Effect of baseplate size on primary glenoid stability and impingement-free range of motion in reverse shoulder arthroplasty
|
|
|
- Shana Jocelin Carpenter
- 5 years ago
- Views:
Transcription
1 Chae et al. BMC Musculoskeletal Disorders 2014, 15:417 RESEARCH ARTICLE Open Access Effect of baseplate size on primary glenoid stability and impingement-free range of motion in reverse shoulder arthroplasty Soo-Won Chae 1, Soung-Yon Kim 2*, Haea Lee 1, Joung-Ro Yon 1, Juneyoung Lee 3 and Seung-Ho Han 4 Abstract Background: Use of a baseplate with a smaller diameter in reverse shoulder arthroplasty is increasing, especially in patients with a small glenoid or glenoid wear. However, the effect of a smaller baseplate on stability of the glenoid component has not been evaluated. Thus, the purpose of this study was to determine whether a smaller baseplate (25 mm) is beneficial to the initial stability of the glenoid component compared to that with a baseplate of a commonly used size (29 mm). Methods: Micromotion of glenoid components attached to 14 scapulae of fresh-frozen cadavers was measured and compared between 25- and 29-mm baseplates in biomechanical testing. Impingement-free range of motion in abduction, adduction, internal rotation, and external rotation was evaluated by using a simulated computer model constructed based on the same fresh-frozen cadavers used in biomechanical testing. Results: Micromotion at the inferior third of the glenoid-glenosphere interface was higher in the 29-mm baseplate group than in the 25-mm baseplate group during both 0.7- and 1-body weight cyclic loading in biomechanical testing. Adduction deficit was smaller, and total impingement-free range of motion from abduction to adduction and rotation were greater in the 25-mm baseplate group than in the 29-mm baseplate group in the simulated computer model. Conclusions: Use of a baseplate with a smaller diameter (25 mm) in reverse shoulder arthroplasty is suitable for improving the primary stability of the glenoid component. With a smaller baseplate, impingement-free range of motion is optimized in a smaller glenoid. Keywords: Reverse shoulder arthroplasty, Smaller baseplate, Biomechanical testing, Simulated computer model Background Since its introduction by Grammont [1,2], reverse shoulder arthroplasty (RSA) has been successful in improving function and pain in patients with massive rotator cuff tear or cuff tear arthropathy [2-4]. Recently, its application has expanded to include rheumatoid arthritis, fracture, failed arthroplasty, and fracture and infection sequelae [5-7]. However, the reported complication rate is still high [8]. Glenoid component loosening, in particular, is known to be a major cause of failure in RSA [9]. There have been several efforts to improve stability of glenoid component * Correspondence: singsingkr@yahoo.co.kr 2 Department of Orthopaedic Surgery, Hallym University, Kangnam Sacred Heart Hospital, Seoul, South Korea Full list of author information is available at the end of the article fixation, including studies of glenoid component design [10,11], glenoid component position [12], and screw fixation [13]. During the RSA procedure, because of glenoid wear or small glenoid size, glenoid surface area, which is required for seating of the baseplate, is sometimes insufficient to fix the commonly used 29-mm-diameter baseplate [14,15]. Surgeons doubt the stability of initial fixation of the baseplate when confronted with this difficulty. Facing this uncertainty, some manufacturers have developed baseplates with a smaller diameter, and their use is increasing, especially among small, female, and Asian patients. However, the effect of a smaller baseplate, the stability of a smaller baseplate compared to that of a baseplate with a commonly used size, has not been examined biomechanically. Thus, the purpose of this study 2014 Chae et al.; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly credited. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Chae et al. BMC Musculoskeletal Disorders 2014, 15:417 Page 2 of 7 was to determine whether a 25-mm baseplate is beneficial to initial stability of the glenoid component and impingement-free range of motion in a relatively small glenoid, compared to that with a 29-mm baseplate. We hypothesized that the smaller 25-mm baseplate would provide better initial fixation stability, lesser micromotion, and more impingement-free range of motion than the commonly used 29-mm baseplate. This was evaluated by comparing micromotion at the glenoid-glenosphere interface in biomechanical testing and impingement-free range of motion in abduction, adduction, internal rotation, and external rotation in a simulated computer model of freshfrozen cadavers with a small glenoid. Methods Biomechanical testing Seven pairs of human scapulae were dissected from 7 fresh-frozen female cadavers with a mean age of 62 years (range, 61 to 65 years) and height less than 160 cm. We selected female donors with a small height because a small glenoid was preferable for our experimental purpose [16]. All cadavers investigated in this study were donated to The Catholic University of Korea by due process of law in Korea with the permission of the individuals prior to death and their family for dissection in educational and research settings. The IRB of The Catholic University of Korea has received AAHRPP accreditation and complies with its ethics. The IRB does not review cadaver studies in which it is not possible to identify the individuals and which do not use personal information. Research involving cadavers, autopsy material or bio-specimens from deceased individuals do not meet the regulatory definitions of human research and do not need IRB review. Our cadaver study complied with these conditions. Specimens showing posttraumatic deformity or degenerative change, such as glenoid wear, based on gross inspection, were excluded. Maximum length of the glenoid from the highest to the lowest point and maximum width of the anteroposterior diameter of the glenoid were measured using a caliper. A Tornier Aequalis Reversed Shoulder Prosthesis (Tornier, Inc., Edina, MN, USA), consisting of a baseplate and glenosphere, was fixed to each scapula according to the standard surgical technique. Specimens were randomly assigned to 2 groups. The control group consisted of 7 scapulae implanted with a 29-mm baseplate and 36-mm glenosphere. The second group consisted of 7 scapulae implanted with a 25-mm baseplate and 36-mm glenosphere. The glenoid was reamed at neutral inclination. The version of the glenoid component was 0, and the baseplate was positioned as inferiorly as possible relative to the scapula while still being fully supported by bone. In the same manner as in clinical surgery, the implantation of the baseplate and glenosphere at neutral inclination was accomplished using the neutral tilt central guide hole included with the prosthesis instrumentation. This guide hole allowed the insertion of a guide pin tilted 0 neutral relative to the glenoid surface. To align the lower border of the baseplate with the inferior glenoid rim, the drill holes were positioned at 11.5 and 9.5 mm above the inferior glenoid rim for the 29- and 25-mm baseplates prior to the glenoid reaming respectively, in compliance with the 12-mm rule described by Kelly et al. [17]. Screw fixation was performed according to the manufacturer s recommended surgical technique. The anterior screw was inserted at a trajectory that was superior and towards the middle of the baseplate. The posterior screw was inserted at a trajectory that was inferior and towards the middle of the baseplate. The inferior screw was positioned into the pillar of the scapula and was generally situated downwards in the vertical axis of the glenoid at an angle of ~20. The superior screw was positioned into the base of the coracoid process and was generally situated superiorly in the vertical axis of the glenoid at an angle of ~20 and anteriorly in the transverse axis of the glenoid at an angle of ~10. We attempted to fix the 25- and 29-mm baseplates in the same directions as the screws. The scapula with the implant was embedded in a rectangular resin block (Lang Dental Manufacturing Co., Inc., Wheeling, IL, USA) so that the glenoid-glenosphere interface was parallel to the floor. The block was then bolted to the mounting plate on a custom-made axialcompressive loading machine. The humeral component of the prosthesis, consisting of a 6-mm polyethylene insert and 36-mm metaphysis and stem, was provisionally affixed to the machine. The specimen was mounted on the axial-compressive loading machine at 60 abduction of the glenoid component to the humeral component (Figure 1a), and 2 compressive cyclic loading modes were applied sequentially through the humeral cup assembly. Cyclic loads of 0.7 body weight (BW) (480 N, 2.5 Hz, 100 cycles) and then that of 1 BW (686 N, 2.5 Hz, 100 cycles) were applied parallel with the long axis of the humeral stem to the center of the glenosphere. We assessed micromotion at the inferior third of the glenoid-glenosphere interface using high-resolution digital imaging [18]. For micromotion analysis, laser markers (1-mm diameter) were engraved on the glenosphere surface prior to implantation such that there was a 3-mm distance between each marker and a 1-mm distance from the rim of the glenosphere. Surface markers (polyvinyl chloride, 2-mm diameter) were affixed with super glue to the adjacent glenoid bone surface near the glenoid-glenosphere interface. A camera was connected by aframetotheresinboxinwhichthescapulawiththeimplant was embedded, and was positioned perpendicular to
3 Chae et al. BMC Musculoskeletal Disorders 2014, 15:417 Page 3 of 7 a b Cyclic Loading Figure 1 Actual experimental setup. (a) The specimen was mounted on a custom-made axial-compressive loading machine. (b) The camera was connected by a frame and positioned perpendicular to the markers where micromotion was measured. the markers where micromotion was measured (Figure 1b). Four surface markers placed at the inferior third of the glenoid-glenosphere interface (one on the surface of the glenoid bone and 3 on the surface of the glenosphere) were used for measuring micromotion during cyclic loading in biomechanical testing (Figure 2a). Micromotion of the glenoid component was defined as the difference in glenoid component displacement from the adjacent glenoid bone surface. Locations of the markers were recorded using a camera (Pearl CCD series; IMI-Technology, San Diego, CA, USA) and 2/3-inch 55-mm telecentric lens (TEC- M55; Computar, NY, USA), and micromotion data were collected using a custom-made LabVIEW graphic interface (National Instruments Corporation, Austin, TX, USA). Micromotion, both parallel (x-axis) and perpendicular (y-axis) to the glenoid-glenosphere interface, was assessed as the hypotenuse of x- and y-axes measured during biomechanical testing (Figure 2b). Simulated computer model Scapulae from the same fresh-frozen cadavers used in biomechanical testing were used for computer model simulation. Computed tomography scans of each scapula were obtained, and 1-mm slices (resolution, mm pixel size) were used to construct 3-dimensional (3D) models using Mimics software (Materialise, Leuven, Belgium). A corresponding 3D prosthesis model consisting of the baseplate (25- or 29-mm) and 36-mm glenosphere was generated by laser scanning (Rexcan 3D Laser Scanner; Solutionix, Seoul, Korea). Point data of the scapula from Mimics and of the implant from the 3D laser scanner were converted into surface data using a reverse engineering program (Rapidform 3D Systems, Inc., Rock Hill, SC, USA). The scapular plane was defined as connecting the most dorsal aspect of the inferior angle, the intersection of the scapular spine and medial border, and the center of the glenoid (intersection of vertical and horizontal glenoid midlines) [14,19]. We computed implantation of the glenoid component into the scapula as the same condition in each group in biomechanical testing. Humeral abduction, adduction, internal rotation, and external rotation in relation to the glenoid in the scapular plane were simulated using SolidWorks 2011 software (SolidWorks Corporation, Concord, MA, USA). a b Figure 2 Micromotion measurement. (a) Four surface markers were placed at the inferior third of the glenoid-glenosphere interface for measuring micromotion. (b) Micromotion was assessed using high-resolution digital imaging.
