THE LOWER EXTREMITIES AMA GUIDES CHAPTER 17
|
|
|
- Annabel Lawson
- 6 years ago
- Views:
Transcription
1 THE LOWER EXTREMITIES AMA GUIDES CHAPTER 17 Tim Mussack Marlene Phillips Bradford & Barthel, LLP AMA Analysis and Ratings Division Bradford & Barthel AMA Analysis and Ratings Division Tim Mussack (916) Marlene Phillips (909)
2 3 Most Frequently Used Chapters Chapters 1 & The Constitution From page 17, in the Introduction to Chapter 2, the Practical Application of the Guides: Two physicians, following the methods of the Guides to evaluate the same patient, should report similar results and reach similar conclusions. Moreover, if the clinical findings are fully described, any knowledgeable observer may check the findings with the Guides criteria. The Almaraz Guzman en banc decision of 9/3/2009: by requiring use of the AMA Guides to determine impairment, the Legislature furthered its expressly stated goal of achieving consistency, uniformity, and objectivity. Chapter Spine Chapter Upper Extremity (UE) Chapter Lower Extremity (LE) 4 2
3 The Lower Extremities Lower extremity impairment values Combining Impairment PD (after adjustment) Methods of Evaluation 5 Chapter 17 The Lower Extremities there are errata 17.1 Principles of Assessment (p ) 17.2 Methods of Assessment (p ) 17.3 LE Impairment Evaluation Procedure Summary and Examples (p ) Impairment evaluations are performed after the injured worker attains MMI 6 3
4 7 Regional Impairment AMA Guides is not jurisdictionally specific for evaluating Permanent Disability The California Schedule for Rating gives additional instructions for rating Permanent Disabilities. Section 1 of the rating schedule is Introduction and Instructions. From page 1-4: "The impairment number identifies the body part, organ system and/ or nature of the injury..." "Under Section 2 of the Permanent Disability Rating Schedule, an appropriate impairment number can be found for most impairments." On page 1-5: "A single injury can result in multiple impairments of several parts of the body. For example, an injury to the arm could result in limited elbow range of motion and shoulder instability..." On page 1-11 of the Schedule: "...'adjusting' refers to adjusting an AMA impairment rating for diminished future earning capacity, occupation, and age." "Impairments of an individual extremity are adjusted and combined at the whole person level with other impairments of the same extremity..." 8 4
5 Impairment Values 100% LE = 40% WPI [LE % x.4 = WPI %] Table 17-3 page % Foot = 70% LE [Foot % x.7 = LE %] 9 Table 17-3 page 527 Conversion Table LE to WPI
6 Combine or Add, and CVC Numbers that are put together for evaluation of impairment/ PD must be either added or combined. When to combine: COMBINE for most situations -- unless specific instructions state to ADD impairment values. The effect/ purpose of combining is that it prevents the combined value from exceeding 100. A + B(1 A) [where A and B are decimal equivalents] When to add: The most notable exception to combining impairments is with the evaluation of range of motion impairment for the same part of the body (for example, right ankle motion) [hand evaluation has unique methodology] 11 Combine or Add, and CVC How to combine: Page 1-11 of the 2005 PDRS: Multiple impairments such as those involving a single part of an extremity, e.g. two impairment involving a shoulder such as shoulder instability and limited range of motion, are combined at the upper extremity level, then converted to whole person impairment and adjusted before being combined with other parts of the same extremity. Impairments with disability numbers in the and series are converted to whole person impairment and adjusted before being combined with any other impairment of the same extremity. Impairments of an individual extremity are adjusted and combined at the whole person [PD] level with other impairments of the same extremity before being combined with impairments of other body parts. For example, an impairment of the left knee and ankle would be combined before further combination with an impairment of the opposing leg or the back
7 13 Chapter Methods of Assessment
8 Methods Used to Evaluate Impairments of the Lower Extremities 15 Table 17-2, page 526 After all potentially impairing conditions have been identified and correct ratings recorded select the most specific method(s) and record the estimated impairment for each. explain in writing why a particular method(s) was chosen. (p. 526)
9 Table 17-2 Typically, one method will adequately characterize the impairment Avoid combining methods that rate the same condition. If more than one method can be used, the method that provides the higher rating should be adopted. (page 527)
10 Interpolation When a Table gives a range for objective findings, and a correlating range for impairment, use interpolation to provide the appropriate value (as shown in Example 17-15, with leg shortening) 19 Method #1 Limb Length Discrepancy X-rays strongly recommended Repeat 3 times 3 averaged to reduce measurement error P
11 Table 17-4 (p. 528) Impairment Due to Limb Discrepancy 21 Shortening due to: Overriding, Malalignment, or Fracture deformities cm (0-1/2 in.) = 5% LE cm (1/2-1 in.) = 10% LE cm (1-1 ½ in.) = 15% LE cm (1 ½ - 2 in.) = 20% LE combine with other functional sequela (p 528)
12 Method #2 Gait Derangement Why is it being used? Should use more specific method Correlating objective findings Read Table 17-5 (p. 529) carefully No combining 23 Table 17-5, p
13 Except as otherwise noted Table 17-5 [is] for full-time gait derangements of persons who are dependent on assistive devices. Not for abnormalities based only on subjective factors, such as pain or sudden giving-way, as with an individual with lowback discomfort who chooses to use a cane to assist in walking Whenever possible, the evaluator should use a more specific method. When the gait method is used, a written rationale should be included in the report. The lower limb impairment percents shown in Table 17-5 stand alone and are not combined with any other impairment evaluation method. As also expressed in the Comment section for Example 17-1 on page 528 of the AMA Guides, Although the individual has a limp (gait abnormality), gait derangement should be used only when no other method is available to rate the person
14 Method #3 Muscle Atrophy (Unilateral) At thigh 10 cm above patella Calf at max level Must compare measurement to opposite, uninjured LE Combine thigh and calf atrophy 27 Atrophy Measurements Compare measurement to opposite member Difference in circumference might be: Swelling Varicose veins Opposite member injured
15 Table 17-6 (p. 530) Impairment Due to Unilateral Leg Muscle Atrophy Mild 29 Example Right tibia fracture MMI Pain free walking Right thigh atrophy = 2 cm Right calf atrophy = 1 cm
16 Impairment? Thigh = 2 cm = 8% LE = 3% WPI Calf = 1 cm = 3% LE = 1% WPI Combine: 8% C 3% = 11 LE Convert: 11% LE = 4% WPI 31 Method #4 Manual Muscle Testing Use Table 17-7 &17-8 (pages ) Note typo - Hip abduction, Grade 3 = 37% LE
17 Table 17-7 (p. 531) Criteria for Grades of Muscle Function of the Lower Extremity 33 Manual Muscle Testing (cont d) Cautions page 531: depends on the examinee s cooperation should be concordant with other signs and medical evidence More than one grade between examiners More than one grade from exam to exam Pain Fear of pain Attributed to deficit of a peripheral nerve
