Practical Management of Lisfranc injuries in Athletes
|
|
|
- Lionel Merritt
- 5 years ago
- Views:
Transcription
1 Practical Management of Lisfranc injuries in Athletes Christian Lattermann, MD * ; Jordan L Goldstein, MD* ; Dane K. Wukich # ; Simon Lee, MD* and Bernard R. Bach Jr., MD 1* *Department of Orthopedic Surgery Rush University Medical Center 1725 W. Harrison Street, Suite 1063; Chicago IL ) Director of Sports Medicine Fellow, Sports Medicine Resident (PGY-3) # Chief of Foot and Ankle Surgery Department of Orthopaedic Surgery University of Pittsburgh Medical Center 1010 Kaufmann Bldg, 3471 Fifth Avenue Pittsburgh PA ADDRESS FOR REPRINTS/CORRESPONDENCE: Bernard R. Bach, Jr., M.D. Division of Sports Medicine Rush University Medical Center 1725 W. Harrison St., Suite 1063 Chicago, IL brbachmd@comcast.net Phone: Fax: Running Title: Practical Management of Lisfranc Injuries
2 Abstract: Foot injuries are common in athletes. Injuries to the midfoot and particularly the Lisfranc joint are less common but have a high risk of ending the athletes season or even career. Lisfranc injuries can be difficult to diagnose and often lead to a disastrous outcome when missed. Team physicians and primary care physicians who see athletic injuries should be vigilant in order not to miss these injuries. Familiarity with the subtle clinical signs of a Lisfranc injury and knowledge of the basic treatment algorithm will help the clinician to better treat these injuries successfully.
3 Introduction: Foot and ankle injuries are among the most common injuries in athletes. Approximately 25% of all sports related injuries are to the foot and ankle. Garrick and Requa showed that 16% of all sports related injuries involve the foot (1). Although less frequent than other athletic injuries, midfoot sprains or Lisfranc joint injuries can be career ending injuries and therefore need to be taken very seriously by the athlete, the trainers, and physicians. The on field diagnosis of Lisfranc injuries is difficult. The athlete usually reports a mechanism of injury similar to an ankle sprain and will often attempt to walk it off. It is not uncommon that the athletic trainer or team physician is not initially involved in the care of this type of injury because the athlete underestimates the severity of the injury and attempts to let the injury resolve with time. The goal of this review is to educate athletic trainers, team physicians, and primary care physicians who see athletes to better recognize and evaluate for Lisfranc joint injuries. Injury mechanism: Mechanisms leading to a Lisfranc injury can roughly be divided into high and low energy injuries. High velocity Lisfranc injuries are commonly seen in high speed motor vehicle accidents. The foot is usually planted on the brake pedal or the floor of the motor vehicle in order to break the forward motion after impact. Most commonly the foot gets forced into hyper plantar flexion with either a valgus or varus component. The energy leading to these injuries usually disrupts the osteo-ligamentous restraints and leads to a dislocation of the Lisfranc joint. This results in gross instability and often causes neurovascular
4 damage. These injuries have a high risk for compartment syndrome due to soft tissue swelling and disruption of the dorsalis pedis artery. While these injuries are commonly seen in the trauma bay of level one and level two trauma centers, they present distinctly differently from the more subtle instability injuries of the Lisfranc joint that occur in athletes after low velocity injuries. Low velocity injuries to the Lisfranc joint typical follow one of two mechanisms. The first is forced hyperplantarflexion of the midfoot that occurs in athletes utilizing foot straps such as surfers, windsurfers, and equestrians. Typically the foot gets trapped in the foot strap and the body falls straight backwards leading to the hyperplantarflexion of the foot. This mechanism is in fact the classic mechanism of Lisfranc injuries as described by Jaques Lisfranc after observing cavalry men fall off their horse with their foot trapped in the foot strap dragging the rider alongside the horse resulting in a slow hyper plantar flexion of the foot. A second mechanism has been described by Shapiro who had looked at football players, particularly linemen (2). He noticed a typical mechanism of injury occuring with the lineman s stance during a block with the foot plantar flexed and the metatarsophalangeal joints maximally dorsiflexed while a force is directed directly down onto the heel (i.e. by a falling player, tackle from behind) which leads to a hyperplantarflexion in the Lisfranc joint and subsequent injury. Several other sports specific mechanism that are variations of the above described mechanisms have been reported such as sliding into fixed bases (baseball) or landing on a fully plantarflexed foot (parachuting).
5 Diagnosis: Whereas these injuries can clinically be easily identified in high velocity type mechanisms due to excessive swelling, ecchymosis, severe pain and midfoot instability, the low velocity type injuries may be very subtle and hard to detect. It is imperative that any athlete who complains about a sprained ankle or foot needs to be thoroughly examined. Distracting injuries such as ankle injuries or fractures may cause the examiner to miss the often more subtle midfoot injuries. The foot must be palpated. Of particular importance are bony landmarks such as the navicular, medial cuneiform, base of the first and fifth metatarsal as well as the space between first and second metatarsal. Any point tenderness in any of these areas is a sign of injury to the midfoot and a Lisfranc injury should be considered. This often times may be difficult due to acute swelling, and as a result may need repeat examination after the swelling improves. Furthermore, the stability of the Lisfranc row can be assessed by passive pro- and supination of the forefoot. Significant pain with this maneuver at the base of the first metatarsal is suspicious for a Lisfranc injury. Another way to test this is to perform a passive dorsiflexion and abduction of the forefoot. This puts strain on the medial column and serves as an apprehension sign if positive. Another delayed clinical sign is a subtle ecchymosis on the plantar aspect of the midfoot. Apart from these subtle signs there may also be gross instability, crepitus or deformity present- even in low velocity type injuries. It is imperative, particularly for the initial evaluation, that both feet are examined since both feet could be involved in the mechanism (windsurfing, parachuting). In addition a full neurovascular exam should be performed of the foot since these injuries can lead to neurovascular injuries which further complicate the outcome and prognosis.
