Indications for surgical reintervention following reverse shoulder arthroplasty: a retrospective audit from 2006 to 2015
|
|
|
- Ada Freeman
- 5 years ago
- Views:
Transcription
1 Du Plessis CP, et al. SA Orthop J 017;16() DOI / /017/v16na South African Orthopaedic Journal SHOULDER Indications for surgical reintervention following reverse shoulder arthroplasty: a retrospective audit from 006 to 015 Du Plessis CP 1, Koch O, Le Roux TLB 3, Janse van Rensburg C 1 MBChB(Stell); Orthopaedic Registrar, University of Pretoria MBChB(Pret), FCS Orth(SA), MMed(Ortho)(Pret); Orthopaedic Surgeon, Department of Orthopaedics, 1 Military Hospital, University of Pretoria 3 MBChB(Pret), FCS Orth(SA), MMed(Ortho)(Pret); Professor and Head of Department, Department of Orthopaedics, 1 Military Hospital, University of Pretoria BSc Actuarial & Financial Mathematics(Pret), BSc(Hons) Mathematical Statistics(Pret); Biostatistician South African Medical Research Council Corresponding author: Dr CP du Plessis, Department of Orthopaedic Surgery, Steve Biko Academic Hospital, Faculty of Health Sciences, University of Pretoria, Private Bag x 33, Pretoria, 000; flipduplessis00@gmail.com; Tel: ; Fax: Abstract Background: Reverse shoulder arthroplasty (RSA) has increased in popularity and its indications have subsequently been expanded. With its increased use, the complication rates have also increased. Complications requiring additional surgeries have the highest morbidity and cost. The aim of this study was to determine the indications for additional surgery following RSA. Methods: All the surgical and clinical notes of patients treated with an RSA at our institution over a nine-year period were retrospectively reviewed. Sixty-seven RSAs met the inclusion criteria and their records were reviewed to assess their indication for surgery, complications, as well as microbiology results if infection was present. Results: Surgical reintervention was required in 16 (3.9%) RSAs. The prevalence was lowest in rotator cuff arthropathy and glenohumeral arthritis (nine RSAs or 18.%), followed by failed hemi- or total shoulder arthroplasty (four RSAs or 36.%) and highest if performed for uncommon conditions (two RSAs or 66.7%). Instability was an early complication, occurring in 10.7% of cases and accounting for 37.8% of all reinterventions. Infection was a late complication, occurring in 6.0% of cases and accounting for 8.6% of all reinterventions. The most common organisms identified were Staphylococcus epididermidis (n=), Escherichia coli (n=3), Staphylococcus aureus (n=) and Klebsiella pneumonia (n=). Conclusions: RSA has the most reliable outcomes if performed for rotator cuff arthropathy and glenohumeral osteoarthritis. Instability and infection are the most common indications for surgical reintervention, and once present, often require repeated surgeries to be successfully treated. These complications should be avoided, as they are major contributors to morbidity and cost. Level of evidence: Level Key words: reverse shoulder arthroplasty, reverse shoulder replacement, complication, reoperation, revision, reintervention Citation: Du Plessis CP, Koch O, Le Roux TLB, Janse van Rensburg C. Indications for surgical reintervention following reverse shoulder arthroplasty: a retrospective audit from 006 to 015. SA Orthop J 017;16(): Editor: Prof Anton Schepers, University of the Witwatersrand Received: April 017 Accepted: July 017 Published: November 017 Copyright: 017 Du Plessis CP, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution Licence, which permits unrestricted use, distribution and reproduction in any medium, provided the original author and source are credited. Funding: No funding was received with respect to this article. Conflict of interest: Drs Du Plessis, Koch and Prof Le Roux declare that they have no conflict of interest. No benefits of any form have or will be received from any commercial party related directly or indirectly to the subject of this article.
2 Du Plessis CP, et al. SA Orthop J 017;16() Page 9 Introduction The French surgeon, Dr Jules-Émile Péan, performed the first shoulder arthroplasty in Although this prosthesis lasted for only two years before it had to be removed, this was a remarkable accomplishment for the time when it was performed. Almost 60 years passed before Neer developed an anatomic prosthesis for hemiarthroplasty of the shoulder in the 1950s. 1 The next development after anatomic shoulder arthroplasties was the non-anatomic reverse shoulder arthroplasty (RSA).,3 In this design the glenoid component is spherical and articulates with the concave humeral component. The result is a new biomechanical environment in which the deltoid muscle can compensate for deficient rotator cuff muscles. 3 Since its approval for use in the United States of America in 003, the use of RSA has sharply increased.,5 The.5-fold increase in the use of shoulder arthroplasties from 000 to 008 is largely attributed to the introduction of RSA. 5 Villacis et al. reported a 70% increase in the use of RSA in the American state of California between 011 and The initial indication for the use of RSA was for elderly patients with severe rotator cuff arthropathy.,5 However, with increased use, the indications for the procedure have been expanded, leading to younger patients also being offered RSA.,6-8 This increased use has been associated with an increased complication rate, which is reported to be.8 68%. 6 The high variability in complication rate can be explained by the inclusion of complications in some studies that are not clinically relevant. Zumstein et al. found that complications leading to revision surgery had a negative effect on the final functional outcome of patients. They defined reintervention as any subsequent surgery on the operated shoulder. This was further divided into reoperations ( interventions requiring any return to the operating room for any reason relating to the shoulder, without altering or replacing any of the components ) and revisions ( surgeries with total or partial exchange or removal of the components ). 9 In the literature currently, reintervention rates range between 5.3 and 15%. 7,9,10 The indications for reinterventions have been investigated by previous authors, but many of the published studies either have a small sample size, 10,11 short follow-up 7,11 or incomplete reporting on their indications for reintervention. 6,11,1 Two notable exceptions to the above are a systematic review by Zumstein et al. 9 and a review article by Boileau. 13 These patients are also typically elderly with multiple co-morbidities that make them unsuitable for repeated high-risk anaesthetics (beach-chair position). 6 Repeated surgical interventions also place a significant monetary burden on the health care system as well as individuals. The purpose of this study was to determine the prevalence of surgical reintervention in RSA, as well as the specific indications for reintervention. Material and methods The records of all patients who had undergone an RSA at our unit between November 006 and September 015 were retrospectively reviewed. Patients were excluded if their RSA was not performed at our unit or if they did not have a minimum follow-up of one year. The following data was recorded: The indication for the RSA and the number of shoulders that had reinterventions (Table I) The indications for surgical reintervention; the number of reinterventions performed; whether it was a reoperation or revision (Figures 1 and ) The interval between reintervention and initial RSA In cases of infection, the microbiology results were retrieved to determine the involved organisms (Table II) Initially the prosthesis was implanted through a deltopectoral approach, but the approach was gradually changed to superolateral due to its improved stability according to the literature.,13 Subscapularis was not routinely repaired and no patients had latissimus dorsi transfers. Patients were operated in the beach-chair position under general anaesthesia, augmented with a regional block if deemed fit by the anaesthesiologist. Wounds were closed over a Porto-Vac suction drain and the shoulder put in an arm immobiliser post-operatively. Multiple fluid samples were taken if infection was suspected and sent in aerobic and anaerobic blood culture bottles for processing. Statistical analysis The descriptive statistics mean, standard deviation, median and range with 95% confidence intervals for continuous variables and proportions with 95% confidence intervals for categorical variables were calculated. The proportions were used to determine the prevalence of surgical reintervention in RSA. The t-test, chi-square and Fisher exact tests were used to test for any associations between categorical variables. Tests were evaluated at 5% level of significance. All analysis was done using STATA 1. Results There were 71 patients that underwent a total of 77 RSAs. Sixty-two patients with a total of 67 RSAs were enrolled in the study. The following patients were excluded: four patients that died of unrelated causes before a one-year follow-up, three patients because of a short follow-up and two patients due to incomplete records. One patient with bilateral replacements had to be excluded. Twenty-five (37.3%) RSAs were performed on the left side and (6.7%) on the right side. Twenty-six prostheses (38.8%) were implanted through a deltopectoral approach and 1 (61.%) through a superolateral approach. Forty-one (61.%) replacements were for females and 6 (38.8%) for males with an average age of 68.7 years (55 85 years). The mean follow-up was 50.8 months (1 17 months). The most common indication for an RSA was rotator cuff arthropathy (n=1, 61.%). A total of 16 (3.8%) replacements required a reintervention (Table I). Seven (10.%) of these had post-operative instability, four (6.0%) infection and five (7.5%) other less common complications (Figure 1). When comparing age (p=0.6), sex (p=0.9) and operated side (p=0.986), there was no statistically significant difference between patients needing a reintervention and those that did not. Table I: Primary indications for RSA showing the number of patients that had surgical reinterventions Primary indication Number of RSA RSA that had reinterventions Rotator cuff arthropathy 1 (61.%) 9 (.0%) Failed hemi shoulder arthroplasty 9 (13.%) 3 (33.3%) Glenohumeral osteoarthritis 8 (11.9%) 0 (0%) Failed ORIF of proximal humeral fractures (6.0%) 1 (5.0%) Miscellaneous 3 (.5%) (66.7%) Failed total shoulder arthroplasty (3.0%) 1 (50.0%) Total (3.9%) The miscellaneous group included an ancient shoulder dislocation, chondrosarcoma and metastatic breast cancer. ORIF = Open Reduction and Internal Fixation. RSA = Reverse Shoulder Arthroplasty
