To diagnose any disease or disorder implies. The Diagnosis and Initial Treatment of Patellofemoral Disorders. A Review Paper
|
|
|
- Amy Lawrence
- 5 years ago
- Views:
Transcription
1 A Review Paper The Diagnosis and Initial Treatment of Patellofemoral Disorders Alan C. Merchant, MD, MS, John P. Fulkerson, MD, and Wayne Leadbetter, MD Abstract Our purpose is to provide simple guidelines for the diagnosis and early care of patellofemoral disorders. Any clinician who treats knee problems, including family practitioners, rheumatologists, orthopedic surgeons, or physical therapists, must know how to make the correct diagnosis, or at least a presumptive diagnosis, at the initial visit. This can avoid unneeded and costly tests, ineffective treatment, and even damaging exercises and unnecessary surgery. The diagnosis of patellofemoral disorders is confusing because they can have many causes. That is, the etiology of patellofemoral disorders is multifactorial. To dispel this confusion and simplify the process, we use a clinical classification based on etiology. Within that framework are 7 key abnormalities or factors that can cause both patellofemoral pain and instability: vastus medialis obliquus deficiency, medial patellofemoral ligament laxity, lateral retinaculum tightness, increased quadriceps angle, hip abductor weakness, patella alta, and trochlear dysplasia. At the initial evaluation, the clinician can assess for these abnormalities through history-taking, physical examination, and standard radiography. Any abnormalities identified, along with their severity, can be used to arrive at a diagnosis, or a presumptive diagnosis, and begin early nonoperative treatment. The clinician does not need magnetic resonance imaging at this point, unless a presumptive diagnosis cannot be made or a more complex problem is suggested. Take-Home Points Patellofemoral disorders should be classified and diagnosed according to specific diagnostic categories (eg, lateral patellar compression syndrome) based on etiology rather than nondescriptive terminology (eg, internal derangement, patellofemoral pain syndrome). Patellofemoral dysplasia defines a spectrum of abnormalities ranging from the mild lateral patellar compression syndrome to the severe recurrent patellar dislocation. There is an inverse relationship between patient activity level and underlying patellofemoral dysplasia. This relationship determines threshold levels for each patient becoming symptomatic. Patients should be examined for 7 physical abnormalities, and if present, in what severity. These 7 are: vastus medialis obliquus deficiency, medial patellofemoral ligament laxity, lateral retinaculum tightness, increased quadriceps angle, hip abductor weakness, patella alta, and trochlear dysplasia. Advanced imaging is rarely, if ever, needed to make a diagnosis or to formulate an initial treatment plan for these common patellofemoral disorders. To diagnose any disease or disorder implies an understanding of the condition s cause(s), which should then lead to a logical treatment plan. For all too long, however, the diagnosis and treatment of patellofemoral disorders have been hampered by diagnoses that lack specific definitions based on etiology. A few of these are: internal derangement, chondromalacia patellae, patellar maltracking, and patellofemoral pain syndrome. To simplify the diagnosis of patellofemoral disorders, we use a clinical classification based on etiology. This system s defined diagnostic categories are useful in identifying probable cause(s), which can be appropriately evaluated and treated (Table). 1 In simple terms, the philosophy of this approach is to try to find out what s wrong, and try to fix it! This clinical classification provides a framework for common patellofemoral conditions that are more easily diagnosed, yet is intentionally Authors Disclosure Statement: The authors report no actual or potential conflict of interest in relation to this article. 68 The American Journal of Orthopedics March/April
2 Table. Clinical Classification of Patellofemoral Disorders a incomplete omitting rare conditions (eg, tumors, metabolic bone disease, neurologic conditions). This allows the focus to fall on the common and frequently misunderstood causes for patellofemoral pain and instability. In this article, we address patellofemoral dysplasia (section II of the Table) and its classification relating to initial evaluation and early treatment. This entity defines a spectrum of abnormalities, ranging from the mild lateral patellar compression syndrome (LPCS) to the moderate chronic subluxation of the patella (CSP) and severe recurrent dislocation of the patella (RDP). Each presumptive diagnosis is suggested by the patient s history and confirmed by physical examination and radiography. Computed tomography (CT), magnetic resonance imaging (MRI), and other advanced imaging modalities are seldom needed to establish a working diagnosis and an initial treatment plan, though they can be important in operative planning for complex cases. Patellofemoral Dysplasia Patellofemoral dysplasia (or extensor mechanism malfunction) is a cluster of physical abnormalities relating to the patellofemoral joint that vary from mild to severe and affect the normal function of that joint. As such, patellofemoral dysplasia itself should be considered on a continuum of mild to severe. To simplify the diagnosis, the clinician should systematically identify these factors and their severity. Armed with this information, the clinician can make the diagnosis and formulate a logical treatment plan for each individual patient. This article focuses on 7 physical abnormalities that are most likely developmental and that can be identified through physical and radiologic examination. When and how each patient with patellofemoral dysplasia becomes symptomatic are determined by 2 key factors: patellofemoral dysplasia severity and activity level (sedentary to strenuous), in an inverse relationship (Figure 1). 2 Their complex interplay determines when a patient exceeds the envelope of function 3 and passes from asymptomatic to symptomatic. Seven Key Patellofemoral Physical Abnormalities Of the 7 commonly identified physical abnormalities that affect the normal functioning of the patellofemoral joint, 5 are discovered by physical examination and 2 by radiography; CT and MRI are seldom needed in the initial evaluation. The most accurate and objective method should be used to assess the presence and severity of each abnormality. I. Trauma (conditions caused by trauma in otherwise normal knee) A. Acute trauma 1. Contusion 2. Fracture a. Patella b. Femoral trochlea c. Proximal tibial epiphyses (tubercle) 3. Patellar dislocation (uncommon in normal knee) 4. Rupture a. Quadriceps tendon b. Patellar tendon B. Repetitive trauma (overuse syndromes) 1. Patellar tendinitis ( jumper s knee ) 2. Quadriceps tendinitis 3. Peripatellar tendinitis (eg, anterior knee pain in adolescents, caused by hamstring contracture) 4. Prepatellar bursitis ( housemaid s knee ) 5. Apophysitis a. Osgood-Schlatter disease b. Sinding-Larsen-Johansson disease C. Late effects of trauma 1. Posttraumatic patellar chondrosis 2. Posttraumatic patellofemoral arthrosis 3. Anterior fat pad syndrome, Hoffa syndrome (posttraumatic fibrosis) 4. Reflex sympathetic dystrophy of patella 5. Patellar osseous dystrophy 6. Acquired patella infera 7. Acquired quadriceps fibrosis II. Patellofemoral dysplasia (or extensor mechanism malfunction) A. Lateral patellar compression syndrome 1. Secondary patellar chondrosis 2. Secondary patellofemoral arthrosis B. Chronic subluxation of patella 1. Secondary patellar chondrosis 2. Secondary patellofemoral arthrosis C. Recurrent dislocation of patella 1. Associated fractures a. Osteochondral (intra-articular) b. Avulsion (extra-articular) 2. Secondary patellar chondrosis 3. Secondary patellofemoral arthrosis D. Chronic dislocation of patella 1. Developmental 2. Acquired III. Idiopathic patellar chondrosis IV. Osteochondritis dissecans A. Patella B. Femoral trochlea V. Synovial plicae (anatomical variants made symptomatic by acute or repetitive trauma) A. Pathologic medial patellar plica ( shelf ) B. Pathologic suprapatellar plica C. Pathologic lateral patellar plica VI. Iatrogenic disorders A. Iatrogenic medial patellar compression syndrome B. Iatrogenic recurrent medial subluxation of patella C. Iatrogenic patella infera a Modified from Arthroscopy. 1 March/April 2017 The American Journal of Orthopedics 69
