Pediatric Neurology Department, Prof. Dr. Alexandru Obregia Psychiatry Clinical Hospital, Bucharest, Romania b
|
|
|
- Barry Malone
- 5 years ago
- Views:
Transcription
1 Mædica - a Journal of Clinical Medicine CASE REPORTS Cohen syndrome a rare genetic cause of hypotonia in children Magdalena BUDISTEANU, MD a,b ; Diana BARCA, MD a ; Sorina Mihaela CHIRIEAC, MD b ; Sanda MAGUREANU, MD a a Pediatric Neurology Department, Prof. Dr. Alexandru Obregia Psychiatry Clinical Hospital, Bucharest, Romania b Medical Genetics Laboratory, Victor Babes National Institute of Pathology, Bucharest, Romania ABSTRACT Cohen syndrome is a rare, genetic condition, recessively inherited, associated with specific facial dysmorphism, global developmental delay, hypotonia and ophthalmic abnormalities. A delay in making the diagnosis commonly occurs, because of the lack of a definitive molecular test and also because of the clinical variability of the syndrome. In this paper we describe four cases of Cohen syndrome, together with a comparison with other cases reported in the literature, in order to further delineate this condition. Key words: Cohen syndrome, hypotonia, dysmorphic features INTRODUCTION Cohen syndrome (MIM ) was first described in 1973 by Cohen et al (1) when they reported three children with a characteristic facial appearance in association with mental retardation, hypotonia, joint laxity, obesity with mid-childhood onset and ocular anomalies. Norio et al (2) reported, in 1984, on a small group of Finnish patients with Cohen syndrome, presenting microcephaly, neutropenia and specific ophthalmic abnormalities, namely high myopia and retinal dystrophy. Consanguinity in the reported families provided support for an autosomal recessive pattern of inheritance. Molecular genetic analysis identified a single major locus for the Cohen syndrome gene, COH1, on the long arm of chromosome 8 (3). Recently, mutations of the COH1 gene were reported in a Northern and Western European cohort of patients with Cohen syndrome, mainly originating from Finland (4). COH1 exhibits various splicing variants containing up to 62 exons and encodes a protein of 4,022 aminoacids, Address for correspondence: Magdalena Budisteanu, MD, Prof. Dr. Alexandru Obregia Psychiatry Clinical Hospital, Berceni Avenue, District 4, Bucharest, Romania address: magda_efrim@yahoo.com 56 Maedica A Journal of Clinical Medicine, Volume 5 No
2 whose domain structure and sequence similarities suggest a role in protein sorting and vesiclemediated protein transport (5). The mouse homologue of COH1 is widely expressed in neurones of the postnatal and adult brain suggesting a role in neuronal differentiation (6). This suggests that COH1 primarily functions in postmitotic cells, which may be the reason for the postnatal microcephaly seen in Cohen syndrome (7). Overall, more than 50 COH1 mutations have been reported in association with Cohen syndrome. Most are termination mutations and predicted to result in a null allele, while missense mutations and larger deletions are less common (7). Kivitie-Kallio and Norio (8) proposed the following features as essential for the diagnosis of Cohen syndrome: (1) non-progressive mental retardation, motor clumsiness, and microcephaly; (2) typical facial features, including wave shaped eyelids, short philtrum, thick hair, and low hairline; (3) childhood hypotonia and joint hyperextensibility; (4) retinochoroidal dystrophy and myopia by 5 years of age; (5) periods of isolated neutropenia. Greater clinical variability is observed in case reports of Cohen syndrome from outside Finland. In 2003, Chandler et al (9) reported a large group of patients with Cohen syndrome from across the UK and assessed their dysmorphic, ophthalmological, hematological, behavioral, and cognitive features. Intra- and interfamilial variability within the clinical spectrum were investigated and the natural history of Cohen syndrome delineated. They linked the diagnosis of Cohen syndrome to the presence of at least two of the following major criteria in a child with significant learning difficulties: (1) facial gestalt, characterized by thick hair, eyebrows and eyelashes, wave shaped, downward slanting palpebral fissures, prominent, beakshaped nose, short, upturned philtrum with grimacing expression on smiling; (2) pigmentary retinopathy; (3) neutropenia (defined as <2 x 109/ L), in association with a number of less specific but supportive criteria, namely: (1) early onset, progressive myopia, (2) microcephaly, (3) truncal obesity with slender extremities, (4) joint hyperextensibility. Recently, Hennies et all (5) reported 26 different mutations in COH1. Their investigation of an ethnically diverse series of patients with Cohen syndrome revealed that, besides developmental delay, myopia and, in particular, the typical facial gestalt were major signs of Cohen syndrome caused by COH1 mutations. COH1 mutations may be present also in patients lacking retinopathy at school age, microcephaly, or neutropenia. A consistent relationship between specific mutations and the severity of Cohen syndrome or the expression of a particular clinical sign has not been observed, with the exception of the mutation c.3348_3349delct, found solely in Finnish patients. These data demonstrated that COH1 is subject to wide allelic heterogeneity, and there seems to be no major mutational hotspot in non-finnish patients with Cohen syndrome (5). Sefert et all (7) demonstrated, also, a broad phenotypic variability. Thus, COH1 mutations may be present in patients with CS lacking either microcephaly or truncal obesity. In all their patients older than 5 years, the severity of myopia was comparable to that reported earlier. Pigmentary retinopathy was not confirmed by retinal examination in two patients who were teenagers at the time of assessments, the authors concluding that, retinopathy present at school age may not to be obligatory for the diagnosis of Cohen syndrome (7). In this paper, we present four children with Cohen syndrome; in addition, to further delineate this condition, we parallel our cases to previous reports. CASES PRESENTATION CASE 1. The patient is an 11-year-old boy admitted to our department for muscular weakness and fatigability. He is the first child of healthy nonconsanguineous parents, born after an uneventful pregnancy, though in pelvic presentation, with a birth weight of g and an Apgar score of 9. His developmental milestones were in normal range, but from the beginning his gait was very difficult, with frequent falls and running difficulties; he presented delayed speech acquisition speaking his first words at 2 years. His general examination showed: weight of 50 kg (Pc 95), height of 143 cm (Pc 50), head circumference of 53 cm (Pc 95); dysmorphic facial features, including a hypotonic facial expression with an open mouth, thick hair, bushy eyebrows, luxuriant eyelashes, downward slanting palpebral fissures, high nasal bridge, a beak-shaped nose, a short, upturned philtrum, malar hypoplasia, thin upper lip, prominent central incisors, truncal obesity, Maedica A Journal of Clinical Medicine, Volume 5 No
3 camptodactyly of the fingers of the left hand, narrow tapering fingers, bilateral genu valgum, talus valgus, dorsal kyphoscoliosis, generalized joint hyperextensibility, small penis. He underwent surgery for ectopic testes. Neurological examination showed generalized muscular hypotonia, difficult, waddling gait, especially on his tips and heels. Laboratory investigations were in the normal range. Psychological evaluation revealed an IQ of 83, with hypoprosexia, slow working rhythm, long answering latency. The ophthalmologic examination showed mild myopia. heels, and she can jump on one leg. Her laboratory tests revealed neutropenia (1.5 x 109/ L). Psychological evaluation showed an IQ of 80, and a slight delay of language development (expressive language for 2 years old). Ophthalmologic examination revealed mild myopia. FIGURE 2. The hands of case 3. The fingers are slender and taper from the proximal interphalangeal joint FIGURE 1. Case 3 showing the characteristic facial appearance CASE 2. The patient is a 3-year-old girl admitted to our department for motor clumsiness and fatigability. She is the younger sister of the first case, born after an uneventful pregnancy, but, as her brother, in pelvic presentation, with a birth weight of 3250 g and an Apgar score of 6, requiring respiratory and feeding assistance for 7 days. She presented a delayed psychomotor development: head control acquisition by 7 months, sitting position by 10 months, walking at 3 years with frequent falls, and her first words at 2 years. Her general examination revealed: weight of 15 kg (Pc 75), height of 113 cm (Pc 25), head circumference of 49 cm (Pc 50), the same dysmorphic facial features as her brother, thick hair, truncal obesity, bilateral