R. Todd Allen, M.D., Ph.D., James P. Tasto, M.D., Jeffrey Cummings, M.D., Catherine M. Robertson, M.D., and David Amiel, Ph.D.
|
|
|
- Barrie Ellis
- 5 years ago
- Views:
Transcription
1 Meniscal Debridement With an Arthroscopic Radiofrequency Wand Versus an Arthroscopic Shaver: Comparative Effects on Menisci and Underlying Articular Cartilage R. Todd Allen, M.D., Ph.D., James P. Tasto, M.D., Jeffrey Cummings, M.D., Catherine M. Robertson, M.D., and David Amiel, Ph.D. Purpose: Meniscal debridement with an arthroscopic radiofrequency (RF) wand versus an arthroscopic shaver and their comparative effects on menisci and underlying articular cartilage were studied. Methods: When repair is not feasible, degenerative or post-traumatic meniscal tears often need debridement. Six fresh bovine knees were harvested, the tibial plateau was dissected free from the femoral articulation and placed in a saline bath at 28 C, with 10% to 15% of the posterior horn of menisci debrided arthroscopically, and the surfaces debrided using a basket punch plus shaver, punch plus RF wand, RF wand alone, and untreated control. Treatment time of each case was 24 seconds at wand power 7. We characterized an injury zone, as well as viability and metabolic activity of meniscal cells and tibial articular cartilage chondrocytes. Results: Chondrocyte viability of the tibial articular surface was 96% to 98%. We saw no differences in viability or injury zone (0 to 150 m) among debrided groups or versus the control for any experimental surface, with no significant difference in metabolic activity in menisci debrided surfaces versus control. Meniscal viability was variable with analyses showing substantial levels (150 to 500 m) of cell death in debrided and control groups. Metabolic activity in treated meniscus was lower than in cartilage specimens. No significant differences were observed among treatment groups versus control. Conclusions: Focal areas of chondrocyte cell death were not seen. Meniscal samples showed cell death (150 to 500 m) throughout the tissue. Clinical Relevance: Debridement of menisci with a bipolar RF wand produces levels of cell injury and death similar to those of debridement with a basket punch mechanical shaver. The RF wand did not harm underlying articular surfaces and produced a precise cut to the meniscal surface. Key Words: Meniscal debridement Radiofrequency wand Arthroscopic shaver Meniscal tear. Although the meniscus is critically important for knee motion, load distribution, and articular congruency, degenerative or post-traumatic tears often From the Department of Orthopaedic Surgery, University of California San Diego (R.T.A., J.P.T., C.M.R., D.A.), La Jolla; and the San Diego Arthroscopy and Sports Medicine Fellowship (J.P.T., J.C.), San Diego, California, U.S.A. Supported by National Institutes of Health Training Grant No. AR07484 and by ArthroCare Corp, Sunnyvale, California. Presented at the Annual Meeting of the Arthroscopy Association of North America, Orlando, Florida, April Address correspondence and reprint requests to David Amiel, Ph.D., Department of Orthopaedic Surgery, University of California San Diego, 9500 Gilman Dr, Dept 0630, San Diego, CA , U.S.A. fshepherd@ucsd.edu; damiel@ucsd.edu 2006 by the Arthroscopy Association of North America /06/ $32.00/0 doi: /j.arthro necessitate debridement or repair. When repair is not feasible, careful debridement, often with an arthroscopic punch and/or shaver, becomes a treatment mainstay. In the majority of cases, significant pain relief can be accomplished. A subset of patients, however, do not respond as well, their pain being either minimally changed or relieved for only a short period of time. Many reasons may account for these less favorable outcomes, but one possibility is that the meniscal debridement itself could have been suboptimal. Limitations to an optimal meniscal debridement can include the arthroscopic instrumentation, the body s repair response or lack of response to partial meniscectomy, the precise amount and location of meniscus debrided to adequately relieve symptoms, patient compliance, and the operative technique. Ample resection without appropriate healing could lead to Arthroscopy: The Journal of Arthroscopic and Related Surgery, Vol 22, No 4 (April), 2006: pp
2 386 R. T. ALLEN ET AL. subsequent meniscus failure, reinjury, and/or articular cartilage damage and early degeneration. To circumvent some of these possibilities, advances in instrumentation and debridement modalities have been explored. One such advance is the introduction of electrosurgical arthroscopy, which has spawned studies on its use for meniscal and cartilage debridement. 1-3 Published reports of electrosurgical devices in arthroscopy began in 1979 for their use in knee synovectomy, 1 with most of the studies using monopolar radiofrequency (RF) energy instruments. Bovie-type monopolar devices dissipate energy from the electrode through the patient to ground at a distant site. This leads to scattering, decreased current density at the point of application, and damage to the surrounding tissues. 1-3 Bipolar devices place both electrodes very close to one another, passing the current only through the tissue in which they are being applied. This leads to increased current density at the treatment site, increasing efficiency, and decreasing damage to adjacent tissue as the wand vaporizes the tissue to which it is applied. Methods of the early electrosurgical studies in arthroscopy dealt mostly with monopolar devices. 3 In essentially all of these studies, laser and electrosurgical devices injured both cartilage and meniscal tissues to variable depths, ranging from nearly undetectable to as much as 1,980 m in depth. 3,4 Studies suggested that monopolar RF energy may produce greater thermal injury on menisci and cartilage than bipolar devices, but in 2002, Vangsness et al. 5 characterized bipolar-induced thermal injury on human meniscal tissues. In their study, thermal injury depth on human menisci averaged 550 m. However, as in many other studies, despite good controls, they observed large variations within experimental groups. There are currently no controlled studies comparing patient outcomes with meniscal debridement using an RF wand versus a mechanical shaver. However, Owens et al. 6 have recently reported a prospective, comparative study for the treatment of grade 2 and 3 patellar chondral lesions, showing that RF treatment produced clinical outcomes superior to debridement with a mechanical shaver. Analysis of the effects of RF wand debridement techniques on tissue at the microscopic level, and correlating this to successful clinical outcomes, may be an even more difficult task. One recent study on cartilage reported that well-controlled RF bipolar wand debridement of cartilage produces a defined margin of chondrocyte death extending approximately 100 to 200 m deep to the treatment area. 2 They also found no significant changes in chondrocyte metabolic activity at the injury site. These findings begin to characterize the injury zone in cartilage beyond the debridement site, but similar studies in the meniscus are lacking. Therefore, the present study was performed (1) because of the large variability of thermal injury reported in the literature during RF wand use and (2) because studies detailing viability and metabolic activity of meniscal cells and chondrocytes at underlying meniscal debridement sites are lacking. In this study, we characterized such parameters, attempting to define a zone of injury following meniscal debridement with a bipolar RF wand in a controlled setting. We hypothesized that no difference exists in cellular viability, metabolic activity, and zone of injury during meniscal debridement with an arthroscopic RF wand versus an arthroscopic shaver. Experimental Model METHODS A validation study has been previously performed for the use of bovine articular cartilage in viability and metabolic activity studies. 2 We have also used 1 surgeon to perform the debridement on the fresh bovine menisci, as close to the operative setting as possible. We observed that chondrocyte viability was preserved in knee joints for a period of 3 to 6 days. In the present study, fresh calf knees were used within 24 hours of death. En bloc knees were stored at 4 C before experimentation. The knee joints were opened under sterile conditions using a medial parapatellar arthrotomy and the tibial plateaus were carefully dissected free from the femoral articulation. Meniscal ligaments, as well as menisci, were kept intact with the tibial plateau. The proximal tibia was cut to allow for adequate submersion of the plateau in an arthroscopic bath. Experiments were performed on 2 bovine knees per experiment (on 3 separate days) using an identical protocol, timing, and sequence of events. In total, 6 fresh bovine knees were carefully dissected, placed in a saline bath at 28 C, and under arthroscopic conditions, approximately 10% to 15% of the posterior horn of each meniscus (except control) was debrided. Per experiment, the 4 surfaces of the 2 knees were carefully labeled as follows (Figs 1 and 2): 1. Knees 1, 3, and 5: Lateral tibial plateau (LTP1) basket punch plus shaver. Medial tibial plateau (MTP2) punch plus RF wand.
3 BIPOLAR RF ON MENISCUS AND CARTILAGE 387 FIGURE 1. Schematic diagram of meniscal treatment areas for each experiment. 2. Knees 2, 4, and 6: Medial tibial plateau (MTP3) RF wand alone. Lateral tibial plateau (LTP4) no treatment, control group. RF Probe and Meniscal Debridement The 2.5-mm 90 wand is a bipolar multi-electrode arthroscopic probe consisting of 7 active electrodes inserted inside an alumina ceramic spacer, placed inside a stainless steel return electrode 2.2 mm in diameter. The tip of the device is oriented at 90 to the 2.4-mm stainless steel shaft. Each active electrode consists of a titanium wire 0.38 mm in diameter and 0.4 mm in length. The ceramic spacer separates the active electrodes from the return by a 2-mm gap. The total time of meniscal treatment, for all modalities, was 24 seconds. The Razorvac (ArthroCare, Sunnyvale, CA) wand power was set at 7 for all studies. Meniscal debridement was carried out in a freehand manner, in the same fashion for each treatment group, by the senior orthopaedist author. In cases where 2 modalities were used, the total time of treatment was still 24 seconds. In all cases, a blunt-ended right-angle hook was used to gently elevate the meniscus before any treatment in an attempt to simulate the floating effect of the posterior horn achieved with fluid during conventional arthroscopy. Basket punch use generally corresponded to punching out about 10% of the posterior horn of the meniscus, allowing us to leave the punched-out and somewhat frayed edges ready for debridement by either the RF wand or the arthroscopic shaver. The FIGURE 2. Gross appearance of calf menisci after treatment by (A) arthroscopic basket punch, (B) arthroscopic basket punch followed by mechanical shaver, and (C) arthroscopic basket punch followed by RF wand. (D) An untreated control meniscus.
