2. Review of Literature
|
|
|
- Logan Milo Martin
- 6 years ago
- Views:
Transcription
1 2. Review of Literature 2.1 Introduction This section provides background information that is pertinent to the dissertation. Gross anatomy of the knee is introduced in terms of human structures, and comparative porcine anatomy is then presented. A description of the function of the anterior cruciate ligament (ACL) follows. Finally, literature related to the incidence, etiology, and treatment of ACL injuries is reviewed. 2.2 Gross Anatomy of the Knee Gross anatomy involves the study of the structure of the body on a macroscopic level. In this section, gross anatomy of the knee is discussed first in terms of human characteristics. Then, comparative porcine anatomy is presented Human Anatomy Except where noted, the following descriptions of the components of the human knee are based on information from Gray s Anatomy [35] Bony Architecture The knee consists of three bony articulations combining to form one joint (Figure 2.1). Two of these connections are condyloid joints, one occurring between each femoral condyle and the related meniscus and tibial condyle. The third articulation, occurring between the patella and femur, is partially arthrodial. Figure 2.1 Bony Architecture of the Knee 3
2 Geoffrey W. Ringer Chapter 2. Review of Literature Femoral Condyles The inferior end of the femur consists of two oblong, convex eminences known as the femoral condyles. On the anterior side, the condyles are extended anteriorly to form a smooth shallow articular depression called the patellar surface. The central part of the patellar surface is typically referred to as the patellofemoral groove. In the posterior direction, the condyles extend to form a deep fossa known as the intercondylar notch. The lateral condyle is the larger of the two in the antero-posterior and transverse directions, while the medial condyle is the larger in the distal direction. This feature allows the lower surfaces of the condyles to lie in the same horizontal plane when the femur is aligned in its natural oblique position. The axes of the condyles from anterior to posterior edges are not parallel; that of the lateral condyle runs nearly antero-posteriorly, while that of the medial condyle is inclined medially Tibial Condyles The superior end of the tibia consists of two large eminences known as the tibial condyles. The lateral condyle is nearly circular, while the medial condyle is oval. In the medio-lateral direction, both condyle surfaces are concave. In the antero-posterior direction, however, the medial condyle surface is concave, while the lateral condyle surface is convex. Located between the condyles are two depressions, the anterior and posterior intercondylar fossae, and a spine, the intercondylar eminence. The anterior surfaces of the condyles meet to form a large flat area. At the inferior edge of this area is the tibial tubercle Patella The patella is a flat, triangular bone located at the front of the knee. The anterior surface is convex and marked with striations. The posterior surface contains a smooth articular area divided into two facets by a vertical ridge, which corresponds to the patellar surface on the femur. Inferior to the articular area is a convex non-articular area. The thick, superior edge of the patella is called the base, and the pointed, inferior edge is called the apex Soft Tissues Soft connective tissues link the three bones in the knee joint (Figure 2.2). The major soft tissues in the knee are: (a) the articular capsule, (b) the quadriceps and patellar tendons, (c) the lateral collateral ligament, (d) the medial collateral ligament, (e) the anterior cruciate ligament, (f) the posterior cruciate ligament, and (g) the lateral and medial menisci.
3 Geoffrey W. Ringer Chapter 2. Review of Literature Articular Capsule Figure 2.2 Soft Tissue of the Knee The articular capsule of the knee is the largest and most extensive in the body. It consists of a strong, thin fibrous synovial membrane which forms a closed sac around the joint. Inseparable bands derived from the fascia lata and from the tendons surrounding the joint are connected throughout almost the entire extent of the synovial membrane to further strengthen the capsule. The inner lining of the synovial membrane consists of a free surface which secretes viscous synovial fluid for lubrication and nutrient supply Quadriceps and Patellar Tendons The quadriceps tendon is the common termination of the four quadriceps femoris muscles and inserts into the base of the patella. Fibers from the central portion of the quadriceps tendon passes over the patella to merge with the patellar tendon. The medial and lateral sections of the quadriceps tendon pass on either side of the patella and blend into the joint capsule to form the medial and lateral patellar retinacula. The patellar tendon inserts into the tibial tubercle to connect the patella and the tibia Lateral Collateral Ligament The lateral collateral ligament is a strong, round fibrous cord attached between the lateral femoral condyle and the lateral side of the fibular head. This ligament has no connections to the lateral meniscus.
4 Geoffrey W. Ringer Chapter 2. Review of Literature Medial Collateral Ligament The medial collateral ligament is a flat fibrous band attached on one end to the medial femoral condyle and on the other end to the medial tibial condyle and medial surface of the tibia. The deep fibers of this ligament adhere to the medial meniscus Anterior Cruciate Ligament The ACL is located in the middle of the joint. The inferior end of the ACL merges with the anterior horn of the medial meniscus and attaches in front of the tibial intercondylar eminence. From this point, the ligament passes in a superior, posterior, and lateral direction to attach to the medial part of the lateral femoral condyle. The fibers of the ACL form three twisted bands: the anteromedial band, the intermediate band, and the posterolateral band [48]. Although the ACL is intracapsular, the synovial fold covers the ligament, thereby maintaining an extrasynovial environment Posterior Cruciate Ligament The posterior cruciate ligament is also located in the middle of the joint, crossing the ACL to form an X. The inferior end of the posterior cruciate ligament blends with the posterior horn of the lateral meniscus and attaches to the tibial posterior intercondylar fossa. From this point, the ligament passes in a superior, anterior, and medial direction to attach to the lateral part of the medial femoral condyle. The fibers of the posterior cruciate ligament form two twisted bands: the anteromedial band, and the posterolateral band [48]. Like the ACL, the posterior cruciate ligament is covered by the synovial fold and is considered to exist in an extrasynovial environment Lateral and Medial Menisci The menisci are two crescent lamellae located between the femoral and tibial condyles. The upper surfaces of the menisci are concave and contact the femoral condyles. The lower surfaces of the menisci are flat and rest on the tibial condyles. The peripheral border of each meniscus is thick, convex, and attached to the interior surface of the joint capsule. The opposite border is thin, concave, and free of connections Comparative Porcine Anatomy Although the overall appearance of the pig is noticeably different from that of the human, gross anatomy of porcine and human knees are similar [12] (Figures 2.3, 2.4). Slight differences between the species do exist. The femur and tibia of the pig are relatively more massive and heavier than human bones. Also, to provide a greater moment arm for the quadriceps tendon, the porcine tibial tubercle protrudes more anteriorly than the human version. Figure 2.3 Skeletal Anatomy of the Porcine Pelvic Limb (Lateral View)
5 Geoffrey W. Ringer Chapter 2. Review of Literature 7 Figure 2.4 Muscular Anatomy of the Porcine Pelvic Limb (Lateral View) Minor soft tissue differences also exist between the porcine and human species. The porcine ACL consists of two distinct morphological units, while the human ligament is only one unit [30,31]. Hence, the porcine ligament contains only two bands: the anteromedial band and the posterolateral band. Function of the ACL in both species is similar. The overall range of motion of the porcine knee is similar to that of the human knee [31]. Range of knee flexion in both species is about 150. However, in the human, full extension occurs at about 0, or when the longitudinal axes of the femur and tibia are approximately parallel. In the pig, full extension corresponds to about 30 human flexion, and full flexion is about Anterior Cruciate Ligament Function Ligaments constrain the relative motion of the bones in the knee joint [11]. The ACL primarily resists anterior tibial displacement through all flexion angles [13,16,28,34,58,80,82]. Secondarily, the ACL resists: (a) hyperextension [29,34], (b) internal and external tibial rotation [29,34,58,84,86], and (c) abduction and adduction [38,58,70] Kinematic Behavior The fibers of the ACL rotate about their insertion sites to control motion of the knee [75]. According to O Connor and Zavatsky [75], Weber and Weber [92] first described the motion of the femur on the tibia during flexion and extension (Figure 2.5). If the femur rolled without sliding, the femoral condyle would lose contact with the tibial plateau at a certain flexion angle. On the other hand, if sliding occurred without rolling, the femur would prematurely contact the tibia, thus limiting motion. Hence, both rolling and sliding must occur during flexion. A four-bar linkage can theoretically model this behavior (Figure 2.6) [74,75]. Because motion of the knee occurs primarily in the sagittal plane, the model assumes the joint to be a two-dimensional single degreeof-freedom linkage. The ACL and PCL are considered to be two of the links, while the tibia and femur are the remaining two links.
