LONG-TERM PARENTERAL NUTRITIONAL SUPPORT AND INTESTINAL ADAPTATION IN CHILDREN WITH SHORT BOWEL SYNDROME: A 25-YEAR EXPERIENCE
|
|
|
- Nickolas Powers
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLES LONG-TERM PARENTERAL NUTRITIONAL SUPPORT AND INTESTINAL ADAPTATION IN CHILDREN WITH SHORT BOWEL SYNDROME: A 25-YEAR EXPERIENCE RUBÉN E. QUIRÓS-TEJEIRA,MD,MARVIN E. AMENT,MD,LAURIE REYEN, RN,FAYE HERZOG,RN, MICHELLE MERJANIAN,MD, NANCY OLIVARES-SERRANO, MD, AND JORGE H. VARGAS, MD Objective To analyze the outcome of children with short bowel syndrome (SBS) who required long-term parenteral nutrition (PN). Study design Retrospective analysis of children (n = 78) with SBS who required PN >3 months from 1975 to Statistics: univariate analysis, Kaplan-Meier method, and Cox proportional regression model were used. Results We identified 78 patients. Survival was better with small bowel length (SBL) >38 cm, intact ileocecal valve (ICV), intact colon, takedown surgery after ostomy (all P <.01), and primary anastomosis (P <.001). PN-associated early persistent cholestatic jaundice (P <.001) and SBL of <15cm (P <.01) were associated with a higher mortality. Intestinal adaptation was less likely if SBL <15 cm (P <.05), ICV was removed, colonic resection was done (both P <.001), >50% of colon was resected (P <.05), and primary anastomosis could not be accomplished (P <.01). Survival was 73% (57), and 77% (44) of survivors had intestinal adaptation. Conclusions SBL, intact ICV, intestinal continuity, and preservation of the colon are important factors for survival and adaptation. Adaptation usually occurred within the first 3 years. Need for long-term PN does not preclude achieving productive adulthood. Patients with ICV even with <15 cm of SBL and patients with SBL >15 cm without ICV have a chance of intestinal adaptation. (J Pediatr 2004;145:157-63) In 1880, Koeberle performed the first reported massive small bowel resection (>200 cm) in a patient who ultimately survived. 1 In 1937, Haymond reported that if >50% of the small bowel was resected the mortality was extremely high. 2 During the late 1960s, parenteral nutrition (PN) became available, improving dramatically the management and outcome of patients with short bowel syndrome (SBS). 3 In 1972, Wilmore s review suggested that without the ileocecal valve (ICV), a jejunoileal segment of $38 cm was needed for intestinal adaptation, and if the ICV was preserved, this might happen with $15 cm of a jejunoileal segment. 4 Today, prolonged survival has allowed us to better understand the adaptation process by the residual small bowel. On the other hand, long-term PN support has brought new clinical and physiological challenges. PN-related morbidity and mortality have been major concerns since the initiation of its use. 5 To learn more about the clinical outcome of children with SBS who required longterm PN support and about their intestinal adaptation, we analyzed the subjects recruited in our 25-year-old home PN program. METHODS We analyzed the complete charts of all children who required PN support at UCLA for more than 3 months from January 1975 to April 2000 (n = 875). We defined SBS as CVC ESLD ICV NEC PN Central venous catheter End-stage liver disease Ileocecal valve Necrotizing enterocolitis Parenteral nutrition SBS SBL SSB USSB VSSB Short bowel syndrome Small bowel length Short small bowel Ultra short small bowel Very short small bowel See editorial, p 147. From the Division of Gastroenterology and Nutrition, UCLA Medical Center, Los Angeles, California; and Section of Pediatric Gastroenterology, Hepatology and Nutrition, Baylor College of Medicine, Houston, Texas. Submitted for publication Mar 17, 2003; last revision received Jan 22, 2004; accepted Feb 17, Reprint requests: Rubén E. Quirós- Tejeira, MD, Baylor College of Medicine, Department of Pediatrics- Gastroenterology & Nutrition, 6621 Fannin St, MC CC , Houston, TX rquiros@bcm.tmc. edu /$ - see front matter Copyright ª 2004 Elsevier Inc. All rights reserved /j.jpeds
2 a residual jejunoileal segment of #75 cm secondary to a surgical resection or congenital malformation. 4 Children were subdivided into three groups according to their jejunoileal segment: (1) Short small bowel (SSB), >38 cm; (2) Very short small bowel (VSSB), 15 to 38 cm; and (3) Ultra short small bowel (USSB), < 15cm. The cited small bowel lengths (SBLs) are the measurements along the antimesenteric border from the ligament of Treitz that were made at the time of surgery; colonic resection and remaining length were obtained from the operative report measurements and descriptions. Intestinal adaptation was defined as the ability to maintain normal growth and fluid and electrolytes balance without the need for PN support. The following data were collected from each patient: sex; date of birth; gestational age; birth weight; PN starting date; proportion of caloric support (enteral versus parenteral); date when PN was stopped; date when central venous catheter (CVC) was placed and removed; cause of SBS; SBL left; resection or not of the ICV; colonic resection; length of colon left; primary anastomosis versus ostomy; date of takedown surgery; date of gastrostomy tube placement and removal; cholecystectomy; evidence of bone disease; CVC-related sepsis; evaluation of sepsis; PN-associated complication (cholestatic jaundice, gallstones, cholecystitis, end-stage liver disease [ESLD], nutritional deficiencies, chronic anemia, deep vein thrombosis or embolus, pancreatitis, diabetes, and muscle cramps); level of education reached; developmental evaluation; marital status; working status; occupation; growth charts; liver function tests; renal function tests; iron studies; complete blood count and differential; electrolytes including calcium, magnesium and phosphorus, albumin, and prealbumin; cause of death; date of death; need for liver/small bowel transplantation; and other comorbidities. Cholestatic jaundice was defined as conjugated bilirubin $2.0 mg/dl (or $34.2 lmol/l). Home PN support, usually cycled at night over 10 to 14 hours, was provided through indwelling Broviac catheters. Catheter insertion and care are standardized, as we previously described. 6 In the adapted children, CVC was usually left for 3 to 6 months after discontinuation of PN, in anticipation of problems that may develop with enteral feeding. The PN solutions, infusion principles, outpatient management, and changes done in our home PN support program at UCLA have been previously described. 7,8 The proportions of nonprotein calories (dextrose and fat emulsion) were customized to individual requirements and tolerance. A comprehensive training period in the hospital was given to parents or guardians because they would be assuming full care and responsibility for CVC and PN at home. The major nutritional criterion for discharge from the hospital was evidence of steady weight gain on cycled PN and, in most instances, some enteral feedings. In all children, the nutritional management includes the establishment of enteral feedings as soon as possible. Even though, the nature of elemental formulas has changed over the past 25 years; the main principle has been the use of a dilute elemental formula or breast milk continuously infused via nasogastric or gastrostomy tube. 9 As intestinal adaptation or decreased stool output occurs, the elemental formula is increased in amount and concentration. and gradually the feeding is changed to boluses. 8 PN is decreased accordingly as growth is closely monitored to ensure a normal pattern. When growth is supported mainly by enteral nutrition, the PN is stopped. About 10% weight loss is accepted during the few months after stopping PN as long as weight is regained and normal growth ensues. Initial enteral nutritional support was defined as the percentage of calories originated from elemental formula in relation to the total amount of calories provided to the child by 2 weeks after the initial surgery. For CVC-related sepsis, we followed our definition and protocol as described. 10 In short, it was defined as an infection where an organism was identified through blood culture from the CVC and other potential sources of infection were ruled out by appropriate tests. 10 Statistics Values are given in percentage, median (range), and mean ± SD. Mean z score for weight and height were calculated to control for age and sex. We performed a univariate analysis of all the variables using v 2 test methods or two-sample t test. The significance of differences in all binary variables in the time to death (death rate) or intestinal adaptation (adaptation rate) was also assessed using the nonparametric log rank test. Survival and intestinal adaptation probabilities were calculated using the Kaplan-Meier method in those variables that were statistically significant. A Cox proportional hazards regression model, after adjusting for highly correlated variables, was used with parameters that were statistically significant after the univariate analysis. A P value <.05 was considered statistically significant. RESULTS We identified 78 patients. Forty-nine were male. PN was started at the median age of 0.6 months ( months). In Table I we compared the characteristics of survivors versus nonsurvivors. We found better survival with SBL >38 cm, intact ICV, whole colon left, primary anastomosis, and takedown surgery after an initial ostomy. Early persistent cholestatic jaundice and SBL < 15cm were associated with higher mortality. These results were duplicated when all binary variables were analyzed by determining the death rate (deaths per 100 person-years) in each category. The only difference was that the diagnosis of necrotizing enterocolitis (NEC) became statistically significant (7.7 ± 2.9 vs 2.6 ± 0.7 deaths per 100 person-years; P <.05). The Kaplan-Meier method was used to analyze these statistically significant variables and two of these variables are presented in Figure 1. We analyzed survivors who had intestinal adaptation versus the ones who did not (Table II). Intestinal adaptation was less likely if SBL < 15 cm, ICV was removed, colonic resection was done, >50% of the colon was resected, and primary anastomosis could not be accomplished. The incidence of PN-associated gallstones/cholecystitis with subsequent 158 Quirós-Tejeira et al The Journal of Pediatrics August 2004