3 Page 30 Du Plessis CP, et al. SA Orthop J 017;16() Reoperations Revisions Dislocations and subluxations (10.%) Surgical site infection (6.0%) Miscellaneous* (3.0%) Haematoma formation Periprosthetic fractures Implant failure Figure 1. The indications for initial reintervention after RSA *Removal of a prominent screw used to ORIF a previous os acromiale now irritating the deltoid muscle and repair of a deltoid muscle tear Reoperations Revisions 0 Dislocations and subluxations (37.8%) Surgical site infection (5.9%) Miscellaneous* (5.%) Haematoma formation (5.%) Periprosthetic fractures (.7%) Implant failure (.7%) Figure. Total number of reinterventions required *Removal of a prominent screw used to ORIF a previous os acromiale now irritating the deltoid muscle and repair of a deltoid muscle tear Table II: Epidemiology of the infective organisms Pathogen No times identified No times identified (%) Patients identified (%) Staphylococcus epididermidis Escherichia coli Staphylococcus aureus Klebsiella pneumonia Candida albicans Streptococcus viridans Stenotrophomonas maltophilia Pseudomonas aeruginosa Enterobacter cloacae Enterococcus faecium More than one organism was identified in five patients (6.5%) A total of 37 reinterventions were performed. Seventeen (5.9%) of these were for surgical-site infection and 1 (37.8%) for instability (Figure ). The reinterventions were not adjusted for the number of times a specific shoulder had to go back to theatre. Surgical reintervention was performed at a mean of 1.8 months (0 67 months). Six of the nine reinterventions that were performed within three months of surgery were for instability. Surgical-site infection (n=) and haematoma formation (n=1) also occurred within three months of RSA. Surgical site infection (n=), deltoid problems (n=), periprosthetic fractures (n=1), instability (n=1) and implant failure (n=1) occurred after three months. Microscopy and culture results revealed a polymicrobial infection in four shoulders and monomicrobial infection in three shoulders. In one case no organism was identified, but this patient was on suppressive antibiotics for five weeks before revision. Escherichia coli, Klebsiella pneumonia and Pseudomonas aeruginosa were the only organisms that occurred in isolation. Staphylococcus epididermidis (n=) was the most commonly isolated organism, followed by E. coli (n=3), Staphylococcus aureus (n=), K. pneumonia (n=) and a number of other pathogens (Table II).
4 Du Plessis CP, et al. SA Orthop J 017;16() Page 31 Discussion RSA has gained in popularity over the last two decades. While it was originally indicated for patients with rotator cuff arthropathy, the indications have been expanded as it became more commonly used. Common indications are rotator cuff arthropathy ( %), glenohumeral osteoarthritis (5.1%), acute proximal humerus fractures ( %), revisions of hemi- or total shoulder arthroplasty (.5 7.6%), rheumatoid arthritis (.9 10%), failed open reduction and internal fixation (ORIF) of proximal humerus fractures (5.%) and tumours (0.8%).,6,7,9,10,1 Similar indications for RSA as mentioned above were found in our cohort, with the exception of rheumatoid arthritis and acute proximal humerus fractures (Table I). The complication rate was lowest if the indication for RSA was rotator cuff arthropathy or glenohumeral osteoarthritis (18.%). When performed as a revision procedure for a failed arthroplasty, the complication rate increased to 36.%. The highest complication rate (66.7%) occurred when RSA was performed for expanded indications, which were an ancient dislocation and tumour-related procedures (Figure 3). Zumstein et al. found that the incidence of all kinds of complications increased from 8.7% for primary RSA to 65.7% for revision cases. 9 Similarly Russo et al. found an increase from 10.8% to 36.8%. 1 This suggests that, although RSA may be a useful method to treat complex shoulder problems, it should be utilised with care in these patients as the best outcomes are seen in patients with primary shoulder pathology. Post-operative instability was the most common complication encountered at 10.% and accounts for 3.8% of all complications. This supports previous findings with instability rates of between. and 31%.,9,13,1 Villacis et al. reported an early dislocation rate (before 90 days) of 1.8% with an increase to 5.5% at two years. 6 In the current study, it was found that dislocation is an early complication with 85.7% (6/7) of the cases presenting within three months of RSA primary surgery. At 66.7% (6/9) it was also the most common complication occurring within three months. Although there is an association between the deltopectoral approach and instability due to subscapularis muscle violation, it could not be confirmed (p=0.557).,13 Instability was found in 7.7% of shoulders operated through a deltopectoral approach, compared to 1.% of those approached through the more commonly used superolateral incision. Technical errors during surgery explain why instability is more frequently an early complication. These include failure to restore adequate soft-tissue tension of the deltoid, incorrect position (version) of the prosthesis, excessive medialisation or inadequate diameter of the glenosphere and not removing tissues inferior to the glenosphere that can cause mechanical impingement. Additionally, failure to recognise and restore humeral and glenoid bone loss as well as not repairing the subscapularis muscle when possible may contribute to instability.,13 Meticulous detail to the above can help to reduce dislocation rates. Fourteen (37.8%) of the reinterventions occurring in seven patients were for instability, indicating that this is a recurrent problem. This supports previous findings indicating that 38 59% of RSA shoulders will remain unstable after reduction. 13 The sample size was too small to determine a relationship between the indication for a RSA and instability. Infection was the second most common complication in our cohort, initially affecting four (6.0%) RSAs and accounting for 5.0% of the complications. A further four cases developed infection after reintervention, two of which followed revisions for instability. One patient required six reinterventions for infection. This suggests that repeated surgeries as well as instability contribute to infection. Infection required the most reinterventions (5.9%), emphasising the difficulty in treating this complication. The post-operative infection rate is reported as 1 10% in the literature and up to 1% after revision surgery.,9,13-16 Risk factors for post-operative infection Figure year-old female with chondrosarcoma of her right proximal humerus successfully treated with a RSA tumour prosthesis are prior failed arthroplasty, multiple surgeries, age less than 65 years, instability, haematoma formation and inadequate dead space management.,15 Infection occurred at a mean of.1 months after RSA, suggesting it is a late complication. This is in keeping with trends seen in the literature where there is an increased incidence of infection after one year.,15,16 The late presentation may be explained by an unrecognised latent low-grade infection sustained during the primary or revision surgery. The organism most commonly identified was S. epididermidis followed by E. coli, S. aureus and K. pneumonia. The most frequently identified bacteria causing infection after RSA in two recent studies were Propionibacterium acnes, S. epididermidis and S. aureus. 15,16 We encountered no cases of P. acnes. This may be due to our local pathogen profile or the prolonged culture that is needed to detect P. acnes.,15 Infection can be avoided by pre-operative chlorhexidine body washes, administrating adequate prophylactic antibiotics within one hour of surgery, using antibiotic-impregnated cement, atraumatic soft-tissue handling and by placing drains to manage the dead space left by the removal of the rotator cuff. Despite all these precautions it must be realised that the elderly population are often poor hosts due to their medical co-morbidities, nutritional status and often very advanced age. This predisposes them to a higher risk of infection. 17 Instability and infection combined accounted for 11 (68.8%) of the patients that required reintervention and 31 (83.8%) of all the reinterventions that were performed, often requiring multiple procedures in the same patient. Periprosthetic fractures, implant failure and haematoma formation that reportedly accounts for 1..0%, 1.8 9% and 3% of complications respectively, were rare in the sample group. 9,1-1 Deltoid problems consisted of a prominent screw after a previous os acromiale ORIF irritating the deltoid muscle, necessitating removal, and a tear in the deltoid muscle requiring repair due to persistent pain. Deltoid injury is a rare complication, accounting for 0.9% of all complications. 13 The pricing of prostheses is one of the big cost drivers in arthroplasty surgery. Revision surgery requires component exchange, and accounted for 1 (56.8%) of the reinterventions performed, indicating the monetary burden on the health care system.
