Description Materials Indications Patient selection factors to be considered include: Contraindications Absolute contraindications include:
|
|
|
- Ira Marsh
- 5 years ago
- Views:
Transcription
1 Description The Patello-Femoral Wave Arthroplasty Systems incorporate a distal femoral trochlear surface articular component that mates to a taper post via a taper interlock, and an all-polyethylene patella component. The prosthesis is intended to be used in cemented arthroplasty. Materials Femoral Component: Cobalt-Chromium Alloy (Co-Cr-Mo) Undersurface Coating: Titanium (CP Ti) Taper Post: Titanium Alloy (Ti-6Al-4V) Patella Component: Ultra-High-Molecular Weight Polyethylene (UHMWPE) Indications Intended to be used in cemented arthroplasty in patients with osteoarthritis limited to the distal patello-femoral joint, patients with a history of patellar dislocation or patellar fracture, and those patients with failed previous surgery (arthroscopy, tibial tubercle elevation, lateral release, etc.) where pain, deformity or dysfunction persists. Patient selection factors to be considered include: 1) Patient s need to obtain pain relief and improve function is significant; 2) Patient s tibio-femoral joint is substantially normal; 3) Patient exhibits no significant mechanical axis deformity; 4) Patient s menisci and cruciates are intact with good joint stability, and good range of motion; and 5) Patient s overall well-being is good, including the ability and willingness to follow instructions and comply with activity restrictions. 6) Failure of previous conservative treatment options in correcting deformity and achieving pain relief. Contraindications Absolute contraindications include: 1) Defects that are not localized. 2) Inflammatory degenerative joint disease, rheumatoid arthritis, infection, sepsis, or osteomyelitis. 3) Patients that have a known sensitivity to materials typically used in orthopedic prosthetic devices or bone cements. 1
2 Relative contraindications include: 1) Uncooperative patient or patient incapable of following preoperative and post-operative instructions. 2) Metabolic disorders, which may impair the formation or healing of bone; osteoporosis. 3) Infections at remote sites, which may spread to the implant site. 4) Rapid joint destruction or bone resorption visible on roentgenogram. 5) Chronic instability or deficient soft tissues and other support structures. 6) Vascular or muscular insufficiency. 7) Inadequate skin, musculotendinous or neurovascular system status. Warnings Improper selection, placement, positioning, alignment, and fixation of the implant components may reduce the service life of the prosthetic components. Inadequate preparation and cleaning of the implant components mating surfaces may result in improper fixation of the device. Improper handling of the implants can produce scratches, nicks or dents that may have adverse clinical effects on mating joint surfaces. Do not modify implants. The surgeon shall be thoroughly familiar with the implants, instruments, and surgical technique prior to performing surgery. When defining offsets of articular surfaces, care should be taken to ensure that instruments are properly aligned and mated with taper in Taper Post. Visually confirm distal tip of Contact Probe is making contact on articular surfaces and free from any soft tissue structures to ensure accuracy. Use light pressure on Contact Probe to slightly indent articular surface at each mapping point, ensuring that the selected implant will be flush or slightly recessed with the articular surface. Prior to placing implant, carefully trim articular cartilage debris around prepared margin. Remove bone particles and lavage thoroughly. To ensure mechanical interlock of the Taper Post and Femoral Component, carefully clean Taper Post taper with provided instruments. All drilling or reaming should be done with vigorous lavage to minimize heat effects to adjacent bone and cartilage tissues. 2
3 Ensure that care is taken to obtain complete and uniform bone cement coverage at implant site. Unsupported components or unevenly supported components may result in implant failure. Accepted practices in post-operative care should be used. The patient is to be instructed and monitored to ensure a reasonable degree of compliance to post-operative instructions and activity restrictions. Excessive activity, impact, and weight gain have been implicated in the reduction of the benefit and service life of prosthetic devices. The Patello-Femoral implants have not been evaluated for safety and compatibility in the MR environment. They have not been tested for heating, migration, or image artifact in the MR environment. The safety of The Patello-Femoral knee implants in the MR environment is unknown. Scanning a patient who has this device may result in patient injury. Precautions Patello-Femoral implants are intended to be fitted and installed with the appropriate Patello-Femoral instrument sets. Use of instruments from other systems may result in improper implant selection, fitting, and placement which could result in implant failure or poor clinical outcome. The instrument set should be regularly inspected for any signs of wear or damage. Do not reuse implants or disposable instruments. The operating surgeon or physician should discuss general risks and potential complications associated with this and any surgical procedure with the patient prior to patient consent. Possible Adverse Effects 1. Material sensitivity reactions. Implantation of foreign material in tissues can result in histological reactions. Particulate wear debris and mild tissue discoloration from metallic components have been noted in other prosthetic devices constructed of similar materials. Some types of wear debris have been associated with osteolysis and implant loosening. 2. Infection or allergic reaction. 3. Loosening, migration or loss of fixation of implant. 4. Fretting and crevice corrosion can occur at the interface between the implant components. 5. Fatigue fracture of the implants as a result of bone resorption around the implant components. 3
4 6. Wear and damage to the implant articulating surface. 7. Wear and damage to the adjacent and opposed articular cartilage surfaces or soft tissue support structures. 8. Intraoperative or postoperative bone fracture. 9. Postoperative pain or incomplete resolution of preoperative symptoms. 10. Periarticular calcification or ossification, with or without impediment of joint mobility. 11. Incomplete range of motion due to improper selection or positioning of components. 12. Transient nerve palsy. 13. Embolism. Sterility The implant components and single use disposable instruments are provided sterile. Metallic prosthetic components are sterilized by exposure to gamma irradiation. Non-metallic prosthetic components are sterilized by gas plasma sterilization. Do not resterilize any components. Do not use components if packaging is opened or damaged. Do not use components if beyond expiration date as indicated on package label. Reuse of single use devices can increase the risk of patient infection and can compromise service life and other performance attributes of these devices. Caution: United States Federal law restricts this device to sale by or on the order of a physician. 4
