Microparticulate Cortical Allograft: An Alternative to Autograft in the Treatment of Osseous Defects
|
|
|
- Dennis Rich
- 5 years ago
- Views:
Transcription
1 The Open Orthopaedics Journal, 2008, 2, Open Access Microparticulate Cortical Allograft: An Alternative to Autograft in the Treatment of Osseous Defects H. Thomas Temple * and Theodore I. Malinin Tissue Bank, Department of Orthopaedics, University of Miami, Miller School of Medicine, Miami, Florida, USA Abstract: Benign bone tumors are commonly diagnosed and treated. Following tumor removal, the defect in the bone can be filled with auto- or allografts, (degradable) bone substitutes or non-degradable polymethylmethacrylate. The ideal substitute for this purpose should provide immediate structural support and readily incorporate into bone over a short period of time. Experimentally, microparticulate allograft has been shown to incorporate quickly in metaphyseal and metadiaphyseal cortico-cancellous defects in primates [1]. Using a combination of small allogeneic cortical graft particles (< 250 μm), bone defects were filled following intralesional excision in 97 consecutive patients with benign and low grade malignant tumors and tumor-like conditions of bone. The clinical results and rate of radiographic incorporation and osseous consolidation were recorded and analyzed. These patients underwent 104 procedures in which osseous defects were packed with microparticulate allograft. The follow-up was from 23 to 49 months. There were 94 (90.3%) closed defects and 10 (9.7%) open defects. The average size of the grafted defect was 42.8 cm 3 ( cm 3 ). Internal fixation was used in 11 of the 104 procedures (10.6 %). Radiographically, incorporation was observed in 91% of patients and consolidation in 60%. There were eleven failures (10.6 %), eight (72 %) due to tumor recurrence. Seven of eight patients with tumor recurrence underwent a second resection and grafting procedure that resulted in allograft incorporation and defect healing. There were two deep infections requiring debridement with retention of the graft; both resolved with satisfactory healing. Both incorporation and consolidation were observed in over 90% of patients with a low rate of complications. The use of small-particle cortical allograft proved to be an effective alternative to autogenous bone graft in patients with metaphyseal and metadiaphyseal surgical bone defects. INTRODUCTION Benign bone tumors and tumor-like conditions of bone are rather common. After these lesions are surgically removed the defects are usually filled with either an autograft, an allograft, a variety of bone substitutes or polymethylmethacrylate. Ideally, the material selected should be both osteoconductive and osteoinductive, it should provide sufficient early mechanical stability, and it should allow the regeneration of normal bone in a short period of time. Advances in surgical technology, during the latter half of the twentieth century, have coincided with an increase in the use of new materials and complex surgical procedures for bone repair [2-6]. Autogenous bone is still considered to be the gold standard for bone grafting. It provides three elements necessary to generate and maintain bone: scaffolding for osteoconduction, growth factors for osteoinduction, and progenitor cells for osteogenesis. Cancellous autograft, however, is in limited supply and its harvesting can result in significant donor site morbidity. Allografts, on the other hand, may not have similar osteoinductive properties to autografts, depending on the way these grafts have been processed. Since the means of preparation and storage, and the structural form of the allograft may significantly affect graft incorporation, its use has been associated with mixed clinical *Address correspondence to this author at the Tissue Bank, Department of Orthopaedics, University of Miami, Miller School of Medicine, Miami, Florida 33101, USA; htemple@med.miami.edu results. Therefore in the past several years, there has been an explosion in the development of bone substitutes, growth factors, and combinations of the two that have made their way to the medical market [3,4]. Well designed clinical trials, however, have not yet demonstrated their efficacy or safety [2]. As the orthopaedic oncologist s ability to achieve local control of bone tumors improves, emphasis is placed on healing of the bone cavity to achieve early function [5, 7]. For most benign tumors, intralesional curetting and bone grafting is the treatment of choice [8]. The materials used to achieve this are: autograft, bone substitutes, cement, and allograft. The usefulness of autograft is limited by availability and donor morbidity. Donor site complications, infection and lateral femoral cutaneous nerve injury, as well as structural insufficiency that can lead to fracture may result in increased patient recovery time, disability, and chronic pain [3]. Furthermore, the residual pain and disability that may result from harvesting cancellous iliac crest bone can be relatively long-lasting. These problems justify continued efforts to find effective bone graft substitutes as alternatives to autografts [4, 9]. Biocompatible substitute materials, such as porous hydroxyapatite, tricalcium phosphate, etc offer the surgeon additional choices in the repair of cavitary long bone defects [3, 6]. The ideal composite synthetic grafts should effectively combine the three salient bone-forming properties / Bentham Open
2 92 The Open Orthopaedics Journal, 2008, Volume 2 Temple and Malinin (osteoinduction, osteoconduction and progenitor cells) [6]. The drawbacks of many substitutes include low biocompatibility, poor restorability, inclusion of processed animal components, inferior handling characteristics, and cost. In clinical practice, incomplete healing has occurred commonly in patients with large lesions [5]. Further investigation, in animal models, evaluating different defect sizes and biomechanical conditions will help to determine the appropriate use for these materials [10, 11]. Polymethymethacrylate (PMMA) has been used to fill large subchondral defects following removal of giant cell tumors.. Once polymerized, PMMA resists axial loading and thus provides immediate structural support. Moreover, the exothermic reaction during polymerization is thought by some to extend the margin of resection. PMMA, however, has no biologic activity and cannot remodel in the face of changing stresses. Therefore, it is less desirable for the treatment of curable lesions when the goal is complete restoration of anatomy and function [12]. Allograft bone has now been used clinically for more than 50 years for various orthopaedic indications [13-16]. Allografts are available in reasonable quantities and are versatile since shape, contour, and mineral density can be altered and tailored to a particular clinical indication. Allograft structure is very important when considering the type of defect and the means by which the graft can be expected to incorporate over time. Materials such as DBM (Demineralized Bone Matrix), DFDBA (Demineralized Freeze-Dried Bone Allograft), allograft paste, powder, chips, strips and putty, all have different mechanical and osteoinductive properties [17-20]. Osteoinductive properties of allograft bone can be altered by many different secondary sterilization techniques. Allograft chips, when used to fill acetabular defects in total hip revision surgery, have shown, in microscopic preparations, to incorporate within 3 weeks [14, 19]. Massive allografts, incompletely incorporate from the periphery inward by a process of creeping substitution [21]. Unpredictable clinical results have been reported with these for a variety of reasons [15, 18]. On the other hand cortical microparticulate allograft incorporates rapidly due to exposed inductive proteins from the large trabecular surface area and interconnected spaces [1, 9]. Furthermore, due to the small particle size, the resorptive phase of bone healing is accelerated. Independent of the type of graft used, the size of graft particles has an important effect on incorporation [1, 22, 23]. Thus, Shapoff, et al. [22] demonstrated increased osteogenesis with small particle, freeze-dried bone allograft when compared to larger particles. However the studies of Syftestad an Urist [23], showed that very small particle sizes (under 125 μm) provided an increase in surface area that enhanced the generation of mechanically-induced free radicals resulting in increased solubility of bone matrix proteins and decreased bone production. Allograft particle size is also related to resistance to shear stresses. In vitro experiments, using morsellised allograft bone, have shown that the graft s mechanical properties improve with increasing normal load and with increasing shear strains (strain hardening) [24]. Further studies were needed to determine the optimal allograft particle size for filling bone defects. These were provided by the experiments on non-human primates and were applied to the present clinical investigation [1, 7]. Optimal osteoconduction is provided by direct apposition between host bone and the implant. The host bone must be viable, the host bone/implant interface must be stable and the implant needs to have a structure (porosity) that allows new bone in-growth. Also important is the fact that optimal incorporation of the graft occurs when histocompatibility differences are minimized by either matching tissue types or by treating the allograft with techniques that reduce immunogenicity [13]. Although freezing significantly reduces antigenicity and thus the inflammatory response it does not reduce it as much as does freeze-drying [7]. Furthermore, although allografts pose a known risk of bacterial contamination and viral transmission, rigorous tissue screening and microbiologic and serologic testing of donor tissue