Angiotensin-Converting Enzyme Inhibitor Induced Small-Bowel Angioedema: Clinical and Imaging Findings in 20 Patients
|
|
|
- Jayson Tate
- 6 years ago
- Views:
Transcription
1 Gastrointestinal Imaging Original Research Scheirey et al. ngiotensin-converting Enzyme Inhibitor and Small-Bowel ngioedema Gastrointestinal Imaging Original Research Christopher D. Scheirey 1 Francis J. Scholz 1 Michael J. Shortsleeve 2 Douglas S. Katz 3 Scheirey CD, Scholz FJ, Shortsleeve MJ, Katz DS Keywords: angioedema, angiotensin-converting enzyme inhibitor, intestinal, small bowel DOI: /JR Received February 15, 2010; accepted after revision December 16, Department of Radiology, Lahey Clinic, 41 Mall Rd, Burlington, M ddress correspondence to C. D. Scheirey (Christopher_Scheirey@lahey.org). 2 Department of Radiology, Mount uburn Hospital, Cambridge, M. 3 Department of Radiology, Winthrop-University Hospital, Mineola, NY. JR 2011; 197: X/11/ merican Roentgen Ray Society ngiotensin-converting Enzyme Inhibitor Induced Small-Bowel ngioedema: Clinical and Imaging Findings in 20 Patients OBJECTIVE. The purpose of this article is to retrospectively review the radiologic and clinical findings in patients with angiotensin-converting enzyme inhibitor (CEI) induced small-bowel angioedema, with an emphasis on CT findings. MTERILS ND METHODS. Imaging findings, with an emphasis on CT, and clinical characteristics of 20 patients (23 presentations) presenting to two institutions emergency departments from 1996 through 2010 with CEI-induced small-bowel angioedema were retrospectively reviewed by two abdominal radiologists who were aware of the diagnosis. Examinations were reviewed in consensus to determine common radiographic findings. RESULTS. Patient age range was years (mean, 56 years). Sixteen of the 20 patients were women, and 15 of 20 were obese. ll had acute onset of severe abdominal pain. The date of the initial episode prompting CT evaluation ranged from 2 days to 10 years after the start of CEI therapy (average, 3.3 years). ll patients underwent abdominal CT examinations while symptomatic; five patients also underwent a small-bowel series. Three patients underwent urgent surgery for presumed small-bowel ischemia. ll patients had resolution of symptoms within 4 days of hospitalization. CT findings included ascites in all patients, small-bowel wall thickening (mean, 1.3 cm), mild dilatation (mean, 2.9 cm), and straightening. There was no small-bowel obstruction. CONCLUSION. CEI-induced small-bowel angioedema should be included in the differential diagnosis when patients receiving CEI therapy present with abdominal complaints and the following combination of findings on CT examination: ascites, small-bowel wall thickening, dilatation without obstruction, and straightening. ngiotensin-converting enzyme inhibitors (CEIs) are a widely used pharmacotherapy to control hypertension. ngioedema is the vascular leakage of serum from small vessels and is the process that induces cutaneous hives. ngioedema induced by CEI therapy is a well-known entity. Many clinicians and radiologists are aware that drug-induced angioedema affects the tongue, throat, face, and other cutaneous sites. Reports of death from laryngeal edema exist [1]. However, many clinicians and, we think, radiologists fail to recognize the causal relationship between CEI therapy and angioedema, especially in the small bowel [2]. Despite articles in the medical and gastrointestinal literature, CEI-induced small-bowel angioedema is rarely reported in the imaging literature; to our knowledge, there are only two individual case reports in the radiographic literature [3, 4]. The CT description of these cas- es overlaps with those of other causes of smallbowel angioedema, including hereditary and idiopathic small-bowel angioedema. Findings described previously of small-bowel angioedema, either related to CEI or not, include segmental bowel-wall thickening with submucosal edema and ascites [3 6]. bdominal presentations include complaints of abdominal pain, diarrhea, nausea, and vomiting [7]. Symptoms are generally self-limited and will resolve with or without cessation of the CEI therapy [8]. If the diagnosis of CEI-induced small-bowel angioedema is not established, recurrences may occur [8, 9]; episodic abdominal pain may result in unnecessary emergency department visits, hospital admissions, radiologic examinations, or even surgical exploration. To increase radiologists awareness of this underrecognized condition and assist in its radiologic detection, we report the clinical and imaging findings of 20 patients (with 23 presentations) with a diagnosis of CEI-induced JR:197, ugust
2 Scheirey et al. small-bowel angioedema, with an emphasis on the CT findings. Materials and Methods retrospective analysis of patients with at least one abdominal and pelvic CT examination and with a diagnosis of CEI-induced small-bowel angioedema was performed. Patient records were from radiology teaching file cases accumulated at two institutions between 1996 and The diagnosis had been made by CT or by clinical or surgical exclusion of other disease processes, in combination with rapid resolution of symptoms. Institutional review board approval was obtained, with waiver of informed consent for retrospective analysis. ll examinations were reviewed by two abdominal radiologists, with an average of 17 years of experience, who were aware of the diagnosis. Three examinations were reviewed on printed film; the rest were reviewed on a PCS workstation. CT scans were reviewed by consensus to determine vascular patency and to subjectively rate the degree of mesenteric edema (i.e., absent, mild, moderate, or severe). The abdominal and pelvic CT images were also reviewed for the presence or absence of ascites. The small bowel was evaluated to determine the location (i.e., duodenal, jejunal, or ileal) of the involved segment, the length of abnormal bowel, and the length of contrast luminal transit. In addition, the luminal caliber and the wall thickness were measured at the most dilated and most thickened segments of small bowel, respectively. The presence or absence of straightening, which we defined as a loop of small bowel that lengthened to occupy greater than either half of the transverse diameter or half of the anteroposterior diameter of the peritoneal cavity, was also evaluated. ll abnormal segments of bowel were also assessed for the presence or absence of the target sign. The smallbowel series, which were performed in five patients, were reviewed for the presence or absence of wall thickening, length of bowel involvement, and the presence or absence of obstruction. One of the two radiologists who examined the radiographic studies also reviewed the patients medical records. Clinical histories and chart notes were reviewed to determine age at initial CT examination, comorbidities, prior angioedema presentations, and initiation and duration of CEI therapy before the development of abdominal symptoms. In addition, chart notes were reviewed to exclude patients with a known diagnosis of Crohn disease, previous radiation therapy, or ongoing infectious gastroenteritis. Emergency department notes were reviewed to determine patient complaints and physical examination findings, as well as concurrent laboratory abnormalities. Hospital notes were reviewed to determine duration of symptoms and hospital course. Results Patients Twenty patients with 23 distinct episodes were identified. Patients ranged in age from 23 to 83 years (mean, 56 years). Thirteen of 20 patients were obese women, two were obese men, and there were five nonobese patients (two men and three women). ll patients had hypertension, 10 had hyperlipidemia, and eight had diabetes. CEI Therapy ll patients were receiving CEI therapy for the treatment of hypertension. Nineteen patients were receiving oral lisinopril therapy at the time of initial presentation (dose range, 5 mg/day to 40 mg twice/day), and one patient was receiving oral enalapril (5 mg/day). Induction of CEI therapy could be documented for a specific time for 14 of 20 patients (for five patients, the start date of therapy was not listed in the chart notes, and for the other patient, chart notes indicated years of lisinopril therapy). In these 14 patients, the date of initial episode prompting CT evaluation ranged from 2 days to 10 years after the start of therapy, with an average of 3.3 years. Three patients presented to the emergency department twice. In one patient who presented twice, we could not document the start date of CEI therapy, but the patient s symptoms resolved while therapy was withheld in the hospital during initial admission, and she presented again 1 week after reinitiation of therapy as an outpatient. The second patient who presented twice had been receiving lisinopril for 1 month, but presented 24 hours after an increase in dose from 5 to 10 mg. The association with the CEI was not recognized, and this patient continued taking her medication until she represented 5 months later; this occurred 24 hours after an additional increase in lisinopril from 10 to 20 mg. In the third patient with two presentations to the emergency department, the initiation of therapy was not indicated. This patient had two different admissions to an outside institution for abdominal pain within 3 months. In seven patients, therapy duration was longer than 1 year, whereas in seven others, therapy duration was less than 1 year. Signs and Symptoms bdominal pain was present in all patients; 17 complained of nausea, 12 of vomiting, and eight of diarrhea. No patient had gastrointestinal bleeding. Of the 23 total episodes, 21 began with abrupt onset of symptoms (duration, 6 72 hours; mean, 29 hours) prompting presentation to the emergency department. One patient had symptoms for 1 week, and another had symptoms for 4 days. Seven of 20 patients reported previous similar abdominal episodes. One had an episode of facial edema 6 months before admission. Physical findings included abdominal tenderness and normoactive bowel sounds in all patients. Fifteen of the patients at presentation had normal vital signs, four had mild systolic hypotension ( mm Hg), and four had mild systolic hypertension ( mm Hg). ll patients were afebrile. t presentation fourteen of the patients had elevated WBC counts (> 10,800 cells/ml), with an overall range of ,000 cells/ml (mean, 12,795 cells/ml). No other common laboratory abnormalities were found. ll patients were admitted to the hospital, and with the exception of the four patients who underwent surgery, all the others were treated conservatively with pain management and IV hydration. Thirteen patients were also given antibiotics because of uncertainty regarding the initial diagnosis. Radiology ll patients underwent IV contrast enhanced CT scans at presentation. Three CT scans were performed on single-slice scanners, and the remaining 20 were performed on MDCT scanners (8 64 detector rows). Nineteen of the 23 CT examinations were performed with standard positive oral contrast agent (for three of the examinations, the patients were unable to tolerate oral contrast agent), and one patient was given water as an oral contrast agent. One patient was given rectal contrast agent in addition to positive oral contrast agent. scitic fluid was present in all patients, with a spectrum in the amount of ascitic fluid encountered (Fig. 1). Twenty CT examinations revealed mild mesenteric edema (Fig. 2), whereas three showed no evidence of mesenteric edema. The visceral vasculature was patent on all examinations. ll CT examinations showed abnormal small bowel with long-segment abnormalities; the involved segment was estimated to be longer than 10 cm, but less than one third the entire length of the small bowel on 21 of the 23 CT examinations. In two patients, more than half of the entire small bowel was involved. Three patients had skip lesions. ll patients had mildly dilated small bowel, with a mean diameter of 2.9 cm (normal, < 2.5 cm) [10] and wall thickening with a mean of 1.3 cm (normal, < 4 mm) [11]. Sixteen of the 20 MDCT scans showed a small-bowel tar- 394 JR:197, ugust 2011