5 Instructions for Use Implantation of the Patello-Femoral Femoral Component 1. With knee in extension, use the Mapping Template to identify the S/I curvature of the trochlear groove. 2a. Select corresponding S/I curvature Sizing Trial and attach the Femoral Pin Guide. Place the 2.5mm Femoral Guide Pin into a cannulated powered drill and advance 2.5mm Femoral Guide Pin until secure in the bone (approximately 10mm deep). 2b. Alternatively, the Offset Drill Guide may be used to place the 2.5mm Femoral Guide Pin. Align the L laser mark to the lateral aspect of the femur. I. Place the yellow Offset Sleeve over the 2.5mm Femoral Guide Pin so the foot of the Offset Sleeve is touching the deepest (medial) portion at the center of the trochlea. Place the Contact Probe over the Offset Sleeve and use light pressure on the Contact Probe to ensure proper contact with the articular surface. 5
6 II. Read the Contact Probe to confirm superior/inferior offsets. Use the Sizing Card to record the average superior/inferior offset. 3. Select the 35mm Central Reamer (5mm) and advance it over the 2.5mm Femoral Guide Pin until the etched mark on the side of the Central Reamer is flush with the medial/lateral facets. 4. Select the Guide Block that corresponds with the S/I curvature value and place onto the trochlear groove. Insert the central portion of the Guide Block into the reamed area and secure the Guide Block onto the femur using the 2.0mm Guide Pins. 6
7 In knees with a dysplastic or flattened trochlea, the Guide Block may not sit flush to the reamed area. Use an osteotome or burr to create slots in the bone to accept the proximal and distal feet of the Guide Block. Creating these slots will allow the Guide Block to sit flush to the reamed area. 5. Assemble the Outer Reamer into the Guide Bushing. Secure the Guide Bushing into the inferior Guide Block bore. Advance the Outer Reamer into the bone until the depth mark on the reamer shaft is reached. Remove assembly and repeat reaming through the superior Guide Block bore. It is critical to keep the Guide Block stable during reaming. Repeat the same sequence for the cannulated Kahuna Tooth Cutter. 7
8 6. With the Kahuna Tooth Cutter in the Guide Bushing at the superior Guide Block bore position, drive the 2.5mm Femoral Guide Pin into bone to create a stable working axis for the Kahuna Reamer (approximately 10mm deep). 7. Remove the Guide Block. Ream over the 2.5mm Femoral Guide Pin with the Kahuna Reamer until reamer bottoms out on the central part of the previously reamed surface. 8
9 8. Assemble the Trial Handle onto the Sizing Trial that corresponds with the S/I curvature value. Place the Sizing Trial into the prepared site. Confirm the fit of the Sizing Trial so that all margins are congruent or recessed to the edge of the surrounding articular surface. Trim the transition areas between the reamed surfaces to ensure the Sizing Trial is fully seated. Fix the Sizing Trial in place using the 2.0mm Guide Pins. 9. Insert the Pilot Drill through the center of the Trial Handle and advance to the laser mark indicated on the Pilot Drill. Leave the Pilot Drill in place and remove the Trial Handle from the Sizing Trial. 9
10 10. Advance the Step Drill over the Pilot Drill until it bottoms out on the back of the Pilot Drill. Remove the Step Drill. 11. Advance the Tap over the Pilot Drill so the end stops when the Pilot Drill is flush to the back of the cannulation in the Tap. Remove the Tap and Pilot Drill. 10
11 12. Apply a small amount of low-viscosity bone cement into the Taper Post bone tunnel. Place the Taper Post into the morse taper of the Trial Handle and attach to the Sizing Trial. Place the Hex Driver through the Trial Handle and advance the Taper Post until the stop on the shaft of the Hex Driver comes in contact with the back of the Trial Handle. Place the Placement Gauge into the Sizing Trial to ensure that the Taper Post is at proper depth to engage the WaveKahuna Femoral Component. 13. An alternative approach to fixation is to pre-assemble the Threadless Stud to the WaveKahuna Femoral Component. Be sure to protect the articular face of the Kahuna Femoral Component by using slight impaction with the mallet to seat the morse taper of the Threadless Stud onto the Kahuna Femoral Component. NOTE: Prepare the Patella Component implant site prior to the final placement of the WaveKahuna Femoral Component. 11
12 14. Prior to placing the WaveKahuna Femoral Component on the Implant Holder, make sure that sufficient suction is present to hold the device on the distal suction cup. Align the WaveKahuna Femoral Component on the Implant Holder. Insert into the taper of the Taper Post. Firmly mallet the Impactor until the WaveKahuna Femoral Component is completely seated. 12
13 Arthrosurface, Inc. 28 Forge Parkway, Franklin, MA tel fax This product is covered by one or more of U.S. Patent Nos.6,520,964; 6,610,067; 6,679,917; other patents and other patents pending. HemiCAP is a trademark of Arthrosurface, Inc. U.S Arthrosurface, Inc. All rights reserved. Printed in the U.S.A. 13 PN REV B
14 Patello-Femoral Wave Arthroplasty Systems Instructions for Use 14
Hip Resurfacing System
 Hip Resurfacing System The Arthrosurface HemiCAP Hip Hemiarthroplasty System restores the articular surface geometry of the femoral head and preserves functional structures using an innovative 3 dimensional
Hip Resurfacing System The Arthrosurface HemiCAP Hip Hemiarthroplasty System restores the articular surface geometry of the femoral head and preserves functional structures using an innovative 3 dimensional
WristMotion Wrist Hemiarthroplasty System Instructions for Use
 WristMotion Wrist Hemiarthroplasty System Instructions for Use Description The Arthrosurface WristMotion Wrist Hemiarthroplasty System consists of a contoured capitate articular implant designed to articulate
WristMotion Wrist Hemiarthroplasty System Instructions for Use Description The Arthrosurface WristMotion Wrist Hemiarthroplasty System consists of a contoured capitate articular implant designed to articulate
Talar Dome System Surgical Technique
 Talar Dome System Surgical Technique CAP TALAR DOME RESURFACING HEMIARTHROPLASTY IMPLANT Surgical Technique Guide Description The HemiCAP Contoured Articular Prosthetic incorporates an articular resurfacing
Talar Dome System Surgical Technique CAP TALAR DOME RESURFACING HEMIARTHROPLASTY IMPLANT Surgical Technique Guide Description The HemiCAP Contoured Articular Prosthetic incorporates an articular resurfacing
Technique Guide Hip Resurfacing System
 Technique Guide Hip Resurfacing System Approximately 5%-18% of all hip arthroplasties are completed on patients with a primary diagnosis of osteonecrosis. Patients are generally younger adults age 35 years
Technique Guide Hip Resurfacing System Approximately 5%-18% of all hip arthroplasties are completed on patients with a primary diagnosis of osteonecrosis. Patients are generally younger adults age 35 years
Technique Guide Wrist Hemiarthroplasty System
 Technique Guide Wrist Hemiarthroplasty System The WristMotion TM Wrist Hemiarthroplasty System restores mobility and maintains native biomechanics using a dual curvature HemiCAPITATE implant that locks
Technique Guide Wrist Hemiarthroplasty System The WristMotion TM Wrist Hemiarthroplasty System restores mobility and maintains native biomechanics using a dual curvature HemiCAPITATE implant that locks
Technique Guide Patello-Femoral Arthroplasty
 Technique Guide Patello-Femoral Arthroplasty The HemiCAP Patello-Femoral Kahuna Arthroplasty System restores the unique articular surface geometry of the Patella and the Femoral Trochlear groove. The HemiCAP
Technique Guide Patello-Femoral Arthroplasty The HemiCAP Patello-Femoral Kahuna Arthroplasty System restores the unique articular surface geometry of the Patella and the Femoral Trochlear groove. The HemiCAP
