Glenoid baseplate fixation using hybrid configurations of locked and unlocked peripheral screws
|
|
|
- Theresa Mills
- 6 years ago
- Views:
Transcription
1 J Orthop Traumatol (2017) 18: DOI /s ORIGINAL ARTICLE Glenoid baseplate fixation using hybrid configurations of locked and unlocked peripheral screws Nathan T. Formaini 1 Nathan G. Everding 1 Jonathan C. Levy 1 Brandon G. Santoni 2 Aniruddh N. Nayak 2 Cooper Wilson 3 Received: 15 March 2016 / Accepted: 28 November 2016 / Published online: 11 January 2017 Ó The Author(s) This article is published with open access at Springerlink.com Abstract Background The use of peripheral locked screws has reduced glenoid baseplate failure rates in reverse shoulder arthroplasty. However, situations may arise when one or more non-locked screws may be preferred. We aimed to determine if different combinations of locked and nonlocked screws significantly alter acute glenoid baseplate fixation in a laboratory setting. Materials and methods Twenty-eight polyurethane trabecular bone surrogates were instrumented with a center screw-type glenoid baseplate and fixated with various combinations of peripheral locked and non-locked screws (1-, 2-, 3- and 4-locked con). Each construct was tested through a 55 arc of abduction motion generating compressive and shear forces across the glenosphere. Baseplate micromotion (lm) was recorded throughout 10,000 cycles for each model. Results All constructs survived 10,000 cycles of loading without catastrophic failure. One test construct in the 1-locked fixation group exhibited a measured micromotion [150 lm (177.6 lm). At baseline (p [ 0.662) and following 10,000 cycles (p [ 0.665), no differences were observed in baseplate micromotion for screw combinations that included one, two, three and four peripheral locked screws. The maximum difference in measured micromotion between the extremes of groups (1-locked and 4-locked) was 29 lm. Conclusions Hybrid peripheral screw fixation using combinations of locked and non-locked screws provides secure glenoid baseplate fixation using a polyurethane bone substitute model. Using a glenosphere with a 10-mm lateralized center of rotation, hybrid baseplate fixation maintains micromotion below the necessary threshold for bony ingrowth. Level of Evidence N/A/, basic science investigation. Keywords Reverse shoulder arthroplasty Glenosphere Glenoid baseplate Hybrid screw fixation Micromotion & Jonathan C. Levy jonlevy@yahoo.com Nathan T. Formaini nateformaini@gmail.com Nathan G. Everding nathan.everding@gmail.com Brandon G. Santoni bsantoni@foreonline.org Holy Cross Orthopedic Institute, 5597 North Dixie Highway, Fort Lauderdale, FL 33334, USA Phillip Spiegel Orthopaedic Research Laboratory, Foundation for Orthopaedic Research and Education, Tampa, USA Department of Orthopaedics and Sports Medicine, University of South Florida, Tampa, USA Introduction Improvements in glenoid baseplate fixation have been critical to the success of the modern reverse shoulder replacement. Recognition of the importance of baseplate tilt [1 3], optimal screw placement [4 9], glenoid reaming techniques [10], peripheral screw fixation [11], baseplate shape and position [9, 12, 13], and introduction of bone ingrowth technologies [13] have contributed to avoiding the catastrophic baseplate failures described using firstgeneration reverse shoulder replacements [14 21]. In combination with improved surgical technique and implant enhancements, baseplate failures are less common [6].
2 222 J Orthop Traumatol (2017) 18: One key modification which helped improve baseplate fixation was the introduction of peripheral locked screws. First tested by Harman et al. [11], locked screw use significantly enhanced baseplate fixation and minimized micromotion at the baseplate-glenoid bone interface. This was also observed in clinical practice. Frankle et al. initially reported an 11% baseplate failure rate using peripheral non-locked 3.5-mm screws [22]. However, in a 5-year follow-up series using the same implant with 5.0-mm peripheral locked screws, the baseplate failure rate was reduced to 0% [23]. This has led most surgeons to utilize locked screws for nearly all peripheral screw fixation opportunities when using a central screw-based baseplate. There are, however, clinical scenarios when a surgeon may prefer to use non-locked peripheral screws. The concept of hybrid fixation, where combinations of locked and non-locked screws are used together, has been a longstanding feature used in locked plate osteosynthesis and has been shown to be biomechanically similar while also providing the potential benefits of compression or aiding with reduction [24 28]. Variations in hybrid peripheral screw combinations have not been tested for reverse shoulder glenoid baseplate fixation. The purpose of this study was to evaluate initial glenoid baseplate fixation using a variety of combinations of locked and non-locked peripheral screws. We hypothesized that glenoid baseplate micromotion would be sufficiently minimized using all combinations of locked and non-locked peripheral screws. Materials and methods Twenty-eight synthetic trabecular bone surrogate cylinders (Sawbones Ò Model # , Rigid Cellular Foam; Pacific Research Laboratories, Vashon, WA, USA) with a nominal density of 0.32 g/cm 3 (ASTM F ) were utilized in the current investigation. This nominal was chosen as an intermediary between poor quality (0.24 g/cm 3 ) and good quality (0.48 g/cm 3 ) cancellous bone used by others in studies of similar scope [33]. Upon receipt of the blocks ( mm) each was machined into cylinders measuring 44.5 mm in diameter and 40 mm in height. This study used the glenoid components of a single reverse shoulder arthroplasty system (RSP Ò ; DJO Global, Austin, TX, USA). The baseplate consists of a single central 6.5-mm lag screw in combination with four peripheral screw holes, which can be used in locked or nonlocked fashion. The underside of the baseplate is coated with hydroxyapatite to facilitate bony ingrowth in vivo. All baseplates were fixed perpendicular to the bone block substitutes. Briefly, a 2.5-mm drill was used to define the trajectory for the baseplate s central screw. A 6.5-mm tap was used to create the threads for the central screw. With the tap still in place, a reamer was used to create the circumferential concavity required to accommodate the underside of the baseplate, which was then inserted and tightened to a maximum torque of 3.5 N-m (Model DID-04 Digital Torque Screwdriver; Imada, Inc. Northbrook, IL, USA). For this study, we evaluated baseplate fixation using four combinations of locked (5-mm diameter) and (3.5-mm diameter) non-locked peripheral screws in seven (n = 7) cylinders per fixation group (1) 1 locked screw? 3 nonlocked screws (1-locked), (2) 2 locked screws? 2 nonlocked screws (2-locked), (3) 3 locked screws? 1 nonlocked screw (3-locked), and (4) 4 locked screws (4- locked). All locked and non-locked screws were the same length as determined by a retrospective analysis of a consecutive series of 100 reverse shoulder arthroplasty surgeries using the same glenoid baseplate. This identified an average peripheral screw length of 21 mm. Thus, 22-mm screws were selected for all locked and non-locked screws. For peripheral screw placement, a 4-in-1 drill guide was used which allows for drilling and placement of screws (after the inner sleeve is removed) in a constant perpendicular orientation to the baseplate. For non-locked and locked peripheral screws, respectively, 2.5 and 4-mm drills were used to define the screw trajectory in the cylinder. On the circular surface of the baseplate-instrumented Sawbones Ò cylinder, one screw hole was arbitrarily defined as superior, with anterior, inferior and posterior orientations defined thereafter in clockwise fashion, thereby mimicking a shoulder s right-sided glenoid orientation (Fig. 1). For the 1-locked screw configuration, the locked peripheral screw was placed in the superior screw hole. In the 2-locked group, locked screws were placed superiorly and inferiorly. Finally, for the 3-locked screw configuration, locked screws were placed superiorly, inferiorly, and posteriorly. Peripheral non-locked screws were advanced to a depth of 22 mm in the foam cylinder and tightened to 0.7 N-m using a torque limiting screw driver. This torque magnitude was determined in pilot experiments and represents the highest, consistently achievable torque in this particular Sawbones Ò block density without loss of nonlocked screw purchase or applied torque. All locked screws were tightened to 2.5 N-m with care taken not to cross the threads. Thereafter, a differential variable reluctance transducer (DVRT) (Model MG-DVRT Ò ; LORD MicroStrain Ò Sensing Systems, Williston, VT, USA) with 3 lm accuracy, was mounted to the instrumented surface of the Sawbones Ò in the inferior/superior direction with a custom-designed attachment rig such that the sensor was in contact with the periphery of the baseplate immediately adjacent to the superior screw hole (Fig. 2). Inferior/superior micromotion was of primary interest given the orientation of the applied loads in our test setup, which were applied to the baseplate in the scapular plane to simulate
3 J Orthop Traumatol (2017) 18: Fig. 1 Position of locked and unlocked screws within the baseplate for each configuration. 1a Baseplate with four locked screws, 2a baseplate with three locked and one unlocked screw, 3a baseplate with two locked and two unlocked screws, 4a baseplate with one locked and three unlocked screws. L locked, U unlocked Fig. 2 The differential variable reluctance transducer (DVRT) placed in direct contact with the inferior aspect of the baseplate abduction and the primary function of reverse shoulders. Out-of-plane micromotion in the anterior/posterior direction was not measured because no shear loads were applied in the axial plane. After screw placement and DVRT attachment, a 32-mm neutral glenosphere (DJO Global, Austin, TX, USA) was impacted onto the baseplate. This glenosphere has a center of rotation 10 mm from the glenoid surface. We adopted a testing methodology identical to our previously published work [37]. Briefly, the instrumented Sawbones Ò cylinder was mounted in a swing arm attached to the torque motor of a servoelectric test frame (Model 800LE; Test Resources, Shakopee, MN, USA). Test specimens were cycled through a 55 arc of motion at 1 Hz, while the test frame s actuator applied a constant 750 N compressive force via a glenosphere size-matched humeral component polyethylene neutral liner, in similar fashion to the methods adopted by previous authors (Fig. 3) [13, 29, 37]. The orientation of the test block was such that the arc of motion occurred in the scapular plane defined by the superior and inferior screw holes of the baseplate, thus serving to approximate a humeral abduction motion relative to a fixed scapula. This loading setup induces a maximum shear force of 346 N at the extremes of the motion arc from neutral (i.e., ±27.5 ) and a 750 N compressive load at the neutral position (Fig. 4).