3 Table I. Characteristics of patients with SBS and PN support (survivors vs nonsurvivors) Background information Surviviors (n = 57) Nonsurvivors (n = 21) P value Sex (M) 63% 62% NS Birth weight (kg) 2.5 ± ± 1.2 NS Prematurity 47% 67% NS (<37 wk GA) Age when PN was 9.4 ± ± 25.9 NS started (mo) * Initial enteral 23% 12% NS nutritional support (mean %) y Primary diagnosis NEC 16% (9) 33% (7) NS Congenital 21% (12) 14% (3) NS malrotation/ volvulus Small bowl atresia 26% (15) 19% (4) NS Gastroschisis 21% (12) 19% (4) NS Others z 16% (9) 14% (3) NS SBL >38 cm 58% 24% < cm 28% 33% NS < 15 cm 14% 43% <.01 Patients with ICV 58% 29% <.01 Colonic resection 42% 71% <.01 >50% of colonic 46% (11/24) 47% (7/15) NS length resected Primary 40% 10% <.001 anastomosis Takedown surgery 94% (32/34) 58% (11/19) <.01 after ostomy Cholecystectomy 18% 38% NS Gastrostomy tube 63% 67% NS placed PN-associated 42% 90% <.001 complications PN-associated early 9% 62% <.001 persistent cholestatic jaundice k Infections per year on PN 1.1 ± ± 1.0 NS GA, Gestational age; NEC, necrotizing enterocolitis; NS, Not statistically significant. Values are given in mean ± SD or percentage. Statistically significant: P <.05. *Median age was 0.6 months for both groups. yestablished by 2 weeks after first surgery. zomphalocele(3), post-surgical intestinal obstruction (3), congenital SBS (3), abdominal trauma (2) and small bowel lymphoma (1). Secondary to gallstones and/or cholecystitis. kearly persistent cholestatic jaundice = cholestatic jaundice that started within the first 3 months on parenteral nutrition and lasted for more than 3 months. Fig 1. Probability of survival in 78 children with SBS based on (A) early persistent cholestatic jaundice and (B) primary anastomosis. cholecystectomy was higher in children who did not have adaptation. When all binary variables were analyzed by determining the adaptation rate (adaptations per 100 person-years) in each category, the same parameters were statistically significant except SBL >38 cm that became statistically significant (54 ± 10.2 versus 8.7 ± 2.2 adaptations per 100 person-years; P <.001). The Kaplan-Meier method was used to analyze these statistically significant variables, and two of them are represented in Figure 2. The shortest SBL of a patient who adapted was 10 cm with ICV. Patients who did not adapt had fewer episodes of CVC-related sepsis per year than the ones who adapted (Table II) even though, as expected, their time on PN support was longer. Long-Term Parenteral Nutritional Support and Intestinal Adaptation in Children with Short Bowel Syndrome: A 25-year Experience 159
4 Table II. Characteristics of patients with SBS and PN Support (adapted vs nonadapted) Background information Adapted (n = 44) Nonadapted (n = 13) P value Age (y) 10.3 ± ± 7.4 NS Sex (M) 66% 54% NS Birth weight (kg) 2.5 ± ± 0.8 NS Prematurity (<37 wk GA) 50% 38% NS Age when PN was 10.3 ± ± 15.6 NS started (mo) * Initial enteral nutritional 24% 20% NS support (mean %) y Primary diagnosis NEC 18% (8) 8% (1) NS Congenital malrotation/ 23% (10) 15% (2) NS volvulus Small bowel atresia(s) 25% (11) 31% (4) NS Gastroschisis 23% (10) 15% (2) NS Others 11% (5) 31% (4) NS SBL >38 cm 64% 38% NS cm 30% 23% NS <15 cm 7% 38% <.05 Patients with ICV 68% 23% <.001 Colonic resection 32% 77% <.001 >50% of colonic length 29% (4/14) 70% (7/10) <.05 resected Primary anastomosis 48% 15% <.01 Takedown surgery after 96% (22/23) 91% (10/11) Ns ostomy Time from first surgery to 6.2 ± ± 35.6 NS ostomy takedown (mo) Cholecystectomy z 11% 38% <.05 Gastrostomy tube placed 61% 69% NS PN-associated complications 36% 62% NS Infections per year 1.3 ± ± 0.5 <.01 Time on PN (y) 2.0 ± ± 7.4 <.001 Mean z score for weight ÿ0.6 ± 1.5 ÿ0.3 ± 0.8 NS Mean z score for height ÿ0.9 ± 1.7 ÿ1.19 ± 1.2 NS Special education 28% 18% NS GA, Gestational age; NEC, necrotizing enterocolitis; NS, not statistically significant. Values are given in mean ± SD or percentage. Statistically significant: P <.05. *Median age was 0.5 months for adapted versus 0.6 months for nonadapted. yestablished by 2 weeks after first surgery. zsecondary to gallstones/cholecystitis. There was no statistical difference in intestinal adaptation between patients with SSB and VSSB with or without ICV, whereas patients with USSB were less likely to adapt if the ICV was resected (Table III). In addition, children with SBL >38 cm spent less time on PN support than the ones with SBL < 38 cm (1.1 ± 1.3 years vs 3.6 ± 3.8 years; P =.01). For the patients with SBL >38 cm, this time was not affected by having or not having an intact ICV (1.2 ± 1.3 years versus Fig 2. Probability of being PN-dependent in 57 children with SBS based on (A) SBL and (B) ICV status. 1.0 ± 1.2 years; P =.82), whereas ICV status was statistically significant for the subjects with SBL < 38 cm (1.8 ± 1.1 years with ICV versus 6.7 ± 4.7 years without ICV; P =.02). Children with SBL >38 cm adapted faster than their counterparts regardless of ICV status, whereas time on PN was significantly affected by ICV status if children s SBLs were < 38 cm. These results demonstrated that having an intact ICV became more crucial for intestinal adaptation as the SBL decreased. In children with ICV who adapted (30/33), 90% (27/30) were adapted by 3 years and the other 3 children were adapted by 5 years postsurgery. In children without ICV who had intestinal adaptation (13/24), 69% (9/13) adapted by 3 years and 1 adapted by 4 years, whereas the other 3 needed more than 5 years of PN before adapting (7.1, 9.9, and 13.5 years). These last 3 children had VSSB. Intestinal adaptation happened in most of these children by 3 years. The following group of children had statistically significant decreased survival rates by Cox proportional hazard regression model: SBL < 15cm (P <.05), lack of primary anastomosis (P <.05), absence of takedown surgery (P <.01), 160 Quirós-Tejeira et al The Journal of Pediatrics August 2004
5 and evidence of PN-associated early persistent cholestatic jaundice (P <.0001). When the same Cox model was used to analyze intestinal adaptation we learned that children with SBL >38cm (P <.01) and with intact ICV (P <.001) were more likely to have intestinal adaptation. Patients with SBL < 15cm and who underwent cholecystectomy (P <.01) were less likely to adapt. In both models, survival and intestinal adaptation, ICV resection was highly correlated with colonic resection. Fifty-seven patients (73%) are alive at a median age of 9.5 years ( years) after a median follow-up of 9 years ( years). PN was discontinued in 44 patients (56%) after a median time of 1 year ( years) at a median age of 1.5 years ( years). Thirteen patients (17%) are still on PN after a median time of 9.5 years ( years) at a median age of 9.6 years ( years). The main causes of death were sepsis (8), liver disease (6), posttransplant complications (2), pneumonias (2), renal disease (1), heart disease (1 who had Down syndrome and congenital heart disease), and unknown etiology (1). Sepsis and liver disease composed 67% of all deaths. One patient had liver transplantation and 2 had combined liver/small bowel transplantation as a result of ESLD. No patient died as a direct consequence of thrombosis and/or lack of venous access. Eleven subjects reached adulthood and 4 of them are still on PN. One patient died as an adult secondary to ESLD. Nine adults finished high school. Four graduated from college, 2 are still in college, and 4 are employed. One adult is married. Concerning the 4 patients on PN: 2 had bone disease, 3 underwent cholecystectomy secondary to symptomatic gallstones, 2 had deep vein thrombosis, and all had normal renal function. Two adults had mild portal fibrosis in their liver biopsy at the time of the cholecystectomy. One patient had abnormal liver function tests. Their mean CVC-related sepsis was 0.2 ± 0.1 episodes per year. The mean z score for height was ÿ0.9 ± 1.7 and the mean z score for weight was ÿ0.4 ± 1.1 for the adapted adults versus a mean z score for height of ÿ1.4 ± 0.9 and a mean z score for weight of ÿ0.6 ± 0.2 for the patients on PN (P =.55 and P =.73, respectively). DISCUSSION The main goal of treatment in SBS is intestinal adaptation while optimizing weight gain and linear growth while trying to maximize enteral nutrition while minimizing parenteral support. This is as much an art as it is a science. Since the late 1960s, PN has had an enormous impact on the accomplishment of these goals. After small bowel resection, the residual intestine becomes dilated, and crypt depth along with villus height increases by mucosal hyperplasia. The overall outcome is an increase of the absorptive capacity of the remaining small intestine. 5,11 The magnitude of the hyperplastic response is directly proportional to the SBL that has been resected. 12 Establishing elemental enteral feedings or feeding with breast milk as soon as possible has been widely accepted as one important controllable variable that may help intestinal Table III. Adaptation of survivors based on SBL and presence or absence of ICV Survivors adaptation SBL With ICV Without ICV P value >38 cm 20/21 8/12 NS cm 7/8 5/8 * NS < 15 cm 3/4 0/4 <.001 NS, Not statistically significant. Statistically significant: P <.05. *A sixth patient came off PN after a liver/small bowel transplantation. adaptation. 8,9,13,14 Unfortunately, in our study too few children were on only breast milk to be able to compare with children on elemental formula. Moreover, the composition of elemental formulas that are available has changed over the past 25 years, which makes this group less homogeneous. In our series, the mean percentage of calories through enteral feeding accomplished by 2 weeks after the first surgery was similar for nonsurvivors or survivors who adapted or not. One problem could be that we look at enteral feedings at one point in time and not continuously. In addition, enteral feeding is not the only variable that affects survival and adaptation because the impact of intraluminal nutrients depends not only on the percentage of calories but also on the ability to maintain enteral nutrition continuously and progressively. 9,14 We found that not only survival but also adaptation are greatly affected by SBL and ICV status. In our series, patients with SBL >38 cm are more likely to survive or adapt with or without ICV. The major impact of an intact ICV is appreciated if the SBL is < 15 cm. SBL has been consistently an important factor to predict intestinal adaptation, 4,8,13-15 whereas the presence of an intact ICV has been a predictor 4,8,15,16 or not a predictor 5,13,14 of who will be able to discontinue PN. What makes the evaluation of the impact of ICV resection so difficult is that it is usually done along with colonic and terminal ileum resections. This was seen in our Cox models, for survival and intestinal adaptation, where ICV and colonic resections were highly correlated. In adults the critical SBL for adaptation is 100 cm, which is different from that for children. 17 Even though, intestinal adaptation is a complex phenomenon; in children the increase of SBL by normal growth, which enhances the capacity for intestinal adaptation, is a crucial factor. This is more significant from birth through aged 3 to 4 years. 18 Ileal resection appears detrimental for the adaptation process. Intestinal adaptation seems to be greater after proximal rather than distal resection. 19 This may be related to a greater adaptive capacity of the ileum, to intrinsic structural and functional differences, or to regional differences in motor and hormonal function such as enteroglucagon. 20 In addition, the transit time of the chyme through the ileum is longer than that through the jejunum because of less vigorous motility that increases the opportunity for nutrients to be absorbed during the adaptation process. 21 Another factor affected by ileal resection is gastric emptying. When the ileum Long-Term Parenteral Nutritional Support and Intestinal Adaptation in Children with Short Bowel Syndrome: A 25-year Experience 161