Lapidus Arthrodesis System Instructions for Use
 Lapidus Arthrodesis System Instructions for Use Description The AlignMATE Lapidus Arthrodesis System consists of bone plates and bone screws (locking, non-locking and interfragmentary), which are intended
Lapidus Arthrodesis System Instructions for Use Description The AlignMATE Lapidus Arthrodesis System consists of bone plates and bone screws (locking, non-locking and interfragmentary), which are intended
Arthroscopically assisted Knee Resurfacing (AKR)
 Arthroscopically assisted Knee Resurfacing (AKR) U The First Meniscal Sparing Knee Resurfacing Preserves meniscus & articular cartilage Maintains soft tissue envelope Inlay components match patient anatomy
Arthroscopically assisted Knee Resurfacing (AKR) U The First Meniscal Sparing Knee Resurfacing Preserves meniscus & articular cartilage Maintains soft tissue envelope Inlay components match patient anatomy
Pinit Plate Small Bone Fusion System Bone Plate & Screw System
 Pinit Plate Small Bone Fusion System Bone Plate & Screw System Description The Pinit Plate Small Bone Fusion System consists of 2-hole bone plates made available in three length options and two thickness
Pinit Plate Small Bone Fusion System Bone Plate & Screw System Description The Pinit Plate Small Bone Fusion System consists of 2-hole bone plates made available in three length options and two thickness
Technique Guide Small Bone Fusion System
 Technique Guide Small Bone Fusion System The Pinit Plate Small Bone Fusion System is a super low profile, modular bone plate and screw system designed to stabilize a bunionectomy with a medial to lateral
Technique Guide Small Bone Fusion System The Pinit Plate Small Bone Fusion System is a super low profile, modular bone plate and screw system designed to stabilize a bunionectomy with a medial to lateral
Technique Guide Toe Hemiarthroplasty
 Technique Guide Toe Hemiarthroplasty The HemiCAP Toe Resurfacing Systems restore the surface geometry of the metatarsal head and preserve functional structures using an innovative 3 dimensional mapping
Technique Guide Toe Hemiarthroplasty The HemiCAP Toe Resurfacing Systems restore the surface geometry of the metatarsal head and preserve functional structures using an innovative 3 dimensional mapping
Technique Guide Toe Hemiarthroplasty
 Technique Guide Toe Hemiarthroplasty The HemiCAP Toe Resurfacing Systems restore the surface geometry of the metatarsal head and preserve functional structures using an innovative 3 dimensional mapping
Technique Guide Toe Hemiarthroplasty The HemiCAP Toe Resurfacing Systems restore the surface geometry of the metatarsal head and preserve functional structures using an innovative 3 dimensional mapping
Technique Guide KISSloc Suture System
 Technique Guide KISSloc Suture System The KISSloc Suture System consists of a strong self-cinching suture assembly, a unique load-dispersing Arrow Plate and procedure specific instrumentation. Simple,
Technique Guide KISSloc Suture System The KISSloc Suture System consists of a strong self-cinching suture assembly, a unique load-dispersing Arrow Plate and procedure specific instrumentation. Simple,
Surgical Technique. Poly UHMWPE. Bio Hyaluronic Acid. Advancing Materials. Advancing Outcomes.
 Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical 2 Assessment 1. Proper implant sizing is determined by placing the appropriate sized trial over the
Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical 2 Assessment 1. Proper implant sizing is determined by placing the appropriate sized trial over the
Glenoid Resurfacing Technique Guide
 Glenoid Resurfacing Technique Guide Restoring the Freedom of Motion 2 Description The HemiCAP Contoured Articular Prosthetic humeral component incorporates an articular resurfacing component and a taper
Glenoid Resurfacing Technique Guide Restoring the Freedom of Motion 2 Description The HemiCAP Contoured Articular Prosthetic humeral component incorporates an articular resurfacing component and a taper
Technique Guide Lapidus Arthrodesis System
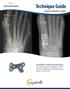 Technique Guide Lapidus Arthrodesis System HVA Angle IMA Angle The AlignMate Lapidus Arthrodesis System features low-profile, anatomically pre-contoured Bone Plates with either a combination of locking
Technique Guide Lapidus Arthrodesis System HVA Angle IMA Angle The AlignMate Lapidus Arthrodesis System features low-profile, anatomically pre-contoured Bone Plates with either a combination of locking
Positioning Sleeve Surgical Technique
 Positioning Sleeve Surgical Technique Surgical Technique The Comprehensive Fracture System offers a unique tool to evaluate and re-establish humeral height, which can be critical to restoring proper biomechanics
Positioning Sleeve Surgical Technique Surgical Technique The Comprehensive Fracture System offers a unique tool to evaluate and re-establish humeral height, which can be critical to restoring proper biomechanics
Surgical Technique. Poly UHMWPE. Bio Hyaluronic Acid. Advancing Materials. Advancing Outcomes.
 Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical 2 Assessment 1. Using the depth probe, determine the appropriate implant size (thickness) for use. The
Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical 2 Assessment 1. Using the depth probe, determine the appropriate implant size (thickness) for use. The
Technique Guide. Primary Stemless Shoulder System
 Technique Guide TM Primary Stemless Shoulder System Anterior Deltopectoral Approach 1. Beachchair position (tilt back to 45 degree angle). 2. Short deltopectoral incision (from coracoid tip to pectoralis
Technique Guide TM Primary Stemless Shoulder System Anterior Deltopectoral Approach 1. Beachchair position (tilt back to 45 degree angle). 2. Short deltopectoral incision (from coracoid tip to pectoralis
Technique Guide Hammertoe Correction System
 Technique Guide Hammertoe Correction System TM The ToeMATE Hammertoe Correction System is an easy to implant bone screw system intended for the correction of hammertoe deformity. It is provided in a complete
Technique Guide Hammertoe Correction System TM The ToeMATE Hammertoe Correction System is an easy to implant bone screw system intended for the correction of hammertoe deformity. It is provided in a complete
Surgical Technique. Poly UHMWPE. Bio Hyaluronic Acid. Advancing Materials. Advancing Outcomes.
 Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical Assessment 1. Proper implant diameter is determined by placing the appropriately sized trial over the
Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical Assessment 1. Proper implant diameter is determined by placing the appropriately sized trial over the
BIOLOX delta Option Ceramic Femoral Head System
 BIOLOX delta Option Ceramic Femoral Head System Product Features and Instructions for Use Knees Hips Extremities Cement and Accessories PMI Technology Product Features BIOLOX delta ceramic heads are composed
BIOLOX delta Option Ceramic Femoral Head System Product Features and Instructions for Use Knees Hips Extremities Cement and Accessories PMI Technology Product Features BIOLOX delta ceramic heads are composed
BIOLOX delta Option Ceramic Femoral Head System. Product Features and Instructions for Use
 BIOLOX delta Option Ceramic Femoral Head System Product Features and Instructions for Use Product Features BIOLOX delta ceramic heads are composed of 75% aluminum oxide and approximately 25% zirconia.
