only an incidence of less than 0.5% even in this setting (1). Torsion after lung transplantation is much more rare with our research revealing only three documented cases before 2009 (2,3,4). In 2009, there was a case series of four patient s published documenting lung torsion status post bilateral lung transplantation (5). Since then there has only been an additional four cases published of torsion after lung transplantation for a total of eleven documented cases with eight of them being in the last six years (6,7,8,9). This suggests lung torsion is becoming an increasingly recognized dreaded complication that can occur after lung transplantation. Given the rarity of lobar torsion after lung transplant, information about this condition comes from the study of the collective case reports, and this discussion will review the prior documented cases as compared to our case. Since torsion is essentially twisting of a lobe or lobes upon its pedicle, the major risk factors for lobar torsion are factors that allow the lung to have increased mobility. This is why the highest reported incidence of lobar torsion is after pneumonectomy. Lung parenchyma is resected and there is relative increased space in the thoracic cavity allowing increased mobility of the remaining lobes of the lung. Thus in this setting fixation of the remaining lobes is routinely performed to decrease the mobility of the respective lobes subsequently decreasing the risk of torsion. However, after transplantation the major risk factors postulated are the normal division of the pulmonary ligament during allograft procurement which normally prevents torsion of the lung around the hilum, size discrepancy between a small donor lung and a relatively larger recipient s thoracic cavity, and the presence of a complete major fissure (3,4). When reviewing the prior eleven cases, the most common risk factor present was the presence of a complete fissure which was documented to be present in six of the eleven cases. Unfortunately, this fact might not have been known in every case, and in our case it is uncertain if there was a complete fissure or not. The complete fissure being one of the most prevalent risk factors is why after lung transplant that the left lobe is thought to torse most frequently because the incidence of complete fissures is highest on the left ranging from 27-82% (6,10). The increased risk associated with discrepancy in size between a small donor lung and a relatively larger chest cavity is easily rationalized because the size discrepancy invariably will allow increased mobility of the lobes which increases the risk for torsion (5). For example, Gilkeson s et al case report was an instance of the donor allograft being significantly smaller than the recipient's hemithorax and was considered to be the major risk factor for torsion (3). In our particular case, the surgeon actually noted that the transplant of the donor lung was technically difficult due to its large size and the patient having a deep right thoracic cavity. Rather too large of a donor lung could play a role is not as easily rationalized. In our case, considering that the right middle lobe of the allograft is what torsed, it seemingly could be related to the patient s deep thoracic cavity and/or too large of a donor lung. Seemingly, after transplantation, the large donor lung starts to re-expand and the resulting increased pressure assumingly could have displaced the right middle lobe more posteriorly allowing it to settle into this patient s deep thoracic cavity. With the resultant displacement of the right middle lobe, the right lower lobe would then be free to move anteriorly. With progressive expansion of the alveoli of the right lung, the right middle lobe would then begin expanding posterior to the right lower lobe and continue to force the right lower lung more anteriorly and cranially torsing the lung counterclockwise. Interestingly there was another case described by Shakoor et al in which the lung allograft was also noted to be large in relation to the patient s chest cavity. Although, in this case there is a confounding factor because a complete minor fissure was also present (6). Either way, size discrepancy between a donor s lung and recipient s chest cavity likely is a major risk factor in the development of torsion after lung transplant. 16
3 Clinical & Imaging Findings: As stated previously, lung torsion occurs when a lung lobe is able to twist around its pedicle. The degree of torsion, rather it is partial or complete, affects the clinical presentation. Partial torsion is when a lobe or lobes rotate around the hilar structures 90 degrees. Complete torsion is when a lobe or lobes rotate around the hilar structures 180 degrees or more. Torsion is a dangerous complication because it results in compromise of the bronchi, arterial blood supply, and venouslymphatic drainage with ensuing ischemia and necrosis of the lung parenchyma. However, the lungs are relatively resistant to infarction secondary to a dual blood supply of from the pulmonary and bronchial circulation. Because of this dual blood supply partial torsion does not quickly result in infarction and necrosis and has more of an insidious clinical presentation with clinical signs that can mimic pneumonia or atelectasis such as chest pain, tachycardia, tachypnea, respiratory insufficiency, fever, and leukocytosis. Additionally, ventilation-perfusion defects are generally equally matched in partial torsion, which means there may be no appreciable alteration in any oxygenation or ventilation. Consequently, as in our case, arterial blood gases may be misleadingly normal (12). In complete torsion the onset of pulmonary gangrene is more rapid and the presentation of chest pain, hemoptysis, and hypoxia is more severe. Considering the variability and nonspecific presentation, a high degree of suspicion is needed in every case. Felson describes the typical findings of lobar torsion on chest radiograph or computed tomography as collapsed or consolidated lobe that occupies an unusual position, abnormal pulmonary vascular pattern often with inverted hilum, bronchial cutoff or distortion, lobar air-trapping, displacement of the hilum in an inappropriate direction relative to the atelectatic lobe involved, and a non-aerated lobe in an unusual position with or without accompanying compensatory hyperinflation of the surrounding lung (11). In every case reviewed from the literature the chest radiograph revealed consolidation which was often confused with atelectasis. In our case, the chest radiograph demonstrated a right lower lung zone consolidation which similar to the other cases was also thought to most likely represent atelectasis. Retrospectively, the consolidation does not fit the normal appearance of atelectasis and signs of right sided volume loss were not present including the minor fissure was not displaced, there was no right sided rib crowding, and the mediastinum was not displaced to the right side (Figure 1). In our case, the combination of a chest radiograph revealing a suspicious opacity, persistent leukocytosis despite antibiotics, worsening acute pulmonary hypertension, and hypoxemia collectively raised clinical concern for lobar torsion. Bronchoscopy is usually the first step in evaluation of a patient status post lung transplant that is having respiratory insufficiency because it can be performed easily and quickly at bedside. Generally bronchoscopy is thought to be highly sensitive in detecting torsion and typical findings include occluded or distorted bronchus without evidence of endobronchial lesion or mucous plugging, abnormal rotation of affected bronchus, and hyperemia of the mucosa. In our case, three bronchoscopies were performed which were all inconclusive and did not