Patellofemoral instability is a common cause of knee
|
|
|
- Avis Rich
- 6 years ago
- Views:
Transcription
1 280 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4): Patella Instability Reuven Minkowitz, M.D., Chris Inzerillo, M.D., and Orrin H. Sherman, M.D. Patellofemoral instability is a common cause of knee pain and disability. Patellar instability can be defined in different ways, 1 the first as a clinical entity or diagnosis of a traumatic dislocation. It can also describe a sign on physical examination, signifying the ability of the patella to be translated out of the trochlear groove of the femur in a passive manner. Furthermore, patellofemoral instability can be a symptom, typically if the knee gives-way as a result of the patella slipping out of the trochlear groove. The relationships between the symptoms, injuries, and diseases of the patellofemoral joint are particularly confusing. 1,2 Addressing the specifics of anatomy, biomechanics, history, physical examination, and radiographic interpretation can shed important light on the treatment options of acute and recurrent patellar dislocation and subluxations. Bony Anatomy The patella is the largest sesamoid bone in the body, and resides within the complex of the quadriceps and patellar tendons. The patella assists in coordinating the forces of these tendons. The patella functions both as a lever and a pulley. As a lever, the patella magnifies the force exerted by the quadriceps on knee extension. As a pulley, the patella redirects the quadriceps force as it undergoes normal lateral Reuven Minkowitz, M.D., was a Chief Resident in the NYU Hospital for Joint Diseases Department of Orthopaedic Surgery, New York, New York. Chris Inzerillo, M.D., was a Fellow in the Sports Medicine Service, NYU Hospital for Joint Diseases Department of Orthopaedic Surgery, NYU Hospital for Joint Diseases, New York, New York. Orrin H. Sherman, M.D., is Associate Professor of Orthopaedic Surgery, New York University School of Medicine, and Chief of the Division of Sports Medicine, NYU Hospital for Joint Diseases Department of Orthopedic Surgery, NYU Medical Center, New York, New York. Correspondence: Orrin Sherman, M.D., Suite 8U, New York University Medical Center, 530 First Avenue, New York, New York tracking during flexion. The lateral trochlear facet, which is normally 1 cm higher than the medial, provides a buttress to lateral patellar subluxation and helps maintain the patella s centered position in the trochlea (Fig. 1). Soft Tissue Anatomy Passive stabilizers are present as uniform restraints of abnormal joint motion. In the patellofemoral joint, these structures include the patellar ligament or patellar retinacular complexes, which include the patellofemoral and patellotibial ligaments. Warren and Marshall 3 published a thorough description of the medial aspect of the knee, basing their description on the dissection of 154 fresh-frozen cadavers. They considered the medial patellofemoral ligament (MPFL), along with the superficial medial collateral ligament (MCL), to be part of layer 2, which is an extracapsular structure. The MPFL is a continuation of the deep retinacular surface of the vastus medialis obliques (VMO) muscle fibers. The patellofemoral ligament extends from the superior medial border of the patella (approximately at the two o clock position on a right knee) and attaches firmly to bone just anterior to the MCL, on the medial epicondyle (Fig. 2). Some superficial fibers of the MPFL can be seen to cross over the epicondyle and blend into the soft tissue posterior to the medial epicondyle. The medial epicondyle is the attachment site for the MCL and the MPFL. The size and thickness of the ligament varies considerably among individuals, but it is relatively constant within a given person. 4,5 The quadriceps functions as a dynamic stabilizer of the patella, while the MPFL acts as a static checkrein to resist lateral translation of the patella. Conlan and colleagues 6 reported that the MPFL contributes an average of 53% of the restraining force against lateral patellar displacement. Desio and associates 5 reported that the MPFL contributes 60% (range, 41% to 80%) of the total restraining force against Minkowits R, Inzerillo C, Sherman O. Patella instability. Bull NYU Hosp Jt Dis. 2007;65(4):
2 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4): Figure 1 Lateral tilt of the patella on an axial view being buttressed by the lateral trochlea. lateral patellar displacement. The patellomeniscal ligament and associated retinacular fibers were also found to be important medial stabilizers, contributing an average of 22% of the total restraining force. The remaining transverse fibers of the medial patellotibial band and ligament were found to be less important restraints to lateral subluxation of the patella. Anatomical studies by Lieb and Berry 7 have shown the contributions of the various portions of the quadriceps muscle to knee extension. They demonstrated that the vastus lateralis pulls laterally to the frontal plane of the femur at an angle of 7 to 10. The vastus medialis is divided into two parts, the vastus medialis longus (with its muscle fibers pulling at 15 to 18 medially) and the vastus medialis obliques (with its muscle fibers pulling at a relatively horizontal 50 to 55 medially). The primary function of the VMO muscle is to stabilize the patella against the lateral pull of the vastus lateralis, making the VMO the dynamic stabilizer of the patella. Biomechanics Stress encountered by the patellofemoral joint can be mathematically defined as the sum of joint reactive force (JRF) divided over the surface area of force distribution. From 0 to 60, the surface area of the patella that comes in contact with the femur enlarges as the knee is increasingly flexed. Beyond 60 of flexion, the studies have been inconclusive. With greater patellofemoral joint loads, the contact surface area is larger between the patella and femur. The location of contact for the patella and femur varies with different degrees of flexion and joint load. At 0, no contact occurs. At early flexion, the distal patella contacts the proximal trochlea. At 90, the superior aspect of the patella contacts the femur as the patella glides further inferiorly. When flexion is greater than 90, the contact area returns to the center of the patella; and when the knee is fully flexed, the inner border of the Figure 2 Image of the medial patellofemoral ligament (black oval) femoral attachment. (From Nomura E. Classification of lesions of the medial patello-femoral ligament in patellar dislocation. Int Orthop (SICOT). 1999;23:262. Copyright 1999 Springer-Verlag, with permission of Springer Science). medial femoral condyle is in contact with the small vertical ridge of the medial facet. 8 Lateral tracking of the patella leads to decreased efficiency of the quadriceps extensor mechanism and increased patellofemoral joint stress. A lateral patellar subluxation of only a few millimeters results in decreased contact surface area between the patellar and trochlear surfaces. Lateral tracking pushes the lateral facet closer to the lateral side of the trochlear groove, thus, creating a greater distance between the medial facet and the medial side of the trochlear groove. The total JRF, distributed over both patellar facets, is now completely transmitted through the lateral patellar facet, increasing lateral facet stress. The result can be pain and chondromalacia. A 2-cm elevation of the tibial tubercle has demonstrated a 50% reduction of the JRF when the knee is flexed to Q Angle Both static and dynamic forces tend to displace the patella laterally. Brattström 10 first described the Q angle (Fig. 3) as an angle formed by the line of pull of the quadriceps mechanism and that of the patellar tendon as they intersect at the center of the patella. Clinically, this angle is represented by the intersection of a line drawn from the anterosuperior iliac spine to the center of the patella, with a second line drawn from the center of the tibial tuberosity to the center of the patella. For this measurement to be accurate, the patella must be centered on the trochlea. In males, the Q angle, normally, is about 8 to 10 ; in females, the normal angle is 15, plus or minus 5. This valgus angle gives a lateral force vector to the patellofemoral joint as the knee is extended. The factors that can increase this Q angle are genu valgum, increased femoral anteversion, external tibial torsion, or a laterally positioned tibial tuberosity. The Q angle also can be increased in a dynamic mode by internally rotating the
3 282 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4): and 59 years of age to 1.5 to 2.0 per 100,000. This study did find that differences in the prevalence of injury based on gender showed a higher average annual risk for females in the second decade, but a higher risk for males in the third decade. Mechanism Two mechanisms of acute lateral patellar dislocations have been proposed. 14 An indirect injury and a direct blow. The indirect mechanism is more common and involves the combination of a strong quadriceps contraction, a flexed and valgus knee position, and an internally rotated femur on an externally rotated tibia. An example of this mechanism is a baseball batter s hind leg when he misses while swinging for a pitched ball. Patients with dislocations frequently have one or more predisposing risk factors (mentioned below). Medial dislocation and subluxation are much less common, usually iatrogenic, and are beyond the scope of this review. Figure 3 Q angle. (From Insall J, Falvo KA, Wise DW. Chondromalacia patellae. A prospective study. J Bone J Surg Am. 1976;58:1, with permission) femur on a fixed tibia, as in a cutting maneuver. Any of these factors that increase the Q angle can be a contributing element in recurrent patellar instability. Acute Patella Dislocation Epidemiology Nietosvaara and coworkers 11 studied the annual incidence of acute patellar dislocations in Finnish children younger than 16 years of age. The investigators found an annual incidence of 43 per 100,000 children. Over a 2-year period, a total of 72 children demonstrated patellar dislocations. Of these, 28 (39%) of the knees had associated osteochondral fractures. Of the 28 osteochondral fractures, 15 had capsular avulsions of the medial patellar margin, and a different 15 had intra-articular fragments from the patella or lateral femoral condyle. The true incidence of acute patellar dislocation in the adult is difficult to discern from the literature. This is primarily due to the lack of population-based prospective studies and a prevalence of retrospective evaluations and case series. 12 The largest North American study to date is that by Atkin and colleagues in They prospectively studied a group of Kaiser Permanente patients from the greater San Diego area of Southern California. The average plan enrollment included more than 360,000 patients, with approximately 1000 of these patients referred each year for evaluation of knee injury. During the three-year study period, 74 patients from this group were diagnosed with primary patellar dislocation. Broken down by age, at 31 per 100,000, the highest annual risk was noted for patients in the second decade. The average annual risk dropped to 11 per 100,000 in the third decade and dropped still further for patients between Pathology (Figs. 4 and 5) Acute lateral patellar dislocation has been associated with medial retinacular injury. As described in an article by Elias and White, 15 Marangi and associates reported on a consecutive series of 74 cases of acute lateral patellar dislocation using MRI. Evidence of medial retinacular injury was seen in 75% (56) of patients. In 44% of knees, complete retinacular disruption was noted near the patellar attachment. Burks and coworkers 16 reported a simulation of patellar dislocation using a cadaveric model. They compared MRI and gross anatomic findings in 10 fresh-frozen cadaveric knees. After MRI imaging, they dissected the medial structures to determine where the ligamentous injury occurred. The MPFL was injured in eight out of the 10 knees. Although the location can vary, the most frequent site found was the femoral attachment of the MPFL. In 2003, Nomura 17 studied 39 consecutive knees with initial lateral patellar dislocation. Articular cartilage injuries were examined using arthroscopy or macroscopic observation. Thirty-seven knees (95%) had articular cartilage injuries of the patellofemoral joint and two knees (5%) had no cartilage injury. In all 37 knees (95%), articular cartilage injuries were observed in the patella, showing that articular cartilage injuries, especially of the patella, seem to be common occurrences after acute patellar dislocation. Physical Exam Acute dislocation of the patella in the adult requires disruption of the medial patellar restraints. Swelling associated with the acute injury is often rapid, and a significant hemarthrosis frequently develops, especially if there is an associated osteochondral fracture. This swelling may mask a persistent lateral subluxation of the patella within the trochlea and may be noted on physical examination. As well, loose chondral or bony fragments may be palpable in the joint, and attached osteochondral fragments may be felt in