4 224 J Orthop Traumatol (2017) 18: Fig. 3 Mechanical testing setup. a Close-up photograph detailing the test block with implanted baseplate and 32 neutral glenosphere loaded through a neutral polyethylene liner. b Photograph detailing testing set up with swing arm, load cell, torque motor, and DVRT Fig. 4 Shear and compressive forces throughout of the 558 arc of simulated abduction motion The continuous analog voltage output from the DVRT was queried at the beginning of testing and every 500 cycles thereafter through 10,000 cycles of loading. The measured voltage was related to baseplate micromotion (lm) using the manufacturer s provided linear calibration coefficient. Here, micromotion was defined as the average of the absolute values of micromotion measured by the DVRT at the arc of motion extremes (?27.5 and ) over 20 loading cycles for each data collection time point. Testing was stopped if catastrophic construct failure was grossly observed. Micromotion data were analyzed using a 2-way ANOVA for intra-group (time) and inter-group (fixation) comparisons and post hoc comparisons were performed with Bonferroni correction at a significance level of The number of test constructs in which micromotion was measured [150 lm threshold commonly accepted for osseous integration was reported. Results All 28 instrumented cylinders survived 10,000 cycles of loading without catastrophic failure. No gross evidence of baseplate subsidence into the test blocks was noted in any specimen. One test construct in the 1-locked fixation group exhibited a measured micromotion [150 lm (177.6 lm) (Table 1). This was observed after 9500 cycles. No
5 J Orthop Traumatol (2017) 18: Table 1 Measured micromotion (lm) at baseline and at 10,000 cycles for each test specimen Test block Hybrid screw fixation group 1-locked 2-locked 3-locked 4-locked Baseline 10,000 cycles Baseline 10,000 cycles Baseline 10,000 cycles Baseline 10,000 cycles Fig. 6 Temporal micromotion plot for all fixation groups lm), or 3-locked fixation groups (72.4 ± 15.3 lm; range lm) (Figs. 5b, 6). Discussion Fig. 5 Mean and standard deviations of measured micromotion (lm) for each testing group at baseline (a) (p = 0.662) and after 10,000 cycles (b) (p = 0.695) constructs in the 2-locked, 3-locked or 4-locked fixation groups exhibited micromotion [150 lm. There was no difference in baseplate micromotion at baseline between any of the fixation groups (p [ 0.662) (Fig. 5a). After 10,000 cycles of loading, the 4-locked fixation group exhibited the lowest measured baseplate micromotion, on average (68.1 ± 15.3 lm; range lm), although this was not significantly different (p [ 0.665) from the 1-locked (97.1 ± 47.2 lm; range lm), 2-locked (76.7 ± 34.5 lm; range Critical to glenoid component survivability of the reverse shoulder replacement is obtaining sufficient initial fixation on the glenoid bone to facilitate osseous integration [4, 6, 11]. Minimization of micromotion\150 lm between an implant and bone has been shown to be optimal in achieving a biologic environment for bone growth onto metal arthroplasty surfaces [30 32]. Extrapolating these findings and applying them to the reverse shoulder glenoid component, numerous attempts have been made at enhancing baseplate fixation with the common goal of limiting micromotion between the glenoid component and the prepared glenoid surface. Over the past 15 years, advancements in surgical technique, implant design modifications, and understanding of scapular anatomy have helped surgeons improve baseplate failure rates. Of these
6 226 J Orthop Traumatol (2017) 18: enhancements, screw fixation has been noted as the most important feature of enhanced fixation [4, 9, 12]. Use of a glenosphere implant with a more lateral center of rotation was met with controversy based on historical implant failures seen with earlier generation implants [14 21]. The first modern reverse shoulder replacement to revisit a more lateralized center of rotation utilized a central screw baseplate and four peripheral non-locked 3.5- mm screws. Using all peripheral non-locked screws, the glenoid baseplate failure rate was 11% [22]. With continued understanding of surgical technique and replacement of the 3.5-mm peripheral non-locked screws with 5.0-mm locked screws, the incidence of glenoid baseplate failures was reduced to 0% in a 5-year minimum follow-up study [33]. This clinical experience validated the mechanical study reported by Harman et al. [11] which showed how peripheral locked screws were superior to non-locked screws at maximizing baseplate fixation \150 lm micromotion threshold. Surgeons have thus gained comfort using a glenoid baseplate with four peripheral locked screws. There are certainly cases where four peripheral locked screws are either not possible or may not be of optimal surgical preference. Included in these scenarios are cases where there is limited bone remaining, such that a screw would capture minimal bone or result in a prominent screw; or cases where a larger locked screw might not be optimal, creating a potential stress riser for an acromion spine fracture [34]. Additionally, there are situations when further glenoid component compression is desirable, which can only be achieved by using a non-locked screw. In these cases, the surgeon may elect to utilize a non-locked screw rather than a locked screw. This concept of hybrid fixation is now commonplace in fracture management using locked plates, but prior to this study had not been tested for applicability in the reverse shoulder replacement glenoid component. Our study results demonstrate that a variety of hybrid peripheral screw combinations can provide sufficient glenoid component fixation using a glenosphere with a more lateral center of rotation. No statistical differences were observed in baseplate micromotion for peripheral screw combinations that included one, two, three and four peripheral locked screws. This was true at initial fixation (p [ 0.662) and following 10,000 cycles (p [ 0.665) using a bone substrate model that simulates poor glenoid bone quality often seen in reverse shoulder arthroplasty patients [13]. In fact, the maximum difference in measured micromotion between the extremes of groups (1-locked and 4-locked) was 29 lm (97 lm and 68 lm, respectively). With increased cyclic loading of the glenosphere, there was increased micromotion seen at the baseplate-bone model interface. However, only one of the 28 tested constructs exhibited micromotion [150 lm threshold within the 10,000 cycles. This specimen utilized a single locked and three non-locked peripheral screws and did not reach this threshold until after 9500 cycles. While we noted no statistically significant differences between fixation groups, the variability in measured micromotion after 10,000 cycles of loading was decreased with an increasing number of locked peripheral screws. Thus, these study findings suggest that (1) hybrid fixation is a reasonable option for surgeons to consider when placing peripheral screws around a central screw baseplate and that (2) maximizing the number of peripheral locked screws, when clinically feasible, may more consistently maintain baseplate fixation through the postoperative rehabilitation course. Furthermore, use of a glenosphere with a center of rotation 10 mm lateral to the glenoid can be utilized with a glenoid baseplate secured with a combination of locked and non-locked screws without compromising the fixation necessary for ingrowth. Several steps were taken to help maintain uniformity of the tested constructs and strengthen the validity of the data. Non-locked screws have the potential to lose fixation during implantation by stripping out. A pilot study was thus performed to evaluate the torque at which peripheral nonlocked screws stripped (documented as a sharp drop in measured torque) within the bone model and lost fixation. All of the peripheral non-locked screws were then implanted within the torque limits observed, ensuring that each screw placed provided similar fixation. Additionally, the orientation of the baseplate was controlled such that the screw orientation remained constant, preventing variability in rigidity based on the orientation of the locked and nonlocked screws. Finally, the central screw baseplates were implanted with an identical maximum torque to ensure that uniform compression was achieved with each tested model. The cyclic loading protocol in this study mimics the stresses that might be observed in vivo and was similar to the technique utilized in our previous work [37] and by Roche et al. [29]. This consisted of a 750 N axial load applied through the humeral component while the glenosphere was rotated about the humeral component in a 55 arc of motion. This loading profile induces a maximum calculated shear force of 346 N and a maximum compressive load of 750 N. The applied compressive load magnitude of 750 N is in good agreement with data published by Bergmann et al. [35] who measured in vivo glenohumeral joint loads during abduction in patients with load/moment measuring total shoulder arthroplasty prostheses. However, the loading approach used here may be considered worst case, as muscle forces in reverse shoulder arthroplasty patients have been reported to vary between 30 and 50% less than in anatomical arthroplasty patients due to a compromised rotator cuff [36]. It was felt that this method of testing would better simulate what would be