5 Page 3 Du Plessis CP, et al. SA Orthop J 017;16() The inherent weaknesses of a retrospective study are acknowledged. However, comprehensive follow-up and recordkeeping with electronically captured theatre and outpatient notes were done. Patients excluded from the study were few and mainly due to unrelated death before minimum follow-up. Our large scope of practice helped minimise selection bias. The relatively small sample size made the assessment of rare complications and comparisons between different groups difficult. The average follow-up was long at 50.8 months, even though the minimum follow-up for inclusion was 1 months. Conclusion Although there has been a tendency to use RSA to treat complex shoulder problems, our data suggests that the outcomes are better when used for primary shoulder pathology such as rotator cuff arthropathy and glenohumeral arthritis. Care should be taken when dealing with other indications, especially if there are other treatment options available. The reintervention rate doubles when treating failed arthroplasty with RSA and increases almost four times when it is used to treat uncommon conditions like ancient dislocations and tumours. Instability is the most common complication and occurs early post-operatively. It is often a recurrent problem. Sepsis is the second most common cause for reintervention but the most difficult to treat, requiring repeated reinterventions. It is a problem that often develops after repeated surgeries, more commonly after reintervention for instability. Once a complication arises that requires reintervention, multiple procedures are often needed, adding to patient morbidity and health care cost. 1. Russo R, Rotonda GD, Ciccarelli M, Cautiero F. Analysis of complications of reverse total shoulder arthroplasty. Joints 015;3: Boileau P. Complications and revision of reverse total shoulder arthroplasty. Orthop Traumatol Surg Res. 016;10:S Bohsali KI, Bois AJ, Wirth MA. Complications of shoulder arthroplasty. J Bone Joint Surg Am. 017;99: Morris BJ, O Connor DP, Torres D, Elkousy HA, Gartsman GM, Edwards TB. Risk factors for periprosthetic infection after reverse shoulder arthroplasty. J Shoulder Elbow Surg. 015;: Jacquot A, Sirveaux F, Roche O, Favard L, Clavert P, Mole D. Surgical management of the infected reversed shoulder arthroplasty: a French multicenter study of reoperation in 3 patients. J Shoulder Elbow Surg. 015;: Wester AL, Dunlop O, Melby KK, Dahel UR, Bruun T. Age-related differences in symptoms, diagnosis and prognosis of bacteremia. BMC Infectious Diseases. 013;13: Compliance with ethics guidelines The ethical committees of our institution as well as the hospital where the research was performed gave approval before the research commenced. References 1. Mehmood A, Everett W. Shoulder replacements: a review. Br J Hosp Med (Lond) 016;77: Grammont P, Trouilloud P, Laffay J Deries X. Etude et realisation d une nouvelle prothese d epaule. Rheumatologie 1987;39: Boileau P, Watkinson DJ, Hatzidakis AM, Balg F. Grammont reverse prosthesis: design, rationale, and biomechanics. J Shoulder Elbow Surg. 005;1:17S-161S.. Cheung E, Willis M, Walker M, Clark R, Frankle MA. Complications in reverse total shoulder arthroplasty. J Am Acad Orthop Surg. 011;19: Kim SH, Wise BL, Zhang Y, Szabo RM. Increasing incidence of shoulder arthroplasty in the United States. J Bone Joint Surg Am. 011;93: Villacis D, Sivasundaram L, Pannell WC, Heckmann N, Omid R, Hatch GF, 3rd. Complication rate and implant survival for reverse shoulder arthroplasty versus total shoulder arthroplasty: results during the initial years. J Shoulder Elbow Surg. 016 Jun;5(6): Groh GI, Groh GM. Complications rates, reoperation rates, and the learning curve in reverse shoulder arthroplasty. J Shoulder Elbow Surg. 01;3: Sershon RA, Van Thiel GS, Lin EC, et al. Clinical outcomes of reverse total shoulder arthroplasty in patients aged younger than 60 years. J Shoulder Elbow Surg. 01;3: Zumstein MA, Pinedo M, Old J, Boileau P. Problems, complications, reoperations, and revisions in reverse total shoulder arthroplasty: a systematic review. J Shoulder Elbow Surg. 011;0: Guery J, Favard L, Sirveaux F, Oudet D, Mole D, Walch G. Reverse total shoulder arthroplasty. Survivorship analysis of eighty replacements followed for five to ten years. J Bone Joint Surg Am. 006;88: Wierks C, Skolasky RL, Ji JH, McFarland EG. Reverse total shoulder replacement: intraoperative and early postoperative complications. Clin Orthop Relat Res. 009;67:5-3.
Clinical Outcomes and Complications during the Learning Curve for Reverse Total Shoulder Arthroplasty: An Analysis of the First 40 Cases
 Original Article Clinics in Orthopedic Surgery 2017;9:213-217 https://doi.org/10.4055/cios.2017.9.2.213 Clinical Outcomes and Complications during the Learning Curve for Reverse Total Shoulder Arthroplasty:
Original Article Clinics in Orthopedic Surgery 2017;9:213-217 https://doi.org/10.4055/cios.2017.9.2.213 Clinical Outcomes and Complications during the Learning Curve for Reverse Total Shoulder Arthroplasty:
Biomechanical concepts of total shoulder replacement. «Shoulder Course» Day 1. Richard W. Nyffeler Orthopädie Sonnenhof Bern. 11. Sept.
 Biomechanical concepts of total shoulder replacement Richard W. Nyffeler Orthopädie Sonnenhof Bern First total shoulder prosthesis Jules Emile Péan, 1830-1898 Monobloc prostheses Charles Neer, 1917-2011
Biomechanical concepts of total shoulder replacement Richard W. Nyffeler Orthopädie Sonnenhof Bern First total shoulder prosthesis Jules Emile Péan, 1830-1898 Monobloc prostheses Charles Neer, 1917-2011
Reverse Total Shoulder Arthroplasty: A New Frontier (of Complications)
 Reverse Total Shoulder Arthroplasty: A New Frontier (of Complications) Emilie Cheung, MD Associate Professor Chief Shoulder Elbow Svc Stanford University Department of Orthopedic Surgery Procedure volumes
Reverse Total Shoulder Arthroplasty: A New Frontier (of Complications) Emilie Cheung, MD Associate Professor Chief Shoulder Elbow Svc Stanford University Department of Orthopedic Surgery Procedure volumes
Why are these shoulder replacements called a reverse prosthesis?
 PATIENT GUIDE TO REVERSE PROSTHESIS Edward G. McFarland MD The Division of Sports Medicine and Shoulder Surgery The Department of Orthopaedic Surgery The Johns Hopkins University Baltimore MD Why are these
PATIENT GUIDE TO REVERSE PROSTHESIS Edward G. McFarland MD The Division of Sports Medicine and Shoulder Surgery The Department of Orthopaedic Surgery The Johns Hopkins University Baltimore MD Why are these
Revision of reversed total shoulder arthroplasty. Indications and outcome
 Farshad et al. BMC Musculoskeletal Disorders 2012, 13:160 RESEARCH ARTICLE Open Access Revision of reversed total shoulder arthroplasty. Indications and outcome Mazda Farshad *, Marion Grögli, Sabrina
Farshad et al. BMC Musculoskeletal Disorders 2012, 13:160 RESEARCH ARTICLE Open Access Revision of reversed total shoulder arthroplasty. Indications and outcome Mazda Farshad *, Marion Grögli, Sabrina
Scapular notching in reverse shoulder arthroplasties: The influence of glenometaphyseal angle
 Orthopaedics & Traumatology: Surgery & Research (2011) 97S, S131 S137 ORIGINAL ARTICLE Scapular notching in reverse shoulder arthroplasties: The influence of glenometaphyseal angle V. Falaise a, C. Levigne
Orthopaedics & Traumatology: Surgery & Research (2011) 97S, S131 S137 ORIGINAL ARTICLE Scapular notching in reverse shoulder arthroplasties: The influence of glenometaphyseal angle V. Falaise a, C. Levigne
Gerald R. Williams, MD
 Reverse Arthroplasty: Is Overutilization a Problem? Gerald R. Williams, MD John M. Fenlin, Jr, MD Professor of Shoulder and Elbow Surgery The Rothman Institute Jefferson Medical College Royalties Conflict
Reverse Arthroplasty: Is Overutilization a Problem? Gerald R. Williams, MD John M. Fenlin, Jr, MD Professor of Shoulder and Elbow Surgery The Rothman Institute Jefferson Medical College Royalties Conflict
)532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY
 )532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE The Midterm Results of the Delta Xtend Reverse Shoulder System: A Five-Year Outcome Study John G. Horneff, MD; Thema A. Nicholson,
)532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE The Midterm Results of the Delta Xtend Reverse Shoulder System: A Five-Year Outcome Study John G. Horneff, MD; Thema A. Nicholson,
Both anatomic (atsa) and reverse (rtsa) total
 S101 Comparison of Outcomes Using Anatomic and Reverse Total Shoulder Arthroplasty Pierre-Henri Flurin, M.D., Yann Marczuk, M.D., Martin Janout, M.D., Thomas W. Wright, M.D., Joseph Zuckerman, M.D., and
S101 Comparison of Outcomes Using Anatomic and Reverse Total Shoulder Arthroplasty Pierre-Henri Flurin, M.D., Yann Marczuk, M.D., Martin Janout, M.D., Thomas W. Wright, M.D., Joseph Zuckerman, M.D., and
0 Introduction (20.9%) [7]
![0 Introduction (20.9%) [7] 0 Introduction (20.9%) [7]](/thumbs/92/108991709.jpg) Chinese Journal of Tissue Engineering Research www.crter.org ( 443000) DOI:10.3969/j.issn.2095-4344.0187 ORCID: 0000-0003-0005-1839() 60 120 2 60 1980 2015 443000 :R318 :A 2017-12-05 3 4 120 60 () 3 (P
Chinese Journal of Tissue Engineering Research www.crter.org ( 443000) DOI:10.3969/j.issn.2095-4344.0187 ORCID: 0000-0003-0005-1839() 60 120 2 60 1980 2015 443000 :R318 :A 2017-12-05 3 4 120 60 () 3 (P
"Stability and Instability of RTSA"
 Orthopedics Update «Reverse Total Shoulder Arthroplasty» Stability and Instability of RTSA A. LÄDERMANN Orthopaedics and Traumatology, La Tour Hospital, Meyrin, Switzerland Orthopaedics and Traumatology,
Orthopedics Update «Reverse Total Shoulder Arthroplasty» Stability and Instability of RTSA A. LÄDERMANN Orthopaedics and Traumatology, La Tour Hospital, Meyrin, Switzerland Orthopaedics and Traumatology,
Disclosures A prospective comparison between reverse and anatomic total shoulder arthroplasty
 Disclosures A prospective comparison between reverse and anatomic total shoulder arthroplasty Tuyen Kiet Micah Naimark, MD Brian T. Feeley, MD Teddy T. Chung Tatiana Gajiu Sarah L. Hall, MA C. Benjamin
Disclosures A prospective comparison between reverse and anatomic total shoulder arthroplasty Tuyen Kiet Micah Naimark, MD Brian T. Feeley, MD Teddy T. Chung Tatiana Gajiu Sarah L. Hall, MA C. Benjamin
Immediate post surgical findings of soft tissue swelling, subcutaneous emphysema, and skin staples for reverse total shoulder arthroplasty.