4 388 R. T. ALLEN ET AL. arthroscopic shaver was used in standard fashion, orienting the guarded portion of the shaver toward the articular cartilage surface during meniscal debridement. During wand debridement, the probe was oriented at approximately 60 to the meniscal surface and the elevated meniscus debrided in a light contact mode, passing at a linear rate of approximately 3 to 5 mm/second across the surface. The tibial articular surface and the menisci were kept submerged in the saline bath during treatment. A fluid-flow system was created during treatments to simulate a normal arthroscopic environment. Despite dedicated attempts to keep each treatment identical from sample to sample, the ultimate control over experimental variability, amount of instrument pressure, and angle of operation of specific debrided areas lies in the hands of the surgeon, just as it does clinically. For this reason the senior orthopaedic surgeon was the only person performing the procedure. Immediately after meniscal debridement, the treatment area was marked and plateaus were placed in normal saline solution until sample sectioning (approximately 15 minutes). A No. 20 scalpel blade was used to carefully dissect meniscal treatment zones and the underlying articular cartilage. Isolated meniscal samples included the entire treatment area plus a surrounding 6- to 8-mm margin to ensure adequate samples for analysis of any potential damage. Cartilage samples directly underlying the debridement site were harvested and comprised at least a 10-mm diameter block. As we and others have previously described, 7 full-thickness cartilage (i.e., from superficial cartilage zone to the deep zone subchondral bone interface of cartilage) was freed from the subchondral bone by sharp dissection, allowing for more precise sectioning of 0.5- to 1.0-mm thick meniscus/cartilage. In fact, because of the relative softness of calf subchondral bone, the 1.0-mm thick sections often contained subchondral bone. At least 6 of these sliced specimens per group were analyzed for viability/injury zone or metabolic activity. Importantly, in numerous previous studies, we have observed no differences in viability/ activity of chondrocytes when cartilage was left on the subchondral bone versus being freed from the subchondral bone. 2,8,9 In radiolabeled 35 SO 4 studies for metabolic activity, it is possible that inclusion of too much healthy cartilage or meniscus beyond the zone of debridement could potentially mask any deleterious effects of treatment. We therefore, as previously described, 2 included a margin of only 3 mm beyond or surrounding the debridement site for metabolic activity/cell viability studies. This was done to standardize sample sizes among groups and to identify possible injury zones more accurately. The 3-mm zone was chosen based on previous reports suggesting that up to 2 mm of cartilage surrounding a treatment zone may sustain injury resulting in chondrocyte death. 10,11 Chondrocyte Viability Debridement zone coronal slices of full-thickness (all 3 zones in depth) articular cartilage and meniscus, 0.5- to 1.0-mm thick, were double stained before confocal laser microscopy, as previously described. 2,7-9 Samples were placed into a solution containing 2,7=- Bis(2-carboxyethyl)-5 (6)-carboxyfluorescein, acetoxymethylester (BCECF-AM), and propidium iodide (PI). BCECF-AM is a fluorescein derivative metabolized by nonspecific esterases in living cell membranes to a green fluorescent product. PI is normally excluded from living cells by the intact cell membrane, but penetrates nonviable cells and intercalates with the DNA and fluoresces red. 12,13 Specimens in solution were placed in a 37 C CO 2 /O 2 incubator for 35 to 40 minutes and then removed for microscopic examination. Each articular cartilage layer (superficial, middle, and deep) was analyzed simultaneously. Specimens were viewed with a Zeiss LSM 510 Laser Confocal Scanning Microscope equipped with krypton and argon lasers (Carl Zeiss, Thornwood, NY). Images were obtained at multiple random locations within the meniscus or cartilage slice using Zeiss Laser Scanning Systems LSM 510 software. At least 5 images were obtained from each region within each specimen and the average of these taken for statistical analysis. Viable green cells and nonviable red cells were counted and viability tabulated by computer software (Image-Pro Plus 4.1; Media Cybernetics, Silver Springs, MD). A magnification of 5 allowed complete visualization of both treatment and adjacent normal zones. LSM 510 software allowed us to superimpose calibrated micrometer measurements into the images studied, thus allowing for calculation of the depth of cell death from the surface. 2 Metabolic Activity via Glycosaminoglycan Synthesis ( 35 SO 4 uptake) Glycosaminoglycan synthesis, as quantified by the amount of radiolabeled sulfate ( 35 SO 4 ) incorporation into the sample tissue/cells, is well described as a marker of cellular metabolic activity. 2,14-17 Specimens designated for metabolic activity were carefully trimmed to include the 2- to 3-mm margins surrounding the debridement zone and then incubated in tissue
5 BIPOLAR RF ON MENISCUS AND CARTILAGE 389 TABLE 1. Meniscus Sulfate Uptake (Metabolic Activity) Meniscal Specimens Metabolic Activity ( 35 SO 4 ) Specimens 1, 3, 5 lateral meniscus (basket/shaver) Specimens 1, 3, 5 medial meniscus (basket/wand) Specimens 2, 4, 6 medial meniscus (wand only) Specimens 2, 4, 6 control lateral meniscus (no treatment) 1, CPM/mg 1, CPM/mg 1, CPM/mg 1, CPM/mg NOTE. Values given as mean SD. culture media containing 5 Ci/mL of 35 SO 4 for 48 hours at 37 C. After incubation, tissue samples were removed, washed with distilled water to remove unincorporated 35 SO 4, then freeze-dried and weighed. The tissue was then hydrolyzed in 1-N NaOH for 2 hours at 65 C and the hydrolysate analyzed in a liquid scintillation spectrometer for quantitation of 35 SO 4 incorporation. 2,14-17 Results were calculated and are reported as counts per minute (cpm) per milligram of dry weight. Slices were taken at random per sample. The mean values are reported in the results of Table 1. Statistical Analysis Data are presented as mean standard deviation. Values were subjected to analysis by either Student t test or analysis of variance for multiple comparisons. Statistical significance was set at P.05. RESULTS Chondrocyte Viability and Metabolic Activity After each meniscal debridement, the articular surface was carefully inspected. It revealed no evidence of scoring or abnormality. Chondrocyte viability was 96% to 98% in all specimens. Cell death occurred primarily in the superficial cartilage zone, as shown in Fig 3. We did not find any focal area of cell death in cartilage beyond the stated 150 m, regardless of treatment group. There was no difference between FIGURE 3. Confocal microscopy of calf articular cartilage underlying each experimental debridement site. Chondrocyte death (indicated by red fluorescing cells, arrows) occurred primarily in the superficial layer (100 m from the surface indicated by the scale in B). Living cells (fluorescing green) represented 96% to 98% of the cell population in all experimental groups. Experimental groups included (A) arthroscopic basket punch plus shaver, (B) arthroscopic basket punch plus wand, (C) RF wand only, and (D) untreated control cartilage. (All images, original objective magnification 5.)
