Genotype±phenotype associations in non-classical steroid 21-hydroxylase de ciency
|
|
|
- Joan White
- 5 years ago
- Views:
Transcription
1 European Journal of Endocrinology (2000) ±403 ISSN CLINICAL STUDY Genotype±phenotype associations in non-classical steroid 21-hydroxylase de ciency Naomi Weintrob, Chaim Brautbar 1, Athalia Pertzelan, Zeev Josefsberg, Zvi Dickerman, Arieh Kauschansky, Pearl Lilos, Dalia Peled, Moshe Phillip and Shoshana Israel 1 Institute for Endocrinology and Diabetes, Schneider Children's Medical Center of Israel, Petah Tiqva and Sackler Faculty of Medicine, Tel Aviv University, Tel Aviv, Israel and 1 Tissue Typing Unit, Hadassah Medical Organization, Jerusalem, Israel (Correspondence should be addressed to N Weintrob, Institute for Endocrinology and Diabetes, Schneider Children's Medical Center of Israel, 14 Kaplan Street, Petah Tiqva 49202, Israel; Fax: ) Abstract Objective: To evaluate whether genotype differences can explain the clinical variability of non-classical steroid 21-hydroxylase de ciency (NC21-OHD) and to determine if genotype is related to ethnic origin. Design: Genotyping for mutations in the steroid 21-hydroxylase (CYP21) gene was performed in 45 unrelated Israeli Jewish patients (nine males) with NC21-OHD (60 min 17-hydroxyprogesterone (17- OHP), 45±386 nmol/l) who were referred for evaluation of postnatal virilization or true precocious/ early puberty. Eleven siblings diagnosed through family screening were genotyped as well. Methods: Patients were divided by genotype into three groups: (A) homozygous or compound heterozygous for the mild mutations (V281L or P30L) (n=29; eight males); (B) compound heterozygous for one mild and one severe mutation (Q318X, I2 splice, I172N) (n=12; no males); (C) mild mutation detected on one allele only (n=4; one male; peak 17-OHP 58±151 nmol/l). We then related the genotype to the ethnic origin, clinical phenotype and hormone level. Since group C was very small, comparisons were made between groups A and B only. Results: At diagnosis, group B tended to be younger ( vs years, P ˆ 0.09), had greater height SDS adjusted for mid-parental height SDS ( vs , P ˆ 0.034), tended to have more advanced bone age SDS ( vs , P ˆ 0.10) and had a higher peak 17-OHP level in response to ACTH stimulation ( vs nmol/l, P < 0.01). Group B also had pubarche and gonadarche at an earlier age ( vs years, P < 0.01 and vs years, P < 0.001, respectively) and a higher rate of precocious puberty (50 vs 17%, P ˆ 0.04). Stepwise logistic regression analysis (excluding males) yielded age at gonadarche as the most signi cant variable differentiating the two groups, with a positive predictive value of 86% for a cut-off of 7.5 years. Conclusions: The ndings suggest that genotype might explain some of the variability in the phenotypic expression of NC21-OHD. Compound heterozygotes for one mild and one severe mutation have a higher peak 17-OHP associated with pubarche and gonadarche at an earlier age and more frequent precocious puberty. Hence, the severity of the enzymatic defect might determine the timing and pattern of puberty. European Journal of Endocrinology ±403 Introduction Congenital adrenal hyperplasia (CAH) denotes a family of disorders due to a defect in cortisol biosynthesis. De cient 21-hydroxylase (CYP21) activity, required to convert 17-hydroxyprogesterone (17-OHP) to 11- deoxycortisol, is the most common cause of CAH and one of the most common genetic inborn errors of metabolism. The disorder has traditionally been divided into three types according to severity of expression. (A) Salt-wasting (SW) and (B) simple virilizing (SV); the more severe SW and SV forms are collectively referred to as classical steroid 21-hydroxylase de ciency (21-OHD), and (C) non-classical (NC21-OHD), which is associated with different degrees of postnatal virilization developing during childhood or at puberty and may be asymptomatic (1). The disorder is inherited as a monogenic autosomal recessive trait. The CYP21 gene and a highly homologous inactive pseudo-gene, CYP21P, are located on the short arm of chromosome 6 within the HLA class III region. CYP21 gene deletion and at least ten sequence aberrations, probably transferred from CYP21P by gene conversion, have been identi ed as causing the different forms of 21-OHD (2). The functional consequences of individual mutations have been studied, and the q 2000 Society of the European Journal of Endocrinology Online version via
2 398 N Weintrob and others EUROPEAN JOURNAL OF ENDOCRINOLOGY (2000) 143 mutations have been classi ed according to the degree of the resultant enzymatic inactivation, so that the genotype can usually predict the clinical phenotype (3, 4). Previous studies have correlated the genotype with the three main forms of the disease, although data on the correlation of the genotype with the various clinical presentations of the non-classical form are lacking. The prevalence of NC21-OHD among Ashkenazi Jews is remarkably high (3.2±3.7%) (5); about 80% carry the mild mutation V281L (6). Screening for CYP21 gene mutations in NC21-OHD in other Jewish ethnic groups has not been done. In this study we screened for CYP21 gene mutations in Jewish patients with NC21-OHD to evaluate whether genotype differences might explain the clinical variability of this disorder and to determine whether there is an association between genotype and ethnic origin. Subjects and methods The genetic study was carried out between 1995 and 1998 in patients who had been followed in our institute since the late 1970s. The study population included 45 unrelated Jewish patients (nine males) with NC21-OHD who were referred for evaluation of postnatal virilization or true precocious/early puberty. The clinical diagnosis of NC21-OHD was based upon presenting signs of postnatal hyperandrogenism and the characteristic 60-min response of 17-OHP to 0.25 mg adrenocorticotropin (ACTH) stimulation (45±386 nmol/l) (7) with normal levels of 11-deoxycortisol. Age at diagnosis ranged from Table 1 Demographic and clinical characteristics of 45 Jewish patients with NC21-OHD. Patients (n ˆ 45) No. (%) Ethnicity* Ashkenazi 24 (53) Sephardic 8 (18) Asian 1 (2) Combined 12 (27) Presenting sign² Precocious pubarche 20 (44) True precocious puberty at diagnosis 12 (27) Clitoromegaly/macrogenitosomia 19 (42)³ PCO-like syndrome 3 (7) Growth acceleration 3 (7) Short nal height + S/P fast puberty 1 (2) Hypertrichosis 1 (2) * By country of origin: Ashkenazi ± Eastern Europe and former USSR; Sephardic ± North Africa, Spain and the Balkans; Asian ± Yemen, Iraq and Iran. ² Most patients had more than one presenting sign. ³ 13/36 females (36%) and 6/9 males (66%). PCO, polycystic ovary; S/P, status post. 0.1 to 17.5 years (median, 7.25). Ethnic origin and clinical signs at presentation are shown in Table 1. For the second part of the study, the genotype and clinical characteristics of 11 affected siblings (six males) detected by family screening were compared with the index case. The study protocol was approved by the Ethics Committee of Rabin Medical Center. We obtained informed consent from the patients and also from the parents of the children who were less than 18 years old. Height of the patients and parents was measured with the Harpenden±Holtain stadiometer. Auxological results were expressed in terms of standard deviation scores (SDS) for age, based on the standards of Tanner & Whitehouse (8). Bone age (BA) was determined according to Greulich & Pyle (9). Height was accepted as the nal height when the increment was < 1 cm over 1 year or when BA was $15 years in girls and $17 years in boys. Clitoris and penile size was measured by sliding caliper. Clitoromegaly and macrogenitosomia were considered when measurements were > 2 S.D. for age and Tanner stage (10, 11). We transformed the measurements of clitoral size made from 1980 to 1992 to the clitoral index published in 1992 (10). Puberty was assessed according to Marshall & Tanner (12, 13). Pubarche was de ned as Tanner 2 for pubic hair (12, 13). The criterion of true puberty was gonadarche: breast buds in girls and a testicular volume reaching 4 ml in boys. True precocious puberty was diagnosed when gonadarche appeared before the age of 8 years in girls and 9 years in boys. When gonadarche was present, a gonadotropin-releasing hormone (GnRH) stimulation test was performed concomitantly with the ACTH test. Plasma 17-OHP and cortisol levels were measured in the morning after an overnight fast before and 60 min after an i.v. bolus of a xed dose of 0.25 mg ACTH (7) (Synacthen, Ciba-Geigy, Basel, Switzerland). Levels of plasma luteinizing hormone (LH) and folliclestimulating hormone (FSH) were measured before and 30 and 60 min after an i.v. bolus of 50 mg/m 2 GnRH (Relisorm; Serono, Aubonne, Switzerland). Pubertal LH response was de ned as $5 IU/l (14). Also determined were basal levels of androstenedione, testosterone, 11- deoxycortisol and estradiol. Measurements were performed by radioimmunoassay (RIA) with commercial kits (17-OHP, cortisol, testosterone, estradiol: DPC, Los Angeles, CA, USA; androstenedione: Buhlman, Basel, Switzerland; 11 deoxycortisol: Sigma, St Louis, MO, USA; LH and FSH: chemiluminescent enzyme immunoassay; DPC). The plasma was separated and stored at 20 8C until assayed. It is noteworthy that we have been using the DPC RIA for determination of 17-OHP and androgen levels since the mid-1980s. Before that, homemade kits were used and ndings were evaluated against norms established in our laboratory for each Tanner stage. Measurements done from the mid-1980s were compared with the norms evaluated by Lashansky et al. (15). For each method, elevated androgen level
