Acute dislocation of the patella: should these patients be operated on more often?
|
|
|
- Laurel Carr
- 5 years ago
- Views:
Transcription
1 Review Article Page 1 of 7 Acute dislocation of the patella: should these patients be operated on more often? Vicente Sanchis-Alfonso 1, Erik Montesinos-Berry 2 1 Department of Orthopaedic Surgery, Hospital Arnau de Vilanova, Valencia, Spain; 2 Agoriaz Orthopaedic Center, Riaz & Clinique CIC, Montreux, Switzerland Contributions: (I) Conception and design: V Sanchis-Alfonso; (II) Administrative support: None; (III) Provision of study materials or patients: None; (IV) Collection and assembly of data: All authors; (V) Data analysis and interpretation: All authors; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Vicente Sanchis-Alfonso, MD, PhD. Department of Orthopaedic Surgery, Hospital Arnau de Vilanova, Valencia, Spain. vicente.sanchis.alfonso@gmail.com. Abstract: Primary patellar dislocations should be operated on more often after the first dislocation. The role of surgery for first-time traumatic patellar dislocations is emerging as a reasonable treatment strategy. In highly active patients under 25 years of age with a pathoanatomy predisposing to recurrent dislocation (trochlear dysplasia associated or not with patella alta) surgical treatment could be considered as a first line of treatment in the first-time patellar dislocation because the recurrence risk is unacceptably high. This recommendation is based on recurrence predictive models after a first-time patella dislocation and in cost effectiveness economic models. Moreover, we must incorporate individual circumstances and preferences (patient s goals such as sports) into the decision protocols. Obviously we need high quality clinical trials describing anatomical abnormalities and medial patellofemoral ligament (MPFL) tear site, ideally multicentric ones, which compare surgical and conservative treatments after a first-time lateral patellar dislocation to definitely answer the question we ask ourselves in this paper. Keywords: Acute dislocation of the patella; conservative treatment; surgical treatment Received: 27 February 2018; Accepted: 05 March 2018; Published: 21 March doi: /aoj View this article at: Background First-time lateral patellar dislocation is a common orthopaedic injury with a high incidence in the general population with a mean of 42 per 100,000 person-years, and particularly in the young female patient aged (108/100,000) (1). Patients who are skeletally immature at the time of the first patellar dislocation have a high rate of recurrent patellar instability with an increment of the redislocation rate with time (2). Moreover, 17% of patients will develop a patellofemoral osteoarthritis (PFOA) 20 years following initial dislocation (2). Sanders et al. (3) have demonstrated that osteochondral injury, recurrent patellar instability, and trochlear dysplasia are associated with the development of PFOA. Therefore, we are faced with a frequent lesion, not self-limited, with potential longterm complications such as anterior knee pain, decrease in the activity level, recurrent dislocation and PFOA, the last being a serious problem with a poor solution in the young patient. The orthopaedic surgeon should be aware of both, the high risk of recurrent dislocation and the risk to develop a PFOA when deciding on the treatment. It is therefore necessary to find the best treatment to avoid these possible outcomes. Typically the first-time lateral patellar dislocation is treated conservatively, except in some very specific cases that we will discuss later. In cases with an acute osteochondral fracture of the trochlea and/or patella that requires surgical treatment (refixation), the tear of the medial patellofemoral ligament (MPFL) will be repaired or reconstructed at the
2 Annals of Joint, 2018 Page 2 of 7 A B Figure 1 Substantial disruption of the MPFL. MPFL injury pattern assessment by MRI. (A) Coronal view; (B) axial view. Laterally subluxated patella. The contralateral patella has a normal alignment. MPFL, medial patellofemoral ligament. A B Figure 2 Large and displaced bone avulsion fracture of the MPFL. (A) Surgical image; (B) CT-3D image. MPFL, medial patellofemoral ligament, same time. Furthermore, in cases with a non-reducible lateral patellar dislocation with rotation as well as in cases with a substantial disruption of the medial patellar stabilizers, MPFL reconstruction would be indicated in the acute phase (Figure 1). Lastly, in those rare cases with a large and displaced bone avulsion fracture of the MPFL, surgical treatment would also be indicated (Figure 2). Controversy Annals of Joint. All rights reserved. remains for the treatment of the rest of the cases and this will be the object of our paper. Our work hypothesis is that the first acute lateral patellar dislocation should be treated surgically more often. To answer the question we ask ourselves in this review article, we are going to follow four different strategies. First we are going to review the literature published about this subject: conservative versus surgical treatment. Some randomized clinical trials (RCT) already analyze this alternative and given the fact that a RCT is the type of study with the highest scientific evidence, we are going to prioritize them but still do a critical reading, which is one of the basic tools of Evidence Based Medicine s (EBM) methodology. Not all the published papers, including those published in high impact factor journals, are quality papers, RCT included. Therefore, all the papers should be analyzed thoroughly in a critical way. For our analysis we are going to focus on the design of the paper and the data provided. We will also perform a critical analysis of systematic reviews with the meta-analyses included, because the quality of a systematic review depends not only on the level of evidence of the papers chosen for the revision but also on the quality of the review. The second strategy to answer the question we ask ourselves in this paper is to critically analyze the studies that examine the probability of recurrence after a first lateral patellar dislocation based on predictive models. The third strategy will be to analyze the goals the patient has. Lastly we are going to analyze the cost-effectiveness economic models. Our goal is to determine which patients with a first aoj.amegroups.com
3 Annals of Joint, 2018 episode of lateral patellar dislocation will be candidates for a surgical treatment and which will not. It is terrifying to read John Ioannidis, from Stanford University, when he states regarding medical literature that: false report probability is likely to exceed 50% for the whole literature (4) or currently, many published research findings are false or exaggerated, and an estimated 85% of research resources are wasted (5). For this reason, we must be very critical when analyzing published studies, and the ones published on the subject we are reviewing are obviously not an exception. The goal of critical analysis is to avoid mistaken conclusions and this is also the final objective of our paper. Decision based on critical analysis of the medical literature where conservative and surgical treatments are compared There are several studies in the medical literature that analyze surgical versus conservative treatment for the firsttime lateral patellar dislocation (6-16). In some of them, the reported patellar dislocation recurrence rates were lower in the surgical treatment group (10,11,13,15,16). However, other authors reported no difference in recurrence rates with operative or non-operative treatment (6-9,12,14). In most of the studies, the functional result is similar in both types of treatment (6-9,11,12,14,16). That is, surgical treatment does not improve the long-term outcomes. Interestingly, Regalado et al. (16) reported an increment of the redislocation rate with time in both types of treatment in adolescents. At 3 years, patients in the operative group had a redislocation rate of 0% versus 35% for the nonoperative group (16). At 6 years of follow-up, the surgical group had a redislocation rate of 33% versus 73% for the non-surgical group (16). Palmu et al. (9), in patients younger than sixteen years of age, reported a similar dislocation recurrence rate of 71% for the non-operative group at the 14-year follow-up but the recurrence rate in the operative group was 67%. These figures would force us to take cautiously the recurrence rates in the studies carried out in the short term. We can conclude that at long-term, surgical stabilization does not reduce the rates of redislocation nor does it produce better subjective functional outcomes. According to Palmu et al. (9) the only significant predictor factor for recurrence was a positive family history of patellar instability. If we analyze in detail the above mentioned studies we can draw several conclusions: (I) the follow-up times are Page 3 of 7 very heterogeneous, so that the recurrence rates are not comparable; (II) the ages of the patients are not comparable in all the studies; (III) the small number of patients in the studies is a limiting factor that could lead to non-detection of statistically significant differences between the groups; (IV) the conservative treatment protocol is not the same in all studies; and (V) the types of surgical treatment are also different (realignment surgery, MPFL repair and MPFL reconstruction). Therefore, it is difficult to draw conclusions when doing systematic reviews with metaanalysis using these studies. Erickson et al. (17) conducted a systematic review of the literature in 2015 to identify meta-analyses comparing nonoperative and operative treatment of patellar dislocations. Meta-analysis quality and level of evidence were assessed. Patients treated operatively had a 24% rate of redislocations, whereas patients treated non-operatively had a 34.6% rate of redislocations (17). No differences in functional outcome scores were seen between both groups. Two out of four meta-analysis had low Oxman-Guyatt scores (<4), which indicates major flaws (17). Thus, according to the best available evidence, operative treatment of the first-time patellar dislocations may result in a lower rate of recurrence of dislocations than nonoperative treatment but does not improve functional outcome scores. Therefore, they conclude that the scientific evidence to recommend surgical treatment is low. When critically analyzing any of the previously mentioned studies we must check if the two groups that we are going to compare are really homogeneous. If they are not, the results are not going to be valid. We will now critically analyze the study by Bitar et al. (13). It is a RCT (level I of evidence) where results after a first lateral patellar dislocation treated with an MPFL reconstruction are compared with the results after a conservative treatment. The authors conclude that the results after a surgical treatment are better than with a conservative treatment after a 2-year follow-up. They observed a high percentage of recurrences in the conservative group (35%) while in the surgical group there were no cases of recurrence. To evaluate function the authors use the Kujala score that is significantly lower in the conservative treatment group (70.8) than in the surgical group (88.9). The authors conclude that the results of surgical treatment far exceed those of non-surgical treatment. However, when thoroughly analyzing the design of this study several questions come to mind. The information on randomization is unclear and therefore there is a risk of selection bias. Moreover, the allocation concealment is also unclear. All of this is