suggest torsion. Then a CT was obtained which demonstrated a consolidated right middle lobe in abnormal posterior position with corresponding anterior displacement of the right lower lobe. There was narrowing of the right middle lobe bronchus with a curvilinear abnormal posteriorly directed course of the right middle lobe bronchus with a corresponding anterior course of the right lower lobe bronchus. These findings are specific for a diagnosis of right middle lobe torsion (Figure 2, 3, 4, 5). Reviewing the other eleven documented cases, similar results were obtained with bronchoscopy not always suggesting torsion. Although this is a very small sample size, bronchoscopy was inferior to CT examination in sensitivity and specificity for lobar torsion. Thus, in these rare cases when patient is not improving clinically and bronchoscopy does not clearly delineate a cause for patient s symptoms, CT scan of the lung should be considered immediately for further characterization. Treatment & Prognosis: After torsion was diagnosed in our case, open thoracotomy was performed which is currently the standard of care. Intraoperatively the decision can be made to perform detorsion or lobectomy which is largely based upon the surgeon s discretion on the viability of the affected lobe. Depending on rather the lung is completely torsed or partially torsed affects the viability of the lung. In patients with complete torsion, the onset of pulmonary gangrene is rapid, and unless immediate surgery is performed, then the lung will not be viable (3). In the eleven cases reviewed after lung transplant, three of them were able to successfully undergo detorsion and all three were alive at follow up. Collin s et al patient had lobectomy and died sixteen months later of other complications (2). Grazia s et al patient had lobectomy and died within two months secondary to severe sepsis and acute respiratory distress (4). Detorsion in itself has inherent risks and the revascularization that occurs may cause an acute release of toxic substances which is typical of ischemic lung reperfusion injury. It was generally thought that if detorsion was not done within the first few hours of torsion than lobectomy was preferred to minimize the risk of reperfusion injury. It was suggested by Velmahos et al after a case that required a subsequent lobectomy after detorsion secondary to reperfusion injury that lobectomy was generally preferred over detorsion (12). Grazia et al concurred that lobectomy is preferred over detorsion in his case report (4). However, Souilamas et al performed detorsion as many as five days after lung transplantation on one of his patient s without any postoperative complications (5). As a rule, patients requiring lung transplant do not have significant quantity of spare pulmonary reserve; thus, detorsion is preferred over lobectomy in cases in which the lung is viable. In our case the patient s right middle lobe was not viable and lobectomy was required (Figure 6). Ultimately, lobar torsion is increasingly recognized as a serious potential complication of lung transplant. The clinical picture is not always clear and a high degree of suspicion is needed to be able to act quickly and possibly avoid infarction and lobectomy. Chest radiographs are very sensitive and 17
4 reveal persistent consolidation that is often confused with atelectasis. It is imperative to recognize if other direct or indirect signs of volume loss are present and if not raise the possibility for lobar torsion. In the limited amount of case reports available, bronchoscopy which is largely considered the best next step in patients with respiratory insufficiency does not have as high of sensitivity as computed tomography in detecting torsion. It is very likely that the advances in high resolution computed tomography scanners now makes this the preferred study after lung transplant in patients with respiratory insufficiency. Overall, if patients have consolidation on chest radiograph with a clinical picture that could be secondary to torsion, a CT scan should be obtained as soon as possible since early recognition increases the likelihood of being able to successfully detorse the lung and avoid lobectomy in these patients with very little pulmonary reserve. Differential Diagnoses: In a patient that is status post lung transplant and is having respiratory insufficiency chest radiograph is the best first step. In cases of lobar torsion an opacity was seen with 100% sensitivity in the reviewed case reports. Unfortunately this is not a specific finding and the opacity was often mistakenly considered to be atelectasis. However, this is understandable because in post-operative patient s atelectasis is very common. The key to avoiding interpreting the opacity as atelectasis is to remember to carefully scrutinize the radiograph for direct and indirect signs of volume loss. Direct signs of volume loss include displacement of the fissures and vascular crowding, and indirect signs of volume loss include elevation of the diaphragm, rib crowding on the side with volume loss, mediastinal shift to the side with volume loss, and hilar displacement towards the expected area of volume loss. If there is an opacity without these signs then we propose you should recommend CT scan if patient is stable to further characterize the opacity which could represent lobar torsion or even pneumonia. However, bronchoscopy has long been considered the next best step. This is reasonable because it can be done quickly at bedside in a patient who might be unstable. In reviewing the prior eleven case reports, bronchoscopy was neither as sensitive nor specific in detecting lobar torsion as computed tomography. In our case three bronchoscopies were performed before computed tomography and none of them suggested lobar torsion. Thus, CT scan should be considered if bronchoscopy is not conclusive for a patient s respiratory insufficiency. Another entity in the differential that could present with respiratory insufficiency in a post- operative patient with a peripheral opacity without signs of volume loss on chest radiograph is pulmonary embolus. If the patient is able to tolerate contrast, then a CT scan with contrast is preferred because a pulmonary embolus is readily diagnosed as filling defects within the pulmonary vasculature, and importantly the lobes of the lung will be in normal anatomical position. In cases of lobar torsion, CT scan will demonstrate a poorly enhancing consolidated lobe or lobes in abnormal anatomic position and possibly tapered obliteration of the proximal pulmonary artery and accompanying bronchus of the involved lobe. CT with contrast would be preferred to assess the vasculature but is not required since the lobes anatomical position and corresponding bronchus can be appreciated without contrast. In reviewing the prior eleven cases, CT was the most sensitive and specific modality used for diagnosis. TEACHING POINT Chest Radiographs are sensitive in the detection of an opacity in patients with torsion but this finding is not specific and often mistaken for atelectasis. Direct and indirect signs of volume loss are the key, and if are not present, CT scan needs to be recommended since it has a high sensitivity and specificity for detecting complications of lung transplant. In lobar torsion early recognition could allow the surgeon to successfully detorse the lung and avoid lobectomy. REFERENCES 1. Van Schil PE, Hendriks JM, Lauwers P. Focus on treatment complications and optimal management surgery. Transl Lung Cancer Res 2014;3(3): PMID: Collins J, Kuhlman JE, Love RB. Acute, life-threatening complications of lung transplantation. Radiographics, 1998; 18(1): 36. PMID: Gilkeson RC, Lange P, Kirby TJ. Lung torsion after lung transplantation: evaluation with helical CT. AJR Am J Roentgenol, 2000; 174(5): PMID: CT scan will be able to reliably further characterize an opacity detected on chest radiograph. In cases of atelectasis there will be consolidation with normal lobar anatomic position that enhances the same as surrounding lung parenchyma. Additionally there will be the same findings of volume loss as seen on chest radiograph. It is important to note air bronchograms are not seen with central bronchial obstruction, but can be seen in subsegmental atelectasis. 4. Grazia TJ, Hodges TN, Cleveland JC Jr., Sheridan BC, Zamora MR. Lobar Torsion Complicating Bilateral Lung Transplantation. J Heart Lung Transplant 2003; 22: PMID: Souilamas R, Couchon S, Hernigou A, Guillemain R, Boussaud V, et al. Management of lobar torsion following lung transplantation. Asian Cardiovasc Thorac Ann 2009; 17(2): PMID: In cases of lobar pneumonia CT scan will demonstrate consolidation and/or ground glass opacities with air bronchograms in a lobe of normal anatomic position. 6. Shakoor H, Murthy S, Mason D, Johnston D, Shah SS, et al. Lobar torsion after lung transplantation a case report and 18