3 EUROPEAN JOURNAL OF ENDOCRINOLOGY (2000) 143 Phenotype±genotype associations in NC21-OHD 399 was de ned as > 2 S.D. from the mean. Since the androgen levels were determined by different methods, we did not compare the absolute levels between groups, but rather the frequency of the patients with elevated androgen levels. Oral hydrocortisone (HC) therapy was instituted when there was evidence of progressive virilization, acceleration of growth, true precocious puberty, advanced BA at diagnosis ($1 S.D. for age) or an increase in DBA/Dage of at least 6 months during follow-up. The dose (7.5± 15 mg/m 2, divided into two to three doses) was adjusted to normalize growth and BA maturation rate (i.e. resume the preacceleration growth curve) and to normalize morning plasma levels of testosterone and androstenedione for age or Tanner stage. Eight girls were treated with i.m. GnRH agonist (3.75 mg/4 weeks; Decapeptyl Depot; Ferring AB, Malmo, Sweden) in addition to HC, for true precocious puberty. The policy of the combined treatment evolved over several years, and therefore this regimen was introduced to only three girls of group B, four girls of group A and one girl of group C; age at start of therapy was 6.7±8.5 years, age at which therapy was stopped was 9.5±12.5 years, and duration of therapy was 1.9± 3.5 years. Genetic analysis The following mutations were sought in the patients, their parents and affected siblings: deletion of 8 bp in exon 3, ve point mutations: P30L exon 1, A/C655G intron 2 (I2 splice), I172N exon 4, V281L exon 7, Q318X exon 8 and a cluster of three point mutations in exon 6 (I236N+V237E+M239K). Blood samples were collected into EDTA and genomic DNA was isolated by the salting out method (16). Identi cation of mutations was performed by the PCR sequence-speci c oligonucleotide probe method. In brief, two sets of primers were used according to Wedell & Luthman (17) with some modi cation. Set one ± CYP11: 5 0 -GGAGCAATAAAG- GAGAAACTGA-3 0 and CYP48A: 5 0 -GAGACTACTCCC- TGCTCTG-3 0. Set two ± CYP1: 5 0 -TTCAGGCGATTC AGGAAGGC-3 0 and CYP48: 5 0 -CAGAGCAGGGAG- TAGTCTC-3 0. The two PCR products were blotted onto nylon membranes and hybridized with sequence speci c oligonucleotide probes which were end-labeled with digoxigenin ddutp (Boehringer Mannheim Biochemicals, Mannheim, Germany). The membranes were then washed with 3 mol/l tetramethylammonium chloride solution at increasing temperatures ranging between 48 8C and 57 8C. Alkaline phosphatase-bound antidigoxigenin was used with the chemiluminescent substrate for alkaline phosphate (CDP star; Boehringer Mannheim) for chemiluminescence detection. The oligonucleotide probes used for detection for wild-type sequence (W) (including two wild-type polymorphic forms, Wa and Wc, for the I2 splice mutations) and mutations (M) were as follows: P30L, W: 5 0 -CCACCTCCCGCCTCTTG-3 0 P30L, M: 5 0 -CCACCTCCTGCCTCTTG-3 0 I2 splice, Wa: 5 0 -AGCCCCCAACTCCTCCTGCA-3 0 I2 splice, Wc: 5 0 -AGCCCCC ACCTCCTCCTGCA-3 0 I2 splice, M: 5 0 -AGCCCCCAGCTCCTCCTGCA-3 0 I172N, W: 5 0 -CAGCATCATCTGTTACCTCA-3 0 I172N, M: 5 0 -CAC ATCGTGGAGATGCAGCT-3 0 cluster E6, W: 5 0 -CACAACGAGGAGAAGCAGCT-3 0 cluster E6, M: 5 0 -CACAACGAGGAGAAGCAGCT-3 0 V281L, W: 5 0 -AAGGGCACGTGCACATGGCT-3 0 V281L, M: 5 0 -AAGGGCACTTGCACATGGCT-3 0 Q318X, W: 5 0 -CAGCGACTGCAGGAGGAGCT-3 0 Q318X, M: 5 0 -GCGACTGTAGGAGGAG-3 0 (Control DNAs for all the mutations analyzed were obtained as a gift from A Wedell.) In patients with homozygous deletion, the primers failed to anneal, and the speci c PCR fragments were not obtained. A third set of primers: CYP5: 5 0 -GGTGCTGAACTCCAAGAGG-3 0 and CYP16: 5 0 -GTCCACAATTTGGATGGACCA-3 0 was used together with the sets above to obtain ampli cation in cases of homozygous deletion as a control for the reaction. Statistics The data were analyzed with the BMPD program (18). Data are presented as means 6 S.D. unless otherwise indicated. Between-group differences were analyzed by ANOVA or ANCOVA, as appropriate. The associations between the clinical and laboratory characteristics and the genotype were analyzed with Pearson's chi-square test or Fisher's exact test, as appropriate. Stepwise logistic regression was applied to estimate the best predictor for differentiating between groups A and B (see below). Results The 90 alleles of the 45 unrelated Jewish subjects with NC21-OHD contained the following disease-causing mutations: 72 (80%) V281L, six (6.7%) I2 splice, four (4.4%) Q318X, two (2.2%) P30L, and two (2.2%) I172N; in four alleles (4.4%), none of the above mutations was detected. Figure 1 shows the genotype distribution among the study patients. Previous studies relating mutations to level of enzymatic activity (19, 20) have shown that the mild mutations (V281L and P30L) result in an enzyme with 20±50% of normal activity, and the severe mutations (I2 splice, Q318X and I172N) in an enzyme with 0±2% of normal activity. Based on these ndings, we divided the patients into three groups: (A) homozygous or compound heterozygous for the mild mutations (n=29; eight males); (B) compound heterozygous for one mild and one severe mutation (n=12; no males); and (C) mild mutation detected on one allele only (n=4; one male; peak 17-OHP 58±151 nmol/l).
4 400 N Weintrob and others EUROPEAN JOURNAL OF ENDOCRINOLOGY (2000) 143 Figure 1 Genotype distribution among 45 patients with NC21-OHD. Table 2 Clinical and laboratory characteristics of the study population by genotype (means6s.d.). Signi cance of Group A Group B Group C difference Parameter (n ˆ 29) (n ˆ 12) (n ˆ 4) (P a ) At diagnosis Age (years) Bone age SDS Height SDS b Basal 17-OHP (nmol/l) NS Peak* 17-OHP (nmol/l) < 0.01 Therapy Starting age (years) HC dose (mg/m 2 per day) NS Puberty Age at pubarche (years) Whole group < 0.01 Females only Age at gonadarche (years) Whole group < Females only Menarche c NS c Final height SDS d NS b Mid-parental height SDS NS Group A ˆ homozygous or compound heterozygous for the mild mutations, group B ˆ compound heterozygous for one mild and one severe mutation and group C ˆ mild mutation (V281L) detected on one allele only. a Between A and B only. b Adjusted for mid-parental height. c No. of girls: 17, 7 and 1 for groups A, B and C respectively. d No. of subjects: 22, 5 and 2 for groups A, B and C respectively. * 60 min after ACTH stimulation. NS, not signi cant.
5 EUROPEAN JOURNAL OF ENDOCRINOLOGY (2000) 143 Phenotype±genotype associations in NC21-OHD 401 Table 3 Frequency of various parameters by genotype. Group A Group B Group C Signi cance of (n ˆ 29) (n ˆ 12) (n ˆ 4) association Parameter No. (%) No. (%) No. (%) (P a ) Gender Male 8 (28) 0 (0) 1 (25) 0.08 Female 21 (72) 12 (100) 3 (75) Ethnicity Ashkenazi 17 (59) 6 (50) 1 (25) NS Sephardic and Oriental 3 (10) 4 (33) 2 (50) Mixed 9 (31) 2 (17) 1 (25) Clitoromegaly/macrogenitosomia 12 (41) 6 (50) 1 (25) NS Precocious puberty at diagnosis* 5 (17) 6 (50) 2 (50) 0.04 Elevated androgens² 21 (72) 11 (92) 3 (75) NS HC therapy 26 (89) 11 (92) 3 (75) NS Group A ˆ homozygous or compound heterozygous for the mild mutations, group B ˆ compound heterozygous for one mild and one severe mutation and group C ˆ mild mutation (V281L) detected on one allele only. a Between A and B only. * Group A, four females and one male; group B, females only. ² Androstenedione and/or testosterone > 2 S.D. for age and pubertal stage. The characteristics of the study population by genotype group are shown in Tables 2 and 3. The correlation of the 17-OHP level to group yielded similar basal levels in groups A and B and a signi cantly lower level in group C (P < 0.05, Bonferroni correction for multiple comparisons) (Table 2); however, mean peak 17-OHP was similar in groups A and C, and signi cantly higher in group B (P < 0.01 for B vs A and B vs C). Because group C was very small, it was excluded from the statistical analysis of the other clinical characteristics. We found that at diagnosis, compared with group A, group B tended to be younger (P ˆ 0.09), had a greater height SDS adjusted for mid-parental height SDS (P ˆ 0.034) and tended to have a more mature BA SDS (P ˆ 0.10). The number of patients with clitoromegaly or macrogenitosomia detected at diagnosis was similar in the two groups, as was the number of patients with elevated androgen levels, the number of treated patients (Table 3) and the dose of HC/m 2 (Table 2). Group B had pubarche and gonadarche (Table 2) at an earlier age than group A (P < 0.01 and P < respectively) and a higher rate of precocious puberty (P ˆ 0.04) (Table 3). Since there were no males in group B, comparisons of age at pubarche and gonadarche were also done separately for girls, and yielded similar results (Table 2). Final height SDS, adjusted for mid-parental height SDS (Table 2), was similar between the two groups, but only 22 patients of group A and ve of group B had reached nal height by the time of the study. Application of stepwise logistic regression analysis (excluding males) using the variables that showed signi cance revealed that age at gonadarche was the most signi cant variable differentiating between the two groups, with a positive predictive value of 86% for a cutoff of 7.5 years. Ethnicity Among the whole cohort, 44 patients (98%), including all patients of Ashkenazi origin, carried at least one allele with the V281L mutation (Fig. 1). Two patients, one of Yemenite origin and the other of mixed Yemenite±Ashkenazi origin, carried the P30L mutation (21). In both cases, the mutation was carried by parents of Yemenite origin. There was no signi cant difference in the ethnic group distribution between group A and group B (Table 3). In group A patients the non-ashkenazi comprised only 10% compared with 59% of Ashkenazi but the difference did not reach statistical signi cance. Family screening Eleven siblings (six males, ve females) of ten families were diagnosed as having NC21-OHD according to 17-OHP response to ACTH stimulation (basal 17-OHP > 8.5 nmol/l, peak 17-OHP > 58 nmol/l). All were diagnosed at an earlier age than their index case owing to the family screening. Eight displayed similar degrees of disease manifestations and three are still asymptomatic at the age of 6.5 (V281L/I2 splice), 7.0 and 9.0 (V281L/V281L) years; we do not yet know if they have the cryptic form or will develop symptoms in the coming years. All siblings shared the same genotype. Six siblings (two of the same family) were homozygous for V281L, three were compound heterozygous for V281L/I2 splice, and two were heterozygous for V281L. A search for the mutations of the index cases among their parents yielded 83 carriers of one mutation (in four parents, no mutation was detected) and three parents (two fathers and one mother) of group 1 patients who were homozygous for V281L; all were Ashkenazi. One father had a history of short stature, and his height was 162 cm. His treated daughter and
