NURSING PRACTICE & SKILL
|
|
|
- Franklin Webster
- 6 years ago
- Views:
Transcription
1 NURSING PRACTICE & SKILL ICD , Authors Carita Caple, RN, BSN, MSHS Eliza Schub, RN, BSN Reviewers Jennifer Kornusky, RN, MS Nursing Practice Council Glendale Adventist Medical Center, Glendale, CA Editor Diane Pravikoff, RN, PhD, FAAN Pneumatic Anti-Shock Garment: Deflating and Removing Link to Skill Competency Checklist Link to Interactive Skill Competency Checklist What Is a Pneumatic Anti-Shock Garment? A pneumatic anti-shock garment (PASG; also known as a military anti-shock garment [MAST] or shock pants) is a device developed to initially stabilize patients with significant trauma of the pelvis or lower extremities by decreasing blood flow to the extremities. PASGs are intended to be used as a temporizing measure (i.e., short-termintervention) until definitive treatment is available. The PASG is distinguished from the nonpneumatic anti-shock garment, which does not use a pump for inflation (for more information, see Nursing Practice and Skill Postpartum Hemorrhage: Applying a Non-Pneumatic Anti-Shock Garment ; and Nursing Practice and Skill Postpartum Hemorrhage: Removing Non-Pneumatic Anti-Shock Garment). The information contained in this Nursing Practice & Skill is intended to present a brief overview of the PASG and is not intended to replace facility protocols, clinician orders, or the coursework and clinical experience necessary to become proficient in applying, removing, or monitoring a patient with a PASG What: A PASG is an inflatable garment with three compartments: abdominal, left leg, and right leg. A pump with a pressure gauge is used to inflate each compartment to the desired pressure in a manner similar to inflating a blood pressure cuff. Once the patient is stabilized or if a complication develops, the PASG is deflated as ordered. The patient is monitored continuously during deflation; rapid reinflation may be necessary, especially if the patient experiences sudden, severe hypotension. For information regarding application of a PASG, see Nursing Practice & Skill Anti-Shock Garment: Applying and Inflating; CINAHL Topic ID Number: T705457) How: PASGs should be applied per institutional or facility protocol. PASGs are never the sole treatment for a patient experiencing hemorrhage other measures (e.g., I.V. fluid resuscitation, medications) are also initiated to help achieve hemodynamic stability. To remove the garment once the patient is stabilized and the treating clinician has issued an order, the nurse slowly deflates it while closely monitoring vital signs. If vital signs remain stable and the treating clinician has ordered garment removal, the PASG is removed; if hypotension develops, it might be necessary to administer I.V. fluids and medications, as prescribed, and to rapidly reinflate the garment to stabilize the patient Where: PASGs are typically used in the prehospital (e.g., at the scene of an accident) or emergency department setting Who: In the prehospital setting, PASGs are applied by paramedics and emergency medical technicians (EMTs) according to institutional protocols. In the hospital setting, emergency department nurses apply PASGs per clinician orders and facility protocols. Depending on the situation and the patient s preference, it may be appropriate to have family members present during placement and use of the PASG March 3, 2017 Published by Cinahl Information Systems, a division of EBSCO Information Services. Copyright 2017, Cinahl Information Systems. All rights reserved. No part of this may be reproduced or utilized in any form or by any means, electronic or mechanical, including photocopying, recording, or by any information storage and retrieval system, without permission in writing from the publisher. Cinahl Information Systems accepts no liability for advice or information given herein or errors/omissions in the text. It is merely intended as a general informational overview of the subject for the healthcare professional. Cinahl Information Systems, 1509 Wilson Terrace, Glendale, CA 91206
2 What Is the Desired Outcome of Removing a Pneumatic Anti-Shock Garment? The desired outcome of deflation and/or removal of the PASG is for the patient to remain physiologically stable and experience no adverse consequences or complications If the patient survives the initial stabilization period, he/she will receive definitive treatment for the condition that necessitated use of the PASG Why Is Successful Removal of a Pneumatic Anti-Shock Garment Important? Successful removal of a PASG is an indication of physiologic stability and readiness of the patient to receive definitive treatment; the garment must be rapidly reinflated and applied if blood pressure drops or other vital sign abnormalities occur Facts and Figures There are very few randomized controlled clinical trials of PASG use During the Vietnam War, the use of a PASG improved the survival of United States soldiers who had severe lower extremity trauma from 0% to 50%. The transport time from the field to the trauma center for these soldiers was approximately 45 minutes via helicopter (Cutler et al., 1971) Use of a PASG in a patient with a chest injury increases the risk for mortality (Cayten et al., 1993; Honigman, 1991) Most adverse effects of PASG use are caused by decreased distal perfusion (Hauswald, 2003) What You Need to Know Before Deflating and Removing a Pneumatic Anti-Shock Garment Use of PASGs is controversial, and protocols outlining the appropriate circumstances for PASG use vary greatly by geographic area, facility, and institution PASGs have been found particularly useful as a means to stabilize patients in war zones The use of PASGs in the civilian setting (i.e., non-war zone environment) has been controversial, with many experts stating that their utility is limited Generally a PASG is ordered when a patient is in decompensated shock I.V. fluids and oxygen should always be administered in conjunction with PASG use to maximize hemodynamic stability hemodynamic status must be monitored throughout the use of PASG and before removing the PASG has a pelvic fracture and hypotension has significant trauma and expected transport time is minutes The nurse s primary responsibilities in removing and deflating a PASG are to complete a thorough patient assessment assess and accurately record the patient s vital signs and physiologic status, and monitor for any complications (for details, see Red Flags, below)adjust the pressure in the PASG compartments according to clinician orders assist in the removal of the PASG Nurses should be familiar with the contraindications to and risks associated with PASG use (for details, see Red Flags, below) Familiarity with all applicable equipment (e.g., PASG, tubing, airflow control valves) is essential Preliminary steps that should be performed before deflating and removing a PASG include the following: Review the facility/unit-specific protocol for PASG deflation and removal, if one is available Review the treating clinician s order for the removal of the PASG Review the patient s medical record for any allergies (e.g., to latex or other substances); use alternative materials, as appropriate Identify a colleague to assist; removal of a PASG may require more than one person, especially if rapid reinflation becomes necessary Gather supplies and equipment necessary to deflate and remove the PASG, as follows: Personal protective equipment (PPE; e.g., nonsterile gloves); use additional PPE (e.g., gown, mask, eye protection) if exposure to body fluids is anticipated Vital signs monitoring equipment, including stethoscope, sphygmomanometer, and a blood pressure cuff of appropriate size for the patient Long spine board or scoop stretcher
