Nutritional support is one of
|
|
|
- Bernadette Grace Harmon
- 6 years ago
- Views:
Transcription
1 Multicenter, prospective, randomized, single-blind study comparing the efficacy and gastrointestinal complications of early jejunal feeding with early gastric feeding in critically ill patients Juan C. Montejo, MD; Teodoro Grau, MD; Jose Acosta, MD; Sergio Ruiz-Santana, MD; Mercé Planas, MD; Abelardo García-de-Lorenzo, MD; Alfonso Mesejo, MD; Manuel Cervera, MD; Carmen Sánchez-Álvarez, MD; Rafael Núñez-Ruiz, MD; Jorge López-Martínez, MD; for the Nutritional and Metabolic Working Group of the Spanish Society of Intensive Care Medicine and Coronary Units Objective: To compare the incidence of enteral nutrition-related gastrointestinal complications, the efficacy of diet administration, and the incidence of nosocomial pneumonia in patients fed in the stomach or in the jejunum. Design: Prospective, randomized multicenter study. Setting: Intensive care units (ICUs) in 11 teaching hospitals. Patients: Critically ill patients who could receive early enteral nutrition more than 5 days. Interventions: Enteral nutrition was started in the first 36 hrs after admission. One group was fed with a nasogastric tube (GEN group) and the other in the jejunum through a dual-lumen nasogastrojejunal tube (JEN group). Measurements and Main Results: Gastrointestinal complications were previously defined. The efficacy of diet administration was calculated using the volume ratio (expressed as the ratio between administered and prescribed volumes). Nosocomial pneumonia was defined according the Centers for Disease Control and Prevention s definitions. One hundred ten patients were included (GEN: 51, JEN: 50). Both groups were comparable in age, gender, Acute Physiology and Chronic Health Evaluation II, and Multiple Organ Dysfunction Score. There were no differences in feeding duration, ICU length of stay, or mortality (43% vs. 38%). The JEN group had lesser gastrointestinal complications (57% vs. 24%, p <.001), mainly because of a lesser incidence of increased gastric residuals (49% vs. 2%, p <.001). Volume ratio was similar in both groups. A post hoc analysis showed that the JEN group had a higher volume ratio at day 7 than the GEN group (68% vs. 82%, p <.03) in patients from ICUs with previous experience in jejunal feeding. Both groups had a similar incidence of nosocomial pneumonia (40% vs. 32%). Conclusions: Gastrointestinal complications are less frequent in ICU patients fed in the jejunum. Nevertheless, it seems to be a necessary learning curve to achieve better results with a postpyloric access. Early enteral nutrition using a nasojejunal route seems not to be an efficacious measure to decrease nosocomial pneumonia in critically ill patients. (Crit Care Med 2002; 30: ) KEY WORDS: enteral nutrition; critical illness; pneumonia; aspiration; intensive care units; intubation; gastrointestinal; prospective studies Nutritional support is one of the routine therapeutic measures in critically ill patients. Some studies have advocated that enteral nutrition is better than parenteral nutrition because it maintains intestinal structure and function, it can limit bacterial translocation, it has a From the Intensive Care Unit (ICU), Hospital Universitario 12 de Octubre, Madrid, Spain (JCM); the ICU, Hospital Universitario Getafe Madrid, Spain (TG); the ICU, Hospital Universitario, Alicante, Spain (JA); the ICU, Hospital Universitario Dr. Negrín, Las Palmas, Spain (SR-S); the ICU, Hospital Universitario Vall d Hebró, Barcelona, Spain (MP); the ICU, Hospital Universitario La Paz, Madrid, Spain (AG-d-L); the ICU, Hospital Universitario Clínico, Valencia, Spain (AM); the ICU, Hospital Universitario Dr Peset, Valencia, Spain (MC); the ICU, Hospital Universitario General, Murcia, Spain (CS-A); the ICU, Hospital Universitario lesser morbidity rate and less severe complications, and it is cheaper (1 3). Also, it has been shown that early enteral nutrition administered to critically ill patients can decrease the number of infectious complications, length of stay, and mortality (4 6). Early enteral nutrition is the treatment of choice with Virgen de la Arrixaca, Murcia, Spain (RN-R); and the ICU, Hospital Universitario Severo Ochoa Leganés, Madrid, Spain (JL-M). Supported, in part, by Novartis Consumer Health (Spain). Novartis Consumer Health (Spain) supplied, at no charge, the dual-lumen tubes used in the study. Funds were dedicated to the statistical analysis. Address requests for reprints to: Juan C Montejo, MD, Hospital Universitario 12 de Octubre, Medicina Intensiva, Carretera de Andalucía Km 5,4, Madrid, Spain. jmontejo@hdoc.insalud.es Copyright 2002 by Lippincott Williams & Wilkins an A level of recommendation for some authors (7). Nevertheless, most of these studies have used a jejunostomy catheter for feedings delivery but most patients are fed via a nasogastric tube in the clinical setting, despite the complications related to this practice (8). As other authors have pointed out (9, 10), our group has shown that enteral nutrition delivered through a nasogastric tube has a high gastrointestinal complication rate, particularly increased gastric residuals (11). This complication leads to underfeeding when using measures to control it (12 14). Moreover, increased gastric residuals could facilitate bronchoaspiration of gastric contents and the appearance of secondary pneumonia. The transpyloric access has been advocated by some authors, using different 796 Crit Care Med 2002 Vol. 30, No. 4
2 methods to avoid the stomach and to better feed the patient (15 17). Enteral feeding through a jejunal tube could decrease the gastrointestinal complication rate, could give more volume of diet, and could decrease the incidence of bronchoaspiration and secondary pneumonia (18). This study has been designed to assess the effectiveness and gastrointestinal complications of early jejunal feeding with a double-lumen nasogastrojejunal tube (Stay-Put, Novartis Consumer Health, Barcelona, Spain) compared with early gastric feeding in critically ill patients. The primary objectives have been the gastrointestinal complication rate and the incidence of nosocomial pneumonia. MATERIALS AND METHODS Protocol. A prospective, multicenter, randomized, single-blind study was performed in 14 intensive care units (ICUs) during 6 months. Patients 18 yrs were enrolled if they would need enteral feeding for 5 days and there were no contraindications for it. The institutional review board of each participating hospital approved the study. Informed consent was obtained from the patients or their relatives. Patients. Adult patients were eligible if they would need enteral nutrition for 5 days in ICU. Patients entered in the study were followed up prospectively until ICU discharge or after 28 days follow-up during the study period. Age, sex, weight, primary diagnosis, Acute Physiology and Chronic Health Evaluation II (APACHE II) score (19) and Multiple Organ Dysfunction Score (MODS) (20) were recorded at admission. Exclusion criteria were anatomical disruptions of the gastrointestinal tract, previous gastrointestinal surgery, or contraindication for enteral nutrition or gastric endoscopy. Tube Placement. Patients were randomly assigned to be fed through a standard nasogastric tube (GEN group) or through a duallumen nasogastrojejunal tube (JEN group) (Stay-Put, Novartis). The nasogastric tube was placed at admission. In the JEN group, the nasogastrojejunal tube was placed in the first 36 hrs after admission by endoscopy, fluoroscopic guidance, blind technique, or by echography. A plain film of the abdomen before diet administration was done to check correct enteral tube placement. Complications related to tube placement were defined previously and registered. Blockage was considered when it was impossible to administer the diet through the Accidental withdrawal was defined as when the tube was removed partially or totally by the patient or during routine care. Dislodgment was considered if there was any radiologic evidence of misplacement of the tubes. If one of these complications was not resolved in Table 1. Randomization profile ICU admissions 1974 Excluded by diagnosis Coronary care and cardiac surgery 1026 Mandatory TPN 237 Eligible patients 711 Not randomized (transpyloric access 395 contraindicated) Eligible 316 Expected EN 5 days 178 EN contraindicated 17 Refused informed consent 20 Randomized 101 Gastric feedings 51 Jejunal feedings 50 ICU, intensive care unit; TPN, total parenteral nutrition; EN, enteral nutrition. Table 2. Patients characteristics the following 24 hrs after detection, the patient was withdrawn from the study. Diet Administration. Caloric requirements and the type of enteral feeding formula were selected by each investigator. Feedings were started in the first 36 hrs after admission and delivered continuously to achieve half of the estimated caloric needs in 24 hrs. The goal was to achieve the calculated caloric requirements in the first 48 hrs of enteral nutrition. Feedings were infused at a constant rate by an infusion pump, and the containers and delivery systems were changed after 24 hrs use. The following data were recorded in accordance with the management protocol: estimated caloric needs, time of first feeding, type of enteral feeding, and duration of their use. The volume ratio, expressed as the ratio between administered and prescribed volumes, was calculated daily as an administration efficacy index. All gastrointestinal complications were recorded prospectively including the number of episodes, day of presentation, and duration according to an established protocol (11). In the JEN group, increased gastric residual was considered when the volume of the gastric aspirated was 300 ml. When detected, the diet was stopped in the next 6 hrs. Reasons