An improved method of supercharged transposed latissimus dorsi flap with the skin paddle for the management of a complicated lumbosacral defect
|
|
|
- Ambrose Wilkins
- 5 years ago
- Views:
Transcription
1 European Review for Medical and Pharmacological Sciences An improved method of supercharged transposed latissimus dorsi flap with the skin paddle for the management of a complicated lumbosacral defect E. CIGNA 1,2, S. MARDINI 1, H.-C. CHEN 1, Ö. ÖZKAN 1, P. SASSU 1, C.J. SALGADO 1, Y.-T. LIEU 1, I. PONZO 2, D. RIBUFFO 2, N. SCUDERI 2 1 Department of Plastic Surgery, and the E-Da Hospital/I-Shou University, Taiwan 2 Department of Plastic and Reconstructive and Aesthetic Surgery, Polyclinic Umberto I, Sapienza University of Rome, Rome, Italy 2015; 19: Abstract. OBJECTIVE: Treatment of nonhealing wounds of lower back often poses a powerful challenge. We present one of the first report of treatment of a lumbosacral defect with a supercharged latissimus dorsi flap with the skin paddle. CASE REPORT: We report a case of a 59 yearold man with myeloma of the sacral spine who underwent radiotherapy and chemotherapy and subsequently, laminectomies and placement of hardware for ongoing paresis and spine instability. Then, he developed an open wound and osteomyelitis of the spine with culture positive tuberculous granulomas. After multiple surgical debridement, he presented to our service and was treated with a single stage debridement followed by the performance of a latissimus dorsi musculocutaneous flap based on paraspinal perforators and supercharged. RESULTS: This solution, allowed for augmentation of blood flow to the muscle with the inferior gluteal artery, provided coverage of the defect resistant to the pressure, and simplified post-operative management of the patient. CONCLUSIONS: Alternative treatment options, including free tissue transfer, posed difficulties in finding suitable recipient vessels near the defect, in inserting the flap so as to restore its original length without compromising blood flow, and in postoperative care of the patient. Treatment of a lumbosacral defect with a supercharged latissimus dorsi flap with the skin paddle may represent a milestone procedure for complicated lower spine wounds. Key Words: Latissimus dorsi flap, Microsurgery, Supercharged flap, Lower back defect, Sacral defect, Pedicled flap, Musculocutaneous flap. Introduction Chronic osteomyelitis of the spine with open wounds of lower back present a reconstructive challenge. A variety of flaps can be used to repair defects in this area, ranging from local cutaneous, muscle and musculocutaneous flaps or perforator flaps to free flaps 1-6. Nevertheless, surgical therapy often fails due to the lack of adequate debridement, provision of soft tissue coverage with inadequate blood supply, and to imperfect postoperative management of the patient. This is particularly true in patients with compromised conditions related to local or systemic factors such as radiation therapy, infection, and compromised immune system. Following the failure of multiple surgical procedures to treat a lower back wound with chronic osteomyelitis, we successfully treated a patient using a latissimus dorsi flap with a large skin paddle that was supercharged in order to optimize blood flow. Case Report (Figure 1) A 59-year-old man with a history of multiple myeloma of the sacral spine surgically treated, resulting in osteomyelitis of the spine and chronic wound, presented to our service after multiple failed attempts at wound debridement and closure. (Figure 1 A) For the initial treatment of the myeloma, the patient received radiotherapy. However, patient s symptoms of lower back pain and progressive lower extremity pareses perstisted. A decompressive laminectomy of L2 through L5 was performed. The patient subsequently de- Corresponding Author: Ida Ponzo, MD; ida.ponzo@hotmail.it 921
2 E. Cigna, S. Mardini, H.-C. Chen, Ö. Özkan, P. Sassu, C.J. Salgado, et al. Figure 1. A 59 year-old man with a lumbosacral defect. 1A, Preoperative view of the wound and markings of the musculocutaenous latissimus dorsi flap. The skin fistulas are marked with arrows. The dotted area shows what is expected to be the extent of the wound under the skin. The parallel lines mark the skin island that was harvested with the flap. 1B, Computerized Tomography demonstrating the extensiveness of the defect, its depth as well as a fistula connecting the spine to the skin (white arrow). 1C, After incising an elliptical area of skin. Note the extent of the wound under the skin, the exposed spinous processes, and the antibiotic beads (cephalad: right side of figure). 1D, The reverse latissimus dorsi musculocutaneous flap after harvest and before clockwise rotation into the defect. Arrows A, B, C, and D point to the thoracodorsal vessels following ligation, the exposed dura following resection of the infected spinous processes, the exposed hardware, and the inferior gluteal vessels respectively. 1E, The flap after complete disinsertion. Two paraspinal perforators are visualized (arrows). Note that the tissue in between these vessels, which might include additional paraspinal perforators, was preserved. 1F, The wound on postoperative day 26 demonstrating complete healing. 922
3 Supercharged transposed latissimus dorsi musculocutaneous flap veloped instability of the spine and infection of the lower back with positive culture of Mycobacterium tuberculosis granulomas. The instability was surgically treated by transpedicle screw fixation from T12 to S1. At that time, antibiotic beads were placed in the wound bed. The patient presented to our service with fever and continuous drainage of the wound. A preoperative CT scan (Figure 1B) showed a large paraspinal defect with apparent skin fìstulas and involvement of lumbar and sacral spinous processes. Intravenous antibiotic therapy was administered and then an extensive debridement of the wound, removal of the spinous processes that were exposed (performed by neurosurgeons) and removal of the beads were performed. The defect was then filled with a latissimus dorsi flap (Figure 1C, 1D, 1E, and 1F). Operative Procedure Marking of the skin island was performed medial to and along the axis of the latissimus dorsi muscle and it measured cm (Figure 1A.) A two team approach was used: one team elevated the right latissimus myocutaneous flap, in the standard fashion, while the other team exposed the left inferior gluteal vessels (Figure1D). After exposure and dissection of the pedicle of the flap, the thoracodorsal artery and the vein were ligated and the muscle was detached from its insertion on the humerus and its origins along the iliac bone and the spine. The flap was then latero-medial elevated. Care was taken to preserve paraspinal perforators, whenever possible. It was rotated clockwise into the defect and the dissection was stopped when adequate mobilization was achieved. We were able to visualize at least two large perforating vessels and we preserved all tissues in, between these vessels (Figures 1D, 1E). After rotating the flap approximately 100 degrees clockwise into the defect, the muscle insertion was placed into the most distal aspect of the wound and the rest of the muscle was used to fill the wound. The flap vessels were anastomized to the inferior gluteal artery and vein. In order to avoid any undue tension, a small area over the distal aspect of the muscle was skin grafted. Suction drainages were placed under the muscle, away from the pedicle; the wound was closed, and the patient was transported to the microsurgical intensive care unit (ICU) in a prone position. It is remarkable that during the dissection, the tissues appeared to be indurated in a way consistent with radiation injury. Postoperative Course The patient was monitored in the microsurgical intensive care unit in a prone position for 5 days before being transferred to the ward. Monitoring of the skin island with doppler checks of the pedicle of the flap was performed. The patient was allowed to lay in a prone as well as right lateral decubitus position for the fìrst 10 days, then he was allowed to lay on the left lateral decubitus position as well, for the following ten days. At postoperative day 20, he was allowed to lay in a supine position and begin ambulating. Intra-operative specimens did not show any evidence of Mycobacterium tuberculosis infection or malignancy. A whole body scan with Tc 99-m MDP was performed at post operative day 20 and was read as negative for osteomyelitis. The patient was discharged on postoperative day 26 ambulating but in unstable health conditions (Figures 1F). At month 4 follow-up, the patient