genu recurvatum, talus valgus, narrow tapering fingers, pes planus, dorsal kyphoscoliosis, generalized joint hyperextensibility. The neurological examination showed generalized muscular hypotonia, difficult, waddling gait, genu recurvatum, and adducted shoulders. She is able to walk on her tips and her C ASE 3. The patient is a boy of 10 year of age, admitted to our department for evaluation of a mild mental retardation. He is the only child of healthy nonconsanguineous parents, born by caesarian operation for pelvic presentation after an uneventful full-term pregnancy, with a birth weight of 3,600 g and an unknown Apgar score; he presented a delayed psychomotor development acquiring head control at 12 months, sitting position by 18 months, walked and spoke his first words at 2 years. He suffered frequent respiratory infections, especially in early childhood. His general examination showed: weight of 50 kg (Pc 97), height of 143 cm (Pc 50), head circumference of 55 cm (Pc 97), dysmorphic facial features, including a hypotonic facial expression with an open mouth, thick hair, bushy eyebrows, luxuriant eyelashes, downward slanting palpebral fissures, high nasal bridge, a short, upturned philtrum, malar hypoplasia, thin upper lip, prominent central incisors, truncal obesity, generalized joint hyperextensibility. Neurological examination revealed generalized muscular hypotonia, clumsiness in fine movements, mild mental retardation. Laboratory tests showed neutropenia (under 2 x 109/ L). Psychological evaluation showed an IQ of 56. Brain CT scan was normal. The ophthalmologic examination revealed mild myopia. 58 Maedica A Journal of Clinical Medicine, Volume 5 No
4 FIGURE 3. Case 3 showing the characteristic body shape of Cohen syndrome: a truncal distribution of body fat, with comparatively slender limbs CASE 4. The patient is a 3-year-old boy, admitted to our clinic for evaluation of a mild psychomotor retardation. He is the only child of healthy nonconsanguineous parents, born after an uneventful pregnancy until the 8 th months, when the diagnosis of placenta praevia was made by ultrasound exam and caesarian operation was performed. The child had a birth weight of 2,250 g, a length of 47 cm, unknown head circumference, and an Apgar score of 5/7, showing neonatal feeding difficulties and hypotonia, necessitating incubation for one month. He had a delayed psychomotor development: head control at 7 months, he sat upright at 10 months, walked at 20 months and said his first words at 18 months. He presented frequent respiratory infections. The general examination revealed: weight of 14 kg (Pc 25), height of 90 cm (Pc 25), head circumference of 49 cm (Pc 2); dysmorphic facial features, including a hypotonic facial expression with open mouth, thick hair, downward slanting palpebral fissures, long, wave-shaped lashes, beak- shaped nose, short philtrum, malar hypoplasia, thin upper lip, prominent central incisors; truncal obesity; generalized joint hyperextensibility; small penis, cryptorchidism. Neurological examination showed generalized muscular hypotonia, clumsiness for fine movements, moderate mental retardation, heteroagresivity, reduced sociability (he prefers to play alone). Laboratory tests showed neutropenia (1.5 x 109/L). Psychological evaluation showed an IQ of 45. CT scan was normal. Ophthalmologic examination revealed mild myopia. Mutations in COH1 are distributed throughout the gene, thus sequencing of the entire gene is needed for confirmation or exclusion of Cohen syndrome diagnosis. The clinical availability of such testing is limited because of the large size of the COH1 gene, thus none of our patients was tested for mutations of COH1 gene. The clinical features of the patients are summarized in Table 1. All patients parents gave their informed consent for the publication of the clinical data of their children. DISCUSSION Three of our patients presented all features proposed by Kivitie-Kallio and Norio (8) as Patient Age (y) Sex OFC percentile Height percentile Weight percentile Neutrophil count (x 10 9 /L) Myopia Hypotonia Mental retardation 1 11 M normal mild F mild M mild F mild TABLE 1. Clinical features of the patients y = years; OFC = occipitofrontal circumference; M = male; F = female; + present; - absent. Speech delay Maedica A Journal of Clinical Medicine, Volume 5 No
5 essential for the diagnosis of Cohen syndrome, whereas in one patient (case 1) we did not find neutropenia (though this feature can be absent). All patients reported here presented some birth difficulties: all were born by caesarian operation, and two of them (cases 2 and 4) had a low Apgar scores. The 4 th case had, also, postnatal feeding and respiratory difficulties. These features could be related to muscular neonatal hypotonia, unnoticed at the time. These aspects were reported by K E Chandler et al. in their study on 33 patients with Cohen syndrome (9): in three cases reduced fetal movements were observed (these reduced fetal movements could explain pelvic presentation noted in all our patients); 85% patients presented feeding difficulties, 56% had neonatal hypotonia, and 21% cases had laryngomalacia. These aspects should be taken into consideration in patients with Cohen syndrome. The hypotonia persisted in all patients, influencing their motor development, and was the reason for which the parents addressed us. The two brothers (cases 1 and 2) had serious skeletal anomalies because of the hypotonia. All our patients showed typical facial features, described above. Two out of three male patients had small penises and cryptorchidism, fact which correlates with the data of Chandler et al.: three of their patients also had cryptorchidism beside the delayed onset of menarche and of pubertal development (over 16 years) recorded in 40% of patients. As a particularity of our cases, none of the 4 children presented microcephaly, in contrast with 90% of the patients reported by Chandler et al.; however, the authors considered that microcephaly, often marked, though characteristic, is not a universal finding. Also microcephaly developed trough life, and after mid-childhood the PC is about 50 th P. Similar to the reports of Hennies et all (5) and Seifert et all (7), none of our patients had retinochoroidal dystrophy, but only mild myopia. It was also proposed that could be two types of this syndrome, one associated with neutropenia, other without it. All children presented delayed speech, including the two with normal intelligence and learning difficulties. Only one child (case 4) had maladaptative behaviour. For last case it is unusual this behaviour, because usually they have cheerful disposition. Cohen syndrome is inherited in an autosomal recessive manner, so the reccurence risk is 25% for the sibs of an affected individual. An early diagnosis is, therefore, very important in order to avoid occurence of two or more sibs with this condition in the same family, like in our first 2 cases. DIFFERENTIAL DIAGNOSIS The diagnosis of Cohen syndrome is often considered within the differential diagnoses of inherited conditions where mental retardation is associated with retinopathy and obesity, for example, Bardet-Biedl (MIM #209900), Alström syndromes (MIM #203800), and Prader- Willi syndrome (MIM #176270) (10). However, the clinical phenotype of these conditions is quite distinct and very different from that of Cohen syndrome. Deafness, diabetes mellitus, and cardiomyopathy are characteristic of Alström syndrome while the patients are usually of normal intellect (11). Postaxial polydactyly and renal dysplasia are diagnostic features of Bardet-Biedl syndrome (12). Prader-Willi syndrome (PWS) is characterized by severe hypotonia and feeding difficulties in early infancy, followed in later infancy or early childhood by excessive eating and obesity. Almost all individuals have some degree of cognitive impairment. A distinctive behavioral phenotype (with temper tantrums, stubbornness, manipulative behavior, and obsessivecompulsive characteristics) is common. Hypogonadism is present in both males and females. PWS is caused by absence of the paternally derived PWS/AS region of chromosome 15 (13). The facial appearance in Cohen syndrome is striking and not easily confused with other syndromic gestalts. However, the beaked nose with overhanging columella is reminiscent of the nasal configuration of Rubenstein-Taybi syndrome (OMIM #180849) in which microcephaly and severe learning disability are also seen (14). Management Management includes the following: Spectacle correction of refractive errors Training as needed for the visually impaired Psychosocial support for affected individuals and their families 60 Maedica A Journal of Clinical Medicine, Volume 5 No