4 Page 4 of 7 Annals of Joint, 2018 important because if randomization is not adequate, the magnification of the effect of the intervention can be increased by 41% (18). If the randomization is not clear, the effect of the intervention can be increased by 30% (18). Furthermore, the absence of hiding the assigning sequence, can by itself magnify the effect of intervention by 21% (19). Moreover, there is a high risk of bias related to lack of blinding. We must note that if there is no double blind the effect of the intervention can be increased by 17% (18). What is more, if we thoroughly analyze the data they provide we can ask ourselves even more questions. Regarding the presence of predisposing factors according to each group, in the non-operative group there were 75% of knees with trochlear bump versus 50% in the reconstruction group. This is very important because trochlear dysplasia is an important risk factor for patellar dislocation recurrence (20,21). If we consider any predisposing factor for patellar instability the percentage in the non-operative group was of 95% vs. 66% in the reconstruction group. We are in fact comparing two groups that are not comparable. Therefore, results cannot be compared either and we must question the results of this study. Moreover, this paper has a duplicate publication (15). This paper was published in 2012 in the American Journal of Sports Medicine (13) and in 2015 in the Brazilian Journal of Orthopaedic Surgery (15). Duplicate publications are a serious problem because they deny other authors the chance to publish their work because of limited journal space. Another problem with duplicate publications is that they can lead to magnifying the results of one of the therapeutic options when a systematic review with metaanalysis is carried out. After a critical revision of the medical literature that compares conservative treatment results to surgical treatment results in a first-time lateral patellar dislocation (6-16), we can conclude that current evidence is not conclusive to recommend one treatment over the other. The quality of the evidence is very low. More studies with the current accepted design quality criteria and with long term results, preferably multicentric trials in order to have a larger number of cases, are necessary. This type of study, today, does not exist. Therefore, we must try to find other reasons to defend a surgical treatment rather than a conservative treatment. Decision based on predictive model analysis and pathoanatomy One reason that could make us decide between the surgical treatment and the conservative treatment is the recurrence risk seen with conservative treatment. The key question is: Can recurrent instability be predicted after a first-time patellar dislocation? The idea would be to identify those risk factors that can predict conservative treatment failure. We believe it would be interesting to analyze recurrent dislocation predictive models after a first episode of lateral patellar dislocation treated conservatively. Following this criterion, patients with a high recurrence risk would be candidates for a surgical treatment after the first lateral patellar dislocation. Nowadays in medicine, it is important to be able to predict future outcomes of treatments. In the past, it was based on the orthopaedic surgeon s experience. Currently, it has been replaced by predictive model analysis, historically used in many business segments and that currently is an important tool in making decisions in orthopaedic surgery. Predictive models, statistical tools that predict a clinical outcome based on at least two points of patient data, can assist in the decision-making process aimed at achieving better clinical outcomes, as well as reducing costs (22). Lewallen et al. (23) in 2013 analyzed what factors predict a lateral patellar dislocation recurrence in pediatric patients and adolescents with a mean age of 15 years (ranging from 9 18 years). They found that success with conservative treatment after a first-time patellar lateral dislocation was 62%, and that almost half of the patients with recurrent lateral patellar dislocation require surgical treatment. However, in skeletally immature patients (open physis) with trochlear dysplasia conservative treatment was successful in only 31% of the cases. Trochlear dysplasia is therefore a risk factor for recurrence of patellar dislocation. The greatest risk of recurrence of dislocation occurs in skeletally immature patients with trochlear dysplasia. The combination of the two factors (trochlear dysplasia and skeletal immaturity) conferred a 69% risk at 5 years (23). The results of this study are in agreement with those of Askenberger et al. (24) who found that trochlear dysplasia is the main anatomic patellar instability risk factor in the skeletally immature children for a primary lateral patellar dislocation. Sillanpää et al. (25) observed that lateral patellar dislocation recurrence was also related to the MPFL tear site after the first dislocation. An MPFL femoral avulsion was associated with a higher probability of recurrence. For this reason, they suggest considering the MPFL tear site when deciding on the treatment for a primary traumatic patellar dislocation. MPFL injury location and pattern can
5 Annals of Joint, 2018 Page 5 of 7 Patella alta Trochlear dysplasia <25 years old 5-year risk of recurrence (%) Yes Yes Yes 70 No Yes Yes 60 Yes No Yes 34 Yes Yes No 30 No No Yes 27 No Yes No 23 Yes No No 11 No No No 9 Figure 3 Clinical tool to evaluate risk of recurrence of patellar dislocation after the first episode (27). Surgical treatment recommended (pink); non-surgical treatment recommended (blue). be assessed by MRI (Figure 1). Jaquith and Parikh (26) performed a study in children and adolescents in order to predict the recurrence of patellar dislocation after a first episode of dislocation. They analyzed four risk factors: trochlear dysplasia, history of contralateral dislocation, skeletal immaturity and a Caton- Deschamps index greater than The recurrence rate with no associated risk factor was 13.8%. However, when one or more risk factors were present the recurrence rate increased considerably. When there was one risk factor present the recurrence rate was 30.1%, with two factors it was 53.6%, with three factors it was 74.8%, and with four it was 88.4%. However, this study is retrospective and therefore other factors such as hyperlaxity, lower limb malalignment or MPFL tear pattern were not included in the predictive model. Lewallen et al. (27) in 2015 analyzed the lateral patellar dislocation recurrence risk after one lateral dislocation in all the ages of patients with this type of problem, not just in children and adolescents like Jaquith and Parikh (26). In Table I you can see the 5-year risk of recurrence based on the associated risk factors. In the first two assumptions (see Figure 3) the authors recommend surgical treatment after one episode of lateral patellar dislocation because the recurrence rate is unacceptably high. In the last 6 cases (see Figure 3) surgical treatment is not recommended as a first line of treatment. Finally, Christensen et al. (28) have found that female patients under eighteen at the time of the first dislocation, trochlear dysplasia, elevated TT-TG distance, and patella alta were at risk for recurrence. To summarize, the pathoanatomy and the predictive models can help us estimate the dislocation recurrence risk after a first episode treated conservatively. This approach can help us with the decision-making for the optimal treatment for a patient with a first-time lateral patellar dislocation. Decision based on patient s goals return to sports at a pre-injury level When deciding on the best treatment for any injury, not only must we consider the best evidence available and/or anatomopathological factors, but also the patient s goals. Among those goals is the return to sports at a pre-injury level. Sport in the current society is so important that the United Nations has declared them a human right: Sport and play are human rights that must be respected and enforced worldwide. Practicing sports will demand more from the knee than a sedentary activity, therefore the joint s stability must be more perfect. The return to sports in adolescents after first-time patellar dislocations has not been well studied. Oliva et al. (29) found that in adolescent athletes with continued patellar instability after initial non-operative treatment, only 9 out of 24 (37.5%) returned to their pre-injury level of activity. Regalado et al. (16) in 2014 found that 80% of the adolescent patients treated surgically after a first-time lateral patellar dislocation achieve an excellent result regarding the return to sports at a pre-injury level. This percentage was only 47% for patients treated conservatively. These studies suggest that for athletic adolescents, surgery increases the probability of a return to sports compared with the conservative treatment. However, Sillanpää et al. (11) found that 72% of young adult patients with a mean age of 20 (ranging years of age) with a first-time lateral patellar dislocation treated surgically returned to sports in comparison with 68% of those treated conservatively.
