CHRONIC PAIN IN INDIVIDUALS with cerebral palsy
|
|
|
- Lorena Ford
- 5 years ago
- Views:
Transcription
1 1431 ORIGINAL ARTICLE Kinematic Determinants of Anterior Knee Pain in Cerebral Palsy: A Case-Control Study Frances T. Sheehan, PhD, Anna Babushkina, MD, Katharine E. Alter, MD ABSTRACT. Sheehan FT, Babushkina A, Alter KE. Kinematic determinants of anterior knee pain in cerebral palsy: a case-control study. Arch Phys Med Rehabil 2012;93: Objective: To quantify the role patellofemoral and tibiofemoral kinematics may play in development of anterior knee pain (AKP) in individuals with cerebral palsy (CP). Design: Case-control. Setting: Clinical research center. Participants: Knees from individuals with diagnosed CP (n 20) and control knees (n 40) were evaluated. Controls were matched for sex and age based on the group average. Matching by height and weight was a secondary priority. Subjects in the control cohort were asymptomatic with no history of lower leg abnormalities, surgery, or major injury. Only individuals who were physically capable of sustaining slow, cyclic knee flexion-extension for 2.5 minutes and had no contraindications to magnetic resonance imaging were enrolled. Both groups were samples of convenience. Interventions: Not applicable. Main Outcome Measures: Three-dimensional patellofemoral and tibiofemoral joint kinematics, acquired during active leg extension, under volitional control. Results: Participants with CP and AKP (n 8) demonstrated significantly greater patellofemoral extension, valgus rotation, and superior and posterior displacement relative to controls and to the subgroup of participants with CP and no AKP (n 12). Patellofemoral extension discriminated AKP in individuals with CP with 100% accuracy. Conclusions: In quantifying the 3-dimensional, in vivo knee joint kinematics during a volitional extension task, kinematic markers that discriminate AKP in individuals with CP were identified. This provides an ability to predict which individuals with CP are most likely to develop AKP and could enable aggressive conservative treatment, aimed at reducing patella alta and excessive patellofemoral extension, to be prescribed before considering surgical options. The current findings will likely lead to improved clinical diagnostics and interventions for individuals with CP, with the ultimate goal of helping maintain, if not improve, functional mobility throughout the lifespan. Key Words: Kinematics; Magnetic resonance imaging; Patellofemoral joint; Rehabilitation; Tibiofemoral joint by the American Congress of Rehabilitation Medicine CHRONIC PAIN IN INDIVIDUALS with cerebral palsy (CP) affects quality of life, 1 limits participation in activities, and reduces function. 2 The overall prevalence of pain in individuals with CP (up to 79%) 1,3-5 is greater than in the general population, and it increases with age. 4 In addition, pain has been identified as a factor in the loss of previously obtained functional mobility skills. 6 For example, the presence of anterior knee pain (AKP) can severely limit ambulation. Idiopathic AKP in the general, active population (often referred to as patellofemoral pain syndrome [PFPS]) is common, constituting 14% to 17% of all injuries presenting to sports injury clinics 7,8 and having a prevalence of 23.7% among midshipman at the U.S. Naval Academy. 9 For individuals with CP, this prevalence is much larger (39%). 4 Despite its prevalence, the causes of AKP remain poorly characterized in individuals with CP. 4,10-13 Most studies evaluating AKP in individuals with CP have focused on static radiographic findings of patellar fragmentation and patella alta, 10,12,13 as well as knee flexion contractures. 10,12 Using incidence rates, such studies have assumed an association between these variables and AKP, but direct correlations have not been documented. Rosenthal and Levine 10 presented some of the earliest research in this area, but found no direct correlation between AKP and knee flexion contractures or patellar pole fragmentation. A recent study 12 categorized 3 groups of children with CP and AKP, with all groups sharing the common traits of patella alta and rectus spasticity. Although this study highlighted potential causes of AKP among individuals with CP, it did not provide an ability to predict AKP. Accurately describing the origins of joint dysfunction and having the ability to predict AKP will likely allow more directed treat- From the Functional and Applied Biomechanics Section, Rehabilitation Medicine Department, National Institutes of Health, Bethesda, MD (Sheehan, Alter); Georgetown University Hospital, Department of Orthopaedic Surgery, Washington, DC (Babushkina); and Mt Washington Pediatric Hospital, an affiliate of Johns Hopkins Health System Corp and University of Maryland Medical System Corp, Baltimore, MD (Alter). Presented in part to the American Academy of Cerebral Palsy and Developmental Medicine, September 23, 2010, Washington, DC; and to the American Society of Biomechanics, August 19, 2010, Providence, RI. Supported by the Intramural Research Program of the National Institutes of Health (NIH), and the Clinical Center at the NIH. No commercial party having a direct financial interest in the results of the research supporting this article has or will confer a benefit on the authors or on any organization with which the authors are associated. Reprint requests to Frances T. Sheehan, PhD, National Institutes of Health, Bldg 10 CRC RM , 10 Center Dr MSC 1604, Bethesda, MD , sheehan@cc.nih.gov. In-press corrected proof published online on May 24, 2012, at /12/ $36.00/0 AKP CP CPC GMFCS MAS_HAM MAS_RF MMT MR NIH PF PFPS TF List of Abbreviations anterior knee pain cerebral palsy cine-phase contrast Gross Motor Function Classification System modified Ashworth scale for the hamstrings modified Ashworth scale for the rectus femoris manual muscle test for the rectus femoris magnetic resonance National Institutes of Health patellofemoral patellofemoral pain syndrome tibiofemoral
2 1432 KNEE KINEMATICS AND PAIN IN CEREBRAL PALSY, Sheehan Table 1: Demographics Demographic Variable Control (n 40) CP (n 20) P Sex (F/M) 20/20 10/ Age 22y3mo 7y3mo 21y8mo 10y1mo.87 Weight (kg) * Height (cm) CP Without Pain (n 12) CP With Pain (n 8) P Sex (F/M) 5/7 5/3.65 Age 19y1mo 8y6mo 25y8mo 11y6mo.19 Weight (kg) Height (cm) GMFCS I (8), II (4) I (1), II (2), III (5).006* level MMT 4 (8), 3 (3), 3 (1) 3 (2), 3 (6).003* MAS_RF 0 (2), 1 (3), 1 (6), 2 (1) 0 (1), 1 (2), 1 (3), 2 (2).77 MAS_HAM 0 (1), 1 (1), 1 (7), 2 (3), 3 (0) 0 (0), 1 (0), 1 (2), 2 (3), 3 (3).12 Diagnosis Hemiplegia (3), diplegia (9), quadriplegia (0) Hemiplegia (0), diplegia (5), quadriplegia (3).04* NOTE. Values are mean SD or as otherwise indicated. The upper portion compares the control and CP cohorts, whereas the lower portion compares the 2 subgroups (CP_pain and CP_noPain) within the CP cohort. For continuous and discrete variables, a 2-tailed Student t test and a 2-tailed 2 test, respectively, were used to test for significance. For categorical data, the number of participants included at each level or score is given in parentheses: sex (M or F), GMFCS (levels of I, II, III, IV, and V), MMT (scores of 0-5), MAS_RF (scores of 0, 1, 1, 2, and 3), MAS_HAM (scores of 0, 1, 1, 2, and 3), Diagnosis (categories of hemiplegia, diplegia, and quadriplegia). Scores of I, 5, 0, and 0 for the GMFCS, MMT, MAS_RF, and MAS_HAM, respectively, indicate the least impaired state. All data are listed for each knee. Abbreviations: CP_noPain cohort, all knees within the CP cohort without chronic AKP; CP_pain cohort, all knees within the CP cohort with chronic AKP 6 mos; F (M), the number of knees within the study from subjects that were (women or girls) or (men or boys). *P.05. ments, which may help preserve functional mobility in individuals with CP. While the etiology of AKP remains poorly characterized in individuals with CP, PFPS has been well studied. The advent of new imaging-based techniques that can accurately quantify 3-dimensional, in vivo patellofemoral (PF) kinematics has rapidly advanced the understanding of PFPS over the last few years It is interesting to note that patella alta has been documented in both the CP 2,10,13,21,22 and PFPS 23,24 populations, with subsets from both populations experiencing patellar dislocation. 12,25 Surprisingly, no study to date has quantified PF kinematics or alignment in individuals with CP and AKP, outside the sagittal plane. An understanding of 3-dimensional PF and tibiofemoral (TF) kinematics in individuals with CP and AKP will likely help elucidate the source of this pain and provide a better understanding of knee joint dysfunction within the CP population. Therefore, the purpose of this study was to quantify the role that knee joint kinematics may play in the development of AKP in individuals with CP and to determine whether these kinematics could discriminate the presence of AKP in a population of individuals with CP. To accomplish this, a novel, dynamic magnetic resonance (MR) imaging technique (cine-phase contrast [CPC]) was used to quantify the in vivo, 3-dimensional knee joint kinematics during a volitional leg extension task in a group of individuals with diagnosed CP, but varying in the reporting of AKP. Three specific hypotheses were tested: (1) PF superior position is greater in individuals with CP who report AKP, in comparison with those who do not; (2) this difference is large enough to enable the prediction of AKP in CP based on a discriminant analysis; and (3) the presence of patella alta in individuals with CP leads to increased lateral shift and tilt, in a manner similar to that documented in PFPS. 24 METHODS In this case-control study, 18 individuals with CP were recruited from local physical medicine and rehabilitation clinics, as well as ongoing National Institutes of Health (NIH) studies. On entering this study, all participants gave written informed consent. If the participant was a minor, written assent was given, with a legal guardian providing written consent. This study was approved by the internal review board of the National Institute of Child Health and Human Development at the NIH. Only individuals who were physically capable of sustaining slow, cyclic knee flexion-extension for 2.5 minutes were accepted into the study. If both lower limbs were involved and time permitted, both knees were scanned, for a total of 20 knees with CP (table 1). Using a physical examination and history, an in-house physiatrist (K.E.A.) recorded the diagnosis (hemiplegia, diplegia, or quadriplegia), the presence of chronic AKP ( 6mo duration), the Gross Motor Function Classification System (GMFCS) level, 26,27 the manual muscle testing score for the knee extensors (MMT), 28 and a Modified Ashworth Scale 29 score for the rectus femoris and hamstrings (MAS_RF and MAS_HAM) for each participant. Each participant was assigned to 1 of 2 subgroups based on the presence of chronic AKP. These 2 groups were referred to as the CP_pain subgroup, which reported chronic AKP 6 months, and the CP_noPain subgroup, which did not. The kinematics of 40 control knees, recruited from ongoing NIH studies, formed the baseline for comparison. These knees were matched for sex and age based on group averages (see table 1). Matching by both height and weight was a secondary priority, as individuals with CP tend to be lighter and shorter than their peers in the general population. All subjects in the control cohort were asymptomatic with no history of lower leg abnormalities, surgery, or major injury. For both cohorts, any subject with contraindications to MR imaging was excluded.