BIOLOX delta Option Ceramic Femoral Head System Product Features and Instructions for Use Product Features BIOLOX delta ceramic heads are composed of 75% aluminum oxide and approximately 25% zirconia.
Important notice: the device(s) can be prescribed and implanted only by a doctor legally authorized to perform this type of surgery.
 rev.10 CAUTION Federal law (USA) restricts this device to sale, by or on the order of a physician. ENGLISH - EVOLIS/GMK KNEE PROSTHESIS - INSTRUCTIONS FOR USE Important notice: the device(s) can be prescribed
rev.10 CAUTION Federal law (USA) restricts this device to sale, by or on the order of a physician. ENGLISH - EVOLIS/GMK KNEE PROSTHESIS - INSTRUCTIONS FOR USE Important notice: the device(s) can be prescribed
Surgical Technique. Poly UHMWPE. Bio Hyaluronic Acid. Advancing Materials. Advancing Outcomes.
 Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Pre-Operative Planning Prior to implantation of the BioPoly RS-Trochlea Implant, pre-operative planning will
Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Pre-Operative Planning Prior to implantation of the BioPoly RS-Trochlea Implant, pre-operative planning will
Comprehensive Reverse Shoulder System Augmented Baseplate
 Comprehensive Reverse Shoulder System Augmented Baseplate Surgical Technique Addendum FPO 1 Comprehensive Reverse Shoulder System Augmented Baseplate Surgical Technique Addendum Adaptive Building on the
Comprehensive Reverse Shoulder System Augmented Baseplate Surgical Technique Addendum FPO 1 Comprehensive Reverse Shoulder System Augmented Baseplate Surgical Technique Addendum Adaptive Building on the
ACETABULAR CUP SURGICAL TECHNIQUE
 ACETABULAR CUP SURGICAL TECHNIQUE ACETABULAR CUP DEVICE INDICATIONS FOR USE The ICONACY I-Hip total hip replacement is indicated for the following conditions: 1. A severely painful and/or disabled hip
ACETABULAR CUP SURGICAL TECHNIQUE ACETABULAR CUP DEVICE INDICATIONS FOR USE The ICONACY I-Hip total hip replacement is indicated for the following conditions: 1. A severely painful and/or disabled hip
SURGICAL TECHNIQUE GUIDE
 DANGER indicates an imminently hazardous situation which, if not avoided, will result in death or serious injury. WARNING indicates a potentially hazardous situation which, if not avoided, could result
DANGER indicates an imminently hazardous situation which, if not avoided, will result in death or serious injury. WARNING indicates a potentially hazardous situation which, if not avoided, could result
CAUTION Federal law (USA) restricts this device to sale, by or on the order of a physician.
 CAUTION Federal law (USA) restricts this device to sale, by or on the order of a physician. ENGLISH Mpact 3D Metal Implants and Augments 3D Metal INSTRUCTION FOR USE Important notice: the device(s) can
CAUTION Federal law (USA) restricts this device to sale, by or on the order of a physician. ENGLISH Mpact 3D Metal Implants and Augments 3D Metal INSTRUCTION FOR USE Important notice: the device(s) can
Regenerex Primary Tibial Tray
 Cruciate Retaining and Posterior Stabilized Surgical Technique Addendum to the Vanguard Complete Knee System Knees Hips Extremities Cement and Accessories PMI Technology Contents Microplasty Knee Instrumentation
Cruciate Retaining and Posterior Stabilized Surgical Technique Addendum to the Vanguard Complete Knee System Knees Hips Extremities Cement and Accessories PMI Technology Contents Microplasty Knee Instrumentation
Taperloc Complete Hip System. Surgical Technique
 Taperloc Complete Hip System Surgical Technique One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide personalized care to one patient. The science and art of medical
Taperloc Complete Hip System Surgical Technique One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide personalized care to one patient. The science and art of medical
CAUTION: Ceramic liners are not approved for use in the United States.
 Total Hip Prostheses, Self-Centering Hip Prostheses and Hemi-Hip Prostheses IMPORTANT: This essential product information sheet does not include all of the information necessary for selection and use of
Total Hip Prostheses, Self-Centering Hip Prostheses and Hemi-Hip Prostheses IMPORTANT: This essential product information sheet does not include all of the information necessary for selection and use of
SURGICAL TECHNIQUE CEMENTED & PRESS-FIT UNIFIED INSTRUMENTATION INTRAOPERATIVE FLEXIBILITY PROVEN BIOMECHANICS
 SURGICAL TECHNIQUE CEMENTED & PRESS-FIT UNIFIED INSTRUMENTATION INTRAOPERATIVE FLEXIBILITY PROVEN BIOMECHANICS INTRODUCTION The Summit Tapered Hip System s comprehensive set of implants and instruments
SURGICAL TECHNIQUE CEMENTED & PRESS-FIT UNIFIED INSTRUMENTATION INTRAOPERATIVE FLEXIBILITY PROVEN BIOMECHANICS INTRODUCTION The Summit Tapered Hip System s comprehensive set of implants and instruments
U2 PSA. Revision Knee. Surgical Protocol
 U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 1 2 Tibial Preparation... 1 2.1 Tibial Canal Preparation... 1 2.2 Proximal Tibial Resection... 2 2.3 Non Offset Tibial
U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 1 2 Tibial Preparation... 1 2.1 Tibial Canal Preparation... 1 2.2 Proximal Tibial Resection... 2 2.3 Non Offset Tibial
Active Articulation. Surgical Technique. Dual Mobility Hip System. Knees Hips Extremities Cement and Accessories PMI Trauma Technology
 Active Articulation Dual Mobility Hip System Surgical Technique Knees Hips Extremities Cement and Accessories PMI Trauma Technology Active Articulation Dual Mobility Hip System Contents Preoperative Planning,
Active Articulation Dual Mobility Hip System Surgical Technique Knees Hips Extremities Cement and Accessories PMI Trauma Technology Active Articulation Dual Mobility Hip System Contents Preoperative Planning,
U2 PSA. Revision Knee. Surgical Protocol
 U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 2 Tibial Preparation... 2.1 Tibial Canal Preparation... 2.2 Proximal Tibial Resection... 2.3 Non Offset Tibial Preparation...
U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 2 Tibial Preparation... 2.1 Tibial Canal Preparation... 2.2 Proximal Tibial Resection... 2.3 Non Offset Tibial Preparation...
Duraloc CONSTRAINED LINER
 SURGICAL TECHNIQUE Duraloc CONSTRAINED LINER A COMPREHENSIVE ACETABULAR REVISION SYSTEM DURALOC CONSTRAINED LINER Introduction Dislocation is the most common postoperative complication in total hip reconstruction.
SURGICAL TECHNIQUE Duraloc CONSTRAINED LINER A COMPREHENSIVE ACETABULAR REVISION SYSTEM DURALOC CONSTRAINED LINER Introduction Dislocation is the most common postoperative complication in total hip reconstruction.
