The Effects of Early Active Motion Rehabilitation after Teno Fixrm Tendon Repair in Zone 11 Flexor Tendon Lacerations of the Hand
|
|
|
- Jasper Alan Marsh
- 5 years ago
- Views:
Transcription
1 The Effects of Early Active Motion Rehabilitation after Teno Fixrm Tendon Repair in Zone 11 Flexor Tendon Lacerations of the Hand Lan Chen A. Study purpose and Rationale The purpose of this study is to evaluate the advantages of an early active motion rehabilitation protocol after flexor tendon repair of the hand with the Teno Fix system. Patients with Zone II flexor tendon lacerations repaired with the Teno Fix system will undergo a rigorous early active motion protocol developed at the New York Orthopedic Hospital, starting post-op day 3. Each patient will be followed and our analysis will focus on range of motion, grip and pinch strength, pain, swelling, and a ftinctional assessment with the DASH (Disabilities of the Arm, Shoulder, and Head) questionnaire. Given that the Teno Fix system offers a stronger and more stable tendon repair construct which allows for earlier mobilization, our hypothesis is that early active motion rehabilitation will lead to a better range of motion of the affected finger while maintaining a low rupture rate. a. Background Repair of flexor tendon injuries of the hand represent a challenge for even the most experienced hand surgeon. Prior to the 1960's, severed tendons were not repaired, instead surgeons chose to graft in tendons as replacements for those injured. Over the last 25 years, an enormous amount of basic research has expanded our knowledge of tendon structure, biomechanics and their response to injury, repair, and rehabilitation, thereby allowing the advent of primary tendon suture methods. The desired outcome is a strong repair that is resistant to rupture and the formation of adhesions. A strong repair permits early mobilization of the digit, a factor that has been correlated with eventual range of motion and functionality. The flexor tendons of the hand are enclosed by a tendon sheath lined by synoviocytes in a parietal and visceral layer that provide a smooth gliding surface for the tendon. Anatomically, the flexor tendons are divided into five zones, with Zone I being the most distal and Zone V the most proximal to the wrist. Overlying the synovial sheath are annular and cruciate pulleys (A I -A5, and C 1-0) that surround the tendon and bring it next to the phalanges for efficient gliding. Loss of portions of these particular digital pulleys may significantly alter the normal integrated balance between the flexor, intrinsic, and extensor tendons and result in diminished digital motion, power, and flexion contrwtures of the interphalangeal (1P) j oints. 2 The degree of difficulty in repairing tendon lacerations differs for each of the zones. Zone 11 lacerations are the most difficult to repair because of their involvement of the sheath and pulleys. The essential contribution to tendon healing and gliding is provided by the sheath's vascular and synovial systems. It is therefore important that the surgeon recognizes their integrity during repair. 3 Flexor lacerations in the finger were once found to perform so poorly after primary 4 repair that the Zone H digital sheath was referred to as a surgical no-mans-land. The historically poor results with Zone II repairs has made it the one that most clinical studies focus on. Small commented that tendon repairs in Zone 11 is widely accepted as the yardstick by which 5 techniques of flexor tendon repairs should be assessed. Restoring ftinction after flexor tendon injuries is one of the greatest challenges to hand surgeons and therapists. Historically, repaired flexor tendons were treated with immobilization. Immobilization reduced suture breakage and protected the repair site because tendon healing had already occurred by the time the subject was allowed to move. However, immobilization led to the formation of adhesions that took away all gliding function of the tendon, leading to contractures and functional disability. 6 Columbia University College of Physicians and Surgeons 1
2 While mobilization is the key to preventing adhesions and achieving maximum ROM, it is at the risk of rupture. In vivo and in vitro studies confirm that mobilization with cyclic tension delivers nutrients more efficiently and promotes better and faster healing7-16. Early motion also decreases the number of adhesions and joint contractures that develop secondary to the formation of scar tissue 17. However, observational studies have shown that most traditional suture techniques do not provide enough strength to allow for safe, early active mobilization. The rupture rate is proportional to the postoperative mobilization regimen for the repaired digit and has been reported in the literature to vary between 3% and 9.4%, depending upon the mobilization scheme used. 18,19 The newly FDA approved Teno Fix tendon repair system was developed to specifically address these difficulties with Zone R flexor tendon repairs. The Teno Fix uses a stainless steel braided suture to approximate the severed tendon edges, and in a randomized controlled clinical trial by B. Su et al, it was shown to have a significantly decreased rupture rate when compared to the traditional suture method (unpublished data). In summary, the Teno Fix produces a stronger and more stable tendon repair construct with the potential to allow for early active mobilization of the repaired digit while minimizing trauma to the vascular and synovial sheath. This translates into minimized adhesions, gap formation, and rupture of the initial repair while allowing fuller, quicker recovery while obviating the need for additional surgeries. Earlier return to ftinction and fewer complications would present a significant advance in the field of flexor tendon surgery. B. Study Design and Statistical Analysis This is a prospective, single arm, blinded study to evaluate the functional outcome of an early active motion rehabilitation protocol after flexor tendon repair of the hand using the newly FDA approved Teno Fix tendon repair system. Eligible patients with single digit or multiple digit flexor tendon lacerations in Zone II of the hand will undergo tendon repair with the Teno Fix system. Occupational/hand therapists and clinical personnel taking post-operative outcome measures (physicians, nurses, etc) will be blinded to the type of rehabilitation program the patient is undergoing. a. Power Analysis The primary outcome measure will be range of motion. The analysis will compare the average range of motion after early active motion rehabilitation using the Teno Fix repair with historical data of 34 cases of Teno Fix flexor tendon repair using a traditional passive motion protocol for the first 3 weeks followed by active flexion at four weeks. Published literature by Silfverskiold et al. indicates that the average range of motion 24 weeks post-surgery for standard passive/active motion rehabilitation is about 157' with a standard deviation of 17'. We estimate that the early active motion protocol will result in a clinically significant 10% increase in the range of motion at six months. Based on this data, a total of 19 digits are needed in the early active motion group to yield a power of 80% at an alpha of Secondary outcome measurements will include pain and swelling, grip and pinch strength, and the Disabilities of the Arm, Shoulder, and Hand (DASH) questionnaire for upper extremity functional ability. Pain in the injured digit(s) will be assessed via a verbal numerical scales designed as an alternative or complement to the categorical and visual analogue scales. Swelling and grip/pinch strength will be clinically measured and compared with an uninjured digit and contralateral hand, respectively. b. Outcome Analysis Range of motion is a continuous variable and it will be assumed that it is normally distributed. Our hypothesis that early active motion rehabilitation will. yield a 10% increase in ROM at 24 weeks when compared to the traditional passive/active rehabilitation, will be tested using the usual two-sample t-test. Range of motion data will also be translated into the Strickland Original Scores at 12 and 24 weeks. The score is calculated as: % of normal active PIP and DIP motion = [(arch of motion at both the PIP and DIPjoint) / 175*] x ' is assumed to the normal combined ROM for the PIP and DIP joints. The percentage scores will be classified into the following categories: Columbia University College of Physicians and Surgeons 2