3 KNEE KINEMATICS AND PAIN IN CEREBRAL PALSY, Sheehan 1433 Fig 1. Experimental setup. Subjects were placed supine within the MR bore. A coil holder stabilized 2 flexible coils medial and lateral to the knee and provided medial-lateral support for the knee. A cushion wedge was placed under the knee and adjusted so that each subject could select his/her own terminal extension angle, which the subject could reach repeatedly and comfortably. An auditory metronome (played through a pair of headphones) provided guidance for the repeated movement (2 beats per cycle at 35 cycles/ min). Subjects were placed supine in an MR imager with the knee bent and supported on a cushioned block (fig 1). The subjects were then asked to cyclically flex and extend their knee while a dynamic CPC MR image set (x,y,z velocity and anatomic images frames) was acquired. Of all the 3-dimensional in vivo techniques for measuring joint kinematics, CPC MR imaging is the most accurate (accuracy 0.3mm 30 ) and the only one that can define both muscular and skeletal kinematics. To establish anatomic coordinate systems, dynamic cine images (anatomic images only) were acquired in 3 axial planes. 31,32 Threedimensional displacements and orientations (fig 2) were defined for both the patella and tibia relative to the femur (PF and TF kinematics, respectively) through integration of the CPC MR velocity data. 33 To account for skeletal size variations across subjects, all displacements were scaled by the ratio of the average epicondylar width from an asymptomatic population (76.9mm 31 ) to the epicondylar width for each individual knee. Scaling, instead of normalization, was used so that the results would be directly comparable to past knee joint kinematic studies that did not use normalization. Data were collected in even temporal increments. To create population averages, each kinematic variable was interpolated to single-degree knee angle increments. All data were presented for the extension portion of the movement only. An individual subject s range of motion depended on the relationship between the leg length and the inner bore dimension, as well as the subject s own physical ability. The experimental setup was adapted to enable subjects to select the terminal extension angle, which they could reach comfortably and repeatedly. Therefore, not all subjects were represented in the average kinematics at all knee angles. Data representing 20% or fewer subjects were eliminated from the group average. Patella alta was defined as a significant (P.05) increase in PF superior displacement. Although this is not the typical measure of patella alta (eg, the Insall-Salvati ratio 34 ), the current method may have more physiologic relevance because the kinematic relationship is defined between the patella and the femur (not tibia) and is measured during volitional exercise with quadriceps activity (not statically). An unpublished preliminary study demonstrated that the value of PF superior displacement (as measured in the current study) in individuals with CP was moderately correlated (r.67, P.02) with the patellophyseal index, a static MR-based index of patella alta that is predictive of contact area and chondral defects. 35 Statistical Methods An a priori power analysis revealed that 10 participants per subgroup (CP_pain and CP_noPain) were needed to have a detectable overall significance (.05, 0.8). This analysis assumed that the same differences in value and variance of PF superior position between the 2 subgroups (CP_pain and CP_noPain) would exist as was found in a previous study 24 between a control cohort (mean SD: mm) and a cohort of individuals with PFPS (mean SD: mm). To simplify the interpretation of the correlations, the full range of motion for each kinematic variable was represented by a single value. The value of a kinematic variable was defined as its magnitude at a 20 knee angle. This was the angle closest to full extension where all subjects were represented. Statistically significant PF and TF kinematic (12 parameters) differences (hypothesis 1) were investigated using a 2-tailed Student t test, assuming unequal variances between (1) the CP and control cohorts; (2) the 2 subgroups within the CP cohort; and (3) each individual CP subgroup and the control population. A Bonferroni-type false discovery rate procedure 36 was used to adjust the P values for the multiple comparisons. Two-tailed chi-square and Student t tests were used to evaluate differences in demographics (see table 1).
4 1434 KNEE KINEMATICS AND PAIN IN CEREBRAL PALSY, Sheehan Fig 2. Three-dimensional PF translations and rotations. The exact directions associated with the 3 movement directions (positive directions: medial, superior, and anterior) are based on establishing a 3-dimensional coordinate system, but can be approximated in 2 dimensions using the anatomic landmarks from which the coordinate system is established. 31 The Po was selected to be the most posterior point on the patella at its midsection in the superior-inferior direction. The Fo was selected to be the deepest point within the femoral sulcus at the level of the femoral epicondylar width. The PF displacements were derived by defining how the patellar origin moved relative to the femoral origin. The rotations are based on an xyz-body fixed Cardan rotation sequence, 54 but can be approximated using anatomic lines (positive rotations: medial tilt, flexion, and varus rotation). The tibial coordinate system was defined in a similar manner, with the tibial origin being the center of the patellar tendon insertion into the tibia, and tibiofemoral internal rotation being positive. Abbreviations: Fo, femoral origin; Po, patellar origin. A discriminant analysis was performed to determine whether the presence of pain in the CP cohort could be predicted (hypothesis 2) using 1 of 3 sets of predicting variables: (1) the value of PF superior displacement; (2) the value of PF extension; and (3) the combined values of PF superior displacement and extension. The predicting variable sets were defined based on the kinematic variables that demonstrated the largest variation from the control population. The Pearson correlation coefficients (CP cohort only) for each PF degree of freedom with each of the other 5 PF degrees of freedom were calculated (hypothesis 3). Spearman correlations were calculated within the CP cohort between the knee joint kinematics and both the presence of AKP and the GMFCS level. In addition, the correlation between each of the PF and TF kinematic variables and each of the other kinematic variables was determined using a Pearson correlation. Statistical significance was set at P.05. RESULTS Quadriceps weakness along with mild to moderate spasticity in both the hamstrings and rectus femoris existed for all participants with CP. No differences in the distribution of the Modified Ashworth Score were found between the subgroups within the CP cohort (CP_pain and CP_noPain) (see table 1). All participants in the CP cohort were ambulatory (GMFCS level ranging from I to III), but the CP_noPain subgroup tended to be higher functioning and stronger. The distribution of functional level (GMFCS level) was not equal among the 2 subgroups, likely because AKP was correlated with the GMFCS level (.65, P.002). The CP cohort weighed less than the control cohort. The first hypothesis (PF superior displacement was greater in individuals with CP who reported pain) was supported (table 2; 12.4mm, P.001). This same result held true when comparing the entire CP cohort to controls (12.9mm, P.001). In addition, PF extension, varus rotation, and posterior displacement were increased in the CP subgroup that reported AKP versus the subgroup that did not. Again, this same result held true when comparing the entire CP cohort to the control cohort. PF lateral translation and tilt were no different between the CP and control cohorts, nor were they different between the 2 subgroups within the CP cohort. Thus, for the entire CP cohort,
5 KNEE KINEMATICS AND PAIN IN CEREBRAL PALSY, Sheehan 1435 Table 2: Kinematics Comparisons of the Values of Each Kinematics Variable Displacement (mm) Rotation (deg) Cohort Medial Superior Anterior Flexion Medial Tilt Varus PF CP vs control * 3.5* 10.0* CP_pain vs control * 6.4* 17.8* * CP_noPain vs control * CP_pain vs * * CP_noPain TF CP vs control * * 0.1 CP_pain vs control * * 0.3 CP_noPain vs control * 0.0 CP_pain vs CP_noPain NOTE. The value of each kinematic variable was defined as its magnitude at a knee angle of 20. Differences are listed between the (1) CP cohort and the controls, (2) the CP_pain subgroup vs the controls, (3) the CP_noPain subgroup vs the controls, and (4) the CP_pain vs the CP_noPain subgroups in the value of PF and TF kinematics (upper and lower portions of the table, respectively). Abbreviations: CP_noPain cohort, all knees within the CP cohort without chronic AKP; CP_pain cohort, all knees within the CP cohort with chronic AKP 6 mos. *P.001; P.05; P.05. patella alta was accompanied by increased PF posterior displacement, extension, and varus, along with increased TF superior displacement and internal rotation. The increased extension and varus rotation caused the superior patellar pole to shift posteriorly and laterally, respectively. These same differences existed in both subgroups (fig 3), but were much larger in the subgroup with AKP for greater than 6 months (CP_pain). PF posterior shift and varus rotation were not significantly greater in the subgroup of knees within the CP cohort that did not have chronic AKP (CP_noPain) than in controls. No significant differences existed between the 2 CP subgroups (CP_pain and CP_noPain) for TF kinematics. The second hypothesis was supported. PF superior displacement could discriminate the presence of AKP within the CP cohort to an accuracy of 80% (fig 4). PF extension alone could better discriminate the presence of AKP within the CP cohort, with an accuracy of 100%. The 2 data points that were closest to the extension discrimination line (1 from each of the subgroups) were 1.3 different from each other, well outside the accuracy and precision limits of the tracking kinematics with CPC MR imaging and larger than the subject repeatability for PF flexion (0.9 ). 30 The third hypothesis (that PF superior displacement was correlated with PF lateral tilt) was not supported, yet correlations between specific PF kinematic variables and other study parameters were found. The existence of AKP was strongly correlated with the value of PF extension (.85, P.001) and superior displacement (.80, P.001), and moderately correlated with the GMFCS level (.65, P.002), PF posterior displacement (.60, P.005), and PF valgus (.51, P.02). The GMFCS level was moderately correlated with both PF extension (.74, P.001) and superior displacement (.61, P.004). The 4 PF kinematic variables that were increased in the CP cohort were all moderately correlated with each other (r.51.72), likely indicating a single source for these variations. The TF kinematic variables did not correlate with any other study variable. DISCUSSION In quantifying the 3-dimensional, in vivo knee joint kinematics during a volitional extension task in individuals with CP, both with and without AKP, this study identified kinematic markers that clearly discriminated AKP in individuals with CP. Interestingly, few studies have even been able to establish a correlation between pain and PF kinematics in the general population, 24 let alone demonstrate an ability to discriminate pain based on PF kinematics. The current study provides evidence that altered PF kinematics are related both to AKP and to functional mobility (GMFCS level). This mirrors recent results that described the relationship between GMFCS level and the incidence of hip displacement as linear. 37 The PF joint, in contrast to the TF joint, is the most affected in the individuals with CP, which agrees with the fact that clinically, individuals with CP frequently have PF joint dysfunction, 16,19,25,27 limited knee extension strength, and spasticity, all of which contribute to long-term mobility impairments. Thus, treatments targeting the altered PF kinematics found within the current CP cohort may best alleviate pain and improve functional mobility. Accurately quantifying 3-dimensional joint function helps improve our clinical understanding of CP 38 by providing new information that will help guide clinicians as they explore and develop therapies and interventions for patients with CP and AKP, with the ultimate goal of reducing pain and minimizing the loss of previously obtained functional mobility skills. 6 The ability to discriminate AKP in the current CP population (hypothesis 2) indicates its likely etiology. It has been reported previously that increased hamstrings spasticity, quadriceps spasticity, and/or quadriceps weakness can, over time, lengthen the patellar tendon, resulting in patella alta. 10,12,13 Patella alta has been reported to result in increased PF contact stress. 39 For the knees within the CP cohort that experienced chronic AKP (CP_pain subgroup), the combination of patella alta and femoral sulcus shape places the patella well outside the femoral sulcus in terminal extension (fig 5). Subsequently, the excessive force within the extensor mechanism rotates (extends) the patella until its posterior edge contacts the femoral shaft. Thus, not only is there excessive contact force, but it is exerted between cartilage and bone, rather than the normal cartilageto-cartilage contact, likely resulting in pain. The knees within the CP cohort that did not have chronic AKP (CP_noPain subgroup) appear to have less force across the extensor mechanics, evidenced by their lower PF superior displacement
6 1436 KNEE KINEMATICS AND PAIN IN CEREBRAL PALSY, Sheehan Fig 3. Comparison of PF kinematics between the CP subgroups. Double arrow lines with 2 asterisks (**) above denote the ranges where there are significant differences between subgroups. The control cohort is represented by a solid line with 1 SD range shown in a shaded area. The CP subgroups without AKP and with pain (CP_noPain and CP_pain) are represented by solid lines with a hollow square symbol and single asterisk, respectively. One SD bar provided every 5. Abbreviations: CP_noPain cohort, all knees within the CP cohort without chronic AKP; CP_pain cohort, all knees within the CP cohort with chronic AKP >6 mos; Disp, displacement; I/S, inferior/superior; L/M, lateral/medial; P/A, posterior/anterior; rot, rotation.