18 Table 17-8, p. 532 Combine Example Method #5 Range of Motion (pages )
19 Use ROM only If it is clear restricted [ROM] has an organic basis Obtain 3 measurements; use greatest Add ROM impairments in joint 37 Figure 17-1 (p. 534) Using a Goniometer to Measure Flexion of the Right Hip
20 Figure 17-2 (p. 534) Neutral Position, Abduction, Adduction of the Right Hip 39 Figure 17-3 (p. 535) Measuring Internal and External Hip Rotation
21 Figure 17-4 (p. 535) Measuring Knee Flexion 41 Figure 17-5 (p. 535)
22 Range of Motion (page 537) Table Hip Table Knee Table Ankle Table Hindfoot Table Ankle/Hindfoot Table Toes (see footnote)
23 Example: Ankle flexion of 6 =? = 6% WPI (15% LE) (Table 17-11, p. 537) Ankle extension of 5 =? = 3% WPI (7% LE) (Table 17-11) 1 cm calf atrophy? = 1% WPI (Table 17-6, p. 530) 45 Impairment? Add flexion + extension = 15% LE + 7% LE = 22% LE = 9% WPI Do not use atrophy (1% WPI) R: 1) Table 17-2 prohibits combining 2) ROM is more generous
24 Range of Motion (continued) Invalid if: Class inconsistency between 2 observers Class inconsistency between exams Pain Fear of pain 47 Method #6 Ankylosis (joint immobility) See text for optimal position values Hip = 50% LE = 20% WPI (p. 538) Knee = 67% LE = 27% WPI (p. 540) Ankle = 14% Foot = 10% LE = 4% WPI (p. 541) Foot = 14% Foot = 10% LE = 4% WPI (p. 542) Toes see Table (page 543)
25 Ankylosis (continued) 1. Determine value for optimal position (text) 2. Use Tables (pages ) for deviation values (malposition increases impairment) 3. Add multiple malpositions for same joint 4. Combine ankylosis of different joints 5. The baseline rating for ankylosis in a neutral position is used only once for each joint Body Part Motion Table Page hip internal rot hip ext rot hip abd hip add knee varus knee valgus knee flex knee int or ext malrotation
26 Body Part Motion Table Page ankle plantar flex or dorsiflexion ankle varus ankle valgus ankle ankle int malrotation ext malrotation ankle tibia-os calcis angle toes ankylosis Method #7 Arthritis
27 Arthritis (cont d) Use x-rays ( standing if possible ) with Table (page 544) ( ) = normal cartilage intervals Compare uninjured opposite member 53 Table 17-31, p
28 Arthritis (cont d) Table Footnote: if (i) direct trauma; (ii) patellofemoral pain (between knee cap and thigh bone/femur), and (iii) crepitation on physical exam; (iv) no joint space narrowing - 2% WPI (5% LE) The knee has a medial and lateral compartment only the more significant loss is used (can be combined with patellofemoral arthritis) 55 Example Right tibia fracture 10 years ago Over years, increase knee pain, occasional swelling Standing x-ray 2 mm cartilage interval
29 Impairment? Cartilage interval (knee) = 2 mm Table? Table (p. 544) Likely amount of cartilage loss? normal = 4 mm WPI? 8% WPI (20% LE) 57 Method #8 Amputations See Table (page 545)
30 Table 17-32, p Method #9 Diagnoses-Based Estimates Table (used in 70-80% of LE cases) Covers 9 regions/conditions 1) Pelvis 2) Hip 3) Femoral Shaft Fracture 4) Knee 5) Malalignment of Tibial Shaft Fracture 6) Ankle 7) Hindfoot 8) Midfoot Deformity 9) Forefoot Deformity
31
32 Hip and Knee Replacements require the use of 2 Tables Hip Replacement: Table and (p. 548, ) Knee Replacement: Table and (p. 549, ) All others: Table (p ) 63 DRE Hip Replacement Add points from Categories a-e (Table 17-34, p. 548) Note that the primary factor is pain Apply to Table (p. 546) (Good, Fair, Poor Results)
33 Table 17-34, p Table 17-35, p
34 Total Hip and/ or Knee Replacement Good Results, pts. 15(37) Fair Results, pts. 20(50) Poor Results, less than 50 pts. 30(75) 67 Method #10 Skin Loss (p. 550)
35 Use Table (p. 550) Full-thickness skin loss: impairment even when the areas are successfully covered with [a] skin graft. Chronic osteomyelitis (bone infection*) too * Usually a bacterial infection of bone/marrow. Resulting inflammation can lead to reduction of blood supply to bone Table (p. 550)
36 Method #11 Peripheral Nerve Injuries (p ) Table maximum impairment values Assessed sensory/ motor deficits are applied Combine with other LE methods except: muscle weakness atrophy gait (p. 552) 71 Dysesthesia Impairment of sensitivity, especially to touch. Altered feelings, such as burning, wetness, electric shock, pins and needles, itching (p. 600)
37 Table (p. 552) 73 Method #12 Causalgia & CRPS (p. 553)
38 CRPS I (RSD) CRPS II (causalgia) characterized by pain, swelling, stiffness, discoloration skeletal demineralization may follow a sprain, fracture or nerve or vascular injury 75 CRPS I (RSD) CRPS II (causalgia) Use Chapter 13 ( Central & Peripheral Nervous System ): Section 13.8 (p ) Section 13.5 (p. 336)
39 to rate [causalgia and RSD], diagnosis is key Diagnosis: rely on clinical findings, threephase bone scan, x-rays, laser Doppler flowmetry, sudomotor reflex Table (p. 496) 77 Table (p. 336)
40 Method #13 Vascular Disorders (p ) 79 Table 17-38, p. 554)
41 Intermittent claudication: cramping or aching in the calves (sometimes the thighs or buttocks) caused by walking; relieved by rest; a manifestation of atherosclerosis (blockage of an artery). It is called intermittent because of the pattern of pain only with walking. Edema: abnormal buildup of fluid in the ankles, feet and legs. Common causes: Prolonged standing Long airplane flights or automobile rides Menstrual periods (for some women) Pregnancy Being overweight Increased age Injury or trauma 81 Summary Multiple potential methods for impairment evaluation Some can be combined; others cannot Combine impairments at the LE impairment level before converting to WPI Cautions regarding the use of Gait Derangement; Strength evaluation
42 Almaraz/ Guzman Almaraz/ Guzman rating not automatic Must be substantial evidence Within four corners of AMA Guides Physician rationale required 2015 DWC Educational Conference Evidence and reasoning 83 Tim Mussack (916) Marlene Phillips (909)
THE SPINE AMA GUIDES CHAPTER 15
 THE SPINE AMA GUIDES CHAPTER 15 Tim Mussack Marlene Phillips Bradford & Barthel, LLP AMA Analysis and Ratings Division HOUSEKEEPING ITEMS To control background noise, all attendees will be muted. Access
THE SPINE AMA GUIDES CHAPTER 15 Tim Mussack Marlene Phillips Bradford & Barthel, LLP AMA Analysis and Ratings Division HOUSEKEEPING ITEMS To control background noise, all attendees will be muted. Access
EVALUATING AMA IMPAIRMENT IN CALIFORNIA. Report Writing Mark Evans, DWC Rater
 EVALUATING AMA IMPAIRMENT IN CALIFORNIA Report Writing Mark Evans, DWC Rater What Makes a Good Report? Identifiers Patient name Claim number Date of injury Date of birth Occupation/duties Introduction/purpose
EVALUATING AMA IMPAIRMENT IN CALIFORNIA Report Writing Mark Evans, DWC Rater What Makes a Good Report? Identifiers Patient name Claim number Date of injury Date of birth Occupation/duties Introduction/purpose
IAIABC 2003 Lower Extremity Impairment Guides Part 4 of the Supplemental Impairment Rating Guides
 IAIABC 2003 Lower Extremity Impairment Guides Part 4 of the Supplemental Impairment Rating Guides Draft 11-03 IAIABC Executive Office 5610 Medical Circle, Suite 24 Madison, WI 53719 Phone: (608) 663-6355
IAIABC 2003 Lower Extremity Impairment Guides Part 4 of the Supplemental Impairment Rating Guides Draft 11-03 IAIABC Executive Office 5610 Medical Circle, Suite 24 Madison, WI 53719 Phone: (608) 663-6355
RECIPES FOR RATINGS !!! A. FIBROMYALGIA: 0% WPI P. 569 B. THORACIC OUTLET SYNDROME 0% WPI P. 569 C. MYOFASCIAL PAIN SYNDROME 0% WPI P.