4 Chae et al. BMC Musculoskeletal Disorders 2014, 15:417 Page 4 of 7 Impingement-free abduction and adduction arc of motion were defined as the arc of motion from the point of inferior impingement to the point of superior impingement on the scapula or acromion [20]. Impingementfree range of motion in internal and external rotation was measured at 60 abduction of the humeral component to the glenoid component. Data analysis Differences in micromotion of the glenoid component during cyclic loading in biomechanical testing and impingement-free range of motion in the simulated computer model between groups were analyzed using Wilcoxon s rank-sum test. Data were presented as means ± SDs. Reported p values were 2-tailed, and values <0.05 were considered to be statistically significant. Results Gross inspection showed that all glenoids had a smaller width than the 29-mm baseplate diameter, as well as insufficient bone stock to fix the anterior or posterior screw for fixation of the 29-mm baseplate (Figure 3). Measurements of glenoid size and screw length are listed in Table 1. The lengths of the anterior, posterior, and superior screws were longer in the 25-mm baseplate group than in the 29-mm baseplate group. Micromotion at the inferior third of the glenoid-glenosphere interface was higher in the 29-mm baseplate group than in the 25-mm baseplate group during both 0.7-BW (34 ± 12 μm and30± 6 μm, respectively p = 0.73) and 1-BW (47 ± 18 μm and 43 ± 10 μm, respectively; p = 0.91) cyclic loading. However, Figure 3 A 29-mm baseplate. This commonly used baseplate (29 mm) is too large to fix on a small glenoid. The arrow indicates insufficient bone stock for screw fixation. Table 1 Measurements of glenoid size and length of screws used for baseplate fixation Variable, mm 25-mm baseplate 29-mm baseplate p value Glenoid length 32.6 ± ± Glenoid width 23.3 ± ± Anterior screw 22.3 ± ± Posterior screw 20.6 ± ± Superior screw 32 ± ± Inferior screw 31.1 ± ± All data are expressed as mean ± SD. no statistically significant difference was evident between groups during the 0.7- or 1-BW cyclic loading. Adduction deficit was smaller in the 25-mm baseplate group than in the 29-mm baseplate group (19.2 ± 4.9 and 22.4 ± 5.7, respectively; p = 0.83), whereas total impingement-free range of motion from abduction to adduction was greater in the 25-mm baseplate group than in the 29-mm baseplate group (64 ± 3.8 and 61.2 ± 3.9, respectively; p = 0.24). Maximum impingement-free abduction was similar between the 25- and 29-mm baseplate groups (83.2 ± 1.9 and 83.6 ± 2.1, respectively; p = 0.48) (Figure 4). Impingement-free range of motion in external rotation was greater in the 25-mm baseplate group than in the 29-mm baseplate group (39 ± 8.1 and 35.4 ± 7.7, respectively; p = 0.20), whereas impingement-free range of motion in internal rotation was similar between the 25- and 29-mm baseplate groups (33.8 ± 5.8 and 33.2 ± 7.0, respectively; p = 1.00). Total impingementfree range of motion in rotation was greater in the 25-mm baseplate group than in the 29-mm baseplate group (72.8 ± 5.3 and 68.6 ± 2.8, respectively; p =0.31) (Figure 5). A statistically significant difference was not observed for these various parameters. Discussion Numerous studies have suggested several methods to increase glenoid component stability and reduce scapular notching, such as glenoid component design [10,11,20-23], positioning [12,24,25], and screw fixation [13,26,27]. Besides glenoid implant factors, another consideration to improve glenoid component fixation is glenoid morphology and size. The glenoid morphology of patients undergoing RSA is heterogeneic in terms of bony deformity, including posterior, superior, global, and anterior wear [14]. Glenoid wear may result in decreased contact surface area and bony support to the baseplate, which may weaken initial stability of glenoid component fixation. Several literatures have reported anatomic measurements of the glenoid. Churchill et al. reported that male glenoid width and height were 27.8 ± 1.6 mm and 37.5 ± 2.2 mm, respectively, while female glenoid width and height were 23.6 ± 1.5 mm and 32.6 ± 1.8 mm, respectively.
5 Chae et al. BMC Musculoskeletal Disorders 2014, 15:417 Page 5 of 7 Figure 4 Simulated computer model based on the same fresh-frozen cadavers used in biomechanical testing. (a) Adduction deficit, maximum impingement-free abduction, and total impingement-free arc of motion in the 25-mm baseplate group. (b) Adduction deficit, maximum impingement-free abduction, and total impingement-free arc of motion in the 29-mm baseplate group. Differences between men and women were found to be significant [16]. Von Schroeder et al. reported that average glenoid dimensions were 29 ± 3 mm (anteroposterior) by 36 ± 4 mm (superoinferior) [28]. Glenoid size, especially in Asian women, is sometimes smaller than the commonly used 29-mm baseplate; therefore, the need for appropriate sizing of the glenoid component has been suggested. Kim et al. reported that in the Korean population, mean glenoid radius of women over 60 years of age was 13.5 ± 1.7 mm; thus it is difficult to insert a 29-mm baseplate (radius, 14.5 mm) in this small glenoid [15]. In small glenoids, the standard glenoid implant (29-mm) is larger than glenoid bone stock, which results in insufficient bone-implant contact and screw fixation, especially of anterior and posterior holes of the baseplate. Initial rigid fixation of the glenoid baseplate is dependent on placement of the screws and glenoid bone stock [10]; insecure initial fixation due to inadequate bony support to the baseplate and screw fixation is likely to result in glenoid loosening and decreased longevity of the RSA. In theory, a smaller diameter baseplate would serve to improve initial glenoid component fixation in terms of Figure 5 Simulated computer model based on the same fresh-frozen cadavers used in biomechanical testing. (a) Impingement-free range of motion in internal rotation, external rotation, and total impingement-free arc of rotation at 60 abduction in the 25-mm baseplate group. (b) Impingement-free range of motion in internal rotation, external rotation, and total impingement-free arc of rotation at 60 abduction in the 29-mm baseplate group.
6 Chae et al. BMC Musculoskeletal Disorders 2014, 15:417 Page 6 of 7 contact surface area and bony support to the baseplate. Clinically, its use has been increasing, especially in small, female, and Asian patients. Middernacht et al. also suggested use of a baseplate with a smaller radius than currently used to avoid scapular notching, considering the varied size of the infraglenoid tubercle. They recommended using a smaller baseplate than is currently available in order to move the center of rotation even lower on the glenoid face [29,30]. Despite several authors suggesting use of a smaller baseplate to reduce scapular notching or to adjust a small glenoid [15,29,30], and its use increasing in smaller patients, the effect of a smaller baseplate with respect to initial fixation strength has not been thoroughly investigated. The present study aimed to clarify whether use of a smaller baseplate (25 mm) is beneficial to improve initial stability of glenoid component fixation in a small glenoid, compared with the commonly used baseplate (29 mm). Our results demonstrated that the smaller baseplate had less micromotion and greater impingement-free range of motion, even though a statistically significant difference was not evident. We postulate that because fixation of a 25-mm baseplate with a 36-mm glenosphere creates an overhang of 5.5 mm, while fixation of a 29-mm baseplate with a 36-mm glenosphere creates an overhang of 3.5 mm, this specific design of the prosthesis may affect adduction deficit as well as total impingement-free range of motion. Based upon our observations, we assumed the shorter length of the anterior, posterior, and superior screws used for the 29-mm baseplate fixation (relative to those used for the 25-mm baseplate fixation) and the insufficient bone stock of the small glenoid for fixation of the larger 29-mm baseplates, particularly for the fixation of the anterior and posterior screws, might influence the biomechanical stability of the 29-mm baseplate on the small glenoid. Some strengths of this study include the use of freshfrozen cadavers reflecting small glenoid morphology and density of cortical and cancellous scapula bone in individuals aged over 60 years. Use of fresh-frozen cadavers with a small glenoid, representing the population in which cuff tear arthropathy commonly occurs, better reflects the anatomic and mechanical properties of glenoid bone, enabling better assessment of glenoid component stability in RSA. In addition, we used digital-image analysis of micromotion in biomechanical testing, which is more reliable than the gauge method [18]. Furthermore, we evaluated the influence of baseplate size in RSA multiply by assessing micromotion in biomechanical testing and impingement-free abduction and adduction arc of motion in a simulated computer model. To our knowledge, no study has assessed stability and impingement-free arc of motion related to micromotion and scapular notching overall. There are some limitations associated with the experimental setup and methodology. First, the 0.7- and 1-BW amounts of loading used in this study could be deemed high considering the forces or load values estimated to occur in the shoulder during normal daily activities [31-33]. In addition, we applied relatively few loading cycles to simulate shoulder mechanics. Considering the high amount of axial-compressive loading forces used in our study, we believe the shorter-duration test might not have influenced the results concerning initial fixation stability of the glenoid component [11,18]. Second, we did not use cadaveric shoulders with rotator cuff arthropathy, which is the most common indication for RSA. In rotator cuff arthropathy, glenohumeral articulation is altered and glenoid wear commonly develops. Third, we assessed glenoid component stability only at an angle of 60 abduction. Different angle of loading condition may affect stability of the glenoid component. Fourth, we evaluated the influence of a smaller baseplate by using one specific type of prosthesis. Different prosthesis designs, such as shape of the baseplate, eccentricity, and curvature of the glenosphere, as well as number or size of screws for fixation, may affect primary stability and/or impingement-free arc of motion in RSA. Finally, stabilizing or destabilizing effects of ligaments, joint capsule, or remaining rotator cuff muscles, which may affect biomechanics in RSA, were not considered. Conclusions This study demonstrated that a smaller baseplate (25 mm) could be suitable for improving the primary stability of the glenoid component as well as impingement-free range of motion in a relatively small glenoid, compared with the commonly used baseplate (29 mm). Use of a smaller baseplate could be optimal in a small glenoid and may make fixation of the glenoid component more stable and may result in more impingement-free range of motion. We believe that further clinical and basic research studies should be performed to assess the influence of baseplate size on the stability of fixation in RSA, considering various designs of the glenoid component. Abbreviation RSA: Reverse shoulder arthroplasty. Competing interests The authors declare that they have no competing interests. Authors contributions SYK conceived of the study, and participated in the design of the study and performed data acquisition, surgical procedures and preparation, writing, and final approval of the manuscript. SWC, HL, JRY and SHH participated in data acquisition and drafting of the manuscript. JL participated in the design of the study and performed the statistical analysis. All authors read and approved the final manuscript. Acknowledgments The authors thank Sang-Hyun Kim, assistant manager of the Catholic Institute for Applied Anatomy, for his technical assistance. This research was supported by the Basic Science Research Program through the National Research Foundation of Korea, funded by the Ministry of Education, Science and Technology ( , ).