7 KNEE KINEMATICS AND PAIN IN CEREBRAL PALSY, Sheehan 1437 Fig 4. Discriminant analysis. PF superior displacement versus PF extension. The participants with CP and AKP (CP_pain) are represented by circular symbols. The participants with CP and no AKP (CP_noPain) are represented by square symbols. The average value of PF superior displacement and extension for the control cohort is represented by a star with lines extending the width and height of the graph. Abbreviations: AK, anterior knee; Disp, displacement. and extension as compared with the knees within the CP cohort that had chronic AKP (CP_pain subgroup). The relatively mild PF extension in this subgroup may actually ameliorate contact stress because it brings more of the patella in contact with the trochlear cartilage. Future work focusing on 3-dimensional PF dynamic contact patterns, areas, and forces in individuals with CP is needed to more fully explore these concepts. Increased PF lateral shift and tilt did not accompany patella alta in this CP cohort (hypothesis 3), but does in the general population with PFPS, 24 indicating that the etiology of kinematic alterations in these 2 groups is likely different (a hypomobile vs a hypermobile patella). In the current CP cohort, there is clearly patellar hypomobility with alta resulting from excessive force in the extensor mechanism, caused by knee flexion contractures and spasticity. Although the patella is free from the constraints of the femoral groove in terminal extension (due to patella alta), the excessive force in the extensor mechanism likely inhibits lateral patellar shift and tilt by pulling the patella posteriorly into the femur. A history of dislocation in children with CP and AKP has been documented, 12 which easily fits with a hypomobile patella, particularly if TF valgus is present. In this situation, the extensor mechanism can be likened to a bowstring, 40 and a slight shift in the PF position can release the bowstring, causing an abrupt and forceful patellar dislocation. In contrast to the CP cohort, otherwise healthy individuals with patella alta and PFPS likely have a hypermobile patella, as patella alta has been correlated with excessive PF lateral tilt and shift 24 and associated with patellar dislocation In such individuals, patella alta is most likely caused by a generalized joint laxity (evidenced by a flexed, not extended patella; see fig 5). In terminal extension, the combined alta and laxity enables the patella to shift and tilt laterally, with extreme shift resulting in dislocation. Thus, unlike the CP cohort, pain in individuals with PFPS is likely the result of (1) reduced contact area, (2) larger patellar movements across the femur, and (3) higher forces required to reengage the patella in the sulcus during early flexion. This unique etiology of pain between the knees within the CP cohort that experienced chronic AKP and knees in the general population with PFPS indicates that clinical interventions aimed at eliminating AKP likely need to be tailored specifically to each group. The current data add more specific insights into which subsets of individuals with CP might benefit from both conservative and surgical intervention by delineating the severity of PF extension and patella alta that appears to lead to AKP within the CP population. Recently, there has been a resurgence of interest in correcting patella alta 44,45 as part of a multilevel surgery The strong correlations between PF extension, patella alta, and the presence of AKP indicate that when severe alta is present, reducing it while lengthening the quadriceps will likely reduce patellar extension, restore cartilage-to-cartilage contact, and thereby relieve AKP. For example, traditionally the spastic or out-of-phase rectus is often treated with transfer surgery. Several studies have demonstrated that the mechanism by which these transfers improve knee function involves reducing the extensor torque rather than a new ability to create flexion torque. Thus, improvements in knee pain after a rectus transfer are likely attributable to both an increase in range of motion and a normalization of PF kinematics. Having an ability to discriminate which individuals with CP are most likely to develop AKP (either directly through quantifying PF kinematics or indirectly through functional assessments such as GMFSC level, which is correlated with PF kinematics and AKP) could enable aggressive conservative treatment aimed at reducing patella alta and excessive PF extension (eg, stretching and mobilization) to be prescribed first. This could help maintain joint function and either delay or eliminate the need to surgically reduce the patella alta and PF extension. Studies evaluating the effects of clinical intervention on 3-dimensional joint kinematics are clearly needed to bring further clarity. Another issue that needs further investigation is the higher levels of tibial internal rotation seen in the CP cohort. Numerous individuals within this cohort clearly demonstrated both internal femoral rotation and external tibial rotation (as measured at the ankle) during ambulation. This discrepancy likely arises because tibial internal rotation was measured at the proximal tibia and distal femur. A twist about the long axis of the tibia could easily enable internal rotation at the knee while the distal tibia and foot remain externally rotated. Study Limitations A limitation of the current study is that nonambulatory individuals with CP (GMFCS levels IV or V) were excluded, as the primary focus of this study was on the movement patterns of the knee joint under volitional control. Although AKP is also reported by nonambulatory individuals, the underlying mechanism of pain in these patients where pain is reported while sitting may be different than that in ambulatory individuals. Thus, the current results and conclusions may not be relevant when treating a more severely affected population. However, it is appropriate to have different assessment tools for different functional levels, as the clinical needs of these groups can differ. A secondary limitation is that CPC MR imaging, as applied to the study of 3-dimensional in vivo joint kinematics, is not a standard clinical tool. Thus, the methodologies are currently not available to most clinicians treating patients. Work is ongoing to improve clinical access to this tool. The moderate correlation between the 2 measures of patella alta, one
8 1438 KNEE KINEMATICS AND PAIN IN CEREBRAL PALSY, Sheehan Fig 5. Visual description of PF extension and patella alta at 20 of knee extension, during active extension. The knee angle was defined as 180. The top row represents a single participant with CP and AKP. This participant had the most severe alta of the entire CP cohort. (A) The CPC MR anatomic image. The PF superior displacement and extension is visually approximated on the image. Patellar extension can be approximated by its 2-dimensional counterpart (the angle between the vector bisecting the anterior and posterior edges of the distal femur and the vector delineating the posterior edge of the patella). The patellar superior position is the superior displacement of the patellar origin relative to the femoral origin (see fig 2) in the femoral coordinate system. (B) A 3-dimensional model of the knee joint for this same individual at 20 knee extension. The patella is not shown so that the contact between the patellar cartilage and femoral shaft can be seen. (C) A CPC MR image for a single control subject with the third highest level of patellar superior position of all the control subjects. (D) A CPC MR image from an otherwise healthy patient with PFPS from a previous study. 24 Of all the patients with PFPS in this previous study, this subject had the second highest level of patella alta. Abbreviations: PF flex, patellofemoral flexion (rotation about the medial-lateral axis); PF SI, patellofemoral superior-inferior displacement. acquired statically and one dynamically, indicates that there is a potential for finding surrogate static MR measures that may provide a similar level of insight into joint dysfunction. Lastly, this relatively small cohort cannot represent the vast number of individuals with CP. Yet, the enrollment of individuals with a specific pathologic disorder was on par with recent work evaluating AKP in individuals with CP. 12 Work is ongoing to determine whether the same relationships between knee joint kinematics, functional mobility, and AKP exist over a larger population of individuals with CP. CONCLUSIONS This study elucidated kinematic markers that could discriminate AKP within a cohort of individuals with CP, and demonstrated clear correlations between AKP, GMFCS, and PF kinematics. In doing so, it has provided new insights into knee dysfunction with implications for clinical management of patients with CP, and has opened numerous pathways for future research. Specifically, treatments that target the excessive PF superior displacement and extension may best alleviate pain and improve functional mobility. As this study focused on the knee joint in isolation, it will be important to expand future studies to incorporate the potential contributing factors at the hip and ankle as well. 53 These study findings will likely lead to improved clinical diagnostics and interventions for this group, with the ultimate aim of helping individuals with CP maintain, if not improve, their functional mobility throughout their lifespan. Acknowledgments: We thank Sara Sadeghi, Abrahm Behnam, MSE, Cris Zampieri-Gallagher, PhD, Bonnie Damaska, and the Diagnostic Radiology Department at the National Institutes of Health for their support and research time.
