Effects of Occlusal Change on the Histology of the Mandibular Condyle Cartilage of Rats. Xinyun Liu. B.D.S., Sun Yat-sen University, 2016
|
|
|
- Ira Ernest Small
- 5 years ago
- Views:
Transcription
1 Effects of Occlusal Change on the Histology of the Mandibular Condyle Cartilage of Rats by Xinyun Liu B.D.S., Sun Yat-sen University, 2016 Submitted to the Graduate Faculty of the School of Dental Medicine in partial fulfillment of the requirements for the degree of Master of Science University of Pittsburgh 2018
2 UNIVERSITY OF PITTSBURGH SCHOOL OF DENTAL MEDICINE This thesis as presented by Xinyun Liu It was defended on August 2, 2018 and approved by Dr. Alejandro Almarza, Associate Professor, Department of Oral Biology Dr. Michael Gold, Professor, Department of Neurobiology Dr. Heather Szabo Rogers, Assistant Professor, Department of Oral Biology Dr. Juan Taboas, Assistant Professor, Department of Oral Biology Thesis Director: Alejandro Almarza, Associate Professor, Department of Oral Biology ii
3 Copyright by Xinyun Liu 2018 iii
4 Effects of Occlusal Change on the Histology of the Mandibular Condyle Cartilage of Rats Xinyun Liu, M.S. University of Pittsburgh, 2018 We have previous data demonstrating that occlusal change in the rabbit results in degeneration of temporomandibular joint (TMJ) condyle, the major moving bone of the TMJ (Henderson, 2015). In the present study, we sought to determine whether comparable changes are observed in a rat model of occlusal change. Composite bite-raising splints (around 1mm) were applied to the left maxillary molars in 14-week-old male Sprague-Dawley rats for 4 weeks in the first batch (n=4) and 14-week-old female Sprague-Dawley rats 6 weeks in the second batch (n=4). Sham splint placement, where the splint was placed and then removed, served as the sham group (n=4) in both batches. At the end of splinting, all the rats were euthanized and histological analysis of the TMJ was carried out on both splinted and contralateral sides of the jaw with Hematoxylin & Eosin (H&E) for cellularity, Safranin-O staining for glycosaminoglycan(gag) and Collagen II immunohistochemistry (IHC) staining. The presence of fibrous zone, proliferation zone, mature zone, hypertrophic zone served as primary tissue boundaries on the condyles ipsi- and contralateral to the splint placement. There did not seem to be a difference between the ipsi- and the contralateral sides after 4 and 6 weeks in sham group. While in the splinted group, there seem to be an increase in GAG on the ipsi- compared to the contralateral side after 4 weeks of splinting. Interestingly, after 6 weeks, the difference seemed less consistent compared to 4 weeks. Meanwhile, there appeared to be no GAG in sham group after 6 weeks. The Collagen II staining showed no significant difference in both sham and splinted group after 4 and 6 weeks. It will be important to iv
5 further characterize the potential changes in other biochemical components of the joint tissue, time course of both the onset and recovery of the changes in the joint, and the extent to which the histological changes correlate with changes in joint sensitivity. v
6 TABLE OF CONTENTS TABLE OF CONTENTS... VI LIST OF FIGURES... VIII ACKNOWLEDGEMENTS... X 1.0 INTRODUCTION HYPOTHESIS MATERIALS AND METHODS UNILATERAL BITE RAISE SAMPLE PROCESSING HISTOLOGY...9 Hematoxylin & Eosin Staining...9 Safranin O staining IMMUNOHISTOCHEMISTRY IMAGES PROCESSING STATISTIC ANALYSIS RESULTS WEEK-OLD MALE RATS SPLINTED FOR 4 WEEKS H&E Staining Safranin O Staining Collagen II Staining WEEKS-OLD FEMALE RATS SPLINTED FOR 6 WEEKS H&E Staining vi
7 Safranin O Staining Collagen II Staining DISCUSSION ANIMAL MODEL HISTOLOGY AND IMMUNOHISTOCHEMISTRY LIMITATIONS AND FUTURE DIRECTIONS CONCLUSION BIBLIOGRAPHY vii
8 LIST OF FIGURES Figure 1. A. Frontal and lateral view of anterior splint B. Histology of rat TMJ showing the condyle cartilage...4 Figure 2. Histology of rabbit TMJ showing the condyle cartilage...4 Figure 3. Unilateral bite raise of the rats....8 Figure 4. Histology showing the ipsi- and contralateral of TMJ discs and condyles in H&E staining of the splinted group Figure 5. Comparison between MCC in sham and splinted group Figure 6. Histology showing the ipsi- and contralateral of TMJ discs and condyles in Safranin O staining of the splinted group Figure 7. Comparison of GAG staining between sham and splinted, ipsi and contralateral sides Figure 8. Histology showing Collagen type II IHC staining of rat s knee Figure 9. Histology showing the ipsi- and contralateral of TMJ discs and condyles in Collagen type II IHC staining of the splinted group Figure 10. Comparison between ipsi- and contralateral side, and sham and splinted group in Collagen type II staining Figure 11. Histology showing the ipsi- and contralateral of TMJ discs and condyles in H&E staining of the splinted group Figure 12. Comparison between MCC thickness in sham and splinted group Figure 13. Histology showing the ipsi- and contralateral of TMJ discs and condyles in H&E staining of the sham and splinted group viii
9 Figure 14. Comparison between ipsi- and contralateral side, and sham and splinted group in GAG staining Figure 15. Histology showing the ipsi- and contralateral of TMJ discs and condyles in Collagen type II IHC staining of the splinted group Figure 16. Comparison between ipsi- and contralateral side, and sham and splinted group in Collagen type II staining ix
10 ACKNOWLEDGEMENTS I would like to thank my advisor, Dr. Alejandro Almarza, who has been supporting me throughout the two years and he is not only our mentor but also our friend. Also, I would like to thank Dr. Michael Gold. As the collaborator of our lab, he always supports us and gives us valuable advice. My research could not be completed without his help. Besides, I also need to thank the TMJ Lab members, Jesse, Adam, John, and Jake, who helped me with problems in research and life. Also, I am thankful to the professors and my colleagues in CCR. It is a great pleasure to work in a courteous and friendly environment. As one of the students in the Oral Biology program, I am sincerely thankful to Dr. Mooney, the former director of our program, who always cares about and think of his students. Last but not least, I am truly grateful to my parents for their love and support. Also, I am thankful to my husband, best friend, colleague---john, he is always there when I need help. x
11 1.0 INTRODUCTION The Temporomandibular joint (TMJ) is a synovial, bilateral, ginglymo-diarthrodial joint, and it is formed by the articulation of the condyle against the glenoid fossa and articular eminence of the temporal bone (Dolwick et al, 1983). It is not only one of the most complicated, but also the most used joint in a human body, which consists of the joint capsule, articular disc, mandibular condyles, articular surface of the temporal bone as well as the muscles and ligaments around the joint (Alomar et al, 2017). The mandibular condyle cartilage (MCC) is the fibrocartilage covers the head of the condyle, which consists of fibrous, proliferative, mature, and hypertrophic and subchondral zones, providing the toleration to compressive force during joint movement. Almost 33% of the population has at least one symptom of temporomandibular joint disorders (TMD), but only 3.6-7% of them seek treatment (Wright et al, 2013). Systematic illness, trauma, and mechanical factors can lead to the degeneration of the TMJ. The excessive or unbalanced mechanical loading may result in the onset and process of osteoarthritis and internal derangement of the TMJ (Tanaka et al, 2008). Furthermore, internal derangement of the TMJ may be induced by excessive or unbalanced stress in the TMJ. According to Wilkes, internal derangement can be separated into five stages. From stage I to stage III, symptoms start from only painless clicking, and headache to frequent joint pain, and mild limited mandibular range motion. These stages show no difference from a healthy joint under X-ray or MRI except for the anterior disc displacement. However, degeneration is evident in the stage VI and V of TMD with deformed or torn disc, and abnormal bone defects of the condyle (Wilkes, 2013). Patients at these stages will suffer from more severe symptoms such as chronic pain and limited mandibular range motion. When the deformation of the disc starts, non-surgical 1
12 treatments might not be as effective as surgical treatments, which including disc repositioning, disc removal, and replacement of the joint with a prosthetic device (Hagandora et al, 2012). To understand the process of TMD or joint degeneration, several animal models have been studied, which can be classified into chemical approaches and surgical/mechanical approaches. Complete Freund s adjuvant (CFA) is one of the chemical approaches used to induce acute inflammation in the TMJ, containing heat-killed Mycobacterium tuberculosis suspended in an oil (Almarza et al, 2011). Mustard oil, formalin and carrageenan are also used as an irritant for provoking pain and inflammation. The mechanical and surgical animal models include disc displacement, condylotomy, disc perforation, discectomy and mechanical perturbation (Almarza et al, 2011). Except for mechanical perturbation, the other models require surgical exposing of the joint cavity, which causes inflammation and introduces an extra variable than expected. Moreover, although chemical approaches and the other mechanical surgeries are sufficient enough to induce hypersensitivity, it does not replicate the slow and sequential development of TMD. For perturbation, one study used the unilateral bite raise by using 1 mm dental composite in six- and nine-week-old Sprague-Dawley rats. After 4 weeks, histology analysis was conducted. The results showed that the expression of proteoglycans increased in ipsilateral side while the treatment-reversal and the sham-operated sham group showed weaker staining intensity, indicating that the increase of the compressive forces in the TMJ (Mao et al, 1998). Another bite raise model was the incisor bite plane in the 7-week-old male Wistar rats. According to the study, the bite raise was prefabricated by the dental composite that covered the upper incisors of the rats with 2 mm interocclusal space between the molars. The biochemical assays, PCR and western blot analysis indicated that protein accumulation and proteoglycan mrna expression were influenced by the change of mechanical loading in the TMJ disc (Nakao et al, 2014). In another anterior splint study, 2