6 Page 6 of 7 Annals of Joint, 2018 Economic decision model The only study published that analyzes the decision-making in an economic model is the one by Nwachukwu et al. (30) in The authors analyze the cost-utility of three different ways of addressing an acute first-time patellar dislocation in adolescents: (I) non-surgical treatment; (II) non-surgical treatment at first, but if an episode of dislocation is repeated again the patient is operated on; and (III) surgical treatment at first. In their analysis, the authors detail both the direct and indirect costs of each therapeutic strategy. Direct costs included direct medical costs: cost of surgery and physical therapy. Indirect costs were calculated from lost productivity associated with caregiver (parental) work absenteeism. Effectiveness was expressed in qualityadjusted life years (QALYs). The authors showed that both immediate surgical treatment and delayed surgery are cost-effective treatment options. Nevertheless, with a perspective of 10 years, immediate surgery provides the most QALY gains and therefore it would be the most cost effective treatment. These findings could have implications for therapeutic decision-making when we see a patient with a first episode of patellar dislocation. Conclusions Based on the data we have analyzed, the answer to the question we ask ourselves in this paper is yes. Primary patellar dislocations should be operated on more often after the first dislocation. We have to think critically and to keep an open mind towards new things. The role of surgery for first-time traumatic patellar dislocations is emerging as a reasonable treatment strategy. In highly active patients under 25 years of age with a pathoanatomy predisposing to recurrent dislocation (trochlear dysplasia associated or not with patella alta) surgical treatment could be considered as a first line of treatment in the first-time patellar dislocation because the recurrence risk is unacceptably high. This recommendation is based on recurrence predictive models after a firsttime patella dislocation and in cost effectiveness economic models. Moreover, we must incorporate individual circumstances and preferences (patient s goals such as sports) into the decision protocols. Obviously we need high quality clinical trials describing anatomical abnormalities and MPFL tear site, ideally multicentric ones, which compare surgical and conservative treatments after a first-time lateral patellar dislocation to definitely answer the question we ask ourselves in this paper. Acknowledgements None. Footnote Conflicts of Interest: The authors have no conflicts of interest to declare. References 1. Gravesen KS, Kallemose T, Blønd L, et al. High incidence of acute and recurrent patellar dislocations: a retrospective nationwide epidemiological study involving primary dislocations. Knee Surg Sports Traumatol Arthrosc [Epub ahead of print]. 2. Sanders TL, Pareek A, Hewett TE, et al. High rate of recurrent patellar dislocation in skeletally immature patients: a long-term population-based study. Knee Surg Sports Traumatol Arthrosc [Epub ahead of print]. 3. Sanders TL, Pareek A, Johnson NR, et al. Patellofemoral Arthritis After Lateral Patellar Dislocation: A Matched Population-Based Analysis. Am J Sports Med 2017; 45: Szucs D, Ioannidis JP. Empirical assessment of published effect sizes and power in the recent cognitive neuroscience and psychology literature. PLoS Biol 2017;15:e Ioannidis JP. How to make more published research true. PLoS Med 2014;11:e Nikku R, Nietosvaara Y, Kallio PE, et al. Operative versus closed treatment of primary dislocation of the patella. Similar 2-year results in 125 randomized patients. Acta Orthop Scand 1997;68: Buchner M, Baudendistel B, Sabo D, et al. Acute traumatic primary patellar dislocation: long-term results comparing conservative and surgical treatment. Clin J Sport Med 2005;15: Christiansen SE, Jakobsen BW, Lund B, et al. Isolated repair of the medial patellofemoral ligament in primary dislocation of the patella: a prospective randomized study. Arthroscopy 2008;24: Palmu S, Kallio PE, Donell ST, et al. Acute patellar dislocation in children and adolescents: a randomized clinical trial. J Bone Joint Surg Am 2008;90: Camanho GL, Viegas Ade C, Bitar AC, et al. Conservative versus surgical treatment for repair of the medial
7 Annals of Joint, 2018 Page 7 of 7 patellofemoral ligament in acute dislocations of the patella. Arthroscopy 2009;25: Sillanpää PJ, Mattila VM, Mäenpää H, et al. Treatment with and without initial stabilizing surgery for primary traumatic patellar dislocation. A prospective randomized study. J Bone Joint Surg Am 2009;91: Apostolovic M, Vukomanovic B, Slavkovic N, et al. Acute patellar dislocation in adolescents: operative versus nonoperative treatment. Int Orthop 2011;35: Bitar AC, Demange MK, D'Elia CO, et al. Traumatic patellar dislocation: nonoperative treatment compared with MPFL reconstruction using patellar tendon. Am J Sports Med 2012;40: Petri M, Liodakis E, Hofmeister M, et al. Operative vs conservative treatment of traumatic patellar dislocation: results of a prospective randomized controlled clinical trial. Arch Orthop Trauma Surg 2013;133: Bitar AC, D'Elia CO, Demange MK, et al. Randomized prospective study on traumatic patellar dislocation: conservative treatment versus reconstruction of the medial patellofemoral ligament using the patellar tendon, with a minimum of two years of follow-up. Rev Bras Ortop 2015;46: Regalado G, Lintula H, Kokki H, et al. Six-year outcome after non-surgical versus surgical treatment of acute primary patellar dislocation in adolescents: a prospective randomized trial. Knee Surg Sports Traumatol Arthrosc 2016;24: Erickson BJ, Mascarenhas R, Sayegh ET, et al. Does Operative Treatment of First-Time Patellar Dislocations Lead to Increased Patellofemoral Stability? A Systematic Review of Overlapping Meta-analyses. Arthroscopy 2015;31: Schulz KF, Chalmers I, Hayes RJ, et al. Empirical evidence of bias. Dimensions of methodological quality associated with estimates of treatment effects in controlled trials. JAMA 1995;273: Pildal J, Hróbjartsson A, Jørgensen KJ, et al. Impact of allocation concealment on conclusions drawn from meta-analyses of randomized trials. Int J Epidemiol 2007;36: Wagner D, Pfalzer F, Hingelbaum S, et al. The influence of risk factors on clinical outcomes following anatomical medial patellofemoral ligament (MPFL) reconstruction using the gracilis tendon. Knee Surg Sports Traumatol Arthrosc 2013;21: Nelitz M, Theile M, Dornacher D, et al. Analysis of failed surgery for patellar instability in children with open growth plates. Knee Surg Sports Traumatol Arthrosc 2012;20: Vogenberg FR. Predictive and Prognostic Models: Implications for Healthcare Decision-Making in a Modern Recession. Am Health Drug Benefits 2009;2: Lewallen LW, McIntosh AL, Dahm DL. Predictors of recurrent instability after acute patellofemoral dislocation in pediatric and adolescent patients. Am J Sports Med 2013;41: Askenberger M, Janarv PM, Finnbogason T, et al. Morphology and Anatomic Patellar Instability Risk Factors in First-Time Traumatic Lateral Patellar Dislocations: A Prospective Magnetic Resonance Imaging Study in Skeletally Immature Children. Am J Sports Med 2017;45: Sillanpää PJ, Peltola E, Mattila VM, et al. Femoral avulsion of the medial patellofemoral ligament after primary traumatic patellar dislocation predicts subsequent instability in men: a mean 7-year nonoperative follow-up study. Am J Sports Med 2009;37: Jaquith BP, Parikh SN. Predictors of Recurrent Patellar Instability in Children and Adolescents After First-time Dislocation. J Pediatr Orthop 2017;37: Lewallen L, McIntosh A, Dahm D. First-time Patellofemoral Dislocation: Risk Factors for Recurrent Instability. J Knee Surg 2015;28: Christensen TC, Sanders TL, Pareek A, et al. Risk Factors and Time to Recurrent Ipsilateral and Contralateral Patellar Dislocations. Am J Sports Med 2017;45: Oliva F, Ronga M, Longo UG, et al. The 3-in-1 procedure for recurrent dislocation of the patella in skeletally immature children and adolescents. Am J Sports Med 2009;37: Nwachukwu BU, So C, Schairer WW, et al. Economic Decision Model for First-Time Traumatic Patellar Dislocations in Adolescents. Am J Sports Med 2017;45: doi: /aoj Cite this article as: Sanchis-Alfonso V, Montesinos-Berry E. Acute dislocation of the patella: should these patients be operated on more often?.