6 If neutropenia is documented, consideration should be given to the use of granulocytecolony stimulating factor (G-CSF). Recurrent infections should be treated per standard therapy; full immunologic evaluation should be considered. Early intervention and physical, occupational, and speech therapy are appropriate to address gross developmental delay, hypotonia, joint hyperextensibility, and motor clumsiness (13). Surveillance Annual ophthalmologic evaluation should assess visual acuity, refractive error, and/or retinal dystrophy. Repeat testing of white blood cell count with differential over time to identify intermittent neutropenia is indicated (13). Prognosis Long term follow up and clinical information on patients older than 40 years are rare in the literature (7). The features characteristic of CS remain in older patients, and can be used in making the diagnosis even at that age (7). Marked deterioration of visual function, and even total blindness, can occur over the age of 50 years (7). Kyphoscoliosis can be observed in patients with CS as teenagers or adults and this tends to be progressive through adult life. As CS patients do not have life threatening disorders and are generally in good health, their life span does not seem to be markedly reduced. CONCLUSION The patients reported in this paper, although presenting most of the characteristic features of Cohen syndrome, had some particularities, such as prenatal and neonatal hypotonia associated with birth difficulties, presence of only a mild myopia (until the data of admittance to our department), absence of microcephaly. It is worthwhile to mention the absence of consangvinous family for all cases. There was a both intra- and interfamilial variability, each case having its own particularities. These aspects underlie the variability within the clinical spectrum of the syndrome. This phenotypic heterogeneity should be taken into account in children with features compatible with Cohen syndrome, in order to facilitate a prompt diagnosis. This is important not only for the patient, who will benefit from the appropriate intervention by a multidisciplinary team, but also for the families who can be accurately counseled regarding the cause, prognosis, and the recurrence risks. Financial support: CNCSIS Grant No REFERENCES 1. Cohen MM Jr, Hall BD, Smith DW A new syndrome with hypotonia, obesity, mental deficiency and facial, oral, ocular and limb anomalies. J Pediatr 1973; 83: Norio R, Raitta C, Lindahl E Further delineation of the Cohen syndrome; report on chorioretinal dystrophy, leukopenia and consanguinity. Clin Genet 1984; 25: Tahvanainen E, Norio R, Karila E et al Cohen syndrome gene assigned to the long arm of chromosome 8 by linkage analysis. Nat Genet 1994; 7: Kolehmainen J, Black GC, Saarinen A et al Cohen syndrome is caused by mutations in a novel gene, COH1, encoding a transmembrane protein with a presumed role in vesiclemediated sorting and intracellular protein transport. Am J Hum Genet 2003; 72: Hennies HC, Rauch A, Seifert W Allelic Heterogeneity in the COH1 Gene Explains Clinical Variability in Cohen Syndrome. Am J Hum Genet 2004; 75: Mochida GH, Rajab A, Eyaid W et al Broader geographical spectrum of Cohen syndrome due to COH1 mutations. J Med Genet e87. Seifert W, Holder-Espinasse M, Spranger S et al Mutational spectrum of COH1 and clinical heterogeneity in Cohen syndrome. J Med Genet 2006; 43: e22 Kivitie-Kallio S, Norio R Cohen syndrome: essential features, natural history, and heterogeneity. Am J Med Genet 2001; 102: Chandler KE, Kidd A, Al-Gazali L et al Diagnostic criteria, clinical characteristics, and natural history of Cohen syndrome. J Med Genet 2003; : Cantani A, Bellioni P, Bamonte G et al Seven hereditary syndromes with pigmentary retinopathy. Clin Pediatr 1985; 24: Michaud JD, Levin AAV, Weksbeerg R et al Natural history of Alström syndrome in early childhood: onset with dilated cardiomyopathy. J Pediatr 1996; 128: Beales PL, Warner AM, Hitman GA et al Bardet-Biedl syndrome: a molecular and phenotypic study of 18 families. J Med Genet 1997; 34:92-98 Falk MJ, Wang H, Traboulsi EI Cohen Syndrome. GeneReviews NCBI Bookshelf. gov/bookshelf/br.fcgi?book=gene&pa rt=cohen Allanson JE Rubenstein-Taybi syndrome: the changing face. Am J Med Genet 1990; suppl 6:38-41 Maedica A Journal of Clinical Medicine, Volume 5 No
C ohen syndrome was first described in 1973 by Cohen et
 233 ORIGINAL ARTICLE Diagnostic criteria, clinical characteristics, and natural history of Cohen syndrome K E Chandler, A Kidd, L Al-Gazali, J Kolehmainen, A-E Lehesjoki, G C M Black, J Clayton-Smith...
233 ORIGINAL ARTICLE Diagnostic criteria, clinical characteristics, and natural history of Cohen syndrome K E Chandler, A Kidd, L Al-Gazali, J Kolehmainen, A-E Lehesjoki, G C M Black, J Clayton-Smith...
To Be Your Local Expert A General Pediatrician s Story
 To Be Your Local Expert A General Pediatrician s Story DDC Clinic mission: To enhance the quality of life for people with special needs caused by rare genetic disorders What Does It Take to Be Your Local
To Be Your Local Expert A General Pediatrician s Story DDC Clinic mission: To enhance the quality of life for people with special needs caused by rare genetic disorders What Does It Take to Be Your Local
Basic Facts About PWS:
 Phone: 800-926-4797 or 941-312-0400 Your membership provides this website - Join Today! Basic Facts About PWS: A Diagnosis and Reference Guide for Physicians and Other Health Professionals What is Prader-Willi
Phone: 800-926-4797 or 941-312-0400 Your membership provides this website - Join Today! Basic Facts About PWS: A Diagnosis and Reference Guide for Physicians and Other Health Professionals What is Prader-Willi
Dysmorphology And The Paediatric Eye. Jill Clayton-Smith Manchester Centre For Genomic Medicine
 Dysmorphology And The Paediatric Eye Jill Clayton-Smith Manchester Centre For Genomic Medicine Why Make A Syndrome Diagnosis? Why did it happen? What does the future hold? How can you treat/manage it?
Dysmorphology And The Paediatric Eye Jill Clayton-Smith Manchester Centre For Genomic Medicine Why Make A Syndrome Diagnosis? Why did it happen? What does the future hold? How can you treat/manage it?
Klinefelter syndrome ( 47, XXY )
 Sex Chromosome Abnormalities, Sex Chromosome Aneuploidy It has been estimated that, overall, approximately one in 400 infants have some form of sex chromosome aneuploidy. A thorough discussion of sex chromosomes
Sex Chromosome Abnormalities, Sex Chromosome Aneuploidy It has been estimated that, overall, approximately one in 400 infants have some form of sex chromosome aneuploidy. A thorough discussion of sex chromosomes
Approach to the Child with Developmental Delay
 Approach to the Child with Developmental Delay Arwa Nasir Department of Pediatrics University of Nebraska Medical Center DISCLOSURE DECLARATION Approach to the Child with Developmental Delay Arwa Nasir
Approach to the Child with Developmental Delay Arwa Nasir Department of Pediatrics University of Nebraska Medical Center DISCLOSURE DECLARATION Approach to the Child with Developmental Delay Arwa Nasir
(i) Family 1. The male proband (1.III-1) from European descent was referred at
 1 Supplementary Note Clinical descriptions of families (i) Family 1. The male proband (1.III-1) from European descent was referred at age 14 because of scoliosis. He had normal development. Physical evaluation
1 Supplementary Note Clinical descriptions of families (i) Family 1. The male proband (1.III-1) from European descent was referred at age 14 because of scoliosis. He had normal development. Physical evaluation
Intrafamilial variation in Cohen syndrome
 Journal of Medical Genetics 1987, 24, 488-492 Intrafamilial variation in Cohen syndrome I D YOUNG AND J R MOORE From the Department of Child Health, University of Leicester, Leicester LE2 7LX. SUMMARY
Journal of Medical Genetics 1987, 24, 488-492 Intrafamilial variation in Cohen syndrome I D YOUNG AND J R MOORE From the Department of Child Health, University of Leicester, Leicester LE2 7LX. SUMMARY
When to suspect Prader Willi Syndrome and how to diagnose it?
 When to suspect Prader Willi Syndrome and how to diagnose it? Dr Chirita-Emandi Adela Dr Dobrescu Andreea Victor Babes University of Medicine and Pahrmacy Timisoara Emergency Hospital for Children Louis
When to suspect Prader Willi Syndrome and how to diagnose it? Dr Chirita-Emandi Adela Dr Dobrescu Andreea Victor Babes University of Medicine and Pahrmacy Timisoara Emergency Hospital for Children Louis
Approach to the Genetic Diagnosis of Neurological Disorders
 Approach to the Genetic Diagnosis of Neurological Disorders Dr Wendy Jones MBBS MRCP Great Ormond Street Hospital for Children National Hospital for Neurology and Neurosurgery What is a genetic diagnosis?
Approach to the Genetic Diagnosis of Neurological Disorders Dr Wendy Jones MBBS MRCP Great Ormond Street Hospital for Children National Hospital for Neurology and Neurosurgery What is a genetic diagnosis?