3 Board straps Airflow control valves (e.g., stopcocks) Deflation valves Pressure gauge Emergency resuscitation equipment and supplies (e.g., crash cart, bag-valve-maskresuscitator, oxygen source and delivery system) How to Remove and Deflate a Pneumatic Anti-Shock Garment Perform hand hygiene and don PPE as appropriate Identify the patient according to facility protocol Establish privacy by closing the door to the patient s room and/or drawing the curtain surrounding the patient s bed Introduce yourself to the patient and family member(s), if present; explain your clinical role in the deflation and removal of a PASG; assess the anxiety level of the patient/family and for knowledge deficits and anxiety regarding removal of the PASG Determine whether the patient/family requires special considerations regarding communication (e.g., due to illiteracy, language barriers, or deafness); make arrangements to meet these needs, if present Use professional certified medical interpreters, either in person or via telephone, when language barriers exist Explain the procedure and its purpose; answer any questions and provide emotional support as needed Maintain in-line spinal immobilization at all times, if indicated Deflate the PASG as ordered when the patient has stabilized or if a complication develops. Perform the following steps to deflate the PASG: Assess and document the patient s vital signs, hemodynamic status, and level of consciousness before initiating deflation Gradually deflate the abdominal compartment while monitoring and documenting the patient s vital signs If the SBP drops more than 5 mm Hg or the heart rate increases by 10 beats/min or more, deflation should be halted and I.V. fluids should be administered, as ordered. If the patient s SBP is not restored, the abdominal compartment should be reinflated Pause for 5 minutes or per facility/unit-specific protocol Gradually deflate one of the leg compartments while monitoring and documenting the patient s vital signs If one of the legs is injured, the compartment containing the uninjured leg should be deflated first If the SBP drops more than 5 mm Hg or the heart rate increases by 10 beats/min or more, deflation should be stopped and I.V. fluids should be administered, as ordered. If the SBP is not restored, the leg compartment should be reinflated Pause for 5 minutes or per facility/unit-specific protocol Gradually deflate the other leg compartment while monitoring and documenting the patient s vital signs If the SBP drops more than 5 mm Hg or the heart rate increases by 10beats/min or more, deflation should be stopped and I.V. fluids should be administered, as ordered. If the SBP is not restored, the leg compartment should be reinflated Monitor the patient s vital signs closely. Sudden and severe hypotension can occur Do not remove the PASG until ordered. Rapid reinflation may be necessary if the patient becomes unstable To remove the PASG, release the Velcro closures; do not use scissors Leave the garment beneath the patient in case reinflation is necessary Discard used procedure materials appropriately; perform hand hygiene Update the patient s plan of care, as appropriate, and document the following information in the patient s medical record: Date and time of PASG deflation and removal Description of the procedure, including amount of supplemental oxygen administered, type and amount of I.V. fluids and blood products infused, and any medications administered Patient assessment information (and the time each element was assessed)regarding vital signs level of pain/anxiety/consciousness pulse oximetry readings Patient s response to use of the PASG Any unexpected outcomes and the interventions performed All patient/family teaching
4 Other Tests, Treatments, or Procedures That Might Be Necessary with Use of a Pneumatic Anti-Shock Garment Imaging studies may be performed to assess the extent of the patient s injuries Use of a PASG can mask a pelvic fracture. The abdominal compartment should be deflated prior to obtaining pelvic X-rays in order to assess for pelvic fractures An electrolyte panel may be ordered before, after, and while the patient is wearing a PASG to identify any electrolyte shifts caused by the PASG that require treatment Vasopressors (e.g., DOPamine), I.V. fluids, oxygen administration, and other measures are often necessary to stabilize the patient Patients often require surgical intervention to definitively treat the underlying condition (e.g., uncontrolled bleeding, pelvic fracture) What to Expect After Deflating and/or Removing a Pneumatic Anti-Shock Garment Following deflation and/or removal of the PASG, the patient will remain physiologically stable and will experience no adverse consequences or complications (see Red Flags, below) If the patient survives the initial stabilization period, he/she will receive definitive treatment for the condition that necessitated use of the PASG Red Flags PASG pressure changes can occur with changes in altitude (e.g., during air transport or ground transport over mountain passes). PASG pressure should be monitored carefully during transport that involves changes in altitude PASG use is absolutely contraindicated in patients with pulmonary edema congestive heart failure penetrating thoracic wounds PASG use is relatively contraindicated in patients impaled by a foreign body with abdominal evisceration who are pregnant. If a PASG is used to treat a pregnant woman, it is suggested that only the leg compartments be inflated. In the event of complications following emptying of the uterus (e.g., abortion complications, ectopic pregnancies, hypocoagulation states, hydatidiform mole bleeding), the entire garment can be utilized to tamponade hemorrhage who have isolated lower-extremity fractures; splinting is preferred for isolated lower-extremity fractures PASGs should be used cautiously in patients with expected transport times > 40 minutes Potential complications of PASG use include skin breakdown compartment syndrome (i.e., compression of muscle, blood vessels, and nerves within a compartment of the body, which leads to tissue necrosis) in the lower extremities metabolic acidosis with prolonged PASG use because lactic acid is released from peripheral tissues decreases in renal perfusion, urine output, and glomerular filtration rate as a result of decreased renal blood flow impaired respiration if the PASG abdominal compartment is incorrectly positioned over the rib cage aggravation of lumbar instability if the abdominal compartment is inflated on a patient who has lumbar instability masking of pelvic fractures increased bleeding as blood pressure increases What Do I Need to Tell the Patient/Patient s Family? Educate about the function of the PASG, that it is a temporary intervention, and that definitive treatment will be performed as soon as possible On discharge from acute care, instruct the patient to seek immediate medical attention for new or worsening signs and symptoms (e.g., pain, swelling, bleeding)