demonstrated complete healing of the wound without any evidence of superficial or deep wound infections. Discussion Small to medium size defects of the lumbosacral region can usually be closed using local cutaneous, muscle or musculocutaneous flaps 5-8. Large defects however require special management due to the size of the defect and the lack of adequate amount of adjacent tissue to the wound that is particularly true when the patient has received preoperative radiation therapy or presents with an infected wound. Bone exposure and hardware represent an even greater challenge and require extensive debridement and provision of well vascularized tissue useful in filling the dead space, providing white blood cells and other immune factors to reach the wound, and in allowing antibiotics to reach critical areas of the wound in high enough concentrations. Regional and distant flaps such as the latissimus dorsi muscle flap in this case, are often used, as they fulfil criteria required for management of such wounds 9. These flaps also have the advantage of not being immediately adjacent to the wound and are therefore not subjected to inflammatory processes and infectious organisms present in the wound 10. Ideally, a local or regional muscle flap such as the gluteus maximus flap 2,11-13 can be used for the reconstruction. Nevertheless, in our case, the location of the wound was slightly too cephalad 923
4 E. Cigna, S. Mardini, H.-C. Chen, Ö. Özkan, P. Sassu, C.J. Salgado, et al. and too large in size and volume and these muscles had also been more directly exposed to the damaging effects of radiation, making them even less viable for transfer. In instances when local flaps are inadequate or have been already used, other regional and distant free flaps are the only available option for wound closure. When dealing with large defects of the lower back, reverse and turnover latissimus dorsi flaps based on the secondary segmental vessels have been reported These flaps have been performed with and without reperfusion of the main pedicle of the flap by the supercharging method 16. Only a few reports have discussed microsurgical free flap methods for the reconstruction of lower back wound ; anyway, when free tissue transfer is opted for, the latissimus dorsi flap based on the thoracodorsal vessels, is the most commonly used flap. This method of reconstruction, although often successful, becomes a significant challenge when the coverage of a lumbosacral wound is required. Two are the main reasons of the increased difficulties: first of all, the paucity of suitable recipient vessels and second, the complexity of postoperative care. Although supercharging a flap does require the use of recipient vessels in the area of the affected region, they do not provide the sole blood supply to the flap. Therefore, the chance of complete flap failure is lessened. Additionally, if occlusion of the supercharged vessels is detected during the postoperative period, exploration and repair can be performed without undergoing any significant ischemia or venous congestion of the flap, by ensuring a dual blood supply. The absence of ideally positioned and sized recipient vessels for microsurgical free tissue transfer, often leads surgeons to use less commonly used vessels (i.e., perforator vessels of the deep femoral system 20, the deep femoral artery 17,21, the inferior or superior 16,19,22,25-27 gluteal vessels, the superficial femoral trunk 28 and the intercostals vessels). Some authors performed staged transfers of the flap using carrier vessels 22,30, and others used more distant vessels bridged with long vein grafts in which an increased risk of thrombosis was observed. In our case, we used the left superior gluteal artery to allow a more comfortable two team approach. Although the vessels appeared to have suffered radiation damages (evident induration and lack of a good plane of dissection around the vessels), the presence of a strong spurt upon transecting the artery encouraged us to use this vessel. Reconstruction of lower back wounds requires proper postoperative care, such as important as adequate preoperative planning and surgical execution. When free tissue transfer is performed, correct positioning of the patient must avoid any compression of the pedicle. Flap circulation has to be carefully monitored, especially during the early postoperative period. Despite all precautions, flap failure may occur and often results in further trouble in these complex kind of patients. Thus, many surgeons opt for conservative methods of wound closure, or attempt primary closure or local flap closure, which often ends up in reconstructive failures and persistent osteomyelitis. Our patient required immediate reconstruction with viable, well vascularized tissue in order to eradicate the osteomyelitis, protect the spinal contents (which were exposed following the debridement) and allow a relatively rapid return to ambulation. A free latissimus dorsi flap was our routine method to achieve this type of outcome 17,21. However, in this case we opted for transposing the latissimus dorsi flap with the skin paddle based on the paraspinal perforators, then to perform microvascular anastomoses of the thoracodorsal vessels to the inferior gluteal vessels in order to enhance the blood flow and augment venous return of the flap. The usual bulge that occurs at the rotation/pivot point was minimized by complete disinsertion of the origin of the muscle along the spine. In order to obtain wound coverage with well vascularized tissue with adequate bulk without worrying about an all or none flap failure phenomenon, we attempted harvest of a latissimus dorsi musculocutaneous flap based on its secondary blood supply. The flap could be placed into the defect with adequate blood flow for flap survival from paraspinal perforators and additional blood flow could be obtained by supercharging the flap using the thoracodorsal vessels. Before performing the microsurgical anastomosis, the flap was inset into the defect and was placed under some tension in order to re-gain the same length of muscle as was present before dis-insertion. This is difficult to reach when the flap is performed as a free flap only, because tension could compress the pedicle and compromise flap perfusion. We often loose at least 20 or 30 percent of flap length when performing closure of back wounds with free flaps due to this phenomenon. By having a dual blood supply and a skin island, there is a higher chance of achieving a successful result, and postoperative monitoring becomes easier. The skin island 924
5 Supercharged transposed latissimus dorsi musculocutaneous flap provides a good way for monitoring flap perfusion. Additionally, the skin provides coverage of this large defect that would otherwise require skin grafting. The skin island over the muscle may also shunt any interruption to venous outflow from certain parts of the muscle in case of temporary occlusion of one of the venous pedicles that could happen in the normal supine position. The presence of intramuscular valves could therefore be bypassed through the skin island whenever this temporary pressure occurs.in selected cases of lower back wounds where the area of rotation of the flap allows wound coverage along with preservation of the secondary blood supply to the latissimus dorsi musculocutaneous flap, this approach assure excellent flap perfusion, decrease in the likelihood of complete flap failure, simplifìed postoperative care and monitoring, the ability to regain the original flap length during the inset and provision of adequate skin for wound coverage without the need for large skin grafts. Conclusions This case is the first report of a successfully supercharged musculocutaneous latissimus dorsi flap used for coverage of a lower back defect. Statement of Interest Each Author certifies that he or she has no commercial associations that might pose a conflict of interest in connection with the submitted article. References 1) MCCRAW JB, PENIX JO, BAKER JW. Repair of major defects of the chest wall and spine with the latissimus dorsi myocutaneous flap. Plast Reconstr Surg 1978; 62: ) HILL HL, BROWN RG, JURKIEWICZ MJ. The transverse lumbosacral back flap. Plast Reconstr Surg 1978; 62: ) HILL C, RIAZ M. A new twist to the myocutaneous turnover flap for closure of a spinal defect. Plast Reconstr Surg 1998; 102: ) KATO H, HASEGAWA M, TAKADA T, TORII S. The lumbar artery perforator based island flap: Anatomical study and case reports. Br J Plast Surg 1999; 52: ) KROLL SS, ROSENFIELD L. Perforator-based flaps for low posterior midline defects. Plast Reconstr Surg 1988; 81: ) KOSHIMA I, MORIGUCHI