9 KNEE KINEMATICS AND PAIN IN CEREBRAL PALSY, Sheehan 1439 References 1. Tuzun EH, Guven DK, Eker L. Pain prevalence and its impact on the quality of life in a sample of Turkish children with cerebral palsy. Disabil Rehabil 2010;32: Murphy KP. The adult with cerebral palsy. Orthop Clin North Am 2010;41: Andersson C, Mattsson E. Adults with cerebral palsy: a survey describing problems, needs, and resources, with special emphasis on locomotion. Dev Med Child Neurol 2001;43: Jahnsen R, Villien L, Aamodt G, Stanghelle JK, Holm I. Musculoskeletal pain in adults with cerebral palsy compared with the general population. J Rehabil Med 2004;36: Parkinson KN, Gibson L, Dickinson HO, Colver AF. Pain in children with cerebral palsy: a cross-sectional multicentre European study. Acta Paediatr 2010;99: Bartlett DJ, Hanna SE, Avery L, Stevenson RD, Galuppi B. Correlates of decline in gross motor capacity in adolescents with cerebral palsy in Gross Motor Function Classification System levels III to V: an exploratory study. Dev Med Child Neurol 2010;52:e Taunton JE, Ryan MB, Clement DB, McKenzie DC, Lloyd-Smith DR, Zumbo BD. A retrospective case-control analysis of 2002 running injuries. Br J Sports Med 2002;36: Iwamoto J, Takeda T, Sato Y, Matsumoto H. Retrospective case evaluation of gender differences in sports injuries in a Japanese sports medicine clinic. Gend Med 2008;5: Boling M, Padua D, Marshall S, Guskiewicz K, Pyne S, Beutler A. Gender differences in the incidence and prevalence of patellofemoral pain syndrome. Scand J Med Sci Sports 2009;20: Rosenthal RK, Levine DB. Fragmentation of the distal pole of the patella in spastic cerebral palsy. J Bone Joint Surg Am 1977;59: Samilson RL, Gill KW. Patello-femoral problems in cerebral palsy. Acta Orthop Belg 1984;50: Senaran H, Holden C, Dabney KW, Miller F. Anterior knee pain in children with cerebral palsy. J Pediatr Orthop 2007;27: Topoleski TA, Kurtz CA, Grogan DP. Radiographic abnormalities and clinical symptoms associated with patella alta in ambulatory children with cerebral palsy. J Pediatr Orthop 2000;20: Campbell SK. Quantifying the effects of interventions for movement disorders resulting from cerebral palsy. J Child Neurol 1996;11(Suppl 1):S Jenkins SE, Harrington ME, Zavatsky AB, O Connor JJ, Theologis TN. Femoral muscle attachment locations in children and adults, and their prediction from clinical measurement. Gait Posture 2003;18: Mackey AH, Walt SE, Lobb GA, Stott NS. Reliability of upper and lower limb three-dimensional kinematics in children with hemiplegia. Gait Posture 2005;22: MacIntyre NJ, Hill NA, Fellows RA, Ellis RE, Wilson DR. Patellofemoral joint kinematics in individuals with and without patellofemoral pain syndrome. J Bone Joint Surg Am 2006;88: Sheehan FT, Derasari A, Brindle TJ, Alter KE. Understanding patellofemoral pain with maltracking in the presence of joint laxity: complete 3D in vivo patellofemoral and tibiofemoral kinematics. J Orthop Res 2009;27: Wilson NA, Sheehan FT. Dynamic in vivo quadriceps lines-ofaction. J Biomech 2010;43: Wilson NA, Press JM, Koh JL, Hendrix RW, Zhang LQ. In vivo noninvasive evaluation of abnormal patellar tracking during squatting in patients with patellofemoral pain. J Bone Joint Surg Am 2009;91: Lotman DB. Knee flexion deformity and patella alta in spastic cerebral palsy. Dev Med Child Neurol 1976;18: Villani C, Billi A, Morico GF, Bonsignore D. A comparative study of the extensor force of the quadriceps between subjects with a normal patella and those with patella alta of neurological pathogenesis. Ital J Orthop Traumatol 1988;14: Hirano A, Fukubayashi T, Ishii T, Ochiai N. Relationship between the patellar height and the disorder of the knee extensor mechanism in immature athletes. J Pediatr Orthop 2001;21: Sheehan FT, Derasari A, Fine KM, Brindle TJ, Alter KE. Q-angle and J-sign: indicative of maltracking subgroups in patellofemoral pain. Clin Orthop Relat Res 2010;468: Powers CM, Ward SR, Fredericson M, Guillet M, Shellock FG. Patellofemoral kinematics during weight-bearing and non-weightbearing knee extension in persons with lateral subluxation of the patella: a preliminary study. J Orthop Sports Phys Ther 2003;33: McCormick A, Brien M, Plourde J, Wood E, Rosenbaum P, McLean J. Stability of the Gross Motor Function Classification System in adults with cerebral palsy. Dev Med Child Neurol 2007;49: Rosenbaum PL, Palisano RJ, Bartlett DJ, Galuppi BE, Russell DJ. Development of the Gross Motor Function Classification System for cerebral palsy. Dev Med Child Neurol 2008;50: Paternostro-Sluga T, Grim-Stieger M, Posch M, et al. Reliability and validity of the Medical Research Council (MRC) scale and a modified scale for testing muscle strength in patients with radial palsy. J Rehabil Med 2008;40: Bohannon RW, Smith MB. Interrater reliability of a modified Ashworth scale of muscle spasticity. Phys Ther 1987;67: Behnam AJ, Herzka DA, Sheehan FT. Assessing the accuracy and precision of musculoskeletal motion tracking using cine-pc MRI on a 3.0T platform. J Biomech 2011;44: Seisler AR, Sheehan FT. Normative three-dimensional patellofemoral and tibiofemoral kinematics: a dynamic, in vivo study. IEEE Trans Biomed Eng 2007;54: Shibanuma N, Sheehan FT, Stanhope SJ. Limb positioning is critical for defining patellofemoral alignment and femoral shape. Clin Orthop Relat Res 2005;434: Sheehan FT, Zajac FE, Drace JE. In vivo tracking of the human patella using cine phase contrast magnetic resonance imaging. J Biomech Eng 1999;121: Grelsamer RP, Meadows S. The modified Insall-Salvati ratio for assessment of patellar height. Clin Orthop Relat Res 1992;282: Ali SA, Helmer R, Terk MR. Patella alta: lack of correlation between patellotrochlear cartilage congruence and commonly used patellar height ratios. AJR Am J Roentgenol 2009;193: Benjamini Y, Hochber Y. Controlling the false discovery rate: a practical and powerful approach to multiple testing. J R Stat Soc Series B Stat Methodol 1995;57: Soo B, Howard JJ, Boyd RN, et al. Hip displacement in cerebral palsy. J Bone Joint Surg Am 2006;88: Sheehan FT, Seisler AR, Alter KE. Three-dimensional in vivo quantification of knee kinematics in cerebral palsy. Clin Orthop Relat Res 2008;466: Singerman R, Davy DT, Goldberg VM. Effects of patella alta and patella infera on patellofemoral contact forces. J Biomech 1994; 27: Jackson AM. Anterior knee pain. J Bone Joint Surg Br 2001;83: Amis AA. Current concepts on anatomy and biomechanics of patellar stability. Sports Med Arthrosc 2007;15: Dejour H, Walch G, Nove-Josserand L, Guier C. Factors of patellar instability: an anatomic radiographic study. Knee Surg Sports Traumatol Arthrosc 1994;2: Escala JS, Mellado JM, Olona M, Gine J, Sauri A, Neyret P. Objective patellar instability: MR-based quantitative assessment
10 1440 KNEE KINEMATICS AND PAIN IN CEREBRAL PALSY, Sheehan of potentially associated anatomical features. Knee Surg Sports Traumatol Arthrosc 2006;14: Roberts WM, Adams JP. The patellar-advancement operation in cerebral palsy. J Bone Joint Surg Am 1953;35: Samilson RL. Current concepts of surgical management of deformities of the lower extremities in cerebral palsy. Clin Orthop Relat Res 1981;158: Joseph B, Reddy K, Varghese RA, Shah H, Doddabasappa SN. Management of severe crouch gait in children and adolescents with cerebral palsy. J Pediatr Orthop 2010;30: Novacheck TF, Stout JL, Gage JR, Schwartz MH. Distal femoral extension osteotomy and patellar tendon advancement to treat persistent crouch gait in cerebral palsy. Surgical technique. J Bone Joint Surg Am 2009;91(Suppl 2): Rodda JM, Graham HK, Nattrass GR, Galea MP, Baker R, Wolfe R. Correction of severe crouch gait in patients with spastic diplegia with use of multilevel orthopaedic surgery. J Bone Joint Surg Am 2006;88: Stout JL, Gage JR, Schwartz MH, Novacheck TF. Distal femoral extension osteotomy and patellar tendon advancement to treat persistent crouch gait in cerebral palsy. J Bone Joint Surg Am 2008;90: Asakawa DS, Blemker SS, Rab GT, Bagley A, Delp SL. Threedimensional muscle-tendon geometry after rectus femoris tendon transfer. J Bone Joint Surg Am 2004;86: Muthusamy K, Seidl AJ, Friesen RM, Carollo JJ, Pan Z, Chang FM. Rectus femoris transfer in children with cerebral palsy: evaluation of transfer site and preoperative indicators. J Pediatr Orthop 2008;28: Ounpuu S, Muik E, Davis RB III, Gage JR, DeLuca PA. Rectus femoris surgery in children with cerebral palsy. Part I: the effect of rectus femoris transfer location on knee motion. J Pediatr Orthop 1993;13: Davis IS, Powers CM. Patellofemoral pain syndrome: proximal, distal, and local factors, an international retreat, April 30-May 2, 2009, Fells Point, Baltimore, MD. J Orthop Sports Phys Ther 2010;40:A1-A Sheehan FT, Mitiguy P. In regards to the ISB recommendations for standardization in the reporting of kinematic data. J Biomech 1999;32:
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes
 Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Patellofemoral Joint. Question? ANATOMY
 Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Correlating Femoral Shape with Patellar Kinematics in Patients with Patellofemoral Pain
 Correlating Femoral Shape with Patellar Kinematics in Patients with Patellofemoral Pain Calista M. Harbaugh, 1 Nicole A. Wilson, 2 Frances T. Sheehan 2 1 University of Michigan, College of Engineering,
Correlating Femoral Shape with Patellar Kinematics in Patients with Patellofemoral Pain Calista M. Harbaugh, 1 Nicole A. Wilson, 2 Frances T. Sheehan 2 1 University of Michigan, College of Engineering,