6 Geoffrey W. Ringer Chapter 2. Review of Literature 8 Figure 2.5 Glide-Roll Relationship of the Knee
7 Geoffrey W. Ringer Chapter 2. Review of Literature Kinetic Behavior Figure 2.6 Four-Bar Linkage Model of the Knee The ACL resists and controls knee motion by developing a tensile force when stretched [75]. Researchers have used indirect [42] and direct methods [53] to determine the force generated in the ACL during various movements Indirect Measurements Researchers described an indirect method based on changes in knee kinematics after ACL transection to estimate ACL force in human cadaver knees [42,89]. A six degree-of-freedom instrumented spatial linkage was used to record relative motion between the femur and tibia as loads were applied to the joint. A load versus length curve was determined by digitizing the ACL insertion sites while performing an anterior drawer test on the specimen with only the ACL intact.
8 Geoffrey W. Ringer Chapter 2. Review of Literature 10 The relative movement between the ACL insertion sites was calculated for the intact knee test, and the load versus length curve was used to determine ACL load throughout the motion Direct Measurements Four methods have been suggested to more directly measure ACL load: using a buckle transducer [1,52,54], bone block transducers [57], modified pressure transducers [41], and a robotic positioning system [27,55,56,81] Buckle Transducer Lewis et al. [53] described the buckle force transducer as consisting of strain gauges mounted on a rectangular metal frame (Figure 2.7). A removable cross-bar is used to place the transducer on a ligament. As the ligament tensile force increases, the bending moment on the frame increases. The output from the strain gauges is calibrated using known ligament forces to permit the measurement of future, unknown loads. Advantages to using buckle transducers to measure ACL force include: (a) The transducer is easily applied directly to the ligament; (b) the transducer directly measures ligament force, not ligament strain; and (c) the transducer is rugged enough to withstand in vivo implantation. Disadvantages of the buckle transducer include: (a) The transducer may contact other surfaces, leading to deceptive results; (b) viscoelastic creep of the ligament may alter the calibration constant after insertion of the transducer; (c) the calibration constant may be affected by stress distribution in the ligament; and (d) the ligament shortening that occurs when applying the transducer may affect the load distribution in the joint Bone Block Transducer Figure 2.7 Buckle Transducer Markolf et al. [57] introduced a method to directly measure force in the in vitro ACL using an externally mounted load cell. A hole was drilled from the anteromedial surface of the tibia in line with the axis of the ACL to a point just below the tibial plateau. Screws were placed in the
9 Geoffrey W. Ringer Chapter 2. Review of Literature 11 subchondral bone under the ACL tibial insertion site. A threaded steel rod centered in a cylindrical liner was inserted into the hole, and acrylic cement was poured into the gap. After the cement had cured, the liner was removed. One end of a three axis load cell was fixed to the body of the tibia, and the other end was attached to the threaded rod in the cement. The bone core was then completed to free the ACL tibial insertion. Hence, the ACL maintained its anatomical position, and all ligament forces during subsequent knee motion were transmitted to the load cell. The authors noted an error in load values of up to nine percent due to motion of the bone plug in the tunnel Modified Pressure Transducer Holden et al. [41] described the use of a modified pressure transducer to measure the in vivo force in the goat ACL during standing, walking, and trotting. A Teflon button was fastened to the diaphragm of the pressure transducer. When the device was implanted into the anteromedial band of the ACL, the ligament fibers pressed the button against the diaphragm. Increasing the axial force of the ligament increased the transverse force against button, and hence, raised the pressure sensed by the transducer. Use of the modified pressure transducer presents similar advantages and disadvantages as the buckle transducer Robotic Positioning System Fujie et al. [27] described the use of a robotic positioning system to study joint kinematics. A 6- axis articulated robotic manipulator with 6 degrees-of-freedom motion controlled the position of a knee via a universal force sensor. Livesay et al. [55,56] used this system to determine the in situ forces in the ACL during knee motion constrained to 1 or 5 degrees-of-freedom. To accomplish this, the intact joint was moved through a range of motion while the universal force sensor monitored the external applied forces and moments. Following transection of the ACL, the robotic manipulator moved the knee precisely through the same path of motion while the universal force sensor again monitored external applied forces and moments. Because the path of motion was identical during both trials, the principle of superposition could be used to determine the force in the ACL during this motion (equal to the difference in external applied forces and moments between the two trials). Sakane et al. [81] used this technique to determine the forces in the bundles of the ACL when an anterior load was applied to the tibia. 2.4 Anterior Cruciate Ligament Injuries Knee injuries are extremely common, and injuries to the ACL constitute a majority of these [40,46]. Research into the incidence and etiology of ACL injuries is reviewed, followed by a discussion of literature describing various treatments for these injuries Incidence and Etiology ACL injuries occur in the general population in large numbers. In 1983, Johnson [47] reported 1.2% of a college entrance population had experienced an injury to the ACL at some time. An estimated 87,500 ACL ruptures occur annually [66]. Hirshman et al. [40] analyzed evaluations of patients that visited the San Diego Kaiser Knee Injury Clinic during a 3 year period. Of 1833 patients with acute knee injuries, 500 involved severe injuries of knee ligaments. Of these 500, 63% concerned the ACL. The majority of these ACL injuries were sports-related; football, baseball, soccer, skiing, and basketball accounted for 52% of the injuries, while other sports accounted for 15%. Vehicular and miscellaneous accidents accounted for the remainder of the injuries.
10 Geoffrey W. Ringer Chapter 2. Review of Literature Treatment Stark [88] attempted one of the earliest reported treatments for an ACL injury. Since that time, a variety of treatments have been suggested, and much controversy surrounds the clinical management of a patient with an ACL injury [3] No Repair Without treatment, the prognosis after an ACL injury may be poor. Based on a study of 223 patients with ACL injuries, Fetto and Marshall [23] declared that the ACL-deficient knee appears to invariably embark upon a course of progressive deterioration and dysfunction. An untreated ACL injury can lead to increased anterior and rotational instabilities and to an increased frequency of meniscal injuries [71]. Researchers noted radiographic changes in 80% and osteoarthritis in 10% of patients with untreated ACL injuries at 14 year follow-up [61]. Noyes et al. [72] evaluated 103 untreated, athletic patients an average of 5.5 years after injury. Eighty-five of the patients participated in sports after injury, and 53 of these sustained a serious reinjury within one year of the initial injury. Only 11 patients reported having no serious limitations with respect to strenuous sports participation. Furthermore, 32 patients reported disability in walking, while 45 reported disability in activities of daily living. Based on a study of patients with lacerated ACLs, Palmer [78] concluded that impromptu healing of a fully ruptured human ACL does not occur. He noted that the ACL had in fact absorbed after injury. A ruptured ACL can disappear entirely within 8 months [91], and possibly as soon as 6 weeks after injury [50]. O Donoghue et al. [77] studied the response of partially and fully transected ACLs in a canine model. The ends of a fully lacerated ACL either retracted or absorbed, and a partially lacerated ACL showed little evidence of healing. The authors suggested that the hostile synovial environment surrounding the injured ligament deterred healing. Similar results have been noted using a rabbit model [39] Effects of Synovial Fluid Researchers have investigated the effect of the synovial environment on ACL and patellar tendon tissues [4]. Ordinarily, a synovial membrane covers the ACL, and separates the ligament from synovial fluid in the joint [6,14]. When the ACL ruptures, the membrane also tears [4]. Synovial fluid then immerses the injured ends of the ligament, and exposes the ligament to potentially destructive enzymes [4]. Following transection, canine ACL displayed an inflammatory response [77]. Synovial fluid also adversely affected ACL fibroblasts in vitro [5]. The number of fibroblasts populating the tissue culture decreased when exposed to synovial fluid. However, Nickerson et al. [69] found that synovial fluid stimulated rabbit ACL cell proliferation in vitro. The authors suggested that different cell types, synovial fluid sources, concentrations, and growth media may have caused the conflicting results. Hence, synovial fluid, under some conditions, may be a source of nutrition to ligament cells [69] Primary Repair Because an injured ACL apparently does not heal spontaneously, practitioners have attempted primary repair [4]. O Donoghue et al. [77] found poor healing in fully transected canine ACLs that were repaired with sutures, although an unpredictable percentage of the ligaments would heal. These results were corroborated using canine and monkey models [18]. Amiel et al. [4] suggested that this phenomenon occurred because the injury model disrupted the ACL at an insertion site.