reduce these risks to theoretical possibilities [13]. The microparticulate allograft is a mixture of mineralized cortical bone particles of a standard combination of sizes between 100 and than 250 microns. This provides an optimal scaffold for delivering osteoinductive growth factors. This preparation has an appropriate 3-dimensional (3-D) structure to serve as an osteoconductive matrix for bone-forming cells. The purpose of this study was to evaluate, in a prospective, consecutive series of patients, the results obtained with freeze-dried small-particle cortical allograft as an alternative for autogenous bone graft in filling bone defects created by tumor ablation. Our hypothesis was that freeze-dried cortical microparticulate allografts would induce healing of bone defects in a manner similar to autografts. Freeze-dried microparticulate allografts were chosen because they were shown to incorporate faster than frozen microparticulate allografts [7]. Likewise cortical bone particulate allografts with particle sizes from 300 to 90 were shown experimentally to produce healing of bone defects in a manner and rate that was identical to that produced by autografts [1]. MATERIALS AND METHODS Ninety seven consecutive patients with benign and low grade malignant bone tumors and tumor-like conditions of bone, aged 12 to 75 years (35.2 years mean), underwent a total of 104 procedures between January 2000 and October There were 53 females (50%) and 44 males (46%) Patients had pre-operative imaging studies that included radiographs, computerized tomography, magnetic resonance imaging and bone scintigraphy when appropriate. Needle biopsies were performed pre-operatively in some patients, but most patients underwent an open biopsy at the time of definitive surgery to confirm the diagnosis. Tumors were classified as benign latent, benign aggressive, and low-grade malignant. The microparticulate cortical bone allograft was prepared by the University of Miami Tissue Bank (Miami, FL) according to a previously described method (7). This allograft was generated from a single donor. Freeze-dried cortical bone particles were less than 250 μm in maximum dimension and over 100 mm in minimum dimension. All bones from which allografts were prepared were excised and processed aseptically. The allografts were processed in compliance with Food and Drug Administration and American Association of Tissue Banks standards. The microparticulate al-
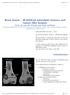
3 Microparticulate Cortical Allograft The Open Orthopaedics Journal, 2008, Volume 2 93 lograft was reconstituted with sterile saline (Fig. 1) or left in its original state, and packed or injected into the defect under fluoroscopy. The graft was injected percutaneously or packed through an open wound. RESULTS Diagnostic categories included: cystic (25), fibrous (15), chondroid (36), giant cell lesions (14), osteomyelitis (1), osteonecrosis (1), osseous tumor (3), lymphoma (1) and cavitary non-union (1) There were 65 benign latent lesions, 27 benign aggressive tumors and 5 low-grade malignant tumors. The most common sites of disease were distal femur, proximal tibia, proximal humerus, pelvis and distal tibia (Table 1). Table 1. Anatomic Locations of Lesions Site Number & Percent Proximal femur 5 (5.2) Distal femur 33 (34%) Proximal tibia 18(18.6) Distal tibia 6 (6.2) Proximal humerus 8 (8.4) Fig. (1). Cortical microparticulate allograft reconstituted with saline. Biplanar radiographs of the operated site were obtained at the time of surgery, and at 6 weeks, 3 months, 6 months and one year after the procedure. The patients were then followed for up to 4 years. In order to assess the incorporation of the bone graft, each radiograph was reviewed by two independent examiners. The following parameters were evaluated: 1) Presence or absence of trabeculae within the grafted defect, 2) Overall bone density, 3) Quality of bone at the border of graft (described as well defined, hazy or invisible), and 4) Bone density within the defect (described as same as, equal to, or less than adjacent normal bone). Incorporation was said to be present if the border between graft and cavity was vague and trabeculae were present at the interface. Consolidation was identified if the border between graft and cavity was not identifiable, trabeculae were present at the interface, and the density of bone graft was the same as that of the adjacent normal bone. Failure was determined to have occurred when a secondary operation to revise the primary bone graft procedure was needed or when there was no radiographic evidence of graft incorporation. The follow-up interval was defined as the period of time from the last operative intervention to the last clinical and radiographic evaluation. In addition to the radiological data, variables analyzed included: patient age, gender, diagnosis, site of disease, defect size, procedure performed, presence or absence of a preoperative fracture, and complications related to surgery. A notation was made about the type of defect, either open or closed. A closed defect was defined as a defect within bone with well contained graft whereas an open defect was generally located on the surface of bone and bordered only by periosteum or muscle. Data was stored and collated on Microsoft Excel software and then transferred to SPSS software for analysis. Distal humerus 3 ( 3.1 ) Proximal radius 1 (1) Distal radius 2 (2) Proximal ulna 1 (1) Distal ulna 2 (2) Phalanx 4 (4) Cuboid 1 (1) Calcaneus 1 (1) Pelvis 6 (6.2) Distal fibula 3 (3.1) Cuneiform 1 (1) Patella 1 (1) Clavicle 1 (1) The mean defect size was 42.8 cm 3 ( cm 3 ). There were 87 (89.7%) closed defects and 10 (10.3%) open defects. In all cases the tumor was curetted; in 44.5% a high speed burr was used, and in 45.5% phenol was applied to extend the margin of resection. The defect was filled with particulate cortical allograft in all cases. Instrumentation was used to stabilize the bone in 11% of cases. Thirteen (13.4%) of 97 patients had a pathologic fracture prior to treatment. The rate of consolidation was 60%, from 6 weeks to 108 weeks, and the rate of incorporation was 91%, from 4 to 68 weeks. There was no statistically significant difference between osseous healing and diagnosis, defect size or site of disease. An example of a patient with a bone cavity filled with microparticulate graft is given in Fig. (2). Eleven procedures, in eleven patients, were considered failures. There were seven patients with recurrent tumors; three with giant cell tumors, two with aneurysmal bone cysts, and one each with a fibroxanthoma and fibrous dysplasia (Table 2).
4 94 The Open Orthopaedics Journal, 2008, Volume 2 Temple and Malinin The average time from the index procedure to tumor recurrence was 9.7 months. All patients, but one underwent a secondary grafting procedure with satisfactory functional and oncologic outcomes. One patient with a giant cell tumor of the distal radius, in addition to having a recurrence, sustained a closed fracture after the index procedure which healed with cast immobilization. In addition, this patient had a soft tissue recurrence following re-excision and grafting. She is free of tumor three years after the bone recurrence and two years six months after the soft tissue recurrence (Fig. 3). The defect is consolidated. Another patient with a giant cell tumor of the distal tibia presented with a recurrence after an incomplete resection at an outside hospital. At the time of treatment for this recurrence, there was a 1 cm defect in the articular cartilage that was filled with a gel foam patch and packed with microparticulate bone allograft. The tumor recurred again after 14 months. At that time, he underwent re-curetting with bone allograft and polymethylmethacrylate packing of the defect. He is free of tumor twenty months following treatment for the second recurrence. Finally, a 44 year old patient with fibrous dysplasia of the proximal femur and with longstanding deformity of the proximal femur complained of persistent pain and inability to walk without assistive devices following curetting and allograft packing. This patient underwent resection of the proximal femur and reconstruction with an un-cemented proximal femoral replacement. Fig. (2). AP radiograph of femur of 23 year old male with an aneurysmal bone cyst involving the subtrochanteric region of the femur following resection and allograft packing. Left: incorporation at 6 weeks. Right: consolidation at 3 months. Table 2. Patients with Tumor Recurrences Case Age Tumor Location Previous Surgery 1 31 Giant cell tumor Distal humerus No Fig. (3A). Post-operative AP radiograph of the wrist of a 51 year old woman with a giant cell tumor of the distal radius who underwent extended curetting and allograft packing. There is extensive bone graft material in the soft tissue Giant cell tumor Distal radius No 3 62 Giant cell tumor Distal tibia Yes 4 18 Aneurysmal bone cyst Proximal radius No 5 14 Aneurysmal bone cyst Distal tibia No 6 12 Fibroxanthoma Distal tibia No 7 44 Fibrous dysplasia Proximal femur Yes Fig. (3B). AP radiograph of the same patient one year later with complete incorporation of the graft material and resorption of the graft in soft tissue. Two patients had deep infections that required operative debridement and antibiotic therapy. In both patients, the infection resolved and the graft was retained and subsequently consolidated. One patient had a cystic chondroblastoma of the calcaneus, and the other had a chondrosarcoma of the pelvis that was resected and instrumented with segmental pedicle screws and plates. In the later case, the allograft was used to fill a large defect between the residual sacrum and the ilium. Two additional patients had prolonged drainage and required oral antibiotics. A third had a stitch abscess that resolved with oral antibiotics and local wound care.