Orthopedic and Surgical Features in Patients with Prader Willi Syndrome
 Orthopedic and Surgical Features in Patients with Prader Willi Syndrome Vlad David, Alexandra Pal Victor Babes University of Medicine and Pharmacy Timisoara Louis Turcanu Emergency Children s Hospital
Orthopedic and Surgical Features in Patients with Prader Willi Syndrome Vlad David, Alexandra Pal Victor Babes University of Medicine and Pharmacy Timisoara Louis Turcanu Emergency Children s Hospital
Case Report MOMO Syndrome with Holoprosencephaly and Cryptorchidism: Expanding the Spectrum of the New Obesity Syndrome
 Case Reports in Genetics Volume 2011, Article ID 839650, 4 pages doi:10.1155/2011/839650 Case Report MOMO Syndrome with Holoprosencephaly and Cryptorchidism: Expanding the Spectrum of the New Obesity Syndrome
Case Reports in Genetics Volume 2011, Article ID 839650, 4 pages doi:10.1155/2011/839650 Case Report MOMO Syndrome with Holoprosencephaly and Cryptorchidism: Expanding the Spectrum of the New Obesity Syndrome
Dysmorphology. Sue White. Diagnostic Dysmorphology, Aase. Victorian Clinical Genetics Services
 Dysmorphology Sue White www.rch.unimelb.edu.au/nets/handbook Diagnostic Dysmorphology, Aase Dysmorphology Assessment Algorithm no Are the features familial? yes Recognised syndrome yes no AD/XL syndrome
Dysmorphology Sue White www.rch.unimelb.edu.au/nets/handbook Diagnostic Dysmorphology, Aase Dysmorphology Assessment Algorithm no Are the features familial? yes Recognised syndrome yes no AD/XL syndrome
Obesity: Physiology, Health and Diseases 5 July Genetic of Obesity
 Obesity: Physiology, Health and Diseases 5 July 2017 Genetic of Obesity Voraluck Phatarakijnirund, MD. Division of Endocrinology Department of Pediatrics Phramongkutklao Hospital Phramongkutklao Colleague
Obesity: Physiology, Health and Diseases 5 July 2017 Genetic of Obesity Voraluck Phatarakijnirund, MD. Division of Endocrinology Department of Pediatrics Phramongkutklao Hospital Phramongkutklao Colleague
Feeding Disorders and Growth in Williams Syndrome
 Feeding Disorders and Growth in Williams Syndrome Sharon M. Greis M.A., CCC/SLP BRS-S and Paige Kaplan M.B.B.Ch. Williams Syndrome Clinic The Children s Hospital of Philadelphia Pediatric Feeding & Swallowing
Feeding Disorders and Growth in Williams Syndrome Sharon M. Greis M.A., CCC/SLP BRS-S and Paige Kaplan M.B.B.Ch. Williams Syndrome Clinic The Children s Hospital of Philadelphia Pediatric Feeding & Swallowing
Senior researcher III/ Head of Research Psychiatry Laboratory Alexandru Obregia Clinical Hospital of Psychiatry
 Europass Curriculum Vitae Personal information First name(s) / Surname(s) Magdalena Budisteanu Address(es) 1 Veronica Micle St., Bucharest, Romania Telephone(s) 0040213349068 Mobile: 0040722929091 Fax(es)
Europass Curriculum Vitae Personal information First name(s) / Surname(s) Magdalena Budisteanu Address(es) 1 Veronica Micle St., Bucharest, Romania Telephone(s) 0040213349068 Mobile: 0040722929091 Fax(es)
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier/Additional Provider
 Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier/Additional Provider TEST DISEASE/CONDITION POPULATION TRIAD Submitting laboratory: Manchester RGC Approved: September 2013
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier/Additional Provider TEST DISEASE/CONDITION POPULATION TRIAD Submitting laboratory: Manchester RGC Approved: September 2013
Abstract. Introduction
 Med. J. Cairo Univ., Vol. 77, No. 1, September: 453-458, 2009 www.medicaljournalofcairouniversity.com Sanjad-Sakati Syndrome: A Rare Autosomal Recessive Disorder of Congenital Hypoparathyroidism-Microcephaly-Mental
Med. J. Cairo Univ., Vol. 77, No. 1, September: 453-458, 2009 www.medicaljournalofcairouniversity.com Sanjad-Sakati Syndrome: A Rare Autosomal Recessive Disorder of Congenital Hypoparathyroidism-Microcephaly-Mental
Alcohol and Pregnancy: What Have We Learned in 37 Years?
 Alcohol and Pregnancy: What Have We Learned in 37 Years? Kenneth Lyons Jones, M.D. Professor of Pediatrics University of California, San Diego School of Medicine La Jolla, CA Generalizations About Phenotype
Alcohol and Pregnancy: What Have We Learned in 37 Years? Kenneth Lyons Jones, M.D. Professor of Pediatrics University of California, San Diego School of Medicine La Jolla, CA Generalizations About Phenotype
Središnja medicinska knjižnica
 Središnja medicinska knjižnica Maradin, M., Fumić, K., Hansikova, H., Tesarova, M., Wenchich, L., Dorner, S., Sarnavka, V., Zeman, J., Barić, I. (2006) Fumaric aciduria: Mild phenotype in a 8-year-old
Središnja medicinska knjižnica Maradin, M., Fumić, K., Hansikova, H., Tesarova, M., Wenchich, L., Dorner, S., Sarnavka, V., Zeman, J., Barić, I. (2006) Fumaric aciduria: Mild phenotype in a 8-year-old
Finding New Friends Down Syndrome. Pedicases
 Finding New Friends Down Syndrome Pedicases Objectives List the diagnostic features of Down syndrome and its associated complications. Describe the role of the clinician in management of Down syndrome,
Finding New Friends Down Syndrome Pedicases Objectives List the diagnostic features of Down syndrome and its associated complications. Describe the role of the clinician in management of Down syndrome,
Faravareh Khordadpoor (PhD in molecular genetics) 1- Tehran Medical Genetics Laboratory 2- Science and research branch, Islamic Azad University
 Faravareh Khordadpoor (PhD in molecular genetics) 1- Tehran Medical Genetics Laboratory 2- Science and research branch, Islamic Azad University 1395 21 مشاوره ژنتیک و نقش آن در پیش گیری از معلولیت ها 20
Faravareh Khordadpoor (PhD in molecular genetics) 1- Tehran Medical Genetics Laboratory 2- Science and research branch, Islamic Azad University 1395 21 مشاوره ژنتیک و نقش آن در پیش گیری از معلولیت ها 20
Unifactorial or Single Gene Disorders. Hanan Hamamy Department of Genetic Medicine and Development Geneva University Hospital
 Unifactorial or Single Gene Disorders Hanan Hamamy Department of Genetic Medicine and Development Geneva University Hospital Training Course in Sexual and Reproductive Health Research Geneva 2011 Single
Unifactorial or Single Gene Disorders Hanan Hamamy Department of Genetic Medicine and Development Geneva University Hospital Training Course in Sexual and Reproductive Health Research Geneva 2011 Single
SWISS SOCIETY OF NEONATOLOGY. Yunis-Varon syndrome
 SWISS SOCIETY OF NEONATOLOGY Yunis-Varon syndrome January 2003 2 Heyland K, Hodler C, Bänziger O, Neonatology, University Children s Hospital of Zurich, Switzerland Swiss Society of Neonatology, Thomas
SWISS SOCIETY OF NEONATOLOGY Yunis-Varon syndrome January 2003 2 Heyland K, Hodler C, Bänziger O, Neonatology, University Children s Hospital of Zurich, Switzerland Swiss Society of Neonatology, Thomas
Phenotypic variability in Angelman syndrome report of two cases
 Mædica - a Journal of Clinical Medicine CASE REPORTS Phenotypic variability in Angelman syndrome report of two cases Magdalena BUDISTEANU a,b, Aurora ARGHIR b, Georgeta CARDOS b, Sorina CHIRIEAC b, Sanda
Mædica - a Journal of Clinical Medicine CASE REPORTS Phenotypic variability in Angelman syndrome report of two cases Magdalena BUDISTEANU a,b, Aurora ARGHIR b, Georgeta CARDOS b, Sorina CHIRIEAC b, Sanda
Genetic test for Bilateral frontoparietal polymicrogyria
 Genetic test for Bilateral frontoparietal polymicrogyria Daniela Pilz, Cardiff UKGTN Genetic testing for neurological conditions; London February 26 th 2013 Region-specific Polymicrogyria (PMG) bilateral
Genetic test for Bilateral frontoparietal polymicrogyria Daniela Pilz, Cardiff UKGTN Genetic testing for neurological conditions; London February 26 th 2013 Region-specific Polymicrogyria (PMG) bilateral
Supplementary Clinical Information
 Supplementary Clinical Information Patient 1 This female was born as the second child of a twin after a pregnancy duration of 32 weeks. The birth was otherwise uncomplicated and her twin brother was healthy.
Supplementary Clinical Information Patient 1 This female was born as the second child of a twin after a pregnancy duration of 32 weeks. The birth was otherwise uncomplicated and her twin brother was healthy.