11 Geoffrey W. Ringer Chapter 2. Review of Literature 13 Cells from the adjoining bone could then produce the healing response. Because more than 80% of ACL ruptures occur in the proximal 20% of the tissue [85], this model does not accurately represent ACL healing in practice [4]. Feagin et al. [21] reported good initial results from the primary repair of 30 ruptured ACLs. Two years after surgery, 25 of 30 patients had good to excellent results. However, in a 5 year followup study of these patients, Feagin and Curl [22] discovered progressive degeneration of the knee. The authors considered these results to be similar to the natural history of the unrepaired ACL. Other researchers have noted similar findings [8,76] Reconstruction Because of the problems associated with the innate healing response and with primary repair of injured ACLs, reconstruction of the ligament for patients with a highly active lifestyle or with functional disability is recommended [10]. Reconstruction involves substituting a graft for the injured ligament [10]. An appropriate replacement for the ACL must be selected, considering the structural and mechanical properties of normal ACL and the graft material [10]. Allografts, autografts, xenografts, and prosthetic devices have been suggested as potential replacement materials [25,26,45,60,90]. It is beyond the scope of this literature review to discuss every type of graft and reconstruction procedure. Because a bone-patellar tendon-bone autograft is arguably the most common structure used for ACL reconstruction [10,45], this procedure is reviewed in detail in the following section Patellar Tendon Autograft ACL reconstruction with a patellar tendon autograft involves replacing the ligament by a graft taken from the injured knee. Except where noted, the following arthroscopic surgical procedure was described by Daniel [20]. An anterior medial incision is made to expose the patellar tendon and its insertion sites. Tissue is dissected along the medial side of the patellar tendon and across the front of the patella. The width of the patellar tendon is then measured. Daniel suggested that the smaller of one-third of the patellar tendon width or 10 mm determines the graft width. However, the width of the graft varies with the surgeon s preference [45]. An outline of the desired graft is drawn on the central portion of the patellar tendon. A scalpel is used to cut around the medial and lateral sides of the graft. A 20 x 9 x 7 mm bone plug from the patella and a 30 x 10 x 10 mm bone plug from the tibia constitute the ends of the graft (Figure 2.8). As with the graft width, the size and shape of the bone plugs vary with the surgeon s preference [45]. Using a sagittal saw, the bone plugs are harvested, thereby freeing the graft. The bone plugs are trimmed so that the patellar end passes through a 9 mm sizer and the tibial end passes through a 10 mm sizer. Sutures are placed in both bone plugs to provide a means to pull the ends of the graft. The graft is wrapped in a saline-soaked cover and fixed under tension for ten minutes to condition the tissue. To connect the graft across the joint, a 10 mm diameter tibial tunnel is drilled from the graft-harvesting incision, and a 9 mm diameter femoral tunnel is drilled from an incision lateral and superior to the knee. Jackson and Lemos [45] described a method in which the femoral tunnel is drilled starting from the interior of the joint. The tibial tunnel is positioned with reference to the anterior side of the anterior tibial spine and to the roof of the intercondylar notch when the knee is in full extension [36]. The femoral tunnel is positioned with reference to the lateral wall and roof of the intercondylar notch and to the posterior cruciate ligament. The surgeon can select a location that corresponds to the center of the ACL femoral attachment or one that is posterior and superior to that point [36]. The graft is pulled by the patellar end sutures through the tibial tunnel and into the femoral tunnel. The bone plug is fixed in the femoral tunnel with an interference screw, or by tying the sutures to a screw and washer (Figures 2.9, 2.10). Tension is applied to the graft by pulling on the sutures in the free
12 Geoffrey W. Ringer Chapter 2. Review of Literature 14 bone plug, and the plug is fixed in the tibial tunnel in a similar manner as the femoral end. The incisions are closed with sutures, and the motion of the knee is tested. If the response is not satisfactory, the graft may be repositioned or retensioned. After a period of healing, the patient may follow a rehabilitation program to help restore normal function and regain muscle strength [79]. Figure 2.8 Bone-Patellar Tendon-Bone Graft Figure 2.9 Completed ACL Reconstruction With Interference Screws
13 Geoffrey W. Ringer Chapter 2. Review of Literature Follow-up Results Figure 2.10 Screw and Washer Fixation of Graft The outcome of reconstruction depends on the graft material selected, as well as other variables, such as graft intraarticular position, graft fixation, and initial graft tension [10]. Follow-up studies of reconstruction patients have reported varying levels of success and are difficult to interpret [33]. Gillquist [33] reviewed studies of follow-up patient examinations and reported the literature showed a substantial number of abnormal results. The literature reported increased knee laxity was frequently noted in patients [33]. Gillquist also reviewed studies that described almost normal or normal knee function in about 75% of patients after various methods of reconstruction.
14 Geoffrey W. Ringer Chapter 2. Review of Literature 16 Because different procedures were expected to yield different results, Gillquist attributed the promising success rates to publication pressures. He suggested surgeons believe the 75% level to be acceptable for publishing a procedure, and may manipulate the statistical analysis of their short-term retrospective follow-up examinations to reach that threshold. Many techniques that are initially advocated, quietly disappear without a demonstration of inefficiency [33]. According to Gillquist, surgeons advocate a procedure until they evaluate mid-term follow-up examinations of patients and find unacceptable results. They then begin to promote a new technique without determining reasons for the inadequacy of the previous method, or even reporting the failure. Because of this phenomenon, Gillquist stressed the need for 10 year prospective studies to analyze reconstruction techniques Biomechanical Changes After implantation, the biomechanical properties of the graft change [68]. Although initially stiffer and stronger than the femur-acl-tibia complex, researchers have shown that the structural properties of the femur-patellar tendon graft-tibia complex drop drastically immediately upon implantation [9,62,63]. The stiffness of the graft complex was determined to be 3% to 15% of a control femur-acl-tibia complex, while the ultimate load was found to be 1% to 7% of the control. The properties improved after a period of healing, but they never approached pre-surgery levels. The specific amount of improvement varied from study to study. Ballock et al. [9] found the graft stiffness and ultimate load to be only 13% and 11% of control, respectively, after 52 weeks. After a healing period of the same duration, McPherson et al. [63] found the graft stiffness and ultimate load to be 35% and 45% of control, respectively. Ballock et al. suggested that the graft may need longer than 1 year to heal properly, but McPherson et al. found the properties decreased during the period between 1 and 2 years postoperative Biochemical Changes Researchers have documented changes of the collagen type and content in the patellar tendon graft over time, indicating a graft remodeling process [3]. Amiel et al. [2] used a rabbit model to study the collagen content in a patellar tendon graft over 30 weeks post-surgery. Type III collagen was detected in the graft as early as 2 weeks, and reached a maximum level at 6 weeks. Type I collagen content decreased during this time to reach a minimum level at 6 weeks. Over the next 24 weeks, the Type III collagen content declined slightly, while the Type I collagen content increased slightly, so that at the completion of the study, the levels of both collagen types in the graft were similar to the amounts in the ACL. Oakes [73] reported collagen fibril diameters based on the analysis of biopsies from 39 human patellar tendon grafts at various times after surgery. The biopsy from a graft that was less than 6 months postoperative contained a large number of small diameter fibrils and none of the large diameter fibrils seen in normal patellar tendon. A similar trend was seen in biopsies from grafts that were from 1 to 5 years postoperative, although the number of larger diameter fibrils increased over time. Biopsies from grafts that were 5 to 9 years postoperative showed an increase in fibrils with a diameter greater than 100 nm Histological Changes Researchers using histological analysis of patellar tendon grafts have detected four stages of transformation: avascular necrosis, revascularization, cellular proliferation, and tissue remodeling [3]. Kleiner et al. [49] studied the early histologic changes in rabbit patellar tendon grafts. Two days postoperative, the researchers noted a decrease in tissue cellularity, and the fibroblasts had become noticeably round. Seven days postoperative, the number of cells further decreased, so that fibroblasts were only noted in the midsubstance sporadically. Fourteen days postoperative, the