5 Note Recent review of the literature has found no updated research evidence on this topic since previous publication on August 7, 2015 References 1. Ali, J., & Duke, K. (1991). Timing and interpretation of the hemodynamic effects of the pneumatic antishock garment. Annals of Emergency Medicine, 20(11), doi: /s (05) (R) 2. Baskerville, J. R. (2009). A blast from the present meets the MAST from the past: Should the pneumatic anti-shock garment ever be used? Emergency Medicine Journal, 26(10), 689. doi: /emj (X) 3. Cayten, C. G., Berendt, B. M., Byrne, D. W., Murphy, J. G., & Moy, F. H. (1993). A study of pneumatic antishock garments in severely hypotensive trauma patients. Journal of Trauma: Injury, Infection, and Critical Care, 34(5), (R) 4. Chang, F. C., Harrison, P. B., Beech, R. R., & Helmer, S. D. (1995). PASG: Does it help in the management of traumatic shock? Journal of Trauma: Injury, Infection, and Critical Care, 39(3), (RCT) 5. Connolly, B., Gerlinger, T., & Pitcher, J. D. (1999). Complete masking of a severe open-book pelvic fracture by a pneumatic antishock garment. Journal of Trauma, 46(2), (C) 6. Cutler, B. S., & Daggett, W. (1971). Application of the "G-suit" to the control of hemorrhage in massive trauma. Annals of Surgery, 173(4), (C) 7. Hauswald, M., & Greene, E. R. (2003). Regional blood flow after pneumatic anti-shock garment inflation. Prehospital Emergency Care, 7(2), doi: /s y (R) 8. Holleran, R. S. (2009). Pneumatic antishock garment. In J. A. Proehl (Ed.), Emergency nursing procedures (4th ed., pp ). St. Louis: Saunders Elsevier. (GI) 9. Honigman, B., Lowenstein, S. R., Moore, E. E., Roweder, K., & Pons, P. (1991). The role of the pneumatic antishock garment in penetrating cardiac wounds. Journal of the American Medical Association, 266(17), doi: /jama (R) 10. Vahedi, M. H., Ayuyao, A. A., Parsa, M. H., & Freeman, H. P. (1995). Pneumatic antishock garment-associated compartment syndrome in uninjured lower extremities. Journal of Trauma: Injury, Infection, and Critical Care, 38(4), (C)
Chapter 20. Learning Objectives. Learning Objectives 9/18/2012. Bleeding and Shock
 Chapter 20 Bleeding and Shock Learning Objectives Describe structure & function of circulatory system Differentiate among arterial, venous, & capillary bleeding Describe methods of emergency medical care
Chapter 20 Bleeding and Shock Learning Objectives Describe structure & function of circulatory system Differentiate among arterial, venous, & capillary bleeding Describe methods of emergency medical care
Bleeding and Shock *** CME Version *** Aaron J. Katz, AEMT-P, CIC
 Bleeding and Shock *** CME Version *** Aaron J. Katz, AEMT-P, CIC www.es26medic.net Circulatory System Composed of heart, blood vessels and blood A closed system Pumps oxygenated blood and nutrients to
Bleeding and Shock *** CME Version *** Aaron J. Katz, AEMT-P, CIC www.es26medic.net Circulatory System Composed of heart, blood vessels and blood A closed system Pumps oxygenated blood and nutrients to
Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: Shock Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: Shock Revised: 11/2013 DEFINITIONS Aerobic metabolism is energy using oxygen into cells. Anaerobic
Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: Shock Revised: 11/2013 DEFINITIONS Aerobic metabolism is energy using oxygen into cells. Anaerobic
Bleeding and Shock. Circulatory System
 Bleeding and Shock Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 Circulatory System Composed of heart, blood vessels and blood A closed system Pumps oxygenated blood and nutrients to body tissues Delivers
Bleeding and Shock Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 Circulatory System Composed of heart, blood vessels and blood A closed system Pumps oxygenated blood and nutrients to body tissues Delivers
Chapter 29 - Chest_and_Abdominal_Trauma
 Introduction to Emergency Medical Care 1 OBJECTIVES 29.1 Define key terms introduced in this chapter. Slides 11, 15, 18, 27 29.2 Describe mechanisms of injury commonly associated with chest injuries. Slides
Introduction to Emergency Medical Care 1 OBJECTIVES 29.1 Define key terms introduced in this chapter. Slides 11, 15, 18, 27 29.2 Describe mechanisms of injury commonly associated with chest injuries. Slides
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Chapter 28. Objectives. Objectives 01/09/2013. Bleeding and Soft-Tissue Trauma
 Chapter 28 Bleeding and Soft-Tissue Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define
Chapter 28 Bleeding and Soft-Tissue Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define
Competency Log Professional Responder Courses
 Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Chapter Goal. Learning Objectives. Chapter 17. Hemorrhage & Shock
 Chapter 17 Hemorrhage & Shock Chapter Goal Use assessment findings to formulate field impression and implement treatment plan for patient with hemorrhage or shock Learning Objectives Describe epidemiology,
Chapter 17 Hemorrhage & Shock Chapter Goal Use assessment findings to formulate field impression and implement treatment plan for patient with hemorrhage or shock Learning Objectives Describe epidemiology,
Introduction (1 of 3)
 Chapter 10 Shock Introduction (1 of 3) Shock (hypoperfusion) means a state of collapse and failure of the cardiovascular system. In the early stages, the body attempts to maintain homeostasis. As shock
Chapter 10 Shock Introduction (1 of 3) Shock (hypoperfusion) means a state of collapse and failure of the cardiovascular system. In the early stages, the body attempts to maintain homeostasis. As shock
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
OSF NORTHERN REGION EMERGENCY MEDICAL SERVICES STANDING MEDICAL ORDERS ILS, ALS. SMO: Adult Pain Management
 OSF NORTHERN REGION EMERGENCY MEDICAL SERVICES STANDING MEDICAL ORDERS ILS, ALS SMO: Adult Pain Management Overview: Objective: Provide a reasonable relief of severe pain to make packaging and transport
OSF NORTHERN REGION EMERGENCY MEDICAL SERVICES STANDING MEDICAL ORDERS ILS, ALS SMO: Adult Pain Management Overview: Objective: Provide a reasonable relief of severe pain to make packaging and transport
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: Shock Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: Shock Revised: 11/2013 (12 questions on trauma exam from this outline) DEFINITIONS Aerobic metabolism
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: Shock Revised: 11/2013 (12 questions on trauma exam from this outline) DEFINITIONS Aerobic metabolism
Pre-hospital Trauma Life Support. Rattiya Banjungam Emergency Physician, Khon Kaen Hospital
 Pre-hospital Trauma Life Support Rattiya Banjungam Emergency Physician, Khon Kaen Hospital Golden principles of Prehospital Trauma Care Golden Hour There is a golden hour if you are critically injured,
Pre-hospital Trauma Life Support Rattiya Banjungam Emergency Physician, Khon Kaen Hospital Golden principles of Prehospital Trauma Care Golden Hour There is a golden hour if you are critically injured,
NURSING PRACTICE & SKILL
 NURSING PRACTICE & SKILL Chemotherapy, Intraperitoneal: Administering What Is Intraperitoneal Chemotherapy Administration? Intraperitoneal (IP) chemotherapy agents are administered to treat cancer within
NURSING PRACTICE & SKILL Chemotherapy, Intraperitoneal: Administering What Is Intraperitoneal Chemotherapy Administration? Intraperitoneal (IP) chemotherapy agents are administered to treat cancer within
3. D Objective: Chapter 4, Objective 4 Page: 79 Rationale: A carbon dioxide level below 35 mmhg indicates hyperventilation.