13 6-week-old female Sprague Dawley rats were splinted for 2, 4, 8,12 and 20 weeks. At each time point, safranin O staining was conducted, which showed decreasing proteoglycan contents in mandibular condyle cartilage as early as 2 weeks after splint placement (Zhang et al, 2016) (Figure 1.1). As one of the glycosylated proteins, proteoglycans are molecules that consists of a protein core which covalently attached by glycosaminoglycans (GAG) side chains (Yanagishita, 1993). GAGs are linear, and highly anionic negatively charged polysaccharides that interact with water molecules resulted from the negative charge. The major biological function of proteoglycans is to provide hydration and swelling pressure to the tissue, enabling it to withstand dynamic compressive forces (Nakano and Scott, 1989; Yanagishita, 1993; Mao, 1998). Aggrecan is a large aggregating proteoglycan that presents along the hypertrophic layer of the MCC (Teramoto et al, 2003). In the rabbit (Henderson et al, 2015), previous data showed that after being splinted for four weeks, the content of GAG decreased in the contralateral splinted condyles compared to the native sham group (Figure 1.2). 3
14 Figure 1 A. Frontal and lateral view of anterior splint B. Histology of rat TMJ showing the condyle cartilage at 10X magnification. (Scale bar=100µm) (Modified from Zhang et al, 2016). Figure 2. Histology of rabbit TMJ showing the condyle cartilage at 10X magnification. A.C. H&E and Safranin-O staining for the sham group; B.D. H&E staining and Safranin-O staining for the splinted group. (Scale bar=100µm) (Modified from Henderson et al, 2015) 4
15 In the present study, our objective is to determine whether comparable changes are observed in an older rat model of occlusal change. We applied the composite bite-raising splints (around 1mm) on the left maxillary molars in 14-week-old male and female Sprague-Dawley rats for 4 and 6 weeks in the splinted group (n=4). After 4 and 6 weeks, all the rats were euthanized and histological analysis of the TMJ was carried out on both splinted and contralateral sides of the jaw. Hematoxylin & Eosin (H&E) was conducted to identify the cell arrangement in mandibular condyle cartilage (MCC) and shape of the mandibular condyle. GAG can be identified by Safranin- O staining. The other biochemical content, Collagen II, will be detected by IHC staining. 5
16 2.0 HYPOTHESIS The GAG layer will be larger in splinted rats in the ipsilateral side of the condyle when compare to the sham group because of the increasing mechanical load caused by the change of occlusion. 6
17 3.0 MATERIALS AND METHODS 3.1 UNILATERAL BITE RAISE In the first batch, 14-week-old male Sprague-Dawley rats were anesthetized for rat cocktail consisting of acepromazine (1.1mg/kg), ketamine (5.5mg/kg) and xylazine (5.5mg/kg). Isoflurane (1.5-2%) was delivered via nose before the injection of the cocktail to induce muscle relaxation. The operating table restricted the mobility of the rat with rubber bands (Figure 3.1). The cotton applicator was used to clean and dry the surface of the maxillary molar of the rats before the application of etching agent (Accu-Spense Acid Etch, Phosphoric Acid 37%). 15 seconds later, the target molars were washed and dried. The adhesive agent (3M ESPE) was used later following by the placement of the composite (Beautifil Flow Plus), which was shaped by the dental instrument and cured with a LED curing light (X-lite). All the sham rats have received the same surgeries as the splinted group, except that the composite was taken off in the last step. Each rat in the splinted group was inspected 7 days after the surgeries to ensure the appliance retention. After 7 days, the splinted rats were inspected once a week. The same surgeries were conducted when the appliance fell off from the maxillary molar in rat 3 and 4 after the splint placement. In the second batch, 14-week-old female Sprague-Dawley rats were treated 3 months later following the same protocol, except that the splinting period was 6 weeks. 7
18 Figure 3. Unilateral bite raise of the rats. A. Splinting operation showing the maxillary molars of the rat. B. Red arrow points to the composite. 3.2 SAMPLE PROCESSING After 4 and 6 weeks, the rats were euthanized in CO2 chamber. A 90-degree angle incision was made along the mandibular ramus and the zygomatic bone. The mandibular fossa, TMJ disc and condyle were preserved by careful dissection. Immunocal (Fisher Scientific, ) was used to demineralize the tissue for 24 hours. After full decalcification, the samples were embedded in OCT compound (Fisher Scientific, E ) and placed in the cold room overnight. Then the samples were frozen in the -80-degree freezer. The sample blocks were sectioned sagittally by Crystat (Microm, HM 505 E) in 10 µm. The slides were preserved in the fridge for further histology and immunohistochemistry. 8
19 3.3 HISTOLOGY Hematoxylin & Eosin Staining After fixation in Acetone (VWR Scientific, EM-AX0116) for 10 minutes, the samples were stained by Harris Hematoxylin (Thermo scientific, ) for 30 seconds and Shandon Eosin- Y (Thermo scientific, ) for 30 seconds. Then the samples were dehydrated through 95% alcohol, 2 changes of absolute alcohol, 5 minutes each, cleared in 2 changes of xylene (Azer scientific, ES609), 5 minutes each and mounted with mounting medium (Thermo Scientific, E ). Safranin O staining Samples were fixed in Acetone (VWR Scientific, EM-AX0116) for 10 minutes before staining. Then 2% fast green (Fisher Scientific, E ) and 1% acidic acid were used for 2 minutes and 10 seconds, followed by 0.5% safranin (Fisher Scientific, E ) for 5 minutes. Then the samples were dehydrated through 95% alcohol, 2 changes of absolute alcohol, 5 minutes each, cleared in 2 changes of xylene (Azer scientific, ES609), 5 minutes each and mounted with mounting medium (Thermo Scientific, E
20 3.4 IMMUNOHISTOCHEMISTRY Frozen-sectioning samples were fixed in Acetone (VWR Scientific, EM-AX0116), washed by PBS buffer (10mM Na3PO4 0.9% PBS, ph=7.5). Then the slides were incubated with 1% hydrogen peroxide (Fisher Scientific, M15829) in 50 ml methanol (Fisher Scientific, A4114) for 30 minutes. After rinsing, the horse serum (Vector Laboratories, PK-4002) was used to block nonspecific binding. Primary antibody (1: 1000, Mouse anti-collagen II, Fisher Scientific, ) was used for 30 minutes. Then the positive slides were incubated with the secondary Horse anti- Mouse antibody (1:400, Vector Laboratories, PK-4002) for 30 minutes. The slides were incubated with ABC reagent (Vector Laboratories, PK-4002) for 30 minutes, and then the slides were stained with DAB substrate (Vector Laboratories, SK-4100) for 2 minutes and washed with tap water. The samples were dehydrated through 95% alcohol, two changes of absolute alcohol, 5 minutes each, cleared in 2 changes of xylene (Azer scientific, ES609), 5 minutes each and mounted with mounting medium (Thermo Scientific, E ). The negative control was exposed to all the steps without the primary antibody. 3.5 IMAGES PROCESSING Image J (NIH image) was used to analyzed the histology and immunohistochemistry. GAG and collagen type II intensity was qualified by the percentage of positive staining area divided by the MCC area between ipsi- and contralateral sides as well as sham and splinted group. The thickness of the MCC was measured at anterior, median and posterior portion. 10
21 3.6 STATISTIC ANALYSIS 15 samples were analyzed (n1=8; n2=7) by student t-test for comparison between ipsi- and contralateral sides in batch 3 and 4 respectively. The differences were identified by the same test between sham and splinted groups. Statistically significant is p<
22 4.0 RESULTS WEEK-OLD MALE RATS SPLINTED FOR 4 WEEKS H&E Staining In Hematoxylin & Eosin staining, the connective tissue was stained in pink, and the nucleus was in purple (Figure 4.1). The MCC consists of fibrous, proliferative, mature, and hypertrophic and subchondral zones from superior to inferior. It can be divided into anterior, median and posterior portion. In H&E staining the five layers were observed on both ipsi- and contralateral side of the MCC with a continuous and complete fibrous layer. In image analysis, there were no statiscally differences in the thickness of the MCC between the anterior, middle and posterior portions between sham and splinted group (Figure 4.2) (p>0.05). 12
23 Figure 4. Histology showing the ipsi- and contralateral of TMJ discs and condyles in H&E staining of the splinted group at 4X magnification (scale bars=500 µm). No histological difference in the cell arrangement of MCC was observed between ipsi- and contralateral side (A-D). 13
24 Figure 5. Comparison between MCC in sham and splinted group. No significant differences between the anterior, middle and posterior portions of the MCC between sham and spl 14
25 Safranin O Staining GAG, the highly anionic side chains of proteoglycans that present on cell surfaces in the extracellular matrix, was stained in red to pink in Safranin O staining while the connective tissue was stained in green (Gandhi, 2008). In the splinted group, there was an increase in safranin-o staining along the mature and hypertrophic layer on the ipsi- compared to the contralateral side, especially on the posterior band of the MCC for most rats (Figure 4.3, A, B). Although GAG was stained faintly in the two rats in the sham group (Figure 4.3, C, D), these did not appear to have a difference in GAG distribution between sides. The other two rats did not stain for GAG (Figure 4.3, E, F). Part of the samples did not have TMJ disc because histology artifacts. In image analysis, splinted group had more GAG than sham group in ipsilateral side (Figure 4.4. A) (p<0.05). The ipsilateral side had more GAG compared to contralateral side in splinted group (p<0.05). In the sham group, there was no difference between the two sides (Figure 4.4. B) (p>0.05). 15
26 Figure 6. Histology showing the ipsi- and contralateral of TMJ discs and condyles in Safranin O staining of the splinted group at 4X magnification (scale bars=500µm). In the splinted group, there was an increase in safranin-o staining along the mature and hypertrophic layer on the ipsilateral side (A, C, E, G) compared to the contralateral side (B, D, F, H). 16