6 402 N Weintrob and others EUROPEAN JOURNAL OF ENDOCRINOLOGY (2000) 143 son with NC21-OHD are 162 and 175 cm respectively, and both are homozygous for V281L. The other father is 167 cm tall and rst shaved at 15 years of age. The mother is 160 cm tall and hirsute. She had menarche at age 13 and three spontaneous pregnancies. Discussion In agreement with previous studies, the majority of our Jewish NC21-OHD patients were of Ashkenazi origin (5, 22) and almost all carried at least one allele with the V281L mutation (4, 6, 23). The P30L mutation (21) was found only in two patients, both of Yemenite origin, probably secondary to founder effect. The distinct genetic background of the Yemenite Jews has been shown in studies of many other inherited disease (24). Our results suggest that some of the variability in the clinical spectrum of NC21-OHD can be explained by genotype differences. The patients with compound heterozygosity for one mild (either V281L or P30L) and one severe (Q318X, I2 splice, I172N) mutation (group B) had a more severe clinical picture than those who carried two mild mutations (group A). At presentation, they were younger (all were diagnosed in the rst decade) and had a greater height SDS adjusted for mid-parental height SDS and slightly more mature BA. They also had earlier age at pubarche and gonadarche, a higher incidence of true central precocious puberty, and a higher peak 17-OHP in response to ACTH stimulation. Thus, even though compound heterozygotes typically exhibit phenotypes corresponding to the less severely affected allele (20, 25), their clinical course seems to be more severe than that of patients carrying two mild mutations. Furthermore, while all the patients of group B presented in the rst decade with either premature/early pubarche, precocious/early puberty, clitoromegaly or growth acceleration, the presentation of group A subjects was much more variable; all the postpubertal patients belonged to this group, as well as the three `asymptomatic' parents who were detected by family screening. The explanations for the phenotypic heterogeneity among individuals carrying the same mutations are still hypothetical and include the presence of other still unidenti ed mutations, the activity of other genes encoding proteins with extra-adrenal 21-hydroxylase activity (26), individual variation in the amount of protein produced (27), differences in intra-adrenal concentrations of progesterone (2), and differences in sensitivity to androgens (28). Our results are in agreement with Rumsby et al. (23) who studied mainly adult females with NC21-OHD and found more frequent oligomenorrhea/amenorrhea and infertility in those with one mild and one severe mutation, and mostly regular menses in those homozygous for the mild mutation. Among our patients were two females, both homozygous for V281L, who presented during adolescence with severe polycystic ovary syndrome with hirsutism and oligomenorrhea. Both resumed regular menses on treatment with low-dose dexamethasone, and one who sought pregnancy conceived on dexamethasone without any additional therapy. Of note is the high frequency (50%) of true central precocious puberty (CPP) among patients with compound heterozygosity for one mild and one severe mutation (group B). True CPP has been described previously in classical 21-OHD (29), NC21-OHD (22), and virilizing adrenal tumors (30), either at presentation or following institution of therapy when the hyperandrogenism resolved. The presentation of CPP associated with hyperandrogenism usually correlates with advanced BA to the range of the pubertal years (29, 30). Our group B patients did tend to have more advanced BA SDS at diagnosis than group A (Table 2), but only three out of six had a BA of > 8 years at gonadarche, which appeared before initiation of therapy, i.e. before androgen suppression. Therefore, it is probably the mildly elevated androgen levels that imitate physiologic adrenarche and prematurely prime the hypothalamic±pituitary±gonadal axis. Since CPP is quite frequently a presenting sign of NC21-OHD (27% in our group), we suggest that the ACTH stimulation test should be added to its evaluation. In four patients with peak 17-OHP levels within the accepted range for NC21-OHD ( nmol/l), a mild mutation (V281L) was detected on one allele only (group C). Their mean basal 17-OHP level was, indeed, signi cantly lower than that of groups A and B (Table 2), but their mean peak 17-OHP level was compatible with NC21-OHD (7) and was similar to that of group A. We did not perform screening for more mutations (R356W, P453S), or direct sequencing to detect rare alleles, owing to technical limitations. In other large studies screening for mutations in patients with clinical and laboratory evidence of 21-OHD (3, 4), mutations were not observed in 5±10% of chromosomes in which they were expected according to the clinical status of the index case. However, sequencing of the CYP21 gene was not done and, therefore, rare mutations might have been missed. Since genotyping for all the mutations described so far, or direct sequencing, is expensive, laborious and restricted to only a few research centers, the diagnosis of 21-OHD de ciency should probably still rely on peak 17-OHP level in response to ACTH stimulation (7, 25). We believe that genotyping is justi ed in patients with NC21-OHD owing to the existence of a subgroup with compound heterozygosity for one mild and one severe mutation. These ndings have important implications for future genetic and prenatal counseling, since prenatal treatment with dexamethasone for fetuses carrying two severe mutations is now feasible (31). Acknowledgements We are grateful to Dr Anna Wedell of Karolinska Hospital, Stockholm, Sweden for providing the initial
7 EUROPEAN JOURNAL OF ENDOCRINOLOGY (2000) 143 Phenotype±genotype associations in NC21-OHD 403 help with the primers; and to Mrs Charlotte Sachs and Mrs Gloria Ginzach of the Editorial Board, Rabin Medical Center, Beilinson Campus, and Oren Moran, for their assistance. References 1 Kohn B, Levine LS, Pollack MS, Pang S, Lorenzen F, Levy D et al. Late onset steroid 21-hydroxylase de ciency: a variant of classical congenital adrenal hyperplasia. Journal of Clinical Endocrinology and Metabolism ± White PC & New MI. Genetic basis of endocrine disease 2: congenital adrenal hyperplasia due to 21-hydroxylase de ciency. Journal of Clinical Endocrinology and Metabolism ±11. 3 Speiser PW, Dupont J, Zhu D, Serrat J, Buegeleisen M, Tusie-Luna MT et al. Disease expression and molecular genotype in congenital adrenal hyperplasia due to 21-hydroxylase de ciency. Journal of Clinical Investigation ± Wedell A, Thilen A, Ritzen EM, Stengler B & Luthman H. Mutational spectrum of the steroid 21-hydroxylase gene in Sweden: implication for genetic diagnosis and association with disease manifestation. Journal of Clinical Endocrinology and Metabolism ± Speiser PW, Dupont B, Rubinstein P, Piazza A, Kastelan A & New MI. High frequency of nonclassic steroid 21-hydroxylase de ciency. American Journal of Human Genetics ± Speiser PW, New MI & White PC. Molecular genetic analysis of nonclassic steroid 21-hydroxylase de ciency associated with HLA-B14,DR1. New England Journal of Medicine ±23. 7 New MI, Lorenzen F, Lerner AJ, Kohn B, Ober eld SE, Pollack MS et al. Genotyping steroid 21-hydroxylase de ciency: hormonal reference data. Journal of Clinical Endocrinology and Metabolism ± Tanner JM & Whitehouse RH. Clinical longitudinal standards for height, weight, height velocity, weight velocity and stages of puberty. Archives of Diseases in Childhood ± Greulich WW & Pyle SI. Radiographic Atlas of Skeletal Development of the Hand and Wrist, edn 2. Stanford, California: Stanford University Press, Sane K & Pescovitz OH. The clitoral index: a determination of clitoral size in normal girls and in girls with abnormal sexual development. Journal of Pediatrics ± Shoenfeld WA. Primary and secondary sexual characteristics. American Journal of Diseases of Childhood ± Marshall WA & Tanner JM. Variation in the pattern of pubertal changes in girls. Archives of Diseases in Childhood ± Marshall WA & Tanner JM. Variation in the pattern of pubertal changes in boys. Archives of Diseases in Childhood ± Dickerman Z, Prager-Lewin R & Laron Z. Response of plasma LH and FSH to synthetic LH-RH in children in various pubertal stages. American Journal of Diseases of Childhood ± Lashansky G, Seanger P, Fishman K, Gautier T, Mayes D, Berg G et al. Normative data for adrenal steroidogenesis in a healthy pediatric population: age- and sex-related changes after adrenocorticotropin stimulation. Journal of Clinical Endocrinology and Metabolism ± Miller SA, Dykes DD & Polesky HF. A simple salting out procedure for extracting DNA from human nucleated cells. Nucleic Acids Research Wedell A & Luthman H. Steroid 21-hydroxylase (P450c21): a new allele and spread of mutations through the pseudogene. Human Genetics ± BMPD Statistical Software. Ed. WJ Dixon. Los Angeles: University of California Press, Tusie-Luna MT, Traktman P & White PC. Determination of functional effects of mutations in the steroid 21-hydroxylase gene (CYP21) using recombinant vaccinia virus. Journal of Biological Chemistry ± Speiser PW & White PC. Congenital adrenal hyperplasia due to steroid 21-hydroxylase de ciency. Clinical Endocrinology ± Tusie-Luna MT, Speiser PW, Dumic M, New MI & White PC. A mutation (Pro-30 to Leu) in CYP21 represents a potential nonclassic steroid 21-hydroxylase de ciency allele. Molecular Endocrinology ± Weintrob N, Dickerman Z, Sprecher E, Galatzer A & Pertzelan A. Non-classical 21-hydroxylase de ciency in infancy and childhood: the effect of time of initiation of therapy on puberty and nal height. European Journal of Endocrinology ± Rumsby G, Avey CJ, Conway GS & Honour JW. Genotype± phenotype analysis in late onset 21-hydroxylase de ciency in comparison to the classical forms. Clinical Endocrinology ± Weingarten MA. Changing Health and Changing Culture, pp 87± 104. New York: Praeger, Wilson RC, Mercado AB, Cheng KC & New MI. Steroid 21- hydroxylase de ciency: genotype may not predict phenotype. Journal of Clinical Endocrinology and Metabolism ± Miller WL. Phenotypic heterogeneity associated with the splicing mutation in congenital adrenal hyperplasia due to 21-hydroxylase de ciency. Journal of Clinical Endocrinology and Metabolism Witchel SF, Bhamidipati DK, Hoffman EP & Cohen JB. Phenotypic heterogeneity associated with the splicing mutation in congenital adrenal hyperplasia due to 21-hydroxylase de ciency. Journal of Clinical Endocrinology and Metabolism ± Kuttenn F, Couillin P, Girard F, Billand L, Vincens M, Boucekkine C et al. Late-onset adrenal hyperplasia in hirsutism. New England Journal of Medicine ± Hirsch-Pescovitz O, Comite F, Cassorla F, Dwyer AJ, Poth MA, Sperling MA et al. True precocious puberty complicating congenital adrenal hyperplasia: treatment with a luteinizing hormone-releasing hormone analog. Journal of Clinical Endocrinology and Metabolism ± Lee PDK, Winter RJ & Green OC. Virilizing adrenocortical tumors in childhood: eight cases and a review of the literature. Pediatrics ± Forest MG, David M & Morel Y. Prenatal diagnosis and treatment of 21-hydroxylase de ciency. The Journal of Steroid Biochemistry and Molecular Biology ±82. Received 2 December 1999 Accepted 1 June 2000
Is basal serum 17-OH progesterone a reliable parameter to predict nonclassical congenital adrenal hyperplasia in premature adrenarche?