7 J Orthop Traumatol (2017) 18: observed clinically rather than the methodologies noted by Harman et al. [11]. Nonetheless, the findings observed in the 4-locked screw group were similar to the findings reported by Harman et al. [11] using the identical 4-peripheral screw baseplate. Limitations of this study relate to the use of polyurethane foam. While efforts were made to simulate the clinical environment, including placement of screws within torque limits, variations in patient bone quality may have different effects on hybrid peripheral screw baseplate fixation strength. Additionally, the screws placed were all within the foam model and did not obtain bi-cortical purchase that may occur in vivo. However, even without bicortical purchase, all but one non-locked baseplate configurations were able to limit micromotion \150 lm through 10,000 cycles. Finally, this study represents the initial fixation obtained by the glenoid baseplate. With the limitations of postoperative rehabilitation protocols, osseous integration of the glenoid baseplate may occur well before the 10,000 cycles tested in this study. Further investigation of the clinical outcomes using hybrid peripheral screw fixation of a central screw baseplate are warranted to validate the findings of this study. In summary, hybrid peripheral screw fixation using combinations of locked and non-locked screws provides secure glenoid baseplate fixation using a polyurethane bone substitute model. Glenospheres with a more lateral center of rotation can be utilized together with a hybrid combination of peripheral glenoid baseplate screws without compromising fixation necessary for ingrowth of bone into the implant. Acknowledgements We would like to acknowledge Kaitlyn Christmas, BS and Andres F. Cabezas, ME for assistance with data collection. This study was funded by a grant from DJO Global. Compliance with ethical standards Conflict of interest This research was supported by a grant from DJO Global (DJO, LLC, Vista, CA, USA). The author, JCL, is a paid consultant for DJO Global and Globus Medical, and receives royalties from DJO Global and Innomed. The author, BGS, is affiliated with a research foundation that received support for this study from DJO Global and also receives additional research support from Stryker Orthopaedics, DJO Global, Arthrex, AO-North America and NIH/ NIBIB. The authors NTF, NGE, ANN, and CW certify that they have no commercial associations (e.g., consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted article. No IRB was required as no human subjects were used. Ethical standards This article does not contain any studies with human participants or animals performed by any of the authors. Informed consent No patient data or information was used in this study. Funding This study was funded by a grant from DJO Global. Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( tivecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. References 1. Gutierrez S, Greiwe RM, Frankle MA, Siegal S, Lee WE 3rd (2007) Biomechanical comparison of component position and hardware failure in the reverse shoulder prosthesis. J Shoulder Elbow Surg 16:S9 S12 2. Gutierrez S, Walker M, Willis M, Pupello DR, Frankle MA (2011) Effects of tilt and glenosphere eccentricity on baseplate/ bone interface forces in a computational model, validated by a mechanical model, of reverse shoulder arthroplasty. J Shoulder Elbow Surg 20: Kwon YW, Forman RE, Walker PS, Zuckerman JD (2010) Analysis of reverse total shoulder joint forces and glenoid fixation. Bull NYU Hosp Jt Dis 68: Chebli C, Huber P, Watling J, Bertelsen A, Bicknell RT, Matsen F 3rd (2008) Factors affecting fixation of the glenoid component of a reverse total shoulder prothesis. J Shoulder Elbow Surg 17: Frankle MA, Teramoto A, Luo ZP, Levy JC, Pupello D (2009) Glenoid morphology in reverse shoulder arthroplasty: classification and surgical implications. J Shoulder Elbow Surg 18: Hoenig MP, Loeffler B, Brown S et al (2010) Reverse glenoid component fixation: is a posterior screw necessary? J Shoulder Elbow Surg 19: Hopkins AR, Hansen UN, Bull AM, Emery R, Amis AA (2008) Fixation of the reversed shoulder prosthesis. J Shoulder Elbow Surg 17: Humphrey CS, Kelly JD 2nd, Norris TR (2008) Optimizing glenosphere position and fixation in reverse shoulder arthroplasty, part two: the three-column concept. J Shoulder Elbow Surg 17: Parsons BO, Gruson KI, Accousti KJ, Klug RA, Flatow EL (2009) Optimal rotation and screw positioning for initial glenosphere baseplate fixation in reverse shoulder arthroplasty. J Shoulder Elbow Surg 18: Sutton LG, Werner FW, Jones AK, Close CA, Nanavati VN (2010) Optimization of glenoid fixation in reverse shoulder arthroplasty using 3-dimensional modeling. J Shoulder Elbow Surg 19: Harman M, Frankle M, Vasey M, Banks S (2005) Initial glenoid component fixation in reverse total shoulder arthroplasty: a biomechanical evaluation. J Shoulder Elbow Surg 14:162S 167S 12. James J, Huffman KR, Werner FW, Sutton LG, Nanavati VN (2012) Does glenoid baseplate geometry affect its fixation in reverse shoulder arthroplasty? J Shoulder Elbow Surg 21: Stroud NJ, DiPaola MJ, Martin BL et al (2013) Initial glenoid fixation using two different reverse shoulder designs with an equivalent center of rotation in a low-density and high-density bone substitute. J Shoulder Elbow Surg 22: Bodey WN, Yeoman PM (1983) Prosthetic arthroplasty of the shoulder. Acta Orthop Scand 54: Coughlin MJ, Morris JM, West WF (1979) The semiconstrained total shoulder arthroplasty. J Bone Joint Surg Am 61:
8 228 J Orthop Traumatol (2017) 18: Fenlin JM Jr (1975) Total glenohumeral joint replacement. Orthop Clin North Am 6: Franklin JL, Barrett WP, Jackins SE, Matsen FA 3rd (1988) Glenoid loosening in total shoulder arthroplasty. Association with rotator cuff deficiency. J Arthroplasty 3: Gerard Y, Leblanc JP, Rousseau B (1973) [A complete shoulder prosthesis]. Chirurgie 99: Kolbel R, Friedebold G (1973) [Shoulder joint replacement]. Arch Orthop Unfallchir 76: Neer CS 2nd, Craig EV, Fukuda H (1983) Cuff-tear arthropathy. J Bone Joint Surg Am 65: Reeves B, Jobbins B, Flowers F, Dowson D, Wright V (1972) Some problems in the development of a total shoulder endoprosthesis. Ann Rheum Dis 31: Frankle M, Siegal S, Pupello D, Saleem A, Mighell M, Vasey M (2005) The reverse shoulder prosthesis for glenohumeral arthritis associated with severe rotator cuff deficiency. A minimum twoyear follow-up study of sixty patients. J Bone Joint Surg Am 87: Cuff D, Pupello D, Virani N, Levy J, Frankle M (2008) Reverse shoulder arthroplasty for the treatment of rotator cuff deficiency. J Bone Joint Surg Am 90: Doornink J, Fitzpatrick DC, Boldhaus S, Madey SM, Bottlang M (2010) Effects of hybrid plating with locked and nonlocked screws on the strength of locked plating constructs in the osteoporotic diaphysis. J Trauma 69: Estes C, Rhee P, Shrader MW, Csavina K, Jacofsky MC, Jacofsky DJ (2008) Biomechanical strength of the Peri-Loc proximal tibial plate: a comparison of all-locked versus hybrid locked/ nonlocked screw configurations. J Orthop Trauma 22: Gardner MJ, Griffith MH, Demetrakopoulos D et al (2006) Hybrid locked plating of osteoporotic fractures of the humerus. J Bone Joint Surg Am 88: Stoffel K, Lorenz KU, Kuster MS (2007) Biomechanical considerations in plate osteosynthesis: the effect of plate-to-bone compression with and without angular screw stability. J Orthop Trauma 21: Sutherland GB, Creekmore T, Mukherjee DP, Ogden AL, Anissian L, Marymont JV (2010) Biomechanics of humerus fracture fixation by locking, cortical, and hybrid plating systems in a cadaver model. Orthopedics 33(8). doi: / Roche CP, Stroud NJ, Flurin PH, Wright TW, Zuckerman JD, DiPaola MJ (2014) Reverse shoulder glenoid baseplate fixation: a comparison of flat-back versus curved-back designs and oval versus circular designs with 2 different offset glenospheres. J Shoulder Elbow Surg 23: Cameron HU, Pilliar RM, MacNab I (1973) The effect of movement on the bonding of porous metal to bone. J Biomed Mater Res 7: Jasty M, Bragdon C, Burke D, O Connor D, Lowenstein J, Harris WH (1997) In vivo skeletal responses to porous-surfaced implants subjected to small induced motions. J Bone Joint Surg Am 79: Pilliar RM, Lee JM, Maniatopoulos C (1986) Observations on the effect of movement on bone ingrowth into porous-surfaced implants. Clin Orthop Relat Res. 208: Cuff D, Clark R, Pupello D, Frankle M (2012) Reverse shoulder arthroplasty for the treatment of rotator cuff deficiency: a concise follow-up, at a minimum of five years, of a previous report. J Bone Joint Surg Am 94: Crosby LA, Hamilton A, Twiss T (2011) Scapula fractures after reverse total shoulder arthroplasty: classification and treatment. Clin Orthop Relat Res 469: Bergmann G, Graichen F, Bender A et al (2011) In vivo glenohumeral joint loads during forward flexion and abduction. J Biomech 44: Terrier A, Reist A, Merlini F, Farron A (2008) Simulated joint and muscle forces in reversed and anatomic shoulder prostheses. J Bone Joint Surg Br 90: Formaini NT, Everding NG, Levy JC, Santoni BG, Nayak AN, Wilson C, Cabezas AF (2015) The effect of glenoid bone loss on reverse shoulder arthroplasty baseplate fixation. J Shoulder Elbow Surg 24(11):e312 e319
Optimal Baseplate Rotational Alignment in Reverse Total Shoulder Arthroplasty: A Three-Dimensional Computer-Aided Design Study.