3 The Diagnosis and Initial Treatment of Patellofemoral Disorders Competitive sports Activity Level Sedentary Mild Asymptomatic Threshold Symptomatic Patellofemoral Dysplasia Severe Figure 1. Diagram shows inverse relationship between severity of patellofemoral dysplasia and patient activity level. Relationship determines when any given patient will cross symptomatic threshold. Reprinted with permission from Operative Arthroscopy. 2 Figure 2. With quadriceps contracted holding knee at 30 flexion and with foot unsupported, deficient vastus medialis obliquus leaves characteristic hollow on medial aspect of knee. Reprinted with permission from Anterior Knee Pain and Patellar Instability. 4 The 7 abnormalities are vastus medialis obliquus (VMO) deficiency, medial patellofemoral ligament (MPFL) laxity, lateral retinaculum (LR) tightness, increased quadriceps (Q) angle, hip abductor weakness, patella alta, and trochlear dysplasia. We list these not in order of importance but in the order in which they are usually encountered during initial evaluation. We advocate for examining both knees including axial patellofemoral radiographs because patellofemoral disorders are frequently bilateral. It is helpful to use an abnormality checklist so none are forgotten. Also useful is a simple shorthand for findings: 0 = normal (no abnormality), 1 = mild abnormality, 2 = moderate abnormality, 3 = severe abnormality, with the right knee always recorded first (R/L). For example, severe left MPFL laxity is recorded as 0/3. Numerical values (eg, Q angles) can be directly recorded in this manner: 14 / Vastus Medialis Obliquus Deficiency VMO deficiency is best seen as the sitting patient actively maintains the unsupported foot and leg at 30 knee flexion. Normally, the VMO inserts into the upper half or third of the medial edge of the patella; a deficient VMO inserts higher into the medial edge of the quadriceps tendon, or it is absent and leaves a characteristic hollow at the medial edge of the patella (Figure 2). 4 Studies using ultrasonography and CT have found significant correlations between VMO abnormalities and anterior knee pain. 5,6 Although there is no simple clinical method of measuring VMO deficiency, clinicians experienced in observing knees can assess VMO deficiency and grade each case mild, moderate, or severe. The VMO deficiency weakens the medial quadriceps vector, increasing the lateral vector, and thereby increases the dynamic Q angle, originally described by Brattström Medial Patellofemoral Ligament Laxity MPFL laxity is assessed with the lateral glide test. Again, the patient sits, but with quadriceps relaxed and foot and leg supported at 30 knee flexion. With the clinician mentally dividing the patella into vertical quadrants and pushing the patella laterally, the normal patella moves about 1 quadrant or 1 fingerbreadth. Severe MPFL laxity often elicits a positive apprehension response during the test. (Tip: Many patients are unable to relax the quadriceps while sitting; therefore, examine them supine and lift the knee into 30 flexion.) Such laxity usually means the MPFL was torn in a previous dislocation and remains elongated, leaving the patella vulnerable to repeated dislocations. The clinician should be alert to the possibility of hyperelastosis (Ehlers-Danlos syndrome) and a hyper-mobile patella. The opposite limb should be evaluated for asymmetric laxity. 3. Lateral Retinaculum Tightness LR tightness is assessed with the medial glide test, again with the quadriceps relaxed and the knee supported at 30 flexion. With a normal LR, the patella can be pushed medially about 1 quadrant or 1 fingerbreadth. Some clinicians prefer the lateral tilt-up test, in which the lateral edge of the patella is lifted up, but this method is more difficult 70 The American Journal of Orthopedics March/April
4 A. C. Merchant et al to quantify, is affected by the cross-sectional shape of the patella, and lacks consistency. 4. Increased Quadriceps Angle The Q angle is one of the most important factors in the normal functioning of the patellofemoral joint. For more than a century, 8 multiple operations have been used successfully to move the tibial tubercle (TT) and patellar ligament from a lateral position to a medial position thereby decreasing the Q angle. It is only logical to measure this angle at every knee examination to check for an abnormal increase, and the degree. The term quadriceps angle, or Q angle, was first used in 1964 by Brattström, 7 who defined it as the supplemental angle to the valgus angle formed by the quadriceps resultant (line of force or vector) + patella + ligamentum patellae. This might be called the dynamic Q angle. With there being no clinical method of measuring the quadriceps line of force, or quadriceps vector, clinicians used a line from the anterior superior iliac spine to the center of the patella, yet still called it the Q angle. By convention, this anatomical Q angle has been accepted as the Q angle. Because the Q angle is the only clinical measurement of TT lateralization at initial evaluation, its measurement should be standardized, accurate, and simple to perform. Placing the patient supine with the lower limb in neutral rotation (patella anterior) and the knee in full extension standardizes the position. In full extension, the tibia reaches its maximum external rotation owing to the terminal screw home mechanism. The clinician should center the patella to the trochlear groove (TG) while measuring the Q angle, as it is the relationship of the TT to the trochlea, not to the patella, that is important. If LR tightness prevents the patella from centering, that fact should be recorded during the medial glide test for LR tightness. For accuracy, the goniometer should have one or more arms long enough to reach the anterior superior iliac spine. A long-armed goniometer is simple to make, and 2 extendable goniometers are commercially available (Figures 3A-3C). Despite the importance of measuring the Q angle, there has been no standard technique. Multiple authors have attempted to define the normal Q angle. In 1999, Post 9 reviewed 7 articles on the topic and found no agreement. Mean normal Q angles varied widely, from 5 to 23 (SD range, ). Grelsamer and colleagues, 10 using a long-armed goniometer and standard technique, A B C Figure 3. (A) Plastic goniometer glued accurately to 22-inch segment of yardstick. (B) Extendable pocket goniometer (GoPro Goniometer, PFJ Solutions). (C) Large extendable goniometer (Lafayette Gollehon Extendable Goniometer, Lafayette Instrument Company). found a mean Q angle of 15.7 for women and 13.3 for men; the small, 2.4 difference between them disappeared when the measurements were corrected for height. Men and women of similar height have similar Q angles. These findings disproved the common misattribution of the differences to the wider female pelvis. Given this confusion and the lack of accuracy in measuring the Q angle, many, if not most, surgeons turned to special CT and MRI scanning techniques to measure the distance of lateralization from TT to TG (TT-TG distance). This technique, by necessity, enforced a standardization not found in the earlier Q angles studies. Patients were positioned supine with the knee fully extended, and patellar position was ignored in favor of the TG. However, recent articles have called into question the accuracy and usefulness of TT-TG distance as an assessment of TT lateralization. As such, standardized measurement of the Q angle remains a simple, inexpensive, and clinically relevant March/April 2017 The American Journal of Orthopedics 71
5 The Diagnosis and Initial Treatment of Patellofemoral Disorders method of assessing TT lateralization. The possible causes of an increased Q angle are valgus limb alignment, internal femoral torsion, external tibial torsion, combined internal femoral and external tibial torsion with foot pronation (the miserable malalignment of James and colleagues 15 ), and a TT-lateralizing proximal tibial malformation. 5. Hip Abductor Weakness The step-down test is easily performed in the office by having the patient stand on a short stool or stair and then slowly step down with the opposite limb to just touch the heel and slowly arise again. A positive test is indicated by the Trendelenburg sign, with the pelvis dropping down and away from the symptomatic supporting limb, the flexing knee collapsing into valgus, and the patient tending to wobble and lack stability (Figure 4). 16 With mild hip abductor weakness, these changes can be subtle, but they may become more severe with increasing weakness. Khayambashi and colleagues 17 found that hip abductor weakness can be a major cause of patellofemoral pain. 6. Patella Alta Patella alta not only allows the patella to escape the confines of the trochlea earlier during active knee extension increasing the risk of patellar dislocation, but also decreases the contact footprint with the trochlea, increasing the patellofemoral joint reaction force and potentially causing patellofemoral pain and even secondary chondrosis. The simplest way to assess patellar height is with a lateral radiograph of the knee. The 3 popular methods (Insall-Salvati, Caton-Deschamps, Blackburn-Peel) all put the normal patellar height ratio at approximately 1:1, ± 20%. Berg and colleagues 18 compared radiologic techniques for measuring patellar height ratio and found that Blackburn-Peel was the most accurate, reliable, and reproducible method. 7. Trochlear Dysplasia Trochlear dysplasia, most simply a flattening of the TG, is perhaps the most important factor effecting normal patellofemoral function. However, it remains the most difficult to correctly address surgically. Senavongse and Amis 19 conducted a cadaveric study demonstrating the prime importance of the TG. They found patellar stability was reduced 30% by releasing the VMO, 49% by cutting the MPFL in full knee extension, and 70% by flattening the trochlea. The most common, successful operations for correcting patellar instability depend on changing other factors that guide patellar excursion to compensate for this trochlear flattening. A B Figure 4. Positive step-down test with pelvis tilting down and away from supporting limb (Trendelenburg sign) and supporting knee collapsing medially into valgus. Reprinted with permission from Pathology and Intervention in Musculoskeletal Rehabilitation. 16 C Figure 5. DeHaven exercises (progressive resistive quadriceps exercises in full extension). (A, B) Weight lifted by arms. (C) Leg fully extended to support weight for full 5 seconds. (D) Weight again supported by arms as knee is flexed to 90 without resistance. Reprinted with permission from The Patellofemoral Joint. 26 D 72 The American Journal of Orthopedics March/April