 The Turkish Journal of Pediatrics 2011; 53: 274-280 Original Is basal serum 17-OH progesterone a reliable parameter to predict nonclassical congenital adrenal hyperplasia in premature adrenarche? E. Nazlı
The Turkish Journal of Pediatrics 2011; 53: 274-280 Original Is basal serum 17-OH progesterone a reliable parameter to predict nonclassical congenital adrenal hyperplasia in premature adrenarche? E. Nazlı
Dr. Nermine Salah El-Din Prof of Pediatrics
 Dr. Nermine Salah El-Din Prof of Pediatrics Diabetes Endocrine Metabolism Pediatric Unit (DEMPU) Children Hospital, Faculty of Medicine Cairo University Congenital adrenal hyperplasia is a common inherited
Dr. Nermine Salah El-Din Prof of Pediatrics Diabetes Endocrine Metabolism Pediatric Unit (DEMPU) Children Hospital, Faculty of Medicine Cairo University Congenital adrenal hyperplasia is a common inherited
Laura Stewart, MD, FRCPC Clinical Associate Professor Division of Pediatric Endocrinology University of British Columbia
 Precocious Puberty Laura Stewart, MD, FRCPC Clinical Associate Professor Division of Pediatric Endocrinology University of British Columbia Faculty Disclosure Faculty: Laura Stewart No relationships with
Precocious Puberty Laura Stewart, MD, FRCPC Clinical Associate Professor Division of Pediatric Endocrinology University of British Columbia Faculty Disclosure Faculty: Laura Stewart No relationships with
Supplemental Data: Detailed Characteristics of Patients with MKRN3. Patient 1 was born after an uneventful pregnancy. She presented in our
 1 2 Supplemental Data: Detailed Characteristics of Patients with MKRN3 Mutations 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 Patient 1 was born after an uneventful pregnancy. She presented
1 2 Supplemental Data: Detailed Characteristics of Patients with MKRN3 Mutations 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 Patient 1 was born after an uneventful pregnancy. She presented
CYP21A2 Mutations Found in Congenital Adrenal Hyperplasia Patients in the California Population
 CYP21A2 Mutations Found in Congenital Adrenal Hyperplasia Patients in the California Population Christopher N. Greene, Ph.D. Newborn Screening and Molecular Biology Branch National Center for Environmental
CYP21A2 Mutations Found in Congenital Adrenal Hyperplasia Patients in the California Population Christopher N. Greene, Ph.D. Newborn Screening and Molecular Biology Branch National Center for Environmental
SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY
 1 SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL SEMINAR: SEX HORMONES PART 1 An Overview What are steroid hormones? Steroid
1 SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL SEMINAR: SEX HORMONES PART 1 An Overview What are steroid hormones? Steroid
Follow-up Study of Adolescent Girls With a History of Premature Pubarche
 JOURNAL OF ADOLESCENT HEALTH 1996;18:301-305 ADOLESCENT HEALTH BRIEF/FELLOWSHIP FORUM Follow-up Study of Adolescent Girls With a History of Premature Pubarche DAPHNE MILLER, M.D., S. JEAN EMANS, M.D.,
JOURNAL OF ADOLESCENT HEALTH 1996;18:301-305 ADOLESCENT HEALTH BRIEF/FELLOWSHIP FORUM Follow-up Study of Adolescent Girls With a History of Premature Pubarche DAPHNE MILLER, M.D., S. JEAN EMANS, M.D.,
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Congenital Adrenal Hyperplasia in Saudi Arabia: The Biochemical Characteristics Nasir A. M.
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Congenital Adrenal Hyperplasia in Saudi Arabia: The Biochemical Characteristics Nasir A. M.
A rapid screening for steroid 21-hydroxylase mutations in patients with congenital adrenal hyperplasia
 HUMAN MUTATION Mutation in Brief #247(1999) Online MUTATION IN BRIEF A rapid screening for steroid 21-hydroxylase mutations in patients with congenital adrenal hyperplasia Klaus Kapelari 1, Zahra Ghanaati
HUMAN MUTATION Mutation in Brief #247(1999) Online MUTATION IN BRIEF A rapid screening for steroid 21-hydroxylase mutations in patients with congenital adrenal hyperplasia Klaus Kapelari 1, Zahra Ghanaati
Characteristics and prevalence of non-classical congenital adrenal hyperplasia with a V281l mutation in patients with premature pubarche
 J Pediatr Endocr Met 2011;24(11-12):965 970 2011 by Walter de Gruyter Berlin Boston. DOI 10.1515/JPEM.2011.354 Characteristics and prevalence of non-classical congenital adrenal hyperplasia with a V281l
J Pediatr Endocr Met 2011;24(11-12):965 970 2011 by Walter de Gruyter Berlin Boston. DOI 10.1515/JPEM.2011.354 Characteristics and prevalence of non-classical congenital adrenal hyperplasia with a V281l
When testes make no testosterone: Identifying a rare cause of 46, XY female phenotype in adulthood
 When testes make no testosterone: Identifying a rare cause of 46, XY female phenotype in adulthood Gardner DG, Shoback D. Greenspan's Basic & Clinical Endocrinology, 10e; 2017 Sira Korpaisarn, MD Endocrinology
When testes make no testosterone: Identifying a rare cause of 46, XY female phenotype in adulthood Gardner DG, Shoback D. Greenspan's Basic & Clinical Endocrinology, 10e; 2017 Sira Korpaisarn, MD Endocrinology
PRENATAL TREATMENT AND FERTILITY OF FEMALE PATIENTS WITH CONGENITAL ADRENAL HYPERPLASIA
 PRENATAL TREATMENT AND FERTILITY OF FEMALE PATIENTS WITH CONGENITAL ADRENAL HYPERPLASIA Nguyen Ngoc Khanh, Vu Chi Dung et al Vietnam Children s Hospital (VCH) Hanoi, Vietnam Outline Intruduction Prenatal
PRENATAL TREATMENT AND FERTILITY OF FEMALE PATIENTS WITH CONGENITAL ADRENAL HYPERPLASIA Nguyen Ngoc Khanh, Vu Chi Dung et al Vietnam Children s Hospital (VCH) Hanoi, Vietnam Outline Intruduction Prenatal
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Puberty and Pubertal Disorders Part 2: Precocious Puberty. These podcasts are designed to give medical students an overview
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Puberty and Pubertal Disorders Part 2: Precocious Puberty. These podcasts are designed to give medical students an overview
Learning Objectives 4/17/2013. Toni Eimicke has no conflicts of interest or disclosures Heather Shanholtz has no conflicts of interest or disclosures
 OVERVIEW OF CONGENITAL ADRENAL HYPERPLASIA PATHOPHYSIOLOGY, LAB INTERPRETATION & MANAGEMENT Presented by: Toni Eimicke, MS, CPNP & Heather J Shanholtz, RN Pediatric Endocrinology Barbara Bush Children
OVERVIEW OF CONGENITAL ADRENAL HYPERPLASIA PATHOPHYSIOLOGY, LAB INTERPRETATION & MANAGEMENT Presented by: Toni Eimicke, MS, CPNP & Heather J Shanholtz, RN Pediatric Endocrinology Barbara Bush Children
Precocious Puberty. Disclosures. No financial disclosures 2/28/2019
 Precocious Puberty Bracha Goldsweig, MD Pediatric Endocrinologist Children s Hospital and Medical Center, Omaha, NE University of Nebraska Medical Center Disclosures No financial disclosures 1 Objectives
Precocious Puberty Bracha Goldsweig, MD Pediatric Endocrinologist Children s Hospital and Medical Center, Omaha, NE University of Nebraska Medical Center Disclosures No financial disclosures 1 Objectives
Topic 3.3 Prevention of ambiguous genitalia by prenatal treatment with dexamethasone in pregnancies at risk for congenital adrenal hyperplasia*
 Pure Appl. Chem., Vol. 75, Nos. 11 12, pp. 2013 2022, 2003. 2003 IUPAC Topic 3.3 Prevention of ambiguous genitalia by prenatal treatment with dexamethasone in pregnancies at risk for congenital adrenal
Pure Appl. Chem., Vol. 75, Nos. 11 12, pp. 2013 2022, 2003. 2003 IUPAC Topic 3.3 Prevention of ambiguous genitalia by prenatal treatment with dexamethasone in pregnancies at risk for congenital adrenal
Clinical Guideline ADRENARCHE MANAGEMENT OF CHILDREN PRESENTING WITH SIGNS OF EARLY ONSET PUBIC HAIR/BODY ODOUR/ACNE
 Clinical Guideline ADRENARCHE MANAGEMENT OF CHILDREN PRESENTING WITH SIGNS OF EARLY ONSET PUBIC HAIR/BODY ODOUR/ACNE Includes guidance for the distinction between adrenarche, precocious puberty and other
Clinical Guideline ADRENARCHE MANAGEMENT OF CHILDREN PRESENTING WITH SIGNS OF EARLY ONSET PUBIC HAIR/BODY ODOUR/ACNE Includes guidance for the distinction between adrenarche, precocious puberty and other
Screening non-classical 21-hydroxylase gene deficiency from patients diagnosed as polycystic ovary syndrome by gene assay HU Jie, JIAO Kai *
 Med J Chin PLA, Vol. 41, No. 3, March 1, 2016 227 21- [ ] (PCOS) 21- (NC-21OHD) 2014 2015 98 PCOS Ferriman-Gallway ( mf-g ) 3 mf-g 0~2 A 3~5 B 6 C30 DNA 5 CYP21A2 8 (ACTH) 30 98 PCOS 5 V281L/920-921insT(P1)
Med J Chin PLA, Vol. 41, No. 3, March 1, 2016 227 21- [ ] (PCOS) 21- (NC-21OHD) 2014 2015 98 PCOS Ferriman-Gallway ( mf-g ) 3 mf-g 0~2 A 3~5 B 6 C30 DNA 5 CYP21A2 8 (ACTH) 30 98 PCOS 5 V281L/920-921insT(P1)
AMBIGUOUS GENITALIA & CONGENITAL ADRENALHYPERPLASIA