Jacques Menetrey, MD, PD. Uniklinik Balgrist. Unité d Orthopédie et Traumatologie du Sport (UOTS)
 Acute patellar dislocation: conservative or surgical treatment Jacques Menetrey, MD, PD Unité d Orthopédie et Traumatologie du Sport (UOTS) Service de chirurgie orthopédique et traumatologie de l appareil
Acute patellar dislocation: conservative or surgical treatment Jacques Menetrey, MD, PD Unité d Orthopédie et Traumatologie du Sport (UOTS) Service de chirurgie orthopédique et traumatologie de l appareil
1 st Time Patella Dislocation When is it best to intervene? The Dilemma. Patellar Dislocation The Issues 3/9/2018. Is there a difference?
 1 st Time Patella Dislocation When is it best to intervene? Jim Bradley MD Clinical Professor UPMC Head Team Physician, Pittsburgh Steelers Consultant Miami Marlins Michael Nickoli MD Orthopaedic Surgery
1 st Time Patella Dislocation When is it best to intervene? Jim Bradley MD Clinical Professor UPMC Head Team Physician, Pittsburgh Steelers Consultant Miami Marlins Michael Nickoli MD Orthopaedic Surgery
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016
 Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
First-Time Patellofemoral Dislocation: Risk Factors for Recurrent Instability
 Special Focus Section 303 First-Time Patellofemoral Dislocation: Risk Factors for Recurrent Instability Laura Lewallen, MD 1 Amy McIntosh, MD 1 Diane Dahm, MD 1 1 Department of Orthopedic Surgery, Mayo
Special Focus Section 303 First-Time Patellofemoral Dislocation: Risk Factors for Recurrent Instability Laura Lewallen, MD 1 Amy McIntosh, MD 1 Diane Dahm, MD 1 1 Department of Orthopedic Surgery, Mayo
Patella Instability 1 st Time Dislocation
 Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery. Restore patella stability.
 Page 1 of 5 Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery Restore patella stability. Restore / improve function. I have no conflicts to declare. 1987
Page 1 of 5 Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery Restore patella stability. Restore / improve function. I have no conflicts to declare. 1987
Where to Draw the Line:
 Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
High incidence of acute and recurrent patellar dislocations: a retrospective nationwide epidemiological study involving primary dislocations
 High incidence of acute and recurrent patellar dislocations: a retrospective nationwide epidemiological study involving 24.154 primary dislocations Kasper Skriver Gravesen, Thomas Kallemose, Lars Blønd,
High incidence of acute and recurrent patellar dislocations: a retrospective nationwide epidemiological study involving 24.154 primary dislocations Kasper Skriver Gravesen, Thomas Kallemose, Lars Blønd,
Lower Extremity Sports Injuries
 Lower Extremity Sports Injuries AAP Musculoskeletal Boot Camp Sigrid F. Wolf, MD Pediatric Sports Medicine Fellow Northwestern University Lurie Children s Hospital Disclosure I have no relevant financial
Lower Extremity Sports Injuries AAP Musculoskeletal Boot Camp Sigrid F. Wolf, MD Pediatric Sports Medicine Fellow Northwestern University Lurie Children s Hospital Disclosure I have no relevant financial
The Role of Medial Patellofemoral Ligament Repair and Imbrication
 A Review Paper The Role of Medial Patellofemoral Ligament Repair and Imbrication Kyle R. Duchman, MD, and Matthew J. Bollier, MD Abstract Repair, reefing, and advancement of the medial patellofemoral ligament
A Review Paper The Role of Medial Patellofemoral Ligament Repair and Imbrication Kyle R. Duchman, MD, and Matthew J. Bollier, MD Abstract Repair, reefing, and advancement of the medial patellofemoral ligament
Patellofemoral Joint. Question? ANATOMY
 Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Where are we now? A little bit of History.. Is menu à la carte relevant in 2019? Medial PatelloFemoral Ligament the Queen of the PF Joint
 Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Personal use only. MRI of the extensor mechanism of the knee. 5 th Musculoskeletal MRI meeting. Falkowski, MD, MHBA
 MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents
 Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents Sheena R. Black, MD, Henry B. Ellis, MD, Philip L. Wilson, MD, David A. Podeszwa, MD LLRS Annual
Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents Sheena R. Black, MD, Henry B. Ellis, MD, Philip L. Wilson, MD, David A. Podeszwa, MD LLRS Annual
PROSPECTIVE AND COMPAR TMENT (MEDIAL PETELLOFEMOR
 ORIGINAL ARTICLE PROSPECTIVE AND COMPAR ARATIVE STUDY BETWEEN CONSERVATIVE AND SURGICAL TREATMENT TMENT (MEDIAL PETELLOFEMOR OFEMORAL LIGAMENT REPAIR) IN PATELL TELLAR ACUTE DISLOCA OCATIONS GILBERTO LUIS
ORIGINAL ARTICLE PROSPECTIVE AND COMPAR ARATIVE STUDY BETWEEN CONSERVATIVE AND SURGICAL TREATMENT TMENT (MEDIAL PETELLOFEMOR OFEMORAL LIGAMENT REPAIR) IN PATELL TELLAR ACUTE DISLOCA OCATIONS GILBERTO LUIS
10/30/18. Disclosures. Recurrent Patellar Instability. Management of Recurrent Patellar Instability
 Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
8/9/2017. Case Based: Beyond Medial Patellofemoral Ligament. Editorial Board AJSM Social Media. Consultant. Not talking about PF pain/chondrosis Rehab
 Case Based: Beyond Medial Patellofemoral Ligament Dr Alan Getgood MD FRCS(Tr&Orth) DipSEM Assistant Professor Orthopaedic Sport Medicine Fellowship Director The Fowler Kennedy Sport Medicine Clinic University
Case Based: Beyond Medial Patellofemoral Ligament Dr Alan Getgood MD FRCS(Tr&Orth) DipSEM Assistant Professor Orthopaedic Sport Medicine Fellowship Director The Fowler Kennedy Sport Medicine Clinic University
Acute patellar dislocation in adults
 CASE STUDY 14 Acute patellar dislocation in adults What are the reasons for the first acute dislocation? How can we document the pathoanatomy? What is our treatment concept? Table CS14 Patellofemoral joint
CASE STUDY 14 Acute patellar dislocation in adults What are the reasons for the first acute dislocation? How can we document the pathoanatomy? What is our treatment concept? Table CS14 Patellofemoral joint
The American Journal of Sports Medicine
 The American Journal of Sports Medicine http://ajs.sagepub.com/ Femoral Avulsion of the Medial Patellofemoral Ligament After Primary Traumatic Patellar Dislocation Predicts Subsequent Instability in Men
The American Journal of Sports Medicine http://ajs.sagepub.com/ Femoral Avulsion of the Medial Patellofemoral Ligament After Primary Traumatic Patellar Dislocation Predicts Subsequent Instability in Men
General Concepts. Growth Around the Knee. Topics. Evaluation
 General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
Introduction. Helmut Wegmann 1 Christoph Würnschimmel 2 Tanja Kraus 2 Georg Singer 1 Robert Eberl 1 Holger Till 1 Matthias Sperl 2
 DOI 10.1007/s00167-017-4425-x KNEE Medial patellofemoral ligament (MPFL) reconstruction in combination with a modified grammont technique leads to favorable mid-term results in adolescents with recurrent
DOI 10.1007/s00167-017-4425-x KNEE Medial patellofemoral ligament (MPFL) reconstruction in combination with a modified grammont technique leads to favorable mid-term results in adolescents with recurrent
Department of Orthopedic Surgery, Ewha Womans University Mokdong Hospital, Seoul, Korea
 Case Report https://doi.org/10.14517/aosm16016 pissn 2289-005X eissn 2289-0068 Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun
Case Report https://doi.org/10.14517/aosm16016 pissn 2289-005X eissn 2289-0068 Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun
No Disclosures. Topics. Pediatric ACL Tears
 Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Pediatric Anterior Cruciate Ligament Injuries Is non operative treatment t t an option?