3 Classification Score Excellent 85%-100% Good 70%-84% Fair 50%-69% Poor < 50% For the 12 and 24 weeks range of motion assessment, a Fisher's exact test will be performed to determine if the distribution of subjects in the treatment and historical control groups are the same across these classifications. C. Study Procedure 1) Baseline examination: After obtaining informed consent, all patients will undergo a baseline exam that includes a medical and orthopedic history and physical examination. 2) Surgical procedure: The surgical procedure will utilize the same anesthesia and surgical approach as in a traditional suture repair of the tendon. The tendon repair will be performed using the standard surgical method for insertion of the Teno Fix device. First, two stainless steel coil anchors will be inserted in the tendon tissue, approximately I cm from the proximal and distal cut ends of the tendon. Next, a multifilament braided stainless steel suture will be passed through the anchors, starting with the distal. anchor. A crimp on the end of the suture will stop the suture from completely passing through the anchor. The tendon edges will be reapproximated, and the suture will be crimped on the proximal side, maintaining the correct length. A single circumferential suture will be used to smooth the reapproximated edges. The placement of this epitendonous suture is a step used in traditional tendon repair to restore contour to the tendon, thus facilitating gliding through the flexor pulley system. Should the investigator determine during the surgery that there is not enough tend on exposure or the tendon is too small in size for use of the Teno FiXTm device, the subject will undergo a standard repair using fourstrand suture technique. Such subjects would be classified as an intraoperative screening failure and would not enter in the study. 3) Postoperative management: After the operation, the hand will be immobilized in a dorsal plaster splint with the wrist and hand in neutral position. On postoperative day 3, patients will be taken out of the splint and started on the New York Orthopedic Hospital Early Active Motion Protocol. They will be asked to hold an appropriate sized dowel allowing for active flexion and extension at the MP joint. VVhile at home patients will do 10 reps of dowel exercise four times per day. Between the exercises, patients' will be in a hand splint and encouraged to perform passive flexion and extension. Each week, the hand therapist will see the patient to evaluate their progress. This regiment will continue for six weeks with progressively decreasing dowel size. 4) Postopgrative evaluation: Patients will be evaluated starting at postoperative day I with the DASH questionnaird to establish a baseline fimctional status of their upper extremity. Outcome measurements will also be taken at week 3, 6, 12, and 24. Outcome measurements will include range of motion and grip/pinch strength at weeks 12 and 24, pain and swelling assessment at postoperative day 1, week 3, 6, 12, and 24, and fimetional assessment with the DASH questionnaires at week 6, 12, and 24 compared to baseline. Safety monitoring throughout the study will include evaluating subjects at each visit for signs and symptoms of tendon rupture, infection, contractures, nerve injury and wound dehiscence. The total follow-up time for each patient is 6 months. Based on prior experience at the New York Orthopedic Hospital, approximately 2 patients with flexor tendon laceration are expected per month. The study is expected to take approximately I year for completion of patient recruitment. D. Study Drugs Columbia University College of Physicians and Surgeons 3
4 none E. Medical Device The Teno FiXTm Tendon Repair System from Ortheon Medical is a surgical anchoring system for soft tissue repair. It received its FDA approval as an implantable device in June 2003 and is currently a commercially available implant intended for the repair of lacerated or severed digital flexor tendons. The device comes as a sterile, preloaded instrument that, when used as directed, implants a stainless steel suture across the area of tendon injury. This core suture is held in place by anchors at its proximal and distal ends. The implantable components (suture, stop beads and anchors) are composed of stainless steel alloy ASTM, similar to suture materials already used in human surgery. The device remains embedded in the tendon substance with little reaction on the tendon surfaces and in successful primary repairs, provides a stronger and more stable repair construct than conventional suture repairs with less rupture and gapping rates, and does not limit interphalangeal joint flexion. The Teno Fix device is well toleirated, does not elicit an inflammatory response, and allows normal histologic tendon healing. It is currently considered an improved alternative to conventional stranded cruciate suture repair. The device is currently available in one size and limits its use in tendons of large enough width to accommodate the stop beads and anchors. F. Study Questionnaires For this study, we will use the Disabilities of the Arm, Shoulder, and Hand (DASH) Survey as a means to measure functional outcome. DASH was created as a joint effort by the American Academy of Orthopedic Surgeons (AAOS), the Council of Musculoskeletal. Specialty Societies, and the Institute for Work and Health.20 The survey contains 30 questions on activities of daily living and pain and is intended to be used to evaluate disability and symptoms in single or multiple disorders of the upper limb at one point or at many points in time. A higher score reflects greater disability. Preliminary work on the DASH showed that it was both reliable and valid. The DASH questionnaire will be used in this study at different points after tendon repair as an assessment of improvement in functional outcome. A suitable measurement of pain for the Teno-FiXTMstudy is a group of verbal numerical scales designed as an alternative or complement to the categorical and visual analogue scales. With these scales, the patient is asked to express numerically the magnitude of the pain. A scale of 0 (no pain) to 10 (worst pain imaginable) showed good correlation with the conventional 10 cm. unmarked horizontal visual analogue scale developed by Huskisson. 21,22 For this study, patients will be asked to assess their own pain on a scale of 0-10 immediately after the operation and at each visit to the therapist up till 6 weeks, and then at 12 and 24 weeks follow-up. Columbia University College of Physicians and Surgeons 4
5 G. Study Subjects Subjects can be male or female, of any race, at least 18 years old, with a lacerated or severed digital flexor digitorum. profimdus tendon with or without concomitant flexor digitorum superficialis injury in Zone 11 of the index, middle, ring, and small finger. The laceration must have occurred within the previous fourteen days, as studies have shown, after 14 days, histologic changes in the tendon appear which can impair tendon healing. Subjects must also have an uninjured contralateral hand and digits that can be used for comparison to the injured hand and injured digits. Exclusion criteria include pregnancy, diabetes mellitus, autoirnmune disorders, documented acquired immunodeficiency complex (AIDS), chronic immunosupressive medications or other conditions that could affect postoperative wound healing.: To minimize confounding outcome measures, subjects with a lack of adequate cutaneous coverage at repair site, concomitant fractures, amputated digits, arthritis of hand, prior hand injury or trauma, congenital hand defects, or other condition(s) that will impair comparative, measurements in the treated hand or the contralateral. control hand, will be excluded. The presence of infected, necrotic or ischemic tissue in the injured hand will also be excluded, along with subjects with known sensitivity or allergy to the metals contained in Teno Fix stainless steel rod: chromium, nickel, copper, cobalt, and iron. If it is determined intraoperatively that the Teno Fix cannot be completed (e.g., insufficient tendon for placement of the Teno FiXTm anchor), the patient will also be excluded. H. Recruitment of Subjects Subjects will be identified and referred by the patient's primary orthopedic surgeon, Dr. Melvin Rosenwasser, after confirmation that the Teno Fix tendon repair system is appropriate for the patient. I. Confidentiality of Study Data Study data will be coded and a unique identifier will be assigned to each subject. All study data will be stored in a locked cabinet in the Department of Orthopedics Trauma Training Center, accessible only to the investigators of the study. J. Potential Conflict of Interest none K. Location of Study The study is a single site study and will be conducted through the Department of Orthopedic Surgery at CPMC. During the postoperative rehabilitation period, patients will be followed by the occupational therapist at CPMC and will return for to CPMC for each subsequent follow-up visit. L. Potential Risks Adverse events in the Teno Fix treatment group include, but are not limited to: rupture of the tendon repair, infection, secondary surgical intervention, adhesions and/or contractures, wound dehiscence, nerve injury, and allergic reaction to the stainless steel suture material. Patient may also experience minimally increased pain and swelling when compared to patients with a less strong, traditional suture repair. Columbia University College of Physicians and Surgeons 5