 AMBIGUOUS GENITALIA & CONGENITAL ADRENALHYPERPLASIA BY Dr Numair Ali sheikh FCPS PGT I Department Of Pediatrics BBH RWP AMBIGUOUS GENITALIA Children born with ambiguous genitalia may be subdivided in to
AMBIGUOUS GENITALIA & CONGENITAL ADRENALHYPERPLASIA BY Dr Numair Ali sheikh FCPS PGT I Department Of Pediatrics BBH RWP AMBIGUOUS GENITALIA Children born with ambiguous genitalia may be subdivided in to
Disorder name: Congenital Adrenal Hyperplasia Acronym: CAH
 Genetic Fact Sheets for Parents Draft Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social issues surrounding
Genetic Fact Sheets for Parents Draft Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social issues surrounding
Reproductive DHEA-S Analyte Information
 Reproductive DHEA-S Analyte Information - 1 - DHEA-S Introduction DHEA-S, DHEA sulfate or dehydroepiandrosterone sulfate, it is a metabolite of dehydroepiandrosterone (DHEA) resulting from the addition
Reproductive DHEA-S Analyte Information - 1 - DHEA-S Introduction DHEA-S, DHEA sulfate or dehydroepiandrosterone sulfate, it is a metabolite of dehydroepiandrosterone (DHEA) resulting from the addition
Medical management of Intersex disorders. Dr. Abdulmoein Al-Agha, Ass. Professor & Consultant Pediatric Endocrinologist KAAUH, Jeddah
 Medical management of Intersex disorders Dr. Abdulmoein Al-Agha, Ass. Professor & Consultant Pediatric Endocrinologist KAAUH, Jeddah Is it a boy or a girl? The birth of an intersex infant is often viewed
Medical management of Intersex disorders Dr. Abdulmoein Al-Agha, Ass. Professor & Consultant Pediatric Endocrinologist KAAUH, Jeddah Is it a boy or a girl? The birth of an intersex infant is often viewed
2.0 Synopsis. Lupron Depot M Clinical Study Report R&D/09/093. (For National Authority Use Only) to Part of Dossier: Name of Study Drug:
 2.0 Synopsis Abbott Laboratories Individual Study Table Referring to Part of Dossier: Name of Study Drug: Volume: Abbott-43818 (ABT-818) leuprolide acetate for depot suspension (Lupron Depot ) Name of
2.0 Synopsis Abbott Laboratories Individual Study Table Referring to Part of Dossier: Name of Study Drug: Volume: Abbott-43818 (ABT-818) leuprolide acetate for depot suspension (Lupron Depot ) Name of
Girls with virilisation in childhood: a diagnostic protocol for investigation
 I Clin Pathol 1997;:379-383 Girls with virilisation in childhood: a diagnostic protocol for investigation 379 Departments of Endocrinology, Chemical Endocrinology and Clinical Biochemistry, St Bartholomew's
I Clin Pathol 1997;:379-383 Girls with virilisation in childhood: a diagnostic protocol for investigation 379 Departments of Endocrinology, Chemical Endocrinology and Clinical Biochemistry, St Bartholomew's
SALSA MLPA KIT P050-B2 CAH
 SALSA MLPA KIT P050-B2 CAH Lot 0510, 0909, 0408: Compared to lot 0107, extra control fragments have been added at 88, 96, 100 and 105 nt. The 274 nt probe gives a higher signal in lot 0510 compared to
SALSA MLPA KIT P050-B2 CAH Lot 0510, 0909, 0408: Compared to lot 0107, extra control fragments have been added at 88, 96, 100 and 105 nt. The 274 nt probe gives a higher signal in lot 0510 compared to
Development of a Multiplex CYP21A2 Genotyping Assay for Congenital Adrenal Hyperplasia Screening
 Development of a Multiplex CYP21A2 Genotyping Assay for Congenital Adrenal Hyperplasia Screening Christopher N. Greene, Ph.D. Newborn Screening and Molecular Biology Branch National Center for Environmental
Development of a Multiplex CYP21A2 Genotyping Assay for Congenital Adrenal Hyperplasia Screening Christopher N. Greene, Ph.D. Newborn Screening and Molecular Biology Branch National Center for Environmental
Congenital Adrenal Hyperplasia
 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. Feingold KR, Anawalt B, Boyce A, et al., editors. Endotext [Internet]. South Dartmouth (MA): MDText.com, Inc.;
NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. Feingold KR, Anawalt B, Boyce A, et al., editors. Endotext [Internet]. South Dartmouth (MA): MDText.com, Inc.;
ORIGINAL ARTICLE Endocrinology, Nutrition & Metabolism INTRODUCTION
 ORIGINAL ARTICLE Endocrinology, Nutrition & Metabolism http://dx.doi.org/10.3346/jkms.2011.26.11.1454 J Korean Med Sci 2011; 26: 1454-1460 Relationships of Basal Level of Serum 17-Hydroxyprogesterone with
ORIGINAL ARTICLE Endocrinology, Nutrition & Metabolism http://dx.doi.org/10.3346/jkms.2011.26.11.1454 J Korean Med Sci 2011; 26: 1454-1460 Relationships of Basal Level of Serum 17-Hydroxyprogesterone with
Paul Hofman. Professor. Paediatrician Endocrinologist Liggins Institute, The University of Auckland, Starship Children Hospital, Auckland
 Professor Paul Hofman Paediatrician Endocrinologist Liggins Institute, The University of Auckland, Starship Children Hospital, Auckland 14:00-14:55 WS #108: Common pubertal variants how to distinguish
Professor Paul Hofman Paediatrician Endocrinologist Liggins Institute, The University of Auckland, Starship Children Hospital, Auckland 14:00-14:55 WS #108: Common pubertal variants how to distinguish
Puberty and Pubertal Disorders. Lisa Swartz Topor, MD, MMSc Pediatric Endocrinology July 2018
 Puberty and Pubertal Disorders Lisa Swartz Topor, MD, MMSc Pediatric Endocrinology July 2018 Objectives Review normal pubertal development Recognize common pubertal disorders Identify recent trends in
Puberty and Pubertal Disorders Lisa Swartz Topor, MD, MMSc Pediatric Endocrinology July 2018 Objectives Review normal pubertal development Recognize common pubertal disorders Identify recent trends in
SEX STERIOD HORMONES I: An Overview. University of PNG School of Medicine & Health Sciences Division of Basic Medical Sciences PBL MBBS III VJ Temple
 SEX STERIOD HORMONES I: An Overview University of PNG School of Medicine & Health Sciences Division of Basic Medical Sciences PBL MBBS III VJ Temple 1 What are the Steroid hormones? Hormones synthesized
SEX STERIOD HORMONES I: An Overview University of PNG School of Medicine & Health Sciences Division of Basic Medical Sciences PBL MBBS III VJ Temple 1 What are the Steroid hormones? Hormones synthesized
IN SUMMARY HST 071 NORMAL & ABNORMAL SEXUAL DIFFERENTIATION Fetal Sex Differentiation Postnatal Diagnosis and Management of Intersex Abnormalities
 Harvard-MIT Division of Health Sciences and Technology HST.071: Human Reproductive Biology Course Director: Professor Henry Klapholz IN SUMMARY HST 071 Title: Fetal Sex Differentiation Postnatal Diagnosis
Harvard-MIT Division of Health Sciences and Technology HST.071: Human Reproductive Biology Course Director: Professor Henry Klapholz IN SUMMARY HST 071 Title: Fetal Sex Differentiation Postnatal Diagnosis
DEFINITION: Masculinization of external genitalia in patients with normal 46XX karyotype.
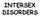 INTERSEX DISORDERS DEFINITION: Masculinization of external genitalia in patients with normal 46XX karyotype. - Degree of masculinization variable: - mild clitoromegaly - complete fusion of labia folds
INTERSEX DISORDERS DEFINITION: Masculinization of external genitalia in patients with normal 46XX karyotype. - Degree of masculinization variable: - mild clitoromegaly - complete fusion of labia folds
Joint AEPCOS/Endocrine Society Update Meeting in ENDO 2017
 Joint AEPCOS/Endocrine Society Update Meeting in Orlando @ ENDO 2017 GUT, MICROBIOME AND FAT: ORIGINS OF PCOS METABOLIC DISEASE? ORANGE COUNTY CONVENTION CENTER, ORLANDO, FL, USA, MARCH 31, 2017 CALL FOR
Joint AEPCOS/Endocrine Society Update Meeting in Orlando @ ENDO 2017 GUT, MICROBIOME AND FAT: ORIGINS OF PCOS METABOLIC DISEASE? ORANGE COUNTY CONVENTION CENTER, ORLANDO, FL, USA, MARCH 31, 2017 CALL FOR
Safe Harbor Statement
 Safe Harbor Statement These slides contain forward-looking statements based on estimates and assumptions by our management that, although we believe to be reasonable, are inherently uncertain. Forward-looking
Safe Harbor Statement These slides contain forward-looking statements based on estimates and assumptions by our management that, although we believe to be reasonable, are inherently uncertain. Forward-looking
PUBERTY. Preetha Krishnamoorthy. Division of Pediatric Endocrinology
 PUBERTY Preetha Krishnamoorthy Division of Pediatric Endocrinology Case 1 8-year-old girl referred for breast development noted by mom What do you want to know? Normal or abnormal? What if this was an
PUBERTY Preetha Krishnamoorthy Division of Pediatric Endocrinology Case 1 8-year-old girl referred for breast development noted by mom What do you want to know? Normal or abnormal? What if this was an
OBJECTIVES. Rebecca McEachern, MD. Puberty: Too early, Too Late or Just Right? Special Acknowledgements. Maryann Johnson M.Ed.