CMA TM Cemented Modular Augmentable. Baseplate. 2 Knee
 CMA TM Cemented Modular Augmentable Baseplate 2 Knee More can be addressed The U2 Cemented Modular Augmentable Baseplate is an optimal solution for tibial bone defect in primary total knee replacement.
CMA TM Cemented Modular Augmentable Baseplate 2 Knee More can be addressed The U2 Cemented Modular Augmentable Baseplate is an optimal solution for tibial bone defect in primary total knee replacement.
Surgical Technique. VISIONAIRE Disposable Instruments for the LEGION Total Knee System
 Surgical Technique VISIONAIRE Disposable Instruments for the LEGION Total Knee System VISIONAIRE and LEGION Disposable instrument technique* Note: All disposable instruments are interchangeable with the
Surgical Technique VISIONAIRE Disposable Instruments for the LEGION Total Knee System VISIONAIRE and LEGION Disposable instrument technique* Note: All disposable instruments are interchangeable with the
Document No Rev. B Pg. 1 of 5 Approvals / Date Title: INSTRUCTIONS FOR USE DJO SURGICAL MODULAR REVISION HIP SYSTEM AND ACETABULAR CAGE
 Document No. 0400-0205 Rev. B Pg. 1 of 5 Approvals / Date Title: INSTRUCTIONS FOR USE DJO SURGICAL MODULAR REVISION HIP SYSTEM AND ACETABULAR CAGE Revision ECO Date ECO Summary of Changes Deann Rector
Document No. 0400-0205 Rev. B Pg. 1 of 5 Approvals / Date Title: INSTRUCTIONS FOR USE DJO SURGICAL MODULAR REVISION HIP SYSTEM AND ACETABULAR CAGE Revision ECO Date ECO Summary of Changes Deann Rector
Cementless Tapered Femoral Stem Surgical technique
 Cementless Tapered Femoral Stem Surgical technique Contents Operative summary 4 Pre-operative planning 5 Femoral neck osteotomy 5 Femoral canal preparation 5 Intra-medullary (IM) reamer 6 Sequential rasping
Cementless Tapered Femoral Stem Surgical technique Contents Operative summary 4 Pre-operative planning 5 Femoral neck osteotomy 5 Femoral canal preparation 5 Intra-medullary (IM) reamer 6 Sequential rasping
Greater Component Accuracy...
 Greater Component Accuracy... StageOne cement spacer molds are designed to provide the surgeon with choices never before offered in two-stage revision knee surgery for an infected total joint. StageOne
Greater Component Accuracy... StageOne cement spacer molds are designed to provide the surgeon with choices never before offered in two-stage revision knee surgery for an infected total joint. StageOne
Surgical Technique. VISIONAIRE FastPak Instruments for the LEGION Total Knee System
 Surgical Technique VISIONAIRE FastPak Instruments for the LEGION Total Knee System VISIONAIRE FastPak for LEGION Instrument Technique* Nota Bene The technique description herein is made available to the
Surgical Technique VISIONAIRE FastPak Instruments for the LEGION Total Knee System VISIONAIRE FastPak for LEGION Instrument Technique* Nota Bene The technique description herein is made available to the
Cementless Tapered Femoral Stem Surgical technique
 Cementless Tapered Femoral Stem Surgical technique Contents Operative summary 4 Pre-operative planning 5 Femoral neck osteotomy 5 Femoral canal preparation 5 Intra-medullary (IM) reamer 6 Sequential rasping
Cementless Tapered Femoral Stem Surgical technique Contents Operative summary 4 Pre-operative planning 5 Femoral neck osteotomy 5 Femoral canal preparation 5 Intra-medullary (IM) reamer 6 Sequential rasping
Progeny Hip Stem. Surgical Protocol and Product Specifications
 Progeny Hip Stem Surgical Protocol and Product Specifications Progeny Hip Stem Introduction With emphasis on maximum stability and ease of use, the StelKast ProgenyTM Hip System provides the surgeon with
Progeny Hip Stem Surgical Protocol and Product Specifications Progeny Hip Stem Introduction With emphasis on maximum stability and ease of use, the StelKast ProgenyTM Hip System provides the surgeon with
Revision A Date:
 Biomet Trauma 56 East Bell Drive P.O. Box 587 Warsaw, Indiana 46581 USA 01-50-4053 Revision A Date: 2016-06 Biomet Unite3D Bridge with OsseoTi Technology ATTENTION OPERATING SURGEON DESCRIPTION Biomet
Biomet Trauma 56 East Bell Drive P.O. Box 587 Warsaw, Indiana 46581 USA 01-50-4053 Revision A Date: 2016-06 Biomet Unite3D Bridge with OsseoTi Technology ATTENTION OPERATING SURGEON DESCRIPTION Biomet
TC-PLUS Primary Knee IMPORTANT MEDICAL INFORMATION SPECIAL NOTE. This Package Insert is for product distributed in the US only.
 TC-PLUS Primary Knee IMPORTANT MEDICAL INFORMATION SPECIAL NOTE This Package Insert is for product distributed in the US only. The component material is provided on the outside carton label. Components
TC-PLUS Primary Knee IMPORTANT MEDICAL INFORMATION SPECIAL NOTE This Package Insert is for product distributed in the US only. The component material is provided on the outside carton label. Components
TaperFill. Surgical Technique
 TaperFill Surgical Technique Table of Contents Indications and Contraindications 3 TaperFill Hip Size Charts 4-5 DJO Surgical 9800 Metric Boulevard Austin, TX (800) 456-8696 www.djosurgical.com Preoperative
TaperFill Surgical Technique Table of Contents Indications and Contraindications 3 TaperFill Hip Size Charts 4-5 DJO Surgical 9800 Metric Boulevard Austin, TX (800) 456-8696 www.djosurgical.com Preoperative
Zimmer NexGen Trabecular Metal Tibial Tray
 Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Give Bone A Solid Hold Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique
Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Give Bone A Solid Hold Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique
Dual Mobility System Evaluation surgical technique
 Trinity Dual Mobility System Evaluation surgical technique Contents Operative summary 4 Overview 5 Operative technique 6 1. Acetabular reaming 6 Reamer guide 6 2. Acetabular shell trial 6 3. Acetabular
Trinity Dual Mobility System Evaluation surgical technique Contents Operative summary 4 Overview 5 Operative technique 6 1. Acetabular reaming 6 Reamer guide 6 2. Acetabular shell trial 6 3. Acetabular
FUSEFORCE. Hand Fixation System SURGICAL TECHNIQUE
 FUSEFORCE Hand Fixation System SURGICAL TECHNIQUE Contents Chapter 1 3 Chapter 2 4 Appendix A 7 Intended Use Surgical Technique Ordering Information Indication Sizing Reference Proper surgical procedures
FUSEFORCE Hand Fixation System SURGICAL TECHNIQUE Contents Chapter 1 3 Chapter 2 4 Appendix A 7 Intended Use Surgical Technique Ordering Information Indication Sizing Reference Proper surgical procedures
Clinical Evaluation Surgical Technique
 Clinical Evaluation Surgical Technique Table of Contents EMPERION Specifications 3 EMPERION Surgical Technique 9 EMPERION Catalog 18 Nota Bene: This technique description herein is made available to the
Clinical Evaluation Surgical Technique Table of Contents EMPERION Specifications 3 EMPERION Surgical Technique 9 EMPERION Catalog 18 Nota Bene: This technique description herein is made available to the
A novel cementless option. Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique
 A novel cementless option Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique Zimmer Trabecular Metal Primary Patella 1 Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique
A novel cementless option Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique Zimmer Trabecular Metal Primary Patella 1 Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique
Precautionary Statement ( )
 Precautionary Statement (21282008) Biomet Sports Medicine, Inc. 21282008 4861 E. Airport Dr. Rev. A Ontario, CA 91761 Date: 06/07 Sleeve and Button Soft Tissue Devices Utilizing ZipLoop Technology ATTENTION
Precautionary Statement (21282008) Biomet Sports Medicine, Inc. 21282008 4861 E. Airport Dr. Rev. A Ontario, CA 91761 Date: 06/07 Sleeve and Button Soft Tissue Devices Utilizing ZipLoop Technology ATTENTION
THE P.F.C. SIGMA FEMORAL ADAPTER. Surgical Technique
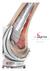 THE P.F.C. SIGMA FEMORAL ADAPTER Surgical Technique Contents P.F.C. Sigma Femoral Adapter and Revision Knee Surgery Introduction 2 Preoperative Planning 2 Overview 3 Surgical Technique Preparation of the
THE P.F.C. SIGMA FEMORAL ADAPTER Surgical Technique Contents P.F.C. Sigma Femoral Adapter and Revision Knee Surgery Introduction 2 Preoperative Planning 2 Overview 3 Surgical Technique Preparation of the
REPIPHYSIS LIMB SALVAGE SYSTEM
 REPIPHYSIS LIMB SALVAGE SYSTEM 150800-0 For additional information please contact the manufacturer or local distributor. M MicroPort Orthopedics Inc. 5677 Airline Rd Arlington, TN 38002 U.S.A. i Y October
REPIPHYSIS LIMB SALVAGE SYSTEM 150800-0 For additional information please contact the manufacturer or local distributor. M MicroPort Orthopedics Inc. 5677 Airline Rd Arlington, TN 38002 U.S.A. i Y October
Ceramic Femoral Heads and Acetabular Cup Liners
 Important Information: Please read prior to use in a clinical setting. The Surgeon should be familiar with the operative technique. Caution: Federal (U.S.A) law restricts this device to sale by or on the
Important Information: Please read prior to use in a clinical setting. The Surgeon should be familiar with the operative technique. Caution: Federal (U.S.A) law restricts this device to sale by or on the
Intramedullary Tibial Preparation
 Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
ESC. Enhanced Stability Liners. Design Rationale & Surgical Technique
 ESC Enhanced Stability Liners Design Rationale & Surgical Technique Choice Without Compromise DePuy Synthes PINNACLE Hip Solutions are designed with a wide range of acetabular cup options, biological and
ESC Enhanced Stability Liners Design Rationale & Surgical Technique Choice Without Compromise DePuy Synthes PINNACLE Hip Solutions are designed with a wide range of acetabular cup options, biological and
Manza Cup HA SURGICAL TECHNIQUE.
 1 PRE-OPERATIVE PLANNING. Preoperative assessment of the appropriate size and position of the acetabular component will provide intraoperative guidance for acetabular reaming. To determine the acetabluar
1 PRE-OPERATIVE PLANNING. Preoperative assessment of the appropriate size and position of the acetabular component will provide intraoperative guidance for acetabular reaming. To determine the acetabluar
Surgical Technique. Hinge Disassembly and Rebuild Technique
 Surgical Technique Hinge Disassembly and Rebuild Technique Revision Knee Arthroplasty Surgical Technique LEGION HK Hinge Knee System Introduction The LEGION HK Hinge Knee System has been designed as an
Surgical Technique Hinge Disassembly and Rebuild Technique Revision Knee Arthroplasty Surgical Technique LEGION HK Hinge Knee System Introduction The LEGION HK Hinge Knee System has been designed as an
Optimum implant geometry
 Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Dual Mobility System Surgical technique
 Trinity Dual Mobility System Surgical technique 2 Contents Operative summary 4 Overview 5 Operative technique 6 1. Acetabular reaming 6 Reamer guide 6 2. Acetabular shell trial 7 3. Acetabular shell implantation
Trinity Dual Mobility System Surgical technique 2 Contents Operative summary 4 Overview 5 Operative technique 6 1. Acetabular reaming 6 Reamer guide 6 2. Acetabular shell trial 7 3. Acetabular shell implantation
Salto Talaris Total Ankle Prosthesis
 Instructions for Use Salto Talaris Total Ankle Prosthesis Federal (USA) law restricts this device to sale by or on the order of a physician. Important The manufacturer recommends that all personnel responsible
Instructions for Use Salto Talaris Total Ankle Prosthesis Federal (USA) law restricts this device to sale by or on the order of a physician. Important The manufacturer recommends that all personnel responsible
Zimmer NexGen MIS Tibial Component. Cemented Surgical Technique IMAGE TO COME
 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique IMAGE TO COME Zimmer NexGen MIS Tibial Component Cemented Surgical Technique 1 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique
Zimmer NexGen MIS Tibial Component Cemented Surgical Technique IMAGE TO COME Zimmer NexGen MIS Tibial Component Cemented Surgical Technique 1 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique
Trabecular Metal Primary Patella
 Trabecular Metal Primary Patella NexGen Complete Knee Solution Surgical Technique Table of Contents Introduction... 2 Prepare the Patella... 2 Patella Reamer Technique... 3 Insetting Technique... 5 Universal
Trabecular Metal Primary Patella NexGen Complete Knee Solution Surgical Technique Table of Contents Introduction... 2 Prepare the Patella... 2 Patella Reamer Technique... 3 Insetting Technique... 5 Universal
INBONE II. Total Ankle System SURGICAL TECHNIQUE SUPPLEMENT TIBIAL REAMING SPECIFICATION
 INBONE II Total Ankle System SURGICAL TECHNIQUE SUPPLEMENT TIBIAL REAMING SPECIFICATION INBONE II Total Ankle System SURGICAL TECHNIQUE SUPPLEMENT Tibial Reaming Specification Contents Chapter 1 4 Product
INBONE II Total Ankle System SURGICAL TECHNIQUE SUPPLEMENT TIBIAL REAMING SPECIFICATION INBONE II Total Ankle System SURGICAL TECHNIQUE SUPPLEMENT Tibial Reaming Specification Contents Chapter 1 4 Product
Signature Personalized Patient Care
 Surgical Technique Acetabular Guide System Contents One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide personalized care to one patient. The science and art of medical
Surgical Technique Acetabular Guide System Contents One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide personalized care to one patient. The science and art of medical
JOINT RULER. Surgical Technique For Knee Joint JRReplacement
 JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
TRK REVISION KNEE Surgical Technique
 1 TRK REVISION KNEE Surgical Technique 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. INTERCONDYLAR RESECTION...... page FEMORAL STEM...... page NON CEMENTED FEMORAL STEM...... page TRIAL FEMORAL COMPONENTS...... page
1 TRK REVISION KNEE Surgical Technique 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. INTERCONDYLAR RESECTION...... page FEMORAL STEM...... page NON CEMENTED FEMORAL STEM...... page TRIAL FEMORAL COMPONENTS...... page
Surgical Technique Guide
 Sacroiliac Joint Fusion System Surgical Technique Guide Moving Life Forward Table of Contents SiCure Implant Overview...2 SiCure System Information...3 X-ray Basics...4 Patient Positioning....5 Surgical