 1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
Damage Control in Abdominal and Pelvic Injuries
 Damage Control in Abdominal and Pelvic Injuries Raul Coimbra, MD, PhD, FACS The Monroe E. Trout Professor of Surgery Surgeon-in Chief UCSD Medical Center Hillcrest Campus Executive Vice-Chairman Department
Damage Control in Abdominal and Pelvic Injuries Raul Coimbra, MD, PhD, FACS The Monroe E. Trout Professor of Surgery Surgeon-in Chief UCSD Medical Center Hillcrest Campus Executive Vice-Chairman Department
CEDR 2018 QCDR Measures for CMS 2018 MIPS Performance Year Reporting
 ACEP19 Emergency Department Utilization of CT for Minor Blunt Head Trauma for Aged 18 Years and Older Percentage of visits for aged 18 years and older who presented with a minor blunt head trauma who had
ACEP19 Emergency Department Utilization of CT for Minor Blunt Head Trauma for Aged 18 Years and Older Percentage of visits for aged 18 years and older who presented with a minor blunt head trauma who had
Shock. William Schecter, MD
 Shock William Schecter, MD The Cell as a furnace O 2 1 mole Glucose Cell C0 2 ATP 38 moles H 2 0 Shock = Inadequate Delivery of 02 and Glucose to the Cell 0 2 Cell ATP 2 moles Lactic Acid Treatment of
Shock William Schecter, MD The Cell as a furnace O 2 1 mole Glucose Cell C0 2 ATP 38 moles H 2 0 Shock = Inadequate Delivery of 02 and Glucose to the Cell 0 2 Cell ATP 2 moles Lactic Acid Treatment of
MIAMI-DADE COLLEGE. Common Course Number: HSC Course Title: Basic Emergency Care. Course Catalog Description:
 Common Course Number: HSC 2400 MIAMI-DADE COLLEGE Course Title: Basic Emergency Care Course Catalog Description: Designed to provide opportunities to develop, practice, and display skills concerning emergency
Common Course Number: HSC 2400 MIAMI-DADE COLLEGE Course Title: Basic Emergency Care Course Catalog Description: Designed to provide opportunities to develop, practice, and display skills concerning emergency
 International Trauma Life Support for Prehospital Care Providers Sixth Edition Patricia M. Hicks, MS, NREMTP Roy Alson, PhD, MD, FACEP Donna Hastings, EMT-P John Emory Campbell, MD, FACEP and Alabama Chapter,
International Trauma Life Support for Prehospital Care Providers Sixth Edition Patricia M. Hicks, MS, NREMTP Roy Alson, PhD, MD, FACEP Donna Hastings, EMT-P John Emory Campbell, MD, FACEP and Alabama Chapter,
Pediatric Trauma Care
 2013 Standard Trauma Care Procedures (Pediatric) Traumatic injuries require prompt care and transportation. Always suspect cervical injury. Note the mechanism of injury and any other condition that may
2013 Standard Trauma Care Procedures (Pediatric) Traumatic injuries require prompt care and transportation. Always suspect cervical injury. Note the mechanism of injury and any other condition that may
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Emergency Care Progress Log
 Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Objectives. Terminology. Shock. Terminology (cont.) Terminology (cont.)
 Objectives Gary Hoertz EMS Division Chief Kootenai Fire and Rescue Department Coeur d Alene, Idaho Terminology Pathophysiology of Shock Stages of Shock Classification of Shock Assessment Treatment Shock
Objectives Gary Hoertz EMS Division Chief Kootenai Fire and Rescue Department Coeur d Alene, Idaho Terminology Pathophysiology of Shock Stages of Shock Classification of Shock Assessment Treatment Shock
Abdomen and Genitalia Injuries. Chapter 28
 Abdomen and Genitalia Injuries Chapter 28 Hollow Organs in the Abdominal Cavity Signs of Peritonitis Abdominal pain Tenderness Muscle spasm Diminished bowel sounds Nausea/vomiting Distention Solid Organs
Abdomen and Genitalia Injuries Chapter 28 Hollow Organs in the Abdominal Cavity Signs of Peritonitis Abdominal pain Tenderness Muscle spasm Diminished bowel sounds Nausea/vomiting Distention Solid Organs
Where Have we Come From, and Where are we Going
 Where Have we Come From, and Where are we Going James Augustine, MD, FACEP Emergency Physician and Fire/EMS Medical Director Naples, Atlanta, and Dayton Clinical Professor, Wright State Univ. Dept of Emergency
Where Have we Come From, and Where are we Going James Augustine, MD, FACEP Emergency Physician and Fire/EMS Medical Director Naples, Atlanta, and Dayton Clinical Professor, Wright State Univ. Dept of Emergency
MASSACHUSETTS DEPARTMENT OF PUBLIC HEALTH OFFICE OF EMERGENCY MEDICAL SERVICES Basic EMT Practical Examination Cardiac Arrest Management
 Basic EMT Practical Examination 6.0 - Cardiac Arrest Management Station 1 RESUSCITATION & DEFIBRILLATION No Point WHILE FUNCTIONING AS FIRST RESCUER: Point 1. Verbalizes or takes body substance isolation
Basic EMT Practical Examination 6.0 - Cardiac Arrest Management Station 1 RESUSCITATION & DEFIBRILLATION No Point WHILE FUNCTIONING AS FIRST RESCUER: Point 1. Verbalizes or takes body substance isolation
1 Chapter 10 Shock 2 Shock Shock: Inadequate State of collapse and failure of the system Leads to inadequate circulation Without adequate blood flow,
 1 Chapter 10 Shock 2 Shock Shock: Inadequate State of collapse and failure of the system Leads to inadequate circulation Without adequate blood flow, cannot get rid of metabolic wastes Results in hypoperfusion
1 Chapter 10 Shock 2 Shock Shock: Inadequate State of collapse and failure of the system Leads to inadequate circulation Without adequate blood flow, cannot get rid of metabolic wastes Results in hypoperfusion
Policies & Procedures. RNSP - RN Procedure. I.D. Number: 1097
 Policies & Procedures Title: ESOPHAGEAL TAMPONADE TUBE (MINNESOTA Tube) ASSISTING WITH INSERTION, CARE OF A PATIENT, ASSISTING WITH REMOVAL RNSP - RN Procedure I.D. Number: 1097 Authorization [x] Nursing
Policies & Procedures Title: ESOPHAGEAL TAMPONADE TUBE (MINNESOTA Tube) ASSISTING WITH INSERTION, CARE OF A PATIENT, ASSISTING WITH REMOVAL RNSP - RN Procedure I.D. Number: 1097 Authorization [x] Nursing
SAN LUIS OBISPO COUNTY EMERGENCY MEDICAL SERVICES AGENCY PREHOSPITAL POLICY
 SAN LUIS OBISPO COUNTY EMERGENCY MEDICAL SERVICES AGENCY PREHOSPITAL POLICY Policy Reference No: 153 [01/08/2013] Formerly Policy No: 201.3 Effective Date: 11/01/2012 Review Date: 03/01/2014 TRAUMA PATIENT
SAN LUIS OBISPO COUNTY EMERGENCY MEDICAL SERVICES AGENCY PREHOSPITAL POLICY Policy Reference No: 153 [01/08/2013] Formerly Policy No: 201.3 Effective Date: 11/01/2012 Review Date: 03/01/2014 TRAUMA PATIENT
PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT
 PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT Board Approved June 2007 Revised December 2009 Revised July 2011 Revised June 2015 435 Hunter Street Fredericksburg, VA 22401
PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT Board Approved June 2007 Revised December 2009 Revised July 2011 Revised June 2015 435 Hunter Street Fredericksburg, VA 22401
Objectives. Shock. Terminology. Terminology Pathophysiology of Shock Stages of Shock Classification of Shock Assessment Treatment Scenario
 Objectives Gary Hoertz EMS Division Chief Kootenai Fire and Rescue Department Coeur d Alene, Idaho Terminology Pathophysiology of Shock Stages of Shock Classification of Shock Assessment Treatment Scenario
Objectives Gary Hoertz EMS Division Chief Kootenai Fire and Rescue Department Coeur d Alene, Idaho Terminology Pathophysiology of Shock Stages of Shock Classification of Shock Assessment Treatment Scenario
Patient Assessment. Chapter 8
 Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
IV Fluids. I.V. Fluid Osmolarity Composition 0.9% NaCL (Normal Saline Solution, NSS) Uses/Clinical Considerations
 IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
Activity Three: Where s the Bleeding?