4 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4): A B Figure 5 Patellar dislocation. A, Anteroposterior view. B, Sunrise view. Figure 4 Axial gradient-echo image (TR/TE, 450/10, Flip angle 30 ) of complete retinacular disruption near the patellar insertion (white arrow). (From Arendt EA. Current concepts of lateral patella dislocation. Clin Sports Med. 2002;21(3):509. Copyright 2002, WB Saunders, with permission from Elsevier.) the medial parapatellar retinaculum. A thorough palpation of the knee should be performed to detect focal areas of maximum tenderness that suggest soft tissue injury. The examiner may find a palpable defect at the medial patellar margin, tenderness along the course of the MPFL and the other medial retinacular ligaments, or tenderness near the medial femoral epicondyle at the MPFL insertion site. Tenderness at the medial femoral condyle may suggest an injury to the MCL of the knee. If significant disruption of the VMO insertion has occurred, there may be a palpable defect at its distal insertion, as well as a visible change in its symmetry. A positive apprehension test at 30 of flexion is the classically described examination finding (Fig. 6). With or without apprehension, the physician may be able to demonstrate increased medial retinacular laxity that is not symmetrical with the contralateral knee. 12 Management Acute dislocations of the patella usually are managed by closed methods. 18 The patella is almost always dislocated laterally; extension of the flexed knee with pressure applied to the lateral margin of the patella results in reduction. After an acute dislocation, the knee is immobilized in a commercial immobilizer with a Jones-type compressive dressing, and crutches are used for ambulation. If a large hemarthrosis is present, causing significant pain and tightness, aspiration under sterile conditions is indicated before the extremity is immobilized. Early short arc (0 to 45 ) range of motion is begun in order to prevent arthrofibrosis and to promote the formation of strong collagen along the lines of stress. Roentgenograms (Fig. 5) should be carefully evaluated to be certain that no osteochondral fragments are displaced within the joint. The patient should be warned of the possibility of future episodes of recurrent patellar subluxation or dislocation. Rehabilitation Quadriceps setting exercises and three sets of 15 to 20 straight leg raises are done four or five times a day during the acute period. Ice is applied for 20 minutes every 2 to 3 hours to reduce swelling. The knee immobilizer and compressive wrap are discontinued approximately 2 to 3 weeks after the acute reaction has resolved. The crutches are discontinued when the patient is able to do straight leg raises with a 5-lb ankle weight and is able to walk with a near normal gait. Rehabilitation should emphasize closed chain exercises, including wall sets, in which the patient squats to approximately 40 while keeping his back flat against the wall for 15 to 20 seconds, for a total of 10 to 15 repetitions. Side and forward step-up exercises using a 6 to 8 inch platform should be performed after the acute inflammatory reaction has resolved. These are followed by short arc leg presses and endurance-type strengthening using a stationary bike and StairMaster or similar stepping machine. The patient can return to sports activity when quadriceps and hamstring muscle strength is normal and sport-specific agility has been regained. Generally, a patellar stabilizing brace is prescribed for the first 2 or 3 months after return to athletic activities. 19 McConnell taping techniques or patellar stabilizing braces have both been commonly used during rehabilitation and when the athlete first returns to sports participation. 13 Although these techniques and braces may serve a protective or proprioceptive function, no outcome studies in the
5 284 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4): literature prove that they reduce the rate of redislocation. 20 Nonoperative Outcomes Redislocation or recurrent subluxation rates after nonoperative treatment have been reported to be as high as 48%. 21 Cofield and Bryan 22 reported that in patients considered athletes, at an average of 5 years after injury, 52% remained unable to return to vigorous sports. Even in more recent literature, there is significant variability among both patient population and treatment methods. Garth and Pomphrey 19 reported on an aggressive, modern rehabilitation protocol in 58 athletically active patients. They began a functional rehabilitation program without antecedent immobilization. At the initial visit, patients were instructed in isometric and isotonic quadriceps strengthening and active and active-assisted range of motion exercises with a stationary bicycle were begun. Patients wore a lateral buttressing knee sleeve, initially for ambulation, until muscle strength was documented to be at least 80% that of the opposite extremity. They reported a return to full activity, with resolution of all significant tenderness, and a return of full isotonic quadriceps strength after, generally, 3 to 8 weeks. Sixty-eight percent of the patients who were treated after acute patellar dislocation without previous symptoms had good or excellent results, with 30% experiencing impairment in athletics. In 2000, Atkin and colleagues 13 studied the early recovery phase (at 6 months); almost 60% of patients continued to have limitations with strenuous activities. These results show that, unfortunately, a large percentage of patients are left with recurring problems of patellofemoral pain and instability. Operative Treatment Operative indications for treatment of an initial dislocation of the patella in the adult continue to be controversial. 23 In the current literature, the most commonly cited indications for operative treatment in the adult without predisposing malalignment include the following: patients with evidence of osteochondral loose bodies, patients with large palpable defects in the VMO insertion, those with obvious tears of the medial peripatellar retinaculum, and those with persistent asymmetrical subluxation. Elite athletes and, more recently, patients thought to have an avulsion of the MPFL are also operative candidates. 24 Use of a realignment procedure assumes that there was an underlying, predisposing malalignment (discussed below). Lateral release is performed if there is an associated tilt. Repair and reconstruction are appropriate if there is an identifiable soft tissue injury. Arthroscopy is usually adequate for a thorough diagnosis and for treating osteochondral injuries and may be used alone or in combination with other procedures. Generally, surgical repair of acute patellar dislocation is best performed within 2 to 3 weeks of injury in order to avoid operating through early scar tissue formation. A diagnostic arthroscopy is utilized to inspect the joint for evidence of soft tissue or capsular injury and to repair or remove osteochondral or chondral loose bodies. The MPFL is external to the synovial layer and, usually, is not visible directly by arthroscopy. Repair of MPFL avulsions or VMO insertional tears is performed through a 4-cm to 6-cm incision just anterior to the medial femoral epicondyle, at the distal edge of the VMO muscle belly. The MPFL is identified confluent with the deep fascia of the VMO and can be demonstrated, usually, to have a direct connection to the superior medial border of the patella. In most of these cases, the MPFL can be found to have avulsed off the femur and may be repaired directly by adhering to bone with suture anchors. Complete intrasubstance tears are repaired with permanent suture. Overlying retinacular tears are then repaired with absorbable suture. If the retinaculum and capsule are disrupted near the patella, this is usually clear from the examination and MRI, and repair is performed through a medial parapatellar incision. In patients without a substantial MPFL, repair can be supplemented with a hamstring graft from the patella to the femoral attachment site of the MPFL. The retinaculum and VMO are also slightly imbricated in the repair. Postoperative treatment consists of progressive weightbearing as tolerated in a postoperative brace, followed by early range of motion and quadriceps strengthening exercises. Regaining flexion can be difficult, even if range of motion is started early. Occasionally, manipulation under anesthesia is required. The athlete is allowed to return to sport-specific training when he or she has regained full, nontender functional range of motion and demonstrates muscular strength equal to 80% to 90% that of the contralateral limb. Return to play follows a demonstration of adequate recovery during functional testing. 12,14 Operative Outcomes In recent reports of operative treatment, rates of recurrence have ranged from 0% to 17% At first glance, these results appear superior to those attained with nonoperative treatment, but few randomized, truly prospective studies have been done. Follow-up is generally limited, the numbers of patients are small, and the operative methods as well as results are varied. Vainionpaa and colleagues 26 reported the results of open repair in 55 patients followed prospectively after their first patellar dislocation. At 2 years, subjective results were good or excellent in 80%, with a redislocation rate of 9%. Sallay and associates 27 reported on 16 patients and found 94% to have had the MPFL avulsed from the femur. Suture repair was performed and, with an average 3-year follow-up, no recurrences were seen; 58% of patients returned to their previous sport. Nikku and Nietosvaara, 28 in 1997, reported on the results of a prospective randomized trial of nonoperative versus operative treatments in 176 consecutive patients, all of whom had sustained primary patellar dislocation. In the group randomized to operative treatment, patients had individually adjusted procedures that consisted of a mixture of medial