for enteral withdrawal were also registered. Outcome Assessment. Primary end points were gastrointestinal complications rate, volume ratio, and ventilator associated pneumonia incidence. Pneumonia was diagnosed according to Centers for Disease Control and Prevention (CDC) criteria (21). MODS at day 5 and at discharge, length of stay, and mortality were also registered. Statistical Analysis. Random numbers were generated by computer for group assignment. Each hospital was the unit of randomization. Sample size was calculated to decrease the nosocomial pneumonia from the 48% infection rate in the GEN group, using the previous data of our group, to 20% in the JEN group. The calculated sample size was 152 patients, with 80% power and 5% significance. An intermediate analysis was done after recruiting 60% of the patients. Statistical analysis was done by intent-to-treat. Continuous data were assessed for normality, and the tests used were two-tailed Student s t-test for normal data and Mann-Whitney for nonnormal distributions. The chi-square test with Yates correction was applied for proportions. Relative risk was calculated for the outcome end points. Data are expressed as mean SD if not quoted otherwise. Statistical analysis was performed by a specialized independent institution. RESULTS A total number of 101 patients (51 GEN group, 50 JEN group) were enrolled during the 1-yr study period (Table 1). Both groups were homogeneous in demographic data and admission severity scores (Table 2). The GEN tube was placed hrs after admission by spontaneous passage. The JEN tube was placed hrs after admission using the blinded technique in 15 patients or using endoscopy (18 patients), fluoroscopic guidance (12 patients), or echography (5 patients). One patient in the GEN group and seven in the JEN group had placement-related complications (p.06). The JEN group had more complications related to tube maintenance (28 vs. 8 patients; p.001). Enteral feeding characteristics are indicated in Table 3. Enteral tube-related complications were responsible for en- No. of patients Men (%) 71 (70) 35 (69) 36 (72).7 Age, yrs APACHE II score MODS score APACHE, Acute Physiologic and Chronic Health Evaluation; MODS, multiple organ dysfunction score. a Patients fed through a standard nasogastric tube; b patients fed through a dual-lumen nasogastrojejunal Crit Care Med 2002 Vol. 30, No
3 teral nutrition withdrawal in nine patients in the JEN group. Enteral nutrition-related gastrointestinal complications were less frequent in the JEN group, with a significant decrease in the incidence of high gastric residuals and a similar rate of the other gastrointestinal complications (Table 4). There were no differences in the caloric intake or in the volume ratio between groups during the complete follow-up (Table 5). Some ICUs had previous experience with the JEN tube used in the study. A post hoc analysis limited to data from the six ICUs with previous experience showed that the JEN group received significantly more calories and had a better volume ratio at day 7 (Table 6). There were no differences in the incidence of nosocomial pneumonia between both groups (Table 7). Also, we were unable to find any differences in ICU length of stay, multiple organ failure score, or mortality (Table 7). DISCUSSION Studies that have assessed the gastric emptying in critically ill patients undergoing mechanical ventilation show that these patients had a marked alteration of normal gastric emptying (22 25). The impaired gastric emptying explains the gastric intolerance to enteral feedings and can justify the use of a double-lumen gastroenteric tube for enteral nutrition. The hypothesis that early enteral nutrition would be more effective when using the transpyloric route if compared with the gastric access is confirmed in this study if we look at the different rate of enteral nutrition-related gastrointestinal complications that we have found. Nevertheless, the absence of increased gastric residuals in the patients who received feedings through the jejunal tube did not result in higher volumes of the administered diet or an increased caloric intake. The potential reasons are the increased frequency of tube-related complications (occlusion, accidental withdrawal, and dislodgment) found in the jejunal group. These complications make it difficult to maintain the caloric intake and are the cause of definitive enteral nutrition withdrawal. This assumption seems to be confirmed by the results coming from the centers with previous experience in the use of this kind of nasogastrojejunal tubes, where we found a Table 3. Enteral nutrition characteristics higher caloric intake in the jejunal group compared with the gastric one. We have been unable to demonstrate that jejunal feedings combined with gastric suction can decrease the incidence of nosocomial pneumonia in critically ill patients compared with the gastric route. Other studies have shown similar results. Montecalvo et al. (26) compared the incidence of nosocomial pneumonia in 38 critically patients randomly assigned to be fed via a gastric tube or a jejunal one placed by gastroscopy. In their study, the group fed by the jejunal route received more calories than the group fed by the gastric route but there were no differences in the incidence of nosocomial pneumonia. A similar study (27) with 44 patients showed also that the transpyloric access led to more caloric intake but the nosocomial pneumonia incidence was similar in both groups. In trauma patients, Kortbeeck et al. (28) studied also the efficacy of the transpyloric route to deliver nutrients compared with the gastric one. By using the transpyloric access, patients achieved the caloric goal earlier than patients fed by the gastric route, but, again, the authors were unable to find any differences in the pneumonia incidence, ICU length of stay, or mortality. According to the similar incidence in All Gen Group a JEN Group b p Value Time of initiation, hrs Duration, days Reasons for withdrawal (%).01 ICU discharge 20 (20) 14 (28) 6 (12) Oral 32 (32) 14 (28) 18 (36) Enteral nutrition complications 4 (4) 3 (6) 1 (2) Enteral tube complications 9 (9) 9 (18) Other complications 2 (2) 2 (4) Terminal illness 2 (2) 1 (2) 1 (2) Death 32 (32) 17 (33) 15 (30) ICU, intensive care unit. Table 4. Gastrointestinal complications of enteral feeding: Patients with one or more complications All (%) GEN Group a (%) JEN Group a p Value Abdominal distention 9 (9) 4 (8) 5 (10).7 Vomiting 6 (6) 2 (4) 4 (8).4 Diarrhea 14 (14) 7 (14) 7 (14).97 Constipation 5 (5) 3 (6) 2 (4) 1 High gastric residuals 26 (25) 25 (49) 1 (2).001 One of these complications 41 (61) 29 (57) 12 (24).001 Table 5. Planned and administered caloric intake Caloric requirements Planned caloric intake at day Administered calories at day Planned caloric intake at day Administered calories at day Volume ratio at day 3, % Volume ratio at day 7, % Mean planned caloric intake Mean administered calories Difference between planned and administered calories Crit Care Med 2002 Vol. 30, No. 4
4 Table 6. Results in intensive care units with previous experience Table 7. Primary outcomes pneumonia indicated in the abovementioned studies, Esparza et al. (29), in a recent study, reported, with an isotopic method, that aspiration rates were no different between gastrically or transpylorically fed critically ill patients. Other studies have not shown the above-indicated superiority of the transpyloric route over the gastric access in terms of caloric intake. In a prospective, randomized study done in 32 critically ill patients, Strong et al. (30) did not show any advantage in time needed to achieve the caloric requirements or in the incidence of nosocomial pneumonia. Another retrospective study (31) also failed in demonstrating advantages in nutritional efficacy (time needed to achieve caloric goals) or in the incidence of nosocomial pneumonia with the transpyloric route. Despite the fact that enteral nutrition is considered to be a risk factor for the development of nosocomial pneumonia in critically ill patients (32, 33), it has not been established whether gastric infusion of feeding formula is accompanied by a Patients Men (%) 44 (73) 20 (67) 24 (80).2 Age, yrs APACHE II score MODS score Enteral nutrition Time of initiation, hrs Duration, days Caloric requirements Administered calories at day Administered calories at day Volume ratio at day 3, % Volume ratio at day 7, % Mean administered calories APACHE, Acute Physiology and Chronic Health Evaluation; MODS, multiple organ dysfunction score. Mortality (%) 41 (41) 22 (43) 19 (38).6 Length of stay, days Nosocomial pneumonia (%) 36 (36) 20 (40) 16 (32).4 MODS score at day (n 46) (n 46) MODS at discharge (n 43) (n 43) MODS, multiple organ dysfunction score. Crit Care Med 2002 Vol. 30, No. 4 greater incidence of pneumonia in comparison with transpyloric infusion of nutrients. Our study does not support the use of any of the two routes, gastric or transpyloric, to decrease the incidence of pneumonia. The trend toward a decreased incidence of pneumonia that we have found in our patients fed by a transpyloric tube is not significant. This would be a problem because of the number of patients studied. As the study by Kortbeeck et al. (28) points out, the number of patients needed to demonstrate a difference of 10% or more in the frequency of nosocomial pneumonia is 400 patients, or even more if we look at our results. Another question to be solved is the criteria used for the diagnosis of mechanical ventilation associated pneumonia. The CDC criteria used in this study could have overestimated the true pneumonia incidence. Nevertheless, these criteria have been applied equally to both groups, and, therefore, it should not be a confounding factor. Other techniques, such as the quantitative