6 M. Potential Benefits Enrollment in the study may be beneficial by assuring close follow-up of patients through their rehabilitation period. By adhering closely to the early active motion protocol, patients may experience early movement of their fingers, as well as an accelerated return to per-operative function and normal activity levels. In addition, future patients may benefit from the results of this early active motion rehabilitation technique after Teno Fix tendon repair. N. Alternative Therapies The Teno Fix tendon repair system is a FDA approved device designed to give improved outcomes of flexor tendon lacerations of the hand when compared to more traditional methods. These alternative methods include other more complicated suturing techniques, which are technically challenging requiring more time in the operating room while necessitating more holes be made in the tendon to repair it. When this occurs, more time may be needed for healing. O. Compensation to Subjects none P. Costs to Subjects Patients will not incur and additional costs due to their participation in the study. Q. Minors as Research Subjects N/A R. Rtadiation or Radioactive Substances Aside from the conventional radiographic imaging to follow the stability of the tendon repair construct and to ascertain the absence of the Teno Fix device migration, no additional radiation exposures are required. S. References 1. Principles of Hand Surgery and Therapy; p Strickland J. Development of flexor tendon surgery: twenty-five years of progress. J Hand Surg 2000; 25A: Silfverskiold K, May E, Tomvall A. Flexor digitorum profundus tendon excursions during controlled motion after flexor tendon repair in zone 11: a prospective clinical study. J Hand Surg. 1992; 17A: Strickland I Flexor tendon injuries: 1. Foundations of treatment. JAm Acad Orthop Surg. 1995;3: Small J, Brennan M, Colville J. Early active mobilisation following flexor tendon repair in zone 2. JHandSurg. 1989;14B: Wang A, Gupta A. Early motion after flexor tendon surgery. Hand Clinics 1996; 12(l): Baktir A, Turk C, Kabak S, Sahin V, Kardas Y. Flexor tendon repair in zone 2 followed by early active mobilization. J Hand Surg. 1996;2 1 B: Columbia University College of Physicians and Surgeons 6
7 8. Peck F, Bucher C, Watson J, Roe A. A comparative study of two methods of controlled mobilization of flexor tendon repairs in zone 2. J Hand Surg. 1998;23B: Kitsis C, Wade P, Krikler S, Parsons N, Nicholls L. Controlled active motion following primary flexor tendon repair: a prospective study over 9 years. J Hand Surg. 1998;23B(34449). 10.Riaz M, Hill C, Khan K, Small J. Long term outcome of early active mobilization following flexor tendon repair in zone 2. JHandSurg. 1999;24B: Lister G, Kleinert H, Kutz J, Atasoy E. Primary flexor tendon repair followed by immediate controlled mobilization. J Hand Surgery. 1977;2: Savage R, Risitano, G. Flexor tendon repair using a "six strand" method of repair and early active mobilisation.jhandsurg. 1989;14B: Olivier L, Assemnacher S, Kendoff D, Schmidt G, Towfigh H, Schmit-Neurerburg K. Results of flexor tendon repair of the hand by the motion-stable wire suture by Towfigh. Arch Orthop Trauma Surg ; 121: Bainbridge L, Robertson C, Gillies D, Elliot D. A comparison of post-operative mobilization of flexor tendon repairs with "passive flexion-active extension" and "controlled active motion" techniques. JHandSurg. 1994;19B: Elliot D, Moiemen N, Flemming A, Harris S, Foster A. The rupture rate of acute flexor tendon repairs mobilized by the controlled active motion regimen. JHandSurg, 1994;19B: So Y, Chow S, Pun W, Luk K, Crosby C, Ng C. Evaluation of results in flexor tendon repair: a 17. Silfverskiold K, May E, Oden A. Factors affecting results after flexor tendon repair in zone II: a multivariate prospective analysis. J Hand Surg. 1992; 1 8A: critical analysis of five methods in ninety-five digits. JHandSurg. 1990;15(2): Bainbridge L, Robertson C, Gillies D, Elliot D. A comparison of post-operative mobilization of flexor tendon repairs with "passive flexion-active extension" and "controlled active motion" techniques. J Hand Surg 1994; 19B: Elliot D, Moiemen N, Flemming A, et al. The rupture rate of acute flexor tendon repairs mobilized by the controlled active motion regimen. J Hand Surg 1994; 19B: Hudak P, Amadio P, Bombardier C, (UECG). TUECG. Development of an upper extremity outcome measure: the DASH (Disabilities of the Arm, Shoulder and Head). Am JInd Med 1996;29: Murphy D, McDonald A, Power C, Unwin A, MacSullivan A. Measurement of pain: a comparison of the visual with a nonvisual analogue scale. The Clinical Journal of Pain. 1988;3: Huskisson E. Measurement of pain. Lancet. 1974;ii: Columbia University College of Physicians and Surgeons 7
FACTORS INFLUENCING THE MANAGEMENT OF THE FLEXOR TENDON INJURIES IN THE HAND
 Basrah Journal of Surgery FACTORS INFLUENCING THE MANAGEMENT OF THE FLEXOR TENDON INJURIES IN THE HAND Avadis F.I.C.M.S. Lecturer in Orthopaedic, Department of Surgery, College of Medicine, and specialist
Basrah Journal of Surgery FACTORS INFLUENCING THE MANAGEMENT OF THE FLEXOR TENDON INJURIES IN THE HAND Avadis F.I.C.M.S. Lecturer in Orthopaedic, Department of Surgery, College of Medicine, and specialist
Interesting Case Series. Zone I Flexor Tendon Injuries
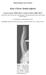 Interesting Case Series Zone I Flexor Tendon Injuries Evgenios Evgeniou, MBBS, MRCS, a and Harriet Walker, MBBS, MRCS b a North Bristol NHS Trust, Bristol, United Kingdom, b Plymouth Hospitals NHS Trust,
Interesting Case Series Zone I Flexor Tendon Injuries Evgenios Evgeniou, MBBS, MRCS, a and Harriet Walker, MBBS, MRCS b a North Bristol NHS Trust, Bristol, United Kingdom, b Plymouth Hospitals NHS Trust,
Hand Therapy Protocols
 Hand Therapy Protocols Post Repair Therapy Protocols Page 1 of 10 Following are representative protocols for each of the three basic approaches to flexor tendon post repair management: immobilization,
Hand Therapy Protocols Post Repair Therapy Protocols Page 1 of 10 Following are representative protocols for each of the three basic approaches to flexor tendon post repair management: immobilization,
Flexor tendon injuries of the hand treated with TenoFix TM : mid-term results
 J Orthopaed Traumatol (2008) 9:201 208 DOI 10.1007/s10195-008-0016-4 ORIGINAL ARTICLE Flexor tendon injuries of the hand treated with TenoFix TM : mid-term results Lorenzo Rocchi Æ Antonio Merolli Æ Andrea
J Orthopaed Traumatol (2008) 9:201 208 DOI 10.1007/s10195-008-0016-4 ORIGINAL ARTICLE Flexor tendon injuries of the hand treated with TenoFix TM : mid-term results Lorenzo Rocchi Æ Antonio Merolli Æ Andrea
11/13/2017. Complications of Flexor Tendon Repair. Brandon E. Earp, M.D. How do we best get there?
 Complications of Flexor Tendon Repair Brandon E. Earp, M.D. Chief of Orthopaedic Surgery Brigham and Women s Faulkner Hospital Vice-Chair of Clinical Operations Brigham and Women s Hospital Frontiers in
Complications of Flexor Tendon Repair Brandon E. Earp, M.D. Chief of Orthopaedic Surgery Brigham and Women s Faulkner Hospital Vice-Chair of Clinical Operations Brigham and Women s Hospital Frontiers in
Andrew B. Stein, MD Boston University Medical Center May 2 & 3, 2016
 Andrew B. Stein, MD Boston University Medical Center andrew.stein@bmc.org Work Related Workshop WorkInjuries Related Injuries Workshop Tendon injuries may be obvious or subtle History (mechanism of injury)
Andrew B. Stein, MD Boston University Medical Center andrew.stein@bmc.org Work Related Workshop WorkInjuries Related Injuries Workshop Tendon injuries may be obvious or subtle History (mechanism of injury)
Reversing PIP Joint Contractures:
 Reversing PIP Joint Contractures: Applicability of the Digit Widget External Fixation System John M. Agee M.D. Reversing PIP Joint Contractures: Applicability of the Digit Widget External Fixation System
Reversing PIP Joint Contractures: Applicability of the Digit Widget External Fixation System John M. Agee M.D. Reversing PIP Joint Contractures: Applicability of the Digit Widget External Fixation System
Clinical Orthopaedic Rehabilitation Volume 1 and 2
 Clinical Orthopaedic Rehabilitation Volume 1 and 2 COURSE DESCRIPTION This program is a practical, clinical guide that provides guidance on the evaluation, differential diagnosis, treatment, and rehabilitation
Clinical Orthopaedic Rehabilitation Volume 1 and 2 COURSE DESCRIPTION This program is a practical, clinical guide that provides guidance on the evaluation, differential diagnosis, treatment, and rehabilitation
Rehabilitation Protocol: Primary Flexor Tendon Repair LHMC Protocol for Zone 1 & 2
 Rehabilitation Protocol: Primary Flexor Tendon Repair LHMC Protocol for Zone 1 & 2 Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington
Rehabilitation Protocol: Primary Flexor Tendon Repair LHMC Protocol for Zone 1 & 2 Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington
SJS. Original Research Article. M. Manninen 1, T. Karjalainen 2, J. Määttä 1, T. Flinkkilä 1
 665544SJS0010.1177/1457496916665544Epidemiology of flexor tendon injuriesm. Manninen, et al. research-article2016 Original Research Article SJS SCANDINAVIAN JOURNAL OF SURGERY Epidemiology of Flexor Tendon
665544SJS0010.1177/1457496916665544Epidemiology of flexor tendon injuriesm. Manninen, et al. research-article2016 Original Research Article SJS SCANDINAVIAN JOURNAL OF SURGERY Epidemiology of Flexor Tendon
AROM of DIP flex/ext, 10 reps hourly.
 BRIGHAM AND WOMEN S HOSPITAL A Teaching Affiliate of Harvard Medical School 75 Francis St. Boston, Massachusetts 02115 Department of Rehabilitation Services Physical Therapy The intent of this protocol
BRIGHAM AND WOMEN S HOSPITAL A Teaching Affiliate of Harvard Medical School 75 Francis St. Boston, Massachusetts 02115 Department of Rehabilitation Services Physical Therapy The intent of this protocol
Swan-Neck Deformity. Introduction. Anatomy
 Swan-Neck Deformity Introduction Normal finger position and movement occur from the balanced actions of many important structures. Ligaments support the finger joints. Muscles hold and move the fingers.
Swan-Neck Deformity Introduction Normal finger position and movement occur from the balanced actions of many important structures. Ligaments support the finger joints. Muscles hold and move the fingers.