6 is resected, the rate of gastric emptying is shortened as a result of the loss of the ileogastric reflex that normally slows it down, diminishing the opportunity for nutrients to be absorbed. 22 This may explain why the children in our study with an intact ICV and part of the terminal ileum tended to adapt better. The role of the colon in intestinal adaptation is an important one. In our study, we found that patients with an intact colon or with >50% of colon were more likely to adapt. In patients with SBS, when undigested nutrients reach the colon it may induce changes that allow the colonic mucosa to enhance its capacity of water and electrolyte absorption as well as modifications that allow absorption of nutrients such as short- and medium-chain fatty acids As more intact nutrients reach the colon, trophic hormones such as enteroglucagon may be stimulated, contributing to the intestinal adaptation process. 26,27 When intestinal continuity is preserved through a primary anastomosis, this colonic exposure to undigested nutrients will take place. As we appreciated in our series, children with primary anastomosis were more likely to adapt. This may be secondary to improvement of water and electrolyte absorption as continuity is conserved and also may be a result of the increased absorptive role that the colon may play after small bowel resection. Increased colonic capacity of water and electrolytes absorption has been demonstrated after jejunal and ileal resection secondary to mucosal hyperplasia. 12,28 In our study, survival was adversely affected by PNassociated early persistent cholestatic jaundice. PN-associated cholestasis will affect the nutritional support because it will enhance nutrient malabsorption precluding advancement of enteral feeding. Furthermore, liver dysfunction and portal hypertension have been shown to be detrimental to the intestinal adaptation process. 29 Even though PN-associated cholestasis is multifactorial, it also could be the consequence of the inability for early restoration of intestinal continuity, which correlates with less severe liver disease. 13 Our study showed that intact ICV was associated with better survival and adaptation rates. The main function of the ICV is to regulate the passage of contents from the small bowel to the cecum and to prevent bacterial reflux from the colon. 30,31 The distal ileum, ICV, and cecum work together as a unit to accomplish this role. 31 By resection of the ICV, malabsorption will occur as a result of alteration of these two mechanisms, causing shortened transit time of nutrients through the small bowel and bacteria overgrowth. 30 The bacterial overgrowth theory has been supported by the use of artificial ICV in enterectomized dogs, causing decrease of the bacterial counts in the small bowel with subsequent improvement of weight loss and dehydration. 32 There was a tendency for more symptomatic gallstones with subsequent cholecystectomy in children who did not adapt. Long-term PN support in association to prolonged periods of fasting and/or ileal resection will cause distorted bile composition and gallbladder stasis, predisposing to gallstone formation. 33 Because pancreato-biliary secretions directly affect the size of the intestinal villi, a decrease in them will diminish the hyperplastic response by the remnant intestinal mucosa, causing further malabsorption and affecting the ability of the small intestine to adapt. 34 Our experience has shown that CVC care improves with time as the CVC may stay in place for more than a decade without major complications. 35 This may explain why the incidence of CVC-related sepsis was lower in patients who did not adapt, since they had a longer overall time on PN. Even though intestinal translocation may account for some CVC septic episodes in children with SBS, 36 our belief is that CVC care is the greatest controllable variable that may be affected by a standard protocol and good technique of CVC care. 10,35,37 Our study showed that need for long-term PN does not preclude achieving productive adulthood with normal heights and weights. Most of our long-term PN patients went through a normal education process. This is consistent with our previous report, where long-term PN children attended normal school and even a school for the mentally gifted. 38 In summary, our overall survival was 73%, with 77% of survivors having intestinal adaptation. SBL, intact ICV, intestinal continuity and preservation of the colon are important factors for survival and adaptation. Adaptation usually occurred within the first 3 years but may take as long as 13.5 years. Early persistent cholestatic jaundice is a predictor of poor outcome. Chronic intestinal failure was present in patients with USSB without ICV. Small bowel transplantation should be considered if such patients develop liver failure or loss of vascular access. Patients with ICV even with USBS and patients with >15 cm of SBL without ICV have a chance of intestinal adaptation. REFERENCES 1. Koeberle E. Resection de deux metres d intestine grele guerison. Bull Acad Med 1881;8: Haymond HE. Massive resection of the small intestine: an analysis of 257 collected cases. Surg Gynecol Obstet 1935;61: Dudrick SJ, Wilmore DW, Vars HM, Rhoads JE. Long-term total parenteral nutrition with growth, development and positive nitrogen balance. Surgery 1968;64: Wilmore DW. Factors correlating with a successful outcome following extensive intestinal resection in newborn infants. J Pediatr 1972;80: Cooper A, Floyd TF, Ross AJ 3rd, Bishop HC, Templeton JM Jr, Ziegler MM. Morbidity and mortality of short-bowel syndrome acquired in infancy: an update. J Pediatr Surg 1984;19: Fonkalsrud EW, Berquist WE, Burke M, Ament ME. Long-term hyperalimentation in children through saphenous central venous catheterization. Am J Surg 1982;143: Cannon RA, Byrne WJ, Ament ME, Gates B, O Connor M, Fonkalsrud EW. Home parenteral nutrition in infants. J Pediatr 1980; 96: Dorney SA, Ament ME, Berquist WE, Vargas JH, Hassall E. Improved survival in very short small bowel of infancy with use of long-term parenteral nutrition. J Pediatr 1985;107: Christie DL, Ament ME. Dilute elemental diet and continuous infusion technique for management of short bowel syndrome. J Pediatr 1975;87: Buchman AL, Moukarzel A, Goodson B, et al. Catheter-related infections associated with home parenteral nutrition and predictive factors for need for catheter removal in their treatment. J Parenter Enteral Nutr 1994;18: Dowling RH. Small bowel adaptation and its regulation. Scand J Gastroenterol 1982;74(suppl): Quirós-Tejeira et al The Journal of Pediatrics August 2004
7 12. Williamson RC, Bauer FL, Ross JS, Malt RA. Proximal enterectomy stimulates distal hyperplasia more than bypass or pancreaticobiliary diversion. Gastroenterology 1978;74: Andorsky DJ, Lund DP, Lillehei CW, et al. Nutritional and other postoperative management of neonates with short bowel syndrome correlates with clinical outcomes. J Pediatr 2001;139: Sondheimer JM, Cadnapaphornchai M, Sontag M, Zerbe GO. Predicting the duration of dependence on parenteral nutrition after neonatal intestinal resection. J Pediatr 1998;132: Goulet OJ, Revillon Y, Jan D, et al. Neonatal short bowel syndrome. J Pediatr 1991;119: Mayr JM, Schober PH, Weissensteiner U, Hollwarth ME. Morbidity and mortality of the short-bowel syndrome. Eur J Pediatr Surg 1999;9: Messing B, Crenn P, Beau P, Boutron-Ruault MC, Rambaud JC, Matuchansky C. Long-term survival and parenteral nutrition dependence in adult patients with the short bowel syndrome. Gastroenterology 1999;117: Siebert JR. Small-intestine length in infants and children. Am J Dis Child 1980;134: Hanson WR, Osborne JW, Sharp JG. Compensation by the residual intestine after intestinal resection in the rat, I: influence of amount of tissue removed. Gastroenterology 1977;72: Thompson JS, Quigley EM, Adrian TE. Factors affecting outcome following proximal and distal intestinal resection in the dog: an examination of the relative roles of mucosal adaptation, motility, luminal factors, and enteric peptides. Dig Dis Sci 1999;44: Summers RW, Kent TH, Osborne JW. Effects of drugs, ileal obstruction, and irradiation on rat gastrointestinal propulsion. Gastroenterology 1970;59: Nylander G. Gastric evacuation and propulsive intestinal motility following resection of the small intestine in the rat. Acta Chir Scand 1967;133: Jeppesen PB, Mortensen PB. The influence of a preserved colon on the absorption of medium chain fat in patients with small bowel resection. Gut 1998;43: Jorgensen J, Holtug K, Jeppesen PB, Mortensen PB. Human rectal absorption of short- and medium-chain C2-C10 fatty acids. Scand J Gastroenterol 1998;33: Sidhu GS, Narasimharao KL, Rani VU, Sarkar AK, Chakravarti RN, Mitra SK. Morphological and functional changes in the gut after massive small bowel resection and colon interposition in rhesus monkeys. Digestion 1984;29: Jacobs LR, Bloom SR, Dowling RH. Response of plasma and tissue levels of enteroglucagon immunoreactivity to intestinal resection, lactation and hyperphagia. Life Sci 1981;29: Miazza BM, Al-Mukhtar MY, Salmeron M, et al. Hyperenteroglucagonaemia and small intestinal mucosal growth after colonic perfusion of glucose in rats. Gut 1985;26: Nundy S, Malamud D, Obertop H, Sczerban J, Malt RA. Onset of cell proliferation in the shortened gut: colonic hyperplasia after ileal resection. Gastroenterology 1977;72: Weber TR, Keller MS. Adverse effects of liver dysfunction and portal hypertension on intestinal adaptation in short bowel syndrome in children. Am J Surg 2002;184: Gazet JC, Kopp J. The surgical significance of the ileocecal junction. Surg 1964;56: Quigley EM, Borody TJ, Phillips SF, et al. Motility of the terminal ileum and ileocecal sphincter in healthy humans. Gastroenterology 1984;87: Ricotta J, Zuidema GD, Gadacz TR, Sadri D. Construction of an ileocecal valve and its role in massive resection of the small intestine. Surg Gynecol Obstet 1981;152: Pitt HA, King W 3rd, Mann LL, et al. Increased risk of cholelithiasis with prolonged total parenteral nutrition. Am J Surg 1983;145: Altmann GG. Influence of bile and pancreatic secretions on the size of the intestinal villi in the rat. Am J Anat 1971;132: Moukarzel AA, Haddad I, Ament ME, et al. 230 patient years of experience with home long-term parenteral nutrition in childhood: natural history and life of central venous catheters. J Pediatr Surg 1994;29: Kurkchubasche AG, Smith SD, Rowe MI. Catheter sepsis in shortbowel syndrome. Arch Surg 1992;127: Maas A, Flament P, Pardou A, Deplano A, Dramaix M, Struelens MJ. Central venous catheter-related bacteraemia in critically ill neonates: risk factors and impact of a prevention programme. J Hosp Infect 1998;40: Vargas JH, Ament ME, Berquist WE. Long-term home parenteral nutrition in pediatrics: ten years of experience in 102 patients. J Pediatr Gastroenterol Nutr 1987;6: Long-Term Parenteral Nutritional Support and Intestinal Adaptation in Children with Short Bowel Syndrome: A 25-year Experience 163
Short Bowel Syndrome: Medical management
 Short Bowel Syndrome: Medical management La Sindrome dell'intestino Corto in età pediatrica Brescia 18 marzo 2011 Jon A.Vanderhoof, M.D. Division of Pediatric GI Harvard Medical School Children s Hospital,
Short Bowel Syndrome: Medical management La Sindrome dell'intestino Corto in età pediatrica Brescia 18 marzo 2011 Jon A.Vanderhoof, M.D. Division of Pediatric GI Harvard Medical School Children s Hospital,
Nutrition Management in GI Diseases
 Nutrition Management in GI Diseases Aryono Hendarto MD Nutrition & Metabolic Diseases Division Department of Child Health Cipto Mangunkusumo Hospital University of Indonesia 1 Patient s Care 1. Drugs 2.