A case with oto-spondylo-mega-epiphyseal-dysplasia (OSMED): the clinical recognition and differential diagnosis
 The Turkish Journal of Pediatrics 2011; 53: 346351 Case A case with otospondylomegaepiphysealdysplasia (OSMED): the clinical recognition and differential diagnosis Kadri Karaer 1, Rasim Özgür Rosti 1,
The Turkish Journal of Pediatrics 2011; 53: 346351 Case A case with otospondylomegaepiphysealdysplasia (OSMED): the clinical recognition and differential diagnosis Kadri Karaer 1, Rasim Özgür Rosti 1,
APPROACH TO A DYSMORPHIC INDIVIDUAL. Denise LM Goh
 APPROACH TO A DYSMORPHIC INDIVIDUAL Denise LM Goh Contents The dysmorphic child Incidence of congenital anomalies Suspicion for diagnosis Approach to the dysmorphic child Problem analysis history hysical
APPROACH TO A DYSMORPHIC INDIVIDUAL Denise LM Goh Contents The dysmorphic child Incidence of congenital anomalies Suspicion for diagnosis Approach to the dysmorphic child Problem analysis history hysical
A CASE OF GIANT AXONAL NEUROPATHY HEMANANTH T SECOND YEAR POST GRADUATE IN PAEDIATRICS INSTITUTE OF SOCIAL PAEDIATRICS GOVERNMENT STANLEY HOSPITAL
 A CASE OF GIANT AXONAL NEUROPATHY HEMANANTH T SECOND YEAR POST GRADUATE IN PAEDIATRICS INSTITUTE OF SOCIAL PAEDIATRICS GOVERNMENT STANLEY HOSPITAL CASE HISTORY Nine year old male child Second born Born
A CASE OF GIANT AXONAL NEUROPATHY HEMANANTH T SECOND YEAR POST GRADUATE IN PAEDIATRICS INSTITUTE OF SOCIAL PAEDIATRICS GOVERNMENT STANLEY HOSPITAL CASE HISTORY Nine year old male child Second born Born
Birth mother Foster carer Other
 PATIENT DETAILS NAME Sex Female Male Other Date of birth (DD/MM/YYYY) / / Age at assessment: Racial/ ethnic background Preferred language Hospital number (if applicable) Referral source, date, provider
PATIENT DETAILS NAME Sex Female Male Other Date of birth (DD/MM/YYYY) / / Age at assessment: Racial/ ethnic background Preferred language Hospital number (if applicable) Referral source, date, provider
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier
 Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name OMIM number for disease 147920 Disease alternative names Please provide any alternative
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name OMIM number for disease 147920 Disease alternative names Please provide any alternative
22q11.2 DELETION SYNDROME. Anna Mª Cueto González Clinical Geneticist Programa de Medicina Molecular y Genética Hospital Vall d Hebrón (Barcelona)
 22q11.2 DELETION SYNDROME Anna Mª Cueto González Clinical Geneticist Programa de Medicina Molecular y Genética Hospital Vall d Hebrón (Barcelona) Genomic disorders GENOMICS DISORDERS refers to those diseases
22q11.2 DELETION SYNDROME Anna Mª Cueto González Clinical Geneticist Programa de Medicina Molecular y Genética Hospital Vall d Hebrón (Barcelona) Genomic disorders GENOMICS DISORDERS refers to those diseases
Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012
 Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012 Hypotonia: reduced tension or resistance to range of motion Localization can be central (brain), peripheral (spinal cord, nerve,
Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012 Hypotonia: reduced tension or resistance to range of motion Localization can be central (brain), peripheral (spinal cord, nerve,
SWISS SOCIETY OF NEONATOLOGY. Raine syndrome: clinical and radiological features of a case from the United Arab Emirates
 SWISS SOCIETY OF NEONATOLOGY Raine syndrome: clinical and radiological features of a case from the United Arab Emirates December 2014 2 Abu Asbeh J, Bystricka A, Qadir M, Nikolay M, Khan J, Neonatal Intensive
SWISS SOCIETY OF NEONATOLOGY Raine syndrome: clinical and radiological features of a case from the United Arab Emirates December 2014 2 Abu Asbeh J, Bystricka A, Qadir M, Nikolay M, Khan J, Neonatal Intensive
Journal of Medical Genetics 1989, 26, syndrome
 Severe Silver-Russell syndrome Journal of Medical Genetics 1989, 26, 447-451 D DONNAI*, E THOMPSONt, J ALLANSONt, AND M BARAITSERt From *the Regional Genetic Service, St Mary's Hospital, Manchester M13
Severe Silver-Russell syndrome Journal of Medical Genetics 1989, 26, 447-451 D DONNAI*, E THOMPSONt, J ALLANSONt, AND M BARAITSERt From *the Regional Genetic Service, St Mary's Hospital, Manchester M13
Section F: Discussing the diagnosis and developing a management plan
 Section E: Formulating a diagnosis Information collected during the diagnostic assessment should be reviewed, ideally in a multi-disciplinary team context, to evaluate the strength of evidence to: Support
Section E: Formulating a diagnosis Information collected during the diagnostic assessment should be reviewed, ideally in a multi-disciplinary team context, to evaluate the strength of evidence to: Support
Prader-Willi Syndrome: an underrecognized
 www.jpnim.com Open Access eissn: 2281-0692 Journal of Pediatric and Neonatal Individualized Medicine 2018;7(1):e070107 doi: 10.7363/070107 Received: 2017 Aug 06; revised: 2017 Aug 24; accepted: 2017 Aug
www.jpnim.com Open Access eissn: 2281-0692 Journal of Pediatric and Neonatal Individualized Medicine 2018;7(1):e070107 doi: 10.7363/070107 Received: 2017 Aug 06; revised: 2017 Aug 24; accepted: 2017 Aug
Neonatal Hypotonia. Encephalopathy acute No encephalopathy. Neurology Chapter of IAP
 The floppy infant assumes a frog legged position. On ventral suspension, the baby can not maintain limb posture against gravity and assumes the position of a rag doll. Encephalopathy acute No encephalopathy
The floppy infant assumes a frog legged position. On ventral suspension, the baby can not maintain limb posture against gravity and assumes the position of a rag doll. Encephalopathy acute No encephalopathy
Systematizing in vivo modeling of pediatric disorders
 Systematizing in vivo modeling of pediatric disorders Nicholas Katsanis, Ph.D. Duke University Medical Center Center for Human Disease Modeling Rescindo Therapeutics www.dukegenes.org Task Force for
Systematizing in vivo modeling of pediatric disorders Nicholas Katsanis, Ph.D. Duke University Medical Center Center for Human Disease Modeling Rescindo Therapeutics www.dukegenes.org Task Force for
Genetic Conditions and Services: An Introduction
 Genetic Conditions and Services: An Introduction Jennifer Roberts, MC, MS, CGC Laboratory Genetics Counselor The Children s Mercy Hospital, 2017 Goals Determine which children/families may benefit from
Genetic Conditions and Services: An Introduction Jennifer Roberts, MC, MS, CGC Laboratory Genetics Counselor The Children s Mercy Hospital, 2017 Goals Determine which children/families may benefit from
FETAL ALCOHOL SYNDROME A SOUTH AFRICAN PERSPECTIVE
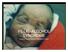 FETAL ALCOHOL SYNDROME A SOUTH AFRICAN PERSPECTIVE Fetal alcohol syndrome is the most common preventable cause of mental retardation in the world (Sampson PD et al.; Teratology (1997); 56:317-326) RISK
FETAL ALCOHOL SYNDROME A SOUTH AFRICAN PERSPECTIVE Fetal alcohol syndrome is the most common preventable cause of mental retardation in the world (Sampson PD et al.; Teratology (1997); 56:317-326) RISK
Quick Reference Guide
 This index may help determine a clinical diagnosis. Fairly common dysmorphic features are listed with corresponding syndromes in which the characteristic is a frequent finding. The syndrome features are
This index may help determine a clinical diagnosis. Fairly common dysmorphic features are listed with corresponding syndromes in which the characteristic is a frequent finding. The syndrome features are
Clinical Summaries. CLN1 Disease, infantile onset and others
 Clinical Summaries CLN1 Disease, infantile onset and others The gene called CLN1 lies on chromosome 1. CLN1 disease is inherited as an autosomal recessive disorder, which means that both chromosomes carry
Clinical Summaries CLN1 Disease, infantile onset and others The gene called CLN1 lies on chromosome 1. CLN1 disease is inherited as an autosomal recessive disorder, which means that both chromosomes carry
Common Genetic syndromes. Dr. E.M. Honey Department Genetics Division Human Genetics University of Pretoria
 Common Genetic syndromes Dr. E.M. Honey Department Genetics Division Human Genetics University of Pretoria Definitions Deformation Malformation Disruption Dysplasia Syndrome Associations Complex Sequences
Common Genetic syndromes Dr. E.M. Honey Department Genetics Division Human Genetics University of Pretoria Definitions Deformation Malformation Disruption Dysplasia Syndrome Associations Complex Sequences
Recognizing Genetic Red Flags in Clinical Evaluations
 Recognizing Genetic Red Flags in Clinical Evaluations ACGME Sub-competencies / Developmental Milestones Addressed Patient Care: Gather essential and accurate information about the patient; Make informed
Recognizing Genetic Red Flags in Clinical Evaluations ACGME Sub-competencies / Developmental Milestones Addressed Patient Care: Gather essential and accurate information about the patient; Make informed
AMERICAN BOARD OF MEDICAL GENETICS AND GENOMICS
 AMERICAN BOARD OF MEDICAL GENETICS AND GENOMICS Logbook Guidelines for Certification in Clinical Genetics and Genomics for the 2017 Examination as of 10/5/2015 Purpose: The purpose of the logbook is to
AMERICAN BOARD OF MEDICAL GENETICS AND GENOMICS Logbook Guidelines for Certification in Clinical Genetics and Genomics for the 2017 Examination as of 10/5/2015 Purpose: The purpose of the logbook is to
SEX-LINKED INHERITANCE. Dr Rasime Kalkan
 SEX-LINKED INHERITANCE Dr Rasime Kalkan Human Karyotype Picture of Human Chromosomes 22 Autosomes and 2 Sex Chromosomes Autosomal vs. Sex-Linked Traits can be either: Autosomal: traits (genes) are located
SEX-LINKED INHERITANCE Dr Rasime Kalkan Human Karyotype Picture of Human Chromosomes 22 Autosomes and 2 Sex Chromosomes Autosomal vs. Sex-Linked Traits can be either: Autosomal: traits (genes) are located
Medical Genetics. Consult and Referral Guidelines
 Medical Genetics Consult and Referral Guidelines HDVCH has developed these consult and referral guidelines as a general reference tool to assist referring physicians with the specialty referral process.