Sacroiliac Joint Fusion System Surgical Technique Guide Moving Life Forward Table of Contents SiCure Implant Overview...2 SiCure System Information...3 X-ray Basics...4 Patient Positioning....5 Surgical
Resurfacing Distal Femur. Orthopaedic Salvage System
 Resurfacing Distal Femur Orthopaedic Salvage System Primary Arthroplasty OSS 3cm Resurfacing Distal Femur Distal Femoral Resection Drill and ream the distal femur in the following sequence: (Figure 1)
Resurfacing Distal Femur Orthopaedic Salvage System Primary Arthroplasty OSS 3cm Resurfacing Distal Femur Distal Femoral Resection Drill and ream the distal femur in the following sequence: (Figure 1)
Enhancing Glenoid Placement. Bigliani/Flatow The Complete Shoulder Solution Cannulated Instruments Surgical Technique
 Enhancing Glenoid Placement Bigliani/Flatow The Complete Shoulder Solution Cannulated Instruments Surgical Technique Bigliani/Flatow The Complete Shoulder Solution Cannulated Instruments 11 Bigliani/Flatow
Enhancing Glenoid Placement Bigliani/Flatow The Complete Shoulder Solution Cannulated Instruments Surgical Technique Bigliani/Flatow The Complete Shoulder Solution Cannulated Instruments 11 Bigliani/Flatow
Technique Guide Glenoid Latarjet System
 Technique Guide Glenoid Latarjet System Glenoid Grafting without the Grief The Glenojet Allograft System was created to replace and augment anterior glenoid bone loss associated with trauma, recurrent
Technique Guide Glenoid Latarjet System Glenoid Grafting without the Grief The Glenojet Allograft System was created to replace and augment anterior glenoid bone loss associated with trauma, recurrent
- October 2013 English
 TOTAL HIP JOINT REPLACEMENT FOR CEMENTED APPLICATIONS FOR THE ATTENTION OF THE OPERATING SURGEON Total hip replacement provides the surgeon with a means of restoring mobility and reducing pain with the
TOTAL HIP JOINT REPLACEMENT FOR CEMENTED APPLICATIONS FOR THE ATTENTION OF THE OPERATING SURGEON Total hip replacement provides the surgeon with a means of restoring mobility and reducing pain with the
Operative Technique Crown Cup Acetabular System
 EXACTECH HIP Operative Technique Crown Cup Acetabular System TABLE OF CONTENTS PRE-OPERATIVE PLANNING... 1 TEMPLATING... 1 INDICATIONS FOR USE... 1 CONTRAINDICATIONS FOR USE... 1 OPERATIVE TECHNIQUE OVERVIEW...
EXACTECH HIP Operative Technique Crown Cup Acetabular System TABLE OF CONTENTS PRE-OPERATIVE PLANNING... 1 TEMPLATING... 1 INDICATIONS FOR USE... 1 CONTRAINDICATIONS FOR USE... 1 OPERATIVE TECHNIQUE OVERVIEW...
Resurfacing Patellar Preparation
 Surgical Technique Resurfacing Patellar Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Resurfacing Patellar preparation Contents Introduction...2 Instrument assembly...3 Resurfacing
Surgical Technique Resurfacing Patellar Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Resurfacing Patellar preparation Contents Introduction...2 Instrument assembly...3 Resurfacing
Enhanced Stability Constrained Liners. Design Rationale Surgical Technique
 Enhanced Stability Constrained Liners Design Rationale Surgical Technique The Pinnacle Acetabular Cup System was designed to maximize the number of options available to the surgeon, and provide those options
Enhanced Stability Constrained Liners Design Rationale Surgical Technique The Pinnacle Acetabular Cup System was designed to maximize the number of options available to the surgeon, and provide those options
TriboFit Hip System. Issue 3 - August 2013 English
 Important Information: Please read prior to use in a clinical setting. The surgeon should be familiar with the operative technique and all the information in this insert. Description: The TriboFit Hip
Important Information: Please read prior to use in a clinical setting. The surgeon should be familiar with the operative technique and all the information in this insert. Description: The TriboFit Hip
For the Attention of the Operating Surgeon: IMPORTANT INFORMATION ON THE MATRIXRIB FIXATION SYSTEM
 For the Attention of the Operating Surgeon: IMPORTANT INFORMATION ON THE MATRIXRIB FIXATION SYSTEM 10/16 GP2685-E-CAN DESCRIPTION The MatrixRIB Fixation System consists of locking plates, locking screws,
For the Attention of the Operating Surgeon: IMPORTANT INFORMATION ON THE MATRIXRIB FIXATION SYSTEM 10/16 GP2685-E-CAN DESCRIPTION The MatrixRIB Fixation System consists of locking plates, locking screws,
Encina Taper Stem. Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA
 Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Table of Contents Introduction 3 Features 4 Surgical Technique 5 Preoperative
Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Table of Contents Introduction 3 Features 4 Surgical Technique 5 Preoperative
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments
 TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Resection Guide System SURGICAL TECHNIQUE RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Resection Guide System SURGICAL TECHNIQUE RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA
Distal Cut First Femoral Preparation
 Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
SURGICAL TECHNIQUE GUIDE TRESTLE. Anterior Cervical Plating System
 SURGICAL TECHNIQUE GUIDE TRESTLE Anterior Cervical Plating System 2 SURGICAL TECHNIQUE GUIDE SURGICAL TECHNIQUE GUIDE System Features Large window enables visualization of graft site and end plates Screw
SURGICAL TECHNIQUE GUIDE TRESTLE Anterior Cervical Plating System 2 SURGICAL TECHNIQUE GUIDE SURGICAL TECHNIQUE GUIDE System Features Large window enables visualization of graft site and end plates Screw
MIS Cemented Tibial Component
 MIS Cemented Tibial Component NexGen Complete Knee Solution Surgical Technique Table of Contents Surgical Exposure... 2 Finish the Tibia... 2 Position Based on Anatomic Landmarks... 3 Lateral Posterior
MIS Cemented Tibial Component NexGen Complete Knee Solution Surgical Technique Table of Contents Surgical Exposure... 2 Finish the Tibia... 2 Position Based on Anatomic Landmarks... 3 Lateral Posterior
ZMR Over-the-Junction Instruments for Revision Hip Arthroplasty. Surgical Technique IMAGE TO COME
 ZMR Over-the-Junction Instruments for Revision Hip Arthroplasty Surgical Technique IMAGE TO COME ZMR Over-the-Junction Instruments for Revision Hip Arthroplasty Introduction The ZMR Over-the-Junction (OTJ)
ZMR Over-the-Junction Instruments for Revision Hip Arthroplasty Surgical Technique IMAGE TO COME ZMR Over-the-Junction Instruments for Revision Hip Arthroplasty Introduction The ZMR Over-the-Junction (OTJ)
TM TM Surgical Technique
 TM TM Surgical Technique TABLE OF CONTENTS Reli SP Spinous Plating System Overview Device Description Implant Features Indications Instruments Access Instruments Preparation Instruments Insertion Instruments
TM TM Surgical Technique TABLE OF CONTENTS Reli SP Spinous Plating System Overview Device Description Implant Features Indications Instruments Access Instruments Preparation Instruments Insertion Instruments
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING.
 LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
MetaFix Ludloff Plate
 Merete MetaFix Ludloff Plate Low Profile Locking Bone Plate System Surgical Technique and Ordering Information - Content - Content 1. Description.................................................. 3 2.
Merete MetaFix Ludloff Plate Low Profile Locking Bone Plate System Surgical Technique and Ordering Information - Content - Content 1. Description.................................................. 3 2.
CONSENSUS ORTHOPEDICS INC. CONSENSUS KNEE SYSTEM
 CONSENSUS ORTHOPEDICS INC. CONSENSUS KNEE SYSTEM IMPORTANT INFORMATION FOR SURGEON: PLEASE READ PRIOR TO IMPLANTING THIS DEVICE IN A CLINICAL SETTING. THE SURGEON SHOULD BE FAMILIAR WITH THE SURGICAL TECHNIQUE.
CONSENSUS ORTHOPEDICS INC. CONSENSUS KNEE SYSTEM IMPORTANT INFORMATION FOR SURGEON: PLEASE READ PRIOR TO IMPLANTING THIS DEVICE IN A CLINICAL SETTING. THE SURGEON SHOULD BE FAMILIAR WITH THE SURGICAL TECHNIQUE.
SURGICAL TECHNIQUE. Alpine Cementless Hip Stem
 SURGICAL TECHNIQUE Alpine Cementless Hip Stem The following technique is a general guide for the instrumentation of the Alpine Cementless Hip Stem. It is expected that the surgeon is already familiar with
SURGICAL TECHNIQUE Alpine Cementless Hip Stem The following technique is a general guide for the instrumentation of the Alpine Cementless Hip Stem. It is expected that the surgeon is already familiar with
Longevity Offset and Oblique Liners. Surgical Technique
 Longevity Offset and Oblique Liners Surgical Technique Longevity Offset & Oblique Liners Surgical Technique 1 Introduction Complete Acetabular System Joint instability is an important issue in both primary
Longevity Offset and Oblique Liners Surgical Technique Longevity Offset & Oblique Liners Surgical Technique 1 Introduction Complete Acetabular System Joint instability is an important issue in both primary
SIDEKICK EZ FRAME EXTERNAL FIXATION SYSTEM The following languages are included in this packet:
 EN SIDEKICK EZ FRAME EXTERNAL FIXATION SYSTEM 149369-0 English (en) The following languages are included in this packet: For additional languages, visit our website www.wmt.com. Then click on the Prescribing
EN SIDEKICK EZ FRAME EXTERNAL FIXATION SYSTEM 149369-0 English (en) The following languages are included in this packet: For additional languages, visit our website www.wmt.com. Then click on the Prescribing
Important Notice to Users in the United States: General Safety Instructions
 SLR-PLUS Revision Stem, SLR-PLUS Revision Stem Lateral Smith & Nephew Orthopaedics AG Oberneuhofstrasse 10d CH-6340 Baar Phone + 41 41 766 22 22 swiss.implants@smith-nephew.com non-sterile cemented non-
SLR-PLUS Revision Stem, SLR-PLUS Revision Stem Lateral Smith & Nephew Orthopaedics AG Oberneuhofstrasse 10d CH-6340 Baar Phone + 41 41 766 22 22 swiss.implants@smith-nephew.com non-sterile cemented non-
Surgical Technique. Cup System
 Surgical Technique Cup System INDICATIONS AND USAGE Indications for the use of the CS2 ACETABULAR CUP SYSTEM must be carefully considered with respect to the patient s entire evaluation and alternative
Surgical Technique Cup System INDICATIONS AND USAGE Indications for the use of the CS2 ACETABULAR CUP SYSTEM must be carefully considered with respect to the patient s entire evaluation and alternative
MICROPORT KNEE SYSTEMS The following languages are included in this packet:
 EN English (en) MICROPORT KNEE SYSTEMS 151251-0 The following languages are included in this packet: For additional languages, visit our website ortho.microport.com Then click on the Prescribing Information
EN English (en) MICROPORT KNEE SYSTEMS 151251-0 The following languages are included in this packet: For additional languages, visit our website ortho.microport.com Then click on the Prescribing Information
Doc. No.: IU/8 for. Rev. No.: 07 ResTOR Prosthesis
 0434 Page 1 of 5 For use by an Accredited Orthopaedic Surgeon only IMPORTANT MEDICAL INFORMATION PURPOSE: The ResTOR system is designed to restore structural skeletal stability and enable functional joint
0434 Page 1 of 5 For use by an Accredited Orthopaedic Surgeon only IMPORTANT MEDICAL INFORMATION PURPOSE: The ResTOR system is designed to restore structural skeletal stability and enable functional joint
Technique Guide. *smith&nephew N8TIVE ACL Anatomic ACL Reconstruction System
 Technique Guide *smith&nephew N8TIVE ACL Anatomic ACL Reconstruction System N8TIVE ACL System The N8TIVE ACL Anatomic Reconstruction System provides a novel and simple approach to ACL repair. The N8TIVE
Technique Guide *smith&nephew N8TIVE ACL Anatomic ACL Reconstruction System N8TIVE ACL System The N8TIVE ACL Anatomic Reconstruction System provides a novel and simple approach to ACL repair. The N8TIVE
Persona. The Personalized Knee. Trabecular Metal Tibia. Surgical Technique
 Persona The Personalized Knee Trabecular Metal Tibia Surgical Technique Table of Contents Resect the Tibia... 4 Size and Finish the Tibia... 4 Trial Fit... 6 Component Implantation... 7 Inserter/Implant
Persona The Personalized Knee Trabecular Metal Tibia Surgical Technique Table of Contents Resect the Tibia... 4 Size and Finish the Tibia... 4 Trial Fit... 6 Component Implantation... 7 Inserter/Implant