15 Geoffrey W. Ringer Chapter 2. Review of Literature 17 tissue midsubstance was acellular; the only fibroblasts in the tissue were observed on the periphery. Amiel et al. [2] studied the histologic changes in rabbit patellar tendon grafts from 2 to 30 weeks postoperative. At 2 weeks postoperative, researchers noted a similar cell distribution to the one identified by Kleiner et al. The tissue crimp was similar to that of normal patellar tendon. Three weeks postoperative, the tissue experienced cellular proliferation, although the relative number of fibroblasts was less than normal patellar tendon. The tissue crimp remained similar to that of normal patellar tendon. Four weeks postoperative, the tissue cellularity had increased and approached that of normal ACL. Tissue crimp at this time was much less distinct. Six weeks postoperative, the tissue was more cellular than either normal patellar tendon or ACL, and the crimp occurred only in some sections. By 30 weeks postoperative, the number of fibroblasts had decreased, so that the cellularity was similar to that of normal ACL. Researchers have noted similar trends in graft remodeling using different animal models, although the duration of each stage varied slightly [7,19]. Rougraff et al. [81] studied histological changes in human patellar tendon grafts ranging from 3 weeks to 6.5 years postoperative. Focal areas of degeneration were present in grafts less than 3 years postoperative, and seemed to be most conspicuous in grafts that were 2 to 10 months postoperative. The degeneration was noted in grafts as late as 30 months postoperative, but none of the grafts that were over 3 years postoperative displayed it. These researchers classified fibroblasts as one of the following shapes: linear, spindle, oblong, or round. Normal patellar tendon was described as containing mostly linear cells. Normal ACL also was described as containing mostly linear cells, but relatively large numbers of spindle and oblong cells were also noted. The 3 week specimen contained spindle cells on the periphery and linear cells in the midsubstance. Spindle and oblong cells were more common than linear cells in the 6 week graft. In grafts older than 2 years, the oblong fibroblasts became much less numerous. Grafts that were older than 3 years contained primarily linear fibroblasts and were similar to normal ACL. The number of fibroblasts in the 6 week graft was twice that of the tissue at implantation. By 4 months, the number of fibroblasts reached eight times that of the tissue at implantation. Over the next 4 years, the number of cells decreased gradually to return to a similar level of normal ACL Graft Position The intraarticular position of the graft determines the change in length of the graft as the knee moves through its full range of motion [36]. Bylski-Austrow et al. [17] found the femoral tunnel position significantly affects graft force as the knee is flexed. Moving the tunnel location anteriorly increased the force, while placing it distally decreased the force. A posterior location decreased the force slightly. A tibial tunnel that is placed too anteriorly can cause graft impingement [43]. Some surgeons try to achieve an isometric placement in which tunnel locations are selected to maintain a constant graft length as the knee moves through its full range of motion [36]. However, researchers have not been able to determine truly isometric sites [65,83,87] Graft Fixation Researchers have demonstrated that failure of a graft shortly after implantation may be due to failure of a fixation site [51,59]. During tensile tests along the tibial axis, Kurosaka et al. [51] found a significantly greater ultimate load when a 9.0 mm diameter interference screw was used versus a suture, screw, and washer fixation. Furthermore, all failures occurred at a fixation site. However, using a similar sized graft, Matthews et al. [59] found no significant difference in ultimate load between the two fixation techniques. Graft failure in this study was more likely to be a tissue rupture instead of fixation site failure. The authors attributed the different findings to strain rate differences. Matthews et al. tested specimens at a strain rate of 51 cm/min., while Kurosaka et al. tested with a strain rate of 180 cm/min. Because the graft is exposed to a variety of strain rates
16 Geoffrey W. Ringer Chapter 2. Review of Literature 18 postoperative, it is not clear which strain rate best approximates in vivo graft failure [59]. Although failure modes were different for the two studies, ultimate loads were similar Graft Pretension Graft pretension affects graft force [17], knee kinematics [15,17,24,37,44,64,67,93], and tissue remodeling [93]. Increasing the pretension in a flexible cable graft from 22 to 44 N led to significantly greater graft forces and posterior tibial displacements at all flexion angles [17]. However, using patellar tendon grafts, Gertel et al. [32] found no significant effect of pretension on knee kinematics or graft force. Yoshiya et al. [93] studied the effects of graft pretension in vivo using a canine model. Patellar tendon grafts were pretensioned to 1 or 39 N. In the immediate postoperative period, significantly greater knee laxity was noted in the lower tensioned group. After a 3 month healing period, however, no significant difference in laxity existed. Furthermore, no significant difference in structural properties was detected, although the authors noted a trend toward greater strength and stiffness in the lower tensioned grafts. After this healing period, the lower tensioned grafts had more vascularity than the higher tensioned grafts. Histologic examination showed the higher tensioned grafts exhibited focal degeneration and collagen fibers were replaced by a myxoid, extracellular matrix. The lower tensioned grafts displayed no apparent degeneration Flexion Angle at Pretensioning Flexion angle when pretensioning the graft affects the magnitude of graft force and knee kinematics [17,32]. Using a flexible cable graft, Bylski-Austrow et al. [17] found pretensioning the graft at 30 flexion significantly increased graft load over a full range of motion as opposed to pretensioning at 0 flexion. The pattern of graft force did not vary between the two groups. Pretensioning the graft at 30 also significantly displaced the tibia posteriorly when compared to pretensioning at 0 flexion. Gertel et al. [32] verified these results using a patellar tendon graft in a cadaveric model.
Knee Joint Anatomy 101
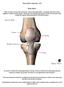 Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
Anterior Cruciate Ligament Surgery
 Anatomy Anterior Cruciate Ligament Surgery Roger Ostrander, MD Andrews Institute Anatomy Anatomy Function Primary restraint to anterior tibial translation Secondary restraint to internal tibial rotation
Anatomy Anterior Cruciate Ligament Surgery Roger Ostrander, MD Andrews Institute Anatomy Anatomy Function Primary restraint to anterior tibial translation Secondary restraint to internal tibial rotation
The Knee Joint By Prof. Dr. Muhammad Imran Qureshi
 The Knee Joint By Prof. Dr. Muhammad Imran Qureshi Structurally, it is the Largest and the most complex joint in the body because of the functions that it performs: Allows mobility (flexion/extension)
The Knee Joint By Prof. Dr. Muhammad Imran Qureshi Structurally, it is the Largest and the most complex joint in the body because of the functions that it performs: Allows mobility (flexion/extension)
Knee: Cruciate Ligaments
 72 Knee: Cruciate Ligaments R. Kent Sanders Sagittal oblique 2.5-mm sequences along the plane of the anterior cruciate ligament (ACL) typically yield three to four images of the ACL, with the first medial
72 Knee: Cruciate Ligaments R. Kent Sanders Sagittal oblique 2.5-mm sequences along the plane of the anterior cruciate ligament (ACL) typically yield three to four images of the ACL, with the first medial
3. Examination of Knee Kinematics In Vitro
 3. Examination of Knee Kinematics In Vitro 3.1 Introduction This chapter details two in vitro studies that were conducted to better understand the kinematic behavior of the knee. First, the role of graft
3. Examination of Knee Kinematics In Vitro 3.1 Introduction This chapter details two in vitro studies that were conducted to better understand the kinematic behavior of the knee. First, the role of graft
Anterior Cruciate Ligament (ACL) Injuries
 Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Medical Diagnosis for Michael s Knee
 Medical Diagnosis for Michael s Knee Introduction The following report mainly concerns the diagnosis and treatment of the patient, Michael. Given that Michael s clinical problem surrounds an injury about
Medical Diagnosis for Michael s Knee Introduction The following report mainly concerns the diagnosis and treatment of the patient, Michael. Given that Michael s clinical problem surrounds an injury about
The Knee. Prof. Oluwadiya Kehinde
 The Knee Prof. Oluwadiya Kehinde www.oluwadiya.sitesled.com The Knee: Introduction 3 bones: femur, tibia and patella 2 separate joints: tibiofemoral and patellofemoral. Function: i. Primarily a hinge joint,
The Knee Prof. Oluwadiya Kehinde www.oluwadiya.sitesled.com The Knee: Introduction 3 bones: femur, tibia and patella 2 separate joints: tibiofemoral and patellofemoral. Function: i. Primarily a hinge joint,
TOTAL KNEE ARTHROPLASTY (TKA)
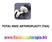 TOTAL KNEE ARTHROPLASTY (TKA) 1 Anatomy, Biomechanics, and Design 2 Femur Medial and lateral condyles Convex, asymmetric Medial larger than lateral 3 Tibia Tibial plateau Medial tibial condyle: concave
TOTAL KNEE ARTHROPLASTY (TKA) 1 Anatomy, Biomechanics, and Design 2 Femur Medial and lateral condyles Convex, asymmetric Medial larger than lateral 3 Tibia Tibial plateau Medial tibial condyle: concave
ACL Reconstruction Cross-Pin Technique
 ACL Reconstruction Cross-Pin Technique Surgical Technique Lonnie E. Paulos, MD Salt Lake City, Utah 325 Corporate Drive Mahwah, NJ 07430 t: 201 831 5000 www.stryker.com A surgeon should always rely on
ACL Reconstruction Cross-Pin Technique Surgical Technique Lonnie E. Paulos, MD Salt Lake City, Utah 325 Corporate Drive Mahwah, NJ 07430 t: 201 831 5000 www.stryker.com A surgeon should always rely on
The Knee. Tibio-Femoral
 The Knee Tibio-Femoral Osteology Distal Femur with Proximal Tibia Largest Joint Cavity in the Body A modified hinge joint with significant passive rotation Technically, one degree of freedom (Flexion/Extension)
The Knee Tibio-Femoral Osteology Distal Femur with Proximal Tibia Largest Joint Cavity in the Body A modified hinge joint with significant passive rotation Technically, one degree of freedom (Flexion/Extension)