 RECIPES FOR RATINGS 1. THE "0% WPI" RATINGS A. FIBROMYALGIA: 0% WPI P. 569 B. THORACIC OUTLET SYNDROME 0% WPI P. 569 C. MYOFASCIAL PAIN SYNDROME 0% WPI P. 569 D. TENDINITIS OF UPPER EXTREMITY 0% WPI P.
RECIPES FOR RATINGS 1. THE "0% WPI" RATINGS A. FIBROMYALGIA: 0% WPI P. 569 B. THORACIC OUTLET SYNDROME 0% WPI P. 569 C. MYOFASCIAL PAIN SYNDROME 0% WPI P. 569 D. TENDINITIS OF UPPER EXTREMITY 0% WPI P.
Basic AMA Impairment Ratings for Chiropractors CE Exam 6 Hours ~ Back to Chiropractic CE Seminars
 Basic AMA Impairment Ratings for Chiropractors CE Exam 6 Hours ~ Back to Chiropractic CE Seminars Simply list your answers (write down letter choice only: in a NUMBERED vertical column and email to: marcusstrutzdc@gmail.com
Basic AMA Impairment Ratings for Chiropractors CE Exam 6 Hours ~ Back to Chiropractic CE Seminars Simply list your answers (write down letter choice only: in a NUMBERED vertical column and email to: marcusstrutzdc@gmail.com
Scar Engorged veins. Size of the foot [In clubfoot, small foot]
![Scar Engorged veins. Size of the foot [In clubfoot, small foot] Scar Engorged veins. Size of the foot [In clubfoot, small foot]](/thumbs/78/77722241.jpg) 6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
SMALL GROUP SESSION 16 January 8 th or 10 th Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination
 SMALL GROUP SESSION 16 January 8 th or 10 th Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination Suggested Readings: Opatrny L. The Healing Touch. Ann Int Med 2002; 137:1003. http://www.annals.org/cgi/reprint/137/12/1003.pdf
SMALL GROUP SESSION 16 January 8 th or 10 th Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination Suggested Readings: Opatrny L. The Healing Touch. Ann Int Med 2002; 137:1003. http://www.annals.org/cgi/reprint/137/12/1003.pdf
QME AMA Impairment Ratings (6hrs) ~ Glenn Crafts, DC ~ Back to Chiropractic CE Seminars
 QME AMA Impairment Ratings (6hrs) ~ Glenn Crafts, DC ~ Back to Chiropractic CE Seminars Instructions: Answer all questions and email answers to: marcusstrutzdc@gmail.com Please DO NOT scan tests or test
QME AMA Impairment Ratings (6hrs) ~ Glenn Crafts, DC ~ Back to Chiropractic CE Seminars Instructions: Answer all questions and email answers to: marcusstrutzdc@gmail.com Please DO NOT scan tests or test
IAIABC 2003 Upper Extremity Impairment Guides Part 3 of the Supplemental Impairment Rating Guides
 IAIABC 2003 Upper Extremity Impairment Guides Part 3 of the Supplemental Impairment Rating Guides Draft 11-03 IAIABC Executive Office 5610 Medical Circle, Suite 14 Madison, WI 53719 Phone: (608) 663-6355
IAIABC 2003 Upper Extremity Impairment Guides Part 3 of the Supplemental Impairment Rating Guides Draft 11-03 IAIABC Executive Office 5610 Medical Circle, Suite 14 Madison, WI 53719 Phone: (608) 663-6355
Chapter 8 8/23/2016. Body Mechanics and Patient Mobility. Introduction to Body Mechanics and Patient Mobility
 Chapter 8 Body Mechanics and Patient Mobility All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Introduction to Body Mechanics and Patient Mobility
Chapter 8 Body Mechanics and Patient Mobility All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Introduction to Body Mechanics and Patient Mobility
BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY
 BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY B.Resseque, D.P.M. ARCH HEIGHT OFF WEIGHTBEARING Evaluate arch height by placing a ruler from the heel to the first metatarsal head Compare arch
BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY B.Resseque, D.P.M. ARCH HEIGHT OFF WEIGHTBEARING Evaluate arch height by placing a ruler from the heel to the first metatarsal head Compare arch
The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the
 The Arthritic Knee The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the medial compartment of the knee, and
The Arthritic Knee The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the medial compartment of the knee, and
Chapter 30 - Musculoskeletal_Trauma
 Introduction to Emergency Medical Care 1 OBJECTIVES 30.1 Define key terms introduced in this chapter. Slides 11 12, 19 20, 22 23, 37 30.2 Describe the anatomy of elements of the musculoskeletal system.
Introduction to Emergency Medical Care 1 OBJECTIVES 30.1 Define key terms introduced in this chapter. Slides 11 12, 19 20, 22 23, 37 30.2 Describe the anatomy of elements of the musculoskeletal system.