7 Chae et al. BMC Musculoskeletal Disorders 2014, 15:417 Page 7 of 7 Author details 1 Department of Mechanical Engineering, Korea University, Seoul, South Korea. 2 Department of Orthopaedic Surgery, Hallym University, Kangnam Sacred Heart Hospital, Seoul, South Korea. 3 Department of Biostatistics, Korea University College of Medicine, Seoul, South Korea. 4 Department of Anatomy, College of Medicine, Chung-Ang University, Seoul, South Korea. Received: 2 August 2014 Accepted: 5 December 2014 Published: 9 December 2014 References 1. Boileau P, Watkinson DJ, Hatzidakis AM, Balg F: Grammont reverse prosthesis: design, rationale, and biomechanics. J Shoulder Elbow Surg 2005, 14(1 Suppl S):147S 161S. 2. Grammont PM, Baulot E: Delta shoulder prosthesis for rotator cuff rupture. Orthopedics 1993, 16(1): Boileau P, Gonzalez JF, Chuinard C, Bicknell R, Walch G: Reverse total shoulder arthroplasty after failed rotator cuff surgery. J Shoulder Elbow Surg 2009, 18(4): Cuff D, Pupello D, Virani N, Levy J, Frankle M: Reverse shoulder arthroplasty for the treatment of rotator cuff deficiency. J Bone Joint Surg Am 2008, 90(6): Boileau P, Watkinson D, Hatzidakis AM, Hovorka I: Neer Award 2005: The Grammont reverse shoulder prosthesis: results in cuff tear arthritis, fracture sequelae, and revision arthroplasty. J Shoulder Elbow Surg 2006, 15(5): Cazeneuve JF, Cristofari DJ: The reverse shoulder prosthesis in the treatment of fractures of the proximal humerus in the elderly. J Bone Joint Surg Br 2010, 92(4): Rittmeister M, Kerschbaumer F: Grammont reverse total shoulder arthroplasty in patients with rheumatoid arthritis and nonreconstructible rotator cuff lesions. J Shoulder Elbow Surg 2001, 10(1): Zumstein MA, Pinedo M, Old J, Boileau P: Problems, complications, reoperations, and revisions in reverse total shoulder arthroplasty: a systematic review. J Shoulder Elbow Surg 2011, 20(1): Hopkins AR, Hansen UN, Bull AM, Emery R, Amis AA: Fixation of the reversed shoulder prosthesis. J Shoulder Elbow Surg 2008, 17(6): Harman M, Frankle M, Vasey M, Banks S: Initial glenoid component fixation in reverse total shoulder arthroplasty: a biomechanical evaluation. J Shoulder Elbow Surg 2005, 14(1 Suppl S):162S 167S. 11. Virani NA, Harman M, Li K, Levy J, Pupello DR, Frankle MA: In vitro and finite element analysis of glenoid bone/baseplate interaction in the reverse shoulder design. J Shoulder Elbow Surg 2008, 17(3): Gutierrez S, Greiwe RM, Frankle MA, Siegal S, Lee WE 3rd: Biomechanical comparison of component position and hardware failure in the reverse shoulder prosthesis. J Shoulder Elbow Surg 2007, 16(3 Suppl):S9 S DiStefano JG, Park AY, Nguyen TQ, Diederichs G, Buckley JM, Montgomery WH 3rd: Optimal screw placement for base plate fixation in reverse total shoulder arthroplasty. J Shoulder Elbow Surg 2011, 20(3): Frankle MA, Teramoto A, Luo ZP, Levy JC, Pupello D: Glenoid morphology in reverse shoulder arthroplasty: classification and surgical implications. J Shoulder Elbow Surg 2009, 18(6): Ji JH, Jeong JY, Song HS, Ok JH, Yang SJ, Jeon BK, Kim TG, Moon YS, Kim YS: Early clinical results of reverse total shoulder arthroplasty in the Korean population. J Shoulder Elbow Surg 2013, 22(8): Churchill RS, Brems JJ, Kotschi H: Glenoid size, inclination, and version: an anatomic study. J Shoulder Elbow Surg 2001, 10(4): Kelly JD 2nd, Humphrey CS, Norris TR: Optimizing glenosphere position and fixation in reverse shoulder arthroplasty, Part One: The twelve-mm rule. J Shoulder Elbow Surg 2008, 17(4): Favre P, Perala S, Vogel P, Fucentese SF, Goff JR, Gerber C, Snedeker JG: In vitro assessments of reverse glenoid stability using displacement gages are misleading - recommendations for accurate measurements of interface micromotion. Clin Biomech (Bristol, Avon) 2011, 26(9): Lewis GS, Armstrong AD: Glenoid spherical orientation and version. J Shoulder Elbow Surg 2011, 20(1): Gutierrez S, Comiskey CA, Luo ZP, Pupello DR, Frankle MA: Range of impingement-free abduction and adduction deficit after reverse shoulder arthroplasty. Hierarchy of surgical and implant-design-related factors. J Bone Joint Surg Am 2008, 90(12): Chou J, Malak SF, Anderson IA, Astley T, Poon PC: Biomechanical evaluation of different designs of glenospheres in the SMR reverse total shoulder prosthesis: range of motion and risk of scapular notching. J Shoulder Elbow Surg 2009, 18(3): Gutierrez S, Walker M, Willis M, Pupello DR, Frankle MA: Effects of tilt and glenosphere eccentricity on baseplate/bone interface forces in a computational model, validated by a mechanical model, of reverse shoulder arthroplasty. J Shoulder Elbow Surg 2011, 20(5): Kowalsky MS, Galatz LM, Shia DS, Steger-May K, Keener JD: The relationship between scapular notching and reverse shoulder arthroplasty prosthesis design. J Shoulder Elbow Surg 2012, 21(10): Nyffeler RW, Werner CM, Gerber C: Biomechanical relevance of glenoid component positioning in the reverse Delta III total shoulder prosthesis. J Shoulder Elbow Surg 2005, 14(5): de Wilde LF, Poncet D, Middernacht B, Ekelund A: Prosthetic overhang is the most effective way to prevent scapular conflict in a reverse total shoulder prosthesis. Acta Orthop 2010, 81(6): Codsi MJ, Iannotti JP: The effect of screw position on the initial fixation of a reverse total shoulder prosthesis in a glenoid with a cavitary bone defect. J Shoulder Elbow Surg 2008, 17(3): Hoenig MP, Loeffler B, Brown S, Peindl R, Fleischli J, Connor P, D Alessandro D: Reverse glenoid component fixation: is a posterior screw necessary? J Shoulder Elbow Surg 2010, 19(4): von Schroeder HP, Kuiper SD, Botte MJ: Osseous anatomy of the scapula. Clin Orthop Relat Res 2001, 383: Middernacht B, De Roo PJ, Van Maele G, De Wilde LF: Consequences of scapular anatomy for reversed total shoulder arthroplasty. Clin Orthop Relat Res 2008, 466(6): Middernacht B, De Wilde L, Mole D, Favard L, Debeer P: Glenosphere disengagement: a potentially serious default in reverse shoulder surgery. Clin Orthop Relat Res 2008, 466(4): Poppen NK, Walker PS: Forces at the glenohumeral joint in abduction. Clin Orthop Relat Res 1978, 135: Terrier A, Reist A, Merlini F, Farron A: Simulated joint and muscle forces in reversed and anatomic shoulder prostheses. J Bone Joint Surg 2008, 90(6): Kontaxis A, Johnson GR: The biomechanics of reverse anatomy shoulder replacement a modelling study. Clin Biomech (Bristol, Avon) 2009, 24(3): doi: / Cite this article as: Chae et al.: Effect of baseplate size on primary glenoid stability and impingement-free range of motion in reverse shoulder arthroplasty. BMC Musculoskeletal Disorders :417. Submit your next manuscript to BioMed Central and take full advantage of: Convenient online submission Thorough peer review No space constraints or color figure charges Immediate publication on acceptance Inclusion in PubMed, CAS, Scopus and Google Scholar Research which is freely available for redistribution Submit your manuscript at
Matthew D. Saltzman, MD a, Deana M. Mercer, MD c, Winston J. Warme, MD b, Alexander L. Bertelsen, PA-C b, Frederick A. Matsen III, MD b, *
 J Shoulder Elbow Surg (2010) 19, 1028-1033 www.elsevier.com/locate/ymse A method for documenting the change in center of rotation with reverse total shoulder arthroplasty and its application to a consecutive
J Shoulder Elbow Surg (2010) 19, 1028-1033 www.elsevier.com/locate/ymse A method for documenting the change in center of rotation with reverse total shoulder arthroplasty and its application to a consecutive
Biomechanical concepts of total shoulder replacement. «Shoulder Course» Day 1. Richard W. Nyffeler Orthopädie Sonnenhof Bern. 11. Sept.
 Biomechanical concepts of total shoulder replacement Richard W. Nyffeler Orthopädie Sonnenhof Bern First total shoulder prosthesis Jules Emile Péan, 1830-1898 Monobloc prostheses Charles Neer, 1917-2011
Biomechanical concepts of total shoulder replacement Richard W. Nyffeler Orthopädie Sonnenhof Bern First total shoulder prosthesis Jules Emile Péan, 1830-1898 Monobloc prostheses Charles Neer, 1917-2011
Optimizing Deltoid Efficiency with Reverse Shoulder Arthroplasty Using a Novel Inset Center of Rotation Glenosphere Design
 S37 Optimizing Deltoid Efficiency with Reverse Shoulder Arthroplasty Using a Novel Inset Center of Rotation Glenosphere Design Christopher P. Roche, M.S., M.B.A., Matthew A. Hamilton, Ph.D., Phong Diep,
S37 Optimizing Deltoid Efficiency with Reverse Shoulder Arthroplasty Using a Novel Inset Center of Rotation Glenosphere Design Christopher P. Roche, M.S., M.B.A., Matthew A. Hamilton, Ph.D., Phong Diep,
Optimal Baseplate Rotational Alignment in Reverse Total Shoulder Arthroplasty: A Three-Dimensional Computer-Aided Design Study.