Do Persons with PFP. PFJ Loading? Biomechanical Factors Contributing to Patellomoral Pain: The Dynamic Q Angle. Patellofemoral Pain: A Critical Review
 Biomechanical Factors Contributing to Patellomoral Pain: The Dynamic Q Angle Division Biokinesiology & Physical Therapy Co Director, oratory University of Southern California Movement Performance Institute
Biomechanical Factors Contributing to Patellomoral Pain: The Dynamic Q Angle Division Biokinesiology & Physical Therapy Co Director, oratory University of Southern California Movement Performance Institute
Where to Draw the Line:
 Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Computational Evaluation of Predisposing Factors to Patellar Dislocation
 Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
BN M BNeurobiomechanics MBNeurobiomechanics
 Fz (% body weight) N Gait Analysis Gait Analysis The following document explains some the content of the gait report (TMP.122) as well as providing key references for the tests used and sources of normal
Fz (% body weight) N Gait Analysis Gait Analysis The following document explains some the content of the gait report (TMP.122) as well as providing key references for the tests used and sources of normal
Research Article. Abstract
 Research Article Total Knee Arthroplasty in Patients With Cerebral Palsy: A Matched Cohort Study to Patients With Osteoarthritis Matthew T. Houdek, MD Chad D. Watts, MD Cody C. Wyles, MD Robert T. Trousdale,
Research Article Total Knee Arthroplasty in Patients With Cerebral Palsy: A Matched Cohort Study to Patients With Osteoarthritis Matthew T. Houdek, MD Chad D. Watts, MD Cody C. Wyles, MD Robert T. Trousdale,
Dynamic Stabilization of the Patellofemoral Joint: Stabilization from above & below
 Dynamic Stabilization of the Patellofemoral Joint: Stabilization from above & below Division Biokinesiology & Physical Therapy Co Director, oratory University of Southern California Movement Performance
Dynamic Stabilization of the Patellofemoral Joint: Stabilization from above & below Division Biokinesiology & Physical Therapy Co Director, oratory University of Southern California Movement Performance
Anterior Knee Pain in Patients with Cerebral Palsy
 Original Article Clinics in Orthopedic Surgery 2014;6:426-431 http://dx.doi.org/10.4055/cios.2014.6.4.426 Anterior Knee Pain in Patients with Cerebral Palsy Young Choi, MD a, Sang Hyeong Lee, MD* a, Chin
Original Article Clinics in Orthopedic Surgery 2014;6:426-431 http://dx.doi.org/10.4055/cios.2014.6.4.426 Anterior Knee Pain in Patients with Cerebral Palsy Young Choi, MD a, Sang Hyeong Lee, MD* a, Chin
Changes in lower limb rotation after soft tissue surgery in spastic diplegia
 Acta Orthopaedica 2010; 81 (2): 245 249 245 Changes in lower limb rotation after soft tissue surgery in spastic diplegia 3-dimensional gait analysis in 28 children Bjørn Lofterød 1 and Terje Terjesen 2
Acta Orthopaedica 2010; 81 (2): 245 249 245 Changes in lower limb rotation after soft tissue surgery in spastic diplegia 3-dimensional gait analysis in 28 children Bjørn Lofterød 1 and Terje Terjesen 2
Management of knee flexion contractures in patients with Cerebral Palsy
 Management of knee flexion contractures in patients with Cerebral Palsy Emmanouil Morakis Orthopaedic Consultant Royal Manchester Children s Hospital 1. Introduction 2. Natural history 3. Pathophysiology
Management of knee flexion contractures in patients with Cerebral Palsy Emmanouil Morakis Orthopaedic Consultant Royal Manchester Children s Hospital 1. Introduction 2. Natural history 3. Pathophysiology
Gait analysis and medical treatment strategy
 Gait analysis and medical treatment strategy Sylvain Brochard Olivier Rémy-néris, Mathieu Lempereur CHU and Pediatric Rehabilitation Centre Brest Course for European PRM trainees Mulhouse, October 22,
Gait analysis and medical treatment strategy Sylvain Brochard Olivier Rémy-néris, Mathieu Lempereur CHU and Pediatric Rehabilitation Centre Brest Course for European PRM trainees Mulhouse, October 22,
Methods Patients A retrospective review of gait studies was conducted for all participants presented to the Motion Analysis
 58 Original article Predictors of outcome of distal rectus femoris transfer surgery in ambulatory children with cerebral palsy Susan A. Rethlefsen a, Galen Kam d, Tishya A.L. Wren a,b,c and Robert M. Kay
58 Original article Predictors of outcome of distal rectus femoris transfer surgery in ambulatory children with cerebral palsy Susan A. Rethlefsen a, Galen Kam d, Tishya A.L. Wren a,b,c and Robert M. Kay
CT Evaluation of Patellar Instability
 CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
AACPDM IC#21 DFEO+PTA 1
 Roles of Distal Femoral Extension Osteotomy and Patellar Tendon Advancement in the Treatment of Severe Persistent Crouch Gait in Adolescents and Young Adults with Cerebral Palsy Instructional Course #21
Roles of Distal Femoral Extension Osteotomy and Patellar Tendon Advancement in the Treatment of Severe Persistent Crouch Gait in Adolescents and Young Adults with Cerebral Palsy Instructional Course #21
PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT. Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology
 PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology PRE OPERATIVE ASSESSMENT RADIOGRAPHS Radiographs are used for assessment and
PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology PRE OPERATIVE ASSESSMENT RADIOGRAPHS Radiographs are used for assessment and
Risk Factors for Hip Displacement in Children With Cerebral Palsy: Systematic Review
 REVIEW ARTICLE Risk Factors for Hip Displacement in Children With Cerebral Palsy: Systematic Review Blazej Pruszczynski, MD,* Julieanne Sees, DO,w and Freeman Miller, MDw Background: When hip displacement
REVIEW ARTICLE Risk Factors for Hip Displacement in Children With Cerebral Palsy: Systematic Review Blazej Pruszczynski, MD,* Julieanne Sees, DO,w and Freeman Miller, MDw Background: When hip displacement
אתגרים ופתרונות ניתוחיים סביב מפרק הברך בילדי CP ד"ר טלי בקר לאורטופדית ילדים,מרכז שניידר לרפואת ילדים
 אתגרים ופתרונות ניתוחיים סביב מפרק הברך בילדי CP היח' ד"ר טלי בקר לאורטופדית ילדים,מרכז שניידר לרפואת ילדים 1 CP- Spectrum of pathology 2 Lower Limb problems in CP Spastic Quadriplegia- Hip,Pelvis, Spine
אתגרים ופתרונות ניתוחיים סביב מפרק הברך בילדי CP היח' ד"ר טלי בקר לאורטופדית ילדים,מרכז שניידר לרפואת ילדים 1 CP- Spectrum of pathology 2 Lower Limb problems in CP Spastic Quadriplegia- Hip,Pelvis, Spine
The Problem of Patellofemoral Pain. The Low Back Pain of the Lower Extremity. Objectives. Christopher M. Powers, PhD, PT, FACSM, FAPTA
 Mechanisms Underlying Patellofemoral Joint Pain: What have we learned over the last 20 years? Professor Co Director, Musculoskeletal Biomechanics Research Laboratory Objectives 1. Highlight recent research
Mechanisms Underlying Patellofemoral Joint Pain: What have we learned over the last 20 years? Professor Co Director, Musculoskeletal Biomechanics Research Laboratory Objectives 1. Highlight recent research
Patella Alta: Lack of Correlation Between Patellotrochlear Cartilage Congruence and Commonly Used Patellar Height Ratios
 Musculoskeletal Imaging Original Research Ali et al. Patella Alta Musculoskeletal Imaging Original Research Syed A. Ali 1 Robert Helmer Michael R. Terk Ali SA, Helmer R, Terk MR Keywords: Insall-Salvati
Musculoskeletal Imaging Original Research Ali et al. Patella Alta Musculoskeletal Imaging Original Research Syed A. Ali 1 Robert Helmer Michael R. Terk Ali SA, Helmer R, Terk MR Keywords: Insall-Salvati
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT *** - Useful in determining mechanism of injury / overuse
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
Discrepancies in Knee Joint Moments Using Common Anatomical Frames Defined by Different Palpable Landmarks
 Journal of Applied Biomechanics, 2008, 24, 185-190 2008 Human Kinetics, Inc. Discrepancies in Knee Joint Moments Using Common Anatomical Frames Defined by Different Palpable Landmarks Dominic Thewlis,
Journal of Applied Biomechanics, 2008, 24, 185-190 2008 Human Kinetics, Inc. Discrepancies in Knee Joint Moments Using Common Anatomical Frames Defined by Different Palpable Landmarks Dominic Thewlis,
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Radiological evaluation of the causes of patellar instability.
 Radiological evaluation of the causes of patellar instability. Poster No.: C-0054 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. M. Spaccesi Pau, D. Pomato, N. CEDOLA; La Plata/AR
Radiological evaluation of the causes of patellar instability. Poster No.: C-0054 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. M. Spaccesi Pau, D. Pomato, N. CEDOLA; La Plata/AR
Chronic patellar dislocation in adults
 CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
10/26/2017. Comprehensive & Coordinated Orthopaedic Management of Children with CP. Objectives. It s all about function. Robert Bruce, MD Sayan De, MD
 Comprehensive & Coordinated Orthopaedic Management of Children with CP Robert Bruce, MD Sayan De, MD Objectives Understand varying levels of intervention are available to optimize function of children
Comprehensive & Coordinated Orthopaedic Management of Children with CP Robert Bruce, MD Sayan De, MD Objectives Understand varying levels of intervention are available to optimize function of children
Personal use only. MRI of the extensor mechanism of the knee. 5 th Musculoskeletal MRI meeting. Falkowski, MD, MHBA
 MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
Multiapical Deformities p. 97 Osteotomy Concepts and Frontal Plane Realignment p. 99 Angulation Correction Axis (ACA) p. 99 Bisector Lines p.