cultures of tracheal Gastrointestinal complications are less frequent in intensive care unit patients fed in the jejunum. aspirates or the use of protected brush catheters, could improve the results but, as other authors have pointed out (34), there are difficulties in unifying the diagnostic criteria of the ventilator-associated pneumonia in multicenter studies. Because the proposed solutions are not implemented in the clinical setting, we thought that clinical diagnoses using objective criteria, such as the CDC recommendations used in our study, are adequate. We can conclude that early placement of a transpyloric tube for enteral nutrition in a nonselected population of critically ill patients is not useful in terms of reducing the incidence of nosocomial pneumonia or increasing nutritional efficacy. Perhaps further studies using other diagnostic criteria of ventilator-associated pneumonia with more patients would demonstrate any difference. Our results support the hypothesis, advanced by other authors (35), that the transpyloric tube is as useful as a nasogastric tube for early enteral nutrition in critically ill patients. Nevertheless, it remains to be established if the transpyloric approach could be effective in selected groups of patients, such as patients who develop high gastric residuals while receiving a diet using the gastric approach. Switching to a transpyloric access when the gastric route fails will be the only way to maintain the enteral nutrition in these cases. Results such as these also indicate that parenteral nutrition must be needed in patients in whom nasogastric or nasojejunal feeding is partially or completely ineffective. REFERENCES 1. Round Table Conference on Metabolic Support of the Critically Ill Patients. Intensive Care Med 1994; 20: ASPEN Board of Directors: Guidelines for the use of parenteral and enteral nutrition in 799
5 adult and paediatric patients. JPEN J Parenter Enteral Nutr 1993; 17:1SA 26SA. 3. Jolliet P, Pichard C, Biolo G, et al: Enteral nutrition in intensive care patients: A practical approach. Intensive Care Med 1998; 24: Grahm TW, Zadrozny DB, Harrington T: The benefits of early jejunal hyperalimentation in the head-injured patient. Neurosurgery 1989; 25: Kudks KA, Croce MA, Fabian TC, et al: Enteral vs parenteral feeding: Effects on septic morbidity following blunt and penetrating abdominal trauma. Ann Surg 1992; 215: Moore FA, Feliciano DV, Andrassy RJ, et al: Early enteral feeding, compared with parenteral, reduces septic complications: The results of a meta-analysis. Ann Surg 1992; 216: Zaloga GP: Early enteral nutritional support improves outcome: Hypothesis or fact? Crit Care Med 1999; 27: Preiser JC, Berre J, Carpentier Y, et al: on behalf of the working group on metabolism and nutrition of the European Society of Intensive Care Medicine. Management of nutrition in European intensive care units: Results of a questionnaire. Intensive Care Med 1999; 52: Heyland D, Cook DJ, Winder B, et al: Enteral nutrition in the critically ill patient: A prospective survey. Crit Care Med 1995; 23: Adam S, Batson S: A study of problems associated with delivery of enteral feeds in critically ill patients in five ICUs in the UK. Intensive Care Med 1996; 23: Montejo J, the Nutritional and Metabolic Working Group of the Spanish Society of Intensive Care Medicine and Coronary Units: Enteral nutrition-related gastrointestinal complications in critically ill patients: A multicenter study. Crit Care Med 1999; 27: Kemper M, Weissman C, Hyman AI: Caloric requirements and supply in critically ill surgical patients. Crit Care Med 1992; 20: Spain DA, McClave SA, Sexton LK, et al: Infusion protocol improves delivery of enteral tube feeding in the critical care unit. JPEN J Parenter Enteral Nutr 1999; 23: De Jonghe B, Appere-De-Vechi C, Fournier M, et al: A prospective survey of nutritional support practices in intensive care unit patients: What is prescribed? What is delivered? Crit Care Med 2001; 29: Baskin WN: Advances in enteral nutrition techniques. Am J Gastroenterol 1992; 87: Kirby DF, Clifton GL, Turner H, et al: Early enteral nutrition after brain injury by percutaneous endoscopic gastrojejunostomy. JPEN J Parenter Enteral Nutr 1991; 15: Zaloga GP: Bedside method for placing small bowel feeding tubes in critically ill patients: A prospective study. Chest 1991; 100: Smith HG, Orlando R: Enteral nutrition: Should we feed the stomach? Crit Care Med 1999; 27: Knaus VA, Draper EA, Wagner DP, et al: APACHE II: A severity of disease classification system. Crit Care Med 1985; 13: Marshall JC, Cook DJ, Christou NV, et al: Multiple Organ Dysfunction Score: A reliable descriptor of a complex clinical outcome. Crit Care Med 1995; 23: Centers for Disease Control: CDC definitions for nosocomial infections, Am Rev Respir Dis 1989; 139: Dive A, Moulart M, Jonard P, et al: Gastroduodenal motility in mechanically ventilated critically ill patients: A manometric study. Crit Care Med 1994; 22: Ibañez J, Peñafiel A, Raurich, et al: Gastroesophageal reflux in intubated patients receiving enteral nutrition: Effect of supine and semirecumbent positions. JPEN J Parenter Enteral Nutr 1992; 16: Ott L, Young B, Phillips R, et al: Altered gastric emptying in the head-injured patient: Relationship to feeding intolerance. J Neurosurg 1991; 74: Heyland DK, Tougas G, King D, et al: Impaired gastric emptying in mechanically ventilated, critically ill patients. Intensive Care Med 1996; 22: Montecalvo MA, Steger KA, Farber HW, et al: Nutritional outcome and pneumonia in critical care patients randomized to gastric versus jejunal tube feedings. Crit Care Med 1992; 20: Kearns PJ, Chin D, Mueller L, et al: The incidence of ventilator-associated pneumonia and success in nutrient delivery with gastric versus small intestinal feeding: A randomized clinical trial. Crit Care Med 2000; 28: Kortbeeck JB, Haigh PI, Doig C: Duodenal versus gastric feeding in ventilated blunt trauma patients: A randomized controlled trial. J Trauma 1999; 46: Esparza J, Boivin M, Hartshorne MF, et al: Equal aspiration rates in gastrically and transpylorically fed critically ill patients. Intensive Care Med 2001; 27: Strong RM, Condon SC, Solinger MR, et al: Equal aspiration rates from postpylorus and intragastric-placed small bore nasoenteric feeding tubes: A randomized, prospective study. JPEN J Parenter Enteral Nutr 1992; 16: Spain DA, DeWeese CG, Reynolds MA, et al: Transpyloric passage of feeding tubes in patients with head injury does not decrease complications. J Trauma 1995; 39: Cook DJ, Walter SD, Cook RJ, et al: Incidence and risk factors for ventilator-associated pneumonia in critically ill patients. Ann Intern Med 1998; 129: Tejada A, Bello S, Chacon E, et al: Risk factors for nosocomial pneumonia in critically ill trauma patients. Crit Care Med 2001; 29: Cook D, Walter S, Freitag A, et al: Adjudicating ventilator-associated pneumonia in a randomized trial of critically ill patients. J Crit Care 1998; 13: Heyland DK: Nutritional support in the critically ill patient: A critical review of the evidence. Crit Care Clin 1998; 14: Crit Care Med 2002 Vol. 30, No. 4
5.3 Strategies to Optimize Delivery and Minimize Risks of EN: Small Bowel Feeding vs. Gastric May 2015
 5.3 Strategies to Optimize Delivery and Minimize Risks of EN: Small Bowel Feeding vs. Gastric May 2015 2015 Recommendation: Based on 16 level 2 studies, small bowel feeding compared to gastric feeding
5.3 Strategies to Optimize Delivery and Minimize Risks of EN: Small Bowel Feeding vs. Gastric May 2015 2015 Recommendation: Based on 16 level 2 studies, small bowel feeding compared to gastric feeding
5.3 Strategies to Optimize Delivery and Minimize Risks of EN: Small Bowel Feeding vs. Gastric February 2014
 5.3 Strategies to Optimize Delivery and Minimize Risks of EN: Small Bowel Feeding vs. Gastric February 2014 2013 Recommendation: Based on 15 level 2 studies, small bowel feeding compared to gastric feeding
5.3 Strategies to Optimize Delivery and Minimize Risks of EN: Small Bowel Feeding vs. Gastric February 2014 2013 Recommendation: Based on 15 level 2 studies, small bowel feeding compared to gastric feeding
Int. Med J Vol. 6 No 1 June 2007 Enteral Nutrition In Intensive Care: Tiger Tube For Small Bowel Feeding In Acute Pancreatitis.
 Page 1 of 6 Int. Med J Vol. 6 No 1 June 2007 Enteral Nutrition In Intensive Care: Tiger Tube For Small Bowel Feeding In Acute Pancreatitis. Case Report Mohd Basri bin Mat Nor. Department of Anaesthesiology
Page 1 of 6 Int. Med J Vol. 6 No 1 June 2007 Enteral Nutrition In Intensive Care: Tiger Tube For Small Bowel Feeding In Acute Pancreatitis. Case Report Mohd Basri bin Mat Nor. Department of Anaesthesiology
Feeding Protocols Enteral or Parenteral. AM Poleÿ 2012
 Practical aspects on Feeding Protocols Enteral or Parenteral AM Poleÿ 2012 Enteral Feeding Facts A reduction in mortality Prophylaxis for stress ulcers Full-strength Time to start enteral nutrition If
Practical aspects on Feeding Protocols Enteral or Parenteral AM Poleÿ 2012 Enteral Feeding Facts A reduction in mortality Prophylaxis for stress ulcers Full-strength Time to start enteral nutrition If
Nutrient intake is considered part of the global resuscitation
 Prospective Randomized Control Trial of Intermittent Versus Continuous Gastric Feeds for Critically Ill Trauma Patients Jana B. A. MacLeod, MD, Jennifer Lefton, RD, CNSD, Doug Houghton, MSN, Christina
Prospective Randomized Control Trial of Intermittent Versus Continuous Gastric Feeds for Critically Ill Trauma Patients Jana B. A. MacLeod, MD, Jennifer Lefton, RD, CNSD, Doug Houghton, MSN, Christina
STRATEGIES TO IMPROVE ENTERAL FEEDING TOLERANCE. IS IT WORTH IT? ENGELA FRANCIS RD(SA)
 STRATEGIES TO IMPROVE ENTERAL FEEDING TOLERANCE. IS IT WORTH IT? ENGELA FRANCIS RD(SA) DEFINITION OF ENTERAL FEEDING INTOLERANCE Gastrointestinal feeding intolerance are usually defined as: High gastric