 Optimal Baseplate Rotational Alignment in Reverse Total Shoulder Arthroplasty: A Three-Dimensional Computer-Aided Design Study. Byron F. Stephens, MD 1, Casey T. Hebert 2, Thomas W. Throckmorton, MD 1,
Optimal Baseplate Rotational Alignment in Reverse Total Shoulder Arthroplasty: A Three-Dimensional Computer-Aided Design Study. Byron F. Stephens, MD 1, Casey T. Hebert 2, Thomas W. Throckmorton, MD 1,
Reverse Total Shoulder Arthroplasty: A New Frontier (of Complications)
 Reverse Total Shoulder Arthroplasty: A New Frontier (of Complications) Emilie Cheung, MD Associate Professor Chief Shoulder Elbow Svc Stanford University Department of Orthopedic Surgery Procedure volumes
Reverse Total Shoulder Arthroplasty: A New Frontier (of Complications) Emilie Cheung, MD Associate Professor Chief Shoulder Elbow Svc Stanford University Department of Orthopedic Surgery Procedure volumes
Assessment of Approximate Glenoid Size in Thai People
 Assessment of Approximate Glenoid Size in Thai People J Med Assoc Thai 2014; 97 (Suppl. 2): S14-S18 Full text. e-journal: http://www.jmatonline.com Pason Phonphok MD*, Nattha Kulkamthorn MD* * Division
Assessment of Approximate Glenoid Size in Thai People J Med Assoc Thai 2014; 97 (Suppl. 2): S14-S18 Full text. e-journal: http://www.jmatonline.com Pason Phonphok MD*, Nattha Kulkamthorn MD* * Division
Accuracy of CT-based measurements of glenoid version for total shoulder arthroplasty
 J Shoulder Elbow Surg (2009) -, 1-6 www.elsevier.com/locate/ymse Accuracy of CT-based measurements of glenoid version for total shoulder arthroplasty Heinz R. Hoenecke Jr., MD*, Juan C. Hermida, MD, Cesar
J Shoulder Elbow Surg (2009) -, 1-6 www.elsevier.com/locate/ymse Accuracy of CT-based measurements of glenoid version for total shoulder arthroplasty Heinz R. Hoenecke Jr., MD*, Juan C. Hermida, MD, Cesar
Assessment of Scapular Morphology and Surgical Technique as Predictors of Notching in Reverse Shoulder Arthroplasty
 An Original Study Assessment of Scapular Morphology and Surgical Technique as Predictors of Notching in Reverse Shoulder Arthroplasty Vani Sabesan, MD, Mark Callanan, MD, Vinay Sharma, BA, and J. Michael
An Original Study Assessment of Scapular Morphology and Surgical Technique as Predictors of Notching in Reverse Shoulder Arthroplasty Vani Sabesan, MD, Mark Callanan, MD, Vinay Sharma, BA, and J. Michael
Scapular notching in reverse shoulder arthroplasties: The influence of glenometaphyseal angle
 Orthopaedics & Traumatology: Surgery & Research (2011) 97S, S131 S137 ORIGINAL ARTICLE Scapular notching in reverse shoulder arthroplasties: The influence of glenometaphyseal angle V. Falaise a, C. Levigne
Orthopaedics & Traumatology: Surgery & Research (2011) 97S, S131 S137 ORIGINAL ARTICLE Scapular notching in reverse shoulder arthroplasties: The influence of glenometaphyseal angle V. Falaise a, C. Levigne
P. Trouilloud M. Gonzalvez P. Martz H. Charles F. Handelberg R. W. Nyffeler E. Baulot DuocentricÒ Group
 DOI 10.1007/s00590-013-1213-2 ORIGINAL ARTICLE Duocentric Ò reversed shoulder prosthesis and Personal Fit Ò templates: innovative strategies to optimize prosthesis positioning and prevent scapular notching
DOI 10.1007/s00590-013-1213-2 ORIGINAL ARTICLE Duocentric Ò reversed shoulder prosthesis and Personal Fit Ò templates: innovative strategies to optimize prosthesis positioning and prevent scapular notching
"Stability and Instability of RTSA"
 Orthopedics Update «Reverse Total Shoulder Arthroplasty» Stability and Instability of RTSA A. LÄDERMANN Orthopaedics and Traumatology, La Tour Hospital, Meyrin, Switzerland Orthopaedics and Traumatology,
Orthopedics Update «Reverse Total Shoulder Arthroplasty» Stability and Instability of RTSA A. LÄDERMANN Orthopaedics and Traumatology, La Tour Hospital, Meyrin, Switzerland Orthopaedics and Traumatology,
Biomechanical Impact of Posterior Glenoid Wear on Anatomic Total Shoulder Arthroplasty
 S5 Biomechanical Impact of Posterior Glenoid Wear on Anatomic Total Shoulder Arthroplasty Christopher P. Roche, M.S., M.B.A., Phong Diep, B.S., Sean G. Grey, M.D., and Pierre-Henri Flurin, M.D. Abstract
S5 Biomechanical Impact of Posterior Glenoid Wear on Anatomic Total Shoulder Arthroplasty Christopher P. Roche, M.S., M.B.A., Phong Diep, B.S., Sean G. Grey, M.D., and Pierre-Henri Flurin, M.D. Abstract
S h o u l d e r Solutions by Tornier C o n v e r T i b l e S h o u l d e r S y S T e m
 S h o u l d e r Solutions by Tornier C o n v e r t i b l e s h o u l d e r s y s t e m C o n v e r t i b l e s h o u l d e r s y s t e m A n a t o m i c Aequalis Ascend Flex - UDZF131 One System. Two Solutions.
S h o u l d e r Solutions by Tornier C o n v e r t i b l e s h o u l d e r s y s t e m C o n v e r t i b l e s h o u l d e r s y s t e m A n a t o m i c Aequalis Ascend Flex - UDZF131 One System. Two Solutions.
Why are these shoulder replacements called a reverse prosthesis?
 PATIENT GUIDE TO REVERSE PROSTHESIS Edward G. McFarland MD The Division of Sports Medicine and Shoulder Surgery The Department of Orthopaedic Surgery The Johns Hopkins University Baltimore MD Why are these
PATIENT GUIDE TO REVERSE PROSTHESIS Edward G. McFarland MD The Division of Sports Medicine and Shoulder Surgery The Department of Orthopaedic Surgery The Johns Hopkins University Baltimore MD Why are these
Evaluating Scapular Notching after Reverse Total Shoulder Arthroplasty
 ORIGINAL ARTICLE Clinics in Shoulder and Elbow Vol. 18, No. 4, December, 2015 http://dx.doi.org/10.5397/cise.2015.18.4.248 CiSE Clinics in Shoulder and Elbow Evaluating Scapular Notching after Reverse
ORIGINAL ARTICLE Clinics in Shoulder and Elbow Vol. 18, No. 4, December, 2015 http://dx.doi.org/10.5397/cise.2015.18.4.248 CiSE Clinics in Shoulder and Elbow Evaluating Scapular Notching after Reverse
Radiology Case Reports. Scapular Spine Stress Fracture as a Complication of Reverse Shoulder Arthroplasty
 Radiology Case Reports Volume 2, Issue 2, 2007 Scapular Spine Stress Fracture as a Complication of Reverse Shoulder Arthroplasty Kimberly J. Burkholz, Catherine C. Roberts, and Steven J. Hattrup We report
Radiology Case Reports Volume 2, Issue 2, 2007 Scapular Spine Stress Fracture as a Complication of Reverse Shoulder Arthroplasty Kimberly J. Burkholz, Catherine C. Roberts, and Steven J. Hattrup We report
Zimmer Patient Specific Instruments (PSI) for Reverse Shoulder Arthroplasty
 Zimmer Patient Specific Instruments (PSI) for Reverse Shoulder Arthroplasty Ryan Krupp, M.D. Norton Orthopaedic Specialists Louisville, KY Anand Murthi, M.D. MedStar Union Memorial Hospital Baltimore,
Zimmer Patient Specific Instruments (PSI) for Reverse Shoulder Arthroplasty Ryan Krupp, M.D. Norton Orthopaedic Specialists Louisville, KY Anand Murthi, M.D. MedStar Union Memorial Hospital Baltimore,
Clinical Outcomes and Complications during the Learning Curve for Reverse Total Shoulder Arthroplasty: An Analysis of the First 40 Cases
 Original Article Clinics in Orthopedic Surgery 2017;9:213-217 https://doi.org/10.4055/cios.2017.9.2.213 Clinical Outcomes and Complications during the Learning Curve for Reverse Total Shoulder Arthroplasty:
Original Article Clinics in Orthopedic Surgery 2017;9:213-217 https://doi.org/10.4055/cios.2017.9.2.213 Clinical Outcomes and Complications during the Learning Curve for Reverse Total Shoulder Arthroplasty:
Scapular Notching. Recognition and Strategies to Minimize Clinical Impact. Gregory P. Nicholson MD, Eric J. Strauss MD, Seth L.
 Clin Orthop Relat Res DOI 10.1007/s11999-010-1720-y SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Scapular Notching Recognition and Strategies to Minimize Clinical Impact Gregory P. Nicholson MD, Eric
Clin Orthop Relat Res DOI 10.1007/s11999-010-1720-y SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Scapular Notching Recognition and Strategies to Minimize Clinical Impact Gregory P. Nicholson MD, Eric
Prosthetic design of reverse shoulder arthroplasty contributes to scapular notching and instability
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v7.i11.738 World J Orthop 2016 November 18; 7(11): 738-745 ISSN 2218-5836 (online)
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v7.i11.738 World J Orthop 2016 November 18; 7(11): 738-745 ISSN 2218-5836 (online)
Influence of Glenosphere Design on Outcomes and Complications of Reverse Arthroplasty: A Systematic Review
 Original Article Clinics in Orthopedic Surgery 2016;8:288-297 http://dx.doi.org/10.4055/cios.2016.8.3.288 Influence of Glenosphere Design on Outcomes and Complications of Reverse Arthroplasty: A Systematic
Original Article Clinics in Orthopedic Surgery 2016;8:288-297 http://dx.doi.org/10.4055/cios.2016.8.3.288 Influence of Glenosphere Design on Outcomes and Complications of Reverse Arthroplasty: A Systematic
Surgical. Technique. AEQUALIS Spherical Base Glenoid. Shoulder Prosthesis.