27 Figure 7. Comparison of GAG staining between sham and splinted, ipsi and contralateral sides. A. Splinted group had more GAG than sham group in ipsilateral side. B. The ipsilateral side had more GAG compared to contralateral in splinted group. In the sham group, there was no difference between the two sides. (p>0.05) 17
28 Collagen II Staining Collagen I and Collagen II are the primary biochemical contents of the articulate cartilage (Figure 4.5). While Collagen I is predominant in the fibrous zone, Collagen II is mainly expressed in the mature and hypertrophic zone (Mizoguchi, 1996). According to the IHC staining, Collagen II was stained in brown along the mature and hypertrophic layer of the MCC in the ipsi- and contralateral side of the sham and splinted group (Figure 4.6. A-D). The image analysis indicated that there was no difference between the ipsi- and contralateral sides, and sham and splinted groups (Figure 4.7) (p>0.05). There was no non-specific staining according to the histology of the negative sham ((Figure 4.6. E, F). Figure 8. Histology showing Collagen type II IHC staining of rat s knee at 4X magnification (scale bars=500 µm). A. Collagen II was stained in brown along the articulate cartilage of femur and tibia. B. There was no non-specific staining in negative sham. 18
29 Figure 9. Histology showing the ipsi- and contralateral of TMJ discs and condyles in Collagen type II IHC staining of the splinted group at 4X magnification (scale bars=500 µm). Collagen II was stained in brown along the mature and hypertrophic layer of the MCC in the ipsi- and contra-lateral side of the splinted and control group (A-D). No difference was observed between the two sides. No non-specific staining can be observed (E, F). 19
30 Figure 10. Comparison between ipsi- and contralateral side, and sham and splinted group in Collagen type II staining. A. No difference in collagen type II staining between ipsi- and contralateral sides; B. No difference in collagen type II staining between sham and splinted groups. (p>0.05) 20
31 WEEKS-OLD FEMALE RATS SPLINTED FOR 6 WEEKS H&E Staining There seemed to be no histological difference in the cell arrangement, and the thickness of MCC between the two sides in both groups (Figure 4.8). One rat in the splinted group died after anesthesia was injected. The image analysis showed that there were no significant differences in MCC thickness between the anterior, middle and posterior portions of the MCC between sham and splinted group (Figure. 4.9) (p>0.05). 21
32 Figure 11. Histology showing the ipsi- and contralateral of TMJ discs and condyles in H&E staining of the splinted group at 4X magnification (scale bars=500 µm). No histological difference in the cell arrangement of MCC was observed between ipsi- and contralateral side, sham and splinted group (A-D). 22
33 Figure 12. Comparison between MCC thickness in sham and splinted group. No significant differences between the anterior, middle and posterior portions of the MCC between sham and splinted group. 23
34 Safranin O Staining In the splinted group, GAG was stained along the mature and hypertrophic layer of the MCC in the ipsi- and contralateral side of the first rat (Figure A, B). Staining was only observed in ipsilateral side of the second rat (Figure C, D). In the third rat, the staining appeared on the opposite side of the condyle (Figure E, F). In the sham group, no staining was detected on both the ipsi- and contralateral side of the condyle (Figure G-H). The image analysis indicated that there was no difference of GAG was found between ipsi- and contralateral side. Overall, splinted group had more GAG than sham group in both ipsi and contralateral side (Figure 4.11) (p>0.05).. 24
35 Figure 13. Histology showing the ipsi- and contralateral of TMJ discs and condyles in H&E staining of the sham and splinted group at 4X magnification (scale bars=500 µm). GAG was stained on both sides of the first rat (A, B). GAG was detected only in ipsilateral side of the second rat (C, D). The staining appeared on the opposite side of the condyle (E, F). No GAG was stained on Sham group. 25
36 Figure 14. Comparison between ipsi- and contralateral side, and sham and splinted group in GAG staining. A. No difference of GAG was found between ipsi- and contralateral side (p>0.05); B. Splinted group had more GAG than sham group in both ipsi and contralateral side (p<0.05). 26
37 Collagen II Staining Both the splinted and sham group showed Collagen II stained along the hypertrophic layer of the MCC (Figure A-D). No histological difference was identified between the ipsi- and contralateral sides of the condyle in both groups. There was no non-specific staining according to the histology of the negative sham group (Figure E, F). In image analysis, there was no difference between ipsi- and contralateral side as well as sham and splinted groups (Figure 4.13) (p>0.05). 27
38 Figure 15. Histology showing the ipsi- and contralateral of TMJ discs and condyles in Collagen type II IHC staining of the splinted group at 4X magnification (scale bars=500 µm). Collagen II stained along the hypertrophic layer of the MCC in splinted and sham group (A-D). No non-specific staining in negative sham group (E, F) 28
39 Figure 16. Comparison between ipsi- and contralateral side, and sham and splinted group in Collagen type II staining. A. No difference in collagen type II staining between ipsi- and contralateral side; B. No difference in collagen type II staining between sham and splinted group. (p>0.05) 29
40 5.0 DISCUSSION 5.1 ANIMAL MODEL Compared to other animal models of degenerative joint disease, splint models had the advantage over the others for the fact that the joint capsule was not penetrated (Henderson, 2015). Incision and mastication are the two main jaw movement of rodents (Nakao, 2015). When the rats obtained food, the splinted rats could only masticate through the ipsilateral side while the maxillary teeth of the contra-lateral side could not form the normal occlusion with the mandibular teeth. Under this circumstance, the mechanical load that MCC received in mastication increased in the ipsilateral side and decreased in the contra-lateral side. Age could be another factor that influenced the distribution of GAG. In Mao s study, the unilateral bite raise was manifested used in in sixand nine-week-old Sprague-Dawley rats (Mao et al, 1998). After 4 weeks of splinting, GAG distribution was different between the two age groups. It may indicate that the adaptability to mechanical loading decreased with age. In the present study, older Sprague-Dawley rats were used, which may eliminate the variable that results from exponential growth in the early 10 weeks. Occlusal splint is designed through detailed study model using articulator for people with TMJ pain and malocclusion (Crout, 2016). Different from unilateral molar splint, it is usually therapeutic, and bilateral, and has a coverage of all the teeth to adjust the occlusion. In comparison, unilateral molar splint changes the occlusion extremely, which can induce dysfunction of the jaw in short period. 30
41 5.2 HISTOLOGY AND IMMUNOHISTOCHEMISTRY The MCC consists of fibrous, proliferative, mature, and hypertrophic and subchondral zones from superior to inferior. According to Henderson et al., after 6 weeks of splinting in the rabbit, the subchondral layer of the fibrocartilage showed loss of GAG (Henderson, 2015). However, Mao et al. found that the unilateral bite in rats increased the thickness of the MCC and GAG after 4 weeks (Mao et al, 1998). In this study, the result of H&E staining in the present study revealed that both 4 and 6 weeks of splinting did not induce cell disarrangement, loss of fibrous layers, and increase thickness in ipsi- and contralateral side of the condyle. Interestingly, there appeared to be an increase in Glycosaminoglycan (GAG) content with splinting that was greater ipsilateral to the splint placement after 4 weeks in the male rats. The distribution of GAG was mostly in the posterior band which is regarded as the major pressure-bearing band, revealing the biochemical content change as well as the beginning of MCC degeneration (Mizoguchi, 1996). In comparison, the safranin O staining after 6 weeks in male rats did not show the same trend between ipsi- and contra-lateral sides. It might indicate that the degeneration is dependent on gender. Meanwhile, it is possible that the distribution of the mechanical force changed resulting from the adaption. In the rabbit, the GAG only appeared on the anterior band of the MCC instead of the posterior band in the rabbit, which was different from GAG staining in the splinted rat, which might indicate that the rabbit adapted the bite raise differently (Henderson et al, 2015). In the sham group, GAG was expected to express along mature and hypertrophic layer. One of the reasons for the absence of GAG is that it might decrease with the growth of the rats, which is consistent with the results from Mao and his colleagues (Mao et al, 1998). It is also possible that the sham surgeries conducted in the sham group caused the decrease of GAG. It could also dissolve during processing and frozen sectioning. 31
42 Collagen II is predominate in the mature and hypertrophic layer of the MCC. According to IHC staining, after 4 weeks and 6 weeks of splinting, no histological difference can be recognized, which indicates that the occlusal change did not influence the concentration and location of collagen II. According to Henderson et al, collagen type II decreased in rabbit with the unilateral splint. The difference suggested that changing occlusion influenced collagen type II between those two species in various ways. 5.3 LIMITATIONS AND FUTURE DIRECTIONS Although there was in increase in Glycosaminoglycan (GAG) content with splinting that was greater ipsilateral to the splint placement in male rats after 4 weeks of splinting, only 4 rats were splinted. In the second batch, the safranin O staining was less consistent and predictable in only 3 female rats. More experimental animals in the future study will increase the statistical power. We are in the process of establishing the splint model in the rats. As such, we are trying to determine an effective splint duration to observe degeneration changes in the condyle, and also determine if gender has an impact. In first batch, the splinting surgery was conducted in female rats for 4 weeks while the second batch was performed in male for six weeks. Therefore, conclusions were made within the same batch. It will be inconclusive to compare batch 1 and batch 2 for the reason that there were 2 variables, which were gender and splinting time. In spite of the fact that there was no histological difference in collagen type II, it is not accurate to conclude that the collagen type II was expressed equally on the MCC based on 32