A Patient s Guide to Adult Finger Fractures
 A Patient s Guide to Adult Finger Fractures 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 1 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Adult Finger Fractures 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 1 DISCLAIMER: The information in this booklet is compiled from a variety
Dynamic treatment for proximal phalangeal fracture of the hand
 Journal of Orthopaedic Surgery 2007;15(2):211-5 Dynamic treatment for proximal phalangeal fracture of the hand G Rajesh, WY Ip, SP Chow, BKK Fung Department of Orthopaedics and Traumatology, University
Journal of Orthopaedic Surgery 2007;15(2):211-5 Dynamic treatment for proximal phalangeal fracture of the hand G Rajesh, WY Ip, SP Chow, BKK Fung Department of Orthopaedics and Traumatology, University
MULTIMEDIA ARTICLES. Mary C. Burns & Brian Derby & Michael W. Neumeister
 HAND (2013) 8:17 22 DOI 10.1007/s11552-012-9488-z MULTIMEDIA ARTICLES Wyndell merritt immediate controlled active motion (ICAM) protocol following extensor tendon repairs in zone IV VII: review of literature,
HAND (2013) 8:17 22 DOI 10.1007/s11552-012-9488-z MULTIMEDIA ARTICLES Wyndell merritt immediate controlled active motion (ICAM) protocol following extensor tendon repairs in zone IV VII: review of literature,
Revisiting the Curtis Procedure for Boutonniere Deformity Correction
 180 Letter to Editor Revisiting the Curtis Procedure for Boutonniere Deformity Correction Lee Seng Khoo*, Vasco Senna-Fernandes Ivo Pitanguy Institute, Rua Dona Mariana 65, Botafogo, Rio De Janeiro, Brazil
180 Letter to Editor Revisiting the Curtis Procedure for Boutonniere Deformity Correction Lee Seng Khoo*, Vasco Senna-Fernandes Ivo Pitanguy Institute, Rua Dona Mariana 65, Botafogo, Rio De Janeiro, Brazil
Flexor Tendon Case Conundrums
 Flexor Tendon Case Conundrums Philly Meeting 2018 Rowena McBeath, MD, PhD Jeffrey A. Greenberg, MD Nancy M. Cannon, OTR, CHT Faculty Rowena McBeath, MD, PhD Yale molecular biochemistry & biophysics John
Flexor Tendon Case Conundrums Philly Meeting 2018 Rowena McBeath, MD, PhD Jeffrey A. Greenberg, MD Nancy M. Cannon, OTR, CHT Faculty Rowena McBeath, MD, PhD Yale molecular biochemistry & biophysics John
Effect of Core Suture Technique and Type on the Gliding Resistance during Cyclic Motion following Flexor Tendon Repair: A Cadaveric Study
 Effect of Core Suture Technique and Type on the Gliding Resistance during Cyclic Motion following Flexor Tendon Repair: A Cadaveric Study Tamami Moriya, 1 Chunfeng Zhao, 1 Toshihiko Yamashita, 2 Kai-Nan
Effect of Core Suture Technique and Type on the Gliding Resistance during Cyclic Motion following Flexor Tendon Repair: A Cadaveric Study Tamami Moriya, 1 Chunfeng Zhao, 1 Toshihiko Yamashita, 2 Kai-Nan
Extensor Tendon Repair Zones II, III, IV
 Zones II, III, IV D. WATTS, MD Indications Lacerations to the central slip, lateral bends and/or triangular ligament Rupture of the central slip in association with a PIP joint volar dislocation Avulsion
Zones II, III, IV D. WATTS, MD Indications Lacerations to the central slip, lateral bends and/or triangular ligament Rupture of the central slip in association with a PIP joint volar dislocation Avulsion
Flexor Tenorrhaphy Using Absorbable Suture Materials
 Flexor Tenorrhaphy Using Absorbable Suture Materials Hyung Joo Kang, Dong Chul Lee, Jin Soo Kim, Sae Hwi Ki, Si Young Roh, Jae Won Yang Department of Plastic and Reconstructive Surgery, Kwang-Myung Sung-Ae
Flexor Tenorrhaphy Using Absorbable Suture Materials Hyung Joo Kang, Dong Chul Lee, Jin Soo Kim, Sae Hwi Ki, Si Young Roh, Jae Won Yang Department of Plastic and Reconstructive Surgery, Kwang-Myung Sung-Ae
Emile N. Brown, MD, and Scott D. Lifchez, MD
 Flexor Pollicis Longus Tendon Rupture After Volar Plating of a Distal Radius Fracture: Pronator Quadratus Plate Coverage May Not Adequately Protect Tendons Emile N. Brown, MD, and Scott D. Lifchez, MD
Flexor Pollicis Longus Tendon Rupture After Volar Plating of a Distal Radius Fracture: Pronator Quadratus Plate Coverage May Not Adequately Protect Tendons Emile N. Brown, MD, and Scott D. Lifchez, MD
Trigger Finger and Trigger Thumb A Patient's Guide to Trigger Finger & Trigger Thumb
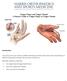 Trigger Finger and Trigger Thumb A Patient's Guide to Trigger Finger & Trigger Thumb Introduction Trigger finger and trigger thumb are conditions affecting the movement of the tendons as they bend the
Trigger Finger and Trigger Thumb A Patient's Guide to Trigger Finger & Trigger Thumb Introduction Trigger finger and trigger thumb are conditions affecting the movement of the tendons as they bend the
Current Practice in Tendon Management
 Current Practice in Tendon Management Handout www.indianahandtoshoulder.com Click on Therapy Flexor Tendons Denver Nancy M. Cannon, OTR, CHT Director Hand to Shoulder Therapy Center Indianapolis, Indiana
Current Practice in Tendon Management Handout www.indianahandtoshoulder.com Click on Therapy Flexor Tendons Denver Nancy M. Cannon, OTR, CHT Director Hand to Shoulder Therapy Center Indianapolis, Indiana
BUNNELL. Expanded product line Customer service Please visit BunnellSplints.com Sizing information on back page WRIST HAND FINGER ORTHOSIS
 Established 1907 WENIGER Exclusive Manufacturer of BUNNELL WRIST HAND FINGER ORTHOSIS STATIC DYNAMIC STATIC PROGRESSIVE POSITIONING LATEX FREE SOFT STRAPS ORTHOSIS FITS RIGHT OR LEFT HAND Expanded product
Established 1907 WENIGER Exclusive Manufacturer of BUNNELL WRIST HAND FINGER ORTHOSIS STATIC DYNAMIC STATIC PROGRESSIVE POSITIONING LATEX FREE SOFT STRAPS ORTHOSIS FITS RIGHT OR LEFT HAND Expanded product
Comparison of Roll Stitch Technique and Core Suture Technique for Extensor Tendon Repair at the Metacarpophalangeal Joint level
 Trauma Mon. 2016 February; 21(1): e24563. Published online 2016 February 6. doi: 10.5812/traumamon.24563 Research Article Comparison of Roll Stitch Technique and Core Suture Technique for Extensor Tendon
Trauma Mon. 2016 February; 21(1): e24563. Published online 2016 February 6. doi: 10.5812/traumamon.24563 Research Article Comparison of Roll Stitch Technique and Core Suture Technique for Extensor Tendon
Structure and Function of the Hand
 Structure and Function of the Hand Some say it takes a village to raise a child, but it takes 19 bones and 19 joints in the hand for it to function smoothly. The Hand Dorsal aspect 2 3 4 The digits are
Structure and Function of the Hand Some say it takes a village to raise a child, but it takes 19 bones and 19 joints in the hand for it to function smoothly. The Hand Dorsal aspect 2 3 4 The digits are
FINGER INJURIES. Chapter 24, pgs ,
 FINGER INJURIES Chapter 24, pgs 727 730, 741 743 1. Demonstrate mastery of anatomical references to the hand and fingers. 2. Compare and contrast Mallet Finger, Swan Neck Deformity and Boutonnière Deformity.
FINGER INJURIES Chapter 24, pgs 727 730, 741 743 1. Demonstrate mastery of anatomical references to the hand and fingers. 2. Compare and contrast Mallet Finger, Swan Neck Deformity and Boutonnière Deformity.
Clinical examination of the wrist, thumb and hand
 Clinical examination of the wrist, thumb and hand 20 CHAPTER CONTENTS Referred pain 319 History 319 Inspection 320 Functional examination 320 The distal radioulnar joint.............. 320 The wrist.......................
Clinical examination of the wrist, thumb and hand 20 CHAPTER CONTENTS Referred pain 319 History 319 Inspection 320 Functional examination 320 The distal radioulnar joint.............. 320 The wrist.......................