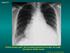
5 review of the literature. Artif Organs 2009; 33(7): PMID: Nguyen J, Maloney J, Kanne JP. Bilateral Whole-lung Torsion After Bilateral Lung Transplantation. Journal of Thoracic Imaging 2011; 26(1): PMID: Lin MW, Huang SC, Kuo SW, Huang PM, Hsu HH, et al. Lobar torsion after lung transplantation. J Formos Med Assoc 2013; 112(2): PMID: Stephens G, Bhagwat K, Pick A, McGiffin D. Lobar Torsion Following Bilateral Lung Transplantation. Journal of Cardiac Surgery 2015; 22(2): PMID: Hayashi K, Aziz A, Ashizawa K, Hayashi H, Nagaoki K, Otsuji H. Radiographic and CT appearance of the major fissures. Radiographics 2001;21: PMID: Felson B. Lung torsion: radiographic findings in nine cases. Radiology, 1987; 162: PMID: Velmahos GC, Frankhouse J, Ciccolo M. Pulmonary torsion of the right upper lobe after right middle lobectomy for a stab wound to the chest. J Trauma 1998; 44(5): PMID: FIGURES Figure 2: 72 year old male with right middle lobe torsion. There is a consolidated right middle lobe (blue star) in an abnormal posterior position with corresponding anterior displacement of the right lower lobe. Additionally, narrowing of the right middle lobe bronchus with a curvilinear abnormal posteriorly directed course of the right middle lobe bronchus (red arrow) is observed coursing posteriorly to the consolidated right middle lobe. The vasculature is not completely evaluated considering the lack of contrast, but these findings are diagnostic of lobar torsion. Figure 1: 72 year old male with right middle lobe torsion. There is right lower lung zone opacity (blue star) on postoperative chest radiograph. Atelectasis is common after lung transplant, and so is at the top of the differential for opacity after transplant. However, indirect signs of volume loss are not present. There is no rib crowding on the right. The most clear indicator though is that the right minor fissure (red arrow) is clearly visualized and is not displaced in the direction of suspected volume loss. Additionally, the mediastinum is not shifted towards the right. Thus, further investigation into the cause of the opacity is required. Figure 3: 72 year old male with right middle lobe torsion. There is abnormal posterior displacement of the consolidated right middle lobe (blue star) with corresponding anterior displacement of the right lower lung. 19
6 Figure 4: 72 year old male with right middle lobe torsion. This is a posterior view of a three dimensional reconstruction that demonstrates the abnormal posterior displacement of the consolidated right middle lobe in red. Etiology Generally it is a complication of lobectomy. It is increasingly recognized as a complication that can occur after lung transplant. It is recognized with a mean of 3.5 days post operation with a range from 1-11 days in the previous documented cases. It can also occur spontaneously or after trauma in rare instances. Incidence The highest incidence is after lobectomy and is considered to be less than 0.5%. After lung transplant there are only eleven previously reported cases. Including our case there are now 12 reported cases. Gender ratio Including our case there is a 5:1 male to female predilection. Age predilection It happens to individuals of all ages after lung transplant. Risk factors The two major identifiable risk factors are: 1) Presence of complete fissure in donor lung. 2) Size discrepancy between a small donor lung and relatively larger thoracic cavity of recipient. Clinical presentation Chest pain, fever, tachycardia, tachypnea, hypoxia, hemoptysis, decreased breath sounds. Laboratory findings Leukocytosis. Arterial blood gas can be surprisingly normal and clinical deterioration with normal abnormal blood gas should raise concern for torsion. Imaging findings Chest Radiograph: Consolidation that is often mistaken for atelectasis but without direct or indirect signs of volume loss present. Computed tomography: Poorly enhancing consolidated lobe of lung in an abnormal anatomic position. There is tapered obliteration of the proximal pulmonary artery and accompanying bronchus of the involved lobe Treatment Detorsion or lobectomy. The surgeon determines the viability of the involved lobe. If it is viable then detorsion can be attempted. If not viable lobectomy is performed. Prognosis Prognosis is generally considered poor; However, of the eleven cases only one patient died within two months secondary to acute respiratory distress syndrome. Table 1: Summary table for pulmonary lobar torsion. Figure 6: 72 year old male with right middle lobe torsion. During thoracotomy an intraoperative image obtained demonstrating a hard, hemorrhagic dark reddish surface of the lung parenchyma of the right middle lobe (blue star) which is compatible with infarct. The right middle lobe was not viable and right middle lobectomy was performed. Figure 5 (left): 72 year old male with right middle lobe torsion. This is a coned in view of the point of interest. The circle clearly delineates right middle lobe bronchial obstruction consistent with the point of torsion of the right middle lobe. 20
7 Lobar Torsion Atelectasis Pneumonia Pulmonary embolism Chest Radiograph Opacification which does not demonstrate the direct and indirect signs of volume loss and can be in an atypical lobar anatomical position. Opacity with direct signs of volume loss including displacement of the fissures and vascular crowding and indirect signs of volume loss on adjacent structures including elevation of the diaphragm, rib crowding on the side with volume loss, mediastinal shift to the side with volume loss, and hilar displacement. Opacification in lobar pattern. Presence of air bronchograms without signs of volume loss. Peripheral opacity without signs of volume loss which is known as the Hampton hump. Sometimes, can also appreciate the Fleishner sign, which is enlargement of a pulmonary artery, or the Westmark sign, which is regional oligemia. Table 2: Differential diagnosis table for pulmonary lobar torsion. CT = computed tomography TID Three times per day ABBREVIATIONS KEYWORDS Lobar torsion; Lung transplant; Complication of Lung Transplant; Atelectasis; Lobectomy Computed Tomography Poorly enhancing consolidated lobe in an abnormal anatomic position. There is tapered obliteration of the proximal pulmonary artery and accompanying bronchus of the involved lobe. Consolidation with enhancement the same as surrounding lung parenchyma. Same findings of volume loss as chest radiograph. It is important to note air bronchograms are not seen with central bronchial obstruction, but air bronchograms are seen in subsegmental atelectasis. Consolidation and/or ground glass opacities with air bronchograms in a lobe of normal anatomic position. CT with contrast demonstrates filling defects in the pulmonary arteries. Additional signs could include enlargement of the pulmonary artery, straightening of the interventricular septum, and an increase in the ratio of right ventricular cavity to left ventricular cavity >1 which all are secondary to increased pulmonary arterial pressure. Additionally, a peripheral wedge shaped opacity that is pleural based with its apex pointing towards the hilum could be seen and is consistent with pulmonary infarction. Online access This publication is online available at: Peer discussion Discuss this manuscript in our protected discussion forum at: Interactivity This publication is available as an interactive article with scroll, window/level, magnify and more features. Available online at Published by EduRad 21
