Flexor tendon injuries of the hand treated with TenoFix TM : mid-term results
|
|
|
- Mercy Washington
- 5 years ago
- Views:
Transcription
1 J Orthopaed Traumatol (2008) 9: DOI /s ORIGINAL ARTICLE Flexor tendon injuries of the hand treated with TenoFix TM : mid-term results Lorenzo Rocchi Æ Antonio Merolli Æ Andrea Genzini Æ Gianfranco Merendi Æ Francesco Catalano Received: 6 October 2007 / Accepted: 19 May 2008 / Published online: 17 July 2008 Springer-Verlag 2008 Abstract Background Recently, the Teno Fix TM device has been detailed in the literature. Conventional stranded cruciate repair requires splinting to protect the sutures from excessive loading, and then, active motion is strongly limited leading to a possible incomplete functional recovery. Materials and methods The authors report on their experience in treating 21 patients presenting primary flexor tendon injuries within the digital sheath in zone 2, in all fingers (including the thumb), at an average follow-up of 16 (range: 6 26) months. Results There were, according to Strickland and Glogovac criteria: 12 excellent; 6 good; 3 fair. Conclusions This new device is practical clinically and can effect strong tendon repairs that withstand early active finger motion, but the best indication is to treat only selected cases of sharp flexor tendon lesions in zone 2. Using this technique it is possible to achieve a quick functional recovery and early return to work. Keywords Flexor tendon injuries New device Metallic suture Early mobilization Introduction Recently, the Teno Fix TM device (Tenofix) has been reported in the literature [1] and the implantation technique is fully explained [2]. This metallic device has been proposed as a practical clinical tool, able to carry out strong tendon repairs effectively, that withstand early active finger motion. Established treatments, like conventional four-stranded cruciate repair, require splinting or pull-out systems to protect the sutures from excessive loading and dehiscence and, in so doing, the active motion is strongly limited for several weeks; this factor may lead to an incomplete functional recovery. Actually, it will be advisable to mobilize the tendon with either passive or active flexion, at the earliest, to prevent adhesions and contractures and the eventual need for tenolysis [3 6]. The authors report on their experience in treating 21 patients presenting primary flexor tendon injuries within the digital sheath in zone 2, using this intratendinous metallic anchoring device. Materials and methods Device and operative procedures L. Rocchi A. Merolli (&) G. Merendi F. Catalano Ortopedia e Chirurgia della Mano, Università Cattolica, Complesso Columbus, via G. Moscati 31, Rome, Italy antonio.merolli@rm.unicatt.it A. Genzini Seconda Divisione di Ortopedia, Azienda Ospedaliera San Giovanni-Addolorata, Rome, Italy The Tenofix (Ortheon Medical, Winter Park, FL, USA) is a stainless steel device (ASTM F138 00) composed of two intratendinous anchor-coil complexes (2.0 mm in diameter and 4.0 mm in length) joined by a multifilament 2-0 stainless steel suture. The anchor-coil complex is composed of a spiraling cork-screw-like coil around a hollow spindle core (Fig. 1a). Two delivery devices are available, one for the proximal anchor and one for the distal anchor.
2 202 J Orthopaed Traumatol (2008) 9: Fig. 1 a The device is composed of two intratendinous anchor-coil complexes joined by a multifilament stainless steel suture. The anchor-coil complex is composed of a spiraling corkscrew-like coil around a hollow spindle core. b Two delivery devices, one for the proximal end, and one for the distal end, are provided; they are assembled with a delivery tube, containing the anchor-coil complex, and a handle. c A radiogram showing the main components of the system: a stainless steel wire connecting the distal (B) and proximal (C) anchor-coil complexes, with a preassembled stop-bead (D) and an opposite stop-bead (A), which are crimped intraoperatively once the device has been put in place Surgical technique Under brachial plexus block anesthesia, after the skin has been incised according to Bruner, the injured tendon stumps are exposed and a longitudinal palmar split is made about 10 mm away from the cut edge (about the same exposure which is required for traditional suture), to accommodate the obturator and the delivery tube, which contains the anchor-coil complex (Fig. 1b). Both proximal and distal stumps can be chosen as the first point of entry, depending on the clinical need. Once the complex has been gently twisted in place, a straight needle with the stainless steel suture and an attached stop-bead is passed through the hole in the core until the bead comes into contact with the complex. The stainless steel suture is passed into the second complex and into a stop-bead allocated into a preloaded crimping instrument using a 22-gauge needle. The tendon stumps are gently redirected into the tendon sheath and under the pulleys and placed together under proper tension until they slightly overlap. Finally, the stopbead is crimped and the excessive stainless steel suture is cut (Fig. 2). The longitudinal tenotomies are sutured by a buried knot, while a continuous epitendinous 6-0 nylon suture at the edge of the stumps completes the repair. Clinical cases The study has been performed in accordance with the ethical standards of the 1964 Declaration of Helsinki. All the patients gave their informed consent. Exclusion criteria Patients were selected according to the following exclusion criteria. Flexor tendon primary repair (within 12 h from injury) was performed with Tenofix on 21 patients [14 males, 7 females; mean age 32 (range: 18 46) years] presenting complete tendon transection by a sharp blade injury in flexor digital sheath zone 2; the subdivision zones defined by Tang [7 9] were followed. Patients with injuries of both flexor tendons or associated injuries (of the vessels or joints) or fractures were excluded. Because of the diameter of the anchors, children as well as adult patients presenting lesions in comparably small-sized fingers (like, most often, the little finger) were excluded from the study. Four kinds of lesions were included: 1. Complete transection of the flexor digitorum profundus (FDP) tendon without concomitant lesion of the
3 J Orthopaed Traumatol (2008) 9: Fig. 2 a FDP injury at zone 2A: the proximal stump was retrieved proximally (A). The anchor and the metallic suture were used to reroute the proximal stump into the digital canal by a Teflon TM guide (B). The suture was performed preserving the A3 pulley (C). b Full extension and full flexion were allowed postoperatively. c Clinical result at 4 weeks flexor digitorum superficialis (FDS) tendon, occurring at zone 2B and 2C. 2. Complete transection of the FDP tendon without concomitant lesion of the FDS tendon, occurring at zone 2A. 3. Complete transection of the FDS alone, occurring at zone 2D. 4. Complete transection of the flexor pollicis longus (FPL) tendon, occurring at zone 2. Regarding the surgical repair of complete transection of the FDS alone occurring at zone 2D (point c-), the authors proposed surgical intervention in young and active patients; the reason is that even if finger motion remains normal when only the FDP is present, the cumulative grip strength is reduced. Assessment Results were assessed after a mean of 16 (range: 6 26) months of follow-up. Clinical end points assessed included a comparison in range of active motion, according to Strickland [5, 6], of the DIP and PIP joints of the finger (Strickland modified Total Active Motion: SmTAM) as well as a recording of the linear measurement of pulp-to-distal-palmar-crease distance [10]. We adopted the Strickland and Glogovac criteria in the documentation of outcome of flexor tendon repair in zones 1 and 2 because we found these criteria (in fact a modified TAM method) to be more practical than TAM where, precisely, only fingers whose total range of active motion is the same as that of the contralateral hand can be rated as excellent. In fact, a varying degree of joint stiffness is always present after tendon repair so that patients gaining an excellent TAM score are rare. With the SmTAM an excellent functional status requires a sufficiently ample total range of active motion, but not necessarily similar to that of the contralateral side [9]. Data about the patients Lesions were treated on the thumb (3 patients), index (11 patients), third (3 patients), fourth (1 patient) and little (3 patients) fingers. The study reports the complete experience of the authors and no patient was lost to follow-up before an end result was determined. The most attainable active digital flexion to the palm was allowed from the first day postoperative, while
4 204 J Orthopaed Traumatol (2008) 9: extension was limited by placing the hand in a plaster with both the wrist and metacarpophalangeal (MCP) joints flexed at 30 until the 14th day postoperation; then the plaster and the skin suture were removed. A dorsal splint in neutral wrist position was applied until the 28th day for limiting wrist extension, while complete active motion of all the fingers was allowed (apart from flexion against resistance and forced passive extension). Outpatient ward clinical controls were made weekly during the first month, then at 2, 6, 12 and 24 months. Anterior and lateral X-ray films, on flexion and extension, were made on the 14th and 60th day post-op, to evaluate the actual sliding and eventual gapping of the tendon, recordable by the position of stainless steel markers placed both proximal and distal to the intratendinous anchors of the device. Results Data about the patients Regarding the 21 patients under study, the results according to SmTAM were as follows: 12 excellent; 6 good; 3 fair at an average follow-up of 16 (range: 6 26) months. Complications Three patients had unsatisfactory results and in two of them the device was removed. All these three patients had a fair score when evaluated by SmTAM. The first patient fell accidentally after surgery provoking a forced hyperextension and the eventual rupture of tendon around the anchors; the device did not rupture but was removed. The second patient required the removal of the device because of a low-grade sepsis that gave persistent pain; the use of Tenofix was probably badly indicated in this patient, which presented a torn and poorly vascularized wound at the time of operation. The third patient was extremely uncooperative and did not follow any rehabilitation program. In the two cases of removal, a traditional four-stranded degradable cruciate repair was performed. Assessment (see Table 1) Complete transection of the FDP tendon without concomitant lesion of the FDS