6 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4): retinacular repair or duplication, adductor magnus tenodesis, and lateral release. In this report of 2-year results, recurrent instability episodes were equivalent, and both function and subjective results were better in the nonoperative group. The investigators felt surgery gave no additional benefit, and it remains to be seen whether long-term follow-up will change their findings. Summary In summary, the literature suggests that two main groups of patients suffer acute dislocation of the patella, those with and those without significant predisposition. In young athletically active adults without previous history of subluxation, who sustain an acute patellar dislocation, the surgeon can focus on addressing specific pathology. It is clear that some patients do well with nonoperative treatment. There is, however, significant enough incidence of occult intra-articular injury that arthroscopic evaluation should be strongly considered in most patients. 2,28,29 In addition, repairing the main medial stabilizer to the patella, the MPFL, may restore patellar stability. Owing to the lack of long-term, prospective study results, however, it continues to be unclear as to whether operative treatment consistently provides significantly improved outcomes, reliably preventing recurrent subluxation or dislocation. Guidelines are as follows: Since it is not possible to predict who will do well with nonoperative treatment, operative treatment should be avoided unless there is a displaced articular surface fragment or any acquired lateral displacement of the patella that is unreduced. Only do an acute release in patients who have a very tight lateral retinaculum associated with imaging evidence of tilt. Avoid excessive medial imbrication, which may overload the medial facet and predispose the patient to medial facet arthrosis. Tear of the MPFL is not always at the adductor tubercle and is frequently multifocal. Obtain preoperative MRI image if acute surgery is planned Recurrent Patellofemoral Instability Risk Factors The typical physical characteristics of the patellar dislocator have been characterized as an adolescent female with ligamentous laxity and multiple developmental anomalies, including trochlear dysplasia, patella alta, and rotational and angular bony alignment. 14 Trochlea dysplasia and patella alta reduce the containment of the patella within the femoral trochlea at any given angle. This contributes directly to the risk of recurrent patellar dislocation by reducing the relative height of the trochlear buttress to the patella. Dysplasia of the lateral femoral condyle can be a contributing factor. Patients with a hypoplastic lateral femoral condyle have lost a bony support that prevents lateral subluxation of the patella from the intercondylar groove. Amis and Dejour 30 reported that simulation of a shallow trochlea in cadaver knees dramatically increases mediolateral patellar mobility. Additional factors that may contribute to recurrent dislocation of the patella include a change in orientation of the fibers of the vastus medialis muscle, atrophy of the vastus medialis, hypertrophy of the vastus lateralis, and generalized ligamentous laxity. In 2004, Fithian and coworkers 31 prospectively followed 189 patients who had a patella dislocation. They found the risk was highest among females 10 to 17 years of age. Patients presenting with a prior history of instability were more likely to be female and were older (median age, 21 years) than first-time dislocators. Fewer first-time dislocators (17%) had episodes of instability during follow-up than patients with a previous history of instability (49%). After adjusting for demographics, patients with a prior history had a seven-fold increase in probability for subsequent instability episodes during follow-up than first time dislocators. Clinical Features History In patients with recurrent dislocation or subluxation of the patella, an accurate history is still one of the most important diagnostic tools. Patients who have recurrent dislocation frequently report diffuse pain about the knee that is aggravated by going up and down stairs or climbing hills. Usually, the pain is located anterior in the knee and often is described as an aching pain with intermittent episodes of sharp, severe pain. A feeling of insecurity in the knee and occasionally of giving way of the knee or the knee going out may be present. Physical Exam Patellar crepitation and swelling of the knee are common. Physical findings include the previously cited factors that contribute to the Q angle. In addition, patellofemoral crepitus may be palpable, and an effusion may be present. Several testing maneuvers are helpful in evaluating patients with recurrent patellar dislocation or subluxation. The patellar grind test is done by applying pressure to the patella and manually displacing it medially, laterally, superiorly, and inferiorly in the trochlear groove. This test reproduces anterior knee pain when a patellofemoral pathological condition is present. In the apprehension test, (Fig. 6) the examiner holds the relaxed knee in 20 to 30 of flexion and manually subluxes the patella laterally. When the test is positive, the patient suddenly complains of pain and resists any further lateral motion of the patella. The same controlled maneuver is done while slowly flexing and extending the patient s knee. The examiner visually divides the patella into four quadrants and passively moves the patella medially and then laterally, measuring the amount of excursion in the patellar quadrants (Fig. 7). This is done with the knee at 0 and at 20 of flexion. Normally, passive patellar glide is one but not more then two quadrants, both
7 286 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4): Figure 6 Apprehension test. (From Walsh WM: Recurrent dislocation of the knee in the adult. In: DeLee J III, Drez D IV, Miller MD (eds): DeLee & Drez s Orthopaedic Sports Medicine: Principles and Practice. (2nd ed). Philadelphia: Saunders, 2003, p Copyright 2003 Saunders, with permission from Elsevier.) Figure 8 Patellar tilt test. In this left knee, the patella can be tilted so that the lateral edge is well anterior to the medial edge. (From Walsh WM: Recurrent dislocation of the knee in the adult. In: DeLee J III, Drez D IV, Miller MD (eds): DeLee & Drez s Orthopaedic Sports Medicine: Principles and Practice. (2nd ed). Philadelphia: Saunders, 2003, p Copyright 2003 Saunders, with permission from Elsevier.) Figure 7 Depiction of two quadrants of lateral translation of the patella. (From Arendt EA. Current concepts of lateral patella dislocation. Clin Sports Med. 2002;21(3):504. Copyright 2002 WB Saunders, with permission from Elsevier.) medially and laterally. Excessive lateral retinacular tightness is indicated by limited medial passive patellar glide and by a negative patellar tilt. The patellar tilt test is done with the knee in extension (Fig. 8). The examiner s fingers are placed along the medial side of the patella and the thumb on the lateral aspect. Inability to raise the lateral facet to the horizontal plane or slightly past indicates excessive lateral retinacular tightness. Dynamic patellar tracking is evaluated with the examiner standing in front of the seated patient while the patient slowly extends the knee. A positive J sign, lateral subluxation of the patella as the knee approaches full extension, indicates some degree of maltracking. Active patellar tracking also should be examined with the knee in the extended relaxed position. The quadriceps is tightened, and motion of the Figure 9 A, Knee in flexion. B and C, Positive J sign, or lateral subluxation of the patella as the knee approaches full extension. (From Walsh WM: Recurrent dislocation of the knee in the adult. In: DeLee J III, Drez D IV, Miller MD (eds): DeLee & Drez s Orthopaedic Sports Medicine: Principles and Practice. (2nd ed). Philadelphia: Saunders, 2003, p Copyright 2003 Saunders, with permission from Elsevier.) patella is examined. Normally, the patella should move more superiorly than laterally (Fig. 9) Tenderness may be palpated at the quadriceps or patellar tendon insertion on the patella or at the medial or lateral
8 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4): retinaculum; defects in the retinaculum also may be palpable. Tenderness along the medial or lateral facets of the patella may be noted on direct palpation of the facet as the patella is manually subluxed and rotated to expose these articular surfaces. This patellar tenderness may indicate a pathological condition of the articular cartilage. Thigh circumferences, measured proximal to the patella, often show quadriceps atrophy on the involved side. With the patient sitting and the knees flexed 90, a lateral or superior position of the patella sometimes can be seen. After careful examination of the uninvolved and injured knees, other joints should be examined for hyperlaxity. Hyperextension of the knees or elbows past 10, ability to touch the thumb passively to the forearm, hyperextension of the metacarpophalangeal joint of the index finger, and multidirectional laxity of the shoulder joint all are indicative of generalized ligamentous laxity. Stanitski 32 found that patients with generalized ligamentous laxity did worse than patients without ligamentous laxity. Imaging Radiographic Exam The AP roentgenogram is of limited use regarding patellofemoral problems. This view may reveal a bipartite patella, which is a variant of normal. Occasionally, an osteochondral fracture of the medial patellar edge can be seen. Loose bodies or osteochondral fractures occasionally are present. The lateral view yields more commonly used information relating to patella alta or excessively low (patella infra or baja) patella. The method of Blumensaat is of historical significance only 33 and related the position of the patella to a line projected along the roof of the intercondylar notch. Investigators such as Insall and Salvati have found the Blumensaat line to be an inexact index of patella alta. In a review of 114 lateral roentgenograms of normal knees, Insall and colleagues 33 found that the length of the patellar tendon (LT) and the diagonal length of the patella (LP) had a ratio of 1.0, with less than 20% variation. They concluded that patella alta is likely to be present if LT exceeds LP by more than 20% (ratio of 1.2 or more) (Fig. 10). The most widely used axial views are those described by Merchant and associates 34 and Laurin and coworkers. 35 In the Merchant technique, the patellofemoral joint is viewed with knees flexed to 45. The radiographic tube is positioned above the knee, with the radiographic plate positioned distal to the knee. These investigators originally described the congruence angle (Fig. 11) and the technique of measuring the angle. The average congruence angle in 100 normal subjects was found to be 6, with a standard deviation of 11. This means that a congruence angle of greater than +16 is abnormal at the 95th percentile. Aglietti and colleagues 36 are credited with providing a more accurate definition of the congruence angle. Their study found an average congruence angle of 8, with a Figure 10 Assessment of patella alta (technique of Insall and Salvati). The ratio of the longest diagonal of the patella to the length of the patellar tendon should be 1.0 ± 20%. (From Walsh WM: Recurrent dislocation of the knee in the adult. In: DeLee J III, Drez D IV, Miller MD (eds): DeLee & Drez s Orthopaedic Sports Medicine: Principles and Practice. (2nd ed). Philadelphia: Saunders, 2003, p Copyright 2003 Saunders, with permission from Elsevier.) Figure 11 Congruence angle of Merchant. Line BO is the bisector of angle ABC. Line BX passes through the lowest point on the median ridge of the patella. Angle OBX is the congruence angle. If line BX falls to the medial side of line BO, the angle is expressed as negative degrees. If it falls to the lateral side of line BO, it is expressed as positive degrees. (From Walsh WM: Recurrent dislocation of the knee in the adult. In: DeLee J III, Drez D IV, Miller MD (eds): DeLee & Drez s Orthopaedic Sports Medicine: Principles and Practice. (2nd ed). Philadelphia: Saunders, 2003, p Copyright 2003 Saunders, with permission from Elsevier.)