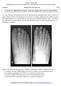
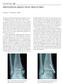
6 Imaging: Standard imaging of the foot should always be done with a minimum of three views of the foot. This includes an A/P, 30 degree oblique and lateral of the foot, weight bearing if tolerated will help to accentuate the deformities. These standard views need to be evaluated for several radiographic tell tale signs. Any fracture of the base of the first three metatarsals is very suspicious for an injury at the Lisfranc joint. Small avulsions at the medial base of the first or second metatarsal suggest disruption of the tarso-metatarsal ligaments (base of first) or the Lisfranc ligament (base of second). In addition to a thorough screening for fresh fractures or avulsions, indirect signs of a Lisfranc-instability should be looked for. The medial cortex of the second metatarsal should line up perfectly with the medial border of the 2 nd cuneiform on an A/P x-ray of the foot. Any displacement of more than 2 mm between the base of the first and second metatarsal in an A/P radiograph of the foot should raise suspicion of a Lisfranc injury. Additionally, the medial cortex of the fourth metatarsal should line up perfectly with the medial border of the lateral cuneiform in the 30 degree oblique x-ray of the foot (Fig 1). Finally, on the non-weight bearing lateral x-ray of the foot there should be no interruption of the dorsal cortical line of the first metatarsal to the medial cuneiform, any displacement is pathologic (Fig 2). Non-weight bearing x-rays of the foot may only raise the suspicion of the examiner and need to be correlated with the clinical findings. If there is any significant tenderness at any of the bony landmarks and non-weigth bearing films are negative it is imperative to obtain a weight bearing A/P and weight bearing lateral. Weight bearing films will usually reveal subtle instabilities not seen on non-weight
7 bearing films. While it is not always practical to obtain weight bearing films of the foot in the initial ER setting, it remains imperative that weight bearing films are performed early on if there is a clinical suspicion with negative non-weight bearing films. The weight bearing film should be the gold standard if the x-rays are obtained in an office setting (Fig 3). If there remains any doubt, either stress views or an MRI can be obtained. The primary utilization of MRI or CT may be helpful in special cases but is not necessary to make the diagnosis. For those patients that present several weeks or months after the injury, a bone scan provides valuable information when the Lisfranc joint shows increased uptake. Increased uptake particularly in the first and second tmt joint is highly suggestive of a Lisfranc injury. Classification: Several classification systems have been described for Lisfranc injuries (3, 4). While most of these classification systems are helpful for the radiographic description of high energy injuries with massive displacement they do not help in the diagnosis or outcome assessment of subtle Lisfranc instabilities as they occur in athletes. Nunley and Vertulla introduced a useful classification for subtle Lisfranc injuries with minimal or no displacement on weight bearing films (5). These injuries are the more likely scenario that a primary care physician or orthopaedic surgeon is going to encounter in an athlete. Nunley utilized three aspects of the patients exam and radiographic findings. He included the ability to weight bear, local point tenderness over the Lisfranc ligament, and medial first TMT joint space as well as the radiographic appearance of the Lisfranc joint. He established three different stages of Lisfranc instability. Patients with a stage one
8 injury were able to weight bear but could not return to play. On exam, they were locally point tender over the medial aspect of the first TMT joint but radiographically, did not show any diastasis of more than two mm between the first and second MT on the A/P weight bearing x-ray of the foot as well as no collapse of the arch as measured by the cuneiform-5 th metatarsal vertical distance. It should be noted, however, that these patients may have a positive bone scan or MRI. Patients with stage two injuries had similar physical findings as patients in group 1 but showed a two to five mm diastasis between the first and second MT on the A/P weight bearing radiograph of the foot. Notably, there was no collapse of the arch in the weight bearing lateral radiograph. Patients with a stage three injury presented with an additional collapse of the longitudinal arch as documented in a lateral radiograph of the foot. Initial Treatment: The initial treatment of any foot injury is elevation and icing. Once the initial on-field treatment has been provided the patient needs to be thoroughly evaluated in an ER or office setting. If the athlete is unable to ambulate without pain she / he needs to remain non-weight bearing until she / he has been evaluated and severe injuries to the foot and ankle have been excluded. Particularly after high energy trauma the foot can show massive swelling that should alert the treating physician or athletic trainer to a possible compartment syndrome. Diagnosis of a foot compartment syndrome is difficult and should be left to an expert. The usual clinical tell tale sign of a compartment syndrome: pain with passive stretch, is not accurate. Fullness of compartments is difficult to assess due to the
9 inaccessibility of the actual muscular compartments. If neurovascular symptoms are described, the compartment syndrome is already established. The evaluating physician should, therefore, be very suspicious if the patient complains of pain out of proportion to physical examination. Pressure measurements have been advocated. Controversy exists regarding pressure measurements in the foot since there is no reliable data concerning baseline pressures in foot compartments. Sequentially inflatable foot pumps used to decrease swelling should be avoided during the initial evaluation period in order to not increase compartment pressures. Non-operative treatment of Lisfranc injuries: Once the diagnosis has been established, the injury grade should be determined. A stage one Lisfranc injury that is functionally stable can be treated conservatively in a well molded non-weight bearing fiberglass cast for 6 weeks. If the patient is pain free to palpation at cast removal a custom molded orthosis should be worn and the patient can gradually return to his sports specific training. If the patient is still point tender then a custom molded weight bearing ankle foot orthosis should be worn for an additional 4 weeks (5). At this point it should be mentioned that any Nunley stage two or three Lisfranc sprain will lead to instability if treated conservatively and non-operative treatment is not recommended. Operative treatment of Lisfranc injuries: Patients with any displacement at the Lisfranc joint (stages 2 or higher) should undergo operative treatment. Intra-operatively, if the Lisfranc joint can be anatomically reduced
10 under fluoroscopy it may be amenable to a percutaneous placement of a screw. If a perfect reduction cannot be obtained an open reduction and internal fixation should be performed in order to restore the Lisfranc joint to a functional unit. The Lisfranc joint can be reduced with a large tenaculum or a towel clip either percutaneously or open. Depending on the severity of the sub / dislocation of the Lisfranc joint, two or three screws can be utilized to stabilize the medial cuneiform against the base of the second metatarsal. If the injury also involves the 4 th and 5 th metatarsals then additional wires need to be placed through the base of the 4 th and 5 th metatarsal into the cuboid and middle cuneiform. Postoperative treatment usually involves a non-weight bearing cast or boot for a minimum of 8 weeks. Between 8 and 12 weeks partial weight bearing is allowed. After 3 months the patient progresses to full weight bearing and should be placed in a custom molded orthosis. Hardware removal may be required in athletes. The recommendation is to remove the hardware at weeks in athletes less than 200 pounds and after 24 weeks in athletes over 200 pounds. In non-athletes the screws may be left in place, additional wires in the 4 th and 5 th metatarsal need to be removed between 8and 12 weeks post-operatively (5). Outcome of Lisfranc injuries in Athletes: Literature on the outcome of Lisfranc injuries in athletes is sparse. Three original studies have been conducted in athletes. One study conducted by Meyer et al. (6) reported about 23 patients who were treated conservatively with good overall outcomes. In his series there were only three patients that radiographically had a diastasis of more than 2 mm
11 between the first and second metatarsal. Interestingly two of these three were initially not diagnosed. These three patients had a prolonged recovery with one of the three continuing to have significant midfoot pain with activity. Shapiro reported about a series of nine athletes with a diastasis between 3 and 5 mm who were treated conservatively (2). The one athlete who had a diastasis of 5 mm was treated operatively and did very well, while the other 8 with a diastatsis of 3mm were treated conservatively with excellent outcome. Nunley, however, reported on about 15 patients, out of which two with even minimal diastasis of 3mm did not do well with conservative management (5). Curtis et al. (7) and Davis et al (8) also report failures and inferior results of non-operative management in athletes with minimal Lisfranc instability. The consequence of missed diagnosis can lead to early arthritis, secondary deformity, arch flattening and chronic pain (4,7,8). Conclusion: Lisfranc injuries are uncommon injuries in athletes that can, however, have grave consequences for the athletes career. A true midfoot sprain involving the Lisfranc joint presenting without any sign of instability in weight bearing x-rays should be regarded as a sprain and should be treated conservatively as outlined above (Table 1). Any instability detected in weight bearing films should be considered for surgical reduction and stabilization in order to avoid prolonged unsuccessful attempts of conservative treatment and long term sequelae. The athlete should also be informed that this injury will sideline them a minimum of 12 to 16 weeks with conservative or operative treatment. Finally it should be stressed that any diagnosis of a Lisfranc sprain that is treated conservatively
12 has to be scrutinized with weight bearing x-rays in order to rule out any subtle instability (Table 1). References: 1. Garrick JG, Requa RK: The epidemiology of foot and ankle injuries in sports. Clin Sports Med 1988; 7: Shapiro MS, Wascher DC, FInerman GA: Rupture of Lisfranc s ligament in athletes. Am J Sports Med 1994; 22(5): QuenuE, Kuss G: Etude sur les luxations du metatarse. Rev Chir Paris 1909; 39: Myerson MS, Fisher RT, Burgess AR, Kenzora JE: Fracture dislocations of the tarsometatarsal joints: end results correlated with pathology and treatment. Foot Ankle 1986;6(5): Nunley JA, Vertullo CJ: Classification, investigation, and management of midfoot sprains: Lisfranc injuries in the athlete. AM J Sports Med 2002; 30(6): Meyer SA, Callaghan JJ, Albright JP, Cowley ET, powell JW: Midfoot sprains in collegiate football players. Am J Sports Med 1994; 22(3): Curtis MJ, Myerson M, Szura B: Tarsometatarsal joint injuires in the athlete. Am J Sports Med 1993; 21: Davies MS, Saxby TS: Intercuneiform instability and the gap sign. Foot Ankle Int 1999; 20:
13 Figure Legend: Figure 1: A/P and oblique non-weight bearing x-ray. The latter A marks the two tangential lines on the first MCP joint. The letter B marks the 2 nd metatarsal cortical line meeting the medial cortex of the middle cuneiform. The circle marks the keystone that is built by the 2 nd metatarsal head as it articulates with the medial and middle cuneiform. The letter C delineates the tangential along the 4 th metatarsal on the oblique radiograph of the foot.