tendon, occurring at zone 2B and 2C Six patients (3 females and 3 males),of a mean age of 31 (range: 19 41) years were treated with a mean follow-up of 12 (range: 6 26) months. The mean SmTAM was 78 (±19 SD)%, with two excellent results in treatment of lesions of the index finger. The mean pulp-to-palm distance achieved was 15 (±14 SD) mm. Adequate functional recovery was obtained after a mean of 33 (±4 SD) days, while they returned to work after a mean of 42 (±12 SD) days. Complete transection of the FDP tendon without concomitant lesion of the FDS tendon, occurring at zone 2A Five patients (3 females and 2 males), of a mean age of 32 (range: 24 38) years were treated with a mean follow-up of 19 (range: 14 25) months. The mean SmTAM was 70 (±16 SD)%: treatment of the index finger had excellent SmTAM; other fingers had a good SmTAM. The mean pulp-to-palm distance achieved was 21 (±11 SD) mm. Adequate functional recovery was obtained after a mean of 28 (±6 SD) days, while return to work occurred after a mean of 34 (±6 SD) days. Use of the device in this zone is strongly related to the exposure available and the dimensions of the site for each patient (Fig. 2). Complete transection of the FDS alone, occurring at zone 2D Four patients (1 female and 3 males), with a mean age of 35 (range: 24 41) years were treated with a mean follow-up of 18 (range: 14 24) months. The mean SmTAM was 92 (±8 SD)% and all the treatments were for the index finger. The mean pulp-to-palm distance achieved was 6 (±7 SD) mm. Adequate functional recovery was obtained after a mean of 26 (±4 SD) days, while return to work occurred after a mean of 32 (±10 SD) days. Table 1 Statistical analysis: data for age and follow-up are reported as a mean and range; all the others are reported as a mean and standard deviation Cases Sex F/M Mean age (years) SmTAM (%) Pulp-to-palm (mm) Follow-up (months) Functional recovery (days) Return to work (days) FDP injuries at zone 2B & C 6 3/3 31 (19 41) 78 (±19) 15 (±14) 12 (6 26) 33 (±4) 42 (±12) FDP injuries at the border 2A 5 3/2 32 (24 38) 70 (±16) 21 (±11) 19 (14 25) 28 (±6) 34 (±6) FDS injuries at zone 2D 4 1/3 35 (24 41) 92 (±8) 6 (±7) 18 (14 24) 26 (±4) 32 (±10) FPL injuries at zone 2 3 0/3 28 (18 45) 92 (±3) 2 (±2) 17(10 24) 21 (±0) 21 (±7) Cumulative results 18 7/11 32 (18 45) 81 (±16) 12 (±12) 16 (6 26) 28 (±6) 34 (±12)
5 J Orthopaed Traumatol (2008) 9: Fig. 3 a FPL injuries at zone 2 (A); the proximal anchor is about to be inserted by the delivery tube which contains the anchor-coil complex (B). b Full extension and full flexion have been documented after 2 weeks, when skin sutures were removed (A B), after 3 weeks (C D). c Full extension has been documented after 91 weeks (21 months) in a bilateral comparison. d Full flexion has been documented after 91 weeks (21 months) in a bilateral comparison Complete transection of the flexor pollicis longus (FPL) tendon, occurring at zone 2 Three patients (3 males), with a mean age of 28 (range: 18 45) years were treated with a mean follow-up of 17 (range: 10 24) months. Treatments of injuries of the flexor pollicis longus at zone 2 had excellent SmTAM, namely 92 (±3 SD)%. The mean pulp-to-palm distance achieved was 2 (±2 SD) mm and adequate functional recovery was obtained after a mean of 21 (±0 SD) days, while return to work occurred after a mean of 21 (±7 SD) days (Fig. 3). Radiological findings Dynamic X-ray films in full flexion and full extension showed that no blockage of the repaired tendon occurred under the pulleys; this proved to be true also for the A4 pulley in distal zone 2A lesions, even if at this level there is more limited space in comparison with more proximal pulleys. Dynamic X-ray films in full flexion and full extension also showed the effective tightening of the tendon suture in the longer term (Fig. 4a, b). Actually, it has to be noted that in 14 cases of the series, the X-ray control after 2 months showed that the anchors have slid around the steel core, closer to the junction site (Fig. 5), than in the beginning; this has been interpreted as a sign of effective tendon scaring, which involves a physiological contracture of the stump tissue, but another possibility may include the displacement of the anchors through repeated contact with the pulley edges; anyway, the latter hypothesis seems to be not
6 206 J Orthopaed Traumatol (2008) 9: Fig. 5 In the majority of cases the X-ray control at 2 months showed the anchors (a) were closer than at the beginning, having slid around the steel core toward the junction site, as noted by the increased distance from the stop-bead (sb); this has been interpreted as a sign of effective tendon scaring, which involves a physiological contracture of the tissue of the stumps Fig. 4 a Dynamic X-ray films, in full extension and full flexion, showed the effective gliding of the tendon suture at 3 weeks. b Dynamic X-ray films, in full extension and full flexion of the same patient after 91 weeks (21 months), showed no variation in gliding supported by cases where anchors were not displaced even after 91 weeks (21 months) (Fig. 4b). Discussion The rationale for the use of Tenofix Treatment of flexor tendon injuries at fingers and recovery of an adequate digital performance following tendon interruption still represent difficult challenges to the orthopedic and hand surgeons [9, 13]. Several different viewpoints persist with regard to the technique of repair, the management of flexor tendon sheath and the postoperative mobilization protocol of the injured finger [3 5, 7, 21]. Many proposed techniques which are adequate in tensile strength are technically demanding and require excessive tendon manipulation and increase the tendon bulk with a high number of strands that cross the repair site [8, 16, 17, 19]. Furthermore, modifying the diameter and shape of tendon cross-section is a cause of vascular impairment and fibrotic adhesions [11]. Achieving excellent results from flexor tendon repair still remains to be difficult. Attention to the details of suture technique and rehabilitation regime is important, but it is also true that significant future improvements are likely to come through new devices and materials able to prevent early gap formation and to allow full function as soon as possible. Strickland wrote in 1995: the most effective method of restoring strength and excursion to repaired tendons involves the use of a strong, gap resistant suture technique followed by the application of controlled motion stress [12]. The objectives of the ideal tendon repair can be summed up as follows: simple and reproducible execution; high resistance from the beginning; small occupancy of the tendon sheath; negligible gap; respect of vascularization, and very early mobilization. It is the opinion of the authors that tendon repair with the Tenofix device seems to satisfy these conditions and presents some advantages in comparison with traditional sutures. In a recent article, a strength analysis and comparison of Tenofix with the widely used modified Kessler suture technique has been conducted on cadaver Achilles tendons [14]. Evaluation of the repairs consisted of tensile strength testing and measurement of the gap formation and peak stressed. Results showed that in the Tenofix repairs the gap formation stress was 67% of the peak tensile stress, in comparison to 29% of the peak stress in the modified Kessler suture. This has been correlated to the elastic property of the synthetic Kessler repair and the
7 J Orthopaed Traumatol (2008) 9: initial tightening of the suture around the tendon fibers. The Tenofix system is nonelastic and it is fully tensioned during installation; this leads to a better gap-resistant repair. In another cadaveric study, where FDP tendons were studied [1] comparing the Tenofix with four-strand 3-0 cruciate suture, energy absorbed up to 2 mm gap was significantly greater for Tenofix, irrespective of the presence or absence of a 5-0 circumferential suture; anyway the load required to create the gap was not different. This kind of suture can then be able, with an unique core passage, to cope with the widely described problems of gapping [15 19]. A final note should be made on the fact that data reported in this paper support the indication, not previously described in the literature, to use the Tenofix device in lesions of the thumb. Advantages The authors noted that it is peculiar to this device that the intratendinous complex inserted in the tendon belly allows the tendon collagen fibers, entangled between the coil and the core, to maintain their physiological elongation, without the excessive twisting and/or constriction, which may occur with the ordinary stranded suture. This is a clear biological advantage in comparison with the vascular interference that can be produced by a traditional suture. Furthermore, the appearance of a well demarcated acellular zone has been evidenced in tied knots, apparently without any correlation with vascularity, casting a shadow on the trend for multistrand locking flexor tendon suture repairs [20]. It is widely known that early mobilization techniques following tendon repair within the digital sheath have improved the final end results. Experimental studies have shown that immediate mobilization favors healing, stimulating at the same time the regeneration of the tendon and the remodeling of the scar [21]. Clinical studies on controlled active motion following primary flexor tendon repair showed best functional results using the methods of earliest active finger mobilization [3 5]. It is an advantage of the Tenofix device to allow an active motion from the first day, with a partial limitation of full extension until the 14th day; this ensures short-term healing and functional recovery. Disadvantages Because of the diameter of the anchors, the device is not applicable to children and adult patients presenting lesions in comparably small-sized fingers, like the little finger. For the risk of infective involvement due to the presence of a metallic device, in our opinion, it is not indicated in treatment of dirty lesions and generally in complex multiple lesions. For want of a good quality of the tissue of the Table 2 Reports from the literature which assessed results by the Strickland and Glogovac criteria in patients treated with multistranded sutures: they are compared with the present serie treated with Tenofix Authors Digits Year of publication stumps receiving the anchors, the device is not indicated in case of fraying cutting lesions. Finally, the need of a full compliance of the patient with the rehabilitation program suggests avoiding the use of the device in the uncooperative patient. All these are clear disadvantages that prevent the use of Tenofix in those clinical occurences. A comparison with previous reports using other repairs A review of the literature on the repair of flexor tendon injuries in zone 2 shows that Tenofix results are in the same range of the best clinical series [9] when SmTAM and percentage of rupture are considered. In Table 2 results reported in the literature, from clinical series where flexor tendon injuries in zone 2 were evaluated by Strickland and Glogovac criteria (SmTAM), are grouped together and compared with our series; the mean values are superimposable. Anyway, it is worth highlighting that Tenofix appears to have a shorter time for functional recovery and for resuming the working activity: i.e., an average of about 30 days in comparison with an average of 60 days from previous reports on multistranded repair [3, 4]. Long-term problems (20 years) % of excellentgood results Cullen et al Thang and Shi Silfverskiod et al Sandow and McMahon Baktir et al Kitsis et al Cumulative Rocchi et al %of rupture They are, obviously, not known yet, because this is a short to middle term follow-up study. Anyway, it is known that the two most important complications of conventional flexor tendon repair are adhesions and dehiscence, which often lead to incomplete functional recovery [21, 22]; they seem to have been avoided in this clinical series by using this new device. Adhesion formation can be limited first of all by increasing the excursion of the repaired tendon throughout the healing period: this is possible using different systems of protection of the suture like the widely known splints of