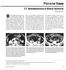
3 ngiotensin-converting Enzyme Inhibitor and Small-Bowel ngioedema Fig. 1 Spectrum of ascites encountered in patient series., Image is of 57-year-old man receiving 10 mg lisinopril who presented with abdominal pain, nausea, and vomiting. Oral and IV contrast-enhanced pelvic CT scan shows least amount of ascites encountered in patient series, with trace ascites (asterisk) adjacent to small bowel in right lower quadrant. Note small-bowel dilatation and relatively mild fold thickening. B, Image is of 43-year-old woman receiving 5 mg lisinopril who presented with abdominal pain, nausea, and vomiting. Oral and IV contrast-enhanced coronal abdominal and pelvic CT reformation shows four-quadrant ascites (asterisks) and long-segment jejunal wall thickening (arrows) with target sign. Fig year-old woman receiving 20 mg lisinopril who presented with abdominal pain and nausea. Oral and IV contrast-enhanced pelvic CT scan shows most pronounced mesenteric edema (arrowhead) encountered in patient series and long-segment jejuno-ileal wall thickening (arrows) with target sign. Subsequent diagnostic laparoscopy 72 hours after admission was normal. get sign with fluid density submucosa (Fig. 3). Distribution of involvement was jejunal only (10/23), ileal only (7/23), and combined jejuno-ileal (6/23). Straightening of the involved segment was present on 10 of the CT examinations (Fig. 4). No other acute visceral organ involvement was present. No patient had evidence of a small-bowel obstruction. In 16 of 19 patients who tolerated oral contrast agent, it extended into the cecum. Follow-up CT scans were performed for two patients. One follow-up CT examination Fig year-old woman receiving 40 mg lisinopril who presented with abdominal pain and vomiting. IV contrast-enhanced pelvic CT scan shows typical target sign (arrow) affecting long segment of ileum, with four-quadrant ascites (asterisk). B was performed within a day for a 46-year-old man and revealed nearly complete resolution of small-bowel abnormalities, although some ascitic fluid remained (Fig. 5). The other follow-up CT examination was performed for a 49-year-old woman, 4 days after initial CT and discontinuation of CEI therapy, and revealed complete resolution of small-bowel thickening and ascites. Five small-bowel follow-through examinations were performed within 72 hours of presentation because of uncertainty regarding the initial diagnosis; two patients had small-bowel series within 24 hours of presentation, one had a small-bowel series 36 hours after presentation, another at 48 hours, and the last at 72 hours after presentation. There was no difference in the appearance of the CT scans in those patients who underwent a barium small-bowel examination, and those patients for whom no small-bowel series was performed. ll five barium examinations revealed long-segment small-bowel involvement with fold thickening and submucosal edema, but without obstruction (Fig. 6). In all patients, clinical symptoms improved within 4 days of hospitalization. In eight of the pain episodes, the diagnosis of CEI-induced small-bowel angioedema was suggested prospectively by the radiologist; in the remaining 15 pain episodes, the association was not made until retrospective review by an abdominal radiologist. Four patients underwent surgical exploration; there was no significant difference in the CT findings of these four patients compared with those who did not undergo surgery. Three patients underwent surgery, in part because the initial interpreting radiologist was Fig year-old woman receiving 5 mg lisinopril who presented with abdominal pain and nausea. Oral and IV contrast-enhanced pelvic CT scan depicts typical long-segment small-bowel edema (arrow) with straightening of small bowel. JR:197, ugust
4 Scheirey et al. unsure of the diagnosis and raised the question of small-bowel ischemia on the basis of the small-bowel wall thickening and ascites; the initial CT interpretation combined with the clinical presentation of severe abdominal pain therefore prompted surgical exploration in these three patients. Two patients, 46- and 83-year-old women, despite CT findings of small-bowel edema and associated ascites, had only mild erythema of the distal ileum at surgery within 24 hours of CT examination. nother 65-year-old woman had a normal laparoscopy approximately 72 after presentation. The fourth patient was taken to surgery despite an initial interpretation suggesting CEI-induced angioedema. This 60-year-old man had atypical increasing pain after admission, which prompted exploration to exclude ischemia, but only mild erythema of the small bowel was seen. None of the patients had a small-bowel biopsy. None of the three patients who presented twice underwent surgery. Fig year-old man receiving 5 mg lisinopril who presented with nausea, diarrhea, and abdominal pain., IV contrast-enhanced abdominal CT scan shows long-segment jejunal thickening (arrows) with target sign and mild mesenteric edema (arrowhead). B, Follow-up oral and IV contrast-enhanced CT scan performed within 24 hours shows nearly complete resolution of small-bowel thickening and mesenteric edema, although trace ascites persists (asterisk). Discussion ngioedema occurs in the skin and mucous membranes [8] and is due to vasodilatation, which leads to serum accumulation in interstitial tissue spaces. lthough the mechanism is not entirely understood, one theory is that CEI-induced angioedema is related to elevated levels of bradykinin, a potent vasodilator and cause of vascular permeability [12]. CEI therapy causes delayed breakdown of bradykinin [13], with intermittent peaks of bradykinin at random time intervals, resulting in angioedema. In 2001, one study estimated that nearly 40 million people worldwide are receiving CEI therapy [14]. CEI-induced angioedema is estimated to occur in approximately % of patients receiving these medications [13], although many researchers think that this entity may be underrecognized [9, 13, 15]. One confounding variable is the time lag between the initiation of therapy and the initial angioedema episode, which may be years [16, 17]. prior retrospective review of all types of angioedema cases documented a median length of 12 months from initiation of CEI therapy before the initial angioedema episode [8]. This is similar to our experience with small-bowel angioedema, with 10 patients presenting at least 8 months after initiation of therapy. Clinical symptoms of intestinal angioedema include abdominal pain, nausea, vomiting, and diarrhea. Pain can be severe and may be mistaken for small-bowel ischemia. Two of our first three patients underwent B surgical exploration to exclude small-bowel ischemia because of severe abdominal pain in the setting of an abnormal CT examination and the lack of a definitive diagnosis. In retrospect, if the association between the CEI therapy and the abnormal CT findings had been recognized, surgery could have been averted. Of interest was the number of obese women in our patient population (65%). Research suggests that estrogen may play a role in some forms of hereditary angioedema [13]. lthough evaluation of all types of CEIinduced angioedema shows no sex predilection [8, 18], for unknown reasons, most reported cases of CEI-induced small-bowel angioedema have occurred in women, possibly underscoring the interaction of estrogens in the pathogenesis of the disease [4]. Initial descriptions of the radiologic appearance of small-bowel angioedema were based on barium studies and included thickened mucosal folds, spiculation, thumbprinting, and separation of adjacent bowel loops [19, 20]. Scattered descriptions of the CT appearance of smallbowel angioedema then appeared in the radiology literature. CT findings included smallbowel wall thickening and ascites [21, 22]. More recently, two case reports of the CT appearance related to CEI-induced angioedema were published; CT findings included ascites and circumferential bowel wall thickening with submucosal edema [3, 4]. lthough these isolated radiology case reports exist, we strongly believe that radiologists should be more attuned Fig year-old woman receiving 5 mg enalapril who presented with nausea, vomiting, and left upper quadrant pain., Oral and IV contrast-enhanced abdominal CT scan depicts marked straightening (arrow) of edematous loop of jejunum, with adjacent ascites (asterisk). B, Small-bowel series performed next morning reveals persistent abnormal segment of jejunum (arrows) with fold thickening, spiculation, and fold separation. Note lack of small-bowel obstruction. Subsequent laparoscopy was negative. B 396 JR:197, ugust 2011