5 Microparticulate Cortical Allograft The Open Orthopaedics Journal, 2008, Volume 2 95 Two patients required re-operations, for a non-union of the femur in one case, and an acetabular fracture in another. The patient with the non-union presented with a large unicameral bone cyst in the inter-trochanteric region of the hip with extension into the sub-trochanteric femur. In addition, he had a displaced pathologic fracture. This patient underwent curetting and allograft bone packing and stabilization with a hip screw and side plate. Due to persistent pain and the radiographic presence of a failure to heal six months post-operatively, this patient underwent removal of the screw and side plate and antegrade intramedually nailing The unicameral cyst was completely healed and the fracture united 8 weeks following the revision procedure. In addition, a 77 year old male, with a protrusio fracture of the pelvis, following chemotherapy and radiation for a non-hodgkin s lymphoma of the hip, underwent total hip arthroplasty and augmentation of the medial acetabular deficiency with microparticulate allograft. He subsequently developed a large medial wall acetabular fracture with a protrusio deformity for which he underwent acetabular cage reconstruction with a large structural allograft. Finally, a 19 year old male with osteonecrosis of the proximal tibia developed regional pain syndrome after curetting and allograft bone grafting of the defect. This resolved two years after the index procedure with non-operative pain management. DISCUSSION Clinical results obtained in this study indicate that freezedried particulate allografts can be safely used for filling of cavitary bone defects. In this study, all allografts were freeze-dried and, during processing, the machine temperature was kept cooler than 50 0 C. The freeze-drying process, removal of fat and marrow elements and standardization of the milling to near exact particle size, resulted in a stronger compacted graft substrate that is more resistant to shear, the usual mode of mechanical failure [24, 25]. These reproducible osteoconductive and osteoinductive properties of the graft produce the uniform clinical results reported in this investigation. Osteoinductive and osteoconductive properties of these grafts were established in laboratory studies [1] Both benign and malignant tumors of bone present diagnostic and therapeutic challenges for the orthopaedic oncologist. The indications for surgical treatment of benign bone tumors and tumor-like lesions depends on the presence or absence of clinical symptoms, the anatomic location of the lesion, and its biological activity. Symptomatic lesions that progressively increase in size and demonstrate radiographic signs of aggressiveness such as deep endosteal scalloping, cortical destruction and periosteal new bone formation, should be considered for biopsy and surgical removal [8]. Despite advanced imaging techniques, including magnetic resonance imaging, fastidious attention to tumor treatment principles, and the availability of allogenic grafts and bone substitutes, control of tumor recurrence and osseous healing can be problematic. Despite extended curetting and the application of phenol for patients with benign aggressive tumors, there were seven tumor recurrences in this series. In six of these patients, salvage was achieved by appropriate surveillance and early intervention by repeated intralesional excision and allograft bone grafting. In the 11 patients with giant cell tumors, there were 3 recurrences (27%). O Donnell [12] reported fifteen recurrent tumors in 60 patients (25%), and Malawer recorded eight recurrent tumors in 103 (7.9%) patients [26]. Although thorough curetting, cryosurgery and the use of a high speed burr extended the intralesional margin of resection these newer techniques have not eliminated the incidence of tumor recurrence. This highlights the fact that neither bone grafting nor the improvement in surgical techniques have solved this problem. We considered the seven cases with tumor recurrence as failures. However, this is not altogether accurate since in six of these patients, treated with re-resection and bone grafting, bone incorporation was complete. Even two patients with deep infections retained and incorporated their grafts. In two cases results with allograft bone were not adequate. The first patient was an elderly man with a lymphoma who underwent chemotherapy and radiotherapy to the acetabulum. He subsequently developed avascular necrosis and a protrusio deformity of the proximal femur. Despite the appearance of graft consolidation after total hip arthroplasty, the patient subsequently developed a fracture of the medial wall requiring revision surgery with a structural allograft and a cage. Although a number of successful grafting procedures using allograft particulate bone have been performed in patients with deficient medial acetabular walls, radiotherapy in this patient more than likely inhibited bone remodeling. Although the patient with fibrous dysplasia underwent internal fixation to augment the proximal femur after curetting and allograft packing, he continued to have pain that may have been more related to his disease than to structural insufficiency. When the oncologic results are separated from the reconstructive results, the later two cases and the two deep infections represent the only true failures of the use of the microparticulate bone allograft in the 97 patients included in this series. In this study, the rate of consolidation was 60% (from 6 to 108 weeks), and incorporation was observed in 91% (from 4 to 68 weeks). In most cases, the short healing period made prolonged cast immobilization unnecessary. Internal fixation was used in only 11% of cases. The microparticulate graft was effective for both closed and open defects and residual graft in the adjacent soft tissue resorbed between 6 weeks and 3 months. The absence of donor morbidity and the rapid rate of incorporation, coupled with a low complication rate, make the microparticulate bone allograft an attractive alternative to autograft. The bone allograft composite used in the study facilitated rapid vascular in-growth. This rapid process of neo-vascularization and incorporation may explain the relative resistance of this graft material to peri-operative bacterial contamination and preservation of the graft in the face of deep infection. The present study was performed with a limited objective. We wanted to find out if replacing autologous bone grafting in patients with cavitary defects following resection of tumors was a sound clinical procedure. It appears it is. Results with autografts are well known. Success rate as also high as it is with a present technique. With success rates as high as these comparisons have little to offer. The literature on the treatment of bone defects created by tumor ablation is
6 96 The Open Orthopaedics Journal, 2008, Volume 2 Temple and Malinin scant. Comparison of results obtained in the present study with those obtained with revision arthroplasty would fall short of the mark, as the procedures and the reasons for performing operation are vastly different. REFERENCES [1] Malinin TI, Carpenter EM, Temple HT. Particulate bone allograft incorporation in regeneration of osseous defects; importance of particle sizes. Open Orthop J 2007; 1: [2] Cornell CN. Proper design of clinical trials for the assessment of bone graft substitutes. Clin Orthop Relat Res 1998; 355 (Suppl): S [3] Johnson KD, Frierson KE, Keller TS, et al. Porous ceramics as bone graft substitutes in long bone defects: a biomechanical, histological, and radiographic analysis. J Orthop Res 1996; 14(3): [4] Marchetti DG. Spinal Leions: Bone and bone substitutes. Eur Spine J 2000; 9(5): [5] Shih HN, Chen YJ, Huang TJ, Hsu KY, Hsu RW. Semistructural allografting in bone defects after curettage. J Surg Oncol 1998; 68(3): [6] Vaccaro AR. The role of the osteoconductive scaffold in synthetic bone graft. [erratum appears in Orthopaedics 2002 Nov; 25(11): 1224]. Orthopaedics 2002; 25(5 Suppl): [7] Malinin T, Temple HT. Comparison of frozen and freeze-dried particulate bone allograft. Cryobiology 2007; 55: [8] Schaser KD, Bail HJ, Haas NP, Melcher I. Treatment concepts of benign bone tumors and tumor-like bone lesions. Chirurg 2002; 73(12): [9] Hall EE, Meffert RM, Hermann JS, Mellonig JT, Cochran DL. Comparison of bioactive glass to demineralized freeze-dried bone allograft in the treatment of intrabony defects around implants in the canine mandible. J Periodontol 1999; 70(5): [10] Wheeler DL, Stokes KE, Hoellrich RG, Chamberland DL, McLoughlin SW. Effect of bioactive glass particle size on osseous regeneration of cancellous defects. J Biomed Mater Res 1998; 41(4): [11] Schepers EJ, Ducheyne P. Bioactive glass particles of narrow size range for the treatment of oral bone defects: a 1-24 month experiment with several materials and particle sizes and size ranges. J Oral Rehabil 1997; 24(3): [12] O'Donnell RJ, Springfield DS, Motwani HK, et al. Recurrence of giant-cell tumors of the long bones after curettage and packing with cement. J Bone Joint Surg Am 1994; 76(12): [13] Malinin TI. Principles of musculoskeletal tissue banking. In: (W.S. Pietrzak Ed) Orthopaedic biology and medicine: Musculoskeletal tissue regeneration. Humana Press, Totowa, N.J. 2008; pp [14] Slooff TJ, Buma P, Schreurs BW, Schimmel JW, Huiskes R, Gardeniers, J. Acetabular and femoral reconstruction with impacted graft and cement. Clin Orthop Relat Res 1996; 324: [15] Bostrom MP, Yang X, Kennan M, Sandhu H, Dicarlo E. An unexpected outcome during testing of commercially available demineralized bone graft materials: how safe are the nonallograft components? Spine 2001; 26(13): [16] Lamerigts N, Schreurs BW, Gardeniers J, et al. Impacted graft incorporation after cemented acetabular revision. Histological evaluation in 8 patients. Acta Orthop Scand 1996; 67(6): [17] Schwartz Z, Mellonig JT, Carnes DL Jr. De la Fontaine J, Cochran DL. Boyan BD. Ability of commercial demineralized freeze-dried bone allograft to induce new bone formation. J Periodontol 1996; 67(9): [18] Nagi ON, Dhillon MS, Reddy VR, Mathur K. Comparison of formalin preserved bone allograft in the form of a paste and as bone chips in fresh femoral shaft fractures with comminution. Singapore Med J 1997; 38(2): [19] Schimmel JW, Buma P, Versleyen D, Huiskes R, Slooff TJ. Acetabular reconstruction with impacted morselized cancellous allografts in cemented hip arthroplasty: a histological and biomechanical study on the goat. J Arthroplasty 1998; 13(4): [20] Tagil M. The morselized and impacted bone graft. Animal experiments on proteins, impaction and load. Acta Orthop Scand Suppl 2000; 290: [21] Enneking WF, Mindell ER. Observations on massive retrieved human allografts. J Bone Joint Surg Am 1991; 73(8): [22] Shapoff CA, Bowers GM, Levy B, Mellonig JT, Yukna RA. The effect of particale size on the osteogenc activity of composite grafts of allogeneic freeze-dried bone and autogenous marrow. J Periodontol 1980; 51: [23] Syftestad G, Urist MR. Degradation of bone matrix morphogenetic activity by pulverization. Clin Orthop Relat Res 1979; 141: [24] Dunlop DG, Brewster NT, Madabhushi SP, Usmani AS, Pankaj P, Howie CR. Techniques to improve the shear strength of impacted bone graft: the effect of particle size and washing of the graft. J Bone Joint Surg Am 2003; 85: [25] Brewster NT, Gillespie WJ, Howie CR, Madabhushi SP. Usmani AS, Fairbarn DR. Mechanical considerations in impaction bone grafting. J Bone Joint Surg Am 1999; 81(1): [26] Malawer MM, Bickels J, Meller I, Buch RG, Henshaw RM, Kollender Y. Cryosurgery in the treatment of giant cell tumor. A longterm followup study. Clin Orthop Relat Res 1999; 359: Received: March 25, 2008 Revised: April 18, 2008 Accepted: April 29, 2008 Temple and Malinin; Licensee Bentham Open. This is an open access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestrictive use, distribution, and reproduction in any medium, provided the original work is properly cited.
Developments in bone grafting in veterinary orthopaedics part one
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Developments in bone grafting in veterinary orthopaedics part one Author : John Innes, Peter Myint Categories : Vets Date
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Developments in bone grafting in veterinary orthopaedics part one Author : John Innes, Peter Myint Categories : Vets Date
BIOACTIVE SYNTHETIC GRAFT
 B U I L D S T R O N G B O N E F A S T Putty Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
B U I L D S T R O N G B O N E F A S T Putty Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
Calcium Phosphate Cement
 Calcium Phosphate Cement Fast-Setting Bone Graft and AutoGraft Extender. * Ossilix is a high performance next generation calcium phosphate cement indicated for filling bony defects in cancellous bone.