JuggerKnot Soft Anchor 1.0 mm Mini
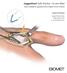 JuggerKnot Soft Anchor 1.0 mm Mini Ulnar Collateral Ligament (UCL) Repair of the Thumb Surgical Technique Surgical Protocols by Mark Rekant, M.D. A. Lee Osterman, M.D. One Surgeon. One Patient. Over 1
JuggerKnot Soft Anchor 1.0 mm Mini Ulnar Collateral Ligament (UCL) Repair of the Thumb Surgical Technique Surgical Protocols by Mark Rekant, M.D. A. Lee Osterman, M.D. One Surgeon. One Patient. Over 1
A Patient s Guide to Biceps Tendon Tears at the Elbow
 A Patient s Guide to Biceps Tendon Tears at the Elbow Introduction The muscles which flex the elbow are the bicep complex. Like all musculoskeletal units, the end connection is a tendon composed of strong,
A Patient s Guide to Biceps Tendon Tears at the Elbow Introduction The muscles which flex the elbow are the bicep complex. Like all musculoskeletal units, the end connection is a tendon composed of strong,
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Svens, B., Ames, E., Burford, K., & Caplash, Y. (2015). Relative active motion programs following extensor tendon repair: A pilot study using a prospective cohort and evaluating
CRITICALLY APPRAISED PAPER (CAP) Svens, B., Ames, E., Burford, K., & Caplash, Y. (2015). Relative active motion programs following extensor tendon repair: A pilot study using a prospective cohort and evaluating
Tensile Strength of Flexor Tendon Repair Using Barbed Suture Material in a Dynamic Ex Vivo Model
 J Hand Microsurg (January June 2012) 4(1):16 20 DOI 10.1007/s12593-012-0063-1 ORIGINAL ARTICLE Tensile Strength of Flexor Tendon Repair Using Barbed Suture Material in a Dynamic Ex Vivo Model Philip H.
J Hand Microsurg (January June 2012) 4(1):16 20 DOI 10.1007/s12593-012-0063-1 ORIGINAL ARTICLE Tensile Strength of Flexor Tendon Repair Using Barbed Suture Material in a Dynamic Ex Vivo Model Philip H.
We perform the vast majority of our flexor HAND/PERIPHERAL NERVE
 HAND/PERIPHERAL NERVE Avoiding Flexor Tendon Repair Rupture with Intraoperative Total Active Movement Examination Amanda Higgins, B.Sc.O.T. Donald H. Lalonde, M.D. Michael Bell, M.D. Daniel McKee, B.Sc.
HAND/PERIPHERAL NERVE Avoiding Flexor Tendon Repair Rupture with Intraoperative Total Active Movement Examination Amanda Higgins, B.Sc.O.T. Donald H. Lalonde, M.D. Michael Bell, M.D. Daniel McKee, B.Sc.
8 Recovering From HAND FRACTURE SURGERY
 8 Recovering From HAND FRACTURE SURGERY Hand fractures are caused by trauma and result in breaking (fracturing) the phalanges or metacarpals. Surgery involves achieving acceptable alignment and providing
8 Recovering From HAND FRACTURE SURGERY Hand fractures are caused by trauma and result in breaking (fracturing) the phalanges or metacarpals. Surgery involves achieving acceptable alignment and providing
Early motion or immobilisation of Hand Fractures? Nikki Burr Consultant Hand Therapist Royal Free Hospital London Mount Vernon Hospital
 Early motion or immobilisation of Hand Fractures? Nikki Burr Consultant Hand Therapist Royal Free Hospital London Mount Vernon Hospital Hand Fractures (distal to carpus) Soft tissue injury with an underlying
Early motion or immobilisation of Hand Fractures? Nikki Burr Consultant Hand Therapist Royal Free Hospital London Mount Vernon Hospital Hand Fractures (distal to carpus) Soft tissue injury with an underlying
Client centered approach to distal radius fracture management. Jared Rasmussen OTR
 Client centered approach to distal radius fracture management Jared Rasmussen OTR Disclosures Sadly, no financial disclosures Objectives Review of anatomy, common fractures of the distal radius, fixation
Client centered approach to distal radius fracture management Jared Rasmussen OTR Disclosures Sadly, no financial disclosures Objectives Review of anatomy, common fractures of the distal radius, fixation
TENDINOSIS: TRIGGER FINGER DE QUERVAIN S TENOSYNOVITIS. Renita Sirisena Mark Puhaindran
 TENDINOSIS: TRIGGER FINGER DE QUERVAIN S TENOSYNOVITIS Renita Sirisena Mark Puhaindran Tendinosis vs Tendinitis Tendinosis: Degeneration of the tendon s collagen Related to chronic use Tendinitis Tendon
TENDINOSIS: TRIGGER FINGER DE QUERVAIN S TENOSYNOVITIS Renita Sirisena Mark Puhaindran Tendinosis vs Tendinitis Tendinosis: Degeneration of the tendon s collagen Related to chronic use Tendinitis Tendon
In Vivo Flexor Tendon Forces Increase with Finger and Wrist Flexion during Active Finger Flexion and Extension
 In Vivo Flexor Tendon Forces Increase with Finger and Wrist Flexion during Active Finger Flexion and Extension Katarzyna Kursa, 1 Lisa Lattanza, 2 Edward Diao, 2 David Rempel 3 1 Department of Bioengineering,
In Vivo Flexor Tendon Forces Increase with Finger and Wrist Flexion during Active Finger Flexion and Extension Katarzyna Kursa, 1 Lisa Lattanza, 2 Edward Diao, 2 David Rempel 3 1 Department of Bioengineering,
JuggerKnot Soft Anchor 1.0 mm Mini
 JuggerKnot Soft Anchor 1.0 mm Mini Ulnar Collateral Ligament (UCL) Repair of the Thumb Surgical Technique Surgical Protocols by Mark Rekant, M.D. A. Lee Osterman, M.D. One Surgeon. One Patient. Over 1
JuggerKnot Soft Anchor 1.0 mm Mini Ulnar Collateral Ligament (UCL) Repair of the Thumb Surgical Technique Surgical Protocols by Mark Rekant, M.D. A. Lee Osterman, M.D. One Surgeon. One Patient. Over 1
JuggerKnot Soft Anchor 1.0 mm Mini. Scapholunate Ligament Repair/Reconstruction. Brochure and Surgical Technique
 JuggerKnot Soft Anchor 1.0 mm Mini Scapholunate Ligament Repair/Reconstruction Brochure and Surgical Technique One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide
JuggerKnot Soft Anchor 1.0 mm Mini Scapholunate Ligament Repair/Reconstruction Brochure and Surgical Technique One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide
Trigger Finger Release
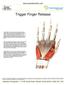 Trigger Finger Release Trigger finger, also known as stenosing tenosynovitis, occurs when one of the tendons responsible for bending a finger or the thumb develops a thickening, known as a nodule, and
Trigger Finger Release Trigger finger, also known as stenosing tenosynovitis, occurs when one of the tendons responsible for bending a finger or the thumb develops a thickening, known as a nodule, and
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Rocchi, L., Merolli, A., Morini, A., Monteleone, G., & Foti, C. (2014). A modified spica-splint in postoperative early-motion management of skier's thumb lesion: A randomized
CRITICALLY APPRAISED PAPER (CAP) Rocchi, L., Merolli, A., Morini, A., Monteleone, G., & Foti, C. (2014). A modified spica-splint in postoperative early-motion management of skier's thumb lesion: A randomized
Dynamic Splinting Devices
 Dynamic Splinting Devices Policy Number: 1.01.500 Last Review: 8/2017 Origination: 8/2003 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for dynamic
Dynamic Splinting Devices Policy Number: 1.01.500 Last Review: 8/2017 Origination: 8/2003 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for dynamic
Phase 1 Maximum Protection 0-4 Weeks
 Dr. Schmidt CMC Arthroplasty When conservative treatment of thumb osteoarthritis fails to control pain surgical treatment may be indicated. The most common surgical technique involves complete resection
Dr. Schmidt CMC Arthroplasty When conservative treatment of thumb osteoarthritis fails to control pain surgical treatment may be indicated. The most common surgical technique involves complete resection
The Adult hand and EB Rachel Box Clinical Specialist St Thomas Hospital
 The Adult hand and EB Rachel Box Clinical Specialist St Thomas Hospital All types of EB affect the Hand. Patients treated often have Junctional, Dystrophic or Recessive Dystrophic EB. Skin, mucosal linings
The Adult hand and EB Rachel Box Clinical Specialist St Thomas Hospital All types of EB affect the Hand. Patients treated often have Junctional, Dystrophic or Recessive Dystrophic EB. Skin, mucosal linings
Objectives. Anatomy Review FDP and FDS Interrelationship. Keys to Successful Treatment
 Flexor Tendon Rehabilitation Joanne Mimm, MPT, CHT University of California, Irvine Irvine, CA February 9-11, 2018 Objectives Understand tendon healing/repair Tensile strength Controlled Stress Rehabilitation
Flexor Tendon Rehabilitation Joanne Mimm, MPT, CHT University of California, Irvine Irvine, CA February 9-11, 2018 Objectives Understand tendon healing/repair Tensile strength Controlled Stress Rehabilitation
Therapy Management PIPJ stiffness. Gemma Willis SUHT
 Therapy Management PIPJ stiffness Gemma Willis SUHT Anatomy Hinge joint with arc of motion 90-100 Surrounded and stabilised by Volar Plate Lateral and accessory collateral ligaments Extensor expansion
Therapy Management PIPJ stiffness Gemma Willis SUHT Anatomy Hinge joint with arc of motion 90-100 Surrounded and stabilised by Volar Plate Lateral and accessory collateral ligaments Extensor expansion
Ascension PIP Post-Operative therapy protocol
 Ascension PIP Post-Operative therapy protocol This brochure summarizes post-operative care guidelines for the Ascension PIP. HUMANITARIAN DEVICE: The Ascension PIP is authorized by Federal law for use
Ascension PIP Post-Operative therapy protocol This brochure summarizes post-operative care guidelines for the Ascension PIP. HUMANITARIAN DEVICE: The Ascension PIP is authorized by Federal law for use
Hand injuries. The metacarpal bones may fracture through the base, shaft or the neck.