8 208 J Orthopaed Traumatol (2008) 9: Kleinert, Duran and others [13]. More easily, the use of the Tenofix device allows the finger immediate active motion with a simple short-time splinting at 30 of flexion. Furthermore, it does not determine modification of the tendon shape, the so-called bulging, nor any reduction of tendon sliding, and its axial disposition does not involve the deep surface of tendon in the suture, respecting the vascular perfusion provided by the vincula vessels. The reparation with this device does not directly involve the extremities of the cut tendon and eliminates knots from the junction site, so that no material interposition is present in the place of fibroblast proliferation. This characteristic also facilitates the closure of the epitenon, which acts like a barrier to the ingrowth of extratendon adhesions, and the reestablishment of the stump s continuity, helping the restoration of tendon metabolism [13, 22]. Despite its increased tensile strength, a stainless steel suture is not usually employed in flexor tendon repair because of its difficult handling and knot tying [15, 16]. Different from the traditional methods, the strength of the repair using Tenofix is not proportional to the numbers of strands that cross the repair site. The absence of multistrands and ligatures around the tendon represents a great advantage in terms of tightness, since it has been demonstrated that flexor tendon repairs usually rupture at the suture knots [17]. Finally, our findings confirm that the strength at 2 months is assured by the tendon healing rather than the device and this accords with the studies that state that between 3 and 6 weeks post-tendon repair, the suture becomes secondary to tendon healing as the primary provider of tensile strength to the tendon wound [22]. Final considerations Based on preliminary results of using Tenofix, we think this new device is practical clinically and can effect strong tendon repairs that withstand early active finger motion and appear to ensure a quicker recovery after surgery. However, in our series, for three patients, treatment with Tenofix was not the right choice owing to giving us results that led to a reoperation rate not lower than those present in recent reports of primary flexor tendon repairs in zone 2. We conclude that there is an indication to treat with Tenofix, selected cases of sharp flexor tendon lesions in zone 2 which, by this technique, may achieve a faster functional recovery and early return to work. Conflict of interest statement Authors do not have any financial relationship with the manufacturer of the device and have the full control of all primary data and agree to allow the journal to review their data if requested. References 1. Su BW, Protopsaltis TS, Koff MF et al (2005) The biomechanical analysis of a tendon fixation device for flexor tendon repair. J Hand Surg 30A: Su BW, Solomons M, Barrow A et al (2005) Device for zone-ii flexor tendon repair: a multicenter, randomised, blinded, clinical trial. J Bone Joint Surg 87A: Kitsis CK, Wade PJ, Krikler SJ (1998) Controlled active motion following primary flexor tendon repair: a prospective study over 9 years. J Hand Surg 23B: Peck FH, Bucher CA, Watson JS (1998) A comparative study of two method of controlled mobilization of flexor tendon repairs in zone 2. J Hand Surg 23B: Strickland JW, Glogovac SV (1980) Digital function following flexor tendon repair in Zone II: A comparison of immobilization and controlled passive motion techniques. J Hand Surg 5A: Strickland JW (1989) Flexor tendon surgery. Part 1: primary flexor tendon repair. J Hand Surg 14B: Tang JB, Shi D (1992) Subdivision of flexor tendon no man s land and different treatment methods in each sub-zone. A preliminary report. Chin Med J 105: Tang JB, Shi D, Gu YQ, Chen JC, Zhou B (1994) Double and multiple looped suture tendon repair. J Hand Surg 19B: Tang JB (2005) Clinical outcomes associated with flexor tendon repair. Hand Clinic 21: Boyes JH (1950) Flexor tendon grafts in the fingers and thumb: an evaluation of end results. J Bone Joint Surg 32A: Strickland JW (1985) Flexor tendon repair. Hand Clinic 1: Strickland JW (1995) Flexor Tendon Injuries: I. Foundation of treatment. J Am Acad Orthop Surg 3: Strickland JW (2000) Development of flexor tendon surgery: twenty-five years of progress. J Hand Surg 25A: Lewis N, Quitkin HM (2003) Strength analysis and comparison of the Teno Fix tendon repair system with the two-strand modified Kessler repair in the Achilles tendon. Foot Ankle Int 24: Robertson GA, Al-Quattan MM (1992) A biomechanical analysis of a new interlock suture for flexor tendon repair. Journal of Hand Surg 17B: Wade PJ, Wetherell RG, Amis AA (1989) Flexor tendon repair: significant gain in strength from the Halsted peripheral suture technique. J Hand Surg 14B: Trail IA, Powell ES, Noble J (1992) The mechanical strength of various suture techniques. J Hand Surg 17B: Seradge H (1983) Elongation of the repair configuration following flexor tendon repair. J Hand Surg 8A: Barrie KA, Tomak SL, Cholewicki J (2001) Effect of suture locking and suture calibre on fatigue strength of flexor tendon repairs. J Hand Surg 26A: Wong JKF, Cerovac S, Ferguson MWJ, McGrouther DA (2006) The Cellular effect of a single interrupted suture on tendon. J Hand Surg 31B: Gelberman RH, Woo SL, Amiel D, Horibe S, Lee D (1990) Influences of flexor sheath continuity and early motion on tendon healing in dogs. J Hand Surg 15A: Ketchum LD (1985) Suture materials and suture techniques used in tendon repair. Hand Clinic 1:43 53
FACTORS INFLUENCING THE MANAGEMENT OF THE FLEXOR TENDON INJURIES IN THE HAND
 Basrah Journal of Surgery FACTORS INFLUENCING THE MANAGEMENT OF THE FLEXOR TENDON INJURIES IN THE HAND Avadis F.I.C.M.S. Lecturer in Orthopaedic, Department of Surgery, College of Medicine, and specialist
Basrah Journal of Surgery FACTORS INFLUENCING THE MANAGEMENT OF THE FLEXOR TENDON INJURIES IN THE HAND Avadis F.I.C.M.S. Lecturer in Orthopaedic, Department of Surgery, College of Medicine, and specialist
The Effects of Early Active Motion Rehabilitation after Teno Fixrm Tendon Repair in Zone 11 Flexor Tendon Lacerations of the Hand
 The Effects of Early Active Motion Rehabilitation after Teno Fixrm Tendon Repair in Zone 11 Flexor Tendon Lacerations of the Hand Lan Chen A. Study purpose and Rationale The purpose of this study is to
The Effects of Early Active Motion Rehabilitation after Teno Fixrm Tendon Repair in Zone 11 Flexor Tendon Lacerations of the Hand Lan Chen A. Study purpose and Rationale The purpose of this study is to
11/13/2017. Complications of Flexor Tendon Repair. Brandon E. Earp, M.D. How do we best get there?
 Complications of Flexor Tendon Repair Brandon E. Earp, M.D. Chief of Orthopaedic Surgery Brigham and Women s Faulkner Hospital Vice-Chair of Clinical Operations Brigham and Women s Hospital Frontiers in
Complications of Flexor Tendon Repair Brandon E. Earp, M.D. Chief of Orthopaedic Surgery Brigham and Women s Faulkner Hospital Vice-Chair of Clinical Operations Brigham and Women s Hospital Frontiers in
Comparison of Roll Stitch Technique and Core Suture Technique for Extensor Tendon Repair at the Metacarpophalangeal Joint level
 Trauma Mon. 2016 February; 21(1): e24563. Published online 2016 February 6. doi: 10.5812/traumamon.24563 Research Article Comparison of Roll Stitch Technique and Core Suture Technique for Extensor Tendon
Trauma Mon. 2016 February; 21(1): e24563. Published online 2016 February 6. doi: 10.5812/traumamon.24563 Research Article Comparison of Roll Stitch Technique and Core Suture Technique for Extensor Tendon
Andrew B. Stein, MD Boston University Medical Center May 2 & 3, 2016
 Andrew B. Stein, MD Boston University Medical Center andrew.stein@bmc.org Work Related Workshop WorkInjuries Related Injuries Workshop Tendon injuries may be obvious or subtle History (mechanism of injury)
Andrew B. Stein, MD Boston University Medical Center andrew.stein@bmc.org Work Related Workshop WorkInjuries Related Injuries Workshop Tendon injuries may be obvious or subtle History (mechanism of injury)
Revisiting the Curtis Procedure for Boutonniere Deformity Correction
 180 Letter to Editor Revisiting the Curtis Procedure for Boutonniere Deformity Correction Lee Seng Khoo*, Vasco Senna-Fernandes Ivo Pitanguy Institute, Rua Dona Mariana 65, Botafogo, Rio De Janeiro, Brazil
180 Letter to Editor Revisiting the Curtis Procedure for Boutonniere Deformity Correction Lee Seng Khoo*, Vasco Senna-Fernandes Ivo Pitanguy Institute, Rua Dona Mariana 65, Botafogo, Rio De Janeiro, Brazil
Two-, Four-, and Six-Strand Zone II Flexor Tendon Repairs: An In Situ Biomechanical Comparison Using a Cadaver Model
 Two-, Four-, and Six-Strand Zone II Flexor Tendon Repairs: An In Situ Biomechanical Comparison Using a Cadaver Model R. Timothy Thurman, MD, San Antonio, TX, Thomas E. Trumble, MD, Douglas P. Hanel, MD,
Two-, Four-, and Six-Strand Zone II Flexor Tendon Repairs: An In Situ Biomechanical Comparison Using a Cadaver Model R. Timothy Thurman, MD, San Antonio, TX, Thomas E. Trumble, MD, Douglas P. Hanel, MD,
Hand injuries. The metacarpal bones may fracture through the base, shaft or the neck.