5 ngiotensin-converting Enzyme Inhibitor and Small-Bowel ngioedema to the association of CEI therapy with smallbowel angioedema. In light of the widespread use of CEI therapy, and the increasing number of CT scans being performed throughout the United States and elsewhere, the scarcity of case reports in the radiology literature suggests that CEI-induced small-bowel angioedema may be underappreciated. Radiologists should recognize the main CT findings in our series, which should prompt radiologists to include small-bowel angioedema related to CEI in the differential diagnosis, in the correct clinical setting: ascites and preservation of luminal transit (i.e., no smallbowel obstruction, including contrast transit to the colon) despite thickening, dilatation, and straightening of the small bowel. There is long-segment involvement of small bowel, with a tendency to affect the jejunum. The majority of cases will have continuous segments of small bowel involved. The affected small bowel typically has marked submucosal edema with the associated target sign [3, 23]. The target sign is produced by alternating enhancement of the mucosa, relatively hypodense submucosa (related to edema), and enhancing serosa [24]. This has previously been described as the hallmark of a benign lesion [6], although there is radiologic overlap with other causes of small-bowel thickening, such as small-bowel ischemia, superior mesenteric and portal vein thrombosis, radiation, vasculitides, Crohn disease, hemorrhage, and infection [6, 24]. However, these other causes often involve tissue damage; the presence of pneumatosis, ulceration, or pronounced mesenteric edema should prompt a search for alternate diagnoses. In our retrospective series, the small-bowel wall was thought to be straightened because it was elongated, as seen in obstruction, but without significant distention. lso, the wall was not as thickened as in severe ischemia or intramural hemorrhage. In ischemia, straightening is accompanied by wall thickening because of intramural blood and edema. In small-bowel obstruction, straightening is related to increased intraluminal pressure. The elongation in CEI-induced small-bowel angioedema is therefore believed to be related to a primary increase in tissue turgor (i.e., stiffening) of the small-bowel wall. We liken this phenomenon to long-segment urticaria of the small-bowel that is, interstitial edema producing adjacent thickening and wall tension, effacing the adjacent wrinkles or folds, and lengthening the affected segment of bowel. On contrast-enhanced CT examinations, the presence of vascular patency will exclude central arterial or venous thrombosis. Crohn disease, vasculitides, and radiation injuries will typically have a longer time course and, often (particularly with radiation enteritis), a characteristic history. In the appropriate clinical setting, the combination of radiographic findings is suggestive of CEI-induced small-bowel angioedema. These patients have abrupt onset as well as quick resolution of symptoms, and all have vascular patency and preservation of bowel motility. However, according to our series, the CT appearance can vary from patient to patient and within each patient, on the basis of the timing of their presentation. The clinical onset and resolution of symptoms can be abrupt, and we think that patients who are not imaged when most symptomatic may have a less pronounced radiographic appearance, which may account for the variability in CT appearance. We wondered whether we could have misdiagnosed gastroenteritis or mild mesenteric ischemia as CEI-induced small-bowel angioedema because 13 patients were given precautionary IV antibiotics at admission. In particular, elevated WBC counts noted in some patients could suggest infectious enteritis. However, we think that the lack of fever in patients with severe pain, prominent ascites, and bowel-wall thickening makes an infectious cause less likely. Similar to our findings, others have documented elevated WBC counts in patients with angioedema [25, 26]. We also believe that the degree of abdominal pain, in some cases prompting surgical exploration, is greater than that encountered with infectious enteritis. Mild mesenteric ischemia was thought to be unlikely, particularly because all visceral vessels were patent and no patient had risk factors for or other clinical features of nonocclusive mesenteric ischemia. There are some limitations to our study. The major limitation is the lack of pathologic proof for any of the cases and the lack of a specific laboratory finding to pinpoint the diagnosis. However, this does not preclude the diagnosis of CEI-induced small-bowel angioedema. lthough CEI-induced smallbowel angioedema remains a diagnosis of exclusion, the constellation of clinical, laboratory, and radiographic findings should direct both radiologists and clinicians to the correct diagnosis. nother limitation is that this is a retrospective evaluation of collected cases, but a prospective study would be very difficult to conduct, given the relatively rare occurrence of CEI-induced small-bowel angioedema. lso, we did not compare our findings to other causes of angioedema, including hereditary or other drug-related angioedema cases. Other case reports have suggested that long-segment wall thickening and ascites may occur in those specific diagnoses [3, 5, 25, 26], although the degree of straightening of small bowel has not been previously described, to our knowledge. lthough we have only discussed the involvement of the small bowel, radiologists should also recognize that both hereditary angioedema and CEI-induced angioedema may involve other portions of the gastrointestinal tract, including the stomach and colon, although no other gastrointestinal tract involvement was encountered in our patients [4, 27 29]. In conclusion, CEI-induced small-bowel angioedema is primarily seen in women and causes severe abdominal pain, mild leukocytosis, and CT findings that may potentially be mistaken for small-bowel ischemia or other diagnoses. Radiologists should be aware of this diagnosis and its radiographic appearance. The findings of ascites, preserved luminal transit, with small-bowel wall thickening, dilatation, and straightening, should prompt radiologists to include CEI-induced smallbowel angioedema in the differential diagnosis. Because the CT findings of bowel edema and symptoms resolve quickly, close clinical follow-up will avert unnecessary surgery or other diagnostic and therapeutic procedures. Early diagnosis should initiate a prompt change in antihypertensive medication. ddendum s this article was going to press, an article was published in the March 2011 issue of JR, briefly describing six MDCT cases of CEI-induced small-bowel angioedema from one institution. The authors noted similar descriptions of the small-bowel appearance as in our cases, with individual smallbowel wall thickness ranging from 4 to 9 mm and lengths of involvement estimated from 20 to 60 cm, without associated lymphadenopathy or bowel obstruction [30]. References 1. Dean DE, Schultz DL, Powers RH. sphyxia due to angiotensin converting enzyme (CE) inhibitor mediated angioedema of the tongue during the treatment of hypertensive heart disease. J Forensic Sci 2001; 46: Zauli D, Contestabile S, Grassi, Bortolotti R, Ballardini G, Bianchi FB. CE-inhibitors and angioedema. J llergy Clin Immunol 2002; 110: De Backer I, De Schepper M, Vandevenne JE, Schoeters P, Michielsen P, Stevens WJ. CT of angio- JR:197, ugust
6 Scheirey et al. edema of the small bowel. JR 2001; 176: Hereditary and acquired angioedema: problems Marmery H, Mirvis SE. ngiotensin-converting and progress: proceedings of the third C1 esterase 23. Wei SC, Fitzgerald K, Maglinte DD. CT find- enzyme inhibitor-induced visceral angioedema. inhibitor deficiency workshop and beyond. J l- ings in small bowel angioedema: a cause of Clin Radiol 2006; 61: lergy Clin Immunol 2004; 114(suppl 3): S51 S131 acute abdominal pain. Emerg Radiol 2007; 5. Fisher J, Fleishman MJ, Hancock D. ngioedema 14. gostoni, Cicardi M. Drug-induced angioede- 13: of the small bowel: CT appearance. JR 2000; 175: Balthazar EJ. CT of the gastrointestinal tract: principles and interpretation. JR 1991; 156: Turcu F, White J, Kulaga ME, Skluth M, Gruss CB. Calcium channel blocker-associated small bowel angioedema. J Clin Gastroenterol 2009; 43: Cicardi M, Zingale LC, Bergamaschini L, gostoni. ngioedema associated with angiotensinconverting enzyme inhibitor use: outcome after switching to a different treatment. rch Intern Med 2004; 164: Brown NJ, Snowden M, Griffin MR. Recurrent angiotensin-converting enzyme inhibitor: associated angioedema. JM 1997; 278: Fukuya T, Hawes DR, Lu CC, Chang PJ, Barloon TJ. CT diagnosis of small-bowel obstruction: efficacy in 60 patients. JR 1992; 158: Desai RK, Tagliabue JR, Wegryn S, Einstein DM. CT evaluation of wall thickening in the alimentary tract. RadioGraphics 1991; 11: Gainer JV, Morrow JD, Loveland, King DJ, Brown NJ. Effect of bradykinin-receptor blockade on the response to angiotensin-convertingenzyme inhibitor in normotensive and hypertensive subjects. N Engl J Med 1998; 339: gostoni, ygoren-pursun E, Binkley KE, et al. ma without urticaria. Drug Saf 2001; 24: Pavletic. Late angioedema caused by CE inhibitors underestimated. m Fam Physician 2002; 66: Pavletic J. ngioedema after long-term use of an angiotensin-converting enzyme inhibitor. J m Board Fam Pract 1997; 10: Orr KK, Myers JR. Intermittent visceral edema induced by long-term enalapril administration. nn Pharmacother 2004; 38: Slater EE, Merrill DD, Guess H, et al. Clinical profile of angioedema associated with angiotensin converting-enzyme inhibition. JM 1988; 260: Pearson KD, Buchignani JS, Shimkin PM, Frank MM. Hereditary angioneurotic edema of the gastrointestinal tract. JR Radium Ther Nucl Med 1972; 116: Ellis K, McConnell DJ. Hereditary angioneurotic edema involving small intestine. Radiology 1969; 92: Ciaccia D, Brazer SR, Baker ME. cquired C1 esterase inhibitor deficiency causing intestinal angioedema: CT appearance. JR 1993; 161: Polger M, Kuhlman JE, Hansen FC 3rd, Fishman EK. Computed tomography of angioedema of small bowel due to reaction to radiographic contrast medium. J Comput ssist Tomogr 1988; 12: 24. Macari M, Megibow J, Balthazar EJ. pattern approach to the abnormal small bowel: observations at MDCT and CT enterography. JR 2007; 188: Byrne TJ, Douglas DD, Landis ME, Heppell JP. Isolated visceral angioedema: an underdiagnosed complication of CE inhibitors? Mayo Clin Proc 2000; 75: bdelmalek MF, Douglas DD. Lisinopril-induced isolated visceral angioedema: review of CE-inhibitor-induced small bowel angioedema. Dig Dis Sci 1997; 42: Eck SL, Morse JH, Janssen D, Emerson SG, Markovitz DM. ngioedema presenting as chronic gastrointestinal symptoms. m J Gastroenterol 1993; 88: Shahzad G, Korsten M, Blatt C, Motwani P. ngiotensin-converting enzyme (CE) inhibitorassociated angioedema of the stomach and small intestine: a case report. Mt Sinai J Med 2006; 73: Tojo, Onozato ML, Fujita T. Repeated subileus due to angioedema during renin-angiotensin system blockade. m J Med Sci 2006; 332: Vallurupalli K, Coakley KJ. MDCT features of angiotensin-converting enzyme inhibitor induced visceral angioedema. JR 2011; 196:833; [web] W405 W JR:197, ugust 2011
MDCT Features of Angiotensin- Converting Enzyme Inhibitor Induced Visceral Angioedema
 Gastrointestinal Imaging Pictorial Essay Vallurupalli and Coakley MDCT of Visceral ngioedema Gastrointestinal Imaging Pictorial Essay Kalyani Vallurupalli 1 Kevin J. Coakley 2 Vallurupalli K, Coakley KJ
Gastrointestinal Imaging Pictorial Essay Vallurupalli and Coakley MDCT of Visceral ngioedema Gastrointestinal Imaging Pictorial Essay Kalyani Vallurupalli 1 Kevin J. Coakley 2 Vallurupalli K, Coakley KJ
Reminder of important clinical lesson: Bad gut feeling: ACE inhibitor induced intest...