A Patient s Guide to Pain Management: Complex Regional Pain Syndrome
 A Patient s Guide to Pain Management: Complex Regional Pain Syndrome Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER:
A Patient s Guide to Pain Management: Complex Regional Pain Syndrome Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER:
Case Studies, Impairment of the Spine in Washington State
 Case Studies, Impairment of the Spine in Washington State NAOEM at Skamania, 2015 25 Sep, 2015 Tim Gilmore, MD Several Slides from this Presentation Borrowed with permission from the Washington State Department
Case Studies, Impairment of the Spine in Washington State NAOEM at Skamania, 2015 25 Sep, 2015 Tim Gilmore, MD Several Slides from this Presentation Borrowed with permission from the Washington State Department
A Patient s Guide to Pain Management: Complex Regional Pain Syndrome
 A Patient s Guide to Pain Management: Complex Regional Pain Syndrome 950 Breckinridge Lane Suite 220 Louisville, KY 40223 Phone: 502.708.2940 DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide to Pain Management: Complex Regional Pain Syndrome 950 Breckinridge Lane Suite 220 Louisville, KY 40223 Phone: 502.708.2940 DISCLAIMER: The information in this booklet is compiled from
Assessment Form Post Polio Syndrome and Late Effects of Polio
 FULL NAME: DATE OF BIRTH: PHONE NUMBER: CURRENT HOME ADDRESS: EMAIL ADDRESS: THERAPIST: REFERRAL SOURCE: CURRENT GP: NEXT OF KIN: ACC/NHI NUMBER: PATIENT GOALS OF TODAY S ASSESSMENT: MAIN PROBLEMS PATIENT
FULL NAME: DATE OF BIRTH: PHONE NUMBER: CURRENT HOME ADDRESS: EMAIL ADDRESS: THERAPIST: REFERRAL SOURCE: CURRENT GP: NEXT OF KIN: ACC/NHI NUMBER: PATIENT GOALS OF TODAY S ASSESSMENT: MAIN PROBLEMS PATIENT
Basics of Soft- Tissue Examination
 Basics of Soft- Tissue Examination Basics of Soft Tissue Exam For practitioners who primarily use their hands to treat the human structure: Examination must include functional tests to determine the type
Basics of Soft- Tissue Examination Basics of Soft Tissue Exam For practitioners who primarily use their hands to treat the human structure: Examination must include functional tests to determine the type
Module Eight. Application of Health Assessment NUR 225. Physical examination of Musculoskeletal System. King Saud University. Collage of Nursing
 King Saud University Collage of Nursing Medical Surgical Nursing depart Application of Health Assessment NUR 225 Module Eight Physical examination of Musculoskeletal System Obtaining a health history Ask
King Saud University Collage of Nursing Medical Surgical Nursing depart Application of Health Assessment NUR 225 Module Eight Physical examination of Musculoskeletal System Obtaining a health history Ask
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY 2017
 BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY 2017 B. RESSEQUE, D.P.M., D.A.B.P.O. Professor, N.Y. College of Podiatric Medicine ARCH HEIGHT OFF WEIGHTBEARING Evaluate arch height by placing
BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY 2017 B. RESSEQUE, D.P.M., D.A.B.P.O. Professor, N.Y. College of Podiatric Medicine ARCH HEIGHT OFF WEIGHTBEARING Evaluate arch height by placing
Musculoskeletal Examination Benchmarks
 Musculoskeletal Examination Benchmarks _ The approach to examining the musculoskeletal system is the same no matter what joint or limb is being examined. The affected and contralateral region should both
Musculoskeletal Examination Benchmarks _ The approach to examining the musculoskeletal system is the same no matter what joint or limb is being examined. The affected and contralateral region should both
SMALL GROUP SESSION 16 January 8 th or 10 th. Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination
 SMALL GROUP SESSION 16 January 8 th or 10 th Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination Suggested Readings: Opatrny L. The Healing Touch. Ann Int Med 2002; 137:1003. http://www.annals.org/cgi/reprint/137/12/1003.pdf
SMALL GROUP SESSION 16 January 8 th or 10 th Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination Suggested Readings: Opatrny L. The Healing Touch. Ann Int Med 2002; 137:1003. http://www.annals.org/cgi/reprint/137/12/1003.pdf
Where should you palpate the pulse of different arteries in the lower limb?
 Where should you palpate the pulse of different arteries in the lower limb? The femoral artery In the femoral triangle, its pulse is easily felt just inferior to the inguinal ligament midway between the
Where should you palpate the pulse of different arteries in the lower limb? The femoral artery In the femoral triangle, its pulse is easily felt just inferior to the inguinal ligament midway between the
SMALL GROUP SESSION 21B February 10 th or February 12 th. Lower Extremity Examination and Ethics Case Discussion
 SMALL GROUP SESSION 21B February 10 th or February 12 th Lower Extremity Examination and Ethics Case Discussion Suggested Readings: Opatrny L. The Healing Touch. Ann Int Med 2002; 137:1003. http://www.annals.org/cgi/reprint/137/12/1003.pdf
SMALL GROUP SESSION 21B February 10 th or February 12 th Lower Extremity Examination and Ethics Case Discussion Suggested Readings: Opatrny L. The Healing Touch. Ann Int Med 2002; 137:1003. http://www.annals.org/cgi/reprint/137/12/1003.pdf
Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles
 1 2 3 4 5 6 7 Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles Striated Skeletal Smooth Anatomy and Physiology of the Musculoskeletal System Skeletal System Skeletal System Functions
1 2 3 4 5 6 7 Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles Striated Skeletal Smooth Anatomy and Physiology of the Musculoskeletal System Skeletal System Skeletal System Functions
LIMB LENGTH DISCREPANCIES
 LIMB LENGTH DISCREPANCIES Jill C Flanagan, MD OBJECTIVES Evaluate the patient with a possible limb length difference (LLD) Understand general treatment principles when managing limb length differences
LIMB LENGTH DISCREPANCIES Jill C Flanagan, MD OBJECTIVES Evaluate the patient with a possible limb length difference (LLD) Understand general treatment principles when managing limb length differences
IFAST Assessment. Name: Date: Sport: Review Health Risk Assessment on initial consult form. List Client Goals (what brings you here?
 IFAST Assessment Name: Date: Sport: Review Health Risk Assessment on initial consult form List Client Goals (what brings you here?) Cardiovascular Measurements Blood Pressure Resting Heart Rate Body Composition
IFAST Assessment Name: Date: Sport: Review Health Risk Assessment on initial consult form List Client Goals (what brings you here?) Cardiovascular Measurements Blood Pressure Resting Heart Rate Body Composition
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT ***
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient - Certain conditions are more prevalent in particular age groups (Hip pain in children may refer to the knee from Legg-Calve-Perthes
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient - Certain conditions are more prevalent in particular age groups (Hip pain in children may refer to the knee from Legg-Calve-Perthes
CHAPTER 8: THE BIOMECHANICS OF THE HUMAN LOWER EXTREMITY
 CHAPTER 8: THE BIOMECHANICS OF THE HUMAN LOWER EXTREMITY _ 1. The hip joint is the articulation between the and the. A. femur, acetabulum B. femur, spine C. femur, tibia _ 2. Which of the following is
CHAPTER 8: THE BIOMECHANICS OF THE HUMAN LOWER EXTREMITY _ 1. The hip joint is the articulation between the and the. A. femur, acetabulum B. femur, spine C. femur, tibia _ 2. Which of the following is
APTA Intro to Identity. The Movement System The Kinesiopathologic Model Movement System Impairment Syndromes of the Knee THE HUMAN MOVEMENT SYSTEM
 The Movement System The Kinesiopathologic Model Movement System Impairment Syndromes of the Knee Shirley Sahrmann, PT, PhD, FAPTA Professor Emerita Statement of Privacy To protect the privacy of the subjects
The Movement System The Kinesiopathologic Model Movement System Impairment Syndromes of the Knee Shirley Sahrmann, PT, PhD, FAPTA Professor Emerita Statement of Privacy To protect the privacy of the subjects