Interpreting thoracic x-ray of the supine immobile patient: Syllabus
 Interpreting thoracic x-ray of the supine immobile patient: Syllabus Johannes Godt Dep. of Radiology and Nuclear Medicine Oslo University Hospital Ullevål NORDTER 2017, Helsinki Content - Why bedside chest
Interpreting thoracic x-ray of the supine immobile patient: Syllabus Johannes Godt Dep. of Radiology and Nuclear Medicine Oslo University Hospital Ullevål NORDTER 2017, Helsinki Content - Why bedside chest
Signs in Chest Radiology
 Signs in Chest Radiology Jonathan H. Chung, MD Disclosures No pertinent disclosures Jonathan H. Chung, MD Assistant Professor Institute t of fadvanced d Biomedical Imaging National Jewish Health Denver,
Signs in Chest Radiology Jonathan H. Chung, MD Disclosures No pertinent disclosures Jonathan H. Chung, MD Assistant Professor Institute t of fadvanced d Biomedical Imaging National Jewish Health Denver,
LOBAR TORSION FOLLOWING LEFT UPPER LOBECTOMY WITH VATS APPROACH: A CASE REPORT
 CASE REPORT LOBAR TORSION FOLLOWING LEFT UPPER LOBECTOMY WITH VATS APPROACH: A CASE REPORT George Kesov, Deyan Yordanov, Ivan Inkov,1,*, Vasil Yordanov, Teodor Badarov, Rumen Asenov, Aleksandra Dimitrova,
CASE REPORT LOBAR TORSION FOLLOWING LEFT UPPER LOBECTOMY WITH VATS APPROACH: A CASE REPORT George Kesov, Deyan Yordanov, Ivan Inkov,1,*, Vasil Yordanov, Teodor Badarov, Rumen Asenov, Aleksandra Dimitrova,
4/16/2017. Learning Objectives. Interpretation of the Chest Radiograph. Components. Production of the Radiograph. Density & Appearance
 Interpretation of the Arthur Jones, EdD, RRT Learning Objectives Identify technical defects in chest radiographs Identify common radiographic abnormalities This Presentation is Approved for 1 CRCE Credit
Interpretation of the Arthur Jones, EdD, RRT Learning Objectives Identify technical defects in chest radiographs Identify common radiographic abnormalities This Presentation is Approved for 1 CRCE Credit
UERMMMC Department of Radiology. Basic Chest Radiology
 UERMMMC Department of Radiology Basic Chest Radiology PHYSICS DENSITIES BONE SOFT TISSUES WATER FAT AIR TELEROENTGENOGRAM Criteria for an Ideal Chest Radiograph 1. Upright 2. Posteroanterior View 3. Full
UERMMMC Department of Radiology Basic Chest Radiology PHYSICS DENSITIES BONE SOFT TISSUES WATER FAT AIR TELEROENTGENOGRAM Criteria for an Ideal Chest Radiograph 1. Upright 2. Posteroanterior View 3. Full
Chest X rays and Case Studies. No disclosures. Outline 5/31/2018. Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital
 Chest X rays and Case Studies Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital No disclosures. Outline Importance of history Densities delineated on radiography An approach
Chest X rays and Case Studies Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital No disclosures. Outline Importance of history Densities delineated on radiography An approach
Bronchial carcinosarcoma
 Bronchial carcinosarcoma Carolina Carcano 1*, Edward Savage 2, Maria Julia Diacovo 3, Jacobo Kirsch 1 1. Division of Radiology, Cleveland Clinic Florida, Weston, Fl, USA 2. Department of Thoracic and Cardiovascular
Bronchial carcinosarcoma Carolina Carcano 1*, Edward Savage 2, Maria Julia Diacovo 3, Jacobo Kirsch 1 1. Division of Radiology, Cleveland Clinic Florida, Weston, Fl, USA 2. Department of Thoracic and Cardiovascular
Chest X-ray Interpretation
 Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
Interesting Cases. Pulmonary
 Interesting Cases Pulmonary 54M with prior history of COPD, hep B/C, and possible history of TB presented with acute on chronic dyspnea, and productive cough Hazy opacity overlying the left hemithorax
Interesting Cases Pulmonary 54M with prior history of COPD, hep B/C, and possible history of TB presented with acute on chronic dyspnea, and productive cough Hazy opacity overlying the left hemithorax
Radiological conference. Left upper lobe collapse. Citation Hong Kong Practitioner, 1998, v. 20 n. 9, p
 Title Radiological conference. Left upper lobe collapse Author(s) Wong, LLS; Peh, WCG Citation Hong Kong Practitioner, 1998, v. 20 n. 9, p. 513-517 Issued Date 1998 URL http://hdl.handle.net/10722/44672
Title Radiological conference. Left upper lobe collapse Author(s) Wong, LLS; Peh, WCG Citation Hong Kong Practitioner, 1998, v. 20 n. 9, p. 513-517 Issued Date 1998 URL http://hdl.handle.net/10722/44672
Bronchial syndrome. Atelectasis Draining bronchus Bronchiectasis
 Bronchial syndrome Atelectasis Draining bronchus Bronchiectasis Etienne Leroy Terquem Pierre L Her SPI / ISP Soutien Pneumologique International / International Support for Pulmonology Atelectasis Consequence
Bronchial syndrome Atelectasis Draining bronchus Bronchiectasis Etienne Leroy Terquem Pierre L Her SPI / ISP Soutien Pneumologique International / International Support for Pulmonology Atelectasis Consequence
10/17/2016. Nuts and Bolts of Thoracic Radiology. Objectives. Techniques
 Nuts and Bolts of Thoracic Radiology October 20, 2016 Carleen Risaliti Objectives Understand the basics of chest radiograph Develop a system for interpreting chest radiographs Correctly identify thoracic
Nuts and Bolts of Thoracic Radiology October 20, 2016 Carleen Risaliti Objectives Understand the basics of chest radiograph Develop a system for interpreting chest radiographs Correctly identify thoracic
Pulmonary Embolism. Thoracic radiologist Helena Lauri
 Pulmonary Embolism Thoracic radiologist Helena Lauri 8.5.2017 Statistics 1-2 out of 1000 adults annually are diagnosed with deep vein thrombosis (DVT) and/or pulmonary embolism (PE) About half of patients
Pulmonary Embolism Thoracic radiologist Helena Lauri 8.5.2017 Statistics 1-2 out of 1000 adults annually are diagnosed with deep vein thrombosis (DVT) and/or pulmonary embolism (PE) About half of patients
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Surgical indications: Non-malignant pulmonary diseases. Punnarerk Thongcharoen
 Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Index. Note: Page numbers of article titles are in boldface type
 Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
An Image Repository for Chest CT
 An Image Repository for Chest CT Francesco Frajoli for the Chest CT in Antibody Deficiency Group An Image Repository for Chest CT he Chest CT in Antibody Deficiency Group is an international and interdisciplinary
An Image Repository for Chest CT Francesco Frajoli for the Chest CT in Antibody Deficiency Group An Image Repository for Chest CT he Chest CT in Antibody Deficiency Group is an international and interdisciplinary
Chest XRay interpretation INTERPRETATIONS Identifications: Name & Date Technical evaluation Basic Interpretations
 Chest XRay interpretation INTERPRETATIONS Identifications: Name & Date Technical evaluation Basic Interpretations TECHNICAL EVALUATION 1. Projection: AP/PA view To differentiate between AP & PA films,