 Immediate post surgical findings of soft tissue swelling, subcutaneous emphysema, and skin staples for reverse total shoulder arthroplasty. REVERSE TOTAL SHOULDER ARTHROPLASTY WITH FRACTURED ACROMION Above:
Immediate post surgical findings of soft tissue swelling, subcutaneous emphysema, and skin staples for reverse total shoulder arthroplasty. REVERSE TOTAL SHOULDER ARTHROPLASTY WITH FRACTURED ACROMION Above:
An evaluation of the radiological changes around the Grammont reverse geometry shoulder arthroplasty after eight to 12 years
 UPPER LIMB An evaluation of the radiological changes around the Grammont reverse geometry shoulder arthroplasty after eight to 12 years B. Melis, M. DeFranco, A. Lädermann, D. Molé, L. Favard, C. Nérot,
UPPER LIMB An evaluation of the radiological changes around the Grammont reverse geometry shoulder arthroplasty after eight to 12 years B. Melis, M. DeFranco, A. Lädermann, D. Molé, L. Favard, C. Nérot,
AJO DO NOT COPY. The low grade of the intrinsic stability of the shoulder. Total Reverse Shoulder Arthroplasty: European Lessons and Future Trends
 A Review Paper Total Reverse Shoulder Arthroplasty: European Lessons and Future Trends Ludwig Seebauer, MD Abstract In the late 1980s, Grammont introduced a new reverse total shoulder arthroplasty (TSA),
A Review Paper Total Reverse Shoulder Arthroplasty: European Lessons and Future Trends Ludwig Seebauer, MD Abstract In the late 1980s, Grammont introduced a new reverse total shoulder arthroplasty (TSA),
Radiology Case Reports. Scapular Spine Stress Fracture as a Complication of Reverse Shoulder Arthroplasty
 Radiology Case Reports Volume 2, Issue 2, 2007 Scapular Spine Stress Fracture as a Complication of Reverse Shoulder Arthroplasty Kimberly J. Burkholz, Catherine C. Roberts, and Steven J. Hattrup We report
Radiology Case Reports Volume 2, Issue 2, 2007 Scapular Spine Stress Fracture as a Complication of Reverse Shoulder Arthroplasty Kimberly J. Burkholz, Catherine C. Roberts, and Steven J. Hattrup We report
Shoulder Arthroplasty. Valentin Lance 3/24/16
 Shoulder Arthroplasty Valentin Lance 3/24/16 Outline Background Pre-operative imaging assessment Total Shoulder Arthroplasty: Standard and Reverse Complications Other shoulder hardware Hemiarthroplasty
Shoulder Arthroplasty Valentin Lance 3/24/16 Outline Background Pre-operative imaging assessment Total Shoulder Arthroplasty: Standard and Reverse Complications Other shoulder hardware Hemiarthroplasty
Making sense of all our measures-inclination, version, subluxation, reaming depth & implant seating
 Thursday - ANATOMIC SHOULDER ARTHROPLASTY 7:00-7:15a Welcome and Introduction of Faculty Athwal, Keener, 7:15-7:22a The ABC s of the Walch Classification Walch 7:22-7:32a How I use x-rays, CT +/- MRI for
Thursday - ANATOMIC SHOULDER ARTHROPLASTY 7:00-7:15a Welcome and Introduction of Faculty Athwal, Keener, 7:15-7:22a The ABC s of the Walch Classification Walch 7:22-7:32a How I use x-rays, CT +/- MRI for
)19( COPYRIGHT 2019 BY THE ARCHIVES OF BONE AND JOINT SURGERY
 )19( COPYRIGHT 2019 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE Failure of Anatomic Total Shoulder Arthroplasty with Revision to Another Anatomic Total Shoulder Arthroplasty Mihir Sheth,
)19( COPYRIGHT 2019 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE Failure of Anatomic Total Shoulder Arthroplasty with Revision to Another Anatomic Total Shoulder Arthroplasty Mihir Sheth,
SSSR. 1. Nov Shoulder Prosthesis. Postoperative Imaging. Florian M. Buck, MD
 Shoulder Prosthesis Postoperative Imaging Florian M. Buck, MD Shoulder Prosthesis Surgical Approach Findings Imaging Modalities Postoperative Problems Shoulder Prosthesis What are we talking about Anatomical
Shoulder Prosthesis Postoperative Imaging Florian M. Buck, MD Shoulder Prosthesis Surgical Approach Findings Imaging Modalities Postoperative Problems Shoulder Prosthesis What are we talking about Anatomical
Optimal Baseplate Rotational Alignment in Reverse Total Shoulder Arthroplasty: A Three-Dimensional Computer-Aided Design Study.
 Optimal Baseplate Rotational Alignment in Reverse Total Shoulder Arthroplasty: A Three-Dimensional Computer-Aided Design Study. Byron F. Stephens, MD 1, Casey T. Hebert 2, Thomas W. Throckmorton, MD 1,
Optimal Baseplate Rotational Alignment in Reverse Total Shoulder Arthroplasty: A Three-Dimensional Computer-Aided Design Study. Byron F. Stephens, MD 1, Casey T. Hebert 2, Thomas W. Throckmorton, MD 1,
Jonathan C. Levy, MD
 Jonathan C. Levy, MD Chief of Orthopedics Program Director, ASES Fellowship Holy Cross Hospital Fort Lauderdale, Florida USA Disclosure: Consultant, Royalties, & Research Support from DJO 72 year old
Jonathan C. Levy, MD Chief of Orthopedics Program Director, ASES Fellowship Holy Cross Hospital Fort Lauderdale, Florida USA Disclosure: Consultant, Royalties, & Research Support from DJO 72 year old
Shoulder Revisions: Why Are We Here?
 Shoulder Revisions: Why Are We Here? Indications for Revision to RSA Mark A. Frankle, MD Kaitlyn N. Christmas, BS Peter Simon, PhD DJO Revision Course 2017 June 2-3 Introduction Reverse shoulder arthroplasty(rsa)
Shoulder Revisions: Why Are We Here? Indications for Revision to RSA Mark A. Frankle, MD Kaitlyn N. Christmas, BS Peter Simon, PhD DJO Revision Course 2017 June 2-3 Introduction Reverse shoulder arthroplasty(rsa)
Instability After Reverse Total Shoulder Arthroplasty: Which Patients Dislocate?