 Optimal Baseplate Rotational Alignment in Reverse Total Shoulder Arthroplasty: A Three-Dimensional Computer-Aided Design Study. Byron F. Stephens, MD 1, Casey T. Hebert 2, Thomas W. Throckmorton, MD 1,
Optimal Baseplate Rotational Alignment in Reverse Total Shoulder Arthroplasty: A Three-Dimensional Computer-Aided Design Study. Byron F. Stephens, MD 1, Casey T. Hebert 2, Thomas W. Throckmorton, MD 1,
Reverse Shoulder Glenoid Loosening
 S12 Reverse Shoulder Glenoid Loosening An Evaluation of the Initial Fixation Associated with Six Different Reverse Shoulder Designs Nick Stroud, M.S., Matthew J. DiPaola, M.D., Pierre-Henri Flurin, M.D.,
S12 Reverse Shoulder Glenoid Loosening An Evaluation of the Initial Fixation Associated with Six Different Reverse Shoulder Designs Nick Stroud, M.S., Matthew J. DiPaola, M.D., Pierre-Henri Flurin, M.D.,
Optimizing Deltoid Efficiency with Reverse Shoulder Arthroplasty Using a Novel Inset Center of Rotation Glenosphere Design
 S37 Optimizing Deltoid Efficiency with Reverse Shoulder Arthroplasty Using a Novel Inset Center of Rotation Glenosphere Design Christopher P. Roche, M.S., M.B.A., Matthew A. Hamilton, Ph.D., Phong Diep,
S37 Optimizing Deltoid Efficiency with Reverse Shoulder Arthroplasty Using a Novel Inset Center of Rotation Glenosphere Design Christopher P. Roche, M.S., M.B.A., Matthew A. Hamilton, Ph.D., Phong Diep,
Biomechanical Impact of Posterior Glenoid Wear on Anatomic Total Shoulder Arthroplasty
 S5 Biomechanical Impact of Posterior Glenoid Wear on Anatomic Total Shoulder Arthroplasty Christopher P. Roche, M.S., M.B.A., Phong Diep, B.S., Sean G. Grey, M.D., and Pierre-Henri Flurin, M.D. Abstract
S5 Biomechanical Impact of Posterior Glenoid Wear on Anatomic Total Shoulder Arthroplasty Christopher P. Roche, M.S., M.B.A., Phong Diep, B.S., Sean G. Grey, M.D., and Pierre-Henri Flurin, M.D. Abstract
Impact of Modeling Assumptions on Stability Predictions in Reverse Shoulder Arthroplasty
 Impact of Modeling Assumptions on Stability Predictions in Reverse Shoulder Arthroplasty Mehul A Dharia*, Jeff Bischoff* *Zimmer Biomet, Warsaw, IN May 17, 2017 Total Shoulder Arthroplasty Shoulder Joint
Impact of Modeling Assumptions on Stability Predictions in Reverse Shoulder Arthroplasty Mehul A Dharia*, Jeff Bischoff* *Zimmer Biomet, Warsaw, IN May 17, 2017 Total Shoulder Arthroplasty Shoulder Joint
Reverse Total Shoulder Arthroplasty: A New Frontier (of Complications)
 Reverse Total Shoulder Arthroplasty: A New Frontier (of Complications) Emilie Cheung, MD Associate Professor Chief Shoulder Elbow Svc Stanford University Department of Orthopedic Surgery Procedure volumes
Reverse Total Shoulder Arthroplasty: A New Frontier (of Complications) Emilie Cheung, MD Associate Professor Chief Shoulder Elbow Svc Stanford University Department of Orthopedic Surgery Procedure volumes
Matthew D. Saltzman, MD a, Deana M. Mercer, MD c, Winston J. Warme, MD b, Alexander L. Bertelsen, PA-C b, Frederick A. Matsen III, MD b, *
 J Shoulder Elbow Surg (2010) 19, 1028-1033 www.elsevier.com/locate/ymse A method for documenting the change in center of rotation with reverse total shoulder arthroplasty and its application to a consecutive
J Shoulder Elbow Surg (2010) 19, 1028-1033 www.elsevier.com/locate/ymse A method for documenting the change in center of rotation with reverse total shoulder arthroplasty and its application to a consecutive
INITIAL FIXATION OF THE TRABECULAR METAL REVERSE SHOULDER GLENOID BASE PLATE IMPLANT
 Copyright 2008 by Zimmer, Inc. INITIAL FIXATION OF THE TRABECULAR METAL REVERSE SHOULDER GLENOID BASE PLATE IMPLANT Matthew L. Mroczkowski M.S. Roy Wiley Background Reverse total shoulder arthroplasty
Copyright 2008 by Zimmer, Inc. INITIAL FIXATION OF THE TRABECULAR METAL REVERSE SHOULDER GLENOID BASE PLATE IMPLANT Matthew L. Mroczkowski M.S. Roy Wiley Background Reverse total shoulder arthroplasty
Correlation of Femoral Component Micromotion to a Physical Test Using an FEA Model.
 Correlation of Femoral Component Micromotion to a Physical Test Using an FEA Model. Robert Davignon, Ananthkrishnan Gopalakrishnan. Stryker Corporation, Parsippany, NJ, USA. Disclosures: R. Davignon: 3A;
Correlation of Femoral Component Micromotion to a Physical Test Using an FEA Model. Robert Davignon, Ananthkrishnan Gopalakrishnan. Stryker Corporation, Parsippany, NJ, USA. Disclosures: R. Davignon: 3A;
Why are these shoulder replacements called a reverse prosthesis?
 PATIENT GUIDE TO REVERSE PROSTHESIS Edward G. McFarland MD The Division of Sports Medicine and Shoulder Surgery The Department of Orthopaedic Surgery The Johns Hopkins University Baltimore MD Why are these
PATIENT GUIDE TO REVERSE PROSTHESIS Edward G. McFarland MD The Division of Sports Medicine and Shoulder Surgery The Department of Orthopaedic Surgery The Johns Hopkins University Baltimore MD Why are these
Comprehensive Reverse Shoulder System Augmented Baseplate
 Comprehensive Reverse Shoulder System Augmented Baseplate Surgical Technique Addendum FPO 1 Comprehensive Reverse Shoulder System Augmented Baseplate Surgical Technique Addendum Adaptive Building on the
Comprehensive Reverse Shoulder System Augmented Baseplate Surgical Technique Addendum FPO 1 Comprehensive Reverse Shoulder System Augmented Baseplate Surgical Technique Addendum Adaptive Building on the
Fixed and Variable Geometry Total Shoulder Arthroplasty
 Fixed and Variable Geometry Total Shoulder Arthroplasty RECOVERY FUNCTION SURVIVORSHIP DePuy believes in an approach to total shoulder replacement that places equal importance on recovery, function and
Fixed and Variable Geometry Total Shoulder Arthroplasty RECOVERY FUNCTION SURVIVORSHIP DePuy believes in an approach to total shoulder replacement that places equal importance on recovery, function and
AEQUALIS PERFORM + REVERSED
 TO R N I E R AEQUALIS PERFORM + REVERSED Glenoid WEDGED AUGMENT SURGIC AL TECHNIQUE Table of Contents: AEQUALIS PERFORM + REVERSED Glenoid...3 Overview...3 Indications/Contraindications...4 Pre-Operative
TO R N I E R AEQUALIS PERFORM + REVERSED Glenoid WEDGED AUGMENT SURGIC AL TECHNIQUE Table of Contents: AEQUALIS PERFORM + REVERSED Glenoid...3 Overview...3 Indications/Contraindications...4 Pre-Operative
Effect of baseplate size on primary glenoid stability and impingement-free range of motion in reverse shoulder arthroplasty
 Chae et al. BMC Musculoskeletal Disorders 2014, 15:417 RESEARCH ARTICLE Open Access Effect of baseplate size on primary glenoid stability and impingement-free range of motion in reverse shoulder arthroplasty
Chae et al. BMC Musculoskeletal Disorders 2014, 15:417 RESEARCH ARTICLE Open Access Effect of baseplate size on primary glenoid stability and impingement-free range of motion in reverse shoulder arthroplasty
Biomechanical concepts of total shoulder replacement. «Shoulder Course» Day 1. Richard W. Nyffeler Orthopädie Sonnenhof Bern. 11. Sept.
 Biomechanical concepts of total shoulder replacement Richard W. Nyffeler Orthopädie Sonnenhof Bern First total shoulder prosthesis Jules Emile Péan, 1830-1898 Monobloc prostheses Charles Neer, 1917-2011
Biomechanical concepts of total shoulder replacement Richard W. Nyffeler Orthopädie Sonnenhof Bern First total shoulder prosthesis Jules Emile Péan, 1830-1898 Monobloc prostheses Charles Neer, 1917-2011
Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty
 Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Challenges of Shoulder Arthroplasty
 Challenges, Complications and Value Jonathan Levy, MD Shoulder & Elbow Surgeon Chief, Orthopaedic Surgery Holy Cross Hospital Medical Director, Holy Cross Orthopaedic Research Institute Director, ASES
Challenges, Complications and Value Jonathan Levy, MD Shoulder & Elbow Surgeon Chief, Orthopaedic Surgery Holy Cross Hospital Medical Director, Holy Cross Orthopaedic Research Institute Director, ASES
SMV Scientific Bone Plate and Screw System Surgical Technique
 SMV Scientific Bone Plate and Screw System Surgical Technique Description: The SMV Scientific Bone Plate and Screw System consists of non-locking plates and bone screw fasteners in a variety of lengths,
SMV Scientific Bone Plate and Screw System Surgical Technique Description: The SMV Scientific Bone Plate and Screw System consists of non-locking plates and bone screw fasteners in a variety of lengths,
what you is back within LOVE arm s reach find out why the exactech shoulder may be right for you
 TOTAL shoulder REPLACEMENT what you is back within LOVE arm s reach find out why the exactech shoulder may be right for you how does your shoulder work? The shoulder is the most mobile joint in the body.
TOTAL shoulder REPLACEMENT what you is back within LOVE arm s reach find out why the exactech shoulder may be right for you how does your shoulder work? The shoulder is the most mobile joint in the body.
SURGICAL TECHNIQUE DUAL-PLATFORM SHOULDER ARTHROPLASTY.
 SURGICAL TECHNIQUE DUAL-PLATFORM SHOULDER ARTHROPLASTY www.fhortho.com SURGICAL TECHNIQUE REFERENCE NUMBERS HUMERAL STEMS REFERENCE DIAMETER HEIGHT 267 360 Ø 06 100 265 102 Ø 08 120 265 103 Ø 08 170 265
SURGICAL TECHNIQUE DUAL-PLATFORM SHOULDER ARTHROPLASTY www.fhortho.com SURGICAL TECHNIQUE REFERENCE NUMBERS HUMERAL STEMS REFERENCE DIAMETER HEIGHT 267 360 Ø 06 100 265 102 Ø 08 120 265 103 Ø 08 170 265
GLENOID SURGICAL TECHNIQUE
 UP. EXTREMITY Dual-Platform Shoulder Prosthesis GLENOID SURGICAL TECHNIQUE ANATOMICAL REVERSE SURGICAL TECHNIQUE REFERENCE NUMBERS HUMERAL STEM REFERENCE DIAMETER HEIGHT 267 360 Ø 06 100 265 102 Ø 08 120
UP. EXTREMITY Dual-Platform Shoulder Prosthesis GLENOID SURGICAL TECHNIQUE ANATOMICAL REVERSE SURGICAL TECHNIQUE REFERENCE NUMBERS HUMERAL STEM REFERENCE DIAMETER HEIGHT 267 360 Ø 06 100 265 102 Ø 08 120
AcUMEDr. Anatomic Midshaft Forearm Plates
 AcUMEDr Anatomic Midshaft Forearm Plates Anatomic Midshaft Forearm Plates Since 1988, Acumed has been designing solutions to the demanding situations facing orthopaedic surgeons, hospitals and their patients.