T, SOEDA S, KAWATA S, OHTA S, IKEDA A. The gluteal perforator-based flap for repair of sacral pressure sores. Plast. Reconstr Surg 1993; 91: ) YANAI A, BANDOH Y, TSUZUKI K. Bilateral gluteal thigh flaps for closure of large defects in the lumbosacral region and perineal region. Plast Reconstr Surg 1991; 88: ) KOMURO Y, TAKATO T, UEDA K, HARII K. Experience with U-shaped gluteal thigh flap for reconstruction of radionecrosis in the sacral region. Ann Plast Surg 1993; 31: ) VESELY J, HYZA P, RANNO R, CIGNA E, MONNI N, STUP- KA I, JUSTAN I, DVORAK Z, NOVAK P, RANNO S. New technique of total phalloplasty with reinnervated latissimus dorsi myocutaneous free flap in female-to-male transsexuals. Ann Plast Surg 2007; 58: ) OZKAN O, CHEN HC, MARDINI S, CIGNA E, HAO SP, HUNG KF, CHEN HS. Microvascular free tissue transfer in patients with hematological disorders. Plast Reconstr Surg 2006; 118: ) PARKASH S, BANERJEE S-N. Gluteus maximus myocutaneous flap cover for sacral radiation ulcers. Aust N Z J Surg 1986; 56: ) STEVENSON TR, POLLOCK RA, ROHRICH RJ, VANDERKOLK CA. The gluteus maximus musculocutaneous island flap: refinements in design and application. Plast Reconstr Surg 1987; 79: ) AY A, AYTEKIN O, AYTEKIN A. Interdigitating fasciocutaneous gluteal V-Y advancement flaps for reconstruction of sacral defects. Ann Plast Surg 2003; 50: ) BOSTWICK J 3RD, SCHEFLAN M, NAHAI F, JURKIEWICZ MJ. The "reverse" latissimus dorsi muscle and musculocutaneous flap: anatomical and clinical considerations. Plast Reconstr Surg 1980; 65: ) STEVENSON TR, ROHRICH RJ, POLLOCK RA, DINGMAN RO, BOSTWICK J 3RD. More experience with the "reverse" latissimus dorsi musculocutaneous flap: precise location of blood supply. Plast Reconstr Surg 1984; 74: ) GIESSWEIN P, CONSTANCE CG, MACKAY DR, MANDERS EK. Supercharged latissimus dorsi muscle flap for coverage of the problem wound in the lower back. Plast Reconstr Surg 1994; 94: ) HUNG SJ, CHEN HC, WEI FC. Free flaps for reconstruction of the lower back and sacral area. Microsurgery 2000; 20: ) MILES WK, CHANG DW, KROLL SS, MILLER MJ, LANGSTEIN HN, REECE GP, EVANS GR, ROBB GL. Reconstruction of large sacral defects following total sacrectomy. Plast Reconstr Surg 2000; 105: ) DI BENEDETTO G, BERTANI A, PALLUA N. The free latissimus dorsi flap revisited: a primary option for coverage of wide recurrent lumbosacral defects. Plast Reconstr Surg 2002; 109: ) CHEN HC, WENG CJ, NOORDHOFF MS. Coverage of multiple extensive pressure sores with a single filleted lower leg myocutaneous free flap. Plast Reconstr Surg 1986; 78:
6 E. Cigna, S. Mardini, H.-C. Chen, Ö. Özkan, P. Sassu, C.J. Salgado, et al. 21) CHEN HC, CHEN HH, CHEN WJ, TANG YB. Chronic osteomyelitis of the spine managed with a free flap of latissimus dorsi. A case report. Spine 1996; 21: ) HARRIS GD, LEWIS VL, NAGLE DJ, EDELSON RJ, KIM PS. Free flap reconstruction of the lower back and posterior pelvis: indications, principles, and techniques. J Reconstr Microsurg 1988; 4: ) ANTHONY JP, RITTER E, MOELLEKEN BR. Utility of the inferior gluteal vessels in free flap coverage of sacral wounds. Ann Plast Surg 1992; 29: ) DANIEL RK, KERRIGAN CL, GARD DA. The great potential of the intercostal flap for torso reconstruction. Plast Reconstr Surg 1978; 61: ) STARK D, TOFIELD JJ, TERRANOVA W, HURLEY D, KENNEY J. The latissimus dorsi free flap for coverage of sacral radiodermatitis in the ambulatory patient. Ann Plast Surg 1987; 19: ) PARK S, KOH KS. Superior gluteal vessel as recipient for free flap reconstruction of lumbosacral defect. Plast Reconstr Surg 1998; 101: ) GOLDBERG JA, BARWICK WJ, LEVIN LS. Restoration of sensation in paraplegia by a sensory innervated plantar fillet free flap. Case report. Paraplegia 1995; 33: ) YAMAMOTO Y, NOHIRA K, SHINTOMI Y, IGAWA H, OHURA T. Reconstruction of recurrent pressure sores using free flaps. J Reconstr Microsurg 1992; 8: ) TAVIN E, SERLETTI JM. Case Report: the intercostals vessels as recipients for a free latissimus dorsi flap to a lumbosacral wound. Plastic Surgery Forum 1996; 19: ) ZHU SX, CHANG BX, LU SB. Free transfer of latissimus dorsi myocutaneous flap using wrist vessels as carriers for the treatment of lumbosacral scar contracture deformity. Eur J Plast Surg 1987; 9: ) SALIBIAN AH, TESORO VR, WOOD DL. Staged transfer of a free microvascular latissimus dorsi myocutaneous flap using saphenous vein grafts. Plast Reconstr Surg 1983; 71: ) NAHAI F, HAGERTY R. One-stage microvascular transfer of a latissimus flap to the sacrum using vein grafts. Plast Reconstr Surg 1986; 77: ) FUDEM GM, MARBLE KR. Latissimus dorsi free flap for sacral wound closure: the world's longest vein grafts for free tissue transfer. Microsurgery 1996; 17: ) KHOURI RK. Avoiding free flap failure. Clin Plast Surg 1992; 19: ) SANTANELLI F, RUBINO C, INNOCENZI D, RIBUFFO D, SCUDERI N. Free flap failure in a patient with a long standing, infected, squamous cell carcinoma. Scand J Plast Reconstr Surg Hand Surg 1994; 28: ) CORMACK GC, LAMBERTY BGH. The arterial anatomy of skin flaps. 2 nd ed. Churchill Livingstone, ) MATHES SJ, NAHAI F. Reconstructive Surgery: Principles, Anatomy, and Technique. London: Churchill Livingstone,
The lumbar artery perforator based island flap: anatomical study and case reports
 British Journal of Plastic Surgery (1999), 52, 541 546 1999 The British Association of Plastic Surgeons The lumbar artery perforator based island flap: anatomical study and case reports H. Kato*, M. Hasegawa,
British Journal of Plastic Surgery (1999), 52, 541 546 1999 The British Association of Plastic Surgeons The lumbar artery perforator based island flap: anatomical study and case reports H. Kato*, M. Hasegawa,
Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps
 e50 Case Report THIEME Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps Shuhei Yoshida, MD 1 Isao Koshima, MD 1 Shogo Nagamatsu, MD 2 Kazunori Yokota, MD 2 Shuji Yamashita,
e50 Case Report THIEME Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps Shuhei Yoshida, MD 1 Isao Koshima, MD 1 Shogo Nagamatsu, MD 2 Kazunori Yokota, MD 2 Shuji Yamashita,
The earlier clinic experience of the reverse-flow anterolateral thigh island flap
 British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect of Upper and Middle Third Leg
 Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
A Retrospective Comparison of Perforator and Rotation Flaps for the Closure of Extensive Stage IV Sacral Pressure Ulcers
 A Retrospective Comparison of Perforator and Rotation Flaps for the Closure of Extensive Stage IV Sacral Pressure Ulcers Masaki Fujioka, MD, PhD; Kenji Hayashida, MD; Sin Morooka, MD; and Hiroto Saijo,
A Retrospective Comparison of Perforator and Rotation Flaps for the Closure of Extensive Stage IV Sacral Pressure Ulcers Masaki Fujioka, MD, PhD; Kenji Hayashida, MD; Sin Morooka, MD; and Hiroto Saijo,
JPRAS Open 3 (2015) 1e5. Contents lists available at ScienceDirect. JPRAS Open. journal homepage:
 JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage
 Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
Case Report The Reverse Latissimus Dorsi Flap for Large Lower Lumbar Defect
 Case Reports in Surgery Volume 2012, Article ID 964625, 5 pages doi:10.1155/2012/964625 Case Report The Reverse Latissimus Dorsi Flap for Large Lower Lumbar Defect Bouraoui Kotti, Olfa Jaidane, Jamel Ben
Case Reports in Surgery Volume 2012, Article ID 964625, 5 pages doi:10.1155/2012/964625 Case Report The Reverse Latissimus Dorsi Flap for Large Lower Lumbar Defect Bouraoui Kotti, Olfa Jaidane, Jamel Ben
Inferior Gluteus Maximus Island Flap for Reconstruction of Ischial Pressure Sores
 Original Article Inferior Gluteus Maximus Island Flap for Reconstruction of Ischial Pressure Sores Yawar Sajjad, 1 Beenish Rahat, 2 Salman Hameed 3 Abstract Surgical management of ischial pressure sores
Original Article Inferior Gluteus Maximus Island Flap for Reconstruction of Ischial Pressure Sores Yawar Sajjad, 1 Beenish Rahat, 2 Salman Hameed 3 Abstract Surgical management of ischial pressure sores
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
Chest wall reconstruction using a combined musculocutaneous anterolateral anteromedial thigh flap
 Free full text on www.ijps.org Case Report DOI: 10.4103/0970-0358.63966 Chest wall reconstruction using a combined musculocutaneous anterolateral anteromedial thigh flap Pearlie W. W. Tan, Chin-Ho Wong,
Free full text on www.ijps.org Case Report DOI: 10.4103/0970-0358.63966 Chest wall reconstruction using a combined musculocutaneous anterolateral anteromedial thigh flap Pearlie W. W. Tan, Chin-Ho Wong,
Anatomical study. Clinical study. R. Ogawa, H. Hyakusoku, M. Murakami, R. Aoki, K. Tanuma* and D. G. Pennington?