 An Original Study Instability After Reverse Total Shoulder Arthroplasty: Which Patients Dislocate? Eric M. Padegimas, MD, Benjamin Zmistowski, MD, Camilo Restrepo, MD, Joseph A. Abboud, MD, Mark D. Lazarus,
An Original Study Instability After Reverse Total Shoulder Arthroplasty: Which Patients Dislocate? Eric M. Padegimas, MD, Benjamin Zmistowski, MD, Camilo Restrepo, MD, Joseph A. Abboud, MD, Mark D. Lazarus,
L. Favard a,, D. Katz b, M. Colmar c, T. Benkalfate d, H. Thomazeau e, S. Emily c WORKSHOPS OF THE SOO (2011, LA BAULE).
 Orthopaedics & Traumatology: Surgery & Research (2012) 98, S41 S47 Available online at www.sciencedirect.com WORKSHOPS OF THE SOO (2011, LA BAULE). ORIGINAL ARTICLE Total shoulder arthroplasty Arthroplasty
Orthopaedics & Traumatology: Surgery & Research (2012) 98, S41 S47 Available online at www.sciencedirect.com WORKSHOPS OF THE SOO (2011, LA BAULE). ORIGINAL ARTICLE Total shoulder arthroplasty Arthroplasty
Convertibilité. Ph. Valenti. Paris Shoulder Unit Clinique Bizet (Paris, France)
 Convertibilité Ph. Valenti Paris Shoulder Unit Clinique Bizet (Paris, France) Disclosures Arthroplasty Consultant : FH orthopaedics receive royalties Arthroscopy Consultant : Zimmer Biomet Arthrex In Last
Convertibilité Ph. Valenti Paris Shoulder Unit Clinique Bizet (Paris, France) Disclosures Arthroplasty Consultant : FH orthopaedics receive royalties Arthroscopy Consultant : Zimmer Biomet Arthrex In Last
MEDICAL POLICY MEDICAL POLICY DETAILS POLICY STATEMENT. Page: 1 of 6
 Page: 1 of 6 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title SHOULDER ARTHROPLASTY (TOTAL, PARTIAL AND REVERSE) Policy Number 7.01.95 Category Technology Assessment Effective Date 6/21/18 Revised
Page: 1 of 6 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title SHOULDER ARTHROPLASTY (TOTAL, PARTIAL AND REVERSE) Policy Number 7.01.95 Category Technology Assessment Effective Date 6/21/18 Revised
The use of the Lima reverse shoulder arthroplasty for the treatment of fracture sequelae of the proximal humerus
 J Orthop Sci (2012) 17:141 147 DOI 10.1007/s00776-011-0185-5 ORIGINAL ARTICLE The use of the Lima reverse shoulder arthroplasty for the treatment of fracture sequelae of the proximal humerus Angel Antonio
J Orthop Sci (2012) 17:141 147 DOI 10.1007/s00776-011-0185-5 ORIGINAL ARTICLE The use of the Lima reverse shoulder arthroplasty for the treatment of fracture sequelae of the proximal humerus Angel Antonio
D Degenerative joint disease, rotator cuff deficiency with, 149 Deltopectoral approach component removal with, 128
 Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
ANATOMIC TOTAL SHOULDER REPLACEMENT:
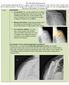 The Shoulder Replacement A total shoulder arthroplasty (TSA) is a surgery to replace the damaged parts of the ball and socket shoulder joint with an artificial prosthesis. The damage to the shoulder can
The Shoulder Replacement A total shoulder arthroplasty (TSA) is a surgery to replace the damaged parts of the ball and socket shoulder joint with an artificial prosthesis. The damage to the shoulder can
Reverse Total Shoulder Arthroplasty: A Review of Results According to Etiology
 1476 COPYRIGHT 2007 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Reverse Total Shoulder Arthroplasty: A Review of Results According to Etiology By Bryan Wall, MD, Laurent Nové-Josserand, MD,
1476 COPYRIGHT 2007 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Reverse Total Shoulder Arthroplasty: A Review of Results According to Etiology By Bryan Wall, MD, Laurent Nové-Josserand, MD,
Reverse Total Shoulder Arthroplasty: Early Outcome and Complication Report
 ORIGINAL ARTICLE Clinics in Shoulder and Elbow Vol. 17, No. 2, June, 2014 http://dx.doi.org/10.5397/cise.2014.17.2.68 CiSE Clinics in Shoulder and Elbow Reverse Total Shoulder Arthroplasty: Early Outcome
ORIGINAL ARTICLE Clinics in Shoulder and Elbow Vol. 17, No. 2, June, 2014 http://dx.doi.org/10.5397/cise.2014.17.2.68 CiSE Clinics in Shoulder and Elbow Reverse Total Shoulder Arthroplasty: Early Outcome
Reversed Revised : What to do when it goes wrong?
 Acta Orthop. Belg., 2014, 80, 314-321 ORIGINAL STUDY Reversed Revised : What to do when it goes wrong? Bart Middernacht, Alexander Van Tongel, Lieven De Wilde From Department of Orthopaedics, University
Acta Orthop. Belg., 2014, 80, 314-321 ORIGINAL STUDY Reversed Revised : What to do when it goes wrong? Bart Middernacht, Alexander Van Tongel, Lieven De Wilde From Department of Orthopaedics, University
Assessment of Scapular Morphology and Surgical Technique as Predictors of Notching in Reverse Shoulder Arthroplasty
 An Original Study Assessment of Scapular Morphology and Surgical Technique as Predictors of Notching in Reverse Shoulder Arthroplasty Vani Sabesan, MD, Mark Callanan, MD, Vinay Sharma, BA, and J. Michael
An Original Study Assessment of Scapular Morphology and Surgical Technique as Predictors of Notching in Reverse Shoulder Arthroplasty Vani Sabesan, MD, Mark Callanan, MD, Vinay Sharma, BA, and J. Michael
Reverse Total Shoulder Arthroplasty Improves Function in Cuff Tear Arthropathy
 Clin Orthop Relat Res (2011) 469:2476 2482 DOI 10.1007/s11999-010-1683-z SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Reverse Total Shoulder Arthroplasty Improves Function in Cuff Tear Arthropathy Betsy
Clin Orthop Relat Res (2011) 469:2476 2482 DOI 10.1007/s11999-010-1683-z SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Reverse Total Shoulder Arthroplasty Improves Function in Cuff Tear Arthropathy Betsy
Balgrist Shoulder Course 2017
 Diagnosis and Management of Infection in Revision Shoulder Arthroplasty Joseph P. Iannotti MD, PhD Maynard Madden Professor and Chairman Orthopaedic and Rheumatologic Institute Cleveland Clinic Conflict
Diagnosis and Management of Infection in Revision Shoulder Arthroplasty Joseph P. Iannotti MD, PhD Maynard Madden Professor and Chairman Orthopaedic and Rheumatologic Institute Cleveland Clinic Conflict
Reverse shoulder arthroplasty for the treatment of three and four part fractures of the proximal humerus in patients older than 75 years old
 Acta Orthop. Belg., 2014, 80, 99-105 ORIGINAL STUDY Reverse shoulder arthroplasty for the treatment of three and four part fractures of the proximal humerus in patients older than 75 years old Aristotelis
Acta Orthop. Belg., 2014, 80, 99-105 ORIGINAL STUDY Reverse shoulder arthroplasty for the treatment of three and four part fractures of the proximal humerus in patients older than 75 years old Aristotelis
Prosthetic design of reverse shoulder arthroplasty contributes to scapular notching and instability
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v7.i11.738 World J Orthop 2016 November 18; 7(11): 738-745 ISSN 2218-5836 (online)
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v7.i11.738 World J Orthop 2016 November 18; 7(11): 738-745 ISSN 2218-5836 (online)
Reverse shoulder arthroplasty : Does reduced medialisation improve radiological and clinical results?