6 A. C. Merchant et al The simplest way to assess trochlear dysplasia is to measure the sulcus angle on an accurate axial view radiograph of the knee at 45 flexion (Merchant view). 20 Dejour and colleagues 21 popularized a technique of assessing and classifying trochlear dysplasia from a true lateral radiograph of the knee, which has the advantage of showing the trochlear at its proximal extent. Davies and colleagues 22 evaluated the Dejour technique, along with patellar tilt, patellar height, and sulcus angle, to identify a rapid and reproducible radiologic feature that would indicate the need for further analysis by other imaging studies (eg, CT, MRI). They found that, if the sulcus angle was normal, analysis of other radiologic features was unlikely to reveal additional useful information. They also showed a correlation of increasing sulcus angle and severity of those other dysplasia features. Merchant and colleagues 20 found a mean normal sulcus angle of 138º (SD, 6º; range, 126º-150º), and Aglietti and colleagues 23 confirmed those findings with nearly identical values (mean, 137º; SD, 6º; range, 116º-151º). Diagnosis and Initial Treatment Plan Patellofemoral disorders generally are divided into patellofemoral pain and instability, but these 2 diagnostic categories are too broad to be useful. Patellofemoral pain is a symptom. Patellofemoral pain syndrome should never be used as a diagnosis because there is no accepted definition for the cluster of findings that customarily defines a syndrome. At initial evaluation, after the easily diagnosed causes of anterior knee pain (eg, prepatellar bursitis, TT apophysitis, patellar and quadriceps tendinitis) have been ruled out, the clinician should consider types of patellofemoral dysplasia for a presumptive diagnosis, which will then lead to a logical treatment program for each identified disorder. With a presumptive diagnosis established, almost all patients suffering from chronic anterior knee pain without history of injury are treated initially with rest, ice, and nonsteroidal anti-inflammatory drugs to restore joint homeostasis. 3 Figure 6. Simple home technique for isometric progressive resistive quadriceps exercises with knee in full extension or straight-leg weight lifting. Reprinted with permission from Operative Orthopedics. 28 Lateral Patellar Compression Syndrome In 1975, Ficat and colleagues 24 described features of what they called syndrome d hyperpression externe de la rotule. Two years later, Ficat and Hungerford 25 defined the syndrome as one in which the patella is well centered in the trochlear sulcus and stable, but in which there is a functional lateralization onto a physiologically and often anatomically predominant lateral facet. Using the tools we have described here, the clinician usually finds the cause(s) of this functional lateralization. Four abnormalities VMO deficiency, LR tightness, increased standardized Q angle, and hip abductor weakness can cause functional lateralization either alone when severe or in combination when mild or moderate. For a presumptive diagnosis of LPCS, initial treatment is nonoperative, and successful in about 90% of patients. It should be obvious that most patients with chronic anterior knee pain have quadriceps atrophy. Physical therapy should be specifically focused on quadriceps strengthening, with absolutely no stress placed on the patellofemoral joint in flexion initially, and on hip abductor strengthening. Progressive resistive isometric quadriceps exercises can be performed with a weight-bench technique (Figures 5A-5D). 26 These isometric progressive resistive quadriceps (DeHaven 27 ) exercises can also be performed with a simple straight-leg weight-lifting program at home (Figure 6). 28 The advantage of isometric quadriceps strengthening is that the knee is in full extension, the patella lies above the trochlea, and there is no patellofemoral joint movement or compression. A patient of average stature can gradually increase quadriceps strength to resist or lift about 20 lb. Progressive hip abductor strengthening can be done in physical therapy or at home using side-lying abductor exercises with ankle weights. DeHaven 27 exercises should be painless when done correctly, but contraindicated in patients March/April 2017 The American Journal of Orthopedics 73
7 The Diagnosis and Initial Treatment of Patellofemoral Disorders with patellar tendinitis, quadriceps tendinitis, TT apophysitis (Osgood-Schlatter s), and anterior fat pad (Hoffa s) syndrome. When appropriate, certain adjunctive modalities for reducing functional lateralization should be tried. Use of McConnell taping and patellar bracing to resist this lateralization can be very helpful. If symptoms persist despite the 20-lb quadriceps goal being achieved and adequate hip abductor strength being demonstrated in a normal step-down test, conservative management has failed. Review and reassessment of the remaining abnormal physical factors (tight LR, increased Q angle) will lead to logical choices in surgical management. Chronic Subluxation of Patella With the use of axial patellofemoral radiographs (Merchant views), 20 the clinician can determine if the patella is well centered in the trochlear sulcus and stable (an important part of the definition of LPCS). If the patient has no symptoms of recurrent instability or patellar dislocation, and these radiographs show a laterally subluxed patella (one not well centered in the trochlea), the diagnosis is most likely CSP, a moderate form of patellofemoral dysplasia (section II of the Table). In addition to the 4 abnormalities used in the diagnosis of LPCS (mentioned earlier), trochlear dysplasia also comes into play in the diagnosis of CSP. Just as the other abnormalities can vary from mild to severe, trochlear dysplasia can vary from mild (slightly shallow sulcus angle) to severe (flat or even convex sulcus angle). As the sulcus becomes shallower, the patella slides more laterally, increasing the likelihood of patellar dislocation. As the patient with CSP gives no history of episodic patellar instability, treatment for CSP is almost identical to that for LPCS, with the primary focus on isometric quadriceps strengthening (DeHaven isometric exercises) 27 and hip abductor muscle strengthening. In the presence of CSP radiographically, it is important to use McConnell taping and/or patellar bracing during muscular strengthening. A patient who achieves 20-lb isometric quadriceps strength, demonstrates a normal step-down test, and is assumed to be asymptomatic can be allowed to return to sports activities with use of a patellar brace. The patient should be counseled that there is an increased risk for patellar dislocation because of this chronic subluxation and the shallower sulcus. As in LPCS, CSP symptoms that persist after dynamic strength is regained may require surgical intervention. The severity of identified abnormal factors (tight LR, increased Q angle, trochlear dysplasia) guides the surgeon in selecting appropriate corrective technique(s). Recurrent Dislocation of Patella Admittedly, given the number and subtlety of abnormal factors, the diagnosis of LPCS as a cause of patellofemoral pain can be challenging. However, RDP is at the opposite end of the spectrum. A history of prior patellar dislocation(s) almost always makes the diagnosis of RDP easier. The patient occasionally complains of a recurrent symptom, the knee going out or giving way, indicating that the diagnosis might be RDP. By carefully asking what the patient was doing and what happened when the knee went out, the clinician may be able to determine if the injury stemmed from sudden patellar pain causing reflex inhibition of the quadriceps or was a true dislocation. Both may be described as going out or giving way. Assessment for the same 7 abnormalities helps establish the diagnosis, a logical treatment plan, and a guide for indicated surgery. The diagnostic focus is MPFL laxity and trochlear