 British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
The gluteal perforator-based flap in repair of pressure sores
 The British Association of Plastic Surgeons (2004) 57, 342 347 CASE REPORTS The gluteal perforator-based flap in repair of pressure sores Çilingir Meltem*, Çelik Esra, Fındık Hasan, Duman Ali Department
The British Association of Plastic Surgeons (2004) 57, 342 347 CASE REPORTS The gluteal perforator-based flap in repair of pressure sores Çilingir Meltem*, Çelik Esra, Fındık Hasan, Duman Ali Department
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps
 Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Using the sac membrane to close the flap donor site in large meningomyeloceles
 The British Association of Plastic Surgeons (2004) 57, 273 277 Using the sac membrane to close the flap donor site in large meningomyeloceles Cengiz Bozkurt a, Selçuk Akın a, *,Şeref Doğan b, Erkut Özdamar
The British Association of Plastic Surgeons (2004) 57, 273 277 Using the sac membrane to close the flap donor site in large meningomyeloceles Cengiz Bozkurt a, Selçuk Akın a, *,Şeref Doğan b, Erkut Özdamar
Pedicled Gluteal Artery Perforator Flap for Sacral and Ischial Pressure Ulcer Reconstruction: Promising Prospects for Mauritius
 UNIVERSITY OF MAURITIUS RESEARCH JOURNAL Volume 17 2011 University of Mauritius, Réduit, Mauritius Pedicled Gluteal Artery Perforator Flap for Sacral and Ischial Pressure Ulcer Reconstruction: Promising
UNIVERSITY OF MAURITIUS RESEARCH JOURNAL Volume 17 2011 University of Mauritius, Réduit, Mauritius Pedicled Gluteal Artery Perforator Flap for Sacral and Ischial Pressure Ulcer Reconstruction: Promising
Role of free tissue transfer in management of chronic venous ulcer
 Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Interesting Case Series. Scalp Reconstruction With Free Latissimus Dorsi Muscle
 Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
THE pedicled flap, commonly used by the plastic surgeon in the reconstruction
 THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study
 Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study Raphael Sinna, MD, a Hassene Hajji, MD, b Quentin Qassemyar,
Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study Raphael Sinna, MD, a Hassene Hajji, MD, b Quentin Qassemyar,
The gastrocnemius with soleus bi-muscle flap
 The British Association of Plastic Surgeons (2004) 57, 77 82 The gastrocnemius with soleus bi-muscle flap Ikuo Hyodo a, *, Bin Nakayama b, Mitsuru Takahashi c, Kazuhiro Toriyama d, Yuzuru Kamei d, Shuhei
The British Association of Plastic Surgeons (2004) 57, 77 82 The gastrocnemius with soleus bi-muscle flap Ikuo Hyodo a, *, Bin Nakayama b, Mitsuru Takahashi c, Kazuhiro Toriyama d, Yuzuru Kamei d, Shuhei
CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion
 CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion Julien Pauchot, MD, PhD, a Emilie Ducroux, MD, b Grégoire Leclerc, MD, a Laurent Obert,
CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion Julien Pauchot, MD, PhD, a Emilie Ducroux, MD, b Grégoire Leclerc, MD, a Laurent Obert,
J. Bryce Olenczak, MD, Matthew G. Stanwix, MD, and Gedge D. Rosson, MD
 CASE REPORT Complex Wound Closure of Partial Sacrectomy Defect With Human Acellular Dermal Matrix and Bilateral V to Y Gluteal Advancement Flaps in a Pediatric Patient J. Bryce Olenczak, MD, Matthew G.
CASE REPORT Complex Wound Closure of Partial Sacrectomy Defect With Human Acellular Dermal Matrix and Bilateral V to Y Gluteal Advancement Flaps in a Pediatric Patient J. Bryce Olenczak, MD, Matthew G.
Versatility of Reverse Sural Artery Flap for Heel Reconstruction
 ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function
 Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function Vinay Gundlapalli, MD, a John W. Gillespie III, MD, b and Chris D. Tzarnas, MD, FACS c a
Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function Vinay Gundlapalli, MD, a John W. Gillespie III, MD, b and Chris D. Tzarnas, MD, FACS c a
Endoscopic assisted harvest of the pedicled pectoralis major muscle flap
 British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
Medical Journal of the Volume 20 Islamic Republic of Iran Number 3 Fall 1385 November Original Articles
 Medical Journal of the Volume 0 Islamic Republic of Iran Number 3 Fall 38 November 00 Original Articles ANATOMY OF THE SUPERFICIAL INFERIOR EPIGASTRIC ARTERY FLAP MAHDI FATHI, M.D., EBRAHIM HATAMIPOUR,
Medical Journal of the Volume 0 Islamic Republic of Iran Number 3 Fall 38 November 00 Original Articles ANATOMY OF THE SUPERFICIAL INFERIOR EPIGASTRIC ARTERY FLAP MAHDI FATHI, M.D., EBRAHIM HATAMIPOUR,
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts
 Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Large thoracolumbar meningomyelocele defects: incidence and clinical experiences with different modalities of latissimus dorsi musculocutaneus flap
 The British Association of Plastic Surgeons (2004) 57, 411 417 Large thoracolumbar meningomyelocele defects: incidence and clinical experiences with different modalities of latissimus dorsi musculocutaneus
The British Association of Plastic Surgeons (2004) 57, 411 417 Large thoracolumbar meningomyelocele defects: incidence and clinical experiences with different modalities of latissimus dorsi musculocutaneus
Clinical Study Combined V-Y Fasciocutaneous Advancement and Gluteus Maximus Muscle Rotational Flaps for Treating Sacral Sores
 BioMed Research International Volume 2016, Article ID 8714713, 8 pages http://dx.doi.org/10.1155/2016/8714713 Clinical Study Combined V-Y Fasciocutaneous Advancement and Gluteus Maximus Muscle Rotational
BioMed Research International Volume 2016, Article ID 8714713, 8 pages http://dx.doi.org/10.1155/2016/8714713 Clinical Study Combined V-Y Fasciocutaneous Advancement and Gluteus Maximus Muscle Rotational
Formation of reconstruction protocol for sacral pressure sore defects
 International Journal of Medical and Health Research ISSN: 2454-9142 Impact Factor: RJIF 5.54 www.medicalsciencejournal.com Volume 4; Issue 8; August 2018; Page No. 18-24 Formation of reconstruction protocol