 Seite 1 von 5 BMJ Case Rep. 2009; 2009: bcr09.2008.0868. Published online 2009 February 27. doi: 10.1136/bcr.09.2008.0868 Reminder of important clinical lesson PMCID: PMC3029297 Bad gut feeling: ACE inhibitor
Seite 1 von 5 BMJ Case Rep. 2009; 2009: bcr09.2008.0868. Published online 2009 February 27. doi: 10.1136/bcr.09.2008.0868 Reminder of important clinical lesson PMCID: PMC3029297 Bad gut feeling: ACE inhibitor
Relationship Between Small Bowel Obstruction and Small Bowel Feces Sign: Four Cases Report
 Case Report Elmer Press Relationship Between Small Bowel Obstruction and Small Bowel Feces Sign: Four Cases Report Altintoprak Fatih a, e, Gunduz Yasemin b, Yalkin Omer c, Gundugdu Kemal c, Serbulent Gokhan
Case Report Elmer Press Relationship Between Small Bowel Obstruction and Small Bowel Feces Sign: Four Cases Report Altintoprak Fatih a, e, Gunduz Yasemin b, Yalkin Omer c, Gundugdu Kemal c, Serbulent Gokhan
Fig. 1. Ileal and jejunal metastases from adenocarcinoma of the lung in 62-year-old male with a clinical history of bloody stool. A.
 507 A B Fig. 1. Ileal and jejunal metastases from adenocarcinoma of the lung in 62-year-old male with a clinical history of bloody stool. A. An intraluminal polypoid mass (arrow) is seen in the dilated
507 A B Fig. 1. Ileal and jejunal metastases from adenocarcinoma of the lung in 62-year-old male with a clinical history of bloody stool. A. An intraluminal polypoid mass (arrow) is seen in the dilated
elical CT plays an important role
 bdominal Imaging Yu et al. Helical CT of cute RLQ Pain Pictorial Essay Jinxing Yu 1 nn S. Fulcher Mary nn Turner Robert. Halvorsen Yu J, Fulcher S, Turner M, Halvorsen R Helical CT Evaluation of cute Right
bdominal Imaging Yu et al. Helical CT of cute RLQ Pain Pictorial Essay Jinxing Yu 1 nn S. Fulcher Mary nn Turner Robert. Halvorsen Yu J, Fulcher S, Turner M, Halvorsen R Helical CT Evaluation of cute Right
Utility of CT enterography in the evaluation of small bowel pathologies
 International Journal of Advances in Medicine Varma RU et al. Int J Adv Med. 2017 Oct;4(5):1328-1332 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20174190
International Journal of Advances in Medicine Varma RU et al. Int J Adv Med. 2017 Oct;4(5):1328-1332 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20174190
General Data. 王 X 村 78 y/o 男性
 General Data 王 X 村 78 y/o 男性 Chief Complaint Vomiting twice this early morning Fever up to 38.9ºC was noted Present Illness (1) Old CVA with left side weakness for more than 10 years and with bed ridden
General Data 王 X 村 78 y/o 男性 Chief Complaint Vomiting twice this early morning Fever up to 38.9ºC was noted Present Illness (1) Old CVA with left side weakness for more than 10 years and with bed ridden
Adult Intussusception: A Complication of Metastatic Melanoma or Primary Malignancy?
 January 2013 Adult Intussusception: A Complication of Metastatic Melanoma or Primary Malignancy? Johanna Sheu, Harvard Medical School Year III 1 Agenda Menu of tests Definition/anatomy/classification Pediatrics
January 2013 Adult Intussusception: A Complication of Metastatic Melanoma or Primary Malignancy? Johanna Sheu, Harvard Medical School Year III 1 Agenda Menu of tests Definition/anatomy/classification Pediatrics
Intestinal Ischemia Versus Intramural Hemorrhage: CT Evaluation
 Michael Macari 1 Hersch Chandarana Emil althazar James abb Received March 27, 2002; accepted after revision July 11, 2002. 1 ll authors: Department of Radiology, bdominal Imaging Section, Tisch Hospital,
Michael Macari 1 Hersch Chandarana Emil althazar James abb Received March 27, 2002; accepted after revision July 11, 2002. 1 ll authors: Department of Radiology, bdominal Imaging Section, Tisch Hospital,
Pneumatosis intestinalis, not always a surgical emergency
 Pneumatosis intestinalis, not always a surgical emergency Poster No.: C-2233 Congress: ECR 2012 Type: Educational Exhibit Authors: E. Vanhoutte, M. Lefere, R. Vanslembrouck, D. Bielen, G. De 1 1 2 1 1
Pneumatosis intestinalis, not always a surgical emergency Poster No.: C-2233 Congress: ECR 2012 Type: Educational Exhibit Authors: E. Vanhoutte, M. Lefere, R. Vanslembrouck, D. Bielen, G. De 1 1 2 1 1
Intramural Fat in the Duodenum and Proximal Small Intestine in Patients with Celiac Disease
 Intramural Fat in eliac Disease Gastrointestinal Imaging linical Observations Francis J. Scholz 1 Spencer. Behr hristopher D. Scheirey Scholz FJ, Behr S, Scheirey D Keywords: abdominal imaging, celiac
Intramural Fat in eliac Disease Gastrointestinal Imaging linical Observations Francis J. Scholz 1 Spencer. Behr hristopher D. Scheirey Scholz FJ, Behr S, Scheirey D Keywords: abdominal imaging, celiac
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 6/23/2012 Radiology Quiz of the Week # 78 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 6/23/2012 Radiology Quiz of the Week # 78 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
ENTEROCOLITIDES CAN YOU TELL THEM APART ON MDCT? Richard M. Gore, MD North Shore University Medical Center University of Chicago Evanston, Illinois
 ENTEROCOLITIDES CAN YOU TELL THEM APART ON MDCT? Richard M. Gore, MD North Shore University Medical Center University of Chicago Evanston, Illinois SCBT/MR 2010 San Diego, California March 8, 2010 13:40-14:00
ENTEROCOLITIDES CAN YOU TELL THEM APART ON MDCT? Richard M. Gore, MD North Shore University Medical Center University of Chicago Evanston, Illinois SCBT/MR 2010 San Diego, California March 8, 2010 13:40-14:00
CT Evaluation of Bowel Wall Thickening. Dr: Adel El Badrawy; M.D. Lecturer of Radio Diagnosis Faculty of Medicine Mansoura University.
 CT Evaluation of Bowel Wall Thickening By Dr: Adel El Badrawy; M.D. Lecturer of Radio Diagnosis Faculty of Medicine Mansoura University. The CT findings of bowel wall thickening includes 1 Degree of thickening.
CT Evaluation of Bowel Wall Thickening By Dr: Adel El Badrawy; M.D. Lecturer of Radio Diagnosis Faculty of Medicine Mansoura University. The CT findings of bowel wall thickening includes 1 Degree of thickening.
Pattern based approach for differential diagnosis of small bowel neoplasms using MDCT
 Pattern based approach for differential diagnosis of small bowel neoplasms using MDCT Poster No.: C-1400 Congress: ECR 2014 Type: Educational Exhibit Authors: P. Bhari Thippeswamy, C. Anuradha, A. Polimood,
Pattern based approach for differential diagnosis of small bowel neoplasms using MDCT Poster No.: C-1400 Congress: ECR 2014 Type: Educational Exhibit Authors: P. Bhari Thippeswamy, C. Anuradha, A. Polimood,
Perforation of a Duodenal Diverticulum. Elective Student S. C.
 Perforation of a Duodenal Diverticulum 2008 4 Elective Student S. C. Case History An elderly male presented to the Emergency Department with abdominal pain. Chief Complaint: Worsening, diffuse abdominal
Perforation of a Duodenal Diverticulum 2008 4 Elective Student S. C. Case History An elderly male presented to the Emergency Department with abdominal pain. Chief Complaint: Worsening, diffuse abdominal
HAE disease fact sheet
 [Insert organization logo and the hae day :-) logo] HAE disease fact sheet Hereditary Angioedema (HAE) is a rare, potentially life threatening inherited disorder with symptoms of severe, painful, and recurring
[Insert organization logo and the hae day :-) logo] HAE disease fact sheet Hereditary Angioedema (HAE) is a rare, potentially life threatening inherited disorder with symptoms of severe, painful, and recurring
Computed tomography (CT) imaging review of small bowel obstruction
 Computed tomography (CT) imaging review of small bowel obstruction Poster No.: C-1602 Congress: ECR 2010 Type: Educational Exhibit Topic: GI Tract - Small Bowel Authors: A. Vousough, D. S. Prasad ; Aberdeen/UK,
Computed tomography (CT) imaging review of small bowel obstruction Poster No.: C-1602 Congress: ECR 2010 Type: Educational Exhibit Topic: GI Tract - Small Bowel Authors: A. Vousough, D. S. Prasad ; Aberdeen/UK,
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
The nontraumatic acute abdomen
 CT features of acute appendicitis: pictorial review Marco ntonio Cura, MD The nontraumatic acute abdomen is one of the most common presentations to the emergency room, with appendicitis being one of the
CT features of acute appendicitis: pictorial review Marco ntonio Cura, MD The nontraumatic acute abdomen is one of the most common presentations to the emergency room, with appendicitis being one of the
Imaging abdominal vascular emergencies. V.Stoynova
 Imaging abdominal vascular emergencies V.Stoynova Abdominal vessels V. Stoynova 2 Acute liver bleeding trauma anticoagulant therapy liver disease : HCC, adenoma, meta, FNH, Hemangioma Diagnosis :CT angiography
Imaging abdominal vascular emergencies V.Stoynova Abdominal vessels V. Stoynova 2 Acute liver bleeding trauma anticoagulant therapy liver disease : HCC, adenoma, meta, FNH, Hemangioma Diagnosis :CT angiography
Computed tomography (CT) imaging review of small bowel obstruction
 Computed tomography (CT) imaging review of small bowel obstruction Poster No.: C-1602 Congress: ECR 2010 Type: Educational Exhibit Topic: GI Tract Authors: A. Vousough, D. S. Prasad ; Aberdeen/UK, Leeds/UK
Computed tomography (CT) imaging review of small bowel obstruction Poster No.: C-1602 Congress: ECR 2010 Type: Educational Exhibit Topic: GI Tract Authors: A. Vousough, D. S. Prasad ; Aberdeen/UK, Leeds/UK
Pitfalls in the CT diagnosis of appendicitis
 The British Journal of Radiology, 77 (2004), 792 799 DOI: 10.1259/bjr/95663370 E 2004 The British Institute of Radiology Pictorial review Pitfalls in the CT diagnosis of appendicitis 1 C D LEVINE, 2 O
The British Journal of Radiology, 77 (2004), 792 799 DOI: 10.1259/bjr/95663370 E 2004 The British Institute of Radiology Pictorial review Pitfalls in the CT diagnosis of appendicitis 1 C D LEVINE, 2 O
Fig year-old man with aortic dissection. Contrast-enhanced
 Pictorial Essay CT Manifestations of owel Ischemia Chung Kuao Chou 1 owel ischemia represents a process of insufficient blood supply of the small or large bowel with the consequences ranging from a transient,
Pictorial Essay CT Manifestations of owel Ischemia Chung Kuao Chou 1 owel ischemia represents a process of insufficient blood supply of the small or large bowel with the consequences ranging from a transient,
Clearing the mind before the "caliber change": Diagnostic algorithm for small bowel obstruction.