6 390 R. T. ALLEN ET AL. TABLE 2. Articular Cartilage Sulfate Uptake (metabolic activity) Tibial Cartilage Specimens Metabolic Activity ( 35 SO 4 ) Specimens 1, 3, 5, LTP1 13,070 8,190 CPM/mg Specimens 1, 3, 5, MTP2 10,110 4,592 CPM/mg Specimens 2, 4, 6, MTP3 12,690 9,932 CPM/mg Specimens 2, 4, 6, LTP4, Control 10, CPM/mg NOTE. Values given as mean SD. Abbreviations: LTP, lateral tibial plateau; MTP, medial tibial plateau. debrided groups and control for any of the experiments, and overall chondrocyte viability ranged from 96% to 98% in each experiment. Importantly, focal areas of chondrocyte death, as might be expected from prolonged RF wand energy in one area and should be readily visible in specimens with such robust viability, were not observed in any specimen. This suggests that meniscal debridement with bipolar RF energy, in this setting, did not significantly extend to underlying cartilage. In general, cartilage had strong sulfate uptake, showing no statistical significance between groups by analysis of variance comparisons (Table 2). Metabolic activity correlates with chondrocyte cell viability. It should be noted that proteoglycan is a fast turnover matrix component in cartilage when compared with collagen and, as expected and observed in this study, it should be much higher in cartilage than in the meniscus (less cellularity and protein synthesis activity in the meniscus). Meniscus Viability and Metabolic Activity Gross inspection of the meniscus showed the types of surfaces remaining after debridement with each device. The RF wand left a distinctly smooth, nondiscolored, and more precise surface, unlike the more textured and irregular surface remaining after shaver debridement. In each specimen analyzed within each treatment group, meniscal viability was variable, similar to previous reports of RF thermal injury depths. 5 Most analyses showed substantial cell death throughout meniscal tissue in both debrided and control groups. A key finding in this study was that specimens from groups undergoing any type of debridement displayed increased numbers of dead cells, most pronounced at debridement sites (Fig 4). Indeed, in each group, treatment with the wand or shaver led to increased levels of cell death beyond the debridement site. Whereas random cell death was noted in each experimental group, the focal death pattern at and beyond debridement sites was not observed in the control specimens. Measurements beyond the site of debridement were typically in the range of 150 to 500 m (Fig 4). Metabolic activity was lower in the meniscus than in the cartilage specimens, but no significant differences were observed among treatment groups versus control. The data are given in Table 1. DISCUSSION The purpose of this study was to compare the effects of bipolar RF energy with those of an arthroscopic shaver and basket punch on meniscal and cartilage cell viability and metabolic activity. These parameters, previously unknown during bipolar RF wand meniscal debridement, were used to characterize a physiologic zone of injury at the site of bipolar wand application. Analysis was both macroscopic and microscopic. Our findings support the hypothesis that no difference exists in these parameters, whether using the RF wand, basket punch, or shaver. Although these data were similar to others in that meniscal injury (and its associated measurements) was variable, we did observe a more pronounced injury zone at debridement sites, regardless of which instrument was used. This injury zone was not found in untreated meniscal samples, despite observing variable levels of random cell death. Thus, in using nonhistologic methods to assess cellular damage, we have for the first time shown that, regardless of debridement device, cellular injury occurs at and beyond debridement sites, and to a similar extent, in fresh calf meniscal tissue. In most reports, meniscal injury from RF energy is based on measuring the depth of a fairly well defined thermal injury pattern of tissue architecture disruption, identified mainly by histologic examination. Why depth of tissue penetration is so important is due in large part to the idea that a certain depth of RF-induced thermal injury produces nonreparable damage or, produces a potentially more harmful or unstable injury to the surrounding tissue. Subsequently, earlier degeneration and failure result. Although tissue changes caused by RF thermal injury are readily observable, histologic analyses may not be predictive of surrounding cellular activity and injury. 2-4 Moreover, there are a number of differences in tissue staining and analysis techniques reported in RF-injured meniscal tissue. These were some of the more important reasons for using the metabolic activity and cell death assessment techniques herein. Another reason was to assess if the variability in mea-
7 BIPOLAR RF ON MENISCUS AND CARTILAGE 391 FIGURE 4. Confocal microscopy of calf menisci following experimental debridement treatment. Experimental groups included (A) arthroscopic basket punch plus shaver, (B) arthroscopic basket punch plus wand, (C) RF wand only, and D) untreated control meniscus. Living cells fluoresce green, while dead cells fluoresce red. (All images, original objective magnification 5. Distance indicated by the 500- m scale.) surements of thermal injury extended to the cellular level, which they appear to do in this study as well. Variability in thermal injury depth, after H&E staining/uptake of formalin-fixed specimens, is a rather consistent finding across the literature in relation to studies using RF energy. In menisci, variability is likely due to differences in staining techniques and injury assessment, quantitative differences, RF wand type, wand power, the surface area of the treatment electrode, contact time of electrode with tissue, and the type of current used. 3,4 A recent report suggests that probe geometry and surface area are 2 of the most critical features in determining how deep RF energy penetrates meniscal tissue. 18 There is, however, some evidence that, despite these levels of thermal injury to the meniscus, it often heals to normal tissue in 6 to 7 months. 3,19 These studies reason that less damage to the meniscus (in an optimal RF debridement) could translate into less postoperative recovery time. Whereas the present study used biochemical means to compare a bipolar wand with a basket punch and shaver, studies evaluating the depth of tissue injury of monopolar and bipolar RF energy give insight into how a shaver may compare with both in regard to cellular injury patterns. In cartilage, evidence suggests that during chondral debridement, bipolar RF energy penetrated cartilage substantially more ( 2 times the depth) than that of monopolar energy. 11 Further, bipolar RF may lead to cartilage thinning, possibly as a result of tissue penetration, predisposing to further mechanical stress, cartilage loss, and degeneration. 20 In regard to the meniscus, RF debridement of ovine menisci showed that monopolar RF energy left a clear demarcation of thermal injury, fibrochondrocyte nuclear pyknosis, and fusion of collagen fibrils. 21 These authors 21 suggest that thermal injury-induced collagen fibril fusion may actually prevent meniscal tear propagation and stabilize a laceration. Chondral RF debridement has been suggested to provide some resistance to abrasion. 22 RF debridement could lead to the same changes of a smoother surface, less resistance to abrasion, and possibly a more stable rim of tissue. In the present study, regardless of whether the meniscal surface was roughened with a basket punch or untouched before debridement, RF treatment left the meniscus and its edges clean, precise, and smooth, unlike the mechanical shaver. In theory, a smoother meniscal surface could produce less pain and an improvement in function. While this was in fact suggested in 2 recent studies on cartilage laser ablation, 23,24 it is clear that a strong dependence on the operative surgeon may exist therein, as well as the potential for iatrogenic wand injury. Furthermore, laser treatments can lead to significant damage to the articular cartilage surface, extending
8 392 R. T. ALLEN ET AL. even into the subchondral bone. 25 It is understood that one important reason for meniscal debridement is to produce a stable rim of tissue while minimizing peripheral damage and maintaining circumferential meniscal integrity. Mechanical shavers are not optimally suited for this, often leaving somewhat roughened, less contoured edges in the less accessible areas of the meniscus during arthroscopy. Moreover, the shaver mechanism may cause trauma to the adjacent meniscal tissues during debridement, possibly predisposing to further or more rapid degenerative changes. 26 In fact, cartilage studies show that debridement with mechanical shavers may remove more tissue than with RF energy ablation. 27 If so, determining the true depth of meniscal cell death and remaining cellular activity may be extremely relevant in trying to predict future tissue stability, damage, or a possible reparative response. In a recent report out of the Hospital for Joint Diseases, debrided human meniscal tissue removed with either an ArthroCare wand at power 3 and 7 or with a mechanical shaver, was assessed histologically. 28 Despite significant increases in thermal tissue penetration from 0.18 to 0.33 mm using a wand power of 3 versus 7, they did not observe any zone of thermal penetration with a shaver or scalpel. In the present study, however, both the viability and metabolic activity of cells at and surrounding the debridement site were not significantly different than the control. Finally, the extent and the zone of meniscus requiring debridement are also important considerations. It is known that the central 66% to 75% of the body of menisci is avascular and limited in its capacity to heal. 29,30 Meniscal tissue can heal within the red zone, largely by fibrochondrocytes and fibroblasts that reintegrate and reinforce debrided areas. In the white zone, ingrowth of fibrochondrocytes, fibroblasts, and other synovial cells are limited in their ability to travel into and repopulate the central meniscal region. If we assume that white zone meniscal tissue will remain essentially as debrided, it seems relevant then to produce a stable, smooth rim of tissue that has optimal cell viability and metabolic activity. In this regard, no significant difference was observed when using a wand, basket punch, or a shaver, implying that they should at least be able to produce similar clinical outcomes. Mechanical shavers have had some success in meniscal debridement in decreasing symptoms, but the complications of iatrogenic cartilage injury, a slightly roughened, less contoured surface, difficulty with precise cutting in difficult operative areas, and possibly overdebridement are all reasons to further define an alternative method. RF energy may be one such method. Despite some evidence in support of monopolar RF meniscal debridement, bipolar RF energy may be of equal or greater benefit. In fact, while both may have some ability to penetrate meniscal tissue and stabilize a tear, the margin of error for meniscal debridement with monopolar RF energy is small and, as suggested, the need to increase parameters during debridement (such as wand power, contact times) would likely produce profoundly negative effects on underlying cartilage surfaces. 21 Cell death and metabolic activity in different RF energy-debrided menisci has not been reported. Unlike studies that attempt to define the depth of penetration of RF monopolar and bipolar devices with specific gram loads and contact times, we have taken a different approach. We have attempted to recreate the clinical setting, then quickly quantify and characterize injury as would occur in vivo during arthroscopy. It is apparent that some inherent variability does exist. However, experiments in this study were performed on fresh calf menisci immediately after harvest from the knee, within 24 hours of death, subsequently performing microscopic analyses on the same day as experimentation. As mentioned, analysis is at a cellular level using confocal laser microscopy and sulfate incorporation assay, rather than at the histologic level. These are among some of the strengths of the current study. Treatment goals of meniscal debridement include taking as little meniscus as possible and leaving as smooth and functional a surface as possible, especially since subsequent degenerative joint changes are directly proportional to the extent of meniscus debrided One weakness of this study is the use of only 1 RF wand device on 1 power setting. Another weakness is the removal of the femoral condyle to gain better access to the meniscus and tibial plateau. In trying to assimilate information and make it as equivalent to the in vivo setting as possible, 1 surgeon performed all of the debridements by hand in a manner consistent with his clinical experience. The fact that 1 device was used, from 1 company and at the same power, is a part of the overall experimental design and study-size constraints. It could be argued that, because of the variability within groups, we could have missed regions of cell death or altered metabolic activity after wand treatments. Through careful study design, meticulous gross and laser microscopy assessments, and by harvesting samples of meniscus and cartilage specifically at the debridement sites, we believe the conclusions of this study accurately represent data on a variety of