dysplasia. Prior lateral dislocation of the patella almost always requires rupture of the normal MPFL. The infrequent exception is a patient with hyper-elasticity of the skin and multiple joints (Ehlers-Danlos syndrome). Trochlear dysplasia is a significant risk factor for patellar dislocation. If the trochlea is normal and there is no MPFL laxity, the diagnosis of RDP should be questioned. If surgery is indicated, the surgeon uses a list of the patient s abnormalities and their severity as a guide in selecting reconstructive techniques. The more abnormalities found and the greater the severity of each, the more techniques are needed to achieve success. Preoperative exercises help speed postoperative recovery by addressing quadriceps and hip abductor weakness. In addition, an active exercise program gives the surgeon insight into the patient s desire for and commitment to recovery. Other physical abnormalities to be considered in preoperative planning include MPFL laxity, LR tightness, increased Q angle, patella alta, and trochlear dysplasia. Surgical tips: 1. When releasing the LR, never cut the vastus lateralis tendon, as this has a high likelihood of causing iatrogenic medial patellar subluxation When medializing the TT, consider compensating for a shallow trochlea by overcorrecting the Q angle to 5 to 10 measured with a surgical goniometer intraoperatively. 74 The American Journal of Orthopedics March/April
8 A. C. Merchant et al Summary Basing clinical classification of disorders on etiology is a simple and effective way to diagnose common patellofemoral conditions. Identifying and rating the severity of patellofemoral dysplasia, using 7 commonly found physical abnormalities, guide the physician to a proper diagnosis and down logical treatment pathways. These principles should be incorporated into the routine evaluation of patellofemoral disorders to optimize diagnosis, formulate a treatment plan, and improve patient outcomes. After all, this is what our patients are asking us to do: Try to find what s wrong, and then try to fix it! Dr. Merchant is Clinical Professor Emeritus, Department of Orthopedic Surgery, Stanford University School of Medicine, Stanford, California. Dr. Fulkerson is an Orthopedic Surgeon, Orthopedic Associates of Hartford, Hartford, Connecticut; Clinical Professor, Department of Orthopedic Surgery, University of Connecticut School of Medicine, Farmington, Connecticut; and President, The Patellofemoral Foundation, Farmington, Connecticut. Dr. Leadbetter is a former Adjunct Clinical Assistant Professor, Uniformed Services University of the Health Sciences, Bethesda, Maryland. Address correspondence to: Alan C. Merchant, MD, MS, ( , kneemd@sbcglobal.net). Am J Orthop. 2017;46(2): Copyright Frontline Medical Communications Inc All rights reserved. References 1. Merchant AC. Classification of patellofemoral disorders. Arthroscopy. 1988;4(4): Merchant AC. Patellofemoral disorders: biomechanics, diagnosis, and nonoperative treatment. In: McGinty JB, Caspari RB, Jackson RW, Poehling GG, eds. Operative Arthroscopy. New York, NY: Raven Press; 1991: Dye SF. The knee as a biologic transmission with an envelope of function: a theory. Clin Orthop Relat Res. 1996;(325): Merchant AC. A philosophy of the patellofemoral joint: a logical clinical approach. In: Sanchis-Alfonso V, ed. Anterior Knee Pain and Patellar Instability. 2nd ed. London, England: Springer; 2011: Jan MH, Lin DH, Lin JJ, Lin CH, Cheng CK, Lin YF. Differences in sonographic characteristics of the vastus medialis obliquus between patients with patellofemoral pain syndrome and healthy adults. Am J Sports Med. 2009;37(9): Pattyn E, Verdonk P, Steyaert A, et al. Vastus medialis obliquus atrophy: does it exist in patellofemoral pain syndrome? Am J Sports Med. 2011;39(7): Brattström H. Shape of the intercondylar groove normally and in recurrent dislocation of the patella. A clinical and x-ray anatomical investigation. Acta Orthop Scand Suppl. 1964;68: Roux D. Luxation habituelle de la rotule: traitement operatoire. Rev Chir Orthop Reparatrice Appar Mot. 1888;8: Post WR. Clinical evaluation of patients with patellofemoral disorders. Arthroscopy. 1999;15(8): Grelsamer RP, Dubey A, Weinstein CH. Men and women have similar Q angles: a clinical and trigonometric evaluation. J Bone Joint Surg Br. 2005;87(11): Skelley N, Friedman M, McGinnis M, Smith C, Hillen T, Matava M. Inter- and intraobserver reliability in the MRI measurement of the tibial tubercle-trochlear groove distance and trochlea dysplasia. Am J Sports Med. 2015;43(4): Tensho K, Akaoka Y, Shimodaira H, et al. What components comprise the measurement of the tibial tuberosity-trochlear groove distance in a patellar dislocation population? J Bone Joint Surg Am. 2015;97(17): Camp CL, Heidenreich MJ, Dahm DL, Stuart MJ, Levy BA, Krych AJ. Individualizing the tibial tubercle-trochlear groove distance: patellar instability ratios that predict recurrent instability. Am J Sports Med. 2016;44(2): Ridley TJ, Hinckel BB, Kruckeberg BM, Agel J, Arendt EA. Anatomical patella instability risk factors on MRI show sensitivity without specificity in patients with patellofemoral instability: a systematic review. JISAKOS. 2016;1(3): James SL, Bates BT, Osternig LR. Injuries to runners. Am J Sports Med. 1978;6(2): Powers CM, Souza RB, Fulkerson JP. Patellofemoral joint. In: Magee DJ, Zachazewski JE, Quillen WS, eds. Pathology and Intervention in Musculoskeletal Rehabilitation. St. Louis, MO: Saunders Elsevier; 2008: Khayambashi K, Mohammadkhani Z, Ghaznavi K, Lyle MA, Powers CM. The effects of isolated hip abductor and external rotator muscle strengthening on pain, health status, and strength in females with patellofemoral pain: a randomized controlled trial. J Orthop Sports Phys Ther. 2012;42(1): Berg EE, Mason SL, Lucas MJ. Patellar height ratios. A comparison of four measurement methods. Am J Sports Med. 1996;24(2): Senavongse W, Amis AA. The effects of articular, retinacular, or muscular deficiencies on patellofemoral joint stability: a biomechanical study in vitro. J Bone Joint Surg Br. 2005;87(4): Merchant AC, Mercer RL, Jacobsen RH, Cool CR. Roentgenographic analysis of patellofemoral congruence. J Bone Joint Surg Am. 1974;56(7): Dejour H, Neyret P, Walch G. Factors in patellar instability. In: Aichroth PM, Cannon WD Jr, Patel DV, eds. Knee Surgery: Current Practice. London, England: Martin Dunitz; Davies AP, Costa ML, Shepstone L, Glasgow MM, Donell S. The sulcus angle and malalignment of the extensor mechanism of the knee. J Bone Joint Surg Br. 2000;82(8): Aglietti P, Insall JN, Cerulli G. Patellar pain and incongruence. I: measurements of incongruence. Clin Orthop Relat Res. 1983;(176): Ficat P, Ficat C, Bailieaux A. External hypertension syndrome of the patella. Its significance in the recognition of arthrosis [in French]. Rev Chir Orthop Reparatrice Appar Mot. 1975;61(1): Ficat P, Hungerford DS. Disorders of the Patellofemoral Joint. Baltimore, MD: Williams & Wilkins; Merchant AC. The lateral compression syndrome. In: Fox JM, Del Pizzo W, eds. The Patellofemoral Joint. New York, NY: McGraw-Hill; 1993: DeHaven KE, Dolan WA, Mayer PJ. Chondromalacia patellae in athletes. Clinical presentation and conservative management. Am J Sports Med. 1979;7(1): Merchant AC. Patellofemoral joint disorders. In: Chapman MW, ed. Operative Orthopedics. Vol 3. Philadelphia, PA: Lippincott; 1988: Sanchis-Alfonso V, Merchant AC. Iatrogenic medial patellar instability: an avoidable injury. Arthroscopy. 2015;31(8): March/April 2017 The American Journal of Orthopedics 75
The Diagnosis and Initial Treatment of Patellofemoral Disorders
 The Diagnosis and Initial Treatment of Patellofemoral Disorders Am J Orthop. 2017 March;46(2):68-75 Authors: Alan C. Merchant, MD, MS John P. Fulkerson, MD Wayne Leadbetter, MD Author Affiliation Disclosures
The Diagnosis and Initial Treatment of Patellofemoral Disorders Am J Orthop. 2017 March;46(2):68-75 Authors: Alan C. Merchant, MD, MS John P. Fulkerson, MD Wayne Leadbetter, MD Author Affiliation Disclosures
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes
 Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Where to Draw the Line:
 Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Joint. Question? ANATOMY
 Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
7/20/14. Patella Instability. Alignment. PF contact areas. Tissue Restraints. Pain. Acute Blunt force trauma Disorders of the Patellafemoral Joint
 Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Peggers Super Summaries: PFJ
 Patellofemoral Joint: ANATOMY: Largest sesamoid ossifying at 3-5 years of age Multiple foci having a sec ossification centre SUPEROLATERAL Helps increase moment arm PATELLOFEMORAL OA Incidence 10% of knee
Patellofemoral Joint: ANATOMY: Largest sesamoid ossifying at 3-5 years of age Multiple foci having a sec ossification centre SUPEROLATERAL Helps increase moment arm PATELLOFEMORAL OA Incidence 10% of knee
Where are we now? A little bit of History.. Is menu à la carte relevant in 2019? Medial PatelloFemoral Ligament the Queen of the PF Joint
 Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
World Medical & Health Games
 Management of Patellofemoral Pain Syndrome João Barroso Orthopaedic department ULS Matosinhos Portugal Introduction Anterior Knee Pain affects 1 in 4 athletes very common! (Knowles et al) Patellofemoral
Management of Patellofemoral Pain Syndrome João Barroso Orthopaedic department ULS Matosinhos Portugal Introduction Anterior Knee Pain affects 1 in 4 athletes very common! (Knowles et al) Patellofemoral
8/9/2017. Case Based: Beyond Medial Patellofemoral Ligament. Editorial Board AJSM Social Media. Consultant. Not talking about PF pain/chondrosis Rehab
 Case Based: Beyond Medial Patellofemoral Ligament Dr Alan Getgood MD FRCS(Tr&Orth) DipSEM Assistant Professor Orthopaedic Sport Medicine Fellowship Director The Fowler Kennedy Sport Medicine Clinic University
Case Based: Beyond Medial Patellofemoral Ligament Dr Alan Getgood MD FRCS(Tr&Orth) DipSEM Assistant Professor Orthopaedic Sport Medicine Fellowship Director The Fowler Kennedy Sport Medicine Clinic University
Personal use only. MRI of the extensor mechanism of the knee. 5 th Musculoskeletal MRI meeting. Falkowski, MD, MHBA
 MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016
 Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Department of Orthopedic Surgery, Ewha Womans University Mokdong Hospital, Seoul, Korea
 Case Report https://doi.org/10.14517/aosm16016 pissn 2289-005X eissn 2289-0068 Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun
Case Report https://doi.org/10.14517/aosm16016 pissn 2289-005X eissn 2289-0068 Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun
Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no
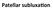 Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
Acute patellar dislocation in adults
 CASE STUDY 14 Acute patellar dislocation in adults What are the reasons for the first acute dislocation? How can we document the pathoanatomy? What is our treatment concept? Table CS14 Patellofemoral joint
CASE STUDY 14 Acute patellar dislocation in adults What are the reasons for the first acute dislocation? How can we document the pathoanatomy? What is our treatment concept? Table CS14 Patellofemoral joint
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force.
 Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
Why does it matter? Patellar Instability 7/23/2018. What is the current operation de jour? Common. Poorly taught. Poorly treated
 Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
10/30/18. Disclosures. Recurrent Patellar Instability. Management of Recurrent Patellar Instability
 Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Patella Instability 1 st Time Dislocation
 Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
The value of weight-bearing functional CT scans
 The value of weight-bearing functional scans In musculoskeletal medicine, advanced imaging like computed axial tomography () scanning, has become invaluable to the evaluation and management of patients
The value of weight-bearing functional scans In musculoskeletal medicine, advanced imaging like computed axial tomography () scanning, has become invaluable to the evaluation and management of patients
Anterior knee pain.
 Anterior knee pain What are the symptoms? Anterior knee pain is very common amongst active adolescents and athletes participating in contact sports. It is one of the most common problems/injuries seen
Anterior knee pain What are the symptoms? Anterior knee pain is very common amongst active adolescents and athletes participating in contact sports. It is one of the most common problems/injuries seen
PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT. Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology
 PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology PRE OPERATIVE ASSESSMENT RADIOGRAPHS Radiographs are used for assessment and
PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology PRE OPERATIVE ASSESSMENT RADIOGRAPHS Radiographs are used for assessment and
Chronic patellar dislocation in adults
 CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
CT Evaluation of Patellar Instability
 CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
Index 377. G GAGS (glycosaminoglycans), 315 Gastrocnemius tightness, 99, 102 Genupath, 104 Glycosaminoglycans. See GAGS Ground surface, 56 57
 Index A Achilles tendonitis/tendinopathy, 257, 259 ACL (anterior cruciate ligament) AKP relating to, 61, 94 injuries, 3, 121, 125 126 reconstruction, 3 4 with bone-patellar tendon-bone autografts, 4 ACL
Index A Achilles tendonitis/tendinopathy, 257, 259 ACL (anterior cruciate ligament) AKP relating to, 61, 94 injuries, 3, 121, 125 126 reconstruction, 3 4 with bone-patellar tendon-bone autografts, 4 ACL
DISCLOSURES. Overview 09/24/2015. Patellofemoral Instability and Treatment Options. I do not have anything to disclose
 Patellofemoral Instability and Treatment Options Gregory Purnell, MD Department of Orthpoaedic Surgery Sports Medicine and Arthroscopy Allegheny Health Network Orthopaedic Surgeon, Pittsburgh Pirates Baseball
Patellofemoral Instability and Treatment Options Gregory Purnell, MD Department of Orthpoaedic Surgery Sports Medicine and Arthroscopy Allegheny Health Network Orthopaedic Surgeon, Pittsburgh Pirates Baseball
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT *** - Useful in determining mechanism of injury / overuse
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
Doron Sher. 160 Belmore Rd, Randwick Burwood Rd, Concord. MBBS, MBiomedE, FRACS FAOrthA
 Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Standard of Care: Patellofemoral Pain Syndrome (PFS)
 Department of Rehabilitation Services Physical Therapy Case Type / Diagnosis: Patellofemoral Pain Syndrome (719.46) Patellofemoral Pain syndrome A general category of anterior knee pain from patella malalignment.
Department of Rehabilitation Services Physical Therapy Case Type / Diagnosis: Patellofemoral Pain Syndrome (719.46) Patellofemoral Pain syndrome A general category of anterior knee pain from patella malalignment.
Patella Instability in Children and Adolescents
 Patella Instability in Children and Adolescents Description Patella Instability is an injury to the kneecap (patella) affecting the joint it forms with the thigh bone (femur) Patella Instability can occur
Patella Instability in Children and Adolescents Description Patella Instability is an injury to the kneecap (patella) affecting the joint it forms with the thigh bone (femur) Patella Instability can occur
CHRONIC PATELLOFEMORAL INSTABILITY
 INSTRUCTIONAL COURSE LECTURE DAVID J. DANDY From Addenbrooke s Hospital, Cambridge, England This article aims to discuss the many causes of patellofemoral instability so that an appropriate stabilisation
INSTRUCTIONAL COURSE LECTURE DAVID J. DANDY From Addenbrooke s Hospital, Cambridge, England This article aims to discuss the many causes of patellofemoral instability so that an appropriate stabilisation
Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff),
 Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff), Consultant Knee Surgeon NHS: The Royal Orthopaedic Hospital & Queen Elizabeth Hospital, Birmingham MRI Knee:
Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff), Consultant Knee Surgeon NHS: The Royal Orthopaedic Hospital & Queen Elizabeth Hospital, Birmingham MRI Knee:
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
5/14/2013. Acute vs Chronic Mechanism of Injury:
 Third Annual Young Athlete Conference: The Lower Extremity February 22, 2013 Audrey Lewis, DPT Acute vs Chronic Mechanism of Injury: I. Direct: blow to the patella II. Indirect: planted foot with a valgus
Third Annual Young Athlete Conference: The Lower Extremity February 22, 2013 Audrey Lewis, DPT Acute vs Chronic Mechanism of Injury: I. Direct: blow to the patella II. Indirect: planted foot with a valgus
PART III Case Studies
 PART III Case Studies Patellofemoral Disorders: Diagnosis and Treatment. Edited by Roland M. Biedert 2004 John Wiley & Sons, Ltd ISBN: 0-470-85011-6 CASE STUDY 1 Unspecific patellofemoral pain What do
PART III Case Studies Patellofemoral Disorders: Diagnosis and Treatment. Edited by Roland M. Biedert 2004 John Wiley & Sons, Ltd ISBN: 0-470-85011-6 CASE STUDY 1 Unspecific patellofemoral pain What do
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
Patello-femoral pain
 Patello-femoral pain Dr Keith Holt Patello-femoral pain describes a spectrum of conditions, beginning with the common mild pain coming from under the knee-cap (patella) and extending up to frank arthritis
Patello-femoral pain Dr Keith Holt Patello-femoral pain describes a spectrum of conditions, beginning with the common mild pain coming from under the knee-cap (patella) and extending up to frank arthritis
A Patient s Guide to Patellofemoral Problems
 A Patient s Guide to Patellofemoral Problems 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Patellofemoral Problems 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety
Please differentiate an internal derangement from an external knee injury.