9 288 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4): A B Figure 12 Measurement of lateral patellofemoral angle. Line YY is drawn across the most anterior portions of the femoral trochlea in the axial view of this left knee. Line XX follows the slope of the lateral patellar facet. A, Demonstration of a normal angle in which the angle opens laterally. B, Demonstration of an abnormal angle with the angle open medially. (From Walsh WM: Recurrent dislocation of the knee in the adult. In: DeLee J III, Drez D IV, Miller MD (eds): DeLee & Drez s Orthopaedic Sports Medicine: Principles and Practice. (2nd ed). Philadelphia: Saunders, 2003, p Copyright 2003 Saunders, with permission from Elsevier.) standard deviation of 6. Laurin and associates 35 described a technique in which the knees are flexed to 20 to 30. The radiographic tube is positioned between the ankles, with the cassette held proximal to the knees by the patient. On this view, these authors defined a lateral patellofemoral angle (Fig. 12). They indicated that, normally, this angle is open laterally, whereas in patients with patellar tilt, the lines used to define the angle are parallel or open medially. Teitge and coworkers 37 described a radiographic technique that can be a helpful adjunctive test for diagnosing patellar instability. They first obtained bilateral axial radiographs of the patellofemoral joints in anatomic position. A constant medial and lateral force was applied to the patella with an instrumented device, and axial radiographs were repeated. They found that a 4 mm increase in medial or lateral patellar excursion, compared with the asymptomatic knee, correlates with patellar instability. These dynamic radiographs are thought to be more reliable than static films. Computed Tomography Inoue and colleagues 38 described a group of patients with minimal subluxation in whom the condition was determined more accurately by using computed tomography (CT) with the knee in full extension. They found that, with the knee extended, the lateral tilt of the patella was more pronounced in patients who had patellar subluxation than in patients of the normal control groups. The patients with patellar subluxation had a lesser degree of abnormality, and the subluxation was not seen with the knee flexed 30 to 45, as is usual in most routine axial views. Another role for CT is identifying lateralization of the tibial tubercle as measured by the distance between the tibial tubercle and the trochlear sulcus. An axial CT image demonstrating the femoral groove is superimposed on an axial image of the tibial tubercle. A line is drawn on this superimposed image between the posterior margins of the femoral condyles. Two lines are drawn perpendicular to this line, one bisecting the femoral trochlear groove (TG) and the other bisecting the anterior tibial tuberosity (ATT). The distance between these two lines determines the extent of lateralization of the tibial tubercle. Values greater than 9 mm have been shown to identify patients with patellofemoral malalignment with a specificity of 95% and a sensitivity of 85%. 39 More recently, Shakespeare and Fick, 40 in 2005, tried to measure theses parameters by clinical exam only. They concluded that examination alone is not reliable and that CT is the only accurate way to measure the ATT-TG distance. Magnetic Resonance Imaging (MRI) Pathologic entities such as chondromalacia, articular cartilage injuries and degeneration, synovial plicae, and patellar tendinitis can be visualized on MRI. Studies similar to those made with CT scans can easily be accomplished with MRI without exposure to radiation, although they involve considerable expense. Recent interest has been generated in the determination of what MRI can show regarding the acute lesion associated with patellar instability, as mentioned above. Among the first to describe this were Sallay and coworkers. 27 They demonstrated how clearly the rupture of the MPFL from the femur could be seen on both sagittal and axial T2-weighted views. Shellock and associates 41 described a medial subluxation of the patella that could be demonstrated only by kinematic MRI of the patellofemoral joint done with the knee at 0, 5, 10, 15, 20, 25, and 30 of flexion. Identifying these subluxations is important, because releasing the lateral side of this patella would make the condition worse. MRI can be helpful in determining the site of retinacular or patellofemoral ligamentous injury if the physical examination is equivocal and surgical repair is contemplated. One must bear in mind that, although these roentgenographic techniques are important in evaluation of the patellofemoral joint, the diagnosis of patellar dislocation or subluxation is made by clinical evaluation and not only by roentgenogram. Conservative Management Surgery is not needed in all patients with patellofemoral malalignment or recurrent subluxation of the patella. Satisfactory results may be achieved with a conservative exercise treatment program. A rehabilitation program to strengthen
10 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4): the quadriceps muscle and VMO is of primary importance. A program similar to that followed after acute dislocation, with the addition of more resistive exercises, can be started early, and a patellar stabilization brace may help prevent chronic recurrent subluxation. Using kinematic MRI, Muhle and coworkers 42 demonstrated no significant effect on patellar tracking when bracing was used. It is unknown whether the brace benefits proprioception as above. Operative Management If clinical improvement with nonoperative treatment has plateaued, operative intervention may be required. Repeated subluxations or dislocations may cause continued apprehension and progressive joint damage. An abnormal patellofemoral articulation, abnormal quadriceps pull, osteochondral free fragments, chondromalacia of the patella, meniscal tears, and degeneration all contribute to progressive deterioration of the knee joint. No single operation is universally successful in correcting recurrent patellar dislocation and subluxation. The operation must be chosen insofar as possible with the needs of the individual patient as the foremost consideration. The extent of the malalignment, the patient s age, the level of activity, and the condition of the joint also are important. Over 100 operations have been described for the treatment of recurrent subluxation or dislocation of the patella. These procedures can generally be divided into categories: 1. Proximal realignment of the extensor mechanism. These procedures alter the medial-lateral position of the patella through manipulation of the soft tissues proximal to its inferior pole. Included in this category are lateral retinacular release, medial plication, vastus medialis obliques advancement, and MPFL repair and reconstruction. 2. Distal realignment of the extensor mechanism. These operations modify the positions of the patella by way of transferring the tibial tuberosity or through surgery on the soft tissues distal to the inferior pole. Most commonly, this method involves medial or anteromedial displacement of the tibial tuberosity. 3. Combined proximal and distal realignment. Proximal Realignment Proximal realignment of the patella is a realignment of the quadriceps muscle to the patella, with or without a lateral release. As emphasized by Insall and colleagues, 33 in 1972, and Insall, 43 in 1982, the operation is not a capsular procedure but rather a quadricepsplasty. Proximal realignment is indicated for patellar instability when the Q angle is the normal range. When the Q angle approaches 20, additional distal realignment should be considered. Further indications are asymmetrical lateral patellar translation at 30, significant trochlear dysplasia, normal or mild tubercle malalignment, and absence of severe medial patella arthrosis. 2,18,41,44 These procedures may be performed by open or mini imbrication, Figure 13 Insall technique of proximal realignment of the patella. A, Medial and lateral vasti are separated from rectus femoris tendon. B, Lateral release is performed; synovium is left intact. C, Completed closure is tight to hold patella securely in femoral groove. D, Remaining medial flap sutured without further overlap. (From Phillips BB: Recurrent dislocations. In: Canal ST (ed): Campbell s Operative Orthopaedics. (10th ed). Philadelphia: Mosby, 2003, p, Copyright 2003 Elsevier. Sources for illustration. A and C redrawn from Insall JN, Aglietti P, Tria AJ Jr: Patellar pain and incongruence. II: Clinical application. Clin Orthop 1983;(176):225-32; B, redrawn from Insall JN, Falvo KA, Wise DW: Chondromalacia patellae. A prospective study. J Bone Joint Surg Am.1976;58;1:1-8. Copyright 1976, The Journal of Bone and Joint Surgery, Inc.; D, redrawn from Insall J, Bullough PG, Burstein AN. Proximal tube realignment of the patella for chondromalacia patellae. Clin Orthop Relat Res. 1979;(144):63-9. All sources, with permission.) as well as arthroscopic medial imbrication. A proximal tube realignment of the patella was described by Insall and associates (Fig. 13). In this technique, the vastus medialis is brought laterally and sutured to the free edge of the vastus lateralis, forming a flattened tube proximal to the patella (Fig. 13). Their results in 53 knees showed 81% excellent or good results and 19% fair or poor.