9 BIPOLAR RF ON MENISCUS AND CARTILAGE 393 modalities on articular cartilage as well as menisci. Studies that compare clinical outcomes of debridement with an RF wand versus a mechanical shaver are needed to determine if short and long-term patient function is significantly different with RF wand treatments. CONCLUSIONS Debridement of menisci with a bipolar RF wand, as may occur during arthroscopy, appears to produce levels of cell injury and death similar to debridement with a mechanical shaver. It did not harm underlying articular surfaces, and appears to produce a precise cut and meniscal surface. REFERENCES 1. Aritomi H, Yamamoto M. A method of arthroscopic surgery: Clinical evaluation of synovectomy with the electric resectorscope and removal of loose bodies in the knee joint. Orthop Clin North Am 1979;10: Ball ST, Tasto JP, Amiel D. Chondrocyte viability and metabolic activity after treatment of bovine articular cartilage with bipolar radiofrequency: An in vitro study. Arthroscopy 2004; 20: Polousky JD, Hedman TP, Vangsness CT. Electrosurgical methods for arthroscopic meniscectomy: A review of the literature. Arthroscopy 2002;16: Miller GK, Drennan DB, Maylahn DJ. The effect of technique on histology of arthroscopic partial meniscectomy with electrosurgery. Arthroscopy 1987;3: Vangsness CT Jr, Polousky JD, Hedman TP. Radiofrequency thermal effects on the human meniscus: An in vitro analysis. Arthroscopy 2002;18: Owens BD, Stickles BJ, Balikian P, Busconi BD. Prospective analysis of radiofrequency versus mechanical debridement of isolated patellar chondral lesions. Arthroscopy 2002;18: Williams SK, Amiel D, Ball ST, et al. Prolonged storage effects on the articular cartilage of fresh human osteochondral allografts. J Bone Joint Surg Am 2003;85: Convery FR, Akeson WH, Amiel D, Meyers MH, Monosov AZ. Long-term survival of chondrocytes in an osteochondral articular cartilage allograft. J Bone Joint Surg Am 1996;78: Lane JG, Massie JB, Ball ST, et al. Follow-up of osteochondral plug transfers in a goat model: A 6-month study. Am J Sports Med 2004;32: Lu Y, Edwards RB, Kalscheur VL, et al. Effect of bipolar radiofrequency energy on human articular cartilage: Comparison of confocal laser microscopy and light microscopy. Arthroscopy 2001;17: Edwards RB III, Lu Y, Nho S, Cole BJ, Markel MD. Thermal chondroplasty of chondromalacic human cartilage. An ex vivo comparison of bipolar and monopolar radiofrequency devices. Am J Sports Med 2002;30: Ohlendorf C, Tomford WW, Mankin HJ. Chondrocyte survival in cryopreserved osteochondral articular cartilage. J Orthop Res 1996;14: Mossberg K, Ericsson M. Detection of doubly stained fluorescent specimens using confocal microscopy. J Microsc 1990;158: Amiel D, Harwood FL, Hoover JA, Meyers M. A histological and biochemical assessment of the cartilage matrix obtained from an in vitro storage of osteochondral allografts. Connective Tissue Res 1989;23: Kim YJ, Sah RL, Grodzinsky AJ, Plaas AHK, Sandy JD. Stimulation of cartilage biosynthesis by dynamic compression: Physical mechanisms. Orthop Trans 1991;15: Sah RL-Y, Grodzinsky AJ, Plaas AHK, Sandy JD. Effects of static and dynamic compression on matrix metabolism in cartilage explants. In: Kuettner K, ed. Articular cartilage and osteoarthritis. Chap 26. New York: Raven, 1992; Sah RL, Chen AC, Grodzinsky AJ, Trippel SB. Differential effects of bfgf and IGF-1 on matrix metabolism in calf and adult bovine cartilage explants. Arch Biochem Biophys 1994; 308: Vangsness CT Jr, Polousky JD, Parkinson AB, Hedman TP. Radiofrequency thermal effects on the human meniscus: An in study of systems with monopolar and bipolar electrodes. Am J Sports Med 2003;31: Bert, JM. Use of an electrocautery loop probe for arthroscopic meniscectomy: A five year experience with results, indications and complications. Arthroscopy 1992;8: Hogan CJ, Diduch DR. Progressive articular cartilage loss following radiofrequency treatment of a partial-thickness lesion. Arthroscopy 2001;17:E24 (available online at Lopez MJ, DeTemple LA, Lu Y, Markel MD. The effects of monopolar radiofrequency energy on intact and lacerated ovine menisci. Arthroscopy 2001;17: Suh JK, Aroen A, Muzzonigro TS, Disilvestro M, Fu FH. Injury and repair of articular cartilage: Related scientific issues. Oper Tech Orthop 1997;7: Lubbers C, Siebert WE. Holmium:YAG-laser-assisted arthroscopy versus conventional methods for treatment of the knee: Two year results of a prospective study. Knee Surg Sports Traumatol Arthrosc 1997;5: Raunest J, Lohnert JH. Arthroscopic cartilage debridement by Excimer laser in chondromalacia of the knee joint: A prospective randomized clinic study. Arch Orthop Trauma Surg 1990; 109: Lane JG, Amiel ME, Greenfield R, Amiel D. Matrix assessment of the articular cartilage surface after chondroplasty with the holmium:yag Laser: A long-term study. Am J Sports Med 2001;29: Kim HK, Moran ME, Salter RB. The potential for regeneration of articular cartilage in defects created by chondral shaving and subchondral abrasion: An experimental investigation in rabbits. J Bone Joint Surg Am 1991;73: Turner AS, Tippett JW, Powers BE, Dewell RD, Mallinckrodt CH. Radiofrequency (electrosurgical) ablation of articular cartilage: A study in sheep. Arthroscopy 1998;14: Jazrawi LM, Chen A, Stein D, Heywood CS, Bernstein A, Steiner G, Rokito A. The effects of radiofrequency bipolar thermal energy on human meniscal tissue. Bull Hosp Jt Dis 2003;61: Newman AP, Daniels AU, Burks RT. Principles and decision making in meniscal surgery. Arthroscopy 1993;9: Awbrey BJ. Arthroscopic management of meniscal injuries. Curr Opin Rheumatol 1993;5: O Meara PM. The basic science of meniscus repair. Orthop Rev 1993;22: Lanzer WL, Komenda G. Changes in articular cartilage after meniscectomy. Clin Orthop 1990;252: Rangger C, Kathrein A, Klestil T, Glotzer W. Partial meniscectomy and osteoarthritis. Sports Med 1997;23:61-68.
Chondrocyte Viability and Metabolic Activity After Treatment of Bovine Articular Cartilage With Bipolar Radiofrequency: An In Vitro Study
 Chondrocyte Viability and Metabolic Activity After Treatment of Bovine Articular Cartilage With Bipolar Radiofrequency: An In Vitro Study David Amiel, Ph.D., Scott T. Ball, M.D., and James P. Tasto, M.D.
Chondrocyte Viability and Metabolic Activity After Treatment of Bovine Articular Cartilage With Bipolar Radiofrequency: An In Vitro Study David Amiel, Ph.D., Scott T. Ball, M.D., and James P. Tasto, M.D.
Thermal chondroplasty using the Smith & Nephew DYONICS GLIDER Articular Cartilage Probe
 Knee Series Technique Guide Thermal chondroplasty using the Smith & Nephew DYONICS GLIDER Articular Cartilage Probe Reviewed by: Dr. James H. Lubowitz, MD Director Taos Orthopaedic Institute Taos, New
Knee Series Technique Guide Thermal chondroplasty using the Smith & Nephew DYONICS GLIDER Articular Cartilage Probe Reviewed by: Dr. James H. Lubowitz, MD Director Taos Orthopaedic Institute Taos, New
Arthroscopic Evaluation of Radiofrequency Chondroplasty of the Knee
 Arthroscopic Evaluation of Radiofrequency Chondroplasty of the Knee Ilya Voloshin,* MD, Kenneth R. Morse, MD, C. Dain Allred, MD, Scott A. Bissell, MD, Michael D. Maloney, MD, and Kenneth E. DeHaven, MD
Arthroscopic Evaluation of Radiofrequency Chondroplasty of the Knee Ilya Voloshin,* MD, Kenneth R. Morse, MD, C. Dain Allred, MD, Scott A. Bissell, MD, Michael D. Maloney, MD, and Kenneth E. DeHaven, MD
Bone&JointAppraisal Vol
 Bone&JointAppraisal Vol 01 No 03 December 2016 COBLATION Chondroplasty Versus Mechanical Debridement: Randomized Controlled Trial with 10-Year Outcomes -Year Four-Year Ten-Year Group A COBLATION technology
Bone&JointAppraisal Vol 01 No 03 December 2016 COBLATION Chondroplasty Versus Mechanical Debridement: Randomized Controlled Trial with 10-Year Outcomes -Year Four-Year Ten-Year Group A COBLATION technology
Meniscus Reconstruction: Trough Surgical Technique
 Meniscus Reconstruction: Trough Surgical Technique Technique Consultant Jeffrey L. Halbrecht, M.D. San Francisco, CA ABOUT THE TROUGH TECHNIQUE The trough technique for meniscal allograft reconstruction
Meniscus Reconstruction: Trough Surgical Technique Technique Consultant Jeffrey L. Halbrecht, M.D. San Francisco, CA ABOUT THE TROUGH TECHNIQUE The trough technique for meniscal allograft reconstruction
Thermal Chondroplasty With Bipolar and Monopolar Radiofrequency Energy: Effect of Treatment Time on Chondrocyte Death and Surface Contouring
 Thermal Chondroplasty With Bipolar and Monopolar Radiofrequency Energy: Effect of Treatment Time on Chondrocyte Death and Surface Contouring Yan Lu, M.D., Ryland B. Edwards III, D.V.M., M.S., Shane Nho,
Thermal Chondroplasty With Bipolar and Monopolar Radiofrequency Energy: Effect of Treatment Time on Chondrocyte Death and Surface Contouring Yan Lu, M.D., Ryland B. Edwards III, D.V.M., M.S., Shane Nho,
Meniscus cartilage replacement with cadaveric
 Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
TREATMENT OF CARTILAGE LESIONS
 TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3
 AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3 1-EMERGENCY CLINICAL HOSPITAL FLOREASCA BUCHAREST 2-EMERGENCY CLINICAL HOSPITAL SFANTUL
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3 1-EMERGENCY CLINICAL HOSPITAL FLOREASCA BUCHAREST 2-EMERGENCY CLINICAL HOSPITAL SFANTUL
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT
 OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
Why the dog? Analogy of the anatomy
 Why the dog? Analogy of the anatomy Surgically Induced canine OA models: Anterior (cranial) cruciate ligament transection model Pond MJ, Nuki G. Ann Rheum Dis 1973 (and > 100 others) Meniscal disruption
Why the dog? Analogy of the anatomy Surgically Induced canine OA models: Anterior (cranial) cruciate ligament transection model Pond MJ, Nuki G. Ann Rheum Dis 1973 (and > 100 others) Meniscal disruption
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Disclosures: C.B. Raub: None. B.C. Hansen: None. T. Yamaguchi: None. M.M. Temple-Wong: None. K. Masuda: None. R.L. Sah: None.