 Hand injuries Metacarpal injuries The metacarpal bones may fracture through the base, shaft or the neck. Shaft fractures; these are caused by direct trauma which may cause transverse # of one or more metacarpal
Hand injuries Metacarpal injuries The metacarpal bones may fracture through the base, shaft or the neck. Shaft fractures; these are caused by direct trauma which may cause transverse # of one or more metacarpal
Flexor Tendon Case Conundrums
 Flexor Tendon Case Conundrums Philly Meeting 2018 Rowena McBeath, MD, PhD Jeffrey A. Greenberg, MD Nancy M. Cannon, OTR, CHT Faculty Rowena McBeath, MD, PhD Yale molecular biochemistry & biophysics John
Flexor Tendon Case Conundrums Philly Meeting 2018 Rowena McBeath, MD, PhD Jeffrey A. Greenberg, MD Nancy M. Cannon, OTR, CHT Faculty Rowena McBeath, MD, PhD Yale molecular biochemistry & biophysics John
Flexor Tenorrhaphy Using Absorbable Suture Materials
 Flexor Tenorrhaphy Using Absorbable Suture Materials Hyung Joo Kang, Dong Chul Lee, Jin Soo Kim, Sae Hwi Ki, Si Young Roh, Jae Won Yang Department of Plastic and Reconstructive Surgery, Kwang-Myung Sung-Ae
Flexor Tenorrhaphy Using Absorbable Suture Materials Hyung Joo Kang, Dong Chul Lee, Jin Soo Kim, Sae Hwi Ki, Si Young Roh, Jae Won Yang Department of Plastic and Reconstructive Surgery, Kwang-Myung Sung-Ae
Hand Therapy Protocols
 Hand Therapy Protocols Post Repair Therapy Protocols Page 1 of 10 Following are representative protocols for each of the three basic approaches to flexor tendon post repair management: immobilization,
Hand Therapy Protocols Post Repair Therapy Protocols Page 1 of 10 Following are representative protocols for each of the three basic approaches to flexor tendon post repair management: immobilization,
Trigger Finger Release
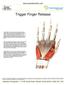 Trigger Finger Release Trigger finger, also known as stenosing tenosynovitis, occurs when one of the tendons responsible for bending a finger or the thumb develops a thickening, known as a nodule, and
Trigger Finger Release Trigger finger, also known as stenosing tenosynovitis, occurs when one of the tendons responsible for bending a finger or the thumb develops a thickening, known as a nodule, and
Ex-Vivo Biomechanical Testing of a Tendon Implant Device for the Repair of Equine Flexor Tendon Lacerations. Elizabeth Jane Barrett
 Ex-Vivo Biomechanical Testing of a Tendon Implant Device for the Repair of Equine Flexor Tendon Lacerations by Elizabeth Jane Barrett A thesis submitted to the Graduate Faculty of Auburn University in
Ex-Vivo Biomechanical Testing of a Tendon Implant Device for the Repair of Equine Flexor Tendon Lacerations by Elizabeth Jane Barrett A thesis submitted to the Graduate Faculty of Auburn University in
Reversing PIP Joint Contractures:
 Reversing PIP Joint Contractures: Applicability of the Digit Widget External Fixation System John M. Agee M.D. Reversing PIP Joint Contractures: Applicability of the Digit Widget External Fixation System
Reversing PIP Joint Contractures: Applicability of the Digit Widget External Fixation System John M. Agee M.D. Reversing PIP Joint Contractures: Applicability of the Digit Widget External Fixation System
Current Practice in Tendon Management
 Current Practice in Tendon Management Handout www.indianahandtoshoulder.com Click on Therapy Flexor Tendons Denver Nancy M. Cannon, OTR, CHT Director Hand to Shoulder Therapy Center Indianapolis, Indiana
Current Practice in Tendon Management Handout www.indianahandtoshoulder.com Click on Therapy Flexor Tendons Denver Nancy M. Cannon, OTR, CHT Director Hand to Shoulder Therapy Center Indianapolis, Indiana
Emile N. Brown, MD, and Scott D. Lifchez, MD
 Flexor Pollicis Longus Tendon Rupture After Volar Plating of a Distal Radius Fracture: Pronator Quadratus Plate Coverage May Not Adequately Protect Tendons Emile N. Brown, MD, and Scott D. Lifchez, MD
Flexor Pollicis Longus Tendon Rupture After Volar Plating of a Distal Radius Fracture: Pronator Quadratus Plate Coverage May Not Adequately Protect Tendons Emile N. Brown, MD, and Scott D. Lifchez, MD
AROM of DIP flex/ext, 10 reps hourly.
 BRIGHAM AND WOMEN S HOSPITAL A Teaching Affiliate of Harvard Medical School 75 Francis St. Boston, Massachusetts 02115 Department of Rehabilitation Services Physical Therapy The intent of this protocol
BRIGHAM AND WOMEN S HOSPITAL A Teaching Affiliate of Harvard Medical School 75 Francis St. Boston, Massachusetts 02115 Department of Rehabilitation Services Physical Therapy The intent of this protocol
Intrinsic muscles palsies of the hand Management of Thumb Opposition with BURKHALTER s Procedure
 Intrinsic muscles palsies of the hand Management of Thumb Opposition with BURKHALTER s Procedure TRUONG LE DAO, MD, IFAAD 1 Burkhalter W.E, Cristhensen R.C, Brown P.W, Extensor Indicis Proprius opponensplasty
Intrinsic muscles palsies of the hand Management of Thumb Opposition with BURKHALTER s Procedure TRUONG LE DAO, MD, IFAAD 1 Burkhalter W.E, Cristhensen R.C, Brown P.W, Extensor Indicis Proprius opponensplasty
Objectives. Anatomy Review FDP and FDS Interrelationship. Keys to Successful Treatment
 Flexor Tendon Rehabilitation Joanne Mimm, MPT, CHT University of California, Irvine Irvine, CA February 9-11, 2018 Objectives Understand tendon healing/repair Tensile strength Controlled Stress Rehabilitation
Flexor Tendon Rehabilitation Joanne Mimm, MPT, CHT University of California, Irvine Irvine, CA February 9-11, 2018 Objectives Understand tendon healing/repair Tensile strength Controlled Stress Rehabilitation
Rehabilitation Protocol: Primary Flexor Tendon Repair LHMC Protocol for Zone 1 & 2
 Rehabilitation Protocol: Primary Flexor Tendon Repair LHMC Protocol for Zone 1 & 2 Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington
Rehabilitation Protocol: Primary Flexor Tendon Repair LHMC Protocol for Zone 1 & 2 Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington
MULTIMEDIA ARTICLES. Mary C. Burns & Brian Derby & Michael W. Neumeister
 HAND (2013) 8:17 22 DOI 10.1007/s11552-012-9488-z MULTIMEDIA ARTICLES Wyndell merritt immediate controlled active motion (ICAM) protocol following extensor tendon repairs in zone IV VII: review of literature,
HAND (2013) 8:17 22 DOI 10.1007/s11552-012-9488-z MULTIMEDIA ARTICLES Wyndell merritt immediate controlled active motion (ICAM) protocol following extensor tendon repairs in zone IV VII: review of literature,
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 The Stiff Hand: Boutonniere & Sylvia Dávila, PT, CHT San Antonio, Texas Extensor Mechanism Central slip inserts into base of the middle phalanx Lateral bands lie dorsal to the PIP joint center of rotation
The Stiff Hand: Boutonniere & Sylvia Dávila, PT, CHT San Antonio, Texas Extensor Mechanism Central slip inserts into base of the middle phalanx Lateral bands lie dorsal to the PIP joint center of rotation
JuggerKnot Soft Anchor 1.0 mm Mini. Scapholunate Ligament Repair/Reconstruction. Brochure and Surgical Technique
 JuggerKnot Soft Anchor 1.0 mm Mini Scapholunate Ligament Repair/Reconstruction Brochure and Surgical Technique One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide
JuggerKnot Soft Anchor 1.0 mm Mini Scapholunate Ligament Repair/Reconstruction Brochure and Surgical Technique One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide
MR: Finger and Thumb Injuries
 MR: Finger and Thumb Injuries Laura W. Bancroft, M.D. Professor of Radiology University of Central Florida Florida State University Outline Normal anatomy of the fingers and thumb MR imaging protocols
MR: Finger and Thumb Injuries Laura W. Bancroft, M.D. Professor of Radiology University of Central Florida Florida State University Outline Normal anatomy of the fingers and thumb MR imaging protocols
Acute Rupture of Flexor Tendons as a Complication of Distal Radius Fracture
 60 pissn : 1226-2102, eissn : 2005-8918 Case Report J Korean Orthop Assoc 2015;50: 60-65 http://dx.doi.org/10.4055/jkoa.2015.50.1.60 www.jkoa.org Acute Rupture of Flexor Tendons as a Complication of Distal
60 pissn : 1226-2102, eissn : 2005-8918 Case Report J Korean Orthop Assoc 2015;50: 60-65 http://dx.doi.org/10.4055/jkoa.2015.50.1.60 www.jkoa.org Acute Rupture of Flexor Tendons as a Complication of Distal
Interesting Case Series. Zone I Flexor Tendon Injuries