43 observation. Therefore, a quantitative method should be considered to compare the biochemical contents between groups. Considering the fact that GAG might dissolve during processing, it is necessary to test other biochemical contents such as Aggrecan to confirm the potential changes. Versican is one of the proteoglycans that mainly located on the fibrous layer and the TMJ disc (Roth, 1997). In our study, we only investigated the biochemical content that expressed in the mature and hypertrophic layer but not in the other layers, where degenerative change could happen. In the first batch, there was no GAG staining in the 14-week-old female rats sham group which only received the surgery but not splinted on the molars. It is possible that the absence of GAG was caused by the splinting surgery. Another sham group without receiving any surgeries should be added to exclude the possible damage of the surgery. A different age group will also be considered because the age of the rats could be a factor in GAG content. Some gaps and tears were seen in the narrow space of the condyles, which was clearly histological artifact. In the future, the tissue could be infiltrated with sucrose first, to then allow full penetration of OCT compound so that smooth tissue will be expected in frozen sectioning. Last but not least, it will be important to further characterize the time course of both the onset and recovery of the changes in the joint, and the extent to which the histological changes correlate with changes in joint sensitivity. 33
44 6.0 CONCLUSION There was an increase in Glycosaminoglycan (GAG) content with splinting that was greater ipsilateral to the splint placement after 4 weeks in the male rats. In female rats which were 14-week-old and splinted for 6 weeks, the result was not consistent with the first batch. More GAG was detected in the splinted group compared to the sham in both batches. Overall, frozen sectioning was successful in obtaining high quality sections without wrinkles or rips. Furthermore, both histology and IHC staining were validated and worked well on the rat condyles. It will be important to further characterize the potential changes in other biochemical components of the joint tissue, for example, Aggrecan, and time course of both the onset and recovery of the changes in the joint, and the extent to which the histological changes correlate with changes in joint sensitivity. 34
45 BIBLIOGRAPHY Almarza, A. J., C. K. Hagandora and S. E. Henderson (2011). "Animal Models of Temporomandibular Joint Disorders: Implications for Tissue Engineering Approaches." Annals of Biomedical Engineering 39(10): Alomar, X., J. Medrano, J. Cabratosa, J. A. Clavero, M. Lorente, I. Serra, J. M. Monill and A. Salvador (2007). "Anatomy of the Temporomandibular Joint." Seminars in Ultrasound, CT and MRI 28(3): DK., C. (2017). "Anatomy of an occlusal splint." Gen Dent 65(2): Hagandora, C. K. and A. J. Almarza (2012). "TMJ Disc Removal:Comparison between Preclinical Studies and Clinical Findings." Journal of Dental Research 91(8): Henderson, S. E., J. R. Lowe, M. A. Tudares, M. S. Gold and A. J. Almarza (2015). "Temporomandibular joint fibrocartilage degeneration from unilateral dental splints." Archives of Oral Biology 60(1): Henderson, S. E., M. A. Tudares, M. S. Gold and A. J. Almarza (2015). "Analysis of pain in the rabbit temporomandibular joint after unilateral splint placement." J Oral Facial Pain Headache. 29(2): Mao, J. J., F. Rahemtulla and P. G. Scott (1998). "Proteoglycan Expression in the Rat Temporomandibular Joint in Response to Unilateral Bite Raise." Journal of Dental Research 77(7): Mizoguchi, I., I. Takahashi, M. Nakamura, Y. Sasano, S. Sato, M. Kagayama and H. Mitani (1996). "An immunohistochemical study of regional differences in the distribution of type I and type II collagens in rat mandibular condylar cartilage." Archives of Oral Biology 41(8): Nakano, H., K. Maki, Y. Shibasaki and A. J. Miller (2004). "Three-dimensional changes in the condyle during development of an asymmetrical mandible in a rat: A microcomputed tomography study." American Journal of Orthodontics and Dentofacial Orthopedics 126(4): S., G. N. and M. R. L. (2008). "The Structure of Glycosaminoglycans and their Interactions with Proteins." Chemical Biology & Drug Design 72(6): Roth, S., K. Müller, D. C. Fischer and K. H. Dannhauer (1997). "Specific properties of the extracellular chondroitin sulphate proteoglycans in the mandibular condylar growth centre in pigs." Archives of Oral Biology 42(1):
46 Tanaka, E., M. S. Detamore and L. G. Mercuri (2008). "Degenerative Disorders of the Temporomandibular Joint: Etiology, Diagnosis, and Treatment." Journal of Dental Research 87(4): Teramoto, M., S. Kaneko, S. Shibata, M. Yanagishita and K. Soma (2003). "Effect of compressive forces on extracellular matrix in rat mandibular condylar cartilage." Journal of Bone and Mineral Metabolism 21(5): Wright, E. F. (2013). Manual of Temporomandibular Disorders, Wiley-Blackwell. Yanagishita, M. (1993). "Function of proteoglygans in extracellular matrix." Acta Pathologica Japonica 43: Zhang, M., H. Wang, J. Zhang, H. Zhang, H. Yang, X. Wan, L. Jing, L. Lu, X. Liu, S. Yu, W. Chang and M. Wang (2016). "Unilateral anterior crossbite induces aberrant mineral deposition in degenerative temporomandibular cartilage in rats." Osteoarthritis and cartilage 24(5):
Temporomandibular Joint. Dr Noman ullah wazir
 Temporomandibular Joint Dr Noman ullah wazir Type of Joint TMJ is a Synovial joint between : The condylar head of the mandible. The mandibular fossa of squamous part of temporal bone. The joint cavity
Temporomandibular Joint Dr Noman ullah wazir Type of Joint TMJ is a Synovial joint between : The condylar head of the mandible. The mandibular fossa of squamous part of temporal bone. The joint cavity
TEMPORO-MANDIBULAR JOINT DISORDERS
 Disclaimer This movie is an educational resource only and should not be used to manage your dental health. All decisions about the management of TMJ Disorders must be made in conjunction with your Dental
Disclaimer This movie is an educational resource only and should not be used to manage your dental health. All decisions about the management of TMJ Disorders must be made in conjunction with your Dental
The Temporomandibular joint: Anatomy, Mechanics, Pathology. Aditya Bahel, DO
 The Temporomandibular joint: Anatomy, Mechanics, Pathology Aditya Bahel, DO Outline Anatomy Mechanics and function Indications for TMJ imaging MR Protocols and pitfalls Pathology Treatment options Anatomy
The Temporomandibular joint: Anatomy, Mechanics, Pathology Aditya Bahel, DO Outline Anatomy Mechanics and function Indications for TMJ imaging MR Protocols and pitfalls Pathology Treatment options Anatomy
Temporomandibular Joint Disorders
 Temporomandibular Joint Disorders Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can cause headaches, ear pain,
Temporomandibular Joint Disorders Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can cause headaches, ear pain,
ANALYSIS OF A JOINT DEGENERATION MODEL AND DEGRADABLE CRANIOFACIAL SCREWS IN THE RABBIT TEMPOROMANDIBULAR JOINT. Sarah Elizabeth Henderson
 ANALYSIS OF A JOINT DEGENERATION MODEL AND DEGRADABLE CRANIOFACIAL SCREWS IN THE RABBIT TEMPOROMANDIBULAR JOINT by Sarah Elizabeth Henderson B.S. in Biomedical Engineering, Bucknell University, 2008 Submitted
ANALYSIS OF A JOINT DEGENERATION MODEL AND DEGRADABLE CRANIOFACIAL SCREWS IN THE RABBIT TEMPOROMANDIBULAR JOINT by Sarah Elizabeth Henderson B.S. in Biomedical Engineering, Bucknell University, 2008 Submitted
TMJ Parametro Classico
 TMJ Parametro Classico Total Temporomandibular Joint Prosthesis 2 Personalized total TMJ replacement system (Parametro Classic & Parametro Saddle ) Patient Information in English This patient information
TMJ Parametro Classico Total Temporomandibular Joint Prosthesis 2 Personalized total TMJ replacement system (Parametro Classic & Parametro Saddle ) Patient Information in English This patient information
Temporomandibular Joint Remodeling for the Treatment of Temporomandibular Joint Disorders - A Clinical Case Study
 The Open Rehabilitation Journal, 2009, 2, 43-49 43 Open Access Temporomandibular Joint Remodeling for the Treatment of Temporomandibular Joint Disorders - A Clinical Case Study Rosita Wurgaft 1 and Ricky
The Open Rehabilitation Journal, 2009, 2, 43-49 43 Open Access Temporomandibular Joint Remodeling for the Treatment of Temporomandibular Joint Disorders - A Clinical Case Study Rosita Wurgaft 1 and Ricky
Functional Lateral Shift of the Mandible Effects on the Expression of ECM in Rat Temporomandibular Cartilage
 Original Article Functional Lateral Shift of the Mandible Effects on the Expression of ECM in Rat Temporomandibular Cartilage Tanapan Wattanachai a ; Ikuo Yonemitsu b ; Sawa Kaneko c ; Kunimichi Soma d
Original Article Functional Lateral Shift of the Mandible Effects on the Expression of ECM in Rat Temporomandibular Cartilage Tanapan Wattanachai a ; Ikuo Yonemitsu b ; Sawa Kaneko c ; Kunimichi Soma d
Anatomy and physiology of Temporomandibular Joint
 Anatomy and physiology of Temporomandibular Joint Temporomandibular joint (TMJ): It is the articulation of the condyle of the mandible, and the inter-articular disc; with the mandibular fossa (glenoid
Anatomy and physiology of Temporomandibular Joint Temporomandibular joint (TMJ): It is the articulation of the condyle of the mandible, and the inter-articular disc; with the mandibular fossa (glenoid
Prosthetic Management of TMJ Disorders
 Prosthetic Management of TMJ Disorders Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Mohd@DrMohdAlfarsi.com @DrMohdAlfarsi DrMohdAlfarsi 056 224 2227 Overview Overview
Prosthetic Management of TMJ Disorders Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Mohd@DrMohdAlfarsi.com @DrMohdAlfarsi DrMohdAlfarsi 056 224 2227 Overview Overview
Muscles of mastication [part 1]
![Muscles of mastication [part 1] Muscles of mastication [part 1]](/thumbs/76/73586850.jpg) Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
Case Report. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System.
 Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
TMJ Joint Replacement System
 TMJ Joint Replacement System Patient Information What is the Temporomandibular Joint (TMJ)? The Temporomandibular Joint is one of the body s most complex joints. It is similar to a ball and socket, but
TMJ Joint Replacement System Patient Information What is the Temporomandibular Joint (TMJ)? The Temporomandibular Joint is one of the body s most complex joints. It is similar to a ball and socket, but
Temporomandibular Joint
 6 Temporomandibular Joint Most human bones are joined with one another. These connections of bones to each other are termed articulations or joints. Some joints are immovable as in the articulations of
6 Temporomandibular Joint Most human bones are joined with one another. These connections of bones to each other are termed articulations or joints. Some joints are immovable as in the articulations of
M. Gonzalez Vazquez; M.Costas; R.Prada; R.Oca; A. Villanueva and G. Tardaguila de la Fuente
 M. Gonzalez Vazquez; M.Costas; R.Prada; R.Oca; A. Villanueva and G. Tardaguila de la Fuente A) Anatomy of temporomandibular joint. closed-mouth position Glenoid fossa Intermediate zone Posterior band Articular
M. Gonzalez Vazquez; M.Costas; R.Prada; R.Oca; A. Villanueva and G. Tardaguila de la Fuente A) Anatomy of temporomandibular joint. closed-mouth position Glenoid fossa Intermediate zone Posterior band Articular
Introduction to Occlusion and Mechanics of Mandibular Movement
 Introduction to Occlusion and Mechanics of Mandibular Movement Dr. Pauline Hayes Garrett Department of Endodontics, Prosthodontics, and Operative Dentistry University of Maryland, Baltimore Assigned reading
Introduction to Occlusion and Mechanics of Mandibular Movement Dr. Pauline Hayes Garrett Department of Endodontics, Prosthodontics, and Operative Dentistry University of Maryland, Baltimore Assigned reading
Temporomandibular Joint Disorders
 Temporomandibular Joint Disorders Temporomandibular Joint : Is a synovial joint located between the condyle (head of the mandible) and the glenoid fossa (inferior surface of the squamous part of Temporal
Temporomandibular Joint Disorders Temporomandibular Joint : Is a synovial joint located between the condyle (head of the mandible) and the glenoid fossa (inferior surface of the squamous part of Temporal
TMJ UNDERSTANDING SYNDROME SPECIAL REPORT By Paul R. White, D.D.S. Special Report: Understanding TMJ Syndrome
 SPECIAL REPORT Special Report: Understanding TMJ Syndrome UNDERSTANDING TMJ SYNDROME By Paul R. White, D.D.S. 804.715.1647 www.smilerichmond.com 804.715.1647 www.smilerichmond.com 1 UNDERSTANDING TMJ SYNDROME
SPECIAL REPORT Special Report: Understanding TMJ Syndrome UNDERSTANDING TMJ SYNDROME By Paul R. White, D.D.S. 804.715.1647 www.smilerichmond.com 804.715.1647 www.smilerichmond.com 1 UNDERSTANDING TMJ SYNDROME
Changes in the temporomandibular joint after mandibular lengthening with different rates of distraction
 Shujuan Zou, DDS, MS Department of Orthodontics Jing Hu, DDS, MS, PhD Dazhang Wang, DDS, FICD Jihua Li, DDS, MS Zhenglong Tang, DDS, MS Department of Oral and Maxillofacial Surgery Huaxi School of Stomatology
Shujuan Zou, DDS, MS Department of Orthodontics Jing Hu, DDS, MS, PhD Dazhang Wang, DDS, FICD Jihua Li, DDS, MS Zhenglong Tang, DDS, MS Department of Oral and Maxillofacial Surgery Huaxi School of Stomatology
ChiroCredit.com Anatomy 226 INSTRUCTIONS/ASSIGNMENT FOR ANATOMICAL DISSECTION:
 ChiroCredit.com Anatomy 226 INSTRUCTIONS/ASSIGNMENT FOR ANATOMICAL DISSECTION: Once you click on the link to open the dissection module, the first thing you need to do is to be sure you can see all the
ChiroCredit.com Anatomy 226 INSTRUCTIONS/ASSIGNMENT FOR ANATOMICAL DISSECTION: Once you click on the link to open the dissection module, the first thing you need to do is to be sure you can see all the
Dr Mohammed Alfarsi Page 1 9 December Principles of Occlusion
 Dr Mohammed Alfarsi Page 1 9 December 2013 Principles of Occlusion Overview: The occlusion is a very large, yet easy to manage once properly understood, topic. Thus, no one handout is enough to fully understand
Dr Mohammed Alfarsi Page 1 9 December 2013 Principles of Occlusion Overview: The occlusion is a very large, yet easy to manage once properly understood, topic. Thus, no one handout is enough to fully understand
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi. E. mail:
 The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
AD2 MEASURES CONDYLE DISPLACEMENT (MCD) MANUAL
 AD2 MEASURES CONDYLE DISPLACEMENT (MCD) MANUAL Dr. Jorge Ayala Puente, DDS* Dr. Gonzalo Gutiérrez Álvarez, DDS* Dr. José Miguel Obach M., DDS Translation: Dr. Barbara Fernández Lübbert, DDS Edited: Dr.
AD2 MEASURES CONDYLE DISPLACEMENT (MCD) MANUAL Dr. Jorge Ayala Puente, DDS* Dr. Gonzalo Gutiérrez Álvarez, DDS* Dr. José Miguel Obach M., DDS Translation: Dr. Barbara Fernández Lübbert, DDS Edited: Dr.
U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health
 T M J D I S O R D E R S U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health CONTENTS 2 4 6 7 8 9 14 WHAT IS THE TEMPOROMANDIBULAR JOINT? WHAT ARE TMJ DISORDERS? WHAT CAUSES TMJ DISORDERS?
T M J D I S O R D E R S U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health CONTENTS 2 4 6 7 8 9 14 WHAT IS THE TEMPOROMANDIBULAR JOINT? WHAT ARE TMJ DISORDERS? WHAT CAUSES TMJ DISORDERS?
Nanomechanical Symptoms in Cartilage Precede Histological Osteoarthritis Signs after the Destabilization of Medial Meniscus in Mice
 Nanomechanical Symptoms in Cartilage Precede Histological Osteoarthritis Signs after the Destabilization of Medial Meniscus in Mice Basak Doyran 1, Wei Tong 2, Qing Li 1, Haoruo Jia 2, Xianrong Zhang 3,
Nanomechanical Symptoms in Cartilage Precede Histological Osteoarthritis Signs after the Destabilization of Medial Meniscus in Mice Basak Doyran 1, Wei Tong 2, Qing Li 1, Haoruo Jia 2, Xianrong Zhang 3,
ORTHOGNATHIC SURGERY
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-16 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-16 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Concepts of occlusion Balanced occlusion. Monoplane occlusion. Lingualized occlusion. Figure (10-1)
 Any contact between teeth of opposing dental arches; usually, referring to contact between the occlusal surface. The static relationship between the incising or masticatory surfaces of the maxillary or
Any contact between teeth of opposing dental arches; usually, referring to contact between the occlusal surface. The static relationship between the incising or masticatory surfaces of the maxillary or
The mandibular condyle fracture is a common mandibular
 ORIGINAL RESEARCH P. Wang J. Yang Q. Yu MR Imaging Assessment of Temporomandibular Joint Soft Tissue Injuries in Dislocated and Nondislocated Mandibular Condylar Fractures BACKGROUND AND PURPOSE: Evaluation
ORIGINAL RESEARCH P. Wang J. Yang Q. Yu MR Imaging Assessment of Temporomandibular Joint Soft Tissue Injuries in Dislocated and Nondislocated Mandibular Condylar Fractures BACKGROUND AND PURPOSE: Evaluation
Joules, Genes, and Behaviors: Degeneration of The Human TMJ
 Joules, Genes, and Behaviors: Degeneration of The Human TMJ Jeffrey C. Nickel, DMD, MSc, PhD Associate Professor University of Missouri-Kansas City Department of Orthodontics and Dentofacial Orthopedics
Joules, Genes, and Behaviors: Degeneration of The Human TMJ Jeffrey C. Nickel, DMD, MSc, PhD Associate Professor University of Missouri-Kansas City Department of Orthodontics and Dentofacial Orthopedics
Total Prosthetic Replacement of the Temporomandibular Joint (TMJ)
 Total Prosthetic Replacement of the Temporomandibular Joint (TMJ) VERSION CONTROL Version: 2.0 Ratified by: Governing Body Date ratified: 13 November 2013 Name of originator/author: Name of responsible
Total Prosthetic Replacement of the Temporomandibular Joint (TMJ) VERSION CONTROL Version: 2.0 Ratified by: Governing Body Date ratified: 13 November 2013 Name of originator/author: Name of responsible
AAO Foundation Awards Final Report
 401 N. Lindbergh Blvd. St. Louis, MO 63141 Tel.: 314.993.1700, #546 Toll Free: 800.424.2841, #546 Fax: 800.708.1364 Cell: 314.283.1983 E-Mail: rhazel@aaortho.org AAO Foundation Awards Final Report In an
401 N. Lindbergh Blvd. St. Louis, MO 63141 Tel.: 314.993.1700, #546 Toll Free: 800.424.2841, #546 Fax: 800.708.1364 Cell: 314.283.1983 E-Mail: rhazel@aaortho.org AAO Foundation Awards Final Report In an
Mixed-reality simulation for orthognathic surgery
 Fushima and Kobayashi Maxillofacial Plastic and Reconstructive Surgery (2016) 38:13 DOI 10.1186/s40902-016-0059-z METHODOLOGY Mixed-reality simulation for orthognathic surgery Kenji Fushima 1* and Masaru
Fushima and Kobayashi Maxillofacial Plastic and Reconstructive Surgery (2016) 38:13 DOI 10.1186/s40902-016-0059-z METHODOLOGY Mixed-reality simulation for orthognathic surgery Kenji Fushima 1* and Masaru
It has been proposed that partially edentulous maxillectomy
 CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
EVALUATION OF LATERAL PTERYGOID MUSCLE IN TEMPOROMANDIBULAR DISORDER PATIENTS - A MRI STUDY. Part I
 EVALUATION OF LATERAL PTERYGOID MUSCLE IN TEMPOROMANDIBULAR DISORDER PATIENTS - A MRI STUDY Part I Authors : Dr. Amol S. Patil, BDS, MDS (ORTHODONTIA) Lecturer, Department of Orthodontics, Bharati Vidyapeeth
EVALUATION OF LATERAL PTERYGOID MUSCLE IN TEMPOROMANDIBULAR DISORDER PATIENTS - A MRI STUDY Part I Authors : Dr. Amol S. Patil, BDS, MDS (ORTHODONTIA) Lecturer, Department of Orthodontics, Bharati Vidyapeeth
Parotid Gland. Parotid Gland. Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible. Medial pterygoid.
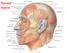 Parotid region Parotid Gland Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible Medial pterygoid Cross section of mandible Masseter D S SCM Parotid Gland Mastoid Process
Parotid region Parotid Gland Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible Medial pterygoid Cross section of mandible Masseter D S SCM Parotid Gland Mastoid Process
Up Date on TMD WHAT IS TMD? Temporomandibular Disorders (TMD)*: Donald Nixdorf DDS, MS
 Up Date on TMD Donald Nixdorf DDS, MS Associate Professor Division of TMD and Orofacial Pain WHAT IS TMD? Temporomandibular Disorders (TMD)*: MUSCLE and JOINT DISORDERS * Temporomandibular Muscle and Joint
Up Date on TMD Donald Nixdorf DDS, MS Associate Professor Division of TMD and Orofacial Pain WHAT IS TMD? Temporomandibular Disorders (TMD)*: MUSCLE and JOINT DISORDERS * Temporomandibular Muscle and Joint
Definition and History of Orthodontics
 In the name of GOD Definition and History of Orthodontics Presented by: Dr Somayeh Heidari Orthodontist Reference: Contemporary Orthodontics Chapter 1 William R. Proffit, Henry W. Fields, David M.Sarver.