 En Face Microscopy of Rabbit Knee Articular Cartilage Following Anterior Cruciate Ligament Transection Reveals Early Matrix Damage, Chondrocyte Loss and Cloning Christopher B. Raub, PhD, Bradley C. Hansen,
En Face Microscopy of Rabbit Knee Articular Cartilage Following Anterior Cruciate Ligament Transection Reveals Early Matrix Damage, Chondrocyte Loss and Cloning Christopher B. Raub, PhD, Bradley C. Hansen,
Osteochondral Transplant Delivery System
 Osteochondral Transplant Delivery System Team Leader: Alex Teague BPAG: David Fiflis Communicator/BWIG: Alex Babinski BSAC: Zach Wodushek Client: Dr. Brian Walczak, DO Advisor: Dr. Tracy Puccinelli, PhD
Osteochondral Transplant Delivery System Team Leader: Alex Teague BPAG: David Fiflis Communicator/BWIG: Alex Babinski BSAC: Zach Wodushek Client: Dr. Brian Walczak, DO Advisor: Dr. Tracy Puccinelli, PhD
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping
 Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
evicore MSK joint surgery procedures requiring prior authorization
 evicore MSK joint surgery procedures requiring prior authorization Moda Health Commercial Group and Individual Members* Updated 1/30/2018 *Check EBT to verify member enrollment in evicore program Radiology
evicore MSK joint surgery procedures requiring prior authorization Moda Health Commercial Group and Individual Members* Updated 1/30/2018 *Check EBT to verify member enrollment in evicore program Radiology
Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status
 # 154134 Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status Jun-Gu Park, Seong-Il Bin, Jong-Min Kim, Bum Sik Lee Department of Orthopaedic Surgery, Asan Medical
# 154134 Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status Jun-Gu Park, Seong-Il Bin, Jong-Min Kim, Bum Sik Lee Department of Orthopaedic Surgery, Asan Medical
KNEE ARTHROSCOPY PATIENT INFORMATION SHEET
 KNEE ARTHROSCOPY PATIENT INFORMATION SHEET Introduction It has been recommended that you undergo an arthroscopy of your knee. This information sheet is designed to explain what is involved in an arthroscopy,
KNEE ARTHROSCOPY PATIENT INFORMATION SHEET Introduction It has been recommended that you undergo an arthroscopy of your knee. This information sheet is designed to explain what is involved in an arthroscopy,
COR. Precision Targeting Cartilage Repair System. Arthroscopic Technique for Repair of Osteochondral Defects
 COR Precision Targeting Cartilage Repair System Arthroscopic Technique for Repair of Osteochondral Defects Planning the Procedure An 18-gauge spinal needle is initially used to plan a perpendicular approach
COR Precision Targeting Cartilage Repair System Arthroscopic Technique for Repair of Osteochondral Defects Planning the Procedure An 18-gauge spinal needle is initially used to plan a perpendicular approach
Resection of bucket-handle tears is one of the most
 Technical Note Arthroscopic Resection of Bucket-Handle Tears With the Help of a Suture Punch: A Simple Technique to Shorten Operating Time Mehmet S. Bı nnet, M.D., İlksen Gürkan, M.D., and Cem Çetı n,
Technical Note Arthroscopic Resection of Bucket-Handle Tears With the Help of a Suture Punch: A Simple Technique to Shorten Operating Time Mehmet S. Bı nnet, M.D., İlksen Gürkan, M.D., and Cem Çetı n,
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
Disclosures: A.G. Bajpayee: None. A.M. Scheu: None. R.M. Porter: None. A.J. Grodzinsky: None.
 Avidin as a Carrier for Drug Delivery into Cartilage: Electrostatic Interactions Enable Rapid Penetration, Enhanced Uptake, and Retention in Rat Knee Joints Ambika Goel Bajpayee 1, Alfredo M. Scheu 2,
Avidin as a Carrier for Drug Delivery into Cartilage: Electrostatic Interactions Enable Rapid Penetration, Enhanced Uptake, and Retention in Rat Knee Joints Ambika Goel Bajpayee 1, Alfredo M. Scheu 2,
Clinical Application of Scaffolds for Partial Meniscus Replacement
 1 Clinical Application of Scaffolds for Partial Meniscus Replacement 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 Cathal&J.&Moran,&MD,&FRCS(Orth)& 1,&Daniel&P&Withers&MB,&FRCS&(Orth)&
1 Clinical Application of Scaffolds for Partial Meniscus Replacement 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 Cathal&J.&Moran,&MD,&FRCS(Orth)& 1,&Daniel&P&Withers&MB,&FRCS&(Orth)&
Torn ACL - Anatomic Footprint ACL Reconstruction
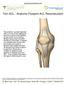 Torn ACL - Anatomic Footprint ACL Reconstruction The anterior cruciate ligament (ACL) is one of four ligaments that are crucial to the stability of your knee. It is a strong fibrous tissue that connects
Torn ACL - Anatomic Footprint ACL Reconstruction The anterior cruciate ligament (ACL) is one of four ligaments that are crucial to the stability of your knee. It is a strong fibrous tissue that connects
Basics of Cartilage Restoration Introduction of TruFit
 Basics of Cartilage Restoration Introduction of TruFit Philip A. Davidson, MD Heiden Orthopaedics Park City, Utah USA Smith & Nephew Seminar London, UK October 2008 Cartilage Restoration A wide realm between..
Basics of Cartilage Restoration Introduction of TruFit Philip A. Davidson, MD Heiden Orthopaedics Park City, Utah USA Smith & Nephew Seminar London, UK October 2008 Cartilage Restoration A wide realm between..
NEW DEVELOPMENTS IN MENISCAL SURGERY
 NEW DEVELOPMENTS IN MENISCAL SURGERY Written by Peter Verdonk, Belgium and Francesco Perdisa, Italy Meniscectomy is one of the most common procedures in orthopaedic surgery, capable of returning the knee
NEW DEVELOPMENTS IN MENISCAL SURGERY Written by Peter Verdonk, Belgium and Francesco Perdisa, Italy Meniscectomy is one of the most common procedures in orthopaedic surgery, capable of returning the knee
Rehabilitation Guidelines for Knee Arthroscopy
 Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE
 In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
Hip, Knee and Shoulder Surgery
 Hip, Knee and Shoulder Surgery Policy Number: MM.06.030 Lines of Business: HMO; PPO; QUEST Integration; Medicare Advantage Section: Surgery Place(s) of Service: Outpatient; Inpatient Original Effective
Hip, Knee and Shoulder Surgery Policy Number: MM.06.030 Lines of Business: HMO; PPO; QUEST Integration; Medicare Advantage Section: Surgery Place(s) of Service: Outpatient; Inpatient Original Effective
The evidence is in...