 1 Puberty: Too early, Too Late or Just Right? Maryann Johnson M.Ed., BSN, RN Special Acknowledgements Rebecca McEachern, MD OBJECTIVES Illustrate basic endocrine system and hormonal pathways Define the
1 Puberty: Too early, Too Late or Just Right? Maryann Johnson M.Ed., BSN, RN Special Acknowledgements Rebecca McEachern, MD OBJECTIVES Illustrate basic endocrine system and hormonal pathways Define the
Lab Activity 36. Principles of Heredity. Portland Community College BI 233
 Lab Activity 36 Principles of Heredity Portland Community College BI 233 Terminology of Chromosomes Homologous chromosomes: A pair, of which you get one from mom, and one from dad. Example: the pair of
Lab Activity 36 Principles of Heredity Portland Community College BI 233 Terminology of Chromosomes Homologous chromosomes: A pair, of which you get one from mom, and one from dad. Example: the pair of
Growth hormone therapy in a girl with Turner syndrome showing a large increase over the initially predicted ht of 4 5
 Disorders of Growth and Puberty: How to Recognize the Normal Variants vs Patients Who Need to be Evaluated Paul Kaplowitz, M.D Pediatric Endocrinology. VCU School of Medicine Interpretation of Growth Charts
Disorders of Growth and Puberty: How to Recognize the Normal Variants vs Patients Who Need to be Evaluated Paul Kaplowitz, M.D Pediatric Endocrinology. VCU School of Medicine Interpretation of Growth Charts
12/27/2013. Kristen Cain, MD FACOG Reproductive Medicine Institute Sanford Health, Fargo ND
 Kristen Cain, MD FACOG Reproductive Medicine Institute Sanford Health, Fargo ND 7% of all women 18-45 Obesity 1/3 of all US women Incidence of PCOS is increasing with increase obesity Obesity Irregular
Kristen Cain, MD FACOG Reproductive Medicine Institute Sanford Health, Fargo ND 7% of all women 18-45 Obesity 1/3 of all US women Incidence of PCOS is increasing with increase obesity Obesity Irregular
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Endocrinology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Endocrinology 1. GOAL: Understand the role of the pediatrician in preventing endocrine dysfunction, and in counseling and
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Endocrinology 1. GOAL: Understand the role of the pediatrician in preventing endocrine dysfunction, and in counseling and
3 year old boy with puberty. Katie Stanley, MD August 1, 2013
 3 year old boy with puberty Katie Stanley, MD August 1, 2013 Initial presentation 3 and 11/12 year old boy with signs of puberty Presented to outside endocrinologist in 2002 with: Pubic hair since 2.5
3 year old boy with puberty Katie Stanley, MD August 1, 2013 Initial presentation 3 and 11/12 year old boy with signs of puberty Presented to outside endocrinologist in 2002 with: Pubic hair since 2.5
BEHAVIORAL STUDIES in children with congenital adrenal
 0013-7227/02/$15.00/0 The Journal of Clinical Endocrinology & Metabolism 87(11):5119 5124 Printed in U.S.A. Copyright 2002 by The Endocrine Society doi: 10.1210/jc.2001-011531 Sex-Typed Toy Play Behavior
0013-7227/02/$15.00/0 The Journal of Clinical Endocrinology & Metabolism 87(11):5119 5124 Printed in U.S.A. Copyright 2002 by The Endocrine Society doi: 10.1210/jc.2001-011531 Sex-Typed Toy Play Behavior
Dr Stella Milsom. Endocrinologist Fertility Associates Auckland. 12:30-12:40 When Puberty is PCO
 Dr Stella Milsom Endocrinologist Fertility Associates Auckland 12:30-12:40 When Puberty is PCO Puberty or Polycystic Ovary Syndrome? Stella Milsom Endocrinologist Auckland DHB, University of Auckland,
Dr Stella Milsom Endocrinologist Fertility Associates Auckland 12:30-12:40 When Puberty is PCO Puberty or Polycystic Ovary Syndrome? Stella Milsom Endocrinologist Auckland DHB, University of Auckland,
Very premature pubarche in girls is not a pubertal variant
 HORMONES 2012, 11(3):356-360 Case report Very premature pubarche in girls is not a pubertal variant Françoise Paris*, 1 Nicolas Kalfa*, 1,2 Pascal Philibert, 1 Claire Jeandel, 1 Laura Gaspari, 1 Charles
HORMONES 2012, 11(3):356-360 Case report Very premature pubarche in girls is not a pubertal variant Françoise Paris*, 1 Nicolas Kalfa*, 1,2 Pascal Philibert, 1 Claire Jeandel, 1 Laura Gaspari, 1 Charles
Audit of Adrenal Function Tests. Kate Davies Senior Lecturer in Children s Nursing London South Bank University London, UK
 Audit of Adrenal Function Tests Kate Davies Senior Lecturer in Children s Nursing London South Bank University London, UK Introduction Audit Overview of adrenal function tests Education Audit why? Explore
Audit of Adrenal Function Tests Kate Davies Senior Lecturer in Children s Nursing London South Bank University London, UK Introduction Audit Overview of adrenal function tests Education Audit why? Explore
3- & 12-Year-Old Sisters with Li-Fraumeni Syndrome KRISTEN DILLARD, M.D. ENDORAMA FEBRUARY 28, 2013
 3- & 12-Year-Old Sisters with Li-Fraumeni Syndrome KRISTEN DILLARD, M.D. ENDORAMA FEBRUARY 28, 2013 Presentation Sisters referred by Peds Oncology to Endo clinic for adrenocortical carcinoma screening
3- & 12-Year-Old Sisters with Li-Fraumeni Syndrome KRISTEN DILLARD, M.D. ENDORAMA FEBRUARY 28, 2013 Presentation Sisters referred by Peds Oncology to Endo clinic for adrenocortical carcinoma screening
Human inherited diseases
 Human inherited diseases A genetic disorder that is caused by abnormality in an individual's DNA. Abnormalities can range from small mutation in a single gene to the addition or subtraction of a whole
Human inherited diseases A genetic disorder that is caused by abnormality in an individual's DNA. Abnormalities can range from small mutation in a single gene to the addition or subtraction of a whole
Obstetrics and Gynecology and of Medicine, The University of Alabama at Birmingham. b Instituto de
 FERTILITY AND STERILITY VOL. 74, NO. 2, AUGUST 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Adrenocortical hyperresponsivity
FERTILITY AND STERILITY VOL. 74, NO. 2, AUGUST 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Adrenocortical hyperresponsivity
A p.p30l MUTATION AT THE CYP21A2 GENE IN MACEDONIAN PATIENTS WITH NONCLASSICAL CONGENITAL ADRENAL HYPERPLASIA
 13 (1), 2010 ORIGINAL ARTICLE A p.p30l MUTATION AT THE CYP21A2 GENE IN MACEDONIAN PATIENTS WITH NONCLASSICAL CONGENITAL ADRENAL HYPERPLASIA Anastasovska V 1, Kocova E 1, Kocova M 1,2, * *Corresponding
13 (1), 2010 ORIGINAL ARTICLE A p.p30l MUTATION AT THE CYP21A2 GENE IN MACEDONIAN PATIENTS WITH NONCLASSICAL CONGENITAL ADRENAL HYPERPLASIA Anastasovska V 1, Kocova E 1, Kocova M 1,2, * *Corresponding
Ambiguous genitalia (Disorders of sex development); is any case in which the external genitalia do not appear completely male or completely female.
 Ambiguous genitalia (Disorders of sex development); is any case in which the external genitalia do not appear completely male or completely female. Disorders of sex development (DSD); True hermaphrodite;
Ambiguous genitalia (Disorders of sex development); is any case in which the external genitalia do not appear completely male or completely female. Disorders of sex development (DSD); True hermaphrodite;
Hyperandrogenism. Dr Jack Biko. MB. BCh (Wits), MMED O & G (Pret), FCOG (SA), Dip Advanced Endoscopic Surgery(Kiel, Germany)
 Hyperandrogenism Dr Jack Biko MB. BCh (Wits), MMED O & G (Pret), FCOG (SA), Dip Advanced Endoscopic Surgery(Kiel, Germany) 2012 Hyperandrogenism Excessive production of androgens Adrenal glands main source
Hyperandrogenism Dr Jack Biko MB. BCh (Wits), MMED O & G (Pret), FCOG (SA), Dip Advanced Endoscopic Surgery(Kiel, Germany) 2012 Hyperandrogenism Excessive production of androgens Adrenal glands main source
ASY-857.1: Synacthen Stimulated 17OH-progesterone Test
 ASY-857.1: Synacthen Stimulated 17OH-progesterone ASY-857.2: Associated Documents a Synacthen Standing Order form (ref 0827/2) G:\Division\NDO\common\ETCProtocols\0827 Standing Order Synacthen 2016.pdf
ASY-857.1: Synacthen Stimulated 17OH-progesterone ASY-857.2: Associated Documents a Synacthen Standing Order form (ref 0827/2) G:\Division\NDO\common\ETCProtocols\0827 Standing Order Synacthen 2016.pdf
Investigation of adrenal functions in patients with idiopathic hyperandrogenemia
 European Journal of Endocrinology (26) 155 37 311 ISSN 84-4643 CLINICAL STUDY Investigation of adrenal functions in patients with idiopathic hyperandrogenemia Hulusi Atmaca, Fatih Tanriverdi 1, Kursad
European Journal of Endocrinology (26) 155 37 311 ISSN 84-4643 CLINICAL STUDY Investigation of adrenal functions in patients with idiopathic hyperandrogenemia Hulusi Atmaca, Fatih Tanriverdi 1, Kursad
Virilisation in siblings secondary to transdermal bioidentical testosterone exposure
 doi:10.1111/jpc.13466 INSTRUCTIVE CASE Virilisation in siblings secondary to transdermal bioidentical testosterone exposure Tony Huynh 1,2 and Catherine I Stewart 3 1 Department of Endocrinology and Diabetes,
doi:10.1111/jpc.13466 INSTRUCTIVE CASE Virilisation in siblings secondary to transdermal bioidentical testosterone exposure Tony Huynh 1,2 and Catherine I Stewart 3 1 Department of Endocrinology and Diabetes,
Adrenarche is the puberty of the adrenal gland. It is
 0163-769X/00/$03.00/0 Endocrine Reviews 21(6): 671 696 Copyright 2000 by The Endocrine Society Printed in U.S.A. Premature Adrenarche Normal Variant or Forerunner of Adult Disease?* LOURDES IBÁÑEZ, JOAN
0163-769X/00/$03.00/0 Endocrine Reviews 21(6): 671 696 Copyright 2000 by The Endocrine Society Printed in U.S.A. Premature Adrenarche Normal Variant or Forerunner of Adult Disease?* LOURDES IBÁÑEZ, JOAN
PCR BASED DIAGNOSIS OF 21-HYDROXYLASE GENE DEFECTS IN SLOVAK PATIENTS WITH CONGENITAL ADRENAL HYPERPLASIA
 ENDOCRINE REGULATIONS, Vol. 34, 65 72, 2000 65 PCR BASED DIAGNOSIS OF 21-HYDROXYLASE GENE DEFECTS IN SLOVAK PATIENTS WITH CONGENITAL ADRENAL HYPERPLASIA L. PINTEROVA, 1 M. GARAMI, 2 Z. PRIBILINCOVA, 3