14 Figure 2: Lateral non-weight bearing radiograph of a right foot. The two lines are the tangentials that define the alignment of the first MCP joint. Any step off along this tangential signifies an instability in the first MCP.
15 Fig 3: Subtle sign of a Lisfranc injury. The left image is a non-weight bearing x-ray showing a minimal displacement (A) that can easily be missed. The right film is a weight bearing film showing a wide gap (B)
16 Table 1: Flow Chart for the Management of Lisfranc Injuries in Athletes
Closed Reduction and Internal Fixation of Lisfranc Fracture Dislocations
 Closed Reduction and Internal Fixation of Lisfranc Fracture Dislocations Anish R. Kadakia, Mark S. Myerson, and Milap Patel Contents Mechanism of Injury... 2 Radiographic Evaluation... 3 Classification...
Closed Reduction and Internal Fixation of Lisfranc Fracture Dislocations Anish R. Kadakia, Mark S. Myerson, and Milap Patel Contents Mechanism of Injury... 2 Radiographic Evaluation... 3 Classification...
Complexities surrounding Lisfranc injuries
 Complexities surrounding Lisfranc injuries Lisfranc injuries are commonly associated with sporting injuries and are easily diagnosed with severe midfoot pain, swelling, deformity and inability to bear
Complexities surrounding Lisfranc injuries Lisfranc injuries are commonly associated with sporting injuries and are easily diagnosed with severe midfoot pain, swelling, deformity and inability to bear
MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium
 MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium Introduction Increasing sports injuries RTA and traumatic injuries
MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium Introduction Increasing sports injuries RTA and traumatic injuries
Hany El-Rashidy and Anand Vora
 Chapter 194 Lisfranc Injuries Chapter 194 Lisfranc Injuries Hany El-Rashidy and Anand Vora 8 ICD-9 CODE 838.03 Lisfranc (Tarsometatarsal) Fracture-Dislocation Key Concepts The Lisfranc joint represents
Chapter 194 Lisfranc Injuries Chapter 194 Lisfranc Injuries Hany El-Rashidy and Anand Vora 8 ICD-9 CODE 838.03 Lisfranc (Tarsometatarsal) Fracture-Dislocation Key Concepts The Lisfranc joint represents
Midfoot - Reduction & Fixation - ORIF - screw fixation - AO Surgery Reference. ORIF - screw fixation
 Midfoot - TMT (Lisfranc) injury 1. Diagnosis ORIF - screw fixation Authors Mechanism of the injury Tarso-metatarsal (Lisfranc) injuries may be caused by direct or indirect forces. Direct forces include
Midfoot - TMT (Lisfranc) injury 1. Diagnosis ORIF - screw fixation Authors Mechanism of the injury Tarso-metatarsal (Lisfranc) injuries may be caused by direct or indirect forces. Direct forces include
Section 3: Foot Subluxations and Dislocations
 Section 3: Foot Subluxations and Dislocations Case Study F: Lisfranc s Midfoot Dislocation Clinical History: J.K. a 28 year old female presents complaining of a painful right foot. She sustained an acute
Section 3: Foot Subluxations and Dislocations Case Study F: Lisfranc s Midfoot Dislocation Clinical History: J.K. a 28 year old female presents complaining of a painful right foot. She sustained an acute
LISFRANC FRACTURE-DISLOCATION
 LISFRANC FRACTURE-DISLOCATION Napoleon at Mont St. Bernard, Jacques-Louis David, 1800, Oil on Canvas, Musee du Louvre, Paris. This is Jacques-Louis David s immortal depiction of a young Napoleon Bonaparte,
LISFRANC FRACTURE-DISLOCATION Napoleon at Mont St. Bernard, Jacques-Louis David, 1800, Oil on Canvas, Musee du Louvre, Paris. This is Jacques-Louis David s immortal depiction of a young Napoleon Bonaparte,
Lisfranc and Midfoot Fracture
 Lisfranc and Midfoot Fracture AO Advanced Principles of Fracture Management Middelfart, 11.-14. april 2016 Overlæge Marianne Vestergaard Lind Traumesektionen Ortopædkirurgisk Klinik Rigshospitalet What
Lisfranc and Midfoot Fracture AO Advanced Principles of Fracture Management Middelfart, 11.-14. april 2016 Overlæge Marianne Vestergaard Lind Traumesektionen Ortopædkirurgisk Klinik Rigshospitalet What
A Ware Injury in Collegiate Athletics- The Lisfranc Fracture-Dislocation
 Journal of Sport Rehabilitation, 1993, 2, 281-286 O 1993 Human Kinetics Publishers, Inc. A Ware Injury in Collegiate Athletics- The Lisfranc Fracture-Dislocation Keith M. Gorse, Graham Johnstone, and Jennifer
Journal of Sport Rehabilitation, 1993, 2, 281-286 O 1993 Human Kinetics Publishers, Inc. A Ware Injury in Collegiate Athletics- The Lisfranc Fracture-Dislocation Keith M. Gorse, Graham Johnstone, and Jennifer
Lisfranc fracture-dislocations. Disclosures. It s just a foot
 Lisfranc fracture-dislocations Gregory J. Della Rocca, MD, PhD, FACS Associate Professor Co-director, Orthopaedic Trauma Service University of Missouri Disclosures Consultant: Synthes, Bioventus Stock
Lisfranc fracture-dislocations Gregory J. Della Rocca, MD, PhD, FACS Associate Professor Co-director, Orthopaedic Trauma Service University of Missouri Disclosures Consultant: Synthes, Bioventus Stock
American Family Physician
 Page 1 of 12 American Family Physician Return to Previous Page Jul 1, 1998 Table of Contents Lisfranc Injury of the Foot: A Commonly Missed Diagnosis KEVIN E. BURROUGHS, M.D, Moses Cone Family Practice
Page 1 of 12 American Family Physician Return to Previous Page Jul 1, 1998 Table of Contents Lisfranc Injury of the Foot: A Commonly Missed Diagnosis KEVIN E. BURROUGHS, M.D, Moses Cone Family Practice
Open Reduction and Internal Fixation to Repair a Lisfranc Injury: A Case Report
 Case Report imedpub Journals http://www.imedpub.com 2015 Abstract Open Reduction and Internal Fixation to Repair a Lisfranc Injury: A Case Report Background: Lisfranc complex consists of bony and ligamentous
Case Report imedpub Journals http://www.imedpub.com 2015 Abstract Open Reduction and Internal Fixation to Repair a Lisfranc Injury: A Case Report Background: Lisfranc complex consists of bony and ligamentous
Complications of missed or untreated Lisfranc injuries
 Foot Ankle Clin N Am 8 (2003) 61 71 Complications of missed or untreated Lisfranc injuries Terry Philbin, DO a,b, *, Gary Rosenberg, MD c, James J. Sferra, MD d a Orthopedic Foot and Ankle, 6200 Cleveland
Foot Ankle Clin N Am 8 (2003) 61 71 Complications of missed or untreated Lisfranc injuries Terry Philbin, DO a,b, *, Gary Rosenberg, MD c, James J. Sferra, MD d a Orthopedic Foot and Ankle, 6200 Cleveland
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/29/2012 Radiology Quiz of the Week # 105 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/29/2012 Radiology Quiz of the Week # 105 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Tarsometatarsal Joint Injuries Review of Clinical Presentation and Surgical Treatment
 Tarsometatarsal Joint Injuries Review of Clinical Presentation and Surgical Treatment S Y Loh, FRCS (Orth)*, J L Soon, MBBS**, W J Verhoeven, FRCS*** *Department of Orthopedic Surgery, Alexandra Hospital,
Tarsometatarsal Joint Injuries Review of Clinical Presentation and Surgical Treatment S Y Loh, FRCS (Orth)*, J L Soon, MBBS**, W J Verhoeven, FRCS*** *Department of Orthopedic Surgery, Alexandra Hospital,
Injuries to the Lisfranc Joint and its Significance for the Patient
 Cronicon OPEN ACCESS EC ORTHOPAEDICS Case Report Injuries to the Lisfranc Joint and its Significance for the Patient Ekkehard Pietsch* Orthopaedic and General Surgeon, The-Expert-Witness.de, Hamburg, Germany
Cronicon OPEN ACCESS EC ORTHOPAEDICS Case Report Injuries to the Lisfranc Joint and its Significance for the Patient Ekkehard Pietsch* Orthopaedic and General Surgeon, The-Expert-Witness.de, Hamburg, Germany
SOFT TISSUE KNEE INJURIES
 SOFT TISSUE KNEE INJURIES Soft tissue injuries of the knee commonly occur in all sports or in any activity that requires sudden changes in activity or movement. The knee is a complex joint and any injury
SOFT TISSUE KNEE INJURIES Soft tissue injuries of the knee commonly occur in all sports or in any activity that requires sudden changes in activity or movement. The knee is a complex joint and any injury