In the name of GOD Definition and History of Orthodontics Presented by: Dr Somayeh Heidari Orthodontist Reference: Contemporary Orthodontics Chapter 1 William R. Proffit, Henry W. Fields, David M.Sarver.
Occlusion in complete denture
 Occlusion in complete denture Occlusion is a concept that is pertinent to all dental patients wheather they have their own teeth or not.it is a term used to describe the contact relationship between the
Occlusion in complete denture Occlusion is a concept that is pertinent to all dental patients wheather they have their own teeth or not.it is a term used to describe the contact relationship between the
Cell Walls, the Extracellular Matrix, and Cell Interactions (part 1)
 14 Cell Walls, the Extracellular Matrix, and Cell Interactions (part 1) Introduction Many cells are embedded in an extracellular matrix which is consist of insoluble secreted macromolecules. Cells of bacteria,
14 Cell Walls, the Extracellular Matrix, and Cell Interactions (part 1) Introduction Many cells are embedded in an extracellular matrix which is consist of insoluble secreted macromolecules. Cells of bacteria,
The future of health is digital
 Dated: XX/XX/XXXX Name: XXXXXXXX XXXXXXXXXXX Birth Date: XX/XX/XXXX Date of scan: XX/XX/XXXX Examination of the anatomical volume: The following structures are reviewed and evaluated for bilateral symmetry,
Dated: XX/XX/XXXX Name: XXXXXXXX XXXXXXXXXXX Birth Date: XX/XX/XXXX Date of scan: XX/XX/XXXX Examination of the anatomical volume: The following structures are reviewed and evaluated for bilateral symmetry,
Anatomy and Physiology. Bones, Sutures, Teeth, Processes and Foramina of the Human Skull
 Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
FOR CMS (MEDICARE) MEMBERS ONLY NATIONAL COVERAGE DETERMINATION (NCD) FOR MAGNETIC RESONANCE IMAGING:
 National Imaging Associates, Inc. Clinical guidelines TEMPOROMANDIBULAR JOINT (TMJ) MRI Original Date: May 23, 2003 Page 1 of 5 CPT Code: 70336 Last Review Date: May 2016 NCD 220.2 MRI Last Effective Date:
National Imaging Associates, Inc. Clinical guidelines TEMPOROMANDIBULAR JOINT (TMJ) MRI Original Date: May 23, 2003 Page 1 of 5 CPT Code: 70336 Last Review Date: May 2016 NCD 220.2 MRI Last Effective Date:
Fixed Twin Blocks. Guidelines for case selection are similar to those for removable Twin Block appliances.
 Fixed Twin Blocks Development of Fixed Twin Blocks Dr Clark has enjoyed the cooperation of Dynaflex in developing the Fixed Twin Block. Six years of clinical testing has confirmed that this technique produces
Fixed Twin Blocks Development of Fixed Twin Blocks Dr Clark has enjoyed the cooperation of Dynaflex in developing the Fixed Twin Block. Six years of clinical testing has confirmed that this technique produces
Outline. Limiting your risk when treating patients with TMD. Temporomandibular Disorders 20/01/2014. TMD diagnosis. Condylar position and TMD risk
 Outline American Association of Orthodontists Limiting your risk when treating patients with TMD Ambra Michelotti michelot@unina.it TMD diagnosis Condylar position and TMD risk Occlusal interference and
Outline American Association of Orthodontists Limiting your risk when treating patients with TMD Ambra Michelotti michelot@unina.it TMD diagnosis Condylar position and TMD risk Occlusal interference and
Treatment Agreement for Oral Appliance Therapy: Temporomandibular Disorder (TMD)
 Treatment Agreement for Oral Appliance Therapy: Temporomandibular Disorder (TMD) What is TMD? Temporomandibular Disorders (TMD) are a group of conditions that cause pain and dysfunction in the jaw joint
Treatment Agreement for Oral Appliance Therapy: Temporomandibular Disorder (TMD) What is TMD? Temporomandibular Disorders (TMD) are a group of conditions that cause pain and dysfunction in the jaw joint
Ibelieve the time has come for the general dentists to
 EARLY ORTHODONTIC TREATMENT Brock Rondeau, D.D.S. I.B.O., D.A.B.C.P., D-A.C.S.D.D., D.A.B.D.S.M., D.A.B.C.D.S.M. Ibelieve the time has come for the general dentists to get serious and educated in an effort
EARLY ORTHODONTIC TREATMENT Brock Rondeau, D.D.S. I.B.O., D.A.B.C.P., D-A.C.S.D.D., D.A.B.D.S.M., D.A.B.C.D.S.M. Ibelieve the time has come for the general dentists to get serious and educated in an effort
Establish a Healthy TMJ
 TW TMJ Establish a Healthy TMJ Prior to Restorative, Orthodontic or Prosthetic Treatment Dr. Brock Rondeau, D.D.S., I.B.O., D.A.B.C.P. Author: Dr. Brock Rondeau is one of North America s most sought after
TW TMJ Establish a Healthy TMJ Prior to Restorative, Orthodontic or Prosthetic Treatment Dr. Brock Rondeau, D.D.S., I.B.O., D.A.B.C.P. Author: Dr. Brock Rondeau is one of North America s most sought after
BIOENGINEERING APPROACH TO UNDERSTANDING TMJ PATHOBIOLOGY
 Clemson University TigerPrints All Dissertations Dissertations 5-2012 BIOENGINEERING APPROACH TO UNDERSTANDING TMJ PATHOBIOLOGY Jonathan Kuo Clemson University, kujo6784@gmail.com Follow this and additional
Clemson University TigerPrints All Dissertations Dissertations 5-2012 BIOENGINEERING APPROACH TO UNDERSTANDING TMJ PATHOBIOLOGY Jonathan Kuo Clemson University, kujo6784@gmail.com Follow this and additional
The America Association of Oral and Maxillofacial Surgeons classify occlusion/malocclusion in to the following three categories:
 Subject: Orthognathic Surgery Policy Effective Date: 04/2016 Revision Date: 07/2018 DESCRIPTION Orthognathic surgery is an open surgical procedure that corrects anomalies or malformations of the lower
Subject: Orthognathic Surgery Policy Effective Date: 04/2016 Revision Date: 07/2018 DESCRIPTION Orthognathic surgery is an open surgical procedure that corrects anomalies or malformations of the lower
Corporate Medical Policy
 Corporate Medical Policy Temporomandibular Joint Dysfunction (TMJD) File Name: Origination: Last CAP Review: Next CAP Review: Last Review: temporomandibular_joint_dysfunction_(tmjd) 1/1996 10/2017 10/2018
Corporate Medical Policy Temporomandibular Joint Dysfunction (TMJD) File Name: Origination: Last CAP Review: Next CAP Review: Last Review: temporomandibular_joint_dysfunction_(tmjd) 1/1996 10/2017 10/2018
Cephalometric Analysis
 Cephalometric Analysis of Maxillary and Mandibular Growth and Dento-Alveolar Change Part III In two previous articles in the PCSO Bulletin s Faculty Files, we discussed the benefits and limitations of
Cephalometric Analysis of Maxillary and Mandibular Growth and Dento-Alveolar Change Part III In two previous articles in the PCSO Bulletin s Faculty Files, we discussed the benefits and limitations of
Answers to Pre-Lab Quiz (p. 171) Answers to Activity Questions
 Answers to Pre-Lab Quiz (p. 171) 1. Holds bones together; allows the rigid skeleton some flexibility so that gross body movements can occur 2. c, amount of movement allowed by the joint 3. synovial 4.
Answers to Pre-Lab Quiz (p. 171) 1. Holds bones together; allows the rigid skeleton some flexibility so that gross body movements can occur 2. c, amount of movement allowed by the joint 3. synovial 4.
Three-dimensional evaluation of TMJ parameters in Class II and Class III patients Zane Krisjane, Ilga Urtane, Gaida Krumina, Katrina Zepa
 Stomatologija, Baltic Dental and Maxillofacial Journal, 11: 32-36, 2009 Three-dimensional evaluation of TMJ parameters in Class II and Class III patients Zane Krisjane, Ilga Urtane, Gaida Krumina, Katrina
Stomatologija, Baltic Dental and Maxillofacial Journal, 11: 32-36, 2009 Three-dimensional evaluation of TMJ parameters in Class II and Class III patients Zane Krisjane, Ilga Urtane, Gaida Krumina, Katrina
Total Knee Replacement
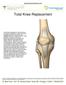 Total Knee Replacement A total knee replacement, also known as total knee arthroplasty, involves removing damaged portions of the knee, and capping the bony surfaces with man-made prosthetic implants.
Total Knee Replacement A total knee replacement, also known as total knee arthroplasty, involves removing damaged portions of the knee, and capping the bony surfaces with man-made prosthetic implants.
Shadeguides Finding the Centric Relation The Kois Deprogrammer
 Maciej Zarow Shadeguides Finding the Centric Relation The Kois Deprogrammer 21 Jun 2018 Finding the centric relation might sometimes seem hard, but with appropriate devices, such as the Kois Deprogrammer
Maciej Zarow Shadeguides Finding the Centric Relation The Kois Deprogrammer 21 Jun 2018 Finding the centric relation might sometimes seem hard, but with appropriate devices, such as the Kois Deprogrammer
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton
 Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
Condylar Movement Assessment is Severe Attrition Patient Undergoing Orthodontic Treatment: Joint Vibrant Analysis Procedure
 Case Report imedpub Journals http://www.imedpub.com Journal of Dental and Craniofacial Research DOI: 10.21767/2576-392X.100004 Condylar Movement Assessment is Severe Attrition Patient Undergoing Orthodontic
Case Report imedpub Journals http://www.imedpub.com Journal of Dental and Craniofacial Research DOI: 10.21767/2576-392X.100004 Condylar Movement Assessment is Severe Attrition Patient Undergoing Orthodontic
Functional anatomy and biomechanics of temporomandibular joint and the far-reaching effects of its disorders
 Journal of Advanced Clinical & Research Insights (2016), 3, 101 106 REVIEW ARTICLE Functional anatomy and biomechanics of temporomandibular joint and the far-reaching effects of its disorders Chaya M.
Journal of Advanced Clinical & Research Insights (2016), 3, 101 106 REVIEW ARTICLE Functional anatomy and biomechanics of temporomandibular joint and the far-reaching effects of its disorders Chaya M.