International Journal of Medical and Health Research ISSN: 2454-9142 Impact Factor: RJIF 5.54 www.medicalsciencejournal.com Volume 4; Issue 8; August 2018; Page No. 18-24 Formation of reconstruction protocol
Anatomical relationship between arteries and veins in the paraumbilical region q
 The British Association of Plastic Surgeons (2003) 56, 552 556 Anatomical relationship between arteries and veins in the paraumbilical region q N. Imanishi a, *, H. Nakajima b, T. Minabe c, H. Chang d,
The British Association of Plastic Surgeons (2003) 56, 552 556 Anatomical relationship between arteries and veins in the paraumbilical region q N. Imanishi a, *, H. Nakajima b, T. Minabe c, H. Chang d,
Reconstruction of the Chest Wall
 HOW TO DO IT Reconstruction of the Chest Wall Reed 0. Dingman, M.D., and Louis C. Argenta, M.D. ABSTRACT Reconstruction of the chest wall can now be accomplished reliably and expeditiously. Past experience
HOW TO DO IT Reconstruction of the Chest Wall Reed 0. Dingman, M.D., and Louis C. Argenta, M.D. ABSTRACT Reconstruction of the chest wall can now be accomplished reliably and expeditiously. Past experience
CHAPTER 16 LOWER EXTREMITY. Amanda K Silva, MD and Warren Ellsworth, MD, FACS
 CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC
 Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Kuwabara, Kaoru; Nonaka, Takashi; H. Citation Journal of Clinical Urology, 7(5),
 NAOSITE: Nagasaki University's Ac Title Author(s) Gluteal-fold adipofascial perforato fistula reconstruction Fujioka, Masaki; Hayashida, Kenji; Kuwabara, Kaoru; Nonaka, Takashi; H Citation Journal of Clinical
NAOSITE: Nagasaki University's Ac Title Author(s) Gluteal-fold adipofascial perforato fistula reconstruction Fujioka, Masaki; Hayashida, Kenji; Kuwabara, Kaoru; Nonaka, Takashi; H Citation Journal of Clinical
CASE REPORT Reconstruction and Characterization of Composite Mandibular Defects Requiring Double Skin Paddle Fibular Free Flaps
 CASE REPORT Reconstruction and Characterization of Composite Mandibular Defects Requiring Double Skin Paddle Fibular Free Flaps Austin M. Badeau, BA, a and Frederic W.-B. Deleyiannis, MD, MPhil, MPH b
CASE REPORT Reconstruction and Characterization of Composite Mandibular Defects Requiring Double Skin Paddle Fibular Free Flaps Austin M. Badeau, BA, a and Frederic W.-B. Deleyiannis, MD, MPhil, MPH b
The free thoracodorsal artery perforator flap in head and neck reconstruction
 European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 167 171 Available online at www.sciencedirect.com TECHNICAL NOTE The free thoracodorsal artery perforator flap in head and neck
European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 167 171 Available online at www.sciencedirect.com TECHNICAL NOTE The free thoracodorsal artery perforator flap in head and neck
Closure of Myelomeningocele Defects Using a Limberg Flap or Direct Repair
 Closure of Myelomeningocele Defects Using a Limberg Flap or Direct Repair Original Article Jung-Hwan Shim 1, Na-Hyun Hwang 1, Eul-Sik Yoon 1, Eun-Sang Dhong 1, Deok-Woo Kim 1, Sang-Dae Kim 2 Departments
Closure of Myelomeningocele Defects Using a Limberg Flap or Direct Repair Original Article Jung-Hwan Shim 1, Na-Hyun Hwang 1, Eul-Sik Yoon 1, Eun-Sang Dhong 1, Deok-Woo Kim 1, Sang-Dae Kim 2 Departments
Clinical teaching/experi ence. Lectures/semina rs/conferences Self-directed. learning. Clinical teaching/experi ence
 Regional Medical Center (The MED) Plastic Surgery PGY-3 By the end of the Plastic Surgery at the MED, the PGY-3 residents are expected to expand and cultivate knowledge and skills developed during previous
Regional Medical Center (The MED) Plastic Surgery PGY-3 By the end of the Plastic Surgery at the MED, the PGY-3 residents are expected to expand and cultivate knowledge and skills developed during previous
Gastrocnemius Muscle Flap Coverage of Chronically= Infected Knee Joints
 Gastrocnemius Muscle Flap Coverage of Chronically= Infected Knee Joints ABSTRACT Chronically infected open knee joints present dif cult problem. Aggressive debridement of chronically infected soft tissue
Gastrocnemius Muscle Flap Coverage of Chronically= Infected Knee Joints ABSTRACT Chronically infected open knee joints present dif cult problem. Aggressive debridement of chronically infected soft tissue
A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction
 A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction In-Soo Baek 1, Jae-Pil You 1, Sung-Mi Rhee 1, Gil-Su Son 2, Deok-Woo Kim 1, Eun-Sang Dhong 1, Seung-Ha
A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction In-Soo Baek 1, Jae-Pil You 1, Sung-Mi Rhee 1, Gil-Su Son 2, Deok-Woo Kim 1, Eun-Sang Dhong 1, Seung-Ha
Progressive Tension Sutures to Prevent Seroma Formation after Latissimus Dorsi Harvest
 Progressive Tension Sutures to Prevent Seroma Formation after Latissimus Dorsi Harvest Jose L. Rios, M.D., Todd Pollock, M.D., and William P. Adams, Jr., M.D. Dallas, Texas The latissimus dorsi muscle
Progressive Tension Sutures to Prevent Seroma Formation after Latissimus Dorsi Harvest Jose L. Rios, M.D., Todd Pollock, M.D., and William P. Adams, Jr., M.D. Dallas, Texas The latissimus dorsi muscle
Interesting Case Series. Reconstruction of Dorsal Wrist Defects
 Interesting Case Series Reconstruction of Dorsal Wrist Defects Maelee Yang, BS, and Joseph Meyerson, MD The Ohio State University Wexner Medical Center, Columbus Correspondence: maelee.yang@osumc.edu Keywords:
Interesting Case Series Reconstruction of Dorsal Wrist Defects Maelee Yang, BS, and Joseph Meyerson, MD The Ohio State University Wexner Medical Center, Columbus Correspondence: maelee.yang@osumc.edu Keywords:
Heel Defect Reconstruction using Local Vascularized Flaps: Results and Clinical Outcomes in 16 Patients
 JFS (P) Kuldeep Singh et al ORIGINL RTICLE 10.5005/jp-journals-10040-1083 Heel Defect Reconstruction using Local Vascularized Flaps: Results and Clinical Outcomes in 16 Patients 1 Kuldeep Singh, 2 Zile
JFS (P) Kuldeep Singh et al ORIGINL RTICLE 10.5005/jp-journals-10040-1083 Heel Defect Reconstruction using Local Vascularized Flaps: Results and Clinical Outcomes in 16 Patients 1 Kuldeep Singh, 2 Zile
ABSTRACT. Key words: Flaps, Adipofascial, Lower limb reconstruction. Khaldoun J. Haddadin, MD*, Samer Y. Haddad, MD. Introduction.