STRATEGIES TO IMPROVE ENTERAL FEEDING TOLERANCE. IS IT WORTH IT? ENGELA FRANCIS RD(SA) DEFINITION OF ENTERAL FEEDING INTOLERANCE Gastrointestinal feeding intolerance are usually defined as: High gastric
AUTHORS: Luisito O. Llido, MD (1), Mariana S. Sioson, MD (1,2), Jesus Fernando Inciong, MD (1), Grace Manuales, MD (1)
 9 Submitted: September 5, 2011 Posted: January 7, 2012 TITLE: Nutrition team supervision on nutrient intake in critical care patients: report of a ten- year experience in the Philippines (years 2000 to
9 Submitted: September 5, 2011 Posted: January 7, 2012 TITLE: Nutrition team supervision on nutrient intake in critical care patients: report of a ten- year experience in the Philippines (years 2000 to
A review on enteral nutrition guidelines for traumatic brain injury
 A review on enteral nutrition guidelines for traumatic brain injury According to the Centers for Disease Control and Prevention, at least 1.7 million people suffer from traumatic brain injury (TBI) every
A review on enteral nutrition guidelines for traumatic brain injury According to the Centers for Disease Control and Prevention, at least 1.7 million people suffer from traumatic brain injury (TBI) every
5.2 Strategies to Optimize Delivery and Minimize Risks of EN: Motility Agents May 2015
 5.2 Strategies to Optimize Delivery and Minimize Risks of EN: Motility Agents May 2015 There were no new randomized controlled trials since the 2009 and 2013 updates and hence there are no changes to the
5.2 Strategies to Optimize Delivery and Minimize Risks of EN: Motility Agents May 2015 There were no new randomized controlled trials since the 2009 and 2013 updates and hence there are no changes to the
[No conflicts of interest]
![[No conflicts of interest] [No conflicts of interest]](/thumbs/86/94144068.jpg) [No conflicts of interest] Patients and staff at: Available evidence pre-calories Three meta-analyses: Gramlich L et al. Does enteral nutrition compared to parenteral nutrition result in better outcomes
[No conflicts of interest] Patients and staff at: Available evidence pre-calories Three meta-analyses: Gramlich L et al. Does enteral nutrition compared to parenteral nutrition result in better outcomes
Wali R Johnson et. al. / International Journal of New Technologies in Science and Engineering Vol. 2, Issue 4, October 2015, ISSN
 Enteral Feeding via Percutaneous Endoscopic Gastrojejunostomy(PEGJ) Tubes Decreases Risk of Aspiration and Tube Dislodgement Related Complications Compared to PEGs. Wali R Johnson, MSIV, L Ray Matthews,
Enteral Feeding via Percutaneous Endoscopic Gastrojejunostomy(PEGJ) Tubes Decreases Risk of Aspiration and Tube Dislodgement Related Complications Compared to PEGs. Wali R Johnson, MSIV, L Ray Matthews,
NO DISCLOSURES 5/9/2015
 Annette Stralovich-Romani, RD, CNSC Adult Critical Care Nutritionist UCSF Medical Center NO DISCLOSURES Incidence & consequences of malnutrition Underfeeding in the ICU Causes/ consequences Nutrition intervention
Annette Stralovich-Romani, RD, CNSC Adult Critical Care Nutritionist UCSF Medical Center NO DISCLOSURES Incidence & consequences of malnutrition Underfeeding in the ICU Causes/ consequences Nutrition intervention
Division of Acute Care Surgery Clinical Practice Policies, Guidelines, and Algorithms: Enteral Nutrition Algorithm Clinical Practice Guideline
 Division of Acute Care Surgery Clinical Practice Policies, Guidelines, and Algorithms: Enteral Nutrition Algorithm Clinical Practice Guideline Original Date: 08/2011 Purpose: To promote the early use of
Division of Acute Care Surgery Clinical Practice Policies, Guidelines, and Algorithms: Enteral Nutrition Algorithm Clinical Practice Guideline Original Date: 08/2011 Purpose: To promote the early use of
Issues in Enteral Feeding: Aspiration
 Issues in Enteral Feeding: Aspiration A webinar for HealthTrust Members February 11, 2019 Co-sponsored by HealthTrust and V NOS Continuing Education Provider Presented by: Kathleen Stoessel, RN, BSN, MS
Issues in Enteral Feeding: Aspiration A webinar for HealthTrust Members February 11, 2019 Co-sponsored by HealthTrust and V NOS Continuing Education Provider Presented by: Kathleen Stoessel, RN, BSN, MS
Current concepts in Critical Care Nutrition
 Current concepts in Critical Care Nutrition Dr.N.Ramakrishnan AB (Int Med), AB (Crit Care), MMM, FACP, FCCP, FCCM Director, Critical Care Services Apollo Hospitals, Chennai Objectives Why? Enteral or Parenteral
Current concepts in Critical Care Nutrition Dr.N.Ramakrishnan AB (Int Med), AB (Crit Care), MMM, FACP, FCCP, FCCM Director, Critical Care Services Apollo Hospitals, Chennai Objectives Why? Enteral or Parenteral
The value of bowel sound assessment in predicting feeding intolerance in critically ill patients
 Crit Care & Shock (2011) 14:65-69 The value of bowel sound assessment in predicting feeding intolerance in critically ill patients Abdullah AlShimemeri, Maram Sakkijha, Samir Haddad, Yaseen Arabi Abstract
Crit Care & Shock (2011) 14:65-69 The value of bowel sound assessment in predicting feeding intolerance in critically ill patients Abdullah AlShimemeri, Maram Sakkijha, Samir Haddad, Yaseen Arabi Abstract
Gastric versus Jejunal Feeding: Evidence or Emotion?
 Carol Rees Parrish, R.D., M.S., Series Editor Gastric versus Jejunal Feeding: Evidence or Emotion? Joe Krenitsky Delivery of enteral feeding into the small bowel has been suggested as a strategy to reduce
Carol Rees Parrish, R.D., M.S., Series Editor Gastric versus Jejunal Feeding: Evidence or Emotion? Joe Krenitsky Delivery of enteral feeding into the small bowel has been suggested as a strategy to reduce
5.5 Strategies to Optimize the Delivery of EN: Use of and Threshold for Gastric Residual Volumes May 2015
 5.5 Strategies to Optimize the Delivery of EN: Use of and Threshold for Gastric Residual Volumes May 2015 2015 Recommendation: Based on 3 level 2 studies, a gastric residual volume of either 250 or 500
5.5 Strategies to Optimize the Delivery of EN: Use of and Threshold for Gastric Residual Volumes May 2015 2015 Recommendation: Based on 3 level 2 studies, a gastric residual volume of either 250 or 500
The Meat and Potatoes of Critical Care Nutrition ROSEMARY KOZAR MD PHD SHOCK TRAUMA UNIVERSITY OF MARYLAND
 The Meat and Potatoes of Critical Care Nutrition ROSEMARY KOZAR MD PHD SHOCK TRAUMA UNIVERSITY OF MARYLAND 2013 Canadian Clinical Practice Guidelines www.criticalcarenutrition.com NEJM March 27, 2014 Use
The Meat and Potatoes of Critical Care Nutrition ROSEMARY KOZAR MD PHD SHOCK TRAUMA UNIVERSITY OF MARYLAND 2013 Canadian Clinical Practice Guidelines www.criticalcarenutrition.com NEJM March 27, 2014 Use
2.0 Early vs. Delayed Nutrient Intake May 2015
 2.0 Early vs. Delayed Nutrient Intake May 2015 There were no new randomized controlled trials since the 2013 update and hence there are no changes to the following summary of evidence. 2013 Recommendation:
2.0 Early vs. Delayed Nutrient Intake May 2015 There were no new randomized controlled trials since the 2013 update and hence there are no changes to the following summary of evidence. 2013 Recommendation:
5.5 Strategies to Optimize the Delivery of EN: Use of and Threshold for Gastric Residual Volumes March 2013
 5.5 Strategies to Optimize the Delivery of EN: Use of and Threshold for Gastric Residual Volumes March 203 NEW SECTION in 203 Recommendation: There are insufficient data to make a recommendation for not
5.5 Strategies to Optimize the Delivery of EN: Use of and Threshold for Gastric Residual Volumes March 203 NEW SECTION in 203 Recommendation: There are insufficient data to make a recommendation for not
Nutrition Supplementation in the ICU
 Nutrition Supplementation in the ICU ROSEMARY KOZAR MD PHD SHOCK TRAUMA UNIVERSITY OF MARYLAND Canadian Clinical Practice Guidelines www.criticalcarenutrition.com NEJM March 27, 2014 1 Use of Enteral vs
Nutrition Supplementation in the ICU ROSEMARY KOZAR MD PHD SHOCK TRAUMA UNIVERSITY OF MARYLAND Canadian Clinical Practice Guidelines www.criticalcarenutrition.com NEJM March 27, 2014 1 Use of Enteral vs
ICU NUTRITION UPDATE : ESPEN GUIDELINES Mirey Karavetian Assistant Professor Zayed University
 ICU NUTRITION UPDATE : ESPEN GUIDELINES 2018 Mirey Karavetian Assistant Professor Zayed University http://www.espen.org/files/espen- Guidelines/ESPEN_Guideline_on_clinical_nutrition_in_-ICU.pdf Medical
ICU NUTRITION UPDATE : ESPEN GUIDELINES 2018 Mirey Karavetian Assistant Professor Zayed University http://www.espen.org/files/espen- Guidelines/ESPEN_Guideline_on_clinical_nutrition_in_-ICU.pdf Medical
A Novel Technique for Post-pyloric Feeding Tube Placement in Critically Ill Patients: A Pilot Study
 Anaesth Intensive Care 2005; 33: 229-234 A Novel Technique for Post-pyloric Feeding Tube Placement in Critically Ill Patients: A Pilot Study R. J. YOUNG*, M. J. CHAPMAN, R. FRASER, R. VOZZO, D. P. CHORLEY**,
Anaesth Intensive Care 2005; 33: 229-234 A Novel Technique for Post-pyloric Feeding Tube Placement in Critically Ill Patients: A Pilot Study R. J. YOUNG*, M. J. CHAPMAN, R. FRASER, R. VOZZO, D. P. CHORLEY**,
5.1 Strategies to Optimize Delivery and Minimize Risks of EN: Feeding Protocols March 2013
 5.1 Strategies to Optimize Delivery and Minimize Risks of EN: Feeding Protocols March 2013 There were no new randomized controlled trials since the 2009 update and hence there are no changes to the following
5.1 Strategies to Optimize Delivery and Minimize Risks of EN: Feeding Protocols March 2013 There were no new randomized controlled trials since the 2009 update and hence there are no changes to the following
Nutrition and Sepsis
 Nutrition and Sepsis Todd W. Rice, MD, MSc Associate Professor of Medicine Vanderbilt University 2017 DNS Symposium June 2, 2017 Case 55 y.o. male COPD, DM, HTN, presents with pneumonia and septic shock.