5 COMMON INJURIES IN THE FOOT & ANKLE
 5 COMMON INJURIES IN THE FOOT & ANKLE MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA MECHANISM OF INJURY HOW DID IT HAPPEN? HIGH ENERGY VS LOW ENERGY DIRECTION OF FORCES INVOLVED LIVING
5 COMMON INJURIES IN THE FOOT & ANKLE MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA MECHANISM OF INJURY HOW DID IT HAPPEN? HIGH ENERGY VS LOW ENERGY DIRECTION OF FORCES INVOLVED LIVING
Foot Injuries. Dr R B Kalia
 Foot Injuries Dr R B Kalia Overview Dramatic impact on the overall health, activity, and emotional status More attention and aggressive management Difficult appendage to study and diagnose. Aim- a stable
Foot Injuries Dr R B Kalia Overview Dramatic impact on the overall health, activity, and emotional status More attention and aggressive management Difficult appendage to study and diagnose. Aim- a stable
Section 4: Tarsal Coalitions
 Case H (Figure 2): PedCat CBCT transverse plane reconstruction of right Lisfranc midfoot dislocation compared to normal left foot. Clinical Relevance of the PedCat Study: The weight bearing CBCT study
Case H (Figure 2): PedCat CBCT transverse plane reconstruction of right Lisfranc midfoot dislocation compared to normal left foot. Clinical Relevance of the PedCat Study: The weight bearing CBCT study
Episode 52 Commonly Missed Uncommon Orthopedic Injuries. Lisfranc Injuries. Drs. Ivy Cheng & Hossein Medhian. Prepared by Dr. Keerat Grewal, Oct 2014
 Prepared by Dr. Keerat Grewal, Oct 2014 Episode 52 Commonly Missed Uncommon Orthopedic Injuries Drs. Ivy Cheng & Hossein Medhian Lisfranc Injuries Q: What is a Lisfranc injury? Lisfranc injuries are a
Prepared by Dr. Keerat Grewal, Oct 2014 Episode 52 Commonly Missed Uncommon Orthopedic Injuries Drs. Ivy Cheng & Hossein Medhian Lisfranc Injuries Q: What is a Lisfranc injury? Lisfranc injuries are a
CASE ONE CASE ONE. RADIAL HEAD FRACTURE Mason Classification. RADIAL HEAD FRACTURE Mechanism of Injury. RADIAL HEAD FRACTURE Imaging
 CASE ONE An eighteen year old female falls during a basketball game, striking her elbow on the court. She presents to your office that day with a painful, swollen elbow that she is unable to flex or extend
CASE ONE An eighteen year old female falls during a basketball game, striking her elbow on the court. She presents to your office that day with a painful, swollen elbow that she is unable to flex or extend
Annual Surgical Conference LisFranc Fractures. Zeeshan S. Husain, DPM, FACFAS, FASPS. Great Lakes Foot and Ankle Institute September 21, 2018
 Annual Surgical Conference 2018 LisFranc Fractures Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Jacques LisFranc 1790 1847 History LisFranc
Annual Surgical Conference 2018 LisFranc Fractures Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Jacques LisFranc 1790 1847 History LisFranc
Unusual fracture combination with Charcot arthropathy and juvenile-onset diabetes
 Injury Extra (2008) 39, 291 295 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/inext CASE REPORT Unusual fracture combination with Charcot arthropathy and juvenile-onset diabetes
Injury Extra (2008) 39, 291 295 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/inext CASE REPORT Unusual fracture combination with Charcot arthropathy and juvenile-onset diabetes
Peggers Super Summaries: Foot Injuries
 Lisfranc Injury ANATOMY Roman arch with recessed 2 nd MT base AP medial side of intermediate cuneiform to 2 nd MT base Oblique medial side of lateral cuneiform with 3 rd MT base and 4 th with medial boarder
Lisfranc Injury ANATOMY Roman arch with recessed 2 nd MT base AP medial side of intermediate cuneiform to 2 nd MT base Oblique medial side of lateral cuneiform with 3 rd MT base and 4 th with medial boarder
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months.
 Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
pedcat Clinical Case Studies
 pedcat Clinical Case Studies C u r v e B e a m 1 7 5 T i t u s A v e, S u i t e 3 0 0 W a r r i n g t o n, P A 1 8 9 7 6 267-4 8 3-8081 w w w. c u r v e b e a m. c o m PedCAT: Clinical Evidence of diagnostic
pedcat Clinical Case Studies C u r v e B e a m 1 7 5 T i t u s A v e, S u i t e 3 0 0 W a r r i n g t o n, P A 1 8 9 7 6 267-4 8 3-8081 w w w. c u r v e b e a m. c o m PedCAT: Clinical Evidence of diagnostic
Ankle Sprains and Their Imitators
 Ankle Sprains and Their Imitators Mark Halstead, MD Dr. Mark Halstead is the Associate Professor of the Departments of Orthopedics and Pediatrics at Washington University School of Medicine; Director of
Ankle Sprains and Their Imitators Mark Halstead, MD Dr. Mark Halstead is the Associate Professor of the Departments of Orthopedics and Pediatrics at Washington University School of Medicine; Director of
One Month Old Neglected Lisfrancs Fracture Dislocation Treated with Wagner's External Fixator and Percutaneous Screw Fixation : A Case Report
 Case Report Journal of Orthopaedic Case Reports 2014 April-June;4(2): Page 42-46 One Month Old Neglected Lisfrancs Fracture Dislocation Treated with Wagner's External Fixator and Percutaneous Screw Fixation
Case Report Journal of Orthopaedic Case Reports 2014 April-June;4(2): Page 42-46 One Month Old Neglected Lisfrancs Fracture Dislocation Treated with Wagner's External Fixator and Percutaneous Screw Fixation
Lower Extremity Dislocations: Management and Triage on the Field
 Lower Extremity Dislocations: Management and Triage on the Field Scott J Tarantino, MD Towson Orthopaedic Associates, Towson, MD None Disclsures Purpose To provide you with knowledge which may guide you
Lower Extremity Dislocations: Management and Triage on the Field Scott J Tarantino, MD Towson Orthopaedic Associates, Towson, MD None Disclsures Purpose To provide you with knowledge which may guide you
Lisfranc injuries. Mikko Kirjavainen, MD, PhD. Department of Orthopaedics and Traumatology Helsinki University Central Hospital, Helsinki Finland
 Lisfranc injuries Mikko Kirjavainen, MD, PhD Department of Orthopaedics and Traumatology Helsinki University Central Hospital, Helsinki Finland Lisfranc injuries are midfoot fracture dislocations. The
Lisfranc injuries Mikko Kirjavainen, MD, PhD Department of Orthopaedics and Traumatology Helsinki University Central Hospital, Helsinki Finland Lisfranc injuries are midfoot fracture dislocations. The
LISFRANC FRACTURE-DISLOCATION IN A FEMALE SOCCER ATHLETE Beth Haddix, DPT 1 Karen Ellis, DPT 2 Estee Saylor-Pavkovich, DPT 3
 IJSPT DIAGNOSTICS CORNER LISFRANC FRACTURE-DISLOCATION IN A FEMALE SOCCER ATHLETE Beth Haddix, DPT 1 Karen Ellis, DPT 2 Estee Saylor-Pavkovich, DPT 3 ABSTRACT Individuals with midfoot injuries may present
IJSPT DIAGNOSTICS CORNER LISFRANC FRACTURE-DISLOCATION IN A FEMALE SOCCER ATHLETE Beth Haddix, DPT 1 Karen Ellis, DPT 2 Estee Saylor-Pavkovich, DPT 3 ABSTRACT Individuals with midfoot injuries may present
Temporary bridge plating of the medial column in Chopart and Lisfranc injuries
 Temporary bridge plating of the medial column in Chopart and Lisfranc injuries by Alaa Mansour DPM 1*, Lawrence Fallat DPM, FACFAS 2 The Foot and Ankle Online Journal 10 (1): 5 Severe traumatic injuries
Temporary bridge plating of the medial column in Chopart and Lisfranc injuries by Alaa Mansour DPM 1*, Lawrence Fallat DPM, FACFAS 2 The Foot and Ankle Online Journal 10 (1): 5 Severe traumatic injuries
11/5/14. I will try to make this painless. Great, a Fracture, Now What? Objectives. Basics for Fracture Workup. Basics for Fracture Workup
 Great, a Fracture, Now What? I will try to make this painless Mary Greve MS, PA-C Department of Orthopedic Surgery Trauma Team University of Iowa Hospitals and Clinics Mary-Greve@uiowa.edu Pager 2121 Objectives
Great, a Fracture, Now What? I will try to make this painless Mary Greve MS, PA-C Department of Orthopedic Surgery Trauma Team University of Iowa Hospitals and Clinics Mary-Greve@uiowa.edu Pager 2121 Objectives
Jeannie Huh, MD Christopher Gross, MD Alex Lampley, MD Samuel B. Adams, MD James K. DeOrio, MD James A. Nunley II, MD Mark E.