ENDOCRINE REGULATIONS, Vol. 34, 65 72, 2000 65 PCR BASED DIAGNOSIS OF 21-HYDROXYLASE GENE DEFECTS IN SLOVAK PATIENTS WITH CONGENITAL ADRENAL HYPERPLASIA L. PINTEROVA, 1 M. GARAMI, 2 Z. PRIBILINCOVA, 3
Reproductive DHEA Analyte Information
 Reproductive DHEA Analyte Information - 1 - DHEA Introduction DHEA (dehydroepiandrosterone), together with other important steroid hormones such as testosterone, DHT (dihydrotestosterone) and androstenedione,
Reproductive DHEA Analyte Information - 1 - DHEA Introduction DHEA (dehydroepiandrosterone), together with other important steroid hormones such as testosterone, DHT (dihydrotestosterone) and androstenedione,
Adrenal Insufficiency During Pregnancy
 Disclosures Adrenal Insufficiency During Pregnancy Research funding from Diurnal Limited via NIH CRADA mechanism Deborah P. Merke, M.D., M.S. Bethesda, MD Outline Primary Adrenal Insufficiency Physiological
Disclosures Adrenal Insufficiency During Pregnancy Research funding from Diurnal Limited via NIH CRADA mechanism Deborah P. Merke, M.D., M.S. Bethesda, MD Outline Primary Adrenal Insufficiency Physiological
Information leaflet for patients and families. Congenital Adrenal Hyperplasia (CAH)
 Information leaflet for patients and families Congenital Adrenal Hyperplasia (CAH) What is CAH? CAH is a disorder causing impaired hormone production from the adrenal glands. Hormones are chemical messengers
Information leaflet for patients and families Congenital Adrenal Hyperplasia (CAH) What is CAH? CAH is a disorder causing impaired hormone production from the adrenal glands. Hormones are chemical messengers
Etiologies of Precocious Puberty: 15-Year Experience in a Tertiary Hospital in Southern Thailand
 Freund Publishing House Ltd., London Journal of Pediatric Endocrinology & Metabolism, 23, 1263-1271 (2010) Etiologies of Precocious Puberty: 15-Year Experience in a Tertiary Hospital in Southern Thailand
Freund Publishing House Ltd., London Journal of Pediatric Endocrinology & Metabolism, 23, 1263-1271 (2010) Etiologies of Precocious Puberty: 15-Year Experience in a Tertiary Hospital in Southern Thailand
Reproductive FSH. Analyte Information
 Reproductive FSH Analyte Information 1 Follicle-stimulating hormone Introduction Follicle-stimulating hormone (FSH, also known as follitropin) is a glycoprotein hormone secreted by the anterior pituitary
Reproductive FSH Analyte Information 1 Follicle-stimulating hormone Introduction Follicle-stimulating hormone (FSH, also known as follitropin) is a glycoprotein hormone secreted by the anterior pituitary
Puberty and Pubertal Disorders Part 3: Delayed Puberty
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Puberty and Pubertal Disorders Part 3: Delayed Puberty These podcasts are designed to give medical students an overview
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Puberty and Pubertal Disorders Part 3: Delayed Puberty These podcasts are designed to give medical students an overview
Congenital adrenal hyperplasia
 [Dermato-Endocrinology 1:2, 87-91; March/April 2009]; 2009 Landes Bioscience Special Focus Review Congenital adrenal hyperplasia Clio Dessinioti* and A.D. Katsambas Department of Dermatology; Andreas Sygros
[Dermato-Endocrinology 1:2, 87-91; March/April 2009]; 2009 Landes Bioscience Special Focus Review Congenital adrenal hyperplasia Clio Dessinioti* and A.D. Katsambas Department of Dermatology; Andreas Sygros
Dexamethasone Treatment of Virilizing Congenital Adrenal Hyperplasia: The Ability to Achieve Normal Growth
 Dexamethasone Treatment of Virilizing Congenital Adrenal Hyperplasia: The Ability to Achieve Normal Growth Scott A. Rivkees, MD*, and John D. Crawford ABSTRACT. Objective. To assess whether treatment of
Dexamethasone Treatment of Virilizing Congenital Adrenal Hyperplasia: The Ability to Achieve Normal Growth Scott A. Rivkees, MD*, and John D. Crawford ABSTRACT. Objective. To assess whether treatment of
The Frequency of Eight Common Point Mutations in CYP21 Gene in Iranian Patients with Congenital Adrenal Hyperplasia
 Iranian Biomedical Journal 12 (1): 49-53 (January 2008) Short Report The Frequency of Eight Common Point Mutations in CYP21 Gene in Iranian Patients with Congenital Adrenal Hyperplasia Ali Ramazani *1,
Iranian Biomedical Journal 12 (1): 49-53 (January 2008) Short Report The Frequency of Eight Common Point Mutations in CYP21 Gene in Iranian Patients with Congenital Adrenal Hyperplasia Ali Ramazani *1,
Leuteinizing hormone responses to leuprolide acetate discriminate between hypogonadotropic hypogonadism and constitutional delay of puberty
 FERTILITY AND STERILITY VOL. 77, NO. 3, MARCH 2002 Copyright 2002 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Leuteinizing hormone
FERTILITY AND STERILITY VOL. 77, NO. 3, MARCH 2002 Copyright 2002 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Leuteinizing hormone
European Journal of Endocrinology (2003) ISSN
 European Journal of Endocrinology (2003) 149 425 432 ISSN 0804-4643 CLINICAL STUDY Pubertal course of persistently short children born small for gestational age (SGA) compared with idiopathic short children
European Journal of Endocrinology (2003) 149 425 432 ISSN 0804-4643 CLINICAL STUDY Pubertal course of persistently short children born small for gestational age (SGA) compared with idiopathic short children
Case. 24 year old female presented to your office complaining of excess hair growth on her face and abdomen. Questions?
 Hirsutism Case 24 year old female presented to your office complaining of excess hair growth on her face and abdomen Questions? Started around puberty with gradual progression Irregular menstrual cycle
Hirsutism Case 24 year old female presented to your office complaining of excess hair growth on her face and abdomen Questions? Started around puberty with gradual progression Irregular menstrual cycle
Provide preventive counseling to parents and patients with specific endocrine conditions about:
 Endocrinology Description: The resident will become familiar with the diagnosis, management, and treatment of endocrine problems. The resident will evaluate patients with a multitude of endocrine problems,
Endocrinology Description: The resident will become familiar with the diagnosis, management, and treatment of endocrine problems. The resident will evaluate patients with a multitude of endocrine problems,
Functional and Structural Studies on CYP21 MUTANTS. in Congenital Adrenal Hyperplasia
 Functional and Structural Studies on CYP21 MUTANTS in Congenital Adrenal Hyperplasia Tiina Robins, M.Sc. Department of Molecular Medicine and Surgery Clinical Genetics Unit, Genetics of Endocrine Disease
Functional and Structural Studies on CYP21 MUTANTS in Congenital Adrenal Hyperplasia Tiina Robins, M.Sc. Department of Molecular Medicine and Surgery Clinical Genetics Unit, Genetics of Endocrine Disease
Prevalence of and markers for the attenuated form of congenital adrenal hyperplasia and hyperprolactinemia masquerading as polycystic ovarian disease*
 FERTILITY AND STERILITY Copyright" 1986 The American Fertility Society Vol. 46, No.2, August 1986 Printed in U.8A. Prevalence of and markers for the attenuated form of congenital adrenal hyperplasia and
FERTILITY AND STERILITY Copyright" 1986 The American Fertility Society Vol. 46, No.2, August 1986 Printed in U.8A. Prevalence of and markers for the attenuated form of congenital adrenal hyperplasia and
Children s Hospital & Research Center Oakland. Endocrinology
 Children s Hospital & Research Center Oakland Endocrinology 5.22 GOAL: Prevention, Counseling and Screening (Endocrine). Understand the role of the pediatrician in preventing endocrine PC, MK, dysfunction,
Children s Hospital & Research Center Oakland Endocrinology 5.22 GOAL: Prevention, Counseling and Screening (Endocrine). Understand the role of the pediatrician in preventing endocrine PC, MK, dysfunction,
Brief Communication Diagnostic Genetics
 Brief Communication Diagnostic Genetics Ann Lab Med 2015;35:535-539 http://dx.doi.org/10.3343/alm.2015.35.5.535 ISSN 2234-3806 eissn 2234-3814 CYP21A2 Mutation Analysis in Korean Patients With Congenital
Brief Communication Diagnostic Genetics Ann Lab Med 2015;35:535-539 http://dx.doi.org/10.3343/alm.2015.35.5.535 ISSN 2234-3806 eissn 2234-3814 CYP21A2 Mutation Analysis in Korean Patients With Congenital
Prof.Dr. Nabil Lymon Head of Internal Medicine Department
 By Prof.Dr. Nabil Lymon Head of Internal Medicine Department Definitions: Hirsutism: Is the presence of terminal hair in androgendependent sites where hair does not normally grow in women. This hair growth
By Prof.Dr. Nabil Lymon Head of Internal Medicine Department Definitions: Hirsutism: Is the presence of terminal hair in androgendependent sites where hair does not normally grow in women. This hair growth
Diagnosing Growth Disorders. PE Clayton School of Medical Sciences, Faculty of Biology, Medicine & Health
 Diagnosing Growth Disorders PE Clayton School of Medical Sciences, Faculty of Biology, Medicine & Health Content Normal pattern of growth and its variation Using growth charts Interpreting auxological
Diagnosing Growth Disorders PE Clayton School of Medical Sciences, Faculty of Biology, Medicine & Health Content Normal pattern of growth and its variation Using growth charts Interpreting auxological
Great Ormond Street Hospital for Children NHS Foundation Trust
 Great Ormond Street Hospital for Children DEPARTMENT OF ENDOCRINOLOGY Great Ormond Street Tel: 2 745 9 Questions answered by Professor Peter Hindmarsh It is true that many centres work differently regarding
Great Ormond Street Hospital for Children DEPARTMENT OF ENDOCRINOLOGY Great Ormond Street Tel: 2 745 9 Questions answered by Professor Peter Hindmarsh It is true that many centres work differently regarding
Dianne Keen-Kim,* Joy B. Redman, Reno U. Alanes, Michele M. Eachus,* Robert C. Wilson, Maria I. New, Jon M. Nakamoto,* and Raymond G.