 DISTALLY BASED ADIPOFASCIAL FLAPS: A VERSATILE FLAP FOR THE RECONSTRUCTION OF LOWER LEG AND PROXIMAL FOOT DEFECTS AT THE ROYAL JORDANIAN REHABILITATION CENTER Khaldoun J. Haddadin, MD*, Samer Y. Haddad,
DISTALLY BASED ADIPOFASCIAL FLAPS: A VERSATILE FLAP FOR THE RECONSTRUCTION OF LOWER LEG AND PROXIMAL FOOT DEFECTS AT THE ROYAL JORDANIAN REHABILITATION CENTER Khaldoun J. Haddadin, MD*, Samer Y. Haddad,
Reconstruction of axillary scar contractures retrospective study of 124 cases over 25 years
 British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
INTRODUCTION. Jong Gyu Kim, Soo Hyang Lee. Original Article
 Comparison of the Multidetector-row Computed Tomographic ngiography xial and Coronal Planes Usefulness for Detecting Thoracodorsal rtery Perforators Original rticle Jong Gyu Kim, Soo Hyang Lee Department
Comparison of the Multidetector-row Computed Tomographic ngiography xial and Coronal Planes Usefulness for Detecting Thoracodorsal rtery Perforators Original rticle Jong Gyu Kim, Soo Hyang Lee Department
Sliding Perforator Island Flap For Covering A Big Lumbosacral Defect
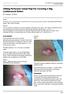 ISPUB.COM The Internet Journal of Plastic Surgery Volume 5 Number 2 Sliding Perforator Island Flap For Covering A Big Lumbosacral Defect R Hussein, S Anis Citation R Hussein, S Anis.. The Internet Journal
ISPUB.COM The Internet Journal of Plastic Surgery Volume 5 Number 2 Sliding Perforator Island Flap For Covering A Big Lumbosacral Defect R Hussein, S Anis Citation R Hussein, S Anis.. The Internet Journal
The progress in microsurgical procedures has led
 Original Article Breast reconstruction with free anterolateral thigh flap Ranjit Raje, Ramesh Chepauk, Kanti Shetty, Rajendra Prasad J. S. Plastic & Reconstructive Services, Department of Surgical Oncology,
Original Article Breast reconstruction with free anterolateral thigh flap Ranjit Raje, Ramesh Chepauk, Kanti Shetty, Rajendra Prasad J. S. Plastic & Reconstructive Services, Department of Surgical Oncology,
Mentosternal Contracture Treated With an Occipito-Scapular Flap in a 5-year-old Boy: A Case Report
 Mentosternal Contracture Treated With an Occipito-Scapular Flap in a 5-year-old Boy: A Case Report Armin Kraus, MD, Hans-Eberhard Schaller, MD, and Hans-Oliver Rennekampff, MD Department for Hand, Plastic,
Mentosternal Contracture Treated With an Occipito-Scapular Flap in a 5-year-old Boy: A Case Report Armin Kraus, MD, Hans-Eberhard Schaller, MD, and Hans-Oliver Rennekampff, MD Department for Hand, Plastic,
T. Rapis, S.N. Zanakis, I.F. Letsa, A.P. Karamanos CLINICAL CASE. Summary. Introduction
 Journal of BUON 8: 397-401, 2003 2003 Zerbinis Medical Publications. Printed in Greece CLINICAL CASE Basal cell carcinoma of the posterior neck, reconstructed with lower trapezius island musculocutaneous
Journal of BUON 8: 397-401, 2003 2003 Zerbinis Medical Publications. Printed in Greece CLINICAL CASE Basal cell carcinoma of the posterior neck, reconstructed with lower trapezius island musculocutaneous
Breast Reconstruction Options
 Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
Abdominal Wall Reconstruction With the Free Tensor Fascia Lata Musculofasciocutaneous Flap Using Intraperitoneal Gastroepiploic Recipient Vessels
 Abdominal Wall Reconstruction With the Free Tensor Fascia Lata Musculofasciocutaneous Flap Using Intraperitoneal Gastroepiploic Recipient Vessels Pierre M. Chevray, MD, PhD* Navin K. Singh, MD The authors
Abdominal Wall Reconstruction With the Free Tensor Fascia Lata Musculofasciocutaneous Flap Using Intraperitoneal Gastroepiploic Recipient Vessels Pierre M. Chevray, MD, PhD* Navin K. Singh, MD The authors
Large full-thickness nasal tip defects after Mohs
 RECONSTRUCTIVE CONUNDRUM Repair of a Large, Exposed-Cartilage Nasal Tip Defect Using Nasalis-Based Subcutaneous Pedicle Flaps and Full-Thickness Skin Grafting DIEGO E. MARRA, MD, EDGAR F. FINCHER, MD,
RECONSTRUCTIVE CONUNDRUM Repair of a Large, Exposed-Cartilage Nasal Tip Defect Using Nasalis-Based Subcutaneous Pedicle Flaps and Full-Thickness Skin Grafting DIEGO E. MARRA, MD, EDGAR F. FINCHER, MD,
Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects
 Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects Joshua L. Levine, M.D., Nassif E. Soueid, M.D., and Robert J. Allen, M.D. New Orleans, La. Background: The use of lateral thoracic
Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects Joshua L. Levine, M.D., Nassif E. Soueid, M.D., and Robert J. Allen, M.D. New Orleans, La. Background: The use of lateral thoracic
Interesting Case Series. Omental Flap for Thoracic Aortic Graft Infection
 Interesting Case Series Omental Flap for Thoracic Aortic Graft Infection Andrew A. Marano, BA, Adam M. Feintisch, MD, and Mark S. Granick, MD Division of Plastic Surgery, Department of Surgery, Rutgers
Interesting Case Series Omental Flap for Thoracic Aortic Graft Infection Andrew A. Marano, BA, Adam M. Feintisch, MD, and Mark S. Granick, MD Division of Plastic Surgery, Department of Surgery, Rutgers
The superior gluteal artery perforator flap: an additional tool in the treatment of sacral pressure sores
 ritish Journal of Plastic Surgery (1999), 52, 385 391 1999 The ritish ssociation of Plastic Surgeons The superior gluteal artery perforator flap: an additional tool in the treatment of sacral pressure
ritish Journal of Plastic Surgery (1999), 52, 385 391 1999 The ritish ssociation of Plastic Surgeons The superior gluteal artery perforator flap: an additional tool in the treatment of sacral pressure
The most common type of breast reconstruction
 BREAST Breast Reconstruction with Perforator Flaps Jay W. Granzow, M.D., M.P.H. Joshua L. Levine, M.D. Ernest S. Chiu, M.D. Maria M. LoTempio, M.D. Robert J. Allen, M.D. New Orleans, La.; Charleston, S.C.;
BREAST Breast Reconstruction with Perforator Flaps Jay W. Granzow, M.D., M.P.H. Joshua L. Levine, M.D. Ernest S. Chiu, M.D. Maria M. LoTempio, M.D. Robert J. Allen, M.D. New Orleans, La.; Charleston, S.C.;
4/30/2010. Options for abdominal wall reconstruction. Scott L. Hansen, MD
 Components Separation Scott L. Hansen, MD University of California, San Francisco Chief, Plastic and Reconstructive Surgery San Francisco General Hospital Overview Options for abdominal wall reconstruction
Components Separation Scott L. Hansen, MD University of California, San Francisco Chief, Plastic and Reconstructive Surgery San Francisco General Hospital Overview Options for abdominal wall reconstruction
1 62, M Biopsy Paget s disease 8/5/92 Perianal skin, None, NED anal canal,
 British Journal of Plastic Surgery (1999), 52, 471 475 1999 The British Association of Plastic Surgeons Reconstruction of perianal skin defect using a V Y advancement of bilateral gluteus maximus musculocutaneous
British Journal of Plastic Surgery (1999), 52, 471 475 1999 The British Association of Plastic Surgeons Reconstruction of perianal skin defect using a V Y advancement of bilateral gluteus maximus musculocutaneous
Flaps vs Grafts. Ronen Avram, MD MSc FRCSC
 Flaps vs Grafts Ronen Avram, MD MSc FRCSC POS Keratoacanthoma is not a malignant tumor! Methods of Reconstruction Reconstructive Ladder Primary closure Primary Delayed Secondary Intention Skin Graft Pedicled
Flaps vs Grafts Ronen Avram, MD MSc FRCSC POS Keratoacanthoma is not a malignant tumor! Methods of Reconstruction Reconstructive Ladder Primary closure Primary Delayed Secondary Intention Skin Graft Pedicled
INTRODUCTION. Toshihiko Satake 1, Jun Sugawara 2, Kazunori Yasumura 1, Taro Mikami 2, Shinji Kobayashi 3, Jiro Maegawa 2. Idea and Innovation
 Mini-Flow-Through Deep Inferior Epigastric Perforator Flap for Breast Reconstruction with Preservation of Both Internal Mammary and Deep Inferior Epigastric Vessels Toshihiko Satake 1, Jun Sugawara 2,
Mini-Flow-Through Deep Inferior Epigastric Perforator Flap for Breast Reconstruction with Preservation of Both Internal Mammary and Deep Inferior Epigastric Vessels Toshihiko Satake 1, Jun Sugawara 2,
A Review of 105 Subscapular-Based Flaps Harvested Using a New Dorsal Decubitus Position: How Far Can We Go?