Calcium Phosphate Cement Fast-Setting Bone Graft and AutoGraft Extender. * Ossilix is a high performance next generation calcium phosphate cement indicated for filling bony defects in cancellous bone.
B U I L D S T R O N G B O N E F A S T
 B U I L D S T R O N G B O N E F A S T Putty MIS Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
B U I L D S T R O N G B O N E F A S T Putty MIS Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
Bone Grafting and Bone Graft Substitutes. Original Author: James Krieg, MD Revision Author: David Hak, MD Last Revision May 2010
 Bone Grafting and Bone Graft Substitutes Original Author: James Krieg, MD Revision Author: David Hak, MD Last Revision May 2010 Bone Graft Function Structural support of articular fracture Tibial plateau
Bone Grafting and Bone Graft Substitutes Original Author: James Krieg, MD Revision Author: David Hak, MD Last Revision May 2010 Bone Graft Function Structural support of articular fracture Tibial plateau
NEW FIXATION STRATEGIES FOR OSTEOPOROTIC BONE
 NEW FIXATION STRATEGIES FOR OSTEOPOROTIC BONE THE PROBLEMS Fixation failure Malunion F 83 yrs 2 Months 6 Months F 81 yrs 3 Months FIXATION AUGMENTATION TECHNIQUES (FATs) Surgical procedures aimed at increasing
NEW FIXATION STRATEGIES FOR OSTEOPOROTIC BONE THE PROBLEMS Fixation failure Malunion F 83 yrs 2 Months 6 Months F 81 yrs 3 Months FIXATION AUGMENTATION TECHNIQUES (FATs) Surgical procedures aimed at increasing
Inion BioRestore. Bone Graft Substitute. Product Overview
 Inion BioRestore Bone Graft Substitute Product Overview Inion BioRestore Introduction Inion BioRestore is a synthetic bone graft substitute, which remodels into bone and is easy to use. Inion BioRestore
Inion BioRestore Bone Graft Substitute Product Overview Inion BioRestore Introduction Inion BioRestore is a synthetic bone graft substitute, which remodels into bone and is easy to use. Inion BioRestore
chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute.
 chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute. Osteoconductive Resorbable Synthetic chronos Bone Void Filler chronos granules and preforms are synthetic, porous, osteoconductive,
chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute. Osteoconductive Resorbable Synthetic chronos Bone Void Filler chronos granules and preforms are synthetic, porous, osteoconductive,
CELLPLEX TCP SYNTHETIC CANCELLOUS BONE
 CELLPLEX TCP SYNTHETIC CANCELLOUS BONE 129257-9 The following languages are included in this packet: English (en) Deutsch (de) Nederlands (nl) Français (fr) Español (es) Italiano (it) Português (pt) -
CELLPLEX TCP SYNTHETIC CANCELLOUS BONE 129257-9 The following languages are included in this packet: English (en) Deutsch (de) Nederlands (nl) Français (fr) Español (es) Italiano (it) Português (pt) -
Radiology Case Reports. Bone Graft Extruded From an Intramedullary Nail Tract in the Tibia. Penelope J. Galbraith, M.D., and Felix S. Chew, M.D.
 Radiology Case Reports Volume 2, Issue 4, 2007 Bone Graft Extruded From an Intramedullary Nail Tract in the Tibia Penelope J. Galbraith, M.D., and Felix S. Chew, M.D. A 33-year-old man presented for follow
Radiology Case Reports Volume 2, Issue 4, 2007 Bone Graft Extruded From an Intramedullary Nail Tract in the Tibia Penelope J. Galbraith, M.D., and Felix S. Chew, M.D. A 33-year-old man presented for follow
MARK D. MURPHEY MD, FACR. Physician-in-Chief, AIRP. Chief, Musculoskeletal Imaging
 ALPHABET SOUP AND CYSTIC LESIONS OF THE BONE MARK D. MURPHEY MD, FACR Physician-in-Chief, AIRP Chief, Musculoskeletal Imaging ALPHABET SOUP AND CYSTIC LESIONS OF THE BONE Giant cell tumor (GCT) Unicameral
ALPHABET SOUP AND CYSTIC LESIONS OF THE BONE MARK D. MURPHEY MD, FACR Physician-in-Chief, AIRP Chief, Musculoskeletal Imaging ALPHABET SOUP AND CYSTIC LESIONS OF THE BONE Giant cell tumor (GCT) Unicameral
Solitary Bone Cyst of the Lunate: A Case Report
 Cronicon OPEN ACCESS ORTHOPAEDICS Case Report Solitary Bone Cyst of the Lunate: A Case Report MihirDesai* and Shivanand Bandekar Department of Orthopedics, Goa Medical College, Goa, India *Corresponding
Cronicon OPEN ACCESS ORTHOPAEDICS Case Report Solitary Bone Cyst of the Lunate: A Case Report MihirDesai* and Shivanand Bandekar Department of Orthopedics, Goa Medical College, Goa, India *Corresponding
Laura M. Fayad, MD. Associate Professor of Radiology, Orthopaedic Surgery & Oncology The Johns Hopkins University
 Society of Pediatric Radiology, May 2013 Laura M. Fayad, MD Associate Professor of Radiology, Orthopaedic Surgery & Oncology The Johns Hopkins University Describes surgical techniques that resect and reconstruct
Society of Pediatric Radiology, May 2013 Laura M. Fayad, MD Associate Professor of Radiology, Orthopaedic Surgery & Oncology The Johns Hopkins University Describes surgical techniques that resect and reconstruct
PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH
 PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH Headline Contents Headline Appendix 4 5 7 8 13 14 Clinical Benefits Self-Forming Porous Scaffold
PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH Headline Contents Headline Appendix 4 5 7 8 13 14 Clinical Benefits Self-Forming Porous Scaffold
In Vivo Evaluation of BioSphere Bioactive Bone Graft Putty: Improved Bone Formation
 In Vivo Evaluation of BioSphere Bioactive Bone Graft : Improved Bone Formation ABSTRACT BioSphere is a novel bone graft product that was developed using spherical particles of bioactive glass with a narrow,
In Vivo Evaluation of BioSphere Bioactive Bone Graft : Improved Bone Formation ABSTRACT BioSphere is a novel bone graft product that was developed using spherical particles of bioactive glass with a narrow,
JMSCR Vol 06 Issue 12 Page December 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i12.140 A Case Report of Recurrent
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i12.140 A Case Report of Recurrent
Bone Void Filler. Callos. The Next Generation in Calcium Phosphate Cement A COLSON ASSOCIATE
 Callos Bone Void Filler The Next Generation in Calcium Phosphate Cement A COLSON ASSOCIATE Callos Calcium Phosphate Cement Callos is a high performance next generation calcium phosphate cement indicated
Callos Bone Void Filler The Next Generation in Calcium Phosphate Cement A COLSON ASSOCIATE Callos Calcium Phosphate Cement Callos is a high performance next generation calcium phosphate cement indicated
Biomaterials Line. MIS Corporation. All Rights Reserved.
 7. Biomaterials Line MIS Corporation. All Rights Reserved. 6. MIS s Quality System complies with international quality standards: ISO 13485: 2003 - Quality Management System for Medical Devices, ISO 9001:
7. Biomaterials Line MIS Corporation. All Rights Reserved. 6. MIS s Quality System complies with international quality standards: ISO 13485: 2003 - Quality Management System for Medical Devices, ISO 9001:
Radiological and histological analysis of synthetic bone grafts in recurring giant cell tumour of bone: a retrospective study
 Journal of Orthopaedic Surgery 2010;18(1):63-7 Radiological and histological analysis of synthetic bone grafts in recurring giant cell tumour of bone: a retrospective study Hiroyuki Hattori, Hiroaki Matsuoka,
Journal of Orthopaedic Surgery 2010;18(1):63-7 Radiological and histological analysis of synthetic bone grafts in recurring giant cell tumour of bone: a retrospective study Hiroyuki Hattori, Hiroaki Matsuoka,
ADVANCED BONE GRAFT SYSTEM OVERVIEW
 ADVANCED BONE GRAFT SYSTEM OVERVIEW NANOSS BIOACTIVE ADVANCED BONE GRAFT Table Of Contents INTRODUCTION System Overview... 1 NANOSS BIOACTIVE COMPONENTS Comparison of nanoss Bioactive and Human Bone...
ADVANCED BONE GRAFT SYSTEM OVERVIEW NANOSS BIOACTIVE ADVANCED BONE GRAFT Table Of Contents INTRODUCTION System Overview... 1 NANOSS BIOACTIVE COMPONENTS Comparison of nanoss Bioactive and Human Bone...
Fibula bone grafting in infected gap non union: A prospective case series
 2019; 3(1): 06-10 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2019; 3(1): 06-10 Received: 03-11-2018 Accepted: 06-12-2018 Dr. Mohammed Nazim M.S (Ortho),
2019; 3(1): 06-10 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2019; 3(1): 06-10 Received: 03-11-2018 Accepted: 06-12-2018 Dr. Mohammed Nazim M.S (Ortho),
The Outcome of Bone Substitute Wedges in Medial Opening High Tibial Osteotomy
 Send Orders for Reprints to reprints@benthamscience.net The Open Orthopaedics Journal, 2013, 7, 373-377 373 Open Access The Outcome of Bone Substitute Wedges in Medial Opening High Tibial Osteotomy N.M.
Send Orders for Reprints to reprints@benthamscience.net The Open Orthopaedics Journal, 2013, 7, 373-377 373 Open Access The Outcome of Bone Substitute Wedges in Medial Opening High Tibial Osteotomy N.M.