 Jeannie Huh, MD Christopher Gross, MD Alex Lampley, MD Samuel B. Adams, MD James K. DeOrio, MD James A. Nunley II, MD Mark E. Easley, MD Duke University Medical Center Durham, NC Disclosures Predictors
Jeannie Huh, MD Christopher Gross, MD Alex Lampley, MD Samuel B. Adams, MD James K. DeOrio, MD James A. Nunley II, MD Mark E. Easley, MD Duke University Medical Center Durham, NC Disclosures Predictors
Hand and wrist emergencies
 Chapter1 Hand and wrist emergencies Carl A. Germann Distal radius and ulnar injuries PEARL: Fractures of the distal radius and ulna are the most common type of fractures in patients younger than 75 years.
Chapter1 Hand and wrist emergencies Carl A. Germann Distal radius and ulnar injuries PEARL: Fractures of the distal radius and ulna are the most common type of fractures in patients younger than 75 years.
AAP Boot Camp KNEE AND ANKLE EXAM
 AAP Boot Camp KNEE AND ANKLE EXAM Disclosures I have no relevant financial relationships with the manufacturers of any commercial products and or providers of commercial services discussed in this CME
AAP Boot Camp KNEE AND ANKLE EXAM Disclosures I have no relevant financial relationships with the manufacturers of any commercial products and or providers of commercial services discussed in this CME
Medical Practice for Sports Injuries and Disorders of the Lower Limb
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Lower Limb JMAJ 48(1): 25 29, 2005 Motonobu NATSUYAMA Chief Surgeon, Department of Orthopedic Surgery, Kantoh
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Lower Limb JMAJ 48(1): 25 29, 2005 Motonobu NATSUYAMA Chief Surgeon, Department of Orthopedic Surgery, Kantoh
Managing Tibialis Posterior Tendon Injuries
 Managing Tibialis Posterior Tendon Injuries by Thomas C. Michaud, DC Published April 1, 2015 by Dynamic Chiropractic Magazine Tibialis posterior is the deepest, strongest, and most central muscle of the
Managing Tibialis Posterior Tendon Injuries by Thomas C. Michaud, DC Published April 1, 2015 by Dynamic Chiropractic Magazine Tibialis posterior is the deepest, strongest, and most central muscle of the
Traumatic Injuries to the Foot and Ankle
 Traumatic Injuries to the Foot and Ankle Dr. Joseph N. Daniel Clinical Associate Professor of Orthopaedic Surgery Foot and Ankle Service, The Rothman Institute Thomas Jefferson University Hospital Philadelphia,
Traumatic Injuries to the Foot and Ankle Dr. Joseph N. Daniel Clinical Associate Professor of Orthopaedic Surgery Foot and Ankle Service, The Rothman Institute Thomas Jefferson University Hospital Philadelphia,
Calcaneus (Heel Bone) Fractures
 Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Tarsometatarsal (Lisfranc) Joint Dislocation
 CHAPTER 106 Tarsometatarsal (Lisfranc) Joint Dislocation Lawrence A. DiDomenico Dawn Y. Stein Fracture dislocations of the tarsal metatarsal (Lisfranc injuries) can be subtle and may be missed in both
CHAPTER 106 Tarsometatarsal (Lisfranc) Joint Dislocation Lawrence A. DiDomenico Dawn Y. Stein Fracture dislocations of the tarsal metatarsal (Lisfranc injuries) can be subtle and may be missed in both
Outcome After Open Reduction and Internal Fixation of Lisfranc Joint Injuries *
 Outcome After Open Reduction and Internal Fixation of Lisfranc Joint Injuries * BY R. S. KUO, M.B.B.S., F.R.A.C.S., N. C. TEJWANI, M.D., C. W. DIGIOVANNI, M.D., S. K. HOLT, M.S.P.H.#, S. K. BENIRSCHKE,
Outcome After Open Reduction and Internal Fixation of Lisfranc Joint Injuries * BY R. S. KUO, M.B.B.S., F.R.A.C.S., N. C. TEJWANI, M.D., C. W. DIGIOVANNI, M.D., S. K. HOLT, M.S.P.H.#, S. K. BENIRSCHKE,
Case Report A Case Report of Isolated Cuboid Nutcracker Fracture
 Case Reports in Orthopedics Volume 2016, Article ID 3264172, 5 pages http://dx.doi.org/10.1155/2016/3264172 Case Report A Case Report of Isolated Cuboid Nutcracker Fracture Takaaki Ohmori, 1,2 Shinichi
Case Reports in Orthopedics Volume 2016, Article ID 3264172, 5 pages http://dx.doi.org/10.1155/2016/3264172 Case Report A Case Report of Isolated Cuboid Nutcracker Fracture Takaaki Ohmori, 1,2 Shinichi
Deltoid and Syndesmosis Ligament Injury of the Ankle Without Fracture
 Deltoid and Syndesmosis Ligament Injury of the Ankle Without Fracture Chris D. Miller, MD, Walter R. Shelton,* MD, Gene R. Barrett, MD, F. H. Savoie, MD, and Andrea D. Dukes, MS From the Mississippi Sports
Deltoid and Syndesmosis Ligament Injury of the Ankle Without Fracture Chris D. Miller, MD, Walter R. Shelton,* MD, Gene R. Barrett, MD, F. H. Savoie, MD, and Andrea D. Dukes, MS From the Mississippi Sports
Case Report Lateral Subtalar Dislocation with Tarsometatarsal Dislocation: A Case Report of a Rare Injury
 Hindawi Case Reports in Orthopedics Volume 2017, Article ID 8090721, 6 pages https://doi.org/10.1155/2017/8090721 Case Report Lateral Subtalar Dislocation with Tarsometatarsal Dislocation: A Case Report
Hindawi Case Reports in Orthopedics Volume 2017, Article ID 8090721, 6 pages https://doi.org/10.1155/2017/8090721 Case Report Lateral Subtalar Dislocation with Tarsometatarsal Dislocation: A Case Report
Review relevant anatomy of the foot and ankle. Learn the approach to examining the foot and ankle
 Objectives Review relevant anatomy of the foot and ankle Learn the approach to examining the foot and ankle Learn the basics of diagnosis and treatment of ankle sprains Overview of other common causes
Objectives Review relevant anatomy of the foot and ankle Learn the approach to examining the foot and ankle Learn the basics of diagnosis and treatment of ankle sprains Overview of other common causes
Burwood Road, Concord Dora Street, Hurstville 119 Lethbridge Street, Penrith 160 Belmore Road, Randwick
 www.orthosports.com.au 47 49 Burwood Road, Concord 29 31 Dora Street, Hurstville 119 Lethbridge Street, Penrith 160 Belmore Road, Randwick Turf Toe Injury By Todd Gothelf Foot, Ankle, Shoulder History