 Acta Orthop. Belg., 2009, 75, 158-166 ORIGINAL STUDY Reverse shoulder arthroplasty : Does reduced medialisation improve radiological and clinical results? Ibrahim KALOUCHE, Nuno SEVIVAS, Abhijeet WAHEGAONKER,
Acta Orthop. Belg., 2009, 75, 158-166 ORIGINAL STUDY Reverse shoulder arthroplasty : Does reduced medialisation improve radiological and clinical results? Ibrahim KALOUCHE, Nuno SEVIVAS, Abhijeet WAHEGAONKER,
Management of arthritis of the shoulder. Omar Haddo Consultant Orthopaedic Surgeon
 Management of arthritis of the shoulder Omar Haddo Consultant Orthopaedic Surgeon Diagnosis Pain - with activity initially. As disease progresses night pain is common and sleep difficult Stiffness trouble
Management of arthritis of the shoulder Omar Haddo Consultant Orthopaedic Surgeon Diagnosis Pain - with activity initially. As disease progresses night pain is common and sleep difficult Stiffness trouble
Evaluating Scapular Notching after Reverse Total Shoulder Arthroplasty
 ORIGINAL ARTICLE Clinics in Shoulder and Elbow Vol. 18, No. 4, December, 2015 http://dx.doi.org/10.5397/cise.2015.18.4.248 CiSE Clinics in Shoulder and Elbow Evaluating Scapular Notching after Reverse
ORIGINAL ARTICLE Clinics in Shoulder and Elbow Vol. 18, No. 4, December, 2015 http://dx.doi.org/10.5397/cise.2015.18.4.248 CiSE Clinics in Shoulder and Elbow Evaluating Scapular Notching after Reverse
Bilateral Anatomic Total Shoulder Arthroplasty Versus Reverse Shoulder Arthroplasty
 Bilateral Anatomic Total Shoulder Arthroplasty Versus Reverse Shoulder Arthroplasty Vaqar Latif, MD; Patrick J. Denard, MD; Allan A. Young, MD; Jean-Pierre Liotard, MD; Gilles Walch, MD abstract Full article
Bilateral Anatomic Total Shoulder Arthroplasty Versus Reverse Shoulder Arthroplasty Vaqar Latif, MD; Patrick J. Denard, MD; Allan A. Young, MD; Jean-Pierre Liotard, MD; Gilles Walch, MD abstract Full article
Integra. Titan Modular Shoulder System, 2.5
 Titan Modular Shoulder System, 2.5 Limit uncertainty with a shoulder implant system that redefines modularity, addresses multiple indications, and allows for reproducible results. Titan Modular Shoulder
Titan Modular Shoulder System, 2.5 Limit uncertainty with a shoulder implant system that redefines modularity, addresses multiple indications, and allows for reproducible results. Titan Modular Shoulder
Are too many reverse TSAs being done? Problems it is causing
 Are too many reverse TSAs being done? Problems it is causing Hithem Rahmi, DO John Itamura, MD The Kerlan Jobe Orthopaedic Clinic Professor of Orthopaedic Surgery Keck School of Medicine University of
Are too many reverse TSAs being done? Problems it is causing Hithem Rahmi, DO John Itamura, MD The Kerlan Jobe Orthopaedic Clinic Professor of Orthopaedic Surgery Keck School of Medicine University of
P. Trouilloud M. Gonzalvez P. Martz H. Charles F. Handelberg R. W. Nyffeler E. Baulot DuocentricÒ Group
 DOI 10.1007/s00590-013-1213-2 ORIGINAL ARTICLE Duocentric Ò reversed shoulder prosthesis and Personal Fit Ò templates: innovative strategies to optimize prosthesis positioning and prevent scapular notching
DOI 10.1007/s00590-013-1213-2 ORIGINAL ARTICLE Duocentric Ò reversed shoulder prosthesis and Personal Fit Ò templates: innovative strategies to optimize prosthesis positioning and prevent scapular notching
Effect of Prosthesis Design on Muscle Length and Moment Arms in Reverse Total Shoulder Arthroplasty
 S31 Effect of Prosthesis Design on Muscle Length and Moment Arms in Reverse Total Shoulder Arthroplasty Matthew A. Hamilton, Ph.D., Christopher P. Roche, M.S., M.B.A., Phong Diep, B.S., Pierre- Henri Flurin,
S31 Effect of Prosthesis Design on Muscle Length and Moment Arms in Reverse Total Shoulder Arthroplasty Matthew A. Hamilton, Ph.D., Christopher P. Roche, M.S., M.B.A., Phong Diep, B.S., Pierre- Henri Flurin,
Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty
 Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
The Irreparable Rotator Cuff Tear:
 The Irreparable Rotator Cuff Tear: Trauma 101: Shoulder Session #2 Brian Grawe, MD Assistant Professor Orthopaedics & Sports Medicine 5/10/2018 Brian Grawe, MD Assistant Professor Phone Number: 513-558-4516
The Irreparable Rotator Cuff Tear: Trauma 101: Shoulder Session #2 Brian Grawe, MD Assistant Professor Orthopaedics & Sports Medicine 5/10/2018 Brian Grawe, MD Assistant Professor Phone Number: 513-558-4516
Percutaneous Fluoroscopic Synovial Biopsy as a New Diagnostic Test for Periprosthetic Infection after Shoulder Arthroplasty: A Feasibility Study
 Percutaneous Fluoroscopic Synovial Biopsy as a New Diagnostic Test for Periprosthetic Infection after Shoulder Arthroplasty: A Feasibility Study J Quon, K Hynes, P Lapner, A Sheikh The Ottawa Hospital
Percutaneous Fluoroscopic Synovial Biopsy as a New Diagnostic Test for Periprosthetic Infection after Shoulder Arthroplasty: A Feasibility Study J Quon, K Hynes, P Lapner, A Sheikh The Ottawa Hospital
Scapular Notching. Recognition and Strategies to Minimize Clinical Impact. Gregory P. Nicholson MD, Eric J. Strauss MD, Seth L.
 Clin Orthop Relat Res DOI 10.1007/s11999-010-1720-y SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Scapular Notching Recognition and Strategies to Minimize Clinical Impact Gregory P. Nicholson MD, Eric
Clin Orthop Relat Res DOI 10.1007/s11999-010-1720-y SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Scapular Notching Recognition and Strategies to Minimize Clinical Impact Gregory P. Nicholson MD, Eric
Optimizing Deltoid Efficiency with Reverse Shoulder Arthroplasty Using a Novel Inset Center of Rotation Glenosphere Design
 S37 Optimizing Deltoid Efficiency with Reverse Shoulder Arthroplasty Using a Novel Inset Center of Rotation Glenosphere Design Christopher P. Roche, M.S., M.B.A., Matthew A. Hamilton, Ph.D., Phong Diep,
S37 Optimizing Deltoid Efficiency with Reverse Shoulder Arthroplasty Using a Novel Inset Center of Rotation Glenosphere Design Christopher P. Roche, M.S., M.B.A., Matthew A. Hamilton, Ph.D., Phong Diep,
Developments in Shoulder Arthroplasty
 Developments in Shoulder Arthroplasty Andrew L. Wallace PhD MFSEM FRCS FRACS Consultant Shoulder Surgeon Glenohumeral Joint Arthritis Relatively uncommon Not as common as hip/knee/hand UK National Joint
Developments in Shoulder Arthroplasty Andrew L. Wallace PhD MFSEM FRCS FRACS Consultant Shoulder Surgeon Glenohumeral Joint Arthritis Relatively uncommon Not as common as hip/knee/hand UK National Joint
Reverse Prostheses in Arthropathies With Cuff Tear
 Clin Orthop Relat Res (2011) 469:2469 2475 DOI 10.1007/s11999-011-1833-y SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Reverse Prostheses in Arthropathies With Cuff Tear Are Survivorship and Function
Clin Orthop Relat Res (2011) 469:2469 2475 DOI 10.1007/s11999-011-1833-y SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Reverse Prostheses in Arthropathies With Cuff Tear Are Survivorship and Function
SHOULDER ARTHROPLASTY (TOTAL, HEMI, REVERSE)/ARTHRODESIS
 evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
Matthew D. Saltzman, MD a, Deana M. Mercer, MD c, Winston J. Warme, MD b, Alexander L. Bertelsen, PA-C b, Frederick A. Matsen III, MD b, *
 J Shoulder Elbow Surg (2010) 19, 1028-1033 www.elsevier.com/locate/ymse A method for documenting the change in center of rotation with reverse total shoulder arthroplasty and its application to a consecutive
J Shoulder Elbow Surg (2010) 19, 1028-1033 www.elsevier.com/locate/ymse A method for documenting the change in center of rotation with reverse total shoulder arthroplasty and its application to a consecutive
Shoulder Replacement Commonly Asked Questions
 Shoulder Replacement Commonly Asked Questions Patrick J Denard, MD Shoulder Specialist 2780 E. Barnett Rd Medford, OR 97530 541-779-6250 Background Information What is the anatomy of the shoulder? The
Shoulder Replacement Commonly Asked Questions Patrick J Denard, MD Shoulder Specialist 2780 E. Barnett Rd Medford, OR 97530 541-779-6250 Background Information What is the anatomy of the shoulder? The
Managing acromial fractures: prevention and treatment, both nonoperative and operative
 Review Article Page 1 of 8 Managing acromial fractures: prevention and treatment, both nonoperative and operative Christopher D. Joyce, Adam J. Seidl Department of Orthopaedics, University of Colorado,
Review Article Page 1 of 8 Managing acromial fractures: prevention and treatment, both nonoperative and operative Christopher D. Joyce, Adam J. Seidl Department of Orthopaedics, University of Colorado,
Influence of Glenosphere Design on Outcomes and Complications of Reverse Arthroplasty: A Systematic Review
 Original Article Clinics in Orthopedic Surgery 2016;8:288-297 http://dx.doi.org/10.4055/cios.2016.8.3.288 Influence of Glenosphere Design on Outcomes and Complications of Reverse Arthroplasty: A Systematic
Original Article Clinics in Orthopedic Surgery 2016;8:288-297 http://dx.doi.org/10.4055/cios.2016.8.3.288 Influence of Glenosphere Design on Outcomes and Complications of Reverse Arthroplasty: A Systematic
Cigna Medical Coverage Policies Musculoskeletal Shoulder Arthroplasty (Total, Hemi, Reverse)/Arthrodesis
 Cigna Medical Coverage Policies Musculoskeletal Shoulder Arthroplasty (Total, Hemi, Reverse)/Arthrodesis Effective January 1, 2016 Instructions for use The following coverage policy applies to health benefit
Cigna Medical Coverage Policies Musculoskeletal Shoulder Arthroplasty (Total, Hemi, Reverse)/Arthrodesis Effective January 1, 2016 Instructions for use The following coverage policy applies to health benefit
Shoulder hemiarthroplasty in the management of humeral head fractures
 Acta Orthop. Belg., 2004, 70, 214-218 ORIGINAL STUDY Shoulder hemiarthroplasty in the management of humeral head fractures Joseph J. CHRISTOFORAKIS, George M. KONTAKIS, Pavlos G. KATONIS, Konstantinos
Acta Orthop. Belg., 2004, 70, 214-218 ORIGINAL STUDY Shoulder hemiarthroplasty in the management of humeral head fractures Joseph J. CHRISTOFORAKIS, George M. KONTAKIS, Pavlos G. KATONIS, Konstantinos
CLINICAL GUIDELINES. CMM-318: Shoulder Arthroplasty/ Replacement/Resurfacing/ Revision/Arthrodesis. Version Effective October 22, 2018
 CLINICAL GUIDELINES CMM-318: / Replacement/Resurfacing/ Revision/Arthrodesis Version 20.0.2018 Effective October 22, 2018 Clinical guidelines for medical necessity review of speech therapy services. CMM-318:
CLINICAL GUIDELINES CMM-318: / Replacement/Resurfacing/ Revision/Arthrodesis Version 20.0.2018 Effective October 22, 2018 Clinical guidelines for medical necessity review of speech therapy services. CMM-318:
Common Shoulder Problems and Treatment Options. Benjamin W. Szerlip D.O. Austin Shoulder Institute
 Common Shoulder Problems and Treatment Options Benjamin W. Szerlip D.O. Austin Shoulder Institute Speaker Disclosure Dr. Szerlip has disclosed that he has no actual or potential conflict of interest in
Common Shoulder Problems and Treatment Options Benjamin W. Szerlip D.O. Austin Shoulder Institute Speaker Disclosure Dr. Szerlip has disclosed that he has no actual or potential conflict of interest in
RCR or rtsa? Massive Rotator Cuff Tears without Arthritis in Patients Older than 65 Reverse Total Shoulder Arthroplasty or Rotator Cuff Repair?