Chest XRay interpretation INTERPRETATIONS Identifications: Name & Date Technical evaluation Basic Interpretations TECHNICAL EVALUATION 1. Projection: AP/PA view To differentiate between AP & PA films,
TB Radiology for Nurses Garold O. Minns, MD
 TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
ISPUB.COM. Rare Cases: Tracheal/bronchial Obstruction. O Wenker, L Moehn, C Portera, G Walsh HISTORY ADMISSION
 ISPUB.COM The Internet Journal of Radiology Volume 1 Number 1 O Wenker, L Moehn, C Portera, G Walsh Citation O Wenker, L Moehn, C Portera, G Walsh.. The Internet Journal of Radiology. 1999 Volume 1 Number
ISPUB.COM The Internet Journal of Radiology Volume 1 Number 1 O Wenker, L Moehn, C Portera, G Walsh Citation O Wenker, L Moehn, C Portera, G Walsh.. The Internet Journal of Radiology. 1999 Volume 1 Number
APICAL SEGMENT OF THE LOWER LOBE IN RESECTIONS FOR BRONCHIECTASIS
 Thorax (1955), 10, 137. THE LATE RESULTS OF THE CONSERVATION OF THE APICAL SEGMENT OF THE LOWER LOBE IN RESECTIONS FOR BRONCHIECTASIS BY E. HOFFMAN From the Regional Thoracic Surgery Centre, Shotley Bridge
Thorax (1955), 10, 137. THE LATE RESULTS OF THE CONSERVATION OF THE APICAL SEGMENT OF THE LOWER LOBE IN RESECTIONS FOR BRONCHIECTASIS BY E. HOFFMAN From the Regional Thoracic Surgery Centre, Shotley Bridge
Parenchyma-sparing lung resections are a potential therapeutic
 Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
X-Rays. Prepared by Prof.Dr. Magda Hassab Allah Assist.lecturer Marwa Al Hady
 X-Rays Prepared by Prof.Dr. Magda Hassab Allah Assist.lecturer Marwa Al Hady CHEST X-RAYS Normal Chest X-ray Comments on chest X ray includes examination of 1- Bony cage (ribs,clavicles &vertebral column
X-Rays Prepared by Prof.Dr. Magda Hassab Allah Assist.lecturer Marwa Al Hady CHEST X-RAYS Normal Chest X-ray Comments on chest X ray includes examination of 1- Bony cage (ribs,clavicles &vertebral column
INDEPENDENT LUNG VENTILATION
 INDEPENDENT LUNG VENTILATION Giuseppe A. Marraro, MD Director Anaesthesia and Intensive Care Department Paediatric Intensive Care Unit Fatebenefratelli and Ophthalmiatric Hospital Milan, Italy gmarraro@picu.it
INDEPENDENT LUNG VENTILATION Giuseppe A. Marraro, MD Director Anaesthesia and Intensive Care Department Paediatric Intensive Care Unit Fatebenefratelli and Ophthalmiatric Hospital Milan, Italy gmarraro@picu.it
Posterior Rectus Sheath Hernia Causing Intermittent Small Bowel Obstruction
 Posterior Rectus Sheath Hernia Causing Intermittent Small Bowel Obstruction Scott Lenobel 1*, Robert Lenobel 2, Joseph Yu 1 1. Department of Radiology, The Ohio State University Wexner Medical Center,
Posterior Rectus Sheath Hernia Causing Intermittent Small Bowel Obstruction Scott Lenobel 1*, Robert Lenobel 2, Joseph Yu 1 1. Department of Radiology, The Ohio State University Wexner Medical Center,
Bronchogenic Carcinoma
 A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
Shedding Light on Neonatal X-rays. Objectives. Indications for X-Rays 5/14/2018
 Shedding Light on Neonatal X-rays Barbara C. Mordue, MSN, NNP-BC Neonatal Nurse Practitioner LLUH Children s Hospital, NICU Objectives Utilize a systematic approach to neonatal x-ray interpretation Identify
Shedding Light on Neonatal X-rays Barbara C. Mordue, MSN, NNP-BC Neonatal Nurse Practitioner LLUH Children s Hospital, NICU Objectives Utilize a systematic approach to neonatal x-ray interpretation Identify
8/14/2017. Objective: correlate radiographic findings of common lung diseases to actual lung pathologic features
 What is that lung disease? Pulmonary Patterns & Correlated Pathology Dr. Russell Tucker, DACVR Objective: correlate radiographic findings of common lung diseases to actual lung pathologic features Improved
What is that lung disease? Pulmonary Patterns & Correlated Pathology Dr. Russell Tucker, DACVR Objective: correlate radiographic findings of common lung diseases to actual lung pathologic features Improved
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress THE LAST GASP II: LUNGS AND THORAX David Holt, BVSc, Diplomate ACVS University of Pennsylvania School of Veterinary
Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress THE LAST GASP II: LUNGS AND THORAX David Holt, BVSc, Diplomate ACVS University of Pennsylvania School of Veterinary
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/23566
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/23566
Chapter 16. Lung Abscess. Mosby items and derived items 2011, 2006 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 16 Lung Abscess 1 EDA PM C AFC RB A B Figure 16-1. Lung abscess. A, Cross-sectional view of lung abscess. B, Consolidation and (C) excessive bronchial secretions are common secondary anatomic alterations
Chapter 16 Lung Abscess 1 EDA PM C AFC RB A B Figure 16-1. Lung abscess. A, Cross-sectional view of lung abscess. B, Consolidation and (C) excessive bronchial secretions are common secondary anatomic alterations
Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600
 Endobronchial valve insertion to reduce lung volume in emphysema Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600 Your responsibility This guidance represents
Endobronchial valve insertion to reduce lung volume in emphysema Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600 Your responsibility This guidance represents
Chapter 21. Flail Chest. Mosby items and derived items 2011, 2006 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 21 Flail Chest 1 Figure 21-1. Flail chest. Double fractures of three or more adjacent ribs produce instability of the chest wall and paradoxical motion of the thorax. Inset, Atelectasis, a common
Chapter 21 Flail Chest 1 Figure 21-1. Flail chest. Double fractures of three or more adjacent ribs produce instability of the chest wall and paradoxical motion of the thorax. Inset, Atelectasis, a common
An Introduction to Radiology for TB Nurses
 An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
Collapse, Crowding, Consolidation, and Contrast: Imaging Findings of Atelectasis on Computed Tomography
 Collapse, Crowding, Consolidation, and Contrast: Imaging Findings of Atelectasis on Computed Tomography Garrana SH 1,2, Desouches SL 1,2, Rosado-de-Christenson ML 1,2, Henry TS 3, Kunin JR 1,2, Walker
Collapse, Crowding, Consolidation, and Contrast: Imaging Findings of Atelectasis on Computed Tomography Garrana SH 1,2, Desouches SL 1,2, Rosado-de-Christenson ML 1,2, Henry TS 3, Kunin JR 1,2, Walker
Complications after lung surgery: CT evaluation
 Complications after lung surgery: CT evaluation Poster No.: C-0855 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: A. Roque Perez, O. Persiva Morenza, D. Varona Porres, E. Pallisa Nuñez,
Complications after lung surgery: CT evaluation Poster No.: C-0855 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: A. Roque Perez, O. Persiva Morenza, D. Varona Porres, E. Pallisa Nuñez,
Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!!
 The lateral chest radiograph: Challenging area around the thoracic aorta!!! Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!! Dong Yoon Han 1, So Youn
The lateral chest radiograph: Challenging area around the thoracic aorta!!! Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!! Dong Yoon Han 1, So Youn
Tests Your Pulmonologist Might Order. Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital
 Tests Your Pulmonologist Might Order Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital BASIC ANATOMY OF THE LUNGS Lobes of Lung 3 lobes on the Right lung 2 lobes on the Left Blood
Tests Your Pulmonologist Might Order Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital BASIC ANATOMY OF THE LUNGS Lobes of Lung 3 lobes on the Right lung 2 lobes on the Left Blood
Case 1. A 35-year-old male presented with fever, cough, and purulent sputum for one week. This was his CXR (Fig. 1.1). What is the diagnosis?