Medical Genetics Consult and Referral Guidelines HDVCH has developed these consult and referral guidelines as a general reference tool to assist referring physicians with the specialty referral process.
Quadriparesis in the Laurence-Moon Biedl-Bardet Syndrome: Case Report
 Paraplegia 29 (1991) 350-354
Paraplegia 29 (1991) 350-354
The Floppy Baby. Clare Betteridge
 The Floppy Baby Clare Betteridge The floppy baby Identification Evaluation Investigation Diagnosis Examples What is a floppy baby? Elbows and knees loosely extended. Head control is usually poor or absent.
The Floppy Baby Clare Betteridge The floppy baby Identification Evaluation Investigation Diagnosis Examples What is a floppy baby? Elbows and knees loosely extended. Head control is usually poor or absent.
Abnormal Facies, Myopia, and Short Stature
 Archives of Disease in Childhood, 1972, 47, 787. Abnormal Facies, Myopia, and Short Stature C. G. KEITH, R. H. DOBBS, D. G. SHAW, and K. COTTRALL From the Queen Elizabeth Hospital for Children, London
Archives of Disease in Childhood, 1972, 47, 787. Abnormal Facies, Myopia, and Short Stature C. G. KEITH, R. H. DOBBS, D. G. SHAW, and K. COTTRALL From the Queen Elizabeth Hospital for Children, London
Neurodevelopmental Disorders
 Neurodevelopmental Disorders Intellectual Disability Disorder Autism Spectrum Disorder (ASD) Attention-Deficit Hyperactivity Disorder (ADD/ADHD) Motor Disorders/Tourette s Disorder Intellectual Disability
Neurodevelopmental Disorders Intellectual Disability Disorder Autism Spectrum Disorder (ASD) Attention-Deficit Hyperactivity Disorder (ADD/ADHD) Motor Disorders/Tourette s Disorder Intellectual Disability
An unusual presentation of Rubinstein-Taybi Syndrome with bilateral postaxial polydactyly
 www.jpnim.com Open Access eissn: 2281-0692 Journal of Pediatric and Neonatal Individualized Medicine 2016;5(2):e050218 doi: 10.7363/050218 Received: 2016 Jun 12; revised: 2016 Jul 04; rerevised: 2016 Jul
www.jpnim.com Open Access eissn: 2281-0692 Journal of Pediatric and Neonatal Individualized Medicine 2016;5(2):e050218 doi: 10.7363/050218 Received: 2016 Jun 12; revised: 2016 Jul 04; rerevised: 2016 Jul
Genetic Disorders. n A genetic disorder is an abnormality
 + GENETIC DISORDERS + Genetic Disorders n A genetic disorder is an abnormality in an individual's DNA. Abnormalities can range from a small mutation in a single gene to the addition or subtraction of an
+ GENETIC DISORDERS + Genetic Disorders n A genetic disorder is an abnormality in an individual's DNA. Abnormalities can range from a small mutation in a single gene to the addition or subtraction of an
Developmental Disabilities. Medical and Psychosocial Aspects Presented by: Dr. Anna Lamikanra
 Developmental Disabilities Medical and Psychosocial Aspects Presented by: Dr. Anna Lamikanra Themes Decreased Independence Social Barriers Communication Difficulties Sexual Issues Limited Vocational Opportunities
Developmental Disabilities Medical and Psychosocial Aspects Presented by: Dr. Anna Lamikanra Themes Decreased Independence Social Barriers Communication Difficulties Sexual Issues Limited Vocational Opportunities
Lab #10: Karyotyping Lab
 Lab #10: Karyotyping Lab INTRODUCTION A karyotype is a visual display of the number and appearance of all chromosomes from a single somatic cell. A normal human karyotype would reveal 46 chromosomes (22
Lab #10: Karyotyping Lab INTRODUCTION A karyotype is a visual display of the number and appearance of all chromosomes from a single somatic cell. A normal human karyotype would reveal 46 chromosomes (22
The global epidemic of obesity
 The global epidemic of obesity Obesity is a genetic disorder Heterogeneity of the genetics of obesity ENVIRONMENT GENE MONOGENIC FORMS -> Early-onset, severe obesity -> Syndromic forms of obesity POLYGENIC
The global epidemic of obesity Obesity is a genetic disorder Heterogeneity of the genetics of obesity ENVIRONMENT GENE MONOGENIC FORMS -> Early-onset, severe obesity -> Syndromic forms of obesity POLYGENIC
CLINICAL HETEROGENEITY OF KABUKI SYNDROME: STUDY OF MOROCCAN PATIENTS
 Int. J. LifeSc. Bt & Pharm. Res. 2012 S Nadifi et al., 2012 Research Paper ISSN 2250-3137 www.ijlbpr.com Vol.1, Issue. 1, January 2012 2012 IJLBPR. All Rights Reserved CLINICAL HETEROGENEITY OF KABUKI
Int. J. LifeSc. Bt & Pharm. Res. 2012 S Nadifi et al., 2012 Research Paper ISSN 2250-3137 www.ijlbpr.com Vol.1, Issue. 1, January 2012 2012 IJLBPR. All Rights Reserved CLINICAL HETEROGENEITY OF KABUKI
RED FLAGS IN DEVELOPMENTAL DELAY. DR. Monika Bajaj Royal London Hospital
 RED FLAGS IN DEVELOPMENTAL DELAY DR. Monika Bajaj Royal London Hospital WHAT I HOPE TO COVER Red Flags in developmental milestones when to refer Cases Red flags to suspect ASD IT IS ABNORMAL IF A CHILD
RED FLAGS IN DEVELOPMENTAL DELAY DR. Monika Bajaj Royal London Hospital WHAT I HOPE TO COVER Red Flags in developmental milestones when to refer Cases Red flags to suspect ASD IT IS ABNORMAL IF A CHILD
Objectives. Genetics and Rett syndrome: As easy as apple pie! Chromosome to gene to protein
 Genetics and Rett syndrome: As easy as apple pie! Victoria Mok Siu M.D., FRCPC, FCCMG ORSA conference Ottawa April 24, 2016 Objectives Review chromosomes and genes Understand s Explore the reasons behind
Genetics and Rett syndrome: As easy as apple pie! Victoria Mok Siu M.D., FRCPC, FCCMG ORSA conference Ottawa April 24, 2016 Objectives Review chromosomes and genes Understand s Explore the reasons behind
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier/Additional Provider
 Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier/Additional Provider TEST DISORDER/CONDITION POPULATION TRIAD Submitting laboratory: Exeter RGC Approved: Sept 2013 1. Disorder/condition
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier/Additional Provider TEST DISORDER/CONDITION POPULATION TRIAD Submitting laboratory: Exeter RGC Approved: Sept 2013 1. Disorder/condition
Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease.
 Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease. Listen Observe Evaluate Test Refer Guide for primary care providers includes: Surveillance Aid: Assessing Weakness
Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease. Listen Observe Evaluate Test Refer Guide for primary care providers includes: Surveillance Aid: Assessing Weakness
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier
 Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name Leber congenital amaurosis OMIM number for disease 204000 Disease alternative
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name Leber congenital amaurosis OMIM number for disease 204000 Disease alternative
Elements of Dysmorphology I. Krzysztof Szczałuba
 Elements of Dysmorphology I Krzysztof Szczałuba 9.05.2016 Common definitions (1) Dysmorphology: recognition and study of birth defects (congenital malformations) and syndromes [David Smith, 1960] Malformation:
Elements of Dysmorphology I Krzysztof Szczałuba 9.05.2016 Common definitions (1) Dysmorphology: recognition and study of birth defects (congenital malformations) and syndromes [David Smith, 1960] Malformation:
CURRENT GENETIC TESTING TOOLS IN NEONATAL MEDICINE. Dr. Bahar Naghavi
 2 CURRENT GENETIC TESTING TOOLS IN NEONATAL MEDICINE Dr. Bahar Naghavi Assistant professor of Basic Science Department, Shahid Beheshti University of Medical Sciences, Tehran,Iran 3 Introduction Over 4000
2 CURRENT GENETIC TESTING TOOLS IN NEONATAL MEDICINE Dr. Bahar Naghavi Assistant professor of Basic Science Department, Shahid Beheshti University of Medical Sciences, Tehran,Iran 3 Introduction Over 4000
What dysmorphologists should keep in mind during evaluation of patients with blepharophimosis and mental disability?
 What dysmorphologists should keep in mind during evaluation of patients with blepharophimosis and mental disability? Aleksandra Jezela-Stanek, M.D., Ph. D. The Children s Memorial Health Institute, Warsaw
What dysmorphologists should keep in mind during evaluation of patients with blepharophimosis and mental disability? Aleksandra Jezela-Stanek, M.D., Ph. D. The Children s Memorial Health Institute, Warsaw
Facts About AS. What is Angelman Syndrome
 What is Angelman Syndrome In 1965, Dr. Harry Angelman, an English physician, first described three children with characteristics now known as the Angelman syndrome (AS). He noted that all had a stiff,
What is Angelman Syndrome In 1965, Dr. Harry Angelman, an English physician, first described three children with characteristics now known as the Angelman syndrome (AS). He noted that all had a stiff,
Medical Advisory Council: Verified
 What is White Sutton Syndrome? White Sutton Syndrome (WHSUS) is a condition characterized by autism and developmental delay and/or intellectual disability, as well as a characteristic facial profile. Children
What is White Sutton Syndrome? White Sutton Syndrome (WHSUS) is a condition characterized by autism and developmental delay and/or intellectual disability, as well as a characteristic facial profile. Children
Genetic Testing for CHARGE Syndrome. Description
 Subject: Genetic Testing for CHARGE Syndrome Page: 1 of 9 Last Review Status/Date: December 2014 Genetic Testing for CHARGE Syndrome Description CHARGE syndrome is a rare genetic condition associated with
Subject: Genetic Testing for CHARGE Syndrome Page: 1 of 9 Last Review Status/Date: December 2014 Genetic Testing for CHARGE Syndrome Description CHARGE syndrome is a rare genetic condition associated with
Case 1 A 65 year old college professor came to the neurology clinic referred by her family physician because of frequent falling. She had a history of
 Peripheral Nervous System Case 1 A 65 year old college professor came to the neurology clinic referred by her family physician because of frequent falling. She had a history of non-insulin dependent diabetes
Peripheral Nervous System Case 1 A 65 year old college professor came to the neurology clinic referred by her family physician because of frequent falling. She had a history of non-insulin dependent diabetes
Section C: Assessing Sentinel Facial Features
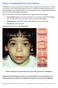 Section C: Assessing Sentinel Facial Features Fetal exposure to alcohol during the first trimester affects development of facial features. The areas most affected are the orbital region (eyes) and mid-face.
Section C: Assessing Sentinel Facial Features Fetal exposure to alcohol during the first trimester affects development of facial features. The areas most affected are the orbital region (eyes) and mid-face.
Genetic diagnosis of limb girdle muscular dystrophy type 2A, A Case Report
 Genetic diagnosis of limb girdle muscular dystrophy type 2A, A Case Report Roshanak Jazayeri, MD, PhD Assistant Professor of Medical Genetics Faculty of Medicine, Alborz University of Medical Sciences
Genetic diagnosis of limb girdle muscular dystrophy type 2A, A Case Report Roshanak Jazayeri, MD, PhD Assistant Professor of Medical Genetics Faculty of Medicine, Alborz University of Medical Sciences
Supplementary Information. Mutations in the Pre-Replication Complex cause Meier-Gorlin syndrome
 Supplementary Information Mutations in the Pre-Replication Complex cause Meier-Gorlin syndrome Louise S. Bicknell, Ernie M.H.F. Bongers, Andrea Leitch, Stephen Brown, Jeroen Schoots, Margaret E. Harley,
Supplementary Information Mutations in the Pre-Replication Complex cause Meier-Gorlin syndrome Louise S. Bicknell, Ernie M.H.F. Bongers, Andrea Leitch, Stephen Brown, Jeroen Schoots, Margaret E. Harley,
Transcript of learning module Developmental delay: a guide for GPs (Dur: 18' 52") You are listening to an audio module from BMJ Learning.
 Transcript of learning module Developmental delay: a guide for GPs (Dur: 18' 52") Contributors: Dianne Cottle and Mitch Blair Available online at: http://learning.bmj.com/ V/O: You are listening to an
Transcript of learning module Developmental delay: a guide for GPs (Dur: 18' 52") Contributors: Dianne Cottle and Mitch Blair Available online at: http://learning.bmj.com/ V/O: You are listening to an
FASD Diagnosis, Intervention, & Prevention
 FASD Diagnosis, Intervention, & Prevention Susan Astley PhD Professor Director Washington State FAS Diagnostic & Prevention Network University of Washington Seattle WA, U.S.A fasdpn.org 07 WA State FAS
FASD Diagnosis, Intervention, & Prevention Susan Astley PhD Professor Director Washington State FAS Diagnostic & Prevention Network University of Washington Seattle WA, U.S.A fasdpn.org 07 WA State FAS
Obesity in Children. JC Opperman
 Obesity in Children JC Opperman Definition The child too heavy for height or length Obvious on inspection 10 to 20% over desirable weight = overweight More than 20% = obese Use percentile charts for the
Obesity in Children JC Opperman Definition The child too heavy for height or length Obvious on inspection 10 to 20% over desirable weight = overweight More than 20% = obese Use percentile charts for the
Supplemental Data: Detailed Characteristics of Patients with MKRN3. Patient 1 was born after an uneventful pregnancy. She presented in our
 1 2 Supplemental Data: Detailed Characteristics of Patients with MKRN3 Mutations 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 Patient 1 was born after an uneventful pregnancy. She presented
1 2 Supplemental Data: Detailed Characteristics of Patients with MKRN3 Mutations 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 Patient 1 was born after an uneventful pregnancy. She presented
BRAIN STEM CASE HISTORIES CASE HISTORY VII
 463 Brain stem Case history BRAIN STEM CASE HISTORIES CASE HISTORY VII A 60 year old man with hypertension wakes one morning with trouble walking. He is feeling dizzy and is sick to his stomach. His wife
463 Brain stem Case history BRAIN STEM CASE HISTORIES CASE HISTORY VII A 60 year old man with hypertension wakes one morning with trouble walking. He is feeling dizzy and is sick to his stomach. His wife
UNIT IX: GENETIC DISORDERS
 UNIT IX: GENETIC DISORDERS Younas Masih Lecturer New Life College Of Nursing Karachi 3/4/2016 1 Objectives By the end of this session the Learners will be able to, 1. Know the basic terms related genetics
UNIT IX: GENETIC DISORDERS Younas Masih Lecturer New Life College Of Nursing Karachi 3/4/2016 1 Objectives By the end of this session the Learners will be able to, 1. Know the basic terms related genetics
World Journal of Pharmaceutical and Life Sciences WJPLS
 wjpls, 2015, Vol. 1, Issue 1, 175-181 Case Reports ISSN 2454-2229 WJPLS www.wjpls.org WAARDENBURG SYNDROME TYPE I A CASE SERIES FROM A SINGLE FAMILY Dr. D. Manikyamba 1*, Dr. S. Chandra Sekhar 2, Dr. G.
wjpls, 2015, Vol. 1, Issue 1, 175-181 Case Reports ISSN 2454-2229 WJPLS www.wjpls.org WAARDENBURG SYNDROME TYPE I A CASE SERIES FROM A SINGLE FAMILY Dr. D. Manikyamba 1*, Dr. S. Chandra Sekhar 2, Dr. G.
1/28/2019. OSF HealthCare INI Care Center Team. Neuromuscular Disease: Muscular Dystrophy. OSF HealthCare INI Care Center Team: Who are we?