Figure 3 Figure 4 Figure 5
 Figure 1 Figure 2 Begin the operation with examination under anesthesia to confirm whether there are any ligamentous instabilities in addition to the posterior cruciate ligament insufficiency. In particular
Figure 1 Figure 2 Begin the operation with examination under anesthesia to confirm whether there are any ligamentous instabilities in addition to the posterior cruciate ligament insufficiency. In particular
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Joints of the Lower Limb II
 Joints of the Lower Limb II Lecture Objectives Describe the components of the knee and ankle joint. List the ligaments associated with these joints and their attachments. List the muscles acting on these
Joints of the Lower Limb II Lecture Objectives Describe the components of the knee and ankle joint. List the ligaments associated with these joints and their attachments. List the muscles acting on these
JOINT RULER. Surgical Technique For Knee Joint JRReplacement
 JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
Torn ACL - Anatomic Footprint ACL Reconstruction
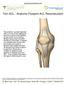 Torn ACL - Anatomic Footprint ACL Reconstruction The anterior cruciate ligament (ACL) is one of four ligaments that are crucial to the stability of your knee. It is a strong fibrous tissue that connects
Torn ACL - Anatomic Footprint ACL Reconstruction The anterior cruciate ligament (ACL) is one of four ligaments that are crucial to the stability of your knee. It is a strong fibrous tissue that connects
ACL AND PCL INJURIES OF THE KNEE JOINT
 ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
Direct Measurement of Graft Tension in Anatomic Versus Non-anatomic ACL Reconstructions during a Dynamic Pivoting Maneuver
 Direct Measurement of Graft Tension in Anatomic Versus Non-anatomic ACL Reconstructions during a Dynamic Pivoting Maneuver Scott A. Buhler 1, Newton Chan 2, Rikin Patel 2, Sabir K. Ismaily 2, Brian Vial
Direct Measurement of Graft Tension in Anatomic Versus Non-anatomic ACL Reconstructions during a Dynamic Pivoting Maneuver Scott A. Buhler 1, Newton Chan 2, Rikin Patel 2, Sabir K. Ismaily 2, Brian Vial
MRI KNEE WHAT TO SEE. Dr. SHEKHAR SRIVASTAV. Sr.Consultant KNEE & SHOULDER ARTHROSCOPY
 MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
Minimally Invasive ACL Surgery
 Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
Anterior Cruciate Ligament Injuries
 Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
Grant H Garcia, MD Sports and Shoulder Surgeon
 What to Expect from your Anterior Cruciate Ligament Reconstruction Surgery A Guide for Patients Grant H Garcia, MD Sports and Shoulder Surgeon Important Contact Information Grant Garcia, MD Wallingford:
What to Expect from your Anterior Cruciate Ligament Reconstruction Surgery A Guide for Patients Grant H Garcia, MD Sports and Shoulder Surgeon Important Contact Information Grant Garcia, MD Wallingford:
Anterolateral Ligament. Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine
 Anterolateral Ligament Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine What in the world? TIME magazine in November 2013 stated: In an age filled with advanced medical techniques like
Anterolateral Ligament Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine What in the world? TIME magazine in November 2013 stated: In an age filled with advanced medical techniques like
To describe he knee joint, ligaments, structure & To list the main features of other lower limb joints
 To describe he knee joint, ligaments, structure & neurovascular supply To demonstrate the ankle joint anatomy To list the main features of other lower limb joints To list main groups of lymph nodes in
To describe he knee joint, ligaments, structure & neurovascular supply To demonstrate the ankle joint anatomy To list the main features of other lower limb joints To list main groups of lymph nodes in
Biomechanics of the Knee. Valerie Nuñez SpR Frimley Park Hospital
 Biomechanics of the Knee Valerie Nuñez SpR Frimley Park Hospital Knee Biomechanics Kinematics Range of Motion Joint Motion Kinetics Knee Stabilisers Joint Forces Axes The Mechanical Stresses to which
Biomechanics of the Knee Valerie Nuñez SpR Frimley Park Hospital Knee Biomechanics Kinematics Range of Motion Joint Motion Kinetics Knee Stabilisers Joint Forces Axes The Mechanical Stresses to which
and K n e e J o i n t Is the most complicated joint in the body!!!!
 K n e e J o i n t K n e e J o i n t Is the most complicated joint in the body!!!! 1-Consists of two condylar joints between: A-The medial and lateral condyles of the femur and The condyles of the tibia
K n e e J o i n t K n e e J o i n t Is the most complicated joint in the body!!!! 1-Consists of two condylar joints between: A-The medial and lateral condyles of the femur and The condyles of the tibia
ANTERIOR CRUCIATE LIGAMENT INJURY
 ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
ACL RECONSTRUCTION HAMSTRING METHOD. Presents ACL RECONSTRUCTION HAMSTRING METHOD. Multimedia Health Education
 HAMSTRING METHOD Presents HAMSTRING METHOD Multimedia Health Education Disclaimer Stephen J. Incavo MD This movie is an educational resource only and should not be used to make a decision on Anterior Cruciate
HAMSTRING METHOD Presents HAMSTRING METHOD Multimedia Health Education Disclaimer Stephen J. Incavo MD This movie is an educational resource only and should not be used to make a decision on Anterior Cruciate
Unicompartmental Knee Resurfacing
 Disclaimer This movie is an educational resource only and should not be used to manage knee pain. All decisions about the management of knee pain must be made in conjunction with your Physician or a licensed
Disclaimer This movie is an educational resource only and should not be used to manage knee pain. All decisions about the management of knee pain must be made in conjunction with your Physician or a licensed
Alternative Design Report
 Alternative Design Report Novel Polysaccharide-derived Fixation Device for Anterior Cruciate Ligament (ACL) Reconstruction Team 13 Derek Holyoak Alexander Werne Benjamin Roberts Clients: Dr. Krystyna Gielo-Perczak
Alternative Design Report Novel Polysaccharide-derived Fixation Device for Anterior Cruciate Ligament (ACL) Reconstruction Team 13 Derek Holyoak Alexander Werne Benjamin Roberts Clients: Dr. Krystyna Gielo-Perczak
AFX. Femoral Implant. System. The AperFix. AM Portal Surgical Technique Guide. with the. The AperFix System with the AFX Femoral Implant
 The AperFix System AFX with the Femoral Implant AM Portal Surgical Technique Guide The Cayenne Medical AperFix system with the AFX Femoral Implant is the only anatomic system for soft tissue ACL reconstruction
The AperFix System AFX with the Femoral Implant AM Portal Surgical Technique Guide The Cayenne Medical AperFix system with the AFX Femoral Implant is the only anatomic system for soft tissue ACL reconstruction
What to Expect from your Anterior Cruciate Ligament (ACL) Reconstruction Surgery A Guide for Patients
 What to Expect from your Anterior Cruciate Ligament (ACL) Reconstruction Surgery A Guide for Patients Sources of Information: http://orthoinfo.aaos.org http://www.orthoinfo.org/informedpatient.cfm http://www.sportsmed.org/patient/
What to Expect from your Anterior Cruciate Ligament (ACL) Reconstruction Surgery A Guide for Patients Sources of Information: http://orthoinfo.aaos.org http://www.orthoinfo.org/informedpatient.cfm http://www.sportsmed.org/patient/
Transtibial PCL Reconstruction. Surgical Technique. Transtibial PCL Reconstruction
 Transtibial PCL Reconstruction Surgical Technique Transtibial PCL Reconstruction The Arthrex Transtibial PCL Reconstruction System includes unique safety features for protecting posterior neurovascular
Transtibial PCL Reconstruction Surgical Technique Transtibial PCL Reconstruction The Arthrex Transtibial PCL Reconstruction System includes unique safety features for protecting posterior neurovascular
Anatomy and Biomechanics
 Introduction Increased participation= increased injury rates Females were found to be 5.4 times more likely to sustain injury than males. And females injured their ACL ad a rate of 7.8 times more than
Introduction Increased participation= increased injury rates Females were found to be 5.4 times more likely to sustain injury than males. And females injured their ACL ad a rate of 7.8 times more than
Technique Guide. *smith&nephew N8TIVE ACL Anatomic ACL Reconstruction System
 Technique Guide *smith&nephew N8TIVE ACL Anatomic ACL Reconstruction System N8TIVE ACL System The N8TIVE ACL Anatomic Reconstruction System provides a novel and simple approach to ACL repair. The N8TIVE
Technique Guide *smith&nephew N8TIVE ACL Anatomic ACL Reconstruction System N8TIVE ACL System The N8TIVE ACL Anatomic Reconstruction System provides a novel and simple approach to ACL repair. The N8TIVE
A Patient s Guide to Knee Anatomy. Stephanie E. Siegrist, MD, LLC
 A Patient s Guide to Knee Anatomy Hands, shoulders, knees and toes (and elbows and ankles, too!) Most bone and joint conditions have several treatment options. The best treatment for you is based on your
A Patient s Guide to Knee Anatomy Hands, shoulders, knees and toes (and elbows and ankles, too!) Most bone and joint conditions have several treatment options. The best treatment for you is based on your
Reconstruction of the Ligaments of the Knee
 Reconstruction of the Ligaments of the Knee Contents ACL reconstruction Evaluation Selection Evolution Graft issues Notchplasty Tunnel issues MCL PCL Posterolateral ligament complex Combined injuries Evaluation
Reconstruction of the Ligaments of the Knee Contents ACL reconstruction Evaluation Selection Evolution Graft issues Notchplasty Tunnel issues MCL PCL Posterolateral ligament complex Combined injuries Evaluation
A Patient s Guide to Knee Anatomy
 A Patient s Guide to Knee Anatomy 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A Patient s Guide to Knee Anatomy 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
Articulations. Articulation. Joint between bones. Does not mean movement! Some joints are immovable; sutures.