 I have no disclosures Pediatric Anterior Cruciate Ligament Injuries Is non operative treatment t t an option? John F. Lovejoy III, MD Chair, Department of Orthopaedics and Sports Medicine Nemours Children
I have no disclosures Pediatric Anterior Cruciate Ligament Injuries Is non operative treatment t t an option? John F. Lovejoy III, MD Chair, Department of Orthopaedics and Sports Medicine Nemours Children
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes
 Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Traumatic Patellar Dislocation and Cartilage Injury A Follow- Up Study of Long-Term Cartilage Deterioration
 Traumatic Patellar Dislocation and Cartilage Injury A Follow- Up Study of Long-Term Cartilage Deterioration Salonen EE 1 M.D., Magga T 2 M.D., Sillanpää PJ 3 M.D. Ph.D., Kiekara T 2 M.D., Ph.D., Mäenpää
Traumatic Patellar Dislocation and Cartilage Injury A Follow- Up Study of Long-Term Cartilage Deterioration Salonen EE 1 M.D., Magga T 2 M.D., Sillanpää PJ 3 M.D. Ph.D., Kiekara T 2 M.D., Ph.D., Mäenpää
Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability
 Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability Two-Year Results of an Algorithm-Based Approach Jason L. Dragoo,* MD, Michael Nguyen, MD, Corey T. Gatewood,
Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability Two-Year Results of an Algorithm-Based Approach Jason L. Dragoo,* MD, Michael Nguyen, MD, Corey T. Gatewood,
Computational Evaluation of Predisposing Factors to Patellar Dislocation
 Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD
 Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD Disclosures Consultant: Smith & Nephew A3 surgical Stockholder: A3 surgical Case Presentation:
Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD Disclosures Consultant: Smith & Nephew A3 surgical Stockholder: A3 surgical Case Presentation:
Clinical Outcomes After the Nonoperative Management of Lateral Patellar Dislocations
 Review Clinical Outcomes After the Nonoperative Management of Lateral Patellar Dislocations A Systematic Review Munim Moiz,* MBBS, BSc, Nick Smith,* BMBS, BMedSci, MSc, PhD, FRCS(Tr&Orth), Toby O. Smith,
Review Clinical Outcomes After the Nonoperative Management of Lateral Patellar Dislocations A Systematic Review Munim Moiz,* MBBS, BSc, Nick Smith,* BMBS, BMedSci, MSc, PhD, FRCS(Tr&Orth), Toby O. Smith,
Knee Case Studies. You might KNEED to know some of this stuff
 Knee Case Studies You might KNEED to know some of this stuff Mark Mildren, MD Specializing in Adult Reconstruction Slocum Center for Orthopedics & Sports Medicine 25 th Annual Orthopedic & Sports Medicine
Knee Case Studies You might KNEED to know some of this stuff Mark Mildren, MD Specializing in Adult Reconstruction Slocum Center for Orthopedics & Sports Medicine 25 th Annual Orthopedic & Sports Medicine
Adult Reconstruction Hip Education Tracks
 Adult Reconstruction Hip Education Tracks Adult Reconstruction Hip Track for the Specialist - HIP1 ICL 281 A Case-based Approach to High Risk Total Hip - When Do I Do Something Differently? ICL 241 The
Adult Reconstruction Hip Education Tracks Adult Reconstruction Hip Track for the Specialist - HIP1 ICL 281 A Case-based Approach to High Risk Total Hip - When Do I Do Something Differently? ICL 241 The
THANK YOU 7/29/2016 DISCLOSURES PATELLOFEMORAL INSTABILITY INTO THE MYSTIC. Skeletally Immature Patients. Anthropology. Epidemiology.
 DETROIT REGIONAL SPORTS MEDICINE SYMPOSIUM THANK YOU Richard Hinton, MD, MPH, MEd, PT Medical and Fellowship Director MedStar Sports Medicine Baltimore / Washington richard.hinton@medstar.net, (410) 554
DETROIT REGIONAL SPORTS MEDICINE SYMPOSIUM THANK YOU Richard Hinton, MD, MPH, MEd, PT Medical and Fellowship Director MedStar Sports Medicine Baltimore / Washington richard.hinton@medstar.net, (410) 554
BAD RESULTS OF CONSERVATIVE TREATMENT OF ACL TEARS IN CHILDREN. Guy BELLIER PARIS France
 BAD RESULTS OF CONSERVATIVE TREATMENT OF ACL TEARS IN CHILDREN Guy BELLIER PARIS France TREATMENT OF ACL TEARS IN CHILDREN CONTROVERSIAL DIAGNOSIS clinical exam X-rays (stress) M.R.I. arthroscopy ACL TEARS
BAD RESULTS OF CONSERVATIVE TREATMENT OF ACL TEARS IN CHILDREN Guy BELLIER PARIS France TREATMENT OF ACL TEARS IN CHILDREN CONTROVERSIAL DIAGNOSIS clinical exam X-rays (stress) M.R.I. arthroscopy ACL TEARS
Patellar instability
 Page 1 of 13 Specific Injuries D Goodwin 1, W Postma 2 * Patellar instability Abstract Introduction Patellar instability is most common among adolescent female athletes, although anyone can be affected.
Page 1 of 13 Specific Injuries D Goodwin 1, W Postma 2 * Patellar instability Abstract Introduction Patellar instability is most common among adolescent female athletes, although anyone can be affected.
Radiological evaluation of the causes of patellar instability.
 Radiological evaluation of the causes of patellar instability. Poster No.: C-0054 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. M. Spaccesi Pau, D. Pomato, N. CEDOLA; La Plata/AR
Radiological evaluation of the causes of patellar instability. Poster No.: C-0054 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. M. Spaccesi Pau, D. Pomato, N. CEDOLA; La Plata/AR
Why does it matter? Patellar Instability 7/23/2018. What is the current operation de jour? Common. Poorly taught. Poorly treated
 Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no
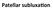 Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
CT Evaluation of Patellar Instability
 CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
7/20/14. Patella Instability. Alignment. PF contact areas. Tissue Restraints. Pain. Acute Blunt force trauma Disorders of the Patellafemoral Joint
 Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Medial Patellofemoral Ligament Reconstruction
 53 Medial Patellofemoral Ligament Reconstruction Hany Elrashidy, Joseph Carney, Najeeb Khan, and Donald C. Fithian CHAPTER DEFINITION Stability of the patellofemoral joint (PFJ) is multifactorial as it
53 Medial Patellofemoral Ligament Reconstruction Hany Elrashidy, Joseph Carney, Najeeb Khan, and Donald C. Fithian CHAPTER DEFINITION Stability of the patellofemoral joint (PFJ) is multifactorial as it
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force.
 Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
Unicompartmental Knee Replacement
 Unicompartmental Knee Replacement Results and Techniques Alexander P. Sah, MD California Orthopaedic Association Meeting Laguna Niguel, CA May 20th, 2011 Overview Why partial knee replacement? - versus
Unicompartmental Knee Replacement Results and Techniques Alexander P. Sah, MD California Orthopaedic Association Meeting Laguna Niguel, CA May 20th, 2011 Overview Why partial knee replacement? - versus
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries
 What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
Knee Contusions and Stress Injuries. Laura W. Bancroft, M.D.
 Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Musculoskeletal Applications for CT. Tal Laor, MD Cincinnati Children s Hospital University of Cincinnati College of Medicine
 Musculoskeletal Applications for CT Tal Laor, MD Cincinnati Children s Hospital University of Cincinnati College of Medicine I have no commercial disclosures. Why CT? Complimentary to other modalities
Musculoskeletal Applications for CT Tal Laor, MD Cincinnati Children s Hospital University of Cincinnati College of Medicine I have no commercial disclosures. Why CT? Complimentary to other modalities
Primary traumatic patellar dislocation
 Tsai et al. Journal of Orthopaedic Surgery and Research 2012, 7:21 REVIEW Primary traumatic patellar dislocation Chun-Hao Tsai 1, Chin-Jung Hsu 1, Chih-Hung Hung 1 and Horng-Chaung Hsu 1,2* Open Access
Tsai et al. Journal of Orthopaedic Surgery and Research 2012, 7:21 REVIEW Primary traumatic patellar dislocation Chun-Hao Tsai 1, Chin-Jung Hsu 1, Chih-Hung Hung 1 and Horng-Chaung Hsu 1,2* Open Access
The value of weight-bearing functional CT scans
 The value of weight-bearing functional scans In musculoskeletal medicine, advanced imaging like computed axial tomography () scanning, has become invaluable to the evaluation and management of patients
The value of weight-bearing functional scans In musculoskeletal medicine, advanced imaging like computed axial tomography () scanning, has become invaluable to the evaluation and management of patients
Patellar instability - An update
 Acta Orthop. Belg., 2017, 83, 367-386 ORIGINAL STUDY Patellar instability - An update Lars Blønd From the Zealand University Hospital, Køge, Department of Orthopedics, Arthroscopic Section, Koege, Denmark
Acta Orthop. Belg., 2017, 83, 367-386 ORIGINAL STUDY Patellar instability - An update Lars Blønd From the Zealand University Hospital, Køge, Department of Orthopedics, Arthroscopic Section, Koege, Denmark
Doron Sher. 160 Belmore Rd, Randwick Burwood Rd, Concord. MBBS, MBiomedE, FRACS FAOrthA
 Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Lateral ligament injuries of the knee
 Knee Surg, Sports Traumatol, Arthrosc (1998) 6:21 25 KNEE Springer-Verlag 1998 Y. Krukhaug A. Mølster A. Rodt T. Strand Lateral ligament injuries of the knee Received: 22 January 1997 Accepted: 20 June
Knee Surg, Sports Traumatol, Arthrosc (1998) 6:21 25 KNEE Springer-Verlag 1998 Y. Krukhaug A. Mølster A. Rodt T. Strand Lateral ligament injuries of the knee Received: 22 January 1997 Accepted: 20 June
Surgical versus conservative treatment for acute first-time anterior shoulder dislocation: the evidence
 J Orthopaed Traumatol (2007) 8:207 213 DOI 10.1007/s10195-007-0095-7 EVIDENCE-BASED MEDICINE SECTION R. Padua R. Bondì L. Bondì A. Campi Surgical versus conservative treatment for acute first-time anterior
J Orthopaed Traumatol (2007) 8:207 213 DOI 10.1007/s10195-007-0095-7 EVIDENCE-BASED MEDICINE SECTION R. Padua R. Bondì L. Bondì A. Campi Surgical versus conservative treatment for acute first-time anterior
Reconstruction of the medial patellofemoral ligament for treatment of patellar instability
 354 Acta Orthopaedica 2008; 79 (3): 354 360 Review Reconstruction of the medial patellofemoral ligament for treatment of patellar instability Martin Lind, Bent W Jakobsen, Bent Lund, and Svend Erik Christiansen
354 Acta Orthopaedica 2008; 79 (3): 354 360 Review Reconstruction of the medial patellofemoral ligament for treatment of patellar instability Martin Lind, Bent W Jakobsen, Bent Lund, and Svend Erik Christiansen
Research Article Long-Term Follow-Up of Nonoperatively and Operatively Treated Acute Primary Patellar Dislocation in Skeletally Immature Patients
 Hindawi Publishing Corporation e Scientific World Journal Volume 2014, Article ID 473281, 8 pages http://dx.doi.org/10.1155/2014/473281 Research Article Long-Term Follow-Up of Nonoperatively and Operatively
Hindawi Publishing Corporation e Scientific World Journal Volume 2014, Article ID 473281, 8 pages http://dx.doi.org/10.1155/2014/473281 Research Article Long-Term Follow-Up of Nonoperatively and Operatively
Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff),
 Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff), Consultant Knee Surgeon NHS: The Royal Orthopaedic Hospital & Queen Elizabeth Hospital, Birmingham MRI Knee:
Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff), Consultant Knee Surgeon NHS: The Royal Orthopaedic Hospital & Queen Elizabeth Hospital, Birmingham MRI Knee:
Chronic patellar dislocation in adults
 CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
Review Article Patellofemoral Joint Instability: A Review of Current Concepts
 Ashdin Publishing Journal of Orthopaedics and Trauma Vol. 6 (2016), Article ID 235979, 8 pages doi:10.4303/jot/235979 ASHDIN publishing Review Article Patellofemoral Joint Instability: A Review of Current
Ashdin Publishing Journal of Orthopaedics and Trauma Vol. 6 (2016), Article ID 235979, 8 pages doi:10.4303/jot/235979 ASHDIN publishing Review Article Patellofemoral Joint Instability: A Review of Current
Retinacular tear knee
 P ford residence southampton, ny Retinacular tear knee The medial patellofemoral ligament (MPFL) helps to keep the kneecap centered along the front of the knee, so that it tracks well during knee movements.
P ford residence southampton, ny Retinacular tear knee The medial patellofemoral ligament (MPFL) helps to keep the kneecap centered along the front of the knee, so that it tracks well during knee movements.
Anterior Cruciate Ligament (ACL) Injuries
 Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Peggers Super Summaries: PFJ
 Patellofemoral Joint: ANATOMY: Largest sesamoid ossifying at 3-5 years of age Multiple foci having a sec ossification centre SUPEROLATERAL Helps increase moment arm PATELLOFEMORAL OA Incidence 10% of knee
Patellofemoral Joint: ANATOMY: Largest sesamoid ossifying at 3-5 years of age Multiple foci having a sec ossification centre SUPEROLATERAL Helps increase moment arm PATELLOFEMORAL OA Incidence 10% of knee
LARS (Ligament Augmentation & Reconstruction System) Literature
 LARS-Related Studies and Papers ACL: 1. Level of Evidence: IV Li, H. et al (2011). Enhancement of the osseointegration of a polyethylene Terephthalate artificial ligament graft in a bone tunnel using 58S
LARS-Related Studies and Papers ACL: 1. Level of Evidence: IV Li, H. et al (2011). Enhancement of the osseointegration of a polyethylene Terephthalate artificial ligament graft in a bone tunnel using 58S
Management of patellofemoral instability in the setting of multiligament knee injury
 Review Article Page 1 of 10 Management of patellofemoral instability in the setting of multiligament knee injury Seth L. Sherman 1, Lasun O. Oladeji 1, John Welsh 2, Zachary J. DiPaolo 1 1 Division of
Review Article Page 1 of 10 Management of patellofemoral instability in the setting of multiligament knee injury Seth L. Sherman 1, Lasun O. Oladeji 1, John Welsh 2, Zachary J. DiPaolo 1 1 Division of
Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini
 Open Access Case report Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini Address: Department of Orthopaedic
Open Access Case report Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini Address: Department of Orthopaedic
Does the patellofemoral joint need articular cartilage? clinical relevance
 Review Article Page 1 of 6 Does the patellofemoral joint need articular cartilage? clinical relevance Lars Blønd 1,2 1 Department of Orthopaedic Surgery, Aleris-Hamlet Parken, Copenhagen, Denmark; 2 Department
Review Article Page 1 of 6 Does the patellofemoral joint need articular cartilage? clinical relevance Lars Blønd 1,2 1 Department of Orthopaedic Surgery, Aleris-Hamlet Parken, Copenhagen, Denmark; 2 Department
Dimensions of the intercondylar notch and the distal femur throughout life
 Dimensions of the intercondylar notch and the distal femur throughout life Poster No.: P-0089 Congress: ESSR 2013 Type: Scientific Exhibit Authors: L. Hirtler, S. Röhrich, F. Kainberger; Vienna/AT Keywords:
Dimensions of the intercondylar notch and the distal femur throughout life Poster No.: P-0089 Congress: ESSR 2013 Type: Scientific Exhibit Authors: L. Hirtler, S. Röhrich, F. Kainberger; Vienna/AT Keywords:
Additions: lumbar spine/spondy. spondy. panners? Elbow dislocation?