 Surgical Technique Shoulder Prosthesis AEQUALIS Spherical Base Glenoid www.tornier.com CONTENTS CONTENTS 1. Subscapularis 2. Anterior capsule 3. Humeral protector 4. Inserting retractors 1. DESIGN FEATURES
Surgical Technique Shoulder Prosthesis AEQUALIS Spherical Base Glenoid www.tornier.com CONTENTS CONTENTS 1. Subscapularis 2. Anterior capsule 3. Humeral protector 4. Inserting retractors 1. DESIGN FEATURES
Shoulder Arthroplasty. Valentin Lance 3/24/16
 Shoulder Arthroplasty Valentin Lance 3/24/16 Outline Background Pre-operative imaging assessment Total Shoulder Arthroplasty: Standard and Reverse Complications Other shoulder hardware Hemiarthroplasty
Shoulder Arthroplasty Valentin Lance 3/24/16 Outline Background Pre-operative imaging assessment Total Shoulder Arthroplasty: Standard and Reverse Complications Other shoulder hardware Hemiarthroplasty
Integra. Titan Modular Shoulder System, 2.5
 Titan Modular Shoulder System, 2.5 Limit uncertainty with a shoulder implant system that redefines modularity, addresses multiple indications, and allows for reproducible results. Titan Modular Shoulder
Titan Modular Shoulder System, 2.5 Limit uncertainty with a shoulder implant system that redefines modularity, addresses multiple indications, and allows for reproducible results. Titan Modular Shoulder
Immediate post surgical findings of soft tissue swelling, subcutaneous emphysema, and skin staples for reverse total shoulder arthroplasty.
 Immediate post surgical findings of soft tissue swelling, subcutaneous emphysema, and skin staples for reverse total shoulder arthroplasty. REVERSE TOTAL SHOULDER ARTHROPLASTY WITH FRACTURED ACROMION Above:
Immediate post surgical findings of soft tissue swelling, subcutaneous emphysema, and skin staples for reverse total shoulder arthroplasty. REVERSE TOTAL SHOULDER ARTHROPLASTY WITH FRACTURED ACROMION Above:
INITIAL FIXATION OF THE TRABECULAR METAL REVERSE SHOULDER GLENOID BASE PLATE IMPLANT
 Copyright 2008 by Zimmer, Inc. INITIAL FIXATION OF THE TRABECULAR METAL REVERSE SHOULDER GLENOID BASE PLATE IMPLANT Matthew L. Mroczkowski M.S. Roy Wiley Background Reverse total shoulder arthroplasty
Copyright 2008 by Zimmer, Inc. INITIAL FIXATION OF THE TRABECULAR METAL REVERSE SHOULDER GLENOID BASE PLATE IMPLANT Matthew L. Mroczkowski M.S. Roy Wiley Background Reverse total shoulder arthroplasty
SSSR. 1. Nov Shoulder Prosthesis. Postoperative Imaging. Florian M. Buck, MD
 Shoulder Prosthesis Postoperative Imaging Florian M. Buck, MD Shoulder Prosthesis Surgical Approach Findings Imaging Modalities Postoperative Problems Shoulder Prosthesis What are we talking about Anatomical
Shoulder Prosthesis Postoperative Imaging Florian M. Buck, MD Shoulder Prosthesis Surgical Approach Findings Imaging Modalities Postoperative Problems Shoulder Prosthesis What are we talking about Anatomical
Impact of Modeling Assumptions on Stability Predictions in Reverse Shoulder Arthroplasty
 Impact of Modeling Assumptions on Stability Predictions in Reverse Shoulder Arthroplasty Mehul A Dharia*, Jeff Bischoff* *Zimmer Biomet, Warsaw, IN May 17, 2017 Total Shoulder Arthroplasty Shoulder Joint
Impact of Modeling Assumptions on Stability Predictions in Reverse Shoulder Arthroplasty Mehul A Dharia*, Jeff Bischoff* *Zimmer Biomet, Warsaw, IN May 17, 2017 Total Shoulder Arthroplasty Shoulder Joint
Effect of Prosthesis Design on Muscle Length and Moment Arms in Reverse Total Shoulder Arthroplasty
 S31 Effect of Prosthesis Design on Muscle Length and Moment Arms in Reverse Total Shoulder Arthroplasty Matthew A. Hamilton, Ph.D., Christopher P. Roche, M.S., M.B.A., Phong Diep, B.S., Pierre- Henri Flurin,
S31 Effect of Prosthesis Design on Muscle Length and Moment Arms in Reverse Total Shoulder Arthroplasty Matthew A. Hamilton, Ph.D., Christopher P. Roche, M.S., M.B.A., Phong Diep, B.S., Pierre- Henri Flurin,
GLENOID SURGICAL TECHNIQUE
 UP. EXTREMITY Dual-Platform Shoulder Prosthesis GLENOID SURGICAL TECHNIQUE ANATOMICAL REVERSE SURGICAL TECHNIQUE REFERENCE NUMBERS HUMERAL STEM REFERENCE DIAMETER HEIGHT 267 360 Ø 06 100 265 102 Ø 08 120
UP. EXTREMITY Dual-Platform Shoulder Prosthesis GLENOID SURGICAL TECHNIQUE ANATOMICAL REVERSE SURGICAL TECHNIQUE REFERENCE NUMBERS HUMERAL STEM REFERENCE DIAMETER HEIGHT 267 360 Ø 06 100 265 102 Ø 08 120
Comprehensive Reverse Shoulder System Augmented Baseplate
 Comprehensive Reverse Shoulder System Augmented Baseplate Surgical Technique Addendum FPO 1 Comprehensive Reverse Shoulder System Augmented Baseplate Surgical Technique Addendum Adaptive Building on the
Comprehensive Reverse Shoulder System Augmented Baseplate Surgical Technique Addendum FPO 1 Comprehensive Reverse Shoulder System Augmented Baseplate Surgical Technique Addendum Adaptive Building on the
The Shoulder. Anatomy and Injuries PSK 4U Unit 3, Day 4
 The Shoulder Anatomy and Injuries PSK 4U Unit 3, Day 4 Shoulder Girdle Shoulder Complex is the most mobile joint in the body. Scapula Clavicle Sternum Humerus Rib cage/thorax Shoulder Girdle It also includes
The Shoulder Anatomy and Injuries PSK 4U Unit 3, Day 4 Shoulder Girdle Shoulder Complex is the most mobile joint in the body. Scapula Clavicle Sternum Humerus Rib cage/thorax Shoulder Girdle It also includes
ANATOMIC TOTAL SHOULDER REPLACEMENT:
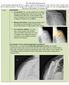 The Shoulder Replacement A total shoulder arthroplasty (TSA) is a surgery to replace the damaged parts of the ball and socket shoulder joint with an artificial prosthesis. The damage to the shoulder can
The Shoulder Replacement A total shoulder arthroplasty (TSA) is a surgery to replace the damaged parts of the ball and socket shoulder joint with an artificial prosthesis. The damage to the shoulder can
 Use of a partial humeral head resurfacing system for management of an osseous mechanic... Page 1 of 12 Int J Shoulder Surg. 2011 Jan-Mar; 5(1): 17 20. doi: 10.4103/0973-6042.80465. PMCID: PMC3109768 Copyright
Use of a partial humeral head resurfacing system for management of an osseous mechanic... Page 1 of 12 Int J Shoulder Surg. 2011 Jan-Mar; 5(1): 17 20. doi: 10.4103/0973-6042.80465. PMCID: PMC3109768 Copyright
Analysis of a retrieved Delta III total shoulder prosthesis
 Analysis of a retrieved Delta III total shoulder prosthesis R. W. Nyffeler, C. M. L. Werner, B. R. Simmen, C. Gerber From the University of Zurich, Zurich, Switzerland A reversed Delta III total shoulder
Analysis of a retrieved Delta III total shoulder prosthesis R. W. Nyffeler, C. M. L. Werner, B. R. Simmen, C. Gerber From the University of Zurich, Zurich, Switzerland A reversed Delta III total shoulder
)532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY
 )532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE The Midterm Results of the Delta Xtend Reverse Shoulder System: A Five-Year Outcome Study John G. Horneff, MD; Thema A. Nicholson,
)532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE The Midterm Results of the Delta Xtend Reverse Shoulder System: A Five-Year Outcome Study John G. Horneff, MD; Thema A. Nicholson,
Reverse Total Shoulder. Dr. Minoo Patel
 Reverse Total Shoulder Dr. Minoo Patel AOA VIC, Lorne, 2011 The role of the rotator cuff Depress and humeral head (against the force of the deltoid) Keep the humeral head co-apted in the glenoid Initiate
Reverse Total Shoulder Dr. Minoo Patel AOA VIC, Lorne, 2011 The role of the rotator cuff Depress and humeral head (against the force of the deltoid) Keep the humeral head co-apted in the glenoid Initiate
Reverse shoulder arthroplasty : Does reduced medialisation improve radiological and clinical results?