 A Review of 105 Subscapular-Based Flaps Harvested Using a New Dorsal Decubitus Position: How Far Can We Go? Laurence S. Paek, MD, a Olivier Boa, MD, a Marc Revol, MD, b Jean-Marie Servant, MD, b Patrick
A Review of 105 Subscapular-Based Flaps Harvested Using a New Dorsal Decubitus Position: How Far Can We Go? Laurence S. Paek, MD, a Olivier Boa, MD, a Marc Revol, MD, b Jean-Marie Servant, MD, b Patrick
Stomal recurrence after total laryngectomy is 1
 CASE REPORT Eben L. Rosenthal, MD, Section Editor ANTEROLATERAL THIGH FREE FLAP FOR TRACHEAL RECONSTRUCTION AFTER PARASTOMAL RECURRENCE Umberto Caliceti, MD, 1 Ottavio Piccin, MD, 1 Ottavio Cavicchi, MD,
CASE REPORT Eben L. Rosenthal, MD, Section Editor ANTEROLATERAL THIGH FREE FLAP FOR TRACHEAL RECONSTRUCTION AFTER PARASTOMAL RECURRENCE Umberto Caliceti, MD, 1 Ottavio Piccin, MD, 1 Ottavio Cavicchi, MD,
Plastic surgery of the breast includes; augmentation, reduction, Plastic Surgery of the Breast. Abstract. Continuing Education Column
 Plastic Surgery of the Breast Keuk Shun Shin, M.D. Keuk SHUN SHIN s Asthetic Plastic Surgery E mail: drsks@drsks.co.kr Abstract Plastic surgery of the breast includes; augmentation, reduction, reconstruction
Plastic Surgery of the Breast Keuk Shun Shin, M.D. Keuk SHUN SHIN s Asthetic Plastic Surgery E mail: drsks@drsks.co.kr Abstract Plastic surgery of the breast includes; augmentation, reduction, reconstruction
Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps
 BREAST SURGERY Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps Joshua L. Levine, MD,* Quintessa Miller, MD, Julie Vasile, MD,* Kamran Khoobehi,
BREAST SURGERY Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps Joshua L. Levine, MD,* Quintessa Miller, MD, Julie Vasile, MD,* Kamran Khoobehi,
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study
 Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
The Use of Perforator-Plus Fasciocutaneous Flaps For Sacral Pressure Ulcer Reconstruction
 Open Journal of Clinical & Medical Case Reports Volume 1 (2015) Issue 2 The Use of Perforator-Plus Fasciocutaneous Flaps For Sacral Pressure Ulcer Reconstruction Jon P VerHalen, MD FACS Adjunct Clinical
Open Journal of Clinical & Medical Case Reports Volume 1 (2015) Issue 2 The Use of Perforator-Plus Fasciocutaneous Flaps For Sacral Pressure Ulcer Reconstruction Jon P VerHalen, MD FACS Adjunct Clinical
A multiple logistic regression analysis of complications following microsurgical breast reconstruction
 Original Article A multiple logistic regression analysis of complications following microsurgical breast reconstruction Samir Rao 1, Ellen C. Stolle 1, Sarah Sher 1, Chun-Wang Lin 1, Bahram Momen 2, Maurice
Original Article A multiple logistic regression analysis of complications following microsurgical breast reconstruction Samir Rao 1, Ellen C. Stolle 1, Sarah Sher 1, Chun-Wang Lin 1, Bahram Momen 2, Maurice
J Wound Management Res 2018 September;14(2):
 J Wound Management Res 2018 September;14(2):132-136 pissn 2586-0402 eissn 2586-0410 Journal of Wound Management and Research Functional and Aesthetic Reconstruction of Shoulder Using Pedicled LD Flap after
J Wound Management Res 2018 September;14(2):132-136 pissn 2586-0402 eissn 2586-0410 Journal of Wound Management and Research Functional and Aesthetic Reconstruction of Shoulder Using Pedicled LD Flap after
Interesting Case Series. Traumatic Thumb Amputation: Case and Review
 Interesting Case Series Traumatic Thumb Amputation: Case and Review Ryan Engdahl, MD, a and Norman Morrison, MD b a Division of Plastic Surgery, New York Presbyterian Hospital, The University Hospital
Interesting Case Series Traumatic Thumb Amputation: Case and Review Ryan Engdahl, MD, a and Norman Morrison, MD b a Division of Plastic Surgery, New York Presbyterian Hospital, The University Hospital
Modern Management of the Open Abdomen A Cautionary Tale. Grand Rounds December 16, 2010 SUNY, Downstate
 Modern Management of the Open Abdomen A Cautionary Tale Grand Rounds December 16, 2010 SUNY, Downstate Case HPI: 41 yo M BIBA; stabbed in left back while walking out of a shopping center. PMH/PSH: GSW
Modern Management of the Open Abdomen A Cautionary Tale Grand Rounds December 16, 2010 SUNY, Downstate Case HPI: 41 yo M BIBA; stabbed in left back while walking out of a shopping center. PMH/PSH: GSW
Masaki Fujioka 1*, Kenji Hayashida 1, Sin Morooka 1, Hiroto Saijo 1 and Takashi Nonaka 2 WORLD JOURNAL OF SURGICAL ONCOLOGY
 Fujioka et al. World Journal of Surgical Oncology 2014, 12:319 WORLD JOURNAL OF SURGICAL ONCOLOGY CASE REPORT Open Access Combined serratus anterior and latissimus dorsi myocutaneous flap for obliteration
Fujioka et al. World Journal of Surgical Oncology 2014, 12:319 WORLD JOURNAL OF SURGICAL ONCOLOGY CASE REPORT Open Access Combined serratus anterior and latissimus dorsi myocutaneous flap for obliteration
Combined tongue flap and V Y advancement flap for lower lip defects
 British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps
 Original Article Breast Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps James L. Mayo, MD Robert J. Allen, MD, FACS Alireza Sadeghi, MD, FACS Background: In cases of bilateral breast
Original Article Breast Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps James L. Mayo, MD Robert J. Allen, MD, FACS Alireza Sadeghi, MD, FACS Background: In cases of bilateral breast
MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION. Adequate speech and swallowing are dependent
 ORIGINAL ARTICLE MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION Shao-Liang Chen, MD, 1 Tim-Mo Chen, MD, 1 Niann-Tzyy Dai, MD, 1 Yi-Jan Hsia, DDS, MDSC, 2 Yaoh-Shiang Lin,
ORIGINAL ARTICLE MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION Shao-Liang Chen, MD, 1 Tim-Mo Chen, MD, 1 Niann-Tzyy Dai, MD, 1 Yi-Jan Hsia, DDS, MDSC, 2 Yaoh-Shiang Lin,
Nanogen Aktiv. Naz Wahab MD, FAAFP, FAPWCA Nexderma
 Nanogen Aktiv Naz Wahab MD, FAAFP, FAPWCA Nexderma Patient BM 75 y.o female with a history of Type 2 Diabetes, HTN, Hypercholesterolemia, Renal insufficiency, Chronic back Pain, who had undergone a L3-L4
Nanogen Aktiv Naz Wahab MD, FAAFP, FAPWCA Nexderma Patient BM 75 y.o female with a history of Type 2 Diabetes, HTN, Hypercholesterolemia, Renal insufficiency, Chronic back Pain, who had undergone a L3-L4
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
Andreas Arkudas¹, Susanne Regus², Alexander Meyer², Werner Lang², Marweh Schmitz¹, Raymund E. Horch¹
 Arkudas et al. Plast Aesthet Res 2018;5:38 DOI: 10.20517/2347-9264.2018.44 Plastic and Aesthetic Research Case Report Open Access Defect reconstruction of the trochanter major after necrotizing fasciitis
Arkudas et al. Plast Aesthet Res 2018;5:38 DOI: 10.20517/2347-9264.2018.44 Plastic and Aesthetic Research Case Report Open Access Defect reconstruction of the trochanter major after necrotizing fasciitis
Distally based anterolateral thigh flap pedicled on the oblique branch of the lateral circumflex femoral artery
 Original Article Page 1 of 8 Distally based anterolateral thigh flap pedicled on the oblique branch of the lateral circumflex femoral artery Yuanbo Liu, Mengqing Zang, Shan Zhu, Bo Chen, Shanshan Li, Bingjian
Original Article Page 1 of 8 Distally based anterolateral thigh flap pedicled on the oblique branch of the lateral circumflex femoral artery Yuanbo Liu, Mengqing Zang, Shan Zhu, Bo Chen, Shanshan Li, Bingjian