Knee Capsular Disorder. ICD-9-CM: Stiffness in joint of lower leg, not elsewhere classified
 1 Knee Capsular Disorder "Knee Capsulitis" ICD-9-CM: 719.56 Stiffness in joint of lower leg, not elsewhere classified Diagnostic Criteria History: Physical Exam: Stiffness Aching with prolonged weight
1 Knee Capsular Disorder "Knee Capsulitis" ICD-9-CM: 719.56 Stiffness in joint of lower leg, not elsewhere classified Diagnostic Criteria History: Physical Exam: Stiffness Aching with prolonged weight
Lecture Notes The LocomotorSystem. W. P. Howlett 2017
 Lecture Notes The LocomotorSystem W. P. Howlett 2017 Symptoms Main Symptoms Pain Stiffness Swelling Weakness The History Joints: involved Pain: onset, precipitating& relievingfactors Stiffness: pattern
Lecture Notes The LocomotorSystem W. P. Howlett 2017 Symptoms Main Symptoms Pain Stiffness Swelling Weakness The History Joints: involved Pain: onset, precipitating& relievingfactors Stiffness: pattern
Applied Functional Science Chain Reaction Skeletal: Real creates Relative. Presented By David Tiberio, Ph.D., PT, FAFS Dean, Gray Institute
 Applied Functional Science Chain Reaction Skeletal: Real creates Relative Presented By David Tiberio, Ph.D., PT, FAFS Dean, Gray Institute 1 How Movement is Created Total body movements are made up of
Applied Functional Science Chain Reaction Skeletal: Real creates Relative Presented By David Tiberio, Ph.D., PT, FAFS Dean, Gray Institute 1 How Movement is Created Total body movements are made up of
PT Final Exam. July 2018 Core Content Review 6 Presented by Mark. Copyright 2018 PT Final Exam
 PT Final Exam July 2018 Core Content Review 6 Presented by Mark A 34 year old male comes to your clinic with reoccurring hamstring tears. Upon examination, the therapist is able to achieve 130 degrees
PT Final Exam July 2018 Core Content Review 6 Presented by Mark A 34 year old male comes to your clinic with reoccurring hamstring tears. Upon examination, the therapist is able to achieve 130 degrees
ANTERIOR KNEE PAIN. Explanation. Causes. Symptoms
 ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
Brennen Lucas, M.D. Advanced Orthopaedic Associates
 Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GUIDELINES FOR REHABILITATION FOLLOWING SURGICAL RECONSTRUCTION
Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GUIDELINES FOR REHABILITATION FOLLOWING SURGICAL RECONSTRUCTION
1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles. Striated Skeletal. Smooth
 1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles Striated Skeletal Smooth 3 Anatomy and Physiology of the Musculoskeletal System 4 Skeletal System 5 Skeletal System Functions
1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles Striated Skeletal Smooth 3 Anatomy and Physiology of the Musculoskeletal System 4 Skeletal System 5 Skeletal System Functions
Evaluation of Gait Mechanics Using Computerized Plantar Surface Pressure Analysis and it s Relation to Common Musculoskeletal Problems
 Evaluation of Gait Mechanics Using Computerized Plantar Surface Pressure Analysis and it s Relation to Common Musculoskeletal Problems Laws of Physics effecting gait Ground Reaction Forces Friction Stored
Evaluation of Gait Mechanics Using Computerized Plantar Surface Pressure Analysis and it s Relation to Common Musculoskeletal Problems Laws of Physics effecting gait Ground Reaction Forces Friction Stored
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
A Syndrome (Pattern) Approach to Low Back Pain. History
 A Syndrome (Pattern) Approach to Low Back Pain Hamilton Hall MD FRCSC Professor, Department of Surgery, University of Toronto Medical Director, CBI Health Group Executive Director, Canadian Spine Society
A Syndrome (Pattern) Approach to Low Back Pain Hamilton Hall MD FRCSC Professor, Department of Surgery, University of Toronto Medical Director, CBI Health Group Executive Director, Canadian Spine Society
Therapeutic Foot Care Certificate Program Part I: Online Home Study Program
 Therapeutic Foot Care Certificate Program Part I: Online Home Study Program 1 Anatomy And Terminology Of The Lower Extremity Joan E. Edelstein, MA, PT, FISPO Associate Professor of Clinical Physical Therapy
Therapeutic Foot Care Certificate Program Part I: Online Home Study Program 1 Anatomy And Terminology Of The Lower Extremity Joan E. Edelstein, MA, PT, FISPO Associate Professor of Clinical Physical Therapy
King Saud University College of Nursing Medical-surgical Nursing
 King Saud University College of Nursing Medical-surgical Nursing 1.Obtaining a health history: Ask about chief complain: History of presence of muscle pain (onset, location, Aggravating and alleviating
King Saud University College of Nursing Medical-surgical Nursing 1.Obtaining a health history: Ask about chief complain: History of presence of muscle pain (onset, location, Aggravating and alleviating
DR. (PROF.) ANIL ARORA MS
 Hip Examination DR. (PROF.) ANIL ARORA MS (Ortho) DNB (Ortho) Dip SIROT (USA) FAPOA (Korea), FIGOF (Germany), FJOA (Japan) Commonwealth Fellow Joint Replacement (Royal National Orthopaedic Hospital, London,
Hip Examination DR. (PROF.) ANIL ARORA MS (Ortho) DNB (Ortho) Dip SIROT (USA) FAPOA (Korea), FIGOF (Germany), FJOA (Japan) Commonwealth Fellow Joint Replacement (Royal National Orthopaedic Hospital, London,
General Procedure and Rules
 General Procedure and Rules PROCEDURE Description: This assessment is a measure of upper extremity (UE) and lower extremity (LE) motor and sensory impairment. Equipment: A chair, bedside table, reflex
General Procedure and Rules PROCEDURE Description: This assessment is a measure of upper extremity (UE) and lower extremity (LE) motor and sensory impairment. Equipment: A chair, bedside table, reflex
Recognizing common injuries to the lower extremity
 Recognizing common injuries to the lower extremity Bones Femur Patella Tibia Tibial Tuberosity Medial Malleolus Fibula Lateral Malleolus Bones Tarsals Talus Calcaneus Metatarsals Phalanges Joints - Knee
Recognizing common injuries to the lower extremity Bones Femur Patella Tibia Tibial Tuberosity Medial Malleolus Fibula Lateral Malleolus Bones Tarsals Talus Calcaneus Metatarsals Phalanges Joints - Knee
Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO
 Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO This handout is for use as a rough guide and study aid. Your instructor may perform certain maneuvers
Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO This handout is for use as a rough guide and study aid. Your instructor may perform certain maneuvers
10/22/15. Running Injury Mechanics. Excessive Pronation. Distribution of Running Injuries. 1. Patellofemoral Pain Syndrome
 Distribution of Running Injuries Metarsalgia/Stress Fx Running Injury Mechanics Irene S. Davis, PhD, PT, FACSM, FAPTA, FASB Dept. PM&R, Harvard Medical School Director, Spaulding National Running Center
Distribution of Running Injuries Metarsalgia/Stress Fx Running Injury Mechanics Irene S. Davis, PhD, PT, FACSM, FAPTA, FASB Dept. PM&R, Harvard Medical School Director, Spaulding National Running Center
Musculoskeletal Examination
 Musculoskeletal Examination Statement of Goals Know how to perform a complete musculoskeletal examination. Learning Objectives A. Describe the anatomy of the musculoskeletal system including the bony structures,
Musculoskeletal Examination Statement of Goals Know how to perform a complete musculoskeletal examination. Learning Objectives A. Describe the anatomy of the musculoskeletal system including the bony structures,
BOW LEGS (GENU VARUM)
 BOW LEGS (GENU VARUM) By Dr John Ebnezar INTRODUCTION Have you noticed how your knees look like? If you observe carefully you will see that both your knees are not parallel but deviated slightly outwards
BOW LEGS (GENU VARUM) By Dr John Ebnezar INTRODUCTION Have you noticed how your knees look like? If you observe carefully you will see that both your knees are not parallel but deviated slightly outwards
Balanced Body Movement Principles
 Balanced Body Movement Principles How the Body Works and How to Train it. Module 3: Lower Body Strength and Power Developing Strength, Endurance and Power The lower body is our primary source of strength,