 Acta Orthop. Belg., 2009, 75, 158-166 ORIGINAL STUDY Reverse shoulder arthroplasty : Does reduced medialisation improve radiological and clinical results? Ibrahim KALOUCHE, Nuno SEVIVAS, Abhijeet WAHEGAONKER,
Acta Orthop. Belg., 2009, 75, 158-166 ORIGINAL STUDY Reverse shoulder arthroplasty : Does reduced medialisation improve radiological and clinical results? Ibrahim KALOUCHE, Nuno SEVIVAS, Abhijeet WAHEGAONKER,
Effectiveness of the surgical torque limiter: a model comparing drill- and hand-based screw insertion into locking plates
 Ioannou et al. Journal of Orthopaedic Surgery and Research (2016) 11:118 DOI 10.1186/s13018-016-0458-y RESEARCH ARTICLE Effectiveness of the surgical torque limiter: a model comparing drill- and hand-based
Ioannou et al. Journal of Orthopaedic Surgery and Research (2016) 11:118 DOI 10.1186/s13018-016-0458-y RESEARCH ARTICLE Effectiveness of the surgical torque limiter: a model comparing drill- and hand-based
The use of the Lima reverse shoulder arthroplasty for the treatment of fracture sequelae of the proximal humerus
 J Orthop Sci (2012) 17:141 147 DOI 10.1007/s00776-011-0185-5 ORIGINAL ARTICLE The use of the Lima reverse shoulder arthroplasty for the treatment of fracture sequelae of the proximal humerus Angel Antonio
J Orthop Sci (2012) 17:141 147 DOI 10.1007/s00776-011-0185-5 ORIGINAL ARTICLE The use of the Lima reverse shoulder arthroplasty for the treatment of fracture sequelae of the proximal humerus Angel Antonio
Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty
 Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
0 Introduction (20.9%) [7]
![0 Introduction (20.9%) [7] 0 Introduction (20.9%) [7]](/thumbs/92/108991709.jpg) Chinese Journal of Tissue Engineering Research www.crter.org ( 443000) DOI:10.3969/j.issn.2095-4344.0187 ORCID: 0000-0003-0005-1839() 60 120 2 60 1980 2015 443000 :R318 :A 2017-12-05 3 4 120 60 () 3 (P
Chinese Journal of Tissue Engineering Research www.crter.org ( 443000) DOI:10.3969/j.issn.2095-4344.0187 ORCID: 0000-0003-0005-1839() 60 120 2 60 1980 2015 443000 :R318 :A 2017-12-05 3 4 120 60 () 3 (P
Proximal Humeral Fractures RSA v HHR. Proximal Humeral Fractures RSA v HHR. Introduction
 Proximal Humeral Fractures RSA v HHR Xavier A. Duralde, MD Peachtree Orthopaedic Clinic Atlanta, GA Proximal Humeral Fractures RSA v HHR Consultant: Smith+Nephew Board of Directors: CORR Introduction Incidence
Proximal Humeral Fractures RSA v HHR Xavier A. Duralde, MD Peachtree Orthopaedic Clinic Atlanta, GA Proximal Humeral Fractures RSA v HHR Consultant: Smith+Nephew Board of Directors: CORR Introduction Incidence
Risks of loosening of a prosthetic glenoid implanted in retroversion
 Risks of loosening of a prosthetic glenoid implanted in retroversion Alain Farron, MD, a Alexandre Terrier, PhD, b and Philippe Büchler, PhD, b Lausanne, Switzerland Osteoarthritis of the shoulder is frequently
Risks of loosening of a prosthetic glenoid implanted in retroversion Alain Farron, MD, a Alexandre Terrier, PhD, b and Philippe Büchler, PhD, b Lausanne, Switzerland Osteoarthritis of the shoulder is frequently
Predicting the Position of the Femoral Head Center
 The Journal of Arthroplasty Vol. 14 No. 1 1999 Predicting the Position of the Femoral Head Center Nobuhiko Sugano, MD, Philip C. Noble, PhD, and Emir Kamaric, MS Abstract: To find an accurate method to
The Journal of Arthroplasty Vol. 14 No. 1 1999 Predicting the Position of the Femoral Head Center Nobuhiko Sugano, MD, Philip C. Noble, PhD, and Emir Kamaric, MS Abstract: To find an accurate method to
Revision of reversed total shoulder arthroplasty. Indications and outcome
 Farshad et al. BMC Musculoskeletal Disorders 2012, 13:160 RESEARCH ARTICLE Open Access Revision of reversed total shoulder arthroplasty. Indications and outcome Mazda Farshad *, Marion Grögli, Sabrina
Farshad et al. BMC Musculoskeletal Disorders 2012, 13:160 RESEARCH ARTICLE Open Access Revision of reversed total shoulder arthroplasty. Indications and outcome Mazda Farshad *, Marion Grögli, Sabrina
TrueSight Personalized Planning & Targeting System. Operative technique
 TrueSight Personalized Planning & Targeting System Operative technique TrueSight Personalized Planning & Targeting System Contents Introduction.... 2 Indications and contraindications... 3 Design rationale...
TrueSight Personalized Planning & Targeting System Operative technique TrueSight Personalized Planning & Targeting System Contents Introduction.... 2 Indications and contraindications... 3 Design rationale...
Structure and Function of the Bones and Joints of the Shoulder Girdle
 Structure and Function of the Bones and Joints of the Shoulder Girdle LEARNING OBJECTIVES: At the end of this laboratory exercise the student will be able to: Palpate the important skeletal landmarks of
Structure and Function of the Bones and Joints of the Shoulder Girdle LEARNING OBJECTIVES: At the end of this laboratory exercise the student will be able to: Palpate the important skeletal landmarks of
An evaluation of the radiological changes around the Grammont reverse geometry shoulder arthroplasty after eight to 12 years
 UPPER LIMB An evaluation of the radiological changes around the Grammont reverse geometry shoulder arthroplasty after eight to 12 years B. Melis, M. DeFranco, A. Lädermann, D. Molé, L. Favard, C. Nérot,
UPPER LIMB An evaluation of the radiological changes around the Grammont reverse geometry shoulder arthroplasty after eight to 12 years B. Melis, M. DeFranco, A. Lädermann, D. Molé, L. Favard, C. Nérot,
Bulletin of the Hospital for Joint Diseases 2013;71(4):284-93
 284 Impact of Inferior Glenoid Tilt, Humeral Retroversion, Bone Grafting, and Design Parameters on Muscle Length and Wrapping in Reverse Shoulder Arthroplasty Christopher P. Roche, M.S., M.B.A., Phong
284 Impact of Inferior Glenoid Tilt, Humeral Retroversion, Bone Grafting, and Design Parameters on Muscle Length and Wrapping in Reverse Shoulder Arthroplasty Christopher P. Roche, M.S., M.B.A., Phong
Posterior Glenoid Wear in Total Shoulder Arthroplasty:
 Posterior Glenoid Wear in Total Shoulder Arthroplasty: Eccentric Anterior Reaming is Superior to Posterior Augment Tim Wang MD, Geoffrey Abrams MD, Anthony Behn MS, Emilie Cheung MD Department of Orthopaedic
Posterior Glenoid Wear in Total Shoulder Arthroplasty: Eccentric Anterior Reaming is Superior to Posterior Augment Tim Wang MD, Geoffrey Abrams MD, Anthony Behn MS, Emilie Cheung MD Department of Orthopaedic
Introduction. Rarely does a single muscle act in isolation at the shoulder complex.
 Shoulder complex 1 Introduction Our study of the upper limb begins with the shoulder complex, a set of four articulations involving the sternum, clavicle, ribs, scapula, and humerus. Rarely does a single
Shoulder complex 1 Introduction Our study of the upper limb begins with the shoulder complex, a set of four articulations involving the sternum, clavicle, ribs, scapula, and humerus. Rarely does a single
SHOULDER JOINT ANATOMY AND KINESIOLOGY
 SHOULDER JOINT ANATOMY AND KINESIOLOGY SHOULDER JOINT ANATOMY AND KINESIOLOGY The shoulder joint, also called the glenohumeral joint, consists of the scapula and humerus. The motions of the shoulder joint
SHOULDER JOINT ANATOMY AND KINESIOLOGY SHOULDER JOINT ANATOMY AND KINESIOLOGY The shoulder joint, also called the glenohumeral joint, consists of the scapula and humerus. The motions of the shoulder joint
DESIGN RATIONALE AND SURGICAL TECHNIQUE
 DESIGN RATIONALE AND SURGICAL TECHNIQUE ANCHOR PEG GLENOID DESIGN RATIONALE In total shoulder arthroplasty, most cases of clinical and radiographic loosening involve failure of the fixation of the glenoid
DESIGN RATIONALE AND SURGICAL TECHNIQUE ANCHOR PEG GLENOID DESIGN RATIONALE In total shoulder arthroplasty, most cases of clinical and radiographic loosening involve failure of the fixation of the glenoid
The Reverse Total Shoulder Arthroplasty
 This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. The Reverse Total Shoulder Arthroplasty Frederick A. Matsen, III, Pascal
This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. The Reverse Total Shoulder Arthroplasty Frederick A. Matsen, III, Pascal
Understanding mechanical trade-offs in changing centers of rotation for reverse shoulder arthroplasty design
 University of Iowa Iowa Research Online Theses and Dissertations Spring 2014 Understanding mechanical trade-offs in changing centers of rotation for reverse shoulder arthroplasty design Vijay Niels Permeswaran
University of Iowa Iowa Research Online Theses and Dissertations Spring 2014 Understanding mechanical trade-offs in changing centers of rotation for reverse shoulder arthroplasty design Vijay Niels Permeswaran
Aequalis -Glenoid. Keeled and Pegged. Surgical Technique
 Aequalis -Glenoid Keeled and Pegged Surgical Technique TABLE OF CONTENTS COMMON OPERATIVE TECHNIQUES FOR THE KEELED AND PEGGED AEQUALIS-GLENOIDS p. 1-3 IMPLANTATION OF THE AEQUALIS KEELED GLENOID p. 4-5
Aequalis -Glenoid Keeled and Pegged Surgical Technique TABLE OF CONTENTS COMMON OPERATIVE TECHNIQUES FOR THE KEELED AND PEGGED AEQUALIS-GLENOIDS p. 1-3 IMPLANTATION OF THE AEQUALIS KEELED GLENOID p. 4-5