11 290 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4): under 15 (Fig. 14); 87% of patients had good to excellent results. The medial patellotibial ligament was also reconstructed using a portion of the autograft. The investigators admitted that the patellotibial ligament may not contribute significant stability, as evidenced by prior anatomic studies. Additionally, although the MPFL reconstruction was performed with a lateral release, they contended, and previous studies support, that lateral release alone would have led to inferior results. Figure 14 The reconstructed medial patellofemoral ligament and the medial patellotibial ligament. (Reprinted from Drez D Jr, Edwards TB, Williams CS. Results of medial patellofemoral ligament reconstruction in the treatment of patellar dislocation. Arthroscopy. 2001;17(3): Copyright 2001, with permission from the Arthroscopy Association of North America.) Halbrecht, 45 in 2001, reported his results of arthroscopic all-inside medial reefing and lateral release. Arthroscopic reefing was performed by percutaneous passage of suture, followed by arthroscopic retrieval and knot tying inside the joint. Ninety-three percent had significant subjective improvement, as well as improvement of the congruence and lateral patellofemoral angle. This procedure is indicated for mild to moderate insufficiency of the MPFL, with a normal Q angle, and without trochlear dysplasia or patella alta. MPFL Reconstruction Since recognition of the important role of the MPFL, techniques have begun to emerge addressing this pathologic process. Hautamaa and colleagues 4 believe that proximal realignment should always repair the MPFL and they demonstrated the effectiveness of this in restoring balance in cadaver knees. Key points to MPFL reconstruction are that isometry is a critical factor and the MPFL should not be over tensioned. In chronic dislocations, reconstruction of the MPFL is performed rather than repair. Avikainen and coworkers 46 presented a technique of augmentation of the MPFL with a strip of adductor magnus tendon. There was one redislocation in 14 patients. Muneta and colleagues 47 reconstructed the MPFL with a double strand gracilis tendon in five cases and an iliotibial band allograft in one. Drez and colleagues, 48 in 2001, presented a series of 19 patients who underwent reconstruction of the MPFL with a lateral release using autogenous hamstrings or iliotibial band and a minimum 2-year follow-up with an average Q angle of Lateral Release The treatment of choice for patellar tilt is an arthroscopic release. This procedure has been shown to be most effective in patients with patellar tilt 49 (as mentioned above). The lateral release does not substantially reduce the active lateral vector of the quadriceps and, therefore, has less satisfactory results in patients with subluxation. Arendt 2 showed that lateral patellar tilt could be a function not only of lateral retinacular tension but also of isolated medial retinacular laxity. Therefore, most investigators 2,49 would recommend that a lateral release be used only when there is residual patellar tilt (a physical examination sign) after restoration of the medial retinacular structures or limited medial passive patellar displacement. The arthroscopic release is performed 5 mm lateral to the patellar border, covering the distance from 1 cm superior to the patella to the anterolateral portal. Hemarthrosis, the most common postoperative complication, inhibits the quadriceps and delays rehabilitation. This can be minimized by using electrocautery and deflating the tourniquet before closure. Distal Realignment Reducing the Q angle by medializing the tibial tubercle insertion has long played a role in patellar realignment surgery. One of the more popular current operations is one that involves medial displacement of the anterior tibial tubercle. This operation was originated and performed by Roux 50 in The principles were modified by Elmslie and published by Trillat and associates. 51 The intent of the operation was to diminish the Q angle and effectively medialize the extensor mechanism to correct lateral tracking of the patella. Current indications for distal realignment are: Increased quadriceps angle or ATT-TG distance, Normal lateral patellar glide (intact MPFL), Static malalignment of patella with tilt, Medial facet arthrosis, and Patella alta. In 1994, Shelbourne and coworkers 52 reported 45 patients with a 2-year follow-up using a modified Elmslie-Trillat procedure for refractory patellar instability (34 knees) or painful patellofemoral syndrome with malalignment (11 knees). The postoperative congruence angle (mean, +3.4 ) was significantly improved when compared with the preoperative value (mean, ). The normal congruence angle is on average -8. Even though their results were better than prior Elmslie-Trillat osteotomies, 51,53 nine knees (20%) had some
12 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4): Figure 15 The direction and extent of the tibial tubercle displacement in the Fulkerson anteriomedialization osteotomy. (From Fulkerson JP, Hungerford DS. Surgical treatment of patellofemoral chondrosis and arthrosis. Disorders of the Patellofemoral Joint. (2nd ed). Baltimore: Williams & Wilkins, 1990, p Copyright 1990 Williams & Wilkins, with permission Lippincott Williams & Wilkins, Wolters Kluwer.) postoperative subluxation. Furthermore, medial tibial tubercle transfer may lead to medial patellofemoral arthrosis. 54 To avoid potential loading of the medial patellar facet or to unload potential damage to patellar articular cartilage in recurrent patellar dislocations, some investigators advocate anteriorization of the tibial tubercle and medialization. Maquet 53 and Bandi 55 first introduced elongation of the extensor lever arm by anterior displacement of the tibial tuberosity. This operation has been modified further by Fulkerson and colleagues. 56 Anteromedial Tibial Tubercle Transfer (Fulkerson Procedure) This procedure corrects the Q angle with medialization of the tibial tubercle and unloads the patellofemoral articulation with anteriorization of the tubercle (Fig. 15). A hinge of bone is maintained intact at the distal tubercle to facilitate healing. After the transfer, the bone pedicle is locked into position with two cortical screws. Patients are made non-weightbearing for 6 to 8 weeks to avoid tibia fracture. Fulkerson and associates 56 reported 93% good and excellent results subjectively and 89% good and excellent results objectively. Trochleoplasty Trochlear dysplasia is identified as a predominant factor in symptomatic patellar dislocation. 57 Trochlear dysplasia, however, is an anomaly that is difficult to correct. A trench type trochleoplasty is technically difficult to perform, and there is concern that there is potential disruption of the cartilage surface or change in contact pressure that may lead to postoperative pain and arthrosis. Clinical outcome seemingly would depend also on the type and shape of the patella, which are factors particularly difficult to simulate and by which to predict an outcome. In 2005, Verdonk and coworkers 58 performed a Henri Dejour trochleoplasty on 13 patients complaining of recurrent patellar dislocations or persistent retropatellar pain due to a dysplastic femoral trochlea. In this technique, the femoral trochlea is deepened by removing the subchondral trochlear bone, followed by incision, impaction, and fixation of the cartilage flange along the trochlear groove. They achieved 77% good to very good subjective results. Although the outcome was not perfect, the patients were satisfied with the procedure. The investigators suggested that this technique might be a valuable alternative in cases of frank trochlear dysplasia associated with persistent retropatellar pain or recurrent patellar dislocations. Combined Proximal and Distal Realignment Indications for a combined proximal and distal procedure are a combination of tubercle malalignment and traumatic incompetency of the medial restraints. Hughston and Walsh 59 reported satisfactory results using a technique for reconstruction of the extensor mechanism that combines many aspects of other procedures. They emphasized the importance of a proximal extensor mechanism reconstruction, including careful placement of the vastus medialis muscle. Distal realignment is indicated for knees in which the Q angle is increased beyond 20 in skeletally mature patients. The surgeon should first correct tubercle malalignment and then reassess patellar tracking, in combination with lateral retinacular release. If patellar tracking is still not corrected and lateral instability is still present, the surgeon should perform medial augmentation or reconstruction of the MPFL. More recently, in 2004, Palmer and colleagues 60 reported their results of a lateral release, a VMO advancement, and an anteromedial tibial tubercle transfer to correct all the abnormalities of patellofemoral maltracking, including patella alta. One hundred seven knees in 84 patients were reviewed, with a mean follow-up of 5.6 years. Seventy-nine percent of patients had a good to excellent functional outcome, and 84% of patients stated they would have the operation again. Two patients with marked generalized ligamentous laxity had recurrent dislocation of the patella. Conclusions Patellofemoral instability can be difficult to treat. Surgical treatment of patellar dislocations both acute and chronic have evolved significantly with the advancement of biomechanical knowledge of patellofemoral restraints and injury patterns identified by physical examination and improved
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes
 Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
7/20/14. Patella Instability. Alignment. PF contact areas. Tissue Restraints. Pain. Acute Blunt force trauma Disorders of the Patellafemoral Joint
 Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016
 Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Patella Instability 1 st Time Dislocation
 Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Why does it matter? Patellar Instability 7/23/2018. What is the current operation de jour? Common. Poorly taught. Poorly treated
 Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Peggers Super Summaries: PFJ
 Patellofemoral Joint: ANATOMY: Largest sesamoid ossifying at 3-5 years of age Multiple foci having a sec ossification centre SUPEROLATERAL Helps increase moment arm PATELLOFEMORAL OA Incidence 10% of knee
Patellofemoral Joint: ANATOMY: Largest sesamoid ossifying at 3-5 years of age Multiple foci having a sec ossification centre SUPEROLATERAL Helps increase moment arm PATELLOFEMORAL OA Incidence 10% of knee
Where to Draw the Line:
 Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Doron Sher. 160 Belmore Rd, Randwick Burwood Rd, Concord. MBBS, MBiomedE, FRACS FAOrthA
 Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Patellofemoral Joint. Question? ANATOMY
 Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Medial Patellofemoral Ligament Reconstruction
 Medial Patellofemoral Ligament Reconstruction 1. Defined a. Reconstruction of the medial patellofemoral ligament in an effort to restore medial patellar stability and reduce chances of lateral dislocation.