 Knee Orthopaedic Tests Sports and Knee Injuries James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Knee Injury Strain, Sprain, Internal Derangement Anatomy of the Knee Please
Knee Orthopaedic Tests Sports and Knee Injuries James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Knee Injury Strain, Sprain, Internal Derangement Anatomy of the Knee Please
Learning Objectives. Epidemiology 7/22/2016. What are the Medical Concerns for the Adolescent Female Athlete? Krystle Farmer, MD July 21, 2016
 What are the Medical Concerns for the Adolescent Female Athlete? Krystle Farmer, MD July 21, 2016 Learning Objectives Discuss why females are different than males in sports- the historical perspective.
What are the Medical Concerns for the Adolescent Female Athlete? Krystle Farmer, MD July 21, 2016 Learning Objectives Discuss why females are different than males in sports- the historical perspective.
Jumper s Knee in Children and Adolescents
 A Patient s Guide to Jumper s Knee in Children and Adolescents 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Jumper s Knee in Children and Adolescents 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
Anterior Knee Pain in Children. Joseph Chorley, MD Associate Professor, Pediatrics Baylor College of Medicine
 Anterior Knee Pain in Children Joseph Chorley, MD Associate Professor, Pediatrics Baylor College of Medicine Goals and Objectives To learn how to care for patients with chronic knee pain To be able to
Anterior Knee Pain in Children Joseph Chorley, MD Associate Professor, Pediatrics Baylor College of Medicine Goals and Objectives To learn how to care for patients with chronic knee pain To be able to
Patellar instability
 Page 1 of 13 Specific Injuries D Goodwin 1, W Postma 2 * Patellar instability Abstract Introduction Patellar instability is most common among adolescent female athletes, although anyone can be affected.
Page 1 of 13 Specific Injuries D Goodwin 1, W Postma 2 * Patellar instability Abstract Introduction Patellar instability is most common among adolescent female athletes, although anyone can be affected.
emoryhealthcare.org/ortho
 COMMON SOCCER INJURIES Oluseun A. Olufade, MD Assistant Professor, Department of Orthopedics and PM&R 1/7/18 GOALS Discuss top soccer injuries and treatment strategies Simplify hip and groin injuries in
COMMON SOCCER INJURIES Oluseun A. Olufade, MD Assistant Professor, Department of Orthopedics and PM&R 1/7/18 GOALS Discuss top soccer injuries and treatment strategies Simplify hip and groin injuries in
General Concepts. Growth Around the Knee. Topics. Evaluation
 General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD
 Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD Disclosures Consultant: Smith & Nephew A3 surgical Stockholder: A3 surgical Case Presentation:
Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD Disclosures Consultant: Smith & Nephew A3 surgical Stockholder: A3 surgical Case Presentation:
Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery. Restore patella stability.
 Page 1 of 5 Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery Restore patella stability. Restore / improve function. I have no conflicts to declare. 1987
Page 1 of 5 Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery Restore patella stability. Restore / improve function. I have no conflicts to declare. 1987
The Knee 20 S1 (2013) S3 S15. Contents lists available at SciVerse ScienceDirect. The Knee
 The Knee 20 S1 (2013) S3 S15 Contents lists available at SciVerse ScienceDirect The Knee Review The contemporary management of anterior knee pain and patellofemoral instability Toby O. Smith, Iain McNamara,
The Knee 20 S1 (2013) S3 S15 Contents lists available at SciVerse ScienceDirect The Knee Review The contemporary management of anterior knee pain and patellofemoral instability Toby O. Smith, Iain McNamara,
W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco
 Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
Do Persons with PFP. PFJ Loading? Biomechanical Factors Contributing to Patellomoral Pain: The Dynamic Q Angle. Patellofemoral Pain: A Critical Review
 Biomechanical Factors Contributing to Patellomoral Pain: The Dynamic Q Angle Division Biokinesiology & Physical Therapy Co Director, oratory University of Southern California Movement Performance Institute
Biomechanical Factors Contributing to Patellomoral Pain: The Dynamic Q Angle Division Biokinesiology & Physical Therapy Co Director, oratory University of Southern California Movement Performance Institute
Imaging in patellofemoral instability is essential to the accurate
 REVIEW ARTICLE Imaging in Patellofemoral Instability: An Abnormality-based Approach Paulo Renato Fernandes Saggin, MD,* Jose Idıĺio Saggin, MD,* and David Dejour, MDw Abstract: Imaging in patellofemoral
REVIEW ARTICLE Imaging in Patellofemoral Instability: An Abnormality-based Approach Paulo Renato Fernandes Saggin, MD,* Jose Idıĺio Saggin, MD,* and David Dejour, MDw Abstract: Imaging in patellofemoral
No Disclosures. Topics. Pediatric ACL Tears
 Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Anterior Cruciate Ligament (ACL)
 Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
Muscle Testing of Knee Extensors. Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department
 Muscle Testing of Knee Extensors Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department Muscle Testing of Knee Extensors othe Primary muscle Quadriceps Femoris -Rectus
Muscle Testing of Knee Extensors Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department Muscle Testing of Knee Extensors othe Primary muscle Quadriceps Femoris -Rectus
BIOMECHANICS OF PATELLA FUNCTION. PETER G. KRAMER, EdD, PT*
 01 96-601 l/86/0806-0301$02.00/0 THE JOURNAL OF ORTHOPAED~C AND SPORTS PHYSICAL THERAPY Copyright 0 1986 by The Orthopaedic and Sports Physical Therapy Sections of the American Physical Therapy Association
01 96-601 l/86/0806-0301$02.00/0 THE JOURNAL OF ORTHOPAED~C AND SPORTS PHYSICAL THERAPY Copyright 0 1986 by The Orthopaedic and Sports Physical Therapy Sections of the American Physical Therapy Association
How do you do exercises for patellar tracking disorder?
 To print: Use your web browser's print feature. Close this window after printing. Patellar Tracking Disorder: Exercises Table of Contents Patellar Tracking Disorder: Exercises Patellar Tracking Disorder:
To print: Use your web browser's print feature. Close this window after printing. Patellar Tracking Disorder: Exercises Table of Contents Patellar Tracking Disorder: Exercises Patellar Tracking Disorder:
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
Computational Evaluation of Predisposing Factors to Patellar Dislocation
 Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
Knee Pain. Pain in the pressure on. the kneecap. well as being supported (retinaculum) quadricep. Abnormal. to the knee. or dislocate.
 Knee Pain in Children and Adolescents Description Pain in the knee can occur from various causess but is usually from increased pressure on the kneecap (patella) or abnormal motion. Softening of the cartilage
Knee Pain in Children and Adolescents Description Pain in the knee can occur from various causess but is usually from increased pressure on the kneecap (patella) or abnormal motion. Softening of the cartilage
Radiological evaluation of the causes of patellar instability.