Bipolar Radial Head System
 Bipolar Radial Head System Katalyst Surgical Technique DESCRIPTION The Katalyst Telescoping Bipolar Radial Head implant restores the support and bearing surface of the radial head in the face of fracture,
Bipolar Radial Head System Katalyst Surgical Technique DESCRIPTION The Katalyst Telescoping Bipolar Radial Head implant restores the support and bearing surface of the radial head in the face of fracture,
Glenoid baseplate fixation using hybrid configurations of locked and unlocked peripheral screws
 J Orthop Traumatol (2017) 18:221 228 DOI 10.1007/s10195-016-0438-3 ORIGINAL ARTICLE Glenoid baseplate fixation using hybrid configurations of locked and unlocked peripheral screws Nathan T. Formaini 1
J Orthop Traumatol (2017) 18:221 228 DOI 10.1007/s10195-016-0438-3 ORIGINAL ARTICLE Glenoid baseplate fixation using hybrid configurations of locked and unlocked peripheral screws Nathan T. Formaini 1
TORNIER AEQUALIS REVERSED II. Shoulder System SURGICAL TECHNIQUE
 TORNIER AEQUALIS REVERSED II Shoulder System SURGICAL TECHNIQUE 2 Table of Contents: Implant Description...4 Implant Indications and Contraindications...6 Surgical Technique...7 Pre-operative Planning...7
TORNIER AEQUALIS REVERSED II Shoulder System SURGICAL TECHNIQUE 2 Table of Contents: Implant Description...4 Implant Indications and Contraindications...6 Surgical Technique...7 Pre-operative Planning...7
AEQUALIS PERFORM + REVERSED
 TO R N I E R AEQUALIS PERFORM + REVERSED Glenoid WEDGED AUGMENT SURGIC AL TECHNIQUE Table of Contents: AEQUALIS PERFORM + REVERSED Glenoid...3 Overview...3 Indications/Contraindications...4 Pre-Operative
TO R N I E R AEQUALIS PERFORM + REVERSED Glenoid WEDGED AUGMENT SURGIC AL TECHNIQUE Table of Contents: AEQUALIS PERFORM + REVERSED Glenoid...3 Overview...3 Indications/Contraindications...4 Pre-Operative
Fixed and Variable Geometry Total Shoulder Arthroplasty
 Fixed and Variable Geometry Total Shoulder Arthroplasty RECOVERY FUNCTION SURVIVORSHIP DePuy believes in an approach to total shoulder replacement that places equal importance on recovery, function and
Fixed and Variable Geometry Total Shoulder Arthroplasty RECOVERY FUNCTION SURVIVORSHIP DePuy believes in an approach to total shoulder replacement that places equal importance on recovery, function and
Does Humeral Component Lateralization in Reverse Shoulder Arthroplasty Affect Rotator Cuff Torque? Evaluation in a Cadaver Model
 Clin Orthop Relat Res (2017) 475:2564 2571 DOI 10.1007/s11999-017-5413-7 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Does Humeral
Clin Orthop Relat Res (2017) 475:2564 2571 DOI 10.1007/s11999-017-5413-7 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Does Humeral
Challenges of Shoulder Arthroplasty
 Challenges, Complications and Value Jonathan Levy, MD Shoulder & Elbow Surgeon Chief, Orthopaedic Surgery Holy Cross Hospital Medical Director, Holy Cross Orthopaedic Research Institute Director, ASES
Challenges, Complications and Value Jonathan Levy, MD Shoulder & Elbow Surgeon Chief, Orthopaedic Surgery Holy Cross Hospital Medical Director, Holy Cross Orthopaedic Research Institute Director, ASES
Anatomy of the Shoulder Girdle. Prof Oluwadiya Kehinde FMCS (Orthop)
 Anatomy of the Shoulder Girdle Prof Oluwadiya Kehinde FMCS (Orthop) www.oluwadiya.com Bony Anatomy Shoulder Complex: Sternum(manubrium) Clavicle Scapula Proximal humerus Manubrium Sterni Upper part of
Anatomy of the Shoulder Girdle Prof Oluwadiya Kehinde FMCS (Orthop) www.oluwadiya.com Bony Anatomy Shoulder Complex: Sternum(manubrium) Clavicle Scapula Proximal humerus Manubrium Sterni Upper part of
Accuracy of Humeral Articular Surface Restoration in a Novel Anatomic Shoulder Arthroplasty Technique and Design: A Cadaveric Study
 Original Scientific Research Accuracy of Humeral Articular Surface Restoration in a Novel Anatomic Shoulder Arthroplasty Technique and Design: A Cadaveric Study Journal of Shoulder and Elbow Arthroplasty
Original Scientific Research Accuracy of Humeral Articular Surface Restoration in a Novel Anatomic Shoulder Arthroplasty Technique and Design: A Cadaveric Study Journal of Shoulder and Elbow Arthroplasty
P V S MEMORIAL HOSPITAL LTD.
 SHOULDER XRAYS Instability Series o True AP (Grashey s) o Axillary o Stryker Notch view o True AP in Internal rotation o Scapular Y view o West Point view for Bony Bankart ( looks like modif axillary view)
SHOULDER XRAYS Instability Series o True AP (Grashey s) o Axillary o Stryker Notch view o True AP in Internal rotation o Scapular Y view o West Point view for Bony Bankart ( looks like modif axillary view)
TORNIER BLUEPRINT. 3D Planning + PSI THE VALUE OF BLUEPRINT
 TORNIER BLUEPRINT D Planning + PSI THE VALUE OF BLUEPRINT BLUEPRINT D Planning + PSI BLUEPRINT D Planning + PSI is a surgeon controlled, automated, D pre-operative planning software with optional patient
TORNIER BLUEPRINT D Planning + PSI THE VALUE OF BLUEPRINT BLUEPRINT D Planning + PSI BLUEPRINT D Planning + PSI is a surgeon controlled, automated, D pre-operative planning software with optional patient
S H O U L D E R Solutions by Tornier. BIO-RSA TM ANGled SURGICAL TECHNIQUE. BIO-RSA Angled. surgical technique
 S H O U L D E R Solutions by Tornier BIO-RSA TM ANGled SURGICAL TECHNIQUE BIO-RSA Angled Bony increased offset - reversed shoulder arthroplasty surgical technique BIO-RSA TM ANGled SURGICAL TECHNIQUE BIO-RSA
S H O U L D E R Solutions by Tornier BIO-RSA TM ANGled SURGICAL TECHNIQUE BIO-RSA Angled Bony increased offset - reversed shoulder arthroplasty surgical technique BIO-RSA TM ANGled SURGICAL TECHNIQUE BIO-RSA
FACTORS AFFECTING THE STABILITY OF REVERSE SHOULDER ARTHROPLASTY
 FACTORS AFFECTING THE STABILITY OF REVERSE SHOULDER ARTHROPLASTY by Allison Loretta Clouthier A thesis submitted to the Department of Mechanical and Materials Engineering In conformity with the requirements
FACTORS AFFECTING THE STABILITY OF REVERSE SHOULDER ARTHROPLASTY by Allison Loretta Clouthier A thesis submitted to the Department of Mechanical and Materials Engineering In conformity with the requirements
Advantages to medialize less
 Advantages to medialize less less RSP? Clinical and radiological results Ph Valenti, D Katz, Ph Sauzieres J Kany, K Elkolti, P Gleyze Paris, Lorient, Toulouse, Lyon, Colmar Delta RSP CTA pseudoparalytic
Advantages to medialize less less RSP? Clinical and radiological results Ph Valenti, D Katz, Ph Sauzieres J Kany, K Elkolti, P Gleyze Paris, Lorient, Toulouse, Lyon, Colmar Delta RSP CTA pseudoparalytic
Reverse Shoulder Glenoid Loosening
 S12 Reverse Shoulder Glenoid Loosening An Evaluation of the Initial Fixation Associated with Six Different Reverse Shoulder Designs Nick Stroud, M.S., Matthew J. DiPaola, M.D., Pierre-Henri Flurin, M.D.,
S12 Reverse Shoulder Glenoid Loosening An Evaluation of the Initial Fixation Associated with Six Different Reverse Shoulder Designs Nick Stroud, M.S., Matthew J. DiPaola, M.D., Pierre-Henri Flurin, M.D.,
Biomechanics of reverse total shoulder arthroplasty
 J Shoulder Elbow Surg (2015) 24, 150-160 www.elsevier.com/locate/ymse REVIEW ARTICLE Biomechanics of reverse total shoulder arthroplasty Jonathan L. Berliner, MD*, Ashton Regalado-Magdos, BS, C. Benjamin
J Shoulder Elbow Surg (2015) 24, 150-160 www.elsevier.com/locate/ymse REVIEW ARTICLE Biomechanics of reverse total shoulder arthroplasty Jonathan L. Berliner, MD*, Ashton Regalado-Magdos, BS, C. Benjamin
TORNIER BIO-RSA. Bony Increased Offset - Reversed Shoulder Arthroplasty SURGICAL TECHNIQUE
 TORNIER BIO-RSA Bony Increased Offset - Reversed Shoulder Arthroplasty SURGICAL TECHNIQUE 2 Table of Contents: Concept...4 Bony Increased Offset Reversed Shoulder Arthroplasty (BIO-RSA ) Concept...4 Surgical
TORNIER BIO-RSA Bony Increased Offset - Reversed Shoulder Arthroplasty SURGICAL TECHNIQUE 2 Table of Contents: Concept...4 Bony Increased Offset Reversed Shoulder Arthroplasty (BIO-RSA ) Concept...4 Surgical
Evaluation of bone impingement prediction in pre-operative planning for shoulder arthroplasty
 4 Evaluation of bone impingement prediction in pre-operative planning for shoulder arthroplasty Peter R. Krekel 1, Paul W. de Bruin 1, Edward R. Valstar 1, Piet M. Rozing 1, Frits H. Post 2, Charl P. Botha
4 Evaluation of bone impingement prediction in pre-operative planning for shoulder arthroplasty Peter R. Krekel 1, Paul W. de Bruin 1, Edward R. Valstar 1, Piet M. Rozing 1, Frits H. Post 2, Charl P. Botha
Technique. Aequalis -Reversed II. Reversed Shoulder Prosthesis.
 Surgical Technique Reversed Shoulder Prosthesis www.tornier.com Proper surgical procedures and techniques are the responsibility of the medical professional. Individual surgeon evaluation of the surgical
Surgical Technique Reversed Shoulder Prosthesis www.tornier.com Proper surgical procedures and techniques are the responsibility of the medical professional. Individual surgeon evaluation of the surgical
SURGICAL TECHNIQUE DUAL-PLATFORM SHOULDER ARTHROPLASTY.