Medial Patellofemoral Ligament Reconstruction 1. Defined a. Reconstruction of the medial patellofemoral ligament in an effort to restore medial patellar stability and reduce chances of lateral dislocation.
W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco
 Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no
 Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
General Concepts. Growth Around the Knee. Topics. Evaluation
 General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force.
 Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT *** - Useful in determining mechanism of injury / overuse
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
Overview Ligament Injuries. Anatomy. Epidemiology Very commonly injured joint. ACL Injury 20/06/2016. Meniscus Tears. Patellofemoral Problems
 Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
No Disclosures. Topics. Pediatric ACL Tears
 Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Chronic patellar dislocation in adults
 CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
World Medical & Health Games
 Management of Patellofemoral Pain Syndrome João Barroso Orthopaedic department ULS Matosinhos Portugal Introduction Anterior Knee Pain affects 1 in 4 athletes very common! (Knowles et al) Patellofemoral
Management of Patellofemoral Pain Syndrome João Barroso Orthopaedic department ULS Matosinhos Portugal Introduction Anterior Knee Pain affects 1 in 4 athletes very common! (Knowles et al) Patellofemoral
Acute patellar dislocation in adults
 CASE STUDY 14 Acute patellar dislocation in adults What are the reasons for the first acute dislocation? How can we document the pathoanatomy? What is our treatment concept? Table CS14 Patellofemoral joint
CASE STUDY 14 Acute patellar dislocation in adults What are the reasons for the first acute dislocation? How can we document the pathoanatomy? What is our treatment concept? Table CS14 Patellofemoral joint
Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD
 Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD Disclosures Consultant: Smith & Nephew A3 surgical Stockholder: A3 surgical Case Presentation:
Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD Disclosures Consultant: Smith & Nephew A3 surgical Stockholder: A3 surgical Case Presentation:
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
10/30/18. Disclosures. Recurrent Patellar Instability. Management of Recurrent Patellar Instability
 Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
DISCLOSURES. Overview 09/24/2015. Patellofemoral Instability and Treatment Options. I do not have anything to disclose
 Patellofemoral Instability and Treatment Options Gregory Purnell, MD Department of Orthpoaedic Surgery Sports Medicine and Arthroscopy Allegheny Health Network Orthopaedic Surgeon, Pittsburgh Pirates Baseball
Patellofemoral Instability and Treatment Options Gregory Purnell, MD Department of Orthpoaedic Surgery Sports Medicine and Arthroscopy Allegheny Health Network Orthopaedic Surgeon, Pittsburgh Pirates Baseball
Medial Patellofemoral Ligament (MPFL) Surgical Technique
 Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
Patellar instability
 Page 1 of 13 Specific Injuries D Goodwin 1, W Postma 2 * Patellar instability Abstract Introduction Patellar instability is most common among adolescent female athletes, although anyone can be affected.
Page 1 of 13 Specific Injuries D Goodwin 1, W Postma 2 * Patellar instability Abstract Introduction Patellar instability is most common among adolescent female athletes, although anyone can be affected.
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
Retinacular tear knee
 P ford residence southampton, ny Retinacular tear knee The medial patellofemoral ligament (MPFL) helps to keep the kneecap centered along the front of the knee, so that it tracks well during knee movements.
P ford residence southampton, ny Retinacular tear knee The medial patellofemoral ligament (MPFL) helps to keep the kneecap centered along the front of the knee, so that it tracks well during knee movements.
Anterior Cruciate Ligament (ACL)
 Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
Ligamentous and Meniscal Injuries: Diagnosis and Management
 Ligamentous and Meniscal Injuries: Diagnosis and Management Daniel K Williams, MD Franciscan Physician Network Orthopedic Specialists September 29, 2017 No Financial Disclosures INTRODUCTION Overview of
Ligamentous and Meniscal Injuries: Diagnosis and Management Daniel K Williams, MD Franciscan Physician Network Orthopedic Specialists September 29, 2017 No Financial Disclosures INTRODUCTION Overview of
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
ACL AND PCL INJURIES OF THE KNEE JOINT
 ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
The patellofemoral joint is the articulation between. Patellofemoral Instability. Brian J. White, M.D., and Orrin H. Sherman, M.D.
 22 Bulletin of the NYU Hospital for Joint Diseases 2009;67(1):22-9 Patellofemoral Instability Brian J. White, M.D., and Orrin H. Sherman, M.D. Abstract This review describes the normal patellofemoral joint
22 Bulletin of the NYU Hospital for Joint Diseases 2009;67(1):22-9 Patellofemoral Instability Brian J. White, M.D., and Orrin H. Sherman, M.D. Abstract This review describes the normal patellofemoral joint
ANTERIOR CRUCIATE LIGAMENT INJURY
 ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
Patient Information & Exercise Folder
 MEDIAL PATELLO-FEMORAL LIGAMENT RECONSTRUCTION Patient Information & Exercise Folder Mr D Raj FRCS (Tr & Orth) Consultant Lower Limb Orthopaedic Surgeon Pilgrim Hospital, Sibsey Road, Boston Lincolnshire
MEDIAL PATELLO-FEMORAL LIGAMENT RECONSTRUCTION Patient Information & Exercise Folder Mr D Raj FRCS (Tr & Orth) Consultant Lower Limb Orthopaedic Surgeon Pilgrim Hospital, Sibsey Road, Boston Lincolnshire
8/9/2017. Case Based: Beyond Medial Patellofemoral Ligament. Editorial Board AJSM Social Media. Consultant. Not talking about PF pain/chondrosis Rehab
 Case Based: Beyond Medial Patellofemoral Ligament Dr Alan Getgood MD FRCS(Tr&Orth) DipSEM Assistant Professor Orthopaedic Sport Medicine Fellowship Director The Fowler Kennedy Sport Medicine Clinic University
Case Based: Beyond Medial Patellofemoral Ligament Dr Alan Getgood MD FRCS(Tr&Orth) DipSEM Assistant Professor Orthopaedic Sport Medicine Fellowship Director The Fowler Kennedy Sport Medicine Clinic University
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
Rehabilitation after Total Elbow Arthroplasty
 Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT. Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology
 PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology PRE OPERATIVE ASSESSMENT RADIOGRAPHS Radiographs are used for assessment and
PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology PRE OPERATIVE ASSESSMENT RADIOGRAPHS Radiographs are used for assessment and
Assessment of Patellar Laxity in the in vitro Native Knee
 Assessment of Patellar Laxity in the in vitro Native Knee By Mark C. Komosa Submitted to the graduate degree program in Bioengineering and the Graduate Faculty of the University of Kansas in partial fulfillment
Assessment of Patellar Laxity in the in vitro Native Knee By Mark C. Komosa Submitted to the graduate degree program in Bioengineering and the Graduate Faculty of the University of Kansas in partial fulfillment
Jia Li 1, Yongqian Li 1, Jingchao Wei 2, Jianzhao Wang 1, Shijun Gao 1 and Yong Shen 1*
 Li et al. Journal of Orthopaedic Surgery and Research 2014, 9:66 RESEARCH ARTICLE Open Access A simple technique for reconstruction of medial patellofemoral ligament with bone-fascia tunnel fixation at
Li et al. Journal of Orthopaedic Surgery and Research 2014, 9:66 RESEARCH ARTICLE Open Access A simple technique for reconstruction of medial patellofemoral ligament with bone-fascia tunnel fixation at
The Knee. Tibio-Femoral
 The Knee Tibio-Femoral Osteology Distal Femur with Proximal Tibia Largest Joint Cavity in the Body A modified hinge joint with significant passive rotation Technically, one degree of freedom (Flexion/Extension)