Nutrition and Sepsis Todd W. Rice, MD, MSc Associate Professor of Medicine Vanderbilt University 2017 DNS Symposium June 2, 2017 Case 55 y.o. male COPD, DM, HTN, presents with pneumonia and septic shock.
Enteral Nutrition: Whom, Why, When, What and Where to Feed?
 Meier RF, Reddy BR, Soeters PB (eds): The Importance of Nutrition as an Integral Part of Disease Management. Nestlé Nutr Inst Workshop Ser, vol 82, pp 53 59, (DOI: 10.1159/000382002) Nestec Ltd., Vevey/S.
Meier RF, Reddy BR, Soeters PB (eds): The Importance of Nutrition as an Integral Part of Disease Management. Nestlé Nutr Inst Workshop Ser, vol 82, pp 53 59, (DOI: 10.1159/000382002) Nestec Ltd., Vevey/S.
Providing Optimal Nutritional Support on the ICU common problems and practical solutions. Pete Turner Specialist Nutritional Support Dietitian
 Providing Optimal Nutritional Support on the ICU common problems and practical solutions Pete Turner Specialist Nutritional Support Dietitian ICU Nutritional Support ACCEPT study showed improved ICU survival
Providing Optimal Nutritional Support on the ICU common problems and practical solutions Pete Turner Specialist Nutritional Support Dietitian ICU Nutritional Support ACCEPT study showed improved ICU survival
Guidelines for the Provision and Assessment of Nutrition Support Therapy in the Pediatric Critically Ill Patient: ASPEN-SCCM 2017
 Number of Patients Guidelines for the Provision and Assessment of Nutrition Support Therapy in the Pediatric Critically Ill Patient: ASPEN-SCCM 2017 Jorge A. Coss-Bu, MD Associate Professor of Pediatrics
Number of Patients Guidelines for the Provision and Assessment of Nutrition Support Therapy in the Pediatric Critically Ill Patient: ASPEN-SCCM 2017 Jorge A. Coss-Bu, MD Associate Professor of Pediatrics
patients : review of advances in last five years Dr. Aditya Jindal
 Enteral nutrition in medical ICU patients : review of advances in last five years Dr. Aditya Jindal Our food should be our medicine and our medicine should be our food. Hippocrates Introduction ti Nutritional
Enteral nutrition in medical ICU patients : review of advances in last five years Dr. Aditya Jindal Our food should be our medicine and our medicine should be our food. Hippocrates Introduction ti Nutritional
Interesting Case Series. Pulmonary Injury Secondary to Feeding Tube Misplacement
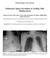 Interesting Case Series Pulmonary Injury Secondary to Feeding Tube Misplacement Thomas R. Resch, MD, Leigh A. Price, MD, and Stephen M. Milner, MBBS, BDS, FRCS (Ed), FACS Johns Hopkins Burn Center, The
Interesting Case Series Pulmonary Injury Secondary to Feeding Tube Misplacement Thomas R. Resch, MD, Leigh A. Price, MD, and Stephen M. Milner, MBBS, BDS, FRCS (Ed), FACS Johns Hopkins Burn Center, The
3.2 Nutritional Prescription of Enteral Nutrition: Achieving Target Dose of Enteral Nutrition March 2013
 . Nutritional Prescription of Enteral Nutrition: Achieving Target Dose of Enteral Nutrition March 01 There were no new randomized controlled trials since the 009 update and hence there are no changes to
. Nutritional Prescription of Enteral Nutrition: Achieving Target Dose of Enteral Nutrition March 01 There were no new randomized controlled trials since the 009 update and hence there are no changes to
Initial efficacy and tolerability of early enteral nutrition with immediate or gradual introduction in intubated patients
 Intensive Care Med (2008) 34:1054 1059 DOI 10.1007/s00134-007-0983-6 ORIGINAL Arnaud Desachy Marc Clavel Albert Vuagnat Sandrine Normand Valérie Gissot Bruno François Initial efficacy and tolerability
Intensive Care Med (2008) 34:1054 1059 DOI 10.1007/s00134-007-0983-6 ORIGINAL Arnaud Desachy Marc Clavel Albert Vuagnat Sandrine Normand Valérie Gissot Bruno François Initial efficacy and tolerability
ESPEN Congress The Hague 2017
 ESPEN Congress The Hague 2017 Using the gut in acute care patients Permissive underfeeding in practice J.-C. Preiser (BE) PERMISSIVE UNDERFEEDING IN PRACTICE ESPEN congress Jean-Charles Preiser, M.D.,
ESPEN Congress The Hague 2017 Using the gut in acute care patients Permissive underfeeding in practice J.-C. Preiser (BE) PERMISSIVE UNDERFEEDING IN PRACTICE ESPEN congress Jean-Charles Preiser, M.D.,
Nutrition. ICU Fellowship Training Radboudumc
 Nutrition ICU Fellowship Training Radboudumc Critical Care MCQ s Nasogastric (NG) and nasojejunal (NJ) feeding tubes: A. Enteral nutrition is associated with a reduced risk of bacterial and toxin translocation.
Nutrition ICU Fellowship Training Radboudumc Critical Care MCQ s Nasogastric (NG) and nasojejunal (NJ) feeding tubes: A. Enteral nutrition is associated with a reduced risk of bacterial and toxin translocation.
3.2 Nutritional Prescription of Enteral Nutrition: Enhanced Dose of Enteral Nutrition May 2015
 . Nutritional Prescription of Enteral Nutrition: Enhanced Dose of Enteral Nutrition May 015 015 Recommendation: Based on 1 level 1 study, level studies and cluster randomized controlled trials, when starting
. Nutritional Prescription of Enteral Nutrition: Enhanced Dose of Enteral Nutrition May 015 015 Recommendation: Based on 1 level 1 study, level studies and cluster randomized controlled trials, when starting
Understanding the benefits of early enteral nutrition in the major trauma patient requiring intensive care: From clinical trials to costs.
 Understanding the benefits of early enteral nutrition in the major trauma patient requiring intensive care: From clinical trials to costs. Dr. Gordon S. Doig Associate Professor in Intensive Care Northern
Understanding the benefits of early enteral nutrition in the major trauma patient requiring intensive care: From clinical trials to costs. Dr. Gordon S. Doig Associate Professor in Intensive Care Northern
Approach to Oral and Enteral Nutrition (PN) in Adults
 Approach to Oral and Enteral Nutrition (PN) in Adults Module 8.3 Topic 8 Techniques of Enteral Nutrition Johann Ockenga Learning Objectives To know about the different types of tubes and access routes;
Approach to Oral and Enteral Nutrition (PN) in Adults Module 8.3 Topic 8 Techniques of Enteral Nutrition Johann Ockenga Learning Objectives To know about the different types of tubes and access routes;
NUTRITION ISSUES IN GASTROENTEROLOGY, SERIES #79. Enteral Feedings in Hospitalized Patients: Early versus Delayed Enteral Nutrition
 Carol Rees Parrish, R.D., M.S., Series Editor Enteral Feedings in Hospitalized Patients: Early versus Delayed Enteral Nutrition by Caitlin S. Curtis, Kenneth A. Kudsk Nutrition support is a cornerstone
Carol Rees Parrish, R.D., M.S., Series Editor Enteral Feedings in Hospitalized Patients: Early versus Delayed Enteral Nutrition by Caitlin S. Curtis, Kenneth A. Kudsk Nutrition support is a cornerstone
ENTERAL NUTRITION IN THE CRITICALLY ILL
 ENTERAL NUTRITION IN THE CRITICALLY ILL 1 Ebb phase Flow phase acute response (catabolic) adoptive response (anabolic) 2 3 Metabolic Response to Stress (catabolic phase) Glucose and Protein Metabolism
ENTERAL NUTRITION IN THE CRITICALLY ILL 1 Ebb phase Flow phase acute response (catabolic) adoptive response (anabolic) 2 3 Metabolic Response to Stress (catabolic phase) Glucose and Protein Metabolism
Oklahoma Dietetic Association. Ainsley Malone, MS, RD, LD, CNSD April, 16, 2008 Permissive Underfeeding: What, Where and Why? Mt.
 The What, Why and When of Permissive Ainsley Malone, MS, RD, CNSD Nutrition Support Team Mt. Carmel West Hospital Mt. Carmel West 500 bed academic center Non-physician based NST Dietitian, pharmacist and
The What, Why and When of Permissive Ainsley Malone, MS, RD, CNSD Nutrition Support Team Mt. Carmel West Hospital Mt. Carmel West 500 bed academic center Non-physician based NST Dietitian, pharmacist and
L.Mageswary Dietitian Hospital Selayang
 L.Mageswary Dietitian Hospital Selayang 14 15 AUG ASMIC 2015 Learning Objectives 1. To understand the importance of nutrition support in ICU 2. To know the right time to feed 3. To understand the indications
L.Mageswary Dietitian Hospital Selayang 14 15 AUG ASMIC 2015 Learning Objectives 1. To understand the importance of nutrition support in ICU 2. To know the right time to feed 3. To understand the indications
Early enteral nutrition in the major trauma patient requiring intensive care: An overview of the evidence.