ALTERNATE OCCLUSAL SCHEMES
 ALTERNATE OCCLUSAL SCHEMES The same basic concepts need to be applied to all occlusal schemes. Some challenges include missing teeth, transposed teeth, crossbites, and anterior open bites. POSTERIOR CROSSBITES
ALTERNATE OCCLUSAL SCHEMES The same basic concepts need to be applied to all occlusal schemes. Some challenges include missing teeth, transposed teeth, crossbites, and anterior open bites. POSTERIOR CROSSBITES
Principle of Occlusion
 Principle of Occlusion Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Overview Principle of Occlusion Overview Principle of Occlusion Point centric Long centric Freedom
Principle of Occlusion Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Overview Principle of Occlusion Overview Principle of Occlusion Point centric Long centric Freedom
Parotid Gland, Temporomandibular Joint and Infratemporal Fossa
 M1 - Anatomy Parotid Gland, Temporomandibular Joint and Infratemporal Fossa Jeff Dupree Sanger 9-057 jldupree@vcu.edu Parotid gland: wraps around the mandible positioned between the mandible and the sphenoid
M1 - Anatomy Parotid Gland, Temporomandibular Joint and Infratemporal Fossa Jeff Dupree Sanger 9-057 jldupree@vcu.edu Parotid gland: wraps around the mandible positioned between the mandible and the sphenoid
TitleTemporomandibular joint ankylosis: Mitarashi, S; Abe, S; Watanabe, H; Author(s) Hashimoto, M; Ide, Y
 TitleTemporomandibular joint ankylosis: Mitarashi, S; Abe, S; Watanabe, H; Author(s) Hashimoto, M; Ide, Y Cranio : the journal of craniomandi Journal 20(1): 67-71 URL http://hdl.handle.net/10130/1098 Right
TitleTemporomandibular joint ankylosis: Mitarashi, S; Abe, S; Watanabe, H; Author(s) Hashimoto, M; Ide, Y Cranio : the journal of craniomandi Journal 20(1): 67-71 URL http://hdl.handle.net/10130/1098 Right
The Position of Anatomical Porion in Different Skeletal Relationships. Tarek. EL-Bialy* Ali. H. Hassan**
 The Position of Anatomical Porion in Different Skeletal Relationships Tarek. EL-Bialy* Ali. H. Hassan** Abstract Previous research has shown that the position of glenoid fossa differs in different skeletal
The Position of Anatomical Porion in Different Skeletal Relationships Tarek. EL-Bialy* Ali. H. Hassan** Abstract Previous research has shown that the position of glenoid fossa differs in different skeletal
HHS Public Access Author manuscript Int J Oral Maxillofac Implants. Author manuscript; available in PMC 2015 March 04.
 Temporomandibular Joint Disorders: A Review of Etiology, Clinical Management, and Tissue Engineering Strategies Meghan K. Murphy, BE a, Regina F. MacBarb, BS a, Mark E. Wong, DDS b, and Kyriacos A. Athanasiou,
Temporomandibular Joint Disorders: A Review of Etiology, Clinical Management, and Tissue Engineering Strategies Meghan K. Murphy, BE a, Regina F. MacBarb, BS a, Mark E. Wong, DDS b, and Kyriacos A. Athanasiou,
Modelling of temporomandibular joint and FEM analysis
 Acta of Bioengineering and Biomechanics Vol. 8, No. 1, 2006 Modelling of temporomandibular joint and FEM analysis MARTINA FRIOVÁ, ZDENK HORÁK, SVATAVA KONVIKOVÁ Laboratory of Biomechanics, Department of
Acta of Bioengineering and Biomechanics Vol. 8, No. 1, 2006 Modelling of temporomandibular joint and FEM analysis MARTINA FRIOVÁ, ZDENK HORÁK, SVATAVA KONVIKOVÁ Laboratory of Biomechanics, Department of
Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle
 Case Report: Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle Dr Anjali Wadhwa, Dr Gaurav Shah, Dr Shweta Sharma, Dr Anand Bhatnagar, Dr Pallavi Malaviya NIMS
Case Report: Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle Dr Anjali Wadhwa, Dr Gaurav Shah, Dr Shweta Sharma, Dr Anand Bhatnagar, Dr Pallavi Malaviya NIMS
8/4/2012. Causes and Cures. Nucleus pulposus. Annulus fibrosis. Vertebral end plate % water. Deforms under pressure
 Causes and Cures Intervertebral discs Facet (zygopophyseal) joints Inter body joints Spinal nerve roots Nerve compression Pathological conditions Video Causes of back pain Nucleus pulposus Annulus fibrosis
Causes and Cures Intervertebral discs Facet (zygopophyseal) joints Inter body joints Spinal nerve roots Nerve compression Pathological conditions Video Causes of back pain Nucleus pulposus Annulus fibrosis
Cartilage. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Cartilage Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology 1 Cartilage is a specialized type of connective tissue designed to give support, bear weight and withstand tension, torsion and
Cartilage Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology 1 Cartilage is a specialized type of connective tissue designed to give support, bear weight and withstand tension, torsion and
SURGICAL - ORTHODONTIC TREATMENT OF CLASS II DIVISION 1 MALOCCLUSION IN AN ADULT PATIENT: A CASE REPORT
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 02 SURGICAL - ORTHODONTIC TREATMENT OF CLASS II DIVISION 1 MALOCCLUSION IN AN ADULT PATIENT: A CASE REPORT Amit Dahiya 1,Minakshi
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 02 SURGICAL - ORTHODONTIC TREATMENT OF CLASS II DIVISION 1 MALOCCLUSION IN AN ADULT PATIENT: A CASE REPORT Amit Dahiya 1,Minakshi
Temporomandibular Joint Treatment
 Temporomandibular Joint Treatment Preamble As stated in the AAMT Position Statement, the Code of Ethics and Standards of Practice governing massage therapy apply to treating the Temporomandibular Joint
Temporomandibular Joint Treatment Preamble As stated in the AAMT Position Statement, the Code of Ethics and Standards of Practice governing massage therapy apply to treating the Temporomandibular Joint
Neuro-Occlusal Rehabilitation: Therapeutic by Direct and Indirect Tracks
 Cronicon OPEN ACCESS EC DENTAL SCIENCE Research Article Neuro-Occlusal Rehabilitation: Therapeutic by Direct and Indirect Tracks Amel Belkhiri* and Latifa Zenati SAAD Dahleb University, 12, rue AEK mechedel,
Cronicon OPEN ACCESS EC DENTAL SCIENCE Research Article Neuro-Occlusal Rehabilitation: Therapeutic by Direct and Indirect Tracks Amel Belkhiri* and Latifa Zenati SAAD Dahleb University, 12, rue AEK mechedel,
Horizontal Jaw Relation
 Horizontal Jaw Relation Horizontal Jaw Relation It is the relationship of the mandible to the maxilla in a horizontal plane. It can also be described as the relationship of the mandible to the maxilla
Horizontal Jaw Relation Horizontal Jaw Relation It is the relationship of the mandible to the maxilla in a horizontal plane. It can also be described as the relationship of the mandible to the maxilla
Skeleton Tedeschi Register (1911) Sex:: M- S. A. Age: 31 years Job:
 Skeleton 1438 Tedeschi Register (1911) Sex:: M- S. A. Age: 31 years Job: Blacksmith Date of death: 9 th of February, 1911 Cause of death: Lung tuberculosis Origin: General Hospital (Padova) Bone Remains
Skeleton 1438 Tedeschi Register (1911) Sex:: M- S. A. Age: 31 years Job: Blacksmith Date of death: 9 th of February, 1911 Cause of death: Lung tuberculosis Origin: General Hospital (Padova) Bone Remains
Joint Health Optimum Flex Plus, Hi- Victory, Yucca, Herbal Respond
 Joint Health Optimum Flex Plus, Hi- Victory, Yucca, Herbal Respond May Educational Webinar 2018 Dr Tania Cubitt Performance Horse Nutrition COMPARATIVE ANATOMY 2 JOINT A joint is defined as a structure
Joint Health Optimum Flex Plus, Hi- Victory, Yucca, Herbal Respond May Educational Webinar 2018 Dr Tania Cubitt Performance Horse Nutrition COMPARATIVE ANATOMY 2 JOINT A joint is defined as a structure
Oral cavity landmarks
 By: Dr. Ahmed Rabah Oral cavity landmarks The knowledge of oral anatomy and physiology will help the operator and provides enough landmarks to act as positive guide during denture construction. This subject
By: Dr. Ahmed Rabah Oral cavity landmarks The knowledge of oral anatomy and physiology will help the operator and provides enough landmarks to act as positive guide during denture construction. This subject
The Effect of the Central Bearing Plate Form on the Fischer Angle
 The Effect of the Central Bearing Plate Form on the Fischer Angle Yasuhiro Kamimura, D.D.S. Kobe City, Japan INTRODUCTION The Fischer angle, which has been defined as "the angle between the inclinations
The Effect of the Central Bearing Plate Form on the Fischer Angle Yasuhiro Kamimura, D.D.S. Kobe City, Japan INTRODUCTION The Fischer angle, which has been defined as "the angle between the inclinations
Bones of the skull & face
 Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Classification of Tempromandibular Disorders
 Classification of Tempromandibular Disorders Defined as any disorder that affects or that is affected by deformity, disease, misalignment, or dysfunction of the tempromandibular articulation. This includes
Classification of Tempromandibular Disorders Defined as any disorder that affects or that is affected by deformity, disease, misalignment, or dysfunction of the tempromandibular articulation. This includes
Archived SECTION 14 - SPECIAL DOCUMENTATION REQUIREMENTS
 SECTION 14 - SPECIAL DOCUMENTATION REQUIREMENTS 14.1 CERTIFICATE OF MEDICAL NECESSITY...2 14.2 OPERATIVE REPORT...2 14.2.A PROCEDURES REQUIRING A REPORT...2 14.3 PRIOR AUTHORIZATION REQUEST...2 14.3.A
SECTION 14 - SPECIAL DOCUMENTATION REQUIREMENTS 14.1 CERTIFICATE OF MEDICAL NECESSITY...2 14.2 OPERATIVE REPORT...2 14.2.A PROCEDURES REQUIRING A REPORT...2 14.3 PRIOR AUTHORIZATION REQUEST...2 14.3.A
Articulators. 5- Wax up and refining the occlusion for dental restorations.