Nutrition Management in GI Diseases Aryono Hendarto MD Nutrition & Metabolic Diseases Division Department of Child Health Cipto Mangunkusumo Hospital University of Indonesia 1 Patient s Care 1. Drugs 2.
Improved survival in a multidisciplinary short bowel syndrome program
 Journal of Pediatric Surgery (2008) 43, 20 24 www.elsevier.com/locate/jpedsurg Improved survival in a multidisciplinary short bowel syndrome program Biren P. Modi a,b, Monica Langer a,b, Y. Avery Ching
Journal of Pediatric Surgery (2008) 43, 20 24 www.elsevier.com/locate/jpedsurg Improved survival in a multidisciplinary short bowel syndrome program Biren P. Modi a,b, Monica Langer a,b, Y. Avery Ching
Minimal Enteral Nutrition
 Abstract Minimal Enteral Nutrition Although parenteral nutrition has been used widely in the management of sick very low birth weight infants, a smooth transition to the enteral route is most desirable.
Abstract Minimal Enteral Nutrition Although parenteral nutrition has been used widely in the management of sick very low birth weight infants, a smooth transition to the enteral route is most desirable.
Management of Short Bowel Syndrome in the Era of Teduglutide. Charlene Compher, PhD, RD University of Pennsylvania
 Management of Short Bowel Syndrome in the Era of Teduglutide Charlene Compher, PhD, RD University of Pennsylvania compherc@nursing.upenn.edu Disclosures Research funding for clinical trials by NPS Pharmaceuticals
Management of Short Bowel Syndrome in the Era of Teduglutide Charlene Compher, PhD, RD University of Pennsylvania compherc@nursing.upenn.edu Disclosures Research funding for clinical trials by NPS Pharmaceuticals
Gastroschisis Sequelae and Management
 Gastroschisis Sequelae and Management Mary Finn Gillian Lieberman, MD Primary Care Radiology Beth Israel Deaconess Medical Center Harvard Medical School April 2014 Outline I. Definition and Epidemiology
Gastroschisis Sequelae and Management Mary Finn Gillian Lieberman, MD Primary Care Radiology Beth Israel Deaconess Medical Center Harvard Medical School April 2014 Outline I. Definition and Epidemiology
PARENTERAL NUTRITION- ASSOCIATED LIVER DISEASE IN CHILDREN
 PARENTERAL NUTRITION- ASSOCIATED LIVER DISEASE IN CHILDREN Praveen Goday MBBS CNSC Associate Professor Pediatric Gastroenterology Medical College of Wisconsin Milwaukee, WI Parenteral Nutrition-Associated
PARENTERAL NUTRITION- ASSOCIATED LIVER DISEASE IN CHILDREN Praveen Goday MBBS CNSC Associate Professor Pediatric Gastroenterology Medical College of Wisconsin Milwaukee, WI Parenteral Nutrition-Associated
Nutritional Requirements in Intestinal Failure
 Nutritional Requirements in Intestinal Failure Christopher Duggan, MD, MPH Center for Nutrition Center for Advanced Intestinal Rehabilitation (CAIR) Division of Gastroenterology, Hepatology and Nutrition
Nutritional Requirements in Intestinal Failure Christopher Duggan, MD, MPH Center for Nutrition Center for Advanced Intestinal Rehabilitation (CAIR) Division of Gastroenterology, Hepatology and Nutrition
Intestinal Rehabilitation and Transplantation
 Intestinal Rehabilitation and Transplantation Joel Lim, MD Associate Professor of Pediatrics Children s Mercy Hospital University of Missouri in Kansas City Objective: Intestinal Failure/Short Bowel Syndrome
Intestinal Rehabilitation and Transplantation Joel Lim, MD Associate Professor of Pediatrics Children s Mercy Hospital University of Missouri in Kansas City Objective: Intestinal Failure/Short Bowel Syndrome
Advances in intestinal Rehabilitation Susan Hill Gastroenterology Consultant
 Advances in intestinal Rehabilitation Susan Hill Gastroenterology Consultant 2 Indication for intravenous nutrition/pn: Intestinal Failure Inability to maintain weight and growth despite adequate enteral
Advances in intestinal Rehabilitation Susan Hill Gastroenterology Consultant 2 Indication for intravenous nutrition/pn: Intestinal Failure Inability to maintain weight and growth despite adequate enteral
Long term home parenteral nutrition or small bowel transplantation? Florence LACAILLE Necker-enfants malades, Paris
 Long term home parenteral nutrition or small bowel transplantation? Florence LACAILLE Necker-enfants malades, Paris Intestinal failure : definitive Ultra-short bowel : ± < 30 cm - valve ± < 20 cm + valve
Long term home parenteral nutrition or small bowel transplantation? Florence LACAILLE Necker-enfants malades, Paris Intestinal failure : definitive Ultra-short bowel : ± < 30 cm - valve ± < 20 cm + valve
Nutritional and other postoperative management
 Nutritional and other postoperative management of neonates with short bowel syndrome correlates with clinical outcomes David J. Andorsky, BA, Dennis P. Lund, MD, Craig W. Lillehei, MD, Tom Jaksic, MD,
Nutritional and other postoperative management of neonates with short bowel syndrome correlates with clinical outcomes David J. Andorsky, BA, Dennis P. Lund, MD, Craig W. Lillehei, MD, Tom Jaksic, MD,
Effect of changing lipid formulation in Parenteral Nutrition in the Newborn Experimental Pathology BSc
 Effect of changing lipid formulation in Parenteral Nutrition in the Newborn Experimental Pathology BSc Word count: 6939 0 CONTENTS Abstract...2 Acknowledgements...3 Introduction...4 Materials and Methods...11
Effect of changing lipid formulation in Parenteral Nutrition in the Newborn Experimental Pathology BSc Word count: 6939 0 CONTENTS Abstract...2 Acknowledgements...3 Introduction...4 Materials and Methods...11
Isolated Liver Transplantation in Infants with End-Stage Liver Disease Due to Short Bowel Syndrome
 LIVER TRANSPLANTATION 12:1062-1066, 2006 ORIGINAL ARTICLE Isolated Liver Transplantation in Infants with End-Stage Liver Disease Due to Short Bowel Syndrome Jean F. Botha, Wendy J. Grant, Clarivet Torres,
LIVER TRANSPLANTATION 12:1062-1066, 2006 ORIGINAL ARTICLE Isolated Liver Transplantation in Infants with End-Stage Liver Disease Due to Short Bowel Syndrome Jean F. Botha, Wendy J. Grant, Clarivet Torres,
Clinical Improvement Following Home Parenteral Nutrition in Pediatric Patients with Intestinal Failure
 ORIGINAL ARTICLE Clinical Improvement Following Home Parenteral Nutrition in Pediatric Patients with Intestinal Failure Yi-Ching Tung, Yen-Hsuan Ni, Hong-Shiee Lai, 1 Der-Yirng Hsieh, 2 Mei-Hwei Chang*
ORIGINAL ARTICLE Clinical Improvement Following Home Parenteral Nutrition in Pediatric Patients with Intestinal Failure Yi-Ching Tung, Yen-Hsuan Ni, Hong-Shiee Lai, 1 Der-Yirng Hsieh, 2 Mei-Hwei Chang*
Morabito A UK. -Royal Manchester Children s Hospital (PABRRU) -Intestinal Failure Unit Salford Royal Hospital
 NON-TRANSPLANT SURGERY IMPROVES OUTCOME IN SHORT BOWEL PATIENTS Morabito A UK -Royal Manchester Children s Hospital (PABRRU) -Intestinal Failure Unit Salford Royal Hospital antonino.morabito@cmft.nhs.uk
NON-TRANSPLANT SURGERY IMPROVES OUTCOME IN SHORT BOWEL PATIENTS Morabito A UK -Royal Manchester Children s Hospital (PABRRU) -Intestinal Failure Unit Salford Royal Hospital antonino.morabito@cmft.nhs.uk
Parenteral Nutrition. Outline. Potential Biomarkers for Use in Intestinal Adaptation. Jejunum is primary site of digestion and absorption
 Outline Potential Biomarkers for Use in Intestinal Adaptation Kelly A. Tappenden, Ph.D., R.D. Professor of Nutrition and GI Physiology 1. Intestinal Adaptation potential regulators 2. Intestinal mucosal
Outline Potential Biomarkers for Use in Intestinal Adaptation Kelly A. Tappenden, Ph.D., R.D. Professor of Nutrition and GI Physiology 1. Intestinal Adaptation potential regulators 2. Intestinal mucosal
Challenges in Pediatric Nutritional Support. Donald E. George, MD
 Challenges in Pediatric Nutritional Support Donald E. George, MD What is so special about Kids They Grow They Change They Explore They Frequently get better What is so special about Kids They require more
Challenges in Pediatric Nutritional Support Donald E. George, MD What is so special about Kids They Grow They Change They Explore They Frequently get better What is so special about Kids They require more
ESPEN Congress Florence 2008
 ESPEN Congress Florence 2008 PN Guidelines presentation PN Guidelines in gastroenterology A. van Gossum (Belgium) ESPEN-Parenteral Guidelines in Gastroenterology André Van Gossum, Eduard Cabre, Xavier
ESPEN Congress Florence 2008 PN Guidelines presentation PN Guidelines in gastroenterology A. van Gossum (Belgium) ESPEN-Parenteral Guidelines in Gastroenterology André Van Gossum, Eduard Cabre, Xavier
Short bowel syndrome after cytoreductive surgery and HIPEC: nutritional considerations
 JBUON 2014; 19(2): 549-553 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Short bowel syndrome after cytoreductive surgery and HIPEC: nutritional
JBUON 2014; 19(2): 549-553 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Short bowel syndrome after cytoreductive surgery and HIPEC: nutritional
SHORT GUT SYNDROME (SGS) : A MANAGEMENT CHALLENGE!