 Journal of Molecular Diagnostics, Vol. 7, No. 2, May 2005 Copyright American Society for Investigative Pathology and the Association for Molecular Pathology Validation and Clinical Application of a Locus-
Journal of Molecular Diagnostics, Vol. 7, No. 2, May 2005 Copyright American Society for Investigative Pathology and the Association for Molecular Pathology Validation and Clinical Application of a Locus-
Prescribing Guidelines Prescribing arrangement for the management of patients transferring from Secondary Care to Primary Care
 Berkshire West Integrated Care System Representing Berkshire West Clinical Commisioning Group Royal Berkshire NHS Foundation Trust Berkshire Healthcare NHS Foundation Trust Berkshire West Primary Care
Berkshire West Integrated Care System Representing Berkshire West Clinical Commisioning Group Royal Berkshire NHS Foundation Trust Berkshire Healthcare NHS Foundation Trust Berkshire West Primary Care
21-Hydroxylase deficiency in Brazil
 Brazilian Journal of Medical and Biological Research (2000) 33: 1211-1216 21OH deficiency in Brazil ISSN 0100-879X 1211 21-Hydroxylase deficiency in Brazil T.A.S.S. Bachega 1, A.E.C. Billerbeck 1, G. Madureira
Brazilian Journal of Medical and Biological Research (2000) 33: 1211-1216 21OH deficiency in Brazil ISSN 0100-879X 1211 21-Hydroxylase deficiency in Brazil T.A.S.S. Bachega 1, A.E.C. Billerbeck 1, G. Madureira
Correlation of Serum Follicular Stimulating Hormone
 Correlation of Serum Follicular Stimulating Hormone (FSH) and Luteinizing Hornone (LH) as Measured by Radioimmunoassay in Disorders of Sexual Development ROBERT PENNY, HARVEY J. GUYDA, ALIcE BAGHDASSARIAN,
Correlation of Serum Follicular Stimulating Hormone (FSH) and Luteinizing Hornone (LH) as Measured by Radioimmunoassay in Disorders of Sexual Development ROBERT PENNY, HARVEY J. GUYDA, ALIcE BAGHDASSARIAN,
Why is my body not changing? Conflicts of interest. Overview 11/9/2015. None
 Why is my body not changing? Murthy Korada Pediatrician, Pediatric Endocrinologist Ridge Meadows Hospital Surrey Memorial Hospital None Conflicts of interest Overview Overview of normal pubertal timing
Why is my body not changing? Murthy Korada Pediatrician, Pediatric Endocrinologist Ridge Meadows Hospital Surrey Memorial Hospital None Conflicts of interest Overview Overview of normal pubertal timing
Case Report Nonclassical Congenital Adrenal Hyperplasia and Pregnancy
 Case Reports in Endocrinology Volume 2015, Article ID 296924, 4 pages http://dx.doi.org/10.1155/2015/296924 Case Report Nonclassical Congenital Adrenal Hyperplasia and Pregnancy Neslihan Cuhaci, 1 Cevdet
Case Reports in Endocrinology Volume 2015, Article ID 296924, 4 pages http://dx.doi.org/10.1155/2015/296924 Case Report Nonclassical Congenital Adrenal Hyperplasia and Pregnancy Neslihan Cuhaci, 1 Cevdet
Linkage and association between HLA and
 Journal of Medical Genetics, 1980, 17, 337-341 Linkage and association between HLA and 21 -hydroxylase deficiency PETER T KLOUDA, RODNEY HARRIS, AND DAVID A PRICE From the Department of Medical Genetics,
Journal of Medical Genetics, 1980, 17, 337-341 Linkage and association between HLA and 21 -hydroxylase deficiency PETER T KLOUDA, RODNEY HARRIS, AND DAVID A PRICE From the Department of Medical Genetics,
Pedigree Analysis Why do Pedigrees? Goals of Pedigree Analysis Basic Symbols More Symbols Y-Linked Inheritance
 Pedigree Analysis Why do Pedigrees? Punnett squares and chi-square tests work well for organisms that have large numbers of offspring and controlled mating, but humans are quite different: Small families.
Pedigree Analysis Why do Pedigrees? Punnett squares and chi-square tests work well for organisms that have large numbers of offspring and controlled mating, but humans are quite different: Small families.
POLYCYSTIC OVARIAN SYNDROME WHERE WE ARE AT IN 2018
 POLYCYSTIC OVARIAN SYNDROME WHERE WE ARE AT IN 2018 PCOS: WHERE WE ARE AT IN 2018 Nancy Arquette, MD Premier Women s Health 6135 Trust Drive #114 Holland, OH 43528 February 3, 2018 Kalahari Resorts ME
POLYCYSTIC OVARIAN SYNDROME WHERE WE ARE AT IN 2018 PCOS: WHERE WE ARE AT IN 2018 Nancy Arquette, MD Premier Women s Health 6135 Trust Drive #114 Holland, OH 43528 February 3, 2018 Kalahari Resorts ME
Department of Pediatrics, Kawasaki Medical School, Kurashiki , Japan 3)
 Endocrine Journal 2014, 61 (6), 629-633 note Uniparental disomy of chromosome 8 leading to homozygosity of a CYP11B1 mutation in a patient with congenital adrenal hyperplasia: Implication for a rare etiology
Endocrine Journal 2014, 61 (6), 629-633 note Uniparental disomy of chromosome 8 leading to homozygosity of a CYP11B1 mutation in a patient with congenital adrenal hyperplasia: Implication for a rare etiology
2-Hypertrichosis:- Hypertrichosis is the
 Hirsutism And Virilization Hirsutism:- Is the development of androgen-dependent dependent terminal body hair in a woman in places in which terminal hair is normally not found, terminal body hairs are the
Hirsutism And Virilization Hirsutism:- Is the development of androgen-dependent dependent terminal body hair in a woman in places in which terminal hair is normally not found, terminal body hairs are the
The prognostic value of acute adrenal suppression and stimulation tests in hyperandrogenic women
 FERTUJTY AND STERILITY Copyright c 1982 The American Fertility Society Vol. 37, No.2, February 198~ Printed in U.SA. The prognostic value of acute adrenal suppression and stimulation tests in hyperandrogenic
FERTUJTY AND STERILITY Copyright c 1982 The American Fertility Society Vol. 37, No.2, February 198~ Printed in U.SA. The prognostic value of acute adrenal suppression and stimulation tests in hyperandrogenic
A. Incorrect! Cells contain the units of genetic they are not the unit of heredity.
 MCAT Biology Problem Drill PS07: Mendelian Genetics Question No. 1 of 10 Question 1. The smallest unit of heredity is. Question #01 (A) Cell (B) Gene (C) Chromosome (D) Allele Cells contain the units of
MCAT Biology Problem Drill PS07: Mendelian Genetics Question No. 1 of 10 Question 1. The smallest unit of heredity is. Question #01 (A) Cell (B) Gene (C) Chromosome (D) Allele Cells contain the units of
European Journal of Endocrinology (1999) ISSN
 European Journal of Endocrinology (1999) 141 132 139 ISSN 0804-4643 CLINICAL STUDY Adrenal 21-hydroxylase gene mutations in Slovenian hyperandrogenic women: evaluation of corticotrophin stimulation and
European Journal of Endocrinology (1999) 141 132 139 ISSN 0804-4643 CLINICAL STUDY Adrenal 21-hydroxylase gene mutations in Slovenian hyperandrogenic women: evaluation of corticotrophin stimulation and
GENDER James Bier
 GENDER 2005-2008 James Bier Objectives 1. State the method of determining gender in several genetic systems. 2. List the three regions of the Y chromosome. 3. Describe the events that promote sexual development
GENDER 2005-2008 James Bier Objectives 1. State the method of determining gender in several genetic systems. 2. List the three regions of the Y chromosome. 3. Describe the events that promote sexual development
Steroid 21-hydroxylase Deficiency in a Newborn Female with Ambiguous Genitalia in Upper Egypt AE Ahmed 1, MH Hassan 2 ABSTRACT
 Steroid 21-hydroxylase Deficiency in a Newborn Female with Ambiguous Genitalia in Upper Egypt AE Ahmed 1, MH Hassan 2 ABSTRACT Congenital adrenal hyperplasia "CAH" is a group of autosomal recessive disorders
Steroid 21-hydroxylase Deficiency in a Newborn Female with Ambiguous Genitalia in Upper Egypt AE Ahmed 1, MH Hassan 2 ABSTRACT Congenital adrenal hyperplasia "CAH" is a group of autosomal recessive disorders
Role of surgical resection in the treatment of hypothalamic hamartomas causing precocious puberty Report of six cases
 Role of surgical resection in the treatment of hypothalamic hamartomas causing precocious puberty Report of six cases Laura Stewart, M.D., F.R.C.P.(C), Paul Steinbok, M.B.B.S., F.R.C.S.(C), and Jorge Daaboul,
Role of surgical resection in the treatment of hypothalamic hamartomas causing precocious puberty Report of six cases Laura Stewart, M.D., F.R.C.P.(C), Paul Steinbok, M.B.B.S., F.R.C.S.(C), and Jorge Daaboul,
Polycystic Ovary Syndrome HEATHER BURKS, MD OU PHYSICIANS REPRODUCTIVE MEDICINE SEPTEMBER 21, 2018
 Polycystic Ovary Syndrome HEATHER BURKS, MD OU PHYSICIANS REPRODUCTIVE MEDICINE SEPTEMBER 21, 2018 Learning Objectives At the conclusion of this lecture, learners should: 1) Know the various diagnostic
Polycystic Ovary Syndrome HEATHER BURKS, MD OU PHYSICIANS REPRODUCTIVE MEDICINE SEPTEMBER 21, 2018 Learning Objectives At the conclusion of this lecture, learners should: 1) Know the various diagnostic
Received April 3, 2007; Accepted September 10, 2007; Released online January 10, 2008
 ORIGINAL The Prevalence of Non-classical Congenital Adrenal Hyperplasia Due to 21-Hydroxylase Deficiency in Greek Women with Hirsutism and Polycystic Ovary Syndrome EFTIHIOS TRAKAKIS 1,2 MD, DEMETRIOS
ORIGINAL The Prevalence of Non-classical Congenital Adrenal Hyperplasia Due to 21-Hydroxylase Deficiency in Greek Women with Hirsutism and Polycystic Ovary Syndrome EFTIHIOS TRAKAKIS 1,2 MD, DEMETRIOS
Summary
 Summary 118 This thesis is focused on the background of elevated levels of FSH in the early follicular phase of women with regular menstrual cycles. In the introduction (chapter 1) we describe the characteristics
Summary 118 This thesis is focused on the background of elevated levels of FSH in the early follicular phase of women with regular menstrual cycles. In the introduction (chapter 1) we describe the characteristics
Usefulness of Ultrasonography in Diagnosing Congenital Adrenal Hyperplasia in Neonates
 Clin Pediatr Endocrinol 1993;2(2):99-105 Copyright (C)1993 by The Japanese Society for Pediatric Endocrinology Usefulness of Ultrasonography in Diagnosing Congenital Adrenal Hyperplasia in Neonates Kunio
Clin Pediatr Endocrinol 1993;2(2):99-105 Copyright (C)1993 by The Japanese Society for Pediatric Endocrinology Usefulness of Ultrasonography in Diagnosing Congenital Adrenal Hyperplasia in Neonates Kunio
Monitoring treatment in congenital adrenal
 Archives of Disease in Childhood, 1989, 64, 1235-1239 Monitoring treatment in congenital adrenal hyperplasia S APPAN, P C HINDMARSH, AND C G D BROOK Endocrine Unit, Middlesex Hospital, London SUMMARY We
Archives of Disease in Childhood, 1989, 64, 1235-1239 Monitoring treatment in congenital adrenal hyperplasia S APPAN, P C HINDMARSH, AND C G D BROOK Endocrine Unit, Middlesex Hospital, London SUMMARY We