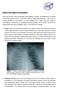 Activity Three: Where s the Bleeding? There are five main sites of potentially fatal bleeding in trauma, remembered by the phrase on the floor and four more. On the floor refers to losing blood externally
Activity Three: Where s the Bleeding? There are five main sites of potentially fatal bleeding in trauma, remembered by the phrase on the floor and four more. On the floor refers to losing blood externally
Objectives. Objectives. Shock. Objectives. Cardiac output. Review of Blood Flow and Perfusion. Review the components of perfusion
 Objectives Shock Review the components of perfusion Cardiac output Perfusion at the capillary level Perfusion and cellular metabolism Aerobic metabolism and energy production Objectives Identify the stages
Objectives Shock Review the components of perfusion Cardiac output Perfusion at the capillary level Perfusion and cellular metabolism Aerobic metabolism and energy production Objectives Identify the stages
CARDIAC ARREST IN SPECIAL CIRCUMSTANCES 2
 CARDIAC ARREST IN SPECIAL CIRCUMSTANCES 2 M1 Objectives To understand how resuscitation techniques should be modified in the special circumstances of: Hypothermia Immersion and submersion Poisoning Pregnancy
CARDIAC ARREST IN SPECIAL CIRCUMSTANCES 2 M1 Objectives To understand how resuscitation techniques should be modified in the special circumstances of: Hypothermia Immersion and submersion Poisoning Pregnancy
Student Guide Module 4: Pediatric Trauma
 Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing
 1 2 3 4 5 6 Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing D-Disability Chief complaint and/or Mechanism
1 2 3 4 5 6 Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing D-Disability Chief complaint and/or Mechanism
L: Cardiovascular. Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 107
 L: Cardiovascular Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 107 Major Competency Area: L Cardiovascular Competency: L-1 Cardiovascular Nursing Date: January
L: Cardiovascular Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 107 Major Competency Area: L Cardiovascular Competency: L-1 Cardiovascular Nursing Date: January
Trauma CT Scanning Protocol
 Northern Trauma Network Trauma CT Scanning Protocol Background Whole body CT (WBCT) has assumed a pivotal position in trauma management. UK trauma is typically described as blunt and blind i.e. blunt trauma
Northern Trauma Network Trauma CT Scanning Protocol Background Whole body CT (WBCT) has assumed a pivotal position in trauma management. UK trauma is typically described as blunt and blind i.e. blunt trauma
CHAPTER 3. The Human Body National Safety Council
 CHAPTER 3 The Human Body The Human Body Composed of many different organs and tissues All parts work together: To sustain life Allow activity Injury or illness impairs functions 3-3 Cranial located in
CHAPTER 3 The Human Body The Human Body Composed of many different organs and tissues All parts work together: To sustain life Allow activity Injury or illness impairs functions 3-3 Cranial located in
ITLS Pediatric Provider Course Basic Pre-Test
 ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
SEMINOLE COUNTY EMS PROVISIONAL EMT SKILLS VERIFICATION
 The following individual has completed the Seminole County EMS Provisional EMT Skills Verification check in the following areas: Oxygen, Airway and Ventilation Skills ALS Assistance Trauma Management Medical
The following individual has completed the Seminole County EMS Provisional EMT Skills Verification check in the following areas: Oxygen, Airway and Ventilation Skills ALS Assistance Trauma Management Medical
CCTC Minnesota Procedure: Minnesota Tube, Assisting with Insertion and Care of Patient
 CCTC Minnesota Procedure: Minnesota Tube, Assisting with Insertion and Care of Patient Purpose: To control bleeding from esophageal or gastric varices that have not responded to medical therapy (ie. Sclerotherapy,
CCTC Minnesota Procedure: Minnesota Tube, Assisting with Insertion and Care of Patient Purpose: To control bleeding from esophageal or gastric varices that have not responded to medical therapy (ie. Sclerotherapy,
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE. MEASURING BLOOD PRESSURE - MANUAL (equ04)
 SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: MEASURING BLOOD PRESSURE - MANUAL Nursing DATE: REVIEWED: PAGES: 2/80 7/17 1 of 5 RESPONSIBILITY: RN, LPN, Patient Care Technician Multi-skilled
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: MEASURING BLOOD PRESSURE - MANUAL Nursing DATE: REVIEWED: PAGES: 2/80 7/17 1 of 5 RESPONSIBILITY: RN, LPN, Patient Care Technician Multi-skilled
ATLS: Initial Assessment and Management. SAUSHEC Medical Student Lecture Series
 ATLS: Initial Assessment and Management SAUSHEC Medical Student Lecture Series Objectives Identify sequence of priorities in assessing the multiply injured patient Apply principles outlined in primary
ATLS: Initial Assessment and Management SAUSHEC Medical Student Lecture Series Objectives Identify sequence of priorities in assessing the multiply injured patient Apply principles outlined in primary
Musculoskeletal System
 CHAPTER 28 Musculoskeletal Injuries Musculoskeletal System Anatomy & Physiology Bones provide framework. Joints allow for bending. Muscles allow for movement. Cartilage provides flexibility. Tendons connect
CHAPTER 28 Musculoskeletal Injuries Musculoskeletal System Anatomy & Physiology Bones provide framework. Joints allow for bending. Muscles allow for movement. Cartilage provides flexibility. Tendons connect
CHAPTER 28 Musculoskeletal Injuries
 CHAPTER 28 Musculoskeletal Injuries Musculoskeletal System Anatomy & Physiology Bones provide framework. Joints allow for bending. Muscles allow for movement. Cartilage provides flexibility. Tendons connect
CHAPTER 28 Musculoskeletal Injuries Musculoskeletal System Anatomy & Physiology Bones provide framework. Joints allow for bending. Muscles allow for movement. Cartilage provides flexibility. Tendons connect
Pilonidal Sinus. Whiston Hospital Warrington Road, Prescot, Merseyside, L35 5DR Telephone:
 Pilonidal Sinus Whiston Hospital Warrington Road, Prescot, Merseyside, L35 5DR Telephone: 0151 426 1600 Author: General Surgery Department: Colorectal Document Number: STHK1059 Version: 002 Review date:
Pilonidal Sinus Whiston Hospital Warrington Road, Prescot, Merseyside, L35 5DR Telephone: 0151 426 1600 Author: General Surgery Department: Colorectal Document Number: STHK1059 Version: 002 Review date:
Scope of Practice Athletic Rehabilitation Therapist, Certified (A.R.T.C.)