 Neuromuscular Disease: Muscular Dystrophy Muscular Dystrophy Association (MDA) and OSF HealthCare Illinois Neurological Institute (INI) Care Center Team The Neuromuscular clinic is a designated MDA Care
Neuromuscular Disease: Muscular Dystrophy Muscular Dystrophy Association (MDA) and OSF HealthCare Illinois Neurological Institute (INI) Care Center Team The Neuromuscular clinic is a designated MDA Care
By: Dr. Doaa Khater Yassin, MM and M.D Paed Sr. specialist of Pediatrics SQUH
 By: Dr. Doaa Khater Yassin, MM and M.D Paed Sr. specialist of Pediatrics SQUH Born SGA with birth weight of 2.4 kg, had IUGR Hospitalized at the age of 2 month with severe dehydration Diagnosed as DKA
By: Dr. Doaa Khater Yassin, MM and M.D Paed Sr. specialist of Pediatrics SQUH Born SGA with birth weight of 2.4 kg, had IUGR Hospitalized at the age of 2 month with severe dehydration Diagnosed as DKA
Hereditary disorders of peroxisomal metabolism.
 Hereditary disorders of peroxisomal metabolism http://www.cytochemistry.net/cell-biology/perox.jpg Peroxisomes single membrane organelles from less than 100 to more than 1000 per eucaryotic cell more than
Hereditary disorders of peroxisomal metabolism http://www.cytochemistry.net/cell-biology/perox.jpg Peroxisomes single membrane organelles from less than 100 to more than 1000 per eucaryotic cell more than
Pathophysiology of the Phenylketonuria
 Problem 4. Pathophysiology of the Phenylketonuria Readings for this problem are found on pages: 79-82, 84, 85-6, 945-6 and 1019 of your Pathophysiology (5 th edition) textbook. (This problem was based
Problem 4. Pathophysiology of the Phenylketonuria Readings for this problem are found on pages: 79-82, 84, 85-6, 945-6 and 1019 of your Pathophysiology (5 th edition) textbook. (This problem was based
DEVELOPMENTAL BEHAVIOURAL REFERRAL
 Date DEVELOPMENTAL BEHAVIOURAL REFERRAL Completed By Role: Paediatrician/GP How long Other professionals involved with the child (e.g. psychologist, OT, speech therapist) Reason for this referral List
Date DEVELOPMENTAL BEHAVIOURAL REFERRAL Completed By Role: Paediatrician/GP How long Other professionals involved with the child (e.g. psychologist, OT, speech therapist) Reason for this referral List
KAT6A Syndrome. rarechromo.org
 KAT6A Syndrome rarechromo.org This leaflet is designed to help families and healthcare professionals looking after people affected by KAT6A syndrome. It contains information about the cause of KAT6A syndrome,
KAT6A Syndrome rarechromo.org This leaflet is designed to help families and healthcare professionals looking after people affected by KAT6A syndrome. It contains information about the cause of KAT6A syndrome,
Dizziness/Balance Questionnaire
 Dizziness/Balance Questionnaire Name: Date: 1. Which of these best describes your dizziness? Please mark only one. A sensation of movement of yourself or the room (spinning, tilting, or wave-like movement)
Dizziness/Balance Questionnaire Name: Date: 1. Which of these best describes your dizziness? Please mark only one. A sensation of movement of yourself or the room (spinning, tilting, or wave-like movement)
and duodenal atresia. Two other families reported may have had the same syndrome. Case reports CASE 1 (III.8, FAMILY 1)
 JMedGenet 1991; 28: 389-394 Autosomal dominant inheritance of abnormalities of the hands and feet with short palpebral fissures, variable microcephaly with learning disability, and oesophageal/duodenal
JMedGenet 1991; 28: 389-394 Autosomal dominant inheritance of abnormalities of the hands and feet with short palpebral fissures, variable microcephaly with learning disability, and oesophageal/duodenal
Correspondence should be addressed to Elichilia R. Shao;
 Hindawi Case Reports in Genetics Volume 2017, Article ID 2348045, 4 pages https://doi.org/10.1155/2017/2348045 Case Report Respiratory Failure due to Severe Obesity and Kyphoscoliosis in a 24-Year-Old
Hindawi Case Reports in Genetics Volume 2017, Article ID 2348045, 4 pages https://doi.org/10.1155/2017/2348045 Case Report Respiratory Failure due to Severe Obesity and Kyphoscoliosis in a 24-Year-Old
Fetal Medicine. Case Presentations. Dr Ermos Nicolaou Fetal Medicine Unit Chris Hani Baragwanath Hospital. October 2003
 Case Presentations Dr Ermos Nicolaou Fetal Medicine Unit Chris Hani Baragwanath Hospital October 2003 Case 1 Ms A M 22year old P0 G1 Referred from Sebokeng Hospital at 36w for polyhydramnios On Ultrasound:
Case Presentations Dr Ermos Nicolaou Fetal Medicine Unit Chris Hani Baragwanath Hospital October 2003 Case 1 Ms A M 22year old P0 G1 Referred from Sebokeng Hospital at 36w for polyhydramnios On Ultrasound:
THE FASD PATHWAY. Dr Patricia D. Jackson SACCH MEETING March 2016
 THE FASD PATHWAY Dr Patricia D. Jackson SACCH MEETING March 2016 Why do we need an FASD Pathway? Other countries recognise this as one of the commonest causes of learning disability In Scotland over the
THE FASD PATHWAY Dr Patricia D. Jackson SACCH MEETING March 2016 Why do we need an FASD Pathway? Other countries recognise this as one of the commonest causes of learning disability In Scotland over the
Red flags for clinical practice - guidance on indicators that your patient may have a genetic condition
 Red flags for clinical practice - guidance on indicators that your patient may have a genetic condition General red flags for clinical practice One or more of these red flags that may indicate a high genetic
Red flags for clinical practice - guidance on indicators that your patient may have a genetic condition General red flags for clinical practice One or more of these red flags that may indicate a high genetic
Seven cases of intellectual disability analysed by genomewide SNP analysis. Rodney J. Scott
 Seven cases of intellectual disability analysed by genomewide SNP analysis Rodney J. Scott Ability to interrogate Genomic Material ~1930 Crude analyses 2012 Highly precise analyses A (very) brief history
Seven cases of intellectual disability analysed by genomewide SNP analysis Rodney J. Scott Ability to interrogate Genomic Material ~1930 Crude analyses 2012 Highly precise analyses A (very) brief history
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on the Approach to Pediatric Anemia and Pallor. These podcasts are designed to give medical students an overview of key
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on the Approach to Pediatric Anemia and Pallor. These podcasts are designed to give medical students an overview of key
Intellectual Disability
 Intellectual Disability Tara Anne Matthews, MD Fellow Kapila Seshadri, MD Associate Professor of Pediatrics UMDNJ Robert Wood Johnson Medical Wednesday November 14, 2012 Intellectual Disability (Mental
Intellectual Disability Tara Anne Matthews, MD Fellow Kapila Seshadri, MD Associate Professor of Pediatrics UMDNJ Robert Wood Johnson Medical Wednesday November 14, 2012 Intellectual Disability (Mental
Stickler syndrome. Geert Mortier, MD, PhD Center for Medical Genetics Ghent University Hospital Ghent, Belgium
 Stickler syndrome Geert Mortier, MD, PhD Center for Medical Genetics Ghent University Hospital Ghent, Belgium Third European Course in Clinical Dysmorphology Rome, November 20-21, 2009 Stickler syndrome
Stickler syndrome Geert Mortier, MD, PhD Center for Medical Genetics Ghent University Hospital Ghent, Belgium Third European Course in Clinical Dysmorphology Rome, November 20-21, 2009 Stickler syndrome
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier
 Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name and description (please provide any alternative names Osteogenesis Imperfecta
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name and description (please provide any alternative names Osteogenesis Imperfecta
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Genetics
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Genetics 1. GOAL: Understand the role of the pediatrician in preventing genetic disease, and in counseling and screening
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Genetics 1. GOAL: Understand the role of the pediatrician in preventing genetic disease, and in counseling and screening
chromosomal anomalies and mental pdf Chapter 8: Chromosomes and Chromosomal Anomalies (PDF) Chromosomal abnormalities -A review - ResearchGate
 DOWNLOAD OR READ : CHROMOSOMAL ANOMALIES AND MENTAL RETARDATION FROM GENOTYPES TO NEUROPSYCHOLOGICAL PHENOTYPES OF GENETIC SYNDROMES AT HIGH INCIDENCEGENOTYPE TO PHENOTYPE PDF EBOOK EPUB MOBI Page 1 Page
DOWNLOAD OR READ : CHROMOSOMAL ANOMALIES AND MENTAL RETARDATION FROM GENOTYPES TO NEUROPSYCHOLOGICAL PHENOTYPES OF GENETIC SYNDROMES AT HIGH INCIDENCEGENOTYPE TO PHENOTYPE PDF EBOOK EPUB MOBI Page 1 Page