The Knee Tibio-Femoral Osteology Distal Femur with Proximal Tibia Largest Joint Cavity in the Body A modified hinge joint with significant passive rotation Technically, one degree of freedom (Flexion/Extension)
5/14/2013. Acute vs Chronic Mechanism of Injury:
 Third Annual Young Athlete Conference: The Lower Extremity February 22, 2013 Audrey Lewis, DPT Acute vs Chronic Mechanism of Injury: I. Direct: blow to the patella II. Indirect: planted foot with a valgus
Third Annual Young Athlete Conference: The Lower Extremity February 22, 2013 Audrey Lewis, DPT Acute vs Chronic Mechanism of Injury: I. Direct: blow to the patella II. Indirect: planted foot with a valgus
Anatomy of the patella :
 PATELLOFEMORAL JOINT REHABILITATION COMPONENTS GREG BENNETT, P.T., DSc. Excel Physical Therapy Anatomy of the patella : Patella is triangular, apex directed downwards Anterior surface gently convex Deep
PATELLOFEMORAL JOINT REHABILITATION COMPONENTS GREG BENNETT, P.T., DSc. Excel Physical Therapy Anatomy of the patella : Patella is triangular, apex directed downwards Anterior surface gently convex Deep
Where are we now? A little bit of History.. Is menu à la carte relevant in 2019? Medial PatelloFemoral Ligament the Queen of the PF Joint
 Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Lower Extremity Sports Injuries
 Lower Extremity Sports Injuries AAP Musculoskeletal Boot Camp Sigrid F. Wolf, MD Pediatric Sports Medicine Fellow Northwestern University Lurie Children s Hospital Disclosure I have no relevant financial
Lower Extremity Sports Injuries AAP Musculoskeletal Boot Camp Sigrid F. Wolf, MD Pediatric Sports Medicine Fellow Northwestern University Lurie Children s Hospital Disclosure I have no relevant financial
Knee Joint Anatomy 101
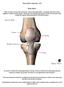 Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
Medial Patellofemoral Ligament Repair/Reconstruction
 Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
Patella Instability in Children and Adolescents
 Patella Instability in Children and Adolescents Description Patella Instability is an injury to the kneecap (patella) affecting the joint it forms with the thigh bone (femur) Patella Instability can occur
Patella Instability in Children and Adolescents Description Patella Instability is an injury to the kneecap (patella) affecting the joint it forms with the thigh bone (femur) Patella Instability can occur
Knee Injury Assessment
 Knee Injury Assessment Clinical Anatomy p. 186 Femur Medial condyle Lateral condyle Femoral trochlea Tibia Intercondylar notch Tibial tuberosity Tibial plateau Fibula Fibular head Patella Clinical Anatomy
Knee Injury Assessment Clinical Anatomy p. 186 Femur Medial condyle Lateral condyle Femoral trochlea Tibia Intercondylar notch Tibial tuberosity Tibial plateau Fibula Fibular head Patella Clinical Anatomy
Prevention and Treatment of Injuries. Anatomy. Anatomy. Chapter 20 The Knee Westfield High School Houston, Texas
 Prevention and Treatment of Injuries Chapter 20 The Knee Westfield High School Houston, Texas Anatomy MCL, Medial Collateral Ligament LCL, Lateral Collateral Ligament PCL, Posterior Cruciate Ligament ACL,
Prevention and Treatment of Injuries Chapter 20 The Knee Westfield High School Houston, Texas Anatomy MCL, Medial Collateral Ligament LCL, Lateral Collateral Ligament PCL, Posterior Cruciate Ligament ACL,
Muscles of the Thigh. 6.1 Identify, describe the attachments of and deduce the actions of the muscles of the thigh: Anterior group
 Muscles of the Thigh 6.1 Identify, describe the attachments of and deduce the actions of the muscles of the thigh: Anterior group Sartorius: This is a long strap like muscle with flattened tendons at each
Muscles of the Thigh 6.1 Identify, describe the attachments of and deduce the actions of the muscles of the thigh: Anterior group Sartorius: This is a long strap like muscle with flattened tendons at each
Please differentiate an internal derangement from an external knee injury.
 Knee Orthopaedic Tests Sports and Knee Injuries James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Knee Injury Strain, Sprain, Internal Derangement Anatomy of the Knee Please
Knee Orthopaedic Tests Sports and Knee Injuries James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Knee Injury Strain, Sprain, Internal Derangement Anatomy of the Knee Please
Anterior Cruciate Ligament Injuries
 Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
DIAGNOSIS AND EARLY MANAGEMENT OF KNEE INJURIES
 DIAGNOSIS AND EARLY MANAGEMENT OF KNEE INJURIES INTRODUCTION: The knee is a common site of athletic injury. The knee injuries can be classified either into traumatic or acute and chronic, with overuse
DIAGNOSIS AND EARLY MANAGEMENT OF KNEE INJURIES INTRODUCTION: The knee is a common site of athletic injury. The knee injuries can be classified either into traumatic or acute and chronic, with overuse
The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the
 The Arthritic Knee The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the medial compartment of the knee, and
The Arthritic Knee The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the medial compartment of the knee, and
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Medial patellofemoral ligament reconstruction using dual patella docking technique
 2018; 4(3): 298-304 ISSN: 2395-1958 IJOS 2018; 4(3): 298-304 2018 IJOS www.orthopaper.com Received: 24-05-2018 Accepted: 25-06-2018 Dr. Ullas Mahesh Assistant Professor, Department of Orthopaedics, Bangalore,
2018; 4(3): 298-304 ISSN: 2395-1958 IJOS 2018; 4(3): 298-304 2018 IJOS www.orthopaper.com Received: 24-05-2018 Accepted: 25-06-2018 Dr. Ullas Mahesh Assistant Professor, Department of Orthopaedics, Bangalore,
Anterior Cruciate Ligament (ACL) Injuries
 Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Disclosures. Outline. The Posterior Cruciate Ligament 5/3/2016
 The Posterior Cruciate Ligament Christopher J. Utz, MD Assistant Professor of Orthopaedic Surgery University of Cincinnati Disclosures I have no disclosures relevant to this topic. Outline 1. PCL Basic
The Posterior Cruciate Ligament Christopher J. Utz, MD Assistant Professor of Orthopaedic Surgery University of Cincinnati Disclosures I have no disclosures relevant to this topic. Outline 1. PCL Basic
Jacques Menetrey, MD, PD. Uniklinik Balgrist. Unité d Orthopédie et Traumatologie du Sport (UOTS)
 Acute patellar dislocation: conservative or surgical treatment Jacques Menetrey, MD, PD Unité d Orthopédie et Traumatologie du Sport (UOTS) Service de chirurgie orthopédique et traumatologie de l appareil
Acute patellar dislocation: conservative or surgical treatment Jacques Menetrey, MD, PD Unité d Orthopédie et Traumatologie du Sport (UOTS) Service de chirurgie orthopédique et traumatologie de l appareil
BASELINE QUESTIONNAIRE (SURGEON)
 SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
Knee Injuries. PSK 4U Mr. S. Kelly North Grenville DHS. Medial Collateral Ligament Sprain
 Knee Injuries PSK 4U Mr. S. Kelly North Grenville DHS Medial Collateral Ligament Sprain Result from either a direct blow from the lateral side in a medial direction or a severe outward twist Greater injury
Knee Injuries PSK 4U Mr. S. Kelly North Grenville DHS Medial Collateral Ligament Sprain Result from either a direct blow from the lateral side in a medial direction or a severe outward twist Greater injury
Case Study: Christopher
 Case Study: Christopher Conditions Treated Anterior Knee Pain, Severe Crouch Gait, & Hip Flexion Contracture Age Range During Treatment 23 Years to 24 Years David S. Feldman, MD Chief of Pediatric Orthopedic
Case Study: Christopher Conditions Treated Anterior Knee Pain, Severe Crouch Gait, & Hip Flexion Contracture Age Range During Treatment 23 Years to 24 Years David S. Feldman, MD Chief of Pediatric Orthopedic
The Lower Limb II. Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa
 The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
These are rehabilitation guidelines for OSU Sports Medicine patients. Please contact us at if you have any questions.