 Additions: lumbar spine/spondy spondy panners? Elbow dislocation? 16 y.o.. female swimmer has had right shoulder pain for the past 6 months. Ultrasound treatment and rest have failed to provide relief.
Additions: lumbar spine/spondy spondy panners? Elbow dislocation? 16 y.o.. female swimmer has had right shoulder pain for the past 6 months. Ultrasound treatment and rest have failed to provide relief.
40 th Annual Symposium on Sports Medicine. Knee Injuries In The Pediatric Athlete. Disclosure
 40 th Annual Symposium on Sports Medicine Travis Murray, MD Assistant Professor University of Texas Health Science Center San Antonio Knee Injuries In The Pediatric Athlete Disclosure Dr. Travis Murray
40 th Annual Symposium on Sports Medicine Travis Murray, MD Assistant Professor University of Texas Health Science Center San Antonio Knee Injuries In The Pediatric Athlete Disclosure Dr. Travis Murray
Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia
 Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia A 4- TO 14-YEAR FOLLOW-UP STUDY F. von Knoch, T. Böhm, M. L. Bürgi, M. von Knoch, H. Bereiter From the Kantonsspital
Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia A 4- TO 14-YEAR FOLLOW-UP STUDY F. von Knoch, T. Böhm, M. L. Bürgi, M. von Knoch, H. Bereiter From the Kantonsspital
Unlocking the locked Knee
 Unlocking the locked Knee Poster No.: P-0027 Congress: ESSR 2013 Type: Scientific Exhibit Authors: J. P. SINGH, S. Srivastava, S. S. BAIJAL ; Gurgaon, Delhi 1 1 2 1 2 NCR/IN, LUCKNOW, UTTAR PRADESH/IN
Unlocking the locked Knee Poster No.: P-0027 Congress: ESSR 2013 Type: Scientific Exhibit Authors: J. P. SINGH, S. Srivastava, S. S. BAIJAL ; Gurgaon, Delhi 1 1 2 1 2 NCR/IN, LUCKNOW, UTTAR PRADESH/IN
Ideal Candidate for Cartilage Restoration. Large or Complex Lesions
 Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Pediatric and Adolescent Sports ACL Injuries
 Pediatric and Adolescent Sports ACL Injuries Stephen K. Aoki, MD Associate Professor University of Utah Department of Orthopaedics Pediatric and Adult Sports Medicine Outline Highlight the following: Differences
Pediatric and Adolescent Sports ACL Injuries Stephen K. Aoki, MD Associate Professor University of Utah Department of Orthopaedics Pediatric and Adult Sports Medicine Outline Highlight the following: Differences
Overview Ligament Injuries. Anatomy. Epidemiology Very commonly injured joint. ACL Injury 20/06/2016. Meniscus Tears. Patellofemoral Problems
 Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
EMERGENCY PITFALLS IN ORTHOPAEDIC TRAUMA. Thierry E. Benaroch, MD, FRCS MCH Trauma Rounds February 9, 2009
 EMERGENCY PITFALLS IN ORTHOPAEDIC TRAUMA Thierry E. Benaroch, MD, FRCS MCH Trauma Rounds February 9, 2009 MORAL OF THE STORY Fracture distal radius and intact ulna W/O radius fracture will most likely
EMERGENCY PITFALLS IN ORTHOPAEDIC TRAUMA Thierry E. Benaroch, MD, FRCS MCH Trauma Rounds February 9, 2009 MORAL OF THE STORY Fracture distal radius and intact ulna W/O radius fracture will most likely
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
Patellofemoral Masterclass
 A unique course dedicated to joint disorders in both young and ageing population CPD applied for 1st-3rd November 2018 LIMITED TO 16 PLACES 1st & 2nd November Scarman Conference Centre, Coventry 3rd November
A unique course dedicated to joint disorders in both young and ageing population CPD applied for 1st-3rd November 2018 LIMITED TO 16 PLACES 1st & 2nd November Scarman Conference Centre, Coventry 3rd November
Classification of Acetabular Cartilage Lesions. Claudio Mella, MD
 Classification of Acetabular Cartilage Lesions Claudio Mella, MD Acetabular cartilage lesions are frequently found during hip arthroscopy. The arthroscopic view offers an exceptional perspective to assess
Classification of Acetabular Cartilage Lesions Claudio Mella, MD Acetabular cartilage lesions are frequently found during hip arthroscopy. The arthroscopic view offers an exceptional perspective to assess
Indications for Medial Patellofemoral Ligament Reconstruction: A Systematic Review
 Original Article Indications for Medial Patellofemoral Ligament Reconstruction: A Systematic Review Marco Yeung, MD 1 Marie-Claude Leblanc, MD, FRCS(C) 1 Olufemi R. Ayeni, MD, MSc, FRCS(C) 1 Moin Khan,
Original Article Indications for Medial Patellofemoral Ligament Reconstruction: A Systematic Review Marco Yeung, MD 1 Marie-Claude Leblanc, MD, FRCS(C) 1 Olufemi R. Ayeni, MD, MSc, FRCS(C) 1 Moin Khan,
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
Grand Rounds from HSS
 winter 2014 Volume 4 Issue 3 Grand Rounds from HSS Management of complex cases Authors Beth E. Shubin Stein, MD Associate Attending Orthopaedic Surgeon Associate Professor of Orthopaedic Surgery Sabrina
winter 2014 Volume 4 Issue 3 Grand Rounds from HSS Management of complex cases Authors Beth E. Shubin Stein, MD Associate Attending Orthopaedic Surgeon Associate Professor of Orthopaedic Surgery Sabrina
Cale A. Jacobs 1, Chaitu S. Malempati 1, Eric C. Makhni 2, Darren L. Johnson 1. Introduction
 Original Article Page 1 of 7 Allograft augmentation of hamstring autografts was not a costeffective treatment option for middle aged patients undergoing primary anterior cruciate ligament reconstruction
Original Article Page 1 of 7 Allograft augmentation of hamstring autografts was not a costeffective treatment option for middle aged patients undergoing primary anterior cruciate ligament reconstruction
Humber. Arthroscopy Knee
 Humber Arthroscopy Knee Intervention Diagnostic & Therapeutic Arthroscopy Knee OPCS Codes W85 Therapeutic endoscopic operations on cavity of knee joint W851 Endoscopic removal of loose body from knee joint
Humber Arthroscopy Knee Intervention Diagnostic & Therapeutic Arthroscopy Knee OPCS Codes W85 Therapeutic endoscopic operations on cavity of knee joint W851 Endoscopic removal of loose body from knee joint
Patella Alta: Lack of Correlation Between Patellotrochlear Cartilage Congruence and Commonly Used Patellar Height Ratios
 Musculoskeletal Imaging Original Research Ali et al. Patella Alta Musculoskeletal Imaging Original Research Syed A. Ali 1 Robert Helmer Michael R. Terk Ali SA, Helmer R, Terk MR Keywords: Insall-Salvati
Musculoskeletal Imaging Original Research Ali et al. Patella Alta Musculoskeletal Imaging Original Research Syed A. Ali 1 Robert Helmer Michael R. Terk Ali SA, Helmer R, Terk MR Keywords: Insall-Salvati
Please differentiate an internal derangement from an external knee injury.