 Massive Rotator Cuff Tears without Arthritis in Patients Older than 65 Reverse Total Shoulder Arthroplasty or Rotator Cuff Repair? JESSE W. ALLERT, MD THOMAS SELLERS, MD PETER SIMON, PHD RACHEL CLARK,
Massive Rotator Cuff Tears without Arthritis in Patients Older than 65 Reverse Total Shoulder Arthroplasty or Rotator Cuff Repair? JESSE W. ALLERT, MD THOMAS SELLERS, MD PETER SIMON, PHD RACHEL CLARK,
Assessment of Approximate Glenoid Size in Thai People
 Assessment of Approximate Glenoid Size in Thai People J Med Assoc Thai 2014; 97 (Suppl. 2): S14-S18 Full text. e-journal: http://www.jmatonline.com Pason Phonphok MD*, Nattha Kulkamthorn MD* * Division
Assessment of Approximate Glenoid Size in Thai People J Med Assoc Thai 2014; 97 (Suppl. 2): S14-S18 Full text. e-journal: http://www.jmatonline.com Pason Phonphok MD*, Nattha Kulkamthorn MD* * Division
Shoulder Injuries: Treatments that Work, Do Not Work, and When ENOUGH is Enough? Mark Ganjianpour, M.D. Beverly Hills, CA April 20, 2012
 Shoulder Injuries: Treatments that Work, Do Not Work, and When ENOUGH is Enough? Mark Ganjianpour, M.D. Beverly Hills, CA April 20, 2012 Multiaxial ball and socket Little Inherent Instability Glenohumeral
Shoulder Injuries: Treatments that Work, Do Not Work, and When ENOUGH is Enough? Mark Ganjianpour, M.D. Beverly Hills, CA April 20, 2012 Multiaxial ball and socket Little Inherent Instability Glenohumeral
What are the options for shoulder replacement today?
 Derek Plausinis, MASC, MD, FRCSC What are the options for shoulder replacement today? Anatomic total shoulder replacement continues to provide excellent outcomes in cases of advanced osteoarthritis, while
Derek Plausinis, MASC, MD, FRCSC What are the options for shoulder replacement today? Anatomic total shoulder replacement continues to provide excellent outcomes in cases of advanced osteoarthritis, while
what you is back within LOVE arm s reach find out why the exactech shoulder may be right for you
 TOTAL shoulder REPLACEMENT what you is back within LOVE arm s reach find out why the exactech shoulder may be right for you how does your shoulder work? The shoulder is the most mobile joint in the body.
TOTAL shoulder REPLACEMENT what you is back within LOVE arm s reach find out why the exactech shoulder may be right for you how does your shoulder work? The shoulder is the most mobile joint in the body.
Not relevant to this presentation.
 Nolan R. May, MD Kearney, NE Heartland Surgery Center, Kearney NE Not relevant to this presentation. 1 What are the indications for total shoulder arthroplasty? What are the differences between total shoulder
Nolan R. May, MD Kearney, NE Heartland Surgery Center, Kearney NE Not relevant to this presentation. 1 What are the indications for total shoulder arthroplasty? What are the differences between total shoulder
Reverse Total Shoulder. Dr. Minoo Patel
 Reverse Total Shoulder Dr. Minoo Patel AOA VIC, Lorne, 2011 The role of the rotator cuff Depress and humeral head (against the force of the deltoid) Keep the humeral head co-apted in the glenoid Initiate
Reverse Total Shoulder Dr. Minoo Patel AOA VIC, Lorne, 2011 The role of the rotator cuff Depress and humeral head (against the force of the deltoid) Keep the humeral head co-apted in the glenoid Initiate
Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
The Deltopectoral Approach for Reverse Shoulder Arthroplasty
 The Deltopectoral Approach for Reverse Shoulder Arthroplasty George M. McCluskey III, MD, and Howard D. Routman, DO Director, St. Francis Shoulder Center, St. Francis Orthopaedic Institute, Columbus, Georgia
The Deltopectoral Approach for Reverse Shoulder Arthroplasty George M. McCluskey III, MD, and Howard D. Routman, DO Director, St. Francis Shoulder Center, St. Francis Orthopaedic Institute, Columbus, Georgia
Massive Rotator Cuff Tears. Rafael M. Williams, MD
 Massive Rotator Cuff Tears Rafael M. Williams, MD Rotator Cuff MRI MRI Small / Partial Thickness Medium Tear Arthroscopic View Massive Tear Fatty Atrophy Arthroscopic View MassiveTears Tear is > 5cm
Massive Rotator Cuff Tears Rafael M. Williams, MD Rotator Cuff MRI MRI Small / Partial Thickness Medium Tear Arthroscopic View Massive Tear Fatty Atrophy Arthroscopic View MassiveTears Tear is > 5cm
Reverse Total Shoulder Arthroplasty Protocol
 General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD
 Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
The Reverse Total Shoulder Arthroplasty
 This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. The Reverse Total Shoulder Arthroplasty Frederick A. Matsen, III, Pascal
This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. The Reverse Total Shoulder Arthroplasty Frederick A. Matsen, III, Pascal
Reverse Shoulder Arthroplasty A Literature Review
 Send Orders for Reprints to reprints@benthamscience.net 366 The Open Orthopaedics Journal, 2013, 7, (Suppl 3: M13) 366-372 Reverse Shoulder Arthroplasty A Literature Review Open Access Aatif Mahmood, Joby
Send Orders for Reprints to reprints@benthamscience.net 366 The Open Orthopaedics Journal, 2013, 7, (Suppl 3: M13) 366-372 Reverse Shoulder Arthroplasty A Literature Review Open Access Aatif Mahmood, Joby
Biomechanical Impact of Posterior Glenoid Wear on Anatomic Total Shoulder Arthroplasty
 S5 Biomechanical Impact of Posterior Glenoid Wear on Anatomic Total Shoulder Arthroplasty Christopher P. Roche, M.S., M.B.A., Phong Diep, B.S., Sean G. Grey, M.D., and Pierre-Henri Flurin, M.D. Abstract
S5 Biomechanical Impact of Posterior Glenoid Wear on Anatomic Total Shoulder Arthroplasty Christopher P. Roche, M.S., M.B.A., Phong Diep, B.S., Sean G. Grey, M.D., and Pierre-Henri Flurin, M.D. Abstract
JRI Thompson Hemiarthroplasty
 JRI ORTHOPAEDICS LTD 18 Churchill Way, 35A Business Park, Chapeltown, Sheffield, S35 2PY, UK Instructions for Use JRI Thompson Hemiarthroplasty Page 1 of 6 English 3 Page 2 of 6 Important Information Please
JRI ORTHOPAEDICS LTD 18 Churchill Way, 35A Business Park, Chapeltown, Sheffield, S35 2PY, UK Instructions for Use JRI Thompson Hemiarthroplasty Page 1 of 6 English 3 Page 2 of 6 Important Information Please
Total Shoulder Arthroplasty
 1 Total Shoulder Arthroplasty Surgical indications and contraindications Anatomical Considerations: Total shoulder arthroplasty surgery involves the replacement of the humeral head and the glenoid articulating
1 Total Shoulder Arthroplasty Surgical indications and contraindications Anatomical Considerations: Total shoulder arthroplasty surgery involves the replacement of the humeral head and the glenoid articulating
Should We Really be Performing HHR for Proximal Humeral Fractures Anymore?