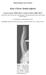 Interesting Case Series Zone I Flexor Tendon Injuries Evgenios Evgeniou, MBBS, MRCS, a and Harriet Walker, MBBS, MRCS b a North Bristol NHS Trust, Bristol, United Kingdom, b Plymouth Hospitals NHS Trust,
Interesting Case Series Zone I Flexor Tendon Injuries Evgenios Evgeniou, MBBS, MRCS, a and Harriet Walker, MBBS, MRCS b a North Bristol NHS Trust, Bristol, United Kingdom, b Plymouth Hospitals NHS Trust,
Ulnar Collateral Ligament Injuries of the Thumb Game Keeper s Thumb A Patient's Guide to Ulnar Collateral Ligament Injuries of the Thumb
 Ulnar Collateral Ligament Injuries of the Thumb Game Keeper s Thumb A Patient's Guide to Ulnar Collateral Ligament Injuries of the Thumb 1 Introduction Injury to the ulnar collateral ligament of the thumb
Ulnar Collateral Ligament Injuries of the Thumb Game Keeper s Thumb A Patient's Guide to Ulnar Collateral Ligament Injuries of the Thumb 1 Introduction Injury to the ulnar collateral ligament of the thumb
SPECIAL ARTICLE. Missed tendon injuries INTRODUCTION
 Archives of Emergency Medicine, 1991, 8, 87-91 SPECIAL ARTICLE Missed tendon injuries H. R. GULY Consultant in A & E, Derriford Hospital, Plymouth INTRODUCTION The timing of the repair of divided tendons
Archives of Emergency Medicine, 1991, 8, 87-91 SPECIAL ARTICLE Missed tendon injuries H. R. GULY Consultant in A & E, Derriford Hospital, Plymouth INTRODUCTION The timing of the repair of divided tendons
A Patient s Guide to Adult Finger Fractures
 A Patient s Guide to Adult Finger Fractures 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 1 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Adult Finger Fractures 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 1 DISCLAIMER: The information in this booklet is compiled from a variety
Effect of Core Suture Technique and Type on the Gliding Resistance during Cyclic Motion following Flexor Tendon Repair: A Cadaveric Study
 Effect of Core Suture Technique and Type on the Gliding Resistance during Cyclic Motion following Flexor Tendon Repair: A Cadaveric Study Tamami Moriya, 1 Chunfeng Zhao, 1 Toshihiko Yamashita, 2 Kai-Nan
Effect of Core Suture Technique and Type on the Gliding Resistance during Cyclic Motion following Flexor Tendon Repair: A Cadaveric Study Tamami Moriya, 1 Chunfeng Zhao, 1 Toshihiko Yamashita, 2 Kai-Nan
SJS. Original Research Article. M. Manninen 1, T. Karjalainen 2, J. Määttä 1, T. Flinkkilä 1
 665544SJS0010.1177/1457496916665544Epidemiology of flexor tendon injuriesm. Manninen, et al. research-article2016 Original Research Article SJS SCANDINAVIAN JOURNAL OF SURGERY Epidemiology of Flexor Tendon
665544SJS0010.1177/1457496916665544Epidemiology of flexor tendon injuriesm. Manninen, et al. research-article2016 Original Research Article SJS SCANDINAVIAN JOURNAL OF SURGERY Epidemiology of Flexor Tendon
Extracapsular Repair Monofilament Nylon Suture
 Extracapsular Repair Monofilament Nylon Suture Management of the ruptured Cranial Cruciate Ligament (CCL) by placing a non-absorbable suture between the lateral fabella and the proximal, cranial tibia
Extracapsular Repair Monofilament Nylon Suture Management of the ruptured Cranial Cruciate Ligament (CCL) by placing a non-absorbable suture between the lateral fabella and the proximal, cranial tibia
Fascial Turn-Down Flap Repair of Chronic Achilles Tendon Rupture
 19 Fascial Turn-Down Flap Repair of Chronic Achilles Tendon Rupture S. Ghosh, P. Laing, and Nicola Maffulli Introduction Fascial turn-down flaps can be used for an anatomic repair of chronic Achilles tendon
19 Fascial Turn-Down Flap Repair of Chronic Achilles Tendon Rupture S. Ghosh, P. Laing, and Nicola Maffulli Introduction Fascial turn-down flaps can be used for an anatomic repair of chronic Achilles tendon
The NBX Non-Bridging External Fixator A Non-Bridging External Fixator/Locking Plate capturing a series of.062mm K-wires and 3mm half-pins that are
 The NBX Non-Bridging External Fixator A Non-Bridging External Fixator/Locking Plate capturing a series of.062mm K-wires and 3mm half-pins that are inserted in a multiplanar and multi-directional fashion
The NBX Non-Bridging External Fixator A Non-Bridging External Fixator/Locking Plate capturing a series of.062mm K-wires and 3mm half-pins that are inserted in a multiplanar and multi-directional fashion
TRIGGER DIGIT, OR stenosing tenosynovitis, isa
 SCIENTIFIC ARTICLE Multiple Pulley Rupture Following Corticosteroid Injection for Trigger Digit: Case Report Cassie Gyuricza, MD, Eva Umoh, BA, Scott W. Wolfe, MD We report a case of pulley rupture following
SCIENTIFIC ARTICLE Multiple Pulley Rupture Following Corticosteroid Injection for Trigger Digit: Case Report Cassie Gyuricza, MD, Eva Umoh, BA, Scott W. Wolfe, MD We report a case of pulley rupture following
PIPR Proximal Interphalangeal Replacement. Operative Technique
 PIPR Proximal Interphalangeal Replacement Operative Technique Contents PIPR Proximal Interphalangeal Replacement Developed in association with Mr I Trail and The Wrightington Hospital. Contents Section
PIPR Proximal Interphalangeal Replacement Operative Technique Contents PIPR Proximal Interphalangeal Replacement Developed in association with Mr I Trail and The Wrightington Hospital. Contents Section
GASTROCNEMIUS TENDON REPAIR VETLIG USING THE STIF CAT 30 SOFT TISSUE INTERNAL FIXATION VETLIG
 VETLIG SOFT TISSUE INTERNAL FIXATION GASTROCNEMIUS TENDON REPAIR USING THE STIF CAT 30 VETLIG A R T I F I C I A L L I G A M E N T S F O R V E T E R I N A R Y U S E VETLIG MANAGEMENT OF CHRONIC GASTROCNEMIUS
VETLIG SOFT TISSUE INTERNAL FIXATION GASTROCNEMIUS TENDON REPAIR USING THE STIF CAT 30 VETLIG A R T I F I C I A L L I G A M E N T S F O R V E T E R I N A R Y U S E VETLIG MANAGEMENT OF CHRONIC GASTROCNEMIUS
PIP Joint Injuries of the Finger A Patient's Guide to PIP Joint Injuries of the Finger
 PIP Joint Injuries of the Finger A Patient's Guide to PIP Joint Injuries of the Finger Introduction We use our hands constantly, placing them in harm's way continuously. Injuries to the finger joints are
PIP Joint Injuries of the Finger A Patient's Guide to PIP Joint Injuries of the Finger Introduction We use our hands constantly, placing them in harm's way continuously. Injuries to the finger joints are
Definition: This problem generally is caused by a size mismatch between the flexor tendon and the first annular (A-1) pulley.
 TRIGGER DIGITS Definition: This problem generally is caused by a size mismatch between the flexor tendon and the first annular (A-1) pulley. Abstract Primary stenosing tenosynovitis is usually idiopathic
TRIGGER DIGITS Definition: This problem generally is caused by a size mismatch between the flexor tendon and the first annular (A-1) pulley. Abstract Primary stenosing tenosynovitis is usually idiopathic
Tendon Injuries of the Hand in Kirikkale, Turkey
 160 Short communication Tendon Injuries of the Hand in Kirikkale, Turkey Elif Sari* Department of Plastic, Reconstructive and Aesthetic Surgery, Faculty of Medicine, Kirikkale University, Kirikkale, Turkey
160 Short communication Tendon Injuries of the Hand in Kirikkale, Turkey Elif Sari* Department of Plastic, Reconstructive and Aesthetic Surgery, Faculty of Medicine, Kirikkale University, Kirikkale, Turkey
Current Practice of Primary Flexor Tendon Repair A Global View
 Current Practice of Primary Flexor Tendon Repair A Global View Jin Bo Tang, MD a, *, Peter C. Amadio, MD b, Martin I. Boyer, MD c, Robert Savage, MS, FRCS d, Chunfeng Zhao, MD b, Michael Sandow, FRCS e,f,
Current Practice of Primary Flexor Tendon Repair A Global View Jin Bo Tang, MD a, *, Peter C. Amadio, MD b, Martin I. Boyer, MD c, Robert Savage, MS, FRCS d, Chunfeng Zhao, MD b, Michael Sandow, FRCS e,f,
WINSTA-R. Distal Radius System
 Distal Radius System Table of Contents Introduction WINSTA-R System 2 Indication 2 Surgical Technique Palmar Access for Radius Plate 3 Dorsal Access for Radius Plate 3 Positioning of the Radius Plate
Distal Radius System Table of Contents Introduction WINSTA-R System 2 Indication 2 Surgical Technique Palmar Access for Radius Plate 3 Dorsal Access for Radius Plate 3 Positioning of the Radius Plate
We perform the vast majority of our flexor HAND/PERIPHERAL NERVE
 HAND/PERIPHERAL NERVE Avoiding Flexor Tendon Repair Rupture with Intraoperative Total Active Movement Examination Amanda Higgins, B.Sc.O.T. Donald H. Lalonde, M.D. Michael Bell, M.D. Daniel McKee, B.Sc.