 Clearing the mind before the "caliber change": Diagnostic algorithm for small bowel obstruction. Poster No.: C-0255 Congress: ECR 2014 Type: Educational Exhibit Authors: C. Santos Montón, D. Oquillas Izquierdo,
Clearing the mind before the "caliber change": Diagnostic algorithm for small bowel obstruction. Poster No.: C-0255 Congress: ECR 2014 Type: Educational Exhibit Authors: C. Santos Montón, D. Oquillas Izquierdo,
Evaluating the CT Diagnosis of Clostridium difficile Colitis: Should CT Guide Therapy?
 Iain D. C. Kirkpatrick 1 Howard M. Greenberg Received April 7, 2000; accepted after revision August 24, 2000. 1 Both authors: Department of Radiology, University of Manitoba, Health Sciences Centre, 820
Iain D. C. Kirkpatrick 1 Howard M. Greenberg Received April 7, 2000; accepted after revision August 24, 2000. 1 Both authors: Department of Radiology, University of Manitoba, Health Sciences Centre, 820
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 09/17/2011 Radiology Quiz of the Week # 38 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 09/17/2011 Radiology Quiz of the Week # 38 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
MESENTERIC ISCHEMIA THE FORGOTTEN DIAGNOSIS. Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, Illinois
 MESENTERIC ISCHEMIA THE FORGOTTEN DIAGNOSIS Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, Illinois SCBT/MR 2010 San Diego, California March 8, 2010 16:00-16:10
MESENTERIC ISCHEMIA THE FORGOTTEN DIAGNOSIS Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, Illinois SCBT/MR 2010 San Diego, California March 8, 2010 16:00-16:10
Which Blunt Trauma Patients Should Be Studied by Abdominal CT?
 MDCT of Bowel and Mesenteric Injury: How Findings Influence Management 4 th Nordic Trauma Radiology Course 2006 4 th Nordic Trauma Radiology Course 2006 Stuart E. Mirvis, M.D., FACR Department of Radiology
MDCT of Bowel and Mesenteric Injury: How Findings Influence Management 4 th Nordic Trauma Radiology Course 2006 4 th Nordic Trauma Radiology Course 2006 Stuart E. Mirvis, M.D., FACR Department of Radiology
Surgical Management of IBD. Val Jefford Grand Rounds October 14, 2003
 Surgical Management of IBD Val Jefford Grand Rounds October 14, 2003 Introduction Important Features Clinical Presentation Evaluation Medical Treatment Surgical Treatment Cases Overview Introduction Two
Surgical Management of IBD Val Jefford Grand Rounds October 14, 2003 Introduction Important Features Clinical Presentation Evaluation Medical Treatment Surgical Treatment Cases Overview Introduction Two
Primary epiploic appendagitis versus omental infarction : The role of MDCT
 Primary epiploic appendagitis versus omental infarction : The role of MDCT e-poster: EE-125 Congress: ESGAR 2010 Type: Educational Exhibit Topic: Diagnostic / Mesentery and Peritoneum Authors: P. Kraniotis,
Primary epiploic appendagitis versus omental infarction : The role of MDCT e-poster: EE-125 Congress: ESGAR 2010 Type: Educational Exhibit Topic: Diagnostic / Mesentery and Peritoneum Authors: P. Kraniotis,
LOOKING FOR AIR IN ALL THE WRONG PLACES Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, IL
 SIGNIFICANCE OF EXTRALUMINAL ABDOMINAL GAS: LOOKING FOR AIR IN ALL THE WRONG PLACES Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, IL SCBT/MR 2012 October 26,
SIGNIFICANCE OF EXTRALUMINAL ABDOMINAL GAS: LOOKING FOR AIR IN ALL THE WRONG PLACES Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, IL SCBT/MR 2012 October 26,
INTRALUMINAL GAS IN NON-PERFORATED ACUTE APPENDICITIS: A predictor of gangrenous appendicitis
 INTRALUMINAL GAS IN NON-PERFORATED ACUTE APPENDICITIS: A predictor of gangrenous appendicitis DM Plata Ariza, MD; E Martínez Chamorro, MD; D Castaño Pardo, MD; M Arroyo López, MD; E Peghini Gavilanes,
INTRALUMINAL GAS IN NON-PERFORATED ACUTE APPENDICITIS: A predictor of gangrenous appendicitis DM Plata Ariza, MD; E Martínez Chamorro, MD; D Castaño Pardo, MD; M Arroyo López, MD; E Peghini Gavilanes,
Colon Ischemia (CI): New Developments and Guidelines for Management. Spectrum of CI
 Colon Ischemia (CI): New Developments and Guidelines for Management Lawrence J. Brandt, MD, MACG Professor of Medicine and Surgery Albert Einstein College of Medicine Emeritus Chief of Gastroenterology
Colon Ischemia (CI): New Developments and Guidelines for Management Lawrence J. Brandt, MD, MACG Professor of Medicine and Surgery Albert Einstein College of Medicine Emeritus Chief of Gastroenterology
Accepted Article. Massive gastrointestinal pneumatosis in a patient with celiac disease and superior mesenteric artery syndrome
 Accepted Article Massive gastrointestinal pneumatosis in a patient with celiac disease and superior mesenteric artery syndrome Aleix Martínez-Pérez, Ramón Trullenque-Juan, Sandra Santarrufina-Martínez,
Accepted Article Massive gastrointestinal pneumatosis in a patient with celiac disease and superior mesenteric artery syndrome Aleix Martínez-Pérez, Ramón Trullenque-Juan, Sandra Santarrufina-Martínez,
CT imaging findings of acute mesenteric ischemia and ischemic colitis. A brief pictorial essay.
 CT imaging findings of acute mesenteric ischemia and ischemic colitis. A brief pictorial essay. Poster No.: C-0750 Congress: ECR 2011 Type: Educational Exhibit Authors: Y. Arias Morales, J. P. Giraldo
CT imaging findings of acute mesenteric ischemia and ischemic colitis. A brief pictorial essay. Poster No.: C-0750 Congress: ECR 2011 Type: Educational Exhibit Authors: Y. Arias Morales, J. P. Giraldo
Emergency MDCT in case of right lower quadrant pain
 Emergency MDCT in case of right lower quadrant pain Poster No.: C-0563 Congress: ECR 2015 Type: Educational Exhibit Authors: M. Lisitskaya, V. Sinitsyn; Moscow/RU Keywords: Abdomen, Emergency, Gastrointestinal
Emergency MDCT in case of right lower quadrant pain Poster No.: C-0563 Congress: ECR 2015 Type: Educational Exhibit Authors: M. Lisitskaya, V. Sinitsyn; Moscow/RU Keywords: Abdomen, Emergency, Gastrointestinal
Images In Gastroenterology
 Images In Gastroenterology Thong-Ngam D, et al. THAI J GASTROENTEROL 2005 Vol. 6 No. 2 May - Aug. 2005 105 Imaging of Gastrointestinal Stromal Tumors Pornpim Fuangtharnthip, M.D. Narumol Hargroove, M.D.
Images In Gastroenterology Thong-Ngam D, et al. THAI J GASTROENTEROL 2005 Vol. 6 No. 2 May - Aug. 2005 105 Imaging of Gastrointestinal Stromal Tumors Pornpim Fuangtharnthip, M.D. Narumol Hargroove, M.D.
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 3, Issue 4 2013 Article 6 Case report: Intussusception of the colon through a colostomy: A rare presentation of colonic intussusception. Dr. Nora Trabulsi Dr.
World Journal of Colorectal Surgery Volume 3, Issue 4 2013 Article 6 Case report: Intussusception of the colon through a colostomy: A rare presentation of colonic intussusception. Dr. Nora Trabulsi Dr.