 Articulations Joint between bones Articulation Does not mean movement Some joints are immovable; sutures. Classification of joints Two questions about joints: 1- How does it move? - functional 2- How is
Articulations Joint between bones Articulation Does not mean movement Some joints are immovable; sutures. Classification of joints Two questions about joints: 1- How does it move? - functional 2- How is
The Knee. Two Joints: Tibiofemoral. Patellofemoral
 Evaluating the Knee The Knee Two Joints: Tibiofemoral Patellofemoral HISTORY Remember the questions from lecture #2? Girth OBSERVATION TibioFemoral Alignment What are the consequences of faulty alignment?
Evaluating the Knee The Knee Two Joints: Tibiofemoral Patellofemoral HISTORY Remember the questions from lecture #2? Girth OBSERVATION TibioFemoral Alignment What are the consequences of faulty alignment?
Your Practice Online
 Your Practice Online Disclaimer P R E S E N T S - PATELLAR TENDON This movie is an educational resource only and should not be used to make a decision on Anterior Cruciate Ligament (ACL) Reconstruction.
Your Practice Online Disclaimer P R E S E N T S - PATELLAR TENDON This movie is an educational resource only and should not be used to make a decision on Anterior Cruciate Ligament (ACL) Reconstruction.
INDIVIDUALISED, ANATOMIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION
 ACL RECONSTRUCTION INDIVIDUALISED, ANATOMIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION Written by Thierry Pauyo, Marcio Bottene Villa Albers and Freddie H. Fu, USA Anterior cruciate ligament (ACL) reconstruction
ACL RECONSTRUCTION INDIVIDUALISED, ANATOMIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION Written by Thierry Pauyo, Marcio Bottene Villa Albers and Freddie H. Fu, USA Anterior cruciate ligament (ACL) reconstruction
STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact)
 STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact) David Drez, Jr., M.D. Clinical Professor of Orthopaedics LSU School of Medicine Financial Disclosure Dr. David Drez has no relevant
STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact) David Drez, Jr., M.D. Clinical Professor of Orthopaedics LSU School of Medicine Financial Disclosure Dr. David Drez has no relevant
Anterior Cruciate Ligament (ACL)
 Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
Human ACL reconstruction
 Human ACL reconstruction current state of the art Rudolph Geesink MD PhD Maastricht The Netherlands Human or canine ACL repair...!? ACL anatomy... right knees! ACL double bundles... ACL double or triple
Human ACL reconstruction current state of the art Rudolph Geesink MD PhD Maastricht The Netherlands Human or canine ACL repair...!? ACL anatomy... right knees! ACL double bundles... ACL double or triple
Copyright 2003 Pearson Education, Inc. publishing as Benjamin Cummings. Dr. Nabil Khouri MD, MSc, Ph.D
 Dr. Nabil Khouri MD, MSc, Ph.D Pelvic Girdle (Hip) Organization of the Lower Limb It is divided into: The Gluteal region The thigh The knee The leg The ankle The foot The thigh and the leg have compartments
Dr. Nabil Khouri MD, MSc, Ph.D Pelvic Girdle (Hip) Organization of the Lower Limb It is divided into: The Gluteal region The thigh The knee The leg The ankle The foot The thigh and the leg have compartments
Hip joint Type: Articulating bones:
 Ana (242 ) Hip joint Type: Synovial, ball & socket Articulating bones: Formed between head of femur and lunate surface of acetabulum of hip bone. Capsule: it is a strong fibrous sleeve connecting the articulating
Ana (242 ) Hip joint Type: Synovial, ball & socket Articulating bones: Formed between head of femur and lunate surface of acetabulum of hip bone. Capsule: it is a strong fibrous sleeve connecting the articulating
Exercise 13. Articulations and Body Movements
 Exercise 13 Articulations and Body Movements Articulations Articulations, or joints, are points where a bone is connected to one or more other bones. Articulations hold the skeleton together. Articulations
Exercise 13 Articulations and Body Movements Articulations Articulations, or joints, are points where a bone is connected to one or more other bones. Articulations hold the skeleton together. Articulations
The AperFix II System
 The AperFix II System A Complete Anatomic Solution Transtibial Surgical Technique 2 AperFix II System Transtibial Surgical Technique Figure 1 A Complete Anatomic Solution The Cayenne Medical AperFix and
The AperFix II System A Complete Anatomic Solution Transtibial Surgical Technique 2 AperFix II System Transtibial Surgical Technique Figure 1 A Complete Anatomic Solution The Cayenne Medical AperFix and
Knee Joint Assessment and General View
 Knee Joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The knee is the largest
Knee Joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The knee is the largest
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
CONTRIBUTING SURGEON. Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD
 CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
Objectives. The BIG Joint. Case 1. Boney Architecture. Presenter Disclosure Information. Common Knee Problems
 3:30 4:15 pm Common Knee Problems SPEAKER Christopher J. Visco, MD Presenter Disclosure Information The following relationships exist related to this presentation: Christopher J. Visco, MD: Speaker s Bureau
3:30 4:15 pm Common Knee Problems SPEAKER Christopher J. Visco, MD Presenter Disclosure Information The following relationships exist related to this presentation: Christopher J. Visco, MD: Speaker s Bureau
Knee Injuries. PSK 4U Mr. S. Kelly North Grenville DHS. Medial Collateral Ligament Sprain
 Knee Injuries PSK 4U Mr. S. Kelly North Grenville DHS Medial Collateral Ligament Sprain Result from either a direct blow from the lateral side in a medial direction or a severe outward twist Greater injury
Knee Injuries PSK 4U Mr. S. Kelly North Grenville DHS Medial Collateral Ligament Sprain Result from either a direct blow from the lateral side in a medial direction or a severe outward twist Greater injury
Revolution. Unicompartmental Knee System
 Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
The Dance Hall by Vincent van Gogh,1888
 The Dance Hall by Vincent van Gogh,1888 Articulations of the pelvic girdle Lumbosacral joints, sacroiliac joints & pubic symphysis The remaining joints of the lower limb Hip joint Knee joint Tibiofibular
The Dance Hall by Vincent van Gogh,1888 Articulations of the pelvic girdle Lumbosacral joints, sacroiliac joints & pubic symphysis The remaining joints of the lower limb Hip joint Knee joint Tibiofibular
Prof. Dr. Ahmed Abdelaziz Professor of Orthopedic Surgery Faculty of Medicine Cairo University
 Comparative study between anatomic single bundle and anatomic double bundle ACL reconstruction Thesis submitted for fulfillment of MD degree in orthopedic surgery By Ahmed Mahmoud Mohamed Gad Assisstant
Comparative study between anatomic single bundle and anatomic double bundle ACL reconstruction Thesis submitted for fulfillment of MD degree in orthopedic surgery By Ahmed Mahmoud Mohamed Gad Assisstant
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
SHOULDER JOINT ANATOMY AND KINESIOLOGY
 SHOULDER JOINT ANATOMY AND KINESIOLOGY SHOULDER JOINT ANATOMY AND KINESIOLOGY The shoulder joint, also called the glenohumeral joint, consists of the scapula and humerus. The motions of the shoulder joint
SHOULDER JOINT ANATOMY AND KINESIOLOGY SHOULDER JOINT ANATOMY AND KINESIOLOGY The shoulder joint, also called the glenohumeral joint, consists of the scapula and humerus. The motions of the shoulder joint
MCL Injuries: When and How to Repair Scott D. Mair, MD
 MCL Injuries: When and How to Repair Scott D. Mair, MD Professor and Team Physician: Orthopaedic Surgery University of Kentucky School of Medicine Disclosure Institution: Research/Education Smith-Nephew