Learning Objectives. Head and Neck Cancer: Post-Treatment Changes. Neck Dissection Classification * Radical neck dissection. Radical Neck Dissection
 Head and Neck Cancer: Post-Treatment Changes Daniel W. Williams III, MD Learning Objectives In patients treated for H/N Cancer: Describe the various types of neck dissections Explain reconstruction techniques
Head and Neck Cancer: Post-Treatment Changes Daniel W. Williams III, MD Learning Objectives In patients treated for H/N Cancer: Describe the various types of neck dissections Explain reconstruction techniques
SCOPE OF PRACTICE PGY-6 PGY-7 PGY-8
 PGY-6 Round on all plastic surgery inpatients every day. Assess progress of patients and identify real or potential problems. Review patients progress with attending physicians daily and participate in
PGY-6 Round on all plastic surgery inpatients every day. Assess progress of patients and identify real or potential problems. Review patients progress with attending physicians daily and participate in
PUT YOUR BEST FOOT FORWARD
 PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases
 J Oral Maxillofac Surg 58:1104-1108, 2000 Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases Yadranko Ducic, MD, FRCS (C),* and Mark Burye, DDS Purpose: This article describes
J Oral Maxillofac Surg 58:1104-1108, 2000 Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases Yadranko Ducic, MD, FRCS (C),* and Mark Burye, DDS Purpose: This article describes
Lower gluteal muscle flap and buttock fascio-cutaneous rotation flap for reconstruction of perineal defects after abdomino-perineal resections
 PRAS3334_proof 31 July 2012 1/6 Journal of Plastic, Reconstructive & Aesthetic Surgery (2012) xx, 1e6 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36
PRAS3334_proof 31 July 2012 1/6 Journal of Plastic, Reconstructive & Aesthetic Surgery (2012) xx, 1e6 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36
W Kuhn MD,l N J Luscher MD,2 R de Roche MD,2 S Krupp MD,3 G A Zach4
 Paraplegia 30 (1992) 396-400 1992 International Medical Society of Paraplegia The neurosensory musculocutaneous tensor fasciae latae flap: long term results W Kuhn MD,l N J Luscher MD,2 R de Roche MD,2
Paraplegia 30 (1992) 396-400 1992 International Medical Society of Paraplegia The neurosensory musculocutaneous tensor fasciae latae flap: long term results W Kuhn MD,l N J Luscher MD,2 R de Roche MD,2
Extended double pedicle free tensor
 e141 Case Report Extended double pedicle free tensor fascia latae myocutaneous flap for abdominal wall reconstruction Dorai A A, Halim A S ABSTRACT Extensive full thickness anterior abdominal wall defects
e141 Case Report Extended double pedicle free tensor fascia latae myocutaneous flap for abdominal wall reconstruction Dorai A A, Halim A S ABSTRACT Extensive full thickness anterior abdominal wall defects
ORIGINAL ARTICLE DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS
 DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS Peddi Manjunath 1, Ramesha K.T 2, Smitha S Segu 3, Jainath 4, Shankarappa M 5 HOW TO CITE THIS ARTICLE: Peddi Manjunath, Ramesha KT, Smitha
DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS Peddi Manjunath 1, Ramesha K.T 2, Smitha S Segu 3, Jainath 4, Shankarappa M 5 HOW TO CITE THIS ARTICLE: Peddi Manjunath, Ramesha KT, Smitha
PARADIGM SPINE. Minimally Invasive Lumbar Fusion. Interlaminar Stabilization
 PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications
 Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications Wan Loong James Mok 1, Yong Chen Por 1, Bien Keem Tan 2 1 Department of Plastic, Reconstructive
Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications Wan Loong James Mok 1, Yong Chen Por 1, Bien Keem Tan 2 1 Department of Plastic, Reconstructive
Hyperbaric oxygen therapy and surgical delay improve flap survival of reverse pedicle flaps for lower third leg and foot reconstruction
 Original Article Plastic and Aesthetic Research Hyperbaric oxygen therapy and surgical delay improve flap survival of reverse pedicle flaps for lower third leg and foot reconstruction Pradeoth Mukundan
Original Article Plastic and Aesthetic Research Hyperbaric oxygen therapy and surgical delay improve flap survival of reverse pedicle flaps for lower third leg and foot reconstruction Pradeoth Mukundan
Breast Restoration Surgery After a mastectomy
 UW MEDICINE PATIENT EDUCATION Breast Restoration Surgery After a mastectomy This handout explains the most common procedures that are used at University of Washington Medical Center (UWMC) to restore a
UW MEDICINE PATIENT EDUCATION Breast Restoration Surgery After a mastectomy This handout explains the most common procedures that are used at University of Washington Medical Center (UWMC) to restore a
Primary closure of the deltopectoral flap-donor site without skin grafting
 Primary closure of the deltopectoral flap-donor site without skin grafting Received: 4/3/2013 Accepted: 14/5/2013 Introduction Reliable and simultaneous reconstruction of head-and-neck defects has been
Primary closure of the deltopectoral flap-donor site without skin grafting Received: 4/3/2013 Accepted: 14/5/2013 Introduction Reliable and simultaneous reconstruction of head-and-neck defects has been
Basics of Flap Design
 Basics of Flap Design Reconstructive Ladder (Mathes & Nahai 1982) Consider the defect, systematically Move from simple to complex Occam s Razor Sutton s Law Ladder is simple, emphasizes closure over form
Basics of Flap Design Reconstructive Ladder (Mathes & Nahai 1982) Consider the defect, systematically Move from simple to complex Occam s Razor Sutton s Law Ladder is simple, emphasizes closure over form
Soft tissue reconstruction with the superior gluteal artery perforator f lap
 Clin Plastic Surg 30 (2003) 371 382 Soft tissue reconstruction with the superior gluteal artery perforator f lap Phillip N. Blondeel, MD, PhD*, Koenraad Van Landuyt, MD, Moustapha Hamdi, MD, Stan J. Monstrey,
Clin Plastic Surg 30 (2003) 371 382 Soft tissue reconstruction with the superior gluteal artery perforator f lap Phillip N. Blondeel, MD, PhD*, Koenraad Van Landuyt, MD, Moustapha Hamdi, MD, Stan J. Monstrey,
Septic Bone and Joint Surgery
 Septic Bone and Joint Surgery Bearbeitet von Reinhard Schnettler 1. Auflage 2010. Buch. 328 S. Hardcover ISBN 978 3 13 149031 5 Format (B x L): 19,5 x 27 cm Weitere Fachgebiete > Medizin > Chirurgie >
Septic Bone and Joint Surgery Bearbeitet von Reinhard Schnettler 1. Auflage 2010. Buch. 328 S. Hardcover ISBN 978 3 13 149031 5 Format (B x L): 19,5 x 27 cm Weitere Fachgebiete > Medizin > Chirurgie >
The fibula osteoseptocutaneous flap with a RECONSTRUCTIVE
 RECONSTRUCTIVE Use of the Soleus Musculocutaneous Perforator for Skin Paddle Salvage of the Fibula Osteoseptocutaneous Flap: Anatomical Study and Clinical Confirmation Chin-Ho Wong, M.R.C.S. Bien-Keem
RECONSTRUCTIVE Use of the Soleus Musculocutaneous Perforator for Skin Paddle Salvage of the Fibula Osteoseptocutaneous Flap: Anatomical Study and Clinical Confirmation Chin-Ho Wong, M.R.C.S. Bien-Keem
Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap.
 Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
BUILDING A. Achieving total reconstruction in a single operation. 70 OCTOBER 2016 // dentaltown.com
 BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