Balanced Body Movement Principles How the Body Works and How to Train it. Module 3: Lower Body Strength and Power Developing Strength, Endurance and Power The lower body is our primary source of strength,
Physical Examination of the Foot & Ankle
 Inspection Standing, feet straight forward facing toward examiner Swelling Deformity Flatfoot (pes planus and hindfoot valgus) High arch (pes cavus and hindfoot varus) Peek-a-boo heel Varus Too many toes
Inspection Standing, feet straight forward facing toward examiner Swelling Deformity Flatfoot (pes planus and hindfoot valgus) High arch (pes cavus and hindfoot varus) Peek-a-boo heel Varus Too many toes
THE EXTREMITY SCREEN MANUAL: A Guide to the Subjective and Objective Outcomes Assessment of the Upper and Lower Extremity
 THE EXTREMITY SCREEN MANUAL: A Guide to the Subjective and Objective Outcomes Assessment of the Upper and Lower Extremity Steven G. Yeomans, DC, FACO INTRODUCTION: Objective screen for the extremities
THE EXTREMITY SCREEN MANUAL: A Guide to the Subjective and Objective Outcomes Assessment of the Upper and Lower Extremity Steven G. Yeomans, DC, FACO INTRODUCTION: Objective screen for the extremities
Arthritic history is similar to that of the hip. Add history of give way and locking, swelling
 KNEE VASU PAI Arthritic history is similar to that of the hip. Add history of give way and locking, swelling INJURY MECHANISM When How Sequence Progress Disability IKDC Activity I - Strenuous activity
KNEE VASU PAI Arthritic history is similar to that of the hip. Add history of give way and locking, swelling INJURY MECHANISM When How Sequence Progress Disability IKDC Activity I - Strenuous activity
Move Better, Feel Better: What Can Physical Therapy Do For You
 Back to Basics Move Better, Feel Better: What Can Physical Therapy Do For You Dr. Stephen Baxter, Dr. Dean Yamanuha Department of Physical Therapy and Rehabilitative Sciences 5/16/2017 Dr. Stephen Baxter
Back to Basics Move Better, Feel Better: What Can Physical Therapy Do For You Dr. Stephen Baxter, Dr. Dean Yamanuha Department of Physical Therapy and Rehabilitative Sciences 5/16/2017 Dr. Stephen Baxter
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY
 Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
AMERICAN RED CROSS FIRST AID RESPONDING TO EMERGENCIES FOURTH EDITION Copyright 2006 by The American National Red Cross All rights reserved.
 Musculoskeletal injuries are most commonly caused by Mechanical forms of energy. Chemicals. Electrical energy. Heat Mechanical energy produces direct, indirect, twisting and contracting forces. Can be
Musculoskeletal injuries are most commonly caused by Mechanical forms of energy. Chemicals. Electrical energy. Heat Mechanical energy produces direct, indirect, twisting and contracting forces. Can be
Differentialdianosis to CRPS Departmentdoctor Bo Biering-Sørensen, Pain Clinic, Neurological Department
 Differentialdianosis to CRPS Departmentdoctor Bo Biering-Sørensen, Pain Clinic, Neurological Department Dato (Sidehoved/fod) Case 1 36 year old man other ethnically background than Danish 2006 Left foot
Differentialdianosis to CRPS Departmentdoctor Bo Biering-Sørensen, Pain Clinic, Neurological Department Dato (Sidehoved/fod) Case 1 36 year old man other ethnically background than Danish 2006 Left foot
ADVANTAGE REPRESENTATIVES Reliable Medical-Legal Observers
 ADVANTAGE REPRESENTATIVES Reliable Medical-Legal Observers PO Box 25978 * Los Angeles, CA 90025-8995 (818) 786-7412 * Fax (818) 786-7413 SAMPLE REPORT CLIENT: ATTORNEY: OBSERVER: EXAMINING PHYSICIAN: Robert
ADVANTAGE REPRESENTATIVES Reliable Medical-Legal Observers PO Box 25978 * Los Angeles, CA 90025-8995 (818) 786-7412 * Fax (818) 786-7413 SAMPLE REPORT CLIENT: ATTORNEY: OBSERVER: EXAMINING PHYSICIAN: Robert
Exam of the Knee and Ankle I HAVE NO FINANCIAL DISCLOSURES RELEVANT TO THIS PRESENTATION
 Exam of the Knee and Ankle I HAVE NO FINANCIAL DISCLOSURES RELEVANT TO THIS PRESENTATION Disclosures I have no relevant financial relationships with the manufacturers of any commercial products and or
Exam of the Knee and Ankle I HAVE NO FINANCIAL DISCLOSURES RELEVANT TO THIS PRESENTATION Disclosures I have no relevant financial relationships with the manufacturers of any commercial products and or
Movement Terminology. The language of movement is designed to allow us to describe how the body moves through space.
 Movement Terminology The language of movement is designed to allow us to describe how the body moves through space. In exercise it allows us to communicate with other movement professionals so we can describe
Movement Terminology The language of movement is designed to allow us to describe how the body moves through space. In exercise it allows us to communicate with other movement professionals so we can describe
Steven Feinberg MD Andrew Sew Hoy MD
 Steven Feinberg MD Andrew Sew Hoy MD COA Conference April 17 th 2010 September 3 rd 2009 PD Rating rebuttable may use any method within the Guides of the Evaluation of Permanent Impairment 5 th Edition
Steven Feinberg MD Andrew Sew Hoy MD COA Conference April 17 th 2010 September 3 rd 2009 PD Rating rebuttable may use any method within the Guides of the Evaluation of Permanent Impairment 5 th Edition
Chapter 10: Flexibility
 Chapter 10: Flexibility Lesson 10.1: Flexibility Facts Self-Assessment 10: Arm, Leg, and Trunk Flexibility Lesson Objectives: Describe the characteristics of flexibility. Explain how you benefit from good
Chapter 10: Flexibility Lesson 10.1: Flexibility Facts Self-Assessment 10: Arm, Leg, and Trunk Flexibility Lesson Objectives: Describe the characteristics of flexibility. Explain how you benefit from good
Flexibility. STRETCH: Kneeling gastrocnemius. STRETCH: Standing gastrocnemius. STRETCH: Standing soleus. Adopt a press up position
 STRETCH: Kneeling gastrocnemius Adopt a press up position Rest one knee on mat with the opposite leg straight Maintain a neutral spine position Push through arms to lever ankle into increased dorsiflexion
STRETCH: Kneeling gastrocnemius Adopt a press up position Rest one knee on mat with the opposite leg straight Maintain a neutral spine position Push through arms to lever ankle into increased dorsiflexion
FUNCTIONAL TESTING GUIDELINES FOR ACL RECONSTRUCTION TESTING INSTRUCTIONS FOR CLINICIANS
 FUNCTIONAL TESTING GUIDELINES FOR ACL RECONSTRUCTION TESTING INSTRUCTIONS FOR CLINICIANS A number of criteria should be met before advanced functional testing of ACL reconstruction or ACL deficient knees
FUNCTIONAL TESTING GUIDELINES FOR ACL RECONSTRUCTION TESTING INSTRUCTIONS FOR CLINICIANS A number of criteria should be met before advanced functional testing of ACL reconstruction or ACL deficient knees
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 2155/14
 WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 2155/14 BEFORE: S. Netten: Vice-Chair HEARING: November 17, 2014 at Toronto Written DATE OF DECISION: January 9, 2015 NEUTRAL CITATION: 2015
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 2155/14 BEFORE: S. Netten: Vice-Chair HEARING: November 17, 2014 at Toronto Written DATE OF DECISION: January 9, 2015 NEUTRAL CITATION: 2015
Non Surgical Management Of Hip And Knee Osteoarthritis Toolkit. Evaluation and Diagnosis of Osteoarthritis in Primary Care
 Non Surgical Management Of Hip And Knee Osteoarthritis Toolkit Evaluation and Diagnosis of Osteoarthritis in Primary Care OA-HxPE-716.indd 1 TABLE OF CONTENTS HISTORY TAKING... 3 EVALUATION OF SUSPECTED
Non Surgical Management Of Hip And Knee Osteoarthritis Toolkit Evaluation and Diagnosis of Osteoarthritis in Primary Care OA-HxPE-716.indd 1 TABLE OF CONTENTS HISTORY TAKING... 3 EVALUATION OF SUSPECTED
AAP Boot Camp KNEE AND ANKLE EXAM
 AAP Boot Camp KNEE AND ANKLE EXAM Disclosures I have no relevant financial relationships with the manufacturers of any commercial products and or providers of commercial services discussed in this CME
AAP Boot Camp KNEE AND ANKLE EXAM Disclosures I have no relevant financial relationships with the manufacturers of any commercial products and or providers of commercial services discussed in this CME
Introduction. What is RSD? Causes of RSD. What Makes Reflex Sympathetic Dystrophy So Complicated?