MCL Injuries: When and How to Repair Scott D. Mair, MD Professor and Team Physician: Orthopaedic Surgery University of Kentucky School of Medicine Disclosure Institution: Research/Education Smith-Nephew
ACL reconstruction. Osteoconductive absorbable interference screws. Unique material. Optimal design. Adapted to different surgical techniques
 ACL reconstruction Osteoconductive absorbable interference screws Unique material Optimal design Adapted to different surgical techniques + complete instrumentation set Controlled resorption Material LIGAFIX
ACL reconstruction Osteoconductive absorbable interference screws Unique material Optimal design Adapted to different surgical techniques + complete instrumentation set Controlled resorption Material LIGAFIX
UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player
 UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player Cheri Drysdale, MEd,, ATC Margot Putukian,, MD Jeffery Bechler,, MD Princeton University How many of you have done an
UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player Cheri Drysdale, MEd,, ATC Margot Putukian,, MD Jeffery Bechler,, MD Princeton University How many of you have done an
UNIT 7 JOINTS. Knee and Ankle Joints DR. ABDEL-MONEM A. HEGAZY
 UNIT 7 JOINTS Knee and Ankle Joints BY DR. ABDEL-MONEM A. HEGAZY (Degree in Bachelor of Medicine and Surgery with honor 1983, Dipl."Gynaecology and Obstetrics "1989, Master "Anatomy and Embryology "1994,
UNIT 7 JOINTS Knee and Ankle Joints BY DR. ABDEL-MONEM A. HEGAZY (Degree in Bachelor of Medicine and Surgery with honor 1983, Dipl."Gynaecology and Obstetrics "1989, Master "Anatomy and Embryology "1994,
The Meniscus. History. Anatomy. Anatomy. Blood Supply. Attachments
 History The Meniscus W. Randall Schultz, MD, MS Austin, TX January 23, 2016 Meniscus originally thought to represent vestigial tissue 1883 first reported meniscal repair (Annandale) Total menisectomy treatment
History The Meniscus W. Randall Schultz, MD, MS Austin, TX January 23, 2016 Meniscus originally thought to represent vestigial tissue 1883 first reported meniscal repair (Annandale) Total menisectomy treatment
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
To classify the joints relative to structure & shape
 To classify the joints relative to structure & shape To describe the anatomy of the hip joint To describe the ankle joint To memorize their blood & nerve supply JOINTS: Joints are sites where skeletal
To classify the joints relative to structure & shape To describe the anatomy of the hip joint To describe the ankle joint To memorize their blood & nerve supply JOINTS: Joints are sites where skeletal
RIGIDfix. Soft Tissue. Surgical Technique for Mitek RIGIDfix ACL Reconstruction PRODUCTS. Daniel J. McKernan, M.D. TISSUE SOFT.
 RIGIDfix A C L C R O S S P I N S Y S T E M Daniel J. McKernan, M.D. Toledo, Ohio SOFT TISSUE Surgical Technique for Mitek RIGIDfix ACL Reconstruction Soft Tissue PRODUCTS SURGICAL TECHNIQUE RIGIDfix A
RIGIDfix A C L C R O S S P I N S Y S T E M Daniel J. McKernan, M.D. Toledo, Ohio SOFT TISSUE Surgical Technique for Mitek RIGIDfix ACL Reconstruction Soft Tissue PRODUCTS SURGICAL TECHNIQUE RIGIDfix A
Joints. Judi Laprade. Illustrations from: Essential Clinical Anatomy 3 rd ed. (ECA3) Moore, K. and Agur, A. Lippincott Williams and Wilkins, 2007
 Slide 1 Joints Judi Laprade Illustrations from: Essential Clinical Anatomy 3 rd ed. (ECA3) Moore, K. and Agur, A. Lippincott Williams and Wilkins, 2007 Grant s Atlas of Anatomy 12 th ed. (GA12) Agur, A.
Slide 1 Joints Judi Laprade Illustrations from: Essential Clinical Anatomy 3 rd ed. (ECA3) Moore, K. and Agur, A. Lippincott Williams and Wilkins, 2007 Grant s Atlas of Anatomy 12 th ed. (GA12) Agur, A.
Joints Outline 8.1 Joints are classified into three structural and three functional categories (p. 251; Table 8.1) A. Joints are classified by
 Joints Outline 8.1 Joints are classified into three structural and three functional categories (p. 251; Table 8.1) A. Joints are classified by structure and by function: Structural classification focuses
Joints Outline 8.1 Joints are classified into three structural and three functional categories (p. 251; Table 8.1) A. Joints are classified by structure and by function: Structural classification focuses
Meniscus Reconstruction: Trough Surgical Technique
 Meniscus Reconstruction: Trough Surgical Technique Technique Consultant Jeffrey L. Halbrecht, M.D. San Francisco, CA ABOUT THE TROUGH TECHNIQUE The trough technique for meniscal allograft reconstruction
Meniscus Reconstruction: Trough Surgical Technique Technique Consultant Jeffrey L. Halbrecht, M.D. San Francisco, CA ABOUT THE TROUGH TECHNIQUE The trough technique for meniscal allograft reconstruction
Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System
 Knee Series Technique Guide Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System Luigi Adriano Pederzini, MD Massimo Tosi, MD Mauro Prandini, MD Luigi Milandri,
Knee Series Technique Guide Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System Luigi Adriano Pederzini, MD Massimo Tosi, MD Mauro Prandini, MD Luigi Milandri,
Current Concepts for ACL Reconstruction
 Current Concepts for ACL Reconstruction David R. McAllister, MD Associate Team Physician UCLA Athletic Department Chief, Sports Medicine Service Professor Department of Orthopaedic Surgery David Geffen
Current Concepts for ACL Reconstruction David R. McAllister, MD Associate Team Physician UCLA Athletic Department Chief, Sports Medicine Service Professor Department of Orthopaedic Surgery David Geffen
ACL Injury: Does It Require Surgery?-OrthoInfo - AAOS
 ACL Injury: Does It Require Surgery?-OrthoInfo - AAOS ACL Injury: Does It Require Surgery? The following article provides in-depth information about treatment for anterior cruciate ligament injuries. The
ACL Injury: Does It Require Surgery?-OrthoInfo - AAOS ACL Injury: Does It Require Surgery? The following article provides in-depth information about treatment for anterior cruciate ligament injuries. The
Anatomy and Physiology 1 Chapter 9 self quiz Pro, Dima Darwish,MD.
 Anatomy and Physiology 1 Chapter 9 self quiz Pro, Dima Darwish,MD. 1) Joints can be classified structurally as A) bony. B) fibrous. C) cartilaginous. D) synovial. E) All of the answers are correct. 2)
Anatomy and Physiology 1 Chapter 9 self quiz Pro, Dima Darwish,MD. 1) Joints can be classified structurally as A) bony. B) fibrous. C) cartilaginous. D) synovial. E) All of the answers are correct. 2)
General Concepts. Growth Around the Knee. Topics. Evaluation
 General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
Total Knee Original System Primary Surgical Technique
 Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
ACL Rehabilitation and Return To Play
 ACL Rehabilitation and Return To Play Seth Gasser, MD Director of Sports Medicine Florida Orthopaedic Institute Introduction Return to Play: the point in recovery from an injury when a person is safely
ACL Rehabilitation and Return To Play Seth Gasser, MD Director of Sports Medicine Florida Orthopaedic Institute Introduction Return to Play: the point in recovery from an injury when a person is safely
UNIT 2 - CHAPTER 8: JOINTS OF THE SKELETAL SYSTEM LEARNING OUTCOMES:
 LEARNING OUTCOMES: 8.1 Introduction 1. List the functions of joints. 2. Explain how joints can be classified according to the type of tissue that binds the bones together and the degree of movement possible
LEARNING OUTCOMES: 8.1 Introduction 1. List the functions of joints. 2. Explain how joints can be classified according to the type of tissue that binds the bones together and the degree of movement possible
THE KNEE JOINT. At a glance. 1. Introduction
 THE KNEE JOINT At a glance As explained in more detail below, the knee is a very complex joint. Owing to its anatomical structure, it is extremely prone not only to injury, but to wear and tear as well.