Chapter 14: Training in Radiology. DDSEP Chapter 1: Question 12
 DDSEP Chapter 1: Question 12 A 52-year-old white male presents for evaluation of sudden onset of abdominal pain and shoulder pain. His past medical history is notable for a history of coronary artery disease,
DDSEP Chapter 1: Question 12 A 52-year-old white male presents for evaluation of sudden onset of abdominal pain and shoulder pain. His past medical history is notable for a history of coronary artery disease,
Nordic Forum - Trauma & Emergency Radiology. Bowel Obstruction: Imaging Update
 Nordic Forum - Trauma & Emergency Radiology Bowel Obstruction: Imaging Update Borut Marincek Institute of Diagnostic Radiology University Hospital Zurich, Switzerland Acute Abdomen Bowel Obstruction Bowel
Nordic Forum - Trauma & Emergency Radiology Bowel Obstruction: Imaging Update Borut Marincek Institute of Diagnostic Radiology University Hospital Zurich, Switzerland Acute Abdomen Bowel Obstruction Bowel
Helical CT Signs in the Diagnosis of Intestinal Ischemia in Small-Bowel Obstruction
 Marc Zalcman 1 Marième Sy 1 Vincent Donckier 2 Jean Closset 2 Daniel Van Gansbeke 1 Received February 17, 2000; accepted after revision May 25, 2000. 1 Department of Radiology, C. U.. Hôpital Erasme, 808,
Marc Zalcman 1 Marième Sy 1 Vincent Donckier 2 Jean Closset 2 Daniel Van Gansbeke 1 Received February 17, 2000; accepted after revision May 25, 2000. 1 Department of Radiology, C. U.. Hôpital Erasme, 808,
Gastrointestinal Metastasis From Primary Lung Cancer: CT Findings and Clinicopathologic Features
 Gastrointestinal Imaging Clinical Observations Kim et al. Gastrointestinal Metastasis of Lung Cancer Gastrointestinal Imaging Clinical Observations So Yeon Kim 1,2 Hyun Kwon Ha 1 Sung Won Park 1 Jun Kang
Gastrointestinal Imaging Clinical Observations Kim et al. Gastrointestinal Metastasis of Lung Cancer Gastrointestinal Imaging Clinical Observations So Yeon Kim 1,2 Hyun Kwon Ha 1 Sung Won Park 1 Jun Kang
Original Report. Stercoral Colitis Leading to Fatal Peritonitis: CT Findings. Gastrointestinal Imaging Heffernan et al. CT of Stercoral Colitis
 Gastrointestinal Imaging Heffernan et al. CT of Stercoral Colitis Cathleen Heffernan 1 H. Leon Pachter 2 lec J. Megibow 1 Michael Macari 1 Hefferman C, Pachter HL, Megibow J, Macari M Received pril 21,
Gastrointestinal Imaging Heffernan et al. CT of Stercoral Colitis Cathleen Heffernan 1 H. Leon Pachter 2 lec J. Megibow 1 Michael Macari 1 Hefferman C, Pachter HL, Megibow J, Macari M Received pril 21,
UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN
 UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN Radiology Enterprises radiologyenterprises@gmail.com www.radiologyenterprises.com STOMACH AND SMALL BOWEL STOMACH AND SMALL BOWEL Swallowed air is a
UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN Radiology Enterprises radiologyenterprises@gmail.com www.radiologyenterprises.com STOMACH AND SMALL BOWEL STOMACH AND SMALL BOWEL Swallowed air is a
ADULT RETROGRADE INTUSSUSCEPTION Brian Tiu Richmond University Medical Center September 3, 2015
 ADULT RETROGRADE INTUSSUSCEPTION Brian Tiu Richmond University Medical Center September 3, 2015 CASE PRESENTATION 41 yo woman presented one day hx abdominal pain, worsening nausea/vomiting denied flatus/bm
ADULT RETROGRADE INTUSSUSCEPTION Brian Tiu Richmond University Medical Center September 3, 2015 CASE PRESENTATION 41 yo woman presented one day hx abdominal pain, worsening nausea/vomiting denied flatus/bm
Objectives. Pediatric Mortality. Another belly pain. Gastroenteritis. Spewing & Pooing Child 4/18/16
 Gastro-tastrophies A Review of Pediatric GI Emergencies Objectives Discuss common presentations of Pediatric Abdominal Pain complaints Discuss work up and physical exam findings Discuss care, management
Gastro-tastrophies A Review of Pediatric GI Emergencies Objectives Discuss common presentations of Pediatric Abdominal Pain complaints Discuss work up and physical exam findings Discuss care, management
ACUTE ABDOMEN IN OLDER CHILDREN. Carlos J. Sivit M.D.
 ACUTE ABDOMEN IN OLDER CHILDREN Carlos J. Sivit M.D. ACUTE ABDOMEN Clinical condition characterized by severe abdominal pain developing over several hours ACUTE ABDOMINAL PAIN Common childhood complaint
ACUTE ABDOMEN IN OLDER CHILDREN Carlos J. Sivit M.D. ACUTE ABDOMEN Clinical condition characterized by severe abdominal pain developing over several hours ACUTE ABDOMINAL PAIN Common childhood complaint
Endometriosis of the Appendix Resulting in Perforated Appendicitis
 27 Endometriosis of the Appendix Resulting in Perforated Appendicitis Toru Hasegawa a Koichi Yoshida b Kazuhiro Matsui c a Department of Obstetrics and Gynecology, Faculty of Medicine, University of Toyama,
27 Endometriosis of the Appendix Resulting in Perforated Appendicitis Toru Hasegawa a Koichi Yoshida b Kazuhiro Matsui c a Department of Obstetrics and Gynecology, Faculty of Medicine, University of Toyama,
ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE. T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar
 ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar LEARNING OBJECTIVES q Through a series of cases illustrate the updated Atlanta symposium
ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar LEARNING OBJECTIVES q Through a series of cases illustrate the updated Atlanta symposium
Posterior Rectus Sheath Hernia Causing Intermittent Small Bowel Obstruction
 Posterior Rectus Sheath Hernia Causing Intermittent Small Bowel Obstruction Scott Lenobel 1*, Robert Lenobel 2, Joseph Yu 1 1. Department of Radiology, The Ohio State University Wexner Medical Center,
Posterior Rectus Sheath Hernia Causing Intermittent Small Bowel Obstruction Scott Lenobel 1*, Robert Lenobel 2, Joseph Yu 1 1. Department of Radiology, The Ohio State University Wexner Medical Center,
Colon ischemia. Bible class 12 September Stefan Christen. ACG Clinical Guideline: Am J Gastroenterol 2015
 Colon ischemia Bible class 12 September 2018 Stefan Christen ACG Clinical Guideline: Am J Gastroenterol 2015 Definition Definition Imbalance between blood supply and metabolic demands of the colonocytes
Colon ischemia Bible class 12 September 2018 Stefan Christen ACG Clinical Guideline: Am J Gastroenterol 2015 Definition Definition Imbalance between blood supply and metabolic demands of the colonocytes
IBD 101. Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition
 IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
Case Report Ileocecal Intussusception due to a Lipoma in an Adult
 Case Reports in Surgery Volume 2012, Article ID 684298, 4 pages doi:10.1155/2012/684298 Case Report Ileocecal Intussusception due to a Lipoma in an Adult Mehmet Bilgin, 1 Huseyin Toprak, 1 Issam Cheikh
Case Reports in Surgery Volume 2012, Article ID 684298, 4 pages doi:10.1155/2012/684298 Case Report Ileocecal Intussusception due to a Lipoma in an Adult Mehmet Bilgin, 1 Huseyin Toprak, 1 Issam Cheikh
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 6, Issue 5 2016 Article 8 Sigmoidocele: A Rare Cause Of Constipation In Males Noor Shah MD Milind Kachare MD Craig Rezac MD Rutgers Robert Wood Johnson Medical
World Journal of Colorectal Surgery Volume 6, Issue 5 2016 Article 8 Sigmoidocele: A Rare Cause Of Constipation In Males Noor Shah MD Milind Kachare MD Craig Rezac MD Rutgers Robert Wood Johnson Medical
Always keep it in the differential
 Acute Appendicitis Lissa C. Sakata and Lindsey Perea 2 Always keep it in the differential Learning Objectives 1. The learner should be able to describe the etiology of acute appendicitis. 2. The learner
Acute Appendicitis Lissa C. Sakata and Lindsey Perea 2 Always keep it in the differential Learning Objectives 1. The learner should be able to describe the etiology of acute appendicitis. 2. The learner
Cecal Volvulus: Case Presentation and Review of CT Findings
 August 2011 Cecal Volvulus: Case Presentation and Review of CT Findings Omar Pardesi, Harvard Medical School Year III Our Patient LD: History & Physical HPI: 28 y.o. female presents with diffuse abdominal
August 2011 Cecal Volvulus: Case Presentation and Review of CT Findings Omar Pardesi, Harvard Medical School Year III Our Patient LD: History & Physical HPI: 28 y.o. female presents with diffuse abdominal
Small-Bowel Obstruction from Adhesive Bands and Matted Adhesions: CT Differentiation
 Gastrointestinal Imaging Original Research Delabrousse et al. CT Diagnosis of the Type of dhesions Causing SO Gastrointestinal Imaging Original Research Eric Delabrousse 1 Jean Lubrano 2 Jérome Jehl 1
Gastrointestinal Imaging Original Research Delabrousse et al. CT Diagnosis of the Type of dhesions Causing SO Gastrointestinal Imaging Original Research Eric Delabrousse 1 Jean Lubrano 2 Jérome Jehl 1
X-ray Corner. Imaging of the Small Bowel. Pantongrag-Brown L. Case 1. A 63-year-old man presented with abdominal pain, nausea and vomiting.