 Early enteral nutrition in the major trauma patient requiring intensive care: An overview of the evidence. Dr. Gordon S. Doig Associate Professor in Intensive Care Northern Clinical School Intensive Care
Early enteral nutrition in the major trauma patient requiring intensive care: An overview of the evidence. Dr. Gordon S. Doig Associate Professor in Intensive Care Northern Clinical School Intensive Care
ASPEN Safe Practices for Enteral Nutrition Therapy
 ASPEN Safe Practices for Enteral Nutrition Therapy Ainsley Malone, MS, RDN, CNSC, FAND, FASPEN Nutrition Support Dietitian Mt. Carmel West Hospital ASPEN Clinical Practice Specialist Disclosure I have
ASPEN Safe Practices for Enteral Nutrition Therapy Ainsley Malone, MS, RDN, CNSC, FAND, FASPEN Nutrition Support Dietitian Mt. Carmel West Hospital ASPEN Clinical Practice Specialist Disclosure I have
Low caloric intake is associated with nosocomial bloodstream infections in patients in the medical intensive care unit*
 Clinical Investigations Low caloric intake is associated with nosocomial bloodstream infections in patients in the medical intensive care unit* Lewis Rubinson, MD; Gregory B. Diette, MD, MHS; Xiaoyan Song,
Clinical Investigations Low caloric intake is associated with nosocomial bloodstream infections in patients in the medical intensive care unit* Lewis Rubinson, MD; Gregory B. Diette, MD, MHS; Xiaoyan Song,
Extremely well tolerated. Feeding shock
 Extremely well tolerated Feeding shock FEEDING DURING CIRCULATORY FAILURE Dr S Omar Chris Hani Baragwanath Hospital Hospital/University of Witwatersrand Introduction Circulatory shock lack of adequate
Extremely well tolerated Feeding shock FEEDING DURING CIRCULATORY FAILURE Dr S Omar Chris Hani Baragwanath Hospital Hospital/University of Witwatersrand Introduction Circulatory shock lack of adequate
Second Generation Enteral Nutrition Feeding Protocols: Taking us the the next level of performance
 Second Generation Enteral Nutrition Feeding Protocols: Taking us the the next level of performance Mr CD 47 renal transplant Severe CAP Septic shock, ARDS, MODs Requires vasopressors for days Admitting
Second Generation Enteral Nutrition Feeding Protocols: Taking us the the next level of performance Mr CD 47 renal transplant Severe CAP Septic shock, ARDS, MODs Requires vasopressors for days Admitting
5.4 Strategies to optimize delivery and minimize risks of Enteral Nutrition: Body position January 31 st, 2009
 5.4 Strategies to optimize delivery and minimize risks of Enteral Nutrition: Body position January 31 st, 2009 Recommendation: Based on 1 level 1 and 1 level 2 study, we recommend that critically ill patients
5.4 Strategies to optimize delivery and minimize risks of Enteral Nutrition: Body position January 31 st, 2009 Recommendation: Based on 1 level 1 and 1 level 2 study, we recommend that critically ill patients
VUMC Multidisciplinary Surgical Critical Care
 VUMC Multidisciplinary Surgical Critical Care Gastrointestinal Stress Ulcer Prophylaxis Guideline: Background: Work by Cooke and colleagues ascribed the risk of overt bleeding to be 4.4% and clinically
VUMC Multidisciplinary Surgical Critical Care Gastrointestinal Stress Ulcer Prophylaxis Guideline: Background: Work by Cooke and colleagues ascribed the risk of overt bleeding to be 4.4% and clinically
/03/ $03.00/0 Vol. 27, No. 5 JOURNAL OF PARENTERAL AND ENTERAL NUTRITION
 0148-6071/03/2705-0355$03.00/0 Vol. 27, No. 5 JOURNAL OF PARENTERAL AND ENTERAL NUTRITION Printed in U.S.A. Copyright 2003 by the American Society for Parenteral and Enteral Nutrition Special Interest
0148-6071/03/2705-0355$03.00/0 Vol. 27, No. 5 JOURNAL OF PARENTERAL AND ENTERAL NUTRITION Printed in U.S.A. Copyright 2003 by the American Society for Parenteral and Enteral Nutrition Special Interest
Pediatric ER Half-day Rounds October 12, 2011 Dr. Karen Bailey
 Pediatric ER Half-day Rounds October 12, 2011 Dr. Karen Bailey Objectives to identify various enteral and vascular access lines what do they look like? indications & contraindications proper placement
Pediatric ER Half-day Rounds October 12, 2011 Dr. Karen Bailey Objectives to identify various enteral and vascular access lines what do they look like? indications & contraindications proper placement
Nutrition Protocol for Intensive Care Beatrice CL Lim et al Letter to the Editor
 416 Letter to the Editor Implementation of a Proactive Nutrition Protocol Improves Enteral Nutrition in Mechanically Ventilated Patients Admitted to the Neuro-Intensive Care Unit Dear Editor, The enteral
416 Letter to the Editor Implementation of a Proactive Nutrition Protocol Improves Enteral Nutrition in Mechanically Ventilated Patients Admitted to the Neuro-Intensive Care Unit Dear Editor, The enteral
Accepted Article. Massive gastrointestinal pneumatosis in a patient with celiac disease and superior mesenteric artery syndrome
 Accepted Article Massive gastrointestinal pneumatosis in a patient with celiac disease and superior mesenteric artery syndrome Aleix Martínez-Pérez, Ramón Trullenque-Juan, Sandra Santarrufina-Martínez,
Accepted Article Massive gastrointestinal pneumatosis in a patient with celiac disease and superior mesenteric artery syndrome Aleix Martínez-Pérez, Ramón Trullenque-Juan, Sandra Santarrufina-Martínez,
Nutritional Management in Enterocutaneous fistula Dr Deepak Govil
 Nutritional Management in Enterocutaneous fistula Dr Deepak Govil MS, PhD (GI Surgery) Senior Consultant Surgical Gastroenterology Indraprastha Apollo Hospital New Delhi What is enterocutaneous fistula
Nutritional Management in Enterocutaneous fistula Dr Deepak Govil MS, PhD (GI Surgery) Senior Consultant Surgical Gastroenterology Indraprastha Apollo Hospital New Delhi What is enterocutaneous fistula
Feeding the septic patient How and when? Masterclass ICU nurses
 Feeding the septic patient How and when? Masterclass ICU nurses Case Male, 60 - No PMH - L 1.74 m and W 85 kg Pneumococcal pneumonia Stable hemodynamics - No AKI MV in prone position (PEEP 16 - FiO2 60%)
Feeding the septic patient How and when? Masterclass ICU nurses Case Male, 60 - No PMH - L 1.74 m and W 85 kg Pneumococcal pneumonia Stable hemodynamics - No AKI MV in prone position (PEEP 16 - FiO2 60%)
WHEN To Initiate Parenteral Nutrition A Frequent Question With New Answers
 WHEN To Initiate Parenteral Nutrition A Frequent Question With New Answers Ainsley Malone, MS, RD, LD, CNSC, FAND, FASPEN Dubai International Nutrition Conference 2018 Disclosures No commercial relationship
WHEN To Initiate Parenteral Nutrition A Frequent Question With New Answers Ainsley Malone, MS, RD, LD, CNSC, FAND, FASPEN Dubai International Nutrition Conference 2018 Disclosures No commercial relationship
E S T A B L I S H I N G N U T R I T I O N I N Y O U R I C U The Need for a Protocol
 E S T A B L I S H I N G N U T R I T I O N I N Y O U R I C U The Need for a Protocol Arthur RH van Zanten, MD PhD Gelderse Vallei Hospital, Ede, The Netherlands Learning objectives Develop an evidence based
E S T A B L I S H I N G N U T R I T I O N I N Y O U R I C U The Need for a Protocol Arthur RH van Zanten, MD PhD Gelderse Vallei Hospital, Ede, The Netherlands Learning objectives Develop an evidence based
ESPEN Congress The Hague 2017
 ESPEN Congress The Hague 2017 Meeting nutritional needs of acute care patients Feeding acute pancreatitis patients J. Luttikhold (NL) FEEDING ACUTE PANCREATITIS PATIENTS Joanna Luttikhold, MD PhD Registrar
ESPEN Congress The Hague 2017 Meeting nutritional needs of acute care patients Feeding acute pancreatitis patients J. Luttikhold (NL) FEEDING ACUTE PANCREATITIS PATIENTS Joanna Luttikhold, MD PhD Registrar
Why You Switched to the Tiger 2 Self-Advancing Nasal Jejunal Feeding Tube
 Why You Switched to the Tiger 2 Self-Advancing Nasal Jejunal Feeding Tube Ease of Use Self-advancing technology minimises hands-on time for clinicians. Requires no additional devices or costly capital
Why You Switched to the Tiger 2 Self-Advancing Nasal Jejunal Feeding Tube Ease of Use Self-advancing technology minimises hands-on time for clinicians. Requires no additional devices or costly capital
Pharmaconutrition in PICU. Gan Chin Seng Paediatric Intensivist UMMC
 Pharmaconutrition in PICU Gan Chin Seng Paediatric Intensivist UMMC Pharmaconutrition in Critical Care Unit Gan Chin Seng Paediatric Intensivist UMMC Definition New concept Treatment with specific nutrients
Pharmaconutrition in PICU Gan Chin Seng Paediatric Intensivist UMMC Pharmaconutrition in Critical Care Unit Gan Chin Seng Paediatric Intensivist UMMC Definition New concept Treatment with specific nutrients