 1 Interpreting Chest X-Rays CASE 1 Fig. 1.1 Case 1. A 35-year-old male presented with fever, cough, and purulent sputum for one week. This was his CXR (Fig. 1.1). What is the diagnosis? CASE 1 Interpreting
1 Interpreting Chest X-Rays CASE 1 Fig. 1.1 Case 1. A 35-year-old male presented with fever, cough, and purulent sputum for one week. This was his CXR (Fig. 1.1). What is the diagnosis? CASE 1 Interpreting
PULMONARY TUBERCULOSIS RADIOLOGY
 PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
ARDS - a must know. Page 1 of 14
 ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
MRSA pneumonia mucus plug burden and the difficult airway
 Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
CASE REPORTS. Idiopathic Unilateral Hyperlucent Lung
 CASE REPORTS Idiopathic Unilateral Hyperlucent Lung The Swyer-James Syndrome J. Judson McNamara, M.D., Harold C. Urschel, M.D., J. H. Arndt, M.D., Herman Ulevitch, M.D., and W. B. Kingsley, M.D. I diopathic
CASE REPORTS Idiopathic Unilateral Hyperlucent Lung The Swyer-James Syndrome J. Judson McNamara, M.D., Harold C. Urschel, M.D., J. H. Arndt, M.D., Herman Ulevitch, M.D., and W. B. Kingsley, M.D. I diopathic
A STUDY OF MORPHOLOGY AND VARIATIONS OF LUNGS IN ADULTS AND FOETUS
 International Journal of Advancements in Research & Technology, Volume 3, Issue 4, April-2014 150 A STUDY OF MORPHOLOGY AND VARIATIONS OF LUNGS IN ADULTS AND FOETUS ZAREENA.SK (assistant professor of anatomy)
International Journal of Advancements in Research & Technology, Volume 3, Issue 4, April-2014 150 A STUDY OF MORPHOLOGY AND VARIATIONS OF LUNGS IN ADULTS AND FOETUS ZAREENA.SK (assistant professor of anatomy)
October 2012 Imaging Case of the Month. Michael B. Gotway, MD Associate Editor Imaging. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 October 2012 Imaging Case of the Month Michael B. Gotway, MD Associate Editor Imaging Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 65-year-old non-smoking woman presented
October 2012 Imaging Case of the Month Michael B. Gotway, MD Associate Editor Imaging Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 65-year-old non-smoking woman presented
Surgery has been proven to be beneficial for selected patients
 Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Lecture Notes. Chapter 16: Bacterial Pneumonia
 Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Respiratory Diseases and Disorders
 Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Thoracostomy: An Update on Imaging Features and Current Surgical Practice
 Thoracostomy: An Update on Imaging Features and Current Surgical Practice Robert D. Ambrosini, MD, PhD, Christopher Gange, MD, Katherine Kaproth-Joslin, MD, PhD, Susan Hobbs, MD, PhD Department of Imaging
Thoracostomy: An Update on Imaging Features and Current Surgical Practice Robert D. Ambrosini, MD, PhD, Christopher Gange, MD, Katherine Kaproth-Joslin, MD, PhD, Susan Hobbs, MD, PhD Department of Imaging
Fariba Rezaeetalab Associate Professor,Pulmonologist
 Fariba Rezaeetalab Associate Professor,Pulmonologist rezaitalabf@mums.ac.ir Patient related risk factors Procedure related risk factors Preoperative risk assessment Risk reduction strategies Age Obesity
Fariba Rezaeetalab Associate Professor,Pulmonologist rezaitalabf@mums.ac.ir Patient related risk factors Procedure related risk factors Preoperative risk assessment Risk reduction strategies Age Obesity
PULMONARY INFARCTS ASSOCIATED WITH BRONCHOGENIC CARCINOMA
 Thor-ax (1954), 9, 304. PULMONARY INFARCTS ASSOCIATED WITH BRONCHOGENIC CARCINOMA W. J. HANBURY, R. J. R. CURETON, AND G. SIMON From St. Bartholomew's Hospital, London BY (RECEIVED FOR PUBLICATION JUNE
Thor-ax (1954), 9, 304. PULMONARY INFARCTS ASSOCIATED WITH BRONCHOGENIC CARCINOMA W. J. HANBURY, R. J. R. CURETON, AND G. SIMON From St. Bartholomew's Hospital, London BY (RECEIVED FOR PUBLICATION JUNE
Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations
 08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
PULMONARY EMBOLISM ANGIOCT (CTA) ASSESSMENT OF VASCULAR OCCLUSION EXTENT AND LOCALIZATION OF EMBOLI 1. BACKGROUND
 JOURNAL OF MEDICAL INFORMATICS & TECHNOLOGIES Vol. 11/2007, ISSN 1642-6037 Damian PTAK * pulmonary embolism, AngioCT, postprocessing techniques, Mastora score PULMONARY EMBOLISM ANGIOCT (CTA) ASSESSMENT
JOURNAL OF MEDICAL INFORMATICS & TECHNOLOGIES Vol. 11/2007, ISSN 1642-6037 Damian PTAK * pulmonary embolism, AngioCT, postprocessing techniques, Mastora score PULMONARY EMBOLISM ANGIOCT (CTA) ASSESSMENT
Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis
 ORIGINAL ARTICLES: Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis Shun-ichi Watanabe, MD, Kenji Suzuki, MD, and Hisao Asamura, MD
ORIGINAL ARTICLES: Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis Shun-ichi Watanabe, MD, Kenji Suzuki, MD, and Hisao Asamura, MD
Lecture Notes. Chapter 2: Introduction to Respiratory Failure
 Lecture Notes Chapter 2: Introduction to Respiratory Failure Objectives Define respiratory failure, ventilatory failure, and oxygenation failure List the causes of respiratory failure Describe the effects
Lecture Notes Chapter 2: Introduction to Respiratory Failure Objectives Define respiratory failure, ventilatory failure, and oxygenation failure List the causes of respiratory failure Describe the effects
PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1).
 PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1). 1 Inform Consent Date: / / dd / Mmm / yyyy 2 Patient identifier: Please enter the 6 digit Patient identification number from your site patient log
PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1). 1 Inform Consent Date: / / dd / Mmm / yyyy 2 Patient identifier: Please enter the 6 digit Patient identification number from your site patient log
Interpretation of the chest radiograph Elizabeth Puddy MB ChB FCARCSI Catherine Hill MB ChB MRCP FRCR
 Interpretation of the chest radiograph Elizabeth Puddy MB ChB FCARCSI Catherine Hill MB ChB MRCP FRCR The traditional technique used in the acquisition and development of a chest radiograph uses methods
Interpretation of the chest radiograph Elizabeth Puddy MB ChB FCARCSI Catherine Hill MB ChB MRCP FRCR The traditional technique used in the acquisition and development of a chest radiograph uses methods
Pulmonary Pathophysiology
 Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Chest Radiology Interpretation: Findings of Tuberculosis
 Chest Radiology Interpretation: Findings of Tuberculosis Get out your laptops, smart phones or other devices pollev.com/chestradiology Case #1 1 Plombage Pneumonia Cancer 2 Reading the TB CXR Be systematic!
Chest Radiology Interpretation: Findings of Tuberculosis Get out your laptops, smart phones or other devices pollev.com/chestradiology Case #1 1 Plombage Pneumonia Cancer 2 Reading the TB CXR Be systematic!
Case of the Day Chest
 Case of the Day Chest Darin White MDCM FRCPC Department of Radiology, Mayo Clinic 76 th Annual Scientific Meeting Canadian Association of Radiologists Montreal, QC April 26, 2013 2013 MFMER slide-1 Disclosures
Case of the Day Chest Darin White MDCM FRCPC Department of Radiology, Mayo Clinic 76 th Annual Scientific Meeting Canadian Association of Radiologists Montreal, QC April 26, 2013 2013 MFMER slide-1 Disclosures
B-I-2 CARDIAC AND VASCULAR RADIOLOGY
 (YEARS 1 3) CURRICULUM FOR RADIOLOGY 13 B-I-2 CARDIAC AND VASCULAR RADIOLOGY KNOWLEDGE To describe the normal anatomy of the heart and vessels including the lymphatic system as demonstrated by radiographs,
(YEARS 1 3) CURRICULUM FOR RADIOLOGY 13 B-I-2 CARDIAC AND VASCULAR RADIOLOGY KNOWLEDGE To describe the normal anatomy of the heart and vessels including the lymphatic system as demonstrated by radiographs,
Tracheal stenosis in infants and children is typically characterized
 Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Restrictive Pulmonary Diseases
 Restrictive Pulmonary Diseases Causes: Acute alveolo-capillary sysfunction Interstitial disease Pleural disorders Chest wall disorders Neuromuscular disease Resistance Pathophysiology Reduced compliance
Restrictive Pulmonary Diseases Causes: Acute alveolo-capillary sysfunction Interstitial disease Pleural disorders Chest wall disorders Neuromuscular disease Resistance Pathophysiology Reduced compliance
The External Anatomy of the Lungs. Prof Oluwadiya KS
 The External Anatomy of the Lungs Prof Oluwadiya KS www.oluwadiya.com Introduction The lungs are the vital organs of respiration Their main function is to oxygenate the blood by bringing inspired air into
The External Anatomy of the Lungs Prof Oluwadiya KS www.oluwadiya.com Introduction The lungs are the vital organs of respiration Their main function is to oxygenate the blood by bringing inspired air into
5/15/2018. Background. Disclosure Statement
 5/15/218 Efficacy of Bronchoscopically-Administered in the Setting of Primary Graft Dysfunction after Lung Transplantation Primary Investigator: Sana Ahmed, PharmD Research Associates: Matthew Soto-Arenall,
5/15/218 Efficacy of Bronchoscopically-Administered in the Setting of Primary Graft Dysfunction after Lung Transplantation Primary Investigator: Sana Ahmed, PharmD Research Associates: Matthew Soto-Arenall,
CASE REPORTS. Inflammatory Polyp of the Bronchus. V. K. Saini, M.S., and P. L. Wahi, M.D.