 Hand injuries Metacarpal injuries The metacarpal bones may fracture through the base, shaft or the neck. Shaft fractures; these are caused by direct trauma which may cause transverse # of one or more metacarpal
Hand injuries Metacarpal injuries The metacarpal bones may fracture through the base, shaft or the neck. Shaft fractures; these are caused by direct trauma which may cause transverse # of one or more metacarpal
CASE REPORT. Distal radius nonunion after volar locking plate fixation of a distal radius fracture: a case report
 Nagoya J. Med. Sci. 79. 551 ~ 557, 2017 doi:10.18999/nagjms.79.4.551 CASE REPORT Distal radius nonunion after volar locking plate fixation of a distal radius fracture: a case report Takaaki Shinohara 1
Nagoya J. Med. Sci. 79. 551 ~ 557, 2017 doi:10.18999/nagjms.79.4.551 CASE REPORT Distal radius nonunion after volar locking plate fixation of a distal radius fracture: a case report Takaaki Shinohara 1
Dr. Brian Klika Sagittal Band Repair / EDC Recentralization Phase 1- Early Protective Phase (Day 1 2 weeks)
 Goals for phase 1 Protect sagittal band repair with constant splinting Minimize scar adhesions and post-operative edema Other Considerations: It is important to prevent full MP joint flexion of the involved
Goals for phase 1 Protect sagittal band repair with constant splinting Minimize scar adhesions and post-operative edema Other Considerations: It is important to prevent full MP joint flexion of the involved
Distal Radius Plate 2.4/2.7 dorsal and volar
 Distal Radius Plate 2.4/2.7 dorsal and volar Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Distal Radius Plate
Distal Radius Plate 2.4/2.7 dorsal and volar Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Distal Radius Plate
PIP Joint Injuries of the Finger A Patient's Guide to PIP Joint Injuries of the Finger
 PIP Joint Injuries of the Finger A Patient's Guide to PIP Joint Injuries of the Finger Introduction We use our hands constantly, placing them in harm's way continuously. Injuries to the finger joints are
PIP Joint Injuries of the Finger A Patient's Guide to PIP Joint Injuries of the Finger Introduction We use our hands constantly, placing them in harm's way continuously. Injuries to the finger joints are
Introduction to Ultrasound Examination of the Hand and upper
 Introduction to Ultrasound Examination of the Hand and upper Emil Dionysian, M.D. Ultrasound of upper ext. Upside Convenient Opens another exam dimension Can be like a stethoscope Helps 3-D D visualization
Introduction to Ultrasound Examination of the Hand and upper Emil Dionysian, M.D. Ultrasound of upper ext. Upside Convenient Opens another exam dimension Can be like a stethoscope Helps 3-D D visualization
Interesting Case Series. Swan-Neck Deformity in Cerebral Palsy
 Interesting Case Series Swan-Neck Deformity in Cerebral Palsy Leyu Chiu, BA, a Nicholas S. Adams, MD, a,b and Paul A. Luce, MD, a,b,c a Michigan State University College of Human Medicine, Grand Rapids,
Interesting Case Series Swan-Neck Deformity in Cerebral Palsy Leyu Chiu, BA, a Nicholas S. Adams, MD, a,b and Paul A. Luce, MD, a,b,c a Michigan State University College of Human Medicine, Grand Rapids,
Dr Klika Proximal & Middle Phalanx Fracture with CRPP
 Dr Klika Proximal & Middle Phalanx Fracture with CRPP Phase 1- Early Protective Phase (0-2 or 3 weeks) Goals for phase 1 Protect healing fracture and surgical fixation Reduce pain & swelling Promote motion
Dr Klika Proximal & Middle Phalanx Fracture with CRPP Phase 1- Early Protective Phase (0-2 or 3 weeks) Goals for phase 1 Protect healing fracture and surgical fixation Reduce pain & swelling Promote motion
HAND INJURY REHAB CONCEPTS AND RETURN TO PLAY
 HAND INJURY REHAB CONCEPTS AND RETURN TO PLAY DAVID COLVIN, PT, DPT, OCS, MS, ATC Presentation Overview Discuss common hand and finger injuries/rehabilitation in baseball UCL of the Thumb Tear Rehab comparisons
HAND INJURY REHAB CONCEPTS AND RETURN TO PLAY DAVID COLVIN, PT, DPT, OCS, MS, ATC Presentation Overview Discuss common hand and finger injuries/rehabilitation in baseball UCL of the Thumb Tear Rehab comparisons
Corporate Medical Policy
 Corporate Medical Policy Continuous Passive Motion in the Home Setting File Name: Origination: Last CAP Review: Next CAP Review: Last Review: continuous_passive_motion_in_the_home_setting 9/1993 6/2018
Corporate Medical Policy Continuous Passive Motion in the Home Setting File Name: Origination: Last CAP Review: Next CAP Review: Last Review: continuous_passive_motion_in_the_home_setting 9/1993 6/2018
Integra. Thumb Joint Replacement PATIENT INFORMATION. with PyroCarbon implants
 Integra Thumb Joint Replacement with PyroCarbon implants PATIENT INFORMATION Anatomy of the Hand The hand is composed of many different bones, muscles and ligaments that allow for a large amount of movement
Integra Thumb Joint Replacement with PyroCarbon implants PATIENT INFORMATION Anatomy of the Hand The hand is composed of many different bones, muscles and ligaments that allow for a large amount of movement
Metacarpophalangeal Joint Implant Arthroplasty REHABILITATION PROTOCOL
 Andrew McNamara, MD The Orthopaedic and Fracture Clinic 1431 Premier Drive Mankato, MN 56001 507-386-6600 Metacarpophalangeal Joint Implant Arthroplasty REHABILITATION PROTOCOL Patient Name: Date: Diagnosis:
Andrew McNamara, MD The Orthopaedic and Fracture Clinic 1431 Premier Drive Mankato, MN 56001 507-386-6600 Metacarpophalangeal Joint Implant Arthroplasty REHABILITATION PROTOCOL Patient Name: Date: Diagnosis:
5/8/2017. Finger Injuries in Football. Tendon Injuries of the Hand and Wrist in Football Steve Kronlage, MD Andrews Institute Gulf Breeze, Florida
 Finger Injuries in Football Tendon Injuries of the Hand and Wrist in Football Steve Kronlage, MD Andrews Institute Gulf Breeze, Florida A jammed finger is an injury (at very least a torn ligament) A swollen
Finger Injuries in Football Tendon Injuries of the Hand and Wrist in Football Steve Kronlage, MD Andrews Institute Gulf Breeze, Florida A jammed finger is an injury (at very least a torn ligament) A swollen
Integra Use of TenoGlide Tendon Protector Sheet to Protect an Extensor Tendon Repair of the Thumb CASE STUDY
 Integra Use of TenoGlide Tendon Protector Sheet to Protect an Extensor Tendon Repair of the Thumb 1 CASE STUDY Use of Integra TenoGlide Tendon Protector Sheet to Protect an Extensor Tendon Repair of the
Integra Use of TenoGlide Tendon Protector Sheet to Protect an Extensor Tendon Repair of the Thumb 1 CASE STUDY Use of Integra TenoGlide Tendon Protector Sheet to Protect an Extensor Tendon Repair of the
SPECIAL ARTICLE. Missed tendon injuries INTRODUCTION
 Archives of Emergency Medicine, 1991, 8, 87-91 SPECIAL ARTICLE Missed tendon injuries H. R. GULY Consultant in A & E, Derriford Hospital, Plymouth INTRODUCTION The timing of the repair of divided tendons
Archives of Emergency Medicine, 1991, 8, 87-91 SPECIAL ARTICLE Missed tendon injuries H. R. GULY Consultant in A & E, Derriford Hospital, Plymouth INTRODUCTION The timing of the repair of divided tendons
Clinical Policy: Mechanical Stretching Devices for Joint Stiffness and Contracture
 Clinical Policy: Mechanical Stretching Devices for Joint Stiffness and Contracture Reference Number: PA.CP.MP.144 Last Review Date: 09/18 Effective Date: 09/18 Coding Implications Revision Log Description
Clinical Policy: Mechanical Stretching Devices for Joint Stiffness and Contracture Reference Number: PA.CP.MP.144 Last Review Date: 09/18 Effective Date: 09/18 Coding Implications Revision Log Description
Definition: This problem generally is caused by a size mismatch between the flexor tendon and the first annular (A-1) pulley.