 OSU Sports Medicine Knee Microfracture Rehabilitation Guidelines These are rehabilitation guidelines for OSU Sports Medicine patients. Please contact us at 614-293-2385 if you have any questions. Rehabilitation
OSU Sports Medicine Knee Microfracture Rehabilitation Guidelines These are rehabilitation guidelines for OSU Sports Medicine patients. Please contact us at 614-293-2385 if you have any questions. Rehabilitation
SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management
 SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management Gauguin Gamboa Australia has always been a nation where emphasis on health and fitness has resulted in an active population engaged
SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management Gauguin Gamboa Australia has always been a nation where emphasis on health and fitness has resulted in an active population engaged
Computational Evaluation of Predisposing Factors to Patellar Dislocation
 Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
A Patient s Guide to Patellofemoral Problems
 A Patient s Guide to Patellofemoral Problems 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Patellofemoral Problems 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety
KNEE MICROFRACTURE CLINICAL PRACTICE GUIDELINE
 KNEE MICROFRACTURE CLINICAL PRACTICE GUIDELINE Progression is time and criterion-based, dependent on soft tissue healing, patient demographics and clinician evaluation. Contact Ohio State Sports Medicine
KNEE MICROFRACTURE CLINICAL PRACTICE GUIDELINE Progression is time and criterion-based, dependent on soft tissue healing, patient demographics and clinician evaluation. Contact Ohio State Sports Medicine
Accelerated Rehabilitation Following ACL-PTG Reconstruction & PCL Reconstruction with Medial Collateral Ligament Repair
 Page 1 of 7 Accelerated Rehabilitation Following ACL-PTG Reconstruction & PCL Reconstruction with Medial Collateral Ligament Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore
Page 1 of 7 Accelerated Rehabilitation Following ACL-PTG Reconstruction & PCL Reconstruction with Medial Collateral Ligament Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore
Anterior Cruciate Ligament Surgery
 Anatomy Anterior Cruciate Ligament Surgery Roger Ostrander, MD Andrews Institute Anatomy Anatomy Function Primary restraint to anterior tibial translation Secondary restraint to internal tibial rotation
Anatomy Anterior Cruciate Ligament Surgery Roger Ostrander, MD Andrews Institute Anatomy Anatomy Function Primary restraint to anterior tibial translation Secondary restraint to internal tibial rotation
Reconstruction of the medial patellofemoral ligament for treatment of patellar instability
 354 Acta Orthopaedica 2008; 79 (3): 354 360 Review Reconstruction of the medial patellofemoral ligament for treatment of patellar instability Martin Lind, Bent W Jakobsen, Bent Lund, and Svend Erik Christiansen
354 Acta Orthopaedica 2008; 79 (3): 354 360 Review Reconstruction of the medial patellofemoral ligament for treatment of patellar instability Martin Lind, Bent W Jakobsen, Bent Lund, and Svend Erik Christiansen
Knee Movement Coordination Deficits. ICD-9-CM: Sprain of cruciate ligament of knee
 1 Knee Movement Coordination Deficits Anterior Cruciate Ligament ACL Tear ICD-9-CM: 844.2 Sprain of cruciate ligament of knee ACL Insufficiency ICD-9-CM: 717.83 Old disruption of anterior cruciate ligament
1 Knee Movement Coordination Deficits Anterior Cruciate Ligament ACL Tear ICD-9-CM: 844.2 Sprain of cruciate ligament of knee ACL Insufficiency ICD-9-CM: 717.83 Old disruption of anterior cruciate ligament
Medical Diagnosis for Michael s Knee
 Medical Diagnosis for Michael s Knee Introduction The following report mainly concerns the diagnosis and treatment of the patient, Michael. Given that Michael s clinical problem surrounds an injury about
Medical Diagnosis for Michael s Knee Introduction The following report mainly concerns the diagnosis and treatment of the patient, Michael. Given that Michael s clinical problem surrounds an injury about
CT Evaluation of Patellar Instability
 CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
Accelerated Rehabilitation Following ACL-PTG Reconstruction with Medial Collateral Ligament Repair
 Page 1 of 7 Accelerated Rehabilitation Following ACL-PTG Reconstruction with Medial Collateral Ligament Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore normal range of
Page 1 of 7 Accelerated Rehabilitation Following ACL-PTG Reconstruction with Medial Collateral Ligament Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore normal range of
MRI KNEE WHAT TO SEE. Dr. SHEKHAR SRIVASTAV. Sr.Consultant KNEE & SHOULDER ARTHROSCOPY
 MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella Treated with a Different Method in Each Knee
 Case Reports in Orthopedics Volume 2015, Article ID 890315, 5 pages http://dx.doi.org/10.1155/2015/890315 Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella
Case Reports in Orthopedics Volume 2015, Article ID 890315, 5 pages http://dx.doi.org/10.1155/2015/890315 Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella
STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact)
 STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact) David Drez, Jr., M.D. Clinical Professor of Orthopaedics LSU School of Medicine Financial Disclosure Dr. David Drez has no relevant
STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact) David Drez, Jr., M.D. Clinical Professor of Orthopaedics LSU School of Medicine Financial Disclosure Dr. David Drez has no relevant
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
Patella Tendon Repair
 Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
Lateral knee injuries
 Created as a free resource by Clinical Edge Based on Physio Edge podcast episode 051 with Matt Konopinski Get your free trial of online Physio education at Orthopaedic timeframes Traditionally Orthopaedic
Created as a free resource by Clinical Edge Based on Physio Edge podcast episode 051 with Matt Konopinski Get your free trial of online Physio education at Orthopaedic timeframes Traditionally Orthopaedic
UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player
 UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player Cheri Drysdale, MEd,, ATC Margot Putukian,, MD Jeffery Bechler,, MD Princeton University How many of you have done an
UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player Cheri Drysdale, MEd,, ATC Margot Putukian,, MD Jeffery Bechler,, MD Princeton University How many of you have done an
Department of Orthopedic Surgery, Ewha Womans University Mokdong Hospital, Seoul, Korea
 Case Report https://doi.org/10.14517/aosm16016 pissn 2289-005X eissn 2289-0068 Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun
Case Report https://doi.org/10.14517/aosm16016 pissn 2289-005X eissn 2289-0068 Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun
Musculoskeletal Examination Benchmarks
 Musculoskeletal Examination Benchmarks _ The approach to examining the musculoskeletal system is the same no matter what joint or limb is being examined. The affected and contralateral region should both
Musculoskeletal Examination Benchmarks _ The approach to examining the musculoskeletal system is the same no matter what joint or limb is being examined. The affected and contralateral region should both
Financial Disclosure. Medial Collateral Ligament
 Matthew Murray, M.D. UTHSCSA Sports Medicine Financial Disclosure Dr. Matthew Murray has no relevant financial relationships with commercial interests to disclose. Medial Collateral Ligament Most commonly
Matthew Murray, M.D. UTHSCSA Sports Medicine Financial Disclosure Dr. Matthew Murray has no relevant financial relationships with commercial interests to disclose. Medial Collateral Ligament Most commonly
Chapter 20 The knee and related structures
 Chapter 20 The knee and related structures Athletic Training Spring 2014 Jihong Park Bones & joints Femur, tibia, fibula, & patella Femur & tibia Weight bearing & muscle attachment Patella functions Anterior
Chapter 20 The knee and related structures Athletic Training Spring 2014 Jihong Park Bones & joints Femur, tibia, fibula, & patella Femur & tibia Weight bearing & muscle attachment Patella functions Anterior
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION FEMORAL CONDYLE REHABILITATION PROGRAM PHASE I - PROTECTION PHASE (WEEKS 0-6) Protection of healing tissue from load and shear forces Decrease pain and effusion
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION FEMORAL CONDYLE REHABILITATION PROGRAM PHASE I - PROTECTION PHASE (WEEKS 0-6) Protection of healing tissue from load and shear forces Decrease pain and effusion
Anterolateral Ligament. Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine
 Anterolateral Ligament Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine What in the world? TIME magazine in November 2013 stated: In an age filled with advanced medical techniques like
Anterolateral Ligament Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine What in the world? TIME magazine in November 2013 stated: In an age filled with advanced medical techniques like
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
Knee Joint Assessment and General View
 Knee Joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The knee is the largest
Knee Joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The knee is the largest
PATELLA INSTABILITY AND REALIGNMENT
 Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando PATELLA INSTABILITY
Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando PATELLA INSTABILITY
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Evaluation of the Knee and Shoulder
 Evaluation of the Knee and Shoulder Karen J. Boselli, MD Northeast Regional Nurse Practitioner Conference May 2018 Knee Overview History Examination Top 5 diagnoses When to image When to refer Pain most
Evaluation of the Knee and Shoulder Karen J. Boselli, MD Northeast Regional Nurse Practitioner Conference May 2018 Knee Overview History Examination Top 5 diagnoses When to image When to refer Pain most
The Knee Joint By Prof. Dr. Muhammad Imran Qureshi
 The Knee Joint By Prof. Dr. Muhammad Imran Qureshi Structurally, it is the Largest and the most complex joint in the body because of the functions that it performs: Allows mobility (flexion/extension)
The Knee Joint By Prof. Dr. Muhammad Imran Qureshi Structurally, it is the Largest and the most complex joint in the body because of the functions that it performs: Allows mobility (flexion/extension)