 SHORT GUT SYNDROME (SGS) : A MANAGEMENT CHALLENGE! Muhammad Saaiq DEPARTMENT OF SURGERY,PIMS, ISLAMABAD. Surgical Grand Round, Pakistan Institute of Medical Sciences (PIMS), Islamabad. September 23, 2005.
SHORT GUT SYNDROME (SGS) : A MANAGEMENT CHALLENGE! Muhammad Saaiq DEPARTMENT OF SURGERY,PIMS, ISLAMABAD. Surgical Grand Round, Pakistan Institute of Medical Sciences (PIMS), Islamabad. September 23, 2005.
What location in the gastrointestinal (GI) tract has tight, or impermeable, junctions between the epithelial cells?
 CASE 32 A 17-year-old boy presents to his primary care physician with complaints of diarrhea for the last 2 days. The patient states that he just returned to the United States after visiting relatives
CASE 32 A 17-year-old boy presents to his primary care physician with complaints of diarrhea for the last 2 days. The patient states that he just returned to the United States after visiting relatives
Enteral and parenteral nutrition in GI failure and short bowel syndrome
 Enteral and parenteral nutrition in GI failure and short bowel syndrome Alastair Forbes University College London Intestinal failure Inadequate functional intestine to allow health to be maintained by
Enteral and parenteral nutrition in GI failure and short bowel syndrome Alastair Forbes University College London Intestinal failure Inadequate functional intestine to allow health to be maintained by
Home Total Parenteral Nutrition for Adults
 Home Total Parenteral Nutrition for Adults Policy Number: Original Effective Date: MM.08.007 05/21/1999 Line(s) of Business: Current Effective Date: PPO, HMO, QUEST Integration 05/27/2016 Section: Home
Home Total Parenteral Nutrition for Adults Policy Number: Original Effective Date: MM.08.007 05/21/1999 Line(s) of Business: Current Effective Date: PPO, HMO, QUEST Integration 05/27/2016 Section: Home
Small-Bowel and colon Transit. Mahsa Sh.Nezami October 2016
 Small-Bowel and colon Transit Mahsa Sh.Nezami October 2016 Dyspeptic symptoms related to dysmotility originating from the small bowel or colon usually include : Abdominal pain Diarrhea Constipation However,
Small-Bowel and colon Transit Mahsa Sh.Nezami October 2016 Dyspeptic symptoms related to dysmotility originating from the small bowel or colon usually include : Abdominal pain Diarrhea Constipation However,
Nutritional Management in Enterocutaneous fistula Dr Deepak Govil
 Nutritional Management in Enterocutaneous fistula Dr Deepak Govil MS, PhD (GI Surgery) Senior Consultant Surgical Gastroenterology Indraprastha Apollo Hospital New Delhi What is enterocutaneous fistula
Nutritional Management in Enterocutaneous fistula Dr Deepak Govil MS, PhD (GI Surgery) Senior Consultant Surgical Gastroenterology Indraprastha Apollo Hospital New Delhi What is enterocutaneous fistula
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abdominal pain, enteral therapy in acute pancreatitis and, 812 Abscess(es), pancreatic, nutritional support for, 814 815 Acute Physiology and
Note: Page numbers of article titles are in boldface type. A Abdominal pain, enteral therapy in acute pancreatitis and, 812 Abscess(es), pancreatic, nutritional support for, 814 815 Acute Physiology and
Fish oil based lipid emulsion s role in transitioning pediatric patients from plant based to combination plant and fish oil based lipid emulsion
 Fish oil based lipid emulsion s role in transitioning pediatric patients from plant based to combination plant and fish oil based lipid emulsion Kayley Liuzzo, PharmD PGY 1 Pharmacy Practice Resident Children
Fish oil based lipid emulsion s role in transitioning pediatric patients from plant based to combination plant and fish oil based lipid emulsion Kayley Liuzzo, PharmD PGY 1 Pharmacy Practice Resident Children
PARENTERAL NUTRITION THERAPY
 UnitedHealthcare Benefits of Texas, Inc. 1. UnitedHealthcare of Oklahoma, Inc. 2. UnitedHealthcare of Oregon, Inc. UnitedHealthcare of Washington, Inc. UnitedHealthcare West BENEFIT INTERPRETATION POLICY
UnitedHealthcare Benefits of Texas, Inc. 1. UnitedHealthcare of Oklahoma, Inc. 2. UnitedHealthcare of Oregon, Inc. UnitedHealthcare of Washington, Inc. UnitedHealthcare West BENEFIT INTERPRETATION POLICY
Different Surgical Techniques in Management of Small Intestinal Atresia in High Risk Neonates
 Annals of Pediatric Surgery Vol 5, No 1, January 2009, PP 31-35 Original Article Different Surgical Techniques in Management of Small Intestinal Atresia in High Risk Neonates Almoutaz A. Eltayeb Pediatric
Annals of Pediatric Surgery Vol 5, No 1, January 2009, PP 31-35 Original Article Different Surgical Techniques in Management of Small Intestinal Atresia in High Risk Neonates Almoutaz A. Eltayeb Pediatric
Radiographic Evaluation of Complications after Jejunoileal Bypass Surgery
 Radiographic Evaluation of Complications after Jejunoileal Bypass Surgery ALBERT A. MOSS, HENRY I. GOLDBERG, AND ROBERT E. KOEHLER A retrospective analysis of 89 patients who underwent jejunoileal bypass
Radiographic Evaluation of Complications after Jejunoileal Bypass Surgery ALBERT A. MOSS, HENRY I. GOLDBERG, AND ROBERT E. KOEHLER A retrospective analysis of 89 patients who underwent jejunoileal bypass
Parenteral and Enteral Nutrition
 Parenteral and Enteral Nutrition Audis Bethea, Pharm.D. Assistant Professor Therapeutics I December 5 & 9, 2003 Parenteral Nutrition Definition process of supplying nutrients via the intravenous route
Parenteral and Enteral Nutrition Audis Bethea, Pharm.D. Assistant Professor Therapeutics I December 5 & 9, 2003 Parenteral Nutrition Definition process of supplying nutrients via the intravenous route
Small Bowel Obstruction after operation in a severely malnourished man. By: Ms Bounmark Phoumesy
 Small Bowel Obstruction after operation in a severely malnourished man By: Ms Bounmark Phoumesy Normal length of GI tract Normal length(achieved by age 9) Small bowel 600cm (Men: 630 cm; Women: 592 cm)
Small Bowel Obstruction after operation in a severely malnourished man By: Ms Bounmark Phoumesy Normal length of GI tract Normal length(achieved by age 9) Small bowel 600cm (Men: 630 cm; Women: 592 cm)
Aggressive Nutrition in Preterm Infants
 Aggressive Nutrition in Preterm Infants Jatinder Bhatia, MD, FAAP Declaration of potential conflicts of interest Regarding this presentation the following relationships could be perceived as potential
Aggressive Nutrition in Preterm Infants Jatinder Bhatia, MD, FAAP Declaration of potential conflicts of interest Regarding this presentation the following relationships could be perceived as potential
Hepatoprotective Therapies for TPN-Associated Cholestasis
 Hepatoprotective Therapies for TPN-Associated Cholestasis Robert A. Cowles, M.D. Department of Surgery Columbia University Medical Center and Morgan Stanley Children s Hospital New York, NY USA For the
Hepatoprotective Therapies for TPN-Associated Cholestasis Robert A. Cowles, M.D. Department of Surgery Columbia University Medical Center and Morgan Stanley Children s Hospital New York, NY USA For the
Definition and Types of Intestinal Failure
 Definition and Types of Intestinal Failure Jeremy Nightingale Consultant Gastroenterologist St Mark s Hospital Intestinal Failure - Definitions Reduction in functioning gut mass below the minimum amount
Definition and Types of Intestinal Failure Jeremy Nightingale Consultant Gastroenterologist St Mark s Hospital Intestinal Failure - Definitions Reduction in functioning gut mass below the minimum amount
Malabsorption: etiology, pathogenesis and evaluation
 Malabsorption: etiology, pathogenesis and evaluation Peter HR Green NORMAL ABSORPTION Coordination of gastric, small intestinal, pancreatic and biliary function Multiple mechanisms Fat protein carbohydrate
Malabsorption: etiology, pathogenesis and evaluation Peter HR Green NORMAL ABSORPTION Coordination of gastric, small intestinal, pancreatic and biliary function Multiple mechanisms Fat protein carbohydrate
Effect of Ileo-Jejunal Intestinal Adaptation
 Tohoku J. exp. Med., 1987, 151, 419-428 Effect of Ileo-Jejunal Intestinal Adaptation Colectomy in Dogs Transposition after Total on IWAO SASAKI, TAKASHI TUCHIYA, HIROO NAITO, YUJI FUNAYAMA, MORIHIKO TODA,
Tohoku J. exp. Med., 1987, 151, 419-428 Effect of Ileo-Jejunal Intestinal Adaptation Colectomy in Dogs Transposition after Total on IWAO SASAKI, TAKASHI TUCHIYA, HIROO NAITO, YUJI FUNAYAMA, MORIHIKO TODA,
Total Parenteral Nutrition and Enteral Nutrition in the Home. Original Policy Date 12:2013