 The evidence is in... Controlled ablation Proven outcomes2,3 WEREWOLF System Supporting healthcare professionals Faster* patient recovery1 RX Better* patient outcomes2,3 RX RX Safe for use on all joint
The evidence is in... Controlled ablation Proven outcomes2,3 WEREWOLF System Supporting healthcare professionals Faster* patient recovery1 RX Better* patient outcomes2,3 RX RX Safe for use on all joint
THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE
 THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE Abstract Spontaneous osteonecrosis of the knee (SPONK) and osteonecrosis in the postoperative knee (ONPK) are
THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE Abstract Spontaneous osteonecrosis of the knee (SPONK) and osteonecrosis in the postoperative knee (ONPK) are
Thermal Chondroplasty of Chondromalacic Human Cartilage
 0363-5465/102/3030-0090$02.00/0 THE AMERICAN JOURNAL OF SPORTS MEDICINE, Vol. 30, No. 1 2002 American Orthopaedic Society for Sports Medicine Thermal Chondroplasty of Chondromalacic Human Cartilage An
0363-5465/102/3030-0090$02.00/0 THE AMERICAN JOURNAL OF SPORTS MEDICINE, Vol. 30, No. 1 2002 American Orthopaedic Society for Sports Medicine Thermal Chondroplasty of Chondromalacic Human Cartilage An
Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of the Tibia
 Case Reports in Orthopedics Volume 2015, Article ID 795759, 5 pages http://dx.doi.org/10.1155/2015/795759 Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of
Case Reports in Orthopedics Volume 2015, Article ID 795759, 5 pages http://dx.doi.org/10.1155/2015/795759 Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of
BIOMECHANICAL MECHANISMS FOR DAMAGE: RETRIEVAL ANALYSIS AND COMPUTATIONAL WEAR PREDICTIONS IN TOTAL KNEE REPLACEMENTS
 Journal of Mechanics in Medicine and Biology Vol. 5, No. 3 (2005) 469 475 c World Scientific Publishing Company BIOMECHANICAL MECHANISMS FOR DAMAGE: RETRIEVAL ANALYSIS AND COMPUTATIONAL WEAR PREDICTIONS
Journal of Mechanics in Medicine and Biology Vol. 5, No. 3 (2005) 469 475 c World Scientific Publishing Company BIOMECHANICAL MECHANISMS FOR DAMAGE: RETRIEVAL ANALYSIS AND COMPUTATIONAL WEAR PREDICTIONS
MSK Covered Services. Musculoskeletal: Joint Metal-on-metal total hip resurfacing, including acetabular and femoral components
 CPT CODE S2118 MSK Covered Services Musculoskeletal: Joint Metal-on-metal total hip resurfacing, including acetabular and femoral components 23000 Removal of subdeltoid calcareous deposits, open 23020
CPT CODE S2118 MSK Covered Services Musculoskeletal: Joint Metal-on-metal total hip resurfacing, including acetabular and femoral components 23000 Removal of subdeltoid calcareous deposits, open 23020
The Meniscus. History. Anatomy. Anatomy. Blood Supply. Attachments
 History The Meniscus W. Randall Schultz, MD, MS Austin, TX January 23, 2016 Meniscus originally thought to represent vestigial tissue 1883 first reported meniscal repair (Annandale) Total menisectomy treatment
History The Meniscus W. Randall Schultz, MD, MS Austin, TX January 23, 2016 Meniscus originally thought to represent vestigial tissue 1883 first reported meniscal repair (Annandale) Total menisectomy treatment
Cartilage Repair Center Brigham and Women s Hospital Harvard Medical School
 Brigham and Women s Hospital Harvard Medical School Safety, feasibility, and radiographic outcomes of the anterior meniscal takedown technique to approach chondral defects on the tibia and posterior femoral
Brigham and Women s Hospital Harvard Medical School Safety, feasibility, and radiographic outcomes of the anterior meniscal takedown technique to approach chondral defects on the tibia and posterior femoral
The Impact of Age on Knee Injury Treatment
 The Impact of Age on Knee Injury Treatment Focus on the Meniscus Dr. Alvin J. Detterline, MD Sports Medicine and Orthopaedic Surgery Towson Orthopaedic Associates University of Maryland St. Joseph Medical
The Impact of Age on Knee Injury Treatment Focus on the Meniscus Dr. Alvin J. Detterline, MD Sports Medicine and Orthopaedic Surgery Towson Orthopaedic Associates University of Maryland St. Joseph Medical
Treatment of meniscal lesions and isolated lesions of the anterior cruciate ligament of the knee in adults
 QUICK REFERENCE GUIDE Treatment of meniscal s and isolated s of the anterior cruciate ligament of the knee in adults June 2008 AIM OF THE GUIDELINES To encourage good practices in the areas of meniscal
QUICK REFERENCE GUIDE Treatment of meniscal s and isolated s of the anterior cruciate ligament of the knee in adults June 2008 AIM OF THE GUIDELINES To encourage good practices in the areas of meniscal
MRI KNEE WHAT TO SEE. Dr. SHEKHAR SRIVASTAV. Sr.Consultant KNEE & SHOULDER ARTHROSCOPY
 MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
Rehabilitation Guidelines for Knee Arthroscopy
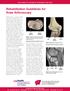 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon
State-of-the-art performance for fast, efficient procedures QUANTUM 2. Controller System for use with COBLATION Wands
 State-of-the-art performance for fast, efficient procedures QUANTUM 2 Controller System for use with COBLATION Wands COBLATION plasma technology How COBLATION technology works The term COBLATION means
State-of-the-art performance for fast, efficient procedures QUANTUM 2 Controller System for use with COBLATION Wands COBLATION plasma technology How COBLATION technology works The term COBLATION means
Chart a course for meniscal preservation
 Chart a course for meniscal preservation 1 The clearly defined value of meniscal preservation A number of studies have been published that clearly define the benefits of preserving as much functional meniscus
Chart a course for meniscal preservation 1 The clearly defined value of meniscal preservation A number of studies have been published that clearly define the benefits of preserving as much functional meniscus
Rakesh Patel, MD 4/9/09
 Rakesh Patel, MD 4/9/09 Chondral Injuries Very common Present in 63-66% patients undergoing arthroscopy 11-19% full-thickness lesions Up to 79% patients with ACL deficient knee have some form of chondral
Rakesh Patel, MD 4/9/09 Chondral Injuries Very common Present in 63-66% patients undergoing arthroscopy 11-19% full-thickness lesions Up to 79% patients with ACL deficient knee have some form of chondral
OSTEOCHONDRAL ALLOGRAFTS AND AUTOGRAFTS IN THE TREATMENT OF FOCAL ARTICULAR CARTILAGE LESIONS
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Effect Of Centralization For Extruded Meniscus Extrusion In A Rat Model
 Effect Of Centralization For Extruded Meniscus Extrusion In A Rat Model Kenichi Kawabata 1, Nobutake Ozeki 1, Hideyuki Koga 1, Yusuke Nakagawa 1, Mio Udo 1, Ryusuke Saito 1, Katsuaki Yanagisawa 1, Toshiyuki
Effect Of Centralization For Extruded Meniscus Extrusion In A Rat Model Kenichi Kawabata 1, Nobutake Ozeki 1, Hideyuki Koga 1, Yusuke Nakagawa 1, Mio Udo 1, Ryusuke Saito 1, Katsuaki Yanagisawa 1, Toshiyuki
BASELINE QUESTIONNAIRE (SURGEON)
 SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
Lateral Meniscus Transplant
 Lateral Meniscus Transplant Using the CONMED Meniscus Allograft Transplant (MAT) Instruments A complete guide to Lateral Meniscus Transplant using the CONMED meniscus allograft transplant Instruments.
Lateral Meniscus Transplant Using the CONMED Meniscus Allograft Transplant (MAT) Instruments A complete guide to Lateral Meniscus Transplant using the CONMED meniscus allograft transplant Instruments.
Partial meniscectomy of tears in the avascular zone remains
 An Original Study Radiofrequency Stimulation for Potential Healing of Meniscal Injuries in the Avascular Zone Christopher S. Lee, MD, MBA, James P. Tasto, MD, Robert M. Healey, BS, MBA, Sakae Sano, MD,
An Original Study Radiofrequency Stimulation for Potential Healing of Meniscal Injuries in the Avascular Zone Christopher S. Lee, MD, MBA, James P. Tasto, MD, Robert M. Healey, BS, MBA, Sakae Sano, MD,
Effects of Meniscus and Defect Size, Location and Orientation on Rim Stress and. Subchondral Bone Contact of Focal Cartilage Defects of the Knee
 Effects of Meniscus and Defect Size, Location and Orientation on Rim Stress and Subchondral Bone Contact of Focal Cartilage Defects of the Knee Undergraduate Research Thesis Presented in Partial Fulfillment
Effects of Meniscus and Defect Size, Location and Orientation on Rim Stress and Subchondral Bone Contact of Focal Cartilage Defects of the Knee Undergraduate Research Thesis Presented in Partial Fulfillment
Knee: Meniscus Back to Basics
 Knee: Meniscus Back to Basics Kyung Jin Suh kyungjin.suh@gmail.com Doctor Radiology, Daegu, KOREA Medial Lateral 7.7 10.2 11.6 9.6 10.6 mm Posterior > Anterior horn 10.6 mm Posterior = Anterior horn Medial
Knee: Meniscus Back to Basics Kyung Jin Suh kyungjin.suh@gmail.com Doctor Radiology, Daegu, KOREA Medial Lateral 7.7 10.2 11.6 9.6 10.6 mm Posterior > Anterior horn 10.6 mm Posterior = Anterior horn Medial
Treatment Options for Articular Cartilage Defects of the Knee
 Innovations Treatment Options for Articular Cartilage Defects of the Knee Alvin J. Detterline Steven Goldberg ernard R. ach, Jr. rian J. Cole The treatment of symptomatic articular cartilage defects of
Innovations Treatment Options for Articular Cartilage Defects of the Knee Alvin J. Detterline Steven Goldberg ernard R. ach, Jr. rian J. Cole The treatment of symptomatic articular cartilage defects of
Introduction to Biomedical Engineering
 Introduction to Biomedical Engineering FW 16/17, AUT Biomechanics of tendons and ligaments G. Rouhi Biomechanics of tendons and ligaments Biomechanics of soft tissues The major soft tissues in musculoskeletal
Introduction to Biomedical Engineering FW 16/17, AUT Biomechanics of tendons and ligaments G. Rouhi Biomechanics of tendons and ligaments Biomechanics of soft tissues The major soft tissues in musculoskeletal
Development of Partial Thickness Articular Cartilage Injury in an Ovine Model
 Development of Partial Thickness Articular Cartilage Injury in an Ovine Model Yan Lu, 1 Mark D. Markel, 1 Carol Swain, 2 Lee D. Kaplan 2 1 Comparative Orthopaedic Research Laboratory, School of Veterinary
Development of Partial Thickness Articular Cartilage Injury in an Ovine Model Yan Lu, 1 Mark D. Markel, 1 Carol Swain, 2 Lee D. Kaplan 2 1 Comparative Orthopaedic Research Laboratory, School of Veterinary
Osteoarthritis. Dr Anthony Feher. With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides
 Osteoarthritis Dr Anthony Feher With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides No Financial Disclosures Number one chronic disability in the United States
Osteoarthritis Dr Anthony Feher With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides No Financial Disclosures Number one chronic disability in the United States
Inside-Out Meniscal Repair Still the Gold Standard?
 Inside-Out Meniscal Repair Still the Gold Standard? ERIC BERKSON, MD MGH SPORTS MEDICINE TEAM PHYSICIAN, BOSTON RED SOX ASSISTANT PROFESSOR, HARVARD MEDICAL SCHOOL JULY 26, 2018 Disclosures Neither I nor
Inside-Out Meniscal Repair Still the Gold Standard? ERIC BERKSON, MD MGH SPORTS MEDICINE TEAM PHYSICIAN, BOSTON RED SOX ASSISTANT PROFESSOR, HARVARD MEDICAL SCHOOL JULY 26, 2018 Disclosures Neither I nor
Is Meniscectomy such a bad thing compared to meniscal repair?