THE KNEE JOINT At a glance As explained in more detail below, the knee is a very complex joint. Owing to its anatomical structure, it is extremely prone not only to injury, but to wear and tear as well.
The Skeletal System. Dr. Naim Kittana Dr. Suhaib Hattab. Faculty of Medicine & Health Sciences An-Najah National University
 The Skeletal System Dr. Naim Kittana Dr. Suhaib Hattab Faculty of Medicine & Health Sciences An-Najah National University 1 Declaration The content and the figures of this seminar were directly adopted
The Skeletal System Dr. Naim Kittana Dr. Suhaib Hattab Faculty of Medicine & Health Sciences An-Najah National University 1 Declaration The content and the figures of this seminar were directly adopted
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments
 TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Resection Guide System SURGICAL TECHNIQUE RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Resection Guide System SURGICAL TECHNIQUE RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA
Original Article A Study on the Results of Reconstructing Posterior Cruciate Ligament Using Graft from Quadriceps Muscle Tendon
 Original Article A Study on the Results of Reconstructing Posterior Cruciate Ligament Using Graft from Quadriceps Muscle Tendon K. Nazem MD*, Kh. Jabalameli MD**, A. Pahlevansabagh MD** Abstract Background:
Original Article A Study on the Results of Reconstructing Posterior Cruciate Ligament Using Graft from Quadriceps Muscle Tendon K. Nazem MD*, Kh. Jabalameli MD**, A. Pahlevansabagh MD** Abstract Background:
UNIT 2 - CHAPTER 8: JOINTS OF THE SKELETAL SYSTEM LEARNING OUTCOMES:
 LEARNING OUTCOMES: 8.1 Types of Joints 1. Explain how joints can be classified according to the type of tissue that binds the bones together and the degree of movement possible at the joint. (p. 268) 2.
LEARNING OUTCOMES: 8.1 Types of Joints 1. Explain how joints can be classified according to the type of tissue that binds the bones together and the degree of movement possible at the joint. (p. 268) 2.
Incidence. Avoiding Complications of ACL Surgery. ACL Complications 6/10/2011. Not if, but when
 Avoiding Complications of ACL Surgery Thomas J. Gill, MD Chief, MGH Sports Medicine Service Dept of Orthopedic Surgery Massachusetts General Hospital Associate Professor of Orthopedic Surgery Harvard Medical
Avoiding Complications of ACL Surgery Thomas J. Gill, MD Chief, MGH Sports Medicine Service Dept of Orthopedic Surgery Massachusetts General Hospital Associate Professor of Orthopedic Surgery Harvard Medical
LARS ACL. Best practice guidelines
 LARS ACL Best practice guidelines LARS ACL Corin is committed to providing up-to-date clinical and educational support to healthcare practitioners worldwide to ensure that best practice guidelines are
LARS ACL Best practice guidelines LARS ACL Corin is committed to providing up-to-date clinical and educational support to healthcare practitioners worldwide to ensure that best practice guidelines are
Biologically-Assisted ACL Reconstruction. Surgical Technique
 Biologically-Assisted ACL Reconstruction Surgical Technique One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide personalized care to one patient. The science and art
Biologically-Assisted ACL Reconstruction Surgical Technique One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide personalized care to one patient. The science and art
HISTORY AND INDICATIONS OF LATERAL TENODESIS IN ATHLETES
 HISTORY AND INDICATIONS OF LATERAL TENODESIS IN ATHLETES Written by Philippe Landreau, Qatar The treatment of anterior cruciate ligament injuries remains challenging in young athletic populations. A residual
HISTORY AND INDICATIONS OF LATERAL TENODESIS IN ATHLETES Written by Philippe Landreau, Qatar The treatment of anterior cruciate ligament injuries remains challenging in young athletic populations. A residual
Disclosures. Outline. The Posterior Cruciate Ligament 5/3/2016
 The Posterior Cruciate Ligament Christopher J. Utz, MD Assistant Professor of Orthopaedic Surgery University of Cincinnati Disclosures I have no disclosures relevant to this topic. Outline 1. PCL Basic
The Posterior Cruciate Ligament Christopher J. Utz, MD Assistant Professor of Orthopaedic Surgery University of Cincinnati Disclosures I have no disclosures relevant to this topic. Outline 1. PCL Basic
The Skeletal System. Dr. Naim Kittana. Faculty of Medicine & Health Sciences An-Najah National University
 The Skeletal System Dr. Naim Kittana Faculty of Medicine & Health Sciences An-Najah National University 1 Declaration The content and the figures of this seminar were directly adopted from the text book
The Skeletal System Dr. Naim Kittana Faculty of Medicine & Health Sciences An-Najah National University 1 Declaration The content and the figures of this seminar were directly adopted from the text book
A Patient s Guide. ACL Injury: Ø Frequently asked questions on injury, Ø Preoperative and postoperative. surgery and recovery.
 ACL Injury: A Patient s Guide Ø Frequently asked questions on injury, surgery and recovery Ø Preoperative and postoperative guidelines Mia S. Hagen, M.D. Assistant Professor Department of Orthopaedics
ACL Injury: A Patient s Guide Ø Frequently asked questions on injury, surgery and recovery Ø Preoperative and postoperative guidelines Mia S. Hagen, M.D. Assistant Professor Department of Orthopaedics
Department of Orthopaedics
 Department of Orthopaedics ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION SURGERY What is the Anterior Cruciate Ligament (ACL)? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilize
Department of Orthopaedics ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION SURGERY What is the Anterior Cruciate Ligament (ACL)? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilize
Knee Injury Assessment
 Knee Injury Assessment Clinical Anatomy p. 186 Femur Medial condyle Lateral condyle Femoral trochlea Tibia Intercondylar notch Tibial tuberosity Tibial plateau Fibula Fibular head Patella Clinical Anatomy
Knee Injury Assessment Clinical Anatomy p. 186 Femur Medial condyle Lateral condyle Femoral trochlea Tibia Intercondylar notch Tibial tuberosity Tibial plateau Fibula Fibular head Patella Clinical Anatomy
Rehabilitation Guidelines for Meniscal Repair
 Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Extracapsular Repair Monofilament Nylon Suture
 Extracapsular Repair Monofilament Nylon Suture Management of the ruptured Cranial Cruciate Ligament (CCL) by placing a non-absorbable suture between the lateral fabella and the proximal, cranial tibia
Extracapsular Repair Monofilament Nylon Suture Management of the ruptured Cranial Cruciate Ligament (CCL) by placing a non-absorbable suture between the lateral fabella and the proximal, cranial tibia
*smith&nephew ENDOBUTTON CL. Knee Series Technique Guide. Fixation System
 Knee Series Technique Guide *smith&nephew ENDOBUTTON CL Fixation System Double Bundle ACL Reconstruction using the Smith & Nephew ACUFEX Director Set for Anatomic ACL Reconstruction French Anatomic ACL-R
Knee Series Technique Guide *smith&nephew ENDOBUTTON CL Fixation System Double Bundle ACL Reconstruction using the Smith & Nephew ACUFEX Director Set for Anatomic ACL Reconstruction French Anatomic ACL-R
Imaging the Athlete s Knee. Peter Lowry, MD Musculoskeletal Radiology University of Colorado
 Imaging the Athlete s Knee Peter Lowry, MD Musculoskeletal Radiology University of Colorado None Disclosures Knee Imaging: Radiographs Can be performed weight-bearing or non-weight-bearing View options
Imaging the Athlete s Knee Peter Lowry, MD Musculoskeletal Radiology University of Colorado None Disclosures Knee Imaging: Radiographs Can be performed weight-bearing or non-weight-bearing View options
5/31/15. The Problem. Every Decade We Change Our Minds The Journey Around the Notch. Life is full of Compromises. 50 years ago..
 The Problem Surgical Treatment of ACL Tears Optimizing Femoral Tunnel Positioning Andrew D. Pearle, MD Associate Attending Orthopedic Surgeon Sports Medicine and Shoulder Service Hospital for Special Surgery
The Problem Surgical Treatment of ACL Tears Optimizing Femoral Tunnel Positioning Andrew D. Pearle, MD Associate Attending Orthopedic Surgeon Sports Medicine and Shoulder Service Hospital for Special Surgery