www.orthosports.com.au 47 49 Burwood Road, Concord 29 31 Dora Street, Hurstville 119 Lethbridge Street, Penrith 160 Belmore Road, Randwick Turf Toe Injury By Todd Gothelf Foot, Ankle, Shoulder History
radiologymasterclass.co.uk
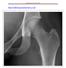 http://radiologymasterclass.co.uk Hip X-ray anatomy - Normal AP (anterior-posterior) Shenton's line is formed by the medial edge of the femoral neck and the inferior edge of the superior pubic ramus Loss
http://radiologymasterclass.co.uk Hip X-ray anatomy - Normal AP (anterior-posterior) Shenton's line is formed by the medial edge of the femoral neck and the inferior edge of the superior pubic ramus Loss
Trainers. Anne-Marie O Connor Musculoskeletal Podiatrist
 Trainers Anne-Marie O Connor Musculoskeletal Podiatrist Agenda Background Tarso-navicular stress fractures Case Study Interventions and research Further Research Anatomy Anatomically, wedged between the
Trainers Anne-Marie O Connor Musculoskeletal Podiatrist Agenda Background Tarso-navicular stress fractures Case Study Interventions and research Further Research Anatomy Anatomically, wedged between the
Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes
 Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes William M Weiss, MD MSc FRCSC Orthopedic Surgery & Rehabilitation Sports Medicine, Arthroscopy & Extremity Reconstruction
Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes William M Weiss, MD MSc FRCSC Orthopedic Surgery & Rehabilitation Sports Medicine, Arthroscopy & Extremity Reconstruction
Merete PlantarMAX Lapidus Plate Surgical Technique. Description of Plate
 Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Commonly Missed Foot and Ankle Conditions. David Miller, DPM AMG Podiatry
 Commonly Missed Foot and Ankle Conditions David Miller, DPM AMG Podiatry Lisfranc Injuries Wide spectrum of injuries High energy Subtle subluxation which could be easily missed injuries Men are 2-4x s
Commonly Missed Foot and Ankle Conditions David Miller, DPM AMG Podiatry Lisfranc Injuries Wide spectrum of injuries High energy Subtle subluxation which could be easily missed injuries Men are 2-4x s
Scar Engorged veins. Size of the foot [In clubfoot, small foot]
![Scar Engorged veins. Size of the foot [In clubfoot, small foot] Scar Engorged veins. Size of the foot [In clubfoot, small foot]](/thumbs/78/77722241.jpg) 6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
Surgical Technique. Customer Service:
 Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Axis Charcot Fixation System in diameters of 5.5, 6.5 and 7.5mm
Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Axis Charcot Fixation System in diameters of 5.5, 6.5 and 7.5mm
Surgery-Ortho. Fractures of the tibia and fibula. Management. Treatment of low energy fractures. Fifth stage. Lec-6 د.
 Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
10 Sports Injuries Not to Miss. Jessica Juntunen, MD Primary Care Sports Medicine
 10 Sports Injuries Not to Miss Jessica Juntunen, MD Primary Care Sports Medicine I have no financial interests or relationships to disclose in regards to this presentation 12 yo RHD male baseball pitcher
10 Sports Injuries Not to Miss Jessica Juntunen, MD Primary Care Sports Medicine I have no financial interests or relationships to disclose in regards to this presentation 12 yo RHD male baseball pitcher
Results of Calcaneal Osteotomy & Flexor Digitorum Longus transfer in Stage II Acquired Flatfoot Deformity
 Results of Calcaneal Osteotomy & Flexor Digitorum Longus transfer in Stage II Acquired Flatfoot Deformity Mr Amit Chauhan Mr Prasad Karpe Ms Maire-claire Killen Mr Rajiv Limaye University Hospital of North
Results of Calcaneal Osteotomy & Flexor Digitorum Longus transfer in Stage II Acquired Flatfoot Deformity Mr Amit Chauhan Mr Prasad Karpe Ms Maire-claire Killen Mr Rajiv Limaye University Hospital of North
The evaluation and management of acute musculoskeletal
 ONLINE EXCLUSIVE George E. Eldayrie, MD; Kristy Smith, MD; Michael Seth Smith, MD, CAQSM, PharmD Department of Community Health and Family Medicine (Drs. Eldayrie and K. Smith) and Department of Orthopedics
ONLINE EXCLUSIVE George E. Eldayrie, MD; Kristy Smith, MD; Michael Seth Smith, MD, CAQSM, PharmD Department of Community Health and Family Medicine (Drs. Eldayrie and K. Smith) and Department of Orthopedics
Fracture and Dislocation of the Carpus ( 1-Jan-1985 )
 In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
Recurrent Fifth Metatarsal Fractures. Carol Frey MD Fellowship Co - Director West Coast Sports Medicine Foundation UCLA Manhattan Beach, California
 Recurrent Fifth Metatarsal Fractures Carol Frey MD Fellowship Co - Director West Coast Sports Medicine Foundation UCLA Manhattan Beach, California General 5th MT fracture fairly common Mechanism: Hindfoot
Recurrent Fifth Metatarsal Fractures Carol Frey MD Fellowship Co - Director West Coast Sports Medicine Foundation UCLA Manhattan Beach, California General 5th MT fracture fairly common Mechanism: Hindfoot
BCCH Emergency Department LOWER LIMB INJURIES Resource pack
 1 BCCH Emergency Department LOWER LIMB INJURIES Resource pack Developed by: Rena Heathcote RN. 2 Knee Injuries The knee joint consists of a variety of structures including: 3 bones (excluding the patella)
1 BCCH Emergency Department LOWER LIMB INJURIES Resource pack Developed by: Rena Heathcote RN. 2 Knee Injuries The knee joint consists of a variety of structures including: 3 bones (excluding the patella)
Copyright 2004, Yoshiyuki Shiratori. All right reserved.
 Ankle and Leg Evaluation 1. History Chief Complaint: A. What happened? B. Is it a sharp or dull pain? C. How long have you had the pain? D. Can you pinpoint the pain? E. Do you have any numbness or tingling?
Ankle and Leg Evaluation 1. History Chief Complaint: A. What happened? B. Is it a sharp or dull pain? C. How long have you had the pain? D. Can you pinpoint the pain? E. Do you have any numbness or tingling?