 Radiological evaluation of the causes of patellar instability. Poster No.: C-0054 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. M. Spaccesi Pau, D. Pomato, N. CEDOLA; La Plata/AR
Radiological evaluation of the causes of patellar instability. Poster No.: C-0054 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. M. Spaccesi Pau, D. Pomato, N. CEDOLA; La Plata/AR
Subluxation of the Patella
 Subluxation of the Patella Alexandra Zaldivar December 15, 2011 2011 Course, Los Angeles Abstract After reading information from the Internet and anatomy books, it becomes very clear why pilates is an
Subluxation of the Patella Alexandra Zaldivar December 15, 2011 2011 Course, Los Angeles Abstract After reading information from the Internet and anatomy books, it becomes very clear why pilates is an
Medial Patellofemoral Ligament Reconstruction
 Medial Patellofemoral Ligament Reconstruction 1. Defined a. Reconstruction of the medial patellofemoral ligament in an effort to restore medial patellar stability and reduce chances of lateral dislocation.
Medial Patellofemoral Ligament Reconstruction 1. Defined a. Reconstruction of the medial patellofemoral ligament in an effort to restore medial patellar stability and reduce chances of lateral dislocation.
Balanced Body Movement Principles
 Balanced Body Movement Principles How the Body Works and How to Train it. Module 3: Lower Body Strength and Power Developing Strength, Endurance and Power The lower body is our primary source of strength,
Balanced Body Movement Principles How the Body Works and How to Train it. Module 3: Lower Body Strength and Power Developing Strength, Endurance and Power The lower body is our primary source of strength,
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Knee Contusions and Stress Injuries. Laura W. Bancroft, M.D.
 Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Anatomy of the patella :
 PATELLOFEMORAL JOINT REHABILITATION COMPONENTS GREG BENNETT, P.T., DSc. Excel Physical Therapy Anatomy of the patella : Patella is triangular, apex directed downwards Anterior surface gently convex Deep
PATELLOFEMORAL JOINT REHABILITATION COMPONENTS GREG BENNETT, P.T., DSc. Excel Physical Therapy Anatomy of the patella : Patella is triangular, apex directed downwards Anterior surface gently convex Deep
William G. Carson, Jr., M.D.
 1 William G. Carson, Jr., M.D. Publications: 1. Carson, W.G., Lowell, W.W. and Whitesides, T.E.: Congenital Elevation of Scapula: Surgical Correction by the Woodward Procedure. Journal of Bone and Joint
1 William G. Carson, Jr., M.D. Publications: 1. Carson, W.G., Lowell, W.W. and Whitesides, T.E.: Congenital Elevation of Scapula: Surgical Correction by the Woodward Procedure. Journal of Bone and Joint
Overview Ligament Injuries. Anatomy. Epidemiology Very commonly injured joint. ACL Injury 20/06/2016. Meniscus Tears. Patellofemoral Problems
 Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
Ligamentous and Meniscal Injuries: Diagnosis and Management
 Ligamentous and Meniscal Injuries: Diagnosis and Management Daniel K Williams, MD Franciscan Physician Network Orthopedic Specialists September 29, 2017 No Financial Disclosures INTRODUCTION Overview of
Ligamentous and Meniscal Injuries: Diagnosis and Management Daniel K Williams, MD Franciscan Physician Network Orthopedic Specialists September 29, 2017 No Financial Disclosures INTRODUCTION Overview of
Dynamic patellar brace: A new orthosis in
 Dynamic patellar brace: A new orthosis in the management of patellofemoral disorders A preliminary report* P. M. PALUMBO, JR., M.D. From the Sports Medicine and Rehabilitation Center of Greater Washington,
Dynamic patellar brace: A new orthosis in the management of patellofemoral disorders A preliminary report* P. M. PALUMBO, JR., M.D. From the Sports Medicine and Rehabilitation Center of Greater Washington,
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Physiotherapy in Recurrent Dislocation of Patella-Wiberg Type II Farzana Alam, Subhadeep Roy Choudhury BPT,
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Physiotherapy in Recurrent Dislocation of Patella-Wiberg Type II Farzana Alam, Subhadeep Roy Choudhury BPT,
(iv) Patellofemoral dysfunction Extensor mechanism malalignment
 Current Orthopaedics (2006) 20, 103 111 Available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/cuor MINI-SYMPOSIUM: SOFT TISSUE KNEE PROBLEMS (iv) Patellofemoral dysfunction Extensor
Current Orthopaedics (2006) 20, 103 111 Available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/cuor MINI-SYMPOSIUM: SOFT TISSUE KNEE PROBLEMS (iv) Patellofemoral dysfunction Extensor
Patellofemoral Pain Syndrome
 What is patellofemoral pain syndrome? Patellofemoral Pain Syndrome Patellofemoral pain syndrome is pain behind the kneecap. It has been given many names, including patellofemoral disorder, patellar malalignment,
What is patellofemoral pain syndrome? Patellofemoral Pain Syndrome Patellofemoral pain syndrome is pain behind the kneecap. It has been given many names, including patellofemoral disorder, patellar malalignment,
Rehabilitation for Patellar Tendinitis (jumpers knee) and Patellofemoral Syndrome (chondromalacia patella)
 Rehabilitation for Patellar Tendinitis (jumpers knee) and Patellofemoral Syndrome (chondromalacia patella) Patellar Tendinitis The most common tendinitis about the knee is irritation of the patellar tendon.
Rehabilitation for Patellar Tendinitis (jumpers knee) and Patellofemoral Syndrome (chondromalacia patella) Patellar Tendinitis The most common tendinitis about the knee is irritation of the patellar tendon.
What is Medial Plica Syndrome?
 What is Medial Plica Syndrome? It is a congenital disorder in which the thin wall of fibrous tissue extends from the synovial capsule of the knee. Pain usually occurs when the synovial capsule becomes
What is Medial Plica Syndrome? It is a congenital disorder in which the thin wall of fibrous tissue extends from the synovial capsule of the knee. Pain usually occurs when the synovial capsule becomes
Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents
 Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents Sheena R. Black, MD, Henry B. Ellis, MD, Philip L. Wilson, MD, David A. Podeszwa, MD LLRS Annual
Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents Sheena R. Black, MD, Henry B. Ellis, MD, Philip L. Wilson, MD, David A. Podeszwa, MD LLRS Annual
The role of Tibial Tubercle Osteotomies in 2017
 ISAKOS ICL #7: How to Strategically Manage Complex Patellar Instability The role of Tibial Tubercle Osteotomies in 2017 Elizabeth A. Arendt, MD Department of Orthopaedic Surgery, University of Minnesota,
ISAKOS ICL #7: How to Strategically Manage Complex Patellar Instability The role of Tibial Tubercle Osteotomies in 2017 Elizabeth A. Arendt, MD Department of Orthopaedic Surgery, University of Minnesota,
40 th Annual Symposium on Sports Medicine. Knee Injuries In The Pediatric Athlete. Disclosure
 40 th Annual Symposium on Sports Medicine Travis Murray, MD Assistant Professor University of Texas Health Science Center San Antonio Knee Injuries In The Pediatric Athlete Disclosure Dr. Travis Murray
40 th Annual Symposium on Sports Medicine Travis Murray, MD Assistant Professor University of Texas Health Science Center San Antonio Knee Injuries In The Pediatric Athlete Disclosure Dr. Travis Murray
Tibial tubercle osteotomy in patello-femoral instability and in patellar height abnormality
 International Orthopaedics (SICOT) (2010) 34:305 309 DOI 10.1007/s00264-009-0929-4 ORIGINAL PAPER Tibial tubercle osteotomy in patello-femoral instability and in patellar height abnormality Jacques H.
International Orthopaedics (SICOT) (2010) 34:305 309 DOI 10.1007/s00264-009-0929-4 ORIGINAL PAPER Tibial tubercle osteotomy in patello-femoral instability and in patellar height abnormality Jacques H.
Patellofemoral Osteoarthritis
 Patellofemoral Osteoarthritis Arthritis of the patellofemoral joint refers to degeneration (wearing out) of the cartilage on the underside of the patella (kneecap) and the trochlea (groove) of the femur.
Patellofemoral Osteoarthritis Arthritis of the patellofemoral joint refers to degeneration (wearing out) of the cartilage on the underside of the patella (kneecap) and the trochlea (groove) of the femur.