 Is Meniscectomy such a bad thing compared to meniscal repair? Jack M. Bert, MD Adjunct Clinical Professor University of Minnesota Minnesota Bone & Joint Specialists, Ltd St. Paul, Minnesota Disclosures
Is Meniscectomy such a bad thing compared to meniscal repair? Jack M. Bert, MD Adjunct Clinical Professor University of Minnesota Minnesota Bone & Joint Specialists, Ltd St. Paul, Minnesota Disclosures
Cartilage Repair Options
 Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Osteochondral regeneration. Getting to the core of the problem.
 Osteochondral regeneration. Getting to the core of the problem. TM TM Bio-mimetic, biointegratable and resorbable Flexible and easy to shape Straightforward one-step procedure Promotes a guided osteo-chondral
Osteochondral regeneration. Getting to the core of the problem. TM TM Bio-mimetic, biointegratable and resorbable Flexible and easy to shape Straightforward one-step procedure Promotes a guided osteo-chondral
PATIENT GUIDE TO CARTILAGE INJURIES
 Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Rehab Considerations: Meniscus
 Rehab Considerations: Meniscus Steve Cox, PT, DPT Department of Orthopaedics School of Medicine University of Texas Health Science Center at San Antonio 1 -Anatomy/ Function/ Injuries -Treatment Options
Rehab Considerations: Meniscus Steve Cox, PT, DPT Department of Orthopaedics School of Medicine University of Texas Health Science Center at San Antonio 1 -Anatomy/ Function/ Injuries -Treatment Options
Technique Guide. *smith&nephew N8TIVE ACL Anatomic ACL Reconstruction System
 Technique Guide *smith&nephew N8TIVE ACL Anatomic ACL Reconstruction System N8TIVE ACL System The N8TIVE ACL Anatomic Reconstruction System provides a novel and simple approach to ACL repair. The N8TIVE
Technique Guide *smith&nephew N8TIVE ACL Anatomic ACL Reconstruction System N8TIVE ACL System The N8TIVE ACL Anatomic Reconstruction System provides a novel and simple approach to ACL repair. The N8TIVE
What Is The Optimal Penetration Depth For "All-Inside" Meniscal Repairs?
 What Is The Optimal Penetration Depth For "All-Inside" Meniscal Repairs? Jeffrey Lue 1, Hugh Jones 2, Jesal Parekh 2, Philip C. Noble 2,3, Patrick McCulloch 1. 1 Methodist Center for Sports Medicine, Houston
What Is The Optimal Penetration Depth For "All-Inside" Meniscal Repairs? Jeffrey Lue 1, Hugh Jones 2, Jesal Parekh 2, Philip C. Noble 2,3, Patrick McCulloch 1. 1 Methodist Center for Sports Medicine, Houston
Resurfacing Patellar Preparation
 Surgical Technique Resurfacing Patellar Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Resurfacing Patellar preparation Contents Introduction...2 Instrument assembly...3 Resurfacing
Surgical Technique Resurfacing Patellar Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Resurfacing Patellar preparation Contents Introduction...2 Instrument assembly...3 Resurfacing
HOW DO WE DIAGNOSE LAMENESS IN YOUR HORSE?
 HOW DO WE DIAGNOSE LAMENESS IN YOUR HORSE? To help horse owners better understand the tools we routinely use at VetweRx to evaluate their horse s soundness, the following section of this website reviews
HOW DO WE DIAGNOSE LAMENESS IN YOUR HORSE? To help horse owners better understand the tools we routinely use at VetweRx to evaluate their horse s soundness, the following section of this website reviews
A Patient s Guide to Meniscal Surgery. William T. Grant, MD
 A Patient s Guide to Meniscal Surgery Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh, PA-C pride themselves
A Patient s Guide to Meniscal Surgery Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh, PA-C pride themselves
Shaw-Ruey Lyu, M.D., Ph.D., and Chia-Chen Hsu, M.D.
 Medial Plicae and Degeneration of the Medial Femoral Condyle Shaw-Ruey Lyu, M.D., Ph.D., and Chia-Chen Hsu, M.D. Purpose: The purpose of this study was to evaluate and analyze the chronological changes
Medial Plicae and Degeneration of the Medial Femoral Condyle Shaw-Ruey Lyu, M.D., Ph.D., and Chia-Chen Hsu, M.D. Purpose: The purpose of this study was to evaluate and analyze the chronological changes
Rehabilitation Guidelines for Meniscal Repair
 Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
H.P. Teng, Y.J. Chou, L.C. Lin, and C.Y. Wong Under general or spinal anesthesia, the knee was flexed gently. In the cases of limited ROM, gentle and
 THE BENEFIT OF ARTHROSCOPY FOR SYMPTOMATIC TOTAL KNEE ARTHROPLASTY Hsiu-Peng Teng, Yi-Jiun Chou, Li-Chun Lin, and Chi-Yin Wong Department of Orthopedic Surgery, Kaohsiung Veterans General Hospital, Kaohsiung,
THE BENEFIT OF ARTHROSCOPY FOR SYMPTOMATIC TOTAL KNEE ARTHROPLASTY Hsiu-Peng Teng, Yi-Jiun Chou, Li-Chun Lin, and Chi-Yin Wong Department of Orthopedic Surgery, Kaohsiung Veterans General Hospital, Kaohsiung,
Meniscus Problems - Torn Meniscus Repair
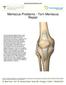 Meniscus Problems - Torn Meniscus Repair The two crescent-shaped menisci in each knee absorb shock, disperse weight, and reduce friction when the knee moves. Activities such as walking or jumping transfer
Meniscus Problems - Torn Meniscus Repair The two crescent-shaped menisci in each knee absorb shock, disperse weight, and reduce friction when the knee moves. Activities such as walking or jumping transfer
Histologic change of cartilage layer of osteochondritis dissecans before and after fixation in the knee
 1 Histologic change of cartilage layer of osteochondritis dissecans before and after fixation in the knee Mitsuo Ochi, M.D. PhD Professor and chairman Department of Orthopaedic Surgery Graduate School
1 Histologic change of cartilage layer of osteochondritis dissecans before and after fixation in the knee Mitsuo Ochi, M.D. PhD Professor and chairman Department of Orthopaedic Surgery Graduate School
Osteochondritis Dissecans
 Osteochondritis Dissecans Introduction Osteochondritis dissecans (OCD) is a problem that affects the knee, mostly at the end of the big bone of the thigh (the femur). A joint surface damaged by OCD doesn't
Osteochondritis Dissecans Introduction Osteochondritis dissecans (OCD) is a problem that affects the knee, mostly at the end of the big bone of the thigh (the femur). A joint surface damaged by OCD doesn't
Classification of Acetabular Cartilage Lesions. Claudio Mella, MD
 Classification of Acetabular Cartilage Lesions Claudio Mella, MD Acetabular cartilage lesions are frequently found during hip arthroscopy. The arthroscopic view offers an exceptional perspective to assess
Classification of Acetabular Cartilage Lesions Claudio Mella, MD Acetabular cartilage lesions are frequently found during hip arthroscopy. The arthroscopic view offers an exceptional perspective to assess
Rehabilitation Guidelines Following Microfracture Procedures to the Knee
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines Following Microfracture Procedures to the Knee There are two types of cartilage in the knee: meniscus and articular. One type of cartilage is the
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines Following Microfracture Procedures to the Knee There are two types of cartilage in the knee: meniscus and articular. One type of cartilage is the
Histopomorphic Evaluation of Radiofrequency Mediated Débridement Chondroplasty
 The Open Orthopaedics Journal, 2010, 4, 211-220 211 Open Access Histopomorphic Evaluation of Radiofrequency Mediated Débridement Chondroplasty Kumkum Ganguly 1, Ian D. McRury 2, Peter M. Goodwin 3, Roy
The Open Orthopaedics Journal, 2010, 4, 211-220 211 Open Access Histopomorphic Evaluation of Radiofrequency Mediated Débridement Chondroplasty Kumkum Ganguly 1, Ian D. McRury 2, Peter M. Goodwin 3, Roy
JMSCR Vol 05 Issue 01 Page January
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.28 Diagnostic Accuracy of Magnetic Resonance
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.28 Diagnostic Accuracy of Magnetic Resonance
Soft tissue biomechanics
 Soft tissue biomechanics Caroline Öhman Pula, 22/06-08 TABLE OF CONTENTS Introduction to soft tissues Tendon and ligaments Introduction Composition Function and structure In vitro testing Stress-strain
Soft tissue biomechanics Caroline Öhman Pula, 22/06-08 TABLE OF CONTENTS Introduction to soft tissues Tendon and ligaments Introduction Composition Function and structure In vitro testing Stress-strain
A Patient s Guide to Osteochondritis Dissecans of the Knee
 A Patient s Guide to Osteochondritis Dissecans of the Knee 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide to Osteochondritis Dissecans of the Knee 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from
Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells,
 What is a Stem Cell? Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells, and so on. These cells can replicate more of their own kind of cell, but they cannot
What is a Stem Cell? Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells, and so on. These cells can replicate more of their own kind of cell, but they cannot
Evaluation & Treatment of the Injured Athlete Autograft OATS versus Osteochondral Allograft Technique: Indications, Problems, Outcomes
 Evaluation & Treatment of the Injured Athlete Autograft OATS versus Osteochondral Allograft Technique: Indications, Problems, Outcomes C H R I S T I A N L AT T E R M A N N C H I E F O F S P O R T S M E
Evaluation & Treatment of the Injured Athlete Autograft OATS versus Osteochondral Allograft Technique: Indications, Problems, Outcomes C H R I S T I A N L AT T E R M A N N C H I E F O F S P O R T S M E
Surgical Technique. Poly UHMWPE. Bio Hyaluronic Acid. Advancing Materials. Advancing Outcomes.
 Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical 2 Assessment 1. Proper implant sizing is determined by placing the appropriate sized trial over the
Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical 2 Assessment 1. Proper implant sizing is determined by placing the appropriate sized trial over the
CASE REPORT GIANT OSTEOCHONDRAL LOOSE BODY OF THE KNEE JOINT
 Journal of Musculoskeletal Research, Vol. 4, No. 2 (2000) 145 149 World Scientific Publishing Company ORIGINAL CASE REPORT ARTICLES GIANT OSTEOCHONDRAL LOOSE BODY OF THE KNEE JOINT Mustafa Yel *,, Mustafa
Journal of Musculoskeletal Research, Vol. 4, No. 2 (2000) 145 149 World Scientific Publishing Company ORIGINAL CASE REPORT ARTICLES GIANT OSTEOCHONDRAL LOOSE BODY OF THE KNEE JOINT Mustafa Yel *,, Mustafa
Radiofrequency energy (RFE) has gained popularity
 Effect of Bipolar Radiofrequency Energy on Human Articular Cartilage: Comparison of Confocal Laser Microscopy and Light Microscopy Yan Lu, M.D., Ryland B. Edwards III, D.V.M., M.S., Vicki L. Kalscheur,
Effect of Bipolar Radiofrequency Energy on Human Articular Cartilage: Comparison of Confocal Laser Microscopy and Light Microscopy Yan Lu, M.D., Ryland B. Edwards III, D.V.M., M.S., Vicki L. Kalscheur,
Original Report. The Reverse Segond Fracture: Association with a Tear of the Posterior Cruciate Ligament and Medial Meniscus
 Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries. Cartilage Surgery. The Knee.
 Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Cartilage Surgery The Knee CARTILAGE INJURY Treatment of cartilage injury remains one of the most significant challenges
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Cartilage Surgery The Knee CARTILAGE INJURY Treatment of cartilage injury remains one of the most significant challenges
Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2, Patrick Smith, M.D. 2, and Larry S. Matthews, M.D. 2
 Skeletal Radiol (1986) 15:27-31 Skeletal Radiology Computed tomography and plain radiography in experimental fracture healing Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2,
Skeletal Radiol (1986) 15:27-31 Skeletal Radiology Computed tomography and plain radiography in experimental fracture healing Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2,
CARTILAGE REPAIR INTRODUCTION. M. BERRUTO and G.M. PERETTI 1,2. Received January 6, Accepted January 8, 2013
 CARTILAGE REPAIR INTRODUCTION M. BERRUTO and G.M. PERETTI 1,2 Gaetano Pini Orthopedic Institute, Milan; 1 Department of Biomedical Sciences for Health, University of Milan, 2 IRCCS Galeazzi Orthopedic
CARTILAGE REPAIR INTRODUCTION M. BERRUTO and G.M. PERETTI 1,2 Gaetano Pini Orthopedic Institute, Milan; 1 Department of Biomedical Sciences for Health, University of Milan, 2 IRCCS Galeazzi Orthopedic
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries
 What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
Retrospective study of cell-free collagen matrix for cartilage repair
 SCIENCE / RESEARCH Survey / Review 515 Andreas Breil-Wirth 1, Lars von Engelhardt 1,2, Stefan Lobner 1, Jörg Jerosch 1 Retrospective study of cell-free collagen matrix for cartilage repair n Study objective:
SCIENCE / RESEARCH Survey / Review 515 Andreas Breil-Wirth 1, Lars von Engelhardt 1,2, Stefan Lobner 1, Jörg Jerosch 1 Retrospective study of cell-free collagen matrix for cartilage repair n Study objective:
SIMITRI STABLE IN STRIDE SURGICAL PROCEDURE
 Copyright 2016 NGD. All rights reserved Neil Embleton, B.Sc., DVM and Veronica Barkowski, DVM Helivet Mobile Surgical Services, Sundre, AB, Canada July 2016 SIMITRI STABLE IN STRIDE SURGICAL PROCEDURE
Copyright 2016 NGD. All rights reserved Neil Embleton, B.Sc., DVM and Veronica Barkowski, DVM Helivet Mobile Surgical Services, Sundre, AB, Canada July 2016 SIMITRI STABLE IN STRIDE SURGICAL PROCEDURE
The Effect of Lateral Meniscal Root Injuries on the Stability of the Anterior Cruciate Ligament Deficient Knee
 The Effect of Lateral Meniscal Root Injuries on the Stability of the Anterior Cruciate Ligament Deficient Knee Charles Vega 1, Jebran Haddad 1, Jerry Alexander 2, Jonathan Gold 2, Theodore Shybut 1, Philip
The Effect of Lateral Meniscal Root Injuries on the Stability of the Anterior Cruciate Ligament Deficient Knee Charles Vega 1, Jebran Haddad 1, Jerry Alexander 2, Jonathan Gold 2, Theodore Shybut 1, Philip
FAI syndrome with or without labral tear.
 Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
New Evidence Suggests that Work Related Knee Pain with Degenerative Complications May Not Require Surgery
 4 th Quarter 2017 New Evidence Suggests that Work Related Knee Pain with Degenerative Complications May Not Require Surgery By: Michael Erdil MD, FACOEM Introduction It is estimated there are approximately
4 th Quarter 2017 New Evidence Suggests that Work Related Knee Pain with Degenerative Complications May Not Require Surgery By: Michael Erdil MD, FACOEM Introduction It is estimated there are approximately
Arthroscopy / MRI Correlation Conference. Department of Radiology, Section of MSK Imaging Department of Orthopedic Surgery 7/19/16
 Arthroscopy / MRI Correlation Conference Department of Radiology, Section of MSK Imaging Department of Orthopedic Surgery 7/19/16 Case 1: 29 YOM with recurrent shoulder dislocations Glenoid Axial T1FS
Arthroscopy / MRI Correlation Conference Department of Radiology, Section of MSK Imaging Department of Orthopedic Surgery 7/19/16 Case 1: 29 YOM with recurrent shoulder dislocations Glenoid Axial T1FS
Discoid lateral meniscus in children and adolescents: a histological study
 Bisicchia et al. Journal of Experimental Orthopaedics (2018) 5:39 https://doi.org/10.1186/s40634-018-0153-5 Journal of Experimental Orthopaedics RESEARCH Open Access Discoid lateral meniscus in children
Bisicchia et al. Journal of Experimental Orthopaedics (2018) 5:39 https://doi.org/10.1186/s40634-018-0153-5 Journal of Experimental Orthopaedics RESEARCH Open Access Discoid lateral meniscus in children
Tibial & Femoral Opening Wedge Osteotomy System. Surgical Technique
 Tibial & Femoral Opening Wedge Osteotomy System Surgical Technique Opening Wedge Osteotomy Tibial & Femoral Opening Wedge Osteotomy 2 Prior to the osteotomy, a diagnostic arthroscopy is performed to verify
Tibial & Femoral Opening Wedge Osteotomy System Surgical Technique Opening Wedge Osteotomy Tibial & Femoral Opening Wedge Osteotomy 2 Prior to the osteotomy, a diagnostic arthroscopy is performed to verify
Knee Cartilage Transplants
 Knee Cartilage Transplants Date of Origin: 3/2005 Last Review Date: 8/23/2017 Effective Date: 8/23/2017 Dates Reviewed: Developed By: Medical Necessity Criteria Committee I. Description Allograft transplants
Knee Cartilage Transplants Date of Origin: 3/2005 Last Review Date: 8/23/2017 Effective Date: 8/23/2017 Dates Reviewed: Developed By: Medical Necessity Criteria Committee I. Description Allograft transplants
Nanomechanical Symptoms in Cartilage Precede Histological Osteoarthritis Signs after the Destabilization of Medial Meniscus in Mice
 Nanomechanical Symptoms in Cartilage Precede Histological Osteoarthritis Signs after the Destabilization of Medial Meniscus in Mice Basak Doyran 1, Wei Tong 2, Qing Li 1, Haoruo Jia 2, Xianrong Zhang 3,
Nanomechanical Symptoms in Cartilage Precede Histological Osteoarthritis Signs after the Destabilization of Medial Meniscus in Mice Basak Doyran 1, Wei Tong 2, Qing Li 1, Haoruo Jia 2, Xianrong Zhang 3,
ARTHROSCOPY INSTRUMENTS- CARE,HANDLING & STERILIZATION. Dr.SHEKHAR SRIVASTAV
 ARTHROSCOPY INSTRUMENTS- CARE,HANDLING & STERILIZATION Dr.SHEKHAR SRIVASTAV Knee & Shoulder Arthroscopy Delhi Institute of Trauma And Orthopedics SANT PARMANAND HOSPITAL,DELHI BASIC ARTHROSCOPY SET-UP
ARTHROSCOPY INSTRUMENTS- CARE,HANDLING & STERILIZATION Dr.SHEKHAR SRIVASTAV Knee & Shoulder Arthroscopy Delhi Institute of Trauma And Orthopedics SANT PARMANAND HOSPITAL,DELHI BASIC ARTHROSCOPY SET-UP
Ferromagnetic Dissection: A Comparison to Electrosurgery
 Ferromagnetic Dissection: A Comparison to Electrosurgery Written by Kim Manwaring, M.D., Chief Medical Officer, Domain Surgical, Inc. Compared to electrosurgery, ferromagnetic dissection achieves superior
Ferromagnetic Dissection: A Comparison to Electrosurgery Written by Kim Manwaring, M.D., Chief Medical Officer, Domain Surgical, Inc. Compared to electrosurgery, ferromagnetic dissection achieves superior