 SURGICAL TECHNIQUE DUAL-PLATFORM SHOULDER ARTHROPLASTY www.fhortho.com SURGICAL TECHNIQUE REFERENCE NUMBERS HUMERAL STEMS REFERENCE DIAMETER HEIGHT 267 360 Ø 06 100 265 102 Ø 08 120 265 103 Ø 08 170 265
SURGICAL TECHNIQUE DUAL-PLATFORM SHOULDER ARTHROPLASTY www.fhortho.com SURGICAL TECHNIQUE REFERENCE NUMBERS HUMERAL STEMS REFERENCE DIAMETER HEIGHT 267 360 Ø 06 100 265 102 Ø 08 120 265 103 Ø 08 170 265
Reverse shoulder arthroplasty for the treatment of three and four part fractures of the proximal humerus in patients older than 75 years old
 Acta Orthop. Belg., 2014, 80, 99-105 ORIGINAL STUDY Reverse shoulder arthroplasty for the treatment of three and four part fractures of the proximal humerus in patients older than 75 years old Aristotelis
Acta Orthop. Belg., 2014, 80, 99-105 ORIGINAL STUDY Reverse shoulder arthroplasty for the treatment of three and four part fractures of the proximal humerus in patients older than 75 years old Aristotelis
Open reduction; plate fixation 1 Principles
 Executive Editor: Peter Trafton Authors: Martin Jaeger, Frankie Leung, Wilson Li Proximal humerus 11-A2 Open reduction, plate fixation Search search... Shortcuts All Preparations All Approaches All Reductions
Executive Editor: Peter Trafton Authors: Martin Jaeger, Frankie Leung, Wilson Li Proximal humerus 11-A2 Open reduction, plate fixation Search search... Shortcuts All Preparations All Approaches All Reductions
Conversion of Anatomic TSA to RSA
 Conversion of Anatomic TSA to RSA Joseph A. Abboud, M.D. Professor of Shoulder and Elbow Surgery Senior Vice-President at the Rothman Institute Philadelphia, PA Disclosures Joseph A. Abboud, MD Depuy Synthes
Conversion of Anatomic TSA to RSA Joseph A. Abboud, M.D. Professor of Shoulder and Elbow Surgery Senior Vice-President at the Rothman Institute Philadelphia, PA Disclosures Joseph A. Abboud, MD Depuy Synthes
Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
Index. B Backslap technique depth assessment, 82, 83 diaphysis distal trocar, 82 83
 Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
AJO DO NOT COPY. The low grade of the intrinsic stability of the shoulder. Total Reverse Shoulder Arthroplasty: European Lessons and Future Trends
 A Review Paper Total Reverse Shoulder Arthroplasty: European Lessons and Future Trends Ludwig Seebauer, MD Abstract In the late 1980s, Grammont introduced a new reverse total shoulder arthroplasty (TSA),
A Review Paper Total Reverse Shoulder Arthroplasty: European Lessons and Future Trends Ludwig Seebauer, MD Abstract In the late 1980s, Grammont introduced a new reverse total shoulder arthroplasty (TSA),
Scapular Notching on Kinematic Simulated Range of Motion After Reverse Shoulder Arthroplasty Is Not the Result of Impingement in Adduction
 Article Scapular Notching on Kinematic Simulated Range of Motion After Reverse Shoulder Arthroplasty Is Not the Result of Impingement in Adduction LAEDERMANN, Alexandre, et al. Abstract Impingement after
Article Scapular Notching on Kinematic Simulated Range of Motion After Reverse Shoulder Arthroplasty Is Not the Result of Impingement in Adduction LAEDERMANN, Alexandre, et al. Abstract Impingement after
Percutaneous Humeral Fracture Repair Surgical Technique
 Percutaneous Humeral Fracture Repair Surgical Technique Percutaneous Pinning Percutaneous Humeral Fracture Repair Closed reduction followed by percutaneous fixation reduces risk from soft tissue dissection
Percutaneous Humeral Fracture Repair Surgical Technique Percutaneous Pinning Percutaneous Humeral Fracture Repair Closed reduction followed by percutaneous fixation reduces risk from soft tissue dissection
Table of Contents. Aequalis-Reversed shoulder prosthesis Biomechanics, indications and contraindications 2
 Table of Contents Aequalis-Reversed shoulder prosthesis Biomechanics, indications and contraindications 2 The Aequalis-Reversed 3 and 4 Surgical technique Pre-operative planning 5 Patient positioning 5
Table of Contents Aequalis-Reversed shoulder prosthesis Biomechanics, indications and contraindications 2 The Aequalis-Reversed 3 and 4 Surgical technique Pre-operative planning 5 Patient positioning 5
Simulator Based Experimental Motion Analysis of 3D Printed Artificial Shoulder Joint Geometries
 EPiC Series in Health Sciences Volume 1, 2017, Pages 82 87 CAOS 2017. 17th Annual Meeting of the International Society for Computer Assisted Orthopaedic Surgery Health Sciences Simulator Based Experimental
EPiC Series in Health Sciences Volume 1, 2017, Pages 82 87 CAOS 2017. 17th Annual Meeting of the International Society for Computer Assisted Orthopaedic Surgery Health Sciences Simulator Based Experimental
Acu-Sinch Repair System. Technical Monograph
 Acu-Sinch Repair System Technical Monograph Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that improve
Acu-Sinch Repair System Technical Monograph Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that improve
Comprehensive Reverse Shoulder System
 Comprehensive Reverse Shoulder System Comprehensive Reverse Shoulder System Simple. Versatile. The Comprehensive Reverse Shoulder System is the next generation reverse shoulder prosthesis, offering unmatched
Comprehensive Reverse Shoulder System Comprehensive Reverse Shoulder System Simple. Versatile. The Comprehensive Reverse Shoulder System is the next generation reverse shoulder prosthesis, offering unmatched
ReUnion RSA Shoulder System
 ReUnion RSA Shoulder System Reverse Surgical Protocol This document is intended to be used by healthcare professionals only. ReUnion RSA Reverse Shoulder Surgical Protocol Table of Contents Surgical Technique
ReUnion RSA Shoulder System Reverse Surgical Protocol This document is intended to be used by healthcare professionals only. ReUnion RSA Reverse Shoulder Surgical Protocol Table of Contents Surgical Technique
Disclosures A prospective comparison between reverse and anatomic total shoulder arthroplasty
 Disclosures A prospective comparison between reverse and anatomic total shoulder arthroplasty Tuyen Kiet Micah Naimark, MD Brian T. Feeley, MD Teddy T. Chung Tatiana Gajiu Sarah L. Hall, MA C. Benjamin
Disclosures A prospective comparison between reverse and anatomic total shoulder arthroplasty Tuyen Kiet Micah Naimark, MD Brian T. Feeley, MD Teddy T. Chung Tatiana Gajiu Sarah L. Hall, MA C. Benjamin
Reverse Prostheses in Arthropathies With Cuff Tear
 Clin Orthop Relat Res (2011) 469:2469 2475 DOI 10.1007/s11999-011-1833-y SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Reverse Prostheses in Arthropathies With Cuff Tear Are Survivorship and Function
Clin Orthop Relat Res (2011) 469:2469 2475 DOI 10.1007/s11999-011-1833-y SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Reverse Prostheses in Arthropathies With Cuff Tear Are Survivorship and Function
Morphometric and Morphological Study of the Glenoid Cavity of Human Scapulae in Rayalaseema Zone of South India and It s Surgical Significance
 Original Research Paper Medical Science Morphometric and Morphological Study of the Glenoid Cavity of Human Scapulae in Rayalaseema Zone of South India and It s Surgical Significance Dr. G. Manoj Kumar
Original Research Paper Medical Science Morphometric and Morphological Study of the Glenoid Cavity of Human Scapulae in Rayalaseema Zone of South India and It s Surgical Significance Dr. G. Manoj Kumar
Biomechanics of Two Reconstruction Techniques for Elbow Ulnar Collateral Ligament Insufficiency
 Biomechanics of Two Reconstruction Techniques for Elbow Ulnar Collateral Ligament Insufficiency Justin E. Chronister, MD 1, Randal P. Morris, BS 2, Clark R. Andersen, MS 2, J. Michael Bennett, MD 3, Thomas
Biomechanics of Two Reconstruction Techniques for Elbow Ulnar Collateral Ligament Insufficiency Justin E. Chronister, MD 1, Randal P. Morris, BS 2, Clark R. Andersen, MS 2, J. Michael Bennett, MD 3, Thomas
Reverse Total Shoulder Arthroplasty: Early Outcome and Complication Report
 ORIGINAL ARTICLE Clinics in Shoulder and Elbow Vol. 17, No. 2, June, 2014 http://dx.doi.org/10.5397/cise.2014.17.2.68 CiSE Clinics in Shoulder and Elbow Reverse Total Shoulder Arthroplasty: Early Outcome
ORIGINAL ARTICLE Clinics in Shoulder and Elbow Vol. 17, No. 2, June, 2014 http://dx.doi.org/10.5397/cise.2014.17.2.68 CiSE Clinics in Shoulder and Elbow Reverse Total Shoulder Arthroplasty: Early Outcome
AEQUALIS TM REVERSED II
 TORNIER AEQUALIS TM REVERSED II SURGICAL TECHNIQUE Tornier Upper Extremities Contents Chapter 1 4 Chapter 2 6 6 6 6 7 24 Appendix A 26 Appendix B 27 Appendix C 35 Implant Description Surgical Technique
TORNIER AEQUALIS TM REVERSED II SURGICAL TECHNIQUE Tornier Upper Extremities Contents Chapter 1 4 Chapter 2 6 6 6 6 7 24 Appendix A 26 Appendix B 27 Appendix C 35 Implant Description Surgical Technique
what you is back within LOVE arm s reach find out why the exactech shoulder may be right for you
 TOTAL shoulder REPLACEMENT what you is back within LOVE arm s reach find out why the exactech shoulder may be right for you how does your shoulder work? The shoulder is the most mobile joint in the body.
TOTAL shoulder REPLACEMENT what you is back within LOVE arm s reach find out why the exactech shoulder may be right for you how does your shoulder work? The shoulder is the most mobile joint in the body.
GB UDRT061 25/07/06 9:30 Page 32. Surgical. Technique. Shoulder Prosthesis. Aequalis-Reversed
 GB UDRT061 25/07/06 9:30 Page 32 Surgical Technique Shoulder Prosthesis Aequalis-Reversed GB UDRT061 25/07/06 9:29 Page 1 Table of Contents Aequalis-Reversed shoulder prosthesis Biomechanics, indications
GB UDRT061 25/07/06 9:30 Page 32 Surgical Technique Shoulder Prosthesis Aequalis-Reversed GB UDRT061 25/07/06 9:29 Page 1 Table of Contents Aequalis-Reversed shoulder prosthesis Biomechanics, indications
A 42-year-old patient presenting with femoral
 Kanda et al. Journal of Medical Case Reports 2015, 9:17 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access A 42-year-old patient presenting with femoral head migration after hemiarthroplasty performed
Kanda et al. Journal of Medical Case Reports 2015, 9:17 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access A 42-year-old patient presenting with femoral head migration after hemiarthroplasty performed
Effects of Scapular Notching and Bone Remodelling on Long-Term Fixation of the Glenoid Component in Reverse Shoulder Arthroplasty.
 Effects of Scapular Notching and Bone Remodelling on Long-Term Fixation of the Glenoid Component in Reverse Shoulder Arthroplasty by Min Zhang A thesis submitted for the degree of Doctor of Philosophy
Effects of Scapular Notching and Bone Remodelling on Long-Term Fixation of the Glenoid Component in Reverse Shoulder Arthroplasty by Min Zhang A thesis submitted for the degree of Doctor of Philosophy