Medial patellofemoral ligament reconstruction using dual patella docking technique
 2018; 4(3): 298-304 ISSN: 2395-1958 IJOS 2018; 4(3): 298-304 2018 IJOS www.orthopaper.com Received: 24-05-2018 Accepted: 25-06-2018 Dr. Ullas Mahesh Assistant Professor, Department of Orthopaedics, Bangalore,
2018; 4(3): 298-304 ISSN: 2395-1958 IJOS 2018; 4(3): 298-304 2018 IJOS www.orthopaper.com Received: 24-05-2018 Accepted: 25-06-2018 Dr. Ullas Mahesh Assistant Professor, Department of Orthopaedics, Bangalore,
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
J oints. CIC Edizioni Internazionali. Patellofemoral malalignment and chondral damage: current concepts. Abstract
 Patellofemoral malalignment and chondral damage: current concepts ClauDIO MaZZOla, DaVIDe MaNtOVaNI Joint Surgery Section, eo Galliera, Genova, Italy Abstract Patellofemoral disorders can be classified
Patellofemoral malalignment and chondral damage: current concepts ClauDIO MaZZOla, DaVIDe MaNtOVaNI Joint Surgery Section, eo Galliera, Genova, Italy Abstract Patellofemoral disorders can be classified
APTA Intro to Identity. The Movement System The Kinesiopathologic Model Movement System Impairment Syndromes of the Knee THE HUMAN MOVEMENT SYSTEM
 The Movement System The Kinesiopathologic Model Movement System Impairment Syndromes of the Knee Shirley Sahrmann, PT, PhD, FAPTA Professor Emerita Statement of Privacy To protect the privacy of the subjects
The Movement System The Kinesiopathologic Model Movement System Impairment Syndromes of the Knee Shirley Sahrmann, PT, PhD, FAPTA Professor Emerita Statement of Privacy To protect the privacy of the subjects
Chapter 20 The knee and related structures
 Chapter 20 The knee and related structures Athletic Training Spring 2014 Jihong Park Bones & joints Femur, tibia, fibula, & patella Femur & tibia Weight bearing & muscle attachment Patella functions Anterior
Chapter 20 The knee and related structures Athletic Training Spring 2014 Jihong Park Bones & joints Femur, tibia, fibula, & patella Femur & tibia Weight bearing & muscle attachment Patella functions Anterior
Assessment of Patellar Laxity in the in vitro Native Knee
 Assessment of Patellar Laxity in the in vitro Native Knee By Mark C. Komosa Submitted to the graduate degree program in Bioengineering and the Graduate Faculty of the University of Kansas in partial fulfillment
Assessment of Patellar Laxity in the in vitro Native Knee By Mark C. Komosa Submitted to the graduate degree program in Bioengineering and the Graduate Faculty of the University of Kansas in partial fulfillment
Patellar Instability. OrthoInfo Patella Instability Page 1 of 5
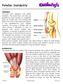 Patellar Instability OVERVIEW You have been diagnosed with patella instability. This means that your knee cap (patella) has been partially or completely going out of place and is not tracking well against
Patellar Instability OVERVIEW You have been diagnosed with patella instability. This means that your knee cap (patella) has been partially or completely going out of place and is not tracking well against
Patellofemoral Pain Syndrome
 Patellofemoral Pain Syndrome This article is also available in Spanish: El síndrome de dolor patelofemoral (Patellofemoral Pain Syndrome) (topic.cfm?topic=a00763). Patellofemoral pain syndrome is a broad
Patellofemoral Pain Syndrome This article is also available in Spanish: El síndrome de dolor patelofemoral (Patellofemoral Pain Syndrome) (topic.cfm?topic=a00763). Patellofemoral pain syndrome is a broad
9/24/2012. Greg Bennett, PT, DSc Excel Physical Therapy Marymount University
 Greg Bennett, PT, DSc Excel Physical Therapy Marymount University Hx often diagnostic Least to most threatening Sx trump exam Develop consistent routine Don t inflame inflamed tissue 1 1. ESTABLISH OR
Greg Bennett, PT, DSc Excel Physical Therapy Marymount University Hx often diagnostic Least to most threatening Sx trump exam Develop consistent routine Don t inflame inflamed tissue 1 1. ESTABLISH OR
Exam of the Knee and Ankle I HAVE NO FINANCIAL DISCLOSURES RELEVANT TO THIS PRESENTATION
 Exam of the Knee and Ankle I HAVE NO FINANCIAL DISCLOSURES RELEVANT TO THIS PRESENTATION Disclosures I have no relevant financial relationships with the manufacturers of any commercial products and or
Exam of the Knee and Ankle I HAVE NO FINANCIAL DISCLOSURES RELEVANT TO THIS PRESENTATION Disclosures I have no relevant financial relationships with the manufacturers of any commercial products and or
Patellofemoral instability is a common cause of knee
 280 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4):280-93 Patella Instability Reuven Minkowitz, M.D., Chris Inzerillo, M.D., and Orrin H. Sherman, M.D. Patellofemoral instability is a common
280 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4):280-93 Patella Instability Reuven Minkowitz, M.D., Chris Inzerillo, M.D., and Orrin H. Sherman, M.D. Patellofemoral instability is a common
The Knee. Clarification of Terms. Osteology of the Knee 7/28/2013. The knee consists of: The tibiofemoral joint Patellofemoral joint
 The Knee Clarification of Terms The knee consists of: The tibiofemoral joint Patellofemoral joint Mansfield, p273 Osteology of the Knee Distal Femur Proximal tibia and fibula Patella 1 Osteology of the
The Knee Clarification of Terms The knee consists of: The tibiofemoral joint Patellofemoral joint Mansfield, p273 Osteology of the Knee Distal Femur Proximal tibia and fibula Patella 1 Osteology of the
Lower Extremity Sports Injuries
 Lower Extremity Sports Injuries AAP Musculoskeletal Boot Camp Sigrid F. Wolf, MD Pediatric Sports Medicine Fellow Northwestern University Lurie Children s Hospital Disclosure I have no relevant financial
Lower Extremity Sports Injuries AAP Musculoskeletal Boot Camp Sigrid F. Wolf, MD Pediatric Sports Medicine Fellow Northwestern University Lurie Children s Hospital Disclosure I have no relevant financial
Common Apophyseal Problems in the Athlete
 Disclosure Common Apophyseal Problems in the Athlete Mark Halstead, MD November 19, 2009 Faculty Disclosure Information In the past 12 months, I have no relevant financial relationships with the manufacturer
Disclosure Common Apophyseal Problems in the Athlete Mark Halstead, MD November 19, 2009 Faculty Disclosure Information In the past 12 months, I have no relevant financial relationships with the manufacturer
42 nd Annual Symposium on Sports Medicine. Knee Injuries In The Pediatric Athlete. Disclosure
 42 nd Annual Symposium on Sports Medicine Travis Murray, MD Assistant Professor University of Texas Health Science Center San Antonio January 23, 2015 Knee Injuries In The Pediatric Athlete Disclosure
42 nd Annual Symposium on Sports Medicine Travis Murray, MD Assistant Professor University of Texas Health Science Center San Antonio January 23, 2015 Knee Injuries In The Pediatric Athlete Disclosure
Recognizing common injuries to the lower extremity
 Recognizing common injuries to the lower extremity Bones Femur Patella Tibia Tibial Tuberosity Medial Malleolus Fibula Lateral Malleolus Bones Tarsals Talus Calcaneus Metatarsals Phalanges Joints - Knee
Recognizing common injuries to the lower extremity Bones Femur Patella Tibia Tibial Tuberosity Medial Malleolus Fibula Lateral Malleolus Bones Tarsals Talus Calcaneus Metatarsals Phalanges Joints - Knee
tibial tubercle of the to 19 Compared pulling on inferior pole patella Cause subsequent pain The injury knee that is
 Osgood-Schlatter Disease Description Osgood Schlatter disease is an inflammatory injury of the growth plate on the tibia (shin bone) just below the level of the knee at the tibial tubercle This disease
Osgood-Schlatter Disease Description Osgood Schlatter disease is an inflammatory injury of the growth plate on the tibia (shin bone) just below the level of the knee at the tibial tubercle This disease
JOINT RULER. Surgical Technique For Knee Joint JRReplacement
 JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