HAND/PERIPHERAL NERVE Avoiding Flexor Tendon Repair Rupture with Intraoperative Total Active Movement Examination Amanda Higgins, B.Sc.O.T. Donald H. Lalonde, M.D. Michael Bell, M.D. Daniel McKee, B.Sc.
Achilles Tendon Rupture: A Biomechanical Evaluation of Varying the Number of Loops in a Physiological Model
 Achilles Tendon Rupture: A Biomechanical Evaluation of Varying the Number of Loops in a Physiological Model Qais Naziri, MD; Preston Grieco, BA; Westley Hayes, MS; Maxwell Weinberg, BS; and Jaime Uribe,
Achilles Tendon Rupture: A Biomechanical Evaluation of Varying the Number of Loops in a Physiological Model Qais Naziri, MD; Preston Grieco, BA; Westley Hayes, MS; Maxwell Weinberg, BS; and Jaime Uribe,
Physical therapy of the wrist and hand
 Physical therapy of the wrist and hand Functional anatomy wrist and hand The wrist includes distal radius, scaphoid, lunate, triquetrum, pisiform, trapezium, trapezoid, capitate, and hamate. The hand includes
Physical therapy of the wrist and hand Functional anatomy wrist and hand The wrist includes distal radius, scaphoid, lunate, triquetrum, pisiform, trapezium, trapezoid, capitate, and hamate. The hand includes
Flexor Tendons. Get a Grip on Flexor Tendons. 1) Click the arrows on the navigation panel at the bottom of the PDF page
 www. treatment2go. com & www. handtherapy. com Flexor Tendons Get a Grip on Flexor Tendons This course has active links. The index is linked so you can just click and go (page 5). To access a website click
www. treatment2go. com & www. handtherapy. com Flexor Tendons Get a Grip on Flexor Tendons This course has active links. The index is linked so you can just click and go (page 5). To access a website click
Intrasynovial flexor tendon injuries and repair
 Digital Comprehensive Summaries of Uppsala Dissertations from the Faculty of Medicine 1307 Intrasynovial flexor tendon injuries and repair SARA EDSFELDT ACTA UNIVERSITATIS UPSALIENSIS UPPSALA 2017 ISSN
Digital Comprehensive Summaries of Uppsala Dissertations from the Faculty of Medicine 1307 Intrasynovial flexor tendon injuries and repair SARA EDSFELDT ACTA UNIVERSITATIS UPSALIENSIS UPPSALA 2017 ISSN
BUNNELL. Expanded product line Customer service Please visit BunnellSplints.com Sizing information on back page WRIST HAND FINGER ORTHOSIS
 Established 1907 WENIGER Exclusive Manufacturer of BUNNELL WRIST HAND FINGER ORTHOSIS STATIC DYNAMIC STATIC PROGRESSIVE POSITIONING LATEX FREE SOFT STRAPS ORTHOSIS FITS RIGHT OR LEFT HAND Expanded product
Established 1907 WENIGER Exclusive Manufacturer of BUNNELL WRIST HAND FINGER ORTHOSIS STATIC DYNAMIC STATIC PROGRESSIVE POSITIONING LATEX FREE SOFT STRAPS ORTHOSIS FITS RIGHT OR LEFT HAND Expanded product
The Rheumatoid Hand Deformities & Management. Dr. Anirudh Sharma Resident Department of Orthopedics
 + The Rheumatoid Hand Deformities & Management Dr. Anirudh Sharma Resident Department of Orthopedics + Why is Rheumatoid Arthritis important? + RA is a very debilitating disease median life expectancy
+ The Rheumatoid Hand Deformities & Management Dr. Anirudh Sharma Resident Department of Orthopedics + Why is Rheumatoid Arthritis important? + RA is a very debilitating disease median life expectancy
Integra Use of TenoGlide Tendon Protector Sheet to Protect an Extensor Tendon Repair of the Thumb CASE STUDY
 Integra Use of TenoGlide Tendon Protector Sheet to Protect an Extensor Tendon Repair of the Thumb 1 CASE STUDY Use of Integra TenoGlide Tendon Protector Sheet to Protect an Extensor Tendon Repair of the
Integra Use of TenoGlide Tendon Protector Sheet to Protect an Extensor Tendon Repair of the Thumb 1 CASE STUDY Use of Integra TenoGlide Tendon Protector Sheet to Protect an Extensor Tendon Repair of the
Classification of Established Volkmann s Ischemic Contracture and the Program for Its Treatment
 10 Classification of Established Volkmann s Ischemic Contracture and the Program for Its Treatment In spite of the advances made in preventive treatment of muscular ischemia at the forearm and hand, there
10 Classification of Established Volkmann s Ischemic Contracture and the Program for Its Treatment In spite of the advances made in preventive treatment of muscular ischemia at the forearm and hand, there
(iii) Twenty questions on tendon injuries in the hand
 Current Orthopaedics (2008) 22, 17 24 Available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/cuor MINI-SYMPOSIUM: HAND TRAUMA (iii) Twenty questions on tendon injuries in the hand
Current Orthopaedics (2008) 22, 17 24 Available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/cuor MINI-SYMPOSIUM: HAND TRAUMA (iii) Twenty questions on tendon injuries in the hand
FINGER INJURIES. Chapter 24, pgs ,
 FINGER INJURIES Chapter 24, pgs 727 730, 741 743 1. Demonstrate mastery of anatomical references to the hand and fingers. 2. Compare and contrast Mallet Finger, Swan Neck Deformity and Boutonnière Deformity.
FINGER INJURIES Chapter 24, pgs 727 730, 741 743 1. Demonstrate mastery of anatomical references to the hand and fingers. 2. Compare and contrast Mallet Finger, Swan Neck Deformity and Boutonnière Deformity.
Dynamic treatment for proximal phalangeal fracture of the hand
 Journal of Orthopaedic Surgery 2007;15(2):211-5 Dynamic treatment for proximal phalangeal fracture of the hand G Rajesh, WY Ip, SP Chow, BKK Fung Department of Orthopaedics and Traumatology, University
Journal of Orthopaedic Surgery 2007;15(2):211-5 Dynamic treatment for proximal phalangeal fracture of the hand G Rajesh, WY Ip, SP Chow, BKK Fung Department of Orthopaedics and Traumatology, University
A Patient s Guide to Adult Thumb Metacarpal Fractures
 A Patient s Guide to Adult Thumb Metacarpal Fractures 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com 1 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Adult Thumb Metacarpal Fractures 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com 1 DISCLAIMER: The information in this booklet is compiled
.org. Tibia (Shinbone) Shaft Fractures. Anatomy. Types of Tibial Shaft Fractures
 Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Tensile Strength of Flexor Tendon Repair Using Barbed Suture Material in a Dynamic Ex Vivo Model
 J Hand Microsurg (January June 2012) 4(1):16 20 DOI 10.1007/s12593-012-0063-1 ORIGINAL ARTICLE Tensile Strength of Flexor Tendon Repair Using Barbed Suture Material in a Dynamic Ex Vivo Model Philip H.
J Hand Microsurg (January June 2012) 4(1):16 20 DOI 10.1007/s12593-012-0063-1 ORIGINAL ARTICLE Tensile Strength of Flexor Tendon Repair Using Barbed Suture Material in a Dynamic Ex Vivo Model Philip H.
Mallet Baseball Finger
 Mallet Baseball Finger Introduction When you think about how much we use our hands, it's not hard to understand why injuries to the fingers are common. Most of these injuries heal without significant problems.
Mallet Baseball Finger Introduction When you think about how much we use our hands, it's not hard to understand why injuries to the fingers are common. Most of these injuries heal without significant problems.
10/10/2014. Structure and Function of the Hand. The Hand. Osteology of the Hand
 Structure and Function of the Hand 19 bones and 19 joints are necessary to produce all the motions of the hand The Hand Dorsal aspect Palmar aspect The digits are numbered 1-5 Thumb = #1 Little finger
Structure and Function of the Hand 19 bones and 19 joints are necessary to produce all the motions of the hand The Hand Dorsal aspect Palmar aspect The digits are numbered 1-5 Thumb = #1 Little finger
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual
 Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Volume 10 Spring 1997 Pages Flexor Tendon Lacerations in the Hand. David R. Steinberg, M.D.