Scott A. Lynch, MD, MPH,FAAFP Assistant Professor
 Scott A. Lynch, MD, MPH,FAAFP Assistant Professor Lynch.Scott@mayo.edu 2015 MFMER 3543652-1 Nutrition in the Hospital Mayo School of Continuous Professional Development 2nd Annual Inpatient Medicine for
Scott A. Lynch, MD, MPH,FAAFP Assistant Professor Lynch.Scott@mayo.edu 2015 MFMER 3543652-1 Nutrition in the Hospital Mayo School of Continuous Professional Development 2nd Annual Inpatient Medicine for
Gastroesophageal Reflux Disease in Infants and Children
 Gastroesophageal Reflux Disease in Infants and Children 4 Marzo 2017 Drssa Chiara Leoni Drssa Valentina Giorgio pediatriagastro@gmail.com valentinagiorgio1@gmail.com Definitions: GER GER is the passage
Gastroesophageal Reflux Disease in Infants and Children 4 Marzo 2017 Drssa Chiara Leoni Drssa Valentina Giorgio pediatriagastro@gmail.com valentinagiorgio1@gmail.com Definitions: GER GER is the passage
11.1 Supplemental Antioxidant Nutrients: Combined Vitamins and Trace Elements April 2013
 . Supplemental Antioxidant Nutrients: Combined Vitamins and Trace Elements April 23 23 Recommendation: Based on 7 level and 7 level 2 studies, the use of supplemental combined vitamins and trace elements
. Supplemental Antioxidant Nutrients: Combined Vitamins and Trace Elements April 23 23 Recommendation: Based on 7 level and 7 level 2 studies, the use of supplemental combined vitamins and trace elements
Interruption of enteral nutrition in the intensive care unit: a single-center survey
 Uozumi et al. Journal of Intensive Care (2017) 5:52 DOI 10.1186/s40560-017-0245-9 RESEARCH Open Access Interruption of enteral nutrition in the intensive care unit: a single-center survey Midori Uozumi
Uozumi et al. Journal of Intensive Care (2017) 5:52 DOI 10.1186/s40560-017-0245-9 RESEARCH Open Access Interruption of enteral nutrition in the intensive care unit: a single-center survey Midori Uozumi
10/3/2012. Pediatric Parenteral Nutrition A Comprehensive Review
 Critical Care Nutrition Foundation for Moving Forward Justine Turner MD PhD Department of Pediatric Gastroenterology and Nutrition University of Alberta I have the following financial relationships to
Critical Care Nutrition Foundation for Moving Forward Justine Turner MD PhD Department of Pediatric Gastroenterology and Nutrition University of Alberta I have the following financial relationships to
ARTICLES ENTERAL FEEDING TOLERANCE IN CRITICALLY ILL PATIENTS PATIENTS AND METHODS
 JCN1102pg000ED 11/6/02 8:08 AM Page 96 96 ENTERAL FEEDING TOLERANCE IN CRITICALLY ILL PATIENTS T E Madiba, A A Haffejee, J Downs, D J J Muckart Objective. To assess tolerance of enteral feeding in intensive
JCN1102pg000ED 11/6/02 8:08 AM Page 96 96 ENTERAL FEEDING TOLERANCE IN CRITICALLY ILL PATIENTS T E Madiba, A A Haffejee, J Downs, D J J Muckart Objective. To assess tolerance of enteral feeding in intensive
Avoidable Causes of Delayed Enteral Nutrition in Critically Ill Children
 ORIGINAL ARTICLE Pediatrics http://dx.doi.org/10.3346/jkms.2013.28.7.1055 J Korean Med Sci 2013; 28: 1055-1059 Avoidable Causes of Delayed Enteral Nutrition in Critically Ill Children Hosun Lee, 1 Shin
ORIGINAL ARTICLE Pediatrics http://dx.doi.org/10.3346/jkms.2013.28.7.1055 J Korean Med Sci 2013; 28: 1055-1059 Avoidable Causes of Delayed Enteral Nutrition in Critically Ill Children Hosun Lee, 1 Shin
Ernährungstherapie des Kritisch Kranken Enteral Parenteral Ganz egal?
 Ernährungstherapie des Kritisch Kranken Enteral Parenteral Ganz egal? PD Dr. med. Claudia Heidegger Service des Soins Intensifs Genf/Schweiz Dresden 11. Juni 2016 Nutrition News Nutrition controversy in
Ernährungstherapie des Kritisch Kranken Enteral Parenteral Ganz egal? PD Dr. med. Claudia Heidegger Service des Soins Intensifs Genf/Schweiz Dresden 11. Juni 2016 Nutrition News Nutrition controversy in
Vanderbilt University Medical Center Trauma ICU Nutrition Management Guidelines
 Vanderbilt University Medical Center Trauma ICU Nutrition Management Guidelines Trauma Critical Care Nutrition Guidelines Clinical judgment may supersede guidelines as patient circumstances warrant ASSESSMENT
Vanderbilt University Medical Center Trauma ICU Nutrition Management Guidelines Trauma Critical Care Nutrition Guidelines Clinical judgment may supersede guidelines as patient circumstances warrant ASSESSMENT
Timing of Parenteral Nutrition
 Timing of Parenteral Nutrition Arun Bansal; MD, FCCM, MRCPCH Professor Pediatric Critical Care PGIMER, Chandigarh, INDIA drarunbansal@gmail.com Malnutrition in Critically Ill Incidence: from 19 32% Associated
Timing of Parenteral Nutrition Arun Bansal; MD, FCCM, MRCPCH Professor Pediatric Critical Care PGIMER, Chandigarh, INDIA drarunbansal@gmail.com Malnutrition in Critically Ill Incidence: from 19 32% Associated
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abdominal pain, enteral therapy in acute pancreatitis and, 812 Abscess(es), pancreatic, nutritional support for, 814 815 Acute Physiology and
Note: Page numbers of article titles are in boldface type. A Abdominal pain, enteral therapy in acute pancreatitis and, 812 Abscess(es), pancreatic, nutritional support for, 814 815 Acute Physiology and
Home Total Parenteral Nutrition for Adults
 Home Total Parenteral Nutrition for Adults Policy Number: Original Effective Date: MM.08.007 05/21/1999 Line(s) of Business: Current Effective Date: PPO, HMO, QUEST Integration 05/27/2016 Section: Home
Home Total Parenteral Nutrition for Adults Policy Number: Original Effective Date: MM.08.007 05/21/1999 Line(s) of Business: Current Effective Date: PPO, HMO, QUEST Integration 05/27/2016 Section: Home
Nutrition care plan. Components and development
 Nutrition care plan Components and development Objectives To define the nutrition care plan To present the components of the nutrition care plan To discuss the different approaches in determining the contents
Nutrition care plan Components and development Objectives To define the nutrition care plan To present the components of the nutrition care plan To discuss the different approaches in determining the contents
Dong Wang, MD, 1,2 Shao-Qin Zheng, MD, 1 Xian-Cai Chen, MD, 2 Shi-Wen Jiang, MD, 3 and
 clinical article J Neurosurg 123:1194 1201, 2015 Comparisons between small intestinal and gastric feeding in severe traumatic brain injury: a systematic review and meta-analysis of randomized controlled
clinical article J Neurosurg 123:1194 1201, 2015 Comparisons between small intestinal and gastric feeding in severe traumatic brain injury: a systematic review and meta-analysis of randomized controlled
Nutritional Support in the Perioperative Period
 Nutritional Support in the Perioperative Period Topic 17 Module 17.3 Nutritional Support in the Perioperative Period Ken Fearon Learning Objectives Understand the principles behind nutritional care for
Nutritional Support in the Perioperative Period Topic 17 Module 17.3 Nutritional Support in the Perioperative Period Ken Fearon Learning Objectives Understand the principles behind nutritional care for
Severe necrotizing pancreatitis. ICU Fellowship Training Radboudumc
 Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
PRACTICE MANAGEMENT GUIDELINES FOR NUTRITIONAL SUPPORT OF THE TRAUMA PATIENT
 PRACTICE MANAGEMENT GUIDELINES FOR NUTRITIONAL SUPPORT OF THE TRAUMA PATIENT The EAST Practice Management Guidelines Workgroup: Danny O. Jacobs, MD, David G. Jacobs, MD, Kenneth A. Kudsk, MD, Frederick
PRACTICE MANAGEMENT GUIDELINES FOR NUTRITIONAL SUPPORT OF THE TRAUMA PATIENT The EAST Practice Management Guidelines Workgroup: Danny O. Jacobs, MD, David G. Jacobs, MD, Kenneth A. Kudsk, MD, Frederick
Prevention of Aspiration
 1 Prevention of Aspiration Scope and Impact of Problem Critically ill patients have an increased risk for aspirating oropharyngeal secretions and regurgitated gastric contents. For those who are tube-fed,
1 Prevention of Aspiration Scope and Impact of Problem Critically ill patients have an increased risk for aspirating oropharyngeal secretions and regurgitated gastric contents. For those who are tube-fed,
Nutrition in critical illness:
 Nutrition in critical illness: from theory to daily practice Aim of the presentation Summarize the guidelines for the provision and assessment of nutrition support therapy in the adult critically ill patient.
Nutrition in critical illness: from theory to daily practice Aim of the presentation Summarize the guidelines for the provision and assessment of nutrition support therapy in the adult critically ill patient.