 Normal Lower Limb Alignment and Joint Orientation p. 1 Mechanical and Anatomic Bone Axes p. 1 Joint Center Points p. 5 Joint Orientation Lines p. 5 Ankle p. 5 Knee p. 5 Hip p. 8 Joint Orientation Angles
Normal Lower Limb Alignment and Joint Orientation p. 1 Mechanical and Anatomic Bone Axes p. 1 Joint Center Points p. 5 Joint Orientation Lines p. 5 Ankle p. 5 Knee p. 5 Hip p. 8 Joint Orientation Angles
Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents
 Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents Sheena R. Black, MD, Henry B. Ellis, MD, Philip L. Wilson, MD, David A. Podeszwa, MD LLRS Annual
Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents Sheena R. Black, MD, Henry B. Ellis, MD, Philip L. Wilson, MD, David A. Podeszwa, MD LLRS Annual
Use of a patella marker to improve tracking of dynamic hip rotation range of motion
 Gait & Posture 27 (2008) 530 534 www.elsevier.com/locate/gaitpost Use of a patella marker to improve tracking of dynamic hip rotation range of motion Tishya A.L. Wren a,b, *, K. Patrick Do a, Reiko Hara
Gait & Posture 27 (2008) 530 534 www.elsevier.com/locate/gaitpost Use of a patella marker to improve tracking of dynamic hip rotation range of motion Tishya A.L. Wren a,b, *, K. Patrick Do a, Reiko Hara
Lower Extremity Orthopedic Surgery in Cerebral Palsy
 Lower Extremity Orthopedic Surgery in Cerebral Palsy Hank Chambers, MD San Diego Children s Hospital San Diego, California Indications Fixed contracture Joint dislocations Shoe wear problems Pain Perineal
Lower Extremity Orthopedic Surgery in Cerebral Palsy Hank Chambers, MD San Diego Children s Hospital San Diego, California Indications Fixed contracture Joint dislocations Shoe wear problems Pain Perineal
Hamstring and psoas length of crouch gait in cerebral palsy: a comparison with induced crouch gait in age- and sex-matched controls
 Rhie et al. Journal of NeuroEngineering and Rehabilitation 2013, 10:10 JOURNAL OF NEUROENGINEERING JNERAND REHABILITATION RESEARCH Open Access Hamstring and psoas length of crouch gait in cerebral palsy:
Rhie et al. Journal of NeuroEngineering and Rehabilitation 2013, 10:10 JOURNAL OF NEUROENGINEERING JNERAND REHABILITATION RESEARCH Open Access Hamstring and psoas length of crouch gait in cerebral palsy:
Mechanisms Underlying Patellofemoral Pain: Lessons Learned over the Past 20 Years. Christopher M. Powers, PT, PhD, FASCM, FAPTA
 Mechanisms Underlying Patellofemoral Pain: Lessons Learned over the Past 20 Years Christopher M. Powers, PT, PhD, FASCM, FAPTA Although recognized as one of the most common lower extremity disorders encountered
Mechanisms Underlying Patellofemoral Pain: Lessons Learned over the Past 20 Years Christopher M. Powers, PT, PhD, FASCM, FAPTA Although recognized as one of the most common lower extremity disorders encountered
Assessment of Patellar Laxity in the in vitro Native Knee
 Assessment of Patellar Laxity in the in vitro Native Knee By Mark C. Komosa Submitted to the graduate degree program in Bioengineering and the Graduate Faculty of the University of Kansas in partial fulfillment
Assessment of Patellar Laxity in the in vitro Native Knee By Mark C. Komosa Submitted to the graduate degree program in Bioengineering and the Graduate Faculty of the University of Kansas in partial fulfillment
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016
 Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Myology of the Knee. PTA 105 Kinesiology
 Myology of the Knee PTA 105 Kinesiology Objectives Describe the planes of motion and axes of rotation of the knee joint Visualize the origins and insertions of the muscles about the knee List the innervations
Myology of the Knee PTA 105 Kinesiology Objectives Describe the planes of motion and axes of rotation of the knee joint Visualize the origins and insertions of the muscles about the knee List the innervations
Ankle Valgus in Cerebral Palsy
 Ankle Valgus in Cerebral Palsy Freeman Miller Contents Introduction... 2 Natural History... 2 Treatment... 3 Diagnostic Evaluations... 3 Indications for Intervention... 3 Outcome of Treatment... 5 Complications
Ankle Valgus in Cerebral Palsy Freeman Miller Contents Introduction... 2 Natural History... 2 Treatment... 3 Diagnostic Evaluations... 3 Indications for Intervention... 3 Outcome of Treatment... 5 Complications
Noninvasive Assessment of Sagittal Knee Kinematics After Total Knee Arthroplasty
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 16 Number 2 Noninvasive Assessment of Sagittal Knee Kinematics After Total Knee Arthroplasty V Chester, E Biden, T Barnhill Citation V Chester,
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 16 Number 2 Noninvasive Assessment of Sagittal Knee Kinematics After Total Knee Arthroplasty V Chester, E Biden, T Barnhill Citation V Chester,
NIH Public Access Author Manuscript Gait Posture. Author manuscript; available in PMC 2008 July 7.
 NIH Public Access Author Manuscript Published in final edited form as: Gait Posture. 2007 October ; 26(4): 546 552. The effect of excessive tibial torsion on the capacity of muscles to extend the hip and
NIH Public Access Author Manuscript Published in final edited form as: Gait Posture. 2007 October ; 26(4): 546 552. The effect of excessive tibial torsion on the capacity of muscles to extend the hip and
Figure 1: Weight bearing apparatus to measure knee contact area.
 Technical note A Device for Inducing Active Lengthening Muscle Contractions for Dynamic MR Imaging Eric Bader, Arinne Lyman, Sarajane Stevens, Christopher Westphal, Darryl Thelen and Amy Silder. Abstract:
Technical note A Device for Inducing Active Lengthening Muscle Contractions for Dynamic MR Imaging Eric Bader, Arinne Lyman, Sarajane Stevens, Christopher Westphal, Darryl Thelen and Amy Silder. Abstract:
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
Influence of surgery involving tendons around the knee joint on ankle motion during gait in patients with cerebral palsy
 Influence of surgery involving tendons around the knee joint on ankle motion during gait in patients with cerebral palsy Seung Yeol Lee, M.D., Ph.D. 1, Kyoung Min Lee, M.D., Ph.D. 2 Soon-Sun Kwon, Ph.D.
Influence of surgery involving tendons around the knee joint on ankle motion during gait in patients with cerebral palsy Seung Yeol Lee, M.D., Ph.D. 1, Kyoung Min Lee, M.D., Ph.D. 2 Soon-Sun Kwon, Ph.D.
5/14/2013. Acute vs Chronic Mechanism of Injury:
 Third Annual Young Athlete Conference: The Lower Extremity February 22, 2013 Audrey Lewis, DPT Acute vs Chronic Mechanism of Injury: I. Direct: blow to the patella II. Indirect: planted foot with a valgus
Third Annual Young Athlete Conference: The Lower Extremity February 22, 2013 Audrey Lewis, DPT Acute vs Chronic Mechanism of Injury: I. Direct: blow to the patella II. Indirect: planted foot with a valgus
Patella position in the trochlea groove: comparison between supine and standing radiographs
 Patella position in the trochlea groove: comparison between supine and standing radiographs Award: Winner Poster No.: P-0098 Congress: ESSR 2014 Type: Authors: Keywords: DOI: Scientific Poster N. Skou,
Patella position in the trochlea groove: comparison between supine and standing radiographs Award: Winner Poster No.: P-0098 Congress: ESSR 2014 Type: Authors: Keywords: DOI: Scientific Poster N. Skou,
Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff),
 Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff), Consultant Knee Surgeon NHS: The Royal Orthopaedic Hospital & Queen Elizabeth Hospital, Birmingham MRI Knee:
Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff), Consultant Knee Surgeon NHS: The Royal Orthopaedic Hospital & Queen Elizabeth Hospital, Birmingham MRI Knee:
Estimating Total Knee Arthroplasty Joint Loads from Kinematics
 Estimating Total Knee Arthroplasty Joint Loads from Kinematics Clare K. Fitzpatrick, Paul Rullkoetter. University of Denver, Denver, CO, USA. Disclosures: C.K. Fitzpatrick: None. P. Rullkoetter: 5; DePuy
Estimating Total Knee Arthroplasty Joint Loads from Kinematics Clare K. Fitzpatrick, Paul Rullkoetter. University of Denver, Denver, CO, USA. Disclosures: C.K. Fitzpatrick: None. P. Rullkoetter: 5; DePuy
Correlation between Knee Kinematics and Patello-femoral Contact Pressure in Total Knee Arthroplasty
 Correlation between Knee Kinematics and Patello-femoral Contact Pressure in Total Knee Arthroplasty Takuya Konno, MD 1, Tomohiro Onodera, MD, PhD 1, Yasuhiko Kasahara, MD, PhD 1, Daisuke Takahashi 1, Norimasa
Correlation between Knee Kinematics and Patello-femoral Contact Pressure in Total Knee Arthroplasty Takuya Konno, MD 1, Tomohiro Onodera, MD, PhD 1, Yasuhiko Kasahara, MD, PhD 1, Daisuke Takahashi 1, Norimasa
Mako Partial Knee Patellofemoral
 Mako Partial Knee Patellofemoral Mako Robotic-Arm Assisted Surgery Surgical reference guide Table of contents Implant compatibility.... 3 Pre-operative implant planning... 4 Intra-operative planning....
Mako Partial Knee Patellofemoral Mako Robotic-Arm Assisted Surgery Surgical reference guide Table of contents Implant compatibility.... 3 Pre-operative implant planning... 4 Intra-operative planning....