 Scope of Practice Athletic Rehabilitation Therapist, Certified (A.R.T.C.) An Athletic Rehabilitation Therapist Certified (A.R.T.C) is an autonomous health care practitioner to whom members of the public
Scope of Practice Athletic Rehabilitation Therapist, Certified (A.R.T.C.) An Athletic Rehabilitation Therapist Certified (A.R.T.C) is an autonomous health care practitioner to whom members of the public
JEFFERSON COLLEGE COURSE SYLLABUS. PAR230 Paramedic Trauma Emergencies. 3 credit hours. Prepared by: Earl Neal Date:
 JEFFERSON COLLEGE COURSE SYLLABUS PAR230 Paramedic Trauma Emergencies 3 credit hours Prepared by: Earl Neal Date: 03-31-2016 Diane Scanga, Director, Public Safety Programs Dena McCaffrey, Ed.D., Dean,
JEFFERSON COLLEGE COURSE SYLLABUS PAR230 Paramedic Trauma Emergencies 3 credit hours Prepared by: Earl Neal Date: 03-31-2016 Diane Scanga, Director, Public Safety Programs Dena McCaffrey, Ed.D., Dean,
Urinary Catheters. Prevalence of Infections
 Urinary Catheterisation Urinary catheterisation is defined as an intervention to enable the emptying of the bladder by insertion of a catheter. Catheters can be short term less than 28 days or long term
Urinary Catheterisation Urinary catheterisation is defined as an intervention to enable the emptying of the bladder by insertion of a catheter. Catheters can be short term less than 28 days or long term
ACUTE CLINICAL MANAGEMENT OF TRAUMA Tina Gaarder, MD, PhD
 ACUTE CLINICAL MANAGEMENT OF TRAUMA Tina Gaarder, MD, PhD Trauma represents a leading cause of disability and preventable death and is mainly affecting people between 15 and 40 years of age, accounting
ACUTE CLINICAL MANAGEMENT OF TRAUMA Tina Gaarder, MD, PhD Trauma represents a leading cause of disability and preventable death and is mainly affecting people between 15 and 40 years of age, accounting
EVALUATION OF SELF LEARNING BASED ON WHO MANUAL SURGICAL CARE AT THE DISTRICT HOSPITAL (SCDH)
 EVALUATION OF SELF LEARNING BASED ON WHO MANUAL SURGICAL CARE AT THE DISTRICT HOSPITAL (SCDH) Note: For the answers, refer to the SCDH Manual. The pages listed below each question will contain the answers,
EVALUATION OF SELF LEARNING BASED ON WHO MANUAL SURGICAL CARE AT THE DISTRICT HOSPITAL (SCDH) Note: For the answers, refer to the SCDH Manual. The pages listed below each question will contain the answers,
Maternal Collapse Guideline
 Maternal Collapse Guideline Guideline Number: 664 Supersedes: Classification Clinical Version No: Date of EqIA: Approved by: Date Approved: Date made active: Review Date: 1 Obstetric Written Documentation
Maternal Collapse Guideline Guideline Number: 664 Supersedes: Classification Clinical Version No: Date of EqIA: Approved by: Date Approved: Date made active: Review Date: 1 Obstetric Written Documentation
CARING FOR YOUR CATHETER AT HOME
 CARING FOR YOUR CATHETER AT HOME After surgery (radical prostatectomy) for prostate cancer you will have a urinary catheter for a short period of time and will need to go home with the catheter still in
CARING FOR YOUR CATHETER AT HOME After surgery (radical prostatectomy) for prostate cancer you will have a urinary catheter for a short period of time and will need to go home with the catheter still in
EMT. Chapter 14 Review
 EMT Chapter 14 Review Review 1. All of the following are common signs and symptoms of cardiac ischemia, EXCEPT: A. headache. B. chest pressure. C. shortness of breath. D. anxiety or restlessness. Review
EMT Chapter 14 Review Review 1. All of the following are common signs and symptoms of cardiac ischemia, EXCEPT: A. headache. B. chest pressure. C. shortness of breath. D. anxiety or restlessness. Review
 TRAUMA LIFE SUPPORT PRE-HOSPITAL EXAMINATION (TLS P) 1. A high-risk bodily fluid for spreading infection is. a. sweat b. saliva c. blood d. urine 2. Items that can be used to reduce the spread of infection
TRAUMA LIFE SUPPORT PRE-HOSPITAL EXAMINATION (TLS P) 1. A high-risk bodily fluid for spreading infection is. a. sweat b. saliva c. blood d. urine 2. Items that can be used to reduce the spread of infection
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device
 I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
CHAPTER 3. The Human Body National Safety Council
 CHAPTER 3 The Human Body Lesson Objectives 1. Describe the primary areas of the body. 2. List the 10 body systems and explain a key function of each. 3. For each body system, describe at least 1 injury
CHAPTER 3 The Human Body Lesson Objectives 1. Describe the primary areas of the body. 2. List the 10 body systems and explain a key function of each. 3. For each body system, describe at least 1 injury
ATI Skills Modules Checklist for Central Venous Access Devices
 For faculty use only Educator s name Score Date ATI Skills Modules Checklist for Central Venous Access Devices Student s name Date Verify order Patient record Assess for procedure need Identify, gather,
For faculty use only Educator s name Score Date ATI Skills Modules Checklist for Central Venous Access Devices Student s name Date Verify order Patient record Assess for procedure need Identify, gather,
You Are the Emergency Medical Responder
 Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
68W COMBAT MEDIC POCKET GUIDE
 GTA 08-05-058 68W COMBAT MEDIC POCKET GUIDE PART I: TRAUMA TREATMENT This publication contains technical information that is for official Government use only. Distribution is limited to U.S. Government
GTA 08-05-058 68W COMBAT MEDIC POCKET GUIDE PART I: TRAUMA TREATMENT This publication contains technical information that is for official Government use only. Distribution is limited to U.S. Government
STANDARDIZED PROCEDURE LUMBAR PUNCTURE (Adult, Peds)
 I. Definition The lumbar puncture (LP) may assist in the diagnosis of meningitis, encephalitis, metastatic carcinomas, brain tumors, leukemia, demyelinating conditions, brain or spinal cord abscesses,
I. Definition The lumbar puncture (LP) may assist in the diagnosis of meningitis, encephalitis, metastatic carcinomas, brain tumors, leukemia, demyelinating conditions, brain or spinal cord abscesses,
Basic Assessment and Treatment of Trauma
 Basic Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls 1.2
Basic Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls 1.2
9/10/2012. Chapter 44. Learning Objectives. Learning Objectives (Cont d) Bleeding
 Chapter 44 Bleeding 1 Learning Objectives Describe the etiology, history, and physical findings of external bleeding Predict hemorrhage on the basis of the patient s mechanism of injury Distinguish between
Chapter 44 Bleeding 1 Learning Objectives Describe the etiology, history, and physical findings of external bleeding Predict hemorrhage on the basis of the patient s mechanism of injury Distinguish between
Muscle spasm Diminished bowel sounds Nausea/vomiting
 3 4 5 6 7 8 9 0 Chapter 8: Abdomen and Genitalia Injuries Abdominal Injuries Abdomen is major body cavity extending from to pelvis. Contains organs that make up digestive, urinary, and genitourinary systems.
3 4 5 6 7 8 9 0 Chapter 8: Abdomen and Genitalia Injuries Abdominal Injuries Abdomen is major body cavity extending from to pelvis. Contains organs that make up digestive, urinary, and genitourinary systems.