Critical illness or major surgery usually results in
 : Improving Outcomes in Multiple Trauma and Gastrointestinal Cancer Resection Rex O. Brown, PharmD, FCCP, BCNSP ABSTRACT Immune-enhancing diets are nutritionally complete enteral nutrition formulations
: Improving Outcomes in Multiple Trauma and Gastrointestinal Cancer Resection Rex O. Brown, PharmD, FCCP, BCNSP ABSTRACT Immune-enhancing diets are nutritionally complete enteral nutrition formulations
8.0 Parenteral Nutrition vs. Standard care May 2015
 8.0 Parenteral Nutrition vs. Standard care May 015 015 Recommendation: Based on 6 level studies, in critically ill patients with an intact gastrointestinal tract, we recommend that parenteral nutrition
8.0 Parenteral Nutrition vs. Standard care May 015 015 Recommendation: Based on 6 level studies, in critically ill patients with an intact gastrointestinal tract, we recommend that parenteral nutrition
Nutritional support is an integral, though often neglected,
 The Journal of TRAUMA Injury, Infection, and Critical Care Clinical Management Update Practice Management Guidelines for Nutritional Support of the Trauma Patient David G. Jacobs, MD, Danny O. Jacobs,
The Journal of TRAUMA Injury, Infection, and Critical Care Clinical Management Update Practice Management Guidelines for Nutritional Support of the Trauma Patient David G. Jacobs, MD, Danny O. Jacobs,
VOLUME-BASED VS. RATE-BASED FEEDING
 VOLUME-BASED VS. RATE-BASED FEEDING Amanda Holyk Critical Care Pharmacist Mount Nittany Medical Center Society of Critical Care Medicine Annual Symposium November 10, 2017 0 Disclosure I have no actual
VOLUME-BASED VS. RATE-BASED FEEDING Amanda Holyk Critical Care Pharmacist Mount Nittany Medical Center Society of Critical Care Medicine Annual Symposium November 10, 2017 0 Disclosure I have no actual
Nutrition therapy in the critical care setting: What is best achievable practice? An international multicenter observational study*
 Continuing Medical Education Article Nutrition therapy in the critical care setting: What is best achievable practice? An international multicenter observational study* Naomi E. Cahill, RD, MSc; Rupinder
Continuing Medical Education Article Nutrition therapy in the critical care setting: What is best achievable practice? An international multicenter observational study* Naomi E. Cahill, RD, MSc; Rupinder
Kombinierte enterale und parenterale Ernährung für welche PatientInnen?
 2014 Kombinierte enterale und parenterale Ernährung für welche PatientInnen? Dr. CP. Heidegger Intensive Care/Geneva claudia-paula.heidegger@hcuge.ch Bern Freitag, 4. April 2014 Nutrition News Worldwide
2014 Kombinierte enterale und parenterale Ernährung für welche PatientInnen? Dr. CP. Heidegger Intensive Care/Geneva claudia-paula.heidegger@hcuge.ch Bern Freitag, 4. April 2014 Nutrition News Worldwide
Nutrition in children with special needs. Dr. Meenakshi J.
 Nutrition in children with special needs Dr. Meenakshi J. 1 Factors affecting growth and nutrition in children with special nutritional factors Inadequate intake primarily related to feeding dysfunction
Nutrition in children with special needs Dr. Meenakshi J. 1 Factors affecting growth and nutrition in children with special nutritional factors Inadequate intake primarily related to feeding dysfunction
Title: Aerophagia due to abdomino-phrenic dyssynergia in a 2-year-old child. Authors: Pablo Ercoli, Belinda García, Enrique del Campo, Sergio Pinillos
 Title: Aerophagia due to abdomino-phrenic dyssynergia in a 2-year-old child Authors: Pablo Ercoli, Belinda García, Enrique del Campo, Sergio Pinillos DOI: 10.17235/reed.2018.5444/2017 Link: PubMed (Epub
Title: Aerophagia due to abdomino-phrenic dyssynergia in a 2-year-old child Authors: Pablo Ercoli, Belinda García, Enrique del Campo, Sergio Pinillos DOI: 10.17235/reed.2018.5444/2017 Link: PubMed (Epub
Nutrition Services at a glance
 Nutrition Services at a glance Ragini Raghuveer, MS, RD, LD/N Systems Clinical Nutrition Manager Linette De Armas, RD, LD/N Clinical Dietitian Melissa Lorenzo, RD, LD/N Clinical Dietitian 1 Learning Objectives
Nutrition Services at a glance Ragini Raghuveer, MS, RD, LD/N Systems Clinical Nutrition Manager Linette De Armas, RD, LD/N Clinical Dietitian Melissa Lorenzo, RD, LD/N Clinical Dietitian 1 Learning Objectives
14-15 Aug ASMIC L.Mageswary Dietitian Hospital Selayang
 14-15 Aug ASMIC 2015 Nurses Role L.Mageswary Dietitian Hospital Selayang Doctor Dietitian Pharmacist Nurse Physiotherapist Occupational therapist Patient Patient Centered Care Patients needs & preferences
14-15 Aug ASMIC 2015 Nurses Role L.Mageswary Dietitian Hospital Selayang Doctor Dietitian Pharmacist Nurse Physiotherapist Occupational therapist Patient Patient Centered Care Patients needs & preferences
THE AUTHOR OF THIS WHAT S NEW IN NUTRITION? OBJECTIVES & OUTLINE EVIDENCE-BASED MEDICINE: PARENTERAL NUTRITION (PN)
 WHAT S NEW IN NUTRITION? Alisha Mutch, Pharm.D., BCPS THE AUTHOR OF THIS PRESENTATION HAS NOTHING TO DISCLOSE. OBJECTIVES & OUTLINE MALNUTRITION OBJECTIVES Indicate when parenteral nutrition (PN) is warranted
WHAT S NEW IN NUTRITION? Alisha Mutch, Pharm.D., BCPS THE AUTHOR OF THIS PRESENTATION HAS NOTHING TO DISCLOSE. OBJECTIVES & OUTLINE MALNUTRITION OBJECTIVES Indicate when parenteral nutrition (PN) is warranted
When to start SPN in critically ill patients? Refereeravond IC
 When to start SPN in critically ill patients? Refereeravond IC Introduction (1) Protein/calorie malnutrition is very frequent in critically ill patients Protein/calorie malnutrition is associated with
When to start SPN in critically ill patients? Refereeravond IC Introduction (1) Protein/calorie malnutrition is very frequent in critically ill patients Protein/calorie malnutrition is associated with
Small bowel feeding and risk of pneumonia in adult critically ill patients: a systematic review and meta-analysis of randomized trials
 Critical Care This Provisional PDF corresponds to the article as it appeared upon acceptance. Copyedited and fully formatted PDF and full text (HTML) versions will be made available soon. Small bowel feeding
Critical Care This Provisional PDF corresponds to the article as it appeared upon acceptance. Copyedited and fully formatted PDF and full text (HTML) versions will be made available soon. Small bowel feeding
Nutritional Support For The Critical Patient Andrea Collins, BBA, LVT, VTS (ECC)
 Nutritional Support For The Critical Patient Andrea Collins, BBA, LVT, VTS (ECC) TOPICS PART 1 Importance Indications for support Nutritional assessment Energy requirements The plan Enteral/Parenteral
Nutritional Support For The Critical Patient Andrea Collins, BBA, LVT, VTS (ECC) TOPICS PART 1 Importance Indications for support Nutritional assessment Energy requirements The plan Enteral/Parenteral
NUTRITION SUPPORT DURING EXTRACORPOREAL MEMBRANE OXYGENATION (ECMO) IN CRITICALLY ILL ADULT PATIENTS. Haley Murrell, March 19, 2015
 NUTRITION SUPPORT DURING EXTRACORPOREAL MEMBRANE OXYGENATION (ECMO) IN CRITICALLY ILL ADULT PATIENTS Haley Murrell, March 19, 2015 Objectives Provide an overview of Extracorporeal Membrane Oxygenation
NUTRITION SUPPORT DURING EXTRACORPOREAL MEMBRANE OXYGENATION (ECMO) IN CRITICALLY ILL ADULT PATIENTS Haley Murrell, March 19, 2015 Objectives Provide an overview of Extracorporeal Membrane Oxygenation
Chapter 29 Gastrointestinal Intubation
 Chapter 29 Gastrointestinal Intubation Intubation Intubation: placement of a tube into a body structure Types of intubation Orogastric: mouth to stomach Nasogastric: nose to stomach Nasointestinal: nose
Chapter 29 Gastrointestinal Intubation Intubation Intubation: placement of a tube into a body structure Types of intubation Orogastric: mouth to stomach Nasogastric: nose to stomach Nasointestinal: nose
MAIN FEATURES. OF THE PEP up PROTOCOL. All patients will receive Peptamen 1.5 initially. All patients will start on Beneprotein
 MAIN FEATURES OF THE PEP up PROTOCOL All patients will receive Peptamen 1.5 initially All patients will start on Beneprotein - 2 packets (14 g) mixed in 120ml water administered bid via NG All patients
MAIN FEATURES OF THE PEP up PROTOCOL All patients will receive Peptamen 1.5 initially All patients will start on Beneprotein - 2 packets (14 g) mixed in 120ml water administered bid via NG All patients
ENTERAL FEEDING GUIDELINES INTRODUCTION
 INTRODUCTION Enteral feeding is defined as the administration of nutrients directly into the gastrointestinal (GI) tract. If the patient is unable to meet his/her nutritional requirements with oral diet/nutritional
INTRODUCTION Enteral feeding is defined as the administration of nutrients directly into the gastrointestinal (GI) tract. If the patient is unable to meet his/her nutritional requirements with oral diet/nutritional
Stressed Out: Evaluating the Need for Stress Ulcer Prophylaxis in the ICU
 Stressed Out: Evaluating the Need for Stress Ulcer Prophylaxis in the ICU Josh Arnold, PharmD PGY1 Pharmacy Resident Pharmacy Grand Rounds November 8, 2016 2016 MFMER slide-1 Objectives Identify the significance
Stressed Out: Evaluating the Need for Stress Ulcer Prophylaxis in the ICU Josh Arnold, PharmD PGY1 Pharmacy Resident Pharmacy Grand Rounds November 8, 2016 2016 MFMER slide-1 Objectives Identify the significance