 Volume 10 Spring 1997 Pages 5-11 Flexor Tendon Lacerations in the Hand David R. Steinberg, M.D. Department of Orthopaedic Surgery, University of Pennsylvania, 8 Penn Tower, 34 and Civic Center Boulevard,
Volume 10 Spring 1997 Pages 5-11 Flexor Tendon Lacerations in the Hand David R. Steinberg, M.D. Department of Orthopaedic Surgery, University of Pennsylvania, 8 Penn Tower, 34 and Civic Center Boulevard,
JuggerKnot Soft Anchor 1.0 mm Mini
 JuggerKnot Soft Anchor 1.0 mm Mini Ulnar Collateral Ligament (UCL) Repair of the Thumb Surgical Technique Surgical Protocols by Mark Rekant, M.D. A. Lee Osterman, M.D. One Surgeon. One Patient. Over 1
JuggerKnot Soft Anchor 1.0 mm Mini Ulnar Collateral Ligament (UCL) Repair of the Thumb Surgical Technique Surgical Protocols by Mark Rekant, M.D. A. Lee Osterman, M.D. One Surgeon. One Patient. Over 1
JuggerKnot Soft Anchor 1.0 mm Mini
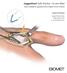 JuggerKnot Soft Anchor 1.0 mm Mini Ulnar Collateral Ligament (UCL) Repair of the Thumb Surgical Technique Surgical Protocols by Mark Rekant, M.D. A. Lee Osterman, M.D. One Surgeon. One Patient. Over 1
JuggerKnot Soft Anchor 1.0 mm Mini Ulnar Collateral Ligament (UCL) Repair of the Thumb Surgical Technique Surgical Protocols by Mark Rekant, M.D. A. Lee Osterman, M.D. One Surgeon. One Patient. Over 1
Distal Radius Plate 2.4/2.7 dorsal and volar
 Distal Radius Plate 2.4/2.7 dorsal and volar Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Distal Radius Plate
Distal Radius Plate 2.4/2.7 dorsal and volar Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Distal Radius Plate
THE 9 FINGER flexor pulleys maintain the course. Quantification of Partial or Complete A4 Pulley Release With FDP Repair in Cadaveric Tendons
 SCIENTIFIC ARTICLE Quantification of Partial or Complete A4 Pulley Release With FDP Repair in Cadaveric Tendons Orrin I. Franko, MD, Nathan M. Lee, BS, John J. Finneran, BA, Matthew C. Shillito, MD, Matthew
SCIENTIFIC ARTICLE Quantification of Partial or Complete A4 Pulley Release With FDP Repair in Cadaveric Tendons Orrin I. Franko, MD, Nathan M. Lee, BS, John J. Finneran, BA, Matthew C. Shillito, MD, Matthew
Introduction to Ultrasound Examination of the Hand and upper
 Introduction to Ultrasound Examination of the Hand and upper Emil Dionysian, M.D. Ultrasound of upper ext. Upside Convenient Opens another exam dimension Can be like a stethoscope Helps 3-D D visualization
Introduction to Ultrasound Examination of the Hand and upper Emil Dionysian, M.D. Ultrasound of upper ext. Upside Convenient Opens another exam dimension Can be like a stethoscope Helps 3-D D visualization
5/8/2017. Finger Injuries in Football. Tendon Injuries of the Hand and Wrist in Football Steve Kronlage, MD Andrews Institute Gulf Breeze, Florida
 Finger Injuries in Football Tendon Injuries of the Hand and Wrist in Football Steve Kronlage, MD Andrews Institute Gulf Breeze, Florida A jammed finger is an injury (at very least a torn ligament) A swollen
Finger Injuries in Football Tendon Injuries of the Hand and Wrist in Football Steve Kronlage, MD Andrews Institute Gulf Breeze, Florida A jammed finger is an injury (at very least a torn ligament) A swollen
Structure and Function of the Hand
 Structure and Function of the Hand Some say it takes a village to raise a child, but it takes 19 bones and 19 joints in the hand for it to function smoothly. The Hand Dorsal aspect 2 3 4 The digits are
Structure and Function of the Hand Some say it takes a village to raise a child, but it takes 19 bones and 19 joints in the hand for it to function smoothly. The Hand Dorsal aspect 2 3 4 The digits are
Metacarpophalangeal Joint Implant Arthroplasty REHABILITATION PROTOCOL
 Andrew McNamara, MD The Orthopaedic and Fracture Clinic 1431 Premier Drive Mankato, MN 56001 507-386-6600 Metacarpophalangeal Joint Implant Arthroplasty REHABILITATION PROTOCOL Patient Name: Date: Diagnosis:
Andrew McNamara, MD The Orthopaedic and Fracture Clinic 1431 Premier Drive Mankato, MN 56001 507-386-6600 Metacarpophalangeal Joint Implant Arthroplasty REHABILITATION PROTOCOL Patient Name: Date: Diagnosis:
Prof Oluwadiya KS FMCS(orthop)
 Prof Oluwadiya KS FMCS(orthop) www.oluwadiya.com Sutures are materials with which two surfaces are kept in apposition. Tensile strength is the measured level of tension that a knotted suture strand can
Prof Oluwadiya KS FMCS(orthop) www.oluwadiya.com Sutures are materials with which two surfaces are kept in apposition. Tensile strength is the measured level of tension that a knotted suture strand can
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Rocchi, L., Merolli, A., Morini, A., Monteleone, G., & Foti, C. (2014). A modified spica-splint in postoperative early-motion management of skier's thumb lesion: A randomized
CRITICALLY APPRAISED PAPER (CAP) Rocchi, L., Merolli, A., Morini, A., Monteleone, G., & Foti, C. (2014). A modified spica-splint in postoperative early-motion management of skier's thumb lesion: A randomized
A Patient s Guide to Adult Thumb Metacarpal Fractures
 A Patient s Guide to Adult Thumb Metacarpal Fractures Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 1 DISCLAIMER: The information
A Patient s Guide to Adult Thumb Metacarpal Fractures Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 1 DISCLAIMER: The information
Surgical Technique. Achilles Tendon Repair Using Conexa Reconstructive Tissue Matrix. conexatm. Surgical Technique Described by Tom Chang, DPM
 Surgical Technique Achilles Tendon Repair Using Conexa Reconstructive Tissue Matrix Surgical Technique Described by Tom Chang, DPM conexatm r e c o n s t r u c t i v e t i s s u e m a t r i x Achilles
Surgical Technique Achilles Tendon Repair Using Conexa Reconstructive Tissue Matrix Surgical Technique Described by Tom Chang, DPM conexatm r e c o n s t r u c t i v e t i s s u e m a t r i x Achilles
Acellular Dermal Matrices for Tendon Sheath Reconstruction: A Novel Method for Pulley Reconstruction and Adhesion Prevention
 Acellular Dermal Matrices for Tendon Sheath Reconstruction: A Novel Method for Pulley Reconstruction and Adhesion Prevention T. JoAnna Nguyen MD, Caroline Yao MD, David A. Kulber MD Division of Plastic
Acellular Dermal Matrices for Tendon Sheath Reconstruction: A Novel Method for Pulley Reconstruction and Adhesion Prevention T. JoAnna Nguyen MD, Caroline Yao MD, David A. Kulber MD Division of Plastic
Interesting Case Series. Swan-Neck Deformity in Cerebral Palsy
 Interesting Case Series Swan-Neck Deformity in Cerebral Palsy Leyu Chiu, BA, a Nicholas S. Adams, MD, a,b and Paul A. Luce, MD, a,b,c a Michigan State University College of Human Medicine, Grand Rapids,
Interesting Case Series Swan-Neck Deformity in Cerebral Palsy Leyu Chiu, BA, a Nicholas S. Adams, MD, a,b and Paul A. Luce, MD, a,b,c a Michigan State University College of Human Medicine, Grand Rapids,
Management of Unstable Metacarpal Fractures with Traversing Kirschner Wiring
 Cronicon OPEN ACCESS EC ORTHOPAEDICS Research Article Tarek Aly* Management of Unstable Metacarpal Fractures with Traversing Kirschner Wiring Department of Orthopedic Surgery, Tanta University School of
Cronicon OPEN ACCESS EC ORTHOPAEDICS Research Article Tarek Aly* Management of Unstable Metacarpal Fractures with Traversing Kirschner Wiring Department of Orthopedic Surgery, Tanta University School of
Acu-Loc Wrist Spanning Plate System. Surgical Technique
 Acu-Loc Wrist Spanning Plate System Surgical Technique Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches
Acu-Loc Wrist Spanning Plate System Surgical Technique Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches
Chapter 24. Arthroscopic Thumb Carpometacarpal Interposition Arthroplasty. Introduction. Operative Technique. Patient Preparation and Positioning
 Chapter 24 Arthroscopic Thumb Carpometacarpal Interposition Arthroplasty Introduction Osteoarthritis in the thumb carpometacarpal (CMC) joint is a common condition, especially in women over 60 years of
Chapter 24 Arthroscopic Thumb Carpometacarpal Interposition Arthroplasty Introduction Osteoarthritis in the thumb carpometacarpal (CMC) joint is a common condition, especially in women over 60 years of
Hand Injuries in Baseball
 Hand Injuries in Baseball Steven S. Shin, MD, MMSc Director of Hand Surgery, Kerlan-Jobe Orthopaedic Clinic Co-Director of Hand Surgery, Cedars-Sinai Health System Los Angeles, California Hand Consultant
Hand Injuries in Baseball Steven S. Shin, MD, MMSc Director of Hand Surgery, Kerlan-Jobe Orthopaedic Clinic Co-Director of Hand Surgery, Cedars-Sinai Health System Los Angeles, California Hand Consultant
Use of Low-profile Palmar Internal Fixation in Digital Replantation
 TECHNIQUE Use of Low-profile Palmar Internal Fixation in Digital Replantation Mark Ross, MBBS, FRACS(Orth),*wz Christof Bollman, MBBS,*wy and Gregory B. Couzens, MBBS, FRACS(Orth)*8 Abstract: There are
TECHNIQUE Use of Low-profile Palmar Internal Fixation in Digital Replantation Mark Ross, MBBS, FRACS(Orth),*wz Christof Bollman, MBBS,*wy and Gregory B. Couzens, MBBS, FRACS(Orth)*8 Abstract: There are
PEDUS-L. Locking Plantar Lapidus Plate
 PEDUS-L Locking Plantar Lapidus Plate Page 1 PEDUS-L - Locking Plantar Lapidus Plate Table of Contents Implants 3 System 4 Operation manual 5 Approach 5 Identification of the TMT 1 joint with a cannula
PEDUS-L Locking Plantar Lapidus Plate Page 1 PEDUS-L - Locking Plantar Lapidus Plate Table of Contents Implants 3 System 4 Operation manual 5 Approach 5 Identification of the TMT 1 joint with a cannula
Conventus CAGE PH Surgical Techniques
 Conventus CAGE PH Surgical Techniques Conventus Orthopaedics The Conventus CAGE PH (PH Cage) is a permanent implant comprised of an expandable scaffold, made from nitinol and titanium, which is deployed
Conventus CAGE PH Surgical Techniques Conventus Orthopaedics The Conventus CAGE PH (PH Cage) is a permanent implant comprised of an expandable scaffold, made from nitinol and titanium, which is deployed
Clinical Orthopaedic Rehabilitation Volume 1 and 2
 Clinical Orthopaedic Rehabilitation Volume 1 and 2 COURSE DESCRIPTION This program is a practical, clinical guide that provides guidance on the evaluation, differential diagnosis, treatment, and rehabilitation
Clinical Orthopaedic Rehabilitation Volume 1 and 2 COURSE DESCRIPTION This program is a practical, clinical guide that provides guidance on the evaluation, differential diagnosis, treatment, and rehabilitation
In Vivo Flexor Tendon Forces Increase with Finger and Wrist Flexion during Active Finger Flexion and Extension
 In Vivo Flexor Tendon Forces Increase with Finger and Wrist Flexion during Active Finger Flexion and Extension Katarzyna Kursa, 1 Lisa Lattanza, 2 Edward Diao, 2 David Rempel 3 1 Department of Bioengineering,
In Vivo Flexor Tendon Forces Increase with Finger and Wrist Flexion during Active Finger Flexion and Extension Katarzyna Kursa, 1 Lisa Lattanza, 2 Edward Diao, 2 David Rempel 3 1 Department of Bioengineering,
Early Elbow Motion Protocol Ligament Repair of the elbow
 499 Blossom Hill Rd, San Jose, Ca 95123 Tel: 408-268-8536 Fax: 408-268-8727 www.handsoncaretherapy.com Early Elbow Motion Protocol Ligament Repair of the elbow EARLY MOTION PROTOCOL 1-3 DAYS POST OP LIGAMENT
499 Blossom Hill Rd, San Jose, Ca 95123 Tel: 408-268-8536 Fax: 408-268-8727 www.handsoncaretherapy.com Early Elbow Motion Protocol Ligament Repair of the elbow EARLY MOTION PROTOCOL 1-3 DAYS POST OP LIGAMENT
Trigger Digits, Mallet Finger & Metacarpal Injuries. Joseph P. McCormick, M.D. Affinity Orthopaedics & Sports Medicine 2013
 Trigger Digits, Mallet Finger & Metacarpal Injuries Joseph P. McCormick, M.D. Affinity Orthopaedics & Sports Medicine 2013 Overview Trigger Digits: diagnosis and treatment Bonus: approach in children Mallet
Trigger Digits, Mallet Finger & Metacarpal Injuries Joseph P. McCormick, M.D. Affinity Orthopaedics & Sports Medicine 2013 Overview Trigger Digits: diagnosis and treatment Bonus: approach in children Mallet
2.4 mm Variable Angle LCP Volar Extra-Articular Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology.