Versatile grafting Solutions
 Versatile grafting Solutions A Canadian company serving Canadian dentists since 1997 Here s why your colleagues are calling us for their bone regeneration needs Founded in 1997 Citagenix has been providing
Versatile grafting Solutions A Canadian company serving Canadian dentists since 1997 Here s why your colleagues are calling us for their bone regeneration needs Founded in 1997 Citagenix has been providing
A 42-year-old patient presenting with femoral
 Kanda et al. Journal of Medical Case Reports 2015, 9:17 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access A 42-year-old patient presenting with femoral head migration after hemiarthroplasty performed
Kanda et al. Journal of Medical Case Reports 2015, 9:17 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access A 42-year-old patient presenting with femoral head migration after hemiarthroplasty performed
Index. orthopedic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Acetabular fractures pediatric, 494 498 classification of, 494 diagnostic imaging of, 494, 496 497 epidemiology of, 494 treatment of, 494 498
Note: Page numbers of article titles are in boldface type. A Acetabular fractures pediatric, 494 498 classification of, 494 diagnostic imaging of, 494, 496 497 epidemiology of, 494 treatment of, 494 498
Cerasorb M DENTAL. O:\Zulassung\Cerasorb Dental Kanada 2013\Texte\Cerasorb M Dental final IFU docx
 Cerasorb M DENTAL Resorbable, pure-phase beta-tricalcium phosphate matrix with interconnecting porosity for bone regeneration for use in dental and maxillofacial surgery DESCRIPTION: Cerasorb M DENTAL
Cerasorb M DENTAL Resorbable, pure-phase beta-tricalcium phosphate matrix with interconnecting porosity for bone regeneration for use in dental and maxillofacial surgery DESCRIPTION: Cerasorb M DENTAL
Treatment of Distal Radius Bone Defects with Injectable Calcium Sulphate Cement
 Treatment of Distal Radius Bone Defects with Injectable Calcium Sulphate Cement Deng Lei, Ma Zhanzhong, Yang Huaikuo, Xue Lei and Yang Gongbo Orthopaedic Department, Beijing XiYuan Hospital, China Academy
Treatment of Distal Radius Bone Defects with Injectable Calcium Sulphate Cement Deng Lei, Ma Zhanzhong, Yang Huaikuo, Xue Lei and Yang Gongbo Orthopaedic Department, Beijing XiYuan Hospital, China Academy
Giant Cell Tumour of the Distal Radius: Wide Resection and Reconstruction by Non-vascularised Proximal Fibular Autograft
 900 Original Article Giant Cell Tumour of the Distal Radius: Wide Resection and Reconstruction by Non-vascularised Proximal Fibular Autograft Ayman Abdelaziz Bassiony, 1 MD Abstract Introduction: Giant
900 Original Article Giant Cell Tumour of the Distal Radius: Wide Resection and Reconstruction by Non-vascularised Proximal Fibular Autograft Ayman Abdelaziz Bassiony, 1 MD Abstract Introduction: Giant
Intercalary Femur and Tibia Segmental Allografts Provide an Acceptable Alternative in Reconstructing Tumor Resections
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 426, pp. 97 102 2004 Lippincott Williams & Wilkins Intercalary Femur and Tibia Segmental Allografts Provide an Acceptable Alternative in Reconstructing
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 426, pp. 97 102 2004 Lippincott Williams & Wilkins Intercalary Femur and Tibia Segmental Allografts Provide an Acceptable Alternative in Reconstructing
CERAMENT BONE VOID FILLER
 CERAMENT BONE VOID FILLER Rapid and complete bone remodeling TM CERAMENT BONE VOID FILLER CERAMENT is an injectable, moldable, drillable and radiopaque bone substitute which provides rapid and complete
CERAMENT BONE VOID FILLER Rapid and complete bone remodeling TM CERAMENT BONE VOID FILLER CERAMENT is an injectable, moldable, drillable and radiopaque bone substitute which provides rapid and complete
DEMINERALIZED BONE MATRIX
 DEMINERALIZED BONE MATRIX DEMINERALIZED BONE MATRIX GRAFT OVERVIEW BioAdapt is a pre-formed demineralized bone matrix (DBM) comprised of 00 percent donated human musculoskeletal tissue. BioAdapt DBM provides
DEMINERALIZED BONE MATRIX DEMINERALIZED BONE MATRIX GRAFT OVERVIEW BioAdapt is a pre-formed demineralized bone matrix (DBM) comprised of 00 percent donated human musculoskeletal tissue. BioAdapt DBM provides
The long term fate of the fibula when used as an intraosseous graft
 Acta Orthop. Belg., 2004, 70, 322-326 The long term fate of the fibula when used as an intraosseous graft Onkar N. NAGI, Mandeep S. DHILLON, Sameer AGGARWAL From the Post Graduate Institute of Medical
Acta Orthop. Belg., 2004, 70, 322-326 The long term fate of the fibula when used as an intraosseous graft Onkar N. NAGI, Mandeep S. DHILLON, Sameer AGGARWAL From the Post Graduate Institute of Medical
RECOVERY. P r o t r u s i o
 RECOVERY P r o t r u s i o TM C a g e RECOVERY P r o t r u s i o TM C a g e Design Features Revision acetabular surgery is a major challenge facing today s total joint revision surgeon. Failed endo/bi-polars,
RECOVERY P r o t r u s i o TM C a g e RECOVERY P r o t r u s i o TM C a g e Design Features Revision acetabular surgery is a major challenge facing today s total joint revision surgeon. Failed endo/bi-polars,
Unicameral bone cysts are benign, fluid-filled cavities
 Endoscopic Surgery for Symptomatic Unicameral Bone Cyst of the Proximal Femur Wataru Miyamoto, M.D., Masato Takao, M.D., Youichi Yasui, M.D., Shinya Miki, M.D., and Takashi Matsushita, M.D. Abstract: Recently,
Endoscopic Surgery for Symptomatic Unicameral Bone Cyst of the Proximal Femur Wataru Miyamoto, M.D., Masato Takao, M.D., Youichi Yasui, M.D., Shinya Miki, M.D., and Takashi Matsushita, M.D. Abstract: Recently,
Orthopedic & Sports Medicine, Bay Care Clinic, 501 N. 10th Street, Manitowoc, WI Procedure. Subtalar arthrodesis
 OSTEOAMP Allogeneic Morphogenetic Proteins Subtalar Nonunions OSTEOAMP Case Report SUBTALAR NONUNIONS Dr. Jason George DeVries and Dr. Brandon M. Scharer Orthopedic & Sports Medicine, Bay Care Clinic,
OSTEOAMP Allogeneic Morphogenetic Proteins Subtalar Nonunions OSTEOAMP Case Report SUBTALAR NONUNIONS Dr. Jason George DeVries and Dr. Brandon M. Scharer Orthopedic & Sports Medicine, Bay Care Clinic,
ctive Bone Bonding Bone Regeneration Osteostimulation*
 www.bonalive.com ctive Bone Bonding Bone Regeneration Osteostimulation* A revolution in bone grafting Osteoconductive bone graft substitute with osteostimulative* properties *non-osteoinductive Before
www.bonalive.com ctive Bone Bonding Bone Regeneration Osteostimulation* A revolution in bone grafting Osteoconductive bone graft substitute with osteostimulative* properties *non-osteoinductive Before
Ankle and subtalar arthrodesis
 OSTEOAMP Allogeneic Morphogenetic Proteins Ankle Nonunions OSTEOAMP Case Report ANKLE NONUNIONS Dr. Jason George DeVries Orthopedic & Sports Medicine, Bay Care Clinic, 501 N. 10th Street, Manitowoc, WI
OSTEOAMP Allogeneic Morphogenetic Proteins Ankle Nonunions OSTEOAMP Case Report ANKLE NONUNIONS Dr. Jason George DeVries Orthopedic & Sports Medicine, Bay Care Clinic, 501 N. 10th Street, Manitowoc, WI
More than bone regeneration. A total solution.
 More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
BONE TRANSPLANTATION IN LIMB SAVING SURGERIES: THE PHILIPPINE EXPERIENCE
 BONE TRANSPLANTATION IN LIMB SAVING SURGERIES: THE PHILIPPINE EXPERIENCE EDWARD HM WANG, MD UP-Musculoskeletal Tumor Unit and Tissue & Bone Bank Dept. of Orthopedics University of the Philippines-Philippine
BONE TRANSPLANTATION IN LIMB SAVING SURGERIES: THE PHILIPPINE EXPERIENCE EDWARD HM WANG, MD UP-Musculoskeletal Tumor Unit and Tissue & Bone Bank Dept. of Orthopedics University of the Philippines-Philippine
synthetic CANCELLOUS BONE technical monograph Presented by Barbara Blum, Ph.D.