 Should We Really be Performing HHR for Proximal Humeral Fractures Anymore? Anthony A. Romeo, MD Professor, Dept. of Orthopaedic Surgery Head, Section of Shoulder and Elbow Rush University Medical Center
Should We Really be Performing HHR for Proximal Humeral Fractures Anymore? Anthony A. Romeo, MD Professor, Dept. of Orthopaedic Surgery Head, Section of Shoulder and Elbow Rush University Medical Center
Reverse Total Shoulder Protocol
 Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
continued TABLE E-1 Potential Predictors of Short-Term Complications and Reoperations* Comparison Group OR 95% CI P Value
 Page 1 of 7 TABLE E-1 Potential Predictors of Short-Term Complications and Reoperations* Pulmonary embolism Charlson comorbidity index 1.2 1.0 to 1.4 0.06 Hospital volume percentile, 40-79 80-100 0.8 0.4
Page 1 of 7 TABLE E-1 Potential Predictors of Short-Term Complications and Reoperations* Pulmonary embolism Charlson comorbidity index 1.2 1.0 to 1.4 0.06 Hospital volume percentile, 40-79 80-100 0.8 0.4
Reverse arthroplasty of the shoulder for treating rotator cuff arthropathy,
 rev bras ortop. 2014;49(3):279 285 www.rbo.org.br Original Article Reverse arthroplasty of the shoulder for treating rotator cuff arthropathy, Marcus Vinicius Galvão Amaral, José Leonardo Rocha de Faria,
rev bras ortop. 2014;49(3):279 285 www.rbo.org.br Original Article Reverse arthroplasty of the shoulder for treating rotator cuff arthropathy, Marcus Vinicius Galvão Amaral, José Leonardo Rocha de Faria,
Index. B Backslap technique depth assessment, 82, 83 diaphysis distal trocar, 82 83
 Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
Results of a stemless reverse shoulder prosthesis at more than 58 months mean without loosening
 J Shoulder Elbow Surg (2013) 22, e1-e6 www.elsevier.com/locate/ymse Results of a stemless reverse shoulder prosthesis at more than 58 months mean without loosening Richard Ballas, MD a, *, Laurent Beguin,
J Shoulder Elbow Surg (2013) 22, e1-e6 www.elsevier.com/locate/ymse Results of a stemless reverse shoulder prosthesis at more than 58 months mean without loosening Richard Ballas, MD a, *, Laurent Beguin,
Comparison of Pegged and Keeled Glenoid Components for Total Shoulder Arthroplasty: A Systematic Review
 Review Article Comparison of Pegged and Keeled Glenoid Components for Total Shoulder Arthroplasty: A Systematic Review Journal of Shoulder and Elbow Arthroplasty Volume 1: 1 7! The Author(s) 2017 Reprints
Review Article Comparison of Pegged and Keeled Glenoid Components for Total Shoulder Arthroplasty: A Systematic Review Journal of Shoulder and Elbow Arthroplasty Volume 1: 1 7! The Author(s) 2017 Reprints
WHAT YOU IS BACK WITHIN ARM S REACH
 YOUR TOTAL SHOULDER REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE WHAT YOU IS BACK WITHIN ARM S REACH Nathan Richardson, MD Orthopedics, Shoulder & Elbow Surgeon Board Certified in
YOUR TOTAL SHOULDER REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE WHAT YOU IS BACK WITHIN ARM S REACH Nathan Richardson, MD Orthopedics, Shoulder & Elbow Surgeon Board Certified in
Revision of total shoulder arthroplasty
 Orthopaedics & Traumatology: Surgery & Research (2013) 99S, S12 S21 Available online at www.sciencedirect.com REVIEW ARTICLE Revision of total shoulder arthroplasty L. Favard Orthopaedic and Trauma Surgery,
Orthopaedics & Traumatology: Surgery & Research (2013) 99S, S12 S21 Available online at www.sciencedirect.com REVIEW ARTICLE Revision of total shoulder arthroplasty L. Favard Orthopaedic and Trauma Surgery,
TORNIER AEQUALIS FX. Shoulder System SYSTEM OVERVIEW
 TORNIER AEQUALIS FX Shoulder System SYSTEM OVERVIEW Simple in design, but used for the most complex fractures Each year, approximately 4 million people in the United States seek medical care for shoulder
TORNIER AEQUALIS FX Shoulder System SYSTEM OVERVIEW Simple in design, but used for the most complex fractures Each year, approximately 4 million people in the United States seek medical care for shoulder
What s New in the Treatment of Proximal Humerus Fractures?
 NHMI Winter Meeting Stowe, VT January 2015 What s New in the Treatment of Proximal Humerus Fractures? John Bell, M.D., M.S. Associate Professor Shoulder and Elbow Surgery Dartmouth-Hitchcock Medical Center
NHMI Winter Meeting Stowe, VT January 2015 What s New in the Treatment of Proximal Humerus Fractures? John Bell, M.D., M.S. Associate Professor Shoulder and Elbow Surgery Dartmouth-Hitchcock Medical Center
Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow.
 Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow. Prepared for The Canadian Orthopaedic Association Contents Executive
Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow. Prepared for The Canadian Orthopaedic Association Contents Executive
Hemiarthroplasty Versus Reverse Total Shoulder Arthroplasty for Acute Proximal Humerus Fractures in Elderly Patients
 Hemiarthroplasty Versus Reverse Total Shoulder Arthroplasty for Acute Proximal Humerus Fractures in Elderly Patients Grant E. Garrigues, MD; Peter S. Johnston, MD; Matthew D. Pepe, MD; Bradford S. Tucker,
Hemiarthroplasty Versus Reverse Total Shoulder Arthroplasty for Acute Proximal Humerus Fractures in Elderly Patients Grant E. Garrigues, MD; Peter S. Johnston, MD; Matthew D. Pepe, MD; Bradford S. Tucker,
Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD
 General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
Proximal Humeral Fractures RSA v HHR. Proximal Humeral Fractures RSA v HHR. Introduction
 Proximal Humeral Fractures RSA v HHR Xavier A. Duralde, MD Peachtree Orthopaedic Clinic Atlanta, GA Proximal Humeral Fractures RSA v HHR Consultant: Smith+Nephew Board of Directors: CORR Introduction Incidence
Proximal Humeral Fractures RSA v HHR Xavier A. Duralde, MD Peachtree Orthopaedic Clinic Atlanta, GA Proximal Humeral Fractures RSA v HHR Consultant: Smith+Nephew Board of Directors: CORR Introduction Incidence
ISSUES FROM AN ORTHOPEDIC PERSPECTIVE
 ISSUES FROM AN ORTHOPEDIC PERSPECTIVE John Brown, MD The Core Institute Objectives: Understand the common orthopedic problems of the geriatric population. Describe the standard treatment algorithms for
ISSUES FROM AN ORTHOPEDIC PERSPECTIVE John Brown, MD The Core Institute Objectives: Understand the common orthopedic problems of the geriatric population. Describe the standard treatment algorithms for
Current designs and trends in reverse shoulder arthroplasty
 Page 1 of 7 Surgical Procedures NP Sachinis*, P Athanasiadou Current designs and trends in reverse shoulder arthroplasty Abstract Introduction The need for finding a suitable treatment for patients suffering
Page 1 of 7 Surgical Procedures NP Sachinis*, P Athanasiadou Current designs and trends in reverse shoulder arthroplasty Abstract Introduction The need for finding a suitable treatment for patients suffering
DESIGN RATIONALE AND SURGICAL TECHNIQUE
 DESIGN RATIONALE AND SURGICAL TECHNIQUE ANCHOR PEG GLENOID DESIGN RATIONALE In total shoulder arthroplasty, most cases of clinical and radiographic loosening involve failure of the fixation of the glenoid
DESIGN RATIONALE AND SURGICAL TECHNIQUE ANCHOR PEG GLENOID DESIGN RATIONALE In total shoulder arthroplasty, most cases of clinical and radiographic loosening involve failure of the fixation of the glenoid
Delta III reverse shoulder arthroplasty in the treatment of complex 3- and 4-part fractures of the proximal humerus: 6 to 42 months of follow up
 Mattiassich et al. BMC Musculoskeletal Disorders 2013, 14:231 RESEARCH ARTICLE Open Access Delta III reverse shoulder arthroplasty in the treatment of complex 3- and 4-part fractures of the proximal humerus:
Mattiassich et al. BMC Musculoskeletal Disorders 2013, 14:231 RESEARCH ARTICLE Open Access Delta III reverse shoulder arthroplasty in the treatment of complex 3- and 4-part fractures of the proximal humerus:
S1 Shoulder. Primary. MDS VERSION 7.0 Shoulder Operation. Form: MDSv7.0 S1 v1.0. Patient Addressograph
 S1 Shoulder Primary Important: Please tick relevant boxes. All component stickers should be affixed to the accompanying Minimum Dataset Form Component Labels Sheet. Please ensure that all sheets are stapled
S1 Shoulder Primary Important: Please tick relevant boxes. All component stickers should be affixed to the accompanying Minimum Dataset Form Component Labels Sheet. Please ensure that all sheets are stapled