 THAI J 42 Imaging of the Small Bowel GASTROENTEROL 2015 X-ray Corner Imaging of the Small Bowel Pantongrag-Brown L Small bowel is the longest tubular organ in the body, about 18-22 feet. It is anchored
THAI J 42 Imaging of the Small Bowel GASTROENTEROL 2015 X-ray Corner Imaging of the Small Bowel Pantongrag-Brown L Small bowel is the longest tubular organ in the body, about 18-22 feet. It is anchored
Improvement of Image Quality with ß-Blocker Premedication on ECG-Gated 16-MDCT Coronary Angiography
 16-MDCT Coronary Angiography Shim et al. 16-MDCT Coronary Angiography Sung Shine Shim 1 Yookyung Kim Soo Mee Lim Received December 1, 2003; accepted after revision June 1, 2004. 1 All authors: Department
16-MDCT Coronary Angiography Shim et al. 16-MDCT Coronary Angiography Sung Shine Shim 1 Yookyung Kim Soo Mee Lim Received December 1, 2003; accepted after revision June 1, 2004. 1 All authors: Department
Journal of Medical Imaging and Radiation Oncology
 Journal of Medical Imaging and Radiation Oncology 62 (2018) 504 511 MEDICAL IMAGING PICTORIAL ESSAY Imaging in pancreas transplantation complications: Temporal classification Paula Gallego Ferrero and
Journal of Medical Imaging and Radiation Oncology 62 (2018) 504 511 MEDICAL IMAGING PICTORIAL ESSAY Imaging in pancreas transplantation complications: Temporal classification Paula Gallego Ferrero and
Gallstone ileus:diagnostic and therapeutic dilemma
 Saurabh et al. 1 CASE SERIES OPEN ACCESS Gallstone ileus:diagnostic and therapeutic dilemma Shireesh Saurabh, Andrew Camerota, Jeffrey Zavotsky ABSTRACT Introduction: Gallstone ileus is a rare complication
Saurabh et al. 1 CASE SERIES OPEN ACCESS Gallstone ileus:diagnostic and therapeutic dilemma Shireesh Saurabh, Andrew Camerota, Jeffrey Zavotsky ABSTRACT Introduction: Gallstone ileus is a rare complication
Imaging Features of Encapsulating Peritoneal Sclerosis in Continuous Ambulatory Peritoneal Dialysis Patients
 Genitourinary Imaging Pictorial Essay Ti et al. Encapsulating Peritoneal Sclerosis in CPD Patients Genitourinary Imaging Pictorial Essay Joanna P. Ti 1 li l-radi 2 Peter J. Conlon 2 Michael J. Lee 1 Martina
Genitourinary Imaging Pictorial Essay Ti et al. Encapsulating Peritoneal Sclerosis in CPD Patients Genitourinary Imaging Pictorial Essay Joanna P. Ti 1 li l-radi 2 Peter J. Conlon 2 Michael J. Lee 1 Martina
children Crohn s disease in MR enterography for GI Complications Microscopy Characterization Primary sclerosing cholangitis Anorectal fistulae
 MR enterography for Crohn s disease in children BOAZ KARMAZYN, MD PEDIATRIC RADIOLOGY ASSOCIATE PROFESSOR Characterization Crohn disease Idiopathic chronic transmural IBD Increasing incidence Age 7/100,000
MR enterography for Crohn s disease in children BOAZ KARMAZYN, MD PEDIATRIC RADIOLOGY ASSOCIATE PROFESSOR Characterization Crohn disease Idiopathic chronic transmural IBD Increasing incidence Age 7/100,000
MISSED FINDINGS IN EMERGENCY RADIOLOGY: CASE BASE SESSION 5 th Nordic Trauma Radiology Course Oslo, Norway
 MISSED FINDINGS IN EMERGENCY RADIOLOGY: CASE BASE SESSION 5 th Nordic Trauma Radiology Course Oslo, Norway K.SHANMUGANATHAN M.D. EASILY MISSED FINDINGS IN EMERGENCY RADIOLOGY OBJECTIVES Commonly missed
MISSED FINDINGS IN EMERGENCY RADIOLOGY: CASE BASE SESSION 5 th Nordic Trauma Radiology Course Oslo, Norway K.SHANMUGANATHAN M.D. EASILY MISSED FINDINGS IN EMERGENCY RADIOLOGY OBJECTIVES Commonly missed
CT imaging of chronic radiation enteritis in surgical and non surgical patients
 CT imaging of chronic radiation enteritis in surgical and non surgical patients Poster No.: C-0334 Congress: ECR 2017 Type: Educational Exhibit Authors: M. Zappa, S. Kemel, C. Bertin, M. Ronot, D. Cazals-Hatem,
CT imaging of chronic radiation enteritis in surgical and non surgical patients Poster No.: C-0334 Congress: ECR 2017 Type: Educational Exhibit Authors: M. Zappa, S. Kemel, C. Bertin, M. Ronot, D. Cazals-Hatem,
CT evaluation of small bowel carcinoid tumors
 CT evaluation of small bowel carcinoid tumors Poster No.: C-0060 Congress: ECR 2015 Type: Educational Exhibit Authors: N. V. V. P. Costa, L. Nascimento, T. Bilhim ; Estoril/PT, PT, 1 2 3 1 2 3 Lisbon/PT
CT evaluation of small bowel carcinoid tumors Poster No.: C-0060 Congress: ECR 2015 Type: Educational Exhibit Authors: N. V. V. P. Costa, L. Nascimento, T. Bilhim ; Estoril/PT, PT, 1 2 3 1 2 3 Lisbon/PT
Medical application of transabdominal ultrasound in gastrointestinal diseases
 Medical application of transabdominal ultrasound in gastrointestinal diseases Hsiu-Po Wang Department of Emergency Medicine National Taiwan University Hospital Real-time ultrasound has become a standard
Medical application of transabdominal ultrasound in gastrointestinal diseases Hsiu-Po Wang Department of Emergency Medicine National Taiwan University Hospital Real-time ultrasound has become a standard
Vomiting in children: The good coordination between radiologists and pediatricians is the key to success
 Vomiting in children: The good coordination between radiologists and pediatricians is the key to success C. Santos Montón 1, M. T. Garzon Guiteria 2, A. Hortal Benito-Sendín 1, K. El Karzazi 1, P. Sanchez
Vomiting in children: The good coordination between radiologists and pediatricians is the key to success C. Santos Montón 1, M. T. Garzon Guiteria 2, A. Hortal Benito-Sendín 1, K. El Karzazi 1, P. Sanchez
IBD 101. Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition
 IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
12 Blueprints Q&A Step 2 Surgery
 12 Blueprints Q&A Step 2 Surgery 34. A 40-year-old female has been referred to you for a recent ER and hospital admission, from which she was given a diagnosis of acute diverticulitis. Treatment at that
12 Blueprints Q&A Step 2 Surgery 34. A 40-year-old female has been referred to you for a recent ER and hospital admission, from which she was given a diagnosis of acute diverticulitis. Treatment at that
Gastrointestinal Tract Imaging. Objectives. Reference. VMB 960 April 6, Stomach Small Intestine Colon. Radiography & Ultrasound
 Gastrointestinal Tract Imaging VMB 960 April 6, 2009 Stomach Small Intestine Colon Objectives Radiography & Ultrasound Contrast Examination of the Small Intestine Reference Chapters 45 47 Pages 750 805
Gastrointestinal Tract Imaging VMB 960 April 6, 2009 Stomach Small Intestine Colon Objectives Radiography & Ultrasound Contrast Examination of the Small Intestine Reference Chapters 45 47 Pages 750 805
Summary and conclusions
 Summary and conclusions 7 Chapter 7 68 Summary and conclusions Chapter 1 provides a general introduction to this thesis focused on the use of ultrasound (US) in children with abdominal problems. The literature
Summary and conclusions 7 Chapter 7 68 Summary and conclusions Chapter 1 provides a general introduction to this thesis focused on the use of ultrasound (US) in children with abdominal problems. The literature
Gastrointestinal Imaging Original Research
 Contrast Enema for Detecting nastomotic Strictures Gastrointestinal Imaging Original Research David Dolinsky 1 Marc S. Levine 1 Stephen E. Rubesin 1 Igor Laufer 1 John L. Rombeau 2 Dolinsky D, Levine MS,
Contrast Enema for Detecting nastomotic Strictures Gastrointestinal Imaging Original Research David Dolinsky 1 Marc S. Levine 1 Stephen E. Rubesin 1 Igor Laufer 1 John L. Rombeau 2 Dolinsky D, Levine MS,
Adult Intussusception
 Bahrain Medical Bulletin, Vol. 27, No. 3, September 2005 Adult Intussusception Suhair Alsaad, MBCHB, CABS, FRCSI* Mariam Al-Muftah, MBCHB** Objectives: Adult intussusception is a rare entity. We present
Bahrain Medical Bulletin, Vol. 27, No. 3, September 2005 Adult Intussusception Suhair Alsaad, MBCHB, CABS, FRCSI* Mariam Al-Muftah, MBCHB** Objectives: Adult intussusception is a rare entity. We present
CT findings of gastric and intestinal anisakiasis as cause of acute abdominal pain
 CT findings of gastric and intestinal anisakiasis as cause of acute abdominal pain Poster No.: C-2258 Congress: ECR 2015 Type: Educational Exhibit Authors: S. Marcos 1, J. Gonzalez 1, L. Sarria Octavio
CT findings of gastric and intestinal anisakiasis as cause of acute abdominal pain Poster No.: C-2258 Congress: ECR 2015 Type: Educational Exhibit Authors: S. Marcos 1, J. Gonzalez 1, L. Sarria Octavio
Peutz Jegher's Syndrome (Gastro-intestinal Polyposis) and Its Complications
 Peutz Jegher's Syndrome (Gastro-intestinal Polyposis) and Its Complications Pages with reference to book, From 154 To 155 Zakiuddin G. Oonwala, Sina Aziz ( Department of Surgery, Dow Medical College and
Peutz Jegher's Syndrome (Gastro-intestinal Polyposis) and Its Complications Pages with reference to book, From 154 To 155 Zakiuddin G. Oonwala, Sina Aziz ( Department of Surgery, Dow Medical College and
Traumatic and Non Traumatic Adrenal Emergencies
 Traumatic and Non Traumatic Adrenal Emergencies Michael N. Patlas, MD, FRCPC (1), Christine O. Menias, MD (2), Douglas S. Katz, MD, FACR (3), Ania Z. Kielar, MD, FRCPC (4), Alla M. Rozenblit, MD (5), Jorge
Traumatic and Non Traumatic Adrenal Emergencies Michael N. Patlas, MD, FRCPC (1), Christine O. Menias, MD (2), Douglas S. Katz, MD, FACR (3), Ania Z. Kielar, MD, FRCPC (4), Alla M. Rozenblit, MD (5), Jorge
ד"ר דוד ירדני המכון לגסטרואנטרולוגיה ומחלות כבד מרכז רפואי סורוקה
 ד"ר דוד ירדני המכון לגסטרואנטרולוגיה ומחלות כבד מרכז רפואי סורוקה Presentaion: S.A is 38 years old. Referred for rectal bleeding investigation. Describes several occasions of bleeding and abdominal pain.
ד"ר דוד ירדני המכון לגסטרואנטרולוגיה ומחלות כבד מרכז רפואי סורוקה Presentaion: S.A is 38 years old. Referred for rectal bleeding investigation. Describes several occasions of bleeding and abdominal pain.