 C E L L P L E X TCP synthetic CANCELLOUS BONE technical monograph Presented by Barbara Blum, Ph.D. TECHNICAL MONOGRAPH CELLPLEX TCP SYNTHETIC CANCELLOUS BONE CELLPLEX TCP synthetic CANCELLOUS BONE introduction
C E L L P L E X TCP synthetic CANCELLOUS BONE technical monograph Presented by Barbara Blum, Ph.D. TECHNICAL MONOGRAPH CELLPLEX TCP SYNTHETIC CANCELLOUS BONE CELLPLEX TCP synthetic CANCELLOUS BONE introduction
BonAlive Clinical Cases
 BonAlive Clinical Cases Inhibition of bacterial growth Osteostimulation* Bioactive bone bonding *Non-osteoinduction BonAlive mechanism of action BonAlive composition: 53% SiO 2, 23% Na 2 O, 20% CaO, 4%
BonAlive Clinical Cases Inhibition of bacterial growth Osteostimulation* Bioactive bone bonding *Non-osteoinduction BonAlive mechanism of action BonAlive composition: 53% SiO 2, 23% Na 2 O, 20% CaO, 4%
CASE REPORT COMPLETE BONE REMODELING AFTER CALCAR RECONSTRUCTION WITH METAL WIRE MESH AND IMPACTION BONE GRAFTING: A CASE REPORT
 Nagoya J. Med. Sci. 75. 287 ~ 293, 2013 CASE REPORT COMPLETE BONE REMODELING AFTER CALCAR RECONSTRUCTION WITH METAL WIRE MESH AND IMPACTION BONE GRAFTING: A CASE REPORT Toshiki Iwase, M.D., Ph.D., Atsushi
Nagoya J. Med. Sci. 75. 287 ~ 293, 2013 CASE REPORT COMPLETE BONE REMODELING AFTER CALCAR RECONSTRUCTION WITH METAL WIRE MESH AND IMPACTION BONE GRAFTING: A CASE REPORT Toshiki Iwase, M.D., Ph.D., Atsushi
Technique Guide. chronos Strip. Osteoconductive betatricalcium phosphate ( -TCP) composite.
 Technique Guide chronos Strip. Osteoconductive betatricalcium phosphate ( -TCP) composite. Table of Contents Introduction chronos Strip 2 Indications and Contraindications 3 Surgical Technique Preparation
Technique Guide chronos Strip. Osteoconductive betatricalcium phosphate ( -TCP) composite. Table of Contents Introduction chronos Strip 2 Indications and Contraindications 3 Surgical Technique Preparation
Lawrence A. DiDomenico, DPM, FACFAS
 Lawrence A. DiDomenico, DPM, FACFAS Adjunct Professor, Kent State University College of Podiatric Medicine, Cleveland, Ohio USA Director, Reconstructive Rearfoot & Ankle Surgical Fellowship, Ankle and
Lawrence A. DiDomenico, DPM, FACFAS Adjunct Professor, Kent State University College of Podiatric Medicine, Cleveland, Ohio USA Director, Reconstructive Rearfoot & Ankle Surgical Fellowship, Ankle and
FDBA(Freeze Dried Bone Allograft) SureOss Cortical Bone - Powder / Chip. OsteOss Cortical with Cancellous Bone - Powder / Chip
 PERIODONTAL Bone & Skin Allograft Products FDBA(Freeze Dried Bone Allograft) SureOss - Powder / Chip OsteOss Cortical with - Powder / Chip DFDBA(Demineralized Freeze Dried Bone Allograft) SureOss -D Demineralized
PERIODONTAL Bone & Skin Allograft Products FDBA(Freeze Dried Bone Allograft) SureOss - Powder / Chip OsteOss Cortical with - Powder / Chip DFDBA(Demineralized Freeze Dried Bone Allograft) SureOss -D Demineralized
Bone Grafting for Total Joint Arthroplasty
 Bone Grafting for Total Joint Arthroplasty 263 14 Bone Grafting for Total Joint Arthroplasty Biology and Clinical Applications Moussa Hamadouche, MD, Daniel A. Oakes, MD, and Daniel J. Berry, MD INTRODUCTION
Bone Grafting for Total Joint Arthroplasty 263 14 Bone Grafting for Total Joint Arthroplasty Biology and Clinical Applications Moussa Hamadouche, MD, Daniel A. Oakes, MD, and Daniel J. Berry, MD INTRODUCTION
Allograft Cortical Strut for Reconstruction of Space-occupying Bone Lesions
 llograft Cortical Strut for Reconstruction of Space-occupying one Lesions Jason C. Tank, MD; Michael F. Vignos, S; Robert J. Wetzel, MD; Scott D. Weiner, MD abstract Full article available online at Healio.com/Orthopedics.
llograft Cortical Strut for Reconstruction of Space-occupying one Lesions Jason C. Tank, MD; Michael F. Vignos, S; Robert J. Wetzel, MD; Scott D. Weiner, MD abstract Full article available online at Healio.com/Orthopedics.
Abstract. Firas T. Ismaeel, Dept. of Surgery, College of Medicine, Tikrit University
 Bone marrow injection in patients with delayed union and non-union of long Firas T. Ismaeel, Dept. of Surgery, College of Medicine, Tikrit University Abstract In the process of bone formation and healing
Bone marrow injection in patients with delayed union and non-union of long Firas T. Ismaeel, Dept. of Surgery, College of Medicine, Tikrit University Abstract In the process of bone formation and healing
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
REGENERATION BY DESIGN
 REGENERATION BY DESIGN ALLOGRAFT, XENOGRAFT, PUTT Y & BIOACTIVE GLASS FOR BONE REGENERATION INSTRUMENTS FOR COLLECTING BONE BARRIER MEMBRANES FOR GUIDED REGENERATION GUIDED IMPLANT TREATMENT Wide Selection
REGENERATION BY DESIGN ALLOGRAFT, XENOGRAFT, PUTT Y & BIOACTIVE GLASS FOR BONE REGENERATION INSTRUMENTS FOR COLLECTING BONE BARRIER MEMBRANES FOR GUIDED REGENERATION GUIDED IMPLANT TREATMENT Wide Selection
Iliac aneurysmal bone cyst treated by cystoscopic controlled curettage
 Accepted February 13th, 2004 Iliac aneurysmal bone cyst treated by cystoscopic controlled curettage Ludwig Schwering¹, Markus Uhl² and Georg W. Herget( )¹ ¹ Department of Orthopaedics and Traumatology,
Accepted February 13th, 2004 Iliac aneurysmal bone cyst treated by cystoscopic controlled curettage Ludwig Schwering¹, Markus Uhl² and Georg W. Herget( )¹ ¹ Department of Orthopaedics and Traumatology,
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT
 OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
Graftys. Cross-selling. Indications. Comparison. Basic Science. Graftys 415 rue Claude Nicolas Ledoux Aix en Provence Cedex 4
 2015 Graftys Cross-selling Indications Comparison Graftys 415 rue Claude Nicolas Ledoux 13854 Aix en Provence Cedex 4 www.graftys.com Basic Science Graftys QuickSet Training 1 Where to use QuickSet? Revision
2015 Graftys Cross-selling Indications Comparison Graftys 415 rue Claude Nicolas Ledoux 13854 Aix en Provence Cedex 4 www.graftys.com Basic Science Graftys QuickSet Training 1 Where to use QuickSet? Revision
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
The injectable, self-setting calcium phosphate bone graft substitute.
 The injectable, self-setting calcium phosphate bone graft substitute. With a porous architecture similar to natural bone. STRUCSURE CP Bone Graft Substitute Because simplicity matters STRUCSURE CP Bone
The injectable, self-setting calcium phosphate bone graft substitute. With a porous architecture similar to natural bone. STRUCSURE CP Bone Graft Substitute Because simplicity matters STRUCSURE CP Bone
Advice sheet for Surgeons and Radiologists. Radiographic appearance of CERAMENT
 Advice sheet for Surgeons and Radiologists Radiographic appearance of CERAMENT The structure and function of CERAMENT CERAMENT is an osteoconductive bone graft substitute which consists of hydroxyapatite
Advice sheet for Surgeons and Radiologists Radiographic appearance of CERAMENT The structure and function of CERAMENT CERAMENT is an osteoconductive bone graft substitute which consists of hydroxyapatite
Trabecular Metal Acetabular Revision System Buttress and Shim Augments Surgical Technique
 Trabecular Metal Acetabular Revision System Buttress and Shim Augments Surgical Technique Trabecular Metal Acetabular Revision System Buttress and Shim Augments 1 Trabecular Metal Acetabular Revision
Trabecular Metal Acetabular Revision System Buttress and Shim Augments Surgical Technique Trabecular Metal Acetabular Revision System Buttress and Shim Augments 1 Trabecular Metal Acetabular Revision
Spine A Preliminary Study of the Efficacy of Beta-Tricalcium Phosphate as a Bone Graft Expander for Instrumented Posterolateral Fusions
 Bibliography Spine Epstein, N.E., A Preliminary Study of the Efficacy of Beta-Tricalcium Phosphate as a Bone Graft Expander for Instrumented Posterolateral Fusions. Journal of Spinal Disorders and Techniques,
Bibliography Spine Epstein, N.E., A Preliminary Study of the Efficacy of Beta-Tricalcium Phosphate as a Bone Graft Expander for Instrumented Posterolateral Fusions. Journal of Spinal Disorders and Techniques,
Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2, Patrick Smith, M.D. 2, and Larry S. Matthews, M.D. 2
 Skeletal Radiol (1986) 15:27-31 Skeletal Radiology Computed tomography and plain radiography in experimental fracture healing Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2,
Skeletal Radiol (1986) 15:27-31 Skeletal Radiology Computed tomography and plain radiography in experimental fracture healing Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2,
Management of infected custom mega prosthesis by Ilizarov method
 International Journal of Research in Medical Sciences Gudaru K et al. Int J Res Med Sci. 2015 Dec;3(12):3874-3878 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Case Report DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20151459
International Journal of Research in Medical Sciences Gudaru K et al. Int J Res Med Sci. 2015 Dec;3(12):3874-3878 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Case Report DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20151459
BIOACTIVE BASICS. Bioactive materials elicit a controlled action and reaction in the physiological environment.