 CASE REPORTS V. K. Saini, M.S., and P. L. Wahi, M.D. I n 1932 Jackson and Jackson [l] first reported a number of clinical cases under the title Benign Tumors of the Trachea and Bronchi with Especial Reference
CASE REPORTS V. K. Saini, M.S., and P. L. Wahi, M.D. I n 1932 Jackson and Jackson [l] first reported a number of clinical cases under the title Benign Tumors of the Trachea and Bronchi with Especial Reference
CT Chest. Verification of an opacity seen on the straight chest X ray
 CT Chest Indications: To assess equivocal plain x-ray findings Staging of lung neoplasm Merastatic workup of extra thoraces malignancies Diagnosis of diffuse lung diseases with HRCT Assessment of bronchietasis
CT Chest Indications: To assess equivocal plain x-ray findings Staging of lung neoplasm Merastatic workup of extra thoraces malignancies Diagnosis of diffuse lung diseases with HRCT Assessment of bronchietasis
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012
 Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by
 24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by diagnosis? ndings, what is the most likely A. Pulmonary sequestration B. Congenital pulmonary airway malformation
24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by diagnosis? ndings, what is the most likely A. Pulmonary sequestration B. Congenital pulmonary airway malformation
Cor pulmonale. Dr hamid reza javadi
 1 Cor pulmonale Dr hamid reza javadi 2 Definition Cor pulmonale ;pulmonary heart disease; is defined as dilation and hypertrophy of the right ventricle (RV) in response to diseases of the pulmonary vasculature
1 Cor pulmonale Dr hamid reza javadi 2 Definition Cor pulmonale ;pulmonary heart disease; is defined as dilation and hypertrophy of the right ventricle (RV) in response to diseases of the pulmonary vasculature
Adam J. Hansen, MD UHC Thoracic Surgery
 Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Neonatal Chest X-Ray Interpretation
 CHAPTER 7 Neonatal Chest X-Ray Interpretation Prof. Praveen Kumar Neonatal unit, Department of Pediatrics, PGIMER, Chandigarh Learning Objectives At the end of this session, you should be able to: 1. Schematically
CHAPTER 7 Neonatal Chest X-Ray Interpretation Prof. Praveen Kumar Neonatal unit, Department of Pediatrics, PGIMER, Chandigarh Learning Objectives At the end of this session, you should be able to: 1. Schematically
Radiologic Features of The Pulmonary Embolus
 January 2003 Radiologic Features of The Pulmonary Embolus Travis McGlothin HMSIII Mr. J is a 51 y.o. male who presented to the BIDMC ED w/ acute onset of: Lft. Hemiparesis slurred speech mild dyspnea mild
January 2003 Radiologic Features of The Pulmonary Embolus Travis McGlothin HMSIII Mr. J is a 51 y.o. male who presented to the BIDMC ED w/ acute onset of: Lft. Hemiparesis slurred speech mild dyspnea mild
Endobronchial valve insertion to reduce lung volume in emphysema
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endobronchial valve insertion to reduce lung volume in emphysema Emphysema is a chronic lung disease that
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endobronchial valve insertion to reduce lung volume in emphysema Emphysema is a chronic lung disease that
Chapter 11 The Respiratory System
 Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
Discussing feline tracheal disease
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Discussing feline tracheal disease Author : ANDREW SPARKES Categories : Vets Date : March 24, 2008 ANDREW SPARKES aims to
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Discussing feline tracheal disease Author : ANDREW SPARKES Categories : Vets Date : March 24, 2008 ANDREW SPARKES aims to
Preoperative assessment for lung resection. RA Dyer
 Preoperative assessment for lung resection RA Dyer 2016 The ideal assessment of operative risk would identify every patient who could safely tolerate surgery. This ideal is probably unattainable... Mittman,
Preoperative assessment for lung resection RA Dyer 2016 The ideal assessment of operative risk would identify every patient who could safely tolerate surgery. This ideal is probably unattainable... Mittman,
ACUTE PULMNARY INFECTIONS: UNDERSTANDING THE CHEST RADIOGRAPH. Leonard E. Swischuk, M.D. University of Texas Medical Branch
 ACUTE PULMNARY INFECTIONS: UNDERSTANDING THE CHEST RADIOGRAPH Leonard E. Swischuk, M.D. University of Texas Medical Branch AUTHOR HAS NOTHING TO DECLARE LEARNING OBJETIVES Understand the pathophysiology
ACUTE PULMNARY INFECTIONS: UNDERSTANDING THE CHEST RADIOGRAPH Leonard E. Swischuk, M.D. University of Texas Medical Branch AUTHOR HAS NOTHING TO DECLARE LEARNING OBJETIVES Understand the pathophysiology
Thorax Lecture 2 Thoracic cavity.