 MP 1.02.01 Total Parenteral Nutrition and Enteral Nutrition in the Home Medical Policy Section Durable Medical Equipment Issue Original Policy Date Last Review Status/Date Return to Medical Policy Index
MP 1.02.01 Total Parenteral Nutrition and Enteral Nutrition in the Home Medical Policy Section Durable Medical Equipment Issue Original Policy Date Last Review Status/Date Return to Medical Policy Index
Strategies for preventing and treating IFALD
 Strategies for preventing and treating IFALD Dr Sue Beath The Liver Unit (including small bowel transplantation) sue.beath@nhs.net Birmingham Children s Hospital Intestinal failure associated liver disease
Strategies for preventing and treating IFALD Dr Sue Beath The Liver Unit (including small bowel transplantation) sue.beath@nhs.net Birmingham Children s Hospital Intestinal failure associated liver disease
Fistuloclysis (distal limb feeding) Dr Alison Culkin Research Dietitian AuSPEN 2015
 Fistuloclysis (distal limb feeding) Dr Alison Culkin Research Dietitian AuSPEN 2015 Overview Consider the evidence Describe the practicalities Present some cases Fistuloclysis/distal limb feeding Infusion
Fistuloclysis (distal limb feeding) Dr Alison Culkin Research Dietitian AuSPEN 2015 Overview Consider the evidence Describe the practicalities Present some cases Fistuloclysis/distal limb feeding Infusion
ESPEN Congress The Hague 2017
 ESPEN Congress The Hague 2017 Meeting nutritional needs of acute care patients Feeding acute pancreatitis patients J. Luttikhold (NL) FEEDING ACUTE PANCREATITIS PATIENTS Joanna Luttikhold, MD PhD Registrar
ESPEN Congress The Hague 2017 Meeting nutritional needs of acute care patients Feeding acute pancreatitis patients J. Luttikhold (NL) FEEDING ACUTE PANCREATITIS PATIENTS Joanna Luttikhold, MD PhD Registrar
MCT AND THE ROLES NUTRITION
 MCT AND THE ROLES NUTRITION Nguyen Hoang Nhut Hoa Department of Nutrition Children's Hospital 2 OBJECTIVES Structure Absorption and metabolic Effects of MCT in the treatment of certain diseases Demand
MCT AND THE ROLES NUTRITION Nguyen Hoang Nhut Hoa Department of Nutrition Children's Hospital 2 OBJECTIVES Structure Absorption and metabolic Effects of MCT in the treatment of certain diseases Demand
PARENTERAL NUTRITION
 PARENTERAL NUTRITION DEFINITION Parenteral nutrition [(PN) or total parenteral nutrition (TPN)] is the intravenous infusion of some or all nutrients for tissue maintenance, metabolic requirements and growth
PARENTERAL NUTRITION DEFINITION Parenteral nutrition [(PN) or total parenteral nutrition (TPN)] is the intravenous infusion of some or all nutrients for tissue maintenance, metabolic requirements and growth
Who Needs Parenteral Nutrition? Is Parenteral Nutrition An Appropriate Intervention?
 Who Needs Parenteral Nutrition? 1 Is Parenteral Nutrition An Appropriate Intervention? Key questions to ask with initial consultation Can the gastrointestinal (GI) tract be utilized? Can the GI tract be
Who Needs Parenteral Nutrition? 1 Is Parenteral Nutrition An Appropriate Intervention? Key questions to ask with initial consultation Can the gastrointestinal (GI) tract be utilized? Can the GI tract be
Corporate Medical Policy
 Corporate Medical Policy Small Bowel, Small Bowel with Liver, or Multivisceral Transplant File Name: Origination: Last CAP Review: Next CAP Last Review: small_bowel_liver_and_multivisceral_transplant 2/1996
Corporate Medical Policy Small Bowel, Small Bowel with Liver, or Multivisceral Transplant File Name: Origination: Last CAP Review: Next CAP Last Review: small_bowel_liver_and_multivisceral_transplant 2/1996
Ashley Robson Canyon Creek Dr. Mckinney, TX 75070
 1 Ashley Robson 2212 Canyon Creek Dr. Mckinney, TX 75070 September 2 nd 2014 Debra Brandon PhD, RN, CCNS, FAAN Duke University School of Nursing Durham, NC Dear Mrs. Brandon- I would like the opportunity
1 Ashley Robson 2212 Canyon Creek Dr. Mckinney, TX 75070 September 2 nd 2014 Debra Brandon PhD, RN, CCNS, FAAN Duke University School of Nursing Durham, NC Dear Mrs. Brandon- I would like the opportunity
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acetate, in pediatric surgical patients, 525 526 Acute respiratory distress syndrome (ARDS), immune-modulating nutrition in, 584 585 Aerobic
Index Note: Page numbers of article titles are in boldface type. A Acetate, in pediatric surgical patients, 525 526 Acute respiratory distress syndrome (ARDS), immune-modulating nutrition in, 584 585 Aerobic
11/4/10 SUPPORTING PREMATURE INFANT NUTRITION WORKSHOP SAM: PREVENT MALNUTRITION 200. Workshop: Preventing extrauterine growth failure
 Jae H Kim MD PhD Lisa Stellwagen MD Division of Neonatology UC San Diego, Medical Center SUPPORTING PREMATURE INFANT NUTRITION WORKSHOP Workshop: Preventing extrauterine growth failure Jae H. Kim, MD,
Jae H Kim MD PhD Lisa Stellwagen MD Division of Neonatology UC San Diego, Medical Center SUPPORTING PREMATURE INFANT NUTRITION WORKSHOP Workshop: Preventing extrauterine growth failure Jae H. Kim, MD,
Slow versus Fast Enteral Feed Advancements in Very Low Birth Weight Infants: A Randomized Controlled Trial. A. Salhotra and S.
 Original Article Slow versus Fast Enteral Feed Advancements in Very Low Birth Weight Infants: A Randomized Controlled Trial A. Salhotra and S. Ramji From the Neonatal Division, Department of Pediatrics,
Original Article Slow versus Fast Enteral Feed Advancements in Very Low Birth Weight Infants: A Randomized Controlled Trial A. Salhotra and S. Ramji From the Neonatal Division, Department of Pediatrics,
INTESTINAL FAILURE, REHABILITATION & TRANSPLANTATION: Indications, Techniques and Outcomes
 INTESTINAL FAILURE, REHABILITATION & TRANSPLANTATION: Indications, Techniques and Outcomes Douglas G. Farmer, MD. Professor of Surgery Director, Intestinal Transplant Program Dumont-UCLA Transplant Center
INTESTINAL FAILURE, REHABILITATION & TRANSPLANTATION: Indications, Techniques and Outcomes Douglas G. Farmer, MD. Professor of Surgery Director, Intestinal Transplant Program Dumont-UCLA Transplant Center
Low Zinc Status and Absorption Exist in Infants with Jejunostomies or Ileostomies Which Persists after Intestinal Repair
 Nutrients 2012, 4, 1273-1281; doi:10.3390/nu4091273 Article OPEN ACCESS nutrients ISSN 2072-6643 www.mdpi.com/journal/nutrients Low Zinc Status and Absorption Exist in Infants with Jejunostomies or Ileostomies
Nutrients 2012, 4, 1273-1281; doi:10.3390/nu4091273 Article OPEN ACCESS nutrients ISSN 2072-6643 www.mdpi.com/journal/nutrients Low Zinc Status and Absorption Exist in Infants with Jejunostomies or Ileostomies
Biliary Atresia. Who is at risk for biliary atresia?
 Biliary Atresia Biliary atresia is a life-threatening condition in infants in which the bile ducts inside or outside the liver do not have normal openings. Bile ducts in the liver, also called hepatic
Biliary Atresia Biliary atresia is a life-threatening condition in infants in which the bile ducts inside or outside the liver do not have normal openings. Bile ducts in the liver, also called hepatic
Chapter 20 The Digestive System Exam Study Questions
 Chapter 20 The Digestive System Exam Study Questions 20.1 Overview of GI Processes 1. Describe the functions of digestive system. 2. List and define the four GI Processes: 20.2 Functional Anatomy of the
Chapter 20 The Digestive System Exam Study Questions 20.1 Overview of GI Processes 1. Describe the functions of digestive system. 2. List and define the four GI Processes: 20.2 Functional Anatomy of the
Home FAQ Archives ABP Topics NeoReviews.org My Bookmarks CME Information Help. Print this Page Add to my Bookmarks Page 3 of 10
 Welcome Kristin Ingstrup [ Logout ] SEARCH Home FAQ Archives ABP Topics NeoReviews.org My Bookmarks CME Information Help Overview Editorial Board My Learning Plan January February March May June July August
Welcome Kristin Ingstrup [ Logout ] SEARCH Home FAQ Archives ABP Topics NeoReviews.org My Bookmarks CME Information Help Overview Editorial Board My Learning Plan January February March May June July August
EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion , version 1.1
 EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion 13.7.2015, version 1.1 III.1. Elements for a Public Summary III.1.1. Overview of disease epidemiology Patients may need parenteral
EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion 13.7.2015, version 1.1 III.1. Elements for a Public Summary III.1.1. Overview of disease epidemiology Patients may need parenteral
following the last documented transfusion; thereafter, evaluate the residual impairment(s).