 Knee Orthopaedic Tests Sports and Knee Injuries James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Knee Injury Strain, Sprain, Internal Derangement Anatomy of the Knee Please
Knee Orthopaedic Tests Sports and Knee Injuries James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Knee Injury Strain, Sprain, Internal Derangement Anatomy of the Knee Please
Surgical treatment of patellar instability can be
 Medial Patellofemoral Ligament Reconstruction Using a Modified Reverse-Loop Technique Nels E. Sampatacos, M.D., and Mark H. Getelman, M.D. Abstract: Medial patellofemoral ligament reconstruction is a commonly
Medial Patellofemoral Ligament Reconstruction Using a Modified Reverse-Loop Technique Nels E. Sampatacos, M.D., and Mark H. Getelman, M.D. Abstract: Medial patellofemoral ligament reconstruction is a commonly
9400 West Higgins Road, Rosemont Illinois January 2017
 Quality Newsletter 9400 West Higgins Road, Rosemont Illinois 60018 847.823.7186 www.aaos.org January 2017 Solicitations Detection and Nonoperative Management of Pediatric Developmental Dysplasia of the
Quality Newsletter 9400 West Higgins Road, Rosemont Illinois 60018 847.823.7186 www.aaos.org January 2017 Solicitations Detection and Nonoperative Management of Pediatric Developmental Dysplasia of the
42 nd Annual Symposium on Sports Medicine. Knee Injuries In The Pediatric Athlete. Disclosure
 42 nd Annual Symposium on Sports Medicine Travis Murray, MD Assistant Professor University of Texas Health Science Center San Antonio January 23, 2015 Knee Injuries In The Pediatric Athlete Disclosure
42 nd Annual Symposium on Sports Medicine Travis Murray, MD Assistant Professor University of Texas Health Science Center San Antonio January 23, 2015 Knee Injuries In The Pediatric Athlete Disclosure
Patellar malalignment: a new method on knee MRI
 DOI 10.1186/s40064-016-3195-0 RESEARCH Open Access Patellar malalignment: a new method on knee MRI Hülya Kurtul Yildiz * and Elif Evrim Ekin Abstract Purpose: The medial patellofemoral ligament (MPFLL)/lateral
DOI 10.1186/s40064-016-3195-0 RESEARCH Open Access Patellar malalignment: a new method on knee MRI Hülya Kurtul Yildiz * and Elif Evrim Ekin Abstract Purpose: The medial patellofemoral ligament (MPFLL)/lateral
The Knee 20 S1 (2013) S3 S15. Contents lists available at SciVerse ScienceDirect. The Knee
 The Knee 20 S1 (2013) S3 S15 Contents lists available at SciVerse ScienceDirect The Knee Review The contemporary management of anterior knee pain and patellofemoral instability Toby O. Smith, Iain McNamara,
The Knee 20 S1 (2013) S3 S15 Contents lists available at SciVerse ScienceDirect The Knee Review The contemporary management of anterior knee pain and patellofemoral instability Toby O. Smith, Iain McNamara,
Clinical outcomes of rehabilitation for patients following lateral patellar dislocation: a systematic review
 Physiotherapy 96 (2010) 269 281 Systematic review Clinical outcomes of rehabilitation for patients following lateral patellar dislocation: a systematic review Toby O. Smith a,c,, Leigh Davies b, Rachel
Physiotherapy 96 (2010) 269 281 Systematic review Clinical outcomes of rehabilitation for patients following lateral patellar dislocation: a systematic review Toby O. Smith a,c,, Leigh Davies b, Rachel
Will She Still Make the WNBA? Sports Injuries & Fractures
 Will She Still Make the WNBA? Sports Injuries & Fractures Aharon Z. Gladstein MD Pediatric Orthopaedic Surgery Pediatric Sports Medicine Sports Injuries Chronic (overuse) Acute Who can be treated in PCP
Will She Still Make the WNBA? Sports Injuries & Fractures Aharon Z. Gladstein MD Pediatric Orthopaedic Surgery Pediatric Sports Medicine Sports Injuries Chronic (overuse) Acute Who can be treated in PCP
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Physiotherapy in Recurrent Dislocation of Patella-Wiberg Type II Farzana Alam, Subhadeep Roy Choudhury BPT,
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Physiotherapy in Recurrent Dislocation of Patella-Wiberg Type II Farzana Alam, Subhadeep Roy Choudhury BPT,
The Society for Patient Centered Orthopedics. Choosing Wisely List. James Rickert, MD 1
 The Society for Patient Centered Orthopedics Choosing Wisely List James Rickert, MD 1 Extremities and Trauma Vertebroplasty Rotator Cuff Repair: For atraumatic (degenerative) tears in patients greater
The Society for Patient Centered Orthopedics Choosing Wisely List James Rickert, MD 1 Extremities and Trauma Vertebroplasty Rotator Cuff Repair: For atraumatic (degenerative) tears in patients greater
Quality Newsletter. OA Hip CPG Approved by BOD. More Quality Links
 Quality Newsletter 9400 West Higgins Road, Rosemont Illinois 60018 847.823.7186 www.aaos.org April 2017 OA Hip CPG Approved by BOD The Clinical Practice Guideline on Management of Osteoarthritis of the
Quality Newsletter 9400 West Higgins Road, Rosemont Illinois 60018 847.823.7186 www.aaos.org April 2017 OA Hip CPG Approved by BOD The Clinical Practice Guideline on Management of Osteoarthritis of the
ORTHOPAEDIC SUMMIT 2016
 Injuries to the Extensor Mechanism Quadriceps & Patellar tendon Pearls and Pitfalls M.Mike Malek, M.D. Washington Orthopaedic and Knee Clinic ORTHOPAEDIC SUMMIT 2016 Las Vegas, Nevada December 8, 2016
Injuries to the Extensor Mechanism Quadriceps & Patellar tendon Pearls and Pitfalls M.Mike Malek, M.D. Washington Orthopaedic and Knee Clinic ORTHOPAEDIC SUMMIT 2016 Las Vegas, Nevada December 8, 2016
Mr Harminder S. Gosal, MBBS, FRCS(Ed), FRCS(Eng), FRCS(Orth)
 Mr Harminder S. Gosal, MBBS, FRCS(Ed), FRCS(Eng), FRCS(Orth) Mr Gosal s undergraduate training was at The London Hospital Medical College. He did his postgraduate training in Leicester, Nottingham, and
Mr Harminder S. Gosal, MBBS, FRCS(Ed), FRCS(Eng), FRCS(Orth) Mr Gosal s undergraduate training was at The London Hospital Medical College. He did his postgraduate training in Leicester, Nottingham, and
Aperture fixation instead of transverse tunnels at the patella for medial patellofemoral ligament reconstruction
 Knee Surg Sports Traumatol Arthrosc (2012) 20:322 326 DOI 10.1007/s00167-011-1582-1 KNEE Aperture fixation instead of transverse tunnels at the patella for medial patellofemoral ligament reconstruction
Knee Surg Sports Traumatol Arthrosc (2012) 20:322 326 DOI 10.1007/s00167-011-1582-1 KNEE Aperture fixation instead of transverse tunnels at the patella for medial patellofemoral ligament reconstruction
Patellofemoral Dislocation and Instability VSM
 Patellofemoral Dislocation and Instability Functions of the Patella Patella functions as the fulcrum of a lever, maximizing flexion & extension with a given quadriceps force Also acts as pulley, changing
Patellofemoral Dislocation and Instability Functions of the Patella Patella functions as the fulcrum of a lever, maximizing flexion & extension with a given quadriceps force Also acts as pulley, changing