 What Makes Reflex Sympathetic Dystrophy So Complicated? Article originally appeared in inmotion Magazine: Volume 14 Issue 5 September/October 2004 Introduction Because this condition is so complex, the
What Makes Reflex Sympathetic Dystrophy So Complicated? Article originally appeared in inmotion Magazine: Volume 14 Issue 5 September/October 2004 Introduction Because this condition is so complex, the
Understanding Leg Anatomy and Function THE UPPER LEG
 Understanding Leg Anatomy and Function THE UPPER LEG The long thigh bone is the femur. It connects to the pelvis to form the hip joint and then extends down to meet the tibia (shin bone) at the knee joint.
Understanding Leg Anatomy and Function THE UPPER LEG The long thigh bone is the femur. It connects to the pelvis to form the hip joint and then extends down to meet the tibia (shin bone) at the knee joint.
Supplemental Information Packet for Classifiers: 2016 DOD WARRIOR GAMES
 FOR TEAM STAFF TRACK and FIELD - Please complete the table below if the athlete has an amputation AMPUTATION TRACK FIELD Below Knee TR4.5 SE6.0 / ST4.5 Above Knee TR4.0 SE5.0 / ST4.0 Double BK or BK &
FOR TEAM STAFF TRACK and FIELD - Please complete the table below if the athlete has an amputation AMPUTATION TRACK FIELD Below Knee TR4.5 SE6.0 / ST4.5 Above Knee TR4.0 SE5.0 / ST4.0 Double BK or BK &
Periarticular knee osteotomy
 Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Dorsal surface-the upper area or top of the foot. Terminology
 It is important to learn the terminology as it relates to feet to properly communicate with referring physicians when necessary and to identify the relationship between the anatomical structure of the
It is important to learn the terminology as it relates to feet to properly communicate with referring physicians when necessary and to identify the relationship between the anatomical structure of the
THE SELECTIVE FUNCTIONAL MOVEMENT ASSESSMENT
 - 33 - THE SELECTIVE FUNCTIONAL MOVEMENT ASSESSMENT SFMA SCORING FP DP Active Cervical Flexion Active Cervical Extension Cervical Rotation Upper Extremity Pattern 1(MRE) Upper Extremity Pattern 2 (LRF)
- 33 - THE SELECTIVE FUNCTIONAL MOVEMENT ASSESSMENT SFMA SCORING FP DP Active Cervical Flexion Active Cervical Extension Cervical Rotation Upper Extremity Pattern 1(MRE) Upper Extremity Pattern 2 (LRF)
The BioMechanics Method
 The BioMechanics Method EXERCISE SOLUTIONS FOR CHRONIC PAIN The Fundamentals of Structural Assessment End of Section Self-Check There are many things that can make conducting a structural assessment more
The BioMechanics Method EXERCISE SOLUTIONS FOR CHRONIC PAIN The Fundamentals of Structural Assessment End of Section Self-Check There are many things that can make conducting a structural assessment more
Iliotibial Band Tendinitis (Runner s Knee)
 Iliotibial Band Tendinitis (Runner s Knee) ANATOMY The iliotibial band (or tract) is a thick band of tissue that starts on the pelvis and upper thigh and passes along the outside of the knee and attaches
Iliotibial Band Tendinitis (Runner s Knee) ANATOMY The iliotibial band (or tract) is a thick band of tissue that starts on the pelvis and upper thigh and passes along the outside of the knee and attaches
Multiapical Deformities p. 97 Osteotomy Concepts and Frontal Plane Realignment p. 99 Angulation Correction Axis (ACA) p. 99 Bisector Lines p.
 Normal Lower Limb Alignment and Joint Orientation p. 1 Mechanical and Anatomic Bone Axes p. 1 Joint Center Points p. 5 Joint Orientation Lines p. 5 Ankle p. 5 Knee p. 5 Hip p. 8 Joint Orientation Angles
Normal Lower Limb Alignment and Joint Orientation p. 1 Mechanical and Anatomic Bone Axes p. 1 Joint Center Points p. 5 Joint Orientation Lines p. 5 Ankle p. 5 Knee p. 5 Hip p. 8 Joint Orientation Angles
Injuries to the Extremities
 Injuries to the Extremities KNOWLEDGE OBJECTIVES 1. List seven signs and symptoms that suggest a serious extremity injury. 2. Describe how to care for injuries to the shoulder, upper arm, and elbow. 3.
Injuries to the Extremities KNOWLEDGE OBJECTIVES 1. List seven signs and symptoms that suggest a serious extremity injury. 2. Describe how to care for injuries to the shoulder, upper arm, and elbow. 3.