 Adult Listings 5.01 Category of Impairments, Digestive System 5.02 Gastrointestinal hemorrhaging from any cause, requiring blood transfusion (with or without hospitalization) of at least 2 units of blood
Adult Listings 5.01 Category of Impairments, Digestive System 5.02 Gastrointestinal hemorrhaging from any cause, requiring blood transfusion (with or without hospitalization) of at least 2 units of blood
Short bowel syndrome: pathophysiological and clinical aspects
 Pathophysiology 6 (1999) 1 19 Review article Short bowel syndrome: pathophysiological and clinical aspects Michael E. Höllwarth * Department of Pediatric Surgery, Uni ersity Klinik für Kinderchirurgie-LKH
Pathophysiology 6 (1999) 1 19 Review article Short bowel syndrome: pathophysiological and clinical aspects Michael E. Höllwarth * Department of Pediatric Surgery, Uni ersity Klinik für Kinderchirurgie-LKH
The Role of Parenteral Nutrition. in PEDIATRIC INTENSIVE CARE UNIT. Dzulfikar DLH. Pediatric Emergency and Intensive Care Unit
 The Role of Parenteral Nutrition in PEDIATRIC INTENSIVE CARE UNIT Dzulfikar DLH Pediatric Emergency and Intensive Care Unit Department of Child Health, Faculty of Medicine Universitas Padjajaran, Hasan
The Role of Parenteral Nutrition in PEDIATRIC INTENSIVE CARE UNIT Dzulfikar DLH Pediatric Emergency and Intensive Care Unit Department of Child Health, Faculty of Medicine Universitas Padjajaran, Hasan
Daniel Hirsch, MD Director of Neonatology Somerset Medical Center Assistant Professor of Pediatrics UMDNJ RWJMS
 Daniel Hirsch, MD Director of Neonatology Somerset Medical Center Assistant Professor of Pediatrics UMDNJ RWJMS Daniel Hirsch, MD Director of Neonatology Somerset Medical Center Assistant Professor of
Daniel Hirsch, MD Director of Neonatology Somerset Medical Center Assistant Professor of Pediatrics UMDNJ RWJMS Daniel Hirsch, MD Director of Neonatology Somerset Medical Center Assistant Professor of
Gastric Residuals in Preterm Infants
 Neonatal Nursing Education Brief: Gastric Residuals in the Preterm Infant https://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/
Neonatal Nursing Education Brief: Gastric Residuals in the Preterm Infant https://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/
GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint
 GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Gastroenterology MOC exam blueprint Based on feedback from physicians that MOC assessments
GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Gastroenterology MOC exam blueprint Based on feedback from physicians that MOC assessments
Dietary management. Dr Alison Culkin Lead Intestinal Failure Dietitian St Mark s Hospital RSM December 2017
 Dietary management Dr Alison Culkin Lead Intestinal Failure Dietitian St Mark s Hospital RSM December 2017 Overview Effect of resection on absorption Evidence for dietary management in short bowel Practicalities
Dietary management Dr Alison Culkin Lead Intestinal Failure Dietitian St Mark s Hospital RSM December 2017 Overview Effect of resection on absorption Evidence for dietary management in short bowel Practicalities
Surgery for Intestinal Failure
 Surgery for Intestinal Failure Kishore Iyer, MBBS, FRCS (Eng), FACS Director, Adult & Pediatric Intestinal Transplantation Associate Professor of Surgery & Pediatrics Mount Sinai School of Medicine New
Surgery for Intestinal Failure Kishore Iyer, MBBS, FRCS (Eng), FACS Director, Adult & Pediatric Intestinal Transplantation Associate Professor of Surgery & Pediatrics Mount Sinai School of Medicine New
Digestive System 7/15/2015. Outline Digestive System. Digestive System
 Digestive System Biology 105 Lecture 18 Chapter 15 Outline Digestive System I. Functions II. Layers of the GI tract III. Major parts: mouth, pharynx, esophagus, stomach, small intestine, large intestine,
Digestive System Biology 105 Lecture 18 Chapter 15 Outline Digestive System I. Functions II. Layers of the GI tract III. Major parts: mouth, pharynx, esophagus, stomach, small intestine, large intestine,
Sustain Follow-up Data Collection Form (Revised 2/4/2014) (both pediatric and adult elements) (Please select) (Please select)
 Patient Information Sustain Follow-up Data Collection Form (Revised 2/4/2014) (both pediatric and adult elements) Visit Date Patient Birth Date -- Gender (please select) What is the nature of this follow-up?
Patient Information Sustain Follow-up Data Collection Form (Revised 2/4/2014) (both pediatric and adult elements) Visit Date Patient Birth Date -- Gender (please select) What is the nature of this follow-up?
Prolonged Neonatal Jaundice
 Prolonged Neonatal Jaundice Ahmed Laving KPA Annual Scientific Conference 2018 Prolonged Jaundice? >6 months >3 months >2 weeks >4 weeks Prolonged Jaundice? >6 months >3 months >2 weeks >4 weeks Case Presentation
Prolonged Neonatal Jaundice Ahmed Laving KPA Annual Scientific Conference 2018 Prolonged Jaundice? >6 months >3 months >2 weeks >4 weeks Prolonged Jaundice? >6 months >3 months >2 weeks >4 weeks Case Presentation
The Digestive System. Chapter 25
 The Digestive System Chapter 25 Introduction Structure of the digestive system A tube that extends from mouth to anus Accessory organs are attached Functions include Ingestion Movement Digestion Absorption
The Digestive System Chapter 25 Introduction Structure of the digestive system A tube that extends from mouth to anus Accessory organs are attached Functions include Ingestion Movement Digestion Absorption
Small bowel atresia. Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families
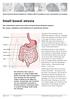 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Small bowel atresia This information sheet from Great Ormond Street Hospital explains the causes, symptoms and treatment
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Small bowel atresia This information sheet from Great Ormond Street Hospital explains the causes, symptoms and treatment
The Digestive System. Chapter
 The Digestive System Chapter 15.1 Functions: mechanical and chemical breakdown of food *absorption of nutrients Consists of alimentary canal and accessory organs Wall of the Alimentary Canal 15.2 Characteristics
The Digestive System Chapter 15.1 Functions: mechanical and chemical breakdown of food *absorption of nutrients Consists of alimentary canal and accessory organs Wall of the Alimentary Canal 15.2 Characteristics
Digestion and Absorption
 Digestion and Absorption Digestion and Absorption Digestion is a process essential for the conversion of food into a small and simple form. Mechanical digestion by mastication and swallowing Chemical digestion
Digestion and Absorption Digestion and Absorption Digestion is a process essential for the conversion of food into a small and simple form. Mechanical digestion by mastication and swallowing Chemical digestion
Continuous tube feeding versus intermittent oral feeding for intermediate position enterostomy in infants
 1 This author s PDF version corresponds to the article as it appeared upon acceptance. Fully formatted PDF versions will be made available soon. Continuous tube feeding versus intermittent oral feeding
1 This author s PDF version corresponds to the article as it appeared upon acceptance. Fully formatted PDF versions will be made available soon. Continuous tube feeding versus intermittent oral feeding
Current concepts in Critical Care Nutrition
 Current concepts in Critical Care Nutrition Dr.N.Ramakrishnan AB (Int Med), AB (Crit Care), MMM, FACP, FCCP, FCCM Director, Critical Care Services Apollo Hospitals, Chennai Objectives Why? Enteral or Parenteral
Current concepts in Critical Care Nutrition Dr.N.Ramakrishnan AB (Int Med), AB (Crit Care), MMM, FACP, FCCP, FCCM Director, Critical Care Services Apollo Hospitals, Chennai Objectives Why? Enteral or Parenteral
Continuous tube feeding versus intermittent oral feeding for intermediate position enterostomy in infants
 Asia Pac J Clin Nutr 2018;27(2):313-317 313 Original Article Continuous tube feeding versus intermittent oral feeding for intermediate position enterostomy in infants Weiwei Jiang MD, Jie Zhang MD, Xiaofeng
Asia Pac J Clin Nutr 2018;27(2):313-317 313 Original Article Continuous tube feeding versus intermittent oral feeding for intermediate position enterostomy in infants Weiwei Jiang MD, Jie Zhang MD, Xiaofeng
LA CHIRURGIA RIABILITATIVA
 LA CHIRURGIA RIABILITATIVA SINDROME DA INTESTINO CORTO: GLI ASPETTI ETICI, L APPROCCIO MEDICO E LE ESIGENZE IN CAMPO NORMATIVO VII CONGRESSO NAZIONALE ASSOCIAZIONE A.N.A.D.P. UN FILO PER LA VITA ONLUS
LA CHIRURGIA RIABILITATIVA SINDROME DA INTESTINO CORTO: GLI ASPETTI ETICI, L APPROCCIO MEDICO E LE ESIGENZE IN CAMPO NORMATIVO VII CONGRESSO NAZIONALE ASSOCIAZIONE A.N.A.D.P. UN FILO PER LA VITA ONLUS
NOTES: The Digestive System (Ch 14, part 2)
 NOTES: The Digestive System (Ch 14, part 2) PANCREAS Structure of the pancreas: The pancreas produces PANCREATIC JUICE that is then secreted into a pancreatic duct. The PANCREATIC DUCT leads to the The
NOTES: The Digestive System (Ch 14, part 2) PANCREAS Structure of the pancreas: The pancreas produces PANCREATIC JUICE that is then secreted into a pancreatic duct. The PANCREATIC DUCT leads to the The
INTESTINAL OBSTRUCTION ESCAPED SURGERY: MECONIUM PLUG
 7 INTESTINAL OBSTRUCTION ESCAPED SURGERY: MECONIUM PLUG Oluwayemi IO 1 *, Ade-Ojo IP 2, Olofinbiyi BA 2 1. Department of Paediatrics, Ekiti State University Teaching Hospital, Ado-Ekiti, Ekiti State, Nigeria