Hypotension / Shock. Adult Medical Section Protocols. Protocol 30
 Hypotension / Shock History Blood loss - vaginal or gastrointestinal bleeding, AAA, ectopic Fluid loss - vomiting, diarrhea, fever nfection Cardiac ischemia (M, CHF) Medications Allergic reaction regnancy
Hypotension / Shock History Blood loss - vaginal or gastrointestinal bleeding, AAA, ectopic Fluid loss - vomiting, diarrhea, fever nfection Cardiac ischemia (M, CHF) Medications Allergic reaction regnancy
ADMINISTRATIVE REQUIREMENT MANUAL EFFECTIVE DATE
 PURPOSE: I. To establish the minimum requirements for a first responder training course in first aid, which all first responders must take, in order to meet the requirements of M.G.L. c. 111, 201 and 105
PURPOSE: I. To establish the minimum requirements for a first responder training course in first aid, which all first responders must take, in order to meet the requirements of M.G.L. c. 111, 201 and 105
Shock. Perfusion. The cardiovascular system s circulation of blood and oxygen to all the cells in different tissues and organs of the body
 Shock Chapter 10 Shock State of collapse and failure of the cardiovascular system Leads to inadequate circulation Without adequate blood flow, cells cannot get rid of metabolic wastes The result- hypoperfusion
Shock Chapter 10 Shock State of collapse and failure of the cardiovascular system Leads to inadequate circulation Without adequate blood flow, cells cannot get rid of metabolic wastes The result- hypoperfusion
Sepsis Awareness and Education
 Sepsis Awareness and Education Meets the updated New York State Department of Health (NYSDOH) requirements for Infection Control and Barrier Precautions coursework Element VII: Sepsis Awareness and Education
Sepsis Awareness and Education Meets the updated New York State Department of Health (NYSDOH) requirements for Infection Control and Barrier Precautions coursework Element VII: Sepsis Awareness and Education
Hemorrhage Control. Chapter 6
 Chapter 6 The hemorrhage that take[s] place when a main artery is divided is usually so rapid and so copious that the wounded man dies before help can reach him. Colonel H. M. Gray, 1919 Stop the Bleeding!
Chapter 6 The hemorrhage that take[s] place when a main artery is divided is usually so rapid and so copious that the wounded man dies before help can reach him. Colonel H. M. Gray, 1919 Stop the Bleeding!
Magnesium Sulphate - Management of Hypertensive Disorders of Pregnancy
 1. Purpose Magnesium sulphate is the anticonvulsant of choice for pre-eclampsia prophylaxis and treatment. This clinical guideline outlines the indications, contraindications, administration and monitoring
1. Purpose Magnesium sulphate is the anticonvulsant of choice for pre-eclampsia prophylaxis and treatment. This clinical guideline outlines the indications, contraindications, administration and monitoring
Homework Assignment Complete and Place in Binder
 Homework Assignment Complete and Place in Binder Chapter # 34/35: Pediatric & Geriatric Emergencies 1. The first month of life after birth is referred to as the: A) neonatal period. B) toddler period.
Homework Assignment Complete and Place in Binder Chapter # 34/35: Pediatric & Geriatric Emergencies 1. The first month of life after birth is referred to as the: A) neonatal period. B) toddler period.
EMERGENCY MEDICAL SERVICES ONLINE COURSE CATALOG. TargetSolutions. Technology with a Purpose
 EMERGENCY MEDICAL SERVICES ONLINE COURSE CATALOG 1 Technology with a Purpose TargetSolutions delivers employee training that helps organizations achieve compliance, mitigate We risk, believe reduce a well-trained
EMERGENCY MEDICAL SERVICES ONLINE COURSE CATALOG 1 Technology with a Purpose TargetSolutions delivers employee training that helps organizations achieve compliance, mitigate We risk, believe reduce a well-trained
Pediatric Patients. BCFPD Paramedic Education Program. EMS Education Paramedic Level
 Pediatric Patients BCFPD Program Basic Considerations Much of the initial patient assessment can be done during visual examination of the scene. Involve the caregiver or parent as much as possible. Allow
Pediatric Patients BCFPD Program Basic Considerations Much of the initial patient assessment can be done during visual examination of the scene. Involve the caregiver or parent as much as possible. Allow
Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test
 Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test Purpose: To provide nurses with on overview of burn injuries in pediatric patients. Learning Objectives:
Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test Purpose: To provide nurses with on overview of burn injuries in pediatric patients. Learning Objectives:
CHAPTER 9. Shock National Safety Council
 CHAPTER 9 Shock Shock Dangerous condition: Not enough oxygen-rich blood reaching vital organs, such as brain and heart Caused by anything that significantly reduces blood flow Life-threatening emergency
CHAPTER 9 Shock Shock Dangerous condition: Not enough oxygen-rich blood reaching vital organs, such as brain and heart Caused by anything that significantly reduces blood flow Life-threatening emergency
Chapter 7 EMERGENCY PLAN AND INITIAL INJURY EVALUATION
 Chapter 7 EMERGENCY PLAN AND INITIAL INJURY EVALUATION Major Concepts. Proper planning of an emergency response is essential for appropriate first aid management of an injury. Anything that can be done
Chapter 7 EMERGENCY PLAN AND INITIAL INJURY EVALUATION Major Concepts. Proper planning of an emergency response is essential for appropriate first aid management of an injury. Anything that can be done
Controversies in Traction Splinting
 Controversies in Traction Splinting Katie Dolbec, MD Department of Surgery Division of Emergency Medicine University of Vermont Medical Center October 19, 2018 Disclosures I have nothing to disclose. History
Controversies in Traction Splinting Katie Dolbec, MD Department of Surgery Division of Emergency Medicine University of Vermont Medical Center October 19, 2018 Disclosures I have nothing to disclose. History
Emergency Room Technician/EMT
 Emergency Room Technician/EMT Directions Please circle a value for each question to provide us and the interested facilities with an assessment of your clinical experience. These values confirm your strengths
Emergency Room Technician/EMT Directions Please circle a value for each question to provide us and the interested facilities with an assessment of your clinical experience. These values confirm your strengths
EMERGENCY CARE at Winona State University
 EMERGENCY CARE at Winona State University The Primary Sports Medicine Team The team generally includes: A. Team Physician B. Certified Athletic Trainer(s) (ATC) C. Athletic Training Student(s) (ATS) D.
EMERGENCY CARE at Winona State University The Primary Sports Medicine Team The team generally includes: A. Team Physician B. Certified Athletic Trainer(s) (ATC) C. Athletic Training Student(s) (ATS) D.