Windswept hip deformity in children with cerebral palsy: a population-based prospective follow-up
 DOI 10.1007/s11832-016-0749-1 ORIGINAL CLINICAL ARTICLE Windswept hip deformity in children with cerebral palsy: a population-based prospective follow-up Gunnar Hägglund 1 Henrik Lauge-Pedersen 1 Måns
DOI 10.1007/s11832-016-0749-1 ORIGINAL CLINICAL ARTICLE Windswept hip deformity in children with cerebral palsy: a population-based prospective follow-up Gunnar Hägglund 1 Henrik Lauge-Pedersen 1 Måns
Kinematic vs. mechanical alignment: What is the difference?
 Kinematic vs. mechanical alignment: What is the difference? In this 4 Questions interview, Stephen M. Howell, MD, explains the potential benefits of 3D alignment during total knee replacement. Introduction
Kinematic vs. mechanical alignment: What is the difference? In this 4 Questions interview, Stephen M. Howell, MD, explains the potential benefits of 3D alignment during total knee replacement. Introduction
Comparison of high-flex and conventional implants for bilateral total knee arthroplasty
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 14 Number 1 Comparison of high-flex and conventional implants for bilateral total knee arthroplasty C Martin-Hernandez, M Guillen-Soriano, A
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 14 Number 1 Comparison of high-flex and conventional implants for bilateral total knee arthroplasty C Martin-Hernandez, M Guillen-Soriano, A
Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery. Restore patella stability.
 Page 1 of 5 Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery Restore patella stability. Restore / improve function. I have no conflicts to declare. 1987
Page 1 of 5 Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery Restore patella stability. Restore / improve function. I have no conflicts to declare. 1987
Knee Contusions and Stress Injuries. Laura W. Bancroft, M.D.
 Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
NexGen Legacy LPS-Flex Knee. Brochure
 NexGen Legacy LPS-Flex Knee Brochure What postoperative range of motion can your TKA patients expect? For patients with the ability and desire to perform For patients with the ability high-flexion activities,
NexGen Legacy LPS-Flex Knee Brochure What postoperative range of motion can your TKA patients expect? For patients with the ability and desire to perform For patients with the ability high-flexion activities,
Unicompartmental Knee Replacement
 Unicompartmental Knee Replacement Results and Techniques Alexander P. Sah, MD California Orthopaedic Association Meeting Laguna Niguel, CA May 20th, 2011 Overview Why partial knee replacement? - versus
Unicompartmental Knee Replacement Results and Techniques Alexander P. Sah, MD California Orthopaedic Association Meeting Laguna Niguel, CA May 20th, 2011 Overview Why partial knee replacement? - versus
Severe crouch gait in spastic diplegia can be prevented
 CHILDREN S ORTHOPAEDICS Severe crouch gait in spastic diplegia can be prevented A POPULATION-BASED STUDY C. Vuillermin, J. Rodda, E. Rutz, B. J. Shore, K. Smith, H. K. Graham From Royal Children s Hospital,
CHILDREN S ORTHOPAEDICS Severe crouch gait in spastic diplegia can be prevented A POPULATION-BASED STUDY C. Vuillermin, J. Rodda, E. Rutz, B. J. Shore, K. Smith, H. K. Graham From Royal Children s Hospital,
APTA Intro to Identity. The Movement System The Kinesiopathologic Model Movement System Impairment Syndromes of the Knee THE HUMAN MOVEMENT SYSTEM
 The Movement System The Kinesiopathologic Model Movement System Impairment Syndromes of the Knee Shirley Sahrmann, PT, PhD, FAPTA Professor Emerita Statement of Privacy To protect the privacy of the subjects
The Movement System The Kinesiopathologic Model Movement System Impairment Syndromes of the Knee Shirley Sahrmann, PT, PhD, FAPTA Professor Emerita Statement of Privacy To protect the privacy of the subjects
Where are we now? A little bit of History.. Is menu à la carte relevant in 2019? Medial PatelloFemoral Ligament the Queen of the PF Joint
 Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
The Knee. Two Joints: Tibiofemoral. Patellofemoral
 Evaluating the Knee The Knee Two Joints: Tibiofemoral Patellofemoral HISTORY Remember the questions from lecture #2? Girth OBSERVATION TibioFemoral Alignment What are the consequences of faulty alignment?
Evaluating the Knee The Knee Two Joints: Tibiofemoral Patellofemoral HISTORY Remember the questions from lecture #2? Girth OBSERVATION TibioFemoral Alignment What are the consequences of faulty alignment?
Masterclass. Tips and tricks for a successful outcome. E. Verhaven, M. Thaeter. September 15th, 2012, Brussels
 Masterclass Tips and tricks for a successful outcome September 15th, 2012, Brussels E. Verhaven, M. Thaeter Belgium St. Nikolaus-Hospital Orthopaedics & Traumatology Ultimate Goal of TKR Normal alignment
Masterclass Tips and tricks for a successful outcome September 15th, 2012, Brussels E. Verhaven, M. Thaeter Belgium St. Nikolaus-Hospital Orthopaedics & Traumatology Ultimate Goal of TKR Normal alignment
Int J Physiother. Vol 1(3), , August (2014) ISSN:
 Int J Physiother. Vol 1(3), 120-126, August (2014) ISSN: 2348-8336 ABSTRACT Sreekar Kumar Reddy.R 1 B. Siva kumar 2 N. Vamsidhar 2 G. Haribabu 3 Background: Patellofemoral pain syndrome is a very common
Int J Physiother. Vol 1(3), 120-126, August (2014) ISSN: 2348-8336 ABSTRACT Sreekar Kumar Reddy.R 1 B. Siva kumar 2 N. Vamsidhar 2 G. Haribabu 3 Background: Patellofemoral pain syndrome is a very common
Anterior knee pain.
 Anterior knee pain What are the symptoms? Anterior knee pain is very common amongst active adolescents and athletes participating in contact sports. It is one of the most common problems/injuries seen
Anterior knee pain What are the symptoms? Anterior knee pain is very common amongst active adolescents and athletes participating in contact sports. It is one of the most common problems/injuries seen
Impact of gait analysis on correction of excessive hip internal rotation in ambulatory children with cerebral palsy: a randomized controlled trial
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE Impact of gait analysis on correction of excessive hip internal rotation in ambulatory children with cerebral palsy: a randomized controlled trial
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE Impact of gait analysis on correction of excessive hip internal rotation in ambulatory children with cerebral palsy: a randomized controlled trial
Hyperpronation of the foot causes many different
 IMMEDIATE CHANGES IN THE QUADRICEPS FEMORIS ANGLE AFTER INSERTION OF AN ORTHOTIC DEVICE D. Robert Kuhn, DC, a Terry R. Yochum, DC, b Anton R. Cherry, c and Sean S. Rodgers c ABSTRACT Objective: To measure
IMMEDIATE CHANGES IN THE QUADRICEPS FEMORIS ANGLE AFTER INSERTION OF AN ORTHOTIC DEVICE D. Robert Kuhn, DC, a Terry R. Yochum, DC, b Anton R. Cherry, c and Sean S. Rodgers c ABSTRACT Objective: To measure
Toe walking gives rise to parental concern. Therefore, toe-walkers are often referred at the 3 years of age.
 IDIOPATHIC TOE WALKING Toe walking is a common feature in immature gait and is considered normal up to 3 years of age. As walking ability improves, initial contact is made with the heel. Toe walking gives
IDIOPATHIC TOE WALKING Toe walking is a common feature in immature gait and is considered normal up to 3 years of age. As walking ability improves, initial contact is made with the heel. Toe walking gives
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY
 SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
FACTS 1. Most need only Gastro aponeurotic release [in positive Silverskiold test]
![FACTS 1. Most need only Gastro aponeurotic release [in positive Silverskiold test] FACTS 1. Most need only Gastro aponeurotic release [in positive Silverskiold test]](/thumbs/83/88335212.jpg) FOOT IN CEREBRAL PALSY GAIT IN CEREBRAL PALSY I True Equinus II Jump gait III Apparent Equinus IV Crouch gait Group I True Equinus Extended hip and knee Equinus at ankle II Jump Gait [commonest] Equinus
FOOT IN CEREBRAL PALSY GAIT IN CEREBRAL PALSY I True Equinus II Jump gait III Apparent Equinus IV Crouch gait Group I True Equinus Extended hip and knee Equinus at ankle II Jump Gait [commonest] Equinus
Muscle Testing of Knee Extensors. Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department
 Muscle Testing of Knee Extensors Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department Muscle Testing of Knee Extensors othe Primary muscle Quadriceps Femoris -Rectus
Muscle Testing of Knee Extensors Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department Muscle Testing of Knee Extensors othe Primary muscle Quadriceps Femoris -Rectus
Knee Capsular Disorder. ICD-9-CM: Stiffness in joint of lower leg, not elsewhere classified
 1 Knee Capsular Disorder "Knee Capsulitis" ICD-9-CM: 719.56 Stiffness in joint of lower leg, not elsewhere classified Diagnostic Criteria History: Physical Exam: Stiffness Aching with prolonged weight
1 Knee Capsular Disorder "Knee Capsulitis" ICD-9-CM: 719.56 Stiffness in joint of lower leg, not elsewhere classified Diagnostic Criteria History: Physical Exam: Stiffness Aching with prolonged weight
British Columbia s Consensus on Hip Surveillance for Children with Cerebral Palsy
 British Columbia s Consensus on Hip Surveillance for Children with Cerebral Palsy Information for Health Care Professionals Caring for Children with Cerebral Palsy 2018 SUMMARY British Columbia s Consensus
British Columbia s Consensus on Hip Surveillance for Children with Cerebral Palsy Information for Health Care Professionals Caring for Children with Cerebral Palsy 2018 SUMMARY British Columbia s Consensus
Knee Joint Anatomy 101
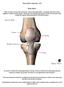 Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
Orthopedic Issues in Children with Special Healthcare Needs