Maximal isokinetic and isometric muscle strength of major muscle groups related to age, body weight, height, and sex in 178 healthy subjects
 Maximal isokinetic and isometric muscle strength of major muscle groups related to age, body weight, height, and sex in 178 healthy subjects Test protocol Muscle test procedures. Prior to each test participants
Maximal isokinetic and isometric muscle strength of major muscle groups related to age, body weight, height, and sex in 178 healthy subjects Test protocol Muscle test procedures. Prior to each test participants
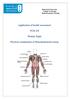
[7] 5-214F - 5 = 06%
![[7] 5-214F - 5 = 06% [7] 5-214F - 5 = 06%](/thumbs/86/93472785.jpg) Craig Andrew Lange craig@pdratings.com Our Document # 1201Taffy (PTP Rating) Impairment & Disability Rating Specialists http://www.pdratings.com/ Voice: (415) 861-4040 / Fax: (415) 276-3741 Luis Pérez-Cordero
Craig Andrew Lange craig@pdratings.com Our Document # 1201Taffy (PTP Rating) Impairment & Disability Rating Specialists http://www.pdratings.com/ Voice: (415) 861-4040 / Fax: (415) 276-3741 Luis Pérez-Cordero
The examination of the painful knee. Maja K Artandi, MD, FACP Clinical Associate Professor of Medicine Stanford University
 The examination of the painful knee Maja K Artandi, MD, FACP Clinical Associate Professor of Medicine Stanford University Objectives of the talk By the end of this talk you will know The important anatomy
The examination of the painful knee Maja K Artandi, MD, FACP Clinical Associate Professor of Medicine Stanford University Objectives of the talk By the end of this talk you will know The important anatomy
Knee Injuries. PSK 4U Mr. S. Kelly North Grenville DHS. Medial Collateral Ligament Sprain
 Knee Injuries PSK 4U Mr. S. Kelly North Grenville DHS Medial Collateral Ligament Sprain Result from either a direct blow from the lateral side in a medial direction or a severe outward twist Greater injury
Knee Injuries PSK 4U Mr. S. Kelly North Grenville DHS Medial Collateral Ligament Sprain Result from either a direct blow from the lateral side in a medial direction or a severe outward twist Greater injury
IMPAIRMENT RATING 5 TH EDITION MODULE III THE UPPER EXTREMITIES AND PAIN
 IMPAIRMENT RATING 5 TH EDITION MODULE III THE UPPER EXTREMITIES AND PAIN PRESENTED BY: RONALD J. WELLIKOFF, D.C., FACC, FICC In conjuction with: The physical examination is the determining factor of a
IMPAIRMENT RATING 5 TH EDITION MODULE III THE UPPER EXTREMITIES AND PAIN PRESENTED BY: RONALD J. WELLIKOFF, D.C., FACC, FICC In conjuction with: The physical examination is the determining factor of a
Ankle Arthritis and Ankle Replacement
 Ankle Arthritis and Ankle Replacement Ryan DeBlis, MD Disclosures I have no disclosures. 1 Diagnosis Ankle arthritis Majority (70%) of patients are post-traumatic (ie, after ankle fracture) Primary arthritis
Ankle Arthritis and Ankle Replacement Ryan DeBlis, MD Disclosures I have no disclosures. 1 Diagnosis Ankle arthritis Majority (70%) of patients are post-traumatic (ie, after ankle fracture) Primary arthritis
.org. Tibia (Shinbone) Shaft Fractures. Anatomy. Types of Tibial Shaft Fractures
 Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
General appearance examination
 Childhood athletic participation has dramatically increased over the past twenty years. Children are being introduced to organised sports at increasingly immature stages of physical development. It is
Childhood athletic participation has dramatically increased over the past twenty years. Children are being introduced to organised sports at increasingly immature stages of physical development. It is
Location of Pain/Symptoms Where do you feel the pain/symptoms? Can you point with one finger to location of pain? Is the pain general or localized?
 Injury Evaluation History A complete and accurate medical history is one of the most important and useful parts of the clinical examination. A complete history consists of past history and a history of
Injury Evaluation History A complete and accurate medical history is one of the most important and useful parts of the clinical examination. A complete history consists of past history and a history of
Pediatric Orthopedics: ``To Refer or Not to Refer``
 Pediatric Orthopedics: ``To Refer or Not to Refer`` Thierry E. Benaroch, MD, FRCS(C) McGill University Health Centre Intoeing Knock knees Bowlegs Flatfeet Toe walking Knee pain Hip click Intoeing Objectives
Pediatric Orthopedics: ``To Refer or Not to Refer`` Thierry E. Benaroch, MD, FRCS(C) McGill University Health Centre Intoeing Knock knees Bowlegs Flatfeet Toe walking Knee pain Hip click Intoeing Objectives
fitting shoes, or repetitive stress. It also frequently arises from unknown causes.
 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353. Website: philip-bayliss.com Morton's Neuroma Morton's Neuroma, also sometimes referred to as plantar Neuroma or intermetatarsal Neuroma,
43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353. Website: philip-bayliss.com Morton's Neuroma Morton's Neuroma, also sometimes referred to as plantar Neuroma or intermetatarsal Neuroma,
A Patient s Guide to Flatfoot Deformity (Pes Planus) in Children
 A Patient s Guide to Flatfoot Deformity (Pes Planus) in Children 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Flatfoot Deformity (Pes Planus) in Children 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled
7 Element Order. elsewhere classified, Spinal stenosis, lumbar region, without neurogenic claudication. Physician signature:
 7 Element Order Medicare national and local policy specify that following completion of the face-to-face examination, the physician or treating practitioner must complete a written order containing seven
7 Element Order Medicare national and local policy specify that following completion of the face-to-face examination, the physician or treating practitioner must complete a written order containing seven
REMEMBER GOOD POSTURE DURING ALL YOUR EXERCISES, AVOID SLOUCHING AS YOUR CURRENT PROGRAM BECOMES EASY SLOWLY INCREASE:
 REMEMBER GOOD POSTURE DURING ALL YOUR EXERCISES, AVOID SLOUCHING Apr 06, 2017 AS YOUR CURRENT PROGRAM BECOMES EASY SLOWLY INCREASE: # OF LAPS YOU ARE WALKING # OF REPITITIONS # OF SECONDS YOU HOLD A STRETCH
REMEMBER GOOD POSTURE DURING ALL YOUR EXERCISES, AVOID SLOUCHING Apr 06, 2017 AS YOUR CURRENT PROGRAM BECOMES EASY SLOWLY INCREASE: # OF LAPS YOU ARE WALKING # OF REPITITIONS # OF SECONDS YOU HOLD A STRETCH
Functional Movement Screen (Cook, 2001)
 Functional Movement Screen (Cook, 2001) TEST 1 DEEP SQUAT Purpose - The Deep Squat is used to assess bilateral, symmetrical, mobility of the hips, knees, and ankles. The dowel held overhead assesses bilateral,
Functional Movement Screen (Cook, 2001) TEST 1 DEEP SQUAT Purpose - The Deep Squat is used to assess bilateral, symmetrical, mobility of the hips, knees, and ankles. The dowel held overhead assesses bilateral,
Diagnostic Imaging Exams
 Guide for Chiropractors Diagnostic Imaging Exams CREATED FOR OUR CHIROPRACTIC PARTNERS This document has been prepared by the specialized, board-certified radiologists who interpret patient exams for Center
Guide for Chiropractors Diagnostic Imaging Exams CREATED FOR OUR CHIROPRACTIC PARTNERS This document has been prepared by the specialized, board-certified radiologists who interpret patient exams for Center
Manage TB Dr. Dina Nair National Institute for Research in Tuberculosis, Chennai. Lecture 07 Clinical manifestations of TB Session 02
 Manage TB Dr. Dina Nair National Institute for Research in Tuberculosis, Chennai Lecture 07 Clinical manifestations of TB Session 02 Hello, welcome to the second session on Clinical manifestations of tuberculosis.
Manage TB Dr. Dina Nair National Institute for Research in Tuberculosis, Chennai Lecture 07 Clinical manifestations of TB Session 02 Hello, welcome to the second session on Clinical manifestations of tuberculosis.
Calcaneus (Heel Bone) Fractures
 Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
A Patient s Guide. ACL Injury: Ø Frequently asked questions on injury, Ø Preoperative and postoperative. surgery and recovery.
 ACL Injury: A Patient s Guide Ø Frequently asked questions on injury, surgery and recovery Ø Preoperative and postoperative guidelines Mia S. Hagen, M.D. Assistant Professor Department of Orthopaedics
ACL Injury: A Patient s Guide Ø Frequently asked questions on injury, surgery and recovery Ø Preoperative and postoperative guidelines Mia S. Hagen, M.D. Assistant Professor Department of Orthopaedics