CHARLOTTE Lisfranc. Recontruction System SURGICAL TECHNIQUE
 CHARLOTTE Lisfranc Recontruction System SURGICAL TECHNIQUE Contents Preface 3 Chapter 1 4 Chapter 2 4 4 4 4 4 Chapter 3 5 5 5 6 6 6 7 7 8 Chapter 4 8 8 9 10 Appendix 10 Introduction Indications and Contraindications
CHARLOTTE Lisfranc Recontruction System SURGICAL TECHNIQUE Contents Preface 3 Chapter 1 4 Chapter 2 4 4 4 4 4 Chapter 3 5 5 5 6 6 6 7 7 8 Chapter 4 8 8 9 10 Appendix 10 Introduction Indications and Contraindications
Therapeutic Foot Care Certificate Program Part I: Online Home Study Program
 Therapeutic Foot Care Certificate Program Part I: Online Home Study Program 1 Anatomy And Terminology Of The Lower Extremity Joan E. Edelstein, MA, PT, FISPO Associate Professor of Clinical Physical Therapy
Therapeutic Foot Care Certificate Program Part I: Online Home Study Program 1 Anatomy And Terminology Of The Lower Extremity Joan E. Edelstein, MA, PT, FISPO Associate Professor of Clinical Physical Therapy
Journal reading. Introduction. Introduction. Ottawa Ankle Rules. Method
 Journal reading Presenter: PGY 林聖傑 Supervisor: Dr. 林俊龍 102.12.23 The accuracy of ultrasound evaluation in foot and ankle trauma Salih Ekinci, MD American Journal of Emergency Medicine 31 (2013) 1551 1555
Journal reading Presenter: PGY 林聖傑 Supervisor: Dr. 林俊龍 102.12.23 The accuracy of ultrasound evaluation in foot and ankle trauma Salih Ekinci, MD American Journal of Emergency Medicine 31 (2013) 1551 1555
Dorsal Multiple Plating Without Routine Transarticular Screws for Fixation of Lisfranc Injury
 Section Editor: Steven F. Harwin, MD Dorsal Multiple Plating Without Routine Transarticular Screws for Fixation of Lisfranc Injury Richard E. Stern, MD; Mathieu ssal, MD bstract: Following a Lisfranc joint
Section Editor: Steven F. Harwin, MD Dorsal Multiple Plating Without Routine Transarticular Screws for Fixation of Lisfranc Injury Richard E. Stern, MD; Mathieu ssal, MD bstract: Following a Lisfranc joint
Clinical evaluation where no obvious fracture a. Squeeze test
 7:43 am The Syndesmotic Injury: From Subtle to Severe Robert B. Anderson, MD Chief, Foot and Ankle Carolinas Medical Center OrthoCarolina (Charlotte, North Carolina) 7:30-8:25 am Symposium 1: Management
7:43 am The Syndesmotic Injury: From Subtle to Severe Robert B. Anderson, MD Chief, Foot and Ankle Carolinas Medical Center OrthoCarolina (Charlotte, North Carolina) 7:30-8:25 am Symposium 1: Management
CHRONIC FOOT PROBLEMS FOOT and ANKLE BASICS
 CHRONIC FOOT PROBLEMS FOOT and ANKLE BASICS ABC s of Comprehensive Musculoskeletal Care December 1 st, 2007 Stephen Pinney MD Chief, UCSF Foot and Ankle Service Chronic problems typically occur gradually
CHRONIC FOOT PROBLEMS FOOT and ANKLE BASICS ABC s of Comprehensive Musculoskeletal Care December 1 st, 2007 Stephen Pinney MD Chief, UCSF Foot and Ankle Service Chronic problems typically occur gradually
SUBTLE CAVUS IN SPORTS INJURIES
 SUBTLE CAVUS IN SPORTS INJURIES MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA NON-NEUROMUSCULAR NORMAL VARIANT: 20-25% INCIDENCE LEDOUX, ET AL. FAI 24, 2003 FOREFOOT-DRIVEN / MORE SUBTLE
SUBTLE CAVUS IN SPORTS INJURIES MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA NON-NEUROMUSCULAR NORMAL VARIANT: 20-25% INCIDENCE LEDOUX, ET AL. FAI 24, 2003 FOREFOOT-DRIVEN / MORE SUBTLE
Disclosures. Syndesmosis Injury. Syndesmosis Ligaments. Objectives. Mark M. Casillas, M.D.
 Disclosures Syndesmosis Injury No relevant disclosures Mark M. Casillas, M.D. 1 Objectives Syndesmosis Ligaments Understand the syndesmosis anatomy and function Classify syndesmosis injuries Describe treatment
Disclosures Syndesmosis Injury No relevant disclosures Mark M. Casillas, M.D. 1 Objectives Syndesmosis Ligaments Understand the syndesmosis anatomy and function Classify syndesmosis injuries Describe treatment
An older systematic review looked at the evidence behind the best approach to evaluate acute knee pain in primary care (Ann Int Med.2003;139:575).
 There is so much we don't know in medicine that could make a difference, and often we focus on the big things, and the little things get forgotten. To highlight some smaller but important issues, we've
There is so much we don't know in medicine that could make a difference, and often we focus on the big things, and the little things get forgotten. To highlight some smaller but important issues, we've
Case. 5 year old with 2 weeks leg pain and now refusing to walk + Fevers, lower leg swelling, warmth Denies and history of trauma or wounds
 Case 5 year old with 2 weeks leg pain and now refusing to walk + Fevers, lower leg swelling, warmth Denies and history of trauma or wounds Exam I: Swelling over entire tibia extending to foot P: Tenderness
Case 5 year old with 2 weeks leg pain and now refusing to walk + Fevers, lower leg swelling, warmth Denies and history of trauma or wounds Exam I: Swelling over entire tibia extending to foot P: Tenderness
Sports Injuries of the Foot and Ankle. Mark McEleney, MD University of Iowa College of Medicine Refresher Course for the Family Physician 4/4/2018
 Sports Injuries of the Foot and Ankle Mark McEleney, MD University of Iowa College of Medicine Refresher Course for the Family Physician 4/4/2018 I. Objectives A. By the end of the lecture attendees will
Sports Injuries of the Foot and Ankle Mark McEleney, MD University of Iowa College of Medicine Refresher Course for the Family Physician 4/4/2018 I. Objectives A. By the end of the lecture attendees will
Outline. Ankle/Foot Anatomy Ankle Sprains Ottawa Ankle Rules DDx: The Sprain That Wasn t
 Ankle Injuries Outline Ankle/Foot Anatomy Ankle Sprains Ottawa Ankle Rules DDx: The Sprain That Wasn t Anatomy: Ankle Mortise Bony Anatomy Lateral Ligament Complex Medial Ligament Complex Ankle Sprains
Ankle Injuries Outline Ankle/Foot Anatomy Ankle Sprains Ottawa Ankle Rules DDx: The Sprain That Wasn t Anatomy: Ankle Mortise Bony Anatomy Lateral Ligament Complex Medial Ligament Complex Ankle Sprains
Goals. Initial management skeletal trauma. Physical Exam ABC OF PRIMARY CARE MEDICINE FRACTURE MANAGEMENT 12/4/2010
 ABC OF PRIMARY CARE MEDICINE FRACTURE MANAGEMENT Brian Feeley, MD UCSF Sports Medicine and Shoulder Surgery Goals Discuss common fractures and initial management, treatment guidelines Let your patients
ABC OF PRIMARY CARE MEDICINE FRACTURE MANAGEMENT Brian Feeley, MD UCSF Sports Medicine and Shoulder Surgery Goals Discuss common fractures and initial management, treatment guidelines Let your patients
Treatment of Acute Traumatic Knee Dislocations
 Treatment of Acute Traumatic Knee Dislocations Angelo J. Colosimo, MD Head Orthopaedic Surgeon University of Cincinnati Athletics Director of Sports Medicine University of Cincinnati Medical Center Associate
Treatment of Acute Traumatic Knee Dislocations Angelo J. Colosimo, MD Head Orthopaedic Surgeon University of Cincinnati Athletics Director of Sports Medicine University of Cincinnati Medical Center Associate
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 11/24/2012 Radiology Quiz of the Week # 100 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 11/24/2012 Radiology Quiz of the Week # 100 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY 2017
 BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY 2017 B. RESSEQUE, D.P.M., D.A.B.P.O. Professor, N.Y. College of Podiatric Medicine ARCH HEIGHT OFF WEIGHTBEARING Evaluate arch height by placing
BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY 2017 B. RESSEQUE, D.P.M., D.A.B.P.O. Professor, N.Y. College of Podiatric Medicine ARCH HEIGHT OFF WEIGHTBEARING Evaluate arch height by placing
Section 6: Preoperative Planning
 Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
A Patient s Guide to Adult-Acquired Flatfoot Deformity
 A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY
 BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY B.Resseque, D.P.M. ARCH HEIGHT OFF WEIGHTBEARING Evaluate arch height by placing a ruler from the heel to the first metatarsal head Compare arch
BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY B.Resseque, D.P.M. ARCH HEIGHT OFF WEIGHTBEARING Evaluate arch height by placing a ruler from the heel to the first metatarsal head Compare arch
Sky Ridge Medical Center, Aspen Building Ridgegate Pkwy., Suite 309 Lone Tree, Colorado Office: Fax:
 ANKLE SPRAIN What is the ATFL? The ankle joint is made up of the tibia, fibula (bones in the lower leg) and the talus (bone below the tibia and fibula). Ligaments in the ankle connect bone to bone and
ANKLE SPRAIN What is the ATFL? The ankle joint is made up of the tibia, fibula (bones in the lower leg) and the talus (bone below the tibia and fibula). Ligaments in the ankle connect bone to bone and
Posterior Tibialis Tendon Dysfunction & Repair
 1 Posterior Tibialis Tendon Dysfunction & Repair Surgical Indications and Considerations Anatomical Considerations: The posterior tibialis muscle arises from the interosseous membrane and the adjacent
1 Posterior Tibialis Tendon Dysfunction & Repair Surgical Indications and Considerations Anatomical Considerations: The posterior tibialis muscle arises from the interosseous membrane and the adjacent
Ankle Ligament Injury: Don t Worry- It s Only a Sprain Wes Jackson MD Orthopaedic Foot & Ankle
 Ankle Ligament Injury: Don t Worry- It s Only a Sprain Wes Jackson MD Orthopaedic Foot & Ankle Outline I. Epidemiology II. Classification and Types of Sprains III. Anatomy IV. Clinical Assessment and Imaging
Ankle Ligament Injury: Don t Worry- It s Only a Sprain Wes Jackson MD Orthopaedic Foot & Ankle Outline I. Epidemiology II. Classification and Types of Sprains III. Anatomy IV. Clinical Assessment and Imaging
Fractures of the Calcaneus
 Fractures of the Calcaneus Anthony T. Sorkin, M.D. Rockford Orthopedic Trauma Service Rajeev Garapati, MD Illinois Bone and Joint Institute Assistant Clinical Professor University of Illinois at Chicago
Fractures of the Calcaneus Anthony T. Sorkin, M.D. Rockford Orthopedic Trauma Service Rajeev Garapati, MD Illinois Bone and Joint Institute Assistant Clinical Professor University of Illinois at Chicago
Burwood Road, Concord Dora Street, Hurstville Lethbridge Street, Penrith 160 Belmore Road, Randwick
 www.orthosports.com.au 47 49 Burwood Road, Concord 29 31 Dora Street, Hurstville 119 121 Lethbridge Street, Penrith 160 Belmore Road, Randwick Update on Syndesmosis Ankle Sprains By Todd Gothelf Foot,
www.orthosports.com.au 47 49 Burwood Road, Concord 29 31 Dora Street, Hurstville 119 121 Lethbridge Street, Penrith 160 Belmore Road, Randwick Update on Syndesmosis Ankle Sprains By Todd Gothelf Foot,
High Ankle Sprains: Diagnosis & Treatment
 High Ankle Sprains: Diagnosis & Treatment Mark J. Mendeszoon, DPM, FACFAS, FACFAOM Precision Orthopaedic Specialties University Regional Hospitals Advanced Foot & Ankle Fellowship- Director It Is Only
High Ankle Sprains: Diagnosis & Treatment Mark J. Mendeszoon, DPM, FACFAS, FACFAOM Precision Orthopaedic Specialties University Regional Hospitals Advanced Foot & Ankle Fellowship- Director It Is Only
Lisfranc Injury: Imaging Findings for this Important but Often-Missed Diagnosis
 Lisfranc Injury: Imaging Findings for this Important but Often-Missed Diagnosis Rajan T. Gupta, MD, a Rakhee P. Wadhwa, MD, b Thomas J. Learch, MD, b and Steven M. Herwick, MD a The Lisfranc injury is
Lisfranc Injury: Imaging Findings for this Important but Often-Missed Diagnosis Rajan T. Gupta, MD, a Rakhee P. Wadhwa, MD, b Thomas J. Learch, MD, b and Steven M. Herwick, MD a The Lisfranc injury is
BUCKS MSK: FOOT AND ANKLE PATHWAY GP MANAGEMENT. Hallux Valgus. Assessment: Early Management. (must be attempted prior to any referral to imsk):
 Hallux Valgus Common condition: affecting around 28% of the adult population. Prevalence increases with age and in females. Observation: Lateral deviation of the great toe. May cause secondary irritation
Hallux Valgus Common condition: affecting around 28% of the adult population. Prevalence increases with age and in females. Observation: Lateral deviation of the great toe. May cause secondary irritation
Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot.
 Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot. Compression technology Variable angle locking technology Anatomic and
Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot. Compression technology Variable angle locking technology Anatomic and
SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT
 C H A P T E R 1 7 SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT William D. Fishco, DPM, MS INTRODUCTION Arthroereisis is a surgical procedure designed to limit the motion of a joint. Subtalar joint arthroereisis
C H A P T E R 1 7 SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT William D. Fishco, DPM, MS INTRODUCTION Arthroereisis is a surgical procedure designed to limit the motion of a joint. Subtalar joint arthroereisis
PRONATION-ABDUCTION FRACTURES
 C H A P T E R 1 2 PRONATION-ABDUCTION FRACTURES George S. Gumann, DPM (The opinions of the author should not be considered as reflecting official policy of the US Army Medical Department.) Pronation-abduction
C H A P T E R 1 2 PRONATION-ABDUCTION FRACTURES George S. Gumann, DPM (The opinions of the author should not be considered as reflecting official policy of the US Army Medical Department.) Pronation-abduction
Radiographic Assessment of Pediatric Foot Alignment: Self-Assessment Module
 1.5 CME AJR Integrative Imaging LIFELONG LEARNING FOR RADIOLOGY Radiographic Assessment of Pediatric Foot Alignment: Self-Assessment Module Mahesh M. Thapa 1,2, Sumit Pruthi 1,2, Felix S. Chew 2 ABSTRACT
1.5 CME AJR Integrative Imaging LIFELONG LEARNING FOR RADIOLOGY Radiographic Assessment of Pediatric Foot Alignment: Self-Assessment Module Mahesh M. Thapa 1,2, Sumit Pruthi 1,2, Felix S. Chew 2 ABSTRACT
Surgical Technique 4.5/8.5MM BEAMING SYSTEM. Customer Service:
 Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The 4.5/8.5 screw system is intended for fixation arthrodesis of
Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The 4.5/8.5 screw system is intended for fixation arthrodesis of
Feet First. Michael K. Cooper, DO FACOFP Family Practice/OMM St John Clinic - Claremore OOA 2018 Annual Convention
 Feet First Michael K. Cooper, DO FACOFP Family Practice/OMM St John Clinic - Claremore OOA 2018 Annual Convention Disclaimer I have no conflict of interest. I am not on any pharmaceutical company payroll
Feet First Michael K. Cooper, DO FACOFP Family Practice/OMM St John Clinic - Claremore OOA 2018 Annual Convention Disclaimer I have no conflict of interest. I am not on any pharmaceutical company payroll
General Concepts. Growth Around the Knee. Topics. Evaluation
 General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
Financial Disclosure. Turf Toe
 Seth O Brien, CP, LP Financial Disclosure Mr. Seth O'Brien has no relevant financial relationships with commercial interests to disclose. Turf Toe Common in athletes playing on firm, artificial turf Forceful
Seth O Brien, CP, LP Financial Disclosure Mr. Seth O'Brien has no relevant financial relationships with commercial interests to disclose. Turf Toe Common in athletes playing on firm, artificial turf Forceful
Introduction. The primary function of the ankle and foot is to absorb shock and impart thrust to the body during walking.
 The ankle 1 Introduction The primary function of the ankle and foot is to absorb shock and impart thrust to the body during walking. OSTEOLOGRY The term ankle refers primarily to the talocrural joint,
The ankle 1 Introduction The primary function of the ankle and foot is to absorb shock and impart thrust to the body during walking. OSTEOLOGRY The term ankle refers primarily to the talocrural joint,
Acute Ankle Injuries, Part 1: Office Evaluation and Management
 t June 08, 2009 Obesity [1] Each acute ankle injury commonly seen in the office has associated with it a mechanism by which it can be injured, trademark symptoms that the patient experiences during the
t June 08, 2009 Obesity [1] Each acute ankle injury commonly seen in the office has associated with it a mechanism by which it can be injured, trademark symptoms that the patient experiences during the