AcUMEDr Anatomic Midshaft Forearm Plates Anatomic Midshaft Forearm Plates Since 1988, Acumed has been designing solutions to the demanding situations facing orthopaedic surgeons, hospitals and their patients.
Zimmer Small Fragment Universal Locking System. Surgical Technique
 Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Open reduction; plate fixation 1 Principles
 Executive Editor: Peter Trafton Authors: Martin Jaeger, Frankie Leung, Wilson Li Proximal humerus 11-A2 Open reduction, plate fixation Search search... Shortcuts All Preparations All Approaches All Reductions
Executive Editor: Peter Trafton Authors: Martin Jaeger, Frankie Leung, Wilson Li Proximal humerus 11-A2 Open reduction, plate fixation Search search... Shortcuts All Preparations All Approaches All Reductions
ANATOMIC TOTAL SHOULDER REPLACEMENT:
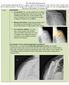 The Shoulder Replacement A total shoulder arthroplasty (TSA) is a surgery to replace the damaged parts of the ball and socket shoulder joint with an artificial prosthesis. The damage to the shoulder can
The Shoulder Replacement A total shoulder arthroplasty (TSA) is a surgery to replace the damaged parts of the ball and socket shoulder joint with an artificial prosthesis. The damage to the shoulder can
Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD
 General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
HUMELOCK II. Cemented + Graft ANATOMICAL and REVERSIBLE if REVISION SURGICAL TECHNIQUE
 TM HUMELOCK II Cemented + Graft ANATOMICAL and REVERSIBLE if REVISION SURGICAL TECHNIQUE CONTENTS - Device descriptionpage 02 - Intended use / indicationspage 03 - Warnings and precautions page 03 - Using
TM HUMELOCK II Cemented + Graft ANATOMICAL and REVERSIBLE if REVISION SURGICAL TECHNIQUE CONTENTS - Device descriptionpage 02 - Intended use / indicationspage 03 - Warnings and precautions page 03 - Using
Accuracy of CT-based measurements of glenoid version for total shoulder arthroplasty
 J Shoulder Elbow Surg (2009) -, 1-6 www.elsevier.com/locate/ymse Accuracy of CT-based measurements of glenoid version for total shoulder arthroplasty Heinz R. Hoenecke Jr., MD*, Juan C. Hermida, MD, Cesar
J Shoulder Elbow Surg (2009) -, 1-6 www.elsevier.com/locate/ymse Accuracy of CT-based measurements of glenoid version for total shoulder arthroplasty Heinz R. Hoenecke Jr., MD*, Juan C. Hermida, MD, Cesar
Surgical. Technique. AEQUALIS Spherical Base Glenoid. Shoulder Prosthesis.
 Surgical Technique Shoulder Prosthesis AEQUALIS Spherical Base Glenoid www.tornier.com CONTENTS CONTENTS 1. Subscapularis 2. Anterior capsule 3. Humeral protector 4. Inserting retractors 1. DESIGN FEATURES
Surgical Technique Shoulder Prosthesis AEQUALIS Spherical Base Glenoid www.tornier.com CONTENTS CONTENTS 1. Subscapularis 2. Anterior capsule 3. Humeral protector 4. Inserting retractors 1. DESIGN FEATURES
Curriculum Vitae. Derek J. Cuff
 Curriculum Vitae Derek J. Cuff Suncoast Orthopaedic Surgery and Sports Medicine 836 Sunset Lake Blvd, Building A Suite 205 Venice, FL 34292 Office:941-485-1505, Email: dcuff001@hotmail.com, web:www.suncoastshoulder-elbow.com
Curriculum Vitae Derek J. Cuff Suncoast Orthopaedic Surgery and Sports Medicine 836 Sunset Lake Blvd, Building A Suite 205 Venice, FL 34292 Office:941-485-1505, Email: dcuff001@hotmail.com, web:www.suncoastshoulder-elbow.com
Effectiveness of the surgical torque limiter: a model comparing drill- and hand-based screw insertion into locking plates
 Ioannou et al. Journal of Orthopaedic Surgery and Research (2016) 11:118 DOI 10.1186/s13018-016-0458-y RESEARCH ARTICLE Effectiveness of the surgical torque limiter: a model comparing drill- and hand-based
Ioannou et al. Journal of Orthopaedic Surgery and Research (2016) 11:118 DOI 10.1186/s13018-016-0458-y RESEARCH ARTICLE Effectiveness of the surgical torque limiter: a model comparing drill- and hand-based
OPTIONAL/ADDITIONAL INSTRUMENTS
 20 Elevated 6320-36-22 20 Elevated Rim Liner, 36mm OD x 22mm ID 6320-80-22 20 Elevated Rim Liner, 80mm OD x 22mm ID 6320-42-26 20 Elevated Rim Liner, 42mm OD x 26mm ID 6320-80-26 20 Elevated Rim Liner,
20 Elevated 6320-36-22 20 Elevated Rim Liner, 36mm OD x 22mm ID 6320-80-22 20 Elevated Rim Liner, 80mm OD x 22mm ID 6320-42-26 20 Elevated Rim Liner, 42mm OD x 26mm ID 6320-80-26 20 Elevated Rim Liner,
Fellowship, Shoulder and Elbow Surgery Mark Frankle, MD Florida Orthopaedic Institute, Tampa, Florida
 JONATHAN C LEVY, MD Fellow of the American Academy of Orthopaedic Surgeons 5597 NORTH DIXIE HIGHWAY FORT LAUDERDALE, FLORIDA 33334 TELEPHONE: (954) 958-4800 JONLEVY123@YAHOO.COM EMPLOYMENT EDUCATION Shoulder
JONATHAN C LEVY, MD Fellow of the American Academy of Orthopaedic Surgeons 5597 NORTH DIXIE HIGHWAY FORT LAUDERDALE, FLORIDA 33334 TELEPHONE: (954) 958-4800 JONLEVY123@YAHOO.COM EMPLOYMENT EDUCATION Shoulder
S h o u l d e r Solutions by Tornier C o n v e r T i b l e S h o u l d e r S y S T e m
 S h o u l d e r Solutions by Tornier C o n v e r t i b l e s h o u l d e r s y s t e m C o n v e r t i b l e s h o u l d e r s y s t e m A n a t o m i c Aequalis Ascend Flex - UDZF131 One System. Two Solutions.
S h o u l d e r Solutions by Tornier C o n v e r t i b l e s h o u l d e r s y s t e m C o n v e r t i b l e s h o u l d e r s y s t e m A n a t o m i c Aequalis Ascend Flex - UDZF131 One System. Two Solutions.
Shoulder Arthroplasty. Valentin Lance 3/24/16
 Shoulder Arthroplasty Valentin Lance 3/24/16 Outline Background Pre-operative imaging assessment Total Shoulder Arthroplasty: Standard and Reverse Complications Other shoulder hardware Hemiarthroplasty
Shoulder Arthroplasty Valentin Lance 3/24/16 Outline Background Pre-operative imaging assessment Total Shoulder Arthroplasty: Standard and Reverse Complications Other shoulder hardware Hemiarthroplasty
Stability at the half pin frame interface on external fixation constructs
 Strat Traum Limb Recon (2016) 11:193 198 DOI 10.1007/s11751-016-0269-z ORIGINAL ARTICLE Stability at the half pin frame interface on external fixation constructs Alexios Dimitrios Iliadis 1 Parag Kumar
Strat Traum Limb Recon (2016) 11:193 198 DOI 10.1007/s11751-016-0269-z ORIGINAL ARTICLE Stability at the half pin frame interface on external fixation constructs Alexios Dimitrios Iliadis 1 Parag Kumar
Humeral SuturePlate. Surgical Technique
 Humeral SuturePlate Surgical Technique The humeral SuturePlate is an anatomically designed, low profile, titanium polyaxial locking plate and screw system. Multiple chamfered suture eyelets along the margin
Humeral SuturePlate Surgical Technique The humeral SuturePlate is an anatomically designed, low profile, titanium polyaxial locking plate and screw system. Multiple chamfered suture eyelets along the margin
Assessment of Approximate Glenoid Size in Thai People
 Assessment of Approximate Glenoid Size in Thai People J Med Assoc Thai 2014; 97 (Suppl. 2): S14-S18 Full text. e-journal: http://www.jmatonline.com Pason Phonphok MD*, Nattha Kulkamthorn MD* * Division
Assessment of Approximate Glenoid Size in Thai People J Med Assoc Thai 2014; 97 (Suppl. 2): S14-S18 Full text. e-journal: http://www.jmatonline.com Pason Phonphok MD*, Nattha Kulkamthorn MD* * Division
Surgical Technique. CONQUEST FN Femoral Neck Fracture System
 Surgical Technique CONQUEST FN Femoral Neck Fracture System Table of Contents Introduction... 3 Indications... 3 Product Overview... 4 Surgical Technique... 5 Patient Positioning... 5 Reduce the Fracture...
Surgical Technique CONQUEST FN Femoral Neck Fracture System Table of Contents Introduction... 3 Indications... 3 Product Overview... 4 Surgical Technique... 5 Patient Positioning... 5 Reduce the Fracture...