 Articulators It is a mechanical device represents the TMJ, maxillary and mandibular arches. It can be used to hold the upper and lower casts according to their relationships to facilitate the purposes
Articulators It is a mechanical device represents the TMJ, maxillary and mandibular arches. It can be used to hold the upper and lower casts according to their relationships to facilitate the purposes
Growth and type-ll collagen expression in the glenoid fossa of the temporomandibular joint during altered loading: a study in the rat
 European Journal of Orthodontics 18 (1996) 3-9 O 1996 European Orthodontic Society Growth and type-ll collagen expression in the glenoid fossa of the temporomandibular joint during altered loading: a study
European Journal of Orthodontics 18 (1996) 3-9 O 1996 European Orthodontic Society Growth and type-ll collagen expression in the glenoid fossa of the temporomandibular joint during altered loading: a study
TOTAL KNEE ARTHROPLASTY (TKA)
 TOTAL KNEE ARTHROPLASTY (TKA) 1 Anatomy, Biomechanics, and Design 2 Femur Medial and lateral condyles Convex, asymmetric Medial larger than lateral 3 Tibia Tibial plateau Medial tibial condyle: concave
TOTAL KNEE ARTHROPLASTY (TKA) 1 Anatomy, Biomechanics, and Design 2 Femur Medial and lateral condyles Convex, asymmetric Medial larger than lateral 3 Tibia Tibial plateau Medial tibial condyle: concave
Methods of determining vertical dimension of occlusion
 Methods of determining vertical dimension of occlusion 1) Pre-extraction records a) Willis gauge This device could used to measure V D O before teeth extraction and then recorded in the patient record.
Methods of determining vertical dimension of occlusion 1) Pre-extraction records a) Willis gauge This device could used to measure V D O before teeth extraction and then recorded in the patient record.
UNIVERSITY OF MEDICINE AND PHARMACY GR. T. POPA - IASI FACULTY OF DENTAL MEDICINE
 UNIVERSITY OF MEDICINE AND PHARMACY GR. T. POPA - IASI FACULTY OF DENTAL MEDICINE ABSTRACT CONTRIBUTIONS OF THREE-DIMENSIONAL IMAGING TO THE DIAGNOSIS AND MANAGEMENT OF CLEFT LIP AND PALATE PhD ADVISOR,
UNIVERSITY OF MEDICINE AND PHARMACY GR. T. POPA - IASI FACULTY OF DENTAL MEDICINE ABSTRACT CONTRIBUTIONS OF THREE-DIMENSIONAL IMAGING TO THE DIAGNOSIS AND MANAGEMENT OF CLEFT LIP AND PALATE PhD ADVISOR,
A Rare Case of Cheerleader Syndrome, Case Report
 47 A Rare Case of Cheerleader Syndrome, Case Report Dr. Ayad AL mudarris, FIBMS (1) and Dr. Shifaa Hussain, MSc (2) (1)Head of Maxillofacial Surgical Department. Al Imamain Al Kadhemain Medical City; (2)
47 A Rare Case of Cheerleader Syndrome, Case Report Dr. Ayad AL mudarris, FIBMS (1) and Dr. Shifaa Hussain, MSc (2) (1)Head of Maxillofacial Surgical Department. Al Imamain Al Kadhemain Medical City; (2)
Oberoi et al Mandibular deviation with MRI
 Original Article DOI: 10.21276/ijchmr.2017.3.1.04 Correlation of Mandibular Deviation with Temporomandibular Joint (MRI) Dimensions between Deviated and Non Deviated Side: An original study Inderpreet
Original Article DOI: 10.21276/ijchmr.2017.3.1.04 Correlation of Mandibular Deviation with Temporomandibular Joint (MRI) Dimensions between Deviated and Non Deviated Side: An original study Inderpreet
Joints Outline 8.1 Joints are classified into three structural and three functional categories (p. 251; Table 8.1) A. Joints are classified by
 Joints Outline 8.1 Joints are classified into three structural and three functional categories (p. 251; Table 8.1) A. Joints are classified by structure and by function: Structural classification focuses
Joints Outline 8.1 Joints are classified into three structural and three functional categories (p. 251; Table 8.1) A. Joints are classified by structure and by function: Structural classification focuses
JAMSS Speed-to-Treat Protocol For treatment of jaw joint and muscle sprain/strain injuries
 JAMSS Speed-to-Treat Protocol For treatment of jaw joint and muscle sprain/strain injuries INTRODUCTION What is Jaw Joint and Muscle Sprain/Strain (JAMSS)? Jaw Joint and Muscle Sprain/Strain (JAMSS) is
JAMSS Speed-to-Treat Protocol For treatment of jaw joint and muscle sprain/strain injuries INTRODUCTION What is Jaw Joint and Muscle Sprain/Strain (JAMSS)? Jaw Joint and Muscle Sprain/Strain (JAMSS) is
Unicompartmental Knee Resurfacing
 Disclaimer This movie is an educational resource only and should not be used to manage knee pain. All decisions about the management of knee pain must be made in conjunction with your Physician or a licensed
Disclaimer This movie is an educational resource only and should not be used to manage knee pain. All decisions about the management of knee pain must be made in conjunction with your Physician or a licensed
Purpose: To review the evolution of Temporomandibular joint TMJ surgery together with the biological evidence for surgical disease
 Stiesch-Scholz M, Kempert J, Wolter S, et al. Comparative prospective study on splint therapy of anterior disc displacement without reduction. J Oral Rehabilitation 2005; 32:474-479. (29 refs.) Purpose:
Stiesch-Scholz M, Kempert J, Wolter S, et al. Comparative prospective study on splint therapy of anterior disc displacement without reduction. J Oral Rehabilitation 2005; 32:474-479. (29 refs.) Purpose:
MRI imaging of the temporo-mandibular joint (TMJ) with regard to degeneration and disk displacement.
 MRI imaging of the temporo-mandibular joint (TMJ) with regard to degeneration and disk displacement. Poster No.: P-0023 Congress: ESSR 2015 Type: Educational Poster Authors: A. Hagenkord; Basel/CH Keywords:
MRI imaging of the temporo-mandibular joint (TMJ) with regard to degeneration and disk displacement. Poster No.: P-0023 Congress: ESSR 2015 Type: Educational Poster Authors: A. Hagenkord; Basel/CH Keywords:
Artigo Original / Original Article
 Artigo Original / Original Article IJD ISSN:1806-146X Mandibular condyle morphology on panoramic radiographs of asymptomatic temporomandibular joints Christiano Oliveira 1 Renata Tarnoschi Bernardo 2 Ana
Artigo Original / Original Article IJD ISSN:1806-146X Mandibular condyle morphology on panoramic radiographs of asymptomatic temporomandibular joints Christiano Oliveira 1 Renata Tarnoschi Bernardo 2 Ana
IJCMR. REVIEW ARTICLE Splint Therapy When And Why? Godwin Clovis Da Costa 1, Meena Aras 2, Vidya Chitre 3, Sanket Sainath Gavhane 4 ABSTRACT
 IJCMR REVIEW ARTICLE When And Why? Godwin Clovis Da Costa 1, Meena Aras 2, Vidya Chitre 3, Sanket Sainath Gavhane 4 ABSTRACT One of the first steps in TMJ disorder treatment for most patients is splint
IJCMR REVIEW ARTICLE When And Why? Godwin Clovis Da Costa 1, Meena Aras 2, Vidya Chitre 3, Sanket Sainath Gavhane 4 ABSTRACT One of the first steps in TMJ disorder treatment for most patients is splint
Active Clinical Treatment Case 48
 Active Clinical Treatment Case 48 Treating Clinicians: Drs. Jung Nam, Scott G. Cohen and Soojin Kim Initial smile Final smile Initial Presentation: January 2004 Age at Initial Presentation: 59 Active Treatment
Active Clinical Treatment Case 48 Treating Clinicians: Drs. Jung Nam, Scott G. Cohen and Soojin Kim Initial smile Final smile Initial Presentation: January 2004 Age at Initial Presentation: 59 Active Treatment
Severe Posterior Open Bite by Posterior Folding of the Retrodiscal Tissue: A Case Report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 10 Ver. V (Oct. 2015), PP 27-31 www.iosrjournals.org Severe Posterior Open Bite by Posterior
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 10 Ver. V (Oct. 2015), PP 27-31 www.iosrjournals.org Severe Posterior Open Bite by Posterior
STRAIGHT TALK about CROOKED TEETH: Key #4, Healthy TMJ Function
 STRAIGHT TALK about CROOKED TEETH: Key #4, Healthy TMJ Function This is fourth in a series of articles by Derek Mahony, BDS, MDSc and S. Kent Lauson, DDS, MS (Orthodontists) Their book was written with
STRAIGHT TALK about CROOKED TEETH: Key #4, Healthy TMJ Function This is fourth in a series of articles by Derek Mahony, BDS, MDSc and S. Kent Lauson, DDS, MS (Orthodontists) Their book was written with
TransForce 2. Arch Developer Appliances Clinical Cases. New Horizons In Orthodontics
 TransForce 2 Arch Developer Appliances Clinical Cases New Horizons In Orthodontics New Horizons In Orthodontics Transverse and Sagittal Arch Development Dr. William Clark has 50 years experience in orthodontic
TransForce 2 Arch Developer Appliances Clinical Cases New Horizons In Orthodontics New Horizons In Orthodontics Transverse and Sagittal Arch Development Dr. William Clark has 50 years experience in orthodontic
Infratemporal fossa: Tikrit University college of Dentistry Dr.Ban I.S. head & neck Anatomy 2 nd y.
 Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
Temporal region. temporal & infratemporal fossae. Zhou Hong Ying Dept. of Anatomy
 Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Symposium on Occlusal Articulation. Mandibular Movement Recordings and Articulator Adjustments Simplified. Harry C. Lundeen, D.D.S.
 Symposium on Occlusal Articulation Mandibular Movement Recordings and Articulator Adjustments Simplified Harry C. Lundeen, D.D.S. Judging from the volume of writing that has appeared in the dental literature
Symposium on Occlusal Articulation Mandibular Movement Recordings and Articulator Adjustments Simplified Harry C. Lundeen, D.D.S. Judging from the volume of writing that has appeared in the dental literature