Kathryn Nuss, MD Associate Trauma Medical Director Associate Director, Emergency Medicine
 Running on Empty Kathryn Nuss, MD Associate Trauma Medical Director Associate Director, Emergency Medicine Nationwide id Children s Hospital Associate Professor, Department of Pediatrics The Ohio State
Running on Empty Kathryn Nuss, MD Associate Trauma Medical Director Associate Director, Emergency Medicine Nationwide id Children s Hospital Associate Professor, Department of Pediatrics The Ohio State
the bleeding won t stop? Liane Manz RN, BScN, CNCC(c) Royal Alexandra Hospital
 What do you do when the bleeding won t stop? Teddie Tanguay RN, MN, NP, CNCC(c) Teddie Tanguay RN, MN, NP, CNCC(c) Liane Manz RN, BScN, CNCC(c) Royal Alexandra Hospital Outline Case study Normal coagulation
What do you do when the bleeding won t stop? Teddie Tanguay RN, MN, NP, CNCC(c) Teddie Tanguay RN, MN, NP, CNCC(c) Liane Manz RN, BScN, CNCC(c) Royal Alexandra Hospital Outline Case study Normal coagulation
1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles. Striated Skeletal. Smooth
 1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles Striated Skeletal Smooth 3 Anatomy and Physiology of the Musculoskeletal System 4 Skeletal System 5 Skeletal System Functions
1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles Striated Skeletal Smooth 3 Anatomy and Physiology of the Musculoskeletal System 4 Skeletal System 5 Skeletal System Functions
Transcutaneous Pacing. Approval: Medical Director James Stubblefield, MD. Approval: EMS Director Michael Petrie
 Transcutaneous Pacing 6091D Low Frequency/High Risk: Transcutaneous Pacing Applies To: Paramedics Effective Approval: Medical Director James Stubblefield, MD Approval: EMS Director Michael Petrie Expires
Transcutaneous Pacing 6091D Low Frequency/High Risk: Transcutaneous Pacing Applies To: Paramedics Effective Approval: Medical Director James Stubblefield, MD Approval: EMS Director Michael Petrie Expires
Shenandoah Co. Fire & Rescue. Injuries to. and Spine. December EMS Training Bill Streett Training Section Chief
 Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
Bachelor of Chinese Medicine Shock
 BCM Year 2 Dr. Irene Ng Jan 28, 2003 9:30 am 1:00 pm Rm 004 UPB Bachelor of Chinese Medicine 2002 2003 Shock Learning objectives Be able to: know the definition of shock know the classification and causes
BCM Year 2 Dr. Irene Ng Jan 28, 2003 9:30 am 1:00 pm Rm 004 UPB Bachelor of Chinese Medicine 2002 2003 Shock Learning objectives Be able to: know the definition of shock know the classification and causes
Resuscitation Checklist
 Resuscitation Checklist Actions if multiple responders are on scene Is resuscitation appropriate? Conditions incompatible with life Advanced decision in place Based on the information available, the senior
Resuscitation Checklist Actions if multiple responders are on scene Is resuscitation appropriate? Conditions incompatible with life Advanced decision in place Based on the information available, the senior
B. high blood pressure. D. hearing impairment. 2. Of the following, the LEAST likely reason for an EMS unit to be called
 CHAPTER 36 Geriatrics HANDOUT 36-2: Evaluating Content Mastery Student s Name EVALUATION CHAPTER 36 QUIZ Write the letter of the best answer in the space provided. 1. Among patients over age 65, almost
CHAPTER 36 Geriatrics HANDOUT 36-2: Evaluating Content Mastery Student s Name EVALUATION CHAPTER 36 QUIZ Write the letter of the best answer in the space provided. 1. Among patients over age 65, almost
Medical NREMT-PTE. NREMT Paramedic Trauma Exam.
 Medical NREMT-PTE NREMT Paramedic Trauma Exam https://killexams.com/pass4sure/exam-detail/nremt-pte Question: 41 Which of the following most accurately describes the finding of jugular venous distension
Medical NREMT-PTE NREMT Paramedic Trauma Exam https://killexams.com/pass4sure/exam-detail/nremt-pte Question: 41 Which of the following most accurately describes the finding of jugular venous distension
Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles
 1 2 3 4 5 6 7 Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles Striated Skeletal Smooth Anatomy and Physiology of the Musculoskeletal System Skeletal System Skeletal System Functions
1 2 3 4 5 6 7 Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles Striated Skeletal Smooth Anatomy and Physiology of the Musculoskeletal System Skeletal System Skeletal System Functions
Titrating Critical Care Medications
 Titrating Critical Care Medications Chad Johnson, MSN (NED), RN, CNCC(C), CNS-cc Clinical Nurse Specialist: Critical Care and Neurosurgical Services E-mail: johnsoc@tbh.net Copyright 2017 1 Learning Objectives
Titrating Critical Care Medications Chad Johnson, MSN (NED), RN, CNCC(C), CNS-cc Clinical Nurse Specialist: Critical Care and Neurosurgical Services E-mail: johnsoc@tbh.net Copyright 2017 1 Learning Objectives
Emergency First Response (EFR) Skills Assessment Sheets V4 June 2017
 Emergency First Response () Skills Assessment Sheets V4 June 2017 Airway management & ventilation Airway management & ventilation Trauma jaw thrust 1 Hand positions 2 Perform jaw thrust / mouth open 3
Emergency First Response () Skills Assessment Sheets V4 June 2017 Airway management & ventilation Airway management & ventilation Trauma jaw thrust 1 Hand positions 2 Perform jaw thrust / mouth open 3
Trauma Alert Step 2 Additions
 Trauma Alert Step 2 Additions MANGLED, DEGLOVED OR PULSELESS EXTREMITY PELVIC INJURY WITH HIGH-RISK MECHANISM OF INJURY Many thanks to Paramedic FTO Justin Bramlette for assembling this training presentation
Trauma Alert Step 2 Additions MANGLED, DEGLOVED OR PULSELESS EXTREMITY PELVIC INJURY WITH HIGH-RISK MECHANISM OF INJURY Many thanks to Paramedic FTO Justin Bramlette for assembling this training presentation
Written 01/09/17 Rewritten 3/29/17 for Interior Regional EMS Symposium
 Written 01/09/17 Rewritten 3/29/17 for Interior Regional EMS Symposium MARIA E. MANDICH MD Fairbanks Memorial Hospital Emergency Department Attending Physician Interior Region EMS Council Medical Director
Written 01/09/17 Rewritten 3/29/17 for Interior Regional EMS Symposium MARIA E. MANDICH MD Fairbanks Memorial Hospital Emergency Department Attending Physician Interior Region EMS Council Medical Director
Describe the influence of pathomechanics on function.
 HPR 219- Introduction to Athletic Training Clinical Examination and Diagnosis (CE) : CE-3 Identify the common congenital and acquired risk factors and causes of musculoskeletal injuries and common illnesses
HPR 219- Introduction to Athletic Training Clinical Examination and Diagnosis (CE) : CE-3 Identify the common congenital and acquired risk factors and causes of musculoskeletal injuries and common illnesses
August 2012 CE. Site code # E Reading the Scene
 August 2012 CE Site code # 107200E-1212 Reading the Scene Prepared by Sharon Hopkins, RN, BSN, EMT-P To view on the Advocate Condell website visit: www.advocatehealth.com/condell/body.cfm?id=422 Date of
August 2012 CE Site code # 107200E-1212 Reading the Scene Prepared by Sharon Hopkins, RN, BSN, EMT-P To view on the Advocate Condell website visit: www.advocatehealth.com/condell/body.cfm?id=422 Date of