7 INTESTINAL OBSTRUCTION ESCAPED SURGERY: MECONIUM PLUG Oluwayemi IO 1 *, Ade-Ojo IP 2, Olofinbiyi BA 2 1. Department of Paediatrics, Ekiti State University Teaching Hospital, Ado-Ekiti, Ekiti State, Nigeria
BALANCING THERAPIES ENTERAL AND PARENTERAL
 BALANCING THERAPIES ENTERAL AND PARENTERAL FINDING BALANCE Luminal Nutrients Intrinsic drive BALANCE Circumstances Intravenous nutrients OBJECTIVES Why focus on adding enteral nutrients? Benefits the patient
BALANCING THERAPIES ENTERAL AND PARENTERAL FINDING BALANCE Luminal Nutrients Intrinsic drive BALANCE Circumstances Intravenous nutrients OBJECTIVES Why focus on adding enteral nutrients? Benefits the patient
Transition from Parenteral to Enteral Nutrition
 Cooke RJ, Vandenplas Y, Wahn U (eds): Nutrition Support for Infants and Children at Risk. Nestlé Nutr Workshop Ser Pediatr Program, vol 59, pp 105 114, Nestec Ltd., Vevey/S. Karger AG, Basel, 2007. Transition
Cooke RJ, Vandenplas Y, Wahn U (eds): Nutrition Support for Infants and Children at Risk. Nestlé Nutr Workshop Ser Pediatr Program, vol 59, pp 105 114, Nestec Ltd., Vevey/S. Karger AG, Basel, 2007. Transition
intrahepatic cholestasis type 1. Citation Pediatric Surgery International, 28
 NAOSITE: Nagasaki University's Ac Title Author(s) Partial internal biliary diversion intrahepatic cholestasis type 1. Mochizuki, Kyoko; Obatake, Masayuki Akiko; Hayashi, Tomayoshi; Okudaira Citation Pediatric
NAOSITE: Nagasaki University's Ac Title Author(s) Partial internal biliary diversion intrahepatic cholestasis type 1. Mochizuki, Kyoko; Obatake, Masayuki Akiko; Hayashi, Tomayoshi; Okudaira Citation Pediatric
Case Discussion. Nutrition in IBD. Rémy Meier MD. Ulcerative colitis. Crohn s disease
 26.08.2017 Case Discussion Nutrition in IBD Crohn s disease Ulcerative colitis Rémy Meier MD Case Presentation 30 years old female, with diarrhea for 3 months Shool frequency 3-4 loose stools/day with
26.08.2017 Case Discussion Nutrition in IBD Crohn s disease Ulcerative colitis Rémy Meier MD Case Presentation 30 years old female, with diarrhea for 3 months Shool frequency 3-4 loose stools/day with
4/23/2015. Linda Steinkrauss, MSN, PNP. No conflicts of interest
 Linda Steinkrauss, MSN, PNP No conflicts of interest 1 5 year old African-American female presented to our Endocrinology Clinic with hypoglycemia Abnormal chromosomes Duplication of 11q13.5-11p14.1 affecting
Linda Steinkrauss, MSN, PNP No conflicts of interest 1 5 year old African-American female presented to our Endocrinology Clinic with hypoglycemia Abnormal chromosomes Duplication of 11q13.5-11p14.1 affecting
SUSTAIN BASELINE DATA COLLECTION FORM. Revised 2/4/2014 (both pediatric and adult data elements) 1. Gestational age at birth ( weeks gestation)
 SUSTAIN BASELINE DATA COLLECTION FORM Patient Demographics Revised 2/4/2014 (both pediatric and adult data elements) Did the patient begin Home PN over 90 days ago? Yes No Date began Home PN Patient Number
SUSTAIN BASELINE DATA COLLECTION FORM Patient Demographics Revised 2/4/2014 (both pediatric and adult data elements) Did the patient begin Home PN over 90 days ago? Yes No Date began Home PN Patient Number
Nutritional Issues in Cholestatic Disease
 THE HOSPITAL FOR SICK CHILDREN Nutritional Issues in Cholestatic Disease NASPGHAN-CPNP Joint Session Binita M. Kamath, MBBChir MRCP MTR Associate Professor Division of Gastroenterology, Hepatology and
THE HOSPITAL FOR SICK CHILDREN Nutritional Issues in Cholestatic Disease NASPGHAN-CPNP Joint Session Binita M. Kamath, MBBChir MRCP MTR Associate Professor Division of Gastroenterology, Hepatology and
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
Why would fatty foods aggravate the patient s RUQ pain? What effect does cholecystokinin (CCK) have on gastric emptying?
 CASE 28 A 43-year-old woman presents to the emergency department with the acute onset of abdominal pain. Her pain is located to the right upper quadrant (RUQ) and radiates to the right shoulder. She reports
CASE 28 A 43-year-old woman presents to the emergency department with the acute onset of abdominal pain. Her pain is located to the right upper quadrant (RUQ) and radiates to the right shoulder. She reports
Introduction to Clinical Nutrition
 M-III Introduction to Clinical Nutrition Donald F. Kirby, MD Chief, Section of Nutrition Division of Gastroenterology 1 Things We Take for Granted Air to Breathe Death Taxes Another Admission Our Next
M-III Introduction to Clinical Nutrition Donald F. Kirby, MD Chief, Section of Nutrition Division of Gastroenterology 1 Things We Take for Granted Air to Breathe Death Taxes Another Admission Our Next
4/15/2014. Nurses Take the Lead to Improve Overall Infant Growth. Improving early nutrition. Problem Identification
 Nurses Take the Lead to Improve Overall Infant Growth Cathy Lee Leon, RN, BSN, MBA, NE-BC California Pacific Medical Center-San Francisco Improving early nutrition Standardized feeding protocol Problem
Nurses Take the Lead to Improve Overall Infant Growth Cathy Lee Leon, RN, BSN, MBA, NE-BC California Pacific Medical Center-San Francisco Improving early nutrition Standardized feeding protocol Problem
Necrotizing Enterocolitis: The Role of the Immune System
 Necrotizing Enterocolitis: The Role of the Immune System Patricia Denning, M.D. Associate Professor in Pediatrics Division of Neonatology Emory University School of Medicine What is NEC? What is NEC? Necrotizing
Necrotizing Enterocolitis: The Role of the Immune System Patricia Denning, M.D. Associate Professor in Pediatrics Division of Neonatology Emory University School of Medicine What is NEC? What is NEC? Necrotizing
Pathology of Intestinal Obstruction. Dr. M. Madhavan, MBBS., MD., MIAC, Professor of Pathology Saveetha Medical College
 Pathology of Intestinal Obstruction Dr. M. Madhavan, MBBS., MD., MIAC, Professor of Pathology Saveetha Medical College Pathology of Intestinal Obstruction Objectives list the causes of intestinal obstruction
Pathology of Intestinal Obstruction Dr. M. Madhavan, MBBS., MD., MIAC, Professor of Pathology Saveetha Medical College Pathology of Intestinal Obstruction Objectives list the causes of intestinal obstruction
Basic Fluid and Electrolytes
 Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
BOWEL LENGTHENING procedures may be beneficial
 Serial Transverse Enteroplasty (STEP): A Novel Bowel Lengthening Procedure By Heung Bae Kim, Dario Fauza, Jennifer Garza, Jung-Tak Oh, Samuel Nurko, and Tom Jaksic Boston, Massachusetts Background/Purpose:
Serial Transverse Enteroplasty (STEP): A Novel Bowel Lengthening Procedure By Heung Bae Kim, Dario Fauza, Jennifer Garza, Jung-Tak Oh, Samuel Nurko, and Tom Jaksic Boston, Massachusetts Background/Purpose:
Anaesthetic considerations and peri-operative risks in patients with liver disease
 Anaesthetic considerations and peri-operative risks in patients with liver disease Dr. C. K. Pandey Professor & Head Department of Anaesthesiology & Critical Care Medicine Institute of Liver and Biliary
Anaesthetic considerations and peri-operative risks in patients with liver disease Dr. C. K. Pandey Professor & Head Department of Anaesthesiology & Critical Care Medicine Institute of Liver and Biliary
A review on enteral nutrition guidelines for traumatic brain injury
 A review on enteral nutrition guidelines for traumatic brain injury According to the Centers for Disease Control and Prevention, at least 1.7 million people suffer from traumatic brain injury (TBI) every
A review on enteral nutrition guidelines for traumatic brain injury According to the Centers for Disease Control and Prevention, at least 1.7 million people suffer from traumatic brain injury (TBI) every
Nutrition in the preterm - current menu Dr Heena Hooker Consulting Neonatal Paediatrician Aga Khan University Hospital, Nairobi
 Nutrition in the preterm - current menu Dr Heena Hooker Consulting Neonatal Paediatrician Aga Khan University Hospital, Nairobi Outline O Background O Challenges in preterm nutrition O Parenteral Nutrition
Nutrition in the preterm - current menu Dr Heena Hooker Consulting Neonatal Paediatrician Aga Khan University Hospital, Nairobi Outline O Background O Challenges in preterm nutrition O Parenteral Nutrition
PAEDIATRIC PARENTERAL NUTRITION. Ezatul Mazuin Ayla binti Mamdooh Waffa Hospital Sultanah Aminah
 PAEDIATRIC PARENTERAL NUTRITION Ezatul Mazuin Ayla binti Mamdooh Waffa Hospital Sultanah Aminah Johor Bahru Malnutrition INTRODUCTION pathologic state of varying severity with clinical features caused
PAEDIATRIC PARENTERAL NUTRITION Ezatul Mazuin Ayla binti Mamdooh Waffa Hospital Sultanah Aminah Johor Bahru Malnutrition INTRODUCTION pathologic state of varying severity with clinical features caused
NUTRITIONAL REQUIREMENTS
 NUTRITION AIMS To achieve growth and nutrient accretion similar to intrauterine rates To achieve best possible neurodevelopmental outcome To prevent specific nutritional deficiencies Target population
NUTRITION AIMS To achieve growth and nutrient accretion similar to intrauterine rates To achieve best possible neurodevelopmental outcome To prevent specific nutritional deficiencies Target population
SIBO
 SIBO What is it? Small Intestinal Bowel Overgrowth A chronic bacterial infection of the small intestine Caused by bad bacteria such as E Coli and Clostridium migrating to the small intestine There is not
SIBO What is it? Small Intestinal Bowel Overgrowth A chronic bacterial infection of the small intestine Caused by bad bacteria such as E Coli and Clostridium migrating to the small intestine There is not