Stability of two versus three peripheral pegs of the glenoid component in modern total shoulder arthroplasty
 International Orthopaedics (SICOT) (2017) 41:2345 2351 DOI 10.1007/s00264-017-3599-7 ORIGINAL ARTICLE Stability of two versus three peripheral pegs of the glenoid component in modern total shoulder arthroplasty
International Orthopaedics (SICOT) (2017) 41:2345 2351 DOI 10.1007/s00264-017-3599-7 ORIGINAL ARTICLE Stability of two versus three peripheral pegs of the glenoid component in modern total shoulder arthroplasty
Reverse Total Shoulder Arthroplasty Protocol
 General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
Biomechanical Performance of Headless Compression Screws: Fixos Ø4.0, 5.0 & 7.0 mm compared to Synthes Ø4.5 & 6.5 mm HCS
 Biomechanical Performance of Headless Compression Screws: ixos Ø4.0, 5.0 & 7.0 mm compared to Synthes Ø4.5 & 6.5 mm HCS M. Vallotton, A. Torcasio PhD Stryker Trauma AG, Selzach, Switzerland Abstract Introduction:
Biomechanical Performance of Headless Compression Screws: ixos Ø4.0, 5.0 & 7.0 mm compared to Synthes Ø4.5 & 6.5 mm HCS M. Vallotton, A. Torcasio PhD Stryker Trauma AG, Selzach, Switzerland Abstract Introduction:
ADDRESSING CLINICAL ISSUES OF CEMENTLESS HIP ARTHROPLASTY
 E C H E L O N P R I M A R Y H I P S Y S T E M P R O D U C T R A T I O N A L E ADDRESSING CLINICAL ISSUES OF CEMENTLESS HIP ARTHROPLASTY Echelon Primary Total Hip System HIGH OFFSET STANDARD OFFSET Cementless
E C H E L O N P R I M A R Y H I P S Y S T E M P R O D U C T R A T I O N A L E ADDRESSING CLINICAL ISSUES OF CEMENTLESS HIP ARTHROPLASTY Echelon Primary Total Hip System HIGH OFFSET STANDARD OFFSET Cementless
NCB Proximal Humerus Plating System
 NCB Proximal Humerus Plating System Surgical Technique The right locking option for tough fractures Disclaimer This document is intended exclusively for experts in the field, i.e. physicians in particular,
NCB Proximal Humerus Plating System Surgical Technique The right locking option for tough fractures Disclaimer This document is intended exclusively for experts in the field, i.e. physicians in particular,
Reverse Shoulder System. Abstracts
 TM Reverse Shoulder System s 2 Contents Introduction 2 Reverse shoulder arthroplasty components and surgical techniques that restore glenohumeralmotion 3 Isometric strength, range of motion, and impairment
TM Reverse Shoulder System s 2 Contents Introduction 2 Reverse shoulder arthroplasty components and surgical techniques that restore glenohumeralmotion 3 Isometric strength, range of motion, and impairment
S U R G I C A L T E C H N I Q U E David A. McQueen, MD Return to Menu
 S U R G I C A L T E C H N I Q U E David A. McQueen, MD TOTAL KNEE INSTRUMENTS Wichita Fusion Nail Introduction...1 Preoperative Planning...2 Surgical Technique...3-8 Wichita Fusion Nail Surgical Technique
S U R G I C A L T E C H N I Q U E David A. McQueen, MD TOTAL KNEE INSTRUMENTS Wichita Fusion Nail Introduction...1 Preoperative Planning...2 Surgical Technique...3-8 Wichita Fusion Nail Surgical Technique
EP A1 (19) (11) EP A1 (12) EUROPEAN PATENT APPLICATION. (43) Date of publication: Bulletin 2012/28
 (19) (12) EUROPEAN PATENT APPLICATION (11) EP 2 474 288 A1 (43) Date of publication: 11.07.2012 Bulletin 2012/28 (51) Int Cl.: A61F 2/40 (2006.01) A61F 2/30 (2006.01) (21) Application number: 11150615.0
(19) (12) EUROPEAN PATENT APPLICATION (11) EP 2 474 288 A1 (43) Date of publication: 11.07.2012 Bulletin 2012/28 (51) Int Cl.: A61F 2/40 (2006.01) A61F 2/30 (2006.01) (21) Application number: 11150615.0
Both anatomic (atsa) and reverse (rtsa) total
 S101 Comparison of Outcomes Using Anatomic and Reverse Total Shoulder Arthroplasty Pierre-Henri Flurin, M.D., Yann Marczuk, M.D., Martin Janout, M.D., Thomas W. Wright, M.D., Joseph Zuckerman, M.D., and
S101 Comparison of Outcomes Using Anatomic and Reverse Total Shoulder Arthroplasty Pierre-Henri Flurin, M.D., Yann Marczuk, M.D., Martin Janout, M.D., Thomas W. Wright, M.D., Joseph Zuckerman, M.D., and
Nailing Stability during Tibia Fracture Early Healing Process: A Biomechanical Study
 Nailing Stability during Tibia Fracture Early Healing Process: A Biomechanical Study Natacha Rosa, Fernão D. Magalhães, Ricardo Simões and António Torres Marques Enhanced Bone Healing in intramedullary
Nailing Stability during Tibia Fracture Early Healing Process: A Biomechanical Study Natacha Rosa, Fernão D. Magalhães, Ricardo Simões and António Torres Marques Enhanced Bone Healing in intramedullary
AxSOS Locking Plate System
 AxSOS Locking Plate System Operative Technique Small Fragment Basic Fragment 1 2 Contents Page 1. Introduction 4 2. Features & Benefits 5 4 and 5mm Compression Plates 5 Reconstruction and 1/3 Tubular Locking
AxSOS Locking Plate System Operative Technique Small Fragment Basic Fragment 1 2 Contents Page 1. Introduction 4 2. Features & Benefits 5 4 and 5mm Compression Plates 5 Reconstruction and 1/3 Tubular Locking
AcUMEDr. Locking Proximal Humeral Plate. PoLARUSr PHPt
 AcUMEDr Locking Proximal Humeral Plate PoLARUSr PHPt PoLARUSr PHPt LOCKING PROXIMAL HUMERAL PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons,
AcUMEDr Locking Proximal Humeral Plate PoLARUSr PHPt PoLARUSr PHPt LOCKING PROXIMAL HUMERAL PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons,
Trilogy Acetabular System
 Trilogy Acetabular System Surgical Technique Versatility in a proven design Trilogy Acetabular System 1 Trilogy Acetabular System Surgical Technique Table of Contents Acetabular Reaming 2 Component Sizing
Trilogy Acetabular System Surgical Technique Versatility in a proven design Trilogy Acetabular System 1 Trilogy Acetabular System Surgical Technique Table of Contents Acetabular Reaming 2 Component Sizing
Effect of Prosthesis Design on Muscle Length and Moment Arms in Reverse Total Shoulder Arthroplasty
 S31 Effect of Prosthesis Design on Muscle Length and Moment Arms in Reverse Total Shoulder Arthroplasty Matthew A. Hamilton, Ph.D., Christopher P. Roche, M.S., M.B.A., Phong Diep, B.S., Pierre- Henri Flurin,
S31 Effect of Prosthesis Design on Muscle Length and Moment Arms in Reverse Total Shoulder Arthroplasty Matthew A. Hamilton, Ph.D., Christopher P. Roche, M.S., M.B.A., Phong Diep, B.S., Pierre- Henri Flurin,
P. Trouilloud M. Gonzalvez P. Martz H. Charles F. Handelberg R. W. Nyffeler E. Baulot DuocentricÒ Group
 DOI 10.1007/s00590-013-1213-2 ORIGINAL ARTICLE Duocentric Ò reversed shoulder prosthesis and Personal Fit Ò templates: innovative strategies to optimize prosthesis positioning and prevent scapular notching
DOI 10.1007/s00590-013-1213-2 ORIGINAL ARTICLE Duocentric Ò reversed shoulder prosthesis and Personal Fit Ò templates: innovative strategies to optimize prosthesis positioning and prevent scapular notching
Surgical Technique. Proximal Humerus Locking Plate
 Surgical Technique Proximal Humerus Locking Plate PERI-LOC Upper Extremity Locked Plating System 3.5mm & 4.5mm Proximal Humerus Locking PlatesCatalog Infor Table of Contents Introduction.........................................................2
Surgical Technique Proximal Humerus Locking Plate PERI-LOC Upper Extremity Locked Plating System 3.5mm & 4.5mm Proximal Humerus Locking PlatesCatalog Infor Table of Contents Introduction.........................................................2
Bulletin of the Hospital for Joint Diseases 2013;71(4):284-93
 284 Impact of Inferior Glenoid Tilt, Humeral Retroversion, Bone Grafting, and Design Parameters on Muscle Length and Wrapping in Reverse Shoulder Arthroplasty Christopher P. Roche, M.S., M.B.A., Phong
284 Impact of Inferior Glenoid Tilt, Humeral Retroversion, Bone Grafting, and Design Parameters on Muscle Length and Wrapping in Reverse Shoulder Arthroplasty Christopher P. Roche, M.S., M.B.A., Phong
Trilogy Acetabular System
 Trilogy Acetabular System Surgical Technique Versatility in a proven design Trilogy Acetabular System 1 Trilogy Acetabular System Surgical Technique Table of Contents Acetabular Reaming 2 Component Sizing
Trilogy Acetabular System Surgical Technique Versatility in a proven design Trilogy Acetabular System 1 Trilogy Acetabular System Surgical Technique Table of Contents Acetabular Reaming 2 Component Sizing
Managing Glenoid Bone Deficiency The Augment Experience in Anatomic and Reverse Shoulder Arthroplasty
 Managing Glenoid Bone Deficiency The Augment Experience in Anatomic and Reverse Shoulder Arthroplasty Publish date: March 5, 2018 Authors: Rowan J. Michael, MD Bradley S. Schoch, MD Joseph J. King, MD
Managing Glenoid Bone Deficiency The Augment Experience in Anatomic and Reverse Shoulder Arthroplasty Publish date: March 5, 2018 Authors: Rowan J. Michael, MD Bradley S. Schoch, MD Joseph J. King, MD
Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
Scapular notching in reverse shoulder arthroplasties: The influence of glenometaphyseal angle
 Orthopaedics & Traumatology: Surgery & Research (2011) 97S, S131 S137 ORIGINAL ARTICLE Scapular notching in reverse shoulder arthroplasties: The influence of glenometaphyseal angle V. Falaise a, C. Levigne
Orthopaedics & Traumatology: Surgery & Research (2011) 97S, S131 S137 ORIGINAL ARTICLE Scapular notching in reverse shoulder arthroplasties: The influence of glenometaphyseal angle V. Falaise a, C. Levigne
Aequalis -Glenoid. Keeled and Pegged. Surgical Technique
 Aequalis -Glenoid Keeled and Pegged Surgical Technique TABLE OF CONTENTS COMMON OPERATIVE TECHNIQUES FOR THE KEELED AND PEGGED AEQUALIS-GLENOIDS p. 1-3 IMPLANTATION OF THE AEQUALIS KEELED GLENOID p. 4-5
Aequalis -Glenoid Keeled and Pegged Surgical Technique TABLE OF CONTENTS COMMON OPERATIVE TECHNIQUES FOR THE KEELED AND PEGGED AEQUALIS-GLENOIDS p. 1-3 IMPLANTATION OF THE AEQUALIS KEELED GLENOID p. 4-5
LCP Distal Humerus Plates
 The anatomic fixation system for the distal humerus with angular stability Surgical technique LCP Locking Compression Plate Contents Indications and contraindications 2 Implants 3 Instruments 5 Preparation
The anatomic fixation system for the distal humerus with angular stability Surgical technique LCP Locking Compression Plate Contents Indications and contraindications 2 Implants 3 Instruments 5 Preparation
Shoulder & Elbow Service, University of Washington Department of Orthopaedics and Sports Medicine
 Reverse Total Shoulder or Delta Shoulder for Shoulder Arthritis Combined with Massive Rotator Cuff Tear and for Failed Conventional Total Shoulder Replacement Follow: shoulderarthritis.blogspot.com For
Reverse Total Shoulder or Delta Shoulder for Shoulder Arthritis Combined with Massive Rotator Cuff Tear and for Failed Conventional Total Shoulder Replacement Follow: shoulderarthritis.blogspot.com For
Percutaneous Humeral Fracture Repair Surgical Technique
 Percutaneous Humeral Fracture Repair Surgical Technique Percutaneous Pinning Percutaneous Humeral Fracture Repair Closed reduction followed by percutaneous fixation reduces risk from soft tissue dissection
Percutaneous Humeral Fracture Repair Surgical Technique Percutaneous Pinning Percutaneous Humeral Fracture Repair Closed reduction followed by percutaneous fixation reduces risk from soft tissue dissection
TORNIER BIO-RSA. Bony Increased Offset - Reversed Shoulder Arthroplasty SURGICAL TECHNIQUE
 TORNIER BIO-RSA Bony Increased Offset - Reversed Shoulder Arthroplasty SURGICAL TECHNIQUE 2 Table of Contents: Concept...4 Bony Increased Offset Reversed Shoulder Arthroplasty (BIO-RSA ) Concept...4 Surgical
TORNIER BIO-RSA Bony Increased Offset - Reversed Shoulder Arthroplasty SURGICAL TECHNIQUE 2 Table of Contents: Concept...4 Bony Increased Offset Reversed Shoulder Arthroplasty (BIO-RSA ) Concept...4 Surgical
2.7 mm/3.5 mm LCP Distal Fibula Plate System. Part of the Synthes locking compression plate (LCP) system.
 2.7 mm/3.5 mm LCP Distal Fibula Plate System. Part of the locking compression plate (LCP) system. Anatomically contoured Multiple screw options for fixedangle support Coaxial holes minimize screw head
2.7 mm/3.5 mm LCP Distal Fibula Plate System. Part of the locking compression plate (LCP) system. Anatomically contoured Multiple screw options for fixedangle support Coaxial holes minimize screw head
Locked plating constructs are creating a challenge for surgeons.
 Locked plating constructs are creating a challenge for surgeons. Three recent studies examining supracondylar femur fractures show concern for the high degree of stiffness of locked plating constructs
Locked plating constructs are creating a challenge for surgeons. Three recent studies examining supracondylar femur fractures show concern for the high degree of stiffness of locked plating constructs
ReUnion RSA Shoulder System
 ReUnion RSA Shoulder System Reverse Surgical Protocol This document is intended to be used by healthcare professionals only. ReUnion RSA Reverse Shoulder Surgical Protocol Table of Contents Surgical Technique
ReUnion RSA Shoulder System Reverse Surgical Protocol This document is intended to be used by healthcare professionals only. ReUnion RSA Reverse Shoulder Surgical Protocol Table of Contents Surgical Technique
Technique Guide. 3.5 mm LCP Periarticular Proximal Humerus Plate. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide 3.5 mm LCP Periarticular Proximal Humerus Plate. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Proximal Humerus Plate 2 AO Principles
Technique Guide 3.5 mm LCP Periarticular Proximal Humerus Plate. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Proximal Humerus Plate 2 AO Principles
TORNIER AEQUALIS REVERSED II. Shoulder System SURGICAL TECHNIQUE
 TORNIER AEQUALIS REVERSED II Shoulder System SURGICAL TECHNIQUE 2 Table of Contents: Implant Description...4 Implant Indications and Contraindications...6 Surgical Technique...7 Pre-operative Planning...7
TORNIER AEQUALIS REVERSED II Shoulder System SURGICAL TECHNIQUE 2 Table of Contents: Implant Description...4 Implant Indications and Contraindications...6 Surgical Technique...7 Pre-operative Planning...7
Dr. John Masonis Charlotte, NC OrthoCarolina. Dr. James Waddell Toronto, Ontario University of Toronto, St. Michael s Hospital
 Design Rationale Design surgeon list Smith & Nephew thanks the following surgeons for their participation as part of the REDAPT Revision Acetabular System design team: Dr. Robert Bourne London, Ontario
Design Rationale Design surgeon list Smith & Nephew thanks the following surgeons for their participation as part of the REDAPT Revision Acetabular System design team: Dr. Robert Bourne London, Ontario
comprehensive Design Rationale shoulder system Knees Hips Extremities Cement and Accessories PMI TEchnology
 comprehensive shoulder system Design Rationale Knees Hips Extremities Cement and Accessories PMI TEchnology . INTRODUCTION The Comprehensive Shoulder System is an evolutionary design based on the successful
comprehensive shoulder system Design Rationale Knees Hips Extremities Cement and Accessories PMI TEchnology . INTRODUCTION The Comprehensive Shoulder System is an evolutionary design based on the successful
 Use of a partial humeral head resurfacing system for management of an osseous mechanic... Page 1 of 12 Int J Shoulder Surg. 2011 Jan-Mar; 5(1): 17 20. doi: 10.4103/0973-6042.80465. PMCID: PMC3109768 Copyright
Use of a partial humeral head resurfacing system for management of an osseous mechanic... Page 1 of 12 Int J Shoulder Surg. 2011 Jan-Mar; 5(1): 17 20. doi: 10.4103/0973-6042.80465. PMCID: PMC3109768 Copyright
Posterior Glenoid Wear in Total Shoulder Arthroplasty:
 Posterior Glenoid Wear in Total Shoulder Arthroplasty: Eccentric Anterior Reaming is Superior to Posterior Augment Tim Wang MD, Geoffrey Abrams MD, Anthony Behn MS, Emilie Cheung MD Department of Orthopaedic
Posterior Glenoid Wear in Total Shoulder Arthroplasty: Eccentric Anterior Reaming is Superior to Posterior Augment Tim Wang MD, Geoffrey Abrams MD, Anthony Behn MS, Emilie Cheung MD Department of Orthopaedic
Integra. Titan Modular Shoulder System, 2.5
 Titan Modular Shoulder System, 2.5 Limit uncertainty with a shoulder implant system that redefines modularity, addresses multiple indications, and allows for reproducible results. Titan Modular Shoulder
Titan Modular Shoulder System, 2.5 Limit uncertainty with a shoulder implant system that redefines modularity, addresses multiple indications, and allows for reproducible results. Titan Modular Shoulder
LCP Distal Tibia Plate
 Surgical Technique LCP Locking Compression Plate Original Instruments and Implants of the Association for the Study of Internal Fixation AO/ASIF Table of contents Indications 3 Implants/Instruments 5 Surgical
Surgical Technique LCP Locking Compression Plate Original Instruments and Implants of the Association for the Study of Internal Fixation AO/ASIF Table of contents Indications 3 Implants/Instruments 5 Surgical
Biomechanics of Two Reconstruction Techniques for Elbow Ulnar Collateral Ligament Insufficiency
 Biomechanics of Two Reconstruction Techniques for Elbow Ulnar Collateral Ligament Insufficiency Justin E. Chronister, MD 1, Randal P. Morris, BS 2, Clark R. Andersen, MS 2, J. Michael Bennett, MD 3, Thomas
Biomechanics of Two Reconstruction Techniques for Elbow Ulnar Collateral Ligament Insufficiency Justin E. Chronister, MD 1, Randal P. Morris, BS 2, Clark R. Andersen, MS 2, J. Michael Bennett, MD 3, Thomas
Anatomical. Redefined.