 Technique Guide 2.4 mm Variable Angle LCP Volar Extra-Articular Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology. Table of Contents Introduction 2.4
Technique Guide 2.4 mm Variable Angle LCP Volar Extra-Articular Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology. Table of Contents Introduction 2.4
REPAIR VERSUS OPEN REPAIR FOR ACUTE
 RETROSPECTIVE ANALYSIS OF MINI-OPEN REPAIR VERSUS OPEN REPAIR FOR ACUTE ACHILLES TENDON RUPTURES Erin E. Klein, DPM, MS Lowell Weil, Jr., DPM, MBA Jeffrey R. Baker, DPM Lowell Scott Weil, Sr., DPM Jessica
RETROSPECTIVE ANALYSIS OF MINI-OPEN REPAIR VERSUS OPEN REPAIR FOR ACUTE ACHILLES TENDON RUPTURES Erin E. Klein, DPM, MS Lowell Weil, Jr., DPM, MBA Jeffrey R. Baker, DPM Lowell Scott Weil, Sr., DPM Jessica
Prospective Morphologic and Dynamic Assessment of Deep Flexor Tendon Healing in Zone II by High-Frequency Ultrasound: Preliminary Experience
 Musculoskeletal Imaging Original Research Puippe et al. High-Frequency Ultrasound ssessment of Deep Flexor Tendon Musculoskeletal Imaging Original Research Prospective Morphologic and Dynamic ssessment
Musculoskeletal Imaging Original Research Puippe et al. High-Frequency Ultrasound ssessment of Deep Flexor Tendon Musculoskeletal Imaging Original Research Prospective Morphologic and Dynamic ssessment
Evaluation of Bioadhesive Mesh Construct to Augment Achilles Tendon Repair in a Rabbit Model
 Evaluation of Bioadhesive Mesh Construct to Augment Achilles Tendon Repair in a Rabbit Model Yan Lu, MD 1, Brett Nemke 1, Jackie Kondratko 1, Vicki kalscheur 1, Gino Bradica 2, Ray Vanderby 1, Mark D.
Evaluation of Bioadhesive Mesh Construct to Augment Achilles Tendon Repair in a Rabbit Model Yan Lu, MD 1, Brett Nemke 1, Jackie Kondratko 1, Vicki kalscheur 1, Gino Bradica 2, Ray Vanderby 1, Mark D.
Study of clinical problems: Mallet injuries
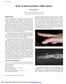 Review Article Study of clinical problems: Mallet injuries Hin-Keung WONG Department of Orthopaedics & Traumatology, Princess Margaret Hospital, Hong Kong SAR INTRODUCTION The extensor mechanism of the
Review Article Study of clinical problems: Mallet injuries Hin-Keung WONG Department of Orthopaedics & Traumatology, Princess Margaret Hospital, Hong Kong SAR INTRODUCTION The extensor mechanism of the
Ascension. Silicone MCP surgical technique. surgical technique Ascension Silicone MCP
 Ascension Silicone MCP surgical technique WW 2 Introduction This manual describes the sequence of techniques and instruments used to implant the Ascension Silicone MCP (FIGURE 1A). Successful use of this
Ascension Silicone MCP surgical technique WW 2 Introduction This manual describes the sequence of techniques and instruments used to implant the Ascension Silicone MCP (FIGURE 1A). Successful use of this
John J Christoforetti, MD Pittsburgh, Pennsylvania
 ARTHROSCOPIC ASSISTED PROXIMAL HAMSTRINGS REPAIR WITH HUMAN ACELLULAR DERMAL ALLOGRAFT PATCH AUGMENTATION FOR REVISION OF FAILED PROXIMAL HAMSTRINGS REPAIR: SHORT TERM CLINICAL AND MRI RESULT John J Christoforetti,
ARTHROSCOPIC ASSISTED PROXIMAL HAMSTRINGS REPAIR WITH HUMAN ACELLULAR DERMAL ALLOGRAFT PATCH AUGMENTATION FOR REVISION OF FAILED PROXIMAL HAMSTRINGS REPAIR: SHORT TERM CLINICAL AND MRI RESULT John J Christoforetti,
Chapter 4: Forearm 4.3 Forearm shaft fractures, transverse (12-D/4)
 AO Manual of ESIN in children s fractures Chapter 4: Forearm 4.3 Forearm shaft fractures, transverse (12-D/4) Title AO Manual of ESIN in children Subtitle Elastic stable intramedullary nailing (ESIN) Author
AO Manual of ESIN in children s fractures Chapter 4: Forearm 4.3 Forearm shaft fractures, transverse (12-D/4) Title AO Manual of ESIN in children Subtitle Elastic stable intramedullary nailing (ESIN) Author
INTERNAL FIXATION OF THE METACARPALS AND PHALANGES P. BURGE
 Riv Chir Mano - Vol. 43 (3) 2006 INTERNL FIXTION OF THE METCRPLS ND PHLNGES P. URGE Nuffield Orthopaedic Centre, Oxford, UK SUMMRY Techniques and instrumentation for open reduction and internal fixation
Riv Chir Mano - Vol. 43 (3) 2006 INTERNL FIXTION OF THE METCRPLS ND PHLNGES P. URGE Nuffield Orthopaedic Centre, Oxford, UK SUMMRY Techniques and instrumentation for open reduction and internal fixation
MULTIFIX S Knotless Implants
 Technique Guide MULTIFIX S Knotless Implants The MULTIFIX S system offers 5.5mm and 6.5mm knotless, all-peek, poundin implants. The system provides multiple fixation options, a streamlined technique, and
Technique Guide MULTIFIX S Knotless Implants The MULTIFIX S system offers 5.5mm and 6.5mm knotless, all-peek, poundin implants. The system provides multiple fixation options, a streamlined technique, and
For treatment of PIP joint flexion contractures. Surgeon s Manual
 For treatment of PIP joint flexion contractures. Maintenance of joint extension depends on identification and treatment of force imbalance causing contracture. Surgeon s Manual Digit Widget External Fixation
For treatment of PIP joint flexion contractures. Maintenance of joint extension depends on identification and treatment of force imbalance causing contracture. Surgeon s Manual Digit Widget External Fixation
Monolateral External Fixation System for Trauma and Orthopaedics
 MEFiSTO Monolateral External Fixation System for Trauma and Orthopaedics Surgical Technique Original Instruments and Implants of the Association for the Study of Internal Fixation AO/ASIF MEFiSTO Table
MEFiSTO Monolateral External Fixation System for Trauma and Orthopaedics Surgical Technique Original Instruments and Implants of the Association for the Study of Internal Fixation AO/ASIF MEFiSTO Table
Surgical Technique. CONQUEST FN Femoral Neck Fracture System
 Surgical Technique CONQUEST FN Femoral Neck Fracture System Table of Contents Introduction... 3 Indications... 3 Product Overview... 4 Surgical Technique... 5 Patient Positioning... 5 Reduce the Fracture...
Surgical Technique CONQUEST FN Femoral Neck Fracture System Table of Contents Introduction... 3 Indications... 3 Product Overview... 4 Surgical Technique... 5 Patient Positioning... 5 Reduce the Fracture...