 BIOACTIVE BASICS Bioactive materials elicit a controlled action and reaction in the physiological environment. Bioglass is a glass ceramic composed of silicon dioxide (SiO 2 ), sodium oxide (Na 2 O), calcium
BIOACTIVE BASICS Bioactive materials elicit a controlled action and reaction in the physiological environment. Bioglass is a glass ceramic composed of silicon dioxide (SiO 2 ), sodium oxide (Na 2 O), calcium
GRAFTON DEMINERALIZED BONE: FIBER TECHNOLOGY AND PERFORMANCE IMPLICATIONS
 GRAFTON DEMINERALIZED BONE: FIBER TECHNOLOGY AND PERFORMANCE IMPLICATIONS Based Upon the Published Source: Martin GJ, Jr., Boden SD, Titus L, Scarborough NL. New formulations of demineralized bone matrix
GRAFTON DEMINERALIZED BONE: FIBER TECHNOLOGY AND PERFORMANCE IMPLICATIONS Based Upon the Published Source: Martin GJ, Jr., Boden SD, Titus L, Scarborough NL. New formulations of demineralized bone matrix
Research Article Evaluation of Amniotic-Derived Membrane Biomaterial as an Adjunct for Repair of Critical Sized Bone Defects
 Advances in Orthopedic Surgery, Article ID 572586, 4 pages http://dx.doi.org/10.1155/2014/572586 Research Article Evaluation of Amniotic-Derived Membrane Biomaterial as an Adjunct for Repair of Critical
Advances in Orthopedic Surgery, Article ID 572586, 4 pages http://dx.doi.org/10.1155/2014/572586 Research Article Evaluation of Amniotic-Derived Membrane Biomaterial as an Adjunct for Repair of Critical
TREATMENT OF CARTILAGE LESIONS
 TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
Metastatic Disease of the Proximal Femur
 CASE REPORT Metastatic Disease of the Proximal Femur WI Faisham, M.Med{Ortho)*, W Zulmi, M.S{Ortho)*, B M Biswal, MBBS** 'Department of Orthopaedic, "Department of Oncology and Radiotherapy, School of
CASE REPORT Metastatic Disease of the Proximal Femur WI Faisham, M.Med{Ortho)*, W Zulmi, M.S{Ortho)*, B M Biswal, MBBS** 'Department of Orthopaedic, "Department of Oncology and Radiotherapy, School of
Innovative Range of Regenerative Solutions
 TM Innovative Range of Regenerative Solutions MIS Implant Technologies Ltd. All rights reserved. Optimal volumes and quality of hard and soft tissue are required to satisfy the goals of oral rehabilitation
TM Innovative Range of Regenerative Solutions MIS Implant Technologies Ltd. All rights reserved. Optimal volumes and quality of hard and soft tissue are required to satisfy the goals of oral rehabilitation
Chondroblastoma associated with aneurysmal cyst of the navicular bone: a case report
 Fang and Chen World Journal of Surgical Oncology 2013, 11:50 WORLD JOURNAL OF SURGICAL ONCOLOGY CASE REPORT Open Access Chondroblastoma associated with aneurysmal cyst of the navicular bone: a case report
Fang and Chen World Journal of Surgical Oncology 2013, 11:50 WORLD JOURNAL OF SURGICAL ONCOLOGY CASE REPORT Open Access Chondroblastoma associated with aneurysmal cyst of the navicular bone: a case report
Product Information. MIS Corporation. All Rights Reserved.
 Product Information MIS Corporation. All Rights Reserved. MIS Warranty: MIS exercises great care and effort in maintaining the superior quality of its products. All MIS products are guaranteed to be free
Product Information MIS Corporation. All Rights Reserved. MIS Warranty: MIS exercises great care and effort in maintaining the superior quality of its products. All MIS products are guaranteed to be free
Comparative Animal Study of OssiMend and Healos 13,14
 Comparative Animal Study of OssiMend and Healos 13,14 Objective This study was conducted to evaluate the use of OssiMend as compared with Healos in combination with autologous bone marrow as a bone grafting
Comparative Animal Study of OssiMend and Healos 13,14 Objective This study was conducted to evaluate the use of OssiMend as compared with Healos in combination with autologous bone marrow as a bone grafting
Original Date: December 2015 Page 1 of 8 FOR CMS (MEDICARE) MEMBERS ONLY
 National Imaging Associates, Inc. Clinical guidelines TOTAL JOINT ARTHROPLASTY -Total Hip Arthroplasty -Total Knee Arthroplasty -Replacement/Revision Hip or Knee Arthroplasty CPT4 Codes: Please refer to
National Imaging Associates, Inc. Clinical guidelines TOTAL JOINT ARTHROPLASTY -Total Hip Arthroplasty -Total Knee Arthroplasty -Replacement/Revision Hip or Knee Arthroplasty CPT4 Codes: Please refer to
Using Animal Models to Help Solve Clinical Problems
 Using Animal Models to Help Solve Clinical Problems -Overview -Epidemiology -Improving the Standards for Initial Wound Care -Use of dual purpose bone grafts -Developing a more relevant animal model Research
Using Animal Models to Help Solve Clinical Problems -Overview -Epidemiology -Improving the Standards for Initial Wound Care -Use of dual purpose bone grafts -Developing a more relevant animal model Research
7/23/2018 DESCRIBING THE FRACTURE. Pattern Open vs closed Location BASIC PRINCIPLES OF FRACTURE MANAGEMENT. Anjan R. Shah MD July 21, 2018.
 BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
Treatment of non-union of forearm bones with a free vascularised cortico - periosteal flap from the medial femoral condyle
 Acta Orthop. Belg., 2009, 75, 611-615 ORIGINAL STUDY Treatment of non-union of forearm bones with a free vascularised cortico - periosteal flap from the medial femoral condyle Luc DE SMET From the University
Acta Orthop. Belg., 2009, 75, 611-615 ORIGINAL STUDY Treatment of non-union of forearm bones with a free vascularised cortico - periosteal flap from the medial femoral condyle Luc DE SMET From the University
Orthobiologics In Orthopaedic Trauma
 Orthobiologics In Orthopaedic Trauma Aaron Nauth, MD, MSc Chair in Fracture Care Research St. Michael s Hospital, University of Toronto Created August 2017 Previous Versions J. Tracy Watson (2007, 2010)
Orthobiologics In Orthopaedic Trauma Aaron Nauth, MD, MSc Chair in Fracture Care Research St. Michael s Hospital, University of Toronto Created August 2017 Previous Versions J. Tracy Watson (2007, 2010)
Bone marrow injection in patients with delayed union and non-union of long bone fractures. Done by Dr.Firas T. Ismaeel
 Bone marrow injection in patients with delayed union and non-union of long bone fractures Done by Dr.Firas T. Ismaeel Abstract Background: In the process of bone formation and healing of fractures, the
Bone marrow injection in patients with delayed union and non-union of long bone fractures Done by Dr.Firas T. Ismaeel Abstract Background: In the process of bone formation and healing of fractures, the
Surgical treatment of aseptic nonunion in long bones: review of 193 cases
 J Orthopaed Traumatol (2007) 8:11 15 DOI 10.1007/s10195-007-0155-z ORIGINAL A. Megaro S. Marchesi U.E. Pazzaglia Surgical treatment of aseptic nonunion in long bones: review of 193 cases Received: 5 September
J Orthopaed Traumatol (2007) 8:11 15 DOI 10.1007/s10195-007-0155-z ORIGINAL A. Megaro S. Marchesi U.E. Pazzaglia Surgical treatment of aseptic nonunion in long bones: review of 193 cases Received: 5 September
chronos Inject. Synthetic Bone Substitute Injectable, Osteoconductive, Resorbable.