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
A Case of Pneumatosis Cystoides Intestinalis Mimicking Intestinal Perforation
 Showa Univ J Med Sci 26 2, 169 173, June 2014 Case Report A Case of Pneumatosis Cystoides Intestinalis Mimicking Intestinal Perforation Takahiro UMEMOTO 1, Yoshikuni HARADA 1, Makiko SAKATA 1, Gaku KIGAWA
Showa Univ J Med Sci 26 2, 169 173, June 2014 Case Report A Case of Pneumatosis Cystoides Intestinalis Mimicking Intestinal Perforation Takahiro UMEMOTO 1, Yoshikuni HARADA 1, Makiko SAKATA 1, Gaku KIGAWA
Burkitt s Lymphoma of the Abdomen: The Northern California Kaiser Permanente Experience
 ISPUB.COM The Internet Journal of Surgery Volume 18 Number 2 Burkitt s Lymphoma of the Abdomen: The Northern California Kaiser Permanente Experience J McClenathan Citation J McClenathan. Burkitt s Lymphoma
ISPUB.COM The Internet Journal of Surgery Volume 18 Number 2 Burkitt s Lymphoma of the Abdomen: The Northern California Kaiser Permanente Experience J McClenathan Citation J McClenathan. Burkitt s Lymphoma
Case Cholecystoduodenal fistula with migrated gallstone leading to gastric outlet obstruction: Bouveret's syndrome
 Case 14613 Cholecystoduodenal fistula with migrated gallstone leading to gastric outlet obstruction: Bouveret's syndrome Eva De Backer 1, Filip Vanhoenacker 2, 3, 4, Adelard De Backer5 1: Ghent University,
Case 14613 Cholecystoduodenal fistula with migrated gallstone leading to gastric outlet obstruction: Bouveret's syndrome Eva De Backer 1, Filip Vanhoenacker 2, 3, 4, Adelard De Backer5 1: Ghent University,
The "whirl sign". Diagnostic accuracy for intestinal volvulus.
 The "whirl sign". Diagnostic accuracy for intestinal volvulus. Poster No.: C-0670 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. Pire, M. Marti, A. Borobia, A. Verón; Madrid/ES Keywords: Abdomen,
The "whirl sign". Diagnostic accuracy for intestinal volvulus. Poster No.: C-0670 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. Pire, M. Marti, A. Borobia, A. Verón; Madrid/ES Keywords: Abdomen,
Internal hernias after laparoscopic Roux-en-Y gastric bypass
 The American Journal of Surgery 188 (2004) 796 800 Scientific paper Internal hernias after laparoscopic Roux-en-Y gastric bypass Ernesto Garza, Jr., M.D., Joseph Kuhn, M.D., David Arnold, M.D., William
The American Journal of Surgery 188 (2004) 796 800 Scientific paper Internal hernias after laparoscopic Roux-en-Y gastric bypass Ernesto Garza, Jr., M.D., Joseph Kuhn, M.D., David Arnold, M.D., William
Nasogastric tube. Stomach. Pylorus. Duodenum 1. Duodenum 2. Duodenum 3. Duodenum 4
 Esophagus Barium Swallow Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum 4
Esophagus Barium Swallow Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum 4
Role of radiology in colo-rectal bleedings. Alban DENYS MD FCIRSE EBIR CHUV LAUSANNE
 Role of radiology in colo-rectal bleedings Alban DENYS MD FCIRSE EBIR CHUV LAUSANNE Epidemiology Lower GI bleeding accounts for 20-25% of all GI bleeding Annual incidence in USA :21-27/100000 Longstreth
Role of radiology in colo-rectal bleedings Alban DENYS MD FCIRSE EBIR CHUV LAUSANNE Epidemiology Lower GI bleeding accounts for 20-25% of all GI bleeding Annual incidence in USA :21-27/100000 Longstreth
Spontaneous Intramural Small-Bowel Hematoma: Imaging Findings and Outcome
 Maher. bbas 1 Joseph M. Collins 2 Kevin W. Olden 3 Received December 10, 2001; accepted after revision May 20, 2002. 1 Department of Surgery, Mayo Clinic, 13400 E. Shea lvd., Scottsdale, Z 85259. 2 Department
Maher. bbas 1 Joseph M. Collins 2 Kevin W. Olden 3 Received December 10, 2001; accepted after revision May 20, 2002. 1 Department of Surgery, Mayo Clinic, 13400 E. Shea lvd., Scottsdale, Z 85259. 2 Department
GENERAL SURGERY FOR SMART PEOPLE JOE NOLD MD, FACS WICHITA SURGICAL SPECIALISTS
 GENERAL SURGERY FOR SMART PEOPLE JOE NOLD MD, FACS WICHITA SURGICAL SPECIALISTS CONFLICTS/DECLARATIONS I have no financial conflicts or declarations I AM always willing to see a consult for you TEXT TOPICS
GENERAL SURGERY FOR SMART PEOPLE JOE NOLD MD, FACS WICHITA SURGICAL SPECIALISTS CONFLICTS/DECLARATIONS I have no financial conflicts or declarations I AM always willing to see a consult for you TEXT TOPICS
A novel plain abdominal radiograph sign to diagnose malrotation with volvulus
 A novel plain abdominal radiograph sign to diagnose malrotation with volvulus Nataraja RM 1, Mahomed AA 1* 1. Department of Paediatric Surgery, Royal Alexandra Hospital for Sick Children, Brighton,UK *
A novel plain abdominal radiograph sign to diagnose malrotation with volvulus Nataraja RM 1, Mahomed AA 1* 1. Department of Paediatric Surgery, Royal Alexandra Hospital for Sick Children, Brighton,UK *
Uncommon conditions in surgical oncology: acute abdomen caused by ileocolic intussusception
 Case Report Uncommon conditions in surgical oncology: acute abdomen caused by ileocolic intussusception Karl Mrak Department of Surgery, Brothers of Mercy Hospital, St. Veit, Glan, Austria Correspondence
Case Report Uncommon conditions in surgical oncology: acute abdomen caused by ileocolic intussusception Karl Mrak Department of Surgery, Brothers of Mercy Hospital, St. Veit, Glan, Austria Correspondence
with susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine
 Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Gastrointestinal Tract. Anatomy of GI Tract. Anatomy of GI Tract. (Effective February 2007) (1%-5%)
 Gastrointestinal Tract (Effective February 2007) (1%-5%) Anatomy of GI Tract Esophagus bulls-eye or target EG junction seen on sagittal scan posterior to left lobe of liver and anterior to aorta Anatomy
Gastrointestinal Tract (Effective February 2007) (1%-5%) Anatomy of GI Tract Esophagus bulls-eye or target EG junction seen on sagittal scan posterior to left lobe of liver and anterior to aorta Anatomy
Citywide Infectious Disease Conference. March 27 th, 2018
 Citywide Infectious Disease Conference March 27 th, 2018 Citywide Show and Tell Case 1 Summary 60 s year old Puerto Rican born man SCC of Esophagus, treated with radiation and chemotherapy and then esophageal
Citywide Infectious Disease Conference March 27 th, 2018 Citywide Show and Tell Case 1 Summary 60 s year old Puerto Rican born man SCC of Esophagus, treated with radiation and chemotherapy and then esophageal
ONE of the most severe complications of diverticulitis of the sigmoid
 CLEVELAND CLINIC QUARTERLY Copyright 1970 by The Cleveland Clinic Foundation Volume 37, July 1970 Printed in U.S.A. Colonic diverticulitis with perforation to region of left hip: a rare complication Report
CLEVELAND CLINIC QUARTERLY Copyright 1970 by The Cleveland Clinic Foundation Volume 37, July 1970 Printed in U.S.A. Colonic diverticulitis with perforation to region of left hip: a rare complication Report
Complicated Meckel`s diverticulum; to be considered as a differential diagnosis in the acute abdominal pain. Ultrasound and MDCT imaging finding
 Complicated Meckel`s diverticulum; to be considered as a differential diagnosis in the acute abdominal pain. Ultrasound and MDCT imaging finding Poster No.: C-0174 Congress: ECR 2013 Type: Educational
Complicated Meckel`s diverticulum; to be considered as a differential diagnosis in the acute abdominal pain. Ultrasound and MDCT imaging finding Poster No.: C-0174 Congress: ECR 2013 Type: Educational
Imaging techniques in the diagnosis, staging and follow up of GI cancers. Moderators: Banke Agarwal, MD and Paul Schultz, MD
 Imaging techniques in the diagnosis, staging and follow up of GI cancers Moderators: Banke Agarwal, MD and Paul Schultz, MD Panelists Axel Grothey, MD Professor of Oncology Division of Medical Oncology
Imaging techniques in the diagnosis, staging and follow up of GI cancers Moderators: Banke Agarwal, MD and Paul Schultz, MD Panelists Axel Grothey, MD Professor of Oncology Division of Medical Oncology
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 3, Issue 4 2013 Article 3 Sigmoidorectal Intussusception Presenting as Prolapse Per Anus in an Adult Venugopal Hg Hasmukh B. Vora Mahendra S. Bhavsar SMT.NHL
World Journal of Colorectal Surgery Volume 3, Issue 4 2013 Article 3 Sigmoidorectal Intussusception Presenting as Prolapse Per Anus in an Adult Venugopal Hg Hasmukh B. Vora Mahendra S. Bhavsar SMT.NHL
Inflammatory Bowel Disease When is diarrhea not just diarrhea?
 Inflammatory Bowel Disease When is diarrhea not just diarrhea? Jackie Kazik, MA, PA C CME Resources CAPA Annual Conference, 2011 Inflammatory Bowel Disease Objectives Discuss what is known about the pathophysiology
Inflammatory Bowel Disease When is diarrhea not just diarrhea? Jackie Kazik, MA, PA C CME Resources CAPA Annual Conference, 2011 Inflammatory Bowel Disease Objectives Discuss what is known about the pathophysiology