 Thorax Lecture 2 Thoracic cavity. Spring 2016 Dr. Maher Hadidi, University of Jordan 1 Enclosed by the thoracic wall. Extends between (thoracic inlet) & (thoracic outlet). Thoracic inlet At root of the
Thorax Lecture 2 Thoracic cavity. Spring 2016 Dr. Maher Hadidi, University of Jordan 1 Enclosed by the thoracic wall. Extends between (thoracic inlet) & (thoracic outlet). Thoracic inlet At root of the
TB Intensive Houston, Texas
 TB Intensive Houston, Texas October 15-17, 17 2013 Diagnosis of TB: Radiology Rosa M Estrada-Y-Martin, MD MSc FCCP October 16, 2013 Rosa M Estrada-Y-Martin, MD MSc FCCP, has the following disclosures to
TB Intensive Houston, Texas October 15-17, 17 2013 Diagnosis of TB: Radiology Rosa M Estrada-Y-Martin, MD MSc FCCP October 16, 2013 Rosa M Estrada-Y-Martin, MD MSc FCCP, has the following disclosures to
Introduction to Chest Radiography
 Introduction to Chest Radiography RSTH 366: DIAGNOSTIC TECHNIQUES Alan Alipoon BS, RCP, RRT Instructor Department of Cardiopulmonary Sciences 1 Introduction Discovered in 1895 by Wilhelm Roentgen Terminology
Introduction to Chest Radiography RSTH 366: DIAGNOSTIC TECHNIQUES Alan Alipoon BS, RCP, RRT Instructor Department of Cardiopulmonary Sciences 1 Introduction Discovered in 1895 by Wilhelm Roentgen Terminology
Table 2: Outcomes measured. Table 1: Intrapleural alteplase instillation therapy protocol
 ORIGINAL RESEARCH ARTICLE Intrapleural F brinolytic Therapy with Alteplase in Empyema Thoracis in Children conducted in the Department of Pediatric critical care and Pulmonology unit at our institution
ORIGINAL RESEARCH ARTICLE Intrapleural F brinolytic Therapy with Alteplase in Empyema Thoracis in Children conducted in the Department of Pediatric critical care and Pulmonology unit at our institution
Pediatric Lung Ultrasound (PLUS) In Diagnosis of Community Acquired Pneumonia (CAP)
 Pediatric Lung Ultrasound (PLUS) In Diagnosis of Community Acquired Pneumonia (CAP) Dr Neetu Talwar Senior Consultant, Pediatric Pulmonology Fortis Memorial Research Institute, Gurugram Study To compare
Pediatric Lung Ultrasound (PLUS) In Diagnosis of Community Acquired Pneumonia (CAP) Dr Neetu Talwar Senior Consultant, Pediatric Pulmonology Fortis Memorial Research Institute, Gurugram Study To compare
Chest X-ray (CXR) Interpretation Brent Burbridge, MD, FRCPC
 Chest X-ray (CXR) Interpretation Brent Burbridge, MD, FRCPC An approach to reviewing a chest x-ray will create a foundation that will facilitate the detection of abnormalities. You should create your own
Chest X-ray (CXR) Interpretation Brent Burbridge, MD, FRCPC An approach to reviewing a chest x-ray will create a foundation that will facilitate the detection of abnormalities. You should create your own
Case N 1. Anterior thoracic paint with increasing dyspnea for few days. No cough. Decrease of cardiac sounds. Courtesy Dr Van den Homberg-Tanzania
 Case N 1 Anterior thoracic paint with increasing dyspnea for few days. No cough. Decrease of cardiac sounds Courtesy Dr Van den Homberg-Tanzania Case N 1 Enlargment of cardiac silhouette. Notice the symetry
Case N 1 Anterior thoracic paint with increasing dyspnea for few days. No cough. Decrease of cardiac sounds Courtesy Dr Van den Homberg-Tanzania Case N 1 Enlargment of cardiac silhouette. Notice the symetry
Radiology of the respiratory disease
 Radiology of the respiratory disease [ Color index: Important Notes Extra ] [ Editing file Feedback Share your notes Shared notes ] Resources: - 435 Slides - 434 Team - 435 Notes Done by: - Mai Alageel
Radiology of the respiratory disease [ Color index: Important Notes Extra ] [ Editing file Feedback Share your notes Shared notes ] Resources: - 435 Slides - 434 Team - 435 Notes Done by: - Mai Alageel
Thoracoplasty for the Management of Postpneumonectomy Empyema
 ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 9 Number 2 Thoracoplasty for the Management of Postpneumonectomy Empyema S Mullangi, G Diaz-Fuentes, S Khaneja Citation S Mullangi,
ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 9 Number 2 Thoracoplasty for the Management of Postpneumonectomy Empyema S Mullangi, G Diaz-Fuentes, S Khaneja Citation S Mullangi,
Imaging of Thoracic Trauma: Tips and Traps. Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania
 Imaging of Thoracic Trauma: Tips and Traps Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania None Disclosures Objectives Describe blunt and penetrating traumatic
Imaging of Thoracic Trauma: Tips and Traps Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania None Disclosures Objectives Describe blunt and penetrating traumatic
Radiation Exposure in Pregnancy. John R. Mayo UNIVERSITY OF BRITISH COLUMBIA
 Radiation Exposure in Pregnancy John R. Mayo UNIVERSITY OF BRITISH COLUMBIA Illustrative Clinical Scenario 32 year old female 34 weeks pregnant with recent onset shortness of breath and central chest pain
Radiation Exposure in Pregnancy John R. Mayo UNIVERSITY OF BRITISH COLUMBIA Illustrative Clinical Scenario 32 year old female 34 weeks pregnant with recent onset shortness of breath and central chest pain
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus
 Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
Variations of Lung Fissures: A Cadaveric Study
 JKIMSU, Vol. 3, No. 1, JanJune 2014 ISSN 22314261 ORIGINAL ARTICLE Variations of Lung Fissures: A Cadaveric Study Ambali Manoj P 1*, Jadhav Surekha D 2, Doshi Medha 1, Patil Raosaheb 1 Roy Priya 1, Desai
JKIMSU, Vol. 3, No. 1, JanJune 2014 ISSN 22314261 ORIGINAL ARTICLE Variations of Lung Fissures: A Cadaveric Study Ambali Manoj P 1*, Jadhav Surekha D 2, Doshi Medha 1, Patil Raosaheb 1 Roy Priya 1, Desai
Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure
 Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure Introduction This pediatric respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure Introduction This pediatric respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Thoracic Surgery; An Overview
 Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
Pediatric High-Resolution Chest CT
 Pediatric High-Resolution Chest CT Alan S. Brody, MD Professor of Radiology and Pediatrics Chief, Thoracic Imaging Cincinnati Children s s Hospital Cincinnati, Ohio, USA Pediatric High-Resolution CT Short
Pediatric High-Resolution Chest CT Alan S. Brody, MD Professor of Radiology and Pediatrics Chief, Thoracic Imaging Cincinnati Children s s Hospital Cincinnati, Ohio, USA Pediatric High-Resolution CT Short
Uniportal video-assisted thoracoscopic surgery segmentectomy
 Case Report on Thoracic Surgery Page 1 of 5 Uniportal video-assisted thoracoscopic surgery segmentectomy John K. C. Tam 1,2 1 Division of Thoracic Surgery, National University Heart Centre, Singapore;
Case Report on Thoracic Surgery Page 1 of 5 Uniportal video-assisted thoracoscopic surgery segmentectomy John K. C. Tam 1,2 1 Division of Thoracic Surgery, National University Heart Centre, Singapore;
FOREIGN BODY ASPIRATION in children. Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital
 FOREIGN BODY ASPIRATION in children Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital How common is choking? About 3,000 people die/year from choking Figure remained unchanged
FOREIGN BODY ASPIRATION in children Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital How common is choking? About 3,000 people die/year from choking Figure remained unchanged
Respiratory Medicine
 Respiratory Medicine This document is based on the handout from the Medicine for Finals course. The notes provided here summarise key aspects, focusing on areas that are popular in clinical examinations.
Respiratory Medicine This document is based on the handout from the Medicine for Finals course. The notes provided here summarise key aspects, focusing on areas that are popular in clinical examinations.
SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I. December 5, 2012
 SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I December 5, 2012 FACULTY COPY GOAL: Describe the basic morphologic and pathophysiologic changes in various conditions
SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I December 5, 2012 FACULTY COPY GOAL: Describe the basic morphologic and pathophysiologic changes in various conditions
Imminent Cardiac Collapse: The Catastrophe You Cannot Afford To Miss
 Imminent Cardiac Collapse: The Catastrophe You Cannot Afford To Miss Presenting Authors Ameya J Baxi, MD (baxi@uthscsa.edu) Carlos Restrepo, MD Disclaimer: We do not have any conflict of interest or financial
Imminent Cardiac Collapse: The Catastrophe You Cannot Afford To Miss Presenting Authors Ameya J Baxi, MD (baxi@uthscsa.edu) Carlos Restrepo, MD Disclaimer: We do not have any conflict of interest or financial