 chronos Inject. Synthetic Bone Substitute Injectable, Osteoconductive, Resorbable. Technique Guide The answer to bone voids Table of contents Introduction 2 Case Study 3 Indications and Contraindications
chronos Inject. Synthetic Bone Substitute Injectable, Osteoconductive, Resorbable. Technique Guide The answer to bone voids Table of contents Introduction 2 Case Study 3 Indications and Contraindications
Methods Used for Reconstruction in Aggressive Bone Tumours: An Early Experience
 ORIGINAL ARTICLE Methods Used for Reconstruction in Aggressive Bone Tumours: An Early Experience K L Pan, FRCS*, S STing, FRCS**, A W K Mohamad, MS (Orth)*, W GLee, FRCS**, C C Wong, FRCS**, A H Rasit,
ORIGINAL ARTICLE Methods Used for Reconstruction in Aggressive Bone Tumours: An Early Experience K L Pan, FRCS*, S STing, FRCS**, A W K Mohamad, MS (Orth)*, W GLee, FRCS**, C C Wong, FRCS**, A H Rasit,
For Commercial products, please refer to the following policy: Preauthorization via Web-Based Tool for Procedures
 Medical Coverage Policy Total Joint Arthroplasty Hip and Knee EFFECTIVE DATE: 08/01/2017 POLICY LAST UPDATED: 06/06/2017 OVERVIEW Joint replacement surgery, also known as arthroplasty, has proved to be
Medical Coverage Policy Total Joint Arthroplasty Hip and Knee EFFECTIVE DATE: 08/01/2017 POLICY LAST UPDATED: 06/06/2017 OVERVIEW Joint replacement surgery, also known as arthroplasty, has proved to be
DRIVING THE FUTURE. About HOSPITAL INNOVATIONS. Strong commitment to healthcare innovation
 idente Catalogue About HOSPITAL INNOVATIONS Since 2008, Hospital Innovations has been supplying a growing range of specialist products for use in orthopaedic and corrective surgery; with an emphasis on
idente Catalogue About HOSPITAL INNOVATIONS Since 2008, Hospital Innovations has been supplying a growing range of specialist products for use in orthopaedic and corrective surgery; with an emphasis on
Wrist Joint Reconstruction With a Vascularized Fibula Free Flap Following Giant Cell Tumor Excision in the Distal Radius
 Wrist Joint Reconstruction With a Vascularized Fibula Free Flap Following Giant Cell Tumor Excision in the Distal Radius Chester J. Mays, BS, a Kyle Ver Steeg, MD, a Saeed Chowdhry, MD, b David Seligson,
Wrist Joint Reconstruction With a Vascularized Fibula Free Flap Following Giant Cell Tumor Excision in the Distal Radius Chester J. Mays, BS, a Kyle Ver Steeg, MD, a Saeed Chowdhry, MD, b David Seligson,
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
The Radiology Assistant : Bone tumor - ill defined osteolytic tumors and tumor-like lesions
 Bone tumor - ill defined osteolytic tumors and tumor-like lesions Henk Jan van der Woude and Robin Smithuis Radiology department of the Onze Lieve Vrouwe Gasthuis, Amsterdam and the Rijnland hospital,
Bone tumor - ill defined osteolytic tumors and tumor-like lesions Henk Jan van der Woude and Robin Smithuis Radiology department of the Onze Lieve Vrouwe Gasthuis, Amsterdam and the Rijnland hospital,
ORS 2015 Annual Meeting (Orthopedic Research Society)
 ORS 2015 Annual Meeting (Orthopedic Research Society) Poster No: 1045 CERAMENT Bone Void Filler Impregnated with Gentamicin Increases Bone Formation and Decreases the Rate of Detectable Infection after
ORS 2015 Annual Meeting (Orthopedic Research Society) Poster No: 1045 CERAMENT Bone Void Filler Impregnated with Gentamicin Increases Bone Formation and Decreases the Rate of Detectable Infection after
Of approximately 2 million long bone fractures
 Proceedings S.Z.P.G.M.I vol: 13(1-2) 1999, pp. 71-75. Treatment of Tibial Non-Union with the Ilizarov Method Pervaiz Iqbal, Muhammad Maq, Hamid Qayum Department of Orthopaedics, Shaikh Zayed Hospital,.
Proceedings S.Z.P.G.M.I vol: 13(1-2) 1999, pp. 71-75. Treatment of Tibial Non-Union with the Ilizarov Method Pervaiz Iqbal, Muhammad Maq, Hamid Qayum Department of Orthopaedics, Shaikh Zayed Hospital,.
CASE STUDY: PRO-DENSE Injectable Regenerative Graft Used to Backfill a Bone Cavity Following Resection of a Giant Cell Tumor
 : PRO-DENSE Used to Backfill a Bone Cavity Following Resection of a Giant Cell Tumor Contributed by: Matthew J. Seidel, MD* Lauren A. Schwartz, NP Scottsdale, AZ *Dr. Seidel is a paid consultant for Wright
: PRO-DENSE Used to Backfill a Bone Cavity Following Resection of a Giant Cell Tumor Contributed by: Matthew J. Seidel, MD* Lauren A. Schwartz, NP Scottsdale, AZ *Dr. Seidel is a paid consultant for Wright
Skeletal System worksheet
 Skeletal System worksheet Name Section A: Intro to Skeletal System The skeletal system performs vital functions that enable us to move through our daily lives. Support - The skeleton provides support and
Skeletal System worksheet Name Section A: Intro to Skeletal System The skeletal system performs vital functions that enable us to move through our daily lives. Support - The skeleton provides support and
Pathophysiology of fracture healing
 Pathophysiology of fracture healing Bone anatomy and biomechanics Fracture patterns Bone healing and blood supply Influence of implants 1 What is the structure of bone? 2 Bone structure Four levels: Chemical
Pathophysiology of fracture healing Bone anatomy and biomechanics Fracture patterns Bone healing and blood supply Influence of implants 1 What is the structure of bone? 2 Bone structure Four levels: Chemical
SPINE BIOMATERIALS Crop Bleed
 A comprehensive guide to biomaterials offered by Posterolateral DBX PUTTY DBX STRIP DBX MIX DBX INJECT chronos Strip chronos Granules chronos Preforms PROCURE CHOICE Marrow Aspiration Kit Bone Marrow Aspiration
A comprehensive guide to biomaterials offered by Posterolateral DBX PUTTY DBX STRIP DBX MIX DBX INJECT chronos Strip chronos Granules chronos Preforms PROCURE CHOICE Marrow Aspiration Kit Bone Marrow Aspiration
Dynamic testing of bone grafts
 Acta of Bioengineering and Biomechanics Vol. 10, No. 4, 2008 Dynamic testing of bone grafts JANUSZ PŁOMIŃSKI 1, ZBIGNIEW WATRAL 2, *, KRZYSZTOF KWIATKOWSKI 1 1 Department of Orthopaedics, Military Medical
Acta of Bioengineering and Biomechanics Vol. 10, No. 4, 2008 Dynamic testing of bone grafts JANUSZ PŁOMIŃSKI 1, ZBIGNIEW WATRAL 2, *, KRZYSZTOF KWIATKOWSKI 1 1 Department of Orthopaedics, Military Medical
Isolated congenital anterolateral bowing of the fibula : A case report with 24 years follow-up
 Acta Orthop. Belg., 2009, 75, 842-846 CASE REPORT Isolated congenital anterolateral bowing of the fibula : A case report with 24 years follow-up Karolien LELIEFELD, Hans VAN DER SLUIJS, Ibo VAN DER HAVEN
Acta Orthop. Belg., 2009, 75, 842-846 CASE REPORT Isolated congenital anterolateral bowing of the fibula : A case report with 24 years follow-up Karolien LELIEFELD, Hans VAN DER SLUIJS, Ibo VAN DER HAVEN
Nonunion of the Femur Treated with Conventional Osteosynthesis Combined with Autogenous and Strut Allogeneic Bone Grafts
 Original Article 268 Nonunion of the Femur Treated with Conventional Osteosynthesis Combined with Autogenous and Strut Allogeneic Bone Grafts Lin-Hsiu Weng, MD; Jun-Wen Wang, MD Background: In this study,
Original Article 268 Nonunion of the Femur Treated with Conventional Osteosynthesis Combined with Autogenous and Strut Allogeneic Bone Grafts Lin-Hsiu Weng, MD; Jun-Wen Wang, MD Background: In this study,
MASTERGRAFT Putty. Technical Guide
 MASTERGRAFT Putty Technical Guide MASTERGRAFT Putty is a malleable-cohesive, osteoconductive scaffold composed of collagen that is physically mixed with resorbable ceramic granules. Mixing Process Collagen
MASTERGRAFT Putty Technical Guide MASTERGRAFT Putty is a malleable-cohesive, osteoconductive scaffold composed of collagen that is physically mixed with resorbable ceramic granules. Mixing Process Collagen
OssiMend Bone Graft Matrix
 OssiMend All-Natural Mineral-Collagen Bone Grafting Matrix Anorganic bone mineral and type I collagen Highly purified, biocompatible matrix Osteoconductive Osteoinductive and Osteogenic in conjunction
OssiMend All-Natural Mineral-Collagen Bone Grafting Matrix Anorganic bone mineral and type I collagen Highly purified, biocompatible matrix Osteoconductive Osteoinductive and Osteogenic in conjunction
A WIDE RANGE OF REGENERATIVE SOLUTIONS
 A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
5/31/2018. Ipsilateral Femoral Neck And Shaft Fractures. Ipsilateral Neck-Shaft Fractures Introduction. Ipsilateral Neck-Shaft Fractures Introduction
 Ipsilateral Femoral Neck And Shaft Fractures Exchange Nailing For Non- Union Donald Wiss MD Cedars-Sinai Medical Center Los Angeles, California Introduction Uncommon Injury Invariably High Energy Trauma
Ipsilateral Femoral Neck And Shaft Fractures Exchange Nailing For Non- Union Donald Wiss MD Cedars-Sinai Medical Center Los Angeles, California Introduction Uncommon Injury Invariably High Energy Trauma
Optimum implant geometry
 Design Rationale Optimum implant geometry Extending the proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Design Rationale Optimum implant geometry Extending the proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
CASE PRESENTATION. Dr. Faseeh Shahab PGY3 Orthopaedic Resident, Khyber Teaching Hospital, Peshawar, PAKISTAN
 CASE PRESENTATION Dr. Faseeh Shahab PGY3 Orthopaedic Resident, Khyber Teaching Hospital, Peshawar, PAKISTAN CASE PRESENTATION - History Ms. SB, 30yo Afghan National Presented with 3 months history of Swelling
CASE PRESENTATION Dr. Faseeh Shahab PGY3 Orthopaedic Resident, Khyber Teaching Hospital, Peshawar, PAKISTAN CASE PRESENTATION - History Ms. SB, 30yo Afghan National Presented with 3 months history of Swelling
Treatment of the benign lytic lesions of the proximal femur with synthetic bone graft
 Zekry et al. Journal of Orthopaedic Surgery and Research (2018) 13:270 https://doi.org/10.1186/s13018-018-0982-z RESEARCH ARTICLE Open Access Treatment of the benign lytic lesions of the proximal femur
Zekry et al. Journal of Orthopaedic Surgery and Research (2018) 13:270 https://doi.org/10.1186/s13018-018-0982-z RESEARCH ARTICLE Open Access Treatment of the benign lytic lesions of the proximal femur