 natomical. Redefined. On two days each year, daylight equals night. Perfect balance is achieved. Such is the power of the quinoxe. Other shoulder systems have claimed anatomical. xactech is raising the
natomical. Redefined. On two days each year, daylight equals night. Perfect balance is achieved. Such is the power of the quinoxe. Other shoulder systems have claimed anatomical. xactech is raising the
Jonathan C. Levy, MD
 Jonathan C. Levy, MD Chief of Orthopedics Program Director, ASES Fellowship Holy Cross Hospital Fort Lauderdale, Florida USA Disclosure: Consultant, Royalties, & Research Support from DJO 72 year old
Jonathan C. Levy, MD Chief of Orthopedics Program Director, ASES Fellowship Holy Cross Hospital Fort Lauderdale, Florida USA Disclosure: Consultant, Royalties, & Research Support from DJO 72 year old
Surgical Technique International Version. Clavicle Locking Plate
 Surgical Technique International Version Clavicle Locking Plate PERI-LOC Upper Extremity Locked Plating System Clavicle Surgical Techniquefor Table of Contents Introduction........................................................2
Surgical Technique International Version Clavicle Locking Plate PERI-LOC Upper Extremity Locked Plating System Clavicle Surgical Techniquefor Table of Contents Introduction........................................................2
WINSTA-C. Clavicle Plating System
 Clavicle Plating System Clinical Advisor Michael Kurer FRCS FRCS (Orth) Consultant Orthopaedic and Shoulder Surgeon North Middlesex University Hospital NHS Trust Table of Contents Introduction Indication
Clavicle Plating System Clinical Advisor Michael Kurer FRCS FRCS (Orth) Consultant Orthopaedic and Shoulder Surgeon North Middlesex University Hospital NHS Trust Table of Contents Introduction Indication
Reverse Shoulder Arthroplasty for the Treatment of Rotator Cuff Deficiency
 1895 COPYRIGHT Ó 2017 BY THE JOURAL OF BOE AD JOIT SURGERY, ICORPORATED Reverse Shouler Arthroplasty for the Treatment of Rotator Cuff Deficiency A Concise Follow-up, at a Minimum of 10 Years, of Previous
1895 COPYRIGHT Ó 2017 BY THE JOURAL OF BOE AD JOIT SURGERY, ICORPORATED Reverse Shouler Arthroplasty for the Treatment of Rotator Cuff Deficiency A Concise Follow-up, at a Minimum of 10 Years, of Previous
Arthroplasty Of The Shoulder
 Arthroplasty Of The Shoulder 1 / 7 2 / 7 3 / 7 Arthroplasty Of The Shoulder About Your Shoulder. Ligaments and tendons hold it together. Ligaments connect the bones, while tendons connect muscles to the
Arthroplasty Of The Shoulder 1 / 7 2 / 7 3 / 7 Arthroplasty Of The Shoulder About Your Shoulder. Ligaments and tendons hold it together. Ligaments connect the bones, while tendons connect muscles to the
3.5 mm LCP Clavicle Hook Plates
 Part of the Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Clavicle Hook Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Clavicle Hook Plates 2 AO Principles 4 Indications
Part of the Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Clavicle Hook Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Clavicle Hook Plates 2 AO Principles 4 Indications
Immediate post surgical findings of soft tissue swelling, subcutaneous emphysema, and skin staples for reverse total shoulder arthroplasty.
 Immediate post surgical findings of soft tissue swelling, subcutaneous emphysema, and skin staples for reverse total shoulder arthroplasty. REVERSE TOTAL SHOULDER ARTHROPLASTY WITH FRACTURED ACROMION Above:
Immediate post surgical findings of soft tissue swelling, subcutaneous emphysema, and skin staples for reverse total shoulder arthroplasty. REVERSE TOTAL SHOULDER ARTHROPLASTY WITH FRACTURED ACROMION Above:
Wichita Fusion Nail Surgical Technique. David A. McQueen, MD
 Wichita Fusion Nail Surgical Technique David A. McQueen, MD The patented design with a dual advantage Generates compression intraoperatively Innovative compression screw (a) locks femoral and tibial components
Wichita Fusion Nail Surgical Technique David A. McQueen, MD The patented design with a dual advantage Generates compression intraoperatively Innovative compression screw (a) locks femoral and tibial components
Design Rationale. ECHELON Primary Hip System
 Design Rationale ECHELON Primary Hip System ECHELON Primary Total Hip System Addressing clinical issues of cementless hip arthroplasty Cementless total hip arthroplasty has provided a proven method of
Design Rationale ECHELON Primary Hip System ECHELON Primary Total Hip System Addressing clinical issues of cementless hip arthroplasty Cementless total hip arthroplasty has provided a proven method of
DESIGN RATIONALE AND SURGICAL TECHNIQUE
 DESIGN RATIONALE AND SURGICAL TECHNIQUE ANCHOR PEG GLENOID DESIGN RATIONALE In total shoulder arthroplasty, most cases of clinical and radiographic loosening involve failure of the fixation of the glenoid
DESIGN RATIONALE AND SURGICAL TECHNIQUE ANCHOR PEG GLENOID DESIGN RATIONALE In total shoulder arthroplasty, most cases of clinical and radiographic loosening involve failure of the fixation of the glenoid
Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer
 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer Surgical Technique 2 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion
Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer Surgical Technique 2 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion
Surgical Technique. Locking Small Fragment Overview
 Surgical Technique Locking Small Fragment Overview PERI-LOC Locked Plating System Locking Small Fragment Overview Surgical Technique Table of contents Product overview... 2 Introduction... 2 Indications...
Surgical Technique Locking Small Fragment Overview PERI-LOC Locked Plating System Locking Small Fragment Overview Surgical Technique Table of contents Product overview... 2 Introduction... 2 Indications...
AEQUALIS TM REVERSED II
 TORNIER AEQUALIS TM REVERSED II SURGICAL TECHNIQUE Tornier Upper Extremities Contents Chapter 1 4 Chapter 2 6 6 6 6 7 24 Appendix A 26 Appendix B 27 Appendix C 35 Implant Description Surgical Technique
TORNIER AEQUALIS TM REVERSED II SURGICAL TECHNIQUE Tornier Upper Extremities Contents Chapter 1 4 Chapter 2 6 6 6 6 7 24 Appendix A 26 Appendix B 27 Appendix C 35 Implant Description Surgical Technique
Variable Angle LCP Locking Technology
 BUILDING ON SUCCESS Variable Angle LCP Locking Technology The Evolution of Plating Technology Round Screw Hole Dynamic Compression Plate Limited-Contact Dynamic Compression Less Invasive Stabilization
BUILDING ON SUCCESS Variable Angle LCP Locking Technology The Evolution of Plating Technology Round Screw Hole Dynamic Compression Plate Limited-Contact Dynamic Compression Less Invasive Stabilization
HUMERISTM. Cementless ANATOMICAL and REVERSIBLE SURGICAL TECHNIQUE
 HUMERISTM Cementless ANATOMICAL and REVERSIBLE Hemi or Total Reversible SURGICAL TECHNIQUE CONTENTS - Device descriptionpage 0 - Intended use / indicationspage 04 - Warnings and precautions page 04 - Anatomical
HUMERISTM Cementless ANATOMICAL and REVERSIBLE Hemi or Total Reversible SURGICAL TECHNIQUE CONTENTS - Device descriptionpage 0 - Intended use / indicationspage 04 - Warnings and precautions page 04 - Anatomical
Surgical Technique Guide PANTERA. Proximal Humerus Fracture Fixation Plate System
 Surgical Technique Guide PANTERA Proximal Humerus Fracture Fixation Plate System Installing the PANTERA is a 4-Step Process: The following technique is designed to optimize the surgical exercise. Step
Surgical Technique Guide PANTERA Proximal Humerus Fracture Fixation Plate System Installing the PANTERA is a 4-Step Process: The following technique is designed to optimize the surgical exercise. Step
Zimmer ITST Intertrochanteric/ Subtrochanteric Fixation System. Abbreviated Surgical Technique
 Zimmer ITST Intertrochanteric/ Subtrochanteric Fixation System Abbreviated Surgical Technique ITST System Abbreviated Surgical Technique Indications The ITST Intramedullary Nail is indicated for use in
Zimmer ITST Intertrochanteric/ Subtrochanteric Fixation System Abbreviated Surgical Technique ITST System Abbreviated Surgical Technique Indications The ITST Intramedullary Nail is indicated for use in
RibLoc U. Chest Wall Plating System. Innovative Solutions for Challenging Thoracic Procedures
 RibLoc U Chest Wall Plating System Innovative Solutions for Challenging Thoracic Procedures RibLoc U Chest Wall Plating System ACUTE Innovations has developed U-shaped plate technology to provide stability
RibLoc U Chest Wall Plating System Innovative Solutions for Challenging Thoracic Procedures RibLoc U Chest Wall Plating System ACUTE Innovations has developed U-shaped plate technology to provide stability
Trilogy Acetabular System
 Trilogy Acetabular System Surgical Technique Versatility in a proven design Trilogy Acetabular System 1 Trilogy Acetabular System Surgical Technique Table of Contents Acetabular Reaming 2 Component Sizing
Trilogy Acetabular System Surgical Technique Versatility in a proven design Trilogy Acetabular System 1 Trilogy Acetabular System Surgical Technique Table of Contents Acetabular Reaming 2 Component Sizing
Comprehensive Reverse Shoulder System
 Comprehensive Reverse Shoulder System Comprehensive Reverse Shoulder System Simple. Versatile. The Comprehensive Reverse Shoulder System is the next generation reverse shoulder prosthesis, offering unmatched
Comprehensive Reverse Shoulder System Comprehensive Reverse Shoulder System Simple. Versatile. The Comprehensive Reverse Shoulder System is the next generation reverse shoulder prosthesis, offering unmatched