 TRIGGER DIGITS Definition: This problem generally is caused by a size mismatch between the flexor tendon and the first annular (A-1) pulley. Abstract Primary stenosing tenosynovitis is usually idiopathic
TRIGGER DIGITS Definition: This problem generally is caused by a size mismatch between the flexor tendon and the first annular (A-1) pulley. Abstract Primary stenosing tenosynovitis is usually idiopathic
Physical therapy of the wrist and hand
 Physical therapy of the wrist and hand Functional anatomy wrist and hand The wrist includes distal radius, scaphoid, lunate, triquetrum, pisiform, trapezium, trapezoid, capitate, and hamate. The hand includes
Physical therapy of the wrist and hand Functional anatomy wrist and hand The wrist includes distal radius, scaphoid, lunate, triquetrum, pisiform, trapezium, trapezoid, capitate, and hamate. The hand includes
Essential intervention No. 3 Oedema control KEY OBJECTIVES. Danger
 Essential intervention No. 3 Oedema control KEY OBJECTIVES To know what causes oedema. To know which kind of oedema needs to be referred for emergency surgery and why. To know the effects of oedema on
Essential intervention No. 3 Oedema control KEY OBJECTIVES To know what causes oedema. To know which kind of oedema needs to be referred for emergency surgery and why. To know the effects of oedema on
Trauma and Immobilization SCAR. Summary: Acute Inflammation & Healing. TRAUMA Wound Healing: Three Phases
 Upper Extremity Stiffness and Contracture After Trauma Phil PT, PhD, FAPTA mcclure@arcadia.edu Trauma and Immobilization SCAR TRAUMA Wound Healing: Three Phases Inflammation (0-5 days) Fibroplasia (Repair,
Upper Extremity Stiffness and Contracture After Trauma Phil PT, PhD, FAPTA mcclure@arcadia.edu Trauma and Immobilization SCAR TRAUMA Wound Healing: Three Phases Inflammation (0-5 days) Fibroplasia (Repair,
Fractures and dislocations of the fingers
 Chapter 1 Fractures and dislocations of the fingers Felix S. Chew, M.D., and Catherine Maldjian, M.D. Case 1 1 Phalangeal tuft avulsion fracture 31-year-old woman injured in a ground-level fall. Lateral
Chapter 1 Fractures and dislocations of the fingers Felix S. Chew, M.D., and Catherine Maldjian, M.D. Case 1 1 Phalangeal tuft avulsion fracture 31-year-old woman injured in a ground-level fall. Lateral
Finger Mobility Deficits Fracture of metacarpal Fracture of phalanx of phalanges
 1 Finger Mobility Deficits ICD-9-CM codes: 715.4 Osteoarthrosis of the hand 815.0 Fracture of metacarpal 816.0 Fracture of phalanx of phalanges ICF codes: Activities and Participation code: d4301 Carrying
1 Finger Mobility Deficits ICD-9-CM codes: 715.4 Osteoarthrosis of the hand 815.0 Fracture of metacarpal 816.0 Fracture of phalanx of phalanges ICF codes: Activities and Participation code: d4301 Carrying
THE 9 FINGER flexor pulleys maintain the course. Quantification of Partial or Complete A4 Pulley Release With FDP Repair in Cadaveric Tendons
 SCIENTIFIC ARTICLE Quantification of Partial or Complete A4 Pulley Release With FDP Repair in Cadaveric Tendons Orrin I. Franko, MD, Nathan M. Lee, BS, John J. Finneran, BA, Matthew C. Shillito, MD, Matthew
SCIENTIFIC ARTICLE Quantification of Partial or Complete A4 Pulley Release With FDP Repair in Cadaveric Tendons Orrin I. Franko, MD, Nathan M. Lee, BS, John J. Finneran, BA, Matthew C. Shillito, MD, Matthew
Fascial Turn-Down Flap Repair of Chronic Achilles Tendon Rupture
 19 Fascial Turn-Down Flap Repair of Chronic Achilles Tendon Rupture S. Ghosh, P. Laing, and Nicola Maffulli Introduction Fascial turn-down flaps can be used for an anatomic repair of chronic Achilles tendon
19 Fascial Turn-Down Flap Repair of Chronic Achilles Tendon Rupture S. Ghosh, P. Laing, and Nicola Maffulli Introduction Fascial turn-down flaps can be used for an anatomic repair of chronic Achilles tendon
INFORMED CONSENT TRIGGER FINGER SURGERY
 . Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only.
. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only.
Acute Rupture of Flexor Tendons as a Complication of Distal Radius Fracture
 60 pissn : 1226-2102, eissn : 2005-8918 Case Report J Korean Orthop Assoc 2015;50: 60-65 http://dx.doi.org/10.4055/jkoa.2015.50.1.60 www.jkoa.org Acute Rupture of Flexor Tendons as a Complication of Distal
60 pissn : 1226-2102, eissn : 2005-8918 Case Report J Korean Orthop Assoc 2015;50: 60-65 http://dx.doi.org/10.4055/jkoa.2015.50.1.60 www.jkoa.org Acute Rupture of Flexor Tendons as a Complication of Distal
Use of Low-profile Palmar Internal Fixation in Digital Replantation
 TECHNIQUE Use of Low-profile Palmar Internal Fixation in Digital Replantation Mark Ross, MBBS, FRACS(Orth),*wz Christof Bollman, MBBS,*wy and Gregory B. Couzens, MBBS, FRACS(Orth)*8 Abstract: There are
TECHNIQUE Use of Low-profile Palmar Internal Fixation in Digital Replantation Mark Ross, MBBS, FRACS(Orth),*wz Christof Bollman, MBBS,*wy and Gregory B. Couzens, MBBS, FRACS(Orth)*8 Abstract: There are
Two-, Four-, and Six-Strand Zone II Flexor Tendon Repairs: An In Situ Biomechanical Comparison Using a Cadaver Model
 Two-, Four-, and Six-Strand Zone II Flexor Tendon Repairs: An In Situ Biomechanical Comparison Using a Cadaver Model R. Timothy Thurman, MD, San Antonio, TX, Thomas E. Trumble, MD, Douglas P. Hanel, MD,
Two-, Four-, and Six-Strand Zone II Flexor Tendon Repairs: An In Situ Biomechanical Comparison Using a Cadaver Model R. Timothy Thurman, MD, San Antonio, TX, Thomas E. Trumble, MD, Douglas P. Hanel, MD,
Prospective Morphologic and Dynamic Assessment of Deep Flexor Tendon Healing in Zone II by High-Frequency Ultrasound: Preliminary Experience
 Musculoskeletal Imaging Original Research Puippe et al. High-Frequency Ultrasound ssessment of Deep Flexor Tendon Musculoskeletal Imaging Original Research Prospective Morphologic and Dynamic ssessment
Musculoskeletal Imaging Original Research Puippe et al. High-Frequency Ultrasound ssessment of Deep Flexor Tendon Musculoskeletal Imaging Original Research Prospective Morphologic and Dynamic ssessment
A new modified Tsuge suture for flexor tendon repairs: the biomechanical analysis and clinical application
 Chen et al. Journal of Orthopaedic Surgery and Research (2014) 9:136 DOI 10.1186/s13018-014-0136-x RESEARCH ARTICLE Open Access A new modified Tsuge suture for flexor tendon repairs: the biomechanical
Chen et al. Journal of Orthopaedic Surgery and Research (2014) 9:136 DOI 10.1186/s13018-014-0136-x RESEARCH ARTICLE Open Access A new modified Tsuge suture for flexor tendon repairs: the biomechanical
Intrinsic muscles palsies of the hand Management of Thumb Opposition with BURKHALTER s Procedure
 Intrinsic muscles palsies of the hand Management of Thumb Opposition with BURKHALTER s Procedure TRUONG LE DAO, MD, IFAAD 1 Burkhalter W.E, Cristhensen R.C, Brown P.W, Extensor Indicis Proprius opponensplasty
Intrinsic muscles palsies of the hand Management of Thumb Opposition with BURKHALTER s Procedure TRUONG LE DAO, MD, IFAAD 1 Burkhalter W.E, Cristhensen R.C, Brown P.W, Extensor Indicis Proprius opponensplasty
Dr. Klika Metacarpal Fracture with CRPP
 Dr. Klika Metacarpal Fracture with CRPP Goals for phase 1 Protect healing fracture and surgical fixation Reduce pain & edema Promote motion in pain-free range If multiple digits are involved, it may be
Dr. Klika Metacarpal Fracture with CRPP Goals for phase 1 Protect healing fracture and surgical fixation Reduce pain & edema Promote motion in pain-free range If multiple digits are involved, it may be
Cubital Tunnel Syndrome
 Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic Health. All decisions about must be made in conjunction with your Physician or a licensed healthcare provider.
Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic Health. All decisions about must be made in conjunction with your Physician or a licensed healthcare provider.
Evaluation of Bioadhesive Mesh Construct to Augment Achilles Tendon Repair in a Rabbit Model
 Evaluation of Bioadhesive Mesh Construct to Augment Achilles Tendon Repair in a Rabbit Model Yan Lu, MD 1, Brett Nemke 1, Jackie Kondratko 1, Vicki kalscheur 1, Gino Bradica 2, Ray Vanderby 1, Mark D.
Evaluation of Bioadhesive Mesh Construct to Augment Achilles Tendon Repair in a Rabbit Model Yan Lu, MD 1, Brett Nemke 1, Jackie Kondratko 1, Vicki kalscheur 1, Gino Bradica 2, Ray Vanderby 1, Mark D.
Ex-Vivo Biomechanical Testing of a Tendon Implant Device for the Repair of Equine Flexor Tendon Lacerations. Elizabeth Jane Barrett
 Ex-Vivo Biomechanical Testing of a Tendon Implant Device for the Repair of Equine Flexor Tendon Lacerations by Elizabeth Jane Barrett A thesis submitted to the Graduate Faculty of Auburn University in
Ex-Vivo Biomechanical Testing of a Tendon Implant Device for the Repair of Equine Flexor Tendon Lacerations by Elizabeth Jane Barrett A thesis submitted to the Graduate Faculty of Auburn University in
MR: Finger and Thumb Injuries
 MR: Finger and Thumb Injuries Laura W. Bancroft, M.D. Professor of Radiology University of Central Florida Florida State University Outline Normal anatomy of the fingers and thumb MR imaging protocols
MR: Finger and Thumb Injuries Laura W. Bancroft, M.D. Professor of Radiology University of Central Florida Florida State University Outline Normal anatomy of the fingers and thumb MR imaging protocols
( 1 ) Ball and socket. Shoulder capsule. Rotator cuff.
 Shoulder Arthroscopy Page ( 1 ) Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word arthroscopy comes from two Greek words, arthro
Shoulder Arthroscopy Page ( 1 ) Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word arthroscopy comes from two Greek words, arthro
The Rheumatoid Hand Deformities & Management. Dr. Anirudh Sharma Resident Department of Orthopedics
 + The Rheumatoid Hand Deformities & Management Dr. Anirudh Sharma Resident Department of Orthopedics + Why is Rheumatoid Arthritis important? + RA is a very debilitating disease median life expectancy
+ The Rheumatoid Hand Deformities & Management Dr. Anirudh Sharma Resident Department of Orthopedics + Why is Rheumatoid Arthritis important? + RA is a very debilitating disease median life expectancy
Endoscopic Carpal Tunnel Release ECTR
 Endoscopic Carpal Tunnel Release ECTR Christophe MATHOULIN Paris, France Historics Paget, 1854 Putnam, 1893 Hunt, 1909 Marie et Foix, 1913 Recommanded surgical release Learmonth, 1933 First reported release
Endoscopic Carpal Tunnel Release ECTR Christophe MATHOULIN Paris, France Historics Paget, 1854 Putnam, 1893 Hunt, 1909 Marie et Foix, 1913 Recommanded surgical release Learmonth, 1933 First reported release
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Integra TenoGlide Tendon Protector Sheet
 Integra Use of TenoGlide Tendon Protector Sheet as an Interface to Protect Extensor Tendons after Removal of Hardware from Multiple Metacarpal Fractures 1 CASE STUDY Use of Integra TenoGlide Tendon Protector
Integra Use of TenoGlide Tendon Protector Sheet as an Interface to Protect Extensor Tendons after Removal of Hardware from Multiple Metacarpal Fractures 1 CASE STUDY Use of Integra TenoGlide Tendon Protector
Ulnar Collateral Ligament Injuries of the Thumb Game Keeper s Thumb A Patient's Guide to Ulnar Collateral Ligament Injuries of the Thumb
 Ulnar Collateral Ligament Injuries of the Thumb Game Keeper s Thumb A Patient's Guide to Ulnar Collateral Ligament Injuries of the Thumb 1 Introduction Injury to the ulnar collateral ligament of the thumb
Ulnar Collateral Ligament Injuries of the Thumb Game Keeper s Thumb A Patient's Guide to Ulnar Collateral Ligament Injuries of the Thumb 1 Introduction Injury to the ulnar collateral ligament of the thumb
Complications of Distal Radius Fractures. How to Treat a Distal Radius Fx 11/13/2017. Michael S. Bednar, M.D. Loyola University Chicago
 Complications of Distal Radius Fractures Michael S. Bednar, M.D. Loyola University Chicago How to Treat a Distal Radius Fx Need to restore motion, begin with uninvolved parts Need to reduce an unreduced
Complications of Distal Radius Fractures Michael S. Bednar, M.D. Loyola University Chicago How to Treat a Distal Radius Fx Need to restore motion, begin with uninvolved parts Need to reduce an unreduced
Flexor Tendons. Get a Grip on Flexor Tendons. 1) Click the arrows on the navigation panel at the bottom of the PDF page
 www. treatment2go. com & www. handtherapy. com Flexor Tendons Get a Grip on Flexor Tendons This course has active links. The index is linked so you can just click and go (page 5). To access a website click
www. treatment2go. com & www. handtherapy. com Flexor Tendons Get a Grip on Flexor Tendons This course has active links. The index is linked so you can just click and go (page 5). To access a website click
Integra. Silicone PIP Implant SURGICAL TECHNIQUE
 Integra Silicone PIP Implant SURGICAL TECHNIQUE Table of Contents Indications For Use...2 Contraindications...2 Warnings and Precautions...2 Surgical Technique Preoperative Assessment... 3 Step 1: Initial
Integra Silicone PIP Implant SURGICAL TECHNIQUE Table of Contents Indications For Use...2 Contraindications...2 Warnings and Precautions...2 Surgical Technique Preoperative Assessment... 3 Step 1: Initial
10/10/2014. Structure and Function of the Hand. The Hand. Osteology of the Hand
 Structure and Function of the Hand 19 bones and 19 joints are necessary to produce all the motions of the hand The Hand Dorsal aspect Palmar aspect The digits are numbered 1-5 Thumb = #1 Little finger
Structure and Function of the Hand 19 bones and 19 joints are necessary to produce all the motions of the hand The Hand Dorsal aspect Palmar aspect The digits are numbered 1-5 Thumb = #1 Little finger
Interesting Case Series. Ring Avulsion Injuries
 Interesting Case Series Ring Avulsion Injuries Matt Jones BMBS, BSc, MRCS, and Sameer Gujral MBChB, BSc, MRCS Department of Plastic Surgery, Royal Devon & Exeter Hospital, Exeter, Devon, England Correspondence:
Interesting Case Series Ring Avulsion Injuries Matt Jones BMBS, BSc, MRCS, and Sameer Gujral MBChB, BSc, MRCS Department of Plastic Surgery, Royal Devon & Exeter Hospital, Exeter, Devon, England Correspondence:
Institute of Reconstructive Surgery, Sofia, Bulgaria
 TRANSPOSITION OF THE LATERAL SLIPS OF THE APONEUROSIS IN TREATMENT OF LONG-STANDING " BOUTONNIERE DEFORMITY " OF THE FINGERS By IVAN MATEV Institute of Reconstructive Surgery, Sofia, Bulgaria RUPTURE of
TRANSPOSITION OF THE LATERAL SLIPS OF THE APONEUROSIS IN TREATMENT OF LONG-STANDING " BOUTONNIERE DEFORMITY " OF THE FINGERS By IVAN MATEV Institute of Reconstructive Surgery, Sofia, Bulgaria RUPTURE of
(iii) Twenty questions on tendon injuries in the hand
 Current Orthopaedics (2008) 22, 17 24 Available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/cuor MINI-SYMPOSIUM: HAND TRAUMA (iii) Twenty questions on tendon injuries in the hand
Current Orthopaedics (2008) 22, 17 24 Available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/cuor MINI-SYMPOSIUM: HAND TRAUMA (iii) Twenty questions on tendon injuries in the hand
Technique Guide. Rotation Correction Plates 1.5 and 2.0. Reposition plates for fractures and osteotomies at the metacarpals and phalanges.
 Technique Guide Rotation Correction Plates 1.5 and 2.0. Reposition plates for fractures and osteotomies at the metacarpals and phalanges. Table of Contents Introduction Rotation Correction Plates 1.5
Technique Guide Rotation Correction Plates 1.5 and 2.0. Reposition plates for fractures and osteotomies at the metacarpals and phalanges. Table of Contents Introduction Rotation Correction Plates 1.5