 Orthopedic Issues in Children with Special Healthcare Needs Kathryn A Keeler, MD Assistant Professor University of Missouri-Kansas City School of Medicine, Department of Orthopaedic Surgery and Department
Orthopedic Issues in Children with Special Healthcare Needs Kathryn A Keeler, MD Assistant Professor University of Missouri-Kansas City School of Medicine, Department of Orthopaedic Surgery and Department
Stability of the Gross Motor Function Classification System after single-event multilevel surgery in children with cerebral palsy
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE Stability of the Gross Motor Function Classification System after single-event multilevel surgery in children with cerebral palsy ERICH RUTZ 1,2,3
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE Stability of the Gross Motor Function Classification System after single-event multilevel surgery in children with cerebral palsy ERICH RUTZ 1,2,3
7/20/14. Patella Instability. Alignment. PF contact areas. Tissue Restraints. Pain. Acute Blunt force trauma Disorders of the Patellafemoral Joint
 Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
CONTROL OF THE BOUNDARY CONDITIONS OF A DYNAMIC KNEE SIMULATOR
 CONTROL OF THE BOUNDARY CONDITIONS OF A DYNAMIC KNEE SIMULATOR J. Tiré 1, J. Victor 2, P. De Baets 3 and M.A. Verstraete 2 1 Ghent University, Belgium 2 Ghent University, Department of Physical Medicine
CONTROL OF THE BOUNDARY CONDITIONS OF A DYNAMIC KNEE SIMULATOR J. Tiré 1, J. Victor 2, P. De Baets 3 and M.A. Verstraete 2 1 Ghent University, Belgium 2 Ghent University, Department of Physical Medicine
Selective Motor Control Assessment of the Lower Extremity in Patients with Spastic Cerebral Palsy
 Overview Selective Motor Control Assessment of the Lower Extremity in Patients with Spastic Cerebral Palsy Marcia Greenberg MS, PT* Loretta Staudt MS, PT* Eileen Fowler PT, PhD Selective Motor Control
Overview Selective Motor Control Assessment of the Lower Extremity in Patients with Spastic Cerebral Palsy Marcia Greenberg MS, PT* Loretta Staudt MS, PT* Eileen Fowler PT, PhD Selective Motor Control
Doron Sher. 160 Belmore Rd, Randwick Burwood Rd, Concord. MBBS, MBiomedE, FRACS FAOrthA
 Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
BIOMECHANICAL MECHANISMS FOR DAMAGE: RETRIEVAL ANALYSIS AND COMPUTATIONAL WEAR PREDICTIONS IN TOTAL KNEE REPLACEMENTS
 Journal of Mechanics in Medicine and Biology Vol. 5, No. 3 (2005) 469 475 c World Scientific Publishing Company BIOMECHANICAL MECHANISMS FOR DAMAGE: RETRIEVAL ANALYSIS AND COMPUTATIONAL WEAR PREDICTIONS
Journal of Mechanics in Medicine and Biology Vol. 5, No. 3 (2005) 469 475 c World Scientific Publishing Company BIOMECHANICAL MECHANISMS FOR DAMAGE: RETRIEVAL ANALYSIS AND COMPUTATIONAL WEAR PREDICTIONS
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Differences in Patellofemoral Kinematics between Weight-Bearing and Non-Weight-Bearing Conditions in Patients with Patellofemoral Pain
 Differences in Patellofemoral Kinematics between Weight-Bearing and Non-Weight-Bearing Conditions in Patients with Patellofemoral Pain Christine E. Draper, 1 Thor F. Besier, 2 Michael Fredericson, 2 Juan
Differences in Patellofemoral Kinematics between Weight-Bearing and Non-Weight-Bearing Conditions in Patients with Patellofemoral Pain Christine E. Draper, 1 Thor F. Besier, 2 Michael Fredericson, 2 Juan
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
Is there a biomechanical explanation for anterior knee pain in patients with patella alta?
 Is there a biomechanical explanation for anterior knee pain in patients with patella alta? INFLUENCE OF PATELLAR HEIGHT ON PATELLOFEMORAL CONTACT FORCE, CONTACT AREA AND CONTACT PRESSURE T. Luyckx, K.
Is there a biomechanical explanation for anterior knee pain in patients with patella alta? INFLUENCE OF PATELLAR HEIGHT ON PATELLOFEMORAL CONTACT FORCE, CONTACT AREA AND CONTACT PRESSURE T. Luyckx, K.
Lateral knee injuries
 Created as a free resource by Clinical Edge Based on Physio Edge podcast episode 051 with Matt Konopinski Get your free trial of online Physio education at Orthopaedic timeframes Traditionally Orthopaedic
Created as a free resource by Clinical Edge Based on Physio Edge podcast episode 051 with Matt Konopinski Get your free trial of online Physio education at Orthopaedic timeframes Traditionally Orthopaedic
The influence of age at single-event multilevel surgery on outcome in children with cerebral palsy who walk with flexed knee gait
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE The influence of age at single-event multilevel surgery on outcome in children with cerebral palsy who walk with flexed knee gait MARTIN ƒvehlýk
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE The influence of age at single-event multilevel surgery on outcome in children with cerebral palsy who walk with flexed knee gait MARTIN ƒvehlýk
Where Is The Natural Flexion-Extension Axis Of The Knee?
 Where Is The Natural Flexion-Extension Axis Of The Knee? Daniel Boguszewski 1, Paul Yang 2, Keith Markolf 1, Frank Petrigliano 1, David McAllister 1. 1 University of California Los Angeles, Los Angeles,
Where Is The Natural Flexion-Extension Axis Of The Knee? Daniel Boguszewski 1, Paul Yang 2, Keith Markolf 1, Frank Petrigliano 1, David McAllister 1. 1 University of California Los Angeles, Los Angeles,
Obesity is associated with reduced joint range of motion (Park, 2010), which has been partially
 INTRODUCTION Obesity is associated with reduced joint range of motion (Park, 2010), which has been partially attributed to adipose tissues around joints limiting inter-segmental rotations (Gilleard, 2007).
INTRODUCTION Obesity is associated with reduced joint range of motion (Park, 2010), which has been partially attributed to adipose tissues around joints limiting inter-segmental rotations (Gilleard, 2007).
THE KNEE SOCIETY VIRTUAL FELLOWSHIP
 THE KNEE SOCIETY VIRTUAL FELLOWSHIP CHAPTER 2: RADIOGRAPHIC EVALUATION OF THE KNEE Radiographic Evaluation of the Knee Presented by: R. Michael Meneghini, MD COPYRIGHT 2016 THE KNEE SOCIETY Disclosures
THE KNEE SOCIETY VIRTUAL FELLOWSHIP CHAPTER 2: RADIOGRAPHIC EVALUATION OF THE KNEE Radiographic Evaluation of the Knee Presented by: R. Michael Meneghini, MD COPYRIGHT 2016 THE KNEE SOCIETY Disclosures
Case Study: Christopher
 Case Study: Christopher Conditions Treated Anterior Knee Pain, Severe Crouch Gait, & Hip Flexion Contracture Age Range During Treatment 23 Years to 24 Years David S. Feldman, MD Chief of Pediatric Orthopedic
Case Study: Christopher Conditions Treated Anterior Knee Pain, Severe Crouch Gait, & Hip Flexion Contracture Age Range During Treatment 23 Years to 24 Years David S. Feldman, MD Chief of Pediatric Orthopedic
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
Iliotibial Band Strain and Force in. Retrospective Iliotibial Band Syndrome. Aspiring Kid, PhD
 Iliotibial Band Strain and Force in Female Runners With and Without Retrospective Iliotibial Band Syndrome Aspiring Kid, PhD FUNCTION OF ILIOTIBIAL BAND Proximally: lateral hip stabilizer Helps prevent
Iliotibial Band Strain and Force in Female Runners With and Without Retrospective Iliotibial Band Syndrome Aspiring Kid, PhD FUNCTION OF ILIOTIBIAL BAND Proximally: lateral hip stabilizer Helps prevent
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO
 Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO This handout is for use as a rough guide and study aid. Your instructor may perform certain maneuvers
Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO This handout is for use as a rough guide and study aid. Your instructor may perform certain maneuvers
CHAPTER 8: THE BIOMECHANICS OF THE HUMAN LOWER EXTREMITY
 CHAPTER 8: THE BIOMECHANICS OF THE HUMAN LOWER EXTREMITY _ 1. The hip joint is the articulation between the and the. A. femur, acetabulum B. femur, spine C. femur, tibia _ 2. Which of the following is
CHAPTER 8: THE BIOMECHANICS OF THE HUMAN LOWER EXTREMITY _ 1. The hip joint is the articulation between the and the. A. femur, acetabulum B. femur, spine C. femur, tibia _ 2. Which of the following is
Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System
 Showa Univ J Med Sci 29 3, 289 296, September 2017 Original Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System Hiroshi TAKAGI 1 2, Soshi ASAI 1, Atsushi
Showa Univ J Med Sci 29 3, 289 296, September 2017 Original Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System Hiroshi TAKAGI 1 2, Soshi ASAI 1, Atsushi
ASSESSING GAIT IN CHILDREN WITH CP: WHAT TO DO WHEN YOU CAN T USE A GAIT LAB
 ASSESSING GAIT IN CHILDREN WITH CP: WHAT TO DO WHEN YOU CAN T USE A GAIT LAB Robert M. Kay, MD Vice Chief, Children s Orthopaedic Center Children s Hospital Los Angeles Professor of Orthopaedic Surgery
ASSESSING GAIT IN CHILDREN WITH CP: WHAT TO DO WHEN YOU CAN T USE A GAIT LAB Robert M. Kay, MD Vice Chief, Children s Orthopaedic Center Children s Hospital Los Angeles Professor of Orthopaedic Surgery
Excessive lateral tracking
 Patellofemoral Kinematics During Weight-earing and Non Weight-earing Knee Extension in Persons With Lateral Subluxation of the Patella: Preliminary Study Christopher M. Powers, PT, PhD 1 Samuel R. Ward,
Patellofemoral Kinematics During Weight-earing and Non Weight-earing Knee Extension in Persons With Lateral Subluxation of the Patella: Preliminary Study Christopher M. Powers, PT, PhD 1 Samuel R. Ward,
JOINT RULER. Surgical Technique For Knee Joint JRReplacement
 JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
Ligamentous and Meniscal Injuries: Diagnosis and Management
 Ligamentous and Meniscal Injuries: Diagnosis and Management Daniel K Williams, MD Franciscan Physician Network Orthopedic Specialists September 29, 2017 No Financial Disclosures INTRODUCTION Overview of
Ligamentous and Meniscal Injuries: Diagnosis and Management Daniel K Williams, MD Franciscan Physician Network Orthopedic Specialists September 29, 2017 No Financial Disclosures INTRODUCTION Overview of
